Headache. Anna Morenkova, MD, PhD Assistant Professor Department of Neurology UC Irvine
|
|
|
- Camron Davidson
- 6 years ago
- Views:
Transcription
1 Headache Anna Morenkova, MD, PhD Assistant Professor Department of Neurology UC Irvine
2 SOURCE OF HEAD PAIN (NOCICEPTIVE STRUCTURES) Intracranial Extracranial arteries of circle of Willis dura, dural arteries large veins and dural venous sinuses pain-sensitive fibers of CN V, IX, X ECA and branches scalp/neck muscles facial skin/nerves mucosa of sinuses and teeth upper C-spine segments STRUCTURES INNERVATED BY TRIGEMINAL NERVE AND UPPER CERVICAL ROOTS
3 Headache Disorders: Classification I. Primary headaches - Migraine - Tension-type headache - Trigeminal autonomic cephalalgias (TAC): cluster headache, paroxysmal hemicrania, SUNCT/SUNA - Other primary headaches II. Secondary headaches - Vascular disorders - Intracranial nonvascular disorders - Head and/or neck trauma - Infection - Disorders of homeostasis (metabolic derangements) - Substance or its withdrawal - Cranium, ENT, teeth and mouth, other facial structures - Psychiatric disorder III. Cranial neuralgias, central or primary facial pain, and other headaches
4 A 39-year old man presents to your office with the abrupt onset severe diffuse headache, nausea and blurred vision. Headache began about 6 hours ago. He tried high dose ibuprofen combined with acetaminophen twice since headache onset with no relief. He has a history of migraine with 2-3 headaches per month that would respond to ibuprofen within 2 hours of use. His blood pressure is 145/70. His examination is normal.
5 Headache High prevalence Presentation to medical attention is either due to headache severity, failure to respond to analgesics, or due to concern of underlying pathology Headache is a frequent presenting symptom in the emergency room Physical examination is often normal >90% of patients have PRIMARY HEADACHE DISORDER History is most important
6 First objective: istinguish primary from secondary headaches Second objective: Establish correct diagnosis of primary headache disorder Third objective: Initiate appropriate abortive and preventive treatment
7 Headaches: Diagnostic Algorithm History and Examination Preliminary diagnosis? Red Flags? NO Primary headache? YES Secondary headache? YES Atypical features? Diagnostic testing
8 Headache features History/Review of systems Diagnostic Criteria Red Flags
9 Headache features Location Quality Severity Time to peak Duration Constant or episodic Frequency Periodicity Onset Associated neurologic symptoms Preceding transient neurologic symptoms (aura) Aggravating and alleviating factors
10 Pertinent Questions History of prior illness Constitutional symptoms Transient neurologic symptoms preceding, associated, or following the headache Medications/supplements (new medications or changes in medication regimen) nitrates hydralazine cialis/viagra beta-agonists stimulants dopamine agonists estrogen
11 SNOOP4 secondary causes (Red Flags) Systemic symptoms/signs: fever, chills, night sweats, myalgia, weight loss (GCA, meningoencephalitis/abscess, malignancy, systemic infection) Neurologic symptoms/signs (focal or global, including changes in behavior or personality; diplopia; transient visual obscurations; pulsatile tinnitus, numbness or weakness in face/limbs, vertigo, loss of balance) Onset after age 50 Onset recent Pattern change (if previous history of headache) 1. Progressive headache with loss of headache-free periods 2. Precipitated by Valsalva: Chiari malformation, structural lesions that obstruct CSF flow, dural CSF leak. Most headaches are worsened by Valsalva. Certain primary headaches may be precipitated by Valsalva (primary cough headache). All headaches that are provoked by Valsalva require imaging to rule out secondary cause. 3. Postural aggravation (worse standing or lying): intracranial hypotension (CSF leak), Chiari, intracranial hypertension (CSF flow obstruction), worse with certain neck movements/position (cervicogenic). 4. Papilledema. Indicates intracranial hypertension. Ask about transient visual obscurations, diplopia, and visual field defects.
12 A 39-year old man presents to your office with the abrupt onset extremely severe diffuse headache, nausea and blurred vision. Headache began about 6 hours ago. When asked, he admits that this is the worst headache he has ever had. He also reports some neck pain and says it feels stiff. He has a history of migraine. What would be the next course of action? 1. Ketorolac i/m injection and antiemetic 2. Sumatriptan s/c injection 3. Arrange for an urgent lumbar puncture 4. Obtain an urgent CT of the head without contrast 5. Start IV hydration with NS * CT of the head is normal. Next step? LP does not show xanthochromia. Next step? CTA h/n is normal. Next step?
13 Thunderclap Headache Severe headache of abrupt onset (peaks within seconds) No warning, as a clap of thunder MUST BE EVALUATED in the Emergency Room
14 Causes of Thunderclap Headache SAH due to cerebral aneurysm or AVM rupture Cervico-cerebral arterial dissection Cerebral venous sinus thrombosis Acute hypertensive crisis Illicit drug use with secondary intracranial hemorrhage or infarction Cerebral reversible vasoconstriction syndrome, posterior reversible encephalopathy syndrome (PRES) Pituitary apoplexy Third ventricle colloid cyst Spontaneous intracranial hypotension (CSF leak) Ischemic or hemorrhagic stroke Primary thunderclap headache (no underlying intracranial pathology after extensive workup)
15
16
17
18
19
20
21 Primary Headaches
22 Primary Headaches 1. Migraine 2. Tension-type headache 3. Trigeminal autonomic cephalalgia (TAC) - Cluster headache - Paroxysmal hemicrania - SUNCT/SUNA 4. Other primary headaches - New Daily Persistent Headache - Hemicrania continua - Primary cough headache - Primary exertional headache - Headache associated with sexual activity - Primary stabbing headache - Hypnic headache
23 An overweight 36-year-old woman presents with 3-4 severe, debilitating headaches per month for the last 2 years. The headaches last 1 to 2 days. They are sometimes localized bifrontally, but more often localized to the right temple, right frontal region, and behind the right eye. There is often bilateral rhinorrhea and congestion associated with her headaches, and sense of pressure over the bridge the nose and sides of the nose. The pain is usually throbbing, but may be pressure-like when not very severe. She has to wear sunglasses and go to a quiet place and lay down because she can t function. She denies any prodrome or auras. What is the most likely diagnosis? 1. Cluster headache 2. Sinus headache 3. Tension-type headache 4. Episodic migraine * 5. Idiopathic intracranial hypertension (pseudotumor cerebri)
24 Migraine 95% of patients presenting in clinical practice with headache have migraine Clinical diagnosis Young age of onset: by age of 40 y.o. 90% of patients with migraine have had their first attack Positive family history (70% have first degree relative with migraine) Prevalence: 12% in general population Women:Men 3:1
25 Migraine: Diagnostic criteria 1. At least 5 attacks fulfilling the following criteria: 2. Attacks lasting 4 to 72 hours (untreated). 3. Any 2 of the following: - Unilateral (at least 40% of migraine sufferers will experience bilateral pain). - Pulsating/throbbing (50% of migraine sufferers will experience nonpulsating pain). - Moderate or severe intensity (mild headaches may still be migraine if other criteria are present). - Aggravated by or causing avoidance of routine physical activity 4. Any 1 of the following: - Photophobia AND phonophobia. - Nausea AND/OR vomiting 5. Not attributed to another disorder
26 probable migraine ( migrainous headache )
27 Migraine headache May switch sides and may become bilateral/diffuse Prodrome (up to 3 days prior to attack): mood changes, decreased energy, yawning, thirst, food craving Pain builds up over 30 min to 2 hrs to peak Cutaneous allodynia develops in most patients during migraine attack
28 Migraine with Aura Aura: transient visual, sensory, or language disturbance or other focal brainstem or cerebral symptoms that precede or accompany the headache Aura occurs in 25% of migraine patients Does not occur with each attack Duration of aura: 5 to 30 minutes Migraine equivalent = acephalgic migraine = migraine aura without headache
29 A 65-year-old woman went on a roller coaster ride. One day later, she began having left-sided retro-orbital daily intermittent throbbing headache lasting from several minutes to several hours. There was no associated sensitivity to light or sound, and no nausea or vomiting. The headache has continued for 3 weeks on-and-off, and today she had what sounds like amaurosis fugax in the left eye ( curtain going down for about 10 seconds). She had rare migraine headaches in her 30 s-40 s. She denies any other symptoms, such as general weakness/fatigue, fevers, chills, weight loss, joint pain, rash. Diagnosis? 1. Migraine with visual aura, status migrainosus 2. Temporal arteritis 3. Internal carotid artery dissection 4. Glaucoma *
30 Aura of migraine: diagnostic criteria At least 2 attacks Aura consisting of at least one of the following, but no motor weakness*: 1. Fully reversible VISUAL symptoms (including positive and/or negative features) 2. Fully reversible SENSORY symptoms (including positive and/or negative symptoms) 3. Fully reversible DYSPHASIC speech disturbance *Migraine with MOTOR deficit is classified as hemiplegic migraine *Migraine with BRAINSTEM SYMPTOMS is classified as basilar-type migraine Duration of typical aura: 5 to 30 minutes (<60 min)
31 Visual Aura
32 Sensory Aura Sensory auras may spread in min from where they started to maximal distribution Slower than sensory seizure spread Much slower than TIA sensory symptoms spread Latent period of few minutes between aura and headache development
33
34 A 65-year-old woman went on a roller coaster ride. One day later, she began having left-sided retro-orbital daily intermittent throbbing headache lasting from several minutes to several hours. There was no associated sensitivity to light or sound, and no nausea or vomiting. The headache has continued for 3 weeks on-andoff, and today she had what sounds like amaurosis fugax in the left eye ( curtain going down for 10 seconds). She had rare migraine headaches in her 30 s-40 s. She feels weak all over, and states that her shoulders have been hurting for at least 6 months. On directed questioning, she endorses to getting tired of chewing, and her jaw hurts. On examination, left temporal scalp area is exquisitely sensitive to touch. Initial brain imaging and vascular imaging has been unremarkable. Diagnosis? 1. Migraine with aura, status migrainosus 2. Temporal arteritis * 3. Internal carotid artery dissection 4. Glaucoma
