Safety and efficacy of a novel polyethylene glycol hydrogel sealant for watertight dural repair
|
|
|
- Shauna Robertson
- 5 years ago
- Views:
Transcription
1 J Neurosurg 106:52 58, 2007 Safety and efficacy of a novel polyethylene glycol hydrogel sealant for watertight dural repair G. REES COSGROVE, M.D., F.R.C.S.C., 1 JOHNNY B. DELASHAW, M.D., 2 J. ANDRE GROTENHUIS, M.D., PH.D., 3 JOHN M. TEW, M.D., 4 HARRY VAN LOVEREN, M.D., 5 ROBERT F. SPETZLER, M.D., 6 TROY PAYNER, M.D., 7 GAIL ROSSEAU, M.D., 8 MARK E. SHAFFREY, M.D., 9 L. NELSON HOPKINS, M.D., 10 RICHARD BYRNE, M.D., 11 AND ALEX NORBASH, M.D Massachusetts General Hospital, Boston, Massachusetts; 2 Oregon Health Sciences University, Portland, Oregon; 3 Radboud University Medical Center, Nijmegen, The Netherlands; 4 University of Cincinnati, Mayfield Clinic, Cincinnati, Ohio; 5 University of South Florida, Tampa General Hospital, Tampa, Florida; 6 Barrow Neurological Institute, Phoenix, Arizona; 7 Indianapolis Neurosurgical Group, Inc., Indianapolis, Indiana; 8 Chicago Institute of Neurosurgery and Neuroresearch, Chicago, Illinois; 9 University of Virginia Health Systems, Charlottesville, Virginia; 10 Department of Neurosurgery, Millard Fillmore Gates Circle Hospital, University at Buffalo, New York; 11 Rush University Medical Center, Chicago, Illinois; and 12 Boston Medical Center, Boston, Massachusetts Object. The authors prospectively evaluated the safety and efficacy of a novel polyethylene glycol (PEG) hydrogel sealant in patients undergoing elective cranial surgery with documented cerebrospinal fluid (CSF) leakage after sutured dural repair. Methods. The PEG hydrogel sealant was used at 11 different study sites in 111 patients with documented intraoperative CSF leakage after neurosurgical dural repair for a variety of conditions. Intraoperative CSF leakage was either spontaneous or induced by a Valsalva maneuver. Patients were monitored for 3 months postoperatively with physical examinations, clinical laboratory analyses, and diagnostic imaging. The PEG hydrogel sealant was 100% effective in stopping CSF leakage in all patients. There were no sealant-related adverse events and all clinical outcomes were consistent with expectations for seriously ill patients undergoing prolonged neurosurgical procedures. Conclusions. The PEG hydrogel sealant provides a safe and effective watertight closure when used as an adjunct to sutured dural repair during cranial surgery. KEY WORDS cerebrospinal fluid leak craniectomy craniotomy dural defect repair polyethelene glycol hydrogel sealant C EREBROSPINAL fluid leakage is one of the most challenging and potentially dangerous complications of cranial surgery. Despite advances in neurosurgical techniques and the development of adjunctive methods to repair dura mater defects, the incidence of postoperative CSF leaks after cranial procedures performed using the infratentorial or supratentorial approaches can be as high as 10 to 27%. 5,10,11,31,38 A metaanalysis of 14 studies documented a postoperative CSF leakage incidence of 10.6% after resection of vestibular schwannomas using suboccipital, translabyrinthine, or middle cranial fossa approaches. 35 In another study in which CT scanning was used to evaluate postoperative subcutaneous and/or subgaleal fluid collections, investigators found the incidence of CSF leakage to be as high as 42%. 6 A true watertight seal in neurosurgery remains an elusive goal despite meticulous dura mater closure, 13,17,40,41 because Abbreviations used in this study: CSF = cerebrospinal fluid; CT = computed tomography; FDA = Food and Drug Administration; PEG = polyethylene glycol. the holes produced by surgical needles preclude a completely watertight repair that can withstand significant intracranial pressure changes. 1,9,21 If the quality of dural closure is improved, complications associated with CSF leakage, including meningitis, pseudomeningoceles, impaired wound healing, and subgaleal fluid collection, could be reduced. 8,37 In several studies, a watertight dural closure prevented CSF leakage and significantly decreased the postoperative occurrence of both positional headaches and pseudomeningoceles. 1,24,27 Effectively sealing dural incisions during surgery is therefore important because it may prevent CSF leakage and related complications. 9,12 Current methods of dural repair include interrupted sutures (possibly using duraplasty to cover significant dural gaps), adhesives, hemostatic agents, and other preparations not specifically approved by the US FDA for dural sealing. In contrast, the PEG hydrogel sealant used in this study was specifically developed to provide a watertight closure as an adjunct to standard methods of dural repair. The PEG hydrogel sealant system involves spraying a synthetic, biocompatible, tissue-adherent PEG hydrogel onto sutured dural incisions to prevent CSF leakage. 52 J. Neurosurg. / Volume 106 / January, 2007
2 Polyethylene glycol hydrogel sealant in CSF leakage We present results from an FDA investigational device exemption study in which we evaluated the safety and effectiveness of a novel hydrogel sealant as an adjunct to sutured dural repair during cranial surgery. The primary efficacy endpoint was to prevent intraoperative CSF leaks after sutured dural repair. The safety evaluation included three months of postoperative monitoring for CSF leaks and adverse events as noted by neurological evaluations, laboratory data, and CT studies. Clinical Material and Methods Study Design This study was a prospective, multicenter, single-arm clinical investigation of patients who underwent elective cranial surgery. Study inclusion criteria included adult patients undergoing elective cranial Class I (clean wound) procedures according to Centers for Disease Control and Prevention criteria. Patients who had undergone prior surgery in the same area, planned penetration of air sinus or mastoid cells, or prior or planned chemotherapy or radiation therapy, or who had preexisting hydrocephalus, external ventricular shunts or drains, preexisting infection, a compromised immune system, uncontrolled diabetes, or renal or hepatic dysfunction were excluded. The respective institutional review boards approved the study at each site, and informed consent was obtained from all patients. Preoperative baseline evaluations were performed within 2 weeks of surgery. Intraoperative inclusion criteria included the inability to create a watertight primary sutured closure due to a spontaneous CSF leak or a leak induced by Valsalva maneuver; a total durotomy equal to or longer than 2 cm; dural margins greater than 3 mm or more from the edges of bone; and a Class I (clean) wound. Patients with dural gaps wider than 2 mm after durotomy closure and those who required synthetic or nonautologous duraplasty materials were excluded. A single-arm study was undertaken because an acceptable control treatment was unavailable, as determined by the FDA. The inclusion of a standard of care control group would have resulted in a heterogeneous population, thus compromising the ability to pool the data. Eligible patients with documented CSF leakage after sutured dural repair were treated with the PEG hydrogel sealant (DuraSeal, Confluent Surgical, Inc., Waltham, MA). After the PEG hydrogel sealant had been applied, patients were assessed for intraoperative CSF leakage from the repaired dura during Valsalva maneuvers that produced average pressures of 20 cm H 2 O for 5 to 10 seconds. If CSF leakage persisted, a second coating of PEG hydrogel sealant was applied and the Valsalva maneuver was repeated. Patients were allowed only two PEG hydrogel applications. If CSF leakage persisted after the second application, conventional management of the leakage was to be instituted at the surgeon s discretion. The wounds were closed in layers according to each institution s standard practice. Subgaleal or subfascial drains were placed by the surgeon as deemed necessary. Prophylactic antibiotic therapy was administered during surgery, and a postoperative course of dexamethasone was prescribed to limit inflammation and swelling. Patients were examined postoperatively within 7 days or at discharge, at 6 weeks ( 2 weeks), and at 3 months ( 2 weeks). J. Neurosurg. / Volume 106 / January, 2007 Safety assessments included the incidence of CSF leaks within 3 months after surgery, as determined by the need for surgical intervention to treat a CSF leak or pseudomeningocele, diagnostic evidence of CSF leakage, or clinical evaluation, including a physical examination of the surgical site. Additional safety assessments included the incidence of adverse events and adverse sealant-related events revealed by physical examination, diagnostic laboratory tests, and neurological assessments (including pain and disability). Adverse events were defined as unfavorable and unintended signs (including abnormal laboratory findings), symptoms, or disease occurring during the study, regardless of its relation to the sealant. Adverse events were classified as mild, moderate, or severe. A Clinical Events Committee of three board-certified neurosurgeons independently reviewed adverse events. Baseline CT images were reviewed for informational purposes, whereas images at the 7-day and 3-month followup examinations were compared to identify evidence of subgaleal or extradural fluid collection and any other clinically significant findings. An image marker (calibrator reference) was printed on all CT scans to provide a perspective of size to the reviewing radiologist, and calipers were used to measure extradural thickness. Using the initial ( 7 days) postoperative CT image, the thickest portion of the hypoattenuating sealant bed was measured and compared with the corresponding anatomical location at the 3-month follow up, when complete hydrogel absorption was expected. 30 Three board-certified neuroradiologists independently reviewed the CT scans. Patient Population Of the 132 patients who met enrollment criteria, 21 patients failed to meet the intraoperative eligibility criteria, and therefore 111 patients (76 women, 35 men; mean age 49 years, range years) were treated with the PEG hydrogel sealant. A majority of patients (53%) were either current smokers or had a history of smoking. A significant percentage of patients had high ( II) American Society of Anesthesiologists Physical Status scores (87% II, 33% III), indicating a large number of patients had severe systemic diseases and comorbidities. The most common indications for surgery included resection of malignant or benign tumors (46%), microvascular decompression (18.9%), aneurysms (10.8%), epilepsy (9%), arteriovenous malformations (6.3%), and Chiari malformations (5.4%). These 111 patients constituted the population from which baseline data were derived and safety evaluations performed. A total of 11 separate centers participated, with an average enrollment of 10 patients per center (median seven patients). Sealant Operation and Mechanism The sealant is provided as a single prepackaged unit with two syringes containing a PEG diluent and a trilysine amine solution, a vial containing end-modified PEG powder with Food, Drugs & Cosmetics Blue No. 1, and a spraying device. To prepare the sealant, the diluent is injected into the powder vial, and the dissolved PEG/dye combination is drawn into the diluent syringe. When mixed, the PEG/dye and amine solutions polymerize to form a strong hydrogel within 2 seconds without detectable heat evolution and without external energy sources. These solutions are simul- 53
