Treatment of multiloculated empyema thoracis using minimally invasive methods
|
|
|
- Kevin Harper
- 5 years ago
- Views:
Transcription
1 O r i g i n a l A r t i c l e Singapore Med J 2010; 51(3) : 242 Treatment of multiloculated empyema thoracis using minimally invasive methods Metin M, Yeginsu A, Sayar A, Alzafer S, Solak O, Ozgul A, Erkorkmaz U, Gürses A Yedikule Chest Disease and Chest Surgery Teaching Hospital, First Chest Surgery Clinic, Istanbul, Metin M, MD Sayar A, MD Gürses A, MD and Chief Surgeon Division of Ozgul A, MD Specialist Thoracic Surgery, Gaziosmanpasa University, School of Medicine, Tokat, Yeginsu A, MD Assistant Professor Biostatistics Erkorkmaz U, MD Assistant Professor Division of, Acibadem Hospital, Bakirkoy, Istanbul, Alzafer S, MD Specialist Thoracic Surgery, Kocatepe University, School of Medicine, Afyon, Solak O, MD Correspondence to: Dr Ali Yeginsu Tel: (90) Fax: (90) yeginsu@ hotmail.com ABSTRACT Introduction : The purpose of this study was to investigate the results of minimally invasive treatment modalities in early stage multiloculated empyema thoracis. Methods: The minimally invasive treatment modalities of 114 patients with Class 5 thoracic empyema were retrospectively reviewed. The patients demographics, symptoms, diagnostic studies, treatment options and complications were evaluated. Results: A total of 47 patients underwent tube thoracostomy, 23 patients underwent fibrinolytic therapy with streptokinase and 44 patients underwent video-assisted thoracoscopic surgery (VATS) deloculation and debridement. No statistical differences were found in the patients age, gender, Gram stain and antibiotherapy before intervention among the groups. Illness days before intervention was significantly longer in the tube thoracostomy group than in the others. The VATS group had a shorter drainage time and hospital stay than the others. The VATS and fibrinolytic therapy groups had lower complication rates and less open decortication requirements than the tube thoracostomy group. Success rates were 66, 95 and 100 percent in the tube thoracostomy, fibrinolytic therapy and VATS groups, respectively. In total, there were 35 patients with complications. The most frequent complication was air space. Two inhospital mortalities occurred. Conclusion : In patients with early stage multiloculated empyema, VATS deloculation and debridement is superior to tube thoracostomy alone and fibrinolitic therapy in reducing drainage time and hospital stay. It has a relatively high success rate without significant morbidity. Therefore, VATS decortication may be recommended as a first-line therapy in early stage multiloculated empyema thoracis. Keywords: decortication, fibrinolytic therapy, empyema, tube thoracostomy, VATS Singapore Med J 2010; 51(3): INTRODUCTION Pleural space infection, or empyema, is a frequently encountered condition that is associated with significant morbidity and mortality. This condition involves three developmental stages. Stage I, the acute or exudative stage, is characterised by a thin serous fluid with minimal debris. Stage II, the fibrinopurulent stage, is characterised by a thicker fluid and thick fibrin strands. The formation of loculations makes chest tube drainage less effective. Stage III, the organising stage, is characterised by a thick fibrous peel and scar formation. (1) Drainage with antibiotherapy has been the primary form of treatment for complicated pleural effusions. If the empyema progresses to the fibropurulent or organised stages, this option may not be sufficient. In this condition, according to the guidelines published by The American College of Chest Physicians, (2) fibrinolytics, video-assisted thoracoscopic surgery (VATS), and open thoracotomy can all be performed as acceptable approaches. Recently, since the improvement of laparoscopic techniques, thoracoscopic surgery has become more effective, and is recommended for the treatment of many thoracic diseases, including empyema, with satisfactory results. The authors have also performed various treatment options for early stage thoracic empyema for many years in our centres. The purpose of this retrospective study was to investigate the effectiveness and outcomes of our minimally invasive surgical treatment options in early stage empyema thoracis. METHODS This was a retrospective review of 114 multiloculated empyema patients surgically treated from January 1995 to December 2007 at our centres. The patients
2 Singapore Med J 2010; 51(3) : 243 demographics, symptoms, diagnostic studies, treatment options and complications were evaluated. Patients who were 18 years of age and had Class 5 empyema were included in this study. Those who were aged < 18 years, unloculated and had cronic empyemas were excluded. A diagnosis of empyema was established if they met the following criteria: existence of gross pus or organisms demonstrated on Gram stain or culture, or all of the tests were positive for ph < 7.2, a glucose level of fluid < 40 mg/l, lactate dehydrogenase above 1,000 IU/ml, protein level above 3 g/ml and white blood cell (WBC) over 15,000 cells/mm 3, and if their physical, radiological and laboratory signs accompanied the relevant clinical picture. (3) The classification of empyema was re-established according to Light s criteria. (4) Class 5 empyema was defined as loculated empyema which had a demonstrated organism on Gram stain or culture, or a ph < 7.0, and/or a glucose level of pleural fluid < 40 mg/l. After radiographic studies were conducted, the initial diagnostic thoracentesis was carried out in all patients. The treatment options were tube thoracostomy (TT) alone, TT plus fibrinolitic therapy (FT), and TT plus VATS, or VATS alone. Between 1995 and 1998, we routinely treated empyema with TT alone and then followed up with the patient. We performed TT plus FT between 1999 and Since 2001, we have been performing VATS whenever loculated empyema was detected. To date, we have performed VATS on nearly all patients with Class 5 loculated empyema, except when there is a strict contraindication for surgery, or in patients unwilling to go through the operation. In these cases, we performed open decortication in case of failure of the main treatment options, in relation to the historical clinical preference. TT indications in our clinics were the presence of pleural fluid that was macroscopically purulent, was positive on culture for bacterial infection, and for bacteria on Gram stain, or that had a ph < 7.2 in a patient with clinical evidence of infection. TTs were carried out in the bedside position and using local anaesthesia. Large bore thoracic tubes (28 32F) were inserted into the pleural space. In case of malpositioning of the tube or inadequate drainage, a second tube was inserted. Tubes were removed when the drainage dropped below 100 ml and the pleural fluid (PF) culture was negative. Intrapleural FT was performed with streptokinase (SK). A single dose of SK 250,000 IU in a 250 ml saline solution was administered daily through the chest tube, and the tube was clamped. After four to six hours, the tube was declamped. SK application was repeated until the drainage dropped below 100 ml and became serous in nature. Table I. Demographics of the patients (n = 114). Demographic Value Mean age ± SD (range) (years) 50 ± 17 (18 89) Male/Female 77/31 Symptoms Fever 91 Dyspnoea 80 Cough 67 Weakness 65 Chest pain 63 Aetiology Pneumonia 90 Tuberculosis 16 Pneumothorax 3 Trauma 3 Iatrogenic 2 Comorbid diseases COPD 8 DM type 2 6 CHI 2 Lung cancer 1 Bacteriology Pseudomonas Aeroginosa 24 Streptococcus Pneumoniae 20 Staphylococcus Aereus 4 Gram stain No staining 43 Gram negative 23 Gram positive 20 COPD: chronic obstructive lung disease; DM: diabetes mellitus; CHI: congestive heart insufficiency VATS for empyema was performed as soon as possible after TT. VATS deloculation and debridement were performed with two or three port entries under general anaesthesia. A single large bore chest tube was inserted at the end of VATS. Open decortication (OD) was not included in the study, as we considered the necessity of open decortication as a treatment failure for noninvasive treatment options in this study. The main criteria for open decortication were inadequate drainage, defined as the presence on a chest radiograph of > 50% of the original amount of pleural fluid, inadequate reexpansion of the lung, defined as the presence on a chest radiograph of > 30% of the hemithorax, and persistent sepsis, defined as the presence of persistent fever (> 38.0 C) and elevated peripheral WBC count (> 11,000/mm 3 ). Illness days before intervention was described as the period between the beginning of the initial symptoms and TT application. Antibiotherapy days before intervention was described as the period between the beginning of antibiotherapy and the main application. Drainage after intervention refers to the drainage period between the main treatment option and chest tube removal. Hospital stay refers to the period between TT application and
