Surgical Neurology International
|
|
|
- Leon Lewis
- 5 years ago
- Views:
Transcription
1 Surgical Neurology International Original Article OPEN ACCESS For entire Editorial Board visit : Two alternative dural sealing techniques in posterior fossa surgery: (Polylactide co glycolide) self adhesive resorbable membrane versus polyethylene glycol hydrogel Marco Schiariti, Francesco Acerbi, Morgan Broggi, Giovanni Tringali, Alberto Raggi 1, Giovanni Broggi 2, Paolo Ferroli Editor: James I. Ausman, MD, PhD University of California, Los Angeles, CA, USA Departments of Neurosurgery, and 1 Neurology, Public Health and Disability Unit, Fondazione Istituto Neurologico Besta, 2 IRCCS Galeazzi, Centro Ricerche di Neuroscienze, Milan, Italy E mail: *Marco Schiariti schiariti.m@istituto besta.it; Francesco Acerbi acerbi.f@istituto besta.it; Morgan Broggi morgan.broggi@istituto besta.it; Giovanni Tringali giovanni.tringali@istituto besta.it; Alberto Raggi gbroggi@gmail.com; Giovanni Broggi paolo.ferroli@istituto besta.it; Paolo Ferroli alberto.raggi@istituto besta.it *Corresponding Author Received: 03 May 14 Accepted: 09 October 14 Published: 03 December 14 This article may be cited as: Schiariti M, Acerbi F, Broggi M, Tringali G, Raggi A, Broggi G, Ferroli P. Two alternative dural sealing techniques in posterior fossa surgery: (Polylactide-co-glycolide) self-adhesive resorbable membrane versus polyethylene glycol hydrogel. Surg Neurol Int 2014;5:171. Available FREE in open access from: Copyright: 2014 Schiariti M. This is an open access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Abstract Background: Post operative cerebrospinal fluid (CSF) leak in posterior fossa surgery remains a significant source of morbidity. TissuePatchDural (TPD), a novel impermeable adhesive membrane, was used to reinforce dural closure. A comparison with one of the most commonly used dural sealing devices, DuraSeal, has been made. Methods: A retrospective, single center study was conducted on 161 patients who underwent elective posterior fossa surgery. On surgeon s opinion, when a primary watertight closure was not possible, they received TPD or DuraSeal to reinforce dural closure. Results: Out of 161 patients analyzed, 115 were treated with TPD and 46 with DuraSeal. The post operative leaks related purely to TPD or DuraSeal failure were recognized in 3 (2.6%) and 5 (10.86%) cases, respectively (P = 0.015). The presence of pre and post operative risk factors was associated with an increased incidence of CSF leak in both groups. TPD showed a better control in patients without these risk factors (P = 0.08). The incidence of CSF leak in patients who underwent posterior fossa surgery by craniectomy was statistically lower in TPD group compared to DuraSeal group (3.22% vs 17.8%, respectively; P = 0.008) Conclusions: TPD seems to be a safe tool for use as an adjunct to standard dural closure in posterior fossa surgery, particularly in patients without pre or post oper ative risk factors, in those who did not develop hydrocephalus, and who underwent craniectomy. The CSF leak rate in TPD group was found to be lower or within the range of the more advanced alternative dural closure strategies, including polyethylene glycol (PEG) based sealant. Access this article online Website: DOI: / Quick Response Code: Key Words: Cerebrospinal fluid leak, dural sealant, DuraSeal, posterior fossa surgery, TissuePatchDural
2 INTRODUCTION Cerebrospinal fluid (CSF) leak still remains a significant source of morbidity in neurosurgery, particularly after posterior fossa surgery. Current treatments aim to promote wound healing by reducing CSF pressure (CSF lumbar drainage or repeated spinal taps) and to prevent infections by administering intravenous antibiotics to the patient. Failure of these treatments potentially requires further surgical intervention. In spite of these treatments, infections, meningitis, encephalitis, and pseudomeningocele formation may complicate the post operative course and result in permanent damage or delay the beginning of adjuvant therapy in oncologic cases. [13] Although technological advances in neurosurgical techniques have reduced the occurrence of post operative CSF leak, the incidence in posterior fossa surgery can be as high as 17%. [8,14,19,20,22,24,33,40,44,48,51,60] Furthermore, the costs related to treating patients affected by this complication have been estimated to be 141% greater than that of patients without a CSF leak. [23] Various approaches have been taken to overcome this issue by the use of a variety of techniques or products to achieve a watertight dural closure. These have included meticulous primary dural closure, lumbar drainage, the use of autologous grafts such as fat or pericranium, dural replacements, Gelfoam (Pfizer, New York, NY, USA), DuraGen (Integra LifeSciences Corporation, Plainsboro, NJ, USA), and fibrin glue, among others. In recent years, DuraSeal (Covidien, Mansfield, MA, USA), a synthetic absorbable hydrogel containing polyethylene glycol (PEG) based polymers, has gained in popularity as a dural sealant. A number of studies have reported a reduction in the incidence of CSF leakage, but only one study considered the incidence of CSF leaks following posterior fossa surgery. [3,10] In this study, Than et al. demonstrated the efficacy of DuraSeal compared to fibrin glue. [59] TissuePatchDural (TPD) (Tissuemed Ltd, Leeds, UK) is a self adhesive, absorbable surgical membrane indicated for adjunctive prevention of CSF leak in neurosurgery. In this retrospective, non randomized, single center study, the authors compared the safety and effectiveness of this novel sealant film (TPD) with DuraSeal, a synthetic liquid formulation, in reducing the incidence of both incisional CSF leak and pseudomeningocele following posterior fossa surgery. MATERIALS AND METHODS Patient population This study is a retrospective, single center clinical investigation conducted on 545 patients who underwent elective posterior fossa surgery in a 30 month period (January 2009-June 2011), with a 6 month follow up period for each patient. Informed consent was obtained from all patients. Pre operative admission criteria included adult patients undergoing clean elective surgical procedures. Previous radiotherapy (RT), previous surgery, and chronic corticosteroid therapy were not considered the exclusion criteria. Intra operative inclusion criteria were a wide cisternal and/or ventricular opening and failure to obtain a watertight primary closure with a standard dural microsuture (leakage evidenced by subdural irrigation of the surgical cavity prior to completion of suturing, followed by Valsalva maneuver and/or positive pressure ventilation to test the completed primary suture closure). On surgeon s opinion, patients received either TPD or DuraSeal to reinforce dural closure. In the period between January 2009 and June 2011, 161 consecutive patients treated at the authors institution and who met the inclusion criteria described above were selected. Of these 161 patients (108 females and 53 males; mean age 45 years, range 8-78 years), 115 were treated with TPD and 46 with DuraSeal. For analysis, patients were stratified according to the presence of: (1) pre operative risk factors, including (a) chronic corticosteroid therapy, b) previous surgery, and (c) radiation therapy; (2) intra operative risk factors, including (a) no dural gap (CSF leakage on Valsalva maneuver and/or positive pressure ventilation), (b) small gap (<5 mm) plugged with muscle or collagen, (c) need for duroplasty); and (3) post operative risks factors, including a) early and (b) late post operative hydrocephalus [Table 1]. All patients underwent daily post operative wound examination in order to assess the occurrence of subgaleal CSF collection, incisional CSF leak, any inflammatory reaction, or wound infection. To monitor post operative complications, a brain CT or MR scan was performed within 48 h in all patients who underwent lesion resection and occipito axial decompression for Chiari malformation. Patients with neurovascular conflicts who underwent microvascular decompression were only scanned if they displayed clinical symptoms. In case of leak or subcutaneous liquid collections, a biochemical testing for β 2 transferrin was performed to confirm CSF presence. The wound was then examined at 2 weeks and 6 months after surgery. In addition, in the period from 2 weeks to 2 months, patients were instructed to contact the hospital in case of wound leak and/or subgaleal collection. Demographic data and operative and outcome data were collected and analyzed. In this study, the term CSF leak was used for both pseudomeningocele and incisional CSF leaks. The etiology of these complications is leakage of CSF from the subarachnoid space into the extradural compartment. When the skin incision has adequately healed, a
3 Table 1: Pre, intra, and post operative risk factors in the 161 patients submitted to surgical procedures for infratentorial pathologies Risk factors Number of patients Proportion of leaks (%) z-test (P value) TPD DuraSeal TPD DuraSeal Pre operative Previous surgery /11 (27.3) (P=0.065) Prior radiation 3 2 c 2/3 (66.6) 1/2 (50) 0.37 (P=0.356) Chronic corticosteroid therapy 4 a 2 d 3/4 (75) 1/2 (50) 0.61 (P=0.271) Post operative Early hydrocephalus 2 1 0/2 (0) 0 (0) NA Delayed hydrocephalus 8 b 4 6/8 (75) 3/4 (75) NA Any pre or post operative Pre and post operative risk factors /20 (35) 4/14 (28.6) 0.39 (P=0.348) No pre operative or post operative risk factor /95 (2.1) 4/32 (12.5) 2.40 (P=0.008) Intra operative No dural gap (CSF leak only after Valsalva) /45 (2.2) 0/9 (0) 0.45 (P=0.326) Small gap<0.5 cm (plugged with muscle or condress) /61 (9.8) 4/30 (13.3) 0.50 (P=0.308) Large gap>0.5 cm (sutured dural substitute) 9 7 2/9 (22.2) 4/7 (57.1) 1.43 (P=0.076) a All submitted to previous surgery and radiotherapy also; b Four of them submitted to previous surgery and radiotherapy also; c One submitted to previous surgery also; d One submitted to previous surgery and radiotherapy also, NA: Not applicable, TPD: Tissuepatchdural, CSF: Cerebrospinal fluid pseudomeningocele may develop; otherwise, an incisional CSF leak may occur. Both situations should be considered as a failure of the dural sealant to prevent CSF from leaking to the extradural compartment. [59] TissuePatchDural TPD [Figure 1] is a sterile, synthetic, self adhesive, absorbable surgical sealant and barrier. It is a thin transparent film available in four different sizes ranging from mm to mm. It is a multilayered device comprising alternate layers of poly (lactide co glycolide) and a proprietary adhesive TissueBond. Poly (lactide co glycolide) is a resorbable membrane that provides reliable strength for temporary wound support. TPD is not a dural replacement/substitute. According to data provided by the manufacturer (Tissuemed Ltd, Leeds, UK) see the product instructions for use), the material achieves its adhesive properties by virtue of the initial tack provided by poly (acrylic acid) and poly (vinyl pyrrolidone) functional groups and longer term adhesion via nucleophilic substitution reaction between N hydroxysuccinimide (NHS) and amines. TPD remains in position while it slowly degrades until substantially reabsorbed facilitating tissue in growth and wound healing. DuraSeal DuraSeal is a synthetic absorbable dural sealant, which can be used to support primary dural closure. As described in the manufacturer s insert, DuraSeal is an US Food and Drug Administration (FDA) approved product that is indicated as an adjunct to sutured dural repair during cranial surgery to provide a watertight closure. More recently, it has received FDA approval for use in spinal Figure 1: TissuePatchDural film ( mm) before (left side) and after activation and adhesion to the sutured dural surface in infratentorial craniotomy (right side) surgery. It contains PEG, a non toxic and biocompatible polymer. When water soluble functionalized PEG is mixed with trilysine (a small molecule amine with reactive linkages), the solutions combine to form the sealant gel that can be sprayed or layered onto the site of dural repair. The cross linking of PEG and trilysine molecules creates a 3 dimensional hydrogel structure that gradually hydrolyzes (water gradually degrades the cross linked bonds in a uniform fashion just like absorbable sutures). According to data provided by the manufacturer, it is cleared from the site in 4-8 weeks, which is enough time to allow healing. Directions and precautions include its avoidance with other hemostatic agents or sealants and the requirement to achieve adequate hemostasis before its application.
