Photocoagulation in proliferative sickle retinopathy:
|
|
|
- Michael Knight
- 5 years ago
- Views:
Transcription
1 British Journal of Ophthalmology, 80, 64, Photocoagulation in proliferative sickle retinopathy: results of a 5-year study PATICK 1. CONDON AND GAHAM. SEJEANT From the Medical esearch Council aboratories, University of the West Indies, Kingston, Jamaica SUMMAY The progress of proliferative sickle retinopathy (PS) in 57 eyes treated by xenon arc photocoagulation has been compared with that in 41 comparison eyes. Angiographic assessment of the treated PS lesions in 54 patients followed up for a mean period of 47 months (range 8- months) revealed cessation of leakage in (81 %), reduction of leakage in 8 (15 %), and no change in 2 (4 %). In the 41 comparison eyes more extensive perfused PS occurred in 25 (60 %), no change in 8 (20), and spontaneous improvement in 8 (20%). Autoinfarction of PS lesions in comparison eyes was observed during the study period in 16 (3 %). Assessed by visual acuity, there was no significant difference between treatment and comparison groups, deterioration of 3 lines or more on the Snellen chart occurring in % of the treated eyes and 5 % of the comparison eyes. Vitreous haemorrhages occurred in 8 (14%) of treated eyes and in 7 (17 %) of the comparison group. The most common complication of photocoagulation was choroidal neovascularisation in the burn area, choroidoretinal neovascularisation (CN) occurring in patients and choroidovitreal neovascularisation (CVN) in 12 patients. In 4 of the latter patients CVN lesions underwent rapid growth and in 4 were associated with vitreous haemorrhages. Other complications in the treated eyes included transient partial third nerve palsies, preretinal haemorrhage, haemorrhage confined to the burn area, vitreous haemorrhage, vitreoretinal traction, and retinal detachment. Statistical limitations of the present study dictate that the results be interpreted with caution. However, the complications of therapy, and the high prevalence of autoinfarction in the comparison eyes, indicate the need for a properly randomised study to define the role, if any, of photocoagulation in the therapy of proliferative sickle retinopathy. Peripheral retinal capillary occlusion in sickle cell disease initiates a sequence of vascular events that may culminate in proliferative sickle retinopathy (PS). Arising from arteriovenous anastomoses at the border of ischaemic retina, arcades of abnormal vessels grow out along the retina or project into the vitreous. As these arcades proliferate, they carry larger blood flows and are supplied by enlarged feeding arterioles and draining venules. These abnormal vessel systems leak fluorescein and plasma and may give rise to vitreous haemorrhage and either traction or rhegmatogenous retinal detachment. The risks of transient or permanent visual impairment have prompted attempts to render these lesions avascular by occluding the feeding arterioles with xenon photocoagulation,'-3 argon laser photocoagulation,3-5 diathermy,2 and cryopexy.6 The techniques and preliminary results of xenon light coagulation in a group of Jamaican patients were reported by Condon and Serjeant,2 and the results in a 5-year follow-up of this group are now presented. Patients and methods Patients were selected from the sickle cell clinic of the University Hospital of the West Indies. Of the 37 patients originally admitted to the study2 33 have been followed up for periods between 30 and months, the remaining 4 patients having defaulted (2) or emigrated (2). Seven patients were added to Correspondence to Dr Graham. Serjeant, Medical the study in March 74, 5 in December 74, 6 in esearch Council aboratories, University of the West August 75, and 6 in January 77, bringing the Indies, Kingston, Jamaica. total of patients to 57. At the last review, in July 832
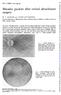
2 Photocoagulation in proliferative sickle retinopathy 78, patient follow-up varied from 8 to months with a mean of 47 0 months. There were 8 patients with homozygous sickle cell (SS) disease, 43 with sickle cell-haemoglobin C (SC) disease, 4 with sickle cell-5+ thalassaemia (Sr+ thalassaemia) and 2 with sickle cell- 3 thalassaemia (Sp' thalassaemia). There were 33 males and 24 females with ages ranging from 13 to 64 years on admission to the study. The criteria used for haematological diagnosis were described by Serjeant7 and involved haemoglobin electrophoresis under alkaline and acid conditions, and quantitation of HbA, to differentiate SS disease from Sp' thalassaemia. Proliferative sickle retinopathy (PS) was present on admission to the study or developed during the study bilaterally in 47 and unilaterally in 10 of the 57 patients. All eyes were treated in patients with unilateral involvement. In those with bilateral involvement the worst affected eye was treated in 41 patients and the less affected eye in 6 patients, in whom visual acuity in the worst eye was <0. The remaining 47 eyes in patients with bilateral involvement were followed up as a comparison group. Ophthalmological assessments as previously described' were made during short-term visits (usually 3 weeks) at approximately yearly intervals by the visiting ophthalmologist (P.I.C.). Techniques of xenon arc photocoagulation using the O'Malley log. I photocoagulator included closure of the feeding arteriole and direct coagulation of the PS lesion.2 The draining venule was not directly coagulated. etrobulbar anaesthesia was induced by injecting 2% xylocaine without epinephrine through a sharp 50 mm 25 g retrobulbar needle. The volume of local anaesthetic was routinely 3 5 ml, but variability in anaesthetic quality occasionally necessitated a volume of 5-6 ml for adequate anaesthesia. The results of treatment were assessed by changes in dye leakage from the treated lesions, changes in visual acuity, and by comparing complications in the treatment and comparison eyes. Post coagulation angiographic assessments were generally performed 4-7 days after treatment. esults A total of 220 PS lesions in the 57 patients were treated by xenon photocoagulation supplemented by diathermy in 8 patients. These included 33 lesions in SS disease (41 lesions/patient), 16 in SC disease (3 lesions/patient), 10 in Sp+ thal (2 5 lesions/patient), and 8 Sp' thal (40 lesions/ patient). The results in terms of fluorescein leakage from the treated PS and complications of therapy Fig. I Fluorescein angiogram of right temporal area in a 17-year-old female with SC disease (case 12) showing PS lesion developing proximal to photocoagulation burn I year earlier. 833 are summarised in Table 1 and the visual acuities at the beginning and end of the study in Table 2. EAKAGE FOM POIFEATIVE ESIONS Closure of feeding vessels and cessation of fluorescein leakage from the treated PS lesions was achieved by one (41 patients) or more (5 patients) treatment sessions in / (87%) patients in whom post-therapy angiograms (4-7 days after treatment) were available. eakage continued despite repeated coagulation in 4 patients (cases 26, 38, 42, 43), and additional therapy was not attempted in 3 patients (cases 7, 30, 41). After successful initial closure fluorescein leakage from retinal lesions recurred in 8 patients, being attributed to reperfusion of the original PS lesion in 3 patients (cases 8, 16, 51) and to the development of new PS lesions (Fig. l) in 5 patients (cases 12, 15,, 31, 57). Further treatment of reperfused lesions was unsuccessfully attempted in 2 patients and not attempted in 1, and treatment of new PS lesions was successful in the 3 patients in which it was attempted. In 2 patients (cases 34, 47) the extreme peripheral location of small PS lesions did not allow attempted closure by the photocoagulator in use, but other lesions in both patients were satisfactorily occluded. Fluorescein angiographic assessment at the end of study periods varying from 8 to months (mean 47 months) was performed in all patients except 2 developing retinal detachment (cases 26.