3 Singapore Med J 2010; 51(3) : 244 Table II. Comparison of the treatment options. Parameter TT (n = 47) SK (n = 23) VATS (n = 44) p-value Mean age ± SD (range) (years) 50 ± 19 (18 88) 55 ± 16 (26 89) 49 ± 15 (18 89) Gender (male/female) 31/16 17/6 26/ Gram stain (Gram /+) 7/20 6/7 10/ Illness day before intervention 7 ± 3 (4 14) 5 ± 1 (2 8) 4 ± 1 (2 8) 0.001* Antibiotherapy day before intervention 8 ± 4 (2 21) 7 ± 4 (1 19) 6 ± 2 (2 14) Drainage day after intervention 11 ± 4 (5 23) 9 ± 3 (5 20) 2 ± 1 (1 3) 0.001* Hospital stay (days) 13 ± 4 (5 25) 11 ± 3 (6 23) 3 ± 1 (1 5) 0.001* Total complication count <0.001* Pleural decortication requirement <0.001* Perioperative mortality NA Multiple comparison: Illness day before intervention: TT vs. SK, p = 0.003*; TT vs. VATS, p = 0.013*; SK vs. VATS, p = Drainage day after intervention: TT vs. SK, p = 0.231; TT vs. VATS, p < 0.001*; SK vs. VATS, p < 0.001* Hospital stay: TT vs. SK, p = 0.209; TT vs. VATS, p < 0.001*; SK vs. VATS, P < 0.001* * denotes statistical significance. SD: standard deviation; TT: tube thoracostomy; SK: streptokinase; VATS: video-assisted thoracoscopic surgery patient discharge. Perioperative mortality rate was defined as the percentage of patients who died of causes related or unrelated to the disease, or operation within 30 days of surgery. The data was expressed as mean ± standard deviation. The categoric variables were expressed by the count and percentage. One way ANOVA was used to compare the continuous variables. Tamhane s T 2 test was used for post hoc comparisons, while the chi-square test was used to compare the categorical variables. A p-value of < 0.05 was considered to be significant. RESULTS A total of 114 Class 5 empyema patients were surgically treated with TT (n = 44), SK (n = 23) or VATS (n = 47). The mean age was 50 ± 16 (range 18 89) years, and the male to female ratio was 80:34. The demographics of the patients are provided in Table II. Fever and dyspnoea were the most frequently encountered symptoms, and pneumonia was the most frequent aetiological source. 50% (43 out of 86) of PF performed Gram stains revealed bacterial isolation. A bacteriologic diagnosis could be made in 48 of the 114 patients (42%) with PF culture. Tuberculosis empyemas was diagnosed with PF tuberculosis culture. The patients demographics are provided in Table I. A total of 84 patients underwent initial TT after diagnosis. In total, 52 chest tubes were introduced among the patients in the TT group and 27 in the SK group. The mean SK application was 5.4 ± 2.4 (range 2 11) days. In the VATS group, 17 patients underwent initial TT to improve their septic condition before VATS, and 30 underwent VATS decortication directly. In total, 17 patients underwent open decortication due to treatment failure. All these patients were in the TT group, and were treated prior to the utilisation of VATS in our centres. No patient required open decortication in the SK and VATS groups. In the TT group, the mean illness time was significantly longer than that of the SK and VATS groups. The mean antibiotherapy time before intervention was 7.3 ± 3.8 (range 1 21) days for all patients. There was no statistical difference in antibiotherapy time among the groups (p = 0.065). However, in the VATS treatment group, the drainage day after intervention and hospital stay were significantly shorter than in the TT and SK groups (p < in both). The TT group had a higher complication rate and more OD requirements than the SK and VATS groups (p < in both). The comparative evaluation of our treatment options is shown in Table II. The success rates for TT, SK and VATS were 66%, 95% and 100%, respectively. The most frequent complication was pleural space (Table III). Two cases of perioperative mortality occurred. One patient died due to sepsis on the 18th day, and the other died because of bronchopleural fistula on the 27th day of hospital stay. 17 patients required OD in the TT group. One patient had pleural haemorrhaging after the second SK instillation, after which SK application was stopped. Out of the 114 patients, 100 were followed up after a mean of 26.1 (range 2 86) months. Two patients in the TT group had recurrent empyema on the sixth and eighth day after chest tube removal. They were treated with OD uneventfully. DISCUSSION This study has shown that VATS deloculation and debridement involves less drainage time, hospitalisation time and morbidity than using TT alone or with FT, in
4 Singapore Med J 2010; 51(3) : 245 the treatment of early stage multiloculated empyema. Between 1995 and 1998, we performed TT alone and followed up with the empyema patients. It was observed that the success rate was low, and that a high rate of open decortication was required among patients with loculated empyema. We then performed SK in patients with loculated empyema immediately after TT. This increased our success rates, and open decortication was no longer required in patients with loculated empyema between 1999 and On the other hand, our drainage time and hospital stay remained as long as that observed with TT alone. Since 2001, we have routinely performed VATS decortication when a diagnosis of loculation results in empyema. An initial chest tube before VATS decortication has been introduced in order to improve the general condition of the patient when required. So far, after VATS decortication applications, our success rate has been 100%, and the hospital stay has been significantly shortened in Class 5 empyema patients. According to Light s classification, (4) antibiotic treatment is sufficient for Class 1 and Class 2 empyema, whereas pleural drainage in addition to antibiotic treatment is recommended for Class 3 and above. We had also routinely conducted TT in patients with Class 5 empyema thoracis in our clinics in the past. Currently, VATS evacuation, deloculation and debridement under general anaesthesia is preferred. We have also performed TT in multiloculated empyema in order to stabilise risky patients, such as in septic conditions and/or in cases with the existence of bronchopleural fistula. Out of the 114 patients, 47 were treated with TT alone, and the success rate was 66%. High failure rates (up to 87%) with conservative treatment have been reported, especially in patients with multiloculated empyema. (5-7) Mandal et al reported a 37% failure rate for TT in his series of 179 patients, where the mortality rate was 11% in the same group, and 26% of the patients had to undergo a second intervention. The overall mortality was 6.7%. (8) Our morbidity and mortality rates for TT alone were 49% and 0.4%, respectively. Eight (18%) patients required a second tube insertion, and 34% of the patients required OD. Our results also highlight the importance of the interval between the onset of symptoms or pleural effusion and intervention on the success of the treatment of empyema. In the TT group, the period of illness days before intervention was longer than that in the SK and VATS groups. This condition may worsen the success rate of TT treatment as compared to the other groups. Many reports have shown that intrapleural FT provides significant benefits in reducing the requirement Table III. Complications after the treatment options. Complications TT SK VATS Air space Air leak > 5 days Atelectasis Bleeding Air-fluid level Wound infection Total TT: tube thoracostomy; SK: streptokinase; VATS: video-assisted thoracoscopic surgery for surgical intervention, and increases the success rate as compared to performing TT alone. (9-11) Success rates of 35% 87% have been reported, even in patients with frank empyema. (11,12) Fibrinolysis is an independent factor for a better outcome. (11) In contrast, Maskell et al reported in a large randomised study that SK instillation did not improve mortality, the rate of surgery or the length of hospital stay in patients with empyema. (13) Our study confirmed that SK instillation is beneficial in reducing the requirement of OD, and increases the success ratio. In our series, FT had to be interrupted in one patient because of haemorrhagic drainage during the second dose, and no patient underwent OD. Our success ratio was 95%. This relatively higher ratio may be due to the time allowed for the re-expansion of the patients lungs before OD was attempted. Although seven patients had obvious pleural space at the time of drainage removal, all had complete re-expansion at the first to third month follow-up. With the advent of VATS, several authors have reported encouraging results for the management of fibrinopurulent Stage II empyema. (14-16) VATS is less invasive than OD and is better accepted by both the referring physician and patient. However, VATS has obvious limitations for the treatment of Stage III disease. Its success rate ranges from 68% 93%. (17) The success rate of VATS is higher in patients with a history shorter than four weeks; however, the requirement of decortication increases in patients with a history of over five weeks. (17) Our success rate was 100%, which was relatively higher than that reported in the literature. This can be explained by the fact that our patients were all early stage multiloculated (Class 5) empyema patients. In patients undergoing a VATS approach to empyema, the conversion thoracotomy rate ranges from 5% 59%. (17,18) The conversion thoracotomy rate is influenced by the aetiology of empyema. In patients with clinical Stage II empyema, the rate has been reported as 55% in postpneumonic, 32% in postraumatic