35 Migraine: Management Education and counseling: reduces anxiety and improves adherence to pharmacologic treatment Migraine diary Trigger avoidance (food, odors) and dietary changes (elimination diets should be avoided) Good hydration Sleep hygiene (weekend headaches) Regular meals and avoidance of fasting Reducing caffeine, alcohol, smoking cessation Medication review and changes Regular exercise nitrates hydralazine cialis/viagra Stress reduction and coping techniques: biofeedback, relaxation training, hypnosis, stimulants cognitive and behavioral training beta-agonists dopamine agonists estrogen
36 Potential Food Triggers Some association of certain food items with migraine Nitrites (hotdogs, preserved cold cuts) Monosodium glutamate (canned food, Chinese food) Aspartam (artificial sweetener) Aged cheeses, fermented food, red wine Chicken liver, pork Chocolate Sweets, nuts, dairy, citrus fruits
37 Pharmacologic treatment Abortive Prophylactic
38 A 34-year-old overweight woman present with a severe migraine headache that began 2 days ago, but is now nearly gone. She has not identified any triggers since these headaches began 2 years ago. She has tried to avoid stress and kept a headache diary prior to a visit with you today. She averages about 5 migraines per month, each lasting up to 1-2 days. What is the best choice of treatment at this time, assuming there are no contraindications? 1. Prescribe sumatriptan and a NSAID to take immediately today to stop her resolving headache 2. Prescribe preventive agent 3. Give IV dihydroergotamine (DHE) infusion today in the office 4. Follow her over the next couple of months before prescribing anything 5. Prescribe sumatriptan to use as needed, as well as preventive agent *
39 Abortive migraine treatment: as early as possible/at onset of aura Simple analgesics Aspirin NSAIDs Acetaminophen Analgesic combination with caffeine (avoid using > 2/week) Triptans Agonists at specific 5-HT receptors 5HT1B agonists: promote vasoconstriction 5HT1D agonists: block release of neuropeptides from perivascular trigeminal afferents Dihydroergotamine (DHE): for prolonged migraine attack/status migrainosus Triptans, DHE: contraindicated in CAD, cerebrovascular disease, peripheral vascular disease, caution in hypertension
40
41 The patient depicted in previous case returns 1 week later. She is now in prolonged, severe headache phase that began 4 days ago. She has missed 2 days of work. Her last triptan dose was 1 day ago. As you examine her head, you find that her right temporal and right frontal regions are exquisitely sensitive to touch. What is the best choice of treatment at this point, assuming there are no contraindications? 1. Increase her preventive medication dose and have her take another triptan 2. Change her preventive agent because it does not appear to be working 3. Give IV dihydroergotamine (DHE) infusion * 4. Change her triptan and have her take one now 5. Proceed with CT of the head without contrast to investigate the dysesthesia found on examination
42 During the office visit, a 46-year-old man with a longstanding history of recurrent headaches is diagnosed for the first time with migraine. He has a history of anxiety, hypertension, hyperlipidemia, smoking, and is noncompliant with medications. Family history is significant for his mother having migraine and his father dying from a heart attack in his mid fifties. If this patient presented to the emergency department at the very onset of a migraine, what would be the least optimal choice of treatment? 1. Sumatriptan 2. Ketorolac * 3. Valproic acid 4. Prochrolperazine 5. IV magnesium
43 Preventive/prophylactic treatment Consider prophylactic treatment if: frequency of headaches > 2 per month frequency and duration of migraines interfere with life style headache duration > 24 hours severe prolonged headaches not responsive to abortive medications, intolerance of abortive medications, contraindications to abortive medications
44 Preventive Treatment Medication selection based on patient s characteristics, comorbidities, and side effect profile of the medications Medications do not exert their effect for at least 2 weeks, most of the time - not sooner than 2 months Doses known to be therapeutic should be reached before failure is considered Ongoing frequent use of analgesics impedes onset of benefit from preventive medication Multiple agents may be necessary
45 Preventive Treatment Beta-blockers: propranolol mg/day Tricyclic antidepressants: amitriptyline (75 mg qhs), nortriptyline, desipramine, imipramine Selective serotonin reuptake inhibitors: Not consistently proven beneficial May cause headaches Anticonvulsants: topiramate, valproate CCB: verapamil mg tid or ER qd Useful in migraine with aura
46 Prophylactic medication selection Comorbid Condition Medication Hypertension Angina Beta blockers, CCB, ACE inhibitor, ARB (candesartan) Beta blockers Stress, anxiety Beta blockers Depression Tricyclic antidepressants, SSRIs Overweight Topiramate Underweight Tricyclic antidepressants Epilepsy Valproic acid, topiramate Bipolar disorder/mania Valproic acid
47
48 A 22-year-old mildly overweight woman presents to the emergency department with increasing frequency of previously diagnosed migraine. Other medical history is unremarkable with exception of mild asthma and recurrent constipation. The attacks are occurring 4 days per week and are lasting the entire day. What would be the best preventive medication to start in this patient? 1. Amitriptyline 2. Propranolol 3. Sumatriptan 4. Topiramate 5. Verapamil *
49 Botulinum toxin type A Proven efficacy in chronic migraine Reduces proinflammatory and vasodilating neuropeptides from nociceptive terminals Reduces or inhibits development of peripheral and central trigeminal sensitization 5 Units in forehead, temporalis, splenius capitis, trapezius muscles into 31 injection sites Effect starts after 7-10 days and lasts 3 months
50 Butterbur extract (Petadolex) DO NOT use parts of plant use only commercially available preparation (Petadolex) Monitoring liver enzymes is recommended
51 A 38-year-old woman complains of frequent headaches for the past 2-3 years. The pain is located in bilateral fronto-temporal areas, described as pressure-like, band-like, tightness. There is no associated sensitivity to light or sound. No associated nausea or vomiting. Headache is not positional. The pain is not aggravated by routine physical activity and she is able to continue with her daily routine with these headaches. Headaches last from several hours to several days and respond fairly well to over-the-counter analgesics. She has had up to 10 headache-days per month for the past several months. She denies any other symptoms, such as vision changes, double vision, tinnitus, vertigo. Her general and neurologic examination is normal, except tenderness of pericranial muscles to palpation. Diagnosis? Treatment? 1. Migraine 2. Sinus headache 3. Pseudotumor cerebri 4. Tension-type headache 5. Psychogenic headache *
52 Tension Type Headache Prevalence: 30-78% Can begin at any age Bilateral, generalized or band-like pressure around the head Frequency: episodic or chronic (> 15 days a month for more than 3 months) With and without pericranial muscle involvement Persistent contraction of the scalp, neck, jaw muscles related to central mechanism Cranio-cervical muscle tenderness
53 Tension type headache: Diagnostic criteria NOT A MIGRAINE : Not unilateral Not throbbing or pulsating Not severe, but mild to moderate Not aggravated/provoked by routine physical activity No photo- AND phonophobia No nausea or vomiting + No other explanation
54 Tension type headache: Treatment Techniques of relaxation (biofeedback), neck massage Medications: 1. Abortive: acetaminophen+isometheptene+dichloralphenazone avoid codeine, propoxyphene, butalbital with caffeine (high potential to cause medication overuse headache) 2. Preventive: amitriptyline is the best choice other TCAs, gabapentin, mirtazapine, topiramate
55 A 46-year-old man presents with episodic headaches. His headaches are described as severe attacks of unilateral pain lasting minutes and associated with ipsilateral droopy eyelid, tearing, redness of the eye, and nasal congestion. He has 1-3 attacks daily or every other day. Some attacks occur during the night, waking him up from sleep typically at 2 a.m. He is agitated and restless during the headache and cannot stay still. The attacks occur in bouts lasting for several weeks up to 4 months, then remit for several months, then return. He has had these headaches for 2 years. Neurologic examination is normal. He was told that during the attacks, his pupil on the side of the headache is smaller compared to the other pupil. Diagnosis? 1. Migraine 2. Hemicrania continua 3. Pseudutumor cerebri 4. Cluster headache 5. Glaucoma *
56 Trigeminal Autonomic Cephalalgias (TACs) 1.Cluster headache 2.Paroxysmal hemicrania 3.SUNCT/SUNA Common features: pain location in the distribution of trigeminal nerve V1 strictly unilateral unilateral ipsilateral cranial autonomic associated symptoms periodicity need to rule out secondary causes: pituitary, hypothalamic, cavernous sinus, trigeminal nerve pathologic process Distinguishing features: attack duration (longest in cluster headache, shortest in SUNCT) and number of attacks a day (highest in SUNCT/SUNA) unique response to medications (abortive and preventive)
57 Cluster Headache Prevalence 1/2000 Men >> women (4.3:1) Onset in 3rd decade of life Most painful recurrent headache ( suicide headache") Unilateral orbital/temporal/supraorbital Throbbing, hot poker in the eye, eye being pushed out Rapid buildup of pain over 5-10 min Attack duration: 15 min-3 hrs Restless patient and prefers to pace 1-8 attacks a day; onset during night or few hours after falling asleep ( alarm headache) Daily or eod attacks in clusters lasting 6-12 weeks followed by remissions for months or years
58 Diagnostic criteria: Cluster Headache A. At least 5 attacks fulfilling B - D B. Severe unilateral orbital, supraorbital and/or temporal pain lasting min untreated C. Headache is associated with at least 1 of the following signs that have to be present on the pain side: 1.Conjunctival injection. 2.Lacrimation. 3.Nasal congestion. 4.Rhinorrhea. 5.Forehead and facial sweating. 6.Miosis. 7.Ptosis. 8.Eyelid edema. D. Frequency of attacks: from 1 every other day to 8 a day.
