Short Communications. Alcoholic Intracerebral Hemorrhage
|
|
|
- Lorraine Crawford
- 5 years ago
- Views:
Transcription
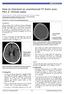
1 Short Communications 1565 Alcoholic Intracerebral Hemorrhage Leon A. Weisberg, MD Six alcoholic patients developed extensive cerebral hemispheric hemorrhages with both intraventricular and subarachnoid blood. All patients had evidence of liver damage, low platelet counts, and abnormal prothrombin and partial thromboplastin times. Four patients presented with seizures; in two of the four, these seizures were initially diagnosed as alcohol withdrawal seizures. Four patients were comatose with lateralizing neurologic deficit; two patients were comatose without lateralizing neurologic deficit, suggesting a metabolic encephalopathy. In one patient there was delayed neurologic deterioration. In all six patients, computed tomography showed large diffuse cerebral hemispheric hemorrhages, prominent intraventricular blood, and breakthrough into the subarachnoid spaces, which was confirmed by necropsy findings. There was marked mass effect but minimal surrounding edema. All six patients died. In three, autopsy showed no evidence of aneurysm, vascular malformation, neoplasm, or amyloid angiopathy and no arteriolar hypertensive changes. (Stroke 1988;19: ) A lcohol has known acute and chronic cardio- ZA vascular effects'- 4 that cause alcoholics to A JL be at risk for stroke. Chronic alcoholics have decreased concentrations of liver-produced coagulation factors and platelet abnormalities that predispose them to hemorrhagic stroke. Chronic alcoholism may cause hypertension, and acute alcoholic episodes may precipitate an acute hypertensive state with return to normotension when the subject stops drinking alcohol. Based on the potential for hypertension and impaired coagulation, hemorrhagic stroke develops with increased frequency in alcoholics. I describe six patients with alcoholic nonhypertensive intracerebral hemorrhages (ICHs) that may have occurred as a consequence of the chronic and/or acute alcoholic state. Case Reports Case 1. A 52-year-old chronic alcoholic woman developed headache and vomiting; she suddenly became unresponsive. Findings were stupor, hyperventilation, left hemiplegia, bilateral Babinski's signs, and a fixed dilated right pupil. Her hemoglobin was 10 g/dl; stool guaiacs were positive. Platelet count was 70,000/mm 3. Her prothrombin time was 14.5 (normal control 12) seconds and her partial thromboplastin time was 38 (normal range 23-34) seconds. She had impaired liver function (SGOT 300 From the Department of Neurology and Psychiatry, Tulane Medical School, the Department of Neurology, Veterans Administration Hospital, and the Department of Neurology, Charity Hospital, New Orleans, Louisiana. Address for correspondence: Leon A. Weisberg, MD, Department of Neurology and Psychiatry, 1430 Tulane Avenue, New Orleans, LA Received November 3, 1987; accepted July 6, IU, SGPT 450 IU, total bilirubin concentration 3.5 mg/dl, alkaline phosphatase value 190 IU). Computed tomography (CT) showed a massive right frontal-parietal hematoma with intraventricular and subarachnoid blood (Figure 1). Despite treatment with mannitol and corticosteroids, she did not improve neurologically; she developed pneumonia and died. Necropsy showed right intracerebral subarachnoid and intraventricular hemorrhage. There was no evidence of aneurysm, arteriovenous malformation, neoplasm, amyloid angiopathy, or hypertensive arteriolar vascular disease. The ICH had broken through into the subarachnoid spaces at multiple points, into the superficial frontal and parietal regions. Case 2. A 45-year-old chronic alcoholic man had been drinking heavily for 2 weeks. He stopped drinking because of abdominal pain. Three days later, he had a generalized seizure; following the seizure, he developed left-sided weakness and became lethargic. During 8 hours, he became comatose and developed left hemiplegia with a fixed dilated right pupil. Laboratory studies showed a hemoglobin concentration of 9.5 g/dl, a white blood cell count of 17,000/mm 3, a total bilirubin concentration of 4.2 mg/dl, a SGOT of 320 IU, a SGPT of 400 IU, and an alkaline phosphatase value of 135 IU. His prothrombin time was 16 (control 11.9) seconds and his partial thromboplastin time was 38 (normal range 23-34) seconds. During a previous admission, he had had a liver biopsy that showed fatty liver. CT showed an extensive right hemispheric hemorrhage (Figure 2) with both intraventricular and subarachnoid blood. He had two seizures, suffered a cardiopulmonary arrest, and died. Necropsy showed a diffuse right ICH. There was
2 1566 Stroke Vol 19, No 12, December 1988 FIGURE 1. Computed tomograms, 52-year-old chronic alcoholic woman (Case 1). Top left: right frontal-parietal hyperdense nonenhancing lesion with (top right) extension into and thalamic region. Bottom left: lateral ventricles are dilated with evidence of ventricular compression by extensive right hemispheric hematoma. Bottom right: intraventricular and cisternal blood. was no evidence of aneurysm, vascular malforma- tion, neoplasm, amyloid angiopathy, or hyperten- sive vascular disease. blood in the lateral ventricles breaking through into the cortical sulcal spaces in multiple regions. There was evidence of transtentorial herniation. There
3 Weisberg Alcoholic Intracerebral Hemorrhage 1567 FIGURE 2. Computed tomograms, 45-year-old chronic alcoholic man (Case 2). Top left: heterogeneous right hemispheric hematoma. Bottom: blood is seen in basal cisternal and sulcal space. Top right: marked right hemispheric mass effect with intraventricular blood. Summary of Clinical Findings The clinical and CT findings in these six patients are summarized in Table 1. Five patients were in their 40s. Five were men and one was a woman. None had a history of hypertension; none had elevated blood pressure when initially examined, and none were hypertensive during their hospital course. All six patients had biopsy evidence of fatty liver or cirrhosis. All were anemic with low platelet counts and abnormal prothrombin and partial thromboplastin times. Four patients initially had seizures; in two, this initial seizure was believed to be an
