ORIGINAL ARTICLE. Computed Tomographic Findings in Patients With Invasive Fungal Sinusitis
|
|
|
- Byron Parsons
- 5 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Computed Tomographic Findings in Patients With Invasive Fungal Sinusitis John M. DelGaudio, MD; Ron E. Swain Jr, MD; Todd T. Kingdom, MD; Susan Muller, DMD; Patricia A. Hudgins, MD Objective: To determine the radiographic findings of computed tomographic (CT) imaging most suggestive of invasive fungal sinusitis (IFS) in an immunocompromised patient population. Design: A retrospective review of patients with a diagnosis of IFS reached with CT and confirmed by histopathologic evaluation. Setting: An academic tertiary care hospital. Patients: Twenty-three immunocompromised patients with confirmed IFS and preoperative CT imaging. Controls were 10 patients with acute myelocytic leukemia and CT evidence of sinusitis but no history of IFS. Outcome Measures: The CT scans were reviewed to identify factors predictive of invasive fungal disease. Parameters evaluated were nasal cavity and sinus soft tissue thickening, the presence of air-fluid levels, bone erosion, extrasinus extension, and unilateral or bilateral nasal cavity and sinus involvement. Results: The CT findings included severe soft tissue edema of the nasal cavity mucosa (turbinates, lateral nasal wall and floor, and septum) in 21 of the 23 patients, sinus mucoperiosteal thickening in 21, bone erosion in 8, orbital invasion in 6, facial soft tissue swelling in 5, and retroantral fat pad thickening in 2. Two patients had air-fluid levels. No patients had intracranial involvement. Unilateral involvement was found in 21 patients, and bilateral involvement in 2. Review of the control group revealed only mild soft tissue edema of the nasal cavity in 2 (P.001), unilateral involvement in 2 (P.001), and evidence of bone erosion or extrasinus soft tissue involvement in none. Conclusions: Most patients do not have classic CT findings of bone erosion or extrasinus extension in the early course of IFS. We found that severe unilateral thickening of the nasal cavity mucosa was the most consistent finding on CT suggestive of underlying IFS, occurring much more frequently in immunocompromised patients with IFS than without IFS. Even though severe nasal cavity soft tissue thickening is much more common in IFS, this is a nonspecific finding that can be seen, to a lesser degree, in all forms of rhinosinusitis. Therefore, the clinician cannot rely solely on CT imaging and must maintain a high index of suspicion when evaluating immunocompromised patients to establish a prompt diagnosis. Early nasal endoscopy with biopsy and initiation of appropriate therapy are necessary to improve prognosis. Arch Otolaryngol Head Neck Surg. 2003;129: From the Departments of Otolaryngology Head & Neck Surgery (Drs DelGaudio, Swain, Kingdom, and Muller), Pathology (Dr Muller), and Radiology (Dr Hudgins), Emory University School of Medicine, Atlanta, Ga. INVASIVE FUNGAL infection of the sinonasal cavities is a disease requiring urgent attention and treatment by the otolaryngologist head and neck surgeon, but it is difficult to diagnose and treat. Essentially, the patients are immunocompromised as a result of systemic chemotherapy and/or bone marrow transplantation, immunosuppressive agents used after solid organ transplantation, acquired immunodeficiency syndrome, or long-term systemic steroid use. Poorly controlled diabetes mellitus, usually with diabetic ketoacidosis, is another common underlying factor in the development of invasive fungal sinusitis (IFS). Protein calorie malnutrition and excessive stored iron can also be predisposing factors in the development of IFS. 1 Although uncommon, IFS has been documented in otherwise healthy individuals. 2,3 Most patients with IFS are already in poor overall physical health as a result of their underlying condition or treatment, and are expected to have a higher mortality rate and poorer prognosis. Leukopenia, especially neutropenia, significantly reduces the inflammatory response, which increases the risk of IFS and may mask some of its early symptoms. These factors contribute to the difficulty in diagnosing and treating the disease, which can progress rapidly and with devastating results. Therefore, early diagnosis is necessary. Treatment usually consists of aggressive surgical debridement and intravenous antifungal therapy. 236
2 The symptoms of IFS, which was first described in the French medical literature in 1885, 4 overlap with those of bacterial sinusitis. They include nasal congestion or obstruction, nasal discharge, facial pain, facial swelling, headache, dental pain, and visual complaints. Anesthesia of the nasal mucosa and/or facial skin is more suggestive of an invasive process such as IFS than of bacterial infection. On physical examination, the most common rhinologic finding is ischemic mucosa. Black eschar is classically described as the hallmark of IFS, but this is a late finding resulting from vascular thrombosis and tissue necrosis. Earlier findings include pale, ischemic mucosa that does not bleed normally with manipulation, mucosal edema, and pain out of proportion to physical findings, likely due to tissue ischemia. Extrasinus extension is usually a late finding. Orbital involvement can present with limitation of extraocular movement, proptosis, and decreased vision. Rapid progression of the disease can occur with involvement of the facial skin, hard and soft palates, retroantral area, and intracranial extension. A classification system with criteria for the diagnosis of IFS has been proposed. 1 de Shazo et al 1 describe 3 forms of IFS, which they classify as follows: granulomatous, acute fulminant, and chronic invasive. They propose that IFS is diagnosed by radiographic evidence of sinusitis and by histopathologically proven hyphal forms within sinus mucosa, submucosa, blood vessels, or bone. 1 Multiple fungal species have been identified in patients with IFS, most commonly Aspergillus and fungi of the order of Mucoraceae, including Rhizopus and Mucor. 1,5 Review of the otolaryngology literature reveals that computed tomographic (CT) findings such as edema of nasal cavity soft tissue, sinus mucoperiosteal thickening, bone erosion, orbital invasion, facial soft tissue swelling, and periantral soft tissue infiltration are all findings suggestive of IFS, 1,5-7 but no radiographic findings have been found to be pathognomonic of IFS. The purpose of this study was to retrospectively review CT scans of patients with histologically proven IFS to determine if specific radiologic characteristics could establish the diagnosis. METHODS Patient Data and Outcomes Patient No. Age, y Diagnosis Pathogen/ Infection A retrospective analysis of patients with a diagnosis of IFS between 1995 and 2001 in the Emory University Hospital system was performed. Only patients with a tissue diagnosis of IFS who, prior to biopsy or debridement, had undergone a CT scan of the sinuses that was available for evaluation were included in this review. Twenty-three patients (12 men and 11 women) met these criteria. Demographic data, underlying diagnosis, identified fungal organism, absolute neutrophil counts, and patient outcomes were reviewed (Table). Most of the patients with leukemia were in the early postoperative period from bone marrow transplantation. All CT studies were reviewed by 1 head and neck radiologist and 2 otolaryngologists. Of the initial 23 scans performed, 11 were coronal views alone, 11 were both axial and coronal views, and 1 was only an axial view. All of the scans were performed with 3-mm-thick sections. Three of the CT scans were performed with contrast, the remaining without contrast. The CT scans were evaluated with both bone and soft tissue window settings. All radiographic and clinical material was retrospectively evaluated. Each CT scan was evaluated for nasal cavity mucosal and soft tissue thickening, sinus mucoperiosteal thickening, osseous erosion, extrasinus extension (ie, orbital and intracranial invasion), facial soft tissue thickening, retroantral fat pad thickening, and unilateral vs bilateral involvement. All 23 patients had been taken to the operating room for nasal endoscopy, histopathologic confirmation of IFS, and debridement. A control group of 10 immunocompromised patients was chosen from an acute myelogenous leukemia database. All of them had a sinus CT scan that showed evidence of sinusitis, but none had a history of IFS. Each was treated for bacterial sinusitis and improved. Their ages ranged from 28 to 70 years, with a mean of 51.8 years. RESULTS ANC, Cells/µL Outcome 1 11 AML Aspergillus 507 Recovered 2 53 HIV Aspergillus 500 Recovered 3 55 IDDM Mucormycosis 500 Recovered 4 22 AML Aspergillus 250 Death 5 53 IDDM Mucormycosis 500 Recovered 6 30 AML Aspergillus 120 Death 7 51 AML/MM Aspergillus 45 Recovered 8 67 IDDM Mucormycosis 500 Recovered 9 38 AML Mucormycosis 96 Recovered Sideroblastic Aspergillus 255 Death anemia HIV Mucormycosis 406 Recovered HIV Aspergillus 500 Recovered HIV Mucormycosis 500 Recovered AML Aspergillus 500 Recovered Renal Aspergillus 500 Recovered Liver transplant Mucormycosis 500 Recovered AML Aspergillus 100 Death IDDM Aspergillus 500 Recovered Malnutrition Mucormycosis 112 Recovered CML Aspergillus 6 Recovered IDDM/NHL Mucormycosis 500 Recovered AML Aspergillus 16 Recovered ALL Aspergillus 500 Recovered Abbreviations: ALL, acute lymphocytic leukemia; AML, acute myelogenous leukemia; ANC, absolute neutrophil count; CML, chronic myelogenous leukemia; HIV, human immunodeficiency virus; IDDM, type 2 (insulin-dependent) diabetes mellitus; MM, multiple myeloma; NHL, non-hodgkin lymphoma. All 23 patients in the study group were immunocompromised and diagnosed as having acute fulminant IFS. The fungal pathogens identified were Aspergillus or Mucormycosis (Table). Absolute neutrophil counts were less than 500/µL in 11 patients and greater than 500/µL in 12 patients. Four patients with persistent IFS died of their underlying medical condition during their hospitalization, and each of them had an absolute neutrophil count of less than 500/µL (Table). Nineteen of the 23 patients were discharged from the hospital after resolution of IFS, with appropriate follow-up from an otolaryngologist. One patient who survived had permanent visual loss. Of the CT findings evaluated, severe thickening of the nasal cavity mucosa and soft tissues, including the turbinates, septum, and nasal floor, was the most common finding, noted in 21 (91%) of the 23 patients (Figure 1 and Figure 2). The nasal cavity soft tissue thickening was uni- 237
