Management of diabetic foot ulcers with a TLC-NOSF wound dressing
|
|
|
- Hilda Clarke
- 6 years ago
- Views:
Transcription
1 Management of diabetic foot ulcers with a TLC-NOSF wound dressing Objective: To evaluate the efficacy, tolerance and acceptability of UrgoStart Contact (Laboratoires URGO), a new wound dressing impregnated with NOSF, as an MMP regulator in the management of neuropathic diabetic foot ulcers. Method: A multicentre, pilot, prospective, non-controlled open-label clinical trial. Adult patients with type 1 or 2 diabetes mellitus, suffering from a grade 1A (Texas classification), uninfected neuropathic foot ulcer, 1 15cm 2 in size and duration 1 24 months (mean 6.7 ± 5.2 months) were included in the study. The primary endpoint was the relative reduction of the wound surface area (%) at the end of the study. Secondary end-points included rate of complete healing, tolerability and acceptability of the dressing. Wound dressing was regularly changed at the investigator s discretion according to the wound status and volume of exudates. Patients were followed up every two weeks for a twelve weeks period. At each visit, patients underwent clinical assessments and ulcer surface area was measured by planimetry and photographs. Results: Thirty-four diabetic patients with a neuropathic foot ulcer were included but only 33 cases were analysed, as data were completely lost for one patient. At baseline, mean surface area was 2.7cm 2. At the 12-week visit, the median surface area reduction was 82.7% (mean reduction 62.7 ± 49.9%) and in 10 of the 33 analysed patients (30%), the wound was healed. Only two out of the seven documented local adverse events were deemed to be related to the tested dressing. According to the nursing staff, acceptability was considered as very satisfactory, particularly conformability and ease of use. Conclusion: The use of the new UrgoStart Contact dressing, combined with offloading and debridement, looks effective to promote the healing process of the neuropathic diabetic foot ulcers, with a good tolerance and acceptability. Declaration of interest: This study was supported by grants from Laboratoires URGO pharmaceutical company. S. Bohbot is an employee of Laboratoires URGO; J.L. Richard has received monetary compensation as a consultant and speaker for Laboratoires URGO. Data management and statistical analysis were carried out by StatMed (Villemoirieu, France). neuropathic diabetic foot ulcers; nano-oligosaccharide factor; wound dressing; multicentre clinical trial J.L. Richard, 1 MD; J. Martini, 2 MD; M.M. Bonello Faraill, 3 MD; J. M Bemba, 4 MD; M. Lepeut, 5 MD; F. Truchetet, 6 MD; S. Ehrler, 7 MD; S. Schuldiner, 1 MD; A. Sauvadet, 8 PhD; S. Bohbot, 8 MD; 1 Department of Nutritional Diseases and Diabetology, Medical Centre, Le Grau du Roi, University Hospital of Nîmes, France; 2 Department of Diabetology, Rangueil University Hospital, Toulouse, France; continued on page 144 Despite many therapeutic advances over the past decades, healing rates of diabetic foot ulcers (DFUs) remain low, impacting on patient quality of life and costs. 1,2 Mechanisms of faulty wound healing in diabetic patients are complex, related to both intrinsic and extrinsic factors. 3 Recently, excessive production of matrix metalloproteases (MMPs), coupled with reduced expression of the tissue inhibitors of MMPs, has been emphasised as a key abnormality within the neuropathic DFU. 3 7 This imbalance may result in excessive degradation of extracellular matrix components, as well as an inappropriate local inflammatory response. A number of medical devices that could reduce MMP activity in the wound bed have been developed, such as collagen/oxidised regenerated cellulose (ORC, Promogran, Systagenix Health Care). However, the results of randomised clinical trials (RCTs) comparing ORC with an inert dressing in both chronic venous ulcers, 8 and in DFUs, 9 were ambiguous, as the percentage of complete wound healing was not significantly different in the Promograntreated patients compared with the control group. A new dressing with anti-mmp properties has now been developed, based on a lipidocolloid technology (TLC) impregnated with nano-oligosaccharide factor (NOSF, UrgoStart Contact; Laboratoires URGO). TLC-NOSF is a dressing made of carboxymethylcellulose particles spread in a petroleum jelly network and impregnated with NOSF over a non-woven non-occlusive soft-adherent polyester layer. On contact with exudate, hydrocolloid particles form a gel that interacts with petroleum jelly to make a lipidocolloid film that creates a moist environment within the wound. This environment is claimed to promote healing and prevents the dressing sticking to the wound. Moreover, the TLC allows 142
2 3 Department of Diabetology, Pasteur University Hospital, Nice, France; 4 Department of Diabetology, Hôtel-Dieu University Hospital, Paris, France; 5 Department of Diabetology, General Hospital, Roubaix, France; 6 Department of Dermatology, Beauregard Hospital, Thionville, France; 7 Department of Rehabilitation, Georges Clemenceau Hospital, Strasbourg; France; 8 R&D Department, Laboratoires URGO, Chenôve, France. jean.louis.richard@ chu-nimes.fr NOSF to recover the whole wound and to interact with MMPs, neutralising their activity. In vitro studies using a dermal equivalent model have shown that TLC-NOSF was able to significantly reduce the activity of some MMPs, such as gelatinases (MMP2 and MMP9) and collagenases (MMP1 and MMP8), that are involved in the chronicity of the DFU. 5 7 Clinically, TLC-NOSF was demonstrated to be significantly more effective in reducing wound surface area of venous leg ulcers compared with ORC in a 12-week European multicentre RCT. 13 To our knowledge, no other RCT about efficacy of TLC-NOSF has been published in the peer-reviewed literature. Based on the evidence of these previous clinical trials, this study aimed to conduct a pilot, openlabel clinical trial to estimate the general performance (efficacy, tolerability and acceptability) of this TLC-NOSF matrix in the local management of DFUs. Method This study was an open-label, non-controlled, pilot study conducted in 14 French hospital departments involved in the management of DFU. All participating centres were chosen because they have expertise on the diabetic foot and manage DFUs in a similar way, including wound debridement and offloading. Participants From May 2008 to June 2009, adult patients (> 18 years) with type 1 or 2 diabetes mellitus were included if they presented with neuropathic foot ulceration, as defined by a Michigan neuropathy screening instrument (MNSI) score > The presenting DFU had to be: 1 15cm 2 in size Located on the forefoot or midfoot Classified as grade 1A, according to the Texas University classification system. 15 In addition, more than 50% of the wound surface had to be covered by granulation tissue. Ischaemia was ruled out by presence of pedal pulses, an ankle brachial pressure index (ABPI) 0.8, a toe systolic pressure > 40mmHg, or a TcPO 2 value > 40mmHg. Wounds with any clinical signs or symptoms of infection were excluded. All patients received detailed information on the study protocol and gave written consent before entering the study. Study protocol Included patients were followed for a maximum of 12 weeks, or until full closure, defined as complete epithelialisation of the wound without drainage. After cleansing the wound with saline, the TLC- NOSF dressing was applied directly to the wound bed, without a secondary dressing. UrgoStart Contact dressing (Laboratoires URGO) is a non-absorbent contact matrix impregnated with NOSF developed from Table 1. Patient characteristics at baseline (n=33) Age (years) 60.5 ± 10.4 (60) [34 78] Gender (female/male) 7 (21%)/26 (79%) BMI (kg/m 2 ) 32.6 ± 6.8 (32.8) [ ] Type of diabetes: Type 1 4 (12%) Type 2 28 (85%) Other type 1 (3.0%) Duration of diabetes (years) 17.5 ± 11.6 (16) [1 45] HbA1c (%) 7.5 ± 1.1 (7.6) [ ] Presence of pedal pulses 28 (85%)* Duration of DFU (months) 6.7 ± 5.2 (5) [1 20] Wound area (cm 2 ) 2.70 ± 2.39 (1.95) [ ] Granulation tissue (%) 88.9 ± 15.3 Surrounding skin: Healthy 10 (30%) Hyperkeratosis 21 (64%) Maceration 4 (12%) Offloading (%) 32 (97%) Local treatment prior baseline: Alginate/Hydrofiber 13 (39%) Greasy gauze/contact layer 12 (36%) Hydrocellular 4 (12%) Silver dressing 2 (6.1%) Hyaluronic acid 2 (6.1%) Results are given as number, or mean ± SD (median) [range]; BMI=body mass index; *In five patients, one or both pedal pulses were not palpable, in three patients ABPI was 0.8, and in another patient TcPO 2 was 47mmHg. The fifth patient had a toe systolic pressure of 190mmHg, likely due to medial arterial calcification; peripheral Doppler ultrasonography was normal TLC. It is indicated for the management of moderate to highly exuding wounds. However, its lipid component makes it non-adherent and usable in the light exuding wounds we treated in this study. Patients were assessed at the hospital centres every 2 weeks. At every follow-up visit, a clinical examination was undertaken by the investigating physician, together with a wound tracing on an acetate sheet and photographs of the DFU, for documenta- 144
