Renal allograft loss in the first post-operative month: causes and consequences
|
|
|
- Dina Parrish
- 5 years ago
- Views:
Transcription
1 Clin Transplant 2012 DOI: /j x ª 2012 John Wiley & Sons A/S. Renal allograft loss in the first post-operative month: causes and consequences Phelan PJ, OÕKelly P, Tarazi M, Tarazi N, Salehmohamed MR, Little DM, Magee C, Conlon PJ. Renal allograft loss in the first post-operative month: causes and consequences. Clin Transplant 2012 DOI: /j x. ª 2012 John Wiley & Sons A/S. Abstract: Early transplant failure is a devastating outcome after kidney transplantation. We report the causes and consequences of deceased donor renal transplant failure in the first 30 d at our center between January 1990 and December Controls were adult deceased donor transplant patients in the same period with an allograft that functioned >30 d. The incidence of early graft failure in our series of 2381 consecutive deceased donor transplants was 4.6% (n = 109). The causes of failure were allograft thrombosis (n = 48; 44%), acute rejection (n = 19; 17.4%), death with a functioning allograft (n = 17; 15.6%), primary non-function (n = 14; 12.8%), and other causes (n = 11; 10.1%). Mean time to allograft failure was 7.3 d. There has been a decreased incidence of all-cause early failure from 7% in 1990 to <1% in Patients who developed early failure had longer cold ischemia times when compared with patients with allografts lasting >30 d (p < 0.001). Early allograft failure was strongly associated with reduced patient survival (p < 0.001). In conclusion, early renal allograft failure is associated with a survival disadvantage, but has thankfully become less common in recent years. Paul J. Phelan a, Patrick OÕKelly a, Munir Tarazi a, Nadim Tarazi a, M. Ridhwaan Salehmohamed a, Dilly M. Little b, Colm Magee a and Peter J. Conlon a Departments of a Nephrology, b Transplantation, Beaumont Hospital, Dublin, Ireland Key words: acute rejection allograft failure allograft thrombosis Corresponding author: Dr. Paul J. Phelan, Department of Nephrology, Beaumont Hospital, Dublin 9, Ireland. Tel.: ; fax: ; paulphel@gmail.com Conflict of interest: The authors have no conflict of interest to declare. Accepted for publication 5 September 2011 Renal allograft loss in the first month post-transplantation is an uncommon, but devastating outcome for patients. It occurs in approximately 5% of first transplants (1) and has a range of etiologies. Vascular accidents, such as thrombosis of a renal vein or artery, are typically early phenomena posttransplantation and usually catastrophic (2, 3). They are frequent causes of early allograft loss accounting for at least a third of all allograft failures within 90 d (2). The reported incidence of allograft thrombosis ranges between 1.6% and 6% (2 4). Other causes include acute rejection, primary non-function, and recurrence of primary disease. Over the last 20 yr, early kidney transplant outcomes have improved significantly (5). Improved technical approaches and new advances in immunosuppression and antibody definition have improved the outcome associated with the procedure (6, 7). Nevertheless, early transplant loss still remains a significant cause of morbidity. The aims of our study were to report the incidence and changing etiology of early renal transplant failure over the past 20 yr at our center. We also sought to compare these patients to those whose allograft functioned for more than one month with respect to patient characteristics and survival. Methods Patients Our institution is the only renal transplantation center in the Republic of Ireland, performing transplants per yr. We conducted a retrospective analysis of all adult ( 18 yr), deceased donor kidney-only transplants between 1 January 1990 and 31 December 2009 and identified those which failed during the first 30 d. Allograft failures were divided into four-yr periods for comparison ( , , , and ). The percentage of pre-emptive transplants increased during the time period from approximately 1% to 8% by A diagnosis of primary non-function was reserved for grafts that were perfused, but never functioned. Also, at least one biopsy was performed to exclude other causes. Patients receiving their fourth and subsequent 1
2 Phelan et al. transplants were excluded from the study as the risk of allograft failure was felt to be exceptionally high. Demographic and outcome data were collected from our prospectively updated transplant database. Transplant operations Transplants were performed in the setting of a negative complement-dependent cytotoxicity (CDC) cross-match and a negative CDC plus flow cytometry cross-match from 2002 onwards. Organs were perfused in-situ using University of Wisconsin solution and generally recovered using cold storage at 4 C. From 2007, machine perfusion was employed for expanded criteria kidneys. Operations were performed using a standard surgical technique with end to side anastomosis to recipient external or common iliac vessels using a Carrel patch. Multiple renal arteries were dealt with using a neo-carrel patch or side to side anastomosis for similar sized arteries. Vena caval extension was routinely used for all right-sided kidneys to obtain additional length for the right renal vein, as described by Chopin et al. (8). Peri-operative heparin prophylaxis against venous thromboembolism was not routinely used nor was intraoperative heparin from 1999 onwards. Transplant isotope scanning was generally performed as a definitive diagnosis if allograft thrombosis was suspected. Regular biopsies were performed if graft function deteriorated. Transplant nephrectomy was performed as soon as a non-correctable graft failure was identified. Panel reactive antibody (PRA) was determined by use of the CDC assay, NIH Basic technique (9). Initial medications Prior to 2005, antibody induction in the form of anti-thymocyte globulin was reserved for high immunological risk patients (highly sensitized, repeat transplants). From 2005, basiliximab induction was routinely administered to all recipients. Initial immunosuppression consisted of a calcineurin inhibitor (cyclosporine [4 mg/kg twice daily; prior to 2001] or tacrolimus [0.1 mg/kg twice daily; 2001 onwards]), an anti-metabolite (azathioprine [2 mg/kg daily; prior to 2002] or mycophenolate mofetil [500 mg twice daily; 2002 onwards]) and steroids. Cyclosporine doses were adjusted to achieve troughs of ng/ml and tacrolimus doses were titrated to troughs of ng/ml in the early post-transplant period. Patients at risk for CMV disease (recipient, donor or both CMV seropositive) received CMV prophylaxis from 1992 onwards. This consisted of acyclovir up until 1998, valaciclovir from 1998 until 2004 and valganciclovir used since then (dosage adjusted for renal function). All patients received co-trimoxazole for Pneumocystosis prophylaxis. Statistical analysis The two groups (allograft survival <30 and >30 d) were compared for patient survival using proportional hazards regression. Patient survival was conducted from the end of 30 d posttransplant and analyzed for first transplants only. Multi-factorial analysis was performed to test for independence of early allograft failure on patient outcome in the presence of several confounding variables. Kaplan Meier methods were used to calculate patient survival and also to determine estimated time to re-transplant for early graft failure. Demographic variables were compared with controls using Pearson chi-square or Wilcoxon rank-sum tests. A p-value of <0.05 was considered to be statistically significant. Results There were 2381 consecutive deceased donor transplants performed during the study period. Two cases of early allograft failure on the fourth or subsequent transplant were excluded. A total of 109 allografts failed within 30 d of transplantation giving an overall incidence of 4.6%. However, the incidence has become less common over time, from >6% in to 1.75% in (Fig. 1). In univariate analysis, patients who developed early failure were older (44.4 vs yr, p = 0.042) and had a longer cold ischemia time (CIT; 23 vs. 20 h; p < 0.001) when compared with patients with allografts lasting >30 d (see Table 1). The mean donor age was higher in the early failure group (40.2 vs yr; p = 0.043) although the percentage of pediatric donors (<18 yr) used was greater (13.0% vs. 10.4%). The early failure group had a lower mean number of HLA mismatches (2.6 vs. 2.9; p = 0.043). In a multivariate model, only cold ischemic time was significantly associated with early allograft failure (Table 2). Etiology of allograft failure The most common cause of early allograft loss was renal vessel thrombosis, occurring in 48 allografts (44% of total early failures). Thirty cases (62.5% of thromboses) were due to venous thrombosis, 11 2
