Gastro-oesophageal reflux (GOR) is a common problem in infants
|
|
|
- Irene Bishop
- 6 years ago
- Views:
Transcription
1 ORIGINAL STUDY Long-Term Outcome of Laparoscopic Nissen Fundoplication Compared with Laparoscopic Thal Fundoplication in Children A Prospective, Randomized Study Rainer Kubiak, MD, James Andrews, MD, and Hugh W. Grant, MD Background: Laparoscopic fundoplication is increasingly performed in pediatric surgery. Many types of fundoplication are performed, each has advantages and disadvantages. To date there has been no prospective randomized study to determine the optimal laparoscopic technique in children. The aim of the study was to compare the long-term outcomes and control of symptoms after laparoscopic Nissen fundoplication with laparoscopic Thal fundoplication in children. Methods: Between July 1998 and April 2007, 175 patients were recruited to this prospective, randomized study. Patients were assessed before the operation and after defined intervals starting at 3 months after surgery. The absolute outcome measure for fundoplication failure was recurrence of symptoms that merited a redofundoplication or insertion of a transgastric jejunostomy. Relative outcome measures were recurrence of symptoms necessitating reintroduction of antireflux medication (ie, intention to treat ) and postoperative complications (eg, postoperative dysphagia). The median follow-up time was 30 months (range, 1 109). This study has been registered with ClinicalTrials.gov (NCT ). Results: Long-term results were available in 167 patients of which 85 underwent a Nissen and 82 a Thal fundoplication. Four patients in the Nissen group (4.7%) and 12 in the Thal group (14.6%) required a redofundoplication. One child in each group developed recurrence of symptoms and had a transgastric jejunostomy performed. The absolute failure rate was significant lower in the Nissen group (n = 5; 5.9%) compared with the Thal group (n = 13; 15.9%) (P = 0.038). The vast majority of these patients (17 of 18) had underlying neurological disorders. The relative failure rate (ie, intention to treat ) was similar in both groups. Nearly one-quarter of patients developed postoperative dysphagia similarly distributed between both groups. However, severe dysphagia requiring endoscopy +/ dilatation was significantly higher in the Nissen group (n = 10, 11.8%) compared with the Thal group (n = 2; 2.4%) (P = 0.020). One of 31 deaths (0.6%) in this series occurred after surgery, but was not directly related to the fundoplication technique. Conclusions: In the long-term a laparoscopic Nissen fundoplication had a significantly lower recurrence rate than a Thal fundoplication, particularly in patients with underlying neurological disorders. There was no significant difference between the 2 types of fundoplication in normal children. There was no significant difference between the need for restarting antireflux medication between both groups because of recurrence of moderate symptoms. The incidence of postoperative dysphagia was similar in the 2 groups, however, significantly more patients in the Nissen group required intervention for se- From the Department of Paediatric Surgery, John Radcliffe Hospital, Headley Way, Headington, Oxford OX3 9DU, United Kingdom. Parts of the study were presented at the 18th Annual Congress for Endosurgery in Children (IPEG), April 22 to 25, 2009; Phoenix, Arizona. Reprints: Rainer Kubiak, MD, Department of Paediatric Surgery, John Radcliffe Hospital, Headley Way, Headington, Oxford OX3 9DU, United Kingdom. rainerkubiak@hotmail.com. Copyright C 2010 by Lippincott Williams & Wilkins ISSN: /11/ DOI: /SLA.0b013e3181fc98a0 vere dysphagia. Overall the perioperative death rate was low even in high-risk patients. (Ann Surg 2011;253:44 49) Gastro-oesophageal reflux (GOR) is a common problem in infants and children. In normal children, GOR is usually self-limiting. In children with disabilities surgical intervention is more frequent as a result of complications (eg, aspiration pneumonia, apneic spells, severe oesophagitis, ulceration, hematemesis). 1 Laparoscopic fundoplication in children was first reported in ,3 The reported benefits compared with open surgery include less postoperative pain, faster recovery, shorter hospital stay, and better cosmesis. 4 The Nissen fundoplication is the most widely performed procedure. 5 However, it is associated with a high incidence of postoperative dysphagia 6,7 and an appreciable recurrence rate in children with disabilities. 8 This is the first prospective, randomized study comparing longterm outcomes after laparoscopic Nissen fundoplication with laparoscopic Thal fundoplication. The purpose of the study was to answer the question of which fundoplication is the most appropriate in children. METHODS Patients and Demography Between July 1998 and April 2007, 175 patients were recruited into this prospective, randomized study at the Department of Paediatric Surgery, John Radcliffe Hospital, Oxford, United Kingdom. Follow-up data was available for 167 patients. The median followup time was 30 months (range, months). All patients were 21 years or less (median 3.1 years, range ) at the time of surgery. Age and sex distributions at the time of operation were similar in both groups, but weight at the time of operation was significantly lower in the Nissen group (Table 1). One-hundred sixteen patients (69.4%) had a variety of underlying neurological disorders (Table 2), 11 had oesophageal pathologies (eg, congenital diaphragmatic hernia or oesophageal atresia) and 40 were classified as normal children without neurological problems or other significant medical conditions contributing to the GOR. STUDY DESIGN Ethical Approval Ethical approval for the study was obtained from the Oxfordshire Research Ethics Committee in 1998 (No. 04.OXA ) and subsequently renewed in 2004 and Inclusion Criteria Inclusion criteria for entry into the study included proven GOR unresponsive to medical treatment, patients who had failed treatment or who had serious complications (eg, apnea, aspiration pneumonia, 44 Annals of Surgery Volume 253, Number 1, January 2011
2 Annals of Surgery Volume 253, Number 1, January 2011 Long-Term Outcome of Laparoscopic TABLE 1. Demography Total (n = 167) Nissen (n = 85) Thal (n = 82) Statistics Male (n = 94) 45 (52.9%) 49 (59.8%) NS Female (n = 73) 40 (47.1%) 33 (40.2%) NS Mean age (OP) 4.6 yrs. (±4.7) 5.5 yrs. (±4.6) NS 5.1 yrs. (±4.7) Weight (OP) 15.9 kg 14.1 kg (±9.5) 17.8 kg (±12.2) P = (±11.0) OP, at time of operation; yrs, years; kg, kilogram; NS, not significant. TABLE 2. Neurologically Impaired Group Characteristics Underlying Condition n Nissen Thal Severe cerebral palsy associated with prematurity and/or birth asphyxia Cerebral palsy, developmental delay and/or syndrome of unknown origin Angelman syndrome 1 1 Cervical medullary astrocytoma 1 1 Chromosome 18 deletion syndrome 1 1 Congenital cytomegalovirus (CMV) infection Congenital toxoplasmosis 1 1 Cornelia de Lange syndrome 1 1 Down syndrome 1 1 Glutaric aciduria type Idiopathic epileptic encephalopathy Leucodystrophy Lissencephaly 2 2 Mitochondrial disease Muscular dystrophy Emery-Dreifuss 1 1 Myelitis/spinal muscular atrophy (SMA) Pfeiffer syndrome 1 1 Rett syndrome Worster Drought syndrome 1 1 Total oesophagitis, failure to thrive), or those who had a hiatus hernia. Gastro-oesophageal reflux was confirmed by a combination of 24- hour ph monitoring, upper gastrointestinal (UGI) swallow and meal, and/or oesophagogastroduodenoscopy (OGD). Exclusion Criteria Patients were excluded if they had had previous antireflux surgery, previous open abdominal surgery, achalasia, if the parents had a preexisting preference for 1 of the procedures, or if parents declined to participate in the study. Eligible participants were identified before surgery. Parents were offered information about the study design, about GOR, about the different operation techniques and they were given written documentation. On the day of admission, informed consent was obtained from the parents. Patients were randomized to undergo a laparoscopic Nissen fundoplication or a laparoscopic Thal fundoplication. Patient Assessment Patients were assessed before surgery and at 3 months, 6 months, 1 year, 2 years, and 5 years postoperatively. Objective criteria included weight, number of chest infections, number of hospital admissions, frequency and severity of vomiting, and recurrence of symptoms. Outcome Measures The absolute outcome measures of failure (or success) of the fundoplication were whether there was recurrence of symptoms sufficiently severe to justify the need for additional revisional surgery (ie, failure of the original surgery), and early death after surgery directly related to the fundoplication technique. The relative outcome measures were the resumption of symptoms bad enough to necessitate the reintroduction of antireflux medication (but not sufficiently bad to require revisional surgery) that is, intention to treat, and postoperative complications (eg, the incidence of postoperative dysphagia). If symptoms recurred the patient was reinvestigated by a combination of 24-hour ph study, UGI-contrast study, and/or OGD. Operative Techniques All operations were performed or supervised by a single surgeon (H.W.G.) in a standardized operative technique the only variation was in the creation of the wrap. A nasogastric tube was inserted by the anesthetist and the patient was placed in a modified Lloyd-Davies, head-up position with the surgeon at the lower end of the table between the patient s legs. Three or 5-mm instruments were used according to the patient s size. A 5 or 10 mm 30 laparoscope was inserted through a periumbilical port. Further ports were placed in the right and left upper quadrants and the liver was retracted using a Nathanson retractor (Cook Medical Bloomington, Indiana) positioned to the left of the falciform ligament in the epigastrium. Pneumoperitoneum pressure ranged from 8 to 12 mm Hg of CO2 according to size. After retraction of the liver, the zona pellucida of the lesser omentum was divided. There was minimal dissection and mobilization of the oesophageal hiatus. Hiatal repair, if necessary, consisted of approximating both crural pillars posteriorly with nonabsorbable 2/0 Ethibond sutures (Ethicon, Johnson & Johnson Medical GmbH, Norderstedt, Germany). In all children 1 suture was placed between the oesophagus and the apex of the oesophageal hiatus to ensure a section of intra-abdominal oesophagus. The only difference between the 2 techniques was the way the fundoplication was created. For the Nissen fundoplication a window was created behind the oesophagogastric junction. The short gastric vessels were only divided if necessary to achieve a tension-free wrap. One 2/0 Ethibond was placed from the fundus to the oesophagus and 3 to 4 2/0 Ethibond were placed from fundus to fundus to create a 2 to 3 cm long 360 posterior wrap around the lower oesophagus. For the Thal fundoplication 9 no posterior window was required. The fundus was sutured anteriorly to the oesophagus in an inverted U -pattern using 7 to 9 (depending on patient size) 2/0 Ethibond sutures, creating a 270 anterior wrap. When necessary a laparoscopically guided gastrostomy button was inserted at the end of the procedure. Sample Size and Statistical Analysis The primary outcome measure for this study was to evaluate the absolute failure rate of each procedure, expressed as the need for revisional surgery due to the recurrence of severe symptoms. A review of the literature undertaken before this study revealed only a few large studies of laparoscopic fundoplication in children. Two studies 4,10 indicated a reoperation rate of 2.6% to 3.4% after shortterm review. In studies reporting the outcome after open antireflux surgery the rate for revisional surgery was 11.8% in neurologically impaired patients 11 and up to 23% after surgery in early infancy. 12 Because of the extreme variability between studies it was estimated that 90 patients were required in each group to demonstrate a C 2010 Lippincott Williams & Wilkins 45