4 1568 Stroke Vol 19, No 12, December 1988 TABLE 1. Clinical and Computed Tomography Findings in Six Patients With Alcoholic Intracerebral Hemorrhage Liver Platelet PT/PTPT Neurologic Case/sex/age dysfunction count (mm" 3 ) (in sec) Seizures deficit l/f/52 Fatty degeneration 70, /38 No Coma, hemiplegia, fixed dilated pupil 2/M/45 3/M/48 4/M/42 5/M/43 6/M/46 Fatty degeneration 80,000 95,000 91,000 15/38 Coma and hemiparesis, delayed progression with dilated pupil 16/40 Coma, hemiplegia 16/40 Coma, no lateralizing signs 110, /37 Coma, no lateralizing signs 130,000 14/37 No Coma, hemiplegia PT/PTPT, prothrombin and partial thromboplastin times; F, female; M, male. Computed tomography findings Parenchymal Ventricular Subarachnoid hematoma blood blood Frontal-parietal, thalamic, Temporal, parietal-frontal Temporal, parietal, frontal, parietal,, thalamic parietal, temporal, temporal, parietal No No alcohol withdrawal seizure, but both patients showed a decreasing level of consciousness with focal deficit. Four of the six patients were comatose without focal deficit, pupillary abnormalities, or abnormal eye movements, suggesting a metabolic encephalopathy. In only one of the six patients was there delayed (8 hours later) neurologic deterioration, which included findings consistent with transtentorial herniation. In this patient necropsy showed evidence of transtentorial herniation and intraventricular bleeding. CT showed a characteristic pattern consisting of widespread cerebral hemispheric hemorrhage that appeared as a mottled, heterogeneous, high-density lesion. There was prominent cortical sulcal space and basal cisternal blood. The subarachnoid space hemorrhage was quite prominent and diffuse. Intraventricular blood was seen in four patients. The hemispheric hemorrhage was associated with marked mass effect. There were CT findings consistent with subfalcine and transtentorial herniation. All six patients died. Autopsy was performed in three patients and showed diffuse and extensive cerebral hemispheric hemorrhage without evidence of an underlying aneurysm, vascular malformation, neoplasm, amyloid angiopathy, or hypertensive disease. Discussion Previous studies have reported that alcohol may predispose to hemorrhagic stroke 5-7 ; chronic alcohol ingestion is associated with hypertension. One study reported that the association of alcohol with stroke is reduced after adjusting for hypertension 8 ; however, in another study alcohol was a major risk factor for ICH despite blood pressure control. 9 The risk of hemorrhagic stroke was directly correlated with the amount of alcohol consumed, and the relation held for subarachnoid hemorrhage and ICH. 510 If alcohol consumption is decreased, the risk of hemorrhagic stroke is reduced. None of these six patients had a history of hypertension or were hypertensive when the ICH developed. My clinical data do not allow me to quantify alcohol consumption with the coagulation disturbances or to compare the risk of hemorrhagic stroke with a control group. If hypertension is not implicated as a major risk factor for hemorrhagic stroke, it is likely that the impaired coagulation mechanism (low platelet count with abnormal prothrombin and partial thromboplastin times) was related to the ICH. The reduced number of platelets and impaired platelet function would weaken the blood vessel wall, and combined with impaired coagulation factors, this predisposes alcoholics to ICH. All these patients had low platelet counts and abnormal prothrombin and partial thromboplastin times. In alcoholics with hepatic damage, there may be decreased concentrations of clotting factors, increased fibrinolysis, and laboratory evidence of disseminated intravascular coagulation." In patients with hypertensive ICH, the characteristic locations include the putamen, thalamus, pons, or cerebellum 12 ; the intracranial bleeding does not usually break through into the subarachnoid space, whereas in nonhypertensive patients with ICH (e.g., aneurysm, vascular malformation, amyloid angiopathy) the hemorrhage is more commonly located in
5 the subcortical hemispheric white matter and breaks through into the subarachnoid spaces In hypertensive ICH, CT shows a homogeneous hyperdense nonenhancing lesion, usually with a surrounding hypodense region representing edema. Although many patients with ICH have erythrocytes in the cerebrospinal fluid, CT rarely shows subarachnoid blood. All six alcoholic patients with cerebral hemispheric hemorrhage showed cisternal and cortical sulcal blood; however, autopsy showed no other identifiable cause of the ICH. In one patient there was delayed neurologic deterioration consistent with transtentorial herniation. Without an early CT at the time the initial neurologic dysfunction developed and a repeat CT after the delayed neurologic deterioration, I could not precisely determine the mechanism of the delayed deterioration. Potential pathologic mechanisms include worsening of the edema, herniation, and intraventricular extension of the bleeding. The infrequent finding of delayed neurologic deterioration in these six alcoholic patients is consistent with the low incidence reported in ICH series Based on the location, size, and the CT pattern of the alcoholic hemorrhage, it is most unlikely that this represented a hemorrhagic contusion or a traumatic ICH. The CT pattern was also not consistent with a hemorrhagic cerebral infarction. The intracranial blood was widely dispersed within the subarachnoid spaces. There was blood in the superficial cortical and subcortical white matter, with extension into the basal ganglia and thalamus. Despite the large size and prominent mass effect (with evidence of subfalcine and transtentorial herniation), surrounding hypodense areas representing edema were not seen. This lack of CT-visualized edema is contrasted with the findings of prominent edema in other large nonalcohol-related ICHs. None of these six alcoholic patients showed multiple ICHs. I suggest that chronic alcohol exposure may lead to massive cerebral hemorrhage. Other studies Weisberg Alcoholic Intracerebral Hemorrhage 1569 using large sample sizes and quantitative features of alcohol ingestion and coagulation may settle the significance of this finding. References 1. Gorelick PB: Alcohol and stroke. Stroke 1987;18: Arkwright PD, Beilin LJ, Rouse 1, Armstrong BK, Vandongen R: Effects of alcohol use and other aspects of lifestyle on blood pressure levels and prevalence of hypertension in a working population. Circulation 1982;66: Gill JS, Zezulka AV, Shipley MJ, Gill SK, Beevers DG: Stroke and alcohol consumption. N Engl J Med 1986; 315: Kagan A, Popper JS, Rhoads GG: Dietary and other risk factors for stroke in Hawaiian Japanese men. Stroke 1985; 16: Donahue RP, Abbott RD, Reed DM.Yano K: Alcohol and hemorrhagic stroke: The Honolulu Heart Program. JAMA 1986;255: Hillbom M, Kaste M: Alcohol intoxication: A risk factor for primary subarachnoid hemorrhage. Neurology 1982; 32: Hillbom M, Kaste M: Does alcohol intoxication precipitate aneurysmal subarachnoid hemorrhage? J Neurol Neurosurg Psychiatry 1981 ;44: Stokes GS: Hypertension and alcohol: Is there a link? J Chronic Dis 1982 ;35: Kozararevic D, Vojvodic N, Dawbir N, McGee D, Racic Z, Gordon T, Zukel W: Frequency of alcohol consumption and morbidity and mortality. The Yugoslavia Cardiovascular Disease Study. Lancet 1980;l: Kagan A, Popper JS, Rhoads GG: Factors related to stroke incidence in Hawaii Japanese men: The Honolulu Heart Study. Stroke 1980;l 1: Cowan DH: Effects of alcoholism on hemostasis. Semin Hematol \9$0;\l: Weisberg LA: Computerized tomography in intracerebral hemorrhage. Arch Neurol 1979;36: McCormick WF, Rosenfield DB: Massive brain hemorrhage: A review of 144 cases and an examination of their causes. Stroke 1973;4: Weisberg LA: Subcortical lobar intracerebral hemorrhage: Clinical-computed tomographic correlations. J Neurol Neurosurg Psychiatry 1985;48: Weisberg LA: Primary putaminal hemorrhage: Clinical-CT correlations (abstract). Neurology 1988;38(suppl 1): 149 KEY WORDS alcoholism cerebral hemorrhage blood coagulation blood platelets
