Accepted Article. Comparative Fracture Risks among US Medicaid Enrollees with and without Systemic. Lupus Erythematosus
|
|
|
- Cory Cox
- 5 years ago
- Views:
Transcription
1 DR. SEOYOUNG C. KIM (Orcid ID : ) Article type : Brief Report Comparative Fracture Risks among US Medicaid Enrollees with and without Systemic Lupus Erythematosus Sara K. Tedeschi, MD, MPH, 1 Seoyoung C. Kim, MD, ScD, 1,2 Hongshu Guan, PhD, 1 Jennifer M. Grossman, MD, 3 Karen H. Costenbader, MD, MPH 1 1 Division of Rheumatology, Immunology and Allergy, Department of Medicine, Brigham and Women s Hospital and Harvard Medical School, Boston, MA 2 Division of Pharmacoepidemiology and Pharmacoeconomics, Department of Medicine, Brigham and Women s Hospital and Harvard Medical School, Boston, MA 3 Division of Rheumatology, Department of Medicine, David Geffen School of Medicine at UCLA, Los Angeles, CA This article has been accepted for publication and undergone full peer review but has not been through the copyediting, typesetting, pagination and proofreading process, which may lead to differences between this version and the Version of Record. Please cite this article as doi: /art.40818
2 Correspondence/Reprint Requests: Sara K. Tedeschi, MD, MPH Brigham and Women s Hospital, Division of Rheumatology, Immunology and Allergy 60 Fenwood Road, Suite 6016 Boston, MA USA stedeschi1@bwh.harvard.edu Phone: Fax: Running head: Fracture risks in SLE FUNDING: This work was supported by the Lupus Foundation of America Career Development Award and the National Institutes of Health L30 AR070514, K24 AR055989, K24 AR CONFLICTS OF INTEREST: The authors declare no conflicts of interest.
3 ABSTRACT Objective: Poor bone health is common in SLE patients. We evaluated fracture risks among low-income SLE and lupus nephritis patients compared to those without SLE. Methods: We performed a cohort study within Medicaid , among SLE patients and age- and sex-matched non-sle comparators. SLE was defined by 3 ICD-9 codes for SLE; lupus nephritis patients additionally had 2 codes for renal disease. The primary outcome was fracture of the pelvis, wrist, hip, or humerus. Demographics, prescriptions, and comorbidities were assessed during the 180-day baseline period. We calculated fracture incidence rates (IR) and 95% confidence intervals (CI) in SLE, lupus nephritis, and non-sle comparator cohorts, and estimated adjusted hazard ratios (HR) for fractures. Sensitivity analyses evaluated the impact of glucocorticoids and comorbidities. We compared subsets of SLE patients with and without lupus nephritis. Results: Among 47,709 SLE patients (19.8% with lupus nephritis) matched to 190,836 non- SLE comparators, mean age was 41.4 years and 92.6% were female. Fracture IR was highest among SLE patients with nephritis (4.60/1,000 person-years). SLE patients had two-fold higher fracture risk than matched comparators (HR 2.09 [95% CI 1.85, 2.37]). Lupus nephritis patients had the greatest fracture risks versus matched comparators (HR 3.06 [2.24, 4.17]), and 1.6 times higher risk than SLE patients without nephritis (HR 1.58 [1.20, 2.07]). Adjustment for glucocorticoid use and comorbidities slightly attenuated risks. Conclusion: Fracture risks were elevated in SLE patients, particularly those with lupus nephritis, compared to matched non-sle Medicaid patients. Elevated risks persisted after adjustment for baseline glucocorticoids and comorbidities.
4 Keywords: SLE, fracture, lupus nephritis INTRODUCTION Poor bone health may occur in systemic lupus erythematosus (SLE) patients for several reasons. High circulating levels of inflammatory cytokines stimulate bone resorption and greater SLE activity has been associated with low bone mineral density. 1 The adverse effects of glucocorticoids on bone health are widely recognized. 2-5 Both the cumulative dose and daily dose of glucocorticoids have been associated with low bone mineral density. Patients with lupus nephritis may be at particularly high risk for fracture due to secondary or tertiary hyperparathyroidism and vitamin D deficiency. SLE typically affects pre-menopausal women who may be at disproportionately high risk for fracture due to these factors. 6 Few large cohort studies have compared fracture risks among SLE patients to age- and sex-matched individuals. 4,7 Fracture risks among racially and ethnically diverse, lowincome SLE patients who are at particularly high risk for SLE complications have not been investigated. Lupus nephritis patients are likely at increased fracture risk, but have not been well studied. 8 We determined fracture incidence rates within a large cohort of lowincome SLE and lupus nephritis patients, compared relative risks for fracture vs. matched comparators, and evaluated subgroups of SLE patients with lupus nephritis and by age.
5 METHODS Data source and study design We performed a cohort study to evaluate fracture incidence rates and relative risks using claims data for adults aged years old enrolled in Medicaid. Medicaid is the US public health insurance program that covers >70 million low-income, racially and ethnically diverse individuals. Claims data were obtained from the Medicaid Analytic extract (MAX) for , provided as billing claims from the 29 most populated states. Data were obtained through a data use agreement with the Center for Medicaid and Medicare Studies providing access to claims data from ; results are presented according to Federal data reporting standards (cell sizes <11 are suppressed). SLE cohort We identified a prevalent SLE cohort defined by 3 ICD-9 codes for SLE (710.0) 30 days apart as in prior work Among SLE patients, lupus nephritis was defined by 2 ICD- 9 codes for nephritis, proteinuria, and/or renal failure 30 days apart on or after the SLE definition The index date was the date fulfilling SLE or lupus nephritis definition. In the event that all required codes occurred within <180 days, the next SLE or nephritis code occurring after 180 days defined the index date.
6 Non-SLE comparator cohort The comparator cohort included Medicaid patients with no ICD-9 codes for SLE during the baseline period, matched 4:1 to SLE patients on index date, age (±1 year), and sex. The index date for non-sle comparators was the date of a claim ±30 days of the index date for matched SLE patients. Baseline and follow-up periods We required a baseline period 180 days prior to and including the index date for all subjects. Follow-up started the day after index date and ended with the first fracture event, Medicaid disenrollment, death, or study period end (12/31/2010). We excluded any patient with fracture during baseline. Assessment of fracture events Pelvis, wrist, hip, and humeral fractures were defined by a claims-based algorithm using diagnosis and procedure codes (positive predictive value [PPV] >90% for each fracture site). 14 We did not include vertebral fractures due to the poor performance of a claims-based algorithm for vertebral fractures (PPV <50%). 15 The primary outcome was the first occurrence of fracture at any of these sites ( any fracture ). The first fracture at each site was a secondary outcome.
7 Covariates Demographics, medications, and comorbidities were assessed during the 180-day baseline period; age was assessed at index date. US Census median household income by zip code was assessed as a marker of socioeconomic status. Race/ethnicity was categorized as White, African-American, Hispanic, or Other (Asian, Native American, or Other). Prescription claims for hydroxychloroquine, azathioprine, mycophenolate mofetil, cyclophosphamide, cyclosporine, tacrolimus, leflunomide, methotrexate or rituximab were treated as binary (ever vs. never during baseline). Mean oral and intravenous glucocorticoid use during baseline were calculated in prednisone equivalents using filled prescription claims, categorized as none (0 mg/day), low-dose (mean prednisone equivalent >0 to <7.5 mg/day), or high-dose (mean prednisone equivalent 7.5 mg/day). 16 The Charlson-Deyo Comorbidity Index indicated the presence/absence of claims for 17 conditions including rheumatic illness, renal disease, and malignancy. We defined end-stage renal disease as 1 ICD-9 code during baseline. Statistical analyses We calculated crude fracture incidence rates (IR) and 95% confidence intervals (CI) in the SLE, lupus nephritis, and non-sle comparator cohorts using Poisson models. The proportional hazards assumption was testing using Schoenfeld residuals. Multivariable Cox regression models estimated hazard ratios (HR) and 95% CI for any fracture and for fractures at each anatomic site, adjusting for age, sex, and race/ethnicity. Sensitivity analyses evaluated the impact of baseline glucocorticoid use on relative fracture risks and adjusted for the Charlson-Deyo Comorbidity Index.
8 In secondary analyses, we evaluated fracture risks among patients with and without lupus nephritis. We compared fracture risks in lupus nephritis patients versus matched non- SLE comparators, and then compared SLE patients with and without lupus nephritis. We compared fracture risks in SLE patients without nephritis to matched non-sle comparators. We also stratified the SLE and non-sle cohorts at <50 vs. 50 years old to compare fracture risks in younger vs. older patients. 7 Analyses were performed using SAS v9.4 (SAS Institute, Cary, N.C). A two-sided p <0.05 was considered significant. The Partners HealthCare Institutional Review Board approved all aspects of the study; formal consent was not required. RESULTS We identified 47,709 SLE patients matched to 190,836 non-sle comparator patients. Lupus nephritis was present in 9,449 (19.8%) patients in the SLE cohort. Baseline characteristics are summarized in Table 1. Mean age in both cohorts was 41.4 years; 92.6% were female. The proportion of African-American patients was higher in the SLE cohort. Glucocorticoid use was uncommon among non-sle comparators (5.7%), while 41.2% of SLE patients were prescribed glucocorticoids. Less than half of the SLE cohort was prescribed hydroxychloroquine. Bisphosphonate prescriptions were very rare and were more frequent in SLE (5.8%) than age- and sex-matched non-sle comparators (0.7%). Fracture incidence rates Among SLE patients, the IR for any fracture was 4.32/1,000 person-years (Table 2). The IR was slightly higher among the subset of SLE patients with lupus nephritis: 4.60/1,000 person-years. Non-SLE patients had a lower IR for any fracture: 2.40/1,000 person-years.
