Hypothermia in Trauma What happens? Hypothermia in the Trauma Patient. Hypothermia in Trauma 10/6/2010
|
|
|
- Gavin Henderson
- 6 years ago
- Views:
Transcription
1 Hypothermia in the Trauma Patient Friend or Foe? Clark Hayward EMTP, AWLS 10/2/10 Hypothermia in Trauma What happens? From the time of injury, trauma itself alters the normal central thermoregulation and blocks the shivering response. Betty J. Tsuei*, Paul A. Kearney, Hypothermia in the trauma patient Injury, Int. J. Care Injured (2004) 35, 7 15 Hypothermia in Trauma Based upon our findings, accidental hypothermia poses a relevant problem in the prehospital treatment of trauma patients. It is not limited to a special season of the year. From: Helm M, Lampl L, Hauke J, Bock KH. Accidental hypothermia in trauma patients. Is it relevant to preclinical emergency treatment? Anaesthesist 1995;44(2): It is estimated that as many as 66% of all trauma patients arrive into the emergency room with hypothermia. Baylor University Medical Center A critical element of trauma care is to prevent hypothermia in the injured patient. 1
2 Objectives Most traditional methods of maintaining trauma patient temperature during prehospital transport appear to be inadequate. From: Watts DD, Roche M, et al. The utility of traditional prehospital interventions in maintaining thermostasis. Prehosp Emerg Care 1999;3(2) Review physiology of thermoregulation Discuss complications of hypothermia in injured patients Discuss the pathophysiology of the Lethal Triad Review current prehospital prevention and treatment Discuss Therapeutic Hypothermia Outcomes Recognize the importance of early identification of at-risk/high susceptibility trauma patients Describe the pathophysiology of the Lethal Triad and its significance in trauma mortality and morbidity Use the knowledge gained to improve outcomes for trauma patients Case Study 04:35 - Dispatched to a rural area for a 34 YO male, self inflicted GSW, patrol enroute. 04:51 - Arrive to find scene secured by PD, male victim supine in parking area of popular local hunting spot, attended by companion (local VFD EMT) holding direct pressure to upper right thigh area. Obvious significant blood loss. 2
3 Case Study Victim states that he leaned his rifle against car and bent over to tighten boots when the rifle fell over and discharged with bullet striking him in right thigh. Case Study You assist with DP and additional dressings while partner applies O2 NRB takes initial vitals and prepares for vascular access. Vital 04:55 LOC = A&O Skin = pale, moist, cool P = 128 R BP = 102/74 R = 26 S Case Study Bleeding continues despite DP and you adjust area of pressure after visualization of wound area, bleeding slows. Partner has gained IV with NS wide open. Pt. is moved to backboard, secured and loaded to stretcher, moved to rig and you begin transport to trauma 05:09. 3
4 Physiology of Thermoregulation Physiology of Thermoregulation Homeostasis requires constant body temp of 98.6F. Humans are tropical animals. Mechanism for losing heat is more efficient than mechanism for retaining heat. Physiology of Thermoregulation Physiology of Thermoregulation Thermoregulation is controlled by 2 primary mechanisms. 1)Hypothalmus 2)Peripheral Thermoreceptors in tissues of skin, muscle, bone. The Hypothalmus is just superior to the Pituitary Gland and monitors blood temp and feedback from peripheral thermoreceptors. 4
5 Temperature Homeostasis Opposition of Heat Loss Hypothalamus Stimulation of sympathetic nervous system if temp below set point of 98.6F. Behavioral responses Wearing clothes when it s cold Leaving cold environment Heat Gain Shivering Non-shivering thermogenesis, metabolism of fats and carbs. Heat Loss Conduction Transfer of heat by direct contact down temperature gradient. Convection Transfer of heat by movement of heated material. (i.e. wind) Radiation Loss of heat from non-insulated areas. H 2 O Evaporation Loss of heat when moisture evaporates from skin. Respiration Populations at Risk for Hypothermia Elderly Very young Intoxicated individuals People involved in cold weather outdoor activities Trauma patients 5
6 Populations at Risk for Hypothermia All those at risk categories can also be trauma patients! Hypothermia Epidemiology Defined as temp <35 O C (<95 O F) >700 die each year in US from hypothermia ½ of those are 65+ years old Individuals at age extremes and those with AMS are at greatest risk Specific Risk Factors Immobility Wet clothing Windchill Lying on a cold surface Any conditions that cause loss of consciousness, immobility, or both (eg., hypoglycemia, seizure disorders, stroke, drug or alcohol intoxication, trauma) are common predisposing factors. Etiology of Hypothermia Accidental Immersion and non-immersion cold exposure Cold, wet, wind ( E-C-C-R-R heat loss) Metabolic Hypoendocrine states (hypothyroid, hypoadrenalism, hypopituitarism) Hypoglycemia Tumor can interfere with thermoregulatory response. Trauma can alter clotting mechanisms 6
7 Etiology of Hypothermia (cont.) Etiology of Hypothermia (cont.) Wernicke s Disease Drug induced Alcohol (majority of hypothermic pt s in US are intoxicated!) Sedatives Tricyclics Insulin Sepsis Severe dermal disease Burns Exfoliative dermatitis Acute incapacitating illness Severe infections DKA Psychotic disorders Other conditions causing impaired thermoregulatory function Resuscitation with room temperature fluid!! Hypothermia Classes Pathophysiology Mild hypothermia (32-35 C)(90-95F) Lethargy Confusion Shivering Loss of fine motor coordination Moderate hypothermia (28-32 C)(82-90F) Delirium Loss of gross motor coordination Severe hypothermia (<28 C)(<82F) Very cold skin Unresponsive Coma Difficulty breathing Abnormal heart rhythms Frozen chest Mild hypothermia (32-35 C) Excitation Phase Between C, most people shiver vigorously from all extremities. As the temperature drops below 34 C, a patient may develop altered judgment, amnesia. Respiratory rate may increase. At 33 C, ataxia and apathy may start. Patients generally are stable hemodynamically and able to compensate for the symptoms. 7
8 Hypothermia Hypothermia Moderate hypothermia (28-32 C) Adynamic phase Oxygen consumption decreases, and the CNS depresses further. Most patients with temperatures of 32 C or lower present in stupor. As the core reaches temperatures of 31 C or below, the body loses its ability to generate heat by shivering. At 30 C, patients become at risk for arrhythmias. Atrial fibrillation and other atrial and ventricular rhythms may present. The pulse continues to slow progressively, and cardiac output is reduced. Between C, pupils may become markedly dilated and minimally responsive to light, a condition that can mimic brain death. Severe hypothermia (<28 C) At 28 C, the body becomes markedly susceptible to ventricular fibrillation and further depression of myocardial contractility. Rigidity Apnea No pulse Areflexia Unresponsiveness Fixed pupils Pathophysiology (cont.) Pathophysiology (cont.) Excitation Phase Sympathetic response (HR, BP, and Cardiac Output all rise). Adynamic Phase HR, CO, BP decrease due to negative ino/chronotropic (force/rate) effects of hypothermia, ECG changes. Hypothermic ECG changes Osborne or J waves T-wave inversion Prolonged PR, QRS, QT intervals Arrhythmias may include bradycardia, slow AF, VF, or asystole 8