Stroke - Intracranial hemorrhage. Dr. Amitesh Aggarwal Associate Professor Department of Medicine
 Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Stroke - Intracranial hemorrhage Dr. Amitesh Aggarwal Associate Professor Department of Medicine Etiology and pathogenesis ICH accounts for ~10% of all strokes 30 day mortality - 35 45% Incidence rates
Primary pontine haemorrhage: clinical and computed tomographic correlations
 Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:346-352 Primary pontine haemorrhage: clinical and computed tomographic correlations LEON A WESBERG From the Department of Neurology and Psychiatry
Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:346-352 Primary pontine haemorrhage: clinical and computed tomographic correlations LEON A WESBERG From the Department of Neurology and Psychiatry
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Intracranial spontaneous hemorrhage mechanisms, imaging and management
 Intracranial spontaneous hemorrhage mechanisms, imaging and management Dora Zlatareva Department of Diagnostic Imaging Medical University, Sofia, Bulgaria Intracranial hemorrhage (ICH) ICH 15% of strokes
Intracranial spontaneous hemorrhage mechanisms, imaging and management Dora Zlatareva Department of Diagnostic Imaging Medical University, Sofia, Bulgaria Intracranial hemorrhage (ICH) ICH 15% of strokes
Hypertensive Haemorrhagic Stroke. Dr Philip Lam Thuon Mine
 Hypertensive Haemorrhagic Stroke Dr Philip Lam Thuon Mine Intracerebral Haemorrhage Primary ICH Spontaneous rupture of small vessels damaged by HBP Basal ganglia, thalamus, pons and cerebellum Amyloid
Hypertensive Haemorrhagic Stroke Dr Philip Lam Thuon Mine Intracerebral Haemorrhage Primary ICH Spontaneous rupture of small vessels damaged by HBP Basal ganglia, thalamus, pons and cerebellum Amyloid
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
Cerebrovascular diseases-2
 Cerebrovascular diseases-2 Primary angiitis of CNS - Other causes of infarction i. Hypercoagulable states ii. Drug-abuse such as amphetamine, heroin and cocain Note - The venous side of the circulation
Cerebrovascular diseases-2 Primary angiitis of CNS - Other causes of infarction i. Hypercoagulable states ii. Drug-abuse such as amphetamine, heroin and cocain Note - The venous side of the circulation
UPSTATE Comprehensive Stroke Center. Neurosurgical Interventions Satish Krishnamurthy MD, MCh
 UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
Starting or Resuming Anticoagulation or Antiplatelet Therapy after ICH: A Neurology Perspective
 Starting or Resuming Anticoagulation or Antiplatelet Therapy after ICH: A Neurology Perspective Cathy Sila MD George M Humphrey II Professor and Vice Chair of Neurology Director, Comprehensive Stroke Center
Starting or Resuming Anticoagulation or Antiplatelet Therapy after ICH: A Neurology Perspective Cathy Sila MD George M Humphrey II Professor and Vice Chair of Neurology Director, Comprehensive Stroke Center
INCREASED INTRACRANIAL PRESSURE
 INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 7: Non traumatic brain haemorrhage
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 7: Non traumatic brain haemorrhage ILOS To list the causes of intracranial haemorrhage. To understand the pathogenesis of each cause.
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 7: Non traumatic brain haemorrhage ILOS To list the causes of intracranial haemorrhage. To understand the pathogenesis of each cause.
ISCHEMIC STROKE IMAGING
 ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
ORIGINAL ARTICLE COMPUTED TOMOGRAPHY EVALUATION OF SPONTANEOUS INTRACRANIAL HAEMORRHAGE
 Available online at www.journalijmrr.com INTERNATIONAL JOURNAL OF MODERN RESEARCH AND REVIEWS IJMRR ISSN: 2347-8314 Int. J. Modn. Res. Revs. Volume 3, Issue 4, pp 647-652, April, 2015 ORIGINAL ARTICLE
Available online at www.journalijmrr.com INTERNATIONAL JOURNAL OF MODERN RESEARCH AND REVIEWS IJMRR ISSN: 2347-8314 Int. J. Modn. Res. Revs. Volume 3, Issue 4, pp 647-652, April, 2015 ORIGINAL ARTICLE
Acute cerebral MCA ischemia with secondary severe head injury and acute intracerebral and subdural haematoma. Case report
 214 Balasa et al - Acute cerebral MCA ischemia Acute cerebral MCA ischemia with secondary severe head injury and acute intracerebral and subdural haematoma. Case report D. Balasa 1, A. Tunas 1, I. Rusu
214 Balasa et al - Acute cerebral MCA ischemia Acute cerebral MCA ischemia with secondary severe head injury and acute intracerebral and subdural haematoma. Case report D. Balasa 1, A. Tunas 1, I. Rusu
Cerebrovascular Disorders. Blood, Brain, and Energy. Blood Supply to the Brain 2/14/11
 Cerebrovascular Disorders Blood, Brain, and Energy 20% of body s oxygen usage No oxygen/glucose reserves Hypoxia - reduced oxygen Anoxia - Absence of oxygen supply Cell death can occur in as little as
Cerebrovascular Disorders Blood, Brain, and Energy 20% of body s oxygen usage No oxygen/glucose reserves Hypoxia - reduced oxygen Anoxia - Absence of oxygen supply Cell death can occur in as little as
Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery
 Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery 2 Stroke Stroke kills almost 130,000 Americans each year. - Third cause of all deaths in Arkansas. - Death Rate is highest in
Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery 2 Stroke Stroke kills almost 130,000 Americans each year. - Third cause of all deaths in Arkansas. - Death Rate is highest in
 www.yassermetwally.com MANAGEMENT OF CEREBRAL HAEMORRHAGE (ICH): A QUICK GUIDE Overview 10% of strokes is caused by ICH. Main Causes: Less than 40 years old: vascular malformations and illicit drug use.
www.yassermetwally.com MANAGEMENT OF CEREBRAL HAEMORRHAGE (ICH): A QUICK GUIDE Overview 10% of strokes is caused by ICH. Main Causes: Less than 40 years old: vascular malformations and illicit drug use.
