Dr, I have pain all over my body!
|
|
|
- Alexina Mosley
- 5 years ago
- Views:
Transcription
1 Dr, I have pain all over my body! Challenges to make the diagnosis in a common elderly complaint Inter-hospital Geriatrics Meeting Speaker: Cheng Jen Ngai Chairperson: Dr. Ip CY Caritas Medical Centre
2 Pain is a common symptom in the elderly 醫生, 我周身唔舒服周身都痛!!
3 Statistics on pain in the elderly 25 50% of community based elders have pain up to 85% of residents in long term care report pain, of which 45 80% is undertreated 20% of the older Americans are taking analgesic medications regularly 63%of those had taken pain medication for more than six months The American Geriatric Society (AGS) Panel on Chronic Pain in Older Persons 2002 Chronic Pain in Cognitively Impaired Elderly: Challenges in Assessment, Diagnosis, and Treatment, By Paula Siciliano
4 Challenges to make the correct diagnosis of pain symptoms Very often, no correct diagnosis could be made, because: We have perception that pain is a normal part of aging and we always assume pain is due to degenerative changes Elderly patient s complaints and history could be nonspecific Pain is a very personal and subjective experience affected by multiple factors, including psychological and social
5 In this presentation A case of an elderly lady who presented with generalized pain No definite diagnosis in the beginning After the diagnosis was made, the patient responded well to the treatment
6 F/ 82 years old Background history Cleansing worker, retired for more than 20 years On CSSA Lived alone Widow, with 2 children, supportive and always visited patient Non smoker, non drinker
7 Pre-morbid functional status Walk with stick Feeding/ Bathing/ Toileting independent Self went out to buy food Personal Emergency Link Service ( 一線通平安鐘服務 ) available at home
8 Past medical history Good past health Sometimes visited GOPD for URTI No regular medications or Chinese medicine taken No known drug allergy
9 Chief complaint Complained pain all over the body since 2/ neck pain 2. low back pain 3. knee pain 4. shoulder pain 5. Headache 6. Hand pain and numbness
10 Nature of the pain Bilateral knee pain after prolonged sitting Neck pain and the LBP, esp at the bilateral para spinal muscle, which increase on movement Bilateral shoulder pain, L>R, which increase on raising the shoulder Headache over bilateral frontal area and vertex, described as shooting pain, each time last for few hours to days Right palm pain and numbness
11 Other symptoms Noticed to have poor appetite Claim subjective weight loss Poor sleep and early morning wakening Deny recent stressful event or depressed mood Deny suicidal idea
12 Other symptoms No hip pain No joint stiffness No muscle weakness complained No rash / joint swelling No history of injury/ trauma
13 Other symptoms No facial pain/ eye pain No visual disturbance No nausea/ vomiting/ photophobia No fever No chest pain/ SOB
14 History of present illness Seek medical advice at GOPD for the headache and generalised pain in 3/2010 Voltaren SR was given, which partially reduces the pain Referred to medical for further management
15 History of present illness Attended medical clinic in 4/2010 Subsequently admitted to the ward on 17/4/2010 for further investigations
16 Physical examinations Afebrile BP:120/55, P:80 GCS:15/15, full orientation Cardiovascular system unremarkable Respiratory system unremarkable Abdominal system unremarkable
17 Physical examinations--cns Tone normal, no tremor Power of upper limbs: 4+/5 (R=L, P=D) Power of lower limbs: 4/5 (R=L, P=D) Reflex normal Sensation grossly normal Gait with stick stable
18 Neck soft Physical examinations : musculoskeletal Paraspinal muscle tenderness Right knee swollen, tender and bony crepitations heard on movement Passive range of movement of shoulder joint and hip joints full No shoulder joint swelling and no sign of subluxations
19 Blood test Hb:11.5, NcNc ALP:84, Cr:74, ca:2.22, PO4:1.06 TSH:1.38 ESR:74, CRP:33
20 Radiological investigations CT brain: No gross intracranial lesion Air fluid level noted at the left maxillary sinus, likely represent sinusitis changes
21 X-ray cervical spine: -Degenerative change with multi-level margical osteophytes formation -The disc spaces and vertebral body heights are preserved
22 X-ray shoulder: -No definite fracture nor dislocation found. The subacromial space is not narrowed -There is no abnormal calcification seen in the soft tissue. No other specific bony lesion detected
23 X-ray knee: -Normal bone density and alignment. -There are degenerative change of both knees with marginal osteophytes. The bilateral patellofemoral joint spaces are narrowed
24 Problems list 1. Multiple joint pain 2. Headache 3.?mood disturbance 4. CT brain showed features of maxillary sinusitis, with increased inflammatory marker of ESR, CRP 5. X ray shows degenerative changes of the joints
25 Diagnosis 1. Cervical spondylosis 2. Osteoarthritis of knee 3. Maxillary sinusitis 4.?tension headache
26 Management Dologesics was given for pain relief SFI glucosamine started for OA knee Physiotherapist was referred for pain relief
27 Progress Bone pain and the headache partially improved after admission Patient discharged on 19/4/2010 Referred to GDH for pain relief and mobility training Referred to ENT for the sinusitis
28 GDH assessment First visit on 9/6/2010 Still complained of multiple joint pain, at the shoulder, neck and the knee On and off headache, but improving Running nose with clear discharge Physical examination unremarkable except degenerative changes at the knee noticed
29 ?depressive symptoms Express sadness about the pain symptoms Complain decreased appetite and weight loss Loss of interest in daily leisure activates No suicidal idea?? Depression/ adjustment disorder
30 Geriatric depression score: 8/15
31 Assessment by physiotherapist Bed mobility and transfer independent Standing under supervision Squatting failed due to the bilateral knee pain Walk with stick independent at ground floor Walk upstairs with rail and stick under supervision 6m walk : 13seconds
32 Assessment by physiotherapist EMS:16/20 BBS:28/56
33 Assessment by occupational therapist Satisfactory hand function Feeding, hygiene independent Toileting, bathing, dressing standby assistance
34 Assessment by occupational therapist Difficulty in stair climbing BI:81/100
35 Assessment by occupational therapist adapted Lawton IADL:38/56
36 Progress Repeated blood test : All normal, except ESR:69, CRP:82 What is the reason for the increase inflammatory marker??
37 What is the diagnosis??polymyalgia rheumatica (PMR) For: There was shoulder pain, neck pain There was systemic symptoms of decrease appetite, weight loss Inflammatory marker was increased Against: X There was no morning joint stiffness which was typical feature of inflammatory pain X The prominent knee pain was not typical feature of PMR
38 What is the diagnosis??degenerative changes in the multiple joints??polymyalgia rheumatica + Degenerative changes in the joints
39 Progress Patient was referred to rheumatology clinic on 11/8/2010 Diagnosis of polymyalgia rheumatica was made Prednisolone 15mg daily was prescribed
40 Progress of symptoms Patient has significant improvement of pain at the follow up 2 weeks later Appetite improved and there was subjective weight gain Mood also improved, she said she felt much happier
