Patients with intralesional hemorrhage in venous malformations: Diagnosis and embolosclerotherapy
|
|
|
- Derek Johns
- 5 years ago
- Views:
Transcription
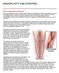
1 Patients with intralesional hemorrhage in venous malformations: Diagnosis and embolosclerotherapy Hui Chen, MD, Xiaoxi Lin, MD, Yunbo Jin, MD, Wei Li, MD, Gang Ma, MD, and Xiaojie Hu, MD, Shanghai, China Purpose: Venous malformations (VMs) are common congenital benign lesions characterized by slow progression. However, intralesional hemorrhage can result in sudden enlargement of the lesions, which, though uncommon clinically, brings difficulties in diagnosis and treatment. The purpose of this study is to explore the clinical features and diagnosis modality of intralesional hemorrhage in VMs and present our experience with embolosclerotherapy. Methods: A series of 16 patients were recruited from May 2003 to February 2007, of which fifteen were males and one was female, aged from five months to 40 years (mean, 11.4 years). The anatomic sites affected included cheek (n 6), upper lid (n 3), neck (n 3), parotid region (n 2), temple (n 1), and upper limb (n 1). The period of enlargement varied from one day to 25 days (mean, 8.4 days). Diagnostic needle aspiration was performed to analyze the internal contents of the masses by macroscopic observation. Magnetic resonance imaging (MRI) was applied to determine the size, location, and extent of the lesions. Two patients received percutaneous venography. Routine blood testing was carried out in all cases. A combination of absolute alcohol and Bleomycin A5 embolosclerotherapy was administered to the patients. The procedure was repeated after 6 to 8 weeks. Outcomes were assessed by MRI measurement and pre and post treatment color photos. Results: All the patients were diagnosed with hemorrhage in VMs. The volume of the localized lesions varied from 3cm 2cm 1cmto8cm 5cm 3 cm. Fourteen patients received embolosclerotherapy in one (n 10) or two (n 4) sessions. Two cases were not treated and the lesions regressed spontaneously with detectable residual lesions. After a mean follow-up of 25 months (range, 3 to 40 months), treatment was considered effective in 12 patients. The complications were minimal including temporary swelling in 14 treated patients and mild fever in two patients. Conclusion: Intralesional hemorrhage in VMs should be distinguished from other lesions in the head and neck region. Diagnostic puncture and MRI are essential for accurate diagnosis. Percutaneous embolosclerotherapy using a combination of absolute ethanol and Bleomycin A5 is a safe and effective treatment of choice. (J Vasc Surg 2009;49: ) Venous malformations (VMs) are common congenital anomalies of vascular morphogenesis. The lesions grow commensurately with the child s development and do not show involution. 1,2 It is uncommon for the lesions to expand suddenly within a few days. However, if intralesional hemorrhage occurs, the lesions may enlarge rapidly, which is quite dissimilar to their natural history. Misdiagnosis or improper treatment may occur if attending physicians are not familiar with this situation. In the past four years, a total of 16 patients with intralesional hemorrhage in VMs were treated in our department. We performed a retrospective study of those cases and confirmed that clinical history, physical examination, diagnostic needle aspiration, and magnetic resonance imaging (MRI) findings were essential to establish a correct diagnosis. Meanwhile, percutaneous embolosclerotherapy using a combination of absolute ethanol and Bleomycin A5 has been performed in our department for the treatment of From the Shanghai Ninth People s Hospital. Competition of interest: none. Reprint requests: Dr. Xiaoxi Lin, Shanghai Ninth People s Hospital, Department of Plastic Surgery, 639# Zhizaoju Rd., Shanghai , China ( linxiaoxi@126.com) /$36.00 Copyright 2009 Published by Elsevier Inc. on behalf of The Society for Vascular Surgery. doi: /j.jvs common VMs (VMs without hemorrhage). The safety and effectiveness of this therapy has been well established. 3 Our aim was to extend the use of this method to treat patients with intralesional hemorrhage in VMs. The purpose of this study was to explore the clinical features, diagnosis, and differential diagnosis of intralesional hemorrhage in VMs and develop an effective treatment method. PATIENTS AND METHODS Patients. From May 2003 to February 2007, 16 patients with intralesional hemorrhage in VMs were included in this study. Those included 15 males and 1 female aged from 5 months to 40 years (mean, 11.4 years). The anatomic sites affected included cheek (n 6), upper lid (n 3), neck (n 3), parotid region (n 2), temple (n 1), and upper limb (n 1). The period of enlargement varied from 1 day to 25 days (mean, 8.4 days). Six patients provided specific trauma histories (blunt trauma in three cases and intensive joint movements in the other three cases). Three patients complained of pre-existing masses before the onset of hemorrhage. At their first visit to the department, diagnostic needle aspiration was performed in all patients to analyze the internal contents of the masses by macroscopic observation. MRI was applied in defining the size, location, and extent 429
2 430 Chen et al JOURNAL OF VASCULAR SURGERY February 2009 Fig 1. a, A 14-year-old boy with a lesion in the left cheek. b, Two years after one treatment. c, A small residual lesion was revealed in MRI (arrow). d, Normal venous blood was aspirated from the residual lesion that was supportive for the diagnosis of intralesional hemorrhage in venous malformations. of the lesions. Two patients received percutaneous venography. Routine blood testing was carried out in all cases. Treatment techniques. Written informed consent was obtained from the patients or their parents before treatment. The first procedure began when the lesions stopped expanding and were stabilized for one week. Six pediatric patients were treated under general anesthesia and the other patients without anesthesia. After preparation of the treatment site with povidoneiodine, 1-2 ml blood was aspirated out of the lesion by a 5 ml-syringe to check for blood again. Then a direct puncture was performed using 21-gauge needles. At each session, 2-6 injection sites were needed according to the size of the lesions. Once the blood returned, 1-3 ml absolute alcohol was injected first, followed by a maximum of 8 mg of bleomycin A5 after 1 to 2 minutes (8 mg dissolved in 4 ml 0.9% sodium chloride). The maximum dose in a single procedure was 0.1 ml/kg for absolute alcohol and 0.2 mg/kg for Bleomycin A5. The treatment was repeated if there was detectable residual mass and confirmed by a direct puncture (venous blood return). The interval between two procedures was 6-8 weeks. Outcome evaluation. MRI and pre- and post-treatment color photos were applied in outcome evaluation. Due to the limited number of cases, we used two categories for outcome evaluation. The treatment was considered effective if the volume of the lesion was reduced 75% (measured by MRI parameters) or significant improvements in appearance were observed and the patient requested no further treatment. The treatment was considered ineffective if the volume of the lesion was reduced 75% or the patient was not satisfied with the improvements in appearance. RESULTS All the patients were diagnosed with intralesional hemorrhage in VMs (Fig 1). No abnormal hematologic findings were observed in routine blood testing. Fifteen patients developed localized lesions and 1 patient had an infiltrating lesion. The volume of the localized lesions varied from 3 cm 2cm 1cmto8cm 5cm 3 cm measured by MRI. The infiltrating lesion was not measured. Fourteen patients received embolosclerotherapy with one (n 10) or two (n 4) procedures. At a mean follow-up of 25 months (range, 3-40 months), treatment was considered effective in 12 patients. Percentage of volume reduction was 82% to 100% (mean, 93%).The patients recovered to nearly normal appearance and asked for no further treatment. Three cases manifested complete resolution of the lesions (Fig 2). In two infantile cases with lesions involving upper eyelids, the treatment was ineffective due to unsatisfactory appearance improvements with a clearance rate of 50% and their parents declined further treatment. Patients follow-up showed stable lesions. The two patients who were not treated were monitored for 4 years and 4 months respectively. The lesions resolved spontaneously after 2 months, but the residual lesions exhibited typical VM features, which corroborated our initial diagnosis (Fig 3). The complications were generally minimal. All treated patients experienced a degree of local swelling that regressed without any therapy after 5 to 10 days. Two patients complained of mild fever that disappeared after 2 days. No major or permanent complications occurred. There was no clinical or MRI evidence of recurrence in the treated cases. DISCUSSION Pathogenesis of intralesional hemorrhage in VMs. Even though the pathogenesis of intralesional hemorrhage in VMs is not well recognized, it may have a close relationship with the abnormal structure of the vascular wall. The VMs are formed by thin-walled channels, deficient in smooth muscle cells and lined by a single layer of endothelium. 4 There are slit-like or interconnected channels dissecting through normal tissues. These veins will dilate over time because of repeated engorgement. 5