9 ECG Changes in Hypothermia Osborn J Wave Localization of ECG Pathology Inferior: leads II, III, and F (called the inferior leads) indicate pathology on the inferior or diaphragmatic surface of the heart. Lateral: Leads I, F, and V5-V6 are called lateral leads. Abnormality in these leads indicates pathology on the lateral, upper surface of the heart. Anterior: Anterior pathology is seen in leads V1-V4, and often in lead I. HYPOTHERMIA In the Trauma Patient Special Considerations 9
10 The Problem Under-recognized Under-treated PHTLS Major Concerns in Trauma Pt. Body temperature A low body temperature could indicate or precipitate syndromes that lead to the death of the patient. Hypothermia in Trauma Hypothermia is an ominous predictor of survival in trauma patients! Once hypothermia occurs it is difficult to correct. Efforts should be started in the field and continued as an integral part of the resuscitation process. Peng RY, Bongard FS 1999 June Journal of the American College of Surgeons Hypothermia in Trauma Devastating consequences of hypothermia in trauma patients: Cardiorespiratory compromise Decreased clotting mechanisms Decreased oxygen delivery Decreased metabolism Acidosis Increased risk of infection 10
11 Adverse Effects of Hypothermia in Trauma Cardiorespiratory Cardiac depression Myocardial ischemia Arrhythmias Peripheral vasoconstriction Impaired tissue oxygen delivery Elevated oxygen consumption during rewarming Blunted response to catecholamines Increased blood viscosity Metabolic acidosis Bleeding diathesis Decreased kinetics of coagulation factors Reduced platelet function Adverse Effects of Hypothermia in Trauma Reduced Clearance of Drugs Decreased hepatic blood flow Decreased hepatic metabolism Decreased renal blood flow Adverse Effects of Hypothermia in Trauma Increased risk of infection Decreased white blood cell number and function Impaired cellular immune response Thermoregulatory vasoconstriction Wound infection Decreased subcutaneous oxygen tension Impaired oxidative killing by neutrophils Decreased collagen deposition Pneumonia Sepsis Insulin resistance with hyperglycemia Consequences of Hypothermia in Trauma The Lethal Triad Hypothermia Acidosis Coagulopathy 11
12 The Lethal Trauma Triad Hypothermia Trauma Pt. Coagulapathy The three mechanisms that contribute to hypothermia-induced coagulopathy in trauma: 1. Platelet Dysfunction 2. Enhanced Fibrinolytic Activity 3. Alteration In Enzyme Functions Hypothermia Trauma Pt. Hypothermia Trauma Pt. Platelet Dysfunction Inhibition of Thromboxane B2 production causes the normal response of platelet aggregation to decrease. The platelets are therefore stored in the spleen and liver, and left unavailable for use. Enhanced Fibrinolytic Activity Trauma-induced hypothermia causes a heparin-like substance to be released, thus causing a disseminated intravascular clotting (DIC)-like syndrome. This is marked by an increase in prothrombin (PT) and partial thromboplastin times (PTT). 12
13 Hypothermia Trauma Pt. Hypothermia Trauma Pt. Alteration In Enzyme Functions Hageman Factor and Thromboplastin are needed to form clots at the site of injured endothelium. Hypothermia alters the function of these enzymes and others, therefore increasing bleeding and clotting times. Coagulopathy Perpetuated Blood transfusions/fluid resuscitation may lead to or exacerbate hypothermia. Silbergleit et al report that room (or ambient) temperature IV fluids, used in resuscitation, increase hypothermia or may actually cause secondary hypothermia in trauma patients. Crystalloids dilute the availability of coagulation factors. The Lethal Trauma Triad Coagulapathy Hypothermia in Trauma Mortality rates of Hypothermic Patients Core temps (T) less than 34C (93F) = 40% less than 33C (91F) = 69% less than 32C (90F) = 100% Whereas mortality if core T is greater than or equal to 34C (93F) = 7% Jurkovich JG, Greiser WB, Luterman A, Curreri PW. Journal of Trauma pgs Hypothermia in trauma victims: an ominous predictor of survival. 13
14 Treatment Prevention! Prevention!! Prevention!!! Treatment Be aggressive Recognize MOI & potential Better to preserve as much warmth as possible If you re losing the battle, treat early Treatment Remove wet clothing Place in warm blankets, hypo wrap etc. Place hypo wrap within vapor barrier Hot packs - neck, axilla, groin 14
15 Rewarming Tx. Rewarming Tx. Methods of Rewarming: Passive Rewarming Active External Rewarming Active Internal Rewarming Passive Rewarming Removal from environment Insulation Active External Rewarming Warm H 2 O Immersion Heating blankets Heated objects Radiant Heat Forced air Active Core Rewarming In-Hospital Inhalation rewarming Heated IV fluids GI tract lavage Bladder lavage Peritoneal lavage Pleural lavage Extracorporeal rewarming Mediastinal lavage Rewarming Tx. Active Rewarming of MILD Hypothermia: Active external methods: Warm blankets Heat packs Warm water immersion (with caution) Active internal methods: Warmed IV fluids Rewarming Tx. Active Rewarming of SEVERE Hypothermia: Active external methods: Warm blankets Heat packs Warm water immersion (with caution) Active internal methods: Warmed IV fluids Warmed, humidified oxygen 15
16 Rewarming Tx. Rewarming Tx. Maintain horizontal position Vertical position may compromise cerebral and systemic perfusion Avoid rough movements and activities Handle victim gently during CPR, intubation, BVM ventilation, vascular access Rewarming of the SEVERE hypothermia patient is best carried out in the Emergency Department using a pre-defined protocol, unless travel time exceeds 15 minutes. Most patients who die during active rewarming die from ventricular fibrillation. Rewarming Issues Rewarming Shock: Occurs due to peripheral reflex vasodilation. Causes the return of cooled blood and metabolic acids from the extremities. May cause a paradoxical afterdrop in the core temperature further worsening hypothermia. After-drop Phenomenon Initial active external rewarming leads to Peripheral vasodilation (BP drops) Cold blood from dilated peripheral vessels carries high lactic acid levels to core vessels Cold acidotic blood causes drop in core temp Temperature drop and acidosis provoke serious arrhythmias 16
17 Rewarming Issues Rewarming Shock: Can be prevented in the prehospital setting by using warmed IV fluids during active rewarming. Pre-Hospital Treatment Devices Portable IV fluid heaters are available in the United States and Canada. Devices fit in-line and are powered by DC power sources. Pre-Hospital Treatment Devices The device is singleuse and remains with the patient in the hospital (both the ED and on the floor). Pre-Hospital Treatment Devices The HOT IV is powered from a Physio-Control battery or from a DC converter plugged in to an AC outlet. 17
18 Pre-Hospital Treatment Devices Pre-Hospital Treatment Devices Charcoal Heater External Heat Source ResQAir Warmed humidified oxygen Benefits of IV Fluid Warming Benefits of IV Fluid Warming Maintains body temps Increases patient comfort Prevents shivering Prevents cold-induced dysrhythmias Decreases hemorrhage in abdominal trauma patients Decreases the incidence of infectious complications in abdominal trauma patients 18