41 Progress of inflammatory markers ESR decreased
42 Progress of inflammatory markers CRP decreased
43 Progress of functional aspects EMS and BBS both improved!!
44 Progress of functional aspects Stair climbing improved BI improved significantly!!
45 Diagnosis The good steroid response also suggests the diagnosis of polymyalgia rheumatica!!
46 Progress In view of good rehabilitation outcome, patient was discharged from GDH on 29/9/2010 Patient now has regular follow up at the rheumatology clinic
47 Polymyalgia rheumatica (PMR) One of the most common: 1. inflammatory rheumatic disease of the elderly 2. indications for long term steroid use in the community Self limiting condition with excellent prognosis if diagnosed promptly Untreated patients often fell unwell and have an impaired quality of life
48 Epidemiology Prevalence increases with increasing age Almost never seen in people under the age of 50 average age of onset is just over 70 The incidence of the disease in patients over 50 is about 100 per % of patients are women Frequency varies by geographical region, highest rates occur in Northern Europe Incidence of PMR is often underestimated Cimmino MA, Zaccaria A. Epidemiology of polymyalgia rheumatica. Clin exp Rheumatol 2000; 18 (4 suppl.20):s9 11
49 Pathogenesis Exact mechanism unknown!! both genetic and environmental factors contribute to disease susceptibility and severity
50 Pathogenesis 1. Environmental factors: particularly infections with Chlamydia, Mycoplasma, parainfluenza virus or parvovirus B19 are believed to be the trigger of the disease 2. Genetic factors: the HLA DRB1 allele is linked to an increased susceptibility and severity of the disease
51 Pathogenesis Genetically predisposed patient Environmental factor, eg: a virus triggers monocyte activation Production of cytokines esp: interleukin 2 and interleukin 6 Induces manifestations of polymyalgia rheumatica
52 Pathogenesis Nonerosive synovitis and tenosynovitis are believed to be responsible for the symtpoms of the disease, and it is found that macrophages and CD4+ T lymphocytes are activated in synovial membranes from the involved joints Evidence of subclinical arterial inflammation can be detected in some patients, with the presence of activated dendritic cells, interleukin 1 and interleukin 4 Polymyalgia rheumatica and giant cell arteritis. Salvarani C; Cantini F; Hunder GG Lancet Jul 19;372(9634):
53 Symptoms and signs Morning stiffness typically lasts at least 30 minutes, with difficulty in activities related to the shoulder and hip, eg: trouble dressing, rising from or turning over in bed Symmetrical shoulder pain (70 to 95 %), hip and neck pain (50 to 70 %), which is worse with movement and may interfere with sleep Muscle tenderness Subjective weakness but the muscle strength is usually normal Decreased active, and sometimes passive, range of motion of the shoulders, neck, and hips Mild and non erosive synovitis and bursitis, especially appears to occur in more peripheral joints, such the knees, wrists, and metacarpophalangeal joints Swelling and pitting edema of the hands, wrists, ankles, and top of the feet, which represent tenosynovitis and synovitis in regional structures Systemic signs and symptoms including malaise, fatigue, depression, anorexia, weight loss, and fever
54 Diagnostic difficulties in polymyalgia rheumatica No gold standard diagnostic test Little sound evidence from randomized controlled trials on which to base diagnosis and management Diagnosis is often made on clinical grounds only, which can lead to diagnostic error It has many non specific features and a wide differential diagnosis Patients complaints could be varied
55 Diagnosis of Polymyalgia Rheumatica Safe Stepped diagnostic process supported by grade B evidence
56 Stepwise approach for management of polymyalgia rheumatica
57 Step I: diagnosis Core inclusion criteria Age >50 years, duration >2 years Bilateral shoulder or pelvic girdle aching, or both Morning stiffness duration of > 45mins Evidence of an acute phrase response **PMR can be diagnosed with normal inflammatory markers, if there is a classic clinical picture and response to steroids. These patients should be referred for specialist assessment
58 Step II: Core exclusion criteria Active infection Active cancer Active giant cell arteritis All 3 conditions could have increase inflammatory markers
59 Differential diagnosis Inflammatory rheumatic disease 1. Rheumatoid arithritis (predominant peripheral joint involved) 2. SLE, vasculitis (multisystem disease) 3. inflammatory myopathy (weakness of muscles with high CK)
60 Differential diagnosis Non inflammatory disease 1. Osteoarthritis 2. Adhesive capsulitis and rotator cuff lesions 3. Drug induced myalgia 4. Chronic pain syndromes/ fibromyalgia (longstanding history, with tender spots) 5. Hypothyroidisam (TSH level ) 6. Metabolic bone disease (PTH, vitamin D level)
61 Investigations Recommended laboratory investigations before commencement of steroid therapy: CBC TSH ESR/ CRP Creatine kinase L/RFT RF Bone profile Dipstick urinalysis Protein electrophioresis CXR
62 Investigations ESR is the most sensitive diagnostic study, but it is not specific CRP is often elevated and may parallel ESR Creatine kinase (CK) is normal and helps to differentiate from polymyositis and other primary myopathic disorders ANA and RF usually normal MRI shoulder joint is not necessary for the diagnosis, it will reveal subacromial and subdeltoid brusitis, glenohumeral joint synovitis
63 Early specialist referral suggested if: Younger patient < 60 years Chronic onset (>2 months) Lack of shoulder involvement Lack of inflammatory stiffness Prominent systemic features, weight loss, night pain, neurological signs Normal or extremely high acute phrase response Features of other rheumatic disease
64 Steps III: treatment Low dose steroids Initial standardized dose of oral prednisolone 15 20mg daily to reduce the inflammatory manifestations Patient reported global improvement of >70% within a week of commencing steroids Normalization of inflammatory markers in 4 weeks A lesser response should prompt the search for an alternative condition
65 Step IV: Follow up If no alternative diagnosis, follow 4 6 weeks was suggested
66 Step IV: Follow up Monitor laboratory investigations CBC ESR, CRP RFT glucose
67 Step IV: Follow up Monitor symptoms of proximal pain morning stiffness diability related to PMR adverse events osteoporotic risk symptoms that may suggest an alternative diagnosis
68 Treatment regime Suggested regime of oral prednisolone: Daily prednisolone 15mg for 3 weeks Then 12.5mg for 3 weeks Then 10mg for 4 6 weeks Then reduction by 1mg every 4 8 weeks or alternate day reductions Usually 1 2 years of treatment is needed, 50 75% of patient can discontinue corticosteroid therapy after 2 years of treatment Kyle V, Hazleman BL. Teatment of polymyalgia rheumatic and giant cell arteritis. II Relation between steroid dosing and steroid associated side effects. Ann Rheum Dis 1989;48:662 6
69 Treatment regime -- alternatives IM methylprednisolone (depomedrone) Used in milder case and can reduce the risk of steroid related complications Initial dose: 120mg every 3 4 weeks Reduce by 20mg every 2 3 months
70 Other considerations bone protection Individuals with high fracture risk: Bisphosphonate with calcium and vitamin D supplementation Other individuals: Calcium and vitamin D supplementation
71 Treatment regime No consistent evidence for an ideal steroid regime suitable for all patients Approach to treatment must be flexible and tailored to the individual Dose adjustment may be required for disease severity, co morbidity, side effects and patient wishes
72 Early specialist referral suggested IF: Incomplete, poorly sustained or nonresponse to corticosteroids Inability to reduce corticosteroids Contraindications to corticosteroid therapy The need for prolonged corticosteroid therapy (> 2 years)
73 Treatment for relapse Relapse is common, in up to 25% of patients, more likely to occur during the initial 18 months of therapy and within 1 year of corticosteroid withdrawal For the 1 st and 2 nd relapse, increase steroids to previous dosage For further relapse, consider immunosupressants e.g. Methotrexate (a dose of 10 mg/wk) Studies show that, Infliximab, a tumour necrosis factor has not shown impressive disease controlling or steroidsparing effects
74 Giant cell Arteritis (GCA) and poylmyalgia rheumatica (PCR) GCA is a common overlapping inflammatory rheumatic diseases with PCR 10% of patients with PMR have GCA 50% of patients with GCA have PMR PMR occurs 3 to 5 fold more frequently than GCA Dasgupta B, Kalke S. Polymyalgia rheumatic. In: Isenberg D, Maddison P, Woo P, Glass D, Breedveld F (eds), Oxford testbook of rheumatology, 3 rd edn. Oxford: Oxford University Press, 2004:977 82
75 Giant cell arteritis (GCA) Systemic, inflammatory, vascular syndrome predominantly affects the cranial branches of arteries arising from the arch of the aorta Major features are due to arterial inflammation and its consequences Chronic vasculitis of large and medium vessels, with granulomatous transmural inflammation histologically T lymphocytes in the vessels produce interferongamma and interleukin 2 Macrophages produce interleukin 1, 6 and transforming growth factor beta
76 Giant cell arteritis (GCA) Incidence is reported as 2.2/ patientyears in UK Mean onset at age of 70, rare before age of 50 Three times more common in females than in males
77 Typical features of GCA Abrupt onset headache (usually temporal) and temporal tenderness Visual disturbance, including diplopia or amaurosis fugax Jaw or tongue claudication Prominence, beading or diminished pulse on examination of the temporal artery Upper cranial nerve palsies Limb claudication or other evidence of largevessel involvement
78 The American College of Rheumatology classification criteria for GCA 1. Age at disease onset >50 years 2. New onset of or new type of localized pain in the head 3. Temporal artery abnormality: temporal artery tenderness to palpation or decreased pulsation, unrelated to arteriosclerosis of cervical arteries 4. Elevated ESR: >50 mm/h 5. Abnormal artery biopsy: vasculitis characterized by a predominance of mononuclear cell infiltration or granulomatous inflammation, usually with multinucleated giant cells GCA if at least three of these five criteria are present (a sensitivity of 93.5% and a specificity of 91.2%)
79 Should we do temporal artery biopsy in all patients with PMR? PMR occurs 3 to 5 fold more frequently than GCA Patients with pure PMR lack the classic findings of GCA such as temporal artery tenderness, headache, jaw pain, visual loss, and evidence of ischemia such as cluadication are very unlikely to have a positive result after temporal biopsy Temporal biopsy is NOT recommended as a routine test Gabriel SE, O Fallon MW, Achkar AA, et al. The use of clinical characteristics to predict the results of temporal aretery biopst among patients with suspected giant cell arteritis. J rheumatol 1995;22:93 6
80 Temporal artery biopsy Always perform the biopsy on the symptomatic side of head If a specific part of the artery is tender, beaded or inflammed, include that area in the biopsy Take at least 2 3cm of the artery Better to include multiple sections because the lesion may be segmental Results of the temporal artery biopsies remain positive after as long as 4 weeks high doses of corticosteroid are administered
81 Duplex ultrasonography Detect the characteristic hypoechoic halo around the affected temporal arteries, representing vessel wall edema, arterial stenosis and occlusion The halo sign had a sensitivity of 69% and specificity of 82%when compared with the biopsy for the diagnosis of giant cell arteritis But it cannot be recommended as a replacement of temporal artery biopsy as it has no prognostic value and it requires high level of expertise
82 Halo sign Halo sign in colour duplex sonography examination in a patient with giant cell arteritis. Hypoechoic area around the temporal artery trunk in longitudinal (upper panel) and transverse (lower panel) views
83 Key point of treatment for giant cell arteritis The dose of prednisolone is much higher than that of PMR! Low dose corticosteroid used in polymyalgia rheumatica is ineffective in giant cell arteritis
84 Guidelines for the management of giant cell arteritis
85 Key point of treatment for giant cell arteritis I. ) Uncomplicated GCA (without visual symptoms): Prednisolone 40 60mg (at least 0.75 mg/kg) daily until resolution of symptoms and laboratory abnormalities
86 Key point of treatment for II. ) Complicated GCA giant cell arteritis 1. Evolving visual loss or history of amaurosis fugax: i.v. methylprednisolone 500mg to 1 g daily for 3 days 2. Established vision loss at least 60mg prednisolone daily to protect the other eye
87 Key point of treatment for In all patients: giant cell arteritis Low dose aspirin 75mg daily (if no contraindications) Bisphosphonates and calcium, vitamin D supplementation Proton pump inhibitor
88 Complications of giant cell arteritis Loss of vision which is often irreversible Scalp necrosis Cerebrovascular accidents Aortic aneurysm, dissection, or stenosis Coronary involvement So, making the diagnosis and have prompt treatment with steroid is important!
