2016 Diabetes Practice Guidelines
|
|
|
- Blaze Pierce
- 5 years ago
- Views:
Transcription
1 2016 Diabetes Practice Guidelines SOURCE(S): 1. American Diabetes Association. Standards of Medical Care in Diabetes Diabetes Care January 2016 Volume 39, Supplement 1. Diagnosis Diabetes can be classified into the following general categories: 1. Type 1 diabetes (due to b-cell destruction, usually leading to absolute insulin deficiency) 2. Type 2 diabetes (due to a progressive insulin secretory defect on the background of insulin resistance) 3. Gestational diabetes mellitus (GDM) (diabetes diagnosed in the second or third trimester of pregnancy that is not clearly overt diabetes) 4. Specific types of diabetes due to other causes, e.g., monogenic diabetes syndromes (such as neonatal diabetes and maturity-onset diabetes of the young [MODY]), diseases of the exocrine pancreas (such as cystic fibrosis), and drug- or chemical-induced diabetes (such as in the treatment of HIV/AIDS or after organ transplantation) Diagnosis is determined by: Fasting Blood Glucose - A fasting blood glucose level of 126 mg/dl or higher ( Fasting is defined as no caloric intake for at least 8 hours.) Random Blood Glucose - A blood glucose level of 200 mg/dl or higher (on 1 or more retests) taken at any time of the day, along with symptoms of diabetes o Blood glucose rather than A1C should be used to diagnose acute onset of type 1 diabetes in individuals with symptoms of hyperglycemia Hemoglobin A1C levels greater than or equal to 6.5% indicate diabetes. Levels between % indicate pre-diabetes. In a patient with classic symptoms of diabetes including polyuria, polydipsia, and unexplained weight loss, a random plasma glucose greater than or equal to 200. Complete history and physical exam o A complete medical evaluation should be performed at the initial visit to: i. Classify diabetes ii. Detect diabetes complications iii. Review previous treatment and risk factor control in patients with established diabetes iv. Assist in formulating a management plan v. Provide a basis for continuing care Testing to detect type 2 diabetes and prediabetes in asymptomatic people should be considered in adults of any age who are overweight or obese (BMI 25 kg/m 2 ) and who have one or more additional risk factors for diabetes. In those without these risk factors, testing should begin at age 45. Approved at 3/20/15 HIQIC 1
2 Testing should be considered in all adults who are overweight (BMI 25 kg/m2*) and have additional risk factors: o Physical inactivity o First-degree relative with diabetes o High-risk race/ethnicity (e.g., African American, Latino, Native American, Asian American, Pacific Islander) o Women who delivered a baby weighing >9 lb or were diagnosed with GDM o Hypertension ( 140/90 mmhg or on therapy for hypertension) o HDL cholesterol level <35 mg/dl (0.90 mmol/l) and/or a triglyceride level >250 mg/dl (2.82 mmol/l) o Women with polycystic ovary syndrome o A1C 5.7%, IGT, or IFG on previous testing o Other clinical conditions associated with insulin resistance (e.g., severe obesity, acanthosis nigricans) o History of CVD In the absence of the above criteria, testing for diabetes should begin at age 45 years. Criteria for Testing for Type 2 diabetes in asymptomatic children and adolescents (age 18 and younger): o Overweight or obese (BMI >85th percentile for age and sex, weight for height >85th percentile, or weight >120% of ideal for height), plus any two of the following risk factors: Family history of type 2 diabetes in first- or second-degree relative Race/ethnicity (Native American, African American, Latino, Asian American, Pacific Islander) Signs of insulin resistance or conditions associated with insulin resistance (acanthosis nigricans, hypertension, dyslipidemia, polycystic ovary syndrome, or small-for-gestationalage birth weight) Maternal history of diabetes or GDM during the child s gestation Age of initiation: age 10 years or at onset of puberty, if puberty occurs at a younger age Frequency: every 3 years Maturity-onset diabetes of the young should be considered in individuals who have mild stable fasting hyperglycemia and multiple family members with diabetes not characteristic of type 1 or type 2 diabetes. o Consider referring individuals with diabetes not typical of type 1 or type 2 diabetes and occurring in successive generations (suggestive of an autosomal dominant pattern of inheritance) to a specialist for further evaluation. Labs: bun/creatinine, thyroid function tests, urine for microalbuminuria, ekg, cholesterol/ triglycerides/ldl Consider screening those with type 1 diabetes for autoimmune disorders (ie/ thyroid dysfunction, celiac disease) as appropriate. Consider assessing for and addressing common comorbid conditions (e.g., depression, obstructive sleep apnea) that may complicate diabetes management. 2
3 Gestational Diabetes: All pregnant women who are between 24 and 28 weeks of gestation should undergo a 75-gram 2-hour oral glucose tolerance test (OGTT). Blood should be drawn for glucose levels at baseline, at 1 hour, and at 2 hours. A woman only needs to have a single abnormal value to be diagnosed with gestational diabetes. o Perform OGTT in the morning after an overnight fast of at least 8 hours o Gestational Diabetes diagnosis: when any one of the following plasma glucose levels are exceeded: o Fasting >92mg/dL o 1 hour >180mg/dL o 2 hours >153mg/dL Screen women with gestational diabetes mellitus for persistent diabetes at 6 12 weeks postpartum, using the oral glucose tolerance test and clinically appropriate nonpregnancy diagnostic criteria. Women with a history of gestational diabetes should have lifelong screening for the development of diabetes or prediabetes at least every three years Women with a history of gestational diabetes who are found to have prediabetes should receive lifestyle interventions or Metformin to prevent diabetes. Screening for Cystic Fibrosis- Related Diabetes (CFRD) Annual screening for CFRD should begin at age 10 in all patients with cystic fibrosis, using glucose tolerance test (not A1C). Patients with CFRD should be treated with insulin to attain individualized glycemic goals. Beginning 5 years after the diagnosis of cystic fibrosis related diabetes, annual monitoring for complications of diabetes is recommended. Prevention or Delay of Type 2 Diabetes Patients with prediabetes should be referred to an intensive diet and physical activity behavioral counseling program targeting loss of 7% of body weight and increasing moderate intensity physical activity (such as brisk walking) to at least 150 minutes / week. Metformin therapy for prevention of Type 2 Diabetes may be considered in those with impaired glucose tolerance (IGT), especially for those with BMI greater than or equal to 35 kg/m, under 60 years of age, and women with prior gestational diabetes mellitus. Screening for and treatment of modifiable risk factors for cardiovascular disease is suggested. Diabetes and self-management education and support programs are appropriate venues for people with prediabetes to receive education and support to develop and maintain behaviors that can prevent or delay the onset of diabetes. 3
4 Treatment Medication Common drugs for treating type II diabetes o Metformin Metformin, if not contraindicated and if tolerated, is the preferred initial pharmacological agent for type 2 diabetes. It is more effective than other type 2 diabetes drugs in reducing blood sugar levels when used alone or in combination with other drugs. In addition, Metformin reduces body weight and improves cholesterol profiles. Metformin is associated with fewer side effects than Sulfonylureas. Some patients with kidney problems should not receive Metformin. If noninsulin monotherapy at maximum tolerated dose does not achieve or maintain the A1C target over 3 months, then add a second oral agent, a glucagon-like peptide 1 receptor agonist, or basal insulin. o Sulfonylurea(glimepiride, glyburide, and tolazamide o Glitazones(rosiglitazone or pioglitazone) o Exenatide (Byetta), pramlintide (Symlin), and liraglutide (Victoza), injectable o Repaglinide (Prandin) and nateglinide (Starlix) o Alpha-glucosidase inhibitors (such as acarbose) o Januvia and saxagliptin (Onglyza). (DPP-4 inhibitor blocker) - works in the pancreas and liver Insulin o Multiple types short acting vs long acting vs mixed o Treatment of choice for type I diabetes and also used for type II diabetes that cannot be well controlled with other medicines o Most individuals with type 1 diabetes should use insulin analogs to reduce hypoglycemia risk o Individuals who have been successfully using continuous subcutaneous insulin infusion should have continued access after they turn 65 years of age. Surgery Bariatric surgery may be considered for adults with BMI 35 kg/m 2 and type 2 diabetes, especially if the diabetes or associated comorbidities are difficult to control with lifestyle and pharmacological therapy. Medications for other risks and complications ACE inhibitors are recommended as: o First choice medicine for treating high blood pressure o Patients who have signs of kidney disease (e.g. microalbuminuria Angiotensin receptor blockers (ARB s) are used when ace inhibitors do not work or are not tolerated Antiplatelets agents o Daily low-dose aspirin is recommended for a majority of adults with diabetes o Clopidogrel (Plavix) may be used when aspirin cannot be given, or after certain cardiac 4
