Role of routine computed tomography in paediatric pleural empyema
|
|
|
- Amos Warren
- 5 years ago
- Views:
Transcription
1 c Additional Methods data are published online only at thorax.bmj.com/content/vol63/ issue10 1 Department of Respiratory Medicine, Great Ormond Street Hospital for Children NHS Trust, London, UK; 2 Portex Anaesthesia, Intensive Therapy and Respiratory Unit, Institute of Child Health, London, UK; 3 Sydney Children s Hospital, Randwick and University of New South Wales, Sydney, Australia; 4 Department of Radiology, Great Ormond Street Hospital for Children NHS Trust, London, UK Correspondence to: Dr S Sonnappa, Portex Anaesthesia, Intensive Therapy and Respiratory Unit, Level 6, Cardiac Wing, Institute of Child Health, 30 Guilford Street, London WC1N 1EH, UK; s.sonnappa@ich.ucl.ac.uk Received 2 December 2007 Accepted 29 April 2008 Published Online First 20 May 2008 Role of routine computed tomography in paediatric pleural empyema A Jaffe, 1,2,3 A D Calder, 4 C M Owens, 4 S Stanojevic, 2 S Sonnappa 1,2 ABSTRACT Background: The incidence of empyema in children is increasing worldwide. While there are emerging data for the best treatment options, there is little evidence to support the imaging modalities used to guide treatment, particularly with regard to the role of routine CT scanning. The aims of this study were to develop a radiological scoring system for paediatric empyema and to assess the utility of routine CT scanning in this disease. Methods: Children with empyema were prospectively enrolled over a 3-year period into a randomised clinical trial of video-assisted thoracoscopic surgery versus percutaneous chest drain insertion and urokinase. All children received a preoperative chest radiograph (CXR), pleural ultrasound scan (USS) and chest CT scan. In the urokinase arm the clinician inserted the drain with USS evidence only and did not have access to the CT scan at the time of insertion to reflect clinical practice. A scoring system was developed for each individual radiological modality and used to compare imaging characteristics of the pleural fluid collection and underlying parenchyma and to assess the utility of USS and CT to predict length of stay after the intervention. Results: Of the 60 subjects recruited, 46 had USS images available for review, 36 had a CT scan which met the inclusion criteria and 31 had all three radiological measurements (CT, USS and CXR) available for analysis. There was substantial interobserver agreement for USS grades (k = 0.709) and moderate agreement for total CT scores (k = 0.520). There were weak correlations between USS grade and total CT score as well as CT loculation and density scores. Of the 25 CXRs showing simple opacification of the underlying parenchyma only, CT demonstrated simple consolidation (n = 14), necrotising pneumonia (n = 7), cavitary necrosis (n = 3) and pneumatoceles (n = 1). No abnormality was detected on CT scanning which directly altered clinical management. Neither the USS score nor the CT score, nor a combination of the two, were able to predict length of hospital stay. Conclusions: CT scanning detects more parenchymal abnormalities than chest radiography. However, the additional information does not alter management and is unable to predict clinical outcome. This suggests that there is no role for the routine use of CT scanning in children if treated with urokinase and percutaneous chest drain. The omission of routine CT scanning in empyema will reduce the exposure of children to unnecessary radiation and reduce costs. Trial registration number: The trial is fully registered with clinicaltrials.gov (ID: NCT ). Although relatively uncommon, the incidence of empyema in children is increasing in many countries. 1 4 The British Thoracic Society (BTS) guidelines on the management of empyema in Paediatric lung disease children highlighted the lack of grade A evidence to inform best management. 5 Since its publication in 2005, this has been increasingly addressed by the publication of prospective randomised controlled studies. 6 7 The BTS guidelines further highlighted the lack of evidence to inform imaging modalities to assist in management. The consensus was that a posterioanterior (or anteroposterior) chest radiograph (CXR) together with a pleural ultrasound scan (USS) should be performed. The expert opinion (level D evidence) was that chest computed tomography (CT) should not be performed routinely but that there may be a role in atypical empyema presentations. If a parapneumonic effusion contains pus it is called an empyema. The American Thoracic Society (ATS) divided the empyema process into three stages: (1) exudative, in which the pleural fluid has a low cell content; (2) fibrinopurulent, in which frank pus is present and fibrin formation begins to cover the pleura with formation of loculations; and (3) organising phase, in which there is thick peel formation by fibroblasts and the pleural space is characterised by very thick exudates with heavy sediment. 8 USS has been used to stage this process in children by demonstrating the presence of septations and to guide management; 9 however, the role of routine CT scanning in guiding management in children with empyema is not known. A major limitation of the radiological data available from adult studies is that they are not applicable to the paediatric population. 10 The disease rarely causes death in children, who are generally healthy before the onset of infection compared with adult empyema which has an estimated mortality of 20%. 11 Management options include the insertion of a drain with or without fibrinolytics, 6 12 limited open decortication 9 or video-assisted thoracoscopic surgery (VATS). In most cases where a surgical approach is taken, a CT scan is performed preoperatively. This is particularly true in VATS where the surgeon requires a road map to provide greater anatomical delineation and better definition of the underlying lung parenchyma to ensure that the placement of the instruments does not cause a bronchopleural fistula. In those centres where children are managed with urokinase and percutaneous chest drain insertion, a CT scan is not routinely performed. There is no consensus on radiological investigations in childhood empyema and practice varies between centres. The aims of this study were to develop a radiological scoring system for childhood empyema and to assess the utility of routine CT chest scanning in paediatric empyema. Thorax 2008;63: doi: /thx
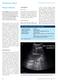
2 METHODS This study formed part of a previously published prospective randomised study comparing VATS with percutaneous drain insertion and urokinase. 6 Subjects were recruited from children aged,16 years referred to our institution, a tertiary paediatric respiratory centre, for further management of complicated parapneumonic effusion over a 3-year period. Preoperative CXR, pleural USS and CT scanning were performed routinely in all patients, irrespective of the treatment group to which they were randomised. However, in order to reflect local standard clinical practice, the CT scans in the VATS group were made available to the surgeons. In the urokinase group the radiologist and paediatrician in charge were aware of the CT image findings; however, at the time of insertion, the clinician inserting the drain did not have the CT information available unless concerns had been raised by the senior clinician or radiologist. The primary clinical outcome measure used for this radiological study was length of stay in hospital following the intervention. The comparisons between CT and both USS and CXR were twofold: (1) we compared the imaging characteristics of the pleural fluid collection itself as defined by USS and CT; and (2) we compared the evaluation of the underlying pulmonary parenchyma as demonstrated on CXR and CT scans as described below. Pleural collections Ultrasound (USS) evaluation Patients were referred for a pleural USS examination before treatment (see online supplement for detailed explanation of methodology). The images were subsequently reviewed by two paediatric radiologists (AC, CMO) blinded to patient data. The effusions were graded according to their internal echostructure using a system based on that described by Kearney et al 15 but with the addition of an extra grade for highly septated effusions with significant solid components (grade 1, anechoic; grade 2, Figure 1 Ultrasound staging of empyema. (A) Grade 1 effusion showing anechoic fluid. (B) Grade 2 effusion showing echoic fluid without septations. (C) Grade 3 effusion showing multiple thick septations. (D) Grade 4 effusion showing multiple septations with solid appearing components comprising more than one-third of the collection. echoic fluid without septation; grade 3, septated effusion; grade 4, septations with solid appearing components comprising more than one-third of the effusion; see fig 1). Scores from both radiologists were used for analysis. CT evaluation CT scans were performed before treatment in all patients. Scans were excluded from analysis if they were performed without intravenous iodinated contrast material as intravenous contrast allows visualisation of pleural inflammation which is not normally possible with a non-contrast enhanced scan. We also excluded scans done at a local hospital prior to admission and transferred with a hard copy or performed following chest drain insertion (see online supplement for detailed explanation of CT methodology). Effusions were graded by fluid density, pleural enhancement, subcostal tissue thickening and loculation/effusion shape (table 1). Effusions were graded as follows: effusion density was taken as the mean of the CT density in Hounsfield units (HU) recorded from three regions of interest drawn in the centre of the thickest portion of the effusion at three contiguous levels measured by one observer (AC): a density of 0 20 scored 0 and a density of.20 scored 1. A cut-off point of 20 HU was chosen as this is generally the accepted upper limit for the density of water-based lesions, for example, in hepatic and renal cysts. The remaining evaluations were performed independently by two paediatric radiologists (AC and CMO). Parietal pleural enhancement recorded a score of 1, and a score of 2 was given for thick pleural enhancement (.2 mm). Thickening of the subcostal tissues was scored similarly. We devised a scoring system to reflect the degree of loculation of the effusion through the assessment of effusion shape: an effusion whose visceral surface paralleled the chest wall scored 0, an effusion with convexity or lobulation of the visceral surface with pleura/pleural fluid thickness between the lobulations of 898 Thorax 2008;63: doi: /thx
