Accidental hypothermia, defined as an unintentional
|
|
|
- Lorena Chapman
- 6 years ago
- Views:
Transcription
1 C l i n i c a l R e v i e w A r t i c l e Accidental Hypothermia Faris A. Khasawneh, MD Asha Thomas, MD Sajan Thomas, MD Accidental hypothermia, defined as an unintentional drop in core body temperature to less than 35 C (95 F), is commonly encountered in emergency departments. In the United States, approximately 700 deaths are attributed to accidental hypothermia each year, 1 3 with approximately half of all hypothermia-related deaths occurring in the elderly. A rise in the incidence of hypothermia has been attributed to increased participation in outdoor activities as well as social problems related to alcoholism, mental illness, and homelessness. 4 Hypothermia is classified based on core body temperature as mild (32 C 35 C), moderate (28 C 32 C), and severe (< 28 C). Management depends on the degree of hypothermia, with severe hypothermia requiring more aggressive treatment (eg, active internal rewarming). Mild hypothermia is not associated with significant mortality; however, the mortality rate associated with moderate to severe hypothermia is 30% to 80%. 5 This article reviews the pathophysiology, etiology, clinical manifestations, and management of accidental hypothermia. thermoregulation Temperature regulation involves loss, conservation, and production of heat and varies in a diurnal fashion within a range of 0.5 C. Body temperature also varies with menstrual cycle by 1 C. 6 Temperature is regulated centrally by the hypothalamus in coordination with peripheral cold and heat receptors. Under normal circumstances, alterations in ambient temperature initiate accommodative changes that maintain core body temperature within a narrow range (0.2 C 0.4 C). Deviations in temperature from a set point are sensed by the hypothalamus, which triggers the initiation of mechanisms that produce, conserve, or dissipate heat. Behavioral responses (eg, moving to a warmer environment, layering of clothes) as well as heat production through shivering and increased basal metabolic rate due to hormonal activity involving thyroxin, cortisol, and epinephrine contribute to changes in core body temperature. The temperature thresholds for sweating and vasodilation, vasoconstriction, nonshivering thermogenesis, and shivering are 37 C, 36.8 C, 36 C, TAKE HOME POINTS Hypothermia is defined as core body temperature less than 35 C. Hypothermia is classified as mild (32 C 35 C), moderate (28 C 32 C), and severe (< 28 C) based on the degree of hypothermia, with clinical signs and symptoms guiding management. Osborn waves, a positive deflection at the ST segment, may be seen on electrocardiography, but this finding is not a pathognomonic feature of hypothermia. Management involves evaluating the patient for a possible cause of hypothermia and rewarming. Passive rewarming is a slow process and should be used in patients with mild hypothermia. Active rewarming is faster and more efficient and should be used in patients with moderate or severe hypothermia or in patients with cardiovascular compromise. A patient should be pronounced dead only when warm and dead. and 35.5 C, respectively. 6 Radiation and conduction contribute to 70% of heat loss. Other methods of heat loss include convection, evaporation of sweat, and respiration. 1,7 ETIOLOGY Hypothermia is the end result of various factors related to disturbances in temperature regulation (Table 1). 1,3,8,9 Decreased basal metabolic rate as seen in Dr. Khasawneh is an internal medicine resident, and Dr. Sajan Thomas is assistant program director of the Internal Medicine Residency Program; both are at Westlake Hospital, Melrose Park, IL. At the time this manuscript was submitted, Dr. Asha Thomas was a chief resident, Westlake Hospital; she is now an attending physician, Rockford Memorial Hospital, Rockford, IL. 16 Hospital Physician December
2 Table 1. Etiology of Accidental Hypothermia Hypoadrenalism Hypothyroidism Hypopituitarism Hypoglycemia Diabetic ketoacidosis Extremes of age (lack of behavioral response and impaired shivering) Skin disorders (burns) Drugs (benzodiazepines, phenothiazine, barbiturates, ethanol) Neurologic (head trauma, stroke, tumors) Sepsis Environmental exposure (cold water immersion, inadequate indoor heating) Iatrogenic (fluid resuscitation, perioperative) hypopituitarism, hypothyroidism, and hypoadrenalism can lead to hypothermia. The presence of a neurologic disorder can lead to altered temperature thresholds, which may result in changes in the behavioral response to hypothermia. Inappropriate behavioral response can occur in patients with head trauma, cerebrovascular accident, and intracranial tumors. Hypothermia also can be caused by environmental factors, medications, and alcohol or can occur along with skin disorders. In the elderly, hypothermia can occur in the setting of an ambient cold environment, such as air conditioning or ice baths, as a result of impaired shivering mechanisms associated with older age. Other factors that place elderly patients at increased risk for hypothermia include a decreased ability to detect temperature changes as well as a decreased ability to generate heat because of reduced lean body mass and impaired mobility. 10 Immersion in cold water also can cause hypothermia, as the heat conductivity of water is 30 times that of air. Medications, such as phenothiazine and sedatives, can decrease the temperature threshold of the hypothalamus and cause impaired behavioral response, leading to hypothermia. 11 Alcohol causes vasodilation of cutaneous blood vessels and impairs the behavioral response to stimuli, increasing the risk for hypothermia. Skin disorders, such as burns, exfoliative disease, and severe psoriasis, may lead to loss of skin (a natural insulator), thereby resulting in hypothermia. 12 When hypothermia is associated with trauma (either blunt or penetrating), the outcome is significantly worse. 13 Iatrogenic causes of hypothermia can be attributed to medications mentioned above, resuscitative intravascular fluids, infusion of blood products, and perioperative anesthetics. It is essential to keep in mind that blood products are preserved at 39.2 F (4 C). 14 Table 2. Clinical Manifestations of Hypothermia Mild hypothermia (32 C 35 C) Confusion Dysarthria Shivering Tachycardia Hypertension Bronchorrhea Cold diuresis Atrial fibrillation Electrolyte imbalances Hyperglycemia Moderate hypothermia (28 C 32 C) Decreasing level of consciousness Dilated pupils Hallucinations Loss of shivering mechanism Bradycardia Cold diuresis Osborn waves (J waves) on electrocardiography Ventricular arrhythmias Severe hypothermia (< 28 C) Coma Loss of reflexes Loss of activity on electroencephalography Bradycardia Oliguria Asystole at < 20 C Apnea at < 24 C Pulmonary edema Osborn waves (J waves) on electrocardiography Adapted with permission from Kempainen RR, Brunette DD. The evaluation and management of accidental hypothermia. Respir Care 2004;49:195. CLINICAL MANIFESTATIONS The clinical manifestations of hypothermia are a spectrum of body responses to loss of heat and decreasing temperature (Table 2). Initially, the body tries to combat hypothermia by conserving heat and increasing catecholamines, thereby producing responses such as tachycardia, tachypnea, and increased blood pressure, cardiac output, and minute ventilation. Although these body responses may maintain core body temperature within the normal range, they result in increased oxygen consumption and shivering. As the patient continues to lose heat, these responses tend to cause fatigue; the patient becomes confused, bradycardic, hypotensive, and cardiac output and metabolic rate decrease. Hospital Physician December