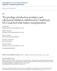
3 Renal allograft loss in the first month 7% 6% 5% 4% 3% 2% AR PNF Other Death Thrombosis 1% 0% Fig. 1. Etiology of early allograft failure as a percentage of total transplants in specified period. Table 1. Patient characteristics (means unless specifies) Variable Early allograft failure group Allograft survival >30 d p-value Recipient 47 (13.4) 44.4 (14.3) age (SD) Donor age (SD) 40.2 (15.4) 37.2 (15.4) Sex (% M) HLA mismatches (SD) 2.6 (1.5) 2.9 (1.4) CIT (SD) 23 (6.6) 20.4 (5.99) <0.001 Diabetes (%) % PRA group a 67.0/11.9/ /13.3/ % First transplant SD, standard deviation; CIT, cold ischemia time. a Panel reactive antibodies (groups 0 10%, 11 49%, %). Table 2. Multivariate model of factors which may influence early allograft loss Variable Odds ratio Odds ratio 95% confidence interval p-value Recipient age (per yr) Donor age (per yr) Male recipient sex Male donor sex HLA mismatches CIT <0.001 PRA group Re-transplant Diabetes mellitus CIT, cold ischemia time. (23%) were due to arterial thrombosis, and in seven cases (14.5%) both vessels were thrombosed. There was no history of venous thromboembolism in 34 patients with eight cases unknown/insufficient data. Of the remaining six cases, three had a pulmonary embolism prior to their transplant, one patient had previously clotted their polytetrafluoroethylene (PTFE) graft when on dialysis and two patients developed a lower limb DVT postnephrectomy. Hemoglobin levels at the time of transplant were similar between patients with an allograft thrombosis (11.4 g/dl; IQR g/dl), patients with other causes of early failure (11.3 g/dl; IQR g/dl), and patients with allograft survival >30 d (11.3 g/dl; IQR g/dl; p = 0.967). Acute rejection was the diagnosis in 19 cases (17.4%). The type of injury was classified as acute cellular rejection (n = 3), antibody-mediated rejection (n = 6), mixed picture (n = 7) and unclassified (n = 3). Death with a functioning allograft occurred in 17 patients (15.6%). The causes of death were cardiovascular (n = 8), sepsis (n = 3), hemorrhage (n = 2), hepatic failure, (n = 1) and unknown (n = 3). Primary nonfunction was the cause in 14 cases (12.8%). Tubular necrosis was the dominant pathological finding in these cases where the transplant never functioned. Eleven allografts (10.1%) failed due to other causes, including transplant hemorrhage (n = 6), sepsis (n = 2), recurrence of primary disease (n = 1), de novo thrombotic microangiopathy (n = 1), and one unknown cause. There was a striking reduction in all-cause early transplant failure and particularly of allograft thrombosis over the study period (see Fig. 1). There were also steep reductions in failures due to acute rejection since
4 Phelan et al. Excluding death with a functioning allograft, 36 transplants failed between implantation and the first post-operative day and 57 had failed within the first week (out of 92 total failures in 30 d). The mean time to all-cause graft failure was 7.3 d. Re-transplantation The median time to re-transplantation in the early allograft failure group was 3.02 yr (see Fig. 2). In total, 71% of patients were eventually re-transplanted. At our center, patients with an early allograft failure may be prioritized for another organ depending on the clinical circumstances (10). If deemed medically suitable, patients can be immediately re-listed and may be offered an ABO-compatible (non-identical) allograft if one becomes available. This occurred in seven patients from this cohort who were re-transplanted prior to hospital discharge. Patient survival In the early graft failure group, survival at 1, 5, 10 and 15 yr after transplant surgery was 84%, 68%, 67%, and 46%, respectively. In the continued allograft function group, the corresponding figures were 98%, 90%, 78%, and 66% (see Fig. 3). A multifactorial model identified death-censored early allograft failure (p < 0.001), presence of diabetes mellitus (p < 0.001), and recipient (p < 0.001) and donor age (p = 0.008) as significant predictors of patient survival (see Table 3). Discussion The most common cause of early renal allograft failure in our series was renal vessel thrombosis % retransplanted after early graft failure Time (years) Fig. 2. Time to re-transplantation in early allograft failure patients. % patient survival Time (years) Early graft failure No early graft failure Fig. 3. Patient survival between the early renal allograft failure group and the controls. Table 3. A multifactorial model of patient survival Variable Hazard ratio Confidence interval p-value Early graft failure <0.001 Recipient age (per yr) <0.001 Male recipient sex HLA mismatches Diabetes mellitus <0.001 Male donor sex Donor age (per yr) PRA group a CIT HLA, human leukocyte antigen; CIT, cold ischaemia time. a Panel reactive antibodies (groups 0 10%, 11 49%, %). which is consistent with other reports (2, 3). In this study, allograft thrombosis was responsible for approximately 44% of all early (<30 d) graft failures and accounted for 52% of causes when death with a functioning graft was excluded. It is also clear from our results that the allograft is most at risk during the first week post-transplantation. In recent years, there has been a decrease in the overall number of early renal allograft failures at our center and a decrease individually in failures due to allograft thrombosis, acute rejection, and primary non-function. The improvement in failures due to acute rejection is assumedly due to more sensitive cross-matching techniques as well as the employment of modern immunosuppression with the introduction of tacrolimus, mycophenolic acid, and more recently antibody induction therapy. The lower rate of allograft thrombosis is encouraging and possibly due to improved surgical technique and cross-matching technologies. The absence of primary non-function as a cause of early allograft loss is difficult to explain, but may be a result of 4
5 Renal allograft loss in the first month more judicious donor selection or perhaps an improved effort to accurately diagnose the cause of organ loss in recent times. Primary allograft thrombosis can be due to donor and recipient factors as well as issues regarding organ recovery and surgical implantation. The donor right kidney has been associated with an increased risk of allograft thrombosis (2). The reason for this has been speculated to be due to the short vein and long artery of the right kidney (11). The short vein may cause problems with positioning of the kidney especially in larger patients. Moreover, the length of the right renal artery can sometimes lead to kinking of the vessel. However, we have recently demonstrated no difference in outcome between left and right deceased donor kidney pairs where vena caval extension was routinely used to provide additional length for the right kidney anastomosis (12), as in this study. Pediatric patients, who were not included in our study, are at increased risk of allograft thrombosis due in part to the small size of the recipient vessels (13). Other technical problems such as vessel torsion or intimal injury during organ procurement may act as a nidus for thrombosis. Due to a lack of precise data, these issues could not be fully explored in our study. The association between prolonged CIT and early allograft failure is not surprising. CIT has long been associated with delayed graft function (DGF). In other series, it was also found that CIT was strongly associated with DGF, with a 23% increase in the risk of DGF for every six h of CIT (p < 0.001) (14). Acute transplant rejection occurred more frequently in the allografts with DGF. A prolonged CIT has also been associated with long-term allograft dysfunction (15) as well as with allograft thrombosis itself (10). Our report reenforces the message to keep CIT as short as possible during kidney transplantation. The mean HLA mismatches were marginally lower in the early graft failure group. This result may be surprising as the importance of HLA matching has been demonstrated in other series (16). The detrimental effect of HLA mismatching in the context of CIT has also been suggested. Connolly et al. (17) showed that zero HLA-DR mismatched grafts showed significantly enhanced survival over those with 1 HLA-DR mismatch at one yr (92.8% vs. 84.5%) and at five yr (88.3% vs. 73.9%), if CIT was <26 h (p = ). However, most of the transplant failures in our series occurred very early and were not immunologically mediated. There is a lack of modern literature on the effect of HLA matching on allograft outcome in the first 30 d. Therefore, the lower degree of HLA mismatching in the early