3 Table 1 CT scoring system for parapneumonic effusions (maximum total score = 8) Fluid density Pleural enhancement Subcostal tissue thickening Loculation/effusion shape Mean density,20 HU Mean density.20 HU HU, Hounsfield units. Absent Present,,2 mm thick.10 mm scored 1, and an effusion whose visceral surface showed lobulations separated by,10 mm of pleural fluid or thickening scored 2 (fig 2). If components of the pleural collection were separated by normal pleura, the effusion scored 3. The individual scores were summated to give one total score and scores from both observers were used for analysis. Pulmonary parenchyma Chest radiograph (CXR) evaluation Posterioanterior CXRs were performed preoperatively in all subjects. The immediate preoperative CXRs were included in the study even if performed at local hospitals before referral to our tertiary unit. Parenchymal changes were classified as simple opacification (including collapse and consolidation with or without air bronchograms) and opacification with cavitation. The CXRs were blindly evaluated by two independent radiologists (AC, CMO) and one paediatric pulmonologist (SS), reporting in consensus, reaching a conclusion by mutual discussion. CT evaluation Pulmonary parenchymal changes were classified in consensus by mutual discussion by two radiologists (AC, CMO) based on the definitions described by Donnelly et al: 16 c Simple collapse or consolidation: homogeneous opacification and enhancement present with or without air bronchograms or with fluid-filled airways. c Pneumatoceles: tubular or cystic areas of air density with thin or imperceptible walls, with no evidence of necrotising pneumonia. c Necrotising pneumonia: ill-defined areas of poorly enhancing lung comprising more than half of consolidated lung. Figure 2 CT shape score. (A) Shape score of 1, effusion showing lobulations with intervening pleural space of.10 mm. (B) Shape score of 2 showing lobulations (arrows) separated by narrow bridge of pleural thickening. Present,.2 mm thick (Score 2) Absent Present,,2 mm thick Present,.2 mm thick (Score 2) c c Simple: Concave medially, parallels chest wall Loculated: convex medially or lobulated with separation of lobulations by.10 mm of fluid/ thickening Incomplete multiloculation: lobulations separated by,10 mm of pleural thickness (Score 2) Complete multiloculation: pockets of fluid separated by normal intervening pleura (Score 3) Cavitary necrosis: necrotising pneumonia containing irregular areas of air density. Pulmonary abscess: well-defined area of intrapulmonary fluid density or cavity with air fluid level, with thick (.2 mm) enhancing wall. Statistical analysis Interobserver reliability for the CT and USS scores between the two observers was assessed using Cohen s kappa (k) with linear weighting. Correlation between USS grade and both the total CT score and the individual component scores were calculated using Kendall s rank correlation. The utility of CT and USS scores to predict the number of days in hospital after the intervention was assessed using multiple linear regression analysis adjusted for intervention (VATS vs urokinase). RESULTS Of the 60 subjects randomised to either VATS or urokinase, 46 had USS images available for review. Thirty-six patients had a CT scan which met the inclusion criteria. Exclusions were as follows: CT performed at local hospital (n = 14); no contrast enhancement due to failure of intravenous access (n = 2); performed with drain in situ (n = 3); unavailable for review (n = 5). Thirty-one patients had all three radiological measurements (CT, USS and CXR) available for analysis. Pleural collection evaluation There was substantial interobserver agreement for USS grades (k = 0.709) and moderate agreement for total CT scores (k = 0.520, tables 2 and 3). Agreement between the two observers for CT scores was strongest for the subcostal thickening (k = 0.568) and pleural enhancement scores Thorax 2008;63: doi: /thx
4 Table 2 Frequency of ultrasound grades by observers (k = 0.709) Observer 2 ultrasound grades Total Observer 1 ultrasound grades Total (k = 0.459). Five of 31 effusions showed increased density (score 1 on density score). The majority of effusions showed pleural enhancement (scores 1 and 2: 20/31 for observer 1 and 25/31 for observer 2). Subcostal tissue thickening was present in a minority (scores 1 and 2: 15/31 for observer 1 and 10/31 for observer 2). The majority of effusions showed some degree of loculation (internal convexity and incomplete multiloculation, scores 1 2, 23/31 for observer 1 and 24/31 for observer 2). However, we did not identify any cases of completely multiloculated collections (score 3 on loculation/shape score) where locules were completely separated from each other by normal intervening pleura. The mean CT score increased across the USS grades for pooled observations (data not shown) with an incremental increase in mean shape, pleural thickening and density score from USS grades 2 4 (only one patient had a USS grade of 1 for each observer). There were weak correlations between USS grade and total CT score as well as the CT loculation score and CT density score (table 4). Despite the positive and statistically significant correlation between USS and CT score, the strength of the relationship is minimal as demonstrated by the low correlation coefficients. Pulmonary parenchyma Twenty-five of the CXRs showed simple opacification of the underlying parenchyma only. Of these, 14 had simple consolidation only, in one case pneumatoceles were present, in seven cases necrotising pneumonia was present and in three cavitary necrosis was present (table 5). Of the six cases with cavitation on the CXR, four showed cavitary necrosis on the CT scan, one showed pneumatoceles and one showed simple consolidation only. No abnormality was detected on CT scanning which directly altered management. In particular, we did not identify any cases of pulmonary abscess although, in several cases, areas of cavitary necrosis were very well defined but lacked an enhancing wall and therefore did not meet our criteria (fig 3). Outcome prediction In the primary study there was no statistically significant difference in length of hospital stay following intervention between the two treatment groups: median difference 0 (95% CI 21 to 2), (p = 0.311). 6 The small sample size in this study precluded comprehensive evaluation of the predictive abilities of the radiographic modalities, although basic multivariable regression adjusted for treatment showed that neither the USS score (geometric slope 1.06 (95% CI 0.72 to 1.59), p = 0.744) nor the CT score (geometric slope 1.09 (95% CI 0.96 to 1.23), p = 0.182) nor a combination of the two (geometric slope 1.08 (95% CI 0.97 to 1.19), p = 0.151) were able to predict length of hospital stay. Patients with CT findings Table 3 Frequency of total CT scores by observer (k = 0.520) Observer 2 total CT scores Total Observer 1 total CT scores Total other than simple consolidation or pneumatoceles did not have a different outcome. Patients in the VATS arm with simple consolidation (n = 7) had a median stay of 5 days (range 4 16) and those with complicated parenchymal disease (n = 7) a median stay of 5 days (range 4 12). Patients in the urokinase arm and simple consolidation (n = 10) had a median stay of 5 days (range 5 9) while those with complicated parenchymal disease (n = 7) had a median stay of 8 days (range 5 16). DISCUSSION We have developed a novel radiological scoring system for children with empyema and demonstrated that CT scans detect more parenchymal changes than CXRs and that no additional abnormality was detected which directly changed clinical management. Furthermore, neither modality alone or in combination was able to predict the clinical outcome and therefore appear to be poor markers of disease severity, albeit these analyses are based on small numbers. These findings suggest no role for routine CT scanning in the management of children with empyema if managed with percutaneous drainage and urokinase. USS is a central investigation in the management of paediatric empyema, offering several key strengths: it is portable, non-invasive, does not use ionising radiation and provides a dynamic assessment of the chest. It is cheap and relatively easy to perform and is able to differentiate pleural fluid from consolidation, estimate the effusion size and guide chest drain placement. It is also able to demonstrate the presence of fibrinous septations within pleural collections CT scanning has several potential strengths as it is able to provide an examination of the entire thorax without being limited by the presence of air or bone compared with USS. It is also able to provide an accurate road map of the pleural space for an operating surgeon. CT can provide an accurate assessment of the pulmonary parenchyma beneath an effusion, the assessment of which is often limited on chest radiography by the presence of pleural fluid. However, CT has many disadvantages: it is unable to detect the presence of fibrinous septations, which are usually too thin and of insufficient density to identify, and requires sedation or anaesthesia in an uncooperative child. The principal weakness of CT, however, is its use of ionising radiation. At our institution the CT dose is estimated to be approximately 115 times that of a CXR, 20 and this may be considerably higher in units not using paediatric dose optimisation. Radiation dose reduction is of particular importance in children as they are more susceptible to the risks of radiation and have a substantially increased lifetime cancer risk compared with the older population following a single CT 900 Thorax 2008;63: doi: /thx
5 Table 4 Correlation coefficients (Kendall s tau) between ultrasound (USS) grade and CT scores from pooled observations Correlation Kendall s tau (95% CI) p Value USS grade vs CT score (0.118 to 0.512) USS grade vs CT density score ( to 0.458) USS grade vs CT pleural enhancement ( to 0.448) score USS grade vs subcostal thickening ( to 0.402) score USS grade vs CT shape score (0.132 to 0.563) scan. 21 A CT examination in a child can thus only be justified if the result is likely to impact on clinical management. This study has shown that, although CT scans were able to detect more detailed parenchymal findings than CXR in our population, no CT scan detected an unexpected abnormality which directly altered clinical management for example, the detection of an unexpected lung abscess requiring prolonged antibiotics 22 or drainage. 23 There are no well validated scoring systems for the severity of empyema measured by CT. Donnelly and Klosterman 24 used a simple 4-point system based on pleural and subcostal fat thickening along with changes in the chest wall. They did not assess the density of pleural fluid or loculation/effusion shape and did not perform independent observations with this system (and hence no measure of interobserver variation was given). This scoring system was unable to distinguish between empyema and transudative effusions. Kearney et al 15 assessed severity of effusions by size, loculation, pleural enhancement, pleural thickening and pleural septation, but did not combine these features into an overall score. In the absence of a validated scoring system, we devised a novel system for scoring CT findings in empyema, based on previously described features of pleural thickening and thickening of subcostal fat, along with assessments of effusion density and loculation. We found only moderate interobserver agreement for this scoring system. This partly reflects a difficulty with all CT scoring systems of reducing a complex three-dimensional dataset to a single score. Some of the components of the score particularly the shape score are quite subjective and hence prone to interobserver variability. We believe the relatively poor level of agreement achieved further highlights the difficulty of using CT as a measure of disease severity in empyema. Furthermore, CT and USS findings do not appear to show a strong relationship, reflecting the very different basis and strengths of these two modalities. Neither the USS grade nor the CT score, nor a combination of the two, was able to predict outcome. There are very few studies which have used radiology to attempt to predict outcome. In a study of 50 children with empyema who underwent either primary or secondary thoracoscopy, the clinical outcome was not predicted by USS when assessed for echogenicity, thickness of the effusion and presence of septations. 