5 procedures or events Statins are generally the preferred lipid lowering drug o For persons with a high cardiovascular risk, the cardiovascular benefits of statin therapy outweigh the risk of side effects Other When choosing glucose-lowering medications for overweight or obese patients with type 2 diabetes, consider their effect on weight. Whenever possible, minimize the medications for comorbid conditions that are associated with weight gain. Chronic Care Model The Chronic Care Model has been shown to be an effective framework for improving the quality of diabetes care. This model includes six core elements for the provision of optimal care of patients with chronic disease. Care should be aligned with components of the Chronic Care Model to ensure productive interactions between a prepared proactive practice team and an informed activated patient. The six core elements include: 1. A delivery system that is more proactive and not reactive where planned visits are coordinated through a team based approach) 2. Self-management support 3. Decision support (basing care on evidence-based, effective care guidelines) 4. Clinical information systems (using registries that can provide patient specific and population-based support to the care team) 5. Community resources and policies (identifying or developing resources to support healthy lifestyles) 6. Health systems (to create a quality oriented culture) Food Insecurity Evaluate hyperglycemia and hypoglycemia in the context of food insecurity, evaluate and propose solutions Homelessness, poor literacy, and poor numeracy often occur with food insecurity, and appropriate resources should be researched and proposed Regular Tests/Exams for Management of Complications Patients should see the physician managing their diabetes every three months. At these visits, the following should occur: o Blood pressure check o Inspection of skin and bones on the feet and legs o Evaluation of sensation on the feet with a Semmes Weinstein filaments Hemoglobin A1C at least twice a year if under control, 4 times a year if not well controlled o Point-of-care testing for A1C provides the opportunity for more timely treatment changes 5
6 Cholesterol risk profile and annually o Lifestyle modification focusing on the reduction of saturated fat, trans fat, and cholesterol intake; increase of n-3 fatty acids, viscous fiber, and plant stanols/sterols; weight loss (if indicated); and increased physical activity should be recommended to improve the lipid profile in patients with diabetes. Retinopathy - annual dilated retinal exam needed Laser photocoagulation therapy is indicated to reduce the risk of vision loss in patients with high risk proliferative diabetic retinopathy (PDR), clinically significant macular edema, and some cases of severe non-proliferative diabetic retinopathy (NPDR). o The presence of retinopathy is not a contraindication to aspirin therapy for cardio-protection, as this therapy does not increase the risk of retinal hemorrhage Blood Pressure To reduce the risk or slow the progress of nephropathy and/or retinopathy, treat hypertension. Target readings for people with diabetes are: 140/90 for many with diabetes 130/80 for those who are younger, have kidney damage, or have heart, cerebrovascular or peripheral vascular disease Microalbuminuria annually to watch for progression to CKD and ESRD o Perform an annual test to assess urine albumin excretion in type 1 diabetic patients with diabetes duration of 5 years or more and in all type 2 diabetics starting at the time of diagnosis. o In the treatment of the non-pregnant patient with micro or macroalbuminuria, either ACE inhibitors or ARBs should be used. o Limited protein diet may improve renal function and is recommended for those with CKD Dental exam and cleaning every six months Foot care o All patients with diabetes should have an annual comprehensive foot examination to identify risk factors predictive of ulcers and amputations. The foot examination should include inspection, assessment of foot pulses, and testing for loss of protective sensation (LOPS) (10-g monofilament plus testing any one of the following: vibration using 128-Hz tuning fork, pinprick sensation, ankle reflexes, or vibration perception threshold). o o Foot ulcers and wound care may require care by a podiatrist, orthopedic or vascular surgeon, or rehabilitation specialist experienced in the management of individuals with diabetes. The risk of ulcers or amputations is increased in people who have the following risk factors: Previous amputation Past foot ulcer history Peripheral neuropathy Foot deformity Peripheral vascular disease Visual impairment Diabetic nephropathy (especially patients on dialysis) Poor glycemic control Cigarette smoking 6
7 Education People with diabetes should receive diabetes self-management education (DSME) and diabetes selfmanagement support (DSMS) when their diabetes is diagnosed and as needed thereafter. Effective selfmanagement and quality of life are the key outcomes of DSME and DSMS and should be measured and monitored as part of care. Diabetes education to help patients acquire the following self-management skills and understanding: Diet and exercise are key components of diabetes management. Potential risks and complications of diabetes. How to test and record blood glucose levels of home How to follow a diabetic diet: o Nutrition therapy is recommended for all people with type 1 and type 2 diabetes as an effective component of the overall treatment plan. o Individuals who have pre-diabetes or diabetes should receive individualized medical nutrition therapy (MNT) as needed to achieve treatment goals, preferably by a registered dietician familiar with the components of diabetes MNT. o Goals of Nutrition Therapy for Adults With Diabetes: 1) To promote and support healthful eating patterns, emphasizing a variety of nutrient-dense foods in appropriate portion sizes, in order to improve overall health and specifically to: Attain individualized glycemic, blood pressure, and lipid goals Achieve and maintain body weight goals Delay or prevent complications of diabetes 2) To address individual nutrition needs based on personal and cultural preferences, health literacy and numeracy, access to healthful food choices, willingness and ability to make behavioral changes, and barriers to change. 3) To maintain the pleasure of eating by providing positive messages about food choices while limiting food choices only when indicated by scientific evidence. 4) To provide the individual with diabetes with practical tools for day-to-day meal planning rather than focusing on individual macronutrients, micronutrients, or single foods. Importance of medication adherence and how to take medications, including insulin How to recognize and treat low and high blood sugar levels: o Treatment of hypoglycemia (plasma glucose <70 mg/dl) requires ingestion of glucose- or carbohydrate-containing foods. o Severe hypoglycemia (where the individual requires the assistance of another person and cannot be treated with oral carbohydrate due to confusion or unconsciousness) should be treated using emergency glucagon kits, which require a prescription. Those in close contact with, or having custodial care of, people with hypoglycemia-prone diabetes (family members, roommates, school personnel, child care providers, correctional institution staff, or coworkers) should be instructed in use of such kits. o Patients should understand situations that increase their risk of hypoglycemia, such as when 7
8 fasting for tests or procedures, during or after intense exercise, and during sleep and that increase the risk of harm to self or others from hypoglycemia, such as with driving. How to adjust insulin for exercise, illness, change in eating, or traveling o Hypoglycemia unawareness or one or more episodes of severe hypoglycemia should trigger reevaluation of the treatment regimen. o In individuals taking insulin and/or insulin secretagogues, physical activity can cause hypoglycemia if medication dose or carbohydrate consumption is not altered. For individuals on these therapies, added carbohydrate should be ingested if pre-exercise glucose levels are <100 mg/dl (5.6 mmol/l). o In the presence of proliferative diabetic retinopathy (PDR) or severe non-pdr (NPDR), vigorous aerobic or resistance exercise may be contraindicated because of the risk of triggering vitreous hemorrhage or retinal detachment How to inspect feet and choose proper footwear o Patients at risk should understand the implications of the loss of protective sensation, the importance of foot monitoring on a daily basis, the proper care of the foot, including nail and skin care, and the selection of appropriate footwear. Patients with visual difficulties, physical constraints preventing movement, or cognitive problems that impair their ability to assess the condition of the foot and to institute appropriate responses will need other people, such as family members, to assist in their o care. All individuals with peripheral neuropathy should wear proper footwear and examine their feet daily to detect lesions early. Anyone with a foot injury or open sore should be restricted to non weight-bearing activities. Importance of annual dilated retinal examination A patient-centered communication style that incorporates patient preferences, assesses literacy and numeracy, and addresses cultural barriers to care should be used. o Include assessment of the patient s psychological and social situation as an ongoing part of the medical management of diabetes Psychosocial screening and follow up may include, but are not limited to, attitudes about the illness, expectations for medical management and outcomes, affect/mood, general and diabetes-related quality of life, resources (financial, social, emotional) and psychiatric history. Routinely screen for psychosocial problems such as depression and diabetes-related distress, anxiety, eating disorders, and cognitive impairment. Older adults (ages 65 or older) with diabetes should be considered a high priority population for depression screening and treatment. Patients with comorbid diabetes and depression should receive a stepwise collaborative care approach for the management of depression. 8
9 Life Style Modifications Weight Reduction Maintain normal body weight (BMI x kg/m 2 ) For weight loss, either low-carbohydrate, low-fat calorie-restricted, or Mediterranean diets may be effective. Diet, physical activity, and behavioral therapy designed to achieve 5% weight loss should be prescribed for overweight and obese patients with type 2 diabetes ready to achieve weight loss Nutrition/Diet Saturated fat less than 7% of total calories trans fats intake should be minimized. Reduction of saturated fat, trans fat, and cholesterol intake, as well as increase of n-3 fatty acids, viscous fiber, and plant stanols/sterols is recommended to improve the lipid profile of patients with diabetes. Carbohydrate monitoring and counting skills Monitoring carbohydrate intake, whether by carbohydrate counting, choices, or experience-based estimation, remains a key strategy in achieving glycemic control. Minimize or eliminate alcohol People with type 1 diabetes should eat at about the same times each day and try to be consistent with the types of food they choose. Exercise Perform at least 150 minutes/week of moderate aerobic physical activity (50-70% of maximum heart rate), spread over at least 3 days per week with no more than 2 consecutive days without exercise. All individuals should be encouraged to limit the amount of time they spend being sedentary by breaking up extended amounts of time (.90 min) spent sitting. In the absence of contraindications, people with type 2 diabetes should be encouraged to perform resistance training at least twice per week. All people with diabetes should check with regular physician and eye doctor before starting an exercise program, as well as make sure they are using proper footwear. Children with diabetes or pre-diabetes should be encouraged to engage in at least 60 minutes of physical activity each day. Decrease other cardiovascular risk factors Stop smoking Note: E-cigarettes are not supported as an alternative to smoking or to facilitate smoking cessation. 9
