Application of the Oral Minimal Model to Korean Subjects with Normal Glucose Tolerance and Type 2 Diabetes Mellitus
|
|
|
- Eunice McKenzie
- 6 years ago
- Views:
Transcription
1 Original Article Others Diabetes Metab J 216;4: pissn eissn DIABETES & METABOLISM JOURNAL Application of the Oral Minimal Model to Korean Subjects with Normal Glucose Tolerance and Type 2 Diabetes Mellitus Min Hyuk Lim 1, Tae Jung Oh 2, Karam Choi 3, Jung Chan Lee 1, Young Min Cho 2, Sungwan Kim 1 Departments of 1 Biomedical Engineering, 2 Internal Medicine, Seoul National University College of Medicine, Seoul, 3 Interdisciplinary Program of Bioengineering, Seoul National University College of Engineering, Seoul, Korea Background: The oral minimal model is a simple, useful tool for the assessment of β-cell function and insulin sensitivity across the spectrum of glucose tolerance, including normal glucose tolerance (), prediabetes, and type 2 diabetes mellitus () in humans. Methods: Plasma glucose, insulin, and C-peptide levels were measured during a 18-minute, 7-g oral glucose tolerance test in 24 Korean subjects with (n=1) and (n=14). The parameters in the computational model were estimated, and the indexes for insulin sensitivity and β-cell function were compared between the and groups. Results: The insulin sensitivity index was lower in the group than the group. The basal index of β-cell responsivity, basal hepatic insulin extraction ratio, and post-glucose challenge hepatic insulin extraction ratio were not different between the and groups. The dynamic, static, and total β-cell responsivity indexes were significantly lower in the group than the group. The dynamic, static, and total disposition indexes were also significantly lower in the group than the group. Conclusion: The oral minimal model can be reproducibly applied to evaluate β-cell function and insulin sensitivity in Koreans. Keywords: Computational method; Disposition index; Glucose tolerance test; Insulin resistance; Oral minimal model; Responsivity index INTRODUCTION The pathophysiology of type 2 diabetes mellitus (), a representative multifactorial disease, is very complex and encompasses decreased β-cell function, unsuppressed α-cell overactivity, increased hepatic glucose production, decreased glucose uptake in the skeletal muscle, increased lipolysis in the adipose tissue, decreased effect of incretin hormones, increased renal glucose reabsorption, and neurotransmitter abnormality [1]. Despite the highly complex nature of glucose homeostasis, there have been continuous efforts to build mathematical models for glucose metabolism using biological variables to predict glucose and insulin responses [2-6]. However, some efforts to adjust numerous variables resulted in an overfitting problem [7]. In this regard, Bergman s minimal model merits by requiring minimal numbers of parameters to estimate β-cell function and insulin sensitivity [8]. Two types of minimal models for the assessment of β-cell Corresponding authors: Sungwan Kim Department of Biomedical Engineering, Seoul National University College of Medicine, 11 Daehak-ro, Jongno-gu, Seoul 38, Korea sungwan@snu.ac.kr Young Min Cho Department of Internal Medicine, Seoul National University College of Medicine, 11 Daehak-ro, Jongno-gu, Seoul 38, Korea ymchomd@snu.ac.kr Received: Jun. 29, 21; Accepted: Aug. 28, 21 This is an Open Access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Copyright 216 Korean Diabetes Association
2 Application of the oral minimal model to Korean subjects function and insulin sensitivity have been developed according to the different routes of glucose administration: intravenous glucose tolerance test (IVGTT) [8] and oral glucose tolerance test (OGTT), or mixed-meal tolerance test [3,9]. The IVGTTbased minimal model consists of glucose and insulin subsystems, where insulin in the plasma compartment passes the endothelium and enters a remote interstitial compartment to exert insulin action. In this model, if plasma insulin levels were solely measured, actual insulin secretion rates (ISRs) might be underestimated owing to the influence of different hepatic extractions of insulin [1]. Therefore, a C-peptide-based model was developed to overcome this shortcoming to estimate more accurate ISRs [11,12]. However, the intravenous administration of glucose is far from the physiologic way of glucose intake, which necessitates further improvement of the model by incorporating the physiology of oral glucose intake [13]. Since the OGTT is the gold standard method to determine glucose tolerance status, glucose, and insulin responses during the OGTT have been incorporated into mathematical models [2,4,14,1]. Among various oral glucose models, the oral minimal model can be easily applied to examine the dynamic physiology of glucose homeostasis, especially during the postprandial period. The oral minimal model comprises three submodels: The glucose minimal model assesses insulin secretion due to intestinal glucose absorption and consequent increases in the plasma glucose levels. The C-peptide minimal model determines how insulin controls the plasma glucose levels. The insulin and C-peptide minimal model was developed based on the C-peptide minimal model to assess the hepatic extraction of insulin. The oral minimal model can also be readily adapted to various situations by modifying its structure. East Asians have a unique pathophysiology of. Compared to their Caucasian counterparts, early β-cell deterioration with relatively preserved insulin sensitivity is characteristic during the pathogenesis of in East Asians [16]. Therefore, it would be meaningful to test whether or not the oral minimal model can be used in the Korean population. In this study, we applied the oral minimal model to Korean subjects with and normal glucose tolerance () to assess β-cell function and insulin sensitivity. METHODS Subjects and ethical statement Our study included 14 patients with and 1 subjects with, aged 18 to 7 years. The patients were diagnosed according to the criteria by the American Diabetes Association and had been treated with either lifestyle modifications or oral antidiabetic drugs. They did not have diabetic complications, such as retinopathy, microalbuminuria, or cardiovascular disease. The study protocol was approved by the Institutional Review Board at the Seoul National University Hospital (registration number: H ) and was in compliance with the Declaration of Helsinki, as revised in 2. Written informed consent was obtained from all of the participants before any study-related procedures. Study procedures Before visiting the Biomedical Research Center at the Seoul National University Hospital, all of the subjects had a 1-week washout period for oral antidiabetic drugs. They also fasted the night before the study day. All of the participants underwent a 18-minute, 7-g OGTT. Venous blood was drawn at, 1, 3, 6, 9, 12, and 18 minutes for the measurement of plasma glucose, insulin, and C-peptide levels. Glucose was measured by a glucose oxidase method (YSI 23 STAT Plus analyzer; Yellow Springs Instruments, Yellow Springs, OH, USA). Insulin (DIAsource, Nivelles, Belgium) and C-peptide (Immunotech, Prague, Czech Republic) concentrations were measured with chemiluminescence immunoassay. The mathematics of the oral minimal model The oral glucose minimal model and the oral C-peptide minimal model were adopted in this study. The oral glucose minimal model has two ordinary differential equations that represent the changes in plasma glucose and insulin concentrations. From previous studies [3,7,17], the following equations were derived: dg(t) = [X(t)] G(t) SG [G(t) Gb]+ Ra(t) G()=Gb dt V, (Equation 1) dx(t) = p2 X(t)+p3 [I(t) Ib], X()= (Equation 2) dt G(t) is the plasma glucose concentration, V is the glucose distribution volume, and SG is the fractional glucose effectiveness for promoting glucose disposal and altering the net hepatic glucose balance (Equation 1). Ra(t) is the glucose appearance rate in plasma following oral glucose intake. X(t) represents Diabetes Metab J 216;4:
3 Lim MH, et al. the insulin action on glucose disposal and glucose production, and b denotes the basal value (Equations 1 and 2). Parameters, such as p2 and p3, are rate constants representing the dynamics and magnitude of insulin action. Namely, p2 is the rate constant in the remote insulin compartment (i.e., interstitial compartment) from which insulin action is derived, and p3 is used for the scaling of the amplitude of insulin action [17]. I(t) is the plasma insulin concentration (Equation 2). These equations describe the glucose response to a given insulin action and the intake of glucose from the gastrointestinal tract. The oral C-peptide minimal model has four ordinary differential equations [3,14]. In this model, C-peptide kinetics is used instead of plasma insulin concentrations for the purpose of reflecting more accurate ISRs. dq1(t) = (k1 + k21) q1(t)+k12 q2(t)+isr(t), d c1(t)= q1(t), q1()= (Equation 3) V dq2(t) = k12 q2(t)+k21 q1(t), q2()= (Equation 4) dt ISR(t)=y(t)+KG dg(t) (Equation ) dt dy(t) 1 = [y(t) β (G(t) Gb)], y()= (Equation 6) dt T Briefly, in Equation 3, q1 and q2 are the increased C-peptide amounts from the basal amounts in the accessible and remote compartments, respectively. ISR means increased C-peptide secretion rates from the basal rates. c1 is the increased C-peptide plasma concentration from the basal level. k1, k12, and k21 are rate constants characterizing C-peptides kinetics. c1 is the increased C-peptide concentration from the basal level, and y(t) is the insulin provision (i.e., the proportion of synthesized insulin reaching the β-cell membrane and ready to be secreted after a delay [T]). KG and β are regarded as dynamic and static parameters, respectively. The oral insulin and C-peptide minimal model is based on the oral C-peptide minimal model; a subsystem for the hepatic extraction of insulin is inserted. The insulin delivery rate (IDR) and hepatic insulin extraction (HE) can be determined in this model [12]. di(t) = n I(t)+IDR(t)/VI, I()=Ib (Equation 7) dt IDR(t)=ISR(t) [1 HE(t)]/VI (Equation 8) In this model, n is the rate constant of insulin elimination, VI is the distribution volume of insulin, and (1 HE) means the fraction of ISR reaching the C-peptide accessible compartment. Parameter estimation Three parameters (SG, p2, and p3) in Equations 1 and 2 were evaluated in the glucose minimal model using clinical data. Their values were obtained by minimizing the nonlinear least square function, which reflects the differences between