3 tion. If necessary, a hospital nurse sharply debrided the wound and, together with the investigator, regularly educated the patient about potential foot problems and the importance of offloading. Between visits, local care was delivered at home by a private nurse, according to instructions from the investigating centre, written on a special leaflet. The investigating clinician decided the frequency of dressing change, according to the quantity of exudate and the wound status. At each dressing change, hospital and private nurses assessed the tolerability and acceptability of the dressing on a 4-point scale, by scoring the following parameters: Ease of application and removal Pain and bleeding on removal Conformability to the wound bed Maceration of the wound Adherence of the dressing to the wound bed. Throughout the study period, each patient received standard foot-care, including offloading. If offloading devices were already worn by the patients before they entered into the study, they were encouraged to continue. All patients but one agreed to wear the offloading device; devices were not standardised, but were those usually prescribed in each centre, mainly half-shoes, known as Barouk s shoes in France. The primary endpoint of the study was the relative reduction of the wound surface area (%) at the end of the study; wound surface area was calculated from the tracings by centralised planimetry, using a digital pen and dedicated software (Stat- Med). Secondary endpoints included healing rate and mean healing time, tolerability and acceptability of the dressing. Statistical analysis The statistical analysis was performed on an intention-to-treat (ITT) basis for both the primary and secondary endpoints of the study. If the patient withdrew or healed before the 12-week treatment period, the analysis took account of the last evaluation available (last observation carried forward). Ethics The study was conducted according to European Good Clinical Practices recommendations, the current French regulations and the principles of the declaration of Helsinki. The study was approved by the local French ethics committee (Comité de Protection des Personnes Sud-Mediterranée) and by the French Health Authority (AFSSAPS; registration no A ). For ethical reasons, the investigating physicians were allowed to discontinue the study and change the dressing if they considered that the wound was aggravating and the TLC-NOSF dressing was Fig 1. Flow of participants through the trial Included in the study (n=34) ITT analysis (n=33) Completed study (n=25) Outcomes: Ulcer healed (n=10) Ulcer not healed (n=15) Not analysed (n=1) no longer indicated; in these case, the dressing was recorded as inappropriate. The type of dressing to replace UrgoStart was left to the investigator s discretion. Results Thirty-four consecutive diabetic patients were included in the study. One patient was excluded from the ITT analysis due to completely missing data; therefore, the ITT analysis took account 33 patients; patient baseline characteristics are shown in Table 1. Each centre included between one and six patients. In five centres, a single patient was included, three centres included two patients, three others included three patients, two centres included four patients, and one centre included six patients. As shown in the Fig 1, 25 patients (76%) completed the study according to the protocol (either fullclosure or 12-week study period). At baseline, mean ulcer surface area was 2.7 ± 2.4cm 2. Coverage of the wound by granulation tissue was 89 ± 15% of the wound surface. At baseline, 97% (n=32) of the patients had an effective offloading system. Healing At the end of the study, 10 DFUs (30%) had healed, seven before the 12-week scheduled period and three on the week 12 visit. Median and mean (± SD) healing times were 58 days and 58.9 ± 25.7 days, respectively. In 24 patients (73%), the wound Reasons: Subjects data completely missing (n=1) Withdrawn (n=8) Reasons: Serious adverse event (n=5) Dressing deemed inappropriate by investigator (n=3) References 1 Snyder, R.J., Hanft, J.R. Diabetic foot ulcers. Effects on QoL, costs, and mortality and the role of standard wound care and advanced-care therapies. Ostomy Wound Manage ; 55: 11, Nabuurs-Franssen, M.H., Huijberts, M.S., Nieuwenhuijzen Kruseman, A.C. et al. Health-related quality of life of diabetic foot ulcer patients and their caregivers. Diabetologia. 2005; 48: 9, Jeffcoate, W.J., Price, P., Harding, K.G. Wound healing and treatments for people with diabetic foot ulcers. Diabetes Metab Res Rev. 2004; 20: (Suppl. 1), S Sibbald, R.G., Woo, K.Y. The biology of chronic foot ulcers in persons with diabetes. Diabetes Metab Res Rev. 2008; 224: (Suppl. 1), S Liu, Y., Min, D., Bolton, T. et al. Increased matrix metalloproteinase-9 predicts poor wound healing in diabetic foot ulcers. Diabetes Care. 2009; 32: 1,
4 6 Lobmann, R., Ambrosch, A., Schultz, G. et al. Expression of matrix-metalloproteinases and inhibitors in the wounds of diabetic and non-diabetic patients. Diabetologia. 2002; 45: 7, Lobmann, R., Zemlin, C., Motzkau, M. et al. Expression of matrix metalloproteinases and growth factors in diabetic foot wounds treated with a protease absorbent dressing. J Diabetes Complications. 2006; 20: 5, Vin, F.L., Téot, L., Meaume, S. The healing properties of Promogran in venous leg ulcers. J Wound Care. 2002; 11: 9, Veves, A., Sheehan, P., Pham, H.T. A randomized controlled trial of Promogran (a collagen/ oxidized regenerated cellulose dressing) vs standard treatment in the management of diabetic foot ulcers. Arch Surg. 2002; 137: 7, Coulomb, B., Couty, L., Fournier, B. et al. A NOSF (nano-oligasaccharide factor) lipido-colloid dressing inhibits MMPs in an in vitro dermal equivalent model. Wound Repair Regen. 2008; 16: 4, A Couty, L., Fournier, B., Laurensou, C. et al. A NOSF (nano-oligasaccharide factor) lipido-colloid dressing stimulates MMPs/TIMPs complexes formation leading to MMPs inhibition in an in vitro dermal equivalent model. Wound Repair Regen. 2009; 17: 4, A64. Reduction of wound area (%) Table 2. General adverse events Description Severity Withdrawn Outcome at end of study Sepsis and acute renal failure Serious (hospitalisation) Yes Unknown Gastroenteritis Serious (hospitalisation) Yes Cured Worsening of the wound Serious (hospitalisation) No Not resolved Probable stroke Serious (death) Yes Cellulitis Serious (hospitalisation) Yes Cured Skin and soft-tissue infection with pus discharge Serious (hospitalisation) Yes Not resolved Conjunctivitis after planed intervention Serious (hospitalisation) No Cured but persistence of for cataract ocular smarting Osteomyelitis of the foot Serious (hospitalisation) No Cured Hypoglycaemic coma Serious (hospitalisation) No Cured Bronchitis Moderate No Cured Tachycardia Mild No Cured Attack of acute gout (left hand) Moderate No Cured Fig 2. Median percentage reduction of ulcer area over the time Table 3. Ease of application/removal of UrgoStart dressing Ease to apply Time (weeks) Ease to remove Very easy 537 (56%) 857 (92%) Easy 378 (39%) 66 (7.1%) Difficult 36 (3.8%) 2 (0.2%) Very difficult 6 (0.6%) 1 (0.1%) Missing data 25 5 Each item was scored by nurses, using a 4-point scale, when dressing was applied (n=982) or removed (n=931) at home or during hospital visits was considered as improving, according to the investigator s judgment, by week 12. At week 12, the median and mean wound surface area were 0.47cm 2 and 0.92 ± 1.47cm 2, respectively. Median reduction of the wound surface area was 82.7% at week 12, compared with baseline surface area, with a mean reduction of 62.7 ± 49.9%. Median percentage reduction in ulcer surface area over the time is shown in Fig 2. In 14 of the 33 patients (42%), wound surface area decreased by more than 50% by week 4. In eight of those patients, the ulcer healed during the 12-week study period, while the surface area decreased by > 95% in four of the six remaining patients. Safety Seven local adverse events were reported over the study duration. Two (maceration) were assessed as possibly or probably related to the dressing, while the five remaining adverse events were judged as not attributable to the dressing (were allergy to a topical cream, occurrence of a phlyctena, occurrence of a new ulcer, foot swelling and skin and softtissue infection). Thirteen general adverse events occurred throughout the study, nine of them serious (Table 2), although none of these were considered to be related to the wound management or dressing by the investigators. In five patients, these serious adverse events led to treatment discontinuation. Four patients recovered with no after-effects and one had only minor local persistent trouble due to chronic conjunctivitis. Finally, three other patients were withdrawn from the trial and switched to another dressing according to the investigator expertise, as the wound was considered to be not responding and the tested dressing 146
