Proceeding of the LAVC Latin American Veterinary Conference Apr , 2012 Lima, Peru
|
|
|
- Abner Wilkerson
- 5 years ago
- Views:
Transcription
1 Close this window to return to IVIS Proceeding of the LAVC Latin American Veterinary Conference Apr , 2012 Lima, Peru Next LAVC Conference: Apr , 2013 Lima, Peru Reprinted in the IVIS website with the permission of the LAVC
2 HEAT STROKE AND HYPOTHERMIA Sergi Serrano, LV DVM DACVECC Connecticut Veterinary Center, the pet E.R. Homeothermic animals need to keep their core temperature within a set range to allow all body systems and reactions to work appropriately and prevent severe damage or even death. Several interlinked mechanisms, ultimately regulated by the thermoregulatory center in the hypothalamus, ensure that a constant temperature is maintained in the face of changing environmental and internal conditions. When these compensatory mechanisms are overwhelmed, body temperature goes over or under the set limits, and a series of deleterious effects can occur. Both heat stroke and hypothermia are common emergency presentations, or can develop whilst the animal is in hospital (particularly hypothermia). A thorough understanding of the temperature preservation mechanisms and the pathophysiologic changes associated with overheating and hypothermia, as well as with rewarming and cooling, are necessary to understand the different therapeutic options, monitoring required and complications. Heat stroke Heat stroke is a condition of extreme hyperthermia resulting from the body s inability to dissipate heat generated by metabolism, exercise, environmental conditions or a combination various or all of these. Core temperature has to be (or has been) above 41ºC (106ºF), and signs of neurological and other organ dysfunction are usually present. Heat stroke can be classified as classical (resulting from exposure to a hot and humid environment) or exertional (associated with intense physical exercise). A combination of both can frequently be encountered, particularly if there has been a lack of acclimatization (such as in working dogs at the beginning of the warm season, or if they move to a warmer area, or in a dog that has been frantically trying to escape from a locked car in the sun). There does not appear to be a direct correlation between core temperature and severity of clinical signs or outcome, nor has a cut-off value for temperature at which prognosis clearly changes been identified. However, time to cooling does seem to have an effect on outcome, suggesting that longer times at a certain temperature might have more detrimental effects than shorter periods at a higher temperature. Due to the paucity of information about heat stroke in small animals, most information is derived from human medicine, and also from experimental models. This information, however, should be interpreted with caution. The canine brain, for instance, has a much higher thermal resistance than the human brain. This may account for neurological signs often being the first to be present in people, and for the higher incidence of neurological damage that people seem to suffer when compared to our patients. In homeothermic animals, heat is produced from metabolism or gained from the environment, and is dissipated by conduction, convection, radiation and evaporation. Conduction occurs when the body is in contact with a cooler surface, and in our patients has a very limited role due to the insulating abilities of the coat. Convection is transference to the air as it passes over the body, such as happens with the wind (or a fan). Radiation is the natural release of heat from the body into the environment. Finally, evaporation is fluid changing to vapor, an endothermic process. Evaporation is the most important process for dissipating heat with environmental temperatures above 32ºC (89.6ºF). In people, it occurs mostly through perspiration. In dogs and cats, perspiration occurs via the footpads, rendering this a largely inefficient heat dissipation method, and evaporation happens through panting instead. With increases in blood temperature of less than 1ºC (1.8ºF), the thermoregulatory center in the hypothalamus is activated, and there is increased delivery of blood to the body surface, as well as increases in cardiac output and minute ventilation, and panting. If the animal becomes dehydrated, evaporation, radiation and convection heat losses are reduced, and thermoregulation is impaired. Although it is easy to assume that heat stroke is more common in areas with high temperatures and humidity, the body can adapt to these environmental conditions through the process called acclimatization, which is partially completed over 10 to 20 days, but might require up to 60 days to be completed. Adaptative mechanisms aim at conservation of water, enhanced cardiovascular performance, salt conservation, increased plasma volume and GFR, and an increase in the resistance to rhabdomyolysis. During heat stroke there is also activation of the Acute Phase Response (APR), which protects against tissue injury and promotes repair. Depending on all the mediators involved, APR can have a combination of protective and destructive effects, as well as inflammatory and/or anti-inflammatory effects. APR has to be exaggerated and inflammatory to be involved in the development of heat stroke. A recently discoverered set of players in the pathophysiology of this condition are the Heat Shock Proteins (HSPs), synthetized by virtually all cell types in response to increased temperatures, that act to help maintain cellular function and structural integrity. Aging, lack of acclimatization and genetic polymorphisms are associated with fewer levels of HSPs, and therefore with increased risk of heat stroke. Genetic predisposition could be one of the reasons for the overrepresentation of certain breeds such as Golden and Labrador Retrievers or Belgian Malinois, although it is unlikely to be the only one. Identifying genetically predisposed patients could allow for
3 prophylactic treatment and ensure that all other risk factors are minimized. NSAIDs, as HSPs up-regulating agents, may play a role in preventing heatstroke, but clinical evidence supporting its use is lacking. The pathophysiology of heat stroke, regardless of the type, has many similarities to sepsis, as the high temperature triggers a systemic inflammatory response which ultimately leads to multiple organ dysfunction syndrome (MODS). In heat stroke, circulatory collapse (including myocardial disfunction), renal failure, ARDS, DIC, rhabdomyolysis, hepatic failure, pancreatitis, and intestinal ischemia are all manifestations of MODS. On presentation, it is important to remember that patients can be hyper, normo or hypothermic, particularly if cooling measures have been started by the owners before presentation. Therefore, heat stroke should not be disregarded in a patient with normal or low core temperature if the history reveals recent exercise or confinment in a hot and humid environment and other clinical and/or clinicopathological findings are compatible. Clinical signs of shock (either in the hyperdynamic or hypodinamic phases), panting and neurological signs including ataxia, blindness, seizures and/or coma, petechiations or echymoses and hemorrhagic diarroea may be obvious on presentation or develop during the initial phases of treatment. Of all the clinical signs, seizures have been associated with increased risk of death. Obesity is not only a predisposing factor but also also a bad prognostic indicator. Clinical pathology usually reveals changes associated with severe hemoconcentration and/or dehydration, as well as azotemia and also commonly hypoglucemia. Hypoglucemia on presentation, particularly if refractory to initial treatment, and increased creatinine after 24 hours (suggesting renal failure) are also risk factors for death. Thrombocytopenia, prolongation of PT and aptt have all also been identified as risk factors for death. Nucleated red blood cells are a common finding, and its presence and number have been recently associated with outcome. More than 18 nrbc /100 WBC have got 91% sensitivity and 88% specificity for death. Therapy must include respiratory and/or ventilatory support (oxygen therapy including intubation and ventilation when required), rapid cooling and fluid therapy to replace volume losses and optimize perfusion. Secondary complications, either present or potential, must be addressed then (hypoglycemia, coagulopathies, ARDS, renal failure). It is important to remember that hypoglucemia is not always present in an animal presenting with seizures, and conversely some animals might be hypothermic and show other neurological signs than seizures (such as depression or coma). Therefore, empirical supplementation with intravenous dextrose should not be attempted and any glucose administration should be guided by the blood glucose concentration. Ideally, cooling should be accomplished by evaporative mechanisms. Wetting the animal with cool water and placing it by a fan is very efficient, as it uses evaporation, conduction and convection. Very cold or ice water baths should be avoided as they cause severe peripheral vasoconstriction and core temperature can therefore increase. It can also cause shivering, which would work towards increasing the temperature. Procedures such as cool gastric lavage, peritoneal lavage or cool water enemas are labor consuming and, although effective at achieving core cooling, they are usually not practical, can interfere with monitoring and make rebound hypothermia more likely. Active cooling should stop between 39.5ºC and 40ºC (103ºF-104ºF) to prevent both shivering and rebound hypothermia. As there is usually a severe water deficit, crystalloids should be the initial fluid of choice. In cases where hypoalbuminemia is severe, colloids can be used once the initial loading with crystalloids has been achieved and volemia is not being maintained. Experimental studies in rats favour small volume resuscitation using hypertonic saline and hydroxyethyl starch. Physical and laboratorial parameters related to perfusion and volume (e.g. PCV and TS, lactate) should be assessed at baseline and frequently thereafter to monitor progression and response to therapy. A urinary catheter should be placed to monitor urine output and allow urine collection for analysis. Cardiac arrhythmias rarely need to be pharmacologically addressed, but if they do, lidocaine is usually effective at controlling them, either as boluses or constant rate infusion. Post-heat stroke arrhythmias are likely to be associated with myocardial damage, and in some studies have been associated with mortality, but this finding has not been consistent across different studies. NSAIDs, as discussed earlier, have HSPs up-regulating effects that could prove beneficial in the management of heatstroke, despite having been traditionally not recommended due to the belief thathypoerthermia is not mediated by the hypothalamus. Although there could be a potential indication as a prophylactic treatment during heat waves or prior to extrenuous exercise, the well-known adverse effects associated with these compounds, both at renal, gastrointestinal and platelet level, would strongly advise against their use in clinical cases. Hyperbaric oxygen therapy has been shown experimentally and in some studies in people to improve outcome by limiting brain and pulmonary damage. These are target organs in human heat stroke, but in dogs they appear to be more resistant and suffer less damage as shown by pathology studies. Mortality in heatstroke ranges from 10-80% in people, and in small animals has been reported to be around 50%, although in the author s experience the mortality rates seem to be lower. Several risk factors, as discussed earlier, have been identified, but as no clear cut-off points for mortality have been found, aggressive therapy should be instituted as soon as possible for any patient presenting with heat stroke. More than half of the fatalities seem to occur during the first 24 hours, and according to one study death is unlikely if the animal survives the first 48 hours, suggesting most lesions can recover if the animal survives the initial period.
