NEUROLEPTIC MALIGNANT SYNDROME : A REPORT OF 2 CASES
|
|
|
- Baldric Cole
- 6 years ago
- Views:
Transcription
1 Chiang Mai Med bull 2005;44(2): Case report NEUROLEPTIC MALIGNANT SYNDROME : A REPORT OF 2 CASES Oranee Sanmaneechai, M.D., Surachai Likasitwattanakul, M.D. Department of Pediatrics, Faculty of Medicine, Chiang Mai University Abstract Neuroleptic malignant syndrome (NMS) is an iatrogenic and potentially fatal complication of neuroleptic medications. It is characterized by fever, altered mental status, muscle rigidity, and autonomic instability. Since these symptoms are non-specific, a high index of suspicious should be made especially in any patients with a history of neuroleptic treatment. The authors report two cases of adolescent girls who developed NMS after the use of neuroleptic medications and stress on prompt recognition and treatment in this condition. Chiang Mai Med Bull 2005;44(2): Keywords: Neuroleptic malignant syndrome, children Neuroleptic malignant syndrome (NMS) is a rare but potentially fatal complication of neuroleptic medications. 1 Its cardinal features are sudden onset of hyperthermia, muscle rigidity, alteration of mental status, and autonomic dysfunction. (1-2) The estimated incidence of NMS in those individuals exposed to neuroleptic medications ranges from 0.07 to 1.4%. (3) NMS has been reported in all age groups and both sexes, but predominantly in young and middle-aged adults. (2,4) Since mortality in this syndrome is as high as 25%, especially when under-recognized, prompt recognition and early treatment are crucial. (5) The authors report 2 adolescent girls who developed NMS after the use of neuroleptic medications. Case report Case 1 A 13-year-old girl, who was blind from retinopathy of prematurity, was admitted to a provincial hospital one month before referral with brief psychotic disorder. A one-week trial of haloperidol at 3 mg /day and artane at 4 mg/day was given without clinical improvement. She was then placed on thioridazine at 150 mg/day and fluoxitin at 10 mg/day. Two weeks after this combination, her consciousness fluctuated between agitation and a decreased level of consciousness. Fever at a peak of 38.5 C and muscle stiffness of the body and limbs were observed. Chlorpromazine, propanolol and diazepam were given Address requests for reprints: Surachai Likasitwattanakul, M.D. Department of Pediatric, Faculty of Medicine, Mahidol University, Bangkok 10330, Thailand. sisli@mahidol.ac.th Received 11 August 2004, and in revised form 1 Decmeber 2004
2 74 Likasitwattanakul S. without clinical improvement, she was then referred to Chiang Mai University Hospital. On admission, her body temperature was 37 C, respiratory rate 36 breaths/min, blood pressure 136/92 mmhg, and pulse rate 100 beats/min. She was restless and verbally unresponsive. Neurological examination revealed generalized hypertonia, lead-pipe rigidity and hyperreflexia. Laboratory findings showed a leukocytosis of 12,000 cells/mm (3) with 74% neutrophils, and serum creatine kinase (CK) of 335 IU/L (normal 0-195). Cerebrospinal fluid examination, and renal and liver function tests were normal. NMS was diagnosed. During the next 24 hours, fluctuation of respiratory rate (20-36 breaths/ min), pulse rate ( beats/min) and blood pressure ( mmhg systolic and mmhg diastolic) were observed. All medications were discontinued, and bromocriptine at 10 mg/day and diphenhydramine at 100 mg/day were started. Her consciousness gradually improved on the third hospital day and the extrapyramidal symptoms improved after one week of treatment. The serum CK decreased to 44 IU/L after two weeks of treatment. Case 2 A previously healthy 12-year-old girl was transferred to our hospital with fever and altered mental status. One day before, she was admitted to a local hospital with hyperventilation syndrome that occurred after having an argument with her mother. After multiple doses of intravenous diazepam for agitation and recurrent hyperventilation syndrome episodes, intramuscular haloperidol at 10 mg was given. Within 2 hours after the injection, her consciousness fluctuated between agitation and no response to verbal command. Fever, muscle rigidity, and lead-pipe rigidity were observed. She was then transferred to Chiang Mai University Hospital. On admission, her body temperature was 38.8 C, pulse 130 beats/min, blood pressure 116/64 mmhg, and respiratory rate 22 breaths/min. Neurological examination revealed resting tremor, generalized hypertonia and lead-pipe rigidity. Laboratory findings showed a leukocytosis of 14,800 cells/mm 3 with 78% neutrophils, and serum CK of 407 IU/L. Other laboratory results, including CSF analysis, renal and liver function tests and electrolyte were normal. Urine heme was positive. Fluctuations of pulse rate were observed during the first 24 hours ( beats/minute). On the basis of these findings, NMS was diagnosed. Soon after admission she developed respiratory failure and needed respiratory support. Bromocriptine at 7.5 mg/day and diphenhydramine at 100 mg/day were administered via nasogastric tube. Intravenous lorazepam was given intermittently for severe agitation. Supportive treatment included intravenous fluid, and alkalinization of the urine to prevent renal failure from myoglobinuria. She developed generalized tonic seizure during admission and was controlled with phenobarbital. Serum CK was initially increased to 1,219 IU/L on day 5 after admission and decreased to 424 on day 10. Her consciousness gradually improved and she was extubated after 5 days of mechanical ventilation. Persistence of extrapyramidal symptoms including oro-facial dystonia and limb rigidity were observed after a 3-week hospital stay. She was discharged from hospital, with bromocriptine and artane prescribed for extrapyramidal symptoms and phenobarbital for seizure control. Rigidity as well as dystonia of oro-facial muscles and limbs improved
3 Neuroleptic maliganant syndrome 75 gradually and no seizures were noted after being discharged. All medications were discontinued within 4 months. Discussion These two cases had all the cardinal features of NMS after receiving conventional neuroleptic drugs. In the first patient, symptoms of NMS occurred within 2 weeks after neuroleptic medication. Since the patient s mental status deteriorated, which could have been caused by worsening of the brief psychotic episode, additional neuroleptic drugs were used. This might have contributed to the full clinical picture of NMS in this patient. In the second patient, symptoms of NMS occurred rather rapidly after an intramuscular injection of haloperidol, which can be seen in up to 16% of patients with NMS. (6) This patient developed several complications from NMS such as rhabdomyolysis, hemoglobinuria and respiratory failure. With supportive care and use of bromocriptine, both patients survived without complications. NMS is a rare, idiosyncratic reaction to neuroleptic medications. (1) The most common drugs that cause NMS are conventional neuroleptic medications (haloperidol, chlorpromazine). (1,2,4) However, atypical neuroleptic medications such as risperidone and olanzapine may also cause this syndrome. (7) The risk of developing NMS among neuroleptic medication users ranges from %. (3) Several cases have been reported from Thailand, however, this condition is still under recognized. (8-10) Factors that increase the risk of NMS are those among patients with psychomotor agitation, higher dose and rapid rate of dosage increase, and parenteral injections. (11) Of the patients who develop NMS, 16% develop NMS features within 24 hours after exposure to neuroleptic medications, 66% by 1 week, and 96% within 30 days. (6) Four prominent clinical features of NMS are hyperthermia, motor symptoms, altered mental status and autonomic instability. (2) Hyperthermia is found in 98% of patients and their temperature peak ranges from 38 C to over 41 C. The most common motor symptoms include lead-pipe rigidity. Other less common features are tremor, bradykinesia, or akinesia that characterize parkinsonian phenotype. Altered mental status ranges from clouding of consciousness to stupor or coma. Autonomic instability manifests by tachycardia, fluctuation of blood pressure and respiratory irregularities. The two most important laboratory findings in NMS are leukocytosis and increased serum CK level. (2,4) Nonspecific leukocytosis with or without left shift ranges from 15,000-30,000/mm. (3) Elevated CK level, which results from muscle injury, ranges from 2,000-15,000 IU/L, but may be lower than 600 IU/L in a few patients. (1) However, the clinical features and severity as well as laboratory findings in NMS vary from patient to patient. Many diagnostic criteria for NMS such as the Diagnostic and Statistical Manual of Mental Disorders, 4 th edition (DSM IV) (3) (Table 1) and Levenson s criteria. (1) (Table 2) are proposed to facilitate the diagnosis of this condition. Differential diagnoses of NMS include central nervous system infection, metabolic encephalopathy, malignant hyperthermia, and serotonin syndrome (SS). (12) Both patients had normal renal and liver function tests, and CSF examination and that excluded CNS infection
