Life Science Journal 2016;13(11) Predictors of MRI Brain Changes in Systemic Lupus Erythematosus Patients
|
|
|
- Mariah Carson
- 5 years ago
- Views:
Transcription
1 Predictors of MRI Brain Changes in Systemic Lupus Erythematosus Patients Yasser El Miedany 1, Sami M Bahlas 2, Yasser M Bawazir 3, Ibtisam M Jali 4 1 Honorary senior clinical lecturer, King's college London, Consultant Rheumatologist, Darent Valley Hospital, Dartford, Kent, England. 2 Professor at king Abdulaziz University, Saudi Arabia 3 Demonstrator at king Abdulaziz University, Saudi Arabia 4 Assistant professor at king Abdulaziz University, Saudi Arabia drelmiedany@rheumatology4u.com, drbahlas@gmail.com, Yasser_bawazir@yahoo.com Dr.das28@gmail.com Abstract: Background: Brain involvement in SLE patients is considered one of the most important, relatively common disease manifestations. The central nervous system affection is associated with more cumulative damage as well as worse prognosis in SLE patients. Objective:1. To assess for the independent clinical / immunological predictors of brain affection in SLE patients as demonstrated by MRI scanning; 2. To investigate the relation between the MRI brain scanning outcome and other disease manifestations as well as management. Methods: A retrospective cohort study which included 88 patients diagnosed to have SLE according to the revised 1981 American College of Rheumatology (ACR) criteria. Disease activity was assessed using SLEDAI. Data regarding age, duration of SLE, neuropsychiatric (NP) manifestations, hypertensive status, and the presence of antiphospholipid antibodies were recorded. The MRI findings were categorized as normal, white and gray matter lesions, mild volume loss, infarction, thrombosis, as well as haemorrhage. Results: White and gray matter MRI changes were prevalent in 49% of the patients. Patterns of MRI brain affection included: 86% had white matter lesions, 19% mild volume loss, 16% had infarction, 13% thrombosis, whereas 8% had haemorrhage. Multivariate logistic regression analysis revealed that hypertension (OR11.8, CI ,(p<.001) and CNS manifestations (OR 10.9, CI , p< 0.003) were independent predictors of the development of brain lesions; whereas the presence of anti-phospholipid antibodies was not (OR: 0.621, 95% CI: ). There was no age difference among the subgroups based on MRI and immunoserological status. Conclusion: Several discrete brainmri patterns were observed in SLE patients suggestive of different pathogenetic mechanisms. White matter hyperintensities, whether distinct or in association with gray matter, were the most prevalent abnormal MRI brain finding in SLE patients. MRI brain changes in SLE patients were independent of the age of patients or the age at the diagnosis. Also they were not influenced by the SLE disease duration; however, they were associated with hypertension and CNS manifestations. [Yasser El Miedany, Sami M Bahlas, Yasser M Bawazir, Ibtisam M Jali. Predictors of MRI Brain Changes in Systemic Lupus Erythematosus Patients. Life Sci J 2016;13(11):24-29]. ISSN: (Print) / ISSN: X (Online) doi: /marslsj Keywords: SLE, MRI, NPSLE, lupus 1. Introduction: In contrast with other autoimmune diseases systemic, neuropsychiatric manifestations is considered one of the diagnostic criteria of systemic lupus erythematosus (SLE). Approximately 30 70% of SLE patients develop neuropsychiatric complications such as cerebrovascular disease, seizures, headaches, cognitive disorders or psychosis [1-3]. In some cases, neuropsychiatric lupus symptoms have been reported in the absence of either immuneserologic activity or other systemic disease manifestations [4]. The adoption of the neuropsychiatric case definitions by the American College of Rheumatology [5] has led to significant developments in the approach utilized to study nervous system affection in SLE patients and categorize homogeneous clusters of SLE patients from multiple studies for comparative research. Systemic lupus erythematosus (SLE) can affect any part of the central nervous system extending from the cerebrum to the cauda eqina, giving rise to diverse neurological manifestations. The patho-etiology of neuropsychiatric lupus (NPSLE) affection is likely to be multifactorial. This may encompass autoimmune antibody production, local production of intrathecal pro-inflammatory cytokines, premature atherosclerosis and microangiopathy [6]. Brain imaging has been reported to be an influential tool which can help to better demonstrate both structural and functional changes in SLE patients [7]. Despite clinically apparent symptoms and signs, imaging may be sometimes out of proportion to the clinical 24
2 manifestations. [8]. Studies attempting to link NPSLE manifestations to underlying SLE-specific pathophysiological processes are ongoing. Early diagnosis of such disorders would have a profound impact, not only on the diagnosis of the condition, but also its management at early stages; which in turn would have a positive impact on the outcomes as well as the patients health related quality of life. This study was carried out, aiming at assessment of the clinical / immunological predictors of brain affection in SLE patients as demonstrated by MRI scanning; and investigate the relation between abnormal MRI brain scanning outcomes and other clinical disease manifestations as well as immune-serologic parameters. 2. Methods: Study: This was a retrospective cohort study design which included 88 among SLE patients. All patients fulfilled the revised 1981 American College of Rheumatology (ACR) criteria for SLE [9]. Local ethical approval for the study was obtained. Patients: Inclusion criteria: Adult patients, more than 18 years old, who have been suffering from SLE and had NPSLE classified according to the 1999 ACR nomenclature and case definitions for NPSLE syndromes [10-12] were included in this work. Exclusion criteria: Patients in whom other concomitant disorders caused the neurological manifestations. Patients diagnosed to have undifferentiated connective tissue disease or overlap syndromes. Clinical Assessment: SLE patients at King Abdulaziz University hospital, were managed and had their disease activity monitored. All of the patients were assessed clinically to assess disease activity using SLEDAI score [13]. Clinical assessment for systemic affection was carried out, as part of the disease activity evaluation, for the patients. Special attention was given to neurological evaluation. History of vascular events such as DVT and pulmonary embolism was recorded. History of abortion or miscarriages was also recorded for every female patient. Blood pressure was taken for every patient. All the patients were managed and monitored according to EULAR recommendations for the management of systemic lupus erythematosus with neuropsychiatric manifestations [14]. Laboratory Assessment: Every patient had a blood test for kidney functions, lipid profile, anti-beta2 glycoprotein I antibodies, Prothrombin and partial thrombin time (PT and PTT). Urine analysis and 24 urine protein was also assessed. Immunology blood profile was carried out for every patient including ANA, anti-dna, lupus anticoagulant, anti-cardiolipinantibodies, anti-beta2 glycoprotein I antibodiesand complements level. MRI scanning: MRI brain was performed for all lupus patients with a GE 1.5 Tesla machine following the standard procedures. MRI included T1-weighted and T2- weighted images, fluid-attenuated inversion recovery (FLAIR) images and diffusion-weighted images. In some patients, gadolinium enhancement was performed on T1-weighted or FLAIR images. Outcome measures: Primary end point: assessment of the clinical / immunological predictors of brain affection in SLE patients as demonstrated by MRI scanning. Secondary outcome: investigate the relation between abnormal MRI brain scanning outcomes and other clinical disease manifestations as well as immune-serologic parameters; and whether it is possible that some of the brain imaging modalities can be useful as biomarkers for SLE-related nervous system damage and also for following treatment response. Statistical analysis: Comparison between patients with MRI abnormalities and those without significant MRI findings was performed using the Mann-Whitney U test, Fisher s exact test and logistic regression analysis where appropriate. Categorical variables were expressed as number and percentage i.e. frequency tables, while quantitative scaled variables are presented as mean and standard deviation. Alpha error was always set at All statistical manipulation and analyses were performed using the 16th version of SPSS. 3. Results: Demographic measures: Mean age in the patients was year. Females were 79/88 (89.8%). Mean disease duration in was 4.2 year months. Table (1) depicts the baseline data of the SLE patients assessed. 11% had NPSLE manifestations at the time of diagnosis, 16% developed them within one year, whereas 73% had NPSLE in 2-4 years. NPSLE manifestations were linked to SLE disease activity in 32%, mediated organ dysfunction in 30%, or secondary phenomenon attributed to infection, medication side-effects or metabolic abnormalities (e.g. uremia) in 25/88 (28.4%). The total spectrum of NPSLE manifestations included headache 55/88 (62.5%), seizures 11/88 (12.5%), cerebrovascular disease 4/88 (4.5%), psychosis 3/88 (3.4%), cranial neuropathy 2/88 (2.2%) movement disorder 1/88 (1.1%) whereas the prevalence of mood disorders and cognitive dysfunction was 63/88 (71.5%). 25