19 Benefits of IV Fluid Warming Having said all that Allows active internal rewarming to begin in the prehospital setting. Less labor-intensive, freeing emergency personnel to manage other, more pressing care needs. Patients who received hot pack rewarming showed a mean increase in body temperature during transport (+1.36 ー F/0.74 ー C), And All other groups (no intervention, passive rewarming, reflective blankets, warmed IV fluids, warmed IV fluid plus reflective blanket) showed a mean decrease in temperature during transport [-0.34 to ー F (-0.2 to -0.4 ー C); p < 0.01] Dorraine D. Watts 1, Margie Roche 2, Ray Tricarico 4, 5, Frank Poole 6, John J. Brown 6, George B. Colson 3, 6, Arthur L. Trask 1 and Samir M. Fakhry 1 The utility of traditional prehospital interventions in maintaining thermostasis 1999, Vol. 3, No. 2, Pages Other hypothermia concerns. Hypothermia complicates prehospital monitoring/treatment capabilities Drug metabolism and elimination are temp dependent Hypothermia prolongs duration of action in some drugs ie. benzos and muscle relaxants Pulse oximitry 19
20 Survival from Hypothermia Other Clinical Issues 59.2º F (15.2º C) - Lowest reported infant survival from accidental exposure. 60.8º F (16º C) - Lowest reported adult survival from accidental exposure. 48.2º F (9º C) - Lowest reported survivor from therapeutic exposure. Hypothermia is common, even in persons with minor trauma. Hypothermia can worsen infectious complications of abdominal trauma. Hypothermic trauma patients suffer increased blood loss compared to normothermic patients. History of Therapeutic Hypothermia What about Therapeutic Hypothermia? 1939-used for pain control in metastatic disease Dr. Temple Fay 1941-Treatment of schizophrenia pioneered use during cardiopulmonary bypass used in management of traumatic brain injury TBI and SCI 20
21 Therapeutic Hypothermia Therapeutic Hypothermia Sudden Cardiac Arrest TBI Therapeutic hypothermia in trauma Shown to be possible beneficial in the absence of significant hemorrhage SCI Back to our Case Study 05:40 - Arrival at trauma center, pt. TOT ED staff with report. Temp on arrival 94F, LOC = unconscious. ED staff provides infused blood products and attempts surgical repair of wound w/o success. Pt. moved to OR at 06:15. Back to our Case Study 15 min into OR procedure pt. goes into VF arrest. After 40 minutes of resusitation pt pronounced 07:22. 21
22 Conclusions Hypothermia in trauma is common. Friend or foe? Generally foe. Conclusions Minimize patient exposure to the environment. Anticipate injury severity and expect hypothermia based on MOI. Rapid assessment and early recognition of severity. Rapid initial treatment/packaging & movement of patient to a warm environment. ALS - warm IV fluids, heat packs, caution with analgesics. Questions? 22
UTSW/BioTel EMS TRAINING BULLETIN January EMS TB Accidental Hypothermia
 UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
UTSW/BioTel EMS TRAINING BULLETIN January 2015 EMS TB 15-001 Accidental Hypothermia Purpose: 1. To provide patient assessment and management guidance to UTSW/BioTel EMS Providers about Accidental Hypothermia
Accidental Hypothermia
 Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
Accidental Hypothermia Gordon G. Giesbrecht, Ph.D., Professor Health Leisure and Human Performance Research Institute University of Manitoba, Winnipeg, Manitoba, Canada, R3T 2N2 Learning Objectives: 1)
Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES. Accidental Hypothermia/Cold Exposure
 Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES Accidental Hypothermia/Cold Exposure Goal: To aid EMS Providers in: the recognition and treatment of systemic effects of accidental hypothermia
Toxins and Environmental: HEAT- and COLD-RELATED EMERGENCIES Accidental Hypothermia/Cold Exposure Goal: To aid EMS Providers in: the recognition and treatment of systemic effects of accidental hypothermia
Cold-Related Illness. Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic
 Cold-Related Illness Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic Hypothermia Frost nip Frostbite Chillbains Trench foot Cold-Related Illness Who gets it? How common? Outdoor
Cold-Related Illness Matthew Gammons, MD Killington Medical Clinic Vermont Orthopaedic Clinic Hypothermia Frost nip Frostbite Chillbains Trench foot Cold-Related Illness Who gets it? How common? Outdoor
DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER
 DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER This tragic recent headline involving Marco Cheseto serves as a grim reminder of the potential devastation inflicted by frostbite and hypothermia
DOCTORS AMPUTATE FROSTBITTEN FEET OFALL-AMERICAN RUNNER This tragic recent headline involving Marco Cheseto serves as a grim reminder of the potential devastation inflicted by frostbite and hypothermia
HYPOTHERMIA IN TRAUMA. Kevin Palmer EMT-P, DiMM
 HYPOTHERMIA IN TRAUMA Kevin Palmer EMT-P, DiMM DISCLOSURE No Financial conflicts of interest Member of the Wilderness Medical Society Diploma in Mountain Medicine Fellowship in the Academy of Wilderness
HYPOTHERMIA IN TRAUMA Kevin Palmer EMT-P, DiMM DISCLOSURE No Financial conflicts of interest Member of the Wilderness Medical Society Diploma in Mountain Medicine Fellowship in the Academy of Wilderness
-Blood Warming- A Hot topic?
 -Blood Warming- A Hot topic? Blaine Kent, MD, FRCPC Associate Professor of Anesthesia Director, Peri-Operative Blood Management Chief, Cardiac Anesthesia Objectives To learn / review the deleterious systemic
-Blood Warming- A Hot topic? Blaine Kent, MD, FRCPC Associate Professor of Anesthesia Director, Peri-Operative Blood Management Chief, Cardiac Anesthesia Objectives To learn / review the deleterious systemic
INDUCED HYPOTHERMIA A Hot Topic. R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences
 INDUCED HYPOTHERMIA A Hot Topic R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences Conflicts of Interest Sadly, we have no financial or industrial conflicts of interest
INDUCED HYPOTHERMIA A Hot Topic R. Darrell Nelson, MD, FACEP Emergency Medicine Wake Forest University Health Sciences Conflicts of Interest Sadly, we have no financial or industrial conflicts of interest
Thermoregulation 2015 WMA
 1 Structure: Temperature sensors Endocrine system Muscles Skin Function: Maintain body core at 37 C Problem: Too little heat Too much heat 2 Normal Body Compensation Heat Response: Vasodilation Sweat Cold
1 Structure: Temperature sensors Endocrine system Muscles Skin Function: Maintain body core at 37 C Problem: Too little heat Too much heat 2 Normal Body Compensation Heat Response: Vasodilation Sweat Cold
Cold Water Shock, Hypothermia and Cardiac Arrest
 Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
Cold Water Shock, Hypothermia and Cardiac Arrest In spring the warm air temperatures lure hibernating humans out of the house. and the waters beckon. While the air temperature may be 60-80 F, the water
Thermal Injury. Thermal Injury Presentation CCFP (EM) Rounds. Topics Hypothermia. Resources Ch Tinitinelli
 Thermal Injury December 17, 2009 Thermal Injury Presentation CCFP (EM) Rounds Dr. Kyle McLaughlin, CCFP (EM) Topics Hypothermia Frostbite Hyperthermia Resources Ch. 191-193 Tinitinelli Multi media http://www.youtube.com/watch?v=x6mq0jftpji&feature=fvsr
Thermal Injury December 17, 2009 Thermal Injury Presentation CCFP (EM) Rounds Dr. Kyle McLaughlin, CCFP (EM) Topics Hypothermia Frostbite Hyperthermia Resources Ch. 191-193 Tinitinelli Multi media http://www.youtube.com/watch?v=x6mq0jftpji&feature=fvsr
INDUCED HYPOTHERMIA. F. Ben Housel, M.D.