3 G. R. Cosgrove et al. taneously sprayed onto the dura mater, where they polymerize to form an adherent and flexible hydrogel sealant capable of withstanding elevated CSF pressure. The PEG hydrogel sealant can be stored at room temperature and can be prepared in 1 to 2 minutes. The blue dye in the dilution helps determine sealant coverage and thickness. The hydrogel retains strength while the dura mater heals and gradually hydrolyzes after 8 weeks. The hydrogel breakdown products, including the PEG molecules, are absorbed and cleared by the kidneys. The synthetic nature of the sealant eliminates any potential for viral transmission or sensitization to animal-derived products. All investigators were thoroughly trained in the use of the DuraSeal system. Statistical Methods Data from all 11 investigative sites were combined because the surgery site was not predictive of key safety or effectiveness parameters, as demonstrated by the ability to pool analyses. All clinically relevant variables were tabulated using descriptive statistics. Categorical variables were summarized using frequencies and percentages. For select variables, Clopper Pearson exact 95% confidence intervals were generated. The Wilcoxon signed-rank test was used to determine statistically significant differences in neurological assessments between baseline and each follow-up visit. The Stuart Maxwell test was used to determine statistically significant differences in clinical laboratory evaluations between baseline and each follow-up visit. Statistical tests were performed using SAS statistical software (Version 8.0; SAS Institute, Cary, NC). Regression analyses were used to create models for predicting pre- and perioperative risk factors associated with postoperative infection. Univariate logistic regression analyses were performed on independent variables to identify clinically important or predictive factors. Multiple regression analyses were then conducted (using either a joint or forward selection technique) in which variables suggested by the univariate analysis (p 0.07) were eligible for inclusion. Surgical Procedures Results A craniotomy was performed in 90 patients (81%), and a craniectomy was performed in 21 patients (19%). The location of the neurological procedure was infratentorial in 53 patients (48%) and supratentorial in 58 patients (52%). The suboccipital surgical approach was used most frequently (41%), followed by the temporal (18%) and frontal (10%) approaches. The mean length of the durotomy was 7.0 cm (range cm). Autologous duraplasty materials were used in 50 patients (45%), most commonly muscle (22%) and then fascia (14%) and pericranium (10%). The mean duration of surgery (the time between skin incision and closure) was 232 minutes (median 205 minutes, range minutes). The duration of surgery was prolonged for a significant proportion of patients; in 38% of patients at least 4 hours was required to complete the surgery and in 92% at least 2 hours was required. Drains were placed in 18% of patients. Sealant Application Following the primary dural suture closure, a spontaneous CSF leak occurred in 67 (60%) of the 111 patients. The remaining 44 patients (40%) required a Valsalva maneuver to generate a CSF leak. The mean pressure achieved during the baseline Valsalva maneuver was 21.4 cm H 2 O (range cm H 2 O). A single PEG hydrogel sealant application was effective in obtaining a watertight closure in 105 patients (95%). Persistent leakage after initial application was present in six patients (5%); one leak (0.9%) was spontaneous, and five (4.5%) were induced by the Valsalva maneuver. All six patients (100%) were treated successfully with a second hydrogel application and did not have a CSF leak after a subsequent Valsalva maneuver. The number of kits used per patient ranged from one to three (median 1 kit). The mean volume of sealant used in the first application was 4.2 ml (range ml). The mean volume of sealant used in the second application was 3.1 ml (range ml). The combined mean total volume of hydrogel sealant used was 4.4 ml (range ml). At the time of sealant application, 95% of the surgeons rated the sealant device as easy or very easy to use. Sealant Efficacy By design, all patients enrolled in the study demonstrated either a spontaneous intraoperative CSF leak or a Valsalva maneuver-induced leak after primary suture closure. After a maximum of two sealant applications no intraoperative CSF leaks were apparent during subsequent Valsalva maneuvers. The PEG hydrogel sealant was therefore 100% effective in creating watertight closures, where none existed previously. Sealant Safety Wound Healing. In the early postoperative period, most patients had some expected local swelling at the incision site. At the 6-week examination, the swelling had resolved in 81% of the patients, and at the 3-month examination, the wounds of all 107 patients (100%) remaining in the study were healed. Postoperative CSF Leaks. Postoperative CSF incisional leaks occurred in one (0.9%) of 111 patients, whereas pseudomeningoceles requiring surgical intervention occurred in three (2.7%) of 111 patients. There were no signs of CSF leaks in 106 (95.5%) of the patients (95% confidence interval %). For the five patients with CSF leakage (incisional or pseudomeningocele), the time to first leakage ranged from 7 to 29 days. All CSF leaks were diagnosed within 4 weeks of surgery. Cerebrospinal fluid rhinorrhea or otorrhea was not observed. The rate of incisional CSF leakage for all infratentorial incisions was 1.9% (one of 53 patients), and was 1.7% (one of 58 patients) for supratentorial incisions. All incisional leaks and pseudomeningoceles were treated successfully by percutaneous aspiration, oversuturing, temporary external drains, permanent internal shunts, or a combination of these procedures. Computed Tomography Scanning. The CT scans obtained in 17 of the 111 patients treated with the PEG hydrogel sealant could not be evaluated comprehensively because the examination was incomplete, the patient was lost to follow up, there was unusual or tangential positioning of the craniotomy site relative to the CT-scan axis precluding orthogonal 54 J. Neurosurg. / Volume 106 / January, 2007
4 Polyethylene glycol hydrogel sealant in CSF leakage measurement of the surgical site, or the bone flap had been removed between the postoperative and follow-up scans. The mean immediate postoperative sealant-bed thickness was 5.7 mm, with a mean follow-up thickness of 1.4 mm at 3 months. Thus, the net reduction of the sealant-bed thickness after the 3-month period averaged 4.3 mm, or 75.4% of the original sealant-bed thickness (Fig. 1). Adverse Events. One patient died of progression of metastatic melanoma 85 days after surgery, and another died of intractable cerebral edema following resection of a glioblastoma multiforme 30 days after surgery. Both deaths were determined by the principal investigator to have been unrelated to the sealant. Two other patients were lost to follow up. At no time during the study did unanticipated adverse events related to the PEG hydrogel sealant occur. The majority (88%) of patients reported that the adverse events were not severe. The serious adverse events included deep infections of the surgical site (7.2%); postoperative fever (5.4%); stroke, cerebrovascular aneurysm, or cerebral hemorrhage (4.5%); cerebral edema (3.6%); hydrocephalus (3.6%); and bacterial meningitis (1.8%). A review of all adverse events by the independent Clinical Events Committee showed that the adverse events were consistent with the patient comorbidities and the nature of the procedures, and were not associated with the PEG hydrogel sealant. A forward multiple logistic regression analysis was performed for deep surgical site infections, evaluating only the independent variables demonstrated by univariate analysis to possibly be associated with infection (p 0.07 based on univariate methods). These variables included the volume of sealant, duration of surgery, length of durotomy, use of intraoperative shunts or drains, and smoking status. Smoking (p = 0.022) and duration of surgery (p = 0.042) were independent predictors for infection. All eight patients with deep wound infections underwent procedures that lasted more than 2 hours, and six of the eight patients (75%) underwent surgeries that lasted longer than 4 hours. Seven of the eight patients (88%) were smokers or had a recent history of smoking, and six patients (75%) had wound drains, incidental sinus penetration, or both. Discussion J. Neurosurg. / Volume 106 / January, 2007 Obtaining a watertight dural closure is a primary objective of neurosurgical practice. Failure to do so often leads to complications related to CSF leaks including meningitis, poor wound healing, and pseudomeningoceles. Primary sutured dural repairs can leak even when using optimal surgical techniques, especially during posterior fossa procedures. Any adjuvant method that can provide a watertight dural closure would be advantageous and desired. Various substances such as fibrin glue, hemostatic agents, and cyanoacrylates have been used for a watertight dural closure but none are currently approved by the FDA for this indication. The PEG hydrogel sealant used in this study seems ideally suited to its task as it is nonbiological and therefore does not transmit viruses. The sealant is biocompatible (and therefore does not interfere with healing), absorbable, flexible, and strongly adherent to tissue. The PEG hydrogel sealant was 100% effective in sealing intraoperative CSF leaks. There were no sealant-related adverse events, and all clinical outcomes were consistent with expectations for seriously ill patients undergoing prolonged neurosurgical procedures. Eight patients (7.2%) experienced deep surgical site infections, and two (1.8%) postoperative incisional CSF leaks. The absence of a uniform standard of care precluded an acceptable control group and forced the design to be a single-arm study. Therefore, relevant literature must be considered to place both the clinical results and the adverse event rates in perspective. Cerebrospinal Fluid Leaks In the present study, a postoperative incisional CSF leak developed in one (1.9%) of the 53 patients with an infratentorial incision and in one (1.7%) of the 58 patients with a supratentorial incision. Both patients had a recent history of hydrocephalus. The treating investigator acknowledged later that the hydrocephalus in the patient with an infratentorial incision was ongoing at the time of the procedure. Three patients had a pseudomeningocele (2.7%) that required surgical intervention. These results compare favorably with the 4 to 30% reported incidence of postoperative CSF leaks in other large surgical series. 