5 Table 4. Acceptability and tolerance of the TLC-NOSF dressing Bleeding on Pain on dressing Maceration Adherence to Exudation Unpleasant dressing removal removal the wound odour Absence 879 (95%) 887 (96%) 671 (73%) 887 (96%) 532 (58%) 864 (94%) Mild 44 (4.8%) 0 (0%) 235 (25%) 37 (4.0%) 366 (40%) 54 (5.9%) Moderate 2 (0.2%) 37 (4.0%) 15 (1.6%) 3 (0.3%) 17 (1.8%) 4 (0.4%) Important 0 (0.0%) 3 (0.3%) 2 (0.2%) 0 (0.0%) 5 (0.5%) 0 (0.0%) Missing data Each item was scored by nurses, using a 4-point scale, when dressing was removed (n=931) at home or during hospital visits Table 5. Conformability of the TLC-NOSF dressing to the wound Conformability Very good 364 (40%) Good 402 (45%) Poor 128 (14%) Very poor 7 (0.8%) Missing data 81 Each item was scored by nurses when the dressing was applied (n=982) no longer adequate. Overall, eight patients (24%) prematurely discontinued the study before the week 12 (Fig 1). Tolerance and acceptability In total, 982 applications of TLC-NOSF dressings were recorded, accounting for 2189 days of treatment, with 931 removals documented. An average of 2.5 dressings were applied per patient per week, equalling one new dressing every 2 days. According to the nurses opinion, application of the dressing was assessed as easy or very easy in 95.6% of cases and its removal in 99.1% (Table 3). Absence of bleeding or pain on removal was recorded in 95.0% and 95.7%, respectively (Table 4). Wound maceration and adherence of the dressing to the wound bed was judged as moderate or important in 1.8% and 0.3%, respectively (Table 4). Finally, conformability of the dressing when applied to the wound was considered as good or very good in 85.0% of cases (Table 5). Discussion The aim of this pilot, open-label clinical trial was to assess the overall performance (efficacy, acceptability and tolerance) of the TLC-NOSF wound dressing in grade 1A neuropathic DFUs. In terms of efficacy, combined with good wound care, including offloading and regular debridement, use of the TLC-NOSF matrix was associated with a median relative reduction in the surface area of 82.7% (mean 62.7 ± 49.9%) by the end of the 12-week follow-up period. Further, 30% of DFUs healed during the 12-week study period and 73% were considered to be improving. The non-controlled design of this pilot clinical trial makes interpretation of the results difficult; however, these preliminary data look encouraging. An indirect comparison with the published data on DFU management has to undertaken very carefully, even if the characteristics of the wounds included in this trial and their prognostic indicators (size, duration, grade and absence of infection) were similar to those reported in other published trials. Despite this, our results seemingly compare favourably with those from the literature. In a systematic review of 10 RCTs, Margolis et al. evaluated the healing rate of neuropathic DFUs treated with a control (gauze or a placebo). 16 The mean healing rate was 24.2% in 450 patients followed up for 12 weeks, and 30.9% for those (n=172) followed up for 20 weeks. All patients in the control groups received good standard wound care, similar to that given in our study. More specifically, the results of our study are similar to those obtained using ORC, another MPP inhibitor. In the study by Vin et al. 8 on non-infected chronic venous leg ulcers measuring between >2cm and 10cm at baseline, the median and mean wound reduction in ORC-treated patients were 54.4 ± 10.9% and 82.4%, respectively. In a RCT comparing ORC and moistened gauze in the management of DFUs, Veves et al. showed a mean percentage of wound reduction of 64.5% in the ORC group. 9 As wound protease activity is thought to have a detrimental effect on growth factors during the healing process, 17 and the TLC-NOSF matrix inhibits MMPs, it is also interesting to compare the 12 Coulomb, B., Couty, L., Fournier, B. et al. Evaluation of a matrix impregnated with NOSF in an in vitro dermal reconstruction model [article in French]. Journal Plaies Cicatrisations. 2008; 13: Schmutz, J.L., Meaume, S., Fays, S. et al. Evaluation of the nano-oligosaccharide factor lipido-colloid matrix, in the local management of venous leg ulcers: results of a randomized controlled trial. Int Wound J. 2008; 5: 2, Feldman, E.L., Stevens, M.J., Thomas, P.K. et al. A practical two-step quantitative clinical and electrophysiological assessment for the diagnosis and staging of diabetic neuropathy. Diabetes Care. 1994; 17: 11, Armstrong, D.G., Lavery, L.A., Harkless, L.B. Validation of a diabetic wound classification system: the contribution of depth, infection and vascular disease to the risk of amputation. Diabetes Care. 1998; 21: 5, Margolis, D.J., Kantor, J., Berlin, J.A. Healing of diabetic neuropathic foot ulcers receiving standard treatment. A meta-analysis. Diabetes Care. 1999; 22: 5, Yager, D.R., Nwomeh, B.C. The proteolytic environment of chronic wounds. Wound Repair Regen. 1999; 7: 6, Smiell, J.M., Wieman, T.J., Steed, D.L. et al. Efficacy and safety of becaplermin (recombinant human platelet-derived growth factor-bb) in patients with nonhealing, lower extremity diabetic ulcers: a combined analysis of four randomized studies. Wound Repair Regen. 1999; 7: 5, Steed, D.L., Diabetic Ulcer Study Group. Clinical evaluation of recombinant human platelet-derived growth factor for the treatment of lower extremity diabetic ulcers. J Vasc Surg. 1995; 21: 1, Embil, J.E., Sibbald, G., Tousignant, J. et al. Recombinant human platelet-derived growth factor-bb (becaplermin) for healing chronic lower extremity diabetic ulcer: an open-label clinical evaluation of efficacy. Wound Repair Regen. 2000; 8: 3,
6 21 Niezgoda, J.A., van Gils, C.C., Frykberg, R.G., Hodde, J.P. Randomized clinical trial comparing OASIS Wound Matrix to Regranex Gel for diabetic ulcers. Adv Skin Wound Care. 2005; 18: (Pt 1), Sheehan, P., Jones, P., Caselli, A. et al. Percent change in wound area of diabetic foot ulcers over a 4-week period is a robust predictor of complete healing in a 12-week prospective trial. Diabetes Care. 2003; 26: 6, Meaume, S., Ourabah, Z., Cartier, H. et al. Evaluation of a lipidocolloid wound dressing in the local management of leg ulcers. J Wound Care. 2005; 14: 7, Part of this study was published in abstract form at the 14th Conférences Plaies et Cicatrisation (CPC), Paris, France, January 2010; at the 20th Conference of the European Wound Management Association (EWMA), Geneva, Switzerland, May 2010 and at the 12th Congress of the German Society of Wound Healing (DFfW), Freiburg, Germany, June results of the present study with those on growth factor therapy in DFUs. Smiell et al. published a combined analysis of four randomised studies that evaluated the effects of a topical platelet-derived growth factor (PDGF) (becaplermin gel, Regranex) in DFUs. 18 Included ulcers were mostly small (median baseline size: 1.5cm 2 ) chronic, uninfected, fullthickness (category III/IV) ulcers, with a sufficient arterial blood supply; therefore, the inclusion criteria were comparable to those of the present study. After 20 weeks of treatment by platelet-derived growth factor (PDGF), the healing rate was estimated to be 50.2%, significantly higher than in the placebo group (36.3%; p=0.007). Despite this, in the first study on PDGF, which involved 118 patients with neuropathic DFUs, 19 while the healing rate was 48% and 25% after 20 weeks of treatment in the PDGF and control group, respectively, this rate decreased to approximately 30% and 10% after 12 weeks of treatment. It is worth noting that this study enrolled diabetic patients with neuropathic ulcers similar to those of our study, except for a larger size (mean and median area 9cm 2 and 4.9cm 2 in the placebo group, respectively and 5.5cm 2 and 3.1cm² in the PDGF-treated group). Moreover, as in the present study, ulcers were sharply debrided and offloaded, as standard treatment protocol. Embil et al. 20 also conducted an open-label study to assess the efficacy of becaplermin in 134 chronic, uninfected, well-perfused, fullthickness (category III/IV) and superficial neuropathic DFUs. Mean ulcer area at baseline (2.71 ± 2.30cm 2 ) was comparable to that in the present study and ulcers were offloaded and regularly debrided, if necessary. Becaplermin gel application resulted in complete healing in 57.5% of patients after 20 weeks of treatment, with a mean time to closure of 63 days. Finally, in a more recent RCT involving 73 patients with grade 1A neuropathic DFUs, 21 the rate of wound closure with becaplermin was 28% after 12 weeks of treatment, with a mean healing time of 73 days. Despite the encouraging results from the studies of Steed 19 and Embil et al., 20 this RCT would suggest using PDGF to heal neuropathic DFUs gives no decisive definite advantages over simpler and less costly approaches, such as dressings. Anecdotally, our study confirms that percentage change in DFU surface area after 4 weeks of treatment is predictive of healing at 12 weeks, as shown by Sheehan et al. 22 Regarding safety, two local adverse events were reported as possibly related to the tested dressing. This low incidence gives evidence for the good tolerance of the matrix, already reported in a previous trial on leg ulcers. 13 Therefore, the addition of the NOSF compound in the neutral TLC seems not to modify the tolerability of the neutral matrix, which has been reported as very satisfactory. 