A prospective comparative study of gentamicin- and amikacin-induced nephrotoxicity in patients with normal baseline renal function
|
|
|
- Catherine Richards
- 6 years ago
- Views:
Transcription
1 doi: /j x ORIGINAL ARTICLE A prospective comparative study of gentamicin- and amikacin-induced nephrotoxicity in patients with normal baseline renal function Waleed M. Sweileh* Clinical Pharmacology, An-Najah National University, Nablus, Palestine Keywords amikacin, gentamicin, nephrotoxicity, renal function Received 4 September 2008; revised 24 November 2008; accepted 22 December 2008 *Correspondence and reprints: waleedsweileh@najah.edu ABSTRACT The aim of this study was to compare the nephrotoxic potential of amikacin (AK) and gentamicin (GM) in patients with normal baseline renal function. This study was a 1-year, non-interventional prospective study of patients administered either GM or AK. The study was carried out at the internal medicine department of Al-Watani governmental study. Nephrotoxicity was defined as a serum creatinine (SCr) increase of 0.5 mg/dl from the basal (normal) SCr level. The two groups (GM, n = 45 and AK, n = 49) were similar in population composition, and underlying pathological and infectious processes requiring antimicrobials. No significant difference in age was found between patients in the GM and AK groups, P = Patients in the GM group received comparatively lower doses than those in the AK group (mean = 2.5 mg/kg/day and 14.4 mg/kg/day, respectively) but the duration of treatment was similar. Sixteen of 45 patients receiving GM (35.6%) and eight of 49 patients receiving AK (16.3%) developed nephrotoxicity, P = Single daily dosing with GM, regardless of the total daily dose, produced less nephrotoxicity than multiple dosing. In contrast, AK given at a total dose of 1 g daily, showed no benefit of single dosing compared with multiple dosing. In patients with initial normal renal function, GM was significantly more nephrotoxic than AK. Multiple dosing of GM was more nephrotoxic than single dosing. AK-induced nephrotoxicity was not significantly dependent on dosing frequency. INTRODUCTION Aminoglycosides are commonly used in everyday clinical practice for the treatment of gram-negative infections [1]. However, aminoglycosides are known to have nephrotoxic activity characterized by tubular necrosis without gross morphological changes in glomerular structures [2]. The most frequently used drugs of the aminoglycoside group include gentamicin (GM) and amikacin (AK). Animal studies suggest that AK induces signs of nephrotoxicity less frequently than GM [3 5]. However, the comparative nephrotoxicity of GM and AK in treated human patients is not fully unequivocal. For example, a study comparing AK and GM nephrotoxicity found that there were no significant differences between AK and GM nephrotoxic potential in matched critically ill patients [6]. A controlled comparison study between GM and AK indicated that AK is effective against severe gram-negative infections and is not more or less nephrotoxic than GM [7]. A comparative study of nephrotoxicity in patients randomly assigned to treatment with AK or GM indicated that AK may be less nephrotoxic than GM in humans [8]. A 4-day study of the effects of GM, tobramycin, and AK on the human kidney revealed that AK induces significantly lower lysosomal overloading and no loss of phospholipase A1 activity compared 515
2 516 W.M. Sweileh with GM [9]. The conclusions of published comparative nephrotoxic studies in hospitalized patients are also complicated by the status of the renal function at the initiation of therapy. Therefore, the following study was carried out to compare the nephrotoxic potential of AK and GM in patients with normal baseline renal function. PATIENTS AND METHODS The study was conducted at Al-Watani hospital, a 100- bed facility located in Nablus city, north Palestine. The hospital is a governmental referral hospital that serves the general population in northern Palestine. The hospital contains all major medical services. There is no specific infectious unit in the hospital and patients with suspected infections are treated in the internal medicine department unit. Aminoglycosides are commonly used in the hospital as empiric therapy and in infections caused by gram-negative bacilli, e.g intra-abdominal, urinary tract and most nosocomial infections. In this non-interventional prospective study we screened all in-patients receiving aminoglycoside treatment, GM or AK, in the ward of internal medicine during a 12-month period. The patients were hospitalized because of infections mainly infections of the respiratory tract, abdomen and urinary tract who had to be administered antibiotics of the aminoglycoside group, GM or AK, by the intravascular route. Inclusion criteria for this study were: patients with initial serum creatinine (SCr) level 1.2 mg/dl, administration of either GM or AK for not less than 5 days, availability of SCr levels obtained before initiation of the treatment and during therapy up until the sixth day of the study and finally, no GM or AK in the previous month. SCr levels were measured daily by laboratory medical technologists by the following method: a sample of 2 ml of venous blood is drawn in a plain test tube and spun for 5 min. Then, 5 ll of serum was taken from the supernatant and treated with picric acid according to the Jaffe method [10]. The intensity of the color was measured at 510 nm which is directly proportional to the SCr concentration. Demographic, clinical and laboratory data and those on medications administered were obtained from the patients medical charts. Information obtained included age, gender, previous hospitalization or aminoglycoside use, presence of other factors predisposing to renal disease (such as diabetes mellitus, hypertension, peripheral vascular disease, and congestive heart failure). SCr was measured at the commencement of the aminoglycoside course in all patients. The outcome of interest was aminoglycoside-induced nephrotoxicity. In this study, nephrotoxicity was defined as an increase in SCr of 0.5 mg/dl from the baseline value. Dose and frequency of aminoglycoside administration were obtained from each patient s medical chart. Administration of aminoglycosides every 24 h was considered as single daily dosing while administration every 8 12 h was considered as multiple daily dosing. Use of potentially nephrotoxic drugs that were given to >10% of the study patients was included in the analysis. Statistical analysis Continuous variables were described using mean ± standard deviation (SD). The proportion of patients developing nephrotoxicity in the study population was expressed as frequency and percentage. The association between nephrotoxicity and the variables of interest was evaluated using the Pearson chi-square or Fishers exact test for categorical variables and the independent Student s t-test for continuous variables. Differences in SCr level between consecutive days were tested using pairedsample t-test. Data analysis and graphics were carried out using SPSS 16 (SPSS Inc., Chicago, IL, USA). RESULTS During the 12-month study period, 94 patients met the inclusion criteria. In the study group, 52 (55.3%) were male and 42 (44.7%) were female. Mean (±SD) age was ± (range ); 46 patients (48.93%) were 65 years old. Forty-five patients (47.9%) received GM, 49 AK (52.1%). Baseline demographic, clinical and laboratory data of the patients are presented in Table I. Nephrotoxicity, defined as an increase of 0.5 mg/dl in SCr from the baseline value was detected in 24 of the 94 patients (25.5%). Univariate analysis of clinical and laboratory risk factors for nephrotoxicity showed that the type of aminoglycoside (P = 0.033), frequency of dosing (P = 0.021), and concomitant diuretic administration (P = 0.004) were statistically linked to nephrotoxicity. Patients on GM and AK were compared. Patients in both groups had comparable characteristics. No significant differences in gender (P = 0.23), age (P = 0.06), initial SCr (P = 0.97), number of co-existing chronic diseases (P = 0.81), and concomitant furosemide administration (P = 0.26) were found between the two groups. The GM group received an average of 2.5 ± 0.94 mg/ kg/day while the AK group received an average of
3 Gentamicin and amikacin comparative nephrotoxicity 517 Table I Baseline demographic, clinical and laboratory data of 94 patients receiving aminoglycosides. Variable Statistics* Gender (male) 52 (55.3) CHF 6 (6.4) HTN 33 (35.1) DM 42 (44.7) Concomitant furosemide 39 (41.5) Gentamicin 45 (47.9) Amikacin 49 (52.1) Gentamicin (total dose) 160 mg/daily 22 (48.9) 240 mg/daily 23 (51.1) Amikacin (total dose) 500 mg/daily 12 (24.5) 1000 mg/daily 27 (55.1) 1500 mg/daily 10 (20.4) Frequency of dosing Single (once daily) 32 (34%) Divided multiple dosing 62 (66%) Age ± SCr level before treatment 0.96 ± 0.23 Duration of hospitalization 8.52 ± 1.52 Nephrotoxicity 24 (25.5) CHF, congestive heart failure; DM, diabetes mellitus; HTN, hypertension. *Statistics are expressed as mean ± SD for continuous variables, and as frequency for categorical variables ± 6.0 mg/kg/day. The difference in dosage was significant (P = 0.001), but the duration of treatment was similar. Sixteen patients of the GM group (35.6%) and eight patients (16.3%) of the AK group experienced nephrotoxicity; the difference was significant (P = 0.033). Table II shows the baseline clinical and demographic characteristics of the GM and AK groups. Gentamicin- and amikacin-induced nephrotoxicity was compared based on SCr levels (Figures 1 and 2). Table II Baseline demographic, clinical and laboratory data of patients receiving either gentamicin or amikacin. Variable GM group AK group P-value Age ± ± Dose (per kg/day) 2.5 ± ± 6.0 < Initial SCr 0.95 ± ± SCr at day ± ± Number of chronic diseases 2.2 ± ± Gender (male) 22 (48.9%) 30 (61.2%) 0.23 Concomitant furosemide 16 (35.6%) 23 (46.9%) 0.26 Single dosing (once daily) 14 (31.1%) 18 (36.7%) 0.57 Nephrotoxicity 16 (35.6%) 8 (16.3%) Bold values are significant at P < The comparison included both the total dose given, frequency, and single vs. multiple dosing. Figure 1 shows that administration of 0.5 or 1.0 g AK once daily or 1.0 g AK in divided multiple dosing did not significantly increase the SCr level for a period of six consecutive days. However, administration of 1.5 g of AK in divided multiple daily dosing significantly induced an increase in SCr level (P = ) at the sixth day of monitoring compared with the baseline SCr level. In the case of GM, single daily dosing with 180 mg/day did not significantly induce a rise in SCr during the 6-day study period. However, single dosing with 240 mg/day induced a significant rise in SCr level at the sixth day compared with the baseline SCr level. Similar effects were obtained with multiple dosing of GM with 160 mg/kg/day. At a dose of 240 mg/day GM in divided multiple dosing, a significant rise in SCr started to appear at the fifth and sixth days. In general, there was a positive correlation between SCr change and dose/kg/day of AK with r = 0.32, P = Stronger correlation was found between dose/kg/day of GM and change in serum creatinine with r = 0.36, P = Finally, within the GM group, there was no significant difference (P = 0.99) in nephrotoxicity between dosing with 160 and 240 mg/day when administered once daily. However, 240 mg/day GM administered in divided multiple dosing produced significantly (P = 0.001) more nephrotoxicity than 160 mg/day administered in divided multiple dosing. Within the AK group, no significant differences in nephrotoxicity were observed between 0.5 gr/day and 1.0 g/day AK regardless of the dosing frequency. DISCUSSION In this study, GM was significantly more nephrotoxic than AK in hospitalized patients with normal baseline renal function despite the fact that AK patients received significantly higher dose per kilogram body weight than those in GM group. This finding cannot be attributed to demographic or baseline clinical characteristics as they were comparable in both groups. Furthermore, the study showed that signs of GM-induced nephrotoxicity became apparent earlier than that of AK-induced nephrotoxicity. Our findings regarding GM- and AK-induced nephrotoxicity are similar to those found by a Spanish study carried out on 65 patients with initial normal renal function. The authors of the Spanish study concluded that in patients with normal renal function, GM was significantly more nephrotoxic than AK [11]. However,
4 518 W.M. Sweileh Figure 1 Changes in serum creatinine level during the 6 days of treatment with gentamicin given in 160 or 240 mg/day as single or in divided multiple dosing. Figure 2 Changes in serum creatinine level during the 6 days of treatment with amikacin given in 500 or 1000 mg/day as single or in divided multiple dosing. in a study carried out to compare nephrotoxicity and ototoxicity between GM and AK among 106 hospitalized patients, the authors used different definitions of nephrotoxicity and found no significant differences in the incidence of nephrotoxicity between the GM and AK treatment arms [8]. The authors also concluded that nephrotoxicity in general is associated with impaired baseline renal function and presence of bacteremia. In a human study comparing lysosomal morphology and function in proximal tubule cells 4 days after AK, GM, and tobramicin administration, GM and tobramicin were found to be significantly more nephrotoxic than AK and netilmicin, and that the nephrotoxicity of AK and netilmicin was comparable [9]. The differences in our
5 Gentamicin and amikacin comparative nephrotoxicity 519 results with those obtained by others could be attributed to the differences in the baseline clinical characteristics between the groups, or to differences in the methodology applied, particularly, the definition of nephrotoxicity. Aminoglycosides are often administered twice or thrice daily. Recently, increasing numbers of experimental and clinical studies have demonstrated that a oncedaily dosing regimen may be at least as effective as, and possibly less toxic than, multiple dosing [12 20]. In the meta-analyses published by Blaser and Konig [12], a total of 24 randomized prospective clinical trials comparing multiple and single daily dosing of AK, GM, netilmicin, or tobramycin were pooled. In most trials, no significant difference between the regimens was detected. The overall analysis of the 3181 patients enrolled in this meta-analysis revealed no significant difference between single and multiple daily dosing. However, there was a trend towards less nephrotoxicity in the once-daily treatment groups. Overall, the Blaser and Konig metaanalysis study indicated that: (i) GM delivered in multiple daily doses was significantly more nephrotoxic than AK; (ii) AK did not show a significant benefit of single daily dosing regarding renal toxicity; and finally (iii) only GM exhibits a benefit from being used once daily. In the experience of the Hartford Hospital, the incidence of nephrotoxicity was reduced from about 4% with conventional dosing to 1.2% with once-daily aminoglycoside regimens [21]. In a study investigating the costs associated with aminoglycoside administration, the authors concluded that once-daily dosing of aminoglycosides saved approximately $ in drugs, supplies and labor for 2200 patients enrolled in the study compared with conventional dosing [22]. The authors further concluded that once-daily dosing with aminoglycosides is cost-effective leading to a reduction of >$ in therapeutic drug-monitoring requests per month for GM [22]. The results of this study indicate that multiple dosing of GM produced more nephrotoxicity than single daily dosing. In case of AK, no differences were observed between single and multiple dosing. These results are in agreement with the overall conclusion of the meta-analysis study mentioned earlier. REFERENCES 1 Drusano G.L., Ambrose P.G., Bhavnani S.M., Bertino J.S., Nafziger A.N., Louie A. Back to the future: using aminoglycosides again and how to dose them optimally. Clin. Infect. Dis. (2007) Review. 2 Martínez-Salgado C., López-Hernández F.J., López-Novoa J.M. Glomerular nephrotoxicity of aminoglycosides. Toxicol. Appl. Pharmacol. (2007) Review. 3 Bonadio M., Maccanti O., Giovannini L. et al. Comparative nephrotoxicity and tissue accumulation of dactimicin, amikacin and gentamicin. Drugs Exp. Clin. Res. (1987) Sairio E., Kasanen A., Kangas L., Nieminen A.L., Nieminen L. The nephrotoxicity and renal accumulation of amikacin, tobramycin and gentamycin in rats, rabbits and guinea pigs. Exp. Pathol. (Jena) (1978) Provoost A.P., Adejuyigbe O., Wolff E.D. Nephrotoxicity of aminoglycosides in young and adult rats. Pediatr. Res. (1985) French M.A., Cerra F.B., Plaut M.E., Schentag J.J. Amikacin and gentamicin accumulation pharmacokinetics and nephrotoxicity in critically ill patients. Antimicrob. Agents Chemother. (1981) Smith C.R., Baughman K.L., Edwards C.Q., Rogers J.F., Lietman P.S. Controlled comparison of amikacin and gentamicin. N. Engl. J. Med. (1977) Lerner S.A., Schmitt B.A., Seligsohn R., Matz G.J. Comparative study of ototoxicity and nephrotoxicity in patients randomly assigned to treatment with amikacin or gentamicin. Am. J. Med. (1986) De Broe M.E., Paulus G.J., Verpooten G.A. et al. Early effects of gentamicin, tobramycin, and amikacin on the human kidney. Kidney Int. (1984) Chromý V., Rozkosná K., Sedlák P. Determination of serum creatinine by Jaffe method and how to calibrate to eliminate matrix interference problems. Clin. Chem. Lab. Med. (2008) Ballesteros J., Northland R., Wolff M. Gentamicin and amikacin nephrotoxicity: comparative study in patients with initially normal renal function. Rev. Med. Chil. (1989) Blaser J., Konig C. Once daily dosing of aminoglycosides. Eur. J. Clin. Microbiol. Infect. Dis. (1995) Galloe A.M., Graudal N., Christensen H.R., Kampmann J.P. Aminoglycosides: single or multiple daily dosing? A metaanalysis on efficacy and safety. Eur. J. Clin. Pharmacol. (1995) Barza M., Ioannidis J.P.A., Cappelleri J.C., Lau J. Single or multiple daily doses of aminoglycosides: a meta-analysis. Br. Med. J. (1996) Ferriols-Lisart R., Alos-Alminana M. Effectiveness and safety of once-daily aminoglycosides: a meta-analysis. Am. J. Health Syst. Pharmacol. (1996) Hatala R., Dinh T., Cook D.J. Once-daily aminoglycoside dosing in immunocompetent adults: a meta-analysis. Ann. Intern. Med. (1996) Munckhof W.J., Grayson M.L., Tumidge J.D. A meta-analysis of studies on the safety and efficacy of aminoglycosides given either once daily or as divided doses. J. Antimicrob. Chemother. (1996) Ali M.Z., Goetz M.B. A meta-analysis of the relative efficacy and toxicity of single daily dosing versus multiple daily dosing of aminoglycosides. Clin. Infect. Dis. (1997)
6 520 W.M. Sweileh 19 Bailey T.C., Little J.R., Littenberg B., Reichley R.M., Dunagan W.C. A meta-analysis of extended-interval dosing versus multiple daily dosing of aminoglycosides. Clin. Infect. Dis. (1997) Hatala R., Dinh T.T., Cook D.J. Single daily dosing of aminoglycosides in immunocompromised adults: a systematic review. Clin. Infect. Dis. (1997) Nicolau D.P., Freeman C.D., Belliveau P.P. et al. Experience with a once-daily aminoglycoside program administered to 2,184 adult patients. Antimicrob. Agents Chemother. (1995) Nicolau D.P., Wu A.H., Finocchiaro S. et al. Once-daily aminoglycoside dosing: impact on requests and costs for therapeutic drug monitoring. Ther. Drug Monit. (1996)
Time Course Analysis of Aminoglycoside - Induced Elevation of Serum Creatinine
 Time Course Analysis of Aminoglycoside - Induced Elevation of Serum Creatinine Waleed M. Sweileh, PhD Associate Professor, Clinical Pharmacology Corresponding author Waleed M. Sweileh, PhD Associate Professor,
Time Course Analysis of Aminoglycoside - Induced Elevation of Serum Creatinine Waleed M. Sweileh, PhD Associate Professor, Clinical Pharmacology Corresponding author Waleed M. Sweileh, PhD Associate Professor,
Aminoglycosides John A. Bosso, Pharm.D.
