Rossetti et al. BMC Ophthalmology 2015, 15:7
|
|
|
- Ambrose Nichols
- 5 years ago
- Views:
Transcription
1 Rossetti et al. BMC Ophthalmology 2015, 15:7 RESEARCH ARTICLE Open Access Comparison of the effects of bimatoprost and a fixed combination of latanoprost and timolol on 24-hour blood and ocular perfusion pressures: the results of a randomized trial Luca Rossetti 1*, Matteo Sacchi 1, Costas H Karabatsas 2, Fotis Topouzis 3, Michele Vetrugno 4, Marco Centofanti 5, Andreas Boehm 6, Christian Vorwerk 7, David Goldblum 8 and Paolo Fogagnolo 1 Abstract Background: To compare the effect of bimatoprost and the fixed combination latanoprost-timolol (LTFC) on 24-hour systolic (SBP) and diastolic (DBP) blood pressure and on 24-hour ocular perfusion pressure (OPP). Methods: 200 patients with glaucoma or ocular hypertension, controlled on the unfixed combination of latanoprost and timolol or eligible for dual therapy being not being fully controlled on monotherapy were enrolled in a randomized, double-masked, placebo-controlled, multicentre clinical trial. They were randomized to LTFC (8 a.m.) or bimatoprost (8 p.m.) and received 24-hour IOP curve at baseline, 6 and 12 weeks (supine and sitting position IOPs were recorded at 8 p.m., midnight, 5 a.m., 8a.m., noon and 4 p.m.). Holter 24-hour blood pressure curve was obtained between weeks 2 and 12. SBP, DBP, OPP were calculated and compared with ANOVA. Rates of diastolic OPP (DPP) 50, 40, 30 mmhg in the 2 groups were calculated and compared using Fisher s test. Results: Mean baseline SBP and DBP were ± 18.3 vs ± 20.1 mmhg (p = 0.1) and 79.1 ± 10.2 vs 78.2 ± 10.1 mmhg (p = 0.4) in the bimatoprost and LTFC groups respectively. Holter SBP was significantly higher for bimatoprost (135.1 mmhg vs mmhg, p = 0.04), while no statistically significant difference in DBP was found. DPP was similar in the 2 groups, and proportions of patients with at least one value of the 24-hour curve 50, 40, 30 mmhg were 94%, 86%, 41% respectively. Conclusions: Bimatoprost and LTFC had similar DBPs and OPPs; SBP was significantly lower with LTFC. In this study, thepercentageof dippers was considerably higher than the one described in previous studies on the role of perfusion pressure in glaucoma. Trial registration: NCT , May 21, Background Primary open angle glaucoma (POAG) is a disease whose pathogenesis is not completely clear [1]. There is evidence that elevated intraocular pressure (IOP) is a strong risk factor for both occurrence and progression of glaucoma [2,3] and also that IOP reduction can be highly protective from worsening of the disease [4]. However, IOP alone can hardly explain all of the pathogenesis of glaucoma and * Correspondence: luca.rossetti@unimi.it 1 Clinica Oculistica, Dipartimento di Medicina, Chirurgia e Odontoiatria, Università di Milano, Ospedale San Paolo, Via di Rudinì 8, Milan, Italy Full list of author information is available at the end of the article the importance of vascular factors, in particular of perfusion pressure (PP), has been ascertained in a number of epidemiologic studies and clinical trials as well [5-8]. Low values of diastolic perfusion pressure (DPP) have been reported to be a major risk factor for the incidence of glaucoma [9,10], and a decreased DPP was found to be a significant predictor for glaucoma progression [11-13]. Yet, the independent role of PP in the pathogenesis of the disease is debated [14]; a further issue is the way PP is calculated and assessed in multivariate analyses together with IOP [15]. Evaluation of both IOP and PP is often a critical point in the context of an epidemiologic study and 2015 Rossetti et al.; licensee BioMed Central. This is an Open Access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly credited. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Rossetti et al. BMC Ophthalmology 2015, 15:7 Page 2 of 7 in a clinical trial as well. Both parameters can, in fact, considerably vary during the 24-hour and can be susceptible to a number of other variables (time point of the day or night, concomitant use of systemic or local drugs, emotional stress during the measurement, etc.). Probably the best way to evaluate IOP rhythm is by means of 24-hour measurements [16-20], while the 24-hour Holter recording is the most appropriate procedure to get an estimate of the systemic blood pressure during a 24-hour period. The effect of beta-blockers and prostaglandin analogues on IOP reduction is well known [21], whereas these drugs effect on PP has been studied only more recently [22,23]. A European multicenter randomized clinical trial was conducted with the aim of comparing the effectiveness and safety of bimatoprost and of the LTFC in lowering IOP in patients with POAG or OH when switched from a non-fixed combination of latanoprost and timolol, and the findings have been published [24]. The objective of this paper was to investigate the effect of these drugs on PP, assess the number of patients at risk due to low DPP despite apparently good IOP control and to calculate the proportion of time in a day when patients were, on average, below PP values that we conventionally consider as potentially safe. Methods The study was carried out at 7 European University Eye Clinics after the approval of the Ethics Committee of the Universities of Milan, Rome, Bari (Italy), Larissa, Thessaloniki (Greece), Dresden, Magdeburg (Germany), Basel (Switzerland). All patients signed a written informed consent form. The patients and the methods of this trial have been described in a previous paper [24]; in this paper, we described in detail the methods for evaluation of IOP and blood pressure and their analyses. Patients inclusion criteria were the following: Inclusion criteria: POAG/PEX or OH patients aged 18 years or more patients controlled (IOP <21 mmhg) on the unfixed combination of latanoprost and timolol for at least 3 months prior to the baseline visit. patients on monotherapy either with latanoprost or timolol eligible for dual therapy (IOP >21 mmhg, or target IOP not reached). Exclusion criteria: contraindications to beta-blockers closed/barely open anterior chamber angles or history of acute angle closure. ocular surgery or argon laser trabeculoplasty within the last 3 months. ocular inflammation/infection occurring within 3 months prior to pre-trial visit. neovascular glaucomas. hypersensitivity to benzalkonium chloride or to any other component of the trial drug solutions. other abnormal ocular condition or symptom preventing the patient from entering the trial. patients on either bimatoprost or the LTFC patients who had undergone refractive surgery inability to adhere to treatment/visit plan. participation in any other clinical trial (i.e., requiring informed consent) within one month prior to pre-study visit. pregnancy, nursing, or, if applicable, not using adequate contraception. any drug known to affect IOP. Study design This was a 12-week, multicentre, randomized, doublemasked study. The trial was conducted in accordance with the ethical principles that have their origins in the Declaration of Helsinki and its amendment of October 2000 (Edinburgh, Scotland), the European Guidelines on Good Clinical Practice (GCP) and the International Conference on Harmonisation (ICH) Guidelines. The trial included five visits: 1) patients were checked for eligibility at the pre-trial screening visit; if potentially eligible, only patients on monotherapy started wash-in medications (unfixed combination of latanoprost and timolol) after the screening visit; 2) baseline visit after at least 6 weeks of wash-in; 3) week 2 visit (safety visit including biomicroscopy, single IOP measurement and evaluation of adverse events); 4) week 6 visit; 5) week 12 visit. At the end of the study (3 weeks after week 12 visit) a safety visit was optional. The baseline visit and the week 6 and 12 visits required hospitalization and patients were evaluated for 24 hours. Patients were hospitalized at 7 pm to undergo a 24-hour IOP assessment. Supine and sitting position IOP was measured at 8 pm, midnight, 5 am, 8 am, noon, and 4 pm; 15 minutes around the time point were allowed. At 8 pm and at 8 am, the study drops were administered by the study personnel. Both 8 a.m. and 8 p.m. tonometric recordings were performed before study drugs were administered. Supine IOP was measured using the handheld Perkins tonometer with the patient resting on a bed for at least minutes. Sitting IOP was measured with the Goldmann applanation tonometer. At each time point IOP was measured twice, and then averaged. If the 2 recordings were not within 2 mmhg a third measurement was taken and the average calculated. All assessments were performed by the same well-trained evaluators different from the study personnel administrating the drugs.
3 Rossetti et al. BMC Ophthalmology 2015, 15:7 Page 3 of 7 On an outpatient basis, the patients underwent a Holter 24-hour blood pressure recording not earlier than 2 weeks after having started the trial medications. Study treatments Patients on monotherapy (either latanoprost or timolol) underwent a wash-in phase lasting 6 weeks. Wash-in treatment consisted in timolol (Timolol XE morning administration) and latanoprost (Xalatan evening administration). After baseline 24-hour evaluation, each patient was allocated to one of the two treatment groups according to a centralized computer-generated randomisation code list prepared and kept at each institute by an independent administrator: 1) LTFC (Xalacom) at 8 am + placebo at 8 pm; 2) placebo at 8 am + bimatoprost (Lumigan) at 8 pm. Identical bottles were used for masking purposes. Definitions The nocturnal period was from 11 pm to 7 am. Perfusion pressure was calculated as blood pressure (systolic, diastolic) minus IOP (taken from the habitual body position readings). During the Holter acquisition, blood pressure was measured every 15 minutes as opposite to IOP, which was measured every 4 hours. For the aims of the study, it was important to consider values which were less affected as possible by disturbing factors (such as sudden awakening, change in body position, exposure to light etc.). In order to use all available BP readings (ideally 96 per patient), we arbitrarily calculated perfusion pressure by subtracting the closest IOP reading to BP. For sake of clarity, considering the period from 10:00 pm to 9:59 am, perfusion pressures for BP collected between 10:00 pm and 1:59 am were calculated using the midnight IOP measurement; from 2:00 am to 5:59, the 4 am IOP reading was subtracted to the singles BP readings, whereas from 6:00 to to 9:59 am, the 8 am IOP reading was used. Statistical analysis Comparisons between treatments and within the 2 treatment groups with baseline were carried out with ANOVA. The following parameters were compared: a. IOP at baseline, at week 6 and week 12; b. IOP difference between baseline and week 12; c. 24-hour diastolic blood pressure (DBP), 24-hour systolic blood pressure (SBP) at the time of Holter acquisition; 24-hour DPP, 24-hour SPP at the time of Holter acquisition; nocturnal DPP, nocturnal SPP at the time of Holter acquisition. The study population (as a whole and for subgroups) was also stratified based on the mean nocturnal DPP (using cut-off values of 50, 45, 40, 35, 30 mmhg). For each cut-off value, mean nocturnal DPP were calculated and compared. Rates of DPP 50, 45, 40, 35, 30 mmhg in the 2 groups were calculated and compared using Fisher s test. In addition, the proportion of time in the day when DPP was below a given cut-off value was calculated. The details of sample size calculation are reported in another paper [24] and were based on the 24-hour mean change in IOP. In the estimates below, the significance level was set to 5% and the power to 80%. The numbers of 81 patients per group (1-sided test) and 102 patients per group (2-sided test) were calculated for a delta of 1.5 mmhg and a standard deviation of 3.8 mmhg. P-values were adjusted for multiple comparisons (Bonferroni corrections). Results A total of 200 patients were enrolled in the trial. All patients completed the study. A protocol violation occurred for two patients: one was treated for a bacterial conjunctivitis and another started a therapy with a systemic betablocker during the study. All data presented in the paper refer to the intention-to-treat analysis. Per-protocol analysis showed very similar results. Patients main characteristics are shown in Table 1. The majority of patients had initial to moderate glaucoma and about 20% of cases had OH. Treatment for systemic hypertension was common and 40% of the whole sample was taking an antihypertensive drug. Results about IOP and PP are reported in Table 2. Very similar IOP levels at baseline and at 12 weeks were found in the 2 groups and no statistically significant difference was shown at any comparison. Baseline (i.e. under the unfixed combination of latanoprost and timolol) mean IOP was 16.3 mmhg (3.3) vs 15.5 mmhg (2.9) in bimatoprost and LTFC groups respectively and similar figures were shown when nocturnal IOPs were analyzed. Table 1 Patients main characteristics Bimatoprost LTFC Total Age, mean (sd) 64.7 (11.5) 67.8 (10.8) Male (%) 55 (54.5) 53 (53.5) POAG/PEX (%) 78 (77) 80 (81) OH (%) 23 (23) 19 (19) MD, mean (sd) 4.2 (2.3 db) 4.6 (2.7 db) CCT, mean (sd) 543 (38 μm) 535 (39 μm) Systemic Drugs Antihypertensives (%) 42 (41) 40 (40) Antidepressants (%) 6 (6) 8 (8) Hypoglycemics oral (%) 11 (11) 13 (13) Cholesterol-lowering drugs (%) 13 (13) 15 (15) Antiarrhythmics (%) 5 (5) 4 (4) LTFC: latanoprost/timolol fixed combination; sd: standard deviation; POAG: primary open-angle glaucoma; PEX pseudoexfoliative glaucoma; OH: ocular hypertension; MD: mean deviation; CCT: central corneal thickness.