 INDUCED HYPOTHERMIA F. Ben Housel, M.D. Historical Use of Induced Hypothermia 1950 s - Moderate hypothermia (30-32º C) in open heart surgery to protect brain against global ischemia 1960-1980 s - Use of
INDUCED HYPOTHERMIA F. Ben Housel, M.D. Historical Use of Induced Hypothermia 1950 s - Moderate hypothermia (30-32º C) in open heart surgery to protect brain against global ischemia 1960-1980 s - Use of
Hypothermia Presentation
 Hypothermia Presentation Thermoregulation Thermal regulation is a balance between heat production and heat loss. Despite marked changes in skin temperature, the body s homeostatic mechanisms are able to
Hypothermia Presentation Thermoregulation Thermal regulation is a balance between heat production and heat loss. Despite marked changes in skin temperature, the body s homeostatic mechanisms are able to
Bill Hall, MD Mesa County EMS System
 Bill Hall, MD Mesa County EMS System Discuss cold related injuries and treatment Discuss hypothermia and treatment Discuss avalanche victim care and considerations Chilblains (Pernio) Trench Foot Frost
Bill Hall, MD Mesa County EMS System Discuss cold related injuries and treatment Discuss hypothermia and treatment Discuss avalanche victim care and considerations Chilblains (Pernio) Trench Foot Frost
All Things Cold: Hypothermia, Altitude Illness and Frostbite. Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine
 All Things Cold: Hypothermia, Altitude Illness and Frostbite Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine Objectives Thermoregulation basics Management of human-sickles
All Things Cold: Hypothermia, Altitude Illness and Frostbite Judith R. Klein, MD, FACEP Assistant Clinical Professor UCSF-SFGH Emergency Medicine Objectives Thermoregulation basics Management of human-sickles
8/20/12. Discuss the importance of thermoregulation in the neonate.
 Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
Sharon Rush MSN NNP-BC Discuss the importance of thermoregulation in the neonate. To maintain correct body temperature range in order to: Reduce oxygen consumption Reduce calorie expenditure Maximize metabolic
THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST
 THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST Heather Harrington RN, BScN, CNCC(c) Clinical Nurse Educator Sunnybrook Health Sciences Centre Objectives Define Therapeutic Hypothermia (TH) Describe current
THERAPEUTIC HYPOTHERMIA POST CARDIAC ARREST Heather Harrington RN, BScN, CNCC(c) Clinical Nurse Educator Sunnybrook Health Sciences Centre Objectives Define Therapeutic Hypothermia (TH) Describe current
Cold Injuries: An Update on Hypothermia and Frostbite
 Cold Injuries: An Update on Hypothermia and Frostbite HYPOTHERMIA Definitions Shell = skin, subcutaneous tissues and extremities; temperature of the shell varies according to environment Core = brain,
Cold Injuries: An Update on Hypothermia and Frostbite HYPOTHERMIA Definitions Shell = skin, subcutaneous tissues and extremities; temperature of the shell varies according to environment Core = brain,
the bleeding won t stop? Liane Manz RN, BScN, CNCC(c) Royal Alexandra Hospital
 What do you do when the bleeding won t stop? Teddie Tanguay RN, MN, NP, CNCC(c) Teddie Tanguay RN, MN, NP, CNCC(c) Liane Manz RN, BScN, CNCC(c) Royal Alexandra Hospital Outline Case study Normal coagulation
What do you do when the bleeding won t stop? Teddie Tanguay RN, MN, NP, CNCC(c) Teddie Tanguay RN, MN, NP, CNCC(c) Liane Manz RN, BScN, CNCC(c) Royal Alexandra Hospital Outline Case study Normal coagulation
Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms. Introduction to the Algorithms
 Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Introduction to the Algorithms Cardiac Arrest Algorithms Prehospital Medication Profiles Perspective regarding the EMT- Intermediate
Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Introduction to the Algorithms Cardiac Arrest Algorithms Prehospital Medication Profiles Perspective regarding the EMT- Intermediate
Hypothermia. d. Severe Hypothermia - core temperature degrees and below (immediately life threatening)
 Hypothermia 1. Hypothermia - "a decrease in the core body temperature to a level at which normal muscular and cerebral functions are impaired." - Medicine for Mountaineering 2. Conditions Leading to Hypothermia
Hypothermia 1. Hypothermia - "a decrease in the core body temperature to a level at which normal muscular and cerebral functions are impaired." - Medicine for Mountaineering 2. Conditions Leading to Hypothermia
Chapter 132 Accidental Hypothermia. Episode Overview. Core Questions. Wisecracks
 Chapter 132 Accidental Hypothermia Episode Overview Passively rewarm patients with temperatures 32-35 degrees Celsius Indications for active rewarming: Cardiovascular instability Temperature < 32 degrees
Chapter 132 Accidental Hypothermia Episode Overview Passively rewarm patients with temperatures 32-35 degrees Celsius Indications for active rewarming: Cardiovascular instability Temperature < 32 degrees
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
-Cardiogenic: shock state resulting from impairment or failure of myocardium
 Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Accidental hypothermia, defined as an unintentional
 C l i n i c a l R e v i e w A r t i c l e Accidental Hypothermia Faris A. Khasawneh, MD Asha Thomas, MD Sajan Thomas, MD Accidental hypothermia, defined as an unintentional drop in core body temperature
C l i n i c a l R e v i e w A r t i c l e Accidental Hypothermia Faris A. Khasawneh, MD Asha Thomas, MD Sajan Thomas, MD Accidental hypothermia, defined as an unintentional drop in core body temperature
ABCDE HOW TO RECOGNISE AND TREAT THE SERIOUSLY ILL CHILD
 ABCDE HOW TO RECOGNISE AND TREAT THE SERIOUSLY ILL CHILD A B C D E Possible Problems Airway obstruction Partial or complete Foreign body Secretions/blood/vomit Infection Swelling e.g. anaphylaxis trauma
ABCDE HOW TO RECOGNISE AND TREAT THE SERIOUSLY ILL CHILD A B C D E Possible Problems Airway obstruction Partial or complete Foreign body Secretions/blood/vomit Infection Swelling e.g. anaphylaxis trauma
THERMOREGULATION 05 JUNE 2013
 THERMOREGULATION 05 JUNE 2013 Lesson Description In this lesson we: Question the need to regulate body temperature in humans Examine the structure and functions of the different parts of the skin Look
THERMOREGULATION 05 JUNE 2013 Lesson Description In this lesson we: Question the need to regulate body temperature in humans Examine the structure and functions of the different parts of the skin Look
Post-Cardiac Arrest Syndrome. MICU Lecture Series
 Post-Cardiac Arrest Syndrome MICU Lecture Series Case 58 y/o female collapses at home, family attempts CPR, EMS arrives and notes VF, defibrillation x 3 with return of spontaneous circulation, brought
Post-Cardiac Arrest Syndrome MICU Lecture Series Case 58 y/o female collapses at home, family attempts CPR, EMS arrives and notes VF, defibrillation x 3 with return of spontaneous circulation, brought
Case Presentation. Cooling. Case Presentation. New Developments in Cardiopulmonary Arrest: Therapeutic Hypothermia in Resuscitation
 New Developments in Cardiopulmonary Arrest: Therapeutic Hypothermia in Resuscitation Michael Sayre, MD Emergency Medicine and LeRoy Essig, MD Pulmonary/Critical Care Medicine Case Presentation 3:40 (+
New Developments in Cardiopulmonary Arrest: Therapeutic Hypothermia in Resuscitation Michael Sayre, MD Emergency Medicine and LeRoy Essig, MD Pulmonary/Critical Care Medicine Case Presentation 3:40 (+
Management Of Medical Emergencies
 Management Of Medical Emergencies U.S. Aging Population 35 million people (12%) 65 years or older Number will increase by nearly 75% by year 2030 The number of people more than 85 years old will approach
Management Of Medical Emergencies U.S. Aging Population 35 million people (12%) 65 years or older Number will increase by nearly 75% by year 2030 The number of people more than 85 years old will approach
Geriatric Emergencies. Lesson Goal. Lesson Objectives 9/10/2012. Introduce ways geriatric patients differ from other patients
 Geriatric Emergencies Lesson Goal Introduce ways geriatric patients differ from other patients Physiologic changes of aging Communication issues Effects of medications Common fears of elderly patients
Geriatric Emergencies Lesson Goal Introduce ways geriatric patients differ from other patients Physiologic changes of aging Communication issues Effects of medications Common fears of elderly patients
Drowning is a leading cause of death and loss of years of life with over 90% of cases occurring in lower- and middle-income countries.