 AMINOGLYCOSIDES Therapeutics/PHRMP-73 Aminoglycoside Mechanism of Action Aminoglycosides bind to 30s ribosomal subunit resulting in mistranslation of mrna thus disrupting protein synthesis. They are rapidly
AMINOGLYCOSIDES Therapeutics/PHRMP-73 Aminoglycoside Mechanism of Action Aminoglycosides bind to 30s ribosomal subunit resulting in mistranslation of mrna thus disrupting protein synthesis. They are rapidly
SBUH Aminoglycoside Dosing Protocol
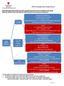 Adult Aminoglycoside Dosing for Gram negative infections prior to available serum levels (Excludes patients with cystic fibrosis, OB GYN patients and surgical prophylaxis) Cr Cl 40 ml/min 5 7 mg/kg INT
Adult Aminoglycoside Dosing for Gram negative infections prior to available serum levels (Excludes patients with cystic fibrosis, OB GYN patients and surgical prophylaxis) Cr Cl 40 ml/min 5 7 mg/kg INT
Back to the Future: Using Aminoglycosides Again and How to Dose Them Optimally
 INVITED ARTICLE ANTIMICROBIAL RESISTANCE George M. Eliopoulos, Section Editor Back to the Future: Using Aminoglycosides Again and How to Dose Them Optimally George L. Drusano, Paul G. Ambrose, Sujata M.
INVITED ARTICLE ANTIMICROBIAL RESISTANCE George M. Eliopoulos, Section Editor Back to the Future: Using Aminoglycosides Again and How to Dose Them Optimally George L. Drusano, Paul G. Ambrose, Sujata M.
Gentamicin - Ototoxicity in children
 Second Meeting of the Subcommittee of the Expert Committee on the Selection and Use of Essential Medicines Geneva, 29 September to 3 October 2008 Gentamicin - Ototoxicity in children Summary Aminoglycosides
Second Meeting of the Subcommittee of the Expert Committee on the Selection and Use of Essential Medicines Geneva, 29 September to 3 October 2008 Gentamicin - Ototoxicity in children Summary Aminoglycosides
Prospective Evaluation of the Effect of an Aminoglycoside Dosing Regimen on Rates of Observed Nephrotoxicity and Ototoxicity
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, July 1999, p. 1549 1555 Vol. 43, No. 7 0066-4804/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Prospective Evaluation of the
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, July 1999, p. 1549 1555 Vol. 43, No. 7 0066-4804/99/$04.00 0 Copyright 1999, American Society for Microbiology. All Rights Reserved. Prospective Evaluation of the
Target Blood Pressure Attainment in Diabetic Hypertensive Patients: Need for more Diuretics? Waleed M. Sweileh, PhD
 Target Blood Pressure Attainment in Diabetic Hypertensive Patients: Need for more Diuretics? Waleed M. Sweileh, PhD Associate Professor, Clinical Pharmacology Corresponding author Waleed M. Sweileh, PhD
Target Blood Pressure Attainment in Diabetic Hypertensive Patients: Need for more Diuretics? Waleed M. Sweileh, PhD Associate Professor, Clinical Pharmacology Corresponding author Waleed M. Sweileh, PhD
Clinical Issues Surrounding Once-Daily Aminoglycoside Dosing in Children
 Butler University Digital Commons @ Butler University Scholarship and Professional Work COPHS College of Pharmacy & Health Sciences 2003 Clinical Issues Surrounding Once-Daily Aminoglycoside Dosing in
Butler University Digital Commons @ Butler University Scholarship and Professional Work COPHS College of Pharmacy & Health Sciences 2003 Clinical Issues Surrounding Once-Daily Aminoglycoside Dosing in
Nephrotoxicity. Pros and Cons of the article: Relationship between Initial Vancomycin
 Pros and Cons of the article: Relationship between Initial Vancomycin Nephrotoxicity among Hospitalized Patients Diane M. Cappelletty, Pharm.D. Associate Professor Pharmacy Practice The University of Toledo
Pros and Cons of the article: Relationship between Initial Vancomycin Nephrotoxicity among Hospitalized Patients Diane M. Cappelletty, Pharm.D. Associate Professor Pharmacy Practice The University of Toledo
Evaluation of Vancomycin Continuous Infusion in Trauma Patients
 OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
OBJECTIVES Evaluation of Vancomycin Continuous Infusion in Trauma Patients Brittany D. Bissell, Pharm.D. PGY-2 Critical Care Pharmacy Resident Jackson Memorial Hospital Miami, Florida Evaluate the potential
TDM of Aminoglycoside Antibiotics
 TDM Lecture 3 5 th Stage TDM of Aminoglycoside Antibiotics The aminoglycoside antibiotics are widely used for the treatment of gram-negative infections, often in combination with a β-lactam antibiotic
TDM Lecture 3 5 th Stage TDM of Aminoglycoside Antibiotics The aminoglycoside antibiotics are widely used for the treatment of gram-negative infections, often in combination with a β-lactam antibiotic
Experience with a Once-Daily Aminoglycoside Program Administered to 2,184 Adult Patients
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Mar. 1995, p. 650 655 Vol. 39, No. 3 0066-4804/95/$04.00 0 Copyright 1995, American Society for Microbiology Experience with a Once-Daily Aminoglycoside Program Administered
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Mar. 1995, p. 650 655 Vol. 39, No. 3 0066-4804/95/$04.00 0 Copyright 1995, American Society for Microbiology Experience with a Once-Daily Aminoglycoside Program Administered
A Meta-Analysis of the Relative Efficacy and Toxicity of Single Daily Dosing Versus Multiple Daily Dosing of Aminoglycosides
 796 A Meta-Analysis of the Relative Efficacy and Toxicity of Single Daily Dosing Versus Multiple Daily Dosing of Aminoglycosides Mirza Zaki Ali and Matthew Bidwell Goetz From the Department ofmedicine,
796 A Meta-Analysis of the Relative Efficacy and Toxicity of Single Daily Dosing Versus Multiple Daily Dosing of Aminoglycosides Mirza Zaki Ali and Matthew Bidwell Goetz From the Department ofmedicine,
Urinary Casts as an Indicator of Renal Tubular Damage
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Oct. 1979, p. 468-474 0066-4804/79/10-0468/07$02.00/0 Vol. 16, No. 4 Urinary Casts as an Indicator of Renal Tubular Damage in Patients Receiving Aminoglycosides JEROME
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, Oct. 1979, p. 468-474 0066-4804/79/10-0468/07$02.00/0 Vol. 16, No. 4 Urinary Casts as an Indicator of Renal Tubular Damage in Patients Receiving Aminoglycosides JEROME
Medication dosing errors in hospitalized patients with renal impairment: a study in Palestine y
 eliminated through the kidney and thus adequate renal function is important to avoid toxicity. The proper dosing of medications for patients with renal impairment can maximize therapeutic efficacy, minimize
eliminated through the kidney and thus adequate renal function is important to avoid toxicity. The proper dosing of medications for patients with renal impairment can maximize therapeutic efficacy, minimize
Prevalence and Risk Factors for Aminoglycoside Nephrotoxicity in Intensive Care Units
 ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, July 2009, p. 2887 2891 Vol. 53, No. 7 0066-4804/09/$08.00 0 doi:10.1128/aac.01430-08 Copyright 2009, American Society for Microbiology. All Rights Reserved. Prevalence
ANTIMICROBIAL AGENTS AND CHEMOTHERAPY, July 2009, p. 2887 2891 Vol. 53, No. 7 0066-4804/09/$08.00 0 doi:10.1128/aac.01430-08 Copyright 2009, American Society for Microbiology. All Rights Reserved. Prevalence
Adult Institutional Pharmacokinetics Protocol
 Adult Institutional Pharmacokinetics Protocol Policy Title: Clinical Pharmacokinetics (PK) Service Policy Policy Statement: It is the policy of UMHC that PK consult orders (for vancomycin or aminoglycosides)
Adult Institutional Pharmacokinetics Protocol Policy Title: Clinical Pharmacokinetics (PK) Service Policy Policy Statement: It is the policy of UMHC that PK consult orders (for vancomycin or aminoglycosides)
Use ideal body weight (IBW) unless actual body weight is less. Use the following equation to calculate IBW:
 Amikacin is a partially restricted (amber) antibiotic for the treatment of infections due to gentamicin resistant Gram negative bacilli or as advised by microbiology. As with other aminoglycosides, therapeutic
Amikacin is a partially restricted (amber) antibiotic for the treatment of infections due to gentamicin resistant Gram negative bacilli or as advised by microbiology. As with other aminoglycosides, therapeutic
Aminoglycosides: What have we learned about toxicity?