23 Serious adverse events were experienced by nine patients (27%), a percentage close to that reported by Embil et al. (22%) in becaplermin-treated patients, 20 and by Smiell et al. 18 in the combined analysis of the four randomised studies (24% in the PDGF-treated group, 25% in the placebo group and 28% in the group treated with good ulcer care alone). Moreover, as in the preceding studies, most of the serious adverse events were related to non-healing DFUs, or diabetic complications, and the majority were considered by the investigators as unrelated to the study dressing. Finally, the dressing was well accepted by both nurses and patients, as its application and removal were judged easy and painless with a good conformability to the wound bed in the majority of cases. Limitations There are a number of limitations of this study. Notwithstanding its non-randomised, non-controlled, non-blinded design, this study included only a small number of patients, despite being a multicentre trial conducted in departments specialised in the management of DFUs. This specialisation could explain in part the difficulty experienced in recruiting patients into the study; those referred to specialised units generally have complicated DFUs, such as infected or ischaemia-associated wounds, while the protocol was aimed at the grade 1A, non-infected, non-ischaemic, superficial wounds. It might be surprising that our study tested TLC-NOSF wound dressing in superficial, mildly exuding ulcers, but these were chronic and recalcitrant, as shown by their long duration (median 5 months) and failure to respond to previous topical treatments. This suggests that these ulcers were stalled in a non-healing phase, possibly due to an excess of MPPs. Another limitation of the study is a possible selection bias, despite including consecutive patients in the study, if they fulfilled the protocol criteria. Finally, as the wounds were not examined by the same observer in a single centre, with some subjective outcomes, and inter-rater reliability was not assessed, a judgment bias may be possible. Despite this, the investigators were part of an experienced staff, very homogeneous in their practice; moreover, at the initiation visit all members involved in the trial were trained. Conclusion This pilot clinical trial suggests that this new impregnated TLC-NOSF matrix (UrgoStart Contact) could be an interesting adjunct in the therapeutic strategy of these chronic wounds. It now remains necessary to consolidate these encouraging preliminary results with clinical data from a randomised controlled trial in patients with more complex and severe neuropathic DFU. 148
Management of diabetic foot ulcers with a TLC-NOSF wound dressing
 Management of diabetic foot ulcers with a TLC-NOSF wound dressing l Objective: To evaluate the efficacy, tolerance and acceptability of UrgoStart Contact (Laboratoires Urgo), a new wound dressing impregnated
Management of diabetic foot ulcers with a TLC-NOSF wound dressing l Objective: To evaluate the efficacy, tolerance and acceptability of UrgoStart Contact (Laboratoires Urgo), a new wound dressing impregnated
The Georgetown Team Approach to Diabetic Limb Salvage: 2013
 The Georgetown Team Approach to Diabetic Limb Salvage: 2013 John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Disclosures: None Need
The Georgetown Team Approach to Diabetic Limb Salvage: 2013 John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Disclosures: None Need
Fibroblast proliferation plays a vital role in helping. Assessing an adherent silicone foam dressing: a clinical evaluation across five NHS trusts
 Assessing an adherent silicone foam dressing: a clinical evaluation across five NHS trusts Abstract The wound contact layer of UrgoTul Absorb Border (Urgo Medical) foam dressing contains a Technology Lipido
Assessing an adherent silicone foam dressing: a clinical evaluation across five NHS trusts Abstract The wound contact layer of UrgoTul Absorb Border (Urgo Medical) foam dressing contains a Technology Lipido
Oxygen is required for normal cellular
 Article The role of topical oxygen therapy in the management of diabetic foot ulcer s in Scotland: round table recommendations Citation: Stang D, Young M, Wilson D et al (18) The role of topical oxygen
Article The role of topical oxygen therapy in the management of diabetic foot ulcer s in Scotland: round table recommendations Citation: Stang D, Young M, Wilson D et al (18) The role of topical oxygen
Diabetic Foot Ulcer Treatment and Prevention
 Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
Diabetic Foot Ulcer Treatment and Prevention Alexander Reyzelman DPM, FACFAS Associate Professor California School of Podiatric Medicine at Samuel Merritt University Diabetic Foot Ulcers One of the most
Evaluation of the nanooligosaccharide
 ORIGINAL ARTICLE Evaluation of the nanooligosaccharide factor lipidocolloid matrix in the local management of venous leg ulcers: results of a randomised, controlled trial Jean-Luc Schmutz, Sylvie Meaume,
ORIGINAL ARTICLE Evaluation of the nanooligosaccharide factor lipidocolloid matrix in the local management of venous leg ulcers: results of a randomised, controlled trial Jean-Luc Schmutz, Sylvie Meaume,
Clinical. Summaries. 3M Tegaderm Matrix Matrix Dressing. Delayed wound healing: A major clinical problem
 3M Tegaderm Matrix Matrix Dressing Clinical Summaries Delayed wound healing: A major clinical problem Chronic wounds have been defined as those that fail to progress through a normal, orderly, and timely
3M Tegaderm Matrix Matrix Dressing Clinical Summaries Delayed wound healing: A major clinical problem Chronic wounds have been defined as those that fail to progress through a normal, orderly, and timely
Dressings do not heal wounds properly selected dressings enhance the body s ability to heal the wound. Progression Towards Healing
 Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Mean percent reduction in ulcer area from baseline at six weeks 62 % SANTYL Ointment + supportive care* + sharp debridement 1 (P<0.
 Evaluating two common adjuncts to sharp debridement in the treatment of diabetic foot ulcers Mean percent reduction in ulcer area from baseline at six weeks 62 % 40 % SANTYL Ointment + supportive care*
Evaluating two common adjuncts to sharp debridement in the treatment of diabetic foot ulcers Mean percent reduction in ulcer area from baseline at six weeks 62 % 40 % SANTYL Ointment + supportive care*
- Conclusion: This study confirmed the very good acceptability and efficacy of Urgotul in the treatment of skin lesions in patients with EB.
 www.journalofwoundcare.com Using Urgotul dressing for the management of epidermolysis bullosa skin lesions VOL 14, NO 10, November 2005 Objective: To evaluate the acceptability, tolerance and efficacy
www.journalofwoundcare.com Using Urgotul dressing for the management of epidermolysis bullosa skin lesions VOL 14, NO 10, November 2005 Objective: To evaluate the acceptability, tolerance and efficacy
1/5. Introduction. Primary endpoint Time to reach readiness for closure by surgical intervention or left for closure by secondary intention
 1/5 Introduction Materials and methods Animal studies show that intermittent NPWT has potential to increase the rate of granulation tissue formation compared with adjustable intermittent (AI) NPWT 1 However,
1/5 Introduction Materials and methods Animal studies show that intermittent NPWT has potential to increase the rate of granulation tissue formation compared with adjustable intermittent (AI) NPWT 1 However,
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management
 An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
An investigation of Cutimed Sorbact as an antimicrobial alternative in wound management G Kammerlander, E Locher, A Suess-Burghart, B von Hallern, P Wipplinger Abstract Background: Antimicrobial dressings
Treatment options for diabetic neuropathic foot ulcers: a cost-effectiveness analysis Kantor J, Margolis D J
 Treatment options for diabetic neuropathic foot ulcers: a cost-effectiveness analysis Kantor J, Margolis D J Record Status This is a critical abstract of an economic evaluation that meets the criteria
Treatment options for diabetic neuropathic foot ulcers: a cost-effectiveness analysis Kantor J, Margolis D J Record Status This is a critical abstract of an economic evaluation that meets the criteria
Prediction of healing for post-operative diabetic foot wounds based on early wound area progression
 Diabetes Care Publish Ahead of Print, published online October 12, 2007 Prediction of healing for post-operative diabetic foot wounds based on early wound area progression Lawrence A Lavery, DPM, MPH 1
Diabetes Care Publish Ahead of Print, published online October 12, 2007 Prediction of healing for post-operative diabetic foot wounds based on early wound area progression Lawrence A Lavery, DPM, MPH 1
Do all foam dressings have the same efficacy in the treatment of chronic wounds? Janice Bianchi, David Gray, John Timmons, Sylvie Meaume
 Do all foam dressings have the same efficacy in the treatment of chronic wounds? The challenge of chronic wounds remains significant both in terms of clinical management, impact on patients and cost to
