Evaluating Medication Use for Continuous Quality Improvement in Diabetes Care
|
|
|
- Dulcie Wells
- 5 years ago
- Views:
Transcription
1 CONTEMPORARY SUBJECT Evaluating Medication Use for Continuous Quality Improvement in Diabetes Care DAVID P. NAU, PhD Continuous quality improvement (CQI) is the structured organizational process for involving personnel in planning and executing a continuous flow of improvements to provide services that meet or exceed expectations. 1 It is integral to the long-term success of managed care organizations (MCOs). Many purchasers of health care, along with accrediting bodies, have encouraged the adoption of the CQI philosophy and its tools. The hope is that CQI will lead to more efficient care as well as better health for members enrolled in health plans. The value of CQI is generally accepted, and consistent with the philosophy of CQI, the methods for measuring quality are undergoing constant evolution. The most common method for evaluating the quality of MCOs is the Health Plan Employer Data and Information Set (HEDIS) from the National Committee for Quality Assurance (NCQA). HEDIS includes performance indicators related to health promotion and the effectiveness of care for selected diseases. These performance indicators offer insight to the quality of care provided by MCOs. The number of performance indicators within HEDIS has expanded over the past several years, and the technical specifications for the indicators have been refined. Reported results and trends in the performance indicators over the past several years suggest that NCQA has been successful in stimulating quality improvement in MCOs 2,3 Nonetheless, HEDIS does have limitations. Kerr and colleagues have pointed out several pitfalls in the use of HEDIS for quality improvement. 4 These pitfalls include the lack of a strong link between many process-oriented measures and outcomes, intermediate outcomes-oriented measures that are not linked to actionable processes, measures that do not target those at highest-risk, the lack of severity adjustment for outcomes measures, and the inability of the measurement system to allow for patient exceptions. These pitfalls in the measurement system limit the utility of HEDIS for quality improvement efforts. Ideally, the current indicators in HEDIS would be supplemented by additional measures of quality that help to pinpoint specific health care processes that need improvement. Author DAVID P. NAU, PhD, is an Assistant Professor, Department of Social and Administrative Sciences, Center for Medication Use, Policy and Economics, University of Michigan College of Pharmacy, Ann Arbor, Michigan. AUTHOR CORRESPONDENCE: David P. Nau, PhD: dnau@umich.edu Copyright 2002, Academy of Managed Care Pharmacy. All rights reserved. Medications are the mainstay of therapy for many chronic diseases. Thus, the medication-use process should be a focal point for CQI initiatives in populations that have diseases such as asthma, diabetes, chronic heart failure, dyslipidemia, or hypertension. While the current HEDIS indicator set does contain a few medication-specific indicators (e.g., beta-blocker treatment following a myocardial infarction and appropriate medications for the treatment of persistent asthma and depression), there are still relatively few indicators targeted specifically on the medicationuse system. One disease state that lacks well-established medication-specific indicators is diabetes mellitus. Quality Measurement for Diabetes For MCOs, the standard for quality measurement in diabetes has been the HEDIS diabetes indicator set. Since 1999, the HEDIS Comprehensive Diabetes Care indicator set has estimated the percentage of health plan members with type 1 and type 2 diabetes who were years old and during the measurement year had (1) a glycosylated hemoglobin (HbA1c) test; (2) poorly controlled HbA1c (HbA1c>9.5%); (3) a cholesterol (LDL-c) test; (4) an LDL-c level less than 130mg/dl; (5) a microalbumin test; and (6) a dilated eye exam. 3 In 2001, NCQA partnered with the American Medical Association and the Joint Commission on Accreditation of Healthcare Organizations to develop a consensus statement on Coordinated Performance Measurement for the Management of Adult Diabetes. 5 This consensus statement proposes quality measures that go beyond the HEDIS reporting set for diabetes. Specifically, it adds indicators related to blood pressure measurement and control, foot exams, office visits, and influenza immunizations. The Veterans Affairs Quality Enhancement Research Initiative is currently testing several indicators for diabetes mellitus, including 2 measures that target the appropriate use of medications for treatment of dyslipidemia and hypertension in persons with diabetes. 4,6 The indicators capture whether appropriate initiation or adjustments of drug therapy occurred for persons with diabetes who had elevated LDL and/or elevated blood pressure. These new measures should enhance the quality improvement efforts of the Department of Veterans Affairs by examining specific provider behaviors that are tightly linked with patient outcomes. Although advancements have been made in quality measurement for diabetes mellitus, there are still relatively few indicators that focus on the use of medications in this population. Although this is a shortcoming of our quality measurement efforts, there may be several reasons for the failure to target medication use in diabetes. For example, initial indicator devel- 378 Journal of Managed Care Pharmacy JMCP September/October 2002 Vol. 8, No. 5
2 TABLE 1 Examples of Medication-Use Indicators for Diabetes Mellitus (DM) Indicator Initiate/Adjust Therapy Definition Population Caveats Diabetes Hypertension* Dyslipidemia* Proportion of patients who had an HbA1c reading above 9.5% in the reporting year and who had initiation or intensification of drug therapy within 3 months of the elevated HbA1c. Proportion of patients with DM who had 2 blood pressure readings > 140/90 mmhg in the reporting year and who had an initiation or intensification of drug therapy within 3 months of the elevated readings. Proportion of patients with DM who had an LDL level > 130mg/dl in the reporting year and who had an initiation or intensification of drug therapy within 3 months of the elevated reading. Patients with an HbA1c reading above 9.5% during the reporting year. Patients with DM who had 2 blood pressure readings > 140/90 mmhg in the reporting year. Patients with DM who had an LDL level > 130mg/dl in the reporting year These indicators do not take into account the other modalities used to treat DM, hypertension or dyslipidemia (e.g., diet, exercise). These indicators would not include patients with DM who have not had a measurement of HbA1c, blood pressure, or lipids. Adherence to Therapy Using administrative claims: The proportion of patients who obtained a supply of medication that would cover at least 90% of days in the assessment period. Using self-reported data: The proportion of patients who reported taking at least 90% of oral antidiabetic drug doses as directed. Patients with an active prescription for oral diabetes medication throughout the reporting year. For patients on multi-drug therapy for diabetes, the first oral antidiabetic agent listed in the drug regimen could be used for analyses in lieu of more complex analyses involving all antidiabetic agents. Monitoring for ADR TZD The proportion of patients dispensed a TZD who had a baseline and follow-up test of serum ALT. Patients prescribed a TZD for at least 2 months The acceptable time frame for tests should be defined by the HMO (e.g., follow-up between 2 and 3 months of initial dispensing of drug). Metformin The proportion of patients dispensed metformin who had a baseline and follow-up test of renal function (serum creatinine) Patients prescribed metformin for at least 2 months. * Adapted from Kerr EA, Krein SL, Vijan S, et al. Am J Managed Care. 2001;7: ADR = Adverse drug reaction. TZD = thiazolidinediones (e.g., rosiglitazone, pioglitazone). opment efforts were often focused on whether appropriate screening and monitoring for conditions occurred (e.g., was the cholesterol and HbA1c checked?). This may have been an appropriate place to start our indicator development efforts since one can t effectively manage a clinical problem if one doesn t know whether the problem exists. However, measuring HbA1c is not enough. We must be making appropriate modifications of therapy to ensure that the HbA1c measurement leads to positive outcomes. There are also challenges to be overcome in data collection when focusing on medication management. Not all managed care patients have a prescription benefit. This limits the feasibility of tracking prescription claims for CQI. Even when prescription claims data are available, the data are often separate from medical claims and need to be merged with other data to provide useful information. Finally, the drug therapy of patients with diabetes is complex, and thus, no simple standard can be applied for which drug is best for each patient. Despite the difficulties in creating valid and reliable indicators for diabetes, it may still be useful for a managed care organization to evaluate the quality of medication management for their members with diabetes. Patients with diabetes often have Vol. 8, No. 5 September/October 2002 JMCP Journal of Managed Care Pharmacy 379