3 Clinical and immunological characteristics: A comparison of disease activity, and medications in NPSLE cohort of patients with MRI changes versus those without MRI changes is shown in Table 2. Serum anti-dna and anti-phospholipid antibodies (including anti-cardiolipin antibodies, antibeta2 glycoprotein I antibodiesand lupus anticoagulant); were not significantly associated with the presence of brain MRI abnormalities (Figure 1). MRI: Figure (2) shows the different MRI brain affection patterns reported in NPSLE patients. White and gray matter MRI changes were prevalent in 67/88 patients (76.2%). Multiple focal white matter hyperintesities was seen in 76.1% SLE patients (51/67) with abnormalities on MRI. White matter hyperintesities were seen in the supratentorial white matter, the brainstem, and in the medullary white matter of the cerebellum. In 10/67 (14.9%) hyperintensities were seen located within the cortical gray matter. All diffuse cortical gray matter hyperintensities showed some involvement of the adjacent white matter, varying from minimal extension to a considerable overlap. There were no significant differences in gender, age at the onset of NPSLE manifestations, or the SLEDAI scores between patients with MRI- versus those without MRI-changes. The SLE disease duration was significantly longer in patients whose MRI showed abnormalities (34.3±11.2 months) than in those without MRI abnormalities (15.8±5.7 months); (p < 0.001). Patterns of MRI brain affection included: 76.2% had white matter lesions(seen on T2-weighted orflair images), 14.9% gray matter lesions, 19.4% mild volume loss, 16.4% had infarction, 13.4% thrombosis, whereas 9% had haemorrhage (figure 2). Predictors of NPSLE: Multivariate logistic regression analysis revealed that hypertension (OR 11.8, CI ,(p<.001) and CNS manifestations (OR 10.7, CI , p< 0.003) were independent predictors of the development of brain lesions; whereas the presence of antiphospholipid antibodies was not (OR: 0.621, 95% CI: ) (table 3). There was no age difference among the subgroups based on MRI and immuneserological status. Table 1: Comparison of demographics and baseline clinical and laboratory data NPSLE patients with MRI changes versus those without MRI changes. Characteristic MRI changes No MRI changes Number of Patients 67 patients 21 patients Age (years) (mean + SD) Disease Duration 4.2 year month 4.3 year month SLEDAI (mean + SD) Prevalence of +ve ANA 92.8% 93.3% ANA: Anti-nuclear antibodystatistical significance was evaluated by Fisher s exact test. Table 2: Comparison of disease activity, and medications in NPSLE cohort of patients with MRI changes versus those without MRI changes. Characteristic MRI changes No MRI changes P-value SLEDAI (mean + SD) NS Cumulative dose of prednisolone (gm +SD) <0.01 Use of antimalarial: (No of patients taking it (%) 65/67 (98.5%) 21/21 (100%) NS Use of immunosuppressive: No of patients (%) 53/67 (79.1%) 17/21 (81.0%) NS Use of cyclophosphamide: No of patients (%) 25/67 (37.3%) 8/21 (38.1%) NS Use of azathioprine: (No of patients (%) 38/67 (56.7%) 12/21 (57.1%) NS Use of methotrexate: (No of patients(%) 7/67 (10.4%) 3/21 (14.3%) NS Use of MycophenolateMofetil: (No of patients 6/67 (9%) 1/21 (4.8%) <0.01 (%) Use of Leflunomide: (No of patients (%) 2/67 (3%) 1/21 (4.8%) NS Changed immunosuppressive dose (No of 51 (76.1%) 13/21 (61.9%) < 0.01 patients) Changed immunosuppressive medication (No. of patients %) 23 (34.3%) 5/21 (23.8%) < 0.01 Statistical significance was evaluated by Mann-Whitney U test. 26
4 Table 3: Multivariable analyses of the predictor of MRI changes in NPSLE patients OR (95% CI) P value Hypertension 11.8 ( ) < CNS manifestations 10.7 ( ) < *Anti-Phospholipids included anticardiolipinantibodies, anti-beta2 glycoprotein I antibodies and/or lupus anticoagulant. Statistical significance was evaluated by Mann-Whitney U test. Figure 1: Association of MRI findings and serum autoantibodies in neuropsychiatric systemic lupus erythematosus. Figure 2: Prevalence of MRI brain affection patterns in NPSLE patients 4. Discussion: In the course of their disease, many SLE patients develop neurologic or psychiatric symptoms. After exclusion of other causes such as concomitant illnesses, infection, or drug side effects, these neuropsychiatric manifestations are attributed to involvement of the nervous system in SLE, which is referred to as neuropsychiatric SLE (NPSLE) [15]. Given the absence of a diagnostic gold standard for NPSLE in clinical practice, NPSLE is a diagnosis per exclusion, usually achieved via case-by-case assessment using clinical, laboratory, and imaging data [16]. Magnetic resonance imaging (MRI) is considered the imaging technique of choice for the 27
5 NPSLE diagnosis [17]. This study was carried out aiming at assessment for the independent clinical / immunological predictors of brain affection in SLE patients as demonstrated by MRI scanning; and to investigate the relation between the MRI brain scanning outcome and other disease manifestations as well as management. Results of this work revealed that the most frequent radiographic finding was the presence of multiple focal white matter hyperintesities. These findings are in concordance with previous studies showing white matter hyperintesities, as the most commonly observed lesions in NPSLE, affecting up to 75% of patients [18,19]. White matter hyperintesities were reported in SLE patients with active NPSLE, in patients with past NPSLE, and in SLE patients without a history of neuropsychiatric events (nonneuropsychiatric SLE) [20, 21]. In this study, no MRI abnormalities were observed in as much as 11% of patients with clinically active NPSLE, with mildsevere symptoms of a wide variety of 1999 ACR defined NPSLE syndromes. These findings agree with the results of previous studies [21, 22]. Results of this work revealed that hypertension and CNS manifestations were independent predictors of the MRI brain lesions development, whereas there was no association with auto-antibodies including anti-dna or anti- phospholipid antibodies. These findings are in agreement with the outcomes of previous studies. De Leeuw et al [23], reported the association between white matter hyperintensities and hypertension. Another study carried out by Arinuma et al [24] reported that, whilst a variety of autoantibodies have been shown to be involved in the pathogenesis of SLE; anti-dna, anti-sm, anti-phospholipids as well as anti-ribosomal P antibodies were not significantly associated with abnormal brain MRI lesions. Even though anti-phospholipid antibodies might cause the irreversible lesions detected on brain MRI, they did not correlate with the presence of the irreversible brain MRI lesions. These findings are of importance in standard clinical practice as it identifies a subgroup of SLE patients who require close monitoring whether clinically or through imaging. In conclusion, MRI correlated significantly with SLE-associated CNS manifestations. Brain involvement in lupus may occur any time in the disease course. Therefore, all SLE patients whether they have neurological manifestations are at risk of brain lesions which could be detected in MRI. Hypertension and CNS manifestations can be used in standard clinical practice to identify a subset of SLE patients prone to develop MRI brain lesions. The occurrence of NPSLE was independent of the patients age, age at the diagnosis of SLE, and was not influenced by the duration of SLE. References: 1. CauliA, MontaldoCP, eltzm, TNurchis P, Sanna G, Garau P, Pala R, Passiu G, Mathieu A. Abnormalities of magnetic resonance imaging of the central nervous system in patients with systemic lupus erythematosus correlate with disease severity. ClinRheumatol 1994; 13: FutrellNS, chultzl, Mrillikan C. Central nervous system disease in patients with systemic lupus erythematosus. N eurology 1992; 42: Van-Dam AP. Diagnosis and pathogenesis of CNS lupus. Rheumatol 1991; Int 11: Harel L, Sandborg C, Lee T, et al. Neuropsychiatric manifestations in pediatric systemic lupus erythematosus and association with antiphospholipid antibodies. J Rheumatol 2006; 33: ACR Ad Hoc Committee on Neuropsychiatric Lupus Nomenclature. The American College of Rheumatology nomenclature and case definitions for neuropsychiatric lupus syndromes. Arthritis Rheum 1999; 42: Hanly JG. Neuropsychiatric lupus. CurrRheumatol Rep 2001; 3: Harirchian M, Saberi H, Najafizadeh S, Ali S. Evaluation of Brain and Cervical MRI Abnormality Rates in Patients With Systemic Lupus Erythematosus With or Without Neurological Manifestations. Iran J Radiol 2011; 8(3): Hanly JG, Urowitz MB, Sanchez-Guerrero J, et al. Neuropsychiatric events at the time of diagnosis of systemic lupus erythematosus: An international inception cohort study. Arthritis Rheum 2007; 56: Ainiala H, Hietaharju A, Loukkola J, et al. Validity of the new American College of Rheumatology criteria for neuropsychiatric lupus syndromes: a population-based evaluation. Arthritis Rheum 2001;45: Luyendijk J, Steens SC, Ouwendijk WJ, et al. Neuropsychiatric systemic lupus erythematosus: lessons learned from magnetic resonance imaging. Arthritis Rheum 2011;63: Steup-Beekman GM, Zirkzee EJ, Cohen D, et al. Neuropsychiatric manifestations in patients with systemic lupus erythematosus: epidemiology and radiology pointing to an immune-mediated cause. Ann Rheum Dis 2013;72(Suppl 2): ii ACR Ad Hoc Committee on Neuropsychiatric Lupus Nomenclature. The American College of Rheumatology nomenclature and case definitions for neuropsychiatric lupus syndromes. Arthritis Rheum 1999;42:
6 13. Gladman DD, Ibañez D, Urowitz MB. Systemic lupus erythematosus disease activity index J Rheumatol. 2002; 29(2): Bertsias GK, Ioannidis JP, Aringer M, et al. EULAR recommendations for the management of systemic lupus erythematosus with neuropsychiatric manifestations: report of a task force of the EULAR standing committee for clinical affairs. Ann Rheum Dis 2010;69: Rood MJ, Breedveld FC, Huizinga TW. The accuracy of diagnosing neuropsychiatric systemic lupus erythematosus in a series of 49 hospitalized patients. ClinExpRheumatol 1999; 17: Hanly JG, Harrison MJ. Management of neuropsychiatric lupus. Best Pract Res ClinRheumatol 2005;19: Sibbitt WL Jr, Sibbitt RR, Brooks WM. Neuroimaging in neuropsychiatric systemic lupus erythematosus [review]. Arthritis Rheum 1999;42: Karassa FB, Ioannidis JP, Boki KA, Touloumi G, Argyropoulou MI, Strigaris KA, et al. Predictors of clinical outcome and radiologic progression in patients with neuropsychiatric manifestations of systemic lupus erythematosus. Am J Med 2000;109: Sanna G, Piga M, Terryberry JW, Peltz MT, Giagheddu S, Satta L, et al. Central nervous system involvement in systemic lupus erythematosus: cerebral imaging and serological profile in patients with and without overt neuropsychiatric manifestations. Lupus 2000;9: Gonzalez-Crespo MR, Blanco FJ, Ramos A, Ciruelo E, Mateo I, Lopez Pino MA, et al. Magnetic resonance imaging of the brain in systemic lupus erythematosus. Br J Rheumatol 1995;34: Appenzeller S, Vasconcelos FA, Li LM, Costallat LT, Cendes F. Quantitative magnetic resonance imaging analyses and clinical significance of hyperintense white matter lesions in systemic lupus erythematosus patients. Ann Neurol 2008;64: Castellino G, Padovan M, Bortoluzzi A, Borrelli M, Feggi L, Caniatti ML, et al. Single photon emission computed tomography and magnetic resonance imaging evaluation in SLE patients with and without neuropsychiatric involvement. Rheumatology (Oxford) 2008;47: De Leeuw FE, de Groot JC, Oudkerk M, Witteman JC, Hofman A, van Gijn J, et al. Hypertension and cerebral white matter lesions in a prospective cohort study. Brain 2002;125: Arinuma Y, Kikuchi H, Wada T, Nagai T et al. Brain MRI in patients with diffuse psychiatric/neuropsychological syndromes in systemic lupus erythematosus. Lupus Science & Medicine 2014;1: e /15/
Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU
 Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU NPSLE represents a diagnostic and therapeutic challenge Wide range
Neuropsychiatric SLE (NPSLE) Dr. MTL NYO FCP(SA), Cert Rheum (Phys) Division of Rheumatology Department of Internal Medicine DGMAH / SMU NPSLE represents a diagnostic and therapeutic challenge Wide range
Evaluation of Symptom-Oriented Selection of Computed Tomography or Magnetic Resonance Imaging for Neuropsychiatric Systemic Lupus Erythematosus
 J Radiol Sci 2015; 40: 75-79 Evaluation of Symptom-Oriented Selection of Computed Tomography or Magnetic Resonance Imaging for Neuropsychiatric Systemic Lupus Erythematosus Hung-Wen Kao 1,2 Chao-Jan Wang
J Radiol Sci 2015; 40: 75-79 Evaluation of Symptom-Oriented Selection of Computed Tomography or Magnetic Resonance Imaging for Neuropsychiatric Systemic Lupus Erythematosus Hung-Wen Kao 1,2 Chao-Jan Wang
Situaciones estresantes en el lupus
 Situaciones estresantes en el lupus Munther A Khamashta MD FRCP PhD Director: Lupus Research Unit Barcelona, Noviembre 2008 What is Lupus? Lupus is a neurological disease and sometimes affects other organs
Situaciones estresantes en el lupus Munther A Khamashta MD FRCP PhD Director: Lupus Research Unit Barcelona, Noviembre 2008 What is Lupus? Lupus is a neurological disease and sometimes affects other organs
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria
 Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Manifestation of Antiphospholipid Syndrome among Saudi patients :examining the applicability of sapporo Criteria Farjah H AlGahtani Associate professor,md,mph Leukemia,Lymphoma in adolescent,thromboembolic
Evaluation of magnetic resonance imaging abnormalities in juvenile onset neuropsychiatric systemic lupus erythematosus
 Clin Rheumatol (2016) 35:2449 2456 DOI 10.1007/s10067-016-3376-9 ORIGINAL ARTICLE Evaluation of magnetic resonance imaging abnormalities in juvenile onset neuropsychiatric systemic lupus erythematosus
Clin Rheumatol (2016) 35:2449 2456 DOI 10.1007/s10067-016-3376-9 ORIGINAL ARTICLE Evaluation of magnetic resonance imaging abnormalities in juvenile onset neuropsychiatric systemic lupus erythematosus
Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience
 Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience References Sanna G, Bertolaccini ML. Neuropsychiatric manifestations
Neuropsychiatric Systemic Lupus Erythematosus (NPSLE) Case presentations and topic discussion The Rheumatology Unit UMMC experience References Sanna G, Bertolaccini ML. Neuropsychiatric manifestations
Development of SLE among Possible SLE Patients Seen in Consultation: Long-Term Follow-Up. Disclosures. Background. Evidence-Based Medicine.
 Development of SLE among Patients Seen in Consultation: Long-Term Follow-Up Abstract # 1699 May Al Daabil, MD Bonnie L. Bermas, MD Alexander Fine Hsun Tsao Patricia Ho Joseph F. Merola, MD Peter H. Schur,
Development of SLE among Patients Seen in Consultation: Long-Term Follow-Up Abstract # 1699 May Al Daabil, MD Bonnie L. Bermas, MD Alexander Fine Hsun Tsao Patricia Ho Joseph F. Merola, MD Peter H. Schur,
Systemic Lupus Erythematosus among Jordanians: A Single Rheumatology Unit Experience
 Systemic Lupus Erythematosus among Jordanians: A Single Rheumatology Unit Experience Ala M. AlHeresh MD* ABSTRACT Objectives: To study the characteristics of Systemic Lupus Erythematosus in Jordan and
Systemic Lupus Erythematosus among Jordanians: A Single Rheumatology Unit Experience Ala M. AlHeresh MD* ABSTRACT Objectives: To study the characteristics of Systemic Lupus Erythematosus in Jordan and
Central Nervous System (CNS) and Lupus: Learn from the Experts. Betty Diamond, M.D. Feinstein Institute for Medical Research
 Central Nervous System (CNS) and Lupus: Learn from the Experts Betty Diamond, M.D. Feinstein Institute for Medical Research Stages in SLE Pathogenesis Crow MK, Arth Res & Tx. 2009 ACR Criteria for the
Central Nervous System (CNS) and Lupus: Learn from the Experts Betty Diamond, M.D. Feinstein Institute for Medical Research Stages in SLE Pathogenesis Crow MK, Arth Res & Tx. 2009 ACR Criteria for the
CHAPTER 2. Early occurrence of neuropsychiatric manifestations in a large cohort of SLE patients
 CHAPTER 2 Early occurrence of neuropsychiatric manifestations in a large cohort of SLE patients G.M. Steup-Beekman 1, B.M.A. Gahrmann 1, B.J. Emmer 2, S.C.A. Steens 2, E.L.E.M. Bollen 3, M.A. van Buchem
CHAPTER 2 Early occurrence of neuropsychiatric manifestations in a large cohort of SLE patients G.M. Steup-Beekman 1, B.M.A. Gahrmann 1, B.J. Emmer 2, S.C.A. Steens 2, E.L.E.M. Bollen 3, M.A. van Buchem
Managing CNS involvement in systemic lupus erythematosus
 Review Managing CNS involvement in systemic lupus erythematosus The occurrence of neuropsychiatric manifestations in systemic lupus erythematosus (NPSLE) represents a diagnostic and therapeutic challenge
Review Managing CNS involvement in systemic lupus erythematosus The occurrence of neuropsychiatric manifestations in systemic lupus erythematosus (NPSLE) represents a diagnostic and therapeutic challenge
Clinical and immunological characteristics of Polish patients with systemic lupus erythematosus
 Original papers Clinical and immunological characteristics of Polish patients with systemic lupus erythematosus Martyna Tomczyk-Socha 1, B E, Hanna Sikorska-Szaflik 2, B E, Marek Frankowski 3, B D, Karolina
