Visual prognosis after panretinal photocoagulation for. Proliferative diabetic retinopathy (PDR)
|
|
|
- Allen Warner
- 5 years ago
- Views:
Transcription
1 Visual prognosis after panretinal photocoagulation for proliferative diabetic retinopathy Toke Bek 1 and Mogens Erlandsen 2 1 Department of Ophthalmology, A rhus University Hospital, A rhus, Denmark 2 Department of Biostatistics, A rhus University, A rhus, Denmark ABSTRACT. Introduction: Proliferative diabetic retinopathy is treated with panretinal photocoagulation, which improves the visual prognosis in this complication considerably. The visual acuity (VA) and grade of retinopathy before treatment are known indicators of the visual prognosis after treatment, but the prognostic value of other clinical background and treatment parameters is unknown. Methods: The study reports predictors for visual outcome identified among retrospective clinical background data and treatment parameters from 4422 panretinal photocoagulation sessions for proliferative diabetic retinopathy in 1013 eyes of 601 patients performed at the Department of Ophthalmology, A rhus University Hospital between 1985 and Results: High pretreatment VA and low age were strong positive predictors of post-treatment VA (p < ). However, diabetes type, diabetes duration and calendar year of treatment showed no influence on post-treatment VA (p = , , and , respectively). The visual prognosis was inversely related to the number of treatment sessions (p = ) and the number of vitrectomies (OR = 2.66 [1.24; 5.69], p = , for more than two operations). However, the visual prognosis was unrelated to any of the other parameters studied. Conclusions: Pretreatment VA, age and the number of panretinal photocoagulation treatment sessions and vitrectomies necessary to halt the disease are indicators of the visual prognosis after panretinal laser photocoagulation for proliferative diabetic retinopathy. Key words: panretinal photocoagulation proliferative diabetic retinopathy visual prognosis Acta Ophthalmol. Scand. 2006: 84: Copyright # Acta Ophthalmol Scand doi: /j x Introduction Proliferative diabetic retinopathy (PDR) is treated with panretinal photocoagulation (PRP), which can improve the visual prognosis in this complication significantly (Diabetic Retinopathy Study Research Group (DRSRG) 1981; Rogell 1983; Blankenship 1991). However, the treatment may also result in adverse effects such as blurring of central vision, visual field constriction, and disturbances in dark adaptation and contrast vision (Lovestam-Adrian et al. 2003). In clinical practice attempts are made to mitigate these adverse effects by decreasing the number of applications or by increasing the interval between treatment sessions (Doft & Blankenship 1982; Liang & Huamonte 1984; Early Treatment Diabetic Retinopathy Study (ETDRS) Research Group 1987). It is generally recommended that PRP should include more than 2000 laser applications, but there is only sparse documentation available to indicate how the treatment should be applied to optimize the positive effects and minimize the adverse effects. Relevant factors might include the number of applications and the length of the time intervals between treatment sessions. Other clinical background parameters such as visual acuity (VA) and the severity of retinopathy have been shown to predict the visual prognosis after PRP (Rand et al. 1985; Kaufman et al. 1989; Kaiser et al. 2000), whereas the influence of parameters such as age, diabetes type and diabetes duration is largely unknown. The present study reports predictors for visual outcome identified among retrospective clinical background data and treatment parameters from 4422 PRP sessions for PDR in 1013 eyes of 601 patients performed at the Department of Ophthalmology, Århus University Hospital between 1985 and Materials and Methods Patients The study is based on data from the database for diabetic retinopathy at 16
2 the Department of Ophthalmology, A rhus University Hospital. This database contains clinical data for all patients who have been screened, examined or treated for diabetic retinopathy in the department since The department treats all the diabetes patients in Århus County (approximately inhabitants) and until 1996 it also treated patients from two neighbouring counties. At the time of data sampling (June 1st, 2002) the database contained information on 7784 diabetes patients, of whom 1991 had type 1 diabetes (defined as those whose age at onset of diabetes was less than 30 years and who required insulin from onset), 5656 had type 2 diabetes (the remaining patients with known age of onset and treatment), and 137 had unknown diabetes type due to lack of information about age of onset and diabetes treatment. The registered laser treatment parameters include number, size, and energy of applications as well as the initials of the treating ophthalmologist. According to the department s routine, astandardspotsizeof500mm wasused and the energy increased until the laser burns produced a definite whitening (ETDRS 1987). In cases with cataract and other media opacities where the energy could not be increased sufficiently to produce a visible burn, a smaller spot size was used. A total of 4613 sessions were registered as having been performed by 73 ophthalmologists. Of these, 48% were performed by one ophthalmologist (the first author), 66% were performed by three ophthalmologists, and 90% were performed by 25 ophthalmologists. Prior to 1994 PRP was carried out by all ophthalmologists in the department, the only guideline being to give at least 2000 laser applications in the retinal periphery when new vessels were detected by ophthalmoscopy or fluorescein angiography. No systematic quality assurance was performed. This resulted in varying treatment strategies and inconsistent registration of treatment parameters. These data were entered into the database post hoc from the patient records. Since 1994 treatment has been performed in a standardized way, preferably in three sessions per eye, by the same ophthalmologist (the first author) or under his supervision, and all patients have been followed up with VA measurement and fundus photography 3 months after treatment. These data have been entered into the database at the time of data collection. At the time of data sampling for this study the database contained information on 4690 PRP sessions in 1484 eyes. Due to incomplete registration before 1994, data were complete for only 4422 treatment sessions in 1013 eyes of 601 patients (253 males, 348 females; 297 type 1 diabetes patients, 297 type 2 diabetes patients, seven patients with unknown diabetes type). The reporting of anonymized data from the database does not require approval from the local scientific ethics committee. Statistical analysis The study was designed to identify predictive parameters for VA after photocoagulation treatment for PDR. However, VA values tended to be clustered in discrete values corresponding to the standard levels on generally used VA charts, which resulted in a non-even distribution unsuitable for standard regression techniques. We therefore used the proportional odds model for ordinal data (McCullagh 1980). In order to do this we introduced five VA categories corresponding to four cutpoints: c 1 ¼ 0.1, c 2 ¼ 0.3, c 3 ¼ 0.5 and c 4 ¼ 0.7. If x ¼ (x 1,...,x p ) denotes the set of explanatory variables, the model for the cumulative odds is: log PrðY <c jjxþ ¼a j x 1 b PrðYc j jxþ 1 x p b p ; j¼1;2;3;4 The model has similarities with an ordinary logistic regression model. For example, the cumulative odds ratio is obtained for one of the covariates (x 1 ) as usual: OR 1 ¼ exp(b l ). The odds ratio compares the odds for a result below the cut-point c j with a result above the cut-point, and each of the four cut-points will yield the same odds ratio. The change of sign of the covariates implies that a negative aˆ-coefficient is associated with an odds ratio >1 (i.e. an increased risk of a bad prognosis). A crucial assumption in the model is that the regression coefficients b ¼ (b 1,...,b p ) do not depend on the category c j, j ¼ 1,2,3,4 (proportional odds assumption). This implies that the interpretation of b ¼ (b 1,...,b p ) does not depend on the particular choice of categories and adjacent categories can be pooled. We used STATA Version 8 to fit the model. As 68% of the patients had been treated in both eyes we had to take account of a possible correlation between eyes in the same patient. This was carried out using the generalized estimation equation principle (GEE) by means of the cluster option in the STATA procedure ologit. The final model was built in a stepwise manner, where the most significant variable among the variables not already in the model was added to the model and the most non-significant variable (if any) was removed. In the initial step only the intercept was included in the model and this procedure was repeated until every variable not included in the model was nonsignificant and every variable in the model was significant. Data identification The following data were used for every included patient. Effect parameter The effect parameter was the VA at the last examination after photocoagulation treatment. The values were assigned to each of five groups defined by the four clinically relevant cutpoints 0.1, 0.3, 0.5 and 0.7. Explanatory parameters Background data Visual acuity immediately before treatment: five groups with cut-points as for the effect parameter, range (n): <0.1 (130); (116); (170); (158), and 0.7 (439). Age at first treatment (years): six groups, range (n): 30 (148); (184); (178); (194); (197), and 71 (112). Diabetes type: two groups, type (n): type 1 (297), type 2 (297). Eleven eyes from seven patients with unknown diabetes type were not included in the analysis. Diabetes duration at first treatment session (years): mean ¼ 18.8; median ¼ 18.6; SD ¼ 11.54, and range Treatment intensity Treatment intensity is a function of both the number of applications given at each treatment session and the time interval between individual sessions. We therefore calculated the area under the curve (AUC) of the 17