4 76 Likasitwattanakul S. and metabolic disturbances. No history of halogenated inhalation anesthetic agent use excluded malignant hyperthermia. SS shares many clinical features with NMS. SS should be a differential diagnosis in the first patient, since she received a combination of antipsychotic drugs a and selective serotonin reuptake inhibitor (SSRI). However, a lack of clinical features for myoclonus, pupillary dilatation and bowel hyperactivity favored a diagnosis of NMS in this patient. In addition, typically, SS develops very quickly, with 75% of patients developing the syndrome during the first 24 hours after initiating or increasing the dosage of an SSRI agent. Although the pathogenesis of NMS is not completely understood, it is believed that the condition is a result of altered central dopamine neurotransmission. (1-2) Medications that block central dopaminergic receptors, such as neuroleptic drugs, are the most common causes of NMS. In addition, sudden discontinuation of dopaminergic drugs could cause NMS, as seen in patients with pakinsonism. (4) Prompt recognition and discontinuation of the offending drugs are a crucial part of management. (5) Symptomatic treatment includes adequate intravenous fluids, antipyretics, correction of metabolic disturbances, and adequate renal and cardiopulmonary support and monitoring. (12) Fever reduction is very important, since it may cause hyperthermia and multiple organs injury. No controlled trial study is available for the use of pharmacologic treatment in this condition. Nevertheless, the most common drugs used in this syndrome are dantrolene and bromocriptine. Dantrolene is a muscle relaxant, which is used for controlling spasticity and hyperthermia. Unfortunately, this medication is not available in Thailand. Table 1. Criteria for diagnosis of NMS (DSM IV) (3) A. The development of severe muscle rigidity and elevated temperature associated with the use of antipsychotic medication. B. Two or more of the following: - Diaphoresis - Elevated blood pressure - Tachycardia - Incontinence - Dysphagia - Mutism - Tremor - Changes in the level of consciousness ranging from confusion to coma - Leukocytosis - Laboratory evidence of muscle injury (e.g. elevated CK). C. The symptoms in criteria A and B are not due to another substance (e.g. phencyclidine), or neurologic or other medical condition (e.g. viral encephalitis). D. The symptoms in criteria A and B are no better accounted for by a mental disorder (e.g. mood disorder with catatonic features). From: Diagnostic and Statistical Manual of Mental Disorders, fourth edition. Washington, DC: American Psychiatry Association; 1994 Table 2. Levenson s clinical criteria for diagnosis of NMS (1) Major manifestations - Fever - Rigidity - Elevated creatinine phosphokinase concentration Minor manifestations - Abnormal arterial pressure - Altered consciousness - Diaphoresis - Leukocytosis The presence of all three major or two major and four minor criteria suggests a high probability of the presence of NMS, if supported by clinical history (e.g. not indicative of malignant hyperthermia).
5 Neuroleptic maliganant syndrome 77 Bromocriptine is a dopaminergic agonist and presumably actis by reversing dopaminergic receptor blockage caused by neuroleptic medications. The initial dose should be 2.5 to 5 mg t.i.d. with an increment of 2.5 mg t.i.d. every 24 hours. Doses of up to 60 mg per day have been used. (12) Side effects of this medication include hypotension, nausea and worsening of psychotic symptoms. Medications should be continued for at least 10 days and up to 2-3 weeks when depot neuroleptics are used after the resolution of the symptoms. (12) Treatment with these medications has shown to improve outcome and shorten the course of NMS. (5,14) Other medications used in NMS are amantadine, levodopa, and benzodiazepine. (2,12) Both beneficial and harm-ful effects from anticholinergic drugs in NMS have been reported. (13) Electroconvulsive treatment has been shown as effective in the treatment of NMS, especially in severe cases that are refractory to medications, when it is difficult to rule out lethal catatonia, or when the underlying conditions are psychotic depression or catatonia. (14) Treatment with ECT is relatively safe and the response may be apparent during early treatment. Symptoms of NMS usually subside 5-10 days after cessation of the medication, but 2-3 times longer with long-acting depot injections. (12) A complication from NMS is rhabdomyolysis, which may cause acute renal failure. It is the most common cause of death in patients with NMS. (5) Respiratory failure may occur from aspiration, pulmonary emboli, septic shock, or decreased chest wall movement from muscle rigidity. (1) Other complications are cardiac failure, arrhythmia, pulmona-ry embolism, and disseminated intravascular coagulation. Death from this syndrome may be as high as 25%, especially when it is unrecognized. 5 Decreased mortality rate may reflect early awareness of this syndrome rather than early treatment. Recurrence of NMS by rechallenging these patients with neuroleptic medications may be as high as 30%. (2) Using less potent drugs at the lowest clinically effective dose, and the time reintroduction starting at least 2 weeks after complete resolution of NMS, can reduce the risk of recurrent NMS. (12) Conclusion Neuroleptic malignant syndrome is a potentially life threatening condition caused by an idiosyncratic reaction to neuroleptic agents. A high index of suspicion is needed to recognize this syndrome, especially in any febrile patients with a history of neuroleptic treatment. Early recognition, discontinuation the offending medications, supportive care and appropriate use of pharmacologic treatment may lead to effective management and decreased morbidity. References 1. Levenson JL. Neuroleptic malignant syndrome. Am J Psychiatry 1985;142: Caroff SN, Mann SC. Neuroleptic malignant syndrome. Med Clin North Am 1993;77: American Psychiatric Association. Diagnostic and statistical manual of mental disorders. Washington DC: American Psychiatric Press, 1994: Guze BH, Baxter LR, Jr. Current concepts. Neuroleptic malignant syndrome. N Engl J Med 1985;313: Shalev A, Hermesh H, Munitz H. Mortality from neuroleptic malignant syndrome. J Clin Psychiatry 1989;50:18-25.
6 78 Likasitwattanakul S. 6. Caroff SN, Mann SC. Neuroleptic malignant syndrome. Psychopharmacol Bull 1988;24: Ananth J, Parameswaran S, Gunatilake S, Burgoyne K, Sidhom T. Neuroleptic malignant syndrome and atypical antipsychotic drugs. J Clin Psychiatry 2004; 65: Kanchanapongkul J. Neuroleptic malignant syndrome: a report of a case and review of the literature. J Med Assoc Thai 1991; 74: Poungvarin N, Prayoonwiwat N, Viriyavejakul A. Neruoleptic malignant syndrome: A case report and review of the literature. Siriraj Hosp Gaz 1993; 74: Kankirawatana P, Raksadawan N. Neuroleptic malignant syndrome. Siriraj Hosp Gaz 1995; 47: Keck PE, Jr., Pope HG, Jr., Cohen BM, McElroy SL, Nierenberg AA. Risk factors for neuroleptic malignant syndrome. A casecontrol study. Arch Gen Psychiatry 1989; 46: Richard IH. Acute, drug-induced, lifethreatening neurological syndromes. The Neurologist 1998; 4: Smego RA, Jr., Durack DT. The neuroleptic malignant syndrome. Arch Intern Med 1982; 142: Trollor JN, Sachdev PS. Electroconvulsive treatment of neuroleptic malignant syndrome: a review and report of cases. Aust N Z J Psychiatry 1999;33: กล มอาการน วโรเลพต ค มาล กแนนท : รายงานผ ป วย 2 ราย อรณ แสนมณ ช ย, พ.บ., ส รช ย ล ขส ทธ ว ฒนก ล, พ.บ. ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร มหาว ทยาล ยเช ยงใหม บทค ดย อ กล มอาการน วโรเลพต ค มาล กแนนท เป นภาวะแทรกซ อนจากการใช ยาท พบได น อยมาก ผ รายงานได รายงานผ ป วยเด ก 2 รายท ม อาการไข ม ระด บสต ส มปช ญญะเปล ยนแปลง ม อาการ เกร งของกล ามเน อ และม ความผ ดปกต ของระบบประสาทเสร ภายหล งได ยาประเภทยากล อม ประสาทหล ก ผ ป วยท งสองรายได การร กษาด วยยาโบรโมคร พท นและการร กษาแบบประค บ- ประคองซ งได ผลด เน องจากผ ป วยท ม ภาวะแทรกซ อนชน ดน อาจจะเส ยช ว ตได ผ รายงานจ งเน น ถ งการท แพทย ใช ยาประเภทน ควรม ความร และสามารถว น จฉ ยภาวะน ได ต งแต เน นๆ ซ งอาจจะ ท าให ผ ป วยรอดช ว ตจากภาวะแทรกซ อนน ได เช ยงใหม เวชสาร 2548;44(2): ค าส าค ญ: กล มอาการน วโรเลพต ค
COALINGA STATE HOSPITAL. Effective Date: August 31, 2006
 COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 717 Effective Date: August 31, 2006 SUBJECT: NEUROLEPTIC MALIGNANT SYNDROME 1. PURPOSE: To provide