19,28,35 In several studies, the development of CSF leaks has been related to the location of the dural incision. Most authors have indicated that CSF leaks develop most frequently in the dependent portion of the skull base region or posterior fossa, 16,34 whereas CSF leaks are relatively uncommon after surgery in supratentorial regions. For example, the incidence of CSF leakage ranges from 15 to 28% in posterior fossa procedures. 20 Sawaya and coworkers 33 used multivariate analysis to establish that major regional complications including CSF leakage were almost six times more likely to occur in infratentorial procedures (Table 1) than in supratentorial procedures (odds ratio 5.84). To explore the relationship of CSF leakage to a location in the dura, we compared the postoperative leakage incidence for infratentorial and supratentorial incisions. In this study the 1.9% incidence of infratentorial incisional leaks compares favorably to those in published reports in which the average is 12 to 14% and as high as 27%. 24,36 In the present study, no CSF leaks followed procedures for vestibular schwannomas. This finding compares favorably with the results of a metaanalysis of acoustic neuroma procedures in which investigators found that leaks occurred in 10.6% of suboccipital, 9.5% of translabyrinthine, and 10.6% of middle cranial fossa surgical procedures (overall rate, 10.6%). 35 Kumar and colleagues 16 prospectively evaluated the use of a bioadhesive as a dural sealant to prevent CSF leakage during 167 craniotomies performed for a variety of reasons, including tumor resection, cyst fenestration, microvascular decompression, and aneurysmal clip placement. Postsurgical CSF leaks, described as fistulas, occurred in two (1.2%) of 167 patients. In the present study we also found two (1.8%) CSF fistulas in 111 patients. A further comparison with the study conducted by Kumar et al. is limited because those authors did not strictly define the diagnosis of CSF leakage and their patients were only followed up once postoperatively after 6 weeks. However, the leakage incidences were similar despite the higher prevalence of infratentorial procedures in the present study (48%) compared with 32% in the study of Kumar, et al. Bejjani and colleagues 4 presented the results of a prospective multicenter evaluation of a dural substitute material in 55
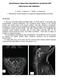
5 G. R. Cosgrove et al. FIG. 1. Computed tomography scans obtained in a 38-year-old woman after resection of a right parietal tumor. The space occupied by the PEG hydrogel sealant can be seen 2 days after surgery (left). At 3 months the extradural void has collapsed (right) due to hydrogel absorption. 51 patients treated primarily for Chiari malformations and tumors. A suboccipital approach was used in 72% of patients. Shunts or drainage catheters were placed in approximately 10% of patients. Apparently fibrin sealant was used to seal the dura in about 30% of patients. The incidence of CSF leakage was 2%, although leakage was not defined. Whether pseudomeningoceles were included in the leakage rate is unknown. Follow up was 1 month or less in 15 of the 51 patients. A report by von Wild 39 provided results of a multicenter evaluation of a dural substitute material in 101 patients undergoing supratentorial (75 patients), infratentorial (20 patients), or thoracic (6 patients) spinal operations. This trial is similar to the present study with respect to the number and type of patients, the clinical diagnosis of leaks, and the distinction between CSF fistulas and CSF leaks. The overall incidence of CSF leakage in the von Wild report (12.9%) was significantly greater than that observed in the present study when pseudomeningocele and incisional leak rates are combined (4.5%, p 0.05, one-tailed Fisher exact test), even though most (75%) of their procedures were supratentorial. Sawamura and coworkers 32 reviewed the surgical records of 509 patients who underwent supratentorial craniotomies, in which 295 patients were treated with a fibrin sealant spray and 214 with other methods of fibrin application. The incidences of postoperative CSF leakage in the two groups were 3.1 and 8.9%, respectively. Although CSF leakage was not defined, all 9 instances of CSF leakage in the fibrin spray group were treated by a subcutaneous needle aspiration with a compression bandage or by lumbar drainage. Additional published reports have focused on specific pathological conditions that represent subsets of patients in the present study. Levy and colleagues 18 reported an 8% CSF leakage incidence (6% leaks and 2% pseudomeningoceles requiring treatment) in 50 children who underwent minicraniotomy for fenestration of temporal arachnoid cysts. In an evaluation by Sarma et al. 31 CSF leaks occurred in 10.9% of patients undergoing primarily frontotemporal or temporal craniotomies for treatment of nonvestibular schwannomas. Eisenberg and coworkers 7 reported a CSF leakage rate of 7.5% (all requiring treatment) in 40 patients undergoing resection of various benign nonmeningeal tumors of the cavernous sinus, primarily using a supratentorial approach. In the present study, 21 patients underwent craniectomies. In this patient subset, no postoperative CSF leak or pseudomeningocele developed. This incidence rate is much smaller than that observed by Gnanalingham and coworkers, 11 who found the incidence of postoperative CSF leakage after craniectomy to be 27%, with 19.6% of the patients experiencing a pseudomeningocele. In summary, the incidence of CSF leaks in the present study is low compared with those cited in published retrospective and prospective reports involving similar procedures, patients, and CSF leakage definitions. Surgical Site Infection In this study, eight patients (7.2%) experienced a deep surgical site infection. Similar to the incidence of postoperative CSF leaks, the only meaningful comparisons of postoperative infection rates are among comparable patients undergoing comparable procedures. A meaningful comparison can be made between the present study and one of the largest prospective studies of neurosurgery-related sepsis. As reported by Narotam and colleagues, neurosurgical patients were evaluated for postoperative infections. Patients were monitored for sepsis 56 J. Neurosurg. / Volume 106 / January, 2007
6 Polyethylene glycol hydrogel sealant in CSF leakage TABLE 1 Reported incidences of CSF leakage following posterior fossa surgery* Authors No. of Focus of CSF Leak & Year Patients Evaluation Rate (%) Patir & Banerji, 179 PF tumors 17.2 (overall) 1990 (9.2 for CSF leaks, 8.0 for pseudomeningocele) Cristante et al., 26 CM-I via suboc cipital craniotomy Narotam et al., 67 not specifically de scribed Anson & 13 various lesions (me- 7.7 Marchand, ningioma, CM-I, 1996 TN) Matthies et al., 134 PF meningiomas re lated to the CPA Vanaclocha & 26 CM-I, cadaveric dura 15.3 for cadaveric dura Saiz-Sapena, vs occipital pericra- group, 0 for occipital 1997 nium & fibrin cranium & fibrin sealant sealant group Manley & 339 PF craniotomies 5.6 Dillon, 2000 Munshi et al., 23 CM-I Alzate et al., 66 CM-I, duraplasty w/ DuraGuard Gnanalingham 84 PF tumors 16.0 et al., 2003 * The CSF leak rates were calculated from the referenced papers based on the CSF leak definition used in the current protocol. Abbreviations: CM-I = Chiari malformation Type I; CPA = cerebellopontine angle; PF = posterior fossa; TN = trigeminal neuralgia. J. Neurosurg. / Volume 106 / January, 2007 postoperatively until discharge, for 4 weeks after surgery (if the patient remained in the hospital), or when the patient returned for follow-up visits. The definition of surgical site infection was based on Centers for Disease Control and Prevention criteria, but the authors also characterized the types of implants (shunts, drains, or other objects in place for more than 24 hours) and surgery lasting longer than 2 hours, which was then classified as clean contaminated. The infection rate strongly correlated with the duration of the surgical procedure in the study of Narotam and colleagues. 26 The infection rate for clean surgery lasting more than 4 hours was 13.4%. In contrast, the infection rate for 2- to 4-hour clean surgery was 5.6%. The rate for clean surgery with an implanted foreign body (including wound drains) was 6%. Finally, the rate for clean surgery (exclusion of all known factors that influence sepsis) was 0.8%. 26 These results are similar to data from the study performed by Korinek, 15 in which the infection rate was 32.5% for patients with surgery lasting longer than 4 hours and the overall infection rate was 4.0%. A similar correlation between the incidence of infection and prolonged surgery was observed in the present study, as noted in the results. Known risk factors were abundant in patients in whom infections in this study developed. Most of the investigational sites were teaching hospitals to which a surgical population requiring complex and prolonged surgical procedures was referred. When compared with surgical procedures of a similar complexity in similar patients, the infection rate in this study is consistent with expected rates from the literature. Computed Tomography Scanning Immediately after surgery the PEG hydrogel sealant was hypointense on CT imaging, reflecting its high water content ( 90%). These results are consistent with those of preclinical studies in which this product was evaluated using magnetic resonance and CT imaging in a canine craniotomy model. 