Reduction of intraocular pressure (IOP) is the only currently
|
|
|
- Amanda Carter
- 5 years ago
- Views:
Transcription
1 ORIGINAL STUDY Long-term 24-hour Intraocular ressure Control With Travoprost Monotherapy in atients With rimary Open-angle Glaucoma Ivano Riva, MD,* Andreas Katsanos, MD, hd,w Irene Floriani, hd,z Elena Biagioli, ScD,z Anastasios G.. Konstas, MD, hd,y Marco Centofanti, MD, hd,8 and Luciano Quaranta, MD, hd* urpose: The aim of the study was to evaluate the long-term 24- hour intraocular pressure (IO) efficacy of travoprost monotherapy in primary open-angle glaucoma patients. atients and Methods: A total of 36 previously untreated primary open-angle glaucoma patients were enrolled in this 5-year study. atients underwent an untreated 24-hour IO evaluation. Subsequently all patients were assigned to topical therapy with travoprost 0.004% eye-drops preserved with benzalkonium chloride (Travatan, Alcon Laboratories Inc., Fort Worth, TX) administered once in the evening (8:00 M) in both eyes. All patients were then scheduled for a 24-hour IO assessment approximately 12 months after the baseline visit. This schedule of follow-up was maintained for the whole duration of the trial. The predetermined range of target IO reduction selected in this cohort of patients ranged between 20% and 30%. Results: A total of 34 patients completed all phases of the investigation. The mean survival time was 57.3 ± 2.0 months and the cumulative survival rate was 0.82 ± 0.6 at 60 months. Travoprost reduced the mean 24-hour IO from 23.4 ± 1.7 mm Hg at baseline to 16.8 ± 2.4 mm Hg (28.4%), 16.8 ± 2.5 mm Hg (28.1%), 16.8 ± 2.4 mm Hg (28.5%), 16.7 ± 2.5 mm Hg (28.6%), and 16.9 ± 2.4 mm Hg (27.8%), respectively at the end of the first, second, third, fourth, and fifth year follow-up. No drug-related serious adverse events were registered during the study. Conclusions: The present study demonstrated the long-term 24- hour efficacy of travoprost for the treatment of primary open-angle glaucoma. Key Words: open-angle glaucoma, prostaglandin analogue, circadian intraocular pressure, travoprost (J Glaucoma 2014;23: ) Received for publication July 11, 2013; accepted March 14, From the *Centre for the Study of Glaucoma, University of Brescia, Brescia; zlaboratory of Clinical Research, IRCCS, Istituto di Ricerche Farmacologiche Mario Negri, Milano; 8DSCMT, University of Tor Vergata, Rome, Italy; wophthalmology Department, University of Ioannina, Ioannina; and yglaucoma Unit, 1st University Department of Ophthalmology, AHEA Hospital, Thessaloniki, Greece. Disclosure: I.R.: Honoraria or travel reimbursement from Alcon, Allergan, MSD, Sooft; A.K.: Travel reimbursement from Alcon and MSD; A.G..K.: Consultant for Alcon, Allergan, MSD and Nicox; L.Q.: Honoraria or travel reimbursement from Alcon, Allergan, MSD, Thea-Farmila, and Bausch & Lomb. I.F., E.B., M.C. declares no conflict of interest. Reprints: Luciano Quaranta, MD, hd, A.O. Spedali Civili di Brescia, Unita` di Oculistica, iazzale Spedali Civili, 1, Brescia 25123, Italy ( quaranta@med.unibs.it). Copyright r 2014 by Lippincott Williams & Wilkins DOI: /IJG Reduction of intraocular pressure (IO) is the only currently available, evidence-based management strategy in patients affected with primary open-angle glaucoma (OAG). Most OAG patients will require lifelong medical therapy to avoid visual loss. The decision to select medical therapy options relies primarily on the efficacy of the available medications in various therapeutic trials. Sadly, most published studies only evaluate the short-term, daytime efficacy of medical therapy. rostaglandin analogues have become a popular firstline therapy option for lowering IO in OAG owing to their superior 24-hour efficacy, 1 6 convenient once-a-day administration, 5 and favorable systemic safety profile. 7 Travoprost is a synthetic prostaglandin F2a analogue that exerts its IO-lowering effect through the prostaglandin F receptors situated at the ciliary muscle 8 and the trabecular meshwork. 9 Travoprost is increasingly becoming a popular first-line monotherapy option for OAG patients 10 as there is cumulative evidence suggesting good quality of shortterm 24-hour IO control with low fluctuation, especially with evening administration However, although several controlled studies have demonstrated the daytime short-term efficacy of travoprost monotherapy, little is currently known about its long-term efficacy. As OAG is a 24-hour, lifelong disease, an ideal antiglaucoma medication should be successful in reducing IO during day and night. 4,17 Importantly, 24-hour studies have confirmed that 24-hour IO monitoring can significantly modify individualized glaucoma care in many glaucoma patients. 18,19 A few 24-hour studies have investigated travoprost efficacy over a period of up to 4 months, 11 13,20 but to date no evidence is available for the long-term 24-hour efficacy of travoprost monotherapy in glaucoma. Therefore, the primary aim of this study was the evaluation of the long-term 24-hour IO efficacy obtained by travoprost monotherapy, used as a first-line therapy during a 5-year follow-up period. A secondary aim was to investigate the survival rate without progression of a OAG cohort treated with travoprost monotherapy. MATERIALS AND METHODS This was a prospective, open label, single-arm study carried out at the Glaucoma Service of the Department of Ophthalmology of the University of Brescia, Italy. The research protocol adhered to the tenets of the Declaration of Helsinki and was approved by the Institutional Review Board of the University of Brescia, Italy. Enrolled patients provided a written informed consent to participate in the trial before any study-related activities were carried out. J Glaucoma Volume 23, Number 8, October/November
2 Riva et al J Glaucoma Volume 23, Number 8, October/November 2014 articipants This study enrolled newly diagnosed, previously untreated OAG patients who exhibited characteristic glaucomatous disc damage and visual field loss between January and November Eligibility criteria were: age above 45 years, no previous ocular surgery other than uncomplicated phacoemulsification cataract surgery performed at least 6 months before entering the study, openangle by gonioscopy (grades III and IV according to the Shaffer classification), untreated IO between 21 and 35 mm Hg at 10:00 AM± 1 hour verified by 2 separate measurements (enrollment IO). Exclusion criteria for ophthalmic conditions were: any type of glaucoma other than OAG; corneal or other anatomic conditions making applanation tonometry unreliable; central corneal thickness r500 mm or Z600 mm; signs or history of macular edema, herpetic, or other ocular inflammatory disease; history of allergy or adverse event related to the study medication; history or suspicion of poor adherence to medical therapy; best-corrected visual acuity <0.4 (Snellen); cup-to-disc ratio >0.7; mean deviation (MD) worse than 15 db in Humphrey 24-2 SITA standard perimetry (Humphrey Visual Field Analyzer; Carl Zeiss Meditec Inc., Dublin, CA); or the possibility of significant visual deterioration and optic nerve damage due to participation to the study according to the principal investigator s judgment. atients were also excluded if they were unable to understand the study procedures, give informed consent, or were using systemic corticosteroids. Assessments During an initial eligibility visit, all qualified patients underwent a detailed ophthalmic examination and their ocular and systemic clinical data were recorded. Study participants were admitted at the University Ophthalmology Clinic of Brescia, Italy, for an untreated 24-hour IO evaluation (baseline visit) with Goldmann tonometry. The IO was recorded at 10:00 AM, 2:00 M, 6:00 M, 10:00 M, 2:00 AM, 6:00 AM, and 10:00 AM (± 1 h). The day before the 24-hour IO assessment, a reliable 24-2 SITA standard visual field test was performed (Humphrey Visual Field Analyzer; Carl Zeiss Meditec Inc.). Subsequently all study patients were assigned to topical therapy with travoprost 0.004% eye-drops preserved with benzalkonium chloride (Travatan, Alcon Laboratories Inc.) administered once in the evening (8:00 M) in both eyes. To ensure that the target IO was reached, according to the principal investigator s judgment, a safety visit was performed approximately 4 weeks after treatment initiation. The predetermined range of target IO reduction selected in this cohort with travoprost monotherapy ranged between 20% and 30%. After this visit, all patients were scheduled for a visit approximately 6 months after the baseline visit at 10:00 AM± 1 hour, as well as a 24-hour IO assessment approximately 12 months after the baseline visit. This schedule of follow-up was maintained for the whole duration of the trial. A comprehensive clinical examination was performed at each visit. Enrolled patients continued on travoprost monotherapy as long as their target IO was successfully maintained. Calibrated Goldmann tonometers were used throughout the duration of the trial by a clinician masked to the previous baseline or treated IO data. Statistics The primary endpoint of the study was the mean 24-hour IO measured at annual intervals. Only 1 eye per patient was included in the analysis. The mean values for 24-hour IO, daytime IO, and nocturnal IO were obtained from every 24-hour IO curve. Areas under the curve (AUCs) were calculated for each variable, using a trapezoidal rule. The trend over time for each variable was evaluated by means of an analysis of variance model for repeated measures, whereas a paired t test was used for comparison of variables at each time-point with baseline values. A Bonferroni approach was adopted to allow for multiple tests: considering an a level of 0.05, statistical significance was set to 0.01, calculating as 0.05 divided for 5 comparisons. In these analyses, the approach of the last value carried forward was applied for patients who did not complete the study. Failure was defined as withdrawal of a patient from the study, due to either failure to reach the target IO set upon enrollment or when reliable evidence of progression existed, necessitating the introduction of adjunctive medical therapy. The percentage of patients meeting target IO at every annual time-point was calculated. The Kaplan-Meier survival method was used to describe the cumulative incidence of travoprost monotherapy failure throughout the 5 years of the study. The mean survival time and cumulative survival rate at 60 months were computed. An intent-totreat approach was applied for the analysis. Univariate Cox regression analysis was performed to evaluate age, MD, pattern standard deviation, baseline 24- hour IO, treated 24-hour IO fluctuation, and treated 24- hour peak IO as risk factors for progression/failure. Treated 24-hour IO fluctuation was defined as the SD of the IOs recorded during the treatment phase of the study and reported in mm Hg. Treated IO peak was defined as the mean of peak IOs (ie, highest point in the range of the 24-hour pressure curve) computed for each 24-hour assessment during the treatment phase of the study. Descriptive statistics were calculated for every variable and variables were compared between nonfailure and failure group of patients using an independent t test. Hazard ratios (HR) for failure were reported for each putative factor in the univariate analysis. RESULTS Thirty-six OAG patients were enrolled in this 5-year study. Thirty-four patients completed all phases of the investigation, whereas 2 patients were lost to follow-up, both at approximately 48 months. Six patients were withdrawn from the study because their target IO could not be reached at some stage, or because of reliable evidence of progression (Fig. 1). Respectively 97.2%, 97.2%, 94.4%, 94.4%, and 94.4% of patients met their target IO at first, second, third, fourth, and fifth year of follow-up. For the whole study population, the mean survival time was 57.3 ± 2.0 months and the cumulative survival rate was 0.82 ± 0.6 at 60 months. Table 1 shows the general features of the patients included. Travoprost reduced the mean 24-hour IO from 23.4 ± 1.7 mm Hg at baseline to 16.8 ± 2.4 mm Hg (28.4%), 16.8 ± 2.5 mm Hg (28.1%), 16.8 ± 2.4 mm Hg (28.5%), 16.7 ± 2.5 mm Hg (28.6%), and 16.9 ± 2.4 mm Hg (27.8%), respectively at the end of the first, second, third, fourth, and fifth year of follow-up (Fig. 2). The mean r 2014 Lippincott Williams & Wilkins