3 Figure 1. Coronal computed tomographic scan showing extensive unilateral left nasal cavity soft tissue thickening of the septum, turbinates, and nasal floor, with complete opacification of the left nasal cavity, in a patient (patient 9) with invasive fungal sinusitis. Right nasal cavity does not display soft tissue thickening. Figure 3. Bone erosion of the left lamina papyracea (arrow) with soft tissue thickening of the lateral nasal and medial canthal areas in a patient with invasive fungal sinusitis (patient 4). Also note the extensive unilateral nasal cavity soft tissue thickening on the left side. Figure 4. Axial soft tissue window demonstrates thickening of the left retroantral fat pad (posterior arrow) and premaxillary soft tissue (anterior arrow) in a patient (patient 23) with invasive fungal sinusitis. Figure 2. Coronal computed tomographic scan showing unilateral nasal cavity and sinus soft tissue thickening of the septum, nasal floor, and lateral wall (arrows) in a patient with invasive fungal sinusitis. The patient (patient 23) had a maxillary antrostomy previously, not associated with his diagnosis of invasive fungal sinusitis. lateral in 21 patients (91%), and was greater than the degree of thickening expected in acute bacterial rhinosinusitis. Sinus mucoperiosteal thickening or opacification was present in 21 (91%), but only 2 had air-fluid levels. Bone erosion was seen in only 8 (35%) (Figure 3). Orbital invasion was found in 6 patients (26%), and 5 (22%) had soft tissue thickening of the face overlying the maxillary sinus. Three of these 5 patients had CT scans with contrast while the other 2 had inflammatory changes visualized with a soft tissue algorithm (Figure 4). Two patients were identified with infiltration of the retroantral fat pad without evidence of bone erosion (Figure 4). No patient in this series had intracranial involvement. All patients were taken to the operating room for biopsy and/or debridement. The most common findings at surgery were mucosal edema and/or pale mucosa. The edematous tissue was hypervascular due to acute inflammation, whereas the pale mucosa had little or no bleeding as a result of tissue ischemia. The presence of necrotic tissue and eschar was an uncommon finding. In the control group, only 2 of 10 patients had nasal cavity soft tissue thickening (Figure 5 and Figure 6), and in these 2 patients the degree of thickening was not nearly as severe as seen in the patients with IFS (Figures 1-4). Only 2 of the patients had unilateral sinonasal involvement. No evidence of bone erosion or extension of infection beyond the sinuses was identified in this control patient group. The differences between the 2 groups in the frequency of nasal cavity soft tissue thickening and of unilateral involvement were statistically significant (P.001). The differences in the frequency of bone erosion or extrasinus extension did not reach statistical significance (P.05). 238
4 Figure 5. Coronal computed tomographic scan of a control patient demonstrating bilateral maxillary air-fluid levels, ethmoid soft tissue thickening, and very mild thickening of the mucosa of the nasal floor (black arrows) and septum (white arrow). Note that the degree of nasal cavity soft tissue thickening is much less than in the patients with invasive fungal sinusitis. COMMENT Figure 6. Coronal computed tomographic scan of control patient demonstrating bilateral ethmoid and maxillary opacification but minimal thickening of the mucosa of the lateral nasal wall (white arrow) and floor (black arrow) and septum. Although many CT findings have been reported as suggestive of IFS, none are definitive. Silverman and Mancuso 6 concluded that infiltration of the periantral fat planes in patients having both noncontrast and contrastenhanced CT scans may represent the earliest imaging evidence of invasive fungal disease. As early as 1993, Som and Curtin 7 described soft tissue changes in a sinus with thickened, reactive bone inflammation, or with associated nasal cavity inflammation, as an early predictor of fungal disease. Nonspecific inflammatory soft tissue changes associated with bone destruction is also described by Gamba et al 8 in patients with IFS. Severe soft tissue thickening of the nasal cavity mucosa and soft tissues, including the turbinates, nasal walls, and septum, was present in 21 of the 23 patients in this study. The degree of nasal cavity inflammation was much higher than would be expected in routine rhinosinusitis in the absence of nasal polyposis (Figures 1-4). Indeed, the degree of edema of the nasal mucosa is especially striking in patients who are neutropenic and, therefore, not expected to display a significant inflammatory response. This finding was rarely present in the control group of immunocompromised patients with sinusitis of nonfungal etiology. In that group, only 2 patients displayed nasal cavity soft tissue thickening and it was much less severe than in the IFS group (Figures 5 and 6). In addition, 21 (91%) of the 23 patients had unilateral nasal mucosal thickening, which is not a typical finding in viral or bacterial rhinosinusitis. Only 2 patients (20%) in the control group displayed unilateral involvement. This severe unilateral nasal mucosal inflammatory process appears to be the most common radiologic characteristic of IFS in the early stages. Although this is a nonspecific finding, in our experience it is identified much more consistently than bone erosion or extrasinus extension, both of which are highly suggestive of IFS. The radiologic findings are consistent with the endoscopic and surgical findings of significant mucosal edema and inflammation surrounding areas of tissue ischemia. Frank tissue and bone necrosis was not commonly seen due to the early diagnosis of IFS in many of these patients. Osseous erosion and extrasinus extension, obvious findings used for the radiologic diagnosis of IFS, are late-stage findings. The use of these 2 criteria alone would result in significant delay in diagnosis. In an immunocompromised patient with sinusitis symptoms, a high index of clinical suspicion, as well as radiographic detection of nasal cavity edema out of proportion to the patient s symptoms, can lead to early detection of IFS. We speculate that our high index of suspicion directly resulted in a cure rate of 83% (19/23) of the patients, a rate higher than that reported for IFS, with mortality reported in the range of 50% to 80%. 9 To completely evaluate the sinuses and surrounding structures, CT scans should be performed at intervals no greater than 3 mm in both the axial and coronal planes. A screening sinus technique, with coronal images only, is not sufficient. Both bone and soft tissue windows should be performed to better evaluate for bone erosion and extrasinus extension, respectively. Intravenous contrast is not usually necessary, although it may be helpful in delineating early orbital or dural enhancement. Although no patient in this series had intracranial involvement, magnetic resonance imaging (MRI) should be obtained as well as neurosurgical evaluation in any patient suspected of having intracranial IFS. Howells and Ramadan 10 propose the use of MRI as the initial radiologic procedure to diagnose IFS in patients at risk because of the nonspecific findings and the underestimation of the disease (compared with MRI and surgical findings) on CT scan. In their series of 4 patients, 2 had intracranial extension on MRI and intraoperatively, but it was missed on CT. Unlike our series, all of their patients had a more advanced disease, with extrasinus symptoms on presentation: 4 of 4 presented with facial swelling, 3 with orbital involvement, and 1 was obtunded. The mortality rate in their series was 100%, attributable to the advanced stage at presentation. 10 In patients with neurologic and orbital symptoms at the time of presentation, the suspicion of IFS 239