failure group (mean 2.6 vs. 2.9) may be a chance occurrence. There was no association between early allograft failure and donor sex, presence of diabetes mellitus, and number of previous transplants. Variables that were significantly associated with decreased patient survival included early allograft loss, presence of diabetes mellitus, and increasing recipient and donor age. These associations are perhaps not surprising, although it does highlight the deleterious effect that an early allograft loss has to the patient. It is clear from the survival curve that the adverse survival effect is evident immediately post-transplant failure. Moreover, reports of mortality with increasing donor age are not consistent with some studies, showing no association between older donor age and patient survival (18, 19) despite expanded criteria donors showing a reduced patient survival (20). Waiting times on the on the renal transplant pool continue to rise (21). In Ireland, the median waiting time was between eight and 15 months depending on blood group, for those with a low level of sensitization, during the period between 2000 and 2005 (22). In this series, the median time to re-transplantation following an early allograft failure was three yrs with almost 30% of patients never getting re-transplanted. During the 1990s, waiting times for renal transplantation in Ireland was generally less than one yr, so it is evident that our early failure patients faced significant barriers to re-transplantation. Despite this, the eventual rate of re-transplantation compares well to other reports (23). It is well recognized that longer waiting times for kidney transplantation translates into shorter patient survival (24). This may explain some of the increased mortality experienced by the early failure patients. There are some limitations to this study. We acknowledge the inherent weaknesses of any retrospective, single center study. Moreover, over the study period, surgical and immunological practices have undoubtedly developed and immunosuppressant agents have been modernized. This can lead to issues when comparing patients from different eras. However, confining the study to one center reduces the confounding effects of multiple surgeons and multiple peri-operative protocols, and the long study period has allowed us to assess the change in the outcome over time. Early renal allograft failure is a catastrophic event for patients and was associated with reduced patient survival. Encouragingly, early transplant failure has become less common in recent years, driven particularly by lower rates of allograft thrombosis and failures due to acute rejection. 5
6 Phelan et al. AuthorsÕ contributions Dr. Paul J. Phelan: wrote article, performed study, study design. Mr. Patrick OÕKelly: analyzed data. Mr. Munir Tarazi, Mr. Nadim Tarazi: collected data, wrote paper. Dr. M. Ridhwaan Salehmohamed: collected data. Ms. Dilly Little, Dr. Colm Magee: critical revision. Prof. Peter J. Conlon: study design, final approval submitted version. References 1. ANZDATA 2008 Report. anzdata/anzdatareport/31streport/ch08txpart1.pdf (accessed 29 April 2010). 2. Bakir N, Sluiter WJ, Ploeg RJ, Van Son WJ, Tegzess AM. Primary renal graft thrombosis. Nephrol Dial Transplant 1996: 11: Penny MJ, Nankivell BJ, Disney AP, Byth K, Chapman JR. Renal graft thrombosis. A survey of 134 consecutive cases. Transplantation 1994: 58: Humar A, Key N, Ramcharan T, Payne WD, Sutherland DER, Matas AJ. Kidney transplants after initial graft loss to vascular thrombosis. Clin Transplant 2001: 15: Hariharan S, Johnson CP, Bresnahan BA, Taranto SE, Mcintosh MJ, Stablein D. Improved graft survival after renal transplantation in the United States, 1988 to N Engl J Med 2000: 342: Risaliti A, Sainz-Barriga M, Baccarani U et al. Surgical complications after kidney transplantation. G Ital Nefrol 2004: 21(Suppl 26): S Barry JM. Current status of renal transplantation. Patient evaluations and outcomes. Urol Clin North Am 2001: 28: Chopin DK, Popov Z, Abbou CC, Auvert JM. Use of vena cava to obtain additional length for the right renal vein during transplantation of cadaveric kidneys. J Urol 1989: 141: Hopkins K. The basic lymphocyte microcytotic tests: standard and AHG enhancement. In Hahn A, Land G, Strothman R eds. ASHI Laboratory Manual. Mt. Laurel, NJ: American Society for Histocompatibility and Immunogenetics, 2000: p.1.c Phelan PJ, Magee C, OÕKelly P, OÕBrien FJ, Little D, Conlon PJ. Immediate re-transplantation following early kidney transplant thrombosis. Nephrology (Carlton) 2011: 16: Merion RM, Calne RY. Allograft renal vein thrombosis. Transplant Proc 1985: 17: Phelan PJ, Shields W, OÕKelly P et al. Left versus right deceased donor renal allograft outcome. Transpl Int 2009: 22: Harmon WE, Stablein D, Alexander SR, Tejani A. Graft thrombosis in pediatric renal transplant recipients. A report of the North American Pediatric Renal Transplant Cooperative Study. Transplantation 1991: 51: Ojo AO, Wolfe RA, Held PJ, Port FK, Schmouder RL. Delayedgraftfunction: riskfactorsandimplicationsforrenal allograft survival. Transplantation 1997: 63: Giblin L, OÕKelly P, Little D et al. A comparison of long-term graft survival rates between the first and second donor kidney transplanted the effect of a longer cold ischaemic time for the second kidney. Am J Transplant 2005: 5: Takemoto SK, Terasaki PI, Gjertson DW, Cecka JM. Twelve yearsõ experience with national sharing of HLAmatched cadaveric kidneys for transplantation. N Engl J Med 2000: 343: Connolly JK, Dyer PA, Martin S, Parrott NR, Pearson RC, Johnston RWG. Importance of minimizing HLA- DR mismatch and cold preservation time in cadaveric renal transplantation. Transplantation 1996: 61: Resende L, Guerra J, Santana A, Mil-Homens C, Abreu F, Da Costa AG. Impact of donor age on renal allograft function and survival. Transplant Proc 2009: 41: Gill J, Bunnapradist S, Danovitch GM, Gjertson D, Gill JS, Cecka M. Outcomes of kidney transplantation from older living donors to older recipients. Am J Kidney Dis 2008: 52: Ojo AO, Hanson JA, Meier-Kriesche H et al. Survival in recipients of marginal cadaveric donor kidneys compared with other recipients and wait-listed transplant candidates. J Am Soc Nephrol 2001: 12: Leichtman AB, Cohen D, Keith D et al. Kidney and pancreas transplantation in the United States, : the HRSA Breakthrough Collaboratives and the 58 DSA Challenge. Am J Transplant 2008: 8(4 Pt 2): Phelan PJ, OÕKelly P, OÕNeill D et al. Analysis of waiting times on Irish renal transplant list. Clin Transplant 2010: 24: Howard RJ, Reed AI, Van Der Werf WJ, Hemming AW, Patton PR, Scornik JC. What happens to renal transplant recipients who lose their grafts? Am J Kidney Dis 2001: 38: Meier-Kriesche HU, Port FK, Ojo AO et al. Effect of waiting time on renal transplant outcome. Kidney Int 2000: 58:
Reduced graft function (with or without dialysis) vs immediate graft function a comparison of long-term renal allograft survival
 Nephrol Dial Transplant (2006) 21: 2270 2274 doi:10.1093/ndt/gfl103 Advance Access publication 22 May 2006 Original Article Reduced graft function (with or without dialysis) vs immediate graft function
Nephrol Dial Transplant (2006) 21: 2270 2274 doi:10.1093/ndt/gfl103 Advance Access publication 22 May 2006 Original Article Reduced graft function (with or without dialysis) vs immediate graft function
J Am Soc Nephrol 14: , 2003
 J Am Soc Nephrol 14: 208 213, 2003 Kidney Allograft and Patient Survival in Type I Diabetic Recipients of Cadaveric Kidney Alone Versus Simultaneous Pancreas/Kidney Transplants: A Multivariate Analysis
J Am Soc Nephrol 14: 208 213, 2003 Kidney Allograft and Patient Survival in Type I Diabetic Recipients of Cadaveric Kidney Alone Versus Simultaneous Pancreas/Kidney Transplants: A Multivariate Analysis
Pancreas After Islet Transplantation: A First Report of the International Pancreas Transplant Registry
 American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
American Journal of Transplantation 2016; 16: 688 693 Wiley Periodicals Inc. Brief Communication Copyright 2015 The American Society of Transplantation and the American Society of Transplant Surgeons doi:
Acute rejection and late renal transplant failure: Risk factors and prognosis
 Nephrol Dial Transplant (2004) 19 [Suppl 3]: iii38 iii42 DOI: 10.1093/ndt/gfh1013 Acute rejection and late renal transplant failure: Risk factors and prognosis Luis M. Pallardo Mateu 1, Asuncio n Sancho
Nephrol Dial Transplant (2004) 19 [Suppl 3]: iii38 iii42 DOI: 10.1093/ndt/gfh1013 Acute rejection and late renal transplant failure: Risk factors and prognosis Luis M. Pallardo Mateu 1, Asuncio n Sancho
Should Pediatric Patients Wait for HLA-DR-Matched Renal Transplants?