Do all foam dressings have the same efficacy in the treatment of chronic wounds? The challenge of chronic wounds remains significant both in terms of clinical management, impact on patients and cost to
INTEGRATED THERAPEUTIC SOLUTIONS TO MANAGE AND PREVENT DIABETIC FOOT ULCERS
 INTEGRATED THERAPEUTIC SOLUTIONS TO MANAGE AND PREVENT DIABETIC FOOT ULCERS UE REMOVE EXU D R IA ER T C D TISS UIL EB ATE AN DB A REMOVE REBUILD REDUCE Cutimed Siltec Sorbact featuring DACC Technology
INTEGRATED THERAPEUTIC SOLUTIONS TO MANAGE AND PREVENT DIABETIC FOOT ULCERS UE REMOVE EXU D R IA ER T C D TISS UIL EB ATE AN DB A REMOVE REBUILD REDUCE Cutimed Siltec Sorbact featuring DACC Technology
A Pilot Study of Oxygen Therapy for Acute Leg Ulcers
 A Pilot Study of Oxygen Therapy for Acute Leg Ulcers Background: The concept of increasing the oxygen concentration in healing wounds developed originally with hyperbaric oxygen therapy and from the fact
A Pilot Study of Oxygen Therapy for Acute Leg Ulcers Background: The concept of increasing the oxygen concentration in healing wounds developed originally with hyperbaric oxygen therapy and from the fact
Cost-effectiveness of becaplermin for nonhealing neuropathic diabetic foot ulcers Sibbald R G, Torrance G, Hux M, Attard C, Milkovich N
 Cost-effectiveness of becaplermin for nonhealing neuropathic diabetic foot ulcers Sibbald R G, Torrance G, Hux M, Attard C, Milkovich N Record Status This is a critical abstract of an economic evaluation
Cost-effectiveness of becaplermin for nonhealing neuropathic diabetic foot ulcers Sibbald R G, Torrance G, Hux M, Attard C, Milkovich N Record Status This is a critical abstract of an economic evaluation
Use of topical negative pressure with a lipidocolloid dressing: results of a clinical evaluation
 Use of topical negative pressure with a lipidocolloid dressing: results of a clinical evaluation Téot L, Lambert L, Ourabah Z, Bey E, Steenman C, Wierzbiecka E, Malikov S, Charles JP, Vives F, Bohbot S
Use of topical negative pressure with a lipidocolloid dressing: results of a clinical evaluation Téot L, Lambert L, Ourabah Z, Bey E, Steenman C, Wierzbiecka E, Malikov S, Charles JP, Vives F, Bohbot S
Your guide to wound debridement and assessment. Michelle Greenwood. Lorraine Grothier. Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust
 Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Your guide to wound debridement and assessment Michelle Greenwood Lead Nurse, Tissue Viability, Walsall Healthcare NHS Trust Lorraine Grothier Clinical Nurse Specialist, Tissue Viability, Central Essex
Patient Care Information
 Patient Care Information A Guide to Healing Diabetic Foot Ulcers Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Dermal Regeneration Matrix Overview Diabetic foot ulcers are
Patient Care Information A Guide to Healing Diabetic Foot Ulcers Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Dermal Regeneration Matrix Overview Diabetic foot ulcers are
An observational evaluation of a new foam adhesive dressing
 An observational evaluation of a new foam adhesive dressing Elizabeth Merlin-Manton, Michelle Greenwood and Adele Linthwaite An observational evaluation of a new foam adhesive dressing Elizabeth Merlin-Manton,
An observational evaluation of a new foam adhesive dressing Elizabeth Merlin-Manton, Michelle Greenwood and Adele Linthwaite An observational evaluation of a new foam adhesive dressing Elizabeth Merlin-Manton,
Regenerative Tissue Matrix in Treatment of Wounds
 Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
Regenerative Tissue Matrix in Treatment of Wounds Learning Objectives Differentiate between reparative and regenerative healing Review surgical techniques for applying a regenerative tissue scaffold to
3M Tegaderm Matrix Matrix Dressing. Conquer Non-healing. Wounds
 Conquer Non-healing Wounds Chronic wounds Chronic wounds have been defined as those that fail to progress through a normal, orderly and timely sequence of repair. Or, wounds that pass through the repair
Conquer Non-healing Wounds Chronic wounds Chronic wounds have been defined as those that fail to progress through a normal, orderly and timely sequence of repair. Or, wounds that pass through the repair
Lower Extremity Wound Evaluation and Treatment
 Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Clinical Policy: EpiFix Wound Treatment
 Clinical Policy: Reference Number: PA.CP.MP.140 Effective Date: 03/18 Last Review Date: 04/18 Coding Implications Revision Log Description EpiFix (MiMedx Group) is dehydrated human amniotic tissue that
Clinical Policy: Reference Number: PA.CP.MP.140 Effective Date: 03/18 Last Review Date: 04/18 Coding Implications Revision Log Description EpiFix (MiMedx Group) is dehydrated human amniotic tissue that
Venous Leg Ulcers. Care for Patients in All Settings
 Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Venous Leg Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a venous leg ulcer. The scope of the standard
Health-related quality of life of diabetic foot ulcer patients and their caregivers
 Diabetologia (2005) 48: 1906 1910 DOI 10.1007/s00125-005-1856-6 ARTICLE M. H. Nabuurs-Franssen. M. S. P. Huijberts. A. C. Nieuwenhuijzen Kruseman. J. Willems. N. C. Schaper Health-related quality of life
Diabetologia (2005) 48: 1906 1910 DOI 10.1007/s00125-005-1856-6 ARTICLE M. H. Nabuurs-Franssen. M. S. P. Huijberts. A. C. Nieuwenhuijzen Kruseman. J. Willems. N. C. Schaper Health-related quality of life
Wound Management. E. Foy White-Chu, MD, CWSP
 Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
Wound Management E. Foy White-Chu, MD, CWSP E. Foy White-Chu, MD, CWSP Assistant Professor, OHSU Wound Medical Director, VAPORHCS List the Four Principles of Wound Bed Preparation Determine safe debridement
Leg ulceration is a common problem, with an
 Clinical evaluation of a dressing with poly absorbent fibres and a silver matrix for managing chronic wounds at risk of infection: a non comparative trial Objective: To assess the efficacy, safety and
Clinical evaluation of a dressing with poly absorbent fibres and a silver matrix for managing chronic wounds at risk of infection: a non comparative trial Objective: To assess the efficacy, safety and
A Post-hoc Analysis of Reduction in Diabetic Foot Ulcer Size at 4 Weeks as a Predictor of Healing by 12 Weeks
 A Post-hoc Analysis of Reduction in Diabetic Foot Ulcer Size at 4 Weeks as a Predictor of Healing by 12 Weeks Robert J. Snyder, DPM, CWS; Matthew Cardinal, ME; Damien M. Dauphinée, DPM, FACFAS, CWS; and
A Post-hoc Analysis of Reduction in Diabetic Foot Ulcer Size at 4 Weeks as a Predictor of Healing by 12 Weeks Robert J. Snyder, DPM, CWS; Matthew Cardinal, ME; Damien M. Dauphinée, DPM, FACFAS, CWS; and
Appropriate Dressing Selection For Treating Wounds
 Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
INTRODUCTION TO WOUND DRESSINGS
 WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
Exudate in the early stages of wound healing
 Products & technology Wound management with the Biatain Silicone foam dressing: A multicentre product evaluation Authors: Hugues Cartier, Simon Barrett, Karen Campbell, Jan Forster, Mike Schmalzbauer,
Products & technology Wound management with the Biatain Silicone foam dressing: A multicentre product evaluation Authors: Hugues Cartier, Simon Barrett, Karen Campbell, Jan Forster, Mike Schmalzbauer,
Setting The setting was a hospital. The economic study was carried out in the USA.
 A cost analysis of a living skin equivalent in the treatment of diabetic foot ulcers Steinberg J, Beusterien K, Plante K, Nordin J, Chaikoff E, Arcona S, Kim J, Belletti D A Record Status This is a critical
A cost analysis of a living skin equivalent in the treatment of diabetic foot ulcers Steinberg J, Beusterien K, Plante K, Nordin J, Chaikoff E, Arcona S, Kim J, Belletti D A Record Status This is a critical
JMSCR Vol 06 Issue 03 Page March 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i3.55 Thesis Paper A Prospective Comparative
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v6i3.55 Thesis Paper A Prospective Comparative
Diabetic Foot Ulcers. Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C. Advanced Practice Nurse / Adult Clinical Nurse Specialist
 Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
Diabetic Foot Ulcers Alex Khan APRN ACNS-BC MSN CWCN CFCN WCN-C Advanced Practice Nurse / Adult Clinical Nurse Specialist Organization of Wound Care Nurses www.woundcarenurses.org Objectives Identify Diabetic/Neuropathic
Advancing the science of wound bed preparation
 Advancing the science of wound bed preparation How Drawtex wound dressing works LevaFiber Technology provides three different types of action. Mechanisms of Action Capillary Action Hydroconductive Action
Advancing the science of wound bed preparation How Drawtex wound dressing works LevaFiber Technology provides three different types of action. Mechanisms of Action Capillary Action Hydroconductive Action
Smart Solutions for Serious Wounds. An advanced bilayer dermal regeneration matrix FDA approved for the treatment of diabetic foot ulcers.