the anticipated and measured points. Among the three parameters in the oral glucose minimal model, glucose effectiveness SG and the ratio of p2 to p3 are important for characterizing the plasma glucose and insulin responses in each subject. Their values can be precisely estimated due to the inherent robustness of the model against errors in which the estimated ratio of p2 to p3 was nearly consistent, if p2 and p3 were respectively overestimated [18]. During this estimation process, all of the parameters were explored based on the reference values [19-21] within the parametric space using optimization techniques. One subject in the group and two subjects in the group were excluded from this calculation via outlier reduction. The function of the absorption rate of glucose into the mesenteric circulation was derived from a previous study [21]. The simulated annealing method in the parametric space for optimization was performed [22]. Because the smooth slopes of curves were important in the calculations, we used simulated responses for estimation. The rate constants (k1, k12, and k21) characterizing the C-peptide kinetics were adapted from a previous study [23]. All of the processes were carried out for each subject using the MATLAB system (The Mathworks Inc., Natick, MA, USA). Calculations Our goals of the calculations were two-fold. Our first goal was to compare the insulin sensitivity (SI) and β-cell function (i.e., basal, dynamic, static, and total responsivity indexes [Φb, Φd, Φs, and Φt]) between the and groups. The second goal was to graphically present the dynamic, static, and total disposition indexes (DIs, DId, and DIt) of the subjects using the DI metric to show the distribution of insulin sensitivity and β-cell responsivity of the and groups. In the oral minimal model, Φb reflects the insulin secretion 31 Diabetes Metab J 216;4:38-317
4 Application of the oral minimal model to Korean subjects at the basal state. Φd and Φs, respectively, correspond to first and second phase of insulin secretion. Φt combines the effects of both Φd and Φs [14]. The indexes SI and Φb, Φd, Φs, and Φt of the subjects were calculated based on the derived parameters. In the glucose minimal model, SI and SG were calculated as follows [24]: SI= p3 V (1 dl/kg/min per pmol/l), SG=p1 (min 1 ) p2 (Equation 9) In the C-peptide minimal model, the β-cell responsivity indexes represent the capacity of the β-cells to release insulin. They were approximated as follows [14,2]: ϕb= k1cpb (1 9 min 1 ) (Equation 1) Gb ϕd=kg (1 9 ) (Equation 11) ϕs=β (1 9 min 1 ) (Equation 12) ϕt=ϕs+ ϕd (Gmax Gb) (1 9 min 1 ) (Equation 13) [G(t) Gb]dt The DId, DIs, and DIt were calculated through multiplying Φd, Φs, and Φt, respectively, by SI. The basal hepatic insulin extraction ratio (HEb) and postglucose challenge hepatic insulin extraction ratio (HEpost) were calculated. T, 18 minutes in this study, is the time reaching the end of the tests [12]. HEb= ISRb IDRb =1 Ib n VI (%) (Equation 14) ISRb ISRb HEpost= T T ISR(t)dt IDR(t)dt T (%) (Equation 1) ISR(t)dt Statistical analysis To compare the variables between the and groups, the Mann-Whitney test, chi-square test, Welch s test, and analysis of covariance for adjusting differences in age were performed. The oral minimal model indexes were log transformed for analysis and back transformed. The Spearman correlation analysis was also used. Prism. (GraphPad, San Diego, CA, USA), R (The R Foundation, Vienna, Austria), and SPSS 19. (IBM Co., Armonk, NY, USA) software were used for statistical analysis. The significance level was set at. for the judgment of intergroup differences. RESULTS The clinical characteristics of the participants are presented in Table 1. The group was older than the group (mean±standard deviation, 3.8±9.4 years vs. 39.8±13. years, P<.19). The fasting glucose levels (146.2±27.6 mg/ dl vs. 92.±4. mg/dl, P<.1) and peak glucose levels during the OGTT (337.±49. mg/dl vs. 17.9±17.1 mg/dl, P<.1) were higher in the group than the group. The group had a longer delay in reaching the peak glucose levels than the group (93.6±18.9 minutes vs. 49.±13. minutes, P<.1). The body weight and body mass indexes were not significantly different between the and groups. Other indexes of insulin secretion or insulin action, such as postprandial C-peptide to glucose ratio (PCGR) [26], Matsuda index [27], and homeostasis model assessment of insulin resistance (HOMA-IR) [28], were compared between the and groups and are shown in Table 1. The PCGR and Matsuda index were higher in the group than the group (2.649±.642 vs. 1.24±.423, P<.1; 8.818±3.26 vs..466±2.814, P=.2, respectively). HOMA-IR was lower in the group than the group (1.2±1.1 vs. 2.3± 1.3, P=.2). Table 1. Clinical characteristics of the subjects Characteristic (n=1) (n=14) P value Sex, male/female 8/2 9/.63 Age, yr 39.8± ± Body weight, kg 66.6± ± Body mass index, kg/m ±3. 24.±3..43 Duration of diabetes mellitus, yr NA 4.7±2.4 NA Fasting plasma glucose, mg/dl 92.± ±27.6 <.1 Peak plasma glucose, mg/dl 17.9± ±49. <.1 Time for peak glucose, min 49.± ±18.9 <.1 PCGR 2.6±.6 1.3±.4 <.1 Matsuda index 8.8±3.3.±2.8.2 HOMA-IR 1.2± ±1.3.2 Values are presented as mean±standard deviation. P values were calculated using the chi-square test or the Mann-Whitney test, where appropriate., normal glucose tolerance;, type 2 diabetes mellitus; NA, not applicable; PCGR, postprandial C-peptide to glucose ratio; HOMA-IR, homeostasis model assessment of insulin resistance. Diabetes Metab J 216;4:
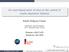
5 Lim MH, et al. Insulin sensitivity SI P=.24 Basal responsivity Φb Age-adjusted P=NS Dynamic sensitivity 1, 1, Φd Age-adjusted P=. A B C Static responsivity Φs Age-adjusted P<.1 D Total secretion index Φt Age-adjusted P<.1 E Basal hepatic extraction ratio (%) HEb P=NS F Post-glucose hepatic extraction ratio (%) HEpost Age-adjusted P=NS G Fig. 1. The indexes for (A) insulin sensitivity (SI) and (B) basal, (C) dynamic, (D) static, and (E) total β-cell responsivity (Φb, Φd, Φs, and Φt), (F) basal hepatic insulin extraction ratio (HEb), and (G) post-glucose challenge hepatic insulin extraction ratio (HEpost). The Mann-Whitney test was used to compare the indexes between the groups., normal glucose tolerance;, type 2 diabetes mellitus; NS, not significant. Insulin sensitivity, β-cell responsivity indexes, and HE ratios Insulin sensitivity and β-cell responsivity indexes were compared between the and groups. As shown in Fig. 1, the group had a higher SI than the group (2.±8.2 [ 1 dl/kg/min per pmol/l] vs. 13.3±11.8 [ 1 dl/kg/min per pmol/l], P=.24). The basal β-cell responsivity index (Φb) was not significantly different between the and groups (2.8±1.2 [ 1 9 min 1 ] vs. 2.9±1.2 [ 1 9 min 1 ], respectively, P=.78, age-adjusted P=.972). The Φd, Φs, and Φt were higher in the group than the group (Φd: 661.7±411.1 [ 1 9 ] vs. 17.9±138.7 [ 1 9 ], P<.1, age-adjusted P=.; Φs: 33.±9.4 [ 1 9 min 1 ] vs. 13.9±6. [ 1 9 min 1 ], P<.1, age-adjusted P<.1; Φt: 41.9±13.2 [ 1 9 min 1 ] vs. 1.±7.2 [ 1 9 min 1 ], P<.1, age-adjusted P<.1, respectively). The HEb was not significantly different between the and groups (.2%±12.91% vs %±9.27%, P=.64). The HEpost appeared to be different between the and groups (49.2%±2.79% vs %±1.72%, P =.28), which lost statistical significance after adjusting for age difference (P=.141). Disposition indexes between and groups The group had significantly lower DId, DIs, and DIt than the group (DId: 2.7±19.9 [ 1 12 dl/kg/min per pmol/ L] vs ±74.6 [ 1 12 dl/kg/min per pmol/l], P=.1, age-adjusted P<.1; DIs: 1.6±1. [ 1 12 dl/kg/min 2 per pmol/l] vs. 6.4±2.8 [ 1 12 dl/kg/min 2 per pmol/l], P<.1, age-adjusted P<.1; DIt: 1.8±1.1 [ 1 12 dl/kg/min 2 per pmol/l] vs. 7.9±3.4 [ 1 12 dl/kg/min 2 per pmol/l], P<.1, age-adjusted P<.1, respectively) (Fig. 2). The hy- 312 Diabetes Metab J 216;4:38-317
6 Application of the oral minimal model to Korean subjects Dynamic disposition index DId DIs DIt Age-adjusted P=.1 1 Age-adjusted P<.1 1 Age-adjusted P<.1 Static disposition index 1 A B C Total disposition index 1 Fig. 2. The (A) dynamic, (B) static, and (C) total disposition indexes (DId, DIs, and DIt) in the patients with type 2 diabetes mellitus () and individuals with normal glucose tolerance (). The Mann-Whitney test was used to compare the indexes between the groups. Insulin sensitivity (SI) DId , Φd A Insulin sensitivity (SI) Fig. 3. Distribution of insulin sensitivity and secretion in the patients with type 2 diabetes () and individuals with normal glucose tolerance (). The hyperbolae for the (A) dynamic, (B) static, (C) and total disposition (DIs, DId, and DIt) indexes are shown for the group (black line and open black circles) and the group (gray line and open gray circles) with a DI metric. Each circle or square represents a single subject. The subjects in each group presumably share the same disposition index, and a tendency toward the leftward and downward positioning in the patients can be observed. Φd, dynamic; Φs, static; Φt, total β-cell responsivity. DIs Φs B Insulin sensitivity (SI) DIt Φt C perbolic relation is shown in the three DI metrics in Fig. 3. The hyperbolic line for the group was located in the leftward and downward region of the group. Correlation between other indexes of insulin secretion or insulin action and oral minimal model indexes As shown in Fig. 4, the PCGR has significant correlation with the dynamic and static responsivity indexes (r=.77, P<.1 and r=.89, P<.1, respectively). The Matsuda index was significantly correlated with insulin sensitivity (r=.1, P=.11), whereas HOMA-IR did not show any significance (r=.21, P=.1). DISCUSSION In this Korean study, SI and β-cell responsivity indexes (Φd, Φs, and Φt) were lower in the patients with than in the individuals with. Compared to the group, insulin sensitivity was 33.9% lower, and the Φd, Φs, and Φt were 74.1%, 8.3%, and 63.3% lower, respectively, in the group. Our results were in line with those of previous studies, showing decreased insulin sensitivity and insulin secretion in Korean patients, which were conducted with the euglycemic hyperinsulinemic clamp method [29], the hyperglycemic clamp method [3], or the IVGTT-based minimal model [31]. Compared to other methods, the oral minimal model has advantages for the separate assessment of insulin sensitivity and dynamic nature of β-cell responsivity simultaneously from a single data set. There are many surrogate measures for insulin sensitivity and/or β-cell function, such as HOMA methods [28], quantitative insulin sensitivity check index (QUICKI) [32], and Matsuda index [27]. Fasting mea- Diabetes Metab J 216;4:
7 Lim MH, et al. 1, r=.77, P<.1 r=.89, P<.1 4 1, 3 Φd Φs PCGR A PCGR B.6 r=.1, P=.11.6 r=.21, P= SI SI Matsuda index C Fig. 4. Correlation analyses between the indexes obtained in the oral minimal model and other indexes of insulin secretion or insulin sensitivity (SI). Spearman correlation analysis was used. Correlations of (A) dynamic (Φd) and (B) static β-cell responsivity (Φs) with postprandial C-peptide to glucose ratio (PCGR) are shown. Correlations of insulin sensitivity (SI) with (C) Matsuda index and (D) homeostasis model assessment of insulin resistance (HOMA-IR) are shown HOMA-IR D sures, such as HOMA-insulin resistance and QUICKI, mainly reflect hepatic insulin sensitivity rather than peripheral insulin sensitivity [33,34]. Because HOMA β-cell function is also derived from fasting data [28], it cannot describe the dynamics of postprandial insulin secretion. In contrast, the SI calculated by the oral minimal model represents not only hepatic but also peripheral insulin sensitivity [3,3,36]. Although the Matsuda index using the mean insulin and glucose responses during the OGTT correlates well with the insulin sensitivity measured by the euglycemic hyperinsulinemic clamp [27], this index is not matched for a measure of β-cell function that reflects the dynamic nature of postprandial insulin secretion. In this regard, the benefits of the oral minimal model are provision of comprehensive measures for insulin sensitivity, β-cell function, and hepatic extraction of insulin. In addition, the indexes obtained from the oral minimal model and other indexes of postchallenge insulin secretion and insulin sensitivity were well correlated. The oral minimal model is simpler than the IVGTT-based minimal model [3,8], which requires much more frequent blood sampling and control for blood glucose concentrations. Therefore, it can be broadly applied for various clinical studies. First, the model can be used to assess characteristics of glucose metabolism in a large number of subjects. A previous study, which enrolled as many as 2 Japanese and Caucasian subjects, showed lower β-cell function and higher insulin sensitivity in the Japanese subjects than the Caucasian subjects [37]. Second, the oral minimal model can be used to assess the effect of antidiabetic drugs on insulin sensitivity and β-cell function, as shown elsewhere [38]. Taken together, the oral minimal model may reduce the burdens of effort in measuring physiologic parameters of glucose homeostasis in various forms of clinical research. The oral minimal model has good expandability and can be 314 Diabetes Metab J 216;4:38-317
8 Application of the oral minimal model to Korean subjects readily modified in an engineering manner. To develop a further upgraded version of the oral minimal model, the incretin effect would be a candidate component to be incorporated in the model. If equations describing the incretin effect [39] were added to the oral minimal model, it could become a more physiologic model. Since a glucagon-adapted model has also been developed [4], it might be useful to assess the glycemic responses to specific antidiabetic drugs and to establish algorithms for the bihormonal artificial pancreas. This study had some limitations. First, in this study, insulin and C-peptide were measured at, 1, and 3 minutes during the first 3 minutes, whereas other studies [14,2] included -, 1-, 2-, and 3-minute samples. Since the insulin response during the first 3 minutes is crucial to determine the dynamic β-cell responsivity index, more frequent measurements would support a more accurate estimation. Second, we did not directly validate the oral minimal model indexes with the values of the hyperglycemic clamp and the euglycemic hyperinsulinemic clamp studies, which are considered the gold standard methods for measuring insulin secretion and SI. Lastly, the subjects with prediabetes, such as impaired fasting glucose or impaired glucose tolerance, were not included in this study. In this study, in accordance with the results of previously published studies using other physiologic methods in Koreans, the insulin sensitivity index, β-cell responsivity indexes, and disposition indexes obtained by the oral minimal model were generally lower in the group than the group. Based on our results, the oral minimal model can also be applied to Koreans to evaluate insulin sensitivity and dynamics of insulin secretion using OGTT data. CONFLICTS OF INTEREST No potential conflict of interest relevant to this article was reported. ACKNOWLEDGMENTS This work was supported by National Research Foundation of Korea (NRF) grants funded by the Korean Government (21 M1A3A3A212636, , and ). REFERENCES 1. Defronzo RA. Banting lecture. From the triumvirate to the ominous octet: a new paradigm for the treatment of type 2 diabetes mellitus. Diabetes 29;8: Brubaker PL, Ohayon EL, D Alessandro LM, Norwich KH. A mathematical model of the oral glucose tolerance test illustrating the effects of the incretins. Ann Biomed Eng 27;3: Cobelli C, Dalla Man C, Toffolo G, Basu R, Vella A, Rizza R. The oral minimal model method. Diabetes 214;63: Cobelli C, Toffolo GM, Dalla Man C, Campioni M, Denti P, Caumo A, Butler P, Rizza R. Assessment of beta-cell function in humans, simultaneously with insulin sensitivity and hepatic extraction, from intravenous and oral glucose tests. Am J Physiol Endocrinol Metab 27;293:E1-1.. Hovorka R, Canonico V, Chassin LJ, Haueter U, Massi-Benedetti M, Orsini Federici M, Pieber TR, Schaller HC, Schaupp L, Vering T, Wilinska ME. Nonlinear model predictive control of glucose concentration in subjects with type 1 diabetes. Physiol Meas 24;2: Lee JC, Kim M, Choi KR, Oh TJ, Kim MY, Cho YM, Kim K, Kim HC, Kim S. In silico evaluation of glucose control protocols for critically ill patients. IEEE Trans Biomed Eng 212;9: James G, Witten D, Hastie T, Tibshirani R. An introduction to statistical learning: with applications in R. New York: Springer; 213. p Bergman RN, Ider YZ, Bowden CR, Cobelli C. Quantitative estimation of insulin sensitivity. Am J Physiol 1979;236:E Staten MA, Kelley DE. Using oral challenge testing to assess insulin action and secretion with mathematical modeling. Diabetes 214;63: Caumo A, Vicini P, Zachwieja JJ, Avogaro A, Yarasheski K, Bier DM, Cobelli C. Undermodeling affects minimal model indexes: insights from a two-compartment model. Am J Physiol 1999;276(6 Pt 1):E Toffolo G, De Grandi F, Cobelli C. Estimation of beta-cell sensitivity from intravenous glucose tolerance test C-peptide data. Knowledge of the kinetics avoids errors in modeling the secretion. Diabetes 199;44: Campioni M, Toffolo G, Basu R, Rizza RA, Cobelli C. Minimal model assessment of hepatic insulin extraction during an oral test from standard insulin kinetic parameters. Am J Diabetes Metab J 216;4:
9 Lim MH, et al. Physiol Endocrinol Metab 29;297:E Basu R, Dalla Man C, Campioni M, Basu A, Klee G, Toffolo G, Cobelli C, Rizza RA. Effects of age and sex on postprandial glucose metabolism: differences in glucose turnover, insulin secretion, insulin action, and hepatic insulin extraction. Diabetes 26;: Breda E, Cavaghan MK, Toffolo G, Polonsky KS, Cobelli C. Oral glucose tolerance test minimal model indexes of beta-cell function and insulin sensitivity. Diabetes 21;: Burattini R, Morettini M. Identification of an integrated mathematical model of standard oral glucose tolerance test for characterization of insulin potentiation in health. Comput Methods Programs Biomed 212;17: Cho YM. Incretin physiology and pathophysiology from an Asian perspective. J Diabetes Investig 21;6: Dalla Man C, Caumo A, Cobelli C. The oral glucose minimal model: estimation of insulin sensitivity from a meal test. IEEE Trans Biomed Eng 22;49: McDonald C, Dunaif A, Finegood DT. Minimal-model estimates of insulin sensitivity are insensitive to errors in glucose effectiveness. J Clin Endocrinol Metab 2;8: Caumo A, Bergman RN, Cobelli C. Insulin sensitivity from meal tolerance tests in normal subjects: a minimal model index. J Clin Endocrinol Metab 2;8: Steil GM, Hwu CM, Janowski R, Hariri F, Jinagouda S, Darwin C, Tadros S, Rebrin K, Saad MF. Evaluation of insulin sensitivity and beta-cell function indexes obtained from minimal model analysis of a meal tolerance test. Diabetes 24;3: Kim M, Oh TJ, Lee JC, Choi K, Kim MY, Kim HC, Cho YM, Kim S. Simulation of oral glucose tolerance tests and the corresponding isoglycemic intravenous glucose infusion studies for calculation of the incretin effect. J Korean Med Sci 214;29: Venkataraman P. Applied optimization with MATLAB programming. 2nd ed. Hoboken: John Wiley & Sons; 29. p Van Cauter E, Mestrez F, Sturis J, Polonsky KS. Estimation of insulin secretion rates from C-peptide levels. Comparison of individual and standard kinetic parameters for C-peptide clearance. Diabetes 1992;41: Dalla Man C, Yarasheski KE, Caumo A, Robertson H, Toffolo G, Polonsky KS, Cobelli C. Insulin sensitivity by oral glucose minimal models: validation against clamp. Am J Physiol Endocrinol Metab 2;289:E Breda E, Toffolo G, Polonsky KS, Cobelli C. Insulin release in impaired glucose tolerance: oral minimal model predicts normal sensitivity to glucose but defective response times. Diabetes 22;1 Suppl 1:S Lee EY, Hwang S, Lee SH, Lee YH, Choi AR, Lee Y, Lee BW, Kang ES, Ahn CW, Cha BS, Lee HC. Postprandial C-peptide to glucose ratio as a predictor of beta-cell function and its usefulness for staged management of type 2 diabetes. J Diabetes Investig 214;: Matsuda M, DeFronzo RA. Insulin sensitivity indices obtained from oral glucose tolerance testing: comparison with the euglycemic insulin clamp. Diabetes Care 1999;22: Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 198;28: Chae BN, Lee SK, Hong EG, Chung YS, Lee KW, Kim HM. The role of insulin secretion and insulin resistance in the development of Korean type 2 diabetes mellitus. J Korean Diabetes Assoc 1998;22: Oh TJ, Park KS, Cho YM. Correlation of the incretin effect with first- and second-phase insulin secretions in Koreans with various glucose tolerance statuses. Clin Endocrinol (Oxf) 21;83: Song J, Oh JY, Sung YA, Pak YK, Park KS, Lee HK. Peripheral blood mitochondrial DNA content is related to insulin sensitivity in offspring of type 2 diabetic patients. Diabetes Care 21; 24: Katz A, Nambi SS, Mather K, Baron AD, Follmann DA, Sullivan G, Quon MJ. Quantitative insulin sensitivity check index: a simple, accurate method for assessing insulin sensitivity in humans. J Clin Endocrinol Metab 2;8: Otten J, Ahren B, Olsson T. Surrogate measures of insulin sensitivity vs the hyperinsulinaemic-euglycaemic clamp: a metaanalysis. Diabetologia 214;7: Reaven GM. What do we learn from measurements of HOMA- IR? Diabetologia 213;6: Dalla Man C, Caumo A, Basu R, Rizza R, Toffolo G, Cobelli C. Measurement of selective effect of insulin on glucose disposal from labeled glucose oral test minimal model. Am J Physiol Endocrinol Metab 2;289:E Man CD, Toffolo G, Basu R, Rizza RA, Cobelli C. Use of labeled oral minimal model to measure hepatic insulin sensitivity. Am J Physiol Endocrinol Metab 28;29:E Moller JB, Dalla Man C, Overgaard RV, Ingwersen SH, Tornoe CW, Pedersen M, Tanaka H, Ohsugi M, Ueki K, Lynge J, Vasconcelos NM, Pedersen BK, Kadowaki T, Cobelli C. Ethnic 316 Diabetes Metab J 216;4:38-317