4 The DuraSeal manufacturer s insert also includes contraindications, warnings, and exclusion criteria concerning its use. One major warning states, Do not apply DuraSeal hydrogel to confined bony structures where nerves are present since neural compression may result due to hydrogel swelling. The hydrogel may swell up to 50% of its size in any dimension. Contraindications to its use include a history of allergy, penetration of an air sinus, renal/hepatic/immune dysfunction, head trauma, and infection; it is also to be avoided with hydrocephalus, a ventricular drain, or lumbar drain. Technique TPD or DuraSeal was used after standard sutured closure of the dura mater, when subdural irrigation and Valsalva maneuver confirmed the presence of a visible CSF leak. When air filled cavities within cranial bones were opened, e.g. mastoid air cells, muscle or wax was used as a sealant. Small dural gaps (<5 mm in diameter), when present, were plugged with muscle (when available) or collagen sheet (Condress ; Abiogen Pharma S.p.A., Ospedaletto (Pi), Italy) before the application of the TPD or DuraSeal, in order to create a barrier to CSF leak and to avoid the adhesion of the sealant to the cerebral tissue. In 16 cases, a large defect in the dura mater was present and required reconstruction with various dural substitutes (Duraform, Codman and Shurtleff, Inc., Berkshire UK; DuraGen, Integra LifeSciences Corporation; Tutopatch, Tutogen Medical GmbH, Neunkirchen, Germany). Care was taken to ensure the dural surface was as dry as possible, with excess blood or fluid removed to avoid premature activation and ensure optimal attachment of both products to the surface of the tissue. When the TPD was applied, wet cottonoids/ swabs were used to soften the film and increase conformability. Gentle digital pressure for at least 60 s assisted the TPD to adhere to the tissue surface by virtue of the bioadhesive properties of TissueBond. Following preparation of the DuraSeal kit (involving hydration of component powder by mixing vials), the reconstituted DuraSeal sealant was applied to the sutured dura via a bespoke syringe provided by the manufacturer. Following sealant application, patients were again assessed for intra operative CSF leakage through the sealed durotomy with a second Valsalva maneuver for 10 s. An intra operative watertight closure was obtained in all patients who received either sealant. The wounds were closed in layers. A subgaleal or subfascial drain was inserted as necessary and prophylactic antibiotic therapy was administered during and after surgery in accordance with standard of care. Statistical analysis Statistical analysis was undertaken using Prism 4 version 4.0a (GraphPad Software, Inc., San Diego, CA, USA). Durotomy size, the requirement for duroplasty or plugging of dural gaps with muscle or collagen, chronic corticosteroid therapy, previous surgery, radiation therapy, and post operative hydrocephalus were all evaluated as variables that had the potential to influence the rate of CSF leak. The two proportion z test was used to assess the difference in proportion of patients developing CSF leak between those in whom TPD or DuraSeal was used. Statistical significance was set at one tailed P < 0.05 level as our hypothesis was that the proportion of patients developing CSF leak should be lower in those patients in whom TPD was used. The following groups were tested: Pre and post operative risk factors, intra operative risk factors, presence of hydrocephalus, and absence of hydrocephalus. Separate analyses were also carried out in patients who underwent different surgical approaches: Proportion of patients with CSF leak was tested in the subgroup of patients that underwent craniotomy or craniectomy. A further separate analysis was also carried out in patients with or without a dural gap after primary closure: Proportion of patients with CSF leak was tested in the subgroup of patients in which TPD or DuraSeal was applied. Finally, we compared the total CSF leak proportion between patients undergoing craniotomy or craniectomy, irrespective of the use of TPD or DuraSeal; in this case, significance was set at two tailed P < 0.05 level as we had no specific hypothesis on the direction of proportions to test. RESULTS TissuePatchDural Overall, TPD was used in 115 posterior fossa surgeries. The mean follow up was 8.4 months (range 4-34 months). CSF leak was detected in 9 (0 incisional leaks and 9 pseudomeningoceles) out of 115 cases (7.8%). CSF leak presented as rhinorrhea in one patient and as subgaleal CSF collection in eight. Table 1 provides baseline patient data including pre operative risk factors (chronic corticosteroid therapy, previous surgery, radiation therapy), intra operative data (durotomy size, requirement for duroplasty or for plugging dural gaps with muscle or collagen), and post operative risk factors (early or delayed hydrocephalus). A significant difference in the proportions was found only for patients who had no pre or post operative risk factors: Those in the TPD group had lower incidence (2.1%) of CSF leak than those in the DuraSeal group (12.5%). In general [Table 2], lower incidence of CSF leak was observed in patients treated with TPD (7.8%) than in those treated with DuraSeal (17.4%). Of the nine patients with a CSF leak, six (5.21%) presented with associated post operative hydrocephalus that was treated using a ventriculo peritoneal shunt (n = 4) or with endoscopic third ventriculostomy (n = 2). We, therefore, concluded that post operative leaks
5 related purely to TPD failure were recognized in 3 out of 115 cases (2.6%). Of these three patients, one patient with a rhinoliquorrhea after a retrosigmoid approach for microvascular decompression required surgical revision, while the other two patients healed with conservative treatment (CSF lumbar drain). There was no significant (P < 0.05) statistical difference in the incidence of CSF leaks between the three risk factor groups (pre, intra, and post operative). Furthermore, in one patient treated with TPD (0.87%), where a dural gap was not visible at the end of dura suturing, a CSF leak was evident in the post operative period. Also, when a definite/visible dural gap was present, despite the use of muscle, condress, or a dural substitute, the incidence of post operative CSF leakage was higher (gap dimension < 0.5 cm = 9.8%; gap > 0.5 cm = 22.2%) [Table 1]. In one patient with no leak, a wound infection was observed and required revision surgery. No correlation with the use of TPD was found. No device related adverse effects were observed. DuraSeal DuraSeal was used in 46 posterior fossa surgeries. The mean follow up was 8.1 months (range 4-34 months). CSF leak was detected in 8 out of 46 cases (17.4%) (2 incisional leaks and 6 pseudomeningoceles) [Table 2]. CSF leak presented consistently as a subgaleal CSF collection. Table 1 provides baseline patient data including pre operative, intra operative, and post operative risk factors. Out of eight patients with a CSF leak, three (6.52%) presented with associated post operative hydrocephalus treated with a ventriculo peritoneal shunt. Therefore, we concluded the post operative leaks related purely to DuraSeal failure were recognized in 5 out of 46 cases (10.86%). Of these five patients, three were treated conservatively (lumbar drain); the other two patients required further surgery due to incisional CSF leaks after microvascular decompression and atlo axial decompression for Arnold Chiari type II disease. No significant difference in CSF leak rate could be found in the three risk factor groups. Of these eight patients, one patient received RT and chronic corticosteroid therapy. No patients with a CSF leak had undergone prior surgery [Table 1]. Furthermore, no patient without a gap at the dural closure presented a CSF leak. As observed in the TPD group, when a dural gap was present, the incidence of CSF leak was higher (gap dimension < 0.5 cm = 13.3%; gap > 0.5 cm = 57.1%) despite the use of muscle, condress, or a dural substitute [Table 1]. No further DuraSeal related adverse effects were observed. Feasibility of TPD application The fragility of TPD means that careful handling of the film is required in certain applications. TPD can be cut to the required shape and size. It can also be applied to confined bone structures without compressive effects. The dural surface requires some preparation before TPD application, to ensure the site is free from excess blood and fluid. Delicate digital pressure for s allows TPD to adhere properly. During the Valsalva maneuver, the integrity of the seal is confirmed under the microscope by checking that the dura is pulsating without fluid leakage. Furthermore, hemostasis is rechecked as there is a risk of dural bone detachment if excessive pressure is applied. The film also adhered to bone surfaces and often oversized TPD was used in order to bridge over the bone edges. Feasibility of DuraSeal application The application of Duraseal was found to be easier than that of TPD. It was delivered as a liquid via a syringe system and onto the sutured dura. The swelling of this hydrogel was taken into account during application, as it is reported to cause compression of neural structures under the dura mater. Typically this mass effect could be observed on post operative MRI scans, although in this series, its presence did not result in any clinical symptoms. Craniectomy vs Craniotomy Table 3 reports the z test results for patients who underwent craniectomy versus craniotomy. There was Table 2: Two proportion z test to assess differences in CSF leak incidence in TPD and DuraSeal total groups, and in patients with or without hydrocephalus TPD (%) DuraSeal (%) z test (P value) Total CSF leak proportion 9/115 (7.8) 8/46 (17.4) z= 1.78 (P=0.038) CSF leak proportion in patients with 6/115 (5.2) 3/46 (6.5) z= 0.33 (P=0.371) hydrocephalus CSF leak proportion in patients without hydrocephalus 3/115 (2.6) 5/46 (10.9) z= 2.18 (P=0.015) TPD: Tissuepatchdural, CSF: Cerebrospinal fluid Table 3: Two proportion z test to assess differences in CSF leak incidence in patients submitted to craniotomy or craniectomy Subgrups CSF leak in subgroups (%) z Total CSF (one tailed P) leak (%) Craniotomy TPD 7/53 (13.2) 0.36 (P=0.359) DuraSeal 3/18 (16.7) Craniectomy TPD 2/62 (3.2) 2.48 (P=0.008) DuraSeal 5/28 (17.9) TPD: Tissuepatchdural, CSF: Cerebrospinal fluid 10/71 (14.1) 7/90 (7.8) z (two tailed P) 1.29 (P=0.197)
6 [Downloaded free from on Monday, December 08, 2014, IP: ] Click here to download free Android application f no statistically significant difference (P = 0.197) in the incidence of CSF leaks in patients who underwent craniectomy compared to craniotomy (7.8% and 14.1%, respectively). Considering the incidence of CSF leak in the craniectomy group, a lower leak rate was observed when TPD was used (3.22% vs 17.8%, respectively; P = 0.008). Parallel to this, no differences were observed in the subgroup of patients that underwent craniotomy (P = 0.359). Comparison between TPD and DuraSeal groups and analysis of specific risk factors CSF leak rate was significantly lower (P = 0.038) in patients treated with TPD (7.8%) than in those treated with DuraSeal (17.4%), specifically in those without hydrocephalus, where the z test was strong (z = 2.18; P = 0.015) The presence of pre operative (chronic corticosteroid therapy, previous surgery, and radiation therapy) or post operative (early and late hydrocephalus) risk factors was associated with a higher incidence of CSF leakage. The difference in proportion was significant only in the TDP group: 35% of patients with pre or post operative risk factors developed CSF leak versus 2.1% of those without risk factors (z = 4.98; P < 0.001). In the DuraSeal group, the proportions were 28.6% and 12.5%, respectively (z = 1.32; P = 0.187). In the TPD group, 11 patients had previous surgery, 3 had prior RT, and 4 received chronic corticosteroid therapy. In addition, two patients presented with early hydrocephalus and eight with late hydrocephalus (four of this cohort had previous surgery and RT). In summary, a total of 20 patients presented with pre and/or post operative risk factors. Seven of these developed a CSF leak (35%). Of the remaining 95 cases without pre and/or post operative risk factors (95), only 2 patients developed a CSF leak (2.1%) [Table 1]. In the DuraSeal group, seven patients had previous surgery, two had received RT (one of them had been also submitted to previous surgery), and two were under chronic corticosteroid therapy (one of these patients had been also submitted to previous surgery and RT). In