3 comorbid conditions such as dyslipidemia, hypertension, and depression. All of these conditions are managed, in part, through the use of drug therapy. Thus, the appropriate management of medication is highly important for achieving optimal outcomes in this population. 7,8 The development of medication-use indicators could facilitate CQI efforts for diabetes by identifying specific prescribing, monitoring, or self-management behaviors that are in need of improvement. Medication-use Indicators for Diabetes There are numerous medication-use indicators that could be constructed for persons with diabetes mellitus. Ideally, the indicators would address various aspects of the medication-use system such as initiation of therapy, selection of drug products, monitoring of therapy, adherence to therapy, and adjustments of therapy. 9 Several examples of indicators are shown in Table 1. Initiation/Adjustment of Therapy The first steps for practitioners in the medication-use system are to diagnose the medical problems exhibited by their patients and to prescribe drugs based upon the diagnoses. Although current HEDIS indicators for diabetes are useful for determining whether practitioners are screening patients for specified problems (e.g., was the HbA1c checked?), they do not provide insight on whether appropriate drug therapy was prescribed in response to the identified problems or adjusted when necessary to achieve the therapeutic goals. Kerr and colleagues have proposed measures that would help to evaluate whether drug therapy was initiated or adjusted in response to elevated LDL or blood pressure in persons with diabetes mellitus. 4 These measures are currently being tested in the Veterans Affairs health system. Adaptations of these measures are represented in Table 1. Selecting the cut-point for each of these indicators is a crucial issue. In one indicator proposed by Kerr and colleagues, an LDL of 130 mg/dl is used as the cutpoint. Patients above this point are identified as being at high risk for cardiovascular events and are thus included in the indicator. This cut-point is consistent with the parameters established in other HEDIS indicators using LDL. 3 Additionally, the American Diabetes Association recommends that drug therapy be initiated in diabetes patients (who do not have preexisting coronary heart disease) when the LDL has exceeded 130 mg/dl. 10 For diabetes patients with preexisting coronary heart disease, the ADA recommends that drug therapy be initiated along with medical nutrition therapy when the LDL exceeds 100 mg/dl. The therapeutic goal for all diabetes patients being treated for dyslipidemia is an LDL<100mg/dl. Although it may be tempting to construct an indicator that identifies the proportion of patients who have not reached the therapeutic goal of LDL<100 mg/dl, this more stringent cut-point may lead to the inappropriate conclusions about the quality of medication use. For example, it may be appropriate for a clinician to choose not to increase the intensity of pharmacological therapy for a diabetes patient with LDL=102 mg/dl. However, it would be more difficult to justify the failure to modify therapy in a diabetes patient with LDL=132 mg/dl. Thus, the cut-point of 130 mg/dl is perhaps less likely to lead to inappropriate categorizations of the quality of therapy. The logic found in Kerr et al. s indicators could be applied to the evaluation of oral antidiabetic drug therapy. If the HbA1c is significantly elevated (>9.5%), then an initiation or adjustment of drug therapy will likely be required to help the patient achieve the therapeutic goal for HbA1c of 6.5%. 11 The cut-point of HbA1c=9.5% is consistent with existing HEDIS indicators and other quality measurement systems. 3,5 Although diet and exercise can also be used to lower HbA1c, most patients with an HbA1c above 9.5% will require drug therapy. For patients who are already taking antidiabetic medications, an HbA1c above 9.5% should signal the need for an adjustment in therapy. Data for constructing the indicators could be obtained through a combination of administrative claims and chart review as specified for the existing HEDIS diabetes indicators. Since chart reviewers are already extracting data on HbA1c, LDL, and blood pressure, they could also determine whether the drug therapy was adjusted within 3 months of the tests. While this would lengthen the time required to complete the chart review, the value of the data may exceed the additional cost for chart review. In a health care system with electronic laboratory data or a system-wide electronic medical record, the electronic medical/laboratory data could be compared to the prescription claims data to determine if a change in medication occurred subsequent to the laboratory test or blood pressure assessment. Adherence to Therapy Oral medications are one of the key factors to glycemic control for many persons with type 2 diabetes. However, many persons find it difficult to adhere to their medication regimen for long periods of time. A recent study found that fewer than 15% of diabetes patients on single-drug therapy maintained ideal adherence throughout a one-year period, while patients on multi-drug therapy for diabetes experienced even lower levels of persistence and adherence. 12 Considering that many patients with type 2 diabetes have other comorbidities (e.g., dyslipidemia, hypertension), the drug regimen for these patients is often very complex and adherence is even more challenging. Many MCOs have implemented disease management strategies that include efforts to enhance patients medication regimen adherence. Because of the high costs of disease management programs and the potentially higher costs of nonadherence, it is important to evaluate whether these programs have led to improvements in patients persistence and adherence. There are many ways in which medication regimen adherence has been measured. 13 The methods that would be most fea- 380 Journal of Managed Care Pharmacy JMCP September/October 2002 Vol. 8, No. 5
4 sible for a managed care organization entail an analysis of prescription claims or a survey of patients. Steiner and Prochazka described several ways in which adherence rates can be calculated from prescription claims data. 14 However, all of these methods rely on having complete and accurate claims data for prescription drugs. While most prescription drug claims are accurate, the quality of the data may not be sufficient to allow valid comparisons between health plans. 15 Additionally, some managed care enrollees may not have complete prescription drug benefits or may be obtaining some medications outside of the prescription benefit. For patients with diabetes, it would also be difficult to estimate an adherence rate for persons using insulin since many patients may adjust their dose based upon their changing need for insulin. Nonetheless, it may be useful to determine whether patients have been obtaining refills of oral medications or blood glucose test strips. The trend in the refill rate for the diabetes population could be tracked over time to determine whether the implementation of new services leads to improvements in medication/strip refill adherence. Surveys of patients can also be used to measure medication regimen adherence. A number of different self-report measures can be used. 13 Some of these measures ask patients to report the number of missed doses over a specified time frame, while others may use visual analog scales or multidimensional scales. 13,16 Some measures are scored as continuous variables (i.e., percent of doses taken) while others convert the data to a dichotomous scale (adherent versus nonadherent). It is also important to recognize that different self-report measures may provide different results when applied to the same patients. 16 Thus, comparisons of adherence rates are only appropriate when using identical adherence measures. An advantage of surveys is that one can also ask patients about the barriers that they encounter in using their medications. This may help to pinpoint common problems encountered by your members with diabetes. Services could then be developed or modified to meet the needs of this population. Repeating the survey on a regular basis could then inform you about whether service modifications actually diminished the barriers to adherence and improved medication use. Although many practitioners may suspect that nonadherent patients would not be truthful on a survey, the existing literature shows that confidential surveys may be reasonably accurate when estimating the adherence rate within a population. 13 Thus, the advantages of patient surveys may outweigh their shortcomings. Monitoring of Drug Therapy One of the most important elements of the medication-use system is the monitoring of drug therapy. Monitoring allows us to determine if the patient is achieving the therapeutic goal and to identify adverse drug reactions. The monitoring of patients progress toward therapeutic goals is already captured by many of the HEDIS diabetes indicators. However, there are no indicators related to monitoring for adverse reactions. Because of the possibility of significant, albeit rare, adverse drug reactions, the manufacturers of metformin have recommended the recurrent monitoring of renal function and the manufacturers of the thiazolidinedione (TZD) class of drugs have developed guidelines for the monitoring of hepatic function Because the occurrence of these problems is rare, it is appropriate to weigh the cost versus benefit of requiring all MCOs to construct indicators regarding the incidence of the adverse events. It could be argued that practitioners should be following the recommended monitoring guidelines for these drugs and that their adherence to the monitoring guidelines is worthy of attention. In health care systems with electronic medical records, it may be cost-effective to measure practitioner adherence to the drug monitoring guidelines for metformin and TZDs. Other Potential Indicators Many other indicators could be selected for the evaluation of the medication use system for diabetes depending on the particular concerns of the MCO. For example, one could measure the proportion of diabetes patients with hypertension who receive an angiotensin-converting enzyme inhibitor (ACEI) or angiotensin receptor blocker (ARB). The ACEI/ARB classes of drugs have been recommended by the American Diabetes Association as first-line therapy for the treatment of hypertension in persons with diabetes due to the ability of these drugs to slow the development or progression of diabetic nephropathy. 