Electrocution is a rare occurrence in adult dogs and
|
|
|
- Arline Emily Watts
- 5 years ago
- Views:
Transcription
1 ELECTROCUTION AND ELECTRICAL CORD INJURY Robert H. Presley, DVM Resident, Small Animal Internal Medicine Douglass K. Macintire, DVM, MS, DACVIM, DACVECC Professor Department of Clinical Sciences College of Veterinary Medicine Auburn University Electrocution is a rare occurrence in adult dogs and cats but is a more common pediatric emergency in veterinary medicine. Electrocution in small animals is most often the result of chewing on electrical cords, although it may rarely occur through exposure to noninsulated wires or downed power lines or from lightning strikes. The type and severity of electrical injury may vary considerably among patients depending on the location on the body and the amperage involved. Amperage is determined by the voltage of the source and the resistance of the animal s body (Ohm s Law: Current in Amperes = Voltage of Source/Resistance). Injury becomes more severe with electrocutions involving either higher voltage or less resistance to electrical flow by the body. Most households in the United States are supplied with both 120V and 240V electrical outlets. Outlets supplied with 240V are reserved for larger appliances, such as clothes dryers or air conditioners. The majority of animal injuries are caused by 120V electrical currents, as these are generally the most common and accessible outlets in the home. Resistance of the body to electrical current also plays a major role in the severity of injury. Dry skin has a very high resistance to electrical flow, thereby allowing less energy to be transferred to the body. However, wet skin or moist mucous membranes (such as the oral cavity) have a low resistance to electrical energy, allowing a high flow of electricity to the tissues and subsequent increased damage. Other factors that must be considered in determining the severity of injury are the type of current involved (AC [alternating current] versus DC [direct current]) and the duration of exposure. AC electricity, which is most common in US households, normally results in more severe injuries at the same amperage than DC electricity. Exposure to AC electricity normally elicits muscular contraction, thus impeding or preventing the animal from releasing the electrical source. Therefore, the exposure time to the electricity is generally much higher than that which occurs with DC, in which muscle tetany does not occur. Damage that occurs from electrocution is mainly derived from two sources: heat generation and electroporation. In cases of high-voltage electrocution, the arcing of electricity from a nearby conductor to the animal s body may generate high-intensity heat. However, most thermal burns are a direct result of electricity passing through the animal s tissues. As electricity flows through tissue, the release of energy causes superheating of intracellular and extracellular fluid, resulting in steam production and necrosis of affected tissue. Damage to this tissue is also propagated by a phenomenon known as electroporation. As the electrical energy travels through tissue, electrical fields disrupt cellular membranes, thus causing osmotic damage to the surrounding cells. The severity of these resultant forces depends on the factors listed above. DIAGNOSTIC CRITERIA Historical Information Gender Predisposition: None. Age Predisposition: Pediatric or young animals are most commonly involved with electrical cord injuries because they are more likely to chew or play with the cords. Breed Predisposition: None Owner Observations: Owners may occasionally witness the incident but are more likely to find their pet in respiratory distress or unconscious near a source of electricity. Exposure to electricity may be evident by the presence of chew marks on a nearby cord or retention of the cord in the animal s mouth as a result of tetanic muscular contraction. Other Historical Considerations/Predispositions: Winter holiday seasons tend to be the most common time of year for electrical injuries to occur, as many households are decorated with low-voltage lighting Questions? Comments? soc.vls@medimedia.com, fax , or post on the Feedback page at 7