3 JOURNAL OF VASCULAR SURGERY Volume 49, Number 2 Chen et al 431 Fig 2. A 3-year-old boy with a lesion in the left cheek. The evident bruise on his left cheek was a sign of subcutaneous hemorrhage. He had no trauma history. a, Before treatment. b, Five months after one session. c, Magnetic resonance imaging revealed a well-defined margin of inhomogenous high-singal intensity area in the left cheek. d, The lesion resolved completely 5 months later. Not all patients have noticeable VMs at birth because in early anomalous veins the blood flow is slow with stable hemodynamics. During puberty or pregnancy, the lesions tend to grow more rapidly, which is stimulated by hormonal effects. However, such sudden enlargement as we have described in this study may not happen during puberty or pregnancy. Trauma is considered to be one of the important factors contributing to sudden growth of the lesions. Intensive movements of the joints have the same effects as blunt trauma, such as temporomandibular joint, shoulder joint, or elbow joint. The clear history of intensive joint movements in our three cases proved this. The blood escapes out of the ruptured veins and accumulates in the adjacent venous sinuses. Not all the VMs have sufficient peripheral drainage according to their anatomy and hemodynamic features. 6 Such blood flow disturbances may change the stable hemodynamics and peripheral drainage of the VMs so that more veins are perfused and dilated rapidly in a short time. The duration of enlargement varied from one to 25 days in our study. If not treated, the expanded lesions would regress gradually, but residual lesions were noticeable. In this study, only 6 patients provided clear trauma histories; the bleeding etiology of the other cases was unknown. The normal routine blood testing excluded hematologic disease that may cause bleeding on the whole. Diagnosis and differential diagnosis. Final diagnosis of the intralesional hemorrhage in venous malformations relied on the combination of the clinical history, clinical presentation, diagnostic needle aspiration, and MRI findings. Clinical history is important to the diagnosis for a sudden enlarged mass. The following three types of signs could be more supportive: clear history of direct blunt
4 432 Chen et al JOURNAL OF VASCULAR SURGERY February 2009 Fig 3. a, A 16-year-old boy had an extensive mass involving his left neck. The mass enlarged abruptly overnight after intense exercises. He was not treated. b, Four months later, the mass had regressed and previous lesion still existed. Small and hard nodules could be felt under the skin (arrow). c, Magnetic resonance imaging revealed numerous phleboliths within the lesion (arrow). trauma to the lesion; pre-existing mass; and self-regressed lesions proven to be VM by long-term follow-up. On physical examination, the lesion presented a localized, prominent, and tense mass at palpation under normal or purple skin. The purple skin was an obvious symptom of subcutaneous hemorrhage. No pulsate or thrill could be detected. Diagnostic needle aspiration was useful to identify whether the lesion was formed by vascular channels. Even without the negative pressure aspiration by a syringe, the blood could flow out from the end of the needle easily. By macroscopic observation, except for being slightly darker in color, the blood had the same characteristics as normal venous blood without any suspicious components. These findings do not occur in solid or cystic tumors. MRI plays a leading role in the diagnosis of different type of vascular anomalies. MRI is powerful in its ability to delineate the extent of the lesions and the relationship to the adjacent tissues and organs, 7,8 which was the most important imaging modality to guide our treatment. In the case of an infiltrating lesion, phleboliths were revealed by MRI that made the diagnosis more convincing. However, it is difficult to distinguish the bleeding VMs from common VMs (VMs without intralesional bleeding), especially large lesions, by MRI. However, MRI can be used to exclude other type of tumors. The most confusing lesions are intralesional bleeding in lymphangiomas. MRI showed a tumor with sharp border, homogenous intensity, a fluid-fluid level, and no signal enhancement. By needle aspiration, the blood is brown to black, viscous but not clotting. In two patients, we performed percutaneous direct puncture phlebography to see whether the bleeding was in VMs or in lymphangiomas. The lesion was proved to be VM due to the emergence of draining veins. Phlebography is used as a road map to guide the treatment of the VMs with high risk, while rarely needed for the differential diagnosis. Other tumors in the head and neck region with similar presentations to bleeding VMs include false aneurysm, branchial cleft cyst, and parotid cyst. False aneurysms may arise following traumatic damage to an artery and are comprised of a slowly expanding blood-filled cavity, which is held around the artery by connective tissue. But generally it is a mass with pulsate and thrill, which is similar to arteriovenous malformations (AVMs) but not to VMs. Branchial cleft cysts and parotid cysts can be distinguished by the findings of cholesterol crystal and positive amylase test for aspirated liquid. Evaluation of combination embolosclerotherapy. In recent years, absolute alcohol has been the most commonly used liquid agent for the percutaneous embolization of VMs. 9 As absolute alcohol can result in severe endothelial denudation and thrombosis immediately, it is the only known and clinically tested effective scleroagent to be able to abrogate endothelial cells, with the prospect of a cure in selected cases A response rate of 74% to 91% with limited to no recurrence has been reported. 10,11,13,14 Bleomycin A5 is a refined ingredient from Bleomycin with more potent antitumor abilities. Bleomycin can produce a sclerosing effect on the endothelial cells of the vessels. Minor complications were reported in the treatment of VMs. 15 Since 2002, we have used the two sclerosing agents in combination in our department. This combination therapy has been proven to be very effective with only minor complications when treating common VMs. 3 Here we have reported that this method was also a treatment of choice for VMs with intralesional bleeding. Most of the bleeding lesions were limited with predictable favorable outcomes. However, because the bleeding lesions were different from non-bleeding ones after all, we could not tell if our method
5 JOURNAL OF VASCULAR SURGERY Volume 49, Number 2 Lee 433 was superior to treatment with single sclerosing agents and further study is warranted. CONCLUSION Intralesional hemorrhage in VMs is uncommon. Accurate diagnosis and differential diagnosis should be based on the history, clinical presentations, diagnositic needle aspiration, and MRI findings. Percutaneous absolute ethanol and Bleomycin A5 embolosclerotherapy is a safe and effective treatment of choice. We would like to thank Nagalakshmi Nadiminty, PhD, (Assistant Professor, Department of Urology and Cancer Center, University of California Davis Medical Center, Sacramento, Calif), Elaine Pinder, PhD, candidate (Graduate Program of Pharmacology and Toxicology, University of California Davis, Davis, Calif), and Siting Feng, MD, PhD, candidate, (Department of Cardiology, Renmin Hospital, Wuhan University, Wuhan, China) for their assistance in the preparation of this manuscript. AUTHOR CONTRIBUTIONS Conception and design: XL Analysis and interpretation: XL, HC Data collection: XL, HC, YJ, WL, GM, XH Writing the article: HC Critical revision of the article: XL, HC, YJ Final approval of the article: XL Statistical analysis: Not applicable Obtained funding: Not applicable Overall responsibility: XL REFERENCES 1. Enjolras O, Mulliken JB. Vascular tumors and vascular malformations (new issues). Adv Dermatol 1997;13: Mulliken JB, Glowacki J. Hemangiomas and vascular malformations in infants and children: a classification based on endothelial characteristics. Plast Reconstr Surg 1982;69: Jin Y, Lin X, Li W, Hu X, Ma G, Wang W. Sclerotherapy after embolization of draining vein: a safe treatment method for venous malformations. J Vasc Surg 2008;47: Claudon M, Upton J, Burrows PE. Diffuse venous malformations of the upper limb: morphologic characterization by MRI and venography. Pediatr Radiol 2001;31: Hein KD, Mulliken JB, Kozakewich HPW, Upton J, Burrows PE. Venous malformations of skeletal muscle. Plast and Reconstr Surg 