20 Although an ACEI or ARB should be considered for every person with diabetes and hypertension, these drugs may not be appropriate for some patients. In order to determine whether care for an individual patient was appropriate, information from the medical record would be required. Consequently, examining only the trend in claims for antihypertensive medications has its limitations. A trend toward increased use of ACEI/ARBs in patients with diabetes and hypertension may indicate improved quality of medication prescribing; however, it is difficult to know the ideal rate of ACEI/ARB utilization without detailed, patient-specific, medical information. Even more indicators could be adapted from the Academy of Managed Care Pharmacy Catalog of Pharmacy Quality Indicators. 21 While the indicators in the catalog are not disease-specific, many of them could be adapted to medication utilization patterns in diabetes. Using the Indicators for CQI Indicators should be a part of a quality improvement program wherein they help to identify areas in need of improvement. They should be selected based upon both the value of the information provided and the feasibility of data collection. 1,22 It may be wise to gradually test and adopt new indicators rather than overwhelm an MCO s staff with a slew of new indicators. Consequently, each organization should prioritize its potential Vol. 8, No. 5 September/October 2002 JMCP Journal of Managed Care Pharmacy 381
5 indicators and select a small number of indicators that will be most useful, while not significantly adding to the burden of data collection. Of the sample indicators listed in Table 1, the most useful indicators may be those related to the initiation/adjustment of therapy. These indicators reflect a highly important element of care and provide actionable information in that they identify a specific provider behavior that can be modified. Additionally, collection of data for these indicators could be integrated with the existing HEDIS data collection. A diabetes quality improvement team within each MCO could respond to the indicator data by identifying the root causes for suboptimal performance and formulating plans for improvement. Potential strategies for improving performance might include (1) the creation or modification of guidelines for the use of diabetes medications, (2) educating providers and patients on the new guidelines, (3) providing performance feedback to individual practitioners, or (4) sending electronic prompts to physicians regarding the potential need for therapy adjustments when lab values exceed predetermined thresholds. By having repeated measurements of indicator data, you can determine whether CQI efforts have led to actual improvements. CQI has been successfully applied in MCOs. 23,24 A collaborative effort of physicians, nurses, pharmacists, patients, data analysts, and other MCO staff can identify opportunities for improvement, formulate and implement plans for improvement, and evaluate the impact of those plans. However, failure to assess key elements of the plan (e.g., medication use) may miss potential explanations for the success or failure of the QI plan. Without valid and actionable data, CQI efforts are hampered. The introduction of HEDIS has led to advances in improvements in the quality of care for persons with diabetes. 2,3 These improvements have mainly pertained to the increased screening and monitoring patients of patients with diabetes. Now it is time to move beyond the initial achievements of HEDIS to examine the ways providers and MCOs respond to the monitoring data. Have adjustments been made in therapy for patients for whom HbA1c is significantly elevated? Has treatment been initiated for patients with elevated blood pressure? Asking questions like these should help to close the loop in the medication use system as more attention is focused on the need to continually manage drug therapy to help patients achieve their therapeutic goals. DISCLOSURES No outside funding supported this study. The author does not have financial disclosures or a conflict of interest. REFERENCES 1. McLaughlin CP, Kaluzny AD. Continuous Quality Improvement in Health Care: Theory, Implementation and Applications. 2nd ed. Gaithersburg, MD: Aspen Publishers; National Committee for Quality Assurance. Quality dividends, Available at: 3. National Committee for Quality Assurance. The state of managed care quality, Available at: 4. Kerr EA, Krein SL, Vijan S, et al. Avoiding pitfalls in chronic disease quality measurement: a case for the next generation of technical quality measures. Am J Managed Care. 2001;7: American Medical Association, Joint Commission on Accreditation of Healthcare Organizations, National Committee for Quality Assurance. Coordinated performance measurement for the management of adult diabetes; April Available at: 6. Veterans Administration. Quality enhancement research initiatitive. Available at: 7. The Diabetes Control and Complications Trial Research Group. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med. 1993;329: UK Prospective Diabetes Study Group. Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet. 1998;352: Hepler CD, Grainger-Rousseau TJ. Pharmaceutical care versus traditional drug treatment. Drugs. 1995;49: American Diabetes Association. Management of dyslipidemia in adults with diabetes. Diabetes Care. 2002;25:S74-S American Association of Clinical Endocrinologists. Medical guidelines for the management of diabetes mellitus, Available at: Dailey G, Kim MS, Lian JF. Patient compliance and persistence with antihyperglycemic drug regimens: evaluation of a Medicaid patient opulation with type 2 diabetes mellitus. Clin Ther. 2001;23: Farmer KC. Methods for measuring and monitoring medication regimen adherence in clinical trials and clinical practice. Clin Ther. 1999;21: Steiner JF, Prochazka AV. The assessment of refill compliance using pharmacy records: Methods, validity, and applications. J Clin Epidemiol. 1997;50: Farris KB, Kaplan B, Kirking DM. Examination of days supply in computerized prescription claims. J Pharmacoepidemiol. 1994;3: Gao X, Nau DP. Congruence of 3 self-report measures of medication adherence among HIV patients. Ann Pharmacother. 2000;34: Bristol-Myers Squibb. Metformin prescribing information. Available at: Takeda Pharmaceuticals America. Actos prescribing information. Available at: GlaxoSmithKline. Avandia prescribing information. Available at: American Diabetes Association. Treatment of hypertension in adults with diabetes. Diabetes Care. 2002;25:S71-S Academy of Managed Care Pharmacy. Catalog of Pharmacy Quality Indicators. Available at: Accessed: August 13, Angaran DM. Selecting, developing, and evaluating indicators. Am J Hosp Pharm. 1991;48: Petitti DB, Dudi J, Contreras R, et al. Evaluation of the effect of performance monitoring and feedback on care process, utilization, and outcome. Diabetes Care. 2000;23: Solberg LI, Kottke TE, Brekke ML. CQI in Managed Care. In: McLaughlin CP, Kaluzny AD, ed. Continuous Quality Improvement in Health Care: Theory, Implications and Applications. Gaithersburg, MD: Aspen Publishers; 1999: Journal of Managed Care Pharmacy JMCP September/October 2002 Vol. 8, No. 5
Clinical and Economic Summary Report. for Employers
 Clinical and Economic Summary Report for Employers Magaly Rodriguez de Bittner, PharmD, CDE, FAPhA Director, P 3 Program Dawn Shojai, PharmD Assistant Director, P 3 Program P 3 Clinical & Economic Summary
Clinical and Economic Summary Report for Employers Magaly Rodriguez de Bittner, PharmD, CDE, FAPhA Director, P 3 Program Dawn Shojai, PharmD Assistant Director, P 3 Program P 3 Clinical & Economic Summary
DIABETES MEASURES GROUP OVERVIEW
 2014 PQRS OPTIONS F MEASURES GROUPS: DIABETES MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN DIABETES MEASURES GROUP: #1. Diabetes: Hemoglobin A1c Poor Control #2. Diabetes: Low Density Lipoprotein (LDL-C)
2014 PQRS OPTIONS F MEASURES GROUPS: DIABETES MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN DIABETES MEASURES GROUP: #1. Diabetes: Hemoglobin A1c Poor Control #2. Diabetes: Low Density Lipoprotein (LDL-C)
Effects of a Community Pharmacist-Based Diabetes Patient-Management Program on Intermediate Clinical Outcome Measures
 RESEARCH Effects of a Community Pharmacist-Based Diabetes Patient-Management Program on Intermediate Clinical Outcome Measures OBJECTIVES: Evaluate a community pharmacist-based diabetes patient-management
RESEARCH Effects of a Community Pharmacist-Based Diabetes Patient-Management Program on Intermediate Clinical Outcome Measures OBJECTIVES: Evaluate a community pharmacist-based diabetes patient-management
SCIENTIFIC STUDY REPORT
 PAGE 1 18-NOV-2016 SCIENTIFIC STUDY REPORT Study Title: Real-Life Effectiveness and Care Patterns of Diabetes Management The RECAP-DM Study 1 EXECUTIVE SUMMARY Introduction: Despite the well-established
PAGE 1 18-NOV-2016 SCIENTIFIC STUDY REPORT Study Title: Real-Life Effectiveness and Care Patterns of Diabetes Management The RECAP-DM Study 1 EXECUTIVE SUMMARY Introduction: Despite the well-established
STARS SYSTEM 5 CATEGORIES
 TMG STARS 2018 1 2 STARS Program Implemented in 2008 by CMS. Tool to inform beneficiaries of quality of various health plans 5-star rating system Used to adjust payments to health plans (bonus to plans
