CLINICAL SCIENCES. Fellow Eye Prognosis in Patients With Severe Visual Field Loss in 1 Eye From Chronic Open-Angle Glaucoma
|
|
|
- Albert Dawson
- 5 years ago
- Views:
Transcription
1 Fellow Eye Prognosis in Patients With Severe Visual Field Loss in 1 Eye From Chronic Open-Angle Glaucoma Philip P. Chen, MD; Anuja Bhandari, FRCOphth CLINICAL SCIENCES Objectives: To examine the prognosis for the fellow eye of patients with severe visual field loss in 1 eye from chronic forms of open-angle glaucoma, and to identify risk factors for visual field progression in such eyes. Methods: Review of 36 patients followed in an academic medical center with monocular severe visual field loss (Advanced Glaucoma Intervention Study score 12) from open-angle glaucoma either at initial Humphrey visual field testing or during follow-up. Change in Advanced Glaucoma Intervention Study visual field score and clinical evaluation were used to determine visual field progression. Kaplan-Meier survival analysis and Cox proportional hazards survival regression were used to estimate visual field progression in fellow eyes and assess possible risk factors. Results: During 67 ± 32 months (mean ± SD), 12 of 36 first-affected eyes (33%) and 6 fellow eyes (17%) had significant visual field progression. The Kaplan-Meier estimate of visual field progression in the fellow eye was 12.4% at 5 years after severe visual field loss in the first eye. Compared with stable fellow eyes, fellow eyes with visual field progression had significantly larger initial cupdisc ratio, smaller between-eyes difference in the initial Advanced Glaucoma Intervention Study score, and lower calculated ocular perfusion pressure. Ocular perfusion pressure was the only variable significantly associated with visual field progression by Cox proportional hazards survival regression (P =.019). During an average of 10.2 years of disease, 2 patients (6%) became bilaterally blind from glaucoma. Conclusions: In this predominantly white population, fellow eyes of patients with severe visual field loss in 1 eye from open-angle glaucoma were not at particularly high risk for further visual field progression, and few patients became bilaterally blind. Fellow eye visual field progression was associated with lower calculated ocular perfusion pressure. Arch Ophthalmol. 2000;118: From the Department of Ophthalmology, University of Washington School of Medicine, Seattle. The authors do not have any proprietary interest in any product mentioned in this article. GLAUCOMA IS a leading cause of blindness in the world. 1,2 Populationbased studies in the United States have found glaucoma to cause 2.5% to 6.3% of bilateral blindness in white patients, 2-5 with levels many times higher in African American patients. 4,6 When automated perimetric data are examined in patients with treated glaucoma, most studies have noted rates of glaucomatous visual field progression ranging from 9% to 30% during periods of 2 to 7 years, 7-18 though others describe higher rates However, these studies are almost entirely based on 1-eye results. Some authors estimate that progression of glaucomatous visual field loss does not frequently result in bilateral blindness during the average course of the disease. 3,23 Prognostic information is important to patients who have severe damage in 1 eye from glaucoma. Grant and Burke 24 reviewed cases of blindness from glaucoma and noted that pairs of eyes tended to behave alike, but outcomes for the fellow eye of patients with severe monocular visual field damage have not been systematically studied. We investigated visual field progression and severe visual field loss in fellow eyes of patients with 1 eye severely damaged from chronic forms of open-angle glaucoma (OAG) to obtain prognostic data and risk factors for fellow eye visual field loss. RESULTS Of 294 patients identified using information from the database on the Humphrey perimeters, 205 (70%) had glaucoma; of these, 36 (18%) fulfilled inclusion criteria (21 men and 15 women). Reasons for exclusion included an AGIS score less than 12 in the worse eye in 66 patients (32%); insufficient follow-up, 64 (31%); other 473
2 PATIENTS, MATERIALS, AND METHODS We reviewed the databases of the Humphrey perimeters (Humphrey Instruments, Dublin, Calif) at the University of Washington Eye Center, Seattle, to identify patients with severe glaucomatous visual field loss in at least 1 eye on program 24-2 or 30-2 perimetry. Our screening criteria included (1) depression of points at least 10 db below normal in at least 3 of 4 quadrants to within 20 of fixation; (2) loss of at least 10 db below normal within 10 of fixation; (3) testing with either the 10-2 program or with a size V stimulus; or (4) testing of only 1 eye. Inclusion criteria included (1) diagnosis of primary OAG (POAG), pseudoexfoliative (PXG), pigmentary, or normal-tension glaucoma (NTG) with open angles documented on gonioscopy; (2) visual acuity and/or visual field loss attributable to glaucoma rather than other causes (media opacity, retinal or vascular disease, nonglaucomatous optic neuropathy, neuro-ophthalmic causes); (3) length of follow-up with Humphrey visual field testing of 2 years or more; (4) visual field tests that fulfilled published criteria for reliability 25 ; and (5) patients without bilaterally severe glaucomatous visual field loss (defined as an Advanced Glaucoma Intervention Study [AGIS] score of 12 or more on a scale of 0-20) 26 at initial visual field testing. We included patients undergoing treatment for NTG because a recent randomized clinical trial provides strong evidence that treated NTG has similar visual field progression rates as treated POAG. 18 Patients medical records were then reviewed for pertinent information: sex, race, diagnosis, age when severe visual field loss was noted in the first eye, ocular history (specifically noting date of glaucoma diagnosis, previous laser or incisional surgery, refractive error [prior to cataract surgery when applicable], medications, and family history of glaucoma), and medical history (specifically noting presence of diabetes mellitus, hypertension, cardiovascular disease, and thyroid disease). Systolic and diastolic blood pressure (BP) measurements were recorded from the clinic notes in the patient s hospital record from the ophthalmology department and other specialty services, and the average was calculated. Ophthalmic data recorded for each eye included visual acuity, disc hemorrhages, medications, and procedures. Not every patient had serial optic disc photographs for review, so cup-disc (C/D) ratios as recorded in the record were used for analysis. Each intraocular pressure (IOP) measurement by Goldmann applanation tonometry was recorded, and the average for each 3-month period was calculated to derive an overall mean IOP. The highest and lowest IOP in the record was noted for each eye. Most patients had target IOPs set by the treating physician(s), generally based on optic nerve appearance, severity of visual field loss, and starting or current IOP. For patients with non-ntg, the target IOP for undamaged eyes (normal visual field test results) was approximately 21 mm Hg; eyes with early damage (early nasal or arcuate damage) had a target IOP in the upper teens; eyes with moderate damage (more dense arcuate and nasal damage, or both superior and inferior damage) had a target IOP in the mid teens; and eyes with advanced damage (very dense superior or inferior damage, with or without involvement of the opposite hemifield) had a target IOP in the low teens. The target IOP for patients with NTG was generally several milligrams of mercury lower than that for patients with non-ntg. Visual acuity throughout follow-up was compared with initial findings, and final visual acuity was considered unchanged if it was within 2 Snellen lines of initial visual acuity. Noncompliance with treatment was noted if the patient admitted poor compliance with medicines, if multiple follow-up visits were missed, or if the treating physician s notes indicated it was a problem. Ocular perfusion pressure was considered equal to two-thirds the mean arterial pressure mean IOP 27 and was calculated using the following formula: [(Mean Systolic Mean Diastolic BP)/3] + (Mean Diastolic BP) 2 3 Mean IOP. Visual field tests were generally obtained yearly, although some patients underwent more frequent testing, and others were tested at slightly greater intervals. In some cases in which the visual acuity in the first-affected eye (hereafter referred to as first eye ) was worse than 20/200, Humphrey visual field testing was not regularly performed in that eye, but the fellow eye continued to be tested regularly. If early improvement in visual field test results (learning effect) was evident, the visual field test used for scoring purposes as the initial test was one obtained after this learning effect had stabilized. Generally, if the clinician considered cataract to be serious, visual field testing was deferred until after cataract extraction, with or without trabeculectomy. For each visual field test, the AGIS score was calculated, and the mean deviation, pattern SD, and corrected pattern SD were recorded. Only visual field tests that met published criteria for reliability 25 and that had a total deviation plot were used. The primary methods used to determine the progression of glaucomatous visual field loss were the following: (1) Comparison of initial and final AGIS scores (AGIS criteria); a change of 4 or more AGIS points was considered to be significant, since fewer than 5% of eyes with glaucomatous visual field loss will show longterm fluctuation of 4 or more AGIS points. 26 A subsequent article has confirmed that a change of 4 or more points will be confirmed on repeated testing in 95% of cases. 17 Although linear regression may be useful in the interpretation of visual field progression, 13,15,16,28 it requires many visual field tests and/or many years of follow-up for it to be valid. 15,16,29 (2) Clinical evaluation, in which visual field progression was the reason for a lowering of the target IOP. Comparison of initial and final Collaborative Initial Glaucoma Treatment Study (CIGTS) scores was also used as a secondary method of examining fellow eye visual field progression. 30 A change in the CIGTS score of 3 or more points was considered to be significant. We assumed this criteria would detect smaller amounts of visual field progression than might be considered significant by AGIS criteria, although no data have been published on long-term fluctuation using this scoring system. All data were entered into a spreadsheet computer program (SPSS 6.1; SPSS, Chicago, Ill). Kaplan-Meier survival analysis was used to estimate rates of visual field progression for fellow eyes. Variables considered to be possible risk factors for visual field progression were examined using the independent samples t test, Fisher exact test, and Cox proportional hazards survival regression with forwardstepwise selection. Results are given as the mean ± SD where applicable. 474