10 Application of the oral minimal model to Korean subjects differences in insulin sensitivity, beta-cell function, and hepatic extraction between Japanese and Caucasians: a minimal model analysis. J Clin Endocrinol Metab 214;99: Alba M, Ahren B, Inzucchi SE, Guan Y, Mallick M, Xu L, O Neill EA, Williams-Herman DE, Kaufman KD, Goldstein BJ. Sitagliptin and pioglitazone provide complementary effects on postprandial glucose and pancreatic islet cell function. Diabetes Obes Metab 213;1: Dalla Man C, Micheletto F, Sathananthan A, Rizza RA, Vella A, Cobelli C. A model of GLP-1 action on insulin secretion in nondiabetic subjects. Am J Physiol Endocrinol Metab 21;298: E Herrero P, Georgiou P, Oliver N, Reddy M, Johnston D, Toumazou C. A composite model of glucagon-glucose dynamics for in silico testing of bihormonal glucose controllers. J Diabetes Sci Technol 213;7: Diabetes Metab J 216;4:
The oral meal or oral glucose tolerance test. Original Article Two-Hour Seven-Sample Oral Glucose Tolerance Test and Meal Protocol
 Original Article Two-Hour Seven-Sample Oral Glucose Tolerance Test and Meal Protocol Minimal Model Assessment of -Cell Responsivity and Insulin Sensitivity in Nondiabetic Individuals Chiara Dalla Man,
Original Article Two-Hour Seven-Sample Oral Glucose Tolerance Test and Meal Protocol Minimal Model Assessment of -Cell Responsivity and Insulin Sensitivity in Nondiabetic Individuals Chiara Dalla Man,
Insulin Secretory Capacity and Insulin Resistance in Korean Type 2 Diabetes Mellitus Patients
 Review Article Endocrinol Metab 2016;31:354-360 http://dx.doi.org/10.3803/enm.2016.31.3.354 pissn 2093-596X eissn 2093-5978 Insulin Secretory Capacity and Insulin Resistance in Korean Type 2 Diabetes Mellitus
Review Article Endocrinol Metab 2016;31:354-360 http://dx.doi.org/10.3803/enm.2016.31.3.354 pissn 2093-596X eissn 2093-5978 Insulin Secretory Capacity and Insulin Resistance in Korean Type 2 Diabetes Mellitus
Agus Kartono, Egha Sabila Putri, Ardian Arif Setiawan, Heriyanto Syafutra and Tony Sumaryada
 American Journal of Applied Sciences Original Research Paper Study of Modified Oral Minimal Model using n-order Decay Rate of Plasma Insulin for the Oral Glucose Tolerance Test in Subjects with Normal,
American Journal of Applied Sciences Original Research Paper Study of Modified Oral Minimal Model using n-order Decay Rate of Plasma Insulin for the Oral Glucose Tolerance Test in Subjects with Normal,
Associations among Body Mass Index, Insulin Resistance, and Pancreatic ß-Cell Function in Korean Patients with New- Onset Type 2 Diabetes
 ORIGINAL ARTICLE korean j intern med 2012;27:66-71 pissn 1226-3303 eissn 2005-6648 Associations among Body Mass Index, Insulin Resistance, and Pancreatic ß-Cell Function in Korean Patients with New- Onset
ORIGINAL ARTICLE korean j intern med 2012;27:66-71 pissn 1226-3303 eissn 2005-6648 Associations among Body Mass Index, Insulin Resistance, and Pancreatic ß-Cell Function in Korean Patients with New- Onset
The Oral Minimal Model Method
 Diabetes Volume 63, April 2014 1203 Claudio Cobelli, 1 Chiara Dalla Man, 1 Gianna Toffolo, 1 Rita Basu, 2 Adrian Vella, 2 and Robert Rizza 2 The Oral Minimal Model Method The simultaneous assessment of
Diabetes Volume 63, April 2014 1203 Claudio Cobelli, 1 Chiara Dalla Man, 1 Gianna Toffolo, 1 Rita Basu, 2 Adrian Vella, 2 and Robert Rizza 2 The Oral Minimal Model Method The simultaneous assessment of
The enteroinsular axis in the pathogenesis of prediabetes and diabetes in humans
 The enteroinsular axis in the pathogenesis of prediabetes and diabetes in humans Young Min Cho, MD, PhD Division of Endocrinology and Metabolism Seoul National University College of Medicine Plasma glucose
The enteroinsular axis in the pathogenesis of prediabetes and diabetes in humans Young Min Cho, MD, PhD Division of Endocrinology and Metabolism Seoul National University College of Medicine Plasma glucose
The Diabetes Epidemic in Korea
 Review Article Endocrinol Metab 2016;31:349-33 http://dx.doi.org/.3803/enm.2016.31.3.349 pissn 2093-96X eissn 2093-978 The Diabetes Epidemic in Korea Junghyun Noh Department of Internal Medicine, Inje
Review Article Endocrinol Metab 2016;31:349-33 http://dx.doi.org/.3803/enm.2016.31.3.349 pissn 2093-96X eissn 2093-978 The Diabetes Epidemic in Korea Junghyun Noh Department of Internal Medicine, Inje
A Composite Model of Glucagon Glucose Dynamics for In Silico Testing of Bihormonal Glucose Controllers
 Journal of Diabetes Science and Technology Volume 7, Issue 4, July 2013 Diabetes Technology Society ORIGINAL ARTICLE A Composite Model of Glucagon Glucose Dynamics for In Silico Testing of Bihormonal Glucose
Journal of Diabetes Science and Technology Volume 7, Issue 4, July 2013 Diabetes Technology Society ORIGINAL ARTICLE A Composite Model of Glucagon Glucose Dynamics for In Silico Testing of Bihormonal Glucose
The Epidemiology of Diabetes in Korea
 Review http://dx.doi.org/10.4093/dmj.2011.35.4.303 pissn 2233-6079 eissn 2233-6087 D I A B E T E S & M E T A B O L I S M J O U R N A L The Epidemiology of Diabetes in Korea Dae Jung Kim Department of Endocrinology
Review http://dx.doi.org/10.4093/dmj.2011.35.4.303 pissn 2233-6079 eissn 2233-6087 D I A B E T E S & M E T A B O L I S M J O U R N A L The Epidemiology of Diabetes in Korea Dae Jung Kim Department of Endocrinology
Obesity and Insulin Resistance According to Age in Newly Diagnosed Type 2 Diabetes Patients in Korea
 https://doi.org/10.7180/kmj.2016.31.2.157 KMJ Original Article Obesity and Insulin Resistance According to Age in Newly Diagnosed Type 2 Diabetes Patients in Korea Ju Won Lee, Nam Kyu Kim, Hyun Joon Park,
https://doi.org/10.7180/kmj.2016.31.2.157 KMJ Original Article Obesity and Insulin Resistance According to Age in Newly Diagnosed Type 2 Diabetes Patients in Korea Ju Won Lee, Nam Kyu Kim, Hyun Joon Park,
IDENTIFICATION OF LINEAR DYNAMIC MODELS FOR TYPE 1 DIABETES: A SIMULATION STUDY
 IDENTIFICATION OF LINEAR DYNAMIC MODELS FOR TYPE 1 DIABETES: A SIMULATION STUDY Daniel A. Finan Howard Zisser Lois Jovanovic Wendy C. Bevier Dale E. Seborg Department of Chemical Engineering University
IDENTIFICATION OF LINEAR DYNAMIC MODELS FOR TYPE 1 DIABETES: A SIMULATION STUDY Daniel A. Finan Howard Zisser Lois Jovanovic Wendy C. Bevier Dale E. Seborg Department of Chemical Engineering University
28 Regulation of Fasting and Post-
 28 Regulation of Fasting and Post- Prandial Glucose Metabolism Keywords: Type 2 Diabetes, endogenous glucose production, splanchnic glucose uptake, gluconeo-genesis, glycogenolysis, glucose effectiveness.
28 Regulation of Fasting and Post- Prandial Glucose Metabolism Keywords: Type 2 Diabetes, endogenous glucose production, splanchnic glucose uptake, gluconeo-genesis, glycogenolysis, glucose effectiveness.
Keywords: Incretins; Oral Glucose Tolerance Test (OGTT); Isoglycemic Intravenous Glucose Infusions (IIGI); Individualized Model INTRODUCTION
 ORIGINAL ARTICLE Endocrinology, Nutrition & Metabolism http://dx.doi.org/10.3346/jkms.2014.29.3.378 J Korean Med Sci 2014; 29: 378-385 Simulation of Oral Glucose Tolerance Tests and the Corresponding Isoglycemic
ORIGINAL ARTICLE Endocrinology, Nutrition & Metabolism http://dx.doi.org/10.3346/jkms.2014.29.3.378 J Korean Med Sci 2014; 29: 378-385 Simulation of Oral Glucose Tolerance Tests and the Corresponding Isoglycemic
Glucose-Insulin Pharmacodynamic Surface Modeling Comparison
 Glucose-Insulin Pharmacodynamic Surface Modeling Comparison J. Geoffrey Chase*, Steen Andreassen.**, Ulrike Pielmeier**, Christopher E. Hann * *Mechanical Eng, Centre for Bio-Engineering, University of
Glucose-Insulin Pharmacodynamic Surface Modeling Comparison J. Geoffrey Chase*, Steen Andreassen.**, Ulrike Pielmeier**, Christopher E. Hann * *Mechanical Eng, Centre for Bio-Engineering, University of
Quantitative indexes of -cell function during graded up&down glucose infusion from C-peptide minimal models
 Am J Physiol Endocrinol Metab 280: E2 E10, 2001. Quantitative indexes of -cell function during graded up&down glucose infusion from C-peptide minimal models GIANNA TOFFOLO, 1 ELENA BREDA, 1 MELISSA K.
Am J Physiol Endocrinol Metab 280: E2 E10, 2001. Quantitative indexes of -cell function during graded up&down glucose infusion from C-peptide minimal models GIANNA TOFFOLO, 1 ELENA BREDA, 1 MELISSA K.
ASSOCIATION OF BMI WITH INSULIN RESISTANCE IN TYPE 2 DIABETES MELLITUS -A STUDY IN LOCAL TELANGANA POPULATION
 - ISSN: 2321-3272 (Print) IJPBS Volume 5 Issue 4 OCT-DEC 2015 130-136 Research Article Biological Sciences ASSOCIATION OF BMI WITH INSULIN RESISTANCE IN TYPE 2 DIABETES MELLITUS -A STUDY IN LOCAL TELANGANA
- ISSN: 2321-3272 (Print) IJPBS Volume 5 Issue 4 OCT-DEC 2015 130-136 Research Article Biological Sciences ASSOCIATION OF BMI WITH INSULIN RESISTANCE IN TYPE 2 DIABETES MELLITUS -A STUDY IN LOCAL TELANGANA
Electronic Supplementary Material to the article entitled Altered pattern of the
 Electronic Supplementary Material to the article entitled Altered pattern of the incretin effect as assessed by modelling in individuals with glucose tolerance ranging from normal to diabetic Integrated
Electronic Supplementary Material to the article entitled Altered pattern of the incretin effect as assessed by modelling in individuals with glucose tolerance ranging from normal to diabetic Integrated
INSULIN IS A key regulator of glucose homeostasis. Insulin
 0021-972X/00/$03.00/0 Vol. 85, No. 7 The Journal of Clinical Endocrinology & Metabolism Printed in U.S.A. Copyright 2000 by The Endocrine Society Quantitative Insulin Sensitivity Check Index: A Simple,
0021-972X/00/$03.00/0 Vol. 85, No. 7 The Journal of Clinical Endocrinology & Metabolism Printed in U.S.A. Copyright 2000 by The Endocrine Society Quantitative Insulin Sensitivity Check Index: A Simple,
Alternative insulin delivery systems: how demanding should the patient be?
