Foreign object ingestion and esophageal food bolus
|
|
|
- Arnold Bennett
- 5 years ago
- Views:
Transcription
1 CURRENT ENDOSCOPIC PRACTICES THE EXPERTS SPEAK Review of food bolus management Hin Hin Ko MD FRCPC, Robert Enns MD FRCPC Foreign object ingestion and esophageal food bolus impactions are common problems faced by gastroenterologists. Fortunately, the majority of ingested foreign objects and food boluses will pass spontaneously. However, 10% to 20% may become lodged in the esophagus or other locations in the gastrointestinal tract and may require nonoperative intervention, and 1% or less will require surgery (1-4). A recent study (5) reported an estimated annual incidence rate of food impactions of 13 episodes per 100,000 in a health maintenance organization population. The overall mortality rate is unknown, but deaths have been rarely reported (6,7). The purpose of the present review is to focus on esophageal food bolus impaction its pathophysiology, clinical presentations, diagnosis and management. PATHOPHYSIOLOGY Food impaction usually occurs as a result of two factors: the state of the esophagus, and the nature of the food that has been swallowed. Previous studies (5), revealed that food bolus impactions have underlying esophageal pathology in 88% to 97% of adult patients evaluated. Benign esophageal stenoses caused by Schatzki (B) rings or by peptic strictures are the most common causes, followed by webs, extrinsic compression, surgical anastomosis, esophagitis and motor disorders such as achalasia. Surprisingly, food bolus impaction is an uncommon presentation for esophageal carcinoma. One other emerging condition that is especially important to recognize is eosinophilic esophagitis. It is commonly found in younger patients presenting with food dysphagia and impaction. A recent study (8) showed that up to 54% of adults who presented with esophageal food impactions over a three-year period had histological evidence of eosinophilic esophagitis. When these underlying esophageal conditions are present and, if food, especially meat, is poorly chewed and swallowed precipitously, acute food impaction can occur. CLINICAL PRESENTATIONS Food bolus impaction usually presents acutely, especially in adults who have had a clear history of ingestion. Impaction at the upper esophageal sphincter is generally easily localized by the patient. However, impaction at sites lower in the esophagus may cause symptoms such as diffuse chest pain or pressure, dysphagia, odynophagia, a sensation of choking, and neck or Dr Hin Hin Ko throat pain (9). Odynophagia may occur as a result of distension of the esophagus by food bolus, but it is also a marker for esophageal injuries such as laceration, abrasion or perforation. Retching and emesis are also very common, and patients sometimes try to self-induce vomiting in an attempt to dislodge the object. Patients with a high-grade esophageal obstruction may experience hypersalivation and may be unable to swallow any liquids, including their own saliva. Respiratory symptoms may result from compression of the trachea by a large food bolus impaction (rare), from aspiration of saliva or food (more common), or complete airway obstruction. Common respiratory symptoms include stridor, coughing, wheezing or choking. DIAGNOSIS Diagnosis of food bolus impaction is rarely a problem because most patients are able to relate the type of food ingested and the approximate time symptoms began. The goal of the initial patient assessment is to determine the stability of the patient, the type of food ingested and time since ingestion, the presence of any complications and the presence of any underlying esophageal conditions or other medical comorbidities. A careful history should inquire of any previous history of dysphagia, food impaction, gastroesophageal reflux disease, known structural esophageal abnormalities and the contents of meals. In general, the patient s localization of food impaction is often unreliable and esophageal dysphagia is more likely to be referred proximally, rather than distally, from the site of obstruction (10,11). The physical examination should focus on the assessment of the patient s stability and any complications from the food bolus impaction. Ventilation, airway compromise and the risk of aspiration should first be assessed. Signs suggestive of perforation include fever, tachycardia, subcutaneous crepitus and swelling of the neck or chest. Esophageal perforation may require surgical intervention, and consultations should not be delayed. Radiographic evaluation is useful to detect any associated complications, such as free mediastinal air from perforation; however, food boluses, including fish or chicken bones, are radiolucent and not readily visualized on plain radiographs. A contrast examination should not be performed because of the risk of aspiration. Division of Gastroenterology, St Paul s Hospital, University of British Columbia, Vancouver, British Columbia Correspondence: Dr Robert Enns, St Paul s Hospital, University of British Columbia, Pacific Gastro Associates, Hornby Street, Vancouver, British Columbia V6Z 2K5. Telephone , fax , renns@interchange.ubc.ca Can J Gastroenterol Vol 22 No 10 October Pulsus Group Inc. All rights reserved 805
2 MANAGEMENT Endoscopy Flexible endoscopy is highly sensitive in detecting food boluses and has the advantage of delivering immediate therapy in most cases. Furthermore, endoscopy can reveal the underlying esophageal pathology leading to the impaction and any associated mucosal damage. Successful management of food bolus impaction is influenced by many factors including the experience and technical skills of the endoscopist, as well as the availability of necessary equipment and accessories. As stated above, flexible endoscopy is the preferred treatment modality for most cases of esophageal food impaction. Furthermore, endoscopic diagnosis and treatment of the underlying pathology can be performed at the same setting. The goal of therapy is to clear the esophagus by either extracting the bolus or moving it into the stomach to prevent any complications. Timing of endoscopy: The timing of endoscopy is dictated by the perceived risks of aspiration and/or perforation. Urgent intervention is indicated when patients are in severe distress. In patients unable to ingest their own secretions, the use of a suction catheter or Yankauer sucker, which can be held by the patient while in a sitting position, is useful while waiting for endoscopic intervention. Patients who have no evidence of high-grade obstruction and who are in no acute distress can be handled less urgently because spontaneous passage of food boluses may occur and endoscopy can be postponed until a more convenient time (1-4). However, endoscopic intervention should not be postponed beyond 24 h from presentation because of the increased risk of complications (12,13). Early removal of the food bolus may minimize the amount of local pressure-induced mucosal damage in the esophagus. Smith and Wong (14) even suggested performing nonurgent endoscopy within the first 6 h to 12 h to increase the likelihood of removing a meat bolus in one piece, before it has a chance to soften. The actual timing of the endoscopy is often delayed a few hours in the early morning until a more convenient endoscopy time (usually 07:00) can be arranged. This seems to be a reasonable approach and, providing that the time for endoscopy fits into the above stated time period, is likely a safe approach. Equipment: Readily available equipment should include appropriately sized endoscopes, overtubes, accessories such as polypectomy snares, rat-tooth and alligator forceps, a Roth retrieval net, Dormia basket, and Magill or Kelly grasping forceps (14). Airway protection: During extraction, it is essential to protect the patient s airway from inadvertent aspiration of saliva and retained esophageal food contents and the food itself. Ideally, assistants should be available to provide oral suctioning and monitor the patient s vital signs. Removal of foreign bodies can be the easiest (requiring simple sedation and insufflation of the esophagus alone) and, at times, the most difficult of procedures. Endotracheal intubation may be needed if the patient is uncooperative or at a high-risk of aspiration. The esophagus should be intubated under direct visualization and any retained secretions in the esophagus should be suctioned to improve visualization and reduce the aspiration risk. Once the food bolus is identified, the endoscopist should decide which technique to use to clear the esophagus and what accessory equipment is needed. Removal techniques: Pushing: There are many reported endoscopic techniques to facilitate removal of food boluses. Considerable disagreement exists concerning whether a bolus 806 should be extracted or pushed into the stomach. Bolus extraction is widely advocated (15-17) and, historically, pushing has been avoided because of the concern for associated distal obstructing lesions, or strictures and increased risk of perforation. However, several authors (5,18-20) have recently advocated using the push technique to guide the esophageal food bolus into the stomach. The push technique is advocated in certain situations such as in patients without a history of dysphagia or those in whom the food bolus is soft or composed of many small fragments, making extraction difficult (1,4,21). Vicari et al (20) reported a 97% success rate using the push technique for acute esophageal food impaction. The push