COALINGA STATE HOSPITAL NURSING POLICY AND PROCEDURE MANUAL SECTION Emergency Procedures POLICY NUMBER: 717 Effective Date: August 31, 2006 SUBJECT: NEUROLEPTIC MALIGNANT SYNDROME 1. PURPOSE: To provide
Chapter 161 Antipsychotics
 Chapter 161 Antipsychotics Episode Overview Extrapyramidal syndromes are a common complication of antipsychotic medications. First line treatment is benztropine or diphenhydramine. Lorazepam is used in
Chapter 161 Antipsychotics Episode Overview Extrapyramidal syndromes are a common complication of antipsychotic medications. First line treatment is benztropine or diphenhydramine. Lorazepam is used in
Neuroleptic Malignant Syndrome, with Attention to Its Occurrence with Atypical Antipsychotic Medication: A Review
 Jefferson Journal of Psychiatry Volume 20 Issue 1 Article 7 December 2006 Neuroleptic Malignant Syndrome, with Attention to Its Occurrence with Atypical Antipsychotic Medication: A Review Sarah Guzofski
Jefferson Journal of Psychiatry Volume 20 Issue 1 Article 7 December 2006 Neuroleptic Malignant Syndrome, with Attention to Its Occurrence with Atypical Antipsychotic Medication: A Review Sarah Guzofski
Neuroleptic malignant syndrome (NMS) was first
 Case Report 576 Severe Neuroleptic Malignant Syndrome: Successful Treatment with High-dose Lorazepam and Diazepam: A Case Report Meng-Chang Tsai, MD; Tiao-Lai Huang, MD Neuroleptic malignant syndrome (NMS)
Case Report 576 Severe Neuroleptic Malignant Syndrome: Successful Treatment with High-dose Lorazepam and Diazepam: A Case Report Meng-Chang Tsai, MD; Tiao-Lai Huang, MD Neuroleptic malignant syndrome (NMS)
Neuroleptic malignant syndrome: Diagnostic and therapeutic dilemmas
 Behavioural Neurology 16 (2005) 9 13 9 IOS Press Neuroleptic malignant syndrome: Diagnostic and therapeutic dilemmas Abebaw Fekadu a, and Jonathan I. Bisson b a St Ann s Hospital, Poole, UK b University
Behavioural Neurology 16 (2005) 9 13 9 IOS Press Neuroleptic malignant syndrome: Diagnostic and therapeutic dilemmas Abebaw Fekadu a, and Jonathan I. Bisson b a St Ann s Hospital, Poole, UK b University
movement disorders for psychiatrists
 Movement disorders for psychiatrists Nandakumar Narayanan Assistant Professor, Neurology University of Iowa Thanks to Dr. Rodnitkzy Funding for my lab National Institutes of Health Carver Medical Trust
Movement disorders for psychiatrists Nandakumar Narayanan Assistant Professor, Neurology University of Iowa Thanks to Dr. Rodnitkzy Funding for my lab National Institutes of Health Carver Medical Trust
Neuroleptic malignant syndrome induced by atypical neuroleptics and responsive to lorazepam. Introduction
 CASE REPORT Neuroleptic malignant syndrome induced by atypical neuroleptics and responsive to lorazepam Adeeb Yacoub Andrew Francis Department of Psychiatry and Behavioral Science, School of Medicine,
CASE REPORT Neuroleptic malignant syndrome induced by atypical neuroleptics and responsive to lorazepam Adeeb Yacoub Andrew Francis Department of Psychiatry and Behavioral Science, School of Medicine,
Neuroleptic malignant syndrome in severe vascular dementia: Diagnostic challenge due to baseline impaired mental status
 www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Neuroleptic malignant syndrome in severe vascular dementia: Diagnostic challenge due to baseline impaired mental status Thein Swe, Akari Thein
www.edoriumjournals.com CASE REPORT PEER REVIEWED OPEN ACCESS Neuroleptic malignant syndrome in severe vascular dementia: Diagnostic challenge due to baseline impaired mental status Thein Swe, Akari Thein
ROS: all remaining ROS negative
 Case # 1 CC: altered mental status HPI: 13 yo male presents with altered metal status. Child`s mother was called by the school nurse to pick her child up from school today due to child`s unusual behavior.
Case # 1 CC: altered mental status HPI: 13 yo male presents with altered metal status. Child`s mother was called by the school nurse to pick her child up from school today due to child`s unusual behavior.
Medicines Management and the Unwell Parkinson s Patient
 Medicines Management and the Unwell Parkinson s Patient Belinda Kessel Geriatrician and Movement Disorder Specialist Princess Royal University Hospital Orpington, Kent The Society for Acute Medicine, 7
Medicines Management and the Unwell Parkinson s Patient Belinda Kessel Geriatrician and Movement Disorder Specialist Princess Royal University Hospital Orpington, Kent The Society for Acute Medicine, 7
A REVIEW OF NEUROLEPTIC MALIGNANT SYNDROME~ INCIDENCE AND FEATURES IN MALTA
 34 Volume VII Issue II 1995 A REVIEW OF NEUROLEPTIC MALIGNANT SYNDROME~ INCIDENCE AND FEATURES IN MALTA A. Grech, JR. 5aliha ABSTRACT: This paper describes Malta's first sample of Neuroleptic Malignant
34 Volume VII Issue II 1995 A REVIEW OF NEUROLEPTIC MALIGNANT SYNDROME~ INCIDENCE AND FEATURES IN MALTA A. Grech, JR. 5aliha ABSTRACT: This paper describes Malta's first sample of Neuroleptic Malignant
Common poly-substance abuse: MDMA, Ketamine, & Methamphetamine Clinical detection and management
 Common poly-substance abuse: MDMA, Ketamine, & Methamphetamine Clinical detection and management Prepared by Dr. S.P. LEUNG Castle Peak Hospital 27th January 2001 Medical practitioner should provide care
Common poly-substance abuse: MDMA, Ketamine, & Methamphetamine Clinical detection and management Prepared by Dr. S.P. LEUNG Castle Peak Hospital 27th January 2001 Medical practitioner should provide care
Delirium. Assessment and Management
 Delirium Assessment and Management Goals and Objectives Participants will: 1. be able to recognize and diagnose the syndrome of delirium. 2. understand the causes of delirium. 3. become knowledgeable about
Delirium Assessment and Management Goals and Objectives Participants will: 1. be able to recognize and diagnose the syndrome of delirium. 2. understand the causes of delirium. 3. become knowledgeable about
When second-generation antipsychotics (SGAs)
 For mass reproduction, content licensing and permissions contact Dowden Health Media. Neuroleptic malignant syndrome: Don t let your guard down yet 88 case reports indicate newer antipsychotics may cause
For mass reproduction, content licensing and permissions contact Dowden Health Media. Neuroleptic malignant syndrome: Don t let your guard down yet 88 case reports indicate newer antipsychotics may cause
Post Cardiac Arrest Care 2015 American Heart Association Guideline Update for CPR and Emergency Cardiovascular Care
 Post Cardiac Arrest Care 2015 American Heart Association Guideline Update for CPR and Emergency Cardiovascular Care รศ.ดร.พญ.ต นหยง พ พานเมฆาภรณ ภาคว ชาว ส ญญ ว ทยา คณะแพทยศาสตร มหาว ทยาล ยเช ยงใหม System
Post Cardiac Arrest Care 2015 American Heart Association Guideline Update for CPR and Emergency Cardiovascular Care รศ.ดร.พญ.ต นหยง พ พานเมฆาภรณ ภาคว ชาว ส ญญ ว ทยา คณะแพทยศาสตร มหาว ทยาล ยเช ยงใหม System
VI.2 Elements for a public summary. VI.2.1 Overview of disease epidemiology
 VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology Incidence and prevalence of target indication Schizophrenia is a mental disorder characterized by a breakdown of thought processes
VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology Incidence and prevalence of target indication Schizophrenia is a mental disorder characterized by a breakdown of thought processes
Elements for a Public Summary
 VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Schizophrenia Schizophrenia is a mental illness with a number of symptoms, including confused or unclear thinking and speech,
VI.2 VI.2.1 Elements for a Public Summary Overview of disease epidemiology Schizophrenia Schizophrenia is a mental illness with a number of symptoms, including confused or unclear thinking and speech,
Pharmaceutical form(s)/strength: 50, 100, 200, 400 mg tablets P-RMS:
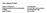 0BCore Safety Profile Active substance: Amisulpride Pharmaceutical form(s)/strength: 50, 100, 200, 400 mg tablets P-RMS: IE/H/PSUR/0017/002 Date of FAR: 28.11.2012 Core Safety Profile [amisulpride] Formulations:
0BCore Safety Profile Active substance: Amisulpride Pharmaceutical form(s)/strength: 50, 100, 200, 400 mg tablets P-RMS: IE/H/PSUR/0017/002 Date of FAR: 28.11.2012 Core Safety Profile [amisulpride] Formulations:
ANTIPSYCHOTICS AGENTS CONVENTIONAL
 ANTIPSYCHOTICS AGENTS CONVENTIONAL Documentation A. FDA approved indications 1. Psychotic Disorder (Haloperidol, Thiothixene) 2. Schizophrenia 3. Bipolar Disorder, Manic (Chlorpromazine) 4. Severe Behavioral
ANTIPSYCHOTICS AGENTS CONVENTIONAL Documentation A. FDA approved indications 1. Psychotic Disorder (Haloperidol, Thiothixene) 2. Schizophrenia 3. Bipolar Disorder, Manic (Chlorpromazine) 4. Severe Behavioral
DEMENTIA and BPSD in PARKINSON'S DISEASE. DR. T. JOHNSON. NOVEMBER 2017.