89 Bring home message Polymyalgia rheumatica is a frequent disorder in the elderly population that can cause severe pain, functional impairment and a reduction in overall quality of life Making the diagnosis of polymyalgia rheumatica and subsequently treating the patient results in rapid and dramatic improvement in the patient s complaints and a return to previous functional status Consider the diagnosis of polymyalgia rheumatica when our patients complain of symptoms of pain and stiffness, with increase in inflammatory marker Always think of giant cell arteritis as the treatment is different
90
9/11/11. Temporal Arteritis. Background. Background. Richard E. Castillo, OD, DO NORTHEASTERN STATE UNIVERSITY Director, Ophthalmic Surgery Service
 Temporal Arteritis Richard E. Castillo, OD, DO NORTHEASTERN STATE UNIVERSITY Director, Ophthalmic Surgery Service 1 Background Giant Cell Arteritis Temporal Arteritis Cranial Arteritis Granulomatous Arteritis
Temporal Arteritis Richard E. Castillo, OD, DO NORTHEASTERN STATE UNIVERSITY Director, Ophthalmic Surgery Service 1 Background Giant Cell Arteritis Temporal Arteritis Cranial Arteritis Granulomatous Arteritis
Dr Kusala S. Gunasekara MBBS(Col),MD(Med),MRCP(UK) Acting Consultant Rheumatologist DGH-Matale
 Dr Kusala S. Gunasekara MBBS(Col),MD(Med),MRCP(UK) Acting Consultant Rheumatologist DGH-Matale Patient 67 yr old female First presentation to the rheumatology unit in May 2013 Referred by GP as the patient
Dr Kusala S. Gunasekara MBBS(Col),MD(Med),MRCP(UK) Acting Consultant Rheumatologist DGH-Matale Patient 67 yr old female First presentation to the rheumatology unit in May 2013 Referred by GP as the patient
BSR and BHPR guidelines for the management of polymyalgia rheumatica
 RHEUMATOLOGY Guidelines Rheumatology 2010;49:186 190 doi:10.1093/rheumatology/kep303a Advance Access publication 12 November 2009 BSR and BHPR guidelines for the management of polymyalgia rheumatica Bhaskar
RHEUMATOLOGY Guidelines Rheumatology 2010;49:186 190 doi:10.1093/rheumatology/kep303a Advance Access publication 12 November 2009 BSR and BHPR guidelines for the management of polymyalgia rheumatica Bhaskar
APPROACH TO PATIENTS WITH POLYARTHRALGIA
 APPROACH TO PATIENTS WITH POLYARTHRALGIA Scott Vogelgesang, MD Division of Immunology University of Iowa No conflicts of interest DEFINITIONS Arthralgia joint pain with no evidence of inflammation Arthritis
APPROACH TO PATIENTS WITH POLYARTHRALGIA Scott Vogelgesang, MD Division of Immunology University of Iowa No conflicts of interest DEFINITIONS Arthralgia joint pain with no evidence of inflammation Arthritis
Polymyalgia, Temporal Arteritis and pineapples
 Polymyalgia, Temporal Arteritis and pineapples Rod Hughes Consultant Rheumatologist Ashford St Peter s Hospital Trust Chertsey Wed 11 th May 2011 Meeting aims Pineapples their significance in disease Defining
Polymyalgia, Temporal Arteritis and pineapples Rod Hughes Consultant Rheumatologist Ashford St Peter s Hospital Trust Chertsey Wed 11 th May 2011 Meeting aims Pineapples their significance in disease Defining
Scintigraphic Findings and Serum Matrix Metalloproteinase 3 and Vascular Endothelial Growth Factor Levels in Patients with Polymyalgia Rheumatica
 The Open General and Internal Medicine Journal, 29, 3, 53-57 53 Open Access Scintigraphic Findings and Serum Matrix Metalloproteinase 3 and Vascular Endothelial Growth Factor Levels in Patients with Polymyalgia
The Open General and Internal Medicine Journal, 29, 3, 53-57 53 Open Access Scintigraphic Findings and Serum Matrix Metalloproteinase 3 and Vascular Endothelial Growth Factor Levels in Patients with Polymyalgia
Objectives. Joint Pain. Case 1. Rheumatology for the Primary MD (Not just your grandmother s disease) 12/4/2010
 Objectives Rheumatology for the Primary MD (Not just your grandmother s disease) Identify when it is appropriate to refer for rheumatologic evaluation Autoimmune/ Inflammatory v. noninflammatory disease
Objectives Rheumatology for the Primary MD (Not just your grandmother s disease) Identify when it is appropriate to refer for rheumatologic evaluation Autoimmune/ Inflammatory v. noninflammatory disease
REFERRAL GUIDELINES: RHEUMATOLOGY
 Outpatient Page 1 1 REFERRAL GUIDELINES: RHEUMATOLOGY Date of birth Demographic Contact details (including mobile phone) Clinical Reason for referral Duration of symptoms Essential Referral Content Referring
Outpatient Page 1 1 REFERRAL GUIDELINES: RHEUMATOLOGY Date of birth Demographic Contact details (including mobile phone) Clinical Reason for referral Duration of symptoms Essential Referral Content Referring
The Joints are Painful & Swollen: Do I give Steroids? Dr Tom Kennedy
 The Joints are Painful & Swollen: Do I give Steroids? Dr Tom Kennedy Learning Objectives When to use an acute rheumatology service Appropriate use of steroids by condition Injection or Oral or Intramuscular
The Joints are Painful & Swollen: Do I give Steroids? Dr Tom Kennedy Learning Objectives When to use an acute rheumatology service Appropriate use of steroids by condition Injection or Oral or Intramuscular
GIANT CELL ARTERITIS. Page 1 of 6 Reproduction of this material requires written permission of the Vasculitis Foundation. Copyright 2018.