25 Similarly, in a prospective randomised study of intrapleural urokinase to treat empyema in children, USS findings were not related to outcome. 12 Kearney et al compared USS and CT scanning in a study of 50 adult patients with parapneumonic effusions. Neither the USS grade nor CT findings of effusion size, pleural thickening or extrapleural fat thickening were able to reliably stage empyema or predict failure of tube drainage. 15 We have previously published data demonstrating no difference in clinical outcome between VATS or treatment with urokinase. However, the VATS group was Table 5 Parenchymal changes detected on CT scan and chest radiograph (CXR) CXR findings CT findings Simple Cavitation Total Simple Pneumatoceles Necrotising pneumonia Cavitary necrosis Abscess Total significantly more expensive, particularly with the addition of a CT scan. 6 Our study data do not support the use of USS, CT or a combination as a means of predicting the outcome from empyema treatment in children, further supporting the view that the role of routine CT scanning in childhood empyema is questionable. In our analysis of parenchymal findings, CT demonstrated potentially important findings of necrotising pneumonia or cavitary necrosis in 10/25 patients with apparently simple collapse or consolidation on the CXR. The finding that CT scanning detects more parenchymal changes than chest radiography supports previous published evidence. Empyema appears to be a common accompaniment to cavitary necrosis Importantly, in our study, patients with cavitary necrosis or necrotising pneumonia on CT scanning in addition to empyema showed no difference in outcome from those with simple consolidation, although the numbers involved are small. This study is subject to several limitations. We recognise that our sample size is small. The initial clinical study was powered to detect a difference of 2 days in the primary outcome measure (number of days in hospital post-intervention) between the two treatment groups and was not powered to detect post hoc differences between radiological modalities. Furthermore, only 31 of the 60 patients recruited had a complete set of valid imaging studies available for review in this study. Of particular note is that 14 patients had CT scans carried out at the local hospital before referral, highlighting the low threshold physicians have for performing CT scans on children with empyema. Figure 3 Well-defined cavitary necrosis. CT image showing welldefined area of non-enhancing lung with cavitation adjacent to empyema. As this area lacks an enhancing wall, this could not be defined as an abscess. Thorax 2008;63: doi: /thx
6 Another limitation is the retrospective nature of our radiological analysis, particularly for USS. USS is a real-time and dynamic examination that can never be fully represented in stored or printed images. The accuracy of our grading is thus open to question. The high level of interobserver variability obtained from independent observations does at least partly validate our methodology. Owing to the retrospective nature of radiological analysis, we were not able to analyse pulmonary parenchymal changes or effusion shape on USS as these require a real-time assessment. A further potential limitation is that we did not directly assess the intervention of CT scanning by randomising subjects to receive CT or not, which we believe would have been unethical. The primary aim of the study was to compare two clinical interventions and the study was designed to reflect standard clinical practice where surgeons routinely request a CT scan before performing VATS, while percutaneous drains are inserted under USS guidance without the need of a CT scan. Nevertheless, we believe that the study design reflects a pragmatic approach and represents the first study to examine the role of routine CT scanning in childhood empyema providing an evidence base for management of this disease. In conclusion, using the novel radiological scoring system, we identified only weak correlation between CT and USS findings in paediatric pleural empyema. Neither CT nor USS provides a reliable means of predicting outcome. Although CT detects additional parenchymal findings to those identifiable on CXR, these do not influence management in the setting of empyema. This study suggests no role for the routine use of CT in the management of pleural empyema in children if treated with percutaneous drainage and urokinase. This approach will reduce the exposure of children to unnecessary radiation and reduce costs. Acknowledgements: The authors thank Dr Robert Dinwiddie, Dr Colin Wallis, Dr Paul Aurora (respiratory paediatricians), Dr Gordon Cohen, Dr Carin van Doorn, Professor Martin Elliott (paediatric thoracic surgeons) and Mr John Cairns. Funding: Research at the Institute of Child Health and Great Ormond Street Hospital for Children NHS Trust benefits from Research and Development funding received from the NHS Executive. Competing interests: AJ is in receipt of an unrestricted grant from GlaxoSmithKline (Belgium) for a study on the epidemiology of childhood empyema in Australia and New Zealand. Ethics approval: The project was approved by the local ethics committee. REFERENCES 1. Rees JH, Spencer DA, Parikh D, et al. Increase in incidence of childhood empyema in West Midlands, UK. Lancet 1997;349: Playfor SD, Smyth AR, Stewart RJ. Increase in incidence of childhood empyema. Thorax 1997;52: Byington CL, Spencer LY, Johnson TA, et al. An epidemiological investigation of a sustained high rate of pediatric parapneumonic empyema: risk factors and microbiological associations. Clin Infect Dis 2002;34: Spencer DA, Iqbal SM, Hasan A, et al. Empyema thoracis is still increasing in UK children. BMJ 2006;332: Balfour-Lynn IM, Abrahamson E, Cohen G, et al. BTS Guidelines for the management of pleural infection in children. Thorax 2005;60(Suppl 1):i Sonnappa S, Cohen G, Owens CM, et al. Comparison of urokinase and videoassisted thoracoscopic surgery for treatment of childhood empyema. Am J Respir Crit Care Med 2006;174: Kurt BA, Winterhalter KM, Connors RH, et al. Therapy of parapneumonic effusions in children: video-assisted thoracoscopic surgery versus conventional thoracostomy drainage. Pediatrics 2006;118:e American Thoracic Society. Management of nontuberculous empyema. Am Rev Respir Dis 1962;85: Carey JA, Hamilton JR, Spencer DA, et al. Empyema thoracis: a role for open thoracotomy and decortication. Arch Dis Child 1998;79: Jaffe A, Balfour-Lynn IM. Management of empyema in children. Pediatr Pulmonol 2005;40: Ferguson AD, Prescott RJ, Selkon JB, et al. The clinical course and management of thoracic empyema. Q J Med 1996;89: Thomson AH, Hull J, Kumar MR, et al. Randomised trial of intrapleural urokinase in the treatment of childhood empyema. Thorax 2002;57: Cohen G, Hjortdal V, Ricci MJ, et al. Primary thoracoscopic treatment of empyema in children. J Thorac Cardiovasc Surg 2003;125: Jaffe A, Cohen G. Thoracic empyema. Arch Dis Child 2003;88: Kearney SE, Davies CW, Davies RJ, et al. Computed tomography and ultrasound in parapneumonic effusions and empyema. Clin Radiol 2000;55: Donnelly LF, Klosterman LA. Cavitary necrosis complicating pneumonia in children: sequential findings on chest radiography. Am J Roentgenol 1998;171: Patel MC, Flower CD. Radiology in the management of pleural disease. Eur Radiol 1997;7: King S, Thomson A. Radiological perspectives in empyema. Br Med Bull 2002;61: Evans AL, Gleeson FV. Radiology in pleural disease: state of the art. Respirology 2004;9: Papaioannou G, Young C, Owens CM. Multidetector row CT for imaging the paediatric tracheobronchial tree. Pediatr Radiol 2007;37: Brenner DJ, Hall EJ. Computed tomography: an increasing source of radiation exposure. N Engl J Med 2007;357: Chan PC, Huang LM, Wu PS, et al. Clinical management and outcome of childhood lung abscess: a 16-year experience. J Microbiol Immunol Infect 2005;38: Coren ME, Ng M, Rubens M, et al. The value of ultrafast computed tomography in the investigation of pediatric chest disease. Pediatr Pulmonol 1998;26: Donnelly LF, Klosterman LA. CT appearance of parapneumonic effusions in children: findings are not specific for empyema. Am J Roentgenol 1997;169: Kalfa N, Allal H, Lopez M, et al. Thoracoscopy in pediatric pleural empyema: a prospective study of prognostic factors. J Pediatr Surg 2006;41: Donnelly LF, Klosterman LA. The yield of CT of children who have complicated pneumonia and noncontributory chest radiography. Am J Roentgenol 1998;170: Ramphul N, Eastham KM, Freeman R, et al. Cavitatory lung disease complicating empyema in children. Pediatr Pulmonol 2006;41: Thorax 2008;63: doi: /thx
Thoracoscopic Management of Complicated Parapneumonic Effusions in Young Children. Saeed Al Hindi, MD, CABS, FRCSI*
 Bahrain Medical Bulletin, Vol. 31, No. 4, December 2009 Thoracoscopic Management of Complicated Parapneumonic Effusions in Young Children Saeed Al Hindi, MD, CABS, FRCSI* Objective: To evaluate the role
Bahrain Medical Bulletin, Vol. 31, No. 4, December 2009 Thoracoscopic Management of Complicated Parapneumonic Effusions in Young Children Saeed Al Hindi, MD, CABS, FRCSI* Objective: To evaluate the role
Alper Toker, MD. VATS decortication. Istanbul University, Istanbul Medical School Department of Thoracic Surgery
 VATS decortication Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery Pleural space infection is a common pathology causing morbidity and mortality. It is a collection
VATS decortication Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery Pleural space infection is a common pathology causing morbidity and mortality. It is a collection
Modern Approaches to Empyema
 Modern Approaches to Empyema Amit Bhargava, MD Attending Thoracic Surgeon Assistant Professor Department of Cardiovascular and Thoracic Surgery 1 Principles of Treatment Adequate drainage Sterilization
Modern Approaches to Empyema Amit Bhargava, MD Attending Thoracic Surgeon Assistant Professor Department of Cardiovascular and Thoracic Surgery 1 Principles of Treatment Adequate drainage Sterilization
EMPYEMA. Catheter Based Treatment vs. VATS. UCHSC Department of Surgery Grand Rounds August 27 th, Jeremy Hedges, M.D.