10 Monitor for symptoms Self-monitoring of blood glucose (SMBG) levels daily Patients who are on insulin pump therapy or multiple insulin injections daily, should perform self-monitoring of blood glucose at least three times a day. Continuous glucose monitoring in conjunction with intensive insulin regimens can be a useful tool to lower A1C in adults at least 25 years of age with type 1 diabetes Insulin-treated patients with hypoglycemia unawareness or an episode of severe hypoglycemia should be advised to raise their glycemic targets to strictly avoid further hypoglycemia for at least several weeks, to partially reverse hypoglycemia unawareness, and to reduce risk of future episodes. When prescribing SMBG, ensure that patients receive ongoing instruction and regular evaluation of SMBG technique, SMBG results, and their ability to use SMBG data to adjust therapy. Check feet every day for sores/ulcers Take blood pressure on a regular basis Immunizations Annually provide an influenza vaccine to all patients with diabetes >6 months of age, if no contraindications are present. Administer pneumococcal polysaccharide vaccine 23 (PPSV23) to all patients with diabetes >2 years of age Adults >65 years of age, if not previously vaccinated, should receive pneumococcal conjugate vaccine 13 (PCV13), followed by PPSV months after initial vaccination. Adults >65 years of age, if previously vaccinated with PPSV23, should receive a follow-up after 12 months with PCV13. Administer hepatitis B vaccination to unvaccinated adults with diabetes who are aged years. Consider administering hepatitis B vaccination to unvaccinated adults with diabetes who are aged 60 years or older. Treatment Goals Effective self-management. Blood sugar should be between 80 and 130 mg per deciliter before meals for adult diabetics, and between 100 and 180 mg per deciliter at bed time for adult diabetics Blood pressure less than 140/90 LDL cholesterol target levels are now driven primarily by risk status rather than specific LDL cholesterol levels 10
11 Triglycerides less than 150 Hemoglobin A1C less than 7% Absence of diabetic foot ulcers Prevention of cardiovascular events Prevention or slowing of diabetic nephropathy, neuropathy, and retinopathy This guideline summary is not intended to replace a clinician s judgment or to establish a protocol for all patients with a particular condition. Some patients will not fit the conditions contemplated by a guideline; moreover, a guideline will rarely establish the only appropriate approach to a problem. The guideline is intended to assist clinicians by providing a framework, based on evidence-based research, for evaluation and treatment of certain medical conditions. 11
12 Previous Updates/References: 1. Standards of Medical Care in Diabetes Diabetes Care January Vol 38 no. supplement 1 S1-S Buse JB, Polonsky KS, Burant CF. Type 2 diabetes mellitus. In: Kronenberg HM, Melmed S, Polonsky KS, Larsen PR. Williams Textbook of Endocrinology. 12th ed. Philadelphia, PA: Saunders Elsevier; 2011:chap Eisenbarth GS, Buse JB. Type 1 diabetes mellitus. In: Kronenberg HM, Melmed S, Polonsky KS, Larsen PR. Williams Textbook of Endocrinology. 12th ed. Philadelphia, PA: Saunders Elsevier; 2011:chap American Diabetes Association. Diagnosis and classification of diabetes mellitus. Diabetes Care Jan;33 Suppl 1:S American Diabetes Association. Executive Summary: Standards of Medical Care in Diabetes Diabetes Care. January 2012 vol. 35 Suppl.I S4-S10. Accessed on September 28, 2012 from 6. American Diabetes Association. Standards of medical care in diabetes Diabetes Care Jan;33 Suppl 1:S American Diabetes Association. Standards of Medical Care in Diabetes Diabetes Care. January 2012 vol. 35:S11-S63. Accessed on September 28, 2012 from 8. American Diabetes Association. Standards of Medical Care in Diabetes Diabetes Care January 2013 vol. 36 no. Supplement 1 S11-S66 9. ADA. IX. Strategies for Improving Diabetes Care. Diabetes Care. 2011;34(suppl 1):S12, Buchwald H, Estok R, Fahrbach K, Banel D, Jensen MD, Pories WJ, Bantle JP, Sledge I. Weight and type 2 diabetes after bariatric surgery: systematic review and metaanalysis. Am J Med Mar;122(3): e In the clinic. Type 2 diabetes. Ann Intern Med. 2007;146:ITC
13 12. Lipsky BA, Berendt AR, Cornia PB, et al.; Infectious Diseases Society of America Infectious Diseases Society of America clinical practice guideline for the diagnosis and treatment of diabetic foot infections. Clin Infect Dis 2012;54:e132 e Oral Drug Treatment of Type 2 Diabetes Mellitus: A Clinical Practice Guideline from the American College of Physicians. Annals of Internal Medicine Feb;156(3):I-36. Accessed on September 28, 2012 from Oral Drug Treatment of Type 2 Diabetes Mellitus: A Clinical Practice Guideline from the American College of Physicians. Annals of Internal Medicine Feb;156(3):I-36. Accessed on September 28, 2012 from 13
Clinical Practice Guidelines for Diabetes Management
 Clinical Practice Guidelines for Diabetes Management Diabetes is a disease in which blood glucose levels are above normal. Over the years, high blood glucose damages nerves and blood vessels, which can
Clinical Practice Guidelines for Diabetes Management Diabetes is a disease in which blood glucose levels are above normal. Over the years, high blood glucose damages nerves and blood vessels, which can
Janice Lazear, DNP, FNP-C, CDE DIAGNOSIS AND CLASSIFICATION OF DIABETES
 Janice Lazear, DNP, FNP-C, CDE DIAGNOSIS AND CLASSIFICATION OF DIABETES Objectives u At conclusion of the lecture the participant will be able to: 1. Differentiate between the classifications of diabetes
Janice Lazear, DNP, FNP-C, CDE DIAGNOSIS AND CLASSIFICATION OF DIABETES Objectives u At conclusion of the lecture the participant will be able to: 1. Differentiate between the classifications of diabetes
Modified version focused on CCNC Quality Measures and Feedback Processes
 Executive Summary: Standards of Medical Care in Diabetes 2010 Modified version focused on CCNC Quality Measures and Feedback Processes See http://care.diabetesjournals.org/content/33/supplement_1/s11.full
Executive Summary: Standards of Medical Care in Diabetes 2010 Modified version focused on CCNC Quality Measures and Feedback Processes See http://care.diabetesjournals.org/content/33/supplement_1/s11.full
Standards of Medical Care In Diabetes
 Standards of Medical Care In Diabetes - 2017 Robert E. Ratner, MD, FACP, FACE Professor of Medicine Georgetown University School of Medicine Disclosed no conflict of interest Standards of Care Professional.diabetes.org/SOC
Standards of Medical Care In Diabetes - 2017 Robert E. Ratner, MD, FACP, FACE Professor of Medicine Georgetown University School of Medicine Disclosed no conflict of interest Standards of Care Professional.diabetes.org/SOC
DIABETES MEASURES GROUP OVERVIEW
 2014 PQRS OPTIONS F MEASURES GROUPS: DIABETES MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN DIABETES MEASURES GROUP: #1. Diabetes: Hemoglobin A1c Poor Control #2. Diabetes: Low Density Lipoprotein (LDL-C)
2014 PQRS OPTIONS F MEASURES GROUPS: DIABETES MEASURES GROUP OVERVIEW 2014 PQRS MEASURES IN DIABETES MEASURES GROUP: #1. Diabetes: Hemoglobin A1c Poor Control #2. Diabetes: Low Density Lipoprotein (LDL-C)
Executive Summary: Standards of Medical Care in Diabetes 2010
 E X E C U T I V E S U M M A R Y Executive Summary: Standards of Medical Care in Diabetes 2010 Current criteria for the diagnosis of diabetes A1C 6.5%: The test should be performed in a laboratory using
E X E C U T I V E S U M M A R Y Executive Summary: Standards of Medical Care in Diabetes 2010 Current criteria for the diagnosis of diabetes A1C 6.5%: The test should be performed in a laboratory using
American Diabetes Association: Standards of Medical Care in Diabetes 2015
 American Diabetes Association: Standards of Medical Care in Diabetes 2015 Synopsis of ADA standards relevant to the 11 th Scope of Work under Task B.2 ASSESSMENT OF GLYCEMIC CONTROL Recommendations: Perform
American Diabetes Association: Standards of Medical Care in Diabetes 2015 Synopsis of ADA standards relevant to the 11 th Scope of Work under Task B.2 ASSESSMENT OF GLYCEMIC CONTROL Recommendations: Perform
Standards of Medical Care in Diabetes 2016
 Standards of Medical Care in Diabetes 2016 Care Delivery Systems 33-49% of patients still do not meet targets for A1C, blood pressure, or lipids. 14% meet targets for all A1C, BP, lipids, and nonsmoking
Standards of Medical Care in Diabetes 2016 Care Delivery Systems 33-49% of patients still do not meet targets for A1C, blood pressure, or lipids. 14% meet targets for all A1C, BP, lipids, and nonsmoking
STATE OF THE STATE: TYPE II DIABETES
 STATE OF THE STATE: TYPE II DIABETES HENRY DRISCOLL, MD, CHIEF of ENDOCRINOLOGY MARSHALL U, CHERTOW DIABETES CENTER, HUNTINGTON VAMC HEATHER VENOY, RD, LD, CDE DIETITIAN, DIABETES EDUCATOR, CHERTOW DIABETES
STATE OF THE STATE: TYPE II DIABETES HENRY DRISCOLL, MD, CHIEF of ENDOCRINOLOGY MARSHALL U, CHERTOW DIABETES CENTER, HUNTINGTON VAMC HEATHER VENOY, RD, LD, CDE DIETITIAN, DIABETES EDUCATOR, CHERTOW DIABETES
Executive Summary: Standards of Medical Care in Diabetes 2009
 Executive Summary Executive Summary: Standards of Medical Care in Diabetes 2009 Current Criteria for the Diagnosis of Diabetes Fasting plasma glucose (FPG) 126 mg/dl (7.0 mmol/l). Fasting is defined as
Executive Summary Executive Summary: Standards of Medical Care in Diabetes 2009 Current Criteria for the Diagnosis of Diabetes Fasting plasma glucose (FPG) 126 mg/dl (7.0 mmol/l). Fasting is defined as
Adult Diabetes Clinician Guide NOVEMBER 2017
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Adult Diabetes Clinician Guide Introduction NOVEMBER 2017 This evidence-based guideline summary is based on the 2017 KP National Diabetes Guideline.