 American Journal of Transplantation 2008; 8: 2056 2061 Wiley Periodicals Inc. C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant
American Journal of Transplantation 2008; 8: 2056 2061 Wiley Periodicals Inc. C 2008 The Authors Journal compilation C 2008 The American Society of Transplantation and the American Society of Transplant
Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function
 ArtIcle Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function Guodong Chen, 1 Jingli Gu, 2 Jiang Qiu, 1 Changxi
ArtIcle Efficacy and Safety of Thymoglobulin and Basiliximab in Kidney Transplant Patients at High Risk for Acute Rejection and Delayed Graft Function Guodong Chen, 1 Jingli Gu, 2 Jiang Qiu, 1 Changxi
Long-term prognosis of BK virus-associated nephropathy in kidney transplant recipients
 Original Article Kidney Res Clin Pract 37:167-173, 2018(2) pissn: 2211-9132 eissn: 2211-9140 https://doi.org/10.23876/j.krcp.2018.37.2.167 KIDNEY RESEARCH AND CLINICAL PRACTICE Long-term prognosis of BK
Original Article Kidney Res Clin Pract 37:167-173, 2018(2) pissn: 2211-9132 eissn: 2211-9140 https://doi.org/10.23876/j.krcp.2018.37.2.167 KIDNEY RESEARCH AND CLINICAL PRACTICE Long-term prognosis of BK
Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
 Wiley Periodicals Inc. C Copyright 2012 The American Society of Transplantation and the American Society of Transplant Surgeons Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
Wiley Periodicals Inc. C Copyright 2012 The American Society of Transplantation and the American Society of Transplant Surgeons Quantification of the Early Risk of Death in Elderly Kidney Transplant Recipients
Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
 Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
Pediatr Transplantation 2013: 17: 436 440 2013 John Wiley & Sons A/S. Pediatric Transplantation DOI: 10.1111/petr.12095 Predictors of cardiac allograft vasculopathy in pediatric heart transplant recipients
The New England Journal of Medicine
 The New England Journal of Medicine Copyright, 2, by the Massachusetts Medical Society VOLUME 342 M ARCH 2, 2 NUMBER 9 IMPROVED GRAFT SURVIVAL AFTER RENAL TRANSPLANTATION IN THE UNITED STATES, 1988 TO
The New England Journal of Medicine Copyright, 2, by the Massachusetts Medical Society VOLUME 342 M ARCH 2, 2 NUMBER 9 IMPROVED GRAFT SURVIVAL AFTER RENAL TRANSPLANTATION IN THE UNITED STATES, 1988 TO
Clinical Study Over Ten-Year Kidney Graft Survival Determinants
 International Nephrology Volume 2012, Article ID 302974, 5 pages doi:10.1155/2012/302974 Clinical Study Over Ten-Year Kidney Graft Survival Determinants Anabela Malho Guedes, 1, 2 Jorge Malheiro, 1 Isabel
International Nephrology Volume 2012, Article ID 302974, 5 pages doi:10.1155/2012/302974 Clinical Study Over Ten-Year Kidney Graft Survival Determinants Anabela Malho Guedes, 1, 2 Jorge Malheiro, 1 Isabel
SELECTED ABSTRACTS. All (n) % 3-year GS 88% 82% 86% 85% 88% 80% % 3-year DC-GS 95% 87% 94% 89% 96% 80%
 SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
Impact of ultrasound examination shortly after kidney transplantation
 Eur Surg (2017) 49:140 144 DOI 10.1007/s10353-017-0467-z Impact of ultrasound examination shortly after kidney transplantation Christoph Schwarz Jakob Mühlbacher Georg A. Böhmig Marin Purtic Eleonore Pablik
Eur Surg (2017) 49:140 144 DOI 10.1007/s10353-017-0467-z Impact of ultrasound examination shortly after kidney transplantation Christoph Schwarz Jakob Mühlbacher Georg A. Böhmig Marin Purtic Eleonore Pablik
COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS
 COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS A COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS KEVIN C. MANGE, M.D.,
COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS A COMPARISON OF THE SURVIVAL OF SHIPPED AND LOCALLY TRANSPLANTED CADAVERIC RENAL ALLOGRAFTS KEVIN C. MANGE, M.D.,
HLA-Matched Kidney Transplantation in the Era of Modern Immunosuppressive Therapy
 HLA-Matched Kidney Transplantation in the Era of Modern Immunosuppressive Therapy Arun Amatya, MD; Sandy Florman, MD; Anil Paramesh, MD; Anup Amatya, PhD Jennifer McGee, MD; Mary Killackey, MD; Quing Ren,
HLA-Matched Kidney Transplantation in the Era of Modern Immunosuppressive Therapy Arun Amatya, MD; Sandy Florman, MD; Anil Paramesh, MD; Anup Amatya, PhD Jennifer McGee, MD; Mary Killackey, MD; Quing Ren,
Should red cells be matched for transfusions to patients listed for renal transplantation?
 Should red cells be matched for transfusions to patients listed for renal transplantation? Dr M.Willicombe Imperial College Renal and Transplant Centre, Hammersmith Hospital Should red cells be matched
Should red cells be matched for transfusions to patients listed for renal transplantation? Dr M.Willicombe Imperial College Renal and Transplant Centre, Hammersmith Hospital Should red cells be matched
Renal Transplant Registry Report 2008
 Renal Transplant Registry Report 28 Contents:. Introduction Page 2. Summary of transplant activity 27-28 Page 2 3. Graft and Patient Survival analysis 989-28 Page 3 4. Acute rejection 989-28 Page 24. Comparison
Renal Transplant Registry Report 28 Contents:. Introduction Page 2. Summary of transplant activity 27-28 Page 2 3. Graft and Patient Survival analysis 989-28 Page 3 4. Acute rejection 989-28 Page 24. Comparison
Echocardiography analysis in renal transplant recipients
 Original Research Article Echocardiography analysis in renal transplant recipients S.A.K. Noor Mohamed 1*, Edwin Fernando 2, 1 Assistant Professor, 2 Professor Department of Nephrology, Govt. Stanley Medical
Original Research Article Echocardiography analysis in renal transplant recipients S.A.K. Noor Mohamed 1*, Edwin Fernando 2, 1 Assistant Professor, 2 Professor Department of Nephrology, Govt. Stanley Medical
OUT OF DATE. Choice of calcineurin inhibitors in adult renal transplantation: Effects on transplant outcomes
 nep_734.fm Page 88 Friday, January 26, 2007 6:47 PM Blackwell Publishing AsiaMelbourne, AustraliaNEPNephrology1320-5358 2006 The Author; Journal compilation 2006 Asian Pacific Society of Nephrology? 200712S18897MiscellaneousCalcineurin
nep_734.fm Page 88 Friday, January 26, 2007 6:47 PM Blackwell Publishing AsiaMelbourne, AustraliaNEPNephrology1320-5358 2006 The Author; Journal compilation 2006 Asian Pacific Society of Nephrology? 200712S18897MiscellaneousCalcineurin
Chapter 6: Transplantation
 Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
The time interval between kidney and pancreas transplantation and the clinical outcomes of pancreas after kidney transplantation
 Clin Transplant 2012: 26: 403 410 DOI: 10.1111/j.1399-0012.2011.01519.x ª 2011 John Wiley & Sons A/S. The time interval between kidney and pancreas transplantation and the clinical outcomes of pancreas
Clin Transplant 2012: 26: 403 410 DOI: 10.1111/j.1399-0012.2011.01519.x ª 2011 John Wiley & Sons A/S. The time interval between kidney and pancreas transplantation and the clinical outcomes of pancreas
BK virus infection in renal transplant recipients: single centre experience. Dr Wong Lok Yan Ivy
 BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
Higher tacrolimus trough levels on days 2 5 post-renal transplant are associated with reduced rates of acute rejection
 Clin Transplant 2009: 23: 462 468 DOI: 10.1111/j.1399-0012.2009.01021.x ª 2009 John Wiley & Sons A/S. Higher tacrolimus trough levels on days 2 5 post-renal transplant are associated with reduced rates
Clin Transplant 2009: 23: 462 468 DOI: 10.1111/j.1399-0012.2009.01021.x ª 2009 John Wiley & Sons A/S. Higher tacrolimus trough levels on days 2 5 post-renal transplant are associated with reduced rates
Literature Review Transplantation
 Literature Review 2010- Transplantation Alexander Wiseman, M.D. Associate Professor, Division of Renal Diseases and Hypertension Medical Director, Kidney and Pancreas Transplant Programs University of
Literature Review 2010- Transplantation Alexander Wiseman, M.D. Associate Professor, Division of Renal Diseases and Hypertension Medical Director, Kidney and Pancreas Transplant Programs University of
Kidney Transplant Outcomes for Prolonged Cold Ischemic Times in the Context of Kidney Paired Donation
 Kidney Transplant Outcomes for Prolonged Cold Ischemic Times in the Context of Kidney Paired Donation by Yayuk Joffres Thesis Submitted in Partial Fulfillment of the Requirements for the Degree of Master
Kidney Transplant Outcomes for Prolonged Cold Ischemic Times in the Context of Kidney Paired Donation by Yayuk Joffres Thesis Submitted in Partial Fulfillment of the Requirements for the Degree of Master
Serum samples from recipients were obtained within 48 hours before transplantation. Pre-transplant
 SDC, Patients and Methods Complement-dependent lymphocytotoxic crossmatch test () Serum samples from recipients were obtained within 48 hours before transplantation. Pre-transplant donor-specific CXM was
SDC, Patients and Methods Complement-dependent lymphocytotoxic crossmatch test () Serum samples from recipients were obtained within 48 hours before transplantation. Pre-transplant donor-specific CXM was
Receiving a Kidney Transplant in the Ninth Decade of Life
 Trends Edmund in Transplant. Huang and 2011;5:121-7 Suphamai Bunnapradist: Receiving a Kidney Transplant in the Ninth Decade of Life Receiving a Kidney Transplant in the Ninth Decade of Life Edmund Huang