3 Figure. An electrocardiogram demonstrating Osborn waves, representing a positive deflection at the ST segment. (Reprinted from Thornton D, Farmer JC. Hypothermia and hyperthermia. In: Parillo JE, Dellinger RP, editors. Critical care medicine: principles of diagnosis and management in the adult. 2nd ed. St. Louis: Mosby; 2002: Copyright 2002, with permission from Elsevier.) Electrocardiographic (ECG) changes seen in patients with mild hypothermia initially include tachycardia, suppression of ventricular ectopy, and prominence of atrial arrhythmias. As hypothermia progresses (ie, moderate hypothermia), bradycardia proceeds to asystole. Asystole has been suggested to be the primary cause of cardiopulmonary arrest due to hypothermia. 10 Additionally, ventricular fibrillation may occur as a result of cardiac stimulation through rewarming, hypocapnia, alkalosis, or physical manipulation. 10 Although not pathognomonic, the ECG in moderate or severe hypothermia may show a J wave or Osborn wave (Figure), which represents a positive deflection at the ST segment. 10,15 These changes are best seen in the lateral leads with increasing amplitude as hypothermia worsens. J wave/osborn waves may also be seen in cases of subarachnoid hemorrhage and intracranial injuries as well as in myocardial ischemia in the absence of hypothermia. Other ECG changes include PR, QRS, and QT prolongation as well as T-wave inversion. 7 Hypothermia-related peripheral vasoconstriction causes cold diuresis, which in turn leads to increased kidney perfusion and the loss of the kidney s ability to concentrate fluids, ultimately resulting in hyperosmolar hypernatremia and oliguria with ensuing hypovolemia. 10 As the kidney starts to fail, acid-base disturbance causes respiratory alkalosis, which progresses to metabolic acidosis and associated hyperkalemia. As the metabolic rate decreases, hypothermia causes reductions in oxygen consumption and carbon dioxide production. A left shift of the oxyhemoglobin dissociation curve with subsequent oxygen delivery impairment and tissue hypoxia is also seen; however, the acidosis and decreased rate of tissue metabolism due to hypothermia compensate for this effect. 10 In trauma patients, hypothermia is associated with coagulopathy, 5,13,16 which is a result of impaired platelet function and thrombocytopenia caused by extravascular sequestration of platelets. Furthermore, as body temperature decreases, coagulation cascade enzymes tend to lose their function. Hypothermia-related coagulopathy cannot be measured by available laboratory tests, as these are performed after heating blood to room temperature. Clinically, coagulopathy might manifest with either bleeding or a hypercoagulable state and thrombus formation. Interestingly, in severe hypothermia, paradoxical undressing may be observed. Although the cause of this phenomenon is not clearly understood, it is thought that cutaneous vascular disturbances result in a false sensation of warmth. 17 Undressing leads to further heat loss and progression of hypothermia. Also, in severe hypothermia, the level of consciousness progressively deteriorates to coma and loss of electroencephalographic activity, which may lead to terminal primitive behaviors (eg, the hide-and-die syndrome). This may explain why some patients who die from hypothermia are found in hidden positions. 17 EVALUATION OF THE PATIENT Managing hypothermic patients can be a challenge because of the absence of a reliable history in most cases. Initially, core body temperature should not be measured with a standard thermometer, which cannot measure temperatures lower than 34.4 C (94 F). 1 Pulmonary artery probe is the most reliable method for measuring core temperature in patients with hypothermia, but it is invasive. Other methods include tympanic membrane probes, rectal probes, and bladder probes. After the diagnosis of hypothermia is made, work-up is individualized based on the suspected cause of hypothermia and the presenting symptoms. Initial laboratory tests should include complete blood count, blood glucose, serum electrolytes, blood urea nitrogen, serum creatinine, arterial blood gas studies, ECG, alcohol level, and toxicology screening, especially in the absence of a reliable history. 3 Other tests to be considered are evaluation for sepsis, endocrine studies, and a coagulation profile. Blood tests might need to be repeated at intervals. Although laboratory results vary with changing temperature, patients with hypothermia should be managed based on results obtained at 37 C, as this is the temperature at which blood testing is conducted in medical laboratories. 16,18 MANAGEMENT Management should be guided by the cause and degree of hypothermia and coexisting conditions. Initially, patients should be rewarmed while looking for a potential cause. If the etiology cannot be determined from 18 Hospital Physician December
4 Table 3. Methods for Rewarming Hypothermic Patients Method Uses/Advantages Disadvantages Passive external rewarming (eg, blankets, humidified heated oxygen by mask) Active external rewarming (eg, forced warmed air, radiant heat, electric/plumbed heat blankets) Active internal rewarming (eg, heated humidified air, warmed intravenous fluids, peritoneal dialysis, closed thoracic lavage, extracorporeal blood rewarming) Noninvasive Useful for mild hypothermia in a previously healthy person Intense monitoring is not needed Useful in mild to moderate hypothermia with cardiovascular stability Can be combined with passive external rewarming Most effective modality Fastest modality Can be used in patients with stable or compromised cardiovascular system A slow process May cause iatrogenic body surface burns Core temperature afterdrop may develop Can be invasive Patient needs to be intensively monitored the patient s presentation, the standard measures for coma patients can be applied (ie, basic airway, breathing, and circulation assessment). In addition, a dextrose solution infusion with thiamine and, if drug overdose is suspected, medications such as naloxone (for opium overdose) or flumezanil (for benzodiazepine overdose) should be considered. Complications can be prevented by avoiding procedures such as nasogastric tube insertion and endotracheal intubation when possible, as these procedures can precipitate ventricular fibrillation. When required, securing the airways and endotracheal intubation are performed using the same guidelines as in nonhypothermic patients. Oxygen therapy may be considered empirically. 7,14 Doppler ultrasonography should be used to check pulses. If this is unavailable, palpate for pulses for 35 to 45 seconds before announcing cardiac arrest as recommended by American Heart Association guidelines. 19 If pulses are present but blood pressure is low, fluid resuscitation is preferred over pressors. Cardiac arrest in hypothermic patients, whether due to asystole or ventricular fibrillation, might be resistant to medical therapy or defibrillation until the patient has been rewarmed. 14 Nonetheless, advanced cardiac life support protocols should be followed initially and, if no response is noted, they should be continued until the patient s core body temperature is above 32 C. Resuscitative efforts have been successful with temperatures as low as 13.7 C. 20 Furthermore, survivors of hypothermia tend not to have the usual adverse hypoxic neurologic sequelae associated with prolonged resuscitation. 18 Rewarming Rewarming can be achieved by different means (Table 3), the choice of which varies based on predisposing factors, degree of hypothermia, and cardiovascular instability. 1,7,8,21 23 Passive external rewarming is used in patients with mild hypothermia without cardiovascular instability. This is a slow process that involves adequate insulation and provision of a warm environment. Passive external rewarming (eg, blankets, humidified heated oxygen by mask) is successful when thermoregulatory mechanisms and endocrine functions are intact. Active external rewarming combined with passive external rewarming is preferred in patients with mild to moderate hypothermia without cardiovascular compromise. Heat is applied directly to the skin by way of forced warmed air, radiant heat, or electric/ plumbed heat blankets. Of these, forced air is the most effective. 11 The efficiency of radiant heat or electric/ plumbed heat blankets varies, as skin perfusion decreases from 200 ml/min/m 2 to 4 ml/min/m 2 in hypothermic patients due to vasoconstriction. 10 Another limitation of using heating blankets is that they do not cover all areas of the body, and therefore heat is exchanged through less than 25% of the total body surface area. Active internal rewarming is the most effective and the fastest modality and is used in cases of moderate to severe hypothermia. In patients without cardiovascular compromise, heated humidified air, warmed intravenous fluids, peritoneal dialysis, and closed thoracic lavage can be used. In patients with cardiovascular compromise, extracorporeal blood rewarming is the modality of choice. This modality raises body temperature by 1 C to 2 C every 5 minutes and can be achieved by using either femoro-femoral bypass or the standard aorto-right atrial bypass. Femoro-femoral bypass is preferred, as it can be established in the emergency department and does not interfere with chest compressions if resuscitation is needed. 21 During rewarming, some complications should be 20 Hospital Physician December
