Recent Exposure to Particulate Matter and C-reactive Protein Concentration in the Multi-Ethnic Study of Atherosclerosis
|
|
|
- Alfred O’Brien’
- 5 years ago
- Views:
Transcription
1 American Journal of Epidemiology Copyright ª 2006 by the Johns Hopkins Bloomberg School of Public Health All rights reserved; printed in U.S.A. Vol. 164, No. 5 DOI: /aje/kwj186 Advance Access publication June 2, 2006 Original Contribution Recent Exposure to Particulate Matter and C-reactive Protein Concentration in the Multi-Ethnic Study of Atherosclerosis A. V. Diez Roux 1, A. H. Auchincloss 1, B. Astor 2, R. G. Barr 3, M. Cushman 4, T. Dvonch 5, D. R. Jacobs, Jr. 6, J. Kaufman 7, X. Lin 8, and P. Samson 9 1 Department of Epidemiology, School of Public Health, University of Michigan, Ann Arbor, MI. 2 Department of Epidemiology, Johns Hopkins Bloomberg School of Public Health, Baltimore, MD. 3 Department of Medicine, College of Physicians and Surgeons, Columbia University, New York, NY. 4 Department of Pathology, University of Vermont, Burlington, VT. 5 Department of Environmental Health Sciences, School of Public Health, University of Michigan, Ann Arbor, MI. 6 Division of Epidemiology and Community Health, School of Public Health, University of Minnesota, Minneapolis, MN. 7 Department of Environmental and Occupational Health Sciences, School of Public Health, University of Washington, Seattle, WA. 8 Department of Biostatistics, School of Public Health, University of Michigan, Ann Arbor, MI. 9 Department of Atmospheric Sciences, School of Engineering, University of Michigan, Ann Arbor, MI. Received for publication August 25, 2005; accepted for publication March 2, Ambient levels of particulate matter have been linked to cardiovascular disease. The mechanisms mediating these associations are poorly understood. One candidate mechanism is inflammation. Using data from the Multi- Ethnic Study of Atherosclerosis ( ), the authors investigated the relation between exposure to particulate matter of less than or equal to 2.5 lm in diameter (PM 2.5 ) and C-reactive protein concentration in 5,634 persons aged years who were free of cardiovascular disease. Data from US Environmental Protection Agency monitors were used to estimate PM 2.5 exposures for the prior day, prior 2 days, prior week, prior 30 days, and prior 60 days. Only the 30-day and 60-day mean exposures showed a weak positive association with C-reactive protein, and confidence intervals were wide: relative increases in C-reactive protein per 10 lg/m 3 of PM 2.5 adjusted for person-level covariates were 3% (95% confidence interval (CI): 2, 10) for a 30-day mean and 4% (95% CI: 3, 11.0) for a 60-day mean. The means of 7-day, 30-day, and 60-day exposures were weakly, positively, and nonsignificantly associated with the odds of C-reactive protein of greater than or equal to 3 mg/liter: adjusted odds ratios were 1.05 (95% CI: 0.96, 1.15), 1.12 (95% CI: 0.98, 1.29), and 1.12 (95% CI: 0.96, 1.32), respectively. Slightly stronger associations were observed in persons without other risk factors for elevated C-reactive protein, but this heterogeneity was not statistically significant. The authors results are not compatible with strong effects of particulate matter exposures on population levels of C-reactive protein. air pollutants, environmental; cardiovascular diseases; inflammation Abbreviations: CI, confidence interval; MESA, Multi-Ethnic Study of Atherosclerosis; PM 2.5, particulate matter of less than or equal to 2.5 lm in diameter; PM 10, particulate matter of less than or equal to 10 lm in diameter. A growing body of work has linked ambient levels of particulate matter to cardiovascular disease morbidity and mortality (1 6), but the mechanisms mediating these associations are still poorly understood. One of several plausible biologic mechanisms linking particulate matter exposure to cardiovascular risk is increased inflammation (7 9). It has Correspondence to Dr. Ana V. Diez Roux, Department of Epidemiology, 1214 South University, Second Floor, Ann Arbor, MI ( adiezrou@umich.edu). 437
2 438 Diez Roux et al. been postulated that the interaction of alveolar macrophages with atmospheric particles results in increased oxidant production and the release of inflammatory mediators (10), which may in turn participate in the development of atherosclerotic disease or the precipitation of clinical events in persons with underlying disease (11). Ultrafine particles may also exert systemic effects through direct passage of particles into the blood circulation (12). Experimental evidence from animal and human studies has shown that exposure to inhaled particles is associated with local inflammatory changes in the lung and may result in a systemic inflammatory response (13 18). However, there is still limited evidence on the extent to which exposure to particulate matter is associated with changes in levels of systemic inflammatory markers in the general population. Although two epidemiologic studies have reported positive associations between recent exposures to particles and markers of the acute phase response such as C-reactive protein and fibrinogen (19, 20), other studies have reported associations limited to the summer months (21), associations present for ambient exposures but not personal exposure (22), positive associations that disappear when highly influential observations are excluded (23), and even negative associations (22). Most prior studies of exposure to particles and inflammatory markers have investigated relatively short lags, ranging from exposures the same day to exposures during the 5 prior days. However, it is plausible that repeated exposures have effects that accumulate over time. The presence of cumulative effects is consistent with recent work showing that exposures occurring more remotely (in some cases during the prior 1 2 months) are associated with all-cause and cardiovascular mortality in time series analyses (24 26), although results regarding the effects of recent and long-term exposures on cardiovascular mortality have not always been consistent (27). No studies have investigated long-term exposures in relation to C-reactive protein levels in population-based samples. Using data from a large, multiethnic, population-based study of atherosclerosis, we investigated the relation between recent exposure to particulate matter of less than or equal to 2.5 lm indiameter(pm 2.5 ) and levels of inflammatory markers. We hypothesized that recent exposure to PM 2.5 would be positively associated with higher C-reactive protein concentration, after adjustment for potential confounders. We also investigated lags ranging from the prior day to the prior 2 months. The confirmation of a relation between air particulate exposure and markers of systemic inflammation would lend support for a mechanistic pathway linking air pollution to cardiovascular disease, and it would also suggest that exposure to particulate matter may be etiologically relevant to other diseases processes in which inflammation may play a causal role. MATERIALS AND METHODS Subjects The Multi-Ethnic Study of Atherosclerosis (MESA) (28) is a longitudinal study supported by the National Heart, Lung, and Blood Institute with the overall goal of identifying risk factors for subclinical atherosclerosis. A total of 6,814 men and women, who identified themselves as White, Black, Hispanic, or Chinese and were aged years and free of clinically apparent cardiovascular disease, were recruited from portions of six US communities: Baltimore City and Baltimore County, Maryland; Chicago, Illinois; Forsyth County, North Carolina; Los Angeles County, California; northern Manhattan and the Bronx, New York; and St. Paul, Minnesota. Each site recruited by randomly selecting potential participants from locally available sources (lists of residents or dwellings) or using random digit dialing. Details of the sampling plan have been previously reported (28). Among those screened and deemed eligible, the participation rate was 59.8 percent. The baseline visit for the cohort (on which these analyses are based) took place between June 2000 and August Measurements and variable definitions Pollutant data were extracted from the US Environmental Protection Agency s Aerometric Information Retrieval System (AIRS) in November 2003 (29). PM 2.5 concentrations were obtained from 24-hour samples, some of which collected data daily, but most of which collected data every third day. For each person, we constructed a set of cumulative exposure measures for the 60 days prior to the day on which blood was drawn. Each daily exposure was based on the monitor nearest to the person s residence with available data on that day. This ensured that complete data were available for most participants but, because most monitors collected data every third day, the monitor from which data were drawn could differ for different days. The mean distance to the nearest monitor was 9 km (distance ranged from 0.45 to 51 km). Five exposure measures were constructed by use of the 60-day lags: prior day, average of prior 2 days, average of prior week, average of prior month, and average of prior 2 months. C-reactive protein was measured in all participants at baseline using a Behring nephelometer II (BNII) automated immunoanalyzer (N High Sensitivity CRP assay; Dade Behring, Inc., Deerfield, Illinois) at the Laboratory for Clinical Biochemistry Research (University of Vermont, Burlington, Vermont). Site and central laboratory quality control procedures are reported elsewhere (28). Intraassay coefficients of variation range from 2.3 to 4.4 percent, and interassay coefficients of variation range from 2.1 to 5.7 percent. C-reactive protein values were highly skewed and were log transformed for analyses. Individual-level variables known to be associated with C-reactive protein concentrations that could also covary with day of visit (and hence with particulate matter levels) were examined as covariates (refer to table 1 for list). Because PM 2.5 concentrations vary by site and site could be associated with C-reactive protein concentrations through other mechanisms, results are also shown after additional adjustment for site. Selected analyses were also repeated for interleukin-6, another inflammatory marker. Interleukin-6 was measured by an ultrasensitive enzyme-linked immunosorbent assay (Quantikine HS human interleukin-6 immunoassay; R&D Systems, Minneapolis, Minnesota).
3 Particulate Matter Exposure and Inflammation 439 TABLE 1. Demographic characteristics, exposure to particulate matter of 2.5 mm in diameter, and C-reactive protein concentrations for the 5,634 participants included in the analyses, Multi-Ethnic Study of Atherosclerosis, Age, years (mean (SD*)) (10.13) % female 52.6 Race/ethnicity (% distribution) Caucasian 40.3 Chinese 12.1 African American 26.5 Hispanic 21.1 Study site (% distribution) Baltimore, MD 15.7 Chicago, IL 18.1 Forsyth County, NC 15.7 Los Angeles, CA 19.0 New York City, NY 16.0 St. Paul, MN 15.5 Self-reported health (% distribution) Poor 0.6 Fair 7.8 Good 40.7 Very good 34.3 Excellent 16.7 Body mass index, kg/m 2 (mean (SD)) (5.37) Diabetes (% distribution)y No 58.5 Impaired glucose tolerance 28.1 Diabetes 13.5 Smoking status (% distribution) Never 50.8 Former 36.8 Current 12.3 Secondhand smoke (% distribution)z None 53.0 At least 1 hour per week 34.7 Current smokers 12.3 Table continues TABLE 1. Continued Physical activity (% distribution) Low 25.1 Medium 47.3 High 27.6 % with arthritis flare within past 2 weeks{ 12.2 % with regular use of any nonsteroidal antiinflammatory drugs, aspirin, or lipid-lowering medications{ 45.4 % with infections within past 2 weeks{ 23.2 PM 2.5,* lg/m 3 (median (25th, 75th percentiles)) Prior day (9.50, 20.90) Prior 2 days# (10.15, 20.35) Prior 7 days# (12.07, 19.70) Prior 30 days# (13.07, 19.22) Prior 60 days# (13.77, 19.08) C-reactive protein, mg/liter (median (25th, 75th percentiles)) 1.84 (0.82, 4.10) * SD, standard deviation; PM 2.5, particulate matter of less than or equal to 2.5 lm in diameter. y American Diabetes Association 2003 criteria: impaired is fasting glucose of mg/dl; diabetic is fasting glucose of 126 mg/dl or takes insulin or oral diabetes medication. z Asked of only noncurrent smokers. Noncurrent smokers missing secondhand smoke information (n ¼ 144) were assigned to no secondhand smoke. Physical activity was based on total minutes per day and categorized into three levels with the lowest level being the lowest quartile, the middle level being the 25th 75th percentiles, and the highest level being the highest quartile. { Persons missing arthritis, medication, or infection information (n ¼ 5, n ¼ 21, or n ¼ 6, respectively) were assigned to no arthritis, no medication, or no infection, respectively. Infection was defined as cold, flu, bronchitis, sinus infection, tooth infection, or urinary tract infection. # Sample sizes for exposures were smaller than for the full sample because of missing data; n ¼ 5,606, 5,510, 5,294, and 5,136 for the prior 2 days, prior 7 days, prior 30 days, and prior 60 days, respectively. Cumulative exposures for copollutants and weather replicated the lagged averaging scheme described for PM 2.5. Data analysis Other gaseous pollutants (sulfur dioxide, nitrogen dioxide, carbon monoxide, and ozone) and weather variables (temperature and dew point temperature) were included as covariates in some models because of their association with PM 2.5 and their potential effects on C-reactive protein concentrations. Nitrogen dioxide and sulfur dioxide daily averages were computed by averaging hourly data if at least 20 hours of data were recorded for a 24-hour period. Ozone and carbon monoxide were represented by the maximum 8-hour running average for a 24-hour period. Measures of daily average temperature, dew point temperature, and sea level barometric pressure were obtained from a National Weather Service monitoring station that was representative of each study area. Scatterplots, LOESS smoothing by SAS/STAT software (SAS Institute, Inc., Cary, North Carolina), and generalized additive models (30) were initially used to investigate the shape of the relation between each of our five measures of exposure and log C-reactive protein concentration. Linear regression was then used to estimate the associations of PM 2.5 exposures with C-reactive protein concentration before and after adjustment for the individual-level covariates, study site, copollutants, and weather. The presence of seasonal trends was investigated by examining seasonal patterns in the residuals of fully adjusted models. We tested for the presence of residual autocorrelation using the Durbin- Watson d statistic.