14 The average cranial space occupied by the sealant decreased from 5.7 mm immediately after surgery to 1.4 mm at 3 months. The sealant is reabsorbed within 8 weeks, 30 and therefore the thickness measured at 3 months is probably a combination of thickened dura and fibrous tissue that filled the void as the sealant was absorbed. These findings support claims of sealant absorption within several months. Conclusions In patients with demonstrated CSF leaks after sutured dural closure, the novel PEG hydrogel sealant used in this study provided a 100% watertight seal in all patients. The exceptionally low overall postoperative incidence of incisional CSF leakage (1.8%), combined with the 0% leak incidence in craniectomies, supports the hypothesis that intraoperative suture line sealing with this PEG hydrogel sealant should decrease the incidence of postoperative CSF leakage. When compared with data from published reports of postoperative CSF leakage among comparable patients and procedures (supratentorial and infratentorial approaches), the results of this study show that the sealant provided a substantial benefit by preventing postoperative CSF leaks after elective craniotomy and craniectomy. Based on the data presented, DuraSeal provides a safe and effective watertight closure when used as an adjunct to sutured dural repair during cranial surgery. Disclosure All investigative sites were provided with grant support from Confluent Surgical, Inc. Dr. Robert Spetzler held a significant equity interest in Confluent Surgical at the time of the study. Craig Van Horne, M.D., Kai Frerichs, M.D., and Robert Friedlander, M.D. served as paid consultants to Confluent Surgical, Inc., as members of the Clinical Events Committee. The three neuroradiologists who reviewed CT images Russell A. Blinder, M.D., Amir A. Zamani, M.D., and Alex Norbash, M.D. served as paid consultants to Confluent Surgical, Inc., for these services. Dr. Norbash was also employed as a company scientific advisor. All financial interest information was submitted to the FDA. References 1. Adams CB: I ve torn it: how to repair it. Br J Neurosurg 9: , Alzate JC, Kothbauer KF, Jallo GI, Epstein FJ: Treatment of Chiari I malformation in patients with and without syringomyelia: a consecutive series of 66 patients. Neurosurg Focus 11(3):E3, Anson JA, Marchand EP: Bovine pericardium for dural grafts: clinical results in 35 patients. Neurosurgery 39: ,
7 G. R. Cosgrove et al. 4. Bejjani GK, Maroon JC, Bost J: DURASIS: a novel dural substitute. Results of a multi-center study. 12th European Congress of Neurosurgery: September 7 12, 2003, Lisbon, Portugal. Bologna, Italy: Medimond SRL, 2003, pp Cristante L, Westphal M, Herrmann HD: Cranio-cervical decompression for Chiari I malformation. A retrospective evaluation of functional outcome with particular attention to the motor deficits. Acta Neurochir (Wien) 130:94 100, Dolenc VV: Comment in Yoshimoto T, Sawamura Y, Houkin K, Abe H: Effectiveness of fibrin glue for preventing postoperative extradural fluid leakage. Neurol Med Chir (Tokyo) 37: 889, Eisenberg MB, Al-Mefty O, DeMonte F, Burson GT: Benign nonmeningeal tumors of the cavernous sinus. Neurosurgery 44: , Eismont FJ, Wiesel SW, Rothman RH: Treatment of dural tears associated with spinal surgery. J Bone Joint Surg Am 63: , Foyt D, Johnson JP, Kirsch AJ, Bruce JN, Wazen JJ: Dural closure with laser tissue welding. Otolaryngol Head Neck Surg 115: , Gnanalingham KK, Lafuente J, Thompson D, Harkness W, Hayward R: MRI study of the natural history and risk factors for pseudomeningocele formation following postfossa surgery in children. Br J Neurosurg 17: , Gnanalingham KK, Lafuente J, Thompson D, Harkness W, Hayward R: Surgical procedures for posterior fossa tumors in children: does craniotomy lead to fewer complications than craniectomy? J Neurosurg 97: , Hadley MN, Martin NA, Spetzler RF, Sonntag VKH, Johnson PC: Comparative transoral dural closure techniques: a canine model. Neurosurgery 22: , Hughes GB, Glassock ME III, Hays JW, Jackson CG, Sismanis A: Cerebrospinal fluid leaks and meningitis following acoustic tumor surgery. Otolaryngol Head Neck Surg 90: , Kacher DF, Frerichs K, Pettit J, Campbell PK, Meunch T, Norbash AM: DuraSeal magnetic resonance and computed tomography imaging: evaluation in a canine craniotomy model. Neurosurgery 58 (Suppl 1): , Korinek AM: Risk factors for neurosurgical site infections after craniotomy: a prospective multicenter study of 2944 patients. The French Study Group of Neurosurgical Infections, the SEHP, and the C-CLIN Paris-Nord. Service Epidemiologie Hygiene et Prevention. Neurosurgery 41: , Kumar A, Maartens NF, Kaye AH: Evaluation of the use of BioGlue in neurosurgical procedures. J Clin Neurosci 10: , Lebowitz RA, Hoffman RA, Roland JT Jr, Cohen NL: Autologous fibrin glue in the prevention of cerebrospinal fluid leak following acoustic neuroma surgery. Am J Otol 16: , Levy ML, Wang M, Aryan HE, Yoo K, Meltzer H: Microsurgical keyhole approach for middle fossa arachnoid cyst fenestration. Neurosurgery 53: , Magliulo G, Sepe C, Varacalli S, Fusconi M: Cerebrospinal fluid leak management following cerebellopontine angle surgery. J Otolaryngol 27: , Manley GT, Dillon W: Acute posterior fossa syndrome following lumbar drainage for treatment of suboccipital pseudomeningocele. Report of three cases. J Neurosurg 92: , Marks P, Koskuba D: Use of a non-penetrating staple device for spinal dural closure. Br J Neurosurg 14:468, Matthies C, Carvalho G, Tatagiba M, Lima M, Samii M: Meningiomas of the cerebellopontine angle. Acta Neurochir Suppl 65: 86 91, Munshi I, Frim D, Stine-Reyes R, Weir BK, Hekmatpanah J, Brown F: Effects of posterior fossa decompression with and without duraplasty on Chiari malformation-associated hydromyelia. Neurosurgery 46: , Muszynski CA, Laurent JP, Cheek WR: Effects of ventricular drainage and dural closure on cerebrospinal fluid leaks after posterior fossa tumor surgery. Pediatr Neurosurg 21: , Narotam PK, van Dellen JR, Bhoola KD: A clinicopathological study of collagen sponge as a dural graft in neurosurgery. J Neurosurg 82: , Narotam PK, van Dellen JR, du Trevou MD, Gouws E: Operative sepsis in neurosurgery: a method of classifying surgical cases. Neurosurgery 34: , Nistor RF, Chiari FM, Maier H, Hehl K: The fixed combination of collagen with components of fibrin adhesive a new hemostyptic agent in skull based procedures. Skull Base Surg 7:23 30, Nutik SL, Korol HW: Cerebrospinal fluid leak after acoustic neuroma surgery. Surg Neurol 43: , Patir R, Banerji AK: Complications related to pre-craniotomy shunts in posterior fossa tumors. Br J Neurosurg 4: , Preul MC, Bichard WD, Spetzler RF: Toward optimal tissue sealants for neurosurgery: use of a novel hydrogel sealant in a canine durotomy repair model. Neurosurgery 53: , Sarma S, Sekhar LN, Schessel DA. Nonvestibular schwannomas of the brain: a 7-year experience. Neurosurgery 50: , Sawamura Y, Asaoka K, Terasaka S, Tada M, Uchida T: Evaluation of application techniques of fibrin sealant to prevent cerebrospinal fluid leakage: a new device for the application of aerosolized fibrin glue. Neurosurgery 44: , Sawaya R, Hammoud M, Schoppa D, Hess KR, Wu SZ, Shi WM, et al: Neurosurgical outcomes in a modern series of 400 craniotomies for treatment of parenchymal tumors. Neurosurgery 42: , Schwaber MK, Netterville JL, Coniglio JU: Complications of skull base surgery. Ear Nose Throat J 70: , Selesnick SH, Liu JC, Jen A, Newman J: The incidence of cerebrospinal fluid leak after vestibular schwannoma surgery. Otol Neurotol 25: , Valtonen HJ, Poe DS, Heilman CB, Tarlov EC: Endoscopically assisted prevention of cerebrospinal fluid leak and suboccipital acoustic neuroma surgery. Am J Otol 18: , Van Calenbergh F, Quintens E, Sciot R, Van Loon J, Gofin J, Plets C: The use of Vicryl Collagen as a dura substitute: a clinical review of 78 surgical cases. Acta Neurochir (Wien) 139: , Vanaclocha V, Saiz-Sapena N: Duraplasty with freeze-dried cadaveric dura versus occipital pericranium for Chiari type I malformation: comparative study. Acta Neurochir (Wien) 139: , von Wild KR: Examination of the safety and efficacy of an absorbable dura matter substitute (Dura Patch) in normal applications in neurosurgery. Surg Neurol 52: , Yasui N: Comment in Yoshimoto T, Sawamura Y, Houkin K, Abe H: Effectiveness of fibrin glue for preventing postoperative extradural fluid leakage. Neurol Med Chir (Tokyo) 37: , Yoshimoto T, Sawamura Y, Houkin K, Abe H: Effectiveness of fibrin glue for preventing postoperative extradural fluid leakage. Neurol Med Chir (Tokyo) 37: , 1997 Manuscript received March 7, Accepted in final form May 17, This paper was presented at the Congress of Neurological Surgeons 55th Annual Meeting, Boston, Massachusetts, October 8 13, Address reprint requests to: G. Rees Cosgrove, M.D., Department of Neurosurgery, Lahey Medical Center, 41 Mall Road, Burlington, Massachusetts g.rees.cosgrove@lahey.org. 58 J. Neurosurg. / Volume 106 / January, 2007
Application of a hydrogel sealant improves watertight closures of duraplasty onlay grafts in a canine craniotomy model
 J Neurosurg 107:642 650, 2007 Application of a hydrogel sealant improves watertight closures of duraplasty onlay grafts in a canine craniotomy model MARK C. PREUL, M.D., 1 PATRICK K. CAMPBELL, PH.D., 2
J Neurosurg 107:642 650, 2007 Application of a hydrogel sealant improves watertight closures of duraplasty onlay grafts in a canine craniotomy model MARK C. PREUL, M.D., 1 PATRICK K. CAMPBELL, PH.D., 2
Management of Cerebrospinal Fluid Leaks After Vestibular Schwannoma Surgery
 Otology & Neurotology 32:1525Y1529 Ó 2011, Otology & Neurotology, Inc. Management of Cerebrospinal Fluid Leaks After Vestibular Schwannoma Surgery *Brannon D. Mangus, *Alejandro Rivas, Mi Jin Yoo, JoAnn
Otology & Neurotology 32:1525Y1529 Ó 2011, Otology & Neurotology, Inc. Management of Cerebrospinal Fluid Leaks After Vestibular Schwannoma Surgery *Brannon D. Mangus, *Alejandro Rivas, Mi Jin Yoo, JoAnn
After a great surgery, why leave anything to chance?