3 Kubiak et al. Annals of Surgery Volume 253, Number 1, January 2011 TABLE 3. Intraoperative Findings at Revisional Surgery in 16 Patients OP-finding (n = 16) Nissen (n = 4) Thal (n = 12) Wrap partially undone (n = 8) 2 6 Hiatus hernia (n = 7) 2 5 Wrap intact, but ineffective 1 (n = 1) OP, at time of operation. 15% difference (12.5% ±7.5%) in the primary outcome measure at a significance level of P < 0.05 and with a power of 90%. Variables were compared using the 2-tailed Student t test, χ 2 test or Fisher exact test where appropriate. Significance was defined as P value 0.05 or less. Data were expressed as median values (range) or mean (± SD) as stated. The SPSS software version11.5 SPSS Inc., Chicago, Illinois for Windows was used for statistical analysis. RESULTS A total of 175 patients were recruited to the study. Long-term results were available in only 167. Of 167 patients 85 underwent a Nissen fundoplication and 82 a Thal fundoplication. One hundred one children (60.5%) had a laparoscopic-assisted gastrostomy performed at the same time: of these the vast majority had underlying neurological problems (n = 94), 3 had oesophageal atresia repair, 2 had cystic fibrosis, 1 had congenital cardiac disease, and 1 had Goldenhar syndrome. A gastrostomy was simultaneously inserted to improve the poor nutritional status in these patients. Four patients required revisional surgery in the Nissen group and 12 patients in the Thal group. One child in each group had severe recurrence of symptoms but the parents declined revisional surgery. Both children had a transgastric jejunostomy inserted. Consequently, the absolute failure rate was 5 in the Nissen group (5.9%) and 13 in the Thal group (15.9%). The Thal fundoplication group had a significantly higher incidence of absolute failure (P = 0.038). The overall absolute failure rate was 10.8% at a median follow-up of 30 months (range, 1 109). Of the 16 patients requiring revision, only 1 child was neurologically normal, whereas all the others had underlying neurological problems (NP). Of the 40 normal children in the study, 18 had a Nissen, and 22 had a Thal fundoplication. The revisional surgery rate in the normal group was low (2.5%), there was no significant difference between Nissen and Thal. The only normal child who required a redo operation had a recurrent hiatus hernia. The Thal wrap was found to be intact. The intraoperative findings at revisional surgery are shown in Table 3. In the Nissen group failure was due to hiatus hernia in 2 patients and due to an undone wrap in another 2. In the Thal group failure was due to hiatus hernia in 5 patients, undone wrap in 6 patients, and due to ineffective wrap (ie, wrap present, but severe reflux) in 1 patient. The reoperation was performed at a median of 16.5 months (range, 3 90) with the highest incidence (69%) being in the first 2 years after fundoplication (Figure 1). At the time of revisional surgery, if the cause of the failure was a hiatus hernia it was repaired; if the Thal wrap had failed a Nissen was fashioned; if the Nissen had failed it was refashioned as a Nissen. Overall, there was no significant difference in the relative failure outcome: 11 patients in the Nissen group (7 with NP, 4 without NP) and 8 in the Thal group (7 with NP, 1 without NP) developed a recurrence of symptoms that was controlled with antireflux medication, that is, intention to treat (Table 4). TABLE 4. Comparison of Relative Failure Rate, Postoperative Dysphagia and Death after Laparoscopic Nissen and Thal Fundoplication Total (n = 167) Nissen (n = 85) Thal (n = 82) Statistics Relative failure 11 (12.9%) 8 (9.8%) NS ( Intention to treat ) (n = 19) Dysphagia (n = 38) 20 (23.5%) 18 (21.9%) NS Severe Dysphagia 10 (11.8%) 2 (2.4%) P = (requiring Endoscopy) (n = 12) Death (n = 31) 21 (24.7%) 10 (12.2%) P = NS, not significant. Postoperative dysphagia occurred in 20 children after Nissen fundoplication (11 with NP, 9 without NP) compared with 18 after Thal fundoplication (7 with NP, 11 without NP). However, severe dysphagia (meriting OGD +/ dilatation) was significantly more common in the Nissen group (n = 10) compared with 2 in the Thal group (P = 0.020) (Table 4). Looking at subgroups: 6 of 18 (33%) normal children who had a Nissen developed severe dysphagia requiring OGD +/ dilatation compared with 1 of 22 (4.5%) in the Thal group. In the neurologically impaired group 4 of 65 (6.2%) who had a Nissen and 1 of 51 (1.9%) after a Thal had significant dysphagia. There were 31 deaths in this study. Only 1 child died as a direct result of a postoperative complication (displaced gastrostomy). This was in a 6-month-old baby girl who had multiple problems including congenital heart disease. Her gastrostomy fell out 3 days postoperatively and it was replaced into the peritoneal cavity. After feeds she developed peritonitis and septicemia requiring relaparotomy. She developed multiorgan failure, required ECMO and died 6 weeks after surgery. All the other deaths, 20 in the Nissen group and 10 in the Thal group, were related to preexisting comorbidities. Figure 2 illustrates the timing of their deaths in relation to surgery. Overall, 30 of 31 patients who died had an underlying neurological disorder. The remaining child had chronic lung disease due to cystic fibrosis and died from overwhelming pneumonia 6 months after a Thal fundoplication. The cause of death was due to respiratory complications in 29 children, multiorgan failure in 1 (the child who died after the gastrostomy complication), and internal volvulus in 1 (6 years after her original surgery). DISCUSSION Although laparoscopic fundoplication is increasingly performed for the treatment of GOR in children, there is no agreement among surgeons as to what is the best antireflux procedure. This is not surprising as fundoplication is a mechanical solution for what is frequently a functional problem (eg, secondary to underlying neuromuscular dysmotility). To date, there has been no prospective, randomized study comparing different fundoplication techiques in children. Most of the studies only report short-term results, and most of the studies involved multiple surgeons and, in some cases, multiple institutions. To overcome these problems we performed a prospective, randomized, controlled study at a single-center, supervised by a single-surgeon performing a standardized procedure, the only variable was the design of the wrap. The main problem in determining the best procedure is the difficulty in defining what is a successful and what is an 46 C 2010 Lippincott Williams & Wilkins
4 Annals of Surgery Volume 253, Number 1, January 2011 Long-Term Outcome of Laparoscopic FIGURE 1. Timing of revisional surgery after laparoscopic fundoplication in 16 patients. unsuccessful outcome. The problem in defining success after antireflux surgery is problematic particularly when dealing with disabled children who may have multiple comorbidities and who may not be able to communicate effectively. Those children cannot verbalize their pain and discomfort. Their muscle tone may change over time, the control of their epilepsy may vary over time, or they may have a degenerative condition. After fundoplication the cessation of vomiting can be considered a success, but retching may persist, or they may experience dysphagia, difficulty with their secretions, and gas bloat. A number of authors have tried to define outcomes symptom scores, 13,14 need for revisional surgery, 4,10 quality of life, 15 and nutritional outcomes. 16 In this study, we chose the need for revisional surgery due to recurrence of GOR symptoms as the primary outcome measure because it was objective and unequivocal and avoided observer bias. In the original study design it was intended to reinvestigate each child with a contrast meal and swallow and with a 24-hour ph study after fundoplication to prove the postoperative outcome in a more objective manner. This was rejected by the Ethics Committee, as a significant number of asymptomatic children would have been subjected to an unnecessary procedure and radiation. Moreover, it has been recognized that there is a poor correlation between these investigations and recurrence of clinical symptoms after fundoplication. 15 Success after fundoplication is not absolute. There may be an improvement in the degree and frequency of vomiting and parents and patients may be satisfied with this result. In this study recurrence of reflux and vomiting were noted in a number of patients. Their symptoms had generally improved after surgery but they still had some of their original symptoms. Antacid therapies (combination of H2 blocker and/or proton pump inhibitors) were started by either the general practitioner (GP) or surgeon, and these patients subsequently had a resolution of symptoms. It is difficult to know what this means in real terms but the intention to treat suggests that the surgical procedure was not entirely effective. There were 11 patients in the Nissen group (12.9%) and 8 in the Thal group (9.8%). There was no statistically significant difference between the 2 groups. This number is comparable with other studies in which the rate of reintroduction of treatment ranged from 3.7 to 21%. 5,7,16,17 The reason for choosing the Thal fundoplication was because the Thal is a partial wrap, it is widely performed and was reported to be a simple and safe operative treatment for GOR in children with fewer perioperative complications and better long-term outcomes. 