5 should be very high. These patients are better evaluated with MRI, although CT is also necessary for defining sinonasal anatomy. Since bone erosion is not a prerequisite for extrasinus extension, likely as a result of perivascular extension through penetrating vessels in the bone, MRI is more sensitive in disclosing intracranial and orbital invasion. 8 In earlier stages of IFS, as demonstrated in our series, CT findings of significant unilateral nasal cavity soft tissue thickening appears to be a consistent finding. At our institution, patients are closely monitored for IFS. Sinus CT scans are not routinely obtained prior to or after bone marrow transplantation. Sinus CT scans are ordered by the hematology or otolaryngology service to evaluate immunocompromised patients with sinonasal symptoms such as facial or nasal pain, headache, nasal obstruction, dental pain, facial swelling and/or paresthesias, or orbital complaints, or to evaluate unexplained fever. Patients with abnormalities on their sinus CT scan are evaluated by a rhinologist with rigid nasal endoscopy under topical anesthesia after decongestion. Biopsy specimens are obtained from areas of mucosal ischemia or necrosis and sent for frozen section analysis. If no mucosal abnormalities are seen but suspicion of IFS remains high, then directed biopsies are performed, particularly on edematous mucosa, either in the office or in the operating room. We recommend that intranasal biopsies be considered early in patients at risk even in the absence of specific nasal findings. 10 Patients with confirmed IFS, and those with negative biopsy results but continued suspicion for IFS, are taken to the operating room for endoscopic examination, biopsy, and debridement. Prior to surgery, systemic antifungal therapy is initiated empirically in neutropenic patients with absolute neutrophil counts below 1000/µL. Granulocyte-monocyte colony-stimulating factor is administered to neutropenic patients when possible to restore normal immune function as early as possible, because return of the immune response is the single most important factor in recovering from IFS. This is reflected in the fact that all 4 patients who died in our series had absolute neutrophil counts of less than 500/µL. Patients are then closely followed up clinically, with frequent endoscopic examinations and periodic debridements as necessary, as well as serial noncontrast CT scans when necessary. As reflected in the 83% recovery rate for patients in our series, early detection and treatment is paramount to obtaining a good outcome. The clinical challenge is identifying patients with invasive fungal disease as early as possible to permit initiation of medical and surgical intervention. However, the ability of the CT scan to detect the early stages of the disease is limited by high sensitivity and low specificity. Our review suggests that severe unilateral nasal cavity soft tissue inflammation is the most consistent early CT finding. Although a nonspecific finding, 21 of our 23 patients with IFS demonstrated nasal cavity edema much more severe than would be expected with routine rhinosinusitis, and 21 had unilateral disease, also unlike patients with viral or bacterial rhinosinusitis. Only 20% of immunocompromised, non-ifs sinusitis patients in the control group had nasal cavity soft tissue thickening and unilateral involvement, and the degree of thickening in these 2 patients was mild compared with the IFS group (Figures 1-5). More extensive changes such as bone erosion, orbital involvement, retroantral fat pad thickening, and facial cellulitis, though highly suggestive of invasive fungal sinusitis, were seen much less frequently, as these are findings more common in more advanced IFS. These findings were absent in the control group. Since 11 of the 23 patients in our series had only coronal CT scans, we could have underestimated the frequency of cases with facial and retroantral soft tissue involvement. We recommend that CT scans be routinely obtained at 3-mm intervals in the axial and coronal planes, using both soft tissue and bone windows. If only the more classic CT findings are used to guide surgical intervention, then a high percentage of cases in the early stages may go undetected. The CT finding of excessive nasal mucosal edema can raise clinical suspicion but cannot definitively diagnose IFS. The diagnosis can only be reliably established with careful clinical evaluation and biopsy. CONCLUSIONS Invasive fungal sinusitis is one of the most challenging infections that otolaryngologists diagnose and treat. Favorable outcomes depend on early diagnosis and aggressive medical and surgical intervention. Unfortunately, there are no standard criteria for the radiographic diagnosis of IFS. Although bone erosion and extrasinus extension are the classic CT findings highly suggestive of IFS in immunocompromised patients, these are usually found late in the course of the disease. The most common early sign of IFS in our patient population is severe unilateral nasal cavity mucosal and soft tissue edema. Although this is a nonspecific finding, in a patient at risk the presence of significant mucosal edema in the nasal cavity should raise the suspicion of a possible invasive fungal infection. Physical examination with biopsy remains the gold standard for diagnosis. The clinician must maintain a high index of suspicion and be vigilant to establish the diagnosis of IFS. Accepted for publication June 27, Corresponding author: John M. DelGaudio, MD, 1365 Clifton Rd NE, Suite 2323A, Atlanta, GA REFERENCES 1. de Shazo RD, O Brien M, Chapin K, Soto-Aguilar M, Gardner L, Swain RE. A new classification and diagnostic criteria for invasive fungal sinusitis. Arch Otolaryngol Head Neck Surg. 1997;123: Sugar AM. Mucormycosis. Clin Infect Dis. 1992;14(suppl): Blitzer A, Lawson W. Fungal infections of the nose and paranasal sinuses, part I. Otolaryngol Clin North Am. 1993;26: Platauf A. Mycosis mucorina. Virchows Arch. 1885;102: Oliveria PJ, Zinreich SJ. Radiology of the nasal cavity and paranasal sinuses. In: Cummings CW, Fredrickson JM, eds. Otolaryngology: Head and Neck Surgery. Vol 2. 3rd ed. St Louis, Mo: Mosby Year Book; 1998: Silverman CS, Mancuso AA. Periantral soft-tissue infiltration and its relevance to the early detection of invasive fungal sinusitis: CT and MR findings. AJNR Am J Neuroradiol. 1998;19: Som PM, Curtin HD. Chronic inflammatory sinonasal diseases including fungal infections: the role of imaging. Radiol Clin North Am. 1993;31: Gamba JL, Woodruff WW, Djang WT, Yeates AE. Craniofacial mucormycosis: assessment with CT. Radiology. 1986;160: Gillespie MB, O Malley BW, Francis HW. An approach to fulminant invasive fungal rhinosinusitis in the immunocompromised host. Arch Otolaryngol Head Neck Surg. 1998;124: Howells RC, Ramadan HH. Usefulness of computed tomography and magnetic resonance in fulminant invasive fungal rhinosinusitis. Am J Rhinol. 2001;15:
Invasive Fungal Rhinosinusitis: A 15-Year Experience With 29 Patients
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Invasive Fungal Rhinosinusitis: A 15-Year Experience With 29 Patients Marcus M. Monroe, MD; Max McLean, BA;
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Invasive Fungal Rhinosinusitis: A 15-Year Experience With 29 Patients Marcus M. Monroe, MD; Max McLean, BA;
Research Article Invasive Fungal Rhinosinusitis versus Bacterial Rhinosinusitis with Orbital Complications: A Case-Control Study
 The Scientific World Journal Volume 2013, Article ID 453297, 5 pages http://dx.doi.org/10.1155/2013/453297 Research Article Invasive Fungal Rhinosinusitis versus Bacterial Rhinosinusitis with Orbital Complications:
The Scientific World Journal Volume 2013, Article ID 453297, 5 pages http://dx.doi.org/10.1155/2013/453297 Research Article Invasive Fungal Rhinosinusitis versus Bacterial Rhinosinusitis with Orbital Complications:
Humans routinely inhale naturally occurring fungal
 SPECIAL TOPICS IN INFECTIOUS DISEASES Managing acute invasive fungal sinusitis Kristina M. Dwyhalo, PA-C; Carrlene Donald, PA-C; Anthony Mendez, PA-C; Joseph Hoxworth, MD ABSTRACT Acute invasive fungal
SPECIAL TOPICS IN INFECTIOUS DISEASES Managing acute invasive fungal sinusitis Kristina M. Dwyhalo, PA-C; Carrlene Donald, PA-C; Anthony Mendez, PA-C; Joseph Hoxworth, MD ABSTRACT Acute invasive fungal
Fungal ball.. Clinical and radiological features DR. AHMED ALTUWAIJRI 1/5/2017
 Fungal ball.. Clinical and radiological features DR. AHMED ALTUWAIJRI 1/5/2017 Fungal Rhinosinusitis (FRS) Rhinosinusitis, is a common disorder affecting approximately 20% of the population at some time
Fungal ball.. Clinical and radiological features DR. AHMED ALTUWAIJRI 1/5/2017 Fungal Rhinosinusitis (FRS) Rhinosinusitis, is a common disorder affecting approximately 20% of the population at some time
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study
 Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Practice patterns regarding noninvasive rhinosinusitis in the immunosuppressed patient population
 Practice patterns regarding noninvasive rhinosinusitis in the immunosuppressed patient population Zara M. Patel, Emory University Journal Title: Allergy & Rhinology Volume: Volume 4, Number 3 Publisher:
Practice patterns regarding noninvasive rhinosinusitis in the immunosuppressed patient population Zara M. Patel, Emory University Journal Title: Allergy & Rhinology Volume: Volume 4, Number 3 Publisher:
Clinical and imagistic correlations in the inflammatory pathology of nasosinusal cavities
 Romanian Journal of Rhinology, Volume 8, No. 29, January-March 2018 ORIGINAL STUDY DOI: 10.2478/rjr-2018-0003 Clinical and imagistic correlations in the inflammatory pathology of nasosinusal cavities Emilia
Romanian Journal of Rhinology, Volume 8, No. 29, January-March 2018 ORIGINAL STUDY DOI: 10.2478/rjr-2018-0003 Clinical and imagistic correlations in the inflammatory pathology of nasosinusal cavities Emilia
MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE
 PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
PROFESSOR DR SALINA HUSAIN DEPUTY HEAD DEPARTMENT OF OTORHINOLARYNGOLOGY-HEAD NECK SURGERY UKM MEDICAL CENTRE MANAGEMENT OF RHINOSINUSITIS IN ADULTS IN PRIMARY CARE CLINICAL PRACTICE GUIDELINES ON MANAGEMENT
Dr.Adel A. Al Ibraheem