2002;110: Puig S, Aref H, Chigot V, Bonin B, Brunelle F. Classification of venous malformations in children and implications for sclerotherapy. Pediatr Radiol 2003;33: Fayad LM, Hazirolan T, Bluemke D, Mitchell S. Vascular malformations in the extremities: emphasis on MR imaging features that guide treatment options. Skeletal Radiol 2006;35: Lee BB, Mattassi R, Loose D, Yakes W, Tasnadi G, Kim HH. Consensus on controversial issues in contemporary diagnosis and management of congenital vascular malformation: Seoul communication. Int J Angiol 2005;13: Puig S, Casati B, Staudenherz A, Paya K. Vascular low-flow malformations in children: current concepts for classification, diagnosis and therapy. Eur J Radiol 2005;53: Lee BB, Kim DI, Huh S, Kim HH, Choo IW, Byun HS, et al. New experiences with absolute ethanol sclerotherapy in the management of a complex form of congenital venous malformation. J Vasc Surg 2001; 33: Lee BB, Do YS, Byun HS, Choo IW, Kim DI, Huh SH. Advanced management of venous malformation with ethanol sclerotherapy: midterm results. J Vasc Surg 2003;37: Yakes WF, Haas DK, Parker SH, Gibson MD, Hopper KD, Mulligan JS, et al. Symptomatic vascular malformations: ethanol embolotherapy. Radiology 1989;170: Goyal M, Causer PA, Armstrong D. Venous vascular malformations in pediatric patients: comparison of results of alcohol sclerotherapy with proposed MR imaging classification. Radiology 2002;223: Mason KP, Michna E, Zurakowski D, Koka BV, Burrows PE. Serum ethanol levels in children and adults after ethanol embolization or sclerotherapy for vascular anomalies. Radiology 2000;217: Zhi K, Wen Y, Li L, Ren W. The role of intralesional Pingyangmycin in the treatment of venous malformation of facial and maxillary region. Int J Pediatr Otorhinolaryngol 2008;72: Submitted May 27, 2008; accepted Aug 20, INVITED COMMENTARY Byung-Boong Lee, MD, Reston, Va In this article, the authors describe the successful management of 16 patients with relatively sudden enlargement of a venous malformation (VM) due to acute hemorrhage. This represents a small subset of patients with VMs since the majority of VMs do not develop intra-lesion hemorrhage. The authors report good results using a combination of ethanol and bleomycin as the sclerosing agent. While the use of the powerful sclerosing agent absolute ethanol is quite well accepted for treating more aggressive arteriovenous malformations, its use in VM is more limited. This is because of serious potential complications reported with its use, including acute complications of nerve palsy or even cardiopulmonary arrest. 1,2 Therefore, many have begun to consider the use of less dangerous sclerosing agents, such as detergent-based foam, especially for less aggressive VMs, including those with transdermal extension in which there is a higher risk for complications from ethanol injection. Although foam sclerotherapy is likely less effective than ethanol, the complication rate is lower, and if VMs recur, or are only partially treated initially, they can be re-treated with foam sclerotherapy with fewer overall complications. The authors attempted to reduce the risk involved with ethanol injection of the VM by mixing it with bleomycin. However, it is difficult to judge the contribution of bleomycin to the overall treatment outcome since the ethanol was given first to block the draining veins; regardless of its amount, there is substantial risk of the vascular spasm induced by the ethanol before bleomycin begins to work, reducing its effective contact with the endothelial cells. Bleomycin was used extensively to various lymphatic malformations (LMs) with excellent result for the macrocystic lesions in particular. 3,4 It still remains a major option when OK-432 (Chugai Pharmaceutical, Tokyo, Japan), also known as picibanil, which is made with attenuated streptococcal exotoxin, is not available for the LM. 5,6 However, we have found bleomycin is generally less effective when the LM is mixed with the VM. Furthermore, the potential concern for pulmonary fibrosis as a long-term complication of bleomycin remains to be answered especially when it is injected to the VM/venous system. This potential long-term concern has led us not to use bleomycin for VM treatment.
Alcohol injections for management of vascular malformations. Clinical case report. Hendro Sudjono Yuwono
 Alcohol injections for management of vascular malformations Clinical case report Hendro Sudjono Yuwono Department of Surgery, School of Medicine, Padjadjaran University Bandung, Indonesia Abstract Vascular
Alcohol injections for management of vascular malformations Clinical case report Hendro Sudjono Yuwono Department of Surgery, School of Medicine, Padjadjaran University Bandung, Indonesia Abstract Vascular
Sclerotherapy after embolization of draining vein: A safe treatment method for venous malformations
 Sclerotherapy after embolization of draining vein: A safe treatment method for venous malformations Yunbo Jin, MD, Xiaoxi Lin, MD, Wei Li, MD, Xiaojie Hu, MD, Gang Ma, andmd, Wei Wang, MD, Shanghai, People
Sclerotherapy after embolization of draining vein: A safe treatment method for venous malformations Yunbo Jin, MD, Xiaoxi Lin, MD, Wei Li, MD, Xiaojie Hu, MD, Gang Ma, andmd, Wei Wang, MD, Shanghai, People
Sonography of soft-tissue vascular lesions
 Sonography of soft-tissue vascular lesions Oscar M. Navarro Associate Professor, University of Toronto Dept. of Diagnostic Imaging, The Hospital for Sick Children Toronto, Canada Declaration of Disclosure
Sonography of soft-tissue vascular lesions Oscar M. Navarro Associate Professor, University of Toronto Dept. of Diagnostic Imaging, The Hospital for Sick Children Toronto, Canada Declaration of Disclosure
From the American Venous Forum
 From the American Venous Forum Predictors of response to percutaneous ethanol sclerotherapy (PES) in patients with venous malformations: Analysis of patient self-assessment and imaging Woo-Sung Yun, MD,
From the American Venous Forum Predictors of response to percutaneous ethanol sclerotherapy (PES) in patients with venous malformations: Analysis of patient self-assessment and imaging Woo-Sung Yun, MD,
DUPLEX-GUIDED FOAM SCLEROTHERAPY FOR THE SYMPTOMATIC VENOUS MALFORMATIONS
 1 Case Report Title of the article: Duplex-guided Foam Sclerotherapy for the Treatment of the Symptomatic Venous Malformations of the face: Report of A Case Brief title Duplex-guided foam sclerotherapy
1 Case Report Title of the article: Duplex-guided Foam Sclerotherapy for the Treatment of the Symptomatic Venous Malformations of the face: Report of A Case Brief title Duplex-guided foam sclerotherapy
Hemangioma of Tongue with Phlebolith: A Rare presentation
 Journal of Government Dental College and Hospital, October 2017, Vol.-04, Issue- 01, P. 20-25 Original article: Hemangioma of Tongue with Phlebolith: A Rare presentation 1 Dr. Jigna S Shah (MDS) 1, 2 Dr.
Journal of Government Dental College and Hospital, October 2017, Vol.-04, Issue- 01, P. 20-25 Original article: Hemangioma of Tongue with Phlebolith: A Rare presentation 1 Dr. Jigna S Shah (MDS) 1, 2 Dr.
Ultrasound of soft-tissue vascular anomalies
 Ultrasound of soft-tissue vascular anomalies Oscar M. Navarro Associate Professor, University of Toronto Dept. of Diagnostic Imaging, The Hospital for Sick Children Toronto, Canada Declaration of Disclosure
Ultrasound of soft-tissue vascular anomalies Oscar M. Navarro Associate Professor, University of Toronto Dept. of Diagnostic Imaging, The Hospital for Sick Children Toronto, Canada Declaration of Disclosure
CHARACTERIZATION OF CONGENITAL VASCULAR MALFORMATION IN THE EXTREMITIES USING WHOLE BODY BLOOD POOL SCINTIGRAPHY AND LYMPHSCINTIGRAPHY
 77 Lymphology 42 (2009) 77-84 CHARACTERIZATION OF CONGENITAL VASCULAR MALFORMATION IN THE EXTREMITIES USING WHOLE BODY BLOOD POOL SCINTIGRAPHY AND LYMPHSCINTIGRAPHY Y.H. Kim, J.Y. Choi, Y.W. Kim, D.I.
77 Lymphology 42 (2009) 77-84 CHARACTERIZATION OF CONGENITAL VASCULAR MALFORMATION IN THE EXTREMITIES USING WHOLE BODY BLOOD POOL SCINTIGRAPHY AND LYMPHSCINTIGRAPHY Y.H. Kim, J.Y. Choi, Y.W. Kim, D.I.
Sclerotherapy for Venous Vascular and Lymphatic Malformations
 Service: Imaging Sclerotherapy for Venous Vascular and Lymphatic Malformations Exceptional healthcare, personally delivered Your doctor has requested that you have sclerotherapy. We hope that the following
Service: Imaging Sclerotherapy for Venous Vascular and Lymphatic Malformations Exceptional healthcare, personally delivered Your doctor has requested that you have sclerotherapy. We hope that the following
Endovascular Therapy for Arteriovenous Malformation
 Endovascular Therapy for Arteriovenous Malformation Wayne F. Yakes, MD Vascular malformations involving the spinal cord are technically challenging clinical entities to diagnosis and ultimately treat.
Endovascular Therapy for Arteriovenous Malformation Wayne F. Yakes, MD Vascular malformations involving the spinal cord are technically challenging clinical entities to diagnosis and ultimately treat.