3 Table 1. Demographics and Characteristics of Patients Studied* Characteristic Age, y 69.5 ± 10.3 (43-81) Follow-up, mo 67.2 ± 31.6 (24-140) No. of visual field tests 7.1 ± 4.5 (3-27) Length of disease, y 10.2 ± 4.6 (2-19) Humphrey Visual Field Test Initial Final Cup-disc ratio First-affected eye 0.83 ± 0.13 ( ) 0.91 ± 0.11 ( ) Fellow eye 0.61 ± 0.21 ( ) 0.69 ± 0.25 ( ) Mean deviation, db First-affected eye 17.9 ± 6.0 ( 2.1 to 27.5) 20.6 ± 4.0 ( 14.4 to 29.7) Fellow eye 6.0 ± 4.8 (+1.3 to 15.6) 7.4 ± 7.4 (+1.9 to 26.1) Pattern SD, db First-affected eye 10.0 ± 2.5 ( ) 10.5 ± 3.0 ( ) Fellow eye 6.4 ± 3.8 ( ) 7.3 ± 4.6 ( ) Corrected pattern SD, db First-affected eye 9.3 ± 3.0 ( ) 10.2 ± 3.2 ( ) Fellow eye 5.5 ± 4.1 ( ) 6.3 ± 9.8 ( ) AGIS score First-affected eye 13.1 ± 4.2 (2-20) 15.2 ± 2.7 (12-20) Fellow eye 4.3 ± 3.9 (0-11) 5.2 ± 5.3 (0-20) *AGIS indicates Advanced Glaucoma Intervention Study; age, age at time of initial visual field test showing first-affected eye severe visual loss. All values are given as mean ± SD (range). types of glaucoma, 13 (6%); confounding ocular disease, 11 (5%); severe visual field loss bilaterally on initial visual field testing, 8 (4%); and consistently unreliable visual field test results, 7 (3%). Thirty patients were white (primarily of Northern European ancestry), 3 were Asian, and 3 were black. Glaucoma diagnoses included POAG in 18 patients; PXG, 14; NTG, 2; and pigmentary glaucoma, 2. Thirteen of 14 patients with PXG were being treated for glaucoma in both eyes. The diagnosis of glaucoma was made between 1979 and 1984 in 9 patients (25%), between 1985 and 1989 in 15 (42%), and in 1990 or later in 12 (33%). A family history of glaucoma in a first-degree relative was known in 10 of 31 patients for whom this information was noted in the medical record. Myopia was noted in 26 of 35 patients for whom this information could be obtained. One patient died after 46 months follow-up. Other demographics and characteristics of the patients studied are given in Table 1. Among first eyes, all 36 had an AGIS score of 12 or more either on initial Humphrey visual field testing (25), or at final visual field testing (11). The first eye to have severe visual field loss from glaucoma was the right eye in 14 patients and the left in 22. Two first eyes had decreased initial visual acuity from glaucoma. First eye visual field progression was noted in 12 patients (33%) in 10 (28%) by AGIS criteria and in 2 (6%) by clinical judgment with a change in AGIS score of 3 points. Progression of visual field loss was confirmed with at least 1 further visual field test in 8 eyes; in 4 eyes, no further testing was obtained. Among first eyes, progression of visual field Proportion of Stable Fellow Eyes Months After First-Affected Eye Severe Visual Field Loss Kaplan-Meier survival plot of visual field progression in fellow eyes from the time of the initial visual field test, which showed severe visual field loss in the first-affected eye. loss was found in 1 of 2 with NTG, in 8 of 18 with POAG, and in 3 of 14 with PXG. Progression of visual field loss in fellow eyes was noted in 6 patients (17%) in 5 (14%) by AGIS criteria and in 1 (3%) by clinical judgment with an increase in AGIS score of 3 points. Five of 6 eyes had a final AGIS score higher than or equal to 12. Visual field progression was confirmed with at least 1 more visual field test in 4 of 6 eyes; in the other 2, no further visual field testing was obtained. The average time between severe visual field loss in first and fellow eyes was 37 ± 28 months. Fellow eye visual field progression was found in 3 eyes with POAG, in 2 with PXG, and in 1 with pigmentary glaucoma. When CIGTS scoring was used, 1 additional eye was found to have visual field progression, but no additional visual field testing was performed to confirm progression. Whether using AGIS or CIGTS scoring, Kaplan-Meier survival analysis estimated visual field progression for fellow eyes to be 12.4% at 5 years after severe visual field loss in the first eye (95% confidence interval, 0.9%-23.9%) (Figure). Four patients had bilateral visual field progression. The Spearman rank correlation coefficient between first and fellow eyes for progression of visual field loss was not significant (R = 0.316; P =.06), but the betweeneye correlation for change in AGIS score was significant (R = 0.495; P =.002). Differences between fellow eyes with and without visual field progression are given in Table 2. The slope of change in mean deviation and pattern SD was significantly steeper in eyes with visual field progression. The initial C/D ratio was significantly larger in fellow eyes with visual field progression (P =.01). The mean IOP was not significantly higher in first and fellow eyes with visual field progression. The range, minimum, and maximum IOP were not significantly different for first or fellow eyes with visual field progression (data not shown). The difference in AGIS score between first and second eyes at initial AGIS testing was significantly smaller in patients with fellow eye visual field progression (P =.04) (Table 2). Notably, the mean ± SD ocular perfusion pressure was significantly lower in fellow eyes with visual field pro- 475
4 Table 2. Comparison of Patients With and Without Fellow Eye Visual Field Progression* Fellow Eye Characteristic Visual Field Characteristic Progression Stable P Age, y 73.0 ± ± Family history of 2 (40) of 5 8 (31) of glaucoma, No. (%) Noncompliance, No. (%) 2 (33) 4 (13).26 Cup-disc ratio 0.78 ± ± Mean IOP, mm Hg First-affected eyes 17.6 ± ± Felow-eyes 18.0 ± ± Systolic BP, mm Hg ± ± Diastolic BP, mm Hg 73.8 ± ± Ocular perfusion 50.2 ± ± pressure, mm Hg Difference in initial AGIS score 4.5 ± ± between first-affected and fellow eye Initial mean deviation, db 8.0 ± ± Slope of mean deviation, db/y 2.2 ± ± Initial pattern SD, db 8.4 ± ± Slope of pattern SD, db/y 0.61 ± ± Initial corrected pattern SD, db 8.0 ± ± Slope of corrected 0.62 ± ± pattern SD, db/y *Age indicates age at time of initial visual field test showing first-affected eye severe visual field loss; IOP, intraocular pressure; BP, blood pressure; and AGIS, Advanced Glaucoma Intervention Study. Values are given as mean ± SD except where indicated. Independent samples 2-tailed t test unless otherwise noted. First-degree relatives; data not recorded for 5 patients. Fisher exact test. P =.019, Cox proportional hazards survival regression. gression compared with nonprogressors (P =.015) (Table 2) and in first eyes of the same patients (50.7 ± 5.6 mm Hg vs 57.6 ± 6.1 mm Hg; P =.02). Cox proportional hazards survival regression revealed increasing ocular perfusion pressure to be the only variable significantly associated with fellow eye stability ( = 0.193; SE = 0.082; relative risk = 0.825; P =.019). This association was essentially unchanged if CIGTS scoring was used to determine visual field progression (relative risk = 0.834; P =.01). Ocular perfusion pressure in first eyes with visual field progression was not significantly lower than in stable first eyes (55.0 ± 8.9 mm Hg vs 57.0 ± 4.8 mm Hg; P =.48). Of 11 fellow eyes with an initial AGIS visual field score of 0, none showed visual field progression, and only 1 eye had any increase in score at all (final score, 1). Visual field progression occured in 3 (30%) of 10 fellow eyes with mild damage (AGIS score, 1-5) and 3 (20%) of 15 fellow eyes with moderate damage (AGIS score, 6-11). These differences were not statistically significant (P =.15). The mean length of disease or follow-up time did not differ significantly between groups or between eyes with visual field progression and stable eyes (first or fellow). Three (4.5%) of 66 eyes improved in AGIS score by 4 or more points during follow-up. None of these patients had dramatic IOP changes during follow-up. No Table 3. Visual Acuity Characteristics* No. (%) Characteristic First-Affected Eyes Fellow Eyes Stable 26 (72) 30 (83) Better 2 (6) 3 (8) Worse 8 (22) 3 (8) *Stable indicates final visual acuity within 2 lines of that at initial visual field testing; better and worse, 3 or more lines better or worse, respectively. other eyes had an improvement in AGIS score of more than 2 points during follow-up. Cataract extraction was performed in 5 patients bilaterally prior to initial visual field testing. During the course of follow-up, cataract extraction was performed bilaterally in 4 patients in the first eye in 3 and in the fellow eye in 1. One patient had a moderate increase in cataract in both eyes, which did not account for the marked progression in visual field loss (AGIS score increase of 16 and 18 points, and worsening of mean deviation by 23 and 24 db, respectively). All other eyes had only mild or stable lens opacities during follow-up. During the average duration of disease of 10.2 years in this group of patients, 56% of first eyes and 25% of fellow eyes underwent incisional glaucoma surgery. No association was found between visual field progression and the number, type, or timing (ie, before or during follow-up) of procedures. Most first and fellow eyes had stable or improved visual acuity during and at final follow-up (Table 3). Reasons for worsened (by 3 or more lines) central visual acuity included glaucoma (3 first eyes); glaucoma with cataract (2 first eyes and 1 fellow eye, including both eyes of the patient with moderate increase in cataracts mentioned in the preceding paragraph); age-related macular degeneration (2 first eyes and 1 fellow eye); and central retinal vein occlusion (1 first eye). One fellow eye had severe visual loss because of suprachoroidal hemorrhage after combined phacoemulsification and trabeculectomy. Among fellow eyes, visual acuity was not worse than 20/60 (only 3 eyes worse than 20/40) throughout the period of visual field follow-up (excluding early postoperative periods) in all but 1 fellow eye, which had reduction of visual acuity from macular degeneration. No visual field tests were used with poor reliability in the presence of reduced central visual acuity. All eyes considered to have severe glaucomatous visual field loss were classified as such prior to the reduction of central visual acuity by the mechanisms listed in this paragraph. If the visual field is judged using the definition of blindness of a concentric visual field defect of 10 db using the Humphrey size III stimulus within 20, 31 then 11 of 36 first eyes were blind at initial visual field testing, and 12 more became blind during follow-up. Among fellow eyes, none were initially blind, and 2 became blind during follow-up, resulting in bilateral blindness in 2 patients. Thus, during the average of 10.2 years of disease, the rate of bilateral blindness was 5.6% among all pa- 476