Intracerebral Hemorrhage
 Review of Primary Intracerebral Hemorrhage Réza Behrouz, DO Assistant Professor of Neurology University of South Florida College of Medicine STROKE 85% ISCHEMIC 15% HEMORRHAGIC HEMORRHAGIC STROKE 1/3 Subarachnoid
Review of Primary Intracerebral Hemorrhage Réza Behrouz, DO Assistant Professor of Neurology University of South Florida College of Medicine STROKE 85% ISCHEMIC 15% HEMORRHAGIC HEMORRHAGIC STROKE 1/3 Subarachnoid
Update in Management of Acute Spontaneous Intracerebral Haemorrhage
 Update in Management of Acute Spontaneous Intracerebral Haemorrhage Aldy S. Rambe Neurology Department, School of Medicine EPIDEMIOLOGY Although ICH represents only about 9% of all stroke, it accounts
Update in Management of Acute Spontaneous Intracerebral Haemorrhage Aldy S. Rambe Neurology Department, School of Medicine EPIDEMIOLOGY Although ICH represents only about 9% of all stroke, it accounts
Acute stroke imaging
 Acute stroke imaging Aims Imaging modalities and differences Why image acute stroke Clinical correlation to imaging appearance What is stroke Classic definition: acute focal injury to the central nervous
Acute stroke imaging Aims Imaging modalities and differences Why image acute stroke Clinical correlation to imaging appearance What is stroke Classic definition: acute focal injury to the central nervous
Cerebral Vascular Diseases. Nabila Hamdi MD, PhD
 Cerebral Vascular Diseases Nabila Hamdi MD, PhD Outline I. Stroke statistics II. Cerebral circulation III. Clinical symptoms of stroke IV. Pathogenesis of cerebral infarcts (Stroke) 1. Ischemic - Thrombotic
Cerebral Vascular Diseases Nabila Hamdi MD, PhD Outline I. Stroke statistics II. Cerebral circulation III. Clinical symptoms of stroke IV. Pathogenesis of cerebral infarcts (Stroke) 1. Ischemic - Thrombotic
Index. C Capillary telangiectasia, intracerebral hemorrhage in, 295 Carbon monoxide, formation of, in intracerebral hemorrhage, edema due to,
 Neurosurg Clin N Am 13 (2002) 395 399 Index Note: Page numbers of article titles are in boldface type. A Age factors, in intracerebral hemorrhage outcome, 344 Albumin, for intracerebral hemorrhage, 336
Neurosurg Clin N Am 13 (2002) 395 399 Index Note: Page numbers of article titles are in boldface type. A Age factors, in intracerebral hemorrhage outcome, 344 Albumin, for intracerebral hemorrhage, 336
2. Subarachnoid Hemorrhage
 Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
Recombinant Factor VIIa for Intracerebral Hemorrhage
 Recombinant Factor VIIa for Intracerebral Hemorrhage January 24, 2006 Justin Lee Pharmacy Resident University Health Network Outline 1. Introduction to patient case 2. Overview of intracerebral hemorrhage
Recombinant Factor VIIa for Intracerebral Hemorrhage January 24, 2006 Justin Lee Pharmacy Resident University Health Network Outline 1. Introduction to patient case 2. Overview of intracerebral hemorrhage
Spontaneous Intracerebral Hemorrhage and Liver Dysfunction
 85 Spontaneous Intracerebral Hemorrhage and Liver Dysfunction Hiroshi Niizuma, MD, Jiro Suzuki, MD, Tsutomu Yonemitsu, MD, and Taisuke Otsuki, MD We evaluated liver function and coagulation parameters
85 Spontaneous Intracerebral Hemorrhage and Liver Dysfunction Hiroshi Niizuma, MD, Jiro Suzuki, MD, Tsutomu Yonemitsu, MD, and Taisuke Otsuki, MD We evaluated liver function and coagulation parameters
Classical CNS Disease Patterns
 Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Neurosurgical Management of Stroke
 Overview Hemorrhagic Stroke Ischemic Stroke Aneurysmal Subarachnoid hemorrhage Neurosurgical Management of Stroke Jesse Liu, MD Instructor, Neurological Surgery Initial management In hospital management
Overview Hemorrhagic Stroke Ischemic Stroke Aneurysmal Subarachnoid hemorrhage Neurosurgical Management of Stroke Jesse Liu, MD Instructor, Neurological Surgery Initial management In hospital management
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE
 THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE * Dr. Sumendra Raj Pandey, Prof. Dr. Liu Pei WU, Dr. Sohan Kumar Sah, Dr. Lalu Yadav, Md. Sadam Husen Haque and Rajan KR. Chaurasiya
THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE * Dr. Sumendra Raj Pandey, Prof. Dr. Liu Pei WU, Dr. Sohan Kumar Sah, Dr. Lalu Yadav, Md. Sadam Husen Haque and Rajan KR. Chaurasiya
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage. By: Shifaa AlQa qa
 CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE
 WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
COMA. DIAH MUSTIKA HW,SpS,KIC INTENSIVE CARE UNIT of EMERGENCY DEPARTMENT
 COMA DIAH MUSTIKA HW,SpS,KIC INTENSIVE CARE UNIT of EMERGENCY DEPARTMENT NAVAL HOSPITAL dr RAMELAN, SURABAYA DEFINITIONS Coma State of unresponsiveness to external or internal stimuli in which a patient
COMA DIAH MUSTIKA HW,SpS,KIC INTENSIVE CARE UNIT of EMERGENCY DEPARTMENT NAVAL HOSPITAL dr RAMELAN, SURABAYA DEFINITIONS Coma State of unresponsiveness to external or internal stimuli in which a patient
Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD.
 Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD. Introduction: Spontaneous intracerebral haemorrhage (SICH) represents one of the most severe
Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD. Introduction: Spontaneous intracerebral haemorrhage (SICH) represents one of the most severe
Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/300 Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm Raja S Vignesh
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/300 Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm Raja S Vignesh
North Oaks Trauma Symposium Friday, November 3, 2017
 Traumatic Intracranial Hemorrhage Aaron C. Sigler, DO, MS Neurosurgery Tulane Neurosciences None Disclosures Overview Anatomy Epidural hematoma Subdural hematoma Cerebral contusions Outline Traumatic ICH
Traumatic Intracranial Hemorrhage Aaron C. Sigler, DO, MS Neurosurgery Tulane Neurosciences None Disclosures Overview Anatomy Epidural hematoma Subdural hematoma Cerebral contusions Outline Traumatic ICH
Supplement Table 1. Definitions for Causes of Death
 Supplement Table 1. Definitions for Causes of Death 3. Cause of Death: To record the primary cause of death. Record only one answer. Classify cause of death as one of the following: 3.1 Cardiac: Death
Supplement Table 1. Definitions for Causes of Death 3. Cause of Death: To record the primary cause of death. Record only one answer. Classify cause of death as one of the following: 3.1 Cardiac: Death
Subarachnoid Hemorrhage (SAH) Disclosures/Relationships. Click to edit Master title style. Click to edit Master title style.