9 Pelvic fractures were the most frequent fracture type in SLE, with an IR 1.72/1,000 personyears and were more frequent in the subset with lupus nephritis (IR 2.23/1,000 person-years). Wrist fractures were the most common fracture type in non-sle comparator patients (IR 1.04/100,000 person-years). Comparative fracture risks SLE patients had a two-fold higher fracture risk compared to age- and sex-matched non-sle comparators (adjusted HR 2.09 [95% CI 1.85, 2.37]) (Table 3). Fracture risk was slightly attenuated after additionally adjusting for baseline glucocorticoid use (HR 1.78 [1.55, 2.05]) and comorbidities (HR 1.74 [1.53, 1.99]). SLE patients were at particularly high risk for hip fracture (HR 3.22 [2.33, 4.46]) and pelvic fracture (HR 2.63 [2.13,3.24]) compared to non-sle patients. Risks for humerus fracture (HR 1.82 [1.34, 2.47]) and wrist fracture (HR 1.57 [1.27, 1.94]) were also elevated in SLE patients vs. non-sle comparators. SLE patients without nephritis had 1.9 times greater risk than their matched comparators. Fracture risks were greatest in the subset of SLE patients with lupus nephritis. Lupus nephritis patients had a three-fold elevated fracture risk compared to matched non-sle patients (HR 3.06 [2.24, 4.17]) (Table 3). SLE patients with nephritis patients had 1.6 times greater fracture risk (HR 1.58 [1.20, 2.07]) than SLE patients without nephritis. Adjusting for baseline glucocorticoid use and comorbidities mildly attenuated this risk. Younger SLE patients had 2.3 times higher fracture risks compared to younger non- SLE patients (HR 2.28 [1.90, 2.74]) (Table 3). Comparative fracture risk in SLE patients was attenuated but remained two-fold elevated after adjusting for baseline glucocorticoids and comorbidities. Among patients aged 50 years, SLE was also associated with a two-fold
10 fracture risk (HR 1.92 [1.61, 2.28]); this risk was mildly attenuated after adjusting for baseline glucocorticoids and comorbidities. DISCUSSION Among >47,000 racially/ethnically diverse SLE patients compared to age- and sexmatched non-sle patients enrolled in Medicaid, we identified a two-fold higher adjusted fracture risk. Fracture risks were particularly elevated among patients with lupus nephritis, with three-fold risk compared to matched non-sle patients and 1.6-fold risk compared to SLE patients without nephritis. Adjustment for glucocorticoid use slightly attenuated fracture risks among SLE patients, consistent with prior literature on the detrimental effects of glucocorticoids on bone health. SLE was associated with a 2.3-fold fracture risk among younger patients, and a 1.9-fold risk among older patients. We identified lupus nephritis patients as a particularly at-risk group for fracture, especially pelvic fracture. Even after adjusting for glucocorticoids and comorbidities (including renal disease), lupus nephritis patients had approximately 2.5-fold elevated fracture risk compared to non-sle patients. Lupus nephritis patients had 1.6 times higher fracture risks compared to SLE patients without nephritis; the risk was essentially unchanged after adjusting for baseline glucocorticoid use. Adjustment for the Charlson-Deyo Comorbidity Index, which includes renal disease, attenuated fracture risks in lupus nephritis reflecting the role that renal disease plays in fracture risk. Medicaid SLE patients had a higher relative risk of incident fracture compared to previous large studies. Wang et al. studied incident hip fractures among ~14,500 Taiwanese SLE patients and ~14,500 non-sle patients, mean age Hip fracture incidence rate was
11 0.86/1,000 person-years, similar to our estimate of 0.76/1,000 person-years. SLE patients had twice the risk of hip fracture compared to non-sle patients (incidence rate ratio [IRR] 2.23) in that study, whereas we detected a three-fold greater risk for hip fracture. Wang et al. identified a six-fold higher risk of hip fracture in SLE patients age <50 compared to agematched comparators, with a wide confidence interval (IRR 6.29 [ ]). SLE patients age <50 in our study had 2.3 times the risk of age-matched comparators, higher than the 1.9- fold relative risk among older SLE patients. Bultink et al. studied incident fractures in ~4,000 SLE patients and ~21,000 matched comparators, mean age 46, seen in general practice clinics in the UK. 4 The incidence rate for fracture of the spine, hip, forearm or humerus was 15.5/1,000 person-years, higher than our observed incidence rate (4.32/1,000 person-years), but our composite outcome did not include spine fractures and did include pelvic fractures. UK SLE patients had 58% higher risk for fracture than comparators (age- and sex- adjusted relative risk [RR] 1.58 [ ]). Adjustment for past fracture and use of glucocorticoids, hydroxychloroquine, calcium/vitamin D supplements, benzodiazepines and proton pump inhibitors attenuated the RR to 1.22 [ ]. Differences in study populations and methodology may explain the slightly higher fracture risks that we observed compared to prior studies. Suboptimal SLE treatment among Medicaid enrollees and poor outcomes in this population, as has been shown in prior work, may have contributed to elevated fracture risks. 11,12 More than 40% of SLE patients in our study used glucocorticoids during the baseline period, and hydroxychloroquine a mainstay of SLE treatment was used by less than half. Based on these practice patterns, it is possible that SLE patients in our cohort had worse bone health due to SLE itself or as a consequence of glucocorticoid use. African-American race was more frequent in the SLE cohort than the non-sle cohort, and was associated with lower fracture risk in multivariable models (data not shown). We chose to include race in our final models because was an important
12 confounder of fracture risk. In contrast to the Bultink et al. study, we did not include spinal (i.e. vertebral) fractures as these are frequently asymptomatic and difficult to detect accurately using claims data. 15 Also in contrast, we elected not to include SLE medications in our primary multivariable model. Glucocorticoids and hydroxychloroquine were very infrequently used in non-sle patients, and we considered them indicators of SLE as well as potential mediators of fracture risk. Adjustment for medications that were more frequently used in SLE patients than non-sle patients likely attenuated fracture risk estimates among SLE patients in the UK. The American College of Rheumatology has published glucocorticoid-induced osteoporosis prevention guidelines, recommending bisphosphonates for patients with longterm glucocorticoid use and moderate or high fracture risks. 16,17 However, renal disease often contraindicates preventive treatment with bisphosphonates. In our study population, bisphosphonate use was infrequent among SLE and non-sle patients and it was unclear if bisphosphonate use would be associated with lower fracture risk due to its biological effect, or higher fracture risk due to confounding by indication (e.g. preferential prescribing to patients perceived to be at highest fracture risk). Therefore we did not include bisphosphonates in our models. We performed this analysis using Medicaid billing data, which have limitations. We were not able to assess history of fracture or covariates prior to the 180-day baseline period. We were also not able to adjust for lifetime exposure to glucocorticoids prior to index date, potentially leading to underestimation of relative risks. Additionally, medication claims data may not reflect the medications or doses patients actually take. For example, patients may have been taking glucocorticoids differently than prescribed at baseline. The fracture algorithm required only one code for pelvic fracture, which may have overestimated pelvic fracture rates in both SLE and non-sle cohorts. 14 We were unable to adjust for calcium and
13 vitamin D due to concern for poor ascertainment, as these are often purchased over-thecounter, nor for frailty, physical activity, and body mass index. We did not have access to bone density measurements so could not determine if these were osteoporotic fractures, but we included anatomic sites that are typical for low-trauma fractures. Our SLE and lupus nephritis cohorts included patients with prevalent disease and we were unable to determine disease duration. We could not assess SLE disease activity. Our SLE cohort had a lower proportion of lupus nephritis cases than other population-based cohorts, likely due to our stringent algorithm requiring at least five ICD-9 codes separate in time, limited duration of follow-up available, and because end-stage renal disease patients in the US often receive insurance through Medicare (not Medicaid). Because we conducted this analysis among Medicaid enrollees, our results may not generalize to other SLE patients with higher socioeconomic status. Our work had several key strengths, including a large sample of >47,000 racially/ethnically diverse SLE patients and age- and sex-matched comparators. We applied established algorithms to identify SLE, lupus nephritis, and fractures at four anatomic sites using billing claims data. While the relative risk for fracture was two- to three-fold elevated in SLE and lupus nephritis patients, absolute fracture rates were moderate. Fracture IRs were of a similar magnitude as in other SLE cohorts, suggesting that claims data are reliable for identifying fragility fractures. We omitted patients with a prior history of fracture, leading to conservative estimates of relative fracture risks. We were able to adjust for both oral and intravenous glucocorticoid use based on filled prescriptions, and other potential confounders. Within a racially and ethnically diverse, low-income Medicaid population, SLE patients had two-fold greater risk for fractures compared to non-sle patients. Greater risk (HR 3.06) was present in the subset of lupus nephritis patients. Glucocorticoid use during the