3 J Glaucoma Volume 23, Number 8, October/November 2014 Long-term 24-hour IO Control With Travoprost FIGURE 1. Kaplan-Meier survival curve for the study cohort on travoprost monotherapy. 24-hour IO and calculated AUCs were significantly lower than baseline untreated values at each annual time-point of evaluation ( < 0.01), whereas no significant differences were found among yearly time-points during follow-up ( > 0.05) (Tables 2, 3). The mean daytime and nocturnal IO values at baseline and at each yearly follow-up time-point are shown in Tables 2 and 3. The trend of daytime and nocturnal IO over time is illustrated in Figure 2. Overall, daytime IO, nocturnal IO, and their respective calculated AUCs, were significantly lower than baseline values at each yearly timepoint analyzed ( < 0.01). No significant difference was documented for these parameters between yearly timepoints during the 5-year follow-up ( > 0.05). No significant differences were detected between nocturnal and diurnal IO reductions induced by travoprost at each annual time-point analyzed ( > 0.05). Univariate Cox regression analyses revealed no significant effect of age ( = 0.53), MD ( = 0.76), pattern standard deviation ( = 0.97), and treated 24-hour IO fluctuation ( = 0.53) upon the risk of failure during the 5- year follow-up period. Only the mean untreated 24-hour IO and treated 24-hour IO peak values were found to be risk factors for predicting travoprost treatment failure (HR: 1.9, < 0.01 and HR: 1.03, < 0.01, respectively) (Table 4). Treatment-related adverse events during the 5-year course of the study are presented in Table 5. The most common travoprost-related adverse events were iris hyperchromia, seen in 10 patients (27.7%) and ocular hyperaemia seen in 3 patients (8.3%). No drug-related serious adverse events were registered during the study. TABLE 1. Characteristics of Studied atients atients (n = 36) Sex (Male/Female) 20/16 seudophakia (n) 21 Mean ± SD Range Age (y) 69 ± IO at enrollment (10 AM±1h) 24.3 ± (mm Hg) Visual field mean deviation at enrollment (db) 5.07 ± IO indicates intraocular pressure. FIGURE 2. The mean 24-hour, diurnal, and nocturnal intraocular pressure at baseline and annual time-points. DISCUSSION Topical therapy for glaucoma should be effective in maintaining a sustained IO reduction over the long term. 21,22 Although travoprost monotherapy has shown a meaningful IO efficacy in the short term, there is limited information on the long-term efficacy (Z12 mo). 23 However, previous clinical trials with latanoprost monotherapy, another prostaglandin analogue, have established a long-lasting daytime hypotensive effect with little evidence of tachyphylaxis, for up to 4 years This is further corroborated by the present long-term 24-hour study, which documented consistent IO efficacy with travoprost monotherapy in OAG patients during the 5-year follow-up period. The present 24-hour investigation observed that a relatively high proportion (82%) of OAG patients reached and maintained a predetermined, individualized target IO reduction between 20% and 30% with travoprost monotherapy during a 5-year follow-up period. Similarly, a multicenter study on OAG patients treated with latanoprost monotherapy reported satisfactory IO control in the vast majority of their patients (86%), but this was with a shorter 2-year follow-up. 29 To the best of our knowledge, this is the first study to monitor the long-term 24-hour IO efficacy with any medication, or therapy option. Interestingly, the efficacy results of the present long-term 24-hour investigation (27.8% to 28.6%) compare well with the available shortterm evidence for travoprost reported to date. A recent meta-analysis by Stewart et al 1 investigating the short-term 24-hour efficacy of topical monotherapy agents reported that travoprost reduced the mean 24-hour IO by 27% from untreated baseline. Further, Konstas et al 11,12 in 2 separate trials reported travoprost to reduce the mean 24- hour IO by 26.7% and 26.3%, respectively. In another short-term study by Orzalesi et al, 13 travoprost reduced the mean 24-hour IO by 27.4%. The short-term 24-hour efficacy reported by these studies is fairly similar to the long-term 24-hour efficacy documented by the present study. It seems that the long-term 24-hour travoprost efficacy is only slightly greater than that reported over the short-term (with up to 3 mo follow-up). ossible reasons for this small difference include the mechanism of action of r 2014 Lippincott Williams & Wilkins 537
4 Riva et al J Glaucoma Volume 23, Number 8, October/November 2014 TABLE 2. Mean 24-hour, Daytime, and Nocturnal IO at Untreated Baseline and During Travoprost-treated Follow-up No. atients at Risk 24-h IO Daytime IO Nocturnal IO Baseline (mm Hg ± SD) ± ± ± mo (mm Hg ± SD) ± 2.4 < ± 2.8 < ± 2.1 < mo (mm Hg ± SD) ± 2.5 < ± 2.6 < ± 2.3 < mo (mm Hg ± SD) ± 2.4 < ± 2.7 < ± 2.2 < mo (mm Hg ± SD) ± 2.5 < ± 2.7 < ± 2.4 < mo (mm Hg ± SD) ± 2.4 < ± 2.7 < ± 2.2 < 0.01 (among yearly time-points) IO indicates intraocular pressure. travoprost, which involves remodeling of the extracellular matrix, hence it is logical to assume a small increase in efficacy after the first few months of treatment. The mean 24-hour IO reduction in patients treated with travoprost was generally stable during the 5 years of the study (Fig. 2). It may be of clinical value that the 24-hour efficacy was quite uniform, without significant differences between the yearly 24-hour IO curves. The long-term consistency of IO lowering may be important in view of the fact that not all classes of antiglaucoma medications have shown persistence in efficacy over the longterm. For example b-blockers are reported to demonstrate a long-term drift, probably due to modifications in the number and affinity of continuously blocked b-adrenergic receptors. 33,34 Considering the slow, insidious nature of functional and anatomic deterioration in glaucoma, persistence of the hypotensive effect should be considered as an advantage of antiglaucoma therapy. In previous 24-hour studies with latanoprost, Quaranta et al 35,36 observed that although this prostaglandin induced a clinically meaningful 24-hour IO reduction, the hypotensive effect was greater during the day, especially 8 to 12 hours after administration, albeit these results were not statistically significant. In the meta-analysis performed by Stewart et al, 1 however, the mean nighttime IO reduction was statistically lower than the daytime IO reduction for latanoprost, but not for travoprost. In the present long-term 24-hour study, although mean nocturnal IO reduction with travoprost was somewhat lower than the mean daytime IO reduction, there was no significant difference between nighttime and daytime efficacy. Travoprost was generally well tolerated and no serious drug-related adverse events were recorded throughout this 5-year study. Treatment-related adverse events were observed in 18 patients (50%) during the course of the study. These adverse events were consistent with those expected with long-term prostaglandin therapy. Hyperpigmentation of the iris was the most common side effect, with a 5-year cumulative prevalence of 27.7%, which was comparable with the 33.4% rate reported in a 5-year study with latanoprost. 37 Importantly, only baseline mean untreated 24-hour IO and treated 24-hour peak IO were found to be significant parameters for predicting failure during the 5-year follow-up of the study. As one would expect, the risk of failure due to insufficient IO lowering increased in those with higher baseline IO. Thus, in OAG patients with higher untreated mean 24-hour IO at diagnosis, stepwise therapy may be warranted earlier. Our study also demonstrated that treated 24-hour peak IO was a risk factor for travoprost monotherapy failure in OAG. This finding may apply for other prostaglandins and other agents, but this should be confirmed with future studies. It is still controversial whether peak 24- hour IO is an independent risk factor for progression in OAG, or other glaucomas. Further, the role of peak 24- hour IO, or mean 24-hour IO has not been adequately evaluated in long-term trials to date. The Advanced Glaucoma Intervention Study demonstrated with single IO measurements over time that a peak IOr18 mm Hg and a mean IO of 12.8 mm Hg were the best combination to prevent progression in patients with advanced OAG. 38 Stewart et al 39 also reported that peak IO is an independent risk factor for progression in treated OAG patients followed-up retrospectively for 5 years. Similarly, a 5-year retrospective study by Hollo et al 40 reported that the TABLE 3. Calculated AUCs for Mean 24-hour, Daytime, and Nighttime IO at Baseline and During Follow-up No. atients at Risk AUC for 24-h IO AUC for Daytime IO AUC for Nocturnal IO Baseline (± SD) ± ± ± mo (± SD) ± 49 < ± 23 < ± 17.2 < mo (± SD) ± 49.1 < ± 22 < ± 18.5 < mo (± SD) ± 48.6 < ± 22.3 < ± 17.5 < mo (± SD) ± 50.4 < ± 22.5 < ± 18.9 < mo (± SD) ± 48.7 < ± 22.6 < ± 18 < 0.01 (among yearly time-points) AUC indicates area under the curve; IO, intraocular pressure r 2014 Lippincott Williams & Wilkins