18,19 In this study, we observed a significantly higher rate of absolute failure after a Thal fundoplication (15.9%) compared with a laparoscopic Nissen fundoplication (5.9%). At the time of revisional surgery there were 6 pure wrap failures in the Thal group compared with 2 in the Nissen group, 5 hiatus hernias in the Thal group compared with 2 in the Nissen group, and 1 additional functional wrap failure in the Thal group necessitating the need for a second antireflux operation. This increased failure rate could be explained by the fact that it is technically more laborious to perform a laparoscopic Thal fundoplication: in the Thal fundoplication the number of sutures is greater and the oesophageal wall thinner so it is easier to make a technical error in the depth of the stitch, if the suture is too superficial it will pull out. In a Nissen fundoplication there are fewer stitches and they are much deeper (as all the sutures go through the stomach wall, fundus to fundus). We are only aware of 4 large retrospective trials comparing different laparoscopic fundoplication techniques in children. They reported a reoperation rate between 2.5 and 11.1% 5,10,16,20 In 2006 Esposito et al 5 observed no statistical significance in outcome between laparoscopic Nissen, Toupet, and Thal procedures in neurologically normal children. Similarly, Chung et al 10 and Steyart et al 16 reported that the Toupet operation was as good as the Nissen with regard to reflux control. The highest incidence of revisional surgery (11.1%) after laparoscopic fundoplication was reported by Esposito et al 20 in 36 infants. There was no difference in outcome between a variety of fundoplication techniques (Toupet, Nissen-Rossetti, Nissen and Lortat- Jacob). In the latter series 20 the rate of associated anomalies was relatively high (41.6%) suggesting that the recurrence rate after antireflux surgery is generally higher in neurologically impaired children. In this series the majority of patients had an underlying neurological disability (69.4%). Of note, all but one of the absolute failures occurred in this group (ie, 17 of 18 patients). Only 1 normal child required revisional surgery, he had a large hiatus hernia that recurred twice but the Thal wrap was intact. In normal children there was no significant difference in the revisional surgery rate between Nissen (0 of 18) and Thal (1 of 22). In this study there was an excess of children with neurological disorders matched toward the Nissen group (65 versus 51 patients in the Thal group). However, bearing in mind the higher failure rate in the Thal group, the increased number of neurologically impaired children in the Nissen group makes the results even more persuasive in favor of the Nissen fundoplication as an antireflux procedure. The larger number of neurologically impaired children in the Nissen group may also explain the significantly lower weight at the time of operation in the Nissen group as one would expect this group of children to have complications necessitating earlier surgery when compared with otherwise normal children. Van der Zee at al. 19 observed the converse: in their retrospective survey comparing 44 children after open Nissen and Thal fundoplication, they observed a significantly better outcome after the Thal C 2010 Lippincott Williams & Wilkins 47
5 Kubiak et al. Annals of Surgery Volume 253, Number 1, January 2011 FIGURE 2. Timing of death after laparoscopic fundoplication in 31 patients. procedure. In their study, there were more mentally impaired children in the Thal group (38.1% versus 17.4% in the Nissen group). 19 Because of the functional nature of GOR, it is important to follow-up patients long-term. In this series, we noted that there was a progressive failure rate overtime (Figure 1). Although the majority of children underwent revisional surgery within 2 years after the first operation, some patients developed late-onset of recurrence and were reoperated up to 8 years later. If we had reported the results of our study a few years earlier the outcome of our study would have been less significant as the majority of late failures occurred in the Thal group. Dysphagia is a significant side-effect of laparoscopic antireflux surgery. 21 The purpose of a fundoplication is to increase the high pressure zone in the lower oesophagus and hence reduce GOR. To achieve this, the fundoplication applies external pressure to the lower oesophagus and this can partially obstruct or impede ante-grade peristalsis in the lower oesophagus. The etiology of the postoperative dysphagia is multi-factorial the type of wrap, the degree of wrap, the tightness of the wrap, torque of the wrap, apposition of the crura, and postoperative edema. Dysphagia is undoubtedly underreported in all pediatric series. In this series, 38 patients (22.8%) experienced at least 1 episode of postoperative dysphagia. In the majority of cases, this was only a temporary problem and the symptoms resolved with time. This phenomenon has been described in the literature. 5,10,15 Mathei et al. 15 suggested that postoperative edema around the lower oesophagus subsequently settles. In our study 10 of 20 patients in the Nissen group experienced sufficiently severe dysphagia that required OGD +/ dilatation compared with 2 of 18 in the Thal group. Of note, severe dysphagia was more often recognized in normal children than in children with other significant neurological disorders. We suspect that neurologically handicapped children experience this side-effect as commonly but cannot communicate the symptoms. Many authors observed a higher rate of dysphagia after a laparoscopic Nissen operation in adults when compared with other fundoplication techniques. 6,7,14,17 Most of the pediatric group of patients cannot verbalize this symptom so the results in children are less conclusive. Chung et al 10 reported a slightly higher rate of dysphagia after a laparoscopic Toupet operation (2.3%) compared with 1.1% after a Nissen procedure, whereas Steyaert et al 16 did not state a significant difference between the Nissen and Toupet techniques in their study with an overall postoperative dysphagia rate of 4.4%. Finally Esposito et al 5 observed a trend, although not statistically significant, toward a higher rate of dysphagia after a laparoscopic Nissen. There are a number of possible reasons why the Nissen fundoplication resulted in more severe and persistent dysphagia in this series. A Nissen fundoplication is a complete 360 wrap, so it is more obstructive than a Thal (which is a partial, 270, anterior wrap). In a Nissen fundoplication, the posterior wrap displaces the oesophagus anteriorly just above the gastrooesophageal junction and causes displacement forwards this does not occur in a Thal fundoplication. There may also be a degree of torque in a Nissen if the fundus is not adequately mobilized this maneuver is not performed in a Thal fundoplication. It is possible to fashion too tight in a Nissen fundoplication this never happens with partial wraps. If there is postoperative edema, it could have more impact when the wrap is circumferential. The long-term cumulative death rate of 18.6% over 9 years was in accordance with the natural history of the underlying medical conditions. 22 Many had life-limiting conditions and all but 2 succumbed to respiratory complications. The excess death rate noted after the Nissen procedure (Figure 2) related to the higher incidence of neurological disability in this group rather than the nature the fundoplication. CONCLUSIONS Overall, in the long-term a laparoscopic Nissen fundoplication had a significantly lower recurrence rate than a Thal fundoplication. In normal patients, there was a low rate of revisional surgery (2.5%) and there was no significant difference between Nissen and Thal. Nissen fundoplication was associated with significantly more severe dysphagia. In normal children our recommendation would be to perform a Thal fundoplication for refractory GOR. In the neurologically impaired group (NP) Nissen fundoplication had a significantly lower recurrence rate than a Thal fundoplication. Our recommendation would be to perform a Nissen fundoplication unless there was evidence of preexisting swallowing problems. In these children a Thal fundoplication might be wiser but the parents should have been counseled about the higher failure rate. The relative failure rate (ie, intention to treat ) was similar after Nissen and Thal fundoplication. Overall the perioperative death rate was low (0.6%), even in high-risk patients. REFERENCES 1. Oldham K, Massey M. Antireflux surgery. In: M Stringer, ed. Pediatric Surgery and Urology: Long Term Outcomes. Philadelphia, PA: Saunders; 1998: Georgeson KE. Laparoscopic gastrostomy and fundoplication. Paediatr Ann. 1993;92: Lobe TE, Schropp KP, Lunsford K. Laparoscopic Nissen fundoplication in childhood. J Pediatr Surg. 1993;28: Rothenberg SS. Experience with 220 consecutive laparoscopic Nissen fundoplications in infants and children. J Pediatr Surg. 1998;33: C 2010 Lippincott Williams & Wilkins
6 Annals of Surgery Volume 253, Number 1, January 2011 Long-Term Outcome of Laparoscopic 5. Esposito C, Montupet P, van der Zee D, et al. Long-term outcome of laparoscopic Nissen, Toupet, and Thal antireflux procedures for neurologically normal children with gastroesophageal reflux disease.surg Endosc. 2006;20: Fernando HC, Luketich JD, Christie NA, et al. Outcomes of laparoscopic Toupet compared to laparoscopic Nissen fundoplication. Surg Endosc. 2002;6: Strate U, Emmermann A, Fibbe C, et al. Laparoscopic fundoplication: Nissen versus Toupet two-year outcome of a prospective randomized study of 200 patients regarding preoperative esophageal mobility. Surg Endosc. 2008;22: Smith CD, Biemann Othersen H, Gogan HJ, et al. Nissen fundoplication in children with profound neurologic disability. Ann Surg. 1992;214: Thal AP. A unified approach to surgical problems of the esophagogastric junction. Ann Surg. 1968;168: Chung DH, Georgeson KE. Fundoplication and gastrostomy. Semin Pediatr Surg. 1998;7: Fonkalsrud EW, Aschraft KW, Coran AG, et al. Surgical treatment of gastroesophageal reflux in children: a combined hospital study of 7,467 patients. Pediatrics. 1998;101: Kubiak R, Spitz L, Kiely EM, et al. Effectiveness of fundoplication in early infancy. J Pediatr Surg. 1999;34: Crhysos E, Tzortzinis A, Tsiaoussis J, et al. Prospective randomized trial comparing Nissen to Nissen-Rossetti technique for laparoscopic fundoplication. Am J Surg. 2001;182: Ludemann R, Watson DI, Jamieson GG, et al. Five years follow-up of a randomized clinical trial of laparoscopic total versus anterior 180 fundoplication. Br J Surg. 2005;92: Mathei J, Coosemans W, Nafteux P, et al. Laparoscopic Nissen fundoplication in infants and children: analysis of 106 consecutive patients with special emphasis in neurologically impaired vs. neurologically normal patients. Surg Endosc. 2008;22: Steyaert H, Al Mohaidly M, Lembo MA, et al. Long-term outcome of laparoscopic Nissen and Toupet fundoplication in normal and neurologically impaired children. Surg Endosc. 2003;17: Zaninotto G, Molena D, Ancona E, et al. A prospective multicenter study on laparoscopic treatment of gastroesophageal reflux disease in Italy. Surg Endosc. 2000;14: Ashcraft KW, Goodwin CD, Amoury RW, et al. Thal fundoplication: a simple and safe operative treatment for gastroesophageal reflux. J Pediatr Surg. 1978;13: Van der Zee DC, Rövekamp MH, Pull ter Gunne AJ, et al. Surgical treatment of reflux esophagitis: Nissen versus Thal procedure. Pediatr Surg Int. 1994;9: Esposito C, Montupet P, Reinberg O. Laparoscopic surgery for gastroesophageal reflux disease during the first year of life. J Pediatr Surg. 2001;36: Pimpalwar A, Najmaldin A. Results of laparoscopic antireflux procedures in neurologically impaired children. Semin Laparosc Surg. 2002;9: Esposito C, van der Zee DC, Settimi A, et al. Risks and benefits of surgical management of gastroesophageal reflux in neurologically impaired children. Surg Endosc. 2003;17: C 2010 Lippincott Williams & Wilkins 49
Unilateral Versus Bilateral Wrap Crural Fixation in Laparoscopic Nissen Fundoplication for Children
 SCIENTIFIC PAPER Unilateral Versus Bilateral Wrap Crural Fixation in Laparoscopic Nissen Fundoplication for Children Mohamed E. Hassan, MD, PhD, FEBPS ABSTRACT Introduction: Gastroesophageal reflux (GERD)
SCIENTIFIC PAPER Unilateral Versus Bilateral Wrap Crural Fixation in Laparoscopic Nissen Fundoplication for Children Mohamed E. Hassan, MD, PhD, FEBPS ABSTRACT Introduction: Gastroesophageal reflux (GERD)
Laparoscopic or Endoscopic Gastrostomy in Children: Comparison of Two Methods. H. STEYAERT, L. CARFAGNA, M.A. LEMBO, E. TREVINO, and J.S.