5 anticipated. During external rewarming, rapid resolution of peripheral vasoconstriction may cause the patient s core temperature to drop (ie, core temperature afterdrop). This effect can be minimized by using minimally invasive active internal rewarming prior to active external rewarming. Another complication related to peripheral rewarming is rewarming shock, which should be managed with fluid resuscitation. Finally, rewarming acidosis occurs as blood flushes lactic acid from hypoxemic peripheries. Terminating Resuscitative Efforts Some believe that patients who appear to be dead after prolonged exposure to cold temperatures should not be considered dead until they are rewarmed to a near-normal core temperature. 23,24 Rewarming efforts should be continued until the core temperature is at least 32 C. Efforts may be discontinued if the patient continues to show no effective cardiac rhythm and remains unresponsive to all resuscitative measures. 25 However, the decision to terminate resuscitative measures should be based on the unique circumstances of each case. 25 CONCLUSION Clinicians should be aware of the clinical signs and symptoms of hypothermia. Documentation of core body temperature using special thermometers is required to diagnose and appropriately classify hypothermia. Active internal rewarming is the most effective method for treating hypothermic patients, but it is invasive. Therefore, passive rewarming and active external rewarming methods should be used in less severe cases of hypothermia in the absence of cardiovascular instability. With proper management, a good outcome can be achieved, even in cases of severe hypothermia. HP Test your knowledge and comprehension of this article with the Clinical Review Quiz on page 22. REFERENCES 1. McCullough L, Arora S. Diagnosis and treatment of hypothermia. Am Fam Physician 2004;70: Hayward JS, Eckerson JD, Kemna D. Thermal and cardiovascular changes during three methods of resuscitation from mild hypothermia. Resuscitation 1984;11: Hypothermia-related deaths Philadelphia, 2001, and United States, Centers for Disease Control and Prevention (CDC). MMWR Morb Mortal Wkly Rep 2003; 52: Aslam AF, Aslam AK, Vasavada BC, et al. Hypothermia: evaluation, electrocardiographic manifestations, and management. Am J Med 2006;119: Hildebrand F, Giannoudis PV, van Griensven M, et al. Pathophysiologic changes and effects of hypothermia on outcome in elective surgery and trauma patients. Am J Surg 2004;187: Ganong WF. Review of medical physiology. 22nd ed. New York: McGraw-Hill Medical; 2005: Wilkey SA. Accidental hypothermia: a case report and focused review. Am J Clin Med 2004;1: Danzl DF, Pozos RS. Accidental hypothermia. N Engl J Med 1994;331: Taguchi A, Kurz A. Thermal management of the patient: where does the patient lose and/or gain temperature? Curr Opin Anaesthesiol 2005;18: Mallet ML. Pathophysiology of accidental hypothermia. QJM 2002;95: Sessler DI. Mild perioperative hypothermia. N Engl J Med 1997;336: Fos LA, Magonet GM, Guidry AF, Judson K. Case study: hypothermia secondary to erythroderma: FP-2. South Med J 2005;98:S Soreide E, Smith CE. Hypothermia in trauma victims friend or foe? Indian J Crit Care Med 2004;8: Kempainen RR, Brunette DD. The evaluation and management of accidental hypothermia. Respir Care 2004; 49: Saadlla H. Images in clinical medicine. Electrocardiographic changes in extreme hypothermia. N Engl J Med 2004;351:e Gentilello LM, Pierson DJ. Trauma critical care. Am J Respir Crit Care Med 2001;163(3 Pt 1): Rothschild MA. Lethal hypothermia: paradoxical undressing and hide-and-die syndrome can produce obscure death scene. Forensic Pathol Rev 2004;1: Walpoth BH, Walpoth-Aslan BN, Mattle HP, et al. Outcome of survivors of accidental deep hypothermia and circulatory arrest treated with extracorporeal blood warming. N Engl J Med 1997;337: American Heart Association guidelines for cardiopulmonary resuscitation and emergency cardiovascular care. Part 10.4: hypothermia. Circulation 2005;112 (Suppl 1): Gilbert M, Busund R, Skagseth A, et al. Resuscitation from accidental hypothermia of 13.7 degrees C with circulatory arrest. Lancet 2000;355: Lazar HL. The treatment of hypothermia. N Engl J Med 1997;337: Sessler DI. Complications and treatment of mild hypothermia. Anesthesiology 2001;95: Steinman AM. Cardiopulmonary resuscitation and hypothermia. Circulation 1986;74(6 Pt 2):IV Southwick FS, Dalglish PH Jr. Recovery after prolonged asystolic cardiac arrest in profound hypothermia. A case report and literature review. JAMA 1980;243: Weinberg AD. Hypothermia. Ann Emerg Med 1993;22 (2 Pt 2): Copyright 2006 by Turner White Communications Inc., Wayne, PA. All rights reserved. Hospital Physician December
Accidental Hypothermia
 Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
Cold-Related Illness. Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic
 Cold-Related Illness Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic Hypothermia Frost nip Frostbite Chillbains Trench foot Cold-Related Illness Who gets it? How common? Outdoor
Cold-Related Illness Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic Hypothermia Frost nip Frostbite Chillbains Trench foot Cold-Related Illness Who gets it? How common? Outdoor
UTSW/BioTel EMS TRAINING BULLETIN January EMS TB Accidental Hypothermia
 UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER
 DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER This tragic recent headline involving Marco Cheseto serves as a grim reminder of the potential devastation inflicted by frostbite and hypothermia
DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER This tragic recent headline involving Marco Cheseto serves as a grim reminder of the potential devastation inflicted by frostbite and hypothermia
Hypothermia Presentation
 Hypothermia Presentation Thermoregulation Thermal regulation is a balance between heat production and heat loss. Despite marked changes in skin temperature, the body s homeostatic mechanisms are able to
Hypothermia Presentation Thermoregulation Thermal regulation is a balance between heat production and heat loss. Despite marked changes in skin temperature, the body s homeostatic mechanisms are able to
Bill Hall, MD Mesa County EMS System
 Bill Hall, MD Mesa County EMS System Discuss cold related injuries and treatment Discuss hypothermia and treatment Discuss avalanche victim care and considerations Chilblains (Pernio) Trench Foot Frost
Bill Hall, MD Mesa County EMS System Discuss cold related injuries and treatment Discuss hypothermia and treatment Discuss avalanche victim care and considerations Chilblains (Pernio) Trench Foot Frost
Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES. Accidental Hypothermia/Cold Exposure
 Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES Accidental Hypothermia/Cold Exposure Goal: To aid EMS Providers in: the recognition and treatment of systemic effects of accidental hypothermia
Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES Accidental Hypothermia/Cold Exposure Goal: To aid EMS Providers in: the recognition and treatment of systemic effects of accidental hypothermia
-Blood Warming- A Hot topic?