Original papers Clinical and immunological characteristics of Polish patients with systemic lupus erythematosus Martyna Tomczyk-Socha 1, B E, Hanna Sikorska-Szaflik 2, B E, Marek Frankowski 3, B D, Karolina
ONE of the following:
 Medical Coverage Policy Belimumab (Benlysta) EFFECTIVE DATE: 01 01 2012 POLICY LAST UPDATED: 11 21 2017 OVERVIEW Belimumab (Benlysta ) is indicated for the treatment of adult patients with active, autoantibody-positive,
Medical Coverage Policy Belimumab (Benlysta) EFFECTIVE DATE: 01 01 2012 POLICY LAST UPDATED: 11 21 2017 OVERVIEW Belimumab (Benlysta ) is indicated for the treatment of adult patients with active, autoantibody-positive,
9/25/2013 SYSTEMIC LUPUS ERYTHEMATOSUS (SLE)
 SYSTEMIC LUPUS ERYTHEMATOSUS (SLE) 1 Other Types of Lupus Discoid Lupus Erythematosus Lupus Pernio --- Sarcoidosis Lupus Vulgaris --- Tuberculosis of the face Manifestations of SLE Fever Rashes Arthritis
SYSTEMIC LUPUS ERYTHEMATOSUS (SLE) 1 Other Types of Lupus Discoid Lupus Erythematosus Lupus Pernio --- Sarcoidosis Lupus Vulgaris --- Tuberculosis of the face Manifestations of SLE Fever Rashes Arthritis
Correlation between Systemic Lupus Erythematosus Disease Activity Index, C3, C4 and Anti-dsDNA Antibodies
 Original Article Correlation between Systemic Lupus Erythematosus Disease Activity Index, C3, C4 and Anti-dsDNA Antibodies Col K Narayanan *, Col V Marwaha +, Col K Shanmuganandan #, Gp Capt S Shankar
Original Article Correlation between Systemic Lupus Erythematosus Disease Activity Index, C3, C4 and Anti-dsDNA Antibodies Col K Narayanan *, Col V Marwaha +, Col K Shanmuganandan #, Gp Capt S Shankar
Committee Approval Date: May 9, 2014 Next Review Date: May 2015
 Medication Policy Manual Policy No: dru248 Topic: Benlysta, belimumab Date of Origin: May 13, 2011 Committee Approval Date: May 9, 2014 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
Medication Policy Manual Policy No: dru248 Topic: Benlysta, belimumab Date of Origin: May 13, 2011 Committee Approval Date: May 9, 2014 Next Review Date: May 2015 Effective Date: June 1, 2014 IMPORTANT
Original Article Role of IL-1β, IL-6, IL-8 and IFN-γ in pathogenesis of central nervous system neuropsychiatric systemic lupus erythematous
 Int J Clin Exp Med 2015;8(9):16658-16663 www.ijcem.com /ISSN:1940-5901/IJCEM0011022 Original Article Role of IL-1β, IL-6, IL-8 and IFN-γ in pathogenesis of central nervous system neuropsychiatric systemic
Int J Clin Exp Med 2015;8(9):16658-16663 www.ijcem.com /ISSN:1940-5901/IJCEM0011022 Original Article Role of IL-1β, IL-6, IL-8 and IFN-γ in pathogenesis of central nervous system neuropsychiatric systemic
CHAPTER 8. TREX1 gene variant in neuropsychiatric SLE
 CHAPTER 8 TREX1 gene variant in neuropsychiatric SLE B. de Vries 1, G.M. Steup-Beekman 2, J. Haan 3,4, E.L.E.M. Bollen 3, J. Luyendijk 5, R.R. Frants 1, G.M. Terwindt 3, M.A. van Buchem 5, T.W.J. Huizinga
CHAPTER 8 TREX1 gene variant in neuropsychiatric SLE B. de Vries 1, G.M. Steup-Beekman 2, J. Haan 3,4, E.L.E.M. Bollen 3, J. Luyendijk 5, R.R. Frants 1, G.M. Terwindt 3, M.A. van Buchem 5, T.W.J. Huizinga
PSYCHIATRIC MANIFESTATIONS IN PEDIATRIC SLE PATIENTS AT SIRIRAJ HOSPITAL BANGKOK, THAILAND
 PSYCHIATRIC MANIFESTATIONS IN PEDIATRIC SLE PATIENTS AT SIRIRAJ HOSPITAL BANGKOK, THAILAND Sasitorn Chantaratin, Prae Wongtangman, Sudrat Sirisakpanit and Vitharon Boon-yasidhi Division of Child and Adolescent
PSYCHIATRIC MANIFESTATIONS IN PEDIATRIC SLE PATIENTS AT SIRIRAJ HOSPITAL BANGKOK, THAILAND Sasitorn Chantaratin, Prae Wongtangman, Sudrat Sirisakpanit and Vitharon Boon-yasidhi Division of Child and Adolescent
Mandana Nikpour 1,2, Murray B Urowitz 1*, Dominique Ibanez 1, Paula J Harvey 3 and Dafna D Gladman 1. Abstract
 RESEARCH ARTICLE Open Access Importance of cumulative exposure to elevated cholesterol and blood pressure in development of atherosclerotic coronary artery disease in systemic lupus erythematosus: a prospective
RESEARCH ARTICLE Open Access Importance of cumulative exposure to elevated cholesterol and blood pressure in development of atherosclerotic coronary artery disease in systemic lupus erythematosus: a prospective
Lupus as a risk factor for cardiovascular disease
 Lupus as a risk factor for cardiovascular disease SØREN JACOBSEN Department Rheumatology, Rigshospitalet Søren Jacobsen Main sponsors: Gigtforeningen Novo Nordisk Fonden Rigshospitalet Disclaimer: Novo
Lupus as a risk factor for cardiovascular disease SØREN JACOBSEN Department Rheumatology, Rigshospitalet Søren Jacobsen Main sponsors: Gigtforeningen Novo Nordisk Fonden Rigshospitalet Disclaimer: Novo
A neuroimaging follow-up study of a patient with juvenile central nervous system systemic lupus erythematosus
 A neuroimaging follow-up study of a patient with juvenile central nervous system systemic lupus erythematosus 11 137 MRI studies on NPSLE A neuroimaging follow-up study of a patient with juvenile central
A neuroimaging follow-up study of a patient with juvenile central nervous system systemic lupus erythematosus 11 137 MRI studies on NPSLE A neuroimaging follow-up study of a patient with juvenile central
Changes in White Matter Microstructure Suggest an Inflammatory Origin of Neuropsychiatric Systemic Lupus Erythematosus
 ARTHRITIS & RHEUMATOLOGY Vol. 68, No. 8, August 2016, pp 1945 1954 DOI 10.1002/art.39653 VC 2016, American College of Rheumatology Changes in White Matter Microstructure Suggest an Inflammatory Origin
ARTHRITIS & RHEUMATOLOGY Vol. 68, No. 8, August 2016, pp 1945 1954 DOI 10.1002/art.39653 VC 2016, American College of Rheumatology Changes in White Matter Microstructure Suggest an Inflammatory Origin
Life Science Journal 2014;11(1)
 Outcome of Systemic Lupus Erythematosus in Hospitalized Patients: A 2-year retrospective analysis Sami M Bahlas 1, Ibtisam Mousa Ali Jali 2, Hosam Mohamed Kamal Atik 3 and Walaa Khaled Aldhahri 4 1 King
Outcome of Systemic Lupus Erythematosus in Hospitalized Patients: A 2-year retrospective analysis Sami M Bahlas 1, Ibtisam Mousa Ali Jali 2, Hosam Mohamed Kamal Atik 3 and Walaa Khaled Aldhahri 4 1 King
Efficacy and Safety of Belimumab in the treatment of Systemic Lupus Erythematosus: a Prospective Multicenter Study.
 1. Title Efficacy and Safety of Belimumab in the treatment of Systemic Lupus Erythematosus: a Prospective Multicenter Study. 2. Background Systemic Lupus Erythematosus (SLE) is a chronic, autoimmune and
1. Title Efficacy and Safety of Belimumab in the treatment of Systemic Lupus Erythematosus: a Prospective Multicenter Study. 2. Background Systemic Lupus Erythematosus (SLE) is a chronic, autoimmune and
Systemic lupus erythematosus (SLE) is a chronic, autoimmune
 115 Focal Neurological Deficits due to a Contrast Enhancing Lesion in a Patient with Systemic Lupus Erythematosus Case report and Review of Literature Sundeep Srikakulam, M.D., and Anca Askanase, M.D.,
115 Focal Neurological Deficits due to a Contrast Enhancing Lesion in a Patient with Systemic Lupus Erythematosus Case report and Review of Literature Sundeep Srikakulam, M.D., and Anca Askanase, M.D.,
INTRODUCTION: Systemic lupus erythematosus (SLE) is the most common multisystemic autoimmune connective tissue disease
 THE SYSTEMIC IRAQI POSTGRADUATE LUPUS ERYTHEMATOSUS MEDICAL JOURNAL Cardiovascular Autonomic Nervous System Dysfunction in Iraqi Systemic Lupus Erythematosus Patients Ziad Shafeek Al-Rawi*, Nizar Abdul
THE SYSTEMIC IRAQI POSTGRADUATE LUPUS ERYTHEMATOSUS MEDICAL JOURNAL Cardiovascular Autonomic Nervous System Dysfunction in Iraqi Systemic Lupus Erythematosus Patients Ziad Shafeek Al-Rawi*, Nizar Abdul
Comparison of the Clinical Manifestations, Brain MRI and Prognosis between NeuroBehçet's Disease and Neuropsychiatric Lupus
 The Korean Journal of Internal Medicine : 22:77-86, 27 Comparison of the Clinical Manifestations, Brain MRI and Prognosis between NeuroBehçet's Disease and Neuropsychiatric Lupus Byung-Sik Cho, M.D., Hyun-Sook
The Korean Journal of Internal Medicine : 22:77-86, 27 Comparison of the Clinical Manifestations, Brain MRI and Prognosis between NeuroBehçet's Disease and Neuropsychiatric Lupus Byung-Sik Cho, M.D., Hyun-Sook
* Autoantibody positive (i.e. antinuclear antibody or ANA titre 1:80 or anti-double stranded (ds) DNA antibody 30 IU/mL)
 Benlysta (belimumab) Policy Number: 5.02.509 Last Review: 05/2018 Origination: 06/2011 Next Review: 05/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Benlysta
Benlysta (belimumab) Policy Number: 5.02.509 Last Review: 05/2018 Origination: 06/2011 Next Review: 05/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Benlysta
Benlysta (belimumab) Prior Authorization Criteria Program Summary
 Benlysta (belimumab) Prior Authorization Criteria Program Summary This prior authorization applies to Commercial, NetResults A series, NetResults F series and Health Insurance Marketplace formularies.
Benlysta (belimumab) Prior Authorization Criteria Program Summary This prior authorization applies to Commercial, NetResults A series, NetResults F series and Health Insurance Marketplace formularies.
What will we discuss today?