 What is giant cell arteritis (GCA)? Giant cell arteritis (GCA) is a form of vasculitis a family of rare disorders characterized by inflammation of the blood vessels, which can restrict blood flow and damage
What is giant cell arteritis (GCA)? Giant cell arteritis (GCA) is a form of vasculitis a family of rare disorders characterized by inflammation of the blood vessels, which can restrict blood flow and damage
Preventing blindness: Ultrasound in Giant cell arteritis
 Preventing blindness: Ultrasound in Giant cell arteritis Elizabeth Jernberg, MD Associate Clinical Professor of Medicine Division of Rheumatology University of Washington Virginia Mason Medical Center
Preventing blindness: Ultrasound in Giant cell arteritis Elizabeth Jernberg, MD Associate Clinical Professor of Medicine Division of Rheumatology University of Washington Virginia Mason Medical Center
Prognosis and management of polymyalgia rheumatica
 Annals of the Rheumatic Diseases, 1981, 40, 1-5 Prognosis and management of polymyalgia rheumatica J. G. JONES AND B. L. HAZLEMAN From Addenbrooke's Hospital, Hills Road, Cambridge SUMMARY Polymyalgia
Annals of the Rheumatic Diseases, 1981, 40, 1-5 Prognosis and management of polymyalgia rheumatica J. G. JONES AND B. L. HAZLEMAN From Addenbrooke's Hospital, Hills Road, Cambridge SUMMARY Polymyalgia
Polymyalgia rheumatica and giant cell arteritis
 Polymyalgia rheumatica and giant cell arteritis What is polymyalgia rheumatica? Polymyalgia rheumatica is a rheumatic disorder associated with moderate-to-severe musculoskeletal pain and stiffness in the
Polymyalgia rheumatica and giant cell arteritis What is polymyalgia rheumatica? Polymyalgia rheumatica is a rheumatic disorder associated with moderate-to-severe musculoskeletal pain and stiffness in the
Rheumatologic Emergencies It s not just swollen joints. Joanne Homik Rheumatologist University of Alberta
 Rheumatologic Emergencies It s not just swollen joints Joanne Homik Rheumatologist University of Alberta Or is it? Disclosures No relevant conflicts of interest regarding the content of this presentation
Rheumatologic Emergencies It s not just swollen joints Joanne Homik Rheumatologist University of Alberta Or is it? Disclosures No relevant conflicts of interest regarding the content of this presentation
Polymyalgia Rheumatica; Giant Cell Arteritis Paul Katzenstein, MD
 Polymyalgia Rheumatica; Giant Cell Arteritis Paul Katzenstein, MD What is it; is it not? How is this thought about, characterized, understood, treated Time honored published clinical experience Clinical
Polymyalgia Rheumatica; Giant Cell Arteritis Paul Katzenstein, MD What is it; is it not? How is this thought about, characterized, understood, treated Time honored published clinical experience Clinical
British Journal of Rheumatology 1991; 30:
 British Journal of Rheumatology 1991; 30:468-470 CASE REPORT CARPAL TUNNEL SYNDROME COMPLICATED BY REFLEX SYMPATHETIC DYSTROPHY SYNDROME BY M.-A. FITZCHARLES AND J.M. ESDAILE Rheumatic Disease Unit, McGill
British Journal of Rheumatology 1991; 30:468-470 CASE REPORT CARPAL TUNNEL SYNDROME COMPLICATED BY REFLEX SYMPATHETIC DYSTROPHY SYNDROME BY M.-A. FITZCHARLES AND J.M. ESDAILE Rheumatic Disease Unit, McGill
Imaging of polymyalgia rheumatica: what the radiologist should know
 Imaging of polymyalgia rheumatica: what the radiologist should know Poster No.: P-0117 Congress: ESSR 2016 Type: Educational Poster Authors: R. Leao, L. C. Zattar-Ramos, E. L. Bizetto, M. F. Correa, M.
Imaging of polymyalgia rheumatica: what the radiologist should know Poster No.: P-0117 Congress: ESSR 2016 Type: Educational Poster Authors: R. Leao, L. C. Zattar-Ramos, E. L. Bizetto, M. F. Correa, M.
Rheumatology Potpourri. Dr. Philip A. Baer Seacourses Asia CME December 2017
 Rheumatology Potpourri Dr. Philip A. Baer Seacourses Asia CME December 2017 Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
Rheumatology Potpourri Dr. Philip A. Baer Seacourses Asia CME December 2017 Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted
ORIGINAL INVESTIGATION
 ORIGINAL INVESTIGATION Corticosteroid Requirements in Polymyalgia Rheumatica Cornelia M. Weyand, MD; James W. Fulbright, MS; Jonathan M. Evans, MD; Gene G. Hunder, MD; Jörg J. Goronzy, MD, PhD Background:
ORIGINAL INVESTIGATION Corticosteroid Requirements in Polymyalgia Rheumatica Cornelia M. Weyand, MD; James W. Fulbright, MS; Jonathan M. Evans, MD; Gene G. Hunder, MD; Jörg J. Goronzy, MD, PhD Background:
Concise guidance: diagnosis and management of giant cell arteritis
 ONISE GUIDANE linical Medicine 2010, Vol 10, No 4: 381 6 oncise guidance: diagnosis and management of giant cell arteritis Bhaskar Dasgupta on behalf of the Giant ell Arteritis Guideline Development Group*
ONISE GUIDANE linical Medicine 2010, Vol 10, No 4: 381 6 oncise guidance: diagnosis and management of giant cell arteritis Bhaskar Dasgupta on behalf of the Giant ell Arteritis Guideline Development Group*
Patient #1. Rheumatoid Arthritis. Rheumatoid Arthritis. 45 y/o female Morning stiffness in her joints >1 hour
 Patient #1 Rheumatoid Arthritis Essentials For The Family Medicine Physician 45 y/o female Morning stiffness in her joints >1 hour Hands, Wrists, Knees, Ankles, Feet Polyarticular, symmetrical swelling
Patient #1 Rheumatoid Arthritis Essentials For The Family Medicine Physician 45 y/o female Morning stiffness in her joints >1 hour Hands, Wrists, Knees, Ankles, Feet Polyarticular, symmetrical swelling
A RARE NEUROLOGICAL PRESENTATION OF SLE. Dr Yoganand M N Dr Prithvi P Nayak
 A RARE NEUROLOGICAL PRESENTATION OF SLE Dr Jayachandra Dr Yoganand M N Dr Prithvi P Nayak Presenter: Dr Shambhavi K R CHIEF COMPLAINTS A 30 year old lady hailing from Nepal presented to OPD with complaints
A RARE NEUROLOGICAL PRESENTATION OF SLE Dr Jayachandra Dr Yoganand M N Dr Prithvi P Nayak Presenter: Dr Shambhavi K R CHIEF COMPLAINTS A 30 year old lady hailing from Nepal presented to OPD with complaints
Giant Cell Arteritis Protocol
 Giant Cell Arteritis Protocol Background Giant cell arteritis (GCA) is a granulomatous vasculitis commonly of the temporal artery associated with polymyalgia rheumatic that classically presents in those
Giant Cell Arteritis Protocol Background Giant cell arteritis (GCA) is a granulomatous vasculitis commonly of the temporal artery associated with polymyalgia rheumatic that classically presents in those
Etiology: Pathogenesis Clinical manifestation Investigation Treatment Prognosis
 Etiology: Pathogenesis Clinical manifestation Investigation Treatment Prognosis JIA is the most common rheumatic disease in childhood and a major cause of chronic disability. Etiology: Unknown, but may
Etiology: Pathogenesis Clinical manifestation Investigation Treatment Prognosis JIA is the most common rheumatic disease in childhood and a major cause of chronic disability. Etiology: Unknown, but may
Mary Derlacki, FNP. No financial relationships to disclose. Office Rheumatology for the Nurse Practitioner. Rheumatoid Arthritis
 Office Rheumatology for the Nurse Practitioner Mary Derlacki, FNP Drs. Cassell and Boren Eugene, OR 541-687-0816 mderlacki@comcast.net No financial relationships to disclose Rheumatoid Arthritis 1% of
Office Rheumatology for the Nurse Practitioner Mary Derlacki, FNP Drs. Cassell and Boren Eugene, OR 541-687-0816 mderlacki@comcast.net No financial relationships to disclose Rheumatoid Arthritis 1% of
Patient with Daily Headache NTERNATIONAL CLASSIFICATION HEADACHE DISORDERS. R. Allan Purdy, MD, FRCPC,FACP. Professor of Medicine (Neurology)
 Patient with Daily Headache NTERNATIONAL CLASSIFICATION of R. Allan Purdy, MD, FRCPC,FACP HEADACHE DISORDERS Professor of Medicine (Neurology) 2nd edition (ICHD-II) Learning Issues Headaches in the elderly
Patient with Daily Headache NTERNATIONAL CLASSIFICATION of R. Allan Purdy, MD, FRCPC,FACP HEADACHE DISORDERS Professor of Medicine (Neurology) 2nd edition (ICHD-II) Learning Issues Headaches in the elderly
A CRP B FBC C LFT D blood culture E uric acid
 1 A 39 year old lady with rheumatoid arthritis is admitted to hospital with a hot, swollen and painful right knee. Which is the most important blood test? A CRP B FBC C LFT D blood culture E uric acid
1 A 39 year old lady with rheumatoid arthritis is admitted to hospital with a hot, swollen and painful right knee. Which is the most important blood test? A CRP B FBC C LFT D blood culture E uric acid
Essential Rheumatology. Dr Ellen Bruce Consultant Rheumatologist CMFT
 Essential Rheumatology Dr Ellen Bruce Consultant Rheumatologist CMFT Saving the best for last! Apparently people recall best the first and last thing they re told. Far too difficult to include everything.