4 Hypothermia Hypothermia is a subnormal body temperature in a homeothermic animal. It can be primary (in an animal with normal heat production and resulting form extremely cold environmental conditions), or secondary (in which heat producing mechanisms are impaired, and can exist with even warm environmental conditions). In clinical practice, most of us have to deal with many more patients suffering from secondary hypothermia than from primary hypothermia. Interestingly, adverse effects are seen at much higher temperatures in patients suffering from secondary hypothermia than in patients suffering from primary hypothermia. Indeed, animals suffering from primary hypothermia as low as 32ºC will only display mild clinical signs such as shivering, piloerection and heat seeking, whilst patients with secondary hypothermia and temperatures below 36.7 can start showing abnorally low MAP and mental depression. Hence the expression it is not dead until it is warm and dead that our human counterparts use as an axiom for accidental hypothermia victims. Therefore, and due to its higher incidence and more severe adverse effects, this presentation will focus mostly on secondary hypothermia. Nevertheless, most of the recommendations and warming procedures can be equally used for cases of primary hypothermia. Primary hypothermia has been classified as Mild (32ºC-37ºC / 90ºF 99ºF), Moderate (28ºC 32ºC / 82ºF 90ºF), Severe (20ºC 28ºC / 68ºF 82ºF) and Profound or Critical (<20ºC / <68ºF). Secondary hypothermia has been classified as Mild (36.7ºC-37.7ºC / 98ºF-99.9ºF), Moderate (35.5ºC- 36.7ºC / 96ºF - 98ºF), Severe (33ºC 35.5ºC / 92ºF 96ºF), and Profound or Critical (< 33ºC / < 92ºF). Under primary hypothermia, asystole rarely occurs above 20ºC / 68ºF. Whilst heat production is a result of cellular metabolism and is ultimately regulated by the hypothalamus, the four basic mechanisms of heat loss have been described above. Hypothermia will occur from increased heat loss, decreased heat production or a combination of both. Whilst in primary hypothermia the body is not able to maintain the critical temperature level or hypothalamic set point, it is not uncommon for mild to moderate secondary hypothermia to be endogenously triggered as a protective mechanism, aiming at decreasing the energetic requirements from vital body systems (such as brain and heart). However this is not the only cause for secondary hypothermia, and even when intentional, secondary hypothermia can carry deleterious effects that far outweigh the beneficial ones. It is also common for secondary hypothermia to be iatrogenic, as associated with procedures under anesthesia. Regardless of the original cause, thermoregulation itself becomes impaired when core temperature falls below 34ºC (94ºF), and a spiral of events (cesation of shivering, peripheral vasodilation, decreased metabolic rate, CNS depression leading to hypothalamic hyporesponsiveness) leads to further heat loss and increased hypothermia. Below 31ºC (88ºF), thermoregulation ceases completely, and without prompt intervention death will be inevitable, particularly in the event of secondary hypothermia. From a metabolic and acid-base point of view, hyperglucemia is common in the initial stages, and frequently progresses to hypoglucemia as the temperature falls further. Initial hypokalemia due to increased urinary losses will lead to hyperkalemia at later stages, and can account for cardiac arrhythmias. Respiratory acidosis (secondary to respiratory and CNS depression) and metabolic acidosis (lactic acidosis secondary to hypoperfusion) commonly coexist. It is difficult to evaluate hemostasis as all tests measure at normal body temperature and therefore do not reflect what is happening in the hypothermic individual. Research reveals that thrombocytopathia is present even with mild to moderate hypothermia, but as with any potential changes in secondary hemostasis, they do not seem to be clinically significant. After an initial response consisting of increasing cardiac output and periperal vasoconstriction, with decreasing temperatures there is a decrease in cardiac contractile response and arteriolar responsiveness which eventually results in hypoperfusion and increased heat loss due to peripheral vasodilatation. Different arrhythmias have been described, including atrial fibrillation, ventricular fibrillation and asystole. In cats, fibrillation seems to be far less common than in dogs and bradycardia usually leads directly to asystole, possibly due to the smaller heart size. Respiratory changes may come not only from hypoventilation but also from concurrent pulmonary edema and pneumonia, which occur commonly and occasionally progress to ARDS. Although there is consistent evidence suggesting that mild hypothermia is neuroprotective and beneficial in the face of several neurological problems (such as head trauma or stroke), caution must be used when examining the data. Most of these come from very well-controlled experimental studies, and in clinical studies in people only mild hypothermia was allowed. Considering that cerebral blood flow has been shown to drop by more than 6% for each degree centigrade (2ºF) below normal core temperature, aggressively cooling brain injured patients or allowing moderate to severe hypothermia in these patients is probably not appropriate and not supported by the existing evidence. Mild hypothermia, however, could be beneficial and might not be addressed immediately if not showing signs of further compromising the patient. Immune function is also impaired with hypothermia, and there is increased risk of infections. In light of abnormal perfusion and drug distribution, however, broad spectrum antibiotic therapy should not be started until
5 temperature has normalised or clinical signs of infection are present. Whenever possible, samples for isolation and culture should be obtained from any wounds, tracheal washes, or other potential infectious foci. The main purpose of treatment is to warm up the patient to the normal clinical range (or at least to mild hypothermia with absence of clinical or laboratorial abnormalities) as soon as possible. However, given the changes in cardiovascular status and body fluids associated with hypothermia, ensuring appropriate fluid ressuscitation is mandatory prior to and during rewarming efforts. Close monitoring is mandatory, as aggressive fluid therapy can increase the risk for complications such as pulmonary edema. Crystalloids are usually the fluid of choice, a replacement fluid should be used, supplemented accordingly with glucose and/or potassium if required. Antiarrhythmics and catecholamines should not be used with moderate to severe hypothermia, as the response to them can be, if any, unpredictable at best. Moreover, most abnormalities will resolve as temperature increases providing volume status is maintained and major electrolyte and acid-base abnormalities are corrected. There are different group methods to warm a patient, which can be chosen based on the severity of the hypothermia and clinical signs, cost and clinician preferences. Regardless of the method used, temperature should be increased at least 1-2 ºC (2ºF-4ºF) per hour, and active rewarming should stop when core temperature reaches 37ºC (98ºF) to prevent rebound pyrexia. Passive surface methods: external covers (blankets, foil, bubble wrap), will prevent further heat loss but not actively warm. These