CLINICAL ARTICLES. An additional analysis of the results of this prospective, Clinical Infectious Diseases 1997;25:811 6
|
|
|
- Kory Powers
- 6 years ago
- Views:
Transcription
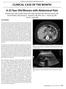
1 811 CLINICAL ARTICLES Differential Prognosis of Gram-Negative Versus Gram-Positive Infected and Sterile Pancreatic Necrosis: Results of a Randomized Trial in Patients with Severe Acute Pancreatitis Treated with Adjuvant Selective Decontamination Ernest J. T. Luiten, Wim C. J. Hop, Johan F. Lange, and Hajo A. Bruining From the Department of Surgery, University Hospital Rotterdam- Dijkzigt; Department of Epidemiology & Biostatistics and Department of Surgery, Erasmus University; and Department of Surgery, St. Clara Hospital, Rotterdam, The Netherlands Results of a previous randomized multicenter trial involving 102 patients with severe acute pancreatitis treated with or without adjuvant selective decontamination (SD) were analyzed additionally with regard to the bacteriologic status of (peri)pancreatic necrosis. The incidence of gramnegative pancreatic infection was significantly reduced in patients treated with SD (P Å.004). Once such an infection develops, mortality increases 15-fold (P õ.001) in comparison with that for patients with sterile necrosis. Among patients in whom only gram-positive infection of pancreatic necrosis was found, there was no significant increase in mortality. These results were similar in both treatment groups. In addition, the hospital stay was significantly longer in cases of gramnegative infected necrosis. The incidence of gram-positive infected necrosis in patients treated with SD did not increase. Gram-negative pancreatic infection can be prevented with adjuvant SD, thereby reducing mortality among patients with severe acute pancreatitis. As infectious complications have become the leading cause to represent an absolute indication for surgery in an effort to of mortality and morbidity in cases of acute necrotizing pancre- reduce mortality [2, 11 14]. atitis, patients in whom devitalized pancreatic and peripancrea- Cultures in cases of infected necrosis most frequently yield tic tissues remain sterile have to be distinguished from others a polymicrobial flora, with a preponderance of gram-negative in whom secondary infection of pancreatic necrosis develops aerobic bacteria in 50% 70% of cultures, suggesting an enteric (i.e., those with sterile vs. infected necrosis). Sterile pancreatic origin [2, 5, 12, 15 19]. Gram-positive aerobes (mainly enteronecrosis, especially in the absence of systemic complications, cocci and staphylococci) are isolated in only 5% 20% of culhas a favorable prognosis, with a reported mortality rate of tures [2, 5, 12, 15 19]. zero to 11% [1 4]. Mortality, which increases sharply with Patients with severe acute pancreatitis in whom infected increasing Ranson or Imrie scores on admission, is related to necrosis exists are usually dealt with as one group, irrespective systemic complications that result in multiple organ failure, of the specific flora cultured. However, because of varying occurring most frequently during the first 2 weeks of illness intrinsic pathogenic potential, the prognosis for patients with [5 10]. infected pancreatic necrosis may differ according to the bacteria cultured. In accordance with results of bacteriological analyses See editorial response by Nathens and Rotstein on pages of infected pancreatic necrosis, two major groups of patients can be distinguished: those with gram-positive infected necrosis and those with gram-negative infected necrosis. This dis- Infected necrosis, on the other hand, occurs later during the tinction between patients with infected pancreatic necrosis has course of the disease, often proves fatal, and is generally agreed not been studied prospectively to date. In a recent controlled clinical trial, selective decontamination (SD) was shown to effectively reduce mortality among patients Received 20 May 1996; revised 4 March with objective signs of severe acute pancreatitis [5]. However, Informed consent was obtained from the patients or their guardians. SD does not prevent gram-positive infection. Subsequent intes- Guidelines for human experimentation of the participating institutions were tinal overgrowth with Enterococcus species, resulting in an followed in the conduct of the clinical research. Reprints or correspondence: Prof. Dr. H. A. Bruining, Department of Surgery, increase in gram-positive infections, has been suggested to be University Hospital Rotterdam-Dijkzigt, Dr. Molewaterplein 40, 3015 a limitation of SD [20]. GD Rotterdam, The Netherlands. An additional analysis of the results of this prospective, Clinical Infectious Diseases 1997;25:811 6 controlled clinical study was performed to evaluate for both 1997 by The University of Chicago. All rights reserved /97/ $03.00 treatment groups (i.e., the SD group and the control group) a
2 812 Luiten et al. CID 1997;25 (October) rotomy and from drainage. They were sent directly to the laboratory and cultured semiquantitatively. If fever (temperature of 39 C) was present, blood cultures were performed. Identifications were made following routine microbiological proce- dures. Pancreatic necrosis, peripancreatic devitalized tissues, and fluid collections were considered sterile in those patients with a nonseptic course and in those with negative cultures. possible difference concerning mortality between (1) patients with either gram-positive infected necrosis or gram-negative pancreatic infection during the course of the disease and (2) patients in whom pancreatic necrosis remained sterile. Patients and Methods Between 22 April 1990 and 19 April 1993, 102 patients with objective signs of severe acute pancreatitis were admitted to 16 participating hospitals. The diagnosis of acute pancreatitis had been established on the basis of clinical examination and elevated plasma levels of serum amylase (ú1,000 IU/L; normal range, IU/L [Phadebas]) or at diagnostic laparotomy (10 patients). All patients had severe acute pancreatitis, ac- cording to a multiple-laboratory-criteria score (Imrie score, 3) and/or a disease-severity grade of D or E (Balthazar grades) determined by contrast-enhanced CT [7, 21]. Bacteriologically proven infected necrosis at the time of randomization was defined as an exclusion criterion. The patients were randomly assigned to receive standard treatment (control group: n Å 52) or the same treatment plus SD (SD group: n Å 50). A 24-hour randomization service was available to randomize patients, with stratification per center. Informed consent was obtained from the patient or relatives by the attending clinician. The SD regimen consisted of oral administration of colistin sulfate (200 mg), amphotericin (500 mg), and norfloxacin (Nor- oxin, Merck & Co., West Point, PA; 50 mg) every 6 hours. A sticky paste containing 2% of the three SD drugs was smeared along the upper and lower gums every 6 hours and at the tracheostomy, if present. The aforementioned daily dose also was given in a rectal enema every day. Surgery Short-term systemic prophylaxis with cefotaxime sodium (Claforan, Hoechst-Roussel Pharmaceuticals, Somerville, NJ; 500 mg) was given every 8 hours until gram-negative bacteria Statistical Analysis were eliminated from the oral cavity and rectum (average, 7.4 Microbiology An ultrasonography or CT-guided fine-needle aspiration (FNA) with subsequent culture was performed if there was clinical suspicion of infected pancreatic necrosis [11]. Clinical suspicion of pancreatic infection was based on the occurrence of fever and leukocytosis (usually lasting at least 2 3 days, during which other sources of infection were excluded), associated with CT findings demonstrating pancreatic necrosis. The microbial flora of the infected pancreas was carefully monitored. Culture specimens of pancreatic and peripancreatic devitalized tissues (i.e., necrosis) were obtained at every lapa- Besides severe intraabdominal hemorrhage or presence of enteric fistulas, reasons for surgery included (1) aspirate cultures that demonstrated development of infected necrosis and (2) rapid deterioration of the patient s condition toward multiple-organ failure that was resistant to exhaustive intensive treatment (SD group, 16 patients; controls, 24). Results of surveil- lance cultures of the digestive tract were not taken into account in the decision to perform a reintervention. The decision to perform either percutaneous drainage or relaparotomy was based on ultrasonographic and CT findings as well as findings from the previous laparotomy. Access to the pancreas was obtained through a median or (preferably) transverse laparotomy. If repeated laparotomies were foreseen, a laparostomy (i.e., ventral open packing of the abdominal cavity) was created, ensuring rapid and easy access to the upper abdominal cavity [12]. Removal of necrotic tissue was mainly performed by means of finger or clamp fraction (i.e., necrosectomy). Infected necrosis is mostly solid, in con- trast with a pancreatic abscess, which represents a localized collection of fluid, often encapsulated, that occurs after the pancreatitis has subsided. days). SD was discontinued as soon as the risk of acquiring a new infection was absent, i.e., the patient was extubated, receiving no supplementary oxygen therapy or infusions, on a regular oral diet, and ambulatory on the ward. A more elaborate outline has been reported previously [5]. Percentages and continuous data were compared between groups by means of Fisher s exact test and Mann-Whitney s test, respectively. Cumulative percentages of patients devel- oping gram-negative or gram-positive infected necrosis, taking into account the length of survival, were assessed by the actuar- ial Kaplan-Meier method and log-rank test. Cox regression was used to evaluate various factors simultaneously with regard to mortality [22]. This method was also used to assess the relationship between the occurrence of pancreatic infections (only gram-negative, only gram-positive, or mixed gramnegative/gram-positive) and mortality [23]. P values given are two-sided, and P Å.05 was considered the limit of significance. Results Of 102 patients with objective signs of severe acute pancreatitis (Imrie score of 3 and/or Balthazar CT score grade of D or E), 50 patients were assigned to the SD group and 52 to