5 Singapore Med J 2010; 51(3) : 246 and 29% in postoperative empyemas. (18) The reported postoperative complication, recurrent empyema and 30-day postoperative mortality rates were 9%, 2.4% and 4%, respectively. (18) Our complication, conversion thoracotomy and mortality rates were 0.7%, 0.0% and 0.0%, respectively. Open surgery is still a method that achieves excellent results in advanced pleural empyema. Although its indications are now limited by its invasive nature, OD by thoracotomy must be the procedure of choice for the treatment of pleural empyema when VATS is not sufficient. Light has advocated that if a sizeable empyema cavity remains after seven days of chest tube drainage, consideration should be given to performing an OD. (4) However, our experience has shown that, particularly in patients with concomitant pneumonic consolidation, lung expansion is not as good as in a healthy lung, even in the absence of pleural thickening. In these patients, waiting and a follow-up period after chest tube removal may be better than early OD in achieving re-expansion of the lung. In 13 of our 25 patients with a pleural cavity, the lungs fully expanded one to two months after the drain removal. In conclusion, in patients with early stage empyema, VATS deloculation and debridement is superior to TT alone and FT in reducing the drainage time and hospital stay. It has a rather high success rate without significant morbidity. Therefore, it may be recommended as a firstline therapy for early stage multiloculated empyemas. REFERENCES 1. Singh M, Singh SK, Chowdhary SK. Management of empyema thoracic in children. Indian Pediatr 2002; 39: Colice GL, Curtis A, Deslauriers J, et al. Medical and surgical treatment of parapneumonic effusions: an evidence-based guideline. Chest. 2000; 118: Deslauriers J, Mehran R. Handbook of perioperative care in general thoracic surgery. Philadelphia: Elsevier; Light RW. A new classification of parapneumonic effusions and empyema. Chest 1995; 108: Solaini L, Prusciano F, Bagioni P. Video-assisted thoracic surgery in the treatment of pleural empyema. Surg Endosc 2007; 21: Striffeler H, Ris HB, Wursten HU, et al. Video-assisted thoracoscopic treatment of pleural empyema, a new therapeutic approach. Eur J Cardiothorac Surg 1994; 8: Lemmer JH, Botham MJ, Orringer MB. Modern management of adult thoracic empyema. J Thorac Cardiovasc Surg 1985; 90: Mandal AK, Thadepalli H, Mandal AK, Chettipally U. Outcome of primary empyema thoracis: therapeutic and microbiologic aspects. Ann Thorac Surg 1998; 66: Cameron R, Davies HR. Intra-pleural fibrinolytic therapy versus conservative management in the treatment of parapneumonic effusions and empyema. Cochrane Database Syst Rev 2004; 1: CD Diacon AH, Theron J, Schuurmans MM, Van de Wal BW, Bolliger CT. Intrapleural streptokinase for empyema and complicated parapneumonic effusions. Am J Respir Crit Care Med 2004; 170: Misthos P, Sepsas E, Konstantinou M, et al. Early use of intrapleural fibrinolytics in the management of postpneumonic empyema. A prospective study. Eur J Cardiothorac Surg 2005; 28: Wait MA, Sharma S, Hohn J, Dal Nogare A. A randomized trial of empyema therapy. Chest 1997; 111: Maskell NA, Davies CW, Nunn AJ, et al; First Multicenter Intrapleural Sepsis Trial (MIST1) Group. UK. Controlled trial of intrapleural streptokinase for pleural infection. N Engl J Med 2005; 352: Cheng YJ, Wu HH, Chou SH, Kao EL. Video-assisted thoracoscopic surgery in the treatment of chronic empyema thoracis. Surg Today 2002; 32: Waller DA, Rengarajan A, Nicholson FH, Rajesh PB. Delayed referral reduces the success of video-assisted thoracoscopic debridement for post-pneumonic empyema. Respir Med 2001; 95: Cassina PC, Hauser M, Hillejan L, Greschuchna D, Stamatis G. Video-assisted thoracoscopy in the treatment of pleural empyema: stage-based management and outcome. J Thorac Cardiovasc Surg 1999; 117: Molnar TF. Current surgical treatment of thoracic empyema in adults. Eur J Cardiothorac Surg 2007; 32: Lardinois D, Gock M, Pezzetta E, et al. Delayed referral and gram-negative organisms increase the conversion thoracotomy rate in patients undergoing video-assisted thoracoscopic surgery for empyema. Ann Thorac Surg 2005; 79:
Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20,
 Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20, 521-525 Empyema thoracis Original Article Singh DR 1, Joshi MR 2, Thapa P 2, Nath S 3 1 Assistant Professor, 2 Lecturer, 3 Professor,
Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20, 521-525 Empyema thoracis Original Article Singh DR 1, Joshi MR 2, Thapa P 2, Nath S 3 1 Assistant Professor, 2 Lecturer, 3 Professor,
Best timing for surgical intervention of empyema. Supervisor: Intern:
 Best timing for surgical intervention of empyema Supervisor: Intern: Brief history 56 y/o male, farmer With anesthesia medication at LMD Admission 30d 7d Dry cough Progressive productive cough with yellow
Best timing for surgical intervention of empyema Supervisor: Intern: Brief history 56 y/o male, farmer With anesthesia medication at LMD Admission 30d 7d Dry cough Progressive productive cough with yellow
Alper Toker, MD. VATS decortication. Istanbul University, Istanbul Medical School Department of Thoracic Surgery
 VATS decortication Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery Pleural space infection is a common pathology causing morbidity and mortality. It is a collection
VATS decortication Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery Pleural space infection is a common pathology causing morbidity and mortality. It is a collection
Modern Approaches to Empyema
 Modern Approaches to Empyema Amit Bhargava, MD Attending Thoracic Surgeon Assistant Professor Department of Cardiovascular and Thoracic Surgery 1 Principles of Treatment Adequate drainage Sterilization
Modern Approaches to Empyema Amit Bhargava, MD Attending Thoracic Surgeon Assistant Professor Department of Cardiovascular and Thoracic Surgery 1 Principles of Treatment Adequate drainage Sterilization
Thoracoscopic Management of Complicated Parapneumonic Effusions in Young Children. Saeed Al Hindi, MD, CABS, FRCSI*
 Bahrain Medical Bulletin, Vol. 31, No. 4, December 2009 Thoracoscopic Management of Complicated Parapneumonic Effusions in Young Children Saeed Al Hindi, MD, CABS, FRCSI* Objective: To evaluate the role
Bahrain Medical Bulletin, Vol. 31, No. 4, December 2009 Thoracoscopic Management of Complicated Parapneumonic Effusions in Young Children Saeed Al Hindi, MD, CABS, FRCSI* Objective: To evaluate the role
EMPYEMA. Catheter Based Treatment vs. VATS. UCHSC Department of Surgery Grand Rounds August 27 th, Jeremy Hedges, M.D.
 EMPYEMA Catheter Based Treatment vs. VATS UCHSC Department of Surgery Grand Rounds August 27 th, 2007 Jeremy Hedges, M.D. OVERVIEW Empyema Pathogenesis Treatment Catheter based treatment Fibrinolytics
EMPYEMA Catheter Based Treatment vs. VATS UCHSC Department of Surgery Grand Rounds August 27 th, 2007 Jeremy Hedges, M.D. OVERVIEW Empyema Pathogenesis Treatment Catheter based treatment Fibrinolytics
Posttraumatic Empyema Thoracis
 Posttraumatic Empyema Thoracis Dr AG Jacobs STEVE BIKO ACADEMIC HOSPITAL, UNIVERSITY OF PRETORIA EMPYEMA THORACIS Derived from Greek word empyein Means pus-producing Refers to accumulation of pus within
Posttraumatic Empyema Thoracis Dr AG Jacobs STEVE BIKO ACADEMIC HOSPITAL, UNIVERSITY OF PRETORIA EMPYEMA THORACIS Derived from Greek word empyein Means pus-producing Refers to accumulation of pus within
Surgical Treatment for Empyema Thoracis: Is Video-Assisted Thoracic Surgery Better Than Thoracotomy?
 Surgical Treatment for Empyema Thoracis: Is Video-Assisted Thoracic Surgery Better Than Thoracotomy? Daniel T. L. Chan, MBBS, Alan D. L. Sihoe, FRCSEd, FCCP, Shun Chan, MBBS, Dickson S. F. Tsang, MBBS,
Surgical Treatment for Empyema Thoracis: Is Video-Assisted Thoracic Surgery Better Than Thoracotomy? Daniel T. L. Chan, MBBS, Alan D. L. Sihoe, FRCSEd, FCCP, Shun Chan, MBBS, Dickson S. F. Tsang, MBBS,
VIDEO-ASSISTED THORACOSCOPY IN THE TREATMENT OF PLEURAL EMPYEMA: STAGE-BASED MANAGEMENT AND OUTCOME
 VIDEO-ASSISTED THORACOSCOPY IN THE TREATMENT OF PLEURAL EMPYEMA: STAGE-BASED MANAGEMENT AND OUTCOME Paolo Claudio Cassina, MD a Markus Hauser, MD, FCCP b Ludger Hillejan, MD a Dieter Greschuchna, MD a
VIDEO-ASSISTED THORACOSCOPY IN THE TREATMENT OF PLEURAL EMPYEMA: STAGE-BASED MANAGEMENT AND OUTCOME Paolo Claudio Cassina, MD a Markus Hauser, MD, FCCP b Ludger Hillejan, MD a Dieter Greschuchna, MD a
Post Pneumonic Empyema: Is There Still a Role for Surgery?
