Epidemiology provides a scientific basis
|
|
|
- Shonda Matthews
- 5 years ago
- Views:
Transcription
1 Reviews/Commentaries/ADA Statements K E L L Y W E S T A W A R D L E C T U R E Diabetes Epidemiology: Guiding Clinical and Public Health Practice The Kelly West Award Lecture, 2006 WILLIAM H. HERMAN, MD, MPH Epidemiology provides a scientific basis for clinical and public health practice. Indeed, epidemiology can be used to guide how we define, diagnose, and screen for diabetes, to describe the present and future burden of diabetes, and to highlight opportunities for intervention. What is diabetes? Diabetes is a group of disorders characterized by high glucose levels that cause unique eye, kidney, and nerve complications and an increased risk for cardiovascular disease. A number of approaches have been used to diagnose diabetes. Some have been based on statistical approaches to defining abnormal or high glucose levels and others on the risk of complications. In populations with a low prevalence of diabetes, glucose levels are normally distributed and diabetes may be defined as glucose levels greater than the mean glucose level plus 2 SDs (Fig. 1A). In the 1950s, Stefan Fajans and Jerome Conn studied large groups of healthy lean individuals without family histories of diabetes, administered oral glucose loads, and measured glucose levels at time intervals following the glucose loads. They observed normal distributions of glucose levels 60, 90, and 120 min after the glucose load and defined abnormal glucose tolerance based on this simple approach (1). In populations with a high prevalence of diabetes, there is a bimodal distribution of glucose levels and diabetes may be defined as glucose levels greater than the antimode (Fig. 1B). Bimodal glucose distributions were first observed among Pima Indians (2), and analyses based on this finding were subsequently used by the National Diabetes Data Group (3) and the American Diabetes Association Expert Committee (4) to establish the fasting and 2-h post glucose load glucose criteria for diabetes. Another approach to diagnosing diabetes looks at the association between glucose level and complications and defines diabetes as glucose levels above the threshold associated with complications (Fig. 1C). The problem with this approach is that there appears to be different glycemic thresholds for different complications. When we examined the prevalence of diabetic retinopathy by decile of fasting plasma glucose and 2-h plasma glucose, we found that the fasting plasma glucose threshold associated with retinopathy was between 108 and 130 mg/dl and that the 2-h plasma glucose threshold was between 155 and 215 mg/dl, consistent with current diagnostic criteria for diabetes (5). More recently, however, the Diabetes Prevention Program Research Group reported that diabetic retinopathy was present in 7.6% of patients with impaired glucose tolerance (IGT) and 12.5% of patients within 6 to 12 months of making the transition from IGT to diabetes (6). Similarly, in a large middle-aged work force, microalbuminuria was present in 4.0% of nondiabetic individuals but in 16.1% of subjects with IGT (7). The slope of the relationship between glucose level and degree of albuminuria increased at 2-h plasma glucose levels between 121 and 166 mg/dl (7). We have previously reported that distal symmetrical peripheral polyneuropathy was present in 6.1% of Egyptian subjects with normal glucose tolerance, 10.0% of those with IGT, and 13.6% of those with newly diagnosed diabetes (8). More recently, Singleton et al. (9) looked at glucose levels in patients with idiopathic painful sensory neuropathy and found that 30 50% had IGT, suggesting that lesser degrees of hyperglycemia may be associated with diabetic neuropathy. Perhaps most importantly, prospective data from 22 European cohorts and nearly 30,000 patients without a history of diabetes followed for up to 11 years demonstrated that the hazard ratio for cardiovascular mortality begins to increase at 2-h plasma glucose levels between 140 and 200 mg/dl (10). Thus, if we define diabetes as hyperglycemia associated with adverse health outcomes and if we consider microvascular, neuropathic, and macrovascular complications, then the 2-h glucose threshold to define diabetes should be at the level currently used to define IGT ( 140 mg/ dl). Defining diabetes at this level would have the advantage of erasing the somewhat arbitrary distinction between IGT and diabetes and would likely promote earlier lifestyle and pharmacologic interventions for glycemic management, more aggressive management of cardiovascular risk factors, and earlier surveillance for microvascular and neuropathic complications. From the University of Michigan Health System, Ann Arbor, Michigan. Address correspondence and reprint requests to William H. Herman, MD, MPH, Stefan S. Fajans/ GlaxoSmithKline Professor of Diabetes, Professor of Internal Medicine and Epidemiology, Director, Michigan Diabetes Research and Training Center, University of Michigan Health System, 3920 Taubman Center, Ann Arbor, MI wherman@umich.edu. Abbreviations: DCCT, Diabetes Control and Complications Trial; DPP, Diabetes Prevention Program; IGT, impaired glucose tolerance; TRIAD, Translating Research Into Action for Diabetes; QALY, qualityadjusted life-year. This lecture was delivered at the 66th Annual Meeting of the American Diabetes Association, Washington, DC, 9 13 June A table elsewhere in this issue shows conventional and Système International (SI) units and conversion factors for many substances. DOI: /dc by the American Diabetes Association. How should we diagnose diabetes? Currently the American Diabetes Association recommends that the oral glucose tolerance test not be used in routine clinical practice (4). Unfortunately, this recommendation illustrates how far diabetologists have strayed from their roots as endocrinologists. Endocrine principles dictate that one should measure the plasma hormone or its principle metabolite and when investigating suspected endocrine underactivity, stimulate hormone pro DIABETES CARE, VOLUME 30, NUMBER 7, JULY 2007
2 Figure 1 Approaches to diagnosing diabetes. A: Glucose level greater than the mean 2 SDs. B: Glucose level more than antimode. C: Glucose level associated with complication. duction. Since diabetes is associated with insulin deficiency and hyperglycemia, endocrine principles would suggest that a stimulated or post glucose load glucose level should distinguish normal from abnormal better than an unstimulated or fasting glucose level. Historically, criteria for the diagnosis of diabetes have relied on post glucose load glucose levels (Table 1). Indeed, the criteria proposed by Fajans and Conn (1) did not use a fasting glucose criterion but relied on 60-, 90-, and 120-min post glucose load values and recommended a 120-min cut point of 140 mg/dl. In 1964, the U.S. Public Health Service criteria for the diagnosis of diabetes included a fasting glucose of 125 mg/dl and a 2-h value of 140 mg/dl (11). Should A1C be used to diagnose diabetes? My answer to this question is no. Even independent of the issues of A1C standardization (12), there are issues related to the sensitivity and accuracy of A1C as a measure of glycemia. When we examined the distributions of fasting plasma glucose, 2-h plasma glucose, and A1C in the Egyptian population and studied the sensitivity of the antimode threshold when specificity was fixed at 99%, fasting plasma glucose was 84% sensitive, 2-h post glucose load glucose was 90% sensitive, and A1C was only 68% sensitive in diagnosing diabetes (5). Another problem with A1C is that there is substantial interindividual variation in A1C that is not explained by glycemia. In nondiabetic individuals, A1C varies markedly among individuals but changes little over time in the same individual (13). Less than 30% of the variance in A1C in nondiabetic subjects with normal glucose levels is explained by fasting or post glucose load glucose levels (14). This unexplained variation in A1C levels in the near-normal range would make it difficult to establish a diagnostic threshold to distinguish normal from abnormal. This problem is compounded by the fact that A1C may differ systematically by race and ethnicity independent of glucose levels. Saaddine et al. (15) looked at A1C levels in nondiabetic individuals 5 24 years of age studied in the National Health and Nutrition Examination Study (NHANES)-3. Even after adjusting for age, sex, education, BMI, and fasting plasma glucose, hemoglobin A1C levels were higher in Hispanics and blacks than Herman in whites. More recently, we analyzed baseline data from the Diabetes Prevention Program (DPP) and from A Diabetes Outcome Progression Trial (ADOPT). In the DPP, in participants over 25 years of age with impaired glucose tolerance, after adjusting for factors including age, sex, BMI, fasting glucose, postprandial glucose, and glucose area under the curve, A1C was higher in Hispanics and blacks than in whites. In ADOPT, in subjects with recently diagnosed type 2 diabetes treated with diet and exercise alone, A1C levels adjusted for age, sex, and BMI were higher in North American Hispanics and blacks than in North American Caucasians in spite of comparable or even lower fasting and post glucose load glucose levels among North American Hispanics and blacks (16). Thus, A1C may not be as sensitive as post glucose load glucose level or even fasting glucose level and may not be valid for diagnosing hyperglycemia among individuals or across racial and ethnic groups. How should we screen for diabetes? How does the choice of cut point and frequency of screening affect the performance of screening tests for diabetes? Is the most sensitive screening test always the best? The answer to this question is again, no (17). To date, most studies of screening for diabetes have examined screening at one point in time (18). If one conceptualizes screening as an ongoing process, it dramatically affects the way one approaches screening. We simulated screening with random plasma glucose using cut points of 100, 130, and 160 mg/dl in the U.S. population years of age without known diabetes (19). We assumed that positive screening tests were followed by oral glucose tolerance tests Table 1 Criteria for abnormal glucose tolerance tests Fajans and Conn (1954) (ref. 1) USPHS (1964) (ref. 11) NDDG (1979) (ref. 3) WHO (1980/1985) (ref. 27) ADA (1997) (ref. 4) Glucose dose 1.75 g/kg IBW* 100 g 75 g 75 g 75 g Fasting min min min min min 125 Criteria for positive test All three At least three Fasting or 120 min and intermediate Fasting or 120 min Fasting or 120 min ADA, American Diabetes Association; NDDG, National Diabetes Data Group; USPHS, U.S. Public Health Service; WHO, World Health Organization. *IBW ideal body weight from Metropolitan Life Insurance Tables. DIABETES CARE, VOLUME 30, NUMBER 7, JULY
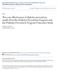