 Aminoglycosides: What have we learned about toxicity? Paul M. Tulkens, MD, PhD Cellular and Molecular Pharmacology Unit & Center for Clinical Pharmacy Catholic University of Louvain, Brussels, Belgium
Aminoglycosides: What have we learned about toxicity? Paul M. Tulkens, MD, PhD Cellular and Molecular Pharmacology Unit & Center for Clinical Pharmacy Catholic University of Louvain, Brussels, Belgium
D DAVID PUBLISHING. 1. Introduction. Kathryn Koliha 1, Julie Falk 1, Rachana Patel 1 and Karen Kier 2
 Journal of Pharmacy and Pharmacology 5 (2017) 607-615 doi: 10.17265/2328-2150/2017.09.001 D DAVID PUBLISHING Comparative Evaluation of Pharmacist-Managed Vancomycin Dosing in a Community Hospital Following
Journal of Pharmacy and Pharmacology 5 (2017) 607-615 doi: 10.17265/2328-2150/2017.09.001 D DAVID PUBLISHING Comparative Evaluation of Pharmacist-Managed Vancomycin Dosing in a Community Hospital Following
AMINOGLYCOSIDES TDM D O N E B Y
 AMINOGLYCOSIDES TDM DONE BY: SARA ALARFAJ 2014 OUTLINE Introduction about Aminoglycosides. Spectrum/uses. TDM Aminoglycosides TDM Pharmacodynamics Pharmacokinetics. Dosing in AG. Sampeling time and Monitoring.
AMINOGLYCOSIDES TDM DONE BY: SARA ALARFAJ 2014 OUTLINE Introduction about Aminoglycosides. Spectrum/uses. TDM Aminoglycosides TDM Pharmacodynamics Pharmacokinetics. Dosing in AG. Sampeling time and Monitoring.
Enzymuria determination in children treated with aminoglycosides drugs
 Human & Experimental Toxicology (2008) 27: 879 882 www.het.sagepub.com treated with aminoglycosides drugs A Mohammadi-Karakani 1,2, S Asgharzadeh-Haghighi 1, M Ghazi-Khansari 2, A Seyed-Ebrahimi 1, A Ghasemi
Human & Experimental Toxicology (2008) 27: 879 882 www.het.sagepub.com treated with aminoglycosides drugs A Mohammadi-Karakani 1,2, S Asgharzadeh-Haghighi 1, M Ghazi-Khansari 2, A Seyed-Ebrahimi 1, A Ghasemi
PHARMONITOR II. Optimisation of aminoglycosides dosage regimen with pharmacokinetics modeling. Pierre Wallemacq
 PHARMONITOR II Optimisation of aminoglycosides dosage regimen with pharmacokinetics modeling Pierre Wallemacq NATIONAL SYMPOSIUM 20 years EEQ Leuven, March 26th 2009 1 Why monitoring of aminoglycosides?
PHARMONITOR II Optimisation of aminoglycosides dosage regimen with pharmacokinetics modeling Pierre Wallemacq NATIONAL SYMPOSIUM 20 years EEQ Leuven, March 26th 2009 1 Why monitoring of aminoglycosides?
A Comparison Of Diagnostic Accuracy Of Cystatin C With Creatinine In The Sample Of Patient Of T2 DM With Diabetic Nephropathy
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. V (July. 2017), PP 53-57 www.iosrjournals.org A Comparison Of Diagnostic Accuracy Of
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. V (July. 2017), PP 53-57 www.iosrjournals.org A Comparison Of Diagnostic Accuracy Of
Patterns of Anti-hypertensive Therapy in Diabetic Patients with and without Reduced Renal Function
 Saudi J Kidney Dis Transpl 2010;21(4):652-659 2010 Saudi Center for Organ Transplantation Saudi Journal of Kidney Diseases and Transplantation Original Article Patterns of Anti-hypertensive Therapy in
Saudi J Kidney Dis Transpl 2010;21(4):652-659 2010 Saudi Center for Organ Transplantation Saudi Journal of Kidney Diseases and Transplantation Original Article Patterns of Anti-hypertensive Therapy in
Pharmacokinetics of daptomycin in a patient with severe renal failure not under dialysis
 AAC Accepts, published online ahead of print on 1 April 2013 Antimicrob. Agents Chemother. doi:10.1128/aac.00230-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 Pharmacokinetics
AAC Accepts, published online ahead of print on 1 April 2013 Antimicrob. Agents Chemother. doi:10.1128/aac.00230-13 Copyright 2013, American Society for Microbiology. All Rights Reserved. 1 Pharmacokinetics
CLINICAL USE OF GLYCOPEPTIDES. Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel
 CLINICAL USE OF GLYCOPEPTIDES Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel Glycopeptides Natural Vancomycin introduced in 1958 Teicoplanin introduced in Europe
CLINICAL USE OF GLYCOPEPTIDES Herbert Spapen Intensive Care Department University Hospital Vrije Universiteit Brussel Glycopeptides Natural Vancomycin introduced in 1958 Teicoplanin introduced in Europe
SAFETY IN THE CATH LAB How to Minimise Contrast Toxicity
 SAFETY IN THE CATH LAB How to Minimise Contrast Toxicity Dr. Vijay Kunadian MBBS, MD, MRCP Senior Lecturer and Consultant Interventional Cardiologist Institute of Cellular Medicine, Faculty of Medical
SAFETY IN THE CATH LAB How to Minimise Contrast Toxicity Dr. Vijay Kunadian MBBS, MD, MRCP Senior Lecturer and Consultant Interventional Cardiologist Institute of Cellular Medicine, Faculty of Medical
Antimicrobial Reference Laboratory
 Antimicrobial Reference Laboratory GUIDELINE RANGES FOR TDM 2018 Andrew Lovering Antimicrobial Reference Laboratory North Bristol NHS Trust Southmead Hospital Bristol, BS10 5NB Guideline Ranges 2018 Aminoglycosides
Antimicrobial Reference Laboratory GUIDELINE RANGES FOR TDM 2018 Andrew Lovering Antimicrobial Reference Laboratory North Bristol NHS Trust Southmead Hospital Bristol, BS10 5NB Guideline Ranges 2018 Aminoglycosides
(telavancin) Healthcare Professional s Guide. Version 2, 4 November 2014
 VIBATIV (telavancin) Healthcare Professional s Guide Version 2, 4 November 2014 1 Table of Contents Introduction... 3 About Vibativ / Therapeutic indications... 3 Antimicrobial spectrum of activity for
VIBATIV (telavancin) Healthcare Professional s Guide Version 2, 4 November 2014 1 Table of Contents Introduction... 3 About Vibativ / Therapeutic indications... 3 Antimicrobial spectrum of activity for
AMINOGLYCOSIDES DOSING AND MONITORING GUIDELINES
 Approved: September 2017 AMINOGLYCOSIDES DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee GENERAL COMMENTS Aminoglycosides (AG) include gentamicin,
Approved: September 2017 AMINOGLYCOSIDES DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee GENERAL COMMENTS Aminoglycosides (AG) include gentamicin,
PHA Spring First Exam. 8 Aminoglycosides (5 points)
 PHA 5128 Spring 2012 First Exam 1 Aminoglycosides (5 points) 2 Aminoglycosides (10 points) 3 Basic Principles (5 points) 4 Basic Principles (5 points) 5 Bioavailability (5 points) 6 Vancomycin (5 points)
PHA 5128 Spring 2012 First Exam 1 Aminoglycosides (5 points) 2 Aminoglycosides (10 points) 3 Basic Principles (5 points) 4 Basic Principles (5 points) 5 Bioavailability (5 points) 6 Vancomycin (5 points)
Relationship between Age and Peripheral White Blood Cell Count in Patients with Sepsis
 IJPM Relationship between Age and Peripheral White Blood Cell Count in Patients with Sepsis Zohreh Aminzadeh 1, Elham Parsa 2 Original Article 1 MD, MPH, Associate Professor, Infectious Disease and Tropical