 Subarachnoid Hemorrhage (SAH) William J. Jones, M.D. Assistant Professor of Neurology Co-Director, UCH Stroke Program Click to edit Master title style Disclosures/Relationships No conflicts of interest
Subarachnoid Hemorrhage (SAH) William J. Jones, M.D. Assistant Professor of Neurology Co-Director, UCH Stroke Program Click to edit Master title style Disclosures/Relationships No conflicts of interest
Giuseppe Micieli Dipartimento di Neurologia d Urgenza IRCCS Fondazione Istituto Neurologico Nazionale C Mondino, Pavia
 Giuseppe Micieli Dipartimento di Neurologia d Urgenza IRCCS Fondazione Istituto Neurologico Nazionale C Mondino, Pavia Charidimou et al, 2012 Pathogenesis of spontaneous and anticoagulationassociated
Giuseppe Micieli Dipartimento di Neurologia d Urgenza IRCCS Fondazione Istituto Neurologico Nazionale C Mondino, Pavia Charidimou et al, 2012 Pathogenesis of spontaneous and anticoagulationassociated
What Are We Going to Do? Fourth Year Meds Clinical Neuroanatomy. Hydrocephalus and Effects of Interruption of CSF Flow. Tube Blockage Doctrine
 Fourth Year Meds Clinical Neuroanatomy Ventricles, CSF, Brain Swelling etc. David A. Ramsay, Neuropathologist, LHSC What Are We Going to Do? Hydrocephalus and some effects of the interruption of CSF flow
Fourth Year Meds Clinical Neuroanatomy Ventricles, CSF, Brain Swelling etc. David A. Ramsay, Neuropathologist, LHSC What Are We Going to Do? Hydrocephalus and some effects of the interruption of CSF flow
Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences
 Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ٢ Level of consciousness is depressed Stuporous patients respond only to repeated
Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ٢ Level of consciousness is depressed Stuporous patients respond only to repeated
Rerupture of intracranial aneurysms: a clinicoanatomic study
 J Neurosurg 67:29-33, 1987 Rerupture of intracranial aneurysms: a clinicoanatomic study ALBERT HIJDRA, M.D., MARINUS VERMEULEN, M.D., JAN VAN GIJN, M.D., AND HANS VAN CREVEL, M.D. Departments ~[ Neurology.
J Neurosurg 67:29-33, 1987 Rerupture of intracranial aneurysms: a clinicoanatomic study ALBERT HIJDRA, M.D., MARINUS VERMEULEN, M.D., JAN VAN GIJN, M.D., AND HANS VAN CREVEL, M.D. Departments ~[ Neurology.
Intracranial Hemorrhage. Objectives. What Do Need to Know?
 Intracranial Hemorrhage What Do Need to Know? Kerry Brega, MD Associate Professor of Neurosurgery University of Colorado Objectives Know the common types of ICH. Know how they can be differentiated. Know
Intracranial Hemorrhage What Do Need to Know? Kerry Brega, MD Associate Professor of Neurosurgery University of Colorado Objectives Know the common types of ICH. Know how they can be differentiated. Know
Acute stroke. Ischaemic stroke. Characteristics. Temporal classification. Clinical features. Interpretation of Emergency Head CT
 Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD
 Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Case Report Isolated Central Sulcus Hemorrhage: A Rare Presentation Most Frequently Associated with Cerebral Amyloid Angiopathy
 Case Reports in Radiology Volume 2012, Article ID 574849, 5 pages doi:10.1155/2012/574849 Case Report Isolated Central Sulcus Hemorrhage: A Rare Presentation Most Frequently Associated with Cerebral Amyloid
Case Reports in Radiology Volume 2012, Article ID 574849, 5 pages doi:10.1155/2012/574849 Case Report Isolated Central Sulcus Hemorrhage: A Rare Presentation Most Frequently Associated with Cerebral Amyloid
Treatment of Acute Hydrocephalus After Subarachnoid Hemorrhage With Serial Lumbar Puncture
 19 Treatment of Acute After Subarachnoid Hemorrhage With Serial Lumbar Puncture Djo Hasan, MD; Kenneth W. Lindsay, PhD, FRCS; and Marinus Vermeulen, MD Downloaded from http://ahajournals.org by on vember,
19 Treatment of Acute After Subarachnoid Hemorrhage With Serial Lumbar Puncture Djo Hasan, MD; Kenneth W. Lindsay, PhD, FRCS; and Marinus Vermeulen, MD Downloaded from http://ahajournals.org by on vember,
11/27/2017. Stroke Management in the Neurocritical Care Unit. Conflict of interest. Karel Fuentes MD Medical Director of Neurocritical Care
 Stroke Management in the Neurocritical Care Unit Karel Fuentes MD Medical Director of Neurocritical Care Conflict of interest None Introduction Reperfusion therapy remains the mainstay in the treatment
Stroke Management in the Neurocritical Care Unit Karel Fuentes MD Medical Director of Neurocritical Care Conflict of interest None Introduction Reperfusion therapy remains the mainstay in the treatment
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases
 How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Carrera J-P, Forrester N, Wang E, et al. Eastern equine encephalitis
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Carrera J-P, Forrester N, Wang E, et al. Eastern equine encephalitis
Chronic Brain-Dead Patients Who Exhibit Lazarus Sign
 CASE REPORT Korean J Neurotrauma 2017;13(2):153-157 pissn 2234-8999 / eissn 2288-2243 https://doi.org/10.13004/kjnt.2017.13.2.153 Chronic Brain-Dead Patients Who Exhibit Lazarus Sign Department of Neurosurgery,
CASE REPORT Korean J Neurotrauma 2017;13(2):153-157 pissn 2234-8999 / eissn 2288-2243 https://doi.org/10.13004/kjnt.2017.13.2.153 Chronic Brain-Dead Patients Who Exhibit Lazarus Sign Department of Neurosurgery,
11/23/2015. Disclosures. Stroke Management in the Neurocritical Care Unit. Karel Fuentes MD Medical Director of Neurocritical Care.
 Stroke Management in the Neurocritical Care Unit Karel Fuentes MD Medical Director of Neurocritical Care Disclosures I have no relevant commercial relationships to disclose, and my presentations will not
Stroke Management in the Neurocritical Care Unit Karel Fuentes MD Medical Director of Neurocritical Care Disclosures I have no relevant commercial relationships to disclose, and my presentations will not
Traumatic brain injuries are caused by external mechanical forces such as: - Falls - Transport-related accidents - Assault
 PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
MRI OF THE THALAMUS. Mohammed J. Zafar, MD, FAAN Kalamazoo, MI
 1 MRI OF THE THALAMUS Mohammed J. Zafar, MD, FAAN Kalamazoo, MI Objectives: The thalamic nuclei can be involved in a wide variety of conditions. A systematic imaging approach would be useful for narrowing
1 MRI OF THE THALAMUS Mohammed J. Zafar, MD, FAAN Kalamazoo, MI Objectives: The thalamic nuclei can be involved in a wide variety of conditions. A systematic imaging approach would be useful for narrowing
ARTERIOVENOUS MALFORMATION OR CONTUSION : A DIAGNOSTIC DILEMMA. Yong Pei Yee, Ibrahim Lutfi Shuaib, Jafri Malin Abdullah*
 Malaysian Journal of Medical Sciences, Vol. 8, No. 2, July 2001 (47-51) CASE REPORT ARTERIOVENOUS MALFORMATION OR CONTUSION : A DIAGNOSTIC DILEMMA Yong Pei Yee, Ibrahim Lutfi Shuaib, Jafri Malin Abdullah*
Malaysian Journal of Medical Sciences, Vol. 8, No. 2, July 2001 (47-51) CASE REPORT ARTERIOVENOUS MALFORMATION OR CONTUSION : A DIAGNOSTIC DILEMMA Yong Pei Yee, Ibrahim Lutfi Shuaib, Jafri Malin Abdullah*
Hemodynamic Disorders, Thrombosis, and Shock. Richard A. McPherson, M.D.
