Institutional repositories
|
|
|
- Dwain Robertson
- 5 years ago
- Views:
Transcription
1 PUBLISHED VERSION Khong, Jwu Jin; Malhotra, Raman; Selva-Nayagam, Dinesh Niranjan; Wormald, Peter-John Efficacy of endoscopic sinus surgery for paranasal sinus mucocele including modified endoscopic Lothrop procedure for frontal sinus mucocele Journal of Laryngology and Otology, 2004; 118(5): Copyright Royal Society of Medicine Press Limited 2004 Originally Published at: PERMISSIONS Institutional repositories 2.4. The author may post the VoR version of the article (in PDF or HTML form) in the Institutional Repository of the institution in which the author worked at the time the article was first submitted, or (for appropriate journals) in PubMed Central or UK PubMed Central or arxiv, no sooner than one year after first publication of the article in the Journal, subject to file availability and provided the posting includes a prominent statement of the full bibliographical details, a copyright notice in the name of the copyright holder (Cambridge University Press or the sponsoring Society, as appropriate), and a link to the online edition of the Journal at Cambridge Journals Online. 23 April
2 The Journal of Laryngology & Otology May 2004, Vol. 118, pp Ef cacy of endoscopic sinus surgery for paranasal sinus mucocele including modi ed endoscopic Lothrop procedure for frontal sinus mucocele Jwu Jin Khong, M.B.B.S., Raman Malhotra, M.B. Ch.B., F.R.C.Ophth., Dinesh Selva, M.B.B.S., F.R.A.C.S., F.R.A.N.Z.C.O., Peter John Wormald*, M.D. F.R.A.C.S., F.R.C.S., F.C.S. (SA) Abstract This study evaluated the ef cacy of the modi ed endoscopic Lothrop procedure (MELP) for complicated frontal mucoceles and endoscopic marsupialization for other paranasal sinus mucoceles. It was a retrospective, consecutive case review of sinus mucoceles treated endoscopically by a single surgeon over a four-year period ( ). There were 41 mucoceles in 28 patients, including 24 frontal, eight frontoethmoidal, three ethmoidal, ve maxillary and one frontal mucocele. Twenty-one patients underwent the modi ed Lothrop procedure for frontal mucoceles, and seven underwent simple drainage and marsupialization for frontoethmoidal, ethmoidal and maxillary mucoceles. At median follow-up of 16 months, all patients had a patent mucocele opening. Patients treated by drainage and marsupialization did not have any complications or mucocele recurrence. All patients treated by the modi ed endoscopic Lothrop procedure had improvement in symptoms and signs. Four patients had minor complications including epistaxis and adhesions and ve required further surgery. The average hospital in-patient stay was days. Endoscopic techniques, including MELP are effective in the short term for the management of complex and simple paranasal sinus mucoceles. MELP has a useful place in the management of mucoceles with a signi cant bony partition from an adjacent sinus or nasal cavity. It is also indicated when the mucocele is associated with loss of lateral support in the sinus with risk of medial-wall collapse of the orbital contents obstructing drainage. Key words: Mucocele; Frontal sinus; Endoscopy; Surgical Procedures, Operative; Paranasal Sinus Disease Introduction Over the past decade, intranasal drainage and marsupialization of mucoceles using endoscopic sinus surgery has emerged as de nitive management, with minimal morbidity and a low recurrence rate. 1 8 Two clinical situations remain a challenge. The rst is where there is signi cant bony separation between the mucocele and the rest of the sinuses or nasal cavity and the mucocele is not bulging into an adjacent sinus or nasal cavity. After marsupialization a circumferential raw area of bone will remain between the mucocele and the sinus or nasal cavity. Due to the circumferential nature of the injury, the opening tends to stenose and the mucocele may recur. The second problem is when the mucocele erodes the oor and/or posterior wall of the frontal sinus. In this situation the mucocele lining is adherent to the orbital periosteum or the dura. Removal of the lining may be dif cult if obliteration of the mucocele is intended and recurrences may occur. The aim of this paper is to evaluate the ef cacy of endoscopic sinus surgery for performing drainage and marsupialization for paranasal sinus mucocele and the ef cacy of the modi ed endoscopic Lothrop procedure (MELP) for complicated frontal sinus mucoceles that have a signi cant bony separation from the nasal cavity and sinuses, and for those mucoceles that have eroded the bone of the orbit or dura. Materials and methods This was a retrospective, consecutive case series of all paranasal sinus mucoceles undergoing endoscopic sinus surgery at the Department of Surgery- Otolaryngology and Ophthalmology, Adelaide and Flinders Universities, over a four-year period between 1998 and A single surgeon (PJW) performed all surgery. Surgical procedures included endoscopic sinus surgery drainage and marsupialization for From the Oculoplastic and Orbital Unit, Department of Ophthalmology, Royal Adelaide Hospital, University of Adelaide, and the Department of Surgery-Otolaryngology, Head and Neck Surgery*, Adelaide and Flinders Universities, Adelaide, Australia. Accepted for publication: 14 February
3 ef cacy of endoscopic sinus surgery for paranasal sinus mucocele 353 uncomplicated paranasal sinus mucoceles (n = 7) and MELP for complicated frontal sinus mucoceles (n.=.21). Intra-operative image guidance (Landmarx, Medtronic Xomed, Jacksonville, Fl, USA) was used in all the MELP procedures and for two of the endoscopic sinus surgery cases. A mucocele was de ned as an expansion of an existing sinus with associated erosion of septations within the sinus and the walls of the sinus. Only patients who ful lled this criterion were included. Patient pro le data consisted of demographic details, past history of sinus surgery, concurrent naso-laryngopharyngeal comorbidities, the mucocele site and pre-operative ndings on computerized tomography (CT) and in some patients magnetic resonance imaging (MRI). All patients underwent a clinical evaluation. Preand post-operative features including ocular and nasal symptoms were chartered. The initial management and follow-up was also recorded. Outcome measures included change in symptoms and signs, patency of the mucocele opening, mucocele recurrence, complications, additional surgery required and duration of hospital stay. Data were recorded on an Excel spreadsheet. Continuous data were analysed using the t-test and described as mean and standard deviation (mean 6 SD). Results and analysis Twenty-eight patients (17 males and 11 females) with 41 paranasal sinus mucoceles underwent endoscopic sinus surgery. The mean age was (range 15 83) years. The median follow-up was 16 (mean 18, range 1 42) months. Sites included frontal (61 per cent), frontoethmoidal (20 per cent), ethmoidal (seven per cent) and maxillary (12 per cent) sinuses. Eight (29 per cent) of patients had multiple mucoceles. Twenty-one (75 per cent) of cases were managed with MELP while seven (25 per cent) of cases required only endoscopic sinus surgery for the management of their mucoceles. Of the 21 cases that underwent MELP, four required concurrent endoscopic sinus surgery. The technique of MELP is described elsewhere. 