4 440 Diez Roux et al. FIGURE 1. Distribution of particulate matter of 2.5 lm in diameter (PM 2.5 ) by study site, Multi-Ethnic Study of Atherosclerosis, Boxes represent the 25th percentile, median, and 75th percentile; box plot whiskers represent the 5th 95th percentiles. Stratified analyses were conducted to investigate if effects differed across site, season (warmer months vs. cooler months), or individual-level variables (age, sex, race/ethnicity, education, self-reported health, diabetes, infection, medication use, and history of asthma, bronchitis, or emphysema). Additive interactions in the log scale (or effect measure modification for relative differences) were tested by including interaction terms in regression models. In order to examine if PM 2.5 exposure was related to C-reactive protein only among persons without other factors strongly related to inflammation, we also repeated the analyses, excluding persons with any of the following characteristics/ conditions: self-reported fair/poor health, impaired glucose tolerance or diabetes, current cigarette smoking, recent arthritis flare, taking antiinflammatory or lipid-lowering medications, or recent infection. We examined the sensitivity of results to alternate ways of estimating exposure by 1) restricting analyses to participants with monitors within 9 km of their home (9 km being the mean distance in our sample) and 2) using the average of all available monitors within the city of residence (defined as 40 km or 25 miles from the centroid of participant residences) as the exposure measure instead of the nearest monitor. In additional sensitivity analyses for a subset of the data, we compared results using the nearest monitor with results obtained by estimating exposure at each residence using inverse distance interpolation and space-time kriging with a separable covariance model (31, 32). These sensitivity analyses were conducted for the site with the greatest within-site variability in exposure (Los Angeles). In secondary analyses, selected (logistic) models were also run using C-reactive protein of greater than or equal to 3 mg/liter (the cutoff used to define high-risk groups on the basis of C-reactive protein concentration) (33) as a binary outcome. Of the 6,814 participants who completed the baseline examination, 6,069 participated in the air pollution study. Of these, 147 were excluded because latitude and longitude coordinates for their address were unavailable, 26 participants were excluded because of missing data on prior day PM 2.5 exposure, and 262 participants were excluded because of missing data on C-reactive protein or key covariates of interest, yielding a total of 5,634 participants (83 percent of the total cohort) for analysis. Analyses of longterm exposures excluded additional participants because of missing exposure data. RESULTS The mean participant was 62 years of age, and 53 percent were female. Additional characteristics of the study sample are shown in table 1. The median PM 2.5 for the set of cumulative exposures investigated ranged from 14.3 lg/m 3 for prior day to 15.9 lg/m 3 for prior 60 days. The median C-reactive protein level was 1.84 mg/liter. Approximately 35 percent of participants had C-reactive protein concentrations of greater than or equal to 3 mg/liter. Median prior day PM 2.5 exposure levels were lowest in St. Paul (10.6 lg/m 3 ) and highest in Los Angeles (18.3 lg/m 3 ) (figure 1). A similar pattern was observed for the mean of the prior 60 days (not shown). Correlations between prior day exposure and other exposures were 0.91, 0.60, 0.43, and 0.36 for prior 2 days, prior 7 days, prior 30 days, and prior 60 days, respectively (all p < 0.001). Other pairwise correlations between exposures lay between this range. Virtually all (99 percent) participants were within 40 km of the centroid for the site. Of the total variance in PM 2.5 measures, the majority (74 87 percent depending on the site) were
5 Particulate Matter Exposure and Inflammation 441 between days (within season), and only a small proportion (7 19 percent) were between monitors within days. C-reactive protein concentrations were positively associated with age, female gender, Hispanic ethnicity, body mass index, diabetes, current smoking status, secondhand smoke, infections, and living in Forsyth County (table 2). Selfreported health, physical activity, and arthritis flare were also associated with C-reactive protein in the expected direction, although differences were not statistically significant. In unadjusted bivariate analyses, there was no evidence of an association between PM 2.5 levels and C-reactive protein concentration. Analyses using generalized additive models (with adjustment for person-level covariates) also revealed no evidence of a clear threshold for the effect of PM 2.5 on C-reactive protein for any of the exposures studied for the range of PM 2.5 levels within which the majority of study participants were found (data available from authors upon request). Table 3 shows relative differences in C-reactive protein per 10-lg/m 3 increase in PM 2.5 for the range of models fitted. Overall, there was no clear evidence of a positive association between PM 2.5 exposure and C-reactive protein concentration for any of the exposures studied. PM 2.5 levels for the prior day, prior 2 days, and prior 7 days were not positively associated with C-reactive protein. In models adjusted for person-level covariates, only the 30-day and 60-day exposures (in some models) showed a positive association with C-reactive protein, but differences were small and all confidence intervals included the null value. Compared with models adjusted for only person-level covariates, site, copollutant, and weather adjustment resulted in associations that were slightly more negative (for prior day, prior 2 days, and prior week) or closer to the null (for prior 30 and 60 days) (table 3). Sensitivity analyses using the study site average as the exposure and restricting the sample to persons within 9 km of a monitor (the mean distance to a monitor in our sample) (table 3) revealed generally similar results. In Los Angeles (the site with the greatest within-site variability in PM 2.5 ), results obtained using inverse distance interpolation and space-time kriging were very similar to those obtained using the nearest monitor for all lags studied (not shown). Plots of residuals from adjusted models against time/season showed no clear evidence of seasonal or time trends. Durbin-Watson d statistics did not indicate the presence of first-order autocorrelation. No consistent associations between particulate matter exposure and C-reactive protein concentrations were observed when selected models for continuous C-reactive protein were repeated for exposures to particulate matter of less than or equal to 10 lm in diameter (PM 10 ) (not shown). Figure 2 shows the relative difference in C-reactive protein per 10-lg/m 3 difference in prior day PM 2.5 for the restricted sample (participants without other risk factors for elevated C-reactive protein) compared with that of all other participants. Although point estimates suggested weakly positive associations with C-reactive protein in the restricted sample for 30- and 60-day mean exposures, tests for interaction were not statistically significant. Of all the other interactions tested (PM 2.5 with age, sex, education, diabetes, smoking, use of medications, history of infection, or history TABLE 2. Adjusted* relative difference in C-reactive protein (mg/liter) for the 5,634 participants included in the analyses, Multi-Ethnic Study of Atherosclerosis, Relative difference 95% confidence interval Age (per 10 years) , 1.12 Gender Female vs. male , 1.63 Race Caucasian Chinese , 0.8 African American , 1.12 Hispanic , 1.24 Study site Chicago, IL Baltimore, MD , 1.11 Forsyth County, NC , 1.30 Los Angeles, CA , 1.21 New York City, NY , 1.00 St. Paul, MN , 1.16 Self-reported health Poor , 2.02 Fair , 1.27 Good , 1.17 Very good , 1.13 Excellent Body mass index (per kg/m 2 ) , 1.09 Diabetes No Impaired glucose tolerance , 1.16 Diabetic , 1.15 Smoking status Never Former , 1.11 Current , 1.55 Secondhand smoke None Any , 1.15 Physical activity Low Medium , 1.01 High , 1.01 Arthritis Flare vs. no flare , 1.14 Medicationsy Use vs. no use , 0.96 Infections in past 2 weeksy Yes vs. no , 1.28 * Each estimate is adjusted for all the other variables in the table. The relative difference indicates the percent increase in mean C-reactive protein associated with the variable in question. For example, a relative difference of 1.5 indicates that C-reactive protein is 50% higher in the exposed than in the unexposed group. y Persons missing medication or infection information (n ¼ 21 or n ¼ 6, respectively) were assigned to no medication or no infection, respectively. Infection was defined as cold, flu, bronchitis, sinus infection, tooth infection, or urinary tract infection.
6 442 Diez Roux et al. TABLE 3. Adjusted relative difference in C-reactive protein (mg/liter) per 10-mg/m 3 increase in particulate matter of 2.5 mm in diameter, Multi-Ethnic Study of Atherosclerosis, Exposure data and adjustment variables Source of exposure data No.* Relative difference 95% confidence interval Prior day Age, gender, racey Nearest monitor 5, , 1.01 All person-level covariatesz Nearest monitor 5, , 1.01 All person-level covariates and site Nearest monitor 5, , 1.01 All person-level covariates, site, copollutants, and weather{ Nearest monitor 5,047# , 1.01 All person-level covariates and site Study site average** 5,572# , 1.01 All person-level covariates and site Nearest, limited to 9 km 2,831# , 1.00 Prior 2 days Age, gender, racey Nearest monitor 5, , 1.00 All person-level covariatesz Nearest monitor 5, , 1.01 All person-level covariates and site Nearest monitor 5, , 1.01 All person-level covariates, site, copollutants, and weather{ Nearest monitor 5,023# , 1.01 All person-level covariates and site Study site average** 5,498# , 1.01 All person-level covariates and site Nearest, limited to 9 km 2,803# , 1.00 Prior 7 days Age, gender, racey Nearest monitor 5, , 1.02 All person-level covariatesz Nearest monitor 5, , 1.04 All person-level covariates and site Nearest monitor 5, , 1.04 All person-level covariates, site, copollutants, and weather{ Nearest monitor 4,913# , 1.04 All person-level covariates and site Study site average** 5,187# , 1.04 All person-level covariates and site Nearest, limited to 9 km 2,237# , 1.06 Prior 30 days Age, gender, racey Nearest monitor 5, , 1.06 All person-level covariatesz Nearest monitor 5, , 1.10 All person-level covariates and site Nearest monitor 5, , 1.10 All person-level covariates, site, copollutants, and weather{ Nearest monitor 4,579# , 1.12 All person-level covariates and site Study site average** 4,307# , 1.12 All person-level covariates and site Nearest, limited to 9 km 925# , 1.34 Prior 60 days Age, gender, racey Nearest monitor 5, , 1.05 All person-level covariatesz Nearest monitor 5, , 1.11 All person-level covariates and site Nearest monitor 5, , 1.11 All person-level covariates, site, copollutants, and weather{ Nearest monitor 4,219# , 1.11 All person-level covariates and site Study site average** 3,813# , 1.13 All person-level covariates and site Nearest, limited to 9 km 369# , 1.73 * For each exposure, all persons with complete data were included. Sample size varies by exposure measure because of missing data. y Model variables: age (1 df), gender (1 df), and race/ethnicity (3 df). z Model variables: age (1 df), gender (1 df), race/ethnicity (3 df), general health status (4 df), body mass index (1 df), diabetes (2 df), cigarette status (2 df), secondhand smoke (1 df), physical activity (2 df), arthritis flare in last 2 weeks (1 df), medications (aspirin, lipids, nonsteroidal antiinflammatory drugs) (1 df), and infections in last 2 weeks (1 df). Model variables: age (1 df), gender (1 df), race/ethnicity (3 df), general health status (4 df), body mass index (1 df), diabetes (2 df), cigarette status (2 df), secondhand smoke (1 df), physical activity (2 df), arthritis flare in last 2 weeks (1 df), medications (aspirin, lipids, nonsteroidal antiinflammatory drugs) (1 df), infections in last 2 weeks (1 df), and study site (5 df). { Model variables: age (1 df), gender (1 df), race/ethnicity (3 df), general health status (4 df), body mass index (1 df), diabetes (2 df), cigarette status (2 df), secondhand smoke (1 df), physical activity (2 df), arthritis flare in last 2 weeks (1 df), medications (aspirin, lipids, nonsteroidal antiinflammatory drugs) (1 df), infections in last 2 weeks (1 df), study site (5 df), sulfur dioxide (1 df), nitrogen dioxide (1 df), carbon monoxide (1 df), ozone (1 df), average temperature (1 df), and dew point temperature (1 df). # Addition of copollutants/weather or study site average or nearest monitor within 9 km resulted in a smaller number of observations because of missing data. ** Based on the average of all monitors within 40 km of the study site centroid.
