Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis
|
|
|
- Jasmine Edwards
- 5 years ago
- Views:
Transcription
1 Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis Ralph Metson, MD; Richard E. Gliklich, MD ORIGINAL ARTICLE Objective: To determine the efficacy of endoscopic surgery for chronic frontal sinusitis. Design: A prospective analysis of established measures of clinical outcome (Chronic Sinusitis Survey and Short Form 36) that was administered to patients before frontal sinus surgery and at intervals of 3 months, 6 months, and 1 year after surgery. Interventions: For limited disease, the frontal recess was opened and the frontal ostium probed or enlarged. For more severe cases, a drill was used to resect the frontal sinus floor and interfrontal septum. Setting: Private and institutional-based practices at an academic medical center. Subjects: Eighty-seven patients who underwent endoscopic surgery for frontal sinusitis, including 24 patients with severe disease who underwent a frontal sinus drillout procedure. Main Outcome Measures: Scores on the Chronic Sinusitis Survey, Short Form 36, and surgical revision rate. Results: Significant improvement in facial pain, nasal drainage, and congestion was observed 1 year after surgery (P.01). Medication use was also significantly reduced during this period (P.01). Quality-of-life measures showed greatest improvement in the domain of social functioning (P.05). Three (12.5%) of 24 patients who underwent a frontal sinus drillout procedure did not respond to surgery secondary to restenosis of the frontal ostium. Conclusions: Although the long-term results of endoscopic surgery for frontal sinusitis are unknown, this approach appears to be effective for most patients and may provide a reasonable alternative to frontal sinus obliteration surgery in selected cases. Arch Otolaryngol Head Neck Surg. 1998;124: From the Department of Otology and Laryngology, Harvard Medical School, Boston, Mass. THE EXTERNAL frontoethmoidectomy described by Lynch 1 in the 1920s and the osteoplastic flap frontal sinus obliteration procedure popularized by Montgomery 2 in the 1960s have been the mainstay of surgical treatment for patients with chronic frontal sinusitis. Since the introduction of endoscopic instrumentation for sinus surgery in the 1980s, a variety of intranasal approaches to the frontal sinus have been described 3-7 that avoid much of the morbidity associated with traditional procedures, including an external incision. Although these endoscopic techniques allow for direct visualization and manipulation within the frontal recess, their efficacy for treatment of more advanced disease remains limited. For severe cases of frontal sinusitis, Draf 8 described an intranasal approach that used a microscope and drill to remove the frontal sinus floor, as well as the superior nasal septum and interfrontal septum. Close et al 9 and Gross et al 10 described a similar technique for treatment of patients with advanced disease, using endoscopic instrumentation to create a large aperture between the frontal sinuses and nasal cavity. This frontal sinus drillout procedure has been compared with that of Lothrop, 11 who in 1914 described a combined external and intranasal approach to resect the frontal sinus floor and septum. Despite the growing popularity of endoscopic techniques for the treatment of frontal sinusitis, the effect of such treatment on sinus-specific symptoms and general health remains largely unknown. The purpose of this study was to develop an endoscopic approach to the frontal sinus based on disease severity and to determine the efficacy of this approach through prospective measures of patient-relevant outcome. This article is also available on our Web site:
2 PATIENTS, MATERIALS, AND METHODS PATIENTS Eighty-seven consecutive patients who underwent endoscopic frontal sinus surgery in our department constitute the study population. All patients underwent preoperative head and neck examination, including nasal endoscopy. Computed tomographic (CT) scans of the sinuses were obtained in coronal and axial views following treatment with a minimum of 3 weeks of antibiotic therapy. These scans were classified as stage 0 through IV according to a CT rating system that has been used previously and demonstrated to be statistically reliable. 12 The following information describes the CT staging system for chronic rhinosinusitis: Stage 0 Less than 2 mm of mucosal thickening on any sinus wall Stage I Unilateral disease or anatomical abnormality Stage II Bilateral ethmoid and/or maxillary sinus disease Stage III Bilateral disease with sphenoid and/or frontal sinus involvement Stage IV Pansinus disease Surgical indications for endoscopic frontal sinusotomy include CT evidence of frontal rhinosinusitis (opacification, air-fluid level, mucocele, or mucosal thickening 2 mm) or recurrent frontal headaches in the presence of radiological or endoscopic evidence of paranasal sinus disease. Sixty-three patients who underwent consecutive endoscopic frontal sinus surgeries in our department between August 1993 and May 1995 were followed up in a prospective fashion. They were administered a rhinosinusitis-specific questionnaire, the Chronic Sinusitis Survey (CSS), 13 and a general health survey, the Short Form 36 (SF- 36), 14 prior to surgery and at 3-, 6-, and 12-month postoperative intervals. Seven patients were lost to follow-up at 6 months and 10 patients at 1 year. The CSS is a 6-item questionnaire that measures 2 areas of patient-relevant outcome: symptoms and medication use. Patients were questioned about the duration of facial pain or headache, postnasal drainage or rhinorrhea, and nasal obstruction or congestion over the preceding 8 weeks. Use of antibiotics, nasal sprays, and other sinus medications were quantified for the same period. The CSS has been studied in populations with chronic rhinosinusitis and shown to have a good reliability and sensitivity to longitudinal clinical change. 13 The SF-36 is a 36-item questionnaire that is divided into 8 subscales of general health: physical functioning, role functioning physical, bodily pain, general health, vitality, social functioning, role functioning emotional, and mental health. The reliability of SF-36 scale scores has been well established. 14 Permission to use the SF-36 form was obtained from the Medical Outcomes Study Trust, Boston, Mass. Scores were tabulated according to published algorithms and normalized to a scale ranging from 0 (worst) to 100 (best). Analysis was performed using the Student t test for comparison of means. Correlations reported reflect Spearman rank correlation statistic. All P values are 2-tailed. A separate analysis was performed on the group of 24 patients who underwent endoscopic drillout of the frontal sinus floor in our department between March 1995 and November Four of these patients had isolated frontal sinus mucoceles with bony expansion into the orbit and displacement of the globe. The other 20 patients presented with frontal sinus opacification or air-fluid levels following previous sinus surgery. Fifteen patients underwent unilateral frontal sinus drillouts, commonly referred to as Draf 2 procedures. 8 The remainder underwent bilateral drillouts using a transseptal technique, similar to the Draf 3 procedure and modified Lothrop procedures. 8,10 All surgeries were performed with patients receiving general anesthesia. SURGICAL TECHNIQUE The endoscopic technique used to treat frontal sinusitis depended on disease severity. In those patients with disease limited to the frontal recess, an anterior ethmoidectomy was performed and obstructing tissue removed from the recess with an angled Blakesley forceps. The frontal ostium was probed in an atraumatic manner with a ball-tipped probe or curved suction cannula to verify patency. Care was taken not to remove normal mucosa or injure tissue at the perimeter of the ostium, since doing so could lead to postoperative adhesion formation with ostial obstruction. When probing within the frontal recess region, sometimes a large supraorbital ethmoid cell was initially mistaken for the frontal sinus. The ostium leading to the supraorbital ethmoid cell was commonly encountered in a posterior and lateral aspect of the frontal recess, whereas the frontal sinus ostium was typically found in a more anterior and medial location. In those patients with more advanced disease, the frontal recess was widely opened with a Hajek forceps using the previously described technique. 5 This maneuver allowed for direct visualization within the recess. Obstructing tissue was cleared from the frontal recess and the ostium was visualized and probed. If the ostium was found to be stenotic (would not allow passage of a 2-mm probe), it was enlarged with a curved frontal sinus curette in an anterior direction to a diameter of approximately 5 mm. In the most severe cases, including frontal sinus mucoceles or frontal sinus opacification following previous surgery with extensive adhesion formation, the ostium was enlarged to at least 10 mm in diameter with a frontal sinus drillout procedure. FRONTAL SINUS DRILLOUT An initial attempt was made to identify the frontal sinus ostium using gentle palpation just behind the anterior attachment of the middle turbinate with a 1-mm ball-tipped probe (Figure 1). Care was taken not to apply excessive force on the probe that could cause inadvertent penetration of the skull base. When the sinus was entered, the probe dropped into an air-containing cavity of the same approximate size and configuration noted on CT scan. It was not uncommon for a large supraorbital ethmoid cell to be initially mistaken for the frontal sinus. The ostium leading to the supraorbital ethmoid cell was usually situated in the posterolateral frontal recess, whereas the frontal sinus ostium was found in a more anteromedial location. Continued on next page 1091