technique requires experience and good judgement. It is generally safe if the endoscope, with insufflation and distension of the esophageal lumen, can be steered successfully beyond the bolus into the stomach. The endoscope can then be pulled back to a position just above the bolus. With the tip of the endoscope, gentle pressure is applied to the bolus, carefully guiding it into the stomach. It is important to push from the right side of the food bolus because in the setting of a hiatus hernia, the gastroesophageal junction has a left turn; pressure from the right then allows a bolus to pass distally (22). A Savary-Gilliard (Cook Medical, USA) dilator push method has also been reported, in which a wire is gently inserted past a food bolus into the stomach under direct visualization. One or two small diameter Savary-Gilliard dilators (28 Fr or 32 Fr catheter) are then passed with subsequent endoscopic examination of the esophagus (18). A retrospective review (18) showed that the pushing technique was successful in 48 patients using the endoscope alone and in 20 patients by Savary-Gilliard dilator push method; however, this method is not usually required in most patients. In instances when the bolus cannot be passed with the endoscope, the push technique may still be attempted; however, the procedure should be stopped if any significant resistance is encountered. Blindly pushing the impacted food bolus with the endoscope is not recommended due to the high incidence of underlying esophageal pathology (4). When gentle pushing is unsuccessful, one can use forceps, snares or baskets (biliary or Roth-type) to attempt breaking the food bolus into smaller pieces for extraction. Extraction: Extraction is the preferred technique when the food bolus is large, firm, contains bones or sharp edges, or the patient is known to have significant stricture. Using a variety of snares, baskets, graspers or forceps, the food bolus can usually be removed in toto in a piecemeal fashion. When using a polypectomy snare, it should be pulled snug against the tip of the endoscope once the food bolus has been successfully ensnared (23). The Roth retrieval net has the added benefit of encompassing the food bolus completely within the net, allowing a firmer grasp and minimizing the risk of dislodging any food fragments in the hypopharynx and airway during the retrieval process. This technique may also result in fewer repeated passes of the endoscope and thus, results in a significantly shorter duration of endoscopy and sedation compared with the use of other instruments (24). If the food bolus is impacted tightly or lodged proximally near the cricopharynx, it can be difficult to grasp with a snare or Roth net. In those instances, many endoscopists prefer to use an endoscopic suction technique. A transparent endoscopic vacuum cap, such as those found in variceal ligation and endoscopic mucosal resection kits, is fit over the endoscope. The Can J Gastroenterol Vol 22 No 10 October 2008
3 continuous suctioning then creates a vacuum between the tip of the endoscope and the foreign body, thereby pulling the food bolus against the cap (25,26). One problem with this technique can be a failure to keep the bolus secured simply by suction, despite using greater suction forces. Patel et al (27) reported modifying the suction cap technique by using a Dormia basket. The basket is advanced into the endoscopic channel through the suction cap. The food bolus is then grasped with the basket, then the endoscope with the suction cap is slowly advanced toward the impaction while the Dormia basket grasping the bolus is carefully pulled toward the endoscope. Once the bolus is inside the suction cap, full suction is applied and the impacted food is extracted by means of this combination method (27). In situations when the bolus has become softer and fragmented, and repeated intubation seems unavoidable, occasional use of an overtube is helpful. After lubrication of the internal and external surfaces, a 44 Fr catheter Maloney dilator (Medovation, USA) is passed through the tube, and the entire unit is guided into the esophagus and the dilator is subsequently removed (28). Use of an overtube offers airway protection and allows for multiple passes of the endoscope during retrieval (29). Younger physicians and trainees may have very little experience with this device because it is required only in very selected cases. Medical therapy A few pharmacological agents may be tried on admission to the emergency room or while preparing for endoscopy. Glucagon is the mainstay pharmacological treatment. It is an endogenous polypeptide secreted from alpha cells in the islets of Langerhans. At pharmacological doses, it relaxes the esophageal smooth muscle and the lower esophageal sphincter, promoting the spontaneous passage of an impacted food bolus (30). Glucagon seems to have very little effect on the motility of the proximal esophagus (31). In a person with normal esophageal anatomy, the resting lower esophageal sphincter pressure decreases by up to 60% after intravenous glucagon administration (30). In one study (30), glucagon given at the time of endoscopy facilitated clearing of the food bolus, probably secondary to its smooth muscle relaxation effect. The success rate for the use of glucagon is reportedly between 12% and 50% (8,32-34). However, glucagon is much less effective in patients with structural abnormalities, such as strictures or rings. Contraindications for the use of glucagon include insulinoma, pheochromocytoma, Zollinger-Ellison syndrome or drug sensitivity. The dose of glucagon normally used is 1 mg to 2 mg intravenously in adults and 0.02 mg/kg to 0.03 mg/kg in children weighing less than 20 kg, with a maximum dose of 0.5 mg. Repeat dosing at 5 min to 10 min is reasonable if needed (35); however, if the first two doses are ineffective, further doses are REFERENCES 1. Webb WA. Management of foreign bodies of the upper gastrointestinal tract. Gastroenterology 1988;1: Henderson CT, Engel J, Schlesinger P. Foreign body ingestion: Review and suggested guidelines for management. Endoscopy 1987;19: Nandi P, Ong GB. Foreign body in the esophagus: Review of 2394 cases. Br J Surg 1979;65: Vizcarrondo FJ, Brady PG, Nord HJ. Foreign bodies of the upper gastrointestinal tract. Gastrointest Endosc 1983;20: Longstreth GF, Longstreth KJ, Yao JF. Esophageal food not indicated (9,35). Glucagon is not a medication free of side effects. It is commonly associated with nausea or vomiting that could be harmful in the presence of a severe impaction and poses a theoretical risk of perforation and aspiration (36). Several gas-forming agents have also been used to treat acute esophageal food impactions. These agents release carbon-dioxide in the esophagus, which raises the intraluminal pressure against a closed upper esophageal sphincter, forcing the bolus into the stomach. Examples of these agents include simethicone, carbonated beverages and a cocktail of tartaric acid and bicarbonate. Success has been reported (37,38), however, complications such as esophageal perforation have also been reported (28). Use of proteolytic enzymes such as papain or chymotrypsin in an attempt to dissolve food boluses have fallen out of favour because of potentially severe complications including esophageal erosion, necrosis and perforation, as well as severe pulmonary complications such as hemorrhagic pulmonary edema if the solution is aspirated (1,39,40). Proteolytic enzyme preparations have no place in the current management of food bolus impaction. Management after food bolus clearance After the food bolus has been removed, endoscopic assessment should be completed. At times, this may be necessary to complete on a different date in a more elective manner, particularly if the patient has been unstable. Patients who have food impactions commonly are found to have underlying esophageal pathologies such as a peptic stricture or Schatzki ring. A decision would have to be made as to whether to dilate the associated stenosis at the same or different sessions. If there is minimal mucosal damage and the bolus has been present for a short period of time, dilation can be performed at the same setting (17,22). However, if there is significant inflammation or mucosal damage, the patient can be placed on acid suppressants and brought back for dilation at a later date. In patients who present with a history of esophageal complaints and have an endoscopic appearance suspicious of eosinophilic esophagitis (eg, linear mucosal furrows, mucosal rings, small-calibre esophagus or characteristic mucosal white exudates), dilation should likely be avoided because it may be associated with a higher incidence of complication and greater likelihood of recurrence (41,42). Unless contraindicated, biopsies of the proximal and distal esophagus should be performed to confirm the diagnosis. SUMMARY Esophageal food impaction is a common emergency faced by gastroenterologists. It is important to know what techniques and instruments are indicated for different situations. Endoscopic treatment is a reliable and safe procedure in skilled, expert hands with a high success rate and low morbidity and mortality. impaction: Epidemiology and therapy. A retrospective, observational study. Gastrointest Endosc 2001;53: Simic MA, Budakov BM. Fatal upper esophageal hemorrhage caused by a previously ingested chicken bone: Case report. Am J Forensic Med Pathol 1988;19: Bennett DR, Baird CJ, Chan KM, et al. Zinc toxicity following massive coin ingestion. Am J Forensic Med Pathol 1997;18: Desai TK, Stecevic V, Chang CH, et al. Association of eosinophilic inflammation with esophageal food impaction in adults. Gastrointest Endosc 2005;61: Can J Gastroenterol Vol 22 No 10 October