 DEMENTIA and BPSD in PARKINSON'S DISEASE. DR. T. JOHNSON. NOVEMBER 2017. Introduction. Parkinson's disease (PD) has been considered largely as a motor disorder. It has been increasingly recognized that
DEMENTIA and BPSD in PARKINSON'S DISEASE. DR. T. JOHNSON. NOVEMBER 2017. Introduction. Parkinson's disease (PD) has been considered largely as a motor disorder. It has been increasingly recognized that
Antipsychotic Use in the Elderly
 Antipsychotic Use in the Elderly Presented by: Fatima M. Ali, PharmD, RPh, BCPS Clinical Consultant Pharmacist MediSystem Pharmacy, Kingston Originally Prepared by: Nicole Tisi BScPhm, RPh ACPR Disclosure
Antipsychotic Use in the Elderly Presented by: Fatima M. Ali, PharmD, RPh, BCPS Clinical Consultant Pharmacist MediSystem Pharmacy, Kingston Originally Prepared by: Nicole Tisi BScPhm, RPh ACPR Disclosure
Elements for a Public Summary. VI.2.1 Overview of disease epidemiology
 VI.2 Elements for a Public Summary VI.2.1 Overview of disease epidemiology Schizophrenia Schizophrenia is a mental disorder often characterized by abnormal social behaviour and failure to recognize what
VI.2 Elements for a Public Summary VI.2.1 Overview of disease epidemiology Schizophrenia Schizophrenia is a mental disorder often characterized by abnormal social behaviour and failure to recognize what
Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy
 Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy Disclaimer: This example is just one of many potential examples of clinician education material that can be provided
Example Clinician Educational Material for Providers of Immune Effector Cellular Therapy Disclaimer: This example is just one of many potential examples of clinician education material that can be provided
EU Risk Management Plan
 6.2 Elements for Public Summary - Abilify 6.2.1 Overview of Disease Epidemiology Bipolar I Disorder Reported prevalence rates for bipolar I disorder differ due to local variations in psychiatric practice,
6.2 Elements for Public Summary - Abilify 6.2.1 Overview of Disease Epidemiology Bipolar I Disorder Reported prevalence rates for bipolar I disorder differ due to local variations in psychiatric practice,
Drugs that poison the elderly
 Drugs that poison the elderly Brent Tipping Sub-specialist Geriatrician and Specialist Physician Division of Geriatric Medicine, Department of Medicine University of the Witwatersrand To treat or not to
Drugs that poison the elderly Brent Tipping Sub-specialist Geriatrician and Specialist Physician Division of Geriatric Medicine, Department of Medicine University of the Witwatersrand To treat or not to
Symbyax (Zyprexa [olanzapine] and Prozac [fluoxetine] combination)
![Symbyax (Zyprexa [olanzapine] and Prozac [fluoxetine] combination) Symbyax (Zyprexa [olanzapine] and Prozac [fluoxetine] combination)](/thumbs/74/70586696.jpg) Symbyax (Zyprexa [olanzapine] and Prozac [fluoxetine] combination) Generic name: Olanzapine and fluoxetine combination Available strengths: 6 mg/25 mg, 6 mg/50 mg, 12 mg/25 mg, 12 mg/50 mg (Zyprexa/Prozac)
Symbyax (Zyprexa [olanzapine] and Prozac [fluoxetine] combination) Generic name: Olanzapine and fluoxetine combination Available strengths: 6 mg/25 mg, 6 mg/50 mg, 12 mg/25 mg, 12 mg/50 mg (Zyprexa/Prozac)
Epilepsy CASE 1 Localization Differential Diagnosis
 2 Epilepsy CASE 1 A 32-year-old man was observed to suddenly become unresponsive followed by four episodes of generalized tonic-clonic convulsions of the upper and lower extremities while at work. Each
2 Epilepsy CASE 1 A 32-year-old man was observed to suddenly become unresponsive followed by four episodes of generalized tonic-clonic convulsions of the upper and lower extremities while at work. Each
PARKINS ON CENTER. Parkinson s Disease: Diagnosis and Management. Learning Objectives: Recognition of PD OHSU. Disclosure Information
 OHSU PARKINS ON CENTER Parkinson s Disease: Diagnosis and Management for Every MD Disclosure Information Grants/Research Support: National Parkinson Foundation, NIH, Michael J. Fox Foundation Consultant:
OHSU PARKINS ON CENTER Parkinson s Disease: Diagnosis and Management for Every MD Disclosure Information Grants/Research Support: National Parkinson Foundation, NIH, Michael J. Fox Foundation Consultant:
Dosing and administration information for ABILIFY MAINTENA (aripiprazole)
 DOSING AND ADMINISTRATION GUIDE Dosing and administration information for ABILIFY MAINTENA (aripiprazole) Approved for deltoid or gluteal administration ABILIFY MAINTENA (aripiprazole) is an atypical antipsychotic
DOSING AND ADMINISTRATION GUIDE Dosing and administration information for ABILIFY MAINTENA (aripiprazole) Approved for deltoid or gluteal administration ABILIFY MAINTENA (aripiprazole) is an atypical antipsychotic
Restlessness, muscle twitches, and diarrhea.
 http://www.medicine-on-line.com Restlessness, twitches & diarrhea: 1/7 Case 062: Restlessness, muscle twitches, and diarrhea. Authors: * Jason Ko MB BS, MRCP # David C Chung MD, FRCPC Affiliations: *Tuen
http://www.medicine-on-line.com Restlessness, twitches & diarrhea: 1/7 Case 062: Restlessness, muscle twitches, and diarrhea. Authors: * Jason Ko MB BS, MRCP # David C Chung MD, FRCPC Affiliations: *Tuen
The Tipping Point. Brita Roy, MD MPH MS F. Stanford Massie Jr., MD
 The Tipping Point Brita Roy, MD MPH MS F. Stanford Massie Jr., MD Learning Objectives 1. To recognize an important cause of fever, somnolence, and rigidity. 2. To appreciate the dangers of polypharmacy.
The Tipping Point Brita Roy, MD MPH MS F. Stanford Massie Jr., MD Learning Objectives 1. To recognize an important cause of fever, somnolence, and rigidity. 2. To appreciate the dangers of polypharmacy.