4 Rossetti et al. BMC Ophthalmology 2015, 15:7 Page 4 of 7 Table 2 Comparison of intraocular, systemic and perfusion pressures (mmhg) in the 2 groups Bimatoprost LTFC p-value Baseline IOP (sd) 16.3 (3.3) 15.5 (2.9) 0.2 Baseline nocturnal IOP (sd) 16.9 (3.6) 16.0 (3.3) 0.3 Baseline SBP (sd) (18.3) (20.1) 0.1 Baseline DBP (sd) 79.1 (10.2) 78.2 (10.1) 0.4 Baseline nocturnal SBP (sd) (13.8) (15.8) 0.3 Baseline nocturnal DBP (sd) 72.7 (7.9) 73.2 (9.5) 0.4 Baseline SPP (sd) (15.7) (16.8) 0.3 Baseline DPP (sd) 62.8 (6.9) 62.7 (8.2) 0.6 Baseline nocturnal SPP (sd) (13.1) (16.4) 0.2 Baseline nocturnal DPP (sd) 55.8 (8.0) 57.2 (12.1) week IOP (sd) 16.1 (2.5) 16.3 (3.7) week nocturnal IOP (sd) 16.1 (2.6) 16.1 (3.9) 0.8 Holter SBP (sd) (16.7) (15.3) 0.04 Holter DBP (sd) 79.5 (8.3) 78.7 (11.8) 0.4 Holter nocturnal SBP (sd) (14.4) (14.5) 0.08 Holter nocturnal DBP (sd) 71.7 (7.9) 70.6 (11.3) 0.2 Holter SPP (sd) (10.8) (15.3) 0.03 Holter DPP (sd) 63.4 (8.0) 62.4 (11.1) 0.1 Holter nocturnal SPP (sd) (14.4) (17.3) 0.07 Holter nocturnal DPP (sd) 55.6 (7.4) 54.5 (12.3) 0.2 LTFC: latanoprost/timolol fixed combination; IOP: intraocular pressure; sd: standard deviation; SBP: systolic blood pressure; DBP: diastolic blood pressure; SPP: systolic perfusion pressure; DPP: diastolic perfusion pressure. Also SBP and DBP were very similar at baseline in the 2 groups and, as expected, were significantly lower during the night (p = 0.01). There was no statistically significant difference between the study drugs for all comparisons but for Holter SBP and SPP that were significantly higher in the group treated with bimatoprost (135.1 mmhg vs mmhg and mmhg vs mmhg in bimatoprost and LTFC groups respectively, p = 0.04, p = 0.03). Figure 1 is showing the proportion of patients who had at least 1 DPP reading below a given cut-off value. More than 90% of the patients had at least one DPP measurement below 50 mmhg, more than 80% below 40 mmhg and about 40% of patients had one reading of 30 mmhg or less. The fraction of time during the 24-hour on which patients remained with DPP below a given cut-off value is reported in Table 3. During the 24-hour curve, these patients were exposed to DPP < 50, 40, 30 mmhg for respectively 3 h 30 ±2h16 (range, 30 ; 10h),1h7 ±1h 2 (0; 5 h 30 ), 10 ±16 (0; 1 h 30 ), being respectively 13.9 ± 9.0 (range, 1; 40), 4.7 ± 4.1 (0; 22), 1.0 ± 1.2 (0; 6) the number of time-points at which DPP fell below the given value. No statistically significant difference was found between the two study treatments. Thirty-eight percent of low DPP values were found during office hours (8 am-4 pm), compared to 62% outside office-hours. Twenty-nine percent of low DPP occurred at night. Discussion The results of this study show that both IOP and PP can be very similar in a group of patients treated with bimatoprost or with LTFC. In fact, with the exception of SBP and SPP that were higher in the group receiving bimatoprost, all other comparisons did not show any statistically significant difference. No major effect of timolol in lowering PP could be evidenced in this trial. As a secondary result, we found that low DPP values were a common finding in our trial population, despite this sample had a very well controlled 24-hour IOP. Nearly all cases had at least one DPP reading below 50 mmhg and 40% below Percentage <50 <45 <40 <35 <30 <25 <20 <15 <10 <5 DPP Figure 1 Percentage of patients showing at least 1 DPP below the given cut-off values.
5 Rossetti et al. BMC Ophthalmology 2015, 15:7 Page 5 of 7 Table 3 Exposure time (during a 24-hour period) to DPP below given cut-off values DPP cut-off Mean (hours, minutes) sd Range <50 mmhg 3 h 30 2h16 30 ;10 h <45 mmhg 2 h 6 1h40 0; 8h <40 mmhg 1 h 7 1h2 0; 5 h 30 <35 mmhg ; 2 h <30 mmhg ; 1 h 30 DPP: diastolic perfusion pressure; sd: standard deviation. 30 mmhg. Furthermore, on average, patients were exposed to a DPP <50 mmhg for more than 3 hours per day. The effect of timolol on PP is debated. A recent 24- hour study found that timolol (both solution and gel formulations) had no relevant effect on BP and PP in patients with POAG [25]. In another clinical trial where the timolol add-on therapy in prostaglandin treated glaucoma patients was evaluated, larger PP fluctuations were recorded after timolol [26]. In another recent prospective cross-over study, timolol was found to cause retinal vascular dysregulation in response to posture change in 30% of the trial sample after 6 weeks of treatment [27]. In our trial, timolol did not seem to have a clinically relevant effect in influencing the 24-hour PP. A secondary, yet important finding of the present trial, was the recording of low nocturnal DPP values in a group of glaucoma patients. The clinical relevance of such a finding is not known but it certainly deserves some discussion. The role of PP in the pathogenesis (and progression) of glaucoma is not completely clear, although large epidemiologic studies have shown that ocular PP is a risk factor for the prevalence, incidence and progression of glaucoma [28-32]. Data from clinical trials seem to confirm the importance of PP: in the Early Manifest Glaucoma Trial (EMGT) [3], patients with low SPP tended to progress faster, and low SSP was a significant predictor of progression with an almost 50% higher risk; a recent report from the Low-pressure Glaucoma Treatment study showed that lower mean ocular perfusion pressure increased the risk for reaching a progression outcome [11]. A high proportion of patients in this trial was exposed to low PP values for a variable amount of time. It is hard to tell whether this risk is clinically relevant; unfortunately, the study was not designed with this objective and the short-term assessment of IOP and PP, the type of patients included (young and not selected according to the risk for low PP) are strongly limiting the possibility of a correct interpretation of our findings. Only long-term clinical trials assessing both visual field progression and 24-hour circadian IOP and PP in high-risk (e.g. older patients, patients treated with evening-dosed systemic anti-hypertensive medications) glaucoma patients will provide a conclusive answer. Other study limitations include: 1. Holter pressures and IOPs were not recorded at the same time; thus, at least potentially, all or some of the PP values that were derived from Holter could be wrong. On the other hand, with such study design Holter readings were not influenced by sudden awakenings that could not be avoided when IOP was measured at night and may result in a better estimate of the true pressures occurring during the sleeping period; 2. Patients in the trial were part of a highly selected population: they had well controlled IOP values, and, belonging to a study group, they probably tended to better adhere to treatment protocol; as a results they were likely to have better IOPs and PPs than the general glaucoma population. This, of course, decreases the generalizability of the findings; 3. The timing of drugs administration that could have influenced our findings: in this trial LTFC was administered in the morning (as suggested when the study was planned) while there is now evidence that it can be more effective when given in the evening [33,34]. The strengths of this study should be also reported. First, at least to our knowledge, this is the biggest randomized clinical trial ever carried out with 24-hour circadian IOP and PP as outcomes in glaucoma patients. Second, the multicentre design and the stability of the IOP profile under the 2 study drugs reinforce the validity of our observations. The vast majority of the evidence about the role of PP in glaucoma comes from large epidemiologic studies or clinical trials where information on IOP is limited to single or few observations. It is reasonable to assume that our study could provide a more accurate estimate of the PPs in a POAG and OH patient population. The true role of IOP variability and, consequently, PP in the pathogenesis of POAG and its progression will remain debated until a reliable tool to assess continuous IOP (and PP) will be clinically available. It seems we are not there yet; surrogate methods, as the one we used in this trial are probably the best options to get an estimate of short-term IOP variability and PP, though, we are aware, still far from perfection. Conclusions In conclusion, low values of DPP are a common findings in glaucoma patients, even when IOP is under optimal control. A significant proportion of such patient can be exposed to risky PP values for a certain amount of time. The clinical meaning of this finding is still to be determined. Competing interests In the past five years, all Authors received reimbursements for participation to meetings and fees for lectures at meetings or advisory boards from Allergan. Allergan did not finance this manuscript (including the article-processing charge). None of the Authors holds or is currently applying for any patents relating to the content of the manuscript.