59 Cluster headache: Management Abortive: High flow O2 (12 L/min 100% O2 via NRM, seated) Sumatriptan: s/c superior to intranasal, s/c and intranasal are superior to oral DHE: intranasal (2 mg) is superior to oral, i/m and s/c Zolmitriptan: intranasal, oral Lidocaine spray or nasal drops (only moderate reduction of pain in less than 30% of patients) Transitional ( bridge ) Course of steroids: 60 mg oral prednisone with rapid taper by 10 mg every 2-3 days over days Ergotamine tartrate orally/rectally to prevent nocturnal attacks DHE: few doses every 6-8 hrs Occipital nerve block Maintenance prophylaxis: Calcium channel blockers (verapamil) mg a day as tid or ER Lithium carbonate 300 mg tid or 450 ER qd Valproic acid mg
60 Paroxysmal Hemicrania(PH) Onset in third decade of life Women >> Men (5:1) Severe unilateral orbital/retroorbital/temporal pain Attack duration: 2-30 minutes Attack frequency > 5 a day Ipsilateral cranial autonomic symptoms Episodic PH: attacks for 4-24 weeks followed by remission periods Chronic PH: daily with multiple discrete attacks without remissions Indomethacin in TID dose (total up to 225 mg/day), diagnosis-defining treatment! May be difficult to distinguish from cluster HA > trial of indomethacin (diagnosis-defining treatment)
61 Onset in fourth decade of life SUNCT/SUNA Men:Women is 3:2 Short-lasting Unilateral Neuralgiform headache with Conjunctival injection and Tearing/Autonomic symptoms Orbital/retroorbital/temporal pain with ipsilateral autonomic symptoms attack duration less than 2 min attack frequency a day Daily or almost daily for weeks/months w/w/o remissions Lamotrigine has best evidence of benefit Rule out pituitary, cavernous sinus pathology, neurovascular conflict (trigeminal neuralgia) Surgical procedures for refractory cases
62 Other Primary Headaches Primary cough headache Primary stabbing headache Primary exertional headache Primary headache associated with F sexual activity Primary thunderclap headache Hypnic headache Hemicrania continua New daily persistent headache
63 Secondary Headaches
64 A 26-year-old obese woman with borderline hypertension presents with worsening headache, which she describes as a bifrontal and bioccipital band-like pressure and pain, variable in intensity - from mild to severe, fluctuating throughout the day. Occasionally, she experiences brief visual loss or graying, especially with straining, which lasts only seconds. On directed questioning, she endorses to occasional mild double vision. Occasionally, she is sensitive to light and sound. She sometimes gets nauseated and vomits when the pain is severe and she feels her vision is becoming increasingly blurred. What do you suspect may be a diagnosis? Diagnostic tests? Treatment? 1. Migraine 2. Psychogenic headache 3. Pseudotumor cerebri 4. Tension-type headache 5. Posterior fossa tumor * CTH > Lumbar puncture + fundoscopic examination > acetazlamide/topiramate > furosemide > CSF diversion procedures (VP shunt, LP shunt, VA shunt), optic nerve sheath fenestration
65 Medication Overuse Headache (MOH) Old term: rebound headache Headache related to overuse of abortive medication for patients with frequent headaches Diagnostic criteria
66 Medication Overuse Headache Opioids, butalbital-based medications, aspirin/acetaminophen/caffeine: highest risk Triptans: moderate risk NSAIDs: lowest risk Treatment
67 Secondary headaches Vascular disorders Intracranial nonvascular disorders Head and/or neck trauma Infection Disorders of homeostasis (metabolic derangements) Substance or its withdrawal Pathology of cranium, ENT, teeth and mouth, other facial structures Psychiatric disorder
68 Headache: classification I. Primary headaches - Migraine - Tension-type headache - Trigeminal autonomic cephalalgias (TAC): cluster headache, paroxysmal hemicrania, SUNCT/SUNA - other primary headaches II. Secondary headaches - Vascular disorders - Intracranial nonvascular disorder - Head and/or neck trauma - Infection - Disorders of homeostasis (metabolic derangements) - Substance or its withdrawal - Cranium, ENT, teeth and mouth, other facial structures - Psychiatric disorder III. Cranial neuralgias, central or primary facial pain, and other headaches
69 Headaches: Diagnostic Algorithm History and Examination Preliminary diagnosis? Red Flag? YES NO Primary headache? Secondary headache Atypical features Diagnostic testing
70 Most headaches are primary Red Flags (SNOOP4) Take home points History and semiology are the most important Diagnostic criteria should be met, otherwise diagnosis is probable migraine, probable cluster headache, etc. Aura: positive and negative symptoms for 5-30 minutes Preventive treatment is critical part of treatment Preventive medication choice is based on comorbidities and side effect profile of the medication Elimination diets are counterproductive Analgesic overuse leads to development of secondary headache - Medication Overuse Headache Brain +/- vascular imaging should be pursued if underlying pathology is suspected Sinus headaches are almost nonexistent Cervicogenic headache can be diagnosed only if pathology is at or above C2-C3 level
71 Thunderclap headache DO NOT IGNORE New onset headache in an adult Change in headache pattern (intensity, frequency, new features, decreased response to analgesics) Nocturnal occurrence or early morning awakening Worsening/precipitation by changes in posture or Valsalva Presence of focal neurologic signs
72 HEADACHE MYTHS Most headaches are secondary Headache is a common initial symptom of stroke Hypertension causes headache Sinus headaches are common Occipital neuralgia is common Cervicogenic headache is due to C4-C7 disc disease Atypical migraine Secondary headache in a patient with underlying primary headache disorder always presents with headache of new pattern Positive Valsalva means secondary headache Medication side effect is a rare cause of headache
73 Questions?
74 Thank you
75 Complications of Migraine 1. Status migrainosus 2. Chronic migraine 3. Persistent aura without infarction 4. Migrainous infarction 5. Migralepsy
Chronic Daily Headaches
 Chronic Daily Headaches ANWARUL HAQ, MD, MRCP(UK), FAHS DIRECTOR BAYLOR HEADACHE CENTER, DALLAS, TEXAS DISCLOSURES: None OBJECTIVES AT THE CONCLUSION OF THIS ACTIVITY, PARTICIPANTS WILL BE ABLE TO: define
Chronic Daily Headaches ANWARUL HAQ, MD, MRCP(UK), FAHS DIRECTOR BAYLOR HEADACHE CENTER, DALLAS, TEXAS DISCLOSURES: None OBJECTIVES AT THE CONCLUSION OF THIS ACTIVITY, PARTICIPANTS WILL BE ABLE TO: define
Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE
 Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE IHS Classification 1989 (updated 2004) Primary Headaches 4 categories Migraine Tension-type Cluster and other trigeminal
Tears of Pain SUNCT and SUNA A/PROFESSOR ARUN AGGARWAL RPAH PAIN MANAGEMENT CENTRE IHS Classification 1989 (updated 2004) Primary Headaches 4 categories Migraine Tension-type Cluster and other trigeminal
Index. Prim Care Clin Office Pract 31 (2004) Note: Page numbers of article titles are in boldface type.