5 tients in the study and 8.7% among 23 who were legally blind in 1 eye. COMMENT Our study shows that patients with severe loss of vision in 1 eye from chronic OAG have a 12.4% risk of significant visual field progression in the fellow eye during a 5-year period (Figure). During follow-up of 67 months, fellow eye visual field progression occured in 6 (17%) of 36 patients, and during 10 years of disease, 2 patients (6%) became bilaterally legally blind from glaucoma. The calculated ocular perfusion pressure was found to be significantly associated with visual field progression in fellow eyes. Reduced ocular perfusion pressure compared with that found in normal eyes has been previously reported in patients with POAG, 32,33 but others have found lower ocular perfusion pressure only in patients with NTG. 34 Trible and Anderson 35 reported that visual field depression during experimental short-term IOP increases was dependent on ocular perfusion pressure. Low BP and a reduction in BP at night (the nocturnal dip ), both of which might be associated with a decrease in ocular perfusion pressure, have been noted in patients with progressive glaucoma, and the nocturnal dip is absent in stable patients. 39,40 We found ocular perfusion pressure to be significantly associated with visual field progression only in fellow eyes, though first eyes with visual field progression also had a lower ocular perfusion pressure than stable first eyes. This may be attributed in part to small sample size, but it is possible that greater severity of damage present on initial visual field testing may increase susceptibility to further damage, despite a higher ocular perfusion pressure (ie, lower IOP). 24 Still, most first eyes of patients with fellow eye visual field progression were considered to have progressed, and these first eyes also had a significantly lower ocular perfusion pressure. Notably, of 23 patients legally blind in 1 eye from OAG either at initial testing or during follow-up, 2 (8.7%) had visual field progression to legal blindness in their fellow eye during a mean disease duration of 10 years. In a community-based study of patients with OAG, Hattenhauer et al 23 found a 9% risk of bilateral blindness at 20 years follow-up among those patients not blind in either eye from glaucoma at diagnosis. Using the same rate of visual field progression for a single eye, these findings are in close agreement with our findings in patients already blind in 1 eye. The time period covered by our study was more recent than the time period in the study by Hattenhauer et al 23 ; although practice patterns may have changed with time and a greater number of treatment options and modalities have been available recently, the results of the 2 studies do not seem to differ greatly. In the present study, 23 the mean follow-up period or disease duration did not differ significantly between eyes with and without visual field progression. Cataract extraction is known to improve automated visual field mean sensitivity in eyes with glaucoma. 41,42 Although several eyes in this study had cataract extraction during follow-up, we believe this had little effect on our findings because the overall improvement is usually small when many preoperative and postoperative visual field test results are compared 41 ; eyes with severe damage from glaucoma generally show little improvement after cataract extraction. 42 In addition, most patients with considerable cataract seemed to have had visual field testing deferred until after cataract extraction. Four patients had bilateral visual field progression. Both eyes of most patients (72%) behaved similarly, with 61% of patients remaining stable and 11% having bilateral progression of visual field loss, though this is a skewed population. The correlation between first and fellow eyes with visual field progression was not significant but might have been if more patients were studied. However, the between-eyes correlation for change in AGIS score was significant. Some of our patients had glaucoma associated with pseudoexfoliation of the lens. Although PXG may clinically seem to be a primarily unilateral disease, 43 all but 1 fellow eye was being treated for glaucoma in our patient group. This study was retrospective and may be limited by incomplete data and bias of selection and reporting. The number of patients studied was relatively small. Nonetheless, patients in similar (predominantly white) populations with severe visual field loss in 1 eye from OAG may be encouraged to know that rates of visual field progression did not seem to be exceptionally high in the fellow eye while under treatment. The rate of bilateral legal blindness was low, and reduction in fellow eye central visual acuity from glaucoma was uncommon. However, visual field progression occurred in many first eyes; when fellow eye visual field progression occurred, the usual result was severe visual field loss, and some patients had bilateral visual field progression despite treatment. Both eyes of 26 patients (72%) in this study behaved similarly, and those with visual field progression in 1 eye must be observed carefully for visual field progression in the fellow eye. Further study is warranted. Accepted for publication November 12, This study was supported in part by an unrestricted departmental grant from Research to Prevent Blindness Inc, New York, NY, and an Association for Research in Vision and Ophthalmology/National Eye Institute Travel Fellowship (Dr Chen). Presented in part at the annual meeting of the Association for Research in Vision and Ophthalmology, Ft Lauderdale, Fla, May 12, Reprints: Phillip P. Chen, MD, Department of Ophthalmology, University of Washington, Box , Seattle, WA REFERENCES 1. Thylefors B, Negrel A-D. The global impact of glaucoma. Bull World Health Org. 1994;72: Quigley HA. Number of people with glaucoma worldwide. Br J Ophthalmol. 1996; 80: Leibowitz HM, Krueger DE, Maunder LR, et al. The Framingham Eye Study monograph. Surv Ophthalmol. 1980;24(suppl): Tielsch JM, Javitt JC, Coleman A, et al. The prevalence of blindness and visual impairment among nursing home residents in Baltimore. N Engl J Med. 1995; 332: Quigley HA, Tielsch JM, Katz J, Sommer A. Rate of progression in open-angle 477
6 glaucoma estimated from cross-sectional prevalence of visual field damage. Am J Ophthalmol. 1996;122: Sommer A, Tielsch JM, Katz J, et al. Racial differences in the cause-specific prevalence of blindness in East Baltimore. N Engl J Med. 1991;325: Holmin C, Krakau CET. Regression analysis of the central visual field in chronic glaucoma cases: a follow-up study using automated perimetry. Acta Ophthalmol. 1982;60: de Natale R, Glaab-Schrems E, Krieglstein GK. The prognosis of glaucoma investigated with computerized perimetry. Doc Ophthalmol. 1984;58: Gloor BP, Vokt BA. Long-term fluctuations versus actual field loss in glaucoma patients. Dev Ophthalmol. 1985;12: Leydhecker W, Gramer E. Long-term studies of visual field changes by means of computerized perimetry (Octopus 201) in eyes with glaucomatous field defects after normalization of the intra-ocular pressure. Int Ophthalmol. 1989;13: Chauhan BC, Drance SM, Douglas GR. The use of visual field indices in detecting changes in the visual field in glaucoma. Invest Ophthalmol Vis Sci. 1990;31: Popovic V, Sjostrand J. Long-term outcome following trabeculectomy, II: visual field survival. Acta Ophthalmol. 1991;69: O Brien C, Schwartz B, Takamoto T, Wu DC. Intraocular pressure and the rate of visualfieldlossinchronicopen-angleglaucoma.amjophthalmol.1991;111: Glaucoma Laser Trial Research Group. The glaucoma laser trial (GLT), 6: treatment group differences in visual field changes. Am J Ophthalmol. 1995;120: Smith SD, Katz J, Quigley HA. Analysis of progressive change in automated visual fields in glaucoma. Invest Ophthalmol Vis Sci. 1996;37: Katz J, Gilbert D, Quigely HA, Sommer A. Estimating progression of visual field loss in glaucoma. Ophthalmology. 1997;104: The AGIS Study Investigators. The Advanced Glaucoma Intervention Study (AGIS), 4: comparison of treatment outcomes within race: 7-year results. Ophthalmology. 1998;105: Collaborative Normal-Tension Glaucoma Study Group. The effectiveness of intraocular pressure reduction in the treatment of normal-tension glaucoma. Am J Ophthalmol. 1998;126: Wilson R, Walker AM, Deuker DK, Crick RP. Risk factors for rate of progression of glaucomatous visual field loss: a computer-based analysis. Arch Ophthalmol. 1982;100: Holmin C, Storr-Paulsen A. The visual field after trabeculectomy: a follow-up study using computerized perimetry. Acta Ophthalmol. 1984;62: Gliklich RE, Steinmann WC, Spaeth GL. Visual field change in low-tension glaucoma over a five-year follow-up. Ophthalmology. 1989;96: Mao LK, Stewart WC, Shields MB. Correlation between intraocular pressure control and progressive glaucomatous damage in primary open-angle glaucoma. Am J Ophthalmol. 1991;111: Hattenhauer MG, Johnson DH, Ing HH, et al. The probability of blindness from open-angle glaucoma. Ophthalmology. 1998;105: Grant WM, Burke JF Jr. Why do some people go blind from glaucoma? Ophthalmology. 1982;89: Anderson DR. Automated Static Perimetry. St Louis, Mo: CV Mosby Co; 1992: The Advanced Glaucoma Intervention Study Investigators. Advanced Glaucoma Intervention Study, 2: visual field test scoring and reliability. Ophthalmology. 1994; 101: Alm A, Bill A. Ocular circulation. In: Moses RA, Hart WM Jr, eds. Adler s Physiology of the Eye: Clinical Application. 8th ed. St Louis, Mo: CV Mosby Co; 1987: Noureddin BN, Poinoosawmy D, Fietzke FW, Hitchings RA. Regression analysis of visual field progression in low tension glaucoma. Br J Ophthalmol. 1991;75: Werner EB, Bishop KI, Koelle J, et al. A comparison of experienced clinical observers and statistical tests in detection of progressive visual field loss in glaucoma using automated perimetry. Arch Ophthalmol. 1988;106: Musch DC, Lichter PR, Guire KE, Standardi CL, CIGTS Study Group. The Collaborative Initial Glaucoma Treatment Study: study design, methods, and baseline characteristics of enrolled patients. Ophthalmology. 1999;106: Walsh JB, Gold A, Charles H, eds. Physicians Desk Reference for Ophthalmology. Montvale, NJ: Medical Economics Data; 1996: Tielsch JM, Katz J, Sommer A, Quigley HA, Javitt JC. Hypertension, perfusion pressure, and primary open-angle glaucoma: a population-based assessment. Arch Ophthalmol. 1995;113: Leske MC, Connell AMS, Wu S-Y, Hyman LG, Schachat AP. Risk factors for open-angle glaucoma: the Barbados Eye Study. Arch Ophthalmol. 1995;113: Pillunat LE, Stodtmeister R, Marquart R, Mattern A. Ocular perfusion pressures in different types of glaucoma. Int Ophthalmol. 1989;13: Trible JR, Anderson DR. Factors associated with intraocular pressure-induced acute visual field depression. Arch Ophthalmol. 1997;115: Reese AB, McGavic JS. Relation of field contraction to blood pressure in chronic primary glaucoma. Arch Ophthalmol. 1942;27: Richler M, Werner EB, Thomas D. Risk factors for progression of visual field defects in medically treated patients with glaucoma. Can J Ophthalmol. 1982;17: Graham Sl, Drance SM, Wijsman K, et al. Ambulatory blood pressure monitoring in glaucoma: the nocturnal dip. Ophthalmology. 1995;102: Hayreh SS, Zimmerman MB, Podhajsky P, Alward WLM. Nocturnal arterial hypotension and its role in optic nerve head and ocular ischemic disorders. Am J Ophthalmol. 1994;117: Harris A, Spaeth G, Wilson R, et al. Nocturnal ophthalmic arterial hemodynamics in primary open-angle glaucoma. J Glaucoma. 1997;6: Smith SD, Katz J, Quigley HA. Effect of cataract extraction on the results of automated perimetry in glaucoma. Arch Ophthalmol. 1997;115: Chen PP, Budenz DL. The effects of cataract extraction on the visual field of eyes with chronic open-angle glaucoma. Am J Ophthalmol. 1998;125: Ritch R. Exfoliation glaucoma. In: Ritch R, Shields MB, Krupin T, eds. The Glaucomas. St Louis, Mo: CV Mosby Co; 1996: Notice to the Authors of Reports From Clinical Trials T he Journal of the American Medical Association ( JAMA) and the Archives of Ophthalmology function as an editorial consortium. With one submission and one set of reviews, your clinical trial manuscript will be considered for publication in both JAMA and the Archives of Ophthalmology. Submit your paper to the journal of your choice according to the appropriate Instructions for Authors and the following guidelines will apply: 1. If your manuscript is accepted by JAMA, it will be considered for an editorial or commentary in JAMA. Your abstract will also be published in the Archives of Ophthalmology with a commentary or editorial. 2. If your manuscript is accepted by the Archives of Ophthalmology, it will be considered for an editorial or commentary in the Archives of Ophthalmology. Your abstract will also be considered for publication in JAMA and may be accompanied by a commentary or editorial in JAMA. 478
Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors
 CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
Present relevant clinical findings of four landmark glaucoma trials OHTS, EMGT, CNTGS and CIGTS.