3 CID 1997;25 (October) Acute Pancreatitis and Selective Decontamination 813 Figure 1. Cumulative percentages over time of patients with infection due to gram-negative bacteria (left) and with gram-positive infection of pancreatic necrosis (right), according to treatment group. In parentheses are numbers of patients at risk. Control group (dotted line), n Å 52; selective decontamination group (solid line), n Å 50. the control group. The groups were well matched with regard without treatment with intravenous antibiotics at the time of to Imrie score (mean for both, 3.2) and Balthazar grade [5]. aspiration. Only 4 of these aspirations (19%) showed presence of bacteria (E. coli, 1; S. epidermidis, 3). Nineteen FNAs (16 Microbiology patients) were done during simultaneous treatment with intravenous antibiotics. Eight of these (42%) showed infection of Twenty-nine of 102 patients (28%) developed infected pan- pancreatic necrosis (Enterobacter species, 1; Klebsiella specreatic necrosis. Pseudomonas aeruginosa (13 patients), Esche- cies, 1; S. epidermidis, 4; enterococci, 4; Staphylococcus richia coli (13), Staphylococcus epidermidis (21), and entero- aureus, 1). Some aspirates contained more than one type of cocci (19) were most frequently isolated; anaerobes (3) were bacteria. found to play only a minor role and were not further analyzed. Infected necrosis occurred in 9 of 50 patients (18%) of the SD group, in comparison with 20 of 52 patients (37%) of the Mortality control group (P Å.03), because of a significant reduction Mortality is significantly reduced among patients treated of gram-negative infected necrosis (SD group, 4 of 50 [8%]; with adjuvant SD [5]. Among patients who survived (n Å 73), controls, 17 of 52 [33%]). Three patients who developed in- the percentage in whom infected necrosis had occurred was fected necrosis had not undergone surgery. Infected necrosis 19% (14 patients), which is significantly (P Å.002) lower than was demonstrated at autopsy (two patients) or by percutaneous the 52% (15) of nonsurvivors (n Å 29) (table 1). To evaluate the drainage (one). impact on mortality of infected pancreatic necrosis developing Figure 1 shows the increasing percentage of patients over during treatment, patients were classified each day according time who developed gram-negative pancreatic infection. The to whether pancreatic necrosis was still sterile or whether only incidence of gram-positive infection of pancreatic necrosis did a gram-positive, only a gram-negative, or a mixed gramnegative/gram-positive not significantly differ between treatment groups (SD group, 9 pancreatic infection had occurred. of 50 [18%]; controls, 16 of 52 [31%]) (figure 1). All patients started in the sterile condition, in accordance The Imrie score at enrollment in the study appeared to correlate with the enrollment criteria. With the use of Cox regression very strongly with the incidence of gram-negative pancre- for both groups, it emerged that in comparison with patients atic necrosis over time, especially in the control group with sterile necrosis, those who acquired only a gram-positive (P õ.001) (figure 2). The Balthazar grade at enrollment in pancreatic infection had a 1.6-fold increased death rate the study also correlated with the incidence of gram-negative (P Å.52). Patients who developed only a gram-negative pan- pancreatic infection, although this correlation was less pro- creatic infection had a 14.4-fold increased death rate nounced (grade C/D, 6 of 48 [12%]; grade E, 14 of 53 [26%]) (P õ.001) in comparison with the rate for those with sterile (with adjustment for treatment group, P Å.03). necrosis. A similarly increased mortality of 15.8-fold Forty FNAs were performed in 25 patients (range, 1 4 per (P õ 0.001) was found for those with mixed gram-negative/ patient). Twenty-one of these FNAs (17 patients) were done gram-positive infected necrosis.
4 814 Luiten et al. CID 1997;25 (October) Figure 2. Cumulative percentages over time of patients with gramnegative infection of pancreatic necrosis in the control group (left) and selective decontamination (SD) group (right), according to Imrie score (I, 0 2; II, 3 4; III, ú4) at enrollment in the study. Control group scores: I, 21 patients; II, 19; III, 12; P trend õ.001. SD group scores: I, 15 patients; II, 22; III, 13; P trend Å.08. Table 2 shows results of multivariate analysis of the relation- between treatment groups. However, a gram-negative pancreatic ship between mortality and the type of pancreatic infection, infection occurred in only four patients in the SD group. taking into account the Imrie score, Balthazar grade, and randomized treatment. This analysis demonstrates that development of a gram-negative infection of pancreatic necrosis during Hospital Stay the course of the disease is an important and ominous sign, The average hospital stay of survivors with gram-negative while there was no significant increase in mortality due to necrosis (8 patients) was 135 days (range, days), which gram-positive pancreatic infection. With these infections taken is significantly higher than the mean values of 55 days (range, into account, there is still an increased death rate among pa days) (P Å.01) and 30 days (range, days) tients with a higher Imrie multifactorial initial assessment. No (P õ.001) for survivors with only gram-positive (6 patients) additional prognostic value was found for the Balthazar grade. or sterile necrosis (59), respectively. Although smaller, the The data in parentheses (table 2) also show that SD decreases difference between hospital stay of survivors with only grammortality when analyzed without consideration of infectious positive infected and sterile necrosis is also significant status. (P Å.004). These results were similar in both treatment groups There was no mortality difference between treatment groups (SD group and controls). for patients without gram-negative infected necrosis (i.e., sterile or only gram-positive), as demonstrated in figure 3 (left panel). After occurrence of a gram-negative pancreatic infection, mortality Discussion was high (13/21; 62%). As shown in figure 3 (right This study demonstrates that mortality increases dramatically panel), survival among these patients did not significantly differ once gram-negative infection of pancreatic necrosis occurs in patients with severe acute pancreatitis. However, if pancreatic necrosis becomes infected with only gram-positive aerobic bac- Table 1. Bacteriologic classification of pancreatic necrosis during teria, mortality is not significantly increased and is comparable the course of the disease in survivors and nonsurvivors. with that among patients in whom pancreatic necrosis remains No. (%) of patients sterile throughout the course of the disease. This is probably because S. epidermidis or enterococci, most frequently isolated Survivors Nonsurvivors in cases of infected necrosis due to a solitary gram-positive Classification (n Å 73) (n Å 29) organism, are less pathogenic in these patients. The overall incidence of secondary infection of pancreatic Sterile 59 (81) 14 (48) Only gram-positive 6 (8) 2 (7) necrosis is 28%. In the control group infected necrosis occurred Only gram-negative 0 4 (14) at a rate of 38%, which has also been described by others [1, Mixed gram-positive/gram-negative 8 (11) 9 (31) 15, 24]. In patients treated with SD, the overall incidence of infected necrosis (18%) was significantly reduced because of NOTE. The percentage of patients with infected pancreatic necrosis among nonsurvivors (15 of 29; 52%) is significantly higher than that among survivors a marked reduction in incidence of gram-negative infected ne- (14 of 73; 19%) (P Å.002). crosis (only 8%, vs. 33% in the control group).
5 CID 1997;25 (October) Acute Pancreatitis and Selective Decontamination 815 Table 2. Results of multivariate analysis of mortality in relation to development of infection of pancreatic necrosis during treatment, baseline Imrie score, baseline Balthazar grade, and randomized treatment. All patients started in the sterile category, in accordance with the enrollment criteria. No. of Relative 95% Confidence limits of Factor deaths* death rate Significance relative death rate Infected pancreatic necrosis Sterile 14/5, Only G/ 2/ , 5.5 Only G0 4/ , 27.1 Mixed G//G0 9/ , 24.5 Imrie score 0 2 1/36 1 (1)...(...) / (10.6).06 (.03) 0.9, / (56.8).001 (.001) 3.9, ú100 Balthazar grade C/D 9/48 1 (1)...(...)... E 20/ (1.3).76 (.38) 0.3, 2.3 Treatment group Controls 18/52 1 (1)...(...)... SD 11/ (0.4).56 (.03) 0.3, 1.8 NOTE. G/ Ågram-positive; G0 Ågram-negative; SD Å selective decontamination. Parentheses around data denote results obtained without allowance for the factor infections (infectious status). Upon enrollment, CT (Balthazer grade) was not performed for one patient. * Per no. of patient-days (up to day 80, i.e., the day number of the last death) after the first occurrence of the infection specified, or per no. of patients for Imrie score, Balthazar grade, or treatment group. In comparison with reference category. Reference category. Not significantly different from each other, but both significantly greater in comparison with Only G/ category value. to the bacteriologic status of pancreatic necrosis was comparable for the SD group and the control group, i.e., once gram- negative infection of pancreatic necrosis occurred, mortality increased considerably in both treatment groups. However, The occurrence of a gram-negative infection of pancreatic necrosis is an ominous sign. Mortality among these patients increases significantly, irrespective of coexistence of a grampositive infection, as shown in this study. Mortality with regard Figure 3. Left, survival from time of enrollment in the study, counting only deaths of patients with sterile or only gram-positive infected pancreatic necrosis, according to treatment group. Tick marks (1) denote deaths after gram-negative infection of pancreatic necrosis. Right, survival after the occurrence of gramnegative infection of pancreatic necrosis, according to treatment group (C Å control group; SD Å selective decontamination group).