4 9. Taylor RB: Esophageal foreign bodies. Emerg Med Clin North Am 1987;5: Johnston B, Castell D. Symptom overview and quality of life. In: Castell D, Richter J, ed. The Esophagus. Philadelphia: Lippincott Williams & Wilkins;2004: Wilcox, CM, Alexander LN, Clark WS. Localization of an obstructing esophageal lesion. Is the patient accurate? Dig Dis Sci 1995;40: Eisen GM, Baron TH, Dominitz JA, et al. Guideline for the management of ingested foreign bodies. Gastrointest Endosc 2002;55: Chaves DM, Ishioka S, Felix VN, et al. Removal of a foreign body from the upper gastrointestinal tract with a flexible endoscope: A prospective study. Endoscopy 2004;36: Smith MT, Wong RKH. Esophageal foreign bodies: Types and techniques for removal. Curr Treat Options Gastroenterol 2006;9: Shaffer RD, Klug T. A comparative study of techniques for esophageal foreign body removal with special emphasis on meat bolus obstruction. Wis Med J 1981;80: Berggreen PJ, Harrison E, Sanowski RA, et al. Techniques and complications of esophageal foreign body extraction in children and adults. Gastrointest Endosc 1993;39: Yeaton P, Peura DA. Foreign bodies. In: Castell DO, Richter JE, eds. The Esophagus, 3rd edn. Philadelphia: Lippincott Williams & Wilkins, 1999: Weinstock LB, Shatz BA, Thyssen SE. Esophageal food bolus obstruction: Evaluation of extraction and modified push techniques in 75 cases. Endoscopy 1999;31: Kozarek R, Ball T, Belic L, et al. Food impaction at a regional referral centre: Should we push? Pull? Or poke? Gastrointest Endosc 1999;49:113 (Abst). 20. Vicari JJ, Johnason JF, Frakes JT. Outcomes of acute esophageal food impaction: Success of the push technique. Gastrointest Endosc 2001;53: Ginsberg G. Management of ingested foreign objects and food bolus impactions. Gastrointest Endosc 1995;41: Webb WA. Management of foreign bodies of the upper gastrointestinal tract: Update. Gastrointest Endosc 1995;41: Webb WW, Taylor MB. Foreign bodies of the upper gastrointestinal tract. In: Taylor MB, ed. Gastrointestinal Emergencies, 2nd edn. Baltimore: Williams & Wilkins, 1997: Neustater B, Barkin JS. Extraction of an esophageal food impaction with a Roth retrieval net. Gastrointest Endosc 1996;43: Pezzi JS, Shiau YF. A method for removing meat impactions from the esophagus. Gastrointest Endosc 1994;40: Nijhawan S, Rai RR, Nepalia S, et al. Suction retrieval of esophageal foreign bodies. Endoscopy 1998;30:S Patel NC, Fry LC, Monkemuller KE. Modified suction cap technique for endoscopic management of esophageal food impaction. Endoscopy 2003;35: Smith MT, Wong RKH. Foreign Bodies. Gastrointest Endosc Clin N Am 2007;17: Guideline for the management of ingested foreign bodies. American Society for Gastrointestinal Endoscopy. Gastrointest Endosc 1995;42: Alaradi O, Bartholomew M, Barkin JS. Upper endoscopy and glucagon: A new technique in the management of acute esophageal food impaction. Am J Gastroenterol 2001;96: Colon V, Grade A, Pulliam G, et al. Effect of doses of glucagon used to treat food impaction on esophageal motor function of normal subjects. Dysphagia 1999;14: Blair SR, Graeber GM, Cruzzavala JL, et al. Current management of esophageal impactions. Chest 1993;104: Brady PG. Esophageal foreign bodies. Gastroenterol Clin North Am 1991;20: Giordano A, Adams G, Boies L, et al. Current management of esophageal foreign bodies. Arch Otolaryngol 1981;107: Lyons MF, Tsuchida AM. Foreign bodies of the gastrointestinal tract. Med Clin North Am 1993;77: Al-Haddad M, Ward EM, Scolapio JS, et al. Glucagon for the relief of esophageal food impaction: Does it really work? Dig Dis Sci 2006;51: Karanjia ND, Rees M. The use of Coca-Cola in the management of bolus obstruction in benign esophageal strictures. Ann R Coll Surg Engl 1993;75: Lee J, Anderson R. Best evidence topic report. Effervescent agents for esophageal food bolus impaction. Emerg Med J 2005;22: Hall ML, Huseby JS. Hemorrhagic pulmonary edema associated with meat tenderizer for esophageal meat impaction. Chest 1988;94: Straumann A, Spichtin HP, Grize L, et al. Natural history of primary eosinophilic esophagitis: A follow-up of 30 adult patients for up to 11.5 years. Gastroenterology 2003;125: Kaplan M, Mutlu EA, Jakate S, et al. Endoscopy in eosinophilic esophagitis: Feline esophagus and perforation risk. Clin Gastroenterol Hepatol 2003;1:433: Vasilopoulos S, Shaker R. Defiant dysphagia: A small-calibre esophagus and refractory benign esophageal strictures. Curr Gastroenterol Rep 2001;3: Can J Gastroenterol Vol 22 No 10 October 2008
5 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Diabetes Research International Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Obesity Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
Managing Foreign Objects in the GI Tract Tips & Tricks
 Managing Foreign Objects in the GI Tract Tips & Tricks STEPHEN LANDRENEAU, MD Take home o Perform emergent endoscopy in cases of: Esophageal obstruction due to food bolus impaction or foreign object. Disk
Managing Foreign Objects in the GI Tract Tips & Tricks STEPHEN LANDRENEAU, MD Take home o Perform emergent endoscopy in cases of: Esophageal obstruction due to food bolus impaction or foreign object. Disk
Foreign Body Management
 Foreign Body Management NYSGE Fellows Summer Course Susana Gonzalez, MD Assistant Professor of Medicine 1 Objectives Timing of endoscopy When? Anatomic location Where? High risk objects What? Choosing
Foreign Body Management NYSGE Fellows Summer Course Susana Gonzalez, MD Assistant Professor of Medicine 1 Objectives Timing of endoscopy When? Anatomic location Where? High risk objects What? Choosing
The Foreign Body. Neil H. Stollman, MD, FACG
 The Foreign Body Neil H. Stollman, MD, FACG Associate Clinical Professor of Medicine University of California San Francisco Chief, Division of Gastroenterology Alta Bates Summit Medical Center, Oakland,
The Foreign Body Neil H. Stollman, MD, FACG Associate Clinical Professor of Medicine University of California San Francisco Chief, Division of Gastroenterology Alta Bates Summit Medical Center, Oakland,
Glucagon Is a Safe and Inexpensive Initial Strategy in Esophageal Food Bolus Impaction
 Dig Dis Sci (2016) 61:841 845 DOI 10.1007/s10620-015-3934-z ORIGINAL ARTICLE Glucagon Is a Safe and Inexpensive Initial Strategy in Esophageal Food Bolus Impaction Jason Haas 1,4 Julia Leo 1 Nimish Vakil
Dig Dis Sci (2016) 61:841 845 DOI 10.1007/s10620-015-3934-z ORIGINAL ARTICLE Glucagon Is a Safe and Inexpensive Initial Strategy in Esophageal Food Bolus Impaction Jason Haas 1,4 Julia Leo 1 Nimish Vakil
Suspected Foreign Body Ingestion
 Teresa Liang Suspected Foreign Body Ingestion 1. General Presentation Background: Of more than 100,000 cases of foreign body ingestion reported each year in the United States, 80% occur in children, with
Teresa Liang Suspected Foreign Body Ingestion 1. General Presentation Background: Of more than 100,000 cases of foreign body ingestion reported each year in the United States, 80% occur in children, with
Use of Magill Forceps to Remove Foreign Bodies in Children
 THIEME Original Article e91 Use of Magill Forceps to Remove Foreign Bodies in Children Murat Oncel, MD 1 Guven Sadi Sunam, MD 1 Cagdas Elsurer, MD 2 Huseyin Yildiran, MD 1 1 Department of Thoracic Surgery,
THIEME Original Article e91 Use of Magill Forceps to Remove Foreign Bodies in Children Murat Oncel, MD 1 Guven Sadi Sunam, MD 1 Cagdas Elsurer, MD 2 Huseyin Yildiran, MD 1 1 Department of Thoracic Surgery,
Fluoroscopy-Guided Endoscopic Removal of Foreign Bodies
 CASE REPORT Clin Endosc 2017;50:197-201 https://doi.org/10.5946/ce.2016.085 Print ISSN 2234-2400 / On-line ISSN 2234-2443 Open Access Fluoroscopy-Guided Endoscopic Removal of Foreign odies Junhwan Kim
CASE REPORT Clin Endosc 2017;50:197-201 https://doi.org/10.5946/ce.2016.085 Print ISSN 2234-2400 / On-line ISSN 2234-2443 Open Access Fluoroscopy-Guided Endoscopic Removal of Foreign odies Junhwan Kim
Acquired pediatric esophageal diseases Imaging approaches and findings. M. Mearadji International Foundation for Pediatric Imaging Aid
 Acquired pediatric esophageal diseases Imaging approaches and findings M. Mearadji International Foundation for Pediatric Imaging Aid Acquired pediatric esophageal diseases The clinical signs of acquired
Acquired pediatric esophageal diseases Imaging approaches and findings M. Mearadji International Foundation for Pediatric Imaging Aid Acquired pediatric esophageal diseases The clinical signs of acquired
Foreign Body Ingested
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Foreign Body Ingested Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Foreign Body Ingested Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should
9/18/2015. Disclosures. Objectives. Dysphagia Sherri Ekobena PA-C. I have no relevant financial interests to disclose I have no conflicts of interest
 Dysphagia Sherri Ekobena PA-C Disclosures I have no relevant financial interests to disclose I have no conflicts of interest Objectives Define what dysphagia is Define types of dysphagia Define studies
Dysphagia Sherri Ekobena PA-C Disclosures I have no relevant financial interests to disclose I have no conflicts of interest Objectives Define what dysphagia is Define types of dysphagia Define studies
(a) (b) Plate 16.1 Esophageal tear after passage of the echoendoscope.