 -Blood Warming- A Hot topic? Blaine Kent, MD, FRCPC Associate Professor of Anesthesia Director, Peri-Operative Blood Management Chief, Cardiac Anesthesia Objectives To learn / review the deleterious systemic
-Blood Warming- A Hot topic? Blaine Kent, MD, FRCPC Associate Professor of Anesthesia Director, Peri-Operative Blood Management Chief, Cardiac Anesthesia Objectives To learn / review the deleterious systemic
8/20/12. Discuss the importance of thermoregulation in the neonate.
 Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
Thermal Injury. Thermal Injury Presentation CCFP (EM) Rounds. Topics Hypothermia. Resources Ch Tinitinelli
 Thermal Injury December 17, 2009 Thermal Injury Presentation CCFP (EM) Rounds Dr. Kyle McLaughlin, CCFP (EM) Topics Hypothermia Frostbite Hyperthermia Resources Ch. 191-193 Tinitinelli Multi media http://www.youtube.com/watch?v=x6mq0jftpji&feature=fvsr
Thermal Injury December 17, 2009 Thermal Injury Presentation CCFP (EM) Rounds Dr. Kyle McLaughlin, CCFP (EM) Topics Hypothermia Frostbite Hyperthermia Resources Ch. 191-193 Tinitinelli Multi media http://www.youtube.com/watch?v=x6mq0jftpji&feature=fvsr
INDUCED HYPOTHERMIA A Hot Topic. R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences
 INDUCED HYPOTHERMIA A Hot Topic R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences Conflicts of Interest Sadly, we have no financial or industrial conflicts of interest
INDUCED HYPOTHERMIA A Hot Topic R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences Conflicts of Interest Sadly, we have no financial or industrial conflicts of interest
Pathophysiology and Cardiac Insights for Targeted Temperature Management in Emergency Medicine and Critical Care
 Pathophysiology and Cardiac Insights for Targeted Temperature Management in Emergency Medicine and Critical Care LINDSAY LEWIS BSN, RN, CCCC Faculty Disclosure I AM CURRENTLY EMPLOYED AS A CLINICAL MANAGER
Pathophysiology and Cardiac Insights for Targeted Temperature Management in Emergency Medicine and Critical Care LINDSAY LEWIS BSN, RN, CCCC Faculty Disclosure I AM CURRENTLY EMPLOYED AS A CLINICAL MANAGER
Drowning is a leading cause of death and loss of years of life with over 90% of cases occurring in lower- and middle-income countries.
 Chapter 145 Drowning Episode Overview: 1) List risk factors for drowning 2) List 5 variables that portend poor outcome 3) Describe the diving reflex 4) Describe the management of a drowning patient with
Chapter 145 Drowning Episode Overview: 1) List risk factors for drowning 2) List 5 variables that portend poor outcome 3) Describe the diving reflex 4) Describe the management of a drowning patient with
INDUCED HYPOTHERMIA. F. Ben Housel, M.D.
 INDUCED HYPOTHERMIA F. Ben Housel, M.D. Historical Use of Induced Hypothermia 1950 s - Moderate hypothermia (30-32º C) in open heart surgery to protect brain against global ischemia 1960-1980 s - Use of
INDUCED HYPOTHERMIA F. Ben Housel, M.D. Historical Use of Induced Hypothermia 1950 s - Moderate hypothermia (30-32º C) in open heart surgery to protect brain against global ischemia 1960-1980 s - Use of
All Things Cold: Hypothermia, Altitude Illness and Frostbite. Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine
 All Things Cold: Hypothermia, Altitude Illness and Frostbite Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine Objectives Thermoregulation basics Management of human-sickles
All Things Cold: Hypothermia, Altitude Illness and Frostbite Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine Objectives Thermoregulation basics Management of human-sickles
Acid-base management during hypothermic CPB alpha-stat and ph-stat models of blood gas interpretation
 Acid-base management during hypothermic CPB alpha-stat and ph-stat models of blood gas interpretation Michael Kremke Department of Anaesthesiology and Intensive Care Aarhus University Hospital, Denmark
Acid-base management during hypothermic CPB alpha-stat and ph-stat models of blood gas interpretation Michael Kremke Department of Anaesthesiology and Intensive Care Aarhus University Hospital, Denmark
Chapter 132 Accidental Hypothermia. Episode Overview. Core Questions. Wisecracks
 Chapter 132 Accidental Hypothermia Episode Overview Passively rewarm patients with temperatures 32-35 degrees Celsius Indications for active rewarming: Cardiovascular instability Temperature < 32 degrees
Chapter 132 Accidental Hypothermia Episode Overview Passively rewarm patients with temperatures 32-35 degrees Celsius Indications for active rewarming: Cardiovascular instability Temperature < 32 degrees
Prehospital Care Bundles
 Prehospital s The MLREMS Prehospital s have been created to provide a simple framework to help EMS providers identify the most critical elements when caring for a patient. These bundles do not replace
Prehospital s The MLREMS Prehospital s have been created to provide a simple framework to help EMS providers identify the most critical elements when caring for a patient. These bundles do not replace
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Hanna K. Al-Makhamreh, M.D., FACC Interventional Cardiologist
 Hanna K. Al-Makhamreh, M.D., FACC Interventional Cardiologist Introduction. Basic Life Support (BLS). Advanced Cardiac Life Support (ACLS). Cardiovascular diseases (CVDs) are the number one cause of death
Hanna K. Al-Makhamreh, M.D., FACC Interventional Cardiologist Introduction. Basic Life Support (BLS). Advanced Cardiac Life Support (ACLS). Cardiovascular diseases (CVDs) are the number one cause of death
The Big Chill: On May 10, 1996, around midnight, the renowned. Accidental Hypothermia
 2.6 hours Continuing Education By Robert Allan Davis, ADN, RN The Big Chill: Accidental Hypothermia How to identify and manage this life-threatening reaction to prolonged exposure. Overview: A potential
2.6 hours Continuing Education By Robert Allan Davis, ADN, RN The Big Chill: Accidental Hypothermia How to identify and manage this life-threatening reaction to prolonged exposure. Overview: A potential
Accidental Hypothermia
 Accidental Hypothermia Doug Brown, MD, FRCPC Emergency Physician Royal Columbian & Eagle Ridge Hospital October, 2013 Objectives 45min lecture, 15min discussion & questions: Inspirational case & overview
Accidental Hypothermia Doug Brown, MD, FRCPC Emergency Physician Royal Columbian & Eagle Ridge Hospital October, 2013 Objectives 45min lecture, 15min discussion & questions: Inspirational case & overview
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH
 Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
Case Presentation. Cooling. Case Presentation. New Developments in Cardiopulmonary Arrest: Therapeutic Hypothermia in Resuscitation
 New Developments in Cardiopulmonary Arrest: Therapeutic Hypothermia in Resuscitation Michael Sayre, MD Emergency Medicine and LeRoy Essig, MD Pulmonary/Critical Care Medicine Case Presentation 3:40 (+
New Developments in Cardiopulmonary Arrest: Therapeutic Hypothermia in Resuscitation Michael Sayre, MD Emergency Medicine and LeRoy Essig, MD Pulmonary/Critical Care Medicine Case Presentation 3:40 (+
Lecture. ALS Algorithm