3 834 Patrick. Condon and Graham. Serjeant Table 1 Clinical details, response to therapy, and complications in treatment group Number Final Series Age/ Eye PS lesions Duration of assessment cases sex treated treated follow up leakage from (D=diathermy) (months) treated PS Homozygous sickle cell disease 1 20 M 2 31 M 3 34 F 4 M 5 48 M 6 4 M 7 56 F 8 57 F (D) S 7 (D) Sickle cell-haemoglobin C disease 13 F M I 11 IS M I (D) F M M F I 16 18F 6(D) M F 2 22 M I M 6 (D) M F F F 6 (D) M M F M M 5 (D) F F M F F M 4 31 M F M M F 3 41 M M F 4 40 F M 4 50 M M F F F M 3 Sickle cell-p+ thalassaemia 52 M 2 M 54 3 F M Sickle cell-p, thalassaemia M M 2 3 (D) No change No change Complications treated eye PVD, CN VT AU, VH, PVD, T 2 VH, CVN 14 3NP, AU, PH, VH (2), VT, CVN 8 HB (2), CN 15 CN 25 HB (2), CN 28 CN 20 3NP, CN - HB, VH, CVN - AU, PH (4), CN 10 HB (2) 27 PVD, EM, CVN CN (2) - ASI, PH (4) CN 17 D, VH 42 HB, CN (2) - CVN _ VH,?CN 11 _ CN 26 HB 16 CVN _ 3NP, HB, D 43 CN (2) 22 CVN (3) 24 3NP, CN - PH, VH (3), PVD, CVN 37 CVN 41 VT, EM - 3NP HB, VH - HB, CVN 21 CN 3 18 PH, CVN AU, PH (5), CN CN CN 3NP, CN 3NP, CVN Case in previous series2 Age indicates age on admission to study. Complications: 3NP = Partial third nerve palsy. AU = Anterior uveitis. ASI = Anterior segment ischaemia. HB = etinal haemorrhage confined to coagulation lesion. PH = Preretinal haemorrhage. VH = Vitreous haemorrhage. VT = Vitreoretinal traction. PVD = Posterior vitreous detachment associated with vitreoretinal traction. EM = Epiretinal membrane. T = etinal tear. D = etinal detachment. CN = Choroidoretinal neovascularisation. CVN = Choroidovitreal neovascularisation. (n) = n as suffix indicates number of lesions
4 Photocoagulation in proliferative sickle retinopathy Table 2 Visual acuity measured on first and last attendance in treatment and control eyes, with probable cause of decreased acuity Visual acuity Genotype Patient Eye Treatyment eye Comparison eye no. treated Start Er;d Start End SS SC S,3+ thal /18 6/12 6/12 6/12 6/18 6/24* 6/18** <0** 6/18 <0** 0** 6/1 8** 6/18* 0 NP No PS No PS No PS No PS CF No PS 6/24 No PS No PS NP 6/ 6/12 NP <0 No PS No PS No PS So' thal /24 NP CF 6/24 NP 0 0** NP <0 6/** *Deterioration in visual acuity of 2 lines or more and ** of 3 lines or more. Abbreviations as in Table 1 except NP = no perception of light; CF = counting fingers; VO Cause of decreased acuity in treatment (comparison) eye () (), (EM) VH, (phthisis bulbi) VH EM (VO) Vo D D (D)? Macular oedema (D) Bilateral VH (Phthisis bulbi) (Choroidal ischaemia) Cataract (VH) = vitreous organisation 835
5 8 Patrick I. Condon and Graham. Serjeanr Fig. 2 Fluorescein angiograms demonstrating development of choroidoretinal neovascularisation in the right temporal area of a 27-year-oldfemale with SC disease (case 27): same vessel junction marked by straight arrow. (a) Initial PS lesion. (b) Two weeks after photocoagulation. (c) Nine months post treatment-major choroidal vessels visible and indicated by curved arrow. (d) Sixteen months post treatment-choroidoretinal neovascularisation. 34) and one who was pregnant (case 15). In the remaining 54 patients leakage from the originally treated PS lesion was considered to have ceased in (81%), improved in 8 (15%), and persisted unchanged in 2 (4%). CHOOIDA NEOVASCUAISATION In 31 patients fluorescein leakage subsequently developed at the site of photocoagulation, all of which showed fine vessel systems within the burn area apparently supplied by choroidal vessels and draining through either choroidal or retinal veins. In patients these abnormal vessels were in the plane of the retina, and their fluorescence was separated from the surrounding normally perfused retina by a margin of nonfluorescence. These lesions were referred to as choroidoretinal neovascularisation (CN), and an example is illustrated in Fig. 2.
6 Photocoagulation in proliferative sickle retin7opathy In 12 patients the abnormal vessel system projected into the vitreous, and fluorescence from these lesions frequently overlay normal retina. These lesions were referred to as choroidovitreal neovascularisation (CVN), and an example is illustrated in Fig. 3. Four of the CVN lesions developed from CN lesions during the period of follow-up, 2 apparently spontaneously and 2 after therapy of the CN lesion. The remaining CN lesions remained flat for follow-up periods of up to 54 months, did not enlarge, and did not give rise to complications. Choroidovitreal neovascularisation, however, underwent rapid enlargement in 5 patients (cases 11,, 22, 28, 33) and was associated with vitreous 837 Fig. 3 Composite fluorescein angiogram depicting choroidovitreal neovascularisation in the left temporal area of a 25-yearold female with SC disease (case 22) 28 months after photocoagulation. ower arrow indicates coagulation site ofprincipal feeder vessels for large PS lesion. Upper arrow indicates site of choriovitreal neovascularisation. haemorrhage in four (cases 10, 11,, 38). Photocoagulation of CN lesions in patients stopped fluorescein leakage in 3 (cases 20, 25, 35) and of CVN lesions in 7 patients stopped leakage in 1 (case 10). HAEMOHAGE Preretinal haemorrhages occurred in 6 patients and were multiple in 3 patients, all of whom had received diathermy. Three patients (cases 20, 24, ) developed haemorrhages in direct relationship to the diathermy burns, and two of these also developed preretinal haemorrhages in remote areas of the same eye. Two patients (cases 11, 52) developed
7 838 preretinal haemorrhages in relation to CVN lesions 4 years after therapy, and 1 patient (case 38) developed two preretinal haemorrhages, one as an extension of a deep retinal haemorrhage, 16 and 26 months after therapy. etinal haemorrhage confined to the burn area occurred in patients. Neither form of haemorrhage extended into the vitreous or affected visual acuity. Vitreous haemorrhage occurred in the treatment eye in 8 patients, 4 of whom had choroidovitreal neovascularisation. In 1 of these (case 10) a limited vitreous haemorrhage occurred during photocoagulation of a CVN lesion, but in the remainder the haemorrhage occurred 11-3 years after therapy. VITEOETINA TACTION Vitreoretinal traction developed or became worse during the study in 7 patients. In 2 patients it was associated with epiretinal membranes and in 4 with posterior vitreous detachments. A retinal tear produced during therapy in one patient (case 8) was successfully sealed by further light coagulation at the same treatment session. etinal detachment occurred in 2 patients both having had retreatment for a persistently perfused PS lesion. In one (case 26) photocoagulation of a darkly pigmented area produced excessive heat release, with fracture of Bruch's membrane and an immediate subretinal haemorrhage which spread to the vitreous. This did not change for 1 month, but 4 months later a gradual blurring of vision occurred, and examination 1 year after the original treatment revealed no red reflex, no observable detail behind the lens, and inaccurate projection of light. The other patient (case 34) had apparently uneventful initial therapy but noted progressive deterioration of vision 1 year later, and examination 3 years after this revealed gross vitreoretinal traction and a total retinal detachment, which was unsuccessfully repaired with vitreoretinal surgery. OTHE COMPICATIONS OF THEAPY Other complications in the treatment group included anterior uveitis, anterior segment ischaemia, partial third nerve palsies, haemorrhage, vitreoretinal changes, and retinal detachment. Anterior uveitis occurred in 4 patients and settled promptly on systemic and topical steroid therapy. Anterior segment ischaemia occurred in 1 patient after scleral diathermy despite care being taken to avoid the long ciliary vessels or detachment of ocular muscles. This complication gradually settled on systemic and topical steroids, but signs of iris atrophy, irregularity of the pupil, and extensive anterior and posterior synechiae remained. Both anterior uveitis and anterior segment ischaemia were Patrick I. Condon and Graham. Serjeant confined to patients treated by scleral diathermy and were not considered complications of photocoagulation. Partial third nerve palsies followed retrobulbar injection of local anaesthetic in 7 patients, all resolving satisfactorily within 2-3 weeks. There was the clinical impression that this complication was more common in patients requiring larger volumes of anaesthetic for effective anaesthesia. BEHAVIOU OF COMPAISON EYE GOUP Of the 47 comparison eyes gross pathology precluded satisfactory longitudinal observations on PS in 6. Four had retinal detachment (cases 8, 35,, 41) and 1 gross vitreous fibrosis (case 22) on admission to the study, and 1 patient (case 5) developed a gross vitreous haemorrhage after initial examination. Of the remaining 41 eyes 10 developed PS for the first time during the study period, and an increase in the number or size of PS lesions occurred in a further 21 patients. Autoinfarcted PS lesions were present on admission to the study in 6 patients and developed during the study in 16, three showing complete autoinfarction of all leaking lesions and 13 a combination of autoinfarction and progression. When angiographic assessments were compared at the beginning and end of the study in the 41 comparison eyes with adequate data, 25 (60%) indicated more extensive perfused PS, 8 (20%) showed no change, and 8 (20%) improved. In 3 of the latter patients PS developed and spontaneously infarcted during the study period. The comparison group showed preretinal haemorrhages in 3 eyes and vitreous haemorrhages in 7 eyes. One vitreous haemorrhage (case 5) followed trauma to an eye with perfused PS, the significance of which was difficult to assess. Visual acuity, measured at the first and last attendance during the study, decreased by 2 lines or more on the Snellen chart in 12/57 (21%) of the treatment group compared to 4/42 (10%) of the comparison group. Deterioration of 3 lines or more occurred in 5 (%) and 2 (5%) respectively and was attributed in the treatment group to retinal detachment (2), vitreous organisation (1), vitreous haemorrhage (1), and possible macular oedema (1), and in the comparison group to vitreous haemorrhage (2). The visual acuity in 1 patient in the treatment group (case ) attributed to possible macular oedema subsequently improved to 6/12. Discussion The abnormal vessel systems that develop at the junction of vascular and avascular retina in sickle cell disease may compromise vision by causing