addition, one patient presented with early hydrocephalus and four with late hydrocephalus. Therefore, a total of 14 patients presented with pre and/or post operative risk factors. Four of these developed a CSF leak (28.6%). Of the remaining 32 cases without pre and/or post operative risk factors, 4 patients developed a CSF leak (12.5%) [Table 1]. On evaluating the influence of pre and post operative risk factors between patients treated with TPD and DuraSeal, we noticed a similar incidence of leakage (35% vs 28.5%, respectively; P = 0.348). In the absence of pre and post operative risk factors, the incidence of CSF leaks in the TPD group was statistically significantly lower (P = 0.008) compared to that in DuraSeal group (2.1% and 12.5%, respectively). Excluding patients with hydrocephalus, the incidence of CSF leak was significantly lower in the TPD group than in the DuraSeal group (2.6% and 10.86%, respectively; P = 0.015) [Table 2]. No statistical differences were found between the two groups with regard to pseudomeningocele, presence of hydrocephalus, or presence of rhinoliquorrea [Table 2]. Considering the size of dural gap (CSF leakage only on Valsalva maneuver, small gap <5 mm plugged with muscle or collagen, large gap >5 mm requiring duroplasty), the absence of a clear dural gap following standard microsuture was associated with prevention of CSF leakage after TPD (z = 1.79; P = 0.036), but not in the subgroup of patients in which DuraSeal was applied (z = 1.53; P = 0.063) [Table 1]. DISCUSSION CSF leak after posterior fossa surgery can occur in 2-17% of cases and remains an unsolved problem since the time of Cushing. [8,12 14,19,20,22,24,33,40,44,48,51,60] This high variability depends on numerous factors such as surgical approach and location, general and local conditions (size and location of dural resection, previous radiation therapy, immunodepression, corticosteroid therapy, uncontrolled diabetes, renal or hepatic dysfunction, etc.), surgical technique, and CSF leak diagnostic methods (radiologic or clinical diagnosis). [3,4,6,9,11,14,16,18,23,30,31,35,39,41,43,50,54,57,63] CSF leak remains a potentially life threatening complication due to the risk of meningoencephalitis. Interventions to treat CSF leaks include repeated surgery, insertion of lumbar drain, and administration of antibiotics to address non healing wounds. All these factors can result in prolonged hospitalization and the cost of CSF leakage has been estimated to be 141% greater than that for uncomplicated cases. [23] Our study showed, consistent with our hypothesis, that the use of TPD was associated with a lower incidence of CSF leak compared to that of DuraSeal in this cohort of patients. Moreover, the use of TPD resulted in a lower probability of developing CSF leak in patients without pre or post operative risk factors, those who did not develop hydrocephalus, and those who underwent craniectomy. Since the early days of neurosurgery, watertight dural closure has been advocated in order to avoid CSF leakage. [21] Although recently it has been claimed that watertight dural closure is not mandatory in supratentorial procedures, direct watertight suturing of the dural defect has been and is generally attempted in every neurosurgical procedure. [2,15] In the elderly, the dura can be particularly fragile and adherent to the bone. Furthermore, when
7 opened, it tends to shrink due to dehydration and as a consequence of using bipolar coagulation. The biochemical features of dura mater make it an elastic membrane where needle piercing creates pinholes. To aid dural sealing under problematic conditions where watertight closure is desirable (but difficult to achieve), different materials have been used alone or in combination [Table 4]. [5,7,10,25,28,46,55,59,61,66 68] The first duraplasty was performed in 1895 by Abbe, who used rubber sheeting for defect closure. [1] Since then, the search for the optimal closure technique has continued and a variety of materials have been proposed, including autografts (fascia, pericranium, fat, and muscle), allografts (such as cadaveric dura), xenografts [processed whole tissues or highly engineered collagen matrices such as pericardium or DuraGen (Integra)], and synthetic grafts [such as polytetrafluoroethylene Gore and Associates Inc., Newark, DE, USA) and polyester urethane (Neuropatch; B. Braun Melsungen AG, Germany)]. [6,14,26,27,29,34,39,42,45,49,56 58,61,64,66] Clinical use has identified various negative effects; for some, the preparation and watertight suturing is time consuming, for others inflammatory and foreign body reaction are common; allografts and autografts can be compromised by disease and are therefore not always available; synthetic dural substitutes are associated with a high percentage of infections and a still high percentage of failure. [32,36,47,58,62,65,66] In addition to grafts, other materials may be used to augment dural closure [Table 4]. Fibrin sealants including Tisseel (Baxter, Deerfield, IL, USA) have been commercially available since the 1990s. They consist of human derived fibrinogen and thrombin and are classified as thromobogenic hemostats designed to treat low level (not severe) of brisk arterial or venous bleeding. [52,53,62] The disadvantages of fibrin sealant include time consuming preparation. Furthermore, there have been reports that fibrin sealants can precipitate acute immune responses; chronically, they are associated with adhesion formation and infection. [23] In recent years, DuraSeal (Covidien), a synthetic absorbable hydrogel containing PEG, has gained popularity. The studies performed have reported a decrease in the incidence of CSF leak compared with that of traditional dural closure techniques [Table 4]. [5,10,59,67] In a prospective study, Cosgrove evaluated the safety and efficacy of DuraSeal in patients undergoing elective cranial surgery with documented CSF leakage after sutured dural repair. [10] The authors reported a safe and effective watertight closure when the DuraSeal was used as an adjunct to sutured dural repair. The post operative incisional CSF leak rate was 1.8%, but in excess of 50% of procedures were supratentorial. The report by Than et al. specifically considered the efficacy of DuraSeal in a series of patients undergoing posterior fossa surgery; in this study, they prospectively collected the data of 100 patients undergoing posterior fossa surgery with this PEG hydrogel to augment the dural closure. [59] These results were compared with a retrospective cohort of 100 patients treated with fibrin glue. The incidence of incisional CSF leak was 2% in the DuraSeal group and 10% in the fibrin glue group (P = 0.03). If one combines the number of patients who had a pseudomeningocele (8 in the DuraSeal group and 5 in the fibrin sealant group; P = 0.4) with those who had an incisional CSF leak (2 and 10 for DuraSeal and fibrin sealant groups, respectively; P = 0.03), there is no difference between the two groups (10 and 15%, respectively; P > 0.5). As highlighted by Steinbok in his reported response to Than s publication, the higher incidence of incisional CSF leaks in the fibrin glue group may be related to the closure type of the skin or of the subcutaneous tissues, and not to the ability of DuraSeal to provide a leak proof seal of the dura. [59] In our study, we were not be able to find any statistical difference between TPD and DuraSeal, including analysis of both incisional CSF leaks and pseudomeningocele together or alone. Table 4: Comparison of studies with different types of dural sealants Author, year Sealant No. of pts % of leakage % High risk pts Site Boogaarts et al., 2005 DuraSeal (out of 41pts) High and low riskprocedures 26 supratentorial 18 infratentorial 2 spinal Cosgrove et al., 2007 DuraSeal High and low riskprocedures 58 supratentorial 53 infratentorial Than et al., 2007 DuraSeal Not specified Posterior fossa Kumar et al., 2003 Bioglue (in twoposterior fossaapproach) Not specified 114 supratentorial 53 infratentorial 41 transsphenoidal 8 spinal Stendel et al., 2008 DuraGen Not specified 165 supratentorial 26 infratentorial Jankowitz et al., 2009 Tisseel Not specified Spine Ferroli et al., 2011 TissuePatchDural (11/119) 36.3 (8/22) of high risk pts 3.1 (3/97) of normal risk pts 22/119 (18.5) high risk cases all patientswith wide cisternal orventricular opening 67 infratentorial 34 supratentorial 18 spinal
8 Boogaarts et al. prospectively treated 46 patients with DuraSeal in combination with autologous materials. [5] Over a 3 month follow up period, they reported one CSF leak following a supratentorial craniotomy and one pseudomeningocele after posterior fossa surgery. There were no infections and no other adverse events related to the hydrogel. In this series, the authors excluded patients affected by hydrocephalus and patients who had a neurosurgical procedure within the previous 12 months, as well as RT or chemotherapy. Furthermore, out of 46 patients, only 18 (39%) patients underwent posterior fossa surgery, with an incidence of CSF leak of 5.5%. In our previous report (Ferroli et al.), we analyzed the influence of pre operative risk factors (chronic corticosteroid therapy, previous surgery, and radiation therapy), intra operative risk factors (size of dural gap), and post operative risks factors (early post operative hydrocephalus) on the appearance of CSF leak. [17] We concluded that the presence of pre operative and post operative risk factors was one of the factors negatively influencing the ability to achieve watertight closure. In fact, of the 22 patients in whom pre and/ or post operative risk factors were present, 8 developed a CSF leak (36.3%). Conversely, in the remaining cases without pre and/or intra operative risk factors, only three patients (3.1%) developed a CSF leak. In the present series, we observed that in the absence of pre and post operative risk factors, TPD had a better protective effect on the CSF leak development. The small size of the two samples and the difference in the sample sizes might explain the lack of statistically significant difference in CSF development in the presence of pre and post operative risk factors. Considering the impact of the risk factors in our previous report, we have excluded patients with post operative hydrocephalus from the analysis. With this exclusion, the incidence of CSF leak (incisional and pseudomeningocele together) was significantly lower in the patients treated with TPD compared to those treated with DuraSeal (2.6% vs 10.9%, respectively; P = 0.015) [Table 1]. In 2002, Gnanalingham et al. analyzed the difference between the complication rates in children who underwent posterior fossa surgery by craniotomy or craniectomy. [22] They reported that craniectomy was associated with an increased incidence of post operative CSF leak (odds ratio 10.8, 95% CI ; P = 0.03). We were not be able to find the same result (P = 0.2) [Table 3]. Interestingly, in the group of patients who underwent craniectomy, the incidence of CSF leak was significantly lower in patients treated with TPD compared to that in whom DuraSeal was used (3.22% vs 17.85%, respectively; P = 0.03) [Table 3], showing a protective effect of TPD. There are clearly some limitations in this study. The sample sizes are small and not matched, and this has an impact on the outcome of the statistical analysis. Furthermore, it is a retrospective evaluation of patients submitted to different procedures by different surgeons in a limited period of time. Despite these limitations, the safety profile of the product is good and no adverse reactions, directly related to TPD, were evident throughout the follow up period. The ability of TPD to achieve watertight closure following use in a population presenting a high risk of CSF leakage is promising. Its non inferiority to DuraSeal, a widely used and FDA approved product, merits further prospective, randomized, multicenter investigations. CONCLUSIONS TPD seems to be safe when used as an adjunct to standard dural closure in posterior fossa surgery, in particular in patients without pre or post operative risk factors, those who did not develop hydrocephalus, and in those who underwent craniectomy. With the intrinsic limitation of this retrospective study, the rate of CSF leak in high risk posterior fossa surgery was found to be within the range of the more advanced alternative dural closure strategies and lower, albeit not statistically significant, than in patients treated with a commonly used PEG based liquid sealant. REFERENCES 1. Abbe R. Rubber tissue for meningeal adhesions. Trans Am Surg Assoc 1895;13: Barth M, Tuettenberg J, Thomé C, Weiss C, Vajkoczy P, Schmiedek P, et al. Is it necessary? A prospective randomized trial in patients with supratentorial craniotomies. Neurosurgery 2008;63 (4 Suppl 2):S Berjano R, Vinas FC, Dujovny M. A review of dural substitutes used in neurosurgery. Crit Rev Neurosurg 1999;9: Biroli F, Fusco M, Bani GG, Signorelli A, Esposito F, de Divitiis O, et al. Novel equine collagen only dural substitute. Neurosurgery 2008;62 (3 Suppl 1):S Boogaarts JD, Grotenhuis JA, Bartels RH, Beems T. Use of a novel absorbable hydrogel for augmentation of dural repair: Results of a preliminary clinical study. Neurosurgery 2005;57 (1 Suppl):S Boop FA, Chadduck WM. Silastic duraplasty in pediatric patients. Neurosurgery 1991;29: Boudreaux B, Zins JE. Treatment of cerebrospinal fluid leaks in high risk patients. J Craniofac Surg 2009;20: Bryce GE, Nedzelski JM, Rowed DW, Rappaport JM. Cerebrospinal fluid leaks and meningitis in acoustic neuroma surgery. Otolaryngol Head Neck Surg 1991;104: Caroli E, Rocchi G, Salvati M, Delfini R. Duraplasty: Our current experience. Surg Neurol 2004;61: Cosgrove GR, Delashaw JB, Grotenhuis JA, Tew JM, van Loveren H, Spetzler RF, et al. Safety and efficacy of a novel polyethylene glycol hydrogel sealant for watertight dural repair. J Neurosurg 2007;106: Costantino PD, Wolpoe ME, Govindaraj S, Chaplin JM, Sen C, Cohen M, et al. Human dural replacement with acellular dermis: Clinical results and a review of the literature. Head Neck 2000;22: Cushing H. Experiences with the cerebellar astrocytomas: A critical review of seventy six cases. Surg Gynecol Obstet 1931;52:
9 13. Cushing H, Surgery of the head. In: Keen WW, editor. Surgery, Its Principles and Practice, Vol 3. Philadelphia: WB Saunders; p Danish SF, Samdani A, Hanna A, Storm P, Sutton L. Experience with acellular human dura and bovine collagen matrix for duraplasty after posterior fossa decompression for Chiari malformations. J Neurosurg 2006;104 (1 Suppl):S Della Puppa A, Rossetto M, Scienza R. Use of a new absorbable sealing film for preventing postoperative cerebrospinal fluid leaks: Remarks on a new approach. Br J Neurosurg 2010;24: Djordjevic Z, Milosavlijevic B. Postoperative cerebrospinal fluid fistulas and their treatment. J Neurosurg Sci 1974;18: Ferroli P, Acerbi F, Broggi M, Schiariti M, Albanese E, Tringali G, et al. A novel impermeable adhesive membrane to reinforce dural closure: A preliminary retrospective study on 119 consecutive high risk patients. World Neurosurg 2013;79: Filippi R, Schwarz M, Voth D, Reisch R, Grunert P, Perneczky A. Bovine pericardium for duraplasty: Clinical results in 32 patients. Neurosurg Rev 2001;24: Fishman AJ, Hoffman RA, Roland JT Jr, Lebowitz RA, Cohen NL. Cerebrospinal fluid drainage in the management of CSF leak following acoustic neuroma surgery. Laryngoscope 1996;106: Fishman AJ, Marrinan MS, Golfinos JG, Cohen NL, Roland JT Jr. Prevention and management of cerebrospinal fluid leak following vestibular schwan noma surgery. Laryngoscope 2004;114: Gardner PA, Kassam AB, Snyderman CH, Carrau RL, Mintz AH, Grahovac S, et al. Outcomes following purely endoscopic, expanded endonasal resection of suprasellar craniopharyngiomas. J Neurosurg 2008;109: Gnanalingham KK, Lafuente J, Thompson D, Harkness W, Hayward R. MRI study of the natural history and risk factors for pseudomeningocele formation following postfossa surgery in children. Br J Neurosurg 2003;17: Grotenhuis JA. Costs of postoperative cerebrospinal fluid leakage: 1 year, retrospective analysis of 412 consecutive nontrauma cases. Surg Neurol 2005;64: Hoffman RA. Cerebrospinal fluid leak following acoustic neuroma removal. Laryngoscope 1994;104: Jankowitz BT, Atteberry DS, Gerszten PC, Karausky P, Cheng BC, Faugh R, et al. Effect of fibrin glue on the prevention of persistent cerebral spinal fluid leakage after incidental durotomy during lumbar spinal surgery Eur Spine J 2009;18: Kline DG. Dural replacement with resorbable collagen. Arch Surg 1965;91: Knopp U, Christmann F, Reusche E, Sepehrnia A. A new collagen biomatrix of equine origin versus a cadaveric dura graft for the repair of dural defects-a comparative animal experimental study. Acta Neurochir (Wien) 2005;147: Kumar A, Maartens NF, Kaye AH. Evaluation of the use of BioGlue in neurosurgical procedures. J Clin Neurosci 2003;10: Laquerriere A, Yun J, Tiollier J, Hemet J, Tadie M. Experimental evaluation of bilayered human collagen as a dural substitute. J Neurosurg 1993;78: Leonetti JP, Anderson D, Marzo S, Moynihan G. Prevention and management of cerebrospinal fluid fistula after transtemporal skull base surgery. Skull Base 2001;11: Maher CO, Anderson RE, McClelland RL, Link MJ. Evaluation of a novel propylene oxide treated collagen material as a dural substitute. J Neurosurg 2003;99: Malliti M, Page P, Gury C, Chomette E, Nataf F, Roux F. Comparison of deep wound infection rates using a synthetic dural substitute (neuro patch) or pericranium graft for dural closure: A clinical review of 1 year. Neurosurgery 2004;54: Mangham CA. Complications of translabyrinthine vs. suboccipital approach for acoustic tumor surgery. Otolaryngol Head Neck Surg 1988;99: Mayfield FH. Autologous fat transplants for the protection and repair of the spinal dura. Clin Neurosurg 1980;27: Messing Jünger AM, Ibáñez J, Calbucci F, Choux M, Lena G, Mohsenipour I, et al. Effectiveness and handling characteristics of a three layer polymer dura substitute: A prospective multicenter clinical study. J Neurosurg 2006;105: Morikawa T. Tissue sealing. Am J Surg 2001;182 (Suppl 2):29 35S. 37. Nakagawa S, Hayashi T, Anegawa S, Nakashima S, Shimokawa S, Furukawa Y. Postoperative infection after duraplasty with expanded polytetrafluoroethylene sheet. Neurol Med Chir (Tokyo) 2003;43: Narotam PK, Jose S, Nathoo N, Taylon C, Vora Y. Collagen matrix (DuraGen) in dural repair: Analysis of a new modified technique. Spine 2004;29: Narotam PK, van Dellen JR, Bhoola KD. A clinicopathological study of collagen sponge as a dural graft in neurosurgery. J Neurosurg 1995;82: Nutik SL, Korol HW. Cerebrospinal fluid leak after acoustic neuroma surgery. Surg Neurol 1995;43: Parízek J, Mericka P, Husek Z, Suba P, Spacek J, Nemecek S, et al. Detailed evaluation of 2959 allogeneic and xenogeneic dense connective tissue grafts (fascia lata, pericardium, and dura mater) used in the course of 20 years for duraplasty in neurosurgery. Acta Neurochir (Wien) 1997;139: Parizek J, Mericka P, Spacek J, Nemecek S, Elias P, Sercl M. Xenogeneic pericardium as a dural substitute in reconstruc tion of suboccipital dura mater in children. J Neurosurg 1989;70: Parízek J, Mericka P. Duraplasty with pretreated freeze dried sterilized human dura mater. Sb Ved Pr Lek Fak Karlovy Univerzity Hradci Kralove 1990;33: Parízek J, Sercl M, Michl A, Mericka P, Nemecek S, Nemecková J, et al. Posterior fossa duraplasty in children: Remarks on surgery and clinical and CT follow up. Childs Nerv Syst 1994;10: Park YK, Tator CH. Prevention of arachnoiditis and postop erative tethering of the spinal cord with Gore Tex surgical membrane: An experimental study with rats. Neurosurgery 1998;42: Pomeranz S, Constatini S, Umansky F. The use of fibrin glue in cerebrospinal fluid leakage. Neurochirurgia (Stuttg) 1991;34: Raul JS, Godard J, Arbez Gindre F, Czorny A. Use of polyes ter urethane (Neuro Patch) as a dural substitute. Prospective study of 70 cases. Neurochirurgie 2003;49: Reyes Moreno I, Verheggen R. Time sparing and effective procedure for dural closure in the posterior fossa using a vicryl mesh (Ethisorb). Neurocirugia (Astur) 2006;17: Rosen DS, Wollman R, Frim DM. Recurrence of symptoms after Chiari decompression and duraplasty with nonautolo gous graft material. Pediatr Neurosurg 2003;38: Sakas DE, Charnvises K, Borges LF, Zervas NT. Biologically inert synthetic dural substitutes. Appraisal of a medical grade aliphatic polyurethane and a polysiloxane carbonate block copolymer. J Neurosurg 1990;73: Samii M, Matthies C. Management of 1000 vestibular schwannomas (acoustic neuromas): Surgical management and results with an emphasis on complications and how to avoid them. Neurosurgery 1997;40: Sawamura Y, Katsuyuki A, Terasaka S. Evaluation of application techniques of fibrin sealant to prevent cerebrospinal fluid leakage: A new device for the application of aerosolized fibrin glue. Neurosurgery 1999;44: Shaffrey CI, Spotnitz WD, Shaffrey ME, Jane JA. Neurosurgical applications of fibrin glue: Augmentation of dural closure in 134 patients. Neurosurgery 1990;26: Shimizu S, Koizumi H, Kurita M, Utsuki S, Oka H, Fujii K. Duraplasty in the posterior fossa using a boat shaped sheet of expanded polytetrafluoroethylene. Neurol Med Chir (Tokyo) 2007;47: Sierra DH, Nissen AJ, Welch J. The use of fibrin glue in intracranial procedures: Preliminary results. Laryngoscope 1990;100: Stendel R, Danne M, Fiss I, Klein I, Schilling A, Hammersen S, et al. Efficacy and safety of a collagen matrix for cranial and spinal dural reconstruction using different fixation techniques. J Neurosurg 2008;109: Tachibana E, Saito K, Fukuta K, Yoshida J. Evaluation of the healing process after dural reconstruction achieved using a free fascial graft. J Neurosurg 2002;96: Thammavaram KV, Benzel EC, Kesterson L. Fascia lata graft as a dural substitute in neurosurgery. South Med J 1990;83: Than KD, Baird CJ, Olivi A. Polyethylene glycol hydrogel dural sealant may reduce incisional cerebrospinal fluid leak after posterior fossa surgery. Neurosurgery 2008;63 (1 Suppl 1):S Tubbs RS, Wellons JC 3 rd, Blount JP, Oakes WJ. Posterior atlanto occipital membrane for duraplasty. Technical note. J Neurosurg 2002;97 (2 Suppl): Turgut M, Erkus M, Tavus N. The effect of fibrin adhesive (Tisseel) on interbody allograft fusion: An experimental study with cats. Acta Neurochir (Wien) 1999;141: van Velthoven V, Clarici G, Auer LM, Fibrin tissue adhesive sealant for the
10 prevention of CSF leakage following transsphenoidal microsurgery. Acta Neurochir (Wien) 1991;109: Vanaclocha V, Saiz Sapena N. Duraplasty with freeze dried cadaveric dura versus occipital pericranium for Chiari type I malformation: Comparative study. Acta Neurochir (Wien) 1997;139: Vargel I, Tuncbilek G, Mavili E, Cila A, Ruacan S, Benli K, et al. Solvent dehydrated calvarial allografts in craniofacial surgery. Plast Reconstr Surg 2004;114: Von Wild KR. Examination of the safety and efficacy of an absorbable dura mater substitute (Dura Patch) in normal ap plications in neurosurgery. Surg Neurol 1999;52: Warren WL, Medary MB, Dureza CD, Bellotte JB, Flannagan PP, Oh MY, et al. Dural repair using acellular human dermis: Experience with 200 cases: Technique assessment. Neurosurgery 2000;46: Weinstein JS, Liu CK, Delashaw JB, Burchiel KJ, van Loveren HR, Vale FL, et al. The safety and effectiveness of a dural sealant system for use with nonautologous duraplasty materials. J Neurosurg 2010;112: Yoshimoto T, Sawamura Y, Houkin K, Abe H. Effectiveness of fibrin glue for preventing postoperative extradural fluid leakage Neurol Med Chir (Tokyo) 1997;37:
Published clinical papers
 Published clinical papers Published clinical papers (Neuro) Use of a new absorbable sealing film for preventing postoperative cerebrospinal fluid leaks: remarks on a new approach. (12 cranial cases) A
Published clinical papers Published clinical papers (Neuro) Use of a new absorbable sealing film for preventing postoperative cerebrospinal fluid leaks: remarks on a new approach. (12 cranial cases) A
Health Sciences University, Diskapi Yildirim Beyazit Training and Research Hospital, Department of Neurosurgery, Ankara, Turkey 2
 DOI: 10.5137/1019-5149.JTN.24432-18.0 Received: 26.07.2018 / Accepted: 30.07.2018 Published Online: 25.03.2019 Original Investigation Turk Neurosurg, 2019 qr code Identification of Risk Factors for Postoperative
DOI: 10.5137/1019-5149.JTN.24432-18.0 Received: 26.07.2018 / Accepted: 30.07.2018 Published Online: 25.03.2019 Original Investigation Turk Neurosurg, 2019 qr code Identification of Risk Factors for Postoperative
Experience with acellular human dura and bovine collagen matrix for duraplasty after posterior fossa decompression for Chiari malformations
 J Neurosurg (1 Suppl Pediatrics) 104:16 20, 2006 Experience with acellular human dura and bovine collagen matrix for duraplasty after posterior fossa decompression for Chiari malformations SHABBAR F. DANISH,
J Neurosurg (1 Suppl Pediatrics) 104:16 20, 2006 Experience with acellular human dura and bovine collagen matrix for duraplasty after posterior fossa decompression for Chiari malformations SHABBAR F. DANISH,
Neurosurgery is complex. DuraGen is the simple choice.