 Pediatric Endosurgery & Innovative Techniques Volume 7, Number 2, 2003 Mary Ann Liebert, Inc. Laparoscopic or Endoscopic Gastrostomy in Children: Comparison of Two Methods H. STEYAERT, L. CARFAGNA, M.A.
Pediatric Endosurgery & Innovative Techniques Volume 7, Number 2, 2003 Mary Ann Liebert, Inc. Laparoscopic or Endoscopic Gastrostomy in Children: Comparison of Two Methods H. STEYAERT, L. CARFAGNA, M.A.
ORIGINAL PAPER. Mesh hiatal reinforcement in laparoscopic Nissen fundoplication for neurologically impaired children is safe and feasible
 Nagoya J. Med. Sci. 79. 427 ~ 433, 2017 doi:10.18999/nagjms.79.4.427 ORIGINAL PAPER Mesh hiatal reinforcement in laparoscopic Nissen fundoplication for neurologically impaired children is safe and feasible
Nagoya J. Med. Sci. 79. 427 ~ 433, 2017 doi:10.18999/nagjms.79.4.427 ORIGINAL PAPER Mesh hiatal reinforcement in laparoscopic Nissen fundoplication for neurologically impaired children is safe and feasible
Combined Experience of Two European Centers
 Minimally Invasive Surgery for Achalasia: Combined Experience of Two European Centers Garzi A, Valla JS*, Molinaro F, Amato G, Messina M. Unit of Pediatric Surgery, University of Siena (Italy) *Lenval
Minimally Invasive Surgery for Achalasia: Combined Experience of Two European Centers Garzi A, Valla JS*, Molinaro F, Amato G, Messina M. Unit of Pediatric Surgery, University of Siena (Italy) *Lenval
Gastrointestinal problems in individuals with CdLS. Peter Gillett Consultant Gastroenterologist RHSC Edinburgh UK Cork 2011
 Gastrointestinal problems in individuals with CdLS Peter Gillett Consultant Gastroenterologist RHSC Edinburgh UK Cork 2011 Major problems Gastro-oesophageal reflux and GORD Swallowing problems and
Gastrointestinal problems in individuals with CdLS Peter Gillett Consultant Gastroenterologist RHSC Edinburgh UK Cork 2011 Major problems Gastro-oesophageal reflux and GORD Swallowing problems and
Nissen fundoplication and gastrostomy in severely neurologically impaired children with gastroesophageal reflux!"#$%&'()*+,-./012&3456!
 Key words: Child; Fundoplication; Gastroesophageal reflux; Mental retardation; Recurrence!!"#!"#!" KM Cheung HW Tse PWT Tse KH Chan Hong Kong Med J 2006;12:282-8 Caritas Medical Centre, 111 Wing Hong Street,
Key words: Child; Fundoplication; Gastroesophageal reflux; Mental retardation; Recurrence!!"#!"#!" KM Cheung HW Tse PWT Tse KH Chan Hong Kong Med J 2006;12:282-8 Caritas Medical Centre, 111 Wing Hong Street,
PAPER. Toupét Fundoplication for Gastroesophageal Reflux in Childhood
 Toupét Fundoplication for Gastroesophageal Reflux in Childhood Thomas R. Weber, MD PAPER Hypothesis: Gastroesophageal reflux (GER) is a common condition in childhood that frequently requires operative
Toupét Fundoplication for Gastroesophageal Reflux in Childhood Thomas R. Weber, MD PAPER Hypothesis: Gastroesophageal reflux (GER) is a common condition in childhood that frequently requires operative
The impact of fibrin glue in the prevention of failure after Nissen fundoplication
 Scandinavian Journal of Surgery 100: 181 18, 011 The impact of fibrin glue in the prevention of failure after Nissen fundoplication T. Rantanen 1,, P. Neuvonen 1, M. Iivonen 1, 3, T. Tomminen 1, N. Oksala
Scandinavian Journal of Surgery 100: 181 18, 011 The impact of fibrin glue in the prevention of failure after Nissen fundoplication T. Rantanen 1,, P. Neuvonen 1, M. Iivonen 1, 3, T. Tomminen 1, N. Oksala
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic insertion of a magnetic titanium ring for gastrooesophageal reflux
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of laparoscopic insertion of a magnetic titanium ring for gastrooesophageal reflux
Combined Collis-Nissen Reconstruction. of the esophagogastric junction at. Mark B. Orringer, M.D., and Herbert Sloan, M.D.
 Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
Combined Collis-Nissen Reconstruction of the Esophagogastric Junction Mark B. Orringer, M.D., and Herbert Sloan, M.D. ABSTRACT Recent reports have indicated that combined Collis-Belsey reconstruction of
Laporoscopic Fundoplication: Not a simple wrap
 BJMP 2009:2(2) 25-29 Original Article Laporoscopic Fundoplication: Not a simple wrap Riaz AA, Kosmoliaptsis V and Meyrick-Thomas J Abstract Introduction Laparoscopic fundoplication (LF) has been emerging
BJMP 2009:2(2) 25-29 Original Article Laporoscopic Fundoplication: Not a simple wrap Riaz AA, Kosmoliaptsis V and Meyrick-Thomas J Abstract Introduction Laparoscopic fundoplication (LF) has been emerging
Clinical Study Management of Gastroesophageal Reflux Disease: A Review of Medical and Surgical Management
 Hindawi Publishing Corporation Minimally Invasive Surgery Volume 2014, Article ID 654607, 5 pages http://dx.doi.org/10.1155/2014/654607 Clinical Study Management of Gastroesophageal Reflux Disease: A Review
Hindawi Publishing Corporation Minimally Invasive Surgery Volume 2014, Article ID 654607, 5 pages http://dx.doi.org/10.1155/2014/654607 Clinical Study Management of Gastroesophageal Reflux Disease: A Review
Role of laparoscopic antireflux surgery in the management of chronic GERD symptoms
 MINI-REVIEW Role of laparoscopic antireflux surgery in the management of chronic GERD symptoms M Anvari. Role of laparoscopic antireflux surgery in the management of chronic GERD symptoms. Can J Gastroenterol
MINI-REVIEW Role of laparoscopic antireflux surgery in the management of chronic GERD symptoms M Anvari. Role of laparoscopic antireflux surgery in the management of chronic GERD symptoms. Can J Gastroenterol
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL. September 17, Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous
 Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Minimal vs extensive esophageal mobilization during laparoscopic fundoplication: a prospective randomized trial
 Journal of Pediatric Surgery (2011) 46, 163 168 www.elsevier.com/locate/jpedsurg Minimal vs extensive during laparoscopic fundoplication: a prospective randomized trial Shawn D. St. Peter a,, Douglas C.
Journal of Pediatric Surgery (2011) 46, 163 168 www.elsevier.com/locate/jpedsurg Minimal vs extensive during laparoscopic fundoplication: a prospective randomized trial Shawn D. St. Peter a,, Douglas C.
Traditionally, surgical antireflux therapy has been
 Laparoscopic Fundoplication Mary Maish, MD and Jeffrey A. Hagen, MD Traditionally, surgical antireflux therapy has been reserved for patients with complicated gastroesophageal reflux disease. The introduction
Laparoscopic Fundoplication Mary Maish, MD and Jeffrey A. Hagen, MD Traditionally, surgical antireflux therapy has been reserved for patients with complicated gastroesophageal reflux disease. The introduction
Hiatal Hernias and Barrett s esophagus. Dr Sajida Ahad Mercy General Surgery
 Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
Symptomatic outcome following laparoscopic anterior 180 partial fundoplication: Our initial experience
 International Journal of Medicine and Medical Sciences Vol. 2(4), pp. 128-132, April 2010 Available online http://www.academicjournals.org/ijmms ISSN 2006-9723 2010 Academic Journals Full Length Research
International Journal of Medicine and Medical Sciences Vol. 2(4), pp. 128-132, April 2010 Available online http://www.academicjournals.org/ijmms ISSN 2006-9723 2010 Academic Journals Full Length Research
Achalasia is a primary esophageal motility disorder of unknown
 Laparoscopic Heller Myotomy for Achalasia Andrew Pierre, MD, MSc Achalasia is a primary esophageal motility disorder of unknown etiology. Pathologically, it is characterized by loss of ganglion cells in
Laparoscopic Heller Myotomy for Achalasia Andrew Pierre, MD, MSc Achalasia is a primary esophageal motility disorder of unknown etiology. Pathologically, it is characterized by loss of ganglion cells in
Gastroesophageal reflux disease (GERD) is the most common
 Laparoscopic Nissen Fundoplication Swee H. Teh, MD, FRCSI, FACS, John G. Hunter, MD, FACS Gastroesophageal reflux disease (GERD) is the most common disorder of the esophagus and gastroesophageal junction,
Laparoscopic Nissen Fundoplication Swee H. Teh, MD, FRCSI, FACS, John G. Hunter, MD, FACS Gastroesophageal reflux disease (GERD) is the most common disorder of the esophagus and gastroesophageal junction,
Gastroesophageal Reflux Disease, Paraesophageal Hernias &
 530.81 553.3 & 530.00 43289, 43659 1043432842, MD Assistant Clinical Professor of Surgery, UH JABSOM Associate General Surgery Program Director Director of Minimally Invasive & Bariatric Surgery Programs
530.81 553.3 & 530.00 43289, 43659 1043432842, MD Assistant Clinical Professor of Surgery, UH JABSOM Associate General Surgery Program Director Director of Minimally Invasive & Bariatric Surgery Programs
Clinical Study Hiatus Hernia Repair with Bilateral Oesophageal Fixation
 Surgery Research and Practice Volume 2015, Article ID 693138, 5 pages http://dx.doi.org/10.1155/2015/693138 Clinical Study Hiatus Hernia Repair with Bilateral Oesophageal Fixation Rajith Mendis, 1 Caran
Surgery Research and Practice Volume 2015, Article ID 693138, 5 pages http://dx.doi.org/10.1155/2015/693138 Clinical Study Hiatus Hernia Repair with Bilateral Oesophageal Fixation Rajith Mendis, 1 Caran
Clinical Study Congenital Paraesophageal Hernia with Intrathoracic Gastric Volvolus in Two Sisters
 International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 856568, 5 pages doi:10.5402/2011/856568 Clinical Study Congenital Paraesophageal Hernia with Intrathoracic Gastric Volvolus
International Scholarly Research Network ISRN Surgery Volume 2011, Article ID 856568, 5 pages doi:10.5402/2011/856568 Clinical Study Congenital Paraesophageal Hernia with Intrathoracic Gastric Volvolus
Nissen Fundoplication
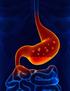 Nissen Fundoplication By Donna Weldon Nissen fundoplication is a surgical procedure used to treat gastroesophageal reflux disease, or GERD, and hiatus hernias. For GERD, is it usually performed when medical
Nissen Fundoplication By Donna Weldon Nissen fundoplication is a surgical procedure used to treat gastroesophageal reflux disease, or GERD, and hiatus hernias. For GERD, is it usually performed when medical
Laparoscopic Nissen Fundoplication in Children: An Initial Experience
 Annals of Pediatric Surgery, Vol 1, No 1, October 2005: PP 10-16 Original Article Laparoscopic Nissen Fundoplication in Children: An Initial Experience Ashraf A. Kabesh *, Fatma Al-Zahraa Abd Al-Bassit
Annals of Pediatric Surgery, Vol 1, No 1, October 2005: PP 10-16 Original Article Laparoscopic Nissen Fundoplication in Children: An Initial Experience Ashraf A. Kabesh *, Fatma Al-Zahraa Abd Al-Bassit
Minimally Invasive Esophagectomy- Valuable. Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006
 Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
Minimally Invasive Esophagectomy- Valuable Jayer Chung, MD University of Colorado Health Sciences Center December 11, 2006 Overview Esophageal carcinoma What is minimally invasive esophagectomy (MIE)?
