CLASSIFICATION OF RENAL DISEASE
|
|
|
- Lesley Fox
- 6 years ago
- Views:
Transcription
1 COMMONWEALTH OF AUSTRALIA Copyright Regulations 1969 WARNING This material has been reproduced and communicated to you by or on behalf of Adelaide University pursuant to Part VB of the Copyright Act 1968 (the Act). The material in this communication may be subject to copyright under the Act. Any further reproduction or communication of this material by you may be the subject of copyright protection under the Act. Do not remove this notice. RENAL PATHOLOGY Dr A. Barbour, Discipline of Pathology, 2008 Copyright University of Adelaide CLASSIFICATION OF RENAL DISEASE Congenital Horseshoe kidney Renal dysplasia Renal agenesis Hereditary Adult polycystic kidney disease Cystic diseases Adult polycystic kidney disease Glomerular diseases Glomerulopathy/glomerulonephritis: many types, primary or secondary Diabetic Amyloidosis Tubular and tubulointerstitial diseases Infective: acute and chronic pyelonephritis Drug or toxin induced Urate nephropathy Nephrocalcinosis Cast nephropathy Analgesic nephropathy Acute tubular necrosis Vascular Changes related to renal artery stenosis Embolism and infarction Changes related to benign and malignant hypertension Vasculitis: e.g. Wegener granulomatosis, microscopic polyangiitis, polyarteritis nodosa Thrombotic microangiopathies Disseminated intravascular coagulation Changes related to urinary tract obstruction Hydronephrosis Renal stones Neoplasia Wilms tumour Renal cell carcinoma Transitional cell carcinoma Pathology of renal transplantation Some diseases fall into more than one group.
2 ARTERIONEPHROSCLEROSIS/BENIGN NEPHROSCLEROSIS Renal vascular and parenchymal changes related to both age and benign hypertension (HT), frequently referred to as benign nephrosclerosis. In those with benign HT, the changes can more specifically be referred to as hypertensive nephrosclerosis. Age related changes: Degenerative changes occur in arterioles with age: haemodynamic stress leads to increased endothelial permeability with deposition of plasma proteins in wall, increased extracellular matrix production and smooth muscle atrophy. The arteriole wall becomes thickened by homogenous eosinophilic glassy material ( hyaline ) and the lumen narrowed: arteriolar hyalinosis/hyaline arteriolosclerosis. Mild medial and intimal fibrosis with replication of the internal elastic lamina occurs in small and medium arteries. Small artery and arteriolar narrowing in kidneys -> chronic ischaemia -> Chronic interstitial inflammation and scarring Tubular atrophy Focal global glomerular sclerosis or obsolescence: wrinkled collapsed mass of glomerular basement membrane surrounded by collagen in Bowman s space. Macroscopically these changes result in a smaller kidney with a thinned cortex and a granular surface, the latter due to depressed areas of atrophy with intervening non-atrophic parenchyma, sometimes with hypertrophied glomeruli. Occur in >50% of those over 60 years of age without HT When severe, these changes can cause chronic renal failure In hypertensive persons, these age related changes become more severe Approx. 15% of patients with benign HT develop renal dysfunction In developed countries HT is estimated to be the cause of 1/4 1/3 of end stage renal disease/chronic renal failure Proteinuria may occur with HT renal disease Hyaline arteriolosclerosis also occurs in diabetics, but due to different mechanisms MALIGNANT NEPHROSCLEROSIS Malignant/accelerated hypertension has different effects in the kidney Hyperplastic arteriolosclerosis ( onion skin endarteritis): oedematous/myxoid intimal expansion with concentric intimal fibrosis Fibrinoid necrosis and thrombosis of small arteries and arterioles -> acute glomerular ischaemia and necrosis -> acute renal failure. The kidneys are swollen with scattered pinpoint haemorrhages GLOMERULAR DISEASE A wide variety of diseases can affect the glomeruli in a variety of different ways i.e. they have different pathogenesis e.g. Ischaemia e.g. in hypertension and diabetes Immunological: glomerulonephritis Metabolic e.g. diabetic glomerulosclerosis Depositions e.g. renal amyloidosis Hereditary GLOMERULONEPHRITIS Immune mediated Antibody and antigen deposition around glomerular capillary basement membranes and/or in mesangium Circulating antibody reacts with endogenous or exogenous antigen already within the glomerulus Deposition of circulating antigen/antibody complexes Mediate damage via a variety of mechanisms e.g. complement activation, cytokine release, inflammatory cell infiltration No organisms Inflammatory cells not seen in all types. These types are often referred to as glomerulopathy or nephropathy rather than glomerulonephritis Many different types/patterns showing different light and electron microscopic changes and immunofluorescence features Light microscopy: variable Proliferation of cells within the glomerulus: endothelial, epithelial and/or mesangial Infiltration by inflammatory cells Deposition of additional mesangial matrix Necrosis Parts or all of glomerulus involved Crescents Electron microscopy: variable location and pattern of electron dense immune deposits Immunofluorescence: variable types and patterns of immunoglobulin and complement deposition Variable clinical presentation, age groups affected, outcome etc May cause various clinical features. Specific GNs can cause one or more of the following (sometimes mixed patterns): Asymptomatic proteinuria (from increased permeability of glomerular filtration membrane) Nephrotic syndrome Asymptomatic haematuria
3 Acute nephritic syndrome (injury to glomerular capillary walls allows leakage of blood cells +/- protein. Hyperplasia of glomerular cells and infiltration by inflammatory cells can result in impaired glomerular blood flow and filtration with renal insufficiency, hypertension and fluid retention). Rapidly progressive nephritis End stage renal disease/chronic renal failure Types of GN include: Acute post infectious (post streptococcal) glomerulonephritis Minimal change disease Membraneous glomerulopathy/nephropathy Focal segmental glomerulosclerosis Membranoproliferative glomerulonephritis IgA nephropathy (diffuse mesangioproliferative) Anti-glomerular basement membrane glomerulonephritis Anti-neutrophil cytoplasmic autoantibody (ANCA) associated glomerulonephritis Crescentic glomerulonephritis Idiopathic (primary) and secondary (occurring in association with a variety of systemic diseases) forms Infection can precipitate a variety of patterns via immunologic mechanisms (not direct infection of glomeruli) Causes of nephrotic syndrome include: minimal change disease, membraneous nephropathy, diabetes mellitus, renal amyloidosis, focal segmental glomerulosclerosis, other Causes of nephritic syndrome include: acute post-infectious GN, membranoproliferative GN, other Examples Acute post-infectious glomerulonephritis Aetiology Generally follows infection with certain strains ( nephritogenic ) of Group A β haemolytic streptococci but other organisms may also be responsible. Immune complexes localise in glomeruli either form in situ or deposit from circulation. Immune complexes activate complement and other inflammatory mediators that attract inflammatory cells and stimulate proliferation of glomerular cells Morphology Light microscopy: enlarged hypercellular glomeruli Infiltration of neutrophils, macrophages Proliferation of endothelial and mesangial cells Immunofluorescence: granular deposits of IgG and complement (C3) on epithelial side of glomerular capillary basement membranes and in the mesangium Electron microscopy: prominent subepithelial dense deposits (subepithelial humps ), also subendothelial and mesangial electron dense immune deposits Clinically Typically in children Arises 1-4 wks after a Streptococcal pharyngitis or skin infection Serum complement levels often low Typically causes nephritic syndrome: results from impaired blood flow though narrowed glomerular capillaries Haematuria +/- proteinuria Oliguria Hypertension Facial oedema >95% recover after several weeks with conservative therapy < 1% have a rapidly progressive course with the development of crescents -> acute renal failure Membranous glomerulonephritis A common cause of nephrotic syndrome in adults Aetiology 85% are idiopathic s arise secondary to other diseases (e.g. SLE, hepatitis B, malaria, certain cancers) or certain drugs All represent a form of chronic immune response to endogenous or exogenous antigens deposited on the subepithelial side of the glomerular capillary basement membranes Morphology Light microscopy: thickening of the glomerular capillary wall (may not be seen early on in the disease course) Immunofluorescence: granular deposits of IgG and complement (C3) along glomerular capillary wall Electron microscopy: irregular electron dense immune deposits on subepithelial side of glomerular capillary basement membrane with intervening deposits of basement membrane material. The progressive ultrastructural changes can be divided into 4 stages. Clinically Causes proteinuria which when severe results in the nephrotic syndrome Nephrotic syndrome Massive proteinuria Hypoalbuminaemia Oedema