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Adult Diabetes Clinician Guide Introduction NOVEMBER 2017 This evidence-based guideline summary is based on the 2017 KP National Diabetes Guideline.
STANDARDS OF MEDICAL CARE IN DIABETES 2014
 STANDARDS OF MEDICAL CARE IN DIABETES 2014 I. CLASSIFICATION AND DIAGNOSIS Classification of Diabetes Type 1 diabetes β-cell destruction Type 2 diabetes Progressive insulin secretory defect Other specific
STANDARDS OF MEDICAL CARE IN DIABETES 2014 I. CLASSIFICATION AND DIAGNOSIS Classification of Diabetes Type 1 diabetes β-cell destruction Type 2 diabetes Progressive insulin secretory defect Other specific
Standards of Medical Care in Diabetes 2018
 Standards of Medical Care in Diabetes 2018 Eric L. Johnson, M.D. Associate Professor University of North Dakota School of Medicine and Health Sciences Assistant Medical Director Altru Diabetes Center Grand
Standards of Medical Care in Diabetes 2018 Eric L. Johnson, M.D. Associate Professor University of North Dakota School of Medicine and Health Sciences Assistant Medical Director Altru Diabetes Center Grand
Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone
 Index Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone Medication GAD glutamic acid decarboxylase GLP-1 glucagon-like peptide 1 NPH neutral
Index Abbreviations DPP-IV dipeptidyl peptidase IV DREAM Diabetes REduction Assessment with ramipril and rosiglitazone Medication GAD glutamic acid decarboxylase GLP-1 glucagon-like peptide 1 NPH neutral
V. N. Karazin Kharkiv National University Department of internal medicine Golubkina E.O., ass. of prof., Shanina I. V., ass. of prof.
 V. N. Karazin Kharkiv National University Department of internal medicine Golubkina E.O., ass. of prof., Shanina I. V., ass. of prof., Macharinskaya O.S., ass. of prof; Supervisor: prof. Yabluchanskiy
V. N. Karazin Kharkiv National University Department of internal medicine Golubkina E.O., ass. of prof., Shanina I. V., ass. of prof., Macharinskaya O.S., ass. of prof; Supervisor: prof. Yabluchanskiy
Standards of Care in Diabetes What's New? Veronica Brady, FNP-BC, PhD, BC-ADM,CDE Karmella Thomas, RD, LD,CDE
 Standards of Care in Diabetes 2016-- What's New? Veronica Brady, FNP-BC, PhD, BC-ADM,CDE Karmella Thomas, RD, LD,CDE Terminology No longer using the term diabetic. Diabetes does not define people. People
Standards of Care in Diabetes 2016-- What's New? Veronica Brady, FNP-BC, PhD, BC-ADM,CDE Karmella Thomas, RD, LD,CDE Terminology No longer using the term diabetic. Diabetes does not define people. People
Dr Aftab Ahmad Consultant Diabetologist at Royal Liverpool University Hospital Regional Diabetes Network Lead
 Dr Aftab Ahmad Consultant Diabetologist at Royal Liverpool University Hospital Regional Diabetes Network Lead Today s Presentation HbA1c & diagnosing Diabetes What is Impaired Glucose & IGR? Implications
Dr Aftab Ahmad Consultant Diabetologist at Royal Liverpool University Hospital Regional Diabetes Network Lead Today s Presentation HbA1c & diagnosing Diabetes What is Impaired Glucose & IGR? Implications
Diabetes Mellitus: Evaluation and Care Management
 Diabetes Mellitus: Evaluation and Care Management Michael King, MD Assistant Professor Residency Program Director University of Kentucky Dept. of Family & Community Medicine Learning Objectives 1. Review
Diabetes Mellitus: Evaluation and Care Management Michael King, MD Assistant Professor Residency Program Director University of Kentucky Dept. of Family & Community Medicine Learning Objectives 1. Review
What s New in the Standards of Medical Care in Diabetes? Dr. Jason Kruse, DO Broadlawns Medical Center
 What s New in the Standards of Medical Care in Diabetes? Dr. Jason Kruse, DO Broadlawns Medical Center Learning Objectives By the end of this presentation, participants should be able to: Discuss updates
What s New in the Standards of Medical Care in Diabetes? Dr. Jason Kruse, DO Broadlawns Medical Center Learning Objectives By the end of this presentation, participants should be able to: Discuss updates
Clinical Practice Guidelines
 Clinical Practice Guidelines Diabetes Objective The purpose is to guide the appropriate diagnosis and management of Diabetes. This guideline is designed to assist the clinician by providing a framework
Clinical Practice Guidelines Diabetes Objective The purpose is to guide the appropriate diagnosis and management of Diabetes. This guideline is designed to assist the clinician by providing a framework
Monthly WellPATH Spotlight November 2016: Diabetes
 Monthly WellPATH Spotlight November 2016: Diabetes DIABETES RISK FACTORS & SELF CARE TIPS Diabetes is a condition in which the body does not produce enough insulin or does not use the insulin produced
Monthly WellPATH Spotlight November 2016: Diabetes DIABETES RISK FACTORS & SELF CARE TIPS Diabetes is a condition in which the body does not produce enough insulin or does not use the insulin produced
Living Well with Diabetes
 Living Well with Diabetes What is diabetes? Diabetes Overview Diabetes is a disorder of the way the body uses food for growth and energy. Most of the food people eat is broken down into glucose, the form
Living Well with Diabetes What is diabetes? Diabetes Overview Diabetes is a disorder of the way the body uses food for growth and energy. Most of the food people eat is broken down into glucose, the form
Standards of Medical Care in Diabetes
 Standards of Medical Care in Diabetes - 2018 1. Improving Care and Promoting Health in Populations Diabetes and Population Health: Recommendations Ensure treatment decisions are timely, rely on evidence-based
Standards of Medical Care in Diabetes - 2018 1. Improving Care and Promoting Health in Populations Diabetes and Population Health: Recommendations Ensure treatment decisions are timely, rely on evidence-based
Vipul Lakhani, MD Oregon Medical Group Endocrinology
 Vipul Lakhani, MD Oregon Medical Group Endocrinology Disclosures None Objectives Be able to diagnose diabetes and assess control Be able to identify appropriate classes of medications for diabetes treatment
Vipul Lakhani, MD Oregon Medical Group Endocrinology Disclosures None Objectives Be able to diagnose diabetes and assess control Be able to identify appropriate classes of medications for diabetes treatment
Chapter 37: Exercise Prescription in Patients with Diabetes
 Chapter 37: Exercise Prescription in Patients with Diabetes American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise testing and prescription (6th ed.). New York:
Chapter 37: Exercise Prescription in Patients with Diabetes American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise testing and prescription (6th ed.). New York:
RCHC Clinical Guidelines Type 2 Diabetes; Adults
 RCHC Clinical Guidelines Type 2 Diabetes; Adults Screening for diabetes in asymptomatic adults 1 Population: Aged > 45 years; Aged < 45 years who are overweight (BMI> 25kg/m 2 ) and have an additional
RCHC Clinical Guidelines Type 2 Diabetes; Adults Screening for diabetes in asymptomatic adults 1 Population: Aged > 45 years; Aged < 45 years who are overweight (BMI> 25kg/m 2 ) and have an additional
The National Diabetes Prevention Program in Washington State March 2012
 The National Diabetes Prevention Program in Washington State March 2012 Session Objectives 1. Overview of pre-diabetes. 2. Describe the Diabetes Prevention Program (DPP). 3. Eligibility for the DPP. 4.