14 baseline accounted for some, but not all, of increased risk. This work underscores the importance of identifying high-risk SLE and lupus nephritis patients for fracture prevention. REFERENCES 1. Lee C, Almagor O, Dunlop DD, Manzi S, Spies S, Chadha AB, et al. Disease damage and low bone mineral density: An analysis of women with systemic lupus erythematosus ever and never receiving corticosteroids. Rheumatology (Oxford) 2006;45: Ramsey-Goldman R, Dunn JE, Huang CF, Dunlop D, Rairie JE, Fitzgerald S, et al. Frequency of fractures in women with systemic lupus erythematosus: Comparison with united states population data. Arthritis Rheum 1999;42: Zonana-Nacach A, Barr SG, Magder LS, Petri M. Damage in systemic lupus erythematosus and its association with corticosteroids. Arthritis Rheum 2000;43: Bultink IE, Harvey NC, Lalmohamed A, Cooper C, Lems WF, van Staa TP, et al. Elevated risk of clinical fractures and associated risk factors in patients with systemic lupus erythematosus versus matched controls: A population-based study in the united kingdom. Osteoporos Int 2014;25: Cramarossa G, Urowitz MB, Su J, Gladman D, Touma Z. Prevalence and associated factors of low bone mass in adults with systemic lupus erythematosus. Lupus 2017;26: Carli L, Tani C, Spera V, Vagelli R, Vagnani S, Mazzantini M, et al. Risk factors for osteoporosis and fragility fractures in patients with systemic lupus erythematosus. Lupus Sci Med 2016;3:e
15 7. Wang SH, Chang YS, Liu CJ, Lai CC, Chen WS, Chen TJ, et al. Association of systemic lupus erythematosus with a higher risk of cervical but not trochanteric hip fracture: A nationwide population-based study. Arthritis Care Res (Hoboken) 2013;65: Le B, Waller JL, Radhakrishnan R, Oh SJ, Kheda MF, Nahman NS, Jr., et al. Osteoporotic fractures in patients with systemic lupus erythematosus and end stage renal disease. Lupus 2018;27: Barbhaiya M, Feldman CH, Guan H, Gomez-Puerta JA, Fischer MA, Solomon DH, et al. Race/ethnicity and cardiovascular events among patients with systemic lupus erythematosus. Arthritis Rheumatol 2017;69: Feldman CH, Marty FM, Winkelmayer WC, Guan H, Franklin JM, Solomon DH, et al. Comparative rates of serious infections among patients with systemic lupus erythematosus receiving immunosuppressive medications. Arthritis Rheumatol 2017;69: Feldman CH, Hiraki LT, Winkelmayer WC, Marty FM, Franklin JM, Kim SC, et al. Serious infections among adult medicaid beneficiaries with systemic lupus erythematosus and lupus nephritis. Arthritis Rheumatol 2015;67: Chen SK, Barbhaiya M, Fischer MA, Guan H, Lin TC, Feldman CH, et al. Lipid testing and statin prescription among medicaid recipients with systemic lupus erythematosus, diabetes mellitus and the general medicaid population. Arthritis Care Res (Hoboken) 2018 Apr 12. doi: /acr [Epub ahead of print] 13. Chibnik LB, Massarotti EM, Costenbader KH. Identification and validation of lupus nephritis cases using administrative data. Lupus 2010;19: Ray WA, Griffin MR, Fought RL, Adams ML. Identification of fractures from computerized medicare files. J Clin Epidemiol 1992;45:
16 15. Curtis JR, Mudano AS, Solomon DH, Xi J, Melton ME, Saag KG. Identification and validation of vertebral compression fractures using administrative claims data. Med Care 2009;47: Grossman JM, Gordon R, Ranganath VK, Deal C, Caplan L, Chen W, et al. American college of rheumatology 2010 recommendations for the prevention and treatment of glucocorticoid-induced osteoporosis. Arthritis Care Res (Hoboken) 2010;62: Buckley L, Guyatt G, Fink HA, Cannon M, Grossman J, Hansen KE, et al american college of rheumatology guideline for the prevention and treatment of glucocorticoid-induced osteoporosis. Arthritis Rheumatol 2017;69:
17
18
19
Disclosures. Evidence Based Medicine. Infections in SLE and LN Patients. Aim
 Serious Infection Rates among Patients with Systemic Lupus Erythematosus Receiving Corticosteroids and Immunosuppressants None Disclosures Candace H. Feldman, MD, MPH 1,2 Linda T. Hiraki, MD, SM, ScD 3
Serious Infection Rates among Patients with Systemic Lupus Erythematosus Receiving Corticosteroids and Immunosuppressants None Disclosures Candace H. Feldman, MD, MPH 1,2 Linda T. Hiraki, MD, SM, ScD 3
AMERICAN COLLEGE OF RHEUMATOLOGY POSITION STATEMENT. Committee on Rheumatologic Care
 AMERICAN COLLEGE OF RHEUMATOLOGY POSITION STATEMENT SUBJECT: PRESENTED BY: FOR DISTRIBUTION TO: Bone Mineral Density Measurement and the Role of Rheumatologists in the Management of Osteoporosis Committee
AMERICAN COLLEGE OF RHEUMATOLOGY POSITION STATEMENT SUBJECT: PRESENTED BY: FOR DISTRIBUTION TO: Bone Mineral Density Measurement and the Role of Rheumatologists in the Management of Osteoporosis Committee
Development of SLE among Possible SLE Patients Seen in Consultation: Long-Term Follow-Up. Disclosures. Background. Evidence-Based Medicine.
 Development of SLE among Patients Seen in Consultation: Long-Term Follow-Up Abstract # 1699 May Al Daabil, MD Bonnie L. Bermas, MD Alexander Fine Hsun Tsao Patricia Ho Joseph F. Merola, MD Peter H. Schur,
Development of SLE among Patients Seen in Consultation: Long-Term Follow-Up Abstract # 1699 May Al Daabil, MD Bonnie L. Bermas, MD Alexander Fine Hsun Tsao Patricia Ho Joseph F. Merola, MD Peter H. Schur,
Mandana Nikpour 1,2, Murray B Urowitz 1*, Dominique Ibanez 1, Paula J Harvey 3 and Dafna D Gladman 1. Abstract
 RESEARCH ARTICLE Open Access Importance of cumulative exposure to elevated cholesterol and blood pressure in development of atherosclerotic coronary artery disease in systemic lupus erythematosus: a prospective
RESEARCH ARTICLE Open Access Importance of cumulative exposure to elevated cholesterol and blood pressure in development of atherosclerotic coronary artery disease in systemic lupus erythematosus: a prospective
Risk of serious infections associated with use of immunosuppressive agents in pregnant women with autoimmune inflammatory conditions: cohor t study
 Risk of serious infections associated with use of immunosuppressive agents in pregnant women with autoimmune inflammatory conditions: cohor t study BMJ 2017; 356 doi: https://doi.org/10.1136/bmj.j895 (Published
Risk of serious infections associated with use of immunosuppressive agents in pregnant women with autoimmune inflammatory conditions: cohor t study BMJ 2017; 356 doi: https://doi.org/10.1136/bmj.j895 (Published
Challenging the Current Osteoporosis Guidelines. Carolyn J. Crandall, MD, MS Professor of Medicine David Geffen School of Medicine at UCLA
 Challenging the Current Osteoporosis Guidelines Carolyn J. Crandall, MD, MS Professor of Medicine David Geffen School of Medicine at UCLA Whom to screen Which test How to diagnose Whom to treat Benefits
Challenging the Current Osteoporosis Guidelines Carolyn J. Crandall, MD, MS Professor of Medicine David Geffen School of Medicine at UCLA Whom to screen Which test How to diagnose Whom to treat Benefits
8/6/2018. Glucocorticoid induced osteoporosis: overlooked and undertreated? Disclosure. Objectives. Overview
 Disclosure Glucocorticoid induced osteoporosis: overlooked and undertreated? I have no financial disclosure relevant to this presentation Tasma Harindhanavudhi, MD Division of Diabetes and Endocrinology
Disclosure Glucocorticoid induced osteoporosis: overlooked and undertreated? I have no financial disclosure relevant to this presentation Tasma Harindhanavudhi, MD Division of Diabetes and Endocrinology
Osteoporosis: A Tale of 3 Task Forces!
 Osteoporosis: A Tale of 3 Task Forces! Robert A. Adler, MD McGuire Veterans Affairs Medical Center Virginia Commonwealth University Richmond, Virginia, USA Disclosures The opinions are those of the speaker
Osteoporosis: A Tale of 3 Task Forces! Robert A. Adler, MD McGuire Veterans Affairs Medical Center Virginia Commonwealth University Richmond, Virginia, USA Disclosures The opinions are those of the speaker
Bone Mass Measurement BONE MASS MEASUREMENT HS-042. Policy Number: HS-042. Original Effective Date: 8/25/2008
 Easy Choice Health Plan, Inc. Harmony Health Plan of Illinois, Inc. Missouri Care, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance of Arizona, Inc. WellCare Health Insurance of Illinois,
Easy Choice Health Plan, Inc. Harmony Health Plan of Illinois, Inc. Missouri Care, Inc. Ohana Health Plan, a plan offered by WellCare Health Insurance of Arizona, Inc. WellCare Health Insurance of Illinois,
Androgen deprivation therapy for treatment of localized prostate cancer and risk of
 Androgen deprivation therapy for treatment of localized prostate cancer and risk of second primary malignancies Lauren P. Wallner, Renyi Wang, Steven J. Jacobsen, Reina Haque Department of Research and
Androgen deprivation therapy for treatment of localized prostate cancer and risk of second primary malignancies Lauren P. Wallner, Renyi Wang, Steven J. Jacobsen, Reina Haque Department of Research and
[If no, skip to question 10.] Y N. 2. Does the member have a diagnosis of Paget s disease of bone? Y N. [If no, skip to question 4.