rely on the animal s ability to generate heat (such as when recovering from anaesthesia), and are iindicated in mild hypothermia with appropriate perfusion status. Active surface warming: heating pads/bottles, circulating air/water, heat lamps, etc. These apply heat to the surface, and can therefore be used for moderate to severe hypothermia, requiring volume support to be provided during rewarming. Close monitoring and caution are to be used to prevent thermal burns and to avoid further heat loss from peripheral vasodilatation. Active core warming: faster and more effective, but also more invasive. Inhaled heated air (which should be humidified), peritoneal or pleural lavage, warm bladder lavages, warm enemas and warm intravenous fluids. These methods will provide central heat, aiming at more rapidly warming the core. They are reserved for severe or critical hypothermia, and although they will prevent dilatation of peripheral arterioles, local changes in vascular tone can result in circulatory compromise. Of all these, warm intravenous fluids (to temperatures up to 42ºC-43ºC / 107ºF- 109ºF) seems to be the least effective. During rewarming and in the immediate post-rewarming period, a series of complications can occur, and prompt recognition and treatment is mandatory to reduce the chances of an adverse outcome. Amongst these complications, the most commonly encountered are cerebral edema, pneumonia, pulmonary edema, pancreatitis, shock gut, hypotension and core temperature afterdrop (although the latter two seem to be clinicallly insignificant in people). Other complications that are more difficult to treat include reperfusion injury and ARDS. There is paucity of data regarding prognosis for primary hypothermia in dogs and cats, but with appropriate therapy many human patients recover with normal full neurological function. As for secondary hypothermia, prognosis is likely to be linked to the underlying cause as well as to both the duration and severity of the hypothermia. No studies have shown an ideal or minimal re-warming rate, and although a rewarming rate of 1-2ºC (2-4ºF) has been deemed safe and effective, considerably faster rates are often advocated and easily reached when using active core warming methods. REFERENCES Johnson SI, McMichael M, White G. Heatstroke in small animal medicine: a clinical practice review. JVECCS 16(2):2006; Bruchim Y, Klement E, Saragusty J, et al. Heat Stroke in Dogs: A retrospective study of 54 cases ( ) and analysis of risk factors for death. J Vet Intern Med 2006;20: Drobatz KJ, Macintire DK. Heat-induced illness in dogs: 42 cases ( ). J Am Vet Med Assoc 1996;209(11): Aroch I, Segev G, Loeb E, Bruchim Y. Peripheral nucleated red blood cells as a prognostic indicator in heatstroke in dogs. J Vet Intern Med 2009;23: Bruchim Y, Loeb E, Saragusty J, Arecho I. Pathological findings in dogs with fatal heatstroke. J Comp Pathol 2009;140: Oncken AK, Kirby R, Rudloff E. Hypothermia in Critically Ill Dogs and Cats. Compendium on Cont Educ Pract Vet 2001;23(6): Epstein E, Anna K. Accidental Hypothermia. British Medical Journal 2006;332: Key words: Heat stroke, Hyperthermia, Cooling, Heat Shock Proteins, Hypothermia, Thermoregulation, Rewarming, Temperature.
HEAT STROKE. Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC
 HEAT STROKE Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC Heat Stroke More Preventable Than Treatable Heat Stroke A form of hyperthermia associated with a systemic inflammatory response leading
HEAT STROKE Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC Heat Stroke More Preventable Than Treatable Heat Stroke A form of hyperthermia associated with a systemic inflammatory response leading
Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida
 Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida Reprinted in the IVIS website with the permission of the NAVC http:/// The North American Veterinary Conference
Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida Reprinted in the IVIS website with the permission of the NAVC http:/// The North American Veterinary Conference
Accidental Hypothermia
 Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
-Blood Warming- A Hot topic?
 -Blood Warming- A Hot topic? Blaine Kent, MD, FRCPC Associate Professor of Anesthesia Director, Peri-Operative Blood Management Chief, Cardiac Anesthesia Objectives To learn / review the deleterious systemic
-Blood Warming- A Hot topic? Blaine Kent, MD, FRCPC Associate Professor of Anesthesia Director, Peri-Operative Blood Management Chief, Cardiac Anesthesia Objectives To learn / review the deleterious systemic
-Cardiogenic: shock state resulting from impairment or failure of myocardium
 Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Hypothermia Presentation
 Hypothermia Presentation Thermoregulation Thermal regulation is a balance between heat production and heat loss. Despite marked changes in skin temperature, the body s homeostatic mechanisms are able to
Hypothermia Presentation Thermoregulation Thermal regulation is a balance between heat production and heat loss. Despite marked changes in skin temperature, the body s homeostatic mechanisms are able to
UTSW/BioTel EMS TRAINING BULLETIN January EMS TB Accidental Hypothermia
 UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
Taking the shock factor out of shock
 Taking the shock factor out of shock Julie Antonellis, BS, LVT, VTS (ECC) Northern Virginia Regional Director for the VALVT Technician Supervisor VCA Animal Emergency Critical Care Business owner Antonellis
Taking the shock factor out of shock Julie Antonellis, BS, LVT, VTS (ECC) Northern Virginia Regional Director for the VALVT Technician Supervisor VCA Animal Emergency Critical Care Business owner Antonellis
Cold-Related Illness. Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic
 Cold-Related Illness Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic Hypothermia Frost nip Frostbite Chillbains Trench foot Cold-Related Illness Who gets it? How common? Outdoor
Cold-Related Illness Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic Hypothermia Frost nip Frostbite Chillbains Trench foot Cold-Related Illness Who gets it? How common? Outdoor
Hypothermia Induction Methods
 Hypothermia Induction Methods Advantages and Disadvantages Xia Luo, M.D. Vice President, Clinical Education ZOLL Corporation Targeted Temperature Management (TTM) Temperature is one of the four vital signs
Hypothermia Induction Methods Advantages and Disadvantages Xia Luo, M.D. Vice President, Clinical Education ZOLL Corporation Targeted Temperature Management (TTM) Temperature is one of the four vital signs
Critical Care of the Post-Surgical Patient
 Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
Critical Care of the Post-Surgical Patient, Dr med vet, DEA, DECVIM-CA Many critically ill patients require surgical treatments. These patients often have multisystem abnormalities during the immediate
CEDR 2018 QCDR Measures for CMS 2018 MIPS Performance Year Reporting
 ACEP19 Emergency Department Utilization of CT for Minor Blunt Head Trauma for Aged 18 Years and Older Percentage of visits for aged 18 years and older who presented with a minor blunt head trauma who had
ACEP19 Emergency Department Utilization of CT for Minor Blunt Head Trauma for Aged 18 Years and Older Percentage of visits for aged 18 years and older who presented with a minor blunt head trauma who had