3 Once the frontal ostium was located, a mediumcutting burr on a long-handled drill was used to widely open the frontal recess by removing bone anterior to the ostium. Any agger nasi cells present were cleared. If the anterior portion of the middle turbinate had not been resected during previous surgery, it was removed, and its anterior attachment to the lateral nasal wall was taken down. After the ostium was exposed and directly visualized, it was enlarged by bone removal along its anterior rim (Figure 2). Care was taken not to drill or injure mucous membrane along the posterior rim of the ostium, since doing so could promote circumferential scar formation. All further drilling was done anterior and superior to the ostium, which serves as a landmark for the posterior limit of resection. Even if the ostium was not identified earlier in the procedure, the inferior aspect of the frontal sinus would eventually be encountered with careful drilling in this location. Any bone removal done prior to identification of the frontal ostium is potentially hazardous because of the proximity of the skull base and should be attempted only by experienced endoscopic surgeons. Nevertheless, so long as bone removal proceeds anterior and superior to the approximate location of the ostium within the frontal recess, penetration of the intracranial cavity remains remote. With excessive bone removal in this location, the surgeon encounters skin of the supraorbital region, rather than spinal fluid. Once the ostium has been adequately enlarged, the interior of the frontal sinus can be visualized with a 30 endoscope that is used for the remainder of the procedure. Removal of the bony sinus floor continues in a lateral direction toward the orbit. The lacrimal bone serves as the lateral limit of resection. The lacrimal sac location can often be verified by movement along the orbital wall seen with palpation over the medial canthal region. With bone removal in a medial direction, the intersinus septum is encountered. If only a unilateral frontal sinus drillout is to be performed, this septum serves as the medial limit of dissection. If a bilateral drillout is to be performed, the intersinus septum is drilled and the contralateral sinus openedthrough a transseptal approach. Visualization and access for bone removal of the frontal sinus floor are greatly facilitated using a transseptal technique that allows for passage of the endoscope and drill through opposite sides of the nose (Figure 3). This technique can be used for both unilateral and bilateral procedures, depending on the amount of bone to be removed. For unilateral drillout, a limited septal defect may be created with a vertical full-thickness incision through septal mucosa and cartilage. When a bilateral drillout is performed, an approximately 2-cm perforation is created with removal of fullthickness septal mucosa and bone where the superior septum attaches to the floor of the frontal sinus (Figure 4). The inferior aspect of the intersinus septum is removed with the drill to create a common opening between both sides of the frontal sinus. The bony floor of the contralateral frontal sinus is then removed by continued enlargement of this medial opening created at the intersinus septum. Alternatively, the frontal ostium can be located and the sinus enlarged from a lateral to medial direction as was done for the initial side. The sinus opening can be further enlarged with bone removal in an anterior direction. The limits of anterior resection depend on the thickness of the anterior flap of bone and the angulation of the drill handle. At the conclusion of surgery, a large common opening should connect both sides of the frontal sinus to each other and the nasal cavity (Figure 5 and Figure 6). Frontal Sinus Probe in Frontal Ostium Nasal Septum Enlarged Frontal Ostium Middle Turbinate Remnant Opened Frontal Recess Anterior Ethmoid Artery Figure 1. Frontal sinus drillout procedure: view of the right nasal cavity after the anterior wall of the frontal recess has been removed and agger nasi cells opened. The frontal sinus ostium is located with gentle palpation along the roof of the frontal recess with a ball-tipped probe. Note the second ostium located just posterior and lateral to the frontal ostium. This opening drains a supraorbital ethmoid cell that can be easily mistaken for a small frontal sinus. The true frontal ostium is usually found in an anterior and medial location within the recess. Figure 2. Once the frontal sinus ostium has been visualized, it is enlarged in an anterior direction with a medium-cutting burr on a long-handled drill. Care is taken not to damage mucosa along the posterior rim of the ostium. For unilateral drillout, bone of the frontal sinus floor is removed in a lateral direction to the orbital wall and in a medial direction to the interfrontal septum. 1092
4 Right Frontal Sinus Interfrontal Septum Enlarged Frontal Ostium Lacrimal Bone Nasal Septum Limited Septectomy Defect Figure 3. Bilateral frontal sinus drillout procedure is performed with a transseptal technique. Resection of the adjacent superior nasal septum enhances surgical access by allowing for passage of the endoscope and drill through opposite sides of the nose. A portion of the interfrontal septum is also resected, and the contralateral frontal sinus is opened. Thick bone overhanging the anterior rim is also drilled. At the completion of the procedure, a large opening connects the frontal sinuses and nasal cavity. RESULTS Among the 63 patients followed up prospectively, there were 25 women and 38 men, with an average age of 46.1 years (age range, years). Fifteen patients (23.8%) had at least 1 comorbidity. Hypertension was most common and was present in 7 patients (11.1%). Sinus CT findings resulted in classification of 35 patients (55.6%) as having stage III and 28 patients (44.4%) as having stage IV disease according to the rating system described earlier. Facial pain and headache were the most commonly reported symptoms, occurring in 100% of patients, followed by nasal congestion in 88.9% and drainage in 85.7%. Pain had been present for the maximum measured duration of 8 consecutive weeks in 28.6% of patients. During this same period, 61.9% of patients had taken at least 1 course of antibiotic treatment, and 71.4% had used nasal corticosteroid sprays. The CSS scores were tabulated using algorithms that normalize results on a scale from 0 to 100, with 100 the best possible score. 13 Preoperative CSS total scores of 46.4 ± 19.5 (mean ± SD) rose to 62.2 ± 18.9 one year following surgery (P.01), as shown in Figure 7. Symptom subscores improved from 36.7 ± 29.2 to 50.1 ± 20.3 (P.01). Similar improvements were observed in patients reports of pain, congestion, and drainage. Medication subscores rose from 55.7 ± 25.9 to 70.6 ± 27.8 during this period (P.01). Comparison of the SF-36 general health survey subscale scores before and 6 months after surgery demonstrated a significant improvement in 4 domains (P.05). The largest improvement was a 13.8% increase in the vitality score, which increased from 57.1 ± 23.8 to 65.0 ± Figure 4. Sagittal view of nasal cavity demonstrates the enlarged frontal sinus opening and septectomy defect present at the completion of surgery. The anterior aspect of the middle turbinate has been resected (dashed line) Other improvements were observed for general health (68.8 ± 20.3 to 71.1 ± 23.0), mental health (75.0 ± 18.9 to 79.2 ± 18.6), and social functioning scores (78.2 ± 27.3 to 85.8 ± 21.9). No significant differences were identified between scores at the 3- and 6-month postoperative testings. One year after surgery, similar improvements were observed for these domains (Table 1), but not all changes remained significant because of a decrease in sample size. Only the social functioning score continued to show a significant improvement (P.05). Figure 8 compares these changes in general health with reported normal values for the general population. 14 Among the group of patients who underwent the frontal sinus drillout procedure, 24 were retrospectively analyzed; there were 18 females and 6 males, with a mean age of 42.7 years (age range, years). Frontal headache was the most common presenting complaint. Four patients with isolated frontal sinus mucoceles expanding into the orbit were classified as having CT stage I disease (Table 2). The other patients demonstrated either frontal sinus opacification without bony expansion (62%) or air-fluid level (21%). Intraoperative frontal sinus cultures were positive for organisms in 8 of 15 patients for whom specimens were sent. Bacteria isolated included Staphylococcus aureus (n = 5), Staphylococcus epidermidis (n = 2), Streptococcus pneumoniae (n = 1), Klebsiella pneumoniae (n = 1), Enterobacter asburia (n = 1), and Alcaligenes xylosoxi (n = 1). A unilateral frontal sinus drillout procedure was performed in 63% of patients. The remainder underwent a bilateral procedure using a transseptal technique. There were no intraoperative complications. All patients were 1093