 Prim Care Clin Office Pract 31 (2004) 441 447 Index Note: Page numbers of article titles are in boldface type. A Abscess, brain, headache in, 388 Acetaminophen for migraine, 406 407 headache from, 369
Prim Care Clin Office Pract 31 (2004) 441 447 Index Note: Page numbers of article titles are in boldface type. A Abscess, brain, headache in, 388 Acetaminophen for migraine, 406 407 headache from, 369
Disclosures. Objectives 6/2/2017
 Classification: Migraine and Trigeminal Autonomic Cephalalgias Lauren Doyle Strauss, DO, FAHS Assistant Professor, Child Neurology Assistant Director, Child Neurology Residency @StraussHeadache No disclosures
Classification: Migraine and Trigeminal Autonomic Cephalalgias Lauren Doyle Strauss, DO, FAHS Assistant Professor, Child Neurology Assistant Director, Child Neurology Residency @StraussHeadache No disclosures
Headache Assessment In Primary Eye Care
 Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
Headache Assessment In Primary Eye Care Spencer Johnson, O.D., F.A.A.O. Northeastern State University Oklahoma College of Optometry johns137@nsuok.edu Course Objectives Review headache classification Understand
A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline. Scottish intercollegiate Guidelines Network SIGN
 A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline Scottish intercollegiate Guidelines Network SIGN November 2008. PETER FRAMPTON MSc MCOptom BAppSc (Optom)(AUS)
A synopsis of: Diagnosis and Management of Headaches in Adults: A national clinical guideline Scottish intercollegiate Guidelines Network SIGN November 2008. PETER FRAMPTON MSc MCOptom BAppSc (Optom)(AUS)
HEADACHES THE RED FLAGS
 HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
Can I send this headache patient home? Dr Nicola Giffin Consultant Neurologist Bath, Nov 2017
 Can I send this headache patient home? Dr Nicola Giffin Consultant Neurologist Bath, Nov 2017 SAH v benign thunderclap headaches Other pathologies not apparent on CT Severe primary headaches: management
Can I send this headache patient home? Dr Nicola Giffin Consultant Neurologist Bath, Nov 2017 SAH v benign thunderclap headaches Other pathologies not apparent on CT Severe primary headaches: management
MIGRAINE UPDATE. Objectives & Disclosures. Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment.
 MIGRAINE UPDATE Karen L. Bremer, MD November 16, 2018 Objectives & Disclosures Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment. Disclosure: I am
MIGRAINE UPDATE Karen L. Bremer, MD November 16, 2018 Objectives & Disclosures Learn techniques used to diagnose headaches. Become familiar with medications used for headache treatment. Disclosure: I am
Headache and Facial Pain. Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology
 Headache and Facial Pain Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology Introduction It is the most common neurologic complain The diagnosis usually
Headache and Facial Pain Mohammed ALEssa MBBS, FRCSC Assistant Professor Consultant Otolaryngology,Head & Neck Surgical Oncology Introduction It is the most common neurologic complain The diagnosis usually
Headache Pain Generators
 Objectives 1. Define the major categories of headache. 2. Take a history directed at characterizing a headache pattern in an individual patient and identify the cause or triggers of the headache. 3. Understand
Objectives 1. Define the major categories of headache. 2. Take a history directed at characterizing a headache pattern in an individual patient and identify the cause or triggers of the headache. 3. Understand
MIGRAINE A MYSTERY HEADACHE
 MIGRAINE A MYSTERY HEADACHE The migraine is a chronic neurological disease that is characterized by moderate to severe episodes of headache that is mostly associated with other central nervous system (CNS)
MIGRAINE A MYSTERY HEADACHE The migraine is a chronic neurological disease that is characterized by moderate to severe episodes of headache that is mostly associated with other central nervous system (CNS)
Strategies in Migraine Care
 Strategies in Migraine Care Julie L. Roth, MD Rhode Island Hospital Assistant Professor, Neurology The Warren Alpert Medical School of Brown University March 28, 2015 Financial Disclosures None. Objectives
Strategies in Migraine Care Julie L. Roth, MD Rhode Island Hospital Assistant Professor, Neurology The Warren Alpert Medical School of Brown University March 28, 2015 Financial Disclosures None. Objectives
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา
 ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
ปวดศ รษะมา 5 ป ก นยาแก ปวดก ย งไม ข น นพ.พาว ฒ เมฆว ช ย โรงพยาบาลนครราชส มา 1 CONTENT 1 2 3 Chronic Daily Headache Medical Overused Headache Management Headaches are one of the most common symptoms List
Outpatient Headache Care Guideline
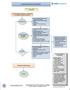 1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
1 Outpatient Care Guideline Inclusion criteria: children > 3 yrs with headaches Is urgent emergency department, neuroimaging, or Neurology consultation indicated? Referral to ED if: New severe headache
Trigeminal Autonomic Cephalalgias. Disclosures. Objectives 6/20/2018. Rashmi Halker Singh, MD FAHS UCNS Review Course June 2018
 Trigeminal Autonomic Cephalalgias Rashmi Halker Singh, MD FAHS UCNS Review Course June 2018 Disclosures Honoraria from Allergan and Amgen for advisory board, Current Neurology and Neuroscience Reports
Trigeminal Autonomic Cephalalgias Rashmi Halker Singh, MD FAHS UCNS Review Course June 2018 Disclosures Honoraria from Allergan and Amgen for advisory board, Current Neurology and Neuroscience Reports
Headache. Section 1. Migraine headache. Clinical presentation
 Section 1 Headache Migraine headache 1 Clinical presentation It is important to recognize just how significant a problem migraine headache is. It has been estimated that migraine affects 11% of the United
Section 1 Headache Migraine headache 1 Clinical presentation It is important to recognize just how significant a problem migraine headache is. It has been estimated that migraine affects 11% of the United
6/4/2018. Headache. Headaches. Headache. Migraine Headaches. Headache. Red Flag signs and symptoms. Imaging CT without contrast.
 Presented by M.D. Shepherd, M.D. OH MY ACHING HEAD! Estimated that one half of the adult population is affected by a headache disorder International Society Classification Primary : Tension s 40% of the
Presented by M.D. Shepherd, M.D. OH MY ACHING HEAD! Estimated that one half of the adult population is affected by a headache disorder International Society Classification Primary : Tension s 40% of the
2) Headache - Dr. Hawar
 2) Headache - Dr. Hawar Headache is caused by traction, displacement, inflammation, vascular spasm, or distention of the painsensitive structures in the head or neck. Isolated involvement of the bony skull,
2) Headache - Dr. Hawar Headache is caused by traction, displacement, inflammation, vascular spasm, or distention of the painsensitive structures in the head or neck. Isolated involvement of the bony skull,
Headache Mary D. Hughes, MD Neuroscience Associates
 Headache Mary D. Hughes, MD Neuroscience Associates Case 1 22 year old female presents with recurrent headaches. She has had headaches for the past 3 years. They start on the right side of her head and
Headache Mary D. Hughes, MD Neuroscience Associates Case 1 22 year old female presents with recurrent headaches. She has had headaches for the past 3 years. They start on the right side of her head and
Faculty Disclosure. Karen L. Bremer, MD. Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest.
 Faculty Disclosure Karen L. Bremer, MD Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest. HEADACHE UPDATE Karen L. Bremer, MD November 10, 2017 karen.bremer@creighton.edu
Faculty Disclosure Karen L. Bremer, MD Dr. Bremer has listed no financial interest/arrangement that would be considered a conflict of interest. HEADACHE UPDATE Karen L. Bremer, MD November 10, 2017 karen.bremer@creighton.edu
HEADACHE: Benign or Severe Dr Gobinda Chandra Roy
 HEADACHE: Benign or Severe Dr Gobinda Chandra Roy Associate Professor, Department of Medicine, Shaheed Suhrawardy Medical College and Hospital Outlines 1. Introduction 2. Classification of headache 3.
HEADACHE: Benign or Severe Dr Gobinda Chandra Roy Associate Professor, Department of Medicine, Shaheed Suhrawardy Medical College and Hospital Outlines 1. Introduction 2. Classification of headache 3.
Classification of headaches
 Classification of headaches Primary headaches OR Idiopathic headaches Secondary headaches OR Symptomatic headaches THE HEADACHE IS ITSELF THE DISEASE NO ORGANIC LESION IN THE BEACKGROUND TREAT THE HEADACHE!
Classification of headaches Primary headaches OR Idiopathic headaches Secondary headaches OR Symptomatic headaches THE HEADACHE IS ITSELF THE DISEASE NO ORGANIC LESION IN THE BEACKGROUND TREAT THE HEADACHE!