3 cumulated number of applications as a function of time. This parameter was divided with the total number of applications the time interval between the first and last treatments to obtain the area fraction (AF). An area fraction close to 0.5 would indicate that treatment had been distributed evenly during the treatment interval (a low treatment intensity), whereas an area fraction close to 0 or 1 would indicate that most of the treatment had been performed during a short period of the treatment interval (a high treatment intensity). Consequently, the following values were defined: Calendar year for starting treatment: three groups, range (n): up to and including 1994 (353); (254), and 1999 onwards (406). Number of treatments per eye: six groups, treatments (n): one (143); two (266); three (312); four (147); five (73), and six and over (70). Total number of laser applications per eye: four groups, applications (n): 2000 (266); (219); (180), and 3001 (348). The interval between each treatment session in days (dt). The number of laser applications at each treatment session (nt). The number of treatment sessions (ns). On the basis of these data the following were calculated as measures of duration and intensity of the treatment: The total time (in days) from the first to last treatment (T): mean ¼ 631; median ¼ 96, and range The total number of laser applications given to each eye (N): mean ¼ 2709; median ¼ 2549, and range The product of total time (days) and total number of laser applications (TA ¼ T N): mean ¼ ; median ¼ , and range The AUC of the number of laser applications and the time interval (days) between examinations (AUC ¼ S n dt): mean ¼ ; median ¼ , and range The treatment intensity as expressed by the area fraction (AF ¼ AUC/TA): mean ¼ 0.45; median ¼ 0.36, and range 0 1. Post-treatment parameters Time of cataract operation: three groups (n): 0 ¼ none or before baseline VA measurement (944); 1 ¼ between last treatment and last VA measurement (33), and 2 ¼ during treatment (36). Number of vitrectomies: three groups (n): none (781); one (198), and two ¼ (64). Time of vitrectomy: three groups (n): 0 ¼ none or after the last VA measurement (781); 1 ¼ within 30 days after baseline VA (78), and 2 ¼ more than 30 days after baseline VA (184). Follow-up time (days) between last VA measurement and last treatment (photocoagulation): median ¼ 136, range Results Background data The change in VA after treatment with PRP is shown in Fig. 1 and Table 1. Both pretreatment VA and age were strong predictors of post-treatment VA (p < for both comparisons). Figure 2 shows the results of the combined model. For increasing pretreatment VA there is a decreasing chance of retaining or improving posttreatment VA with increasing age. However, diabetes type, diabetes duration and calendar year of treatment show no influence on post-treatment VA (p ¼ , and , respectively). After Treatment variables In the statistical analysis a correction was made for the interactions found between the treatment variables. Consequently, the visual prognosis was inversely related to the number of treatment sessions (p ¼ ) and the number of vitrectomies (OR ¼ 2.66 [1.24; 5.69], p ¼ , for more than two operations). However, the visual prognosis was unrelated to the total number of treatment sessions (p ¼ ), laser applications (p ¼ ), the intensity of the laser treatment (p ¼ ), or any of the other parameters studied. Discussion The present study is the first to report the influence of treatment parameters and clinical background data other than VA and retinopathy grade on the visual prognosis after panretinal laser photocoagulation for proliferative diabetic retinopathy (Rand et al. 1985; Kaufman et al. 1989; Kaiser et al. 2000). The weaknesses of the study lie in its retrospective design and the fact that many ophthalmologists were involved in the treatment. However, all ophthalmologists followed the generally recommended guidelines for the treatment of PDR. Furthermore, there was no difference between the results of patients treated before 1994 or after Visual acuity Before Fig. 1. Visual acuity before and after treatment for each person included. Visual acuity values <1/60 have been truncated to zero. A clustering of values corresponding to the discrete levels of standard VA charts can be seen. 18
4 Table 1. The number of treated eyes according to visual acuity before treatment and at follow-up. Before treatment After treatment < Total < Total this time, when treatment was almost exclusively performed by one person. This confirms recent data showing that the pattern of visual loss secondary to diabetic retinopathy in A rhus County did not change when the treatment pattern was standardized around 1994 (Jeppesen & Bek 2004). Finally, although the clinical data and treatment parameters were incomplete for the first years of the studied period, and the excluded patients (n ¼ 471) were on average slightly (2.2 years) older (p ¼ 0.064) than those included, there was no difference between the two groups with regard to diabetes duration (p ¼ ). Therefore, the shortcomings of the retrospective design can be assumed to be of little importance to the interpretation of the results, and are greatly outbalanced by the large patient material, which included all patients treated in the county over a long time period. Visual acuity only measures limited aspects of visual function, and a number of visual modalities known to be affected by retinal laser photocoagulation, such as contrast vision Probability Improved or unchanged visual acuity (Lovestam-Adrian et al. 2000), visual fields (Pahor 1998) and adaptation (Mantyjarvi 1989), were not assessed by this parameter. Therefore, the visual prognosis reported in the present study may not fully cover the complaints experienced by the patients. However, VA is generally a good indicator of reading capability and other central visual functions and is measured routinely in clinical practice, which makes it suitable as an effect parameter by which to evaluate therapeutic intervention in diabetic retinopathy. The study confirmed existing evidence that pretreatment VA is an indicator of the visual prognosis after PRP for PDR (Rand et al. 1985; Kaiser et al. 2000). However, the treatment parameters were found not to have affected VA at the time of follow-up, implying that the visual blurring and other acute adverse effects known to be prevalent immediately after treatment had disappeared (Doft & Blankenship 1982). These results are encouraging but also point to the necessity of treating PDR before retinal damage has occurred. As has Age VA0.05 VA0.2 VA0.4 VA0.6 VA0.9 Fig. 2. The probability of preserving or improving VA after panretinal photocoagulation as a function of age for different pretreatment VA levels. been shown previously, the grade of PDR is also an important clinical predictor of visual outcome after treatment (Rand et al. 1985; Kaufman et al. 1989; Kaiser et al. 2000). In the present study this parameter could not be systematically and consistently evaluated as data were not available for the period before 1992 when the department s screening clinic for diabetic retinopathy was launched. The data confirm the clinical practice of informing patients that treatment will not improve vision, but that the VA may at best be preserved at the level it had reached before treatment. In addition to this it was found that the risk of experiencing a loss in VA secondary to panretinal laser photocoagulation increases significantly with age, and this increased risk is most pronounced when pretreatment VA was high. This emphasizes the need for special information about the risks of PRP in older age groups. The results demonstrate that neither the total number of laser applications, the time period over which the treatment was given, nor the treatment intensity were related to the visual prognosis after panretinal laser photocoagulation for PRP. This extends the findings of other authors who found no difference in visual prognosis after single versus multiple treatment sessions (Doft & Blankenship 1982). The findings also argue against assessing the progression and effect of the treatment on the basis of the number of given laser applications and indicate that the visual blurring that can be experienced after extensive treatment mostly disappears after some period of recovery. It has been clinically routine to augment the treatment until a sufficient clinical response has been reached, which is probably the cause of the poor visual prognosis in patients who were subjected to many photocoagulation sessions and many vitrectomies. These patients also had low pretreatment VA and the increased number of treatments therefore indicates that their disease was of a severe grade which needed extensive treatment (Kaiser et al. 2000). Therefore, it may be concluded that the major determining factor for amount and intensity of treatment should be the observed clinical response (Rogell 1983). In conclusion, the study has shown that, in addition to retinopathy stage, 19