TMG STARS 2018 1 2 STARS Program Implemented in 2008 by CMS. Tool to inform beneficiaries of quality of various health plans 5-star rating system Used to adjust payments to health plans (bonus to plans
2017 Diabetes. Program Evaluation. Our mission is to improve the health and quality of life of our members
 2017 Diabetes Program Evaluation Our mission is to improve the health and quality of life of our members Diabetes Program Evaluation Program Title: Diabetes Program Evaluation Period: January 1, 2017 December
2017 Diabetes Program Evaluation Our mission is to improve the health and quality of life of our members Diabetes Program Evaluation Program Title: Diabetes Program Evaluation Period: January 1, 2017 December
Achieving Quality and Value in Chronic Care Management
 The Burden of Chronic Disease One of the greatest burdens on the US healthcare system is the rapidly growing rate of chronic disease. These statistics illustrate the scope of the problem: Nearly half of
The Burden of Chronic Disease One of the greatest burdens on the US healthcare system is the rapidly growing rate of chronic disease. These statistics illustrate the scope of the problem: Nearly half of
Measure Owner Designation. AMA-PCPI is the measure owner. NCQA is the measure owner. QIP/CMS is the measure owner. AMA-NCQA is the measure owner
 2011 EHR Measure Specifications The specifications listed in this document have been updated to reflect clinical practice guidelines and applicable health informatics standards that are the most current
2011 EHR Measure Specifications The specifications listed in this document have been updated to reflect clinical practice guidelines and applicable health informatics standards that are the most current
A Clinical Context Report
 Type 2 Diabetes in Practice An Expert Commentary with Silvio E. Inzucchi, MD A Clinical Context Report Clinical Context: Type 2 Diabetes in Practice Expert Commentary Jointly Sponsored by: and Clinical
Type 2 Diabetes in Practice An Expert Commentary with Silvio E. Inzucchi, MD A Clinical Context Report Clinical Context: Type 2 Diabetes in Practice Expert Commentary Jointly Sponsored by: and Clinical
Measuring and Improving Quality in Accountable Care Organizations
 Measuring and Improving Quality in Accountable Care Organizations Joachim Roski, PhD MPH Fellow, Economic Studies Managing Director, High Value Healthcare Initiative Overview ACOs and health care reform
Measuring and Improving Quality in Accountable Care Organizations Joachim Roski, PhD MPH Fellow, Economic Studies Managing Director, High Value Healthcare Initiative Overview ACOs and health care reform
2015 Diabetes. Program Evaluation. Our mission is to improve the health and quality of life of our members
 2015 Diabetes Program Evaluation Our mission is to improve the health and quality of life of our members Diabetes Care Program Evaluation Program Title: Diabetes Care Program Evaluation Period: January
2015 Diabetes Program Evaluation Our mission is to improve the health and quality of life of our members Diabetes Care Program Evaluation Program Title: Diabetes Care Program Evaluation Period: January
Target Blood Pressure Attainment in Diabetic Hypertensive Patients: Need for more Diuretics? Waleed M. Sweileh, PhD
 Target Blood Pressure Attainment in Diabetic Hypertensive Patients: Need for more Diuretics? Waleed M. Sweileh, PhD Associate Professor, Clinical Pharmacology Corresponding author Waleed M. Sweileh, PhD
Target Blood Pressure Attainment in Diabetic Hypertensive Patients: Need for more Diuretics? Waleed M. Sweileh, PhD Associate Professor, Clinical Pharmacology Corresponding author Waleed M. Sweileh, PhD
QUALITY IMPROVEMENT Section 9
 Quality Improvement Program The Plan s Quality Improvement Program serves to improve the health of its members through emphasis on health maintenance, education, diagnostic testing and treatment. The Quality
Quality Improvement Program The Plan s Quality Improvement Program serves to improve the health of its members through emphasis on health maintenance, education, diagnostic testing and treatment. The Quality
Int. J. Pharm. Sci. Rev. Res., 36(1), January February 2016; Article No. 06, Pages: JNC 8 versus JNC 7 Understanding the Evidences
 Research Article JNC 8 versus JNC 7 Understanding the Evidences Anns Clara Joseph, Karthik MS, Sivasakthi R, Venkatanarayanan R, Sam Johnson Udaya Chander J* RVS College of Pharmaceutical Sciences, Coimbatore,
Research Article JNC 8 versus JNC 7 Understanding the Evidences Anns Clara Joseph, Karthik MS, Sivasakthi R, Venkatanarayanan R, Sam Johnson Udaya Chander J* RVS College of Pharmaceutical Sciences, Coimbatore,
Together 2 Goal Campaign Measurement Specifications American Medical Group Foundation Version 1.0 February 23, 2016
 Together 2 Goal Campaign Measurement Specifications American Medical Group Foundation Version 1.0 February 23, 2016 1. Purpose The purpose of this document is to provide guidance to participating medical
Together 2 Goal Campaign Measurement Specifications American Medical Group Foundation Version 1.0 February 23, 2016 1. Purpose The purpose of this document is to provide guidance to participating medical
CME/CE QUIZ CME/CE QUESTIONS
 CME/CE QUIZ CME/CE QUESTIONS Continuing Medical Education Accreditation The University of Cincinnati College of Medicine designates this educational activity for a maximum of two (2) AMA PRA Category 1
CME/CE QUIZ CME/CE QUESTIONS Continuing Medical Education Accreditation The University of Cincinnati College of Medicine designates this educational activity for a maximum of two (2) AMA PRA Category 1
Table of Contents. Page 2 of 20
 Page 1 of 20 Table of Contents Table of Contents... 2 NMHCTOD Participants... 3 Introduction... 4 Methodology... 5 Types of Data Available... 5 Diabetes in New Mexico... 7 HEDIS Quality Indicators for
Page 1 of 20 Table of Contents Table of Contents... 2 NMHCTOD Participants... 3 Introduction... 4 Methodology... 5 Types of Data Available... 5 Diabetes in New Mexico... 7 HEDIS Quality Indicators for
The Role of Health Information Technology in Implementing Disease Management Programs
 The Role of Health Information Technology in Implementing Disease Management Programs Donald F. Wilson, MD Medical Director Quality Insights of Pennsylvania May 11, 2006 Statewide Combined Topic Average
The Role of Health Information Technology in Implementing Disease Management Programs Donald F. Wilson, MD Medical Director Quality Insights of Pennsylvania May 11, 2006 Statewide Combined Topic Average
Identifying the Barriers for Access to Care and Treatment for Arterial Hypertension and Diabetes in Lima, Peru
 Identifying the Barriers for Access to Care and Treatment for Arterial Hypertension and Diabetes in Lima, Peru Executive Summary María Kathia Cárdenas, Dulce Morán, David Beran & Jaime Miranda Identifying
Identifying the Barriers for Access to Care and Treatment for Arterial Hypertension and Diabetes in Lima, Peru Executive Summary María Kathia Cárdenas, Dulce Morán, David Beran & Jaime Miranda Identifying
Disclosures. Diabetes and Cardiovascular Risk Management. Learning Objectives. Atherosclerotic Cardiovascular Disease
 Disclosures Diabetes and Cardiovascular Risk Management Tony Hampton, MD, MBA Medical Director Advocate Aurora Operating System Advocate Aurora Healthcare Downers Grove, IL No conflicts or disclosures
Disclosures Diabetes and Cardiovascular Risk Management Tony Hampton, MD, MBA Medical Director Advocate Aurora Operating System Advocate Aurora Healthcare Downers Grove, IL No conflicts or disclosures
Primary Care Pharmacist Integration and Reimbursement Models
 Primary Care Pharmacist Integration and Reimbursement Models May 20, 2015 MODERATOR: Marie Smith, PharmD Palmer Professor and Assistant Dean, Practice and Public Policy Partnerships, UConn School of Pharmacy
Primary Care Pharmacist Integration and Reimbursement Models May 20, 2015 MODERATOR: Marie Smith, PharmD Palmer Professor and Assistant Dean, Practice and Public Policy Partnerships, UConn School of Pharmacy
American Diabetes Association 2018 Guidelines Important Notable Points
 American Diabetes Association 2018 Guidelines Important Notable Points The Standards of Medical Care in Diabetes-2018 by ADA include the most current evidencebased recommendations for diagnosing and treating
American Diabetes Association 2018 Guidelines Important Notable Points The Standards of Medical Care in Diabetes-2018 by ADA include the most current evidencebased recommendations for diagnosing and treating
Care Facilitation Quality Improvement Report
 Disease Management Program Clinical Outcomes for Reporting Period: 2006 Diabetes 100.0% 90.0% % of participants with diabetes 80.0% 70.0% 60.0% 50.0% 40.0% 30.0% 20.0% 10.0% 0.0% % participants with at
Disease Management Program Clinical Outcomes for Reporting Period: 2006 Diabetes 100.0% 90.0% % of participants with diabetes 80.0% 70.0% 60.0% 50.0% 40.0% 30.0% 20.0% 10.0% 0.0% % participants with at
Condition/Procedure Measure Compliance Criteria Reference Attribution Method
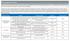 Premium Specialty: Cardiology Credentialed Specialties include: Cardiac Diagnostic, Cardiology, Cardiovascular Disease, Clinical Cardiac Electrophysiology, and Interventional Cardiology This document is
Premium Specialty: Cardiology Credentialed Specialties include: Cardiac Diagnostic, Cardiology, Cardiovascular Disease, Clinical Cardiac Electrophysiology, and Interventional Cardiology This document is
Adult Diabetes Clinician Guide NOVEMBER 2017
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Adult Diabetes Clinician Guide Introduction NOVEMBER 2017 This evidence-based guideline summary is based on the 2017 KP National Diabetes Guideline.