3 Kelly West Award Lecture, 2006 Figure 2 Cumulative true and false positives. Reprinted with permission from ref. 19. and looked at 1-, 3-, and 5-year screening intervals over 15 years. The most sensitive screening test, a random plasma glucose of 100 mg/dl, resulted in very few falsenegative tests, 500,000 after the first screen. Using the least sensitive test, a random plasma glucose of 160 mg/dl, left 4 million people undetected after the first screen. With repeated screenings, performance improved and false-negative tests decreased with all approaches except with the least sensitive test performed least frequently. Figure 2 shows the cumulative true positive and false-positive test results. The most sensitive test, a fasting plasma glucose of 100 mg/dl applied annually, resulted in the most true positive cases detected, but over the course of 15 years, all approaches except the least sensitive screening test performed least frequently resulted in similar numbers of true positive cases detected ( million). In contrast, there was a huge difference in the number of false-positive tests. The random plasma glucose of 100 mg/dl performed annually resulted in almost 486 million false-positive tests over 15 years. Use of a test with moderate sensitivity but high specificity such as a random plasma glucose with a cut point of 130 mg/dl every 3 years provided a good yield (17.3 million true positive tests) and substantially reduced the number of falsepositive screening tests requiring follow-up (46.5 million false-positive tests over 15 years). There has also been interest in developing multivariate models to screen for diabetes. These have included equations to predict future risk of diabetes and equations to predict prevalent undiagnosed diabetes. We developed a multivariate model using age, sex, BMI, random plasma glucose, and postprandial time to identify people at increased risk for prevalent undiagnosed diabetes (20). Other investigators using Dutch (21), English (22), Danish (23), and Indian popula- Table 2 Models to screen for prevalent diabetes Author Ref. Population Variables Sensitivity (%) Specificity (%) AUC (%) Tabaei 20 Egyptian Age, sex, BMI, RPG, PP time Baan 21 Dutch Age, sex, BMI, BP Griffin 22 U.K. Age, sex, BMI, BP, steroids, smoking, FH Glumer 23 Danish Age, sex, BMI, BP, physical activity, FH Ramachandran 24 Indian Age, BMI, waist circumference, physical activity, FH AUC, area under the curve; BP, blood pressure; FH, family history of diabetes; PP time, postprandial time; RPG, random plasma glucose DIABETES CARE, VOLUME 30, NUMBER 7, JULY 2007
4 Herman Table 3 Strategies to prevent diabetes and its complications, 1980 Problem Interventions % Preventable Preventable cases/year Type 2 diabetes Diet and exercise ,000 Stroke Blood pressure 85 19,000 Coronary heart disease Blood pressure, smoking, lipids 45 38,000 Peripheral vascular disease Blood pressure, smoking 60 24,000 Blindness Laser 60 3,500 End-stage renal disease Blood pressure 50 2,000 Amputations Blood pressure, smoking, glycemia 50 15,000 Adapted with permission from ref. 30. tions (24) have developed similar screening models (Table 2). In general, equations that do not include glucose measures have not performed as well as those that have in predicting prevalent undiagnosed diabetes. What is the present and future burden of diabetes? Epidemiologic modeling can also be used to define the present and future burden of diabetes. In the early 1980s, we critically reviewed the descriptive epidemiology of type 1 and type 2 diabetes and made projections of the future burden of diabetes (25). We estimated that in the U.S. in 1980 there were 19,000 new cases of type 1 diabetes and 19,000 deaths per year. We predicted that the prevalence of type 1 diabetes would remain relatively stable. In contrast, we estimated that there were 590,000 new cases of type 2 diabetes per year and 304,000 deaths. Based upon this simple model, we projected that the prevalence of type 2 diabetes would increase by 6% per year in the U.S. and estimated that by 2000, 15 million Americans would be diagnosed with diabetes. Centers for Disease Control surveillance data have confirmed these projections (26). Subsequently, we worked with the World Health Organization to project the number of persons over the age of 20 with diabetes in the world in the years 1995, 2000, and 2025 (27). In these analyses, we defined diabetes using both fasting and 2-h post glucose load glucose levels, considered both diagnosed and previously undiagnosed diabetes, and generated estimates by applying age- and sexspecific diabetes prevalence rates from more than 100 communities in 38 countries to current and future population projections obtained from the United Nations Population Division. For developed countries, we assumed that diabetes prevalence rates applied nationwide and for developing countries that the rural rate was one-half the urban rate. We further assumed that for countries lacking prevalence estimates, those of the ethnically and socioeconomically most similar countries applied and that age, sex, and urban- and rural-specific diabetes prevalence rates remained constant over time. Based on the conservative assumption that population growth, aging, and urbanization capture present and future trends in diabetes frequency, we projected that the number of adults with diabetes worldwide would increase 122% from 135 million to 300 million. The number of adults with diabetes would increase by 42% in developed countries, from 51 million to 72 million, and 170% in developing countries, from 84 million to 228 million. Unfortunately, empirical data have again largely confirmed these projections. In a cross-sectional study of diabetes in Egypt performed in the early 1990s, we found that the prevalence of obesity was lower in men living in rural areas and in poor urban areas and higher in men living in higher socioeconomic urban areas. The highest prevalence of obesity was in women living in the lower socioeconomic areas of Cairo. The prevalence of diabetes in adults in Egypt ranged from 5% in rural communities in the Nile delta to 10% in lower socioeconomic areas of Cairo and over 20% in higher socioeconomic areas in Cairo (28). More recently, studies of diabetes in Arab Americans in Dearborn, Michigan, have demonstrated an epidemic of diabetes with diabetes prevalence rates of 16% in women and 20% in men, rates very similar to those seen in persons living in the higher socioeconomic areas of Cairo (29). What should be done? Diabetes is an enormous and growing problem fueled by changing population demographics, urbanization, and lifestyle factors. What should be done? In the early 1980s, we examined the descriptive epidemiology of diabetes and highlighted areas where interventions, if systematically applied, could impact health (Table 3) (30). We estimated that diet and exercise could prevent up to 50% of type 2 diabetes or almost 300,000 cases of diabetes per year, with a substantial impact on downstream complications, comorbidities, and cost. The other striking finding from this analysis was that cardiovascular disease was the major cause of morbidity and mortality in diabetes (30). The DPP has established that the incidence of type 2 diabetes can be delayed or prevented by 58% with an intensive lifestyle intervention (31). The efficacy of lifestyle intervention has been confirmed by trials from Finland (32), China (33), and India (34). The Diabetes Control and Complications Trial (DCCT) showed that improved glycemic control reduced the risk of clinically meaningful retinopathy, nephropathy, and neuropathy in type 1 diabetes (35). Perhaps even more exciting are the recent results of the Epidemiology of Diabetes Interventions and Complications (EDIC) study, an epidemiologic follow-up of the DCCT cohort. At the end of the DCCT, intensive therapy patients had an A1C of 7% and standard therapy patients an A1C of 9%. Standard therapy patients were introduced to intensive therapy, and over 5 years of follow-up, the difference in A1C between intensive and conventional therapy patients diminished so that all patients had A1Cs of slightly less than 8%. Among patients with no evidence of diabetic retinopathy or diabetic nephropathy at study end, there was a persistent, beneficial effect of previous intensive therapy on microvascular complications (36 38). DIABETES CARE, VOLUME 30, NUMBER 7, JULY
5 Kelly West Award Lecture, 2006 Figure 3 Annual direct medical costs (A) and health utility scores (B) in a man progressing from IGT to diabetes with complications. BP, blood pressure. The cumulative incidence of nonfatal myocardial infarction, stroke, and death from cardiovascular disease, although not different at the end of the DCCT, was also reduced by 57% at 11 years of follow-up (39). So, clinical trials have demonstrated the feasibility of preventing diabetes and its complications, and epidemiologic follow-up has shown the importance of early aggressive glycemic management. What is the cost-effectiveness of diabetes prevention? To address the cost-effectiveness of diabetes prevention, the DPP Research Group performed a prospective economic analysis that adopted a health system perspective and looked at cost per qualityadjusted life-year (QALY) gained over a lifetime (40). Interventions were assessed as they were implemented in the DPP, and sensitivity analyses were performed by age and to assess the interventions as they might be implemented in routine clinical practice (40). Empiric data on costs, quality of life, and health outcomes were prospectively collected in the DPP (41,42). To project costs, quality of life, and health outcomes over the lifetime of an individual, we developed a cost model, a quality of life model, and a type 2 diabetes model. The cost model was developed with information from a large number of patients with type 2 diabetes (43). Demographic and disease state variables were assessed with questionnaires and medical chart review, and costs were assessed with HMO insurance claims. Similarly we developed a diabetes quality of life model (44). Demographic and disease state variables were assessed with a questionnaire, and health utilities were assessed with the same multiattribute utility model used in the DPP. Figure 3 illustrates the models with the annual direct medical costs and health utility scores for a man progressing from IGT to diabetes with complications. In the DPP, the annual direct medical costs of IGT treatment and other medical care were $1,400 per person per year. The model demonstrated that when the person developed diabetes, complications, or comorbidities, costs increased (Fig. 3A). Similarly, in the DPP, the health utility score for a man with IGT treated with placebo was The model demonstrated that the health utility score for a man with diabetes treated with diet and exercise was 0.69 and that quality of life decreased with additional treatments, complications, and comorbidities (Fig. 3B). The third part of the simulation was a Markov model that followed the DPP patient cohort from diagnosis of IGT to diabetes to death. IGT transition probabilities were based on the DPP (40). Diabetes, microvascular, and macrovascular transition probabilities were based on the UK Prospective Diabetes Study (UKPDS) and other studies in the literature (40). In this analysis, we assumed a 10-year time interval between DPP onset and UKPDS clinical diagnosis of type 2 diabetes (40). The model tracked costs, QALYs, disease progression, five complications, and survival. Compared with the placebo intervention, the metformin and lifestyle interventions both delayed the time to development of diabetes and reduced the cumulative incidence of diabetes (Fig. 4). The metformin intervention increased the time to which half of the people developed diabetes by 3.4 years relative to the placebo intervention, and the lifestyle intervention increased the time by 11.1 years. Metformin reduced the cumulative incidence of diabetes by 8% (from 83 to 75%) and the lifestyle intervention by 20% (from 83 to 63%). Not surprisingly, the interventions increased cost but, by delaying or preventing the development of diabetes, reduced the cumulative incidence of complications and comorbidities and increased length of life. Over a life DIABETES CARE, VOLUME 30, NUMBER 7, JULY 2007