2 PREVENTING ELECTRICAL CORD INJURIES Electrical cords should be kept out of reach of animals in the home. During holiday seasons, animals should be kept out of areas with a large amount of decorations, and decorations should be unplugged from wall outlets when animals are unsupervised. Electric heating pads or lamps should be avoided with puppies or kittens. Not only are these items a shock hazard, they may also cause direct thermal burns. Water blankets are a much safer alternative. (i.e., Halloween or Christmas decorations, Christmas trees) that is not normally present in the animal s environment. Also, the winter holidays are a major time of year when puppies or kittens are introduced into homes. Physical Examination Findings Thermal burns: Although burns may be found at any point of contact, they are most commonly found in the oral cavity or commissures of the lips. The severity of these burns may range from mild hyperemia to full-thickness or third-degree burns. Cardiac arrhythmias: Severity and type of arrhythmia vary according to the intensity of electrical exposure. High-amperage current may result in asystole, which often may be converted with cardiopulmonary cerebral resuscitation (CPCR). Lower-amperage current, like that in most household exposures, commonly results in ventricular dysrhythmia or fibrillation. Most presenting animals are tachycardic, although some patients may develop bradycardia as a result of decompensatory shock or hyperkalemia. Respiratory distress: Patients may exhibit apnea, tachypnea, and/or cyanosis. These signs may be a result of neurogenic pulmonary edema, facial or nasopharyngeal edema, or tetanic contraction of the diaphragmatic musculature. Harsh lung sounds or crackles are commonly heard on auscultation. If pulmonary edema occurs, it normally develops within the first few minutes after the electrical shock but may continue to progress over the first 12 to 24 hours. Neurologic disorders: Impaired consciousness, focal muscular tremors, seizures, paresis, or paralysis may be present. Pain. Alterations in blood pressure: Hypertension may be present in patients secondary to pain and/or hyper- dynamic shock; the latter may progress to hypovolemic shock and subsequent hypotension. Hyperthermia. Laboratory Findings Routine complete blood counts and serum chemistries are usually within normal limits. Hypoxia (partial pressure of arterial oxygen, < 90 mm Hg) and/or respiratory acidosis (partial pressure of arterial carbon dioxide, > 40 mm Hg) may occur with development of neurogenic pulmonary edema. Hyperkalemia may occur secondary to tissue necrosis and rhabdomyolysis. Myoglobinemia and/or myoglobinuria. Hemoglobinemia and/or hemoglobinuria. Hypoproteinemia may occur in patients with severe burns. Other Diagnostic Findings Electrocardiogram (ECG): Such abnormalities as sinus tachycardia, ventricular arrhythmias or fibrillation, or heart conduction blockade may be present. Thoracic radiography: May reveal alveolar consolidation, consistent with neurogenic pulmonary edema. This consolidation normally initiates in the caudodorsal lung fields but may progress to other lung lobes. Skull and/or dental radiography: Damage or fractures to teeth and/or mandible may be evident. These may be the result of direct electrical burns or trauma related to tetanic contracture of the masticatory muscles. Abdominal radiography and ultrasonography: May reveal the presence of generalized intestinal ileus secondary to electrical dysrhythmia. Summary of Diagnostic Criteria Diagnosis may be confirmed with owner observation of electrocution. Presence of oral thermal burns may be suggestive but is not diagnostic. Neurogenic pulmonary edema in a young animal is also supportive of electrical cord injury. Differential Diagnosis Oral cavity lesions secondary to electrical burns: Chemical burns. Nonelectrical direct-heat burns. Flame burns. Pulmonary edema: Seizures. Head trauma. Upper airway obstruction. 8 O C T O B E R V O L U M E 7. 9