 Lecture ALS Algorithm 1 Learning outcomes The ALS algorithm Treatment of shockable and non-shockable rhythms Potentially reversible causes of cardiac arrest 2 Adult ALS Algorithm 3 To confirm cardiac arrest
Lecture ALS Algorithm 1 Learning outcomes The ALS algorithm Treatment of shockable and non-shockable rhythms Potentially reversible causes of cardiac arrest 2 Adult ALS Algorithm 3 To confirm cardiac arrest
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Hypothermia in Trauma What happens? Hypothermia in the Trauma Patient. Hypothermia in Trauma 10/6/2010
 Hypothermia in the Trauma Patient Friend or Foe? Clark Hayward EMTP, AWLS 10/2/10 Hypothermia in Trauma What happens? From the time of injury, trauma itself alters the normal central thermoregulation and
Hypothermia in the Trauma Patient Friend or Foe? Clark Hayward EMTP, AWLS 10/2/10 Hypothermia in Trauma What happens? From the time of injury, trauma itself alters the normal central thermoregulation and
Cold Water Shock, Hypothermia and Cardiac Arrest
 Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
2. General Cardiac Arrest Protocol Medical Newborn/Neonatal. Protocol 8-3 Resuscitation 4. Medical Supraventricular
 PEDIATRIC CARDIAC SECTION: Pediatric Cardiovascular Emergencies REVISED: 06/2017 Section 8 1. Cardiac Arrest Unknown Rhythm (i.e. Protocol 8-1 BLS) 2. General Cardiac Arrest Protocol 8-2 3. Medical Newborn/Neonatal
PEDIATRIC CARDIAC SECTION: Pediatric Cardiovascular Emergencies REVISED: 06/2017 Section 8 1. Cardiac Arrest Unknown Rhythm (i.e. Protocol 8-1 BLS) 2. General Cardiac Arrest Protocol 8-2 3. Medical Newborn/Neonatal
Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms. Introduction to the Algorithms
 Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Introduction to the Algorithms Cardiac Arrest Algorithms Prehospital Medication Profiles Perspective regarding the EMT- Intermediate
Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Introduction to the Algorithms Cardiac Arrest Algorithms Prehospital Medication Profiles Perspective regarding the EMT- Intermediate
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC
 Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Thermoregulation 2015 WMA
 1 Structure: Temperature sensors Endocrine system Muscles Skin Function: Maintain body core at 37 C Problem: Too little heat Too much heat 2 Normal Body Compensation Heat Response: Vasodilation Sweat Cold
1 Structure: Temperature sensors Endocrine system Muscles Skin Function: Maintain body core at 37 C Problem: Too little heat Too much heat 2 Normal Body Compensation Heat Response: Vasodilation Sweat Cold
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT.
 HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
Advanced Resuscitation - Adult
 C02A Resuscitation 2017-03-23 17 years & older Office of the Medical Director Advanced Resuscitation - Adult Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia Algorithm
C02A Resuscitation 2017-03-23 17 years & older Office of the Medical Director Advanced Resuscitation - Adult Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia Algorithm
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 6.1 Define key terms introduced in this chapter. Slides 11, 15, 17, 26, 27, 31, 33, 37, 40 42, 44, 45, 51, 58 6.2 Describe the basic roles and structures
Introduction to Emergency Medical Care 1 OBJECTIVES 6.1 Define key terms introduced in this chapter. Slides 11, 15, 17, 26, 27, 31, 33, 37, 40 42, 44, 45, 51, 58 6.2 Describe the basic roles and structures
In-hospital Care of the Post-Cardiac Arrest Patient. David A. Pearson, MD, FACEP, FAAEM Associate Program Director Department of Emergency Medicine
 In-hospital Care of the Post-Cardiac Arrest Patient David A. Pearson, MD, FACEP, FAAEM Associate Program Director Department of Emergency Medicine Disclosures I have no financial interest, arrangement,
In-hospital Care of the Post-Cardiac Arrest Patient David A. Pearson, MD, FACEP, FAAEM Associate Program Director Department of Emergency Medicine Disclosures I have no financial interest, arrangement,
Hypothermia Induction Methods
 Hypothermia Induction Methods Advantages and Disadvantages Xia Luo, M.D. Vice President, Clinical Education ZOLL Corporation Targeted Temperature Management (TTM) Temperature is one of the four vital signs
Hypothermia Induction Methods Advantages and Disadvantages Xia Luo, M.D. Vice President, Clinical Education ZOLL Corporation Targeted Temperature Management (TTM) Temperature is one of the four vital signs
Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen
 Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen utilization The effects of shock are initially reversible
Shock is defined as a state of cellular and tissue hypoxia due to : reduced oxygen delivery and/or increased oxygen consumption or inadequate oxygen utilization The effects of shock are initially reversible
03RC1- Greif. Temperature Monitoring. Robert Greif - 1 -
 03RC1- Greif Temperature Monitoring Robert Greif Department of Anaesthesiology and Pain Therapy, University Hospital Bern, Inselspital Bern, Switzerland Small decreases of core body temperature during
03RC1- Greif Temperature Monitoring Robert Greif Department of Anaesthesiology and Pain Therapy, University Hospital Bern, Inselspital Bern, Switzerland Small decreases of core body temperature during
THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST
 THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST Heather Harrington RN, BScN, CNCC(c) Clinical Nurse Educator Sunnybrook Health Sciences Centre Objectives Define Therapeutic Hypothermia (TH) Describe current
THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST Heather Harrington RN, BScN, CNCC(c) Clinical Nurse Educator Sunnybrook Health Sciences Centre Objectives Define Therapeutic Hypothermia (TH) Describe current
Neurotrauma: The Place for Cooling
 Neurotrauma: The Place for Cooling Cooling: to achieve hypothermia History, evidence, open questions Cooling: to achieve normothermia Evidence, open questions Cooling: Practical Aspects Hypothermia: History
Neurotrauma: The Place for Cooling Cooling: to achieve hypothermia History, evidence, open questions Cooling: to achieve normothermia Evidence, open questions Cooling: Practical Aspects Hypothermia: History
SHOCK. Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital
 SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University
 Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida
 Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida Reprinted in the IVIS website with the permission of the NAVC http:/// The North American Veterinary Conference
Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida Reprinted in the IVIS website with the permission of the NAVC http:/// The North American Veterinary Conference
Advanced Resuscitation - Child
 C02C Resuscitation 2017-03-23 1 up to 10 years Office of the Medical Director Advanced Resuscitation - Child Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia Algorithm
C02C Resuscitation 2017-03-23 1 up to 10 years Office of the Medical Director Advanced Resuscitation - Child Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia Algorithm