6 Rossetti et al. BMC Ophthalmology 2015, 15:7 Page 6 of 7 None of the Authors has non-financial competing interests. Authors contributions LR: conceived of the study, and participated in its design and coordination, participated in the sequence alignment and drafted the manuscript. MS: participated in the sequence alignment and drafted the manuscript. CHK: conceived of the study, and participated in its design and coordination, participated in the sequence alignment and drafted the manuscript. FT: conceived of the study, and participated in its design and coordination, participated in the sequence alignment and drafted the manuscript. MV: participated in study design and coordination. MC: participated in study design and coordination. AB: participated in study design and coordination. CV: conceived of the study, and participated in its design and coordination, participated in the sequence alignment and drafted the manuscript. DG: participated in study design and coordination. PF: conceived of the study, performed the statistical analysis, and participated in its design and coordination, participated in the sequence alignment and drafted the manuscript. All authors read and approved the final manuscript. Acknowledgements This study was presented at ARVO, Fort Lauderdale FL, May This study was funded by an unrestricted grant from Allergan, Inc. Author details 1 Clinica Oculistica, Dipartimento di Medicina, Chirurgia e Odontoiatria, Università di Milano, Ospedale San Paolo, Via di Rudinì 8, Milan, Italy. 2 Department of Ophthalmology, University of Thessaly School of Medicine, Larissa, Greece. 3 Department of Ophthalmology, School of Medicine, Aristotle University of Thessaloniki, American Hellenic Educational Progressive Association (AHEPA) Hospital, Thessaloniki, Greece. 4 Anthea Hospital, GVM Care and Research, Bari, Italy. 5 DSCMT Università di Roma Tor Vergata ; IRCCS Fondazione G.B. Bietti, Rome, Italy. 6 University Hospital Carl Gustav Carus Dresden, Technical University Dresden, Dresden, Germany. 7 Augenklinik der Otto von Guericke Universität Magdeburg, Magdeburg, Germany. 8 Department of Ophthalmology, University Hospital Basel, University Basel, Basel, Switzerland. Received: 28 April 2014 Accepted: 10 January 2015 Published: 22 January 2015 References 1. Casson RJ, Chidlow G, Wood JP, Crowston JG, Goldberg I. Definition of glaucoma: clinical and experimental concepts. Clin Exp Ophthalmol. 2012;40: De Moraes CG, Demirel S, Gardiner SK, Liebmann JM, Cioffi GA, Ritch R, et al. Effect of treatment on the rate of visual field change in the ocular hypertension treatment study observation group. Invest Ophthalmol Vis Sci. 2012;53: Leske MC, Heijl A, Hyman L, Bengtsson B, Dong L, Yang Z, et al. Predictors of long-term progression in the early manifest glaucoma trial. Ophthalmology. 2007;114: Maier PC, Funk J, Schwarzer G, Antes G, Falck-Ytter YT. Treatment of ocular hypertension and open angle glaucoma: meta-analysis of randomised controlled trials. BMJ. 2005;331(7509): Zheng Y, Wong TY, Mitchell P, Friedman DS, He M, Aung T. Distribution of ocular perfusion pressure and its relationship with open-angle glaucoma: the singapore malay eye study. Invest Ophthalmol Vis Sci. 2010;51: Memarzadeh F, Ying-Lai M, Chung J, Azen SP, Varma R, Los Angeles Latino Eye Study Group. Blood pressure, perfusion pressure, and open-angle glaucoma: the Los Angeles Latino Eye Study. Invest Ophthalmol Vis Sci. 2010;51: Leske MC. Ocular perfusion pressure and glaucoma: clinical trial and epidemiologic findings. Curr Opin Ophthalmol. 2009;20: Hulsman CA, Vingerling JR, Hofman A, Witteman JC, de Jong PT. Blood pressure, arterial stiffness, and open-angle glaucoma: the Rotterdam study. Arch Ophthalmol. 2007;125: Bonomi L, Marchini G, Marraffa M, Bernardi P, Morbio R, Varotto A. Vascular risk factors for primary open angle glaucoma: the Egna-Neumarkt Study. Ophthalmology. 2000;107: Leske MC, Wu SY, Hennis A, Honkanen R, Nemesure B, BESs Study Group. Risk factors for incident open-angle glaucoma: the Barbados Eye Studies. Ophthalmology. 2008;115: De Moraes CG, Liebmann JM, Greenfield DS, Gardiner SK, Ritch R, Krupin T, et al. Risk factors for visual field progression in the low-pressure glaucoma treatment study. Am J Ophthalmol. 2012;154: Okumura Y, Yuki K, Tsubota K. Low diastolic blood pressure is associated with the progression of normal-tension glaucoma. Ophthalmologica. 2012;228: Janulevičiene I, Ehrlich R, Siesky B, Nedzelskienė I, Harris A. Evaluation of hemodynamic parameters as predictors of glaucoma progression. J Ophthalmol. 2011;2011: Ramdas WD, Wolfs RC, Hofman A, de Jong PT, Vingerling JR, Jansonius NM. Ocular perfusion pressure and the incidence of glaucoma: real effect or artifact? The Rotterdam Study. Invest Ophthalmol Vis Sci. 2011;52: Khawaja AP, Crabb DP, Jansonius NM. The role of ocular perfusion pressure in glaucoma cannot Be studied with multivariable regression analysis applied to surrogates. Invest Ophthalmol Vis Sci. 2013;54: Mosaed S, Liu JH, Weinreb RN. Correlation between office and peak nocturnal intraocular pressures in healthy subjects and glaucoma patients. Am J Ophthalmol. 2005;139: Fogagnolo P, Orzalesi N, Ferreras A, Rossetti L. The circadian curve of intraocular pressure: can we estimate its characteristics during office hours? Invest Ophthalmol Vis Sci. 2009;50: Quaranta L, Katsanos A, Russo A, Riva I. 24-hour intraocular pressure and ocular perfusion pressure in glaucoma. Surv Ophthalmol. 2013;58: Quaranta L, Konstas AG, Rossetti L, Garcia-Feijoo J, O'Brien C, Nasr MB, et al. Untreated 24-h intraocular pressures measured with Goldmann applanation tonometry vs nighttime supine pressures with Perkins applanation tonometry. Eye (Lond). 2010;24: Konstas AG, Quaranta L, Mikropoulos DG, Nasr MB, Russo A, Jaffee HA, et al. Peak intraocular pressure and glaucomatousprogressioninprimary open-angle glaucoma. J Ocul Pharmacol Ther. 2012;28: van der Valk R, Webers CA, Schouten JS, Zeegers MP, Hendrikse F, Prins MH. Intraocular pressure-lowering effects of all commonly used glaucoma drugs: a meta-analysis of randomized clinical trials. Ophthalmology. 2005;112: Quaranta L, Gandolfo F, Turano R, Rovida F, Pizzolante T, Musig A, et al. Effects of topical hypotensive drugs on circadian IOP, blood pressure, and calculated diastolic ocular perfusion pressure in patients with glaucoma. Invest Ophthalmol Vis Sci. 2006;47: Orzalesi N, Rossetti L, Bottoli A, Fogagnolo P. Comparison of the effects of latanoprost, travoprost, and bimatoprost on circadian intraocular pressure in patients with glaucoma or ocular hypertension. Ophthalmology. 2006;113: Rossetti L, Karabatsas CH, Topouzis F, Vetrugno M, Centofanti M, Boehm A, et al. Comparison of the effects of bimatoprost and a fixed combination of latanoprost and timolol on circadian intraocular pressure. Ophthalmology. 2007;114: Quaranta L, Katsanos A, Floriani I, Riva I, Russo A, Konstas AG. Circadian intraocular pressure and blood pressure reduction with timolol 0.5% solution and timogel 0.1% in patients with primary open-angle glaucoma. J Clin Pharmacol. 2012;52: Januleviciene I, Siaudvytyte L, Diliene V, Barsauskaite R, Paulaviciute-Baikstiene D, Siesky B, et al. Comparison of intraocular pressure, blood pressure, ocular perfusion pressure and blood flow fluctuations during dorzolamide versus timolol add-on therapy in prostaglandin analogue treated glaucoma subjects. Pharmaceuticals. 2012;5: Feke GT, Rhee DJ, Turalba AV, Pasquale LR. Effects of dorzolamide-timolol and brimonidine-timolol on retinal vascular autoregulation and ocular perfusion pressure in primary open angle glaucoma. J Ocul Pharmacol Ther. 2013;29: Costa VP, Jimenez-Roman J, Carrasco FG, Lupinacci A, Harris A. Twenty-fourhour ocular perfusion pressure in primary open-angle glaucoma. Br J Ophthalmol. 2010;94: Cherecheanu AP, Garhofer G, Schmidl D, Werkmeister R, Schmetterer L. Ocular perfusion pressure and ocular blood flow in glaucoma. Curr Opin Pharmacol. 2013;13: Leske MC, Wu SY, Hennis A, Honkanen R, Nemesure B. Risk factors for incident open-angle glaucoma: the Barbados Eye Studies. Ophthalmology. 2008;115: Quigley HA, West SK, Rodriguez J, Munoz B, Klein R, Snyder R. The prevalence of glaucoma in a population-based study of Hispanic subjects: Proyecto VER. Arch Ophthalmol. 2001;119: Topouzis F, Wilson MR, Harris A, Founti P, Yu F, Anastasopoulos E, et al. Association of open-angle glaucoma with perfusion pressure status in the Thessaloniki Eye Study. Am J Ophthalmol. 2013;155:
7 Rossetti et al. BMC Ophthalmology 2015, 15:7 Page 7 of Diestelhorst M, Larsson LI, European Latanoprost Fixed Combination Study Group. A 12 week study comparing the fixed combination of latanoprost and timolol with the concomitant use of the individual components in patients with open angle glaucoma and ocular hypertension. Br J Ophthalmol. 2004;88: Diestelhorst M, Larsson LI, European-Canadian Latanoprost Fixed Combination Study Group. A 12-week, randomized, double-masked, multicenter study of the fixed combination of latanoprost and timolol in the evening versus the individual components. Ophthalmology. 2006;113:70 6. doi: / Cite this article as: Rossetti et al.: Comparison of the effects of bimatoprost andafixedcombinationoflatanoprostandtimololon24-hourbloodand ocular perfusion pressures: the results of a randomized trial. BMC Ophthalmology :7. Submit your next manuscript to BioMed Central and take full advantage of: Convenient online submission Thorough peer review No space constraints or color figure charges Immediate publication on acceptance Inclusion in PubMed, CAS, Scopus and Google Scholar Research which is freely available for redistribution Submit your manuscript at
Intraocular pressure (IOP) is the main risk factor for the
 The Circadian Curve of Intraocular Pressure: Can We Estimate Its Characteristics during Office Hours? Paolo Fogagnolo, 1 Nicola Orzalesi, 2 Antonio Ferreras, 3,4 and Luca Rossetti 2 PURPOSE. To verify
The Circadian Curve of Intraocular Pressure: Can We Estimate Its Characteristics during Office Hours? Paolo Fogagnolo, 1 Nicola Orzalesi, 2 Antonio Ferreras, 3,4 and Luca Rossetti 2 PURPOSE. To verify
24-hour IOP fluctuation: myth or reality?