 Chapter 145 Drowning Episode Overview: 1) List risk factors for drowning 2) List 5 variables that portend poor outcome 3) Describe the diving reflex 4) Describe the management of a drowning patient with
Chapter 145 Drowning Episode Overview: 1) List risk factors for drowning 2) List 5 variables that portend poor outcome 3) Describe the diving reflex 4) Describe the management of a drowning patient with
Update on Sudden Cardiac Death and Resuscitation
 Update on Sudden Cardiac Death and Resuscitation Ashish R. Panchal, MD, PhD Medical Director Center for Emergency Medical Services Assistant Professor Clinical Department of Emergency Medicine The Ohio
Update on Sudden Cardiac Death and Resuscitation Ashish R. Panchal, MD, PhD Medical Director Center for Emergency Medical Services Assistant Professor Clinical Department of Emergency Medicine The Ohio
Chapter 12. Temperature Regulation
 Chapter 12 Temperature Regulation Temperature Regulation Body core temperature regulation Critical for: Cellular structures Metabolic pathways Too high Protein structure of cells destroyed Too low Slowed
Chapter 12 Temperature Regulation Temperature Regulation Body core temperature regulation Critical for: Cellular structures Metabolic pathways Too high Protein structure of cells destroyed Too low Slowed
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #9 Heat Emergencies
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #9 Heat Emergencies As EMS providers we are called to treat several medical conditions. Heart Attacks,
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #9 Heat Emergencies As EMS providers we are called to treat several medical conditions. Heart Attacks,
Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida
 Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida Reprinted in the IVIS website with the permission of the NAVC http:/// The North American Veterinary Conference
Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida Reprinted in the IVIS website with the permission of the NAVC http:/// The North American Veterinary Conference
Ac#ve, ECMO or locally available alterna#ves. invasive warming. Ini#ally: Ac#ve noninvasive or minimally
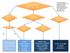 Suspected Hypothermia Temp
Suspected Hypothermia Temp
11/8/2017. Notice. Road Map
 Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
Notice All EMS Live@Nite presentations will be recorded (both audio and video) and available for public viewing online. By participating in EMS Live@Nite, you consent to audio and video recording and its/their
CHILL OUT! Induced Hypothermia: Challenges & Successes in the
 CHILL OUT! Induced Hypothermia: Challenges & Successes in the ICU Colleen Bell RN, BS, CCRN, Donna Brault RN, BSN, CCRN, Cathy Patnode RN, BSN, CCRN Champlain Valley Physician Hospital November 2012 Objectives
CHILL OUT! Induced Hypothermia: Challenges & Successes in the ICU Colleen Bell RN, BS, CCRN, Donna Brault RN, BSN, CCRN, Cathy Patnode RN, BSN, CCRN Champlain Valley Physician Hospital November 2012 Objectives
3. D Objective: Chapter 4, Objective 4 Page: 79 Rationale: A carbon dioxide level below 35 mmhg indicates hyperventilation.
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
By: M.A Jafari MD EM Specialist Shahid Sadoughi Hospital
 By: M.A Jafari MD EM Specialist Shahid Sadoughi Hospital Cold weather was an important factor in second world war. Factors Influencing the Likelihood of Cold Injuries Temperature, Cold acclimatization,
By: M.A Jafari MD EM Specialist Shahid Sadoughi Hospital Cold weather was an important factor in second world war. Factors Influencing the Likelihood of Cold Injuries Temperature, Cold acclimatization,
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Update on Sudden Cardiac Death and Resuscitation
 Update on Sudden Cardiac Death and Resuscitation Ashish R. Panchal, MD, PhD Medical Director Center for Emergency Medical Services Assistant Professor Clinical Department of Emergency Medicine The Ohio
Update on Sudden Cardiac Death and Resuscitation Ashish R. Panchal, MD, PhD Medical Director Center for Emergency Medical Services Assistant Professor Clinical Department of Emergency Medicine The Ohio
New Therapeutic Hypothermia Techniques
 New Therapeutic Hypothermia Techniques Joseph P. Ornato, MD, FACP, FACC, FACEP Professor & Chairman, Emergency Medicine Virginia Commonwealth University Health System Richmond, VA Medical Director Richmond
New Therapeutic Hypothermia Techniques Joseph P. Ornato, MD, FACP, FACC, FACEP Professor & Chairman, Emergency Medicine Virginia Commonwealth University Health System Richmond, VA Medical Director Richmond
People maintain normal body temperature despite variations in both their metabolic activity and Ambient temperature Homeothermic animals (hot blooded)
 People maintain normal body temperature despite variations in both their metabolic activity and Ambient temperature Homeothermic animals (hot blooded) Animals with body temperature changes with environmental
People maintain normal body temperature despite variations in both their metabolic activity and Ambient temperature Homeothermic animals (hot blooded) Animals with body temperature changes with environmental
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH
 Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
Care of the Deteriorating Patient in Recovery NADIA TICEHURST : CLINICAL NURSE EDUCATOR PERI ANAESTHETICS BENDIGO HEALTH Intended learning outcomes Describe the components of a comprehensive clinician
Financial Disclosure. Objectives 9/24/2018
 Hemorrhage and Transfusion Adjuncts in the Setting of Damage Control Joseph Cuschieri, MD FACS Professor of Surgery, University of Washington Adjunct Professor of Orthopedics and Neurosurgery, University
Hemorrhage and Transfusion Adjuncts in the Setting of Damage Control Joseph Cuschieri, MD FACS Professor of Surgery, University of Washington Adjunct Professor of Orthopedics and Neurosurgery, University
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
Patient Case. Post cardiac arrest pathophysiology 10/19/2017. Disclosure. Objectives. Patient Case-TM
 Disclosure TARGETED TEMPERATURE MANAGEMENT POST CARDIAC ARREST I have nothing to disclose concerning possible financial or personal relationships with commercial entities that may have a direct or indirect
Disclosure TARGETED TEMPERATURE MANAGEMENT POST CARDIAC ARREST I have nothing to disclose concerning possible financial or personal relationships with commercial entities that may have a direct or indirect
Induced Hypothermia for Cardiac Arrest. Heather Hand RN,CCRN,CNRN,ATCN,LNC
 Induced Hypothermia for Cardiac Arrest Heather Hand RN,CCRN,CNRN,ATCN,LNC Cardiac Arrest Epidemiology 400,000 arrests / year in U.S.A 3 / 4 Out-of-hospital 1 / 4 In-hospital survival to hospital 1-5% discharge