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #9 Heat Emergencies
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #9 Heat Emergencies As EMS providers we are called to treat several medical conditions. Heart Attacks,
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #9 Heat Emergencies As EMS providers we are called to treat several medical conditions. Heart Attacks,
Proceeding of the LAVECCS
 Close this window to return to IVIS Proceeding of the LAVECCS Congreso Latinoamericano de Emergencia y Cuidados Intensivos Ju1. 28-30, 2011 Santiago de Chile, Chile www.laveccs.org Reprinted in IVIS with
Close this window to return to IVIS Proceeding of the LAVECCS Congreso Latinoamericano de Emergencia y Cuidados Intensivos Ju1. 28-30, 2011 Santiago de Chile, Chile www.laveccs.org Reprinted in IVIS with
Overview. Physiology of Heat Stress Causal factors Heat Disorders & Health Effects Control
 Overview Physiology of Heat Stress Causal factors Heat Disorders & Health Effects Control 1 Causal Factors Age, weight, degree of physical fitness Degree of acclimatization, metabolism Intercurrent illnesses
Overview Physiology of Heat Stress Causal factors Heat Disorders & Health Effects Control 1 Causal Factors Age, weight, degree of physical fitness Degree of acclimatization, metabolism Intercurrent illnesses
DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER
 DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER This tragic recent headline involving Marco Cheseto serves as a grim reminder of the potential devastation inflicted by frostbite and hypothermia
DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER This tragic recent headline involving Marco Cheseto serves as a grim reminder of the potential devastation inflicted by frostbite and hypothermia
HYPOTHERMIA IN TRAUMA. Kevin Palmer EMT-P, DiMM
 HYPOTHERMIA IN TRAUMA Kevin Palmer EMT-P, DiMM DISCLOSURE No Financial conflicts of interest Member of the Wilderness Medical Society Diploma in Mountain Medicine Fellowship in the Academy of Wilderness
HYPOTHERMIA IN TRAUMA Kevin Palmer EMT-P, DiMM DISCLOSURE No Financial conflicts of interest Member of the Wilderness Medical Society Diploma in Mountain Medicine Fellowship in the Academy of Wilderness
Cold Water Shock, Hypothermia and Cardiac Arrest
 Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
Thermoregulation 2015 WMA
 1 Structure: Temperature sensors Endocrine system Muscles Skin Function: Maintain body core at 37 C Problem: Too little heat Too much heat 2 Normal Body Compensation Heat Response: Vasodilation Sweat Cold
1 Structure: Temperature sensors Endocrine system Muscles Skin Function: Maintain body core at 37 C Problem: Too little heat Too much heat 2 Normal Body Compensation Heat Response: Vasodilation Sweat Cold
THERMOREGULATION 05 JUNE 2013
 THERMOREGULATION 05 JUNE 2013 Lesson Description In this lesson we: Question the need to regulate body temperature in humans Examine the structure and functions of the different parts of the skin Look
THERMOREGULATION 05 JUNE 2013 Lesson Description In this lesson we: Question the need to regulate body temperature in humans Examine the structure and functions of the different parts of the skin Look
Ac#ve, ECMO or locally available alterna#ves. invasive warming. Ini#ally: Ac#ve noninvasive or minimally
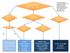 Suspected Hypothermia Temp
Suspected Hypothermia Temp
Chapter 12. Temperature Regulation
 Chapter 12 Temperature Regulation Temperature Regulation Body core temperature regulation Critical for: Cellular structures Metabolic pathways Too high Protein structure of cells destroyed Too low Slowed
Chapter 12 Temperature Regulation Temperature Regulation Body core temperature regulation Critical for: Cellular structures Metabolic pathways Too high Protein structure of cells destroyed Too low Slowed
INDUCED HYPOTHERMIA. F. Ben Housel, M.D.
 INDUCED HYPOTHERMIA F. Ben Housel, M.D. Historical Use of Induced Hypothermia 1950 s - Moderate hypothermia (30-32º C) in open heart surgery to protect brain against global ischemia 1960-1980 s - Use of
INDUCED HYPOTHERMIA F. Ben Housel, M.D. Historical Use of Induced Hypothermia 1950 s - Moderate hypothermia (30-32º C) in open heart surgery to protect brain against global ischemia 1960-1980 s - Use of
8/20/12. Discuss the importance of thermoregulation in the neonate.
 Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
Induced Hypothermia for Cardiac Arrest. Heather Hand RN,CCRN,CNRN,ATCN,LNC
 Induced Hypothermia for Cardiac Arrest Heather Hand RN,CCRN,CNRN,ATCN,LNC Cardiac Arrest Epidemiology 400,000 arrests / year in U.S.A 3 / 4 Out-of-hospital 1 / 4 In-hospital survival to hospital 1-5% discharge
Induced Hypothermia for Cardiac Arrest Heather Hand RN,CCRN,CNRN,ATCN,LNC Cardiac Arrest Epidemiology 400,000 arrests / year in U.S.A 3 / 4 Out-of-hospital 1 / 4 In-hospital survival to hospital 1-5% discharge
HEAT EMERGENCIES. Objectives. Dehydration and Heat Stroke. Definitions. Epidemiology. Epidemiology 4/5/2017
 Objectives HEAT EMERGENCIES Dehydration and Heat Stroke Define heat emergencies Appreciate the impact dehydration has on heat emergencies. Differentiate between heat stroke and other heat emergencies Describe
Objectives HEAT EMERGENCIES Dehydration and Heat Stroke Define heat emergencies Appreciate the impact dehydration has on heat emergencies. Differentiate between heat stroke and other heat emergencies Describe
3/6/2017. Endovascular Selective Cerebral Hypothermia First-in-Human Experience
 Endovascular Selective Cerebral Hypothermia First-in-Human Experience Ronald Jay Solar, Ph.D. San Diego, CA 32 nd Annual Snowmass Symposium March 5-10, 2017 Introduction Major limitations in acute ischemic
Endovascular Selective Cerebral Hypothermia First-in-Human Experience Ronald Jay Solar, Ph.D. San Diego, CA 32 nd Annual Snowmass Symposium March 5-10, 2017 Introduction Major limitations in acute ischemic
Sepsis Awareness and Education
 Sepsis Awareness and Education Meets the updated New York State Department of Health (NYSDOH) requirements for Infection Control and Barrier Precautions coursework Element VII: Sepsis Awareness and Education
Sepsis Awareness and Education Meets the updated New York State Department of Health (NYSDOH) requirements for Infection Control and Barrier Precautions coursework Element VII: Sepsis Awareness and Education
SYSTEM-WIDE POLICY & PROCEDURE MANUAL. Policy Title: Hypothermia Post Cardiac Arrest Policy Number: PC-124. President & CEO Page 1 of 9
 Approved By: President & CEO Date Page 1 of 9 POLICY: PURPOSE: To define and describe the implementation of induced hypothermia post cardiac arrest and the nursing assessment and interventions required
Approved By: President & CEO Date Page 1 of 9 POLICY: PURPOSE: To define and describe the implementation of induced hypothermia post cardiac arrest and the nursing assessment and interventions required
Neurotrauma: The Place for Cooling
 Neurotrauma: The Place for Cooling Cooling: to achieve hypothermia History, evidence, open questions Cooling: to achieve normothermia Evidence, open questions Cooling: Practical Aspects Hypothermia: History
Neurotrauma: The Place for Cooling Cooling: to achieve hypothermia History, evidence, open questions Cooling: to achieve normothermia Evidence, open questions Cooling: Practical Aspects Hypothermia: History
What would be the response of the sympathetic system to this patient s decrease in arterial pressure?