 Journal for Modeling in Ophthalmology 2016; 2:103-109 Review article 24-hour IOP fluctuation: myth or reality? Luciano Quaranta 1, Ivano Riva 1, Francesco Oddone 2 1 Department of Medical and Surgical
Journal for Modeling in Ophthalmology 2016; 2:103-109 Review article 24-hour IOP fluctuation: myth or reality? Luciano Quaranta 1, Ivano Riva 1, Francesco Oddone 2 1 Department of Medical and Surgical
Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study
 Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study James H. Peace, M.D. 1, Casey K. Kopczynski, Ph.D. 2, and Theresa Heah, M.D. 2 1 Inglewood, CA 2
Ocular Hypotensive Efficacy of Netarsudil Ophthalmic Solution 0.02% Over a 24-Hour Period: A Pilot Study James H. Peace, M.D. 1, Casey K. Kopczynski, Ph.D. 2, and Theresa Heah, M.D. 2 1 Inglewood, CA 2
Page 1. Robert P. Wooldridge, OD, FAAO
 Robert P. Wooldridge, OD, FAAO I have received support from the following companies Alcon, Allergan, Biotissue, Centervue, EyeiC, Oculus, Optovue, Synemed, 46 yo WM referred as glaucoma suspect MH: no
Robert P. Wooldridge, OD, FAAO I have received support from the following companies Alcon, Allergan, Biotissue, Centervue, EyeiC, Oculus, Optovue, Synemed, 46 yo WM referred as glaucoma suspect MH: no
Relation & Association of Mean Ocular Perfusion Pressure in Primary Open Angle Glaucoma
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 5 Ver. XII (May. 2017), PP 54-58 www.iosrjournals.org Relation & Association of Mean Ocular
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 5 Ver. XII (May. 2017), PP 54-58 www.iosrjournals.org Relation & Association of Mean Ocular
24-h Efficacy of Glaucoma Treatment Options
 Adv Ther (2016) 33:481 517 DOI 10.1007/s12325-016-0302-0 REVIEW 24-h Efficacy of Glaucoma Treatment Options Anastasios G. P. Konstas. Luciano Quaranta. Banu Bozkurt. Andreas Katsanos. Julian Garcia-Feijoo.
Adv Ther (2016) 33:481 517 DOI 10.1007/s12325-016-0302-0 REVIEW 24-h Efficacy of Glaucoma Treatment Options Anastasios G. P. Konstas. Luciano Quaranta. Banu Bozkurt. Andreas Katsanos. Julian Garcia-Feijoo.
M Diestelhorst, L-I Larsson,* for The European Latanoprost Fixed Combination Study Group...
 199 SCIENTIFIC REPORT A 12 week study comparing the fixed combination of latanoprost and timolol with the concomitant use of the individual components in patients with open angle glaucoma and ocular hypertension
199 SCIENTIFIC REPORT A 12 week study comparing the fixed combination of latanoprost and timolol with the concomitant use of the individual components in patients with open angle glaucoma and ocular hypertension
The role of IOP levels in determining the onset and progression
 Effects of Topical Hypotensive Drugs on Circadian IOP, Blood Pressure, and Calculated Diastolic Ocular Perfusion Pressure in Patients with Glaucoma Luciano Quaranta, Federico Gandolfo, Raffaele Turano,
Effects of Topical Hypotensive Drugs on Circadian IOP, Blood Pressure, and Calculated Diastolic Ocular Perfusion Pressure in Patients with Glaucoma Luciano Quaranta, Federico Gandolfo, Raffaele Turano,
Review Article The Association between Primary Open-Angle Glaucoma and Blood Pressure: Two Aspects of Hypertension and Hypotension
 BioMed Research International Volume 2015, Article ID 827516, 7 pages http://dx.doi.org/10.1155/2015/827516 Review Article The Association between Primary Open-Angle Glaucoma and Blood Pressure: Two Aspects
BioMed Research International Volume 2015, Article ID 827516, 7 pages http://dx.doi.org/10.1155/2015/827516 Review Article The Association between Primary Open-Angle Glaucoma and Blood Pressure: Two Aspects
24-hour Intraocular Pressure and Ocular Perfusion Pressure in Glaucoma
 SURVEY OF OPHTHALMOLOGY VOLUME 58 NUMBER 1 JANUARY FEBRUARY 2013 MAJOR REVIEW 24-hour Intraocular Pressure and Ocular Perfusion Pressure in Glaucoma Luciano Quaranta, MD, PhD, 1 Andreas Katsanos, MD, PhD,
SURVEY OF OPHTHALMOLOGY VOLUME 58 NUMBER 1 JANUARY FEBRUARY 2013 MAJOR REVIEW 24-hour Intraocular Pressure and Ocular Perfusion Pressure in Glaucoma Luciano Quaranta, MD, PhD, 1 Andreas Katsanos, MD, PhD,
Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 611-615 Effect of brimonidine on intraocular pressure in normal tension glaucoma: A short term clinical trial S.A. GANDOLFI, L. CIMINO, P.
Ocular Perfusion Pressure and Its Association with Primary Open Angle Glaucoma in Patients with Systemic Hypertension
 ARC Journal of Ophthalmology Volume, Issue,, PP -9 www.arcjournals.org Ocular Perfusion Pressure and Its Association with Primary Open Angle Glaucoma in Patients with Dr. Sandhya. R, MBBS, MS, DNB, (FRCS),
ARC Journal of Ophthalmology Volume, Issue,, PP -9 www.arcjournals.org Ocular Perfusion Pressure and Its Association with Primary Open Angle Glaucoma in Patients with Dr. Sandhya. R, MBBS, MS, DNB, (FRCS),
Glaucoma: NOT just IOP, Think DPP, OMG!
 Glaucoma: NOT just IOP, Think DPP, OMG! Bruce E. Onofrey, OD, RPh, FAAO Professor, Univ. Houston Exec. Director Continuing Education Programs I m a clinician, so let s talk patients TWO Patients ( a priest
Glaucoma: NOT just IOP, Think DPP, OMG! Bruce E. Onofrey, OD, RPh, FAAO Professor, Univ. Houston Exec. Director Continuing Education Programs I m a clinician, so let s talk patients TWO Patients ( a priest
Meta-analysis of timolol on diurnal and nighttime intraocular pressure and blood pressure
 Eur J Ophthalmol 2010; 20 ( 6) : 1035-1041 Original Article Meta-analysis of timolol on diurnal and nighttime intraocular pressure and blood pressure Princeton Wen-Yuan Lee 1, Aoife Doyle 1, Jeanette A.
Eur J Ophthalmol 2010; 20 ( 6) : 1035-1041 Original Article Meta-analysis of timolol on diurnal and nighttime intraocular pressure and blood pressure Princeton Wen-Yuan Lee 1, Aoife Doyle 1, Jeanette A.
4/06/2013. Medication Observation POAG. Proportion. Native American 0.1% 0.4%
 Clinical Research in Glaucoma: Putting Science into Practice J. James Thimons, O.D., FAAO Chairman, National Glaucoma Society www.nationalglaucomasociety.org Ocular Hypertension Treatment Study (OHTS)
Clinical Research in Glaucoma: Putting Science into Practice J. James Thimons, O.D., FAAO Chairman, National Glaucoma Society www.nationalglaucomasociety.org Ocular Hypertension Treatment Study (OHTS)
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma
 Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
Role of Central Corneal Thickness in Circadian Intraocular Pressure Fluctuations among Patients with Primary Open Angle Glaucoma Mohannad Albdour MD*, Karanjit Kooner MD, PHD** ABSTRACT Objectives: To
Abbreviated Update: Ophthalmic Glaucoma Agents
 Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-945-5220 Fax 503-947-1119 Abbreviated Update: Ophthalmic Glaucoma Agents Month/Year
Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-945-5220 Fax 503-947-1119 Abbreviated Update: Ophthalmic Glaucoma Agents Month/Year
Blood Pressure, Perfusion Pressure, and Open-Angle Glaucoma: The Los Angeles Latino Eye Study METHODS. Design
 Clinical and Epidemiologic Research Blood Pressure, Perfusion Pressure, and Open-Angle Glaucoma: The Los Angeles Latino Eye Study Farnaz Memarzadeh, 1 Mei Ying-Lai, 2 Jessica Chung, 2 Stanley P. Azen,
Clinical and Epidemiologic Research Blood Pressure, Perfusion Pressure, and Open-Angle Glaucoma: The Los Angeles Latino Eye Study Farnaz Memarzadeh, 1 Mei Ying-Lai, 2 Jessica Chung, 2 Stanley P. Azen,
The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters.
 A Study of the Safety and Efficacy of Travoprost 0.004%/Timolol 0.5% Ophthalmic Solution Compared to Latanoprost 0.005% and Timolol 0.5% Dosed Concomitantly in Patients with Open-Angle Glaucoma or Ocular
A Study of the Safety and Efficacy of Travoprost 0.004%/Timolol 0.5% Ophthalmic Solution Compared to Latanoprost 0.005% and Timolol 0.5% Dosed Concomitantly in Patients with Open-Angle Glaucoma or Ocular
Clinical Research in Glaucoma
 Clinical Research in Glaucoma J. James Thimons, O.D., FAAO Chairman, National Glaucoma Society www.nationalglaucomasociety.org Ocular Hypertension Treatment Study (OHTS) Primary Goals Evaluate the safety
Clinical Research in Glaucoma J. James Thimons, O.D., FAAO Chairman, National Glaucoma Society www.nationalglaucomasociety.org Ocular Hypertension Treatment Study (OHTS) Primary Goals Evaluate the safety
BJO Online First, published on September 1, 2009 as /bjo
 BJO Online First, published on September 1, 2009 as 10.1136/bjo.2009.158071 Efficacy and Tolerability of Bimatoprost versus Travoprost in Patients Previously on Latanoprost: a 3-Month, Randomised, Masked-Evaluator,
BJO Online First, published on September 1, 2009 as 10.1136/bjo.2009.158071 Efficacy and Tolerability of Bimatoprost versus Travoprost in Patients Previously on Latanoprost: a 3-Month, Randomised, Masked-Evaluator,
Circadian variations in central corneal thickness and intraocular pressure in patients with glaucoma
 SCIENTIFIC REPORT Circadian variations in central corneal thickness and intraocular pressure in patients with glaucoma P Fogagnolo, L Rossetti, F Mazzolani, N Orzalesi... Br J Ophthalmol ;9:. doi: 1.113/bjo.5.795
SCIENTIFIC REPORT Circadian variations in central corneal thickness and intraocular pressure in patients with glaucoma P Fogagnolo, L Rossetti, F Mazzolani, N Orzalesi... Br J Ophthalmol ;9:. doi: 1.113/bjo.5.795
LONG TERM IOP LOWERING EFFICACY OF BIMATOPROST/TIMOLOL FIXED COMBINATION: A 12 MONTH PROSPECTIVE STUDY
 LONG TERM IOP LOWERING EFFICACY OF BIMATOPROST/TIMOLOL FIXED COMBINATION: A 12 MONTH PROSPECTIVE STUDY LEQUEU I, THEUWIS K *1, ABEGAzO PINTO L *1,2, VANDEWALLE E 1,3, STALMANS I 1,3 ABSTRACT Purpose: To
LONG TERM IOP LOWERING EFFICACY OF BIMATOPROST/TIMOLOL FIXED COMBINATION: A 12 MONTH PROSPECTIVE STUDY LEQUEU I, THEUWIS K *1, ABEGAzO PINTO L *1,2, VANDEWALLE E 1,3, STALMANS I 1,3 ABSTRACT Purpose: To
Efficacy and Tolerability of Latanoprost 0.005% in Treatment of Primary Open Angle Glaucoma (POAG)
 Original Article Efficacy and Tolerability of Latanoprost.5% in Treatment of Primary Open Angle Glaucoma (POAG) Muhammad Imran Janjua, Saira Bano, Ali Raza Pak J Ophthalmol 217, Vol. 33, No. 3.....................................................................................................