4 Hyperlipidaemia Course variable. Progresses over many years to chronic renal failure in 25% CHRONIC RENAL FAILURE Major cause of death from renal disease. Gradual and progressive loss of the ability of the kidneys to excrete wastes, concentrate urine and conserve electrolytes. Clinically Fluid & electrolytes: dehydration, oedema, hyperkalaemia, metabolic acidosis Cardiopulmonary: hypertension, CCF, uraemic pericarditis Ca, PO 4 and bone: hypocalcaemia, secondary hyperparathyroidism, renal osteodystrophy Neuromuscular: myopathy, peripheral neuropathy Gastrointestinal: nausea and vomiting Haematologic: anaemia Dermatologic: sallow skin, pruritus Causes of end stage renal disease: diabetes mellitus 40%, HT 26-38%, glomerulonephritis 12-16%, polycystic kidney 3%, urologic conditions 3%, other In some cases, nephron loss due to the primary disease may lead to increased filtration and hypertrophy in remaining glomeruli, increasing their risk of secondary injury and glomerulosclerosis, leading to proteinuria and further impairment of renal function. Macroscopic features depend on the underlying disease. The kidneys in chronic renal failure from HT and glomerulonephritis are generally small with granular surfaces, often with small cysts Chronic pyelonephritis small kidneys, U shaped cortical scars overlying abnormal calyces Dialysis also affects the morphologic findings > atrophy and cysts Diabetic kidneys may be normal in size or enlarged, the surface is granular related to underlying vascular disease. Kidneys may be small due to hypertensive changes. In adult polycystic kidney disease, the kidneys are enlarged with numerous cysts. Occasionally diagnostic features may still be seen histologically. Irrespective of initial causes, eventually all 4 compartments (glomeruli, vessels, tubules, interstitium) become damaged sclerosis/fibrosis of glomeruli, tubular atrophy, interstitial fibrosis and variable interstitial inflammation, thickened arterioles and small arteries URINARY TRACT INFECTION Cystitis Common Bladder acutely inflamed Usually caused by Gram negative bacteria from the gut Most common in women due to proximity of urethral orifice to anus, certain bacteria are able to adhere to urethral mucosa Patients develop dysuria, haematuria, cloudy urine Acute pyelonephritis Acute suppurative inflammation of the renal tubules, interstitium and pelvis and calyces caused by infection Tends to primarily involve upper and lower poles intrarenal reflux more common in these areas as the compound papillae at the upper and lower poles allow increased pressure and urinary fluid (and infection) to be transmitted into the overlying parenchyma more readily than the simple papillae (which can close under increased pressure) in the mid-regions. Caused by Gram negative bacilli from the gut in 85% of cases. E. coli most common. Other: Proteus, Enterobacter, Klebsiella species, Strep. faecalis 2 routes by which bacteria can reach the kidney Ascending infection from the bladder is most common (95% of cases) Predisposing factors include Urinary obstruction e.g. benign prostatic hyperplasia Instrumentation Vesicoureteric reflux (due to congenital anatomic anomaly usually in males) Pregnancy Impaired immune system e.g. diabetes mellitus Neurogenic bladder in e.g. paraplegia or diabetes Renal stones Haematogenous (5 % of cases) From distant foci of infection e.g. in infective endocarditis In the immunosuppressed or debilitated patient Often with non-enteric organisms including fungi and Staph. aureus Histologically: acute inflammation is typically in the interstitium and tubules, get tubular damage and microabscess formation. Glomerular infiltrates of neutrophils may be seen in haematogenous infection. Macroscopically: kidney swollen, erythematous, microabscesses, mucosa of pyelocalyceal system is erythematous. Clinically: patients develop fever, malaise (i.e. systemic symptoms), loin pain, haematuria, dysuria, cloudy urine. Creatinine generally normal unless volume depleted or pre-existing renal disease. Presence of granular leukocyte casts in urine proves renal involvement in infection (casts formed in renal tubules).
5 Potential complications Papillary necrosis - mainly in diabetics and in those with urinary tract obstruction. May lead to acute renal failure Pyonephrosis - seen in near or total obstruction. Pus fills the renal pelvis, calyces and ureter Perinephric abscess: extension of infection through the renal capsule into adjacent tissue Chronic pyelonephritis An important cause of chronic renal failure when affecting both kidneys Chronic tubulointerstitial inflammation and damage with renal scarring. Pyelocalyceal damage is required for diagnosis. Some have a history of infections but not all. Kidneys are small and demonstrate fine and coarse cortical scarring, the coarse scars often overly blunted or deformed calyces May have an insidious onset -> renal insufficiency. Polyuria and nocturia. Proteinuria may be present. Caused by recurrent infection, sometimes subclinical, often related to underlying obstruction and/or vesicoureteric reflux, leading to chronic inflammation and scarring Reflux nephropathy: Uncertain if reflux itself can lead to scarring or whether concomitant bacterial infection is required. NEPHROLITHIASIS Stones may form anywhere within the urinary tract but the kidney is the most common site Affects 5-10% of people; M >F Some cases have a familial predisposition Cause and pathogenesis 4 main types Calcium: most common, usually a mix of Ca ++ oxalate and Ca ++ phosphate Most related to hypercalciuria, without hypercalcaemia s related to underlying disease causing hypercalcaemia (e.g. hyperparathyroidism) or to hyperuricosuria, acting as a nucleus for the deposition of calcium, or to hyperoxaluria So called triple stones: magnesium ammonium phosphate Largely follow infection by urea-splitting bacteria e.g. Proteus which convert urea to ammonia and thus make the urine alkaline, causing the precipitation of magnesium ammonium phosphate Form some of the largest stones Uric acid stones Common in patients with hyperuricaemia (and gout) s may have excessively acidic urine Cysteine stones Genetic defect in the renal reabsorption of amino acids including cysteine Stones are caused by a variable combination of an increased concentration of the stone s constituents within the urine to a level of supersaturation, changes in urinary ph and volume, the presence of factors that act as nuclei for the deposition of crystals and the deficiency of inhibitors of crystal formation. Clinical course May not cause any problems Smaller stones are more hazardous because they may pass into the ureter and cause spasm renal colic (severe pain) and ureteric obstruction Larger stones more likely to stay within the renal pelvis and may cause hydronephrosis Haematuria Predisposition to infection URINARY TRACT OBSTRUCTION Increases susceptibility to infection and stone formation If unrelieved will lead to hydronephrosis (dilated renal pelvis and calyces) and permanent renal parenchymal atrophy (from pressure impairing blood supply in parenchyma), and chronic renal failure if bilateral Causes Congenital anomalies Stones Prostatic enlargement (hyperplasia or malignancy) tumours obstructing ureters Pregnancy Progressive dilation of pyelocalyceal system, flattening of the papillae and thinning of the parenchyma. ADULT POLYCYSTIC KIDNEY DISEASE There are a number of different cystic diseases of the kidney, including congenital and inherited ones that have different appearances. Adult polycystic kidney disease is the commonest, apart from scattered small sporadic simple cysts that are very common. Genetic disorder inherited in autosomal dominant fashion A small proportion of cases arise from spontaneous mutations Most cases due to mutations of PKD1 gene on chromosome 16 The kidneys develop cysts that arise from tubular epithelium that subsequently cause pressure atrophy of adjacent tissue Patients typically present by middle age with hypertension, chronic renal failure, loin pain, haematuria, renal infections and/or stones.