6 816 Luiten et al. CID 1997;25 (October) mortality in the treatment group was significantly reduced 3. Rattner DW, Legemate DA, Lee MJ, Muelles PR, Warshaw AL. Early surgical debridement of pancreatic necrosis is beneficial irrespective of among patients treated with adjuvant SD (table 2), a finding infection. Am J Surg 1992;163: that was also published previously [5]. 4. Roscher R, Beger HG. Bacterial infection of pancreatic necrosis. In: Beger Consequently, SD reduces mortality among patients with HG, Büchler M, eds. Acute pancreatitis: research and clinical management. severe acute pancreatitis because of a significant reduction in Berlin: Springer-Verlag, 1987: the development of gram-negative infection of pancreatic neof 5. Luiten EJT, Hop WCJ, Lange JF, Bruining HA. Controlled clinical trial selective decontamination for the treatment of severe acute pancreati- crosis. This is accomplished by reduction of gram-negative tis. Ann Surg 1995;222: intestinal colonization, leading to reduced gram-negative bacte- 6. Karimgani I, Porter KA, Langevin RE, Banks PA. Prognostic factors in rial translocation into the pancreatic necrosis. However, SD sterile pancreatic necrosis. Gastroenterology 1992;103: is not useful for patients in whom gram-negative pancreatic 7. Blamey SL, Imrie CW, O Neill J, Gilmour WH, Carter DC. Prognostic factors in acute pancreatitis. Gut 1984;25: infection already exists or develops during SD administration, 8. Ranson JHC. Etiological and prognostic factors in human acute pancreatias is demonstrated in this study. tis: a review. Am J Gastroenterol 1982;77: It has been suggested that overgrowth and translocation of 9. Steinberg W, Tenner S. Acute pancreatitis. N Engl J Med 1994;330:1198 gram-positive bacteria, i.e., enterococci or staphylococci, may 210. be a drawback of SD [20, 25]. Our results do not support 10. Wilson C, Imrie CW. Systemic effects of acute pancreatitis In: Johnson CD, Imrie CW, eds. Pancreatic disease. London: Springer-Verlag, 1991: this hypothesis. Neither intestinal overgrowth nor increased incidence of gram-positive infected necrosis has been found in 11. Gerzof SG, Banks PA, Robbins AH, et al. Early diagnosis of pancreatic our study. Deaths due to unexplained gram-positive sepsis infection by computed tomography guided aspiration. Gastroenterol- along with positive blood cultures (two patients) and otherwise- ogy 1987;93: Bradley EL III. Management of infected necrosis by open drainage. Ann documented sterile necrosis at time of death were equally di- Surg 1987;206: vided among the SD group and controls. However, these possi- 13. Ranson JHC. The role of surgery in the management of acute pancreatitis. ble hazards demand strict indications and careful bacteriologic Ann Surg 1990;211: surveillance, as is the case for any kind of antibiotic regimen. 14. Beger HG. Surgery in acute pancreatitis. Hepatogastroenterology 1991; The development of gram-negative infection of devitalized 38: Beger HG, Bittner R, Block S, Büchler M. Bacterial contamination of tissues in and around the pancreas is, apart from the Imrie pancreatic necrosis: A prospective clinical study. Gastroenterology score, the most important parameter determining outcome. 1986;91: Gram-negative pancreatic infection can be minimized with adcreatitis. 16. Widdison AL, Karanjia ND. Pancreatic infection complicating acute panjuvant SD, thereby reducing mortality among patients with Br J Surg 1993;80: Pederzoli P, Bassi C, Vesentini S, et al. Retroperitoneal and peritoneal severe acute pancreatitis. drainage and lavage in the treatment of severe necrotizing pancreatitis. Surg Gynecol Obstet 1990;170: Bittner R, Block S, Büchler M, Beger HG. Pancreatic abscess and infected Acknowledgments pancreatic necrosis. Different local septic complications in acute pancreatitis. Dig Dis Sci 1987;32: The authors thank Dr. C. W. Imrie, Consultant Surgeon of the 19. Bradley EL III. Operative management of acute pancreatitis: ventral open University Department of Surgery and Division of Surgery of the packing. Hepatogastroenterology 1991;38: Royal Infirmary, Glasgow, United Kingdom, and Dr. H. Ph. Endtz, 20. Jackson RJ, Smith SD, Rowe MI. Selective bowel decontamination results in gram-positive translocation. J Surg Res 1990;48: of the Department of Clinical Microbiology of the University Hos- 21. Balthazar EJ, Ranson JHC, Naidich DP, Megibow AJ, Caccavale R, Coopital Rotterdam-Dijkzigt, for their support and critical review of per MM. Acute pancreatitis: prognostic value of CT. Radiology 1985; the manuscript. 156: Cox DR. Regression models and life tables. J R Stat Soc B 1972;34: References 23. Hop WCJ, van Buuren HR. A method to evaluate changes in prognostic status during follow-up, illustrated by an assessment of the effect of a 1. Beger HG, Büchler M, Bittner R, Block S, Nevalainen T, Roscher R. rebleed in patients with oesophageal variceal bleeding. Comput Biol Necrosectomy and postoperative local lavage in necrotizing pancreatitis. Med 1989;19: Br J Surg 1988;75: Smadja C, Bismuth H. Pancreatic debridement in acute necrotizing pancre- 2. Bradley EL III, Allen K. A prospective longitudinal study of observation atitis: an obsolete procedure? Br J Surg 1986;73: versus surgical intervention in the management of necrotizing pancreati- 25. Webb CH. Antibiotic resistance associated with selective decontamination tis. Am J Surg 1991;161: of the digestive tract. J Hosp Infect 1992;22:1 5.
Antibiotic Therapy for Prophylaxis of Infection in Severe Pancreatitis is Overrated. Jessica Yu, R2 10/26/09
 Antibiotic Therapy for Prophylaxis of Infection in Severe Pancreatitis is Overrated Jessica Yu, R2 10/26/09 Of 12 with pancreatitis 15% will get necrosis Of these, 40-70% progress to infection week 2-3
Antibiotic Therapy for Prophylaxis of Infection in Severe Pancreatitis is Overrated Jessica Yu, R2 10/26/09 Of 12 with pancreatitis 15% will get necrosis Of these, 40-70% progress to infection week 2-3
Prophylactic Antibiotics in Severe Acute Pancreatitis: Antibiotics are good. Karen Lo R 3 University of Colorado Oct 11, 2010
 Prophylactic Antibiotics in Severe Acute Pancreatitis: Antibiotics are good Karen Lo R 3 University of Colorado Oct 11, 2010 Overview Pancreas: The History Pancreas: The Organ The Disease Pathogenesis
Prophylactic Antibiotics in Severe Acute Pancreatitis: Antibiotics are good Karen Lo R 3 University of Colorado Oct 11, 2010 Overview Pancreas: The History Pancreas: The Organ The Disease Pathogenesis
Imaging Techniques for Acute Necrotizing Pancreatitis: Multidetector Computed Tomography
 AISP - 29 th National Congress. Bologna (Italy). September 15-17, 2005. Imaging Techniques for Acute Necrotizing Pancreatitis: Multidetector Computed Tomography Lucia Calculli 1, Raffaele Pezzilli 2, Riccardo
AISP - 29 th National Congress. Bologna (Italy). September 15-17, 2005. Imaging Techniques for Acute Necrotizing Pancreatitis: Multidetector Computed Tomography Lucia Calculli 1, Raffaele Pezzilli 2, Riccardo
University of Colorado
 University of Colorado Dept. of Surgery Grand Rounds Prophylactic Antibiotics in Severe Acute Pancreatitis Eduardo Gonzalez, PGY2 Mortality from Acute Pancreatitis SAP 1 - >30% necrosis - SBP2.0,
University of Colorado Dept. of Surgery Grand Rounds Prophylactic Antibiotics in Severe Acute Pancreatitis Eduardo Gonzalez, PGY2 Mortality from Acute Pancreatitis SAP 1 - >30% necrosis - SBP2.0,
PROGNOSTIC VALUE OF EARLY CT IN PATIENTS WITH ACUTE PANCREATITIS
 Analele Universităţii din Oradea, Fascicula Protecţia Mediului Vol. XXIII, 2014 PROGNOSTIC VALUE OF EARLY CT IN PATIENTS WITH ACUTE PANCREATITIS Osiceanu Adrian*, Osiceanu Alina,Maghiar Traian Teodor *University
Analele Universităţii din Oradea, Fascicula Protecţia Mediului Vol. XXIII, 2014 PROGNOSTIC VALUE OF EARLY CT IN PATIENTS WITH ACUTE PANCREATITIS Osiceanu Adrian*, Osiceanu Alina,Maghiar Traian Teodor *University
Fungal Infections in Patients with Severe Acute Pancreatitis and the Use of Prophylactic Therapy
 MAJOR ARTICLE Fungal Infections in Patients with Severe Acute Pancreatitis and the Use of Prophylactic Therapy Jan J. De Waele, 1 D. Vogelaers, 2 S. Blot, 1 and F. Colardyn 1 1 Intensive Care Unit and
MAJOR ARTICLE Fungal Infections in Patients with Severe Acute Pancreatitis and the Use of Prophylactic Therapy Jan J. De Waele, 1 D. Vogelaers, 2 S. Blot, 1 and F. Colardyn 1 1 Intensive Care Unit and
THE CLINICAL course of severe
 ORIGINAL ARTICLE Improved Prediction of Outcome in Patients With Severe Acute Pancreatitis by the APACHE II Score at 48 Hours After Hospital Admission Compared With the at Admission Arif A. Khan, MD; Dilip
