ICHD 3 Guide to use and key definitions ASHS UCNS Board Review. Morris Levin Chief, Division of Headache Medicine Department of Neurology, UCSF
|
|
|
- Oswald Hawkins
- 5 years ago
- Views:
Transcription
1 ICHD 3 Guide to use and key definitions ASHS UCNS Board Review Morris Levin Chief, Division of Headache Medicine Department of Neurology, UCSF
2 Disclosures for Dr. Morris Levin Consultant: Supernus, Upsher-Smith, Lilly, Amgen, Allergan, Alder, Teva Royalties: Oxford University Press, Anadem Publishing, Wiley Blackwell, Castle Connolly Publishing, UCSF Office of Innovation
3 History International classification of headache disorder, 1st edition (ICHD-1) in 1988 ICHD-2 in 2004 ICHD-3 beta in 2013 ICHD-3 in 2018* *Based on 4 years of input including field testing and research aimed at increasing precision and accuracy ICHD 3
4 Painful structures in the head (neck) Dura Dural veins and arteries Intracran arteries V,VII,IX,X,C1-3 Periosteum Scalp Scalp muscles Scalp vessels Sinuses Eyes Ears Teeth, TMJ Carotids, vertebrals C-spine periost Cerv musc
5 Painful structures in the head (neck) Not painful Parenchyma Pia, arachnoid Skull Ventricles
6 ICHD III Basic Organization Part 1: Primary headaches Part 2: Secondary headaches Part 3: Cranial Neuralgias, etc. The Appendix
7 ICHD III The Appendix: 1. Suggested criteria for possible new entities 2. Alternative diagnostic criteria for certain categories (pending evidence) 3. Some previously accepted disorders which have not been supported by evidence
8 ICHD III Part 1: Primary headaches (no other causative disorder) 1. Migraine 2. Tension-type Headache 3. Cluster and its relatives (TACs) 4. Other primary headaches exertional, hypnic headache, NDPH, et al
9 Migraine 1.1 Migraine without aura Diagnostic criteria: A. At least five attacks1 fulfilling criteria B D B. Headache attacks lasting 4 72 hours (when untreated or unsuccessfully treated) C. Headache has at least two of the following four characteristics: 1. unilateral location 2. pulsating quality 3. moderate or severe pain intensity 4. aggravation by or causing avoidance of routine physical activity D. During headache at least one of the following: 1. nausea and/or vomiting 2. photophobia and phonophobia
10 1.2 Migraine with Aura ICHD 3 b A. At least two attacks fulfilling criteria B and C B. One or more of the following fully reversible aura symptoms: 1. visual 2. sensory 3. speech and/or language 4. motor 5. brainstem 6. retinal C. At least 2 of the following 4 characteristics: 1. at least one aura symptom spreads gradually over 5 minutes and/or two or more aura symptoms occur in succession 2. each individual aura symptom lasts 5-60 minutes 3. at least one aura symptom is unilateral 4. the aura is accompanied, or followed within 60 minutes, by HA D. Not better accounted for by another ICHD-3 diagnosis.
11 New Definition of 1.2 Migraine with Aura ICHD 3 Final A. At least two attacks fulfilling criteria B and C B. One or more of the following fully reversible aura symptoms: 1. visual 2. sensory 3. speech and/or language 4. motor 5. brainstem 6. retinal C. At least three of the following six characteristics: 1. at least one aura symptom spreads gradually over 5 minutes 2. two or more aura symptoms occur in succession 3. each individual aura symptom lasts 5-60 minutes 4. at least one aura symptom is unilateral 5. at least one aura symptom is positive 6. the aura is accompanied, or followed within 60 minutes, by headache D. Not better accounted for by another ICHD-3 diagnosis.
12 New Definition of Migraine with Aura (new) 1.2 criteria performed much better in distinguishing MA from TIA ICHD is dynamic
13 1.2 Migraine with typical aura A. Attacks fulfilling criteria for 1.2 Migraine with aura and criterion B below B. Aura with both of the following: 1. fully reversible visual, sensory and/or speech/ language symptoms 2. no motor, brainstem or retinal symptoms.
14 Migraine with Aura ICHD III Migraine with aura Migraine with typical aura Migraine with brainstem aura Hemiplegic Migraine Retinal migraine With headache Without headaches
15 1.2.4 Retinal migraine A. At least 2 attacks fulfilling criteria B and C B. Aura of fully reversible monocular positive and/or negative visual phenomena confirmed during an attack by either or both of the following: 1. clinical visual field examination 2. patient s drawing of a monocular field defect C. 2 of the following 3 characteristics: 1. aura spreads gradually over 5 min 2. aura symptoms last 5-60 min 3. aura accompanied or followed in <60 min by headache
16 Retinal migraine v. Binocular aura The typical migraine visual aura is a binocular visual disturbance. Most patients describe the disturbance as monocular as it tends to occur in either the right or left visual field, which they interpret as occurring in the eye on the side of the disturbance. It is present with eyes open or closed. Careful questioning almost always reveals that it occurs as a binocular phenomenon.
17 Retinal migraine v. Binocular aura How to tell if symptoms are emanating from one eye or are homonymous? If positive phenomena are emanating from one retina e.g. closing that eye will NOT eliminate them If negative phenomena are emanating from one retina, closing that eye will eliminate them. But negative phenomena emanating from one retina may not have been noticed in the first place if that is not the dominant eye.
18 1.2.4 Retinal migraine A. At least 2 attacks fulfilling criteria B and C B. Aura of fully reversible monocular positive and/or negative visual phenomena confirmed during an attack by either or both of the following: 1. clinical visual field examination 2. patient s drawing of a monocular field defect C. 2 of the following 3 characteristics: 1. aura spreads gradually over 5 min 2. aura symptoms last 5-60 min 3. aura accompanied or followed in <60 min by headache D. Not better accounted for by another ICHD-3 diagnosis, and other causes of amaurosis fugax excluded
19 1.2.2 Migraine with brainstem aura A. At least 2 attacks fulfilling criteria B and C below, and criteria C and D for Migraine with typical aura B. Aura of fully reversible visual, sensory and/or speech/language symptoms, but not motor or retinal C. 2 of the following brainstem symptoms: 1. dysarthria 2. vertigo 3. tinnitus 4. hypacusis 5. diplopia 6. ataxia 7. decr level of consc Richter, F et al. Enhanced neuronal excitability in adult rat brainstem causes widespread repetitive brainstem depolarizations. Jnl Cereb Blood Flow Metab 2012; 32: Noseda, R, & Burstein, R (2013). Migraine pathophysiology: anatomy of the trigeminovascular pathway and associated neurological symptoms, cortical spreading depression, sensitization, and modulation of pain. PAIN 2013, 154, S44-S53. descendent modulation of the brainstem trigeminovasc system from CSD projected to brainstem via descending neuronal pathways
20 1.2.2 Migraine with brainstem aura A. At least 2 attacks fulfilling criteria B and C below, and criteria C and D for Migraine with typical aura B. Aura of fully reversible visual, sensory and/or speech/language symptoms, but not motor or retinal C. 2 of the following brainstem symptoms: 1. dysarthria 2. vertigo 3. tinnitus 4. hypacusis 5. diplopia 6. ataxia 7. decr level of consc Richter, F et al. Enhanced neuronal excitability in adult rat brainstem causes widespread repetitive brainstem depolarizations. Jnl Cereb Blood Flow Metab 2012; 32: Noseda, R, & Burstein, R (2013). Migraine pathophysiology: anatomy of the trigeminovascular pathway and associated neurological symptoms, cortical spreading depression, sensitization, and modulation of pain. PAIN 2013, 154, S44-S53. descendent modulation of the brainstem trigeminovasc system from CSD projected to brainstem via descending neuronal pathways
21 A1.6.5 Vestibular migraine a proposed migraine subtype A. At least five episodes fulfilling criteria C and D B. A current or past history of 1.1 Migraine without aura or 1.2 Migraine with aura1 C. Vestibular symptoms of moderate or severe intensity, lasting between 5 minutes and 72 hours D. At least 50% of episodes are associated with at least one of the following three migrainous features: 1. headache with at least two of the following four: a)unilat location b) pulsating quality c) moderate or severe intensity d) aggravation by routine activity 2. photophobia and phonophobia 3. visual aura
22 Migraine with Aura ICHD III Migraine with typical aura With headache Without headaches Migraine with aura Migraine with brainstem aura Migraine with hemiplegia Retinal migraine Vestibular migraine
23 Menstrual migraine is not listed in the ICHD3 considered a trigger But: Appendix A1.1.1 Pure menst mig without aura A1.1.2 Menstrually related mig without aura A1.1.3 Non-menst mig without aura
24 Chronic migraine defined as migraine or strongly suspected migraine on >15d/mo ICHD3 1.3 Chronic Migraine A. Headache on 15 d/mo for >3 mo B. In a patient who has had 5 attacks fulfilling criteria for 1.1 Migraine without aura or 1.2 Migraine with aura C. On 8 d/mo for >3 mo fulfilling any of the following: 1. criteria C and D for 1.1 Migraine without aura 2. criteria B and C for 1.2 Migraine with aura 3. believed by the patient to be migraine at onset and relieved by a triptan or ergot derivative D. Not better accounted for by another ICHD-3 diagnosis
25 Imaging studies support the distinction between EM and CM Maniyar, FH et al. Functional imaging in Chronic Migraine. Curr Headache and Pain Reports, Increasing frequency of migraine attacks is associated with changes in key brainstem areas, basal ganglia and various cortical areas involved in pain. Schwedt, T, et al Headache 2015 Accurate subclassification of individuals into lower and higher frequency subgroups via measurements of cortical thickness (and other measurements in temporal pole, anterior cingulate cortex, superior temporal lobe, entorhinal cortex, medial orbital frontal gyrus, and pars triangularis. Threshold = 15 days per month
26 1.2.3 Hemiplegic migraine A. At least 2 attacks fulfilling criteria B and C B. Aura consisting of both of the following: 1. fully reversible motor weakness; 2. fully reversible visual, sensory and/or speech/language symptoms C. 2 of the following 4 characteristics: 1. 1 aura symptom spreads gradually over 5 min, and/or 2 symptoms occur in succession 2. each individual non-motor aura symptom lasts 5-60 min, and motor symptoms last <72 h 3. 1 aura symptom is unilateral 4. aura accompanied or followed in <60 min by headache D. Not better accounted for by another ICHD-3 diagnosis, and TIA excluded
27 Familial hemiplegic migraine (FHM) A. Fulfils criteria for Hemiplegic migraine B. At least one first- or second-degree relative has had attacks fulfilling criteria for Hemiplegic migraine Mutations in the CACNA1A, ATP1A2, SCN1A, genes which code for ion transport channel proteins PRRT2 gene mutation can also cause FHM also benign familial infantile convulsions and kinesiogenic dystonia
28 Familial hemiplegic migraine (FHM) FHM1 - CACNA1A gene (coding for a Ca channel) on chrom 19 FHM2 - ATP1A2 gene (coding for a K/Na-ATPase) on chrom 1 FHM3 - SCN1A gene (coding for a Na channel) on chrom 2. FHM very often presents with brainstem symptoms in addition to typical aura symptoms Headache almost always occurs. Rarely, during FHM attacks, disturbances of consciousness (including coma), confusion, fever and CSF pleocytosis can occur.