9 Patients symptoms and signs were summarized and categorized, according to the procedure they underwent, into the endoscopic sinus surgery and MELP subgroups (Table I). Frontal pain (57.1 per cent), nasal obstruction (57.1 per cent) and rhinorrhoea (42.9 per cent) were the main presenting symptoms in the endoscopic sinus surgery subgroup as compared to frontal pain (71.4 per cent), headache (52.4 per cent), nasal obstruction (38.1 per cent) and posterior nasal drip (38.1 per cent) in the MELP subgroup. Two patients from the endoscopic sinus surgery subgroup and one from the MELP subgroup had a palpable mass on presentation. Medial canthus masses were correlated with the presence of frontoethmoidal mucoceles and gingivobuccal sulcus swelling was associated with a left maxillary mucocele. One case with a frontal mucopyocele presented with progressive reduction of vision to 6/18, ptosis and periorbital swelling as a result of orbital cellulitis complicated by preseptal abscess. His visual acuity returned to 6/6 within two weeks of the MELP procedure. In the endoscopic sinus surgery patient group, none had signi cant separation of their mucoceles from the nasal cavity or the sinuses on imaging. Most patients had extension of the mucocele into the orbit (71 per cent) and nearly half (43 per cent) had globe displacement. Two patients had erosion of the medial orbital wall and the orbital roof. In the MELP patient group, 10 (48 per cent) had orbital extension and eight (38 per cent) had globe displacement. Eleven (52 per cent) patients had a thick bony wall separating the mucocele from the sinuses and the nasal cavity. Two of the frontal sinus mucoceles were located laterally (Figure 1(a)) and two were located superiorly in the frontal sinus. Erosion of the orbital wall and skull base was present in 10 (48 per cent) patients (Figure 1(b) and 1(c)). These included four patients with dehiscence of the posterior table of the frontal sinus, six with orbital roof erosion, two with erosion of the medial orbital wall, one with erosion of the lamina papyracea and three with intracranial extension (Table II). Prior ENT history and co-morbidities are summarized in Table III. Treatment outcome All patients treated by endoscopic sinus surgery alone had a patent sinus ostia. None required additional surgery. One had minor epistaxis after the procedure. Symptoms ESS group (n) n = 7 TABLE I presenting symptoms and signs MELP group (n) n = 21 Signs ESS group (n) n = 7 MELP group (n) n = 21 Diplopia 2 (28.6%) 5 (23.8%) Visual loss 0 (. %) 1 (4.8%) Epiphora 1 (14.3%) 1 (4.8%) Non-axial proptosis 2 (28.6%) 3 (14.3%) Frontal pain 4 (57.1%) 15 (71.4%) Globe displacement 3 (42.9%) 8 (38.1%) Headache 2 (28.6%) 11 (52.4%) Lid swelling 2 (28.6%) 7 (33.3%) Rhinorrhoea 3 (42.9%) 7 (33.3%) Vitreochoroidal fold 0 (. %) 1 (4.8%) Nasal obstruction 4 (57.1%) 8 (38.1%) Palpable mass-medial canthus (2), gingivobuccal sulcus (1) 2 (28.6%) 1 (4.8%) Post nasal drip 2 (28.6%) 8 (38.1%) Subcutaneous air 0 (. %) 1 (4.8%) Anosmia 2 (28.6%) 1 (4.8%) Ptosis 0 (. %) 1 (4.8%)
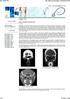
4 354 j. j. khong, r. malhotra, d. selva, p. j. wormald Fig. 1(a) Coronal computerized tomographic image showing bilateral frontal mucoceles. The left frontal mucocele is located laterally and separate from the nasal cavity. In the MELP group, two patients had stenosis of their frontal ostium requiring revision surgery to reestablish a widely patent frontal ostium. These frontal ostia have subsequently remained patent and the patients asymptomatic. One patient needed toileting of the frontal ostium at one month to clear crusts and debris from the marsupialized mucocele ostium. Self-limiting complications were recorded in three cases in the MELP patient group. These were minor epistaxis, adhesions between the middle turbinate and lateral nasal wall and adhesions between the middle turbinate and septum. Nine patients, ( ve from the MELP group and four from the endoscopic sinus surgery group) had incomplete resolution of symptoms. Their nasal symptoms were attributable to ongoing nasal and sinuses pathology including chronic fungal sinusitis and recurrent nasal polyposis. Residual symptoms include headache, rhinorrhoea, nasal obstructions, frontal pain and posterior nasal drip. The median duration of in-patient stay was two (mean , range one to six) days. Twelve patients were managed as day cases and six patients stayed overnight after the procedure. Those that remained as in-patients for longer did so for nonmedical reasons (patients lived too far for immediate out-patient follow up). Fig. 1(b) Coronal image demonstrates bilateral orbital roof destruction and intraorbital extension, which resulted in right lateral globe displacement and left inferior globe displacement. Fig. 1(c) Axial image showing anterior and posterior frontal sinus table destruction and intracranial extension bilaterally. Discussion Mucoceles are expansile masses originating in the sinuses usually presenting with frontal headache, nasal obstruction and eye signs such as globe displacement, diplopia, proptosis, lid swelling, palpable mass and at times reduced vision and ptosis. 10,11 Scarring of the sinus opening is the most common cause for mucocele formation. The frontal and ethmoidal sinuses were the most commonly involved, which re ects the predisposition for their small sinus openings to be damaged during sinus surgery or trauma, or by repeated infections with subsequent obstruction and mucocele formation. Most patients (93 per cent) in our series had prior sinus surgery (86 per cent), chronic sinusitis (79 per cent) or trauma (seven per cent). Endoscopic management of mucoceles protruding into the other sinuses or nasal cavity has been the accepted treatment for years. 1 8 Our results con rm the success of treating uncomplicated mucoceles with standard endoscopic sinus surgery techniques. However, mucoceles presenting with a signi cant bony separation from the other sinuses or nasal cavity are more complex and dif cult to manage. This bony divide needs to be removed by a drill so that a large enough opening is created into the mucocele that will stay patent in the long term. In this series MELP provided short-term successful management of these complex patients. The alternative to drilling away this bone is to approach the mucocele via external incisions, remove its entire lining and obliterate it with fat. A survey of contemporary practices in the United Kingdom showed that while many surgeons routinely performed endoscopic sinus surgery, 54 per cent
5 x x x x ef cacy of endoscopic sinus surgery for paranasal sinus mucocele 355 TABLE II pre-operative imaging ndings CT ndings ESS group (n) n = 7 MELP group (n) n = 21 Intra-orbital extension 5 (71.4%) 10 (47.6%) Globe displacement 3 (42.9%) 8 (38.1%) Separation of mucocele from sinuses and nasal cavity 0 (. %) 11 (52.4%) Erosion of the orbital wall and/or skull base 2 (28.6%) 10 (47.6%) of surgeons would still rely on the external approach for frontal sinus mucocele and pyocele. 12 However, if the mucocele has eroded the orbital roof or skull base and there is extensive apposition of mucocele mucosa on the orbital periosteum or dura, complete removal of the mucosa is very dif cult. If mucosa remains and the sinus is obliterated then recurrence of the mucocele is likely. 7 The follow up of an obliterated sinus can also be unreliable as imaging may not be able to distinguish an obliterated sinus from a recurrent mucocele 1,7 In addition, it has been shown that the mucosa of a mucocele do not lose normal respiratory epithelium 13,14 and follow-up endoscopic examination has also found well-mucosalized cavities after mucocele marsupialization. 4 These ndings suggest that there is no added bene t in attempting to remove the mucocele lining if it is closely applied to either the orbital periosteum or dura. MELP provides the largest possible access to the frontal sinuses 9,15 and allows mucoceles based in the lateral regions of the frontal sinus to be accessed and opened as widely as possible. This wide access improves the potential success rate of maintaining a patent opening into the mucocele. This study showed that MELP was used successfully to open 11 mucoceles separated from the nasal cavity and sinuses and 10 mucoceles with signi cant erosion of either the orbital roof or skull base. Two patients required revisions due to mucocele recurrences but all currently have patent ostia. While the authors acknowledge that the follow-up period is still relatively short, MELP has proved to be a reliable alternative for the management of dif cult and complex mucoceles of the frontal sinuses. MELP has a useful place in the management of mucoceles This paper evaluates the outcome from a modified endoscopic Lothrop procedure for frontal sinus and marsupialization for other paranasal sinus mucoceles in 28 patients At 16 months follow up all patients had adequate drainage of their mucoceles Four patients, all of whom had Lothrop procedures, had minor complications The paper concludes that endoscopic procedures for paranasal sinus mucoceles are effective in the short to medium term separated from the nasal and sinus cavity by a thick bony divide. In addition MELP is also indicated when the mucocele is associated with loss of lateral support in the sinus with risk of medial-wall collapse of the orbital contents obstructing drainage. These recommendations augment those of previous authors that most paranasal sinus mucoceles can be successfully managed by endoscopic marsupialization into the nasal cavity. 