Essential Rheumatology Dr Ellen Bruce Consultant Rheumatologist CMFT Saving the best for last! Apparently people recall best the first and last thing they re told. Far too difficult to include everything.
Musculoskeletal Referral Guidelines
 Musculoskeletal Referral Guidelines Introduction These guidelines have been developed to provide an integrated musculoskeletal service. They are based on reasonable clinical practice and will initially
Musculoskeletal Referral Guidelines Introduction These guidelines have been developed to provide an integrated musculoskeletal service. They are based on reasonable clinical practice and will initially
Professor Helen Danesh-Meyer. Eye Institute Auckland
 Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Professor Helen Danesh-Meyer Eye Institute Auckland Bitten by Ophthalmology Emergencies Helen Danesh-Meyer, MBChB, MD, FRANZCO Sir William and Lady Stevenson Professor of Ophthalmology Head of Glaucoma
Osteoarthritis. Rheumatology Update. Gout 1/17/2013
 Osteoarthritis Rheumatology Update Richard Zweig, MD January, 2013 Degeneration of cartilage over time accompanied by increase in bone density and bone formation around the joint Risks include: aging,
Osteoarthritis Rheumatology Update Richard Zweig, MD January, 2013 Degeneration of cartilage over time accompanied by increase in bone density and bone formation around the joint Risks include: aging,
Polymyalgia rheumatica and temporal arteritis: evidence and guidelines for diagnosis and management in older people
 Age and Ageing 2003; 32: 370 374 Age and Ageing Vol. 32 No. 4 # 2003, British Geriatrics Society. All rights reserved. REVIEW Polymyalgia rheumatica and temporal arteritis: evidence and guidelines for
Age and Ageing 2003; 32: 370 374 Age and Ageing Vol. 32 No. 4 # 2003, British Geriatrics Society. All rights reserved. REVIEW Polymyalgia rheumatica and temporal arteritis: evidence and guidelines for
Polymyalgia rheumatica and temporal arteritis: evidence and guidelines for diagnosis and management in older people
 Age and Ageing 2003; 32: 370 374 Age and Ageing Vol. 32 No. 4 # 2003, British Geriatrics Society. All rights reserved. REVIEW Polymyalgia rheumatica and temporal arteritis: evidence and guidelines for
Age and Ageing 2003; 32: 370 374 Age and Ageing Vol. 32 No. 4 # 2003, British Geriatrics Society. All rights reserved. REVIEW Polymyalgia rheumatica and temporal arteritis: evidence and guidelines for
Hths 2231 Laboratory 13 Alterations in Musculoskeletal
 Watch Movie: Osteoporosis Answer the movie questions on the worksheet. Complete activities 1-4. Activity #1: Click on the website link in activity 1 to review the structure and function of bone. Activity
Watch Movie: Osteoporosis Answer the movie questions on the worksheet. Complete activities 1-4. Activity #1: Click on the website link in activity 1 to review the structure and function of bone. Activity
Vasculitis local: systemic
 Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated 2- infectious
Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated 2- infectious
CAN WE REPLACE TEMPORAL ARTERY BIOPSY WITH CRANIAL ULTRASOUND FOR THE DIAGNOSIS OF GIANT CELL ARTERITIS?
 CAN WE REPLACE TEMPORAL ARTERY BIOPSY WITH CRANIAL ULTRASOUND FOR THE DIAGNOSIS OF GIANT CELL ARTERITIS? Adam P. Croft (ST3 Rheumatology) Susan Mollan, Paresh Jobunputra Speaker has no disclosures TAB
CAN WE REPLACE TEMPORAL ARTERY BIOPSY WITH CRANIAL ULTRASOUND FOR THE DIAGNOSIS OF GIANT CELL ARTERITIS? Adam P. Croft (ST3 Rheumatology) Susan Mollan, Paresh Jobunputra Speaker has no disclosures TAB
History Taking and the Musculoskeletal Examination
 History Taking and the Musculoskeletal Examination Introduction A thorough rheumatologic assessment is performed within the context of a good general evaluation of the patient. The patient should be undressed
History Taking and the Musculoskeletal Examination Introduction A thorough rheumatologic assessment is performed within the context of a good general evaluation of the patient. The patient should be undressed
Rheumatoid Arthritis
 Rheumatoid Arthritis Rheumatoid arthritis (RA) is an autoimmune disease that causes chronic inflammation of the joints. Autoimmune diseases are illnesses that occur when the body's tissues are mistakenly
Rheumatoid Arthritis Rheumatoid arthritis (RA) is an autoimmune disease that causes chronic inflammation of the joints. Autoimmune diseases are illnesses that occur when the body's tissues are mistakenly
RHEUMATOLOGY OVERVIEW. Carmelita J. Colbert, MD Assistant Professor of Medicine Division of Rheumatology Loyola University Medical Center
 RHEUMATOLOGY OVERVIEW Carmelita J. Colbert, MD Assistant Professor of Medicine Division of Rheumatology Loyola University Medical Center What is Rheumatology? Medical science devoted to the rheumatic diseases
RHEUMATOLOGY OVERVIEW Carmelita J. Colbert, MD Assistant Professor of Medicine Division of Rheumatology Loyola University Medical Center What is Rheumatology? Medical science devoted to the rheumatic diseases
Original Date: December 2015 Page 1 of 8 FOR CMS (MEDICARE) MEMBERS ONLY
 National Imaging Associates, Inc. Clinical guidelines TOTAL JOINT ARTHROPLASTY -Total Hip Arthroplasty -Total Knee Arthroplasty -Replacement/Revision Hip or Knee Arthroplasty CPT4 Codes: Please refer to
National Imaging Associates, Inc. Clinical guidelines TOTAL JOINT ARTHROPLASTY -Total Hip Arthroplasty -Total Knee Arthroplasty -Replacement/Revision Hip or Knee Arthroplasty CPT4 Codes: Please refer to
Paul Allan Regional Clinical Lead - South. Lumbar Spine. Assessment & Differential Diagnosis
 Paul Allan Regional Clinical Lead - South Lumbar Spine Assessment & Differential Diagnosis Aims Refresh lumbar spine anatomy Red flags Discuss common pathologies seen in general practice Subjective and
Paul Allan Regional Clinical Lead - South Lumbar Spine Assessment & Differential Diagnosis Aims Refresh lumbar spine anatomy Red flags Discuss common pathologies seen in general practice Subjective and
Types of osteoarthritis
 ARTHRITIS Osteoarthritis is a degenerative joint disease is the most common joint disorder. It is a frequent part of aging and is an important cause of physical disability in persons older than 65 years
ARTHRITIS Osteoarthritis is a degenerative joint disease is the most common joint disorder. It is a frequent part of aging and is an important cause of physical disability in persons older than 65 years
SAMPLE. Osteopathy and Back pain a safe and effective approach
 Osteopathy and Back pain a safe and effective approach Back pain will affect 8 out of 10 people at some point in their life - mild or severe, acute or chronic. Common causes of back pain include: heavy
Osteopathy and Back pain a safe and effective approach Back pain will affect 8 out of 10 people at some point in their life - mild or severe, acute or chronic. Common causes of back pain include: heavy
Case Presentation VASCULITIS. Case Presentation. Case Presentation. Vasculitis
 Case Presentation VASCULITIS The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
Case Presentation VASCULITIS The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
Rheumatoid Arthritis
 Rheumatoid Arthritis Introduction Rheumatoid arthritis is a fairly common joint disease that affects up to 2 million Americans. Rheumatoid arthritis is one of the most debilitating forms of arthritis.
Rheumatoid Arthritis Introduction Rheumatoid arthritis is a fairly common joint disease that affects up to 2 million Americans. Rheumatoid arthritis is one of the most debilitating forms of arthritis.
Orthopaedic Shoulder (and Anatomical Arm) Referral Guidelines
 Orthopaedic ( Anatomical Arm) Referral Guidelines Austin Health Orthopaedic Clinic holds weekly multidisciplinary meetings to discuss plan the treatment of patients with Orthopaedic Fracture conditions.