High-Flow Vascular Malformation of Ear: A Case Report
 256 Ear high-flow vascular malformation Case Report High-Flow Vascular Malformation of Ear: A Case Report Ankit Gupta 1*, Shyam Gupta 1, Akhil Kumar 2, Sameek Bhattacharaya 1, Manoj Jha 1, Vinay Tiwari
256 Ear high-flow vascular malformation Case Report High-Flow Vascular Malformation of Ear: A Case Report Ankit Gupta 1*, Shyam Gupta 1, Akhil Kumar 2, Sameek Bhattacharaya 1, Manoj Jha 1, Vinay Tiwari
Angiographic features of rapidly involuting congenital hemangioma (RICH)
 Pediatr Radiol (2003) 33: 15 19 DOI 10.1007/s00247-002-0726-3 CASE REPORT Orhan Konez Patricia E. Burrows John B. Mulliken Steven J. Fishman Harry P.W. Kozakewich Angiographic features of rapidly involuting
Pediatr Radiol (2003) 33: 15 19 DOI 10.1007/s00247-002-0726-3 CASE REPORT Orhan Konez Patricia E. Burrows John B. Mulliken Steven J. Fishman Harry P.W. Kozakewich Angiographic features of rapidly involuting
Hamburg Classification: Vascular Malformation
 1 2 Hamburg Classification: Vascular Malformation 9 3 Dirk A. Loose and Raul E. Mattassi 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 AU1 Vascular malformations occur
1 2 Hamburg Classification: Vascular Malformation 9 3 Dirk A. Loose and Raul E. Mattassi 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 AU1 Vascular malformations occur
Original Article Study on new classification and treatment of vascular malformations in the extremities
 Int J Clin Exp Med 2018;11(4):4021-4029 www.ijcem.com /ISSN:1940-5901/IJCEM0072003 Original Article Study on new classification and treatment of vascular malformations in the extremities Xuejian Liu, Hailin
Int J Clin Exp Med 2018;11(4):4021-4029 www.ijcem.com /ISSN:1940-5901/IJCEM0072003 Original Article Study on new classification and treatment of vascular malformations in the extremities Xuejian Liu, Hailin
Young patient with swelling of mandible
 HR J Young patient with swelling of mandible, p. 66-71 Clinical Case - Test Yourself Interventional Young patient with swelling of mandible Nikolaos Galanakis 1, Maria Papadaki 2, Dimitrios Tsetis 1 1
HR J Young patient with swelling of mandible, p. 66-71 Clinical Case - Test Yourself Interventional Young patient with swelling of mandible Nikolaos Galanakis 1, Maria Papadaki 2, Dimitrios Tsetis 1 1
Direct percutaneous ethanol instillation for treatment of venous malformation in the face and neck
 British Journal of Plastic Surgery (2005) 58, 1073 1078 Direct percutaneous ethanol instillation for treatment of venous malformation in the face and neck Chih-Hsien Lee, Shyi-Gen Chen* Division of Plastic
British Journal of Plastic Surgery (2005) 58, 1073 1078 Direct percutaneous ethanol instillation for treatment of venous malformation in the face and neck Chih-Hsien Lee, Shyi-Gen Chen* Division of Plastic
PEDIATRICS WK 3 HEAD AND NECK ALISON WALLACE MD, PHD
 PEDIATRICS WK 3 HEAD AND NECK ALISON WALLACE MD, PHD Topics 1. Cervical lymphadenopathy 2. Lymphatic malformation 3. Thyroglossal duct cysts 4. Branchial cleft cysts 5. Thyroid masses CASE 1 Case 1 A 2
PEDIATRICS WK 3 HEAD AND NECK ALISON WALLACE MD, PHD Topics 1. Cervical lymphadenopathy 2. Lymphatic malformation 3. Thyroglossal duct cysts 4. Branchial cleft cysts 5. Thyroid masses CASE 1 Case 1 A 2
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Vascular malformations and their management
 Information for patients Vascular malformations and their management Introduction This leaflet tells you about the condition known as vascular malformation, including venous malformation, arteriovenous
Information for patients Vascular malformations and their management Introduction This leaflet tells you about the condition known as vascular malformation, including venous malformation, arteriovenous
Comment je réponds au clinicien qui me demande de classer (selon ISSVA) une tache de naissance?
 Comment je réponds au clinicien qui me demande de classer (selon ISSVA) une tache de naissance? Ph. Clapuyt, L. Boon Cliniques universitaires saint Luc Université catholique de Louvain 1200 Bruxelles Les
Comment je réponds au clinicien qui me demande de classer (selon ISSVA) une tache de naissance? Ph. Clapuyt, L. Boon Cliniques universitaires saint Luc Université catholique de Louvain 1200 Bruxelles Les
Clinical effects and safety of interventional therapy for parenchyma vascular malformation
 Clinical effects and safety of interventional therapy for parenchyma vascular malformation M.J. Cai 1, W.X. Liang 2, W.W. Mai 1, W.L. He 1 and H.X. Kuang 1 1 Department of Radiology, The Third Affiliated
Clinical effects and safety of interventional therapy for parenchyma vascular malformation M.J. Cai 1, W.X. Liang 2, W.W. Mai 1, W.L. He 1 and H.X. Kuang 1 1 Department of Radiology, The Third Affiliated
Ultrasound imaging of vascular anomalies: pearls and pitfalls
 Ultrasound imaging of vascular anomalies: pearls and pitfalls Oscar Navarro, MD Dept. of Medical Imaging, University of Toronto Dept. of Diagnostic Imaging, The Hospital for Sick Children Declaration of
Ultrasound imaging of vascular anomalies: pearls and pitfalls Oscar Navarro, MD Dept. of Medical Imaging, University of Toronto Dept. of Diagnostic Imaging, The Hospital for Sick Children Declaration of
GLUT-1: an extra diagnostic tool to differentiate between haemangiomas and vascular malformations q
 The British Association of Plastic Surgeons (2005) 58, 348 352 GLUT-1: an extra diagnostic tool to differentiate between haemangiomas and vascular malformations q J. Leon-Villapalos a, K. Wolfe b, L. Kangesu
The British Association of Plastic Surgeons (2005) 58, 348 352 GLUT-1: an extra diagnostic tool to differentiate between haemangiomas and vascular malformations q J. Leon-Villapalos a, K. Wolfe b, L. Kangesu
INFECTION. HIV Infection DWI
 HIV Infection INFECTION DWI Fig Axial CT and MRI images show multiple enlarged lymph nodes in the neck as well as in the parotid gland bilaterally. These nodes were suppurative with positive diffusion.
HIV Infection INFECTION DWI Fig Axial CT and MRI images show multiple enlarged lymph nodes in the neck as well as in the parotid gland bilaterally. These nodes were suppurative with positive diffusion.