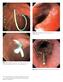 Plate 16.1 Esophageal tear after passage of the echoendoscope. Plate 11.1 Prophylactic pancreatic duct stents. 3-Fr, 4-cm long single-pigtail stent. 5-Fr, 3-cm long flanged stent. Plate 16.2 Esophageal
Plate 16.1 Esophageal tear after passage of the echoendoscope. Plate 11.1 Prophylactic pancreatic duct stents. 3-Fr, 4-cm long single-pigtail stent. 5-Fr, 3-cm long flanged stent. Plate 16.2 Esophageal
Dysphagia. Conflicts of Interest
 Dysphagia Bob Kizer MD Assistant Professor of Medicine Creighton University School of Medicine August 25, 2018 Conflicts of Interest None 1 Which patient does not need an EGD as the first test? 1. 50 year
Dysphagia Bob Kizer MD Assistant Professor of Medicine Creighton University School of Medicine August 25, 2018 Conflicts of Interest None 1 Which patient does not need an EGD as the first test? 1. 50 year
Historical perspective
 Raj Santharam, MD GI Associates, LLC Clinical Assistant Professor of Medicine Medical College of Wisconsin Historical perspective FFS first widespread use in the early 1970 s Expansion of therapeutic techniques
Raj Santharam, MD GI Associates, LLC Clinical Assistant Professor of Medicine Medical College of Wisconsin Historical perspective FFS first widespread use in the early 1970 s Expansion of therapeutic techniques
EGD. John M. Wo, M.D. University of Louisville July 3, 2008
 EGD John M. Wo, M.D. University of Louisville July 3, 2008 Different Ways to do an EGD Which scope? Pediatric, regular, jumbo EGD endoscope or pediatric colonoscope Transnasal vs. transoral insertion Sedation
EGD John M. Wo, M.D. University of Louisville July 3, 2008 Different Ways to do an EGD Which scope? Pediatric, regular, jumbo EGD endoscope or pediatric colonoscope Transnasal vs. transoral insertion Sedation
Esophageal injuries. 新光急診張志華醫師 Facebook.com/jack119
 Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic Pre-test 2 Which contrast agent
Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic Pre-test 2 Which contrast agent
Gastroesophageal Reflux Disease in Infants and Children
 Gastroesophageal Reflux Disease in Infants and Children 4 Marzo 2017 Drssa Chiara Leoni Drssa Valentina Giorgio pediatriagastro@gmail.com valentinagiorgio1@gmail.com Definitions: GER GER is the passage
Gastroesophageal Reflux Disease in Infants and Children 4 Marzo 2017 Drssa Chiara Leoni Drssa Valentina Giorgio pediatriagastro@gmail.com valentinagiorgio1@gmail.com Definitions: GER GER is the passage
Esophageal injuries. Pre-test /11/10. 新光急診張志華醫師 Facebook.com/jack119. O What is the most common cause of esophageal injuries?
 Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 O What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic 1 Pre-test 2 O Which contrast
Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 O What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic 1 Pre-test 2 O Which contrast
Information Technology Solutions
 2016 2014 CPT Esophagoscopy Changes - Gastroenterology CPT Changes Information Technology Solutions ASGE LOGO AND INFO Esophagogastroduodenoscopy CPT Codes 43235-43270 The American Society for Gastrointestinal
2016 2014 CPT Esophagoscopy Changes - Gastroenterology CPT Changes Information Technology Solutions ASGE LOGO AND INFO Esophagogastroduodenoscopy CPT Codes 43235-43270 The American Society for Gastrointestinal
REMOVAL OF IMPACTED DENTURES WITH POLYPECTOMY SNARE
 JMBR: A Peer-review Journal of Biomedical Sciences June 2012, Vol. 11 No.1 pp 14-19 REMOVAL OF IMPACTED DENTURES WITH POLYPECTOMY SNARE *OKUGBO SU, **OKORO E, ***KESIEME E ABSTRACT Impacted dentures have
JMBR: A Peer-review Journal of Biomedical Sciences June 2012, Vol. 11 No.1 pp 14-19 REMOVAL OF IMPACTED DENTURES WITH POLYPECTOMY SNARE *OKUGBO SU, **OKORO E, ***KESIEME E ABSTRACT Impacted dentures have
Chapter 14: Training in Radiology. DDSEP Chapter 1: Question 12
 DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
Icd 10 code for distal esophageal stricture Address Submit
 Icd 10 code for distal esophageal stricture Email Address Submit If an EGD is performed with a biopsy, and then the physician removes the scope and performs an Esophageal Dilation by unguided sound, it
Icd 10 code for distal esophageal stricture Email Address Submit If an EGD is performed with a biopsy, and then the physician removes the scope and performs an Esophageal Dilation by unguided sound, it
Barrett s Esophagus. lining of the lower esophagus that bears his name (i.e., Barrett's esophagus). We now
 Shamika Johnson Anatomy & Physiology 206 April 20, 2010 Barrett s Esophagus What is Barrett s Esophagus? Norman Barrett was a pathologist. In 1950, he described an abnormality in the lining of the lower
Shamika Johnson Anatomy & Physiology 206 April 20, 2010 Barrett s Esophagus What is Barrett s Esophagus? Norman Barrett was a pathologist. In 1950, he described an abnormality in the lining of the lower
Swallowed Foreign Body
 Swallowed Foreign Body Page 1 of 5 INTRODUCTION Swallowed foreign bodies can be divided into five distinct groups: 1 Small blunt objects 2 Large blunt objects 3 Potentially poisonous objects 4 Sharp objects
Swallowed Foreign Body Page 1 of 5 INTRODUCTION Swallowed foreign bodies can be divided into five distinct groups: 1 Small blunt objects 2 Large blunt objects 3 Potentially poisonous objects 4 Sharp objects
Esophageal foreign bodies 1
 European Journal of Cardio-thoracic Surgery 13 (1998) 494 499 Esophageal foreign bodies 1 A. Al-Qudah*, S. Daradkeh, M. Abu- Khalaf Sections of Thoracic And General Surgery, Department of Surgery, Jordan
European Journal of Cardio-thoracic Surgery 13 (1998) 494 499 Esophageal foreign bodies 1 A. Al-Qudah*, S. Daradkeh, M. Abu- Khalaf Sections of Thoracic And General Surgery, Department of Surgery, Jordan
 P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
P R E S E N T S Dr. Mufa T. Ghadiali is skilled in all aspects of General Surgery. His General Surgery Services include: General Surgery Advanced Laparoscopic Surgery Surgical Oncology Gastrointestinal
Dysphagia. A Problem Swallowing Foods or Liquids
 Dysphagia A Problem Swallowing Foods or Liquids What Is Dysphagia? If you have a problem swallowing foods or liquids, you may have dysphagia. It has a number of causes. Your doctor can find out what is
Dysphagia A Problem Swallowing Foods or Liquids What Is Dysphagia? If you have a problem swallowing foods or liquids, you may have dysphagia. It has a number of causes. Your doctor can find out what is
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City
 Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
Sreeni Jonnalagadda, MD., FASGE Professor of Medicine, UMKC Director of Interventional Endoscopy Saint Luke s Hospital, Kansas City Peptic stricture Shtki Schatzki s ring Esophageal cancer Radiation therapy