 Diabetologia (1997) 4: S97 S11 Springer-Verlag 1997 Alternative insulin delivery systems: how demanding should the patient be? K.S. Polonsky, M. M. Byrne, J. Sturis Department of Medicine, The University
Diabetologia (1997) 4: S97 S11 Springer-Verlag 1997 Alternative insulin delivery systems: how demanding should the patient be? K.S. Polonsky, M. M. Byrne, J. Sturis Department of Medicine, The University
In-Silico Trials for Glucose Control in Hospitalized Patients with Type 2 Diabetes
 ORIGINAL ARTICLE Endocrinology, Nutrition & Metabolism http://dx.doi.org/1.3346/jkms.216.31.2.231 J Korean Med Sci 216; 31: 231-239 In-Silico Trials for Glucose Control in Hospitalized Patients with Type
ORIGINAL ARTICLE Endocrinology, Nutrition & Metabolism http://dx.doi.org/1.3346/jkms.216.31.2.231 J Korean Med Sci 216; 31: 231-239 In-Silico Trials for Glucose Control in Hospitalized Patients with Type
Standardized Thyroid Cancer Mortality in Korea between 1985 and 2010
 Original Article Endocrinol Metab 2014;29:530-535 http://dx.doi.org/10.3803/enm.2014.29.4.530 pissn 2093-596X eissn 2093-5978 Standardized Thyroid Cancer Mortality in Korea between 1985 and 2010 Yun Mi
Original Article Endocrinol Metab 2014;29:530-535 http://dx.doi.org/10.3803/enm.2014.29.4.530 pissn 2093-596X eissn 2093-5978 Standardized Thyroid Cancer Mortality in Korea between 1985 and 2010 Yun Mi
Dynamic Modeling of Exercise Effects on Plasma Glucose and Insulin Levels
 Journal of Diabetes Science and Technology Volume 1, Issue 3, May 2007 Diabetes Technology Society SYMPOSIUM Dynamic Modeling of Exercise Effects on Plasma Glucose and Insulin Levels Anirban, M.S., and
Journal of Diabetes Science and Technology Volume 1, Issue 3, May 2007 Diabetes Technology Society SYMPOSIUM Dynamic Modeling of Exercise Effects on Plasma Glucose and Insulin Levels Anirban, M.S., and
Adapting to insulin resistance in obesity: role of insulin secretion and clearance
 Diabetologia (218) 61:681 687 https://doi.org/1.17/s125-17-4511- ARTICLE Adapting to insulin resistance in obesity: role of insulin secretion and clearance Sang-Hee Jung 1 & Chan-Hee Jung 2 & Gerald M.
Diabetologia (218) 61:681 687 https://doi.org/1.17/s125-17-4511- ARTICLE Adapting to insulin resistance in obesity: role of insulin secretion and clearance Sang-Hee Jung 1 & Chan-Hee Jung 2 & Gerald M.
Active Insulin Infusion Using Fuzzy-Based Closed-loop Control
 Active Insulin Infusion Using Fuzzy-Based Closed-loop Control Sh. Yasini, M. B. Naghibi-Sistani, A. Karimpour Department of Electrical Engineering, Ferdowsi University of Mashhad, Mashhad, Iran E-mail:
Active Insulin Infusion Using Fuzzy-Based Closed-loop Control Sh. Yasini, M. B. Naghibi-Sistani, A. Karimpour Department of Electrical Engineering, Ferdowsi University of Mashhad, Mashhad, Iran E-mail:
Back Stepping SMC for Blood Glucose Control of Type-1 Diabetes Mellitus Patients
 Back Stepping SMC for Blood Glucose Control of Type-1 Diabetes Mellitus Patients Deirdre D. Sylvester and Ravindra K. Munje K.K. Wagh Institute of Engineering Education and Research, Nashik-4003, (M.S.),
Back Stepping SMC for Blood Glucose Control of Type-1 Diabetes Mellitus Patients Deirdre D. Sylvester and Ravindra K. Munje K.K. Wagh Institute of Engineering Education and Research, Nashik-4003, (M.S.),
BARIATRIC SURGERY AND TYPE 2 DIABETES MELLITUS
 BARIATRIC SURGERY AND TYPE 2 DIABETES MELLITUS George Vl Valsamakis European Scope Fellow Obesity Visiting iti Associate Prof Warwick Medical School Diabetes is an increasing healthcare epidemic throughout
BARIATRIC SURGERY AND TYPE 2 DIABETES MELLITUS George Vl Valsamakis European Scope Fellow Obesity Visiting iti Associate Prof Warwick Medical School Diabetes is an increasing healthcare epidemic throughout
Insulin Administration for People with Type 1 diabetes
 Downloaded from orbit.dtu.dk on: Nov 17, 1 Insulin Administration for People with Type 1 diabetes Boiroux, Dimitri; Finan, Daniel Aaron; Poulsen, Niels Kjølstad; Madsen, Henrik; Jørgensen, John Bagterp
Downloaded from orbit.dtu.dk on: Nov 17, 1 Insulin Administration for People with Type 1 diabetes Boiroux, Dimitri; Finan, Daniel Aaron; Poulsen, Niels Kjølstad; Madsen, Henrik; Jørgensen, John Bagterp
A Closed-loop Artificial Pancreas based on MPC: human-friendly identification and automatic meal disturbance rejection
 Proceedings of the 17th World Congress The International Federation of Automatic Control Seoul, Korea, July 6-11, 8 A Closed-loop Artificial Pancreas based on MPC: human-friendly identification and automatic
Proceedings of the 17th World Congress The International Federation of Automatic Control Seoul, Korea, July 6-11, 8 A Closed-loop Artificial Pancreas based on MPC: human-friendly identification and automatic
Clinical Overview of Combination Therapy with Sitagliptin and Metformin
 Clinical Overview of Combination Therapy with Sitagliptin and Metformin 1 Contents Pathophysiology of type 2 diabetes and mechanism of action of sitagliptin Clinical data overview of sitagliptin: Monotherapy
Clinical Overview of Combination Therapy with Sitagliptin and Metformin 1 Contents Pathophysiology of type 2 diabetes and mechanism of action of sitagliptin Clinical data overview of sitagliptin: Monotherapy
A Minimal C-Peptide Sampling Method to Capture Peak and Total Prehepatic Insulin Secretion in Model-Based Experimental Insulin Sensitivity Studies
 Journal of Diabetes Science and Technology Volume 3, Issue 4, July 29 Diabetes Technology Society ORIGINAL ARTICLES A Minimal C-Peptide Sampling Method to Capture Peak and Total Prehepatic Insulin Secretion
Journal of Diabetes Science and Technology Volume 3, Issue 4, July 29 Diabetes Technology Society ORIGINAL ARTICLES A Minimal C-Peptide Sampling Method to Capture Peak and Total Prehepatic Insulin Secretion
Elevated serum levels of visfatin in gestational diabetes: a comparative study across various degrees of glucose tolerance
 Diabetologia (2007) 50:1033 1037 DOI 10.1007/s00125-007-0610-7 SHORT COMMUNICATION Elevated serum levels of visfatin in gestational diabetes: a comparative study across various degrees of glucose tolerance
Diabetologia (2007) 50:1033 1037 DOI 10.1007/s00125-007-0610-7 SHORT COMMUNICATION Elevated serum levels of visfatin in gestational diabetes: a comparative study across various degrees of glucose tolerance
A Proportional-Derivative Endogenous Insulin Secretion model with an Adapted Gauss Newton Approach
 A Proportional-Derivative Endogenous Insulin Secretion model with an Adapted Gauss Newton Approach Nor Azlan Othman, Paul D. Docherty, Nor Salwa Damanhuri and J. Geoffrey Chase Department of Mechanical
A Proportional-Derivative Endogenous Insulin Secretion model with an Adapted Gauss Newton Approach Nor Azlan Othman, Paul D. Docherty, Nor Salwa Damanhuri and J. Geoffrey Chase Department of Mechanical
Relationship between insulin resistance, obesity and serum prostate-specific antigen levels in healthy men
 400 Original Article Asian Journal of Andrology (2010) 12: 400 404 2010 AJA, SIMM & SJTU All rights reserved 1008-682X/10 $ 32.00 www.nature.com/aja Relationship between insulin resistance, obesity and
400 Original Article Asian Journal of Andrology (2010) 12: 400 404 2010 AJA, SIMM & SJTU All rights reserved 1008-682X/10 $ 32.00 www.nature.com/aja Relationship between insulin resistance, obesity and
la prise en charge du diabète de
 N21 XIII Congrès National de Diabétologie, 29 mai 2011, Alger Intérêt et place des Anti DPP4 dans la prise en charge du diabète de type 2 Nicolas PAQUOT, MD, PhD CHU Sart-Tilman, Université de Liège Belgique
N21 XIII Congrès National de Diabétologie, 29 mai 2011, Alger Intérêt et place des Anti DPP4 dans la prise en charge du diabète de type 2 Nicolas PAQUOT, MD, PhD CHU Sart-Tilman, Université de Liège Belgique
Chief of Endocrinology East Orange General Hospital
 Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
Epidemiologic characteristics of cervical cancer in Korean women
 Review Article J Gynecol Oncol Vol. 25, No. 1:70-74 pissn 2005-0380 eissn 2005-0399 Epidemiologic characteristics of cervical cancer in Korean women Hyun-Joo Seol, Kyung-Do Ki, Jong-Min Lee Department
Review Article J Gynecol Oncol Vol. 25, No. 1:70-74 pissn 2005-0380 eissn 2005-0399 Epidemiologic characteristics of cervical cancer in Korean women Hyun-Joo Seol, Kyung-Do Ki, Jong-Min Lee Department
Outline Insulin-Glucose Dynamics a la Deterministic models Biomath Summer School and Workshop 2008 Denmark
 Outline Insulin-Glucose Dynamics a la Deterministic models Biomath Summer School and Workshop 2008 Denmark Seema Nanda Tata Institute of Fundamental Research Centre for Applicable Mathematics, Bangalore,
Outline Insulin-Glucose Dynamics a la Deterministic models Biomath Summer School and Workshop 2008 Denmark Seema Nanda Tata Institute of Fundamental Research Centre for Applicable Mathematics, Bangalore,
David C. Polidori, 1 Richard N. Bergman, 2 Stephanie T. Chung, 3 and Anne E. Sumner 3
 1556 Diabetes Volume 65, June 2016 David C. Polidori, 1 Richard N. Bergman, 2 Stephanie T. Chung, 3 and Anne E. Sumner 3 Hepatic and Extrahepatic Insulin Clearance Are Differentially Regulated: Results
1556 Diabetes Volume 65, June 2016 David C. Polidori, 1 Richard N. Bergman, 2 Stephanie T. Chung, 3 and Anne E. Sumner 3 Hepatic and Extrahepatic Insulin Clearance Are Differentially Regulated: Results
A Practical Approach to Prescribe The Amount of Used Insulin of Diabetic Patients
 A Practical Approach to Prescribe The Amount of Used Insulin of Diabetic Patients Mehran Mazandarani*, Ali Vahidian Kamyad** *M.Sc. in Electrical Engineering, Ferdowsi University of Mashhad, Iran, me.mazandarani@gmail.com
A Practical Approach to Prescribe The Amount of Used Insulin of Diabetic Patients Mehran Mazandarani*, Ali Vahidian Kamyad** *M.Sc. in Electrical Engineering, Ferdowsi University of Mashhad, Iran, me.mazandarani@gmail.com
Patients characteristics associated with better glycemic response to teneligliptin and metformin therapy in type 2 diabetes: a retrospective study
 International Journal of Advances in Medicine Gadge PV et al. Int J Adv Med. 2018 Apr;5(2):424-428 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20181082
International Journal of Advances in Medicine Gadge PV et al. Int J Adv Med. 2018 Apr;5(2):424-428 http://www.ijmedicine.com pissn 2349-3925 eissn 2349-3933 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3933.ijam20181082
Analysis of glucose-insulin-glucagon interaction models.