6 Herman Figure 4 Cumulative incidence of diabetes. Reprinted with permission from ref. 40. time, the metformin intervention was the most expensive, the lifestyle intervention intermediate, and the placebo intervention the least expensive. Compared with the placebo intervention, the lifestyle intervention cost about $635 more over a lifetime and the metformin intervention almost $4,000 more over a lifetime. Because they developed the fewest complications and lived the longest, individuals in the lifestyle intervention group experienced the most QALYs. Those receiving metformin experienced fewer QALYs, and those in the placebo group experienced the fewest QALYs. Compared with the placebo group, individuals in the lifestyle intervention gained about 0.57 QALYs and those receiving metformin 0.13 QALYs. The cost per QALY for the lifestyle intervention was about $1,000 and that for metformin about $31,000. Other investigators have examined the cost-effectiveness of lifestyle intervention for diabetes prevention. Caro et al. (45) used data from the Finnish Diabetes Prevention Study and the DPP to simulate diabetes prevention and Palmer et al. (46) looked at diabetes prevention from a number of European perspectives. They, like us, found lifestyle intervention to be very cost-effective for diabetes prevention. In contrast, Eddy et al. (47) used the Archimedes model and found lifestyle intervention not to be cost-effective for diabetes prevention. Their published report shows a cost per QALY gained of almost $63,000 for lifestyle intervention and $36,000 for the metformin intervention. It is unclear why the two simulations provided similar estimates of the costeffectiveness of the metformin intervention with such dissimilar estimates for the cost-effectiveness of the lifestyle intervention, but at least two factors may explain this difference. One difference relates to assumptions regarding intervention costs. In our simulations, we assumed that the lifestyle intervention stopped at the onset of diabetes. In contrast, Eddy et al. assumed that the lifestyle intervention continued for the duration of the simulation. Costs are greater if people with diabetes continue to receive the lifestyle intervention and there is no impact on diabetes prevention; thus, the apparent cost-effectiveness is reduced. The second issue relates to the progression of diabetes and its complications. The DPP simulations and the Archimedes simulations projected a similar cumulative incidence of diabetes in patients receiving the lifestyle intervention (63 vs. 61%, respectively). In contrast, the cumulative incidence of complications was much higher in the DPP simulation than in the Archimedes simulation (for example, 39% cumulative incidence of myocardial infarction vs. 10%), and mortality was extremely low in the Archimedes simulation (11% mortality at 30 years follow-up, mean attained age 81 years). If diabetes is not associated with complications or adverse health outcomes, there is no benefit to preventing diabetes. From a single payer perspective, we still believe that intensive lifestyle intervention for diabetes represents a good value for money and should become clinical and public health practice in the U.S. What can be done? We now have treatments to prevent diabetes and its complications. How can they be translated into routine clinical practice to reduce the burden of diabetes? Again, epidemiology can provide answers. Translating Research Into Action for Diabetes (TRIAD) is a Centers for Disease Control and National Institutes of Health funded prospective observational study looking at diabetes care in managed care (48). TRIAD has focused on how DIABETES CARE, VOLUME 30, NUMBER 7, JULY
7 Kelly West Award Lecture, 2006 health plan and provider group structure and organization affect the processes and outcomes of diabetes care. TRIAD has demonstrated that for-profit and not-forprofit health plans seem to have comparable processes of care (49), groups that compensate physicians by salary and reward quality and patient satisfaction have better processes of care (50), and plans that have high cost-sharing in terms of co-payments and out-of-pocket costs have lower levels of preventive care (51). Referral management does not appear to be associated with worse processes of care (52) and intensity of disease management, including use of registries, physician reminders, and profiling, and care management is associated with better processes of care but may not be associated with better intermediate outcomes (53). As a part of TRIAD, we have also had the opportunity to implement a population-based intervention for diabetes. In April 2004, the University of Michigan announced a major initiative to promote the health and well-being of the University community by removing financial barriers to proven-effective, evidencebased interventions. Initially, this has included waiving or reducing co-payments for antidiabetic, antihypertensive, antidepressant, and lipid-lowering medications and for diabetic eye exams for University of Michigan employees and their dependents with diabetes with the hope of improving processes of care, outcomes of care, health-related quality of life, and productivity. Over the next couple of years, we ll be working to evaluate this program. If translated into practice, such health system interventions may reduce the burden of diabetes and its complications. References 1. Fajans SS, Conn JW: Prediabetes, subclinical diabetes, and latent clinical diabetes: Interpretation, diagnosis and treatment. In On the Nature and Treatment of Diabetes. Leibel BS, Wrenshall GA, Eds. New York, 1965, p Bennett PH, Rushforth NB, Miller M, Lecompte PM: Epidemiologic studies of diabetes in Pima Indians. Recent Prog Horm Res 32: , National Diabetes Data Group: Classification and diagnosis of diabetes mellitus and other categories of glucose intolerance. Diabetes 28: , Expert Committee on the Diagnosis and Classification of Diabetes Mellitus: Report of the Expert Committee on the Diagnosis and Classification of Diabetes Mellitus. Diabetes Care 20: , Engelgau MM, Thompson TJ, Herman WH, Boyle JP, Aubert RE, Kenny SJ, Badran A, Sous ES, Ali MA: Comparison of fasting and 2-hour glucose and HbA1C levels for diagnosing diabetes. Diabetes Care 20: , Hamman RF: Retinopathy in recent-onset diabetes and persons at high risk of diabetes in the Diabetes Prevention Program. Late-breaking abstract presented at the 65th Annual Meeting of the American Diabetes Association, June 2005, at the San Diego Convention Center, San Diego, California 7. Metcalf PA, Baker JR, Scragg RKR, Dryson E, Scott AJ, Wild CJ: Microalbuminuria in a middle-aged workforce. Diabetes Care 16: , Herman WH, Aubert RE, Engelgau MM, Thompson TJ, Ali MA, Sous ES, Hegazy M, Badran A, Kenny SJ, Gunter EW, Malarcher AM, Brechner RJ, Wetterhall SF, DeStefano F, Smith PJ, Habib M, abd el Shakour S, Ibrahim AS, Behairy EME: Diabetes mellitus in Egypt: glycaemic control and microvascular and neuropathic complications. Diabet Med 15: , Singleton JR, Smith AG, Bromberg MB: Increased prevalence of impaired glucose tolerance in patients with painful sensory neuropathy. Diabetes Care 24: , The DECODE Study Group: Is the current definition for diabetes relevant to mortality risk from all causes and cardiovascular and noncardiovascular diseases? Diabetes Care 26: , Remein QR, Wilkerson HLC: The efficiency of screening tests for diabetes. J Chronic Dis 13:6 21, Little RR, Rohlfing CL, Wiedmeyer HM, Myers GL, Sacks DB, Goldstein DE, for the NGSP Steering Committee: The national glycohemoglobin standardization program: a five-year progress report. Clin Chem 47: , Meigs JB, Nathan DM, Cupples LA, Wilson PW, Singer DE: Tracking of glycated hemoglobin in the original cohort of the Framingham-Heart Study. J Clin Epidemiol 49: , Yudkin JS, Forrest RD, Jackson CA, Ryle AJ, Davie S, Gould BJ: Unexplained variability of glycated hemoglobin in non-diabetic subjects not related to glycaemia. Diabetologia 33: , Saaddine JB, Fagot-Campagna A, Rolka D, Narayan KMV, Geiss L, Eberhardt M, Flegal KM: Distribution of HbA 1C levels for children and young adults in the U.S.: Third National Health and Nutrition Examination Survey. Diabetes Care 25: , Viberti G, Lachin J, Holman R, Zinman B, Haffner S, Kravitz B, Heise MA, Jones NP, O Neill MC, Freed MI, Kahn SE, Herman WH, for ADOPT Study Group: A Diabetes Outcome Progression Trial (ADOPT): baseline characteristics of type 2 diabetic patients in North America and Europe. Diabet Med 23: , Engelgau MM, Venkat Narayan KM, Herman WH: Screening for type 2 diabetes. Diabetes Care 23: , CDC Diabetes Cost-Effectiveness Study Group: Screening for type 2 diabetes: Is it cost-effective? JAMA 280: , Johnson SL, Tabaei BP, Herman WH: The efficacy and cost of alternative strategies for systematic screening for type 2 diabetes in the U.S. population years of age. Diabetes Care 28: , Tabaei BP, Herman WH: A multivariate logistic regression equation to screen for diabetes: development and validation. Diabetes Care 25: , Baan CA, Ruige JB, Stolk RP, Witteman JCM, Dekker JM, Heine RJ, Feskens EJM: Performance of a predictive model to identify undiagnosed diabetes in a health care setting. Diabetes Care 22: , Griffin SJ, Little PS, Hales CN, Kinmonth AL, Wareham NJ: Diabetes risk score: towards earlier detection of type 2 diabetes in general practice. Diabete Metab Res Rev 16: , Glumer C, Carstensen B, Sandbaek A, Lauritzen T, Jorgensen T, Borch-Johnsen K: A Danish diabetes risk score for targeted screening: the Inter99 Study. Diabetes Care 27: , Ramachandran A, Snehalatha C, Vijay V, Wareham NJ, Colaguiri S: Derivation and validation of diabetes risk score for urban Asian Indians. Diabetes Res and Clinical Practice 70:63 70, Herman WH, Sinnock P, Brenner E, Brimberry JL, Langford D, Nakashima A, Sepe SJ, Teutsch SM, Mazze RS: An epidemiologic model for diabetes mellitus: incidence, prevalence, and mortality. Diabetes Care 4: , Centers for Disease Control and Prevention: National Diabetes Surveillance System: Prevalence of Diabetes: Number (in Millions) of Persons With Diagnosed Diabetes, United States, [article online]. Available from gov/diabetes/statistics/prev/national/fig persons.htm. Accessed 18 May King H, Aubert RE, Herman WH: Global burden of diabetes, : prevalence, numerical estimates, and projections. Diabetes Care 21: , Herman WH, Ali MA, Aubert RE, Engelgau MM, Kenny SJ, Gunter EW, Malarcher AM, Brechner RJ, Wetterhall SF, DeStefano F, Thompson TJ, Smith PJ, Badran A, Sous ES, Habib M, Hegazy M, abd el Shakour S, Ibrahim AS, el Moneim 1918 DIABETES CARE, VOLUME 30, NUMBER 7, JULY 2007