6 Extra-renal manifestations include intracranial berry/saccular aneurysms, colonic diverticula, mitral valve prolapse and (asymptomatic) cysts in the liver, spleen and pancreas. RENAL CELL CARCINOMA (RCC) 1-3% of all solid organ cancers More common in males than females Middle age and older Predisposing factors Tobacco: incidence is doubled in cigarette smokers Von Hippel-Lindau syndrome (hereditary) hereditary forms Genetics In most cases of RCC there are abnormalities involving one allele of the VHL gene (on chromosome 3), a tumour suppressor gene Morphology Usually well circumscribed lesion, 3 to 15 cm in diameter, composed of variegated yellow-grey-white tissue +/- necrosis+/- haemorrhage +/- cystic change May fungate through into the pyelocalyceal system or invade the renal vein Histologically there are various types. The most common type shows cells with abundant clear or granular cytoplasm containing glycogen (clear cell carcinoma). May show marked nuclear atypia and sarcomatoid change Histologic grading: Fuhrman system - 4 grades Clinical course Classically: loin pain, haematuria, abdominal mass Constitutional symptoms include fever, malaise, loss of weight Tumour may be silent until it reaches a large size RCC can cause a variety of paraneoplastic syndromes such as Polycythaemia Hypercalcaemia Hypertension Commonly gives rise to metastases in the absence of local signs The lungs are the most common sites of metastases, followed by bone
Histopathology: Glomerulonephritis and other renal pathology
 Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
Histopathology: Glomerulonephritis and other renal pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you
A clinical syndrome, composed mainly of:
 Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Nephritic syndrome We will discuss: 1)Nephritic syndrome: -Acute postinfectious (poststreptococcal) GN -IgA nephropathy -Hereditary nephritis 2)Rapidly progressive GN (RPGN) A clinical syndrome, composed
Chapter 20 Diseases of the kidney:
 Chapter 20 Diseases of the kidney: 1. Which of the following is seen in Nephrotic syndrome (2000, 2004) (a) Albumin is lost in the urine, while other globulins are unaffected (b) Early hypertension (c)
Chapter 20 Diseases of the kidney: 1. Which of the following is seen in Nephrotic syndrome (2000, 2004) (a) Albumin is lost in the urine, while other globulins are unaffected (b) Early hypertension (c)
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
QUESTION 53 Endothelial cell pathology on renal biopsy is most characteristic of which one of the following diagnoses? A. Pre-eclampsia B. Haemolytic uraemic syndrome C. Lupus nephritis D. Immunoglobulin
Alterations of Renal and Urinary Tract Function
 Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
Alterations of Renal and Urinary Tract Function Chapter 29 Urinary Tract Obstruction Urinary tract obstruction is an interference with the flow of urine at any site along the urinary tract The obstruction
Glomerular diseases mostly presenting with Nephritic syndrome
 Glomerular diseases mostly presenting with Nephritic syndrome 1 The Nephritic Syndrome Pathogenesis: proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls escape of RBCs
Glomerular diseases mostly presenting with Nephritic syndrome 1 The Nephritic Syndrome Pathogenesis: proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls escape of RBCs
Renal Disease. Please refer to the assignment page Three online modules TBLs
 Renal Disease Please refer to the assignment page Three online modules TBLs 1 Renal Embryology 2 Lab Tests UA CBC Enzymes Creatinine Creatinine clearance Ammonia Abs C Bx 3 BUN Creatinine Creatinine Clearance
Renal Disease Please refer to the assignment page Three online modules TBLs 1 Renal Embryology 2 Lab Tests UA CBC Enzymes Creatinine Creatinine clearance Ammonia Abs C Bx 3 BUN Creatinine Creatinine Clearance
Histopathology: Hypertension and diabetes in the kidney These presentations are to help you identify basic histopathological features.
 Histopathology: Hypertension and diabetes in the kidney These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need
Histopathology: Hypertension and diabetes in the kidney These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need
Dr Ian Roberts Oxford. Oxford Pathology Course 2010 for FRCPath Illustration-Cellular Pathology. Oxford Radcliffe NHS Trust
 Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing proteinuria & haematuria Highlight diagnostic pitfalls Nephrotic
Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing proteinuria & haematuria Highlight diagnostic pitfalls Nephrotic
Glomerular pathology in systemic disease
 Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Glomerular pathology in systemic disease Lecture outline Lupus nephritis Diabetic nephropathy Glomerulonephritis Associated with Bacterial Endocarditis and Other Systemic Infections Henoch-Schonlein Purpura
Functions of the kidney:
 Diseases of renal system : Normal anatomy of renal system : Each human adult kidney weighs about 150 gm, the ureter enters the kidney at the hilum, it dilates into a funnel-shaped cavity, the pelvis, from
Diseases of renal system : Normal anatomy of renal system : Each human adult kidney weighs about 150 gm, the ureter enters the kidney at the hilum, it dilates into a funnel-shaped cavity, the pelvis, from
CYSTIC DISEASES of THE KIDNEY. Dr. Nisreen Abu Shahin
 CYSTIC DISEASES of THE KIDNEY Dr. Nisreen Abu Shahin 1 Types of cysts 1-Simple Cysts 2-Dialysis-associated acquired cysts 3-Autosomal Dominant (Adult) Polycystic Kidney Disease 4-Autosomal Recessive (Childhood)
CYSTIC DISEASES of THE KIDNEY Dr. Nisreen Abu Shahin 1 Types of cysts 1-Simple Cysts 2-Dialysis-associated acquired cysts 3-Autosomal Dominant (Adult) Polycystic Kidney Disease 4-Autosomal Recessive (Childhood)
Glomerular pathology-2 Nephritic syndrome. Dr. Nisreen Abu Shahin
 Glomerular pathology-2 Nephritic syndrome Dr. Nisreen Abu Shahin 1 The Nephritic Syndrome Pathogenesis: inflammation proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls
Glomerular pathology-2 Nephritic syndrome Dr. Nisreen Abu Shahin 1 The Nephritic Syndrome Pathogenesis: inflammation proliferation of the cells in glomeruli & leukocytic infiltrate Injured capillary walls
Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome.
 Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome. Azotemia and Urinary Abnormalities Disturbances in urine volume oliguria, anuria, polyuria Abnormalities of urine sediment red
Disorders of the kidney. Urine analysis. Nephrotic and nephritic syndrome. Azotemia and Urinary Abnormalities Disturbances in urine volume oliguria, anuria, polyuria Abnormalities of urine sediment red
Some renal vascular disorders
 Some renal vascular disorders Introduction Nearly all diseases of the kidney involve the renal blood vessels secondarily We will discuss: -Hypertension (arterionephrosclerosis in benign HTN & hyperplastic
Some renal vascular disorders Introduction Nearly all diseases of the kidney involve the renal blood vessels secondarily We will discuss: -Hypertension (arterionephrosclerosis in benign HTN & hyperplastic
DIABETES MELLITUS. Kidney in systemic diseases. Slower the progression: Pathology: Patients with diabetes mellitus are prone to other renal diseases:
 Kidney in systemic diseases Dr. Badri Paudel The kidneys may be directly involved in a number of multisystem diseases or secondarily affected by diseases of other organs. Involvement may be at a prerenal,
Kidney in systemic diseases Dr. Badri Paudel The kidneys may be directly involved in a number of multisystem diseases or secondarily affected by diseases of other organs. Involvement may be at a prerenal,
Advanced Concept of Nursing- II UNIT-VI Advance Nursing Management of Genitourinary (GU) Diseases.