 EMPYEMA Catheter Based Treatment vs. VATS UCHSC Department of Surgery Grand Rounds August 27 th, 2007 Jeremy Hedges, M.D. OVERVIEW Empyema Pathogenesis Treatment Catheter based treatment Fibrinolytics
EMPYEMA Catheter Based Treatment vs. VATS UCHSC Department of Surgery Grand Rounds August 27 th, 2007 Jeremy Hedges, M.D. OVERVIEW Empyema Pathogenesis Treatment Catheter based treatment Fibrinolytics
Outcomes & Clinical Trials Update: Empyema & NEC
 Outcomes & Clinical Trials Update: Empyema & NEC American Pediatric Surgical Association Outcomes & Clinical Trials Committee Fizan Abdullah, Chair Saleem Islam, Vice Chair Gudrun Aspelund Catherine C.
Outcomes & Clinical Trials Update: Empyema & NEC American Pediatric Surgical Association Outcomes & Clinical Trials Committee Fizan Abdullah, Chair Saleem Islam, Vice Chair Gudrun Aspelund Catherine C.
Treatment approaches for empyema in children
 PAEDIATRIC RESPIRATORY REVIEWS (2007) 8, 164 170 CME REVIEW Treatment approaches for empyema in children Samatha Sonnappa 1, * and Adam Jaffe 2 1 Portex Respiratory Unit, Great Ormond Street Hospital and
PAEDIATRIC RESPIRATORY REVIEWS (2007) 8, 164 170 CME REVIEW Treatment approaches for empyema in children Samatha Sonnappa 1, * and Adam Jaffe 2 1 Portex Respiratory Unit, Great Ormond Street Hospital and
Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20,
 Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20, 521-525 Empyema thoracis Original Article Singh DR 1, Joshi MR 2, Thapa P 2, Nath S 3 1 Assistant Professor, 2 Lecturer, 3 Professor,
Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20, 521-525 Empyema thoracis Original Article Singh DR 1, Joshi MR 2, Thapa P 2, Nath S 3 1 Assistant Professor, 2 Lecturer, 3 Professor,
Empyema in Australia (and related Soapbox topics)
 Empyema in Australia (and related Soapbox topics) Adam Jaffe School of Women s and Children s Health, Sydney Children s Hospital Introduction Relatively rare < 1% pneumonias empyema Strachan R, Jaffé A.
Empyema in Australia (and related Soapbox topics) Adam Jaffe School of Women s and Children s Health, Sydney Children s Hospital Introduction Relatively rare < 1% pneumonias empyema Strachan R, Jaffé A.
Best timing for surgical intervention of empyema. Supervisor: Intern:
 Best timing for surgical intervention of empyema Supervisor: Intern: Brief history 56 y/o male, farmer With anesthesia medication at LMD Admission 30d 7d Dry cough Progressive productive cough with yellow
Best timing for surgical intervention of empyema Supervisor: Intern: Brief history 56 y/o male, farmer With anesthesia medication at LMD Admission 30d 7d Dry cough Progressive productive cough with yellow
Trust Guideline for the management of Parapneumonic Effusion in children
 A clinical guideline recommended for use For Use in: By: For: Division responsible for document: Buxton ward, Children s Assessment Unit (CAU) All staff Children with parapneumonic effusion Women and Children
A clinical guideline recommended for use For Use in: By: For: Division responsible for document: Buxton ward, Children s Assessment Unit (CAU) All staff Children with parapneumonic effusion Women and Children
Pediatric Lung Ultrasound (PLUS) In Diagnosis of Community Acquired Pneumonia (CAP)
 Pediatric Lung Ultrasound (PLUS) In Diagnosis of Community Acquired Pneumonia (CAP) Dr Neetu Talwar Senior Consultant, Pediatric Pulmonology Fortis Memorial Research Institute, Gurugram Study To compare
Pediatric Lung Ultrasound (PLUS) In Diagnosis of Community Acquired Pneumonia (CAP) Dr Neetu Talwar Senior Consultant, Pediatric Pulmonology Fortis Memorial Research Institute, Gurugram Study To compare
The Management of Paediatric Empyema
 HK J Paediatr (new series) 2009;14:16-21 The Management of Paediatric Empyema AA YOUSEF, A JAFFE Abstract Key words Empyema is a recognised complication of bacterial pneumonia in children. It is a very
HK J Paediatr (new series) 2009;14:16-21 The Management of Paediatric Empyema AA YOUSEF, A JAFFE Abstract Key words Empyema is a recognised complication of bacterial pneumonia in children. It is a very
MANAGEMENT OF RETAINED HAEMOTHORAX DR AG JACOBS PRINCIPAL SPECIALIST DEPARTMENT OF CARDIO THORACIC SURGERY UNIVERSITY OF PRETORIA
 MANAGEMENT OF RETAINED HAEMOTHORAX DR AG JACOBS PRINCIPAL SPECIALIST DEPARTMENT OF CARDIO THORACIC SURGERY UNIVERSITY OF PRETORIA MANAGEMENT OF RETAINED HAEMOTHORAX Retained Haemothorax Definition: Failure
MANAGEMENT OF RETAINED HAEMOTHORAX DR AG JACOBS PRINCIPAL SPECIALIST DEPARTMENT OF CARDIO THORACIC SURGERY UNIVERSITY OF PRETORIA MANAGEMENT OF RETAINED HAEMOTHORAX Retained Haemothorax Definition: Failure
Bacterial pneumonia with associated pleural empyema pleural effusion
 EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
EMPYEMA Synonyms : - Parapneumonic effusion - Empyema thoracis - Bacterial pneumonia - Pleural empyema, pleural effusion - Lung abscess - Complicated parapneumonic effusions (CPE) 1 Bacterial pneumonia
Table 2: Outcomes measured. Table 1: Intrapleural alteplase instillation therapy protocol
 ORIGINAL RESEARCH ARTICLE Intrapleural F brinolytic Therapy with Alteplase in Empyema Thoracis in Children conducted in the Department of Pediatric critical care and Pulmonology unit at our institution
ORIGINAL RESEARCH ARTICLE Intrapleural F brinolytic Therapy with Alteplase in Empyema Thoracis in Children conducted in the Department of Pediatric critical care and Pulmonology unit at our institution
Post Pneumonic Empyema: Is There Still a Role for Surgery?
 Post Pneumonic Empyema: Is There Still a Role for Surgery? M. Blair Marshall, MD Ismael Matus, MD Chief, Thoracic Surgery Interventional Pulmonary Professor of Surgery Medicine MedStar Georgetown University
Post Pneumonic Empyema: Is There Still a Role for Surgery? M. Blair Marshall, MD Ismael Matus, MD Chief, Thoracic Surgery Interventional Pulmonary Professor of Surgery Medicine MedStar Georgetown University
Interventional radiology treatment of empyema and lung abscesses
 PAEDIATRIC RESPIRATORY REVIEWS (2008) 9, 77 84 CME ARTICLE Interventional radiology treatment of empyema and lung abscesses Mark J. Hogan* and Brian D. Coley Nationwide Children s Hospital and The Ohio
PAEDIATRIC RESPIRATORY REVIEWS (2008) 9, 77 84 CME ARTICLE Interventional radiology treatment of empyema and lung abscesses Mark J. Hogan* and Brian D. Coley Nationwide Children s Hospital and The Ohio
Comparison of Urokinase and Video-assisted Thoracoscopic Surgery for Treatment of Childhood Empyema
 Comparison of Urokinase and Video-assisted Thoracoscopic Surgery for Treatment of Childhood Empyema Samatha Sonnappa, Gordon Cohen, Catherine M. Owens, Carin van Doorn, John Cairns, Sanja Stanojevic, Martin
Comparison of Urokinase and Video-assisted Thoracoscopic Surgery for Treatment of Childhood Empyema Samatha Sonnappa, Gordon Cohen, Catherine M. Owens, Carin van Doorn, John Cairns, Sanja Stanojevic, Martin
Thoracostomy: An Update on Imaging Features and Current Surgical Practice
 Thoracostomy: An Update on Imaging Features and Current Surgical Practice Robert D. Ambrosini, MD, PhD, Christopher Gange, MD, Katherine Kaproth-Joslin, MD, PhD, Susan Hobbs, MD, PhD Department of Imaging
Thoracostomy: An Update on Imaging Features and Current Surgical Practice Robert D. Ambrosini, MD, PhD, Christopher Gange, MD, Katherine Kaproth-Joslin, MD, PhD, Susan Hobbs, MD, PhD Department of Imaging
Imaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT findings
 Imaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT findings Poster No.: C-2067 Congress: ECR 2017 Type: Educational Exhibit Authors: J. M. Almeida, N. Antunes, C. Leal, L. Figueiredo ; Lisboa/PT,
Imaging of Pleural Effusion: Comparing Ultrasound, X-Ray and CT findings Poster No.: C-2067 Congress: ECR 2017 Type: Educational Exhibit Authors: J. M. Almeida, N. Antunes, C. Leal, L. Figueiredo ; Lisboa/PT,
Advances in the Management of Empyema
 Advances in the Management of Empyema RCP Update in Respiratory Medicine 26 th January 2017 Najib M Rahman Associate Professor of Respiratory Medicine University of Oxford najib.rahman@ndm.ox.ac.uk Financial