 C.J. in t Veld Analysis of glucose-insulin-glucagon interaction models. Bachelor thesis August 1, 2017 Thesis supervisor: dr. V. Rottschäfer Leiden University Mathematical Institute Contents 1 Introduction
C.J. in t Veld Analysis of glucose-insulin-glucagon interaction models. Bachelor thesis August 1, 2017 Thesis supervisor: dr. V. Rottschäfer Leiden University Mathematical Institute Contents 1 Introduction
Factors Associated with Long-Term Oral Hypoglycemic Agent Responsiveness in Korean Patients with Type 2 Diabetes Mellitus
 Original Article doi: 10.4093/dmj.2011.35.3.282 pissn 2233-6079 eissn 2233-6087 D I A B E T E S & M E T A B O L I S M J O U R N A L Factors Associated with Long-Term Oral Hypoglycemic Agent Responsiveness
Original Article doi: 10.4093/dmj.2011.35.3.282 pissn 2233-6079 eissn 2233-6087 D I A B E T E S & M E T A B O L I S M J O U R N A L Factors Associated with Long-Term Oral Hypoglycemic Agent Responsiveness
Pathogenesis of Type 2 Diabetes
 9/23/215 Multiple, Complex Pathophysiological Abnmalities in T2DM incretin effect gut carbohydrate delivery & absption pancreatic insulin secretion pancreatic glucagon secretion HYPERGLYCEMIA? Pathogenesis
9/23/215 Multiple, Complex Pathophysiological Abnmalities in T2DM incretin effect gut carbohydrate delivery & absption pancreatic insulin secretion pancreatic glucagon secretion HYPERGLYCEMIA? Pathogenesis
Young Seok Song 1, You-Cheol Hwang 2, Hong-Yup Ahn 3, Cheol-Young Park 1
 Comparison of the Usefulness of the Updated Homeostasis Model Assessment (HOMA2) with the Original HOMA1 in the Prediction of Type 2 Diabetes Mellitus in Koreans Young Seok Song 1, You-Cheol Hwang 2, Hong-Yup
Comparison of the Usefulness of the Updated Homeostasis Model Assessment (HOMA2) with the Original HOMA1 in the Prediction of Type 2 Diabetes Mellitus in Koreans Young Seok Song 1, You-Cheol Hwang 2, Hong-Yup
Glucagon secretion in relation to insulin sensitivity in healthy subjects
 Diabetologia (2006) 49: 117 122 DOI 10.1007/s00125-005-0056-8 ARTICLE B. Ahrén Glucagon secretion in relation to insulin sensitivity in healthy subjects Received: 4 July 2005 / Accepted: 12 September 2005
Diabetologia (2006) 49: 117 122 DOI 10.1007/s00125-005-0056-8 ARTICLE B. Ahrén Glucagon secretion in relation to insulin sensitivity in healthy subjects Received: 4 July 2005 / Accepted: 12 September 2005
Assessment of insulin sensitivity and beta-cell function from measurements in the fasting state and during an oral glucose tolerance test
 Diabetologia 2000) 43: 1507±1511 Ó Springer-Verlag 2000 Assessment of insulin sensitivity and beta-cell function from measurements in the fasting state and during an oral glucose tolerance test M. Albareda
Diabetologia 2000) 43: 1507±1511 Ó Springer-Verlag 2000 Assessment of insulin sensitivity and beta-cell function from measurements in the fasting state and during an oral glucose tolerance test M. Albareda
An integrated glucose-insulin model to describe oral glucose tolerance test data in healthy volunteers
 Title: An integrated glucose-insulin model to describe oral glucose tolerance test data in healthy volunteers Authors: Hanna E. Silber 1, Nicolas Frey 2 and Mats O. Karlsson 1 Address: 1 Department of
Title: An integrated glucose-insulin model to describe oral glucose tolerance test data in healthy volunteers Authors: Hanna E. Silber 1, Nicolas Frey 2 and Mats O. Karlsson 1 Address: 1 Department of
Dipeptidyl Peptidase-4 Inhibition by Vildagliptin and the Effect on Insulin Secretion and Action in Response to Meal Ingestion in Type 2 Diabetes
 Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Dipeptidyl Peptidase-4 Inhibition by Vildagliptin and the Effect on Insulin Secretion and Action in Response to Meal
Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Dipeptidyl Peptidase-4 Inhibition by Vildagliptin and the Effect on Insulin Secretion and Action in Response to Meal
A switching based PID technique for blood glucose control.
 Biomedical Research 2017; 28 (19): 8477-8483 ISSN 0970-938X www.biomedres.info A switching based PID technique for blood glucose control. Muhammad Hamayun Qammar Kayani, Kainat Naeem Malik, Shaban Ahmad,
Biomedical Research 2017; 28 (19): 8477-8483 ISSN 0970-938X www.biomedres.info A switching based PID technique for blood glucose control. Muhammad Hamayun Qammar Kayani, Kainat Naeem Malik, Shaban Ahmad,
Physician-Directed Diabetes Education without a Medication Change and Associated Patient Outcomes
 Original Article Clinical Care/Education Diabetes Metab J 2017;41:187-194 https://doi.org/10.4093/dmj.2017.41.3.187 pissn 2233-6079 eissn 2233-6087 DIABETES & METABOLISM JOURNAL Physician-Directed Diabetes
Original Article Clinical Care/Education Diabetes Metab J 2017;41:187-194 https://doi.org/10.4093/dmj.2017.41.3.187 pissn 2233-6079 eissn 2233-6087 DIABETES & METABOLISM JOURNAL Physician-Directed Diabetes
The necessity of identifying the basal glucose set-point in the IVGTT for patients with Type 2 Diabetes
 Othman et al. BioMedical Engineering OnLine (215) 14:18 DOI 1.1186/s12938-15-15-7 RESEARCH Open Access The necessity of identifying the basal glucose set-point in the IVGTT for patients with Type 2 Diabetes
Othman et al. BioMedical Engineering OnLine (215) 14:18 DOI 1.1186/s12938-15-15-7 RESEARCH Open Access The necessity of identifying the basal glucose set-point in the IVGTT for patients with Type 2 Diabetes
Clinical Characteristics of People with Newly Diagnosed Type 2 Diabetes between 2015 and 2016: Difference by Age and Body Mass Index
 Original Article Epidemiology Diabetes Metab J 218;42:137-146 https://doi.org/1.493/dmj.218.42.2.137 pissn 2233-679 eissn 2233-687 DIABETES & METABOLISM JOURNAL Clinical Characteristics of People with
Original Article Epidemiology Diabetes Metab J 218;42:137-146 https://doi.org/1.493/dmj.218.42.2.137 pissn 2233-679 eissn 2233-687 DIABETES & METABOLISM JOURNAL Clinical Characteristics of People with
Changing Clinical Characteristics according to Insulin Resistance and Insulin Secretion in Newly Diagnosed Type 2 Diabetic Patients in Korea
 Original Article Epidemiology Diabetes Metab J 2015 Forthcoming. Posted online 2015 pissn 2233-6079 eissn 2233-6087 DIABETES & METABOLISM JOURNAL Changing Clinical Characteristics according to Insulin
Original Article Epidemiology Diabetes Metab J 2015 Forthcoming. Posted online 2015 pissn 2233-6079 eissn 2233-6087 DIABETES & METABOLISM JOURNAL Changing Clinical Characteristics according to Insulin
An integrated glucose homeostasis model of glucose, insulin, C-peptide, GLP-1, GIP and glucagon in healthy subjects and patients with type 2 diabetes
 An integrated glucose homeostasis model of glucose, insulin, C-peptide, GLP-1, GIP and glucagon in healthy subjects and patients with type 2 diabetes Oskar Alskär, Jonatan Bagger, Rikke Røge, Kanji Komatsu,
An integrated glucose homeostasis model of glucose, insulin, C-peptide, GLP-1, GIP and glucagon in healthy subjects and patients with type 2 diabetes Oskar Alskär, Jonatan Bagger, Rikke Røge, Kanji Komatsu,
A model of GLP-1 action on insulin secretion in nondiabetic subjects
 Am J Physiol Endocrinol Metab 298: E1115 E1121, 21. First published February 23, 21; doi:1.1152/ajpendo.75.29. A model of GLP-1 action on insulin secretion in nondiabetic subjects Chiara Dalla Man, 1 Francesco
Am J Physiol Endocrinol Metab 298: E1115 E1121, 21. First published February 23, 21; doi:1.1152/ajpendo.75.29. A model of GLP-1 action on insulin secretion in nondiabetic subjects Chiara Dalla Man, 1 Francesco
Achieving Open-loop Insulin Delivery using ITM Designed for T1DM Patients
 I. J. Computer Network and Information Security, 2012, 1, 52-58 Published Online February 2012 in MECS (http://www.mecs-press.org/) DOI: 10.5815/ijcnis.2012.01.07 Achieving Open-loop Insulin Delivery using
I. J. Computer Network and Information Security, 2012, 1, 52-58 Published Online February 2012 in MECS (http://www.mecs-press.org/) DOI: 10.5815/ijcnis.2012.01.07 Achieving Open-loop Insulin Delivery using
Glycemia Prediction in Critically Ill Patients Using an Adaptive Modeling Approach
 Journal of Diabetes Science and Technology Volume 1, Issue 3, May 2007 Diabetes Technology Society SYMPOSIUM Glycemia Prediction in Critically Ill Patients Using an Adaptive Modeling Approach Tom, M.Sc.,
Journal of Diabetes Science and Technology Volume 1, Issue 3, May 2007 Diabetes Technology Society SYMPOSIUM Glycemia Prediction in Critically Ill Patients Using an Adaptive Modeling Approach Tom, M.Sc.,
GLP 1 agonists Winning the Losing Battle. Dr Bernard SAMIA. KCS Congress: Impact through collaboration
 GLP 1 agonists Winning the Losing Battle Dr Bernard SAMIA KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email: kcardiacs@gmail.com Web: www.kenyacardiacs.org Disclosures I have
GLP 1 agonists Winning the Losing Battle Dr Bernard SAMIA KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email: kcardiacs@gmail.com Web: www.kenyacardiacs.org Disclosures I have
A mathematical model of glucose-insulin interaction
 Science Vision www.sciencevision.org Science Vision www.sciencevision.org Science Vision www.sciencevision.org Science Vision www.sciencevision.org the alpha and beta cells of the pancreas respectively.
Science Vision www.sciencevision.org Science Vision www.sciencevision.org Science Vision www.sciencevision.org Science Vision www.sciencevision.org the alpha and beta cells of the pancreas respectively.