29 Sporadic hemiplegic migraine A. Fulfils criteria for Hemiplegic migraine B. No first- or second-degree relative has had attacks fulfilling criteria for Hemiplegic migraine 50% of hemiplegic migraine Ddx for all forms of HM TIAs, HANDL (HA, Neuro deficits and CSF lymphocytosis)
30 Complications of migraine Status migrainosis unremitting for >72 hours pain and/or associated sx are debilitating Persistent aura without infarction >1 week with nl MRI Migrainous infaction Aura sx >1 hour, MRI shows stroke in approp area
31 Pediatric migraine and syndromes Migraine in childhood 2-72 h Recurrent GI disturbance discomfort or nausea/vom Cyc vom ( ) and Abd mig ( ) both include pain and nauseas; differences: CV age 3-5 and inv vom 4x/h up to 10 days AM age 7-10, and inv less vomiting, up to 3 d Benign Paroxysmal Vertigo (not BPPV) brief unprovoked attacks of vertigo, may be accomp by N/V (r/u sz, mass) Benign Paroxysmal Torticollis attacks of head tilt in infant or young child
32 Tension type headache Tension HA Muscle contraction headache Tension-type headache
33 2.1 Infrequent episodic TTH A. At least 10 episodes of headache occurring on <1 d/mo (<12 d/y) and fulfilling criteria B-D B. Lasting from 30 min to 7 d C. 2 of the following 4 characteristics: 1. bilateral location 2. pressing or tightening (non-pulsating) quality 3. mild or moderate intensity 4. not aggravated by routine physical activity D. Both of the following: 1. no nausea or vomiting 2. no more than one of photophobia or phonophobia E. Not better accounted for by another ICHD-3 diagnosis
34 A2. TTH A. Episodes of headache fulfilling one of the tension type headache criteria B. Lasting from 30 min to 7 d C. 3 of the following 4 characteristics: 1. bilateral location 2. pressing or tightening (non-pulsating) quality 3. mild or moderate intensity 4. not aggravated by routine physical activity D. No nausea or vomiting; No photophobia or phonophobia E. Not better accounted for by another ICHD-3 diagnosis more specific, less likely to diagnose mild migraine Migraine TTHA
35 2.2 Frequent episodic TTH A. At least 10 episodes occurring on 1-14 d/mo for >3 mo ( 12 and <180 d/y) and fulfilling criteria B-D B. Lasting from 30 min to 7 d C. 2 of the following 4 characteristics: 1. bilateral location 2. pressing or tightening (non-pulsating) quality 3. mild or moderate intensity 4. not aggravated by routine physical activity D. Both of the following: 1. no nausea or vomiting 2. no more than one of photophobia or phonophobia E. Not better accounted for by another ICHD-3 diagnosis
36 2.3 Chronic TTH A. Headache occurring on 15 d/mo on average for >3 mo ( 180 d/y), fulfilling criteria B-D B. Lasting hours to days, or unremitting C. 2 of the following 4 characteristics: 1. bilateral location 2. pressing/tightening (non-pulsating) quality 3. mild or moderate intensity 4. not aggravated by routine physical activity D. Both of the following: 1. not >1 of photophobia, phonophobia, mild nausea 2. neither moderate or severe nausea nor vomiting E. Not better accounted for by another ICHD-3 diagnosis
37 TTHA still subdivided by presence/absence of muscle tenderness Infrequent (<1/mo), Freq (1-14 d/mo), CTTH (>15 d/mo) Each category subdivided with or w/o pericranial tenderness. And still no clear evidence for etiopathology
38 3. Trigeminal autonomic cephalalgias (TACs) 3.1 Cluster headache 3.2 Paroxysmal hemicrania 3.3 Short-lasting unilateral neuralgiform headache. 3.4 Hemicrania continua All are unilateral, supposedly accompanied by restlessness and accompanied by cranial autonomic sx. But are they related?
39 3.1 Cluster headache A.At least 5 attacks fulfilling criteria B-D B.Severe or very severe unilateral orbital, supraorbital and/or temporal pain lasting min (when untreated) C.Either or both of the following: 1. 1 of the following ipsilateral symptoms or signs: a) conjunctival injection and/or lacrimation; b) nasal congestion and/or rhinorrhoea; c) eyelid oedema; d) fore-head and facial sweating; e) forehead and facial flushing; f) sensation of fullness in the ear; g) miosis and/or ptosis 2. a sense of restlessness or agitation D. Frequency from 1/2 d to 8/d for > half the time when active E. Not better accounted for by another ICHD-3 diagnosis
40 3.1 Cluster headache Episodic cluster headache A. Attacks fulfilling criteria for 3.1 Cluster headache and occurring in bouts (cluster periods) B. 2 cluster periods lasting 7 d to 1 y (when untreated) and separated by pain-free remission periods of 1 mo Chronic cluster headache A. Attacks fulfilling criteria for 3.1 Cluster headache and criterion B below B. Occurring without a remission period, or with remissions lasting <1 mo, for 1 y
41 3.2 Paroxysmal hemicrania A.At least 20 attacks fulfilling criteria B-E B.Severe unilateral orbital, supraorbital and/or temporal pain lasting 2-30 min C. 1 of the following ipsilateral symptoms or signs: 1. conjunctival injection and/or lacrimation 2. nasal congestion and/or rhinorrhoea 3. eyelid oedema 4. forehead and facial sweating 5. forehead and facial flushing 6. sensation of fullness in the ear 7. miosis and/or ptosis D. Frequency >5/d for > half the time E.Prevented absolutely by therapeutic doses of indomethacin F. Not better accounted for by another ICHD-3 diagnosis
42 3.2 Paroxysmal hemicrania Episodic paroxysmal hemicrania A. Attacks fulfilling criteria for 3.2 Paroxysmal hemicrania and occurring in bouts B. 2 bouts lasting 7d to 1 y (when untreated) and separated by pain-free remission periods of 1 mo Chronic paroxysmal hemicrania A. Attacks fulfilling criteria for 3.2 Paroxysmal hemicrania B. Occurring without a remission period, or with remission periods lasting <1 mo, for 1 y
43 3.3 Short-lasting unilateral neuralgiform headache attacks (SUN) A.At least 20 attacks fulfilling criteria B-D B.Moderate or severe unilateral head pain, with orbital, supraorbital, temporal and/or other trigeminal distribution, lasting s and occurring as single stabs, series of stabs or in a saw-tooth pattern C. 1 of the following ipsilateral cranial autonomic symptoms or signs: 1. conjunctival injection and/or lacrimation; 2. nasal congestion and/or rhinorrhoea; 3. eyelid oedema; 4. forehead and facial sweating; 5. forehead and facial flushing; 6. sensation of fullness in the ear; 7. miosis and/or ptosis D. Frequency 1/d for > half the time when active E.Not better accounted for by another ICHD-3 diagnosis
44 3.3 Short-lasting unilateral neuralgiform headache attacks Short-lasting unilateral neuralgiform headache attacks with conjunctival injection and tearing (SUNCT) 3.3.2Short lasting unilateral neuralgiform headache attacks with cranial autonomic symptoms, but with conjunctival injection or tearing or neither) (SUNA) Either can be episodic or chronic Episodic - 7d to 1 y and separated by pain-free remission periods of 1 mo Chronic - Occurring without a remission period, or with remissions lasting <1 mo, and continuing for 1 y
45 3.4 Hemicrania continua A.Unilateral headache fulfilling criteria B-D B.Present >3 mo, with exacerbations of moderate or greater intensity C.Either or both of the following: 1. 1 of the following ipsilateral symptoms or signs: a) conjunctival injection and/or lacrimation; b) nasal congestion and/or rhinorrhoea; c) eyelid oedema; d) fore-head and facial sweating; e) forehead and facial flushing; f) sensation of fullness in the ear; g) miosis and/or ptosis 2. a sense of restlessness or agitation, or aggravation of pain by movement D. Responds absolutely to therapeutic doses of indomethacin E. Not better accounted for by another ICHD-3 diagnosis
46 3.4 Hemicrania continua Hemicrania continua, remitting subtype A. Headache fulfilling criteria for 3.4 Hemicrania continua, and criterion B below B. Headache is not daily or continuous, but interrupted by remission periods of 1 d without treatment Hemicrania continua, unremitting subtype A. Headache fulfilling criteria for 3.4 Hemicrania continua, and criterion B below B. Headache is daily and continuous for 1 y, without remission periods of 1 d
47 TAC s: Duration decreases with name length HC Months-Yrs Cluster min Paroxysmal Hemicrania 2-30 min Short-lasting unilateral neuralgiform headaches sec
48 4. Other primary headache disorders 4.1 Primary cough headache 4.2 Primary exercise headache 4.3 Primary headache associated with sexual activity 4.4 Primary thunderclap headache 4.5 Cold-stimulus headache 4.6 External pressure headache 4.7 Primary stabbing headache 4.8 Nummular headache 4.9 Hypnic headache 4.10 New daily persistent headache (NDPH)