 Smart Solutions for Serious Wounds An advanced bilayer dermal regeneration matrix FDA approved for the treatment of diabetic foot ulcers. A New Approach to Diabetic Foot Ulcer Care Supported by Over Two
Smart Solutions for Serious Wounds An advanced bilayer dermal regeneration matrix FDA approved for the treatment of diabetic foot ulcers. A New Approach to Diabetic Foot Ulcer Care Supported by Over Two
A Prospective Study of Negative Pressure Wound Therapy With Integrated Irrigation for the Treatment of Diabetic Foot Ulcers
 A Prospective Study of Negative Pressure Wound Therapy With Integrated Irrigation for the Treatment of Diabetic Foot Ulcers Charles M. Zelen, DPM, FACFAS, a,b Brian Stover, DPM, a David Nielson, DPM, a,b
A Prospective Study of Negative Pressure Wound Therapy With Integrated Irrigation for the Treatment of Diabetic Foot Ulcers Charles M. Zelen, DPM, FACFAS, a,b Brian Stover, DPM, a David Nielson, DPM, a,b
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated April 7,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Use of an Acellular Regenerative Tissue Matrix Over Chronic Wounds
 Use of an Acellular Regenerative Tissue Matrix Over Chronic Wounds D. Heath Stacey, MD Northwest Arkansas Center for Plastic Surgery, Fayetteville, Ark Correspondence: dheathstacey@gmail.com Keywords:
Use of an Acellular Regenerative Tissue Matrix Over Chronic Wounds D. Heath Stacey, MD Northwest Arkansas Center for Plastic Surgery, Fayetteville, Ark Correspondence: dheathstacey@gmail.com Keywords:
Hyperbarics in Diabetic Wound Care. Aurel Mihai, MD & Brian Kline, MD
 Hyperbarics in Diabetic Wound Care Aurel Mihai, MD & Brian Kline, MD Presentation Outline The Scope of the Problem Important Definitions Standard Wound Care Hyperbaric Oxygen as an Adjunct Diabetic Foot
Hyperbarics in Diabetic Wound Care Aurel Mihai, MD & Brian Kline, MD Presentation Outline The Scope of the Problem Important Definitions Standard Wound Care Hyperbaric Oxygen as an Adjunct Diabetic Foot
Case study: A targeted approach to healing complex wounds using the geko device.
 Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Case study: A targeted approach to healing complex wounds using the geko device. Authors: Mr Sameh Dimitri Consultant Vascular and Endovascular Surgeon MSc FRCS (Eng Edin) Nikki Pavey Physiotherapist at
Increased Matrix Metalloproteinase-9 Predicts Poor Wound Healing in Diabetic Foot Ulcers
 Diabetes Care Publish Ahead of Print, published online October 3, 2008 MMP-9 Predicts Wound Healing Increased Matrix Metalloproteinase-9 Predicts Poor Wound Healing in Diabetic Foot Ulcers Yu Liu, MD 1,
Diabetes Care Publish Ahead of Print, published online October 3, 2008 MMP-9 Predicts Wound Healing Increased Matrix Metalloproteinase-9 Predicts Poor Wound Healing in Diabetic Foot Ulcers Yu Liu, MD 1,
SDMA Categorisation of Wound Care and Associated Products
 Version 7 - February 2015 TAPES AND TRADITIONAL DRESSINGS Traditional Wound Dressings Wound Dressings Packs Swabs Swabs Swab Products Adhesive Tapes Taping Sheets Absorbent Wadding Absorbent Dressings
Version 7 - February 2015 TAPES AND TRADITIONAL DRESSINGS Traditional Wound Dressings Wound Dressings Packs Swabs Swabs Swab Products Adhesive Tapes Taping Sheets Absorbent Wadding Absorbent Dressings
The primary function of low-adherence wound contact
 S35 Product focus S35 A multicentre clinical evaluation of silicone wound contact layer in daily practice Abstract Objective To evaluate clinically the performance of, a silicone-based primary contact
S35 Product focus S35 A multicentre clinical evaluation of silicone wound contact layer in daily practice Abstract Objective To evaluate clinically the performance of, a silicone-based primary contact
Adjunctive Therapies: The Use of Skin Substitutes and Growth Factors in Venous Leg Ulceration (VLU)
 Adjunctive Therapies: The Use of Skin Substitutes and Growth Factors in Venous Leg Ulceration (VLU) Sami Khan, MD FACS Associate Professor of Surgery Division of Plastic and Reconstructive Surgery SUNY-Stony
Adjunctive Therapies: The Use of Skin Substitutes and Growth Factors in Venous Leg Ulceration (VLU) Sami Khan, MD FACS Associate Professor of Surgery Division of Plastic and Reconstructive Surgery SUNY-Stony
Wound Dressing. Choosing the Right Dressing
 Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
STUDY. complication of diabetes, affecting 12% to 15% of patients. during their lifetime. 1,2 Diabetic foot ulcers (DFUs) impair quality
 STUDY Advanced Biological Therapies for Diabetic Foot Ulcers Robert S. Kirsner, MD, PhD; Robert Warriner, MD; Michelle Michela, MS; Laure Stasik, BA; Katherine Freeman, PhD Objective: To assess the clinical
STUDY Advanced Biological Therapies for Diabetic Foot Ulcers Robert S. Kirsner, MD, PhD; Robert Warriner, MD; Michelle Michela, MS; Laure Stasik, BA; Katherine Freeman, PhD Objective: To assess the clinical
Equine Pericardium Collagen Wound Dressing in the Treatment of the Neuropathic Diabetic Foot Wound
 ORIGINAL ARTICLES Equine Pericardium Collagen Wound Dressing in the Treatment of the Neuropathic Diabetic Foot Wound A Pilot Study John G. Fleischli, DPM* Terese J. Laughlin, DPM* Jeffery W. Fleischli,
ORIGINAL ARTICLES Equine Pericardium Collagen Wound Dressing in the Treatment of the Neuropathic Diabetic Foot Wound A Pilot Study John G. Fleischli, DPM* Terese J. Laughlin, DPM* Jeffery W. Fleischli,
A comprehensive study on effect of collagen dressing in diabetic foot ulcer
 Original Research Article A comprehensive study on effect of collagen dressing in diabetic foot ulcer Sivakumar 1, S. Shanmugam 2* 1 Associate Professor, 2 Senior Assistant Professor Department of General
Original Research Article A comprehensive study on effect of collagen dressing in diabetic foot ulcer Sivakumar 1, S. Shanmugam 2* 1 Associate Professor, 2 Senior Assistant Professor Department of General
Many patients with chronic wounds. Case reports. The use of Prontosan in combination with Askina Calgitrol : an independent case series
 Case reports The use of Prontosan in combination with Askina Calgitrol : an independent case series Author: Liezl Naude Many patients with chronic wounds will develop infection (Landis et al, 2007; Sibbald
Case reports The use of Prontosan in combination with Askina Calgitrol : an independent case series Author: Liezl Naude Many patients with chronic wounds will develop infection (Landis et al, 2007; Sibbald
Compression bandaging remains the basis of venous
 CLINICAL EVALUATION Evaluation of Urgotul plus K-Four compression for venous leg ulcers J Smith, J Hill, S Barrett, W Hayes, P Kirby, S Walsh, E Gittins, F Whitehurst, R Cooper Compression bandaging remains
CLINICAL EVALUATION Evaluation of Urgotul plus K-Four compression for venous leg ulcers J Smith, J Hill, S Barrett, W Hayes, P Kirby, S Walsh, E Gittins, F Whitehurst, R Cooper Compression bandaging remains
WOUND CARE. By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare
 WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. MTG Review Decision Document
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Centre for Health Technology Evaluation MTG Review Decision Document Review of MTG5: The MIST Therapy system for the promotion of wound healing This guidance
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Centre for Health Technology Evaluation MTG Review Decision Document Review of MTG5: The MIST Therapy system for the promotion of wound healing This guidance
QUICK GUIDE SNAP THERAPY SYSTEM
 QUICK GUIDE SNAP THERAPY SYSTEM Clinical Pathway to SNAP System Full holistic assessment of patient and wound Is the wound type indicated for NPWT use without contraindications 1? SNAP System is indicated
QUICK GUIDE SNAP THERAPY SYSTEM Clinical Pathway to SNAP System Full holistic assessment of patient and wound Is the wound type indicated for NPWT use without contraindications 1? SNAP System is indicated
DIABETES AND THE AT-RISK LOWER LIMB:
 DIABETES AND THE AT-RISK LOWER LIMB: Shawn M. Cazzell Disclosure of Commercial Support: Dr. Shawn Cazzell reports the following financial relationships: Speakers Bureau: Organogenesis Grants/Research Support:
DIABETES AND THE AT-RISK LOWER LIMB: Shawn M. Cazzell Disclosure of Commercial Support: Dr. Shawn Cazzell reports the following financial relationships: Speakers Bureau: Organogenesis Grants/Research Support:
Cost and dressing evaluation of hydrofiber and alginate dressings in the management of community-based patients with chronic leg ulceration
 Cost and dressing evaluation of hydrofiber and alginate dressings in the management of community-based patients with chronic leg ulceration Harding K G, Price P, Robinson B, Thomas S, Hofman D Record Status
Cost and dressing evaluation of hydrofiber and alginate dressings in the management of community-based patients with chronic leg ulceration Harding K G, Price P, Robinson B, Thomas S, Hofman D Record Status
AWMA MODULE ACCREDITATION. Module Five: The High Risk Foot (Including the Diabetic Foot)
 AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
AWMA MODULE ACCREDITATION Module Five: The High Risk Foot (Including the Diabetic Foot) Introduction - The Australian Wound Management Association Education & Professional Development Sub Committee-(AWMA
CASE 1: TYPE-II DIABETIC FOOT ULCER
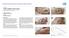 CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
Manuscript received: August 1, 2011 Accepted in final form: March 30, DOI: /j X x
 A randomized, controlled, double-blind prospective trial with a Lipido-Colloid Technology-Nano-OligoSaccharide Factor wound dressing in the local management of venous leg ulcers Sylvie Meaume, MD 1 ; François
A randomized, controlled, double-blind prospective trial with a Lipido-Colloid Technology-Nano-OligoSaccharide Factor wound dressing in the local management of venous leg ulcers Sylvie Meaume, MD 1 ; François
P. P.2-7 P R A C T I C A L
 P R A T I A L O U R S E The use of hyaluronic acid derivatives in the treatment of long-term non-healing wounds Systematic review and meta-analysis of RSs (randomized controlled studies) J. Voigt and V.