 CASE 51 A 62-year-old man undergoes surgery to correct a herniated disc in his spine. The patient is thought to have an uncomplicated surgery until he complains of extreme abdominal distention and pain
CASE 51 A 62-year-old man undergoes surgery to correct a herniated disc in his spine. The patient is thought to have an uncomplicated surgery until he complains of extreme abdominal distention and pain
Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES. Accidental Hypothermia/Cold Exposure
 Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES Accidental Hypothermia/Cold Exposure Goal: To aid EMS Providers in: the recognition and treatment of systemic effects of accidental hypothermia
Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES Accidental Hypothermia/Cold Exposure Goal: To aid EMS Providers in: the recognition and treatment of systemic effects of accidental hypothermia
THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST
 THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST Heather Harrington RN, BScN, CNCC(c) Clinical Nurse Educator Sunnybrook Health Sciences Centre Objectives Define Therapeutic Hypothermia (TH) Describe current
THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST Heather Harrington RN, BScN, CNCC(c) Clinical Nurse Educator Sunnybrook Health Sciences Centre Objectives Define Therapeutic Hypothermia (TH) Describe current
Salicylate (Aspirin) Ingestion California Poison Control Background 1. The prevalence of aspirin-containing analgesic products makes
 Salicylate (Aspirin) Ingestion California Poison Control 1-800-876-4766 Background 1. The prevalence of aspirin-containing analgesic products makes these agents, found in virtually every household, common
Salicylate (Aspirin) Ingestion California Poison Control 1-800-876-4766 Background 1. The prevalence of aspirin-containing analgesic products makes these agents, found in virtually every household, common
Thermal Injury. Thermal Injury Presentation CCFP (EM) Rounds. Topics Hypothermia. Resources Ch Tinitinelli
 Thermal Injury December 17, 2009 Thermal Injury Presentation CCFP (EM) Rounds Dr. Kyle McLaughlin, CCFP (EM) Topics Hypothermia Frostbite Hyperthermia Resources Ch. 191-193 Tinitinelli Multi media http://www.youtube.com/watch?v=x6mq0jftpji&feature=fvsr
Thermal Injury December 17, 2009 Thermal Injury Presentation CCFP (EM) Rounds Dr. Kyle McLaughlin, CCFP (EM) Topics Hypothermia Frostbite Hyperthermia Resources Ch. 191-193 Tinitinelli Multi media http://www.youtube.com/watch?v=x6mq0jftpji&feature=fvsr
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
All Things Cold: Hypothermia, Altitude Illness and Frostbite. Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine
 All Things Cold: Hypothermia, Altitude Illness and Frostbite Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine Objectives Thermoregulation basics Management of human-sickles
All Things Cold: Hypothermia, Altitude Illness and Frostbite Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine Objectives Thermoregulation basics Management of human-sickles
Regulation of Body Temperature. Ass. Prof. Dr. ADEL AMRAN DEPARTMENT OF PHYSIOLOGY
 Regulation of Body Temperature Ass. Prof. Dr. ADEL AMRAN DEPARTMENT OF PHYSIOLOGY objectives heat gain heat loss discuss the mechanisms by which the body gains or loses heat in a variety of healthy or
Regulation of Body Temperature Ass. Prof. Dr. ADEL AMRAN DEPARTMENT OF PHYSIOLOGY objectives heat gain heat loss discuss the mechanisms by which the body gains or loses heat in a variety of healthy or
2. A drop in core temperature induced thermogenesis. A drop in core temperature initiates:
 Get Adobe Flash player Introduction to Cold: Only in rare instances do people exercise at very low body temperatures (Brooks, 2009). Due to the combination of increased metabolism duirng exercise and the
Get Adobe Flash player Introduction to Cold: Only in rare instances do people exercise at very low body temperatures (Brooks, 2009). Due to the combination of increased metabolism duirng exercise and the
Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE
 Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE In critically ill patients: too little fluid Low preload,
Fluids in Sepsis: How much and what type? John Fowler, MD, FACEP Kent Hospital, İzmir Eisenhower Medical Center, USA American Hospital Dubai, UAE In critically ill patients: too little fluid Low preload,
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University
 Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
SHOCK. Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital
 SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
Proceedings of the Congreso Ecuatoriano de Especialidades Veterinarias CEEV Nov , 2011 Quito, Ecuador
 Close this window to return to IVIS www.ivis.org Proceedings of the Congreso Ecuatoriano de Especialidades Veterinarias CEEV 2011 Nov. 15-17, 2011 Quito, Ecuador Reprinted in IVIS with the permission of
Close this window to return to IVIS www.ivis.org Proceedings of the Congreso Ecuatoriano de Especialidades Veterinarias CEEV 2011 Nov. 15-17, 2011 Quito, Ecuador Reprinted in IVIS with the permission of
Update on Sudden Cardiac Death and Resuscitation
 Update on Sudden Cardiac Death and Resuscitation Ashish R. Panchal, MD, PhD Medical Director Center for Emergency Medical Services Assistant Professor Clinical Department of Emergency Medicine The Ohio
Update on Sudden Cardiac Death and Resuscitation Ashish R. Panchal, MD, PhD Medical Director Center for Emergency Medical Services Assistant Professor Clinical Department of Emergency Medicine The Ohio
INTRAVENOUS FLUID THERAPY. Tom Heaps Consultant Acute Physician
 INTRAVENOUS FLUID THERAPY Tom Heaps Consultant Acute Physician LEARNING OBJECTIVES 1. Crystalloids vs colloids 2. Balanced vs non-balanced solutions 3. Composition of various IV fluids 4. What is normal
INTRAVENOUS FLUID THERAPY Tom Heaps Consultant Acute Physician LEARNING OBJECTIVES 1. Crystalloids vs colloids 2. Balanced vs non-balanced solutions 3. Composition of various IV fluids 4. What is normal
Unrestricted. Dr ppooransari fellowship of perenatalogy
 Unrestricted Dr ppooransari fellowship of perenatalogy Assessment of severity of hemorrhage Significant drops in blood pressure are generally not manifested until substantial bleeding has occurred, and
Unrestricted Dr ppooransari fellowship of perenatalogy Assessment of severity of hemorrhage Significant drops in blood pressure are generally not manifested until substantial bleeding has occurred, and
Rhonda Dixon, DVM Section Head, Emergency and Critical Care Sugar Land Veterinary Specialty and Emergency
 Rhonda Dixon, DVM Section Head, Emergency and Critical Care Sugar Land Veterinary Specialty and Emergency Traumatic Brain Injury Causes Pathophysiology Neurologic assessment Therapeutic Approach Status
Rhonda Dixon, DVM Section Head, Emergency and Critical Care Sugar Land Veterinary Specialty and Emergency Traumatic Brain Injury Causes Pathophysiology Neurologic assessment Therapeutic Approach Status
LESSON 2. Section I. GENERAL INFORMATION 2-1. WHY IS IT IMPORTANT TO KNOW THE PATIENT'S TEMPERATURE?