5 pretreatment VA and age are the most significant predictors of visual prognosis after panretinal photocoagulation for proliferative diabetic retinopathy. The effect of the treatment should be adjusted after the clinical response and is independent of the number of laser applications, the time interval and the intensity of the treatment. References Blankenship GW (1991): Fifteen-year argon laser and xenon photocoagulation results of Bascom Palmer Eye Institute s patients participating in the Diabetic Retinopathy Study. Ophthalmology 98 (2): Diabetic Retinopathy Study Research Group (DRSRG) (1981): Photocoagulation treatment of proliferative diabetic retinopathy. Clinical applications of Diabetic Retinopathy Study (DRS) findings. DRS Report no. 8. Ophthalmology 88 (7): Doft BH & Blankenship GW (1982): Single versus multiple treatment sessions of argon laser panretinal photocoagulation for proliferative diabetic retinopathy. Ophthalmology 89: Early Treatment Diabetic Retinopathy Study (ETDRS) Research Group (1987): Techniques for scatter and local photocoagulation treatment of diabetic retinopathy: Early Treatment Diabetic Retinopathy Study Report no. 3. Int Clin Ophthalmol 274: Jeppesen P & Bek T (2004): The occurrence and causes of blindness in diabetes patients in Århus County Denmark Acta Ophthalmol Scand 82: Kaiser RS, Maguire MG, Grunwald JE et al. (2000): One-year outcomes of panretinal photocoagulation in proliferative diabetic retinopathy. Am J Ophthalmol 129 (2): Kaufman SC, Ferris FL, Seigel DG, Davis MD & DeMers DL (1989): Factors associated with visual outcome after photocoagulation for diabetic retinopathy. Invest Ophthalmol Vis Sci 30 (1): Liang JC & Huamonte FU (1984): Reduction of immediate complications after panretinal photocoagulation. Retina 4: Lovestam-Adrian M, Agardh CD, Torffvit T & Agardh E (2003): Type 1 diabetes patients with severe non-proliferative retinopathy may benefit from panretinal photocoagulation. Acta Ophthalmol Scand 81 (3): Lovestam-Adrian M, Svendenius N & Agardh E (2000): Contrast sensitivity and visual recovery time in diabetic patients treated with panretinal photocoagulation. Acta Ophthalmol Scand 78 (6): Mantyjarvi M (1989): Colour vision and dark adaptation in diabetic patients after photocoagulation. Acta Ophthalmol 67 (2): McCullagh P (1980): Regression models for ordinal data (with discussion). J R Statist Soc 42: Pahor D (1998): Visual field loss after argon laser panretinal photocoagulation in diabetic retinopathy: full- versus mild-scatter coagulation. Int Ophthalmol 22 (5): Rand LI, Ederer F, Prud homme G, Canner P & the Diabetic Retinopathy Study Research Group (DRSRG) (1985): Factors influencing the development of visual loss in diabetic retinopathy. DRS Report no. 3. Invest Ophthalmol Vis Sci 26: Rogell GD (1983): Incremental panretinal photocoagulation. Results in treating proliferative diabetic retinopathy. Retina 3 (4): Received on March 12th, Accepted on August 2nd, Correspondence: Toke Bek Professor and Chairman Department of Ophthalmology Århus University Hospital DK-8000 Århus C Denmark Tel: þ Fax: þ toke.bek@mail.tele.dk 20
Long-Term Visual Outcome in Proliferative Diabetic Retinopathy Patients After Panretinal Photocoagulation
 Long-Term Visual Outcome in Proliferative Diabetic Retinopathy Patients After Panretinal Photocoagulation Murat Dogru, Makoto Nakamura, Masanori Inoue and Misao Yamamoto Department of Ophthalmology, Kobe
Long-Term Visual Outcome in Proliferative Diabetic Retinopathy Patients After Panretinal Photocoagulation Murat Dogru, Makoto Nakamura, Masanori Inoue and Misao Yamamoto Department of Ophthalmology, Kobe
Factors Associated with Visual Outcome after Photocoagulation for Diabetic Retinopathy
 Investigative Ophthalmology & Visual Science, Vol. 30, No. 1, January 1989 Copyright Association for Research in Vision and Ophthalmology Factors Associated with Visual Outcome after Photocoagulation for
Investigative Ophthalmology & Visual Science, Vol. 30, No. 1, January 1989 Copyright Association for Research in Vision and Ophthalmology Factors Associated with Visual Outcome after Photocoagulation for
Extensive argon laser photocoagulation in the
 British Journal of Ophthalmology, 1989, 73, 197-201 Extensive argon laser photocoagulation in the treatment of proliferative diabetic retinopathy G W AYLWARD, R V PEARSON, J D JAGGER, AND A M HAMILTON
British Journal of Ophthalmology, 1989, 73, 197-201 Extensive argon laser photocoagulation in the treatment of proliferative diabetic retinopathy G W AYLWARD, R V PEARSON, J D JAGGER, AND A M HAMILTON
Type 1 diabetes patients with severe non-proliferative retinopathy may benefit from panretinal photocoagulation.
 Type 1 diabetes patients with severe non-proliferative retinopathy may benefit from panretinal photocoagulation. Lövestam-Adrian, Monica; Agardh, Carl-David; Torffvit, Ole; Agardh, Elisabet Published in:
Type 1 diabetes patients with severe non-proliferative retinopathy may benefit from panretinal photocoagulation. Lövestam-Adrian, Monica; Agardh, Carl-David; Torffvit, Ole; Agardh, Elisabet Published in:
optic disc neovascularisation
 British Journal of Ophthalmology, 1979, 63, 412-417 A comparative study of argon laser and krypton laser in the treatment of diabetic optic disc neovascularisation W. E. SCHULENBURG, A. M. HAMILTON, AND
British Journal of Ophthalmology, 1979, 63, 412-417 A comparative study of argon laser and krypton laser in the treatment of diabetic optic disc neovascularisation W. E. SCHULENBURG, A. M. HAMILTON, AND
Comparative electroretinograms in argon laser
 British Journal of Ophthalmology, 1983, 67, 520-525 Comparative electroretinograms in argon laser and xenon arc panretinal photocoagulation JAMES C. LIANG,' GERALD A. FISHMAN,' FELIPE U. HUAMONTE,' AND
British Journal of Ophthalmology, 1983, 67, 520-525 Comparative electroretinograms in argon laser and xenon arc panretinal photocoagulation JAMES C. LIANG,' GERALD A. FISHMAN,' FELIPE U. HUAMONTE,' AND
Diabetes & Your Eyes
 Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
Diabetic Retinopathy: Recent Advances in Treatment and Treatment Approaches
 Diabetic Retinopathy: Recent Advances in Treatment and Treatment Approaches Dr. David Wong Associate Professor Retina Specialist, Department of Ophthalmology & Vision Sciences, University of Toronto, Canada
Diabetic Retinopathy: Recent Advances in Treatment and Treatment Approaches Dr. David Wong Associate Professor Retina Specialist, Department of Ophthalmology & Vision Sciences, University of Toronto, Canada
Efficacy of principle-guided laser treatment in diabetic retinopathy.
 Biomedical Research 2017; 28 (6): 2566-2570 ISSN 0970-938X www.biomedres.info Efficacy of 4-2-1 principle-guided laser treatment in diabetic retinopathy. Ding Xu 1, Chun-Xia Li 2, Chun Zhao 1, Wan-Cheng
Biomedical Research 2017; 28 (6): 2566-2570 ISSN 0970-938X www.biomedres.info Efficacy of 4-2-1 principle-guided laser treatment in diabetic retinopathy. Ding Xu 1, Chun-Xia Li 2, Chun Zhao 1, Wan-Cheng
Diabetic retinopathy (DR) progressively
 FOCUS ON DIABETIC MACULAR EDEMA * Frederick L. Ferris III, MD ABSTRACT The current state of treatment for diabetic macular edema (DME) is focused on slowing the rate of vision loss through assessment of
FOCUS ON DIABETIC MACULAR EDEMA * Frederick L. Ferris III, MD ABSTRACT The current state of treatment for diabetic macular edema (DME) is focused on slowing the rate of vision loss through assessment of
Diagnosis and treatment of diabetic retinopathy. Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City
 Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
OCT Assessment of the Vitreoretinal Relationship in CSME
 December 2007 Sonia Rani John et al. - IFIS 375 ORIGINAL ARTICLE OCT Assessment of the Vitreoretinal Relationship in CSME Dr. Manoj S. DNB FRCS, Dr. Unnikrishnan Nair MS DO FRCS, Dr. Gargi Sathish MS Introduction
December 2007 Sonia Rani John et al. - IFIS 375 ORIGINAL ARTICLE OCT Assessment of the Vitreoretinal Relationship in CSME Dr. Manoj S. DNB FRCS, Dr. Unnikrishnan Nair MS DO FRCS, Dr. Gargi Sathish MS Introduction
Study of 189 Cases of Diabetic Retinopathy at CMC Larkana
 Original Article Study of 189 Cases of Diabetic Retinopathy at CMC Larkana Shahid Jamal Siddiqui, Sayed Imtiaz Ali Shah, Abdul Qadir Shaikh, Mohammed Yousuf Depar, Safder Ali Abbassi Pak J Ophthalmol 2007,
Original Article Study of 189 Cases of Diabetic Retinopathy at CMC Larkana Shahid Jamal Siddiqui, Sayed Imtiaz Ali Shah, Abdul Qadir Shaikh, Mohammed Yousuf Depar, Safder Ali Abbassi Pak J Ophthalmol 2007,
The Diabetic Retinopathy Clinical Research Network. Management of DME in Eyes with PDR
 The Diabetic Retinopathy Clinical Research Network Management of DME in Eyes with PDR 1 What Has Been Learned? Diabetic Retinopathy Treatment Protocol F: Results suggest that clinically meaningful differences
The Diabetic Retinopathy Clinical Research Network Management of DME in Eyes with PDR 1 What Has Been Learned? Diabetic Retinopathy Treatment Protocol F: Results suggest that clinically meaningful differences
The Human Eye. Cornea Iris. Pupil. Lens. Retina
 The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
Diabetic Retinopathy. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Abnormalities of the retinal veins are. loops and reduplications in diabetic retinopathy. Prevalence, distribution, and pattern of development
 Venous loops and reduplications in diabetic retinopathy Prevalence, distribution, and pattern of development Toke Bek Department of Ophthalmology, Århus University Hospital, DK-8000 Århus C, Denmark ABSTRACT.