 Rhinology Chair Weekly Activity Dr.Adel A. Al Ibraheem www.rhinologychair.org conference@rhinologychair.org Rhinology Chair Introduction: It is important to classify and stage nasal polyposis. ( decide
Rhinology Chair Weekly Activity Dr.Adel A. Al Ibraheem www.rhinologychair.org conference@rhinologychair.org Rhinology Chair Introduction: It is important to classify and stage nasal polyposis. ( decide
A descriptive study of the patients with orbital complication of acute and chronic sinusitis
 International Journal of Otorhinolaryngology and Head and Neck Surgery Pullarat AN et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Jul;4(4):990-996 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
International Journal of Otorhinolaryngology and Head and Neck Surgery Pullarat AN et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Jul;4(4):990-996 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937
Rhinosinusitis. John Ramey, MD Joseph Russell, MD
 Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
Rhinosinusitis John Ramey, MD Joseph Russell, MD Disclosure Statement RSFH as a continuing medical education provider, accredited by the South Carolina Medical Association, it is the policy of RSFH to
Mucor Mycosis maxilla with palatal destruction An Interesting Case Report with Literature Review
 ISSN 2250-0359 Volume 3 Issue 3.5 2013 Mucor Mycosis maxilla with palatal destruction An Interesting Case Report with Literature Review 1 Balasubramanian Thiagarajan 2 Venkatesan Ulaganathan 1 Stanley
ISSN 2250-0359 Volume 3 Issue 3.5 2013 Mucor Mycosis maxilla with palatal destruction An Interesting Case Report with Literature Review 1 Balasubramanian Thiagarajan 2 Venkatesan Ulaganathan 1 Stanley
Fungal-related diseases of the nasal cavity and paranasal sinuses
 Published April 16, 2015 as 10.3174/ajnr.A4298 ORIGINAL RESEARCH HEAD & NECK Acute Invasive Fungal Rhinosinusitis: A Comprehensive Update of CT Findings and Design of an Effective Diagnostic Imaging Model
Published April 16, 2015 as 10.3174/ajnr.A4298 ORIGINAL RESEARCH HEAD & NECK Acute Invasive Fungal Rhinosinusitis: A Comprehensive Update of CT Findings and Design of an Effective Diagnostic Imaging Model
Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities
 10.5005/jp-journals-10013-1141 H Verma et al ORIGINAL ARTICLE Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities H Verma, Rijuneeta, AK Gupta, A Chakrabarti
10.5005/jp-journals-10013-1141 H Verma et al ORIGINAL ARTICLE Allergic Fungal Rhinosinusitis Involving Frontal Sinus: A Prospective Study comparing Surgical Modalities H Verma, Rijuneeta, AK Gupta, A Chakrabarti
Provider Led Entity. CDI Quality Institute PLE Rhinosinusitis AUC 12/04/2018
 Provider Led Entity CDI Quality Institute PLE Rhinosinusitis AUC 12/04/2018 Appropriateness of advanced imaging procedures* in patients with rhinosinusitis and the following clinical presentations or diagnoses:
Provider Led Entity CDI Quality Institute PLE Rhinosinusitis AUC 12/04/2018 Appropriateness of advanced imaging procedures* in patients with rhinosinusitis and the following clinical presentations or diagnoses:
NASAL SEPTUM ADENOID CYSTIC CARCINOMA: A CASE REPORT
 NASAL SEPTUM ADENOID CYSTIC CARCINOMA: A CASE REPORT Shu-Yu Tai, 1 Chen-Yu Chien, 2 Chih-Feng Tai, 2,4 Wen-Rei Kuo, 2,4 Wan-Ting Huang, 3 and Ling-Feng Wang 2,4 Departments of 1 Family Medicine, 2 Otolaryngology
NASAL SEPTUM ADENOID CYSTIC CARCINOMA: A CASE REPORT Shu-Yu Tai, 1 Chen-Yu Chien, 2 Chih-Feng Tai, 2,4 Wen-Rei Kuo, 2,4 Wan-Ting Huang, 3 and Ling-Feng Wang 2,4 Departments of 1 Family Medicine, 2 Otolaryngology
Sphenoid rhinosinusitis associated with abducens nerve palsy Case report
 Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Romanian Journal of Rhinology, Volume 8, No. 30, April-June 2018 CASE REPORT Sphenoid rhinosinusitis associated with abducens nerve palsy Case report Lucian Lapusneanu 1, Marlena Radulescu 1, Florin Ghita
Extranodal Natural Killer/T-Cell Lymphoma Nasal Type: Detection by Computed Tomography Features
 The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. Extranodal Natural Killer/T-Cell Lymphoma Nasal Type: Detection by Computed Tomography Features Yin-Ping
The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. Extranodal Natural Killer/T-Cell Lymphoma Nasal Type: Detection by Computed Tomography Features Yin-Ping
Histopathology of Nasal Masses
 ORIGINAL ARTICLE Histopathology of Nasal Masses 1 Hemant Chopra, 2 Kapil Dua, 3 Neha Chopra, 4 Vikrant Mittal AIJCR Histopathology of Nasal Masses 1 Professor and Head, Dayanand Medical College, Ludhiana,
ORIGINAL ARTICLE Histopathology of Nasal Masses 1 Hemant Chopra, 2 Kapil Dua, 3 Neha Chopra, 4 Vikrant Mittal AIJCR Histopathology of Nasal Masses 1 Professor and Head, Dayanand Medical College, Ludhiana,
JMSCR Vol 05 Issue 09 Page September 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i9.52 Relationship of Agger Nasi Cell and Uncinate
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i9.52 Relationship of Agger Nasi Cell and Uncinate
1. BRIEF DESCRIPTION OF TRAINING
 RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
Medical Mycology Case Reports
 Medical Mycology Case Reports 1 (2012) 107 111 Contents lists available at SciVerse ScienceDirect Medical Mycology Case Reports journal homepage: www.elsevier.com/locate/mmcr Granulomatous invasive fungal
Medical Mycology Case Reports 1 (2012) 107 111 Contents lists available at SciVerse ScienceDirect Medical Mycology Case Reports journal homepage: www.elsevier.com/locate/mmcr Granulomatous invasive fungal
Clinical Study of Fungal Granulomatous Diseases
 International Journal of Advances in Health Sciences (IJHS) ISSN 2349-7033 Vol2, Issue5, 2015, pp665-669 http://www.ijhsonline.com Review Article Clinical Study of Fungal Granulomatous Diseases Sunil Pai
International Journal of Advances in Health Sciences (IJHS) ISSN 2349-7033 Vol2, Issue5, 2015, pp665-669 http://www.ijhsonline.com Review Article Clinical Study of Fungal Granulomatous Diseases Sunil Pai
COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY
 COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY John M. DelGaudio, MD Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology-Head and Neck Surgery Emory University School
COMPLICATIONS IN ENDOSCOPIC SINUS SURGERY John M. DelGaudio, MD Professor and Vice Chair Chief of Rhinology and Sinus Surgery Department of Otolaryngology-Head and Neck Surgery Emory University School
Functional Endoscopic Sinus Surgery
 WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
WHAT IS FUNCTIONAL ENDOSCOPIC SINUS SURGERY (FESS)? The nasal telescope has greatly changes the evaluation and treatment of rhino-sinusitis. This instrument, which provides a view of the structures in
Sinusitis & its complication. MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University
 Sinusitis & its complication MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University Definition Types Clinical manifestation Complications Diagnosis
Sinusitis & its complication MOHAMMED ALESSA MBBS,FRCSC Assistant Professor,Consultant Otolaryngology, Head & Neck Surgery King Saud University Definition Types Clinical manifestation Complications Diagnosis
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS
 MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
MANAGEMENT OF RHINOSINUSITIS IN ADOLESCENTS AND ADULTS Ministry of Health Malaysia Malaysian Society of Otorhinolaryngologist - Head & Neck Surgeons (MS)-HNS) Academy of Medicine Malaysia KEY MESSAGES
Frontal sinus disease continues to be one of the great
 Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Orbital facia. Periororbital facia Orbital septum Bulbar facia Muscular facia
 Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
Anatomy Orbital facia Periororbital facia Orbital septum Bulbar facia Muscular facia Physiology of symptoms 1) Proptosis ( exophthalmos) Pseudoproptosis Axial Non axial Pulsating Positional Intermittent
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
 Measure #334: Adult Sinusitis: More than One Computerized Tomography (CT) Scan Within 90 Days for Chronic Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2016 PQRS OPTIONS
Measure #334: Adult Sinusitis: More than One Computerized Tomography (CT) Scan Within 90 Days for Chronic Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2016 PQRS OPTIONS
Review Article The Prevalence of Concha Bullosa and Nasal Septal Deviation and Their Relationship to Maxillary Sinusitis by Volumetric Tomography
 Hindawi Publishing Corporation International Journal of Dentistry Volume 2010, Article ID 404982, 5 pages doi:10.1155/2010/404982 Review Article The Prevalence of and Nasal Septal Deviation and Their Relationship
Hindawi Publishing Corporation International Journal of Dentistry Volume 2010, Article ID 404982, 5 pages doi:10.1155/2010/404982 Review Article The Prevalence of and Nasal Septal Deviation and Their Relationship
Communication issue - What should the radiologist report before functional endoscopic sinus surgery
 Communication issue - What should the radiologist report before functional endoscopic sinus surgery Poster No.: C-0509 Congress: ECR 2015 Type: Educational Exhibit Authors: A. M. Dobra 1, C. A. Badiu 1,
Communication issue - What should the radiologist report before functional endoscopic sinus surgery Poster No.: C-0509 Congress: ECR 2015 Type: Educational Exhibit Authors: A. M. Dobra 1, C. A. Badiu 1,
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
ORIGINAL ARTICLE RELATIONSHIP OF CONCHA BULLOSA WITH OSTEOMEATAL UNIT BLOCKAGE. TOMOGRAPHIC STUDY IN 200 PATIENTS.