Trends Edmund in Transplant. Huang and 2011;5:121-7 Suphamai Bunnapradist: Receiving a Kidney Transplant in the Ninth Decade of Life Receiving a Kidney Transplant in the Ninth Decade of Life Edmund Huang
En-Bloc Kidney Transplantation in the United States: An Analysis of United Network of Organ Sharing (UNOS) Data from 1987 to 2003
 American Journal of Transplantation 2005; 5: 1513 1517 Blackwell Munksgaard Copyright C Blackwell Munksgaard 2005 doi: 10.1111/j.1600-6143.2005.00878.x En-Bloc Kidney Transplantation in the United States:
American Journal of Transplantation 2005; 5: 1513 1517 Blackwell Munksgaard Copyright C Blackwell Munksgaard 2005 doi: 10.1111/j.1600-6143.2005.00878.x En-Bloc Kidney Transplantation in the United States:
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Lefaucheur C, Loupy A, Vernerey D, et al. Antibody-mediated
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Lefaucheur C, Loupy A, Vernerey D, et al. Antibody-mediated
NAPRTCS Annual Transplant Report
 North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2010 Annual Transplant Report This is a privileged communication not for publication. TABLE OF CONTENTS PAGE I INTRODUCTION 1 II
North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2010 Annual Transplant Report This is a privileged communication not for publication. TABLE OF CONTENTS PAGE I INTRODUCTION 1 II
Downloaded from ismj.bpums.ac.ir at 20: on Friday March 22nd 2019
 - ( ) - -. :. ( ) :.. :... :. : // : -// : Email :Kazem_an@modares.ac.ir /..().(). ) (HLA.(). ( ) ( ). ) () ( ) ( () () () ( ). ().().().().().() (). / / / /..().. / / : (LDL). SPSS) SPSS STATA. (Inc,
- ( ) - -. :. ( ) :.. :... :. : // : -// : Email :Kazem_an@modares.ac.ir /..().(). ) (HLA.(). ( ) ( ). ) () ( ) ( () () () ( ). ().().().().().() (). / / / /..().. / / : (LDL). SPSS) SPSS STATA. (Inc,
Donor Scoring System for Cadaveric Renal Transplantation
 American Journal of Transplantation 2001; 1: 162 170 Copyright C Munksgaard 2001 Munksgaard International Publishers ISSN 1600-6135 Donor Scoring System for Cadaveric Renal Transplantation Scott L. Nyberg
American Journal of Transplantation 2001; 1: 162 170 Copyright C Munksgaard 2001 Munksgaard International Publishers ISSN 1600-6135 Donor Scoring System for Cadaveric Renal Transplantation Scott L. Nyberg
Donor and Recipient Age and the Allocation of Deceased Donor Kidneys for Transplantation
 Donor and Recipient Age and the Allocation of Deceased Donor Kidneys for Transplantation July 26, 2006 Donor and Recipient Age and the Allocation of Deceased Donor Kidneys for Transplantation A paper prepared
Donor and Recipient Age and the Allocation of Deceased Donor Kidneys for Transplantation July 26, 2006 Donor and Recipient Age and the Allocation of Deceased Donor Kidneys for Transplantation A paper prepared
Management of Rejection
 Management of Rejection I have no disclosures Disclosures (relevant or otherwise) Deborah B Adey, MD Professor of Medicine University of California, San Francisco Kidney and Pancreas Transplant Center
Management of Rejection I have no disclosures Disclosures (relevant or otherwise) Deborah B Adey, MD Professor of Medicine University of California, San Francisco Kidney and Pancreas Transplant Center
Article. Simultaneous Pancreas Kidney Transplant versus Other Kidney Transplant Options in Patients with Type 2 Diabetes
 Article Simultaneous Pancreas Kidney Transplant versus Other Kidney Transplant Options in Patients with Type 2 Diabetes Alexander C. Wiseman* and Jane Gralla Summary Background and objectives Current organ
Article Simultaneous Pancreas Kidney Transplant versus Other Kidney Transplant Options in Patients with Type 2 Diabetes Alexander C. Wiseman* and Jane Gralla Summary Background and objectives Current organ
Chronic Kidney Disease (CKD) Stages. CHRONIC KIDNEY DISEASE Treatment Options. Incident counts & adjusted rates, by primary diagnosis Figure 2.
 Chronic Kidney Disease (CKD) Stages Stage 1 GFR > 90 (evidence of renal disease) Stage 2 GFR 60-89 Stage 3 GFR 30-59 Stage 4 GFR 15-29 Stage 5 GFR
Chronic Kidney Disease (CKD) Stages Stage 1 GFR > 90 (evidence of renal disease) Stage 2 GFR 60-89 Stage 3 GFR 30-59 Stage 4 GFR 15-29 Stage 5 GFR
Mycophenolate mofetil in low-risk renal transplantation in patients receiving no cyclosporine: a single-centre experience
 840 O.A. Raheem et al. Nephrol Dial Transplant (2012) 27: 840 844 doi: 10.1093/ndt/gfr263 Advance Access publication 28 May 2011 Mycophenolate mofetil in low-risk renal transplantation in patients receiving
840 O.A. Raheem et al. Nephrol Dial Transplant (2012) 27: 840 844 doi: 10.1093/ndt/gfr263 Advance Access publication 28 May 2011 Mycophenolate mofetil in low-risk renal transplantation in patients receiving
Paired Donation. Andrew Bradley Rachel Johnson Joanne Allen Susan V Fuggle. Cambridge University NHS Hospitals NHS Foundation trust
 Paired Donation Andrew Bradley Rachel Johnson Joanne Allen Susan V Fuggle Cambridge University NHS Hospitals NHS Foundation trust Showing a preference 1860 John Calcott Horsley UK Living Donor kidney transplant
Paired Donation Andrew Bradley Rachel Johnson Joanne Allen Susan V Fuggle Cambridge University NHS Hospitals NHS Foundation trust Showing a preference 1860 John Calcott Horsley UK Living Donor kidney transplant
Heart Transplant: State of the Art. Dr Nick Banner
 Heart Transplant: State of the Art Dr Nick Banner Heart Transplantation What is achieved Current challenges Donor scarcity More complex recipients Long-term limitations Non-specific Pharmacological Immunosuppression
Heart Transplant: State of the Art Dr Nick Banner Heart Transplantation What is achieved Current challenges Donor scarcity More complex recipients Long-term limitations Non-specific Pharmacological Immunosuppression
NAPRTCS Annual Transplant Report
 North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2014 Annual Transplant Report This is a privileged communication not for publication. TABLE OF CONTENTS PAGE II TRANSPLANTATION Section
North American Pediatric Renal Trials and Collaborative Studies NAPRTCS 2014 Annual Transplant Report This is a privileged communication not for publication. TABLE OF CONTENTS PAGE II TRANSPLANTATION Section
Kidney Transplantation
 Kidney Transplantation Current Kidney Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr Current Kidney
Kidney Transplantation Current Kidney Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr Current Kidney
Kidney Transplant Outcomes In Elderly Patients. Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania
 Kidney Transplant Outcomes In Elderly Patients Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania Case Discussion 70 year old Asian male, neuropsychiatrist, works full
Kidney Transplant Outcomes In Elderly Patients Simin Goral MD University of Pennsylvania Medical Center Philadelphia, Pennsylvania Case Discussion 70 year old Asian male, neuropsychiatrist, works full
A Risk Prediction Model for Delayed Graft Function in Deceased Donor Kidney Transplantation
 Trends in Transplant. 2011;5:13-22 William D. Irish: Delayed Graft Function Risk Model A Risk Prediction Model for Delayed Graft Function in Deceased Donor Kidney Transplantation William D. Irish Health
Trends in Transplant. 2011;5:13-22 William D. Irish: Delayed Graft Function Risk Model A Risk Prediction Model for Delayed Graft Function in Deceased Donor Kidney Transplantation William D. Irish Health
Overview. Evaluation of Potential Kidney Transplant Recipients. Projected Years of Life in Patients with ESRD
 Evaluation of Potential Kidney Transplant Recipients Donald E. Hricik MD Professor of Medicine and Chief, Division of Nephrology and Hypertension University Hospitals Case Medical Center Conflict of Interest
Evaluation of Potential Kidney Transplant Recipients Donald E. Hricik MD Professor of Medicine and Chief, Division of Nephrology and Hypertension University Hospitals Case Medical Center Conflict of Interest
Renal Data from the Arab World
 Saudi J Kidney Dis Transpl 2011;22(4):818-824 2011 Saudi Center for Organ Transplantation Saudi Journal of Kidney Diseases and Transplantation Renal Data from the Arab World Why does Kidney Allograft Fail?
Saudi J Kidney Dis Transpl 2011;22(4):818-824 2011 Saudi Center for Organ Transplantation Saudi Journal of Kidney Diseases and Transplantation Renal Data from the Arab World Why does Kidney Allograft Fail?
Early Postoperative Urine Flow Predicts Delayed Graft Function Irrespective of Diuretic Use
 Early Postoperative Urine Flow Predicts Delayed Graft Function Irrespective of Diuretic Use Sunil Bhandari, PhD, FRCP * David Eisinger, MD, FRACS Josette Eris, PhD, FRACP * *Department of Transplant Medicine,
Early Postoperative Urine Flow Predicts Delayed Graft Function Irrespective of Diuretic Use Sunil Bhandari, PhD, FRCP * David Eisinger, MD, FRACS Josette Eris, PhD, FRACP * *Department of Transplant Medicine,
Diabetes Mellitus GUIDELINES UNGRADED SUGGESTIONS FOR CLINICAL CARE IMPLEMENTATION AND AUDIT BACKGROUND
 Diabetes Mellitus Date written: November 2011 Author: Scott Campbell GUIDELINES a. We recommend that diabetes should not on its own preclude a patient from being considered for kidney transplantation (1D).
Diabetes Mellitus Date written: November 2011 Author: Scott Campbell GUIDELINES a. We recommend that diabetes should not on its own preclude a patient from being considered for kidney transplantation (1D).