Venous loops and reduplications in diabetic retinopathy Prevalence, distribution, and pattern of development Toke Bek Department of Ophthalmology, Århus University Hospital, DK-8000 Århus C, Denmark ABSTRACT.
CLINICAL SCIENCES. Results After Lens Extraction in Patients With Diabetic Retinopathy. Early Treatment Diabetic Retinopathy Study Report Number 25
 CLINICAL SCIENCES Results After Lens Extraction in Patients With Diabetic Retinopathy Early Treatment Diabetic Retinopathy Study Report Number 25 Emily Y. Chew, MD; William E. Benson, MD; Nancy A. Remaley,
CLINICAL SCIENCES Results After Lens Extraction in Patients With Diabetic Retinopathy Early Treatment Diabetic Retinopathy Study Report Number 25 Emily Y. Chew, MD; William E. Benson, MD; Nancy A. Remaley,
A Patient s Guide to Diabetic Retinopathy
 Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Downloaded from:
 Evans, JR; Michelessi, M; Virgili, G (2014) Laser photocoagulation for proliferative diabetic retinopathy. Cochrane Database Syst Rev, 11. CD011234. ISSN 1469-493X DOI: 10.1002/14651858.CD011234.pub2 Downloaded
Evans, JR; Michelessi, M; Virgili, G (2014) Laser photocoagulation for proliferative diabetic retinopathy. Cochrane Database Syst Rev, 11. CD011234. ISSN 1469-493X DOI: 10.1002/14651858.CD011234.pub2 Downloaded
Diabetic Retinopathy Frequently Asked Questions
 Diabetic Retinopathy Frequently Asked Questions Q.Who is at risk of diabetic retinopathy? Diabetic retinopathy is a highly vascularised eye complication of both insulin dependent and non-insulin dependent
Diabetic Retinopathy Frequently Asked Questions Q.Who is at risk of diabetic retinopathy? Diabetic retinopathy is a highly vascularised eye complication of both insulin dependent and non-insulin dependent
Diabetic Management beyond traditional risk factors and LDL-C control: Can we improve macro and microvascular risks?
 Retinopathy Diabetes has a negative effect on eyes in many ways, increasing the risk of cataracts for example, but the most common and serious ocular complication of diabetes is retinopathy. Diabetic retinopathy
Retinopathy Diabetes has a negative effect on eyes in many ways, increasing the risk of cataracts for example, but the most common and serious ocular complication of diabetes is retinopathy. Diabetic retinopathy
Clinical biomicroscopy versus fluorescein angiography: Effectiveness and sensitivity in detecting diabetic retinopathy
 European Journal of Ophthalmology / Vol. 17 no. 1, 2007 / pp. 84-88 Clinical biomicroscopy versus fluorescein angiography: Effectiveness and sensitivity in detecting diabetic retinopathy S.S. KHALAF, M.D.
European Journal of Ophthalmology / Vol. 17 no. 1, 2007 / pp. 84-88 Clinical biomicroscopy versus fluorescein angiography: Effectiveness and sensitivity in detecting diabetic retinopathy S.S. KHALAF, M.D.
Progression of diabetic retinopathy after cataract extraction
 BritishlournalofOphthalmology, 1991,75,547-551 Ophthalmology Department, Kaplan Hospital, Rehovot, affiliated with the Hebrew University-Hadassah Medical School, Jerusalem, Israel A Pollock S Dotan M Oliver
BritishlournalofOphthalmology, 1991,75,547-551 Ophthalmology Department, Kaplan Hospital, Rehovot, affiliated with the Hebrew University-Hadassah Medical School, Jerusalem, Israel A Pollock S Dotan M Oliver
Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema
 Original Research Article Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema Neha Kantilal Desai 1,*, Somesh Vedprakash Aggarwal 2, Sonali
Original Research Article Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema Neha Kantilal Desai 1,*, Somesh Vedprakash Aggarwal 2, Sonali
PART 1: GENERAL RETINAL ANATOMY
 PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
Multi-spot laser coagulation with the VISULAS 532s VITE : A comparative study of 101 procedures
 Multi-spot laser coagulation with the VISULAS 532s VITE : A comparative study of 11 procedures A single-center clinical study comparing treatment workflow and patient comfort of multi-spot laser photocoagulation
Multi-spot laser coagulation with the VISULAS 532s VITE : A comparative study of 11 procedures A single-center clinical study comparing treatment workflow and patient comfort of multi-spot laser photocoagulation
INTRODUCTION. Trans Am Ophthalmol Soc 2010;108:62-76
 INTERPRETING THICKNESS CHANGES IN THE DIABETIC MACULA: THE PROBLEM OF SHORT- TERM VARIATION IN OPTICAL COHERENCE TOMOGRAPHY MEASURED MACULAR THICKENING (AN AMERICAN OPHTHALMOLOGICAL SOCIETY THESIS) BY
INTERPRETING THICKNESS CHANGES IN THE DIABETIC MACULA: THE PROBLEM OF SHORT- TERM VARIATION IN OPTICAL COHERENCE TOMOGRAPHY MEASURED MACULAR THICKENING (AN AMERICAN OPHTHALMOLOGICAL SOCIETY THESIS) BY
Diabetes mellitus: A risk factor affecting visual outcome in branch retinal vein occlusion
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 648-652 Diabetes mellitus: A risk factor affecting visual outcome in branch retinal vein occlusion J. SWART 1,2, J.W. REICHERT-THOEN 1, M.S.
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 648-652 Diabetes mellitus: A risk factor affecting visual outcome in branch retinal vein occlusion J. SWART 1,2, J.W. REICHERT-THOEN 1, M.S.
Clinically Significant Macular Edema (CSME)
 Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Diabetes, particularly diabetic retinopathy, is
 Chapter 14 Vision Disorders in Diabetes Ronald Klein, MD, MPH, and Barbara E.K. Klein, MD, MPH SUMMARY Diabetes, particularly diabetic retinopathy, is the leading cause of new cases of blindness in people
Chapter 14 Vision Disorders in Diabetes Ronald Klein, MD, MPH, and Barbara E.K. Klein, MD, MPH SUMMARY Diabetes, particularly diabetic retinopathy, is the leading cause of new cases of blindness in people
Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and
 British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
Effects of an Intravitreal Bevacizumab Injection Combined With Panretinal Photocoagulation on High-Risk Proliferative Diabetic Retinopathy
 Korean Journal of Ophthalmology 2009;23:266-272 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.4.266 Effects of an Intravitreal Bevacizumab Injection Combined With Panretinal Photocoagulation on High-Risk
Korean Journal of Ophthalmology 2009;23:266-272 ISSN : 1011-8942 DOI : 10.3341/kjo.2009.23.4.266 Effects of an Intravitreal Bevacizumab Injection Combined With Panretinal Photocoagulation on High-Risk
Clinical Trials in Diabetic Retinopathy. Harry W. Flynn Jr., M.D. Nidhi Relhan Batra, M.D.