49 4. Other primary headache disorders 4.1 Primary cough headache sudden with cough or Valsalva 1 sec-2 h 4.2 Primary exercise headache during or after sustained exercise <48 h 4.3 Primary headache associated with sexual activity - Either or both : 1. increasing in intensity with increasing sexual excitement 2. abrupt explosive intensity just before or with orgasm
50 4.4 Primary thunderclap headache Diagnostic criteria: A. Severe head pain B. Abrupt onset, reaching maximum intensity in <1 minute C. Lasting for 5 minutes D. Not better accounted for by another ICHD-3 diagnosis
51 4.4 Primary thunderclap headache Ddx: Subarachnoid hemorrhage Intracerebral hemorrhage Pituitary Apoplexy 3 rd ventric colloid cyst Cerebral Venous Thrombosis Arterial Dissection CNS Vasculitis, RCVS Intracranial hypotension Primary Thunderclap Headache Sex related Headache Meningitis Acute Sinusitis Unruptured AVM, aneurysm ICHD 3: Evidence that Thunderclap headache exists as a primary condition is poor; the search for an underlying cause should be expedited and expected ICHD 3
52 4. Other primary headache disorders 4.5 Cold-stimulus HA ingest or inhale, resolves < 30 min 4.6 External pressure HA pressure (hat) or traction (pony-tail) resolves in 1 h 4.7 Primary stabbing HA jabs and jolts 10sec-2 min 4.8 Nummular HA 1-6 cm, usually parietal, local tenderness, allodynia 4.9 Hypnic HA during sleep, USUALLY over age 50, lasting 15 min-4 h, no autonomic sx
53 4. Other primary headache disorders 4.5 Cold-stimulus HA ingest or inhale, resolves < 30 min 4.6 External pressure HA pressure (hat) or traction (pony-tail) resolves in 1 h 4.7 Primary stabbing HA jabs and jolts 10sec-2 min 4.8 Nummular HA 1-6 cm, usually parietal, local tenderness, allodynia 4.9 Hypnic HA during sleep, USUALLY over age 50, lasting 15 min-4 h, no autonomic sx
54 ICHD III 4.10 New Daily Persistent Headache A. Persistent headache B. Distinct and clearly remembered onset, with pain becoming continuous and unremitting within 24 hours C. Present for >3 months D. Not better accounted for by another ICHD-3 diagnosis. Ddx exacerbation of preexisting Primary HA, Hemicrania continua, medication overuse headache
55 New Daily Persistent Headache Description: A daily or very frequent headache of abrupt onset. The pain and associated features may resemble chronic migraine or chronic tension-type headache, or have elements of both. A discrete entity? A mixed group? Is there evidence for the self limiting subtype and the refractory subtype
56 Lingering classification questions in migraine and primary headaches Is motor aura critically different from other auras How to diagnose/classify auras which persist beyond an hour but do not persist beyond 1 week (persistent aura 1.4.2) And what is the basis for long term persistent aura without stroke? Chapter 3 similarities v. differences Is the SUNCT / SUNA distinction relevant? NDPH
57 Many primary headaches can be seen as overlapping sets? Other primary headaches Migraine TTHA Cluster Other TACs
58 ICHD III Part 2: Secondary headaches (caused by another disorder) 5. Posttraumatic 6. Vascular disease 7. Nonvasc intracranial pathology e.g. mass, pressure 8. Substances 9. CNS infection 10. Homeostatic disorder 11. Cranial, neck, EENT, sinuses, teeth, jaw 12. Psychiatric
59 ICHD Challenges with Secondary Headaches Morphology of HA is not necessarily diagnostic Location of pain is not necessarily diagnostic Presence of pathology is not necessarily diagnostic Multiple sources of pain coexist in many patients - relative contributions? Pain may not resolve when cause is gone
60 Lingering questions in 2 o Headaches Post-traumatic headache require emergence within 7 days IIH retained requirement for OP>250 ( 280 in obese children) CSF leak or hypovolemic headaches retained requirement for OP<60 (not included positionality) Are day limit differences meaningful in MOH? Are there interpatient differences? Are only migraineurs prone? What constitutes acceptable causes (and treatment targets) for cervicogenic headache? Are there persistent HA s following resolution of viral meningitis or encephalitis (Not classified in ICHD3) Does HIV cause HA? (Not classified in ICHD3)
61 5.1 Persistent headache attributed to traumatic injury to the head A. Any headache fulfilling criteria C and D B. Traumatic injury to the head has occurred C. Headache is reported to have developed within 7 d after one of the following: 1. the injury to the head 2. regaining of consciousness following the injury 3. discontinuation of medication(s) that impair ability to sense or report headache following the injury D. Headache persists for >3 mo after injury to the head E. Not better accounted for by another ICHD-3 diagnosis
62 5.3 Persistent headache attributed to whiplash A. Any headache fulfilling criteria C and D B. Whiplash, associated at the time with neck pain and/or headache, has occurred C. Headache has developed within 7 d after whiplash D. Headache persists for >3 mo after whiplash E. Not better accounted for by another ICHD-3 diagnosis
63 Idiopathic Intracranial Hypertension A. New headache, or a significant worsening of a preexisting headache, fulfilling criterion C B. Both: 1. IIH has been diagnosed 2. CSF pressure > 250 mm (>280 mm in obese children) C. Either or both of the following: 1. headache has developed or significantly worsened in temporal relation to the intracranial hypotension, or led to its discovery 2. headache is accompanied by either or both of the following: a) pulsatile tinnitus b) papilloedema
64 Intracranial Hypotension HA A. Any headache fulfilling criterion C B. Low CSF pressure (<60 mm CSF) and/or evidence of CSF leakage on imaging C. Headache has developed in temporal relation to the low CSF pressure or CSF leakage, or led to its discovery D. Not better accounted for by another ICHD-III diagnosis post LP CSF fistula SIH
65 Intracranial Hypotension HA MUCH worse upon arising Antecedent LP, surgery, barotrauma Goal Responds to targeted blood patch Not part of the definition
66 Imaging clues to SIH also not in dx criteria Subdural collections Brain sag Dural enhancement
67 Drugs, substances and headaches Exposure to NO donors, CO, Ethanol, Cocaine, Histamine, CGRP, pressor Overuse of - Ergots, Triptans, analgesics, opioids, combination meds Withdrawal from - caffeine, opioid, estrogen
68 8.2 Medication-overuse headache (MOH) A. Headache occurring on 15 d/mo in a patient with a pre-existing headache disorder B. Regular overuse for >3 mo of one or more drugs that can be taken for acute and/or symptomatic treatment of headache C. Not better accounted for by another ICHD-3 diagnosis
69 8.2 Medication-overuse headache (MOH) Ergotamine-overuse headache (10 d/mo use) Triptan-overuse headache (10d/mo) Simple analgesic-overuse headache (15d/mo) Opioid-overuse headache (10d/mo) Combination -analgesic-overuse headache (10d/mo) MOH attributed to multiple drug classes not individually overused (10d/mo) MOH headache attributed to unverified overuse of multiple drug classes (10d/mo) MOH attributed to other medication (10d/mo)
70 Distinguishing CM, CTTH & MOH Still difficult, and using ICHD3 one could diagnose all 3 in one patient very easily e.g. 23 headache per month 8 mig, 7 thought by patient to be mig, and 8 tension type If patient is overusing analgesic/abortive med and fulfills CM supposed to diagnose both and judge after med overuse has resolved
71 9. Infections and Headaches Headaches can be induced by many acute and chronic infections If a chronic infection: Chronic HA, e.g. Chronic headache attrib to intracranial parasitic infection If infec has resolved but HA persists: Persistent HA, e.g. Persistent HA attrib to past meningoencephalitis But no category for HA due to HIV, or persistent HA after Mono infection
72 Homeostasis and Headaches 10.1 Headache attributed to hypoxia and/or hypercapnia High-altitude headache Headache attributed to aeroplane travel Diving headache Sleep apnoea headache 10.2 Dialysis headache 10.3 Headache attributed to arterial hypertension Headache attributed to phaeochromocytoma Headache attributed to hypertensive crisis w/o hypertensive encephalopathy Headache attributed to hypertensive encephalopathy Headache attributed to pre-eclampsia or eclampsia Headache attributed to autonomic dysreflexia 10.4 Headache attributed to hypothyroidism 10.5 Headache attributed to fasting 10.6 Cardiac cephalalgia