 Autoimmune diseases What will we discuss today? Introduction to autoimmune diseases Some examples Introduction to autoimmune diseases Chronic Sometimes relapsing Progressive damage Epitope spreading more
Autoimmune diseases What will we discuss today? Introduction to autoimmune diseases Some examples Introduction to autoimmune diseases Chronic Sometimes relapsing Progressive damage Epitope spreading more
CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution
 CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution Poster No.: C-2723 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro
CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution Poster No.: C-2723 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro
The Diagnosis of Lupus
 The Diagnosis of Lupus LUPUSUK 2017 This information booklet has been produced by LUPUS UK 2017 LUPUS UK LUPUS UK is the registered national charity for people with systemic lupus erythematosus (SLE) and
The Diagnosis of Lupus LUPUSUK 2017 This information booklet has been produced by LUPUS UK 2017 LUPUS UK LUPUS UK is the registered national charity for people with systemic lupus erythematosus (SLE) and
ARD Online First, published on August 19, 2010 as /ard Recommendations
 ARD Online First, published on August 19, 2010 as 10.1136/ard.2010.130476 Recommendations Additional data (supplementary tables) are published online only. To view these fi les please visit the journal
ARD Online First, published on August 19, 2010 as 10.1136/ard.2010.130476 Recommendations Additional data (supplementary tables) are published online only. To view these fi les please visit the journal
Pattern of Systemic Lupus Erythematosus in Tabuk, Saudi Arabia
 Original article: Pattern of Systemic Lupus Erythematosus in Tabuk, Saudi Arabia Abdullah ALYOUSSUF 1, Bashar ALASSAR 2, Osama MOHAMMED*, 1, Hyder MIRGHANI 1, Palanisamy Amirthalingam 3 1Department of
Original article: Pattern of Systemic Lupus Erythematosus in Tabuk, Saudi Arabia Abdullah ALYOUSSUF 1, Bashar ALASSAR 2, Osama MOHAMMED*, 1, Hyder MIRGHANI 1, Palanisamy Amirthalingam 3 1Department of
Key words: antiphospholipid syndrome, trombosis, pathogenesis
 26. XI,. 4/2011,.,..,..,., -..,,. 2GPI. -,.,,., -,, -, -,,,,, IL-1, IL-2, IL-6, IL-8, IL-12, IL-10, TNF, INF-. :,, N. Stoilov, R. Rashkov and R. Stoilov. ANTIPHOSPHOLIPID SYNDROME HISTORICAL DATA, ETI-
26. XI,. 4/2011,.,..,..,., -..,,. 2GPI. -,.,,., -,, -, -,,,,, IL-1, IL-2, IL-6, IL-8, IL-12, IL-10, TNF, INF-. :,, N. Stoilov, R. Rashkov and R. Stoilov. ANTIPHOSPHOLIPID SYNDROME HISTORICAL DATA, ETI-
UPDATES ON PEDIATRIC SLE
 UPDATES ON PEDIATRIC SLE BY ANGELA MIGOWA, PEDIATRIC RHEUMATOLOGIST/SENIOR INSTRUCTOR AKUHN MBCHB-UON, MMED-AKUHN,PEDIATRIC RHEUMATOLOGY- MCGILL UNIVERSITY HEALTH CENTRE ROSA PARKS OBJECTIVES RECOGNIZE
UPDATES ON PEDIATRIC SLE BY ANGELA MIGOWA, PEDIATRIC RHEUMATOLOGIST/SENIOR INSTRUCTOR AKUHN MBCHB-UON, MMED-AKUHN,PEDIATRIC RHEUMATOLOGY- MCGILL UNIVERSITY HEALTH CENTRE ROSA PARKS OBJECTIVES RECOGNIZE
Ischemic Stroke in Critically Ill Patients with Malignancy
 Ischemic Stroke in Critically Ill Patients with Malignancy Jeong-Am Ryu 1, Oh Young Bang 2, Daesang Lee 1, Jinkyeong Park 1, Jeong Hoon Yang 1, Gee Young Suh 1, Joongbum Cho 1, Chi Ryang Chung 1, Chi-Min
Ischemic Stroke in Critically Ill Patients with Malignancy Jeong-Am Ryu 1, Oh Young Bang 2, Daesang Lee 1, Jinkyeong Park 1, Jeong Hoon Yang 1, Gee Young Suh 1, Joongbum Cho 1, Chi Ryang Chung 1, Chi-Min
Seizure disorders in systemic lupus erythematosus results from an international, prospective, inception cohort study
 Seizure disorders in systemic lupus erythematosus results from an international, prospective, inception cohort study John G Hanly, Dalhousie University Murray B Urowitz, University of Toronto Li Su, University
Seizure disorders in systemic lupus erythematosus results from an international, prospective, inception cohort study John G Hanly, Dalhousie University Murray B Urowitz, University of Toronto Li Su, University
Role of MRI in acute disseminated encephalomyelitis
 Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Abnormal Brain Diffusivity in Patients with Neuropsychiatric Systemic Lupus Erythematosus
 AJNR Am J Neuroradiol 24:850 854, May 2003 Abnormal Brain Diffusivity in Patients with Neuropsychiatric Systemic Lupus Erythematosus Gerlof P. Th. Bosma, Tom W. J. Huizinga, Simon P. Mooijaart, and Mark
AJNR Am J Neuroradiol 24:850 854, May 2003 Abnormal Brain Diffusivity in Patients with Neuropsychiatric Systemic Lupus Erythematosus Gerlof P. Th. Bosma, Tom W. J. Huizinga, Simon P. Mooijaart, and Mark
Supplemental Figures and Legends
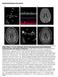 Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Supplemental Figures and Legends Online Figure 1. 18 year old female with SLE and acute homonymous hemianopsia, confusional state, and cognitive dysfunction. A. This TEE four chamber view demonstrates
Late onset systemic lupus erythematosus in southern Chinese. Citation Annals Of The Rheumatic Diseases, 1998, v. 57 n. 7, p.
 Title Late onset systemic lupus erythematosus in southern Chinese Author(s) Ho, CTK; Mok, CC; Lau, CS; Wong, RWS Citation Annals Of The Rheumatic Diseases, 1998, v. 57 n. 7, p. 437-440 Issued Date 1998
Title Late onset systemic lupus erythematosus in southern Chinese Author(s) Ho, CTK; Mok, CC; Lau, CS; Wong, RWS Citation Annals Of The Rheumatic Diseases, 1998, v. 57 n. 7, p. 437-440 Issued Date 1998
THE CARDIOVASCULAR INFLAMMATORY CONTINUUM DR AB MAHARAJ
 THE CARDIOVASCULAR INFLAMMATORY CONTINUUM DR AB MAHARAJ Disclosures: On National Advisory Boards of: (1) Pfizer Pharmaceuticals (2) MSD (3) Roche Pharmaceuticals (4) Abbott International: AfME Rheumatology
THE CARDIOVASCULAR INFLAMMATORY CONTINUUM DR AB MAHARAJ Disclosures: On National Advisory Boards of: (1) Pfizer Pharmaceuticals (2) MSD (3) Roche Pharmaceuticals (4) Abbott International: AfME Rheumatology
High Impact Rheumatology
 High Impact Rheumatology Systemic Lupus Erythematosus Bernard Rubin, DO MPH Case 1: History A 45-year-old woman presents with severe dyspnea and cough. She was in excellent health until 4 weeks ago when
High Impact Rheumatology Systemic Lupus Erythematosus Bernard Rubin, DO MPH Case 1: History A 45-year-old woman presents with severe dyspnea and cough. She was in excellent health until 4 weeks ago when
Original Article MRI Brain in Rheumatic Patients Pak Armed Forces Med J 2015; 65(4):
 Original Article Brain in Rheumatic Patients Pak Armed Forces Med J 0; 6(4): 0-4 PATTERN OF BRAIN ABNORMALITIES IN RHEUMATIC PATIENTS WITH NEUROLOGICAL INVOLVEMENT: A TERTIARY CARE TEACHING HOSPITAL EXPERIENCE
Original Article Brain in Rheumatic Patients Pak Armed Forces Med J 0; 6(4): 0-4 PATTERN OF BRAIN ABNORMALITIES IN RHEUMATIC PATIENTS WITH NEUROLOGICAL INVOLVEMENT: A TERTIARY CARE TEACHING HOSPITAL EXPERIENCE
Lupus (2014) 23,
 (2014) 23, 10 19 http://lup.sagepub.com PAPER In vivo evaluation of brain damage in the course of systemic lupus erythematosus using magnetic resonance spectroscopy, perfusion-weighted and diffusion-tensor
(2014) 23, 10 19 http://lup.sagepub.com PAPER In vivo evaluation of brain damage in the course of systemic lupus erythematosus using magnetic resonance spectroscopy, perfusion-weighted and diffusion-tensor
Redgrave JN, Coutts SB, Schulz UG et al. Systematic review of associations between the presence of acute ischemic lesions on
 6. Imaging in TIA 6.1 What type of brain imaging should be used in suspected TIA? 6.2 Which patients with suspected TIA should be referred for urgent brain imaging? Evidence Tables IMAG1: After TIA/minor
6. Imaging in TIA 6.1 What type of brain imaging should be used in suspected TIA? 6.2 Which patients with suspected TIA should be referred for urgent brain imaging? Evidence Tables IMAG1: After TIA/minor
Advanced Magnetic Resonance Imaging of the brain in patients treated with TNF-alpha blocking agents
 Chapter 3 Advanced Magnetic Resonance Imaging of the brain in patients treated with TNF-alpha blocking agents AE van der Bijl, BJ Emmer, FC Breedveld, HAM Middelkoop, CK Jurgens, MA van Buchem, TWJ Huizinga,
Chapter 3 Advanced Magnetic Resonance Imaging of the brain in patients treated with TNF-alpha blocking agents AE van der Bijl, BJ Emmer, FC Breedveld, HAM Middelkoop, CK Jurgens, MA van Buchem, TWJ Huizinga,
Patrick R Wood, MD Fellow, Rheumatology University of Colorado
 Patrick R Wood, MD Fellow, Rheumatology University of Colorado Discuss an unusual case of CNS calcification encountered on an academic VA rheumatology service Summarize bilateral striatopallidodentate
Patrick R Wood, MD Fellow, Rheumatology University of Colorado Discuss an unusual case of CNS calcification encountered on an academic VA rheumatology service Summarize bilateral striatopallidodentate