 Course title: The Glaucoma Compass Course length: 1 hour +/- 31 slides Corse Description: Even with the technology and available information, glaucoma decision making can still be confusing. How should
Course title: The Glaucoma Compass Course length: 1 hour +/- 31 slides Corse Description: Even with the technology and available information, glaucoma decision making can still be confusing. How should
Rate and Amount of Visual Loss in 102 Patients with Open-Angle Glaucoma Followed Up for at Least 15 Years
 Rate and Amount of Visual Loss in 102 Patients with Open-Angle Glaucoma Followed Up for at Least 15 Years Tarek M. Eid, MD, 1 George L. Spaeth, MD, 2 Anya Bitterman, MD, 3 William C. Steinmann, MD, MSc
Rate and Amount of Visual Loss in 102 Patients with Open-Angle Glaucoma Followed Up for at Least 15 Years Tarek M. Eid, MD, 1 George L. Spaeth, MD, 2 Anya Bitterman, MD, 3 William C. Steinmann, MD, MSc
Variability of Automated Visual Fields in Clinically Stable Glaucoma Patients
 Investigative Ophthalmology & Visual Science, Vol. 30, No. 6, June 1989 Copyright Association for Research in Vision and Ophthalmology Variability of Automated Visual Fields in Clinically Stable Glaucoma
Investigative Ophthalmology & Visual Science, Vol. 30, No. 6, June 1989 Copyright Association for Research in Vision and Ophthalmology Variability of Automated Visual Fields in Clinically Stable Glaucoma
21st Century Visual Field Testing
 Supplement to Supported by an educational grant from Carl Zeiss Meditec, Inc. Winter 2011 21st Century Visual Field Testing the Evolution Continues 21st Century Visual Field Testing 21st Century Visual
Supplement to Supported by an educational grant from Carl Zeiss Meditec, Inc. Winter 2011 21st Century Visual Field Testing the Evolution Continues 21st Century Visual Field Testing 21st Century Visual
T he retinal ganglion cells of different sizes have distinct
 604 CLINICAL SCIENCE Agreement between frequency doubling perimetry and static perimetry in eyes with high tension glaucoma and normal tension glaucoma S Kogure, Y Toda, D Crabb, K Kashiwagi, F W Fitzke,
604 CLINICAL SCIENCE Agreement between frequency doubling perimetry and static perimetry in eyes with high tension glaucoma and normal tension glaucoma S Kogure, Y Toda, D Crabb, K Kashiwagi, F W Fitzke,
Is NTG different from POAG?
 Is NTG different from POAG? Sunita Radhakrishnan, M.D Glaucoma Center of San Francisco Glaucoma Research and Education Group Subset of POAG 1 Connective tissue structure within ONH Ganglion cell susceptibility
Is NTG different from POAG? Sunita Radhakrishnan, M.D Glaucoma Center of San Francisco Glaucoma Research and Education Group Subset of POAG 1 Connective tissue structure within ONH Ganglion cell susceptibility
Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma
 Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma Chiharu Matsumoto, Shiroaki Shirato, Mai Haneda, Hiroko Yamashiro
Study of Retinal Nerve Fiber Layer Thickness Within Normal Hemivisual Field in Primary Open-Angle Glaucoma and Normal-Tension Glaucoma Chiharu Matsumoto, Shiroaki Shirato, Mai Haneda, Hiroko Yamashiro
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Conversion of Ocular Hypertensives into Glaucoma: A Retrospective Study Aditi Singh 1, Shibi
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Conversion of Ocular Hypertensives into Glaucoma: A Retrospective Study Aditi Singh 1, Shibi
CLINICAL SCIENCES. Glaucoma Monitoring in a Clinical Setting
 CLINICAL SCIENCES Glaucoma Monitoring in a Clinical Setting Glaucoma Progression Analysis vs Nonparametric Progression Analysis in the Groningen Longitudinal Glaucoma Study Christiaan Wesselink, MD; Govert
CLINICAL SCIENCES Glaucoma Monitoring in a Clinical Setting Glaucoma Progression Analysis vs Nonparametric Progression Analysis in the Groningen Longitudinal Glaucoma Study Christiaan Wesselink, MD; Govert
STANDARD AUTOMATED PERIMETRY IS A GENERALLY
 Comparison of Long-term Variability for Standard and Short-wavelength Automated Perimetry in Stable Glaucoma Patients EYTAN Z. BLUMENTHAL, MD, PAMELA A. SAMPLE, PHD, LINDA ZANGWILL, PHD, ALEXANDER C. LEE,
Comparison of Long-term Variability for Standard and Short-wavelength Automated Perimetry in Stable Glaucoma Patients EYTAN Z. BLUMENTHAL, MD, PAMELA A. SAMPLE, PHD, LINDA ZANGWILL, PHD, ALEXANDER C. LEE,
Glaucoma surgery with or without adjunctive antiproliferatives in normal tension glaucoma: 2 Visual field progression
 696 Glaucoma Unit, Moorfields Eye Hospital, City Road, London EC1V 2PD, UK W L Membrey C Bunce D P Poinoosawmy F W Fitzke R A Hitchings Correspondence to: R A Hitchings roger.hitchings@virgin.net Accepted
696 Glaucoma Unit, Moorfields Eye Hospital, City Road, London EC1V 2PD, UK W L Membrey C Bunce D P Poinoosawmy F W Fitzke R A Hitchings Correspondence to: R A Hitchings roger.hitchings@virgin.net Accepted
CLINICAL SCIENCES. Screening for Glaucoma With Frequency-Doubling Technology and Damato Campimetry
 CLINICAL SCIENCES Screening for Glaucoma With Frequency-Doubling Technology and Damato Campimetry Noriko Yamada, MD; Philip P. Chen, MD; Richard P. Mills, MD; Martha M. Leen, MD; Marc F. Lieberman, MD;
CLINICAL SCIENCES Screening for Glaucoma With Frequency-Doubling Technology and Damato Campimetry Noriko Yamada, MD; Philip P. Chen, MD; Richard P. Mills, MD; Martha M. Leen, MD; Marc F. Lieberman, MD;
Research Article Optic Disc Hemorrhage after Phacoemulsification in Patients with Glaucoma
 ISRN Ophthalmology, Article ID 574054, 5 pages http://dx.doi.org/10.1155/2014/574054 Research Article Optic Disc Hemorrhage after Phacoemulsification in Patients with Glaucoma Karine D. Bojikian, Daniel
ISRN Ophthalmology, Article ID 574054, 5 pages http://dx.doi.org/10.1155/2014/574054 Research Article Optic Disc Hemorrhage after Phacoemulsification in Patients with Glaucoma Karine D. Bojikian, Daniel
CLINICAL SCIENCES. Steven L. Mansberger, MD; Pamela A. Sample, PhD; Linda Zangwill, PhD; Robert N. Weinreb, MD
 CLINICAL SCIENCES Achromatic and Short-Wavelength Automated Perimetry in Patients With Glaucomatous Large Cups Steven L. Mansberger, MD; Pamela A. Sample, PhD; Linda Zangwill, PhD; Robert N. Weinreb, MD
CLINICAL SCIENCES Achromatic and Short-Wavelength Automated Perimetry in Patients With Glaucomatous Large Cups Steven L. Mansberger, MD; Pamela A. Sample, PhD; Linda Zangwill, PhD; Robert N. Weinreb, MD
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma
 Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
Intro to Glaucoma/2006
 Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
Glaucoma Burden in a Public Sector Hospital
 Original Article Glaucoma Burden in a Public Sector Hospital P.S Mahar, M Aamir Shahzad Pak J Ophthalmol 28, Vol. 24 No. 3...............................................................................