8 Photocoagulation in proliferative sickle retinopathy vitreous haemorrhage and/or retinal detachment. endering these lesions avascular appears logical, and their characteristic anatomy, with feeding arterioles and draining veins, makes them amenable to closure by localised coagulation. Xenon arc, argon laser, diathermy, and cryopexy have been employed, the present study using the xenon arc with supplemental diathermy in some cases. The procedure included coagulation of the feeding arterioles after their identification by fluorescein angiography, followed by coagulation of the proliferative lesion. Coagulation of the veins was not performed. The method and details of treatment of 33 patients in this series have been previously published.2 These methods are capable of stopping perfusion in most proliferative lesions. Condon and Serjeant2 achieved closure in 1% of eyes treated with predominantly xenon arc and Goldbaum et al.3 reported similar results in eyes using either xenon or argon photocoagulation. However, the follow-up periods in these studies were relatively short, ranging from 2 weeks to 21 years. The initial closure rate of 87% in the present study is similar to that in earlier series, 3 patients continuing to leak despite repeated photocoagulation. The development of fluorescein leakage from vessel networks developing within the burn area complicated angiographic assessment of continued closure during follow-up. Noted initially as 'spot leakage' within the photocoagulation scar, fine networks of vessels developed, fed from the choroidal vessels and draining into either the retinal or choroidal veins. Two patterns of this choroidal neovascularisation were apparent. The term choroidoretinal neovascularisation (CN) was used to describe vessel systems which lay flat in the plane of the retina and was not intended to imply anastomoses between choroidal and retinal circulations, although they frequently occurred. These lesions produced fluorescence within the burn area, which was usually separated by a margin of nonfluorescence from surrounding normally perfused retina. This abnormality has not been previously reported but has been noted elsewhere (Dr ee Jampol, personal communication). Throughout follow-up periods up to 54 months these abnormal vessels generally did not enlarge or give rise to complications. The term choroidovitreal neovascularisation (CVN) was applied to vessel systems which invaded the vitreous and were originally reported as complications of argon laser therapy.5 The high prevalence of CVNs in the present study (22%) indicates that this is also a common complication with the xenon arc. These lesions tended to show progressive enlargement, and the association with vitreous 83 haemorrhage in 4 patients suggested that their natural history may be less benign than that of the CN. Further coagulation therapy of these lesions was attempted in 7 patients, successfully stopping perfusion in 1, and it was interesting to note that rapid vitreous extension of a CVN in 1 patient was associated with decreased dye leakage compatible with spontaneous autoinfarction. The aetiology of these lesions is unclear, though presumably related to breaks in Bruch's membrane caused by excessive energy release in the pigment epithelial layer. eporting this complication following argon laser therapy, Goldbaum et al.3 attributed it to the high energy density associated with small (50-100,um) burn sizes and suggested that this complication did not occur with larger burns ( plm). These authors did not observe this complication with xenon arc therapy, in contrast to our own experience. Different techniques may have contributed to these different conclusions, Goldbaum et al.3 limiting coagulation to the feeding vessels whereas the PS lesion was also coagulated in the present study. Since on several occasions a small apparently innocuous PS lesion was replaced, after therapy, by a larger potentially serious CVN, this complication must be avoided if xenon arc photocoagulation is to play a part in the management of PS lesions in these patients. Certain complications attended repeated photocoagulation. Increased organisation and rigidity of the vitreous body with subsequent traction on the internal limiting membrane of the retina of the posterior pole occurred in 7 patients, 6 of whom had had 2 or more treatment sessions. Posterior vitreous detachment occurred in 4 patients, but traction retinal detachment was not observed. In 1 patient with 4 treatment sessions gross vitreous fibrotic changes occurred with vitreoretinal traction and recurrent vitreous haemorrhages originating in the choroid or deep retina peripheral to the coagulated area. etreatment of a darkly pigmented area in another resulted in retinal detachment and blindness. To diminish these dangers the minimally effective power of the coagulator should be used in retreatment of pigmented areas. Other complications related to therapy included transient partial third nerve palsies, anterior uveitis and anterior segment ischaemia, and haemorrhages. The duration of burn with the xenon arc photocoagulator used ( seconds), necessitated the routine use of retrobulbar anaesthesia. Partial third nerve palsies which developed in 7 patients were probably related to the volume or siting of retrobulbar injections and all resolved satisfactorily. Anterior uveitis and anterior segment ischaemia were confined to patients receiving diathermy and
9 840 should probably not be considered complications o1 xenon arc photocoagulation. Multiple preretinal haemorrhages were also confined to the diathermy group. A single preretinal haemorrhage developed in 2 patients after xenon arc photocoagulation, but neither these nor the retinal haemorrhages confined to the burn area were of clinical significance. Experience in the treated group must be compared with the behaviour of PS in the comparison group during the study. Development or progression of PS in 31 comparison eyes must be balanced against evidence of autoinfarction in 17 patients and complete cure in 3. Furthermore the rapid progression in some patients was not reflected in deteriorating visual acuity. There is some evidence that the most rapid progression of PS occurs in the year age group, which includes 27 (47%) patients in the present study, and it is therefore possible that longer term follow-up will be associated with more complete regression of PS. In terms of visual acuity measured at the first and last attendance there was no significant difference between treatment and comparison groups over a mean 4-year follow-up period. In terms of vitreous haemorrhage an episode occurred in every 26-4 years of observation in the treatment group compared to 21 4 years of observation in the comparison group. However, the failure to demonstrate a difference between treatment and comparison groups must be treated with caution in view of the statistical limitations of the study. When the study was started in 73, it was felt that the response to xenon arc photocoagulation in this condition was Patrick I. Condon and Graham. Serjeant sufficiently unknown to justify treating only the worst affected eye. More data are now available, and if the problems of choroidal neovascularisation can be avoided there is a need for a proper randomly controlled trial of xenon arc therapy in PS. With the realisation of the high prevalence of spontaneous autoinfarction, this study is especially necessary to define the role, if any, of photocoagulation in the therapy of these lesions. eferences I Goldberg MF. Treatment of proliferative sickle retinopathy. Trans Am Acad Ophthalmol Otolaryngol 71; 75: Condon PI, Serjeant G. Photocoagulation and diathermy in the treatment of proliferative sickle retinopathy. Br J Ophthalmol 74; 57: Goldbaum MH, Goldberg MF, Nagpal K, Asdourian GK, Galinos SO. Proliferative sickle retinopathy. In: 'Esperance FA, ed. Current Diagnosis and Management of Chorio-retinal Diseases. St ouis: Mosby, 77: Goldberg MF, Acacio I. Argon laser photocoagulation of proliferative sickle retinopathy. Arch Ophthalmol 73; 30: Galinos SO, Asdourian GK, Woolf MB, Goldberg MF, Busse BJ. Choroido-vitreal neovascularisation after argon laser photocoagulation. Arch Ophthalmol 75; 3: ee CB, Woolf MB, Galinos SO, Goldbaum MH, Stevens TS, Goldberg MF. Cryotherapy of proliferative sickle retinopathy. Part 1. Single freeze-thaw cycle. Ann Ophthalmol 75; 7: Serjeant G. The Clinical Features of Sickle Cell Disease. Amsterdam: North Holland, 74: Condon PI, Serjeant G. Ocular findings in hemoglobin SC disease in Jamaica. Am J Ophthalmol 72; 74: Condon PI, Serjeant G. The behaviour of untreated proliferative sickle retinopathy. Br J Ophthalmol 80; 64: Br J Ophthalmol: first published as 10.11/bjo on 1 November 80. Downloaded from on July 2018 by guest. Protected by copyright.
Ocular findings in children with sickle
 Brit. J. Ophthal. (I 974) 58, 644 Ocular findings in children with sickle cell haemoglobin C disease in Jamaica PATRICK I. CONDON, ROBERT GRAY, AND GRAHAM R. SERJEANT From the Medical Research Council,
Brit. J. Ophthal. (I 974) 58, 644 Ocular findings in children with sickle cell haemoglobin C disease in Jamaica PATRICK I. CONDON, ROBERT GRAY, AND GRAHAM R. SERJEANT From the Medical Research Council,
Retinal photocoagulation for proliferative sickle cell retinopathy: A prospective clinical trial with new sea fan classification
 European Journal of Ophthalmology / Vol. 18 no. 2, 2008 / pp. 248-254 Retinal photocoagulation for proliferative sickle cell retinopathy: A prospective clinical trial with new sea fan classification D.