IJPM Relationship between Age and Peripheral White Blood Cell Count in Patients with Sepsis Zohreh Aminzadeh 1, Elham Parsa 2 Original Article 1 MD, MPH, Associate Professor, Infectious Disease and Tropical
The Art and Science of Diuretic therapy
 The Art and Science of Diuretic therapy Dr. Fayez EL Shaer Associate Professour of cardiology Consultant cardiologist MD, MSc, PhD, CBNC, NBE FESC, ACCP, FASNC,HFA KKUH, KFCC Heart failure: fluid overload
The Art and Science of Diuretic therapy Dr. Fayez EL Shaer Associate Professour of cardiology Consultant cardiologist MD, MSc, PhD, CBNC, NBE FESC, ACCP, FASNC,HFA KKUH, KFCC Heart failure: fluid overload
Learning Objectives. How big is the problem? ACUTE KIDNEY INJURY
 ACUTE KIDNEY INJURY Karen Innocent, DNP, RN, CRNP, ANP-BC, CMSRN Executive Director, Continuing Education Wolters Kluwer Health, Inc May 2016 Orlando FL Learning Objectives Identify the risk factors and
ACUTE KIDNEY INJURY Karen Innocent, DNP, RN, CRNP, ANP-BC, CMSRN Executive Director, Continuing Education Wolters Kluwer Health, Inc May 2016 Orlando FL Learning Objectives Identify the risk factors and
GENTAMICIN: GUIDELINES FOR ONCE DAILY USAGE IN ADULT AND PAEDIATRIC SETTINGS GENTAMICIN: GUIDELINES FOR ONCE DAILY USAGE IN ADULT AND PAEDIATRIC
 GENTAMICIN: GUIDELINES FOR ONCE DAILY USAGE IN ADULT AND PAEDIATRIC SETTINGS 1 1 Gentamicin: Guidelines for Once Daily Usage in Adult and Paediatric Settings These guidelines were designed by the Gentamicin
GENTAMICIN: GUIDELINES FOR ONCE DAILY USAGE IN ADULT AND PAEDIATRIC SETTINGS 1 1 Gentamicin: Guidelines for Once Daily Usage in Adult and Paediatric Settings These guidelines were designed by the Gentamicin
ORIGINAL ARTICLE DOI: (e) ISSN Online: (p) ISSN Print: Anand Kumar Singh 1, Poonam Verma 2. Sciences, Dehradun
 ORIGINAL ARTICLE CLINICAL ASSESSMENT OF NEPHROTOXICITY ASSOCIATED WITH VANCOMYCIN TROUGH CONCENTRATIONS DURING TREATMENT OF DEEP-SEATED INFECTIONS: A RETROSPECTIVE ANALYSIS Anand Kumar Singh 1, Poonam
ORIGINAL ARTICLE CLINICAL ASSESSMENT OF NEPHROTOXICITY ASSOCIATED WITH VANCOMYCIN TROUGH CONCENTRATIONS DURING TREATMENT OF DEEP-SEATED INFECTIONS: A RETROSPECTIVE ANALYSIS Anand Kumar Singh 1, Poonam
Policy: Created: 2/11/2015; Approved: Adult Pharmacokinetic Dosing and Monitoring- Vancomycin Dosing
 ProMedica Health System Clinical Interdepartmental Policy and Procedure: Section: Policy: Date: Subject: Pharmacy Created: 2/11/2015; Approved: Adult Pharmacokinetic Dosing and Monitoring- Vancomycin Dosing
ProMedica Health System Clinical Interdepartmental Policy and Procedure: Section: Policy: Date: Subject: Pharmacy Created: 2/11/2015; Approved: Adult Pharmacokinetic Dosing and Monitoring- Vancomycin Dosing
Antimicrobial practice. Monitoring serum concentrations for once-daily netilmicin dosing regimens
 Journal of Antimicrobial Chemotherapy (1994) 33, 341348 Antimicrobial practice Monitoring serum concentrations for oncedaily netilmicin dosing regimens Jurg Blasei*'*, Christian* KSnig*, HansPeter Simmen*
Journal of Antimicrobial Chemotherapy (1994) 33, 341348 Antimicrobial practice Monitoring serum concentrations for oncedaily netilmicin dosing regimens Jurg Blasei*'*, Christian* KSnig*, HansPeter Simmen*
Professor of Chemotherapy Department of Preclinical and Clinical Pharmacology University of Florence
 Professor of Chemotherapy Department of Preclinical and Clinical Pharmacology University of Florence Researching field Pharmacokinetics, Pharmacodynamics of antimicrobial, antifungal and antitumoral drugs
Professor of Chemotherapy Department of Preclinical and Clinical Pharmacology University of Florence Researching field Pharmacokinetics, Pharmacodynamics of antimicrobial, antifungal and antitumoral drugs
A Survey of Extended-Interval Aminoglycoside Dosing Practices in United States Adult Cystic Fibrosis Programs
 A Survey of Extended-Interval Aminoglycoside Dosing Practices in United States Adult Cystic Fibrosis Programs William A Prescott Jr PharmD INTRODUCTION: The Cystic Fibrosis Foundation recently deemed the
A Survey of Extended-Interval Aminoglycoside Dosing Practices in United States Adult Cystic Fibrosis Programs William A Prescott Jr PharmD INTRODUCTION: The Cystic Fibrosis Foundation recently deemed the
Effect of piperacillin/tazobactam restriction on usage and rates of acute renal failure
 Journal of Medical Microbiology (2016), 65, 195 199 DOI 10.1099/jmm.0.000211 Effect of piperacillin/tazobactam restriction on usage and rates of acute renal failure Michael A. Lorenz, 1,2 Ryan P. Moenster
Journal of Medical Microbiology (2016), 65, 195 199 DOI 10.1099/jmm.0.000211 Effect of piperacillin/tazobactam restriction on usage and rates of acute renal failure Michael A. Lorenz, 1,2 Ryan P. Moenster
Clinical Guidelines for Use of Antibiotics. VANCOMYCIN (Adult)
 VANCOMYCIN (Adult) Please always prescribe VANCOMYCIN in the Variable Dose Antibiotic section of the EPMA SUPPLEMENTARY drug chart (and add a placeholder on the electronic drug chart). 1 Background Vancomycin
VANCOMYCIN (Adult) Please always prescribe VANCOMYCIN in the Variable Dose Antibiotic section of the EPMA SUPPLEMENTARY drug chart (and add a placeholder on the electronic drug chart). 1 Background Vancomycin
Outline. How should we do TDM? Does the evidence support TDM outcomes
 Overcoming Barriers to TDM: Information and the TDM Renaissance How to integrate PK intelligence with routine clinical data Alexander A. Vinks, PharmD, PhD, FCP Professor, Director Pediatric Pharmacology
Overcoming Barriers to TDM: Information and the TDM Renaissance How to integrate PK intelligence with routine clinical data Alexander A. Vinks, PharmD, PhD, FCP Professor, Director Pediatric Pharmacology
Recognizing and Treating Patients with the Cardio-Renal Syndrome
 Recognizing and Treating Patients with the Cardio-Renal Syndrome Joachim H. Ix, MD, MAS, FASN Professor of Medicine Chief; Division of Nephrology-Hypertension University of California San Diego 1 Conflicts
Recognizing and Treating Patients with the Cardio-Renal Syndrome Joachim H. Ix, MD, MAS, FASN Professor of Medicine Chief; Division of Nephrology-Hypertension University of California San Diego 1 Conflicts
Terapia della candidiasi addomaniale
 Verona 16 marzo 2018 Terapia della candidiasi addomaniale Pierluigi Viale Infectious Disease Unit Teaching Hospital S. Orsola Malpighi Bologna INTRA ABDOMINAL CANDIDIASIS open questions a single definition
Verona 16 marzo 2018 Terapia della candidiasi addomaniale Pierluigi Viale Infectious Disease Unit Teaching Hospital S. Orsola Malpighi Bologna INTRA ABDOMINAL CANDIDIASIS open questions a single definition
Initiating Aminoglycosides Safely. Last updated: July 2016, Version 5 Questions/Comments?