Original Article Glaucoma Burden in a Public Sector Hospital P.S Mahar, M Aamir Shahzad Pak J Ophthalmol 28, Vol. 24 No. 3...............................................................................
Citation for published version (APA): Wesselink, C. (2017). Glaucoma care optimised in an ageing population [Groningen]: Rijksuniversiteit Groningen
![Citation for published version (APA): Wesselink, C. (2017). Glaucoma care optimised in an ageing population [Groningen]: Rijksuniversiteit Groningen Citation for published version (APA): Wesselink, C. (2017). Glaucoma care optimised in an ageing population [Groningen]: Rijksuniversiteit Groningen](/thumbs/90/102866625.jpg) University of Groningen Glaucoma care optimised in an ageing population Wesselink, Christiaan IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
University of Groningen Glaucoma care optimised in an ageing population Wesselink, Christiaan IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
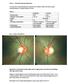 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND PACHYMETRY. POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
LUP. Lund University Publications Institutional Repository of Lund University
 LUP Lund University Publications Institutional Repository of Lund University This is an author produced version of a paper published in Ophthalmology. This paper has been peerreviewed but does not include
LUP Lund University Publications Institutional Repository of Lund University This is an author produced version of a paper published in Ophthalmology. This paper has been peerreviewed but does not include
Retrospective analysis of risk factors for late presentation of chronic glaucoma
 24 Glaxo Department of Ophthalmic Epidemiology, Moorfields Eye Hospital, City Road, London EC1V 2PD S Fraser C Bunce R Wormald Correspondence to: Mr S G Fraser. Accepted for publication 31 July 1998 Retrospective
24 Glaxo Department of Ophthalmic Epidemiology, Moorfields Eye Hospital, City Road, London EC1V 2PD S Fraser C Bunce R Wormald Correspondence to: Mr S G Fraser. Accepted for publication 31 July 1998 Retrospective
Collaboration in the care of glaucoma patients and glaucoma suspects. Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012
 Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
Collaboration in the care of glaucoma patients and glaucoma suspects Barry Emara MD FRCS(C) Nico Ristorante November 29, 2012 Goals of Collaboration Patient-centred and evidence based approach Timely access
Clinical Study Visual Field Loss Morphology in High- and Normal-Tension Glaucoma
 Journal of Ophthalmology Volume 2012, Article ID 327326, 8 pages doi:10.1155/2012/327326 Clinical Study Visual Field Loss Morphology in High- and Normal-Tension Glaucoma Michele Iester, 1, 2 Fabio De Feo,
Journal of Ophthalmology Volume 2012, Article ID 327326, 8 pages doi:10.1155/2012/327326 Clinical Study Visual Field Loss Morphology in High- and Normal-Tension Glaucoma Michele Iester, 1, 2 Fabio De Feo,
VISUAL FIELD TESTING OCCUpies
 CLINICAL SCIENCES Prediction of Glaucomatous Visual Field Loss by Extrapolation of Linear Trends Boel Bengtsson, PhD; Vincent Michael Patella, OD; Anders Heijl, MD, PhD Objective: To investigate how well
CLINICAL SCIENCES Prediction of Glaucomatous Visual Field Loss by Extrapolation of Linear Trends Boel Bengtsson, PhD; Vincent Michael Patella, OD; Anders Heijl, MD, PhD Objective: To investigate how well
LABORATORY SCIENCES. Spatial and Temporal Processing of Threshold Data for Detection of Progressive Glaucomatous Visual Field Loss
 LABORATORY SCIENCES Spatial and Temporal Processing of Threshold Data for Detection of Progressive Glaucomatous Visual Field Loss Paul G. D. Spry, PhD; Chris A. Johnson, PhD; Alex B. Bates; Andrew Turpin,
LABORATORY SCIENCES Spatial and Temporal Processing of Threshold Data for Detection of Progressive Glaucomatous Visual Field Loss Paul G. D. Spry, PhD; Chris A. Johnson, PhD; Alex B. Bates; Andrew Turpin,
4/06/2013. Medication Observation POAG. Proportion. Native American 0.1% 0.4%
 Clinical Research in Glaucoma: Putting Science into Practice J. James Thimons, O.D., FAAO Chairman, National Glaucoma Society www.nationalglaucomasociety.org Ocular Hypertension Treatment Study (OHTS)
Clinical Research in Glaucoma: Putting Science into Practice J. James Thimons, O.D., FAAO Chairman, National Glaucoma Society www.nationalglaucomasociety.org Ocular Hypertension Treatment Study (OHTS)
Messages From the Advanced Glaucoma Intervention Study
 Landmark Studies Section editor: Ronald L. Fellman, MD Take-Home Messages From the Advanced Glaucoma Intervention Study By Leon W. Herndon, MD, and Daniel B. Moore, MD I tasked Leon W. Herndon, MD, and
Landmark Studies Section editor: Ronald L. Fellman, MD Take-Home Messages From the Advanced Glaucoma Intervention Study By Leon W. Herndon, MD, and Daniel B. Moore, MD I tasked Leon W. Herndon, MD, and
Misleading Statistical Calculations in Faradvanced Glaucomatous Visual Field Loss
 Misleading Statistical Calculations in Faradvanced Glaucomatous Visual Field Loss Eytan Z. Blumenthal, MD, Ruthy Sapir-Pichhadze, MD Objective: In this study, the capability of statistical analysis indices
Misleading Statistical Calculations in Faradvanced Glaucomatous Visual Field Loss Eytan Z. Blumenthal, MD, Ruthy Sapir-Pichhadze, MD Objective: In this study, the capability of statistical analysis indices
Ocular hypertension is present in approximately 8%
 ORIGINAL STUDY The Probability of Glaucoma From Ocular Hypertension Determined by Ophthalmologists in Comparison to a Risk Calculator Steven L. Mansberger, MD, MPH and George A. Cioffi, MD Objective: To
ORIGINAL STUDY The Probability of Glaucoma From Ocular Hypertension Determined by Ophthalmologists in Comparison to a Risk Calculator Steven L. Mansberger, MD, MPH and George A. Cioffi, MD Objective: To
Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1
 Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1 By: Andrew Kemp, OD, Marcus Gonzales, OD, FAAO, Joe DeLoach, OD, FAAO, and Zanna Kruoch, OD FAAO Background Glaucoma is a range of conditions
Targeting Intraocular Pressure in Glaucoma: a Teaching Case Report 1 By: Andrew Kemp, OD, Marcus Gonzales, OD, FAAO, Joe DeLoach, OD, FAAO, and Zanna Kruoch, OD FAAO Background Glaucoma is a range of conditions
Central corneal thickness and vascular risk factors in normal tension glaucoma
 Central corneal thickness and vascular risk factors in normal tension glaucoma Aoife Doyle, Ahmed Bensaid and Yves Lachkar L Institut du Glaucome, Fondation Hoˆpital St. Joseph, Paris, France ABSTRACT.
Central corneal thickness and vascular risk factors in normal tension glaucoma Aoife Doyle, Ahmed Bensaid and Yves Lachkar L Institut du Glaucome, Fondation Hoˆpital St. Joseph, Paris, France ABSTRACT.
Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography
 Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
Original Article Philippine Journal of OPHTHALMOLOGY Retinal Nerve Fiber Layer Measurements in Myopia Using Optical Coherence Tomography Dennis L. del Rosario, MD and Mario M. Yatco, MD University of Santo
Surgery for normal tension glaucoma
 42 British Journal of Ophthalmology 1995; 79: 42-46 ORIGINAL ARTICLES - Clinical science Moorfields Eye Hospital, City Road, London EClV 2PD R A Hitchings J Wu D Poinoosawmy A McNaught Correspondence to:
42 British Journal of Ophthalmology 1995; 79: 42-46 ORIGINAL ARTICLES - Clinical science Moorfields Eye Hospital, City Road, London EClV 2PD R A Hitchings J Wu D Poinoosawmy A McNaught Correspondence to:
GLAUCOMA SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES
 SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
SUMMARY BENCHMARKS FOR PREFERRED PRACTICE PATTERN GUIDELINES Introduction These are summary benchmarks for the Academy s Preferred Practice Pattern (PPP) guidelines. The Preferred Practice Pattern series
NIH Public Access Author Manuscript Arch Ophthalmol. Author manuscript; available in PMC 2014 March 26.