European Journal of Ophthalmology / Vol. 18 no. 2, 2008 / pp. 248-254 Retinal photocoagulation for proliferative sickle cell retinopathy: A prospective clinical trial with new sea fan classification D.
optic disc neovascularisation
 British Journal of Ophthalmology, 1979, 63, 412-417 A comparative study of argon laser and krypton laser in the treatment of diabetic optic disc neovascularisation W. E. SCHULENBURG, A. M. HAMILTON, AND
British Journal of Ophthalmology, 1979, 63, 412-417 A comparative study of argon laser and krypton laser in the treatment of diabetic optic disc neovascularisation W. E. SCHULENBURG, A. M. HAMILTON, AND
Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and
 British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
Photocoagulation of disciform macular lesions
 British Journal of Ophthalmology, 1979, 63, 669-673 Photocoagulation of disciform macular lesions with krypton laser A. C. BIRD AND R. H. B. GREY From the Institute of Ophthalmology, Moorfields Eye Hospital,
British Journal of Ophthalmology, 1979, 63, 669-673 Photocoagulation of disciform macular lesions with krypton laser A. C. BIRD AND R. H. B. GREY From the Institute of Ophthalmology, Moorfields Eye Hospital,
Panretinal photocoagulation in central retinal vein
 British Journal of Ophthalmology, 1977, 61, 741-753 Panretinal photocoagulation in central retinal vein occlusion: a randomised controlled clinical study L. LAATIKAINEN, E. M. KOHNER, D. KHOURY, AND R.
British Journal of Ophthalmology, 1977, 61, 741-753 Panretinal photocoagulation in central retinal vein occlusion: a randomised controlled clinical study L. LAATIKAINEN, E. M. KOHNER, D. KHOURY, AND R.
Iris atrophy in sickle cell disease
 British Journal of Ophthalmology, 1986, 70, 516-521 R W ACHESON,' S M FORD,' G H MAUDE,' R W LYNESS,2 AND G R SERJEANT From the 'Medical Research Council Laboratories (Jamaica), University ofthe West Indies,
British Journal of Ophthalmology, 1986, 70, 516-521 R W ACHESON,' S M FORD,' G H MAUDE,' R W LYNESS,2 AND G R SERJEANT From the 'Medical Research Council Laboratories (Jamaica), University ofthe West Indies,
Michael P. Blair, MD Retina Consultants, Ltd Libertyville/Des Plaines, Illinois Clinical Associate University of Chicago 17 October 2015
 Michael P. Blair, MD Retina Consultants, Ltd Libertyville/Des Plaines, Illinois Clinical Associate University of Chicago 17 October 2015 So What Parts of the Eye Retina are Affected by VHL Neural tissue
Michael P. Blair, MD Retina Consultants, Ltd Libertyville/Des Plaines, Illinois Clinical Associate University of Chicago 17 October 2015 So What Parts of the Eye Retina are Affected by VHL Neural tissue
Introduction How the eye works
 1 Introduction Diabetic retinopathy is a condition that can cause permanent loss of eyesight and even blindness. It is a major cause of loss of vision. But if a person with diabetes receives proper eye
1 Introduction Diabetic retinopathy is a condition that can cause permanent loss of eyesight and even blindness. It is a major cause of loss of vision. But if a person with diabetes receives proper eye
New vessel formation in retinal branch vein occlusion
 Brit. 7. Ophthal. (I 976) 6o, 8io New vessel formation in retinal branch vein occlusion JOHN S. SHILLING AND EVA M. KOHNER From the Retinal Diagnostic Unit, Moorfields Eye Hospital, London Neovascularization
Brit. 7. Ophthal. (I 976) 6o, 8io New vessel formation in retinal branch vein occlusion JOHN S. SHILLING AND EVA M. KOHNER From the Retinal Diagnostic Unit, Moorfields Eye Hospital, London Neovascularization
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Large capillary aneurysms secondary to retinal venous obstruction
 British Journal of Ophthalmology, 1981, 65, 36-41 Large capillary aneurysms secondary to retinal venous obstruction JOEL SCHULMAN, LEE M. JAMPOL, AND MORTON F. GOLDBERG From the University of Illinois
British Journal of Ophthalmology, 1981, 65, 36-41 Large capillary aneurysms secondary to retinal venous obstruction JOEL SCHULMAN, LEE M. JAMPOL, AND MORTON F. GOLDBERG From the University of Illinois
Retinal pigment epithelial detachments in the elderly:
 British Journal of Ophthalmology, 1985, 69, 397-403 Retinal pigment epithelial detachments in the elderly: classification and outcome A G CASSWELL, D KOHEN, AND A C BIRD From Moorfields Eye Hospital, City
British Journal of Ophthalmology, 1985, 69, 397-403 Retinal pigment epithelial detachments in the elderly: classification and outcome A G CASSWELL, D KOHEN, AND A C BIRD From Moorfields Eye Hospital, City
Extensive argon laser photocoagulation in the
 British Journal of Ophthalmology, 1989, 73, 197-201 Extensive argon laser photocoagulation in the treatment of proliferative diabetic retinopathy G W AYLWARD, R V PEARSON, J D JAGGER, AND A M HAMILTON
British Journal of Ophthalmology, 1989, 73, 197-201 Extensive argon laser photocoagulation in the treatment of proliferative diabetic retinopathy G W AYLWARD, R V PEARSON, J D JAGGER, AND A M HAMILTON
PART 1: GENERAL RETINAL ANATOMY
 PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
 measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
ZEISS AngioPlex OCT Angiography. Clinical Case Reports
 Clinical Case Reports Proliferative Diabetic Retinopathy (PDR) Case Report 969 PROLIFERATIVE DIABETIC RETINOPATHY 1 1-year-old diabetic female presents for follow-up of proliferative diabetic retinopathy
Clinical Case Reports Proliferative Diabetic Retinopathy (PDR) Case Report 969 PROLIFERATIVE DIABETIC RETINOPATHY 1 1-year-old diabetic female presents for follow-up of proliferative diabetic retinopathy
Late retinal reattachment
 :British Journal of Ophthalmology, 1981, 65, 142-146 Late retinal reattachment S. N. KOKOLAKIS, L. BRAVO, AND A. H. CHIGNELL From the Ophthalmic Department, St Thomas's Hospital, London SEI SUMMARY Six
:British Journal of Ophthalmology, 1981, 65, 142-146 Late retinal reattachment S. N. KOKOLAKIS, L. BRAVO, AND A. H. CHIGNELL From the Ophthalmic Department, St Thomas's Hospital, London SEI SUMMARY Six
Diabetic Retinopathy
 Diabetic Retinopathy Diabetes can be classified into type 1 diabetes mellitus and type 2 diabetes mellitus, formerly known as insulin-dependent diabetes mellitus, and non-insulin diabetes mellitus, respectively.
Diabetic Retinopathy Diabetes can be classified into type 1 diabetes mellitus and type 2 diabetes mellitus, formerly known as insulin-dependent diabetes mellitus, and non-insulin diabetes mellitus, respectively.