5 J Glaucoma Volume 23, Number 8, October/November 2014 Long-term 24-hour IO Control With Travoprost TABLE 4. Descriptive Statistics for Variables Included in Univariate Cox Regression Analyses and Hazard Ratio for Failure Nonfailure (30 atients) Failure (6 atients) (Nonfailure vs. Failure) Hazard Ratio (95% CI) Age ± ± (0.89-1) 0.53 Mean deviation 5.06 ± ± ( ) 0.76 attern standard deviation 3.08 ± ± ( ) 0.97 Mean 24-h IO at baseline ± ± 2.65 < ( ) < 0.01 IO fluctuation 1.30 ± ± ( ) 0.53 Treated 24 h IO peak ± ± 0.89 < (1-1.05) < % CI indicates 95% confidence interval; IO, intraocular pressure. peak IO and the mean IO are independent risk factors for progression in treated exfoliative glaucoma patients. These results are not consistent with other studies investigating the role of peak IO established with single IO measurements over a long-term follow-up, in which peak IO was not found to be an independent risk factor for progression To date only one previous study 44 analyzed retrospectively the effect of 24-hour peak IO on long-term progression in OAG. In that study 24-hour peak IO was documented to be an independent risk factor for progression, and a 24-hour peak IO below 18 mm Hg ensured a 78% nonprogression rate in treated OAG patients after 5 years of follow-up. Similarly, in the present prospective study that used travoprost monotherapy, stable patients exhibited a mean treated 24-hour IO peak of 17.8 ± 1.01 mm Hg, whereas progressive patients (who were withdrawn from the study) demonstrated a mean treated 24-hour peak IO of 19.4 ± 0.89 mm Hg ( < 0.01). A limitation of this study is the relatively small sample size. This is due to significant difficulties in enrolling a large cohort of patients with a long follow-up for 24-hour monitoring. Small sample size could have limited the power of statistical analysis, especially regarding the evaluation of parameters as risk factors for failure. Further, progression was evaluated by the principal investigator and relied upon a number of clinical criteria (eg, visual field, optic disc appearance, etc.) and not by a masked observer relying on visual fields, or disc photographs. This approach, however, reflects standard clinical practice used in an academic glaucoma service. Our results apply only to OAG and not to other glaucomas that may be more difficult to control with monotherapy (eg, exfoliative glaucoma, chronic angleclosure glaucoma, etc.). It should also be noted that because our participants had mild OAG, the results might not necessarily apply to patients with more advanced disease whose IO may be less likely to be controlled with travoprost monotherapy. Another limitation of the study was the incomplete assessor masking: the clinician who performed the IO measurements knew that the patient was a participant of a long-term travoprost efficacy study TABLE 5. Adverse Events During the Study Related to Travoprost Therapy N (%) Iris hyperpigmentation 10 (27.7) Ocular hyperemia 3 (8.3) Foreign body sensation 2 (5.5) Hypertrichosis 2 (5.5) Skin hyperpigmentation 1 (2.7) but was masked to the previous baseline or treated IO data. Although the importance of compliance with medication was stressed to all patients in each visit, no formal method of compliance assessment was used in this study. Such methodology reflects the norm in medium and longterm drug efficacy studies, as well as the real life situation in typical academic glaucoma centers. Despite these limitations, our long-term study has demonstrated that travoprost monotherapy can consistently control the 24-hour IO in a significant proportion of OAG patients. Future research is needed to evaluate the long-term 24-hour efficacy of all therapy options in glaucoma. Such evidence may optimize glaucoma care and reduce the rate of glaucomatous visual loss. REFERENCES 1. Stewart WC, Konstas AG, Nelson LA, et al. Meta-analysis of 24- hour intraocular pressure studies evaluating the efficacy of glaucoma medicines. Ophthalmology. 2008;115: , e Konstas AG, Kozobolis V, Katsimpris IE, et al. Efficacy and safety of latanoprost versus travoprost in exfoliative glaucoma patients. Ophthalmology. 2007;114: Yan DB, Battista RA, Haidich AB, et al. Comparison of morning versus evening dosing and 24-h post-dose efficacy of travoprost compared with latanoprost in patients with openangle glaucoma. Curr Med Res Opin. 2008;24: Quaranta L, Katsanos A, Russo A, et al. 24-hour intraocular pressure and ocular perfusion pressure in glaucoma. Surv Ophthalmol. 2013;58: Aptel F, Cucherat M, Denis. Efficacy and tolerability of prostaglandin analogs: a meta-analysis of randomized controlled clinical trials. J Glaucoma. 2008;17: Quaranta L, Biagioli E, Riva I, et al. rostaglandin analogs and timolol-fixed versus unfixed combinations or monotherapy for open-angle glaucoma: a systematic review and metaanalysis. J Ocul harmacol Ther. 2013;29: Hollo G. The side effects of the prostaglandin analogues. Expert Opin Drug Saf. 2007;6: Sharif NA, Kelly CR, Crider JY. Agonist activity of bimatoprost, travoprost, latanoprost, unoprostone isopropyl ester and other prostaglandin analogs at the cloned human ciliary body F prostaglandin receptor. J Ocul harmacol Ther. 2002;18: Sharif NA, Kelly CR, Crider JY. Human trabecular meshwork cell responses induced by bimatoprost, travoprost, unoprostone, and other F prostaglandin receptor agonist analogues. Invest Ophthalmol Vis Sci. 2003;44: Aptel F, Denis. Balancing efficacy and tolerability of prostaglandin analogues and prostaglandin-timolol fixed combinations in primary open-angle glaucoma. Curr Med Res Opin. 2011;27: Konstas AG, Mikropoulos D, Haidich AB, et al. Twenty-fourhour intraocular pressure control with the travoprost/timolol maleate fixed combination compared with travoprost when r 2014 Lippincott Williams & Wilkins 539
6 Riva et al J Glaucoma Volume 23, Number 8, October/November 2014 both are dosed in the evening in primary open-angle glaucoma. Br J Ophthalmol. 2009;93: Konstas AG, Mikropoulos D, Kaltsos K, et al. 24-hour intraocular pressure control obtained with evening- versus morning-dosed travoprost in primary open-angle glaucoma. Ophthalmology. 2006;113: Orzalesi N, Rossetti L, Bottoli A, et al. Comparison of the effects of latanoprost, travoprost, and bimatoprost on circadian intraocular pressure in patients with glaucoma or ocular hypertension. Ophthalmology. 2006;113: rzydryga JT, Egloff C. Intraocular pressure lowering efficacy of travoprost. Eur J Ophthalmol. 2004;14: Franks WA, Renard J, Cunliffe IA, et al. A 6-week, doublemasked, parallel-group study of the efficacy and safety of travoprost 0.004% compared with latanoprost 0:005%/timolol 0.5% in patients with primary open-angle glaucoma or ocular hypertension. Clin Ther. 2006;28: Kumar RS, Istiantoro VW, Hoh ST, et al. Efficacy and safety of a systematic switch from latanoprost to travoprost in patients with glaucoma. J Glaucoma. 2007;16: Konstas AG, Mikropoulos DG, Irkec M. Open-angle glaucoma and ocular perfusion. Br J Ophthalmol. 2010;94: Hughes E, Spry, Diamond J. 24-hour monitoring of intraocular pressure in glaucoma management: a retrospective review. J Glaucoma. 2003;12: Barkana Y, Anis S, Liebmann J, et al. Clinical utility of intraocular pressure monitoring outside of normal office hours in patients with glaucoma. Arch Ophthalmol. 2006;124: Yildirim N, Sahin A, Gultekin S. The effect of latanoprost, bimatoprost, and travoprost on circadian variation of intraocular pressure in patients with open-angle glaucoma. J Glaucoma. 2008;17: Friedman DS, Wolfs RC, O Colmain BJ, et al. revalence of open-angle glaucoma among adults in the United States. Arch Ophthalmol. 2004;122: Leske MC, Wu SY, Honkanen R, et al. Nine-year incidence of open-angle glaucoma in the Barbados Eye Studies. Ophthalmology. 2007;114: Netland A, Landry T, Sullivan EK, et al. Travoprost compared with latanoprost and timolol in patients with open-angle glaucoma or ocular hypertension. Am J Ophthalmol. 2001;132: Alm A, Widengard I. Latanoprost: experience of 2-year treatment in Scandinavia. Acta Ophthalmol Scand. 2000;78: Costagliola C, Del rete A, Verolino M, et al. Effect of 0.005% latanoprost once daily on intraocular pressure in glaucomatous patients not adequately controlled by beta-blockers twice daily: a 3-year follow-up. Experience and incidence of side effects in a prospective study on 76 patients. Graefes Arch Clin Exp Ophthalmol. 2002;240: Watson G. Latanoprost. Two years experience of its use in the United Kingdom. Latanoprost Study Group. Ophthalmology. 1998;105: Kashiwagi K, Tsumura T, Tsukahara S. Long-term effects of latanoprost monotherapy on intraocular pressure in Japanese glaucoma patients. J Glaucoma. 2008;17: Fristrom B, Uusitalo H. A randomized, 36-month, postmarketing efficacy and tolerability study in Sweden and Finland of latanoprost versus non-prostaglandin therapy in patients with glaucoma or ocular hypertension. Acta Ophthalmol. 2010;88: Hedman K, Watson G, Alm A. The effect of latanoprost on intraocular pressure during 2 years of treatment. Surv Ophthalmol. 2002;47(suppl 1):S65 S Nilsson SF, Drecoll E, Lutjen-Drecoll E, et al. The prostanoid E2 receptor agonist butaprost increases uveoscleral outflow in the cynomolgus monkey. Invest Ophthalmol Vis Sci. 2006; 47: Weinreb RN, Kashiwagi K, Kashiwagi F, et al. rostaglandins increase matrix metalloproteinase release from human ciliary smooth muscle cells. Invest Ophthalmol Vis Sci. 1997;38: Weinreb RN, Toris CB, Gabelt BT, et al. Effects of prostaglandins on the aqueous humor outflow pathways. Surv Ophthalmol. 2002;47(suppl 1):S53 S Boger W III. Shortterm escape and longterm drift. The dissipation effects of the beta adrenergic blocking agents. Surv Ophthalmol. 1983;28(suppl): Gandolfi SA. Restoring sensitivity to timolol after long-term drift in primary open-angle glaucoma. Invest Ophthalmol Vis Sci. 1990;31: Quaranta L, Gandolfo F, Turano R, et al. Effects of topical hypotensive drugs on circadian IO, blood pressure, and calculated diastolic ocular perfusion pressure in patients with glaucoma. Invest Ophthalmol Vis Sci. 2006;47: Quaranta L, Miglior S, Floriani I, et al. Effects of the timololdorzolamide fixed combination and latanoprost on circadian diastolic ocular perfusion pressure in glaucoma. Invest Ophthalmol Vis Sci. 2008;49: Alm A, Schoenfelder J, McDermott J. A 5-year, multicenter, open-label, safety study of adjunctive latanoprost therapy for glaucoma. Arch Ophthalmol. 2004;122: The AGIS investigators. The Advanced Glaucoma Intervention Study (AGIS): 7. The relationship between control of intraocular pressure and visual field deterioration. Am J Ophthalmol. 2000;130: Stewart WC, Day DG, Jenkins JN, et al. Mean intraocular pressure and progression based on corneal thickness in primary open-angle glaucoma. J Ocul harmacol Ther. 2006; 22: Hollo G, Quaranta L, Cvenkel B, et al. Risk factors associated with progression in exfoliative glaucoma patients. Ophthalmic Res. 2012;47: Seong GJ, Rho SH, Kim CS, et al. otential benefit of intraocular pressure reduction in normal-tension glaucoma in South Korea. J Ocul harmacol Ther. 2009;25: Jonas JB, Budde WM, Stroux A, et al. Diurnal intraocular pressure profiles and progression of chronic open-angle glaucoma. Eye (Lond). 2007;21: Stewart WC, Kolker AE, Sharpe ED, et al. Long-term progression at individual mean intraocular pressure levels in primary open-angle and exfoliative glaucoma. Eur J Ophthalmol. 2008;18: Konstas AG, Quaranta L, Mikropoulos DG, et al. eak intraocular pressure and glaucomatous progression in primary open-angle glaucoma. J Ocul harmacol Ther. 2012; 28: r 2014 Lippincott Williams & Wilkins
effect of previous argon laser trabeculoplasty
 Graefe s Arch Clin Exp Ophthalmol (2006) 244: 1073 1076 CLINICAL INVESTIGATION DOI 10.1007/s00417-005-0198-x Esther Arranz-Marquez Miguel A. Teus Effect of previous argon laser trabeculoplasty on the ocular
Graefe s Arch Clin Exp Ophthalmol (2006) 244: 1073 1076 CLINICAL INVESTIGATION DOI 10.1007/s00417-005-0198-x Esther Arranz-Marquez Miguel A. Teus Effect of previous argon laser trabeculoplasty on the ocular
24-hour IOP fluctuation: myth or reality?