PRESCRIBING PRACTICE IN DELIRIUM. John Warburton Critical Care Pharmacist
 PRESCRIBING PRACTICE IN DELIRIUM John Warburton Critical Care Pharmacist Learning outcomes Modifiable medication risk factors for delirium An appreciation of contributing factors modifiable with medicines
PRESCRIBING PRACTICE IN DELIRIUM John Warburton Critical Care Pharmacist Learning outcomes Modifiable medication risk factors for delirium An appreciation of contributing factors modifiable with medicines
More information about Cymbalta is available in the current edition of MPR.
 www.empr.com Clinical ALERT Dear Healthcare Professional, At MPR we strive to bring you important drug information in a timely fashion. In keeping with this goal, we are pleased to bring you this CLINICAL
www.empr.com Clinical ALERT Dear Healthcare Professional, At MPR we strive to bring you important drug information in a timely fashion. In keeping with this goal, we are pleased to bring you this CLINICAL
B Kessel - BGS Aut 2009
 www.bgsmds.org.uk www.bgsmdslive.org/ Fifth British Geriatrics Society Movement Disorders Section Award medical, nursing and therapy students are invited to submit an essay title can we change outcomes
www.bgsmds.org.uk www.bgsmdslive.org/ Fifth British Geriatrics Society Movement Disorders Section Award medical, nursing and therapy students are invited to submit an essay title can we change outcomes
A rating scale for neuroleptic malignant syndrome
 Psychiatry Research 135 (2005) 249 256 www.elsevier.com/locate/psychres A rating scale for neuroleptic malignant syndrome Perminder S. Sachdev* School of Psychiatry, University of New South Wales, Sydney,
Psychiatry Research 135 (2005) 249 256 www.elsevier.com/locate/psychres A rating scale for neuroleptic malignant syndrome Perminder S. Sachdev* School of Psychiatry, University of New South Wales, Sydney,
COLCHICINE MYOTOXICITY : A CASE REPORT
 Chiang Mai Med Bull 2004;47(2):87-92. Case report COLCHICINE MYOTOXICITY : A CASE REPORT Suttinee Sripotong, M.D., Suparaporn Wangkaew, M.D., Nuntana Kasitanon, M.D., Worawit Louthreno, M.D. Division of
Chiang Mai Med Bull 2004;47(2):87-92. Case report COLCHICINE MYOTOXICITY : A CASE REPORT Suttinee Sripotong, M.D., Suparaporn Wangkaew, M.D., Nuntana Kasitanon, M.D., Worawit Louthreno, M.D. Division of
Antidepressants: Prof. Riyadh Al_Azzawi F.R.C.Psych
 Antidepressants: Prof. Riyadh Al_Azzawi F.R.C.Psych A. Heterocyclic antidepressants: (tricyclic and tetracyclic ), e.g.amitryptaline,imipramine. B. Monoamine oxidase inhibitors(m.a.o.i), e.g.phenelzine.
Antidepressants: Prof. Riyadh Al_Azzawi F.R.C.Psych A. Heterocyclic antidepressants: (tricyclic and tetracyclic ), e.g.amitryptaline,imipramine. B. Monoamine oxidase inhibitors(m.a.o.i), e.g.phenelzine.
Olanzapine and ECT combined therapy in a refractory catatonic subtype schizophrenia. Pedro Gomes de Alvarenga* Sérgio Paulo Rigonatti**
 Case report Olanzapine and ECT combined therapy in a refractory catatonic subtype schizophrenia patient with previous neuroleptic malignant syndrome episodes Pedro Gomes de Alvarenga* Sérgio Paulo Rigonatti**
Case report Olanzapine and ECT combined therapy in a refractory catatonic subtype schizophrenia patient with previous neuroleptic malignant syndrome episodes Pedro Gomes de Alvarenga* Sérgio Paulo Rigonatti**
DELIRIUM. Approach and Management
 DELIRIUM Approach and Management By Dr. K.S. Jacob, Professor of Psychiatry and Dr. Anju Kuruvilla, Professor of Psychiatry, Christian Medical College, Vellore. Based on a chapter in the book Psychiatric
DELIRIUM Approach and Management By Dr. K.S. Jacob, Professor of Psychiatry and Dr. Anju Kuruvilla, Professor of Psychiatry, Christian Medical College, Vellore. Based on a chapter in the book Psychiatric
CT SCANS OF ABDOMINAL TRAUMA IN CHILDREN
 Chiang Mai Med Bull 2005;44(1):35-41. Original article CT SCANS OF ABDOMINAL TRAUMA IN CHILDREN Nuttaya Pattamapaspong, M.D., Pannee Visrutaratna, M.D., Wittanee na ChiangMai, M.D. Department of Radiology,
Chiang Mai Med Bull 2005;44(1):35-41. Original article CT SCANS OF ABDOMINAL TRAUMA IN CHILDREN Nuttaya Pattamapaspong, M.D., Pannee Visrutaratna, M.D., Wittanee na ChiangMai, M.D. Department of Radiology,
An Approach to the Pharmacotherapy of Neuroleptic Malignant Syndrome
 Complicated case histories Key Words: neuroleptic malignant syndrome, pharmacotherapy, dantrolene, bromocriptine, amantadine, benzodiazepines, severity An Approach to the Pharmacotherapy of Neuroleptic
Complicated case histories Key Words: neuroleptic malignant syndrome, pharmacotherapy, dantrolene, bromocriptine, amantadine, benzodiazepines, severity An Approach to the Pharmacotherapy of Neuroleptic
Periodic catatonia with long-term treatment: a case report
 Chen and Huang BMC Psychiatry (2017) 17:337 DOI 10.1186/s12888-017-1497-6 CASE REPORT Open Access Periodic catatonia with long-term treatment: a case report Ruei-An Chen and Tiao-Lai Huang * Abstract Background:
Chen and Huang BMC Psychiatry (2017) 17:337 DOI 10.1186/s12888-017-1497-6 CASE REPORT Open Access Periodic catatonia with long-term treatment: a case report Ruei-An Chen and Tiao-Lai Huang * Abstract Background:
Antipsychotic dose escalation as a trigger for Neuroleptic Malignant Syndrome (NMS): literature review and case series report
 Langan et al. BMC Psychiatry 2012, 12:214 DATABASE Open Access Antipsychotic dose escalation as a trigger for Neuroleptic Malignant Syndrome (NMS): literature review and case series report Julie Langan
Langan et al. BMC Psychiatry 2012, 12:214 DATABASE Open Access Antipsychotic dose escalation as a trigger for Neuroleptic Malignant Syndrome (NMS): literature review and case series report Julie Langan
Clinical Presentations of Bipolar Disorder in Children and Adolescents
 Clinical Presentations of Bipolar Disorder in Children and Adolescents J Med Assoc Thai 2014; 97 (2): 179-83 Full text. e-journal: http://www.jmatonline.com Nida Limsuwan MD* * Department of Psychiatry,
Clinical Presentations of Bipolar Disorder in Children and Adolescents J Med Assoc Thai 2014; 97 (2): 179-83 Full text. e-journal: http://www.jmatonline.com Nida Limsuwan MD* * Department of Psychiatry,
The PI includes important warnings and precautions. It states (in pertinent part):
 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration Rockville, MD 20857 TRANSMITTED BY FACSIMILE James L. Gaskill, PharmD Director Promotional Regulatory Affairs AstraZeneca
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration Rockville, MD 20857 TRANSMITTED BY FACSIMILE James L. Gaskill, PharmD Director Promotional Regulatory Affairs AstraZeneca
Management of Severe Agitation
 Management of Severe Agitation Key Points 1. The management of the severely agitated or violent patient embraces psychological, physical and pharmacological approaches. 2. Psychological methods focus on
Management of Severe Agitation Key Points 1. The management of the severely agitated or violent patient embraces psychological, physical and pharmacological approaches. 2. Psychological methods focus on
L : Line and Tube อ นตรายป องก นได จากการให สารน า
 L : Line and Tube อ นตรายป องก นได จากการให สารน า รศ.นพ.กว ศ กด จ ตตว ฒนร ตน ภาคว ชาศ ลยศาสตร คณะแพทยศาสตร มหาว ทยาล ยเช ยงใหม 3 rd Mini Conference: ความปลอดภ ยในผ ป วย ร วมด วย ช วยได ท กคน ว นท 13-14
L : Line and Tube อ นตรายป องก นได จากการให สารน า รศ.นพ.กว ศ กด จ ตตว ฒนร ตน ภาคว ชาศ ลยศาสตร คณะแพทยศาสตร มหาว ทยาล ยเช ยงใหม 3 rd Mini Conference: ความปลอดภ ยในผ ป วย ร วมด วย ช วยได ท กคน ว นท 13-14
( delirium ) 15%- ( extrapyramidal syndrome ) risperidone olanzapine ( extrapyramidal side effect ) olanzapine ( Delirium Rating Scale, DRS )
 2005 6 48-52 Olanzapine 30% ( delirium 5%- Haloperidol ( extrapyramidal syndrome risperidone ( extrapyramidal side effect ( Delirium Rating Scale, DRS ( Delirium ( Olanzapine ( Delirium Rating Scale, DRS
2005 6 48-52 Olanzapine 30% ( delirium 5%- Haloperidol ( extrapyramidal syndrome risperidone ( extrapyramidal side effect ( Delirium Rating Scale, DRS ( Delirium ( Olanzapine ( Delirium Rating Scale, DRS