3 Inhaled toxins. Drug toxicity. Smoke inhalation. Near-drowning. Pulmonary contusions (trauma). Pneumonia. Congenital heart disease with congestive failure. TREATMENT RECOMMENDATIONS Initial Treatment At Time of Electrical Cord Exposure Source of electricity should be shut off, preferably at the electrical panel although the cord may be unplugged from the outlet if conditions permit. Owner or observer should be warned against touching the animal while electricity is still on, as contact could result in spread of the electrical current and electrocution of the person trying to render aid. If the patient is not breathing or is in asystole, CPCR should be started by the owner as quickly as possible. Initial Treatment In the Emergency Clinic Patient s cardiovascular and respiratory status should be evaluated quickly. If no heartbeat is auscultated, CPCR should be initiated immediately. If the patient is unconscious or in respiratory distress, the airway should be evaluated for patency and supplemental oxygen should be provided. Intubation of the patient should be considered if excessive pharyngeal edema or cyanosis is present. Correction of hypovolemic shock should also be initiated. Crystalloids should be used cautiously if pulmonary edema is suspected or present. If possible, the initial bolus should not exceed 20 ml/kg. Colloidal support may be a more appropriate choice to help correct hypovolemic shock in these cases. Hetastarch can be administered in increments of 5 ml/kg up to 20 ml/kg until pulse quality and blood pressure improve. Alternative/Optional Treatments/Therapy Furosemide: 1 to 2 mg/kg IV q6 8h as needed to reduce pulmonary edema. Although this may be beneficial, the use of this medication is controversial. Further discussion is located in the Checkpoints section. $ Positive-pressure mechanical ventilation may be required for patients with severe respiratory distress unresponsive to oxygen supplementation. $$ $$$ CHECKPOINTS Pulmonary edema resulting from electrocution is classified as neurogenic pulmonary edema. The true pathophysiology is currently unknown, but it is believed to be a result of direct vascular barotrauma. Exaggerated increases in sympathetic tone during electrocution (and other pathologic events, such as seizures and head trauma) result in severe vasoconstriction of the pulmonary vasculature. This vasoconstriction produces a substantial increase in pulmonary hydrostatic pressure. Pulmonary edema then forms as a direct result of extravasation of fluid into the alveoli and from hypertension-induced vascular endothelial damage. Benefit from the use of diuretics, such as furosemide, is controversial in patients with neurogenic pulmonary edema. Although pulmonary edema may develop during the initial event, no true fluid volume overload or prolonged pulmonary hypertension occurs. Therefore, the use of diuretics may actually potentiate hypovolemia. This is especially true in patients with severe endothelial damage because increased vascular permeability leads to protein and fluid losses into the alveoli. In most cases, however, furosemide has proven to be beneficial. Although its major mechanism of action occurs at the ascending loop of Henle, furosemide has also been found to have a direct effect on the alveoli. It is believed that furosemide acts on alveolar cells, causing an active pumping of fluid from the airspaces. Therefore, its benefit on pulmonary edema is also direct, not simply a reduction in systemic fluid volume and hydrostatic pressure. Bronchodilators may also be of benefit with respiratory distress: Terbutaline: 0.01 mg/kg SC q6 8h. $ Aminophylline: 6 11 mg/kg IV q8h. $ Albuterol: mg/kg PO q12h. $ Colloidal support (hetastarch, plasma, 10% human albumin) may be useful in cases of severe burns, in which hypoproteinemia may be a complication. Hetastarch: 20 ml/kg/day IV as a constant-rate infusion. $ 10% Human albumin: 1.5 ml/kg/day IV as a constant-rate infusion over 4 6 hours. $ Plasma: ml/kg/day IV as a constant-rate infusion over 4 6 hours. $ STANDARDS of CARE: EMERGENCY AND CRITICAL CARE MEDICINE 9
4 Antiarrythmogenics: Rarely needed in electrical injury but may be required in patients with severe arrhythmias. $ Antiseizure medication: Midazolam or diazepam (0.5 mg/kg IV or rectally) as needed to control seizures. $ Supportive Treatment Supplemental oxygen should be implemented in cases of respiratory distress from pulmonary edema. Nasal oxygen or oxygen-cage therapy normally provides an oxygen concentration of 40%. However, if the patient remains in distress or blood gas values continue to remain unacceptable (partial pressure of arterial oxygen, < 60 mm Hg or partial pressure of arterial carbon dioxide, > 60 mm Hg), nasotracheal oxygen or intubation with mechanical ventilatory support should be considered. $$ $$$ Antibiotics may be necessary, especially with extensive thermal