16,17 This study adds to the number of publications advocating endoscopic sinus surgery as a safe and effective approach for mucocele management. 8,16,17 Har et al. 8 reported the largest series of 103 patients (108 mucoceles) with a median follow-up of 4.7 years and a recurrence rate of 0.9 per cent. This also represents the longest follow up for endoscopically managed mucoceles. However, signi cantly longer follow up is necessary to fully evaluate outcomes. Recurrence of mucocele after osteoplastic and obliteration procedures was 19 per cent (nine out Prior ENT history and co-morbidities TABLE III prior ent history and co-morbidities SM group Number of patients (n) MELP group Number of patients (n) Chronic sinusitis 6 (85.7%) 16 (76.1%) Fungal sinusitis 0 (. %) 7 (33.3%) Nasal polyposis 0 (. %) 8 (38.1%) Previous endoscopic sinus surgery 4 (57.1%) 7 (33.3%) Previous sinus surgery external approach 3 (42.9%) 14 (66.7%) Facial trauma-facial fracture, anterior and posterior table frontal sinus fracture 0 (. %) 2 (9.5%) Prior neurosurgery temporal craniectomy for trigeminal rhizotomy (1), craniotomy with infected bone aps (1), frontal meningioma excision (1), bilateral cranialization (1) 0 (. %) 4 (19.0%) Paranasal obstructive lesion-osteoma (1), inverting papilloma (1), large midline frontal cell (1) 1 (14.3%) 2 (9.52%) Asthma 1 (14.3%) 5 (23.8%) Pyomucocele 0 (. %) 1 (4.8%)
6 356 j. j. khong, r. malhotra, d. selva, p. j. wormald of 47 patients) in a retrospective study 18 whereas in two endoscopic series, 1,5 the recurrence rate was zero per cent with minimal complications. It is important to note that in the latter two studies, patients thought not suitable for an entirely endoscopic approach due to complex sinus anatomy were managed with an external approach or a combined endoscopic and external approach. However, despite the addition of an external incision, the principle of mucocele marsupialization into the nasal cavity was maintained and obliteration was rarely performed. In conclusion, MELP should be considered as an alternative to external obliteration for the treatment of complex frontal mucoceles. Endoscopic marsupialization should be considered the rst line treatment for simple paranasal sinus mucoceles. References 1 Kennedy DW, Josephson JS, Zinreich SJ, Mattox DE, Goldsmith MM. Endoscopic sinus surgery for mucoceles: a viable alternative. Laryngoscope 1989;99: Schaefer SD, Close LG. Endoscopic management of frontal sinus disease. Laryngoscope 1990;100: Benninger MS, Marks S. The endoscopic management of sphenoid and ethmoid mucoceles with orbital and intranasal extension. Rhinology 1995;33: Har-El G, Balwally AN, Lucente FE. Sinus mucoceles: is marsupialization enough? Otolaryngol Head Neck Surg 1997;117: Lund VJ. Endoscopic management of paranasal sinus mucocoeles. J Laryngol Otol 1998;112: Ikeda K, Takahashi C, Oshima T, Suzuki H, Satake M, Hidaka H et al. Endonasal endoscopic marsupialization of paranasal sinus mucoceles. Am J Rhinol 2000;14: Har-El G. Transnasal endoscopic management of frontal mucoceles. Otolaryngol Clin North Am 2001;34: Har-El G. Endoscopic management of 108 sinus mucoceles. Laryngoscope 2001;111: Wormald PJ. Salvage frontal sinus surgery: the endoscopic modi ed Lothrop procedure. Laryngoscope 2003;113: Rootman J, Allen L. Structural lesions. In: Rootman J, ed. Diseases of the Orbit, 2nd edn, Philadelphia: Lippincott Williams & Wilkins, 2003; Haik BG, Amedee RG. Ophthalmic manifestations of mucoceles. In: Bosniak S, ed. Principles and Practice of Ophthalmic Plastic and Reconstructive Surgery. Philadelphia: WB Saunders, 1996; Molony NC, Ah-See K, Rachmanidou A, Draf W. A survey of contemporary management of frontal sinus disease in the United Kingdom. Eur Arch Otorhinolaryngol 2000;257: Lund VJ. Fronto-ethmoidal mucocoeles: A histopathological analysis. J Laryngol Otol 1991;105: Har-El G, DiMaio T. Histologic and physiologic studies of marsupialized sinus mucoceles. J Otolaryngol 2000;29: Gross CW, Harrison SE. The modi ed Lothrop procedure: indications, results, and complications. (Review) Otolaryngol Clin North Am 2001;34: Beasley NJ, Jones NS. Paranasal sinus mucoceles: modern management. Am J Rhinol 1995;9: Conboy PJ, Jones NS. The place of endoscopic sinus surgery in the treatment of paranasal sinus mucocoeles. Clin Otolaryngol 2003;28: Bordley JE, Bosley WR. Mucoceles of the frontal sinus: causes and treatment. Ann Otol Rhinol Laryngol 1973;82: Address for correspondence: Professor Peter John Wormald, Department of Surgery Otolaryngology Head and Neck Surgery, Queen Elizabeth Hospital, 28 Woodville Road, Woodville South, Adelaide, SA 5011, Australia. Fax: peterjwormald@adelaide.edu.au Professor P. J. Wormald takes responsibility for the integrity of the content of the paper. Competing interests: None declared
Endoscopic Management Of A Giant Ethmoid Mucocele
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
Mucocele of paranasal sinuses
 From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
Frontal Sinus Mucocele After Osteoplastic Flap Surgery: Case Report
 Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550013 Volume 1, Issue 3 Case Report Frontal Sinus Mucocele After Osteoplastic Flap Surgery: Case Report Peter Catalano, MD * and Michael
Archives of Clinical and Medical Case Reports doi: 10.26502/acmcr.96550013 Volume 1, Issue 3 Case Report Frontal Sinus Mucocele After Osteoplastic Flap Surgery: Case Report Peter Catalano, MD * and Michael
Frontal Sinus Drillout (Modified Lothrop Procedure): Long-Term Results in 204 Patients
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Frontal Sinus Drillout (Modified Lothrop Procedure): Long-Term Results in 204 Patients Jonathan Y. Ting,
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Frontal Sinus Drillout (Modified Lothrop Procedure): Long-Term Results in 204 Patients Jonathan Y. Ting,
Ethmoid mucocele and post traumatic nasal deformity
 Ethmoid mucocele and post traumatic nasal deformity Abdullah Musleh, Hefni Montaser Abdelazeem Department of Otolaryngology, Head and Neck Surgery, Armed Forces Hospital, South Region, Saudi Arabia shahrani99@hotmail.com
Ethmoid mucocele and post traumatic nasal deformity Abdullah Musleh, Hefni Montaser Abdelazeem Department of Otolaryngology, Head and Neck Surgery, Armed Forces Hospital, South Region, Saudi Arabia shahrani99@hotmail.com
Traditional open surgery for advanced benign nasal tumours in an era of endoscopy: review of 38 cases.
 Traditional open surgery for advanced benign nasal tumours in an era of endoscopy: review of 38 cases. Akeem O Lasisi* and Aderemi A Adeosun Department of Otorhinolaryngology College of Medicine, University
Traditional open surgery for advanced benign nasal tumours in an era of endoscopy: review of 38 cases. Akeem O Lasisi* and Aderemi A Adeosun Department of Otorhinolaryngology College of Medicine, University
Mucoceles of the paranasal sinus are epithelial lesions
 Rev Bras Otorrinolaringol. V.70, n.6, 850-4, nov./dec. 2004 ARTIGO DE REVISÃO CASE REPORT Frontoethmoidal mucoceles: a case report and literature review Andy de Oliveira Vicente 1, Adriana Gonzaga Chaves
Rev Bras Otorrinolaringol. V.70, n.6, 850-4, nov./dec. 2004 ARTIGO DE REVISÃO CASE REPORT Frontoethmoidal mucoceles: a case report and literature review Andy de Oliveira Vicente 1, Adriana Gonzaga Chaves
Destructive Giant Maxillary Sinus Mucocele: A Case Report
 Destructive Giant Maxillary Sinus Mucocele: A Vahit Mutlu 1, Ozgur Yoruk 1, Ozalkan Ozkan 2 1 Atatürk University Faculty of Medicine, Department of Ears, Nose and Throat, Erzurum, Turkey 2 Erzincan University
Destructive Giant Maxillary Sinus Mucocele: A Vahit Mutlu 1, Ozgur Yoruk 1, Ozalkan Ozkan 2 1 Atatürk University Faculty of Medicine, Department of Ears, Nose and Throat, Erzurum, Turkey 2 Erzincan University
Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis
 Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis Ralph Metson, MD; Richard E. Gliklich, MD ORIGINAL ARTICLE Objective: To determine the efficacy of endoscopic surgery for chronic frontal sinusitis.