 Neurosurgery is complex. is the simple choice. Family of Grafts Dural Regeneration Matrix Keep Closure Simple. A Breakthrough in Dural Repair A Pioneer in Dural Regeneration Matrices For almost forty years,
Neurosurgery is complex. is the simple choice. Family of Grafts Dural Regeneration Matrix Keep Closure Simple. A Breakthrough in Dural Repair A Pioneer in Dural Regeneration Matrices For almost forty years,
The Synthetic Self-Adhesive Barrier to Cerebrospinal Fluid Leaks
 The Synthetic SelfAdhesive Barrier to Cerebrospinal Fluid Leaks TissuePatchl has a fused multilaminate structure containing patented reactive polymers for chemical bonding to tissue surface, and a nonadhesive
The Synthetic SelfAdhesive Barrier to Cerebrospinal Fluid Leaks TissuePatchl has a fused multilaminate structure containing patented reactive polymers for chemical bonding to tissue surface, and a nonadhesive
Safety and efficacy of a novel polyethylene glycol hydrogel sealant for watertight dural repair
 J Neurosurg 106:52 58, 2007 Safety and efficacy of a novel polyethylene glycol hydrogel sealant for watertight dural repair G. REES COSGROVE, M.D., F.R.C.S.C., 1 JOHNNY B. DELASHAW, M.D., 2 J. ANDRE GROTENHUIS,
J Neurosurg 106:52 58, 2007 Safety and efficacy of a novel polyethylene glycol hydrogel sealant for watertight dural repair G. REES COSGROVE, M.D., F.R.C.S.C., 1 JOHNNY B. DELASHAW, M.D., 2 J. ANDRE GROTENHUIS,
Management of Cerebrospinal Fluid Leaks After Vestibular Schwannoma Surgery
 Otology & Neurotology 32:1525Y1529 Ó 2011, Otology & Neurotology, Inc. Management of Cerebrospinal Fluid Leaks After Vestibular Schwannoma Surgery *Brannon D. Mangus, *Alejandro Rivas, Mi Jin Yoo, JoAnn
Otology & Neurotology 32:1525Y1529 Ó 2011, Otology & Neurotology, Inc. Management of Cerebrospinal Fluid Leaks After Vestibular Schwannoma Surgery *Brannon D. Mangus, *Alejandro Rivas, Mi Jin Yoo, JoAnn
After a great surgery, why leave anything to chance?
 HyperBranch Medical Technology, Inc. creates innovative medical devices using synthetic hydrogels with novel tunable properties for use as surgical sealants in general and specialty surgery. The products
HyperBranch Medical Technology, Inc. creates innovative medical devices using synthetic hydrogels with novel tunable properties for use as surgical sealants in general and specialty surgery. The products
Restoration not just repair
 DURAGEN ENGLISH Restoration not just repair r e g e n e r at i v e t e c h n o l o g y PRODUCTS FOR SALE IN EUROPE, MIDDLE-EAST and AFRICA ONLY. More than a graft DuraGen is a matrix for repair of the
DURAGEN ENGLISH Restoration not just repair r e g e n e r at i v e t e c h n o l o g y PRODUCTS FOR SALE IN EUROPE, MIDDLE-EAST and AFRICA ONLY. More than a graft DuraGen is a matrix for repair of the
Application of a hydrogel sealant improves watertight closures of duraplasty onlay grafts in a canine craniotomy model
 J Neurosurg 107:642 650, 2007 Application of a hydrogel sealant improves watertight closures of duraplasty onlay grafts in a canine craniotomy model MARK C. PREUL, M.D., 1 PATRICK K. CAMPBELL, PH.D., 2
J Neurosurg 107:642 650, 2007 Application of a hydrogel sealant improves watertight closures of duraplasty onlay grafts in a canine craniotomy model MARK C. PREUL, M.D., 1 PATRICK K. CAMPBELL, PH.D., 2
DuraMatrix Collagen Dura Substitute Membrane. Manufactured by: Collagen Matrix, Inc., Franklin Lakes, New Jersey
 DuraMatrix Collagen Dura Substitute Membrane Manufactured by: Collagen Matrix, Inc., Franklin Lakes, New Jersey What is DuraMatrix? Onlay or Sutured Implantation Balanced Implant Resorption vs. Host Tissue
DuraMatrix Collagen Dura Substitute Membrane Manufactured by: Collagen Matrix, Inc., Franklin Lakes, New Jersey What is DuraMatrix? Onlay or Sutured Implantation Balanced Implant Resorption vs. Host Tissue
At the conclusion of craniotomy procedures, it is
 J Neurosurg 120:278 284, 2014 AANS, 2014 The incidence of complications in elective cranial neurosurgery associated with dural closure material Clinical article Brian P. Walcott, M.D., 1 Jonathan B. Neal,
J Neurosurg 120:278 284, 2014 AANS, 2014 The incidence of complications in elective cranial neurosurgery associated with dural closure material Clinical article Brian P. Walcott, M.D., 1 Jonathan B. Neal,
SYNTHECEL Dura Repair. Assurance and Versatility for Dura Reconstruction.
 SYNTHECEL Dura Repair Assurance and Versatility for Dura Reconstruction. SYNTHECEL Dura Repair is an assured and versatile solution for your dura reconstruction needs. Clinically proven One product choice
SYNTHECEL Dura Repair Assurance and Versatility for Dura Reconstruction. SYNTHECEL Dura Repair is an assured and versatile solution for your dura reconstruction needs. Clinically proven One product choice
BioGlue Surgical Adhesive as a Dural Sealant in Neurosurgery Clinical Needs and Surgical Technique
 BioGlue Surgical Adhesive as a Dural Sealant in Neurosurgery Clinical Needs and Surgical Technique Massimo Miscusi, MD, PhD Assistant Professor of Neurosurgery, Sapienza University of Rome, Rome, Italy
BioGlue Surgical Adhesive as a Dural Sealant in Neurosurgery Clinical Needs and Surgical Technique Massimo Miscusi, MD, PhD Assistant Professor of Neurosurgery, Sapienza University of Rome, Rome, Italy
The Incidence of Cerebrospinal Fluid Leak after Vestibular Schwannoma Surgery
 Otology & Neurotology 25:387 393 2004, Otology & Neurotology, Inc. The Incidence of Cerebrospinal Fluid Leak after Vestibular Schwannoma Surgery Samuel H. Selesnick, Jeffrey C. Liu, Albert Jen, and Jason
Otology & Neurotology 25:387 393 2004, Otology & Neurotology, Inc. The Incidence of Cerebrospinal Fluid Leak after Vestibular Schwannoma Surgery Samuel H. Selesnick, Jeffrey C. Liu, Albert Jen, and Jason
Durotomies with CSF leakage are one of the most
 CASE REPORT J Neurosurg Spine 28:181 185, 2018 A novel duraplasty technique following fenestration of a massive lumbar arachnoid cyst in a patient with scoliosis: technical case report Matthew T. Neal,
CASE REPORT J Neurosurg Spine 28:181 185, 2018 A novel duraplasty technique following fenestration of a massive lumbar arachnoid cyst in a patient with scoliosis: technical case report Matthew T. Neal,
got you covered. Codman s The global leader in neurosurgery is your one-stop, comprehensive source for proven, market-leading dural repair solutions.