 Initiating Aminoglycosides Safely Last updated: July 2016, Version 5 Questions/Comments? Email Mark.McIntyre@uhn.ca Click orange buttons to navigate protocol. Index: Aminoglycoside Dosing Algorithms Objective
Initiating Aminoglycosides Safely Last updated: July 2016, Version 5 Questions/Comments? Email Mark.McIntyre@uhn.ca Click orange buttons to navigate protocol. Index: Aminoglycoside Dosing Algorithms Objective
ZIN EN ONZIN VAN ANTIBIOTICASPIEGELS BIJ NEONATEN
 ZIN EN ONZIN VAN ANTIBIOTICASPIEGELS BIJ NEONATEN Anne Smits Fellow neonatologie UZ Leuven Use of antibiotics in neonates 50 European hospitals 23 non-european hospitals Countries n = 14 n = 9 Pediatric
ZIN EN ONZIN VAN ANTIBIOTICASPIEGELS BIJ NEONATEN Anne Smits Fellow neonatologie UZ Leuven Use of antibiotics in neonates 50 European hospitals 23 non-european hospitals Countries n = 14 n = 9 Pediatric
EVALUATION OF THE ROLE OF NEPHROTOXIC DRUGS IN CONTRAST INDUCED
 EVALUATION OF THE ROLE OF NEPHROTOXIC DRUGS IN CONTRAST INDUCED NEPHROPATHY (CIN) Dr. SIRISHA.A POST GRADUATE KAMINENI INSTITUTE OF MEDICAL SCIENCES NARKETPALLY, TELANGANA INTRODUCTION Contrast-induced
EVALUATION OF THE ROLE OF NEPHROTOXIC DRUGS IN CONTRAST INDUCED NEPHROPATHY (CIN) Dr. SIRISHA.A POST GRADUATE KAMINENI INSTITUTE OF MEDICAL SCIENCES NARKETPALLY, TELANGANA INTRODUCTION Contrast-induced
VANCOMYCIN DOSING AND MONITORING GUIDELINES
 VANCOMYCIN DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee Approved: May 2017 GENERAL COMMENTS Vancomycin is a glycopeptide antibiotic with bactericidal
VANCOMYCIN DOSING AND MONITORING GUIDELINES NB Provincial Health Authorities Anti-Infective Stewardship Committee Approved: May 2017 GENERAL COMMENTS Vancomycin is a glycopeptide antibiotic with bactericidal
BSWH Pharmacist Continuing Education PART 5: Pharmacotherapy and Pharmacokinetics in Adults: Aminoglycosides and Vancomycin
 BSWH Pharmacist Continuing Education 2015 PART 5: Pharmacotherapy and Pharmacokinetics in Adults: Aminoglycosides and Vancomycin Objectives Define basic pharmacodynamic and pharmacokinetic principles Describe
BSWH Pharmacist Continuing Education 2015 PART 5: Pharmacotherapy and Pharmacokinetics in Adults: Aminoglycosides and Vancomycin Objectives Define basic pharmacodynamic and pharmacokinetic principles Describe
EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING
 EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING Commentary provided by: Julie Hall, MHS, MT (ASCP) Assistant Dean, College of Health Professions Assistant Professor, Medical Laboratory Science Grand Valley
EDUCATIONAL COMMENTARY VANCOMYCIN MONITORING Commentary provided by: Julie Hall, MHS, MT (ASCP) Assistant Dean, College of Health Professions Assistant Professor, Medical Laboratory Science Grand Valley
Management of New-Onset Proteinuria in the Ambulatory Care Setting. Akinlolu Ojo, MD, PhD, MBA
 Management of New-Onset Proteinuria in the Ambulatory Care Setting Akinlolu Ojo, MD, PhD, MBA Urine dipstick results Negative Trace between 15 and 30 mg/dl 1+ between 30 and 100 mg/dl 2+ between 100 and
Management of New-Onset Proteinuria in the Ambulatory Care Setting Akinlolu Ojo, MD, PhD, MBA Urine dipstick results Negative Trace between 15 and 30 mg/dl 1+ between 30 and 100 mg/dl 2+ between 100 and
Pivotal Role of Renal Function in Acute Heart failure
 Pivotal Role of Renal Function in Acute Heart failure Doron Aronson MD, FESC Department of Cardiology RAMBAM Health Care Campus Haifa, Israel Classification and definitions of cardiorenal syndromes CRS
Pivotal Role of Renal Function in Acute Heart failure Doron Aronson MD, FESC Department of Cardiology RAMBAM Health Care Campus Haifa, Israel Classification and definitions of cardiorenal syndromes CRS
This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data.
 abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data. The synopsis
abcd Clinical Study Synopsis for Public Disclosure This clinical study synopsis is provided in line with Boehringer Ingelheim s Policy on Transparency and Publication of Clinical Study Data. The synopsis
Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2017
 i Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2017 Jessica R. Spencer and Uzo Chukwuma Approved for public release. Distribution is unlimited. The
i Annual Surveillance Summary: Pseudomonas aeruginosa Infections in the Military Health System (MHS), 2017 Jessica R. Spencer and Uzo Chukwuma Approved for public release. Distribution is unlimited. The
Aminoglycosides as an antibiotic class maintain
 SURGICAL INFECTIONS Volume 17, Number 3, 2016 ª Mary Ann Liebert, Inc. DOI: 10.1089/sur.2015.276 An Argument for the Use of Aminoglycosides in the Empiric Treatment of Ventilator-Associated Pneumonia Addison
SURGICAL INFECTIONS Volume 17, Number 3, 2016 ª Mary Ann Liebert, Inc. DOI: 10.1089/sur.2015.276 An Argument for the Use of Aminoglycosides in the Empiric Treatment of Ventilator-Associated Pneumonia Addison
Cystatin C: A New Approach to Improve Medication Dosing
 Cystatin C: A New Approach to Improve Medication Dosing Erin Frazee Barreto, PharmD, MSc, FCCM Assistant Professor of Pharmacy and Medicine Kern Scholar, Center for the Science of Health Care Delivery
Cystatin C: A New Approach to Improve Medication Dosing Erin Frazee Barreto, PharmD, MSc, FCCM Assistant Professor of Pharmacy and Medicine Kern Scholar, Center for the Science of Health Care Delivery
Optimal Use of Iodinated Contrast Media In Oncology Patients. Focus on CI-AKI & cancer patient management
 Optimal Use of Iodinated Contrast Media In Oncology Patients Focus on CI-AKI & cancer patient management Dr. Saritha Nair Manager-Medical Affairs-India & South Asia GE Healthcare Context Cancer patients
Optimal Use of Iodinated Contrast Media In Oncology Patients Focus on CI-AKI & cancer patient management Dr. Saritha Nair Manager-Medical Affairs-India & South Asia GE Healthcare Context Cancer patients
Antimicrobial Reference Laboratory
 Antimicrobial Reference Laboratory GUIDELINE RANGES FOR TDM 2016-17 Andrew Lovering Antimicrobial Reference Laboratory North Bristol NHS Trust Southmead Hospital Bristol, BS10 5NB UK Aminoglycosides Gentamicin
Antimicrobial Reference Laboratory GUIDELINE RANGES FOR TDM 2016-17 Andrew Lovering Antimicrobial Reference Laboratory North Bristol NHS Trust Southmead Hospital Bristol, BS10 5NB UK Aminoglycosides Gentamicin
A Study To Evaluate The Efficacy Of Tolvaptan In Correction Of Hyponatremia And Its Effect On..
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 5 Ver. 11 (May. 2018), PP 29-34 www.iosrjournals.org A Study To Evaluate The Efficacy Of Tolvaptan
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 5 Ver. 11 (May. 2018), PP 29-34 www.iosrjournals.org A Study To Evaluate The Efficacy Of Tolvaptan
Prospective audit and feedback of piperacillin-tazobactam use in a 1115 bed acute care hospital
 Prospective audit and feedback of piperacillin-tazobactam use in a 1115 bed acute care hospital Final Results Nathan Beahm, BSP, PharmD(student) September 10, 2016 Objectives Review background information
Prospective audit and feedback of piperacillin-tazobactam use in a 1115 bed acute care hospital Final Results Nathan Beahm, BSP, PharmD(student) September 10, 2016 Objectives Review background information
Citation: Sorkhi H, Raheleh Behzadi, Joghtaei N, et al. Glomerular filtration rate determination by
 Original Article Caspian J Intern Med 2018; 9(3):290-295 DOI: 10.22088/cjim.9.3.290 Glomerular filtration rate determination by creatinine and cystatin-c in patients with acute pyelonephritis Hadi Sorkhi
Original Article Caspian J Intern Med 2018; 9(3):290-295 DOI: 10.22088/cjim.9.3.290 Glomerular filtration rate determination by creatinine and cystatin-c in patients with acute pyelonephritis Hadi Sorkhi
Contrast Induced Nephropathy
 Contrast Induced Nephropathy O CIAKI refers to an abrupt deterioration in renal function associated with the administration of iodinated contrast media O CIAKI is characterized by an acute (within 48 hours)
Contrast Induced Nephropathy O CIAKI refers to an abrupt deterioration in renal function associated with the administration of iodinated contrast media O CIAKI is characterized by an acute (within 48 hours)
Clinical Comparison of Cefotaxime with Gentamicin plus Clindamycin in the Treatment of Peritonitis and Other Soft-Tissue Infections
 REVIEWS OF INFECTIOUS DISEASES. VOL. 4, SUPPLEMENT. SEPTEMBER-OCTOBER 982 982 by The University of Chicago. All rights reserved. 062-0886/82/0405-022$02.00 Clinical Comparison of with Gentamicin plus Clindamycin
REVIEWS OF INFECTIOUS DISEASES. VOL. 4, SUPPLEMENT. SEPTEMBER-OCTOBER 982 982 by The University of Chicago. All rights reserved. 062-0886/82/0405-022$02.00 Clinical Comparison of with Gentamicin plus Clindamycin
Approved by: SMG Origination Date: 06/14 Expiration Date: 06/17 Review Date: Revision Date: POLICY and PROCEDURE Archived Date: Page 1 of 14
 POLICY and PROCEDURE Archived Date: Page 1 of 14 PURPOSE In order to provide consistent and optimal vancomycin and aminoglycoside dosing and monitoring, a pharmacokinetic (PK) service will be provided
POLICY and PROCEDURE Archived Date: Page 1 of 14 PURPOSE In order to provide consistent and optimal vancomycin and aminoglycoside dosing and monitoring, a pharmacokinetic (PK) service will be provided
Risk factors and prevention counter measures of nosocomial infection in hospitalized children.