73 10.6 Cardiac Cephalgia classification saves lives!!! Acute myocardial ischaemia has been demonstrated Evidence of causation -- at least 2 of the following: 1.headache has developed in temporal relation to the onset of acute myocardial ischaemia 2. HA worsens with ischemia and/or improves with resolution of ischemia 3.headache has at least two of the following four characteristics: a)moderate to severe intensity b)accompanied by nausea c) not accompanied by photophobia or phonophobia d)aggravated by exertion 4.headache is relieved by nitroglycerine or derivatives of it
74 11.3 Cervicogenic Headache Clinical and/or imaging evidence of a disorder or lesion within the cervical spine or soft tissues of the neck, known to be able to cause headache Evidence of causation -- at least two of the following: 1. headache has developed in temporal relation to the onset of the cervical disorder or appearance of the lesion 2. headache has significantly improved or resolved in parallel with improvement in or resolution of the cervical disorder or lesion 3. cervical range of motion is reduced and headache is made significantly worse by provocative manœuvres 4. headache is abolished following diagnostic blockade of a cervical structure or its nerve supply
75 Cervicogenic Headache Unaccepted causes in ICHD3 Upper cervical radiculopathy A Myofascial pain A11.2.5
76 Psychiatric causes of Headache 12.1 Somatization Psychosis 12A12. Headache attributed to psychiatric disorder A12.3 Headache attributed to depressive disorder A12.4 Headache attributed to separation anxiety disorder A12.5 Headache attributed to panic disorder A12.6 Headache attributed to specific phobia A12.7 Headache attributed to social anxiety disorder (social phobia) A12.8 Headache attributed to generalized anxiety disorder A12.9 Headache attributed to post-traumatic stress disorder (PTSD)
77 Part 3 Painful cranial neuropathies and other facial pain Trigeminal nerve pain is organized differently and is the model for other neuropathies like GN and nervus intermedius neuralgia Trigeminal Neuropathy Painful trigeminal neuropathy
78 Part 3 Painful cranial neuropathies and other facial pain Trigeminal Pain TN - unilateral, lancinating (though may have some aching too) Classical TN (due to vasc compression) Secondary - e.g. mass, MS Idiopathic (no vasc comp or lesion found) Painful trigeminal neuropathy - continuous, burning and or pins and needles, sensation change or allodynia or both Zoster PHN Traumatic other idiopathic
79 Part 3 Painful cranial neuropathies etc 13.2 Glossopharyngeal neuralgia, neuropathy 13.3 Nervus intermedius neuralgia, neuropathy 13.4 Occipital neuralgia 13.5 Neck-tongue syndrome 13.6 Painful optic neuritis 13.7 Ischemic ocular motor nerve 13.8 Tolosa Hunt syndrome 13.9 Paratrigeminal oculosympathetic (Raeder s) syndrome Recurrent painful ophthalmoplegic neuropathy Burning mouth syndrome (BMS) Persistent idiopathic facial pain (PIFP) Central neuropathic pain
80 Can some primary and secondary headaches can be seen as overlapping sets? Other primary headaches Migraine TTHA Cluster Other TACs
81 What s New in the Appendix? A1.3.1 Chronic migraine with pain free periods A1.3.2 Chronic migraine with continuous pain A1.4.5 Migraine aura status A Infantile Colic A Vestibular migraine A 4.11 Epicrania fugax zig-zag HA A5.1, 5.2 Delayed PTH A7.11 Post-electroconvulsive therapy (ECT) headache A7.12 Persistent post-intracranial disorder headache A 7.13 Ictal Epileptic Headache
82 What s New in the Appendix? A9.3 Headache attributed to HIV infection Headache attributed to aeroplane travel A10.9 Headache attributed to travel to space A10.10 Coat hanger pain attributed to orthostatic (postural) hypotension A Headache attributed to upper cervical radiculopathy A Headache attributed to myofascial pain in the cervical muscles A Headache attributed to pathology of the nasal mucosa, turbinates or septum
Disclosures. Objectives 6/2/2017
 Classification: Migraine and Trigeminal Autonomic Cephalalgias Lauren Doyle Strauss, DO, FAHS Assistant Professor, Child Neurology Assistant Director, Child Neurology Residency @StraussHeadache No disclosures
Classification: Migraine and Trigeminal Autonomic Cephalalgias Lauren Doyle Strauss, DO, FAHS Assistant Professor, Child Neurology Assistant Director, Child Neurology Residency @StraussHeadache No disclosures
Classification and WHO ICD-10NA Codes
 Classification and WHO ICD-10NA Codes IHS WHO Diagnosis ICHD-II ICD-10NA [and aetiological ICD-10 code for secondary headache disorders] code code 1. [G43] Migraine 1.1 [G43.0] Migraine without aura 1.2
Classification and WHO ICD-10NA Codes IHS WHO Diagnosis ICHD-II ICD-10NA [and aetiological ICD-10 code for secondary headache disorders] code code 1. [G43] Migraine 1.1 [G43.0] Migraine without aura 1.2
UCNS Course A Review of ICHD-3b
 UCNS Course A Review of ICHD-3b Andrew D. Hershey, M.D., Ph.D., FAHS Endowed Chair and Director of Neurology Director, Cincinnati Children s Headache Center Professor of Neurology and Pediatrics University
UCNS Course A Review of ICHD-3b Andrew D. Hershey, M.D., Ph.D., FAHS Endowed Chair and Director of Neurology Director, Cincinnati Children s Headache Center Professor of Neurology and Pediatrics University
Chronic Daily Headaches
 Chronic Daily Headaches ANWARUL HAQ, MD, MRCP(UK), FAHS DIRECTOR BAYLOR HEADACHE CENTER, DALLAS, TEXAS DISCLOSURES: None OBJECTIVES AT THE CONCLUSION OF THIS ACTIVITY, PARTICIPANTS WILL BE ABLE TO: define
Chronic Daily Headaches ANWARUL HAQ, MD, MRCP(UK), FAHS DIRECTOR BAYLOR HEADACHE CENTER, DALLAS, TEXAS DISCLOSURES: None OBJECTIVES AT THE CONCLUSION OF THIS ACTIVITY, PARTICIPANTS WILL BE ABLE TO: define
Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE
 Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE IHS Classification 1989 (updated 2004) Primary Headaches 4 categories Migraine Tension-type Cluster and other trigeminal
Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE IHS Classification 1989 (updated 2004) Primary Headaches 4 categories Migraine Tension-type Cluster and other trigeminal
By Nathan Hall Associate Editor
 By Nathan Hall Associate Editor 34 Practical Neurology March 2005 These new rules may change the definition of head pain, but some practitioners may find the new guidelines themselves to be a source of
By Nathan Hall Associate Editor 34 Practical Neurology March 2005 These new rules may change the definition of head pain, but some practitioners may find the new guidelines themselves to be a source of
A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline. Scottish intercollegiate Guidelines Network SIGN
 A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline Scottish intercollegiate Guidelines Network SIGN November 2008. PETER FRAMPTON MSc MCOptom BAppSc (Optom)(AUS)
A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline Scottish intercollegiate Guidelines Network SIGN November 2008. PETER FRAMPTON MSc MCOptom BAppSc (Optom)(AUS)
Trigeminal Autonomic Cephalalgias. Disclosures. Objectives 6/20/2018. Rashmi Halker Singh, MD FAHS UCNS Review Course June 2018
 Trigeminal Autonomic Cephalalgias Rashmi Halker Singh, MD FAHS UCNS Review Course June 2018 Disclosures Honoraria from Allergan and Amgen for advisory board, Current Neurology and Neuroscience Reports
Trigeminal Autonomic Cephalalgias Rashmi Halker Singh, MD FAHS UCNS Review Course June 2018 Disclosures Honoraria from Allergan and Amgen for advisory board, Current Neurology and Neuroscience Reports
Headache Master School Japan-Osaka 2016 II. Management of refractory headaches Case Presentation 2. SUNCT/SUNA: concept, management and prognosis
 Headache Master School Japan-Osaka 2016 II. Management of refractory headaches Case Presentation 2. SUNCT/SUNA: concept, management and prognosis Noboru Imai(Department of Neurology, Japanese Red Cross
Headache Master School Japan-Osaka 2016 II. Management of refractory headaches Case Presentation 2. SUNCT/SUNA: concept, management and prognosis Noboru Imai(Department of Neurology, Japanese Red Cross
GENERAL APPROACH AND CLASSIFICATION OF HEADACHES