7 Particulate Matter Exposure and Inflammation 443 FIGURE 2. Relative differences (with 95% confidence intervals) in C-reactive protein (mg/liter) per 10-lg/m 3 increase in particulate matter of 2.5 lm in diameter for different exposure periods in a restricted sample without risk factors for elevated C-reactive protein and in the rest of the sample, adjusted for person-level covariates, Multi-Ethnic Study of Atherosclerosis, The restricted sample (20%, n ¼ 1,123) are nonsmokers without a history of recent infection or arthritis, in good to excellent health, with normal glucose, and who are not taking antiinflammatory medications; others are the participants not in the restricted sample. Analyses were adjusted for age, gender, race/ethnicity, general health status, body mass index, diabetes, cigarette smoking, secondhand smoke, physical activity, arthritis flare, medications, and infections. The p values for interaction between exposure and sample group (restricted vs. other) were 0.4, 0.7, 0.8, 0.4, and 0.8 for the prior day, prior 2 days, prior 7 days, prior 30 days, and prior 60 days, respectively. of lung disease), only season revealed statistically significant interactions consistently across lags. Associations were generally negative for the warm season (March August) and null or weakly positive for the cool season (September February) (relative difference per 10-lg/m 3 increase in PM 2.5 : 0.95 (95 percent confidence interval (CI): 0.92, 0.99) and 1.01 (95 percent CI: 0.97, 1.05) for prior day exposure in warm and cool seasons, respectively, and 0.92 (95 percent CI: 0.80, 1.05) and 1.06 (95 percent CI: 0.93, 1.21) for 60-day exposure in warm and cool seasons, respectively). In analyses with C-reactive protein of greater than or equal to 3 mg/liter as a dichotomous outcome, weak positive associations between PM 2.5 exposures and C-reactive protein were observed for some of the models for prior 7-, 30-, and 60-day means, but confidence intervals were wide and included the null value (table 4). In most cases, adjustment for site, copollutants, and weather resulted in estimates even closer to the null. Associations of PM 2.5 exposures with the odds of C-reactive protein of greater than or equal to 3 mg/ liter appeared to be stronger or present only in participants without other risk factors for elevated C-reactive protein, but tests for interaction did not achieve statistical significance (figure 3). No positive associations between particulate matter exposures were observed when selected analyses were repeated using interleukin-6 as the outcome. DISCUSSION We found no consistent evidence that recent exposure to PM 2.5 levels is positively associated with C-reactive protein concentration in a population-based sample. Of the five exposure measures investigated (prior day, prior 2 days, prior week, prior 30 days, and prior 60 days), only the 30-day and 60-day mean exposures showed the expected positive association in analyses of log C-reactive protein as a continuous outcome (3 4 percent increase per 10-lg/m 3 difference in PM 2.5 in models adjusted for person-level covariates). The mean 7-, 30-, and 60-day exposures were weakly, positively, and nonsignificantly associated with the odds of C-reactive protein of greater than or equal to 3 mg/liter after adjustment for person-level covariates (increased odds ranging from 5 percent to 12 percent depending on the model).
8 444 Diez Roux et al. TABLE 4. Odds ratios of C-reactive protein of 3 mg/liter per 10-mg/m 3 increase in particulate matter of 2.5 mm in diameter, Multi-Ethnic Study of Atherosclerosis, Exposure data and adjustment variables No. Odds ratio 95% confidence interval Prior day Age, gender, race* 5, , 1.03 All person-level covariatesy 5, , 1.04 All person-level covariates and sitez 5, , 1.02 All person-level covariates, site, copollutants, and weather 5, , 0.99 Prior 2 days Age, gender, race* 5, , 1.04 All person-level covariatesy 5, , 1.06 All person-level covariates and sitez 5, , 1.04 All person-level covariates, site, copollutants, and weather 5, , 1.04 Prior 7 days Age, gender, race* 5, , 1.10 All person-level covariatesy 5, , 1.15 All person-level covariates and sitez 5, , 1.12 All person-level covariates, site, copollutants, and weather 4, , 1.14 Prior 30 days Age, gender, race* 5, , 1.18 All person-level covariatesy 5, , 1.29 All person-level covariates and sitez 5, , 1.29 All person-level covariates, site, copollutants, and weather 4, , 1.40 Prior 60 days Age, gender, race* 5, , 1.17 All person-level covariatesy 5, , 1.32 All person-level covariates and sitez 5, , 1.31 All person-level covariates, site, copollutants, and weather 4, , 1.34 * Model variables: age (1 df), gender (1 df), and race/ethnicity (3 df). y Model variables: age (1 df), gender (1 df), race/ethnicity (3 df), general health status (4 df), body mass index (1 df), diabetes (2 df), cigarette status (2 df), secondhand smoke (1 df), physical activity (2 df), arthritis flare in last 2 weeks (1 df), medications (aspirin, lipids, nonsteroidal antiinflammatory drugs) (1 df), and infections in last 2 weeks (1 df). z Model variables: age (1 df), gender (1 df), race/ethnicity (3 df), general health status (4 df), body mass index (1 df), diabetes (2 df), cigarette status (2 df), secondhand smoke (1 df), physical activity (2 df), arthritis flare in last 2 weeks (1 df), medications (aspirin, lipids, nonsteroidal antiinflammatory drugs) (1 df), infections in last 2 weeks (1 df), and study site (5 df). Model variables: age (1 df), gender (1 df), race/ethnicity (3 df), general health status (4 df), body mass index (1 df), diabetes (2 df), cigarette status (2 df), secondhand smoke (1 df), physical activity (2 df), arthritis flare in last 2 weeks (1 df), medications (aspirin, lipids, nonsteroidal antiinflammatory drugs) (1 df), infections in last 2 weeks (1 df), study site (5 df), sulfur dioxide (1 df), nitrogen dioxide (1 df), carbon monoxide (1 df), ozone (1 df), average temperature (1 df), and dew point temperature (1 df). Associations were of small magnitude and became even weaker after additional adjustment for site, copollutants, and weather, and confidence intervals of all estimates included the null value. Although stratified analyses suggested stronger associations in persons without other risk factors for elevated C-reactive protein, this heterogeneity was not statistically significant. We also found no evidence of associations between particulate matter exposures and interleukin-6 (not shown). Prior evidence regarding the relation between short-term exposures to particulate matter and C-reactive protein concentration is not entirely consistent. In one of the largest
9 Particulate Matter Exposure and Inflammation 445 FIGURE 3. Odds ratios (with 95% confidence intervals) of C-reactive protein of 3 mg/liter per 10-lg/m 3 increase in particulate matter of 2.5 lm in diameter for different exposure periods in a restricted sample without risk factors for elevated C-reactive protein and in the rest of the sample, adjusted for person-level covariates, Multi-Ethnic Study of Atherosclerosis, The restricted sample (20%, n ¼ 1,123) are nonsmokers without a history of recent infection or arthritis, in good to excellent health, with normal glucose, and who are not taking antiinflammatory medications; others are the participants not in the restricted sample. Analyses were adjusted for age, gender, race/ethnicity, general health status, body mass index, diabetes, cigarette smoking, secondhand smoke, physical activity, arthritis flare, medications, and infections. p values for interaction between exposure and sample group (restricted vs. other) were 0.5, 0.5, 0.5, 0.3, and 0.6 for the prior day, prior 2 days, prior 7 days, prior 30 days, and prior 60 days, respectively. studies to date, Peters et al. (19) found that contemporaneous and recent (5 prior days) exposures to total suspended particulates were associated with C-reactive protein concentration in a sample of 631 men with two repeated measures. C-reactive protein increased 0.88 mg/liter for each 26-lg/m 3 increase in the previous 5-day average level of total suspended particulates. Seaton et al. (22) found positive associations between recent (up to 3-day) city-level exposures to PM 10 and C-reactive protein (147 percent increase in C-reactive protein per 100-lg/m 3 increase in PM 10 )in a sample of 112 persons with multiple repeated measures over 18 months, although no associations were observed for person-level measures of exposure. Pope et al. (23) found a positive association between recent (up to 3-day) PM 2.5 exposure and C-reactive protein in 88 subjects with a mean of 2.8 repeated measures, but this association disappeared when one influential subject was removed from the sample. One prior study has reported increases in interleukin-6 associated with PM 10 exposure during an acute episode of air pollution in a sample of 30 healthy volunteers, but the magnitude of the increase in PM 10 studied (from 40 lg/m 3 to 125 lg/m 3 ) was much greater than the variation observed in our sample (10). An advantage of our study over prior work is the large sample size, as well as the geographic and demographic diversity of the sample. Although there was limited within-site spatial variability in PM 2.5, at least as reflected by ambient monitors, our analyses rely more on day-to-day variability than on between-site or within-site variability. However, it is possible that the range of values present in our sample did not allow us to detect important threshold effects at the higher end of the particulate matter distribution. In a comparison of the magnitude of PM 2.5 exposure with US Environmental Protection Agency National Ambient Air Quality Standards, almost half (47 percent) of the sample had prior day PM 2.5 levels that exceeded the annual standard of 15 lg/m 3, although less than 1 percent had prior day PM 2.5 levels that exceeded the 24-hour standard of 65 lg/m 3. Two prior studies based on ambient monitoring that reported an association between exposure to particulate matter and C-reactive protein may have contrasted more extreme values by studying an air pollution episode (19)