 NIH Public Access Author Manuscript Published in final edited form as: Arch Ophthalmol. 2010 March ; 128(3): 276 287. doi:10.1001/archophthalmol.2010.20. Delaying Treatment of Ocular Hypertension: The
NIH Public Access Author Manuscript Published in final edited form as: Arch Ophthalmol. 2010 March ; 128(3): 276 287. doi:10.1001/archophthalmol.2010.20. Delaying Treatment of Ocular Hypertension: The
Intraocular pressure, systemic blood pressure, and
 g i MEDICAL MONTEFIORE MLDK'\?TA L.,PA British Journal of Ophthalmology, 1987, 71, 245-249 Intraocular pressure, systemic blood pressure, and age: a correlational study MICHAEL SCHULZER' AND STEPHEN M
g i MEDICAL MONTEFIORE MLDK'\?TA L.,PA British Journal of Ophthalmology, 1987, 71, 245-249 Intraocular pressure, systemic blood pressure, and age: a correlational study MICHAEL SCHULZER' AND STEPHEN M
Practical approach to medical management of glaucoma DR. RATHINI LILIAN DAVID
 Practical approach to medical management of glaucoma DR. RATHINI LILIAN DAVID Glaucoma is one of the major causes of visual loss worldwide. The philosophy of glaucoma management is to preserve the visual
Practical approach to medical management of glaucoma DR. RATHINI LILIAN DAVID Glaucoma is one of the major causes of visual loss worldwide. The philosophy of glaucoma management is to preserve the visual
Retinal nerve fiber layer thickness in Indian eyes with optical coherence tomography
 Original articles in Indian eyes with optical coherence tomography Malik A, Singh M, Arya SK, Sood S, Ichhpujani P Department of Ophthalmology Government Medical College and Hospital, Sector 32, Chandigarh,
Original articles in Indian eyes with optical coherence tomography Malik A, Singh M, Arya SK, Sood S, Ichhpujani P Department of Ophthalmology Government Medical College and Hospital, Sector 32, Chandigarh,
Trabeculectomy is an effective method for lowering
 ORIGINAL STUDY Refractive Outcome of Cataract Surgery in Eyes With Prior Trabeculectomy: Risk Factors for Postoperative Myopia Oliver L. Yeh, MD, Karine D. Bojikian, MD, Mark A. Slabaugh, MD, and Philip
ORIGINAL STUDY Refractive Outcome of Cataract Surgery in Eyes With Prior Trabeculectomy: Risk Factors for Postoperative Myopia Oliver L. Yeh, MD, Karine D. Bojikian, MD, Mark A. Slabaugh, MD, and Philip
Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective cohort study
 Nesaratnam et al. BMC Ophthalmology (2015) 15:17 DOI 10.1186/s12886-015-0007-1 RESEARCH ARTICLE Open Access Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective
Nesaratnam et al. BMC Ophthalmology (2015) 15:17 DOI 10.1186/s12886-015-0007-1 RESEARCH ARTICLE Open Access Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective
Micro-Invasive Glaucoma Surgery (Aqueous Stents)
 Micro-Invasive Glaucoma Surgery (Aqueous Stents) Policy Number: Original Effective Date: MM.06.029 02/01/2019 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2019 Section:
Micro-Invasive Glaucoma Surgery (Aqueous Stents) Policy Number: Original Effective Date: MM.06.029 02/01/2019 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2019 Section:
Glaucoma Related Morbidity at A Tertiary Care Eye Hospital
 Glaucoma Related Morbidity at A Tertiary Care Eye Hospital AKHTAR F., ALI M. Al-Shifa Trust Eye Hospital, Rawalpindi Correspondence to: Dr. Farah Akhtar, Consultant Glaucoma House # 217, St. 49, F10/4,
Glaucoma Related Morbidity at A Tertiary Care Eye Hospital AKHTAR F., ALI M. Al-Shifa Trust Eye Hospital, Rawalpindi Correspondence to: Dr. Farah Akhtar, Consultant Glaucoma House # 217, St. 49, F10/4,
NERVE FIBER LAYER THICKNESS IN NORMALS AND GLAUCOMA PATIENTS
 Nerve fiber layer thickness in normals and glaucoma patients 403 NERVE FIBER LAYER THICKNESS IN NORMALS AND GLAUCOMA PATIENTS HIROTAKA SUZUMURA, KAYOKO HARASAWA, AKIKO KOBAYASHI and NARIYOSHI ENDO Department
Nerve fiber layer thickness in normals and glaucoma patients 403 NERVE FIBER LAYER THICKNESS IN NORMALS AND GLAUCOMA PATIENTS HIROTAKA SUZUMURA, KAYOKO HARASAWA, AKIKO KOBAYASHI and NARIYOSHI ENDO Department
Lifetime Risk of Blindness in Open-Angle Glaucoma.
 Lifetime Risk of Blindness in Open-Angle Glaucoma. Peters, Dorothea; Bengtsson, Boel; Heijl, Anders Published in: American Journal of Ophthalmology DOI: 10.1016/j.ajo.2013.05.027 2013 Link to publication
Lifetime Risk of Blindness in Open-Angle Glaucoma. Peters, Dorothea; Bengtsson, Boel; Heijl, Anders Published in: American Journal of Ophthalmology DOI: 10.1016/j.ajo.2013.05.027 2013 Link to publication
GLAUCOMA EVOLUTION IN PATIENTS WITH DIABETES
 Rev. Med. Chir. Soc. Med. Nat., Iaşi 2014 vol. 118, no. 3 SURGERY ORIGINAL PAPERS GLAUCOMA EVOLUTION IN PATIENTS WITH DIABETES Nicoleta Anton Apreutesei¹, D. Chiselita²*, O. I. Motas ¹ University of Medicine
Rev. Med. Chir. Soc. Med. Nat., Iaşi 2014 vol. 118, no. 3 SURGERY ORIGINAL PAPERS GLAUCOMA EVOLUTION IN PATIENTS WITH DIABETES Nicoleta Anton Apreutesei¹, D. Chiselita²*, O. I. Motas ¹ University of Medicine
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,100 116,000 120M Open access books available International authors and editors Downloads Our
Glaucoma Clinical Update. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
Glaucoma Clinical Update Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Objectives Understand the different categories of glaucoma Recognize the symptoms and signs of open angle and angle-closure
Introduction. Paulo de Tarso Ponte Pierre-Filho, 1 Rui Barroso Schimiti, 1 Jose Paulo Cabral de Vasconcellos 1 and Vital Paulino Costa 1,2
 ACTA OPHTHALMOLOGICA SCANDINAVICA 2006 Sensitivity and specificity of frequency-doubling technology, tendency-oriented perimetry, SITA Standard and SITA Fast perimetry in perimetrically inexperienced individuals
ACTA OPHTHALMOLOGICA SCANDINAVICA 2006 Sensitivity and specificity of frequency-doubling technology, tendency-oriented perimetry, SITA Standard and SITA Fast perimetry in perimetrically inexperienced individuals
International Journal Of Basic And Applied Physiology
 A STUDY TO CORRELATE OPTIC CUP/DISC RATIO WITH VISUAL FIELD DEFECTS IN PRIMARY OPEN ANGLE GLAUCOMA Nilay B. Patel, Jayendrasinh M. Jadeja 2, Purvi Bhagat, Jagdeepkaur S. Dani 4, Arjunkumar Jakasania Harsiddh
A STUDY TO CORRELATE OPTIC CUP/DISC RATIO WITH VISUAL FIELD DEFECTS IN PRIMARY OPEN ANGLE GLAUCOMA Nilay B. Patel, Jayendrasinh M. Jadeja 2, Purvi Bhagat, Jagdeepkaur S. Dani 4, Arjunkumar Jakasania Harsiddh
EPIDEMIOLOGY AND BIOSTATISTICS
 Incidence of Open-Angle Glaucoma The Barbados Eye Studies EPIDEMIOLOGY AND BIOSTATISTICS M. Cristina Leske, MD, MPH; Anthea M. S. Connell, FRCS, FRCOphth; Suh-Yuh Wu, MA; Barbara Nemesure, PhD; Xiaowei
Incidence of Open-Angle Glaucoma The Barbados Eye Studies EPIDEMIOLOGY AND BIOSTATISTICS M. Cristina Leske, MD, MPH; Anthea M. S. Connell, FRCS, FRCOphth; Suh-Yuh Wu, MA; Barbara Nemesure, PhD; Xiaowei
Is Posner Schlossman Syndrome Benign?
 Is Posner Schlossman Syndrome Benign? Aliza Jap, FRCS (G), 1 Meenakshi Sivakumar, FRCS (Ed), M Med (Ophth), 2, Soon-Phaik Chee, FRCS (Ed), FRCOphth 2 Purpose: To determine the clinical course of patients
Is Posner Schlossman Syndrome Benign? Aliza Jap, FRCS (G), 1 Meenakshi Sivakumar, FRCS (Ed), M Med (Ophth), 2, Soon-Phaik Chee, FRCS (Ed), FRCOphth 2 Purpose: To determine the clinical course of patients
Science & Technologies
 STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
STANDARD COMPUTERIZED PERIMETRY IN FUNCTION OF DIAGNOSTIC GLAUCOMA Iljaz Ismaili, 1 Gazepov Strahil, 2, Goshevska Dashtevska Emilija 1 1 University Eye Clinic,Skopje 2 Clinical Hospital, Shtip Abstract
Micro-Invasive Glaucoma Surgery (Aqueous Stents)
 Micro-Invasive Glaucoma Surgery (Aqueous Stents) Policy Number: Original Effective Date: MM.06.029 02/01/2019 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2019 Section:
Micro-Invasive Glaucoma Surgery (Aqueous Stents) Policy Number: Original Effective Date: MM.06.029 02/01/2019 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 02/01/2019 Section:
CLINICAL SCIENCES. The Ocular Hypertension Treatment Study
 CLINICAL SCIENCES The Ocular Hypertension Treatment Study Topical Medication Delays or Prevents Primary Open-angle Glaucoma in African American Individuals Eve J. Higginbotham, MD; Mae O. Gordon, PhD;
CLINICAL SCIENCES The Ocular Hypertension Treatment Study Topical Medication Delays or Prevents Primary Open-angle Glaucoma in African American Individuals Eve J. Higginbotham, MD; Mae O. Gordon, PhD;
Financial Disclosure. Visual Field Interpretation RELIABILITY VISUAL FIELD INTERPRETATION IN GLAUCOMA METHODS OF DATA PRESENTATION
 VISUAL FIELD INTERPRETATION IN GLAUCOMA Danica J. Marrelli, OD, FAAO University of Houston College of Optometry Financial Disclosure I have received speaking and/or consulting fees from: Aerie Pharmaceutical
VISUAL FIELD INTERPRETATION IN GLAUCOMA Danica J. Marrelli, OD, FAAO University of Houston College of Optometry Financial Disclosure I have received speaking and/or consulting fees from: Aerie Pharmaceutical
Glaucoma surgery with or without adjunctive antiproliferatives in normal tension glaucoma: 1 Intraocular pressure control and complications
 586 Glaucoma Unit, Moorfields Eye Hospital, City Road, London ECV 2PD W L Membrey D P Poinoosawmy C Bunce R A Hitchings Correspondence to: R A Hitchings Roger.Hitchings@virgin.net Accepted for publication
586 Glaucoma Unit, Moorfields Eye Hospital, City Road, London ECV 2PD W L Membrey D P Poinoosawmy C Bunce R A Hitchings Correspondence to: R A Hitchings Roger.Hitchings@virgin.net Accepted for publication
Research Article Long-Term Clinical Course of Normal-Tension Glaucoma: 20 Years of Experience
 Hindawi Ophthalmology Volume 2017, Article ID 2651645, 6 pages https://doi.org/10.1155/2017/2651645 Research Article Long-Term Clinical Course of Normal-Tension Glaucoma: 20 Years of Experience Sang Wook
Hindawi Ophthalmology Volume 2017, Article ID 2651645, 6 pages https://doi.org/10.1155/2017/2651645 Research Article Long-Term Clinical Course of Normal-Tension Glaucoma: 20 Years of Experience Sang Wook
Landmark Glaucoma Studies
 Landmark Glaucoma Studies: How They Affect Our Management Strategies Today Disclosures None By: Alex Kabiri, O.D. & Devin Singh, O.D. Course Goals 1. Review series of glaucoma studies that: Evaluate when
Landmark Glaucoma Studies: How They Affect Our Management Strategies Today Disclosures None By: Alex Kabiri, O.D. & Devin Singh, O.D. Course Goals 1. Review series of glaucoma studies that: Evaluate when
Prevalence Of Primary Open Angle Glaucoma in Diabetic Patients
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. III (June. 2017), PP 147-151 www.iosrjournals.org Prevalence Of Primary Open Angle Glaucoma
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. III (June. 2017), PP 147-151 www.iosrjournals.org Prevalence Of Primary Open Angle Glaucoma
NIH Public Access Author Manuscript Br J Ophthalmol. Author manuscript; available in PMC 2014 November 01.