 Post Pneumonic Empyema: Is There Still a Role for Surgery? M. Blair Marshall, MD Ismael Matus, MD Chief, Thoracic Surgery Interventional Pulmonary Professor of Surgery Medicine MedStar Georgetown University
Post Pneumonic Empyema: Is There Still a Role for Surgery? M. Blair Marshall, MD Ismael Matus, MD Chief, Thoracic Surgery Interventional Pulmonary Professor of Surgery Medicine MedStar Georgetown University
Bacterial pneumonia with associated pleural empyema pleural effusion
 EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
The use of thrombolytics in the management of complex pleural fluid collections
 Original Article The use of thrombolytics in the management of complex pleural fluid collections Jessica Heimes 1, Hannah Copeland 2, Aditya Lulla 3, Marjulin Duldulao 4, Khaled Bahjri 5, Salman Zaheer
Original Article The use of thrombolytics in the management of complex pleural fluid collections Jessica Heimes 1, Hannah Copeland 2, Aditya Lulla 3, Marjulin Duldulao 4, Khaled Bahjri 5, Salman Zaheer
Complicated parapneumonic effusion and empyema thoracis: Microbiologic and therapeutic aspects
 Respiratory Medicine (2006) 100, 286 291 Complicated parapneumonic effusion and empyema thoracis: Microbiologic and therapeutic aspects Duygu Ozol, Sibel Oktem, Erturk Erdinc Department of Chest Disease,
Respiratory Medicine (2006) 100, 286 291 Complicated parapneumonic effusion and empyema thoracis: Microbiologic and therapeutic aspects Duygu Ozol, Sibel Oktem, Erturk Erdinc Department of Chest Disease,
Surgery should be the first line of treatment for empyemaresp_1677
 202..207 PRO/CON DEBATE Surgery should be the first line of treatment for empyemaresp_1677 IOANNIS E. PETRAKIS, 1 JOHN E. HEFFNER 2 * AND JEFFREY S. KLEIN 3 1 Department of General and Thoracic Surgery,
202..207 PRO/CON DEBATE Surgery should be the first line of treatment for empyemaresp_1677 IOANNIS E. PETRAKIS, 1 JOHN E. HEFFNER 2 * AND JEFFREY S. KLEIN 3 1 Department of General and Thoracic Surgery,
Parapneumonic effusions are a common problem
 Proceeding S.Z.P.G.M.I. vol: 20(2): pp. 9-3, 200. Intrapleural Streptokinase in Management of Complicated Parapneumonic Effusion and Empyema Kamran Hameed, Ahmad Hasan Banjer, Mohammad Abdul-Aziz Siddiqui
Proceeding S.Z.P.G.M.I. vol: 20(2): pp. 9-3, 200. Intrapleural Streptokinase in Management of Complicated Parapneumonic Effusion and Empyema Kamran Hameed, Ahmad Hasan Banjer, Mohammad Abdul-Aziz Siddiqui
Surgical decortication as the first-line treatment for pleural empyema
 Shin et al General Thoracic Surgical decortication as the first-line treatment for pleural empyema Jung Ar Shin, MD, a Yoon Soo Chang, MD, PhD, a Tae Hoon Kim, MD, PhD, b Seok Jin Haam, MD, c Hyung Jung
Shin et al General Thoracic Surgical decortication as the first-line treatment for pleural empyema Jung Ar Shin, MD, a Yoon Soo Chang, MD, PhD, a Tae Hoon Kim, MD, PhD, b Seok Jin Haam, MD, c Hyung Jung
A review of the management of complex para-pneumonic effusion in adults
 Review Article A review of the management of complex para-pneumonic effusion in adults Vikas Koppurapu, Nikhil Meena Department of Internal Medicine, University of Arkansas for Medical Sciences, Little
Review Article A review of the management of complex para-pneumonic effusion in adults Vikas Koppurapu, Nikhil Meena Department of Internal Medicine, University of Arkansas for Medical Sciences, Little
Table 2: Outcomes measured. Table 1: Intrapleural alteplase instillation therapy protocol
 ORIGINAL RESEARCH ARTICLE Intrapleural F brinolytic Therapy with Alteplase in Empyema Thoracis in Children conducted in the Department of Pediatric critical care and Pulmonology unit at our institution
ORIGINAL RESEARCH ARTICLE Intrapleural F brinolytic Therapy with Alteplase in Empyema Thoracis in Children conducted in the Department of Pediatric critical care and Pulmonology unit at our institution
Outcomes & Clinical Trials Update: Empyema & NEC
 Outcomes & Clinical Trials Update: Empyema & NEC American Pediatric Surgical Association Outcomes & Clinical Trials Committee Fizan Abdullah, Chair Saleem Islam, Vice Chair Gudrun Aspelund Catherine C.
Outcomes & Clinical Trials Update: Empyema & NEC American Pediatric Surgical Association Outcomes & Clinical Trials Committee Fizan Abdullah, Chair Saleem Islam, Vice Chair Gudrun Aspelund Catherine C.
aacp consensus statement
 aacp consensus statement Medical and Surgical Treatment of Parapneumonic Effusions* An Evidence-Based Guideline Gene L. Colice, MD, FCCP; Anne Curtis, MD; Jean Deslauriers, MD; John Heffner, MD, FCCP;
aacp consensus statement Medical and Surgical Treatment of Parapneumonic Effusions* An Evidence-Based Guideline Gene L. Colice, MD, FCCP; Anne Curtis, MD; Jean Deslauriers, MD; John Heffner, MD, FCCP;
MANAGEMENT OF RETAINED HAEMOTHORAX DR AG JACOBS PRINCIPAL SPECIALIST DEPARTMENT OF CARDIO THORACIC SURGERY UNIVERSITY OF PRETORIA
 MANAGEMENT OF RETAINED HAEMOTHORAX DR AG JACOBS PRINCIPAL SPECIALIST DEPARTMENT OF CARDIO THORACIC SURGERY UNIVERSITY OF PRETORIA MANAGEMENT OF RETAINED HAEMOTHORAX Retained Haemothorax Definition: Failure
MANAGEMENT OF RETAINED HAEMOTHORAX DR AG JACOBS PRINCIPAL SPECIALIST DEPARTMENT OF CARDIO THORACIC SURGERY UNIVERSITY OF PRETORIA MANAGEMENT OF RETAINED HAEMOTHORAX Retained Haemothorax Definition: Failure
Thoracotomy and decortication in empyema: Clinical spectrum and outcome
 Original Article Thoracotomy and decortication in empyema: Clinical spectrum and outcome Shrestha KP*, Adhikari S**, Pokhrel DP*** *Associate Professor, **DM Resident, ***Professor NAMS ABSTRACT INTRODUCTION:
Original Article Thoracotomy and decortication in empyema: Clinical spectrum and outcome Shrestha KP*, Adhikari S**, Pokhrel DP*** *Associate Professor, **DM Resident, ***Professor NAMS ABSTRACT INTRODUCTION:
Advances in the Management of Empyema
 Advances in the Management of Empyema RCP Update in Respiratory Medicine 26 th January 2017 Najib M Rahman Associate Professor of Respiratory Medicine University of Oxford najib.rahman@ndm.ox.ac.uk Financial
Advances in the Management of Empyema RCP Update in Respiratory Medicine 26 th January 2017 Najib M Rahman Associate Professor of Respiratory Medicine University of Oxford najib.rahman@ndm.ox.ac.uk Financial
Empyema Thoracis* Therapeutic Management and Outcome
 Empyema Thoracis* Therapeutic Management and Outcome Gregory P. LeMense, MD; Charlie Strange, MD, FCCP; and Steven A. Sahn, MD, FCCP Study objective: We evaluated treatment and outcome of patients with
Empyema Thoracis* Therapeutic Management and Outcome Gregory P. LeMense, MD; Charlie Strange, MD, FCCP; and Steven A. Sahn, MD, FCCP Study objective: We evaluated treatment and outcome of patients with
Videothoracoscopy in Pleural Empyema Following Methicillin-Resistant Staphylococcus aureus (MRSA) Lung Infection
 Short Communication TheScientificWorldJOURNAL (2009) 9, 723 728 ISSN 1537-744X; DOI 10.1100/tsw.2009.91 Videothoracoscopy in Pleural Empyema Following Methicillin-Resistant Staphylococcus aureus (MRSA)
Short Communication TheScientificWorldJOURNAL (2009) 9, 723 728 ISSN 1537-744X; DOI 10.1100/tsw.2009.91 Videothoracoscopy in Pleural Empyema Following Methicillin-Resistant Staphylococcus aureus (MRSA)
Guidelines/Guidance/CAP/ Hospitalized Child. PHM Boot Camp 2014 Jay Tureen, MD June 19, 2014
 Guidelines/Guidance/CAP/ Hospitalized Child PHM Boot Camp 2014 Jay Tureen, MD June 19, 2014 CAP in Children: Epi Greatest cause of death in children worldwide Estimated > 2 M deaths in children In developed
Guidelines/Guidance/CAP/ Hospitalized Child PHM Boot Camp 2014 Jay Tureen, MD June 19, 2014 CAP in Children: Epi Greatest cause of death in children worldwide Estimated > 2 M deaths in children In developed
Review of video-assisted thoracoscopy in children
 Review Article Review of video-assisted thoracoscopy in children S N Oak, S V Parelkar, K V SatishKumar, R Pathak, B H Ramesh, S Sudhir, M Keshav Department of Pediatric Surgery, TNMC and BYL Nair Hospital,
Review Article Review of video-assisted thoracoscopy in children S N Oak, S V Parelkar, K V SatishKumar, R Pathak, B H Ramesh, S Sudhir, M Keshav Department of Pediatric Surgery, TNMC and BYL Nair Hospital,
Treatment of Loculated Pleural Effusions with Transcatheter Intracavitary Urokinase
 941 Treatment of Loculated Pleural Effusions with Transcatheter Intracavitary Urokinase Jeffrey S. Moulton1 Surgical thoracostomy tube placement and radiologically guided catheter drainage Patrick Timothy
941 Treatment of Loculated Pleural Effusions with Transcatheter Intracavitary Urokinase Jeffrey S. Moulton1 Surgical thoracostomy tube placement and radiologically guided catheter drainage Patrick Timothy
ABDULHAMEED AZIZ, 1 JEFFREY M. HEALEY, 1 FAISAL QURESHI, 1 TIMOTHY D. KANE, 1 GEOFFREY KURLAND, 2 MICHAEL GREEN, 3 and DAVID J.