Significance of Anti-C1q Antibodies in Patients with Systemic Lupus Erythematosus as A Marker of Disease Activity and Lupus Nephritis
 THE EGYPTIAN JOURNAL OF IMMUNOLOGY Vol. 23 (1), 2016 Page: 00-00 Significance of Anti-C1q Antibodies in Patients with Systemic Lupus Erythematosus as A Marker of Disease Activity and Lupus Nephritis 1
THE EGYPTIAN JOURNAL OF IMMUNOLOGY Vol. 23 (1), 2016 Page: 00-00 Significance of Anti-C1q Antibodies in Patients with Systemic Lupus Erythematosus as A Marker of Disease Activity and Lupus Nephritis 1
Policy. Section: Medicine Effective Date: January 15, 2015 Subsection: Pathology/Laboratory Original Policy Date: December 5, 2014 Subject:
 Last Review Status/Date: December 2014 Page: 1 of 10 Summary Systemic lupus erythematosus (SLE) is an autoimmune connective tissue disease that can be difficult to diagnose because patients often present
Last Review Status/Date: December 2014 Page: 1 of 10 Summary Systemic lupus erythematosus (SLE) is an autoimmune connective tissue disease that can be difficult to diagnose because patients often present
Supplementary Figure Legends
 Supplementary Figure Legends Supplementary Figure 1. Comparison of RNP IC-mediated NET formation. Quantification of DNA release induced by ICs consisting of SmRNP combined with SLE IgG 961 (n = 10), 1032
Supplementary Figure Legends Supplementary Figure 1. Comparison of RNP IC-mediated NET formation. Quantification of DNA release induced by ICs consisting of SmRNP combined with SLE IgG 961 (n = 10), 1032
Pediatric systemic lupus erythematosus
 REVIEW Pediatric systemic lupus erythematosus Earl Silverman Professor of Pediatrics & Immunology, Division of Rheumatology, Hospital for Sick Children, Toronto, Ontario, Canada Tel.: +1 416 813 6249;
REVIEW Pediatric systemic lupus erythematosus Earl Silverman Professor of Pediatrics & Immunology, Division of Rheumatology, Hospital for Sick Children, Toronto, Ontario, Canada Tel.: +1 416 813 6249;
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Successful Use of Intensive Immunosuppressive Therapy for Treating Simultaneously Occurring Cerebral Lesions and Pulmonary Arterial Hypertension in a Patient with Systemic Lupus Erythematosus
CASE REPORT Successful Use of Intensive Immunosuppressive Therapy for Treating Simultaneously Occurring Cerebral Lesions and Pulmonary Arterial Hypertension in a Patient with Systemic Lupus Erythematosus
Cha pter 6. Perfusion MRI in Neuro-Psychiatric Systemic Lupus Erythemathosus
 Cha pter 6 Perfusion MRI in Neuro-Psychiatric Systemic Lupus Erythemathosus B. J. Emmer 1, M. J. van Osch 1, O. Wu 2, G. M. Steup-Beekman 3, S. C. Steens 1, T. W. Huizinga 3, M. A. van Buchem 1, J. van
Cha pter 6 Perfusion MRI in Neuro-Psychiatric Systemic Lupus Erythemathosus B. J. Emmer 1, M. J. van Osch 1, O. Wu 2, G. M. Steup-Beekman 3, S. C. Steens 1, T. W. Huizinga 3, M. A. van Buchem 1, J. van
Autoantibodies in the Idiopathic Inflammatory Myopathies
 Autoantibodies in the Idiopathic Inflammatory Myopathies Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic Rochester, MN The Myositis Association Annual Conference St. Louis, MO Sept. 25,
Autoantibodies in the Idiopathic Inflammatory Myopathies Steven R. Ytterberg, M.D. Division of Rheumatology Mayo Clinic Rochester, MN The Myositis Association Annual Conference St. Louis, MO Sept. 25,
Horizon Scanning Centre May Tabalumab for systemic lupus erythematosus SUMMARY NIHR HSC ID: 5581
 Horizon Scanning Centre May 2014 Tabalumab for systemic lupus erythematosus SUMMARY NIHR HSC ID: 5581 This briefing is based on information available at the time of research and a limited literature search.
Horizon Scanning Centre May 2014 Tabalumab for systemic lupus erythematosus SUMMARY NIHR HSC ID: 5581 This briefing is based on information available at the time of research and a limited literature search.
Association between microscopic brain damage as indicated by Magnetization Transfer Imaging and anticardiolipin antibodies in neuropsychiatric SLE
 CHAPTER 7 Association between microscopic brain damage as indicated by Magnetization Transfer Imaging and anticardiolipin antibodies in neuropsychiatric SLE S.C.A. Steens 1, G.P.Th. Bosma 1, G.M. Steup-Beekman
CHAPTER 7 Association between microscopic brain damage as indicated by Magnetization Transfer Imaging and anticardiolipin antibodies in neuropsychiatric SLE S.C.A. Steens 1, G.P.Th. Bosma 1, G.M. Steup-Beekman
Psychosis due to systemic lupus erythematosus: characteristics and long-term outcome of this rare manifestation of the disease
 Rheumatology 2008;47:1498 1502 Advance Access publication 25 July 2008 doi:10.1093/rheumatology/ken260 Psychosis due to systemic lupus erythematosus: characteristics and long-term outcome of this rare
Rheumatology 2008;47:1498 1502 Advance Access publication 25 July 2008 doi:10.1093/rheumatology/ken260 Psychosis due to systemic lupus erythematosus: characteristics and long-term outcome of this rare
February 2016, Volume: 8, Issue: 2, Pages: , DOI:
 Electronic Physician (ISSN: 2008-5842) http://www.ephysician.ir February 2016, Volume: 8, Issue: 2, Pages: 1874-1879, DOI: http://dx.doi.org/10.19082/1874 Pulmonary embolism in an adolescent girl with
Electronic Physician (ISSN: 2008-5842) http://www.ephysician.ir February 2016, Volume: 8, Issue: 2, Pages: 1874-1879, DOI: http://dx.doi.org/10.19082/1874 Pulmonary embolism in an adolescent girl with
Association of anti-mcv autoantibodies with SLE (Systemic Lupus Erythematosus) overlapping with various syndromes
 International Journal of Medicine and Medical Sciences Vol. () pp. 21-214, June 211 Available online http://www.academicjournals.org/ijmms ISSN 2-972 211 Academic Journals Full Length Research Paper Association
International Journal of Medicine and Medical Sciences Vol. () pp. 21-214, June 211 Available online http://www.academicjournals.org/ijmms ISSN 2-972 211 Academic Journals Full Length Research Paper Association
Noninfectious Causes of Fever in 128 Patients with Systemic Lupus Erythematosus
 Iran J Public Health, Vol. 48, No.1, Jan 2019, pp.62-68 Original Article Noninfectious Causes of Fever in 128 Patients with Systemic Lupus Erythematosus Feng GUO 1, Jianmei CHEN 1, Yu XIE 1, *Xueping ZHOU
Iran J Public Health, Vol. 48, No.1, Jan 2019, pp.62-68 Original Article Noninfectious Causes of Fever in 128 Patients with Systemic Lupus Erythematosus Feng GUO 1, Jianmei CHEN 1, Yu XIE 1, *Xueping ZHOU
Study of Neuropsychiatric Manifestations and Immunological Markers in Systemic Lupus Erythematosus
 Study of Neuropsychiatric Manifestations and Immunological Markers in Systemic Lupus Erythematosus Hafez N 1, Soltan L 1, Abo Ray AA 2, Hamdy M 1 Departments of Neuropsychiatry 1, Internal Medicine 2,
Study of Neuropsychiatric Manifestations and Immunological Markers in Systemic Lupus Erythematosus Hafez N 1, Soltan L 1, Abo Ray AA 2, Hamdy M 1 Departments of Neuropsychiatry 1, Internal Medicine 2,
Intracranial lesion as onset symptom in a patient with early undifferentiated connective tissue disease: a case report
 Du et al. BMC Neurology (2017) 17:85 DOI 10.1186/s12883-017-0868-4 CASE REPORT Open Access Intracranial lesion as onset symptom in a patient with early undifferentiated connective tissue disease: a case
Du et al. BMC Neurology (2017) 17:85 DOI 10.1186/s12883-017-0868-4 CASE REPORT Open Access Intracranial lesion as onset symptom in a patient with early undifferentiated connective tissue disease: a case
Serum interleukin 27: a possible biomarker of pediatric systemic lupus erythematosus
 Egypt J Pediatr Allergy Immunol 2013;11(1):15-21. Original article Serum interleukin 27: a possible biomarker of pediatric systemic lupus erythematosus Background: Systemic lupus erythematosus (SLE) is
Egypt J Pediatr Allergy Immunol 2013;11(1):15-21. Original article Serum interleukin 27: a possible biomarker of pediatric systemic lupus erythematosus Background: Systemic lupus erythematosus (SLE) is
Rheumatoid Arthritis. Manish Relan, MD FACP RhMSUS Arthritis & Rheumatology Care Center. Jacksonville, FL (904)
 Rheumatoid Arthritis Manish Relan, MD FACP RhMSUS Arthritis & Rheumatology Care Center. Jacksonville, FL (904) 503-6999. 1 Disclosures Speaker Bureau: Abbvie 2 Objectives Better understand the pathophysiology
Rheumatoid Arthritis Manish Relan, MD FACP RhMSUS Arthritis & Rheumatology Care Center. Jacksonville, FL (904) 503-6999. 1 Disclosures Speaker Bureau: Abbvie 2 Objectives Better understand the pathophysiology
Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus
 CM&R Rapid Release. Published online ahead of print February 26, 2009 as doi:10.3121/cmr.2008.828 Original Research Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus José María Calvo-Romero,
CM&R Rapid Release. Published online ahead of print February 26, 2009 as doi:10.3121/cmr.2008.828 Original Research Anticardiolipin Antibodies in Patients With Type 2 Diabetes Mellitus José María Calvo-Romero,