 HyperBranch Medical Technology, Inc. creates innovative medical devices using synthetic hydrogels with novel tunable properties for use as surgical sealants in general and specialty surgery. The products
HyperBranch Medical Technology, Inc. creates innovative medical devices using synthetic hydrogels with novel tunable properties for use as surgical sealants in general and specialty surgery. The products
The Incidence of Cerebrospinal Fluid Leak after Vestibular Schwannoma Surgery
 Otology & Neurotology 25:387 393 2004, Otology & Neurotology, Inc. The Incidence of Cerebrospinal Fluid Leak after Vestibular Schwannoma Surgery Samuel H. Selesnick, Jeffrey C. Liu, Albert Jen, and Jason
Otology & Neurotology 25:387 393 2004, Otology & Neurotology, Inc. The Incidence of Cerebrospinal Fluid Leak after Vestibular Schwannoma Surgery Samuel H. Selesnick, Jeffrey C. Liu, Albert Jen, and Jason
Restoration not just repair
 DURAGEN ENGLISH Restoration not just repair r e g e n e r at i v e t e c h n o l o g y PRODUCTS FOR SALE IN EUROPE, MIDDLE-EAST and AFRICA ONLY. More than a graft DuraGen is a matrix for repair of the
DURAGEN ENGLISH Restoration not just repair r e g e n e r at i v e t e c h n o l o g y PRODUCTS FOR SALE IN EUROPE, MIDDLE-EAST and AFRICA ONLY. More than a graft DuraGen is a matrix for repair of the
Iatrogenic lumbar Pseudomeningocele: A case report and review of literature
 Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
Available online at Available online at: www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2016, 5, 1:153-157 Iatrogenic lumbar Pseudomeningocele: A case report
DuraMatrix Collagen Dura Substitute Membrane. Manufactured by: Collagen Matrix, Inc., Franklin Lakes, New Jersey
 DuraMatrix Collagen Dura Substitute Membrane Manufactured by: Collagen Matrix, Inc., Franklin Lakes, New Jersey What is DuraMatrix? Onlay or Sutured Implantation Balanced Implant Resorption vs. Host Tissue
DuraMatrix Collagen Dura Substitute Membrane Manufactured by: Collagen Matrix, Inc., Franklin Lakes, New Jersey What is DuraMatrix? Onlay or Sutured Implantation Balanced Implant Resorption vs. Host Tissue
Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma
 Open Access Case Report DOI: 10.7759/cureus.2217 Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma Abdurrahman Raeiq 1 1.
Open Access Case Report DOI: 10.7759/cureus.2217 Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma Abdurrahman Raeiq 1 1.
Durotomies with CSF leakage are one of the most
 CASE REPORT J Neurosurg Spine 28:181 185, 2018 A novel duraplasty technique following fenestration of a massive lumbar arachnoid cyst in a patient with scoliosis: technical case report Matthew T. Neal,
CASE REPORT J Neurosurg Spine 28:181 185, 2018 A novel duraplasty technique following fenestration of a massive lumbar arachnoid cyst in a patient with scoliosis: technical case report Matthew T. Neal,
Neurosurgery is complex. DuraGen is the simple choice.
 Neurosurgery is complex. is the simple choice. Family of Grafts Dural Regeneration Matrix Keep Closure Simple. A Breakthrough in Dural Repair A Pioneer in Dural Regeneration Matrices For almost forty years,
Neurosurgery is complex. is the simple choice. Family of Grafts Dural Regeneration Matrix Keep Closure Simple. A Breakthrough in Dural Repair A Pioneer in Dural Regeneration Matrices For almost forty years,
Fleece-Bound Tissue Sealing in Microvascular Decompression
 DOI: 10.5137/1019-5149.JTN.17462-16.2 Received: 01.03.2016 / Accepted: 20.04.2016 Published Online: 23.08.2016 Original Investigation Fleece-Bound Tissue Sealing in Microvascular Decompression Levent TANRIKULU
DOI: 10.5137/1019-5149.JTN.17462-16.2 Received: 01.03.2016 / Accepted: 20.04.2016 Published Online: 23.08.2016 Original Investigation Fleece-Bound Tissue Sealing in Microvascular Decompression Levent TANRIKULU
Results of Surgery of Cerebellopontine angle Tumors
 Original Article Iranian Journal of Otorhinolaryngology, Vol. 27(1), Serial No.78, Jan 2015 Abstract Results of Surgery of Cerebellopontine angle Tumors Faramarz Memari 1, * Fatemeh Hassannia 1, Seyed
Original Article Iranian Journal of Otorhinolaryngology, Vol. 27(1), Serial No.78, Jan 2015 Abstract Results of Surgery of Cerebellopontine angle Tumors Faramarz Memari 1, * Fatemeh Hassannia 1, Seyed
5.5. RETROSIGMOID APPROACH
 5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
SURGICAL PROCEDURES OPERATIONS ON THE NERVOUS SYSTEM
 98100 Hypothermia - when employed, basic fee for any procedure on nervous system... 25 25 BRAIN Astrocytoma, oligodendroglioma, glioblastoma or metastatic tumour Craniotomy plus excision 98130 - supratentorial...
98100 Hypothermia - when employed, basic fee for any procedure on nervous system... 25 25 BRAIN Astrocytoma, oligodendroglioma, glioblastoma or metastatic tumour Craniotomy plus excision 98130 - supratentorial...
Adult - Cerebrovascular. Adult - Cranio-Cervical Junction. Adult - Epilepsy. Adult - Hydrocephalus
 list for SET and IMG Neurosurgery Adult - Cerebrovascular Aneurysm - Clipping: Anterior circulation Aneurysm - Clipping: Posterior circulation AVM excision Carotid endarterectomy Carotid trapping Cavernoma
list for SET and IMG Neurosurgery Adult - Cerebrovascular Aneurysm - Clipping: Anterior circulation Aneurysm - Clipping: Posterior circulation AVM excision Carotid endarterectomy Carotid trapping Cavernoma
Meningioma tumor. Meningiomas are named according to their location (Fig. 1) and cause various symptoms: > 1
 Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
Department of Neurological Surgery
 Department of Neurological Surgery CAT 1 A Basic Privileges: Patient management, including H & Ps and diagnostic and therapeutic treatments, procedures and interventions, Requiring a level of training
Department of Neurological Surgery CAT 1 A Basic Privileges: Patient management, including H & Ps and diagnostic and therapeutic treatments, procedures and interventions, Requiring a level of training
The translabyrinthine approach to the cerebellopontine
 Neurosurg Focus 33 (3):E17, 2012 Fascial sling technique for dural reconstruction after translabyrinthine resection of acoustic neuroma: technical note James K. Liu, M.D., 1 3 Smruti K. Patel, B.A., 1
Neurosurg Focus 33 (3):E17, 2012 Fascial sling technique for dural reconstruction after translabyrinthine resection of acoustic neuroma: technical note James K. Liu, M.D., 1 3 Smruti K. Patel, B.A., 1
Kiyoshi Ito, MD, Tatsuro Aoyama, MD, Takuya Nakamura, MD, Yoshiki Hanaoka, MD, Tetsuyoshi Horiuchi, MD, and Kazuhiro Hongo, MD
 technical note J Neurosurg Spine 25:620 625, 2016 Novel dural incision and closure procedure for preventing postoperative cerebrospinal fluid leakage during the surgical removal of dumbbell-shaped spinal
technical note J Neurosurg Spine 25:620 625, 2016 Novel dural incision and closure procedure for preventing postoperative cerebrospinal fluid leakage during the surgical removal of dumbbell-shaped spinal
DIANE MUELLER, N.D., R.N., C-F.N.P., AND JOHN J. ORO, M.D.