 NIH Public Access Author Manuscript Published in final edited form as: Br J Ophthalmol. 2014 November ; 98(11): 1551 1554. doi:10.1136/bjophthalmol-2013-304393. Optic Nerve Head Morphology in Glaucoma
NIH Public Access Author Manuscript Published in final edited form as: Br J Ophthalmol. 2014 November ; 98(11): 1551 1554. doi:10.1136/bjophthalmol-2013-304393. Optic Nerve Head Morphology in Glaucoma
Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India
 Original article: Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India 1Dr. Apala Bhattacharya, 2 Dr Gautam Bhaduri,
Original article: Central Corneal Thickness-An important variable for prognostication in Primary Open Angle glaucoma; A Kolkata based study in Eastern India 1Dr. Apala Bhattacharya, 2 Dr Gautam Bhaduri,
Baseline Visual Field Characteristics in the Ocular Hypertension Treatment Study
 Baseline Visual Field Characteristics in the Ocular Hypertension Treatment Study Chris A. Johnson, PhD, 1 John L. Keltner, MD, 2 Kimberly E. Cello, BS, 2 Mary Edwards, BS, 2 Michael A. Kass, MD, 3 Mae
Baseline Visual Field Characteristics in the Ocular Hypertension Treatment Study Chris A. Johnson, PhD, 1 John L. Keltner, MD, 2 Kimberly E. Cello, BS, 2 Mary Edwards, BS, 2 Michael A. Kass, MD, 3 Mae
Fluctuations on the Humphrey and Octopus Perimeters
 May 987 Vol. 28/ Investigative Ophthalmology & Visual Science A Journal of Dosic and Clinical Research Articles Fluctuations on the and Perimeters Randall S. Drenton and William A. Argus Fluctuation of
May 987 Vol. 28/ Investigative Ophthalmology & Visual Science A Journal of Dosic and Clinical Research Articles Fluctuations on the and Perimeters Randall S. Drenton and William A. Argus Fluctuation of
Landmark Tube Trials
 SECTION EDITOR: BARBARA SMIT, MD, PhD Landmark Tube Trials A review of key findings from recent multicenter randomized clinical trials involving tube shunts. BY AMBIKA HOGUET, MD, AND STEVEN J. GEDDE,
SECTION EDITOR: BARBARA SMIT, MD, PhD Landmark Tube Trials A review of key findings from recent multicenter randomized clinical trials involving tube shunts. BY AMBIKA HOGUET, MD, AND STEVEN J. GEDDE,
Efficacy of latanoprost in management of chronic angle closure glaucoma. Kumar S 1, Malik A 2 Singh M 3, Sood S 4. Abstract
 Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
The Role of the RNFL in the Diagnosis of Glaucoma
 Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
Chapter 1. The Role of the RNFL in the Diagnosis of Glaucoma Introduction Glaucoma is an optic neuropathy characterized by a loss of of retinal ganglion cells and their axons, the Retinal Nerve Fiber Layer
Quantification of Glaucomatous Visual Field Defects with Automated Perimetry
 Quantification of Glaucomatous Visual Field Defects with Automated Perimetry J. Flammer,* 5. M. Drance,f L. Augusriny,* and A. Funkhouser* A method to quantify different glaucomatous visual field defects
Quantification of Glaucomatous Visual Field Defects with Automated Perimetry J. Flammer,* 5. M. Drance,f L. Augusriny,* and A. Funkhouser* A method to quantify different glaucomatous visual field defects
Detection of glaucoma in a cohort of chinese subjects with systemic hypertension. Gangwani, RA; Chan, J; Lee, J; Kwong, A; Lai, JSM
 Title Detection of glaucoma in a cohort of chinese subjects with systemic hypertension Author(s) Gangwani, RA; Chan, J; Lee, J; Kwong, A; Lai, JSM Citation Ophthalmology, 2013, v. 2013, article no. 463710
Title Detection of glaucoma in a cohort of chinese subjects with systemic hypertension Author(s) Gangwani, RA; Chan, J; Lee, J; Kwong, A; Lai, JSM Citation Ophthalmology, 2013, v. 2013, article no. 463710
PREVALENCE OF GLAUCOMA AMONG FISHERMEN COMMUNITY OF MUNDRA TALUKA OF KUTCH DISTRICT- A CROSS- SECTIONAL STUDY
 ORIGINAL RESEARCH PREVALENCE OF GLAUCOMA AMONG FISHERMEN COMMUNITY OF MUNDRA TALUKA OF KUTCH DISTRICT- A CROSS- SECTIONAL STUDY Sanjay Upadhyay 1, Jayantilal Shah 2 1 Assistant Professor, 2 Associate Professor,
ORIGINAL RESEARCH PREVALENCE OF GLAUCOMA AMONG FISHERMEN COMMUNITY OF MUNDRA TALUKA OF KUTCH DISTRICT- A CROSS- SECTIONAL STUDY Sanjay Upadhyay 1, Jayantilal Shah 2 1 Assistant Professor, 2 Associate Professor,
Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial
 Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial Boel Bengtsson, PhD, 1 M. Cristina Leske, MD, MPH, 2 Leslie Hyman, PhD, 2 Anders Heijl, MD, PhD, 1 Early
Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial Boel Bengtsson, PhD, 1 M. Cristina Leske, MD, MPH, 2 Leslie Hyman, PhD, 2 Anders Heijl, MD, PhD, 1 Early
Relation & Association of Mean Ocular Perfusion Pressure in Primary Open Angle Glaucoma
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 5 Ver. XII (May. 2017), PP 54-58 www.iosrjournals.org Relation & Association of Mean Ocular
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 5 Ver. XII (May. 2017), PP 54-58 www.iosrjournals.org Relation & Association of Mean Ocular
DR.RUPNATHJI( DR.RUPAK NATH )
 34. Screening for Glaucoma Burden of Suffering RECOMMENDATION There is insufficient evidence to recommend for or against routine screening for intraocular hypertension or glaucoma by primary care clinicians.
34. Screening for Glaucoma Burden of Suffering RECOMMENDATION There is insufficient evidence to recommend for or against routine screening for intraocular hypertension or glaucoma by primary care clinicians.
Characteristics of Frequency-of-Seeing Curves in Normal Subjects, Patients With Suspected Glaucoma, and Patients With Glaucoma
 Characteristics of Frequency-of-Seeing Curves in Normal Subjects, Patients With Suspected Glaucoma, and Patients With Glaucoma Balwantray C. Chauhan* James D. Tompkins,-\ Raymond P. LeBlanc* and Terry
Characteristics of Frequency-of-Seeing Curves in Normal Subjects, Patients With Suspected Glaucoma, and Patients With Glaucoma Balwantray C. Chauhan* James D. Tompkins,-\ Raymond P. LeBlanc* and Terry
Diurnal IOP fluctuation: not an independent risk factor for glaucomatous visual field loss in high-risk ocular hypertension.