Mathematical model of standard oral glucose tolerance test for characterization of insulin potentiation in health
 Università Politecnica delle Marche Scuola di Dottorato di Ricerca in Scienze dell Ingegneria Curriculum in Elettromagnetismo e Bioingegneria ----------------------------------------------------------------------------------------
Università Politecnica delle Marche Scuola di Dottorato di Ricerca in Scienze dell Ingegneria Curriculum in Elettromagnetismo e Bioingegneria ----------------------------------------------------------------------------------------
Management of Type 2 Diabetes
 Management of Type 2 Diabetes Pathophysiology Insulin resistance and relative insulin deficiency/ defective secretion Not immune mediated No evidence of β cell destruction Increased risk with age, obesity
Management of Type 2 Diabetes Pathophysiology Insulin resistance and relative insulin deficiency/ defective secretion Not immune mediated No evidence of β cell destruction Increased risk with age, obesity
SIMULATIONS OF A MODEL-BASED FUZZY CONTROL SYSTEM FOR GLYCEMIC CONTROL IN DIABETES
 Bulletin of the Transilvania University of Braşov Vol. 8 (57) No. 2-2015 Series I: Engineering Sciences SIMULATIONS OF A MODEL-BASED FUZZY CONTROL SYSTEM FOR GLYCEMIC CONTROL IN DIABETES C. BOLDIȘOR 1
Bulletin of the Transilvania University of Braşov Vol. 8 (57) No. 2-2015 Series I: Engineering Sciences SIMULATIONS OF A MODEL-BASED FUZZY CONTROL SYSTEM FOR GLYCEMIC CONTROL IN DIABETES C. BOLDIȘOR 1
Observer-Based State Feedback for Enhanced Insulin Control of Type I Diabetic Patients
 98 The Open Biomedical Engineering Journal, 211, 5, 98-19 Open Access Observer-Based State Feedback for Enhanced Insulin Control of Type I Diabetic Patients Ali Hariri 1, * and Le Yi Wang 2 1 DTE Energy,
98 The Open Biomedical Engineering Journal, 211, 5, 98-19 Open Access Observer-Based State Feedback for Enhanced Insulin Control of Type I Diabetic Patients Ali Hariri 1, * and Le Yi Wang 2 1 DTE Energy,
Cordoba 01/02/2008. Slides Professor Pierre LEFEBVRE
 Cordoba 01/02/2008 Slides Professor Pierre LEFEBVRE Clinical Research in Type 2 Diabetes : Current Status and Future Approaches Pierre Lefèbvre* University of Liège Belgium Granada, Spain, February 2008
Cordoba 01/02/2008 Slides Professor Pierre LEFEBVRE Clinical Research in Type 2 Diabetes : Current Status and Future Approaches Pierre Lefèbvre* University of Liège Belgium Granada, Spain, February 2008
Computational assessment of insulin secretion and insulin sensitivity from 2-h oral glucose tolerance tests for clinical use for type 2 diabetes
 J Physiol Sci (211) 61:321 33 DOI 1.17/s12576-11-153-z ORIGINAL PAPER Computational assessment of insulin secretion and insulin sensitivity from 2-h oral glucose tolerance tests for clinical use for type
J Physiol Sci (211) 61:321 33 DOI 1.17/s12576-11-153-z ORIGINAL PAPER Computational assessment of insulin secretion and insulin sensitivity from 2-h oral glucose tolerance tests for clinical use for type
Characteristics Predictive for a Successful Switch from Insulin Analogue Therapy to Oral Hypoglycemic Agents in Patients with Type 2 Diabetes
 Original Article Yonsei Med J 2016 Nov;57(6):1395-1403 pissn: 0513-5796 eissn: 1976-2437 Characteristics Predictive for a Successful Switch from Insulin Analogue Therapy to Oral Hypoglycemic Agents in
Original Article Yonsei Med J 2016 Nov;57(6):1395-1403 pissn: 0513-5796 eissn: 1976-2437 Characteristics Predictive for a Successful Switch from Insulin Analogue Therapy to Oral Hypoglycemic Agents in
Prandial Insulin Dosing Using Run-to-Run Control 2,3
 Emerging Treatments and Technologies O R I G I N A L A R T I C L E Prandial Insulin Dosing Using Run-to-Run Control Application of clinical data and medical expertise to define a suitable performance metric
Emerging Treatments and Technologies O R I G I N A L A R T I C L E Prandial Insulin Dosing Using Run-to-Run Control Application of clinical data and medical expertise to define a suitable performance metric
Scope. History. History. Incretins. Incretin-based Therapy and DPP-4 Inhibitors
 Plasma Glucose (mg/dl) Plasma Insulin (pmol/l) Incretin-based Therapy and Inhibitors Scope Mechanism of action ผศ.ดร.นพ.ว ระเดช พ ศประเสร ฐ สาขาว ชาโภชนว ทยาคล น ก ภาคว ชาอาย รศาสตร คณะแพทยศาสตร มหาว ทยาล
Plasma Glucose (mg/dl) Plasma Insulin (pmol/l) Incretin-based Therapy and Inhibitors Scope Mechanism of action ผศ.ดร.นพ.ว ระเดช พ ศประเสร ฐ สาขาว ชาโภชนว ทยาคล น ก ภาคว ชาอาย รศาสตร คณะแพทยศาสตร มหาว ทยาล
Treating Type 2 Diabetes with Bariatric Surgery. Goal of Treating T2DM. Remission of T2DM with Bariatric
 Treating Type 2 Diabetes with Bariatric Surgery Number (in Millions) of Persons with Diagnosed Diabetes, United States, 198 25 The number of Americans with diabetes increased from 5.6 to 15.8 million Guilherme
Treating Type 2 Diabetes with Bariatric Surgery Number (in Millions) of Persons with Diagnosed Diabetes, United States, 198 25 The number of Americans with diabetes increased from 5.6 to 15.8 million Guilherme
Carbohydrate Ratio Optimization and Adaptation Algorithm. Supplementary Figure 1. Schematic showing components of the closed-loop system.
 Basal Profile Adaptation Algorithm Carbohydrate Ratio Optimization and Adaptation Algorithm Supplementary Figure 1. Schematic showing components of the closed-loop system. The insulin pump and Dexcom G4
Basal Profile Adaptation Algorithm Carbohydrate Ratio Optimization and Adaptation Algorithm Supplementary Figure 1. Schematic showing components of the closed-loop system. The insulin pump and Dexcom G4
Independent measures of insulin secretion and insulin sensitivity during the same test: the glucagon insulin tolerance test
 Original Article doi: 10.1111/j.1365-2796.2008.01921.x Independent measures of insulin secretion and insulin sensitivity during the same test: the glucagon insulin tolerance test M. Dorkhan 1, D. Tripathy
Original Article doi: 10.1111/j.1365-2796.2008.01921.x Independent measures of insulin secretion and insulin sensitivity during the same test: the glucagon insulin tolerance test M. Dorkhan 1, D. Tripathy
Importance of quantifying insulin secretion in relation to insulin sensitivity to accurately assess beta cell function in clinical studies
 European Journal of Endocrinology (2004) 150 97 104 ISSN 0804-4643 REVIEW Importance of quantifying insulin secretion in relation to insulin sensitivity to accurately assess beta cell function in clinical
European Journal of Endocrinology (2004) 150 97 104 ISSN 0804-4643 REVIEW Importance of quantifying insulin secretion in relation to insulin sensitivity to accurately assess beta cell function in clinical
Glucose Clamp Algorithms and Insulin Time-Action Profiles. B. Wayne Bequette, Ph.D.
 Journal of Diabetes Science and Technology Volume 3, Issue 5, September 2009 Diabetes Technology Society SYMPOSIUM Glucose Clamp Algorithms and Insulin Time-Action Profiles B. Wayne, Ph.D. Abstract Motivation:
Journal of Diabetes Science and Technology Volume 3, Issue 5, September 2009 Diabetes Technology Society SYMPOSIUM Glucose Clamp Algorithms and Insulin Time-Action Profiles B. Wayne, Ph.D. Abstract Motivation:
METABOLISM CLINICAL AND EXPERIMENTAL XX (2011) XXX XXX. available at Metabolism.
 METABOLISM CLINICAL AND EXPERIMENTAL XX (211) XXX XXX available at www.sciencedirect.com Metabolism www.metabolismjournal.com Estimation of prehepatic insulin secretion: comparison between standardized
METABOLISM CLINICAL AND EXPERIMENTAL XX (211) XXX XXX available at www.sciencedirect.com Metabolism www.metabolismjournal.com Estimation of prehepatic insulin secretion: comparison between standardized
Real-Time State Estimation and Long-Term Model Adaptation: A Two-Sided Approach toward Personalized Diagnosis of Glucose and Insulin Levels
 Journal of Diabetes Science and Technology Volume 6, Issue 5, September 202 Diabetes Technology Society ORIGINAL ARTICLE Real-Time State Estimation and Long-Term Model Adaptation: A Two-Sided Approach
Journal of Diabetes Science and Technology Volume 6, Issue 5, September 202 Diabetes Technology Society ORIGINAL ARTICLE Real-Time State Estimation and Long-Term Model Adaptation: A Two-Sided Approach
Specific insulin and proinsulin in normal glucose tolerant first-degree relatives of NIDDM patients
 Brazilian Journal of Medical and Biological Research (1999) 32: 67-72 Insulin and proinsulin in first-degree relatives of NIDDM ISSN 1-879X 67 Specific insulin and proinsulin in normal glucose tolerant
Brazilian Journal of Medical and Biological Research (1999) 32: 67-72 Insulin and proinsulin in first-degree relatives of NIDDM ISSN 1-879X 67 Specific insulin and proinsulin in normal glucose tolerant
Insulin Control System for Diabetic Patients by Using Adaptive Controller
 J. Basic. Appl. Sci. Res., 1(10)1884-1889, 2011 2011, TextRoad Publication ISSN 2090-4304 Journal of Basic and Applied Scientific Research www.textroad.com Insulin Control System for Diabetic Patients
J. Basic. Appl. Sci. Res., 1(10)1884-1889, 2011 2011, TextRoad Publication ISSN 2090-4304 Journal of Basic and Applied Scientific Research www.textroad.com Insulin Control System for Diabetic Patients
Smith Predictor Sliding Mode Closed-loop Glucose Controller in Type 1 Diabetes
 Smith Predictor Sliding Mode Closed-loop Glucose Controller in Type 1 Diabetes Amjad Abu-Rmileh Winston Garcia-Gabin Research group on Statistics, Applied Economics and Health (GRECS), University of Girona,
Smith Predictor Sliding Mode Closed-loop Glucose Controller in Type 1 Diabetes Amjad Abu-Rmileh Winston Garcia-Gabin Research group on Statistics, Applied Economics and Health (GRECS), University of Girona,
Insulin resistance might play an important
 Pathophysiology/Complications O R I G I N A L A R T I C L E Quantitative Insulin Sensitivity Check Index and the Reciprocal Index of Homeostasis Model Assessment in Normal Range Weight and Moderately Obese
Pathophysiology/Complications O R I G I N A L A R T I C L E Quantitative Insulin Sensitivity Check Index and the Reciprocal Index of Homeostasis Model Assessment in Normal Range Weight and Moderately Obese