 RELATIONSHIP OF CONCHA BULLOSA WITH OSTEOMEATAL UNIT BLOCKAGE. TOMOGRAPHIC STUDY IN 200 PATIENTS. Shrikrishna B H 1, Jyothi A C 2, Sanjay G 3, Sandeep Samson G 4. 1. Associate Professor, Department of
RELATIONSHIP OF CONCHA BULLOSA WITH OSTEOMEATAL UNIT BLOCKAGE. TOMOGRAPHIC STUDY IN 200 PATIENTS. Shrikrishna B H 1, Jyothi A C 2, Sanjay G 3, Sandeep Samson G 4. 1. Associate Professor, Department of
Atlas of the Vasculitic Syndromes
 CHAPTER e40 Atlas of the Vasculitic Syndromes Carol A. Langford Anthony S. Fauci Diagnosis of the vasculitic syndromes is usually based upon characteristic histologic or arteriographic findings in a patient
CHAPTER e40 Atlas of the Vasculitic Syndromes Carol A. Langford Anthony S. Fauci Diagnosis of the vasculitic syndromes is usually based upon characteristic histologic or arteriographic findings in a patient
Bilateral blindness due to acute isolated sphenoid sinusitis- is it reversible? A. Case Report
 ISSN: 2250-0359 Volume 5 Issue 3 2015 Bilateral blindness due to acute isolated sphenoid sinusitis- is it reversible? A Case Report Roshan Kumar Verma Naresh K panda PGIMER, Chandigarh, India ABSTRACT
ISSN: 2250-0359 Volume 5 Issue 3 2015 Bilateral blindness due to acute isolated sphenoid sinusitis- is it reversible? A Case Report Roshan Kumar Verma Naresh K panda PGIMER, Chandigarh, India ABSTRACT
Pott s Puffy Tumor. Shahad Almohanna 15/1/2018
 Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
Syndromes of invasive fungal sinusitis
 Medical Mycology 2009, 47 (Supplement 1), S309S314 Syndromes of invasive fungal sinusitis RICHARD D. DESHAZO University of Mississippi Medical Center, Department of Medicine, Jackson, Mississippi, USA
Medical Mycology 2009, 47 (Supplement 1), S309S314 Syndromes of invasive fungal sinusitis RICHARD D. DESHAZO University of Mississippi Medical Center, Department of Medicine, Jackson, Mississippi, USA
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Endoscopic Management Of A Giant Ethmoid Mucocele
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
The Nose and Sinuses. Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital
 The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
The Nose and Sinuses Ophir Ilan, MD, PhD Department of Otolaryngology/Head&Neck surgery Hadassah University Hospital Nasal Mucociliary System Function of the Nasal Mucosa warming and humidifying the
2017 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Efficiency
 Measure #334: Adult Sinusitis: More than One Computerized Tomography (CT) Scan Within 90 Days for Chronic Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2017 OPTIONS
Measure #334: Adult Sinusitis: More than One Computerized Tomography (CT) Scan Within 90 Days for Chronic Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2017 OPTIONS
The advent of high-resolution computerized tomography
 An anatomic classification of the ethmoidal bulla REUBEN C. SETLIFF, III, MD, PETER J. CATALANO, MD, FACS, LISA A. CATALANO, MPH, and CHAD FRANCIS, BA, Sioux Falls, South Dakota, and Burlington, Massachusetts
An anatomic classification of the ethmoidal bulla REUBEN C. SETLIFF, III, MD, PETER J. CATALANO, MD, FACS, LISA A. CATALANO, MPH, and CHAD FRANCIS, BA, Sioux Falls, South Dakota, and Burlington, Massachusetts
INTERNATIONAL JOURNAL OF PHARMACEUTICAL RESEARCH AND BIO-SCIENCE
 INTERNATIONAL JOURNAL OF PHARMACEUTICAL RESEARCH AND BIO-SCIENCE RHINOCEREBRAL MUCORMYCOSIS DUE TO RHIZOPUS IN A RECENTLY DIAGNOSED DIABETIC FEMALE: A CASE REPORT KULKARNI KV 1, PATHAK NP 2 1. Assistant
INTERNATIONAL JOURNAL OF PHARMACEUTICAL RESEARCH AND BIO-SCIENCE RHINOCEREBRAL MUCORMYCOSIS DUE TO RHIZOPUS IN A RECENTLY DIAGNOSED DIABETIC FEMALE: A CASE REPORT KULKARNI KV 1, PATHAK NP 2 1. Assistant
Conventional Sinus Surgery Vs Fess
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 7 Ver. III (July. 2017), PP 44-51 www.iosrjournals.org Conventional Sinus Surgery Vs Fess *
ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS
 From the SelectedWorks of Balasubramanian Thiagarajan July 1, 2012 ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/51/
From the SelectedWorks of Balasubramanian Thiagarajan July 1, 2012 ROLE OF ANATOMICAL OBSTRUCTION IN THE PATHOGENESIS OF CHRONIC SINUSITIS Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/51/
Imaging of the Paranasal Sinuses
 14. Sommerschule Imaging of the Paranasal Sinuses Bettlach 24.08.2018 Christoph Schlegel Conventional Radiology NNH-Status: okzipito-frontal: frontal sinus, anterior ethmoid okzipito-nasal : maxillary
14. Sommerschule Imaging of the Paranasal Sinuses Bettlach 24.08.2018 Christoph Schlegel Conventional Radiology NNH-Status: okzipito-frontal: frontal sinus, anterior ethmoid okzipito-nasal : maxillary
SINUSITIS. HAVAS ENT CLINICS Excellence in otolaryngology
 JULY 2015 SINUSITIS WHAT IS IT? WHAT SHOULD YOU DO? WHAT WORKS? THOMAS E HAVAS MBBS (SYD) MD (UNSW) FRCSE, FRACS, FACS CONJOINT ASSOCIATE PROFESSOR UNSW OTOLARNGOLOGY HEAD AND NECK SURGERY HAVAS ENT CLINICS
JULY 2015 SINUSITIS WHAT IS IT? WHAT SHOULD YOU DO? WHAT WORKS? THOMAS E HAVAS MBBS (SYD) MD (UNSW) FRCSE, FRACS, FACS CONJOINT ASSOCIATE PROFESSOR UNSW OTOLARNGOLOGY HEAD AND NECK SURGERY HAVAS ENT CLINICS
Case Report Chronic Invasive Nongranulomatous Fungal Rhinosinusitis in Immunocompetent Individuals
 Case Reports in Otolaryngology Volume 2016, Article ID 6854121, 7 pages http://dx.doi.org/10.1155/2016/6854121 Case Report Chronic Invasive Nongranulomatous Fungal Rhinosinusitis in Immunocompetent Individuals
Case Reports in Otolaryngology Volume 2016, Article ID 6854121, 7 pages http://dx.doi.org/10.1155/2016/6854121 Case Report Chronic Invasive Nongranulomatous Fungal Rhinosinusitis in Immunocompetent Individuals
A CONTRIBUTION TO THE ETIOPATHOGENESIS, DIAGNOSIS AND MANAGEMENT OF SINONASAL INVERTED PAPILLOMAS
 UNIVERSITY OF MEDICINE AND PHARMACY OF TÂRGU MUREȘ ROMANIA A CONTRIBUTION TO THE ETIOPATHOGENESIS, DIAGNOSIS AND MANAGEMENT OF SINONASAL INVERTED PAPILLOMAS PhD THESIS ABSTRACT PhD Student Viorel Emanoil
UNIVERSITY OF MEDICINE AND PHARMACY OF TÂRGU MUREȘ ROMANIA A CONTRIBUTION TO THE ETIOPATHOGENESIS, DIAGNOSIS AND MANAGEMENT OF SINONASAL INVERTED PAPILLOMAS PhD THESIS ABSTRACT PhD Student Viorel Emanoil
Kathleen R. Fink, MD Virginia Mason Medical Center. 6 th Nordic Emergency Radiology Course 2017
 Kathleen R. Fink, MD Virginia Mason Medical Center 6 th Nordic Emergency Radiology Course 2017 Disclosure My spouse has a financial relationship with a commercial organization that may have a direct or
Kathleen R. Fink, MD Virginia Mason Medical Center 6 th Nordic Emergency Radiology Course 2017 Disclosure My spouse has a financial relationship with a commercial organization that may have a direct or
National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488
 National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488 Date: September 1997 Page 1 of 5 LIMITED OR LOCALIZED FOLLOW UP - SINUS CT 76380 Guideline
National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488 Date: September 1997 Page 1 of 5 LIMITED OR LOCALIZED FOLLOW UP - SINUS CT 76380 Guideline
Pathophysiology and Etiology