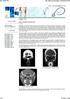
5 Figure 5. Computed tomographic scans of the sinus both before (left) and after (right) surgery demonstrate successful eradication of frontal sinusitis following a bilateral drillout procedure. Figure 6. View with 30 endoscope looking up into the frontal sinuses 6 weeks after a bilateral drillout procedure. discharged within 24 hours of surgery. As an expected result of the surgery, a permanent superior septal perforation occurred in the 9 patients who underwent the bilateral drillout procedure. The only morbidity associated with this perforation was increased crust formation, requiring more intensive postoperative cleaning and follow-up. Patients who underwent unilateral frontal sinusotomy required no more than 2 visits for crust removal, whereas those who underwent the transseptal bilateral drillout procedure typically required crust removal on a weekly basis for up to 1 month following surgery. Postoperative follow-up ranged from 12 to 32 months, with a mean of 22.7 months. Although most patients obtained postoperative relief from their frontal discomfort, 3 patients (12.5%) were considered surgical failures and required frontal sinus obliteration with abdominal fat to relieve their headaches. Each of these patients had undergone a unilateral drillout procedure. They all developed recurrent frontal headaches within 6 weeks of their procedure, and a repeated CT scan demonstrated persistent frontal sinus opacification. A bilateral drillout technique could have been performed as an alternative to obliteration surgery in these cases; however, we chose to proceed directly to the obliterative procedure because of its known longterm success rate. The first surgical failure involved a 44-year-old man who had undergone 2 previous endoscopic sinus surgeries, as well as an external trephination for chronic frontal sinusitis. Because of persistent headaches and left frontal sinus opacification shown on a CT scan, he was referred for a left frontal sinus drillout procedure. Intraoperative cultures grew S epidermidis. His headaches recurred within 1 month of surgery, and a repeated CT scan showed persistent sinus opacification, prompting frontal sinus obliteration surgery. The second patient who did not respond to the frontal drillout procedure was a 45-year-old woman who was referred for persistent frontal headaches following 2 endoscopic sinus surgeries. Her first procedure was an endoscopic ethmoidectomy; the second was a left endoscopic frontal sinusotomy. Because preoperative cultures had grown Pseudomonas aeruginosa, she received 3 weeks of intravenous antibiotic therapy at home following her left frontal sinus drillout procedure. Frontal headaches returned, and she underwent obliteration surgery 7 months following the drillout procedure. The most rapid failure involved a 41-year-old woman who had undergone a left external frontoethmoidectomy (Lynch procedure) 3 years earlier. Three weeks after unilateral frontal sinus drillout, she reported a recurrence of her preoperative headaches that did not resolve with antibiotic therapy. Absence of lateral bony support from previous surgery was thought to be a contributing factor to soft tissue collapse and early failure. Subsequent patients who have presented with frontal sinus opacification following a unilateral Lynch procedure have been treated with a bilateral drillout technique to decrease the likelihood of a similar occurrence. Those pa- 1094
6 80 Before Surgery After Surgery Before Surgery After Surgery Normative Worst Best Symptom Medication Total Best Worst PF RP BP VT GH RE MH SF Subscales Figure 7. Mean scores for Chronic Sinusitis Survey demonstrate significant improvement in symptoms of pain, congestion, and drainage 1 year after endoscopic frontal sinus surgery. Medication use was also significantly reduced. Figure 8. Mean scores for Short Form 36 survey 14 show effect of frontal sinus surgery on domains of general health compared with published normative values. PF indicates physical functioning; RP, role functioning physical; BP, bodily pain; VT, vitality; GH, general health; RE, role functioning emotional; MH, mental health; and SF, social functioning. Table 1. Data Before and 1 Year After Endoscopic Surgery for Frontal Sinusitis* Short Form 36 Subscales Before Surgery After Surgery Physical functioning 90.1 ± ± 14.6 Role functioning physical 68.9 ± ± 35.6 Bodily pain 52.4 ± ± 19.1 Vitality 57.5 ± ± 21.9 General health 70.7 ± ± 21.2 Role functioning emotional 87.3 ± ± 23.2 Mental health 76.5 ± ± 16.1 Social functioning 81.7 ± ± 14.7 *All data are presented as mean ± SD scores. P.05. tients who have presented with disease following bilateral Lynch procedures have proceeded directly to obliteration surgery. COMMENT Table 2. Clinical Data for 24 Patients Who Underwent Endoscopic Frontal Sinus Drillout Procedure* Characteristics No. (%) Mean age, y 42.7 Sex Male 6 (25) Female 18 (75) CT stage I 4 (17) III 15 (62) IV 5 (21) CT findings Air-fluid level 5 (21) Opacification 15 (62) Mucocele with bony expansion 4 (17) Previous sinus surgeries 0 4 (17) 1 6 (25) 2 9 (37) 3 5 (21) Drillout technique Unilateral (left/right) 4/11 (17/46) Bilateral 9 (37) Ancillary procedures Septoplasty 17 (70) Maxillary antrostomy 6 (25) Sphenoidotomy 3 (12) *CT indicates computed tomographic. See the Patients, Materials, and Methods section for an explanation of the staging system. Surgical intervention for frontal sinusitis is indicated in patients unresponsive to medical therapy. In this study, endoscopic surgery for frontal rhinosinusitis resulted in significant improvement in both sinusitis-specific and general health status. The CSS symptom scores improved 37% 1 year after surgery. The CSS medication scores improved by 25%, indicating a significant reduction in the use of medications following surgery. These improvements are less than those previously reported for surgery of the ethmoid, maxillary, and sphenoid sinuses, 15,16 confirming clinical suspicion that disease of the frontal sinus is more refractory to therapy than that of the other paranasal sinuses. Nevertheless, the improvements seen in this cohort of patients with frontal sinusitis are both statistically and clinically significant (P.05). Quality-of-life measures demonstrated improvement in the domains of vitality, general health, mental health, and social functioning following surgery. However, compared with normative population data, patients with frontal sinusitis following surgery continue to report more bodily pain and fatigue than the general US population. This finding indicates that frontal sinusitis is a chronic disease that is ameliorated but often not cured with endoscopic intervention. Furthermore, these results demonstrate the importance of evaluating both disease-specific symptoms and general health measures when studying treatment outcomes for this disease. The endoscopic approach we used to treat frontal sinusitis was based on disease severity. When obstructing tissue was restricted to the frontal recess, surgery was limited to clearing the recess and probing the frontal ostium to ensure patency. When disease extended to within the ostium or sinus, the frontal recess was opened and the ostium inspected with direct visualization to clear obstructing tissue. If the ostium was found to be stenotic, it was enlarged with a curette in an anterior direction. 1095
7 In the most severe cases, patients with expanding mucoceles and those who were not helped with previous frontal sinus surgery, a frontal sinus drillout procedure was performed. A modification of the Draf and endoscopic Lothrop procedures 8,9,17 used a transseptal approach to remove the floor of the frontal sinuses and provide a wide aperture for intranasal drainage. In contrast to the technique of Close et al, 9 the middle turbinates were resected to allow for wide lateral exposure with incorporation of the natural frontal ostia into the surgical opening. When disease was limited to 1 side, a unilateral drillout was performed. This procedure used a vertical incision in the nasal septum to allow for passage of instruments through both sides of the nasal cavity without compromising the integrity of the septum. When a bilateral procedure was performed, a superior septectomy facilitated access to the frontal sinus floor and interfrontal septum. The resultant septal perforation resulted in increased crust formation during the immediate postoperative period, but no associated long-term sequelae were noted. The failure rate of 12.5% found for frontal sinus drillout will undoubtedly increase with longer patient followup. It is interesting to note that all 3 drillout failures occurred in patients who underwent unilateral procedures. This finding may reflect the smaller sinusotomy aperture created with a unilateral approach. A bilateral drillout procedure creates a surgical opening that is twice the size and may be less susceptible to postoperative closure. Becker et al 18 reported no ostial closure in 14 patients who underwent bilateral frontal drillout with a mean follow-up of 9 months; however, frontal headaches recurred in 2 patients (14.3%). Close et al 9 reported symptoms of recurrent rhinosinusitis in 1 of 7 patients who underwent frontal sinus drillout who had been followed up for at least 3 months for a similar short-term failure rate of 14.3%. One of the patients developed a cerebrospinal fluid leak that was repaired intraoperatively. Unlike external approaches to reestablish frontal sinus drainage, endoscopic surgery creates an enlarged ostium that is bounded on all sides by bone. Thus, soft tissue collapse with reobstruction of nasofrontal drainage, a common cause of recurrent rhinosinusitis following Lynch frontoethmoidectomy, is avoided. 