![[If no, skip to question 10.] Y N. 2. Does the member have a diagnosis of Paget s disease of bone? Y N. [If no, skip to question 4. [If no, skip to question 10.] Y N. 2. Does the member have a diagnosis of Paget s disease of bone? Y N. [If no, skip to question 4.](/thumbs/86/94943423.jpg) Pharmacy Prior Authorization AETA BETTER HEALTH EW JERSE (MEDICAID) Zoledronic Acid (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information,
Pharmacy Prior Authorization AETA BETTER HEALTH EW JERSE (MEDICAID) Zoledronic Acid (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information,
Risk of Fractures Following Cataract Surgery in Medicare Beneficiaries
 Risk of Fractures Following Cataract Surgery in Medicare Beneficiaries Victoria L. Tseng, MD, Fei Yu, PhD, Flora Lum, MD, Anne L. Coleman, MD, PhD JAMA. 2012;308(5):493-501 Background Visual impairment
Risk of Fractures Following Cataract Surgery in Medicare Beneficiaries Victoria L. Tseng, MD, Fei Yu, PhD, Flora Lum, MD, Anne L. Coleman, MD, PhD JAMA. 2012;308(5):493-501 Background Visual impairment
Prevalence of vertebral fractures on chest radiographs of elderly African American and Caucasian women
 Osteoporos Int (2011) 22:2365 2371 DOI 10.1007/s00198-010-1452-6 ORIGINAL ARTICLE Prevalence of vertebral fractures on chest radiographs of elderly African American and Caucasian women D. Lansdown & B.
Osteoporos Int (2011) 22:2365 2371 DOI 10.1007/s00198-010-1452-6 ORIGINAL ARTICLE Prevalence of vertebral fractures on chest radiographs of elderly African American and Caucasian women D. Lansdown & B.
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Bucholz EM, Butala NM, Ma S, Normand S-LT, Krumholz HM. Life
Glucocorticoid Use in Patients With Systemic Lupus Erythematosus: Association Between Dose and Health Care Utilization and Costs
 Arthritis Care & Research Vol. 67, No. 8, August 2015, pp 1086 1094 DOI 10.1002/acr.22574 VC 2015, American College of Rheumatology ORIGINAL ARTICLE Glucocorticoid Use in Patients With Systemic Lupus Erythematosus:
Arthritis Care & Research Vol. 67, No. 8, August 2015, pp 1086 1094 DOI 10.1002/acr.22574 VC 2015, American College of Rheumatology ORIGINAL ARTICLE Glucocorticoid Use in Patients With Systemic Lupus Erythematosus:
3. Has bone specific alkaline phosphatase level increased OR does the member have symptoms related to active Paget s?
 Pharmacy Prior Authorization AETA BETTER HEALTH VIRGIIA CCC PLUS and MEDALLIO/FAMIS 4.0 Zoledronic Acid (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review
Pharmacy Prior Authorization AETA BETTER HEALTH VIRGIIA CCC PLUS and MEDALLIO/FAMIS 4.0 Zoledronic Acid (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review
Side Effects May Include (F031)
 Side Effects May Include (F031) American Academy of Dermatology 3/1/2019 Nicole Fett MD MSCE Associate Professor of Dermatology Oregon Health and Science University Conflicts of Interest and Disclosures
Side Effects May Include (F031) American Academy of Dermatology 3/1/2019 Nicole Fett MD MSCE Associate Professor of Dermatology Oregon Health and Science University Conflicts of Interest and Disclosures
Intensification to triple therapy non-biologic disease-modifying antirheumatic drugs for rheumatoid arthritis in the United States from 2009 to 2014
 Brief Report DOI 10.1002/art.39617 Intensification to triple therapy non-biologic disease-modifying antirheumatic drugs for rheumatoid arthritis in the United States from 2009 to 2014 Jeffrey A. Sparks,
Brief Report DOI 10.1002/art.39617 Intensification to triple therapy non-biologic disease-modifying antirheumatic drugs for rheumatoid arthritis in the United States from 2009 to 2014 Jeffrey A. Sparks,
Committee Approval Date: May 9, 2014 Next Review Date: May 2015
 Medication Policy Manual Policy No: dru248 Topic: Benlysta, belimumab Date of Origin: May 13, 2011 Committee Approval Date: May 9, 2014 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
Medication Policy Manual Policy No: dru248 Topic: Benlysta, belimumab Date of Origin: May 13, 2011 Committee Approval Date: May 9, 2014 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
No Association between Calcium Channel Blocker Use and Confirmed Bleeding Peptic Ulcer Disease
 American Journal of Epidemiology Copyright 1998 by The Johns Hopkins University School of Hygiene and Public Health All rights reserved Vol. 148, No. 4 Printed in U.S.A. A BRIEF ORIGINAL CONTRIBUTION No
American Journal of Epidemiology Copyright 1998 by The Johns Hopkins University School of Hygiene and Public Health All rights reserved Vol. 148, No. 4 Printed in U.S.A. A BRIEF ORIGINAL CONTRIBUTION No
LONGITUDINAL TREATMENT PATTERNS AND ASSOCIATED OUTCOMES IN PATIENTS WITH NEWLY DIAGNOSED SYSTEMIC LUPUS ERYTHEMATOSUS. Hong Kan 7/12/2016
 LONGITUDINAL TREATMENT PATTERNS AND ASSOCIATED OUTCOMES IN PATIENTS WITH NEWLY DIAGNOSED SYSTEMIC LUPUS ERYTHEMATOSUS Hong Kan 7/12/2016 1 Acknowledgements Research conceptualization and design, programming
LONGITUDINAL TREATMENT PATTERNS AND ASSOCIATED OUTCOMES IN PATIENTS WITH NEWLY DIAGNOSED SYSTEMIC LUPUS ERYTHEMATOSUS Hong Kan 7/12/2016 1 Acknowledgements Research conceptualization and design, programming
Switching Treatment Between Mycophenolate Mofetil and Azathioprine in Lupus Patients: Indications and Outcomes
 Arthritis Care & Research Vol. 66, No. 12, December 2014, pp 1905 1909 DOI 10.1002/acr.22364 2014, American College of Rheumatology ORIGINAL ARTICLE Switching Treatment Between Mycophenolate Mofetil and
Arthritis Care & Research Vol. 66, No. 12, December 2014, pp 1905 1909 DOI 10.1002/acr.22364 2014, American College of Rheumatology ORIGINAL ARTICLE Switching Treatment Between Mycophenolate Mofetil and
Integrating Effectiveness and Safety Outcomes in the Assessment of Treatments
 Integrating Effectiveness and Safety Outcomes in the Assessment of Treatments Jessica M. Franklin Instructor in Medicine Division of Pharmacoepidemiology & Pharmacoeconomics Brigham and Women s Hospital
Integrating Effectiveness and Safety Outcomes in the Assessment of Treatments Jessica M. Franklin Instructor in Medicine Division of Pharmacoepidemiology & Pharmacoeconomics Brigham and Women s Hospital
Parathyroid Hormone Analogs
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.36 Subject: Parathyroid Hormone Analogs Page: 1 of 6 Last Review Date: September 15, 2017 Parathyroid
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.30.36 Subject: Parathyroid Hormone Analogs Page: 1 of 6 Last Review Date: September 15, 2017 Parathyroid
Catch the HEDIS Buzz!
 Catch the HEDIS Buzz! Focus Area: Osteoporosis Management in Women Who Had a Fracture Date: October 2014 HEDIS Performance Score In 2013, Humana At Home associates did a great job of promoting Osteoporosis
Catch the HEDIS Buzz! Focus Area: Osteoporosis Management in Women Who Had a Fracture Date: October 2014 HEDIS Performance Score In 2013, Humana At Home associates did a great job of promoting Osteoporosis
Incidence and Risk of Alcohol Use Disorders by Age, Gender and Poverty Status: A Population-Based-10 Year Follow-Up Study
 Incidence and Risk of Alcohol Use Disorders by Age, Gender and Poverty Status: A Population-Based-10 Year Chun-Te Lee 1,2, Chiu-Yueh Hsiao 3, Yi-Chyan Chen 4,5, Oswald Ndi Nfor 6, Jing-Yang Huang 6, Lee
Incidence and Risk of Alcohol Use Disorders by Age, Gender and Poverty Status: A Population-Based-10 Year Chun-Te Lee 1,2, Chiu-Yueh Hsiao 3, Yi-Chyan Chen 4,5, Oswald Ndi Nfor 6, Jing-Yang Huang 6, Lee
Prescribing of anti-osteoporotic therapies following the use of Proton Pump Inhibitors in general practice
 Prescribing of anti-osteoporotic therapies following the use of Proton Pump Inhibitors in general practice B. McGowan, K. Bennett, J. Feely Department of Pharmacology & Therapeutics, Trinity Centre for
Prescribing of anti-osteoporotic therapies following the use of Proton Pump Inhibitors in general practice B. McGowan, K. Bennett, J. Feely Department of Pharmacology & Therapeutics, Trinity Centre for
Designing a Community-Based Intervention to Improve the Health of Medically-Underserved Women with Systemic Lupus Erythematosus
 Designing a Community-Based Intervention to Improve the Health of Medically-Underserved Women with Systemic Lupus Erythematosus Candace H Feldman MD, MPH Patricia Fraser MD Melanie Zibit MEd, MBA Derrick
Designing a Community-Based Intervention to Improve the Health of Medically-Underserved Women with Systemic Lupus Erythematosus Candace H Feldman MD, MPH Patricia Fraser MD Melanie Zibit MEd, MBA Derrick
Cervical neoplasia in systemic lupus erythematosus: a nationwide study.