Vascular Remodelling in Pancreas Transplantation
 Vascular Remodelling in Pancreas Transplantation Prof Steve White Consultant HPB/Transplant Surgeon The Freeman Hospital Newcastle President Elect EPITA European Pancreas Transplants Pancreas Transplants
Vascular Remodelling in Pancreas Transplantation Prof Steve White Consultant HPB/Transplant Surgeon The Freeman Hospital Newcastle President Elect EPITA European Pancreas Transplants Pancreas Transplants
Clinical Study Different Impact of Pretransplant Anti-HLA Antibodies Detected by Luminex in Highly Sensitized Renal Transplanted Patients
 BioMed Research International Volume 2013, Article ID 738404, 5 pages http://dx.doi.org/10.1155/2013/738404 Clinical Study Different Impact of Pretransplant Anti-HLA Antibodies Detected by Luminex in Highly
BioMed Research International Volume 2013, Article ID 738404, 5 pages http://dx.doi.org/10.1155/2013/738404 Clinical Study Different Impact of Pretransplant Anti-HLA Antibodies Detected by Luminex in Highly
Strategies for Desensitization
 Strategies for Desensitization Olwyn Johnston MB, MRCPI, MD, MHSc BC Nephrology Day October 8 th 2010 Pre-transplant crossmatch (CMX) with donor lymphocytes has been standard of practice Positive CDC CXM
Strategies for Desensitization Olwyn Johnston MB, MRCPI, MD, MHSc BC Nephrology Day October 8 th 2010 Pre-transplant crossmatch (CMX) with donor lymphocytes has been standard of practice Positive CDC CXM
UEMS & EBS: DIVISION OF TRANSPLANT SURGERY
 CURRICULUM AND SYLLABUS TRANSPLANTATION Module 1: Multi-organ retrieval Ability to evaluate donor suitability Ability to retrieve abdominal organs for transplantation Evaluation of donor/ organs suitability
CURRICULUM AND SYLLABUS TRANSPLANTATION Module 1: Multi-organ retrieval Ability to evaluate donor suitability Ability to retrieve abdominal organs for transplantation Evaluation of donor/ organs suitability
Induction Immunosuppressive Therapy in the Elderly Kidney Transplant Recipient in the United States
 Article Induction Immunosuppressive Therapy in the Elderly Kidney Transplant Recipient in the United States Jagbir Gill,* Marcelo Sampaio, John S. Gill,* James Dong,* Hung-Tien Kuo, Gabriel M. Danovitch,
Article Induction Immunosuppressive Therapy in the Elderly Kidney Transplant Recipient in the United States Jagbir Gill,* Marcelo Sampaio, John S. Gill,* James Dong,* Hung-Tien Kuo, Gabriel M. Danovitch,
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/29755 holds various files of this Leiden University dissertation. Author: Moes, Dirk Jan Alie Roelof Title: Optimizing immunosuppression with mtor inhibitors
Cover Page The handle http://hdl.handle.net/1887/29755 holds various files of this Leiden University dissertation. Author: Moes, Dirk Jan Alie Roelof Title: Optimizing immunosuppression with mtor inhibitors
Clinical correlates, outcomes and healthcare costs associated with early mechanical ventilation after kidney transplantation
 The American Journal of Surgery (2013) 206, 686-692 Association of Women Surgeons: Clinical Science Clinical correlates, outcomes and healthcare costs associated with early mechanical ventilation after
The American Journal of Surgery (2013) 206, 686-692 Association of Women Surgeons: Clinical Science Clinical correlates, outcomes and healthcare costs associated with early mechanical ventilation after
Thromboembolic Risk Factors in Patients Undergoing Kidney Transplant: Implication of Abnormally Short Activated Partial Thromboplastin Time
 396 Annals of Clinical & Laboratory Science, vol. 33, no. 4, 2003 Thromboembolic Risk Factors in Patients Undergoing Kidney Transplant: Implication of Abnormally Short Activated Partial Thromboplastin
396 Annals of Clinical & Laboratory Science, vol. 33, no. 4, 2003 Thromboembolic Risk Factors in Patients Undergoing Kidney Transplant: Implication of Abnormally Short Activated Partial Thromboplastin
Steroid Minimization: Great Idea or Silly Move?
 Steroid Minimization: Great Idea or Silly Move? Disclosures I have financial relationship(s) within the last 12 months relevant to my presentation with: Astellas Grants ** Bristol Myers Squibb Grants,
Steroid Minimization: Great Idea or Silly Move? Disclosures I have financial relationship(s) within the last 12 months relevant to my presentation with: Astellas Grants ** Bristol Myers Squibb Grants,
Progress in Pediatric Kidney Transplantation
 Send Orders for Reprints to reprints@benthamscience.net The Open Urology & Nephrology Journal, 214, 7, (Suppl 2: M2) 115-122 115 Progress in Pediatric Kidney Transplantation Jodi M. Smith *,1 and Vikas
Send Orders for Reprints to reprints@benthamscience.net The Open Urology & Nephrology Journal, 214, 7, (Suppl 2: M2) 115-122 115 Progress in Pediatric Kidney Transplantation Jodi M. Smith *,1 and Vikas
ORIGINAL ARTICLE. Received April 30, 2007; accepted June
 LIVER TRANSPLANTATION 13:1405-1413, 2007 ORIGINAL ARTICLE Human Leukocyte Antigen and Adult Living- Donor Liver Transplantation Outcomes: An Analysis of the Organ Procurement and Transplantation Network
LIVER TRANSPLANTATION 13:1405-1413, 2007 ORIGINAL ARTICLE Human Leukocyte Antigen and Adult Living- Donor Liver Transplantation Outcomes: An Analysis of the Organ Procurement and Transplantation Network
Metabolic Control Improves Long-Term Renal Allograft and Patient Survival in Type 1 Diabetes
 Metabolic Control Improves Long-Term Renal Allograft and Patient Survival in Type 1 Diabetes Christian Morath,* Martin Zeier,* Bernd Döhler, Jan Schmidt, Peter P. Nawroth, and Gerhard Opelz Departments
Metabolic Control Improves Long-Term Renal Allograft and Patient Survival in Type 1 Diabetes Christian Morath,* Martin Zeier,* Bernd Döhler, Jan Schmidt, Peter P. Nawroth, and Gerhard Opelz Departments
Le migliori strategie immunosoppressive per il paziente con re-trapianto Prof. Maurizio Salvadori FIRENZE
 Le migliori strategie immunosoppressive per il paziente con re-trapianto Prof. Maurizio Salvadori FIRENZE Best Therapy for Kidney Re- Transplantation? PREVENTION!!!! Registries CTS OPTN UNOS USRDS SRTR
Le migliori strategie immunosoppressive per il paziente con re-trapianto Prof. Maurizio Salvadori FIRENZE Best Therapy for Kidney Re- Transplantation? PREVENTION!!!! Registries CTS OPTN UNOS USRDS SRTR
IV.13 Analysis of patient and graft survival. Guidelines. Commentary on Guidelines IV.13: Analysis of patient and graft survival
 60 SECTION IV: Long-term management of the transplant recipient IV.13 Analysis of patient and graft survival Guidelines A. It is important for a transplant unit to follow-up on the results of their transplant
60 SECTION IV: Long-term management of the transplant recipient IV.13 Analysis of patient and graft survival Guidelines A. It is important for a transplant unit to follow-up on the results of their transplant
Mary Keogan, on Mary behalf Keogan of all in NHISSOT On behalf of all in NHISSOT. 4th April 2014
 Solid Organ Transplantation How the Lab Contributes to Improved Patient Outcomes Mary Keogan, on Mary behalf Keogan of all in NHISSOT On behalf of all in NHISSOT 4th April 2014 Solid Organ Transplantation
Solid Organ Transplantation How the Lab Contributes to Improved Patient Outcomes Mary Keogan, on Mary behalf Keogan of all in NHISSOT On behalf of all in NHISSOT 4th April 2014 Solid Organ Transplantation
Intruduction PSI MODE OF ACTION AND PHARMACOKINETICS
 Multidisciplinary Insights on Clinical Guidance for the Use of Proliferation Signal Inhibitors in Heart Transplantation Andreas Zuckermann, MD et al. Department of Cardio-Thoracic Surgery, Medical University
Multidisciplinary Insights on Clinical Guidance for the Use of Proliferation Signal Inhibitors in Heart Transplantation Andreas Zuckermann, MD et al. Department of Cardio-Thoracic Surgery, Medical University
Transplantation in highly sensitised patients treated with intravenous immunoglobulin and Rituximab
 ORIGINAL ARTICLE Advance Access publication 1 February 2010 Transplantation in highly sensitised patients treated with intravenous immunoglobulin and Rituximab Ana Carina Ferreira 1, Sandra Brum 1, Vasco
ORIGINAL ARTICLE Advance Access publication 1 February 2010 Transplantation in highly sensitised patients treated with intravenous immunoglobulin and Rituximab Ana Carina Ferreira 1, Sandra Brum 1, Vasco
Morbidity and Mortality After Living Kidney Donation, : Survey of United States Transplant Centers