 SURGICAL INFECTIONS Volume 9, Number 3, 2008 Mary Ann Liebert, Inc. DOI: 10.1089/sur.2007.025 Comparative Analysis of Chest Tube Thoracostomy and Video-Assisted Thoracoscopic Surgery in Empyema and Parapneumonic
SURGICAL INFECTIONS Volume 9, Number 3, 2008 Mary Ann Liebert, Inc. DOI: 10.1089/sur.2007.025 Comparative Analysis of Chest Tube Thoracostomy and Video-Assisted Thoracoscopic Surgery in Empyema and Parapneumonic
Guideline for management of children & adolescents with pleural empyema
 CHILD AND ADOLESCENT HEALTH SERVICE PRINCESS MARGARET HOSPITAL FOR CHILDREN Guideline for management of children & adolescents with pleural empyema This guideline provides an evidence-based framework for
CHILD AND ADOLESCENT HEALTH SERVICE PRINCESS MARGARET HOSPITAL FOR CHILDREN Guideline for management of children & adolescents with pleural empyema This guideline provides an evidence-based framework for
Surgical versus non-surgical management for pleural empyema(protocol)
 Cochrane Database of Systematic Reviews Surgical versus non-surgical management for pleural empyema(protocol) ChinTY,ReddenMD,HsuCCT,vanDrielML ChinTY,ReddenMD,HsuCCT,vanDrielML. Surgical versus non-surgical
Cochrane Database of Systematic Reviews Surgical versus non-surgical management for pleural empyema(protocol) ChinTY,ReddenMD,HsuCCT,vanDrielML ChinTY,ReddenMD,HsuCCT,vanDrielML. Surgical versus non-surgical
Diagnostic Approach to Pleural Effusion
 Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
Case Report Intrapleural administration of DNase alone for pleural empyema
 Int J Clin Exp Med 2015;8(11):22011-22015 www.ijcem.com /ISSN:1940-5901/IJCEM0016173 Case Report Intrapleural administration of DNase alone for pleural empyema Vladimir Bobek 1,2,3, Andrzej Majewski 4,
Int J Clin Exp Med 2015;8(11):22011-22015 www.ijcem.com /ISSN:1940-5901/IJCEM0016173 Case Report Intrapleural administration of DNase alone for pleural empyema Vladimir Bobek 1,2,3, Andrzej Majewski 4,
Fibrinolytic Therapy in Complicated Parapneumonic Effusions and Empyema
 Fibrinolytic Therapy in Complicated Parapneumonic Effusions and Empyema MS Barthwal Pulmonologist and Medical Specialist, Department of Respiratory Medicine, Military Hospital (Cardio Thoracic Center),
Fibrinolytic Therapy in Complicated Parapneumonic Effusions and Empyema MS Barthwal Pulmonologist and Medical Specialist, Department of Respiratory Medicine, Military Hospital (Cardio Thoracic Center),
Accepted Manuscript. Current State of the Art for the Surgical Management of empyema thoracis. K. Robert Shen, M.D.
 Accepted Manuscript Current State of the Art for the Surgical Management of empyema thoracis K. Robert Shen, M.D. PII: S0022-5223(18)32919-2 DOI: https://doi.org/10.1016/j.jtcvs.2018.11.006 Reference:
Accepted Manuscript Current State of the Art for the Surgical Management of empyema thoracis K. Robert Shen, M.D. PII: S0022-5223(18)32919-2 DOI: https://doi.org/10.1016/j.jtcvs.2018.11.006 Reference:
PAPER. Video-Assisted Thoracic Surgery in the Treatment of Posttraumatic Empyema
 PAPER Video-Assisted Thoracic Surgery in the Treatment of Posttraumatic Empyema Lynette A. Scherer, MD; Felix D. Battistella, MD; John T. Owings, MD; Michael M. Aguilar, MD Background: Video-assisted thoracic
PAPER Video-Assisted Thoracic Surgery in the Treatment of Posttraumatic Empyema Lynette A. Scherer, MD; Felix D. Battistella, MD; John T. Owings, MD; Michael M. Aguilar, MD Background: Video-assisted thoracic
Surgical treatment of empyema in children
 Surgical treatment of empyema in children Jacques Janson Pierre Goussard Cardiothoracic Surgery, Paediatric Pulmonology Tygerberg Academic Hospital University of Stellenbosch Pleural space Netter, Frank
Surgical treatment of empyema in children Jacques Janson Pierre Goussard Cardiothoracic Surgery, Paediatric Pulmonology Tygerberg Academic Hospital University of Stellenbosch Pleural space Netter, Frank
V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY
 V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY Kharkov Regional Centre of Cardiovascular surgery V.N. Karazin Kharkov National University Department of Internal Medicine Pleural empyema Abduyeva F.M., MD, PhD
V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY Kharkov Regional Centre of Cardiovascular surgery V.N. Karazin Kharkov National University Department of Internal Medicine Pleural empyema Abduyeva F.M., MD, PhD
Paediatric Empyema: A Case Report and Literature Review
 Case reports Paediatric Empyema: A Case Report and Literature Review S. J. PARSONS, E. FENTON, M. WILLIAMS Department of Paediatrics, Royal Hobart Hospital, Hobart, TASMANIA ABSTRACT Objective: To present
Case reports Paediatric Empyema: A Case Report and Literature Review S. J. PARSONS, E. FENTON, M. WILLIAMS Department of Paediatrics, Royal Hobart Hospital, Hobart, TASMANIA ABSTRACT Objective: To present
RETROSPECTIVE COMPARISON OF EMPYEMA THORACIS IN HIV INFECTED AND NON-INFECTED PATIENTS WITH REGARDS TO AETIOLOGY AND OUTCOMES
 RETROSPECTIVE COMPARISON OF EMPYEMA THORACIS IN HIV INFECTED AND NON-INFECTED PATIENTS WITH REGARDS TO AETIOLOGY AND OUTCOMES Dr Grace Helga Kaye-Eddie A research report submitted to the Faculty of Health
RETROSPECTIVE COMPARISON OF EMPYEMA THORACIS IN HIV INFECTED AND NON-INFECTED PATIENTS WITH REGARDS TO AETIOLOGY AND OUTCOMES Dr Grace Helga Kaye-Eddie A research report submitted to the Faculty of Health
EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC CHANGES
 Trakia Journal of Sciences, Vol. 3, No. 2, pp 61-65, 2005 Copyright 2005 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC
Trakia Journal of Sciences, Vol. 3, No. 2, pp 61-65, 2005 Copyright 2005 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC
Interventional radiology treatment of empyema and lung abscesses
 PAEDIATRIC RESPIRATORY REVIEWS (2008) 9, 77 84 CME ARTICLE Interventional radiology treatment of empyema and lung abscesses Mark J. Hogan* and Brian D. Coley Nationwide Children s Hospital and The Ohio
PAEDIATRIC RESPIRATORY REVIEWS (2008) 9, 77 84 CME ARTICLE Interventional radiology treatment of empyema and lung abscesses Mark J. Hogan* and Brian D. Coley Nationwide Children s Hospital and The Ohio
Review Article Management of Infectious Processes of the Pleural Space: A Review
 Pulmonary Medicine Volume 2012, Article ID 816502, 10 pages doi:10.1155/2012/816502 Review Article Management of Infectious Processes of the Pleural Space: A Review Ankur Girdhar, Adil Shujaat, and Abubakr
Pulmonary Medicine Volume 2012, Article ID 816502, 10 pages doi:10.1155/2012/816502 Review Article Management of Infectious Processes of the Pleural Space: A Review Ankur Girdhar, Adil Shujaat, and Abubakr
@ERSpublications Does pleural irrigation improve pleural fluid drainage and resolution of sepsis in pleural infection?