UVEITIS IN GENERAL. Information for patients UVEITIS CLINIC WHAT IS UVEITIS? MAIN CATEGORIES OF UVEITIS
 Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
Information for patients UVEITIS CLINIC UVEITIS IN GENERAL WHAT IS UVEITIS? The uvea is a name given to the pigmented layer of tissue inside the eye. When all or part of the uvea becomes inflamed, the
Retina Conference. Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014
 Retina Conference Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014 Subjective CC/HPI: 64 year old Caucasian female referred by outside ophthalmologist
Retina Conference Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014 Subjective CC/HPI: 64 year old Caucasian female referred by outside ophthalmologist
Treatment of diabetic maculopathy by
 Brit. J. Ophthal. (1974) 58, 85 Treatment of diabetic maculopathy by argon-laser S. MERIN, L. YANKO, AND M. IVRY From the Department of Ophthalmology, Hadassah University Hospital, Jerusalem, Israel Diabetic
Brit. J. Ophthal. (1974) 58, 85 Treatment of diabetic maculopathy by argon-laser S. MERIN, L. YANKO, AND M. IVRY From the Department of Ophthalmology, Hadassah University Hospital, Jerusalem, Israel Diabetic
Diabetes & Your Eyes
 Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
VITREOUS FLOATERS AND PHOTOPSIA AS PREDICTORS OF VITREORETINAL PATHOLOGY
 Basrah Journal Of Surgery VITREOUS FLOATERS AND PHOTOPSIA AS PREDICTORS OF VITREORETINAL PATHOLOGY Salah Zuhair Al-Asadi MB,ChB, FRCS, FIBMS, Lecturer of Ophthalmology, College of Medicine, University
Basrah Journal Of Surgery VITREOUS FLOATERS AND PHOTOPSIA AS PREDICTORS OF VITREORETINAL PATHOLOGY Salah Zuhair Al-Asadi MB,ChB, FRCS, FIBMS, Lecturer of Ophthalmology, College of Medicine, University
Retinal dialysis. procedures. The purpose of the present paper is to report the results of treatment of 62
 Brit. J. Ophthal. (I973) 57, 572 Retinal dialysis A. H. CHIGNELL Moorfields Eye Hospital, City Road, London, E.C. i Retinal dialysis is an important cause of retinal detachment and subsequent reduction
Brit. J. Ophthal. (I973) 57, 572 Retinal dialysis A. H. CHIGNELL Moorfields Eye Hospital, City Road, London, E.C. i Retinal dialysis is an important cause of retinal detachment and subsequent reduction
Diabetic Retinopathy A Presentation for the Public
 Diabetic Retinopathy A Presentation for the Public Ray M. Balyeat, MD The Eye Institute Tulsa, Oklahoma The Healthy Eye Light rays enter the eye through the cornea, pupil and lens. These light rays are
Diabetic Retinopathy A Presentation for the Public Ray M. Balyeat, MD The Eye Institute Tulsa, Oklahoma The Healthy Eye Light rays enter the eye through the cornea, pupil and lens. These light rays are
RETINAL CONDITIONS RETINAL CONDITIONS
 GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
Trabeculectomy combined with cataract extraction: a follow-up study
 British Journal of Ophthalmology, 1980, 64, 720-724 Trabeculectomy combined with cataract extraction: a follow-up study R. S. EDWARDS From the Birmingham and Midland Eye Hospital, Church Street, Birmingham
British Journal of Ophthalmology, 1980, 64, 720-724 Trabeculectomy combined with cataract extraction: a follow-up study R. S. EDWARDS From the Birmingham and Midland Eye Hospital, Church Street, Birmingham
The Human Eye. Cornea Iris. Pupil. Lens. Retina
 The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
GENERAL INFORMATION DIABETIC EYE DISEASE
 GENERAL INFORMATION DIABETIC EYE DISEASE WHAT IS DIABETIC EYE DISEASE? Diabetic eye disease is a term used to describe the common eye complications seen in people with diabetes. It includes: Diabetic retinopathy
GENERAL INFORMATION DIABETIC EYE DISEASE WHAT IS DIABETIC EYE DISEASE? Diabetic eye disease is a term used to describe the common eye complications seen in people with diabetes. It includes: Diabetic retinopathy
Diabetic retinopathy damage to the blood vessels in the retina. Cataract clouding of the eye s lens. Cataracts develop at an earlier age in people
 Diabetic Retinopathy What is diabetic eye disease? Diabetic eye disease refers to a group of eye problems that people with diabetes may face as a complication of diabetes. All can cause severe vision loss
Diabetic Retinopathy What is diabetic eye disease? Diabetic eye disease refers to a group of eye problems that people with diabetes may face as a complication of diabetes. All can cause severe vision loss
Ultrasonic examination in severe diabetic eye disease
 British Journal of Ophthalmology, 1979, 63, 533-538 Ultrasonic examination in severe diabetic eye disease DAVID McLEOD AND MARIE RESTORI From the Department of Ultrasound, Moorfields Eye Hospital, City
British Journal of Ophthalmology, 1979, 63, 533-538 Ultrasonic examination in severe diabetic eye disease DAVID McLEOD AND MARIE RESTORI From the Department of Ultrasound, Moorfields Eye Hospital, City
THE OCULAR histoplasmosis
 CLINICAL SCIENCES Reactivation of Inflammatory Lesions in Ocular Histoplasmosis David Callanan, MD; Gary E. Fish, MD, JD; Rajiv Anand, MD Background: Active inflammation has not been traditionally associated
CLINICAL SCIENCES Reactivation of Inflammatory Lesions in Ocular Histoplasmosis David Callanan, MD; Gary E. Fish, MD, JD; Rajiv Anand, MD Background: Active inflammation has not been traditionally associated
Vascular changes in the iris in chronic
 Vascular changes in the iris in chronic anterior uveitis LEILA LAATIKAINEN From the Department of Ophthalmology, University of Helsinki, Finland British Journal of Ophthalmology, 1979, 63, 145-149 SUMMARY
Vascular changes in the iris in chronic anterior uveitis LEILA LAATIKAINEN From the Department of Ophthalmology, University of Helsinki, Finland British Journal of Ophthalmology, 1979, 63, 145-149 SUMMARY
Purtscher s retinopathy: A case of severe bilateral visual loss due to chest compression
 O P E N A C C E S S Case study Purtscher s retinopathy: A case of severe bilateral visual loss due to chest compression Shakeel P Hashim, Maha M El Shafei, Zakia M Al Ansari Hamad Medical Corporation,
O P E N A C C E S S Case study Purtscher s retinopathy: A case of severe bilateral visual loss due to chest compression Shakeel P Hashim, Maha M El Shafei, Zakia M Al Ansari Hamad Medical Corporation,
Royal Berkshire Hospital Dunedin Hospital. Prince Charles Eye Unit Pi Princess Margaret Hospital
 Vitreoretinal Surgery Mr Vaughan Tanner www.tanner-eyes.co.uk eyes Reading Royal Berkshire Hospital Dunedin Hospital Windsor Prince Charles Eye Unit Pi Princess Margaret Hospital Success rates VR surgery
Vitreoretinal Surgery Mr Vaughan Tanner www.tanner-eyes.co.uk eyes Reading Royal Berkshire Hospital Dunedin Hospital Windsor Prince Charles Eye Unit Pi Princess Margaret Hospital Success rates VR surgery
Long-Term Visual Outcome in Proliferative Diabetic Retinopathy Patients After Panretinal Photocoagulation
 Long-Term Visual Outcome in Proliferative Diabetic Retinopathy Patients After Panretinal Photocoagulation Murat Dogru, Makoto Nakamura, Masanori Inoue and Misao Yamamoto Department of Ophthalmology, Kobe
Long-Term Visual Outcome in Proliferative Diabetic Retinopathy Patients After Panretinal Photocoagulation Murat Dogru, Makoto Nakamura, Masanori Inoue and Misao Yamamoto Department of Ophthalmology, Kobe
The use of a high-intensity laser to create an anastomotic
 Case Report 866 Laser Chorioretinal Venous Anastomosis for Progressive Nonischemic Central Retinal Vein Occlusion Chih-Hsin Chen, MD; Chien-Hsiung Lai 1, MD; Hsi-Kung Kuo, MD The use of high or medium-intensity
Case Report 866 Laser Chorioretinal Venous Anastomosis for Progressive Nonischemic Central Retinal Vein Occlusion Chih-Hsin Chen, MD; Chien-Hsiung Lai 1, MD; Hsi-Kung Kuo, MD The use of high or medium-intensity
Ophthalmology Macular Pathways
 Ophthalmology Macular Pathways Age related Macular Degeneration Diabetic Macular Oedema Macular Oedema secondary to Central Retinal Macular Oedema secondary to Branch Retinal CNV associated with pathological
Ophthalmology Macular Pathways Age related Macular Degeneration Diabetic Macular Oedema Macular Oedema secondary to Central Retinal Macular Oedema secondary to Branch Retinal CNV associated with pathological
Evolution of the retinal black sunburst in sickling haemoglobinopathies
 Brit. 7. Ophthal. (I975) 59, 710 Evolution of the retinal black sunburst in sickling haemoglobinopathies GEORGE ASDOURIAN, KRISHAN C. NAGPAL, MICHAEL GOLDBAUM, DIMITRIOS PATRIANAKOS, MORTON F. GOLDBERG,
Brit. 7. Ophthal. (I975) 59, 710 Evolution of the retinal black sunburst in sickling haemoglobinopathies GEORGE ASDOURIAN, KRISHAN C. NAGPAL, MICHAEL GOLDBAUM, DIMITRIOS PATRIANAKOS, MORTON F. GOLDBERG,
New classification of peripheral retinal vascular changes in sickle cell disease
 Bnrtish Journal ofophthalmology 1994; 78: 681-689 Medical Research Council Laboratories (Jamaica) University of the West Indies, Kingston, Jamaica A D Penman P Thomas G R Serjeant The Royal Hallamshire
Bnrtish Journal ofophthalmology 1994; 78: 681-689 Medical Research Council Laboratories (Jamaica) University of the West Indies, Kingston, Jamaica A D Penman P Thomas G R Serjeant The Royal Hallamshire
A Patient s Guide to Diabetic Retinopathy
 Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Diabetic Retinopathy. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS
 ORIGINAL ARTICLE ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS Aggarwal Somesh VP 1, Shah Sonali N 2, Bharwada Rekha M 3,
ORIGINAL ARTICLE ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS Aggarwal Somesh VP 1, Shah Sonali N 2, Bharwada Rekha M 3,
Brampton Hurontario Street Brampton, ON L6Y 0P6
 Diabetic Retinopathy What is Diabetic Retinopathy Diabetic retinopathy is one of the leading causes of blindness world-wide. Diabetes damages blood vessels in many organs of the body including the eyes.
Diabetic Retinopathy What is Diabetic Retinopathy Diabetic retinopathy is one of the leading causes of blindness world-wide. Diabetes damages blood vessels in many organs of the body including the eyes.
Retinal Tear and Detachment
 Retinal Tear and Detachment Introduction The retina is the layer of tissue in the back of the eye that is responsible for vision. It is attached to the choroid tissue, which supplies the retina with blood.