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Adult Diabetes Clinician Guide Introduction NOVEMBER 2017 This evidence-based guideline summary is based on the 2017 KP National Diabetes Guideline.
Moving to an A1C-Based Screening & Diagnosis of Diabetes. By Prof.M.Assy Diabetes&Endocrinology unit
 Moving to an A1C-Based Screening & Diagnosis of Diabetes By Prof.M.Assy Diabetes&Endocrinology unit is the nonenzymatic glycated product of the hemoglobin beta-chain at the valine terminal residue. Clin
Moving to an A1C-Based Screening & Diagnosis of Diabetes By Prof.M.Assy Diabetes&Endocrinology unit is the nonenzymatic glycated product of the hemoglobin beta-chain at the valine terminal residue. Clin
MEASURING CARE QUALITY
 MEASURING CARE QUALITY Region December 2013 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
MEASURING CARE QUALITY Region December 2013 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
Clinical Quality Measures Summary of Upcoming Enhancements
 Upcoming coding enhancements will impact the logic behind the clinical quality indicators applicable to your practice specialty. Please refer to this grid for a summary of the coding enhancements and some
Upcoming coding enhancements will impact the logic behind the clinical quality indicators applicable to your practice specialty. Please refer to this grid for a summary of the coding enhancements and some
2012 Diabetes. Program Evaluation. Our mission is to improve the health and quality of life of our members
 2012 Diabetes Program Evaluation Our mission is to improve the health and quality of life of our members Diabetes Program Evaluation Program Title: Diabetes Program Evaluation Period: January 1, 2012 December
2012 Diabetes Program Evaluation Our mission is to improve the health and quality of life of our members Diabetes Program Evaluation Program Title: Diabetes Program Evaluation Period: January 1, 2012 December
Learning Objectives. Impact of Diabetes II UPDATES IN TYPE 2 DIABETES. David Doriguzzi, PA-C
 UPDATES IN TYPE 2 DIABETES David Doriguzzi, PA-C Learning Objectives Upon completion of this educational activity, the participant should be able to: Overcome barriers and attitudes that limit Clinician/Patient
UPDATES IN TYPE 2 DIABETES David Doriguzzi, PA-C Learning Objectives Upon completion of this educational activity, the participant should be able to: Overcome barriers and attitudes that limit Clinician/Patient
PATIENT-IMPACT SCORECARD
 UNDERSTANDING THE GSC PATIENT-IMPACT SCORECARD What is the GSC Patient-Impact Scorecard? The GSC Patient-Impact Scorecard shows pharmacy performance scores for GSC patients during the period indicated.
UNDERSTANDING THE GSC PATIENT-IMPACT SCORECARD What is the GSC Patient-Impact Scorecard? The GSC Patient-Impact Scorecard shows pharmacy performance scores for GSC patients during the period indicated.
DISCLOSURE PHARMACIST OBJECTIVES 9/30/2014 JNC 8: A REVIEW OF THE LONG-AWAITED/MUCH-ANTICIPATED HYPERTENSION GUIDELINES. I have nothing to disclose.
 JNC 8: A REVIEW OF THE LONG-AWAITED/MUCH-ANTICIPATED HYPERTENSION GUIDELINES Tiffany Dickey, PharmD Assistant Professor, UAMS COP Clinical Pharmacy Specialist, Mercy Hospital Northwest AR DISCLOSURE I
JNC 8: A REVIEW OF THE LONG-AWAITED/MUCH-ANTICIPATED HYPERTENSION GUIDELINES Tiffany Dickey, PharmD Assistant Professor, UAMS COP Clinical Pharmacy Specialist, Mercy Hospital Northwest AR DISCLOSURE I
2016 General Practice/Family Practice Preferred Specialty Measure Set
 1 0059 5 0081 41 N/A 50 N/A 65 0069, EHR 66 0002, EHR Effective Clinical Care Effective Clinical Care Effective Clinical Care Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%): Percentage of patients
1 0059 5 0081 41 N/A 50 N/A 65 0069, EHR 66 0002, EHR Effective Clinical Care Effective Clinical Care Effective Clinical Care Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%): Percentage of patients
CLINICAL PROCESS IMPROVEMENT INITIATIVE (CPII) EFFICIENCY REPORT EXPLANATION January 4, 2016
 CLINICAL PROCESS IMPROVEMENT INITIATIVE (CPII) EFFICIENCY REPORT EXPLANATION January 4, 2016 WHAT IS AN EPISODE OF CARE? An episode of care is a grouping of a patient s health care claims for a unique
CLINICAL PROCESS IMPROVEMENT INITIATIVE (CPII) EFFICIENCY REPORT EXPLANATION January 4, 2016 WHAT IS AN EPISODE OF CARE? An episode of care is a grouping of a patient s health care claims for a unique
2016 Internal Medicine Preferred Specialty Measure Set
 1 0059 Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%): Percentage of patients 18-75 years of age with diabetes who had hemoglobin A1c > 9.0% during the measurement period 5 0081 Registry, EHR, 9 0105
1 0059 Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%): Percentage of patients 18-75 years of age with diabetes who had hemoglobin A1c > 9.0% during the measurement period 5 0081 Registry, EHR, 9 0105
Consensus Core Set: ACO and PCMH / Primary Care Measures Version 1.0
 Consensus Core Set: ACO and PCMH / Primary Care s 0018 Controlling High Blood Pressure patients 18 to 85 years of age who had a diagnosis of hypertension (HTN) and whose blood pressure (BP) was adequately
Consensus Core Set: ACO and PCMH / Primary Care s 0018 Controlling High Blood Pressure patients 18 to 85 years of age who had a diagnosis of hypertension (HTN) and whose blood pressure (BP) was adequately
Quality ID #119 (NQF 0062): Diabetes: Medical Attention for Nephropathy National Quality Strategy Domain: Effective Clinical Care
 Quality ID #119 (NQF 0062): Diabetes: Medical Attention for Nephropathy National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS F INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process
Quality ID #119 (NQF 0062): Diabetes: Medical Attention for Nephropathy National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS F INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE: Process
Why is Earlier and More Aggressive Treatment of T2 Diabetes Better?
 Blood glucose (mmol/l) Why is Earlier and More Aggressive Treatment of T2 Diabetes Better? Disclosures Dr Kennedy has provided CME, been on advisory boards or received travel or conference support from:
Blood glucose (mmol/l) Why is Earlier and More Aggressive Treatment of T2 Diabetes Better? Disclosures Dr Kennedy has provided CME, been on advisory boards or received travel or conference support from:
PCMH 2018 Enrollment and Update August 25, 2017
 PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
The BlueCompare SM Physician Designation Program
 The BlueCompare SM Physician Designation Program Continuing escalation of health care costs has driven premiums and medical expenses to higher and higher levels each year, motivating employers and consumers
The BlueCompare SM Physician Designation Program Continuing escalation of health care costs has driven premiums and medical expenses to higher and higher levels each year, motivating employers and consumers
Diabetes Prevalence and Health Care Utilization in MaineCare. FY2003 Report
 Prevalence and Health Care Utilization in MaineCare FY2003 Report August, 2004 Table of Contents Executive Summary 1 Introduction 3 Methods 7 Results 9 Discussion 22 Tables 25 Appendix: Methods 36 References
Prevalence and Health Care Utilization in MaineCare FY2003 Report August, 2004 Table of Contents Executive Summary 1 Introduction 3 Methods 7 Results 9 Discussion 22 Tables 25 Appendix: Methods 36 References
Diabetes affects 25.8 million people in the United
 Impact of Clinical Pharmacy Services on Outcomes and Costs for Indigent Patients With Diabetes Marissa Escobar Quinones, PharmD, CDE; Margaret Youngmi Pio, PharmD, BCPS, CDE; Diem Hong Chow, PharmD, CDE;
Impact of Clinical Pharmacy Services on Outcomes and Costs for Indigent Patients With Diabetes Marissa Escobar Quinones, PharmD, CDE; Margaret Youngmi Pio, PharmD, BCPS, CDE; Diem Hong Chow, PharmD, CDE;
Diabetes Quality Improvement Initiative
 Diabetes Quality Improvement Initiative Community Care of North Carolina 2300 Rexwoods Drive, Ste. 100 Raleigh, NC 27607 (919) 745-2350 www.communitycarenc.org 2007 Background The Clinical Directors of
Diabetes Quality Improvement Initiative Community Care of North Carolina 2300 Rexwoods Drive, Ste. 100 Raleigh, NC 27607 (919) 745-2350 www.communitycarenc.org 2007 Background The Clinical Directors of
Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable?
 Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable? Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of
Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable? Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of
Diabetic Dyslipidemia
 Diabetic Dyslipidemia Dr R V S N Sarma, M.D., (Internal Medicine), M.Sc., (Canada), Consultant Physician Cardiovascular disease (CVD) is a significant cause of illness, disability, and death among individuals
Diabetic Dyslipidemia Dr R V S N Sarma, M.D., (Internal Medicine), M.Sc., (Canada), Consultant Physician Cardiovascular disease (CVD) is a significant cause of illness, disability, and death among individuals
The Many Faces of T2DM in Long-term Care Facilities
 The Many Faces of T2DM in Long-term Care Facilities Question #1 Which of the following is a risk factor for increased hypoglycemia in older patients that may suggest the need to relax hyperglycemia treatment
The Many Faces of T2DM in Long-term Care Facilities Question #1 Which of the following is a risk factor for increased hypoglycemia in older patients that may suggest the need to relax hyperglycemia treatment
Clinical Practice Guidelines for Diabetes Management
 Clinical Practice Guidelines for Diabetes Management Diabetes is a disease in which blood glucose levels are above normal. Over the years, high blood glucose damages nerves and blood vessels, which can
Clinical Practice Guidelines for Diabetes Management Diabetes is a disease in which blood glucose levels are above normal. Over the years, high blood glucose damages nerves and blood vessels, which can
Pharmacy Partnership to Improve Patient Outcomes
 Pharmacy Partnership to Improve Patient Outcomes Minnesota Rural Health Conference Session 2B Ryan M. Harden, MD MS Kendra Metz, Pharm D Sarah Nelson, MD June 25, 2018 Involved Partners Involved Partners
Pharmacy Partnership to Improve Patient Outcomes Minnesota Rural Health Conference Session 2B Ryan M. Harden, MD MS Kendra Metz, Pharm D Sarah Nelson, MD June 25, 2018 Involved Partners Involved Partners
Diabetes Mellitus: Implications of New Clinical Trials and New Medications
 Diabetes Mellitus: Implications of New Clinical Trials and New Medications Estimates of Diagnosed Diabetes in Adults, 2005 Alka M. Kanaya, MD Asst. Professor of Medicine UCSF, Primary Care CME October
Diabetes Mellitus: Implications of New Clinical Trials and New Medications Estimates of Diagnosed Diabetes in Adults, 2005 Alka M. Kanaya, MD Asst. Professor of Medicine UCSF, Primary Care CME October
Long-Term Care Updates
 Long-Term Care Updates August 2015 By Darren Hein, PharmD Hypertension is a clinical condition in which the force of blood pushing on the arteries is higher than normal. This increases the risk for heart
Long-Term Care Updates August 2015 By Darren Hein, PharmD Hypertension is a clinical condition in which the force of blood pushing on the arteries is higher than normal. This increases the risk for heart
Non-insulin treatment in Type 1 DM Sang Yong Kim
 Non-insulin treatment in Type 1 DM Sang Yong Kim Chosun University Hospital Conflict of interest disclosure None Committee of Scientific Affairs Committee of Scientific Affairs Insulin therapy is the mainstay
Non-insulin treatment in Type 1 DM Sang Yong Kim Chosun University Hospital Conflict of interest disclosure None Committee of Scientific Affairs Committee of Scientific Affairs Insulin therapy is the mainstay
Status of the CKD and ESRD treatment: Growth, Care, Disparities
 Status of the CKD and ESRD treatment: Growth, Care, Disparities United States Renal Data System Coordinating Center An J. Collins, MD FACP Director USRDS Coordinating Center Robert Foley, MB Co-investigator
Status of the CKD and ESRD treatment: Growth, Care, Disparities United States Renal Data System Coordinating Center An J. Collins, MD FACP Director USRDS Coordinating Center Robert Foley, MB Co-investigator
2019 COLLECTION TYPE: MIPS CLINICAL QUALITY MEASURES (CQMS) MEASURE TYPE: Process
 Quality ID #119 (NQF 0062): Diabetes: Medical Attention for Nephropathy National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Management of Chronic Conditions 2019 COLLECTION
Quality ID #119 (NQF 0062): Diabetes: Medical Attention for Nephropathy National Quality Strategy Domain: Effective Clinical Care Meaningful Measure Area: Management of Chronic Conditions 2019 COLLECTION
Participants in the Program
 Type 2 Diabetes Performance Improvement Initiative: Chart Reviews Participants in the Program 318 clinicians have registered 192 have started the program 126 have started their initial chart review 26
Type 2 Diabetes Performance Improvement Initiative: Chart Reviews Participants in the Program 318 clinicians have registered 192 have started the program 126 have started their initial chart review 26
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications
 HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications Fidelis SecureCare strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications Fidelis SecureCare strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
Long-Term Care Updates
 Long-Term Care Updates January 2019 By Kristina Nikl, PharmD Several recent studies evaluating the management of diabetes in older adults have concluded that 25-52% of elderly patients are currently being
Long-Term Care Updates January 2019 By Kristina Nikl, PharmD Several recent studies evaluating the management of diabetes in older adults have concluded that 25-52% of elderly patients are currently being
Clinical Guidelines for the Pharmacologic Treatment of Schizophrenia
 Clinical Guidelines for the Pharmacologic Treatment of Community Behavioral Health (CBH) is committed to working with our provider partners to continuously improve the quality of behavioral healthcare
Clinical Guidelines for the Pharmacologic Treatment of Community Behavioral Health (CBH) is committed to working with our provider partners to continuously improve the quality of behavioral healthcare
Key Quality of Care Measures. Blue Cross Blue Shield of Michigan Traditional, PPO and POS Members. Fourth Quarter 2003
 Key Quality of Care Measures Blue Cross Blue Shield of Michigan Traditional, PPO and POS Members Fourth Quarter 2003 Blue Cross Blue Shield of Michigan is a nonprofit corporation and independent licensee
Key Quality of Care Measures Blue Cross Blue Shield of Michigan Traditional, PPO and POS Members Fourth Quarter 2003 Blue Cross Blue Shield of Michigan is a nonprofit corporation and independent licensee
Managing Diabetes for Improved Health and Economic Outcomes
 Managing Diabetes for Improved Health and Economic Outcomes Based on a presentation by David McCulloch, MD Presentation Summary The contribution of postprandial glucose to diabetes progression and diabetes-related
Managing Diabetes for Improved Health and Economic Outcomes Based on a presentation by David McCulloch, MD Presentation Summary The contribution of postprandial glucose to diabetes progression and diabetes-related
The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only.