 Cervical neoplasia in systemic lupus erythematosus: a nationwide study. Hjalmar Wadström, Elizabeth V Arkema, Christopher Sjöwall, Johan Askling and Julia F Simard Journal Article Original Publication:
Cervical neoplasia in systemic lupus erythematosus: a nationwide study. Hjalmar Wadström, Elizabeth V Arkema, Christopher Sjöwall, Johan Askling and Julia F Simard Journal Article Original Publication:
ORIGINAL ARTICLE. Abstract. Introduction. Daijun Kirigaya 1,2, Takeo Nakayama 2, Tatsuro Ishizaki 2, Shunya Ikeda 3 and Toshihiko Satoh 4
 ORIGINAL ARTICLE Management and Treatment of Osteoporosis in Patients Receiving Long-term Glucocorticoid Treatment: Current Status of Adherence to Clinical Guidelines and Related Factors Daijun Kirigaya
ORIGINAL ARTICLE Management and Treatment of Osteoporosis in Patients Receiving Long-term Glucocorticoid Treatment: Current Status of Adherence to Clinical Guidelines and Related Factors Daijun Kirigaya
CASE 1 WHY IS IT IMPORTANT TO TREAT? FACTS CONCERNS
 4:30-5:15pm Ask the Expert: Osteoporosis SPEAKERS Silvina Levis, MD OSTEOPOROSIS - FACTS 1:3 older women and 1:5 older men will have a fragility fracture after age 50 After 3 years of treatment, depending
4:30-5:15pm Ask the Expert: Osteoporosis SPEAKERS Silvina Levis, MD OSTEOPOROSIS - FACTS 1:3 older women and 1:5 older men will have a fragility fracture after age 50 After 3 years of treatment, depending
Benlysta. Benlysta (belimumab) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 Subject: Benlysta Page: 1 of 5 Last Review Date: December 3, 2015 Benlysta Description Benlysta (belimumab)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 Subject: Benlysta Page: 1 of 5 Last Review Date: December 3, 2015 Benlysta Description Benlysta (belimumab)
Index. Rheum Dis Clin N Am 32 (2006) Note: Page numbers of article titles are in boldface type.
 Rheum Dis Clin N Am 32 (2006) 775 780 Index Note: Page numbers of article titles are in boldface type. A AACE (American Association of Clinical Endocrinologists), bone mineral density recommendations of,
Rheum Dis Clin N Am 32 (2006) 775 780 Index Note: Page numbers of article titles are in boldface type. A AACE (American Association of Clinical Endocrinologists), bone mineral density recommendations of,
Osteoporosis as a Focus for Practice Improvement
 Osteoporosis as a Focus for Practice Improvement Karen E. Hansen, M.D. Assistant Professor of Medicine Rheumatology and Endocrine Sections University of Wisconsin Madison, WI Postmenopausal Osteoporosis
Osteoporosis as a Focus for Practice Improvement Karen E. Hansen, M.D. Assistant Professor of Medicine Rheumatology and Endocrine Sections University of Wisconsin Madison, WI Postmenopausal Osteoporosis
Osteoporosis/Fracture Prevention
 Osteoporosis/Fracture Prevention NATIONAL GUIDELINE SUMMARY This guideline was developed using an evidence-based methodology by the KP National Osteoporosis/Fracture Prevention Guideline Development Team
Osteoporosis/Fracture Prevention NATIONAL GUIDELINE SUMMARY This guideline was developed using an evidence-based methodology by the KP National Osteoporosis/Fracture Prevention Guideline Development Team
Benlysta. Benlysta (belimumab) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.99.01 Subject: Benlysta Page: 1 of 5 Last Review Date: June 22, 2018 Benlysta Description Benlysta (belimumab)
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.99.01 Subject: Benlysta Page: 1 of 5 Last Review Date: June 22, 2018 Benlysta Description Benlysta (belimumab)
Module 5 - Speaking of Bones Osteoporosis For Health Professionals: Fracture Risk Assessment. William D. Leslie, MD MSc FRCPC
 Module 5 - Speaking of Bones Osteoporosis For Health Professionals: Fracture Risk Assessment William D. Leslie, MD MSc FRCPC Case #1 Age 53: 3 years post-menopause Has always enjoyed excellent health with
Module 5 - Speaking of Bones Osteoporosis For Health Professionals: Fracture Risk Assessment William D. Leslie, MD MSc FRCPC Case #1 Age 53: 3 years post-menopause Has always enjoyed excellent health with
Trends in Glucocorticoid-Induced Osteoporosis Management Among Seniors in Ontario,
 Trends in Glucocorticoid-Induced Osteoporosis Management Among Seniors in Ontario, 1996-2012 Jordan M Albaum 1, Linda E Lévesque 2, Andrea S Gershon 3, Yan Yun Liu 1, Suzanne M Cadarette 1 1 Leslie Dan
Trends in Glucocorticoid-Induced Osteoporosis Management Among Seniors in Ontario, 1996-2012 Jordan M Albaum 1, Linda E Lévesque 2, Andrea S Gershon 3, Yan Yun Liu 1, Suzanne M Cadarette 1 1 Leslie Dan
Market Access CTR Summary
 Market Access CTR Summary Study No.: BEL114246 Title: Efficacy of Belimumab Treatment in a Subpopulation of Systemic Lupus Erythematosus (SLE) Patients: A Pooled Analysis of the HGS1006-C1056 (BLISS-52)
Market Access CTR Summary Study No.: BEL114246 Title: Efficacy of Belimumab Treatment in a Subpopulation of Systemic Lupus Erythematosus (SLE) Patients: A Pooled Analysis of the HGS1006-C1056 (BLISS-52)
Incidence and Mortality after Proximal Humerus Fractures Over 50 Years of Age in South Korea: National Claim Data from 2008 to 2012
 J Bone Metab 2015;22:17-21 http://dx.doi.org/10.11005/jbm.2015.22.1.17 pissn 2287-6375 eissn 2287-7029 Original Article Incidence and Mortality after Proximal Humerus Fractures Over 50 s of Age in South
J Bone Metab 2015;22:17-21 http://dx.doi.org/10.11005/jbm.2015.22.1.17 pissn 2287-6375 eissn 2287-7029 Original Article Incidence and Mortality after Proximal Humerus Fractures Over 50 s of Age in South
Official Positions on FRAX
 196 96 DEPLIANT 3,5x8,5.indd 1 2010 Official Positions on FRAX 21.03.11 11:45 Interpretation and Use of FRAX in Clinical Practice from the International Society for Clinical Densitometry and International
196 96 DEPLIANT 3,5x8,5.indd 1 2010 Official Positions on FRAX 21.03.11 11:45 Interpretation and Use of FRAX in Clinical Practice from the International Society for Clinical Densitometry and International
Product: Denosumab (AMG 162) Clinical Study Report: month Primary Analysis Date: 21 November 2016 Page 1
 Date: 21 November 2016 Page 1 2. SYNOPSIS Name of Sponsor: Amgen Inc., Thousand Oaks, CA, USA Name of Finished Product: Prolia Name of Active Ingredient: denosumab Title of Study: Randomized, Double-blind,
Date: 21 November 2016 Page 1 2. SYNOPSIS Name of Sponsor: Amgen Inc., Thousand Oaks, CA, USA Name of Finished Product: Prolia Name of Active Ingredient: denosumab Title of Study: Randomized, Double-blind,
Ankle fractures are one of
 Elevated Risks of Ankle Fracture Surgery in Patients With Diabetes Nelson F. SooHoo, MD, Lucie Krenek, MD, Michael Eagan, MD, and David S. Zingmond, MD, PhD Ankle fractures are one of the most common types
Elevated Risks of Ankle Fracture Surgery in Patients With Diabetes Nelson F. SooHoo, MD, Lucie Krenek, MD, Michael Eagan, MD, and David S. Zingmond, MD, PhD Ankle fractures are one of the most common types
Effective Health Care
 Number 12 Effective Health Care Comparative Effectiveness of Treatments To Prevent Fractures in Men and Women With Low Bone Density or Osteoporosis Executive Summary Background Osteoporosis is a systemic
Number 12 Effective Health Care Comparative Effectiveness of Treatments To Prevent Fractures in Men and Women With Low Bone Density or Osteoporosis Executive Summary Background Osteoporosis is a systemic
Chapter 2: Identification and Care of Patients With CKD
 Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Chapter 2: Identification and Care of Patients With CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Racial Variation In Quality Of Care Among Medicare+Choice Enrollees
 Racial Variation In Quality Of Care Among Medicare+Choice Enrollees Black/white patterns of racial disparities in health care do not necessarily apply to Asians, Hispanics, and Native Americans. by Beth
Racial Variation In Quality Of Care Among Medicare+Choice Enrollees Black/white patterns of racial disparities in health care do not necessarily apply to Asians, Hispanics, and Native Americans. by Beth
The Cost-Effectiveness of Bisphosphonates in Postmenopausal Women Based on Individual Long-Term Fracture Risks
 Volume ** Number ** ** VALUE IN HEALTH The Cost-Effectiveness of Bisphosphonates in Postmenopausal Women Based on Individual Long-Term Fracture Risks Tjeerd-Peter van Staa, MD, MA, PhD, 1,2 John A. Kanis,