Retinal Tear and Detachment Introduction The retina is the layer of tissue in the back of the eye that is responsible for vision. It is attached to the choroid tissue, which supplies the retina with blood.
Retinal Detachment PATIENT EDUCATION
 Retinal Detachment PATIENT EDUCATION What is Retinal Detachment (RD)? Retina is the light-sensitive layer at the back of the eye that converts light images into nerve impulses that are relayed to the brain
Retinal Detachment PATIENT EDUCATION What is Retinal Detachment (RD)? Retina is the light-sensitive layer at the back of the eye that converts light images into nerve impulses that are relayed to the brain
Prophylaxis of retinal detachment
 Brit. J. Ophthal. (I973) 57, 291 Communications Prophylaxis of retinal detachment A. H. CHIGNELL AND J. SHILLING Moorfields Eye Hospital, City Road, London, E.C. i. The detection of conditions which may
Brit. J. Ophthal. (I973) 57, 291 Communications Prophylaxis of retinal detachment A. H. CHIGNELL AND J. SHILLING Moorfields Eye Hospital, City Road, London, E.C. i. The detection of conditions which may
Autosomal dominant exudative vitreoretinopathy
 British Journal of Ophthalmology, 1980, 64, 112-120 R. R. OBER, A. C. BIRD, A. M. HAMILTON, AND K. SEHMI From the Institute of Ophthalmology, Moorfields Eye Hospital, City Road, London SUMMARY Twelve affected
British Journal of Ophthalmology, 1980, 64, 112-120 R. R. OBER, A. C. BIRD, A. M. HAMILTON, AND K. SEHMI From the Institute of Ophthalmology, Moorfields Eye Hospital, City Road, London SUMMARY Twelve affected
Facts About Diabetic Eye Disease
 Facts About Diabetic Eye Disease Points to Remember 1. Diabetic eye disease comprises a group of eye conditions that affect people with diabetes. These conditions include diabetic retinopathy, diabetic
Facts About Diabetic Eye Disease Points to Remember 1. Diabetic eye disease comprises a group of eye conditions that affect people with diabetes. These conditions include diabetic retinopathy, diabetic
Bilateral nodular sarcoid choroiditis with vitreous haemorrhage
 British Journal of Ophthalmology, 1984, 68, 660-666 Bilateral nodular sarcoid choroiditis with vitreous haemorrhage LAURENCE S. STONE AND MARTIN EHRENBERG From the Departments of Ophthalmology, Eye Research
British Journal of Ophthalmology, 1984, 68, 660-666 Bilateral nodular sarcoid choroiditis with vitreous haemorrhage LAURENCE S. STONE AND MARTIN EHRENBERG From the Departments of Ophthalmology, Eye Research
FRANZCO, MD, MBBS. Royal Darwin Hospital
 Diabetes and Eye By Dr. Nishantha Wijesinghe FRANZCO, MD, MBBS Consultant Ophthalmologist Royal Darwin Hospital 98% of Diabetics do not need to suffer from severe visual loss Yet Diabetic eye disease is
Diabetes and Eye By Dr. Nishantha Wijesinghe FRANZCO, MD, MBBS Consultant Ophthalmologist Royal Darwin Hospital 98% of Diabetics do not need to suffer from severe visual loss Yet Diabetic eye disease is
SCREENING FOR OPHTHALMIC MANIFESTATIONS OF SICKLE CELL DISEASE IN THE UNITED KINGDOM
 SCREENING FOR OPHTHALMIC MANIFESTATIONS OF SICKLE CELL DISEASE IN THE UNITED KINGDOM D. KENTl, R. ARYA2, W. A. ACLIMANDOSl, A. J. BELLINGHAM2 and A. C. BIRD3 London SUMMARY There are marked variations
SCREENING FOR OPHTHALMIC MANIFESTATIONS OF SICKLE CELL DISEASE IN THE UNITED KINGDOM D. KENTl, R. ARYA2, W. A. ACLIMANDOSl, A. J. BELLINGHAM2 and A. C. BIRD3 London SUMMARY There are marked variations
Prognosis for rubeosis iridis following central
 British Journal of Ophthalmology, 1979, 63, 735-743 Prognosis for rubeosis iridis following central retinal vein occlusion STEPHEN H. SINCLAIR AND EVANGELOS S. GRAGOUDAS From the Eye Research Institute
British Journal of Ophthalmology, 1979, 63, 735-743 Prognosis for rubeosis iridis following central retinal vein occlusion STEPHEN H. SINCLAIR AND EVANGELOS S. GRAGOUDAS From the Eye Research Institute
EyePACS Grading System (Part 3): Detecting Proliferative (Neovascular) Diabetic Retinopathy. George Bresnick MD MPA Jorge Cuadros OD PhD
 EyePACS Grading System (Part 3): Detecting Proliferative (Neovascular) Diabetic Retinopathy George Bresnick MD MPA Jorge Cuadros OD PhD Anatomy of the eye: 3 Normal Retina Retinal Arcades Macula Optic
EyePACS Grading System (Part 3): Detecting Proliferative (Neovascular) Diabetic Retinopathy George Bresnick MD MPA Jorge Cuadros OD PhD Anatomy of the eye: 3 Normal Retina Retinal Arcades Macula Optic
UNDERSTAND MORE ABOUT UVEITIS UVEITIS
 UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
UNDERSTAND MORE ABOUT UVEITIS UVEITIS Uveitis What is uveitis? Uveitis is inflammation of the uvea, the middle layer of your eye. The eye is shaped much like a tennis ball, with three different layers
Acute posterior vitreous detachment: the predictive value of vitreous pigment and symptomatology
 1264 Vitreo-Retinal Unit, Department of Ophthalmology, St Thomas s Hospital, Lambeth Palace Road, London SE1 7EH, UK V Tanner D Harle JTan T H Williamson A H Chignell Audit Department, Royal College of
1264 Vitreo-Retinal Unit, Department of Ophthalmology, St Thomas s Hospital, Lambeth Palace Road, London SE1 7EH, UK V Tanner D Harle JTan T H Williamson A H Chignell Audit Department, Royal College of
Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion
 Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion Hiroki Fujita, Kyoko Ohno-Matsui, Soh Futagami and Takashi Tokoro Department of Visual Science, Tokyo Medical
Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion Hiroki Fujita, Kyoko Ohno-Matsui, Soh Futagami and Takashi Tokoro Department of Visual Science, Tokyo Medical
surgery Macular puckers after retinal detachment and loss of the macular reflex with a greyish appearance of the macula
 Brit. J. Ophthal. (97 ) 55, 451 Macular puckers after retinal detachment surgery W. S. HAGLER AND UPAL ATURALYA* From the Department of Ophthalmology, Emory University School of Medicine, and Emory University
Brit. J. Ophthal. (97 ) 55, 451 Macular puckers after retinal detachment surgery W. S. HAGLER AND UPAL ATURALYA* From the Department of Ophthalmology, Emory University School of Medicine, and Emory University
RETINAL DETACHMENT AT THE POSTERIOR POLE*
 Brit. J. Ophthal. (1958) 42, 749. RETINAL DETACHMENT AT THE POSTERIOR POLE* BY CALBERT I. PHILLIPSt Institute of Ophthalmology, University oflondon THE common feature of the cases to be described in this
Brit. J. Ophthal. (1958) 42, 749. RETINAL DETACHMENT AT THE POSTERIOR POLE* BY CALBERT I. PHILLIPSt Institute of Ophthalmology, University oflondon THE common feature of the cases to be described in this
Diabetes and Eye Health more than meets the eye Vision Initiative - in association with PSA
 Diabetes and Eye Health more than meets the eye Vision Initiative - in association with PSA Vision 2020 Australia Vision Initiative RANZCO & OAA (Vic) Proud members of Vision 2020 Australia Outline Vision
Diabetes and Eye Health more than meets the eye Vision Initiative - in association with PSA Vision 2020 Australia Vision Initiative RANZCO & OAA (Vic) Proud members of Vision 2020 Australia Outline Vision
Central serous chorioretinopathy (CSCR) was
 Case Report 777 Perfluorocarbon Liquid-Assisted External Drainage in the Management of Central Serous Chorioretinopathy with Bullous Serous Retinal Detachment Hung-Chiao Chen, MD; Jau-Der Ho, MD; San-Ni
Case Report 777 Perfluorocarbon Liquid-Assisted External Drainage in the Management of Central Serous Chorioretinopathy with Bullous Serous Retinal Detachment Hung-Chiao Chen, MD; Jau-Der Ho, MD; San-Ni
Diabetic Retinopathy
 Diabetic Retinopathy Diabetes mellitus is one of the leading causes of irreversible blindness worldwide. In the United States, it is the most common cause of blindness in people younger than 65 years.