Advances in the Management of Empyema RCP Update in Respiratory Medicine 26 th January 2017 Najib M Rahman Associate Professor of Respiratory Medicine University of Oxford najib.rahman@ndm.ox.ac.uk Financial
Guideline for management of children & adolescents with pleural empyema
 CHILD AND ADOLESCENT HEALTH SERVICE PRINCESS MARGARET HOSPITAL FOR CHILDREN Guideline for management of children & adolescents with pleural empyema This guideline provides an evidence-based framework for
CHILD AND ADOLESCENT HEALTH SERVICE PRINCESS MARGARET HOSPITAL FOR CHILDREN Guideline for management of children & adolescents with pleural empyema This guideline provides an evidence-based framework for
PULMONARY TUBERCULOSIS RADIOLOGY
 PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
PULMONARY TUBERCULOSIS RADIOLOGY RADIOLOGICAL MODALITIES Medical radiophotography Radiography Fluoroscopy Linear (conventional) tomography Computed tomography Pulmonary angiography, bronchography Ultrasonography,
Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit
 Page1 Original Article NJR 2011;1(1):1 7;Available online at www.nranepal.org Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit S
Page1 Original Article NJR 2011;1(1):1 7;Available online at www.nranepal.org Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit S
Posttraumatic Empyema Thoracis
 Posttraumatic Empyema Thoracis Dr AG Jacobs STEVE BIKO ACADEMIC HOSPITAL, UNIVERSITY OF PRETORIA EMPYEMA THORACIS Derived from Greek word empyein Means pus-producing Refers to accumulation of pus within
Posttraumatic Empyema Thoracis Dr AG Jacobs STEVE BIKO ACADEMIC HOSPITAL, UNIVERSITY OF PRETORIA EMPYEMA THORACIS Derived from Greek word empyein Means pus-producing Refers to accumulation of pus within
Pediatric complicated pneumonia: Diagnosis and management of empyema CPS Podcast
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Pediatric complicated pneumonia: Diagnosis and management of empyema. These podcasts are designed to give medical students
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Pediatric complicated pneumonia: Diagnosis and management of empyema. These podcasts are designed to give medical students
The use of thrombolytics in the management of complex pleural fluid collections
 Original Article The use of thrombolytics in the management of complex pleural fluid collections Jessica Heimes 1, Hannah Copeland 2, Aditya Lulla 3, Marjulin Duldulao 4, Khaled Bahjri 5, Salman Zaheer
Original Article The use of thrombolytics in the management of complex pleural fluid collections Jessica Heimes 1, Hannah Copeland 2, Aditya Lulla 3, Marjulin Duldulao 4, Khaled Bahjri 5, Salman Zaheer
Diagnostic Approach to Pleural Effusion
 Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
A simple weighted scoring system to guide surgical decisionmaking in patients with parapneumonic pleural effusion
 Original Article A simple weighted scoring system to guide surgical decisionmaking in patients with parapneumonic pleural effusion Che-Chia Chang 1,2, Tzu-Ping Chen 1, Chi-Hsiao Yeh 1, Pin-Fu Huang 1,
Original Article A simple weighted scoring system to guide surgical decisionmaking in patients with parapneumonic pleural effusion Che-Chia Chang 1,2, Tzu-Ping Chen 1, Chi-Hsiao Yeh 1, Pin-Fu Huang 1,
Top Tips for Pleural Disease in 2012
 Top Tips for Pleural Disease in 2012 The unilateral pleural effusion on the Post Take Ward Round Pleural Effusion on CXR Bedside ultrasound + Pleural aspirate Empyema Nil evidence infection Admit IV antibiotics
Top Tips for Pleural Disease in 2012 The unilateral pleural effusion on the Post Take Ward Round Pleural Effusion on CXR Bedside ultrasound + Pleural aspirate Empyema Nil evidence infection Admit IV antibiotics
Surgical treatment of empyema in children
 Surgical treatment of empyema in children Jacques Janson Pierre Goussard Cardiothoracic Surgery, Paediatric Pulmonology Tygerberg Academic Hospital University of Stellenbosch Pleural space Netter, Frank
Surgical treatment of empyema in children Jacques Janson Pierre Goussard Cardiothoracic Surgery, Paediatric Pulmonology Tygerberg Academic Hospital University of Stellenbosch Pleural space Netter, Frank
Treatment of multiloculated empyema thoracis using minimally invasive methods
 O r i g i n a l A r t i c l e Singapore Med J 2010; 51(3) : 242 Treatment of multiloculated empyema thoracis using minimally invasive methods Metin M, Yeginsu A, Sayar A, Alzafer S, Solak O, Ozgul A, Erkorkmaz
O r i g i n a l A r t i c l e Singapore Med J 2010; 51(3) : 242 Treatment of multiloculated empyema thoracis using minimally invasive methods Metin M, Yeginsu A, Sayar A, Alzafer S, Solak O, Ozgul A, Erkorkmaz
V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY
 V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY Kharkov Regional Centre of Cardiovascular surgery V.N. Karazin Kharkov National University Department of Internal Medicine Pleural empyema Abduyeva F.M., MD, PhD
V.N. KARAZIN KHARKOV NATIONAL UNIVERSITY Kharkov Regional Centre of Cardiovascular surgery V.N. Karazin Kharkov National University Department of Internal Medicine Pleural empyema Abduyeva F.M., MD, PhD
Diagnostic accuracy, safety and utilisation of respiratory physician-delivered thoracic ultrasound
 < Additional methods, figures and tables are published online only. To view these files please visit the journal online http:// thorax.bmj.com/content/vol65/ issue5 1 Oxford Centre for Respiratory Medicine
< Additional methods, figures and tables are published online only. To view these files please visit the journal online http:// thorax.bmj.com/content/vol65/ issue5 1 Oxford Centre for Respiratory Medicine
Parapneumonic effusions are a common problem
 Proceeding S.Z.P.G.M.I. vol: 20(2): pp. 9-3, 200. Intrapleural Streptokinase in Management of Complicated Parapneumonic Effusion and Empyema Kamran Hameed, Ahmad Hasan Banjer, Mohammad Abdul-Aziz Siddiqui
Proceeding S.Z.P.G.M.I. vol: 20(2): pp. 9-3, 200. Intrapleural Streptokinase in Management of Complicated Parapneumonic Effusion and Empyema Kamran Hameed, Ahmad Hasan Banjer, Mohammad Abdul-Aziz Siddiqui
Computed tomography of the chest: I. Basic principles
 BJA Education, 15 (6): 299 304 (2015) doi: 10.1093/bjaceaccp/mku063 Advance Access Publication Date: 2 February 2015 Matrix reference 1A03, 2A12 Computed tomography of the chest: I. Basic principles P
BJA Education, 15 (6): 299 304 (2015) doi: 10.1093/bjaceaccp/mku063 Advance Access Publication Date: 2 February 2015 Matrix reference 1A03, 2A12 Computed tomography of the chest: I. Basic principles P
Review of video-assisted thoracoscopy in children
 Review Article Review of video-assisted thoracoscopy in children S N Oak, S V Parelkar, K V SatishKumar, R Pathak, B H Ramesh, S Sudhir, M Keshav Department of Pediatric Surgery, TNMC and BYL Nair Hospital,
Review Article Review of video-assisted thoracoscopy in children S N Oak, S V Parelkar, K V SatishKumar, R Pathak, B H Ramesh, S Sudhir, M Keshav Department of Pediatric Surgery, TNMC and BYL Nair Hospital,
aacp consensus statement
 aacp consensus statement Medical and Surgical Treatment of Parapneumonic Effusions* An Evidence-Based Guideline Gene L. Colice, MD, FCCP; Anne Curtis, MD; Jean Deslauriers, MD; John Heffner, MD, FCCP;
aacp consensus statement Medical and Surgical Treatment of Parapneumonic Effusions* An Evidence-Based Guideline Gene L. Colice, MD, FCCP; Anne Curtis, MD; Jean Deslauriers, MD; John Heffner, MD, FCCP;
EUROPEAN ASSOCIATION OF VETERINARY DIAGNOSTIC IMAGING EUROPEAN COLLEGE OF VETERINARY DIAGNOSTIC IMAGING
 EISAGOGIKO EUROPEAN ASSOCIATION OF VETERINARY DIAGNOSTIC IMAGING EUROPEAN COLLEGE OF VETERINARY DIAGNOSTIC IMAGING ARISTOTLE UNIVERSITY OF THESSALONIKI SCHOOL OF VETERINARY MEDICINE SECTION OF RADIOLOGY
EISAGOGIKO EUROPEAN ASSOCIATION OF VETERINARY DIAGNOSTIC IMAGING EUROPEAN COLLEGE OF VETERINARY DIAGNOSTIC IMAGING ARISTOTLE UNIVERSITY OF THESSALONIKI SCHOOL OF VETERINARY MEDICINE SECTION OF RADIOLOGY
Accepted Manuscript. Current State of the Art for the Surgical Management of empyema thoracis. K. Robert Shen, M.D.