10 446 Diez Roux et al. or by purposely sampling high and low air pollution days (23), although at least one study has reported associations even at relatively low levels of PM 2.5 exposures (34). We relied on the existing ambient air-monitoring network to characterize exposures. Outdoor concentrations have been shown to be reasonable proxies for personal exposure to particles of outdoor origin (35, 36). Indoor exposures (such as those from passive smoking and wood-burning stoves and fireplaces) are important contributors to personal particle exposure and are not captured by the outdoor measurements. However, in order to be confounders of the effects we were interested in estimating, these indoor exposures would have to be associated with ambient levels on the day of the clinic examination, which is unlikely. Moreover, our results were adjusted for passive smoking, which is likely to be the major contributor to indoor exposures in the populations we studied. The existing literature has characterized personal exposures based on monitor measurements averaged over very large areas: within a county (37), within a metropolitan area (38, 39), or within a city (40). Single representative monitors located in the center of a city have also been used (22, 41). We used data from the monitors closest to each participant s residence. Thirty-eight percent of study participants were not employed at the time of the survey (retired and not working, unemployed, or homemakers). In addition, over 75 percent of our participants reported spending 60 percent of their time either in their home or within 1 mile (1.6 km) of their home. This suggests that assignment of exposure based on place of residence is reasonable. We tested the sensitivity of our results to alternate ways of estimating exposure and found similar results when analyses were restricted to participants with monitors within 9 km of their home and when the exposure measure was based on the average of all available measurements within the study area. The high withinsite correlation of monitor PM 2.5 measures suggests that the results are unlikely to be highly sensitive to alternate methods, such as averaging over the specific areas within which participants are likely to move in the course of a usual day. The results were also robust to alternative interpolation methods. There is little a priori knowledge on which to base hypotheses regarding the relevant lags expected between exposure to particulate matter and effects on inflammatory markers. Circulating C-reactive protein has a plasma halflife of only 19 hours and can be upregulated rapidly, within hours, during an acute-phase response (42). Human and animal experimental studies have found that an inflammatory response occurs 6 36 hours after exposure to particles (13 16). This evidence suggests that short-term lags are likely to be especially relevant for C-reactive protein. Pope et al. (23) found that concurrently measured PM 2.5 was more strongly associated with C-reactive protein than were measures lagged 1 or 2 days, although an effect almost comparable with the concurrent day was observed for the average of the 3 days prior. Peters et al. (19) found that levels of C-reactive protein were positively associated with levels of total suspended particulates on the day of the examination. However, similar or slightly stronger associations were observed for total suspended particulates measured on the prior day and for the mean of the prior 5 days, suggesting longer-term cumulative effects. In our analyses, the only weakly positive (albeit not statistically significant) associations were observed for the longer lags. Zanobetti et al. (43) recently reported a positive association between prior 60-day PM 2.5 exposure and C-reactive protein concentration in a large population sample: C-reactive protein increased 7.7 percent per 10-lg/m 3 increase in PM 2.5 (95 percent CI: 0.96, 14.96). Given the relatively short half-life of C-reactive protein, it is difficult to reconcile the presence of long-term exposure effects with the absence of effects for shorter lags. An alternative explanation for associations with longer-term exposure periods is that the averaging process reduces measurement error and hence increases the ability to detect associations. Similarly to some prior studies of air pollution exposures and inflammatory markers (20, 21, 41), our analyses are based on a single measure of C-reactive protein on each person. Therefore, inferences are based on between-person as opposed to within-person comparisons. This raises the possibility that associations (or the lack thereof) could result from confounding by individual-level characteristics. Our analyses controlled for a large set of variables associated with C-reactive protein levels. Analyses of residuals revealed no evidence of seasonal patterns or residual autocorrelation in adjusted models. It is therefore unlikely that our null findings are the result of individual-level confounding. Studies of repeated measures, however, which allow inferences to be drawn by within-person comparisons, do have greater power for detecting associations with exposures that change over time while holding time-independent individuallevel factors constant (44). Repeated-measures analyses based on the MESA cohort will be possible as additional follow-up becomes available. Measurement error in our exposure estimates may have biased results toward the null. More detailed assessment of personal exposures (involving activity diaries and additional monitoring both indoors and outdoors) currently planned for the MESA cohort will allow much more precise measurement of personal exposures. It is also plausible that improved measurement of specific components of PM 2.5 (such as ultrafine particles or transition metals) may enhance our ability to detect effects on systemic inflammation (9). In any case, our results make it unlikely that a systemic inflammatory response explains the short-term effects of recent exposures observed in time-series analyses, which also rely exclusively on monitor data. Inconsistent results regarding the relation between ambient particulate matter mass and markers of systemic inflammation, plus persistent questions on the extent to which inflammation is a risk factor, risk marker, or simply a correlate of atherosclerosis (45), suggest that other mechanistic pathways linking particulate matter exposures to cardiovascular events need to be explored. ACKNOWLEDGMENTS MESA is supported by contracts N01-HC through N01-HC and by contract N01-HC from the
11 Particulate Matter Exposure and Inflammation 447 National Heart, Lung, and Blood Institute. This work was supported by grant R (A. D. R.) from the Environmental Protection Agency. The authors thank the other investigators and staff of the MESA study for their valuable contributions. A full list of participating MESA investigators and institutions can be found at Conflict of interest: none declared. REFERENCES 1. Morris RD. Airborne particulates and hospital admissions for cardiovascular disease: a quantitative review of the evidence. Environ Health Perspect 2001;109(suppl 4): Samet JM, Dominici F, Curriero FC, et al. Fine particulate air pollution and mortality in 20 U.S. cities, N Engl J Med 2000;343: Dockery DW. Epidemiologic evidence of cardiovascular effects of particulate air pollution. Environ Health Perspect 2001;109(suppl 4): Dockery DW, Pope CA 3rd, Xu X, et al. An association between air pollution and mortality in six U.S. cities. N Engl J Med 1993;329: Pope CA 3rd, Burnett RT, Thun MJ, et al. Lung cancer, cardiopulmonary mortality, and long-term exposure to fine particulate air pollution. JAMA 2002;287: Pope CA 3rd, Thun MJ, Namboodiri MM, et al. Particulate air pollution as a predictor of mortality in a prospective study of U.S. adults. Am J Respir Crit Care Med 1995;151: Seaton A, MacNee W, Donaldson K, et al. Particulate air pollution and acute health effects. Lancet 1995;345: Frampton MW. Systemic and cardiovascular effects of airway injury and inflammation: ultrafine particle exposure in humans. Environ Health Perspect 2001;109(suppl 4): Donaldson K, Stone V, Seaton A, et al. Ambient particle inhalation and the cardiovascular system: potential mechanisms. Environ Health Perspect 2001;109(suppl 4): van Eeden SF, Tan WC, Suwa T, et al. Cytokines involved in the systemic inflammatory response induced by exposure to particulate matter air pollutants (PM 10 ). Am J Respir Crit Care Med 2001;164: Ridker PM, Morrow DA. C-reactive protein, inflammation, and coronary risk. Cardiol Clin 2003;21: Nemmar A, Hoylaerts MF, Hoet PH, et al. Possible mechanisms of the cardiovascular effects of inhaled particles: systemic translocation and prothrombotic effects. Toxicol Lett 2004;149: Gardner SY, Lehmann JR, Costa DL. Oil fly ash-induced elevation of plasma fibrinogen levels in rats. Toxicol Sci 2000; 56: Salvi S, Blomberg A, Rudell B, et al. Acute inflammatory responses in the airways and peripheral blood after short-term exposure to diesel exhaust in healthy human volunteers. Am J Respir Crit Care Med 1999;159: Salvi SS, Nordenhall C, Blomberg A, et al. Acute exposure to diesel exhaust increases IL-8 and GRO-alpha production in healthy human airways. Am J Respir Crit Care Med 2000; 161: Ghio AJ, Kim C, Devlin RB. Concentrated ambient air particles induce mild pulmonary inflammation in healthy human volunteers. Am J Respir Crit Care Med 2000;162: Clarke RW, Catalano PJ, Koutrakis P, et al. Urban air particulate inhalation alters pulmonary function and induces pulmonary inflammation in a rodent model of chronic bronchitis. Inhal Toxicol 1999;11: Clarke RW, Coull B, Reinisch U, et al. Inhaled concentrated ambient particles are associated with hematologic and bronchoalveolar lavage changes in canines. Environ Health Perspect 2000;108: Peters A, Frohlich M, Doring A, et al. Particulate air pollution is associated with an acute phase response in men; results from the MONICA-Augsburg Study. Eur Heart J 2001;22: Schwartz J. Air pollution and blood markers of cardiovascular risk. Environ Health Perspect 2001;109(suppl 3): Pekkanen J, Brunner EJ, Anderson HR, et al. Daily concentrations of air pollution and plasma fibrinogen in London. Occup Environ Med 2000;57: Seaton A, Soutar A, Crawford V, et al. Particulate air pollution and the blood. Thorax 1999;54: Pope CA 3rd, Hansen ML, Long RW, et al. Ambient particulate air pollution, heart rate variability, and blood markers of inflammation in a panel of elderly subjects. Environ Health Perspect 2004;112: Zanobetti A, Schwartz J, Samoli E, et al. The temporal pattern of mortality responses to air pollution: a multicity assessment of mortality displacement. Epidemiology 2002;13: Zanobetti A, Schwartz J, Samoli E, et al. The temporal pattern of respiratory and heart disease mortality in response to air pollution. Environ Health Perspect 2003;111: Dominici F, McDermott A, Zeger SL, et al. Airborne particulate matter and mortality: timescale effects in four US cities. Am J Epidemiol 2003;157: Goodman PG, Dockery DW, Clancy L. Cause-specific mortality and the extended effects of particulate pollution and temperature exposure. Environ Health Perspect 2004;112: Bild DE, Bluemke DA, Burke GL, et al. Multi-Ethnic Study of Atherosclerosis: objectives and design. Am J Epidemiol 2002;156: Office of Air Quality Planning and Standards. AIRS (Aerometric Information Retrieval System). (Database). Research Triangle Park, NC: US Environmental Protection Agency, ( 30. Hastie T, Tibshirani R. Generalized additive models for medical research. Stat Methods Med Res 1995;4: Haas TC. Local prediction of a spatio-temporal process with an application to wet sulfate deposition. J Am Stat Assoc 1995;90: Kyriakidis PC, Journel AG. Stochastic modeling of atmospheric pollution: a spatial time-series framework. Park II: application to monitoring monthly sulfate deposition over Europe. Atmos Environ 2001;35: Ridker PM. Clinical application of C-reactive protein for cardiovascular disease detection and prevention. Circulation 2003;107: Riediker M, Cascio WE, Griggs TR, et al. Particulate matter exposure in cars is associated with cardiovascular effects in healthy young men. Am J Respir Crit Care Med 2004;169: Janssen NA, Hoek G, Brunekreef B, et al. Personal sampling of particles in adults: relation among personal, indoor, and outdoor air concentrations. Am J Epidemiol 1998;147: Dockery DW, Spengler JD. Indoor-outdoor relationships of respirable sulfates and particles. Atmos Environ 1981;15: Liao D, Duan Y, Whitsel EA, et al. Association of higher levels of ambient criteria pollutants with impaired cardiac autonomic control: a population-based study. Am J Epidemiol 2004; 159:
Long-term Exposure to Ambient Particulate Matter and Prevalence of Subclinical Atherosclerosis in the Multi-Ethnic Study of Atherosclerosis
 American Journal of Epidemiology Advance Access published January 27, 2008 American Journal of Epidemiology ª 2008 The Authors This is an Open Access article distributed under the terms of the Creative