ORIGINAL ARTICLE Improved Prediction of Outcome in Patients With Severe Acute Pancreatitis by the APACHE II Score at 48 Hours After Hospital Admission Compared With the at Admission Arif A. Khan, MD; Dilip
Timing of intervention in acute pancreatitis
 Postgrad Med J (1993) 69, 509-515 The Fellowship of Postgraduate Medicine, 1993 Review Article Timing of intervention in acute pancreatitis C.D. Johnson University Surgical Unit, F Level, Centre Block,
Postgrad Med J (1993) 69, 509-515 The Fellowship of Postgraduate Medicine, 1993 Review Article Timing of intervention in acute pancreatitis C.D. Johnson University Surgical Unit, F Level, Centre Block,
ORIGINAL ARTICLE. Pancreatic Infection in Severe Pancreatitis
 ORIGINAL ARTICLE Pancreatic Infection in Severe Pancreatitis The Role of Fungus and Multiresistant Organisms Beat Gloor, MD; Christophe A. Müller, MD; Matthias Worni, MS; Philip F. Stahel, MD; Claudio
ORIGINAL ARTICLE Pancreatic Infection in Severe Pancreatitis The Role of Fungus and Multiresistant Organisms Beat Gloor, MD; Christophe A. Müller, MD; Matthias Worni, MS; Philip F. Stahel, MD; Claudio
DEBRIDEMENT OR FORMAL RESECTION OF THE
 HPB Surgery, 1993, Vol. 6, pp. 255-262 Reprints available directly from the publisher Photocopying permitted by license only (C) 1993 Harwood Academic Publishers GmbH Printed in the United States of America
HPB Surgery, 1993, Vol. 6, pp. 255-262 Reprints available directly from the publisher Photocopying permitted by license only (C) 1993 Harwood Academic Publishers GmbH Printed in the United States of America
Role of Early Multisystem Organ Failure as Major Risk Factor for Pancreatic Infections and Death in Severe Acute Pancreatitis
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1053 1061 Role of Early Multisystem Organ Failure as Major Risk Factor for Pancreatic Infections and Death in Severe Acute Pancreatitis BETTINA M. RAU,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2006;4:1053 1061 Role of Early Multisystem Organ Failure as Major Risk Factor for Pancreatic Infections and Death in Severe Acute Pancreatitis BETTINA M. RAU,*
Patients With Severe Acute Pancreatitis Should Be More Often Treated In An Intensive Care Department
 ISPUB.COM The Internet Journal of Emergency and Intensive Care Medicine Volume 6 Number 2 Patients With Severe Acute Pancreatitis Should Be More Often Treated In An Intensive Care Department M Dinis-Ribeiro,
ISPUB.COM The Internet Journal of Emergency and Intensive Care Medicine Volume 6 Number 2 Patients With Severe Acute Pancreatitis Should Be More Often Treated In An Intensive Care Department M Dinis-Ribeiro,
Clinical profile, degree of severity and underlying factors of acute pancreatitis among a group of Bangladeshi patients
 Clinical profile, degree of severity and underlying factors of acute pancreatitis among a group of Bangladeshi patients Indrajit Kumar Datta 1, Md Nazmul Haque 1, Tareq M Bhuiyan 2 Original Article 1 Deaprtment
Clinical profile, degree of severity and underlying factors of acute pancreatitis among a group of Bangladeshi patients Indrajit Kumar Datta 1, Md Nazmul Haque 1, Tareq M Bhuiyan 2 Original Article 1 Deaprtment
AMERICAN JOURNAL OF BIOLOGICAL AND PHARMACEUTICAL RESEARCH
 AMERICAN JOURNAL OF BIOLOGICAL AND PHARMACEUTICAL RESEARCH e-issn - 2348-2184 Print ISSN - 2348-2176 Journal homepage: www.mcmed.us/journal/ajbpr ABDOMINAL ABSCESS A SEQUEL OF EXPLORATORY LAPAROTOMY FOR
AMERICAN JOURNAL OF BIOLOGICAL AND PHARMACEUTICAL RESEARCH e-issn - 2348-2184 Print ISSN - 2348-2176 Journal homepage: www.mcmed.us/journal/ajbpr ABDOMINAL ABSCESS A SEQUEL OF EXPLORATORY LAPAROTOMY FOR
Acute Pancreatitis. Falk Symposium 161 Dresden
 Acute Pancreatitis Falk Symposium 161 Dresden 12.10.2007 Incidence of Acute Pancreatitis (Malmö) Lindkvist B, et al Clin Gastroenterol Hepatol 2004;2:831-837 Gallstones Alcohol AGA Medical Position Statement
Acute Pancreatitis Falk Symposium 161 Dresden 12.10.2007 Incidence of Acute Pancreatitis (Malmö) Lindkvist B, et al Clin Gastroenterol Hepatol 2004;2:831-837 Gallstones Alcohol AGA Medical Position Statement
Review. The role of infection in acute pancreatitis
 Gut 1999;45:311 316 311 Review The role of infection in acute pancreatitis Acute pancreatitis can be a mild, transitory illness or a severe, rapidly fatal disease. About 80% of cases of the disease are
Gut 1999;45:311 316 311 Review The role of infection in acute pancreatitis Acute pancreatitis can be a mild, transitory illness or a severe, rapidly fatal disease. About 80% of cases of the disease are
ISF criteria (International sepsis forum consensus conference of infection in the ICU) Secondary peritonitis
 Appendix with supplementary material. This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Supplementary Tables Table S1. Definitions
Appendix with supplementary material. This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. Supplementary Tables Table S1. Definitions
Severe and Tertiary Peritonitis
 Severe and Tertiary Peritonitis Addison K. May, MD FACS Professor of Surgery and Anesthesiology Division of Trauma and Surgical Critical Care Vanderbilt University Medical Center PS204: The Bad Infections:
Severe and Tertiary Peritonitis Addison K. May, MD FACS Professor of Surgery and Anesthesiology Division of Trauma and Surgical Critical Care Vanderbilt University Medical Center PS204: The Bad Infections:
JMSCR Vol 05 Issue 06 Page June 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i6.76 A Comparative Study of Assessment of Different
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i6.76 A Comparative Study of Assessment of Different
Assessments of Severity and Management of Acute Pancreatitis Based on the Santorini Consensus Conference Report
 Assessments of Severity and Management of Acute Pancreatitis Based on the Santorini Consensus Conference Report Christos Dervenis 1 st Department of Surgery, Konstantopoulion, Agia Olga Hospital. Athens,
Assessments of Severity and Management of Acute Pancreatitis Based on the Santorini Consensus Conference Report Christos Dervenis 1 st Department of Surgery, Konstantopoulion, Agia Olga Hospital. Athens,
Multidetector CT evaluation of acute pancreatitis and its complications and its correlation with clinical outcome
 INTERNATIONAL JOURNAL OF CURRENT RESEARCH IN BIOLOGY AND MEDICINE ISSN: 2455-944X www.darshanpublishers.com DOI:10.22192/ijcrbm Volume 3, Issue 1-2018 Original Research Article Multidetector CT evaluation
INTERNATIONAL JOURNAL OF CURRENT RESEARCH IN BIOLOGY AND MEDICINE ISSN: 2455-944X www.darshanpublishers.com DOI:10.22192/ijcrbm Volume 3, Issue 1-2018 Original Research Article Multidetector CT evaluation
Severe necrotizing pancreatitis. ICU Fellowship Training Radboudumc
 Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Acute pancreatitis (AP) is a potentially lethal disease with
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:1089 1094 Primary Conservative Treatment Results in Mortality Comparable to Surgery in Patients With Infected Pancreatic Necrosis PRAMOD KUMAR GARG,* MANIK
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:1089 1094 Primary Conservative Treatment Results in Mortality Comparable to Surgery in Patients With Infected Pancreatic Necrosis PRAMOD KUMAR GARG,* MANIK
Prophylactic Antibiotics in Severe Acute Pancreatitis: An Unnecessary And Potentially Dangerous Therapy. John Stringham, MD October 11, 2010
 Prophylactic Antibiotics in Severe Acute Pancreatitis: An Unnecessary And Potentially Dangerous Therapy John Stringham, MD October 11, 2010 Necrotizing Pancreatitis Occurs in approximately 20% of all cases
Prophylactic Antibiotics in Severe Acute Pancreatitis: An Unnecessary And Potentially Dangerous Therapy John Stringham, MD October 11, 2010 Necrotizing Pancreatitis Occurs in approximately 20% of all cases
Treatment of febrile neutropenia in patients with neoplasia
 Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
Treatment of febrile neutropenia in patients with neoplasia George Samonis MD, PhD Medical Oncologist Infectious Diseases Specialist Professor of Medicine The University of Crete, Heraklion,, Crete, Greece
ACG Clinical Guideline: Management of Acute Pancreatitis
 ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
ACG Clinical Guideline: Management of Acute Pancreatitis Scott Tenner, MD, MPH, FACG 1, John Baillie, MB, ChB, FRCP, FACG 2, John DeWitt, MD, FACG 3 and Santhi Swaroop Vege, MD, FACG 4 1 State University
Mild. Moderate. Severe
 2012 Revised Atlanta Classification Acute pancreatitis Classified based on absence or presence of local and/or systemic complications Mild Acute Pancreatits Moderate Severe P. A. Banks, T. L. Bollen, C.