 Biomedical Research 2017; 28 (21): 9429-9433 ISSN 0970-938X www.biomedres.info Risk factors and prevention counter measures of nosocomial infection in hospitalized children. Xiuzhen Zhao 1*, Li Feng 2,
Biomedical Research 2017; 28 (21): 9429-9433 ISSN 0970-938X www.biomedres.info Risk factors and prevention counter measures of nosocomial infection in hospitalized children. Xiuzhen Zhao 1*, Li Feng 2,
Young Hyo Kim, Hong Lyeol Lee, Kyu-Sung Kim, Hoseok Choi, Jeong Seok Choi, Seung Ho Shin
 Int. Adv. Otol. 2011; 7:(1) 91-95 ORIGINAL ARTICLE Young Hyo Kim, Hong Lyeol Lee, Kyu-Sung Kim, Hoseok Choi, Jeong Seok Choi, Seung Ho Shin Department of Otorhinolaryngology-Head & Neck Surgery, Inha University
Int. Adv. Otol. 2011; 7:(1) 91-95 ORIGINAL ARTICLE Young Hyo Kim, Hong Lyeol Lee, Kyu-Sung Kim, Hoseok Choi, Jeong Seok Choi, Seung Ho Shin Department of Otorhinolaryngology-Head & Neck Surgery, Inha University
Setting The setting was hospital and the economic analysis was carried out in the Netherlands.
 Impact of goal-oriented and model-based clinical pharmacokinetic dosing of aminoglycosides on clinical outcome: a cost-effectiveness analysis van Lent-Evers N A, Mathot R A, Geus W P, van Hout B A, Vinks
Impact of goal-oriented and model-based clinical pharmacokinetic dosing of aminoglycosides on clinical outcome: a cost-effectiveness analysis van Lent-Evers N A, Mathot R A, Geus W P, van Hout B A, Vinks
How and why to measure renal function in patients with liver disease?
 ow and why to measure renal function in patients with liver disease? P. Angeli, Dept. of Medicine, Unit of Internal Medicine and epatology (), University of Padova (Italy) pangeli@unipd.it 10th Paris epatology
ow and why to measure renal function in patients with liver disease? P. Angeli, Dept. of Medicine, Unit of Internal Medicine and epatology (), University of Padova (Italy) pangeli@unipd.it 10th Paris epatology
Supplementary Data. Supplementary Table S2. Antiretroviral Therapies Taken with Ledipasvir/Sofosbuvir
 Supplementary Data Statistical Analysis Due to the limited number of patients with acute kidney injury and concern for model overfitting, covariates included in multivariable logistic regression analyses
Supplementary Data Statistical Analysis Due to the limited number of patients with acute kidney injury and concern for model overfitting, covariates included in multivariable logistic regression analyses
Validity of the use of Schwartz formula against creatinine clearance in the assessment of renal functions in children
 Validity of the use of Schwartz formula against creatinine clearance in the assessment of renal functions in children *H W Dilanthi 1, G A M Kularatnam 1, S Jayasena 1, E Jasinge 1, D B D L Samaranayake
Validity of the use of Schwartz formula against creatinine clearance in the assessment of renal functions in children *H W Dilanthi 1, G A M Kularatnam 1, S Jayasena 1, E Jasinge 1, D B D L Samaranayake
Assessment of Therapeutic Drug Monitoring of Vancomycin in Elderly Patients According to New Guidelines
 Original Article Clinical Chemistry Ann Lab Med 2014;34:1-6 http://dx.doi.org/10.3343/alm.2014.34.1.1 ISSN 2234-3806 eissn 2234-3814 Assessment of Therapeutic Drug Monitoring of Vancomycin in Elderly Patients
Original Article Clinical Chemistry Ann Lab Med 2014;34:1-6 http://dx.doi.org/10.3343/alm.2014.34.1.1 ISSN 2234-3806 eissn 2234-3814 Assessment of Therapeutic Drug Monitoring of Vancomycin in Elderly Patients
Morbid Obesity: Multi system Considerations for Acute Care
 Morbid Obesity: Multi system Considerations for Acute Care BRENDA ENGLER, MSN, ACNP BC, CCRN GEISINGER MEDICAL CENTER Disclosures None 1 Obesity Statistics 30 % of the adult population of Pennsylvania
Morbid Obesity: Multi system Considerations for Acute Care BRENDA ENGLER, MSN, ACNP BC, CCRN GEISINGER MEDICAL CENTER Disclosures None 1 Obesity Statistics 30 % of the adult population of Pennsylvania
Learning Objectives. Bilateral Vestibular Loss. Bilateral Vestibular Loss. Diagnosis of vestibulotoxicity is usually easy
 Learning Objectives Bilateral Vestibular Loss Learn how to recognize bilateral vestibular loss Learn treatment of bilateral vestibular loss Timothy C. Hain, M.D. Northwestern University Medical School
Learning Objectives Bilateral Vestibular Loss Learn how to recognize bilateral vestibular loss Learn treatment of bilateral vestibular loss Timothy C. Hain, M.D. Northwestern University Medical School
Invokana (canagliflozin) NEW INDICATION REVIEW
 Invokana (canagliflozin) NEW INDICATION REVIEW Introduction Brand name: Invokana Generic name: Canagliflozin Pharmacological class: Sodium-glucose cotransporter 2 (SGLT2) inhibitor Strength and Formulation:
Invokana (canagliflozin) NEW INDICATION REVIEW Introduction Brand name: Invokana Generic name: Canagliflozin Pharmacological class: Sodium-glucose cotransporter 2 (SGLT2) inhibitor Strength and Formulation:
Vancomycin Drug Class 1
 Drug Class 1 Antibiotic glycopeptide Spectrum 1 Cross Sensitivities / Allergies 1 Refer to product monograph for complete spectrum Gram positive pathogens (e.g., S. aureus, Enterococcus, S. viridans, methicillinresistant
Drug Class 1 Antibiotic glycopeptide Spectrum 1 Cross Sensitivities / Allergies 1 Refer to product monograph for complete spectrum Gram positive pathogens (e.g., S. aureus, Enterococcus, S. viridans, methicillinresistant
Human Creatinine Urinary Detection Kit
 Human Creatinine Urinary CATALOG NO: IRAAKT2509 Detection Kit LOT NO: SAMPLE INTENDED USE The Urinary Creatinine kit is designed to quantitatively measure creatinine present in urine samples. BACKGROUND
Human Creatinine Urinary CATALOG NO: IRAAKT2509 Detection Kit LOT NO: SAMPLE INTENDED USE The Urinary Creatinine kit is designed to quantitatively measure creatinine present in urine samples. BACKGROUND
Chapter 2: Identification and Care of Patients With CKD
 Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Bioequivalence Studies of Two Formulations of Famciclovir Tablets by HPLC Method
 Asian Journal of Chemistry Vol. 19, No. 6 (2007), 4245-4250 Bioequivalence Studies of Two Formulations of Famciclovir Tablets by HPLC Method K.V. SUBRAHMANYAM*, P. MOHANRAJ, P. SANDHYARANI, V.S. SARAVANAN
Asian Journal of Chemistry Vol. 19, No. 6 (2007), 4245-4250 Bioequivalence Studies of Two Formulations of Famciclovir Tablets by HPLC Method K.V. SUBRAHMANYAM*, P. MOHANRAJ, P. SANDHYARANI, V.S. SARAVANAN
VetScan UA Urine Analyzer Clinical Performance Larry Lem, PhD & Andrew Rosenfeld, DVM, ABVP
 VetScan UA Urine Analyzer Clinical Performance Larry Lem, PhD & Andrew Rosenfeld, DVM, ABVP Abstract Background: The VetScan UA urine strip reader is an analyzer designed to provide semi-quantitative and
VetScan UA Urine Analyzer Clinical Performance Larry Lem, PhD & Andrew Rosenfeld, DVM, ABVP Abstract Background: The VetScan UA urine strip reader is an analyzer designed to provide semi-quantitative and
Comparison of Meropenem with Ceftazidime as Monotherapy of Cancer Patients with Chemotherapy induced Febrile Neutropenia
 Comparison of Meropenem with Ceftazidime as Monotherapy of Cancer Patients with Chemotherapy induced Febrile Neutropenia I. Malik ( National Cancer lnsititute, Karachi ) Shaharyar (, Department of Radiotherapy
Comparison of Meropenem with Ceftazidime as Monotherapy of Cancer Patients with Chemotherapy induced Febrile Neutropenia I. Malik ( National Cancer lnsititute, Karachi ) Shaharyar (, Department of Radiotherapy