P R A T I A L O U R S E The use of hyaluronic acid derivatives in the treatment of long-term non-healing wounds Systematic review and meta-analysis of RSs (randomized controlled studies) J. Voigt and V.
2008 American Medical Association and National Committee for Quality Assurance. All Rights Reserved. CPT Copyright 2007 American Medical Association
 Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
Chronic Wound Care ASPS #1: Use of wound surface culture technique in patients with chronic skin ulcers (overuse measure) This measure may be used as an Accountability measure Clinical Performance Measure
A comprehensive study on effect of recombinant human epidermal growth factor gel in diabetic foot ulcer
 Original Research Article A comprehensive study on effect of recombinant human epidermal growth factor gel in diabetic foot ulcer S Vijayalakshmi * Associate Professor, Department of General Surgery, Govt.
Original Research Article A comprehensive study on effect of recombinant human epidermal growth factor gel in diabetic foot ulcer S Vijayalakshmi * Associate Professor, Department of General Surgery, Govt.
Wound Healing Community Outreach Service
 Wound Healing Community Outreach Service Wound Management Education Plan January 2011 December 2011 Author: Michelle Gibb Nurse Practitioner Wound Management Wound Healing Community Outreach Service Institute
Wound Healing Community Outreach Service Wound Management Education Plan January 2011 December 2011 Author: Michelle Gibb Nurse Practitioner Wound Management Wound Healing Community Outreach Service Institute
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
Efficacy of two compression systems in the management of VLUs: results of a European RCT
 journal of wound care W C vo l u m e 2 1. n u m b e r 1 1. n ov e m b e r 2 0 1 2??? C Efficacy of two compression systems in the management of VLUs: results of a European RCT I. Lazareth, 1 MD; C. Moffatt,
journal of wound care W C vo l u m e 2 1. n u m b e r 1 1. n ov e m b e r 2 0 1 2??? C Efficacy of two compression systems in the management of VLUs: results of a European RCT I. Lazareth, 1 MD; C. Moffatt,
Lower Extremity Venous Disease (LEVD)
 Lower Extremity Venous Disease (LEVD) Lower Extremity Venous Disease (LEVD) Wounds Etiology Lower extremity venous leg ulcers are caused by chronic venous hypertension. Failure of valves in the veins or
Lower Extremity Venous Disease (LEVD) Lower Extremity Venous Disease (LEVD) Wounds Etiology Lower extremity venous leg ulcers are caused by chronic venous hypertension. Failure of valves in the veins or
Aetiology Macroangiopathy occurs mainly distally ie Popliteal artery There is arterial wall calcification Microangiopathy is less common
 DIABETIC FOOT Facts 5% of the population is diabetic 12% of diabetic admissions are with foot problems 1/3rd of diabetic foot ulcerations are neuropathic, 1/3rd are ischaemic and 1/3 are of a mixed in
DIABETIC FOOT Facts 5% of the population is diabetic 12% of diabetic admissions are with foot problems 1/3rd of diabetic foot ulcerations are neuropathic, 1/3rd are ischaemic and 1/3 are of a mixed in
CASE STUDIES SERIES 2017
 INTERNATIONAL CASE STUDIES Case studies evaluation: BIOSORB Gelling Fibre Dressing in moderate to highly exuding wounds CASE STUDIES SERIES 2017 PUBLISHED BY: Wounds International 1.01 Cargo Works 1 2
INTERNATIONAL CASE STUDIES Case studies evaluation: BIOSORB Gelling Fibre Dressing in moderate to highly exuding wounds CASE STUDIES SERIES 2017 PUBLISHED BY: Wounds International 1.01 Cargo Works 1 2
Authors' objectives To assess the value of treatments for foot ulcers in patients with Type 2 diabetes mellitus.
 A systematic review of foot ulcer in patients with Type 2 diabetes mellitus - II: treatment Mason J, O'Keeffe C, Hutchinson A, McIntosh A, Young R, Booth A Authors' objectives To assess the value of treatments
A systematic review of foot ulcer in patients with Type 2 diabetes mellitus - II: treatment Mason J, O'Keeffe C, Hutchinson A, McIntosh A, Young R, Booth A Authors' objectives To assess the value of treatments
a,b and the annual cost of diabetic neuropathy is estimated to be $10.91 billion in the United States alone. 3
 eplasty: Vol. 11 A Prospective Study of Negative Pressure Wound Therapy With Integrated Charles M. Zelen, DPM,, FACFAS a,b Brian Stover, DPM, a Professional Education and b esearch Institute, oanoke, Department
eplasty: Vol. 11 A Prospective Study of Negative Pressure Wound Therapy With Integrated Charles M. Zelen, DPM,, FACFAS a,b Brian Stover, DPM, a Professional Education and b esearch Institute, oanoke, Department
Advazorb. Hydrophilic foam dressing range
 Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Advazorb Hydrophilic foam dressing range Advazorb A comprehensive range of patient friendly, absorbent foam dressings Non-adhesive and atraumatic silicone adhesive options Designed to manage exudate whilst
Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types. Summary
 Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
ULCERS 1/12/ million diabetics in the US (2012) Reamputation Rate 26.7% at 1 year 48.3% at 3 years 60.7% at 5 years
 Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Jay Christensen D.P.M Advanced Foot and Ankle of Wisconsin 2-4% of the population at any given time will have ulcers 0.06-0.20% of the total population Average age of patients 70 years increased as more
Diabetic Foot Ulcers. A guide to help minimise pain, trauma and stress
 Diabetic Foot Ulcers A guide to help minimise pain, trauma and stress From day one, Safetac was about less pain to patients. It s an easy story it does not stick to the wound, so it does not damage or
Diabetic Foot Ulcers A guide to help minimise pain, trauma and stress From day one, Safetac was about less pain to patients. It s an easy story it does not stick to the wound, so it does not damage or
HydroTherapy: A simple approach to Wound Management
 Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
Copyright Paul Hartmann Pty Ltd material may not be reproduced or used without written permission HydroTherapy: A simple approach to Wound Management HARTMANN Education Agenda Agenda Acute vs Chronic wounds:
Diabetic/Neuropathic Foot Ulcer Assessment Guide South West Regional Wound Care Program Last Updated June 10,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Jonathan Brown Assignment 2 November 11, 2010
 1 Jonathan Brown Assignment 2 November 11, 2010 2 The Effectiveness of Removable Walking Casts and Total Contact Casts in Decreasing Healing Times of Diabetic Foot Ulcers Prepared by: jonathan.brown@gbcpando.com
1 Jonathan Brown Assignment 2 November 11, 2010 2 The Effectiveness of Removable Walking Casts and Total Contact Casts in Decreasing Healing Times of Diabetic Foot Ulcers Prepared by: jonathan.brown@gbcpando.com
Leg ulcer assessment and management
 Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Leg ulceration The views expressed in this presentation are solely those of the presenter and do not necessarily represent the views of Smith & Nephew. Smith & Nephew does not guarantee the accuracy or
Pressure Ulcers: 3 Keys to Pressure Ulcer Management. Evidence Based Prevention & Management. I have no financial conflicts of interest
 Pressure Ulcers: Evidence Based Prevention & Management Madhuri Reddy, MD MSc I have no financial conflicts of interest I have nothing to disclose financially 3 Keys to Pressure Ulcer Management 1 3 Keys
Pressure Ulcers: Evidence Based Prevention & Management Madhuri Reddy, MD MSc I have no financial conflicts of interest I have nothing to disclose financially 3 Keys to Pressure Ulcer Management 1 3 Keys
Taking up the challenge neuroischaemic diabetic foot ulcers
 Taking up the challenge neuroischaemic diabetic foot ulcers Galea E ABSTRACT Diabetic patients are at a high risk of amputations with most of these debilitating and life-threatening procedures being preceded
Taking up the challenge neuroischaemic diabetic foot ulcers Galea E ABSTRACT Diabetic patients are at a high risk of amputations with most of these debilitating and life-threatening procedures being preceded
Reality TV Managing patients in the real world. Wounds UK Harrogate 2009
 Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
Reality TV Managing patients in the real world Wounds UK Harrogate 2009 Reality TV Managing patients in the real world Brenda M King Nurse Consultant Tissue Viability Sheffield PCT Harrogate 2009 Familiar
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists
 EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
EVALUATION OF THE VASCULAR STATUS OF DIABETIC WOUNDS Travis Littman, MD NorthWest Surgical Specialists Nothing To Disclosure DISCLOSURES I have no outside conflicts of interest, financial incentives, or
The Great Debate: Offloading Diabetic Foot Ulcers: TCC vs. CAM Walkers Gregory A Bohn, MD MAPWCA, ABPM/UHMS
 The Great Debate: Offloading Diabetic Foot Ulcers: TCC vs. CAM Walkers Gregory A Bohn, MD MAPWCA, ABPM/UHMS Department of Surgery Central Michigan School of Medicine Tawas, Michigan Disclosures Medical/Scientific
The Great Debate: Offloading Diabetic Foot Ulcers: TCC vs. CAM Walkers Gregory A Bohn, MD MAPWCA, ABPM/UHMS Department of Surgery Central Michigan School of Medicine Tawas, Michigan Disclosures Medical/Scientific
Equine Pericardium as a Biological Covering for the Treatment of Diabetic Foot Wounds
 ORIGINAL ARTICLES Equine Pericardium as a Biological Covering for the Treatment of Diabetic Foot Wounds A Prospective Study Jeffery H. Alexander, DPM* David A. Yeager, DPM Dean S. Stern, DPM* Carlo A.