 1 Clinical Trials in Diabetic Retinopathy 2018 Harry W. Flynn Jr., M.D. Nidhi Relhan Batra, M.D. Bascom Palmer Eye Institute 900 N.W. 17th Street Miami, FL 33136 Phone: (305) 326-6118 Fax: (305) 326-6417
1 Clinical Trials in Diabetic Retinopathy 2018 Harry W. Flynn Jr., M.D. Nidhi Relhan Batra, M.D. Bascom Palmer Eye Institute 900 N.W. 17th Street Miami, FL 33136 Phone: (305) 326-6118 Fax: (305) 326-6417
In its initial report, the Early Treatment Diabetic Retinopathy. A Severity Scale for Diabetic Macular Edema Developed from ETDRS Data
 A Severity Scale for Diabetic Macular Edema Developed from ETDRS Data Ronald E. Gangnon, 1,2 Matthew D. Davis, 3 Larry D. Hubbard, 3 Lloyd M. Aiello, 4 Emily Y. Chew, 5 Frederick L. Ferris III, 5 Marian
A Severity Scale for Diabetic Macular Edema Developed from ETDRS Data Ronald E. Gangnon, 1,2 Matthew D. Davis, 3 Larry D. Hubbard, 3 Lloyd M. Aiello, 4 Emily Y. Chew, 5 Frederick L. Ferris III, 5 Marian
Retinopathy in a diabetic population
 Kathmandu University Medical Journal (2007), Vol. 5, No. 2, Issue 18, 204-209 Retinopathy in a diabetic population Shrestha S 1, Malla OK 2, Karki DB 3, Byanju RN 4 2 Fellow of NAMS, 3 Professor, NAMS,
Kathmandu University Medical Journal (2007), Vol. 5, No. 2, Issue 18, 204-209 Retinopathy in a diabetic population Shrestha S 1, Malla OK 2, Karki DB 3, Byanju RN 4 2 Fellow of NAMS, 3 Professor, NAMS,
Brampton Hurontario Street Brampton, ON L6Y 0P6
 Diabetic Retinopathy What is Diabetic Retinopathy Diabetic retinopathy is one of the leading causes of blindness world-wide. Diabetes damages blood vessels in many organs of the body including the eyes.
Diabetic Retinopathy What is Diabetic Retinopathy Diabetic retinopathy is one of the leading causes of blindness world-wide. Diabetes damages blood vessels in many organs of the body including the eyes.
Andrew J. Barkmeier, MD; Benjamin P. Nicholson, MA; Levent Akduman, MD
 c l i n i c a l s c i e n c e Effectiveness of Laser Photocoagulation in Clinically Significant Macular Edema With Focal Versus Diffuse Parafoveal Thickening on Optical Coherence Tomography Andrew J. Barkmeier,
c l i n i c a l s c i e n c e Effectiveness of Laser Photocoagulation in Clinically Significant Macular Edema With Focal Versus Diffuse Parafoveal Thickening on Optical Coherence Tomography Andrew J. Barkmeier,
Diabetic Retinopathy A Presentation for the Public
 Diabetic Retinopathy A Presentation for the Public Ray M. Balyeat, MD The Eye Institute Tulsa, Oklahoma The Healthy Eye Light rays enter the eye through the cornea, pupil and lens. These light rays are
Diabetic Retinopathy A Presentation for the Public Ray M. Balyeat, MD The Eye Institute Tulsa, Oklahoma The Healthy Eye Light rays enter the eye through the cornea, pupil and lens. These light rays are
VISUAL OUTCOME IN DIABETIC MACULAR EDEMA AFTER GRID LASER TREATMENT
 The Professional Medical Journal DOI: 10.17957/TPMJ/16.2856 ORIGINAL PROF-2856 VISUAL OUTCOME IN DIABETIC MACULAR EDEMA AFTER GRID LASER TREATMENT 1. MBBS.FCPS Assistant Professor Ophthalmology Independent
The Professional Medical Journal DOI: 10.17957/TPMJ/16.2856 ORIGINAL PROF-2856 VISUAL OUTCOME IN DIABETIC MACULAR EDEMA AFTER GRID LASER TREATMENT 1. MBBS.FCPS Assistant Professor Ophthalmology Independent
MANAGING DIABETIC RETINOPATHY. <Your Hospital Name> <Your Logo>
 MANAGING DIABETIC RETINOPATHY It s difficult living with Diabetes Mellitus. Ask any diabetic... Their lives are centered around meal plans, glucose levels, and insulin
MANAGING DIABETIC RETINOPATHY It s difficult living with Diabetes Mellitus. Ask any diabetic... Their lives are centered around meal plans, glucose levels, and insulin
04/06/2015. Documentation Do s and Don ts In The Retina Practice. Financial Disclosure. Documentation Dos and Don ts
 Documentation Do s and Don ts In The Retina Practice William T. Koch, COA, COE, CPC Administrative Director Director of Billing Operations The Retina Institute St. Louis, Missouri Advisory Boards Allergan
Documentation Do s and Don ts In The Retina Practice William T. Koch, COA, COE, CPC Administrative Director Director of Billing Operations The Retina Institute St. Louis, Missouri Advisory Boards Allergan
Diabetic Retinopathy Screening in Hong Kong. Dr. Rita Gangwani M.S, FRCS (Ophth), FCOphth(HK), FHKAM Eye Institute, The University of Hong Kong
 Diabetic Retinopathy Screening in Hong Kong Dr. Rita Gangwani M.S, FRCS (Ophth), FCOphth(HK), FHKAM Eye Institute, The University of Hong Kong Co-Investigators Prof. David Wong Prof. Sarah McGhee Dr. Wico
Diabetic Retinopathy Screening in Hong Kong Dr. Rita Gangwani M.S, FRCS (Ophth), FCOphth(HK), FHKAM Eye Institute, The University of Hong Kong Co-Investigators Prof. David Wong Prof. Sarah McGhee Dr. Wico
The retinal renin-angiotensin system: implications for therapy in diabetic retinopathy
 (2002) 16, S42 S46 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh : implications for therapy in diabetic retinopathy AK Sjølie 1 and N Chaturvedi 2 1 Department
(2002) 16, S42 S46 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh : implications for therapy in diabetic retinopathy AK Sjølie 1 and N Chaturvedi 2 1 Department
Diabetic retinopathy damage to the blood vessels in the retina. Cataract clouding of the eye s lens. Cataracts develop at an earlier age in people
 Diabetic Retinopathy What is diabetic eye disease? Diabetic eye disease refers to a group of eye problems that people with diabetes may face as a complication of diabetes. All can cause severe vision loss
Diabetic Retinopathy What is diabetic eye disease? Diabetic eye disease refers to a group of eye problems that people with diabetes may face as a complication of diabetes. All can cause severe vision loss
Preparing for laser treatment for diabetic retinopathy and maculopathy
 Preparing for laser treatment for diabetic retinopathy and maculopathy Information for patients Preparing for laser treatment for diabetic retinopathy and maculopathy. This leaflet sets out to answer the
Preparing for laser treatment for diabetic retinopathy and maculopathy Information for patients Preparing for laser treatment for diabetic retinopathy and maculopathy. This leaflet sets out to answer the
A Study on Multi Stages of Diabetic Retinopathy among Diabetic Patients in Puducherry - Using Markov Chain Model Approach
 Advances in Applied Mathematical Biosciences. ISSN 2248-9983 Volume 3, Number 1 (2012), pp. 49-55 International Research Publication House http://www.irphouse.com A Study on Multi Stages of Diabetic Retinopathy
Advances in Applied Mathematical Biosciences. ISSN 2248-9983 Volume 3, Number 1 (2012), pp. 49-55 International Research Publication House http://www.irphouse.com A Study on Multi Stages of Diabetic Retinopathy
 measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
Diabetic Retinopathy
 Diabetic Retinopathy Overview This presentation covers the following topics: Definitions Epidemiology of diabetic retinopathy Evidence for public health approaches Screening for diabetic retinopathy Health
Diabetic Retinopathy Overview This presentation covers the following topics: Definitions Epidemiology of diabetic retinopathy Evidence for public health approaches Screening for diabetic retinopathy Health
Facts About Diabetic Eye Disease
 Facts About Diabetic Eye Disease Points to Remember 1. Diabetic eye disease comprises a group of eye conditions that affect people with diabetes. These conditions include diabetic retinopathy, diabetic
Facts About Diabetic Eye Disease Points to Remember 1. Diabetic eye disease comprises a group of eye conditions that affect people with diabetes. These conditions include diabetic retinopathy, diabetic
Longitudinal study of a cohort of people with diabetes screened by the Exeter Diabetic Retinopathy Screening Programme
 (2002) 16, 140 145 2002 Nature Publishing Group All rights reserved 1470-269X/02 $25.00 www.nature.com/eye CLINICAL STUDY Longitudinal study of a cohort of people with diabetes screened by the Exeter Diabetic
(2002) 16, 140 145 2002 Nature Publishing Group All rights reserved 1470-269X/02 $25.00 www.nature.com/eye CLINICAL STUDY Longitudinal study of a cohort of people with diabetes screened by the Exeter Diabetic
Diabetes Care 24: , 2001
 Pathophysiology/Complications O R I G I N A L A R T I C L E Prevalence and Significance of Retinopathy in Subjects With Type 1 Diabetes of Less Than 5 Years Duration Screened for the Diabetes Control and
Pathophysiology/Complications O R I G I N A L A R T I C L E Prevalence and Significance of Retinopathy in Subjects With Type 1 Diabetes of Less Than 5 Years Duration Screened for the Diabetes Control and
JMSCR Vol. 03 Issue 08 Page August 2015
 www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x DOI: http://dx.doi.org/10.18535/jmscr/v3i8.05 Study of Prevalence of Diabetic Retinopathy in Already Confirmed Diabetic Patients Who Were
www.jmscr.igmpublication.org Impact Factor 3.79 ISSN (e)-2347-176x DOI: http://dx.doi.org/10.18535/jmscr/v3i8.05 Study of Prevalence of Diabetic Retinopathy in Already Confirmed Diabetic Patients Who Were
Tuberous sclerosis presenting as atypical aggressive retinal astrocytoma with proliferative retinopathy and vitreous haemorrhage
 Case Report Brunei Int Med J. 2015; 11 (1): 49-53 Tuberous sclerosis presenting as atypical aggressive retinal astrocytoma with proliferative retinopathy and vitreous haemorrhage Pui Ling TANG and Mae-Lynn
Case Report Brunei Int Med J. 2015; 11 (1): 49-53 Tuberous sclerosis presenting as atypical aggressive retinal astrocytoma with proliferative retinopathy and vitreous haemorrhage Pui Ling TANG and Mae-Lynn
N lar complication of diabetes mellitus. Diabetic iris neovascularization. Natural history and treatment. Subjects and Methods
 Diabetic iris neovascularization. Natural history and treatment Jose FernandezVigo, Juan Castro and Ana Macarro Department of Ophthalmology, School of Medicine, University of Extremadura, Spain ABSTRACT.