ORIGINAL INVESTIGATION
 ORIGINAL INVESTIGATION High Impact of Antiphospholipid Syndrome on Irreversible Organ Damage and Survival of Patients With Systemic Lupus Erythematosus Guillermo Ruiz-Irastorza, MD, PhD; Maria-Victoria
ORIGINAL INVESTIGATION High Impact of Antiphospholipid Syndrome on Irreversible Organ Damage and Survival of Patients With Systemic Lupus Erythematosus Guillermo Ruiz-Irastorza, MD, PhD; Maria-Victoria
Insights into the DX of Pediatric SLE
 Insights into the DX of Pediatric SLE Dr. John H. Yost Pediatric Rheumatology Children s Hospital at Dartmouth Assistant Professor of Medicine Geisel School of Medicine at Dartmouth john.h.yost@hitchcock.org
Insights into the DX of Pediatric SLE Dr. John H. Yost Pediatric Rheumatology Children s Hospital at Dartmouth Assistant Professor of Medicine Geisel School of Medicine at Dartmouth john.h.yost@hitchcock.org
Clinical Commissioning Policy Statement: Rituximab For Systemic Lupus Erythematosus (SLE) December Reference : NHSCB/A3C/1b
 Clinical Commissioning Policy Statement: Rituximab For Systemic Lupus Erythematosus (SLE) December 2012 Reference : NHSCB/A3C/1b NHS Commissioning Board Clinical Commissioning Policy Statement: Rituximab
Clinical Commissioning Policy Statement: Rituximab For Systemic Lupus Erythematosus (SLE) December 2012 Reference : NHSCB/A3C/1b NHS Commissioning Board Clinical Commissioning Policy Statement: Rituximab
Brain tissue and white matter lesion volume analysis in diabetes mellitus type 2
 Brain tissue and white matter lesion volume analysis in diabetes mellitus type 2 C. Jongen J. van der Grond L.J. Kappelle G.J. Biessels M.A. Viergever J.P.W. Pluim On behalf of the Utrecht Diabetic Encephalopathy
Brain tissue and white matter lesion volume analysis in diabetes mellitus type 2 C. Jongen J. van der Grond L.J. Kappelle G.J. Biessels M.A. Viergever J.P.W. Pluim On behalf of the Utrecht Diabetic Encephalopathy
Newer classification criteria 2010:How adequate is this to classify Rheumatoid Arthritis?
 Newer classification criteria 2010:How adequate is this to classify Rheumatoid Arthritis? DR MD MATIUR RAHMAN MBBS, MD, FCPS, FACR, Fellow APLAR Associate Professor, Medicine SSMC & Mitford Hospital New
Newer classification criteria 2010:How adequate is this to classify Rheumatoid Arthritis? DR MD MATIUR RAHMAN MBBS, MD, FCPS, FACR, Fellow APLAR Associate Professor, Medicine SSMC & Mitford Hospital New
Elevated BLyS levels in patients with systemic lupus erythematosus: Associated factors and responses to belimumab
 (2016) 25, 346 354 http://lup.sagepub.com PAPER Elevated BLyS levels in patients with systemic lupus erythematosus: Associated factors and responses to belimumab DA Roth 1, A Thompson 2, Y Tang 2*, AE
(2016) 25, 346 354 http://lup.sagepub.com PAPER Elevated BLyS levels in patients with systemic lupus erythematosus: Associated factors and responses to belimumab DA Roth 1, A Thompson 2, Y Tang 2*, AE
Anti β 2. -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With Antiphospholipid Syndrome
 Coagulation and Transfusion Medicine / PREDICTIVE VALUE OF ANTIPHOSPHOLIPID ANTIBODIES Anti β -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With
Coagulation and Transfusion Medicine / PREDICTIVE VALUE OF ANTIPHOSPHOLIPID ANTIBODIES Anti β -Glycoprotein I and Antiphosphatidylserine Antibodies Are Predictors of Arterial Thrombosis in Patients With
Prevalence of Abnormal Ankle Brachial Index in Iraqi Patients with Systemic Lupus Erythematosus
 ANKLE THE IRAQI BRACHIAL POSTGRADUATE INDEX MEDICAL IN SYSTEMIC JOURNAL LUPUS ERYTHEMATOSUS Prevalence of Abnormal Ankle Brachial Index in Iraqi Patients with Systemic Lupus Erythematosus Ziad S. Al-Rawi*,
ANKLE THE IRAQI BRACHIAL POSTGRADUATE INDEX MEDICAL IN SYSTEMIC JOURNAL LUPUS ERYTHEMATOSUS Prevalence of Abnormal Ankle Brachial Index in Iraqi Patients with Systemic Lupus Erythematosus Ziad S. Al-Rawi*,
Lupus and Your Kidneys. Michael P. Madaio, MD Professor of Medicine Chairman of Medicine Medical College of Georgia Augusta, Georgia
 Lupus and Your Kidneys Michael P. Madaio, MD Professor of Medicine Chairman of Medicine Medical College of Georgia Augusta, Georgia Kidney Inflammation and Abnormal Function as a Result of Lupus (Lupus
Lupus and Your Kidneys Michael P. Madaio, MD Professor of Medicine Chairman of Medicine Medical College of Georgia Augusta, Georgia Kidney Inflammation and Abnormal Function as a Result of Lupus (Lupus
Autoimmune diseases. SLIDE 3: Introduction to autoimmune diseases Chronic
 SLIDE 3: Introduction to autoimmune diseases Chronic Autoimmune diseases Sometimes relapsing : and remitting. which means that they present as attacks Progressive damage Epitope spreading more and more
SLIDE 3: Introduction to autoimmune diseases Chronic Autoimmune diseases Sometimes relapsing : and remitting. which means that they present as attacks Progressive damage Epitope spreading more and more
VII EULAR Scientifically Endorsed Course on. Pisa, Italy May 3rd - 8th, Course Chairmen Stefano Bombardieri, Marta Mosca
 VII EULAR Scientifically Endorsed Course on Pisa, Italy May 3rd - 8th, 2015 Course Chairmen Stefano Bombardieri, Marta Mosca Scientific Secretariat: Chiara Tani Organizing Secretariat: Luisa Marconcini,
VII EULAR Scientifically Endorsed Course on Pisa, Italy May 3rd - 8th, 2015 Course Chairmen Stefano Bombardieri, Marta Mosca Scientific Secretariat: Chiara Tani Organizing Secretariat: Luisa Marconcini,
J. van Aken* H. van Dongen* S. le Cessie F.C. Breedveld T.W.J. Huizinga. * both authors contributed equally
 CHAPTER Comparison of long term outcome of patients with rheumatoid arthritis presenting with undifferentiated arthritis or with rheumatoid arthritis: an observational cohort study J. van Aken* H. van
CHAPTER Comparison of long term outcome of patients with rheumatoid arthritis presenting with undifferentiated arthritis or with rheumatoid arthritis: an observational cohort study J. van Aken* H. van
Clinical features and mortality in Chinese with lupus nephritis and neuropsychiatric lupus: A 124-patient study
 ORIGINAL ARTICLE Clinical features and mortality in Chinese with lupus nephritis and neuropsychiatric lupus: A 124-patient study Min Feng, Jun Lv, Sha Fu, Bo Liu, Ying Tang, Xia Wan, Peifen Liang, Yuchun
ORIGINAL ARTICLE Clinical features and mortality in Chinese with lupus nephritis and neuropsychiatric lupus: A 124-patient study Min Feng, Jun Lv, Sha Fu, Bo Liu, Ying Tang, Xia Wan, Peifen Liang, Yuchun
SYSTEMIC LUPUS ERYTHEMATOSUS: CURRENT CONCEPTS AND CLINICAL PEARLS. Dr Sheila Vasoo Consultant Division of Rheumatology NUHS
 SYSTEMIC LUPUS ERYTHEMATOSUS: CURRENT CONCEPTS AND CLINICAL PEARLS Dr Sheila Vasoo Consultant Division of Rheumatology NUHS Listen to the Patient Concepts Diagnosis Immunopathogenesis Clinical Pearls Disease
SYSTEMIC LUPUS ERYTHEMATOSUS: CURRENT CONCEPTS AND CLINICAL PEARLS Dr Sheila Vasoo Consultant Division of Rheumatology NUHS Listen to the Patient Concepts Diagnosis Immunopathogenesis Clinical Pearls Disease
Association of Global Brain Damage and Clinical Functioning in Neuropsychiatric Systemic Lupus Erythematosus
 ARTHRITIS & RHEUMATISM Vol. 46, No. 10, 2002, pp 2665 2672 DOI 10.1002/art.10574 2002, American College of Rheumatology Association of Global Brain Damage and Clinical Functioning in Neuropsychiatric Systemic
ARTHRITIS & RHEUMATISM Vol. 46, No. 10, 2002, pp 2665 2672 DOI 10.1002/art.10574 2002, American College of Rheumatology Association of Global Brain Damage and Clinical Functioning in Neuropsychiatric Systemic
Systemic Lupus Erythematosus
 Systemic Lupus Erythematosus Marc C. Hochberg, MD, MPH Professor of Medicine and Head, Division of Rheumatology University of Maryland School of Medicine CASE: HISTORY A 26-year-old woman is seen for migratory
Systemic Lupus Erythematosus Marc C. Hochberg, MD, MPH Professor of Medicine and Head, Division of Rheumatology University of Maryland School of Medicine CASE: HISTORY A 26-year-old woman is seen for migratory
Review. Undifferentiated connective tissue diseases (UCTD): A review of the literature and a proposal for preliminary classification criteria
 Fibrinolysis in joint inflammation / M. Del Rosso et al. Review REVIEW Undifferentiated connective tissue diseases (UCTD): A review of the literature and a proposal for preliminary classification criteria
Fibrinolysis in joint inflammation / M. Del Rosso et al. Review REVIEW Undifferentiated connective tissue diseases (UCTD): A review of the literature and a proposal for preliminary classification criteria
Living with Lupus: An Insider s Perspective
 Living with Lupus: An Insider s Perspective Pamela Thorpe, MD, FACP Lupus Foundation of America, Inc. Philadelphia Tri-State Chapter Volunteer May 2014 My Own Story Is it Lupus Yet? The What What is this?