 ORIGINAL ARTICLE RESPIRATORY INFECTIONS Pleural irrigation trial (PIT): a randomised controlled trial of pleural irrigation with normal saline versus standard care in patients with pleural infection Clare
ORIGINAL ARTICLE RESPIRATORY INFECTIONS Pleural irrigation trial (PIT): a randomised controlled trial of pleural irrigation with normal saline versus standard care in patients with pleural infection Clare
Factors predictive of the failure of medical treatment in patients with pleural infection
 ORIGINAL ARTICLE Korean J Intern Med 2014;29:603-612 Factors predictive of the failure of medical treatment in patients with pleural infection Sung-Kyoung Kim 1, Chul Ung Kang 2, So Hyang Song 1, Deog
ORIGINAL ARTICLE Korean J Intern Med 2014;29:603-612 Factors predictive of the failure of medical treatment in patients with pleural infection Sung-Kyoung Kim 1, Chul Ung Kang 2, So Hyang Song 1, Deog
Intrapleural Fibrinolytic Therapy in Complicated Parapneumonic Effusion and Empyema: Present Status
 Review Article Intrapleural Fibrinolytic Therapy in Complicated Parapneumonic Effusion and Empyema: Present Status Col (Dr) M.S. Barthwal Department of Pulmonary Medicine, Military Hospital, Namkum, Ranchi,
Review Article Intrapleural Fibrinolytic Therapy in Complicated Parapneumonic Effusion and Empyema: Present Status Col (Dr) M.S. Barthwal Department of Pulmonary Medicine, Military Hospital, Namkum, Ranchi,
Management of Pleural Effusion
 Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
Trust Guideline for the management of Parapneumonic Effusion in children
 A clinical guideline recommended for use For Use in: By: For: Division responsible for document: Buxton ward, Children s Assessment Unit (CAU) All staff Children with parapneumonic effusion Women and Children
A clinical guideline recommended for use For Use in: By: For: Division responsible for document: Buxton ward, Children s Assessment Unit (CAU) All staff Children with parapneumonic effusion Women and Children
Fibrinolytic treatment of complicated pediatric thoracic empyemas with intrapleural streptokinase
 European Journal of Cardio-thoracic Surgery 26 (2004) 503 507 www.elsevier.com/locate/ejcts Fibrinolytic treatment of complicated pediatric thoracic empyemas with intrapleural streptokinase Gülşen Ekingen*,
European Journal of Cardio-thoracic Surgery 26 (2004) 503 507 www.elsevier.com/locate/ejcts Fibrinolytic treatment of complicated pediatric thoracic empyemas with intrapleural streptokinase Gülşen Ekingen*,
Management of Pleural Empyema Using VATS with Jet-Lavage System
 Journal of Surgery 2018; 6(5): 135-139 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20180605.15 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Management of Pleural Empyema Using VATS
Journal of Surgery 2018; 6(5): 135-139 http://www.sciencepublishinggroup.com/j/js doi: 10.11648/j.js.20180605.15 ISSN: 2330-0914 (Print); ISSN: 2330-0930 (Online) Management of Pleural Empyema Using VATS
Alfonso Fiorelli 1, Francesco Caronia 2, Aldo Prencipe 3, Mario Santini 1, Brendon Stiles 4. Evidenced-Based Clinical Problem Solving Article
 Evidenced-Based Clinical Problem Solving Article The role of video-assisted thoracoscopic surgery for management of symptomatic pleural effusion after coronary artery bypass surgery: a best evidence topic
Evidenced-Based Clinical Problem Solving Article The role of video-assisted thoracoscopic surgery for management of symptomatic pleural effusion after coronary artery bypass surgery: a best evidence topic
Immediate Drainage Is Not Required for All Patients with Complicated Parapneumonic Effusions*
 Immediate Drainage Is Not Required for All Patients with Complicated Parapneumonic Effusions* Herbert A. Berger; M.D.;t and Melvin L. Morganroth, M.D., F.C.C.P.t We retrospectively investigated if the
Immediate Drainage Is Not Required for All Patients with Complicated Parapneumonic Effusions* Herbert A. Berger; M.D.;t and Melvin L. Morganroth, M.D., F.C.C.P.t We retrospectively investigated if the
Effectiveness and Risks Associated With Intrapleural Alteplase by Means of Tube Thoracostomy
 Effectiveness and Risks Associated With Intrapleural Alteplase by Means of Tube Thoracostomy Sharon Ben-Or, MD, Richard H. Feins, MD, Nirmal K. Veeramachaneni, MD, and Benjamin E. Haithcock, MD Division
Effectiveness and Risks Associated With Intrapleural Alteplase by Means of Tube Thoracostomy Sharon Ben-Or, MD, Richard H. Feins, MD, Nirmal K. Veeramachaneni, MD, and Benjamin E. Haithcock, MD Division
UAMS MEDICAL CENTER TRAUMA SERVICES MANUAL. REVIEWED: New PAGE: 1 of 7. RECOMMENDATION(S): Dr. Michael Sutherland APPROVAL: 04/28/2016
 REVIEWED: New PAGE: 1 of 7 PURPOSE: To provide guidelines for the evaluation and management of patients with traumatic chest wall injury including rib fractures, sternal fractures, hemothorax and retained
REVIEWED: New PAGE: 1 of 7 PURPOSE: To provide guidelines for the evaluation and management of patients with traumatic chest wall injury including rib fractures, sternal fractures, hemothorax and retained
A simple weighted scoring system to guide surgical decisionmaking in patients with parapneumonic pleural effusion
 Original Article A simple weighted scoring system to guide surgical decisionmaking in patients with parapneumonic pleural effusion Che-Chia Chang 1,2, Tzu-Ping Chen 1, Chi-Hsiao Yeh 1, Pin-Fu Huang 1,
Original Article A simple weighted scoring system to guide surgical decisionmaking in patients with parapneumonic pleural effusion Che-Chia Chang 1,2, Tzu-Ping Chen 1, Chi-Hsiao Yeh 1, Pin-Fu Huang 1,
Complicated parapneumonic effusion and empyema thoracis: microbiology and predictors of adverse outcomes
 O R I G I N A L A R T I C L E KY Tsang WS Leung Veronica L Chan Alsa WL Lin CM Chu Key words Empyema, pleural; Fibrinolytic agents; Guidelines; Pleural effusion; Pneumonia; Thoracic cavity Hong Kong Med
O R I G I N A L A R T I C L E KY Tsang WS Leung Veronica L Chan Alsa WL Lin CM Chu Key words Empyema, pleural; Fibrinolytic agents; Guidelines; Pleural effusion; Pneumonia; Thoracic cavity Hong Kong Med
Pleural infection. CME Respiratory medicine. Investigations. Clinical features. Chest x-ray. Pleural ultrasound
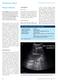 Clinical Medicine 2012, Vol 12, No 1: 82 6 Pleural infection John M Wrightson, clinical research fellow and respiratory specialist registrar, Oxford Pleural Unit, Churchill Hospital, Oxford and NIHR Oxford
Clinical Medicine 2012, Vol 12, No 1: 82 6 Pleural infection John M Wrightson, clinical research fellow and respiratory specialist registrar, Oxford Pleural Unit, Churchill Hospital, Oxford and NIHR Oxford
Empyema in Australia (and related Soapbox topics)
 Empyema in Australia (and related Soapbox topics) Adam Jaffe School of Women s and Children s Health, Sydney Children s Hospital Introduction Relatively rare < 1% pneumonias empyema Strachan R, Jaffé A.
Empyema in Australia (and related Soapbox topics) Adam Jaffe School of Women s and Children s Health, Sydney Children s Hospital Introduction Relatively rare < 1% pneumonias empyema Strachan R, Jaffé A.
Empyema following pulmonary resection. What is difficult management? รศ.นพ. ธ รว ทย พ นธ ช ยเพชร
 Empyema following pulmonary resection. What is difficult management? รศ.นพ. ธ รว ทย พ นธ ช ยเพชร Post lung resection empyema Post lobectomy 0.01-2.00% Post-pneumonectomy 2-16% Rt>Lt., mortality 10% Residual
Empyema following pulmonary resection. What is difficult management? รศ.นพ. ธ รว ทย พ นธ ช ยเพชร Post lung resection empyema Post lobectomy 0.01-2.00% Post-pneumonectomy 2-16% Rt>Lt., mortality 10% Residual
Management of postpneumonic empyemas in children
 European Journal of Cardio-thoracic Surgery 25 (2004) 1072 1078 www.elsevier.com/locate/ejcts Management of postpneumonic empyemas in children Cemal Ozcelik a, *, Refik Ülkü a, Serdar Onat a, Zerrin Ozcelik
European Journal of Cardio-thoracic Surgery 25 (2004) 1072 1078 www.elsevier.com/locate/ejcts Management of postpneumonic empyemas in children Cemal Ozcelik a, *, Refik Ülkü a, Serdar Onat a, Zerrin Ozcelik
Pleural Space Infections: Microbiologic And Fluid Characteristics In 84 Patients. J Porcel, P Vázquez, M Vives, A Nogués, M Falguera, A Manonelles
 ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 3 Number 1 Pleural Space Infections: Microbiologic And Fluid Characteristics In 84 Patients J Porcel, P Vázquez, M Vives, A Nogués, M Falguera,
ISPUB.COM The Internet Journal of Pulmonary Medicine Volume 3 Number 1 Pleural Space Infections: Microbiologic And Fluid Characteristics In 84 Patients J Porcel, P Vázquez, M Vives, A Nogués, M Falguera,
Pneumothorax lecture no. 3
 Pneumothorax lecture no. 3 Is accumulation of air in a pleural space or accumulation of extra pulmonary air within the chest, Is uncommon during childhood, may result from external trauma, iatrogenic,
Pneumothorax lecture no. 3 Is accumulation of air in a pleural space or accumulation of extra pulmonary air within the chest, Is uncommon during childhood, may result from external trauma, iatrogenic,