 Sinusitis Pathophysiology and Etiology Sinusitis is inflammation of the mucosa of one or more sinuses. It can be either acute chronic. Chronic sinusitis is diagnosed if symptoms are present for more than
Sinusitis Pathophysiology and Etiology Sinusitis is inflammation of the mucosa of one or more sinuses. It can be either acute chronic. Chronic sinusitis is diagnosed if symptoms are present for more than
Invasive Aspergillosis Associated Bacterial Infection in the Nasal Septum After Sphenoid Sinus Surgery
 Case Report Korean J Otorhinolaryngol-Head Neck Surg 2018;61(10):541-5 / pissn 2092-5859 / eissn 2092-6529 https://doi.org/10.3342/kjorl-hns.2017.17657 Invasive Aspergillosis Associated Bacterial Infection
Case Report Korean J Otorhinolaryngol-Head Neck Surg 2018;61(10):541-5 / pissn 2092-5859 / eissn 2092-6529 https://doi.org/10.3342/kjorl-hns.2017.17657 Invasive Aspergillosis Associated Bacterial Infection
Controversies surrounding categorization of fungal sinusitis
 Controversies surrounding categorization of fungal sinusitis Arunaloke Chakrabarti Professor,Department of Medical Microbiology Center for Advanced Research in Medical Mycology Postgraduate Institute of
Controversies surrounding categorization of fungal sinusitis Arunaloke Chakrabarti Professor,Department of Medical Microbiology Center for Advanced Research in Medical Mycology Postgraduate Institute of
Spheno-Ethmoidectomy
 Diagnostic and Therapeutic Endoscopy, Vol. 5, pp. 1-8 Reprints available directly from the publisher Photocopying permitted by license only (C) 1998 OPA (Overseas Publishers Association) N.V. Published
Diagnostic and Therapeutic Endoscopy, Vol. 5, pp. 1-8 Reprints available directly from the publisher Photocopying permitted by license only (C) 1998 OPA (Overseas Publishers Association) N.V. Published
Malignant growth Maxilla management an analysis
 ISSN: 2250-0359 Volume 3 Issue 2 2013 Malignant growth Maxilla management an analysis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Malignant tumors involving maxilla
ISSN: 2250-0359 Volume 3 Issue 2 2013 Malignant growth Maxilla management an analysis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Malignant tumors involving maxilla
FOR CMS (MEDICARE) MEMBERS ONLY NATIONAL COVERAGE DETERMINATION (NCD) FOR COMPUTED TOMOGRAPHY:
 National Imaging Associates, Inc. Clinical guidelines SINUS & MAXILLOFACIAL AREA CT LIMITED OR LOCALIZED FOLLOW UP SINUS CT Original Date: September 1997 Page 1 of 5 CPT Codes: 70486, 70487, 70488, 76380
National Imaging Associates, Inc. Clinical guidelines SINUS & MAXILLOFACIAL AREA CT LIMITED OR LOCALIZED FOLLOW UP SINUS CT Original Date: September 1997 Page 1 of 5 CPT Codes: 70486, 70487, 70488, 76380
Presentation of Invasive Fungal Rhinosinusitis in Sudanese Children: A Report of Four Cases
 Volume 13, Issue no. 2, DOI 10.18502/sjms.v13i2.2643 Production and Hosting by Knowledge E Case Report Presentation of Invasive Fungal Rhinosinusitis in Sudanese Children: A Report of Four Cases Faculty
Volume 13, Issue no. 2, DOI 10.18502/sjms.v13i2.2643 Production and Hosting by Knowledge E Case Report Presentation of Invasive Fungal Rhinosinusitis in Sudanese Children: A Report of Four Cases Faculty
Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision
 THIEME Original Research 73 Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision Jan Alessandro Socher 1 Jonas Mello 2 Barbara Batista Baltha 2 1 Department of Otorhinolaryngology,
THIEME Original Research 73 Tomographical Findings in Adult Patients Undergoing Endoscopic Sinus Surgery Revision Jan Alessandro Socher 1 Jonas Mello 2 Barbara Batista Baltha 2 1 Department of Otorhinolaryngology,
Chronic Sinusitis. Acute Sinusitis. Sinusitis. Anatomy of the Paranasal Sinuses. Sinusitis. Medical Topics - Sinusitis
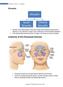 1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
1 Acute Chronic is the inflammation of the inner lining of the parnasal sinuses due to infection or non-infectious causes such as allergies or environmental pullutants. If the inflammation lasts more than
ORIGINAL ARTICLE. Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the Anterior Ethmoid
 Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the nterior Ethmoid Long-term Results ORIGINL RTICLE Toru Kikawada, MD; Masao Fujigaki, MD; Mikino
Extended Endoscopic Frontal Sinus Surgery to Interrupted Nasofrontal Communication Caused by Scarring of the nterior Ethmoid Long-term Results ORIGINL RTICLE Toru Kikawada, MD; Masao Fujigaki, MD; Mikino
Incidence of accessory ostia in patients with chronic maxillary sinusitis
 International Journal of Otorhinolaryngology and Head and Neck Surgery Ghosh P et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Mar;4(2):443-447 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original
International Journal of Otorhinolaryngology and Head and Neck Surgery Ghosh P et al. Int J Otorhinolaryngol Head Neck Surg. 2018 Mar;4(2):443-447 http://www.ijorl.com pissn 2454-5929 eissn 2454-5937 Original
Inter-Observer and Intra-Observer Variability In the Assessment of The Paranasal Sinuses Radiographs
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 5 Number 2 Inter-Observer and Intra-Observer Variability In the Assessment of The Paranasal Sinuses Radiographs A Norie, R Ahmad, W Liew, M
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 5 Number 2 Inter-Observer and Intra-Observer Variability In the Assessment of The Paranasal Sinuses Radiographs A Norie, R Ahmad, W Liew, M
, Aspergillus A. terreus. 4 Candida albicans. 2 Otomycosis. , Histoplasmosis Paracoccidiomycosis
 Jpn. J. Med. Mycol. Vol. 44, 277 283, 2003 ISSN 0916 4804 1 2 2 1 2, Aspergillus A. terreus, A. flavus, A. niger, Candida,. A. terreus,, CT, fungus ball, drainage,, Key words: otolaryngologic mycosis,
Jpn. J. Med. Mycol. Vol. 44, 277 283, 2003 ISSN 0916 4804 1 2 2 1 2, Aspergillus A. terreus, A. flavus, A. niger, Candida,. A. terreus,, CT, fungus ball, drainage,, Key words: otolaryngologic mycosis,
Mucin-Related Rhinosinusitis YOUSEF ALJATHLANY ORL-HNS RESIDENT
 Mucin-Related Rhinosinusitis YOUSEF ALJATHLANY ORL-HNS RESIDENT Free PPT Click to add title This PowerPoint Template has clean and neutral design that can be adapted to any content and meets various market
Mucin-Related Rhinosinusitis YOUSEF ALJATHLANY ORL-HNS RESIDENT Free PPT Click to add title This PowerPoint Template has clean and neutral design that can be adapted to any content and meets various market
9/18/2018. Disclosures. Objectives
 Is It Really Acute Bacterial Rhinosinusitis? Assessment, Differential Diagnosis and Management of Common Sinonasal Symptoms Kristina Haralambides, MS, RN, FNP-C Disclosures The content of this presentation
Is It Really Acute Bacterial Rhinosinusitis? Assessment, Differential Diagnosis and Management of Common Sinonasal Symptoms Kristina Haralambides, MS, RN, FNP-C Disclosures The content of this presentation
FUNGAL RHINOSINUSITIS: A RETROSPECTIVE ANALYSIS OF CLINICOPATHOLOGIC FEATURES AND TREATMENT OUTCOMES AT RAMATHIBODI HOSPITAL
 SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH FUNGAL RHINOSINUSITIS: A RETROSPECTIVE ANALYSIS OF CLINICOPATHOLOGIC FEATURES AND TREATMENT OUTCOMES AT RAMATHIBODI HOSPITAL Pannathat Soontrapa 1, Noppadol Larbcharoensub