 Journal for Modeling in Ophthalmology 2016; 2:103-109 Review article 24-hour IOP fluctuation: myth or reality? Luciano Quaranta 1, Ivano Riva 1, Francesco Oddone 2 1 Department of Medical and Surgical
Journal for Modeling in Ophthalmology 2016; 2:103-109 Review article 24-hour IOP fluctuation: myth or reality? Luciano Quaranta 1, Ivano Riva 1, Francesco Oddone 2 1 Department of Medical and Surgical
24-h Efficacy of Glaucoma Treatment Options
 Adv Ther (2016) 33:481 517 DOI 10.1007/s12325-016-0302-0 REVIEW 24-h Efficacy of Glaucoma Treatment Options Anastasios G. P. Konstas. Luciano Quaranta. Banu Bozkurt. Andreas Katsanos. Julian Garcia-Feijoo.
Adv Ther (2016) 33:481 517 DOI 10.1007/s12325-016-0302-0 REVIEW 24-h Efficacy of Glaucoma Treatment Options Anastasios G. P. Konstas. Luciano Quaranta. Banu Bozkurt. Andreas Katsanos. Julian Garcia-Feijoo.
Changes in Trend of Newly Prescribed Anti-Glaucoma Medications in Recent Nine Years in a Japanese Local Community
 The Open Ophthalmology Journal,, 4, 7-7 Open Access Changes in Trend of Newly Prescribed Anti-Glaucoma Medications in Recent Nine Years in a Japanese Local Community Kenji Kashiwagi Department of Community
The Open Ophthalmology Journal,, 4, 7-7 Open Access Changes in Trend of Newly Prescribed Anti-Glaucoma Medications in Recent Nine Years in a Japanese Local Community Kenji Kashiwagi Department of Community
Efficacy of latanoprost in management of chronic angle closure glaucoma. Kumar S 1, Malik A 2 Singh M 3, Sood S 4. Abstract
 Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
VI.2.2 Summary of treatment benefits
 EU-Risk Management Plan for Bimatoprost V01 aetiology), both OAG and ACG can be secondary conditions. Secondary glaucoma refers to any case in which another disorder (e.g. injury, inflammation, vascular
EU-Risk Management Plan for Bimatoprost V01 aetiology), both OAG and ACG can be secondary conditions. Secondary glaucoma refers to any case in which another disorder (e.g. injury, inflammation, vascular
Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial
 Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial Boel Bengtsson, PhD, 1 M. Cristina Leske, MD, MPH, 2 Leslie Hyman, PhD, 2 Anders Heijl, MD, PhD, 1 Early
Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial Boel Bengtsson, PhD, 1 M. Cristina Leske, MD, MPH, 2 Leslie Hyman, PhD, 2 Anders Heijl, MD, PhD, 1 Early
Regional Institute of Ophthalmology, Indira Gandhi Institute of Medical Sciences, Patna, India 2
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(5):399-407 http://dx.doi.org/10.3341/kjo.2014.28.5.399 Original Article Comparing the Efficacy of (0.005%), Bimatoprost (0.03%), Travoprost
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(5):399-407 http://dx.doi.org/10.3341/kjo.2014.28.5.399 Original Article Comparing the Efficacy of (0.005%), Bimatoprost (0.03%), Travoprost
Meta-analysis of timolol on diurnal and nighttime intraocular pressure and blood pressure
 Eur J Ophthalmol 2010; 20 ( 6) : 1035-1041 Original Article Meta-analysis of timolol on diurnal and nighttime intraocular pressure and blood pressure Princeton Wen-Yuan Lee 1, Aoife Doyle 1, Jeanette A.
Eur J Ophthalmol 2010; 20 ( 6) : 1035-1041 Original Article Meta-analysis of timolol on diurnal and nighttime intraocular pressure and blood pressure Princeton Wen-Yuan Lee 1, Aoife Doyle 1, Jeanette A.
Patients with ocular hypertension or
 ... REPORTS... An Economic Analysis of Switching to Latanoprost from a β-blocker or Adding Brimonidine or Latanoprost to a β-blocker in Open-Angle Glaucoma or Ocular Hypertension William C. Stewart, MD;
... REPORTS... An Economic Analysis of Switching to Latanoprost from a β-blocker or Adding Brimonidine or Latanoprost to a β-blocker in Open-Angle Glaucoma or Ocular Hypertension William C. Stewart, MD;
The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters.
 A Study of the Safety and Efficacy of Travoprost 0.004%/Timolol 0.5% Ophthalmic Solution Compared to Latanoprost 0.005% and Timolol 0.5% Dosed Concomitantly in Patients with Open-Angle Glaucoma or Ocular
A Study of the Safety and Efficacy of Travoprost 0.004%/Timolol 0.5% Ophthalmic Solution Compared to Latanoprost 0.005% and Timolol 0.5% Dosed Concomitantly in Patients with Open-Angle Glaucoma or Ocular
A Short-term Study of the Additive Effect of Latanoprost 0.005% and Brimonidine 0.2%
 A Short-term Study of the Additive Effect of Latanoprost 0.005% and Brimonidine 0.2% Haydar Erdoğan, İlker Toker, Mustafa Kemal Arıcı, Ahmet Aygen and Ayşen Topalkara Department of Ophthalmology, School
A Short-term Study of the Additive Effect of Latanoprost 0.005% and Brimonidine 0.2% Haydar Erdoğan, İlker Toker, Mustafa Kemal Arıcı, Ahmet Aygen and Ayşen Topalkara Department of Ophthalmology, School
4/06/2013. Medication Observation POAG. Proportion. Native American 0.1% 0.4%
 Clinical Research in Glaucoma: Putting Science into Practice J. James Thimons, O.D., FAAO Chairman, National Glaucoma Society www.nationalglaucomasociety.org Ocular Hypertension Treatment Study (OHTS)
Clinical Research in Glaucoma: Putting Science into Practice J. James Thimons, O.D., FAAO Chairman, National Glaucoma Society www.nationalglaucomasociety.org Ocular Hypertension Treatment Study (OHTS)
M Diestelhorst, L-I Larsson,* for The European Latanoprost Fixed Combination Study Group...
 199 SCIENTIFIC REPORT A 12 week study comparing the fixed combination of latanoprost and timolol with the concomitant use of the individual components in patients with open angle glaucoma and ocular hypertension
199 SCIENTIFIC REPORT A 12 week study comparing the fixed combination of latanoprost and timolol with the concomitant use of the individual components in patients with open angle glaucoma and ocular hypertension
Latanoprost 0.005% v/s Timolol Maleate 0.5% Pressure Lowering Effect in Primary Open Angle Glaucoma
 Original Article Latanoprost 0.005% v/s Timolol Maleate 0.5% Pressure Lowering Effect in Primary Open Angle Glaucoma Arshad Ali Lodhi, Khalid Iqbal Talpur, Mahtab Alam Khanzada Pak J Ophthalmol 2008, Vol.
Original Article Latanoprost 0.005% v/s Timolol Maleate 0.5% Pressure Lowering Effect in Primary Open Angle Glaucoma Arshad Ali Lodhi, Khalid Iqbal Talpur, Mahtab Alam Khanzada Pak J Ophthalmol 2008, Vol.
Managing the Patient with POAG
 Managing the Patient with POAG Vision Institute Annual Fall Conference Mitchell W. Dul, OD, MS, FAAO mdul@sunyopt.edu Richard J. Madonna, MA, OD, FAAO rmadonna@sunyopt.edu Ocular Hypertension (OHT) Most
Managing the Patient with POAG Vision Institute Annual Fall Conference Mitchell W. Dul, OD, MS, FAAO mdul@sunyopt.edu Richard J. Madonna, MA, OD, FAAO rmadonna@sunyopt.edu Ocular Hypertension (OHT) Most
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma
 Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
Pooling Data from Similar Randomized Clinical Trials Comparing Latanoprost with Timolol; Medical Results and Statistical Aspects
 Comprehensive Summaries of Uppsala Dissertations from the Faculty of Medicine 1235 Pooling Data from Similar Randomized Clinical Trials Comparing Latanoprost with Timolol; Medical Results and Statistical
Comprehensive Summaries of Uppsala Dissertations from the Faculty of Medicine 1235 Pooling Data from Similar Randomized Clinical Trials Comparing Latanoprost with Timolol; Medical Results and Statistical
Efficacy and Safety of Latanoprost Eye Drops for Glaucoma Treatment: A 1-Year Study in Japan
 Efficacy and Safety of Latanoprost Eye Drops for Glaucoma Treatment: A 1-Year Study in Japan Masanobu Suzuki,* Hiromu K. Mishima,* Kanjiro Masuda, Makoto Araie, Yoshiaki Kitazawa and Ikuo Azuma *Department
Efficacy and Safety of Latanoprost Eye Drops for Glaucoma Treatment: A 1-Year Study in Japan Masanobu Suzuki,* Hiromu K. Mishima,* Kanjiro Masuda, Makoto Araie, Yoshiaki Kitazawa and Ikuo Azuma *Department
BJO Online First, published on September 1, 2009 as /bjo
 BJO Online First, published on September 1, 2009 as 10.1136/bjo.2009.158071 Efficacy and Tolerability of Bimatoprost versus Travoprost in Patients Previously on Latanoprost: a 3-Month, Randomised, Masked-Evaluator,
BJO Online First, published on September 1, 2009 as 10.1136/bjo.2009.158071 Efficacy and Tolerability of Bimatoprost versus Travoprost in Patients Previously on Latanoprost: a 3-Month, Randomised, Masked-Evaluator,
Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study
 Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study James H. Peace, M.D. 1, Casey K. Kopczynski, Ph.D. 2, and Theresa Heah, M.D. 2 1 Inglewood, CA 2
Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study James H. Peace, M.D. 1, Casey K. Kopczynski, Ph.D. 2, and Theresa Heah, M.D. 2 1 Inglewood, CA 2
Intraocular pressure (IOP) is the main risk factor for the
 The Circadian Curve of Intraocular Pressure: Can We Estimate Its Characteristics during Office Hours? Paolo Fogagnolo, 1 Nicola Orzalesi, 2 Antonio Ferreras, 3,4 and Luca Rossetti 2 PURPOSE. To verify
The Circadian Curve of Intraocular Pressure: Can We Estimate Its Characteristics during Office Hours? Paolo Fogagnolo, 1 Nicola Orzalesi, 2 Antonio Ferreras, 3,4 and Luca Rossetti 2 PURPOSE. To verify
Glaucoma Disease Progression Role of Intra Ocular Pressure. Is Good Enough, Low Enough?