Diabetic Retinopathy Diabetes mellitus is one of the leading causes of irreversible blindness worldwide. In the United States, it is the most common cause of blindness in people younger than 65 years.
Age-Related Macular Degeneration (AMD)
 Age-Related Macular Degeneration (AMD) What is the Macula? What is Dry AMD (Age-related Macular Degeneration)? Dry AMD is an aging process that causes accumulation of waste product under the macula leading
Age-Related Macular Degeneration (AMD) What is the Macula? What is Dry AMD (Age-related Macular Degeneration)? Dry AMD is an aging process that causes accumulation of waste product under the macula leading
Development and classification of rubeosis iridis
 British Journal of Ophthalmology, 1979, 63, 150-156 Development and classification of rubeosis iridis in diabetic eye disease LEILA LAATIKAINEN From the Department of Ophthalmology, University of Helsinki,
British Journal of Ophthalmology, 1979, 63, 150-156 Development and classification of rubeosis iridis in diabetic eye disease LEILA LAATIKAINEN From the Department of Ophthalmology, University of Helsinki,
When optical coherence tomography (OCT)
 Macular Imaging: SD-OCT in nterior Segment Surgical Practice Many pathologic processes of the macula can be visualized or quantified only with this modality. y Steven G. Safran, MD When optical coherence
Macular Imaging: SD-OCT in nterior Segment Surgical Practice Many pathologic processes of the macula can be visualized or quantified only with this modality. y Steven G. Safran, MD When optical coherence
Mild NPDR. Moderate NPDR. Severe NPDR
 Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
NEOVASCULAR GLAUCOMA IN A NIGERIAN AFRICAN POPULATION
 October 2006 E AST AFRICAN MEDICAL JOURNAL 559 East African Medical Journal Vol. 83 No. 10 October 2006 NEOVASCULAR GLAUCOMA IN A NIGERIAN AFRICAN POPULATION: A.O. Ashaye, FWACS, MSc, Department of Ophthalmology,
October 2006 E AST AFRICAN MEDICAL JOURNAL 559 East African Medical Journal Vol. 83 No. 10 October 2006 NEOVASCULAR GLAUCOMA IN A NIGERIAN AFRICAN POPULATION: A.O. Ashaye, FWACS, MSc, Department of Ophthalmology,
DIABETIC VITRECTOMY INDICATIONS AND TECHNIQUES. steve charles
 DIABETIC VITRECTOMY INDICATIONS AND TECHNIQUES steve charles Traction Retinal Detachment Macula involved TRD TRD with rhegmatogenous component even if extra-macular TTRD Extra-Macular TRD should be observed
DIABETIC VITRECTOMY INDICATIONS AND TECHNIQUES steve charles Traction Retinal Detachment Macula involved TRD TRD with rhegmatogenous component even if extra-macular TTRD Extra-Macular TRD should be observed
Information for Patients undergoing Intravitreal Triamcinolone Acetonide (Kenalog) Injection
 Information for Patients undergoing Intravitreal Triamcinolone Acetonide (Kenalog) Injection Kenalog/SS/ST/04.2012/v1.1 review 05.2013 Page 1 Introduction Your doctor has found that you have leakage of
Information for Patients undergoing Intravitreal Triamcinolone Acetonide (Kenalog) Injection Kenalog/SS/ST/04.2012/v1.1 review 05.2013 Page 1 Introduction Your doctor has found that you have leakage of
Information for Patients. Vitrectomy
 Manchester Royal Eye Hospital Vitreoretinal Services Information for Patients Vitrectomy Your eye doctor has advised you that you require vitrectomy surgery. This leaflet gives you information that will
Manchester Royal Eye Hospital Vitreoretinal Services Information for Patients Vitrectomy Your eye doctor has advised you that you require vitrectomy surgery. This leaflet gives you information that will
ISPUB.COM. Photopsia post flu: A case of MEWDS. S Baisakhiya, S Dulani, S Lele INTRODUCTION CASE HISTORY
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 1 Photopsia post flu: A case of MEWDS S Baisakhiya, S Dulani, S Lele Citation S Baisakhiya, S Dulani, S Lele. Photopsia
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 1 Photopsia post flu: A case of MEWDS S Baisakhiya, S Dulani, S Lele Citation S Baisakhiya, S Dulani, S Lele. Photopsia
COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY
 Original Article COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY Aggarwal Somesh V 1, Shah Sonali N 2, Bharwada Rekha
Original Article COMPARISON OF INTRAVITREAL TRIAMCINOLONE INJECTION VS LASER PHOTOCOAGULATION IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETIC RETINOPATHY Aggarwal Somesh V 1, Shah Sonali N 2, Bharwada Rekha
Bilateral common carotid occlusion with hypoxic ocular sequelae
 Brit. J. Ophthal. (1971) 55, 383 Bilateral common carotid occlusion with hypoxic ocular sequelae C. T. HART AND S. HAWORTH Cheltenham A patient is described who was referred with anterior uveitis; following
Brit. J. Ophthal. (1971) 55, 383 Bilateral common carotid occlusion with hypoxic ocular sequelae C. T. HART AND S. HAWORTH Cheltenham A patient is described who was referred with anterior uveitis; following
Comparative electroretinograms in argon laser
 British Journal of Ophthalmology, 1983, 67, 520-525 Comparative electroretinograms in argon laser and xenon arc panretinal photocoagulation JAMES C. LIANG,' GERALD A. FISHMAN,' FELIPE U. HUAMONTE,' AND
British Journal of Ophthalmology, 1983, 67, 520-525 Comparative electroretinograms in argon laser and xenon arc panretinal photocoagulation JAMES C. LIANG,' GERALD A. FISHMAN,' FELIPE U. HUAMONTE,' AND
Insertion of an epiretinal prosthesis for retinitis pigmentosa
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Insertion of an epiretinal prosthesis for retinitis pigmentosa Retinitis pigmentosa is a disease that affects
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Insertion of an epiretinal prosthesis for retinitis pigmentosa Retinitis pigmentosa is a disease that affects
OCT Assessment of the Vitreoretinal Relationship in CSME
 December 2007 Sonia Rani John et al. - IFIS 375 ORIGINAL ARTICLE OCT Assessment of the Vitreoretinal Relationship in CSME Dr. Manoj S. DNB FRCS, Dr. Unnikrishnan Nair MS DO FRCS, Dr. Gargi Sathish MS Introduction
December 2007 Sonia Rani John et al. - IFIS 375 ORIGINAL ARTICLE OCT Assessment of the Vitreoretinal Relationship in CSME Dr. Manoj S. DNB FRCS, Dr. Unnikrishnan Nair MS DO FRCS, Dr. Gargi Sathish MS Introduction
Tuberous sclerosis presenting as atypical aggressive retinal astrocytoma with proliferative retinopathy and vitreous haemorrhage
 Case Report Brunei Int Med J. 2015; 11 (1): 49-53 Tuberous sclerosis presenting as atypical aggressive retinal astrocytoma with proliferative retinopathy and vitreous haemorrhage Pui Ling TANG and Mae-Lynn
Case Report Brunei Int Med J. 2015; 11 (1): 49-53 Tuberous sclerosis presenting as atypical aggressive retinal astrocytoma with proliferative retinopathy and vitreous haemorrhage Pui Ling TANG and Mae-Lynn
Disease-Specific Fluorescein Angiography
 Ruth E. Picchiottino, CRA Disease-Specific Fluorescein Angiography 15 Disease-Specific Fluorescein Angiography Recommendations for tailoring retinal fluorescein angiography to diabetic retinopathy, macular
Ruth E. Picchiottino, CRA Disease-Specific Fluorescein Angiography 15 Disease-Specific Fluorescein Angiography Recommendations for tailoring retinal fluorescein angiography to diabetic retinopathy, macular
Retinal detachment When to see a doctor How retinal detachment occurs
 Retinal detachment Retinal detachment describes an emergency situation in which a thin layer of tissue (the retina) at the back of the eye pulls away from its normal position. Retinal detachment separates
Retinal detachment Retinal detachment describes an emergency situation in which a thin layer of tissue (the retina) at the back of the eye pulls away from its normal position. Retinal detachment separates
Spontaneous Regression of Neovascularization at the Disc in Diabetic Retinopathy
 Korean J Ophthalmol Vol. 18:41-46, 2004 Spontaneous Regression of Neovascularization at the Disc in Diabetic Retinopathy Jae Ryong Han, MD, Won Kyung Ju, MD, In Won Park, MD Department of Ophthalmology,
Korean J Ophthalmol Vol. 18:41-46, 2004 Spontaneous Regression of Neovascularization at the Disc in Diabetic Retinopathy Jae Ryong Han, MD, Won Kyung Ju, MD, In Won Park, MD Department of Ophthalmology,