Diagnosis and Management of Parapneumonic Effusions and Empyema
 CLINICAL PRACTICE Ellie J. C. Goldstein, Section Editor INVITED ARTICLE Diagnosis and Management of Parapneumonic Effusions and Empyema Steve A. Sahn Division of Pulmonary, Critical Care, Allergy, and
CLINICAL PRACTICE Ellie J. C. Goldstein, Section Editor INVITED ARTICLE Diagnosis and Management of Parapneumonic Effusions and Empyema Steve A. Sahn Division of Pulmonary, Critical Care, Allergy, and
A 50-year-old male with fever, cough, dyspnoea, chest pain, weight loss and night sweats
 Petru Emil Muntean muntean.petruemil@yahoo.com Pulmonology, Spitalul Clinic Judetean Mures, Targu Mures, Romania. A 50-year-old male with fever, cough, dyspnoea, chest pain, weight loss and night sweats
Petru Emil Muntean muntean.petruemil@yahoo.com Pulmonology, Spitalul Clinic Judetean Mures, Targu Mures, Romania. A 50-year-old male with fever, cough, dyspnoea, chest pain, weight loss and night sweats
The diagnosis and management of pneumothorax
 Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Top Tips for Pleural Disease in 2012
 Top Tips for Pleural Disease in 2012 The unilateral pleural effusion on the Post Take Ward Round Pleural Effusion on CXR Bedside ultrasound + Pleural aspirate Empyema Nil evidence infection Admit IV antibiotics
Top Tips for Pleural Disease in 2012 The unilateral pleural effusion on the Post Take Ward Round Pleural Effusion on CXR Bedside ultrasound + Pleural aspirate Empyema Nil evidence infection Admit IV antibiotics
Management of pleural infection in adults: British Thoracic Society pleural disease guideline 2010
 1 Oxford Centre for Respiratory Medicine, Churchill Hospital Site, Oxford Radcliffe Hospital, Oxford, UK 2 Department of Respiratory Medicine, Royal Berkshire Hospital, Reading, UK Correspondence to Dr
1 Oxford Centre for Respiratory Medicine, Churchill Hospital Site, Oxford Radcliffe Hospital, Oxford, UK 2 Department of Respiratory Medicine, Royal Berkshire Hospital, Reading, UK Correspondence to Dr
Outcome and mortality analysis in complicated parapneumonic effusion and empyema
 International Journal of Clinical Trials Arivudainambi VP. Int J Clin Trials. 2017 Nov;4(4):176-183 http://www.ijclinicaltrials.com pissn 2349-3240 eissn 2349-3259 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3259.ijct20174208
International Journal of Clinical Trials Arivudainambi VP. Int J Clin Trials. 2017 Nov;4(4):176-183 http://www.ijclinicaltrials.com pissn 2349-3240 eissn 2349-3259 Original Research Article DOI: http://dx.doi.org/10.18203/2349-3259.ijct20174208
Thoraxdrainage SGP Jahresversammlung 2016, Lausanne
 Thoraxdrainage SGP Jahresversammlung 2016, Lausanne Dr. med. Lukas Kern a bit of history (incomplete.) a bit of physiology (basic ) indication data guidelines a bit of history (incomplete.) a bit of physiology
Thoraxdrainage SGP Jahresversammlung 2016, Lausanne Dr. med. Lukas Kern a bit of history (incomplete.) a bit of physiology (basic ) indication data guidelines a bit of history (incomplete.) a bit of physiology
Pediatric complicated pneumonia: Diagnosis and management of empyema CPS Podcast
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Pediatric complicated pneumonia: Diagnosis and management of empyema. These podcasts are designed to give medical students
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Pediatric complicated pneumonia: Diagnosis and management of empyema. These podcasts are designed to give medical students
APPROACH TO PLEURAL EFFUSIONS. Raed Alalawi, MD, FCCP
 APPROACH TO PLEURAL EFFUSIONS Raed Alalawi, MD, FCCP CASE 65-year-old woman with H/O breast cancer presented with a 1 week H/O progressively worsening exersional dyspnea. Physical exam: Diminished breath
APPROACH TO PLEURAL EFFUSIONS Raed Alalawi, MD, FCCP CASE 65-year-old woman with H/O breast cancer presented with a 1 week H/O progressively worsening exersional dyspnea. Physical exam: Diminished breath
Complex Thoracoscopic Resections for Locally Advanced Lung Cancer
 Complex Thoracoscopic Resections for Locally Advanced Lung Cancer Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery,
Complex Thoracoscopic Resections for Locally Advanced Lung Cancer Duke Thoracoscopic Lobectomy Workshop March 21, 2018 Thomas A. D Amico MD Gary Hock Professor of Surgery Section Chief, Thoracic Surgery,
CONTRIBUTIONS TO THE COMPLEX MEDICO-SURGICAL TREATMENT OF PLEURAL SPACE DISEASES DOCTORAL THESIS
 UNIVERSITY OF MEDICINE AND PHARMACY FROM TÂRGU-MUREŞ DOCTORAL SCHOOL CONTRIBUTIONS TO THE COMPLEX MEDICO-SURGICAL TREATMENT OF PLEURAL SPACE DISEASES DOCTORAL THESIS Scientific Supervisor Prof. Dr. Alexandru-Mihail
UNIVERSITY OF MEDICINE AND PHARMACY FROM TÂRGU-MUREŞ DOCTORAL SCHOOL CONTRIBUTIONS TO THE COMPLEX MEDICO-SURGICAL TREATMENT OF PLEURAL SPACE DISEASES DOCTORAL THESIS Scientific Supervisor Prof. Dr. Alexandru-Mihail
Empyema thoracis: Surgical management in children
 Review Article Full text online at http://www.jiaps.com Empyema thoracis: Surgical management in children Prema Menon, Ravi Prakash Kanojia, K. L. N. Rao Department of Pediatric Surgery, Advanced Pediatric
Review Article Full text online at http://www.jiaps.com Empyema thoracis: Surgical management in children Prema Menon, Ravi Prakash Kanojia, K. L. N. Rao Department of Pediatric Surgery, Advanced Pediatric
P leural empyema continues to be a serious problem
 1009 ORIGINAL ARTICLE Empyema thoracis: a 10-year comparative review of hospitalised children from south Asia A K Baranwal, M Singh, R K Marwaha, L Kumar... See end of article for authors affiliations...
1009 ORIGINAL ARTICLE Empyema thoracis: a 10-year comparative review of hospitalised children from south Asia A K Baranwal, M Singh, R K Marwaha, L Kumar... See end of article for authors affiliations...
Espace. It could complicate pneumonia, Empyema Thoracis in Zaria; a Preliminary Report
 Empyema Thoracis in Zaria; a Preliminary Report SA Edaigbini* IZ Delia* MB Aminu* N Anumenechi* SS Audu** Division of Cardiothoracic Surgery* Department of Surgery Department of Orthopaedic Surgery** Ahmadu
Empyema Thoracis in Zaria; a Preliminary Report SA Edaigbini* IZ Delia* MB Aminu* N Anumenechi* SS Audu** Division of Cardiothoracic Surgery* Department of Surgery Department of Orthopaedic Surgery** Ahmadu
Role of medical Thoracoscopy in the Management of Multiloculated Empyema
 Sumalani et al. BMC Pulmonary Medicine (2018) 18:179 https://doi.org/10.1186/s12890-018-0745-y RESEARCH ARTICLE Role of medical Thoracoscopy in the Management of Multiloculated Empyema Kamran Khan Sumalani
Sumalani et al. BMC Pulmonary Medicine (2018) 18:179 https://doi.org/10.1186/s12890-018-0745-y RESEARCH ARTICLE Role of medical Thoracoscopy in the Management of Multiloculated Empyema Kamran Khan Sumalani
Malignant Effusions. Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital
 Malignant Effusions Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital Malignant Effusions Definition: Presence of malignant cells in the pleural space 75% are caused by
Malignant Effusions Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital Malignant Effusions Definition: Presence of malignant cells in the pleural space 75% are caused by
A Repeat Case of Idiopathic Spontaneous Hemothorax
 Case Report A Repeat Case of Idiopathic Spontaneous Hemothorax Felix R. Gaw, MD Jack H. Bloch, MD, PhD, FACS Nolan J. Anderson, MD, FACS Spontaneous hemothorax, a collection of blood in the pleural cavity
Case Report A Repeat Case of Idiopathic Spontaneous Hemothorax Felix R. Gaw, MD Jack H. Bloch, MD, PhD, FACS Nolan J. Anderson, MD, FACS Spontaneous hemothorax, a collection of blood in the pleural cavity
ORIGINAL ARTICLES PROFILE AND OUTCOME OF PATIENTS REFERRED FOR THORACIC EMPYEMA IN BLOEMFONTEIN, SOUTH AFRICA. p ATIENTS AND METHODS
 ORGNAL ARTCLES PROFLE AND OUTCOME OF PATENTS REFERRED FOR THORACC EMPYEMA N BLOEMFONTEN, SOUTH AFRCA Marius J Swart Objective. To establish the profile and outcome of patients referred to the Department
ORGNAL ARTCLES PROFLE AND OUTCOME OF PATENTS REFERRED FOR THORACC EMPYEMA N BLOEMFONTEN, SOUTH AFRCA Marius J Swart Objective. To establish the profile and outcome of patients referred to the Department
Microbiological Prevalence in Empyema Thoracis in a Tertiary Care Centre in North India
 ISSN: 2319-7706 Special Issue-1 (2015) pp. 182-188 http://www.ijcmas.com Original Research Article Microbiological Prevalence in Empyema Thoracis in a Tertiary Care Centre in North India Prakhar Gupta*,
ISSN: 2319-7706 Special Issue-1 (2015) pp. 182-188 http://www.ijcmas.com Original Research Article Microbiological Prevalence in Empyema Thoracis in a Tertiary Care Centre in North India Prakhar Gupta*,
Current Management of Postpneumonectomy Bronchopleural Fistula
 Current Management of Postpneumonectomy Bronchopleural Fistula Shaf Keshavjee MD MSc FRCSC FACS Surgeon-in-Chief, University Health Network James Wallace McCutcheon Chair in Surgery Professor, Division