Analysis of Intravenous Glucose Tolerance Test Data Using Parametric and Nonparametric Modeling: Application to a Population at Risk for Diabetes
 Journal of Diabetes Science and Technology Volume 7, Issue 4, July 2013 Diabetes Technology Society ORIGINAL ARTICLE Analysis of Intravenous Glucose Tolerance Test Data Using Parametric and Nonparametric
Journal of Diabetes Science and Technology Volume 7, Issue 4, July 2013 Diabetes Technology Society ORIGINAL ARTICLE Analysis of Intravenous Glucose Tolerance Test Data Using Parametric and Nonparametric
An event-based point of view on the control of insulin-dependent diabetes
 An event-based point of view on the control of insulin-dependent diabetes Brigitte Bidégaray-Fesquet Laboratoire Jean Kuntzmann Univ. Grenoble Alpes, France Réunion e-baccuss September 4th 20 Réunion e-baccuss,
An event-based point of view on the control of insulin-dependent diabetes Brigitte Bidégaray-Fesquet Laboratoire Jean Kuntzmann Univ. Grenoble Alpes, France Réunion e-baccuss September 4th 20 Réunion e-baccuss,
VIRTUAL PATIENTS DERIVED FROM THE
 VIRTUAL PATIENTS DERIVED FROM THE CARELINK DATABASE Benyamin Grosman PhD Senior Principle Scientist Medtronic Diabetes WHY VIRTUAL PATIENT MODELING? Reduce the cost of clinical trials Use models in conjunction
VIRTUAL PATIENTS DERIVED FROM THE CARELINK DATABASE Benyamin Grosman PhD Senior Principle Scientist Medtronic Diabetes WHY VIRTUAL PATIENT MODELING? Reduce the cost of clinical trials Use models in conjunction
Comparison of Oral Glucose Insulin Sensitivity with Other Insulin Sensitivity Surrogates from Oral Glucose Tolerance Tests in Chinese
 4 Original Article Comparison of Oral Glucose Insulin Sensitivity with Other Insulin Sensitivity Surrogates from Oral Glucose Tolerance Tests in Chinese Chung-Ze Wu 1 MD Dee Pei 2 MD Ching-Chieh Su 2 MD
4 Original Article Comparison of Oral Glucose Insulin Sensitivity with Other Insulin Sensitivity Surrogates from Oral Glucose Tolerance Tests in Chinese Chung-Ze Wu 1 MD Dee Pei 2 MD Ching-Chieh Su 2 MD
Nutrition Journal. Open Access. Abstract
 Nutrition Journal BioMed Central Research Indices of insulin sensitivity and secretion from a standard liquid meal test in subjects with type 2 diabetes, impaired or normal fasting glucose Kevin C Maki*
Nutrition Journal BioMed Central Research Indices of insulin sensitivity and secretion from a standard liquid meal test in subjects with type 2 diabetes, impaired or normal fasting glucose Kevin C Maki*
A Dynamic Model with Structured Recurrent Neural Network to Predict Glucose-Insulin Regulation of Type 1 Diabetes Mellitus
 Proceedings of the 9th International Symposium on Dynamics and Control of Process Systems (DYCOPS 1), Leuven, Belgium, July 5-7, 1 Mayuresh Kothare, Moses Tade, Alain Vande Wouwer, Ilse Smets (Eds.) MoAT1.1
Proceedings of the 9th International Symposium on Dynamics and Control of Process Systems (DYCOPS 1), Leuven, Belgium, July 5-7, 1 Mayuresh Kothare, Moses Tade, Alain Vande Wouwer, Ilse Smets (Eds.) MoAT1.1
The Identifiable Virtual Patient Model: Comparison of Simulation and Clinical Closed-Loop Study Results
 Journal of Diabetes Science and Technology Volume 6, Issue 2, March 202 Diabetes Technology Society ORIGINAL ARTICLE The Identifiable Virtual Patient Model: Comparison of Simulation and Clinical Closed-Loop
Journal of Diabetes Science and Technology Volume 6, Issue 2, March 202 Diabetes Technology Society ORIGINAL ARTICLE The Identifiable Virtual Patient Model: Comparison of Simulation and Clinical Closed-Loop
Causal Modeling of the Glucose-Insulin System in Type-I Diabetic Patients J. Fernandez, N. Aguilar, R. Fernandez de Canete, J. C.
 Causal Modeling of the Glucose-Insulin System in Type-I Diabetic Patients J. Fernandez, N. Aguilar, R. Fernandez de Canete, J. C. Ramos-Diaz Abstract In this paper, a simulation model of the glucoseinsulin
Causal Modeling of the Glucose-Insulin System in Type-I Diabetic Patients J. Fernandez, N. Aguilar, R. Fernandez de Canete, J. C. Ramos-Diaz Abstract In this paper, a simulation model of the glucoseinsulin
OGTT-Derived Measures of Insulin Sensitivity Are Confounded by Factors Other Than Insulin Sensitivity Itself
 University of Pennsylvania ScholarlyCommons Departmental Papers (Vet) School of Veterinary Medicine 9-6-2012 OGTT-Derived Measures of Insulin Sensitivity Are Confounded by Factors Other Than Insulin Sensitivity
University of Pennsylvania ScholarlyCommons Departmental Papers (Vet) School of Veterinary Medicine 9-6-2012 OGTT-Derived Measures of Insulin Sensitivity Are Confounded by Factors Other Than Insulin Sensitivity
A study on the effects of exercise motivation of the elderly people on euphoria
 Original Article Journal of Exercise Rehabilitation 2017;13(4):387-392 A study on the effects of exercise motivation of the elderly people on euphoria Ah-Ra Oh 1, Eun-Surk Yi 2, * 1 Department of Physical
Original Article Journal of Exercise Rehabilitation 2017;13(4):387-392 A study on the effects of exercise motivation of the elderly people on euphoria Ah-Ra Oh 1, Eun-Surk Yi 2, * 1 Department of Physical
Validation of a novel index to assess insulin resistance of adipose tissue lipolytic activity in. obese subjects
 Validation of a novel index to assess insulin resistance of adipose tissue lipolytic activity in obese subjects Elisa Fabbrini, MD, PhD; Faidon Magkos, PhD; Caterina Conte, MD; Bettina Mittendorfer, PhD;
Validation of a novel index to assess insulin resistance of adipose tissue lipolytic activity in obese subjects Elisa Fabbrini, MD, PhD; Faidon Magkos, PhD; Caterina Conte, MD; Bettina Mittendorfer, PhD;
Exenatide Treatment for 6 Months Improves Insulin Sensitivity in Adults With Type 1 Diabetes
 666 Diabetes Care Volume 37, March 2014 CLIN CARE/EDUCATION/NUTRITION/PSYCHOSOCIAL Exenatide Treatment for 6 Months Improves Insulin Sensitivity in Adults With Type 1 Diabetes Gayatri Sarkar, 1 May Alattar,
666 Diabetes Care Volume 37, March 2014 CLIN CARE/EDUCATION/NUTRITION/PSYCHOSOCIAL Exenatide Treatment for 6 Months Improves Insulin Sensitivity in Adults With Type 1 Diabetes Gayatri Sarkar, 1 May Alattar,
Accurate Measurement of Postprandial Glucose Turnover: Why Is It Difficult and How Can It Be Done (Relatively) Simply?
 Diabetes Volume 65, May 2016 1133 Robert A. Rizza, 1 Gianna Toffolo, 2 and Claudio Cobelli 2 Accurate Measurement of Postprandial Glucose Turnover: Why Is It Difficult and How Can It Be Done (Relatively)
Diabetes Volume 65, May 2016 1133 Robert A. Rizza, 1 Gianna Toffolo, 2 and Claudio Cobelli 2 Accurate Measurement of Postprandial Glucose Turnover: Why Is It Difficult and How Can It Be Done (Relatively)
Insulin Secretion and Sensitivity during Oral Glucose Tolerance Test in Korean Lean Elderly Women
 J Korean Med Sci 2001; 16: 592-7 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences Insulin Secretion and Sensitivity during Oral Glucose Tolerance Test in Korean Lean Elderly Women Impaired
J Korean Med Sci 2001; 16: 592-7 ISSN 1011-8934 Copyright The Korean Academy of Medical Sciences Insulin Secretion and Sensitivity during Oral Glucose Tolerance Test in Korean Lean Elderly Women Impaired
Trends in the Diabetes Epidemic in Korea
 Review Article Endocrinol Metab 15;3:142-146 http://dx.doi.org/1.383/enm.15.3.2.142 pissn 93-596X eissn 93-5978 Trends in the Diabetes Epidemic in Korea Kyoung Hwa Ha 1,2, Dae Jung Kim 1,2 1 Department
Review Article Endocrinol Metab 15;3:142-146 http://dx.doi.org/1.383/enm.15.3.2.142 pissn 93-596X eissn 93-5978 Trends in the Diabetes Epidemic in Korea Kyoung Hwa Ha 1,2, Dae Jung Kim 1,2 1 Department
Week 3, Lecture 5a. Pathophysiology of Diabetes. Simin Liu, MD, ScD
 Week 3, Lecture 5a Pathophysiology of Diabetes Simin Liu, MD, ScD General Model of Peptide Hormone Action Hormone Plasma Membrane Activated Nucleus Cellular Trafficking Enzymes Inhibited Receptor Effector
Week 3, Lecture 5a Pathophysiology of Diabetes Simin Liu, MD, ScD General Model of Peptide Hormone Action Hormone Plasma Membrane Activated Nucleus Cellular Trafficking Enzymes Inhibited Receptor Effector
Individuals with impaired fasting glucose (IFG) have
 Original Article Pathogenesis of Pre-Diabetes Mechanisms of Fasting and Postprandial Hyperglycemia in People With Impaired Fasting Glucose and/or Impaired Glucose Tolerance Gerlies Bock, 1 Chiara Dalla
Original Article Pathogenesis of Pre-Diabetes Mechanisms of Fasting and Postprandial Hyperglycemia in People With Impaired Fasting Glucose and/or Impaired Glucose Tolerance Gerlies Bock, 1 Chiara Dalla
Tutorial ADAPT Case study 1. Data sampling / error model. Yared Paalvast Yvonne Rozendaal
 Tutorial ADAPT 13.15 17.00 Yared Paalvast (t.paalvast@umcg.nl) Yvonne Rozendaal (y.j.w.rozendaal@tue.nl) Case study 1. Data sampling / error model 1.1 Visualize raw data (dataset1a.mat) time data: t concentration
Tutorial ADAPT 13.15 17.00 Yared Paalvast (t.paalvast@umcg.nl) Yvonne Rozendaal (y.j.w.rozendaal@tue.nl) Case study 1. Data sampling / error model 1.1 Visualize raw data (dataset1a.mat) time data: t concentration
Estimates of Insulin Sensitivity Using Glucose and C-Peptide From the Hyperglycemia and Adverse Pregnancy Outcome Glucose Tolerance Test
 Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Estimates of Insulin Sensitivity Using Glucose and C-Peptide From the Hyperglycemia and Adverse Pregnancy Outcome Glucose
Clinical Care/Education/Nutrition/Psychosocial Research O R I G I N A L A R T I C L E Estimates of Insulin Sensitivity Using Glucose and C-Peptide From the Hyperglycemia and Adverse Pregnancy Outcome Glucose
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Diabetes: Definition Pathophysiology Treatment Goals. By Scott Magee, MD, FACE
 Diabetes: Definition Pathophysiology Treatment Goals By Scott Magee, MD, FACE Disclosures No disclosures to report Definition of Diabetes Mellitus Diabetes Mellitus comprises a group of disorders characterized
Diabetes: Definition Pathophysiology Treatment Goals By Scott Magee, MD, FACE Disclosures No disclosures to report Definition of Diabetes Mellitus Diabetes Mellitus comprises a group of disorders characterized