2012 Revised Atlanta Classification Acute pancreatitis Classified based on absence or presence of local and/or systemic complications Mild Acute Pancreatits Moderate Severe P. A. Banks, T. L. Bollen, C.
Reinterventions belong to complications
 Reinterventions belong to complications Pancreatic surgery is the archetypus of complex abdominal surgery Mortality (1-4%) and morbidity (7-60%) rates are relevant even at high volume centres Reinterventions
Reinterventions belong to complications Pancreatic surgery is the archetypus of complex abdominal surgery Mortality (1-4%) and morbidity (7-60%) rates are relevant even at high volume centres Reinterventions
Management of necrotizing pancreatitis and its outcome in a secondary healthcare institution
 International Surgery Journal Karim T et al. Int Surg J. 2017 Mar;4(3):1049-1054 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20170860
International Surgery Journal Karim T et al. Int Surg J. 2017 Mar;4(3):1049-1054 http://www.ijsurgery.com pissn 2349-3305 eissn 2349-2902 Original Research Article DOI: http://dx.doi.org/10.18203/2349-2902.isj20170860
Surveillance of Surgical Site Infection in Surgical Hospital Wards in Bulgaria,
 International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 01 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.701.361
International Journal of Current Microbiology and Applied Sciences ISSN: 2319-7706 Volume 7 Number 01 (2018) Journal homepage: http://www.ijcmas.com Original Research Article https://doi.org/10.20546/ijcmas.2018.701.361
Use of Vacuum-assisted Wound Closure to Manage Limb Wounds in Patients Suffering from Acute Necrotizing Fasciitis
 Original Article Use of Vacuum-assisted Wound Closure to Manage Limb Wounds in Patients Suffering from Acute Necrotizing Fasciitis Wen-Shyan Huang, Shang-Chin Hsieh, Chun-Sheng Hsieh, Jen-Yu Schoung and
Original Article Use of Vacuum-assisted Wound Closure to Manage Limb Wounds in Patients Suffering from Acute Necrotizing Fasciitis Wen-Shyan Huang, Shang-Chin Hsieh, Chun-Sheng Hsieh, Jen-Yu Schoung and
Case-Matched Comparison of the Retroperitoneal Approach With Laparotomy for Necrotizing Pancreatitis
 World J Surg (2007) 31:1635 1642 DOI 10.1007/s00268-007-9083-6 Case-Matched Comparison of the Retroperitoneal Approach With Laparotomy for Necrotizing Pancreatitis Hjalmar C. van Santvoort Æ Marc G. Besselink
World J Surg (2007) 31:1635 1642 DOI 10.1007/s00268-007-9083-6 Case-Matched Comparison of the Retroperitoneal Approach With Laparotomy for Necrotizing Pancreatitis Hjalmar C. van Santvoort Æ Marc G. Besselink
Emergency Surgery Course Graz, March ACUTE PANCREATITIS. Carlos Mesquita Coimbra
 ACUTE PANCREATITIS Carlos Mesquita Coimbra ESSENTIALS (1) AP occurs when digestive enzymes become activated while still in the pancreas, causing inflammation repeated bouts of AP can lead to chronic pancreatitis
ACUTE PANCREATITIS Carlos Mesquita Coimbra ESSENTIALS (1) AP occurs when digestive enzymes become activated while still in the pancreas, causing inflammation repeated bouts of AP can lead to chronic pancreatitis
The New England Journal of Medicine. Review Article
 The New England Journal of Medicine Review Article Current Concepts ACUTE NECROTIZING PANCREATITIS TODD H. BARON, M.D., AND DESIREE E. MORGAN, M.D. ACUTE pancreatitis may be clinically mild or severe.
The New England Journal of Medicine Review Article Current Concepts ACUTE NECROTIZING PANCREATITIS TODD H. BARON, M.D., AND DESIREE E. MORGAN, M.D. ACUTE pancreatitis may be clinically mild or severe.
A Comparative Study of Different Predictive Severity Scoring Systems for Acute Pancreatitis in Relation To Outcome A Prospective Study
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 12 Ver. 2 (December. 2018), PP 01-09 www.iosrjournals.org A Comparative Study of Different
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 12 Ver. 2 (December. 2018), PP 01-09 www.iosrjournals.org A Comparative Study of Different
Pancreatic Benign April 27, 2016
 Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Disclosures. Extra-hepatic Biliary Disease and the Pancreas. Objectives. Pancreatitis 10/3/2018. No relevant financial disclosures to report
 Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Extra-hepatic Biliary Disease and the Pancreas Disclosures No relevant financial disclosures to report Jeffrey Coughenour MD FACS Clinical Associate Professor of Surgery and Emergency Medicine Division
Clinical Comparison of Cefotaxime with Gentamicin plus Clindamycin in the Treatment of Peritonitis and Other Soft-Tissue Infections
 REVIEWS OF INFECTIOUS DISEASES. VOL. 4, SUPPLEMENT. SEPTEMBER-OCTOBER 982 982 by The University of Chicago. All rights reserved. 062-0886/82/0405-022$02.00 Clinical Comparison of with Gentamicin plus Clindamycin
REVIEWS OF INFECTIOUS DISEASES. VOL. 4, SUPPLEMENT. SEPTEMBER-OCTOBER 982 982 by The University of Chicago. All rights reserved. 062-0886/82/0405-022$02.00 Clinical Comparison of with Gentamicin plus Clindamycin
EARLY PREDICTION OF SEVERITY AND OUTCOME OF ACUTE SEVERE PANCREATITIS
 Original Article EARLY PREDICTION OF SEVERITY AND OUTCOME OF ACUTE SEVERE PANCREATITIS Syed Sagheer Hussian Shah 1, M. Ali Ansari 2, Shazia Ali 3 ABSTRACT Objective: To establish the value of APACHE II
Original Article EARLY PREDICTION OF SEVERITY AND OUTCOME OF ACUTE SEVERE PANCREATITIS Syed Sagheer Hussian Shah 1, M. Ali Ansari 2, Shazia Ali 3 ABSTRACT Objective: To establish the value of APACHE II
Management of Acute Pancreatitis
 Management of Acute Pancreatitis A Clinical Practice Guideline developed by the University of Toronto s Best Practice in Surgery JA Greenberg, M Bawazeer, J Hsu, J Marshall, JO Friedrich, A Nathens, N
Management of Acute Pancreatitis A Clinical Practice Guideline developed by the University of Toronto s Best Practice in Surgery JA Greenberg, M Bawazeer, J Hsu, J Marshall, JO Friedrich, A Nathens, N
GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT
 GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT Name & Title Of Author: Dr Linda Jewes, Consultant Microbiologist Date Amended: December 2016 Approved by Committee/Group: Drugs & Therapeutics
GASTRO-INTESTINAL TRACT INFECTIONS - ANTIMICROBIAL MANAGEMENT Name & Title Of Author: Dr Linda Jewes, Consultant Microbiologist Date Amended: December 2016 Approved by Committee/Group: Drugs & Therapeutics
VIDEO ASSISTED RETROPERITONEAL DEBRIDEMENT IN HUGE INFECTED PANCREATIC PSEUDOCYST
 Trakia Journal of Sciences, Vol. 13, Suppl. 2, pp 102-106, 2015 Copyright 2015 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) doi:10.15547/tjs.2015.s.02.022 ISSN 1313-3551
Trakia Journal of Sciences, Vol. 13, Suppl. 2, pp 102-106, 2015 Copyright 2015 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) doi:10.15547/tjs.2015.s.02.022 ISSN 1313-3551
ABSTRACT. KEY WORDS antibiotics; prophylaxis; hysterectomy
 Infectious Diseases in Obstetrics and Gynecology 8:230-234 (2000) (C) 2000 Wiley-Liss, Inc. Wound Infection in Gynecologic Surgery Aparna A. Kamat,* Leo Brancazio, and Mark Gibson Department of Obstetrics
Infectious Diseases in Obstetrics and Gynecology 8:230-234 (2000) (C) 2000 Wiley-Liss, Inc. Wound Infection in Gynecologic Surgery Aparna A. Kamat,* Leo Brancazio, and Mark Gibson Department of Obstetrics
ACUTE PANCREATITIS IN BERGEN, NORWAY
 Scandinavian Journal of Surgery 93: 29 33, 2004 ACUTE PANCREATITIS IN BERGEN, NORWAY A study on incidence, etiology and severity H. Gislason 2, A. Horn 1, D. Hoem 1, Å. Andrén-Sandberg 1, A. K. Imsland
Scandinavian Journal of Surgery 93: 29 33, 2004 ACUTE PANCREATITIS IN BERGEN, NORWAY A study on incidence, etiology and severity H. Gislason 2, A. Horn 1, D. Hoem 1, Å. Andrén-Sandberg 1, A. K. Imsland
ORIGINAL ARTICLE. Potential Harmful Effect of Iodinated Intravenous Contrast Medium on the Clinical Course
 ORIGINAL ARTICLE Potential Harmful Effect of Iodinated Intravenous Contrast Medium on the Clinical Course of Mild Acute Pancreatitis Ramón Carmona-Sánchez, MD; Luis Uscanga, MD; Paulina Bezaury-Rivas,
ORIGINAL ARTICLE Potential Harmful Effect of Iodinated Intravenous Contrast Medium on the Clinical Course of Mild Acute Pancreatitis Ramón Carmona-Sánchez, MD; Luis Uscanga, MD; Paulina Bezaury-Rivas,
Surgical Management of Acute Pancreatitis
 Surgical Management of Acute Pancreatitis Steven J. Hughes, MD, FACS Cracchiolo Family Professor of Surgery and Chief, General Surgery Overview Biliary pancreatitis a cost effective algorithm Key concepts
Surgical Management of Acute Pancreatitis Steven J. Hughes, MD, FACS Cracchiolo Family Professor of Surgery and Chief, General Surgery Overview Biliary pancreatitis a cost effective algorithm Key concepts
Efficacy of antibiotic penetration into pancreatic necrosis
 HPB, 2006; 8: 43/48 Efficacy of antibiotic penetration into pancreatic necrosis W. OTTO, K. KOMORZYCKI & M. KRAWCZYK Department of General, Transplantation & Liver Surgery, Medical University of Warsaw,
HPB, 2006; 8: 43/48 Efficacy of antibiotic penetration into pancreatic necrosis W. OTTO, K. KOMORZYCKI & M. KRAWCZYK Department of General, Transplantation & Liver Surgery, Medical University of Warsaw,
Supplementary Materials to the Manuscript: Polymorphisms in TNF-α Increase Susceptibility to
 Supplementary Materials to the Manuscript: Polymorphisms in TNF-α Increase Susceptibility to Intra-abdominal Candida Infection in High Risk Surgical ICU Patients A. Wójtowicz, Ph.D. 1, F. Tissot, M.D.