Headache Master School Japan-Osaka 2016 II. Management of refractory headaches Case Presentation 2. SUNCT/SUNA: concept, management and prognosis
 Headache Master School Japan-Osaka 2016 II. Management of refractory headaches Case Presentation 2. SUNCT/SUNA: concept, management and prognosis Noboru Imai(Department of Neurology, Japanese Red Cross
Headache Master School Japan-Osaka 2016 II. Management of refractory headaches Case Presentation 2. SUNCT/SUNA: concept, management and prognosis Noboru Imai(Department of Neurology, Japanese Red Cross
Headache. Susan Hickenbottom MD, MS February 24, 2015
 Headache Susan Hickenbottom MD, MS February 24, 2015 Epidemiology One of most common complaints in primary care 90% of US population 50% at least one severe 25% recurrent disabling attacks 5% chronic daily
Headache Susan Hickenbottom MD, MS February 24, 2015 Epidemiology One of most common complaints in primary care 90% of US population 50% at least one severe 25% recurrent disabling attacks 5% chronic daily
A case of a patient with chronic headache. Focus on Migraine. None related to the presentation Grants to conduct clinical trials from: Speaker bureau:
 Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
Chronic Daily Headache Bassel F. Shneker, MD, MBA Associate Professor Vice Chair, OSU Neurology The Ohio State University Wexner Medical Center Financial Disclosures None related to the presentation Grants
By Nathan Hall Associate Editor
 By Nathan Hall Associate Editor 34 Practical Neurology March 2005 These new rules may change the definition of head pain, but some practitioners may find the new guidelines themselves to be a source of
By Nathan Hall Associate Editor 34 Practical Neurology March 2005 These new rules may change the definition of head pain, but some practitioners may find the new guidelines themselves to be a source of
HMFP Comprehensive Headache Center Department of Anesthesia, Critical Care and Pain Medicine Beth Israel Deaconess Medical Center Instructor in
 HMFP Comprehensive Headache Center Department of Anesthesia, Critical Care and Pain Medicine Beth Israel Deaconess Medical Center Instructor in Anesthesia and Neurology Harvard Medical School Limited time
HMFP Comprehensive Headache Center Department of Anesthesia, Critical Care and Pain Medicine Beth Israel Deaconess Medical Center Instructor in Anesthesia and Neurology Harvard Medical School Limited time
Overview INTRODUCTION 3/15/2018. Headache Emergencies. Other way to differentiate between them? Is there an easy way to differentiate between them?
 Overview Headache Emergencies Primary versus Secondary headache disorder Red flags 4 cases of unusual headache emergencies Disclaimer: we will not talk about brain bleed as patients usually go the ED.
Overview Headache Emergencies Primary versus Secondary headache disorder Red flags 4 cases of unusual headache emergencies Disclaimer: we will not talk about brain bleed as patients usually go the ED.
Neurological Dilemmas in Primary Care
 Neurological Dilemmas in Primary Care David Clark, DO dclark@oregonneurology.com When to test? How to test? Pitfalls in testing? When to treat? How to treat? How long to treat? Neurological Dilemmas Seizure
Neurological Dilemmas in Primary Care David Clark, DO dclark@oregonneurology.com When to test? How to test? Pitfalls in testing? When to treat? How to treat? How long to treat? Neurological Dilemmas Seizure
GENERAL APPROACH AND CLASSIFICATION OF HEADACHES
 GENERAL APPROACH AND CLASSIFICATION OF HEADACHES CLASSIFICATION Headache is one of the most common medical complaints. Most of the population will have experienced headache, and over 5% will seek medical
GENERAL APPROACH AND CLASSIFICATION OF HEADACHES CLASSIFICATION Headache is one of the most common medical complaints. Most of the population will have experienced headache, and over 5% will seek medical
10/31/2017 PRIMARY CARE AND HEADACHE DISCLOSURES WHERE DO THOSE WITH HEADACHE SEEK MEDICAL CARE? Primary Care 67%
 PRIMARY CARE AND HEADACHE Sonja Potrebic MD PhD Regional Headache Specialist Kaiser LAMC 1 WHERE DO THOSE WITH HEADACHE SEEK MEDICAL CARE? Column1 Primary Care 67% Primary Care Headache Specialty Other
PRIMARY CARE AND HEADACHE Sonja Potrebic MD PhD Regional Headache Specialist Kaiser LAMC 1 WHERE DO THOSE WITH HEADACHE SEEK MEDICAL CARE? Column1 Primary Care 67% Primary Care Headache Specialty Other
HEADACHE Transient discomfort, chronic nuisance, or looming disaster?
 HEADACHE Transient discomfort, chronic nuisance, or looming disaster? Hussien H. Rizk, MD Cairo University Medical School ١ Headache Second most common o symptom (after pain) Migraine alone afflicts 12
HEADACHE Transient discomfort, chronic nuisance, or looming disaster? Hussien H. Rizk, MD Cairo University Medical School ١ Headache Second most common o symptom (after pain) Migraine alone afflicts 12
I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation.
 I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation. In 1962, Bille published landmark epidemiologic survey of headache among 9,000 school
I have no financial relationships to disclose. I will not discuss investigational use of medication in my presentation. In 1962, Bille published landmark epidemiologic survey of headache among 9,000 school
How could I be having migraine when I don't have a headache?
 Migraine Your doctor thinks you may have migraine. Classic migraine attacks start with visual symptoms (often zig-zag colored lights or flashes of light expanding to one side over 10-30 minutes) followed
Migraine Your doctor thinks you may have migraine. Classic migraine attacks start with visual symptoms (often zig-zag colored lights or flashes of light expanding to one side over 10-30 minutes) followed
WHY IS MIGRAINE IMPORTANT
 WHY IS MIGRAINE IMPORTANT Migraine is a complex disorder characterized by recurrent episodes of headache, most often unilateral and in some cases associated with visual or sensory symptoms collectively
WHY IS MIGRAINE IMPORTANT Migraine is a complex disorder characterized by recurrent episodes of headache, most often unilateral and in some cases associated with visual or sensory symptoms collectively
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
Cluster headache (CH): epidemiology, classification and clinical picture
 Cluster headache (CH): epidemiology, classification and clinical picture Toomas Toomsoo, M.D. Head of the Center of Neurology East Tallinn Central Hospital 1 INTRODUCTION Cluster headache - known as trigeminal
Cluster headache (CH): epidemiology, classification and clinical picture Toomas Toomsoo, M.D. Head of the Center of Neurology East Tallinn Central Hospital 1 INTRODUCTION Cluster headache - known as trigeminal
Primary Care Adult Headache Management Pathway (formerly North West Headache Management Guideline for Adults) Version 1.0
 Primary Care Adult Headache Management Pathway (formerly rth West Headache Management Guideline for Adults) Version 1.0 1 VERSION CONTROL Version Date Amendments made Version 1.0 October 2018 Reformatted
Primary Care Adult Headache Management Pathway (formerly rth West Headache Management Guideline for Adults) Version 1.0 1 VERSION CONTROL Version Date Amendments made Version 1.0 October 2018 Reformatted
HEADACHE. Dr Nick Pendleton. September Headache
 HEADACHE Dr Nick Pendleton September 2017 Headache Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache Raised ICP
HEADACHE Dr Nick Pendleton September 2017 Headache Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache Raised ICP
25/09/2018 HEADACHE. Dr Nick Pendleton
 HEADACHE Dr Nick Pendleton September 2018 1 Small Group Work Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache
HEADACHE Dr Nick Pendleton September 2018 1 Small Group Work Tension Type Headache Cranial Nerve Examination Migraine Migraine Treatment Medication Overuse Headache Headache Red Flags Sinusitis Headache
Headache Syndrome. Karen Alvarez, D.O Nemours Children s Specialty Care Jacksonville, FL
 Headache Syndrome Karen Alvarez, D.O Nemours Children s Specialty Care Jacksonville, FL What is a headache? A headache or cephalgia is defined as pain anywhere in the region of head or neck Where does
Headache Syndrome Karen Alvarez, D.O Nemours Children s Specialty Care Jacksonville, FL What is a headache? A headache or cephalgia is defined as pain anywhere in the region of head or neck Where does
Classification and WHO ICD-10NA Codes
 Classification and WHO ICD-10NA Codes IHS WHO Diagnosis ICHD-II ICD-10NA [and aetiological ICD-10 code for secondary headache disorders] code code 1. [G43] Migraine 1.1 [G43.0] Migraine without aura 1.2
Classification and WHO ICD-10NA Codes IHS WHO Diagnosis ICHD-II ICD-10NA [and aetiological ICD-10 code for secondary headache disorders] code code 1. [G43] Migraine 1.1 [G43.0] Migraine without aura 1.2
Headache. Headache Case. Migraine Headache. Eric Kraus, MD. Types» Without aura (common)» With aura (classic)
 Headache Eric Kraus, MD Headache Case This 23 year-old female has headaches behind the right eye that cause her to lay down in a quiet room. They have a throbbing quality and she may vomit. Migraine Headache
Headache Eric Kraus, MD Headache Case This 23 year-old female has headaches behind the right eye that cause her to lay down in a quiet room. They have a throbbing quality and she may vomit. Migraine Headache
FINANCIAL DISCLOSURE. No relevant financial relationships
 Sleep and Headache Paul Mathew, MD, FAHS Director of Continuing Medical Education John R. Graham Headache Center Brigham & Women s Hospital Director of Headache Medicine Cambridge Health Alliance Harvard
Sleep and Headache Paul Mathew, MD, FAHS Director of Continuing Medical Education John R. Graham Headache Center Brigham & Women s Hospital Director of Headache Medicine Cambridge Health Alliance Harvard
Lynda J. Krasenbaum, MSN, ANP BC. Associate Director New York Headache Center
 Diagnosing Headache in Adults and Adolescents Lynda J. Krasenbaum, MSN, ANP BC Associate Director New York Headache Center New York, New York Learning Objectives Understand the diagnostic challenges of
Diagnosing Headache in Adults and Adolescents Lynda J. Krasenbaum, MSN, ANP BC Associate Director New York Headache Center New York, New York Learning Objectives Understand the diagnostic challenges of
PREVALENCE BY HEADACHE TYPE
 CLINICAL CLUES AND CLINICAL RULES: PRIMARY VS SECONDARY HEADACHE * Based on a presentation by David W. Dodick, MD ABSTRACT Headache is a common condition, accounting for many specialist office visits annually.