 Neurosurg Focus 18 (2):ECP2, 2005 Prospective analysis of self-perceived quality of life before and after posterior fossa decompression in 112 patients with Chiari malformation with or without syringomyelia
Neurosurg Focus 18 (2):ECP2, 2005 Prospective analysis of self-perceived quality of life before and after posterior fossa decompression in 112 patients with Chiari malformation with or without syringomyelia
MANAGEMENT OF CSF. Steven D. Schaefer, MD, FACS. Department of Otolaryngology New York Eye and Ear Infirmary
 MANAGEMENT OF CSF RHINORRHEA, MENIGIOCELES, Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York Eye and Ear Infirmary New York Medical College Anatomy and Physiology
MANAGEMENT OF CSF RHINORRHEA, MENIGIOCELES, Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York Eye and Ear Infirmary New York Medical College Anatomy and Physiology
CURRICULUM VITAE. SPR in Neurosurgery North Thames Rotation Scheme. 1. Royal Free Hospital RFH ( ; 18 months ) Specialist Registrar
 CURRICULUM VITAE Name Title Present Position Address : -Jesus Lafuente : -MD, FRCSEd, PhD : -CONSULTANT NEUROSURGEON : -HOSPÌTAL DEL MAR PASEO MARITIMO 23 BARCELONA 08003 E-mail : jlbspine@gmail.com Phone
CURRICULUM VITAE Name Title Present Position Address : -Jesus Lafuente : -MD, FRCSEd, PhD : -CONSULTANT NEUROSURGEON : -HOSPÌTAL DEL MAR PASEO MARITIMO 23 BARCELONA 08003 E-mail : jlbspine@gmail.com Phone
Minimally invasive subpial tonsillectomy for Chiari I decompression
 Acta Neurochir (2016) 158:1807 1811 DOI 10.1007/s00701-016-2877-2 HOW I DO IT - NEUROSURGICAL TECHNIQUES Minimally invasive subpial tonsillectomy for Chiari I decompression Jeffrey S. Beecher 1 Yong Liu
Acta Neurochir (2016) 158:1807 1811 DOI 10.1007/s00701-016-2877-2 HOW I DO IT - NEUROSURGICAL TECHNIQUES Minimally invasive subpial tonsillectomy for Chiari I decompression Jeffrey S. Beecher 1 Yong Liu
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts
 Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts Exceptional healthcare, personally delivered Ventriculo-Peritoneal/ Lumbo-Peritoneal Shunts What is hydrocephalus? Hydrocephalus is the build up of an excess
Cranial Postoperative Site: MR Imaging Appearance
 27 Cranial Postoperative Site: MR Imaging Appearance Charles F. Lanzieri1 Mark Larkins2 Andrew Mancall 1 Ronald Lorig 1 Paul M. Duchesneau 1 Scott A. Rosenbloom 1 Meredith A. Weinstein 1 The ability to
27 Cranial Postoperative Site: MR Imaging Appearance Charles F. Lanzieri1 Mark Larkins2 Andrew Mancall 1 Ronald Lorig 1 Paul M. Duchesneau 1 Scott A. Rosenbloom 1 Meredith A. Weinstein 1 The ability to
Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery
 Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery The Review Committee has made the following changes to the CPT code mappings: The following previously untracked CPT codes
Case Log Mapping Update: April 2018 Review Committee for Neurological Surgery The Review Committee has made the following changes to the CPT code mappings: The following previously untracked CPT codes
Unintended durotomy during degenerative lumbar spine surgery (Incidence and management)
 Original Article Unintended durotomy during degenerative lumbar spine surgery * Ali T. AbdulWahid** Ammar Salah*** FRCS MBChB, FIBMS MBChB, FIBMS Fac Med Baghdad 2014 Vol.56, No.4 Received: Sept., 2014
Original Article Unintended durotomy during degenerative lumbar spine surgery * Ali T. AbdulWahid** Ammar Salah*** FRCS MBChB, FIBMS MBChB, FIBMS Fac Med Baghdad 2014 Vol.56, No.4 Received: Sept., 2014
Original Policy Date
 MP 7.01.66 Auditory Brainstem Implant Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy
MP 7.01.66 Auditory Brainstem Implant Medical Policy Section Surgery Issue 12/2013 Original Policy Date 12/2013 Last Review Status/Date Reviewed with literature search/12/2013 Return to Medical Policy
CURRICULUM VITAE. 99 West Martial Ave Lafayette, LA Resident in Neurosurgery, Department of Surgery, University of Chicago
 CURRICULUM VITAE NAME Ilyas Munshi Date of Birth September 5, 1971 Citizenship Address USA Office 99 West Martial Ave Lafayette, LA 70508 Telephone 337-234-5344 Fax 337-234-5311 E-mail ilyasgmunshi@yahoo.com
CURRICULUM VITAE NAME Ilyas Munshi Date of Birth September 5, 1971 Citizenship Address USA Office 99 West Martial Ave Lafayette, LA 70508 Telephone 337-234-5344 Fax 337-234-5311 E-mail ilyasgmunshi@yahoo.com
POSTOPERATIVE CHRONIC SUBDURAL HEMATOMA FOLLOWING CLIP- PING SURGERY
 Nagoya postoperative Med. J., chronic subdural hematoma after aneurysmal clipping 13 POSTOPERATIVE CHRONIC SUBDURAL HEMATOMA FOLLOWING CLIP- PING SURGERY TAKAYUKI OHNO, M.D., YUSUKE NISHIKAWA, M.D., KIMINORI
Nagoya postoperative Med. J., chronic subdural hematoma after aneurysmal clipping 13 POSTOPERATIVE CHRONIC SUBDURAL HEMATOMA FOLLOWING CLIP- PING SURGERY TAKAYUKI OHNO, M.D., YUSUKE NISHIKAWA, M.D., KIMINORI
Bone flap preservation in abdominal wall after decompressive craniectomy in head injury: A single institute experience
 DOI: 10.2478/romneu-2018-0063 Article Bone flap preservation in abdominal wall after decompressive craniectomy in head injury: A single institute experience Pavan Kumar, Ashok Kumar, Gaurav Jaiswal, Tarun
DOI: 10.2478/romneu-2018-0063 Article Bone flap preservation in abdominal wall after decompressive craniectomy in head injury: A single institute experience Pavan Kumar, Ashok Kumar, Gaurav Jaiswal, Tarun
Surgical Neurology International
 Surgical Neurology International Original Article OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Two alternative dural sealing techniques in posterior fossa surgery:
Surgical Neurology International Original Article OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Two alternative dural sealing techniques in posterior fossa surgery:
SYNTHECEL Dura Repair. Assurance and Versatility for Dura Reconstruction.
 SYNTHECEL Dura Repair Assurance and Versatility for Dura Reconstruction. SYNTHECEL Dura Repair is an assured and versatile solution for your dura reconstruction needs. Clinically proven One product choice
SYNTHECEL Dura Repair Assurance and Versatility for Dura Reconstruction. SYNTHECEL Dura Repair is an assured and versatile solution for your dura reconstruction needs. Clinically proven One product choice
Utilizing real-time contrast medium to detect the fistula of giant spinal arachnoid cyst and treat with minimal invasive surgery
 Ying et al. BMC Surgery (2019) 19:11 https://doi.org/10.1186/s12893-019-0475-y CASE REPORT Open Access Utilizing real-time contrast medium to detect the fistula of giant spinal arachnoid cyst and treat
Ying et al. BMC Surgery (2019) 19:11 https://doi.org/10.1186/s12893-019-0475-y CASE REPORT Open Access Utilizing real-time contrast medium to detect the fistula of giant spinal arachnoid cyst and treat
The Synthetic Self-Adhesive Barrier to Cerebrospinal Fluid Leaks
 The Synthetic SelfAdhesive Barrier to Cerebrospinal Fluid Leaks TissuePatchl has a fused multilaminate structure containing patented reactive polymers for chemical bonding to tissue surface, and a nonadhesive
The Synthetic SelfAdhesive Barrier to Cerebrospinal Fluid Leaks TissuePatchl has a fused multilaminate structure containing patented reactive polymers for chemical bonding to tissue surface, and a nonadhesive
CSF Leaks. Abnormal communication between the subarachnoid space and the tympanomastoid space or nasal cavity. Presenting symptoms:
 CSF Leaks Steven Wright, M.D. Faculty Advisor: Matthew Ryan, M.D. The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation January 5, 2005 CSF Leaks Abnormal communication
CSF Leaks Steven Wright, M.D. Faculty Advisor: Matthew Ryan, M.D. The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation January 5, 2005 CSF Leaks Abnormal communication
Revision Surgery for Vestibular Schwannomas
 528 Original Article Kevin A. Peng 1 Brian S. Chen 3 Mark B. Lorenz 2 Gregory P. Lekovic 1 Marc S. Schwartz 1 William H. Slattery 1 Eric P. Wilkinson 1 1 House Clinic, Los Angeles, California, United States
528 Original Article Kevin A. Peng 1 Brian S. Chen 3 Mark B. Lorenz 2 Gregory P. Lekovic 1 Marc S. Schwartz 1 William H. Slattery 1 Eric P. Wilkinson 1 1 House Clinic, Los Angeles, California, United States
Spontaneous intracranial hypotension syndrome with extracranial vein dilatation
 Spontaneous intracranial hypotension syndrome with extracranial vein dilatation C. Heine 1, H. Altinova 1, T. Pietilä 1, LC Stavrinou 1 1. Department of Neurosurgery, Evangelical Hospital Bielefeld, Germany
Spontaneous intracranial hypotension syndrome with extracranial vein dilatation C. Heine 1, H. Altinova 1, T. Pietilä 1, LC Stavrinou 1 1. Department of Neurosurgery, Evangelical Hospital Bielefeld, Germany
Supratentorial cerebral arteriovenous malformations : a clinical analysis
 Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Neurosurgery Review. Mudit Sharma, MD May 16 th, 2008
 Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Health Sciences University, Diskapi Yildirim Beyazit Training and Research Hospital, Department of Neurosurgery, Ankara, Turkey 2
 DOI: 10.5137/1019-5149.JTN.24432-18.0 Received: 26.07.2018 / Accepted: 30.07.2018 Published Online: 25.03.2019 Original Investigation Turk Neurosurg, 2019 qr code Identification of Risk Factors for Postoperative
DOI: 10.5137/1019-5149.JTN.24432-18.0 Received: 26.07.2018 / Accepted: 30.07.2018 Published Online: 25.03.2019 Original Investigation Turk Neurosurg, 2019 qr code Identification of Risk Factors for Postoperative
doi: /j.issn
 19 34 20150820 Chinese Journal of Tissue Engineering Research August 20, 2015 Vol.19, No.34 ( 830002) 1 12 2 (XYDCX2014185) 2008 6 2013 6 2 266 126 5.56% 12 () 12 12 2472 h 48 h 812 d 9.5 d 2 714 d 3 1981
19 34 20150820 Chinese Journal of Tissue Engineering Research August 20, 2015 Vol.19, No.34 ( 830002) 1 12 2 (XYDCX2014185) 2008 6 2013 6 2 266 126 5.56% 12 () 12 12 2472 h 48 h 812 d 9.5 d 2 714 d 3 1981
Experience with acellular human dura and bovine collagen matrix for duraplasty after posterior fossa decompression for Chiari malformations
 J Neurosurg (1 Suppl Pediatrics) 104:16 20, 2006 Experience with acellular human dura and bovine collagen matrix for duraplasty after posterior fossa decompression for Chiari malformations SHABBAR F. DANISH,