 Glaucoma Disease Progression Role of Intra Ocular Pressure Is Good Enough, Low Enough? Glaucoma Diseases Progression Key Considerations Good number of patients may be diagnosed only after some damage the
Glaucoma Disease Progression Role of Intra Ocular Pressure Is Good Enough, Low Enough? Glaucoma Diseases Progression Key Considerations Good number of patients may be diagnosed only after some damage the
Abbreviated Update: Ophthalmic Glaucoma Agents
 Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-945-5220 Fax 503-947-1119 Abbreviated Update: Ophthalmic Glaucoma Agents Month/Year
Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-945-5220 Fax 503-947-1119 Abbreviated Update: Ophthalmic Glaucoma Agents Month/Year
Treatments on the Horizon
 Latanoprostene bunod (Vesneo) Treatments on the Horizon Dominick L Opitz, OD, FAAO Associate Professor Illinois College of Optometry Valeant (B+L) Nitrous oxide-donating prostaglandin F2-alpha analogue
Latanoprostene bunod (Vesneo) Treatments on the Horizon Dominick L Opitz, OD, FAAO Associate Professor Illinois College of Optometry Valeant (B+L) Nitrous oxide-donating prostaglandin F2-alpha analogue
Elevated intraocular pressure (IOP) is a major risk factor for
 Glaucoma Twenty-Four Hour Pattern of Intraocular Pressure in Untreated Patients with Ocular Hypertension Tomas M. Grippo, 1,2 John H. K. Liu, 1 Nazlee Zebardast, 2 Taylor B. Arnold, 3 Grant H. Moore, 1
Glaucoma Twenty-Four Hour Pattern of Intraocular Pressure in Untreated Patients with Ocular Hypertension Tomas M. Grippo, 1,2 John H. K. Liu, 1 Nazlee Zebardast, 2 Taylor B. Arnold, 3 Grant H. Moore, 1
Efficacy and Tolerability of Latanoprost 0.005% in Treatment of Primary Open Angle Glaucoma (POAG)
 Original Article Efficacy and Tolerability of Latanoprost.5% in Treatment of Primary Open Angle Glaucoma (POAG) Muhammad Imran Janjua, Saira Bano, Ali Raza Pak J Ophthalmol 217, Vol. 33, No. 3.....................................................................................................
Original Article Efficacy and Tolerability of Latanoprost.5% in Treatment of Primary Open Angle Glaucoma (POAG) Muhammad Imran Janjua, Saira Bano, Ali Raza Pak J Ophthalmol 217, Vol. 33, No. 3.....................................................................................................
Latanoprost ophthalmic solution in the treatment of open angle glaucoma or raised intraocular pressure: a review
 REVIEW Latanoprost ophthalmic solution in the treatment of open angle glaucoma or raised intraocular pressure: a review Andrea Russo Ivano Riva Teodoro Pizzolante Federico Noto Luciano Quaranta Cattedra
REVIEW Latanoprost ophthalmic solution in the treatment of open angle glaucoma or raised intraocular pressure: a review Andrea Russo Ivano Riva Teodoro Pizzolante Federico Noto Luciano Quaranta Cattedra
Original Article Intraocular Pressure Lowering Effect Pak Armed Forces Med J 2015; 65(1): 94-8
 Original Article Intraocular Pressure Lowering Effect Pak Armed Forces Med J 2015; 65(1): 94-8 COMPARISON OF INTRAOCULAR PRESSURE LOWERING EFFECT OF LATANOPROST AND TIMOLOL COMBINATION VERSUS LATANOPROST
Original Article Intraocular Pressure Lowering Effect Pak Armed Forces Med J 2015; 65(1): 94-8 COMPARISON OF INTRAOCULAR PRESSURE LOWERING EFFECT OF LATANOPROST AND TIMOLOL COMBINATION VERSUS LATANOPROST
Building a Major Ophthalmic Pharmaceutical Company. Aerie Pharmaceuticals, Inc. Company Overview June 2-3, 2015
 Building a Major Ophthalmic Pharmaceutical Company Aerie Pharmaceuticals, Inc. Company Overview June 2-3, 2015 1 Important Information Any discussion of the potential use or expected success of our product
Building a Major Ophthalmic Pharmaceutical Company Aerie Pharmaceuticals, Inc. Company Overview June 2-3, 2015 1 Important Information Any discussion of the potential use or expected success of our product
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
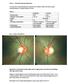 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Original Article. Abstract. Introduction. C Olali, G Malietzis, S Ahmed, E Samaila 1, M Gupta
 Original Article Real-life experience study of the safety and efficacy of travoprost 0.004% / timoptol 0.50% fixed combination ophthalmic solution in intraocular pressure control C Olali, G Malietzis,
Original Article Real-life experience study of the safety and efficacy of travoprost 0.004% / timoptol 0.50% fixed combination ophthalmic solution in intraocular pressure control C Olali, G Malietzis,
[TRAVOPROST] 40 MICROGRAMS/ML, EYE DROPS, SOLUTION RISK MANAGEMENT PLAN. TRAVOPR-v
![[TRAVOPROST] 40 MICROGRAMS/ML, EYE DROPS, SOLUTION RISK MANAGEMENT PLAN. TRAVOPR-v [TRAVOPROST] 40 MICROGRAMS/ML, EYE DROPS, SOLUTION RISK MANAGEMENT PLAN. TRAVOPR-v](/thumbs/94/119684929.jpg) [TRAVOPROST] 40 MICROGRAMS/ML, EYE DROPS, SOLUTION RISK MANAGEMENT PLAN TRAVOPR-v2-270214 VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology Studies estimated that 3-6 million people
[TRAVOPROST] 40 MICROGRAMS/ML, EYE DROPS, SOLUTION RISK MANAGEMENT PLAN TRAVOPR-v2-270214 VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology Studies estimated that 3-6 million people
The role of IOP levels in determining the onset and progression
 Effects of Topical Hypotensive Drugs on Circadian IOP, Blood Pressure, and Calculated Diastolic Ocular Perfusion Pressure in Patients with Glaucoma Luciano Quaranta, Federico Gandolfo, Raffaele Turano,
Effects of Topical Hypotensive Drugs on Circadian IOP, Blood Pressure, and Calculated Diastolic Ocular Perfusion Pressure in Patients with Glaucoma Luciano Quaranta, Federico Gandolfo, Raffaele Turano,
ROBERT L. SHIELDS, M.D. GLAUCOMA SURGERY AND TREATMENT
 1 CURRICULUM VITAE ROBERT L. SHIELDS, M.D. GLAUCOMA SURGERY AND TREATMENT University of Colorado Health Eye Center Cherry Creek 2000 South Colorado Boulevard Annex Building, Suite 100 Denver, Colorado
1 CURRICULUM VITAE ROBERT L. SHIELDS, M.D. GLAUCOMA SURGERY AND TREATMENT University of Colorado Health Eye Center Cherry Creek 2000 South Colorado Boulevard Annex Building, Suite 100 Denver, Colorado
24-hour Intraocular Pressure and Ocular Perfusion Pressure in Glaucoma
 SURVEY OF OPHTHALMOLOGY VOLUME 58 NUMBER 1 JANUARY FEBRUARY 2013 MAJOR REVIEW 24-hour Intraocular Pressure and Ocular Perfusion Pressure in Glaucoma Luciano Quaranta, MD, PhD, 1 Andreas Katsanos, MD, PhD,
SURVEY OF OPHTHALMOLOGY VOLUME 58 NUMBER 1 JANUARY FEBRUARY 2013 MAJOR REVIEW 24-hour Intraocular Pressure and Ocular Perfusion Pressure in Glaucoma Luciano Quaranta, MD, PhD, 1 Andreas Katsanos, MD, PhD,
Restoring Sensitivity to Timolol After Long-Term Drift in Primary Open-Angle Glaucoma
 Investigative Ophthalmology & Visual Science, Vol., No. 2, February 90 Copyright Association for esearch in Vision and Ophthalmology estoring Sensitivity to Timolol After ong-term Drift in Primary Open-Angle
Investigative Ophthalmology & Visual Science, Vol., No. 2, February 90 Copyright Association for esearch in Vision and Ophthalmology estoring Sensitivity to Timolol After ong-term Drift in Primary Open-Angle
F Honrubia, 1 J García-Sánchez, 2 V Polo, 1 J M Martínez de la Casa, 2 J Soto 3. Clinical science
 1 Ophthalmology Service, Hospital Miguel Servet, Zaragoza, Spain; 2 Ophthalmology Service, Hospital Clínico, Madrid, Spain; 3 Medical Unit, Pfizer Spain, Madrid, Spain Correspondence to: Dr J Soto, Medical
1 Ophthalmology Service, Hospital Miguel Servet, Zaragoza, Spain; 2 Ophthalmology Service, Hospital Clínico, Madrid, Spain; 3 Medical Unit, Pfizer Spain, Madrid, Spain Correspondence to: Dr J Soto, Medical
Practical approach to medical management of glaucoma DR. RATHINI LILIAN DAVID
 Practical approach to medical management of glaucoma DR. RATHINI LILIAN DAVID Glaucoma is one of the major causes of visual loss worldwide. The philosophy of glaucoma management is to preserve the visual
Practical approach to medical management of glaucoma DR. RATHINI LILIAN DAVID Glaucoma is one of the major causes of visual loss worldwide. The philosophy of glaucoma management is to preserve the visual
Harvey B DuBiner 1* and Douglas A Hubatsch 2