CLINICAL CLUES AND CLINICAL RULES: PRIMARY VS SECONDARY HEADACHE * Based on a presentation by David W. Dodick, MD ABSTRACT Headache is a common condition, accounting for many specialist office visits annually.
Pause for thought. Dr Jane Anderson Consultant Neurologist
 Pause for thought Dr Jane Anderson Consultant Neurologist Which is the top cause of years lived with disability worldwide? 1. COPD 2. Low Back pain 3. Diabetes 4. Migraine with medication overuse headache
Pause for thought Dr Jane Anderson Consultant Neurologist Which is the top cause of years lived with disability worldwide? 1. COPD 2. Low Back pain 3. Diabetes 4. Migraine with medication overuse headache
Diagnosis of Primary Headache Syndromes. Gerald W. Smetana, M.D. Division of General Medicine Beth Israel Deaconess Medical Center
 Diagnosis of Primary Headache Syndromes Gerald W. Smetana, M.D. Division of General Medicine Beth Israel Deaconess Medical Center Goals Distinguish primary from secondary headaches Recognize typical histories
Diagnosis of Primary Headache Syndromes Gerald W. Smetana, M.D. Division of General Medicine Beth Israel Deaconess Medical Center Goals Distinguish primary from secondary headaches Recognize typical histories
Do you suffer from Headaches? - November/Dec 2011
 Do you suffer from Headaches? - November/Dec 2011 Inside this month's issue Headaches Acute single headaches Recurring Headaches: Migraine What causes Migraine? Treatments for migraine & prevention Headaches
Do you suffer from Headaches? - November/Dec 2011 Inside this month's issue Headaches Acute single headaches Recurring Headaches: Migraine What causes Migraine? Treatments for migraine & prevention Headaches
How do we treat migraine? New SIGN Guidelines
 How do we treat migraine? New SIGN Guidelines Managing your migraine Migraine Trust, Edinburgh 2018 Callum Duncan Consultant Neurologist Aberdeen Royal Infirmary Chair SIGN Guideline 155 Premonitory Mood
How do we treat migraine? New SIGN Guidelines Managing your migraine Migraine Trust, Edinburgh 2018 Callum Duncan Consultant Neurologist Aberdeen Royal Infirmary Chair SIGN Guideline 155 Premonitory Mood
Chronic Migraine in Primary Care. December 11 th, 2017 Werner J. Becker University of Calgary
 Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
Chronic Migraine in Primary Care December 11 th, 2017 Werner J. Becker University of Calgary Disclosures Faculty: Werner J. Becker Relationships with commercial interests: Grants/Research Support: Clinical
ADVANCES IN MIGRAINE MANAGEMENT
 ADVANCES IN MIGRAINE MANAGEMENT Joanna Girard Katzman, M.D.MSPH Assistant Professor, Dept. of Neurology Project ECHO, Chronic Pain Program University of New Mexico Outline Migraine throughout the decades
ADVANCES IN MIGRAINE MANAGEMENT Joanna Girard Katzman, M.D.MSPH Assistant Professor, Dept. of Neurology Project ECHO, Chronic Pain Program University of New Mexico Outline Migraine throughout the decades
11/10/2017. THE BRIDGE Course Objectives. THE BRIDGE Course Objectives
 THE BRIDGE Course Objectives Describe clinical characteristics associated with migraine diagnosis in adult and pediatric populations. Identify barriers and risk factors impacting the clinical course of
THE BRIDGE Course Objectives Describe clinical characteristics associated with migraine diagnosis in adult and pediatric populations. Identify barriers and risk factors impacting the clinical course of
Headache. Luke Bennetto Consultant Neurologist Engineers House 13 th September 2016
 Headache Luke Bennetto Consultant Neurologist Engineers House 13 th September 2016 Contents General thoughts Primary headache Secondary headache I want to curl up in a cave and die I want to drill a
Headache Luke Bennetto Consultant Neurologist Engineers House 13 th September 2016 Contents General thoughts Primary headache Secondary headache I want to curl up in a cave and die I want to drill a
Case Presentation. Case Presentation. Case Presentation. Truths about Headaches (2017) Most headaches were muscle-tension headaches
 Agenda Case presentation Migraine Morphology Primary and Premonitory Phase Secondary Headache Aura Headache Primer on Pain Medication Overuse Headache Case Presentation RT is a 25 year old woman with daily
Agenda Case presentation Migraine Morphology Primary and Premonitory Phase Secondary Headache Aura Headache Primer on Pain Medication Overuse Headache Case Presentation RT is a 25 year old woman with daily
Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert
 Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert Childhood headache: Is it really difficult to manage? It shouldn t be... But it can be...
Ishaq Abu Arafeh Consultant Paediatrician Royal Hospital for Children, Glasgow Forth Valley Royal Hospital, Larbert Childhood headache: Is it really difficult to manage? It shouldn t be... But it can be...
Back Pain. John W. Engstrom, MD December 15, Disclosures. A Primary Care Approach to Headache. Headache Goals
 Disclosures Nothing to declare --- or --- Significant ownership interests Consulting, speaker bureaus, honorarium, grants Link to Harrison s Chapter on Headache: http://ucsfneuroresidency.com/public_html/educati
Disclosures Nothing to declare --- or --- Significant ownership interests Consulting, speaker bureaus, honorarium, grants Link to Harrison s Chapter on Headache: http://ucsfneuroresidency.com/public_html/educati
Chapter 2 Diagnosis of Trigeminal Autonomic Cephalalgias
 Chapter 2 Diagnosis of Trigeminal Autonomic Cephalalgias Mark J. Stillman Introduction The trigeminal autonomic cephalalgias (TACs) refer to a specific group of primary headaches characterized by unilaterality,
Chapter 2 Diagnosis of Trigeminal Autonomic Cephalalgias Mark J. Stillman Introduction The trigeminal autonomic cephalalgias (TACs) refer to a specific group of primary headaches characterized by unilaterality,
Adult with headache. Problem-specific video guides to diagnosing patients and helping them with management and prevention
 Adult with headache Problem-specific video guides to diagnosing patients and helping them with management and prevention London Strategic Clinical Networks London Neuroscience Strategic Clinical Network
Adult with headache Problem-specific video guides to diagnosing patients and helping them with management and prevention London Strategic Clinical Networks London Neuroscience Strategic Clinical Network
July 2012 Target Population. Adult patients 18 years or older in primary care settings.