2/2/14 INTRODUCTION. Vascular Anomalies: An Introduction to Classification and Coordination of Care. VASCULAR ANOMALIES: History and Classification
 INTRODUCTION Vascular Anomalies: An Introduction to Classification and Coordination of Care Cindy Kerr,RN,MSN,CPNP Erin Spera,RN,MSN,CPNP Mary Beth Sylvia,RN,MS,FNP-BC 1in 3 newborns has a vascular birthmark
INTRODUCTION Vascular Anomalies: An Introduction to Classification and Coordination of Care Cindy Kerr,RN,MSN,CPNP Erin Spera,RN,MSN,CPNP Mary Beth Sylvia,RN,MS,FNP-BC 1in 3 newborns has a vascular birthmark
2. Subarachnoid Hemorrhage
 Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
Traumatic Arteriovenous Malformation of Cheek: A Case Report and Review of Literature
 10.5005/jp-journals-10003-1138 CASE REPORT Traumatic Arteriovenous Malformation of Cheek: A Case Report and Review of Literature Vadisha Srinivas Bhat, Rajeshwary Aroor, B Satheesh Kumar Bhandary, Shama
10.5005/jp-journals-10003-1138 CASE REPORT Traumatic Arteriovenous Malformation of Cheek: A Case Report and Review of Literature Vadisha Srinivas Bhat, Rajeshwary Aroor, B Satheesh Kumar Bhandary, Shama
Sinus and Cerebral Vein Thrombosis
 Sinus and Cerebral Vein Thrombosis A Summary Sinus and cerebral vein clots are uncommon. They can lead to severe headaches, confusion, and stroke-like symptoms. They may lead to bleeding into the surrounding
Sinus and Cerebral Vein Thrombosis A Summary Sinus and cerebral vein clots are uncommon. They can lead to severe headaches, confusion, and stroke-like symptoms. They may lead to bleeding into the surrounding
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Classification des Malformations vasculaires
 Classification des Malformations vasculaires Gilles Soulez, MD, MSc, FSIR Professeur Titulaire et Chairman Dpt Radiologie, Radio-Oncologie et Medecine Nucléaire Université de Montréal Basic principles
Classification des Malformations vasculaires Gilles Soulez, MD, MSc, FSIR Professeur Titulaire et Chairman Dpt Radiologie, Radio-Oncologie et Medecine Nucléaire Université de Montréal Basic principles
Swelling. Size: measure exact size in cm using a tape measure (measure longitudinal and transverse axis and if possible the depth)
 Swelling Inspection Site: exact anatomic position Number: single or multiple Shape: spherical, oval, kidney-shaped or irregular Size: measure exact size in cm using a tape measure (measure longitudinal
Swelling Inspection Site: exact anatomic position Number: single or multiple Shape: spherical, oval, kidney-shaped or irregular Size: measure exact size in cm using a tape measure (measure longitudinal
Rare case of a Congenital Arteriovenous malformation (Park Weber angiodysplasia) around the elbow with median nerve compression
 ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Rare case of a Congenital Arteriovenous malformation (Park Weber angiodysplasia) around the elbow with median nerve compression S
ISPUB.COM The Internet Journal of Orthopedic Surgery Volume 14 Number 1 Rare case of a Congenital Arteriovenous malformation (Park Weber angiodysplasia) around the elbow with median nerve compression S
Treatment of venous malformations direct injection with ethanol
 Treatment of venous malformations direct injection with ethanol by Paula IC Shireman, M_D, Walter J. McCarthy, MD, James S. T. Yao, MD, PhD, and Robert L. Vogelzang, MD, Chicago, Ill. Purpose: Venous malformations
Treatment of venous malformations direct injection with ethanol by Paula IC Shireman, M_D, Walter J. McCarthy, MD, James S. T. Yao, MD, PhD, and Robert L. Vogelzang, MD, Chicago, Ill. Purpose: Venous malformations
TREATMENT OF VENOUS MALFORMATIONS COMPARISON TO LYMPHATIC MALFORMATIONS
 139 Lymphology 41 (2008) 139-146 TREATMENT OF VENOUS MALFORMATIONS COMPARISON TO LYMPHATIC MALFORMATIONS M. Schumacher, U. Ernemann, A. Berlis, J. Weber Department of Neuroradiology, University Hospital
139 Lymphology 41 (2008) 139-146 TREATMENT OF VENOUS MALFORMATIONS COMPARISON TO LYMPHATIC MALFORMATIONS M. Schumacher, U. Ernemann, A. Berlis, J. Weber Department of Neuroradiology, University Hospital
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Supplementary Online Content
 Supplementary Online Content Yu W, Jin Y, Yang J, et al. Occurrence of bruise, hematoma, and pain in upper blepharoplasty using blunt-needle vs sharp-needle anesthetic injection in upper blepharoplasty:
Supplementary Online Content Yu W, Jin Y, Yang J, et al. Occurrence of bruise, hematoma, and pain in upper blepharoplasty using blunt-needle vs sharp-needle anesthetic injection in upper blepharoplasty:
Distinguishing high-flow from low-flow vascular malformations using maximum intensity projection images in dynamic magnetic resonance angiography
 Distinguishing high-flow from low-flow vascular malformations using maximum intensity projection images in dynamic magnetic resonance angiography Poster No.: C-2297 Congress: ECR 2016 Type: Scientific
Distinguishing high-flow from low-flow vascular malformations using maximum intensity projection images in dynamic magnetic resonance angiography Poster No.: C-2297 Congress: ECR 2016 Type: Scientific
Fluoroscopy-guided foam sclerotherapy with sodium morrhuate for peripheral venous malformations: Preliminary experience
 Fluoroscopy-guided foam sclerotherapy with sodium morrhuate for peripheral venous malformations: Preliminary experience Long Li, MD, a Jie Feng, MD, b Xin-Qiao Zeng, BMed, c and Yan-Hao Li, MD, a Guangzhou,
Fluoroscopy-guided foam sclerotherapy with sodium morrhuate for peripheral venous malformations: Preliminary experience Long Li, MD, a Jie Feng, MD, b Xin-Qiao Zeng, BMed, c and Yan-Hao Li, MD, a Guangzhou,
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
Endovascular Management of Head and Neck Vascular Malformations
 Curr Otorhinolaryngol Rep (2014) 2:273 284 DOI 10.1007/s40136-014-0053-x PEDIATRIC VASCULAR MALFORMATIONS OF THE HEAD AND NECK (R ELLURU, SECTION EDITOR) Endovascular Management of Head and Neck Vascular
Curr Otorhinolaryngol Rep (2014) 2:273 284 DOI 10.1007/s40136-014-0053-x PEDIATRIC VASCULAR MALFORMATIONS OF THE HEAD AND NECK (R ELLURU, SECTION EDITOR) Endovascular Management of Head and Neck Vascular
V. CENTRAL NERVOUS SYSTEM TRAUMA
 V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
Abdomen Sonography Examination Content Outline
 Abdomen Sonography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 Anatomy, Perfusion, and Function Pathology, Vascular Abnormalities, Trauma, and Postoperative Anatomy
Abdomen Sonography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 Anatomy, Perfusion, and Function Pathology, Vascular Abnormalities, Trauma, and Postoperative Anatomy
Carotid Cavernous Fistula
 Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
Treatment of Venous Malformations with Ethanolamine Oleate
 20 th Congress of AAPS Treatment of Venous Malformations with Ethanolamine Oleate Bijoy Krishna Das 1 and Shafiqul Hoque, 2 1 Department of Paediatric Surgery, Gono-Shasthaya Samaj Vittik Medical College,
20 th Congress of AAPS Treatment of Venous Malformations with Ethanolamine Oleate Bijoy Krishna Das 1 and Shafiqul Hoque, 2 1 Department of Paediatric Surgery, Gono-Shasthaya Samaj Vittik Medical College,
Interventional Radiology, Shanghai Ninth People s Hospital, Shanghai Jiao Tong University School of Medicine, Shanghai, People s Republic of China.
 ORIGINAL ARTICLE Direct intralesional ethanol sclerotherapy of extensive venous malformations with oropharyngeal involvement after a temporary tracheotomy in the head and neck: Initial results Deming Wang,
ORIGINAL ARTICLE Direct intralesional ethanol sclerotherapy of extensive venous malformations with oropharyngeal involvement after a temporary tracheotomy in the head and neck: Initial results Deming Wang,
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
ORIGINAL RESEARCH. Abstract
 ORIGINAL RESEARCH Ultrasound-guided Intralesional Bleomycin Injection (IBI) for Treatment of Cutaneous Hemangiomas and Vascular Malformations Yousuf Memon 1 *, Nuzhat Irfan Malik 1, Naveed Anjum 2, S.
ORIGINAL RESEARCH Ultrasound-guided Intralesional Bleomycin Injection (IBI) for Treatment of Cutaneous Hemangiomas and Vascular Malformations Yousuf Memon 1 *, Nuzhat Irfan Malik 1, Naveed Anjum 2, S.
Explaining All of the Options for AVM: Cerebral Arteriovenous Malformation
 Explaining All of the Options for AVM: Cerebral Arteriovenous Malformation Recorded on: November 19, 2012 Bernard Bendok, M.D. Director of the Neurointerventional Program Northwestern Memorial Hospital
Explaining All of the Options for AVM: Cerebral Arteriovenous Malformation Recorded on: November 19, 2012 Bernard Bendok, M.D. Director of the Neurointerventional Program Northwestern Memorial Hospital
PACKAGE LEAFLET: INFORMATION FOR THE USER. Fibrovein 3%, 1%, 0.5% and 0.2% Solution for Injection Sodium tetradecyl sulphate
 PACKAGE LEAFLET: INFORMATION FOR THE USER Fibrovein 3%, 1%, 0.5% and 0.2% Solution for Injection Sodium tetradecyl sulphate Read all of this leaflet carefully before you start using this medicine. Keep
PACKAGE LEAFLET: INFORMATION FOR THE USER Fibrovein 3%, 1%, 0.5% and 0.2% Solution for Injection Sodium tetradecyl sulphate Read all of this leaflet carefully before you start using this medicine. Keep
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage. By: Shifaa AlQa qa
 CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
PDF hosted at the Radboud Repository of the Radboud University Nijmegen
 PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/066/5
PDF hosted at the Radboud Repository of the Radboud University Nijmegen The following full text is a publisher's version. For additional information about this publication click this link. http://hdl.handle.net/066/5
Congenital Neck Masses C. Stefan Kénel-Pierre, MD
 Congenital Neck Masses C. Stefan Kénel-Pierre, MD SUNY-LICH Medical Center Department of Surgery Case Presentation xx year old male presents with sudden onset left lower neck swelling x 1 week Denies pain,
Congenital Neck Masses C. Stefan Kénel-Pierre, MD SUNY-LICH Medical Center Department of Surgery Case Presentation xx year old male presents with sudden onset left lower neck swelling x 1 week Denies pain,
Surgical indications: Non-malignant pulmonary diseases. Punnarerk Thongcharoen
 Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
General Imaging. Imaging modalities. Incremental CT. Multislice CT Multislice CT [ MDCT ]
![General Imaging. Imaging modalities. Incremental CT. Multislice CT Multislice CT [ MDCT ] General Imaging. Imaging modalities. Incremental CT. Multislice CT Multislice CT [ MDCT ]](/thumbs/76/74079340.jpg) General Imaging Imaging modalities Conventional X-rays Ultrasonography [ US ] Computed tomography [ CT ] Radionuclide imaging Magnetic resonance imaging [ MRI ] Angiography conventional, CT,MRI Interventional
General Imaging Imaging modalities Conventional X-rays Ultrasonography [ US ] Computed tomography [ CT ] Radionuclide imaging Magnetic resonance imaging [ MRI ] Angiography conventional, CT,MRI Interventional
Vascular Malformations: A Review
 58 Vascular Malformations: A Review Joshua A. Cox, MD 1 Erica Bartlett, MD 1 Edward I. Lee, MD 1 1 Division of Plastic Surgery, Baylor College of Medicine, Houston, Texas Semin Plast Surg 2014;28:58 63.