Management Of Medical Emergencies
 Management Of Medical Emergencies U.S. Aging Population 35 million people (12%) 65 years or older Number will increase by nearly 75% by year 2030 The number of people more than 85 years old will approach
Management Of Medical Emergencies U.S. Aging Population 35 million people (12%) 65 years or older Number will increase by nearly 75% by year 2030 The number of people more than 85 years old will approach
Patient Case. Post cardiac arrest pathophysiology 10/19/2017. Disclosure. Objectives. Patient Case-TM
 Disclosure TARGETED TEMPERATURE MANAGEMENT POST CARDIAC ARREST I have nothing to disclose concerning possible financial or personal relationships with commercial entities that may have a direct or indirect
Disclosure TARGETED TEMPERATURE MANAGEMENT POST CARDIAC ARREST I have nothing to disclose concerning possible financial or personal relationships with commercial entities that may have a direct or indirect
Regulation of Body Temperature. Ass. Prof. Dr. ADEL AMRAN DEPARTMENT OF PHYSIOLOGY
 Regulation of Body Temperature Ass. Prof. Dr. ADEL AMRAN DEPARTMENT OF PHYSIOLOGY objectives heat gain heat loss discuss the mechanisms by which the body gains or loses heat in a variety of healthy or
Regulation of Body Temperature Ass. Prof. Dr. ADEL AMRAN DEPARTMENT OF PHYSIOLOGY objectives heat gain heat loss discuss the mechanisms by which the body gains or loses heat in a variety of healthy or
Resuscitation in Special Situations what s new
 Resuscitation in Special Situations what s new Asc. Prof. Dr. Serkan Şener Acıbadem University, School of Medicine Department of Emergency Medicine Acıbadem Ankara Hospital Objectives To understand the
Resuscitation in Special Situations what s new Asc. Prof. Dr. Serkan Şener Acıbadem University, School of Medicine Department of Emergency Medicine Acıbadem Ankara Hospital Objectives To understand the
The ALS Algorithm and Post Resuscitation Care
 The ALS Algorithm and Post Resuscitation Care CET - Ballarat Health Services Valid from 1 st July 2018 to 30 th June 2020 2 Defibrillation Produces simultaneous mass depolarisation of myocardial cells
The ALS Algorithm and Post Resuscitation Care CET - Ballarat Health Services Valid from 1 st July 2018 to 30 th June 2020 2 Defibrillation Produces simultaneous mass depolarisation of myocardial cells
Accidental Hypothermia. Peter Paal, MD, Associate Professor DESA, EDIC
 Accidental Hypothermia Peter Paal, MD, Associate Professor DESA, EDIC Conflict of interest Ambu Covidien Genericon Jolife Laerdal Larnygeal Mask Company Ratiopharm VBM 2 Innsbruck 3 Innsbruck 4 Innsbruck
Accidental Hypothermia Peter Paal, MD, Associate Professor DESA, EDIC Conflict of interest Ambu Covidien Genericon Jolife Laerdal Larnygeal Mask Company Ratiopharm VBM 2 Innsbruck 3 Innsbruck 4 Innsbruck
PEDIATRIC CARDIAC RHYTHM DISTURBANCES. -Jason Haag, CCEMT-P
 PEDIATRIC CARDIAC RHYTHM DISTURBANCES -Jason Haag, CCEMT-P General: CARDIAC RHYTHM DISTURBANCES - More often the result and not the cause of acute cardiovascular emergencies - Typically the end result
PEDIATRIC CARDIAC RHYTHM DISTURBANCES -Jason Haag, CCEMT-P General: CARDIAC RHYTHM DISTURBANCES - More often the result and not the cause of acute cardiovascular emergencies - Typically the end result
Temperature Monitoring Locations: For TEMP 01, any temperature measurement coming from a physiologic monitor will suffice (peripheral or core).
 Measure Abbreviation: TEMP 01 Measure Description: Percentage of cases that active warming was administered by the anesthesia provider. NQS Domain: Effective Clinical Care Measure Type: Process Scope:
Measure Abbreviation: TEMP 01 Measure Description: Percentage of cases that active warming was administered by the anesthesia provider. NQS Domain: Effective Clinical Care Measure Type: Process Scope:
Geriatric Emergencies. Lesson Goal. Lesson Objectives 9/10/2012. Introduce ways geriatric patients differ from other patients
 Geriatric Emergencies Lesson Goal Introduce ways geriatric patients differ from other patients Physiologic changes of aging Communication issues Effects of medications Common fears of elderly patients
Geriatric Emergencies Lesson Goal Introduce ways geriatric patients differ from other patients Physiologic changes of aging Communication issues Effects of medications Common fears of elderly patients
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Chapter 12. Temperature Regulation
 Chapter 12 Temperature Regulation Temperature Regulation Body core temperature regulation Critical for: Cellular structures Metabolic pathways Too high Protein structure of cells destroyed Too low Slowed
Chapter 12 Temperature Regulation Temperature Regulation Body core temperature regulation Critical for: Cellular structures Metabolic pathways Too high Protein structure of cells destroyed Too low Slowed
Instruct patient and caregivers: Need for constant monitoring Potential complications of drug therapy
 Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
SYSTEM-WIDE POLICY & PROCEDURE MANUAL. Policy Title: Hypothermia Post Cardiac Arrest Policy Number: PC-124. President & CEO Page 1 of 9
 Approved By: President & CEO Date Page 1 of 9 POLICY: PURPOSE: To define and describe the implementation of induced hypothermia post cardiac arrest and the nursing assessment and interventions required
Approved By: President & CEO Date Page 1 of 9 POLICY: PURPOSE: To define and describe the implementation of induced hypothermia post cardiac arrest and the nursing assessment and interventions required
Update on Sudden Cardiac Death and Resuscitation
 Update on Sudden Cardiac Death and Resuscitation Ashish R. Panchal, MD, PhD Medical Director Center for Emergency Medical Services Assistant Professor Clinical Department of Emergency Medicine The Ohio
Update on Sudden Cardiac Death and Resuscitation Ashish R. Panchal, MD, PhD Medical Director Center for Emergency Medical Services Assistant Professor Clinical Department of Emergency Medicine The Ohio
Chapter 24 Vital Signs. Copyright 2011 Wolters Kluwer Health Lippincott Williams & Wilkins
 Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara
 Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials
 Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
HEAT STROKE. Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC
 HEAT STROKE Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC Heat Stroke More Preventable Than Treatable Heat Stroke A form of hyperthermia associated with a systemic inflammatory response leading
HEAT STROKE Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC Heat Stroke More Preventable Than Treatable Heat Stroke A form of hyperthermia associated with a systemic inflammatory response leading
Ac#ve, ECMO or locally available alterna#ves. invasive warming. Ini#ally: Ac#ve noninvasive or minimally
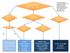 Suspected Hypothermia Temp
Suspected Hypothermia Temp
3. D Objective: Chapter 4, Objective 4 Page: 79 Rationale: A carbon dioxide level below 35 mmhg indicates hyperventilation.