 Guideline for Primary Care Management of Headache in Adults July 2012 Target Population Adult patients 18 years or older in primary care settings. Exclusions: This guideline does not provide recommendations
Guideline for Primary Care Management of Headache in Adults July 2012 Target Population Adult patients 18 years or older in primary care settings. Exclusions: This guideline does not provide recommendations
Atypical presentations of cluster headache
 Blackwell Science, LtdOxford, UKCHACephalalgia0333-1024Blackwell Science, 200222Original ArticleAtypical presentations in cluster headachetd Rozen Atypical presentations of cluster headache TD Rozen Department
Blackwell Science, LtdOxford, UKCHACephalalgia0333-1024Blackwell Science, 200222Original ArticleAtypical presentations in cluster headachetd Rozen Atypical presentations of cluster headache TD Rozen Department
UCNS Course A Review of ICHD-3b
 UCNS Course A Review of ICHD-3b Andrew D. Hershey, M.D., Ph.D., FAHS Endowed Chair and Director of Neurology Director, Cincinnati Children s Headache Center Professor of Neurology and Pediatrics University
UCNS Course A Review of ICHD-3b Andrew D. Hershey, M.D., Ph.D., FAHS Endowed Chair and Director of Neurology Director, Cincinnati Children s Headache Center Professor of Neurology and Pediatrics University
Controlling Migraine Pain
 Migraine Stats Controlling Migraine Pain Alan Zacharias, M.D. Associated Neurologists, Boulder Community Health 303-622-3365 Women 15% Men 5% Usually starts in 2 nd and 3 rd Decade Major Impact on days
Migraine Stats Controlling Migraine Pain Alan Zacharias, M.D. Associated Neurologists, Boulder Community Health 303-622-3365 Women 15% Men 5% Usually starts in 2 nd and 3 rd Decade Major Impact on days
Update on Diagnosis and Management of Migraines
 Update on Diagnosis and Management of Migraines Joel J. Heidelbaugh, MD, FAAFP, FACG Clinical Professor Departments of Family Medicine and Urology University of Michigan Learning Objectives To distinguish
Update on Diagnosis and Management of Migraines Joel J. Heidelbaugh, MD, FAAFP, FACG Clinical Professor Departments of Family Medicine and Urology University of Michigan Learning Objectives To distinguish
Headaches in Pregnancy Before, During, and After
 Headaches in Pregnancy Before, During, and After Robert Kaniecki, MD Director, UPMC Headache Center Assistant Professor of Neurology University of Pittsburgh Headaches and Pregnancy Pre-pregnancy counseling
Headaches in Pregnancy Before, During, and After Robert Kaniecki, MD Director, UPMC Headache Center Assistant Professor of Neurology University of Pittsburgh Headaches and Pregnancy Pre-pregnancy counseling
Clinical case. Clinical case 3/15/2018 OVERVIEW. Refractory headaches and update on novel treatment. Refractory headache.
 OVERVIEW Refractory headaches and update on novel treatment Definition of refractory headache Treatment approach Medications Neuromodulation In the pipeline Juliette Preston, MD OHSU Headache Center Refractory
OVERVIEW Refractory headaches and update on novel treatment Definition of refractory headache Treatment approach Medications Neuromodulation In the pipeline Juliette Preston, MD OHSU Headache Center Refractory
HEADACHES AND MIGRAINES
 HEADACHES AND MIGRAINES CONTENT CREATED BY Learn more at www.health.harvard.edu TALK WITH YOUR DOCTOR Table of Contents Whether this is your first visit or a follow-up, answer these questions for your
HEADACHES AND MIGRAINES CONTENT CREATED BY Learn more at www.health.harvard.edu TALK WITH YOUR DOCTOR Table of Contents Whether this is your first visit or a follow-up, answer these questions for your
Headaches. Mini Medical School. November 10, A. Laine Green MSc, MD FRCP(C) Assistant Professor Department of Medicine (Neurology)
 Headaches. Mini Medical School. November 10, 2016 A. Laine Green MSc, MD FRCP(C) Assistant Professor Department of Medicine (Neurology) Artist Agnes Cecile Disclosures I have received an honorarium from
Headaches. Mini Medical School. November 10, 2016 A. Laine Green MSc, MD FRCP(C) Assistant Professor Department of Medicine (Neurology) Artist Agnes Cecile Disclosures I have received an honorarium from
The trigeminal autonomic cephalalgias (TACs) are a group of. Cluster Headache and Other Trigeminal Autonomic Cephalalgias By Mark Burish, MD, PhD
 Downloaded from https://journals.lww.com/continuum by SruuCyaLiGD/095xRqJ2PzgDYuM98ZB494KP9rwScvIkQrYai2aioRZDTyulujJ/fqPksscQKqke3QAnIva1ZqwEKekuwNqyUWcnSLnClNQLfnPrUdnEcDXOJLeG3sr/HuiNevTSNcdMFp1i4FoTX9EXYGXm/fCfrbTavvQSUHUH4eazE11ptLzgCyEpzDoF
Downloaded from https://journals.lww.com/continuum by SruuCyaLiGD/095xRqJ2PzgDYuM98ZB494KP9rwScvIkQrYai2aioRZDTyulujJ/fqPksscQKqke3QAnIva1ZqwEKekuwNqyUWcnSLnClNQLfnPrUdnEcDXOJLeG3sr/HuiNevTSNcdMFp1i4FoTX9EXYGXm/fCfrbTavvQSUHUH4eazE11ptLzgCyEpzDoF
Headaches in the Pediatric Emergency Dept
 Headaches in Children February 23, 2011 Jinny Tavee, MD Associate Professor Neuromuscular Center Cleveland Clinic Foundation Cleveland, OH 1 Headaches in the Pediatric Emergency Dept Burton Gutierrez Kan
Headaches in Children February 23, 2011 Jinny Tavee, MD Associate Professor Neuromuscular Center Cleveland Clinic Foundation Cleveland, OH 1 Headaches in the Pediatric Emergency Dept Burton Gutierrez Kan
OH, MY ACHING HEAD! I HAVE NO DISCLOSURES OR CONFLICTS OF INTERESTS TO DECLARE MANAGING HEADACHE IN THE OUTPATIENT SETTING SECONDARY HEADACHES
 1 JUSTIN A. OSSMAN, MD CHATTANOOGA FAMILY MEDICINE UPDATE OH, MY ACHING HEAD! MANAGING HEADACHE IN THE OUTPATIENT SETTING 2 I HAVE NO DISCLOSURES OR CONFLICTS OF INTERESTS TO DECLARE OBJECTIVES International
1 JUSTIN A. OSSMAN, MD CHATTANOOGA FAMILY MEDICINE UPDATE OH, MY ACHING HEAD! MANAGING HEADACHE IN THE OUTPATIENT SETTING 2 I HAVE NO DISCLOSURES OR CONFLICTS OF INTERESTS TO DECLARE OBJECTIVES International
Goals. Primary Headache Syndromes. One-Year Prevalence of Common Headache Disorders
 Goals One-Year Prevalence of Common Headache Disorders Impact of primary headache syndromes Non pharmacologic Rx of migraine individualized to patient triggers Complementary and alternative Rx of migraine
Goals One-Year Prevalence of Common Headache Disorders Impact of primary headache syndromes Non pharmacologic Rx of migraine individualized to patient triggers Complementary and alternative Rx of migraine
PAEDIATRIC ACUTE CARE GUIDELINE. Headache. This document should be read in conjunction with this DISCLAIMER
 Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
Princess Margaret Hospital for Children PAEDIATRIC ACUTE CARE GUIDELINE Scope (Staff): Scope (Area): All Emergency Department Clinicians Emergency Department This document should be read in conjunction
HEADACHE: Prevalence and Impact
 Mod 2 Headaches HEADACHE: Prevalence and Impact PREVALENCE 18-25 % women have headaches 6-10 % men have headaches 5% of women have headaches more than 15 days per month 112 million bedridden days per year
Mod 2 Headaches HEADACHE: Prevalence and Impact PREVALENCE 18-25 % women have headaches 6-10 % men have headaches 5% of women have headaches more than 15 days per month 112 million bedridden days per year
Migraine Management. Jane Melling Headache nurse Mater Misericordiae Hospital
 Migraine Management Jane Melling Headache nurse Mater Misericordiae Hospital Migraine facts Among the most common disorders of the nervous system 3 rd most prevalent medical disorder on the planet (lancet
Migraine Management Jane Melling Headache nurse Mater Misericordiae Hospital Migraine facts Among the most common disorders of the nervous system 3 rd most prevalent medical disorder on the planet (lancet
Current Migraine Treatment Therapy. Daniel Kassicieh, DO, FAAN
 Current Migraine Treatment Therapy Daniel Kassicieh, DO, FAAN Migraine a Disease Process Migraines are a chronic disease process similar to many other chronic medical conditions Migraine has a low mortality
Current Migraine Treatment Therapy Daniel Kassicieh, DO, FAAN Migraine a Disease Process Migraines are a chronic disease process similar to many other chronic medical conditions Migraine has a low mortality
Managing Headache in Acute Medicine. Ben Lovell Consultant Physician in Acute Medicine University College London Hospital
 Managing Headache in Acute Medicine Ben Lovell Consultant Physician in Acute Medicine University College London Hospital Some ED headache stats Arrive by ambulance 31% Median age 39 Worst ever headache
Managing Headache in Acute Medicine Ben Lovell Consultant Physician in Acute Medicine University College London Hospital Some ED headache stats Arrive by ambulance 31% Median age 39 Worst ever headache
Çiçek Wöber-Bingöl HEADACHE UNIT FOR CHILDREN AND ADOLESCENCE
 Headache in children and adolescents Çiçek Wöber-Bingöl HEADACHE UNIT FOR CHILDREN AND ADOLESCENCE Dept. of Psychiatry of Childhood and Adolescence Medical University of Vienna, Vienna, Austria Impact
Headache in children and adolescents Çiçek Wöber-Bingöl HEADACHE UNIT FOR CHILDREN AND ADOLESCENCE Dept. of Psychiatry of Childhood and Adolescence Medical University of Vienna, Vienna, Austria Impact
ONZETRA XSAIL (sumatriptan) nasal powder
 ONZETRA XSAIL (sumatriptan) nasal powder Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
ONZETRA XSAIL (sumatriptan) nasal powder Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Pharmacy
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, II. Management of Refractory Headaches
 Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
Headache Master School Japan-Osaka 2016 (HMSJ-Osaka2016) October 23, 2016 II. Management of Refractory Headaches Case presentation 1: A case of intractable daily-persistent headache Keio University School
Treatment of Primary Headache Syndromes
 Presenter Disclosure Information 2:45 3:45pm Treatment of Primary Headache Syndromes SPEAKER Gerald W. Smetana, MD The following relationships exist related to this presentation: Gerald W.Smetana, MD,
Presenter Disclosure Information 2:45 3:45pm Treatment of Primary Headache Syndromes SPEAKER Gerald W. Smetana, MD The following relationships exist related to this presentation: Gerald W.Smetana, MD,