58 Vascular Malformations: A Review Joshua A. Cox, MD 1 Erica Bartlett, MD 1 Edward I. Lee, MD 1 1 Division of Plastic Surgery, Baylor College of Medicine, Houston, Texas Semin Plast Surg 2014;28:58 63.
The Leeds Teaching Hospitals NHS Trust Thyroid lobectomy
 n The Leeds Teaching Hospitals NHS Trust Thyroid lobectomy Information for patients having surgery at Leeds General Infirmary This leaflet provides information on having a thyroid lobectomy, reasons for
n The Leeds Teaching Hospitals NHS Trust Thyroid lobectomy Information for patients having surgery at Leeds General Infirmary This leaflet provides information on having a thyroid lobectomy, reasons for
Treatment of tongue cavernous haemangioma with direct puncture and sclerotization with ethanol
 case report 75 Treatment of tongue cavernous haemangioma with direct puncture and sclerotization with ethanol Tomaz Seruga, Jernej Lucev, Marko Jevsek Radiology Department, University Medical Centre Maribor,
case report 75 Treatment of tongue cavernous haemangioma with direct puncture and sclerotization with ethanol Tomaz Seruga, Jernej Lucev, Marko Jevsek Radiology Department, University Medical Centre Maribor,
Large Cavernous Hemangioma of the Subscapularis Muscle - A Case Report
 CASE REPORT Clinics in Shoulder and Elbow Vol. 17, No. 4, December, 2014 http://dx.doi.org/10.5397/cise.2014.17.4.185 CiSE Clinics in Shoulder and Elbow Large Cavernous Hemangioma of the Subscapularis
CASE REPORT Clinics in Shoulder and Elbow Vol. 17, No. 4, December, 2014 http://dx.doi.org/10.5397/cise.2014.17.4.185 CiSE Clinics in Shoulder and Elbow Large Cavernous Hemangioma of the Subscapularis
Interventional Treatment VTE: Radiologic Approach
 Interventional Treatment VTE: Radiologic Approach Hae Giu Lee, MD Professor, Dept of Radiology Seoul St. Mary s Hospital The Catholic University of Korea Introduction Incidence High incidence: 250,000-1,000,000/year
Interventional Treatment VTE: Radiologic Approach Hae Giu Lee, MD Professor, Dept of Radiology Seoul St. Mary s Hospital The Catholic University of Korea Introduction Incidence High incidence: 250,000-1,000,000/year
Lung sequestration and Scimitar syndrome
 Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
Lung sequestration and Scimitar syndrome Imaging approaches M. Mearadji International Foundation for Pediatric Imaging Aid Rotterdam, The Netherlands Pulmonary sequestration Pulmonary sequestration (PS)
SCLEROTHERAPY. Cosmetic purposes to improve the appearance of varicose and spider veins
 SCLEROTHERAPY Sclerotherapy effectively treats varicose and spider veins. It's often considered the treatment of choice for small varicose veins. Sclerotherapy involves injecting a solution directly into
SCLEROTHERAPY Sclerotherapy effectively treats varicose and spider veins. It's often considered the treatment of choice for small varicose veins. Sclerotherapy involves injecting a solution directly into
Coronary Arteriovenous Malformation presenting as Acute Myocardial Infarction. Choon Ta NG, Aaron WONG, Foong-Koon CHEAH, Chi Keong CHING
 Coronary Arteriovenous Malformation presenting as Acute Myocardial Infarction Choon Ta NG, Aaron WONG, Foong-Koon CHEAH, Chi Keong CHING The patient 49 year old Male presented with Chest tightness x 1
Coronary Arteriovenous Malformation presenting as Acute Myocardial Infarction Choon Ta NG, Aaron WONG, Foong-Koon CHEAH, Chi Keong CHING The patient 49 year old Male presented with Chest tightness x 1
Case Report. A Surgical Case of Venous Aneurysm of the Cephalic Vein. with Unique Clinicopathological Findings for Venous Dissection
 Case Report A Surgical Case of Venous Aneurysm of the Cephalic Vein with Unique Clinicopathological Findings for Venous Dissection Takashi Kobata, 1 Sohsuke Yamada, 2,3* Ken-ichi Mizutani, 2 Nozomu Kurose,
Case Report A Surgical Case of Venous Aneurysm of the Cephalic Vein with Unique Clinicopathological Findings for Venous Dissection Takashi Kobata, 1 Sohsuke Yamada, 2,3* Ken-ichi Mizutani, 2 Nozomu Kurose,
Percutaneous sclerotherapy for venous malformations in the extremities: clinical outcomes and predictors of patient satisfaction
 Nakamura et al. SpringerPlus 2014, 3:520 a SpringerOpen Journal RESEARCH Open Access Percutaneous sclerotherapy for venous malformations in the extremities: clinical outcomes and predictors of patient
Nakamura et al. SpringerPlus 2014, 3:520 a SpringerOpen Journal RESEARCH Open Access Percutaneous sclerotherapy for venous malformations in the extremities: clinical outcomes and predictors of patient
Hemangiomas and Other Vascular Tumors
 facebook.com/cincykidsrad Hemangiomas and Other Vascular Tumors Disclosures No relevant financial disclosures Bernadette L. Koch, M.D. Departments of Radiology and Pediatrics Cincinnati Children s Hospital
facebook.com/cincykidsrad Hemangiomas and Other Vascular Tumors Disclosures No relevant financial disclosures Bernadette L. Koch, M.D. Departments of Radiology and Pediatrics Cincinnati Children s Hospital
Conflict of Interest: none. Neonatal Airway Masses. Neonatal Respiratory Papillomatosis. Paul J. Samuels, MD
 Paul J. Samuels, MD Professor of Anesthesiology and Pediatrics Director of Education Cincinnati Children s Hospital Cincinnati, Ohio Conflict of Interest: none Neonatal Respiratory Papillomatosis Caused
Paul J. Samuels, MD Professor of Anesthesiology and Pediatrics Director of Education Cincinnati Children s Hospital Cincinnati, Ohio Conflict of Interest: none Neonatal Respiratory Papillomatosis Caused
Management of the Low-Flow Head and Neck Vascular Malformations in Children: the Sclerotherapy Protocol
 Original Article 97 Management of the Low-Flow Head and Neck Vascular Malformations in Children: the Sclerotherapy Protocol Michael Leung 1 Ling Leung 1 Dickson Fung 2 Wai-lun Poon 2 Clarence Liu 1 Kenneth
Original Article 97 Management of the Low-Flow Head and Neck Vascular Malformations in Children: the Sclerotherapy Protocol Michael Leung 1 Ling Leung 1 Dickson Fung 2 Wai-lun Poon 2 Clarence Liu 1 Kenneth
Update on Pediatric Vascular Tumors
 Update on Pediatric Vascular Tumors Jim Treat, MD Associate Professor of Clinical Pediatrics and Dermatology No Relevant Conflicts of Interest PHOTOGRAPHY & VIDEOTAPING ARE STRICTLY PROHIBITED IN ALL EDUCATIONAL
Update on Pediatric Vascular Tumors Jim Treat, MD Associate Professor of Clinical Pediatrics and Dermatology No Relevant Conflicts of Interest PHOTOGRAPHY & VIDEOTAPING ARE STRICTLY PROHIBITED IN ALL EDUCATIONAL
The Surgical Treatment of Migraine Headaches
 The Surgical Treatment of Migraine Headaches Being migraine-free for 11 years has been a dream come true. I live my life now with a freedom that I hadn t known for more than 23 years. Kathy Where is the
The Surgical Treatment of Migraine Headaches Being migraine-free for 11 years has been a dream come true. I live my life now with a freedom that I hadn t known for more than 23 years. Kathy Where is the
Love your legs again Varicose Veins
 Love your legs again Varicose Veins Veins are the vessels that return blood to the heart once it has circulated through the body (as opposed to arteries, which carry oxygen-rich blood from the heart to
Love your legs again Varicose Veins Veins are the vessels that return blood to the heart once it has circulated through the body (as opposed to arteries, which carry oxygen-rich blood from the heart to
The Efficacy of Polidocanol foam Sclerotherapy in Treatment of Infantile Hemangioma and Slow-Flow Vascular Malformation
 The Efficacy of Polidocanol foam Sclerotherapy in Treatment of Infantile Hemangioma and Slow-Flow Vascular Malformation Suhail Ibraheem Kadhum, B.D.S. (1) Thair Abdul Lateef, B.D.S., H.D.D., F.I.B.M.S.