3 In this series, the earliest failure occurred in a patient who had undergone a previous Lynch procedure. Frontal headaches with sinus opacification recurred within 1 month of drillout. In a report of 12 patients who underwent removal of the frontal sinus floor, superior nasal septum, and interfrontal septum with an operating microscope, Draf 8 described his only complication as postoperative mucocele formation in patients who had undergone prior surgery on the frontal sinus through an external approach. It appears that patients who have undergone previous external procedures may be at increased risk for recurrent frontal sinusitis following an endoscopic drillout procedure. We now favor a bilateral drillout technique to ensure the largest surgical opening possible in all patients who present with frontal sinusitis following a Lynch procedure, even those with unilateral disease. Patients who have not responded to bilateral Lynch procedures proceed directly to frontal sinus obliteration surgery. The 4 patients in this series who presented with isolated frontal sinus mucoceles were all successfully treated with the unilateral drillout procedure. This procedure appears to offer a satisfactory alternative to frontal sinus obliteration surgery for such patients. In the case of revision surgery, the frontal sinus drillout procedure also appears to provide a safe alternative to external procedures. With a short-term success rate of more than 80%, the drillout technique provides most patients with immediate symptomatic relief. However, this success rate will undoubtedly decrease with longer patient followup. Additional studies are needed to determine the longterm efficacy of this procedure. For those patients who develop recurrent disease, frontal sinus obliteration remains a viable treatment option. Accepted for publication May 21, Reprints: Ralph Metson, MD, Zero Emerson Place, Boston, MA REFERENCES 1. Lynch RC. The technique of a radical frontal sinus operation which has given me the best results. Laryngoscope. 1921;31: Montgomery WW. Osteoplastic frontal sinus operation: coronal incision. Ann Otol Rhinol Laryngol. 1965;74: Perko D. Endoscopic surgery of the frontal sinus without external approach. Rhinology. 1989;27: Schaefer SD, Close LG. Endoscopic management of frontal sinus disease. Laryngoscope. 1990;100: Loury MC. Endoscopic frontal recess and frontal sinus ostium dissection. Laryngoscope. 1993;103: Wigand M, Hoseman W. Endoscopic surgery for frontal sinusitis and its complications. Am J Rhinol. 1991;73: Metson R. Endoscopic treatment of frontal sinusitis. Laryngoscope. 1992;102: Draf W. Endonasal micro-endoscopic frontal sinus surgery: the Fulda concept. Op Tech Otolaryngol Head Neck Surg. 1991;2: Close LG, Lee NK, Leach JL, Manning SC. Endoscopic resection of the intranasal frontal sinus floor. Ann Otol Rhinol Laryngol. 1994;103: Gross WE, Gross CW, Becker D, Moore D, Phillips D. Modified transnasal endoscopic Lothrop procedure as an alternative to frontal sinus obliteration. Otolaryngol Head Neck Surg. 1995;113: Lothrop HA. Frontal sinus suppuration. Ann Surg. 1914;59: Metson R, Gliklich RE, Stankiewicz JA, et al. A comparison of sinus computerized tomography staging systems. Otolaryngol Head Neck Surg. 1997;117: Gliklich RE, Metson R. Techniques for outcomes research in chronic sinusitis. Laryngoscope. 1995;105: Ware JE, ed. The SF-36 Health Survey Manual and Interpretation Guide. Boston, Mass: Nimrod Press; Gliklich RE, Metson R. The effect of sinus surgery on quality of life. Otolaryngol Head Neck Surg. 1997;117: Metson R, Gliklich RE. Endoscopic treatment of sphenoid sinusitis. Otolaryngol Head Neck Surg. 1996;114: Gross CW, Gross WE, Becker DG. Modified transnasal endoscopic Lothrop procedure: frontal drillout. Op Tech Otolaryngol Head Neck Surg. 1995;6: Becker DG, Moore D, Lindsey WH, Gross WE, Gross CW. Modified transnasal endoscopic Lothrop procedure: further considerations. Laryngoscope. 1995; 105:
Frontal Sinus Drillout (Modified Lothrop Procedure): Long-Term Results in 204 Patients
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Frontal Sinus Drillout (Modified Lothrop Procedure): Long-Term Results in 204 Patients Jonathan Y. Ting,
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Frontal Sinus Drillout (Modified Lothrop Procedure): Long-Term Results in 204 Patients Jonathan Y. Ting,
ORIGINAL ARTICLE. Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the Anterior Ethmoid
 Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the nterior Ethmoid Long-term Results ORIGINL RTICLE Toru Kikawada, MD; Masao Fujigaki, MD; Mikino
Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the nterior Ethmoid Long-term Results ORIGINL RTICLE Toru Kikawada, MD; Masao Fujigaki, MD; Mikino
Frontal sinus disease continues to be one of the great
 Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Endoscopic Management Of A Giant Ethmoid Mucocele
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
REVISION ENDOSCOPIC FRONTAL SINUSOTOMY WITH MUCOPERIOSTEAL FLAP ADVANCEMENT
 CURRENT CONCEPTS IN THE SURGICAL MANAGEMENT OF FRONTAL SINUS DISEASE 00304665/01 $15.00 +.OO REVISION ENDOSCOPIC FRONTAL SINUSOTOMY WITH MUCOPERIOSTEAL FLAP ADVANCEMENT The Frontal Sinus Rescue Procedure
CURRENT CONCEPTS IN THE SURGICAL MANAGEMENT OF FRONTAL SINUS DISEASE 00304665/01 $15.00 +.OO REVISION ENDOSCOPIC FRONTAL SINUSOTOMY WITH MUCOPERIOSTEAL FLAP ADVANCEMENT The Frontal Sinus Rescue Procedure
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013
 FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
ORIGINAL ARTICLE. Computed Tomographic Staging and the Fate of the Dependent Sinuses in Revision Endoscopic Sinus Surgery
 Computed Tomographic Staging and the Fate of the Dependent es in Revision Endoscopic Surgery Neil Bhattacharyya, MD ORIGINAL ARTICLE Objectives: To determine the patterns of disease recurrence in chronic
Computed Tomographic Staging and the Fate of the Dependent es in Revision Endoscopic Surgery Neil Bhattacharyya, MD ORIGINAL ARTICLE Objectives: To determine the patterns of disease recurrence in chronic
Functional Endoscopic Sinus Surgery
 WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
Chronic Frontal Rhinosinusitis: Diagnosis and Management
 Chapter Chronic Frontal Rhinosinusitis: Diagnosis and Management Core Messages Despite significant advances in surgical techniques, technology, and knowledge of pathophysiology, management of chronic frontal
Chapter Chronic Frontal Rhinosinusitis: Diagnosis and Management Core Messages Despite significant advances in surgical techniques, technology, and knowledge of pathophysiology, management of chronic frontal
Radiological anatomy of frontal sinus By drtbalu
 2009 Radiological anatomy of frontal sinus By drtbalu Anatomy of frontal sinus is highly variable. Precise understanding of these variables will help a surgeon to avoid unnecessary complications during
2009 Radiological anatomy of frontal sinus By drtbalu Anatomy of frontal sinus is highly variable. Precise understanding of these variables will help a surgeon to avoid unnecessary complications during
Anatomical Analysis of the Frontal Recess Cells in Endoscopic Sinus Surgery An Indian Perspective
 ORIGINAL ARTICLE Anatomical Analysis of the Frontal Recess Cells in Endoscopic Sinus Surgery An Indian Perspective 1 Dhingra Shruti, 2 Agarwal AK, 3 Passey JC, 4 Kaul JM 1 Resident, Department of Otolaryngology
ORIGINAL ARTICLE Anatomical Analysis of the Frontal Recess Cells in Endoscopic Sinus Surgery An Indian Perspective 1 Dhingra Shruti, 2 Agarwal AK, 3 Passey JC, 4 Kaul JM 1 Resident, Department of Otolaryngology
The surgical approach to the sphenoid sinus continues to
 A comparison of two sphenoidotomy approaches using a novel computerized tomography grading system Heitham Gheriani, F.R.C.S.C., F.R.C.S.I., David Flamer, B.Sc., Trent Orton, M.D., Brad Mechor, F.R.C.S.C.,
A comparison of two sphenoidotomy approaches using a novel computerized tomography grading system Heitham Gheriani, F.R.C.S.C., F.R.C.S.I., David Flamer, B.Sc., Trent Orton, M.D., Brad Mechor, F.R.C.S.C.,
Reasons for Failure and Surgical Revisions. Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology
 Reasons for Failure and Surgical Revisions Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology Medical College of Georgia of Georgia Regents University Department of Otolaryngology / Head
Reasons for Failure and Surgical Revisions Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology Medical College of Georgia of Georgia Regents University Department of Otolaryngology / Head
Surgical Risk Factors for Recurrence of Inverted Papilloma
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Surgical Risk Factors for Recurrence of Inverted Papilloma David Y. Healy Jr., MD, CDR, MC, USN; Nipun Chhabra,
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Surgical Risk Factors for Recurrence of Inverted Papilloma David Y. Healy Jr., MD, CDR, MC, USN; Nipun Chhabra,
Imaging Anatomy in Revision Sinus Surgery