Supplementary Materials to the Manuscript: Polymorphisms in TNF-α Increase Susceptibility to Intra-abdominal Candida Infection in High Risk Surgical ICU Patients A. Wójtowicz, Ph.D. 1, F. Tissot, M.D.
VAP Prevention bundles
 VAP Prevention bundles Dr. Shafiq A.Alimad MD Head of medical department at USTH YICID workshop, 15-12-2014 Care Bundles What are they & why use them? What are Care Bundles? Types of Care Bundles available
VAP Prevention bundles Dr. Shafiq A.Alimad MD Head of medical department at USTH YICID workshop, 15-12-2014 Care Bundles What are they & why use them? What are Care Bundles? Types of Care Bundles available
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist. Alireza Sedarat, MD UCLA Division of Digestive Diseases
 Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Lumen Apposing Metal Stents: Expanding the Role of the Interventional Endoscopist Alireza Sedarat, MD UCLA Division of Digestive Diseases Disclosures Consultant for Boston Scientific and Olympus Corporation
Terapia della candidiasi addomaniale
 Verona 16 marzo 2018 Terapia della candidiasi addomaniale Pierluigi Viale Infectious Disease Unit Teaching Hospital S. Orsola Malpighi Bologna INTRA ABDOMINAL CANDIDIASIS open questions a single definition
Verona 16 marzo 2018 Terapia della candidiasi addomaniale Pierluigi Viale Infectious Disease Unit Teaching Hospital S. Orsola Malpighi Bologna INTRA ABDOMINAL CANDIDIASIS open questions a single definition
U Nordic Forum - Trauma & Emergency Radiology. Lecture Objectives. MDCT in Acute Pancreatitis. Acute Pancreatitis: Etiologies
 Nordic Forum - Trauma & Emergency Radiology Lecture Objectives MDCT in Acute Pancreatitis Borut Marincek Institute of Diagnostic Radiology niversity Hospital Zurich, Switzerland To describe the role of
Nordic Forum - Trauma & Emergency Radiology Lecture Objectives MDCT in Acute Pancreatitis Borut Marincek Institute of Diagnostic Radiology niversity Hospital Zurich, Switzerland To describe the role of
The Bile Duct (and Pancreas) and the Physician
 The Bile Duct (and Pancreas) and the Physician Javaid Iqbal Consultant in Gastroenterology and Pancreato-biliary Medicine University Hospital South Manchester Not so common?! Two weeks 38 ERCP s 20 15
The Bile Duct (and Pancreas) and the Physician Javaid Iqbal Consultant in Gastroenterology and Pancreato-biliary Medicine University Hospital South Manchester Not so common?! Two weeks 38 ERCP s 20 15
Bacteraemia in patients receiving human cadaveric
 J. clin. Path., 1971, 24, 295-299 Bacteraemia in patients receiving human cadaveric renal transplants D. A. LEIGH1 From the Department of Bacteriology, The Wright-Fleming Institute, St Mary's Hospital,
J. clin. Path., 1971, 24, 295-299 Bacteraemia in patients receiving human cadaveric renal transplants D. A. LEIGH1 From the Department of Bacteriology, The Wright-Fleming Institute, St Mary's Hospital,
The Clinical Significance of Blood Cultures. Presented BY; Cindy Winfrey, MSN, RN, CIC, DON- LTC TM, VA- BC TM
 The Clinical Significance of Blood Cultures Presented BY; Cindy Winfrey, MSN, RN, CIC, DON- LTC TM, VA- BC TM OVERVIEW Blood cultures are considered an important laboratory tool used to diagnose serious
The Clinical Significance of Blood Cultures Presented BY; Cindy Winfrey, MSN, RN, CIC, DON- LTC TM, VA- BC TM OVERVIEW Blood cultures are considered an important laboratory tool used to diagnose serious
UK guidelines for the management of acute pancreatitis
 UK guidelines for the management of acute pancreatitis Gut 2005;54;1-9 doi:10.1136/gut.2004.057026 Updated information and services can be found at: http://gut.bmjjournals.com/cgi/content/full/54/suppl_3/iii1
UK guidelines for the management of acute pancreatitis Gut 2005;54;1-9 doi:10.1136/gut.2004.057026 Updated information and services can be found at: http://gut.bmjjournals.com/cgi/content/full/54/suppl_3/iii1
Online Supplement for:
 Online Supplement for: INFLUENCE OF COMBINED INTRAVENOUS AND TOPICAL ANTIBIOTIC PROPHYLAXIS ON THE INCIDENCE OF INFECTIONS, ORGAN DYSFUNCTIONS, AND MORTALITY IN CRITICALLY ILL SURGICAL PATIENTS A PROSPECTIVE,
Online Supplement for: INFLUENCE OF COMBINED INTRAVENOUS AND TOPICAL ANTIBIOTIC PROPHYLAXIS ON THE INCIDENCE OF INFECTIONS, ORGAN DYSFUNCTIONS, AND MORTALITY IN CRITICALLY ILL SURGICAL PATIENTS A PROSPECTIVE,
Acute Diverticulitis. Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh
 Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
Acute Diverticulitis Andrew B. Peitzman, MD Mark M. Ravitch Professor of Surgery University of Pittsburgh Focus today: when to operate n Recurrent, uncomplicated diverticulitis; after how many episodes?
Review article. Prevention of severe change in acute pancreatitis: prediction and prevention. Hans G. Beger, Bettina Rau, and Rainer Isenmann
 J Hepatobiliary Pancreat Surg (2001) 8:140 147 Review article Prevention of severe change in acute pancreatitis: prediction and prevention Hans G. Beger, Bettina Rau, and Rainer Isenmann Department of
J Hepatobiliary Pancreat Surg (2001) 8:140 147 Review article Prevention of severe change in acute pancreatitis: prediction and prevention Hans G. Beger, Bettina Rau, and Rainer Isenmann Department of
Comprehensive Study of Acute Pancreatitis (Diagnosis, Disease Course, and Clinical Management): A Retrospective and Prospective Study
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/449 Comprehensive Study of Acute Pancreatitis (Diagnosis, Disease Course, and Clinical Management): A Retrospective
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/449 Comprehensive Study of Acute Pancreatitis (Diagnosis, Disease Course, and Clinical Management): A Retrospective
Interventions in Acute Pancreatitis
 382 Medicine Update 65 Interventions in Acute Pancreatitis RAKESH TANDON Acute pancreatitis (AP) is a medical emergency presenting usually with acute abdominal pain associated with nausea and vomiting,
382 Medicine Update 65 Interventions in Acute Pancreatitis RAKESH TANDON Acute pancreatitis (AP) is a medical emergency presenting usually with acute abdominal pain associated with nausea and vomiting,
A prospective audit against national standards of the presentation and management of acute pancreatitis in the South of England
 Gut 2000;46:29 24 29 University Surgical Unit (86), Southampton General Hospital, Tremona Rd, Southampton, Hampshire SO6 6YD, UK SKCToh S Phillips C D Johnson Correspondence to: Mr Johnson. Accepted for
Gut 2000;46:29 24 29 University Surgical Unit (86), Southampton General Hospital, Tremona Rd, Southampton, Hampshire SO6 6YD, UK SKCToh S Phillips C D Johnson Correspondence to: Mr Johnson. Accepted for
CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement
 CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement Evidence-Based Assessment of Diagnostic Tests for Ventilator- Associated Pneumonia* Executive Summary Ronald F. Grossman, MD, FCCP; and Alan Fein, MD,
CHEST VOLUME 117 / NUMBER 4 / APRIL, 2000 Supplement Evidence-Based Assessment of Diagnostic Tests for Ventilator- Associated Pneumonia* Executive Summary Ronald F. Grossman, MD, FCCP; and Alan Fein, MD,
PFIZER INC. THERAPEUTIC AREA AND FDA APPROVED INDICATIONS: See USPI
 PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
PFIZER INC. These results are supplied for informational purposes only. Prescribing decisions should be made based on the approved package insert. For publications based on this study, see associated bibliography.