American Journal of Epidemiology Advance Access published January 27, 2008 American Journal of Epidemiology ª 2008 The Authors This is an Open Access article distributed under the terms of the Creative
Overview of Key Ozone Epidemiology Literature
 Overview of Key Ozone Epidemiology Literature Julie E. Goodman, Ph.D., DABT, ACE, ATS Ozone Webinar Texas Commission on Environmental Quality March 20, 2015 Epidemiology The study of the causes, distribution,
Overview of Key Ozone Epidemiology Literature Julie E. Goodman, Ph.D., DABT, ACE, ATS Ozone Webinar Texas Commission on Environmental Quality March 20, 2015 Epidemiology The study of the causes, distribution,
ORIGINAL INVESTIGATION. C-Reactive Protein Concentration and Incident Hypertension in Young Adults
 ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
Air Quality: What an internist needs to know
 Air Quality: What an internist needs to know Robert Paine, M.D. Pulmonary and Critical Care Medicine University of Utah School of Medicine Program for Air Quality, Health and Society February, 2017 October
Air Quality: What an internist needs to know Robert Paine, M.D. Pulmonary and Critical Care Medicine University of Utah School of Medicine Program for Air Quality, Health and Society February, 2017 October
APPENDIX AVAILABLE ON THE HEI WEB SITE
 APPENDIX AVAILABLE ON THE HEI WEB SITE Research Report 178 National Particle Component Toxicity (NPACT) Initiative Report on Cardiovascular Effects Sverre Vedal et al. Section 1: NPACT Epidemiologic Study
APPENDIX AVAILABLE ON THE HEI WEB SITE Research Report 178 National Particle Component Toxicity (NPACT) Initiative Report on Cardiovascular Effects Sverre Vedal et al. Section 1: NPACT Epidemiologic Study
Intermediate Methods in Epidemiology Exercise No. 4 - Passive smoking and atherosclerosis
 Intermediate Methods in Epidemiology 2008 Exercise No. 4 - Passive smoking and atherosclerosis The purpose of this exercise is to allow students to recapitulate issues discussed throughout the course which
Intermediate Methods in Epidemiology 2008 Exercise No. 4 - Passive smoking and atherosclerosis The purpose of this exercise is to allow students to recapitulate issues discussed throughout the course which
COMPARISON OF THE NUMBER OF ULTRA-FINE PARTICLES AND THE MASS OF FINE PARTICLES WITH RESPIRATORY SYMPTOMS IN ASTHMATICS
 PII: S0003-4878(96)00128-7 Ann. occup. Hyg., Vol. 41, Supplement 1, pp. 19-23, 1997 1997 Published by Elsevier Science Ltd on behalf of BOHS Printed in Great Britain. All rights reserved 0003-4878/97 $17.00
PII: S0003-4878(96)00128-7 Ann. occup. Hyg., Vol. 41, Supplement 1, pp. 19-23, 1997 1997 Published by Elsevier Science Ltd on behalf of BOHS Printed in Great Britain. All rights reserved 0003-4878/97 $17.00
Fine or ultrafine particulate matter (PM) is a mixture of solid and liquid particles, including
 Special Contribution Health Effects of Ambient Particulate Matter Dong Chun Shin, MD Department of Preventive Medicine, Yonsei University College of Medicine Email : dshin5@yumc.yonsei.ac.kr J Korean Med
Special Contribution Health Effects of Ambient Particulate Matter Dong Chun Shin, MD Department of Preventive Medicine, Yonsei University College of Medicine Email : dshin5@yumc.yonsei.ac.kr J Korean Med
Hotspot Analysis For Examining The Association Between Spatial Air Pollutants And Asthma In New York State, USA Using Kernel Density Estimation (KDE)
 Hotspot Analysis For Examining The Association Between Spatial Air Pollutants And Asthma In New York State, USA Using Kernel Density Estimation (KDE) Francis Tuluri 1, Amit Kr. Gorai 2, Aaron James 1 1
Hotspot Analysis For Examining The Association Between Spatial Air Pollutants And Asthma In New York State, USA Using Kernel Density Estimation (KDE) Francis Tuluri 1, Amit Kr. Gorai 2, Aaron James 1 1
SGRQ Questionnaire assessing respiratory disease-specific quality of life. Questionnaire assessing general quality of life
 SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
SUPPLEMENTARY MATERIAL e-table 1: Outcomes studied in present analysis. Outcome Abbreviation Definition Nature of data, direction indicating adverse effect (continuous only) Clinical outcomes- subjective
Atmospheric particulate matter and hospital admission due to lower respiratory tract infection: a
 Med J Chin PLA, Vol. 41, No. 2, February 1, 2016 123 (PM 10 /PM 2.5 ) [ ] Pearson logistic Pearson PM 2.5 PM 10 SO 2 NO 2 CO O 3 PM 2.5 5d PM 10 10 g/m 3 OR (95%CI) 1.010(1.005~1.015) 1.006(1.003~1.009)
Med J Chin PLA, Vol. 41, No. 2, February 1, 2016 123 (PM 10 /PM 2.5 ) [ ] Pearson logistic Pearson PM 2.5 PM 10 SO 2 NO 2 CO O 3 PM 2.5 5d PM 10 10 g/m 3 OR (95%CI) 1.010(1.005~1.015) 1.006(1.003~1.009)
Acute and chronic exposure to urban air
 Eur Respir J 2009; 34: 316 323 DOI: 10.1183/09031936.00138908 CopyrightßERS Journals Ltd 2009 Acute effects of outdoor air pollution on forced expiratory volume in 1 s: a panel study of schoolchildren
Eur Respir J 2009; 34: 316 323 DOI: 10.1183/09031936.00138908 CopyrightßERS Journals Ltd 2009 Acute effects of outdoor air pollution on forced expiratory volume in 1 s: a panel study of schoolchildren
Association of Higher Levels of Ambient Criteria Pollutants with Impaired Cardiac Autonomic Control: A Population-based Study
 American Journal of Epidemiology Copyright 2004 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 159, No. 8 Printed in U.S.A. DOI: 10.1093/aje/kwh109 Association of Higher
American Journal of Epidemiology Copyright 2004 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 159, No. 8 Printed in U.S.A. DOI: 10.1093/aje/kwh109 Association of Higher
ASSESSING AMBIENT FINE PARTICULATE MATTER EXPOSURE AND ASSOCIATIONS WITH CORONARY ARTERY CALCIFICATION
 ASSESSING AMBIENT FINE PARTICULATE MATTER EXPOSURE AND ASSOCIATIONS WITH CORONARY ARTERY CALCIFICATION by Ryan Tyler Rubright BS, Furman University, 2009 Submitted to the Graduate Faculty of the Department
ASSESSING AMBIENT FINE PARTICULATE MATTER EXPOSURE AND ASSOCIATIONS WITH CORONARY ARTERY CALCIFICATION by Ryan Tyler Rubright BS, Furman University, 2009 Submitted to the Graduate Faculty of the Department
Health effects of (particulate) air pollution
 Health effects of (particulate) air pollution Peter Hoet Ben Nemery Jan Emmerechts Katrien Luyts Ernesto Alfaro-Moreno Dorota Napierska K.U.Leuven Pneumology, Lung Toxicology Air pollution and Health Introduction
Health effects of (particulate) air pollution Peter Hoet Ben Nemery Jan Emmerechts Katrien Luyts Ernesto Alfaro-Moreno Dorota Napierska K.U.Leuven Pneumology, Lung Toxicology Air pollution and Health Introduction
Increases in Heart Rate during an Air Pollution Episode
 American Journal of Epidemiology Copyright 1999 by The Johns Hopkins University School of Hygiene and Public Health All rights reserved Vol. 150, 10 Printed In U.S.A. Increases in Rate during an Air Pollution
American Journal of Epidemiology Copyright 1999 by The Johns Hopkins University School of Hygiene and Public Health All rights reserved Vol. 150, 10 Printed In U.S.A. Increases in Rate during an Air Pollution
AIR POLLUTION AND EMERGENCY DEPARTMENT VISITS FOR DEPRESSION IN EDMONTON, CANADA
 International Journal of Occupational Medicine and Environmental Health 2007;20(3):241 245 DOI 10.2478/v10001-007-0024-2 AIR POLLUTION AND EMERGENCY DEPARTMENT VISITS FOR DEPRESSION IN EDMONTON, CANADA
International Journal of Occupational Medicine and Environmental Health 2007;20(3):241 245 DOI 10.2478/v10001-007-0024-2 AIR POLLUTION AND EMERGENCY DEPARTMENT VISITS FOR DEPRESSION IN EDMONTON, CANADA
Bad Things and the Heart
 Bad Things and the Heart K A T H L E E N M H E I N T Z, D. O., F A C C A S S I S T A N T P R O F E S S O R O F M E D I C I N E D I V I S I O N O F C A R D I O L O G Y C O O P E R M E D I C A L S C H O
Bad Things and the Heart K A T H L E E N M H E I N T Z, D. O., F A C C A S S I S T A N T P R O F E S S O R O F M E D I C I N E D I V I S I O N O F C A R D I O L O G Y C O O P E R M E D I C A L S C H O
Diesel Exhaust: Health Effects. Research Needs
 Diesel Exhaust: Health Effects and Research Needs Eric Garshick, MD, MOH Assistant Professor of Medicine VA Boston Healthcare System Channing Laboratory, Brigham and Womens Hospital Harvard Medical School
Diesel Exhaust: Health Effects and Research Needs Eric Garshick, MD, MOH Assistant Professor of Medicine VA Boston Healthcare System Channing Laboratory, Brigham and Womens Hospital Harvard Medical School
Health effects of wood burning. Dr. M.E. Gerlofs-Nijland RIVM, The Netherlands
 Health effects of wood burning Dr. M.E. Gerlofs-Nijland RIVM, The Netherlands 1 Outline Introduction wood smoke and particulate matter In vitro cell culture studies In vivo animal studies Comparison effects
Health effects of wood burning Dr. M.E. Gerlofs-Nijland RIVM, The Netherlands 1 Outline Introduction wood smoke and particulate matter In vitro cell culture studies In vivo animal studies Comparison effects
t air pollution Peter Hoet Ben Nemery
 Health effects of (particulate) t air pollution Peter Hoet Ben Nemery Tim Nawrot Jan Emmerechts Katrien Luyts Ernesto Alfaro Moreno Dorota Napierska K.U.Leuven Pneumology, Lung Toxicology Air pollution
Health effects of (particulate) t air pollution Peter Hoet Ben Nemery Tim Nawrot Jan Emmerechts Katrien Luyts Ernesto Alfaro Moreno Dorota Napierska K.U.Leuven Pneumology, Lung Toxicology Air pollution
A ir pollution is a major public health problem resulting
 780 CHRONIC OBSTRUCTIVE PULMONARY DISEASE Temporal relationship between air pollutants and hospital admissions for chronic obstructive pulmonary disease in Hong Kong Fanny W S Ko, Wilson Tam, Tze Wai Wong,
780 CHRONIC OBSTRUCTIVE PULMONARY DISEASE Temporal relationship between air pollutants and hospital admissions for chronic obstructive pulmonary disease in Hong Kong Fanny W S Ko, Wilson Tam, Tze Wai Wong,
Increased asthma medication use in association with ambient fine and ultrafine particles
 Eur Respir J 2002; 20: 691 702 DOI: 10.1183/09031936.02.01402001 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 Increased asthma medication
Eur Respir J 2002; 20: 691 702 DOI: 10.1183/09031936.02.01402001 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2002 European Respiratory Journal ISSN 0903-1936 Increased asthma medication
Asthma and air pollution: health effects and prevention
 Asthma and air pollution: health effects and prevention FuyuenYip PhD, MPH Air Pollution and Respiratory Health Branch Division of Environmental Hazards and Health Effects National Center for Environmental
Asthma and air pollution: health effects and prevention FuyuenYip PhD, MPH Air Pollution and Respiratory Health Branch Division of Environmental Hazards and Health Effects National Center for Environmental
Air pollution and population health: a global challenge
 Environ Health Prev Med (2008) 13:94 101 DOI 10.1007/s12199-007-0018-5 REVIEW Air pollution and population health: a global challenge Bingheng Chen Æ Haidong Kan Received: 14 September 2007 / Accepted:
Environ Health Prev Med (2008) 13:94 101 DOI 10.1007/s12199-007-0018-5 REVIEW Air pollution and population health: a global challenge Bingheng Chen Æ Haidong Kan Received: 14 September 2007 / Accepted:
Air Pollution and Heart Health
 Air Pollution and Heart Health Wayne E. Cascio, MD, FACC, FAHA Director, Environmental Public Health Division National Health and Environmental Effects Research Laboratory Disclosure of Conflicts of Interest
Air Pollution and Heart Health Wayne E. Cascio, MD, FACC, FAHA Director, Environmental Public Health Division National Health and Environmental Effects Research Laboratory Disclosure of Conflicts of Interest