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
SHOCK Susanna Hilda Hutajulu, MD, PhD
 SHOCK Susanna Hilda Hutajulu, MD, PhD Div Hematology and Medical Oncology Department of Internal Medicine Universitas Gadjah Mada Yogyakarta Outline Definition Epidemiology Physiology Classes of Shock
SHOCK Susanna Hilda Hutajulu, MD, PhD Div Hematology and Medical Oncology Department of Internal Medicine Universitas Gadjah Mada Yogyakarta Outline Definition Epidemiology Physiology Classes of Shock
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
Post-Cardiac Arrest Syndrome. MICU Lecture Series
 Post-Cardiac Arrest Syndrome MICU Lecture Series Case 58 y/o female collapses at home, family attempts CPR, EMS arrives and notes VF, defibrillation x 3 with return of spontaneous circulation, brought
Post-Cardiac Arrest Syndrome MICU Lecture Series Case 58 y/o female collapses at home, family attempts CPR, EMS arrives and notes VF, defibrillation x 3 with return of spontaneous circulation, brought
The cold never bother me anymore. R2 Wariya Vongchaiudomchoke & R2 Pichchaporn Praserdvigai Supervisor: Aj. Aphichat Suphathamwit
 The cold never bother me anymore R2 Wariya Vongchaiudomchoke & R2 Pichchaporn Praserdvigai Supervisor: Aj. Aphichat Suphathamwit Is that really true? Frozen by Walt Disney Animation Studios, 2013 Definition
The cold never bother me anymore R2 Wariya Vongchaiudomchoke & R2 Pichchaporn Praserdvigai Supervisor: Aj. Aphichat Suphathamwit Is that really true? Frozen by Walt Disney Animation Studios, 2013 Definition
HYPOTHERMIA IN TRAUMA. Kevin Palmer EMT-P, DiMM
 HYPOTHERMIA IN TRAUMA Kevin Palmer EMT-P, DiMM DISCLOSURE No Financial conflicts of interest Member of the Wilderness Medical Society Diploma in Mountain Medicine Fellowship in the Academy of Wilderness
HYPOTHERMIA IN TRAUMA Kevin Palmer EMT-P, DiMM DISCLOSURE No Financial conflicts of interest Member of the Wilderness Medical Society Diploma in Mountain Medicine Fellowship in the Academy of Wilderness
Update on Sudden Cardiac Death and Resuscitation
 Update on Sudden Cardiac Death and Resuscitation Ashish R. Panchal, MD, PhD Medical Director Center for Emergency Medical Services Assistant Professor Clinical Department of Emergency Medicine The Ohio
Update on Sudden Cardiac Death and Resuscitation Ashish R. Panchal, MD, PhD Medical Director Center for Emergency Medical Services Assistant Professor Clinical Department of Emergency Medicine The Ohio
4/5/2018. Update on Sepsis NIKHIL JAGAN PULMONARY AND CRITICAL CARE CREIGHTON UNIVERSITY. I have no financial disclosures
 Update on Sepsis NIKHIL JAGAN PULMONARY AND CRITICAL CARE CREIGHTON UNIVERSITY I have no financial disclosures 1 Objectives Why do we care about sepsis Understanding the core measures by Centers for Medicare
Update on Sepsis NIKHIL JAGAN PULMONARY AND CRITICAL CARE CREIGHTON UNIVERSITY I have no financial disclosures 1 Objectives Why do we care about sepsis Understanding the core measures by Centers for Medicare
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of
 Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Induced Hypothermia for Cardiac Arrest. Heather Hand RN,CCRN,CNRN,ATCN,LNC
 Induced Hypothermia for Cardiac Arrest Heather Hand RN,CCRN,CNRN,ATCN,LNC Cardiac Arrest Epidemiology 400,000 arrests / year in U.S.A 3 / 4 Out-of-hospital 1 / 4 In-hospital survival to hospital 1-5% discharge
Induced Hypothermia for Cardiac Arrest Heather Hand RN,CCRN,CNRN,ATCN,LNC Cardiac Arrest Epidemiology 400,000 arrests / year in U.S.A 3 / 4 Out-of-hospital 1 / 4 In-hospital survival to hospital 1-5% discharge
IN HOSPITAL CARDIAC ARREST AND SEPSIS
 IN HOSPITAL CARDIAC ARREST AND SEPSIS MARGARET DISSELKAMP, MD OVERVIEW Background Epidemiology of in hospital cardiac arrest (IHCA) Use a case scenario to introduce new guidelines Review surviving sepsis
IN HOSPITAL CARDIAC ARREST AND SEPSIS MARGARET DISSELKAMP, MD OVERVIEW Background Epidemiology of in hospital cardiac arrest (IHCA) Use a case scenario to introduce new guidelines Review surviving sepsis
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Cold Injuries: Frostbite and Hypothermia. Michael White MD,FACS Director Detroit Receiving Hospital Wayne State University
 Cold Injuries: Frostbite and Hypothermia Michael White MD,FACS Director Detroit Receiving Hospital Wayne State University Objectives of Talk Describe the incidence and characteristics of Frostbite injury
Cold Injuries: Frostbite and Hypothermia Michael White MD,FACS Director Detroit Receiving Hospital Wayne State University Objectives of Talk Describe the incidence and characteristics of Frostbite injury
table of contents pediatric treatment guidelines
 table of contents pediatric treatment guidelines P1 PEDIATRIC PATIENT CARE...70 P2 APPARENT LIFE-THREATENING EVENT (ALTE)...71 P3 CARDIAC ARREST INITIAL CARE AND CPR...72 73 P4 NEONATAL CARE AND RESUSCITATION...74
table of contents pediatric treatment guidelines P1 PEDIATRIC PATIENT CARE...70 P2 APPARENT LIFE-THREATENING EVENT (ALTE)...71 P3 CARDIAC ARREST INITIAL CARE AND CPR...72 73 P4 NEONATAL CARE AND RESUSCITATION...74
Basic Fluid and Electrolytes
 Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Written 01/09/17 Rewritten 3/29/17 for Interior Regional EMS Symposium
 Written 01/09/17 Rewritten 3/29/17 for Interior Regional EMS Symposium MARIA E. MANDICH MD Fairbanks Memorial Hospital Emergency Department Attending Physician Interior Region EMS Council Medical Director
Written 01/09/17 Rewritten 3/29/17 for Interior Regional EMS Symposium MARIA E. MANDICH MD Fairbanks Memorial Hospital Emergency Department Attending Physician Interior Region EMS Council Medical Director
Cardiopulmonary Resuscitation in Adults
 Cardiopulmonary Resuscitation in Adults Fatma Özdemir, MD Emergency Deparment of Uludag University Faculty of Medicine OVERVIEW Introduction Pathophysiology BLS algorithm ALS algorithm Post resuscitation
Cardiopulmonary Resuscitation in Adults Fatma Özdemir, MD Emergency Deparment of Uludag University Faculty of Medicine OVERVIEW Introduction Pathophysiology BLS algorithm ALS algorithm Post resuscitation
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02
 PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