 In The Name of God (A PROJECT OF NEW LIFE COLLEGE OF NURSING KARACHI) Advanced Concept of Nursing- II UNIT-VI Advance Nursing Management of Genitourinary (GU) Diseases. Shahzad Bashir RN, BScN, DCHN,MScN
In The Name of God (A PROJECT OF NEW LIFE COLLEGE OF NURSING KARACHI) Advanced Concept of Nursing- II UNIT-VI Advance Nursing Management of Genitourinary (GU) Diseases. Shahzad Bashir RN, BScN, DCHN,MScN
Overview of glomerular diseases
 Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
Overview of glomerular diseases *Endothelial cells are fenestrated each fenestra: 70-100nm in diameter Contractile, capable of proliferation, makes ECM & releases mediators *Glomerular basement membrane
RENAL HISTOPATHOLOGY
 RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
RENAL HISTOPATHOLOGY Peter McCue, M.D. Department of Pathology, Anatomy & Cell Biology Sidney Kimmel Medical College There are no conflicts of interest. 1 Goals and Objectives! Goals Provide introduction
Dr P Sigwadi 30 May 2012
 Dr P Sigwadi 30 May 2012 Introduction Haematuria Positive blood on urine dipstick 5 red blood cells/ microliter of urine Prevalence Gross haematuria ( macroscopic) 0.13 % Microscopic- 1.5% Haematuria +
Dr P Sigwadi 30 May 2012 Introduction Haematuria Positive blood on urine dipstick 5 red blood cells/ microliter of urine Prevalence Gross haematuria ( macroscopic) 0.13 % Microscopic- 1.5% Haematuria +
Glomerular Pathology- 1 Nephrotic Syndrome. Dr. Nisreen Abu Shahin
 Glomerular Pathology- 1 Nephrotic Syndrome Dr. Nisreen Abu Shahin The Nephrotic Syndrome a clinical complex resulting from glomerular disease & includes the following: (1) massive proteinuria (3.5 gm /day
Glomerular Pathology- 1 Nephrotic Syndrome Dr. Nisreen Abu Shahin The Nephrotic Syndrome a clinical complex resulting from glomerular disease & includes the following: (1) massive proteinuria (3.5 gm /day
Renal Pathology 1: Glomerulus. With many thanks to Elizabeth Angus PhD for EM photographs
 Renal Pathology 1: Glomerulus With many thanks to Elizabeth Angus PhD for EM photographs Anatomy of the Kidney http://www.yalemedicalgroup.org/stw/page.asp?pageid=stw028980 The Nephron http://www.beltina.org/health-dictionary/nephron-function-kidney-definition.html
Renal Pathology 1: Glomerulus With many thanks to Elizabeth Angus PhD for EM photographs Anatomy of the Kidney http://www.yalemedicalgroup.org/stw/page.asp?pageid=stw028980 The Nephron http://www.beltina.org/health-dictionary/nephron-function-kidney-definition.html
DISEASES AFFECTING TUBULES AND INTERSTITIUM
 DISEASES AFFECTING TUBULES AND INTERSTITIUM Acute tubular injury (ATI) Pyelonephritis Drug-induced tubulointerstitial nephritis (TIN) Myeloma cast NP Renal stones Urinary outflow obstruction: hydronephrosis
DISEASES AFFECTING TUBULES AND INTERSTITIUM Acute tubular injury (ATI) Pyelonephritis Drug-induced tubulointerstitial nephritis (TIN) Myeloma cast NP Renal stones Urinary outflow obstruction: hydronephrosis
Dr Ian Roberts Oxford
 Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing renal failure Highlight diagnostic pitfalls. Crescentic GN: renal
Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Present the basic diagnostic features of the commonest conditions causing renal failure Highlight diagnostic pitfalls. Crescentic GN: renal
Diseases of the Kidney. Janos Vasko
 Diseases of the Kidney Janos Vasko Congenital anomalies Glomerular diseases Tubulointerstitial diseases Infections Vascular diseases Stones Tumours POLYCYSTIC KIDNEY DISEASE INFANTILE TYPE ADULT TYPE Autosomal
Diseases of the Kidney Janos Vasko Congenital anomalies Glomerular diseases Tubulointerstitial diseases Infections Vascular diseases Stones Tumours POLYCYSTIC KIDNEY DISEASE INFANTILE TYPE ADULT TYPE Autosomal
GLOMERULAR TUBULAR/INTERSTITIAL BLOOD VESSELS
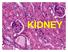 KIDNEY RENAL PATHOLOGY NORMAL CONGENITAL CYSTS GLOMERULAR TUBULAR/INTERSTITIAL BLOOD VESSELS OBSTRUCTION TUMORS 1. Renal Vein 2. Renal Artery 3. Renal Calyx 4. Medullary Pyramid 5. Renal Cortex 6. Segmental
KIDNEY RENAL PATHOLOGY NORMAL CONGENITAL CYSTS GLOMERULAR TUBULAR/INTERSTITIAL BLOOD VESSELS OBSTRUCTION TUMORS 1. Renal Vein 2. Renal Artery 3. Renal Calyx 4. Medullary Pyramid 5. Renal Cortex 6. Segmental
Dr Ian Roberts Oxford. Oxford Pathology Course 2010 for FRCPath Illustration-Cellular Pathology. Oxford Radcliffe NHS Trust
 Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Plan of attack: Diagnostic approach to the renal biopsy Differential diagnosis of the clinical syndromes of renal disease Microscopy Step
Dr Ian Roberts Oxford Oxford Pathology Course 2010 for FRCPath Plan of attack: Diagnostic approach to the renal biopsy Differential diagnosis of the clinical syndromes of renal disease Microscopy Step
Glomerulonephritis. Dr Rodney Itaki Anatomical Pathology Discipline.