Pharmacologic Treatment of Parkinson s Disease. Nicholas J. Silvestri, M.D. Associate Professor of Neurology
 + Pharmacologic Treatment of Parkinson s Disease Nicholas J. Silvestri, M.D. Associate Professor of Neurology + Disclosures n NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT + Learning
+ Pharmacologic Treatment of Parkinson s Disease Nicholas J. Silvestri, M.D. Associate Professor of Neurology + Disclosures n NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT + Learning
พรช ย ก งว ฒนก ล ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร จ ฬาลงกรณ มหาว ทยาล ย
 พรช ย ก งว ฒนก ล ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร จ ฬาลงกรณ มหาว ทยาล ย We are detectives. Frame of thought Clinical or Lab Medical vs. Surgical Supportive care only? Refer? Frame of thought Onset Clinical
พรช ย ก งว ฒนก ล ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร จ ฬาลงกรณ มหาว ทยาล ย We are detectives. Frame of thought Clinical or Lab Medical vs. Surgical Supportive care only? Refer? Frame of thought Onset Clinical
Drug Therapy of Parkinsonism. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Drug Therapy of Parkinsonism Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Parkinsonism is a progressive neurological disorder of muscle movement, usually
Drug Therapy of Parkinsonism Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Parkinsonism is a progressive neurological disorder of muscle movement, usually
Cases Report: Clavicular Fractures after Hook-Plate Fixation Surgery
 บทความทบทวนผ ป วย (Case review) Cases Report: Clavicular Fractures after Hook-Plate Fixation Surgery Thitinut Dilokhuttakarn 1, Ronnachit Boonprasert 1, Chaturong Pornrattanamaneewong 2 1 Department of
บทความทบทวนผ ป วย (Case review) Cases Report: Clavicular Fractures after Hook-Plate Fixation Surgery Thitinut Dilokhuttakarn 1, Ronnachit Boonprasert 1, Chaturong Pornrattanamaneewong 2 1 Department of
Risk Evaluation and Mitigation Strategy (REMS): Cytokine release syndrome and neurological toxicities
 Risk Evaluation and Mitigation Strategy (REMS): Cytokine release syndrome and neurological toxicities A REMS is a program required by the FDA to manage known or potential serious risks associated with
Risk Evaluation and Mitigation Strategy (REMS): Cytokine release syndrome and neurological toxicities A REMS is a program required by the FDA to manage known or potential serious risks associated with
srmp DK/H/2440/ /DC aripiprazole
 srmp DK/H/2440/001-004/DC aripiprazole VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology Schizophrenia is a mental disorder affecting about 7 per thousand of the adult population,
srmp DK/H/2440/001-004/DC aripiprazole VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology Schizophrenia is a mental disorder affecting about 7 per thousand of the adult population,
Section I: EPS and NMS Nauman Ashraf, M.D. Section II: Serotonin Syndrome and Seizure Disorders Constanza Martinez, M.D.
 Pharmacologic Induced Movement & Neurologic Disorders Section I: EPS and NMS Nauman Ashraf, M.D. Section II: Serotonin Syndrome and Seizure Disorders Constanza Martinez, M.D. Pharmacologic Induced Movement
Pharmacologic Induced Movement & Neurologic Disorders Section I: EPS and NMS Nauman Ashraf, M.D. Section II: Serotonin Syndrome and Seizure Disorders Constanza Martinez, M.D. Pharmacologic Induced Movement
Chapter 17. Psychoses. Classifications of Psychoses. Schizophrenia. Factors Attributed to Development of Psychoses
 Chapter 17 Psychoses Drugs for Psychoses Delusions Hallucinations Illusions Paranoia Upper Saddle River, New Jersey 07458 All rights reserved. Classifications of Psychoses Acute episode Chronic episode
Chapter 17 Psychoses Drugs for Psychoses Delusions Hallucinations Illusions Paranoia Upper Saddle River, New Jersey 07458 All rights reserved. Classifications of Psychoses Acute episode Chronic episode
ICU Delirium in Infants & Children: Cause for Concern or False Alarm. Objectives
 ICU Delirium in Infants & Children: Cause for Concern or False Alarm Peter (Pete) N. Johnson, Pharm.D., BCPS, BCPPS, FPPAG Associate Professor of Pharmacy Practice University of Oklahoma College of Pharmacy
ICU Delirium in Infants & Children: Cause for Concern or False Alarm Peter (Pete) N. Johnson, Pharm.D., BCPS, BCPPS, FPPAG Associate Professor of Pharmacy Practice University of Oklahoma College of Pharmacy
Summary of the risk management plan (RMP) for Aripiprazole Mylan Pharma (aripiprazole)
 EMA/370707/2016 Summary of the risk management plan (RMP) for Aripiprazole Mylan Pharma (aripiprazole) This is a summary of the risk management plan (RMP) for Aripiprazole Mylan Pharma, which details the
EMA/370707/2016 Summary of the risk management plan (RMP) for Aripiprazole Mylan Pharma (aripiprazole) This is a summary of the risk management plan (RMP) for Aripiprazole Mylan Pharma, which details the
THIOTHIXENE. THERAPEUTICS Brands Navane see index for additional brand names. Generic? Yes
 THIOTHIXENE THERAPEUTICS Brands Navane see index for additional brand names Generic? Yes Class Conventional antipsychotic (neuroleptic, thioxanthene, dopamine 2 antagonist) Commonly Prescribed for (bold
THIOTHIXENE THERAPEUTICS Brands Navane see index for additional brand names Generic? Yes Class Conventional antipsychotic (neuroleptic, thioxanthene, dopamine 2 antagonist) Commonly Prescribed for (bold
FDA Approves Deltoid Injection Site for Abilify Maintena (aripiprazole) for extendedrelease injectable suspension in the Treatment of Schizophrenia
 FOR IMMEDIATE RELEASE FDA Approves Deltoid Injection Site for Abilify Maintena (aripiprazole) for extendedrelease injectable suspension in the Treatment of Schizophrenia Patients being treated for schizophrenia
FOR IMMEDIATE RELEASE FDA Approves Deltoid Injection Site for Abilify Maintena (aripiprazole) for extendedrelease injectable suspension in the Treatment of Schizophrenia Patients being treated for schizophrenia
Key Points. Angus DC: Crit Care Med 29:1303, 2001
 Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
Medication Audit Checklist- Antipsychotics - Atypical
 Medication Audit checklist Page 1 of 7 10-2018 Audit number: Client number: Ordering Provider: INDICATIONS 1) Disorders with psychotic symptoms (schizophrenia, schizoaffective disorder, manic disorders,
Medication Audit checklist Page 1 of 7 10-2018 Audit number: Client number: Ordering Provider: INDICATIONS 1) Disorders with psychotic symptoms (schizophrenia, schizoaffective disorder, manic disorders,
Case Files of the Program in Medical Toxicology at Brown University: Amantadine Withdrawal and the Neuroleptic Malignant Syndrome
 Toxicology Case Files Case Files of the Program in Medical Toxicology at Brown University: Amantadine Withdrawal and the Neuroleptic Malignant Syndrome Eric J. Brantley, MD a, Jamieson V. Cohn, MD a, Kavita
Toxicology Case Files Case Files of the Program in Medical Toxicology at Brown University: Amantadine Withdrawal and the Neuroleptic Malignant Syndrome Eric J. Brantley, MD a, Jamieson V. Cohn, MD a, Kavita
AMANTREL Capsules (Amantadine hydrochloride)
 Published on: 10 Jul 2014 AMANTREL Capsules (Amantadine hydrochloride) Composition AMANTREL Capsules Each capsule contains: Amantadine Hydrochloride equivalent to Amantadine. 100 mg Dosage Form Capsule
Published on: 10 Jul 2014 AMANTREL Capsules (Amantadine hydrochloride) Composition AMANTREL Capsules Each capsule contains: Amantadine Hydrochloride equivalent to Amantadine. 100 mg Dosage Form Capsule
Pharmacologic Treatment of Parkinson s Disease. Nicholas J. Silvestri, M.D. Assistant Professor of Neurology
 + Pharmacologic Treatment of Parkinson s Disease Nicholas J. Silvestri, M.D. Assistant Professor of Neurology + Overview n Brief review of Parkinson s disease (PD) n Clinical manifestations n Pathophysiology