The National Diabetes Prevention Program in Washington State March 2012 Session Objectives 1. Overview of pre-diabetes. 2. Describe the Diabetes Prevention Program (DPP). 3. Eligibility for the DPP. 4.
Diabetes Summary of Medical Guidelines
 Diabetes Summary of Medical Guidelines Key concepts in setting glycemic controls: goals should be individualized; certain populations (children, pregnant women, and elderly) require special considerations;
Diabetes Summary of Medical Guidelines Key concepts in setting glycemic controls: goals should be individualized; certain populations (children, pregnant women, and elderly) require special considerations;
Diabetes Update: Diabetes Management In Primary Care. Jonathon M. Firnhaber, MD, FAAFP
 Diabetes Update: Diabetes Management In Primary Care Jonathon M. Firnhaber, MD, FAAFP Learning objectives 1. Critically evaluate the evidence emerging within diabetes research as it applies to recommendations
Diabetes Update: Diabetes Management In Primary Care Jonathon M. Firnhaber, MD, FAAFP Learning objectives 1. Critically evaluate the evidence emerging within diabetes research as it applies to recommendations
American Diabetes Association Standards of Medical Care in Diabetes 2017: Focus on Complications
 American Diabetes Association Standards of Medical Care in Diabetes 2017: Focus on Complications Juan Pablo Frias, M.D., FACE President and CEO, National Research Institute, Los Angeles, CA Clinical Faculty,
American Diabetes Association Standards of Medical Care in Diabetes 2017: Focus on Complications Juan Pablo Frias, M.D., FACE President and CEO, National Research Institute, Los Angeles, CA Clinical Faculty,
Diabetes Review Chris Paras, D.O. Assistant Prof of Medicine, NYIT & Touro COM Designated Institutional Official & Assoc. Clinical Dean, Brookdale
 Diabetes Review Chris Paras, D.O. Assistant Prof of Medicine, NYIT & Touro COM Designated Institutional Official & Assoc. Clinical Dean, Brookdale University Hospital Diabetes Care 2018 Jan; 41 Objectives
Diabetes Review Chris Paras, D.O. Assistant Prof of Medicine, NYIT & Touro COM Designated Institutional Official & Assoc. Clinical Dean, Brookdale University Hospital Diabetes Care 2018 Jan; 41 Objectives
RISK FACTORS OR COMPLICATIONS AND RECOMMENDED TREATMENT GOALS AND FREQUENCY OF EVALUATION FOR ADULTS WITH DIABETES
 RISK FACTORS OR COMPLICATIONS AND RECOMMENDED TREATMENT GOALS AND FREQUENCY OF EVALUATION FOR ADULTS WITH DIABETES Risk Factors or Complications Glycemic Control Fasting & Capillary Plasma Glucose Anti-platelet
RISK FACTORS OR COMPLICATIONS AND RECOMMENDED TREATMENT GOALS AND FREQUENCY OF EVALUATION FOR ADULTS WITH DIABETES Risk Factors or Complications Glycemic Control Fasting & Capillary Plasma Glucose Anti-platelet
Diabetes is a chronic illness that requires
 P O S I T I O N S T A T E M E N T Standards of Medical Care for Patients With Diabetes Mellitus AMERICAN DIABETES ASSOCIATION Diabetes is a chronic illness that requires continuing medical care and patient
P O S I T I O N S T A T E M E N T Standards of Medical Care for Patients With Diabetes Mellitus AMERICAN DIABETES ASSOCIATION Diabetes is a chronic illness that requires continuing medical care and patient
Diabetes is a chronic illness that
 Standards of Medical Care for Patients With Diabetes Mellitus Originally approved 1988. Most recent review/revision, October 2001 Abridged from Diabetes Care 25:213 229, 2002. Full text of this position
Standards of Medical Care for Patients With Diabetes Mellitus Originally approved 1988. Most recent review/revision, October 2001 Abridged from Diabetes Care 25:213 229, 2002. Full text of this position
Metabolic Syndrome. Shon Meek MD, PhD Mayo Clinic Florida Endocrinology
 Metabolic Syndrome Shon Meek MD, PhD Mayo Clinic Florida Endocrinology Disclosure No conflict of interest No financial disclosure Does This Patient Have Metabolic Syndrome? 1. Yes 2. No Does This Patient
Metabolic Syndrome Shon Meek MD, PhD Mayo Clinic Florida Endocrinology Disclosure No conflict of interest No financial disclosure Does This Patient Have Metabolic Syndrome? 1. Yes 2. No Does This Patient
Am I at Risk for Type 2 Diabetes?
 Am I at Risk for Type Diabetes? Taking Steps to Lower Your Risk of Getting Diabetes On this page: What is type diabetes? Can type diabetes be prevented? What are the signs and symptoms of type diabetes?
Am I at Risk for Type Diabetes? Taking Steps to Lower Your Risk of Getting Diabetes On this page: What is type diabetes? Can type diabetes be prevented? What are the signs and symptoms of type diabetes?
STANDARDS OF MEDICAL CARE IN DIABETES 2012
 STANDARDS OF MEDICAL CARE IN DIABETES 2012 Section Table of Contents ADA Evidence Grading System of Clinical Recommendations Slide No. I. Classification and Diagnosis 4-11 II. Testing for Diabetes in Asymptomatic
STANDARDS OF MEDICAL CARE IN DIABETES 2012 Section Table of Contents ADA Evidence Grading System of Clinical Recommendations Slide No. I. Classification and Diagnosis 4-11 II. Testing for Diabetes in Asymptomatic
Objectives. Objectives. Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015
 Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015 Presentation downloaded from http://ce.unthsc.edu Objectives Understand that the obesity epidemic is also affecting children and adolescents
Alejandro J. de la Torre, MD Cook Children s Hospital May 30, 2015 Presentation downloaded from http://ce.unthsc.edu Objectives Understand that the obesity epidemic is also affecting children and adolescents
Presenter Disclosure Information
 Prediabetes & Type 2 Diabetes Prevention Cari Ritter, PA-C Presenter Disclosure Information In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure
Prediabetes & Type 2 Diabetes Prevention Cari Ritter, PA-C Presenter Disclosure Information In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure
Guiding Principles. for Diabetes Care: For Health Care. Providers
 Guiding Principles N A T I O N A L for Diabetes Care: D I A B E T E S For Health Care E D U C A T I O N Providers P R O G R A M The National Diabetes Education Program (NDEP) has developed these Guiding
Guiding Principles N A T I O N A L for Diabetes Care: D I A B E T E S For Health Care E D U C A T I O N Providers P R O G R A M The National Diabetes Education Program (NDEP) has developed these Guiding
Diabetes Overview. Basics of Diabetes
 Diabetes Overview Basics of Diabetes Objectives Review the prevalence of diabetes, how it develops and the risk of developing diabetes Review diabetes diagnosis Identify the key areas of medically managing
Diabetes Overview Basics of Diabetes Objectives Review the prevalence of diabetes, how it develops and the risk of developing diabetes Review diabetes diagnosis Identify the key areas of medically managing
Screening for diabetes
 Screening for diabetes Peggy Odegard, Pharm.D, BCPS, CDE What are your risks? 1 Diabetes Mellitus A problem with glucose regulation type 1= pancreas cannot produce insulin so total insulin deficiency,
Screening for diabetes Peggy Odegard, Pharm.D, BCPS, CDE What are your risks? 1 Diabetes Mellitus A problem with glucose regulation type 1= pancreas cannot produce insulin so total insulin deficiency,
The American Diabetes
 Standards of Medical Care in Diabetes 2015 Abridged for Primary Care Providers American Diabetes Association This is an abridged version of the American Diabetes Association Position Statement: Standards
Standards of Medical Care in Diabetes 2015 Abridged for Primary Care Providers American Diabetes Association This is an abridged version of the American Diabetes Association Position Statement: Standards
Standards of Medical Care in Diabetes 2019 Abridged for Primary Care Providers