Current Management of Postpneumonectomy Bronchopleural Fistula Shaf Keshavjee MD MSc FRCSC FACS Surgeon-in-Chief, University Health Network James Wallace McCutcheon Chair in Surgery Professor, Division
Role of routine computed tomography in paediatric pleural empyema
 c Additional Methods data are published online only at http:// thorax.bmj.com/content/vol63/ issue10 1 Department of Respiratory Medicine, Great Ormond Street Hospital for Children NHS Trust, London, UK;
c Additional Methods data are published online only at http:// thorax.bmj.com/content/vol63/ issue10 1 Department of Respiratory Medicine, Great Ormond Street Hospital for Children NHS Trust, London, UK;
Persistent Spontaneous Pneumothorax for Four Years: A Case Report
 303) Persistent Spontaneous Pneumothorax for Four Years: A Case Report Mizuno Y., Iwata H., Shirahashi K., Matsui M., Takemura H. Department of General and Cardiothoracic Surgery, Graduate School of Medicine,
303) Persistent Spontaneous Pneumothorax for Four Years: A Case Report Mizuno Y., Iwata H., Shirahashi K., Matsui M., Takemura H. Department of General and Cardiothoracic Surgery, Graduate School of Medicine,
The Eloesser flap thoracostomy window was initially described
 Eloesser Flap Thoracostomy Window Chadrick E. Denlinger, MD Department of Surgery, Medical University of South Carolina and the Ralph H. Johnson VA Medical Center, Charleston, South Carolina. Address reprint
Eloesser Flap Thoracostomy Window Chadrick E. Denlinger, MD Department of Surgery, Medical University of South Carolina and the Ralph H. Johnson VA Medical Center, Charleston, South Carolina. Address reprint
Treatment approaches for empyema in children
 PAEDIATRIC RESPIRATORY REVIEWS (2007) 8, 164 170 CME REVIEW Treatment approaches for empyema in children Samatha Sonnappa 1, * and Adam Jaffe 2 1 Portex Respiratory Unit, Great Ormond Street Hospital and
PAEDIATRIC RESPIRATORY REVIEWS (2007) 8, 164 170 CME REVIEW Treatment approaches for empyema in children Samatha Sonnappa 1, * and Adam Jaffe 2 1 Portex Respiratory Unit, Great Ormond Street Hospital and
Case Presentation Surgery Grand Round. Amid Keshavarzi, MD UCHSC 4/9/2006
 Case Presentation Surgery Grand Round Amid Keshavarzi, MD UCHSC 4/9/2006 Case Presentation 12 y/o female Presented to OSH after accidental swallowing of plastic fork in the bus, CXR/AXR form OSH did not
Case Presentation Surgery Grand Round Amid Keshavarzi, MD UCHSC 4/9/2006 Case Presentation 12 y/o female Presented to OSH after accidental swallowing of plastic fork in the bus, CXR/AXR form OSH did not
Thoracostomy: An Update on Imaging Features and Current Surgical Practice
 Thoracostomy: An Update on Imaging Features and Current Surgical Practice Robert D. Ambrosini, MD, PhD, Christopher Gange, MD, Katherine Kaproth-Joslin, MD, PhD, Susan Hobbs, MD, PhD Department of Imaging
Thoracostomy: An Update on Imaging Features and Current Surgical Practice Robert D. Ambrosini, MD, PhD, Christopher Gange, MD, Katherine Kaproth-Joslin, MD, PhD, Susan Hobbs, MD, PhD Department of Imaging
Comparative Study for the Efficacy of Small Bore Catheter in the Patients with Iatrogenic Pneumothorax
 Korean J Thorac Cardiovasc Surg 20;44:48-422 ISSN: 2233-60X (Print) ISSN: 2093-656 (Online) Clinical Research http://dx.doi.org/0.5090/kjtcs.20.44.6.48 Comparative Study for the Efficacy of Small Bore
Korean J Thorac Cardiovasc Surg 20;44:48-422 ISSN: 2233-60X (Print) ISSN: 2093-656 (Online) Clinical Research http://dx.doi.org/0.5090/kjtcs.20.44.6.48 Comparative Study for the Efficacy of Small Bore
Tissue Plasminogen Activator for the Treatment of Parapneumonic Effusions in Pediatric Patients
 Tissue Plasminogen Activator for the Treatment of Parapneumonic Effusions in Pediatric Patients Emily N. Israel 1,2 and Allison B. Blackmer 1,2, * 1 Department of Pharmacy Services, University of Michigan
Tissue Plasminogen Activator for the Treatment of Parapneumonic Effusions in Pediatric Patients Emily N. Israel 1,2 and Allison B. Blackmer 1,2, * 1 Department of Pharmacy Services, University of Michigan
Empyema due to Klebsiella pneumoniae
 Thorax (1967), 22, 170. Empyema due to Klebsiella pneumoniae J. M. REID, R. S. BARCLAY, J. G. STEVENSON, T. M. WELSH, AND N. McSWAN From thle Cardio-thoracic Unit, Mearnskirk Hospital, Renifrewshire Three
Thorax (1967), 22, 170. Empyema due to Klebsiella pneumoniae J. M. REID, R. S. BARCLAY, J. G. STEVENSON, T. M. WELSH, AND N. McSWAN From thle Cardio-thoracic Unit, Mearnskirk Hospital, Renifrewshire Three
A recurrent empyema with peripheral bronchopleural fistulas treated by retrograde bronchial sealing with Gore Tex plugs: a case report
 Case Report A recurrent empyema with peripheral bronchopleural fistulas treated by retrograde bronchial sealing with Gore Tex plugs: a case report Jin-Young Ahn 1, Dohun Kim 2, Jong-Myeon Hong 2, Si-Wook
Case Report A recurrent empyema with peripheral bronchopleural fistulas treated by retrograde bronchial sealing with Gore Tex plugs: a case report Jin-Young Ahn 1, Dohun Kim 2, Jong-Myeon Hong 2, Si-Wook
Pleural Fluid Analysis: Back to Basics
 Pleural Fluid Analysis: Back to Basics Tonya L. Page, MSN, RN, ACNP-BC Patrick A. Laird, DNP, RN, ACNP-BC 70 y/o female with complaints of shortness of breath and orthopnea for 1 month. Symptoms have worsened
Pleural Fluid Analysis: Back to Basics Tonya L. Page, MSN, RN, ACNP-BC Patrick A. Laird, DNP, RN, ACNP-BC 70 y/o female with complaints of shortness of breath and orthopnea for 1 month. Symptoms have worsened
Removal of Chest Tube to Diagnose Pneumothorax Pak Armed Forces Med J 2017; 67 (4):
 Open Access Original Article Removal of Chest Tube to Diagnose Pneumothorax Pak Armed Forces Med J 2017; 67 (4): 641-45 CLINICAL ASSESSMENT COMPARED WITH CHEST-X-RAY AFTER REMOVAL OF CHEST TUBE TO DIAGNOSE
Open Access Original Article Removal of Chest Tube to Diagnose Pneumothorax Pak Armed Forces Med J 2017; 67 (4): 641-45 CLINICAL ASSESSMENT COMPARED WITH CHEST-X-RAY AFTER REMOVAL OF CHEST TUBE TO DIAGNOSE
Complications During and One Month after Surgery in the Patients Who Underwent Thoracoscopic Surgery
 Available online at www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 8:305-309 Complications During and One Month after Surgery in the Patients Who
Available online at www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 8:305-309 Complications During and One Month after Surgery in the Patients Who
ORIGINAL ARTICLE. Characteristics of the patients undergoing surgical treatment for pneumothorax: A descriptive study
 554 Characteristics of the patients undergoing surgical treatment for pneumothorax: A descriptive study Muharrem Cakmak, Melih Yuksel, Mehmet Nail Kandemir ORIGINAL ARTICLE Abstract Objective: To identify
554 Characteristics of the patients undergoing surgical treatment for pneumothorax: A descriptive study Muharrem Cakmak, Melih Yuksel, Mehmet Nail Kandemir ORIGINAL ARTICLE Abstract Objective: To identify
Infection of the pleural space with the formation of. Effects of Streptokinase and Deoxyribonuclease on Viscosity of Human Surgical and Empyema Pus*
 Effects of Streptokinase and Deoxyribonuclease on Viscosity of Human Surgical and Empyema Pus* Graham Simpson, MD; David Roomes, MB, ChB; and Mal Heron, PhD Study objective: To investigate the effects
Effects of Streptokinase and Deoxyribonuclease on Viscosity of Human Surgical and Empyema Pus* Graham Simpson, MD; David Roomes, MB, ChB; and Mal Heron, PhD Study objective: To investigate the effects
A comparison between two types of indwelling pleural catheters for management of malignant pleural effusions
 Original Article A comparison between two types of indwelling pleural catheters for management of malignant pleural effusions Sushilkumar Satish Gupta 1, Charalampos S. Floudas 2, Abhinav B. Chandra 3
Original Article A comparison between two types of indwelling pleural catheters for management of malignant pleural effusions Sushilkumar Satish Gupta 1, Charalampos S. Floudas 2, Abhinav B. Chandra 3
Pus in the thorax: management of empyema and lung abscess
 : management of empyema and lung abscess James Walters MBBS MRCP Noeleen Foley MB BCH BAO MRCPI MD FRCP Matthew Molyneux MBBS FRCA Matrix reference 3G00 Key points Thoracic ultrasound before pleural procedures
: management of empyema and lung abscess James Walters MBBS MRCP Noeleen Foley MB BCH BAO MRCPI MD FRCP Matthew Molyneux MBBS FRCA Matrix reference 3G00 Key points Thoracic ultrasound before pleural procedures
Contemporary outcomes of surgical management of complex thoracic infections
 Original Article Contemporary outcomes of surgical management of complex thoracic infections Ian C. Bostock 1, Fariha Sheikh 1, Timothy M. Millington 1,2, David J. Finley 1,2, Joseph D. Phillips 1,2 1
Original Article Contemporary outcomes of surgical management of complex thoracic infections Ian C. Bostock 1, Fariha Sheikh 1, Timothy M. Millington 1,2, David J. Finley 1,2, Joseph D. Phillips 1,2 1