Oesophageal Disorders
 Oesophageal Disorders Anatomy Upper sphincter Oesophageal body Diaphragm Lower sphincter Gastric Cardia Symptoms Of Oesophageal Disorders Dysphagia Odynophagia Heartburn Atypical Chest Pain Regurgitation
Oesophageal Disorders Anatomy Upper sphincter Oesophageal body Diaphragm Lower sphincter Gastric Cardia Symptoms Of Oesophageal Disorders Dysphagia Odynophagia Heartburn Atypical Chest Pain Regurgitation
Endoscopic management of foreign bodies in the upper gastrointestinal tract: An analysis of 846 cases in China
 EXPERIMENTAL AND THERAPEUTIC MEDICINE 15: 1257-1262, 2018 Endoscopic management of foreign bodies in the upper gastrointestinal tract: An analysis of 846 cases in China FANGFANG YUAN 1,2, XIAOWEI TANG
EXPERIMENTAL AND THERAPEUTIC MEDICINE 15: 1257-1262, 2018 Endoscopic management of foreign bodies in the upper gastrointestinal tract: An analysis of 846 cases in China FANGFANG YUAN 1,2, XIAOWEI TANG
Owen Dickinson. Consultant in Endoscopy & Interventional Radiology. Upper GI Stenting. Rotherham Foundation Trust
 Owen Dickinson Consultant in Endoscopy & Interventional Radiology Upper GI Stenting Rotherham Foundation Trust Owen Dickinson Consultant in Endoscopy & Interventional Radiology Rotherham Foundation Trust
Owen Dickinson Consultant in Endoscopy & Interventional Radiology Upper GI Stenting Rotherham Foundation Trust Owen Dickinson Consultant in Endoscopy & Interventional Radiology Rotherham Foundation Trust
Tools of the Gastroenterologist: Introduction to GI Endoscopy
 Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
Tools of the Gastroenterologist: Introduction to GI Endoscopy Objectives Endoscopy Upper endoscopy Colonoscopy Endoscopic retrograde cholangiopancreatography (ERCP) Endoscopic ultrasound (EUS) Endoscopic
KIDS PUT THINGS IN THE CRAZIEST PLACES...
 KIDS PUT THINGS IN THE CRAZIEST PLACES... YOU CAN T MAKE ME EAT MY DINNER! 2 year old observed to stuff corn up right nostril Judith Klein, MD FACEP Assistant Professor of Emergency Medicine UCSF-SFGH
KIDS PUT THINGS IN THE CRAZIEST PLACES... YOU CAN T MAKE ME EAT MY DINNER! 2 year old observed to stuff corn up right nostril Judith Klein, MD FACEP Assistant Professor of Emergency Medicine UCSF-SFGH
Management of foreign body ingestion and food bolus impaction in children: a retrospective analysis of 675 cases
 The Turkish Journal of Pediatrics 2011; 53: 381-387 Original Management of foreign body ingestion and food bolus impaction in children: a retrospective analysis of 675 cases Dimitris Antoniou, George Christopoulos-Geroulanos
The Turkish Journal of Pediatrics 2011; 53: 381-387 Original Management of foreign body ingestion and food bolus impaction in children: a retrospective analysis of 675 cases Dimitris Antoniou, George Christopoulos-Geroulanos
University College Hospital. Achalasia. Gastrointestinal Services Division Physiology Unit
 University College Hospital Achalasia Gastrointestinal Services Division Physiology Unit Author: Dr Anton Emmanuel, Consultant Gastroenterologist First published: September 2012 Last review date: February
University College Hospital Achalasia Gastrointestinal Services Division Physiology Unit Author: Dr Anton Emmanuel, Consultant Gastroenterologist First published: September 2012 Last review date: February
Endoscopic Treatment of Luminal Perforations and Leaks
 Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Endoscopic Treatment of Luminal Perforations and Leaks Ali A. Siddiqui, MD Professor of Medicine Director of Interventional Endoscopy Jefferson Medical College Philadelphia, PA When Do You Suspect a Luminal
Case Report Complete Obstruction of Endotracheal Tube in an Infant with a Retropharyngeal and Anterior Mediastinal Abscess
 Hindawi Case Reports in Pediatrics Volume 2017, Article ID 1848945, 4 pages https://doi.org/10.1155/2017/1848945 Case Report Complete Obstruction of Endotracheal Tube in an Infant with a Retropharyngeal
Hindawi Case Reports in Pediatrics Volume 2017, Article ID 1848945, 4 pages https://doi.org/10.1155/2017/1848945 Case Report Complete Obstruction of Endotracheal Tube in an Infant with a Retropharyngeal
Esophageal Eosinophilia and Eosinophilic Esophagitis. Bible Class 09. Mai 2018
 Esophageal Eosinophilia and Eosinophilic Esophagitis Bible Class 09. Mai 2018 61 yo male No upper-gi symptoms Gastroscopy vor bariatric Operation Lesion: Papilloma Histology of the surrounding mucosa:
Esophageal Eosinophilia and Eosinophilic Esophagitis Bible Class 09. Mai 2018 61 yo male No upper-gi symptoms Gastroscopy vor bariatric Operation Lesion: Papilloma Histology of the surrounding mucosa:
INTRODUCTION TO UPPER ENDOSCOPY
 INTRODUCTION TO UPPER ENDOSCOPY Satish Nagula, MD Associate Professor of Medicine Icahn School of Medicine at Mount Sinai NYSGE First Year Fellows Course July 14, 2018 Early endoscopes 1805: Bozzini Lichtleiter
INTRODUCTION TO UPPER ENDOSCOPY Satish Nagula, MD Associate Professor of Medicine Icahn School of Medicine at Mount Sinai NYSGE First Year Fellows Course July 14, 2018 Early endoscopes 1805: Bozzini Lichtleiter
The effect of sodium phosphate enema in patients ingested foreign bodies: a prospective, randomized trial
 Vol.2, No.11, 1294-1298 (2010) doi:10.4236/health.2010.211192 Health The effect of sodium phosphate enema in patients ingested foreign bodies: a prospective, randomized trial Sodium phosphate enema in
Vol.2, No.11, 1294-1298 (2010) doi:10.4236/health.2010.211192 Health The effect of sodium phosphate enema in patients ingested foreign bodies: a prospective, randomized trial Sodium phosphate enema in
Understanding GERD. & Stretta Therapy. GERD (gĕrd): Gastroesophageal Reflux Disease
 Understanding GERD & Stretta Therapy GERD (gĕrd): Gastroesophageal Reflux Disease What is GERD? When the muscle between your stomach and esophagus is weak, stomach contents like acid or bile can reflux
Understanding GERD & Stretta Therapy GERD (gĕrd): Gastroesophageal Reflux Disease What is GERD? When the muscle between your stomach and esophagus is weak, stomach contents like acid or bile can reflux
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
Eosinophilic Esophagitis (EoE)
 Eosinophilic Esophagitis (EoE) 01.06.2016 EoE: immune-mediated disorder food or environmental antigens => Th2 inflammatory response. Key cytokines: IL-4, IL-5, and IL-13 stimulate the production of eotaxin-3
Eosinophilic Esophagitis (EoE) 01.06.2016 EoE: immune-mediated disorder food or environmental antigens => Th2 inflammatory response. Key cytokines: IL-4, IL-5, and IL-13 stimulate the production of eotaxin-3
Myogenic Control. Esophageal Motility. Enteric Nervous System. Alimentary Tract Motility. Determinants of GI Tract Motility.