Orthopaedic ( Anatomical Arm) Referral Guidelines Austin Health Orthopaedic Clinic holds weekly multidisciplinary meetings to discuss plan the treatment of patients with Orthopaedic Fracture conditions.
Rheumatoid arthritis
 Rheumatoid arthritis 1 Definition Rheumatoid arthritis is one of the most common inflammatory disorders affecting the population worldwide. It is a systemic inflammatory disease which affects not only
Rheumatoid arthritis 1 Definition Rheumatoid arthritis is one of the most common inflammatory disorders affecting the population worldwide. It is a systemic inflammatory disease which affects not only
Facet syndrome in the cervical (upper) spine
 Dr. Michael J Walls, MD 320 Thomas More Parkway. Ste 202 Crestview Hills, KY 41017 Phone: (859) 331-0956 Facet syndrome in the cervical (upper) spine Cervical facet syndrome, also known as cervical facet
Dr. Michael J Walls, MD 320 Thomas More Parkway. Ste 202 Crestview Hills, KY 41017 Phone: (859) 331-0956 Facet syndrome in the cervical (upper) spine Cervical facet syndrome, also known as cervical facet
Pain Management Questionnaire
 In order to make the most of your visit, we require this form to be completed to the best of your ability and sent to the Pain Management Clinic a copy should be shared with your Primary Care Provider
In order to make the most of your visit, we require this form to be completed to the best of your ability and sent to the Pain Management Clinic a copy should be shared with your Primary Care Provider
Rafik Girgis. Consultant Ophthalmic Surgeon ( Cataract & Primary Care)
 Rafik Girgis Consultant Ophthalmic Surgeon ( Cataract & Primary Care) Blepharitis Is a very common condition which usually bilateral & symmetrical. The main types are: Anterior, posterior or mixed Complications:
Rafik Girgis Consultant Ophthalmic Surgeon ( Cataract & Primary Care) Blepharitis Is a very common condition which usually bilateral & symmetrical. The main types are: Anterior, posterior or mixed Complications:
Rheumatoid Arthritis. Marge Beckman FALU, FLMI Vice President RGA Underwriting Quarterly Underwriting Meeting March 24, 2011
 Rheumatoid Arthritis Marge Beckman FALU, FLMI Vice President RGA Underwriting Quarterly Underwriting Meeting March 24, 2011 The security of experience. The power of innovation. www.rgare.com Case Study
Rheumatoid Arthritis Marge Beckman FALU, FLMI Vice President RGA Underwriting Quarterly Underwriting Meeting March 24, 2011 The security of experience. The power of innovation. www.rgare.com Case Study
VASCULITIS. Case Presentation. Case Presentation
 VASCULITIS Case Presentation The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
VASCULITIS Case Presentation The patient is a 24 year old woman who presented to the emergency room with left-sided weakness. She was confused and complained of a severe headache. She was noted to have
Date of Admission: [DATE]. Date of Discharge:
![Date of Admission: [DATE]. Date of Discharge: Date of Admission: [DATE]. Date of Discharge:](/thumbs/74/71277118.jpg) Date of Admission: [DATE]. Date of Discharge: History of Present Illness: Mr. [NAME] AKA [NAME] is a 31-year-old male who presents to the [PLACE] Trauma Surgery Service as a moderate trauma on [DATE] following
Date of Admission: [DATE]. Date of Discharge: History of Present Illness: Mr. [NAME] AKA [NAME] is a 31-year-old male who presents to the [PLACE] Trauma Surgery Service as a moderate trauma on [DATE] following
New Practice Member Paperwork
 Cornerstone Family Chiropractic Health Information Form 928.237.9477 www.cfc4familyhealth.com 2225 E State Route 69 Suite A Prescott, AZ 86301 New Practice Member Paperwork This form is for adults only.
Cornerstone Family Chiropractic Health Information Form 928.237.9477 www.cfc4familyhealth.com 2225 E State Route 69 Suite A Prescott, AZ 86301 New Practice Member Paperwork This form is for adults only.
Patient Name: Date of Birth:
 Patient Name: Date of Birth: Marital Status: Single Married Divorced Widowed Height: Referring Doctor: Weight: Primary Care Dr.: Preferred Pharmacy:(name/address) ALLERGIES: Do you have any drug allergies?
Patient Name: Date of Birth: Marital Status: Single Married Divorced Widowed Height: Referring Doctor: Weight: Primary Care Dr.: Preferred Pharmacy:(name/address) ALLERGIES: Do you have any drug allergies?
PAEDIATRIC VASCULITIS
 PAEDIATRIC VASCULITIS Lawrence Owino Okong o, Mmed (UoN); Mphil. (UCT). Lecturer, Department of Paediatrics and Child Health, University of Nairobi. Paediatrician/ Rheumatologist. OUTLINE Introduction
PAEDIATRIC VASCULITIS Lawrence Owino Okong o, Mmed (UoN); Mphil. (UCT). Lecturer, Department of Paediatrics and Child Health, University of Nairobi. Paediatrician/ Rheumatologist. OUTLINE Introduction
General appearance examination
 Childhood athletic participation has dramatically increased over the past twenty years. Children are being introduced to organised sports at increasingly immature stages of physical development. It is
Childhood athletic participation has dramatically increased over the past twenty years. Children are being introduced to organised sports at increasingly immature stages of physical development. It is
A patient reported outcome measure for Giant Cell Arteritis UHBristol Research Showcase Tuesday 31st October 2017
 A patient reported outcome measure for Giant Cell Arteritis UHBristol Research Showcase Tuesday 31st October 2017 Joanna Robson Consultant Senior Lecturer in Rheumatology UHBristol University of the West
A patient reported outcome measure for Giant Cell Arteritis UHBristol Research Showcase Tuesday 31st October 2017 Joanna Robson Consultant Senior Lecturer in Rheumatology UHBristol University of the West
Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis
 Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis The program consisted of manual therapy twice per week (eg, soft tissue and neural The components of the Boot Camp Program
Therapeutic Exercise And Manual Therapy For Persons With Lumbar Spinal Stenosis The program consisted of manual therapy twice per week (eg, soft tissue and neural The components of the Boot Camp Program
Vasculitis local: systemic
 Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated inflammation
Vasculitis Inflammation of the vessel wall. Signs and symptoms: 1- local: according to the involved tissue 2- systemic:(fever, myalgia, arthralgias, and malaise) Pathogenesis 1- immune-mediated inflammation
Discussion Questions WHAT ARE SOME POSSIBLE CAUSES OF HER PAIN? WHAT ELSE WOULD YOU LIKE TO KNOW
 CLINICAL CASES Case: Ms. FM Case: Ms. FM Ms. FM is a 37-year-old school teacher Under your care for 10 years Unremarkable past history Was in minor car accident 4 months ago Has had progressive generalized
CLINICAL CASES Case: Ms. FM Case: Ms. FM Ms. FM is a 37-year-old school teacher Under your care for 10 years Unremarkable past history Was in minor car accident 4 months ago Has had progressive generalized
Neurological Dilemmas in Primary Care
 Neurological Dilemmas in Primary Care David Clark, DO dclark@oregonneurology.com When to test? How to test? Pitfalls in testing? When to treat? How to treat? How long to treat? Neurological Dilemmas Seizure
Neurological Dilemmas in Primary Care David Clark, DO dclark@oregonneurology.com When to test? How to test? Pitfalls in testing? When to treat? How to treat? How long to treat? Neurological Dilemmas Seizure
4 2 Osteoarthritis 1
 Osteoarthritis 1 Osteoarthritis ( OA) Osteoarthritis is a chronic disease and the most common of all rheumatological disorders. It particularly affects individuals over the age of 65 years. The prevalence
Osteoarthritis 1 Osteoarthritis ( OA) Osteoarthritis is a chronic disease and the most common of all rheumatological disorders. It particularly affects individuals over the age of 65 years. The prevalence
Guide to Understanding and Managing Arthritis
 Guide to Understanding and Managing Arthritis The content in this guide is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician
Guide to Understanding and Managing Arthritis The content in this guide is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician
Exclude referred pain from the neck, diaphragm, heart, lungs, & polymyalgia rheumatica YES. NSAIDs/analgesics as required
 Shoulder Pain Clinical Presentation info for GPs who refer into PAH more info History and Examination Exclude referred pain from the neck, diaphragm, heart, lungs, & polymyalgia rheumatica more info for
Shoulder Pain Clinical Presentation info for GPs who refer into PAH more info History and Examination Exclude referred pain from the neck, diaphragm, heart, lungs, & polymyalgia rheumatica more info for
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH)
 A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) 6565 Fannin Street Houston, TX 77030 Phone: 713-790-3333 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Diffuse Idiopathic Skeletal Hyperostosis (DISH) 6565 Fannin Street Houston, TX 77030 Phone: 713-790-3333 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging
 Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging These guidelines have been issued in conjunction with the Royal College of Radiology referral
Salisbury Foundation Trust Radiology Department Referral Guidelines for Primary Care: Musculoskeletal Imaging These guidelines have been issued in conjunction with the Royal College of Radiology referral
Topics in Disability. Case Studies
 Topics in Disability Case Studies Individual vs Group Disability Underwriting, group vs individual Definition of disability Duration of disability period Difference in contract language Case #1 52 year
Topics in Disability Case Studies Individual vs Group Disability Underwriting, group vs individual Definition of disability Duration of disability period Difference in contract language Case #1 52 year
BSR and BHPR guidelines for the management of polymyalgia rheumatica
 RHEUMATOLOGY Guidelines doi:10.1093/rheumatology/kep303b BSR and BHPR guidelines for the management of polymyalgia rheumatica Bhaskar Dasgupta 1, Frances A. Borg 1, Nada Hassan 1, Kevin Barraclough 2,
RHEUMATOLOGY Guidelines doi:10.1093/rheumatology/kep303b BSR and BHPR guidelines for the management of polymyalgia rheumatica Bhaskar Dasgupta 1, Frances A. Borg 1, Nada Hassan 1, Kevin Barraclough 2,
SUMMARY DECISION NO. 1058/98. Fibromyalgia.