 Hemodynamic Disorders, Thrombosis, and Shock Richard A. McPherson, M.D. Edema The accumulation of abnormal amounts of fluid in intercellular spaces of body cavities. Inflammation and release of mediators
Hemodynamic Disorders, Thrombosis, and Shock Richard A. McPherson, M.D. Edema The accumulation of abnormal amounts of fluid in intercellular spaces of body cavities. Inflammation and release of mediators
HAEMORRHAGIA Bleeding
 HAEMORRHAGIA Bleeding Cassification Size Location pathomechanism Hematoma: external or may be enclosed within a tissue petechiae : 1-2 mm hemorrhages into skin, mucous membranes, or serosal surfaces increased
HAEMORRHAGIA Bleeding Cassification Size Location pathomechanism Hematoma: external or may be enclosed within a tissue petechiae : 1-2 mm hemorrhages into skin, mucous membranes, or serosal surfaces increased
For Emergency Doctors. Dr Suzanne Smallbane November 2011
 For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
Vascular Malformations of the Brain: A Review of Imaging Features and Risks
 Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
An Introduc+on to Stroke
 An Introduc+on to Stroke Elizabeth Huntoon MS, MD Assistant Professor Department of Physical Medicine and Rehabilita>on Vanderbilt University School of Medicine Defini+on Sudden focal neurologic deficit
An Introduc+on to Stroke Elizabeth Huntoon MS, MD Assistant Professor Department of Physical Medicine and Rehabilita>on Vanderbilt University School of Medicine Defini+on Sudden focal neurologic deficit
Hemorrhagic Stroke. Team Members: Nawaf Aldarwish, Rawan Alqahtani, Talal AlTukhaim, Fatima Altassan.
 Hemorrhagic Stroke Objectives: Introduction Etiology Pathophysiology Clinical presentation Diagnosis and Imaging Treatment Team Members: Nawaf Aldarwish, Rawan Alqahtani, Talal AlTukhaim, Fatima Altassan.
Hemorrhagic Stroke Objectives: Introduction Etiology Pathophysiology Clinical presentation Diagnosis and Imaging Treatment Team Members: Nawaf Aldarwish, Rawan Alqahtani, Talal AlTukhaim, Fatima Altassan.
Supratentorial cerebral arteriovenous malformations : a clinical analysis
 Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Strokes in young adults are relatively uncommon;
 Stroke in Young Adults Heather Bevan, MD, Khema Sharma, MD, and Walter Bradley, DM, FRCP Strokes in young adults are uncommon and often a diagnostic challenge. A retrospective study of strokes due to intracerebral
Stroke in Young Adults Heather Bevan, MD, Khema Sharma, MD, and Walter Bradley, DM, FRCP Strokes in young adults are uncommon and often a diagnostic challenge. A retrospective study of strokes due to intracerebral
Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes
 Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes By Sheila Smith, MD Swedish Medical Center 1 Disclosures I have no disclosures 2 Course Objectives Review significance and differential
Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes By Sheila Smith, MD Swedish Medical Center 1 Disclosures I have no disclosures 2 Course Objectives Review significance and differential
Case Report. Herpes simplex virus encephalitis presenting as frontal lobe hemorrhage
 1 Case Report Herpes simplex virus encephalitis presenting as frontal lobe hemorrhage Authors: Shila, MD, *Jessica Erfan, MPAS, PA-C, Ray Bogitch, MD, Jefferson T. Miley, MD Department of Neurology, Dell
1 Case Report Herpes simplex virus encephalitis presenting as frontal lobe hemorrhage Authors: Shila, MD, *Jessica Erfan, MPAS, PA-C, Ray Bogitch, MD, Jefferson T. Miley, MD Department of Neurology, Dell
CEREBROVASCULAR DISEASES. By: Shifaa AlQa qa
 CEREBROVASCULAR DISEASES By: Shifaa AlQa qa Cerebrovascular diseases Brain disorders caused by pathologic processes involving blood vessels 3 pathogenic mechanisms (1) thrombotic occlusion, (2) embolic
CEREBROVASCULAR DISEASES By: Shifaa AlQa qa Cerebrovascular diseases Brain disorders caused by pathologic processes involving blood vessels 3 pathogenic mechanisms (1) thrombotic occlusion, (2) embolic
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
Imaging PRES syndrome: typical, atypical and follow up findings.
 Imaging PRES syndrome: typical, atypical and follow up findings. Poster No.: C-2361 Congress: ECR 2013 Type: Educational Exhibit Authors: P. Borrego Jimenez, A. Villalba Gutiérrez, M. Á. López Pino, P.
Imaging PRES syndrome: typical, atypical and follow up findings. Poster No.: C-2361 Congress: ECR 2013 Type: Educational Exhibit Authors: P. Borrego Jimenez, A. Villalba Gutiérrez, M. Á. López Pino, P.
8/29/2011. Brain Injury Incidence: 200/100,000. Prehospital Brain Injury Mortality Incidence: 20/100,000
 Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Thrombolytic therapy should be the first line treatment in acute ishchemic stroke. We are against it!!