J Neurosurg (1 Suppl Pediatrics) 104:16 20, 2006 Experience with acellular human dura and bovine collagen matrix for duraplasty after posterior fossa decompression for Chiari malformations SHABBAR F. DANISH,
Analysing the Effect of Early Acetazolamide Administration on Patients with A High Risk of Permanent Cerebrospinal Fluid Leakage
 ORIGINAL REPORT Analysing the Effect of Early Acetazolamide Administration on Patients with A High Risk of Permanent Cerebrospinal Fluid Leakage Saeid Abrishamkar, Nima Khalighinejad, and Payam Moein Department
ORIGINAL REPORT Analysing the Effect of Early Acetazolamide Administration on Patients with A High Risk of Permanent Cerebrospinal Fluid Leakage Saeid Abrishamkar, Nima Khalighinejad, and Payam Moein Department
Cranio-cervical decompression. Information for patients Neurosurgery
 Cranio-cervical decompression Information for patients Neurosurgery page 2 of 12 What is a cranio-cervical decompression? A cranio-cervical decompression is an operation involving the back of the head
Cranio-cervical decompression Information for patients Neurosurgery page 2 of 12 What is a cranio-cervical decompression? A cranio-cervical decompression is an operation involving the back of the head
The Management of Cerebrospinal Fluid Leak After Anterior Cervical Decompression Surgery. Copyrighted Material
 The Management of Cerebrospinal Fluid Leak After Anterior Cervical Decompression Surgery Jiliang Zhai, MD; Ripul R. Panchal, DO; Ye Tian, MD; Shujie Wang, PhD; Lijuan Zhao, RN abstract Cerebrospinal fluid
The Management of Cerebrospinal Fluid Leak After Anterior Cervical Decompression Surgery Jiliang Zhai, MD; Ripul R. Panchal, DO; Ye Tian, MD; Shujie Wang, PhD; Lijuan Zhao, RN abstract Cerebrospinal fluid
Intracranial hypotension secondary to spinal CSF leak: diagnosis
 Intracranial hypotension secondary to spinal CSF leak: diagnosis Spinal cerebrospinal fluid (CSF) leak is an important and underdiagnosed cause of new onset headache that is treatable. Cerebrospinal fluid
Intracranial hypotension secondary to spinal CSF leak: diagnosis Spinal cerebrospinal fluid (CSF) leak is an important and underdiagnosed cause of new onset headache that is treatable. Cerebrospinal fluid
Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience
 80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
2/20/2019 BRAIN DISSECTION CODING AND DOCUMENTATION OBJECTIVES INTRODUCTION
 BRAIN DISSECTION CODING AND DOCUMENTATION Diana R. Phelps, CPC, CPC-I, CEMC OBJECTIVES Identify general structure of the human brain Describe how the different parts work Recognized the two hemispheres
BRAIN DISSECTION CODING AND DOCUMENTATION Diana R. Phelps, CPC, CPC-I, CEMC OBJECTIVES Identify general structure of the human brain Describe how the different parts work Recognized the two hemispheres
BioGlue Surgical Adhesive as a Dural Sealant in Neurosurgery Clinical Needs and Surgical Technique
 BioGlue Surgical Adhesive as a Dural Sealant in Neurosurgery Clinical Needs and Surgical Technique Massimo Miscusi, MD, PhD Assistant Professor of Neurosurgery, Sapienza University of Rome, Rome, Italy
BioGlue Surgical Adhesive as a Dural Sealant in Neurosurgery Clinical Needs and Surgical Technique Massimo Miscusi, MD, PhD Assistant Professor of Neurosurgery, Sapienza University of Rome, Rome, Italy
Published clinical papers
 Published clinical papers Published clinical papers (Neuro) Use of a new absorbable sealing film for preventing postoperative cerebrospinal fluid leaks: remarks on a new approach. (12 cranial cases) A
Published clinical papers Published clinical papers (Neuro) Use of a new absorbable sealing film for preventing postoperative cerebrospinal fluid leaks: remarks on a new approach. (12 cranial cases) A
Brain Meninges, Ventricles and CSF
 Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Surgical dural tears: Prevalence and updated management protocol based on 1359 lumbar vertebra interventions
 Orthopaedics & Traumatology: Surgery & Research (2012) 98, 879 886 Available online at www.sciencedirect.com ORIGINAL ARTICLE Surgical dural tears: Prevalence and updated management protocol based on 1359
Orthopaedics & Traumatology: Surgery & Research (2012) 98, 879 886 Available online at www.sciencedirect.com ORIGINAL ARTICLE Surgical dural tears: Prevalence and updated management protocol based on 1359
Acoustic Neuroma. Presenting Signs and Symptoms of an Acoustic Neuroma:
 Acoustic Neuroma An acoustic neuroma is a benign tumor which arises from the nerves behind the inner ear and which may affect hearing and balance. The incidence of symptomatic acoustic neuroma is estimated
Acoustic Neuroma An acoustic neuroma is a benign tumor which arises from the nerves behind the inner ear and which may affect hearing and balance. The incidence of symptomatic acoustic neuroma is estimated
INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT. G. Tamburrini, Rome
 INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT G. Tamburrini, Rome Incidence 2% of occasional neuroradiological findings From clinical studies (1960 s): 0.4-1% of intracranial space occupying
INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT G. Tamburrini, Rome Incidence 2% of occasional neuroradiological findings From clinical studies (1960 s): 0.4-1% of intracranial space occupying
Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male
 Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Neurosurgical Techniques
 Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN
 A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
A NOVEL CAUSE FOR CAUDA- EQUINA SYNDROME WITH A NEW RADIOLOGICAL SIGN W Singleton, D Ramnarine, N Patel, C Wigfield Department of Neurological Surgery, Frenchay Hospital, Bristol, UK Introduction We present
Guidelines in the management of neural tube defects and hydrocephalus
 Guidelines in the management of neural tube defects and hydrocephalus Dominic Venne, MD, MSc, FRCSC, Division of Neurosurgery Sheikh Khalifa Medical City Abu Dhabi, UAE 1. Introduction: Neural tube defects
Guidelines in the management of neural tube defects and hydrocephalus Dominic Venne, MD, MSc, FRCSC, Division of Neurosurgery Sheikh Khalifa Medical City Abu Dhabi, UAE 1. Introduction: Neural tube defects
Neurosurgery. Neurosurgery
 Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Neurosurgery Neurosurgery Neurosurgery Telephone Numbers: Appointment: 202-476-3020 Fax: 202-476-3091 Administration: 202-476-3020 Evenings and Weekends: 202-476-5000 Robert Keating, MD, Chief The Division
Surgical techniques and procedures for cerebrovascular surgery. Surgery for the AVF at the cranio-cervical junction and high cervical spine
 VS-1 Surgery for the AVF at the cranio-cervical junction and high cervical spine Hiroyuki Kinouchi University of Yamanashi, Department of Neurosurgery Dural AVFs have been recognized as common type of
VS-1 Surgery for the AVF at the cranio-cervical junction and high cervical spine Hiroyuki Kinouchi University of Yamanashi, Department of Neurosurgery Dural AVFs have been recognized as common type of
Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries. Goes to 6N
 Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries Goes to 6N Burr holes and Craniotomies for hemorrhage, tumors, trauma, debulking Goes
Procedures commonly seen at Vanderbilt Medical Center PACU s: Cervical, thoracic, lumbar, and sacral spine surgeries Goes to 6N Burr holes and Craniotomies for hemorrhage, tumors, trauma, debulking Goes
Disclosures. Dr. Hall is a paid consultant to the American College of Surgeons (ACS) as Associate Director of ACS-NSQIP
 Does Routine Drainage of the Operative Bed following Elective Distal Pancreatectomy reduce Complications? An Analysis of the ACS-NSQIP Pancreatectomy Demonstration Project Stephen W. Behrman, MD 1, Ben
Does Routine Drainage of the Operative Bed following Elective Distal Pancreatectomy reduce Complications? An Analysis of the ACS-NSQIP Pancreatectomy Demonstration Project Stephen W. Behrman, MD 1, Ben
Unilateral extended suboccipital approach for a C1 dumbbell schwanoma
 38 Gorgan et al Unilateral extended suboccipital approach for a C1 dumbbell schwanoma Unilateral extended suboccipital approach for a C1 dumbbell schwanoma R.M. Gorgan, Angela Neacşu, A. Giovani Clinical
38 Gorgan et al Unilateral extended suboccipital approach for a C1 dumbbell schwanoma Unilateral extended suboccipital approach for a C1 dumbbell schwanoma R.M. Gorgan, Angela Neacşu, A. Giovani Clinical
Perioperative Management Of Extra-Ventricular Drains (EVD)
 Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
CSF Rhinorrhoea after Transsphenoidal Surgery
 ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 CSF Rhinorrhoea after Transsphenoidal Surgery E Elgamal Citation E Elgamal. CSF Rhinorrhoea after Transsphenoidal Surgery. The Internet
ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 CSF Rhinorrhoea after Transsphenoidal Surgery E Elgamal Citation E Elgamal. CSF Rhinorrhoea after Transsphenoidal Surgery. The Internet
North Oaks Trauma Symposium Friday, November 3, 2017
 + Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
+ Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
Microsurgery for ruptured cerebellar arteriovenous malformations
 European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
Original Article Surgical Management of Tentorial Meningiomas: Analysis of 14 Cases Experience
 Egyptian Journal of Neurosurgery Volume 29 / No. 1 / January - March 2014 39-44 Original Article Surgical Management of Tentorial Meningiomas: Analysis of 14 Cases Experience Ahmed M Zaater*, Mohamed I
Egyptian Journal of Neurosurgery Volume 29 / No. 1 / January - March 2014 39-44 Original Article Surgical Management of Tentorial Meningiomas: Analysis of 14 Cases Experience Ahmed M Zaater*, Mohamed I
At the conclusion of craniotomy procedures, it is
 J Neurosurg 120:278 284, 2014 AANS, 2014 The incidence of complications in elective cranial neurosurgery associated with dural closure material Clinical article Brian P. Walcott, M.D., 1 Jonathan B. Neal,
J Neurosurg 120:278 284, 2014 AANS, 2014 The incidence of complications in elective cranial neurosurgery associated with dural closure material Clinical article Brian P. Walcott, M.D., 1 Jonathan B. Neal,
got you covered. Codman s The global leader in neurosurgery is your one-stop, comprehensive source for proven, market-leading dural repair solutions.