 American Journal of Transplantation 2003; 3: 830 834 Copyright # Blackwell Munksgaard 2003 Blackwell Munksgaard ISSN 1600-6135 Morbidity and Mortality After Living Kidney Donation, 1999 2001: Survey of
American Journal of Transplantation 2003; 3: 830 834 Copyright # Blackwell Munksgaard 2003 Blackwell Munksgaard ISSN 1600-6135 Morbidity and Mortality After Living Kidney Donation, 1999 2001: Survey of
Repeat Organ Transplantation in the United States,
 American Journal of Transplantation 2007; 7 (Part 2): 1424 1433 Blackwell Munksgaard No claim to original US government works Journal compilation C 2007 The American Society of Transplantation and the
American Journal of Transplantation 2007; 7 (Part 2): 1424 1433 Blackwell Munksgaard No claim to original US government works Journal compilation C 2007 The American Society of Transplantation and the
Our Experiences in Kidney Transplantation and Monitoring of Kidney Graft Outcomes
 & Our Experiences in Kidney Transplantation and Monitoring of Kidney Graft Outcomes Rašić Senija¹*, Džemidžić Jasminka¹, Aganović Kenana¹, Aganović Damir², Prcić Alden² 1. Institute of Nephrology, Clinical
& Our Experiences in Kidney Transplantation and Monitoring of Kidney Graft Outcomes Rašić Senija¹*, Džemidžić Jasminka¹, Aganović Kenana¹, Aganović Damir², Prcić Alden² 1. Institute of Nephrology, Clinical
Effects of HLA-Matched Blood Transfusion for Patients Awaiting Renal Transplantation
 CLINICAL AND TRANSLATIONAL RESEARCH Effects of HLA-Matched Blood Transfusion for Patients Awaiting Renal Transplantation Bernadette A. Magee, 1,4 Jeanie Martin, 1 Miceal P. Cole, 1 Kieran G. Morris, 2
CLINICAL AND TRANSLATIONAL RESEARCH Effects of HLA-Matched Blood Transfusion for Patients Awaiting Renal Transplantation Bernadette A. Magee, 1,4 Jeanie Martin, 1 Miceal P. Cole, 1 Kieran G. Morris, 2
Outpatient Management of Delayed Graft Function Is Associated With Reduced Length of Stay Without an Increase in Adverse Events
 American Journal of Transplantation 2016; 16: 1604 1611 Wiley Periodicals Inc. Brief Communication Copyright 2016 The American Society of Transplantation and the American Society of Transplant Surgeons
American Journal of Transplantation 2016; 16: 1604 1611 Wiley Periodicals Inc. Brief Communication Copyright 2016 The American Society of Transplantation and the American Society of Transplant Surgeons
Rejection after simultaneous pancreas kidney transplantation
 Nephrol Dial Transplant (2005) 20 [Suppl 2]: ii11 ii17 doi:10.1093/ndt/gfh1077 Rejection after simultaneous pancreas kidney transplantation Helmut Arbogast 1, Jacques Malaise 3, Wolf-Dieter Illner 1, Anwar
Nephrol Dial Transplant (2005) 20 [Suppl 2]: ii11 ii17 doi:10.1093/ndt/gfh1077 Rejection after simultaneous pancreas kidney transplantation Helmut Arbogast 1, Jacques Malaise 3, Wolf-Dieter Illner 1, Anwar
Allocation of deceased donor kidneys. Phil Clayton NSW Renal Group 14 June 2012
 Allocation of deceased donor kidneys Phil Clayton NSW Renal Group 14 June 2012 Outline Why study kidney allocation? Equity vs utility Current Australian model Previous work in Australia US allocation research
Allocation of deceased donor kidneys Phil Clayton NSW Renal Group 14 June 2012 Outline Why study kidney allocation? Equity vs utility Current Australian model Previous work in Australia US allocation research
journal of medicine The new england
 The new england journal of medicine established in 1812 february 5, 2004 vol. 350 no. 6 Effect of Changing the Priority for HLA Matching on the Rates and Outcomes of Kidney Transplantation in Minority
The new england journal of medicine established in 1812 february 5, 2004 vol. 350 no. 6 Effect of Changing the Priority for HLA Matching on the Rates and Outcomes of Kidney Transplantation in Minority
Date: 23 June Context and policy issues:
 Title: Basiliximab for Immunosuppression During a Calcineurin Inhibitor Holiday in Renal Transplant Patients with Acute Renal Dysfunction: Guidelines for Use and a Clinical and Cost-Effectiveness Review
Title: Basiliximab for Immunosuppression During a Calcineurin Inhibitor Holiday in Renal Transplant Patients with Acute Renal Dysfunction: Guidelines for Use and a Clinical and Cost-Effectiveness Review
The recovery status from delayed graft function can predict long-term outcome after deceased donor kidney transplantation
 www.nature.com/scientificreports Received: 5 June 2017 Accepted: 6 October 2017 Published: xx xx xxxx OPEN The recovery status from delayed graft function can predict long-term outcome after deceased donor
www.nature.com/scientificreports Received: 5 June 2017 Accepted: 6 October 2017 Published: xx xx xxxx OPEN The recovery status from delayed graft function can predict long-term outcome after deceased donor
The New Kidney Allocation System: What You Need to Know. Anup Patel, MD Clinical Director Renal and Pancreas Transplant Division Barnabas Health
 The New Kidney Allocation System: What You Need to Know Anup Patel, MD Clinical Director Renal and Pancreas Transplant Division Barnabas Health ~6% of patients die each year on the deceased donor waiting
The New Kidney Allocation System: What You Need to Know Anup Patel, MD Clinical Director Renal and Pancreas Transplant Division Barnabas Health ~6% of patients die each year on the deceased donor waiting
Kidney Transplantation in the Elderly. Kristian Heldal, MD, PhD Telemark Hospital Trust, Skien, Norway and University of Oslo
 Kidney Transplantation in the Elderly Kristian Heldal, MD, PhD Telemark Hospital Trust, Skien, Norway and University of Oslo Agenda Background: Age and chronic kidney disease End stage kidney disease:
Kidney Transplantation in the Elderly Kristian Heldal, MD, PhD Telemark Hospital Trust, Skien, Norway and University of Oslo Agenda Background: Age and chronic kidney disease End stage kidney disease:
Ten-year survival of second kidney transplants: Impact of immunologic factors and renal function at 12 months
 Kidney International, Vol. 64 (2003), pp. 674 680 Ten-year survival of second kidney transplants: Impact of immunologic factors and renal function at 12 months STÉPHANIE COUPEL, MAGALI GIRAL-CLASSE, GEORGES
Kidney International, Vol. 64 (2003), pp. 674 680 Ten-year survival of second kidney transplants: Impact of immunologic factors and renal function at 12 months STÉPHANIE COUPEL, MAGALI GIRAL-CLASSE, GEORGES
Immunopathology of T cell mediated rejection
 Immunopathology of T cell mediated rejection Ibrahim Batal MD Columbia University College of Physicians & Surgeons New York, NY, USA Overview Pathophysiology and grading of TCMR TCMR is still a significant
Immunopathology of T cell mediated rejection Ibrahim Batal MD Columbia University College of Physicians & Surgeons New York, NY, USA Overview Pathophysiology and grading of TCMR TCMR is still a significant
Living Donor Kidney Versus Simultaneous Pancreas-Kidney Transplant in Type I Diabetics: An Analysis of the OPTN/UNOS Database
 Living Donor Kidney Versus Simultaneous Pancreas-Kidney Transplant in Type I Diabetics: An Analysis of the OPTN/UNOS Database Brian Y. Young,* Jagbir Gill,* Edmund Huang, Steven K. Takemoto, Bishoy Anastasi,*
Living Donor Kidney Versus Simultaneous Pancreas-Kidney Transplant in Type I Diabetics: An Analysis of the OPTN/UNOS Database Brian Y. Young,* Jagbir Gill,* Edmund Huang, Steven K. Takemoto, Bishoy Anastasi,*
Peter Chang,* Jagbir Gill,* James Dong,* Caren Rose,* Howard Yan,* David Landsberg,* Edward H. Cole, and John S. Gill*
 Article Living Donor Age and Kidney Allograft Half-Life: Implications for Living Donor Paired Exchange Programs Peter Chang,* Jagbir Gill,* James Dong,* Caren Rose,* Howard Yan,* David Landsberg,* Edward
Article Living Donor Age and Kidney Allograft Half-Life: Implications for Living Donor Paired Exchange Programs Peter Chang,* Jagbir Gill,* James Dong,* Caren Rose,* Howard Yan,* David Landsberg,* Edward
Wait List Management. John J. Friedewald, Darshika Chhabra, and Baris Ata. The US Transplant System. National Wait List
 Wait List Management John J. Friedewald, Darshika Chhabra, and Baris Ata 4 Abbreviations CDC Centers for Disease Control and Prevention CPRAs Calculated panel reactive antibodies DCD Donation after cardiac
Wait List Management John J. Friedewald, Darshika Chhabra, and Baris Ata 4 Abbreviations CDC Centers for Disease Control and Prevention CPRAs Calculated panel reactive antibodies DCD Donation after cardiac
Table S1. Clinical outcomes of the acceptable mismatch allocation model.