8 el Behairy A: Diabetes mellitus in Egypt: risk factors and prevalence. Diabet Med 12: , Jaber LA, Brown MB, Hammad A, Nowak SN, Zhu Q, Ghafoor A, Herman WH: Epidemiology of diabetes among Arab Americans. Diabetes Care 26: , Herman WH, Teutsch SM, Geiss LS: The Carter Center of Emory University: closing the gap: the problem of diabetes mellitus in the United States. Diabetes Care 8: , Diabetes Prevention Program Research Group: Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. N Engl J Med 346: , Tuomilehto J, Lindstrom J, Eriksson JG, Valle TT, Hamalainen H, Ilanne-Parikka P, Keinanen-Kiukaanniemi S, Laakso M, Louheranta A, Rastas M, Salminen V, Uusitupa M, for the Finnish Diabetes Prevention Study Group: Prevention of type 2 diabetes mellitus by changes in lifestyle among subjects with impaired glucose tolerance. N Engl J Med 344: , Pan XR, Li GW, Hu YH, Wang JX, Yang WY, An ZX, Hu ZX, Lin J, Xiao JZ, Cao HB, Liu PA, Jiang XG, Jiang YY, Wang JP, Zheng H, Zhang H, Bennett PH, Howard BV: Effects of diet and exercise in preventing NIDDM in people with impaired glucose tolerance: the Da Qing IGT and Diabetes Study. Diabetes Care 20: , Ramachandran A, Snehalatha C, Mary S, Mukesh B, Bhaskar AD, Vijay V, Indian Diabetes Prevention Programme (IDPP): The Indian Diabetes Prevention Programme shows that lifestyle modification and metformin prevent type 2 diabetes in Asian Indian subjects with impaired glucose tolerance (IDPP-1). Diabetologia 49: , The Diabetes Control and Complications Trial Research Group: The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med 329: , The Diabetes Control and Complications Trial/Epidemiology of Diabetes Interventions and Complications (DCCT/EDIC) Research Group: Retinopathy and nephropathy in patients with type 1 diabetes four years after a trial of intensive therapy. N Engl J Med 342: , The Diabetes Control and Complications Trial (DCCT)/Epidemiology of Diabetes Interventions and Complications (EDIC) Research Group: Effect of intensive therapy on the microvascular complications of type 1 diabetes mellitus. JAMA 287: , The Diabetes Control and Complications Trial (DCCT)/Epidemiology of Diabetes Interventions and Complications (EDIC) Research Group: Sustained effect of intensive treatment of type 1 diabetes mellitus on development and progression of diabetic nephropathy. JAMA 290: , The Diabetes Control and Complications Trial/Epidemiology of Diabetes Interventions and Complications (DCCT/EDIC) Research Group: Intensive diabetes treatment and cardiovascular disease in patients with type 1 diabetes. N Engl J Med 353: , Herman WH, Hoerger TJ, Brandle M, Hicks K, Sorensen S, Zhang P, Hamman RF, Ackermann RT, Engelgau MM, Ratner RE: The cost-effectiveness of lifestyle modification or metformin in preventing type 2 diabetes in adults with impaired glucose tolerance. Ann Intern Med 142: , Herman WH, Brandle M, Zhang P, Williamson DF, Matulik MJ, Ratner RE, Lachin JM, Engelgau MM: The Diabetes Prevention Program Research Group: costs associated with the primary prevention of type 2 diabetes mellitus in the Diabetes Prevention Program. Diabetes Care 26:36 47, Herman WH, Brandle M, Zhang P, Williamson DF, Matulik MJ, Ratner RE, Lachin JM, Engelgau MM, the Diabetes Prevention Program Research Group: Within-trial cost-effectiveness of lifestyle intervention or metformin for the primary prevention of type 2 diabetes. Diabetes Care 26: , Brandle M, Zhou H, Smith BRK, Marriott D, Burke R, Tabaei BP, Brown MB, Herman WH: The direct medical cost of type 2 diabetes mellitus. Diabetes Care 26: , Coffey JT, Brandle M, Zhou H, Marriott D, Burke R, Tabaei BP, Engelgau MM, Kaplan R, Herman WH: Valuing healthrelated quality of life in diabetes. Diabetes Care 25: , Caro JJ, Getsios D, Caro I, Klittich WS, O Brien JA: Economic evaluation of therapeutic interventions to prevent type 2 diabetes in Canada. Diabet Med 21: , Palmer AJ, Roze S, Valentine WJ, Spinas Herman GA, Shaw JE, Zimmet PZ: Intensive lifestyle changes or metformin in patients with impaired glucose tolerance: Modeling the long-term health economic implications of the Diabetes Prevention Program in Australia, France, Germany, Switzerland, and the United Kingdom. Clinical Therapeutics 26: , Eddy DM, Schlessinger L, Kahn R: Clinical outcomes and cost-effectiveness of strategies for managing people at high risk for diabetes. Ann Intern Med 143: , TRIAD Study Group: The Translating Research Into Action for Diabetes (TRIAD) study: a multicenter study of diabetes in managed care. Diabetes Care 25: , Kim C, Williamson DF, Mangione CM, Safford MM, Selby JV, Marrero DG, Curb JD, Thompson TJ, Narayan KM, Herman WH, the TRIAD Study Group: Managed care organization and the quality of diabetes care: the Translating Research Into Action for Diabetes (TRIAD) study. Diabetes Care 27: , Ettner SL, Thompson TJ, Stevens MR, Mangione CM, Kim C, Neil Steers W, Goewey J, Brown AF, Chung RS, Venkat Narayan KM, the TRIAD Study Group: Are physician reimbursement strategies associated with processes of care and patient satisfaction for patients with diabetes in managed care? Health Serv Res 41: , Karter AJ, Stevens MR, Herman WH, Ettner S, Marrero DG, Safford MM, Engelgau MM, Curb JD, Brown AF, the TRIAD Study Group: Out-of-pocket costs and diabetes preventive services: the Translating Research Into Action for Diabetes (TRIAD) study. Diabetes Care 26: , Kim C, Williamson DF, Herman WH, Safford MM, Selby JV, Marrero DG, Curb JD, Thompson TJ, Narayan KM, Mangione CM, the TRIAD Study Group: Referral management and the care of patients with diabetes: the Translating Research Into Action for Diabetes (TRIAD) study. Am J Manag Care 10: , Mangione CM, Gerzoff RB, Williamson DF, Steers WN, Kerr EA, Brown AF, Waitzfelder BE, Marrero DG, Dudley RA, Kim C, Herman W, Thompson TJ, Safford MM, Selby JV, the TRIAD Study Group: The association between quality of care and the intensity of diabetes disease management programs. Ann Intern Med 145: , 2006 DIABETES CARE, VOLUME 30, NUMBER 7, JULY
The Efficacy and Cost of Alternative Strategies for Systematic Screening for Type 2 Diabetes in the U.S. Population Years of Age
 Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E The Efficacy and Cost of Alternative Strategies for Systematic Screening for Type 2 Diabetes in the U.S. Population 45 74
Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E The Efficacy and Cost of Alternative Strategies for Systematic Screening for Type 2 Diabetes in the U.S. Population 45 74
A simple tool for detecting undiagnosed diabetes and pre-diabetes
 Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Diabetes Risk Calculator A simple tool for detecting undiagnosed diabetes and pre-diabetes KENNETH E. HEIKES, PHD 1 DAVID M. EDDY, MD, PHD
Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Diabetes Risk Calculator A simple tool for detecting undiagnosed diabetes and pre-diabetes KENNETH E. HEIKES, PHD 1 DAVID M. EDDY, MD, PHD
DIABETES RISK CALCULATOR: A Simple Tool for Detecting Undiagnosed Diabetes and Prediabetes
 Diabetes Care Publish Ahead of Print, published online March 3, 2008 DIABETES RISK CALCULATOR: A Simple Tool for Detecting Undiagnosed Diabetes and Prediabetes Kenneth E. Heikes PhD, Archimedes, Inc. David
Diabetes Care Publish Ahead of Print, published online March 3, 2008 DIABETES RISK CALCULATOR: A Simple Tool for Detecting Undiagnosed Diabetes and Prediabetes Kenneth E. Heikes PhD, Archimedes, Inc. David
Diabetes Care 25: , 2002
 Emerging Treatments and Technologies O R I G I N A L A R T I C L E A Multivariate Logistic Regression Equation to Screen for Diabetes Development and validation BAHMAN P. TABAEI, MPH 1 WILLIAM H. HERMAN,
Emerging Treatments and Technologies O R I G I N A L A R T I C L E A Multivariate Logistic Regression Equation to Screen for Diabetes Development and validation BAHMAN P. TABAEI, MPH 1 WILLIAM H. HERMAN,
Asian Journal of Medical and Biological Research ISSN (Print) (Online)
 , 458-463; doi: 10.3329/ajmbr.v2i3.30118 Asian Journal of Medical and Biological Research ISSN 2411-4472 (Print) 2412-5571 (Online) www.ebupress.com/journal/ajmbr Article Management and treatment patterns
, 458-463; doi: 10.3329/ajmbr.v2i3.30118 Asian Journal of Medical and Biological Research ISSN 2411-4472 (Print) 2412-5571 (Online) www.ebupress.com/journal/ajmbr Article Management and treatment patterns
Projection of Diabetes Burden Through 2050
 Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E Projection of Diabetes Burden Through 2050 Impact of changing demography and disease prevalence in the U.S. JAMES P. BOYLE,
Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E Projection of Diabetes Burden Through 2050 Impact of changing demography and disease prevalence in the U.S. JAMES P. BOYLE,
A Simplified Indian Diabetes Risk Score for Screening for Undiagnosed Diabetic Subjects
 Original Article# A Simplified Indian Diabetes Risk Score for Screening for Undiagnosed Diabetic Subjects V Mohan*, R Deepa*, M Deepa*, S Somannavar*, M Datta** Abstract Aim : The aim of this study was
Original Article# A Simplified Indian Diabetes Risk Score for Screening for Undiagnosed Diabetic Subjects V Mohan*, R Deepa*, M Deepa*, S Somannavar*, M Datta** Abstract Aim : The aim of this study was
Diabetes Day for Primary Care Clinicians Advances in Diabetes Care
 Diabetes Day for Primary Care Clinicians Advances in Diabetes Care Elliot Sternthal, MD, FACP, FACE Chair New England AACE Diabetes Day Planning Committee Welcome and Introduction This presentation will:
Diabetes Day for Primary Care Clinicians Advances in Diabetes Care Elliot Sternthal, MD, FACP, FACE Chair New England AACE Diabetes Day Planning Committee Welcome and Introduction This presentation will:
Impact of the population at risk of diabetes on projections of diabetes burden in the United States: an epidemic on the way
 Diabetologia (2007) 50:934 940 DOI 10.1007/s00125-006-0528-5 ARTICLE Impact of the population at risk of diabetes on projections of diabetes burden in the United States: an epidemic on the way A. G. Mainous
Diabetologia (2007) 50:934 940 DOI 10.1007/s00125-006-0528-5 ARTICLE Impact of the population at risk of diabetes on projections of diabetes burden in the United States: an epidemic on the way A. G. Mainous
FAMILY SUPPORT IS ASSOCIATED WITH SUCCESS IN ACHIEVING WEIGHT LOSS IN A GROUP LIFESTYLE INTERVENTION FOR DIABETES PREVENTION IN ARAB AMERICANS
 FAMILY SUPPORT IS ASSOCIATED WITH SUCCESS IN ACHIEVING WEIGHT LOSS IN A GROUP LIFESTYLE INTERVENTION FOR DIABETES PREVENTION IN ARAB AMERICANS Objective: We have recently shown the feasibility of a community-based,
FAMILY SUPPORT IS ASSOCIATED WITH SUCCESS IN ACHIEVING WEIGHT LOSS IN A GROUP LIFESTYLE INTERVENTION FOR DIABETES PREVENTION IN ARAB AMERICANS Objective: We have recently shown the feasibility of a community-based,
Diabetes: Staying Two Steps Ahead. The prevalence of diabetes is increasing. What causes Type 2 diabetes?
 Focus on CME at the University of University Manitoba of Manitoba : Staying Two Steps Ahead By Shagufta Khan, MD; and Liam J. Murphy, MD The prevalence of diabetes is increasing worldwide and will double
Focus on CME at the University of University Manitoba of Manitoba : Staying Two Steps Ahead By Shagufta Khan, MD; and Liam J. Murphy, MD The prevalence of diabetes is increasing worldwide and will double
An Evaluation of Cost Sharing to Finance a Diet and Physical Activity Intervention to Prevent Diabetes
 Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E An Evaluation of Cost Sharing to Finance a Diet and Physical Activity Intervention to Prevent Diabetes RONALD T. ACKERMANN,
Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E An Evaluation of Cost Sharing to Finance a Diet and Physical Activity Intervention to Prevent Diabetes RONALD T. ACKERMANN,
The Metabolic Syndrome: Is It A Valid Concept? YES
 The Metabolic Syndrome: Is It A Valid Concept? YES Congress on Diabetes and Cardiometabolic Health Boston, MA April 23, 2013 Edward S Horton, MD Joslin Diabetes Center Harvard Medical School Boston, MA
The Metabolic Syndrome: Is It A Valid Concept? YES Congress on Diabetes and Cardiometabolic Health Boston, MA April 23, 2013 Edward S Horton, MD Joslin Diabetes Center Harvard Medical School Boston, MA
Diabetes. Health Care Disparities: Medical Evidence. A Constellation of Complications. Every 24 hours.