 Chapter 1 Imaging Anatomy in Revision Sinus Surgery Ramon E. Figueroa 1 Core Messages An intimate knowledge of sinus anatomy and a clear understanding of the baseline postsurgical anatomy are required
Chapter 1 Imaging Anatomy in Revision Sinus Surgery Ramon E. Figueroa 1 Core Messages An intimate knowledge of sinus anatomy and a clear understanding of the baseline postsurgical anatomy are required
A Computer-Assisted Anatomical Study of the Nasofrontal Region
 The Laryngoscope Lippincott Williams & Wilkins, Inc., Philadelphia 2001 The American Laryngological, Rhinological and Otological Society, Inc. A Computer-Assisted Anatomical Study of the Nasofrontal Region
The Laryngoscope Lippincott Williams & Wilkins, Inc., Philadelphia 2001 The American Laryngological, Rhinological and Otological Society, Inc. A Computer-Assisted Anatomical Study of the Nasofrontal Region
Mucocele of paranasal sinuses
 From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
Sphenoid rhinosinusitis associated with abducens nerve palsy Case report
 Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
A Targeted Endoscopic Approach to Chronic Isolated Frontal Sinusitis
 Otolaryngology Head and Neck Surgery (2006) 134, 28-32 ORIGINAL RESEARCH A Targeted Endoscopic Approach to Chronic Isolated Frontal Sinusitis Roee Landsberg, MD, Yoram Segev, MD, Michael Friedman, MD,
Otolaryngology Head and Neck Surgery (2006) 134, 28-32 ORIGINAL RESEARCH A Targeted Endoscopic Approach to Chronic Isolated Frontal Sinusitis Roee Landsberg, MD, Yoram Segev, MD, Michael Friedman, MD,
Study of success rates in endoscopic dacryocystorhinostomy with and without stenting. dacryocystorhinostomy with and
 Original Research Article Study of success rates in endoscopic dacryocystorhinostomy with and without stenting Kirti Ambani 1, Niraj Suri 2, Hiren Parmar 3* 1 Assistant Professor, ENT Department, GMERS
Original Research Article Study of success rates in endoscopic dacryocystorhinostomy with and without stenting Kirti Ambani 1, Niraj Suri 2, Hiren Parmar 3* 1 Assistant Professor, ENT Department, GMERS
The advent of high-resolution computerized tomography
 An anatomic classification of the ethmoidal bulla REUBEN C. SETLIFF, III, MD, PETER J. CATALANO, MD, FACS, LISA A. CATALANO, MPH, and CHAD FRANCIS, BA, Sioux Falls, South Dakota, and Burlington, Massachusetts
An anatomic classification of the ethmoidal bulla REUBEN C. SETLIFF, III, MD, PETER J. CATALANO, MD, FACS, LISA A. CATALANO, MPH, and CHAD FRANCIS, BA, Sioux Falls, South Dakota, and Burlington, Massachusetts
Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities
 10.5005/jp-journals-10013-1141 H Verma et al ORIGINAL ARTICLE Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities H Verma, Rijuneeta, AK Gupta, A Chakrabarti
10.5005/jp-journals-10013-1141 H Verma et al ORIGINAL ARTICLE Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities H Verma, Rijuneeta, AK Gupta, A Chakrabarti
COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY
 COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY John M. DelGaudio, MD Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology-Head and Neck Surgery Emory University School
COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY John M. DelGaudio, MD Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology-Head and Neck Surgery Emory University School
Conventional Sinus Surgery Vs Fess
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
1. BRIEF DESCRIPTION OF TRAINING
 RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
Boundaries Septum Turbinates & Meati Lamellae Drainage Pathways Variants
 The Fastest 20 Minutes in Michelle A. Michel, MD Professor of Radiology and Otolaryngology Medical College of Wisconsin, Milwaukee Overview Nasal cavity Anterior skull base Ostiomeatal complex Frontal
The Fastest 20 Minutes in Michelle A. Michel, MD Professor of Radiology and Otolaryngology Medical College of Wisconsin, Milwaukee Overview Nasal cavity Anterior skull base Ostiomeatal complex Frontal
Intranasal location of lacrimal sac in Thai cadavers
 Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
The Outside-In Approach to the Modified Endoscopic Lothrop Procedure
 The Laryngoscope VC 2012 The American Laryngological, Rhinological and Otological Society, Inc. The Outside-In Approach to the Modified Endoscopic Lothrop Procedure David Chin, MBBS; Kornkiat Snidvongs,
The Laryngoscope VC 2012 The American Laryngological, Rhinological and Otological Society, Inc. The Outside-In Approach to the Modified Endoscopic Lothrop Procedure David Chin, MBBS; Kornkiat Snidvongs,
Fracture frontal bone and its management
 From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K.
 05 Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K. Gananathan Introduction...75 General Principles...76 Tips and Tricks in Ventral
05 Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K. Gananathan Introduction...75 General Principles...76 Tips and Tricks in Ventral
Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision
 THIEME Original Research 73 Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision Jan Alessandro Socher 1 Jonas Mello 2 Barbara Batista Baltha 2 1 Department of Otorhinolaryngology,
THIEME Original Research 73 Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision Jan Alessandro Socher 1 Jonas Mello 2 Barbara Batista Baltha 2 1 Department of Otorhinolaryngology,
PROBLEM RECOMMENDATION
 PREVENTION (MINIMIZING) IN ENDOSCOPIC Steven D. Schaefer, MD Professor and Chair Department of Otolaryngology PREVENTION AND Intraoperative Hemorrhage Loss of Orientation Inability to Identify/Preserve
PREVENTION (MINIMIZING) IN ENDOSCOPIC Steven D. Schaefer, MD Professor and Chair Department of Otolaryngology PREVENTION AND Intraoperative Hemorrhage Loss of Orientation Inability to Identify/Preserve
History of Frontal Sinus Surgery
 Chapter History of Frontal Sinus Surgery Core Messages With over two centuries of scientific description of frontal sinus surgery, the optimal procedure remains unclear Balancing concerns of eradication
Chapter History of Frontal Sinus Surgery Core Messages With over two centuries of scientific description of frontal sinus surgery, the optimal procedure remains unclear Balancing concerns of eradication
Extended Draf IIb Procedures in the Treatment of Frontal Sinus Pathology
 Original rticle linical and Experimental Otorhinolaryngology Vol. 8, No. 1: 34-38, March 2015 http://dx.doi.org/10.3342/ceo.2015.8.1.34 pissn 1976-8710 eissn 2005-0720 Extended raf IIb Procedures in the
Original rticle linical and Experimental Otorhinolaryngology Vol. 8, No. 1: 34-38, March 2015 http://dx.doi.org/10.3342/ceo.2015.8.1.34 pissn 1976-8710 eissn 2005-0720 Extended raf IIb Procedures in the
ISSN X (Print) Research Article. *Corresponding author Dr.V. Krishna Chaitanya
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(1G):508-513 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(1G):508-513 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
ORIGINAL ARTICLE. Toru Kikawada, MD; Takeo Nonoda, MD; Mariko Matsumoto, MD; Mikino Kikura, MD; Keiko Kikawada, MD
 ORIGINAL ARTILE Treatment of Intractable iseased Tissue in the Maxillary Sinus After Endoscopic Sinus Surgery With High-Pressure Water Jet and Preservation of the Periosteum Toru Kikawada, M; Takeo Nonoda,
ORIGINAL ARTILE Treatment of Intractable iseased Tissue in the Maxillary Sinus After Endoscopic Sinus Surgery With High-Pressure Water Jet and Preservation of the Periosteum Toru Kikawada, M; Takeo Nonoda,
Frontal Sinus Mucocele After Osteoplastic Flap Surgery: Case Report
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550013 Volume 1, Issue 3 Case Report Frontal Sinus Mucocele After Osteoplastic Flap Surgery: Case Report Peter Catalano, MD * and Michael
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550013 Volume 1, Issue 3 Case Report Frontal Sinus Mucocele After Osteoplastic Flap Surgery: Case Report Peter Catalano, MD * and Michael
Consumer summary. Endoscopic modified Lothrop procedure for the. treatment of chronic frontal sinusitis
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Endoscopic modified Lothrop procedure for the treatment of chronic frontal sinusitis (The report
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Endoscopic modified Lothrop procedure for the treatment of chronic frontal sinusitis (The report
Communication issue - What should the radiologist report before functional endoscopic sinus surgery
 Communication issue - What should the radiologist report before functional endoscopic sinus surgery Poster No.: C-0509 Congress: ECR 2015 Type: Educational Exhibit Authors: A. M. Dobra 1, C. A. Badiu 1,
Communication issue - What should the radiologist report before functional endoscopic sinus surgery Poster No.: C-0509 Congress: ECR 2015 Type: Educational Exhibit Authors: A. M. Dobra 1, C. A. Badiu 1,
Institutional repositories
 PUBLISHED VERSION Khong, Jwu Jin; Malhotra, Raman; Selva-Nayagam, Dinesh Niranjan; Wormald, Peter-John Efficacy of endoscopic sinus surgery for paranasal sinus mucocele including modified endoscopic Lothrop
PUBLISHED VERSION Khong, Jwu Jin; Malhotra, Raman; Selva-Nayagam, Dinesh Niranjan; Wormald, Peter-John Efficacy of endoscopic sinus surgery for paranasal sinus mucocele including modified endoscopic Lothrop
The International Frontal Sinus Anatomy Classification (IFAC) and Classification of the Extent of Endoscopic Frontal...