GASTRO-OESOPHAGEAL REFLUX DR RONALDA DELACY
 GASTRO-OESOPHAGEAL REFLUX DR RONALDA DELACY DEFINITIONS GERD -Involuntary, effortless passage of gastric contents into the oesophagus +/-ejected from the mouth resulting in troublesome symptoms or complications
GASTRO-OESOPHAGEAL REFLUX DR RONALDA DELACY DEFINITIONS GERD -Involuntary, effortless passage of gastric contents into the oesophagus +/-ejected from the mouth resulting in troublesome symptoms or complications
Information leaflet for parents/carers. Fundoplication
 Information leaflet for parents/carers Fundoplication Introduction Your child has gastro oesophageal reflux disease (GORD), which is where acid from the stomach leaks up into the oesophagus (gullet). It
Information leaflet for parents/carers Fundoplication Introduction Your child has gastro oesophageal reflux disease (GORD), which is where acid from the stomach leaks up into the oesophagus (gullet). It
The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control
 ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
ORIGINAL ARTICLES The Combined Collis-Nissen Operation: Early Assessment of Reflwx Control Mark B. Orringer, M.D., and Jay S. Orringer, M.D. ABSTRACT This report summarizes the clinical experience with
POSTOPERATIVE CONGENITAL ESOPHAGEAL ATRESIA COMPLICATIONS: A REVIEW
 CHILDREN S HOSPITAL II POSTOPERATIVE CONGENITAL ESOPHAGEAL ATRESIA COMPLICATIONS: A REVIEW Dr. Nguyen Thuy Hanh Ngan Neonatal Department CONTENTS 1. Background 2. Classification 3. Management 4. Complications
CHILDREN S HOSPITAL II POSTOPERATIVE CONGENITAL ESOPHAGEAL ATRESIA COMPLICATIONS: A REVIEW Dr. Nguyen Thuy Hanh Ngan Neonatal Department CONTENTS 1. Background 2. Classification 3. Management 4. Complications
ORIGINAL ARTICLE. Myriam J. Curet, MD, FACS; Robert K. Josloff, MD; Othmar Schoeb, MD; Karl A. Zucker, MD
 ORIGINAL ARTICLE Laparoscopic Reoperation for Failed Antireflux Procedures Myriam J. Curet, MD, FACS; Robert K. Josloff, MD; Othmar Schoeb, MD; Karl A. Zucker, MD Background: Laparoscopic fundoplication
ORIGINAL ARTICLE Laparoscopic Reoperation for Failed Antireflux Procedures Myriam J. Curet, MD, FACS; Robert K. Josloff, MD; Othmar Schoeb, MD; Karl A. Zucker, MD Background: Laparoscopic fundoplication
Paraoesophageal Hernia
 Paraoesophageal Hernia Grand Round Adam Cichowitz Surgical Registrar Paraoesophageal Hernia Type of hiatal hernia Transdiaphragmatic migration of abdominal content gastric fundus gastric body pylorus colon
Paraoesophageal Hernia Grand Round Adam Cichowitz Surgical Registrar Paraoesophageal Hernia Type of hiatal hernia Transdiaphragmatic migration of abdominal content gastric fundus gastric body pylorus colon
Gastro-oesophageal reflux related cough and its response to laparoscopic fundoplication
 Thorax 1998;53:963 968 963 Departments of Medicine and Surgery, McMaster University, St Joseph s Hospital, Hamilton, Ontario, Canada L8N 4A6 C J Allen M Anvari Correspondence to: Dr C Allen. Received 10
Thorax 1998;53:963 968 963 Departments of Medicine and Surgery, McMaster University, St Joseph s Hospital, Hamilton, Ontario, Canada L8N 4A6 C J Allen M Anvari Correspondence to: Dr C Allen. Received 10
Minimally Invasive Esophagectomy
 Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
Minimally Invasive Esophagectomy M A R K B E R R Y, M D A S S O C I AT E P R O F E S S O R D E PA R T M E N T OF C A R D I O T H O R A C I C S U R G E R Y S TA N F O R D U N I V E R S I T Y S E P T E M
PeriOperative Concerns for Anti Reflux Procedure Patients
 PeriOperative Concerns for Anti Reflux Procedure Patients Kevin Gillian, M.D., F.A.C.S. VHC Heartburn Center Director GERD word association Heartburn Chest pain Spicy food Tums Purple pills How big a problem
PeriOperative Concerns for Anti Reflux Procedure Patients Kevin Gillian, M.D., F.A.C.S. VHC Heartburn Center Director GERD word association Heartburn Chest pain Spicy food Tums Purple pills How big a problem
SURGERY LAPAROSCOPIC ANTI-REFLUX (GORD) SURGERY
 LAPAROSCOPIC ANTI-REFLUX (GORD) If you suffer from heartburn, your surgeon may have recommended Laparoscopic Anti-reflux Surgery to treat this condition, technically referred to as Gastro-oesophageal Reflux
LAPAROSCOPIC ANTI-REFLUX (GORD) If you suffer from heartburn, your surgeon may have recommended Laparoscopic Anti-reflux Surgery to treat this condition, technically referred to as Gastro-oesophageal Reflux
Acquired pediatric esophageal diseases Imaging approaches and findings. M. Mearadji International Foundation for Pediatric Imaging Aid
 Acquired pediatric esophageal diseases Imaging approaches and findings M. Mearadji International Foundation for Pediatric Imaging Aid Acquired pediatric esophageal diseases The clinical signs of acquired
Acquired pediatric esophageal diseases Imaging approaches and findings M. Mearadji International Foundation for Pediatric Imaging Aid Acquired pediatric esophageal diseases The clinical signs of acquired
Paraesophageal Hernia
 Paraesophageal Hernia Inderpal (Netu) S. Sarkaria, M.D. Vice Chairman, Clinical Affairs Director, Robotic Thoracic Surgery Co-Director, Esophageal and Lung Surgery Institute Speaker/Education: Intuitive
Paraesophageal Hernia Inderpal (Netu) S. Sarkaria, M.D. Vice Chairman, Clinical Affairs Director, Robotic Thoracic Surgery Co-Director, Esophageal and Lung Surgery Institute Speaker/Education: Intuitive
2 Paraesophageal Hiatus Hernia
 2 Paraesophageal Hiatus Hernia Luigi Bonavina Pearls and Pitfalls Paraesophageal (type II) hiatus hernia represents a distinct anatomic and clinic entity requiring a unique therapeutic strategy, and is
2 Paraesophageal Hiatus Hernia Luigi Bonavina Pearls and Pitfalls Paraesophageal (type II) hiatus hernia represents a distinct anatomic and clinic entity requiring a unique therapeutic strategy, and is
Medical Policy Manual. Topic: Gastric Reflux Surgery Date of Origin: November Section: Surgery Last Reviewed Date: March 2014
 Medical Policy Manual Topic: Gastric Reflux Surgery Date of Origin: November 2012 Section: Surgery Last Reviewed Date: March 2014 Policy No: 186 Effective Date: May 1, 2014 IMPORTANT REMINDER Medical Policies
Medical Policy Manual Topic: Gastric Reflux Surgery Date of Origin: November 2012 Section: Surgery Last Reviewed Date: March 2014 Policy No: 186 Effective Date: May 1, 2014 IMPORTANT REMINDER Medical Policies
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)?
 WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
Laparoscopic Nissen fundoplication consecutive cases
 Gut 1996; 38: 487-491 487 Laparoscopic Nissen fundoplication - 200 consecutive cases University of Queensland Department of Surgery, Princess Alexandra Hospital, Queensland, Australia D C Gotley B M Smithers
Gut 1996; 38: 487-491 487 Laparoscopic Nissen fundoplication - 200 consecutive cases University of Queensland Department of Surgery, Princess Alexandra Hospital, Queensland, Australia D C Gotley B M Smithers
Interventional procedures guidance Published: 16 December 2015 nice.org.uk/guidance/ipg540
 Electrical stimulation of the lower oesophageal sphincter for treating gastro-oesophageal reflux disease Interventional procedures guidance Published: 16 December 2015 nice.org.uk/guidance/ipg540 Your
Electrical stimulation of the lower oesophageal sphincter for treating gastro-oesophageal reflux disease Interventional procedures guidance Published: 16 December 2015 nice.org.uk/guidance/ipg540 Your
Oesophageal Disorders
 Oesophageal Disorders Anatomy Upper sphincter Oesophageal body Diaphragm Lower sphincter Gastric Cardia Symptoms Of Oesophageal Disorders Dysphagia Odynophagia Heartburn Atypical Chest Pain Regurgitation
Oesophageal Disorders Anatomy Upper sphincter Oesophageal body Diaphragm Lower sphincter Gastric Cardia Symptoms Of Oesophageal Disorders Dysphagia Odynophagia Heartburn Atypical Chest Pain Regurgitation
Post-Prandial Trouble! KPA 2017 Nutrition pre-congress case Presentation Dr. Esther Kimani. Facilitator- Dr. A. Laving. 25/04/2017
 Post-Prandial Trouble! KPA 2017 Nutrition pre-congress case Presentation Dr. Esther Kimani. Facilitator- Dr. A. Laving. 25/04/2017 Biodata. Name- I.M.M. Age-6 years Gender- female Referred to the Paediatric
Post-Prandial Trouble! KPA 2017 Nutrition pre-congress case Presentation Dr. Esther Kimani. Facilitator- Dr. A. Laving. 25/04/2017 Biodata. Name- I.M.M. Age-6 years Gender- female Referred to the Paediatric
Congenital hiatus hernia: A case series. Department of Pediatric Surgery, Afyon Kocatepe University Faculty of Medicine, Afyonkarahisar, Turkey
 Orıgınal Article PEDIATRIC SURGERY North Clin Istanb 2018 doi: 10.14744/nci.2017.58672 UNCORRECTED PROOF Congenital hiatus hernia: A case series Didem Baskin Embleton, 1 Ahmet Ali Tuncer, 1 Mehmet Surhan
Orıgınal Article PEDIATRIC SURGERY North Clin Istanb 2018 doi: 10.14744/nci.2017.58672 UNCORRECTED PROOF Congenital hiatus hernia: A case series Didem Baskin Embleton, 1 Ahmet Ali Tuncer, 1 Mehmet Surhan
Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES
 SAGES Society of American Gastrointestinal and Endoscopic Surgeons https://www.sages.org Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Author : SAGES Webmaster Surgery for Heartburn
SAGES Society of American Gastrointestinal and Endoscopic Surgeons https://www.sages.org Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Author : SAGES Webmaster Surgery for Heartburn
Nissen Hiatal Hernia Rep& Problems of Recurrence &d. Continued Symptoms. R. D. Henderson, M.B.
 Nissen Hiatal Hernia Rep& Problems of Recurrence &d R. D. Henderson, M.B. Continued Symptoms ABSTRACT The standard Nissen operation is the most effective method of reflux control. However, the procedure
Nissen Hiatal Hernia Rep& Problems of Recurrence &d R. D. Henderson, M.B. Continued Symptoms ABSTRACT The standard Nissen operation is the most effective method of reflux control. However, the procedure
ORIGINAL ARTICLE. Laparoscopic Nissen Fundoplication With Prosthetic Hiatal Closure Reduces Postoperative Intrathoracic Wrap Herniation
 ORIGINAL ARTICLE Laparoscopic Nissen Fundoplication With Prosthetic Hiatal Closure Reduces Postoperative Intrathoracic Wrap Herniation Preliminary Results of a Prospective Randomized Functional and Clinical
ORIGINAL ARTICLE Laparoscopic Nissen Fundoplication With Prosthetic Hiatal Closure Reduces Postoperative Intrathoracic Wrap Herniation Preliminary Results of a Prospective Randomized Functional and Clinical
Persistence of a Gastrocutaneous Fistula after gastrostomy removal in children: Incidence and predictive factors
 Persistence of a Gastrocutaneous Fistula after gastrostomy removal in children: Incidence and predictive factors by Anne-Sophie MASSY et Olivier REINBERG* Department of Pediatric Surgery, University Hospital
Persistence of a Gastrocutaneous Fistula after gastrostomy removal in children: Incidence and predictive factors by Anne-Sophie MASSY et Olivier REINBERG* Department of Pediatric Surgery, University Hospital
ORIGINAL ARTICLE. Laparoscopic Refundoplication With Prosthetic Hiatal Closure for Recurrent Hiatal Hernia After Primary Failed Antireflux Surgery
 ORIGINL RTICLE Laparoscopic Refundoplication With Prosthetic Hiatal Closure for Recurrent Hiatal Hernia fter Primary Failed ntireflux Surgery Frank. Granderath, MD; Thomas Kamolz, PhD; Ursula M. Schweiger,
ORIGINL RTICLE Laparoscopic Refundoplication With Prosthetic Hiatal Closure for Recurrent Hiatal Hernia fter Primary Failed ntireflux Surgery Frank. Granderath, MD; Thomas Kamolz, PhD; Ursula M. Schweiger,
Mehmet Melek 1 and Ufuk Cobanoglu Introduction. 2. Material and Method
 Gastroenterology Research and Practice Volume 2011, Article ID 527323, 4 pages doi:10.1155/2011/527323 Methodology Report A New Technique in Primary Repair of Congenital Esophageal Atresia Preventing Anastomotic
Gastroenterology Research and Practice Volume 2011, Article ID 527323, 4 pages doi:10.1155/2011/527323 Methodology Report A New Technique in Primary Repair of Congenital Esophageal Atresia Preventing Anastomotic
MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER AUGMENTATION FOR THE TREATMENT OF GASTROESOPHAGEAL REFLUX DISEASE (GERD)
 MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial
MEDICAL POLICY SUBJECT: MAGNETIC ESOPHAGEAL RING/ MAGNETIC SPHINCTER PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria do not apply. If a commercial
Anatomical failure following laparoscopic antireflux surgery (LARS); does it really matter?
 The Royal College of Surgeons of England GASTROINTESTINAL SURGERY doi 10.1308/003588410X12518836440126 Anatomical failure following laparoscopic antireflux surgery (LARS); does it really matter? N DUNNE
The Royal College of Surgeons of England GASTROINTESTINAL SURGERY doi 10.1308/003588410X12518836440126 Anatomical failure following laparoscopic antireflux surgery (LARS); does it really matter? N DUNNE
Back to Basics: What Imaging Test should I order? Jeanne G. Hill, M.D. Pediatric Radiology Medical University of South Carolina
 Back to Basics: What Imaging Test should I order? Jeanne G. Hill, M.D. Pediatric Radiology Medical University of South Carolina Disclosure Neither I nor any member of my immediate family has a relevant
Back to Basics: What Imaging Test should I order? Jeanne G. Hill, M.D. Pediatric Radiology Medical University of South Carolina Disclosure Neither I nor any member of my immediate family has a relevant
Technical Guidance for Surgical Workload Audit and Research Database: Anti Reflux Surgery V1.0
 Technical Guidance for Surgical Workload Audit and Research Database: Anti Reflux Surgery V1.0 Contents 1. The Indicators... 3 1.1. Activity Volume... 3 3.2. Average Length of Stay (Days)... 3 3.3. 2/7/30
Technical Guidance for Surgical Workload Audit and Research Database: Anti Reflux Surgery V1.0 Contents 1. The Indicators... 3 1.1. Activity Volume... 3 3.2. Average Length of Stay (Days)... 3 3.3. 2/7/30
PAPER. Is the Use of a Bougie Necessary for Laparoscopic Nissen Fundoplication?
 PAPER Is the Use of a Bougie Necessary for Laparoscopic Nissen Fundoplication? Yuri W. Novitsky, MD; Kent W. Kercher, MD; Mark P. Callery, MD; Donald R. Czerniach, MD; John J. Kelly, MD; Demetrius E. M.
PAPER Is the Use of a Bougie Necessary for Laparoscopic Nissen Fundoplication? Yuri W. Novitsky, MD; Kent W. Kercher, MD; Mark P. Callery, MD; Donald R. Czerniach, MD; John J. Kelly, MD; Demetrius E. M.
Early View Article: Online published version of an accepted article before publication in the final form.
 Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title:
Early View Article: Online published version of an accepted article before publication in the final form. Journal Name: Journal of Case Reports and Images in Surgery Type of Article: Case Report Title:
Quality of Life Comparing Dor and Toupet After Heller Myotomy for Achalasia
 SCIENTIFIC PAPER Quality of Life Comparing Dor and Toupet After Heller Myotomy for Achalasia Jonathan M. Tomasko, MD, Toms Augustin, MD, Tung T. Tran, MD, Randy S. Haluck, MD, FACS, Ann M. Rogers, MD,
SCIENTIFIC PAPER Quality of Life Comparing Dor and Toupet After Heller Myotomy for Achalasia Jonathan M. Tomasko, MD, Toms Augustin, MD, Tung T. Tran, MD, Randy S. Haluck, MD, FACS, Ann M. Rogers, MD,
Hiatal hernias may be classified. hiatal hernia DESCRIPTION AND IDENTIFICATION. This article is the first in a twopart series about these somewhat
 paraesophagealh hiatal hernia Leslie K Browder, MD, and Alex G Little, MD DESCRIPTION AND IDENTIFICATION Hiatal hernias may be classified as four types. The most common, Type I, may present as gastroesophageal
paraesophagealh hiatal hernia Leslie K Browder, MD, and Alex G Little, MD DESCRIPTION AND IDENTIFICATION Hiatal hernias may be classified as four types. The most common, Type I, may present as gastroesophageal
Surgical Evaluation for Benign Esophageal Disease. Kimberly Howard, PA-C, MHS Duke University Medical Center April 7, 2018
 Surgical Evaluation for Benign Esophageal Disease Kimberly Howard, PA-C, MHS Duke University Medical Center April 7, 2018 Disclosures No disclosures relevant to this presentation. Objectives (for CME purposes)
Surgical Evaluation for Benign Esophageal Disease Kimberly Howard, PA-C, MHS Duke University Medical Center April 7, 2018 Disclosures No disclosures relevant to this presentation. Objectives (for CME purposes)
Left diaphragmmatic eventration with gastric volvulus: Laparoscopic mesh repair of left diaphragmatic eventration
 JMSR Dr. Lakshmikanth T Case Report Left diaphragmmatic eventration with gastric volvulus: Laparoscopic mesh repair of left diaphragmatic eventration Lakshmikanth T 1 and Sanjeeva Rao K 1 1 Department
JMSR Dr. Lakshmikanth T Case Report Left diaphragmmatic eventration with gastric volvulus: Laparoscopic mesh repair of left diaphragmatic eventration Lakshmikanth T 1 and Sanjeeva Rao K 1 1 Department
Effective Health Care
 Effective Health Care Comparative Effectiveness of Management Strategies for Gastroesophageal Reflux Disease Executive Summary Background Gastroesophageal reflux disease (GERD), defined as weekly heartburn
Effective Health Care Comparative Effectiveness of Management Strategies for Gastroesophageal Reflux Disease Executive Summary Background Gastroesophageal reflux disease (GERD), defined as weekly heartburn
34th Annual Toronto Thoracic Surgery Refresher Course
 34th Annual Toronto Thoracic Surgery Refresher Course TREATMENT OPTIONS FOR ACHALASIA Dr. Carmine Simone Director, Intensive Care Unit Head, Division of Critical Care Departments of Medicine and Surgery
34th Annual Toronto Thoracic Surgery Refresher Course TREATMENT OPTIONS FOR ACHALASIA Dr. Carmine Simone Director, Intensive Care Unit Head, Division of Critical Care Departments of Medicine and Surgery
Single Center Experience with Gastrostomy Insertion in Pediatric Patients: A 10-Year Review
 pissn: 2234-8646 eissn: 2234-8840 https://doi.org/10.5223/pghn.2017.20.1.34 Pediatr Gastroenterol Hepatol Nutr 2017 March 20(1):34-40 Original Article PGHN Single Center Experience with Gastrostomy Insertion
pissn: 2234-8646 eissn: 2234-8840 https://doi.org/10.5223/pghn.2017.20.1.34 Pediatr Gastroenterol Hepatol Nutr 2017 March 20(1):34-40 Original Article PGHN Single Center Experience with Gastrostomy Insertion
Putting Chronic Heartburn On Ice
 Putting Chronic Heartburn On Ice Over the years, gastroesophageal reflux disease has proven to be one of the most common complaints facing family physicians. With quicker diagnosis, this pesky ailment
Putting Chronic Heartburn On Ice Over the years, gastroesophageal reflux disease has proven to be one of the most common complaints facing family physicians. With quicker diagnosis, this pesky ailment
PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
 Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
LAPAROSCOPIC HELLER MYOTOMY WITH FUNDOPLICATION FOR ACHALASIA
 LAPAROSCOPIC HELLER MYOTOMY WITH FUNDOPLICATION FOR ACHALASIA I-Rue Lai, 1 Wei-Jei Lee, 1,2 and Ming-Te Huang 2 Background and Purpose: Laparoscopic Heller cardiomyotomy for the treatment of achalasia
LAPAROSCOPIC HELLER MYOTOMY WITH FUNDOPLICATION FOR ACHALASIA I-Rue Lai, 1 Wei-Jei Lee, 1,2 and Ming-Te Huang 2 Background and Purpose: Laparoscopic Heller cardiomyotomy for the treatment of achalasia
Enteral Feeding Access: Your BFF or Frenemy?
 Enteral Feeding Access: Your BFF or Frenemy? Elizabeth Hood, APN/CPNP The Ann and Robert H. Lurie Children s Hospital of Chicago Chicago, IL Disclosure Information No disclosures to report Objectives The
Enteral Feeding Access: Your BFF or Frenemy? Elizabeth Hood, APN/CPNP The Ann and Robert H. Lurie Children s Hospital of Chicago Chicago, IL Disclosure Information No disclosures to report Objectives The
Gastroesophageal Reflux Disease in Infants and Children
 Gastroesophageal Reflux Disease in Infants and Children 4 Marzo 2017 Drssa Chiara Leoni Drssa Valentina Giorgio pediatriagastro@gmail.com valentinagiorgio1@gmail.com Definitions: GER GER is the passage
Gastroesophageal Reflux Disease in Infants and Children 4 Marzo 2017 Drssa Chiara Leoni Drssa Valentina Giorgio pediatriagastro@gmail.com valentinagiorgio1@gmail.com Definitions: GER GER is the passage
Causes of Long-Term Dysphagia After Laparoscopic Nissen Fundoplication
 SCIENTIFIC PAPER Causes of Long-Term Dysphagia After Laparoscopic Nissen Fundoplication Kazuyoshi Sato, MD, PhD, Ziad T. Awad, MD, Charles J. Filipi, MD, Mohamed A. Selima, MD, Judd E. Cummings, Steve
SCIENTIFIC PAPER Causes of Long-Term Dysphagia After Laparoscopic Nissen Fundoplication Kazuyoshi Sato, MD, PhD, Ziad T. Awad, MD, Charles J. Filipi, MD, Mohamed A. Selima, MD, Judd E. Cummings, Steve
Gastric transposition in infants and children
 DOI 10.1007/s00383-010-2736-9 REVIEW ARTICLE Gastric transposition in infants and children Robert A. Cowles Arnold G. Coran Accepted: 6 September 2010 Ó Springer-Verlag 2010 Abstract The loss of esophageal
DOI 10.1007/s00383-010-2736-9 REVIEW ARTICLE Gastric transposition in infants and children Robert A. Cowles Arnold G. Coran Accepted: 6 September 2010 Ó Springer-Verlag 2010 Abstract The loss of esophageal
Role of Prolene Mesh in the repair of Recurrent Congenital Inguinal Hernia: a Pilot Study
 Annals of Pediatric Surgery, Vol 5, No 1, January, 2009, PP 11-15 Original Article Role of Prolene Mesh in the repair of Recurrent Congenital Inguinal Hernia: a Pilot Study Ehab El-Shafei Pediatric Surgery
Annals of Pediatric Surgery, Vol 5, No 1, January, 2009, PP 11-15 Original Article Role of Prolene Mesh in the repair of Recurrent Congenital Inguinal Hernia: a Pilot Study Ehab El-Shafei Pediatric Surgery
Gastrointestinal Imaging Clinical Observations
 Esophageal Motility Disorders After Laparoscopic Nissen Fundoplication Gastrointestinal Imaging Clinical Observations Natasha E. Wehrli 1 Marc S. Levine 1 Stephen E. Rubesin 1 David A. Katzka 2 Igor Laufer
Esophageal Motility Disorders After Laparoscopic Nissen Fundoplication Gastrointestinal Imaging Clinical Observations Natasha E. Wehrli 1 Marc S. Levine 1 Stephen E. Rubesin 1 David A. Katzka 2 Igor Laufer
! "! # $% : 2000!!,!!&/ +& # )012.A C 'B " ;BDB
 *! "! # $% :.) '(,(!.( 112 ', " # '- : # +( 2000!!,!!/ + # )012!! 5!-.0( +( 1 ' 4 32005 +!% 9!! 38! 9, 5 : $. 67.+ ;2 8 3'( 3$0$!!>$- (%66) $= 1% '7 4 78-18 +( - ' :< #( @; 36, 3? / +.(%34) 42!, B : 7
*! "! # $% :.) '(,(!.( 112 ', " # '- : # +( 2000!!,!!/ + # )012!! 5!-.0( +( 1 ' 4 32005 +!% 9!! 38! 9, 5 : $. 67.+ ;2 8 3'( 3$0$!!>$- (%66) $= 1% '7 4 78-18 +( - ' :< #( @; 36, 3? / +.(%34) 42!, B : 7
Gastro-Oesophageal Reflux Disease Information Sheet
 Gastro-Oesophageal Reflux Disease Information Sheet Gastro-Oesophageal Reflux Disease This sheet gives you information about Gastro-Oesophageal Reflux Disease & Fundoplication Surgery What is gastro-oesophageal
Gastro-Oesophageal Reflux Disease Information Sheet Gastro-Oesophageal Reflux Disease This sheet gives you information about Gastro-Oesophageal Reflux Disease & Fundoplication Surgery What is gastro-oesophageal
Outcomes After Minimally Invasive Reoperation for Gastroesophageal Reflux Disease
 Outcomes After Minimally Invasive Reoperation for Gastroesophageal Reflux Disease James D. Luketich, MD, Hiran C. Fernando, FRCS, FRCSEd, Neil A. Christie, FRCS(C), Percival O. Buenaventura, MD, Sayeed
Outcomes After Minimally Invasive Reoperation for Gastroesophageal Reflux Disease James D. Luketich, MD, Hiran C. Fernando, FRCS, FRCSEd, Neil A. Christie, FRCS(C), Percival O. Buenaventura, MD, Sayeed
DISCLAIMER. No Conflict of Interest
 DISCLAIMER No Conflict of Interest EXCLAIMER No Interest in Conflict GORD IS SURGICAL John Dunn, FRACS Laparoscopy Auckland GOD IS SURGICAL He taua ano ta te kai (Even food can attack) PATHOGENESIS Failure
DISCLAIMER No Conflict of Interest EXCLAIMER No Interest in Conflict GORD IS SURGICAL John Dunn, FRACS Laparoscopy Auckland GOD IS SURGICAL He taua ano ta te kai (Even food can attack) PATHOGENESIS Failure
Trans-oral anterior fundoplication: 5-year follow-up of pilot study
 DOI 10.1007/s00464-015-4142-9 and Other Interventional Techniques Trans-oral anterior fundoplication: 5-year follow-up of pilot study Aviel Roy-Shapira 1 Amol Bapaye 2 Suhas Date 2 Rajendra Pujari 2 Shivangi
DOI 10.1007/s00464-015-4142-9 and Other Interventional Techniques Trans-oral anterior fundoplication: 5-year follow-up of pilot study Aviel Roy-Shapira 1 Amol Bapaye 2 Suhas Date 2 Rajendra Pujari 2 Shivangi
The Physician as Medical Illustrator
 The Physician as Medical Illustrator Francois Luks Arlet Kurkchubasche Division of Pediatric Surgery Wednesday, December 9, 2015 Week 5 A good picture is worth a 1,000 bad ones How to illustrate an operation
The Physician as Medical Illustrator Francois Luks Arlet Kurkchubasche Division of Pediatric Surgery Wednesday, December 9, 2015 Week 5 A good picture is worth a 1,000 bad ones How to illustrate an operation
POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS BENEFIT VARIATIONS DISCLAIMER CODING INFORMATION REFERENCES POLICY HISTORY
 Original Issue Date (Created): November 26, 2013 Most Recent Review Date (Revised): November 26, 2013 Effective Date: April 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS
Original Issue Date (Created): November 26, 2013 Most Recent Review Date (Revised): November 26, 2013 Effective Date: April 1, 2014 POLICY PRODUCT VARIATIONS DESCRIPTION/BACKGROUND RATIONALE DEFINITIONS
gastro-oesophageal reflux
 Archives of Disease in Childhood, 1985, 60, 743-747 Results and complications of surgery for gastro-oesophageal reflux L SPITZ AND J KIRTANE Department of Paediatric Surgery, Hospital for Sick Children,
Archives of Disease in Childhood, 1985, 60, 743-747 Results and complications of surgery for gastro-oesophageal reflux L SPITZ AND J KIRTANE Department of Paediatric Surgery, Hospital for Sick Children,
Gastroplasty with Partial or Total Plication for Gastroesophageal Reflux: Manometric and ph-metric Postoperative Studies
 Gastroplasty with Partial or Total Plication for Gastroesophageal Reflux: Manometric and ph-metric Postoperative Studies Francisco Paris, M.D., Manuel Tomas-Ridocci, M.D., Adolfo Benages, M.D., Angel G.