 Codman s got you covered. The global leader in neurosurgery is your one-stop, comprehensive source for proven, market-leading dural repair solutions. AN INTEGRA LIFESCIENCES COMPANY The Leader in Dural
Codman s got you covered. The global leader in neurosurgery is your one-stop, comprehensive source for proven, market-leading dural repair solutions. AN INTEGRA LIFESCIENCES COMPANY The Leader in Dural
5.5. RETROSIGMOID APPROACH
 5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
Kiyoshi Ito, MD, Tatsuro Aoyama, MD, Takuya Nakamura, MD, Yoshiki Hanaoka, MD, Tetsuyoshi Horiuchi, MD, and Kazuhiro Hongo, MD
 technical note J Neurosurg Spine 25:620 625, 2016 Novel dural incision and closure procedure for preventing postoperative cerebrospinal fluid leakage during the surgical removal of dumbbell-shaped spinal
technical note J Neurosurg Spine 25:620 625, 2016 Novel dural incision and closure procedure for preventing postoperative cerebrospinal fluid leakage during the surgical removal of dumbbell-shaped spinal
The translabyrinthine approach to the cerebellopontine
 Neurosurg Focus 33 (3):E17, 2012 Fascial sling technique for dural reconstruction after translabyrinthine resection of acoustic neuroma: technical note James K. Liu, M.D., 1 3 Smruti K. Patel, B.A., 1
Neurosurg Focus 33 (3):E17, 2012 Fascial sling technique for dural reconstruction after translabyrinthine resection of acoustic neuroma: technical note James K. Liu, M.D., 1 3 Smruti K. Patel, B.A., 1
Fleece-Bound Tissue Sealing in Microvascular Decompression
 DOI: 10.5137/1019-5149.JTN.17462-16.2 Received: 01.03.2016 / Accepted: 20.04.2016 Published Online: 23.08.2016 Original Investigation Fleece-Bound Tissue Sealing in Microvascular Decompression Levent TANRIKULU
DOI: 10.5137/1019-5149.JTN.17462-16.2 Received: 01.03.2016 / Accepted: 20.04.2016 Published Online: 23.08.2016 Original Investigation Fleece-Bound Tissue Sealing in Microvascular Decompression Levent TANRIKULU
Iatrogenic lumbar Pseudomeningocele: A case report and review of literature
 Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
Evaluation of efficacy and biocompatibility of a novel semisynthetic collagen matrix as a dural onlay graft in a large animal model
 Acta Neurochir (2011) 153:2241 2250 DOI 10.1007/s00701-011-1059-5 EXPERIMENTAL RESEARCH Evaluation of efficacy and biocompatibility of a novel semisynthetic collagen matrix as a dural onlay graft in a
Acta Neurochir (2011) 153:2241 2250 DOI 10.1007/s00701-011-1059-5 EXPERIMENTAL RESEARCH Evaluation of efficacy and biocompatibility of a novel semisynthetic collagen matrix as a dural onlay graft in a
Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience
 80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
Adult - Cerebrovascular. Adult - Cranio-Cervical Junction. Adult - Epilepsy. Adult - Hydrocephalus
 list for SET and IMG Neurosurgery Adult - Cerebrovascular Aneurysm - Clipping: Anterior circulation Aneurysm - Clipping: Posterior circulation AVM excision Carotid endarterectomy Carotid trapping Cavernoma
list for SET and IMG Neurosurgery Adult - Cerebrovascular Aneurysm - Clipping: Anterior circulation Aneurysm - Clipping: Posterior circulation AVM excision Carotid endarterectomy Carotid trapping Cavernoma
CSF Rhinorrhoea after Transsphenoidal Surgery
 ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 CSF Rhinorrhoea after Transsphenoidal Surgery E Elgamal Citation E Elgamal. CSF Rhinorrhoea after Transsphenoidal Surgery. The Internet
ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 CSF Rhinorrhoea after Transsphenoidal Surgery E Elgamal Citation E Elgamal. CSF Rhinorrhoea after Transsphenoidal Surgery. The Internet
MANAGEMENT OF CSF. Steven D. Schaefer, MD, FACS. Department of Otolaryngology New York Eye and Ear Infirmary
 MANAGEMENT OF CSF RHINORRHEA, MENIGIOCELES, Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York Eye and Ear Infirmary New York Medical College Anatomy and Physiology
MANAGEMENT OF CSF RHINORRHEA, MENIGIOCELES, Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York Eye and Ear Infirmary New York Medical College Anatomy and Physiology
Skullbase Lesions. Skullbase Surgery Open vs endoscopic. Choice Of Surgical Approaches 12/28/2015. Skullbase Surgery: Evolution
 Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
PRO-DENSE BONE GRAFT SUBSTITUTE
 PRO-DENSE BONE GRAFT SUBSTITUTE 152917-0 The following languages are included in this packet: For additional languages, visit our website www.wright.com. Then click on the option. For additional information
PRO-DENSE BONE GRAFT SUBSTITUTE 152917-0 The following languages are included in this packet: For additional languages, visit our website www.wright.com. Then click on the option. For additional information
Surgical Neurology International
 Surgical Neurology International OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: James I. Ausman, MD, PhD University of California, Los Angeles, CA, USA Original
Surgical Neurology International OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor: James I. Ausman, MD, PhD University of California, Los Angeles, CA, USA Original
Guidelines in the management of neural tube defects and hydrocephalus
 Guidelines in the management of neural tube defects and hydrocephalus Dominic Venne, MD, MSc, FRCSC, Division of Neurosurgery Sheikh Khalifa Medical City Abu Dhabi, UAE 1. Introduction: Neural tube defects
Guidelines in the management of neural tube defects and hydrocephalus Dominic Venne, MD, MSc, FRCSC, Division of Neurosurgery Sheikh Khalifa Medical City Abu Dhabi, UAE 1. Introduction: Neural tube defects
Integra. TenoGlide Tendon Protector Sheet SURGICAL TECHNIQUE
 Integra TenoGlide Tendon Protector Sheet SURGICAL TECHNIQUE Table of Contents Description...2 Indications...2 Contraindications...2 Surgical Technique...4 Step 1 Surgical Approach...4 Step 2 Remove TenoGlide
Integra TenoGlide Tendon Protector Sheet SURGICAL TECHNIQUE Table of Contents Description...2 Indications...2 Contraindications...2 Surgical Technique...4 Step 1 Surgical Approach...4 Step 2 Remove TenoGlide
doi: /j.issn
 19 34 20150820 Chinese Journal of Tissue Engineering Research August 20, 2015 Vol.19, No.34 ( 830002) 1 12 2 (XYDCX2014185) 2008 6 2013 6 2 266 126 5.56% 12 () 12 12 2472 h 48 h 812 d 9.5 d 2 714 d 3 1981
19 34 20150820 Chinese Journal of Tissue Engineering Research August 20, 2015 Vol.19, No.34 ( 830002) 1 12 2 (XYDCX2014185) 2008 6 2013 6 2 266 126 5.56% 12 () 12 12 2472 h 48 h 812 d 9.5 d 2 714 d 3 1981
CURRICULUM VITAE. SPR in Neurosurgery North Thames Rotation Scheme. 1. Royal Free Hospital RFH ( ; 18 months ) Specialist Registrar
 CURRICULUM VITAE Name Title Present Position Address : -Jesus Lafuente : -MD, FRCSEd, PhD : -CONSULTANT NEUROSURGEON : -HOSPÌTAL DEL MAR PASEO MARITIMO 23 BARCELONA 08003 E-mail : jlbspine@gmail.com Phone
CURRICULUM VITAE Name Title Present Position Address : -Jesus Lafuente : -MD, FRCSEd, PhD : -CONSULTANT NEUROSURGEON : -HOSPÌTAL DEL MAR PASEO MARITIMO 23 BARCELONA 08003 E-mail : jlbspine@gmail.com Phone
Surgical dural tears: Prevalence and updated management protocol based on 1359 lumbar vertebra interventions
 Orthopaedics & Traumatology: Surgery & Research (2012) 98, 879 886 Available online at www.sciencedirect.com ORIGINAL ARTICLE Surgical dural tears: Prevalence and updated management protocol based on 1359
Orthopaedics & Traumatology: Surgery & Research (2012) 98, 879 886 Available online at www.sciencedirect.com ORIGINAL ARTICLE Surgical dural tears: Prevalence and updated management protocol based on 1359
Pichayen Duangthongpon MD*, Chaiwit Thanapaisal MD*, Amnat Kitkhuandee MD*, Kowit Chaiciwamongkol MD**, Vilaiwan Morthong MD**
 The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
Neurosurgery Review. Mudit Sharma, MD May 16 th, 2008
 Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN
 A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
Middle Turbinate Mucosal Flap in Endoscopic Skull Base Reconstruction
 DOI: 10.5137/1019-5149.JTN.6250-12.0 Received: 30.03.2012 / Accepted: 14.05.2012 Original Investigation Middle Turbinate Mucosal Flap in Endoscopic Skull Base Reconstruction Xuejian WANG, Xiaobiao Zhang,
DOI: 10.5137/1019-5149.JTN.6250-12.0 Received: 30.03.2012 / Accepted: 14.05.2012 Original Investigation Middle Turbinate Mucosal Flap in Endoscopic Skull Base Reconstruction Xuejian WANG, Xiaobiao Zhang,
Lyoplant Onlay. Adding another layer of confidence to every procedure. Aesculap Neurosurgery
 Adding another layer of confidence to every procedure Aesculap Neurosurgery Adding another layer of confidence to every procedure For more than 140 years, Aesculap Neurosurgery has developed products that
Adding another layer of confidence to every procedure Aesculap Neurosurgery Adding another layer of confidence to every procedure For more than 140 years, Aesculap Neurosurgery has developed products that
ORIGINAL ARTICLE. Choice of Graft Material and Postoperative Healing in Endoscopic Repair of Cerebrospinal Fluid Leak
 ONLINE FIRST ORIGINAL ARTICLE Choice of Material and Postoperative Healing in Endoscopic Repair of Cerebrospinal Fluid Leak Kara K. Prickett, MD; Sarah K. Wise, MD; John M. DelGaudio, MD Objective: To
ONLINE FIRST ORIGINAL ARTICLE Choice of Material and Postoperative Healing in Endoscopic Repair of Cerebrospinal Fluid Leak Kara K. Prickett, MD; Sarah K. Wise, MD; John M. DelGaudio, MD Objective: To
NovoSorb BTM. A unique synthetic biodegradable wound scaffold. Regenerating tissue. Changing lives.
 NovoSorb BTM A unique synthetic biodegradable wound scaffold Regenerating tissue. Changing lives. Overview NovoSorb BTM is a unique synthetic biodegradable wound scaffold that delivers good cosmetic and
NovoSorb BTM A unique synthetic biodegradable wound scaffold Regenerating tissue. Changing lives. Overview NovoSorb BTM is a unique synthetic biodegradable wound scaffold that delivers good cosmetic and
POSTOPERATIVE CHRONIC SUBDURAL HEMATOMA FOLLOWING CLIP- PING SURGERY
 Nagoya postoperative Med. J., chronic subdural hematoma after aneurysmal clipping 13 POSTOPERATIVE CHRONIC SUBDURAL HEMATOMA FOLLOWING CLIP- PING SURGERY TAKAYUKI OHNO, M.D., YUSUKE NISHIKAWA, M.D., KIMINORI
Nagoya postoperative Med. J., chronic subdural hematoma after aneurysmal clipping 13 POSTOPERATIVE CHRONIC SUBDURAL HEMATOMA FOLLOWING CLIP- PING SURGERY TAKAYUKI OHNO, M.D., YUSUKE NISHIKAWA, M.D., KIMINORI
CSF Leaks. Abnormal communication between the subarachnoid space and the tympanomastoid space or nasal cavity. Presenting symptoms:
 CSF Leaks Steven Wright, M.D. Faculty Advisor: Matthew Ryan, M.D. The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation January 5, 2005 CSF Leaks Abnormal communication
CSF Leaks Steven Wright, M.D. Faculty Advisor: Matthew Ryan, M.D. The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation January 5, 2005 CSF Leaks Abnormal communication
RapidSorb Resorbable Tacks. Resorbable Fixation System.
 RapidSorb Resorbable Tacks. Resorbable Fixation System. Fast Safe Resorbable Drill Press Fixed Table of Contents Introduction Overview 2 Indications and Contraindications 4 RapidSorb 5 Surgical Technique
RapidSorb Resorbable Tacks. Resorbable Fixation System. Fast Safe Resorbable Drill Press Fixed Table of Contents Introduction Overview 2 Indications and Contraindications 4 RapidSorb 5 Surgical Technique
Surgical Privileges Form: "Neurosurgery" Clinical Privileges Request. Requested (To be completed by the applicant) Not Recommended (For committee use)
 Surgical Form: Clinical Request "Neurosurgery" Applicant s Name:. License No. (If Any):... Date:... Scope of Practice:. Facility:.. Place of Work:. the applicant) CATEGORY I: Core : 1. Interpretation of
Surgical Form: Clinical Request "Neurosurgery" Applicant s Name:. License No. (If Any):... Date:... Scope of Practice:. Facility:.. Place of Work:. the applicant) CATEGORY I: Core : 1. Interpretation of
Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery
 Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery The Review Committee has made the following changes to the CPT code mappings: The following previously untracked CPT codes
Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery The Review Committee has made the following changes to the CPT code mappings: The following previously untracked CPT codes
Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma
 Open Access Case Report DOI: 10.7759/cureus.2217 Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma Abdurrahman Raeiq 1 1.
Open Access Case Report DOI: 10.7759/cureus.2217 Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma Abdurrahman Raeiq 1 1.