 SUMMARY DECISION NO. 1058/98 Fibromyalgia. The worker suffered a wrist injury in 1984. The worker appealed a decision of the Appeals Officer denying entitlement for fibromyalgia. Considering the evidence
SUMMARY DECISION NO. 1058/98 Fibromyalgia. The worker suffered a wrist injury in 1984. The worker appealed a decision of the Appeals Officer denying entitlement for fibromyalgia. Considering the evidence
When is it Rheumatoid Arthritis When to Refer
 When is it Rheumatoid Arthritis When to Refer Nancy A. Brown, DO Spring 2015 When is it Rheumatoid Arthritis When to Refer Learning objectives To review the definition and epidemiology of Rheumatoid Arthritis
When is it Rheumatoid Arthritis When to Refer Nancy A. Brown, DO Spring 2015 When is it Rheumatoid Arthritis When to Refer Learning objectives To review the definition and epidemiology of Rheumatoid Arthritis
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME
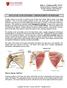 ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
ROTATOR CUFF INJURIES / IMPINGEMENT SYNDROME Shoulder injuries are common in patients across all ages, from young, athletic people to the aging population. Two of the most common problems occur in the
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abatacept, for rheumatoid arthritis, 789 Acetaminophen, for low back pain, 735 Acupuncture for fibromyalgia, 753 for low back pain, 738
Index Note: Page numbers of article titles are in boldface type. A Abatacept, for rheumatoid arthritis, 789 Acetaminophen, for low back pain, 735 Acupuncture for fibromyalgia, 753 for low back pain, 738
CME for Family Medicine Specialists. Evelyn Sutton, MD, FRCPC, FACP November 17, 2018
 CME for Family Medicine Specialists Evelyn Sutton, MD, FRCPC, FACP November 17, 2018 Disclosures Received $ from Advisory Board Consultant: Amgen, Abvie, Pfizer, Actelion, Lilly, Grants: Arthritis Society,
CME for Family Medicine Specialists Evelyn Sutton, MD, FRCPC, FACP November 17, 2018 Disclosures Received $ from Advisory Board Consultant: Amgen, Abvie, Pfizer, Actelion, Lilly, Grants: Arthritis Society,
Joint Injuries and Disorders
 Joint Injuries and Disorders Introduction A joint is where two or more bones come together. Your joints include the knees, hips, elbows and shoulders. There are many types of joint disorders, including
Joint Injuries and Disorders Introduction A joint is where two or more bones come together. Your joints include the knees, hips, elbows and shoulders. There are many types of joint disorders, including
HEADACHES THE RED FLAGS
 HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
HEADACHES THE RED FLAGS FAYYAZ AHMED CONSULTANT NEUROLOGIST HON. SENIOR LECTURER HULL YORK MEDICAL SCHOOL SECONDARY VS PRIMARY HEADACHES COMMON SECONDARY HEADACHES UNCOMMON BUT SERIOUS SECONDARY HEADACHES
PUFF THE MAGIC DRAGON
 PUFF THE MAGIC DRAGON AN UNUSUAL CASE OF A PUFFY FACE MA ACP Annual Scientific Meeting Gurbir Gill, M.D., PGY-3 (Associate) George M. Abraham, MD, MPH, FACP Department of Medicine, Saint Vincent Hospital,
PUFF THE MAGIC DRAGON AN UNUSUAL CASE OF A PUFFY FACE MA ACP Annual Scientific Meeting Gurbir Gill, M.D., PGY-3 (Associate) George M. Abraham, MD, MPH, FACP Department of Medicine, Saint Vincent Hospital,
HISTORY OF PRESENT ILLNESS A. TELL US ABOUT YOUR PAIN PROBLEM
 1 UT Health Austin Comprehensive Pain Management New Patient Questionnaire Thank you for scheduling a visit with the Comprehensive Pain Management Care Team. The responses you provide to these questions
1 UT Health Austin Comprehensive Pain Management New Patient Questionnaire Thank you for scheduling a visit with the Comprehensive Pain Management Care Team. The responses you provide to these questions
Physician Approach to MSK Complains in Elderly. Dr Tjan Soon Yin, Consultant and Deputy Head, TTSH Rehab Medicine
 Physician Approach to MSK Complains in Elderly Dr Tjan Soon Yin, Consultant and Deputy Head, TTSH Rehab Medicine Impact of MSK Conditions Neuro-musculoskeletal and cardiorespiratory systems determines
Physician Approach to MSK Complains in Elderly Dr Tjan Soon Yin, Consultant and Deputy Head, TTSH Rehab Medicine Impact of MSK Conditions Neuro-musculoskeletal and cardiorespiratory systems determines
Mr. OA: Case Presentation
 CLINICAL CASES Case 1: Mr. OA OA Mr. OA: Case Presentation 62-year-old lawyer Mild left knee pain for 3 month, but became worse 1 week ago No swelling 1 week earlier: 2-hour walk in the countryside 2 days
CLINICAL CASES Case 1: Mr. OA OA Mr. OA: Case Presentation 62-year-old lawyer Mild left knee pain for 3 month, but became worse 1 week ago No swelling 1 week earlier: 2-hour walk in the countryside 2 days
ABACAVIR HYPERSENSITIVITY REACTION
 ABACAVIR HYPERSENSITIVITY REACTION Key Risk Minimisation Points: Abacavir Hypersensitivity Reaction (HSR) Abacavir is associated with a risk for hypersensitivity reactions (HSR) characterised by fever
ABACAVIR HYPERSENSITIVITY REACTION Key Risk Minimisation Points: Abacavir Hypersensitivity Reaction (HSR) Abacavir is associated with a risk for hypersensitivity reactions (HSR) characterised by fever
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING
 AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
Blindness In An Elderly Woman
 Blindness In An Elderly Woman A 74 y/o woman with a chief complaint of: a cloud in front of my right eye and I can t t see through it Symptoms began 24 hours prior to examination. Visual loss was painless
Blindness In An Elderly Woman A 74 y/o woman with a chief complaint of: a cloud in front of my right eye and I can t t see through it Symptoms began 24 hours prior to examination. Visual loss was painless
Please fill out the following form in as much detail as possible. Please Print. Name. Address. City State Zip. Home Phone Office Phone.