 The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only. Please note that the results reported in any single trial may not reflect the overall
The clinical trial information provided in this public disclosure synopsis is supplied for informational purposes only. Please note that the results reported in any single trial may not reflect the overall
Metformin should be considered in all patients with type 2 diabetes unless contra-indicated
 November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
November 2001 N P S National Prescribing Service Limited PPR fifteen Prescribing Practice Review PPR Managing type 2 diabetes For General Practice Key messages Metformin should be considered in all patients
egfr > 50 (n = 13,916)
 Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Saxagliptin and Cardiovascular Risk in Patients with Type 2 Diabetes Mellitus and Moderate or Severe Renal Impairment: Observations from the SAVOR-TIMI 53 Trial Supplementary Table 1. Characteristics according
Combination treatment for T2DM
 Combination treatment for T2DM Date of approval: December 2016 SAGLB.DIA.16.08.0657 Abbreviations ADA: American Diabetes Association CVD: Cardiovascular disease DPP-4: Dipeptidyl Peptidase-4 EASD: European
Combination treatment for T2DM Date of approval: December 2016 SAGLB.DIA.16.08.0657 Abbreviations ADA: American Diabetes Association CVD: Cardiovascular disease DPP-4: Dipeptidyl Peptidase-4 EASD: European
Clinical Approach to Achieving Treatment Targets: Case Vignette Discussion
 Clinical Approach to Achieving Treatment Targets: Case Vignette Discussion Om P. Ganda, MD; Kirit Tolia, MD, FACE Postcardiac Follow-up in a 66-Year-Old Man Slide 1. Dr. Ganda: Now we will present a case
Clinical Approach to Achieving Treatment Targets: Case Vignette Discussion Om P. Ganda, MD; Kirit Tolia, MD, FACE Postcardiac Follow-up in a 66-Year-Old Man Slide 1. Dr. Ganda: Now we will present a case
RESEARCH. J Manag Care Pharm. 2006;12(8): ABSTRACT
 RESEARCH Physician Conformity and Patient Adherence to ACE Inhibitors and ARBs in Patients With Diabetes, With and Without Renal Disease and Hypertension, in a Medicaid Managed Care Organization CATHERINE
RESEARCH Physician Conformity and Patient Adherence to ACE Inhibitors and ARBs in Patients With Diabetes, With and Without Renal Disease and Hypertension, in a Medicaid Managed Care Organization CATHERINE
Barriers to Achieving A1C Targets: Clinical Inertia and Hypoglycemia. KM Pantalone Endocrinology
 Barriers to Achieving A1C Targets: Clinical Inertia and Hypoglycemia KM Pantalone Endocrinology Disclosures Speaker Bureau AstraZeneca, Merck, Novo Nordisk, Sanofi Consultant Novo Nordisk, Eli Lilly, Merck
Barriers to Achieving A1C Targets: Clinical Inertia and Hypoglycemia KM Pantalone Endocrinology Disclosures Speaker Bureau AstraZeneca, Merck, Novo Nordisk, Sanofi Consultant Novo Nordisk, Eli Lilly, Merck
Diabetes Overview. How Food is Digested
 Diabetes Overview You are The Teacher, The Coach and the Fan Pathophysiology of Diabetes Complications Know the Numbers Treatment Can Good Control Make a Difference? Can Tight Control Be too Tight? How
Diabetes Overview You are The Teacher, The Coach and the Fan Pathophysiology of Diabetes Complications Know the Numbers Treatment Can Good Control Make a Difference? Can Tight Control Be too Tight? How
Oral Antihyperglycemic Medication Nonadherence and Subsequent Hospitalization Among Individuals With Type 2 Diabetes
 Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E Oral Antihyperglycemic Medication Nonadherence and Subsequent Hospitalization Among Individuals With Type 2 Diabetes DENYS
Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E Oral Antihyperglycemic Medication Nonadherence and Subsequent Hospitalization Among Individuals With Type 2 Diabetes DENYS
Guidelines for Improving the Care of the Older Person with Diabetes Mellitus
 Guidelines for Improving the Care of the Older Person with Diabetes Mellitus California Healthcare Foundation/American Geriatrics Society Panel on Improving Care for Elders with Diabetes This guideline
Guidelines for Improving the Care of the Older Person with Diabetes Mellitus California Healthcare Foundation/American Geriatrics Society Panel on Improving Care for Elders with Diabetes This guideline
High-quality diabetes care can
 Development and Evolution of a Primary Care Based Diabetes Disease Management Program Robb Malone, PharmD, CDE, CPP; Betsy Bryant Shilliday, PharmD, CDE, CPP; Timothy J. Ives, PharmD, MPH; and Michael
Development and Evolution of a Primary Care Based Diabetes Disease Management Program Robb Malone, PharmD, CDE, CPP; Betsy Bryant Shilliday, PharmD, CDE, CPP; Timothy J. Ives, PharmD, MPH; and Michael
Setting The setting was not explicitly stated. The economic study was carried out in the UK.
 Cost-effectiveness of rosiglitazone combination therapy for the treatment of type 2 diabetes mellitus in the UK Beale S, Bagust A, Shearer A T, Martin A, Hulme L Record Status This is a critical abstract
Cost-effectiveness of rosiglitazone combination therapy for the treatment of type 2 diabetes mellitus in the UK Beale S, Bagust A, Shearer A T, Martin A, Hulme L Record Status This is a critical abstract
Diabetes and Hypertension
 Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
PEER REVIEW HISTORY ARTICLE DETAILS TITLE (PROVISIONAL)
 PEER REVIEW HISTORY BMJ Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form (see an example) and are provided with free text boxes to
PEER REVIEW HISTORY BMJ Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form (see an example) and are provided with free text boxes to
Thiazolidinedione Step Therapy Program
 Thiazolidinedione Step Therapy Program Policy Number: 5.01.580 Last Review: 7/2018 Origination: 07/2014 Next Review: 7/2019 LoB: ACA Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide
Thiazolidinedione Step Therapy Program Policy Number: 5.01.580 Last Review: 7/2018 Origination: 07/2014 Next Review: 7/2019 LoB: ACA Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide
Diabetes and the Heart
 Diabetes and the Heart Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 6, 2012 Outline Screening for diabetes in patients with CAD Screening for CAD in patients with
Diabetes and the Heart Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 6, 2012 Outline Screening for diabetes in patients with CAD Screening for CAD in patients with
The University of Mississippi School of Pharmacy
 LONG TERM PERSISTENCE WITH ACEI/ARB THERAPY AFTER ACUTE MYOCARDIAL INFARCTION: AN ANALYSIS OF THE 2006-2007 MEDICARE 5% NATIONAL SAMPLE DATA Lokhandwala T. MS, Yang Y. PhD, Thumula V. MS, Bentley J.P.
LONG TERM PERSISTENCE WITH ACEI/ARB THERAPY AFTER ACUTE MYOCARDIAL INFARCTION: AN ANALYSIS OF THE 2006-2007 MEDICARE 5% NATIONAL SAMPLE DATA Lokhandwala T. MS, Yang Y. PhD, Thumula V. MS, Bentley J.P.
Clinical Study Synopsis
 Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
Clinical Study Synopsis This Clinical Study Synopsis is provided for patients and healthcare professionals to increase the transparency of Bayer's clinical research. This document is not intended to replace
2018 MIPS Reporting Family Medicine
 2018 MIPS Reporting Family Medicine Quality Reporting Requirements: Report on 6 quality measures or a specialty measure set Include at least ONE outcome or high-priority measure Report on patients of All-Payers
2018 MIPS Reporting Family Medicine Quality Reporting Requirements: Report on 6 quality measures or a specialty measure set Include at least ONE outcome or high-priority measure Report on patients of All-Payers
The Global Agenda for the Prevention of Diabetes: Research Opportunities
 The Global Agenda for the Prevention of Diabetes: Research Opportunities William H. Herman, MD, MPH Stefan S. Fajans/GlaxoSmithKline Professor of Diabetes Professor of Internal Medicine and Epidemiology
The Global Agenda for the Prevention of Diabetes: Research Opportunities William H. Herman, MD, MPH Stefan S. Fajans/GlaxoSmithKline Professor of Diabetes Professor of Internal Medicine and Epidemiology
DICE Study Backgrounder
 DICE Study Backgrounder Diabetes In Canada Evaluation (DICE), the largest diabetes study of its kind in Canada, examines the management and control of type 2 diabetes in the Canadian family practice setting.
DICE Study Backgrounder Diabetes In Canada Evaluation (DICE), the largest diabetes study of its kind in Canada, examines the management and control of type 2 diabetes in the Canadian family practice setting.