 Accepted Manuscript Current State of the Art for the Surgical Management of empyema thoracis K. Robert Shen, M.D. PII: S0022-5223(18)32919-2 DOI: https://doi.org/10.1016/j.jtcvs.2018.11.006 Reference:
Accepted Manuscript Current State of the Art for the Surgical Management of empyema thoracis K. Robert Shen, M.D. PII: S0022-5223(18)32919-2 DOI: https://doi.org/10.1016/j.jtcvs.2018.11.006 Reference:
A Practical Approach to Ultrasound Assessment of Respiratory Distress
 A Practical Approach to Ultrasound Assessment of Respiratory Distress Yanick Beaulieu, MD, FRCPC Director, Bedside Ultrasound Curriculum Division of Cardiology and Critical Care Hôpital du Sacré-Coeur
A Practical Approach to Ultrasound Assessment of Respiratory Distress Yanick Beaulieu, MD, FRCPC Director, Bedside Ultrasound Curriculum Division of Cardiology and Critical Care Hôpital du Sacré-Coeur
Guidelines/Guidance/CAP/ Hospitalized Child. PHM Boot Camp 2014 Jay Tureen, MD June 19, 2014
 Guidelines/Guidance/CAP/ Hospitalized Child PHM Boot Camp 2014 Jay Tureen, MD June 19, 2014 CAP in Children: Epi Greatest cause of death in children worldwide Estimated > 2 M deaths in children In developed
Guidelines/Guidance/CAP/ Hospitalized Child PHM Boot Camp 2014 Jay Tureen, MD June 19, 2014 CAP in Children: Epi Greatest cause of death in children worldwide Estimated > 2 M deaths in children In developed
ABDULHAMEED AZIZ, 1 JEFFREY M. HEALEY, 1 FAISAL QURESHI, 1 TIMOTHY D. KANE, 1 GEOFFREY KURLAND, 2 MICHAEL GREEN, 3 and DAVID J.
 SURGICAL INFECTIONS Volume 9, Number 3, 2008 Mary Ann Liebert, Inc. DOI: 10.1089/sur.2007.025 Comparative Analysis of Chest Tube Thoracostomy and Video-Assisted Thoracoscopic Surgery in Empyema and Parapneumonic
SURGICAL INFECTIONS Volume 9, Number 3, 2008 Mary Ann Liebert, Inc. DOI: 10.1089/sur.2007.025 Comparative Analysis of Chest Tube Thoracostomy and Video-Assisted Thoracoscopic Surgery in Empyema and Parapneumonic
Definitions and diagnostic implications of terms used in the chest radiograph and lung ultrasound diagnoses of pneumonia.
 Supplementary 1 Definitions and diagnostic implications of terms used in the chest radiograph and lung ultrasound diagnoses of pneumonia. Imaging finding Definition Implication CR Consolidation Interstitial
Supplementary 1 Definitions and diagnostic implications of terms used in the chest radiograph and lung ultrasound diagnoses of pneumonia. Imaging finding Definition Implication CR Consolidation Interstitial
EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC CHANGES
 Trakia Journal of Sciences, Vol. 3, No. 2, pp 61-65, 2005 Copyright 2005 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC
Trakia Journal of Sciences, Vol. 3, No. 2, pp 61-65, 2005 Copyright 2005 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC
Computed tomography in children with community-acquired pneumonia
 Pediatr Radiol (2017) 47:1431 1440 DOI 10.1007/s00247-017-3891-0 MINISYMPOSIUM: IMAGING PNEUMONIA Computed tomography in children with community-acquired pneumonia Savvas Andronikou 1,2 & Pierre Goussard
Pediatr Radiol (2017) 47:1431 1440 DOI 10.1007/s00247-017-3891-0 MINISYMPOSIUM: IMAGING PNEUMONIA Computed tomography in children with community-acquired pneumonia Savvas Andronikou 1,2 & Pierre Goussard
VIDEO-ASSISTED THORACOSCOPY IN THE TREATMENT OF PLEURAL EMPYEMA: STAGE-BASED MANAGEMENT AND OUTCOME
 VIDEO-ASSISTED THORACOSCOPY IN THE TREATMENT OF PLEURAL EMPYEMA: STAGE-BASED MANAGEMENT AND OUTCOME Paolo Claudio Cassina, MD a Markus Hauser, MD, FCCP b Ludger Hillejan, MD a Dieter Greschuchna, MD a
VIDEO-ASSISTED THORACOSCOPY IN THE TREATMENT OF PLEURAL EMPYEMA: STAGE-BASED MANAGEMENT AND OUTCOME Paolo Claudio Cassina, MD a Markus Hauser, MD, FCCP b Ludger Hillejan, MD a Dieter Greschuchna, MD a
Surgical versus non-surgical management for pleural empyema(protocol)
 Cochrane Database of Systematic Reviews Surgical versus non-surgical management for pleural empyema(protocol) ChinTY,ReddenMD,HsuCCT,vanDrielML ChinTY,ReddenMD,HsuCCT,vanDrielML. Surgical versus non-surgical
Cochrane Database of Systematic Reviews Surgical versus non-surgical management for pleural empyema(protocol) ChinTY,ReddenMD,HsuCCT,vanDrielML ChinTY,ReddenMD,HsuCCT,vanDrielML. Surgical versus non-surgical
Chapter. Imaging of Pneumonia in Children. Introduction. Chest X-ray and Common Infective Agents. School Age Children
 content Chapter 11 Winnie CW Chu Introduction Chest X-ray and Common Infective Agents School Age Children Computed Tomography and Common Infective Agents Utility of Computed Tomography Evaluation of Persistent
content Chapter 11 Winnie CW Chu Introduction Chest X-ray and Common Infective Agents School Age Children Computed Tomography and Common Infective Agents Utility of Computed Tomography Evaluation of Persistent
MANAGEMENT RECOMMENDATIONS
 1 MANAGEMENT RECOMMENDATIONS 1. Adrenal masses!!!!!!! page 2 2. Liver Masses!!!!!!! page 3 3. Obstetric US Soft Markers for Aneuploidy!! pages 4-6 4. Ovarian and Adnexal Cysts!!!!! pages 7-10 5. Pancreatic
1 MANAGEMENT RECOMMENDATIONS 1. Adrenal masses!!!!!!! page 2 2. Liver Masses!!!!!!! page 3 3. Obstetric US Soft Markers for Aneuploidy!! pages 4-6 4. Ovarian and Adnexal Cysts!!!!! pages 7-10 5. Pancreatic
Indwelling Pleural Catheters in Malignant and Non-Malignant Disease
 Indwelling Catheters in Malignant and Non-Malignant Disease 20th Hellenic Conference November 2011 Najib Rahman Clinical Lecturer Oxford Centre for Respiratory Medicine University of Oxford, UK Najib.rahman@ndm.ox.ac.uk
Indwelling Catheters in Malignant and Non-Malignant Disease 20th Hellenic Conference November 2011 Najib Rahman Clinical Lecturer Oxford Centre for Respiratory Medicine University of Oxford, UK Najib.rahman@ndm.ox.ac.uk
This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors.
 This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. - Figure S1: The four quadrant approach lung ultrasound at the bedside. * The anterolateral
This appendix was part of the submitted manuscript and has been peer reviewed. It is posted as supplied by the authors. - Figure S1: The four quadrant approach lung ultrasound at the bedside. * The anterolateral
Surgical decortication as the first-line treatment for pleural empyema
 Shin et al General Thoracic Surgical decortication as the first-line treatment for pleural empyema Jung Ar Shin, MD, a Yoon Soo Chang, MD, PhD, a Tae Hoon Kim, MD, PhD, b Seok Jin Haam, MD, c Hyung Jung
Shin et al General Thoracic Surgical decortication as the first-line treatment for pleural empyema Jung Ar Shin, MD, a Yoon Soo Chang, MD, PhD, a Tae Hoon Kim, MD, PhD, b Seok Jin Haam, MD, c Hyung Jung
Videothoracoscopy in Pleural Empyema Following Methicillin-Resistant Staphylococcus aureus (MRSA) Lung Infection
 Short Communication TheScientificWorldJOURNAL (2009) 9, 723 728 ISSN 1537-744X; DOI 10.1100/tsw.2009.91 Videothoracoscopy in Pleural Empyema Following Methicillin-Resistant Staphylococcus aureus (MRSA)
Short Communication TheScientificWorldJOURNAL (2009) 9, 723 728 ISSN 1537-744X; DOI 10.1100/tsw.2009.91 Videothoracoscopy in Pleural Empyema Following Methicillin-Resistant Staphylococcus aureus (MRSA)
Malignant Effusions. Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital
 Malignant Effusions Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital Malignant Effusions Definition: Presence of malignant cells in the pleural space 75% are caused by
Malignant Effusions Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital Malignant Effusions Definition: Presence of malignant cells in the pleural space 75% are caused by
Pleural Empyema Joseph Junewick, MD FACR
 Pleural Empyema Joseph Junewick, MD FACR 03/19/2010 History Teenager with persistent fever and cough. Pneumonia diagnosed 1 week ago. Diagnosis Pleural Empyema Additional Clinical Surgery-Clear fluid with
Pleural Empyema Joseph Junewick, MD FACR 03/19/2010 History Teenager with persistent fever and cough. Pneumonia diagnosed 1 week ago. Diagnosis Pleural Empyema Additional Clinical Surgery-Clear fluid with
Lung ultrasound in the critically ill patient Pleural Effusions
 Lung ultrasound in the critically ill patient Pleural Effusions Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville, Florida
Lung ultrasound in the critically ill patient Pleural Effusions Rohit Patel, MD University of Florida Health Director, Critical Care Ultrasound Surgical ICU Center for Intensive Care Gainesville, Florida
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus. Lung
 Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Lung ASUM Quality CCPU Syllabi Released: 21 March 2013 Approved by: CEO Lung Purpose: This unit is designed to cover the theoretical and practical
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Lung ASUM Quality CCPU Syllabi Released: 21 March 2013 Approved by: CEO Lung Purpose: This unit is designed to cover the theoretical and practical
TB Radiology for Nurses Garold O. Minns, MD
 TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
TB Nurse Case Management Salina, Kansas March 31-April 1, 2010 TB Radiology for Nurses Garold O. Minns, MD April 1, 2010 TB Radiology for Nurses Highway Patrol Training Center Salina, KS April 1, 2010
Pneumothorax Post CT-guided Fine Needle Aspiration Biopsy for Lung Nodules: Our Experience in King Hussein Medical Center