Volume ** Number ** ** VALUE IN HEALTH The Cost-Effectiveness of Bisphosphonates in Postmenopausal Women Based on Individual Long-Term Fracture Risks Tjeerd-Peter van Staa, MD, MA, PhD, 1,2 John A. Kanis,
Assessment of the risk of osteoporotic fractures in Prof. J.J. Body, MD, PhD CHU Brugmann Univ. Libre de Bruxelles
 Assessment of the risk of osteoporotic fractures in 2008 Prof. J.J. Body, MD, PhD CHU Brugmann Univ. Libre de Bruxelles Estimated lifetime fracture risk in 50-year-old white women and men Melton et al.;
Assessment of the risk of osteoporotic fractures in 2008 Prof. J.J. Body, MD, PhD CHU Brugmann Univ. Libre de Bruxelles Estimated lifetime fracture risk in 50-year-old white women and men Melton et al.;
ONE of the following:
 Medical Coverage Policy Belimumab (Benlysta) EFFECTIVE DATE: 01 01 2012 POLICY LAST UPDATED: 11 21 2017 OVERVIEW Belimumab (Benlysta ) is indicated for the treatment of adult patients with active, autoantibody-positive,
Medical Coverage Policy Belimumab (Benlysta) EFFECTIVE DATE: 01 01 2012 POLICY LAST UPDATED: 11 21 2017 OVERVIEW Belimumab (Benlysta ) is indicated for the treatment of adult patients with active, autoantibody-positive,
A Population-Based Study of the Effectiveness of Bisphosphonates at Reducing Hip Fractures among High Risk Women
 A Population-Based Study of the Effectiveness of Bisphosphonates at Reducing Hip Fractures among High Risk Women APHA Conference Washington, DC November 2, 2011 Presenter Disclosures Kathy Schneider, PhD
A Population-Based Study of the Effectiveness of Bisphosphonates at Reducing Hip Fractures among High Risk Women APHA Conference Washington, DC November 2, 2011 Presenter Disclosures Kathy Schneider, PhD
Table S1. Read and ICD 10 diagnosis codes for polymyalgia rheumatica and giant cell arteritis
 SUPPLEMENTARY MATERIAL TEXT Text S1. Multiple imputation TABLES Table S1. Read and ICD 10 diagnosis codes for polymyalgia rheumatica and giant cell arteritis Table S2. List of drugs included as immunosuppressant
SUPPLEMENTARY MATERIAL TEXT Text S1. Multiple imputation TABLES Table S1. Read and ICD 10 diagnosis codes for polymyalgia rheumatica and giant cell arteritis Table S2. List of drugs included as immunosuppressant
Estimating Medicaid Costs for Cardiovascular Disease: A Claims-based Approach
 Estimating Medicaid Costs for Cardiovascular Disease: A Claims-based Approach Presented by Susan G. Haber, Sc.D 1 ; Boyd H. Gilman, Ph.D. 1 1 RTI International Presented at The 133rd Annual Meeting of
Estimating Medicaid Costs for Cardiovascular Disease: A Claims-based Approach Presented by Susan G. Haber, Sc.D 1 ; Boyd H. Gilman, Ph.D. 1 1 RTI International Presented at The 133rd Annual Meeting of
Pharmacy Management Drug Policy
 SUBJECT: - Forteo (teriparatide), Prolia (denosumab), Tymlos (abaloparatide), Boniva injection (Ibandronate) POLICY NUMBER: Pharmacy-35 EFFECTIVE DATE: 9/07 LAST REVIEW DATE: 10/15/2018 If the member s
SUBJECT: - Forteo (teriparatide), Prolia (denosumab), Tymlos (abaloparatide), Boniva injection (Ibandronate) POLICY NUMBER: Pharmacy-35 EFFECTIVE DATE: 9/07 LAST REVIEW DATE: 10/15/2018 If the member s
Increased risk of death in African American patients with end-stage renal disease secondary to lupus
 Clin Kidney J (2014) 7: 40 44 doi: 10.1093/ckj/sft157 Advance Access publication 2 January 2014 Original Article Increased risk of death in patients with end-stage renal disease secondary to lupus Sangeeta
Clin Kidney J (2014) 7: 40 44 doi: 10.1093/ckj/sft157 Advance Access publication 2 January 2014 Original Article Increased risk of death in patients with end-stage renal disease secondary to lupus Sangeeta
Osteoporosis: A Tale of 3 Task Forces!
 Osteoporosis: A Tale of 3 Task Forces! Robert A. Adler, MD McGuire Veterans Affairs Medical Center Virginia Commonwealth University Richmond, Virginia, USA Disclosures The opinions are those of the speaker
Osteoporosis: A Tale of 3 Task Forces! Robert A. Adler, MD McGuire Veterans Affairs Medical Center Virginia Commonwealth University Richmond, Virginia, USA Disclosures The opinions are those of the speaker
Osteoporosis Screening and Treatment in Type 2 Diabetes
 Osteoporosis Screening and Treatment in Type 2 Diabetes Ann Schwartz, PhD! Dept. of Epidemiology and Biostatistics! University of California San Francisco! October 2011! Presenter Disclosure Information
Osteoporosis Screening and Treatment in Type 2 Diabetes Ann Schwartz, PhD! Dept. of Epidemiology and Biostatistics! University of California San Francisco! October 2011! Presenter Disclosure Information
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Prada D, Zhong J, Colicino E, et al. Association
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Prada D, Zhong J, Colicino E, et al. Association
Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments
 Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments Prepared for: American Hospital Association April 4, 2019 Berna Demiralp,
Comparison of Medicare Fee-for-Service Beneficiaries Treated in Ambulatory Surgical Centers and Hospital Outpatient Departments Prepared for: American Hospital Association April 4, 2019 Berna Demiralp,
HEALTH DISPARITIES AMONG ADULTS IN OHIO
 OHIO MEDICAID ASSESSMENT SURVEY 2012 Taking the pulse of health in Ohio HEALTH DISPARITIES AMONG ADULTS IN OHIO Amy K. Ferketich, PhD 1 Ling Wang, MPH 1 Timothy R. Sahr, MPH, MA 2 1The Ohio State University
OHIO MEDICAID ASSESSMENT SURVEY 2012 Taking the pulse of health in Ohio HEALTH DISPARITIES AMONG ADULTS IN OHIO Amy K. Ferketich, PhD 1 Ling Wang, MPH 1 Timothy R. Sahr, MPH, MA 2 1The Ohio State University
Addressing Healthcare Disparities in Autoimmune Disease: A Focus On Systemic Lupus Erythematosus in the USA
 Addressing Healthcare Disparities in Autoimmune Disease: A Focus On Systemic Lupus Erythematosus in the USA by Halima Moncrieffe, PhD halima.moncrieffe@cchmc.org Center for Autoimmune Genomics & Etiology,
Addressing Healthcare Disparities in Autoimmune Disease: A Focus On Systemic Lupus Erythematosus in the USA by Halima Moncrieffe, PhD halima.moncrieffe@cchmc.org Center for Autoimmune Genomics & Etiology,
Pharmacy Management Drug Policy
 SUBJECT: - Forteo (teriparatide), Prolia (denosumab), Tymlos (abaloparatide) POLICY NUMBER: Pharmacy-35 EFFECTIVE DATE: 9/07 LAST REVIEW DATE: 9/29/2017 If the member s subscriber contract excludes coverage
SUBJECT: - Forteo (teriparatide), Prolia (denosumab), Tymlos (abaloparatide) POLICY NUMBER: Pharmacy-35 EFFECTIVE DATE: 9/07 LAST REVIEW DATE: 9/29/2017 If the member s subscriber contract excludes coverage
BONIVA (ibandronate sodium)
 BONIVA (ibandronate sodium) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
BONIVA (ibandronate sodium) Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices
Children s Oral Health and Access to Dental Care in the United States
 Children s Oral Health and Access to Dental Care in the United States Bruce Dye, DDS, MPH Institute of Medicine Oral Health Access to Services Meeting: 4 March 2010 U.S. DEPARTMENT OF HEALTH AND HUMAN
Children s Oral Health and Access to Dental Care in the United States Bruce Dye, DDS, MPH Institute of Medicine Oral Health Access to Services Meeting: 4 March 2010 U.S. DEPARTMENT OF HEALTH AND HUMAN
Erythrocyte-bound C4d in combination with complement and autoantibody status for the monitoring of SLE
 To cite: Merrill JT, Petri MA, Buyon J, et al. Erythrocytebound C4d in combination with complement and autoantibody status for the monitoring of SLE. Lupus Science & Medicine 2018;5:e000263. doi:10.1136/
To cite: Merrill JT, Petri MA, Buyon J, et al. Erythrocytebound C4d in combination with complement and autoantibody status for the monitoring of SLE. Lupus Science & Medicine 2018;5:e000263. doi:10.1136/
Case identification of patients at risk for an osteoporotic fracture
 Identifying Patients With Osteoporosis or at Risk for Osteoporotic Fractures Yong Chen, MD, PhD; Leslie R. Harrold, MD, MPH; Robert A. Yood, MD; Terry S. Field, DSc; and Becky A. Briesacher, PhD Case identification
Identifying Patients With Osteoporosis or at Risk for Osteoporotic Fractures Yong Chen, MD, PhD; Leslie R. Harrold, MD, MPH; Robert A. Yood, MD; Terry S. Field, DSc; and Becky A. Briesacher, PhD Case identification
AETNA BETTER HEALTH Prior Authorization guideline for Injectable Osteoporosis Agents
 AETNA BETTER HEALTH Prior Authorization guideline for Injectable Osteoporosis Agents Injectable Osteoporosis Agents Forteo (teriparatide); zoledronic acid Prolia (denosumab)] Authorization guidelines For