 GENERAL APPROACH AND CLASSIFICATION OF HEADACHES CLASSIFICATION Headache is one of the most common medical complaints. Most of the population will have experienced headache, and over 5% will seek medical
GENERAL APPROACH AND CLASSIFICATION OF HEADACHES CLASSIFICATION Headache is one of the most common medical complaints. Most of the population will have experienced headache, and over 5% will seek medical
HEADACHES THE RED FLAGS
 HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
Headache Assessment In Primary Eye Care
 Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
Section la. Migraine and other headache syndromes. Migraine. Other headache syndromes G44
 Section la Migraine and other headache syndromes Overview of categories dealing with migraine, other headache syndromes, and neuralgia of cranial nerves, in accordance with the ICD-NA, second edition G43
Section la Migraine and other headache syndromes Overview of categories dealing with migraine, other headache syndromes, and neuralgia of cranial nerves, in accordance with the ICD-NA, second edition G43
Can I send this headache patient home? Dr Nicola Giffin Consultant Neurologist Bath, Nov 2017
 Can I send this headache patient home? Dr Nicola Giffin Consultant Neurologist Bath, Nov 2017 SAH v benign thunderclap headaches Other pathologies not apparent on CT Severe primary headaches: management
Can I send this headache patient home? Dr Nicola Giffin Consultant Neurologist Bath, Nov 2017 SAH v benign thunderclap headaches Other pathologies not apparent on CT Severe primary headaches: management
Headache Pain Generators
 Objectives 1. Define the major categories of headache. 2. Take a history directed at characterizing a headache pattern in an individual patient and identify the cause or triggers of the headache. 3. Understand
Objectives 1. Define the major categories of headache. 2. Take a history directed at characterizing a headache pattern in an individual patient and identify the cause or triggers of the headache. 3. Understand
Chapter 2 Diagnosis of Trigeminal Autonomic Cephalalgias
 Chapter 2 Diagnosis of Trigeminal Autonomic Cephalalgias Mark J. Stillman Introduction The trigeminal autonomic cephalalgias (TACs) refer to a specific group of primary headaches characterized by unilaterality,
Chapter 2 Diagnosis of Trigeminal Autonomic Cephalalgias Mark J. Stillman Introduction The trigeminal autonomic cephalalgias (TACs) refer to a specific group of primary headaches characterized by unilaterality,
2) Headache - Dr. Hawar
 2) Headache - Dr. Hawar Headache is caused by traction, displacement, inflammation, vascular spasm, or distention of the painsensitive structures in the head or neck. Isolated involvement of the bony skull,
2) Headache - Dr. Hawar Headache is caused by traction, displacement, inflammation, vascular spasm, or distention of the painsensitive structures in the head or neck. Isolated involvement of the bony skull,
A case of a patient with chronic headache. Focus on Migraine. None related to the presentation Grants to conduct clinical trials from: Speaker bureau:
 Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
HEADACHE: Benign or Severe Dr Gobinda Chandra Roy
 HEADACHE: Benign or Severe Dr Gobinda Chandra Roy Associate Professor, Department of Medicine, Shaheed Suhrawardy Medical College and Hospital Outlines 1. Introduction 2. Classification of headache 3.
HEADACHE: Benign or Severe Dr Gobinda Chandra Roy Associate Professor, Department of Medicine, Shaheed Suhrawardy Medical College and Hospital Outlines 1. Introduction 2. Classification of headache 3.
Index. Prim Care Clin Office Pract 31 (2004) Note: Page numbers of article titles are in boldface type.
 Prim Care Clin Office Pract 31 (2004) 441 447 Index Note: Page numbers of article titles are in boldface type. A Abscess, brain, headache in, 388 Acetaminophen for migraine, 406 407 headache from, 369
Prim Care Clin Office Pract 31 (2004) 441 447 Index Note: Page numbers of article titles are in boldface type. A Abscess, brain, headache in, 388 Acetaminophen for migraine, 406 407 headache from, 369
Differential Diagnosis of Orthostatic Headache
 Differential Diagnosis of Orthostatic Headache MORRIS LEVIN, MD PROFESSOR OF NEUROLOGY CHIEF, DIVISION OF HEADACHE MEDICINE, UCSF Disclosures Consulting for Amgen, Lilly, Allergan, Supernus, Pernix No
Differential Diagnosis of Orthostatic Headache MORRIS LEVIN, MD PROFESSOR OF NEUROLOGY CHIEF, DIVISION OF HEADACHE MEDICINE, UCSF Disclosures Consulting for Amgen, Lilly, Allergan, Supernus, Pernix No
11/10/2017. THE BRIDGE Course Objectives. THE BRIDGE Course Objectives
 THE BRIDGE Course Objectives Describe clinical characteristics associated with migraine diagnosis in adult and pediatric populations. Identify barriers and risk factors impacting the clinical course of
THE BRIDGE Course Objectives Describe clinical characteristics associated with migraine diagnosis in adult and pediatric populations. Identify barriers and risk factors impacting the clinical course of
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา
 ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
Cluster headache (CH): epidemiology, classification and clinical picture
 Cluster headache (CH): epidemiology, classification and clinical picture Toomas Toomsoo, M.D. Head of the Center of Neurology East Tallinn Central Hospital 1 INTRODUCTION Cluster headache - known as trigeminal
Cluster headache (CH): epidemiology, classification and clinical picture Toomas Toomsoo, M.D. Head of the Center of Neurology East Tallinn Central Hospital 1 INTRODUCTION Cluster headache - known as trigeminal
Pause for thought. Dr Jane Anderson Consultant Neurologist
 Pause for thought Dr Jane Anderson Consultant Neurologist Which is the top cause of years lived with disability worldwide? 1. COPD 2. Low Back pain 3. Diabetes 4. Migraine with medication overuse headache
Pause for thought Dr Jane Anderson Consultant Neurologist Which is the top cause of years lived with disability worldwide? 1. COPD 2. Low Back pain 3. Diabetes 4. Migraine with medication overuse headache
Lynda J. Krasenbaum, MSN, ANP BC. Associate Director New York Headache Center
 Diagnosing Headache in Adults and Adolescents Lynda J. Krasenbaum, MSN, ANP BC Associate Director New York Headache Center New York, New York Learning Objectives Understand the diagnostic challenges of
Diagnosing Headache in Adults and Adolescents Lynda J. Krasenbaum, MSN, ANP BC Associate Director New York Headache Center New York, New York Learning Objectives Understand the diagnostic challenges of
Diagnosing headache. The clinician should approach the diagnosis of. Secondary headache. Primary headache. Blue and red flag headaches
 Headache THEME Diagnosing headache BACKGROUND A systematic approach to the diagnosis of primary and secondary headache disorders requires the measurement of the frequency and the duration of headache.
Headache THEME Diagnosing headache BACKGROUND A systematic approach to the diagnosis of primary and secondary headache disorders requires the measurement of the frequency and the duration of headache.
Headache and Facial Pain. Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology
 Headache and Facial Pain Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology Introduction It is the most common neurologic complain The diagnosis usually
Headache and Facial Pain Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology Introduction It is the most common neurologic complain The diagnosis usually
Headache Mary D. Hughes, MD Neuroscience Associates
 Headache Mary D. Hughes, MD Neuroscience Associates Case 1 22 year old female presents with recurrent headaches. She has had headaches for the past 3 years. They start on the right side of her head and
Headache Mary D. Hughes, MD Neuroscience Associates Case 1 22 year old female presents with recurrent headaches. She has had headaches for the past 3 years. They start on the right side of her head and
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
PREVALENCE BY HEADACHE TYPE
 CLINICAL CLUES AND CLINICAL RULES: PRIMARY VS SECONDARY HEADACHE * Based on a presentation by David W. Dodick, MD ABSTRACT Headache is a common condition, accounting for many specialist office visits annually.
CLINICAL CLUES AND CLINICAL RULES: PRIMARY VS SECONDARY HEADACHE * Based on a presentation by David W. Dodick, MD ABSTRACT Headache is a common condition, accounting for many specialist office visits annually.