Neurosurgical Techniques
 Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Over one hundred years ago Hans Chiari first published
 J Neurosurg Pediatrics 8:000 000, 8:177 183, 2011 Complications following decompression of Chiari malformation Type I in children: dural graft or sealant? Clinical article Stephen R. Parker, M.D., M.P.H.,
J Neurosurg Pediatrics 8:000 000, 8:177 183, 2011 Complications following decompression of Chiari malformation Type I in children: dural graft or sealant? Clinical article Stephen R. Parker, M.D., M.P.H.,
Utilizing real-time contrast medium to detect the fistula of giant spinal arachnoid cyst and treat with minimal invasive surgery
 Ying et al. BMC Surgery (2019) 19:11 https://doi.org/10.1186/s12893-019-0475-y CASE REPORT Open Access Utilizing real-time contrast medium to detect the fistula of giant spinal arachnoid cyst and treat
Ying et al. BMC Surgery (2019) 19:11 https://doi.org/10.1186/s12893-019-0475-y CASE REPORT Open Access Utilizing real-time contrast medium to detect the fistula of giant spinal arachnoid cyst and treat
Surgical management of diastatic linear skull fractures in infants
 Surgical management of diastatic linear skull fractures in infants JOHN B. THOMPSON, M.D., THOMAS H. MASON, M.D., GERALD L. HAINES, M.D., AND ROBERT J. CASSIDY, M.D. Divisions of Neurosurgery and Neurology,
Surgical management of diastatic linear skull fractures in infants JOHN B. THOMPSON, M.D., THOMAS H. MASON, M.D., GERALD L. HAINES, M.D., AND ROBERT J. CASSIDY, M.D. Divisions of Neurosurgery and Neurology,
Ventricles, CSF & Meninges. Steven McLoon Department of Neuroscience University of Minnesota
 Ventricles, CSF & Meninges Steven McLoon Department of Neuroscience University of Minnesota 1 Coffee Hour Thursday (Sept 14) 8:30-9:30am Surdyk s Café in Northrop Auditorium Stop by for a minute or an
Ventricles, CSF & Meninges Steven McLoon Department of Neuroscience University of Minnesota 1 Coffee Hour Thursday (Sept 14) 8:30-9:30am Surdyk s Café in Northrop Auditorium Stop by for a minute or an
Brain Meninges, Ventricles and CSF
 Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
External Ventricular Drainage & Lumbar Drainage Procedure and Care. Amey R. Savardekar Assistant Professor Neurosurgery, NIMHANS.
 External Ventricular Drainage & Lumbar Drainage Procedure and Care. Amey R. Savardekar Assistant Professor Neurosurgery, NIMHANS. External Ventricular Drain Indications: Therapeutic (To relieve raised
External Ventricular Drainage & Lumbar Drainage Procedure and Care. Amey R. Savardekar Assistant Professor Neurosurgery, NIMHANS. External Ventricular Drain Indications: Therapeutic (To relieve raised
While performing cranial surgery, it is of utmost
 J Neurosurg 121:735 744, 2014 AANS, 2014 Risk factors for postoperative CSF leakage after elective craniotomy and the efficacy of fleece-bound tissue sealing against dural suturing alone: a randomized
J Neurosurg 121:735 744, 2014 AANS, 2014 Risk factors for postoperative CSF leakage after elective craniotomy and the efficacy of fleece-bound tissue sealing against dural suturing alone: a randomized
Idiopathic cervical syringomyelia can be associated. Pediatric Chiari malformation Type 0: a 12-year institutional experience.
 J Neurosurg J Neurosurg Pediatrics Pediatrics 8:000 000, 8:1 5, 2011 Pediatric Chiari malformation Type 0: a 12-year institutional experience Clinical article Joshua J. Chern, M.D., Ph.D., Amber J. Gordon,
J Neurosurg J Neurosurg Pediatrics Pediatrics 8:000 000, 8:1 5, 2011 Pediatric Chiari malformation Type 0: a 12-year institutional experience Clinical article Joshua J. Chern, M.D., Ph.D., Amber J. Gordon,
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts
 Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
SURGICAL PROCEDURES OPERATIONS ON THE NERVOUS SYSTEM
 98100 Hypothermia - when employed, basic fee for any procedure on nervous system... 25 25 BRAIN Astrocytoma, oligodendroglioma, glioblastoma or metastatic tumour Craniotomy plus excision 98130 - supratentorial...
98100 Hypothermia - when employed, basic fee for any procedure on nervous system... 25 25 BRAIN Astrocytoma, oligodendroglioma, glioblastoma or metastatic tumour Craniotomy plus excision 98130 - supratentorial...
The Management of Cerebrospinal Fluid Leak After Anterior Cervical Decompression Surgery. Copyrighted Material
 The Management of Cerebrospinal Fluid Leak After Anterior Cervical Decompression Surgery Jiliang Zhai, MD; Ripul R. Panchal, DO; Ye Tian, MD; Shujie Wang, PhD; Lijuan Zhao, RN abstract Cerebrospinal fluid
The Management of Cerebrospinal Fluid Leak After Anterior Cervical Decompression Surgery Jiliang Zhai, MD; Ripul R. Panchal, DO; Ye Tian, MD; Shujie Wang, PhD; Lijuan Zhao, RN abstract Cerebrospinal fluid
Minimally invasive subpial tonsillectomy for Chiari I decompression
 Acta Neurochir (2016) 158:1807 1811 DOI 10.1007/s00701-016-2877-2 HOW I DO IT - NEUROSURGICAL TECHNIQUES Minimally invasive subpial tonsillectomy for Chiari I decompression Jeffrey S. Beecher 1 Yong Liu
Acta Neurochir (2016) 158:1807 1811 DOI 10.1007/s00701-016-2877-2 HOW I DO IT - NEUROSURGICAL TECHNIQUES Minimally invasive subpial tonsillectomy for Chiari I decompression Jeffrey S. Beecher 1 Yong Liu
Two-Stage Management of Mega Occipito Encephalocele
 Two-Stage Management of Mega Occipito Encephalocele CASE REPORT A I Mardzuki*, J Abdullah**, G Ghazaime*, A R Ariff!'*, M Ghazali* *Department of Neurosciences, **Department of Radiology, Hospital Universiti
Two-Stage Management of Mega Occipito Encephalocele CASE REPORT A I Mardzuki*, J Abdullah**, G Ghazaime*, A R Ariff!'*, M Ghazali* *Department of Neurosciences, **Department of Radiology, Hospital Universiti
OHSU Neurological Surgery Education. Neurosurgical Basics. Copyright Oregon Health & Science University Department of Neurological Surgery
 OHSU Neurological Surgery Education Neurosurgical Basics Chapter 1 Basic Principles: Cranial Three-Point Head Fixation Proper and safe application of a three-point rigid cranial fixation device provides
OHSU Neurological Surgery Education Neurosurgical Basics Chapter 1 Basic Principles: Cranial Three-Point Head Fixation Proper and safe application of a three-point rigid cranial fixation device provides
Unilateral extended suboccipital approach for a C1 dumbbell schwanoma
 38 Gorgan et al Unilateral extended suboccipital approach for a C1 dumbbell schwanoma Unilateral extended suboccipital approach for a C1 dumbbell schwanoma R.M. Gorgan, Angela Neacşu, A. Giovani Clinical
38 Gorgan et al Unilateral extended suboccipital approach for a C1 dumbbell schwanoma Unilateral extended suboccipital approach for a C1 dumbbell schwanoma R.M. Gorgan, Angela Neacşu, A. Giovani Clinical
Management of Cerebrospinal Fluid Leaks
 Management of Cerebrospinal Fluid Leaks J Trauma. 2001;51:S29 S33. I. RECOMMENDATIONS A. Standards The available data are not sufficient to support a treatment Standard for management of cerebrospinal
Management of Cerebrospinal Fluid Leaks J Trauma. 2001;51:S29 S33. I. RECOMMENDATIONS A. Standards The available data are not sufficient to support a treatment Standard for management of cerebrospinal
DMF Page 63. Description
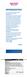 DMF Page 60 DMF Page 61 DMF Page 62 4 GB Description The SPONGOSTAN Absorbable Haemostatic Gelatin Powder is a sterile, water-insoluble, porcine gelatin absorbable powder intended for haemostatic use by
DMF Page 60 DMF Page 61 DMF Page 62 4 GB Description The SPONGOSTAN Absorbable Haemostatic Gelatin Powder is a sterile, water-insoluble, porcine gelatin absorbable powder intended for haemostatic use by
Bone flap preservation in abdominal wall after decompressive craniectomy in head injury: A single institute experience
 DOI: 10.2478/romneu-2018-0063 Article Bone flap preservation in abdominal wall after decompressive craniectomy in head injury: A single institute experience Pavan Kumar, Ashok Kumar, Gaurav Jaiswal, Tarun
DOI: 10.2478/romneu-2018-0063 Article Bone flap preservation in abdominal wall after decompressive craniectomy in head injury: A single institute experience Pavan Kumar, Ashok Kumar, Gaurav Jaiswal, Tarun
Integra. PriMatrix Dermal Repair Scaffold PATIENT INFORMATION. Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1
 Integra PriMatrix Dermal Repair Scaffold PATIENT INFORMATION Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Your Path to Recovery Your health care provider has chosen to use
Integra PriMatrix Dermal Repair Scaffold PATIENT INFORMATION Questions? Contact us: Clinician: Phone #: In case of emergency, dial 9-1-1 Your Path to Recovery Your health care provider has chosen to use
PRO-DENSE Bone Graft Substitute The following languages are included in this packet:
 EN PRO-DENSE Bone Graft Substitute 133486-11 The following languages are included in this packet: English (en) For additional languages, visit our website www.wmt.com Then click on the Prescribing Information
EN PRO-DENSE Bone Graft Substitute 133486-11 The following languages are included in this packet: English (en) For additional languages, visit our website www.wmt.com Then click on the Prescribing Information
Results of Surgery of Cerebellopontine angle Tumors
 Original Article Iranian Journal of Otorhinolaryngology, Vol. 27(1), Serial No.78, Jan 2015 Abstract Results of Surgery of Cerebellopontine angle Tumors Faramarz Memari 1, * Fatemeh Hassannia 1, Seyed
Original Article Iranian Journal of Otorhinolaryngology, Vol. 27(1), Serial No.78, Jan 2015 Abstract Results of Surgery of Cerebellopontine angle Tumors Faramarz Memari 1, * Fatemeh Hassannia 1, Seyed
Spontaneous intracranial hypotension syndrome with extracranial vein dilatation
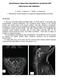 Spontaneous intracranial hypotension syndrome with extracranial vein dilatation C. Heine 1, H. Altinova 1, T. Pietilä 1, LC Stavrinou 1 1. Department of Neurosurgery, Evangelical Hospital Bielefeld, Germany
Spontaneous intracranial hypotension syndrome with extracranial vein dilatation C. Heine 1, H. Altinova 1, T. Pietilä 1, LC Stavrinou 1 1. Department of Neurosurgery, Evangelical Hospital Bielefeld, Germany
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Cerebrospinal fluid leaks are a significant concern
 Neurosurg Focus 32 (6):E8, 2012 Repair of middle fossa cerebrospinal fluid leaks using a novel combination of materials: technical note Cedric D. Shorter, M.D., 1 David E. Connor Jr., D.O., 1 Jai Deep
Neurosurg Focus 32 (6):E8, 2012 Repair of middle fossa cerebrospinal fluid leaks using a novel combination of materials: technical note Cedric D. Shorter, M.D., 1 David E. Connor Jr., D.O., 1 Jai Deep
Pedicled Nasoseptal Flap as Final Layer of Reconstruction for Skull Base Defects
 Med. J. Cairo Univ., Vol. 79, No. 2, June: 123-128, 2011 www.medicaljournalofcairouniversity.com Pedicled Nasoseptal Flap as Final Layer of Reconstruction for Skull Base Defects SAMEH M. AMIN, M.D.*; AHMED
Med. J. Cairo Univ., Vol. 79, No. 2, June: 123-128, 2011 www.medicaljournalofcairouniversity.com Pedicled Nasoseptal Flap as Final Layer of Reconstruction for Skull Base Defects SAMEH M. AMIN, M.D.*; AHMED
Department of Neurological Surgery
 Department of Neurological Surgery CAT 1 A Basic Privileges: Patient management, including H & Ps and diagnostic and therapeutic treatments, procedures and interventions, Requiring a level of training
Department of Neurological Surgery CAT 1 A Basic Privileges: Patient management, including H & Ps and diagnostic and therapeutic treatments, procedures and interventions, Requiring a level of training
Case Report Primary Dural Repair in Minimally Invasive Spine Surgery
 Case Reports in Medicine Volume 2013, Article ID 876351, 6 pages http://dx.doi.org/10.1155/2013/876351 Case Report Primary Dural Repair in Minimally Invasive Spine Surgery Raqeeb M. Haque, Sohaib Z. Hashmi,
Case Reports in Medicine Volume 2013, Article ID 876351, 6 pages http://dx.doi.org/10.1155/2013/876351 Case Report Primary Dural Repair in Minimally Invasive Spine Surgery Raqeeb M. Haque, Sohaib Z. Hashmi,
INSTRUCTIONS FOR USE FOR:
 INSTRUCTIONS FOR USE FOR: en English INSTRUCTIONS FOR USE GORE ENFORM PREPERITONEAL BIOMATERIAL Carefully read all instructions prior to use. Observe all instructions, warnings, and precautions noted throughout.