AETNA BETTER HEALTH Prior Authorization guideline for Injectable Osteoporosis Agents Injectable Osteoporosis Agents Forteo (teriparatide); zoledronic acid Prolia (denosumab)] Authorization guidelines For
Chapter 2: Identification and Care of Patients with CKD
 Chapter 2: Identification and Care of Patients with CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Chapter 2: Identification and Care of Patients with CKD Over half of patients in the Medicare 5% sample (aged 65 and older) had at least one of three diagnosed chronic conditions chronic kidney disease
Review. Healthcare quality in systemic lupus erythematosus: using Donabedian s conceptual framework to understand what we know
 Review Healthcare quality in systemic lupus erythematosus: using Donabedian s conceptual framework to understand what we know Healthcare quality improvement has the potential to reduce the striking disparities
Review Healthcare quality in systemic lupus erythematosus: using Donabedian s conceptual framework to understand what we know Healthcare quality improvement has the potential to reduce the striking disparities
Bisphosphonates in the Management of. Myeloma Bone Disease
 Bisphosphonates in the Management of Myeloma Bone Disease James R. Berenson, MD Medical & Scientific Director Institute for Myeloma & Bone Cancer Research Los Angeles, CA Myeloma Bone Disease Myeloma cells
Bisphosphonates in the Management of Myeloma Bone Disease James R. Berenson, MD Medical & Scientific Director Institute for Myeloma & Bone Cancer Research Los Angeles, CA Myeloma Bone Disease Myeloma cells
Direct healthcare costs of hip, vertebral, and nonhip, non-vertebral fractures.
 Thomas Jefferson University Jefferson Digital Commons College of Population Health Faculty Papers Jefferson College of Population Health 12-1-2009 Direct healthcare costs of hip, vertebral, and nonhip,
Thomas Jefferson University Jefferson Digital Commons College of Population Health Faculty Papers Jefferson College of Population Health 12-1-2009 Direct healthcare costs of hip, vertebral, and nonhip,
Use of DXA / Bone Density in the Care of Your Patients. Brenda Lee Holbert, M.D. Associate Professor Senior Staff Radiologist
 Use of DXA / Bone Density in the Care of Your Patients Brenda Lee Holbert, M.D. Associate Professor Senior Staff Radiologist Important Websites Resources for Clinicians and Patients www.nof.org www.iofbonehealth.org
Use of DXA / Bone Density in the Care of Your Patients Brenda Lee Holbert, M.D. Associate Professor Senior Staff Radiologist Important Websites Resources for Clinicians and Patients www.nof.org www.iofbonehealth.org
Racial and Socioeconomic Disparities in Appendicitis
 Racial and Socioeconomic Disparities in Appendicitis Steven L. Lee, MD Chief of Pediatric Surgery, Harbor-UCLA Associate Clinical Professor of Surgery and Pediatrics David Geffen School of Medicine at
Racial and Socioeconomic Disparities in Appendicitis Steven L. Lee, MD Chief of Pediatric Surgery, Harbor-UCLA Associate Clinical Professor of Surgery and Pediatrics David Geffen School of Medicine at
Effect of mycophenolate mofetil on the white blood cell count and the frequency of infection in systemic lupus erythematosus.
 Thomas Jefferson University Jefferson Digital Commons Department of Medicine Faculty Papers Department of Medicine 10-22-2015 Effect of mycophenolate mofetil on the white blood cell count and the frequency
Thomas Jefferson University Jefferson Digital Commons Department of Medicine Faculty Papers Department of Medicine 10-22-2015 Effect of mycophenolate mofetil on the white blood cell count and the frequency
Elevated BLyS levels in patients with systemic lupus erythematosus: Associated factors and responses to belimumab
 (2016) 25, 346 354 http://lup.sagepub.com PAPER Elevated BLyS levels in patients with systemic lupus erythematosus: Associated factors and responses to belimumab DA Roth 1, A Thompson 2, Y Tang 2*, AE
(2016) 25, 346 354 http://lup.sagepub.com PAPER Elevated BLyS levels in patients with systemic lupus erythematosus: Associated factors and responses to belimumab DA Roth 1, A Thompson 2, Y Tang 2*, AE
Are glucocorticoid-induced osteoporosis recommendations sufficient to determine antiosteoporotic treatment for patients with rheumatoid arthritis?
 ORIGINAL ARTICLE Korean J Intern Med 2014;29:509-515 Are glucocorticoid-induced osteoporosis recommendations sufficient to determine antiosteoporotic treatment for patients with rheumatoid arthritis? Joo-Hyun
ORIGINAL ARTICLE Korean J Intern Med 2014;29:509-515 Are glucocorticoid-induced osteoporosis recommendations sufficient to determine antiosteoporotic treatment for patients with rheumatoid arthritis? Joo-Hyun
INHALED AND NASAL CORTICOSTEROID USE AND THE RISK OF FRACTURE. Online data supplement.
 INHALED AND NASAL CORTICOSTEROID USE AND THE RISK OF FRACTURE. Online data supplement. Samy Suissa, PhD, Marc Baltzan, MD, MSc, Richard Kremer, MD, Pierre Ernst, MD, MSc 26 METHODS Source of data We used
INHALED AND NASAL CORTICOSTEROID USE AND THE RISK OF FRACTURE. Online data supplement. Samy Suissa, PhD, Marc Baltzan, MD, MSc, Richard Kremer, MD, Pierre Ernst, MD, MSc 26 METHODS Source of data We used
10-Year Mortality of Older Acute Myocardial Infarction Patients Treated in U.S. Community Practice
 10-Year Mortality of Older Acute Myocardial Infarction Patients Treated in U.S. Community Practice Ajar Kochar, MD on behalf of: Anita Y. Chen, Puza P. Sharma, Neha J. Pagidipati, Gregg C. Fonarow, Patricia
10-Year Mortality of Older Acute Myocardial Infarction Patients Treated in U.S. Community Practice Ajar Kochar, MD on behalf of: Anita Y. Chen, Puza P. Sharma, Neha J. Pagidipati, Gregg C. Fonarow, Patricia
Alcohol Consumption and Mortality Risks in the U.S. Brian Rostron, Ph.D. Savet Hong, MPH
 Alcohol Consumption and Mortality Risks in the U.S. Brian Rostron, Ph.D. Savet Hong, MPH 1 ABSTRACT This study presents relative mortality risks by alcohol consumption level for the U.S. population, using
Alcohol Consumption and Mortality Risks in the U.S. Brian Rostron, Ph.D. Savet Hong, MPH 1 ABSTRACT This study presents relative mortality risks by alcohol consumption level for the U.S. population, using
Supplementary Online Content
 Supplementary Online Content Pincus D, Ravi B, Wasserstein D. Association between wait time and 30-day mortality in adults undergoing hip fracture surgery. JAMA. doi: 10.1001/jama.2017.17606 eappendix
Supplementary Online Content Pincus D, Ravi B, Wasserstein D. Association between wait time and 30-day mortality in adults undergoing hip fracture surgery. JAMA. doi: 10.1001/jama.2017.17606 eappendix
Erythropoiesis-stimulating Agent Use among Patients with Lupus Nephritis Approaching End-stage Renal Disease
 Erythropoiesis-stimulating Agent Use among Patients with Lupus Nephritis Approaching End-stage Renal Disease The Harvard community has made this article openly available. Please share how this access benefits
Erythropoiesis-stimulating Agent Use among Patients with Lupus Nephritis Approaching End-stage Renal Disease The Harvard community has made this article openly available. Please share how this access benefits
Medha Barbhaiya 1*, Yan Dong 2, Jeffrey A. Sparks 1, Elena Losina 1,3, Karen H. Costenbader 1 and Jeffrey N. Katz 1,3
 Barbhaiya et al. BMC Musculoskeletal Disorders (2017) 18:268 DOI 10.1186/s12891-017-1626-x RESEARCH ARTICLE Open Access Administrative Algorithms to identify Avascular necrosis of bone among patients undergoing
Barbhaiya et al. BMC Musculoskeletal Disorders (2017) 18:268 DOI 10.1186/s12891-017-1626-x RESEARCH ARTICLE Open Access Administrative Algorithms to identify Avascular necrosis of bone among patients undergoing
Discontinuation and restarting in patients on statin treatment: prospective open cohort study using a primary care database
 open access Discontinuation and restarting in patients on statin treatment: prospective open cohort study using a primary care database Yana Vinogradova, 1 Carol Coupland, 1 Peter Brindle, 2,3 Julia Hippisley-Cox
open access Discontinuation and restarting in patients on statin treatment: prospective open cohort study using a primary care database Yana Vinogradova, 1 Carol Coupland, 1 Peter Brindle, 2,3 Julia Hippisley-Cox
Thank you for agreeing to give us a statement on your organisation s view of the technology and the way it should be used in the NHS.