 DuBiner and Hubatsch BMC Ophthalmology 2014, 14:151 RESEARCH ARTICLE Open Access Late-day intraocular pressure lowering efficacy and tolerability of travoprost 0.004% versus bimatoprost 0.01% in patients
DuBiner and Hubatsch BMC Ophthalmology 2014, 14:151 RESEARCH ARTICLE Open Access Late-day intraocular pressure lowering efficacy and tolerability of travoprost 0.004% versus bimatoprost 0.01% in patients
Clinical effectiveness and safety of brimonidine (0.2%) versus Dorzolamide (2.0%) in primary open angle
 ISSN: 2231-3354 Received on: 07-10-2011 Revised on: 13:10:2011 Accepted on: 21-10-2011 Clinical effectiveness and safety of brimonidine (0.2%) versus Dorzolamide (2.0%) in primary open angle Sharma Neetu,
ISSN: 2231-3354 Received on: 07-10-2011 Revised on: 13:10:2011 Accepted on: 21-10-2011 Clinical effectiveness and safety of brimonidine (0.2%) versus Dorzolamide (2.0%) in primary open angle Sharma Neetu,
Research Article Long-Term Clinical Course of Normal-Tension Glaucoma: 20 Years of Experience
 Hindawi Ophthalmology Volume 2017, Article ID 2651645, 6 pages https://doi.org/10.1155/2017/2651645 Research Article Long-Term Clinical Course of Normal-Tension Glaucoma: 20 Years of Experience Sang Wook
Hindawi Ophthalmology Volume 2017, Article ID 2651645, 6 pages https://doi.org/10.1155/2017/2651645 Research Article Long-Term Clinical Course of Normal-Tension Glaucoma: 20 Years of Experience Sang Wook
Xalatan and Xalatan /betablocker fixed combination : role in glaucoma therapy
 Xalatan and Xalatan /betablocker fixed combination : role in glaucoma therapy Grant McLaren St John Eye Hospital Division of Ophthalmology University of Witwatersrand Johannesburg South Africa 1 Goals
Xalatan and Xalatan /betablocker fixed combination : role in glaucoma therapy Grant McLaren St John Eye Hospital Division of Ophthalmology University of Witwatersrand Johannesburg South Africa 1 Goals
Clinical Research in Glaucoma
 Clinical Research in Glaucoma J. James Thimons, O.D., FAAO Chairman, National Glaucoma Society www.nationalglaucomasociety.org Ocular Hypertension Treatment Study (OHTS) Primary Goals Evaluate the safety
Clinical Research in Glaucoma J. James Thimons, O.D., FAAO Chairman, National Glaucoma Society www.nationalglaucomasociety.org Ocular Hypertension Treatment Study (OHTS) Primary Goals Evaluate the safety
Science & Technologies. UNWANTED SIDE EFFECTS OF TRAVOPROST Gazepov Strahil 1, Iljaz Ismaili 2, Goshevska Dashtevska Emilija 2
 UNWANTED SIDE EFFECTS OF TRAVOPROST Gazepov Strahil 1, Iljaz Ismaili 2, Goshevska Dashtevska Emilija 2 1 Clinical Hospital, Shtip 2 University Eye Clinic,Skopje Introduction: Glaucoma is a chronical progressive
UNWANTED SIDE EFFECTS OF TRAVOPROST Gazepov Strahil 1, Iljaz Ismaili 2, Goshevska Dashtevska Emilija 2 1 Clinical Hospital, Shtip 2 University Eye Clinic,Skopje Introduction: Glaucoma is a chronical progressive
Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors
 CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
Glaucoma: NOT just IOP, Think DPP, OMG!
 Glaucoma: NOT just IOP, Think DPP, OMG! Bruce E. Onofrey, OD, RPh, FAAO Professor, Univ. Houston Exec. Director Continuing Education Programs I m a clinician, so let s talk patients TWO Patients ( a priest
Glaucoma: NOT just IOP, Think DPP, OMG! Bruce E. Onofrey, OD, RPh, FAAO Professor, Univ. Houston Exec. Director Continuing Education Programs I m a clinician, so let s talk patients TWO Patients ( a priest
IOP measurements: 8.00 am (trough drug levels) and am (peak drug levels)(2 hours post dose)
 This overview of 2% eye drops was presented by Dr. Ravin N. Das, at Hotel Satya Ashoka, on 19-6-2004 in place of Dr. H. S. Ray due to unforseen circumstances. This dinner meeting was sponsored by Cipla
This overview of 2% eye drops was presented by Dr. Ravin N. Das, at Hotel Satya Ashoka, on 19-6-2004 in place of Dr. H. S. Ray due to unforseen circumstances. This dinner meeting was sponsored by Cipla
COMPARISON OF IOP LOWERING EFFICACY BRIMONIDINE-TIMOLOL VERSUS DORZOLAMIDE-TIMOLOL FIXED COMBINATION THERAPY
 COMPARISON OF IOP LOWERING EFFICACY BRIMONIDINE-TIMOLOL VERSUS DORZOLAMIDE-TIMOLOL FIXED COMBINATION THERAPY DR. HIDAYATULLA KHAN, M.S. (Ophthalmology) SILVER CRESCENT EYE HOSPITAL Noorkhan Bazar, Hyderabad
COMPARISON OF IOP LOWERING EFFICACY BRIMONIDINE-TIMOLOL VERSUS DORZOLAMIDE-TIMOLOL FIXED COMBINATION THERAPY DR. HIDAYATULLA KHAN, M.S. (Ophthalmology) SILVER CRESCENT EYE HOSPITAL Noorkhan Bazar, Hyderabad
3/31/2019. Role of IOP. Role of IOP. Role of IOP. Role of IOP. Evaluation of glaucoma has changed Why hasn t treatment?
 Glaucoma Update ROLE FOR RHOPRESSA Gregory D. Searcy, M.D. 1857: German ophthalmologist Albrecht Van Graefe concluded all glaucomatous optic disc excavation is associated with high IOP based on the only
Glaucoma Update ROLE FOR RHOPRESSA Gregory D. Searcy, M.D. 1857: German ophthalmologist Albrecht Van Graefe concluded all glaucomatous optic disc excavation is associated with high IOP based on the only
Sustainability of Intraocular Pressure Reduction of Travoprost Ophthalmic Solution in Subjects with Normal Tension Glaucoma
 Adv Ther (2016) 33:435 446 DOI 10.1007/s12325-016-0297-6 ORIGINAL RESEARCH Sustainability of Intraocular Pressure Reduction of Travoprost Ophthalmic Solution in Subjects with Normal Tension Glaucoma Tomoko
Adv Ther (2016) 33:435 446 DOI 10.1007/s12325-016-0297-6 ORIGINAL RESEARCH Sustainability of Intraocular Pressure Reduction of Travoprost Ophthalmic Solution in Subjects with Normal Tension Glaucoma Tomoko
Preservative-Free Tafluprost % in the Treatment of Patients with Glaucoma and Ocular Hypertension
 Adv Ther (211) 28(7):575-585. DOI 1.17/s12325-11-38-9 ORIGINAL RESEARCH Preservative-Free Tafluprost.15% in the Treatment of Patients with Glaucoma and Ocular Hypertension Carl Erb Ines Lanzl Seid-Fatima
Adv Ther (211) 28(7):575-585. DOI 1.17/s12325-11-38-9 ORIGINAL RESEARCH Preservative-Free Tafluprost.15% in the Treatment of Patients with Glaucoma and Ocular Hypertension Carl Erb Ines Lanzl Seid-Fatima
Present relevant clinical findings of four landmark glaucoma trials OHTS, EMGT, CNTGS and CIGTS.
 Course title: The Glaucoma Compass Course length: 1 hour +/- 31 slides Corse Description: Even with the technology and available information, glaucoma decision making can still be confusing. How should
Course title: The Glaucoma Compass Course length: 1 hour +/- 31 slides Corse Description: Even with the technology and available information, glaucoma decision making can still be confusing. How should
Switch from BAK-preserved to preservative-free latanoprost decreases anterior chamber flare in POAG patients
 https://doi.org/10.1007/s10792-017-0792-z ORIGINAL PAPER Switch from BAK-preserved to preservative-free latanoprost decreases anterior chamber flare in POAG patients Ph. A. Kestelyn. Ph. G. Kestelyn. D.
https://doi.org/10.1007/s10792-017-0792-z ORIGINAL PAPER Switch from BAK-preserved to preservative-free latanoprost decreases anterior chamber flare in POAG patients Ph. A. Kestelyn. Ph. G. Kestelyn. D.
Class Update with New Drug Evaluation: Glaucoma Drugs
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Research Article Twenty-Four-Hour Variation of Intraocular Pressure in Primary Open-Angle Glaucoma Treated with Triple Eye Drops
 Hindawi Ophthalmology Volume 2017, Article ID 4398494, 6 pages https://doi.org/10.15/2017/4398494 Research Article Twenty-Four-Hour Variation of Intraocular Pressure in Primary Open-Angle Glaucoma Treated
Hindawi Ophthalmology Volume 2017, Article ID 4398494, 6 pages https://doi.org/10.15/2017/4398494 Research Article Twenty-Four-Hour Variation of Intraocular Pressure in Primary Open-Angle Glaucoma Treated
Glaucoma. Glaucoma. Optic Disc Cupping
 Glaucoma What is Glaucoma? Bruce James A group of diseases in which damage to the optic nerve occurs as a result of intraocualar pressure being above the physiological norm for that eye Stoke Mandeville
Glaucoma What is Glaucoma? Bruce James A group of diseases in which damage to the optic nerve occurs as a result of intraocualar pressure being above the physiological norm for that eye Stoke Mandeville
Diurnal IOP fluctuation: not an independent risk factor for glaucomatous visual field loss in high-risk ocular hypertension.