 Myogenic Control Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Basic Electrical Rythym: intrinsic rhythmic fluctuation of smooth muscle membrane potential
Myogenic Control Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Basic Electrical Rythym: intrinsic rhythmic fluctuation of smooth muscle membrane potential
Esophageal Motility. Alimentary Tract Motility
 Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions Mixing Allows for greater
Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions Mixing Allows for greater
Two Cases of Colonoscopic Retrieval of a Foreign Body in Children: A Button Battery and an Open Safety Pin
 pissn: 2234-8646 eissn: 2234-8840 https://doi.org/10.5223/pghn.2017.20.3.204 Pediatr Gastroenterol Hepatol Nutr 2017 September 20(3):204-209 Case Report PGHN Two Cases of Colonoscopic Retrieval of a Foreign
pissn: 2234-8646 eissn: 2234-8840 https://doi.org/10.5223/pghn.2017.20.3.204 Pediatr Gastroenterol Hepatol Nutr 2017 September 20(3):204-209 Case Report PGHN Two Cases of Colonoscopic Retrieval of a Foreign
David Markowitz, MD. Physicians and Surgeons
 Esophageal Motility David Markowitz, MD Columbia University, College of Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions
Esophageal Motility David Markowitz, MD Columbia University, College of Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions
Surgical aspects of dysphagia
 Dysphagia Why is dysphagia important? Surgery Surgical aspects of dysphagia Adrian P. Ireland aireland@eircom.net Academic RCSI Department of Surgery, Beaumont Hospital Why important Definitons Swallowing
Dysphagia Why is dysphagia important? Surgery Surgical aspects of dysphagia Adrian P. Ireland aireland@eircom.net Academic RCSI Department of Surgery, Beaumont Hospital Why important Definitons Swallowing
Eosinophilic Esophagitis. Another Reason Not to Swallow
 Eosinophilic Esophagitis Another Reason Not to Swallow Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or
Eosinophilic Esophagitis Another Reason Not to Swallow Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form or
Study of aerodigestive tract foreign bodies
 Original article Study of aerodigestive tract foreign bodies 1Dr Durga Prasad. G, 2 Dr Ravi Kumar Raju M, 3 Dr M A N Murty, 4 Dr Rahul Singh 1P.G Resident, KIMS & RF, Amalapuram 2 Prof. of ENT, KIMS &
Original article Study of aerodigestive tract foreign bodies 1Dr Durga Prasad. G, 2 Dr Ravi Kumar Raju M, 3 Dr M A N Murty, 4 Dr Rahul Singh 1P.G Resident, KIMS & RF, Amalapuram 2 Prof. of ENT, KIMS &
Case Report Foreign Body Moves Retrograde through Ileocecal Valve during Colonoscopy
 Hindawi Case Reports in Gastrointestinal Medicine Volume 2017, Article ID 8707959, 4 pages https://doi.org/10.1155/2017/8707959 Case Report Foreign Body Moves Retrograde through Ileocecal Valve during
Hindawi Case Reports in Gastrointestinal Medicine Volume 2017, Article ID 8707959, 4 pages https://doi.org/10.1155/2017/8707959 Case Report Foreign Body Moves Retrograde through Ileocecal Valve during
Diarrhea may be: Acute (short-term, usually lasting several days), which is usually related to bacterial or viral infections.
 Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
Pediatric Gastroenterology Conditions Evaluated and Treated Having a child suffer with abdominal pain, chronic eating problems, or other gastrointestinal disorders can be a very trying time for a parent.
SASKATCHEWAN REGISTERED NURSES ASSOCIATION
 DEFINITION Reflux of gastric contents into the esophagus, which results in esophageal irritation or inflammation. IMMEDIATE CONSULTATION REQUIRED IN THE FOLLOWING SITUATIONS Dysphagia (solid food, progressive)
DEFINITION Reflux of gastric contents into the esophagus, which results in esophageal irritation or inflammation. IMMEDIATE CONSULTATION REQUIRED IN THE FOLLOWING SITUATIONS Dysphagia (solid food, progressive)
Case Report A Rare Case of Hypopharyngeal Screw Migration after Spine Stabilization with Plating
 Case Reports in Otolaryngology Volume 2013, Article ID 475285, 4 pages http://dx.doi.org/10.1155/2013/475285 Case Report A Rare Case of Hypopharyngeal Screw Migration after Spine Stabilization with Plating
Case Reports in Otolaryngology Volume 2013, Article ID 475285, 4 pages http://dx.doi.org/10.1155/2013/475285 Case Report A Rare Case of Hypopharyngeal Screw Migration after Spine Stabilization with Plating
Radiology. Gastrointestinal. Transient Intraluminal Diverticulum of the Esophagus: A Significant Flow Artifact. Farooq P. Agha
 Gastrointest Radiol 9:9%103 (1984) Gastrointestinal Radiology 9 Springer-Verlag 1984 Transient Intraluminal Diverticulum of the Esophagus: A Significant Flow Artifact Farooq P. Agha Department of Radiology,
Gastrointest Radiol 9:9%103 (1984) Gastrointestinal Radiology 9 Springer-Verlag 1984 Transient Intraluminal Diverticulum of the Esophagus: A Significant Flow Artifact Farooq P. Agha Department of Radiology,
Tracheoesophageal Fistula and Esophageal Atresia
 Patient and Family Education Tracheoesophageal Fistula and Esophageal Atresia What is tracheoesophageal fistula? The word fistula means abnormal connection. Tracheoesophageal fistula (TEF) is a condition
Patient and Family Education Tracheoesophageal Fistula and Esophageal Atresia What is tracheoesophageal fistula? The word fistula means abnormal connection. Tracheoesophageal fistula (TEF) is a condition
Esophageal Perforation
 Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease
 ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease Philip O. Katz MD 1, Lauren B. Gerson MD, MSc 2 and Marcelo F. Vela MD, MSCR 3 1 Division of Gastroenterology, Einstein
ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease Philip O. Katz MD 1, Lauren B. Gerson MD, MSc 2 and Marcelo F. Vela MD, MSCR 3 1 Division of Gastroenterology, Einstein
TRACHEOBRONCHIAL FOREIGN BODY REMOVAL ADVICE IN DOGS AND CATS
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk TRACHEOBRONCHIAL FOREIGN BODY REMOVAL ADVICE IN DOGS AND CATS Author : MIKE STAFFORD-JOHNSON, MIKE MARTIN Categories : Vets
Vet Times The website for the veterinary profession https://www.vettimes.co.uk TRACHEOBRONCHIAL FOREIGN BODY REMOVAL ADVICE IN DOGS AND CATS Author : MIKE STAFFORD-JOHNSON, MIKE MARTIN Categories : Vets
A study of clinical and endoscopic findings in benign strictures of middle and lower thirds of esophagus
 Original article A study of clinical and endoscopic findings in benign strictures of middle and lower thirds of esophagus 1Dr. Varsha S. Dabadghao, 2 Dr. Arjun Lal Kakrani 1Associate Professor, Department
Original article A study of clinical and endoscopic findings in benign strictures of middle and lower thirds of esophagus 1Dr. Varsha S. Dabadghao, 2 Dr. Arjun Lal Kakrani 1Associate Professor, Department
Benchmarking For Colonoscopy. Technology and Technique to Improve Adenoma Detection
 Benchmarking For Colonoscopy Technology and Technique to Improve Adenoma Detection Objectives 1. Review the latest data on performance characteristics and efficacy for colon cancer prevention 2. Highlight
Benchmarking For Colonoscopy Technology and Technique to Improve Adenoma Detection Objectives 1. Review the latest data on performance characteristics and efficacy for colon cancer prevention 2. Highlight
Translaryngeal tracheostomy
 Translaryngeal tracheostomy Issued: August 2013 NICE interventional procedure guidance 462 guidance.nice.org.uk/ipg462 NICE has accredited the process used by the NICE Interventional Procedures Programme
Translaryngeal tracheostomy Issued: August 2013 NICE interventional procedure guidance 462 guidance.nice.org.uk/ipg462 NICE has accredited the process used by the NICE Interventional Procedures Programme
Non-Surgical Management of Gastroduodenal Fistula Caused by Ingested Neodymium Magnets
 pissn: 2234-8646 eissn: 2234-8840 https://doi.org/10.5223/pghn.2018.21.4.336 Pediatr Gastroenterol Hepatol Nutr 2018 October 21(4):336-340 Case Report PGHN Non-Surgical Management of Gastroduodenal Fistula
pissn: 2234-8646 eissn: 2234-8840 https://doi.org/10.5223/pghn.2018.21.4.336 Pediatr Gastroenterol Hepatol Nutr 2018 October 21(4):336-340 Case Report PGHN Non-Surgical Management of Gastroduodenal Fistula
GIT RADIOLOGY. Water-soluble contrast media (e.g. gastrograffin) are the other available agents.which doesn t cause inflammatory peritonitis..