 See discussions, stats, and author profiles for this publication at: https://www.researchgate.net/publication/298902054 The International Frontal Sinus Anatomy Classification (IFAC) and Classification
See discussions, stats, and author profiles for this publication at: https://www.researchgate.net/publication/298902054 The International Frontal Sinus Anatomy Classification (IFAC) and Classification
Chapter Five. 1 of 8 11/3/2008 2:52 PM.
 1 of 8 11/3/2008 2:52 PM Email : myousefmian@hotmail.com Chapter Five FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
1 of 8 11/3/2008 2:52 PM Email : myousefmian@hotmail.com Chapter Five FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
Endoscopic septoplasty
 Endoscopic septoplasty Claudiu Manea, MD, PhD University of Medicine and Pharmacy Carol Davila, Bucharest, Romania Septal deviation is a common clinical finding in patients reporting nasal obstruction.
Endoscopic septoplasty Claudiu Manea, MD, PhD University of Medicine and Pharmacy Carol Davila, Bucharest, Romania Septal deviation is a common clinical finding in patients reporting nasal obstruction.
Imaging of the Paranasal Sinuses
 14. Sommerschule Imaging of the Paranasal Sinuses Bettlach 24.08.2018 Christoph Schlegel Conventional Radiology NNH-Status: okzipito-frontal: frontal sinus, anterior ethmoid okzipito-nasal : maxillary
14. Sommerschule Imaging of the Paranasal Sinuses Bettlach 24.08.2018 Christoph Schlegel Conventional Radiology NNH-Status: okzipito-frontal: frontal sinus, anterior ethmoid okzipito-nasal : maxillary
JMSCR Vol 05 Issue 09 Page September 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i9.52 Relationship of Agger Nasi Cell and Uncinate
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i9.52 Relationship of Agger Nasi Cell and Uncinate
Anatomical Variants in Frontal Recess Region and their Impact on Frontal Sinus Surgery in Chronic Sinusitis
 American Journal of Health Research 2015; 3(3): 140-145 Published online April 23, 2015 (http://www.sciencepublishinggroup.com/j/ajhr) doi: 10.11648/j.ajhr.20150303.15 ISSN: 2330-8788 (Print); ISSN: 2330-8796
American Journal of Health Research 2015; 3(3): 140-145 Published online April 23, 2015 (http://www.sciencepublishinggroup.com/j/ajhr) doi: 10.11648/j.ajhr.20150303.15 ISSN: 2330-8788 (Print); ISSN: 2330-8796
Transnasal Endoscopic Sinonasal Surgery
 Reda kamel, Cadaveric dissection 1 Transnasal Endoscopic Sinonasal Surgery Cadaver Dissection Guide For Endoscopic Sinus Surgery Cairo University Egypt Reda Kamel Professor of Rhinology Cairo University
Reda kamel, Cadaveric dissection 1 Transnasal Endoscopic Sinonasal Surgery Cadaver Dissection Guide For Endoscopic Sinus Surgery Cairo University Egypt Reda Kamel Professor of Rhinology Cairo University
A comprehensive study on complications of endoscopic sinus surgery
 International Journal of Otorhinolaryngology and Head and Neck Surgery Shyras JAD et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Jul;3(3):472-477 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
International Journal of Otorhinolaryngology and Head and Neck Surgery Shyras JAD et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Jul;3(3):472-477 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
Mucoceles of the paranasal sinus are epithelial lesions
 Rev Bras Otorrinolaringol. V.70, n.6, 850-4, nov./dec. 2004 ARTIGO DE REVISÃO CASE REPORT Frontoethmoidal mucoceles: a case report and literature review Andy de Oliveira Vicente 1, Adriana Gonzaga Chaves
Rev Bras Otorrinolaringol. V.70, n.6, 850-4, nov./dec. 2004 ARTIGO DE REVISÃO CASE REPORT Frontoethmoidal mucoceles: a case report and literature review Andy de Oliveira Vicente 1, Adriana Gonzaga Chaves
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery FACIAL FRACTURES
 Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
ENDOSCOPIC ENDONASAL SURGERY FOR RESECTION OF BENIGN SINONASAL TUMORS: EXPERIENCE WITH 107 PATIENTS
 Arch Iranian Med 2006; 9 (3): 244 249 Original Article ENDOSCOPIC ENDONASAL SURGERY FOR RESECTION OF BENIGN SINONASAL TUMORS: EXPERIENCE WITH 107 PATIENTS Mohammad-Hossein Baradaranfar MD, Payman Dabirmoghaddam
Arch Iranian Med 2006; 9 (3): 244 249 Original Article ENDOSCOPIC ENDONASAL SURGERY FOR RESECTION OF BENIGN SINONASAL TUMORS: EXPERIENCE WITH 107 PATIENTS Mohammad-Hossein Baradaranfar MD, Payman Dabirmoghaddam
Dr.Adel A. Al Ibraheem
 Rhinology Chair Weekly Activity Dr.Adel A. Al Ibraheem www.rhinologychair.org conference@rhinologychair.org Rhinology Chair Introduction: It is important to classify and stage nasal polyposis. ( decide
Rhinology Chair Weekly Activity Dr.Adel A. Al Ibraheem www.rhinologychair.org conference@rhinologychair.org Rhinology Chair Introduction: It is important to classify and stage nasal polyposis. ( decide
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Variation in frontal cells in relation to chronic frontal sinusitis
 International Journal of Current Research in Medical Sciences ISSN: 244-71 P-ISJN: A472-04, E -ISJN: A472-01 www.ijcrims.com Original Research Article Volume, Issue 1-2019 DOI: http://dx.doi.org/10.22192/ijcrms.2019.0.01.00
International Journal of Current Research in Medical Sciences ISSN: 244-71 P-ISJN: A472-04, E -ISJN: A472-01 www.ijcrims.com Original Research Article Volume, Issue 1-2019 DOI: http://dx.doi.org/10.22192/ijcrms.2019.0.01.00
Original Article Comparison of different surgical approaches of functional endoscopic sinus surgery on patients with chronic rhinosinusitis
 Int J Clin Exp Med 2014;7(6):1585-1591 www.ijcem.com /ISSN:1940-5901/IJCEM0000315 Original Article Comparison of different surgical approaches of functional endoscopic sinus surgery on patients with chronic
Int J Clin Exp Med 2014;7(6):1585-1591 www.ijcem.com /ISSN:1940-5901/IJCEM0000315 Original Article Comparison of different surgical approaches of functional endoscopic sinus surgery on patients with chronic
Recalcitrant chronic rhinosinusitis. Difficulties in diagnosis and treatment Videler, W.J.M.
 UvA-DARE (Digital Academic Repository) Recalcitrant chronic rhinosinusitis. Difficulties in diagnosis and treatment Videler, W.J.M. Link to publication Citation for published version (APA): Videler, W.
UvA-DARE (Digital Academic Repository) Recalcitrant chronic rhinosinusitis. Difficulties in diagnosis and treatment Videler, W.J.M. Link to publication Citation for published version (APA): Videler, W.
The Honrubia Technique of Balloon Sinuplasty for the Improvement of Symptoms in Chronic Sinusitis. Patients. Vincent Honrubia MD, FACS
 The Honrubia Technique of Balloon Sinuplasty for the Improvement of Symptoms in Chronic Sinusitis Patients Vincent Honrubia MD, FACS Allyssa Cantu, PA-S Sharon Gelman, MEd, PA-S Rachel Tsai, BS Director,
The Honrubia Technique of Balloon Sinuplasty for the Improvement of Symptoms in Chronic Sinusitis Patients Vincent Honrubia MD, FACS Allyssa Cantu, PA-S Sharon Gelman, MEd, PA-S Rachel Tsai, BS Director,
ORIGINAL ARTICLE RELATIONSHIP OF CONCHA BULLOSA WITH OSTEOMEATAL UNIT BLOCKAGE. TOMOGRAPHIC STUDY IN 200 PATIENTS.