 Diurnal IOP fluctuation: not an independent risk factor for glaucomatous visual field loss in high-risk ocular hypertension. Bengtsson, Boel; Heijl, Anders Published in: Graefe's Archive for Clinical and
Diurnal IOP fluctuation: not an independent risk factor for glaucomatous visual field loss in high-risk ocular hypertension. Bengtsson, Boel; Heijl, Anders Published in: Graefe's Archive for Clinical and
Financial Disclosure. Prostaglandin Analogs (PGs) The Glaucoma Grab Bag: Practical Guidelines for Effective Glaucoma Therapy
 The Glaucoma Grab Bag: Practical Guidelines for Effective Glaucoma Therapy Danica J. Marrelli, OD, FAAO University of Houston College of Optometry Financial Disclosure I have received I have received speaking
The Glaucoma Grab Bag: Practical Guidelines for Effective Glaucoma Therapy Danica J. Marrelli, OD, FAAO University of Houston College of Optometry Financial Disclosure I have received I have received speaking
Primary open-angle glaucoma (OAG) is a chronic ocular
 ORIGINAL STUDY Ocular Hypotensive Effect of ONO-9054, an EP 3 /FP Receptor Agonist: Results of a Randomized, Placebocontrolled, Dose Escalation Study Alon Harris, MS, PhD, FARVO,* Caroline L. Ward, PhD,
ORIGINAL STUDY Ocular Hypotensive Effect of ONO-9054, an EP 3 /FP Receptor Agonist: Results of a Randomized, Placebocontrolled, Dose Escalation Study Alon Harris, MS, PhD, FARVO,* Caroline L. Ward, PhD,
LONG TERM IOP LOWERING EFFICACY OF BIMATOPROST/TIMOLOL FIXED COMBINATION: A 12 MONTH PROSPECTIVE STUDY
 LONG TERM IOP LOWERING EFFICACY OF BIMATOPROST/TIMOLOL FIXED COMBINATION: A 12 MONTH PROSPECTIVE STUDY LEQUEU I, THEUWIS K *1, ABEGAzO PINTO L *1,2, VANDEWALLE E 1,3, STALMANS I 1,3 ABSTRACT Purpose: To
LONG TERM IOP LOWERING EFFICACY OF BIMATOPROST/TIMOLOL FIXED COMBINATION: A 12 MONTH PROSPECTIVE STUDY LEQUEU I, THEUWIS K *1, ABEGAzO PINTO L *1,2, VANDEWALLE E 1,3, STALMANS I 1,3 ABSTRACT Purpose: To
Effect of a Single Drop of Latanoprost on Intraocular Pressure and Blood-Aqueous Barrier Permeability in Patients with Uveitis
 Kobe J. Med. Sci., Vol. 48, No. 6, pp. 153-159, 2002 Effect of a Single Drop of Latanoprost on Intraocular Pressure and Blood-Aqueous Barrier Permeability in Patients with Uveitis YOSHIAKI KIUCHI, KOJI
Kobe J. Med. Sci., Vol. 48, No. 6, pp. 153-159, 2002 Effect of a Single Drop of Latanoprost on Intraocular Pressure and Blood-Aqueous Barrier Permeability in Patients with Uveitis YOSHIAKI KIUCHI, KOJI
East and North Hertfordshire treatment pathway for primary open angle glaucoma and ocular hypertension in adults
 East and North Hertfordshire treatment pathway for primary open angle glaucoma and ocular hypertension in adults Introduction Glaucoma is a group of eye diseases causing optic nerve damage. In most cases
East and North Hertfordshire treatment pathway for primary open angle glaucoma and ocular hypertension in adults Introduction Glaucoma is a group of eye diseases causing optic nerve damage. In most cases
The improvement in perimetric results occurring over
 ORIGINAL STUDY Learning Effect of Humphrey Matrix Frequency Doubling Technology Perimetry in Patients With Ocular Hypertension Marco Centofanti, MD, PhD,*w Paolo Fogagnolo, MD,w Francesco Oddone, MD,w
ORIGINAL STUDY Learning Effect of Humphrey Matrix Frequency Doubling Technology Perimetry in Patients With Ocular Hypertension Marco Centofanti, MD, PhD,*w Paolo Fogagnolo, MD,w Francesco Oddone, MD,w
Rossetti et al. BMC Ophthalmology 2015, 15:7
 Rossetti et al. BMC Ophthalmology 2015, 15:7 RESEARCH ARTICLE Open Access Comparison of the effects of bimatoprost and a fixed combination of latanoprost and timolol on 24-hour blood and ocular perfusion
Rossetti et al. BMC Ophthalmology 2015, 15:7 RESEARCH ARTICLE Open Access Comparison of the effects of bimatoprost and a fixed combination of latanoprost and timolol on 24-hour blood and ocular perfusion
National Institute for Health and Clinical Excellence. Glaucoma. Guideline Consultation Comments Table. 29 September November 2008
 National Institute for Health and Clinical Excellence Glaucoma Guideline Consultation Comments Table 29 September 2008 24 November 2008 Stat us Organisa tion Order no. Version Page no Line no/se ction
National Institute for Health and Clinical Excellence Glaucoma Guideline Consultation Comments Table 29 September 2008 24 November 2008 Stat us Organisa tion Order no. Version Page no Line no/se ction
Elements for a public summary. Overview of disease epidemiology
 VI.2 VI.2.1 Elements for a public summary Overview of disease epidemiology Glaucoma is an eye disease that can result in damage to the optic nerve and loss of vision (blindness). It is the major cause
VI.2 VI.2.1 Elements for a public summary Overview of disease epidemiology Glaucoma is an eye disease that can result in damage to the optic nerve and loss of vision (blindness). It is the major cause
PRACTICAL APPROACH TO MEDICAL MANAGEMENT OF GLAUCOMA
 PRACTICAL APPROACH TO MEDICAL MANAGEMENT OF GLAUCOMA DR. RAVI THOMAS, DR. RAJUL PARIKH, DR. SHEFALI PARIKH IJO MAY 2008 PRESENTER AT JDOS : DR. RAHUL SHUKLA T.N. SHUKLA EYE HOSPITAL TERMINOLOGY POAG: PRIMARY
PRACTICAL APPROACH TO MEDICAL MANAGEMENT OF GLAUCOMA DR. RAVI THOMAS, DR. RAJUL PARIKH, DR. SHEFALI PARIKH IJO MAY 2008 PRESENTER AT JDOS : DR. RAHUL SHUKLA T.N. SHUKLA EYE HOSPITAL TERMINOLOGY POAG: PRIMARY
Innovations in Glaucoma Drug Delivery What the Future Holds. Justin Schweitzer, OD, FAAO Vance Thompson Vision Sioux Falls, South Dakota
 Innovations in Glaucoma Drug Delivery What the Future Holds Justin Schweitzer, OD, FAAO Vance Thompson Vision Sioux Falls, South Dakota Allergan Glaukos Bausch and Lomb Bio- Tissue Alcon TearScience Reichert
Innovations in Glaucoma Drug Delivery What the Future Holds Justin Schweitzer, OD, FAAO Vance Thompson Vision Sioux Falls, South Dakota Allergan Glaukos Bausch and Lomb Bio- Tissue Alcon TearScience Reichert
Collaboration in the care of glaucoma patients and glaucoma suspects. Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012
 Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC)
 Guidelines for the medical treatment of chronic open angle glaucoma and ocular hypertension Summary: DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) Diagnosis and management of ocular hypertension (OHT)
Guidelines for the medical treatment of chronic open angle glaucoma and ocular hypertension Summary: DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) Diagnosis and management of ocular hypertension (OHT)
WARNING LETTER DEPARTMENT OF HEALTH & HUMAN SERVICES TRANSMITTED BY FACSIMILE
 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration Rockville, MD 20857 TRANSMITTED BY FACSIMILE David E.I. Pyott President and Chief Executive Officer PO Box 19534
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration Rockville, MD 20857 TRANSMITTED BY FACSIMILE David E.I. Pyott President and Chief Executive Officer PO Box 19534
Elements for a public summary. VI.2.1 Overview of disease epidemiology
 VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology Studies estimated that 3-6 million people in the United States alone, including 4-10% of the population older than 40 years, have
VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology Studies estimated that 3-6 million people in the United States alone, including 4-10% of the population older than 40 years, have
CLINICAL SCIENCES. Fellow Eye Prognosis in Patients With Severe Visual Field Loss in 1 Eye From Chronic Open-Angle Glaucoma
 Fellow Eye Prognosis in Patients With Severe Visual Field Loss in 1 Eye From Chronic Open-Angle Glaucoma Philip P. Chen, MD; Anuja Bhandari, FRCOphth CLINICAL SCIENCES Objectives: To examine the prognosis
Fellow Eye Prognosis in Patients With Severe Visual Field Loss in 1 Eye From Chronic Open-Angle Glaucoma Philip P. Chen, MD; Anuja Bhandari, FRCOphth CLINICAL SCIENCES Objectives: To examine the prognosis
Sponsor. Generic Drug Name. Trial Indications. Protocol Number. Protocol Title. Clinical Trial Phase. Study Start/End Dates. Reason for Termination
 Sponsor Alcon Research, Ltd. Generic Drug Name Travoprost/timolol maleate Trial Indications Open-angle glaucoma or ocular hypertension Protocol Number C-09-007 Protocol Title An Evaluation of Patient Reported
Sponsor Alcon Research, Ltd. Generic Drug Name Travoprost/timolol maleate Trial Indications Open-angle glaucoma or ocular hypertension Protocol Number C-09-007 Protocol Title An Evaluation of Patient Reported
GLAUCOMA IS CHARACTERIZED BY OPTIC NEUROPathy
 Polyquaternium-1 Preserved Travoprost 0.003% or Benzalkonium Chloride Preserved Travoprost 0.004% for Glaucoma and Ocular Hypertension JAMES H. PEACE, PETER AHLBERG, MATHIAS WAGNER, JOHN M. LIM, DAVID
Polyquaternium-1 Preserved Travoprost 0.003% or Benzalkonium Chloride Preserved Travoprost 0.004% for Glaucoma and Ocular Hypertension JAMES H. PEACE, PETER AHLBERG, MATHIAS WAGNER, JOHN M. LIM, DAVID
CLINICAL SCIENCES. Comparison of the Early Effects of Brimonidine and Apraclonidine as Topical Ocular Hypotensive Agents
 Comparison of the Early Effects of Brimonidine and Apraclonidine as Topical Ocular Hypotensive Agents Todd L. Maus, MD; Cherie Nau; Richard F. Brubaker, MD CLINICAL SCIENCES Objective: To compare the mechanism
Comparison of the Early Effects of Brimonidine and Apraclonidine as Topical Ocular Hypotensive Agents Todd L. Maus, MD; Cherie Nau; Richard F. Brubaker, MD CLINICAL SCIENCES Objective: To compare the mechanism
Evaluating visual field over time is a key element in the
 The Effects of Intraocular Pressure Reduction on Perimetric Variability in Glaucomatous Eyes Paolo Fogagnolo, 1 Andrew McNaught, 2 Marco Centofanti, 1,3 Luca Rossetti, 4 and Nicola Orzalesi 4 PURPOSE.
The Effects of Intraocular Pressure Reduction on Perimetric Variability in Glaucomatous Eyes Paolo Fogagnolo, 1 Andrew McNaught, 2 Marco Centofanti, 1,3 Luca Rossetti, 4 and Nicola Orzalesi 4 PURPOSE.