Induced Hypothermia for Cardiac Arrest Heather Hand RN,CCRN,CNRN,ATCN,LNC Cardiac Arrest Epidemiology 400,000 arrests / year in U.S.A 3 / 4 Out-of-hospital 1 / 4 In-hospital survival to hospital 1-5% discharge
Cardiovascular Emergencies. Chapter 12
 Cardiovascular Emergencies Chapter 12 Cardiovascular Emergencies Cardiovascular disease (CVD) claimed 931,108 lives in the US during 2001. 2,551 per day Almost two people per minute! CVD accounts for 38.5%
Cardiovascular Emergencies Chapter 12 Cardiovascular Emergencies Cardiovascular disease (CVD) claimed 931,108 lives in the US during 2001. 2,551 per day Almost two people per minute! CVD accounts for 38.5%
12/1/2009. Chapter 19: Hemorrhage. Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system Internal hemorrhage
 Chapter 19: Hemorrhage Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system External hemorrhage Internal hemorrhage Associated with higher morbidity and mortality than
Chapter 19: Hemorrhage Hemorrhage and Shock Occurs when there is a disruption or leak in the vascular system External hemorrhage Internal hemorrhage Associated with higher morbidity and mortality than
LESSON 2. Section I. GENERAL INFORMATION 2-1. WHY IS IT IMPORTANT TO KNOW THE PATIENT'S TEMPERATURE?
 LESSON 2 Section I. GENERAL INFORMATION 2-1. WHY IS IT IMPORTANT TO KNOW THE PATIENT'S TEMPERATURE? a. To Determine the Cause of the Patient's Condition. When a person becomes ill, one of the first things
LESSON 2 Section I. GENERAL INFORMATION 2-1. WHY IS IT IMPORTANT TO KNOW THE PATIENT'S TEMPERATURE? a. To Determine the Cause of the Patient's Condition. When a person becomes ill, one of the first things
Acid-base management during hypothermic CPB alpha-stat and ph-stat models of blood gas interpretation
 Acid-base management during hypothermic CPB alpha-stat and ph-stat models of blood gas interpretation Michael Kremke Department of Anaesthesiology and Intensive Care Aarhus University Hospital, Denmark
Acid-base management during hypothermic CPB alpha-stat and ph-stat models of blood gas interpretation Michael Kremke Department of Anaesthesiology and Intensive Care Aarhus University Hospital, Denmark
ENVIRONMENTAL EMERGENCIES REVIEW WITH CASE STUDIES. Justin Astafan, EMT-P, CIC
 ENVIRONMENTAL EMERGENCIES REVIEW WITH CASE STUDIES Justin Astafan, EMT-P, CIC NYS EMT-P NYS CIC 17 years in the fire and ems profession Work both career and volunteer side Worked for commercial and notfor
ENVIRONMENTAL EMERGENCIES REVIEW WITH CASE STUDIES Justin Astafan, EMT-P, CIC NYS EMT-P NYS CIC 17 years in the fire and ems profession Work both career and volunteer side Worked for commercial and notfor
Therapeutic hypothermia
 INDUCED HYPOTHERMIA Dr. Attilla Kiss M.D. Acting Medical Director Emergency Services EMS Medical Director St. John Medical Center OBJECTIVES Define and explain Induced Hypothermia Discuss both pre-hospital
INDUCED HYPOTHERMIA Dr. Attilla Kiss M.D. Acting Medical Director Emergency Services EMS Medical Director St. John Medical Center OBJECTIVES Define and explain Induced Hypothermia Discuss both pre-hospital
Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest. Objectives: U.S. stats
 Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest Nicole L. Kupchik RN, MN, CCNS CCRN-CMC Clinical Nurse Specialist Harborview Medical Center Seattle, WA Objectives: At the
Post-Resuscitation Care: Optimizing & Improving Outcomes after Cardiac Arrest Nicole L. Kupchik RN, MN, CCNS CCRN-CMC Clinical Nurse Specialist Harborview Medical Center Seattle, WA Objectives: At the
Therapeutic Hypothermia
 Objectives Overview Therapeutic Hypothermia Nerissa U. Ko, MD, MAS UCSF Department of Neurology Critical Care Medicine and Trauma June 4, 2011 Hypothermia as a neuroprotectant Proven indications: Adult
Objectives Overview Therapeutic Hypothermia Nerissa U. Ko, MD, MAS UCSF Department of Neurology Critical Care Medicine and Trauma June 4, 2011 Hypothermia as a neuroprotectant Proven indications: Adult
Hypothermia: The Science and Recommendations (In-hospital and Out)
 Hypothermia: The Science and Recommendations (In-hospital and Out) L. Kristin Newby, MD, MHS Professor of Medicine Duke University Medical Center Chair, Council on Clinical Cardiology, AHA President, Society
Hypothermia: The Science and Recommendations (In-hospital and Out) L. Kristin Newby, MD, MHS Professor of Medicine Duke University Medical Center Chair, Council on Clinical Cardiology, AHA President, Society
Hypothermia Induction Methods
 Hypothermia Induction Methods Advantages and Disadvantages Xia Luo, M.D. Vice President, Clinical Education ZOLL Corporation Targeted Temperature Management (TTM) Temperature is one of the four vital signs
Hypothermia Induction Methods Advantages and Disadvantages Xia Luo, M.D. Vice President, Clinical Education ZOLL Corporation Targeted Temperature Management (TTM) Temperature is one of the four vital signs
Accidental Hypothermia. Peter Paal, MD, Associate Professor DESA, EDIC
 Accidental Hypothermia Peter Paal, MD, Associate Professor DESA, EDIC Conflict of interest Ambu Covidien Genericon Jolife Laerdal Larnygeal Mask Company Ratiopharm VBM 2 Innsbruck 3 Innsbruck 4 Innsbruck
Accidental Hypothermia Peter Paal, MD, Associate Professor DESA, EDIC Conflict of interest Ambu Covidien Genericon Jolife Laerdal Larnygeal Mask Company Ratiopharm VBM 2 Innsbruck 3 Innsbruck 4 Innsbruck
Restore adequate respiratory and circulatory conditions. Reduce pain
 Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
Pre-hospital management of the trauma patient is best performed by an integrated team focused on minimizing the time from injury to definitive care at an appropriate trauma center. Dispatchers, first responders,
Hypothermia & Local Cold Injuries
 Sacred Heart Medical Center and Children s Hospital Hypothermia & Local Cold Injuries Objectives Types of heat loss Describe mechanisms of injury for hypothermia and local cold injuries Discuss pre-hospital
Sacred Heart Medical Center and Children s Hospital Hypothermia & Local Cold Injuries Objectives Types of heat loss Describe mechanisms of injury for hypothermia and local cold injuries Discuss pre-hospital
Hypothermia & Local Cold Injuries
 Sacred Heart Medical Center and Children s Hospital Hypothermia & Local Cold Injuries Objectives Types of heat loss Describe mechanisms of injury for hypothermia and local cold injuries Discuss pre-hospital
Sacred Heart Medical Center and Children s Hospital Hypothermia & Local Cold Injuries Objectives Types of heat loss Describe mechanisms of injury for hypothermia and local cold injuries Discuss pre-hospital
Energy Metabolism and Body Temperature