INSTRUCTIONS FOR USE FOR: en English INSTRUCTIONS FOR USE GORE ENFORM PREPERITONEAL BIOMATERIAL Carefully read all instructions prior to use. Observe all instructions, warnings, and precautions noted throughout.
Rotational Pericranial Flap for Repair of Refractory Posterior Fossa
 Rotational Pericranial Flap for Repair of Refractory Posterior Fossa Pseudomeningocele Rajiv Saigal 1, Arnau Benet 2, William Hoffman 3, Lawrence R. Lustig 4, Steven W. Cheung 4, Michael McDermott 5 Corresponding
Rotational Pericranial Flap for Repair of Refractory Posterior Fossa Pseudomeningocele Rajiv Saigal 1, Arnau Benet 2, William Hoffman 3, Lawrence R. Lustig 4, Steven W. Cheung 4, Michael McDermott 5 Corresponding
GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D.
 J Neurosurg 47:590-595, 1977 Subgaleal shunt for temporary ventricle decompression and subdural drainage GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D. Division of Neurological Surgery, University of Iowa
J Neurosurg 47:590-595, 1977 Subgaleal shunt for temporary ventricle decompression and subdural drainage GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D. Division of Neurological Surgery, University of Iowa
Unintended durotomy during degenerative lumbar spine surgery (Incidence and management)
 Original Article Unintended durotomy during degenerative lumbar spine surgery * Ali T. AbdulWahid** Ammar Salah*** FRCS MBChB, FIBMS MBChB, FIBMS Fac Med Baghdad 2014 Vol.56, No.4 Received: Sept., 2014
Original Article Unintended durotomy during degenerative lumbar spine surgery * Ali T. AbdulWahid** Ammar Salah*** FRCS MBChB, FIBMS MBChB, FIBMS Fac Med Baghdad 2014 Vol.56, No.4 Received: Sept., 2014
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Pediatric Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Pediatric Neurosurgery Pediatric neurosurgeons
Introduction to Neurosurgical Subspecialties: Pediatric Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Pediatric Neurosurgery Pediatric neurosurgeons
/ 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66
 1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
1425 / 66 / 66 nano-hydroxyapatite/polyamide-66 n-ha/pa66 2011 1 10 20 n-ha/pa66 8 12 22 80 51 1 24 4 L 4 5 8 L 5 S 1 9 L 4 S 1 3 3 5 9 3 X CT Oswestry ODI SF-36 20 6 9 7 3 d 3 6 P < 0.01P > 0.05 3 9 4
Peri-Radicular Fibrosis After Lumbar Surgery: Is There Any Help?
 Research Article imedpub Journals http://www.imedpub.com Spine Research DOI: 10.21767/2471-8173.100002 Peri-Radicular Fibrosis After Lumbar Surgery: Is There Any Help? Iñaki Arrotegui Department of Neurosurgery,
Research Article imedpub Journals http://www.imedpub.com Spine Research DOI: 10.21767/2471-8173.100002 Peri-Radicular Fibrosis After Lumbar Surgery: Is There Any Help? Iñaki Arrotegui Department of Neurosurgery,
Cranial Postoperative Site: MR Imaging Appearance
 27 Cranial Postoperative Site: MR Imaging Appearance Charles F. Lanzieri1 Mark Larkins2 Andrew Mancall 1 Ronald Lorig 1 Paul M. Duchesneau 1 Scott A. Rosenbloom 1 Meredith A. Weinstein 1 The ability to
27 Cranial Postoperative Site: MR Imaging Appearance Charles F. Lanzieri1 Mark Larkins2 Andrew Mancall 1 Ronald Lorig 1 Paul M. Duchesneau 1 Scott A. Rosenbloom 1 Meredith A. Weinstein 1 The ability to
Application Guide for Full-Thickness Wounds
 Application Guide for Full-Thickness Wounds PriMatrix Dermal Repair Scaffold PriMatrix Ag Antimicrobial Dermal Repair Scaffold Application Guide for Full Thickness Wounds PriMatrix is a unique dermal repair
Application Guide for Full-Thickness Wounds PriMatrix Dermal Repair Scaffold PriMatrix Ag Antimicrobial Dermal Repair Scaffold Application Guide for Full Thickness Wounds PriMatrix is a unique dermal repair
Revision Surgery for Vestibular Schwannomas
 528 Original Article Kevin A. Peng 1 Brian S. Chen 3 Mark B. Lorenz 2 Gregory P. Lekovic 1 Marc S. Schwartz 1 William H. Slattery 1 Eric P. Wilkinson 1 1 House Clinic, Los Angeles, California, United States
528 Original Article Kevin A. Peng 1 Brian S. Chen 3 Mark B. Lorenz 2 Gregory P. Lekovic 1 Marc S. Schwartz 1 William H. Slattery 1 Eric P. Wilkinson 1 1 House Clinic, Los Angeles, California, United States
Ossification of the posterior longitudinal ligament
 Neurosurg Focus 30 (3):E13, 2011 Management of cerebrospinal fluid leaks after anterior decompression for ossification of the posterior longitudinal ligament: a review of the literature Marcus Mazur, M.D.,
Neurosurg Focus 30 (3):E13, 2011 Management of cerebrospinal fluid leaks after anterior decompression for ossification of the posterior longitudinal ligament: a review of the literature Marcus Mazur, M.D.,
Nature and Science 2017;15(7) Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus
 Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus Mohamed Mahmoud Abohashima; Ahmed Mohamed Hasan Salem; Magdy Asaad El-Hawary Neurosurgery department, Faculty of Medicine, Al-azhar
Surgical Options for Treatment of Posterior Fossa Tumors with Hydrocephalus Mohamed Mahmoud Abohashima; Ahmed Mohamed Hasan Salem; Magdy Asaad El-Hawary Neurosurgery department, Faculty of Medicine, Al-azhar
Analysing the Effect of Early Acetazolamide Administration on Patients with A High Risk of Permanent Cerebrospinal Fluid Leakage
 ORIGINAL REPORT Analysing the Effect of Early Acetazolamide Administration on Patients with A High Risk of Permanent Cerebrospinal Fluid Leakage Saeid Abrishamkar, Nima Khalighinejad, and Payam Moein Department
ORIGINAL REPORT Analysing the Effect of Early Acetazolamide Administration on Patients with A High Risk of Permanent Cerebrospinal Fluid Leakage Saeid Abrishamkar, Nima Khalighinejad, and Payam Moein Department
Original Article Incidental Durotomy during Lumbar Spine Surgery: Management and Complications. A Retrospective Review
 Egyptian Journal of Neurosurgery Volume 3 / No. 2 / April June 206 9-24 Original Article Incidental Durotomy during Lumbar Spine Surgery: Management and Complications. A Retrospective Review Shafik El
Egyptian Journal of Neurosurgery Volume 3 / No. 2 / April June 206 9-24 Original Article Incidental Durotomy during Lumbar Spine Surgery: Management and Complications. A Retrospective Review Shafik El
Pathologies, Procedures and Room Set-Up
 Pathologies, Procedures and Room Set-Up Degenerative diseases - arthritis, osteoperosis Most common cause for neck pain and back pain Herniated disks or bulging disk Commonly occur at L4-5, L5-S1 Spinal
Pathologies, Procedures and Room Set-Up Degenerative diseases - arthritis, osteoperosis Most common cause for neck pain and back pain Herniated disks or bulging disk Commonly occur at L4-5, L5-S1 Spinal
Case Report Gigant Transethmoidal Meningoencephalocele Operated by Full Endonasal Endoscopic Approach: Case Report
 Case Reports in Medicine Volume 2012, Article ID 763259, 4 pages doi:10.1155/2012/763259 Case Report Gigant Transethmoidal Meningoencephalocele Operated by Full Endonasal Endoscopic Approach: Case Report
Case Reports in Medicine Volume 2012, Article ID 763259, 4 pages doi:10.1155/2012/763259 Case Report Gigant Transethmoidal Meningoencephalocele Operated by Full Endonasal Endoscopic Approach: Case Report
Risk factors for Ventriculoperitoneal shunting in children with posterior fossa tumor
 Risk factors for Ventriculoperitoneal shunting in children with posterior fossa tumor Raed M Aljubour, MD *, Ahmed K Alomari, MD*, Awni F Musharbash, MD** ABSTRACT Objectives: To investigate the Predictors
Risk factors for Ventriculoperitoneal shunting in children with posterior fossa tumor Raed M Aljubour, MD *, Ahmed K Alomari, MD*, Awni F Musharbash, MD** ABSTRACT Objectives: To investigate the Predictors
Technique Guide. SynPOR Porous Polyethylene Implants. For craniofacial and orbital augmentation and reconstruction.
 Technique Guide SynPOR Porous Polyethylene Implants. For craniofacial and orbital augmentation and reconstruction. Table of Contents Introduction SynPOR Porous Polyethylene Implants 2 Indications and Contraindications
Technique Guide SynPOR Porous Polyethylene Implants. For craniofacial and orbital augmentation and reconstruction. Table of Contents Introduction SynPOR Porous Polyethylene Implants 2 Indications and Contraindications
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Antonio De la Cruz, MD 27th Alexandria International Combined ORL Congress Alexandria, Egypt April 8, 2009
 ACOUSTIC NEUROMA TREATMENT OPTIONS 2009 27 th Alexandria International Combined ORL Congress Alexandria, Egypt April 10, 2009 AntonioDelaCruz Cruz, MD House Ear Institute Los Angeles, California Antonio
ACOUSTIC NEUROMA TREATMENT OPTIONS 2009 27 th Alexandria International Combined ORL Congress Alexandria, Egypt April 10, 2009 AntonioDelaCruz Cruz, MD House Ear Institute Los Angeles, California Antonio
DuraMatrix portfolio. Restore with confidence
 DuraMatrix portfolio Restore with confidence History Since 2003, Stryker has partnered with Collagen Matrix, Inc. to provide our customers with quality products that are safe and effective in the restoration
DuraMatrix portfolio Restore with confidence History Since 2003, Stryker has partnered with Collagen Matrix, Inc. to provide our customers with quality products that are safe and effective in the restoration
Incidental durotomy during spine surgery occurs in. Computed tomography guided epidural patching of postoperative cerebrospinal fluid leaks
 J Neurosurg Spine 21:805 810, 2014 AANS, 2014 Computed tomography guided epidural patching of postoperative cerebrospinal fluid leaks Clinical article Frank Mihlon, M.D., Peter G. Kranz, M.D., Andreia
J Neurosurg Spine 21:805 810, 2014 AANS, 2014 Computed tomography guided epidural patching of postoperative cerebrospinal fluid leaks Clinical article Frank Mihlon, M.D., Peter G. Kranz, M.D., Andreia
Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan
 Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Occipital flattening in the infant skull
 Occipital flattening in the infant skull Kant Y. Lin, M.D., Richard S. Polin, M.D., Thomas Gampper, M.D., and John A. Jane, M.D., Ph.D. Departments of Plastic Surgery and Neurological Surgery, University
Occipital flattening in the infant skull Kant Y. Lin, M.D., Richard S. Polin, M.D., Thomas Gampper, M.D., and John A. Jane, M.D., Ph.D. Departments of Plastic Surgery and Neurological Surgery, University