Late ocular manifestations in neonatal herpes simplex infection
 British Journal of Ophthalmology, 1977, 61, 608-616 Late ocular manifestations in neonatal herpes simplex infection AHTI TARKKANEN AND LEILA LAATIKAINEN From the Helsinki University Eye Hospital SUMMARY
British Journal of Ophthalmology, 1977, 61, 608-616 Late ocular manifestations in neonatal herpes simplex infection AHTI TARKKANEN AND LEILA LAATIKAINEN From the Helsinki University Eye Hospital SUMMARY
Haemorrhagic glaucoma
 Brit. j. Ophthal. (I97I) 55, 444 Haemorrhagic glaucoma Comparative study in diabetic and nondiabetic patients P. H. MADSEN From the Departments of Ophthalmology and Internal Medicine, the University Hospital,
Brit. j. Ophthal. (I97I) 55, 444 Haemorrhagic glaucoma Comparative study in diabetic and nondiabetic patients P. H. MADSEN From the Departments of Ophthalmology and Internal Medicine, the University Hospital,
Clinical Case Presentation. Branch Retinal Vein Occlusion. Sarita M. Registered Nurse Whangarei Base Hospital
 Clinical Case Presentation on Branch Retinal Vein Occlusion Sarita M. Registered Nurse Whangarei Base Hospital Introduction Case Study Pathogenesis Clinical Features Investigations Treatment Follow-up
Clinical Case Presentation on Branch Retinal Vein Occlusion Sarita M. Registered Nurse Whangarei Base Hospital Introduction Case Study Pathogenesis Clinical Features Investigations Treatment Follow-up
Irreversible visual loss in Waldenstrom's macroglobulinaemia
 British Journal of Ophthalmology, 1983, 67, 102-106 Irreversible visual loss in Waldenstrom's macroglobulinaemia EDGAR L. THOMAS, R. JOSEPH OLK, MAURIE MARKMAN, HAYDEN BRAINE, AND ARNALL PATZ From the
British Journal of Ophthalmology, 1983, 67, 102-106 Irreversible visual loss in Waldenstrom's macroglobulinaemia EDGAR L. THOMAS, R. JOSEPH OLK, MAURIE MARKMAN, HAYDEN BRAINE, AND ARNALL PATZ From the
Studies on intravitreal blood vessels. II. Effectiveness of xenon arc and argon laser photocoagulation in blood vessel closure
 Studies on intravitreal blood vessels. II. Effectiveness of xenon arc and argon laser photocoagulation in blood vessel closure Gholam A. Peyman, Jeff E. Koziol, Donald R. Sanders, and Joseph K. Vlchek
Studies on intravitreal blood vessels. II. Effectiveness of xenon arc and argon laser photocoagulation in blood vessel closure Gholam A. Peyman, Jeff E. Koziol, Donald R. Sanders, and Joseph K. Vlchek
OAKLEIGH EYE CENTRE. THE EYE Before looking at diabetic retinopathy it is important to understand what the healthy eye looks like and how it works.
 ABN: 80 836 359 971 Dr Mark Steiner 345 799X 135 Warrigal Road Dr Helen Steiner 292 419A OAKLEIGH VIC 3166 Tel: 03 9568 7706 Fax: 03 9568 4498 E-Mail: oakeye13@bigpond.com DIABETIC RETINOPATHY DIABETES
ABN: 80 836 359 971 Dr Mark Steiner 345 799X 135 Warrigal Road Dr Helen Steiner 292 419A OAKLEIGH VIC 3166 Tel: 03 9568 7706 Fax: 03 9568 4498 E-Mail: oakeye13@bigpond.com DIABETIC RETINOPATHY DIABETES
Visual outcome after silicone oil removal and recurrent retinal detachment repair
 Visual outcome after silicone oil removal and recurrent retinal detachment repair CHRISTINA J. FLAXEL, SUZANNE M. MITCHELL, G. WILLIAM AYLWARD c.j. Flaxel GW. Aylward Moorfields Eye Hospital City Road
Visual outcome after silicone oil removal and recurrent retinal detachment repair CHRISTINA J. FLAXEL, SUZANNE M. MITCHELL, G. WILLIAM AYLWARD c.j. Flaxel GW. Aylward Moorfields Eye Hospital City Road
Retinal Vein Occlusion (RVO) Treatment pathway- Northeast England. Retinal Vein Occlusion (RVO) with Macular oedema (MO)
 Retinal Vein Occlusion (RVO) Treatment pathway- Northeast England (Royal Victoria Infirmary, Sunderland Eye Infirmary, James Cook University Hospital, Darlington Memorial Hospital, University Hospital
Retinal Vein Occlusion (RVO) Treatment pathway- Northeast England (Royal Victoria Infirmary, Sunderland Eye Infirmary, James Cook University Hospital, Darlington Memorial Hospital, University Hospital
Patient Information Cataract Surgery
 Patient Information Cataract Surgery Introduction This leaflet has been written to help you understand more about surgery for a cataract. It explains what the operation involves, the benefits and risks
Patient Information Cataract Surgery Introduction This leaflet has been written to help you understand more about surgery for a cataract. It explains what the operation involves, the benefits and risks
Clinically Significant Macular Edema (CSME)
 Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Coagulative necrosis in a malignant melanoma of the choroid at the macula with extensive subretinal hemorrhage
 Coagulative necrosis in a malignant melanoma of the choroid at the macula with extensive subretinal hemorrhage Robert D. Yee, Robert Y. Foos, and Bradley R. Straatsma The authors present a case report
Coagulative necrosis in a malignant melanoma of the choroid at the macula with extensive subretinal hemorrhage Robert D. Yee, Robert Y. Foos, and Bradley R. Straatsma The authors present a case report
Recalcitrant Diabetic Macular Oedema: Therapeutic Options
 December 2007 A. Giridhar et al. - Recalcitrant DME 451 CONSULTATION S E C T I O N Recalcitrant Diabetic Macular Oedema: Therapeutic Options Dr. Cyrus M Shroff 1, Dr. N S Muralidhar 2, Dr. R Narayanan
December 2007 A. Giridhar et al. - Recalcitrant DME 451 CONSULTATION S E C T I O N Recalcitrant Diabetic Macular Oedema: Therapeutic Options Dr. Cyrus M Shroff 1, Dr. N S Muralidhar 2, Dr. R Narayanan
epitheliopathy associated with diffuse retinal vasculitis
 British Journal of Ophthalmology, 1986, 70, 255-259 Acute posterior multifocal placoid pigment epitheliopathy associated with diffuse retinal vasculitis and late haemorrhagic macular detachment MAKOTO
British Journal of Ophthalmology, 1986, 70, 255-259 Acute posterior multifocal placoid pigment epitheliopathy associated with diffuse retinal vasculitis and late haemorrhagic macular detachment MAKOTO
Medical Retina 2011 Nicholas Lee
 Medical Retina 2011 Nicholas Lee 1 Diabetic Retinopathy Epidemiology 1000 registered blind each year 2% diabetics registered as blind (8% of all Blind Registrations) 42% with Mild Background DR will progress
Medical Retina 2011 Nicholas Lee 1 Diabetic Retinopathy Epidemiology 1000 registered blind each year 2% diabetics registered as blind (8% of all Blind Registrations) 42% with Mild Background DR will progress
Outline. Outline. Vitreous Development & Anatomy OPT - 243
 2010 OPT - 243 Vitreous Disorders & Vitreoretinal Disorders of the Posterior Pole I Leo Semes, OD, FAAO 100% 0% 0% 0% 0% Which of these gives the best resolution for studying vitreoretinal disorders of
2010 OPT - 243 Vitreous Disorders & Vitreoretinal Disorders of the Posterior Pole I Leo Semes, OD, FAAO 100% 0% 0% 0% 0% Which of these gives the best resolution for studying vitreoretinal disorders of
MANAGING DIABETIC RETINOPATHY. <Your Hospital Name> <Your Logo>
 MANAGING DIABETIC RETINOPATHY It s difficult living with Diabetes Mellitus. Ask any diabetic... Their lives are centered around meal plans, glucose levels, and insulin
MANAGING DIABETIC RETINOPATHY It s difficult living with Diabetes Mellitus. Ask any diabetic... Their lives are centered around meal plans, glucose levels, and insulin
Scrub In. What is the function of vitreous humor? What does the pupil do when exposed to bright light? a. Maintain eye shape and provide color vision
 Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Scrub In What is the function of vitreous humor? a. Maintain eye shape and provide color vision b. Maintain eye shape and refract light rays c. Provide night vision and color vision d. Provide night vision
Photodynamic therapy (PDT) for Central Serous Retinopathy (CSR)/ Polypoidal Choroidal Vasculopathy (PCV)
 Photodynamic therapy (PDT) for Central Serous Retinopathy (CSR)/ Polypoidal Choroidal Vasculopathy (PCV) About photodynamic therapy for Retinal Conditions The macula is the central part of the retina at
Photodynamic therapy (PDT) for Central Serous Retinopathy (CSR)/ Polypoidal Choroidal Vasculopathy (PCV) About photodynamic therapy for Retinal Conditions The macula is the central part of the retina at