7 City Air Monitoring Study (7CAM), March-April 2004.
 7 City Air Monitoring Study (7CAM), March-April 24. Andrew Hyland, PhD Mark Travers Department of Health Behavior Roswell Park Cancer Institute James Repace, Msc Repace Associates, Inc. and Visiting Assistant
7 City Air Monitoring Study (7CAM), March-April 24. Andrew Hyland, PhD Mark Travers Department of Health Behavior Roswell Park Cancer Institute James Repace, Msc Repace Associates, Inc. and Visiting Assistant
The Relationship Between Blood Pressure and C-Reactive Protein in the Multi-Ethnic Study of Atherosclerosis (MESA)
 Journal of the American College of Cardiology Vol. 46, No. 10, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2005.07.050
Journal of the American College of Cardiology Vol. 46, No. 10, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2005.07.050
Epidemiological analyses throughout the world have
 Increased Particulate Air Pollution and the Triggering of Myocardial Infarction Annette Peters, PhD; Douglas W. Dockery, ScD; James E. Muller, MD; Murray A. Mittleman, MD, DrPH Background Elevated concentrations
Increased Particulate Air Pollution and the Triggering of Myocardial Infarction Annette Peters, PhD; Douglas W. Dockery, ScD; James E. Muller, MD; Murray A. Mittleman, MD, DrPH Background Elevated concentrations
Composition of PM 2.5 in the Urban Atmosphere Overall Episode PM 10>50μg/m 3
 Why worry about PM 2.5 and Black Carbon? Dr Ian S Mudway MRC-PHE Centre for Environment & Health, King s College London Composition of PM 2.5 in the Urban Atmosphere Overall Episode PM 10>50μg/m 3 Yin
Why worry about PM 2.5 and Black Carbon? Dr Ian S Mudway MRC-PHE Centre for Environment & Health, King s College London Composition of PM 2.5 in the Urban Atmosphere Overall Episode PM 10>50μg/m 3 Yin
GUIDANCE ON METHODOLOGY FOR ASSESSMENT OF FOREST FIRE INDUCED HEALTH EFFECTS
 GUIDANCE ON METHODOLOGY FOR ASSESSMENT OF FOREST FIRE INDUCED HEALTH EFFECTS David M. Mannino Air Pollution and Respiratory Health Branch Division of Environmental Hazards and Health Effects National Center
GUIDANCE ON METHODOLOGY FOR ASSESSMENT OF FOREST FIRE INDUCED HEALTH EFFECTS David M. Mannino Air Pollution and Respiratory Health Branch Division of Environmental Hazards and Health Effects National Center
US power plant carbon standards and clean air and health co-benefits
 US power plant carbon standards and clean air and health co-benefits Emissions Modeling For each scenario, we used emissions output from ICF International s Integrated Planning Model (IPM) conducted by
US power plant carbon standards and clean air and health co-benefits Emissions Modeling For each scenario, we used emissions output from ICF International s Integrated Planning Model (IPM) conducted by
What are the Human Health Effects of Air Pollution?
 What are the Human Health Effects of Air Pollution? Dr. Judy Guernsey Department of Community Health and Epidemiology Dalhousie University Nova Scotia Department of Environment and Labour Outdoor Air Quality
What are the Human Health Effects of Air Pollution? Dr. Judy Guernsey Department of Community Health and Epidemiology Dalhousie University Nova Scotia Department of Environment and Labour Outdoor Air Quality
Insulin, Insulin Resistance, and Exposure to Ambient Particulate Matter Air Pollution
 Insulin, Insulin Resistance, and Exposure to Ambient Particulate Matter Air Pollution Archana P. Lamichhane, PhD Research Assistant Professor University of North Carolina, Chapel Hill WHI Investigator
Insulin, Insulin Resistance, and Exposure to Ambient Particulate Matter Air Pollution Archana P. Lamichhane, PhD Research Assistant Professor University of North Carolina, Chapel Hill WHI Investigator
Temporal variability and health effects of air pollutants in epidemiological shortterm
 Temporal variability and health effects of air pollutants in epidemiological shortterm studies Dr. Regina Pickford Beijing, 29.06.2016 Environmental Science Center, University of Augsburg, Augsburg, Germany
Temporal variability and health effects of air pollutants in epidemiological shortterm studies Dr. Regina Pickford Beijing, 29.06.2016 Environmental Science Center, University of Augsburg, Augsburg, Germany
Urban air pollution, and asthma and COPD hospital emergency room visits
 See Editorial, page 574 c Tables S1, S2 and S3, figs S1 and S2, and supplementary data are published online only at http://thorax.bmj.com/content/ vol63/issue7 1 Environmental Epidemiology Unit, National
See Editorial, page 574 c Tables S1, S2 and S3, figs S1 and S2, and supplementary data are published online only at http://thorax.bmj.com/content/ vol63/issue7 1 Environmental Epidemiology Unit, National
Traffic Air Pollution and Mortality Rate Advancement Periods
 American Journal of Epidemiology Copyright 2004 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 160, No. 2 Printed in U.S.A. DOI: 10.1093/aje/kwh181 Traffic Air Pollution
American Journal of Epidemiology Copyright 2004 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 160, No. 2 Printed in U.S.A. DOI: 10.1093/aje/kwh181 Traffic Air Pollution
Epidemiological studies on health effects of ambient fine and ultrafine particles
 Epidemiological studies on health effects of ambient fine and ultrafine particles Francesco Forastiere Department of Epidemiology, Rome E Health Authority, Rome, Italy Outline What are (urban air) ultrafines?
Epidemiological studies on health effects of ambient fine and ultrafine particles Francesco Forastiere Department of Epidemiology, Rome E Health Authority, Rome, Italy Outline What are (urban air) ultrafines?
The Framingham Coronary Heart Disease Risk Score
 Plasma Concentration of C-Reactive Protein and the Calculated Framingham Coronary Heart Disease Risk Score Michelle A. Albert, MD, MPH; Robert J. Glynn, PhD; Paul M Ridker, MD, MPH Background Although
Plasma Concentration of C-Reactive Protein and the Calculated Framingham Coronary Heart Disease Risk Score Michelle A. Albert, MD, MPH; Robert J. Glynn, PhD; Paul M Ridker, MD, MPH Background Although
Author s response to reviews
 Author s response to reviews Title: Short-term effects of ambient fine particulate matter pollution on hospital visits for chronic obstructive pulmonary disease in Beijing, China Authors: Yaohua Tian (yaohua_tian@bjmu.edu.com)
Author s response to reviews Title: Short-term effects of ambient fine particulate matter pollution on hospital visits for chronic obstructive pulmonary disease in Beijing, China Authors: Yaohua Tian (yaohua_tian@bjmu.edu.com)
I n the past decade, a number of epidemiological studies have
 RESEARCH REPORT Short-term effects of particulate air pollution on cardiovascular diseases in eight European cities A Le Tertre, S Medina, E Samoli, B Forsberg, P Michelozzi, A Boumghar, J M Vonk, A Bellini,
RESEARCH REPORT Short-term effects of particulate air pollution on cardiovascular diseases in eight European cities A Le Tertre, S Medina, E Samoli, B Forsberg, P Michelozzi, A Boumghar, J M Vonk, A Bellini,
Biomed Environ Sci, 2014; 27(11):
 Biomed Environ Sci, 2014; 27(11): 833-840 833 Original Article Association between Ambient Air Pollution and Outpatient Visits for Acute Bronchitis in a Chinese City * GUO Li Juan 1,2,6,, ZHAO Ang 3,,
Biomed Environ Sci, 2014; 27(11): 833-840 833 Original Article Association between Ambient Air Pollution and Outpatient Visits for Acute Bronchitis in a Chinese City * GUO Li Juan 1,2,6,, ZHAO Ang 3,,
Supplementary Online Content
 Supplementary Online Content Berhane K, Chang C-C, McConnell R, et al. Association of changes in air quality with bronchitic symptoms in children in California, 1993-2012. JAMA. doi:10.1001/jama.2016.3444
Supplementary Online Content Berhane K, Chang C-C, McConnell R, et al. Association of changes in air quality with bronchitic symptoms in children in California, 1993-2012. JAMA. doi:10.1001/jama.2016.3444
High concentrations of particulate air pollution have been
 ORIGINAL ARTICLE Who is Sensitive to the Effects of Particulate Air Pollution on Mortality? A Case-Crossover Analysis of Effect Modifiers Thomas F. Bateson * and Joel Schwartz * Background: Populations
ORIGINAL ARTICLE Who is Sensitive to the Effects of Particulate Air Pollution on Mortality? A Case-Crossover Analysis of Effect Modifiers Thomas F. Bateson * and Joel Schwartz * Background: Populations
THE ASSOCIATION BETWEEN AIR POLLUTIONS AND RESPIRATORY DISEASES : STUDY IN THAILAND
 THE ASSOCIATION BETWEEN AIR POLLUTIONS AND RESPIRATORY DISEASES : STUDY IN THAILAND Anongsin Danpaiboon 1 *, Phongtape Wiwatthadate 2, ChannarongChaisuwan 2,Warungarn Kosawang 3 and Petsawat Kankum 4 1
THE ASSOCIATION BETWEEN AIR POLLUTIONS AND RESPIRATORY DISEASES : STUDY IN THAILAND Anongsin Danpaiboon 1 *, Phongtape Wiwatthadate 2, ChannarongChaisuwan 2,Warungarn Kosawang 3 and Petsawat Kankum 4 1
Elderly humans exposed to concentrated air pollution particles have decreased heart rate variability
 Eur Respir J ; : Suppl. 4, 76s 8s DOI:.8/996..44 Printed in UK all rights reserved Copyright #ERS Journals Ltd European Respiratory Journal ISSN 94-85 Elderly humans exposed to concentrated air pollution
Eur Respir J ; : Suppl. 4, 76s 8s DOI:.8/996..44 Printed in UK all rights reserved Copyright #ERS Journals Ltd European Respiratory Journal ISSN 94-85 Elderly humans exposed to concentrated air pollution
Low birthweight and respiratory disease in adulthood: A population-based casecontrol
 Page 26 of 36 Online Data Supplement Low birthweight and respiratory disease in adulthood: A population-based casecontrol study Eric C. Walter, MD; William J. Ehlenbach, MD; David L. Hotchkin, MD, Jason
Page 26 of 36 Online Data Supplement Low birthweight and respiratory disease in adulthood: A population-based casecontrol study Eric C. Walter, MD; William J. Ehlenbach, MD; David L. Hotchkin, MD, Jason
T he short term effect of particulate air pollutants on the
 1of12 ELECTRONIC PAPER Particulate air pollution and panel studies in children: a systematic review D J Ward, J G Ayres... See end of article for authors affiliations... Correspondence to: Professor J
1of12 ELECTRONIC PAPER Particulate air pollution and panel studies in children: a systematic review D J Ward, J G Ayres... See end of article for authors affiliations... Correspondence to: Professor J
Lecture Outline. Biost 517 Applied Biostatistics I. Purpose of Descriptive Statistics. Purpose of Descriptive Statistics
 Biost 517 Applied Biostatistics I Scott S. Emerson, M.D., Ph.D. Professor of Biostatistics University of Washington Lecture 3: Overview of Descriptive Statistics October 3, 2005 Lecture Outline Purpose
Biost 517 Applied Biostatistics I Scott S. Emerson, M.D., Ph.D. Professor of Biostatistics University of Washington Lecture 3: Overview of Descriptive Statistics October 3, 2005 Lecture Outline Purpose
Acute evects of urban air pollution on respiratory health of children with and without chronic respiratory symptoms
 802 Environmental and Occupational Health Group, University of Wageningen, The Netherlands S C van der Zee G Hoek B Brunekreef Department of Epidemiology and Statistics, University of Groningen, The Netherlands