SOUTHEAST ASIAN J TROP MED PUBLIC HEALTH FUNGAL RHINOSINUSITIS: A RETROSPECTIVE ANALYSIS OF CLINICOPATHOLOGIC FEATURES AND TREATMENT OUTCOMES AT RAMATHIBODI HOSPITAL Pannathat Soontrapa 1, Noppadol Larbcharoensub
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013
 FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
FRONTAL SINUPLASTY P R E P A R E D A N D P R E S E N T E D B Y : D R. Y A H Y A F A G E E H R 4 16/ 12/ 2013 ANATOMY: FRONTAL SINUS Not present at birth Starts developing at 4 years Radiographically visualized
 www.oralradiologists.com CONE BEAM CT REPORT CASE ---- Case Information Referring Doctor: - Patient Name: - Scan Date: December 1, 2015 Patient DOB: - Reason for Exam: - Study Details: icat Flex, 160x160x112
www.oralradiologists.com CONE BEAM CT REPORT CASE ---- Case Information Referring Doctor: - Patient Name: - Scan Date: December 1, 2015 Patient DOB: - Reason for Exam: - Study Details: icat Flex, 160x160x112
ISSN: Volume 4 Issue CHOLESTEROL GRANULOMA: AN UNCOMMON CLINICAL ENTITY OF THE MAXILLARY SINUS
 ISSN: 2250-0359 Volume 4 Issue 4 2014 CHOLESTEROL GRANULOMA: AN UNCOMMON CLINICAL ENTITY OF THE MAXILLARY SINUS Sunita Singh Sonia Chhabra Pansi Gupta Priya Malik Pt B.D. Sharma PGIMS, Rohtak, Haryana
ISSN: 2250-0359 Volume 4 Issue 4 2014 CHOLESTEROL GRANULOMA: AN UNCOMMON CLINICAL ENTITY OF THE MAXILLARY SINUS Sunita Singh Sonia Chhabra Pansi Gupta Priya Malik Pt B.D. Sharma PGIMS, Rohtak, Haryana
A case of malignant mucormycosis in a diabetic
 Case report A case of malignant mucormycosis in a diabetic Dr. P.K. Satpathy, Dr. P.M. Diggikar, Dr. A. Patil, Dr. Priyanka Zagade, Dr. Mukund Wasekar, Dr. T. Venu Babu, Dr. Deepak Baldania. Name of Institute/College:
Case report A case of malignant mucormycosis in a diabetic Dr. P.K. Satpathy, Dr. P.M. Diggikar, Dr. A. Patil, Dr. Priyanka Zagade, Dr. Mukund Wasekar, Dr. T. Venu Babu, Dr. Deepak Baldania. Name of Institute/College:
The future of health is digital
 Dated: XX/XX/XXXX Name: XXXXXXXX XXXXXXXXXXX Birth Date: XX/XX/XXXX Date of scan: XX/XX/XXXX Examination of the anatomical volume: The following structures are reviewed and evaluated for bilateral symmetry,
Dated: XX/XX/XXXX Name: XXXXXXXX XXXXXXXXXXX Birth Date: XX/XX/XXXX Date of scan: XX/XX/XXXX Examination of the anatomical volume: The following structures are reviewed and evaluated for bilateral symmetry,
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Anatomical Study of the Middle Meatus with Emphasis to the Maxillary Ostium and Their Clinical
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Anatomical Study of the Middle Meatus with Emphasis to the Maxillary Ostium and Their Clinical
Citation Hong Kong Practitioner, 1996, v. 18 n. 12, p
 Title Radiological conference. Frontal sinus osteoma complicated by pneumocephalus Author(s) Fung, WT; Peh, WCG Citation Hong Kong Practitioner, 1996, v. 18 n. 12, p. 658-662 Issued Date 1996 URL http://hdl.handle.net/10722/44655
Title Radiological conference. Frontal sinus osteoma complicated by pneumocephalus Author(s) Fung, WT; Peh, WCG Citation Hong Kong Practitioner, 1996, v. 18 n. 12, p. 658-662 Issued Date 1996 URL http://hdl.handle.net/10722/44655
Septic Cavernous Sinus Thrombosis: An Unusual and Fatal Disease
 ORIGINAL ARTICLE Septic Cavernous Sinus Thrombosis: An Unusual and Fatal Disease Huan-Wen Chen, Chan-Ping Su, 1 Deng-Huang Su, 2 Huan-Wu Chen, 3 Yee-Chun Chen 4,5 * Background: Septic cavernous sinus thrombosis
ORIGINAL ARTICLE Septic Cavernous Sinus Thrombosis: An Unusual and Fatal Disease Huan-Wen Chen, Chan-Ping Su, 1 Deng-Huang Su, 2 Huan-Wu Chen, 3 Yee-Chun Chen 4,5 * Background: Septic cavernous sinus thrombosis
Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study
 Abhishek Ramadhin REVIEW ARTICLE 10.5005/jp-journals-10013-1246 Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study Abhishek Ramadhin ABSTRACT There
Abhishek Ramadhin REVIEW ARTICLE 10.5005/jp-journals-10013-1246 Evaluation of the Change in Recent Diagnostic Criteria of Chronic Rhinosinusitis: A Cross-sectional Study Abhishek Ramadhin ABSTRACT There
Radiological anatomy of frontal sinus By drtbalu
 2009 Radiological anatomy of frontal sinus By drtbalu Anatomy of frontal sinus is highly variable. Precise understanding of these variables will help a surgeon to avoid unnecessary complications during
2009 Radiological anatomy of frontal sinus By drtbalu Anatomy of frontal sinus is highly variable. Precise understanding of these variables will help a surgeon to avoid unnecessary complications during
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Efficiency
 Quality ID #333: Adult Sinusitis: Computerized Tomography (CT) for Acute Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
Quality ID #333: Adult Sinusitis: Computerized Tomography (CT) for Acute Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY
OSTEITIS IN CRS. Rhinology Chair Meeting presented by Amal Binhazza a
 OSTEITIS IN CRS Rhinology Chair Meeting presented by Amal Binhazza a ROAD MAP Definition. pathophysiology. Diagnosis. Grading systems. Clinical implications. Management. OSTEITIS Presence of new bone formation,
OSTEITIS IN CRS Rhinology Chair Meeting presented by Amal Binhazza a ROAD MAP Definition. pathophysiology. Diagnosis. Grading systems. Clinical implications. Management. OSTEITIS Presence of new bone formation,
Allergic fungal rhinosinusitis: detection of fungal DNA in sinus aspirate using polymerase chain reaction
 1- Allergic fungal rhinosinusitis: detection of fungal DNA in sinus aspirate using polymerase chain reaction Abstract Objective: This study investigated allergic fungal rhinosinusitis cases, and aimed
1- Allergic fungal rhinosinusitis: detection of fungal DNA in sinus aspirate using polymerase chain reaction Abstract Objective: This study investigated allergic fungal rhinosinusitis cases, and aimed
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations
 White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
White Paper: Balloon Sinuplasty for Chronic Sinusitis, The Latest Recommendations For Health Plans, Medical Management Organizations and TPAs Executive Summary Despite recent advances in instrumentation
CASE REPORT A CASE OF RHINO-ORBITAL MUCORMYCOSIS IN A PATIENT WITH UNCONTROLLED TYPE 2 DIABETES MELLITUS
 A CASE OF RHINO-ORBITAL MUCORMYCOSIS IN A PATIENT WITH UNCONTROLLED TYPE 2 DIABETES MELLITUS Vikas L 1, Ranjith V 2, Riyaz Ahmed 3, Surakshith T.K 4 HOW TO CITE THIS ARTICLE: Vikas L, Ranjith V, Riyaz
A CASE OF RHINO-ORBITAL MUCORMYCOSIS IN A PATIENT WITH UNCONTROLLED TYPE 2 DIABETES MELLITUS Vikas L 1, Ranjith V 2, Riyaz Ahmed 3, Surakshith T.K 4 HOW TO CITE THIS ARTICLE: Vikas L, Ranjith V, Riyaz
The role of plain radiographs in the diagnosis of chronic maxillary rhinosinusitis in adults
 The role of plain radiographs in the diagnosis of chronic maxillary rhinosinusitis in adults *Kolo ES Department of Otorhinolaryngology, Bayero University Kano/Aminu Kano Teaching Hospital, Kano, Nigeria
The role of plain radiographs in the diagnosis of chronic maxillary rhinosinusitis in adults *Kolo ES Department of Otorhinolaryngology, Bayero University Kano/Aminu Kano Teaching Hospital, Kano, Nigeria