Original Article Efficacy and Tolerability of Latanoprost.5% in Treatment of Primary Open Angle Glaucoma (POAG) Muhammad Imran Janjua, Saira Bano, Ali Raza Pak J Ophthalmol 217, Vol. 33, No. 3.....................................................................................................
53 year old woman attends your practice for routine exam. She has no past medical history or family history of note.
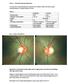 Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Case 1 Normal Tension Glaucoma 53 year old woman attends your practice for routine exam. She has no past medical history or family history of note. Table 1. Right Eye Left Eye Visual acuity 6/6 6/6 Ishihara
Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial
 Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial Boel Bengtsson, PhD, 1 M. Cristina Leske, MD, MPH, 2 Leslie Hyman, PhD, 2 Anders Heijl, MD, PhD, 1 Early
Fluctuation of Intraocular Pressure and Glaucoma Progression in the Early Manifest Glaucoma Trial Boel Bengtsson, PhD, 1 M. Cristina Leske, MD, MPH, 2 Leslie Hyman, PhD, 2 Anders Heijl, MD, PhD, 1 Early
Research Article Long-Term Clinical Course of Normal-Tension Glaucoma: 20 Years of Experience
 Hindawi Ophthalmology Volume 2017, Article ID 2651645, 6 pages https://doi.org/10.1155/2017/2651645 Research Article Long-Term Clinical Course of Normal-Tension Glaucoma: 20 Years of Experience Sang Wook
Hindawi Ophthalmology Volume 2017, Article ID 2651645, 6 pages https://doi.org/10.1155/2017/2651645 Research Article Long-Term Clinical Course of Normal-Tension Glaucoma: 20 Years of Experience Sang Wook
Primary open-angle glaucoma (POAG) is a chronic optic
 Clinical and Epidemiologic Research Physical Activity and Ocular Perfusion Pressure: The EPIC-Norfolk Eye Study Jennifer L.Y. Yip, 1,2 David C. Broadway, 3 Robert Luben, 1 David F. Garway-Heath, 2 Shabina
Clinical and Epidemiologic Research Physical Activity and Ocular Perfusion Pressure: The EPIC-Norfolk Eye Study Jennifer L.Y. Yip, 1,2 David C. Broadway, 3 Robert Luben, 1 David F. Garway-Heath, 2 Shabina
Reduction of intraocular pressure (IOP) is the only currently
 ORIGINAL STUDY Long-term 24-hour Intraocular ressure Control With Travoprost Monotherapy in atients With rimary Open-angle Glaucoma Ivano Riva, MD,* Andreas Katsanos, MD, hd,w Irene Floriani, hd,z Elena
ORIGINAL STUDY Long-term 24-hour Intraocular ressure Control With Travoprost Monotherapy in atients With rimary Open-angle Glaucoma Ivano Riva, MD,* Andreas Katsanos, MD, hd,w Irene Floriani, hd,z Elena
Elevated intraocular pressure (IOP) is a major risk factor for
 Glaucoma Twenty-Four Hour Pattern of Intraocular Pressure in Untreated Patients with Ocular Hypertension Tomas M. Grippo, 1,2 John H. K. Liu, 1 Nazlee Zebardast, 2 Taylor B. Arnold, 3 Grant H. Moore, 1
Glaucoma Twenty-Four Hour Pattern of Intraocular Pressure in Untreated Patients with Ocular Hypertension Tomas M. Grippo, 1,2 John H. K. Liu, 1 Nazlee Zebardast, 2 Taylor B. Arnold, 3 Grant H. Moore, 1
East and North Hertfordshire treatment pathway for primary open angle glaucoma and ocular hypertension in adults
 East and North Hertfordshire treatment pathway for primary open angle glaucoma and ocular hypertension in adults Introduction Glaucoma is a group of eye diseases causing optic nerve damage. In most cases
East and North Hertfordshire treatment pathway for primary open angle glaucoma and ocular hypertension in adults Introduction Glaucoma is a group of eye diseases causing optic nerve damage. In most cases
effect of previous argon laser trabeculoplasty
 Graefe s Arch Clin Exp Ophthalmol (2006) 244: 1073 1076 CLINICAL INVESTIGATION DOI 10.1007/s00417-005-0198-x Esther Arranz-Marquez Miguel A. Teus Effect of previous argon laser trabeculoplasty on the ocular
Graefe s Arch Clin Exp Ophthalmol (2006) 244: 1073 1076 CLINICAL INVESTIGATION DOI 10.1007/s00417-005-0198-x Esther Arranz-Marquez Miguel A. Teus Effect of previous argon laser trabeculoplasty on the ocular
Evolution of the Definition of Primary Open-Angle Glaucoma
 OCULAR BLOOD FLOW IN GLAUCOMA MANAGEMENT AHMED HOSSAM ABDALLA PROFESSOR AND HEAD OF OPHTHALMOLOGY DEPARTEMENT ALEXANDRIA UNIVERSITY Evolution of the Definition of Primary Open-Angle Glaucoma Former definition
OCULAR BLOOD FLOW IN GLAUCOMA MANAGEMENT AHMED HOSSAM ABDALLA PROFESSOR AND HEAD OF OPHTHALMOLOGY DEPARTEMENT ALEXANDRIA UNIVERSITY Evolution of the Definition of Primary Open-Angle Glaucoma Former definition
Glaucoma Disease Progression Role of Intra Ocular Pressure. Is Good Enough, Low Enough?
 Glaucoma Disease Progression Role of Intra Ocular Pressure Is Good Enough, Low Enough? Glaucoma Diseases Progression Key Considerations Good number of patients may be diagnosed only after some damage the
Glaucoma Disease Progression Role of Intra Ocular Pressure Is Good Enough, Low Enough? Glaucoma Diseases Progression Key Considerations Good number of patients may be diagnosed only after some damage the
Practical approach to medical management of glaucoma DR. RATHINI LILIAN DAVID
 Practical approach to medical management of glaucoma DR. RATHINI LILIAN DAVID Glaucoma is one of the major causes of visual loss worldwide. The philosophy of glaucoma management is to preserve the visual
Practical approach to medical management of glaucoma DR. RATHINI LILIAN DAVID Glaucoma is one of the major causes of visual loss worldwide. The philosophy of glaucoma management is to preserve the visual
Research Article Twenty-Four-Hour Variation of Intraocular Pressure in Primary Open-Angle Glaucoma Treated with Triple Eye Drops
 Hindawi Ophthalmology Volume 2017, Article ID 4398494, 6 pages https://doi.org/10.15/2017/4398494 Research Article Twenty-Four-Hour Variation of Intraocular Pressure in Primary Open-Angle Glaucoma Treated
Hindawi Ophthalmology Volume 2017, Article ID 4398494, 6 pages https://doi.org/10.15/2017/4398494 Research Article Twenty-Four-Hour Variation of Intraocular Pressure in Primary Open-Angle Glaucoma Treated
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND PACHYMETRY. POLICY NUMBER: CATEGORY: Technology Assessment
 MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
MEDICAL POLICY SUBJECT: CORNEAL ULTRASOUND,, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial product, including
Relationship between Intra Ocular Pressure and Some Risk Factors, In Northern Iran
 Available online at www.ijmrhs.com ISSN : 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 4:104-110 Relationship between Intra Ocular Pressure and Some Risk Factors, In
Available online at www.ijmrhs.com ISSN : 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 4:104-110 Relationship between Intra Ocular Pressure and Some Risk Factors, In
Keeping Up with the Chaglasian s: Pearls for Glaucoma Cases
 Keeping Up with the Chaglasian s: Pearls for Glaucoma Cases Disclosure Michael Chaglasian has the following disclosures: 1. Advisory Board: Allergan, Alcon, B+L, Carl Zeiss, 2. Research Support: Topcon
Keeping Up with the Chaglasian s: Pearls for Glaucoma Cases Disclosure Michael Chaglasian has the following disclosures: 1. Advisory Board: Allergan, Alcon, B+L, Carl Zeiss, 2. Research Support: Topcon
Glaucoma is the third leading cause of blindness worldwide
 Hypertension as an Independant Risk Factor for Primary Open-Angle Glaucoma: A Review Boluwaji A. Ogunyemi, BSc, MD Candidate 2013, Faculty of Medicine, Memorial University of Newfoundland Abstract Glaucoma
Hypertension as an Independant Risk Factor for Primary Open-Angle Glaucoma: A Review Boluwaji A. Ogunyemi, BSc, MD Candidate 2013, Faculty of Medicine, Memorial University of Newfoundland Abstract Glaucoma
Regional Institute of Ophthalmology, Indira Gandhi Institute of Medical Sciences, Patna, India 2
 pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(5):399-407 http://dx.doi.org/10.3341/kjo.2014.28.5.399 Original Article Comparing the Efficacy of (0.005%), Bimatoprost (0.03%), Travoprost
pissn: 1011-8942 eissn: 2092-9382 Korean J Ophthalmol 2014;28(5):399-407 http://dx.doi.org/10.3341/kjo.2014.28.5.399 Original Article Comparing the Efficacy of (0.005%), Bimatoprost (0.03%), Travoprost
Systemic Hypertension as a Risk Factor for Open-Angle Glaucoma: A Meta-Analysis of Population-Based Studies
 Systemic Hypertension as a Risk Factor for Open-Angle Glaucoma: A Meta-Analysis of Population-Based Studies Hyoung Won Bae 1, Naeun Lee 1,3, Hye Sun Lee 2, Samin Hong 1, Gong Je Seong 1, Chan Yun Kim 1
Systemic Hypertension as a Risk Factor for Open-Angle Glaucoma: A Meta-Analysis of Population-Based Studies Hyoung Won Bae 1, Naeun Lee 1,3, Hye Sun Lee 2, Samin Hong 1, Gong Je Seong 1, Chan Yun Kim 1
ROBERT L. SHIELDS, M.D. GLAUCOMA SURGERY AND TREATMENT
 1 CURRICULUM VITAE ROBERT L. SHIELDS, M.D. GLAUCOMA SURGERY AND TREATMENT University of Colorado Health Eye Center Cherry Creek 2000 South Colorado Boulevard Annex Building, Suite 100 Denver, Colorado
1 CURRICULUM VITAE ROBERT L. SHIELDS, M.D. GLAUCOMA SURGERY AND TREATMENT University of Colorado Health Eye Center Cherry Creek 2000 South Colorado Boulevard Annex Building, Suite 100 Denver, Colorado
Changes in Trend of Newly Prescribed Anti-Glaucoma Medications in Recent Nine Years in a Japanese Local Community
 The Open Ophthalmology Journal,, 4, 7-7 Open Access Changes in Trend of Newly Prescribed Anti-Glaucoma Medications in Recent Nine Years in a Japanese Local Community Kenji Kashiwagi Department of Community
The Open Ophthalmology Journal,, 4, 7-7 Open Access Changes in Trend of Newly Prescribed Anti-Glaucoma Medications in Recent Nine Years in a Japanese Local Community Kenji Kashiwagi Department of Community
Efficacy of selective laser trabeculoplasty for normal tension glaucoma: 1 year results. Citation BMC Ophthalmology, 2015, v. 15, article no.