 Standards of Medical Care in Diabetes 2019 Abridged for Primary Care Providers American Diabetes Association This is an abridged version of the American Diabetes Association s Standards of Medical Care
Standards of Medical Care in Diabetes 2019 Abridged for Primary Care Providers American Diabetes Association This is an abridged version of the American Diabetes Association s Standards of Medical Care
Diabetes Updates. Disclosures
 Diabetes Updates Dr. Thanh D. Hoang, DO, FACP, FACE Walter Reed National Military Medical Center Associate Professor of Medicine Uniformed Services University of the Health Sciences March 2018 Disclosures
Diabetes Updates Dr. Thanh D. Hoang, DO, FACP, FACE Walter Reed National Military Medical Center Associate Professor of Medicine Uniformed Services University of the Health Sciences March 2018 Disclosures
Clinical Practice Guideline Key Points
 Clinical Practice Guideline Key Points Clinical Practice Guideline 2008 Key Points Diabetes Mellitus Provided by: Highmark Endocrinology Clinical Quality Improvement Committee In accordance with Highmark
Clinical Practice Guideline Key Points Clinical Practice Guideline 2008 Key Points Diabetes Mellitus Provided by: Highmark Endocrinology Clinical Quality Improvement Committee In accordance with Highmark
Pre-diabetes. Pharmacological Approaches to Delay Progression to Diabetes
 Pre-diabetes Pharmacological Approaches to Delay Progression to Diabetes Overview Definition of Pre-diabetes Risk Factors for Pre-diabetes Clinical practice guidelines for diabetes Management, including
Pre-diabetes Pharmacological Approaches to Delay Progression to Diabetes Overview Definition of Pre-diabetes Risk Factors for Pre-diabetes Clinical practice guidelines for diabetes Management, including
AUGUST 25-27, 2017 UPDATE & BOARD REVIEW. acofp INTENSIVE. Diabetes Review. Colleen Cagno, MD INNOVATIVE COMPREHENSIVE HANDS-ON
 acofp INTENSIVE UPDATE & BOARD REVIEW AUGUST 25-27, 2017 Loews Chicago O'Hare Hotel Rosemont, IL INNOVATIVE COMPREHENSIVE HANDS-ON Diabetes Review Colleen Cagno, MD acofp Am eric an College of Osteopathi
acofp INTENSIVE UPDATE & BOARD REVIEW AUGUST 25-27, 2017 Loews Chicago O'Hare Hotel Rosemont, IL INNOVATIVE COMPREHENSIVE HANDS-ON Diabetes Review Colleen Cagno, MD acofp Am eric an College of Osteopathi
In providing the best care for
 An Evaluation of the Current Type 2 Diabetes Guidelines: Where They Converge and Diverge Evelyn Tan, PharmD, Jennifer Polello, MPA, MCES, and Lisa J. Woodard, PharmD, MP In providing the best care for
An Evaluation of the Current Type 2 Diabetes Guidelines: Where They Converge and Diverge Evelyn Tan, PharmD, Jennifer Polello, MPA, MCES, and Lisa J. Woodard, PharmD, MP In providing the best care for
Multiple Small Feedings of the Mind: Diabetes. Sonja K Fredrickson, MD, BC-ADM March 7, 2014
 Multiple Small Feedings of the Mind: Diabetes Sonja K Fredrickson, MD, BC-ADM March 7, 2014 Question 1: Setting A1c Goals Describe the evidence based approach to determining the target HgbA1c in different
Multiple Small Feedings of the Mind: Diabetes Sonja K Fredrickson, MD, BC-ADM March 7, 2014 Question 1: Setting A1c Goals Describe the evidence based approach to determining the target HgbA1c in different
Standards of Medical Care for Patients With Diabetes Mellitus
 Standards of Medical Care for Patients With Diabetes Mellitus American Diabetes Association Originally approved 1988. Most recent review/revision, October 2002. Abridged from Diabetes Care 26 (Suppl. 1):S33
Standards of Medical Care for Patients With Diabetes Mellitus American Diabetes Association Originally approved 1988. Most recent review/revision, October 2002. Abridged from Diabetes Care 26 (Suppl. 1):S33
Personal Diabetes Passport
 Personal Diabetes Passport Contact information: Name: Physician: Diabetes Education Centre: Dietitian: Ophthalmologist: Chiropodist: Type of Diabetes: Type 1 (T1DM) Increased risk for diabetes Type 2(T2DM)
Personal Diabetes Passport Contact information: Name: Physician: Diabetes Education Centre: Dietitian: Ophthalmologist: Chiropodist: Type of Diabetes: Type 1 (T1DM) Increased risk for diabetes Type 2(T2DM)
Wayne Gravois, MD August 6, 2017
 Wayne Gravois, MD August 6, 2017 Americans with Diabetes (Millions) 40 30 Source: National Diabetes Statistics Report, 2011, 2017 Millions 20 10 0 1980 2009 2015 2007 - $174 Billion 2015 - $245 Billion
Wayne Gravois, MD August 6, 2017 Americans with Diabetes (Millions) 40 30 Source: National Diabetes Statistics Report, 2011, 2017 Millions 20 10 0 1980 2009 2015 2007 - $174 Billion 2015 - $245 Billion
Diabetes in Pregnancy
 Diabetes in Pregnancy Ebony Boyce Carter, MD, MPH Division of Maternal Fetal Medicine Washington University School of Medicine Disclosures I have no financial disclosures to report. Objectives Review the
Diabetes in Pregnancy Ebony Boyce Carter, MD, MPH Division of Maternal Fetal Medicine Washington University School of Medicine Disclosures I have no financial disclosures to report. Objectives Review the
Diabetes is a chronic illness that requires
 P O S I T I O N S T A T E M E N T Standards of Medical Care in Diabetes 2006 AMERICAN DIABETES ASSOCIATION CONTENTS I. CLASSIFICATION AND DIAGNOSIS, p. S4 A. Classification B. Diagnosis II. SCREENING FOR
P O S I T I O N S T A T E M E N T Standards of Medical Care in Diabetes 2006 AMERICAN DIABETES ASSOCIATION CONTENTS I. CLASSIFICATION AND DIAGNOSIS, p. S4 A. Classification B. Diagnosis II. SCREENING FOR
Common Diabetes-related Terms
 Common Diabetes-related Terms A1C An A1C test measures a person's average blood glucose level over two to three months. Hemoglobin is the part of a red blood cell that carries oxygen to the cells and sometimes
Common Diabetes-related Terms A1C An A1C test measures a person's average blood glucose level over two to three months. Hemoglobin is the part of a red blood cell that carries oxygen to the cells and sometimes
Diabetes Mellitus II CPG
 1 Diabetes Mellitus II CPG Candidates for Screening Integrated Complex Care Patients: Check Yearly Prediabetes: Check Yearly No Diabetes Mellitus (DM) Risk Factors: Check at Age 45, Repeat Every 3 Years
1 Diabetes Mellitus II CPG Candidates for Screening Integrated Complex Care Patients: Check Yearly Prediabetes: Check Yearly No Diabetes Mellitus (DM) Risk Factors: Check at Age 45, Repeat Every 3 Years
Objectives 10/11/2013. Diabetes- The Real Cost of Sugar. Diabetes 101: What is Diabetes. By Ruth Nekonchuk RD CDE LMNT
 Diabetes- The Real Cost of Sugar By Ruth Nekonchuk RD CDE LMNT Objectives To explain diabetes To explain the risks of diabetes To enumerate the cost of diabetes to our country To enumerate the cost of
Diabetes- The Real Cost of Sugar By Ruth Nekonchuk RD CDE LMNT Objectives To explain diabetes To explain the risks of diabetes To enumerate the cost of diabetes to our country To enumerate the cost of
Vishwanath Pattan Endocrinology Wyoming Medical Center
 Vishwanath Pattan Endocrinology Wyoming Medical Center Disclosure Holdings in Tandem Non for this Training Introduction In the United States, 5 to 6 percent of pregnancies almost 250,000 women are affected
Vishwanath Pattan Endocrinology Wyoming Medical Center Disclosure Holdings in Tandem Non for this Training Introduction In the United States, 5 to 6 percent of pregnancies almost 250,000 women are affected
Physical Activity/Exercise Prescription with Diabetes
 Physical Activity/Exercise Prescription with Diabetes B R AD H I NTERMEYER C E P A C SM S A NFORD H E ALTH C A RDIAC R E H AB A N D D I ABE TES E XE RCISE The adoption and maintenance of physical activity
Physical Activity/Exercise Prescription with Diabetes B R AD H I NTERMEYER C E P A C SM S A NFORD H E ALTH C A RDIAC R E H AB A N D D I ABE TES E XE RCISE The adoption and maintenance of physical activity
Am I at Risk for Type 2 Diabetes?