Osteomeatal unit OMU
 20074724752 CT Osteomeatal unitomu Assessment of the Relationship between Odontogenic Maxillary Sinusitis and Findings in the Ostiomeatal Unit on Coronal CT Images Miya Kato, Takashi Kaneda, Masataka Kato,
20074724752 CT Osteomeatal unitomu Assessment of the Relationship between Odontogenic Maxillary Sinusitis and Findings in the Ostiomeatal Unit on Coronal CT Images Miya Kato, Takashi Kaneda, Masataka Kato,
Actinomycosis and aspergillosis in the nose of a diabetic: A case report
 Volume 2 Issue 3 2012 ISSN 2250-0359 Actinomycosis and aspergillosis in the nose of a diabetic: A case report 1 Meenu Khurana Cherian 1*, Rajarajeswari 2 1 Department of ENT, Gulf Medical College Hospital
Volume 2 Issue 3 2012 ISSN 2250-0359 Actinomycosis and aspergillosis in the nose of a diabetic: A case report 1 Meenu Khurana Cherian 1*, Rajarajeswari 2 1 Department of ENT, Gulf Medical College Hospital
The Role of Computed Tomography in the Evaluation of Paranasal Sinuses Lesions
 ORIGINAL ARTICLE The Role of Computed Tomography in the Evaluation of Paranasal Sinuses Lesions Bhumikaben P. Suthar 1 *, Divya Vaidya 2, Pukhraj P. Suthar 3. 1 Assistant Professor, 2 Third Year Resident,
ORIGINAL ARTICLE The Role of Computed Tomography in the Evaluation of Paranasal Sinuses Lesions Bhumikaben P. Suthar 1 *, Divya Vaidya 2, Pukhraj P. Suthar 3. 1 Assistant Professor, 2 Third Year Resident,
Destructive Giant Maxillary Sinus Mucocele: A Case Report
 Destructive Giant Maxillary Sinus Mucocele: A Vahit Mutlu 1, Ozgur Yoruk 1, Ozalkan Ozkan 2 1 Atatürk University Faculty of Medicine, Department of Ears, Nose and Throat, Erzurum, Turkey 2 Erzincan University
Destructive Giant Maxillary Sinus Mucocele: A Vahit Mutlu 1, Ozgur Yoruk 1, Ozalkan Ozkan 2 1 Atatürk University Faculty of Medicine, Department of Ears, Nose and Throat, Erzurum, Turkey 2 Erzincan University
Study of correlation between patient symptomatology and incidental paranasal sinus abnormalities detected on CT & MRI Brain imaging
 Original article Study of correlation between patient symptomatology and incidental paranasal sinus abnormalities detected on CT & MRI Brain imaging 1 DR. SHAIKH IMRAN NIZAMUDDIN, 2 DR. Y.P.SACHDEV*, 3
Original article Study of correlation between patient symptomatology and incidental paranasal sinus abnormalities detected on CT & MRI Brain imaging 1 DR. SHAIKH IMRAN NIZAMUDDIN, 2 DR. Y.P.SACHDEV*, 3
The Relation between Anatomical Variations of Osteomeatal Complex & Nasal Structures and Chronic Sinusitis by Computed Tomography
 International Journal of Medical Imaging 2015; 3(2): 16-20 Published online March 6, 2015 (http://www.sciencepublishinggroup.com/j/ijmi) doi: 10.11648/j.ijmi.20150302.12 ISSN: 2330-8303 (Print); ISSN:
International Journal of Medical Imaging 2015; 3(2): 16-20 Published online March 6, 2015 (http://www.sciencepublishinggroup.com/j/ijmi) doi: 10.11648/j.ijmi.20150302.12 ISSN: 2330-8303 (Print); ISSN:
ENT Infections. Case 1. Diagnosis. Marlene L. Durand, M.D. Mass. General Hospital Mass. Eye & Ear Infirmary
 ENT Infections Marlene L. Durand, M.D. Mass. General Hospital Mass. Eye & Ear Infirmary Case 1 18 yr-old patient presents with L eyelid swelling, redness, and pain. He was well until 10 days ago, when
ENT Infections Marlene L. Durand, M.D. Mass. General Hospital Mass. Eye & Ear Infirmary Case 1 18 yr-old patient presents with L eyelid swelling, redness, and pain. He was well until 10 days ago, when
Crista galli sinusitis a radiological impression or a real clinical entity
 Romanian Journal of Rhinology, Vol. 6, No. 23, July - September 2016 ORIGINAL STUDY Crista galli sinusitis a radiological impression or a real clinical entity Claudiu Manea 1,2, Ranko Mladina 3 1 CESITO
Romanian Journal of Rhinology, Vol. 6, No. 23, July - September 2016 ORIGINAL STUDY Crista galli sinusitis a radiological impression or a real clinical entity Claudiu Manea 1,2, Ranko Mladina 3 1 CESITO
Retrospective Analysis of Patients with Allergy Sinusitis
 Original article: Retrospective Analysis of Patients with Allergy Sinusitis G.S. Thalor Senior Specialist (MS) (department of Oto Rhino Laryngology), Govt. S.K. Hospital, Sikar, Rajasthan, India. Corresponding
Original article: Retrospective Analysis of Patients with Allergy Sinusitis G.S. Thalor Senior Specialist (MS) (department of Oto Rhino Laryngology), Govt. S.K. Hospital, Sikar, Rajasthan, India. Corresponding
Clinical study of fungal sinusitis
 International Journal of Otorhinolaryngology and Head and Neck Surgery Waghray J. Int J Otorhinolaryngol Head Neck Surg. 28 Sep;4():7-32 http://www.ijorl.com pissn 24-929 eissn 24-937 Original Research
International Journal of Otorhinolaryngology and Head and Neck Surgery Waghray J. Int J Otorhinolaryngol Head Neck Surg. 28 Sep;4():7-32 http://www.ijorl.com pissn 24-929 eissn 24-937 Original Research
ORIGINAL ARTICLE. Computed Tomographic Staging and the Fate of the Dependent Sinuses in Revision Endoscopic Sinus Surgery
 Computed Tomographic Staging and the Fate of the Dependent es in Revision Endoscopic Surgery Neil Bhattacharyya, MD ORIGINAL ARTICLE Objectives: To determine the patterns of disease recurrence in chronic
Computed Tomographic Staging and the Fate of the Dependent es in Revision Endoscopic Surgery Neil Bhattacharyya, MD ORIGINAL ARTICLE Objectives: To determine the patterns of disease recurrence in chronic
Index. K Keratectomy, 213
 Index A Acute bacterial rhinosinusitis (ABRS), 76, 78 Acute rhinosinusitis (ARS), 77 83 diagnostic symptoms, 75 direct and indirect costs, 75 pathophysiology, 76, 77 sinonasal inflammationin, 75 treatment
Index A Acute bacterial rhinosinusitis (ABRS), 76, 78 Acute rhinosinusitis (ARS), 77 83 diagnostic symptoms, 75 direct and indirect costs, 75 pathophysiology, 76, 77 sinonasal inflammationin, 75 treatment
Experience with malignant tumours of the maxillary sinus in the Department of Otolaryngology Universiti Kebangsaan Malaysia, Kuala Lumpur
 Med. J. Malaysia Vol. 44 No. 1 March 1989 Experience with malignant tumours of the maxillary sinus in the Department of Otolaryngology Universiti Kebangsaan Malaysia, Kuala Lumpur S. Lokman, MD (UKMalaysia)
Med. J. Malaysia Vol. 44 No. 1 March 1989 Experience with malignant tumours of the maxillary sinus in the Department of Otolaryngology Universiti Kebangsaan Malaysia, Kuala Lumpur S. Lokman, MD (UKMalaysia)
The Incidence of Concha Bullosa and Its Association with Chronic Rhinosinusitis Deviated Nasal Septum and Osteomeatal Complex Obstruction
 1 Bahrain Medical Bulletin, Vol. 33, No. 4, December 2011 The Incidence of Concha Bullosa and Its Association with Chronic Rhinosinusitis Deviated Nasal Septum and Osteomeatal Complex Obstruction Fatma
1 Bahrain Medical Bulletin, Vol. 33, No. 4, December 2011 The Incidence of Concha Bullosa and Its Association with Chronic Rhinosinusitis Deviated Nasal Septum and Osteomeatal Complex Obstruction Fatma
CHRONIC RHINOSINUSITIS IN ADULTS
 CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
CHRONIC RHINOSINUSITIS IN ADULTS SCOPE OF THE PRACTICE GUIDELINE This clinical practice guideline is for use by the Philippine Society of Otolaryngology-Head and Neck Surgery. It covers the diagnosis and