ORIGINAL ARTICLES Equine Pericardium as a Biological Covering for the Treatment of Diabetic Foot Wounds A Prospective Study Jeffery H. Alexander, DPM* David A. Yeager, DPM Dean S. Stern, DPM* Carlo A.
Case study: Young athlete suffering from PTS recovers from traumatic foot ulcer, following use of the geko TM device.
 Case study: Young athlete suffering from PTS recovers from traumatic foot ulcer, following use of the geko TM device.... Subject 34-year-old male, ex professional rugby player. Wound Type Lower left leg
Case study: Young athlete suffering from PTS recovers from traumatic foot ulcer, following use of the geko TM device.... Subject 34-year-old male, ex professional rugby player. Wound Type Lower left leg
W C. Quality of life in patients with leg ulcers: results from CHALLENGE, a double-blind randomised controlled trial ??? journal of wound care
 journal of wound care C W C VOLUME 26. NUMBER 7. JULY 2017??? Quality of life in patients with leg ulcers: results from CHALLENGE, a double-blind randomised controlled trial *S. Meaume, 1 MD, Dermatologist
journal of wound care C W C VOLUME 26. NUMBER 7. JULY 2017??? Quality of life in patients with leg ulcers: results from CHALLENGE, a double-blind randomised controlled trial *S. Meaume, 1 MD, Dermatologist
Description. Section: Medicine Effective Date: April 15, 2015 Subsection: Medicine Original Policy Date: September 13, 2012 Subject:
 Last Review Status/Date: March 2015 Description Page: 1 of 6 Low-frequency ultrasound (US) in the kilohertz (KHz) range may improve wound healing. Several noncontact devices have received regulatory approval
Last Review Status/Date: March 2015 Description Page: 1 of 6 Low-frequency ultrasound (US) in the kilohertz (KHz) range may improve wound healing. Several noncontact devices have received regulatory approval
Emerging Use of Topical Biologics in Limb Salvage Role of Activated Collagen in Multimodality Treatment
 9 th Annual New Cardiovascular Horizons New Orleans September 12, 2008 Emerging Use of Topical Biologics in Limb Salvage Role of Activated Collagen in Multimodality Treatment Gary M. Rothenberg, DPM, CDE,
9 th Annual New Cardiovascular Horizons New Orleans September 12, 2008 Emerging Use of Topical Biologics in Limb Salvage Role of Activated Collagen in Multimodality Treatment Gary M. Rothenberg, DPM, CDE,
Case Study 2 - Mr J. Medical history
 Case Study 2 - Mr J A 54 year-old male was referred to the podiatrist at Coast Provincial General Hospital Diabetic Clinic, for management of active foot disease. The patient s presenting complaint was
Case Study 2 - Mr J A 54 year-old male was referred to the podiatrist at Coast Provincial General Hospital Diabetic Clinic, for management of active foot disease. The patient s presenting complaint was
Diabetic Foot Ulcers. Care for Patients in All Settings
 Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
Diabetic Foot Ulcers Care for Patients in All Settings Summary This quality standard focuses on care for people who have developed or are at risk of developing a diabetic foot ulcer. The scope of the standard
DRESSING SELECTION. Rebecca Aburn MN NP Candidate
 DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
DRESSING SELECTION Rebecca Aburn MN NP Candidate Should be individually tailored in conjunction with the patient to meet their individual needs. WOUND MANAGEMENT: Comprehensive health assessment Wound
Wound Classification. Overview
 Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Overview Jeffrey A. Niezgoda, MD FACHM, MAPWCA, CHWS Review of Initial Wound Care Consultation Rational for Classification Wound Appearance Wound Etiology Management Algorithms Initial Wound Care Consult
Silver Dressings. Sajida Khatri PrescQIPP Primary Care Lead.
 Silver Dressings Sajida Khatri PrescQIPP Primary Care Lead www.prescqipp.info Available at: www.prescqipp.info/silverdressings 2 Introduction PrescQIPP Silver dressings bulletin published in March 2014
Silver Dressings Sajida Khatri PrescQIPP Primary Care Lead www.prescqipp.info Available at: www.prescqipp.info/silverdressings 2 Introduction PrescQIPP Silver dressings bulletin published in March 2014
HIGH- VOLTAGE PULSED CURRENT (HVPC) ELECTRICAL STIMULATION FOR TREATMENT OF DIABETIC FOOT ULCER (DFU) - A REVIEW
 Review Article Allied Science International Journal of Pharma and Bio Sciences ISSN 0975-6299 HIGH- VOLTAGE PULSED CURRENT (HVPC) ELECTRICAL STIMULATION FOR TREATMENT OF DIABETIC FOOT ULCER (DFU) - A REVIEW
Review Article Allied Science International Journal of Pharma and Bio Sciences ISSN 0975-6299 HIGH- VOLTAGE PULSED CURRENT (HVPC) ELECTRICAL STIMULATION FOR TREATMENT OF DIABETIC FOOT ULCER (DFU) - A REVIEW
Diabetic foot ulcers (DFUs) are difficult to. Treatment of diabetic foot ulcers with dehydrated amniotic membrane allograft: a prospective case series
 Treatment of diabetic foot ulcers with dehydrated amniotic membrane allograft: a prospective case series Objective: A diabetic foot ulcer (DFU) is one of the many potential complications associated with
Treatment of diabetic foot ulcers with dehydrated amniotic membrane allograft: a prospective case series Objective: A diabetic foot ulcer (DFU) is one of the many potential complications associated with
Granulox Update on evidence and science
 Update on evidence and science New clinical data in DFU wounds Retrospective cohort evaluation Site: Southtees, UK Main Inclusion criteria: DFU, < wound size reduction in 4 weeks Verum Group: Standard
Update on evidence and science New clinical data in DFU wounds Retrospective cohort evaluation Site: Southtees, UK Main Inclusion criteria: DFU, < wound size reduction in 4 weeks Verum Group: Standard
IPM Wound Gel Bio A New High Concentration (2.5%) Hyaluronic Acid (HA) Based Gel Treatment of Chronic Wounds
 IPM Wound Gel Bio A New High Concentration (2.5%) Hyaluronic Acid (HA) Based Gel Treatment of Chronic Wounds Part 1 of 3 Chronic wounds: widely considered to be stuck in the inflammatory phase Hyaluronic
IPM Wound Gel Bio A New High Concentration (2.5%) Hyaluronic Acid (HA) Based Gel Treatment of Chronic Wounds Part 1 of 3 Chronic wounds: widely considered to be stuck in the inflammatory phase Hyaluronic