 Health Care Disparities: Medical Evidence Diabetes Effects 2.8 Million People in US 7% of the US Population Sixth Leading Cause of Death Kenneth J. Steier, DO, MBA, MPH, MHA, MGH Dean of Clinical Education
Health Care Disparities: Medical Evidence Diabetes Effects 2.8 Million People in US 7% of the US Population Sixth Leading Cause of Death Kenneth J. Steier, DO, MBA, MPH, MHA, MGH Dean of Clinical Education
The cost-effectiveness of diabetes prevention: results from the Diabetes Prevention Program and the Diabetes Prevention Program Outcomes Study
 Himmelfarb Health Sciences Library, The George Washington University Health Sciences Research Commons GW Biostatistics Center George Washington University Biostatistics Center 2015 The cost-effectiveness
Himmelfarb Health Sciences Library, The George Washington University Health Sciences Research Commons GW Biostatistics Center George Washington University Biostatistics Center 2015 The cost-effectiveness
The Global Agenda for the Prevention of Diabetes: Research Opportunities
 The Global Agenda for the Prevention of Diabetes: Research Opportunities William H. Herman, MD, MPH Stefan S. Fajans/GlaxoSmithKline Professor of Diabetes Professor of Internal Medicine and Epidemiology
The Global Agenda for the Prevention of Diabetes: Research Opportunities William H. Herman, MD, MPH Stefan S. Fajans/GlaxoSmithKline Professor of Diabetes Professor of Internal Medicine and Epidemiology
Although the prevalence and incidence of type 2 diabetes mellitus
 n clinical n Validating the Framingham Offspring Study Equations for Predicting Incident Diabetes Mellitus Gregory A. Nichols, PhD; and Jonathan B. Brown, PhD, MPP Background: Investigators from the Framingham
n clinical n Validating the Framingham Offspring Study Equations for Predicting Incident Diabetes Mellitus Gregory A. Nichols, PhD; and Jonathan B. Brown, PhD, MPP Background: Investigators from the Framingham
Microvascular Disease in Type 1 Diabetes
 Microvascular Disease in Type 1 Diabetes Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of Miami Miller School of Medicine The Course
Microvascular Disease in Type 1 Diabetes Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of Miami Miller School of Medicine The Course
Hemoglobin A1C and diabetes diagnosis: The Rancho Bernardo Study
 Diabetes Care Publish Ahead of Print, published online October 16, 2009 Hemoglobin A1c and diabetes Hemoglobin A1C and diabetes diagnosis: The Rancho Bernardo Study Running Title: Hemoglobin A1c and diabetes
Diabetes Care Publish Ahead of Print, published online October 16, 2009 Hemoglobin A1c and diabetes Hemoglobin A1C and diabetes diagnosis: The Rancho Bernardo Study Running Title: Hemoglobin A1c and diabetes
Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis
 CLINICAL RESEARCH STUDY Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis Gregory A. Nichols, PhD, Teresa A. Hillier, MD, MS, Jonathan B. Brown, PhD, MPP Center for Health Research, Kaiser
CLINICAL RESEARCH STUDY Normal Fasting Plasma Glucose and Risk of Type 2 Diabetes Diagnosis Gregory A. Nichols, PhD, Teresa A. Hillier, MD, MS, Jonathan B. Brown, PhD, MPP Center for Health Research, Kaiser
Diabetes Mellitus Type 2 Evidence-Based Drivers
 This module is supported by an unrestricted educational grant by Aventis Pharmaceuticals Education Center. Copyright 2003 1 Diabetes Mellitus Type 2 Evidence-Based Drivers Driver One: Reducing blood glucose
This module is supported by an unrestricted educational grant by Aventis Pharmaceuticals Education Center. Copyright 2003 1 Diabetes Mellitus Type 2 Evidence-Based Drivers Driver One: Reducing blood glucose
Considerable evidence has been presented on the increased. Assessing Risk for Development of Diabetes in Young Adults
 Assessing Risk for Development of Diabetes in Young Adults Arch G. Mainous III, PhD Vanessa A. Diaz, MD, MS Charles J. Everett, PhD Department of Family Medicine, Medical University of South Carolina,
Assessing Risk for Development of Diabetes in Young Adults Arch G. Mainous III, PhD Vanessa A. Diaz, MD, MS Charles J. Everett, PhD Department of Family Medicine, Medical University of South Carolina,
Managing Diabetes for Improved Health and Economic Outcomes
 Managing Diabetes for Improved Health and Economic Outcomes Based on a presentation by David McCulloch, MD Presentation Summary The contribution of postprandial glucose to diabetes progression and diabetes-related
Managing Diabetes for Improved Health and Economic Outcomes Based on a presentation by David McCulloch, MD Presentation Summary The contribution of postprandial glucose to diabetes progression and diabetes-related
Isolated Post-challenge Hyperglycemia: Concept and Clinical Significance
 CLINICAL PRACTICE Isolated Post-challenge Hyperglycemia: Concept and Clinical Significance John MF. Adam*, Daniel Josten** ABSTRACT The American Diabetes Association has strongly recommended that fasting
CLINICAL PRACTICE Isolated Post-challenge Hyperglycemia: Concept and Clinical Significance John MF. Adam*, Daniel Josten** ABSTRACT The American Diabetes Association has strongly recommended that fasting
follow-up data from the UKPDS reported reduction in both microvascular and macrovascular complications in the intensive treatment arm. 11 A meta-analy
 COMMENTARY SCREENING FOR TYPE 2 DIABETES MELLITUS Back to Wilson and Jungner: 10 Good Reasons to Screen for Type 2 Diabetes Mellitus ANN M. SHEEHY, MD, MS; DOUGLAS B. COURSIN, MD; AND ROBERT A. GABBAY,
COMMENTARY SCREENING FOR TYPE 2 DIABETES MELLITUS Back to Wilson and Jungner: 10 Good Reasons to Screen for Type 2 Diabetes Mellitus ANN M. SHEEHY, MD, MS; DOUGLAS B. COURSIN, MD; AND ROBERT A. GABBAY,
P. G. Lee 1,7, L. N. McEwen 1, B. Waitzfelder 2, U. Subramanian 3, A. J. Karter 4, C. M. Mangione 5 and W. H. Herman 1,6. Abstract.
 Short Report: Care Delivery Is the physical functioning of older adults with diabetes associated with the processes and outcomes of care? Evidence from Translating Research Into Action for Diabetes (TRIAD)
Short Report: Care Delivery Is the physical functioning of older adults with diabetes associated with the processes and outcomes of care? Evidence from Translating Research Into Action for Diabetes (TRIAD)
Why is Earlier and More Aggressive Treatment of T2 Diabetes Better?
 Blood glucose (mmol/l) Why is Earlier and More Aggressive Treatment of T2 Diabetes Better? Disclosures Dr Kennedy has provided CME, been on advisory boards or received travel or conference support from:
Blood glucose (mmol/l) Why is Earlier and More Aggressive Treatment of T2 Diabetes Better? Disclosures Dr Kennedy has provided CME, been on advisory boards or received travel or conference support from:
The Burden of the Diabetic Heart
 The Burden of the Diabetic Heart Dr. Ghaida Kaddaha (MBBS, MRCP-UK, FRCP-london) Diabetes Unit Rashid Hospital Dubai U.A.E Risk of CVD in Diabetes Morbidity and mortality from CVD is 2-4 fold higher than
The Burden of the Diabetic Heart Dr. Ghaida Kaddaha (MBBS, MRCP-UK, FRCP-london) Diabetes Unit Rashid Hospital Dubai U.A.E Risk of CVD in Diabetes Morbidity and mortality from CVD is 2-4 fold higher than
Eugene Barrett M.D., Ph.D. University of Virginia 6/18/2007. Diagnosis and what is it Glucose Tolerance Categories FPG
 Diabetes Mellitus: Update 7 What is the unifying basis of this vascular disease? Eugene J. Barrett, MD, PhD Professor of Internal Medicine and Pediatrics Director, Diabetes Center and GCRC Health System
Diabetes Mellitus: Update 7 What is the unifying basis of this vascular disease? Eugene J. Barrett, MD, PhD Professor of Internal Medicine and Pediatrics Director, Diabetes Center and GCRC Health System
Type 2 diabetes in the United
 Diabetes Risk Assessment in Latinas: Effectiveness of a Brief Diabetes Risk Questionnaire for Detecting Prediabetes in a Community-Based Sample Adam B. Scanlan, 1 Catarina M. Maia, 1 Alberly Perez, 1 Carol
Diabetes Risk Assessment in Latinas: Effectiveness of a Brief Diabetes Risk Questionnaire for Detecting Prediabetes in a Community-Based Sample Adam B. Scanlan, 1 Catarina M. Maia, 1 Alberly Perez, 1 Carol
Creating Policy to Promote and Support Individual Change. Ann Albright, PhD, RD
 Creating Policy to Promote and Support Individual Change Ann Albright, PhD, RD Director, Division of Diabetes Translation Centers for Disease Control and Prevention The findings and conclusions in this
Creating Policy to Promote and Support Individual Change Ann Albright, PhD, RD Director, Division of Diabetes Translation Centers for Disease Control and Prevention The findings and conclusions in this
ORIGINAL INVESTIGATION. Prediction of Incident Diabetes Mellitus in Middle-aged Adults
 ORIGINAL INVESTIGATION Prediction of Incident Diabetes Mellitus in Middle-aged Adults The Framingham Offspring Study Peter W. F. Wilson, MD; James B. Meigs, MD, MPH; Lisa Sullivan, PhD; Caroline S. Fox,
ORIGINAL INVESTIGATION Prediction of Incident Diabetes Mellitus in Middle-aged Adults The Framingham Offspring Study Peter W. F. Wilson, MD; James B. Meigs, MD, MPH; Lisa Sullivan, PhD; Caroline S. Fox,
It is well known that obesity, unbalanced
 D I A B E T E S P R O G R E S S I O N, P R E V E N T I O N, A N D T R E A T M E N T Nonpharmacologic Therapy and Exercise in the Prevention of Type 2 Diabetes JAAKKO TUOMILEHTO, MD, MPOLSC, PHD OBJECTIVE
D I A B E T E S P R O G R E S S I O N, P R E V E N T I O N, A N D T R E A T M E N T Nonpharmacologic Therapy and Exercise in the Prevention of Type 2 Diabetes JAAKKO TUOMILEHTO, MD, MPOLSC, PHD OBJECTIVE
Physical activity and the metabolic syndrome in elderly German men and women: Results from the population based KORA survey
 Diabetes Care Publish Ahead of Print, published online December 15, 2008 Physical activity and the metabolic syndrome in elderly German men and women: Results from the population based KORA survey Valerie
Diabetes Care Publish Ahead of Print, published online December 15, 2008 Physical activity and the metabolic syndrome in elderly German men and women: Results from the population based KORA survey Valerie
A1C Cut Points to Define Various Glucose Intolerance Groups in Asian Indians
 Epidemiology/Health Services Research O R I G I N A L A R T I C L E A1C Cut Points to Define Various Glucose Intolerance Groups in Asian Indians VISWANATHAN MOHAN, MD, PHD 1 VENKATARAMAN VIJAYACHANDRIKA,