 NATIONAL DIABETES INFORMATION CLEARINGHOUSE Am I at Risk for Type 2 Diabetes? Taking Steps to Lower Your Risk of Getting Diabetes U.S. Department of Health and Human Services National Institutes of Health
NATIONAL DIABETES INFORMATION CLEARINGHOUSE Am I at Risk for Type 2 Diabetes? Taking Steps to Lower Your Risk of Getting Diabetes U.S. Department of Health and Human Services National Institutes of Health
Guideline for Management of Type 2 Diabetes Mellitus: Kingdome of Bahrain Ministry of Health 2016
 Guideline for Management of Type 2 Diabetes Mellitus: Kingdome of Bahrain Ministry of Health 2016 1. Screening and diagnosis: Detection type 2 Diabetes are usually based on a two-step approach: Step 1:
Guideline for Management of Type 2 Diabetes Mellitus: Kingdome of Bahrain Ministry of Health 2016 1. Screening and diagnosis: Detection type 2 Diabetes are usually based on a two-step approach: Step 1:
Joslin Diabetes Center Joslin Diabetes Forum 2013: The Impact of Comorbidities on Glucose Control Scenario 2: Reduced Renal Function
 Scenario 2: Reduced Renal Function 62 y.o. white man with type 2 diabetes for 18 years Hypertension and hypercholesterolemia Known proliferative retinopathy Current medications: Metformin 1000 mg bid Glyburide
Scenario 2: Reduced Renal Function 62 y.o. white man with type 2 diabetes for 18 years Hypertension and hypercholesterolemia Known proliferative retinopathy Current medications: Metformin 1000 mg bid Glyburide
Exercise and Type 1 Diabetes
 Exercise and Type 1 Diabetes QuickTime and a decompressor are needed to see this picture. 1 Characteristics of Type 1 & Type 2 Diabetes Mellitus ACE Mtng 2011 Rate of New Cases of Type 1 & Type 2 Diabetes
Exercise and Type 1 Diabetes QuickTime and a decompressor are needed to see this picture. 1 Characteristics of Type 1 & Type 2 Diabetes Mellitus ACE Mtng 2011 Rate of New Cases of Type 1 & Type 2 Diabetes
Diabetes 2013: Achieving Goals Through Comprehensive Treatment. Session 2: Individualizing Therapy
 Diabetes 2013: Achieving Goals Through Comprehensive Treatment Session 2: Individualizing Therapy Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism
Diabetes 2013: Achieving Goals Through Comprehensive Treatment Session 2: Individualizing Therapy Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism
Prediabetes 101. What is it and what can I do about it? Intermountainhealthcare.org/diabetes
 Prediabetes 101 What is it and what can I do about it? Patient Education Intermountainhealthcare.org/diabetes What do you already know about prediabetes? Fact or Fiction? There are often no symptoms of
Prediabetes 101 What is it and what can I do about it? Patient Education Intermountainhealthcare.org/diabetes What do you already know about prediabetes? Fact or Fiction? There are often no symptoms of
Diabetes and the Heart
 Diabetes and the Heart Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 6, 2012 Outline Screening for diabetes in patients with CAD Screening for CAD in patients with
Diabetes and the Heart Jeffrey Boord, MD, MPH Advances in Cardiovascular Medicine Kingston, Jamaica December 6, 2012 Outline Screening for diabetes in patients with CAD Screening for CAD in patients with
Donna Tomky, MSN, C-ANP, CDE, FAADE Albuquerque, New Mexico
 Donna Tomky, MSN, C-ANP, CDE, FAADE Albuquerque, New Mexico Presented in Collaboration with New Mexico Health Care Takes On Diabetes Discuss the burden and challenges prediabetes presents in New Mexico.
Donna Tomky, MSN, C-ANP, CDE, FAADE Albuquerque, New Mexico Presented in Collaboration with New Mexico Health Care Takes On Diabetes Discuss the burden and challenges prediabetes presents in New Mexico.
DIABETES. A growing problem
 DIABETES A growing problem Countries still grappling with infectious diseases such as tuberculosis, HIV/AIDS and malaria now face a double burden of disease Major social and economic change has brought
DIABETES A growing problem Countries still grappling with infectious diseases such as tuberculosis, HIV/AIDS and malaria now face a double burden of disease Major social and economic change has brought
Management of Pregestational and Gestational Diabetes Mellitus
 Background and Prevalence Management of Pregestational and Gestational Diabetes Mellitus Pregestational Diabetes - 8 million women in the US are affected, complicating 1% of all pregnancies. Type II is
Background and Prevalence Management of Pregestational and Gestational Diabetes Mellitus Pregestational Diabetes - 8 million women in the US are affected, complicating 1% of all pregnancies. Type II is
Treating Patients with PRE- DIABETES David Doriguzzi, PA-C First Valley Medical Group. Learning Objectives. Background
 Treating Patients with PRE- DIABETES David Doriguzzi, PA-C First Valley Medical Group Learning Objectives To accurately make the diagnosis of pre-diabetes/metabolic syndrome To understand the prevalence
Treating Patients with PRE- DIABETES David Doriguzzi, PA-C First Valley Medical Group Learning Objectives To accurately make the diagnosis of pre-diabetes/metabolic syndrome To understand the prevalence
Diabetes Mellitus Type 2
 Diabetes Mellitus Type 2 What is it? Diabetes is a common health problem in the U.S. and the world. In diabetes, the body does not use the food it digests well. It is hard for the body to use carbohydrates
Diabetes Mellitus Type 2 What is it? Diabetes is a common health problem in the U.S. and the world. In diabetes, the body does not use the food it digests well. It is hard for the body to use carbohydrates
Diabetes Mellitus: A Cardiovascular Disease
 Diabetes Mellitus: A Cardiovascular Disease Nestoras Mathioudakis, M.D. Assistant Professor of Medicine Division of Endocrinology, Diabetes, & Metabolism September 30, 2013 1 The ABCs of cardiovascular
Diabetes Mellitus: A Cardiovascular Disease Nestoras Mathioudakis, M.D. Assistant Professor of Medicine Division of Endocrinology, Diabetes, & Metabolism September 30, 2013 1 The ABCs of cardiovascular
Diabetes School October 2016
 Diabetes School October 2016 Name Change- Why? Shorter Has my name in it Emphasizes a major part of the practice Still see non-research patients Novo Nordisk Lilly sanofi aventis! Thank You to our LucasResearch
Diabetes School October 2016 Name Change- Why? Shorter Has my name in it Emphasizes a major part of the practice Still see non-research patients Novo Nordisk Lilly sanofi aventis! Thank You to our LucasResearch
The American Diabetes
 Standards of Medical Care in Diabetes 2016 Abridged for Primary Care Providers American Diabetes Association This is an abridged version of the American Diabetes Association Position Statement: Standards
Standards of Medical Care in Diabetes 2016 Abridged for Primary Care Providers American Diabetes Association This is an abridged version of the American Diabetes Association Position Statement: Standards
Understanding the Diabetes Care Process Pfizer Medical Affairs
 Understanding the Diabetes Care Process Pfizer Medical Affairs Overview of Diabetes 1 Diabetes is a group of metabolic diseases characterized by hyperglycemia resulting from defects in insulin secretion,
Understanding the Diabetes Care Process Pfizer Medical Affairs Overview of Diabetes 1 Diabetes is a group of metabolic diseases characterized by hyperglycemia resulting from defects in insulin secretion,
Type 2 Diabetes Mellitus 2011
 2011 Michael T. McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetes Mellitus Diagnosis 2011 Diabetes Mellitus Fasting Glucose
2011 Michael T. McDermott MD Director, Endocrinology and Diabetes Practice University of Colorado Hospital Michael.mcdermott@ucdenver.edu Diabetes Mellitus Diagnosis 2011 Diabetes Mellitus Fasting Glucose
Update on Diabetes Standards-What Community Physicians Should Know. Kevin Miller D.O.
 Update on Diabetes Standards-What Community Physicians Should Know. Kevin Miller D.O. Know The ABC Targets A1C BP LDL Cholesterol AACE Recommendations for A1C Testing A1C levels may be misleading in several
Update on Diabetes Standards-What Community Physicians Should Know. Kevin Miller D.O. Know The ABC Targets A1C BP LDL Cholesterol AACE Recommendations for A1C Testing A1C levels may be misleading in several
American Diabetes Association Standards of Medical Care in Diabetes 2018: Latest Updates
 American Diabetes Association Standards of Medical Care in Diabetes 2018: Latest Updates Juan Pablo Frias, MD President and CEO, National Research Institute, Los Angeles, CA Clinical Faculty, University
American Diabetes Association Standards of Medical Care in Diabetes 2018: Latest Updates Juan Pablo Frias, MD President and CEO, National Research Institute, Los Angeles, CA Clinical Faculty, University
Diabetes and Hypertension
 Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
Diabetes and Hypertension M.Nakhjvani,M.D Tehran University of Medical Sciences 20-8-96 Hypertension Common DM comorbidity Prevalence depends on diabetes type, age, BMI, ethnicity Major risk factor for
Diagnosis of Diabetes
 Diagnosis of Diabetes National Diabetes Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is diabetes? Diabetes is a disease in which levels of blood
Diagnosis of Diabetes National Diabetes Information Clearinghouse U.S. Department of Health and Human Services NATIONAL INSTITUTES OF HEALTH What is diabetes? Diabetes is a disease in which levels of blood
Individualizing Type 2 Diabetes Management. Cynthia Gerstenlauer, ANP-BC, GCNS-BC, CDE, CCD
 Individualizing Type 2 Diabetes Management Cynthia Gerstenlauer, ANP-BC, GCNS-BC, CDE, CCD Harsh Statistics 30.3 million (9.4% of population) in US had DM in 2015 The percent of population with DM increases
Individualizing Type 2 Diabetes Management Cynthia Gerstenlauer, ANP-BC, GCNS-BC, CDE, CCD Harsh Statistics 30.3 million (9.4% of population) in US had DM in 2015 The percent of population with DM increases
Diabetes Mellitus (DM) - Dr Hiren Patt
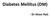 Diabetes Mellitus (DM) - Dr Hiren Patt What is DM? FPG 2-Hour PG on OGTT Diabetes Mellitus Diabetes Mellitus 126 mg/dl 100 mg/dl Impaired Fasting Glucose 200 mg/dl 140 mg/dl Impaired Glucose Tolerance
Diabetes Mellitus (DM) - Dr Hiren Patt What is DM? FPG 2-Hour PG on OGTT Diabetes Mellitus Diabetes Mellitus 126 mg/dl 100 mg/dl Impaired Fasting Glucose 200 mg/dl 140 mg/dl Impaired Glucose Tolerance
Rick Fox M.A Health and Wellness Specialist
 Metabolic Diseases Rick Fox M.A Health and Wellness Specialist Metabolic Diseases Metabolism is the process your body uses to get or make energy from the food you eat. Food is made up of proteins, carbohydrates
Metabolic Diseases Rick Fox M.A Health and Wellness Specialist Metabolic Diseases Metabolism is the process your body uses to get or make energy from the food you eat. Food is made up of proteins, carbohydrates
NEW SA DIABETES GUIDELINES
 Earn 3 CPD Points online 2017 SEMDSA diabetes management guidelines The updated 2017 South African guidelines for the management of type 2 diabetes mellitus were launched on 5 May at the 52 nd congress
Earn 3 CPD Points online 2017 SEMDSA diabetes management guidelines The updated 2017 South African guidelines for the management of type 2 diabetes mellitus were launched on 5 May at the 52 nd congress
Section 1: 1: Trends. Section 2: 2: Comparisons to to Overall Portland Area Area Results for for
 Section 1: 1: Trends 1 Patients in the Diabetes Register 2 Gender of Patients with Diabetes 2 Age of Patients with Diabetes 3 Diabetes Type 3 Duration of Diabetes 4 Weight Control 5 Hemoglobin A1c 6 Blood
Section 1: 1: Trends 1 Patients in the Diabetes Register 2 Gender of Patients with Diabetes 2 Age of Patients with Diabetes 3 Diabetes Type 3 Duration of Diabetes 4 Weight Control 5 Hemoglobin A1c 6 Blood
Diabetes is usually a lifelong (chronic) disease in which there are high levels of sugar in the blood.