 Glomerulonephritis Dr Rodney Itaki Anatomical Pathology Discipline. University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology Gross anatomy Ref: Goggle Images Microanatomy
Glomerulonephritis Dr Rodney Itaki Anatomical Pathology Discipline. University of Papua New Guinea School of Medicine & Health Sciences Division of Pathology Gross anatomy Ref: Goggle Images Microanatomy
AN APPROACH TO HEMATURIA. Dr Saima Ali
 AN APPROACH TO HEMATURIA Dr Saima Ali Definition Microscopic hematuria hematuria is defined as the presence of 5 or more RBCs per high-power field in 3 of 3 consecutive centrifuged specimens obtained at
AN APPROACH TO HEMATURIA Dr Saima Ali Definition Microscopic hematuria hematuria is defined as the presence of 5 or more RBCs per high-power field in 3 of 3 consecutive centrifuged specimens obtained at
Renal tumors of adults
 Renal tumors of adults Urinary Tract Tumors 2%-3% of all cancers in adults. The most common malignant tumor of the kidney is renal cell carcinoma. Tumors of the lower urinary tract are twice as common
Renal tumors of adults Urinary Tract Tumors 2%-3% of all cancers in adults. The most common malignant tumor of the kidney is renal cell carcinoma. Tumors of the lower urinary tract are twice as common
Membranoproliferative Glomerulonephritis
 Membranoproliferative Glomerulonephritis MPGN is characterizedby alterations in the GBM and mesangium and by proliferation of glomerular cells. 5% to 10% of cases of 1ry nephrotic syndrome in children
Membranoproliferative Glomerulonephritis MPGN is characterizedby alterations in the GBM and mesangium and by proliferation of glomerular cells. 5% to 10% of cases of 1ry nephrotic syndrome in children
Pathology of Hypertension
 2016-03-07 Pathology of Hypertension Honghe Zhang honghezhang@zju.edu.cn Tel:88208199 Department of Pathology ❶ Genetic predisposition ❷ Dietary factors ❸ Environmental factors ❹ Others Definition and
2016-03-07 Pathology of Hypertension Honghe Zhang honghezhang@zju.edu.cn Tel:88208199 Department of Pathology ❶ Genetic predisposition ❷ Dietary factors ❸ Environmental factors ❹ Others Definition and
Ordering Physician. Collected REVISED REPORT. Performed. IgG IF, Renal MCR. Lambda IF, Renal MCR. C1q IF, Renal. MCR Albumin IF, Renal MCR
 RenalPath Level IV Wet Ts IgA I Renal IgM I Renal Kappa I Renal Renal Bx Electron Microscopy IgG I Renal Lambda I Renal C1q I Renal C3 I Renal Albumin I Renal ibrinogen I Renal Mayo Clinic Dept. of Lab
RenalPath Level IV Wet Ts IgA I Renal IgM I Renal Kappa I Renal Renal Bx Electron Microscopy IgG I Renal Lambda I Renal C1q I Renal C3 I Renal Albumin I Renal ibrinogen I Renal Mayo Clinic Dept. of Lab
Nephrology - the study of the kidney. Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system
 Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Acute flank pain in children: Imaging considerations
 Acute flank pain in children: Imaging considerations Carlos J. Sivit MD Rainbow Babies and Children s Hospital Case Western Reserve School of Medicine Flank pain Results from distention of ureter or renal
Acute flank pain in children: Imaging considerations Carlos J. Sivit MD Rainbow Babies and Children s Hospital Case Western Reserve School of Medicine Flank pain Results from distention of ureter or renal
Urinary tract pathology Renal syndromes Acute nephritic syndrome syndrome includes oliguria hematuria proteinuria edema hypertension typically occurs
 Urinary tract Structure [Figs. 13-1, 13-2] Kidneys (left and right) cortex (glomeruli and tubules) medulla (tubules, loops of Henle, and collecting ducts) calices and pelvis forming the collecting system
Urinary tract Structure [Figs. 13-1, 13-2] Kidneys (left and right) cortex (glomeruli and tubules) medulla (tubules, loops of Henle, and collecting ducts) calices and pelvis forming the collecting system
Crescentic Glomerulonephritis (RPGN)
 Crescentic Glomerulonephritis (RPGN) Background Rapidly progressive glomerulonephritis (RPGN) is defined as any glomerular disease characterized by extensive crescents (usually >50%) as the principal histologic
Crescentic Glomerulonephritis (RPGN) Background Rapidly progressive glomerulonephritis (RPGN) is defined as any glomerular disease characterized by extensive crescents (usually >50%) as the principal histologic
Surgical Pathology Report
 Louisiana State University Health Sciences Center Department of Pathology Shreveport, Louisiana Accession #: Collected: Received: Reported: 6/1/2012 09:18 6/2/2012 09:02 6/2/2012 Patient Name: Med. Rec.
Louisiana State University Health Sciences Center Department of Pathology Shreveport, Louisiana Accession #: Collected: Received: Reported: 6/1/2012 09:18 6/2/2012 09:02 6/2/2012 Patient Name: Med. Rec.
Dr. Rai Muhammad Asghar Head of Paediatric Department BBH Rawalpindi
 Dr. Rai Muhammad Asghar Head of Paediatric Department BBH Rawalpindi Acute Post streptococcal Glomerulonephritis Sudden onset of Gross hematuria Edema Hypertension Renal insufficiency Cause of AGN Post
Dr. Rai Muhammad Asghar Head of Paediatric Department BBH Rawalpindi Acute Post streptococcal Glomerulonephritis Sudden onset of Gross hematuria Edema Hypertension Renal insufficiency Cause of AGN Post
ESRD Dialysis Prevalence - One Year Statistics
 Age Group IL Other Total 00-04 12 1 13 05-09 5 2 7 10-14 15 1 16 15-19 55 2 57 20-24 170 10 180 25-29 269 14 283 30-34 381 9 390 35-39 583 14 597 40-44 871 20 891 45-49 1,119 20 1,139 50-54 1,505 35 1,540
Age Group IL Other Total 00-04 12 1 13 05-09 5 2 7 10-14 15 1 16 15-19 55 2 57 20-24 170 10 180 25-29 269 14 283 30-34 381 9 390 35-39 583 14 597 40-44 871 20 891 45-49 1,119 20 1,139 50-54 1,505 35 1,540
Mr PA. Clinical assessment of hydration. Poor urine output Sunken eyes Moistness of mucosa Cool peripheries Reduction in weight Postural hypotension
 X Anthony Warrens Mr PA 54 years old Previously well Went to Thailand Developed serious diarrhoea and vomiting two days before coming home 24 hours after return, still unwell GP found: urea 24 mmol/l creatinine
X Anthony Warrens Mr PA 54 years old Previously well Went to Thailand Developed serious diarrhoea and vomiting two days before coming home 24 hours after return, still unwell GP found: urea 24 mmol/l creatinine
Renal Cystic Disease. Dr H Bierman
 Renal Cystic Disease Dr H Bierman Objectives Be able to diagnose renal cystic disease Genetic / non-genetic Be able to describe patterns of various renal cystic disease on routine imaging studies Be able
Renal Cystic Disease Dr H Bierman Objectives Be able to diagnose renal cystic disease Genetic / non-genetic Be able to describe patterns of various renal cystic disease on routine imaging studies Be able
Excretory urography (EU) or IVP US CT & radionuclide imaging
 Excretory urography (EU) or IVP US CT & radionuclide imaging MRI arteriography studies requiring catherization or direct puncture of collecting system EU & to a lesser extent CT provide both functional
Excretory urography (EU) or IVP US CT & radionuclide imaging MRI arteriography studies requiring catherization or direct puncture of collecting system EU & to a lesser extent CT provide both functional
Index. electron microscopy, 81 immunofluorescence microscopy, 80 light microscopy, 80 Amyloidosis clinical setting, 185 etiology/pathogenesis,
 A Acute antibody-mediated rejection (Acute AMR) clinical features, 203 clinicopathologic correlations, 206 pathogenesis, 205 206 204 205 light microscopy, 203 204 Acute cellular rejection (ACR) clinical
A Acute antibody-mediated rejection (Acute AMR) clinical features, 203 clinicopathologic correlations, 206 pathogenesis, 205 206 204 205 light microscopy, 203 204 Acute cellular rejection (ACR) clinical
PATTERNS OF RENAL INJURY
 PATTERNS OF RENAL INJURY Normal glomerulus podocyte Glomerular capillaries electron micrograph THE CLINICAL SYNDROMES 1. The Nephrotic Syndrome 2. The Acute Nephritic Syndrome 3. Rapidly Progressive Glomerulonephritis
PATTERNS OF RENAL INJURY Normal glomerulus podocyte Glomerular capillaries electron micrograph THE CLINICAL SYNDROMES 1. The Nephrotic Syndrome 2. The Acute Nephritic Syndrome 3. Rapidly Progressive Glomerulonephritis
Basic Urinary Tract Anatomy and Histology
 Basic Urinary Tract Anatomy and Histology The two kidneys are located in the retroperitoneum on either side of the vertebral bladder and the contraction of the detrusor muscle. Any mechanical barrier,
Basic Urinary Tract Anatomy and Histology The two kidneys are located in the retroperitoneum on either side of the vertebral bladder and the contraction of the detrusor muscle. Any mechanical barrier,
Urinary system. Urinary system
 INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
INTRODUCTION. Several organs system Produce urine and excrete it from the body Maintenance of homeostasis. Components. two kidneys, produce urine; two ureters, carry urine to single urinary bladder for
Interesting case seminar: Native kidneys Case Report:
 Interesting case seminar: Native kidneys Case Report: Proximal tubulopathy and light chain deposition disease presented as severe pulmonary hypertension with right-sided cardiac dysfunction and nephrotic
Interesting case seminar: Native kidneys Case Report: Proximal tubulopathy and light chain deposition disease presented as severe pulmonary hypertension with right-sided cardiac dysfunction and nephrotic
27-Apr-15 1 UAF ANOMALIES OF DEVELOPMENT RENAL SYSTEM - 1 DR. MUHAMMAD TARIQ JAVED UAF UAF
 RENAL SYSTEM - 1 DR. MUHAMMAD TARIQ JAVED Professor, Department of Pathology, Faculty of Veterinary Science, University of Agriculture, Faisalabad, Pakistan. Email: mtjaved@uaf.edu.pk RENAL AGENESIS Renal
RENAL SYSTEM - 1 DR. MUHAMMAD TARIQ JAVED Professor, Department of Pathology, Faculty of Veterinary Science, University of Agriculture, Faisalabad, Pakistan. Email: mtjaved@uaf.edu.pk RENAL AGENESIS Renal
The Urinary System Pathology. Dr. Methaq Mueen د.ميثاق معين
 The Urinary System Pathology Dr. Methaq Mueen د.ميثاق معين objectives To Know normal anatomy physiology and histology of renal system To discuss Kidney pathology: congenital, cystic disease, Glmerular
The Urinary System Pathology Dr. Methaq Mueen د.ميثاق معين objectives To Know normal anatomy physiology and histology of renal system To discuss Kidney pathology: congenital, cystic disease, Glmerular
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
WSC , Conference 9, Case 1. Tissue from a nyala.
 WSC 2009-2010, Conference 9, Case 1. Tissue from a nyala. MICROSCOPIC DESCRIPTION: Heart, atrium (1 pt.): Approximately 40% of the atrial myocardium is replaced by areas of fibrous connective tissue (1
WSC 2009-2010, Conference 9, Case 1. Tissue from a nyala. MICROSCOPIC DESCRIPTION: Heart, atrium (1 pt.): Approximately 40% of the atrial myocardium is replaced by areas of fibrous connective tissue (1
THE URINARY SYSTEM. The cases we will cover are:
 THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
THE URINARY SYSTEM The focus of this week s lab will be pathology of the urinary system. Diseases of the kidney can be broken down into diseases that affect the glomeruli, tubules, interstitium, and blood
RaDaR Inclusion and Exclusion Criteria. Diagnosis Inclusion Criteria Exclusion Criteria. Alport Syndrome definite or probable
 Alport Syndrome and Type IV collagenopathies APRT Deficiency Alport Syndrome definite or probable Alport carrier definite or probable Thin basement membrane nephropathy APRT Deficiency confirmed Abolished
Alport Syndrome and Type IV collagenopathies APRT Deficiency Alport Syndrome definite or probable Alport carrier definite or probable Thin basement membrane nephropathy APRT Deficiency confirmed Abolished
CHRONIC KIDNEY DISEASE (CKD)
 CHRONIC KIDNEY DISEASE (CKD) CKD implies longstanding (more than 3 months), and usually progressive, impairment in renal function. In many instances, no effective means are available to reverse the primary
CHRONIC KIDNEY DISEASE (CKD) CKD implies longstanding (more than 3 months), and usually progressive, impairment in renal function. In many instances, no effective means are available to reverse the primary
URINARY SYSTEM CHAPTER 28 I ANATOMY OF THE URINARY SYSTEM. Student Name
 Student Name CHAPTER 28 URINARY SYSTEM L iving produces wastes. Wherever people live or work or play, wastes accumulate. To keep these areas healthy, there must be a method of disposing of these wastes
Student Name CHAPTER 28 URINARY SYSTEM L iving produces wastes. Wherever people live or work or play, wastes accumulate. To keep these areas healthy, there must be a method of disposing of these wastes
Renal pathophysiology.
 Renal pathophysiology basa.konecna@gmail.com Outline Intro basic structure & physiology Nephrotic syndrome Nephritic syndrome Acute renal failure Chronic kidney disease Gross structure and location Kidney
Renal pathophysiology basa.konecna@gmail.com Outline Intro basic structure & physiology Nephrotic syndrome Nephritic syndrome Acute renal failure Chronic kidney disease Gross structure and location Kidney
Lung diseases of Vascular Origin. By: Shefaa Qa qqa
 Lung diseases of Vascular Origin By: Shefaa Qa qqa Pulmonary Hypertension Pulmonary hypertension is defined as a mean pulmonary artery pressure greater than or equal to 25 mm Hg at rest. Based on underlying
Lung diseases of Vascular Origin By: Shefaa Qa qqa Pulmonary Hypertension Pulmonary hypertension is defined as a mean pulmonary artery pressure greater than or equal to 25 mm Hg at rest. Based on underlying
NEPHRITIC SYNDROME. By Dr Mai inbiek
 NEPHRITIC SYNDROME By Dr Mai inbiek Nephritic Syndrome The nephritic Syndrome is a clinical complex, usually of acute onset. Is caused by inflammatory lesions of glomeruli. Characterized by; 1) Hematuria
NEPHRITIC SYNDROME By Dr Mai inbiek Nephritic Syndrome The nephritic Syndrome is a clinical complex, usually of acute onset. Is caused by inflammatory lesions of glomeruli. Characterized by; 1) Hematuria
Elevated Serum Creatinine, a simplified approach
 Elevated Serum Creatinine, a simplified approach Primary Care Update Creighton University School of Medicine. April 27 th, 2018 Disclosure Slide I have no disclosures and have no conflicts with this presentation.
Elevated Serum Creatinine, a simplified approach Primary Care Update Creighton University School of Medicine. April 27 th, 2018 Disclosure Slide I have no disclosures and have no conflicts with this presentation.
Renal. Pathology. Kris%ne Kra*s, M.D.
 Renal Pathology Kris%ne Kra*s, M.D. Renal Pathology Outline Introductory stuff Glomerular diseases Tubular and inters%%al diseases Diseases involving blood vessels Cys%c diseases Tumors Renal Pathology
Renal Pathology Kris%ne Kra*s, M.D. Renal Pathology Outline Introductory stuff Glomerular diseases Tubular and inters%%al diseases Diseases involving blood vessels Cys%c diseases Tumors Renal Pathology
The Excretory System
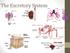 The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
ACUTE GLOMERULONEPHRITIS. IAP UG Teaching slides
 ACUTE GLOMERULONEPHRITIS 1 Definition Etiology Pathology/pathogenesis Risk factors Clinical Presentation Investigation Differential Diagnosis Management Outcome/Prognosis Indication for Renal Biopsy Summary
ACUTE GLOMERULONEPHRITIS 1 Definition Etiology Pathology/pathogenesis Risk factors Clinical Presentation Investigation Differential Diagnosis Management Outcome/Prognosis Indication for Renal Biopsy Summary
Non-protein nitrogenous substances (NPN)
 Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
Non-protein nitrogenous substances (NPN) A simple, inexpensive screening test a routine urinalysis is often the first test conducted if kidney problems are suspected. A small, randomly collected urine
URINARY SYSTEM I. Kidneys II. Nephron Unit and Urine Formation
 URINARY SYSTEM I. Kidneys A. Location and Structure 1. Retroperitoneal 2. Between T12 and L3 3. Rt. kidney slightly lower 4. Two bean shaped organs 5. Adrenal gland 6. Internal construction a. Renal cortex
URINARY SYSTEM I. Kidneys A. Location and Structure 1. Retroperitoneal 2. Between T12 and L3 3. Rt. kidney slightly lower 4. Two bean shaped organs 5. Adrenal gland 6. Internal construction a. Renal cortex
Analgesic and NSAID-induced Kidney Disease
 Analgesic and NSAID-induced Kidney Disease Edited by J.H.STEWART Associate Dean, Western Clinical School University of Sydney, Australia Oxford New York Tokyo Melbourne OXFORD UNIVERSITY PRESS 1993 CONTENTS
Analgesic and NSAID-induced Kidney Disease Edited by J.H.STEWART Associate Dean, Western Clinical School University of Sydney, Australia Oxford New York Tokyo Melbourne OXFORD UNIVERSITY PRESS 1993 CONTENTS
HYPERTENSIVE VASCULAR DISEASE
 HYPERTENSIVE VASCULAR DISEASE Cutoffs in diagnosing hypertension in clinical practice sustained diastolic pressures >90 mm Hg, or sustained systolic pressures >140 mm Hg Malignant hypertension A small
HYPERTENSIVE VASCULAR DISEASE Cutoffs in diagnosing hypertension in clinical practice sustained diastolic pressures >90 mm Hg, or sustained systolic pressures >140 mm Hg Malignant hypertension A small
CHAPTER 2. Primary Glomerulonephritis
 2nd Report of the PRIMARY GLOMERULONEPHRITIS CHAPTER 2 Primary Glomerulonephritis Sunita Bavanandan Lee Han Wei Lim Soo Kun 21 PRIMARY GLOMERULONEPHRITIS 2nd Report of the 2.1 Introduction This chapter
2nd Report of the PRIMARY GLOMERULONEPHRITIS CHAPTER 2 Primary Glomerulonephritis Sunita Bavanandan Lee Han Wei Lim Soo Kun 21 PRIMARY GLOMERULONEPHRITIS 2nd Report of the 2.1 Introduction This chapter
1. Disorders of glomerular filtration
 RENAL DISEASES 1. Disorders of glomerular filtration 2. Nephrotic syndrome 3. Disorders of tubular transport 4. Oliguria and polyuria 5. Nephrolithiasis 6. Disturbances of renal blood flow 7. Acute renal
RENAL DISEASES 1. Disorders of glomerular filtration 2. Nephrotic syndrome 3. Disorders of tubular transport 4. Oliguria and polyuria 5. Nephrolithiasis 6. Disturbances of renal blood flow 7. Acute renal
Interpretation of Renal Transplant Biopsy. Arthur H. Cohen Wake Forest University School of Medicine Winston-Salem, North Carolina USA
 Interpretation of Renal Transplant Biopsy Arthur H. Cohen Wake Forest University School of Medicine Winston-Salem, North Carolina USA Renal Transplant Biopsies Tissue Processing Ideal world process as
Interpretation of Renal Transplant Biopsy Arthur H. Cohen Wake Forest University School of Medicine Winston-Salem, North Carolina USA Renal Transplant Biopsies Tissue Processing Ideal world process as
Approach to Glomerular Diseases: Clinical Presentation Nephrotic Syndrome Nephritis
 GLOMERULONEPHRITIDES Vivette D Agati Jai Radhakrishnan Approach to Glomerular Diseases: Clinical Presentation Nephrotic Syndrome Nephritis Heavy Proteinuria Renal failure Low serum Albumin Hypertension
GLOMERULONEPHRITIDES Vivette D Agati Jai Radhakrishnan Approach to Glomerular Diseases: Clinical Presentation Nephrotic Syndrome Nephritis Heavy Proteinuria Renal failure Low serum Albumin Hypertension
2014 /2018 ERA-EDTA PRD Code ERA-EDTA PRD code 1996 ERA-EDTA. SNOMED CT concept identifier Convert ERA-EDTA Primary Renal Diagnosis (PRD) Term
 Convert Primary Renal Diagnosis (PRD) Term ERA_EDTA diagnosis 3380 901.1.C 90 Acute kidney injury Acute Renal Failure 14669001 Miscellaneous renal disorders 3398 901.2.C 90 Acute kidney injury due to hypovolaemia
Convert Primary Renal Diagnosis (PRD) Term ERA_EDTA diagnosis 3380 901.1.C 90 Acute kidney injury Acute Renal Failure 14669001 Miscellaneous renal disorders 3398 901.2.C 90 Acute kidney injury due to hypovolaemia
RaDaR Inclusion and Exclusion Criteria. Diagnosis Inclusion Criteria Exclusion Criteria. Alport Syndrome definite or probable
 Alport Syndrome and Type IV collagenopathies APRT Deficiency Alport Syndrome definite or probable Alport carrier definite or probable Thin basement membrane nephropathy APRT Deficiency confirmed Abolished
Alport Syndrome and Type IV collagenopathies APRT Deficiency Alport Syndrome definite or probable Alport carrier definite or probable Thin basement membrane nephropathy APRT Deficiency confirmed Abolished
Dr. Najla a Aldaoud. Omar Ayman Khasawneh
 Pathology 1 Congenital & Cystic diseases of the kidney Dr. Najla a Aldaoud Omar Ayman Khasawneh 1 P a g e Slides are included بسم هللا الرحمن الرحيم Today is our first pathology lectures, Dr Najla' will
Pathology 1 Congenital & Cystic diseases of the kidney Dr. Najla a Aldaoud Omar Ayman Khasawneh 1 P a g e Slides are included بسم هللا الرحمن الرحيم Today is our first pathology lectures, Dr Najla' will
Nephritic vs. Nephrotic Syndrome
 Page 1 of 18 Nephritic vs. Nephrotic Syndrome Terminology: Glomerulus: A network of blood capillaries contained within the cuplike end (Bowman s capsule) of a nephron. Glomerular filtration rate: The rate
Page 1 of 18 Nephritic vs. Nephrotic Syndrome Terminology: Glomerulus: A network of blood capillaries contained within the cuplike end (Bowman s capsule) of a nephron. Glomerular filtration rate: The rate
Chapter 1. Incidence of End Stage Kidney Disease. Contents:
 Chapter 1 Incidence of End Stage Kidney Disease Contents: Incidence of End Stage Kidney Disease 1-1 Stock and Flow 1-2 Incident patients 1-3 Incident Rates 1-3 Late Referral 1-7 Co-Morbidities 1-9 Primary
Chapter 1 Incidence of End Stage Kidney Disease Contents: Incidence of End Stage Kidney Disease 1-1 Stock and Flow 1-2 Incident patients 1-3 Incident Rates 1-3 Late Referral 1-7 Co-Morbidities 1-9 Primary
CHAPTER 2 NEW PATIENTS COMMENCING TREATMENT IN 2007
 CHAPTER 2 NEW PATIENTS COMMENCING TREATMENT IN 27 Stephen McDonald Leonie Excell Hannah Dent NEW PATIENTS ANZDATA Registry 28 Report Figure 2.1 Annual Intake of New Patients 23-27 (Number Per Million Population)
CHAPTER 2 NEW PATIENTS COMMENCING TREATMENT IN 27 Stephen McDonald Leonie Excell Hannah Dent NEW PATIENTS ANZDATA Registry 28 Report Figure 2.1 Annual Intake of New Patients 23-27 (Number Per Million Population)
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
PRINCIPLE OF URINALYSIS
 PRINCIPLE OF URINALYSIS Vanngarm Gonggetyai Objective Can explain : the abnormalities detected in urine Can perform : routine urinalysis Can interprete : the results of urinalysis Examination of urine
PRINCIPLE OF URINALYSIS Vanngarm Gonggetyai Objective Can explain : the abnormalities detected in urine Can perform : routine urinalysis Can interprete : the results of urinalysis Examination of urine
Case Presentation VASCULITIS. Case Presentation. Case Presentation. Vasculitis
 Case Presentation VASCULITIS The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
Case Presentation VASCULITIS The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
PATHOLOGY OF THE URINARY SYSTEM Dr. Ameer Dhahir Part one
 PATHOLOGY OF THE URINARY SYSTEM Dr. Ameer Dhahir Part one Objectives: Defining certain clinical terms related to urinary disorders. Describing the pathogenesis of glomerular diseases Defining certain clinical
PATHOLOGY OF THE URINARY SYSTEM Dr. Ameer Dhahir Part one Objectives: Defining certain clinical terms related to urinary disorders. Describing the pathogenesis of glomerular diseases Defining certain clinical
ERA-EDTA ERA-EDTA Primary Renal Diagnosis (PRD) Term ERA-EDTA PRD classification SNOMED CT PRD Code 1/1/2015
 1003 Adult nephrotic syndrome - no histology Immunological Glomerulopathy 52254009 1019 Nephrotic syndrome of childhood - steroid sensitive - no histology Immunological Glomerulopathy 445119005 1026 Congenital
1003 Adult nephrotic syndrome - no histology Immunological Glomerulopathy 52254009 1019 Nephrotic syndrome of childhood - steroid sensitive - no histology Immunological Glomerulopathy 445119005 1026 Congenital
Pathophysiology of Cardiovascular System. Dr. Hemn Hassan Othman, PhD
 Pathophysiology of Cardiovascular System Dr. Hemn Hassan Othman, PhD hemn.othman@univsul.edu.iq What is the circulatory system? The circulatory system carries blood and dissolved substances to and from
Pathophysiology of Cardiovascular System Dr. Hemn Hassan Othman, PhD hemn.othman@univsul.edu.iq What is the circulatory system? The circulatory system carries blood and dissolved substances to and from
Monoclonal Gammopathies and the Kidney. Tibor Nádasdy, MD The Ohio State University, Columbus, OH
 Monoclonal Gammopathies and the Kidney Tibor Nádasdy, MD The Ohio State University, Columbus, OH Monoclonal gammopathy of renal significance (MGRS) Biopsies at OSU (n=475) between 2007 and 2016 AL or AH
Monoclonal Gammopathies and the Kidney Tibor Nádasdy, MD The Ohio State University, Columbus, OH Monoclonal gammopathy of renal significance (MGRS) Biopsies at OSU (n=475) between 2007 and 2016 AL or AH
Tumors of kidney and urinary bladder
 Tumors of kidney and urinary bladder Overview of kidney tumors Benign and malignant Of the benign: papillary adenoma -cortical -small (0.5cm) -in 40% of population -clinically insignificant The most common
Tumors of kidney and urinary bladder Overview of kidney tumors Benign and malignant Of the benign: papillary adenoma -cortical -small (0.5cm) -in 40% of population -clinically insignificant The most common
Lab 3, case 1. Is this an example of nephrotic or nephritic syndrome? Why? Which portion of the nephron would you expect to be abnormal?
 Lab 3, case 1 12-year-old Costa Rican boy is brought into clinic by his parents because of dark brownish-red urine over the last 24 hours. The family has been visiting friends in Indianapolis for two weeks.
Lab 3, case 1 12-year-old Costa Rican boy is brought into clinic by his parents because of dark brownish-red urine over the last 24 hours. The family has been visiting friends in Indianapolis for two weeks.
VASCULITIS. Case Presentation. Case Presentation
 VASCULITIS Case Presentation The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
VASCULITIS Case Presentation The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
Excretory System. Biology 2201
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System. Excretory System
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
CHAPTER 2 PRIMARY GLOMERULONEPHRITIS
 CHAPTER 2 Sunita Bavanandan Lim Soo Kun 19 5th Report of the 2.1: Introduction This chapter covers the main primary glomerulonephritis that were reported to the MRRB from the years 2005-2012. Minimal change
CHAPTER 2 Sunita Bavanandan Lim Soo Kun 19 5th Report of the 2.1: Introduction This chapter covers the main primary glomerulonephritis that were reported to the MRRB from the years 2005-2012. Minimal change
Case Presentation Turki Al-Hussain, MD
 Case Presentation Turki Al-Hussain, MD Director, Renal Pathology Chapter Saudi Society of Nephrology & Transplantation Consultant Nephropathologist & Urological Pathologist Department of Pathology & Laboratory
Case Presentation Turki Al-Hussain, MD Director, Renal Pathology Chapter Saudi Society of Nephrology & Transplantation Consultant Nephropathologist & Urological Pathologist Department of Pathology & Laboratory
the urinary system pathology Dr. Fairoz A Eltorgman
 the urinary system pathology Dr. Fairoz A Eltorgman Tumors of the renal pelvis & kidney Benign tumors of the renal pelvis: Hemangioma Leiomyoma Malignant tumors: Transitional cell carcinoma Squamous cell
the urinary system pathology Dr. Fairoz A Eltorgman Tumors of the renal pelvis & kidney Benign tumors of the renal pelvis: Hemangioma Leiomyoma Malignant tumors: Transitional cell carcinoma Squamous cell
C3 GLOMERULOPATHIES. Budapest Nephrology School Zoltan Laszik
 C3 GLOMERULOPATHIES Budapest Nephrology School 8.30.2018. Zoltan Laszik 1 Learning Objectives Familiarize with the pathogenetic mechanisms of glomerular diseases Learn the pathologic landscape and clinical
C3 GLOMERULOPATHIES Budapest Nephrology School 8.30.2018. Zoltan Laszik 1 Learning Objectives Familiarize with the pathogenetic mechanisms of glomerular diseases Learn the pathologic landscape and clinical
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
renoprotection therapy goals 208, 209
 Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
Urinary system disorders Chapter 29
 Urinary system disorders Chapter 29 1 The Nephron Anatomy 2 Physiology 1.25 L per minute blood flow 25% of Cardiac Output Kidney compensates if one is lost - 2 weeks 3 Urine Formation 1. Filtration 2.
Urinary system disorders Chapter 29 1 The Nephron Anatomy 2 Physiology 1.25 L per minute blood flow 25% of Cardiac Output Kidney compensates if one is lost - 2 weeks 3 Urine Formation 1. Filtration 2.
Urinary System. Dr. Thorson
 Urinary System Dr. Thorson Lesson Objectives Upon completion of this lesson, students should be able to Define and spell the terms to learn for this chapter. Describe the purpose and function of the urinary
Urinary System Dr. Thorson Lesson Objectives Upon completion of this lesson, students should be able to Define and spell the terms to learn for this chapter. Describe the purpose and function of the urinary
Histopathology: Vascular pathology
 Histopathology: Vascular pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need to learn about these
Histopathology: Vascular pathology These presentations are to help you identify basic histopathological features. They do not contain the additional factual information that you need to learn about these
LECTURE IN INTERNAL MEDICINE PROPAEDEUTICS 2017/2018
 SIGNS AND SYMPTOMS OF URINARY SYSTEM DISEASES (urinary syndrome, nephrotic syndrome, nephritic syndrome, urinary tract obstruction syndrome, hypertensive syndrome) LECTURE IN INTERNAL MEDICINE PROPAEDEUTICS
SIGNS AND SYMPTOMS OF URINARY SYSTEM DISEASES (urinary syndrome, nephrotic syndrome, nephritic syndrome, urinary tract obstruction syndrome, hypertensive syndrome) LECTURE IN INTERNAL MEDICINE PROPAEDEUTICS
ATHEROSCLEROSIS. Secondary changes are found in other coats of the vessel wall.
 ATHEROSCLEROSIS Atherosclerosis Atherosclerosis is a disease process affecting the intima of the aorta and large and medium arteries, taking the form of focal thickening or plaques of fibrous tissue and
ATHEROSCLEROSIS Atherosclerosis Atherosclerosis is a disease process affecting the intima of the aorta and large and medium arteries, taking the form of focal thickening or plaques of fibrous tissue and