STANDARD AUTOMATED PERIMETRY IS A GENERALLY
 Comparison of Long-term Variability for Standard and Short-wavelength Automated Perimetry in Stable Glaucoma Patients EYTAN Z. BLUMENTHAL, MD, PAMELA A. SAMPLE, PHD, LINDA ZANGWILL, PHD, ALEXANDER C. LEE,
Comparison of Long-term Variability for Standard and Short-wavelength Automated Perimetry in Stable Glaucoma Patients EYTAN Z. BLUMENTHAL, MD, PAMELA A. SAMPLE, PHD, LINDA ZANGWILL, PHD, ALEXANDER C. LEE,
Joao F. Lopes 1*, Douglas A. Hubatsch 2 and Patricia Amaris 3
 Lopes et al. BMC Ophthalmology (2015) 15:166 DOI 10.1186/s12886-015-0151-7 RESEARCH ARTICLE Open Access Effect of benzalkonium chloride free travoprost on intraocular pressure and ocular surface symptoms
Lopes et al. BMC Ophthalmology (2015) 15:166 DOI 10.1186/s12886-015-0151-7 RESEARCH ARTICLE Open Access Effect of benzalkonium chloride free travoprost on intraocular pressure and ocular surface symptoms
Factors Associated With Visual Field Progression in Cirrus Optical Coherence Tomography-guided Progression Analysis: A Topographic Approach
 ORIGINAL STUDY Factors Associated With Visual Field Progression in Cirrus Optical Coherence Tomography-guided Progression Analysis: A Topographic Approach Joong Won Shin, MD, Kyung Rim Sung, MD, PhD, Jiyun
ORIGINAL STUDY Factors Associated With Visual Field Progression in Cirrus Optical Coherence Tomography-guided Progression Analysis: A Topographic Approach Joong Won Shin, MD, Kyung Rim Sung, MD, PhD, Jiyun
Messages From the Advanced Glaucoma Intervention Study
 Landmark Studies Section editor: Ronald L. Fellman, MD Take-Home Messages From the Advanced Glaucoma Intervention Study By Leon W. Herndon, MD, and Daniel B. Moore, MD I tasked Leon W. Herndon, MD, and
Landmark Studies Section editor: Ronald L. Fellman, MD Take-Home Messages From the Advanced Glaucoma Intervention Study By Leon W. Herndon, MD, and Daniel B. Moore, MD I tasked Leon W. Herndon, MD, and
Class Update: Ophthalmic Glaucoma Agents
 Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-945-5220 Fax 503-947-1119 Class Update: Ophthalmic Glaucoma Agents Month/Year
Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-945-5220 Fax 503-947-1119 Class Update: Ophthalmic Glaucoma Agents Month/Year
Persistency and clinical outcomes associated with latanoprost and beta-blocker monotherapy: Evidence from a European retrospective cohort study
 European Journal of Ophthalmology / Vol. 13 / Suppl. 4, 2003 / pp. S21-S29 Persistency and clinical outcomes associated with latanoprost and beta-blocker monotherapy: Evidence from a European retrospective
European Journal of Ophthalmology / Vol. 13 / Suppl. 4, 2003 / pp. S21-S29 Persistency and clinical outcomes associated with latanoprost and beta-blocker monotherapy: Evidence from a European retrospective
MODERN DIAGNOSTICS AND TREATMENT OF GLAUCOMA
 Semmelweis University, Ph.D. School, Clinical Sciences, Ophthalmology Head of Program: Ildikó Süveges, M.D., Ph.D., D.Sc. Tutor: Gábor Holló, M.D., Ph.D. MODERN DIAGNOSTICS AND TREATMENT OF GLAUCOMA Ph.D.
Semmelweis University, Ph.D. School, Clinical Sciences, Ophthalmology Head of Program: Ildikó Süveges, M.D., Ph.D., D.Sc. Tutor: Gábor Holló, M.D., Ph.D. MODERN DIAGNOSTICS AND TREATMENT OF GLAUCOMA Ph.D.
Comparison of Intraocular Pressure Lowering Effect of Travoprost and Timolol / Dorzolamide Combination in Primary Open Angle Glaucoma
 Original Article Comparison of Intraocular Pressure Lowering Effect of Travoprost and Timolol / Dorzolamide Combination in Primary Open Angle Glaucoma Farooq Khan, Mubashir Rehman, Omar Ilyas, Mohammad
Original Article Comparison of Intraocular Pressure Lowering Effect of Travoprost and Timolol / Dorzolamide Combination in Primary Open Angle Glaucoma Farooq Khan, Mubashir Rehman, Omar Ilyas, Mohammad
Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1
 Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1 By: Andrew Kemp, OD, Marcus Gonzales, OD, FAAO, Joe DeLoach, OD, FAAO, and Zanna Kruoch, OD FAAO Background Glaucoma is a range of conditions
Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1 By: Andrew Kemp, OD, Marcus Gonzales, OD, FAAO, Joe DeLoach, OD, FAAO, and Zanna Kruoch, OD FAAO Background Glaucoma is a range of conditions
L atanoprost, a prostaglandin (PG) F2α related compound, is
 297 CLINICAL SCIENCE Effect of non-steroidal anti-inflammatory ophthalmic solution on intraocular pressure reduction by latanoprost K Kashiwagi, S Tsukahara... See end of article for authors affiliations...
297 CLINICAL SCIENCE Effect of non-steroidal anti-inflammatory ophthalmic solution on intraocular pressure reduction by latanoprost K Kashiwagi, S Tsukahara... See end of article for authors affiliations...
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND PACHYMETRY. POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
The second most common causes of blindness worldwide. ( after cataract) The commonest cause of irreversible blindness in the world Estimated that 3%
 The second most common causes of blindness worldwide. ( after cataract) The commonest cause of irreversible blindness in the world Estimated that 3% of our population age > 40 have glaucoma In the past:
The second most common causes of blindness worldwide. ( after cataract) The commonest cause of irreversible blindness in the world Estimated that 3% of our population age > 40 have glaucoma In the past:
SUPPLEMENTARY INFORMATION
 SUPPLEMENTARY INFORMATION Contents METHODS... 2 Inclusion and exclusion criteria... 2 Supplementary table S1... 2 Assessment of abnormal ocular signs and symptoms... 3 Supplementary table S2... 3 Ocular
SUPPLEMENTARY INFORMATION Contents METHODS... 2 Inclusion and exclusion criteria... 2 Supplementary table S1... 2 Assessment of abnormal ocular signs and symptoms... 3 Supplementary table S2... 3 Ocular
INTRODUCTION S. HERDENER, D. HAFIZOVIC, M. PACHE, S. LAUTEBACH, J. FUNK. University Eye Hospital, Freiburg - Germany
 European Journal of Ophthalmology / Vol. 18 no. 1, 2008 / pp. 39-43 Is the PASCAL -Tonometer suitable for measuring intraocular pressure in clinical routine? Long- and short-term reproducibility of dynamic
European Journal of Ophthalmology / Vol. 18 no. 1, 2008 / pp. 39-43 Is the PASCAL -Tonometer suitable for measuring intraocular pressure in clinical routine? Long- and short-term reproducibility of dynamic
Glaucoma: target intraocular pressures and current treatments James McAllister FRCS, FRCOphth
 Glaucoma: target intraocular pressures and current treatments James McAllister FRCS, FRCOphth Skyline Imaging Ltd Our Drug review of glaucoma management describes the use of target intraocular pressures
Glaucoma: target intraocular pressures and current treatments James McAllister FRCS, FRCOphth Skyline Imaging Ltd Our Drug review of glaucoma management describes the use of target intraocular pressures
Evolution of the Definition of Primary Open-Angle Glaucoma
 OCULAR BLOOD FLOW IN GLAUCOMA MANAGEMENT AHMED HOSSAM ABDALLA PROFESSOR AND HEAD OF OPHTHALMOLOGY DEPARTEMENT ALEXANDRIA UNIVERSITY Evolution of the Definition of Primary Open-Angle Glaucoma Former definition
OCULAR BLOOD FLOW IN GLAUCOMA MANAGEMENT AHMED HOSSAM ABDALLA PROFESSOR AND HEAD OF OPHTHALMOLOGY DEPARTEMENT ALEXANDRIA UNIVERSITY Evolution of the Definition of Primary Open-Angle Glaucoma Former definition
The treatment benefit of latanoprost has not been studied in the following populations/patients:
 6.1. ELEMENTS FOR A PUBLIC SUMMARY 6.1.1. Overview of Disease Epidemiology Glaucoma is the second leading cause of blindness worldwide, and affects about 66.8 million people worldwide i,ii. Glaucoma can
6.1. ELEMENTS FOR A PUBLIC SUMMARY 6.1.1. Overview of Disease Epidemiology Glaucoma is the second leading cause of blindness worldwide, and affects about 66.8 million people worldwide i,ii. Glaucoma can
STARTING IN THE 1960s, epidemiological. Reduction of Intraocular Pressure and Glaucoma Progression. Results From the Early Manifest Glaucoma Trial
 CLINICAL SCIENCES Reduction of Intraocular Pressure and Glaucoma Progression Results From the Early Manifest Glaucoma Trial Anders Heijl, MD, PhD; M. Cristina Leske, MD, MPH; Bo Bengtsson, MD, PhD; Leslie
CLINICAL SCIENCES Reduction of Intraocular Pressure and Glaucoma Progression Results From the Early Manifest Glaucoma Trial Anders Heijl, MD, PhD; M. Cristina Leske, MD, MPH; Bo Bengtsson, MD, PhD; Leslie
Aerie Pharmaceuticals, Inc. Additional Rhopressa Rocket 1 Analyses and Path Forward
 Aerie Pharmaceuticals, Inc. Additional Rhopressa Rocket 1 Analyses and Path Forward May 7, 2015 1 Important Information Any discussion of the potential use or expected success of our product candidates
Aerie Pharmaceuticals, Inc. Additional Rhopressa Rocket 1 Analyses and Path Forward May 7, 2015 1 Important Information Any discussion of the potential use or expected success of our product candidates
The Utility of the Monocular Trial
 The Utility of the Monocular Trial Data from the Ocular Hypertension Treatment Study Anjali M. Bhorade, MD, MSCI, 1 Bradley S. Wilson, MA, 1 Mae O. Gordon, PhD, 1 Paul Palmberg, MD, PhD, 2 Robert N. Weinreb,
The Utility of the Monocular Trial Data from the Ocular Hypertension Treatment Study Anjali M. Bhorade, MD, MSCI, 1 Bradley S. Wilson, MA, 1 Mae O. Gordon, PhD, 1 Paul Palmberg, MD, PhD, 2 Robert N. Weinreb,
Provocative testing for primary open-angle glaucoma in "senior citizens" Norman Ballin* and Bernard Becker
 Provocative testing for primary open-angle glaucoma in "senior citizens" Norman Ballin* and Bernard Becker A group of "senior citizens" was studied with respect to applanation pressures, water-provocative
Provocative testing for primary open-angle glaucoma in "senior citizens" Norman Ballin* and Bernard Becker A group of "senior citizens" was studied with respect to applanation pressures, water-provocative