 LESSON 2 Section I. GENERAL INFORMATION 2-1. WHY IS IT IMPORTANT TO KNOW THE PATIENT'S TEMPERATURE? a. To Determine the Cause of the Patient's Condition. When a person becomes ill, one of the first things
LESSON 2 Section I. GENERAL INFORMATION 2-1. WHY IS IT IMPORTANT TO KNOW THE PATIENT'S TEMPERATURE? a. To Determine the Cause of the Patient's Condition. When a person becomes ill, one of the first things
ENVIRONMENTAL EMERGENCIES
 Joanna Jakubaszko-Jabłońska ENVIRONMENTAL EMERGENCIES Chair of Emergency Medicine Wroclaw Medical University Emergency treatment of near-drowning victims Clinical findings: The victim may present with
Joanna Jakubaszko-Jabłońska ENVIRONMENTAL EMERGENCIES Chair of Emergency Medicine Wroclaw Medical University Emergency treatment of near-drowning victims Clinical findings: The victim may present with
CrackCast Episode 8 Brain Resuscitation
 CrackCast Episode 8 Brain Resuscitation Episode Overview: 1) Describe 6 therapeutic interventions for the post-arrest brain 2) List 5 techniques for initiating therapeutic hypothermia 3) List 4 mechanisms
CrackCast Episode 8 Brain Resuscitation Episode Overview: 1) Describe 6 therapeutic interventions for the post-arrest brain 2) List 5 techniques for initiating therapeutic hypothermia 3) List 4 mechanisms
Patient Case. Post cardiac arrest pathophysiology 10/19/2017. Disclosure. Objectives. Patient Case-TM
 Disclosure TARGETED TEMPERATURE MANAGEMENT POST CARDIAC ARREST I have nothing to disclose concerning possible financial or personal relationships with commercial entities that may have a direct or indirect
Disclosure TARGETED TEMPERATURE MANAGEMENT POST CARDIAC ARREST I have nothing to disclose concerning possible financial or personal relationships with commercial entities that may have a direct or indirect
ANESTHETIZING DISEASED PATIENTS: URINARY; NEUROLOGICAL; TRAUMATIZED
 ANESTHETIZING DISEASED PATIENTS: URINARY; NEUROLOGICAL; TRAUMATIZED Lyon Lee DVM PhD DACVA Patients with Urinary Tract Diseases General considerations Three main factors to consider in anesthetizing urinary
ANESTHETIZING DISEASED PATIENTS: URINARY; NEUROLOGICAL; TRAUMATIZED Lyon Lee DVM PhD DACVA Patients with Urinary Tract Diseases General considerations Three main factors to consider in anesthetizing urinary
Bill Hall, MD Mesa County EMS System
 Bill Hall, MD Mesa County EMS System Discuss cold related injuries and treatment Discuss hypothermia and treatment Discuss avalanche victim care and considerations Chilblains (Pernio) Trench Foot Frost
Bill Hall, MD Mesa County EMS System Discuss cold related injuries and treatment Discuss hypothermia and treatment Discuss avalanche victim care and considerations Chilblains (Pernio) Trench Foot Frost
HEAT PRODUCTION HEAT DISSIPATION
 Heat Illness Shaylon Rettig, MD, MBA HEAT PRODUCTION Heat is a byproduct of the metabolic process Muscle contributes the largest amount of heat produced at rest Muscle work increases heat production Fever
Heat Illness Shaylon Rettig, MD, MBA HEAT PRODUCTION Heat is a byproduct of the metabolic process Muscle contributes the largest amount of heat produced at rest Muscle work increases heat production Fever
Hypovolemic Shock: Regulation of Blood Pressure
 CARDIOVASCULAR PHYSIOLOGY 81 Case 15 Hypovolemic Shock: Regulation of Blood Pressure Mavis Byrne is a 78-year-old widow who was brought to the emergency room one evening by her sister. Early in the day,
CARDIOVASCULAR PHYSIOLOGY 81 Case 15 Hypovolemic Shock: Regulation of Blood Pressure Mavis Byrne is a 78-year-old widow who was brought to the emergency room one evening by her sister. Early in the day,
Prehospital Care Bundles
 Prehospital s The MLREMS Prehospital s have been created to provide a simple framework to help EMS providers identify the most critical elements when caring for a patient. These bundles do not replace
Prehospital s The MLREMS Prehospital s have been created to provide a simple framework to help EMS providers identify the most critical elements when caring for a patient. These bundles do not replace
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT.
 HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
Seizures Emergency Treatment
 Seizures Emergency Treatment Emergency Seizures SEIZURE CLASSIFICATION Cluster seizures - 2 or more generalized convulsive seizures in 24 hours Simon R. Platt BVM&S MRCVS Dipl. ACVIM (Neurology) Dipl.ECVN
Seizures Emergency Treatment Emergency Seizures SEIZURE CLASSIFICATION Cluster seizures - 2 or more generalized convulsive seizures in 24 hours Simon R. Platt BVM&S MRCVS Dipl. ACVIM (Neurology) Dipl.ECVN
Staging Sepsis for the Emergency Department: Physician
 Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
Staging Sepsis for the Emergency Department: Physician Sepsis Continuum 1 Sepsis Continuum SIRS = 2 or more clinical criteria, resulting in Systemic Inflammatory Response Syndrome Sepsis = SIRS + proven/suspected
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal compartment syndrome, as complication of fluid resuscitation, 331 338 abdominal perfusion pressure, 332 fluid restriction practice
Index Note: Page numbers of article titles are in boldface type. A Abdominal compartment syndrome, as complication of fluid resuscitation, 331 338 abdominal perfusion pressure, 332 fluid restriction practice
The Pharmacology of Hypotension: Vasopressor Choices for HIE patients. Keliana O Mara, PharmD August 4, 2018
 The Pharmacology of Hypotension: Vasopressor Choices for HIE patients Keliana O Mara, PharmD August 4, 2018 Objectives Review the pathophysiology of hypotension in neonates Discuss the role of vasopressors
The Pharmacology of Hypotension: Vasopressor Choices for HIE patients Keliana O Mara, PharmD August 4, 2018 Objectives Review the pathophysiology of hypotension in neonates Discuss the role of vasopressors
INDUCED HYPOTHERMIA A Hot Topic. R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences
 INDUCED HYPOTHERMIA A Hot Topic R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences Conflicts of Interest Sadly, we have no financial or industrial conflicts of interest
INDUCED HYPOTHERMIA A Hot Topic R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences Conflicts of Interest Sadly, we have no financial or industrial conflicts of interest
Drowning is a leading cause of death and loss of years of life with over 90% of cases occurring in lower- and middle-income countries.