 RELATIONSHIP OF CONCHA BULLOSA WITH OSTEOMEATAL UNIT BLOCKAGE. TOMOGRAPHIC STUDY IN 200 PATIENTS. Shrikrishna B H 1, Jyothi A C 2, Sanjay G 3, Sandeep Samson G 4. 1. Associate Professor, Department of
RELATIONSHIP OF CONCHA BULLOSA WITH OSTEOMEATAL UNIT BLOCKAGE. TOMOGRAPHIC STUDY IN 200 PATIENTS. Shrikrishna B H 1, Jyothi A C 2, Sanjay G 3, Sandeep Samson G 4. 1. Associate Professor, Department of
ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS
 From the SelectedWorks of Balasubramanian Thiagarajan July 1, 2012 ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/51/
From the SelectedWorks of Balasubramanian Thiagarajan July 1, 2012 ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/51/
SINUS SURGERY. Dr Zenia Chow MBBS(hons), FRACS
 SINUS SURGERY Dr Zenia Chow MBBS(hons), FRACS Facial Plastic & Reconstructive Surgeon Otolaryngology, Head and Neck Surgeon ENDOSCOPIC SINUS SURGERY/FESS What are sinuses The sinuses are a connected system
SINUS SURGERY Dr Zenia Chow MBBS(hons), FRACS Facial Plastic & Reconstructive Surgeon Otolaryngology, Head and Neck Surgeon ENDOSCOPIC SINUS SURGERY/FESS What are sinuses The sinuses are a connected system
EVALUATION OF PATIENT'S OUTCOME AFTER ENDOSCOPIC SINUS SURGERY
 Basrah Journal Of Surgery Bas J Surg, September, 16, 2010 EVALUATION OF PATIENT'S OUTCOME AFTER ENDOSCOPIC SINUS SURGERY Hiwa A Abdulkareem MB.ChB, FICMS, CABS(ENT); Teaching Hospital; University of Sulaimania.
Basrah Journal Of Surgery Bas J Surg, September, 16, 2010 EVALUATION OF PATIENT'S OUTCOME AFTER ENDOSCOPIC SINUS SURGERY Hiwa A Abdulkareem MB.ChB, FICMS, CABS(ENT); Teaching Hospital; University of Sulaimania.
Pott s Puffy Tumor. Shahad Almohanna 15/1/2018
 Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
Skull Base Danger Zones in FESS
 Skull Base Danger Zones in FESS Poster No.: C-2278 Congress: ECR 2014 Type: Educational Exhibit Authors: L. Renza Lozada, R. Carreño Gonzalez, G. Quintana Sanchez, 1 2 1 1 1 2 R. E. Figueroa ; Malaga/ES,
Skull Base Danger Zones in FESS Poster No.: C-2278 Congress: ECR 2014 Type: Educational Exhibit Authors: L. Renza Lozada, R. Carreño Gonzalez, G. Quintana Sanchez, 1 2 1 1 1 2 R. E. Figueroa ; Malaga/ES,
This Page Intentionally Left Blank
 This Page Intentionally Left Blank ISBN: 0-8247-0743-5 Marcel Dekker, Inc., and the author make no warranty with regard to the accompanying software, its accuracy, or its suitability for any purpose other
This Page Intentionally Left Blank ISBN: 0-8247-0743-5 Marcel Dekker, Inc., and the author make no warranty with regard to the accompanying software, its accuracy, or its suitability for any purpose other
DIFFICULT-TO-TREAT CHRONIC
 MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
MANAGEMENT STRATEGIES FOR DIFFICULT-TO-TREAT CHRONIC RHINOSINUSITIS DR ZULKEFLI HUSSEIN CONSULTANT EAR NOSE & THROAT SURGEON PANTAI HOSPITAL PENANG DISCLAIMER Nothing to disclose PENANG ISLAND, MALAYSIA
Endoscopic Sinus Surgery in the Pediatric Age Group
 Endoscopic Sinus Surgery in the Pediatric Age Group Scott C. Manning Endoscopic Sinus Surgical Preparation and Technique Surgical Risks Every decision for therapy involves a risk-benefit analysis and a
Endoscopic Sinus Surgery in the Pediatric Age Group Scott C. Manning Endoscopic Sinus Surgical Preparation and Technique Surgical Risks Every decision for therapy involves a risk-benefit analysis and a
Inverted papilloma of the nasal cavity and paranasal sinuses: a study of 20 cases
 Original article: Inverted papilloma of the nasal cavity and paranasal sinuses: a study of 20 cases 1 Dr. Vijay Kumar Kalra, 2 Dr. Samar Pal Singh Yadav, 3 Dr. Swati 1Assistant Professor, 2 Senior Professor
Original article: Inverted papilloma of the nasal cavity and paranasal sinuses: a study of 20 cases 1 Dr. Vijay Kumar Kalra, 2 Dr. Samar Pal Singh Yadav, 3 Dr. Swati 1Assistant Professor, 2 Senior Professor
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE The XprESS Multi-Sinus Dilation System for the treatment of 1 Technology 1.1 Description of the technology The XprESS
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE The XprESS Multi-Sinus Dilation System for the treatment of 1 Technology 1.1 Description of the technology The XprESS
Assessing symptoms of empty nose syndrome in patients following sinonasal and anterior skull base resection
 Research Article Page 1 of 5 Assessing symptoms of empty nose syndrome in patients following sinonasal and anterior skull base resection Joel Hardman 1,2, Julie Ahn 3, Arjuna Nirmalananda 2 1 University
Research Article Page 1 of 5 Assessing symptoms of empty nose syndrome in patients following sinonasal and anterior skull base resection Joel Hardman 1,2, Julie Ahn 3, Arjuna Nirmalananda 2 1 University
Learner Objectives. Overview. Minimally Invasive Sinus Surgery: What is the data for Balloon Catheter Dilation 7/31/2017
 Minimally Invasive Sinus Surgery: What is the data for Balloon Catheter Dilation David M. Poetker, MD Christopher M. Long, MD Rhinology and Sinus Surgery Medical College of Wisconsin Thank you to Susan
Minimally Invasive Sinus Surgery: What is the data for Balloon Catheter Dilation David M. Poetker, MD Christopher M. Long, MD Rhinology and Sinus Surgery Medical College of Wisconsin Thank you to Susan
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study
 Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Nasal region. cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?
 Nasal region skull bones: nasal and frontal processes of maxilla cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?) 1 Nasal cavity Roof
Nasal region skull bones: nasal and frontal processes of maxilla cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?) 1 Nasal cavity Roof
Spheno-Ethmoidectomy
 Diagnostic and Therapeutic Endoscopy, Vol. 5, pp. 1-8 Reprints available directly from the publisher Photocopying permitted by license only (C) 1998 OPA (Overseas Publishers Association) N.V. Published
Diagnostic and Therapeutic Endoscopy, Vol. 5, pp. 1-8 Reprints available directly from the publisher Photocopying permitted by license only (C) 1998 OPA (Overseas Publishers Association) N.V. Published
Surgical Management of Sinusitis (What About Balloons?) Relative Indications for Sinus Surgery in Children
 Surgical Management of Sinusitis (What About Balloons?) Andrew N. Goldberg M.D. Andrew H. Murr M.D. Michael J. Cunningham, M.D. Department of Otolaryngology and Communication Enhancement Children s Hospital
Surgical Management of Sinusitis (What About Balloons?) Andrew N. Goldberg M.D. Andrew H. Murr M.D. Michael J. Cunningham, M.D. Department of Otolaryngology and Communication Enhancement Children s Hospital
Functional Endoscopic Sinus Surgery
 Page 1 of 9 Today News Reference Education Log In Register Functional Endoscopic Sinus Surgery Author: Ankit Patel, MD; Chief Editor: Arlen D Meyers, MD, MBA more... Updated: Apr 30, 2012 Overview Introduction
Page 1 of 9 Today News Reference Education Log In Register Functional Endoscopic Sinus Surgery Author: Ankit Patel, MD; Chief Editor: Arlen D Meyers, MD, MBA more... Updated: Apr 30, 2012 Overview Introduction
Skull Base Volume 12 Month. Patients. Anterior/Midline. Pituitary CSF Leak. Lateral. Craniocervical Junction
 UC SF 2 11/7/2009 Skull Base Surgery in 2009 Ivan El-Sayed MD, FACS Director- Otolaryngology Minimally Invasive Skull Base Surgery Program Department Otolaryngology-Head and Neck Surgery University of
UC SF 2 11/7/2009 Skull Base Surgery in 2009 Ivan El-Sayed MD, FACS Director- Otolaryngology Minimally Invasive Skull Base Surgery Program Department Otolaryngology-Head and Neck Surgery University of
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations
 White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
Anatomical Variations in Osteomeatal Complex among Patients undergoing Functional Endoscopic Sinus Surgery
 V Narendrakumar, V Subramanian Original article 10.5005/jp-journals-10013-1259 Anatomical Variations in Osteomeatal Complex among Patients undergoing Functional Endoscopic Sinus Surgery 1 V Narendrakumar,
V Narendrakumar, V Subramanian Original article 10.5005/jp-journals-10013-1259 Anatomical Variations in Osteomeatal Complex among Patients undergoing Functional Endoscopic Sinus Surgery 1 V Narendrakumar,
Destructive Giant Maxillary Sinus Mucocele: A Case Report