Clinical Outcome of Endoscopic Surgery for Frontal Sinusitis Ralph Metson, MD; Richard E. Gliklich, MD ORIGINAL ARTICLE Objective: To determine the efficacy of endoscopic surgery for chronic frontal sinusitis.
Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities
 10.5005/jp-journals-10013-1141 H Verma et al ORIGINAL ARTICLE Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities H Verma, Rijuneeta, AK Gupta, A Chakrabarti
10.5005/jp-journals-10013-1141 H Verma et al ORIGINAL ARTICLE Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities H Verma, Rijuneeta, AK Gupta, A Chakrabarti
Frontal sinus disease continues to be one of the great
 Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Large Frontal Sinus Mucopyocele
 AIJCR 10.5005/jp-journals-10013-1173 CASE REPORT Anirudh Shukla, Vivek Dudeja ABSTRACT A mucocele is an epithelial-lined, mucus-containing sac completely filling the sinus and capable of expansion. This
AIJCR 10.5005/jp-journals-10013-1173 CASE REPORT Anirudh Shukla, Vivek Dudeja ABSTRACT A mucocele is an epithelial-lined, mucus-containing sac completely filling the sinus and capable of expansion. This
Surgical Risk Factors for Recurrence of Inverted Papilloma
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Surgical Risk Factors for Recurrence of Inverted Papilloma David Y. Healy Jr., MD, CDR, MC, USN; Nipun Chhabra,
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Surgical Risk Factors for Recurrence of Inverted Papilloma David Y. Healy Jr., MD, CDR, MC, USN; Nipun Chhabra,
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Malignant growth Maxilla management an analysis
 ISSN: 2250-0359 Volume 3 Issue 2 2013 Malignant growth Maxilla management an analysis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Malignant tumors involving maxilla
ISSN: 2250-0359 Volume 3 Issue 2 2013 Malignant growth Maxilla management an analysis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Malignant tumors involving maxilla
Inverted papilloma of the nasal cavity and paranasal sinuses: a study of 20 cases
 Original article: Inverted papilloma of the nasal cavity and paranasal sinuses: a study of 20 cases 1 Dr. Vijay Kumar Kalra, 2 Dr. Samar Pal Singh Yadav, 3 Dr. Swati 1Assistant Professor, 2 Senior Professor
Original article: Inverted papilloma of the nasal cavity and paranasal sinuses: a study of 20 cases 1 Dr. Vijay Kumar Kalra, 2 Dr. Samar Pal Singh Yadav, 3 Dr. Swati 1Assistant Professor, 2 Senior Professor
The Outside-In Approach to the Modified Endoscopic Lothrop Procedure
 The Laryngoscope VC 2012 The American Laryngological, Rhinological and Otological Society, Inc. The Outside-In Approach to the Modified Endoscopic Lothrop Procedure David Chin, MBBS; Kornkiat Snidvongs,
The Laryngoscope VC 2012 The American Laryngological, Rhinological and Otological Society, Inc. The Outside-In Approach to the Modified Endoscopic Lothrop Procedure David Chin, MBBS; Kornkiat Snidvongs,
National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488
 National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488 Date: September 1997 Page 1 of 5 LIMITED OR LOCALIZED FOLLOW UP - SINUS CT 76380 Guideline
National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488 Date: September 1997 Page 1 of 5 LIMITED OR LOCALIZED FOLLOW UP - SINUS CT 76380 Guideline
Chronic Frontal Rhinosinusitis: Diagnosis and Management
 Chapter Chronic Frontal Rhinosinusitis: Diagnosis and Management Core Messages Despite significant advances in surgical techniques, technology, and knowledge of pathophysiology, management of chronic frontal
Chapter Chronic Frontal Rhinosinusitis: Diagnosis and Management Core Messages Despite significant advances in surgical techniques, technology, and knowledge of pathophysiology, management of chronic frontal
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013
 FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
Imaging of the Paranasal Sinuses
 14. Sommerschule Imaging of the Paranasal Sinuses Bettlach 24.08.2018 Christoph Schlegel Conventional Radiology NNH-Status: okzipito-frontal: frontal sinus, anterior ethmoid okzipito-nasal : maxillary
14. Sommerschule Imaging of the Paranasal Sinuses Bettlach 24.08.2018 Christoph Schlegel Conventional Radiology NNH-Status: okzipito-frontal: frontal sinus, anterior ethmoid okzipito-nasal : maxillary
Introduction. Ophthalmic manifestations can result from a myriad of Non Sinogenic and Sinogenic Disease :
 Ophthalmic Manifestations of Paranasal Sinus Disease; A Clinical Grading System Surayie Al Dousary, MD Associate Professor Director Rhinology Research Chair & Fatma Al Anazy, MD Associate Professor Rhinology
Ophthalmic Manifestations of Paranasal Sinus Disease; A Clinical Grading System Surayie Al Dousary, MD Associate Professor Director Rhinology Research Chair & Fatma Al Anazy, MD Associate Professor Rhinology
Recalcitrant chronic rhinosinusitis. Difficulties in diagnosis and treatment Videler, W.J.M.
 UvA-DARE (Digital Academic Repository) Recalcitrant chronic rhinosinusitis. Difficulties in diagnosis and treatment Videler, W.J.M. Link to publication Citation for published version (APA): Videler, W.
UvA-DARE (Digital Academic Repository) Recalcitrant chronic rhinosinusitis. Difficulties in diagnosis and treatment Videler, W.J.M. Link to publication Citation for published version (APA): Videler, W.
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE The XprESS Multi-Sinus Dilation System for the treatment of 1 Technology 1.1 Description of the technology The XprESS
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Medical technology guidance SCOPE The XprESS Multi-Sinus Dilation System for the treatment of 1 Technology 1.1 Description of the technology The XprESS
Chapter Five. 1 of 8 11/3/2008 2:52 PM.
 1 of 8 11/3/2008 2:52 PM Email : myousefmian@hotmail.com Chapter Five FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
1 of 8 11/3/2008 2:52 PM Email : myousefmian@hotmail.com Chapter Five FRONT COVER Introduction Acknowledgement CHAPTERS Chapter One Chapter Two Chapter Three Chapter Four Chapter Five Chapter Six Chapter
JMSCR Vol 05 Issue 09 Page September 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i9.52 Relationship of Agger Nasi Cell and Uncinate
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i9.52 Relationship of Agger Nasi Cell and Uncinate
A Computer-Assisted Anatomical Study of the Nasofrontal Region
 The Laryngoscope Lippincott Williams & Wilkins, Inc., Philadelphia 2001 The American Laryngological, Rhinological and Otological Society, Inc. A Computer-Assisted Anatomical Study of the Nasofrontal Region
The Laryngoscope Lippincott Williams & Wilkins, Inc., Philadelphia 2001 The American Laryngological, Rhinological and Otological Society, Inc. A Computer-Assisted Anatomical Study of the Nasofrontal Region
Anatomical Analysis of the Frontal Recess Cells in Endoscopic Sinus Surgery An Indian Perspective
 ORIGINAL ARTICLE Anatomical Analysis of the Frontal Recess Cells in Endoscopic Sinus Surgery An Indian Perspective 1 Dhingra Shruti, 2 Agarwal AK, 3 Passey JC, 4 Kaul JM 1 Resident, Department of Otolaryngology
ORIGINAL ARTICLE Anatomical Analysis of the Frontal Recess Cells in Endoscopic Sinus Surgery An Indian Perspective 1 Dhingra Shruti, 2 Agarwal AK, 3 Passey JC, 4 Kaul JM 1 Resident, Department of Otolaryngology
ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA
 ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA Anthony Po-Wing Yuen, FRCS, 1 Yiu Wah Fan, FRCS, 2 Ching Fai Fung, FRCS, 2 Kwan Ngai Hung, FRCS 2 1 Division of Otorhinolaryngology,
ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA Anthony Po-Wing Yuen, FRCS, 1 Yiu Wah Fan, FRCS, 2 Ching Fai Fung, FRCS, 2 Kwan Ngai Hung, FRCS 2 1 Division of Otorhinolaryngology,
1. BRIEF DESCRIPTION OF TRAINING
 RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
The advent of high-resolution computerized tomography
 An anatomic classification of the ethmoidal bulla REUBEN C. SETLIFF, III, MD, PETER J. CATALANO, MD, FACS, LISA A. CATALANO, MPH, and CHAD FRANCIS, BA, Sioux Falls, South Dakota, and Burlington, Massachusetts
An anatomic classification of the ethmoidal bulla REUBEN C. SETLIFF, III, MD, PETER J. CATALANO, MD, FACS, LISA A. CATALANO, MPH, and CHAD FRANCIS, BA, Sioux Falls, South Dakota, and Burlington, Massachusetts
Citation Hong Kong Practitioner, 1996, v. 18 n. 12, p
 Title Radiological conference. Frontal sinus osteoma complicated by pneumocephalus Author(s) Fung, WT; Peh, WCG Citation Hong Kong Practitioner, 1996, v. 18 n. 12, p. 658-662 Issued Date 1996 URL http://hdl.handle.net/10722/44655
Title Radiological conference. Frontal sinus osteoma complicated by pneumocephalus Author(s) Fung, WT; Peh, WCG Citation Hong Kong Practitioner, 1996, v. 18 n. 12, p. 658-662 Issued Date 1996 URL http://hdl.handle.net/10722/44655
Sphenoid rhinosinusitis associated with abducens nerve palsy Case report
 Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Allergic Fungal Rhinosinusitis
 Allergic Fungal Rhinosinusitis My Published Experience 1999-2018 Prof. Surayie H Al Dousary Professor of Rhinology Rhinology research Chair Director KSU Rhinology fellowship Program Director KSU Rhinology
Allergic Fungal Rhinosinusitis My Published Experience 1999-2018 Prof. Surayie H Al Dousary Professor of Rhinology Rhinology research Chair Director KSU Rhinology fellowship Program Director KSU Rhinology
ORIGINAL ARTICLE. Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the Anterior Ethmoid
 Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the nterior Ethmoid Long-term Results ORIGINL RTICLE Toru Kikawada, MD; Masao Fujigaki, MD; Mikino
Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the nterior Ethmoid Long-term Results ORIGINL RTICLE Toru Kikawada, MD; Masao Fujigaki, MD; Mikino
Fracture frontal bone and its management
 From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
ORIGINAL ARTICLE RELATIONSHIP OF CONCHA BULLOSA WITH OSTEOMEATAL UNIT BLOCKAGE. TOMOGRAPHIC STUDY IN 200 PATIENTS.
 RELATIONSHIP OF CONCHA BULLOSA WITH OSTEOMEATAL UNIT BLOCKAGE. TOMOGRAPHIC STUDY IN 200 PATIENTS. Shrikrishna B H 1, Jyothi A C 2, Sanjay G 3, Sandeep Samson G 4. 1. Associate Professor, Department of
RELATIONSHIP OF CONCHA BULLOSA WITH OSTEOMEATAL UNIT BLOCKAGE. TOMOGRAPHIC STUDY IN 200 PATIENTS. Shrikrishna B H 1, Jyothi A C 2, Sanjay G 3, Sandeep Samson G 4. 1. Associate Professor, Department of
Boundaries Septum Turbinates & Meati Lamellae Drainage Pathways Variants
 The Fastest 20 Minutes in Michelle A. Michel, MD Professor of Radiology and Otolaryngology Medical College of Wisconsin, Milwaukee Overview Nasal cavity Anterior skull base Ostiomeatal complex Frontal
The Fastest 20 Minutes in Michelle A. Michel, MD Professor of Radiology and Otolaryngology Medical College of Wisconsin, Milwaukee Overview Nasal cavity Anterior skull base Ostiomeatal complex Frontal
ORIGINAL ARTICLE. Group Chandler Maloney. First Inflammatory oedema Preseptal cellulitis. Second Orbital Cellulitis Subperiosteal abscess
 ORBITAL MANIFESTATIONS OF SINUS DISEASE T. Jyothirmayi 1, V. Meenakshi 2, M. Deepika 3 HOW TO CITE THIS ARTICLE: T. Jyothirmayi, V. Meenakshi, M. Deepika. Orbital Manifestations of Sinus Disease. Journal
ORBITAL MANIFESTATIONS OF SINUS DISEASE T. Jyothirmayi 1, V. Meenakshi 2, M. Deepika 3 HOW TO CITE THIS ARTICLE: T. Jyothirmayi, V. Meenakshi, M. Deepika. Orbital Manifestations of Sinus Disease. Journal
Conventional Sinus Surgery Vs Fess
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
ORIGINAL ARTICLE. Computed Tomographic Staging and the Fate of the Dependent Sinuses in Revision Endoscopic Sinus Surgery
 Computed Tomographic Staging and the Fate of the Dependent es in Revision Endoscopic Surgery Neil Bhattacharyya, MD ORIGINAL ARTICLE Objectives: To determine the patterns of disease recurrence in chronic
Computed Tomographic Staging and the Fate of the Dependent es in Revision Endoscopic Surgery Neil Bhattacharyya, MD ORIGINAL ARTICLE Objectives: To determine the patterns of disease recurrence in chronic
Bilateral blindness due to acute isolated sphenoid sinusitis- is it reversible? A. Case Report
 ISSN: 2250-0359 Volume 5 Issue 3 2015 Bilateral blindness due to acute isolated sphenoid sinusitis- is it reversible? A Case Report Roshan Kumar Verma Naresh K panda PGIMER, Chandigarh, India ABSTRACT
ISSN: 2250-0359 Volume 5 Issue 3 2015 Bilateral blindness due to acute isolated sphenoid sinusitis- is it reversible? A Case Report Roshan Kumar Verma Naresh K panda PGIMER, Chandigarh, India ABSTRACT
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study
 Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Learn Connect Succeed. JCAHPO Regional Meetings 2017
 Learn Connect Succeed JCAHPO Regional Meetings 2017 Financial Disclosure Evaluation and Treatment of Orbital Cellulitis Thomas E. Johnson, M.D. Bascom Palmer Eye Institute University of Miami School of
Learn Connect Succeed JCAHPO Regional Meetings 2017 Financial Disclosure Evaluation and Treatment of Orbital Cellulitis Thomas E. Johnson, M.D. Bascom Palmer Eye Institute University of Miami School of
ENDOSCOPIC ENDONASAL SURGERY FOR RESECTION OF BENIGN SINONASAL TUMORS: EXPERIENCE WITH 107 PATIENTS
 Arch Iranian Med 2006; 9 (3): 244 249 Original Article ENDOSCOPIC ENDONASAL SURGERY FOR RESECTION OF BENIGN SINONASAL TUMORS: EXPERIENCE WITH 107 PATIENTS Mohammad-Hossein Baradaranfar MD, Payman Dabirmoghaddam
Arch Iranian Med 2006; 9 (3): 244 249 Original Article ENDOSCOPIC ENDONASAL SURGERY FOR RESECTION OF BENIGN SINONASAL TUMORS: EXPERIENCE WITH 107 PATIENTS Mohammad-Hossein Baradaranfar MD, Payman Dabirmoghaddam
Mucoceles of the Paranasal Sinuses November 22, 2010
 TITLE: Mucoceles of the Paranasal Sinuses SOURCE: Grand Rounds Presentation, The University of Texas Medical Branch, Department of Otolaryngology DATE: November 22, 2010 MEDICAL STUDENT: Ashley Agan, MSIV
TITLE: Mucoceles of the Paranasal Sinuses SOURCE: Grand Rounds Presentation, The University of Texas Medical Branch, Department of Otolaryngology DATE: November 22, 2010 MEDICAL STUDENT: Ashley Agan, MSIV
COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY
 COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY John M. DelGaudio, MD Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology-Head and Neck Surgery Emory University School
COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY John M. DelGaudio, MD Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology-Head and Neck Surgery Emory University School
REVISION ENDOSCOPIC FRONTAL SINUSOTOMY WITH MUCOPERIOSTEAL FLAP ADVANCEMENT
 CURRENT CONCEPTS IN THE SURGICAL MANAGEMENT OF FRONTAL SINUS DISEASE 00304665/01 $15.00 +.OO REVISION ENDOSCOPIC FRONTAL SINUSOTOMY WITH MUCOPERIOSTEAL FLAP ADVANCEMENT The Frontal Sinus Rescue Procedure
CURRENT CONCEPTS IN THE SURGICAL MANAGEMENT OF FRONTAL SINUS DISEASE 00304665/01 $15.00 +.OO REVISION ENDOSCOPIC FRONTAL SINUSOTOMY WITH MUCOPERIOSTEAL FLAP ADVANCEMENT The Frontal Sinus Rescue Procedure
Study of success rates in endoscopic dacryocystorhinostomy with and without stenting. dacryocystorhinostomy with and
 Original Research Article Study of success rates in endoscopic dacryocystorhinostomy with and without stenting Kirti Ambani 1, Niraj Suri 2, Hiren Parmar 3* 1 Assistant Professor, ENT Department, GMERS
Original Research Article Study of success rates in endoscopic dacryocystorhinostomy with and without stenting Kirti Ambani 1, Niraj Suri 2, Hiren Parmar 3* 1 Assistant Professor, ENT Department, GMERS
Reasons for Failure and Surgical Revisions. Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology
 Reasons for Failure and Surgical Revisions Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology Medical College of Georgia of Georgia Regents University Department of Otolaryngology / Head
Reasons for Failure and Surgical Revisions Stil Kountakis, MD, PhD Professor and Chief, Division of Rhinology Medical College of Georgia of Georgia Regents University Department of Otolaryngology / Head
Learner Objectives. Overview. Minimally Invasive Sinus Surgery: What is the data for Balloon Catheter Dilation 7/31/2017
 Minimally Invasive Sinus Surgery: What is the data for Balloon Catheter Dilation David M. Poetker, MD Christopher M. Long, MD Rhinology and Sinus Surgery Medical College of Wisconsin Thank you to Susan
Minimally Invasive Sinus Surgery: What is the data for Balloon Catheter Dilation David M. Poetker, MD Christopher M. Long, MD Rhinology and Sinus Surgery Medical College of Wisconsin Thank you to Susan
The International Frontal Sinus Anatomy Classification (IFAC) and Classification of the Extent of Endoscopic Frontal...
 See discussions, stats, and author profiles for this publication at: https://www.researchgate.net/publication/298902054 The International Frontal Sinus Anatomy Classification (IFAC) and Classification
See discussions, stats, and author profiles for this publication at: https://www.researchgate.net/publication/298902054 The International Frontal Sinus Anatomy Classification (IFAC) and Classification
Spheno-Ethmoidectomy
 Diagnostic and Therapeutic Endoscopy, Vol. 5, pp. 1-8 Reprints available directly from the publisher Photocopying permitted by license only (C) 1998 OPA (Overseas Publishers Association) N.V. Published
Diagnostic and Therapeutic Endoscopy, Vol. 5, pp. 1-8 Reprints available directly from the publisher Photocopying permitted by license only (C) 1998 OPA (Overseas Publishers Association) N.V. Published
Consumer summary. Endoscopic modified Lothrop procedure for the. treatment of chronic frontal sinusitis
 ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Endoscopic modified Lothrop procedure for the treatment of chronic frontal sinusitis (The report
ASERNIP S Australian Safety and Efficacy Register of New Interventional Procedures Surgical Consumer summary Endoscopic modified Lothrop procedure for the treatment of chronic frontal sinusitis (The report
Epidemiology 3002). Epidemiology and Pathophysiology
 Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Dr.Adel A. Al Ibraheem
 Rhinology Chair Weekly Activity Dr.Adel A. Al Ibraheem www.rhinologychair.org conference@rhinologychair.org Rhinology Chair Introduction: It is important to classify and stage nasal polyposis. ( decide
Rhinology Chair Weekly Activity Dr.Adel A. Al Ibraheem www.rhinologychair.org conference@rhinologychair.org Rhinology Chair Introduction: It is important to classify and stage nasal polyposis. ( decide
Pediatric Endoscopic Sinus Surgery in a Tertiary Government Hospital: Patient Profile and Surgical Indications
 Philippine Journal Of Otolaryngology-Head And Neck Surgery Vol. 4 No. January June ichael Joseph C. David, D Gil. Vicente, D, Antonio H. Chua, D, Jose R. Reyes emorial edical Center St. Luke s edical Center
Philippine Journal Of Otolaryngology-Head And Neck Surgery Vol. 4 No. January June ichael Joseph C. David, D Gil. Vicente, D, Antonio H. Chua, D, Jose R. Reyes emorial edical Center St. Luke s edical Center
Radiological anatomy of frontal sinus By drtbalu
 2009 Radiological anatomy of frontal sinus By drtbalu Anatomy of frontal sinus is highly variable. Precise understanding of these variables will help a surgeon to avoid unnecessary complications during
2009 Radiological anatomy of frontal sinus By drtbalu Anatomy of frontal sinus is highly variable. Precise understanding of these variables will help a surgeon to avoid unnecessary complications during
Three-Dimensional Volumetric Display of the Nasal Ostiomeatal Channels and Paranasal Sinuses
 Downloaded from www.ajronline.org by 37.44.202.192 on 12/22/17 from IP address 37.44.202.192. Copyright RRS. For personal use only; all rights reserved Three-Dimensional Volumetric Display of the Nasal
Downloaded from www.ajronline.org by 37.44.202.192 on 12/22/17 from IP address 37.44.202.192. Copyright RRS. For personal use only; all rights reserved Three-Dimensional Volumetric Display of the Nasal
A descriptive study of the patients with orbital complication of acute and chronic sinusitis
 International Journal of Otorhinolaryngology and Head and Neck Surgery Pullarat AN et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Jul;4(4):990-996 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
International Journal of Otorhinolaryngology and Head and Neck Surgery Pullarat AN et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Jul;4(4):990-996 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
A comprehensive study on complications of endoscopic sinus surgery
 International Journal of Otorhinolaryngology and Head and Neck Surgery Shyras JAD et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Jul;3(3):472-477 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
International Journal of Otorhinolaryngology and Head and Neck Surgery Shyras JAD et al. Int J Otorhinolaryngol Head Neck Surg. 2017 Jul;3(3):472-477 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures Alice Z.
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures Alice Z.
Proptosis due to otolaryngology causes a study
 From the SelectedWorks of Balasubramanian Thiagarajan March 29, 2013 Proptosis due to otolaryngology causes a study Balasubramanian Thiagarajan Srikamakshi Kothandaraman Available at: https://works.bepress.com/drtbalu/11/
From the SelectedWorks of Balasubramanian Thiagarajan March 29, 2013 Proptosis due to otolaryngology causes a study Balasubramanian Thiagarajan Srikamakshi Kothandaraman Available at: https://works.bepress.com/drtbalu/11/
Pictorial review of extraconal and osseous orbital pathology - what can be found 'around' the orbits?
 Pictorial review of extraconal and osseous orbital pathology - what can be found 'around' the orbits? Poster No.: C-2011 Congress: ECR 2013 Type: Educational Exhibit Authors: M. Meissnitzer, T. Meissnitzer,
Pictorial review of extraconal and osseous orbital pathology - what can be found 'around' the orbits? Poster No.: C-2011 Congress: ECR 2013 Type: Educational Exhibit Authors: M. Meissnitzer, T. Meissnitzer,
Isolated sphenoid inflammatory diseases
 International Journal of Otorhinolaryngology and Head and Neck Surgery http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original Research Article DOI: http://dx.doi.org/10.18203/issn.2454-5929.ijohns20183688
International Journal of Otorhinolaryngology and Head and Neck Surgery http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original Research Article DOI: http://dx.doi.org/10.18203/issn.2454-5929.ijohns20183688
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery FACIAL FRACTURES
 Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
POST-TRAUMATIC FRONTAL SWELLING WITH PROPTOSIS AND DIPLOPIA
 CASE REPORT Sabari R 1, Singh SP 2, Reddy N 3 Fig.1 can encroach on the orbit with ocular displacement and proptosis. They are a common cause of long standing unilateral proptosis[4]. Ocular motility disturbance,
CASE REPORT Sabari R 1, Singh SP 2, Reddy N 3 Fig.1 can encroach on the orbit with ocular displacement and proptosis. They are a common cause of long standing unilateral proptosis[4]. Ocular motility disturbance,
Original Article Effect of lamina papyracea ingression on orbito-ocular complications after functional endoscopic sinus surgery
 Int J Clin Exp Med 2016;9(6):10317-10321 www.ijcem.com /ISSN:1940-5901/IJCEM0025371 Original Article Effect of lamina papyracea ingression on orbito-ocular complications after functional endoscopic sinus
Int J Clin Exp Med 2016;9(6):10317-10321 www.ijcem.com /ISSN:1940-5901/IJCEM0025371 Original Article Effect of lamina papyracea ingression on orbito-ocular complications after functional endoscopic sinus
Communication issue - What should the radiologist report before functional endoscopic sinus surgery
 Communication issue - What should the radiologist report before functional endoscopic sinus surgery Poster No.: C-0509 Congress: ECR 2015 Type: Educational Exhibit Authors: A. M. Dobra 1, C. A. Badiu 1,
Communication issue - What should the radiologist report before functional endoscopic sinus surgery Poster No.: C-0509 Congress: ECR 2015 Type: Educational Exhibit Authors: A. M. Dobra 1, C. A. Badiu 1,
Pott s Puffy Tumor. Shahad Almohanna 15/1/2018
 Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
The surgical approach to the sphenoid sinus continues to
 A comparison of two sphenoidotomy approaches using a novel computerized tomography grading system Heitham Gheriani, F.R.C.S.C., F.R.C.S.I., David Flamer, B.Sc., Trent Orton, M.D., Brad Mechor, F.R.C.S.C.,
A comparison of two sphenoidotomy approaches using a novel computerized tomography grading system Heitham Gheriani, F.R.C.S.C., F.R.C.S.I., David Flamer, B.Sc., Trent Orton, M.D., Brad Mechor, F.R.C.S.C.,
Invasive Fungal Rhinosinusitis: A 15-Year Experience With 29 Patients
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Invasive Fungal Rhinosinusitis: A 15-Year Experience With 29 Patients Marcus M. Monroe, MD; Max McLean, BA;
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Invasive Fungal Rhinosinusitis: A 15-Year Experience With 29 Patients Marcus M. Monroe, MD; Max McLean, BA;
Allergic fungal rhinosinusitis: detection of fungal DNA in sinus aspirate using polymerase chain reaction
 1- Allergic fungal rhinosinusitis: detection of fungal DNA in sinus aspirate using polymerase chain reaction Abstract Objective: This study investigated allergic fungal rhinosinusitis cases, and aimed
1- Allergic fungal rhinosinusitis: detection of fungal DNA in sinus aspirate using polymerase chain reaction Abstract Objective: This study investigated allergic fungal rhinosinusitis cases, and aimed
Intranasal location of lacrimal sac in Thai cadavers
 Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
FRONTO-ETHMOIDAL MUCOCOELE AS A CAUSE OF UNILATERAL PROPTOSIS*t
 Brit. J. Ophthal. (1968) 52, 833 FRONTO-ETHMOIDAL MUCOCOELE AS A CAUSE OF UNILATERAL PROPTOSIS*t BY P. W. R. M. ALBERTI, H. F. MARSHALL, AND J. I. MUNRO BLACK Royal Victoria Infirmary, Newcastle upon Tyne
Brit. J. Ophthal. (1968) 52, 833 FRONTO-ETHMOIDAL MUCOCOELE AS A CAUSE OF UNILATERAL PROPTOSIS*t BY P. W. R. M. ALBERTI, H. F. MARSHALL, AND J. I. MUNRO BLACK Royal Victoria Infirmary, Newcastle upon Tyne
ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS
 From the SelectedWorks of Balasubramanian Thiagarajan July 1, 2012 ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/51/
From the SelectedWorks of Balasubramanian Thiagarajan July 1, 2012 ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/51/
Research Article Expanded Endoscopic Endonasal Treatment of Primary Intracranial Tumors within the Paranasal Sinuses
 ISRN Minimally Invasive Surgery Volume 2013, Article ID 129780, 5 pages http://dx.doi.org/10.1155/2013/129780 Research Article Expanded Endoscopic Endonasal Treatment of Primary Intracranial Tumors within
ISRN Minimally Invasive Surgery Volume 2013, Article ID 129780, 5 pages http://dx.doi.org/10.1155/2013/129780 Research Article Expanded Endoscopic Endonasal Treatment of Primary Intracranial Tumors within
ISSN X (Print) Research Article. *Corresponding author Dr.V. Krishna Chaitanya
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(1G):508-513 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(1G):508-513 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Provider Led Entity. CDI Quality Institute PLE Rhinosinusitis AUC 12/04/2018
 Provider Led Entity CDI Quality Institute PLE Rhinosinusitis AUC 12/04/2018 Appropriateness of advanced imaging procedures* in patients with rhinosinusitis and the following clinical presentations or diagnoses:
Provider Led Entity CDI Quality Institute PLE Rhinosinusitis AUC 12/04/2018 Appropriateness of advanced imaging procedures* in patients with rhinosinusitis and the following clinical presentations or diagnoses:
Orbital Complications of Sinogenic Origin: A Case Study of 20 Patients
 World Articles of Ear, Nose and Throat ---------------------Page 1 Orbital Complications of Sinogenic Origin: A Case Study of 20 Patients Authors: Shrinivas Shripatrao Chavan*, Sunil D.Deshmukh**, Vasant
World Articles of Ear, Nose and Throat ---------------------Page 1 Orbital Complications of Sinogenic Origin: A Case Study of 20 Patients Authors: Shrinivas Shripatrao Chavan*, Sunil D.Deshmukh**, Vasant
Inflammation of the paranasal sinuses is a common
 Case Report 5 Concomitant ilateral Orbital and rain bscesses-unusual Complications of Pediatric Rhinosinusitis Shiang-Fu Huang, MD; Ta-Jen Lee, MD; Kuang-Lin Lin, MD Rhinosinusitis is a common medical
Case Report 5 Concomitant ilateral Orbital and rain bscesses-unusual Complications of Pediatric Rhinosinusitis Shiang-Fu Huang, MD; Ta-Jen Lee, MD; Kuang-Lin Lin, MD Rhinosinusitis is a common medical
FRONTAL SINUS FRACTURES February 1995
 TITLE: FRONTAL SINUS FRACTURES SOURCE: Dept. of Otolaryngology, UTMB, Grand Rounds DATE: February 22, 1995 RESIDENT PHYSICIAN: Kelly D. Sweeney, M.D. FACULTY: Brian P. Driscoll, M.D. SERIES EDITOR: Francis
TITLE: FRONTAL SINUS FRACTURES SOURCE: Dept. of Otolaryngology, UTMB, Grand Rounds DATE: February 22, 1995 RESIDENT PHYSICIAN: Kelly D. Sweeney, M.D. FACULTY: Brian P. Driscoll, M.D. SERIES EDITOR: Francis
Major orbital complications of endoscopic sinus surgery
 598 Moorfields Eye Hospital, London EC1V 2PD, UK C Rene G E Rose R Lenthall I Moseley Correspondence to: Mr G E Rose, Orbital Clinic, Moorfields Eye Hospital, City Road, London EC1V 2PD, UK Accepted 20
598 Moorfields Eye Hospital, London EC1V 2PD, UK C Rene G E Rose R Lenthall I Moseley Correspondence to: Mr G E Rose, Orbital Clinic, Moorfields Eye Hospital, City Road, London EC1V 2PD, UK Accepted 20
A Targeted Endoscopic Approach to Chronic Isolated Frontal Sinusitis
 Otolaryngology Head and Neck Surgery (2006) 134, 28-32 ORIGINAL RESEARCH A Targeted Endoscopic Approach to Chronic Isolated Frontal Sinusitis Roee Landsberg, MD, Yoram Segev, MD, Michael Friedman, MD,
Otolaryngology Head and Neck Surgery (2006) 134, 28-32 ORIGINAL RESEARCH A Targeted Endoscopic Approach to Chronic Isolated Frontal Sinusitis Roee Landsberg, MD, Yoram Segev, MD, Michael Friedman, MD,
Ophthalmic Manifestations in ENT Diseases & Surgical Procedures
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 11, Issue 4 (Nov.- Dec. 2013), PP 87-92 Ophthalmic Manifestations in ENT Diseases & Surgical Procedures
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 11, Issue 4 (Nov.- Dec. 2013), PP 87-92 Ophthalmic Manifestations in ENT Diseases & Surgical Procedures
Endoscopic transnasal orbital decompression for thyrotoxic orbitopathy
 Key words: Endoscopes; Exophthalmos; Keratitis; Orbital diseases; Thyrotoxicosis "# " APW Yuen KYW Kwan E Chan AWC Kung KSL Lam Hong Kong Med J 2002;8:406-10 Queen Mary Hospital, 102 Pokfulam Road, Hong
Key words: Endoscopes; Exophthalmos; Keratitis; Orbital diseases; Thyrotoxicosis "# " APW Yuen KYW Kwan E Chan AWC Kung KSL Lam Hong Kong Med J 2002;8:406-10 Queen Mary Hospital, 102 Pokfulam Road, Hong
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations
 White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
Anatomical Variations in Osteomeatal Complex among Patients undergoing Functional Endoscopic Sinus Surgery
 V Narendrakumar, V Subramanian Original article 10.5005/jp-journals-10013-1259 Anatomical Variations in Osteomeatal Complex among Patients undergoing Functional Endoscopic Sinus Surgery 1 V Narendrakumar,
V Narendrakumar, V Subramanian Original article 10.5005/jp-journals-10013-1259 Anatomical Variations in Osteomeatal Complex among Patients undergoing Functional Endoscopic Sinus Surgery 1 V Narendrakumar,
Treatment Options for Chronic Sinusitis
 Treatment Options for Chronic Sinusitis Jesse Ryan, M.D. Assistant Professor Head and Neck Surgery & Reconstruction Department of Otolaryngology January 17, 2019 Disclosures I have no financial relationship
Treatment Options for Chronic Sinusitis Jesse Ryan, M.D. Assistant Professor Head and Neck Surgery & Reconstruction Department of Otolaryngology January 17, 2019 Disclosures I have no financial relationship
Clinical and imagistic correlations in the inflammatory pathology of nasosinusal cavities
 Romanian Journal of Rhinology, Volume 8, No. 29, January-March 2018 ORIGINAL STUDY DOI: 10.2478/rjr-2018-0003 Clinical and imagistic correlations in the inflammatory pathology of nasosinusal cavities Emilia
Romanian Journal of Rhinology, Volume 8, No. 29, January-March 2018 ORIGINAL STUDY DOI: 10.2478/rjr-2018-0003 Clinical and imagistic correlations in the inflammatory pathology of nasosinusal cavities Emilia
PROBLEM RECOMMENDATION
 PREVENTION (MINIMIZING) IN ENDOSCOPIC Steven D. Schaefer, MD Professor and Chair Department of Otolaryngology PREVENTION AND Intraoperative Hemorrhage Loss of Orientation Inability to Identify/Preserve
PREVENTION (MINIMIZING) IN ENDOSCOPIC Steven D. Schaefer, MD Professor and Chair Department of Otolaryngology PREVENTION AND Intraoperative Hemorrhage Loss of Orientation Inability to Identify/Preserve
Computerised tomographic profile of ethmoid roof on basis of keros classification among ethnic Kashmiri s
 International Journal of Otorhinolaryngology and Head and Neck Surgery Salroo IN et al. Int J Otorhinolaryngol Head Neck Surg. 2016 Jan;2(1):1-5 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Research
International Journal of Otorhinolaryngology and Head and Neck Surgery Salroo IN et al. Int J Otorhinolaryngol Head Neck Surg. 2016 Jan;2(1):1-5 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Research
Imaging Anatomy in Revision Sinus Surgery
 Chapter 1 Imaging Anatomy in Revision Sinus Surgery Ramon E. Figueroa 1 Core Messages An intimate knowledge of sinus anatomy and a clear understanding of the baseline postsurgical anatomy are required
Chapter 1 Imaging Anatomy in Revision Sinus Surgery Ramon E. Figueroa 1 Core Messages An intimate knowledge of sinus anatomy and a clear understanding of the baseline postsurgical anatomy are required
Surgical Management of Sinusitis (What About Balloons?) Relative Indications for Sinus Surgery in Children
 Surgical Management of Sinusitis (What About Balloons?) Andrew N. Goldberg M.D. Andrew H. Murr M.D. Michael J. Cunningham, M.D. Department of Otolaryngology and Communication Enhancement Children s Hospital
Surgical Management of Sinusitis (What About Balloons?) Andrew N. Goldberg M.D. Andrew H. Murr M.D. Michael J. Cunningham, M.D. Department of Otolaryngology and Communication Enhancement Children s Hospital
Malignant Non-Hodgkin's Lymphomas of the Nose and Paranasal Sinuses
 Mcd, J. Malaysia Vol. 43 No. 1 March 1988 Malignant Non-Hodgkin's Lymphomas of the Nose and Paranasal Sinuses JOHN TAN, MBBS, FRCSEd HUSAIN SAID, FRCS (Edin and Glasgow) S.M. CHONG DCP(London), MRCPath,
Mcd, J. Malaysia Vol. 43 No. 1 March 1988 Malignant Non-Hodgkin's Lymphomas of the Nose and Paranasal Sinuses JOHN TAN, MBBS, FRCSEd HUSAIN SAID, FRCS (Edin and Glasgow) S.M. CHONG DCP(London), MRCPath,
The Nose and Sinuses. Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital
 The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
Skullbase Lesions. Skullbase Surgery Open vs endoscopic. Choice Of Surgical Approaches 12/28/2015. Skullbase Surgery: Evolution
 Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Is the Classical Classification of Aspergillosis of the Paranasal Sinuses to non invasive and invasive still valid or not?
 Bahrain Medical Bulletin, Vol.24, No.3, September 2002 Is the Classical Classification of Aspergillosis of the Paranasal Sinuses to non invasive and invasive still valid or not? Abdul Aziz Ashoor (FA-HNO)*
Bahrain Medical Bulletin, Vol.24, No.3, September 2002 Is the Classical Classification of Aspergillosis of the Paranasal Sinuses to non invasive and invasive still valid or not? Abdul Aziz Ashoor (FA-HNO)*
JMSCR Vol 04 Issue 05 Page May 2016
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i5.25 Radiologic Variations of Nose and Paranasal
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 5.88 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: http://dx.doi.org/10.18535/jmscr/v4i5.25 Radiologic Variations of Nose and Paranasal