+ Pharmacologic Treatment of Parkinson s Disease Nicholas J. Silvestri, M.D. Assistant Professor of Neurology + Overview n Brief review of Parkinson s disease (PD) n Clinical manifestations n Pathophysiology
Practical. Septic shock resuscitation ไชยร ตน เพ มพ ก ล พบ. ภาคว ชาอาย รศาสตร คณะแพทยศาสตร ศ ร ราชพยาบาล
 Practical Septic shock resuscitation ไ ไชยร ตน เพ มพ ก ล พบ. ภาคว ชาอาย รศาสตร คณะแพทยศาสตร ศ ร ราชพยาบาล ประช มว ชาการ 101 ป อาย รศาสตร ศ ร ราช 6 ก มภาพ นธ 2561 Early recognition Early resuscitation Early
Practical Septic shock resuscitation ไ ไชยร ตน เพ มพ ก ล พบ. ภาคว ชาอาย รศาสตร คณะแพทยศาสตร ศ ร ราชพยาบาล ประช มว ชาการ 101 ป อาย รศาสตร ศ ร ราช 6 ก มภาพ นธ 2561 Early recognition Early resuscitation Early
The Agitated. Older Patient: old. What To Do? Michelle Gibson, MD, CCFP Presented at Brockville General Hospital Rounds, May 2003
 Focus on CME at Queen s University Focus on CME at Queen s University The Agitated The Older Patient: What To Do? Michelle Gibson, MD, CCFP Presented at Brockville General Hospital Rounds, May 2003 Both
Focus on CME at Queen s University Focus on CME at Queen s University The Agitated The Older Patient: What To Do? Michelle Gibson, MD, CCFP Presented at Brockville General Hospital Rounds, May 2003 Both
Psychopharmacology in the Emergency Room. Michael D. Jibson, M.D., Ph.D. Associate Professor of Psychiatry University of Michigan
 Psychopharmacology in the Emergency Room Michael D. Jibson, M.D., Ph.D. Associate Professor of Psychiatry University of Michigan Pretest 1. Appropriate target symptoms for emergency room medication treatment
Psychopharmacology in the Emergency Room Michael D. Jibson, M.D., Ph.D. Associate Professor of Psychiatry University of Michigan Pretest 1. Appropriate target symptoms for emergency room medication treatment
Delirium. Dr. Lesley Wiesenfeld. Deputy Psychiatrist in Chief, Mount Sinai Hospital. Dr. Carole Cohen
 Delirium Dr. Lesley Wiesenfeld Deputy Psychiatrist in Chief, Mount Sinai Hospital Dr. Carole Cohen Department of Psychiatry, University of Toronto and Sunnybrook Health Sciences Centre Case Study Mrs B
Delirium Dr. Lesley Wiesenfeld Deputy Psychiatrist in Chief, Mount Sinai Hospital Dr. Carole Cohen Department of Psychiatry, University of Toronto and Sunnybrook Health Sciences Centre Case Study Mrs B
Cambridge University Press Effective Treatments in Psychiatry Peter Tyrer and Kenneth R. Silk Excerpt More information
 Organic disorders 1 Delirium Based on Delirium by Laura Gage and David K. Conn in Effective Treatments in Psychiatry, Cambridge University Press, 2008 Introduction Delirium needs treatment for both its
Organic disorders 1 Delirium Based on Delirium by Laura Gage and David K. Conn in Effective Treatments in Psychiatry, Cambridge University Press, 2008 Introduction Delirium needs treatment for both its
Parkinson s Disease. Sirilak yimcharoen
 Parkinson s Disease Sirilak yimcharoen EPIDEMIOLOGY ~1% of people over 55 years Age range 35 85 years peak age of onset is in the early 60s ~5% of cases characterized by an earlier age of onset (typically
Parkinson s Disease Sirilak yimcharoen EPIDEMIOLOGY ~1% of people over 55 years Age range 35 85 years peak age of onset is in the early 60s ~5% of cases characterized by an earlier age of onset (typically
Clozapine-induced concordant agranulocytosis
 Ó 2001 Martin Dunitz Ltd International Journal of Psychiatry in Clinical Practice 2001 Volume 5 Pages 71 ± 73 71 Clozapine-induced concordant agranulocytosis in monozygotic twins J HORAÂ C Ï EK, J LIBIGER,
Ó 2001 Martin Dunitz Ltd International Journal of Psychiatry in Clinical Practice 2001 Volume 5 Pages 71 ± 73 71 Clozapine-induced concordant agranulocytosis in monozygotic twins J HORAÂ C Ï EK, J LIBIGER,
Dosing & Administration
 Dosing & Administration REAL LIFE. REAL RESULTS. INDICATION INVEGA SUSTENNA (paliperidone palmitate) is indicated for the treatment of: Schizophrenia. Schizoaffective disorder as monotherapy and as an
Dosing & Administration REAL LIFE. REAL RESULTS. INDICATION INVEGA SUSTENNA (paliperidone palmitate) is indicated for the treatment of: Schizophrenia. Schizoaffective disorder as monotherapy and as an
Shared Care Guideline for Olanzapine (Zyprexa )
 Shared Care Guideline for Olanzapine (Zyprexa ) Development Process This guidance has been produced by Sarah Hudson Lead Pharmacist SWYPFT following an AMBER classification status of Olanzapine by the
Shared Care Guideline for Olanzapine (Zyprexa ) Development Process This guidance has been produced by Sarah Hudson Lead Pharmacist SWYPFT following an AMBER classification status of Olanzapine by the
Neuroleptic malignant syndrome in the
 Postgrad Med J 1997; 73: 779-784 ( The Fellowship of Postgraduate Medicine, 1997 HIV medicine Summary Patients infected by the human immunodeficiency virus are predisposed to many infectious and noninfectious
Postgrad Med J 1997; 73: 779-784 ( The Fellowship of Postgraduate Medicine, 1997 HIV medicine Summary Patients infected by the human immunodeficiency virus are predisposed to many infectious and noninfectious
Successful treatment of catatonic syndrome in bipolar I disorder adding aripiprazole to ECT: A case report
 Eur. J. Psychiat. Vol. 26, N. 3, (169-173) 2012 Short report Keywords: Catatonia; Aripiprazole; Second generation antipsychotics; ECT; Bipolar disorder. Successful treatment of catatonic syndrome in bipolar
Eur. J. Psychiat. Vol. 26, N. 3, (169-173) 2012 Short report Keywords: Catatonia; Aripiprazole; Second generation antipsychotics; ECT; Bipolar disorder. Successful treatment of catatonic syndrome in bipolar
Risk Factors in Neuroleptic Malignant Syndrome
 INDIAN JOURNAL OF PSYCHIATRY, 2003. 45 (I). 30-35 Risk Factors in Neuroleptic Malignant Syndrome VINAY GUPTA, RAKESH MAGON. B.P. MISHRA.G.B.S.SIDHU. RANJIV MAHAJAN ABSTRACT Neuroleptic malignant syndrome
INDIAN JOURNAL OF PSYCHIATRY, 2003. 45 (I). 30-35 Risk Factors in Neuroleptic Malignant Syndrome VINAY GUPTA, RAKESH MAGON. B.P. MISHRA.G.B.S.SIDHU. RANJIV MAHAJAN ABSTRACT Neuroleptic malignant syndrome
Antipsychotic Medications
 TRAIL: Team Review of EVIDENCE REVIEW & RECOMMENDATIONS FOR LTC Behavioural and psychological symptoms of dementia (BPSD) refer to the non-cognitive symptoms of disturbed perception, thought content, mood
TRAIL: Team Review of EVIDENCE REVIEW & RECOMMENDATIONS FOR LTC Behavioural and psychological symptoms of dementia (BPSD) refer to the non-cognitive symptoms of disturbed perception, thought content, mood
Parkinson s Disease. Gillian Sare
 Parkinson s Disease Gillian Sare Outline Reminder about PD Parkinson s disease in the inpatient Surgical patients with PD Patients who cannot swallow End of life care Parkinson s disease PD is the second
Parkinson s Disease Gillian Sare Outline Reminder about PD Parkinson s disease in the inpatient Surgical patients with PD Patients who cannot swallow End of life care Parkinson s disease PD is the second
Hyperkinetic movement disorders are. Hyperkinetic Movement Disorders. Cases in Movement Disorders. James case. About Tom
 Hyperkinetic Movement Disorders Sarah Furtado, MD, PhD, FRCPC James case A mother brings her son James, 10, to your office because of repetitive sniffing sounds and repetitive eye blinking. This sniffing
Hyperkinetic Movement Disorders Sarah Furtado, MD, PhD, FRCPC James case A mother brings her son James, 10, to your office because of repetitive sniffing sounds and repetitive eye blinking. This sniffing
Trial No.: RIS-USA-102 Clinical phase: III
 SYNOPSIS Trial identification and protocol summary Company: Johnson & Johnson Pharmaceutical Research and Development, a division of Janssen Pharmaceutica, N.V. Finished product: Risperdal Active ingredient:
SYNOPSIS Trial identification and protocol summary Company: Johnson & Johnson Pharmaceutical Research and Development, a division of Janssen Pharmaceutica, N.V. Finished product: Risperdal Active ingredient:
SECTION 9 : MANAGEMENT OF MOVEMENT DISORDERS AND EXTRAPYRAMIDAL SIDE EFFECTS