IFT1 Interfacility Transfer of STEMI Patients. IFT2 Interfacility Transfer of Intubated Patients. IFT3 Interfacility Transfer of Stroke Patients
 IFT1 Interfacility Transfer of STEMI Patients IFT2 Interfacility Transfer of Intubated Patients IFT3 Interfacility Transfer of Stroke Patients Interfacility Transfer Guidelines IFT 1 TRANSFER INTERFACILITY
IFT1 Interfacility Transfer of STEMI Patients IFT2 Interfacility Transfer of Intubated Patients IFT3 Interfacility Transfer of Stroke Patients Interfacility Transfer Guidelines IFT 1 TRANSFER INTERFACILITY
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #9 Heat Emergencies
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #9 Heat Emergencies As EMS providers we are called to treat several medical conditions. Heart Attacks,
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #9 Heat Emergencies As EMS providers we are called to treat several medical conditions. Heart Attacks,
UNDERSTANDING YOUR ECG: A REVIEW
 UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Proceeding of the LAVC Latin American Veterinary Conference Apr , 2012 Lima, Peru
 Close this window to return to IVIS www.ivis.org Proceeding of the LAVC Latin American Veterinary Conference Apr. 23-26, 2012 Lima, Peru Next LAVC Conference: Apr. 22-25, 2013 Lima, Peru Reprinted in the
Close this window to return to IVIS www.ivis.org Proceeding of the LAVC Latin American Veterinary Conference Apr. 23-26, 2012 Lima, Peru Next LAVC Conference: Apr. 22-25, 2013 Lima, Peru Reprinted in the
Pediatric advanced life support. Management of decreased conscious level in children. Virgi ija Žili skaitė 2017
 Pediatric advanced life support. Management of decreased conscious level in children Virgi ija Žili skaitė 2017 Life threatening conditions: primary assessment, differential diagnostics and emergency care.
Pediatric advanced life support. Management of decreased conscious level in children Virgi ija Žili skaitė 2017 Life threatening conditions: primary assessment, differential diagnostics and emergency care.
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Preparing for your upcoming PALS course
 IU Health PALS Study Guide Preparing for your upcoming PALS course UPDATED November 2016 Course Curriculum: 2015 American Heart Association (AHA) Guidelines for Pediatric Advanced Life Support (PALS) AHA
IU Health PALS Study Guide Preparing for your upcoming PALS course UPDATED November 2016 Course Curriculum: 2015 American Heart Association (AHA) Guidelines for Pediatric Advanced Life Support (PALS) AHA
Critical Care of the Post-Surgical Patient
 Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
THERMOREGULATION 05 JUNE 2013
 THERMOREGULATION 05 JUNE 2013 Lesson Description In this lesson we: Question the need to regulate body temperature in humans Examine the structure and functions of the different parts of the skin Look
THERMOREGULATION 05 JUNE 2013 Lesson Description In this lesson we: Question the need to regulate body temperature in humans Examine the structure and functions of the different parts of the skin Look
Yolo County Health & Human Services Agency
 Yolo County Health & Human Services Agency Kristin Weivoda EMS Administrator John S. Rose, MD, FACEP Medical Director DATE: December 28, 2017 TO: Yolo County Providers and Agencies FROM: Yolo County EMS
Yolo County Health & Human Services Agency Kristin Weivoda EMS Administrator John S. Rose, MD, FACEP Medical Director DATE: December 28, 2017 TO: Yolo County Providers and Agencies FROM: Yolo County EMS
Chapter 13. Learning Objectives. Learning Objectives 9/11/2012. Poisonings, Overdoses, and Intoxications
 Chapter 13 Poisonings, Overdoses, and Intoxications Learning Objectives Discuss use of activated charcoal in treatment of poisonings List treatment options for acetaminophen overdose List clinical manifestations
Chapter 13 Poisonings, Overdoses, and Intoxications Learning Objectives Discuss use of activated charcoal in treatment of poisonings List treatment options for acetaminophen overdose List clinical manifestations
Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest. Objectives: U.S. stats
 Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest Nicole L. Kupchik RN, MN, CCNS CCRN-CMC Clinical Nurse Specialist Harborview Medical Center Seattle, WA Objectives: At the
Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest Nicole L. Kupchik RN, MN, CCNS CCRN-CMC Clinical Nurse Specialist Harborview Medical Center Seattle, WA Objectives: At the
ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments
 ADENOSINE Paroxysmal SVT 1 st Dose 6 mg rapid IV 2 nd & 3 rd Doses 12 mg rapid IV push Follow each dose with rapid bolus of 20 ml NS May cause transient heart block or asystole. Side effects include chest
ADENOSINE Paroxysmal SVT 1 st Dose 6 mg rapid IV 2 nd & 3 rd Doses 12 mg rapid IV push Follow each dose with rapid bolus of 20 ml NS May cause transient heart block or asystole. Side effects include chest
Objectives. Birth Depression Management. Birth Depression Terms
 Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Objectives Birth Depression Management Regional Perinatal Outreach Program 2016 Understand the terms and the clinical characteristics of birth depression. Be familiar with the evidence behind therapeutic
Other 12-Lead ECG Findings
 Other 12-Lead ECG Findings Left Atrial Enlargement Left atrial enlargement is illustrated by increased P wave duration in lead II, top ECG, and by the prominent negative P terminal force in lead V1, bottom
Other 12-Lead ECG Findings Left Atrial Enlargement Left atrial enlargement is illustrated by increased P wave duration in lead II, top ECG, and by the prominent negative P terminal force in lead V1, bottom
Z19.2 Cross Reference to Patient Care Maps & Clinical Care Procedures
 2017-04-07 Old version G1 Code of Ethics G2 Scope and Function G3 Scene Assessment G4 Triage G5 Primary Survey G6 Shock G7 Load and Go G8 Secondary Survey G9 Unconscious Patient G10A Obstructed Airway
2017-04-07 Old version G1 Code of Ethics G2 Scope and Function G3 Scene Assessment G4 Triage G5 Primary Survey G6 Shock G7 Load and Go G8 Secondary Survey G9 Unconscious Patient G10A Obstructed Airway