NQF Measure Number & PQRI Implementation Number
 Title NQF Steward s Adult Weight Screening and Follow-Up Hypertension: Blood Pressure ment Preventive Care and Screening Pair: a. Tobacco Use Assessment, b. Tobacco Cessation Intervention with a calculated
Title NQF Steward s Adult Weight Screening and Follow-Up Hypertension: Blood Pressure ment Preventive Care and Screening Pair: a. Tobacco Use Assessment, b. Tobacco Cessation Intervention with a calculated
Keywords: Type 2 DM, lipid profile, metformin, glimepiride ABSTRACT
 Human Journals Research Article September 2015 Vol.:4, Issue:2 All rights are reserved by K. Saravanan et al. Effects of Monotherapy and Combination Therapy Involving Metformin and Glimepiride on HbA1c
Human Journals Research Article September 2015 Vol.:4, Issue:2 All rights are reserved by K. Saravanan et al. Effects of Monotherapy and Combination Therapy Involving Metformin and Glimepiride on HbA1c
Boosting the Value of Lab Testing: How HEDIS Uses Lab
 Boosting the Value of Lab Testing: How HEDIS Uses Lab Cindy Ottone, MHA Director HEDIS Policy All materials 2009, National Committee for Quality Assurance Overview What is NCQA and HEDIS? How are measures
Boosting the Value of Lab Testing: How HEDIS Uses Lab Cindy Ottone, MHA Director HEDIS Policy All materials 2009, National Committee for Quality Assurance Overview What is NCQA and HEDIS? How are measures
Balancing Glycemic Overtreatment and Undertreatment for Seniors: An Out of Range (OOR) Population Health Safety Measure
 Balancing Glycemic Overtreatment and Undertreatment for Seniors: An Out of Range (OOR) Population Health Safety Measure Leonard Pogach, 1,2 Orysya Soroka, 1 Chin Lin Tseng, 1,2 Miriam Maney, 1 and David
Balancing Glycemic Overtreatment and Undertreatment for Seniors: An Out of Range (OOR) Population Health Safety Measure Leonard Pogach, 1,2 Orysya Soroka, 1 Chin Lin Tseng, 1,2 Miriam Maney, 1 and David
Presenter Disclosure Information
 Prediabetes & Type 2 Diabetes Prevention Cari Ritter, PA-C Presenter Disclosure Information In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure
Prediabetes & Type 2 Diabetes Prevention Cari Ritter, PA-C Presenter Disclosure Information In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure
Effect of Drug Therapy on HEDIS Measurements of HbA 1c Control In Diabetes Patients
 Effect of Drug Therapy on HEDIS Measurements of HbA 1c Control In Diabetes Patients Gary Bazalo, MS, MBA 1 ; Richard Weiss, MS 1 ; Nathaniel Clark, MD 2 ; Berhanu Alemayehu, PhD 3 ; Felicia Forma 3 ; Garrett
Effect of Drug Therapy on HEDIS Measurements of HbA 1c Control In Diabetes Patients Gary Bazalo, MS, MBA 1 ; Richard Weiss, MS 1 ; Nathaniel Clark, MD 2 ; Berhanu Alemayehu, PhD 3 ; Felicia Forma 3 ; Garrett
Title: DreamTel; Diabetes Risk Evaluation and Management Tele-monitoring Study
 Author's response to reviews Title: DreamTel; Diabetes Risk Evaluation and Management Tele-monitoring Study Authors: Sheldon Tobe (sheldon.tobe@sunnybrook.ca) Joan Wentworth (jwentworth@miwayawinhealth.org)
Author's response to reviews Title: DreamTel; Diabetes Risk Evaluation and Management Tele-monitoring Study Authors: Sheldon Tobe (sheldon.tobe@sunnybrook.ca) Joan Wentworth (jwentworth@miwayawinhealth.org)
Your Partnership in Health Report: Chronic Conditions ABC Company and Kaiser Permanente
 Your Partnership in Health Report: s ABC Company and Kaiser Permanente Measurement Period: JUL-01-2012 through JUN-30-2013 Report Date: DEC-31-2013 Commercial All Members Partnership in Health (PIH) reports:
Your Partnership in Health Report: s ABC Company and Kaiser Permanente Measurement Period: JUL-01-2012 through JUN-30-2013 Report Date: DEC-31-2013 Commercial All Members Partnership in Health (PIH) reports:
Key Elements in Managing Diabetes
 Key Elements in Managing Diabetes Presentor Disclosure No conflicts of interest to disclose Presented by Susan Cotey, RN, CDE Lennon Diabetes Center Stephanie Tubbs Jones Health Center Cleveland Clinic
Key Elements in Managing Diabetes Presentor Disclosure No conflicts of interest to disclose Presented by Susan Cotey, RN, CDE Lennon Diabetes Center Stephanie Tubbs Jones Health Center Cleveland Clinic
Getting Hypertension Under Control
 Getting Hypertension Under Control Learning Objectives EXPLAIN the factors involved in patient medication non-adherence. OUTLINE the results of studies focusing on medication adherence issues in patients
Getting Hypertension Under Control Learning Objectives EXPLAIN the factors involved in patient medication non-adherence. OUTLINE the results of studies focusing on medication adherence issues in patients
An estimated 20.8 million Americans 7% of the population
 Provider Organization Performance Assessment Utilizing Diabetes Physician Recognition Program Bruce Wall, MD, MMM; Evelyn Chiao, PharmD; Craig A. Plauschinat, PharmD, MPH; Paul A. Miner, PharmD; James
Provider Organization Performance Assessment Utilizing Diabetes Physician Recognition Program Bruce Wall, MD, MMM; Evelyn Chiao, PharmD; Craig A. Plauschinat, PharmD, MPH; Paul A. Miner, PharmD; James
Hedis Behavioral Health Measures
 Hedis Behavioral Health Measures Generating better health outcomes and improving HEDIS scores is a positive outcome for everyone. Magellan Complete Care is offering support by providing the details of
Hedis Behavioral Health Measures Generating better health outcomes and improving HEDIS scores is a positive outcome for everyone. Magellan Complete Care is offering support by providing the details of
Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone
 Index Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone Medication GAD glutamic acid decarboxylase GLP-1 glucagon-like peptide 1 NPH neutral
Index Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone Medication GAD glutamic acid decarboxylase GLP-1 glucagon-like peptide 1 NPH neutral
Patient Education. intermountainhealthcare.org/diabetes. BG Tracker. for people with diabetes MONITORING BLOOD GLUCOSE
 Patient Education intermountainhealthcare.org/diabetes Tracker for people with diabetes MONITORING BLOOD GLUCOSE Title Case My name/phone: Contact numbers: Healthcare provider: Diabetes educator: Pharmacy:
Patient Education intermountainhealthcare.org/diabetes Tracker for people with diabetes MONITORING BLOOD GLUCOSE Title Case My name/phone: Contact numbers: Healthcare provider: Diabetes educator: Pharmacy:
The Asheville Program. John Miall
 The Asheville Program John Miall It s s the System That Needs Care Over half of all healthcare via managed care Largest increase in 6 years in costs It s evolution not revolution Giving patients the resources
The Asheville Program John Miall It s s the System That Needs Care Over half of all healthcare via managed care Largest increase in 6 years in costs It s evolution not revolution Giving patients the resources
Clinical Therapeutics/Volume 33, Number 1, 2011
 Clinical Therapeutics/Volume 33, Number 1, 2011 Concurrent Control of Blood Glucose, Body Mass, and Blood Pressure in Patients With Type 2 Diabetes: An Analysis of Data From Electronic Medical Records
Clinical Therapeutics/Volume 33, Number 1, 2011 Concurrent Control of Blood Glucose, Body Mass, and Blood Pressure in Patients With Type 2 Diabetes: An Analysis of Data From Electronic Medical Records
Quality ID #1 (NQF 0059): Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%) National Quality Strategy Domain: Effective Clinical Care
 Quality ID #1 (NQF 0059): Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%) National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE:
Quality ID #1 (NQF 0059): Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%) National Quality Strategy Domain: Effective Clinical Care 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY MEASURE TYPE:
Commenting draft report: NQF-endorsed measures for Primary Care and Chronic Illness, Spring 2018
 Memo July 31, 2018 To: NQF members and the public From: NQF staff Re: Background Commenting draft report: NQF-endorsed measures for Primary Care and Chronic Illness, Spring 2018 This report reflects the
Memo July 31, 2018 To: NQF members and the public From: NQF staff Re: Background Commenting draft report: NQF-endorsed measures for Primary Care and Chronic Illness, Spring 2018 This report reflects the
Cost-Effective Process to Improve Drug Adherence for Medicare 5-Star
 Cost-Effective Process to Improve Drug Adherence for Medicare 5-Star HEALTH ALLIANCE PLAN Presented by Vanita K. Pindolia, Pharm.D. VP, Ambulatory Clinical Pharmacy Programs_PCM Medicare 5-Star Rating
Cost-Effective Process to Improve Drug Adherence for Medicare 5-Star HEALTH ALLIANCE PLAN Presented by Vanita K. Pindolia, Pharm.D. VP, Ambulatory Clinical Pharmacy Programs_PCM Medicare 5-Star Rating
Collaborative Hypertension Case Management by Registered Nurses and Clinical Pharmacy Specialists within the Patient Aligned Care Teams (PACT) Model
 Collaborative Hypertension Case Management by Registered Nurses and Clinical Pharmacy Specialists within the Patient Aligned Care Teams (PACT) Model Jessica L. O Neill, Pharm.D 1, Tori L. Cunningham, Pharm.D
Collaborative Hypertension Case Management by Registered Nurses and Clinical Pharmacy Specialists within the Patient Aligned Care Teams (PACT) Model Jessica L. O Neill, Pharm.D 1, Tori L. Cunningham, Pharm.D