MIGRAINE CLASSIFICATION
 MIGRAINE CLASSIFICATION Nada Šternić At most, only 30% of migraineurs have classic aura The same patient may have migraine headache without aura, migraine headache with aura as well as migraine aura without
MIGRAINE CLASSIFICATION Nada Šternić At most, only 30% of migraineurs have classic aura The same patient may have migraine headache without aura, migraine headache with aura as well as migraine aura without
MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache
 MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache Measure Description Percentage of patients age 18 years old and older with a diagnosis of primary headache
MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache Measure Description Percentage of patients age 18 years old and older with a diagnosis of primary headache
Overview INTRODUCTION 3/15/2018. Headache Emergencies. Other way to differentiate between them? Is there an easy way to differentiate between them?
 Overview Headache Emergencies Primary versus Secondary headache disorder Red flags 4 cases of unusual headache emergencies Disclaimer: we will not talk about brain bleed as patients usually go the ED.
Overview Headache Emergencies Primary versus Secondary headache disorder Red flags 4 cases of unusual headache emergencies Disclaimer: we will not talk about brain bleed as patients usually go the ED.
The trigeminal autonomic cephalalgias (TACs) are a group of. Cluster Headache and Other Trigeminal Autonomic Cephalalgias By Mark Burish, MD, PhD
 Downloaded from https://journals.lww.com/continuum by SruuCyaLiGD/095xRqJ2PzgDYuM98ZB494KP9rwScvIkQrYai2aioRZDTyulujJ/fqPksscQKqke3QAnIva1ZqwEKekuwNqyUWcnSLnClNQLfnPrUdnEcDXOJLeG3sr/HuiNevTSNcdMFp1i4FoTX9EXYGXm/fCfrbTavvQSUHUH4eazE11ptLzgCyEpzDoF
Downloaded from https://journals.lww.com/continuum by SruuCyaLiGD/095xRqJ2PzgDYuM98ZB494KP9rwScvIkQrYai2aioRZDTyulujJ/fqPksscQKqke3QAnIva1ZqwEKekuwNqyUWcnSLnClNQLfnPrUdnEcDXOJLeG3sr/HuiNevTSNcdMFp1i4FoTX9EXYGXm/fCfrbTavvQSUHUH4eazE11ptLzgCyEpzDoF
Outpatient Headache Care Guideline
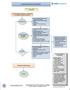 1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
6/4/2018. Headache. Headaches. Headache. Migraine Headaches. Headache. Red Flag signs and symptoms. Imaging CT without contrast.
 Presented by M.D. Shepherd, M.D. OH MY ACHING HEAD! Estimated that one half of the adult population is affected by a headache disorder International Society Classification Primary : Tension s 40% of the
Presented by M.D. Shepherd, M.D. OH MY ACHING HEAD! Estimated that one half of the adult population is affected by a headache disorder International Society Classification Primary : Tension s 40% of the
Measure Components Numerator Statement
 MEASURE #5: OVERUSE OF OPIOID CONTAINING MEDICATIONS FOR PRIMARY HEADACHE DISORDERS Headache For Quality Improvement Only. Not to be used for Public Reporting or Accountability Measure Description Percentage
MEASURE #5: OVERUSE OF OPIOID CONTAINING MEDICATIONS FOR PRIMARY HEADACHE DISORDERS Headache For Quality Improvement Only. Not to be used for Public Reporting or Accountability Measure Description Percentage
Headache. Luke Bennetto Consultant Neurologist Engineers House 13 th September 2016
 Headache Luke Bennetto Consultant Neurologist Engineers House 13 th September 2016 Contents General thoughts Primary headache Secondary headache I want to curl up in a cave and die I want to drill a
Headache Luke Bennetto Consultant Neurologist Engineers House 13 th September 2016 Contents General thoughts Primary headache Secondary headache I want to curl up in a cave and die I want to drill a
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, II. Management of Refractory Headaches
 Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
Headache. Section 1. Migraine headache. Clinical presentation
 Section 1 Headache Migraine headache 1 Clinical presentation It is important to recognize just how significant a problem migraine headache is. It has been estimated that migraine affects 11% of the United
Section 1 Headache Migraine headache 1 Clinical presentation It is important to recognize just how significant a problem migraine headache is. It has been estimated that migraine affects 11% of the United
HEADACHE Transient discomfort, chronic nuisance, or looming disaster?
 HEADACHE Transient discomfort, chronic nuisance, or looming disaster? Hussien H. Rizk, MD Cairo University Medical School ١ Headache Second most common o symptom (after pain) Migraine alone afflicts 12
HEADACHE Transient discomfort, chronic nuisance, or looming disaster? Hussien H. Rizk, MD Cairo University Medical School ١ Headache Second most common o symptom (after pain) Migraine alone afflicts 12
Classification of headaches
 Classification of headaches Jasna Zidverc Trajković Headache center Headache in adults: 1-year prevalence 13.4 Kryst 35.9 Miranda 28.7 Jaillard 87.3 O Brien 63.1 Wiehe 37.3 Lavados 59.7 Schwartz 76.0 Boardman
Classification of headaches Jasna Zidverc Trajković Headache center Headache in adults: 1-year prevalence 13.4 Kryst 35.9 Miranda 28.7 Jaillard 87.3 O Brien 63.1 Wiehe 37.3 Lavados 59.7 Schwartz 76.0 Boardman
Nicolas Bianchi M.D. May 15th, 2012
 Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Headache Classifica-on
 Headache Classifica-on 2 Tension-Type Headache Criteria -Infrequent episodic tension-type headache- A. At least 10 episodes occurring on < 1 day per month on average (< 12 days per year) and fulfilling
Headache Classifica-on 2 Tension-Type Headache Criteria -Infrequent episodic tension-type headache- A. At least 10 episodes occurring on < 1 day per month on average (< 12 days per year) and fulfilling
HEADACHE. Dr Nick Pendleton. September Headache
 HEADACHE Dr Nick Pendleton September 2017 Headache Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache Raised ICP
HEADACHE Dr Nick Pendleton September 2017 Headache Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache Raised ICP
25/09/2018 HEADACHE. Dr Nick Pendleton
 HEADACHE Dr Nick Pendleton September 2018 1 Small Group Work Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache
HEADACHE Dr Nick Pendleton September 2018 1 Small Group Work Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache
FINANCIAL DISCLOSURE. No relevant financial relationships
 Sleep and Headache Paul Mathew, MD, FAHS Director of Continuing Medical Education John R. Graham Headache Center Brigham & Women s Hospital Director of Headache Medicine Cambridge Health Alliance Harvard
Sleep and Headache Paul Mathew, MD, FAHS Director of Continuing Medical Education John R. Graham Headache Center Brigham & Women s Hospital Director of Headache Medicine Cambridge Health Alliance Harvard
Managing Headache in Acute Medicine. Ben Lovell Consultant Physician in Acute Medicine University College London Hospital
 Managing Headache in Acute Medicine Ben Lovell Consultant Physician in Acute Medicine University College London Hospital Some ED headache stats Arrive by ambulance 31% Median age 39 Worst ever headache
Managing Headache in Acute Medicine Ben Lovell Consultant Physician in Acute Medicine University College London Hospital Some ED headache stats Arrive by ambulance 31% Median age 39 Worst ever headache
Chronic Migraine in Primary Care. December 11 th, 2017 Werner J. Becker University of Calgary
 Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
Specific Objectives A. Topics to be lectured and discussed at the plenary sessions
 Specific Objectives A. Topics to be lectured and discussed at the plenary sessions 0. Introduction: Good morning ICHD-III! Let s start at the very beginning. When you read you begin with A-B-C, so when
Specific Objectives A. Topics to be lectured and discussed at the plenary sessions 0. Introduction: Good morning ICHD-III! Let s start at the very beginning. When you read you begin with A-B-C, so when
Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert
 Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert Childhood headache: Is it really difficult to manage? It shouldn t be... But it can be...
Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert Childhood headache: Is it really difficult to manage? It shouldn t be... But it can be...
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
Painless, progressive weakness Could this be Motor Neurone Disease?
 APPENDIX 1 Painless, progressive weakness Could this be Motor Neurone Disease? 1. Does the patient have one or more of these? Bulbar features Limb features Respiratory features Cognitive features (rare)
APPENDIX 1 Painless, progressive weakness Could this be Motor Neurone Disease? 1. Does the patient have one or more of these? Bulbar features Limb features Respiratory features Cognitive features (rare)
Atypical presentations of cluster headache
 Blackwell Science, LtdOxford, UKCHACephalalgia0333-1024Blackwell Science, 200222Original ArticleAtypical presentations in cluster headachetd Rozen Atypical presentations of cluster headache TD Rozen Department
Blackwell Science, LtdOxford, UKCHACephalalgia0333-1024Blackwell Science, 200222Original ArticleAtypical presentations in cluster headachetd Rozen Atypical presentations of cluster headache TD Rozen Department
It s Always a Stroke; Except For When It s Not..
 It s Always a Stroke; Except For When It s Not.. TREVOR PHINNEY, D.O. Disclosures No Relevant Disclosures 1 Objectives Discuss variables of differential diagnosis for stroke Review when to TPA and when
It s Always a Stroke; Except For When It s Not.. TREVOR PHINNEY, D.O. Disclosures No Relevant Disclosures 1 Objectives Discuss variables of differential diagnosis for stroke Review when to TPA and when
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Suspected neurological conditions: clinical questions
 Suspected neurological clinical questions For questions on signs and symptoms, the committee wanted to consider any studies that determine whether a certain sign or symptom accompanying a main presenting
Suspected neurological clinical questions For questions on signs and symptoms, the committee wanted to consider any studies that determine whether a certain sign or symptom accompanying a main presenting
Intracranial hypotension secondary to spinal CSF leak: diagnosis
 Intracranial hypotension secondary to spinal CSF leak: diagnosis Spinal cerebrospinal fluid (CSF) leak is an important and underdiagnosed cause of new onset headache that is treatable. Cerebrospinal fluid
Intracranial hypotension secondary to spinal CSF leak: diagnosis Spinal cerebrospinal fluid (CSF) leak is an important and underdiagnosed cause of new onset headache that is treatable. Cerebrospinal fluid
Embriologically, The head is formed from the first two cervical segments (except the mandible, which is formed by the third). The first and second
 Embriologically, The head is formed from the first two cervical segments (except the mandible, which is formed by the third). The first and second cervical vertebra are also derived from these two segments.
Embriologically, The head is formed from the first two cervical segments (except the mandible, which is formed by the third). The first and second cervical vertebra are also derived from these two segments.
Primary Care Adult Headache Management Pathway (formerly North West Headache Management Guideline for Adults) Version 1.0
 Primary Care Adult Headache Management Pathway (formerly rth West Headache Management Guideline for Adults) Version 1.0 1 VERSION CONTROL Version Date Amendments made Version 1.0 October 2018 Reformatted
Primary Care Adult Headache Management Pathway (formerly rth West Headache Management Guideline for Adults) Version 1.0 1 VERSION CONTROL Version Date Amendments made Version 1.0 October 2018 Reformatted
Diagnosis of Primary Headache Syndromes. Gerald W. Smetana, M.D. Division of General Medicine Beth Israel Deaconess Medical Center
 Diagnosis of Primary Headache Syndromes Gerald W. Smetana, M.D. Division of General Medicine Beth Israel Deaconess Medical Center Goals Distinguish primary from secondary headaches Recognize typical histories
Diagnosis of Primary Headache Syndromes Gerald W. Smetana, M.D. Division of General Medicine Beth Israel Deaconess Medical Center Goals Distinguish primary from secondary headaches Recognize typical histories
An Overview of MOH. ALAN M. Rapoport, M.D. Clinical Professor of Neurology The David Geffen School of Medicine at UCLA Los Angeles, California
 An Overview of MOH IHS ASIAN HA MASTERS SCHOOL MARCH 24, 2013 ALAN M. Rapoport, M.D. Clinical Professor of Neurology The David Geffen School of Medicine at UCLA Los Angeles, California President-Elect
An Overview of MOH IHS ASIAN HA MASTERS SCHOOL MARCH 24, 2013 ALAN M. Rapoport, M.D. Clinical Professor of Neurology The David Geffen School of Medicine at UCLA Los Angeles, California President-Elect
MIGRAINE A MYSTERY HEADACHE
 MIGRAINE A MYSTERY HEADACHE The migraine is a chronic neurological disease that is characterized by moderate to severe episodes of headache that is mostly associated with other central nervous system (CNS)
MIGRAINE A MYSTERY HEADACHE The migraine is a chronic neurological disease that is characterized by moderate to severe episodes of headache that is mostly associated with other central nervous system (CNS)
Mark W. Green, MD, FAAN
 Mark W. Green, MD, FAAN Professor of Neurology, Anesthesiology, and Rehabilitation Medicine Director of Headache and Pain Medicine Icahn School of Medicine at Mt Sinai New York Pain-sensitive structures
Mark W. Green, MD, FAAN Professor of Neurology, Anesthesiology, and Rehabilitation Medicine Director of Headache and Pain Medicine Icahn School of Medicine at Mt Sinai New York Pain-sensitive structures
Headaches. Mini Medical School. November 10, A. Laine Green MSc, MD FRCP(C) Assistant Professor Department of Medicine (Neurology)
 Headaches. Mini Medical School. November 10, 2016 A. Laine Green MSc, MD FRCP(C) Assistant Professor Department of Medicine (Neurology) Artist Agnes Cecile Disclosures I have received an honorarium from
Headaches. Mini Medical School. November 10, 2016 A. Laine Green MSc, MD FRCP(C) Assistant Professor Department of Medicine (Neurology) Artist Agnes Cecile Disclosures I have received an honorarium from
COMPLEXITIES OF MIGRAINE HEADACHES
 COMPLEXITIES OF MIGRAINE HEADACHES Michael A. Rogawski, MD, PhD Professor and Chair Department of Neurology University of California, Davis Sacramento, CA MICHAEL A. ROGAWSKI, MD, PHD Disclosures Research/Grants:
COMPLEXITIES OF MIGRAINE HEADACHES Michael A. Rogawski, MD, PhD Professor and Chair Department of Neurology University of California, Davis Sacramento, CA MICHAEL A. ROGAWSKI, MD, PHD Disclosures Research/Grants:
with susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine
 Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Vertigo. Tunde Magyar MD, PhD
 Vertigo Tunde Magyar MD, PhD What could be reffered to as dizziness by the patient? Rotational vertigo Sense of instability Ataxia of gait Disturbance of vision Loss of contact with surroundings Nausea
Vertigo Tunde Magyar MD, PhD What could be reffered to as dizziness by the patient? Rotational vertigo Sense of instability Ataxia of gait Disturbance of vision Loss of contact with surroundings Nausea
Cambridge Pocket Clinicians
 Headache Cambridge Pocket Clinicians Cambridge Pocket Clinicians provide practical, portable, note-based guidance for medical trainees, junior doctors, residents, and those from outside the field seeking
Headache Cambridge Pocket Clinicians Cambridge Pocket Clinicians provide practical, portable, note-based guidance for medical trainees, junior doctors, residents, and those from outside the field seeking
Primary Headache Prevalence % (95% CI) Migraine without aura 9 (7-9) Migraine with aura 6 (5-8)
 Primary Headache Prevalence % (95% CI) Migraine without aura 9 (7-9) Migraine with aura 6 (5-8) Episodic tension-type headache 66 (62-69) Chronic tension-type headache 3 (2-5) Cluster headache 0.1 (0 1)
Primary Headache Prevalence % (95% CI) Migraine without aura 9 (7-9) Migraine with aura 6 (5-8) Episodic tension-type headache 66 (62-69) Chronic tension-type headache 3 (2-5) Cluster headache 0.1 (0 1)
Neurological Dilemmas in Primary Care
 Neurological Dilemmas in Primary Care David Clark, DO dclark@oregonneurology.com When to test? How to test? Pitfalls in testing? When to treat? How to treat? How long to treat? Neurological Dilemmas Seizure
Neurological Dilemmas in Primary Care David Clark, DO dclark@oregonneurology.com When to test? How to test? Pitfalls in testing? When to treat? How to treat? How long to treat? Neurological Dilemmas Seizure
Headaches need not be a headache for optometrists
 Headaches need not be a headache for optometrists C-19309 O/D Tina Kipioti, MD, FRCSEd Of all the painful states that afflict humans, headache (cephalalgia) is the most common. According to a large study,
Headaches need not be a headache for optometrists C-19309 O/D Tina Kipioti, MD, FRCSEd Of all the painful states that afflict humans, headache (cephalalgia) is the most common. According to a large study,
The NIHSS score is 4 (considering 2 pts for the ataxia involving upper and lower limbs.
 Neuroscience case 5 1. Speech comprehension, ability to speak, and word use were normal in Mr. Washburn, indicating that aphasia (cortical language problem) was not involved. However, he did have a problem
Neuroscience case 5 1. Speech comprehension, ability to speak, and word use were normal in Mr. Washburn, indicating that aphasia (cortical language problem) was not involved. However, he did have a problem
Paediatric headaches. Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services. Brevity, levity, repetition
 Paediatric headaches Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services Brevity, levity, repetition Paediatric)headache?)! Headache!in!children!is!not!that!common.!The!question!is!which!headaches!do!I!
Paediatric headaches Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services Brevity, levity, repetition Paediatric)headache?)! Headache!in!children!is!not!that!common.!The!question!is!which!headaches!do!I!
Dr Jo-Anne Pon. Consultant Ophthalmologist and Oculoplastic Surgeon Southern Eye Specialists Christchurch
 Dr Jo-Anne Pon Consultant Ophthalmologist and Oculoplastic Surgeon Southern Eye Specialists Christchurch 12:15-12:30 Visual Migraines to be Worried About Visual Migraines To Be Worried About Jo-Anne Pon
Dr Jo-Anne Pon Consultant Ophthalmologist and Oculoplastic Surgeon Southern Eye Specialists Christchurch 12:15-12:30 Visual Migraines to be Worried About Visual Migraines To Be Worried About Jo-Anne Pon
What could be reffered to as dizziness by the patient?