burns. Broad-spectrum antibiotic therapy should be considered. Anaerobic coverage is very important with full-thickness or extensive oral lesions. $ Pain control is also warranted for patients with thermal burns. Opioids are generally the drugs of choice. However, combination drug therapy may be beneficial in patients with severe burns. In dehydrated animals, NSAIDs or glucocorticoids should be avoided or used with extreme caution. Hydromorphone: mg/kg IM, IV, or SC q2 6h. $ Fentanyl: 5 µg/kg bolus IV followed by 5 10 µg/kg/hr IV as a constant-rate infusion. $ Buprenorphine: mg/kg IM, IV, or SC q6 12h. $ Wound care must also be provided. The topic of burn wound management is beyond the scope of this article, although a few points should be considered. Application of chilled sterile saline or cool compresses to burn wounds within 2 hours of the injury helps decrease residual heat, thereby reducing the overall area of tissue destruction. However, the patient must be continuously monitored to prevent development of hypothermia. Topical antibiotics should be applied to the wounds to aid in prevention of bacterial contamination. $ $$ Nutritional support is also critical in patients with extensive burns. To heal adequately, animals with large burn wounds require approximately two to three times their normal caloric needs. For inappetent patients or those with oral burns, other means of delivering nutrients (e.g., nasoesophageal or esophagostomy tubes) should be considered. $ $$ Patient Monitoring Blood gas values and pulse oximetry should be monitored closely over the first 24 to 48 hours to ensure adequate tissue oxygenation and pulmonary function. Serial ECGs or telemetry should be performed to monitor for arrhythmias. Thoracic radiographs should be taken at presentation and every 24 hours thereafter to monitor pulmonary edema. Renal values (blood urea nitrogen, creatinine, urine specific gravity, and urine output) should be monitored to evaluate adequate hydration. Patients should also be monitored for pigmenturia (hemoglobinuria, myoglobinuria) as diuresis may be required to prevent renal tubular toxicity in the face of massive tissue damage. Creatine kinase and serum potassium levels should be evaluated to monitor for hyperkalemia if extensive muscle damage has occurred from thermal burns. Colloidal oncotic pressure, albumin, and total serum protein should also be monitored in patients with large areas of skin necrosis because large amounts of protein are lost in denuded areas. Home Management Home monitoring of patients with electrocution or electrical cord injury is quite variable depending on the type and location of the injury. Milestones/Recovery Time Frames With proper therapy, pulmonary edema usually subsides within 72 hours. Recovery time for thermal burns is quite variable, depending on the size and location of the injuries. Treatment Contraindications Overzealous crystalloid administration should be avoided because it may potentiate pulmonary edema. Colloids may be a better choice in patients with pulmonary edema. Use of corticosteroids is controversial in the therapy of hypovolemic shock and may increase the risk of infection, especially with burn wounds. PROGNOSIS Favorable Criteria Low-amperage electrocution. Low total body surface area of wounds. 10 O C T O B E R V O L U M E 7. 9
5 Thermal burns affecting only the epidermis. Lack of pulmonary edema or resolution of edema within first 24 hours. Unfavorable Criteria Continued respiratory distress with supplemental oxygen and/or requirement of positive-pressure mechanical ventilation. Thermal burns covering more than 50% of total body surface area. Development of uncontrollable cardiac arrhythmias. Continued seizure activity despite therapy. RECOMMENDED READING Faggella AM: Electrical cord and smoke inhalation injuries, in Morgan RV (ed): Handbook of Small Animal Practice. Philadelphia, WB Saunders, 1998, pp Hedlund CS: Surgery of the integumentary system, in Fossum TW (ed): Small Animal Surgery, ed 2. St. Louis, Mosby, 2002, pp Macintire DK: Pediatric emergencies. Proc WVC:125, Macintire DK, Drobatz KJ, Haskins SC, Saxon WD: Manual of Small Animal Emergency and Critical Care Medicine. Philadelphia, Lippincott Williams & Wilkins, 2005, pp Plunkett SJ: Emergency Procedures for the Small Animal Veterinarian, ed 2. Philadelphia, WB Saunders, 2001, pp STANDARDS of CARE: EMERGENCY AND CRITICAL CARE MEDICINE 11