Epidemiology/Health Services Research O R I G I N A L A R T I C L E A1C Cut Points to Define Various Glucose Intolerance Groups in Asian Indians VISWANATHAN MOHAN, MD, PHD 1 VENKATARAMAN VIJAYACHANDRIKA,
Strategies for the prevention of type 2 diabetes and cardiovascular disease
 European Heart Journal Supplements (2005) 7 (Supplement D), D18 D22 doi:10.1093/eurheartj/sui025 Strategies for the prevention of type 2 diabetes and cardiovascular disease Jaakko Tuomilehto 1,2,3 *, Jaana
European Heart Journal Supplements (2005) 7 (Supplement D), D18 D22 doi:10.1093/eurheartj/sui025 Strategies for the prevention of type 2 diabetes and cardiovascular disease Jaakko Tuomilehto 1,2,3 *, Jaana
Diabetes mellitus is diagnosed and characterized by chronic hyperglycemia. The effects of
 Focused Issue of This Month Early Diagnosis of Diabetes Mellitus Hyun Shik Son, MD Department of Internal Medicine, The Catholic University of Korea College of Medicine E - mail : sonhys@gmail.com J Korean
Focused Issue of This Month Early Diagnosis of Diabetes Mellitus Hyun Shik Son, MD Department of Internal Medicine, The Catholic University of Korea College of Medicine E - mail : sonhys@gmail.com J Korean
Within-Trial Cost-Effectiveness of Lifestyle Intervention or Metformin for the Primary Prevention of Type 2 Diabetes
 Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E Within-Trial Cost-Effectiveness of Lifestyle Intervention or Metformin for the Primary Prevention of Type 2 Diabetes THE
Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E Within-Trial Cost-Effectiveness of Lifestyle Intervention or Metformin for the Primary Prevention of Type 2 Diabetes THE
American Academy of Insurance Medicine
 American Academy of Insurance Medicine October 2012 Dr. Alison Moy Liberty Mutual Dr. John Kirkpatrick Thrivent Financial for Lutherans 1 59 year old male, diagnosed with T2DM six months ago Nonsmoker
American Academy of Insurance Medicine October 2012 Dr. Alison Moy Liberty Mutual Dr. John Kirkpatrick Thrivent Financial for Lutherans 1 59 year old male, diagnosed with T2DM six months ago Nonsmoker
Initiating Insulin in Primary Care for Type 2 Diabetes Mellitus. Dr Manish Khanolkar, Diabetologist, Auckland Diabetes Centre
 Initiating Insulin in Primary Care for Type 2 Diabetes Mellitus Dr Manish Khanolkar, Diabetologist, Auckland Diabetes Centre Outline How big is the problem? Natural progression of type 2 diabetes What
Initiating Insulin in Primary Care for Type 2 Diabetes Mellitus Dr Manish Khanolkar, Diabetologist, Auckland Diabetes Centre Outline How big is the problem? Natural progression of type 2 diabetes What
Type 2 diabetes affects 18% to 20% of people more
 Reduction in Use of Healthcare Services With Combination Sulfonylurea and Rosiglitazone: Findings From the Rosiglitazone Early vs SULfonylurea Titration (RESULT) Study William H. Herman, MD, MPH; Riad
Reduction in Use of Healthcare Services With Combination Sulfonylurea and Rosiglitazone: Findings From the Rosiglitazone Early vs SULfonylurea Titration (RESULT) Study William H. Herman, MD, MPH; Riad
Risk Scores for Type 2 Diabetes Can Be Applied in Some Populations but Not All STEPHEN COLAGIURI, MD ON BEHALF OF THE DETECT-2 COLLABORATION
 Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Risk Scores for Type 2 Diabetes Can Be Applied in Some Populations but Not All CHARLOTTE GLÜMER, MD, PHD 1 DORTE VISTISEN, MSC, PHD 1 KNUT
Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Risk Scores for Type 2 Diabetes Can Be Applied in Some Populations but Not All CHARLOTTE GLÜMER, MD, PHD 1 DORTE VISTISEN, MSC, PHD 1 KNUT
Metabolic Syndrome Update The Metabolic Syndrome: Overview. Global Cardiometabolic Risk
 Metabolic Syndrome Update 21 Marc Cornier, M.D. Associate Professor of Medicine Division of Endocrinology, Metabolism & Diabetes University of Colorado Denver Denver Health Medical Center The Metabolic
Metabolic Syndrome Update 21 Marc Cornier, M.D. Associate Professor of Medicine Division of Endocrinology, Metabolism & Diabetes University of Colorado Denver Denver Health Medical Center The Metabolic
A multivariate logistic regression equation to screen for dysglycaemia: development and validation
 A multivariate logistic regression equation to screen for Oxford, DME Diabetic 0742-3071 Blackwell 21 Original Dysglycaemia UK Article article Medicine Publishing, screening Ltd. 2004 equation B. P. Tabaei
A multivariate logistic regression equation to screen for Oxford, DME Diabetic 0742-3071 Blackwell 21 Original Dysglycaemia UK Article article Medicine Publishing, screening Ltd. 2004 equation B. P. Tabaei
Long-term trends in cardiorespiratory fitness and the incidence of type 2. diabetes
 Diabetes Care Publish Ahead of Print, published online March 9, 2010 Long-term trends in fitness and diabetes Long-term trends in cardiorespiratory fitness and the incidence of type 2 diabetes Running
Diabetes Care Publish Ahead of Print, published online March 9, 2010 Long-term trends in fitness and diabetes Long-term trends in cardiorespiratory fitness and the incidence of type 2 diabetes Running
TAHFA-South Texas HFMA Fall Symposium. Tuesday, October 17, from 10:45 AM 11:35 AM.
 1 TAHFA-South Texas HFMA Fall Symposium Tuesday, October 17, from 10:45 AM 11:35 AM. Dr. Anil T. Mangla, MS., PhD., MPH., FRSPH Director of Public Health and Associate Professor of Biomedical Science 2
1 TAHFA-South Texas HFMA Fall Symposium Tuesday, October 17, from 10:45 AM 11:35 AM. Dr. Anil T. Mangla, MS., PhD., MPH., FRSPH Director of Public Health and Associate Professor of Biomedical Science 2
DIABETES. A growing problem
 DIABETES A growing problem Countries still grappling with infectious diseases such as tuberculosis, HIV/AIDS and malaria now face a double burden of disease Major social and economic change has brought
DIABETES A growing problem Countries still grappling with infectious diseases such as tuberculosis, HIV/AIDS and malaria now face a double burden of disease Major social and economic change has brought
Lifetime Risk of Cardiovascular Disease Among Individuals with and without Diabetes Stratified by Obesity Status in The Framingham Heart Study
 Diabetes Care Publish Ahead of Print, published online May 5, 2008 Lifetime Risk of Cardiovascular Disease Among Individuals with and without Diabetes Stratified by Obesity Status in The Framingham Heart
Diabetes Care Publish Ahead of Print, published online May 5, 2008 Lifetime Risk of Cardiovascular Disease Among Individuals with and without Diabetes Stratified by Obesity Status in The Framingham Heart
IN THE UNITED STATES, IT IS A GRAVE FACT THAT 75%
 Original Research Achievable Cost Saving and Cost-Effective Thresholds for Diabetes Prevention Lifestyle Interventions in People Aged 65 Years and Older: A Single-Payer Perspective Jennifer M. Anderson,
Original Research Achievable Cost Saving and Cost-Effective Thresholds for Diabetes Prevention Lifestyle Interventions in People Aged 65 Years and Older: A Single-Payer Perspective Jennifer M. Anderson,
Why Do We Care About Prediabetes?
 Why Do We Care About Prediabetes? Complications of Diabetes Diabetic Retinopathy Leading cause of blindness in adults 1,2 Diabetic Nephropathy Leading cause of Kidney failure Stroke 2- to 4-fold increase
Why Do We Care About Prediabetes? Complications of Diabetes Diabetic Retinopathy Leading cause of blindness in adults 1,2 Diabetic Nephropathy Leading cause of Kidney failure Stroke 2- to 4-fold increase
Prevention of diabetes and its associated
 Metabolic Syndrome/Insulin Resistance Syndrome/Pre-Diabetes O R I G I N A L A R T I C L E Identifying Individuals at High Risk for Diabetes The Atherosclerosis Risk in Communities study MARIA INÊS SCHMIDT,
Metabolic Syndrome/Insulin Resistance Syndrome/Pre-Diabetes O R I G I N A L A R T I C L E Identifying Individuals at High Risk for Diabetes The Atherosclerosis Risk in Communities study MARIA INÊS SCHMIDT,
Diabetes risk perception and intention to adopt healthy lifestyles among primary care patients
 Diabetes Care Publish Ahead of Print, published online July 10, 2009 Primary care patients diabetes risk perception Diabetes risk perception and intention to adopt healthy lifestyles among primary care
Diabetes Care Publish Ahead of Print, published online July 10, 2009 Primary care patients diabetes risk perception Diabetes risk perception and intention to adopt healthy lifestyles among primary care
In 1997, nearly 16 million people in
 Reviews/Commentaries/Position Statements T E C H N I C A L R E V I E W Screening for Type 2 Diabetes MICHAEL M. ENGELGAU, MD, MS K.M. VENKAT NARAYAN, MD, MPH, MBA WILLIAM H. HERMAN, MD, MPH In 1997, nearly
Reviews/Commentaries/Position Statements T E C H N I C A L R E V I E W Screening for Type 2 Diabetes MICHAEL M. ENGELGAU, MD, MS K.M. VENKAT NARAYAN, MD, MPH, MBA WILLIAM H. HERMAN, MD, MPH In 1997, nearly
Prevalence, Diagnosis, and Treatment of Impaired Fasting Glucose and Impaired Glucose Tolerance in Nondiabetic U.S. Adults
 Epidemiology/Health Services Research O R I G I N A L A R T I C L E Prevalence, Diagnosis, and Treatment of Impaired Fasting Glucose and Impaired Glucose Tolerance in Nondiabetic U.S. Adults AMRITA KARVE,
Epidemiology/Health Services Research O R I G I N A L A R T I C L E Prevalence, Diagnosis, and Treatment of Impaired Fasting Glucose and Impaired Glucose Tolerance in Nondiabetic U.S. Adults AMRITA KARVE,
Michigan s Diabetes Crisis: Today and Future Trends. Dr. William Rowley Institute for Alternative Futures
 Michigan s Diabetes Crisis: Today and Future Trends Dr. William Rowley Institute for Alternative Futures 1 What s Happening to Our Children? During their lifetimes: 1/2 will become obese 1 in 3 males &
Michigan s Diabetes Crisis: Today and Future Trends Dr. William Rowley Institute for Alternative Futures 1 What s Happening to Our Children? During their lifetimes: 1/2 will become obese 1 in 3 males &
The clinical and economic benefits of better treatment of adult Medicaid beneficiaries with diabetes
 The clinical and economic benefits of better treatment of adult Medicaid beneficiaries with diabetes September, 2017 White paper Life Sciences IHS Markit Introduction Diabetes is one of the most prevalent
The clinical and economic benefits of better treatment of adult Medicaid beneficiaries with diabetes September, 2017 White paper Life Sciences IHS Markit Introduction Diabetes is one of the most prevalent
Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable?
 Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable? Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of
Diabetes Guidelines in View of Recent Clinical Trials Are They Still Applicable? Jay S. Skyler, MD, MACP Division of Endocrinology, Diabetes, and Metabolism and Diabetes Research Institute University of
The American Diabetes Association estimates
 DYSLIPIDEMIA, PREDIABETES, AND TYPE 2 DIABETES: CLINICAL IMPLICATIONS OF THE VA-HIT SUBANALYSIS Frank M. Sacks, MD* ABSTRACT The most serious and common complication in adults with diabetes is cardiovascular
DYSLIPIDEMIA, PREDIABETES, AND TYPE 2 DIABETES: CLINICAL IMPLICATIONS OF THE VA-HIT SUBANALYSIS Frank M. Sacks, MD* ABSTRACT The most serious and common complication in adults with diabetes is cardiovascular
How to Reduce CVD Complications in Diabetes?
 How to Reduce CVD Complications in Diabetes? Chaicharn Deerochanawong M.D. Diabetes and Endocrinology Unit Department of Medicine Rajavithi Hospital, Ministry of Public Health Framingham Heart Study 30-Year
How to Reduce CVD Complications in Diabetes? Chaicharn Deerochanawong M.D. Diabetes and Endocrinology Unit Department of Medicine Rajavithi Hospital, Ministry of Public Health Framingham Heart Study 30-Year
Reduced 10-year Risk of CHD in Patients who Participated in Communitybased DPP: The DEPLOY Pilot Study
 Diabetes Care Publish Ahead of Print, published online December 23, 2008 Reduced 10-year CHD Risk: DEPLOY Pilot Study Reduced 10-year Risk of CHD in Patients who Participated in Communitybased DPP: The
Diabetes Care Publish Ahead of Print, published online December 23, 2008 Reduced 10-year CHD Risk: DEPLOY Pilot Study Reduced 10-year Risk of CHD in Patients who Participated in Communitybased DPP: The
Risks and benefits of weight loss: challenges to obesity research
 European Heart Journal Supplements (2005) 7 (Supplement L), L27 L31 doi:10.1093/eurheartj/sui083 Risks and benefits of weight loss: challenges to obesity research Donna Ryan* Pennington Biomedical Research
European Heart Journal Supplements (2005) 7 (Supplement L), L27 L31 doi:10.1093/eurheartj/sui083 Risks and benefits of weight loss: challenges to obesity research Donna Ryan* Pennington Biomedical Research
A COMPREHENSIVE REPORT ISSUED BY THE AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS IN PARTNERSHIP WITH:
 A COMPREHENSIVE REPORT ISSUED BY THE AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS IN PARTNERSHIP WITH: Amputee Coalition of America Mended Hearts National Federation of the Blind National Kidney Foundation
A COMPREHENSIVE REPORT ISSUED BY THE AMERICAN ASSOCIATION OF CLINICAL ENDOCRINOLOGISTS IN PARTNERSHIP WITH: Amputee Coalition of America Mended Hearts National Federation of the Blind National Kidney Foundation
Translation of the Diabetes Prevention Program: the U.S. National Diabetes Prevention Program
 Translation of the Diabetes Prevention Program: the U.S. National Diabetes Prevention Program Kris Ernst, RN, CDE Division of Diabetes Translation Centers for Disease Control and Prevention kce0@cdc.gov
Translation of the Diabetes Prevention Program: the U.S. National Diabetes Prevention Program Kris Ernst, RN, CDE Division of Diabetes Translation Centers for Disease Control and Prevention kce0@cdc.gov
New Guidelines for the Diagnosis of Diabetes Mellitus
 New Guidelines for the Diagnosis of Diabetes Mellitus Joely Straseski, PhD, DABCC, FACB Assistant Professor and Medical Director Endocrinology and Automated Core Laboratory University of Utah and ARUP
New Guidelines for the Diagnosis of Diabetes Mellitus Joely Straseski, PhD, DABCC, FACB Assistant Professor and Medical Director Endocrinology and Automated Core Laboratory University of Utah and ARUP
Glucose and CV disease
 Glucose and CV disease Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic, electronic,
Glucose and CV disease Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic, electronic,
Overweight is defined as a body mass
 THE DANGEROUS LIAISON: WEIGHT GAIN AND ITS ASSOCIATED COMORBIDITIES * Zachary T. Bloomgarden, MD ABSTRACT Overweight and obesity have tangible physical consequences that affect mortality and economics,
THE DANGEROUS LIAISON: WEIGHT GAIN AND ITS ASSOCIATED COMORBIDITIES * Zachary T. Bloomgarden, MD ABSTRACT Overweight and obesity have tangible physical consequences that affect mortality and economics,
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Study on Prevalence of Pre-Diabetes in Urban Area of Mumbai and Its Association with Various
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Study on Prevalence of Pre-Diabetes in Urban Area of Mumbai and Its Association with Various
DICE Study Backgrounder
 DICE Study Backgrounder Diabetes In Canada Evaluation (DICE), the largest diabetes study of its kind in Canada, examines the management and control of type 2 diabetes in the Canadian family practice setting.
DICE Study Backgrounder Diabetes In Canada Evaluation (DICE), the largest diabetes study of its kind in Canada, examines the management and control of type 2 diabetes in the Canadian family practice setting.
Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting glucose: The Rancho Bernardo Study
 Diabetes Care Publish Ahead of Print, published online June 9, 2009 Serum uric acid and incident DM2 Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting
Diabetes Care Publish Ahead of Print, published online June 9, 2009 Serum uric acid and incident DM2 Serum uric acid levels improve prediction of incident Type 2 Diabetes in individuals with impaired fasting
Sensory Function and Albumin Excretion According to Diagnostic Criteria for Diabetes
 Metabolic Syndrome/Insulin Resistance Syndrome/Pre-Diabetes O R I G I N A L A R T I C L E Sensory Function and Albumin Excretion According to Diagnostic Criteria for Diabetes JAY M. SOSENKO, MD 1,2 MARTHA
Metabolic Syndrome/Insulin Resistance Syndrome/Pre-Diabetes O R I G I N A L A R T I C L E Sensory Function and Albumin Excretion According to Diagnostic Criteria for Diabetes JAY M. SOSENKO, MD 1,2 MARTHA
This article identifies key challenges in incorporating costs
 ARENAS OF APPLICATION Using Costs in Cost-Effectiveness Models for Chronic Diseases Lessons From Diabetes Thomas J. Hoerger, PhD From the RTI-UNC Center of Excellence in Health Promotion Economics, RTI
ARENAS OF APPLICATION Using Costs in Cost-Effectiveness Models for Chronic Diseases Lessons From Diabetes Thomas J. Hoerger, PhD From the RTI-UNC Center of Excellence in Health Promotion Economics, RTI
Should pregnant women be excluded from community based lifestyle intervention trial?- a case study
 Should pregnant women be excluded from community based lifestyle intervention trial?- a case study Elezebeth Mathews, Ph.D., MPH Assistant Professor Department of Public Health and Community Medicine Central
Should pregnant women be excluded from community based lifestyle intervention trial?- a case study Elezebeth Mathews, Ph.D., MPH Assistant Professor Department of Public Health and Community Medicine Central
Diabetes Mellitus: A Cardiovascular Disease
 Diabetes Mellitus: A Cardiovascular Disease Nestoras Mathioudakis, M.D. Assistant Professor of Medicine Division of Endocrinology, Diabetes, & Metabolism September 30, 2013 1 The ABCs of cardiovascular
Diabetes Mellitus: A Cardiovascular Disease Nestoras Mathioudakis, M.D. Assistant Professor of Medicine Division of Endocrinology, Diabetes, & Metabolism September 30, 2013 1 The ABCs of cardiovascular
Source of effectiveness data The effectiveness data were derived from a review or synthesis of completed studies.
 Cost effectiveness of ACE inhibitor treatment for patients with Type 1 diabetes mellitus Dong F B, Sorensen S W, Manninen D L, Thompson T J, Narayan V, Orians C E, Gregg E W, Eastman R C, Dasbach E J,
Cost effectiveness of ACE inhibitor treatment for patients with Type 1 diabetes mellitus Dong F B, Sorensen S W, Manninen D L, Thompson T J, Narayan V, Orians C E, Gregg E W, Eastman R C, Dasbach E J,
Diabetes: What is the scope of the problem?
 Diabetes: What is the scope of the problem? Elizabeth R. Seaquist MD Division of Endocrinology and Diabetes Department of Medicine Director, General Clinical Research Center Pennock Family Chair in Diabetes
Diabetes: What is the scope of the problem? Elizabeth R. Seaquist MD Division of Endocrinology and Diabetes Department of Medicine Director, General Clinical Research Center Pennock Family Chair in Diabetes
Type 1 diabetes, although the most common
 ADDRESSING THE 21ST CENTURY DIABETES EPIDEMIC * Based on a presentation by David M. Nathan, MD ABSTRACT Type 2 diabetes is an epidemic disorder. Although its complications can be treated, prevented, or
ADDRESSING THE 21ST CENTURY DIABETES EPIDEMIC * Based on a presentation by David M. Nathan, MD ABSTRACT Type 2 diabetes is an epidemic disorder. Although its complications can be treated, prevented, or
Screening for prediabetes and type 2 diabetes in dental offices
 Journal of Public Health Dentistry. ISSN 0022-4006 Screening for prediabetes and type 2 diabetes in dental offices William H. Herman, MD, MPH 1,2 ; George W. Taylor, DMD, MPH, DrPH 3 ; Jed J. Jacobson,
Journal of Public Health Dentistry. ISSN 0022-4006 Screening for prediabetes and type 2 diabetes in dental offices William H. Herman, MD, MPH 1,2 ; George W. Taylor, DMD, MPH, DrPH 3 ; Jed J. Jacobson,
It is estimated that 79 million
 Speaking to Patients About Diabetes Risk: Is Terminology Important? Valentina D. Tarasova, MD, Jaime A. Caballero, MD, Paul Turner, PhD, and Silvio E. Inzucchi, MD It is estimated that 79 million people
Speaking to Patients About Diabetes Risk: Is Terminology Important? Valentina D. Tarasova, MD, Jaime A. Caballero, MD, Paul Turner, PhD, and Silvio E. Inzucchi, MD It is estimated that 79 million people
A Computer Simulation Model of Diabetes Progression, Quality of Life, and Cost
 Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E A Computer Simulation Model of Diabetes Progression, Quality of Life, and Cost HONGHONG ZHOU, PHD 1 DEANNA J.M. ISAMAN,
Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E A Computer Simulation Model of Diabetes Progression, Quality of Life, and Cost HONGHONG ZHOU, PHD 1 DEANNA J.M. ISAMAN,
Update on Diabetes. Ketan Dhatariya. Why it s Not Just About Glucose Lowering Any More. Consultant in Diabetes NNUH
 Update on Diabetes Why it s Not Just About Glucose Lowering Any More Ketan Dhatariya Consultant in Diabetes NNUH The Story So Far.. DCCT Retinopathy Neuropathy Nephropathy Intensive glucose control in
Update on Diabetes Why it s Not Just About Glucose Lowering Any More Ketan Dhatariya Consultant in Diabetes NNUH The Story So Far.. DCCT Retinopathy Neuropathy Nephropathy Intensive glucose control in
Objectives 10/11/2013. Diabetes- The Real Cost of Sugar. Diabetes 101: What is Diabetes. By Ruth Nekonchuk RD CDE LMNT
 Diabetes- The Real Cost of Sugar By Ruth Nekonchuk RD CDE LMNT Objectives To explain diabetes To explain the risks of diabetes To enumerate the cost of diabetes to our country To enumerate the cost of
Diabetes- The Real Cost of Sugar By Ruth Nekonchuk RD CDE LMNT Objectives To explain diabetes To explain the risks of diabetes To enumerate the cost of diabetes to our country To enumerate the cost of
COMMUNITY SCREENING FOR PRE-DIABETES AND DIABETES USING HBA1C LEVELS IN HIGH-RISK AFRICAN AMERICANS AND LATINOS
 COMMUNITY SCREENING FOR PRE-DIABETES AND DIABETES USING HBA1C LEVELS IN HIGH-RISK AFRICAN AMERICANS AND LATINOS Objective: To evaluate community screening using HbA1c levels in high risk African Americans
COMMUNITY SCREENING FOR PRE-DIABETES AND DIABETES USING HBA1C LEVELS IN HIGH-RISK AFRICAN AMERICANS AND LATINOS Objective: To evaluate community screening using HbA1c levels in high risk African Americans
Copyright 2017 by Sea Courses Inc.