 1 of 15 12/30/2012 10:52 PM PubMed Health. A service of the National Library of Medicine, National Institutes of Health. A.D.A.M. Medical Encyclopedia. Atlanta (GA): A.D.A.M.; 2011. Diabetes Last reviewed:
1 of 15 12/30/2012 10:52 PM PubMed Health. A service of the National Library of Medicine, National Institutes of Health. A.D.A.M. Medical Encyclopedia. Atlanta (GA): A.D.A.M.; 2011. Diabetes Last reviewed:
UPDATED APRIL 26, 2018 This slide deck contains content created, reviewed, and approved by the American Diabetes Association. You are free to use the
 UPDATED APRIL 26, 2018 This slide deck contains content created, reviewed, and approved by the American Diabetes Association. You are free to use the slides in presentations without further permission
UPDATED APRIL 26, 2018 This slide deck contains content created, reviewed, and approved by the American Diabetes Association. You are free to use the slides in presentations without further permission
Diabetes for CNAs. This course has been awarded two (2.0) contact hours. This course expires on August 31, 2017.
 Diabetes for CNAs This course has been awarded two (2.0) contact hours. This course expires on August 31, 2017. Copyright 2005 by RN.com. All Rights Reserved. Reproduction and distribution of these materials
Diabetes for CNAs This course has been awarded two (2.0) contact hours. This course expires on August 31, 2017. Copyright 2005 by RN.com. All Rights Reserved. Reproduction and distribution of these materials
Application of the Diabetes Algorithm to a Patient
 Application of the Diabetes Algorithm to a Patient Apply knowledge gained from this activity to improve disease management and outcomes for patients with T2DM and obesity Note: The cases in this deck represent
Application of the Diabetes Algorithm to a Patient Apply knowledge gained from this activity to improve disease management and outcomes for patients with T2DM and obesity Note: The cases in this deck represent
Quick Reference Guide
 2013 Clinical Practice Guidelines Quick Reference Guide (Updated November 2016) 416569-16 guidelines.diabetes.ca diabetes.ca 1-800-BANTING (226-8464) Copyright 2016 Canadian Diabetes Association SCREENING
2013 Clinical Practice Guidelines Quick Reference Guide (Updated November 2016) 416569-16 guidelines.diabetes.ca diabetes.ca 1-800-BANTING (226-8464) Copyright 2016 Canadian Diabetes Association SCREENING
Addressing Addressing Challenges in Type 2 Challenges in Type 2 Diabetes Diabetes Speaker:
 Addressing Challenges in Type 2 Diabetes Geneva Briggs, PharmD,, BCPS Addressing Challenges in Type 2 Diabetes Speaker: Dr. Geneva Clark Briggs, a board-certified Pharmacotherapy Specialist, received her
Addressing Challenges in Type 2 Diabetes Geneva Briggs, PharmD,, BCPS Addressing Challenges in Type 2 Diabetes Speaker: Dr. Geneva Clark Briggs, a board-certified Pharmacotherapy Specialist, received her
2018 Standard of Medical Care Diabetes and Pregnancy
 2018 Standard of Medical Care Diabetes and Pregnancy 2018 Standard of Medical Care Diabetes and Pregnancy Marjorie Cypress does not have any relevant financial relationships with any commercial interests
2018 Standard of Medical Care Diabetes and Pregnancy 2018 Standard of Medical Care Diabetes and Pregnancy Marjorie Cypress does not have any relevant financial relationships with any commercial interests
PREDIABETES TESTING SERVICES
 PREDIABETES TESTING SERVICES ASSESSING DIABETES RISK IN ASYMPTOMATIC ADULTS Depending upon population characteristics, up to 70% of individuals with prediabetes will ultimately progress to diabetes at
PREDIABETES TESTING SERVICES ASSESSING DIABETES RISK IN ASYMPTOMATIC ADULTS Depending upon population characteristics, up to 70% of individuals with prediabetes will ultimately progress to diabetes at
第十五章. Diabetes Mellitus
 Diabetes-1/9 第十五章 Diabetes Mellitus 陳曉蓮醫師 2/9 - Diabetes 羅東博愛醫院 Management of Diabetes mellitus A. DEFINITION OF DIABETES MELLITUS Diabetes Mellitus is characterized by chronic hyperglycemia with disturbances
Diabetes-1/9 第十五章 Diabetes Mellitus 陳曉蓮醫師 2/9 - Diabetes 羅東博愛醫院 Management of Diabetes mellitus A. DEFINITION OF DIABETES MELLITUS Diabetes Mellitus is characterized by chronic hyperglycemia with disturbances
associated with serious complications, but reduce occurrences with preventive measures
 Wk 9. Management of Clients with Diabetes Mellitus 1. Diabetes Mellitus body s inability to metabolize carbohydrates, fats, proteins hyperglycemia associated with serious complications, but reduce occurrences
Wk 9. Management of Clients with Diabetes Mellitus 1. Diabetes Mellitus body s inability to metabolize carbohydrates, fats, proteins hyperglycemia associated with serious complications, but reduce occurrences
Harmonizing the ADA, AACE and other Guidelines in the Treatment of the Patient with Diabetes Mellitus. Angel L Comulada, MD, FACE Endocrinologist
 Harmonizing the ADA, AACE and other Guidelines in the Treatment of the Patient with Diabetes Mellitus Angel L Comulada, MD, FACE Endocrinologist 2 Disclosure Angel L Comulada, MD, FACE, CCD Has received
Harmonizing the ADA, AACE and other Guidelines in the Treatment of the Patient with Diabetes Mellitus Angel L Comulada, MD, FACE Endocrinologist 2 Disclosure Angel L Comulada, MD, FACE, CCD Has received
Primary and Secondary Prevention of Cardiovascular Disease. Frank J. Green, M.D., F.A.C.C. St. Vincent Medical Group
 Primary and Secondary Prevention of Cardiovascular Disease Frank J. Green, M.D., F.A.C.C. St. Vincent Medical Group AHA Diet and Lifestyle Recommendations Balance calorie intake and physical activity to
Primary and Secondary Prevention of Cardiovascular Disease Frank J. Green, M.D., F.A.C.C. St. Vincent Medical Group AHA Diet and Lifestyle Recommendations Balance calorie intake and physical activity to
Type 1 Diabetes-Pathophysiology, Diagnosis, and Long-Term Complications. Alejandro J de la Torre Pediatric Endocrinology 10/17/2014
 Type 1 Diabetes-Pathophysiology, Diagnosis, and Long-Term Complications Alejandro J de la Torre Pediatric Endocrinology 10/17/2014 Objectives Understand the pathophysiology of Type 1 diabetes. Be familiar
Type 1 Diabetes-Pathophysiology, Diagnosis, and Long-Term Complications Alejandro J de la Torre Pediatric Endocrinology 10/17/2014 Objectives Understand the pathophysiology of Type 1 diabetes. Be familiar
Prediabetes & Type 2 Diabetes Prevention. Jacob M. Haus, PHD
 Prediabetes & Type 2 Diabetes Prevention Jacob M. Haus, PHD Disclosures In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure to the participants:
Prediabetes & Type 2 Diabetes Prevention Jacob M. Haus, PHD Disclosures In compliance with the accrediting board policies, the American Diabetes Association requires the following disclosure to the participants:
