The Acetazolamide Challenge: Imaging Techniques Designed to Evaluate Cerebral Blood Flow Reserve
|
|
|
- Buddy Stone
- 5 years ago
- Views:
Transcription
1 803 The Acetazolamide Challenge: Imaging Techniques Designed to Evaluate Cerebral Blood Flow Reserve Jeffrey Rogg 1 Michael Rutigliano 2 Howard Yonas 3 David W. Johnson 4 Susan Pentheny 4 Richard E. Latchaw 3 Cerebral blood flow was analyzed by the stable xenon (Xe)/CT scanning technique in 29 patients with significant vascular lesions before and after administration of an acetazolamide (Diamox) vasodilatory challenge. Three response types were identified: I, normal flow before Diamox with flow augmentation after Diamox; II, low flow before Diamox with flow augmentation after Diamox; and Ill, low or normal flow before Diamox with no augmentation or decreased flow after Diamox. Twenty-four percent of the patients studied qualified for category Ill. We believe that patients in this category represent a group of individuals without blood flow reserve whose clinical management should include careful consideration of their hemodynamic status. The XejCT scanning technique with the addition of Diamox flow challenge is a clinically accessible and effective method for assessing cerebral blood flow and blood flow reserve. This article appears in the July/August 1989 issue of AJNR and the September 1989 issue of AJR. Received June 24, 1988; revision requested August 22, 1988; revision received November 11, 1988; accepted December 5, Department of Radiology, Brown University School of Medicine, Rhode Island Hospital, Providence, Rl University of Pittsburgh School of Medicine, Pittsburgh, PA Department of Radiology and Neurological Surgery, University of Pittsburgh School of Medicine, Pittsburgh, PA Address reprint requests to H. Yonas. 4 Department of Radiology, University of Pittsburgh School of Medicine, Pittsburgh, PA AJNR 10: , July/August /89/ American Society of Neuroradiology The development of a clinically accessible means to identify patients with neurologic symptoms caused by transient focal or global low cerebral blood flow (CBF) has important potential therapeutic implications [1-3]. Signs and symptoms of decreased cerebrovascular reserves and episodic low CBF are generally nonspecific and may be difficult to recognize [4). Angiography is imprecise in establishing the diagnosis because this technology is unable to provide the physiologic information necessary to assess the adequacy of primary or collateral regional blood supply [5). Ideally, this analysis is performed by positron emission tomography (PET), which requires the measurement of both CBF and metabolism [6, 7). PET is, however, available at relatively few centers. This article describes the use of stable xenon (Xe)/CT performed before and after a vasodilatory challenge to identify patients with low cerebral blood flow and blood flow reserve. The strategy we followed was derived in part from PET studies that determined that the cerebral arteries maintain CBF in response to decreased perfusion pressure by dilatation [2]. After vessels are maximally dilated, any further compromise in perfusion pressure results in a progressive decrease in blood flow and an accompanying increase in oxygen extraction. When this condition, termed "misery perfusion " [3], has been achieved, additional vasodilatory challenges would not be expected to augment flow. When CBF falls below 20 ml/1 00 gjmin in normal cortical tissue, metabolism and neurologic function become compromised as the regional oxygen and glucose supply to the brain is expended [8, 9). Although local cerebral blood flow values may be reduced by proximal vascular compromise and inadequate supply, CBF can also be reduced by decreased metabolic demand caused by either neuronal loss or deafferentation. Therefore, a single measurement of CBF, regardless of the method-xe-133, single photon emission CT (SPECT), or stable XefCT -does not give nonspecific information in this regard. However, the addition of a second measurement obtained during a vasodilatory challenge can assess whether territorial reserves have been compromised. That is, CBF augmentation would not be expected in regions that already
2 804 ROGG ET AL. AJNR:10, July/August 1989 TABLE 1: Summary of Clinical Histories, Significant Vascular Anatomy by Doppler or Angiographic Investigation, and Categorization by Xe Diamox Analysis in 29 Patients Case Significant Pre-pC02/ Baseline Cerebral Clinical History Age No. Vascular Anatomy Post-pC02 Blood Flow Xe Diamox L hemiparesis R MCA occlusion 59 39/30 Focal R MCA No change Ill expressive distr.; low flow aphasia 2 L facial and upper R ICA occlusion; 78 38/30 Diffuse low Diffuse increase II extremity weak- bilateral moderness; symptoms ate VA related to de- creased blood pressure 3 Transient L L ICA occlusion 55 31/27 Focal L ICA distr.; No change Ill hemisphere low flow symptoms 4 L hemisphere TIAs 74 38/32 Normal Diffuse increase after endarterectomy 5 L TIA R & L VA steno /30 Diffuse low Diffuse increase II sis 6 Aphasia R ICA occlusion 64 32/24 Normal Diffuse increase I 7 Syncope L ICA occlusion 37/32 Normal Diffuse increase I 8 R hemiparesis L ICA occlusion, 66 30/28 Focal R MCA No change Ill 80-90%; R ICA distr.; low flow 9 L carotid bruit Doppler 80% L 50 39/37 Normal Diffuse increase ICA 10 Transient R hemi- Doppler severe L 57 42/40 Focal L MCA de- Unchanged Ill paresis & ex- ICA creased flow pressive aphasia 11 Transient R hemi % L ICA 66 34/24 Normal Diffuse increase paresis 12 L occipital infarct; >80% L ICA 54 42/34 Normal Diffuse increase light-headed- ; >80% ness L subclavian ; R subclavian ocelusion 13 RCVA R ICA occlusion 63 30/26 Low flow R ACA; Diffuse increase II R MCA distr. 14 Transient R hemi- >70% L ICA 32/28 Periinfarct; normal Diffuse increase paresis & aphasia 15 Syncope R ICA occlusion 41/38 Normal Diffuse increase 16 Episodic dizziness >70% L & R VA 67 36/30 Normal Diffuse increase 17 Asymptomatic L ICA occlusion 66 30/27 Global low flow Diffuse increase II 18 Asymptomatic L ICA & RICA 60 36/30 Global low flow Diffuse increase II occlusion 19 R hemiparesis; L MCA occlusion Low normal flow Diffuse increase L caudate (periinfarct) except in infarction infarct 20 Vertigo L ICA, RICA, 70 Global low Diffuse increase II R VA occlusion; L EC-IC bypass 21 R hemisphere R ICA occlusion Focal low R ICA Focal low R ICA Ill TIAs; R amau- R ICA distr. flow distr. rosis fugax 22 R amaurosis fugax L ICA occl; R VA 64 35/28 Diffuse low flow Diffuse increase occl; RICA pseudoocclusion 23 R amaurosis fugax RICA 80% 54 35/26 Normal Diffuse increase ; R subclavian ocelusion 24 R hemiparesis > 80% L ICA ste /28 Low normal Diffuse increase nos is Type
3 AJNR :10, July/August 1989 XejCT OF CEREBRAL BLOOD FLOW 805 Table 1-Continued Case No Clinical History Vertigo L carotid bruit R amaurosis fugax L bruit; old MCA infarct L upper extremity weakness Significant Vascular Anatomy Doppler; R ICA 90% L ICA L ICA & RICA occlusion; 80% L VA ; 60% R VA 99% L ICA ; 50% R ICA 99% RICA ; L ICA occlusion; 50% L & R VA Age Pre-pC02/ Post-pC02 32/32 Baseline Cerebral Blood Flow Diffuse low flow Normal Diffuse low flow Focal low flow (periinfarct) Normal Xe Diamox Focal low Diffuse increase Diffuse increase Diffuse increase Focal decrease (R ICA distr.) Type Ill II Ill Type: I = normal baseline with post-diamox flow augmentation; II = low-flow baseline with post-diamox augmentation; Ill = low or normal baseline with no response or decreased flow post-diamox. Low = 20-35, normal = 35-60, high = > 60 (as defined in text). Note.-ACA = anterior cerebral artery; MCA = middle cerebral artery; PCA = posterior cerebral artery; subclav = subclavian artery; VA = vertebral artery; ICA = internal carotid artery; R = right; L = left; EC-IC = extracranial to intracranial; TIA = transient ischemic attack; CVA = cerebrovascular accident. have maximum vasodilation, while augmentation would be expected in regions with reduced CBF secondary to decreased metabolic demand. On the basis of this theory, some investigators have measured CBF before and after a flow challenge to identify patients with "misery perfusion. " Various methods have been used to create a flow challenge: (1) elevating or lowering blood pressure, (2) having patients inhale a 3-5% carbon dioxide mixture, or, more recently, (3) administering an IV acetazolamide (Diamox) bolus [9-12]. Acetazolamide is easy to administer, safe, and provokes a predictably potent vasodilatory challenge [13-15]. The specific action of the drug that causes vasodilation is unclear, but it is believed that vasodilation is mediated by the drug's inhibition of carbonic anhydrase [12, 13]. The vasodilatory effect appears to be localized to the brain [13, 15, 16], and the activity of the drug remains potent despite baseline increased tissue levels of pc02 [13, 14]. The degree of CBF augmentation found in the normal individual has ranged from 70-90% [12, 13]. With advancing age, activated flows may not increase as dramatically, but flow symmetry will remain preserved [12]. Materials and Methods CBF was determined by the Xe/CT CBF method. The XefCT method is a relatively new CBF technology that provides tomographic, quantitative CBF information with direct anatomic correlation: This methodology has been addressed in detail previously [1, 17-19]. XefCT CBF with an acetazolamide challenge can be performed on an outpatient as well as inpatient basis. The average time to complete a double CBF study-before and 20 min after the administration of General Electric Medical Systems, Milwaukee, WI. TABLE 2: Cerebral Blood Flow* Analysis in Four Representative Cases: The Effect of Diamox by Vascular Territory R ACA L ACA R MCA L MCA R PCA L PCA Type I Baseline Case 26 Diamox % Change 35% 43% 37% 29% 30% 39% Type II Baseline Case 27 Diamox %Change 43% 73% 31 % 50% 65% 60% Type II Baseline Case 28 Diamox %Change 35% 28% 23% 35% 29% 27% Type Ill Baseline Case 29 Diamox %Change 1% -11% -5% 18% 0% 23% Cerebral blood flow measured as mlf100 gfmin. Note.-R = right; L = left; ACA = anterior cerebral artery; MCA = middle cerebral artery; PCA = posterior cerebral artery. acetazolamide-is 60 to 90 min. Patient cooperation is required for this study, which also demands direct involvement of a health care professional. Immediately after the initial CBF study, 1 g of IV acetazolamide is administered. The second study is begun 20 min after drug delivery. Typically, acetazolamide results in a reduction of measured end tidal C02 (see Table 1) without alteration of vital signs or other associated symptoms. We studied 29 patients with significant vascular disease diagnosed by either noninvasive studies or angiography. Twenty-three individuals had at least one significantly stenosed or occluded carotid artery, and 12 had occlusion in two or more major vessels (Table 1 ). Three patients were asymptomatic and underwent these studies because they were found to have a carotid bruit. Twenty-six patients had experienced transient ischemic attacks (TIAs) or fixed neurologic compromise. The latter patients were studied at least 3 weeks after a stroke. This allowed time for the recoupling of CBF and metabolism to occur.
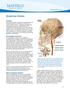
4 806 ROGG ET AL. AJNR:10, July/August 1989 We compared pre- and postacetazolamide CBF studies by using standard contrast-mode software and region-of-interest density software for blood flow analysis (see Fig. 1 ). In the contrast mode, all values above the designated flow level are displayed as white, and all values below as black (see Figs. 2E and 2F). Regions of interest for regional cerebral blood flow (rcbf) were consistent with vascular territories reported by Damasio [20]. Pre- and postacetazolamide blood flow maps were compared for evidence of flow change in corresponding vascular territories. We generally considered rcbf to be within normal limits when flows ranged between 35 and 60 mlf 100 gfmin. Acceptable limits of normal were somewhat dependent on patient age, however, as flows of 35 ml/1 00 gfmin were considered low in a 20-year-old but acceptable in an 80-year-old. An rcbf between 20 and 35 was generally considered low; an rcbf greater than 60 was generally considered elevated. Results The results are summarized in Table 1. This table provides clinical information and significant vascular anatomy for each of the 29 patients in the study. All patients had at least one major vessel with greater than 50%. Twelve (41 %) had multivessel disease. pc02 values are provided to demonstrate that Diamox was physiologically active, blocking carbonic anhydrase and thereby decreasing pc02 in all cases. Three basic types of responses to Diamox are defined: type I, normal CBF before Diamox with flow augmentation after Diamox; type II, diffuse or focal low CBF before Diamox with augmentation after Diamox; type Ill, low or normal CBF before Diamox with no response or decreased CBF after Diamox. Thirteen patients (45%) had a type I response, nine patients (31 %) had a type II response, and seven patients (24%) had a type Ill response. The following four cases are representative of each response type and are described in greater detail in Table 2. A B Type I (case 26, Table 1 ): A 69-year-old man was evaluated after being diagnosed, during a routine physical examination, as having an asymptomatic left carotid bruit. Noninvasive studies showed severe of his left internal carotid artery (ICA). Angiography confirmed 80-90% at the origin of the proximal left ICA; the remainder of the intracranial vasculature and the circle of Willis were normal. A CT scan (Fig. 1 A) was unremarkable, and the baseline XefCT CBF study (Fig. 1 B) was normal. Flow was symmetrical in all territories, with most values ranging between 45 and 55 mlf 1 00 gjmin. Twenty minutes after the patient received 1 g of IV acetazolamide, we performed a second CBF study (Fig. 1 C), which showed an average flow increase of 36% in all vascular territories (Table 2). Type II (case 27, Table 1 ): A 63-year-old woman presented with a sudden onset of blindness in the right eye that resolved partially over the next 6 weeks. Angiography demonstrated 90% at the origin of the left common carotid artery and occlusion of the left internal carotid artery (ICA). The right ICA also was occluded, and the right external carotid artery was moderately stenotic at its origin. The origin of the left vertebral artery had an 80%, and the origin of the right vertebral artery had 50-60%. Collateral supply to the right ICA siphon was supplied by ethmoidal vessels. In addition to flow from the right ICA, the right anterior cerebral artery (ACA) and middle cerebral artery (MCA) also received collateral flow through the right posterior communicating artery and leptomeningeal collaterals from the right posterior cerebral distributions. The baseline XefCT CBF study demonstrated lower flow values bilaterally than would be expected in a 63-year-old person (a mean of 29, Table 2). The introduction of acetazolamide, however, caused a symmetrical flow augmentation of 55% (up to 44.9 mlf1 00 gjmin). Type II (case 28, Table 1 ): A 42-year-old man presented with an asymptomatic bruit found after a significant left hemic Fig. 1.-A-C, Case 26. XefCT scans demonstrate a representative type I normal scan series. A, The middle of the usual three levels selected for evaluation. B, Baseline XefCT image with superimposed vascular territory map and region of interest blood flows (ml/100 gfmin). C, Repeat Xe fct CBF evaluation after Diamox (1 g IV). Flow augmentation has occurred in all vascular territories.
5 AJNR :1 0, July/August 1989 XejCT OF CEREBRAL BLOOD FLOW 807 sphere, closed head injury. His examination revealed a mild residual expressive aphasia. CT images disclosed an area of encephalomalacia in the left middle cerebral artery distribution, consistent with a remote infarction (Fig. 2A). Angiography demonstrated 99% at the origin of the left ICA and 50% at the origin of the right ICA. Collateral flow to the left hemisphere occurred by retrograde ophthalmic artery flow to the carotid siphon, and by posterior communicating artery and leptomeningeal collaterals from the posterior circulation. The baseline XejCT CBF study showed an area of hypoperfusion corresponding to the site of previous infarction, but also showed compromised flow values in the remainder of the left middle cerebral artery (Figs. 2B, 2E, and Table 2). After receiving 1 g of acetazolamide, there was an increase of CBF in all territories, including the region immediately posterior to the infarction within the distal distribution of the middle cerebral artery (Figs. 2C, 2F, and Table 2). Type Ill (case 29, Table 1): A 55-year-old man presented with left upper extremity weakness and left facial paresis of recent onset. An angiogram defined a 95% at the proximal right ICA, and complete occlusion of the left ICA. The left and right anterior and middle cerebral arteries were supplied by the stenotic right ICA. The left middle cerebral artery was supplied by collateral vessels from the left external A 8 c Fig. 2.-A-F, Case 28. Xe/CT scans demonstrate a representative type II scan series. A shows an area of encephalomalacia in left frontoparietal region from a previous infarction. The level above, D, appears normal. In 8 and E, Xe/CT shows that the area of decreased CBF is greater than that expected from plain CT. Flows are decreased in the left frontal and midparietal regions anterior and posterior to the old infarction, as well as in the frontoparietal region above the site of the infarct. In C and F, Post-Diamox flow augmentation is seen in periinfarct zone at level of, and cephalad to, the known area of encephalomalacia. E and F were filmed at a level of 20 (white= flow greater than 20 ml/100 gfmin) to accentuate flow differences before and after Diamox.
6 808 ROGG ET AL. AJNR:1 0, July/August 1989 carotid and left posterior cerebral arteries. The origins of both vertebral arteries were moderately stenotic. A CT scan was unremarkable (Fig. 3A). The baseline XejCT CBF study disclosed normal baseline flow values within all territories, but with mild asymmetry (R < L) (Figs. 38, 3C, and Table 2). After the addition of acetazolamide, flow remained unchanged or decreased in all right anterior circulation territories and in the left anterior cerebral artery territory (Figs. 30, 3E, and Table 2). Discussion The diagnostic utility and specificity provided by the use of acetazolamide as a vasodilatory challenge were suggested by Vorstrup et al. [21 ], who used Xe-133 with SPECT imaging to evaluate patients before and after extracranial-intracranial bypass operations [21, 22]. These researchers noted postoperative augmentation of resting CBF in only one of the 13 patients with preoperative regional hypoperfusion; this patient was also the only patient in the study whose CBF was not increased after preoperative acetazolamide flow challenge. These findings support the contention that acetazolamide flow challenge can identify those patients who already have maximal vasodilation and minimal flow reserves. On the basis of our experience, we defined three types of responses to an acetazolamide challenge: I, an increase in normal baseline flow values; II, an increase in focal or diffuse low flow values; and Ill, no change or a decrease in low or normal flow values. Type Ill is the only group that would A 8 c D E F Fig. 3.-A-F, Case 29. Xe{CT scans demonstrate a representative type Ill scan series. A shows a baseline CT with low-normal right hemispheric CBF (8) on baseline Xe{CT scans. C displays the CBF data shown in B at a flow threshold of 20 ml/1 00 gfmin. The post-diamox (0 and E) scans demonstrate decreased CBF from baseline in right and left anterior cerebral and right middle cerebral artery territories. F, obtained 48 hr after xenon evaluation, shows massive area of infarction corresponding to region of predicted CBF compromise.
7 AJNR :1 0, July/August 1989 XefCT OF CEREBRAL BLOOD FLOW 809 include the single patient reported by Vorstrup et al. [21] and the group with "misery perfusion" reported by Baron et al. [3]. Each of these categories is represented by one or two of the cases described earlier. Case 26 is an example of type 1: normal baseline CBF that increased significantly after the administration of acetazolamide. This patient is typical of many patients (13 of 29) we studied who had normal flow despite angiographic evidence of significant or occlusion. Cases 27 and 28 exemplify type II : diffuse or focal low flow in baseline studies but with maintained reserves of CBF as demonstrated by the ability to augment flow with acetazolamide. Nine of our 29 patients fell into this group. Although angiography suggested that the supply of blood was severely compromised in case 27, the patient's retention of blood flow reserves suggested that the low flow areas were appropriate to the decreased demand. The patient's absence of further symptoms while on anticoagulation therapy in the 6 months following this assessment supports our assumption of an embolic origin of her symptoms. Case 28 illustrates reduced CBF, and presumably reduced metabolism, due to deafferentation. Figure 2B shows a region with relatively low flow posterior to the CT-defined infarction, despite the relatively normal appearance of this region on the CT images. After acetazolamide administration, the flow in this area increased, providing evidence for adequate availability of blood flow, but reduced demand. The presence of a larger area of flow and metabolic disturbance than suggested by the CT-defined injury has been widely reported [23]. Case 29 represents type Ill, low or normal baseline flow values that decreased in a potentially compromised vascular distribution after the patient received acetazolamide, despite an elevation of CBF in other areas. This finding suggested that there is little potential for collateral flow to the portion of the brain that angiography has shown to be supplied preferentially by the right ICA. If the right ICA were further compromised, the patient would be at a significant risk of sustaining a massive infarct [24]. The patient was scheduled for emergency right carotid endarterectomy but before this could be performed, 36 hr after the study, the predictive value of the acetazolamide challenge was substantiated by the onset of a massive stroke in the territory of the right middle cerebral artery (Fig. 3F). Seven (24%) of our 29 patients with significant occlusive vascular disease were in this category. Despite angiographic andfor noninvasive evidence of significant occlusive vascular disease, 76% of the patients studied by XefCT CBF had, at rest, flow values that increased significantly with acetazolamide. This finding is consistent with earlier reports that emphasize the imprecision of existing anatomic methods for predicting hemodynamic compromise [5], and is supported by Sullivan et al. [13], who found that 40% of patients with significant vascular disease on angiography had normal CBF when given an acetazolamide flow challenge and studied by Xe-133 scintillation counting. The tudies of Vorstrup and others along with our own limited experience indicate that patients who have type Ill responses are those most likely to benefit from medical or surgical efforts to augment CBF delivery. Although the international study of extracranial-intracranial bypass operations suggested that flow augmentation procedures were not of significant clinical benefit [25, 26], a recent review of that study suggests that a subgroup of critically flow-dependent patients may have been excluded [27]. Our experience indicates that the XefCT CBF technique combined with a challenge of flow reserve is a useful clinical means to identify a hemodynamically compromised subgroup of individuals who may have transient symptoms due to a marginal basal level of perfusion that transiently drops to a level inadequate to maintain function. Once such persons are identified, future studies are needed to define their prognosis and determine whether they may benefit from either medical or surgical approaches. In summary, we believe that Xe/CT CBF measurements used with an acetazolamide challenge provide an objective, clinically accessible method of assessing cerebral blood flow and blood flow reserve. REFERENCES 1. Yonas H, Gur D, Good B, et al. Stable xenon CT blood flow mapping for evaluation of patients with extracranial-intracranial bypass surgery. J Neurosurg 1985;62 : Grubb RL Jr, Ratcheson R, Raichic M, et al. Regional cerebral blood flow and cerebral oxygen utilization in superficial temporal middle cerebral artery anastomosis patients. Acta Neural Scand 1979;60: Baron JC, Sausser MG, Rex A, et al. Reversal of focal "misery perfusion syndrome" by extra- intracranial arterial bypass in hemodynamic cerebral ischemia: a case study with 0-15 positron emission tomography. Stroke 1981;12: Kistler PJ, Popper AH, Heres RC. Therapy of ischemic cerebral vascular disease due to atherothrombosis. N Eng/ J Med 1984;311 :22-34, 1984; 311 : Latchaw RE, Ausman Jl, Lee M. Superficial temporal-middle cerebral artery bypass: a detailed analysis of multiple pre- and post-operative angiograms in 40 consecutive patients. J Neurosurg 1979;51 : Lebrun-Grandie P, Baron JC, Soussaline F, et al. Coupling between regional blood flow and oxygen utilization in the normal human brain: a study with positron tomography and oxygen-15. Arch Neural 1986;4: Lenzi GL, Frackowiak RS, Jones T. Cerebral oxygen metabolism and blood flow in human cerebral ischemic infarction. J Cereb Blood Flow Metab 1982;2: Jones TH, Morawetz RB, Crowell RM, et al. Thresholds of focal cerebral ischemia in awake monkeys. J Neurosurg 1981;54: Yonas H, Gur D, Claassen D, Wolfson SK Jr, Moossy J. Stable xenonenhanced computed tomography in the study of clinical and pathologic correlates of focal ischemia in baboons.. Stroke 1988;19: Norrving B, Bengt N, Risberg J. rc BF in patients with carotid occlusion; resting and hypercapnic flow related to collateral pattern. Stroke 1982;13: Grubb Rl, Reichle ME, Erchling JO, et al. The effects of changes in PaC02 on cerebral blood volume, blood flow and vascular mean transit time. Stroke 1974;5: Aauge A, Thoresen M, Walle L. Changes in cerebral blood flow during hyperventilation and C02-breathing measured transcranially in humans by pulsed bidirectional ultrasound Doppler blood velocity meter. Acta Physiol Scand 1980;110: Sullivan HG, Kingsbury TB, Morgan MS, et al. The rcbf response to Diamox in norm al subjects and cerebrovascular disease patients. J Neurosurg 1987;67: Hauge A, Nicolaysen G, Thoresen M. Acute effects of acetazolamide on cerebral blood flow in man. Acta Physiol Scand 1983;117: Cotev S, Lee J, Severinghaus JW. The effects of acetazolamide on cerebral blood flow and cerebral tissue PC02. Anesthesiology 1968;29 : Macri JJ, Politoff A, Rubin R, Dixon R, Rail D. Preferential vasoconstrictor properties of acetazolamide on the arteries of the choroid plexus. lnt J
8 810 ROGG ET AL. AJNR:10, July/August 1989 Neuropharmaco/ 1966;5 : Gur D, Wolfsen SK, Yonas H, et al. Progress in cerebrovascular disease: local cerebral blood flow by xenon-enhanced CT. Stroke 1982;13: Yonas H, Good WF, Gur D, et al. Mapping cerebral blood flow by xenonenhanced computed tomography: clinical experience. Radiology 1984; 152: Yonas H, Wolfson SK Jr, Gur D, et al. Clinical experience with the use of xenon-enhanced CT blood flow mapping in cerebral vascular disease. Stroke 1984;15: Damasio H. A computed tomographic guide to the identification of cerebral vascular territories. Arch Neuro/1983;40: Vorstrup S, Paulson OB, Lassen NA. How to identify hemodynamic cases. In: Spetzler, Carter, Selman, Martin, eds. Cerebral revascularization for stroke. New York: Theme-Stratton, Batjer HH, Devous MD, Purdy PD, et al. Improvement in regional cerebral blood flow and cerebral vasoreactivity after extracranial-intracranial arterial bypass. Neurosurgery 1988; 22: Kuhl DE, Phelps ME, Kowell AP, Metter EJ, Selin C, Winter J. Effects of stroke on local cerebral metabolism and perfusion: mapping by emission computed tomography of '"FOG and 13 NH 3. Ann Neuro/1980;8: Yonas H, Steed D, Latchaw R, Gur D, Peitzman A, Webster M. Relief of nonhemispheric symptoms in low flow states by anterior circulation revascularization: a physiologic approach. J Vase Surg 1987;5: EC/IC Bypass Study Group. Failure of extracranial-intracranial arterial bypass to reduce the risk of ischemic stroke. N Eng/ J Med 1985; 313: Plum F. Extracranial-intracranial arterial bypass and cerebral vascular disease. N Eng/ J Med 1985;313: Sundt TM Jr. Was the international randomized trial of ECfiC arterial bypass representative of the population at risk? N Eng/ J Med 1987; 316:
Balloon Test Occlusion of the Internal Carotid Artery with Stable Xenon/CT Cerebral Blood Flow Imaging
 533 Balloon Test Occlusion of the Internal Carotid Artery with Stable Xenon/CT Cerebral Blood Flow Imaging S. M. Erba 1 J. A. Horton 1 R. E. Latchaw 1 H. Yonas 2 L. Sekhar2 V. Schramm 3 S. Pentheny1 We
533 Balloon Test Occlusion of the Internal Carotid Artery with Stable Xenon/CT Cerebral Blood Flow Imaging S. M. Erba 1 J. A. Horton 1 R. E. Latchaw 1 H. Yonas 2 L. Sekhar2 V. Schramm 3 S. Pentheny1 We
Compromised cerebral blood flow reactivity is a predictor of stroke in patients with symptomatic carotid artery occlusive disease
 Compromised cerebral blood flow reactivity is a predictor of stroke in patients with symptomatic carotid artery occlusive disease Marshall W. Webster, MD, Michel S. Makaroun, MD, David L. Steed, MD, Holly
Compromised cerebral blood flow reactivity is a predictor of stroke in patients with symptomatic carotid artery occlusive disease Marshall W. Webster, MD, Michel S. Makaroun, MD, David L. Steed, MD, Holly
Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography
 Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography Kazumi Kimura, Yoichiro Hashimoto, Teruyuki Hirano, Makoto Uchino, and Masayuki Ando PURPOSE: To determine
Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography Kazumi Kimura, Yoichiro Hashimoto, Teruyuki Hirano, Makoto Uchino, and Masayuki Ando PURPOSE: To determine
Acetazolamide enhanced single photon emission computed tomography (SPECT) evaluation of cerebral perfusion before and after carotid endarterectomy
 Acetazolamide enhanced single photon emission computed tomography (SPECT) evaluation of cerebral perfusion before and after carotid endarterectomy Dolores F. Cikrit, MD, Robert W. Butt, MD, Michael C.
Acetazolamide enhanced single photon emission computed tomography (SPECT) evaluation of cerebral perfusion before and after carotid endarterectomy Dolores F. Cikrit, MD, Robert W. Butt, MD, Michael C.
Cerebral Hemodynamic Change in the Child and the Adult With Moyamoya Disease
 272 Cerebral Hemodynamic Change in the Child and the Adult With Moyamoya Disease Yasuo Kuwabara, MD, Yuichi Ichiya, MD, Makoto Otsuka, MD, Takashi Tahara, MD, Ranjan Gunasekera, MD, Kanehiro Hasuo, MD,
272 Cerebral Hemodynamic Change in the Child and the Adult With Moyamoya Disease Yasuo Kuwabara, MD, Yuichi Ichiya, MD, Makoto Otsuka, MD, Takashi Tahara, MD, Ranjan Gunasekera, MD, Kanehiro Hasuo, MD,
Hasan T. Ozgur, T. Kent Walsh, Anthony Masaryk, Joachim F. Seeger, Walter Williams, Elizabeth Krupinski, Miguel Melgar, and Enrique Labadie
 AJNR Am J Neuroradiol :98 96, May 00 Correlation of Cerebrovascular Reserve as Measured by Acetazolamide-challenged SPECT with Angiographic Flow Patterns and Intra- or Extracranial Arterial Stenosis Hasan
AJNR Am J Neuroradiol :98 96, May 00 Correlation of Cerebrovascular Reserve as Measured by Acetazolamide-challenged SPECT with Angiographic Flow Patterns and Intra- or Extracranial Arterial Stenosis Hasan
I n patients with occlusion of the internal carotid artery
 1697 PAPER Pattern of collaterals, type of infarcts, and haemodynamic impairment in carotid artery occlusion H Yamauchi, T Kudoh, K Sugimoto, M Takahashi, Y Kishibe, H Okazawa... See Editorial Commentary,
1697 PAPER Pattern of collaterals, type of infarcts, and haemodynamic impairment in carotid artery occlusion H Yamauchi, T Kudoh, K Sugimoto, M Takahashi, Y Kishibe, H Okazawa... See Editorial Commentary,
Chronic middle cerebral artery (MCA) occlusion as a cause
 ORIGINAL RESEARCH M. Tanaka E. Shimosegawa K. Kajimoto Y. Kimura H. Kato N. Oku M. Hori K. Kitagawa J. Hatazawa Chronic Middle Cerebral Artery Occlusion: A Hemodynamic and Metabolic Study with Positron-Emission
ORIGINAL RESEARCH M. Tanaka E. Shimosegawa K. Kajimoto Y. Kimura H. Kato N. Oku M. Hori K. Kitagawa J. Hatazawa Chronic Middle Cerebral Artery Occlusion: A Hemodynamic and Metabolic Study with Positron-Emission
Since the introduction of extracranial-intracranial (ECIC)
 ORIGINAL RESEARCH A. Nakamizo T. Inoue Y. Kikkawa K. Uda Y. Hirata K. Okamura M. Yasaka Y. Okada Postoperative Evaluation of Changes in Extracranial-Intracranial Bypass Graft Using Superficial Temporal
ORIGINAL RESEARCH A. Nakamizo T. Inoue Y. Kikkawa K. Uda Y. Hirata K. Okamura M. Yasaka Y. Okada Postoperative Evaluation of Changes in Extracranial-Intracranial Bypass Graft Using Superficial Temporal
Stroke/TIA. Tom Bedwell
 Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
Arterial Occlusion Following Anastomosis of the Superficial Temporal Artery to Middle Cerebral Artery
 Arterial Occlusion Following Anastomosis of the Superficial Temporal Artery to Middle Cerebral Artery 91 ANTHONY J. FURLAN, M.D., JOHN R. LITTLE, M.D., AND DONALD F. DOHN, M.D. SUMMARY Symptoms of cerebral
Arterial Occlusion Following Anastomosis of the Superficial Temporal Artery to Middle Cerebral Artery 91 ANTHONY J. FURLAN, M.D., JOHN R. LITTLE, M.D., AND DONALD F. DOHN, M.D. SUMMARY Symptoms of cerebral
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
[ 15 0]H 2 0 Positron Emission Tomography Determination of Cerebral Blood Flow during Balloon Test Occlusion of the Internal Carotid Artery
![[ 15 0]H 2 0 Positron Emission Tomography Determination of Cerebral Blood Flow during Balloon Test Occlusion of the Internal Carotid Artery [ 15 0]H 2 0 Positron Emission Tomography Determination of Cerebral Blood Flow during Balloon Test Occlusion of the Internal Carotid Artery](/thumbs/84/91207644.jpg) [ 15 0]H 2 0 Positron Emission Tomography Determination of Cerebral Blood Flow during Balloon Test Occlusion of the Internal Carotid Artery James A. Brunberg, Kirk A. Frey, Joseph A. Horton, John P. Deveikis,
[ 15 0]H 2 0 Positron Emission Tomography Determination of Cerebral Blood Flow during Balloon Test Occlusion of the Internal Carotid Artery James A. Brunberg, Kirk A. Frey, Joseph A. Horton, John P. Deveikis,
Estimation of Cerebrovascular Reactivity Using Transcranial Doppler, Including the Use of Breath-Holding as the Vasodilatory Stimulus
 668 Estimation of Cerebrovascular Reactivity Using Transcranial Doppler, Including the Use of Breath-Holding as the Vasodilatory Stimulus H.S. Markus, MRCP, and M.J.G. Harrison, FRCP Background and Purpose:
668 Estimation of Cerebrovascular Reactivity Using Transcranial Doppler, Including the Use of Breath-Holding as the Vasodilatory Stimulus H.S. Markus, MRCP, and M.J.G. Harrison, FRCP Background and Purpose:
INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU
 CEREBRAL BYPASS An Innovative Treatment for Arteritis INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU CASE 1 q 1 year old girl -recurrent seizure, right side limb weakness, excessive cry and irritability.
CEREBRAL BYPASS An Innovative Treatment for Arteritis INSTITUTE OF NEUROSURGERY & DEPARTMENT OF PICU CASE 1 q 1 year old girl -recurrent seizure, right side limb weakness, excessive cry and irritability.
Effect of Chronic Middle Cerebral Artery Stenosis on the Local Cerebral Hemodynamics
 24 Effect of Chronic Middle Cerebral Artery Stenosis on the Local Cerebral Hemodynamics HIROAKI NARITOMI, M.D.,* TOHRU SAWADA, M.D.,t YOSHIHIRO KURIYAMA, M.D.,t HIDEKAZU KINUGAWA, M.D.,t TAKAJI KANEKO,
24 Effect of Chronic Middle Cerebral Artery Stenosis on the Local Cerebral Hemodynamics HIROAKI NARITOMI, M.D.,* TOHRU SAWADA, M.D.,t YOSHIHIRO KURIYAMA, M.D.,t HIDEKAZU KINUGAWA, M.D.,t TAKAJI KANEKO,
Double STA-MCA Anatomosis for Bilateral Carotid Occlusion
 Double STA-MCA Anatomosis for Bilateral Carotid Occlusion -Case Report and Literature Review- Sandra vuignier 1, Kenji Kanamaru 2, Tomohiro Araki 2 1 Department of Neurosurgery, Nagoya University School
Double STA-MCA Anatomosis for Bilateral Carotid Occlusion -Case Report and Literature Review- Sandra vuignier 1, Kenji Kanamaru 2, Tomohiro Araki 2 1 Department of Neurosurgery, Nagoya University School
Blood Supply. Allen Chung, class of 2013
 Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
Guidelines for Ultrasound Surveillance
 Guidelines for Ultrasound Surveillance Carotid & Lower Extremity by Ian Hamilton, Jr, MD, MBA, RPVI, FACS Corporate Medical Director BlueCross BlueShield of Tennessee guidelines for ultrasound surveillance
Guidelines for Ultrasound Surveillance Carotid & Lower Extremity by Ian Hamilton, Jr, MD, MBA, RPVI, FACS Corporate Medical Director BlueCross BlueShield of Tennessee guidelines for ultrasound surveillance
TABLES. Table 1 Terminal vessel aneurysms. Table. Aneurysm location. Bypass flow** Symptoms Strategy Bypass recipient. Age/ Sex.
 Table TABLES Table 1 Terminal vessel aneurysms Age/ Sex Aneurysm location Symptoms Strategy Bypass recipient Recipient territory Recipient territory flow* Cut flow Bypass flow** Graft Patent postop F/U
Table TABLES Table 1 Terminal vessel aneurysms Age/ Sex Aneurysm location Symptoms Strategy Bypass recipient Recipient territory Recipient territory flow* Cut flow Bypass flow** Graft Patent postop F/U
MMD is a rare cerebrovascular disease first described by
 ORIGINAL RESEARCH M.A. Mogensen P. Karzmark P.D. Zeifert J. Rosenberg M. Marks G.K. Steinberg L.J. Dorfman Neuroradiologic Correlates of Cognitive Impairment in Adult Moyamoya Disease BACKGROUND AND PURPOSE:
ORIGINAL RESEARCH M.A. Mogensen P. Karzmark P.D. Zeifert J. Rosenberg M. Marks G.K. Steinberg L.J. Dorfman Neuroradiologic Correlates of Cognitive Impairment in Adult Moyamoya Disease BACKGROUND AND PURPOSE:
Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke
 Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke Tetsuyoshi Horiuchi, Junpei Nitta, Shigetoshi Ishizaka, Kohei Kanaya, Takao Yanagawa, and Kazuhiro Hongo. Department of Neurosurgery,
Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke Tetsuyoshi Horiuchi, Junpei Nitta, Shigetoshi Ishizaka, Kohei Kanaya, Takao Yanagawa, and Kazuhiro Hongo. Department of Neurosurgery,
Neuro Quiz 29 Transcranial Doppler Monitoring
 Verghese Cherian, MD, FFARCSI Penn State Hershey Medical Center, Hershey Quiz Team Shobana Rajan, M.D Suneeta Gollapudy, M.D Angele Marie Theard, M.D Neuro Quiz 29 Transcranial Doppler Monitoring This
Verghese Cherian, MD, FFARCSI Penn State Hershey Medical Center, Hershey Quiz Team Shobana Rajan, M.D Suneeta Gollapudy, M.D Angele Marie Theard, M.D Neuro Quiz 29 Transcranial Doppler Monitoring This
Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report
 Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report BY JIRI J. VITEK, M.D., JAMES H. HALSEY, JR., M.D., AND HOLT A. McDOWELL, M.D. Abstract: Occlusion of All Four
Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report BY JIRI J. VITEK, M.D., JAMES H. HALSEY, JR., M.D., AND HOLT A. McDOWELL, M.D. Abstract: Occlusion of All Four
Carotid Embolectomy and Endarterectomy for Symptomatic Complete Occlusion of the Carotid Artery as a Rescue Therapy in Acute Ischemic Stroke
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
The severity of neurologic deficits associated with
 Effect of Internal Carotid Artery Occlusion on Intracranial Hemodynamics Transcranial Doppler Evaluation and Clinical Correlation 589 Peter A. Schneider, MD, Mary E. Rossman, RVT, Eugene F. Bernstein,
Effect of Internal Carotid Artery Occlusion on Intracranial Hemodynamics Transcranial Doppler Evaluation and Clinical Correlation 589 Peter A. Schneider, MD, Mary E. Rossman, RVT, Eugene F. Bernstein,
History of revascularization
 History of revascularization Author (year) Kredel, 1942 Woringer& Kunlin, 1963 Donaghy& Yasargil, 1968 Loughheed 1971 Kikuchini & Karasawa1973 Karasawa, 1977 Story, 1978 Sundt, 1982 EC/IC bypass study
History of revascularization Author (year) Kredel, 1942 Woringer& Kunlin, 1963 Donaghy& Yasargil, 1968 Loughheed 1971 Kikuchini & Karasawa1973 Karasawa, 1977 Story, 1978 Sundt, 1982 EC/IC bypass study
Recanalization of Chronic Carotid Artery Occlusion Objective Improvement Of Cerebral Perfusion
 Recanalization of Chronic Carotid Artery Occlusion Objective Improvement Of Cerebral Perfusion Paul Hsien-Li Kao, MD Assistant Professor National Taiwan University Medical School and Hospital ICA stenting
Recanalization of Chronic Carotid Artery Occlusion Objective Improvement Of Cerebral Perfusion Paul Hsien-Li Kao, MD Assistant Professor National Taiwan University Medical School and Hospital ICA stenting
Assessment of Cerebrovascular Reserve before and after STA-MCA Bypass Surgery by SPECT and SPM Analysis
 Assessment of Cerebrovascular Reserve before and after STA-MCA Bypass Surgery by SPECT and SPM Analysis Joo-Hyun O, MD 1 Kyung-Sool Jang, MD 2 Ie-Ryung Yoo, MD 1 Sung-Hoon Kim, MD 1 Soo-Kyo Chung, MD 1
Assessment of Cerebrovascular Reserve before and after STA-MCA Bypass Surgery by SPECT and SPM Analysis Joo-Hyun O, MD 1 Kyung-Sool Jang, MD 2 Ie-Ryung Yoo, MD 1 Sung-Hoon Kim, MD 1 Soo-Kyo Chung, MD 1
Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery
 2011 65 4 239 245 Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery a* a b a a a b 240 65 4 2011 241 9 1 60 10 2 62 17 3 67 2 4 64 7 5 69 5 6 71 1 7 55 13 8 73 1
2011 65 4 239 245 Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery a* a b a a a b 240 65 4 2011 241 9 1 60 10 2 62 17 3 67 2 4 64 7 5 69 5 6 71 1 7 55 13 8 73 1
Carotid artery stenting for long CTO and pseudo occlusion of carotid artery -2 case reports-
 Carotid artery stenting for long CTO and pseudo occlusion of carotid artery -2 case reports- Katsutoshi Takayama, MD, Ph.D Department of Radiology and Interventional Neuroradiology Ishinkai Yao General
Carotid artery stenting for long CTO and pseudo occlusion of carotid artery -2 case reports- Katsutoshi Takayama, MD, Ph.D Department of Radiology and Interventional Neuroradiology Ishinkai Yao General
Overview Blood supply of the brain What is moyamoya disease? > 1
 Moyamoya Disease Overview Moyamoya disease is caused by blocked arteries at the base of the brain. The name "moyamoya" means "puff of smoke" in Japanese and describes the appearance of tiny vessels that
Moyamoya Disease Overview Moyamoya disease is caused by blocked arteries at the base of the brain. The name "moyamoya" means "puff of smoke" in Japanese and describes the appearance of tiny vessels that
Relief of nonhemispheric symptoms in low flow states by anterior circulation revascularization: A physiologic approach
 Relief of nonhemispheric symptoms in low flow states by anterior circulation revascularization: A physiologic approach Howard Yonas, M.D., David L. Steed, M.D., Richard E. Latchaw, M.D., David Gur, Sc.D.,
Relief of nonhemispheric symptoms in low flow states by anterior circulation revascularization: A physiologic approach Howard Yonas, M.D., David L. Steed, M.D., Richard E. Latchaw, M.D., David Gur, Sc.D.,
Amaurosis fugax: some aspects of management
 Journal of Neurology, Neurosurgery, and Psvchiatry 1982;45:1-6 Amaurosis fugax: some aspects of management PJ PARKIN, BE KENDALL, J MARSHALL, WI McDONALD From the National Hospital for Nervous Diseases,
Journal of Neurology, Neurosurgery, and Psvchiatry 1982;45:1-6 Amaurosis fugax: some aspects of management PJ PARKIN, BE KENDALL, J MARSHALL, WI McDONALD From the National Hospital for Nervous Diseases,
Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature
 Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Romanian Neurosurgery Volume XXXI Number 3 2017 July-September Article Moyamoya Syndrome with contra lateral DACA aneurysm: First Case report with review of literature Ashish Kumar Dwivedi, Pradeep Kumar,
Lecture Outline: 1/5/14
 John P. Karis, MD Lecture Outline: Provide a clinical overview of stroke: Risk Prevention Diagnosis Intervention Illustrate how MRI is used in the diagnosis and management of stroke. Illustrate how competing
John P. Karis, MD Lecture Outline: Provide a clinical overview of stroke: Risk Prevention Diagnosis Intervention Illustrate how MRI is used in the diagnosis and management of stroke. Illustrate how competing
This quiz is being published on behalf of the Education Committee of the SNACC.
 Quiz 48 Cerebrovascular Atherosclerotic Disease Shobana Rajan, M.D. Associate Director of Neuroanesthesia, Vice Chair of Education, Allegheny Health Network. Quiz team; Suneeta Gollapudy M.D, Angele Marie
Quiz 48 Cerebrovascular Atherosclerotic Disease Shobana Rajan, M.D. Associate Director of Neuroanesthesia, Vice Chair of Education, Allegheny Health Network. Quiz team; Suneeta Gollapudy M.D, Angele Marie
Neurosurg Focus 5 (5):Article 4, 1998
 Neurosurg Focus 5 (5):Article 4, 1998 Multiple combined indirect procedure for the surgical treatment of children with moyamoya disease. A comparison with single indirect anastomosis with direct anastomosis
Neurosurg Focus 5 (5):Article 4, 1998 Multiple combined indirect procedure for the surgical treatment of children with moyamoya disease. A comparison with single indirect anastomosis with direct anastomosis
Article. Ilkay Uzunca, MD, Talip Asil, MD, Kemal Balci, MD, Ufuk Utku, MD
 Article Evaluation of Vasomotor Reactivity by Transcranial Doppler Sonography in Patients With Acute Stroke Who Have Symptomatic Intracranial and Extracranial Stenosis Ilkay Uzunca, MD, Talip Asil, MD,
Article Evaluation of Vasomotor Reactivity by Transcranial Doppler Sonography in Patients With Acute Stroke Who Have Symptomatic Intracranial and Extracranial Stenosis Ilkay Uzunca, MD, Talip Asil, MD,
The phenomenon of unilateral loss of vision in
 554 Short Communication Bilateral Loss of Vision in Bright Light David 0. Wiebers, MD, Jerry W. Swanson, MD, Terrence L. Cascino, MD, and Jack P. Whisnant, MD We describe four patients with episodic bilateral
554 Short Communication Bilateral Loss of Vision in Bright Light David 0. Wiebers, MD, Jerry W. Swanson, MD, Terrence L. Cascino, MD, and Jack P. Whisnant, MD We describe four patients with episodic bilateral
Occlusio Supra Occlusionem: Intracranial Occlusions Following Carotid Thrombosis as Diagnosed by Cerebral Angiography
 Occlusio Supra Occlusionem: Intracranial Occlusions Following Carotid Thrombosis as Diagnosed by Cerebral Angiography BY B. ALBERT RING, M.D. Abstract: Occlusio Supra Occlusionem: Intracranial Occlusions
Occlusio Supra Occlusionem: Intracranial Occlusions Following Carotid Thrombosis as Diagnosed by Cerebral Angiography BY B. ALBERT RING, M.D. Abstract: Occlusio Supra Occlusionem: Intracranial Occlusions
PAPER F National Collaborating Centre for Chronic Conditions at the Royal College of Physicians
 6.3 Early carotid imaging in acute stroke or TIA Evidence Tables IMAG4: Which patients with suspected stroke/tia should be referred for urgent carotid imaging? Reference Ahmed AS, Foley E, Brannigan AE
6.3 Early carotid imaging in acute stroke or TIA Evidence Tables IMAG4: Which patients with suspected stroke/tia should be referred for urgent carotid imaging? Reference Ahmed AS, Foley E, Brannigan AE
TIA AND STROKE. Topics/Order of the day 1. Topics/Order of the day 2 01/08/2012
 Charles Ashton Medical Director TIA AND STROKE Topics/Order of the day 1 What Works? Clinical features of TIA inc the difference between Carotid and Vertebral territories When is a TIA not a TIA TIA management
Charles Ashton Medical Director TIA AND STROKE Topics/Order of the day 1 What Works? Clinical features of TIA inc the difference between Carotid and Vertebral territories When is a TIA not a TIA TIA management
Disclosures. CREST Trial: Summary. Lecture Outline 4/16/2015. Cervical Atherosclerotic Disease
 Disclosures Your Patient Has Carotid Bulb Stenosis and a Tandem Intracranial Stenosis: How Do SAMMPRIS and Other Evidence Inform Your Treatment? UCSF Vascular Symposium 2015 Steven W. Hetts, MD Associate
Disclosures Your Patient Has Carotid Bulb Stenosis and a Tandem Intracranial Stenosis: How Do SAMMPRIS and Other Evidence Inform Your Treatment? UCSF Vascular Symposium 2015 Steven W. Hetts, MD Associate
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Asymptomatic Occlusion of an Internal Carotid Artery in a Hospital Population: Determined by Directional Doppler Ophthalmosonometry
 Asymptomatic Occlusion of an Internal Carotid Artery in a Hospital Population: Determined by Directional Doppler Ophthalmosonometry BY MARK L. DYKEN, M.D.,* J. FREDERICK DOEPKER, JR., RICHARD KIOVSKY,
Asymptomatic Occlusion of an Internal Carotid Artery in a Hospital Population: Determined by Directional Doppler Ophthalmosonometry BY MARK L. DYKEN, M.D.,* J. FREDERICK DOEPKER, JR., RICHARD KIOVSKY,
Assessment Of Collateral Pathways In Acute Ischemic Cerebrovascular Stroke Using A Mansour Grading Scale; A New Scale, A Pilot Study
 ISPUB.COM The Internet Journal of Interventional Medicine Volume 3 Number 1 Assessment Of Collateral Pathways In Acute Ischemic Cerebrovascular Stroke Using A Mansour Grading Scale; A New Scale, A Pilot
ISPUB.COM The Internet Journal of Interventional Medicine Volume 3 Number 1 Assessment Of Collateral Pathways In Acute Ischemic Cerebrovascular Stroke Using A Mansour Grading Scale; A New Scale, A Pilot
Occlusion or severe stenosis of the carotid artery and its
 ORIGINAL RESEARCH S. Xie L.H. Hui J.X. Xiao X.D. Zhang Q. Peng Detecting Misery Perfusion in Unilateral Steno- Occlusive Disease of the Internal Carotid Artery or Middle Cerebral Artery by MR Imaging BACKGROUND
ORIGINAL RESEARCH S. Xie L.H. Hui J.X. Xiao X.D. Zhang Q. Peng Detecting Misery Perfusion in Unilateral Steno- Occlusive Disease of the Internal Carotid Artery or Middle Cerebral Artery by MR Imaging BACKGROUND
Alan Barber. Professor of Clinical Neurology University of Auckland
 Alan Barber Professor of Clinical Neurology University of Auckland Presented with L numbness & slurred speech 2 episodes; 10 mins & 2 hrs Hypertension Type II DM Examination P 80/min reg, BP 160/95, normal
Alan Barber Professor of Clinical Neurology University of Auckland Presented with L numbness & slurred speech 2 episodes; 10 mins & 2 hrs Hypertension Type II DM Examination P 80/min reg, BP 160/95, normal
CEA and cerebral protection Volodymyr labinskyy, MD
 CEA and cerebral protection Volodymyr labinskyy, MD VA Hospital 7/26/2012 63 year old male presents for the vascular evaluation s/p TIA in January 2012 PMH: HTN, long term active smoker, Hep C PSH: None
CEA and cerebral protection Volodymyr labinskyy, MD VA Hospital 7/26/2012 63 year old male presents for the vascular evaluation s/p TIA in January 2012 PMH: HTN, long term active smoker, Hep C PSH: None
How to manage the left subclavian and left vertebral artery during TEVAR
 How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine
 Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
occlusions. Cerebral perfusion is driven fundamentally by regional cerebral
 Appendix Figures Figure A1. Hemodynamic changes that may occur in major anterior circulation occlusions. Cerebral perfusion is driven fundamentally by regional cerebral perfusion pressure (CPP). In response
Appendix Figures Figure A1. Hemodynamic changes that may occur in major anterior circulation occlusions. Cerebral perfusion is driven fundamentally by regional cerebral perfusion pressure (CPP). In response
Policies and Statements D16. Intracranial Cerebrovascular Ultrasound
 Policies and Statements D16 Intracranial Cerebrovascular Ultrasound SECTION 1: INSTRUMENTATION Policies and Statements D16 Intracranial Cerebrovascular Ultrasound May 2006 (Reaffirmed July 2007) Essential
Policies and Statements D16 Intracranial Cerebrovascular Ultrasound SECTION 1: INSTRUMENTATION Policies and Statements D16 Intracranial Cerebrovascular Ultrasound May 2006 (Reaffirmed July 2007) Essential
CT perfusion in Moyamoya disease
 CT perfusion in Moyamoya disease Poster No.: C-1726 Congress: ECR 2015 Type: Scientific Exhibit Authors: K. C. Lam, C. P. Tsang, K. K. Wong, R. LEE ; HK, Hong Kong/HK Keywords: Hemodynamics / Flow dynamics,
CT perfusion in Moyamoya disease Poster No.: C-1726 Congress: ECR 2015 Type: Scientific Exhibit Authors: K. C. Lam, C. P. Tsang, K. K. Wong, R. LEE ; HK, Hong Kong/HK Keywords: Hemodynamics / Flow dynamics,
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al.
 ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
ANASTAMOSIS FOR BRAIN STEM ISCHEMIA/Khodadad et al. visualization of the posterior inferior cerebellar artery. The patient, now 11 months post-operative, has shown further neurological improvement since
PTA 106 Unit 1 Lecture 3
 PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
Moyamoya disease is an idiopathic progressive occlusive
 ORIGINAL RESEARCH K.H. Kang H.S. Kim S.Y. Kim Quantitative Cerebrovascular Reserve Measured by Acetazolamide-Challenged Dynamic CT Perfusion in Ischemic Adult Moyamoya Disease: Initial Experience with
ORIGINAL RESEARCH K.H. Kang H.S. Kim S.Y. Kim Quantitative Cerebrovascular Reserve Measured by Acetazolamide-Challenged Dynamic CT Perfusion in Ischemic Adult Moyamoya Disease: Initial Experience with
Although moyamoya disease, a rare cerebrovascular occlusive
 Renal Artery Lesions in Patients With Moyamoya Disease Angiographic Findings Ichiro Yamada, MD; Yoshiro Himeno, MD; Yoshiharu Matsushima, MD; Hitoshi Shibuya, MD Background and Purpose Renal artery lesions
Renal Artery Lesions in Patients With Moyamoya Disease Angiographic Findings Ichiro Yamada, MD; Yoshiro Himeno, MD; Yoshiharu Matsushima, MD; Hitoshi Shibuya, MD Background and Purpose Renal artery lesions
NEURORADIOLOGY DIL part 4
 NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
CT INTERPRETATION COURSE
 CT INTERPRETATION COURSE Refresher Course ASTRACAT October 2012 Stroke is a Clinical Diagnosis A clinical syndrome characterised by rapidly developing clinical symptoms and/or signs of focal loss of cerebral
CT INTERPRETATION COURSE Refresher Course ASTRACAT October 2012 Stroke is a Clinical Diagnosis A clinical syndrome characterised by rapidly developing clinical symptoms and/or signs of focal loss of cerebral
Transorbital blood flow sound recordings have the
 397 Noninvasive Detection of Intracranial Vascular Lesions by Recording Blood Flow Sounds Yasushi Kurokawa, MD; Seisho Abiko, MD; Kohsaku Watanabe, MD Background and Purpose Transorbital blood flow sound
397 Noninvasive Detection of Intracranial Vascular Lesions by Recording Blood Flow Sounds Yasushi Kurokawa, MD; Seisho Abiko, MD; Kohsaku Watanabe, MD Background and Purpose Transorbital blood flow sound
Hyperperfusion syndrome after MCA embolectomy a rare complication?
 ISSN 1507-6164 DOI: 10.12659/AJCR.889672 Received: 2013.08.13 Accepted: 2013.09.11 Published: 2013.11.29 Hyperperfusion syndrome after MCA embolectomy a rare complication? Authors Contribution: Study Design
ISSN 1507-6164 DOI: 10.12659/AJCR.889672 Received: 2013.08.13 Accepted: 2013.09.11 Published: 2013.11.29 Hyperperfusion syndrome after MCA embolectomy a rare complication? Authors Contribution: Study Design
Case Report Cerebral Hyperperfusion Syndrome following Protected Carotid Artery Stenting
 Case Reports in Vascular Medicine Volume 2013, Article ID 207602, 4 pages http://dx.doi.org/10.1155/2013/207602 Case Report Cerebral Hyperperfusion Syndrome following Protected Carotid Artery Stenting
Case Reports in Vascular Medicine Volume 2013, Article ID 207602, 4 pages http://dx.doi.org/10.1155/2013/207602 Case Report Cerebral Hyperperfusion Syndrome following Protected Carotid Artery Stenting
Protokollanhang zur SPACE-2-Studie Neurology Quality Standards
 Protokollanhang zur SPACE-2-Studie Neurology Quality Standards 1. General remarks In contrast to SPACE-1, the neurological center participating in the SPACE-2 trial will also be involved in the treatment
Protokollanhang zur SPACE-2-Studie Neurology Quality Standards 1. General remarks In contrast to SPACE-1, the neurological center participating in the SPACE-2 trial will also be involved in the treatment
Basilar artery stenosis with bilateral cerebellar strokes on coumadin
 Qaisar A. Shah, MD Patient Profile 68 years old female with a history of; Basilar artery stenosis with bilateral cerebellar strokes on coumadin Diabetes mellitus Hyperlipidemia Hypertension She developed
Qaisar A. Shah, MD Patient Profile 68 years old female with a history of; Basilar artery stenosis with bilateral cerebellar strokes on coumadin Diabetes mellitus Hyperlipidemia Hypertension She developed
Any vascular studies performed should be as a result of, or to complement, a thorough patient evaluation and neurological examination.
 National Imaging Associates, Inc. Clinical guidelines NON-INVASIVE CEREBROVASCULAR ARTERIALS TUDIES Original Date: October 2015 Page 1 of 8 FOR CMS (MEDICARE) MEMBERS ONLY CPT4 Codes: Please refer to page
National Imaging Associates, Inc. Clinical guidelines NON-INVASIVE CEREBROVASCULAR ARTERIALS TUDIES Original Date: October 2015 Page 1 of 8 FOR CMS (MEDICARE) MEMBERS ONLY CPT4 Codes: Please refer to page
Interventions in the Management of Acute Stroke. Dr Md Shafiqul Islam Associate Professor Neurosurgery Dhaka Medical College Hospital
 Interventions in the Management of Acute Stroke Dr Md Shafiqul Islam Associate Professor Neurosurgery Dhaka Medical College Hospital Acute stroke intervention Number of stroke patients increasing day by
Interventions in the Management of Acute Stroke Dr Md Shafiqul Islam Associate Professor Neurosurgery Dhaka Medical College Hospital Acute stroke intervention Number of stroke patients increasing day by
Moyamoya disease is an unusual form of chronic, occlusive
 Angiographic Dilatation and Branch Extension of the Anterior Choroidal and Posterior Communicating Arteries Are Predictors of Hemorrhage in Adult Moyamoya Patients Motohiro Morioka, MD; Jun-Ichiro Hamada,
Angiographic Dilatation and Branch Extension of the Anterior Choroidal and Posterior Communicating Arteries Are Predictors of Hemorrhage in Adult Moyamoya Patients Motohiro Morioka, MD; Jun-Ichiro Hamada,
Poststenotic Flow and Intracranial Hemodynamics in Patients with Carotid Stenosis: Transoral Carotid Ultrasonography Study
 AJNR Am J Neuroradiol 26:76 81, January 2005 Poststenotic Flow and Intracranial Hemodynamics in Patients with Carotid Stenosis: Transoral Carotid Ultrasonography Study Masahiro Kamouchi, Kazuhiro Kishikawa,
AJNR Am J Neuroradiol 26:76 81, January 2005 Poststenotic Flow and Intracranial Hemodynamics in Patients with Carotid Stenosis: Transoral Carotid Ultrasonography Study Masahiro Kamouchi, Kazuhiro Kishikawa,
Title. Author(s) 黒田, 敏 ; 川堀, 真人 ; 宮本, 倫行 ; 笹森, 徹 ; 遠藤, 将吾 ; 中山, 若樹 ; 石川, 達哉. Citation 脳卒中の外科, 37(5): Issue Date Doc URL.
 Title 側頭葉から後頭葉にかけて高度の虚血を有するもやもや病に対する脳血行再建術 Author(s) 黒田, 敏 ; 川堀, 真人 ; 宮本, 倫行 ; 笹森, 徹 ; 遠藤, 将吾 ; 中山, 若樹 ; 石川, 達哉 Citation 脳卒中の外科, 37(5): 345-349 Issue Date 2009 Doc URL http://hdl.handle.net/2115/70929
Title 側頭葉から後頭葉にかけて高度の虚血を有するもやもや病に対する脳血行再建術 Author(s) 黒田, 敏 ; 川堀, 真人 ; 宮本, 倫行 ; 笹森, 徹 ; 遠藤, 将吾 ; 中山, 若樹 ; 石川, 達哉 Citation 脳卒中の外科, 37(5): 345-349 Issue Date 2009 Doc URL http://hdl.handle.net/2115/70929
/ / / / / / Hospital Abstraction: Stroke/TIA. Participant ID: Hospital Code: Multi-Ethnic Study of Atherosclerosis
 Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Imaging Acute Stroke and Cerebral Ischemia
 Department of Radiology University of California San Diego Imaging Acute Stroke and Cerebral Ischemia John R. Hesselink, M.D. Causes of Stroke Arterial stenosis Thrombosis Embolism Dissection Hypotension
Department of Radiology University of California San Diego Imaging Acute Stroke and Cerebral Ischemia John R. Hesselink, M.D. Causes of Stroke Arterial stenosis Thrombosis Embolism Dissection Hypotension
Brain SPECT Used to Evaluate Vasospasm After Subarachnoid Hemorrhage. Correlation with Angiography and Transcranial Doppler
 CLINICAL NUCLEAR MEDICINE Volume 26, Number 2, pp 125 130 2001, Lippincott Williams & Wilkins Brain SPECT Used to Evaluate Vasospasm After Subarachnoid Hemorrhage Correlation with Angiography and Transcranial
CLINICAL NUCLEAR MEDICINE Volume 26, Number 2, pp 125 130 2001, Lippincott Williams & Wilkins Brain SPECT Used to Evaluate Vasospasm After Subarachnoid Hemorrhage Correlation with Angiography and Transcranial
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS. 73 year old NS right-handed male applicant for $1 Million life insurance
 MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
FIRST COAST SERVICE OPTIONS FLORIDA MEDICARE PART B LOCAL COVERAGE DETERMINATION
 FIRST COAST SERVICE OPTIONS FLORIDA MEDICARE PART B LOCAL COVERAGE DETERMINATION CPT/HCPCS Codes 93875 Non-invasive physiologic studies of extracranial arteries, complete bilateral study (eg, periorbital
FIRST COAST SERVICE OPTIONS FLORIDA MEDICARE PART B LOCAL COVERAGE DETERMINATION CPT/HCPCS Codes 93875 Non-invasive physiologic studies of extracranial arteries, complete bilateral study (eg, periorbital
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS. 73 year old NS right-handed male applicant for $1 Million Life Insurance
 MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
MORTALITY AND MORBIDITY RISK FROM CAROTID ARTERY ATHEROSCLEROSIS October 17, 2012 AAIM Triennial Conference, San Diego Robert Lund, MD What Is The Risk? 73 year old NS right-handed male applicant for $1
Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis
 HOSPITAL CHRONICLES 2008, 3(3): 136 140 ORIGINAL ARTICLE Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis Antonios Polydorou, MD Hemodynamic
HOSPITAL CHRONICLES 2008, 3(3): 136 140 ORIGINAL ARTICLE Subclavian and Vertebral Artery Angioplasty - Vertebro-basilar Insufficiency: Clinical Aspects and Diagnosis Antonios Polydorou, MD Hemodynamic
TRANSCRANIAL DOPPLER ULTRASOUND INTRODUCTION TO TCD INTERPRETATION
 TRANSCRANIAL DOPPLER ULTRASOUND INTRODUCTION TO TCD INTERPRETATION ---Rune Aaslid First TCD Publication 1982 WHAT IS TCD? Uses 2 MHz pulsed Doppler ultrasound Passes through cranial windows Provides information
TRANSCRANIAL DOPPLER ULTRASOUND INTRODUCTION TO TCD INTERPRETATION ---Rune Aaslid First TCD Publication 1982 WHAT IS TCD? Uses 2 MHz pulsed Doppler ultrasound Passes through cranial windows Provides information
Spasm of the extracranial internal carotid artery resulting from blunt trauma demonstrated by angiography
 Spasm of the extracranial internal carotid artery resulting from blunt trauma demonstrated by angiography Case report ELISHA S. GURDJIAN, M.D., BLAISE AUDET, M.D., RENATO W. SIBAYAN, M.D., AND LLYWELLYN
Spasm of the extracranial internal carotid artery resulting from blunt trauma demonstrated by angiography Case report ELISHA S. GURDJIAN, M.D., BLAISE AUDET, M.D., RENATO W. SIBAYAN, M.D., AND LLYWELLYN
Cerebral hyperperfusion syndrome after carotid angioplasty
 case report Cerebral hyperperfusion syndrome after carotid angioplasty Zoran Miloševič 1, Bojana Žvan 2, Marjan Zaletel 2, Miloš Šurlan 1 1 Institute of Radiology, 2 University Neurology Clinic, University
case report Cerebral hyperperfusion syndrome after carotid angioplasty Zoran Miloševič 1, Bojana Žvan 2, Marjan Zaletel 2, Miloš Šurlan 1 1 Institute of Radiology, 2 University Neurology Clinic, University
Assessment of intracranial hemodynamics in carotid artery disease by transcranial Doppler ultrasound
 J Neurosurg 63:890-898,1985 Assessment of intracranial hemodynamics in carotid artery disease by transcranial Doppler ultrasound KARL-FREDRIK LINDEGAARD, M.D., S~REN JACOB BAKKE, M.D., PETER GROLIMUND,
J Neurosurg 63:890-898,1985 Assessment of intracranial hemodynamics in carotid artery disease by transcranial Doppler ultrasound KARL-FREDRIK LINDEGAARD, M.D., S~REN JACOB BAKKE, M.D., PETER GROLIMUND,
ACUTE ISCHEMIC STROKE. Current Treatment Approaches for Acute Ischemic Stroke
 ACUTE ISCHEMIC STROKE Current Treatment Approaches for Acute Ischemic Stroke EARLY MANAGEMENT OF ACUTE ISCHEMIC STROKE Rapid identification of a stroke Immediate EMS transport to nearest stroke center
ACUTE ISCHEMIC STROKE Current Treatment Approaches for Acute Ischemic Stroke EARLY MANAGEMENT OF ACUTE ISCHEMIC STROKE Rapid identification of a stroke Immediate EMS transport to nearest stroke center
Anastomosis of the superficial temporal artery to the distal anterior cerebral artery with interposed cephalic vein graft
 J Neurosurg 58~25-429, 1983 Anastomosis of the superficial temporal artery to the distal anterior cerebral artery with interposed cephalic vein graft Case report RYOJI ISHII, M.D., TETSUO KOIKE, M.D.,
J Neurosurg 58~25-429, 1983 Anastomosis of the superficial temporal artery to the distal anterior cerebral artery with interposed cephalic vein graft Case report RYOJI ISHII, M.D., TETSUO KOIKE, M.D.,
Intracranial vascular anastomosis using the microanastomotic system
 J Neurosurg 89:676 681, 1998 Intracranial vascular anastomosis using the microanastomotic system Technical note DAVID W. NEWELL, M.D., ANDREW T. DAILEY, M.D., AND STEPHEN L. SKIRBOLL, M.D. Department of
J Neurosurg 89:676 681, 1998 Intracranial vascular anastomosis using the microanastomotic system Technical note DAVID W. NEWELL, M.D., ANDREW T. DAILEY, M.D., AND STEPHEN L. SKIRBOLL, M.D. Department of
positron emission tomography PET
 020-8505 19-1 1-3) positron emission tomography PET PET PET single photon emission computed tomography SPECT acetazolamide 4-10) magnetic resonance imaging MRI MRI 11,12) MRI perfusion weighted imaging
020-8505 19-1 1-3) positron emission tomography PET PET PET single photon emission computed tomography SPECT acetazolamide 4-10) magnetic resonance imaging MRI MRI 11,12) MRI perfusion weighted imaging
Percutaneous Transluminal Angioplasty and Stenting for Chronic Total Occlusion of Intracranial Carotid Artery A Case Report
 www.centauro.it Interventional Neuroradiology 12: 263-268, 2006 Percutaneous Transluminal Angioplasty and Stenting for Chronic Total Occlusion of Intracranial Carotid Artery A Case Report H. ISHIHARA,
www.centauro.it Interventional Neuroradiology 12: 263-268, 2006 Percutaneous Transluminal Angioplasty and Stenting for Chronic Total Occlusion of Intracranial Carotid Artery A Case Report H. ISHIHARA,
Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke
 Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
PFO closure group total no. PFO closure group no. of males
 Suppl Table. Characteristics of the five trials included in this meta-analysis. Trial name Device used for Definition of medical Primary Endpoint group total no. group no. of males group age (yrs) group
Suppl Table. Characteristics of the five trials included in this meta-analysis. Trial name Device used for Definition of medical Primary Endpoint group total no. group no. of males group age (yrs) group
Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note
 Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note Saleem I. Abdulrauf, M.D., F.A.C.S. 1 ABSTRACT The management of complex skull base tumors
Extracranial-to-Intracranial Bypass Using Radial Artery Grafting for Complex Skull Base Tumors: Technical Note Saleem I. Abdulrauf, M.D., F.A.C.S. 1 ABSTRACT The management of complex skull base tumors
Internal Carotid Artery Occlusion: Clinical and Therapeutic Implications
 94 Internal Carotid Artery Occlusion: Clinical and Therapeutic Implications VIVIAN U. FRITZ, M.D., CHRIS L. VOLL, M.D., AND LEWIS J. LEVIEN, M.D., PH.D. Downloaded from http://ahajournals.org by on November
94 Internal Carotid Artery Occlusion: Clinical and Therapeutic Implications VIVIAN U. FRITZ, M.D., CHRIS L. VOLL, M.D., AND LEWIS J. LEVIEN, M.D., PH.D. Downloaded from http://ahajournals.org by on November
Carotid Revascularization
 Options for Carotid Disease Carotid Revascularization Wayne Causey, MD 2 nd Year Vascular Surgery Fellow Best medical therapy, Carotid Endarterectomy, and Carotid Stenting Who benefits from best medical
Options for Carotid Disease Carotid Revascularization Wayne Causey, MD 2 nd Year Vascular Surgery Fellow Best medical therapy, Carotid Endarterectomy, and Carotid Stenting Who benefits from best medical
Acute Ischemic Stroke Imaging. Ronald L. Wolf, MD, PhD Associate Professor of Radiology
 Acute Ischemic Stroke Imaging Ronald L. Wolf, MD, PhD Associate Professor of Radiology Title of First Slide of Substance An Illustrative Case 2 Disclosures No financial disclosures Off-label uses of some
Acute Ischemic Stroke Imaging Ronald L. Wolf, MD, PhD Associate Professor of Radiology Title of First Slide of Substance An Illustrative Case 2 Disclosures No financial disclosures Off-label uses of some
Applicable Neuroradiology
 For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
In cerebral embolism, recanaiization occurs very
 680 Case Reports Recanaiization of Intracranial Carotid Occlusion Detected by Duplex Carotid Sonography Haruhiko Hoshino, MD, Makoto Takagi, MD, Ikuo Takeuchi, MD, Tsugio Akutsu, MD, Yasuyuki Takagi, MD,
680 Case Reports Recanaiization of Intracranial Carotid Occlusion Detected by Duplex Carotid Sonography Haruhiko Hoshino, MD, Makoto Takagi, MD, Ikuo Takeuchi, MD, Tsugio Akutsu, MD, Yasuyuki Takagi, MD,
Case Conference: Neuroradiology. Case 1: Tumor Case 1: 22yo F w/ HA and prior Seizures
 Case Conference: Neuroradiology Case 1: 22yo F w/ HA and prior Seizures David E. Rex, MD, PhD Stanford University Hospital Department of Radiology Case 1: Tumor Most likely gangiloglioma, oligodendroglioma,
Case Conference: Neuroradiology Case 1: 22yo F w/ HA and prior Seizures David E. Rex, MD, PhD Stanford University Hospital Department of Radiology Case 1: Tumor Most likely gangiloglioma, oligodendroglioma,
ISPUB.COM. Transcranial Doppler: An Overview of its Clinical Applications. A Alexandrov, M Joseph INTRODUCTION SICKLE CELL DISEASE
 ISPUB.COM The Internet Journal of Neuromonitoring Volume 1 Number 1 Transcranial Doppler: An Overview of its Clinical Applications A Alexandrov, M Joseph Citation A Alexandrov, M Joseph. Transcranial Doppler:
ISPUB.COM The Internet Journal of Neuromonitoring Volume 1 Number 1 Transcranial Doppler: An Overview of its Clinical Applications A Alexandrov, M Joseph Citation A Alexandrov, M Joseph. Transcranial Doppler:
The contribution of the external carotid artery to cerebral perfusion in carotid disease
 The contribution of the external carotid artery to cerebral perfusion in carotid disease Shirley J. Fearn, PhD, FRCS, Andrew J. Picton, BSc, Andrew J. Mortimer, MD, FRCA, Andrew D. Parry, MBChB, FRCS,
The contribution of the external carotid artery to cerebral perfusion in carotid disease Shirley J. Fearn, PhD, FRCS, Andrew J. Picton, BSc, Andrew J. Mortimer, MD, FRCA, Andrew D. Parry, MBChB, FRCS,