 GIT RADIOLOGY Imaging techniques-general principles: Contrast examinations: Barium sulphate is the best contrast for GIT (with good mucosal coating & excellent opacification & being inert); but is contraindicated
GIT RADIOLOGY Imaging techniques-general principles: Contrast examinations: Barium sulphate is the best contrast for GIT (with good mucosal coating & excellent opacification & being inert); but is contraindicated
CPT COD1NG UPDATES Gastroenterology CPT Advisors
 2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
2014 CPT COD1NG UPDATES Gastroenterology CPT Advisors Joel V. Brill, MD, AGA CPT Advisor Daniel C. DeMarco, MD, ACG CPT Advisor Glenn D. Littenberg, MD, ASGE CPT Advisor The American College of Gastroenterology
Retrieval Devices MA KIN G A D IFFER EN C E T O H EA L T H
 Retrieval Devices For over 25 years the ROTH NET retriever has been the go to device for physicians around the world and this expanded range, coupled with the rest of our portfolio has created a dynamic
Retrieval Devices For over 25 years the ROTH NET retriever has been the go to device for physicians around the world and this expanded range, coupled with the rest of our portfolio has created a dynamic
pthaigastro.org Caustic injury The 5 th Pediatric GI Days Pediatric GI & Liver Emergency : Current Practical Management
 The 5 th Pediatric GI Days Pediatric GI & Liver Emergency : Current Practical Management Caustic injury Phisek Yimyaem Pediatric Department, Khon Kaen Regional Hospital 18 July 2013 Outlines Introduction
The 5 th Pediatric GI Days Pediatric GI & Liver Emergency : Current Practical Management Caustic injury Phisek Yimyaem Pediatric Department, Khon Kaen Regional Hospital 18 July 2013 Outlines Introduction
Roth Net Speciality Retrieval M AKI N G A DIF F ERENC E TO HEAL TH
 Roth Net Speciality Retrieval M AKI N G A DIF F ERENC E TO HEAL TH 2 Retrieval Devices PlatinumTM Universal Select Mini Polyp Maxi Mini Enteroscopic 00711050/1052/1053/1162 00711155 00715050/5060 00711169/1170
Roth Net Speciality Retrieval M AKI N G A DIF F ERENC E TO HEAL TH 2 Retrieval Devices PlatinumTM Universal Select Mini Polyp Maxi Mini Enteroscopic 00711050/1052/1053/1162 00711155 00715050/5060 00711169/1170
Danis Procedure Pack - BASIC
 Danis Procedure Pack - BASIC Manufactured by: ELLA CS, s.r.o. Milady Horákové 504 500 06 Hradec Králové 6 Czech Republic Phone: +420 49 527 91 11 Fax: +420 49 526 56 55 E-mail: volenec@ellacs.eu Danis
Danis Procedure Pack - BASIC Manufactured by: ELLA CS, s.r.o. Milady Horákové 504 500 06 Hradec Králové 6 Czech Republic Phone: +420 49 527 91 11 Fax: +420 49 526 56 55 E-mail: volenec@ellacs.eu Danis
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
Introduction to Emergency Medical Care 1 OBJECTIVES 8.1 Define key terms introduced in this chapter. Slides 12 15, 21, 24, 31-34, 39, 40, 54 8.2 Describe the anatomy and physiology of the upper and lower
Achalasia and Laparoscopic Heller Myotomy
 1 Monterey County Surgical Associates 2 Upper Ragsdale Drive, Bldg B, Suite 230 Monterey, CA 93940 Phone: (831) 649-0808 Fax: (831) 649-8795 Mark Vierra, MD Achalasia and Laparoscopic Heller Myotomy Introduction
1 Monterey County Surgical Associates 2 Upper Ragsdale Drive, Bldg B, Suite 230 Monterey, CA 93940 Phone: (831) 649-0808 Fax: (831) 649-8795 Mark Vierra, MD Achalasia and Laparoscopic Heller Myotomy Introduction
Discussing feline tracheal disease
 Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
Vet Times The website for the veterinary profession https://www.vettimes.co.uk Discussing feline tracheal disease Author : ANDREW SPARKES Categories : Vets Date : March 24, 2008 ANDREW SPARKES aims to
Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
Dysphagia after EA repair. Disclosure. Learning objectives 9/17/2013
 Dysphagia after EA repair Christophe Faure, M.D. Professor of Pediatrics, Division of Pediatric Gastroenterology, Sainte-Justine University Health Center, Université de Montréal, Montréal, QC, Canada christophe.faure@umontreal.ca
Dysphagia after EA repair Christophe Faure, M.D. Professor of Pediatrics, Division of Pediatric Gastroenterology, Sainte-Justine University Health Center, Université de Montréal, Montréal, QC, Canada christophe.faure@umontreal.ca
A CURIOUS CASE OF HYPERTENSIVE LES. Erez Hasnis Department of Gastroenterology Rambam Health Care Campus
 A CURIOUS CASE OF HYPERTENSIVE LES Erez Hasnis Department of Gastroenterology Rambam Health Care Campus CASE DESCRIPTION 63yo, F, single, attending nurse. PMH includes T2DM (Sitagliptin/Metformin), Hyperlipidemia
A CURIOUS CASE OF HYPERTENSIVE LES Erez Hasnis Department of Gastroenterology Rambam Health Care Campus CASE DESCRIPTION 63yo, F, single, attending nurse. PMH includes T2DM (Sitagliptin/Metformin), Hyperlipidemia
THORACIC SURGERY: Dysphagia. Dr. Robert Zeldin Dr. John Dickie Dr. Carmine Simone. Thoracic Surgery Toronto East General Hospital
 THORACIC SURGERY: Dysphagia Dr. Robert Zeldin Dr. John Dickie Dr. Carmine Simone Thoracic Surgery Toronto East General Hospital Objectives Definitions Common causes Investigations Treatment options Anatomy
THORACIC SURGERY: Dysphagia Dr. Robert Zeldin Dr. John Dickie Dr. Carmine Simone Thoracic Surgery Toronto East General Hospital Objectives Definitions Common causes Investigations Treatment options Anatomy
Gastroenterology. Certification Examination Blueprint. Purpose of the exam
 Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
Gastroenterology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified gastroenterologist
PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
 Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
Patient Information published on: 03/2004 by the Society of American Gastrointestinal and Endoscopic Surgeons (SAGES) PATIENT INFORMATION FROM YOUR SURGEON & SAGES Laparoscopic Anti-Reflux (GERD) Surgery
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Foreign body ingestions occur
 Navid Dehghani, MD, FRCRC, Jeffrey P. Ludemann, MDCM, FRCSC Ingested foreign bodies in children: BC Children s Hospital emergency room protocol Clinicians should be aware of the dangers presented by disc
Navid Dehghani, MD, FRCRC, Jeffrey P. Ludemann, MDCM, FRCSC Ingested foreign bodies in children: BC Children s Hospital emergency room protocol Clinicians should be aware of the dangers presented by disc
Achalasia is a rare disease with an annual incidence estimated REVIEWS. Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:1020 1024 REVIEWS Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia BOUDEWIJN F. KESSING, ALBERT J. BREDENOORD, and ANDRÉ J. P. M. SMOUT
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:1020 1024 REVIEWS Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia BOUDEWIJN F. KESSING, ALBERT J. BREDENOORD, and ANDRÉ J. P. M. SMOUT
Module 2 Heartburn Glossary
 Absorption Antacids Antibiotic Module 2 Heartburn Glossary Barrett s oesophagus Bloating Body mass index Burping Chief cells Colon Digestion Endoscopy Enteroendocrine cells Epiglottis Epithelium Absorption
Absorption Antacids Antibiotic Module 2 Heartburn Glossary Barrett s oesophagus Bloating Body mass index Burping Chief cells Colon Digestion Endoscopy Enteroendocrine cells Epiglottis Epithelium Absorption
Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012
 Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012 Esophageal Leiomyoma Introduction Case presentation Operative video Discussion Esophageal Leiomyoma Benign tumors of the