 CASE NO. Please fill out the following form in as much detail as possible. Please Print Date Name Address City State Zip Home Phone Office Phone E-mail Address Age Date of Birth Occupation Sex (M) (F)
CASE NO. Please fill out the following form in as much detail as possible. Please Print Date Name Address City State Zip Home Phone Office Phone E-mail Address Age Date of Birth Occupation Sex (M) (F)
Fran Pulver, MD - PM&R Laurie Bell, PT - Physical Therapy Gregg Weidner, MD - Anesthesia Steven Severyn, MD, MBA, MSS - Anesthesia
 Fran Pulver, MD - PM&R Laurie Bell, PT - Physical Therapy Gregg Weidner, MD - Anesthesia Steven Severyn, MD, MBA, MSS - Anesthesia Case Presentation-Fibromyalgia 30 year old female Chief complaint of back
Fran Pulver, MD - PM&R Laurie Bell, PT - Physical Therapy Gregg Weidner, MD - Anesthesia Steven Severyn, MD, MBA, MSS - Anesthesia Case Presentation-Fibromyalgia 30 year old female Chief complaint of back
Medicare Regulations for Chiropractors. Presented by Clinic Pro Software Inc. Marilyn K. Gard. CEO, MBA
 Medicare Regulations for Chiropractors Presented by Clinic Pro Software Inc. Marilyn K. Gard. CEO, MBA Use AT modifier which means active treatment. Claims submitted for Chiropractic manipulative treatment
Medicare Regulations for Chiropractors Presented by Clinic Pro Software Inc. Marilyn K. Gard. CEO, MBA Use AT modifier which means active treatment. Claims submitted for Chiropractic manipulative treatment
Ultrasound in Rheumatology
 Arthritis Research UK Primary Care Centre Winner of a Queen s Anniversary Prize For Higher and Further Education 2009 Ultrasound in Rheumatology Alison Hall Consultant MSK Sonographer/Research Fellow Primary
Arthritis Research UK Primary Care Centre Winner of a Queen s Anniversary Prize For Higher and Further Education 2009 Ultrasound in Rheumatology Alison Hall Consultant MSK Sonographer/Research Fellow Primary
Dr Ng Swee Cheng Senior Consultant Khoo Teck Puat Hospital
 Dr Ng Swee Cheng Senior Consultant Khoo Teck Puat Hospital 1. Soft Tissue Rheumatism 2. Myofascial Pain 3. Neurovascular compression Syndromes 4. Complex Regional Pain Syndromes Tendinitis, tenosynovitis
Dr Ng Swee Cheng Senior Consultant Khoo Teck Puat Hospital 1. Soft Tissue Rheumatism 2. Myofascial Pain 3. Neurovascular compression Syndromes 4. Complex Regional Pain Syndromes Tendinitis, tenosynovitis
Clinical Commissioning Policy Proposition: Tocilizumab for Giant cell arteritis (adults)
 Clinical Commissioning Policy Proposition: Tocilizumab for Giant cell arteritis (adults) Version Number: NHS England A13X12/01 Information Reader Box (IRB) to be inserted on inside front cover for documents
Clinical Commissioning Policy Proposition: Tocilizumab for Giant cell arteritis (adults) Version Number: NHS England A13X12/01 Information Reader Box (IRB) to be inserted on inside front cover for documents
Polymyalgia Rheumatica: A Challenging Diagnosis in Elderly Patients-Case Reports
 Annals of Geriatric Medicine and Research AGMR 2017;21(4):210-214 Case Report https://doi.org/10.4235/agmr.2017.21.4.210 Print ISSN 2508-4798 On-line ISSN 2508-4909 www.e-agmr.org Polymyalgia Rheumatica:
Annals of Geriatric Medicine and Research AGMR 2017;21(4):210-214 Case Report https://doi.org/10.4235/agmr.2017.21.4.210 Print ISSN 2508-4798 On-line ISSN 2508-4909 www.e-agmr.org Polymyalgia Rheumatica:
Initial Visit Forms. Life in Motion Chiropractic & Wellness 6139 Route 96 -Suite 1 Farmington, NY (585)
 Initial Visit Forms 6139 Route 96 -Suite 1 Patient Name: Patient Intake Form Name: Date: Address: City: State: Zip: Home #: ( ) Cell #: ( ) Work #: ( ) E-mail: Preferred method of contact: Date of Birth:
Initial Visit Forms 6139 Route 96 -Suite 1 Patient Name: Patient Intake Form Name: Date: Address: City: State: Zip: Home #: ( ) Cell #: ( ) Work #: ( ) E-mail: Preferred method of contact: Date of Birth:
Primary Care Adult Headache Management Pathway (formerly North West Headache Management Guideline for Adults) Version 1.0
 Primary Care Adult Headache Management Pathway (formerly rth West Headache Management Guideline for Adults) Version 1.0 1 VERSION CONTROL Version Date Amendments made Version 1.0 October 2018 Reformatted
Primary Care Adult Headache Management Pathway (formerly rth West Headache Management Guideline for Adults) Version 1.0 1 VERSION CONTROL Version Date Amendments made Version 1.0 October 2018 Reformatted
Patient Name: Date of Birth: Preferred Pharmacy: (name/location/phone #)
 Patient Name: Date of Birth: Referring Doctor: Primary Care Dr: Preferred Pharmacy: (name/location/phone #) CURRENT MEDICATIONS: Please list all Medication Dose Frequency 1 2 3 4 5 6 7 8 9 10 11 12 13
Patient Name: Date of Birth: Referring Doctor: Primary Care Dr: Preferred Pharmacy: (name/location/phone #) CURRENT MEDICATIONS: Please list all Medication Dose Frequency 1 2 3 4 5 6 7 8 9 10 11 12 13
DIAGNOSTIC EVALUATION OF CERVICAL VS. SHOULDER PAIN: A PHYSIATRIST S PERSPECTIVE
 Russ Cantrell, M.D. Physical Medicine and Rehabilitation Orthopedic Sports Medicine and Spine Care Institute DIAGNOSTIC EVALUATION OF CERVICAL VS. SHOULDER PAIN: A PHYSIATRIST S PERSPECTIVE PHYSIATRIST
Russ Cantrell, M.D. Physical Medicine and Rehabilitation Orthopedic Sports Medicine and Spine Care Institute DIAGNOSTIC EVALUATION OF CERVICAL VS. SHOULDER PAIN: A PHYSIATRIST S PERSPECTIVE PHYSIATRIST
On alert for giant cell arteritis
 1.0 ANCC CONTACT HOUR On alert for giant cell arteritis By Vincent M. Vacca, Jr., MSN, RN, CCRN, SCRN, ENLS, and Isabel Argento, BSN, RN ALSO KNOWN AS temporal arteritis, giant cell arteritis (GCA) is
1.0 ANCC CONTACT HOUR On alert for giant cell arteritis By Vincent M. Vacca, Jr., MSN, RN, CCRN, SCRN, ENLS, and Isabel Argento, BSN, RN ALSO KNOWN AS temporal arteritis, giant cell arteritis (GCA) is
DISEASES AND DISORDERS
 DISEASES AND DISORDERS 9. 53 10. Rheumatoid arthritis 59 11. Spondyloarthropathies 69 12. Connective tissue diseases 77 13. Osteoporosis and metabolic bone disease 95 14. Crystal arthropathies 103 15.
DISEASES AND DISORDERS 9. 53 10. Rheumatoid arthritis 59 11. Spondyloarthropathies 69 12. Connective tissue diseases 77 13. Osteoporosis and metabolic bone disease 95 14. Crystal arthropathies 103 15.
 www.fisiokinesiterapia.biz Peak onset between 20 and 30 years Form of spondyloarthritis (cause inflammation around site of ligament insertion into bone) and association with HLA-B27 Prevalence as high
www.fisiokinesiterapia.biz Peak onset between 20 and 30 years Form of spondyloarthritis (cause inflammation around site of ligament insertion into bone) and association with HLA-B27 Prevalence as high
Upper limb injuries II. Traumatology RHS 231 Dr. Einas Al-Eisa
 Upper limb injuries II Traumatology RHS 231 Dr. Einas Al-Eisa Capsulitis = inflammatory lesion of the glenohumeral joint capsule leading to: thickening and loss of joint volume painful stiffness of the
Upper limb injuries II Traumatology RHS 231 Dr. Einas Al-Eisa Capsulitis = inflammatory lesion of the glenohumeral joint capsule leading to: thickening and loss of joint volume painful stiffness of the
RHEUMATIC FEVER AND POST-STREPTOCOCCAL REACTIVE ARTHRITIS
 www.pediatric-rheumathology.printo.it RHEUMATIC FEVER AND POST-STREPTOCOCCAL REACTIVE ARTHRITIS What is it? Rheumatic fever has been defined as a disease triggered by infection caused by streptococcus.
www.pediatric-rheumathology.printo.it RHEUMATIC FEVER AND POST-STREPTOCOCCAL REACTIVE ARTHRITIS What is it? Rheumatic fever has been defined as a disease triggered by infection caused by streptococcus.
Neck Pain Guide. Understanding Causes, Treatment and Prevention
 Neck Pain Guide Understanding Causes, Treatment and Prevention Neck pain may be more than a nuisance; it could be a symptom of an underlying condition. Use this guide to help you understand common causes
Neck Pain Guide Understanding Causes, Treatment and Prevention Neck pain may be more than a nuisance; it could be a symptom of an underlying condition. Use this guide to help you understand common causes