 SECTION 9 : MANAGEMENT OF MOVEMENT DISORDERS AND EXTRAPYRAMIDAL SIDE EFFECTS Formulary and Prescribing Guidelines 9.1 Introduction Movement disorders and extrapyramidal side effects can manifest in the
SECTION 9 : MANAGEMENT OF MOVEMENT DISORDERS AND EXTRAPYRAMIDAL SIDE EFFECTS Formulary and Prescribing Guidelines 9.1 Introduction Movement disorders and extrapyramidal side effects can manifest in the
Sepsis Awareness and Education
 Sepsis Awareness and Education Meets the updated New York State Department of Health (NYSDOH) requirements for Infection Control and Barrier Precautions coursework Element VII: Sepsis Awareness and Education
Sepsis Awareness and Education Meets the updated New York State Department of Health (NYSDOH) requirements for Infection Control and Barrier Precautions coursework Element VII: Sepsis Awareness and Education
Catatonia a forgotten but not extinct condition
 NACT meeting 2016 Catatonia a forgotten but not extinct condition Tom G. Bolwig Professor emeritus, dr.med University of Copenhagen What is Catatonia? Catatonia is a motor dysregulation syndrome among
NACT meeting 2016 Catatonia a forgotten but not extinct condition Tom G. Bolwig Professor emeritus, dr.med University of Copenhagen What is Catatonia? Catatonia is a motor dysregulation syndrome among
Talking to Patients and Their Families
 Talking to Patients and Their Families About Clozapine The Care Transitions Network National Council for Behavioral Health Montefiore Medical Center Northwell Health New York State Office of Mental Health
Talking to Patients and Their Families About Clozapine The Care Transitions Network National Council for Behavioral Health Montefiore Medical Center Northwell Health New York State Office of Mental Health
Rapid Tranquillisation for adolescent, adults and older people Medicines management team July 2014
 Rapid Tranquillisation for adolescent, adults and older people Medicines management team July 2014 A definition of rapid tranquillisation (RT) The use of medicines to quickly control extreme agitation,
Rapid Tranquillisation for adolescent, adults and older people Medicines management team July 2014 A definition of rapid tranquillisation (RT) The use of medicines to quickly control extreme agitation,
THE ROLE OF CYP2D6 AND TAQI A POLYMORPHISMS IN MALIGNANT NEUROLEPTIC SYNDROME: TWO CASE REPORTS WITH THREE EPISODES
 Psychiatria Danubina, 2010; Vol. 22, No. 1, pp 114 425 Medicinska naklada - Zagreb, Croatia Conference paper THE ROLE OF CYP2D6 AND TAQI A POLYMORPHISMS IN MALIGNANT NEUROLEPTIC SYNDROME: TWO CASE REPORTS
Psychiatria Danubina, 2010; Vol. 22, No. 1, pp 114 425 Medicinska naklada - Zagreb, Croatia Conference paper THE ROLE OF CYP2D6 AND TAQI A POLYMORPHISMS IN MALIGNANT NEUROLEPTIC SYNDROME: TWO CASE REPORTS
Mellaril (thioridazine)
 Generic name: Thioridazine Available strengths: 10 mg, 25 mg, 50 mg, 100 mg, 200 mg tablets; 30 mg/ml, 100 mg/ml oral concentrate Available in generic: Yes Drug class: First-generation (conventional) antipsychotic
Generic name: Thioridazine Available strengths: 10 mg, 25 mg, 50 mg, 100 mg, 200 mg tablets; 30 mg/ml, 100 mg/ml oral concentrate Available in generic: Yes Drug class: First-generation (conventional) antipsychotic
Dean Olsen, DO Director, Medical Education and Emergency Medicine Residency Nassau University Medical Center Faculty, New York City Poison Control
 Dean Olsen, DO Director, Medical Education and Emergency Medicine Residency Nassau University Medical Center Faculty, New York City Poison Control Center Professor, Toxicology NYIT College of Osteopathic
Dean Olsen, DO Director, Medical Education and Emergency Medicine Residency Nassau University Medical Center Faculty, New York City Poison Control Center Professor, Toxicology NYIT College of Osteopathic
Antipsychotic Drugs Toxicity (Neuroleptic)
 Antipsychotic Drugs Toxicity (Neuroleptic) Royal Medical Services Emergency Senior Specialist King Hussein Medical City Neuroleptic: A term that refers to the effects of Antipsychotic drugs on a patient,
Antipsychotic Drugs Toxicity (Neuroleptic) Royal Medical Services Emergency Senior Specialist King Hussein Medical City Neuroleptic: A term that refers to the effects of Antipsychotic drugs on a patient,
Supplementary Online Content
 Supplementary Online Content Hocker SE, Britton JW, Mandrekar JN, Wijdicks EFM, Rabinstein AA. Predictors of outcome in refractory status epilepticus. Arch Neurol. Published online October 8, 2012. doi:10.1001/archneurol.2012.1697.
Supplementary Online Content Hocker SE, Britton JW, Mandrekar JN, Wijdicks EFM, Rabinstein AA. Predictors of outcome in refractory status epilepticus. Arch Neurol. Published online October 8, 2012. doi:10.1001/archneurol.2012.1697.
SHARED CARE GUIDELINE
 SHARED CARE GUIDELINE Title: Shared Care Guideline for the prescribing and monitoring of Antipsychotics for the treatment of Schizophrenia and psychotic symptoms in children and adolescents Scope: Pennine
SHARED CARE GUIDELINE Title: Shared Care Guideline for the prescribing and monitoring of Antipsychotics for the treatment of Schizophrenia and psychotic symptoms in children and adolescents Scope: Pennine
Neurostorm: Modern understanding and nomenclature. Mitch Stanek RN, CBIS Charge Nurse/Infection Preventionist On With Life
 Neurostorm: Modern understanding and nomenclature Mitch Stanek RN, CBIS Charge Nurse/Infection Preventionist On With Life Despite its significant clinical impact, the scientific literature on this syndrome
Neurostorm: Modern understanding and nomenclature Mitch Stanek RN, CBIS Charge Nurse/Infection Preventionist On With Life Despite its significant clinical impact, the scientific literature on this syndrome
Commonly encountered medications and their side effects - what the generalist needs to know
 Commonly encountered medications and their side effects - what the generalist needs to know Jeremy Cosgrove Consultant Neurologist Leeds Teaching Hospitals NHS Trust Outline: Parkinson s medications and
Commonly encountered medications and their side effects - what the generalist needs to know Jeremy Cosgrove Consultant Neurologist Leeds Teaching Hospitals NHS Trust Outline: Parkinson s medications and
Neuroleptic malignant syndrome: A review of the clinical/diagnostic features and report of a case without fever
 GLOBAL JOURNAL OF MEDICINE AND PUBLIC HEALTH Neuroleptic malignant syndrome: A review of the clinical/diagnostic features and report of a case without fever Okwudili Obayi *1, Monday Igwe 1, Christian
GLOBAL JOURNAL OF MEDICINE AND PUBLIC HEALTH Neuroleptic malignant syndrome: A review of the clinical/diagnostic features and report of a case without fever Okwudili Obayi *1, Monday Igwe 1, Christian
What Team Members Other Than Prescribers Need To Know About Antipsychotics
 What Team Members Other Than Prescribers Need To Know About Antipsychotics The Care Transitions Network National Council for Behavioral Health Montefiore Medical Center Northwell Health New York State
What Team Members Other Than Prescribers Need To Know About Antipsychotics The Care Transitions Network National Council for Behavioral Health Montefiore Medical Center Northwell Health New York State
DELIRIUM IN ICU: Prevention and Management. Milind Baldi
 DELIRIUM IN ICU: Prevention and Management Milind Baldi Contents Introduction Risk factors Assessment Prevention Management Introduction Delirium is a syndrome characterized by acute cerebral dysfunction
DELIRIUM IN ICU: Prevention and Management Milind Baldi Contents Introduction Risk factors Assessment Prevention Management Introduction Delirium is a syndrome characterized by acute cerebral dysfunction
ADVERSE REACTIONS
 HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use SYMBYAX safely and effectively. See full prescribing information for SYMBYAX. SYMBYAX (olanzapine
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use SYMBYAX safely and effectively. See full prescribing information for SYMBYAX. SYMBYAX (olanzapine