Diabetic iris neovascularization. Natural history and treatment Jose FernandezVigo, Juan Castro and Ana Macarro Department of Ophthalmology, School of Medicine, University of Extremadura, Spain ABSTRACT.
Diabetic Retinopathy
 Diabetic Retinopathy Diabetes can be classified into type 1 diabetes mellitus and type 2 diabetes mellitus, formerly known as insulin-dependent diabetes mellitus, and non-insulin diabetes mellitus, respectively.
Diabetic Retinopathy Diabetes can be classified into type 1 diabetes mellitus and type 2 diabetes mellitus, formerly known as insulin-dependent diabetes mellitus, and non-insulin diabetes mellitus, respectively.
Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient
 Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient Rova Virgana FK Unpad Pusat Mata Nasional RS Mata Cicendo Bandung Eye Center (Hospital and Clinic) PIT IDI Jabar 2018 Keys Facts from WHO
Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient Rova Virgana FK Unpad Pusat Mata Nasional RS Mata Cicendo Bandung Eye Center (Hospital and Clinic) PIT IDI Jabar 2018 Keys Facts from WHO
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Multivariate Analysis of Intravitreal Injection of Anti-VEGF Bevacizumab in the Treatment
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Multivariate Analysis of Intravitreal Injection of Anti-VEGF Bevacizumab in the Treatment
Diabetic Retinopathy What You Should Know. U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health National Eye Institute
 Diabetic Retinopathy What You Should Know U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health National Eye Institute The National Eye Institute (NEI) conducts and supports research
Diabetic Retinopathy What You Should Know U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health National Eye Institute The National Eye Institute (NEI) conducts and supports research
Diabetic Retinopathy: Managing the Extremes. J. Michael Jumper, MD West Coast Retina
 Diabetic Retinopathy: Managing the Extremes J. Michael Jumper, MD West Coast Retina Case 1: EC 65 y.o. HM No vision complaints Meds: Glyburide Metformin Pioglitazone Va: 20/20 OU 20/20 Case 2: HS 68 y.o.
Diabetic Retinopathy: Managing the Extremes J. Michael Jumper, MD West Coast Retina Case 1: EC 65 y.o. HM No vision complaints Meds: Glyburide Metformin Pioglitazone Va: 20/20 OU 20/20 Case 2: HS 68 y.o.
Diabetic Retinopathy WHAT IS DIABETIC RETINOPATHY? WHAT CAUSES DIABETIC RETINOPATHY? WHAT ARE THE STAGES OF DIABETIC RETINOPATHY?
 Diabetic Retinopathy WHAT IS DIABETIC RETINOPATHY? Diabetic retinopathy affects 8 million Americans with diabetes. A leading cause of blindness in American adults, it is caused by damage to the small blood
Diabetic Retinopathy WHAT IS DIABETIC RETINOPATHY? Diabetic retinopathy affects 8 million Americans with diabetes. A leading cause of blindness in American adults, it is caused by damage to the small blood
Diabetic Retinopatathy
 Diabetic Retinopatathy Jay M. Haynie, OD, FAAO Financial Disclosure I have received honoraria or am on the advisory board for the following companies: Carl Zeiss Meditec Arctic DX Macula Risk Advanced
Diabetic Retinopatathy Jay M. Haynie, OD, FAAO Financial Disclosure I have received honoraria or am on the advisory board for the following companies: Carl Zeiss Meditec Arctic DX Macula Risk Advanced
Measures have been taken, by the Utah Department of Health, Bureau of Health Promotions, to ensure no conflict of interest in this activity.
 Measures have been taken, by the Utah Department of Health, Bureau of Health Promotions, to ensure no conflict of interest in this activity. CNE/CPE/CEU s are available for this live webinar. You must
Measures have been taken, by the Utah Department of Health, Bureau of Health Promotions, to ensure no conflict of interest in this activity. CNE/CPE/CEU s are available for this live webinar. You must
MAGNITUDE OF DIABETIC EYE DISEASE IN INDIA
 Dear Doctor This booklet contains information about your role as a physician in preventing blindness in your diabetic patients. You are the first point of contact for your diabetic patients. You see them
Dear Doctor This booklet contains information about your role as a physician in preventing blindness in your diabetic patients. You are the first point of contact for your diabetic patients. You see them
Diabetic Retinopathy Clinical Research Network
 Diabetic Retinopathy Clinical Research Network Prompt Panretinal Photocoagulation Versus Intravitreal Ranibizumab with Deferred Panretinal Photocoagulation for Proliferative Diabetic Retinopathy (Protocol
Diabetic Retinopathy Clinical Research Network Prompt Panretinal Photocoagulation Versus Intravitreal Ranibizumab with Deferred Panretinal Photocoagulation for Proliferative Diabetic Retinopathy (Protocol
Widefield Retinal Imaging with Auto Fluorescence Technology in the Optometric Practice
 Widefield Retinal Imaging with Auto Fluorescence Technology in the Optometric Practice This course will define ultra-widefield retinal imaging and autofluorescence for the attendee. Will show how it is
Widefield Retinal Imaging with Auto Fluorescence Technology in the Optometric Practice This course will define ultra-widefield retinal imaging and autofluorescence for the attendee. Will show how it is
Use of Scanning Laser Ophthalmoscope Microperimetry in Clinically Significant Macular Edema in Type 2 Diabetes Mellitus
 Use of Scanning Laser Ophthalmoscope Microperimetry in Clinically Significant Macular Edema in Type 2 Diabetes Mellitus Fumihiko Mori, Satoshi Ishiko, Norihiko Kitaya, Taiichi Hikichi, Eiichi Sato, Akira
Use of Scanning Laser Ophthalmoscope Microperimetry in Clinically Significant Macular Edema in Type 2 Diabetes Mellitus Fumihiko Mori, Satoshi Ishiko, Norihiko Kitaya, Taiichi Hikichi, Eiichi Sato, Akira
Diabetologia 9 by Springer-Verlag 1978
 Diabetologia 15, 105-111 (1978) Diabetologia 9 by Springer-Verlag 1978 Diabetic Retinopathy and Pregnancy J. Cassar, Eva M. Kohner, A. M. Hamilton, H. Gordon 1, and G. F. Joplin The Endocrine Unit and
Diabetologia 15, 105-111 (1978) Diabetologia 9 by Springer-Verlag 1978 Diabetic Retinopathy and Pregnancy J. Cassar, Eva M. Kohner, A. M. Hamilton, H. Gordon 1, and G. F. Joplin The Endocrine Unit and
Medical Retina 2011 Nicholas Lee
 Medical Retina 2011 Nicholas Lee 1 Diabetic Retinopathy Epidemiology 1000 registered blind each year 2% diabetics registered as blind (8% of all Blind Registrations) 42% with Mild Background DR will progress
Medical Retina 2011 Nicholas Lee 1 Diabetic Retinopathy Epidemiology 1000 registered blind each year 2% diabetics registered as blind (8% of all Blind Registrations) 42% with Mild Background DR will progress
Use of Eye Care Services among Type 2 Diabetic Patients in Laguna
 Original Article Philippine Journal of OPHTHALMOLOGY Use of Eye Care Services among Type 2 Diabetic Patients in Laguna Glenn Carandang, MD, MPH, 1,2, Maria Victoria Rondaris, MD, MPH, 3, and Genejane Adarlo,
Original Article Philippine Journal of OPHTHALMOLOGY Use of Eye Care Services among Type 2 Diabetic Patients in Laguna Glenn Carandang, MD, MPH, 1,2, Maria Victoria Rondaris, MD, MPH, 3, and Genejane Adarlo,
Marcus Gonzales, OD, FAAO Cedar Springs Eye Clinic
 Marcus Gonzales, OD, FAAO Cedar Springs Eye Clinic 25.6 million adults 11.3% of the adult population 10.9 million adults 65 years and older 26.9% of this age population 79 million people are Pre-diabetic!!