 Chapter 145 Drowning Episode Overview: 1) List risk factors for drowning 2) List 5 variables that portend poor outcome 3) Describe the diving reflex 4) Describe the management of a drowning patient with
Chapter 145 Drowning Episode Overview: 1) List risk factors for drowning 2) List 5 variables that portend poor outcome 3) Describe the diving reflex 4) Describe the management of a drowning patient with
SHOCK Susanna Hilda Hutajulu, MD, PhD
 SHOCK Susanna Hilda Hutajulu, MD, PhD Div Hematology and Medical Oncology Department of Internal Medicine Universitas Gadjah Mada Yogyakarta Outline Definition Epidemiology Physiology Classes of Shock
SHOCK Susanna Hilda Hutajulu, MD, PhD Div Hematology and Medical Oncology Department of Internal Medicine Universitas Gadjah Mada Yogyakarta Outline Definition Epidemiology Physiology Classes of Shock
Post Cardiac Arrest Care. From : 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care
 Post Cardiac Arrest Care From : 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Initial Objectives of Post cardiac Arrest Care Optimize cardiopulmonary
Post Cardiac Arrest Care From : 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Initial Objectives of Post cardiac Arrest Care Optimize cardiopulmonary
HYPOVOLEMIA AND HEMORRHAGE UPDATE ON VOLUME RESUSCITATION HEMORRHAGE AND HYPOVOLEMIA DISTRIBUTION OF BODY FLUIDS 11/7/2015
 UPDATE ON VOLUME RESUSCITATION HYPOVOLEMIA AND HEMORRHAGE HUMAN CIRCULATORY SYSTEM OPERATES WITH A SMALL VOLUME AND A VERY EFFICIENT VOLUME RESPONSIVE PUMP. HOWEVER THIS PUMP FAILS QUICKLY WITH VOLUME
UPDATE ON VOLUME RESUSCITATION HYPOVOLEMIA AND HEMORRHAGE HUMAN CIRCULATORY SYSTEM OPERATES WITH A SMALL VOLUME AND A VERY EFFICIENT VOLUME RESPONSIVE PUMP. HOWEVER THIS PUMP FAILS QUICKLY WITH VOLUME
Understanding the pediatric patient and basics of pediatric emergencies. Dr. Alenka Hrovat Vernik DrVetMed PhD MRCVS
 Understanding the pediatric patient and basics of pediatric emergencies Dr. Alenka Hrovat Vernik DrVetMed PhD MRCVS Stages of development Neonatal period - from birth till 3 rd -4 th week Weaning period
Understanding the pediatric patient and basics of pediatric emergencies Dr. Alenka Hrovat Vernik DrVetMed PhD MRCVS Stages of development Neonatal period - from birth till 3 rd -4 th week Weaning period
Case Presentation. Cooling. Case Presentation. New Developments in Cardiopulmonary Arrest: Therapeutic Hypothermia in Resuscitation
 New Developments in Cardiopulmonary Arrest: Therapeutic Hypothermia in Resuscitation Michael Sayre, MD Emergency Medicine and LeRoy Essig, MD Pulmonary/Critical Care Medicine Case Presentation 3:40 (+
New Developments in Cardiopulmonary Arrest: Therapeutic Hypothermia in Resuscitation Michael Sayre, MD Emergency Medicine and LeRoy Essig, MD Pulmonary/Critical Care Medicine Case Presentation 3:40 (+
Acid-base management during hypothermic CPB alpha-stat and ph-stat models of blood gas interpretation
 Acid-base management during hypothermic CPB alpha-stat and ph-stat models of blood gas interpretation Michael Kremke Department of Anaesthesiology and Intensive Care Aarhus University Hospital, Denmark
Acid-base management during hypothermic CPB alpha-stat and ph-stat models of blood gas interpretation Michael Kremke Department of Anaesthesiology and Intensive Care Aarhus University Hospital, Denmark
Lecture Notes. Chapter 9: Smoke Inhalation Injury and Burns
 Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Key Points. Angus DC: Crit Care Med 29:1303, 2001
 Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
Sepsis Key Points Sepsis is the combination of a known or suspected infection and an accompanying systemic inflammatory response (SIRS) Severe sepsis is sepsis with acute dysfunction of one or more organ
12/1/2009. Chapter 19: Hemorrhage. Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system Internal hemorrhage
 Chapter 19: Hemorrhage Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system External hemorrhage Internal hemorrhage Associated with higher morbidity and mortality than
Chapter 19: Hemorrhage Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system External hemorrhage Internal hemorrhage Associated with higher morbidity and mortality than
Current State of Pediatric Sepsis. Jason Clayton, MD PhD Pediatric Critical Care 9/19/2018
 Current State of Pediatric Sepsis Jason Clayton, MD PhD Pediatric Critical Care 9/19/2018 Objectives Review the history of pediatric sepsis Review the current definition of pediatric sepsis Review triage
Current State of Pediatric Sepsis Jason Clayton, MD PhD Pediatric Critical Care 9/19/2018 Objectives Review the history of pediatric sepsis Review the current definition of pediatric sepsis Review triage
2.5 HEALTH AND SAFETY
 2.5 HEALTH AND SAFETY 2.5.1 Fundamentals of Heat Illness Prevention and Management (a) A Certified Athletic Trainer or 1 st Responder MUST be in attendance at all football practices and games. (b) The
2.5 HEALTH AND SAFETY 2.5.1 Fundamentals of Heat Illness Prevention and Management (a) A Certified Athletic Trainer or 1 st Responder MUST be in attendance at all football practices and games. (b) The
Initial Resuscitation of Sepsis & Septic Shock
 Initial Resuscitation of Sepsis & Septic Shock Dr. Fatema Ahmed MD (Critical Care Medicine) FCPS (Medicine) Associate professor Dept. of Critical Care Medicine BIRDEM General Hospital Is Sepsis a known
Initial Resuscitation of Sepsis & Septic Shock Dr. Fatema Ahmed MD (Critical Care Medicine) FCPS (Medicine) Associate professor Dept. of Critical Care Medicine BIRDEM General Hospital Is Sepsis a known
SHOCK. Pathophysiology
 SHOCK Dr. Ahmed Saleem FICMS TUCOM / 3rd Year / 2015 Shock is the most common and therefore the most important cause of death of surgical patients. Death may occur rapidly due to a profound state of shock,
SHOCK Dr. Ahmed Saleem FICMS TUCOM / 3rd Year / 2015 Shock is the most common and therefore the most important cause of death of surgical patients. Death may occur rapidly due to a profound state of shock,
Sepsis is an important issue. Clinician s decision-making capability. Guideline recommendations
 Surviving Sepsis Campaign: International Guidelines for Management of Severe Sepsis and Septic Shock: 2012 Clinicians decision-making capability Guideline recommendations Sepsis is an important issue 8.7%
Surviving Sepsis Campaign: International Guidelines for Management of Severe Sepsis and Septic Shock: 2012 Clinicians decision-making capability Guideline recommendations Sepsis is an important issue 8.7%
Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest. Objectives: U.S. stats
 Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest Nicole L. Kupchik RN, MN, CCNS CCRN-CMC Clinical Nurse Specialist Harborview Medical Center Seattle, WA Objectives: At the
Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest Nicole L. Kupchik RN, MN, CCNS CCRN-CMC Clinical Nurse Specialist Harborview Medical Center Seattle, WA Objectives: At the
Vasoactive Medications. Matthew J. Korobey Pharm.D., BCCCP Critical Care Clinical Specialist Mercy St. Louis
 Vasoactive Medications Matthew J. Korobey Pharm.D., BCCCP Critical Care Clinical Specialist Mercy St. Louis Objectives List components of physiology involved in blood pressure Review terminology related
Vasoactive Medications Matthew J. Korobey Pharm.D., BCCCP Critical Care Clinical Specialist Mercy St. Louis Objectives List components of physiology involved in blood pressure Review terminology related
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC
 Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Hypothermia in Neonates with HIE TARA JENDZIO, DNP(C), RN, RNC-NIC Objectives 1. Define Hypoxic-Ischemic Encephalopathy (HIE) 2. Identify the criteria used to determine if an infant qualifies for therapeutic
Shock Quiz! By Clare Di Bona
 Shock Quiz! By Clare Di Bona Test Question What is Mr Burns full legal name? Answer Charles Montgomery Plantagenet Schicklgruber Burns. (Season 22, episode 11) Question 1. What is the definition of shock?
Shock Quiz! By Clare Di Bona Test Question What is Mr Burns full legal name? Answer Charles Montgomery Plantagenet Schicklgruber Burns. (Season 22, episode 11) Question 1. What is the definition of shock?
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Accelerated intravascular coagulation and fibrinolysis (AICF) in liver disease, 390 391 Acid suppression in liver disease, 403 404 ACLF.
Index Note: Page numbers of article titles are in boldface type. A Accelerated intravascular coagulation and fibrinolysis (AICF) in liver disease, 390 391 Acid suppression in liver disease, 403 404 ACLF.