 Destructive Giant Maxillary Sinus Mucocele: A Vahit Mutlu 1, Ozgur Yoruk 1, Ozalkan Ozkan 2 1 Atatürk University Faculty of Medicine, Department of Ears, Nose and Throat, Erzurum, Turkey 2 Erzincan University
Destructive Giant Maxillary Sinus Mucocele: A Vahit Mutlu 1, Ozgur Yoruk 1, Ozalkan Ozkan 2 1 Atatürk University Faculty of Medicine, Department of Ears, Nose and Throat, Erzurum, Turkey 2 Erzincan University
Allergic fungal rhinosinusitis: detection of fungal DNA in sinus aspirate using polymerase chain reaction
 1- Allergic fungal rhinosinusitis: detection of fungal DNA in sinus aspirate using polymerase chain reaction Abstract Objective: This study investigated allergic fungal rhinosinusitis cases, and aimed
1- Allergic fungal rhinosinusitis: detection of fungal DNA in sinus aspirate using polymerase chain reaction Abstract Objective: This study investigated allergic fungal rhinosinusitis cases, and aimed
Canine Fossa Puncture for Severe Maxillary Disease in Unilateral Chronic Sinusitis With Nasal Polyp
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Canine Fossa Puncture for Severe Maxillary Disease in Unilateral Chronic Sinusitis With Nasal Polyp Jang
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Canine Fossa Puncture for Severe Maxillary Disease in Unilateral Chronic Sinusitis With Nasal Polyp Jang
Epidemiology 3002). Epidemiology and Pathophysiology
 Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
By: Abdulrahman A. Al-Humaizi Rhinology Fellow, F2
 20.03.2017 By: Abdulrahman A. Al-Humaizi Rhinology Fellow, F2 Objectives Introduction Materials and methods Results Discussion Literature Review Conclusion Introduction Topical delivery to the paranasal
20.03.2017 By: Abdulrahman A. Al-Humaizi Rhinology Fellow, F2 Objectives Introduction Materials and methods Results Discussion Literature Review Conclusion Introduction Topical delivery to the paranasal
Evaluation With Acoustic Rhinometry of Patients Undergoing Sinonasal Surgery
 ORIGINAL ARTICLE Evaluation With Acoustic Rhinometry of Patients Undergoing Sinonasal Surgery R L A Raja Ahmad, MS (ORL)*, B S Gendeh, MS (ORL)** Department of Otolaryngology-Head & Neck Surgery, Kulliyyah
ORIGINAL ARTICLE Evaluation With Acoustic Rhinometry of Patients Undergoing Sinonasal Surgery R L A Raja Ahmad, MS (ORL)*, B S Gendeh, MS (ORL)** Department of Otolaryngology-Head & Neck Surgery, Kulliyyah
Treatment of Maxillary Sinusitis Using the SinuSys Vent-Os Sinus Dilation System
 WHITE PAPER Treatment of Maxillary Sinusitis Using the SinuSys Vent-Os Sinus Dilation System Jerome Hester, MD Chief Medical Officer SinuSys Corporation Palo Alto, California USA Introduction Establishment
WHITE PAPER Treatment of Maxillary Sinusitis Using the SinuSys Vent-Os Sinus Dilation System Jerome Hester, MD Chief Medical Officer SinuSys Corporation Palo Alto, California USA Introduction Establishment
Endoscopic medial maxillectomy
 Operative Techniques in Otolaryngology (2010) 21, 111-116 Endoscopic medial maxillectomy Kelly Cunningham, MD, Kevin C. Welch, MD From the Department of Otolaryngology - Head and Neck Surgery, Loyola University
Operative Techniques in Otolaryngology (2010) 21, 111-116 Endoscopic medial maxillectomy Kelly Cunningham, MD, Kevin C. Welch, MD From the Department of Otolaryngology - Head and Neck Surgery, Loyola University
MedStar Health considers Septoplasty-Rhinoplasty medically necessary for the following indications:
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.038.MH Septoplasty-Rhinoplasty This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar CareFirst
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.038.MH Septoplasty-Rhinoplasty This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar CareFirst
Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures Alice Z.
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures Alice Z.
7. Results of Endoscopic Sinus Surgery. Overall Assessment and Evaluation Criteria
 7. Results of Endoscopic Sinus Surgery Overall Assessment and Evaluation Criteria If several means of treatment of a group of diseases are available a comparison of the results with respect to several
7. Results of Endoscopic Sinus Surgery Overall Assessment and Evaluation Criteria If several means of treatment of a group of diseases are available a comparison of the results with respect to several
Extranodal Natural Killer/T-Cell Lymphoma Nasal Type: Detection by Computed Tomography Features
 The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. Extranodal Natural Killer/T-Cell Lymphoma Nasal Type: Detection by Computed Tomography Features Yin-Ping
The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. Extranodal Natural Killer/T-Cell Lymphoma Nasal Type: Detection by Computed Tomography Features Yin-Ping
Chapter Six. 1 of 6 11/3/2008 2:21 PM.
 1 of 6 11/3/2008 2:21 PM Email : myousefmian@hotmail.com Chapter Six FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
1 of 6 11/3/2008 2:21 PM Email : myousefmian@hotmail.com Chapter Six FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
Role of Modified Endoscopic Medial Maxillectomy in Persistent Chronic Maxillary Sinusitis
 THIEME Original Research 159 Role of Modified Endoscopic Medial Maxillectomy in Persistent Chronic Maxillary Sinusitis Ponnaiah Thulasidas 1 Venkatraman Vaidyanathan 2 1 Department of Otolaryngology Head
THIEME Original Research 159 Role of Modified Endoscopic Medial Maxillectomy in Persistent Chronic Maxillary Sinusitis Ponnaiah Thulasidas 1 Venkatraman Vaidyanathan 2 1 Department of Otolaryngology Head
ISSN X (Print) B. G Nagara, Nagamangala Taluk, Mandya District, Karnataka, Karnataka, India
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2016; 4(2C):489-493 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2016; 4(2C):489-493 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Traditional open surgery for advanced benign nasal tumours in an era of endoscopy: review of 38 cases.
 Traditional open surgery for advanced benign nasal tumours in an era of endoscopy: review of 38 cases. Akeem O Lasisi* and Aderemi A Adeosun Department of Otorhinolaryngology College of Medicine, University
Traditional open surgery for advanced benign nasal tumours in an era of endoscopy: review of 38 cases. Akeem O Lasisi* and Aderemi A Adeosun Department of Otorhinolaryngology College of Medicine, University
Crista galli sinusitis a radiological impression or a real clinical entity
 Romanian Journal of Rhinology, Vol. 6, No. 23, July - September 2016 ORIGINAL STUDY Crista galli sinusitis a radiological impression or a real clinical entity Claudiu Manea 1,2, Ranko Mladina 3 1 CESITO
Romanian Journal of Rhinology, Vol. 6, No. 23, July - September 2016 ORIGINAL STUDY Crista galli sinusitis a radiological impression or a real clinical entity Claudiu Manea 1,2, Ranko Mladina 3 1 CESITO
See the corresponding editorial in this issue, pp J Neurosurg 116: , 2012
 See the corresponding editorial in this issue, pp 529 530. J Neurosurg 116:531 535, 2012 Cranialization of the frontal sinus the final remedy for refractory chronic frontal sinusitis Clinical article J.
See the corresponding editorial in this issue, pp 529 530. J Neurosurg 116:531 535, 2012 Cranialization of the frontal sinus the final remedy for refractory chronic frontal sinusitis Clinical article J.
CHRONIC RHINOSINUSITIS IN ADULTS
 CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
Incidence of accessory ostia in patients with chronic maxillary sinusitis
 International Journal of Otorhinolaryngology and Head and Neck Surgery Ghosh P et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Mar;4(2):443-447 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original
International Journal of Otorhinolaryngology and Head and Neck Surgery Ghosh P et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Mar;4(2):443-447 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original
ISSN: Volume 4 Issue Role of Modified Endoscopic Medial Maxillectomy in persistent chronic maxillary. sinusitis
 ISSN: 2250-0359 Volume 4 Issue 3 2014 Role of Modified Endoscopic Medial Maxillectomy in persistent chronic maxillary sinusitis Thulasidas P ¹ Venkatraman V ² ¹ Sinus and Nose Hospital, Chennai, India,
ISSN: 2250-0359 Volume 4 Issue 3 2014 Role of Modified Endoscopic Medial Maxillectomy in persistent chronic maxillary sinusitis Thulasidas P ¹ Venkatraman V ² ¹ Sinus and Nose Hospital, Chennai, India,