 Thrombolytic therapy should be the first line treatment in acute ishchemic stroke We are against it!! 85% of strokes are ischaemic, and related to blockage of an artery by a blood clot, so potential treatments
Thrombolytic therapy should be the first line treatment in acute ishchemic stroke We are against it!! 85% of strokes are ischaemic, and related to blockage of an artery by a blood clot, so potential treatments
O F the many complications that may. Supratentorial intracerebral hemorrhage following posterior fossa surgery
 J Neurosurg 49:881-886, 1978 Supratentorial intracerebral hemorrhage following posterior fossa surgery STEPHEN J. HAINES, M.D., JOSEPH C. MAROON, M.D., AND PETER J. JANNETTA, M.D. Department of Neurological
J Neurosurg 49:881-886, 1978 Supratentorial intracerebral hemorrhage following posterior fossa surgery STEPHEN J. HAINES, M.D., JOSEPH C. MAROON, M.D., AND PETER J. JANNETTA, M.D. Department of Neurological
Acute Ischaemic Stroke
 Acute Ischaemic Stroke CT or MR SCA READIG FORM SCA ID: DATE OF READIG: SCA QUALIT: Good Moderate Poor Comment: READER ID: TPE OF SCA: CT: Without contrast: With contrast: MR: Diffusion: Perfusion ote
Acute Ischaemic Stroke CT or MR SCA READIG FORM SCA ID: DATE OF READIG: SCA QUALIT: Good Moderate Poor Comment: READER ID: TPE OF SCA: CT: Without contrast: With contrast: MR: Diffusion: Perfusion ote
HYPERTENSIVE ENCEPHALOPATHY
 HYPERTENSIVE ENCEPHALOPATHY Reversible posterior leukoencephalopathy syndrome Cause Renal disease Pheochromocytoma Disseminated vasculitis Eclampsia Acute toxemia Medications & illicit drugs (cocaine)
HYPERTENSIVE ENCEPHALOPATHY Reversible posterior leukoencephalopathy syndrome Cause Renal disease Pheochromocytoma Disseminated vasculitis Eclampsia Acute toxemia Medications & illicit drugs (cocaine)
Stroke in the ED. Dr. William Whiteley. Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian
 Stroke in the ED Dr. William Whiteley Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian 2016 RCP Guideline for Stroke RCP guidelines for acute ischaemic stroke
Stroke in the ED Dr. William Whiteley Scottish Senior Clinical Fellow University of Edinburgh Consultant Neurologist NHS Lothian 2016 RCP Guideline for Stroke RCP guidelines for acute ischaemic stroke
IV. Cerebrovascular diseases
 IV. Cerebrovascular diseases - Cerebrovascular disease denotes brain disorders caused by pathologic processes involving the blood vessels. - The three main pathogenic mechanisms are: 1. Thrombotic occlusion
IV. Cerebrovascular diseases - Cerebrovascular disease denotes brain disorders caused by pathologic processes involving the blood vessels. - The three main pathogenic mechanisms are: 1. Thrombotic occlusion
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
Marc Norman, Ph.D. - Do Not Use without Permission 1. Cerebrovascular Accidents. Marc Norman, Ph.D. Department of Psychiatry
 Cerebrovascular Accidents Marc Norman, Ph.D. Department of Psychiatry Neuropsychiatry and Behavioral Medicine Neuropsychology Clinical Training Seminar 1 5 http://www.nlm.nih.gov/medlineplus/ency/images/ency/fullsize/18009.jpg
Cerebrovascular Accidents Marc Norman, Ph.D. Department of Psychiatry Neuropsychiatry and Behavioral Medicine Neuropsychology Clinical Training Seminar 1 5 http://www.nlm.nih.gov/medlineplus/ency/images/ency/fullsize/18009.jpg
V. CENTRAL NERVOUS SYSTEM TRAUMA
 V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
PROGNOSTIC FACTORS IN GANGLIONIC AND THAL4MIC HAEMORRBAGES: A CLINICAL AND RADIOLOGICAL STUDY
 PROGNOSTIC FACTORS IN GANGLIONIC AND THAL4MIC HAEMORRBAGES: A CLINICAL AND RADIOLOGICAL STUDY Pages with reference to book, From 62 To 64 Aziz Badruddin Sonawalla, Zaigham Abbas, Mohammed Ataullah Khan
PROGNOSTIC FACTORS IN GANGLIONIC AND THAL4MIC HAEMORRBAGES: A CLINICAL AND RADIOLOGICAL STUDY Pages with reference to book, From 62 To 64 Aziz Badruddin Sonawalla, Zaigham Abbas, Mohammed Ataullah Khan
Pontine haemorrhage: a clinical analysis of 26 cases
 Journal of Neurology, Neurosurgery, and Psychiatry 1985;48:658-662 Pontine haemorrhage: a clinical analysis of 26 cases SHOJI MASIYAMA, HIROSHI NIIZUMA, JIRO SUZUKI From the Division ofneurosurgery, Institute
Journal of Neurology, Neurosurgery, and Psychiatry 1985;48:658-662 Pontine haemorrhage: a clinical analysis of 26 cases SHOJI MASIYAMA, HIROSHI NIIZUMA, JIRO SUZUKI From the Division ofneurosurgery, Institute
Updated Ischemic Stroke Guidelines นพ.ส ชาต หาญไชยพ บ ลย ก ล นายแพทย ทรงค ณว ฒ สาขาประสาทว ทยา สถาบ นประสาทว ทยา กรมการแพทย กระทรวงสาธารณส ข
 Updated Ischemic Stroke Guidelines นพ.ส ชาต หาญไชยพ บ ลย ก ล นายแพทย ทรงค ณว ฒ สาขาประสาทว ทยา สถาบ นประสาทว ทยา กรมการแพทย กระทรวงสาธารณส ข Emergency start at community level: Prehospital care Acute stroke
Updated Ischemic Stroke Guidelines นพ.ส ชาต หาญไชยพ บ ลย ก ล นายแพทย ทรงค ณว ฒ สาขาประสาทว ทยา สถาบ นประสาทว ทยา กรมการแพทย กระทรวงสาธารณส ข Emergency start at community level: Prehospital care Acute stroke
Disclosure. + Outline. Case-based approach to neurological emergencies that might present to the ED
 Kathleen R. Fink, MD University of Washington 5 th Nordic Emergency Radiology Course May 21, 2015 Disclosure My spouse receives research salary support from: Bracco BayerHealthcare Guerbet Outline Case-based
Kathleen R. Fink, MD University of Washington 5 th Nordic Emergency Radiology Course May 21, 2015 Disclosure My spouse receives research salary support from: Bracco BayerHealthcare Guerbet Outline Case-based
An Introduction to Imaging the Brain. Dr Amy Davis
 An Introduction to Imaging the Brain Dr Amy Davis Common reasons for imaging: Clinical scenarios: - Trauma (NICE guidelines) - Stroke - Tumours - Seizure - Neurological degeneration memory, motor dysfunction,
An Introduction to Imaging the Brain Dr Amy Davis Common reasons for imaging: Clinical scenarios: - Trauma (NICE guidelines) - Stroke - Tumours - Seizure - Neurological degeneration memory, motor dysfunction,
The management of ICH when to operate when not to?