Gastroplasty with Partial or Total Plication for Gastroesophageal Reflux: Manometric and ph-metric Postoperative Studies Francisco Paris, M.D., Manuel Tomas-Ridocci, M.D., Adolfo Benages, M.D., Angel G.
Magnetic Esophageal Ring to Treat Gastroesophageal Reflux Disease (GERD)
 Medical Policy Manual Surgery, Policy No. 190 Magnetic Esophageal Ring to Treat Gastroesophageal Reflux Disease (GERD) Next Review: January 2019 Last Review: January 2018 Effective: March 1, 2018 IMPORTANT
Medical Policy Manual Surgery, Policy No. 190 Magnetic Esophageal Ring to Treat Gastroesophageal Reflux Disease (GERD) Next Review: January 2019 Last Review: January 2018 Effective: March 1, 2018 IMPORTANT
Repair of giant paraesophageal hernias, once considered a
 Robotic-Assisted Giant Paraesophageal Hernia Repair and Nissen Fundoplication Justin Karush, DO *, and Inderpal S. Sarkaria, MD, FACS Repair of giant paraesophageal hernias, once considered a relatively
Robotic-Assisted Giant Paraesophageal Hernia Repair and Nissen Fundoplication Justin Karush, DO *, and Inderpal S. Sarkaria, MD, FACS Repair of giant paraesophageal hernias, once considered a relatively
Complications of Intrathoraac Nissen Fundoplication
 Complications of Intrathoraac Nissen Fundoplication Kamal A. Mansour, M.D., Harry G. Burton, M.D., Joseph I. Miller, Jr., M.D., and Charles R. Hatcher, Jr., M.D. ABSTRACT This report details our experience
Complications of Intrathoraac Nissen Fundoplication Kamal A. Mansour, M.D., Harry G. Burton, M.D., Joseph I. Miller, Jr., M.D., and Charles R. Hatcher, Jr., M.D. ABSTRACT This report details our experience
G astro-oesophageal reflux (GOR) refers to
 1047 REVIEW Outcomes of fundoplication: causes for concern, newer options E Hassall... Antireflux surgery has been a mainstay of treatment for gastro-oesophageal reflux disease in children for some 40
1047 REVIEW Outcomes of fundoplication: causes for concern, newer options E Hassall... Antireflux surgery has been a mainstay of treatment for gastro-oesophageal reflux disease in children for some 40
AATS Focus on Thoracic Surgery: Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017?
 AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
Traditional surgical treatment of large diaphragmatic. Laparoscopic Repair of Large Paraesophageal Hiatal Hernia
 Laparoscopic Repair of Large Paraesophageal Hiatal Hernia Peter S. Dahlberg, MD, Claude Deschamps, MD, Daniel L. Miller, MD, Mark S. Allen, MD, Francis C. Nichols, MD, and Peter C. Pairolero, MD Division
Laparoscopic Repair of Large Paraesophageal Hiatal Hernia Peter S. Dahlberg, MD, Claude Deschamps, MD, Daniel L. Miller, MD, Mark S. Allen, MD, Francis C. Nichols, MD, and Peter C. Pairolero, MD Division
Case Study. The 4-year journey of feeding intolerance of an enterally-fed child from 9 months of age. Synopsis. Introduction/Overview
 Case Study The 4-year journey of feeding intolerance of an enterally-fed child from 9 months of age Library image Emma Liesl Silbernagl, Clinical lead HEN Dietitian, Home Enteral Nutrition Team, Lewisham
Case Study The 4-year journey of feeding intolerance of an enterally-fed child from 9 months of age Library image Emma Liesl Silbernagl, Clinical lead HEN Dietitian, Home Enteral Nutrition Team, Lewisham
Enteral Tube Feeding in Paediatric Mitochondrial Diseases
 www.nature.com/scientificreports Received: 6 April 2017 Accepted: 23 November 2017 Published: xx xx xxxx OPEN Enteral Tube Feeding in Paediatric Mitochondrial Diseases Han Som Choi & Young-Mock Lee We
www.nature.com/scientificreports Received: 6 April 2017 Accepted: 23 November 2017 Published: xx xx xxxx OPEN Enteral Tube Feeding in Paediatric Mitochondrial Diseases Han Som Choi & Young-Mock Lee We
Gastro esophageal reflux disease DR. AMMAR I. ABDUL-LATIF
 Gastro esophageal reflux disease )GERD( DR. AMMAR I. ABDUL-LATIF GERD DEFINITION EPIDEMIOLOGY CAUSES PATHOGENESIS SIGNS &SYMPTOMS COMPLICATIONS DIAGNOSIS TREATMENT Definition Montreal consensus defined
Gastro esophageal reflux disease )GERD( DR. AMMAR I. ABDUL-LATIF GERD DEFINITION EPIDEMIOLOGY CAUSES PATHOGENESIS SIGNS &SYMPTOMS COMPLICATIONS DIAGNOSIS TREATMENT Definition Montreal consensus defined
The Influence of Operation Technique on Long-Term Results of Achalasia Treatment
 56 :56-60 The Influence of Operation Technique on Long-Term Results of Achalasia Treatment Mindaugas Kiudelis, Kristina Mechonosina, Antanas Mickevičius, Almantas Maleckas, Žilvinas Endzinas Department
56 :56-60 The Influence of Operation Technique on Long-Term Results of Achalasia Treatment Mindaugas Kiudelis, Kristina Mechonosina, Antanas Mickevičius, Almantas Maleckas, Žilvinas Endzinas Department
Description. Section: Medicine Effective Date: January 15, 2015 Subsection: Original Policy Date: December 6, 2013 Subject: Page: 1 of 7
 Last Review Status/Date: December 2014 Page: 1 of 7 Description Esophageal achalasia is characterized by prolonged occlusion of the lower esophageal sphincter (LES) and reduced peristaltic activity, making
Last Review Status/Date: December 2014 Page: 1 of 7 Description Esophageal achalasia is characterized by prolonged occlusion of the lower esophageal sphincter (LES) and reduced peristaltic activity, making
Lung Function Abnormalities Following Repaired Esophageal Atresia and Tracheoesophageal Fistula
 Bahrain Medical Bulletin, Vol. 27, No.4, December 2005 Lung Function Abnormalities Following Repaired Esophageal Atresia and Tracheoesophageal Fistula Hanaa Banjar, MD, FRCPC* Introduction: Esophageal
Bahrain Medical Bulletin, Vol. 27, No.4, December 2005 Lung Function Abnormalities Following Repaired Esophageal Atresia and Tracheoesophageal Fistula Hanaa Banjar, MD, FRCPC* Introduction: Esophageal
L ANELLO MAGNETICO NELLA TERAPIA DEL REFLUSSO
 L ANELLO MAGNETICO NELLA TERAPIA DEL REFLUSSO GASTROESOFAGEO Greta Saino University of Milan Department of Biomedical Sciences for Health Division of General Surgery IRCCS Policlinico San Donato TOP TEN
L ANELLO MAGNETICO NELLA TERAPIA DEL REFLUSSO GASTROESOFAGEO Greta Saino University of Milan Department of Biomedical Sciences for Health Division of General Surgery IRCCS Policlinico San Donato TOP TEN
A Novel Endoscopic Treatment for Achalasia Is the POEM mightier than the sword?
 A Novel Endoscopic Treatment for Achalasia Is the POEM mightier than the sword? Pavlos Kaimakliotis, MD Department of Gastroenterology Lahey Hospital and Medical Center Assistant Professor of Medicine
A Novel Endoscopic Treatment for Achalasia Is the POEM mightier than the sword? Pavlos Kaimakliotis, MD Department of Gastroenterology Lahey Hospital and Medical Center Assistant Professor of Medicine
Magnetic Esophageal Sphincter Augmentation to Treat Gastroesophageal Reflux Disease (GERD)
 Magnetic Esophageal Sphincter Augmentation to Treat Gastroesophageal Reflux Disease (GERD) Policy Number: 7.01.137 Last Review: 02/2018 Origination: 02/2014 Next Review: 02/2019 Policy Blue Cross and Blue
Magnetic Esophageal Sphincter Augmentation to Treat Gastroesophageal Reflux Disease (GERD) Policy Number: 7.01.137 Last Review: 02/2018 Origination: 02/2014 Next Review: 02/2019 Policy Blue Cross and Blue
4/24/2015. History of Reflux Surgery. Recent Innovations in the Surgical Treatment of Reflux
 Recent Innovations in the Surgical Treatment of Reflux Scott Carpenter, DO, FACOS, FACS Mercy Hospital Ardmore Ardmore, OK History of Reflux Surgery - 18 th century- first use of term heartburn - 1934-
Recent Innovations in the Surgical Treatment of Reflux Scott Carpenter, DO, FACOS, FACS Mercy Hospital Ardmore Ardmore, OK History of Reflux Surgery - 18 th century- first use of term heartburn - 1934-