Hong Kong Society of Upper Gastrointestinal Surgeons CLINICAL MEETING 29 NOV 2012 Esophageal Leiomyoma Introduction Case presentation Operative video Discussion Esophageal Leiomyoma Benign tumors of the
Combined Experience of Two European Centers
 Minimally Invasive Surgery for Achalasia: Combined Experience of Two European Centers Garzi A, Valla JS*, Molinaro F, Amato G, Messina M. Unit of Pediatric Surgery, University of Siena (Italy) *Lenval
Minimally Invasive Surgery for Achalasia: Combined Experience of Two European Centers Garzi A, Valla JS*, Molinaro F, Amato G, Messina M. Unit of Pediatric Surgery, University of Siena (Italy) *Lenval
Esophageal stricture causes and pattern of presentation at Ibn Sina Specialized Hospital Abstract Introduction: Methods: Results and discussion:
 bü z ÇtÄ TÜà väx causes and pattern of presentation at Ibn Sina Specialized Hospital Mohammed Osman El Hassan Gadour 1 and Hayder Hussein Elamin 2 Abstract Introduction: The aim of this study is to evaluate
bü z ÇtÄ TÜà väx causes and pattern of presentation at Ibn Sina Specialized Hospital Mohammed Osman El Hassan Gadour 1 and Hayder Hussein Elamin 2 Abstract Introduction: The aim of this study is to evaluate
Indian Journal of Basic and Applied Medical Research; December 2015: Vol.-5, Issue- 1, P
 Original article A study of clinical profile and therapeutic efficacy of esophageal dilatation with Savary- Gilliard dilators in benign strictures of middle and lower thirds of esophagus,without the use
Original article A study of clinical profile and therapeutic efficacy of esophageal dilatation with Savary- Gilliard dilators in benign strictures of middle and lower thirds of esophagus,without the use
Endoscopic Management of Perforations
 Endoscopic Management of Perforations Gregory G. Ginsberg, MD Professor of Medicine University of Pennsylvania Perelman School of Medicine Gastroenterology Division Executive Director of Endoscopic Services
Endoscopic Management of Perforations Gregory G. Ginsberg, MD Professor of Medicine University of Pennsylvania Perelman School of Medicine Gastroenterology Division Executive Director of Endoscopic Services
ReShape Integrated Dual Balloon System Procedure Manual
 ReShape Integrated Dual Balloon System Procedure Manual 1 TABLE OF CONTENTS Introduction... 3 Product Description... 3 Overview... 3 Component description... 4 Intragastric Balloon... 4 Placement Catheter...
ReShape Integrated Dual Balloon System Procedure Manual 1 TABLE OF CONTENTS Introduction... 3 Product Description... 3 Overview... 3 Component description... 4 Intragastric Balloon... 4 Placement Catheter...
Gastric Signet-Ring Cell Carcinoma: Unilateral Lower Extremity Lymphoedema as the Presenting Feature
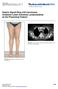 Clinical Image TheScientificWorldJOURNAL (2007) 7, 1189 1192 ISSN 1537-744X; DOI 10.1100/tsw.2007.199 Gastric Signet-Ring Cell Carcinoma: Unilateral Lower Extremity Lymphoedema as the Presenting Feature
Clinical Image TheScientificWorldJOURNAL (2007) 7, 1189 1192 ISSN 1537-744X; DOI 10.1100/tsw.2007.199 Gastric Signet-Ring Cell Carcinoma: Unilateral Lower Extremity Lymphoedema as the Presenting Feature
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to
 1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
1 Chapter 40 Advanced Airway Management 2 Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only. In
Having a PEG tube inserted
 Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
Having a PEG tube inserted This information leaflet is for patients who are having a PEG (Percutaneous Endoscopic Gastrostomy) tube inserted. It explains what is involved, what to expect and what significant
Chapter 40 Advanced Airway Management
 1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
1 2 3 4 5 Chapter 40 Advanced Airway Management Advanced Airway Management The advanced airway management techniques discussed in this chapter are to introduce the EMT-B student to these procedures only.
GERD. Gastroesophageal reflux disease, or GERD, occurs when acid from the. stomach backs up into the esophagus. Normally, food travels from the
 GERD What is GERD? Gastroesophageal reflux disease, or GERD, occurs when acid from the stomach backs up into the esophagus. Normally, food travels from the mouth, down through the esophagus and into the
GERD What is GERD? Gastroesophageal reflux disease, or GERD, occurs when acid from the stomach backs up into the esophagus. Normally, food travels from the mouth, down through the esophagus and into the
Correspondence should be addressed to Justin Cochrane;
 Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 794282, 4 pages http://dx.doi.org/10.1155/2015/794282 Case Report Acute on Chronic Pancreatitis Causing a Highway to the Colon with Subsequent
Case Reports in Gastrointestinal Medicine Volume 2015, Article ID 794282, 4 pages http://dx.doi.org/10.1155/2015/794282 Case Report Acute on Chronic Pancreatitis Causing a Highway to the Colon with Subsequent
Eosinophilic Esophagitis: Extraesophageal Manifestations
 Eosinophilic Esophagitis: Extraesophageal Manifestations Karen B. Zur, MD Director, Pediatric Voice Program Associate Director, Center for Pediatric Airway Disorders The Children s Hospital of Philadelphia
Eosinophilic Esophagitis: Extraesophageal Manifestations Karen B. Zur, MD Director, Pediatric Voice Program Associate Director, Center for Pediatric Airway Disorders The Children s Hospital of Philadelphia
Stenting for Esophageal Cancer Technical Issues and Outcomes
 Stenting for Esophageal Cancer Technical Issues and Outcomes Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Disclosures Research and Educational
Stenting for Esophageal Cancer Technical Issues and Outcomes Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Disclosures Research and Educational
Research Article Balloon Dilatation of Pediatric Subglottic Laryngeal Stenosis during the Artificial Apneic Pause: Experience in 5 Children
 BioMed Research International, Article ID 397295, 4 pages http://dx.doi.org/10.1155/2014/397295 Research Article Balloon Dilatation of Pediatric Subglottic Laryngeal Stenosis during the Artificial Apneic
BioMed Research International, Article ID 397295, 4 pages http://dx.doi.org/10.1155/2014/397295 Research Article Balloon Dilatation of Pediatric Subglottic Laryngeal Stenosis during the Artificial Apneic
Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES
 SAGES Society of American Gastrointestinal and Endoscopic Surgeons https://www.sages.org Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Author : SAGES Webmaster Surgery for Heartburn
SAGES Society of American Gastrointestinal and Endoscopic Surgeons https://www.sages.org Laparoscopic Anti-Reflux (GERD) Surgery Patient Information from SAGES Author : SAGES Webmaster Surgery for Heartburn
INVESTIGATIONS OF GASTROINTESTINAL DISEAS
 INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
INVESTIGATIONS OF GASTROINTESTINAL DISEAS Lecture 1 and 2 دز اسماعيل داود فرع الطب كلية طب الموصل Radiological tests of structure (imaging) Plain X-ray: May shows soft tissue outlines like liver, spleen,
UMC HEALTH SYSTEM Lubbock, Texas :
 Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
Consent for Commonly Performed Procedures in the Adult Critical Care Units I, the undersigned, understand that the adult intensive and intermediate care units ( critical care units ) are places where seriously