 Title Efficacy of selective laser trabeculoplasty for normal tension glaucoma: 1 year results Author(s) Lee, WYJ; Ho, WL; Chan, JC; Lai, JS Citation BMC Ophthalmology, 2015, v. 15, article no. 1 Issued
Title Efficacy of selective laser trabeculoplasty for normal tension glaucoma: 1 year results Author(s) Lee, WYJ; Ho, WL; Chan, JC; Lai, JS Citation BMC Ophthalmology, 2015, v. 15, article no. 1 Issued
CLINICAL SCIENCES. Effect of Central Corneal Thickness, Corneal Curvature, and Axial Length on Applanation Tonometry
 CLINICAL SCIENCES Effect of Central Corneal Thickness, Corneal Curvature, and Axial Length on Applanation Tonometry Markus Kohlhaas, MD; Andreas G. Boehm, MD; Eberhard Spoerl, PhD; Antje Pürsten, Dipl-Ing
CLINICAL SCIENCES Effect of Central Corneal Thickness, Corneal Curvature, and Axial Length on Applanation Tonometry Markus Kohlhaas, MD; Andreas G. Boehm, MD; Eberhard Spoerl, PhD; Antje Pürsten, Dipl-Ing
Glaucoma is the leading cause of blindness worldwide
 ORIGINAL STUDY Relationship Between Serum Glucose Levels and Intraocular Pressure, a Population-based Cross-sectional Study Eytan Cohen, MD,*wz Michal Kramer, MD,zy Tzippy Shochat, MSC,8 Elad Goldberg,
ORIGINAL STUDY Relationship Between Serum Glucose Levels and Intraocular Pressure, a Population-based Cross-sectional Study Eytan Cohen, MD,*wz Michal Kramer, MD,zy Tzippy Shochat, MSC,8 Elad Goldberg,
Generics are Cheaper and Just as Effective
 Disclosures Generics are Cheaper and Just as Effective Robert L. Stamper, MD UCSF Department of Ophthalmology No current pharmaceutical industry connections Data & Safety Monitor for Cypass - Chair - Transcend
Disclosures Generics are Cheaper and Just as Effective Robert L. Stamper, MD UCSF Department of Ophthalmology No current pharmaceutical industry connections Data & Safety Monitor for Cypass - Chair - Transcend
Efficacy of latanoprost in management of chronic angle closure glaucoma. Kumar S 1, Malik A 2 Singh M 3, Sood S 4. Abstract
 Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
Original article Efficacy of latanoprost in management of chronic angle closure glaucoma Kumar S 1, Malik A 2 Singh M 3, Sood S 4 1 Associate Professor, 2 Assistant Professor, 4 Professor, Department of
Long-term perimetric fluctuation in patients with different stages of glaucoma
 Long-term perimetric fluctuation in patients with different stages of glaucoma Paolo Fogagnolo, Chiara Sangermani, Francesco Oddone, Paolo Frezzotti, Michele Iester, Michele Figus, Antonio Ferreras, Simona
Long-term perimetric fluctuation in patients with different stages of glaucoma Paolo Fogagnolo, Chiara Sangermani, Francesco Oddone, Paolo Frezzotti, Michele Iester, Michele Figus, Antonio Ferreras, Simona
A Short-term Study of the Additive Effect of Latanoprost 0.005% and Brimonidine 0.2%
 A Short-term Study of the Additive Effect of Latanoprost 0.005% and Brimonidine 0.2% Haydar Erdoğan, İlker Toker, Mustafa Kemal Arıcı, Ahmet Aygen and Ayşen Topalkara Department of Ophthalmology, School
A Short-term Study of the Additive Effect of Latanoprost 0.005% and Brimonidine 0.2% Haydar Erdoğan, İlker Toker, Mustafa Kemal Arıcı, Ahmet Aygen and Ayşen Topalkara Department of Ophthalmology, School
MODERN DIAGNOSTICS AND TREATMENT OF GLAUCOMA
 Semmelweis University, Ph.D. School, Clinical Sciences, Ophthalmology Head of Program: Ildikó Süveges, M.D., Ph.D., D.Sc. Tutor: Gábor Holló, M.D., Ph.D. MODERN DIAGNOSTICS AND TREATMENT OF GLAUCOMA Ph.D.
Semmelweis University, Ph.D. School, Clinical Sciences, Ophthalmology Head of Program: Ildikó Süveges, M.D., Ph.D., D.Sc. Tutor: Gábor Holló, M.D., Ph.D. MODERN DIAGNOSTICS AND TREATMENT OF GLAUCOMA Ph.D.
Introduction. Although the intraocular pressure is considered firstly the main risk factor in the emerging and evolution of glaucoma and,
 Romanian Journal of Ophthalmology, Volume 59, Issue 3, July-September 2015. pp:141-147 GENERAL ARTICLE THE ROLE OF SYSTEMIC BLOOD PRESSURE IN GLAUCOMA PROGRESSION Silvia Mariana Chiotoroiu*, Oana Stefaniu**,
Romanian Journal of Ophthalmology, Volume 59, Issue 3, July-September 2015. pp:141-147 GENERAL ARTICLE THE ROLE OF SYSTEMIC BLOOD PRESSURE IN GLAUCOMA PROGRESSION Silvia Mariana Chiotoroiu*, Oana Stefaniu**,
South East London Area Prescribing Committee Chronic Open Angle Glaucoma and Ocular Hypertension Treatment Pathway
 Proceed to 2 nd line treatment if further reduction in IOP required and there is good response to PGAs or (& no South East London Area Prescribing Committee Chronic Open Angle Glaucoma and Ocular Hypertension
Proceed to 2 nd line treatment if further reduction in IOP required and there is good response to PGAs or (& no South East London Area Prescribing Committee Chronic Open Angle Glaucoma and Ocular Hypertension
Comparison of Intraocular Pressure Fluctuations Measured by Goldmann Applanation Tonometer and Pulsatile Ocular Blood Flow Analyser
 International journal of Biomedical science ORIGINAL ARTICLE Comparison of Intraocular Pressure Fluctuations Measured by Goldmann Applanation Tonometer and Pulsatile Ocular Blood Flow Analyser Ingrida
International journal of Biomedical science ORIGINAL ARTICLE Comparison of Intraocular Pressure Fluctuations Measured by Goldmann Applanation Tonometer and Pulsatile Ocular Blood Flow Analyser Ingrida
Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective cohort study
 Nesaratnam et al. BMC Ophthalmology (2015) 15:17 DOI 10.1186/s12886-015-0007-1 RESEARCH ARTICLE Open Access Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective
Nesaratnam et al. BMC Ophthalmology (2015) 15:17 DOI 10.1186/s12886-015-0007-1 RESEARCH ARTICLE Open Access Pre-operative intraocular pressure does not influence outcome of trabeculectomy surgery: a retrospective
PRACTICAL APPROACH TO MEDICAL MANAGEMENT OF GLAUCOMA
 PRACTICAL APPROACH TO MEDICAL MANAGEMENT OF GLAUCOMA DR. RAVI THOMAS, DR. RAJUL PARIKH, DR. SHEFALI PARIKH IJO MAY 2008 PRESENTER AT JDOS : DR. RAHUL SHUKLA T.N. SHUKLA EYE HOSPITAL TERMINOLOGY POAG: PRIMARY
PRACTICAL APPROACH TO MEDICAL MANAGEMENT OF GLAUCOMA DR. RAVI THOMAS, DR. RAJUL PARIKH, DR. SHEFALI PARIKH IJO MAY 2008 PRESENTER AT JDOS : DR. RAHUL SHUKLA T.N. SHUKLA EYE HOSPITAL TERMINOLOGY POAG: PRIMARY
F Honrubia, 1 J García-Sánchez, 2 V Polo, 1 J M Martínez de la Casa, 2 J Soto 3. Clinical science
 1 Ophthalmology Service, Hospital Miguel Servet, Zaragoza, Spain; 2 Ophthalmology Service, Hospital Clínico, Madrid, Spain; 3 Medical Unit, Pfizer Spain, Madrid, Spain Correspondence to: Dr J Soto, Medical
1 Ophthalmology Service, Hospital Miguel Servet, Zaragoza, Spain; 2 Ophthalmology Service, Hospital Clínico, Madrid, Spain; 3 Medical Unit, Pfizer Spain, Madrid, Spain Correspondence to: Dr J Soto, Medical
Long Term Efficacy of Repeat Treatment with SLT: Seven Years Follow up
 Long Term Efficacy of Repeat Treatment with SLT: Seven Years Follow up Lawrence F. Jindra, MD Columbia University Winthrop University Hospital Disclosure Speaker has independently conducted and financed
Long Term Efficacy of Repeat Treatment with SLT: Seven Years Follow up Lawrence F. Jindra, MD Columbia University Winthrop University Hospital Disclosure Speaker has independently conducted and financed
Trans Am Ophthalmol Soc 2015;113:T6[1-13] by the American Ophthalmological Society.