 The management of ICH when to operate when not to? Intracranial Hemorrhage High Incidence o Accounts for 10-15% of all strokes 1,2,5 o 80,000 cases in US; 2 million WW 2,5 o Incidence doubles for African-
The management of ICH when to operate when not to? Intracranial Hemorrhage High Incidence o Accounts for 10-15% of all strokes 1,2,5 o 80,000 cases in US; 2 million WW 2,5 o Incidence doubles for African-
PACT module. Traumatic Brain Injury. Intensive Care Training Program Radboud University Medical Centre Nijmegen
 PACT module Traumatic Brain Injury Intensive Care Training Program Radboud University Medical Centre Nijmegen Severe traumatic brain injury Leading cause of morbidity/mortality among young individuals
PACT module Traumatic Brain Injury Intensive Care Training Program Radboud University Medical Centre Nijmegen Severe traumatic brain injury Leading cause of morbidity/mortality among young individuals
Head Injury and Early Signs of Tentorial Herniation
 Refer to: Hoff JT, Spetzler R, Winestock D: Head injury and early signs of tentorial herniation-a management dilemma. West J Med 128:112-116, Feb 1978 Head Injury and Early Signs of Tentorial Herniation
Refer to: Hoff JT, Spetzler R, Winestock D: Head injury and early signs of tentorial herniation-a management dilemma. West J Med 128:112-116, Feb 1978 Head Injury and Early Signs of Tentorial Herniation
Stroke in the Emergency Room: What do we need to know?
 Stroke in the Emergency Room: What do we need to know? Salah G. Keyrouz, MD, FAHA March 10, 2012 Stroke in the Emergency Room: What do we need to know? Disclosure: None 2 1 Outline Definition Introduction
Stroke in the Emergency Room: What do we need to know? Salah G. Keyrouz, MD, FAHA March 10, 2012 Stroke in the Emergency Room: What do we need to know? Disclosure: None 2 1 Outline Definition Introduction
Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins
 ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
Role of MRI in acute disseminated encephalomyelitis
 Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Lothian Audit of the Treatment of Cerebral Haemorrhage (LATCH)
 1. INTRODUCTION Stroke physicians, emergency department doctors, and neurologists are often unsure about which patients they should refer for neurosurgical intervention. Early neurosurgical evacuation
1. INTRODUCTION Stroke physicians, emergency department doctors, and neurologists are often unsure about which patients they should refer for neurosurgical intervention. Early neurosurgical evacuation
Standardize comprehensive care of the patient with severe traumatic brain injury
 Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Management of Patients with Severe Traumatic Brain Injury (GCS < 9) ADULT Practice Management Guideline Contact: Trauma
Postinfarction Seizures. A Clinical Study. Sudha R. Gupta, MD, Mohammad H. Naheedy, MD, Dean Elias, MD, and Frank A. Rubino, MD
 4 Postinfarction Seizures A Clinical Study Sudha R. Gupta, MD, Mohammad H. Naheedy, MD, Dean Elias, MD, and Frank A. Rubino, MD We retrospectively studied 90 patients with postinfarction to determine the
4 Postinfarction Seizures A Clinical Study Sudha R. Gupta, MD, Mohammad H. Naheedy, MD, Dean Elias, MD, and Frank A. Rubino, MD We retrospectively studied 90 patients with postinfarction to determine the
INTRACEREBRAL HAEMORRHAGE:
 INTRACEREBRAL HAEMORRHAGE: WHAT IS THE CAUSE? Prof. Charlotte Cordonnier Head, Department of neurology & stroke centre Director, Lille haemorrhagic stroke research program Lille University Hospital France
INTRACEREBRAL HAEMORRHAGE: WHAT IS THE CAUSE? Prof. Charlotte Cordonnier Head, Department of neurology & stroke centre Director, Lille haemorrhagic stroke research program Lille University Hospital France
Overview of Stroke: Etiologies, Demographics, Syndromes, and Outcomes. Alex Abou-Chebl, MD, FSVIN Medical Director, Stroke Baptist Health Louisville
 Overview of Stroke: Etiologies, Demographics, Syndromes, and Outcomes Alex Abou-Chebl, MD, FSVIN Medical Director, Stroke Baptist Health Louisville Disclosure Statement of Financial Interest Within the
Overview of Stroke: Etiologies, Demographics, Syndromes, and Outcomes Alex Abou-Chebl, MD, FSVIN Medical Director, Stroke Baptist Health Louisville Disclosure Statement of Financial Interest Within the
Disclosure Statement: Dr. Knoefel has nothing to disclose
 Stroke Janice E. Knoefel, MD, MPH Professor of Medicine & Neurology University of New Mexico Geriatrics/Extended Care (retired) New Mexico VA Healthcare System Albuquerque, NM Disclosure Statement: Dr.
Stroke Janice E. Knoefel, MD, MPH Professor of Medicine & Neurology University of New Mexico Geriatrics/Extended Care (retired) New Mexico VA Healthcare System Albuquerque, NM Disclosure Statement: Dr.
Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage
 Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
Int J Clin Exp Med 2016;9(8):15921-15927 www.ijcem.com /ISSN:1940-5901/IJCEM0022273 Original Article CT grouping and microsurgical treatment strategies of hypertensive cerebellar hemorrhage Xielin Tang
Clinical Analysis of Risk Factors Affecting Rebleeding in Patients with an Aneurysm. Gab Teug Kim, M.D.
 / 119 = Abstract = Clinical Analysis of Risk Factors Affecting Rebleeding in Patients with an Aneurysm Gab Teug Kim, M.D. Department of Emergency Medicine, College of Medicine, Dankook University, Choenan,
/ 119 = Abstract = Clinical Analysis of Risk Factors Affecting Rebleeding in Patients with an Aneurysm Gab Teug Kim, M.D. Department of Emergency Medicine, College of Medicine, Dankook University, Choenan,
Neuropathology lecture series. III. Neuropathology of Cerebrovascular Disease. Physiology of cerebral blood flow
 Neuropathology lecture series III. Neuropathology of Cerebrovascular Disease Physiology of cerebral blood flow Brain makes up only 2% of body weight Percentage of cardiac output: 15-20% Percentage of O
Neuropathology lecture series III. Neuropathology of Cerebrovascular Disease Physiology of cerebral blood flow Brain makes up only 2% of body weight Percentage of cardiac output: 15-20% Percentage of O
GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE
 2018 UPDATE QUICK SHEET 2018 American Heart Association GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE A Summary for Healthcare Professionals from the American Heart Association/American
2018 UPDATE QUICK SHEET 2018 American Heart Association GUIDELINES FOR THE EARLY MANAGEMENT OF PATIENTS WITH ACUTE ISCHEMIC STROKE A Summary for Healthcare Professionals from the American Heart Association/American
Herpes Simplex Encephalitis Complicated by Cerebral Hemorrhage during Acyclovir Therapy
 CASE REPORT Herpes Simplex Encephalitis Complicated by Cerebral Hemorrhage during Acyclovir Therapy Yukinori Harada and Yuuta Hara Abstract Herpes simplex encephalitis (HSE) can be complicated by adverse
CASE REPORT Herpes Simplex Encephalitis Complicated by Cerebral Hemorrhage during Acyclovir Therapy Yukinori Harada and Yuuta Hara Abstract Herpes simplex encephalitis (HSE) can be complicated by adverse