 Codman s got you covered. The global leader in neurosurgery is your one-stop, comprehensive source for proven, market-leading dural repair solutions. AN INTEGRA LIFESCIENCES COMPANY The Leader in Dural
Codman s got you covered. The global leader in neurosurgery is your one-stop, comprehensive source for proven, market-leading dural repair solutions. AN INTEGRA LIFESCIENCES COMPANY The Leader in Dural
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage
 Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
HIROSHI NAKAGUCHI, M.D., PH.D., TAKEO TANISHIMA, M.D., PH.D., Clinical Material and Methods
 J Neurosurg 93:791 795, 2000 Relationship between drainage catheter location and postoperative recurrence of chronic subdural hematoma after burr-hole irrigation and closed-system drainage HIROSHI NAKAGUCHI,
J Neurosurg 93:791 795, 2000 Relationship between drainage catheter location and postoperative recurrence of chronic subdural hematoma after burr-hole irrigation and closed-system drainage HIROSHI NAKAGUCHI,
Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan
 Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Original Article Postoperative Surgical Site Infection after Incisional Hernia Repair: Link to Previous Surgical Site Infection? Zulfiqar Ali, AG Rehan ABSTRACT Objective: Aim of the study was to determine
Occipital flattening in the infant skull
 Occipital flattening in the infant skull Kant Y. Lin, M.D., Richard S. Polin, M.D., Thomas Gampper, M.D., and John A. Jane, M.D., Ph.D. Departments of Plastic Surgery and Neurological Surgery, University
Occipital flattening in the infant skull Kant Y. Lin, M.D., Richard S. Polin, M.D., Thomas Gampper, M.D., and John A. Jane, M.D., Ph.D. Departments of Plastic Surgery and Neurological Surgery, University
Curriculum Vitae. Date March 1, Contact Information
 Curriculum Vitae Mark S. Greenberg, MD, FAANS Associate Professor, Department of Neurosurgery and Brain Repair University of South Florida, Morsani College of Medicine Date March 1, 2018 Contact Information
Curriculum Vitae Mark S. Greenberg, MD, FAANS Associate Professor, Department of Neurosurgery and Brain Repair University of South Florida, Morsani College of Medicine Date March 1, 2018 Contact Information
Application of neuronavigation in Neurosurgery at King Hussein Medical Center, Jordan
 Keeping up with technology Application of neuronavigation in Neurosurgery at King Hussein Medical Center, Jordan Abdullah al-akayleh Department of Neuosurgery, King Hussean Medical Center, Jordan. ABSTRACT
Keeping up with technology Application of neuronavigation in Neurosurgery at King Hussein Medical Center, Jordan Abdullah al-akayleh Department of Neuosurgery, King Hussean Medical Center, Jordan. ABSTRACT
A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES
 A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES Takahiro Tsutsumimoto, Mutsuki Yui, Masashi Uehara, Hiroki Ohba, Hiroshi Ohta, Hidemi
A PROSPECTIVE STUDY OF INCIDENTAL DURAL TEARS IN MICROENDOSCOPIC LUMBAR DECOMPRESSION SURGERY: INCIDENCE AND OUTCOMES Takahiro Tsutsumimoto, Mutsuki Yui, Masashi Uehara, Hiroki Ohba, Hiroshi Ohta, Hidemi
Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature
 Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature Anand Sharma 1, Arti Sharma 2, Yashbir Dewan 1 1 Artemis
Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature Anand Sharma 1, Arti Sharma 2, Yashbir Dewan 1 1 Artemis
Spontaneous intracranial hypotension The first 1111 patients: A practical approach
 Spontaneous intracranial hypotension The first 1111 patients: A practical approach WOUTER I. SCHIEVINK, M.D. Professor of Neurosurgery Department of Neurosurgery, Cedars-Sinai Medical Center Los Angeles,
Spontaneous intracranial hypotension The first 1111 patients: A practical approach WOUTER I. SCHIEVINK, M.D. Professor of Neurosurgery Department of Neurosurgery, Cedars-Sinai Medical Center Los Angeles,
Skullbase Lesions. Skullbase Surgery Open vs endoscopic. Choice Of Surgical Approaches 12/28/2015. Skullbase Surgery: Evolution
 Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Pediatric and adult Chiari malformation Type I surgical series : a review of demographics, operative treatment, and outcomes
 PEDIATRICS literature review Pediatric and adult Chiari malformation Type I surgical series 1965 2013: a review of demographics, operative treatment, and outcomes aska arnautovic, bsc, 1 bruno splavski,
PEDIATRICS literature review Pediatric and adult Chiari malformation Type I surgical series 1965 2013: a review of demographics, operative treatment, and outcomes aska arnautovic, bsc, 1 bruno splavski,
Pichayen Duangthongpon MD*, Chaiwit Thanapaisal MD*, Amnat Kitkhuandee MD*, Kowit Chaiciwamongkol MD**, Vilaiwan Morthong MD**
 The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
Chiari Malformations. Google. Objectives Seventh Annual NKY TBI Conference 3/22/13. Kerry R. Crone, M.D.
 Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Chiari Malformations Kerry R. Crone, M.D. Professor of Neurosurgery and Pediatrics University of Cincinnati College of Medicine University of Cincinnati Medical Center Cincinnati Children s Hospital Medical
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score
 Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score Mehdi Abouzari, Marjan Asadollahi, Hamideh Aleali Amir-Alam Hospital, Medical Sciences/University of Tehran, Tehran, Iran Introduction
Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score Mehdi Abouzari, Marjan Asadollahi, Hamideh Aleali Amir-Alam Hospital, Medical Sciences/University of Tehran, Tehran, Iran Introduction
T HERE is an unusual and interesting variety of craniosynostosis in
 SURGICAL TREATMENT OF CONGENITAL ANOMALIES OF THE CORONAL AND METOPIC SUTURES TECHNICAL NOTE DONALD D. MATSON, M.D. Neurosurgical Service, The Children's Medical Center, and Deparlment of Surgery, Itarvard
SURGICAL TREATMENT OF CONGENITAL ANOMALIES OF THE CORONAL AND METOPIC SUTURES TECHNICAL NOTE DONALD D. MATSON, M.D. Neurosurgical Service, The Children's Medical Center, and Deparlment of Surgery, Itarvard
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 3/12/2011 Radiology Quiz of the Week # 11 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 3/12/2011 Radiology Quiz of the Week # 11 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
With advances in microsurgical techniques and the. Staged resection of large vestibular schwannomas. Clinical article
 J Neurosurg 116:1126 1133, 2012 Staged resection of large vestibular schwannomas Clinical article Ahmed M. Raslan, M.D., 1 James K. Liu, M.D., 3 Sean O. McMenomey, M.D., 1,2 and Johnny B. Delashaw Jr.,
J Neurosurg 116:1126 1133, 2012 Staged resection of large vestibular schwannomas Clinical article Ahmed M. Raslan, M.D., 1 James K. Liu, M.D., 3 Sean O. McMenomey, M.D., 1,2 and Johnny B. Delashaw Jr.,
GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D.
 J Neurosurg 47:590-595, 1977 Subgaleal shunt for temporary ventricle decompression and subdural drainage GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D. Division of Neurological Surgery, University of Iowa
J Neurosurg 47:590-595, 1977 Subgaleal shunt for temporary ventricle decompression and subdural drainage GEORGE E. PERRET, M.D., AND CARL J. GRAF, M.D. Division of Neurological Surgery, University of Iowa
Management of Cerebrospinal Fluid Leaks
 Management of Cerebrospinal Fluid Leaks J Trauma. 2001;51:S29 S33. I. RECOMMENDATIONS A. Standards The available data are not sufficient to support a treatment Standard for management of cerebrospinal
Management of Cerebrospinal Fluid Leaks J Trauma. 2001;51:S29 S33. I. RECOMMENDATIONS A. Standards The available data are not sufficient to support a treatment Standard for management of cerebrospinal
NON MALIGNANT BRAIN TUMOURS Facilitator. Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol
 NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report
 Neurosurg Focus 5 (3):Article 9, 1998 Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report Dean Chou, M.D., Prakash Sampath, M.D., and Henry Brem, M.D. Departments of Neurological
Neurosurg Focus 5 (3):Article 9, 1998 Hemorrhagic vestibular schwannoma: an unusual clinical entity Case report Dean Chou, M.D., Prakash Sampath, M.D., and Henry Brem, M.D. Departments of Neurological
Incidental durotomy in lumbar spine surgery - incidence, risk factors and management
 20 Adam et al Incidental durotomy in lumbar spine surgery Incidental durotomy in lumbar spine surgery - incidence, risk factors and management D. Adam 1,3, T. Papacocea 2,3, R. Iliescu 3, I. Hornea 3,
20 Adam et al Incidental durotomy in lumbar spine surgery Incidental durotomy in lumbar spine surgery - incidence, risk factors and management D. Adam 1,3, T. Papacocea 2,3, R. Iliescu 3, I. Hornea 3,
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Pediatric Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Pediatric Neurosurgery Pediatric neurosurgeons
Introduction to Neurosurgical Subspecialties: Pediatric Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Pediatric Neurosurgery Pediatric neurosurgeons
Capt. Nazim ATA Aerospace Medicine Specialist Turkish Air Force AAMIMO 2013
 F-15 Pilot with ACOUSTIC NEUROMA Capt. Nazim ATA Aerospace Medicine Specialist Turkish Air Force AAMIMO 2013 Disclosure Information 84 th Annual AsMA Scientific Meeting Nazim ATA I have no financial relationships
F-15 Pilot with ACOUSTIC NEUROMA Capt. Nazim ATA Aerospace Medicine Specialist Turkish Air Force AAMIMO 2013 Disclosure Information 84 th Annual AsMA Scientific Meeting Nazim ATA I have no financial relationships
Surgical management of diastatic linear skull fractures in infants
 Surgical management of diastatic linear skull fractures in infants JOHN B. THOMPSON, M.D., THOMAS H. MASON, M.D., GERALD L. HAINES, M.D., AND ROBERT J. CASSIDY, M.D. Divisions of Neurosurgery and Neurology,
Surgical management of diastatic linear skull fractures in infants JOHN B. THOMPSON, M.D., THOMAS H. MASON, M.D., GERALD L. HAINES, M.D., AND ROBERT J. CASSIDY, M.D. Divisions of Neurosurgery and Neurology,