802 Environmental and Occupational Health Group, University of Wageningen, The Netherlands S C van der Zee G Hoek B Brunekreef Department of Epidemiology and Statistics, University of Groningen, The Netherlands
Both elevated blood pressure (BP) and ambient particle exposure
 Hypertension Ambient Pollution and Blood Pressure in Cardiac Rehabilitation Patients Antonella Zanobetti, PhD; Marina Jacobson Canner, MA; Peter H. Stone, MD; Joel Schwartz, PhD; David Sher, BA; Elizabeth
Hypertension Ambient Pollution and Blood Pressure in Cardiac Rehabilitation Patients Antonella Zanobetti, PhD; Marina Jacobson Canner, MA; Peter H. Stone, MD; Joel Schwartz, PhD; David Sher, BA; Elizabeth
IMPACT OF THE AMBIENT AIR PM2.5 ON CARDIOVASCULAR DISEASES OF ULAANBAATAR RESIDENTS
 Altangerel Enkhjargal 1*, Badrakhyn Burmaajav 2 1 Ach Medical University, Ulaanbaatar, Mongolia * Сorresponding author; e-mail: ajargal8@gmail.com 2 Mongolian Academia of Medical Sciences, Ulaanbaatar,
Altangerel Enkhjargal 1*, Badrakhyn Burmaajav 2 1 Ach Medical University, Ulaanbaatar, Mongolia * Сorresponding author; e-mail: ajargal8@gmail.com 2 Mongolian Academia of Medical Sciences, Ulaanbaatar,
Chronic kidney disease (CKD) has received
 Participant Follow-up in the Kidney Early Evaluation Program (KEEP) After Initial Detection Allan J. Collins, MD, FACP, 1,2 Suying Li, PhD, 1 Shu-Cheng Chen, MS, 1 and Joseph A. Vassalotti, MD 3,4 Background:
Participant Follow-up in the Kidney Early Evaluation Program (KEEP) After Initial Detection Allan J. Collins, MD, FACP, 1,2 Suying Li, PhD, 1 Shu-Cheng Chen, MS, 1 and Joseph A. Vassalotti, MD 3,4 Background:
New York State Department of Health Center for Environmental Health
 New York State Department of Health Center for Environmental Health March 2002 Evaluation of Asthma and Other Respiratory Hospital Admissions among Residents of ZIP Codes 14043 and 14227, Cheektowaga,
New York State Department of Health Center for Environmental Health March 2002 Evaluation of Asthma and Other Respiratory Hospital Admissions among Residents of ZIP Codes 14043 and 14227, Cheektowaga,
S hort term increases in concentrations of airborne
 718 ORIGINAL ARTICLE Short term effects of particulate matter on cause specific mortality: effects of lags and modification by city characteristics A Zeka, A Zanobetti, J Schwartz... See end of article
718 ORIGINAL ARTICLE Short term effects of particulate matter on cause specific mortality: effects of lags and modification by city characteristics A Zeka, A Zanobetti, J Schwartz... See end of article
Coronary Calcium Predicts Events Better With Absolute Calcium Scores Than Age-Sex-Race/Ethnicity Percentiles
 Journal of the American College of Cardiology Vol. 53, No. 4, 2009 2009 by the American College of Cardiology Foundation ISSN 0735-1097/09/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.07.072
Journal of the American College of Cardiology Vol. 53, No. 4, 2009 2009 by the American College of Cardiology Foundation ISSN 0735-1097/09/$36.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.07.072
Annette Peters. Research Needs for Aerosols and Health
 Research Needs for Aerosols and Health Annette Peters Helmholtz Zentrum München, Institute of Epidemiology, Neuherberg, Germany Harvard School of Public Health, Department of Environmental Health, Boston,
Research Needs for Aerosols and Health Annette Peters Helmholtz Zentrum München, Institute of Epidemiology, Neuherberg, Germany Harvard School of Public Health, Department of Environmental Health, Boston,
Air Pollution and Respiratory Symptoms: Results from Three Panel Studies in Bangkok, Thailand
 Air Pollution and Respiratory Symptoms: Results from Three Panel Studies in Bangkok, Thailand Nuntavarn Vichit-Vadakan, 1 Bart D. Ostro, 2 Lauraine G. Chestnut, 3 David M. Mills, 3 Wichai Aekplakorn, 1
Air Pollution and Respiratory Symptoms: Results from Three Panel Studies in Bangkok, Thailand Nuntavarn Vichit-Vadakan, 1 Bart D. Ostro, 2 Lauraine G. Chestnut, 3 David M. Mills, 3 Wichai Aekplakorn, 1
Comparison of fine particulate matter and ozone levels in zip code areas of New York City with different child asthma burdens
 Environmental Exposure and Health 23 Comparison of fine particulate matter and ozone levels in zip code areas of New York City with different child asthma burdens M. Solorzano 1, J. Stingone 2, A. R. Rentas
Environmental Exposure and Health 23 Comparison of fine particulate matter and ozone levels in zip code areas of New York City with different child asthma burdens M. Solorzano 1, J. Stingone 2, A. R. Rentas
The Effects of Air Pollution on Cardiovascular and Respiratory Causes of Emergency Admission
 107 Emergency (2014); 2 (3): 107-114 ORIGINAL RESEARCH The Effects of Air Pollution on Cardiovascular and Respiratory Causes of Emergency Admission Ali Mohammad Shahi 1, Ali Omraninava 1, Mitra Goli 2,
107 Emergency (2014); 2 (3): 107-114 ORIGINAL RESEARCH The Effects of Air Pollution on Cardiovascular and Respiratory Causes of Emergency Admission Ali Mohammad Shahi 1, Ali Omraninava 1, Mitra Goli 2,
Air Pollution and Hospital Admissions for Respiratory Disease in Certain Areas of Korea
 J Occup Health 2000; 42: 185 191 Journal of Occupational Health Air Pollution and Hospital Admissions for Respiratory Disease in Certain Areas of Korea Belong CHO 1, Jaewook CHOI 2 and Yong-Tae YUM 2 1
J Occup Health 2000; 42: 185 191 Journal of Occupational Health Air Pollution and Hospital Admissions for Respiratory Disease in Certain Areas of Korea Belong CHO 1, Jaewook CHOI 2 and Yong-Tae YUM 2 1
AN EVALUATION OF THE INDOOR/OUTDOOR AIR POLLUTION AND RESPIRATORY HEALTH OF FARMERS LIVING IN RURAL AREAS OF ANHUI PROVINCE, CHINA
 AN EVALUATION OF THE INDOOR/OUTDOOR AIR POLLUTION AND RESPIRATORY HEALTH OF FARMERS LIVING IN RURAL AREAS OF ANHUI PROVINCE, CHINA X-C Pan 1*, Z Dong 2, L Wang 3 and W Yue 1 1 Dept. of Occupational and
AN EVALUATION OF THE INDOOR/OUTDOOR AIR POLLUTION AND RESPIRATORY HEALTH OF FARMERS LIVING IN RURAL AREAS OF ANHUI PROVINCE, CHINA X-C Pan 1*, Z Dong 2, L Wang 3 and W Yue 1 1 Dept. of Occupational and
An Overview of Asthma - Diagnosis and Treatment
 An Overview of Asthma - Diagnosis and Treatment Definition of Asthma: Asthma is a common chronic disease of children and adults. Nationally, more than 1 in 14 Americans report having asthma and as many
An Overview of Asthma - Diagnosis and Treatment Definition of Asthma: Asthma is a common chronic disease of children and adults. Nationally, more than 1 in 14 Americans report having asthma and as many
Acute effects of air pollution on respiratory health of 50±70 yr old adults
 Eur Respir J 2000; 15: 700±709 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2000 European Respiratory Journal ISSN 0903-1936 Acute effects of air pollution on respiratory health of 50±70
Eur Respir J 2000; 15: 700±709 Printed in UK ± all rights reserved Copyright #ERS Journals Ltd 2000 European Respiratory Journal ISSN 0903-1936 Acute effects of air pollution on respiratory health of 50±70
Health Effects of Ambient Air Pollution
 Health Effects of Ambient Air Pollution Jennifer L. Peel, PhD, MPH jennifer.peel@colostate.edu Department of Environmental and Radiological Health Sciences Colorado State University Fort Collins, CO 5/18/2010
Health Effects of Ambient Air Pollution Jennifer L. Peel, PhD, MPH jennifer.peel@colostate.edu Department of Environmental and Radiological Health Sciences Colorado State University Fort Collins, CO 5/18/2010
STATE ENVIRONMENTAL HEALTH INDICATORS COLLABORATIVE (SEHIC) CLIMATE AND HEALTH INDICATORS
 STATE ENVIRONMENTAL HEALTH INDICATORS COLLABORATIVE (SEHIC) CLIMATE AND HEALTH INDICATORS Category: Indicator: Health Outcome Indicators Allergic Disease MEASURE DESCRIPTION Measure: Time scale: Measurement
STATE ENVIRONMENTAL HEALTH INDICATORS COLLABORATIVE (SEHIC) CLIMATE AND HEALTH INDICATORS Category: Indicator: Health Outcome Indicators Allergic Disease MEASURE DESCRIPTION Measure: Time scale: Measurement
Advanced IPD meta-analysis methods for observational studies
 Advanced IPD meta-analysis methods for observational studies Simon Thompson University of Cambridge, UK Part 4 IBC Victoria, July 2016 1 Outline of talk Usual measures of association (e.g. hazard ratios)
Advanced IPD meta-analysis methods for observational studies Simon Thompson University of Cambridge, UK Part 4 IBC Victoria, July 2016 1 Outline of talk Usual measures of association (e.g. hazard ratios)
Supplementary Online Content
 Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
Supplementary Online Content Regan EA, Lynch DA, Curran-Everett D, et al; Genetic Epidemiology of COPD (COPDGene) Investigators. Clinical and radiologic disease in smokers with normal spirometry. Published
Attitudes Toward Smoking Restrictions in Work Sites, Restaurants, and Bars Among North Carolinians. Abstract
 ORIGINAL ARTICLE Attitudes Toward Smoking Restrictions in Work Sites, Restaurants, and Bars Among North Carolinians Rachel Loflin Maguire, Jason Brinkley, Christopher Mansfield Abstract Background Public
ORIGINAL ARTICLE Attitudes Toward Smoking Restrictions in Work Sites, Restaurants, and Bars Among North Carolinians Rachel Loflin Maguire, Jason Brinkley, Christopher Mansfield Abstract Background Public
London, UK. Daily time series for cardiovascular hospital admissions and previous day's air pollution in. Lipfert.' The diagnosis of the cause of
 Occupational and Environmental Medicine 1997;54:535-540 Department of Public Health Sciences, St George's Hospital Medical School, London, UK J D Poloniecki R W Atkinson A P de Leon H R Anderson Correspondence
Occupational and Environmental Medicine 1997;54:535-540 Department of Public Health Sciences, St George's Hospital Medical School, London, UK J D Poloniecki R W Atkinson A P de Leon H R Anderson Correspondence
Tobacco Program Evaluation Group
 Tobacco Program Evaluation Group Smoking pollution in gaming venues before and after the Colorado Clean Indoor Air Act Prepared for the State Tobacco Education & Prevention Partnership, Colorado Department
Tobacco Program Evaluation Group Smoking pollution in gaming venues before and after the Colorado Clean Indoor Air Act Prepared for the State Tobacco Education & Prevention Partnership, Colorado Department
A Case-Crossover Study of Fine Particulate Matter Air Pollution and Onset of Congestive Heart Failure Symptom Exacerbation Leading to Hospitalization
 American Journal of Epidemiology Copyright ª 2006 by the Johns Hopkins Bloomberg School of Public Health All rights reserved; printed in U.S.A. Vol. 164, No. 5 DOI: 10.1093/aje/kwj206 Advance Access publication
American Journal of Epidemiology Copyright ª 2006 by the Johns Hopkins Bloomberg School of Public Health All rights reserved; printed in U.S.A. Vol. 164, No. 5 DOI: 10.1093/aje/kwj206 Advance Access publication
BASED ON SEVERAL SEVERE AIR
 ORIGINAL CONTRIBUTION Lung Cancer, Cardiopulmonary Mortality, and Long-term Exposure to Fine Particulate Air Pollution C. Arden Pope III, PhD Richard T. Burnett, PhD Michael J. Thun, MD Eugenia E. Calle,
ORIGINAL CONTRIBUTION Lung Cancer, Cardiopulmonary Mortality, and Long-term Exposure to Fine Particulate Air Pollution C. Arden Pope III, PhD Richard T. Burnett, PhD Michael J. Thun, MD Eugenia E. Calle,