 Energy Metabolism and Body Temperature Hui-ping Wang( 王会平 ), PhD Dept. of Physiology, Zhejiang University School of Medicine wanghuiping@zju.edu.cn Part I Energy metabolism Definition The metabolic processes
Energy Metabolism and Body Temperature Hui-ping Wang( 王会平 ), PhD Dept. of Physiology, Zhejiang University School of Medicine wanghuiping@zju.edu.cn Part I Energy metabolism Definition The metabolic processes
CEDR 2018 QCDR Measures for CMS 2018 MIPS Performance Year Reporting
 ACEP19 Emergency Department Utilization of CT for Minor Blunt Head Trauma for Aged 18 Years and Older Percentage of visits for aged 18 years and older who presented with a minor blunt head trauma who had
ACEP19 Emergency Department Utilization of CT for Minor Blunt Head Trauma for Aged 18 Years and Older Percentage of visits for aged 18 years and older who presented with a minor blunt head trauma who had
Mild. Moderate. Severe. 32 to to and below
 Mohamud Daya MD, MS Mild 32 to 34 Moderate 28 to 32 Severe 28 and below Jon Rittenberger Shervin Ayati Protocol Development Committee Hypothermia Working Group Lynn Wittwer Jon Jui John Stouffer Scott
Mohamud Daya MD, MS Mild 32 to 34 Moderate 28 to 32 Severe 28 and below Jon Rittenberger Shervin Ayati Protocol Development Committee Hypothermia Working Group Lynn Wittwer Jon Jui John Stouffer Scott
Prehospital Resuscitation for the 21 st Century Simulation Case. VF/Asystole
 Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Accidental Hypothermia
 Accidental Hypothermia Doug Brown, MD, FRCPC Emergency Physician Royal Columbian & Eagle Ridge Hospital October, 2013 Objectives 45min lecture, 15min discussion & questions: Inspirational case & overview
Accidental Hypothermia Doug Brown, MD, FRCPC Emergency Physician Royal Columbian & Eagle Ridge Hospital October, 2013 Objectives 45min lecture, 15min discussion & questions: Inspirational case & overview
CrackCast Episode 8 Brain Resuscitation
 CrackCast Episode 8 Brain Resuscitation Episode Overview: 1) Describe 6 therapeutic interventions for the post-arrest brain 2) List 5 techniques for initiating therapeutic hypothermia 3) List 4 mechanisms
CrackCast Episode 8 Brain Resuscitation Episode Overview: 1) Describe 6 therapeutic interventions for the post-arrest brain 2) List 5 techniques for initiating therapeutic hypothermia 3) List 4 mechanisms
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02
 PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
Post-Arrest Care: Beyond Hypothermia
 Post-Arrest Care: Beyond Hypothermia Damon Scales MD PhD Department of Critical Care Medicine Sunnybrook Health Sciences Centre University of Toronto Disclosures CIHR Physicians Services Incorporated Main
Post-Arrest Care: Beyond Hypothermia Damon Scales MD PhD Department of Critical Care Medicine Sunnybrook Health Sciences Centre University of Toronto Disclosures CIHR Physicians Services Incorporated Main
Pathophysiology and Cardiac Insights for Targeted Temperature Management in Emergency Medicine and Critical Care
 Pathophysiology and Cardiac Insights for Targeted Temperature Management in Emergency Medicine and Critical Care LINDSAY LEWIS BSN, RN, CCCC Faculty Disclosure I AM CURRENTLY EMPLOYED AS A CLINICAL MANAGER
Pathophysiology and Cardiac Insights for Targeted Temperature Management in Emergency Medicine and Critical Care LINDSAY LEWIS BSN, RN, CCCC Faculty Disclosure I AM CURRENTLY EMPLOYED AS A CLINICAL MANAGER
Case Scenario 3: Shock and Sepsis
 Name: Molly Boyle 1. Define the term shock (Lewis textbook): Shock is a syndrome characterized by decreased perfusion and impaired metabolism. Shock can have a number of causes that result in damage to
Name: Molly Boyle 1. Define the term shock (Lewis textbook): Shock is a syndrome characterized by decreased perfusion and impaired metabolism. Shock can have a number of causes that result in damage to
1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D.
 1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D. Sacral-coccygeal 2. A 36-year-old male sustains blunt force thoracic
1. In a rear-impact motor vehicle crash, which area of the spine is most susceptible to injury? A. Cervical B. Thoracic C. Lumbar D. Sacral-coccygeal 2. A 36-year-old male sustains blunt force thoracic
2017 Northern Mine Rescue Contest Written Exam (First Aid Competition)
 2017 Northern Mine Rescue Contest Written Exam (First Aid Competition) 2017 2010 June 5, 2017 Findley Lake, New York 2017 Northern Mine Rescue Contest Written Exam First Aid Competition Directions: Fill
2017 Northern Mine Rescue Contest Written Exam (First Aid Competition) 2017 2010 June 5, 2017 Findley Lake, New York 2017 Northern Mine Rescue Contest Written Exam First Aid Competition Directions: Fill
Cold Injuries: Frostbite and Hypothermia. Michael White MD,FACS Director Detroit Receiving Hospital Wayne State University
 Cold Injuries: Frostbite and Hypothermia Michael White MD,FACS Director Detroit Receiving Hospital Wayne State University Objectives of Talk Describe the incidence and characteristics of Frostbite injury
Cold Injuries: Frostbite and Hypothermia Michael White MD,FACS Director Detroit Receiving Hospital Wayne State University Objectives of Talk Describe the incidence and characteristics of Frostbite injury
Overview. Physiology of Heat Stress Causal factors Heat Disorders & Health Effects Control
 Overview Physiology of Heat Stress Causal factors Heat Disorders & Health Effects Control 1 Causal Factors Age, weight, degree of physical fitness Degree of acclimatization, metabolism Intercurrent illnesses
Overview Physiology of Heat Stress Causal factors Heat Disorders & Health Effects Control 1 Causal Factors Age, weight, degree of physical fitness Degree of acclimatization, metabolism Intercurrent illnesses
You Are the Emergency Medical Responder
 Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
CPR What Works, What Doesn t
 Resuscitation 2017 ECMO and ECLS April 1, 2017 Corey M. Slovis, M.D. Vanderbilt University Medical Center Metro Nashville Fire Department Nashville International Airport Nashville, TN Circulation 2013;128:417-35
Resuscitation 2017 ECMO and ECLS April 1, 2017 Corey M. Slovis, M.D. Vanderbilt University Medical Center Metro Nashville Fire Department Nashville International Airport Nashville, TN Circulation 2013;128:417-35
Management of the Trauma Patient. Elizabeth R Benjamin MD PhD Trauma and Surgical Critical Care Critical Care Symposium April 20, 2015
 Management of the Trauma Patient Elizabeth R Benjamin MD PhD Trauma and Surgical Critical Care Critical Care Symposium April 20, 2015 Saturday Night 25 yo M s/p high speed MVC Hypotensive in the ED, altered
Management of the Trauma Patient Elizabeth R Benjamin MD PhD Trauma and Surgical Critical Care Critical Care Symposium April 20, 2015 Saturday Night 25 yo M s/p high speed MVC Hypotensive in the ED, altered