The Efficacy of Polidocanol foam Sclerotherapy in Treatment of Infantile Hemangioma and Slow-Flow Vascular Malformation Suhail Ibraheem Kadhum, B.D.S. (1) Thair Abdul Lateef, B.D.S., H.D.D., F.I.B.M.S.
Diagnostic imaging of cervical vascular malformations
 Diagnostic imaging of cervical vascular malformations Poster No.: C-0781 Congress: ECR 2013 Type: Educational Exhibit Authors: A. Llanes Rivada, D. Dualde-Beltrán, L. Ariño Montaner, J. 1 2 1 1 1 1 1 Joudanin
Diagnostic imaging of cervical vascular malformations Poster No.: C-0781 Congress: ECR 2013 Type: Educational Exhibit Authors: A. Llanes Rivada, D. Dualde-Beltrán, L. Ariño Montaner, J. 1 2 1 1 1 1 1 Joudanin
How varicose veins occur
 Varicose veins are a very common problem, generally appearing as twisting, bulging rope-like cords on the legs, anywhere from groin to ankle. Spider veins are smaller, flatter, red or purple veins closer
Varicose veins are a very common problem, generally appearing as twisting, bulging rope-like cords on the legs, anywhere from groin to ankle. Spider veins are smaller, flatter, red or purple veins closer
Percutaneous endovenous treatment of congenital extratruncular venous malformations with an ultrasound-guided and 810-nm diode laser
 Percutaneous endovenous treatment of congenital extratruncular venous malformations with an ultrasound-guided and 810-nm diode laser XinWu Lu, PhD, MD, Kaichuang Ye, MD, Huihua Shi, MD, Weimin Li, MD,
Percutaneous endovenous treatment of congenital extratruncular venous malformations with an ultrasound-guided and 810-nm diode laser XinWu Lu, PhD, MD, Kaichuang Ye, MD, Huihua Shi, MD, Weimin Li, MD,
World Journal of Surgical Research
 Case Report World Journal of Surgical Research Open Access A Rare Case of Servelle Martorelle Syndrome- Extensive Angio-osteohypotrophic Lesion of Upper Limb Ankur Bhatnagar 1, Mayuresh Deshpande 1, V
Case Report World Journal of Surgical Research Open Access A Rare Case of Servelle Martorelle Syndrome- Extensive Angio-osteohypotrophic Lesion of Upper Limb Ankur Bhatnagar 1, Mayuresh Deshpande 1, V
Vascular Malformations of the Head & Neck
 Vascular Malformations of the Head & Neck Jared Steinklein, MD Lenox Hill Hospital The New York Head & Neck Institute Vascular Birthmark Institute of New York Disclosures The presenter has no financial
Vascular Malformations of the Head & Neck Jared Steinklein, MD Lenox Hill Hospital The New York Head & Neck Institute Vascular Birthmark Institute of New York Disclosures The presenter has no financial
Vessel malformation vascular malformation vascular malformation vascular malformation Vascular malformation vascular malformations
 A vascular malformation is another type of birthmark, or congenital (present at birth) growth, made up of arteries, veins, capillaries, or lymphatic vessels. There are several different types of malformations
A vascular malformation is another type of birthmark, or congenital (present at birth) growth, made up of arteries, veins, capillaries, or lymphatic vessels. There are several different types of malformations
Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury
 Chin J Radiol 2005; 30: 173-177 173 Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury HUI-YI CHEN 1 YING-SHYUAN LI 1 CHUNG-HO CHEN 1
Chin J Radiol 2005; 30: 173-177 173 Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury HUI-YI CHEN 1 YING-SHYUAN LI 1 CHUNG-HO CHEN 1
Sclerosing Agents: Tips & Tricks Session: Liquid Embolics
 Sclerosing Agents: Tips & Tricks Session: Liquid Embolics Jeffrey S. Pollak, M.D. Robert I. White, Jr., M.D. Professor of Interventional Radiology Yale University School of Medicine Department of Radiology
Sclerosing Agents: Tips & Tricks Session: Liquid Embolics Jeffrey S. Pollak, M.D. Robert I. White, Jr., M.D. Professor of Interventional Radiology Yale University School of Medicine Department of Radiology
Interesting Case Series. Ganglion Cyst of the Peroneus Longus
 Interesting Case Series Ganglion Cyst of the Peroneus Longus Andrew A. Marano, BA, Paul J. Therattil, MD, Dare V. Ajibade, MD, PhD, MPH, and Ramazi O. Datiashvili, MD, PhD Division of Plastic and Reconstructive
Interesting Case Series Ganglion Cyst of the Peroneus Longus Andrew A. Marano, BA, Paul J. Therattil, MD, Dare V. Ajibade, MD, PhD, MPH, and Ramazi O. Datiashvili, MD, PhD Division of Plastic and Reconstructive
Lymphangiomas (LMs) are uncommon
 Case Report Paediatrica Indonesiana VOLUME 57 September 2017 Number 5 Preoperative intralesional injection of triamcinolone acetonide for a large head and neck lymphangioma in a baby: a case report Julius
Case Report Paediatrica Indonesiana VOLUME 57 September 2017 Number 5 Preoperative intralesional injection of triamcinolone acetonide for a large head and neck lymphangioma in a baby: a case report Julius
Ultrasound-guided polidocanol foam sclerotherapy for treating venous malformations
 Received: 21 October 2016 Revised: 22 May 2017 Accepted: 22 May 2017 DOI: 10.1002/jcu.22546 RESEARCH ARTICLE Ultrasound-guided polidocanol foam sclerotherapy for treating venous malformations Subhash Kumar
Received: 21 October 2016 Revised: 22 May 2017 Accepted: 22 May 2017 DOI: 10.1002/jcu.22546 RESEARCH ARTICLE Ultrasound-guided polidocanol foam sclerotherapy for treating venous malformations Subhash Kumar
External Jugular Vein Vascular Malformation: Sonographic and MR Imaging Appearances
 AJNR Am J Neuroradiol 25:338 342, February 2004 Case Report External Jugular Vein Vascular Malformation: Sonographic and MR Imaging Appearances Anil T. Ahuja, Hok-Yuen Yuen, Ka-Tak Wong, Ann D. King, Victor
AJNR Am J Neuroradiol 25:338 342, February 2004 Case Report External Jugular Vein Vascular Malformation: Sonographic and MR Imaging Appearances Anil T. Ahuja, Hok-Yuen Yuen, Ka-Tak Wong, Ann D. King, Victor
The field of vascular anomalies has been obscured. Intralesional Sclerotherapy with Polidocanol in the Management of Head and Neck Vascular Lesions
 Main Article Intralesional Sclerotherapy with Polidocanol in the Management of Head and Neck Vascular Lesions Arindam Das, 1 Anindita Sengupta, 2 Debashis Ghosh, 2 Deepjoy Bose, 1 Subhadip Dhara, 2 Arunabha
Main Article Intralesional Sclerotherapy with Polidocanol in the Management of Head and Neck Vascular Lesions Arindam Das, 1 Anindita Sengupta, 2 Debashis Ghosh, 2 Deepjoy Bose, 1 Subhadip Dhara, 2 Arunabha
A Giant Hydronephrotic Kidney with Ureteropelvic Junction Obstruction with Blunt Renal Trauma in a Boy
 A Giant Hydronephrotic Kidney with Ureteropelvic Junction Obstruction with Blunt Renal Trauma in a Boy BY JUNYA TSURUKIRI, HIDEFUMI SANO, YOSUKE TANAKA, TAKAO SATO, HIROKAZU TAGUCHI Abstract An 18-year-old
A Giant Hydronephrotic Kidney with Ureteropelvic Junction Obstruction with Blunt Renal Trauma in a Boy BY JUNYA TSURUKIRI, HIDEFUMI SANO, YOSUKE TANAKA, TAKAO SATO, HIROKAZU TAGUCHI Abstract An 18-year-old
Neuroform Microdelivery Stent System
 Neuroform Microdelivery Stent System Patient Information Booklet TABLE OF CONTENTS What is the Purpose of This Booklet?...2 What is a Wide Neck, Intracranial Aneurysm?...2 What is the Treatment for Wide
Neuroform Microdelivery Stent System Patient Information Booklet TABLE OF CONTENTS What is the Purpose of This Booklet?...2 What is a Wide Neck, Intracranial Aneurysm?...2 What is the Treatment for Wide
Vascular Tumors in Children and Adults. Thuy Phung, MD, PhD Houston Methodist Hospital Texas Children s Hospital Baylor College of Medicine
 Vascular Tumors in Children and Adults Thuy Phung, MD, PhD Houston Methodist Hospital Texas Children s Hospital Baylor College of Medicine What are these lesions? (Marcelo Hochman, MD) What are these lesions?