Three Cases of Liver Abscesses Complicated with Colon Cancer without Liver Metastasis: Importance of Screening for Digestive Disease
 CASE REPORT Three Cases of Liver Abscesses Complicated with Colon Cancer without Liver Metastasis: Importance of Screening for Digestive Disease Atsushi Hiraoka 1, Yoshimasa Yamashita 1, Kazuhiro Uesugi
CASE REPORT Three Cases of Liver Abscesses Complicated with Colon Cancer without Liver Metastasis: Importance of Screening for Digestive Disease Atsushi Hiraoka 1, Yoshimasa Yamashita 1, Kazuhiro Uesugi
Acute Pancreatitis:
 American College of Gastroenterology 2014 Acute Pancreatitis Scott Tenner, MD, MPH, FACG Clinical Professor of Medicine State University of New York Health Sciences Center Director, Brooklyn Gastroenterology
American College of Gastroenterology 2014 Acute Pancreatitis Scott Tenner, MD, MPH, FACG Clinical Professor of Medicine State University of New York Health Sciences Center Director, Brooklyn Gastroenterology
Effects of probiotics in the treatment of alcoholic hepatitis: randomized controlled multicenter study
 Effects of probiotics in the treatment of alcoholic hepatitis: randomized controlled multicenter study Lactobacillus subtilis/streptococcus faecium Lactobacillus rhamnosus R0011/acidophilus R0052 Ki Tae
Effects of probiotics in the treatment of alcoholic hepatitis: randomized controlled multicenter study Lactobacillus subtilis/streptococcus faecium Lactobacillus rhamnosus R0011/acidophilus R0052 Ki Tae
Positioning Biologics in Ulcerative Colitis
 Positioning Biologics in Ulcerative Colitis Bruce E. Sands, MD, MS Acting Chief, Gastrointestinal Unit Massachusetts General Hospital Associate Professor of Medicine Harvard Medical School Sequential Therapies
Positioning Biologics in Ulcerative Colitis Bruce E. Sands, MD, MS Acting Chief, Gastrointestinal Unit Massachusetts General Hospital Associate Professor of Medicine Harvard Medical School Sequential Therapies
Whether culture positivity and Perforation-operation interval affects mortality in perforation peritonitis?: Experiences of a Rural Medical College
 Original article: Whether culture positivity and Perforation-operation interval affects mortality in perforation peritonitis?: Experiences of a Rural Medical College Dr Aslam A Shivani, Dr Vinod V Prabhu,
Original article: Whether culture positivity and Perforation-operation interval affects mortality in perforation peritonitis?: Experiences of a Rural Medical College Dr Aslam A Shivani, Dr Vinod V Prabhu,
Aerobic bacteria isolated from diabetic septic wounds
 Aerobic bacteria isolated from diabetic septic wounds Eithar Mohammed Mahgoub*, Mohammed Elfatih A. Omer Faculty of Pharmacy, Omdurman Islamic University Department of Pharmaceutical Microbiology, Omdurman
Aerobic bacteria isolated from diabetic septic wounds Eithar Mohammed Mahgoub*, Mohammed Elfatih A. Omer Faculty of Pharmacy, Omdurman Islamic University Department of Pharmaceutical Microbiology, Omdurman
Routine endotracheal cultures for the prediction of sepsis in ventilated babies
 Archives of Disease in Childhood, 1989, 64, 34-38 Routine endotracheal cultures for the prediction of sepsis in ventilated babies T A SLAGLE, E M BIFANO, J W WOLF, AND S J GROSS Department of Pediatrics,
Archives of Disease in Childhood, 1989, 64, 34-38 Routine endotracheal cultures for the prediction of sepsis in ventilated babies T A SLAGLE, E M BIFANO, J W WOLF, AND S J GROSS Department of Pediatrics,
Randomized Controlled Trials in Pancreatic Diseases. James Buxbaum MD University of Southern California Los Angeles County Hospital
 Randomized Controlled Trials in Pancreatic Diseases James Buxbaum MD University of Southern California Los Angeles County Hospital Randomized Trials in Pancreatic Diseases Focus acute pancreatitis Challenges
Randomized Controlled Trials in Pancreatic Diseases James Buxbaum MD University of Southern California Los Angeles County Hospital Randomized Trials in Pancreatic Diseases Focus acute pancreatitis Challenges
The recurrent nature of adhesive small bowel obstruction
 FEATURE Long-term Prognosis After Operation for Adhesive Small Bowel Obstruction Bjørg-Tilde Svanes Fevang, MD,* Jonas Fevang, MD, PhD,* Stein Atle Lie, MSc, PhD, Odd Søreide, MD, PhD, FRCS, FACS,* Knut
FEATURE Long-term Prognosis After Operation for Adhesive Small Bowel Obstruction Bjørg-Tilde Svanes Fevang, MD,* Jonas Fevang, MD, PhD,* Stein Atle Lie, MSc, PhD, Odd Søreide, MD, PhD, FRCS, FACS,* Knut
Antimicrobial prophylaxis in liver transplant A multicenter survey endorsed by the European Liver and Intestine Transplant Association
 Antimicrobial prophylaxis in liver transplant A multicenter survey endorsed by the European Liver and Intestine Transplant Association Els Vandecasteele, Jan De Waele, Dominique Vandijck, Stijn Blot, Dirk
Antimicrobial prophylaxis in liver transplant A multicenter survey endorsed by the European Liver and Intestine Transplant Association Els Vandecasteele, Jan De Waele, Dominique Vandijck, Stijn Blot, Dirk
Guillain-Barré Syndrome
 Guillain-Barré Syndrome A Laboratory Perspective Laura Dunn Biomedical Scientist (Trainee Healthcare Scientist) Diagnosis of GBS GBS is generally diagnosed on clinical grounds Basic laboratory studies
Guillain-Barré Syndrome A Laboratory Perspective Laura Dunn Biomedical Scientist (Trainee Healthcare Scientist) Diagnosis of GBS GBS is generally diagnosed on clinical grounds Basic laboratory studies
SWISS SOCIETY OF NEONATOLOGY. Spontaneous intestinal perforation or necrotizing enterocolitis?
 SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
SWISS SOCIETY OF NEONATOLOGY Spontaneous intestinal perforation or necrotizing enterocolitis? June 2004 2 Stocker M, Berger TM, Neonatal and Pediatric Intensive Care Unit, Children s Hospital of Lucerne,
Influence of Obesity on the Severity and Clinical Outcome of Acute Pancreatitis
 Gut and Liver, Vol. 5, No. 3, September 2011, pp. 335-339 ORiginal Article Influence of Obesity on the Severity and Clinical Outcome of Acute Pancreatitis Keun Young Shin, Wan Suk Lee, Duk Won Chung, Jun
Gut and Liver, Vol. 5, No. 3, September 2011, pp. 335-339 ORiginal Article Influence of Obesity on the Severity and Clinical Outcome of Acute Pancreatitis Keun Young Shin, Wan Suk Lee, Duk Won Chung, Jun
Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任
 Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任 A Positive Blood Culture Clinically Important Organism Failure of host defenses to contain an infection at its primary focus Failure of the physician to effectively eradicate,
Blood culture 壢新醫院 病理檢驗科 陳啟清技術主任 A Positive Blood Culture Clinically Important Organism Failure of host defenses to contain an infection at its primary focus Failure of the physician to effectively eradicate,
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE. T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar
 ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
ACUTE PANCREATITIS: NEW CLASSIFICATION OF AN OLD FOE T Barrow, A Nasrullah, S Liong, V Rudralingam, S A Sukumar LEARNING OBJECTIVES q Through a series of cases illustrate the updated Atlanta symposium
Acute Necrotizing Pancreatitis: Laboratory, Clinical, and Imaging Findings as Predictors of Patient Outcome
 Gastrointestinal Imaging Original Research Brand et al. Acute Necrotizing Pancreatitis Gastrointestinal Imaging Original Research Michael Brand 1 Andrea Götz 1 Florian Zeman 2 Gundula Behrens 3 Michael
Gastrointestinal Imaging Original Research Brand et al. Acute Necrotizing Pancreatitis Gastrointestinal Imaging Original Research Michael Brand 1 Andrea Götz 1 Florian Zeman 2 Gundula Behrens 3 Michael
Joint Trust Management of Acute Severe Pancreatitis in Adults
 A clinical guideline recommended for use For Use in: By: For: Division responsible for document: All clinical areas (as a reference for screening) ITU/HDU (for definitive care) All medical staff likely
A clinical guideline recommended for use For Use in: By: For: Division responsible for document: All clinical areas (as a reference for screening) ITU/HDU (for definitive care) All medical staff likely
Gram Negative Bacillary Brain Abscess: Clinical Features And Therapeutic Outcome
 ISPUB.COM The Internet Journal of Neurosurgery Volume 4 Number 2 Gram Negative Bacillary Brain Abscess: Clinical Features And Therapeutic Outcome F Huda, V Sharma, W Ali, M Rashid Citation F Huda, V Sharma,
ISPUB.COM The Internet Journal of Neurosurgery Volume 4 Number 2 Gram Negative Bacillary Brain Abscess: Clinical Features And Therapeutic Outcome F Huda, V Sharma, W Ali, M Rashid Citation F Huda, V Sharma,
Management of Acute Pancreatitis and its Complications Aspirus Grand Rounds June 6, 2017 Eric A. Johnson MD
 Management of Acute Pancreatitis and its Complications Aspirus Grand Rounds June 6, 2017 Eric A. Johnson MD Disclosure: None In accordance with the Standards of the Wisconsin Medical Society, all those
Management of Acute Pancreatitis and its Complications Aspirus Grand Rounds June 6, 2017 Eric A. Johnson MD Disclosure: None In accordance with the Standards of the Wisconsin Medical Society, all those
ORIGINAL ARTICLE. organ dysfunction syndrome is paralleled
 ORIGINAL ARTICLE Early Physiological Response to Intensive Care as a Clinically Relevant Approach to Predicting the Outcome in Severe Acute Pancreatitis Richard Flint, MBChB; John A. Windsor, MBChB, MD,
ORIGINAL ARTICLE Early Physiological Response to Intensive Care as a Clinically Relevant Approach to Predicting the Outcome in Severe Acute Pancreatitis Richard Flint, MBChB; John A. Windsor, MBChB, MD,
A Retrospective & Prospective Comprehensive Study of Acute Pancreatitis (Diagnosis, Course & Managment)
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. X (May. 2016), PP 15-19 www.iosrjournals.org A Retrospective & Prospective Comprehensive
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 5 Ver. X (May. 2016), PP 15-19 www.iosrjournals.org A Retrospective & Prospective Comprehensive
Blood cultures in ED. Dr Sebastian Chang MBBS FACEM
 Blood cultures in ED Dr Sebastian Chang MBBS FACEM Why do we care about blood cultures? blood cultures are the most direct method for detecting bacteraemia in patients a positive blood culture: 1. can
Blood cultures in ED Dr Sebastian Chang MBBS FACEM Why do we care about blood cultures? blood cultures are the most direct method for detecting bacteraemia in patients a positive blood culture: 1. can
Severe β-lactam allergy. Alternative (use for mild-moderate β-lactam allergy) therapy
 Recommended Empirical Antibiotic Regimens for MICU Patients Notes: The antibiotic regimens shown are general guidelines and should not replace clinical judgment. Always assess for antibiotic allergies.
Recommended Empirical Antibiotic Regimens for MICU Patients Notes: The antibiotic regimens shown are general guidelines and should not replace clinical judgment. Always assess for antibiotic allergies.
Acute pancreatitis Case reports. Clinical problems. Use of antibiotics? (P 1 & 2) Surgical treatment of AP? (P 3 & 4)
 Case reports Clinical problems Use of antibiotics? (P 1 & 2) Surgical treatment of AP? (P 3 & 4) Case reports Case 1 Case 1 Patient KD History M, 63 y Obesity BMI 30.3 kg/m 2 Gallbladder stones No concomitant
Case reports Clinical problems Use of antibiotics? (P 1 & 2) Surgical treatment of AP? (P 3 & 4) Case reports Case 1 Case 1 Patient KD History M, 63 y Obesity BMI 30.3 kg/m 2 Gallbladder stones No concomitant
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sprung CL, Annane D, Keh D, et al. Hydrocortisone therapy for
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Sprung CL, Annane D, Keh D, et al. Hydrocortisone therapy for
HOSPITAL INFECTION CONTROL
 HOSPITAL INFECTION CONTROL Objectives To be able to define hospital acquired infections discuss the sources and routes of transmission of infections in a hospital describe methods of prevention and control
HOSPITAL INFECTION CONTROL Objectives To be able to define hospital acquired infections discuss the sources and routes of transmission of infections in a hospital describe methods of prevention and control
CLINICAL CASE OF THE MONTH. A 35 Year Old Woman with Abdominal Pain
 CASE REPORT JOURNAL OF THE LOUISIANA STATE MEDICAL SOCIETY CLINICAL CASE OF THE MONTH A 35 Year Old Woman with Abdominal Pain Melissa Spera, MD, Camille Thelin, MD, Abby Gandolfi, MD, Nicholas Clayton,
CASE REPORT JOURNAL OF THE LOUISIANA STATE MEDICAL SOCIETY CLINICAL CASE OF THE MONTH A 35 Year Old Woman with Abdominal Pain Melissa Spera, MD, Camille Thelin, MD, Abby Gandolfi, MD, Nicholas Clayton,
URINARY TRACT INFECTIONS 3 rd Y Med Students. Prof. Dr. Asem Shehabi Faculty of Medicine, University of Jordan
 URINARY TRACT INFECTIONS 3 rd Y Med Students Prof. Dr. Asem Shehabi Faculty of Medicine, University of Jordan Urinary Tract Infections-1 Normal urine is sterile.. It contains fluids, salts, and waste products,
URINARY TRACT INFECTIONS 3 rd Y Med Students Prof. Dr. Asem Shehabi Faculty of Medicine, University of Jordan Urinary Tract Infections-1 Normal urine is sterile.. It contains fluids, salts, and waste products,
ESPEN Congress The Hague 2017
 ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
ESPEN Congress The Hague 2017 Meeting nutritional needs of acute care patients Feeding acute pancreatitis patients J. Luttikhold (NL) FEEDING ACUTE PANCREATITIS PATIENTS Joanna Luttikhold, MD PhD Registrar
Complicated surgical infections
 Complicated surgical infections JASLYN DOSHI ID ADVANCED TRAINEE, WESTMEAD HOPC 46 F admitted 13 th March 2017 Epigastric pain Vomiting Diarrhoea Background Gastric banding 2009 Vomiting since last year
Complicated surgical infections JASLYN DOSHI ID ADVANCED TRAINEE, WESTMEAD HOPC 46 F admitted 13 th March 2017 Epigastric pain Vomiting Diarrhoea Background Gastric banding 2009 Vomiting since last year
Correspondence should be addressed to Justin Cochrane;
 Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 794282, 4 pages http://dx.doi.org/10.1155/2015/794282 Case Report Acute on Chronic Pancreatitis Causing a Highway to the Colon with Subsequent
Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 794282, 4 pages http://dx.doi.org/10.1155/2015/794282 Case Report Acute on Chronic Pancreatitis Causing a Highway to the Colon with Subsequent
5. Use of antibiotics, which disturbs balance of normal flora. 6. Poor nutritional status.
 Microbiology Chapter 5 Introduction to Pathogens 5:1 Changing Patterns of Disease In the past 100 years, since the discovery of the Germ Theory of Disease was accepted: We have learned that microbes cause
Microbiology Chapter 5 Introduction to Pathogens 5:1 Changing Patterns of Disease In the past 100 years, since the discovery of the Germ Theory of Disease was accepted: We have learned that microbes cause
Abstract. J Pak Med Assoc
 Intraprostatic Tissue Infection in Catheterised Patients in comparison to Controls A. N. Talpur, A. T. Hasan, M. A. Sheikh Department of Urological Surgery and Transplantation, Jinnah Postraduate Medical
Intraprostatic Tissue Infection in Catheterised Patients in comparison to Controls A. N. Talpur, A. T. Hasan, M. A. Sheikh Department of Urological Surgery and Transplantation, Jinnah Postraduate Medical
Morbidity & Mortality Conference Downstate Medical Center. Daniel Kaufman, MD
 Morbidity & Mortality Conference Downstate Medical Center University Case Presentation Hospital of Brooklyn Daniel Kaufman, MD Necrotizing Fasciitis and Soft- Tissue Infections Necrotizing Fasciitis Deep
Morbidity & Mortality Conference Downstate Medical Center University Case Presentation Hospital of Brooklyn Daniel Kaufman, MD Necrotizing Fasciitis and Soft- Tissue Infections Necrotizing Fasciitis Deep
Comparative study of different modalities of treatment of liver abscess
 Comparative study of different modalities of treatment of liver abscess Original Research Article ISSN: 2394-0026 (P) A comparative study of different modalities of treatment of liver abscesss Alpesh B.
Comparative study of different modalities of treatment of liver abscess Original Research Article ISSN: 2394-0026 (P) A comparative study of different modalities of treatment of liver abscesss Alpesh B.