 Table S1. Clinical outcomes of the acceptable mismatch allocation model. Recipient Age PRA Waiting Time (months) HLA mismatch (A/B/DR) HLAMatchmaker acceptable mismatch (years) (%) Actual Simulation Change
Table S1. Clinical outcomes of the acceptable mismatch allocation model. Recipient Age PRA Waiting Time (months) HLA mismatch (A/B/DR) HLAMatchmaker acceptable mismatch (years) (%) Actual Simulation Change
Kidney transplantation 2016: current status and potential challenges
 Kidney transplantation 2016: current status and potential challenges 15/12/2016 BVN-SBN : State-of-the-Art on Kidney Transplantation Patrick Peeters Ghent University Hospital, Belgium Challenges in 2016
Kidney transplantation 2016: current status and potential challenges 15/12/2016 BVN-SBN : State-of-the-Art on Kidney Transplantation Patrick Peeters Ghent University Hospital, Belgium Challenges in 2016
Transplant Nephrology Update: Focus on Outcomes and Increasing Access to Transplantation
 Transplant Nephrology Update: Focus on Outcomes and Increasing Access to Transplantation Titte R Srinivas, MD, FAST Medical Director, Kidney and Pancreas Transplant Programs Objectives: Describe trends
Transplant Nephrology Update: Focus on Outcomes and Increasing Access to Transplantation Titte R Srinivas, MD, FAST Medical Director, Kidney and Pancreas Transplant Programs Objectives: Describe trends
Kidney Transplant in the Elderly. Robert Santella, M.D., F.A.C.P.
 Kidney Transplant in the Elderly! Robert Santella, M.D., F.A.C.P. Incident Rate of ESRD by Age Age 75+ 65-74 From US Renal Data System, 2012 Should there be an age limit? Various guidelines: Canadian,
Kidney Transplant in the Elderly! Robert Santella, M.D., F.A.C.P. Incident Rate of ESRD by Age Age 75+ 65-74 From US Renal Data System, 2012 Should there be an age limit? Various guidelines: Canadian,
Obesity in renal transplantation
 Obesity in renal transplantation Date written: November 2011 Author: Christine Russell GUIDELINES a. We recommend that obesity should not on its own preclude a patient from being considered for kidney
Obesity in renal transplantation Date written: November 2011 Author: Christine Russell GUIDELINES a. We recommend that obesity should not on its own preclude a patient from being considered for kidney
Emerging Drug List EVEROLIMUS
 Generic (Trade Name): Manufacturer: Everolimus (Certican ) Novartis Pharmaceuticals NO. 57 MAY 2004 Indication: Current Regulatory Status: Description: Current Treatment: Cost: Evidence: For use with cyclosporine
Generic (Trade Name): Manufacturer: Everolimus (Certican ) Novartis Pharmaceuticals NO. 57 MAY 2004 Indication: Current Regulatory Status: Description: Current Treatment: Cost: Evidence: For use with cyclosporine
PENILE TRANSPLANTATION SURGERY
 PENILE TRANSPLANTATION SURGERY First successful penile transplant was performed at Tygerberg Academic Hospital on 11 December 2014 by a team of plastic surgeons and urologists The patient was 21 years
PENILE TRANSPLANTATION SURGERY First successful penile transplant was performed at Tygerberg Academic Hospital on 11 December 2014 by a team of plastic surgeons and urologists The patient was 21 years
Innovation In Transplantation:
 Innovation In Transplantation: Improving outcomes Thomas C. Pearson Department of Surgery Emory Transplant Center CHOA Symposium October 22, 2016 Disclosures Belatacept preclinical and clinical trial were
Innovation In Transplantation: Improving outcomes Thomas C. Pearson Department of Surgery Emory Transplant Center CHOA Symposium October 22, 2016 Disclosures Belatacept preclinical and clinical trial were
What is the Best Induction Immunosuppression Regimen in Kidney Transplantation? Richard Borrows: Queen Elizabeth Hospital Birmingham
 What is the Best Induction Immunosuppression Regimen in Kidney Transplantation? Richard Borrows: Queen Elizabeth Hospital Birmingham SYMPHONY Study Ekberg et al. NEJM 2008 Excluded: DCD kidneys; CIT>30hours;
What is the Best Induction Immunosuppression Regimen in Kidney Transplantation? Richard Borrows: Queen Elizabeth Hospital Birmingham SYMPHONY Study Ekberg et al. NEJM 2008 Excluded: DCD kidneys; CIT>30hours;
Kidney and Pancreas Transplantation in the United States,
 American Journal of Transplantation 2006; 6 (Part 2): 1153 1169 Blackwell Munksgaard No claim to original US government works Journal compilation C 2006 The American Society of Transplantation and the
American Journal of Transplantation 2006; 6 (Part 2): 1153 1169 Blackwell Munksgaard No claim to original US government works Journal compilation C 2006 The American Society of Transplantation and the
Why Do We Need New Immunosuppressive Agents
 Why Do We Need New Immunosuppressive Agents 1 Reducing acute rejection rates has not transplanted into better long-term graft survival Incidence of early acute rejection episodes by era Relative risk for
Why Do We Need New Immunosuppressive Agents 1 Reducing acute rejection rates has not transplanted into better long-term graft survival Incidence of early acute rejection episodes by era Relative risk for
A Lifetime of Allograft Function with Kidneys from Older Donors
 A Lifetime of Allograft Function with Kidneys from Older Donors Caren Rose,* Elke Schaeffner, Ulrich Frei, Jagbir Gill,* and John S. Gill* *Division of Nephrology, University of British Columbia, Vancouver,
A Lifetime of Allograft Function with Kidneys from Older Donors Caren Rose,* Elke Schaeffner, Ulrich Frei, Jagbir Gill,* and John S. Gill* *Division of Nephrology, University of British Columbia, Vancouver,
Transplantation in Australia and New Zealand
 Transplantation in Australia and New Zealand Matthew D. Jose MBBS (Adel), FRACP, FASN, PhD (Monash), AFRACMA Professor of Medicine, UTAS Renal Physician, Royal Hobart Hospital Overview CKD in Australia
Transplantation in Australia and New Zealand Matthew D. Jose MBBS (Adel), FRACP, FASN, PhD (Monash), AFRACMA Professor of Medicine, UTAS Renal Physician, Royal Hobart Hospital Overview CKD in Australia
MORTALITY IN PATIENTS ON DIALYSIS AND TRANSPLANT RECIPIENTS
 MORTALITY IN PATIENTS ON DIALYSIS AND TRANSPLANT RECIPIENTS COMPARISON OF MORTALITY IN ALL PATIENTS ON DIALYSIS, PATIENTS ON DIALYSIS AWAITING TRANSPLANTATION, AND RECIPIENTS OF A FIRST CADAVERIC TRANSPLANT
MORTALITY IN PATIENTS ON DIALYSIS AND TRANSPLANT RECIPIENTS COMPARISON OF MORTALITY IN ALL PATIENTS ON DIALYSIS, PATIENTS ON DIALYSIS AWAITING TRANSPLANTATION, AND RECIPIENTS OF A FIRST CADAVERIC TRANSPLANT
The privilege of induction avoidance and calcineurin inhibitors withdrawal in 2 haplotype HLA matched white kidney transplantation
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 The privilege of induction avoidance and calcineurin inhibitors withdrawal in 2 haplotype HLA matched white
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2017 The privilege of induction avoidance and calcineurin inhibitors withdrawal in 2 haplotype HLA matched white
Expanded Criteria Recipients: Are there any Limits
 Expanded Criteria Recipients: Are there any Limits Andreas Paul, MD, MSc, FRCS Department of General-, Visceral- and Transplant Surgery, University Hospital Essen Ruhr Area 5.200 000 inhabitants University
Expanded Criteria Recipients: Are there any Limits Andreas Paul, MD, MSc, FRCS Department of General-, Visceral- and Transplant Surgery, University Hospital Essen Ruhr Area 5.200 000 inhabitants University
Impact of graft implantation order on graft survival in simultaneous pancreas kidney transplantation
 Transplant International ORIGINAL ARTICLE Impact of graft implantation order on graft survival in simultaneous pancreas kidney transplantation Nadja Niclauss, Beno^ıt Bedat, Philippe Morel, Axel Andres,
Transplant International ORIGINAL ARTICLE Impact of graft implantation order on graft survival in simultaneous pancreas kidney transplantation Nadja Niclauss, Beno^ıt Bedat, Philippe Morel, Axel Andres,
Desensitization in Kidney Transplant. James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver
 Desensitization in Kidney Transplant James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver Organ Shortage Currently there are >90,000 patients on the kidney
Desensitization in Kidney Transplant James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver Organ Shortage Currently there are >90,000 patients on the kidney