Marcus Gonzales, OD, FAAO Cedar Springs Eye Clinic 25.6 million adults 11.3% of the adult population 10.9 million adults 65 years and older 26.9% of this age population 79 million people are Pre-diabetic!!
PROGRESSION OF DIABETIC RETINOPATHY FOLLOWING CATARACT SURGERY
 PROGRESSION OF DIABETIC RETINOPATHY FOLLOWING CATARACT SURGERY Yayan Heryanto, Iwan Sovani, Arief Kartasasmita, Erwin Iskandar, Djonggi Panggabean. Dept. of Ophthalmology Medical Faculty Unpad, Cicendo
PROGRESSION OF DIABETIC RETINOPATHY FOLLOWING CATARACT SURGERY Yayan Heryanto, Iwan Sovani, Arief Kartasasmita, Erwin Iskandar, Djonggi Panggabean. Dept. of Ophthalmology Medical Faculty Unpad, Cicendo
Diabetic Eye Disease
 Manchester Royal Eye Hospital Medical Retinal Services Information for Patients Diabetic Eye Disease This leaflet sets out to answer some of your questions about diabetic eye disease. You may wish to discuss
Manchester Royal Eye Hospital Medical Retinal Services Information for Patients Diabetic Eye Disease This leaflet sets out to answer some of your questions about diabetic eye disease. You may wish to discuss
Study of correlation of severity of diabetic retinopathy with levels of haemogloelbin A1c in patients with type II Diabetes Mellitus
 Original article: Study of correlation of severity of diabetic retinopathy with levels of haemogloelbin A1c in patients with type II Diabetes Mellitus 1Dr Apoorva*, 2 Dr Sabhia Jan 1Senior Resident, 2
Original article: Study of correlation of severity of diabetic retinopathy with levels of haemogloelbin A1c in patients with type II Diabetes Mellitus 1Dr Apoorva*, 2 Dr Sabhia Jan 1Senior Resident, 2
THE ROLE OF anti-vegf IN DIABETIC RETINOPATHY AND AGE RELATED MACULAR DEGENERATION
 THE ROLE OF anti-vegf IN DIABETIC RETINOPATHY AND AGE RELATED MACULAR DEGENERATION MOESTIDJAB DEPARTMENT OF OPHTHALMOLOGY SCHOOL OF MEDICINE AIRLANGGA UNIVERSITY DR SOETOMO HOSPITAL SURABAYA INTRODUCTION
THE ROLE OF anti-vegf IN DIABETIC RETINOPATHY AND AGE RELATED MACULAR DEGENERATION MOESTIDJAB DEPARTMENT OF OPHTHALMOLOGY SCHOOL OF MEDICINE AIRLANGGA UNIVERSITY DR SOETOMO HOSPITAL SURABAYA INTRODUCTION
Preoperative Electroretinogram and Postoperative Visual Outcome in Patients with Diabetic Vitreous Hemorrhage
 Preoperative Electroretinogram and Postoperative Visual Outcome in Patients with Diabetic Vitreous Hemorrhage Takashi Hiraiwa*, Naoichi Horio*, Hiroko Terasaki*, Toshimitsu Suzuki*, Etsuko Yamamoto*, Masayuki
Preoperative Electroretinogram and Postoperative Visual Outcome in Patients with Diabetic Vitreous Hemorrhage Takashi Hiraiwa*, Naoichi Horio*, Hiroko Terasaki*, Toshimitsu Suzuki*, Etsuko Yamamoto*, Masayuki
Accidental foveal burn following pan retinal photocoagulation and its long-term outcome
 www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Accidental foveal burn following pan retinal photocoagulation and its long-term outcome Khan Perwez, Pandey Kankambari, Khan Lubna, Saxena
www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Accidental foveal burn following pan retinal photocoagulation and its long-term outcome Khan Perwez, Pandey Kankambari, Khan Lubna, Saxena
The beneficial effects of focal photocoagulation for clinically
 Retinal Function in Diabetic Macular Edema after Focal Laser Photocoagulation Vivienne C. Greenstein, 1 Haifan Chen, 1 Donald C. Hood, 2 Karen Holopigian, 1 William Seiple, 1 and Ronald E. Carr 1 PURPOSE.
Retinal Function in Diabetic Macular Edema after Focal Laser Photocoagulation Vivienne C. Greenstein, 1 Haifan Chen, 1 Donald C. Hood, 2 Karen Holopigian, 1 William Seiple, 1 and Ronald E. Carr 1 PURPOSE.
Central Mersey Diabetic Retinopathy Screening Programme. Referring patients for Diabetic Retinopathy Screening
 Central Mersey Diabetic Retinopathy Screening Programme Referring patients for Diabetic Retinopathy Screening Information for GPs in Halton & St Helens, Knowsley and Warrington PCT Version: June 2008 Review
Central Mersey Diabetic Retinopathy Screening Programme Referring patients for Diabetic Retinopathy Screening Information for GPs in Halton & St Helens, Knowsley and Warrington PCT Version: June 2008 Review
Diabetic Retinopathy Clinical Research Network
 Diabetic Retinopathy Clinical Research Network An Observational Study of the Development of Diabetic Macular Edema Following Scatter Laser Photocoagulation Version 1.4 June 24, 2005 PRP Obs Study Protocol
Diabetic Retinopathy Clinical Research Network An Observational Study of the Development of Diabetic Macular Edema Following Scatter Laser Photocoagulation Version 1.4 June 24, 2005 PRP Obs Study Protocol
CHAPTER 8 EVALUATION OF FUNDUS IMAGE ANALYSIS SYSTEM
 CHAPTER 8 EVALUATION OF FUNDUS IMAGE ANALYSIS SYSTEM Diabetic retinopathy is very common retinal disease associated with diabetes. Efforts to prevent diabetic retinopathy though have yielded some results;
CHAPTER 8 EVALUATION OF FUNDUS IMAGE ANALYSIS SYSTEM Diabetic retinopathy is very common retinal disease associated with diabetes. Efforts to prevent diabetic retinopathy though have yielded some results;
04/11/2014. Retina Coding and Reimbursement 101. Financial Disclosure. Chief Complaint
 Retina Coding and Reimbursement 101 William T. Koch, COA, COE, CPC Administrative Director Director of Billing Operations The Retina Institute St. Louis, Missouri Advisory Boards Allergan Genentech Regeneron
Retina Coding and Reimbursement 101 William T. Koch, COA, COE, CPC Administrative Director Director of Billing Operations The Retina Institute St. Louis, Missouri Advisory Boards Allergan Genentech Regeneron
Treatment of Diabetic Macular Edema without Intravitreal injections
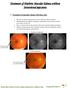 Treatment of Diabetic Macular Edema without Intravitreal injections 1. Treatment of macular edema with laser only This 60 year old female presented on 02-01-2007 for retinal evaluation. She had proliferative
Treatment of Diabetic Macular Edema without Intravitreal injections 1. Treatment of macular edema with laser only This 60 year old female presented on 02-01-2007 for retinal evaluation. She had proliferative
Original Policy Date
 MP 9.03.08 Photocoagulation of Macular Drusen Medical Policy Section Miscellaneous Policies Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return
MP 9.03.08 Photocoagulation of Macular Drusen Medical Policy Section Miscellaneous Policies Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return
Appropriate Statistical Methods to Account for Similarities in Binary Outcomes Between Fellow Eyes
 Appropriate Statistical Methods to Account for Similarities in Binary Outcomes Between Fellow Eyes Joanne Katz,* Scott Zeger,-\ and Kung-Yee Liangf Purpose. Many ocular measurements are more alike between
Appropriate Statistical Methods to Account for Similarities in Binary Outcomes Between Fellow Eyes Joanne Katz,* Scott Zeger,-\ and Kung-Yee Liangf Purpose. Many ocular measurements are more alike between
Macular function assessed with mferg before and after panretinal photocoagulation in patients with proliferative diabetic retinopathy.