Mild. Moderate. Severe. 32 to to and below
 Mohamud Daya MD, MS Mild 32 to 34 Moderate 28 to 32 Severe 28 and below Jon Rittenberger Shervin Ayati Protocol Development Committee Hypothermia Working Group Lynn Wittwer Jon Jui John Stouffer Scott
Mohamud Daya MD, MS Mild 32 to 34 Moderate 28 to 32 Severe 28 and below Jon Rittenberger Shervin Ayati Protocol Development Committee Hypothermia Working Group Lynn Wittwer Jon Jui John Stouffer Scott
State of Florida Systemic Supportive Care Guidelines. Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology
 State of Florida Systemic Supportive Care Guidelines Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. FEN 1. What intravenous fluids should be initiated upon admission
State of Florida Systemic Supportive Care Guidelines Michael D. Weiss, M.D. Associate Professor of Pediatrics Division of Neonatology I. FEN 1. What intravenous fluids should be initiated upon admission
SHOCK. May 12, 2011 Body and Disease
 SHOCK May 12, 2011 Body and Disease Shock Definition of shock Pathophysiology Types of shock Management of shock Shock Definition? Shock What the Duke Community would have experienced if Gordon Hayward
SHOCK May 12, 2011 Body and Disease Shock Definition of shock Pathophysiology Types of shock Management of shock Shock Definition? Shock What the Duke Community would have experienced if Gordon Hayward
Chapter 3 MAKING THE DECISION TO TRANSFUSE
 Chapter 3 MAKING THE DECISION TO TRANSFUSE PRACTICE POINTS Determine the best treatment for the patient which may include transfusion. Treat the cause of cytopenia (anaemia or thrombocytopenia) or plasma
Chapter 3 MAKING THE DECISION TO TRANSFUSE PRACTICE POINTS Determine the best treatment for the patient which may include transfusion. Treat the cause of cytopenia (anaemia or thrombocytopenia) or plasma
INTRODUCTION: DEFINITION OF HEAT ILLNESS:
 Coastal Carolina University Athletic Training Department Policy and Procedure Manual Exertional Heat Illness Management Fluid Replacement/Rehydration Protocol Revised/Reviewed 3/2013 INTRODUCTION: The
Coastal Carolina University Athletic Training Department Policy and Procedure Manual Exertional Heat Illness Management Fluid Replacement/Rehydration Protocol Revised/Reviewed 3/2013 INTRODUCTION: The
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit
 Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
Information Often Given to the Nurse at the Time of Admission to the Postanesthesia Care Unit * Patient s name and age * Surgical procedure and type of anesthetic including drugs used * Other intraoperative
BREAK 11:10-11:
 1. Sepsis Tom Heaps 09:30-10:20 2. Oncological Emergencies Clare Pollard 10:20-11:10 ------------------------ BREAK 11:10-11:30 ------------------------ 3. Diabetic Ketoacidosis Tom Heaps 11:30-12:20 4.
1. Sepsis Tom Heaps 09:30-10:20 2. Oncological Emergencies Clare Pollard 10:20-11:10 ------------------------ BREAK 11:10-11:30 ------------------------ 3. Diabetic Ketoacidosis Tom Heaps 11:30-12:20 4.
Shock. Shao Mian Emergency Department,Zhongshan Hospital
 Shock Shao Mian Emergency Department,Zhongshan Hospital What is shock THE BEGINNINGS OF UNDERSTANDING: THE LATE 19TH CENTURY THE AGE OF REASON: 1890 1925 THE MODERN ERA: BLALOCK S EPIPHANY POSTMODERNISM:
Shock Shao Mian Emergency Department,Zhongshan Hospital What is shock THE BEGINNINGS OF UNDERSTANDING: THE LATE 19TH CENTURY THE AGE OF REASON: 1890 1925 THE MODERN ERA: BLALOCK S EPIPHANY POSTMODERNISM:
Hypothermia in Trauma What happens? Hypothermia in the Trauma Patient. Hypothermia in Trauma 10/6/2010
 Hypothermia in the Trauma Patient Friend or Foe? Clark Hayward EMTP, AWLS 10/2/10 Hypothermia in Trauma What happens? From the time of injury, trauma itself alters the normal central thermoregulation and
Hypothermia in the Trauma Patient Friend or Foe? Clark Hayward EMTP, AWLS 10/2/10 Hypothermia in Trauma What happens? From the time of injury, trauma itself alters the normal central thermoregulation and
Shock Management. Seyed Tayeb Moradian MSc, Critical Care Nursing Ph.D Candidate. PDF created with pdffactory Pro trial version
 Shock Management Seyed Tayeb Moradian MSc, Critical Care Nursing Ph.D Candidate Definition of Shock The definition of shock does not involve low blood pressure, rapid pulse or cool clammy skin - these
Shock Management Seyed Tayeb Moradian MSc, Critical Care Nursing Ph.D Candidate Definition of Shock The definition of shock does not involve low blood pressure, rapid pulse or cool clammy skin - these
Heat-related illnesses are prevalent in human and veterinary. Heatstroke: Thermoregulation, Pathophysiology, and Predisposing Factors
 3 CE Credits Heatstroke: Thermoregulation, Pathophysiology, and Predisposing Factors Carey Hemmelgarn, DVM Kristi Gannon, DVM, DACVECC Oradell Animal Hospital Paramus, New Jersey Abstract: Heatstroke is
3 CE Credits Heatstroke: Thermoregulation, Pathophysiology, and Predisposing Factors Carey Hemmelgarn, DVM Kristi Gannon, DVM, DACVECC Oradell Animal Hospital Paramus, New Jersey Abstract: Heatstroke is
Heat-related illnesses can affect people
 Scott Kinkade, MD, EdD; Megan Warhol, DO Department of Family and Community Medicine, University of Missouri School of Medicine, Columbia (Dr. Kinkade); SSMHealth Troy, Mo (Dr. Warhol) Kinkades@health.
Scott Kinkade, MD, EdD; Megan Warhol, DO Department of Family and Community Medicine, University of Missouri School of Medicine, Columbia (Dr. Kinkade); SSMHealth Troy, Mo (Dr. Warhol) Kinkades@health.
Proceeding of the LAVC Latin American Veterinary Conference Oct , 2011 Lima, Peru
 Close this window to return to IVIS www.ivis.org Proceeding of the LAVC Latin American Veterinary Conference Oct. 24-26, 2011 Lima, Peru Next LAVC Conference: Apr. 24-26, 2012 Lima, Peru Reprinted in the
Close this window to return to IVIS www.ivis.org Proceeding of the LAVC Latin American Veterinary Conference Oct. 24-26, 2011 Lima, Peru Next LAVC Conference: Apr. 24-26, 2012 Lima, Peru Reprinted in the
Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy
 Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy A 44 year old female undergoing 10 hour Cytoreductive (CRS) procedure followed by Hyperthermic Intraperitoneal Chemotherapy (HIPEC).
Cytoreductive Surgery and Hyperthermic Intraperitoneal Chemotherapy A 44 year old female undergoing 10 hour Cytoreductive (CRS) procedure followed by Hyperthermic Intraperitoneal Chemotherapy (HIPEC).
Instituting preventive warming measures for patients who are normothermic. A variety of measures may be used, unless contraindicated.
 Patient Warmer Perioperative Hypothermia specifies that a preoperative patient management assessment should include: Identification of a patient s risk factors for unplanned perioperative hypothermia Measurement
Patient Warmer Perioperative Hypothermia specifies that a preoperative patient management assessment should include: Identification of a patient s risk factors for unplanned perioperative hypothermia Measurement
Failure of the circulation to maintain Tissue cellular. Tissue hypoperfusion Cellular hypoxia SHOCK. Perfusion
 Shock SHOCK Failure of the circulation to maintain Tissue cellular Perfusion Organs Syndrome RR
Shock SHOCK Failure of the circulation to maintain Tissue cellular Perfusion Organs Syndrome RR
Heat Illness in Children
 Heat Illness in Children Charles G. Macias MD, MPH Baylor College of Medicine Attending Physician, Texas Children s Hospital Emergency Department Houston, Texas Scope of the problem Heat stroke mortality
Heat Illness in Children Charles G. Macias MD, MPH Baylor College of Medicine Attending Physician, Texas Children s Hospital Emergency Department Houston, Texas Scope of the problem Heat stroke mortality