 Appendix I - Thank you for agreeing to give us a statement on your organisation s view of the technology and the way it should be used in the NHS. Healthcare professionals can provide a unique perspective
Appendix I - Thank you for agreeing to give us a statement on your organisation s view of the technology and the way it should be used in the NHS. Healthcare professionals can provide a unique perspective
Osteoporosis and Rheumatic Diseases
 Osteoporosis and Rheumatic Diseases This is an area which is often neglected and is a burden too heavy to be carried by the weakened bones! There is an increased risk of osteoporosis (OP) in rheumatic
Osteoporosis and Rheumatic Diseases This is an area which is often neglected and is a burden too heavy to be carried by the weakened bones! There is an increased risk of osteoporosis (OP) in rheumatic
Section I Project Leader: Michael P. Catalino Credentials: MD, DO, MS. Male Female Date of birth: 6/24/1987 NC medical license no.
 North Carolina Spine Society Tel: 919-833-3836 PO Box 27167 Fax: 919-833-2023 Raleigh, NC 27611 ncspine@ncmedsoc.org Section I Project Leader: Michael P. Catalino Credentials: MD, DO, MS Male Female Date
North Carolina Spine Society Tel: 919-833-3836 PO Box 27167 Fax: 919-833-2023 Raleigh, NC 27611 ncspine@ncmedsoc.org Section I Project Leader: Michael P. Catalino Credentials: MD, DO, MS Male Female Date
Benlysta (belimumab) Prior Authorization Criteria Program Summary
 Benlysta (belimumab) Prior Authorization Criteria Program Summary This prior authorization applies to Commercial, NetResults A series, NetResults F series and Health Insurance Marketplace formularies.
Benlysta (belimumab) Prior Authorization Criteria Program Summary This prior authorization applies to Commercial, NetResults A series, NetResults F series and Health Insurance Marketplace formularies.
Chapter 10: Dialysis Providers
 Chapter 10: Dialysis Providers In 2014 the two largest dialysis organizations, Fresenius and DaVita, collectively treated 69% of patients in 65% of all dialysis units (Figure 10.2). Nearly 90% of all dialysis
Chapter 10: Dialysis Providers In 2014 the two largest dialysis organizations, Fresenius and DaVita, collectively treated 69% of patients in 65% of all dialysis units (Figure 10.2). Nearly 90% of all dialysis
Submission to the National Institute for Clinical Excellence on
 Submission to the National Institute for Clinical Excellence on Strontium ranelate for the prevention of osteoporotic fractures in postmenopausal women with osteoporosis by The Society for Endocrinology
Submission to the National Institute for Clinical Excellence on Strontium ranelate for the prevention of osteoporotic fractures in postmenopausal women with osteoporosis by The Society for Endocrinology
Interpreting DEXA Scan and. the New Fracture Risk. Assessment. Algorithm
 Interpreting DEXA Scan and the New Fracture Risk Assessment Algorithm Prof. Samir Elbadawy *Osteoporosis affect 30%-40% of women in western countries and almost 15% of men after the age of 50 years. Osteoporosis
Interpreting DEXA Scan and the New Fracture Risk Assessment Algorithm Prof. Samir Elbadawy *Osteoporosis affect 30%-40% of women in western countries and almost 15% of men after the age of 50 years. Osteoporosis
Chapter 6: Healthcare Expenditures for Persons with CKD
 Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
Chapter 6: Healthcare Expenditures for Persons with CKD In this 2017 Annual Data Report (ADR), we introduce information from the Optum Clinformatics DataMart for persons with Medicare Advantage and commercial
Osteoporosis and Lupus. Andrew Ruthberg, MD University Rheumatologists
 Osteoporosis and Lupus Andrew Ruthberg, MD University Rheumatologists 1 Forget the medical terminology (osteoporosis, osteopenia, low bone mass, DEXA, DXA, T score etc) The bottom line is that you don
Osteoporosis and Lupus Andrew Ruthberg, MD University Rheumatologists 1 Forget the medical terminology (osteoporosis, osteopenia, low bone mass, DEXA, DXA, T score etc) The bottom line is that you don
DXA When to order? How to interpret? Dr Nikhil Tandon Department of Endocrinology and Metabolism All India Institute of Medical Sciences New Delhi
 DXA When to order? How to interpret? Dr Nikhil Tandon Department of Endocrinology and Metabolism All India Institute of Medical Sciences New Delhi Clinical Utility of Bone Densitometry Diagnosis (DXA)
DXA When to order? How to interpret? Dr Nikhil Tandon Department of Endocrinology and Metabolism All India Institute of Medical Sciences New Delhi Clinical Utility of Bone Densitometry Diagnosis (DXA)
Fractures: Epidemiology and Risk Factors. Osteoporosis in Men (more this afternoon) 1/5 men over age 50 will suffer osteoporotic fracture 7/16/2009
 Fractures: Epidemiology and Risk Factors Mary L. Bouxsein, PhD Department of Orthopaedic Surgery Beth Israel Deaconess Medical Center Harvard Medical School, Boston, MA Outline Fracture incidence and impact
Fractures: Epidemiology and Risk Factors Mary L. Bouxsein, PhD Department of Orthopaedic Surgery Beth Israel Deaconess Medical Center Harvard Medical School, Boston, MA Outline Fracture incidence and impact
Supplementary Material*
 Supplementary Material* Park LS, Tate JP, Sigel K, Brown ST, Crothers K, Gibert C, et al. Association of Viral Suppression With Lower AIDS-Defining and Non AIDS-Defining Cancer Incidence in HIV-Infected
Supplementary Material* Park LS, Tate JP, Sigel K, Brown ST, Crothers K, Gibert C, et al. Association of Viral Suppression With Lower AIDS-Defining and Non AIDS-Defining Cancer Incidence in HIV-Infected
Assessment and management of glucocorticoid-induced osteoporosis
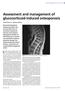 PRESCRIBING IN PRACTICE n Assessment and management of glucocorticoid-induced osteoporosis Gerald Tracey and Tehseen Ahmed Glucocorticoid-induced osteoporosis (GIO) is the most prevalent form of secondary
PRESCRIBING IN PRACTICE n Assessment and management of glucocorticoid-induced osteoporosis Gerald Tracey and Tehseen Ahmed Glucocorticoid-induced osteoporosis (GIO) is the most prevalent form of secondary
RESEARCH. Predicting risk of osteoporotic fracture in men and women in England and Wales: prospective derivation and validation of QFractureScores
 Predicting risk of osteoporotic fracture in men and women in England and Wales: prospective derivation and validation of QFractureScores Julia Hippisley-Cox, professor of clinical epidemiology and general
Predicting risk of osteoporotic fracture in men and women in England and Wales: prospective derivation and validation of QFractureScores Julia Hippisley-Cox, professor of clinical epidemiology and general
Learning Objectives. Controversies in Osteoporosis Prevention and Management. Etiology. Presenter Disclosure Information. Epidemiology.
 12:45 1:30pm Controversies in Osteoporosis Prevention and Management SPEAKER Carolyn Crandall, MD, MS Presenter Disclosure Information The following relationships exist related to this presentation: Carolyn
12:45 1:30pm Controversies in Osteoporosis Prevention and Management SPEAKER Carolyn Crandall, MD, MS Presenter Disclosure Information The following relationships exist related to this presentation: Carolyn
Coordinator of Post Professional Programs Texas Woman's University 1
 OSTEOPOROSIS Update 2007-2008 April 26, 2008 How much of our BMD is under our control (vs. genetics)? 1 2 Genetic effects on bone loss: longitudinal twin study (Makovey, 2007) Peak BMD is under genetic
OSTEOPOROSIS Update 2007-2008 April 26, 2008 How much of our BMD is under our control (vs. genetics)? 1 2 Genetic effects on bone loss: longitudinal twin study (Makovey, 2007) Peak BMD is under genetic
Carolyn J. Crandall, MD, MS On behalf of the WHI Bone SIG
 Carolyn J. Crandall, MD, MS On behalf of the WHI Bone SIG Background One half of all postmenopausal women will have an osteoporosis related fracture during their lifetimes. Background Low body weight is
Carolyn J. Crandall, MD, MS On behalf of the WHI Bone SIG Background One half of all postmenopausal women will have an osteoporosis related fracture during their lifetimes. Background Low body weight is