![Trans Am Ophthalmol Soc 2015;113:T6[1-13] by the American Ophthalmological Society. Trans Am Ophthalmol Soc 2015;113:T6[1-13] by the American Ophthalmological Society.](/thumbs/85/92235589.jpg) OCULAR PERFUSION PRESSURE VS ESTIMATED TRANS LAMINA CRIBROSA PRESSURE DIFFERENCE IN GLAUCOMA: THE CENTRAL INDIA EYE AND MEDICAL STUDY (AN AMERICAN OPHTHALMOLOGICAL SOCIETY THESIS) By Jost B. Jonas MD,
OCULAR PERFUSION PRESSURE VS ESTIMATED TRANS LAMINA CRIBROSA PRESSURE DIFFERENCE IN GLAUCOMA: THE CENTRAL INDIA EYE AND MEDICAL STUDY (AN AMERICAN OPHTHALMOLOGICAL SOCIETY THESIS) By Jost B. Jonas MD,
SUPPLEMENTARY INFORMATION
 SUPPLEMENTARY INFORMATION Contents METHODS... 2 Inclusion and exclusion criteria... 2 Supplementary table S1... 2 Assessment of abnormal ocular signs and symptoms... 3 Supplementary table S2... 3 Ocular
SUPPLEMENTARY INFORMATION Contents METHODS... 2 Inclusion and exclusion criteria... 2 Supplementary table S1... 2 Assessment of abnormal ocular signs and symptoms... 3 Supplementary table S2... 3 Ocular
Circadian Variation in Arterial Blood Pressure and Glaucomatous Optic Neuropathy A Systematic Review and Meta-Analysis
 State of the Art Circadian Variation in Arterial Blood Pressure and Glaucomatous Optic Neuropathy A Systematic Review and Meta-Analysis Andrea Bowe, 1 Michael Grünig, 1 Jens Schubert, 1 Münevver Demir,
State of the Art Circadian Variation in Arterial Blood Pressure and Glaucomatous Optic Neuropathy A Systematic Review and Meta-Analysis Andrea Bowe, 1 Michael Grünig, 1 Jens Schubert, 1 Münevver Demir,
Volume 9; Number 6 May 2015 PRESCRIBING FOR CHRONIC OPEN ANGLE GLAUCOMA (COAG) AND OCULAR HYPERTENSION (OHT)
 Greater East Midlands Commissioning Support Unit in association with Lincolnshire Clinical Commissioning Groups, Lincolnshire Community Health Services, United Lincolnshire Hospitals Trust and Lincolnshire
Greater East Midlands Commissioning Support Unit in association with Lincolnshire Clinical Commissioning Groups, Lincolnshire Community Health Services, United Lincolnshire Hospitals Trust and Lincolnshire
National Institute for Health and Clinical Excellence. Glaucoma. Guideline Consultation Comments Table. 29 September November 2008
 National Institute for Health and Clinical Excellence Glaucoma Guideline Consultation Comments Table 29 September 2008 24 November 2008 Stat us Organisa tion Order no. Version Page no Line no/se ction
National Institute for Health and Clinical Excellence Glaucoma Guideline Consultation Comments Table 29 September 2008 24 November 2008 Stat us Organisa tion Order no. Version Page no Line no/se ction
True IOP No Doubt Facts and Figures Figures. Ziemer Ophthalmic Systems AG a Ziemer Group Company Allmendstrasse 11 CH-2562 Port, Switzerland
 True IOP No Doubt Facts and Figures Figures and Facts Ziemer Ophthalmic Systems AG a Ziemer Group Company Allmendstrasse 11 CH-2562 Port, Switzerland There is increasing evidence that DCT measures IOP
True IOP No Doubt Facts and Figures Figures and Facts Ziemer Ophthalmic Systems AG a Ziemer Group Company Allmendstrasse 11 CH-2562 Port, Switzerland There is increasing evidence that DCT measures IOP
Pressure lowering effect of fixed combination and unfixed- combination of latanoprost and timolol in Asian population
 Clinical Medicine Research 2012; 1(1) : 7-12 Published online December 30, 2012 (http://www.sciencepublishinggroup.com/j/cmr) doi: 10.11648/j.cmr.20120101.12 Pressure lowering effect of fixed combination
Clinical Medicine Research 2012; 1(1) : 7-12 Published online December 30, 2012 (http://www.sciencepublishinggroup.com/j/cmr) doi: 10.11648/j.cmr.20120101.12 Pressure lowering effect of fixed combination
INTRODUCTION S. HERDENER, D. HAFIZOVIC, M. PACHE, S. LAUTEBACH, J. FUNK. University Eye Hospital, Freiburg - Germany
 European Journal of Ophthalmology / Vol. 18 no. 1, 2008 / pp. 39-43 Is the PASCAL -Tonometer suitable for measuring intraocular pressure in clinical routine? Long- and short-term reproducibility of dynamic
European Journal of Ophthalmology / Vol. 18 no. 1, 2008 / pp. 39-43 Is the PASCAL -Tonometer suitable for measuring intraocular pressure in clinical routine? Long- and short-term reproducibility of dynamic
Latanoprost 0.005% v/s Timolol Maleate 0.5% Pressure Lowering Effect in Primary Open Angle Glaucoma
 Original Article Latanoprost 0.005% v/s Timolol Maleate 0.5% Pressure Lowering Effect in Primary Open Angle Glaucoma Arshad Ali Lodhi, Khalid Iqbal Talpur, Mahtab Alam Khanzada Pak J Ophthalmol 2008, Vol.
Original Article Latanoprost 0.005% v/s Timolol Maleate 0.5% Pressure Lowering Effect in Primary Open Angle Glaucoma Arshad Ali Lodhi, Khalid Iqbal Talpur, Mahtab Alam Khanzada Pak J Ophthalmol 2008, Vol.
Clinical Study Evaluation of the New Digital Goldmann Applanation Tonometer for Measuring Intraocular Pressure
 Ophthalmology, Article ID 461681, 5 pages http://dx.doi.org/1.1155/214/461681 Clinical Study Evaluation of the New Digital Goldmann Applanation Tonometer for Measuring Intraocular Pressure Yuta Sakaue,
Ophthalmology, Article ID 461681, 5 pages http://dx.doi.org/1.1155/214/461681 Clinical Study Evaluation of the New Digital Goldmann Applanation Tonometer for Measuring Intraocular Pressure Yuta Sakaue,
Long Term Care Formulary RS 14. RESTRICTED STATUS Topical Medical Treatment of Glaucoma 1 of 5
 RESTRICTED STATUS Topical Medical Treatment of Glaucoma 1 of 5 PREAMBLE Significance: Glaucoma occurs in 1-2% of white people aged over 40 years, rising to 5% at 70 years and exponentially with advancing
RESTRICTED STATUS Topical Medical Treatment of Glaucoma 1 of 5 PREAMBLE Significance: Glaucoma occurs in 1-2% of white people aged over 40 years, rising to 5% at 70 years and exponentially with advancing
IOP measurements: 8.00 am (trough drug levels) and am (peak drug levels)(2 hours post dose)
 This overview of 2% eye drops was presented by Dr. Ravin N. Das, at Hotel Satya Ashoka, on 19-6-2004 in place of Dr. H. S. Ray due to unforseen circumstances. This dinner meeting was sponsored by Cipla
This overview of 2% eye drops was presented by Dr. Ravin N. Das, at Hotel Satya Ashoka, on 19-6-2004 in place of Dr. H. S. Ray due to unforseen circumstances. This dinner meeting was sponsored by Cipla
Present relevant clinical findings of four landmark glaucoma trials OHTS, EMGT, CNTGS and CIGTS.
 Course title: The Glaucoma Compass Course length: 1 hour +/- 31 slides Corse Description: Even with the technology and available information, glaucoma decision making can still be confusing. How should
Course title: The Glaucoma Compass Course length: 1 hour +/- 31 slides Corse Description: Even with the technology and available information, glaucoma decision making can still be confusing. How should
Effects of Argon Laser Trabeculoplasty in the Early Manifest Glaucoma Trial. Heijl, Anders; Peters, Dorothea; Leske, M Christina; Bengtsson, Boel
 Effects of Argon Laser Trabeculoplasty in the Early Manifest Glaucoma Trial. Heijl, Anders; Peters, Dorothea; Leske, M Christina; Bengtsson, Boel Published in: American Journal of Ophthalmology DOI: 10.1016/j.ajo.2011.04.036
Effects of Argon Laser Trabeculoplasty in the Early Manifest Glaucoma Trial. Heijl, Anders; Peters, Dorothea; Leske, M Christina; Bengtsson, Boel Published in: American Journal of Ophthalmology DOI: 10.1016/j.ajo.2011.04.036
LUP. Lund University Publications Institutional Repository of Lund University
 LUP Lund University Publications Institutional Repository of Lund University This is an author produced version of a paper published in Ophthalmology. This paper has been peerreviewed but does not include
LUP Lund University Publications Institutional Repository of Lund University This is an author produced version of a paper published in Ophthalmology. This paper has been peerreviewed but does not include
Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors
 CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
CLINICAL INVESTIGATIONS Spontaneous Intraocular Pressure Reduction in Normal-Tension Glaucoma and Associated Clinical Factors Akihiro Oguri, Tetsuya Yamamoto and Yoshiaki Kitazawa Department of Ophthalmology,
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 28 May 2008
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 28 May 2008 COSOPT 20 mg/5 mg/ml, eye drops, solution in single dose container Box of 60 0.2 ml single dose containers
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 28 May 2008 COSOPT 20 mg/5 mg/ml, eye drops, solution in single dose container Box of 60 0.2 ml single dose containers
Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University.
 Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University. Although the clinical picture of glaucoma is well described, the exact mechanism leading to this specific type of damage to the optic
Dr Taha Abdel Monein Labib Professor of Eye Surgery Cairo University. Although the clinical picture of glaucoma is well described, the exact mechanism leading to this specific type of damage to the optic
The improvement in perimetric results occurring over
 ORIGINAL STUDY Learning Effect of Humphrey Matrix Frequency Doubling Technology Perimetry in Patients With Ocular Hypertension Marco Centofanti, MD, PhD,*w Paolo Fogagnolo, MD,w Francesco Oddone, MD,w
ORIGINAL STUDY Learning Effect of Humphrey Matrix Frequency Doubling Technology Perimetry in Patients With Ocular Hypertension Marco Centofanti, MD, PhD,*w Paolo Fogagnolo, MD,w Francesco Oddone, MD,w
University of Groningen
 University of Groningen Ocular Perfusion Pressure and the Incidence of Glaucoma Ramdas, Wishal D.; Wolfs, Roger C. W.; Hofman, Albert; de Jong, Paulus T. V. M.; Vingerling, Johannes R.; Jansonius, Nomdo
University of Groningen Ocular Perfusion Pressure and the Incidence of Glaucoma Ramdas, Wishal D.; Wolfs, Roger C. W.; Hofman, Albert; de Jong, Paulus T. V. M.; Vingerling, Johannes R.; Jansonius, Nomdo
International Journal of Biological & Medical Research
 Int J Biol Med Res. 2013; 4(4) :3637-3641 Int J Biol Med Res Volume 3, Issue 1, Jan 2012 www.biomedscidirect.com BioMedSciDirect Publications Contents lists available at BioMedSciDirect Publications International
Int J Biol Med Res. 2013; 4(4) :3637-3641 Int J Biol Med Res Volume 3, Issue 1, Jan 2012 www.biomedscidirect.com BioMedSciDirect Publications Contents lists available at BioMedSciDirect Publications International
Clinical Discussions in Glaucoma
 Clinical Discussions in Glaucoma Joseph W. Sowka, OD, FAAO, Diplomate Professor of Optometry Nova Southeastern University, College of Optometry 3200 South University Drive Fort Lauderdale, Florida 33328
Clinical Discussions in Glaucoma Joseph W. Sowka, OD, FAAO, Diplomate Professor of Optometry Nova Southeastern University, College of Optometry 3200 South University Drive Fort Lauderdale, Florida 33328
WARNING LETTER DEPARTMENT OF HEALTH & HUMAN SERVICES TRANSMITTED BY FACSIMILE
 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration Rockville, MD 20857 TRANSMITTED BY FACSIMILE David E.I. Pyott President and Chief Executive Officer PO Box 19534
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration Rockville, MD 20857 TRANSMITTED BY FACSIMILE David E.I. Pyott President and Chief Executive Officer PO Box 19534
Class Update: Ophthalmic Glaucoma Agents
 Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-945-5220 Fax 503-947-1119 Class Update: Ophthalmic Glaucoma Agents Month/Year
Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-945-5220 Fax 503-947-1119 Class Update: Ophthalmic Glaucoma Agents Month/Year
Original Article. Abstract. Introduction. C Olali, G Malietzis, S Ahmed, E Samaila 1, M Gupta
 Original Article Real-life experience study of the safety and efficacy of travoprost 0.004% / timoptol 0.50% fixed combination ophthalmic solution in intraocular pressure control C Olali, G Malietzis,
Original Article Real-life experience study of the safety and efficacy of travoprost 0.004% / timoptol 0.50% fixed combination ophthalmic solution in intraocular pressure control C Olali, G Malietzis,
Harvey B DuBiner 1* and Douglas A Hubatsch 2
 DuBiner and Hubatsch BMC Ophthalmology 2014, 14:151 RESEARCH ARTICLE Open Access Late-day intraocular pressure lowering efficacy and tolerability of travoprost 0.004% versus bimatoprost 0.01% in patients
DuBiner and Hubatsch BMC Ophthalmology 2014, 14:151 RESEARCH ARTICLE Open Access Late-day intraocular pressure lowering efficacy and tolerability of travoprost 0.004% versus bimatoprost 0.01% in patients
Correlating central corneal thickness and intraocular pressure in ocular hypertension and glaucoma
 VOL. 3 NO. 1 PHILIPPINE JOURNAL OF Ophthalmology JANUARY ORIGINAL ARTICLE JUNE 07 Jonathan G. Soriano, MD 1 Ma. Margarita L. Lat-Luna, MD 1, 3 Patricia M. Khu, MD 1, 1 Department of Ophthalmology and Visual
VOL. 3 NO. 1 PHILIPPINE JOURNAL OF Ophthalmology JANUARY ORIGINAL ARTICLE JUNE 07 Jonathan G. Soriano, MD 1 Ma. Margarita L. Lat-Luna, MD 1, 3 Patricia M. Khu, MD 1, 1 Department of Ophthalmology and Visual
The Uniocular Drug Trial and Second-Eye Response to Glaucoma Medications
 The Uniocular Drug Trial and Second-Eye Response to Glaucoma Medications Tony Realini, MD, 1 Robert D. Fechtner, MD, 2 Sean-Paul Atreides, MD, 3 Stephen Gollance, MD 2 Purpose: To determine if the intraocular
The Uniocular Drug Trial and Second-Eye Response to Glaucoma Medications Tony Realini, MD, 1 Robert D. Fechtner, MD, 2 Sean-Paul Atreides, MD, 3 Stephen Gollance, MD 2 Purpose: To determine if the intraocular
Managing the Patient with POAG
 Managing the Patient with POAG Vision Institute Annual Fall Conference Mitchell W. Dul, OD, MS, FAAO mdul@sunyopt.edu Richard J. Madonna, MA, OD, FAAO rmadonna@sunyopt.edu Ocular Hypertension (OHT) Most
Managing the Patient with POAG Vision Institute Annual Fall Conference Mitchell W. Dul, OD, MS, FAAO mdul@sunyopt.edu Richard J. Madonna, MA, OD, FAAO rmadonna@sunyopt.edu Ocular Hypertension (OHT) Most
Received: 17 October 2011; in revised form: 7 March 2012 / Accepted: 19 March 2012 / Published: 21 March 2012
 Pharmaceuticals 2012, 5, 325-338; doi:10.3390/ph5030325 Article OPEN ACCESS Pharmaceuticals ISSN 1424-8247 www.mdpi.com/journal/pharmaceuticals Comparison of Intraocular Pressure, Blood Pressure, Ocular
Pharmaceuticals 2012, 5, 325-338; doi:10.3390/ph5030325 Article OPEN ACCESS Pharmaceuticals ISSN 1424-8247 www.mdpi.com/journal/pharmaceuticals Comparison of Intraocular Pressure, Blood Pressure, Ocular
Changes in medical and surgical treatments of glaucoma between 1997 and 2003 in France
 European Journal of Ophthalmology / Vol. 17 no. 4, 2007 / pp. 521-527 Changes in medical and surgical treatments of glaucoma between 1997 and 2003 in France P.-A. KENIGSBERG PAK Santé, Paris - France PURPOSE.
European Journal of Ophthalmology / Vol. 17 no. 4, 2007 / pp. 521-527 Changes in medical and surgical treatments of glaucoma between 1997 and 2003 in France P.-A. KENIGSBERG PAK Santé, Paris - France PURPOSE.
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Conversion of Ocular Hypertensives into Glaucoma: A Retrospective Study Aditi Singh 1, Shibi
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Conversion of Ocular Hypertensives into Glaucoma: A Retrospective Study Aditi Singh 1, Shibi
Elements for a Public Summary. Overview of disease epidemiology
 VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Epidemiology of the disease Incidence and prevalence Increased pressure in the eye occurs in more than 100 million people, and
VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Epidemiology of the disease Incidence and prevalence Increased pressure in the eye occurs in more than 100 million people, and
EPIDEMIOLOGY AND BIOSTATISTICS. Incident Open-Angle Glaucoma and Blood Pressure
 EPIDEMIOLOGY AND BIOSTATISTICS Incident Open-Angle Glaucoma and Blood Pressure M. Cristina Leske, MD, MPH; Suh-Yuh Wu, MA; Barbara Nemesure, PhD; Anselm Hennis, MRCP(UK), PhD; for the Barbados Eye Studies
EPIDEMIOLOGY AND BIOSTATISTICS Incident Open-Angle Glaucoma and Blood Pressure M. Cristina Leske, MD, MPH; Suh-Yuh Wu, MA; Barbara Nemesure, PhD; Anselm Hennis, MRCP(UK), PhD; for the Barbados Eye Studies
CHARTING THE NEW COURSE FOR MIGS
 CHARTING THE NEW COURSE FOR MIGS SEE WHAT S ON THE HORIZON CyPass Micro-Stent the next wave in micro-invasive glaucoma surgery. MICRO-INVASIVE GLAUCOMA SURGERY (MIGS) OFFERS A REVOLUTIONARY APPROACH TO
CHARTING THE NEW COURSE FOR MIGS SEE WHAT S ON THE HORIZON CyPass Micro-Stent the next wave in micro-invasive glaucoma surgery. MICRO-INVASIVE GLAUCOMA SURGERY (MIGS) OFFERS A REVOLUTIONARY APPROACH TO
ALTHOUGH OCULAR hypertension
 EPIDEMIOLOGY AND BIOSTATISTICS Association of Demographic, Familial, Medical, and Ocular Factors With Intraocular Pressure LeAnn M. Weih, PhD; Bickol N. Mukesh, PhD; Catherine A. McCarty, PhD; Hugh R.
EPIDEMIOLOGY AND BIOSTATISTICS Association of Demographic, Familial, Medical, and Ocular Factors With Intraocular Pressure LeAnn M. Weih, PhD; Bickol N. Mukesh, PhD; Catherine A. McCarty, PhD; Hugh R.
GLAUCOMA (2006) PHILIPPINE GLAUCOMA SOCIETY
 GLAUCOMA (2006) PHILIPPINE GLAUCOMA SOCIETY CPM 9 TH EDITION Philippine Glaucoma Society (PGS) Correspondence to: Eye Referral Center, T. M. Kalaw Street, Ermita, Manila Telephone: 524-7119/525-9360 Mobile:
GLAUCOMA (2006) PHILIPPINE GLAUCOMA SOCIETY CPM 9 TH EDITION Philippine Glaucoma Society (PGS) Correspondence to: Eye Referral Center, T. M. Kalaw Street, Ermita, Manila Telephone: 524-7119/525-9360 Mobile:
GLAUCOMA EVOLUTION IN PATIENTS WITH DIABETES
 Rev. Med. Chir. Soc. Med. Nat., Iaşi 2014 vol. 118, no. 3 SURGERY ORIGINAL PAPERS GLAUCOMA EVOLUTION IN PATIENTS WITH DIABETES Nicoleta Anton Apreutesei¹, D. Chiselita²*, O. I. Motas ¹ University of Medicine
Rev. Med. Chir. Soc. Med. Nat., Iaşi 2014 vol. 118, no. 3 SURGERY ORIGINAL PAPERS GLAUCOMA EVOLUTION IN PATIENTS WITH DIABETES Nicoleta Anton Apreutesei¹, D. Chiselita²*, O. I. Motas ¹ University of Medicine
Science & Technologies. UNWANTED SIDE EFFECTS OF TRAVOPROST Gazepov Strahil 1, Iljaz Ismaili 2, Goshevska Dashtevska Emilija 2
 UNWANTED SIDE EFFECTS OF TRAVOPROST Gazepov Strahil 1, Iljaz Ismaili 2, Goshevska Dashtevska Emilija 2 1 Clinical Hospital, Shtip 2 University Eye Clinic,Skopje Introduction: Glaucoma is a chronical progressive
UNWANTED SIDE EFFECTS OF TRAVOPROST Gazepov Strahil 1, Iljaz Ismaili 2, Goshevska Dashtevska Emilija 2 1 Clinical Hospital, Shtip 2 University Eye Clinic,Skopje Introduction: Glaucoma is a chronical progressive
Supplementary Online Content
 Supplementary Online Content Lin H-C, Stein JD, Nan B, et al. Association of geroprotective effects of metformin and risk of open-angle glaucoma in persons with diabetes mellitus. JAMA Ophthalmol. Published
Supplementary Online Content Lin H-C, Stein JD, Nan B, et al. Association of geroprotective effects of metformin and risk of open-angle glaucoma in persons with diabetes mellitus. JAMA Ophthalmol. Published
Pooling Data from Similar Randomized Clinical Trials Comparing Latanoprost with Timolol; Medical Results and Statistical Aspects
 Comprehensive Summaries of Uppsala Dissertations from the Faculty of Medicine 1235 Pooling Data from Similar Randomized Clinical Trials Comparing Latanoprost with Timolol; Medical Results and Statistical
Comprehensive Summaries of Uppsala Dissertations from the Faculty of Medicine 1235 Pooling Data from Similar Randomized Clinical Trials Comparing Latanoprost with Timolol; Medical Results and Statistical