 What could be reffered to as dizziness by the patient? Rotational vertigo Sense of instability Ataxia of gait Disturbance of vision Loss of contact with surroundings Nausea Loss of memory Loss of confidence
What could be reffered to as dizziness by the patient? Rotational vertigo Sense of instability Ataxia of gait Disturbance of vision Loss of contact with surroundings Nausea Loss of memory Loss of confidence
Headache. Karen Thaxter
 Headache Karen Thaxter An eight year old girl is taken to her paediatrician because she has been complaining of almost daily pain at the back of her head for the past 4 months. She states that each headache
Headache Karen Thaxter An eight year old girl is taken to her paediatrician because she has been complaining of almost daily pain at the back of her head for the past 4 months. She states that each headache
Case Presentation. Case Presentation. Case Presentation. Truths about Headaches (2017) Most headaches were muscle-tension headaches
 Agenda Case presentation Migraine Morphology Primary and Premonitory Phase Secondary Headache Aura Headache Primer on Pain Medication Overuse Headache Case Presentation RT is a 25 year old woman with daily
Agenda Case presentation Migraine Morphology Primary and Premonitory Phase Secondary Headache Aura Headache Primer on Pain Medication Overuse Headache Case Presentation RT is a 25 year old woman with daily
continuing medical education
 In collaboration with Jeddah Primary Care CME unit This is a CME (Continuing Medical Education) article. It is presented to you in collaboration with the Middle East CME organizations. Self-test answers
In collaboration with Jeddah Primary Care CME unit This is a CME (Continuing Medical Education) article. It is presented to you in collaboration with the Middle East CME organizations. Self-test answers
Identification of Painful Tissue Orthopaedic Examination DX 612. James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic
 Identification of Painful Tissue Orthopaedic Examination DX 612 James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Generalized Pain Description Joint pain may be constant
Identification of Painful Tissue Orthopaedic Examination DX 612 James J. Lehman, DC, MBA, DABCO University of Bridgeport College of Chiropractic Generalized Pain Description Joint pain may be constant
Headache Why headaches hurt When to see a doctor Diagnosing your headache
 Headache Why headaches hurt Information about touch, pain, temperature, and vibration in the head and neck is sent to the brain by the trigeminal nerve, one of 12 pairs of cranial nerves that start at
Headache Why headaches hurt Information about touch, pain, temperature, and vibration in the head and neck is sent to the brain by the trigeminal nerve, one of 12 pairs of cranial nerves that start at
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Alveolar osteitis (dry socket), periodontal pain due to, 436 Aphthous stomatitis, recurrent, mucosal pain due to, 439 440 Arthrocentesis/arthroscopy,
Index Note: Page numbers of article titles are in boldface type. A Alveolar osteitis (dry socket), periodontal pain due to, 436 Aphthous stomatitis, recurrent, mucosal pain due to, 439 440 Arthrocentesis/arthroscopy,
doi: /brain/awl202 Brain (2006), 129,
 doi:10.1093/brain/awl202 Brain (2006), 129, 2746 2760 Short-lasting unilateral neuralgiform headache attacks with conjunctival injection and tearing (SUNCT) or cranial autonomic features (SUNA) a prospective
doi:10.1093/brain/awl202 Brain (2006), 129, 2746 2760 Short-lasting unilateral neuralgiform headache attacks with conjunctival injection and tearing (SUNCT) or cranial autonomic features (SUNA) a prospective
HEADACHE: Prevalence and Impact
 Mod 2 Headaches HEADACHE: Prevalence and Impact PREVALENCE 18-25 % women have headaches 6-10 % men have headaches 5% of women have headaches more than 15 days per month 112 million bedridden days per year
Mod 2 Headaches HEADACHE: Prevalence and Impact PREVALENCE 18-25 % women have headaches 6-10 % men have headaches 5% of women have headaches more than 15 days per month 112 million bedridden days per year
Headache: Update and Review
 UCSF Advances in Internal Medicine 2017 Headache: Update and Review Disclosures Consulting for Allergan, Amgen, Lilly, Supernus Royalties from Anadem, Oxford Univ Press, Castle Connolly, Wiley-Blackwell
UCSF Advances in Internal Medicine 2017 Headache: Update and Review Disclosures Consulting for Allergan, Amgen, Lilly, Supernus Royalties from Anadem, Oxford Univ Press, Castle Connolly, Wiley-Blackwell
Vascular Disorders. Nervous System Disorders (Part B-1) Module 8 -Chapter 14. Cerebrovascular disease S/S 1/9/2013
 Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
Nervous System Disorders (Part B-1) Module 8 -Chapter 14 Overview ACUTE NEUROLOGIC DISORDERS Vascular Disorders Infections/Inflammation/Toxins Metabolic, Endocrinologic, Nutritional, Toxic Neoplastic Traumatic
Controversy One: Headache and Disability. Robert Shapiro, MD, PhD University of Vermont
 Controversy One: Headache and Disability Robert Shapiro, MD, PhD University of Vermont Southern Headache Society Orlando, FL, Sept 21, 2013 Disclosures Consulting within the past 12 months: Transcept Pharmaceuticals
Controversy One: Headache and Disability Robert Shapiro, MD, PhD University of Vermont Southern Headache Society Orlando, FL, Sept 21, 2013 Disclosures Consulting within the past 12 months: Transcept Pharmaceuticals
Sudden Headache and visual disturbances in a young woman
 Sudden Headache and visual disturbances in a young woman A. Soupart, MD, PhD Department of Internal Medicine BSIM, December 12, 2014 48 years old woman with Sudden Headache 7/2014 * Admitted for Headache
Sudden Headache and visual disturbances in a young woman A. Soupart, MD, PhD Department of Internal Medicine BSIM, December 12, 2014 48 years old woman with Sudden Headache 7/2014 * Admitted for Headache
Chief Complaint. History. History of Similar Episodes. A 10 Year-Old Boy With Headache
 A 10 Year-Old Boy With Headache Chief Complaint Recent Advances in Neurology 2013 10 year-old boy presented with his fifth lifetime bout of left-sided head pain followed by diplopia. Amy A. Gelfand, MD
A 10 Year-Old Boy With Headache Chief Complaint Recent Advances in Neurology 2013 10 year-old boy presented with his fifth lifetime bout of left-sided head pain followed by diplopia. Amy A. Gelfand, MD
PREVIEW ONLY 28/08/2013. Andrew Ellis. Professor Michael J Fulham. This webinar will begin in the next few minutes
 This webinar will begin in the next few minutes Need technical support for this live event? Please call 1800 006 293, then press 1 NOTE: You will be initially asked for the email address associated with
This webinar will begin in the next few minutes Need technical support for this live event? Please call 1800 006 293, then press 1 NOTE: You will be initially asked for the email address associated with
5. Headache. and/or neck trauma. attributed to moderate. head injury. Glasgow Coma Scale x/15. ICHD II- Chaps 5&6 Posttraumatic and Vascular Headaches
 Diagnosis and Classification of Secondary Headaches Part 1 Posttraumatic and Vascular Morris Levin, MD Associate Professor of Medicine (Neurology) Associate Professor of Psychiatry Dartmouth Medical School
Diagnosis and Classification of Secondary Headaches Part 1 Posttraumatic and Vascular Morris Levin, MD Associate Professor of Medicine (Neurology) Associate Professor of Psychiatry Dartmouth Medical School
PAEDIATRIC ACUTE CARE GUIDELINE. Headache. This document should be read in conjunction with this DISCLAIMER
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Secondary Headaches: A Strategic Approach. Emerg Med 40(4):18, 2008
 Secondary Headaches: A Strategic Approach Emerg Med 40(4):18, 2008 Headaches are common complaints in the emergency department, but the causes of secondary headaches are often misdiagnosed. The authors
Secondary Headaches: A Strategic Approach Emerg Med 40(4):18, 2008 Headaches are common complaints in the emergency department, but the causes of secondary headaches are often misdiagnosed. The authors
Faculty Disclosure. Karen L. Bremer, MD. Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest.
 Faculty Disclosure Karen L. Bremer, MD Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest. HEADACHE UPDATE Karen L. Bremer, MD November 10, 2017 karen.bremer@creighton.edu
Faculty Disclosure Karen L. Bremer, MD Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest. HEADACHE UPDATE Karen L. Bremer, MD November 10, 2017 karen.bremer@creighton.edu
Differentiating Migraine from Other Headache Types to Target Treatment Peter J. Goadsby, MD, PhD
 Differentiating Migraine from Other Headache Types to Target Treatment Peter J. Goadsby, MD, PhD University of California, San Francisco San Francisco, CA King's College London London, England Learning
Differentiating Migraine from Other Headache Types to Target Treatment Peter J. Goadsby, MD, PhD University of California, San Francisco San Francisco, CA King's College London London, England Learning
I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation.
 I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation. In 1962, Bille published landmark epidemiologic survey of headache among 9,000 school
I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation. In 1962, Bille published landmark epidemiologic survey of headache among 9,000 school
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