Vascular Tumors in Children and Adults Thuy Phung, MD, PhD Houston Methodist Hospital Texas Children s Hospital Baylor College of Medicine What are these lesions? (Marcelo Hochman, MD) What are these lesions?
Marc Norman, Ph.D. - Do Not Use without Permission 1. Cerebrovascular Accidents. Marc Norman, Ph.D. Department of Psychiatry
 Cerebrovascular Accidents Marc Norman, Ph.D. Department of Psychiatry Neuropsychiatry and Behavioral Medicine Neuropsychology Clinical Training Seminar 1 5 http://www.nlm.nih.gov/medlineplus/ency/images/ency/fullsize/18009.jpg
Cerebrovascular Accidents Marc Norman, Ph.D. Department of Psychiatry Neuropsychiatry and Behavioral Medicine Neuropsychology Clinical Training Seminar 1 5 http://www.nlm.nih.gov/medlineplus/ency/images/ency/fullsize/18009.jpg
ANGIOPLASTY AND STENTING
 ANGIOPLASTY AND STENTING What is angioplasty and stenting? During an angioplasty, your vascular surgeon inflates a small balloon inside a narrowed blood vessel. This balloon helps to widen your blood vessel
ANGIOPLASTY AND STENTING What is angioplasty and stenting? During an angioplasty, your vascular surgeon inflates a small balloon inside a narrowed blood vessel. This balloon helps to widen your blood vessel
Soft tissue venous malformations may cause musculoskeletal
 ORIGINAL ARTICLE Toe-Walking Attributable to Venous Malformation of the Calf Muscle Benjamin G. Domb, MD,* A. Jay Khanna, MD, * Sally E. Mitchell, MD and Frank J. Frassica, MD* Abstract: Soft tissue venous
ORIGINAL ARTICLE Toe-Walking Attributable to Venous Malformation of the Calf Muscle Benjamin G. Domb, MD,* A. Jay Khanna, MD, * Sally E. Mitchell, MD and Frank J. Frassica, MD* Abstract: Soft tissue venous
CASE REPORT Blocking of the Lymphatic Vessel in Lymphedema
 CASE REPORT Blocking of the Lymphatic Vessel in Lymphedema Hisako Hara, MD, and Makoto Mihara, MD Department of Lymphatic and Reconstructive Surgery, Saiseikai Kawaguchi General Hospital, Saitama, Japan
CASE REPORT Blocking of the Lymphatic Vessel in Lymphedema Hisako Hara, MD, and Makoto Mihara, MD Department of Lymphatic and Reconstructive Surgery, Saiseikai Kawaguchi General Hospital, Saitama, Japan
Head and Neck Vascular Lesions: Characterization of the Flow Pattern by the Use of Three-Phase CT
 Head and Neck Vascular Lesions: Characterization of the Flow Pattern by the Use of Three-Phase CT Chang-Woo Ryu, MD 1 Jae Kyun Kim, MD 2 Sang Joon Kim, MD 3 Jeong Hyun Lee, MD 3 Jeoung Hyun Kim, MD 3 Hong
Head and Neck Vascular Lesions: Characterization of the Flow Pattern by the Use of Three-Phase CT Chang-Woo Ryu, MD 1 Jae Kyun Kim, MD 2 Sang Joon Kim, MD 3 Jeong Hyun Lee, MD 3 Jeoung Hyun Kim, MD 3 Hong
Endo- aneurysmorrhaphy of a giant aneurysm of the subclavian vein
 Endo- aneurysmorrhaphy of a giant aneurysm of the subclavian vein Ahmed Afifi, Ahmed ElGuindy, Mahmoud Farouk, Magdi H Yacoub* * m.yacoub@imperial.ac.uk DOI: http://dx.doi.org/10.5339/gcsp.2012.13 ISSN:
Endo- aneurysmorrhaphy of a giant aneurysm of the subclavian vein Ahmed Afifi, Ahmed ElGuindy, Mahmoud Farouk, Magdi H Yacoub* * m.yacoub@imperial.ac.uk DOI: http://dx.doi.org/10.5339/gcsp.2012.13 ISSN:
Management of arteriovenous malformations: A multidisciplinary approach
 Management of arteriovenous malformations: A multidisciplinary approach Byung-Boong Lee, MD, PhD, FACS, Y. S. Do, MD, Wayne Yakes, MD, D. I. Kim, MD, Raul Mattassi, MD, and W. S. Hyon, MD, Seoul, Korea
Management of arteriovenous malformations: A multidisciplinary approach Byung-Boong Lee, MD, PhD, FACS, Y. S. Do, MD, Wayne Yakes, MD, D. I. Kim, MD, Raul Mattassi, MD, and W. S. Hyon, MD, Seoul, Korea
Originally Posted: November 15, 2014 BRUIT IN THE GROIN
 Originally Posted: November 15, 2014 BRUIT IN THE GROIN Resident(s): Donald ML Tse, MD Attending(s): KT Tan, MD Program/Dept(s): University Health Network/Mount Sinai Hospital, Toronto, ON, Canada CHIEF
Originally Posted: November 15, 2014 BRUIT IN THE GROIN Resident(s): Donald ML Tse, MD Attending(s): KT Tan, MD Program/Dept(s): University Health Network/Mount Sinai Hospital, Toronto, ON, Canada CHIEF
Features compression after open and endovascular operation in vascular malformation
 Features compression after open and endovascular operation in vascular malformation Sapelkin Sergey Institute of Surgery named A.V. Vishnevsky, Moscow, Russia 21.10.2017 CIRC Meeting, Grassau AV-malformations:
Features compression after open and endovascular operation in vascular malformation Sapelkin Sergey Institute of Surgery named A.V. Vishnevsky, Moscow, Russia 21.10.2017 CIRC Meeting, Grassau AV-malformations:
Vascular Ehlers- Danlos in the pediatric population
 Vascular Ehlers- Danlos in the pediatric population Shaine A. Morris, MD, MPH Pediatric Cardiology Texas Children s Hospital, Baylor College of Medicine Objectives Learn what Vascular EDS is, and how it
Vascular Ehlers- Danlos in the pediatric population Shaine A. Morris, MD, MPH Pediatric Cardiology Texas Children s Hospital, Baylor College of Medicine Objectives Learn what Vascular EDS is, and how it
INTERNAL JUGULAR VEIN PHLEBECTASIA PRESENTING WITH HOARSENESS OF VOICE.
 ISSN: 2250-0359 VOLUME 4 ISSUE 2 2014 INTERNAL JUGULAR VEIN PHLEBECTASIA PRESENTING WITH HOARSENESS OF VOICE. Sohini Chakraborty,Pranab Kumar Dey Amrita Roy Kolkatta Medical College India Abstract:- Internal
ISSN: 2250-0359 VOLUME 4 ISSUE 2 2014 INTERNAL JUGULAR VEIN PHLEBECTASIA PRESENTING WITH HOARSENESS OF VOICE. Sohini Chakraborty,Pranab Kumar Dey Amrita Roy Kolkatta Medical College India Abstract:- Internal