 Diurnal IOP fluctuation: not an independent risk factor for glaucomatous visual field loss in high-risk ocular hypertension. Bengtsson, Boel; Heijl, Anders Published in: Graefe's Archive for Clinical and
Diurnal IOP fluctuation: not an independent risk factor for glaucomatous visual field loss in high-risk ocular hypertension. Bengtsson, Boel; Heijl, Anders Published in: Graefe's Archive for Clinical and
Noel de Jesus Atienza, MD, MSc and Joseph Anthony Tumbocon, MD
 Original Article Philippine Journal of OPHTHALMOLOGY Diagnostic Accuracy of the Optical Coherence Tomography in Assessing Glaucoma Among Filipinos. Part 1: Categorical Outcomes Based on a Normative Database
Original Article Philippine Journal of OPHTHALMOLOGY Diagnostic Accuracy of the Optical Coherence Tomography in Assessing Glaucoma Among Filipinos. Part 1: Categorical Outcomes Based on a Normative Database
Ganglion cell complex scan in the early prediction of glaucoma
 Original article in the early prediction of glaucoma Ganekal S Nayana Super Specialty Eye Hospital and Research Center, Davangere, Karnataka, India Abstract Objective: To compare the macular ganglion cell
Original article in the early prediction of glaucoma Ganekal S Nayana Super Specialty Eye Hospital and Research Center, Davangere, Karnataka, India Abstract Objective: To compare the macular ganglion cell
11/30/2009. Glaukosis: ancient greek term meaning sparkling or shining appearance of pupil
 Normal Ocular Anatomy Glaucoma Dr Sunil Deokule, MD Asst. Prof and Glaucoma Specialist University of Kentucky Definition Glaukosis: ancient greek term meaning sparkling or shining appearance of pupil Optic
Normal Ocular Anatomy Glaucoma Dr Sunil Deokule, MD Asst. Prof and Glaucoma Specialist University of Kentucky Definition Glaukosis: ancient greek term meaning sparkling or shining appearance of pupil Optic
CLINICAL SCIENCES. Comparison of Glaucoma Diagnostic Capabilities of Cirrus HD and Stratus Optical Coherence Tomography
 CLINICAL SCIENCES Comparison of Glaucoma Diagnostic Capabilities of Cirrus HD and Stratus Optical Coherence Tomography Seong Bae Park, MD; Kyung Rim Sung, MD, PhD; Sung Yong Kang, MD; Kyung Ri Kim, BS;
CLINICAL SCIENCES Comparison of Glaucoma Diagnostic Capabilities of Cirrus HD and Stratus Optical Coherence Tomography Seong Bae Park, MD; Kyung Rim Sung, MD, PhD; Sung Yong Kang, MD; Kyung Ri Kim, BS;
STARTING IN THE 1960s, epidemiological. Reduction of Intraocular Pressure and Glaucoma Progression. Results From the Early Manifest Glaucoma Trial
 CLINICAL SCIENCES Reduction of Intraocular Pressure and Glaucoma Progression Results From the Early Manifest Glaucoma Trial Anders Heijl, MD, PhD; M. Cristina Leske, MD, MPH; Bo Bengtsson, MD, PhD; Leslie
CLINICAL SCIENCES Reduction of Intraocular Pressure and Glaucoma Progression Results From the Early Manifest Glaucoma Trial Anders Heijl, MD, PhD; M. Cristina Leske, MD, MPH; Bo Bengtsson, MD, PhD; Leslie
Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study
 Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study James H. Peace, M.D. 1, Casey K. Kopczynski, Ph.D. 2, and Theresa Heah, M.D. 2 1 Inglewood, CA 2
Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study James H. Peace, M.D. 1, Casey K. Kopczynski, Ph.D. 2, and Theresa Heah, M.D. 2 1 Inglewood, CA 2
Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University.
 Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University. Although the clinical picture of glaucoma is well described, the exact mechanism leading to this specific type of damage to the optic
Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University. Although the clinical picture of glaucoma is well described, the exact mechanism leading to this specific type of damage to the optic
Pit-like changes of the optic nerve head
 Pit-like changes of the optic nerve head in open-angle glaucoma British Journal of Ophthalmology, 1978, 62, 389-393 RONALD L. RADIUS, A. EDWARD MAUMENEE, AND WILLIAM R. GREEN From the Wilmer Ophthalmologic
Pit-like changes of the optic nerve head in open-angle glaucoma British Journal of Ophthalmology, 1978, 62, 389-393 RONALD L. RADIUS, A. EDWARD MAUMENEE, AND WILLIAM R. GREEN From the Wilmer Ophthalmologic
Randomised controlled trial comparing the effect of brimonidine and timolol on visual field loss after acute primary angle closure
 88 EXTENDED REPORT Randomised controlled trial comparing the effect of brimonidine and timolol on visual field loss after acute primary angle closure T Aung, F T S Oen, H-T Wong, Y-H Chan, B-K Khoo, Y-P
88 EXTENDED REPORT Randomised controlled trial comparing the effect of brimonidine and timolol on visual field loss after acute primary angle closure T Aung, F T S Oen, H-T Wong, Y-H Chan, B-K Khoo, Y-P
Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
 Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
Med. J. Cairo Univ., Vol. 83, No. 2, September: 67-72, 2015 www.medicaljournalofcairouniversity.net Macular Ganglion Cell Complex Measurement Using Spectral Domain Optical Coherence Tomography in Glaucoma
T he extent of damage to the optic nerve caused by nonarteritic
 1274 EXTENDED REPORT Frequency doubling technology perimetry in non-arteritic ischaemic optic neuropathy with altitudinal defects C A Girkin, G McGwin Jr, J DeLeon-Ortega... See end of article for authors
1274 EXTENDED REPORT Frequency doubling technology perimetry in non-arteritic ischaemic optic neuropathy with altitudinal defects C A Girkin, G McGwin Jr, J DeLeon-Ortega... See end of article for authors
Glaucoma at a tertiary referral eye hospital in Nepal
 Original article Glaucoma at a tertiary referral eye hospital in Nepal Paudyal I 1,Thapa S S 1, Paudyal G 2, Gurung R 2, Ruit S 2 1 Nepal Glaucoma Eye Clinic, Tilganga Institute of Ophthalmology, Kathmandu,
Original article Glaucoma at a tertiary referral eye hospital in Nepal Paudyal I 1,Thapa S S 1, Paudyal G 2, Gurung R 2, Ruit S 2 1 Nepal Glaucoma Eye Clinic, Tilganga Institute of Ophthalmology, Kathmandu,
Discrimination between normal and glaucomatous eyes with visual field and scanning laser polarimetry measurements
 586 Glaucoma Service, Department of Ophthalmology, University of Campinas, Campinas, Brazil R Lauande-Pimentel R A Carvalho H C Oliveira D C Gonçalves L M Silva V P Costa Glaucoma Service, Department of
586 Glaucoma Service, Department of Ophthalmology, University of Campinas, Campinas, Brazil R Lauande-Pimentel R A Carvalho H C Oliveira D C Gonçalves L M Silva V P Costa Glaucoma Service, Department of
CHAPTER 13 CLINICAL CASES INTRODUCTION
 2 CHAPTER 3 CLINICAL CASES INTRODUCTION The previous chapters of this book have systematically presented various aspects of visual field testing and is now put into a clinical context. In this chapter,
2 CHAPTER 3 CLINICAL CASES INTRODUCTION The previous chapters of this book have systematically presented various aspects of visual field testing and is now put into a clinical context. In this chapter,
Scanning Laser Polarimetry in Patients with Acute Attack of Primary Angle Closure
 Scanning Laser Polarimetry in Patients with Acute Attack of Primary Angle Closure Jimmy S. M. Lai*, Clement C. Y. Tham, Jonathan C. H. Chan*, Nelson K. F. Yip, Wilson W. T. Tang, Patrick S. H. Li*, Jane
Scanning Laser Polarimetry in Patients with Acute Attack of Primary Angle Closure Jimmy S. M. Lai*, Clement C. Y. Tham, Jonathan C. H. Chan*, Nelson K. F. Yip, Wilson W. T. Tang, Patrick S. H. Li*, Jane
The Uniocular Drug Trial and Second-Eye Response to Glaucoma Medications
 The Uniocular Drug Trial and Second-Eye Response to Glaucoma Medications Tony Realini, MD, 1 Robert D. Fechtner, MD, 2 Sean-Paul Atreides, MD, 3 Stephen Gollance, MD 2 Purpose: To determine if the intraocular
The Uniocular Drug Trial and Second-Eye Response to Glaucoma Medications Tony Realini, MD, 1 Robert D. Fechtner, MD, 2 Sean-Paul Atreides, MD, 3 Stephen Gollance, MD 2 Purpose: To determine if the intraocular
3/16/2018. Perimetry
 Perimetry The normal visual field extends further away from fixation temporally and inferiorly than superiorly and nasally. From the center of the retina this sensitivity decreases towards the periphery,
Perimetry The normal visual field extends further away from fixation temporally and inferiorly than superiorly and nasally. From the center of the retina this sensitivity decreases towards the periphery,
glaucoma and ocular hypertension
 British Journal of Ophthalmology, 1980, 64, 852-857 Colour vision in patients with chronic simple glaucoma and ocular hypertension D. POINOOSAWMY, S. NAGASUBRAMANIAN, AND J. GLOSTER From the Glaucoma Unit,
British Journal of Ophthalmology, 1980, 64, 852-857 Colour vision in patients with chronic simple glaucoma and ocular hypertension D. POINOOSAWMY, S. NAGASUBRAMANIAN, AND J. GLOSTER From the Glaucoma Unit,
ALTHOUGH OCULAR hypertension
 EPIDEMIOLOGY AND BIOSTATISTICS Association of Demographic, Familial, Medical, and Ocular Factors With Intraocular Pressure LeAnn M. Weih, PhD; Bickol N. Mukesh, PhD; Catherine A. McCarty, PhD; Hugh R.
EPIDEMIOLOGY AND BIOSTATISTICS Association of Demographic, Familial, Medical, and Ocular Factors With Intraocular Pressure LeAnn M. Weih, PhD; Bickol N. Mukesh, PhD; Catherine A. McCarty, PhD; Hugh R.
Clinical Significance of Serum Antibody Against Neuron-Specific Enolase in Glaucoma Patients
 Clinical Significance of Serum Antibody Against Neuron-Specific Enolase in Glaucoma Patients Yoko Ikeda,* Ikuyo Maruyama,, Mitsuru Nakazawa and Hiroshi Ohguro *Department of Ophthalmology, Kyoto Prefectural
Clinical Significance of Serum Antibody Against Neuron-Specific Enolase in Glaucoma Patients Yoko Ikeda,* Ikuyo Maruyama,, Mitsuru Nakazawa and Hiroshi Ohguro *Department of Ophthalmology, Kyoto Prefectural
9/25/2017 CASE. 67 years old On 2 topical meds since 3 years. Rx: +3.0 RE LE
 CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
CASE 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115 LE IOP : 17 RE 19 LE CD: 0.5 RE 0.6 LE 1 67 years old On 2 topical meds since 3 years Rx: +3.0 /-0.5@65 RE +2.5/-0.5@115
Correlation of Blue Chromatic Macular Sensitivity with Optic Disc Change in Early Glaucoma Patients
 Correlation of Blue Chromatic Macular Sensitivity with Optic Disc Change in Early Glaucoma Patients Yoshio Yamazaki, Kenji Mizuki, Fukuko Hayamizu and Chizuru Tanaka Department of Ophthalmology, Nihon
Correlation of Blue Chromatic Macular Sensitivity with Optic Disc Change in Early Glaucoma Patients Yoshio Yamazaki, Kenji Mizuki, Fukuko Hayamizu and Chizuru Tanaka Department of Ophthalmology, Nihon