Aminoglycosides. Not orally absorbed. Interact with negatively charged lipopolysaccharide on Gram- cell wall. Aminoglycoside properties
 Aminoglycosides Tobramycin Kanamycin H2N Gentamicin Amikacin NHCOCHCH2CH2NH2 OH Aminoglycosides made of linked sugars. Decorated with many OH and NH2 groups, which render these compounds positively charged
Aminoglycosides Tobramycin Kanamycin H2N Gentamicin Amikacin NHCOCHCH2CH2NH2 OH Aminoglycosides made of linked sugars. Decorated with many OH and NH2 groups, which render these compounds positively charged
Treatment of febrile neutropenia in patients with neoplasia
 Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
Use of Antihypertensive Medications in Patients with type -2 Diabetes in Ajman, UAE
 Use of Antihypertensive Medications in Patients with type -2 Diabetes in Ajman, UAE ORIGINAL ARTICLE Mohammed Arifulla 1, Lisha Jenny John 1, Jayadevan Sreedharan 2, Jayakumary Muttappallymyalil 3, Jenny
Use of Antihypertensive Medications in Patients with type -2 Diabetes in Ajman, UAE ORIGINAL ARTICLE Mohammed Arifulla 1, Lisha Jenny John 1, Jayadevan Sreedharan 2, Jayakumary Muttappallymyalil 3, Jenny
egfr > 50 (n = 13,916)
 Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Adult Inpatient Antibiogram. Antimicrobial Susceptibilities of Frequently Recovered Clinical Isolates. January to December 2016
 Adult Inpatient Antibiogram Antimicrobial Susceptibilities of Frequently Recovered Clinical Isolates January to December 2016 Department of Pathology Camille Hamula, PhD Director, Clinical Microbiology
Adult Inpatient Antibiogram Antimicrobial Susceptibilities of Frequently Recovered Clinical Isolates January to December 2016 Department of Pathology Camille Hamula, PhD Director, Clinical Microbiology
Pseudomonas aeruginosa
 JOURNAL OF CLINICAL MICROBIOLOGY, July 1983, p. 16-164 95-1137/83/716-5$2./ Copyright C) 1983, American Society for Microbiology Vol. 18, No. 1 A Three-Year Study of Nosocomial Infections Associated with
JOURNAL OF CLINICAL MICROBIOLOGY, July 1983, p. 16-164 95-1137/83/716-5$2./ Copyright C) 1983, American Society for Microbiology Vol. 18, No. 1 A Three-Year Study of Nosocomial Infections Associated with
Vancomycin-associated nephrotoxicity, a case control study
 Master Thesis in Medicine, Nr 859 Vancomycin-associated nephrotoxicity, a case control study Student Tutor Pr. Thierry Buclin, PD MER Div. of Clinical Pharmacology, CHUV Co-tutor Nicolas Widmer Div. of
Master Thesis in Medicine, Nr 859 Vancomycin-associated nephrotoxicity, a case control study Student Tutor Pr. Thierry Buclin, PD MER Div. of Clinical Pharmacology, CHUV Co-tutor Nicolas Widmer Div. of
THE AMINOGLYCOSIDE ANTIBIOTICS
 4 THE AMINOGLYCOSIDE ANTIBIOTICS INTRODUCTION The aminoglycoside antibiotics are widely used for the treatment of severe gram-negative infections such as pneumonia or bacteremia, often in combination with
4 THE AMINOGLYCOSIDE ANTIBIOTICS INTRODUCTION The aminoglycoside antibiotics are widely used for the treatment of severe gram-negative infections such as pneumonia or bacteremia, often in combination with
Sang Ling Wu, MD, Wei Li, MD, PhD, Alice Wells, MT(ASCP), and Amitava Dasgupta, PhD
 Clinical Chemistry / DIGOXIN-LIKE AND DIGITOXIN-LIKE IMMUNOREACTIVE SUBSTANCES IN ELDERLY PEOPLE Digoxin-Like and Digitoxin-Like Immunoreactive Substances in Elderly People Impact on Therapeutic Drug Monitoring
Clinical Chemistry / DIGOXIN-LIKE AND DIGITOXIN-LIKE IMMUNOREACTIVE SUBSTANCES IN ELDERLY PEOPLE Digoxin-Like and Digitoxin-Like Immunoreactive Substances in Elderly People Impact on Therapeutic Drug Monitoring
Tobi Frymark Hillary Leech Rob Mullen Tracy Schooling Rebecca Venediktov Beverly Wang
 Evidence-Based Systematic Review: Drug-Induced Hearing Loss Gentamicin Tobi Frymark Hillary Leech Rob Mullen Tracy Schooling Rebecca Venediktov Beverly Wang National Center for Evidence-Based Practice
Evidence-Based Systematic Review: Drug-Induced Hearing Loss Gentamicin Tobi Frymark Hillary Leech Rob Mullen Tracy Schooling Rebecca Venediktov Beverly Wang National Center for Evidence-Based Practice
Trust Guideline for the Use of Parenteral Vancomycin and Teicoplanin in Adults
 A clinical guideline recommended for use: In: By: For: Division responsible for document: Key words: Names of document authors: Job titles of document authors: Name of document author s Line Manager: Job
A clinical guideline recommended for use: In: By: For: Division responsible for document: Key words: Names of document authors: Job titles of document authors: Name of document author s Line Manager: Job
Fungi GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER NUMBER 53: Author Moi Lin Ling, MBBS, FRCPA, CPHQ, MBA
 GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER NUMBER 53: Fungi Author Moi Lin Ling, MBBS, FRCPA, CPHQ, MBA Chapter Editor Ziad A. Memish, MD, FRCPC, FACP Cover heading - Topic Outline Topic outline
GUIDE TO INFECTION CONTROL IN THE HOSPITAL CHAPTER NUMBER 53: Fungi Author Moi Lin Ling, MBBS, FRCPA, CPHQ, MBA Chapter Editor Ziad A. Memish, MD, FRCPC, FACP Cover heading - Topic Outline Topic outline
Drug dosing in Extremes of Weight
 Drug dosing in Extremes of Weight The Plump & Heavy versus The Skinny & Light Maria Minerva P. Calimag, MD, MSc, PhD, DPBA, FPSECP PROFESSOR Departments of Pharmacology, Anesthesiology and Clinical Epidemiology
Drug dosing in Extremes of Weight The Plump & Heavy versus The Skinny & Light Maria Minerva P. Calimag, MD, MSc, PhD, DPBA, FPSECP PROFESSOR Departments of Pharmacology, Anesthesiology and Clinical Epidemiology
Joint Trust Guideline for the Use of Intravenous Vancomycin in Paediatrics
 A clinical guideline recommended For use in: All clinical areas where vancomycin is prescribed for Children aged 1 month to 16 years By: All medical, nursing, pharmacy, microbiology and phlebotomy paediatric
A clinical guideline recommended For use in: All clinical areas where vancomycin is prescribed for Children aged 1 month to 16 years By: All medical, nursing, pharmacy, microbiology and phlebotomy paediatric
Sponsor / Company: Sanofi Drug substance(s): Insulin Glargine (HOE901) Insulin Glulisine (HMR1964)
 These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert in the country of prescription. Sponsor / Company: Sanofi Drug substance(s):
Aminoglycosides. Uses: Treatment of serious gram-negative systemic infections and some grampositive
 Aminoglycosides Uses: Treatment of serious gram-negative systemic infections and some grampositive infections such as infective endocarditis. Disadvantage: aminoglycosides are their association with nephrotoxicity
Aminoglycosides Uses: Treatment of serious gram-negative systemic infections and some grampositive infections such as infective endocarditis. Disadvantage: aminoglycosides are their association with nephrotoxicity
Acute Kidney Injury. Amandeep Khurana, MD Southwest Kidney Institute
 Acute Kidney Injury Amandeep Khurana, MD Southwest Kidney Institute 66 yr white male w/ DM, HTN, CAD admitted to an OSH w/ E Coli UTI on 7/24/16, developed E Coli bacteremia and Shock (on vaso + levo)
Acute Kidney Injury Amandeep Khurana, MD Southwest Kidney Institute 66 yr white male w/ DM, HTN, CAD admitted to an OSH w/ E Coli UTI on 7/24/16, developed E Coli bacteremia and Shock (on vaso + levo)