Effects of Restaurant and Bar Smoking Regulations on Exposure to Environmental Tobacco Smoke Among Massachusetts Adults
 Effects of Restaurant and Bar Smoking Regulations on Exposure to Environmental Tobacco Smoke Among Massachusetts Adults Alison B. Albers, PhD, Michael Siegel, MD, MPH, Debbie M. Cheng, PhD, Nancy A. Rigotti,
Effects of Restaurant and Bar Smoking Regulations on Exposure to Environmental Tobacco Smoke Among Massachusetts Adults Alison B. Albers, PhD, Michael Siegel, MD, MPH, Debbie M. Cheng, PhD, Nancy A. Rigotti,
Air pollution and hospital admissions for respiratory conditions in Rome, Italy
 Eur Respir J 2001; 17: 1143 1150 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 Air pollution and hospital admissions for respiratory conditions
Eur Respir J 2001; 17: 1143 1150 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 Air pollution and hospital admissions for respiratory conditions
A comprehensive review of European epidemiological studies on particulate matter exposure and health
 A comprehensive review of European epidemiological studies on particulate matter exposure and health Prepared for CONCAWE s Special Task Force on Health Effects of Air Pollution (H/STF-27) by: E. Negri
A comprehensive review of European epidemiological studies on particulate matter exposure and health Prepared for CONCAWE s Special Task Force on Health Effects of Air Pollution (H/STF-27) by: E. Negri
Chapter 1: CKD in the General Population
 Chapter 1: CKD in the General Population Overall prevalence of CKD (Stages 1-5) in the U.S. adult general population was 14.8% in 2011-2014. CKD Stage 3 is the most prevalent (NHANES: Figure 1.2 and Table
Chapter 1: CKD in the General Population Overall prevalence of CKD (Stages 1-5) in the U.S. adult general population was 14.8% in 2011-2014. CKD Stage 3 is the most prevalent (NHANES: Figure 1.2 and Table
BIOSTATISTICAL METHODS
 BIOSTATISTICAL METHODS FOR TRANSLATIONAL & CLINICAL RESEARCH PROPENSITY SCORE Confounding Definition: A situation in which the effect or association between an exposure (a predictor or risk factor) and
BIOSTATISTICAL METHODS FOR TRANSLATIONAL & CLINICAL RESEARCH PROPENSITY SCORE Confounding Definition: A situation in which the effect or association between an exposure (a predictor or risk factor) and
Short-term Associations between Ambient Air Pollutants and Pediatric Asthma Emergency Department Visits
 Short-term Associations between Ambient Air Pollutants and Pediatric Asthma Emergency Department Visits Matthew J. Strickland 1, Lyndsey A. Darrow 1, Mitchel Klein 1, W. Dana Flanders 2, Jeremy A. Sarnat
Short-term Associations between Ambient Air Pollutants and Pediatric Asthma Emergency Department Visits Matthew J. Strickland 1, Lyndsey A. Darrow 1, Mitchel Klein 1, W. Dana Flanders 2, Jeremy A. Sarnat
Relation between Ambient Air Quality and Selected Birth Defects, Seven County Study, Texas,
 American Journal of Epidemiology Copyright ª 2005 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 162, No. 3 Printed in U.S.A. DOI: 10.1093/aje/kwi189 Relation between Ambient
American Journal of Epidemiology Copyright ª 2005 by the Johns Hopkins Bloomberg School of Public Health All rights reserved Vol. 162, No. 3 Printed in U.S.A. DOI: 10.1093/aje/kwi189 Relation between Ambient
Smoke gets in your lungs. Assoc Prof Peter Franklin University of Western Australia Environmental Health Directorate, EHD
 Smoke gets in your lungs Assoc Prof Peter Franklin University of Western Australia Environmental Health Directorate, EHD Conflict of Interest Conflict of Interest I have an open fireplace Wood smoke is
Smoke gets in your lungs Assoc Prof Peter Franklin University of Western Australia Environmental Health Directorate, EHD Conflict of Interest Conflict of Interest I have an open fireplace Wood smoke is
Ecologic Studies. Ecologic fallacy
 E R I C N O T E B O O K S E R I E S Second Edition Ecologic Studies Second Edition Authors: Lorraine K. Alexander, DrPH Brettania Lopes, MPH Kristen Ricchetti-Masterson, MSPH Karin B. Yeatts, PhD, MS Ecologic
E R I C N O T E B O O K S E R I E S Second Edition Ecologic Studies Second Edition Authors: Lorraine K. Alexander, DrPH Brettania Lopes, MPH Kristen Ricchetti-Masterson, MSPH Karin B. Yeatts, PhD, MS Ecologic
Human Evidence: Environment and Gestational Diabetes
 Human Evidence: Environment and Gestational Diabetes Candace A. Robledo, PhD, MPH Assistant Professor, Department of Behavioral & Community Health Director, MPH Maternal & Child Health Concentration candace.robledo@unthsc.edu
Human Evidence: Environment and Gestational Diabetes Candace A. Robledo, PhD, MPH Assistant Professor, Department of Behavioral & Community Health Director, MPH Maternal & Child Health Concentration candace.robledo@unthsc.edu
The Association of Air Pollution With the Patients Visits to the Department of Respiratory Diseases
 Elmer ress Original Article J Clin Med Res. 2015;7(7):551-555 The Association of Air Pollution With the Patients Visits to the Department of Respiratory Diseases Yanran Cai a, Yumeng Shao a, Chenggang
Elmer ress Original Article J Clin Med Res. 2015;7(7):551-555 The Association of Air Pollution With the Patients Visits to the Department of Respiratory Diseases Yanran Cai a, Yumeng Shao a, Chenggang
Patterns of adolescent smoking initiation rates by ethnicity and sex
 ii Tobacco Control Policies Project, UCSD School of Medicine, San Diego, California, USA C Anderson D M Burns Correspondence to: Dr DM Burns, Tobacco Control Policies Project, UCSD School of Medicine,
ii Tobacco Control Policies Project, UCSD School of Medicine, San Diego, California, USA C Anderson D M Burns Correspondence to: Dr DM Burns, Tobacco Control Policies Project, UCSD School of Medicine,
Air Pollution and Wheeze in the Fresno Asthmatic Children s Environment Study
 Air Pollution and Wheeze in the Fresno Asthmatic Children s Environment Study Jennifer Mann and the FACES Team Valley Air Conference June 9, Fresno, CA 1 Sponsors California Air Resources Board (2000-2005)
Air Pollution and Wheeze in the Fresno Asthmatic Children s Environment Study Jennifer Mann and the FACES Team Valley Air Conference June 9, Fresno, CA 1 Sponsors California Air Resources Board (2000-2005)
Fire Smoke and Human Health: How we share what we know
 Fire Smoke and Human Health: How we share what we know Dona Upson, MD Associate Professor, UNM, NMVAHCS Pulmonary, Critical Care & Sleep Medicine American Lung Association & American Thoracic Society Slides
Fire Smoke and Human Health: How we share what we know Dona Upson, MD Associate Professor, UNM, NMVAHCS Pulmonary, Critical Care & Sleep Medicine American Lung Association & American Thoracic Society Slides
N owadays, people cannot evade the global problem of
 350 ORIGINAL ARTICLE Long term effects of exposure to automobile exhaust on the pulmonary function of female adults in Tokyo, Japan K Sekine, M Shima, Y Nitta, M Adachi... See end of article for authors
350 ORIGINAL ARTICLE Long term effects of exposure to automobile exhaust on the pulmonary function of female adults in Tokyo, Japan K Sekine, M Shima, Y Nitta, M Adachi... See end of article for authors
Biases in clinical research. Seungho Ryu, MD, PhD Kanguk Samsung Hospital, Sungkyunkwan University
 Biases in clinical research Seungho Ryu, MD, PhD Kanguk Samsung Hospital, Sungkyunkwan University Learning objectives Describe the threats to causal inferences in clinical studies Understand the role of
Biases in clinical research Seungho Ryu, MD, PhD Kanguk Samsung Hospital, Sungkyunkwan University Learning objectives Describe the threats to causal inferences in clinical studies Understand the role of
Analytical Methods: the Kidney Early Evaluation Program (KEEP) The Kidney Early Evaluation program (KEEP) is a free, community based health
 Analytical Methods: the Kidney Early Evaluation Program (KEEP) 2000 2006 Database Design and Study Participants The Kidney Early Evaluation program (KEEP) is a free, community based health screening program
Analytical Methods: the Kidney Early Evaluation Program (KEEP) 2000 2006 Database Design and Study Participants The Kidney Early Evaluation program (KEEP) is a free, community based health screening program
Li Liu, Li-Ya Yu, Hui-Juan Mu, Li-Ying Xing, Yan-Xia Li, Guo-Wei Pan. Introduction
 Review Article Shape of concentration-response curves between long-term particulate matter exposure and morbidities of chronic bronchitis: a review of epidemiological evidence Li Liu, Li-Ya Yu, Hui-Juan
Review Article Shape of concentration-response curves between long-term particulate matter exposure and morbidities of chronic bronchitis: a review of epidemiological evidence Li Liu, Li-Ya Yu, Hui-Juan
85% of Tobacco Smoke is Invisible a confirmation of previous claims.
 85% of Tobacco Smoke is Invisible a confirmation of previous claims. Ivan L Gee 1, Sean Semple 2,3, Adrian Watson 4 and Andrea Crossfield 5. Author Affiliations: 1 Faculty of Health and Applied Social
85% of Tobacco Smoke is Invisible a confirmation of previous claims. Ivan L Gee 1, Sean Semple 2,3, Adrian Watson 4 and Andrea Crossfield 5. Author Affiliations: 1 Faculty of Health and Applied Social
EFFECT OF SMOKING ON BODY MASS INDEX: A COMMUNITY-BASED STUDY
 ORIGINAL ARTICLE. EFFECT OF SMOKING ON BODY MASS INDEX: A COMMUNITY-BASED STUDY Pragti Chhabra 1, Sunil K Chhabra 2 1 Professor, Department of Community Medicine, University College of Medical Sciences,
ORIGINAL ARTICLE. EFFECT OF SMOKING ON BODY MASS INDEX: A COMMUNITY-BASED STUDY Pragti Chhabra 1, Sunil K Chhabra 2 1 Professor, Department of Community Medicine, University College of Medical Sciences,
Diabetes Care Publish Ahead of Print, published online February 25, 2010
 Diabetes Care Publish Ahead of Print, published online February 25, 2010 Undertreatment Of Mental Health Problems In Diabetes Undertreatment Of Mental Health Problems In Adults With Diagnosed Diabetes
Diabetes Care Publish Ahead of Print, published online February 25, 2010 Undertreatment Of Mental Health Problems In Diabetes Undertreatment Of Mental Health Problems In Adults With Diagnosed Diabetes
Chicago Air Monitoring Study. Mark Travers, MS Andrew Hyland, PhD Department of Health Behavior Roswell Park Cancer Institute
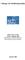 Chicago Air Monitoring Study Mark Travers, MS Andrew Hyland, PhD Department of Health Behavior Roswell Park Cancer Institute October 2005 Executive Summary Indoor air quality was assessed in 10 Chicago
Chicago Air Monitoring Study Mark Travers, MS Andrew Hyland, PhD Department of Health Behavior Roswell Park Cancer Institute October 2005 Executive Summary Indoor air quality was assessed in 10 Chicago
T here are a growing number of epidemiological studies
 515 ORIGINAL ARTICLE Occupational exposure to particulate air pollution and mortality due to ischaemic heart disease and cerebrovascular disease Kjell Torén, Ingvar A Bergdahl, Tohr Nilsson, Bengt Järvholm...
515 ORIGINAL ARTICLE Occupational exposure to particulate air pollution and mortality due to ischaemic heart disease and cerebrovascular disease Kjell Torén, Ingvar A Bergdahl, Tohr Nilsson, Bengt Järvholm...