Hanna K. Al-Makhamreh, M.D., FACC Interventional Cardiologist
 Hanna K. Al-Makhamreh, M.D., FACC Interventional Cardiologist Introduction. Basic Life Support (BLS). Advanced Cardiac Life Support (ACLS). Cardiovascular diseases (CVDs) are the number one cause of death
Hanna K. Al-Makhamreh, M.D., FACC Interventional Cardiologist Introduction. Basic Life Support (BLS). Advanced Cardiac Life Support (ACLS). Cardiovascular diseases (CVDs) are the number one cause of death
Algorithm Focus. Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms. Perspective regarding the EMT- Intermediate algorithms
 Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Algorithms for the Conscious Patient Prehospital Medication Profiles Algorithm Focus Bradycardia Acute Pulmonary Edema and Shock Hypothermia
Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Algorithms for the Conscious Patient Prehospital Medication Profiles Algorithm Focus Bradycardia Acute Pulmonary Edema and Shock Hypothermia
ENVIRONMENTAL EMERGENCIES
 SECTION: Environmental Emergencies REVISED: 06/2015 Section 5 1. Environmental Hypothermia Protocol 5-1 2. Environmental Heat Exposure/Heat Protocol 5-2 Exhaustion Environmental Heat Stroke 3. Injury Bites
SECTION: Environmental Emergencies REVISED: 06/2015 Section 5 1. Environmental Hypothermia Protocol 5-1 2. Environmental Heat Exposure/Heat Protocol 5-2 Exhaustion Environmental Heat Stroke 3. Injury Bites
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara
 Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
Guslihan Dasa Tjipta Division of Perinatology Department of Child Health Medical School University of Sumatera Utara 1 Definition Perinatal asphyxia is a fetus/newborn, due to: is an insult to the Lack
High Risk + Challenging Trauma Cases. Hawaii. Topics 1/27/2014. David Thompson, MD, MPH. Head injury in the anticoagulated patient.
 High Risk + Challenging Trauma Cases David Thompson, MD, MPH Hawaii Topics Head injury in the anticoagulated patient Shock recognition Case 1: Head injury HPI: 57 yo male w/ PMH atrial fibrillation, on
High Risk + Challenging Trauma Cases David Thompson, MD, MPH Hawaii Topics Head injury in the anticoagulated patient Shock recognition Case 1: Head injury HPI: 57 yo male w/ PMH atrial fibrillation, on
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: Shock Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: Shock Revised: 11/2013 DEFINITIONS Aerobic metabolism is energy using oxygen into cells. Anaerobic
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: Shock Revised: 11/2013 DEFINITIONS Aerobic metabolism is energy using oxygen into cells. Anaerobic
Neurotrauma: The Place for Cooling
 Neurotrauma: The Place for Cooling Cooling: to achieve hypothermia History, evidence, open questions Cooling: to achieve normothermia Evidence, open questions Cooling: Practical Aspects Hypothermia: History
Neurotrauma: The Place for Cooling Cooling: to achieve hypothermia History, evidence, open questions Cooling: to achieve normothermia Evidence, open questions Cooling: Practical Aspects Hypothermia: History
Heat Illness in Children
 Heat Illness in Children Charles G. Macias MD, MPH Baylor College of Medicine Attending Physician, Texas Children s Hospital Emergency Department Houston, Texas Scope of the problem Heat stroke mortality
Heat Illness in Children Charles G. Macias MD, MPH Baylor College of Medicine Attending Physician, Texas Children s Hospital Emergency Department Houston, Texas Scope of the problem Heat stroke mortality
SHOCK. Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital
 SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
Objectives. Terminology. Shock. Terminology (cont.) Terminology (cont.)
 Objectives Gary Hoertz EMS Division Chief Kootenai Fire and Rescue Department Coeur d Alene, Idaho Terminology Pathophysiology of Shock Stages of Shock Classification of Shock Assessment Treatment Shock
Objectives Gary Hoertz EMS Division Chief Kootenai Fire and Rescue Department Coeur d Alene, Idaho Terminology Pathophysiology of Shock Stages of Shock Classification of Shock Assessment Treatment Shock
Objectives. Shock. Terminology. Terminology Pathophysiology of Shock Stages of Shock Classification of Shock Assessment Treatment Scenario
 Objectives Gary Hoertz EMS Division Chief Kootenai Fire and Rescue Department Coeur d Alene, Idaho Terminology Pathophysiology of Shock Stages of Shock Classification of Shock Assessment Treatment Scenario
Objectives Gary Hoertz EMS Division Chief Kootenai Fire and Rescue Department Coeur d Alene, Idaho Terminology Pathophysiology of Shock Stages of Shock Classification of Shock Assessment Treatment Scenario
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 6.1 Define key terms introduced in this chapter. Slides 11, 15, 17, 26, 27, 31, 33, 37, 40 42, 44, 45, 51, 58 6.2 Describe the basic roles and structures
Introduction to Emergency Medical Care 1 OBJECTIVES 6.1 Define key terms introduced in this chapter. Slides 11, 15, 17, 26, 27, 31, 33, 37, 40 42, 44, 45, 51, 58 6.2 Describe the basic roles and structures
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT
 PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
PRE-HOSPITAL PATIENT CARE PROTOCOLS BASIC LIFE SUPPORT/ADVANCED LIFE SUPPORT Board Approved June 2007 Revised December 2009 Revised July 2011 Revised June 2015 435 Hunter Street Fredericksburg, VA 22401
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders
 C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
Chapter 13. Learning Objectives. Learning Objectives 9/11/2012. Poisonings, Overdoses, and Intoxications
 Chapter 13 Poisonings, Overdoses, and Intoxications Learning Objectives Discuss use of activated charcoal in treatment of poisonings List treatment options for acetaminophen overdose List clinical manifestations
Chapter 13 Poisonings, Overdoses, and Intoxications Learning Objectives Discuss use of activated charcoal in treatment of poisonings List treatment options for acetaminophen overdose List clinical manifestations
Naloxone Intranasal EMT OPTIONAL SKILL. Cell Phones and Pagers. Course Outline 09/2017
 EMT OPTIONAL SKILL Naloxone Intranasal Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. Course Outline Introduction and Overview
EMT OPTIONAL SKILL Naloxone Intranasal Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. Course Outline Introduction and Overview
Prehospital Care Bundles
 Prehospital s The MLREMS Prehospital s have been created to provide a simple framework to help EMS providers identify the most critical elements when caring for a patient. These bundles do not replace
Prehospital s The MLREMS Prehospital s have been created to provide a simple framework to help EMS providers identify the most critical elements when caring for a patient. These bundles do not replace