1. On how many days in the last 3 months did you miss work or school because of your headaches?
 The Migraine Disability Assessment Test The MIDAS (Migraine Disability Assessment) questionnaire was put together to help you measure the impact your headaches have on your life. The information on this
The Migraine Disability Assessment Test The MIDAS (Migraine Disability Assessment) questionnaire was put together to help you measure the impact your headaches have on your life. The information on this
HEADACHE. Primary vs Secondary Headaches SNOOP4. Classification of Primary Headaches. Novel Approaches to Diagnosis and Treatment.
 HEADACHE Novel Approaches to Diagnosis and Treatment Primary vs Secondary Headaches SNOOP4 S - systemic signs and symptoms (fever, weight loss) or secondary risk factors (HIV, cancer) N - neurological
HEADACHE Novel Approaches to Diagnosis and Treatment Primary vs Secondary Headaches SNOOP4 S - systemic signs and symptoms (fever, weight loss) or secondary risk factors (HIV, cancer) N - neurological
Pediatric Grand Rounds UT Health San Antonio 2/10/2017
 Jose Luis Aceves, M.D. has no relationships with commercial companies to disclose. Jose Luis Aceves, M.D. Clinical Associate Professor Department of Pediatrics at UTHSCSA At the end of this presentation
Jose Luis Aceves, M.D. has no relationships with commercial companies to disclose. Jose Luis Aceves, M.D. Clinical Associate Professor Department of Pediatrics at UTHSCSA At the end of this presentation
Headache Why headaches hurt When to see a doctor Diagnosing your headache
 Headache Why headaches hurt Information about touch, pain, temperature, and vibration in the head and neck is sent to the brain by the trigeminal nerve, one of 12 pairs of cranial nerves that start at
Headache Why headaches hurt Information about touch, pain, temperature, and vibration in the head and neck is sent to the brain by the trigeminal nerve, one of 12 pairs of cranial nerves that start at
Neuralgias tend to be sudden, brief, intermittent severe, stabbing or lightning pains or electric shock sensations.
 Neuralgia is the term used to describe pain arising from a nerve. There are many different neuralgias which have been described in the medical literature, but I will only touch upon a few more common ones.
Neuralgia is the term used to describe pain arising from a nerve. There are many different neuralgias which have been described in the medical literature, but I will only touch upon a few more common ones.
Paediatric headaches. Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services. Brevity, levity, repetition
 Paediatric headaches Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services Brevity, levity, repetition Paediatric)headache?)! Headache!in!children!is!not!that!common.!The!question!is!which!headaches!do!I!
Paediatric headaches Dr Jaycen Cruickshank Director of Clinical Training Ballarat Health Services Brevity, levity, repetition Paediatric)headache?)! Headache!in!children!is!not!that!common.!The!question!is!which!headaches!do!I!
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: occipital_nerve_stimulation 8/2010 5/2017 5/2018 5/2017 Description of Procedure or Service Occipital nerve
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: occipital_nerve_stimulation 8/2010 5/2017 5/2018 5/2017 Description of Procedure or Service Occipital nerve
11. HEADACHE 1. Pablo Lapuerta, MD, Steven Asch, MD, MPH, and Kenneth Clark, MD, MPH
 11. HEADACHE 1 Pablo Lapuerta, MD, Steven Asch, MD, MPH, and Kenneth Clark, MD, MPH We identified articles on the evaluation and management of headache by conducting a MEDLINE search of English language
11. HEADACHE 1 Pablo Lapuerta, MD, Steven Asch, MD, MPH, and Kenneth Clark, MD, MPH We identified articles on the evaluation and management of headache by conducting a MEDLINE search of English language
Understanding. Migraine. Amy, diagnosed in 1989, with her family.
 Understanding Migraine Amy, diagnosed in 1989, with her family. What Is a Migraine? A migraine is a recurring moderate to severe headache. The pain usually occurs on one side of the head. It is typically
Understanding Migraine Amy, diagnosed in 1989, with her family. What Is a Migraine? A migraine is a recurring moderate to severe headache. The pain usually occurs on one side of the head. It is typically
MIGRAINE ASSOCIATION OF IRELAND
 MIGRAINE ASSOCIATION OF IRELAND HEADACHE IN MEN: THE FACTS This leaflet was composed by Paolo Rossi M.D., Ph.D. of the European Headache Alliance to mark European Migraine Day of Action 2014. Why a leaflet
MIGRAINE ASSOCIATION OF IRELAND HEADACHE IN MEN: THE FACTS This leaflet was composed by Paolo Rossi M.D., Ph.D. of the European Headache Alliance to mark European Migraine Day of Action 2014. Why a leaflet
Common Headaches. Types and Natural Treatments
 Common Headaches Types and Natural Treatments by Heidi Fritz, MA, ND Bolton Naturopathic Clinic 64 King St W, Bolton, Ontario, L7E1C7 www.boltonnaturopathic.ca Three Common Types of Headaches Headaches
Common Headaches Types and Natural Treatments by Heidi Fritz, MA, ND Bolton Naturopathic Clinic 64 King St W, Bolton, Ontario, L7E1C7 www.boltonnaturopathic.ca Three Common Types of Headaches Headaches
Migraine Clinical Guideline
 Migraine Clinical Guideline Definition: Migraine refers to a chronic neurological disorder characterized by episodic attacks often in association with enhanced sensitivity of the nervous system and activation
Migraine Clinical Guideline Definition: Migraine refers to a chronic neurological disorder characterized by episodic attacks often in association with enhanced sensitivity of the nervous system and activation
MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache
 MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache Measure Description Percentage of patients age 18 years old and older with a diagnosis of primary headache
MEASURE #4: Overuse of Barbiturate Containing Medications for Primary Headache Disorders Headache Measure Description Percentage of patients age 18 years old and older with a diagnosis of primary headache
Diagnosing headache. The clinician should approach the diagnosis of. Secondary headache. Primary headache. Blue and red flag headaches
 Headache THEME Diagnosing headache BACKGROUND A systematic approach to the diagnosis of primary and secondary headache disorders requires the measurement of the frequency and the duration of headache.
Headache THEME Diagnosing headache BACKGROUND A systematic approach to the diagnosis of primary and secondary headache disorders requires the measurement of the frequency and the duration of headache.
CHRONIC HEADACHES IN CHILDHOOD
 CHRONIC HEADACHES IN CHILDHOOD EDWIN LIU, MD PEDIATRIC NEUROLOGISTS OF PALM BEACH PEDIATRIC SLEEP CENTERS OF FLORIDA ASSISTANT CLINICAL PROFESSOR FSU ASSISTANT CLINICAL PROFESSOR NOVA SOUTHEASTERN PEDIATRIC
CHRONIC HEADACHES IN CHILDHOOD EDWIN LIU, MD PEDIATRIC NEUROLOGISTS OF PALM BEACH PEDIATRIC SLEEP CENTERS OF FLORIDA ASSISTANT CLINICAL PROFESSOR FSU ASSISTANT CLINICAL PROFESSOR NOVA SOUTHEASTERN PEDIATRIC
Headache Management in Primary Care Dr Niranjanan Nirmalananthan Consultant Neurologist
 Headache Management in Primary Care Dr Niranjanan Nirmalananthan Consultant Neurologist Wednesday 10 th of April 2019 Summary Why does it matter? Classification and diagnosis Who to refer / scan? Serious
Headache Management in Primary Care Dr Niranjanan Nirmalananthan Consultant Neurologist Wednesday 10 th of April 2019 Summary Why does it matter? Classification and diagnosis Who to refer / scan? Serious
Managing Headache in General Practice 2nd Edition
 1 Managing Headache in General Practice 2nd Edition Dr Raeburn Forbes Consultant Neurologist November 2012 Email: elaine.johnston@southerntrust.hscni.net Department of Neurology Craigavon Area Hospital
1 Managing Headache in General Practice 2nd Edition Dr Raeburn Forbes Consultant Neurologist November 2012 Email: elaine.johnston@southerntrust.hscni.net Department of Neurology Craigavon Area Hospital