 Macular function assessed with mferg before and after panretinal photocoagulation in patients with proliferative diabetic retinopathy. Lövestam Adrian, Monica; Andréasson, Sten; Ponjavic, Vesna Published
Macular function assessed with mferg before and after panretinal photocoagulation in patients with proliferative diabetic retinopathy. Lövestam Adrian, Monica; Andréasson, Sten; Ponjavic, Vesna Published
CENTENE PHARMACY AND THERAPEUTICS NEW DRUG REVIEW 2Q17 April May
 BRAND NAME Lucentis GENERIC NAME ranibizumab MANUFACTURER Genentech, Inc. DATE OF APPROVAL June 30, 2006 PRODUCT LAUNCH DATE July 13, 2006 REVIEW TYPE Review type 1 (RT1): New Drug Review Full review of
BRAND NAME Lucentis GENERIC NAME ranibizumab MANUFACTURER Genentech, Inc. DATE OF APPROVAL June 30, 2006 PRODUCT LAUNCH DATE July 13, 2006 REVIEW TYPE Review type 1 (RT1): New Drug Review Full review of
Understanding Diabetic Retinopathy
 Understanding Diabetic Retinopathy What Is Diabetic Retinopathy? Diabetes damages blood vessels in the rear of the eye. This condition is called diabetic retinopathy. It can lead to vision loss or blindness.
Understanding Diabetic Retinopathy What Is Diabetic Retinopathy? Diabetes damages blood vessels in the rear of the eye. This condition is called diabetic retinopathy. It can lead to vision loss or blindness.
Predictors of postoperative bleeding after vitrectomy for vitreous hemorrhage in patients with diabetic retinopathy
 ORIGINAL ARTICLE Predictors of postoperative bleeding after vitrectomy for vitreous hemorrhage in patients with diabetic retinopathy Saori Motoda 1, Nobuhiko Shiraki 2, Takuma Ishihara 3, Hirokazu Sakaguchi
ORIGINAL ARTICLE Predictors of postoperative bleeding after vitrectomy for vitreous hemorrhage in patients with diabetic retinopathy Saori Motoda 1, Nobuhiko Shiraki 2, Takuma Ishihara 3, Hirokazu Sakaguchi
When is eye screening performed
 Why is a regular ophthalmological exam critical in VHL Screening Department of Ophthalmology, University of South Florida VHLA Family Meeting in Tampa 2017 Screening is the testing of individuals at risk
Why is a regular ophthalmological exam critical in VHL Screening Department of Ophthalmology, University of South Florida VHLA Family Meeting in Tampa 2017 Screening is the testing of individuals at risk
CONDITIONAL REGRESSION MODELS TRANSIENT STATE SURVIVAL ANALYSIS
 CONDITIONAL REGRESSION MODELS FOR TRANSIENT STATE SURVIVAL ANALYSIS Robert D. Abbott Field Studies Branch National Heart, Lung and Blood Institute National Institutes of Health Raymond J. Carroll Department
CONDITIONAL REGRESSION MODELS FOR TRANSIENT STATE SURVIVAL ANALYSIS Robert D. Abbott Field Studies Branch National Heart, Lung and Blood Institute National Institutes of Health Raymond J. Carroll Department
Diabetic Learning Event: Diabetic Eye Screening and Retinopathy- Samantha Mann & Mark Frost
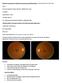 Diabetic Learning Event: Diabetic Eye Screening and Retinopathy- Samantha Mann & Mark Frost Case 1 : 63 yr-old Caucasian woman with type-2 Diabetes for 8 years Ex-smoker Hypertension- 5 years FH: father
Diabetic Learning Event: Diabetic Eye Screening and Retinopathy- Samantha Mann & Mark Frost Case 1 : 63 yr-old Caucasian woman with type-2 Diabetes for 8 years Ex-smoker Hypertension- 5 years FH: father
Risk Factors for High-Risk Proliferative Diabetic Retinopathy and Severe Visual Loss: Early Treatment Diabetic Retinopathy Study Report #18
 Risk Factors for High-Risk Proliferative Diabetic Retinopathy and Severe Visual Loss: Early Treatment Diabetic Retinopathy Study Report #18 Matthew D. Davis, 1 Marian R. Fisher, 1 Ronald E. Gangnon, 1
Risk Factors for High-Risk Proliferative Diabetic Retinopathy and Severe Visual Loss: Early Treatment Diabetic Retinopathy Study Report #18 Matthew D. Davis, 1 Marian R. Fisher, 1 Ronald E. Gangnon, 1
Retinal photocoagulation for proliferative sickle cell retinopathy: A prospective clinical trial with new sea fan classification
 European Journal of Ophthalmology / Vol. 18 no. 2, 2008 / pp. 248-254 Retinal photocoagulation for proliferative sickle cell retinopathy: A prospective clinical trial with new sea fan classification D.
European Journal of Ophthalmology / Vol. 18 no. 2, 2008 / pp. 248-254 Retinal photocoagulation for proliferative sickle cell retinopathy: A prospective clinical trial with new sea fan classification D.
Treatment of diabetic maculopathy by
 Brit. J. Ophthal. (1974) 58, 85 Treatment of diabetic maculopathy by argon-laser S. MERIN, L. YANKO, AND M. IVRY From the Department of Ophthalmology, Hadassah University Hospital, Jerusalem, Israel Diabetic
Brit. J. Ophthal. (1974) 58, 85 Treatment of diabetic maculopathy by argon-laser S. MERIN, L. YANKO, AND M. IVRY From the Department of Ophthalmology, Hadassah University Hospital, Jerusalem, Israel Diabetic
Jay M. Haynie, O.D.; F.A.A.O. Olympia Tacoma Renton Kennewick Washington
 Jay M. Haynie, O.D.; F.A.A.O. Olympia Tacoma Renton Kennewick Washington I Jay M. Haynie, OD, FAAO have received honoraria from the following companies: Reichert Technologies Notal Vision Carl Zeiss Meditec
Jay M. Haynie, O.D.; F.A.A.O. Olympia Tacoma Renton Kennewick Washington I Jay M. Haynie, OD, FAAO have received honoraria from the following companies: Reichert Technologies Notal Vision Carl Zeiss Meditec
Retinal pigment epithelial detachments in the elderly:
 British Journal of Ophthalmology, 1985, 69, 397-403 Retinal pigment epithelial detachments in the elderly: classification and outcome A G CASSWELL, D KOHEN, AND A C BIRD From Moorfields Eye Hospital, City
British Journal of Ophthalmology, 1985, 69, 397-403 Retinal pigment epithelial detachments in the elderly: classification and outcome A G CASSWELL, D KOHEN, AND A C BIRD From Moorfields Eye Hospital, City
Andalusian Programme for Diabetes
 Andalusian Programme for Diabetes Diabetic Retinopathy Screening Programme in Andalusia Francisco José Sánchez Laguna MSc Health Informatics Diabetic Retinopathy High prevalence. Socioeconomic impact.
Andalusian Programme for Diabetes Diabetic Retinopathy Screening Programme in Andalusia Francisco José Sánchez Laguna MSc Health Informatics Diabetic Retinopathy High prevalence. Socioeconomic impact.
Front Line Diabetic Retinopathy What Not to Miss and Why
 Front Line Diabetic Retinopathy What Not to Miss and Why David M Brown MD FACS Clinical Professor of Ophthalmology Blanton Eye Institute, Houston Methodist Hospital Baylor College of Medicine Retina Consultants
Front Line Diabetic Retinopathy What Not to Miss and Why David M Brown MD FACS Clinical Professor of Ophthalmology Blanton Eye Institute, Houston Methodist Hospital Baylor College of Medicine Retina Consultants
Spatial distribution of early red lesions is a risk factor for development of vision-threatening diabetic retinopathy
 Diabetologia (2017) 60:2361 2367 DOI 10.1007/s00125-017-4424-y ARTICLE Spatial distribution of early red lesions is a risk factor for development of vision-threatening diabetic retinopathy Giovanni Ometto
Diabetologia (2017) 60:2361 2367 DOI 10.1007/s00125-017-4424-y ARTICLE Spatial distribution of early red lesions is a risk factor for development of vision-threatening diabetic retinopathy Giovanni Ometto