Living with Lupus: An Insider s Perspective Pamela Thorpe, MD, FACP Lupus Foundation of America, Inc. Philadelphia Tri-State Chapter Volunteer May 2014 My Own Story Is it Lupus Yet? The What What is this?
Gender Differences in the Clinical and Serological Features of Systemic Lupus Erythematosus in Malaysian Patients
 o ORIGINAL ARTICLE Gender Differences in the Clinical and Serological Features of Systemic Lupus Erythematosus in Malaysian Patients M R Azizah, MBBCh*, S S Ainol, MMed**, N C T Kong, MRCP***, Y Normaznah,
o ORIGINAL ARTICLE Gender Differences in the Clinical and Serological Features of Systemic Lupus Erythematosus in Malaysian Patients M R Azizah, MBBCh*, S S Ainol, MMed**, N C T Kong, MRCP***, Y Normaznah,
THE KIDNEY AND SLE LUPUS NEPHRITIS
 THE KIDNEY AND SLE LUPUS NEPHRITIS JACK WATERMAN DO FACOI 2013 NEPHROLOGY SIR RICHARD BRIGHT TERMINOLOGY RENAL INSUFFICIENCY CKD (CHRONIC KIDNEY DISEASE) ESRD (ENDSTAGE RENAL DISEASE) GLOMERULONEPHRITIS
THE KIDNEY AND SLE LUPUS NEPHRITIS JACK WATERMAN DO FACOI 2013 NEPHROLOGY SIR RICHARD BRIGHT TERMINOLOGY RENAL INSUFFICIENCY CKD (CHRONIC KIDNEY DISEASE) ESRD (ENDSTAGE RENAL DISEASE) GLOMERULONEPHRITIS
ENFERMEDADES AUTOINMUNES SISTÉMICAS. Dr. J. María Pego Reigosa
 ENFERMEDADES AUTOINMUNES SISTÉMICAS Dr. J. María Pego Reigosa ABSTRACT NUMBER: 888 PHASE 3 TRIAL RESULTS WITH BLISIBIMOD, A SELECTIVE INHIBITOR OF B-CELL ACTIVATING FACTOR, IN SUBJECTS WITH MODERATE-TO-SEVERE
ENFERMEDADES AUTOINMUNES SISTÉMICAS Dr. J. María Pego Reigosa ABSTRACT NUMBER: 888 PHASE 3 TRIAL RESULTS WITH BLISIBIMOD, A SELECTIVE INHIBITOR OF B-CELL ACTIVATING FACTOR, IN SUBJECTS WITH MODERATE-TO-SEVERE
Summary Article: Lupus (Systemic Lupus Erythematosus) from Harvard Medical School Health Topics A-Z
 Topic Page: Systemic Lupus Erythematosus Summary Article: Lupus (Systemic Lupus Erythematosus) from Harvard Medical School Health Topics A-Z What Is It? Lupus is thought to develop when the immune system
Topic Page: Systemic Lupus Erythematosus Summary Article: Lupus (Systemic Lupus Erythematosus) from Harvard Medical School Health Topics A-Z What Is It? Lupus is thought to develop when the immune system
CTD-related Lung Disease
 13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
13 th Cambridge Chest Meeting King s College, Cambridge April 2015 Imaging of CTD-related Lung Disease Dr Sujal R Desai King s College Hospital, London Disclosure Statement No Disclosures / Conflicts of
AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid
 AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid PLASMABLAST PROLIFERATION IS ASSOCIATED WITH TLR7 POLYMORPHISMS AND UPREGULATION OF
AMPLIADO SÍNDROME ANTIFOSFOLÍPIDO SÍNDROME DE SJÖGREN María José Cuadrado Lozano Clínica Universidad de Navarra-Madrid PLASMABLAST PROLIFERATION IS ASSOCIATED WITH TLR7 POLYMORPHISMS AND UPREGULATION OF
MR Imaging of Systemic Lupus Erythematosus Involving the Brain
 197 MR Imaging of Systemic Lupus Erythematosus Involving the Brain lex M. isen' Trygve O. Gabrielsen' W. Joseph McCune 2 Focal lesions were demonstrated on magnetic resonance (MR) imaging in eight patients
197 MR Imaging of Systemic Lupus Erythematosus Involving the Brain lex M. isen' Trygve O. Gabrielsen' W. Joseph McCune 2 Focal lesions were demonstrated on magnetic resonance (MR) imaging in eight patients
Imaging the Premature Brain- New Knowledge
 Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Diffusion-weighted imaging and ADC mapping in the differentiation of intraventricular brain tumors
 Diffusion-weighted imaging and ADC mapping in the differentiation of intraventricular brain tumors Poster No.: C-2652 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: M. Gavrilov, T.
Diffusion-weighted imaging and ADC mapping in the differentiation of intraventricular brain tumors Poster No.: C-2652 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro Authors: M. Gavrilov, T.
Neuropsychiatric manifestations are commonly. Neuropsychiatric Syndromes in Systemic Lupus Erythematosus: A Meta-Analysis SLE
 SLE Neuropsychiatric Syndromes in Systemic Lupus Erythematosus: A Meta-Analysis Avraham Unterman, MD,*, Johannes E.S. Nolte, MD,*, Mona Boaz, PhD,, Maya Abady, MPT, Yehuda Shoenfeld, MD,*, and Gisele Zandman-Goddard,
SLE Neuropsychiatric Syndromes in Systemic Lupus Erythematosus: A Meta-Analysis Avraham Unterman, MD,*, Johannes E.S. Nolte, MD,*, Mona Boaz, PhD,, Maya Abady, MPT, Yehuda Shoenfeld, MD,*, and Gisele Zandman-Goddard,
Antiphospholipid Syndrome Handbook
 Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, Oier Ateka-Barrutia, and Munther A. Khamashta Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, MD, PhD Lupus Research Unit The Rayne
Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, Oier Ateka-Barrutia, and Munther A. Khamashta Antiphospholipid Syndrome Handbook Maria Laura Bertolaccini, MD, PhD Lupus Research Unit The Rayne
LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS LUPUS 101 SLE SUBSETS AUTOIMMUNE DISEASE 11/4/2013 HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS
 LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
LUPUS 101 LUPUS CAN DO EVERYTHING, BUT NOT EVERYTHING IS LUPUS HOWARD HAUPTMAN, MD IDIOPATHIC DISCOID LUPUS SLE SUBSETS SUBACUTE CUTANEOUS LUPUS DRUG INDUCED LUPUS NEONATAL LUPUS LATE ONSET LUPUS ANTI-PHOSPHOLIPID
A RARE NEUROLOGICAL PRESENTATION OF SLE. Dr Yoganand M N Dr Prithvi P Nayak
 A RARE NEUROLOGICAL PRESENTATION OF SLE Dr Jayachandra Dr Yoganand M N Dr Prithvi P Nayak Presenter: Dr Shambhavi K R CHIEF COMPLAINTS A 30 year old lady hailing from Nepal presented to OPD with complaints
A RARE NEUROLOGICAL PRESENTATION OF SLE Dr Jayachandra Dr Yoganand M N Dr Prithvi P Nayak Presenter: Dr Shambhavi K R CHIEF COMPLAINTS A 30 year old lady hailing from Nepal presented to OPD with complaints
Definition Chronic autoimmune disease The body s immune system starts attacking itself Can affect most organs and tissues in the body Brain, lungs, he
 LIVING WITH SYSTEMIC LUPUS ERYTHEMATOSUS Stacy Kennedy, M.D.,M.B.A. Rowan Diagnostic Clinic Salisbury, N.C. May 11, 2013 Agenda What is lupus Who is affected Causes of lupus Symptoms and organ involvement
LIVING WITH SYSTEMIC LUPUS ERYTHEMATOSUS Stacy Kennedy, M.D.,M.B.A. Rowan Diagnostic Clinic Salisbury, N.C. May 11, 2013 Agenda What is lupus Who is affected Causes of lupus Symptoms and organ involvement