 Pre-Diabetes: Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic, electronic, or mechanical,
Pre-Diabetes: Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or by any means graphic, electronic, or mechanical,
EPID 712/DIABETES EPIDEMIOLOGY. Monday Friday/8:30 AM to 12:00 Noon/Room and Building
 EPID 712/DIABETES EPIDEMIOLOGY Monday Friday/8:30 AM to 12:00 Noon/Room and Building Professor: Coordinator: William H. Herman, MD, MPH wherman@umich.edu (734) 936 8279 Office Hours: By Appointment Laura
EPID 712/DIABETES EPIDEMIOLOGY Monday Friday/8:30 AM to 12:00 Noon/Room and Building Professor: Coordinator: William H. Herman, MD, MPH wherman@umich.edu (734) 936 8279 Office Hours: By Appointment Laura
Glycemic Control Patterns and Kidney Disease Progression among Primary Care Patients with Diabetes Mellitus
 ORIGINAL RESEARCH Glycemic Control Patterns and Kidney Disease Progression among Primary Care Patients with Diabetes Mellitus Doyle M. Cummings, PharmD, Lars C. Larsen, MD, Lisa Doherty, MD, MPH, C. Suzanne
ORIGINAL RESEARCH Glycemic Control Patterns and Kidney Disease Progression among Primary Care Patients with Diabetes Mellitus Doyle M. Cummings, PharmD, Lars C. Larsen, MD, Lisa Doherty, MD, MPH, C. Suzanne
WILL YOU USE HBA1C TO SCREEN & MONITOR DIABETES? Dr. Amany Mousa
 WILL YOU USE HBA1C TO SCREEN & MONITOR DIABETES? Dr. Amany Mousa Diabetes is clinically well defined by glycation of proteins 1. True 2. false So far, diabetes has been defined as a clinical condition
WILL YOU USE HBA1C TO SCREEN & MONITOR DIABETES? Dr. Amany Mousa Diabetes is clinically well defined by glycation of proteins 1. True 2. false So far, diabetes has been defined as a clinical condition
Fasting Glucose, Obesity, and Metabolic Syndrome as Predictors of Type 2 Diabetes: The Cooper Center Longitudinal Study
 Fasting Glucose, Obesity, and Metabolic Syndrome as Predictors of Type 2 Diabetes: The Cooper Center Longitudinal Study Laura F. DeFina, MD,* Gloria Lena Vega, PhD,Þ David Leonard, PhD,Þ and Scott M. Grundy,
Fasting Glucose, Obesity, and Metabolic Syndrome as Predictors of Type 2 Diabetes: The Cooper Center Longitudinal Study Laura F. DeFina, MD,* Gloria Lena Vega, PhD,Þ David Leonard, PhD,Þ and Scott M. Grundy,
Diabetes Care 26: , 2003
 Epidemiology/Health Services/Pyschosocial Research O R I G I N A L A R T I C L E The Direct Medical Cost of Type 2 Diabetes MICHAEL BRANDLE, MD 1 HONGHONG ZHOU, MS 2 BARBARA R.K. SMITH, MHSA 1 DEANNA MARRIOTT,
Epidemiology/Health Services/Pyschosocial Research O R I G I N A L A R T I C L E The Direct Medical Cost of Type 2 Diabetes MICHAEL BRANDLE, MD 1 HONGHONG ZHOU, MS 2 BARBARA R.K. SMITH, MHSA 1 DEANNA MARRIOTT,
Welcome and Introduction
 Welcome and Introduction This presentation will: Define obesity, prediabetes, and diabetes Discuss the diagnoses and management of obesity, prediabetes, and diabetes Explain the early risk factors for
Welcome and Introduction This presentation will: Define obesity, prediabetes, and diabetes Discuss the diagnoses and management of obesity, prediabetes, and diabetes Explain the early risk factors for
The Florida Diabetes Master Clinician Program: Facilitating Increased Quality and Significant Cost Savings for Diabetic Patients
 The Florida Diabetes Master Clinician Program: Facilitating Increased Quality and Significant Cost Savings for Diabetic Patients Edward Shahady, MD, ABCL, ABFM, FAAFP Up to 10% of Americans > 20 years
The Florida Diabetes Master Clinician Program: Facilitating Increased Quality and Significant Cost Savings for Diabetic Patients Edward Shahady, MD, ABCL, ABFM, FAAFP Up to 10% of Americans > 20 years
Pre Diabetes Screening in Primary Care
 University of San Diego Digital USD Doctor of Nursing Practice Final Manuscripts Theses and Dissertations Spring 5-21-2016 Pre Diabetes Screening in Primary Care Christine Rieger crieger@sandiego.edu Follow
University of San Diego Digital USD Doctor of Nursing Practice Final Manuscripts Theses and Dissertations Spring 5-21-2016 Pre Diabetes Screening in Primary Care Christine Rieger crieger@sandiego.edu Follow
Diabetes risk scores and death: predictability and practicability in two different populations
 Diabetes risk scores and death: predictability and practicability in two different populations Short Report David Faeh, MD, MPH 1 ; Pedro Marques-Vidal, MD, PhD 2 ; Michael Brändle, MD 3 ; Julia Braun,
Diabetes risk scores and death: predictability and practicability in two different populations Short Report David Faeh, MD, MPH 1 ; Pedro Marques-Vidal, MD, PhD 2 ; Michael Brändle, MD 3 ; Julia Braun,
Changing the Course of Diabetes: Turning Hope into Reality
 Indian Health Service Special Diabetes Program for Indians 2014 Report to Congress Changing the Course of Diabetes: Turning Hope into Reality In response to the burgeoning diabetes epidemic among American
Indian Health Service Special Diabetes Program for Indians 2014 Report to Congress Changing the Course of Diabetes: Turning Hope into Reality In response to the burgeoning diabetes epidemic among American
ORIGINAL INVESTIGATION. Performance of Screening Questionnaires and Risk Scores for Undiagnosed Diabetes
 ORIGINAL INVESTIGATION Performance of Screening Questionnaires and Risk Scores for Undiagnosed Diabetes The KORA Survey 2000 Wolfgang Rathmann, MD, MSPH; Stephan Martin, MD; Burkhard Haastert, PhD; Andrea
ORIGINAL INVESTIGATION Performance of Screening Questionnaires and Risk Scores for Undiagnosed Diabetes The KORA Survey 2000 Wolfgang Rathmann, MD, MSPH; Stephan Martin, MD; Burkhard Haastert, PhD; Andrea
Long-Term Care Updates
 Long-Term Care Updates January 2019 By Kristina Nikl, PharmD Several recent studies evaluating the management of diabetes in older adults have concluded that 25-52% of elderly patients are currently being
Long-Term Care Updates January 2019 By Kristina Nikl, PharmD Several recent studies evaluating the management of diabetes in older adults have concluded that 25-52% of elderly patients are currently being
T he prevalence of type 2 diabetes
 Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Two-Step Approach for the Prediction of Future Type 2 Diabetes Risk MUHAMMAD A. ABDUL-GHANI, MD, PHD 1 TAMAM ABDUL-GHANI, MSC 1 MICHAEL P.
Cardiovascular and Metabolic Risk O R I G I N A L A R T I C L E Two-Step Approach for the Prediction of Future Type 2 Diabetes Risk MUHAMMAD A. ABDUL-GHANI, MD, PHD 1 TAMAM ABDUL-GHANI, MSC 1 MICHAEL P.
There really is an epidemic of type 2 diabetes
 Diabetologia (2005) 48: 1459 1463 DOI 10.1007/s00125-005-1843-y FOR DEBATE S. Colagiuri. K. Borch-Johnsen. C. Glümer. D. Vistisen There really is an epidemic of type 2 diabetes Received: 22 December 2004
Diabetologia (2005) 48: 1459 1463 DOI 10.1007/s00125-005-1843-y FOR DEBATE S. Colagiuri. K. Borch-Johnsen. C. Glümer. D. Vistisen There really is an epidemic of type 2 diabetes Received: 22 December 2004
Performance of Recommended Screening Tests for Undiagnosed Diabetes and Dysglycemia
 Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E Performance of Recommended Screening Tests for Undiagnosed Diabetes and Dysglycemia DEBORAH B. ROLKA, MS 1 K. M. VENKAT
Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E Performance of Recommended Screening Tests for Undiagnosed Diabetes and Dysglycemia DEBORAH B. ROLKA, MS 1 K. M. VENKAT
Diabetes Care 26: , 2003
 Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E The Risk Score A practical tool to predict type 2 diabetes risk JAANA LINDSTRÖM, MSC 1 JAAKKO TUOMILEHTO, MD, PHD 1,2 OBJECTIVE
Epidemiology/Health Services/Psychosocial Research O R I G I N A L A R T I C L E The Risk Score A practical tool to predict type 2 diabetes risk JAANA LINDSTRÖM, MSC 1 JAAKKO TUOMILEHTO, MD, PHD 1,2 OBJECTIVE
Detecting Type 2 diabetes and impaired glucose regulation using glycated hemoglobin in different populations
 Detecting Type 2 diabetes and impaired glucose regulation using glycated hemoglobin in different populations Practice Points Samiul A Mostafa 1, Kamlesh Khunti2, Balasubramanian Thiagarajan Srinivasan1,
Detecting Type 2 diabetes and impaired glucose regulation using glycated hemoglobin in different populations Practice Points Samiul A Mostafa 1, Kamlesh Khunti2, Balasubramanian Thiagarajan Srinivasan1,