 Pneumothorax Post CT-guided Fine Needle Aspiration Biopsy for Lung Nodules: Our Experience in King Hussein Medical Center Ala Qayet MD*, Laith Obaidat MD**, Mazin Al-Omari MD*, Ashraf Al-Tamimi MD^, Ahmad
Pneumothorax Post CT-guided Fine Needle Aspiration Biopsy for Lung Nodules: Our Experience in King Hussein Medical Center Ala Qayet MD*, Laith Obaidat MD**, Mazin Al-Omari MD*, Ashraf Al-Tamimi MD^, Ahmad
An Introduction to Radiology for TB Nurses
 An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
An Introduction to Radiology for TB Nurses Garold O. Minns, MD September 14, 2017 TB Nurse Case Management September 12 14, 2017 EXCELLENCE EXPERTISE INNOVATION Garold O. Minns, MD has the following disclosures
Management of Pleural Effusion
 Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
Role of medical Thoracoscopy in the Management of Multiloculated Empyema
 Sumalani et al. BMC Pulmonary Medicine (2018) 18:179 https://doi.org/10.1186/s12890-018-0745-y RESEARCH ARTICLE Role of medical Thoracoscopy in the Management of Multiloculated Empyema Kamran Khan Sumalani
Sumalani et al. BMC Pulmonary Medicine (2018) 18:179 https://doi.org/10.1186/s12890-018-0745-y RESEARCH ARTICLE Role of medical Thoracoscopy in the Management of Multiloculated Empyema Kamran Khan Sumalani
Case Report Intrapleural administration of DNase alone for pleural empyema
 Int J Clin Exp Med 2015;8(11):22011-22015 www.ijcem.com /ISSN:1940-5901/IJCEM0016173 Case Report Intrapleural administration of DNase alone for pleural empyema Vladimir Bobek 1,2,3, Andrzej Majewski 4,
Int J Clin Exp Med 2015;8(11):22011-22015 www.ijcem.com /ISSN:1940-5901/IJCEM0016173 Case Report Intrapleural administration of DNase alone for pleural empyema Vladimir Bobek 1,2,3, Andrzej Majewski 4,
Parapneumonic pleural effusion: early versus late thoracoscopy
 J Bras Pneumol. 2017;43(5):344-350 http://dx.doi.org/10.1590/s1806-37562016000000261 OIGINAL ATICLE Parapneumonic pleural effusion: early versus late thoracoscopy odrigo omualdo Pereira 1, Cristina Gonçalves
J Bras Pneumol. 2017;43(5):344-350 http://dx.doi.org/10.1590/s1806-37562016000000261 OIGINAL ATICLE Parapneumonic pleural effusion: early versus late thoracoscopy odrigo omualdo Pereira 1, Cristina Gonçalves
ARTICLE. most common reasons for hospitalization in childhood. 1 Up to 50% of children
 ARTICLE The Long-term Outcomes of Pediatric Pleural Empyema A Prospective Study Eyal Cohen, MD, MSc; Sanjay Mahant, MD, MSc; Sharon D. Dell, MD; Jeffrey Traubici, MD; Alejandra Ragone, MD; Anu Wadhwa,
ARTICLE The Long-term Outcomes of Pediatric Pleural Empyema A Prospective Study Eyal Cohen, MD, MSc; Sanjay Mahant, MD, MSc; Sharon D. Dell, MD; Jeffrey Traubici, MD; Alejandra Ragone, MD; Anu Wadhwa,
ARDS - a must know. Page 1 of 14
 ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
ARDS - a must know Poster No.: C-1683 Congress: ECR 2016 Type: Authors: Keywords: DOI: Educational Exhibit M. Cristian; Turda/RO Education and training, Edema, Acute, Localisation, Education, Digital radiography,
The diagnosis and management of pneumothorax
 Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
JMSCR Vol 04 Issue 10 Page October 2016
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i10.08 Ultrasound and CT Evaluation of Pleural
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i10.08 Ultrasound and CT Evaluation of Pleural
Current Management of Postpneumonectomy Bronchopleural Fistula
 Current Management of Postpneumonectomy Bronchopleural Fistula Shaf Keshavjee MD MSc FRCSC FACS Surgeon-in-Chief, University Health Network James Wallace McCutcheon Chair in Surgery Professor, Division
Current Management of Postpneumonectomy Bronchopleural Fistula Shaf Keshavjee MD MSc FRCSC FACS Surgeon-in-Chief, University Health Network James Wallace McCutcheon Chair in Surgery Professor, Division
BTS guidelines for the management of pleural infection in children
 i1 BTS GUIDELINES BTS guidelines for the management of pleural infection in children I M Balfour-Lynn, E Abrahamson, G Cohen, J Hartley, S King, D Parikh, D Spencer, A H Thomson, D Urquhart, on behalf
i1 BTS GUIDELINES BTS guidelines for the management of pleural infection in children I M Balfour-Lynn, E Abrahamson, G Cohen, J Hartley, S King, D Parikh, D Spencer, A H Thomson, D Urquhart, on behalf
Introduction to transthoracic ultrasound for the pulmonologist
 Review Introduction to transthoracic ultrasound for the pulmonologist Clementine Bostantzoglou 1, Charalampos Moschos 2 1 7 th Pulmonary Department, Sotiria Hospital for Chest Diseases, Athens, Greece
Review Introduction to transthoracic ultrasound for the pulmonologist Clementine Bostantzoglou 1, Charalampos Moschos 2 1 7 th Pulmonary Department, Sotiria Hospital for Chest Diseases, Athens, Greece
How to do it: ultrasoundguided
 How to do it: ultrasoundguided pleural biopsy Background Malignancy is the cause of 40,000 pleural effusions in the UK and 175,000 in the USA [1], with pleural fluid cytology able to diagnose, at best,
How to do it: ultrasoundguided pleural biopsy Background Malignancy is the cause of 40,000 pleural effusions in the UK and 175,000 in the USA [1], with pleural fluid cytology able to diagnose, at best,
TB Intensive Houston, Texas
 TB Intensive Houston, Texas October 15-17, 17 2013 Diagnosis of TB: Radiology Rosa M Estrada-Y-Martin, MD MSc FCCP October 16, 2013 Rosa M Estrada-Y-Martin, MD MSc FCCP, has the following disclosures to
TB Intensive Houston, Texas October 15-17, 17 2013 Diagnosis of TB: Radiology Rosa M Estrada-Y-Martin, MD MSc FCCP October 16, 2013 Rosa M Estrada-Y-Martin, MD MSc FCCP, has the following disclosures to
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus. Lung
 Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Lung Page 1 of 8 01/17 Lung Syllabus Purpose: This unit is designed to cover the theoretical and practical curriculum for lung ultrasound in
Certificate in Clinician Performed Ultrasound (CCPU) Syllabus Lung Page 1 of 8 01/17 Lung Syllabus Purpose: This unit is designed to cover the theoretical and practical curriculum for lung ultrasound in
Fibrinolytic treatment of complicated pediatric thoracic empyemas with intrapleural streptokinase
 European Journal of Cardio-thoracic Surgery 26 (2004) 503 507 www.elsevier.com/locate/ejcts Fibrinolytic treatment of complicated pediatric thoracic empyemas with intrapleural streptokinase Gülşen Ekingen*,
European Journal of Cardio-thoracic Surgery 26 (2004) 503 507 www.elsevier.com/locate/ejcts Fibrinolytic treatment of complicated pediatric thoracic empyemas with intrapleural streptokinase Gülşen Ekingen*,
Information for Patients
 Having a Percutaneous Drainage Information for Patients In this leaflet: Introduction 2 What is a percutaneous drainage?..... 2 Why do I need a percutaneous drainage?.....2 Are there any risks?....2 What
Having a Percutaneous Drainage Information for Patients In this leaflet: Introduction 2 What is a percutaneous drainage?..... 2 Why do I need a percutaneous drainage?.....2 Are there any risks?....2 What
UAMS MEDICAL CENTER TRAUMA SERVICES MANUAL. REVIEWED: New PAGE: 1 of 7. RECOMMENDATION(S): Dr. Michael Sutherland APPROVAL: 04/28/2016
 REVIEWED: New PAGE: 1 of 7 PURPOSE: To provide guidelines for the evaluation and management of patients with traumatic chest wall injury including rib fractures, sternal fractures, hemothorax and retained
REVIEWED: New PAGE: 1 of 7 PURPOSE: To provide guidelines for the evaluation and management of patients with traumatic chest wall injury including rib fractures, sternal fractures, hemothorax and retained
Pneumothorax lecture no. 3
 Pneumothorax lecture no. 3 Is accumulation of air in a pleural space or accumulation of extra pulmonary air within the chest, Is uncommon during childhood, may result from external trauma, iatrogenic,
Pneumothorax lecture no. 3 Is accumulation of air in a pleural space or accumulation of extra pulmonary air within the chest, Is uncommon during childhood, may result from external trauma, iatrogenic,
Management of pleural infection in adults: British Thoracic Society pleural disease guideline 2010
 1 Oxford Centre for Respiratory Medicine, Churchill Hospital Site, Oxford Radcliffe Hospital, Oxford, UK 2 Department of Respiratory Medicine, Royal Berkshire Hospital, Reading, UK Correspondence to Dr
1 Oxford Centre for Respiratory Medicine, Churchill Hospital Site, Oxford Radcliffe Hospital, Oxford, UK 2 Department of Respiratory Medicine, Royal Berkshire Hospital, Reading, UK Correspondence to Dr
Efficacy of ultrasonography and computed tomography in differentiating transudate from exudate in patients with pleural effusion
 Efficacy of ultrasonography and computed tomography in differentiating transudate from exudate in patients with pleural effusion Purpose: To evaluate USG and CT imaging findings in differentiating transudative
Efficacy of ultrasonography and computed tomography in differentiating transudate from exudate in patients with pleural effusion Purpose: To evaluate USG and CT imaging findings in differentiating transudative
OBJECTIVES. Solitary Solid Spiculated Nodule. What would you do next? Case Based Discussion: State of the Art Management of Lung Nodules.
 Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Organ Imaging : September 25 2015 OBJECTIVES Case Based Discussion: State of the Art Management of Lung Nodules Dr. Elsie T. Nguyen Dr. Kazuhiro Yasufuku 1. To review guidelines for follow up and management
Study of clinical profile, etiological bacterial agents and outcome in pediatric patients of empyema
 Original article: Study of clinical profile, etiological bacterial agents and outcome in pediatric patients of empyema A.M. Lingayat, P.R. Wankhade Department of Pediatrics, Government Medical College,
Original article: Study of clinical profile, etiological bacterial agents and outcome in pediatric patients of empyema A.M. Lingayat, P.R. Wankhade Department of Pediatrics, Government Medical College,
Risk of Pneumothorax in Post Lung Biopsy Patients: Is Short-Term Monitoring Necessary?
 Risk of Pneumothorax in Post Lung Biopsy Patients: Is Short-Term Monitoring Necessary? Poster No.: C-1852 Congress: ECR 2011 Type: Authors: Keywords: DOI: Scientific Exhibit R. Hayter, T. Berkmen; New
Risk of Pneumothorax in Post Lung Biopsy Patients: Is Short-Term Monitoring Necessary? Poster No.: C-1852 Congress: ECR 2011 Type: Authors: Keywords: DOI: Scientific Exhibit R. Hayter, T. Berkmen; New
tomography Assessment of bronchiectasis by computed Reid' into three types-cystic, varicose, andcylindrical.
 Thorax 1985;40:920-924 Assessment of bronchiectasis by computed tomography IM MOOTOOSAMY, RH REZNEK, J OSMAN, RSO REES, MALCOLM GREEN From the Departments of Diagnostic Radiology and Chest Medicine, St
Thorax 1985;40:920-924 Assessment of bronchiectasis by computed tomography IM MOOTOOSAMY, RH REZNEK, J OSMAN, RSO REES, MALCOLM GREEN From the Departments of Diagnostic Radiology and Chest Medicine, St
@ERSpublications Does pleural irrigation improve pleural fluid drainage and resolution of sepsis in pleural infection?
 ORIGINAL ARTICLE RESPIRATORY INFECTIONS Pleural irrigation trial (PIT): a randomised controlled trial of pleural irrigation with normal saline versus standard care in patients with pleural infection Clare
ORIGINAL ARTICLE RESPIRATORY INFECTIONS Pleural irrigation trial (PIT): a randomised controlled trial of pleural irrigation with normal saline versus standard care in patients with pleural infection Clare
Pleural infection. CME Respiratory medicine. Investigations. Clinical features. Chest x-ray. Pleural ultrasound
 Clinical Medicine 2012, Vol 12, No 1: 82 6 Pleural infection John M Wrightson, clinical research fellow and respiratory specialist registrar, Oxford Pleural Unit, Churchill Hospital, Oxford and NIHR Oxford
Clinical Medicine 2012, Vol 12, No 1: 82 6 Pleural infection John M Wrightson, clinical research fellow and respiratory specialist registrar, Oxford Pleural Unit, Churchill Hospital, Oxford and NIHR Oxford
Excavated pulmonary nodule: steps to diagnosis?
 Excavated pulmonary nodule: steps to diagnosis? Poster No.: C-1044 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit W. Mnari, M. MAATOUK, A. Zrig, B. Hmida, M. GOLLI; Monastir/ TN Metastases,
Excavated pulmonary nodule: steps to diagnosis? Poster No.: C-1044 Congress: ECR 2014 Type: Authors: Keywords: DOI: Educational Exhibit W. Mnari, M. MAATOUK, A. Zrig, B. Hmida, M. GOLLI; Monastir/ TN Metastases,
Surgical Treatment for Empyema Thoracis: Is Video-Assisted Thoracic Surgery Better Than Thoracotomy?
 Surgical Treatment for Empyema Thoracis: Is Video-Assisted Thoracic Surgery Better Than Thoracotomy? Daniel T. L. Chan, MBBS, Alan D. L. Sihoe, FRCSEd, FCCP, Shun Chan, MBBS, Dickson S. F. Tsang, MBBS,
Surgical Treatment for Empyema Thoracis: Is Video-Assisted Thoracic Surgery Better Than Thoracotomy? Daniel T. L. Chan, MBBS, Alan D. L. Sihoe, FRCSEd, FCCP, Shun Chan, MBBS, Dickson S. F. Tsang, MBBS,
Causes of pleural effusion and its imaging approach in pediatrics. M. Mearadji International Foundation for Pediatric Imaging Aid
 Causes of pleural effusion and its imaging approach in pediatrics M. Mearadji International Foundation for Pediatric Imaging Aid Pleural fluid A tiny amount of fluid in the pleural cavity is physiological.
Causes of pleural effusion and its imaging approach in pediatrics M. Mearadji International Foundation for Pediatric Imaging Aid Pleural fluid A tiny amount of fluid in the pleural cavity is physiological.
Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule
 Case Report on Aerodigestive Endoscopy Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule Jennifer L. Sullivan 1, Michael G. Martin 2, Benny Weksler 1 1 Division of
Case Report on Aerodigestive Endoscopy Navigational bronchoscopy-guided dye marking to assist resection of a small lung nodule Jennifer L. Sullivan 1, Michael G. Martin 2, Benny Weksler 1 1 Division of
Are extra-colonic findings on CT colonogram clinically significant? A review of 758 consecutive cases
 Are extra-colonic findings on CT colonogram clinically significant? A review of 758 consecutive cases Lynn WR 1, Vadhwana B 1, Borgstein R 2, Demetriou G 1, Nair MS 1, Meleagros L 1, Bell DJ 2 1 Department
Are extra-colonic findings on CT colonogram clinically significant? A review of 758 consecutive cases Lynn WR 1, Vadhwana B 1, Borgstein R 2, Demetriou G 1, Nair MS 1, Meleagros L 1, Bell DJ 2 1 Department
Surgical decision making in NEC
 Surgical decision making in NEC (the role of ultrasound) Nigel Hall Associate Professor of Paediatric Surgery University of Southampton Consultant Paediatric and Neonatal Surgeon Southampton Children s
Surgical decision making in NEC (the role of ultrasound) Nigel Hall Associate Professor of Paediatric Surgery University of Southampton Consultant Paediatric and Neonatal Surgeon Southampton Children s
Accuracy of lung ultrasonography in diagnosis of community acquired pneumonia in hospitalized children as compared to chest x-ray
 International Journal of Contemporary Pediatrics Tirdia PR et al. Int J Contemp Pediatr. 2016 Aug;3(3):1026-1031 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Research Article DOI: http://dx.doi.org/10.18203/2349-3291.ijcp20162385
International Journal of Contemporary Pediatrics Tirdia PR et al. Int J Contemp Pediatr. 2016 Aug;3(3):1026-1031 http://www.ijpediatrics.com pissn 2349-3283 eissn 2349-3291 Research Article DOI: http://dx.doi.org/10.18203/2349-3291.ijcp20162385
Empyema thoracis: Surgical management in children
 Review Article Full text online at http://www.jiaps.com Empyema thoracis: Surgical management in children Prema Menon, Ravi Prakash Kanojia, K. L. N. Rao Department of Pediatric Surgery, Advanced Pediatric
Review Article Full text online at http://www.jiaps.com Empyema thoracis: Surgical management in children Prema Menon, Ravi Prakash Kanojia, K. L. N. Rao Department of Pediatric Surgery, Advanced Pediatric
Horizon Scanning Technology Summary. Magnetic resonance angiography (MRA) imaging for the detection of coronary artery disease
 Horizon Scanning Technology Summary National Horizon Scanning Centre Magnetic resonance angiography (MRA) imaging for the detection of coronary artery disease April 2007 This technology summary is based
Horizon Scanning Technology Summary National Horizon Scanning Centre Magnetic resonance angiography (MRA) imaging for the detection of coronary artery disease April 2007 This technology summary is based
Paediatric Empyema: A Case Report and Literature Review
 Case reports Paediatric Empyema: A Case Report and Literature Review S. J. PARSONS, E. FENTON, M. WILLIAMS Department of Paediatrics, Royal Hobart Hospital, Hobart, TASMANIA ABSTRACT Objective: To present
Case reports Paediatric Empyema: A Case Report and Literature Review S. J. PARSONS, E. FENTON, M. WILLIAMS Department of Paediatrics, Royal Hobart Hospital, Hobart, TASMANIA ABSTRACT Objective: To present
Bedside Sonographic Diagnosis of Pneumothorax in Pediatric Patients: A Preliminary Report Chia-Wang Tang 1, Kai-Sheng Hsieh 1 1
 ORIGINAL ARTICLE Bedside Sonographic Diagnosis of in Pediatric Patients: A Preliminary Report Chia-Wang Tang 1, Kai-Sheng Hsieh 1 1 Division of Pediatric Pulmonology, Department of Pediatrics, Kaohsiung
ORIGINAL ARTICLE Bedside Sonographic Diagnosis of in Pediatric Patients: A Preliminary Report Chia-Wang Tang 1, Kai-Sheng Hsieh 1 1 Division of Pediatric Pulmonology, Department of Pediatrics, Kaohsiung
Interventional Pulmonology
 Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