STANDARDS of CARE. Smoke inhalation has been reported relatively EMERGENCY AND CRITICAL CARE MEDICINE SMOKE INHALATION TOXICITY
 Peer Reviewed JULY 2006 STANDARDS of CARE EMERGENCY AND CRITICAL CARE MEDICINE VOL 8.6 FROM THE PUBLISHER OF COMPENDIUM SMOKE INHALATION TOXICITY Jeffery P. Simmons, DVM, MS Visiting Assistant Professor
Peer Reviewed JULY 2006 STANDARDS of CARE EMERGENCY AND CRITICAL CARE MEDICINE VOL 8.6 FROM THE PUBLISHER OF COMPENDIUM SMOKE INHALATION TOXICITY Jeffery P. Simmons, DVM, MS Visiting Assistant Professor
-Cardiogenic: shock state resulting from impairment or failure of myocardium
 Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
Shock chapter Shock -Condition in which tissue perfusion is inadequate to deliver oxygen, nutrients to support vital organs, cellular function -Affects all body systems -Classic signs of early shock: Tachycardia,tachypnea,restlessness,anxiety,
HEAT STROKE. Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC
 HEAT STROKE Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC Heat Stroke More Preventable Than Treatable Heat Stroke A form of hyperthermia associated with a systemic inflammatory response leading
HEAT STROKE Lindsay VaughLindsay Vaughn, DVM, DACVECCDVM, DACVECC Heat Stroke More Preventable Than Treatable Heat Stroke A form of hyperthermia associated with a systemic inflammatory response leading
Restrictive Cardiomyopathy in Cats (a Type of Heart-Muscle Disease) Basics
 Restrictive Cardiomyopathy in Cats (a Type of Heart-Muscle Disease) Basics OVERVIEW The heart of the cat is composed of four chambers; the top two chambers are the left and right atria and the bottom two
Restrictive Cardiomyopathy in Cats (a Type of Heart-Muscle Disease) Basics OVERVIEW The heart of the cat is composed of four chambers; the top two chambers are the left and right atria and the bottom two
Lecture Notes. Chapter 2: Introduction to Respiratory Failure
 Lecture Notes Chapter 2: Introduction to Respiratory Failure Objectives Define respiratory failure, ventilatory failure, and oxygenation failure List the causes of respiratory failure Describe the effects
Lecture Notes Chapter 2: Introduction to Respiratory Failure Objectives Define respiratory failure, ventilatory failure, and oxygenation failure List the causes of respiratory failure Describe the effects
PALS Pulseless Arrest Algorithm.
 PALS Pulseless Arrest Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Bradycardia Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Tachycardia Algorithm. Kleinman M
PALS Pulseless Arrest Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Bradycardia Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Tachycardia Algorithm. Kleinman M
Non-cardiogenic pulmonary oedema
 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2012 Non-cardiogenic pulmonary oedema Glaus, T M Posted at the Zurich Open
Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich www.zora.uzh.ch Year: 2012 Non-cardiogenic pulmonary oedema Glaus, T M Posted at the Zurich Open
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 46 Caring for Clients with Burns Types of Burns Thermal Dry heat flame Moist heat steam or hot liquid
Taking the shock factor out of shock
 Taking the shock factor out of shock Julie Antonellis, BS, LVT, VTS (ECC) Northern Virginia Regional Director for the VALVT Technician Supervisor VCA Animal Emergency Critical Care Business owner Antonellis
Taking the shock factor out of shock Julie Antonellis, BS, LVT, VTS (ECC) Northern Virginia Regional Director for the VALVT Technician Supervisor VCA Animal Emergency Critical Care Business owner Antonellis
ELECTRICAL INJURY 9/21/2015 I HAVE NO DISCLOSURES WE HAVE OBTAINED APPROVAL FOR USE OF IDENTIFIABLE PATIENT PHOTOS
 ELECTRICAL INJURY SAMUEL P. MANDELL, MD, MPH ASSISTANT PROFESSOR OF SURGERY UNIVERSITY OF WASHINGTON SEPTEMBER 28, 2015 I HAVE NO DISCLOSURES WE HAVE OBTAINED APPROVAL FOR USE OF IDENTIFIABLE PATIENT PHOTOS
ELECTRICAL INJURY SAMUEL P. MANDELL, MD, MPH ASSISTANT PROFESSOR OF SURGERY UNIVERSITY OF WASHINGTON SEPTEMBER 28, 2015 I HAVE NO DISCLOSURES WE HAVE OBTAINED APPROVAL FOR USE OF IDENTIFIABLE PATIENT PHOTOS
Rhonda Dixon, DVM Section Head, Emergency and Critical Care Sugar Land Veterinary Specialty and Emergency
 Rhonda Dixon, DVM Section Head, Emergency and Critical Care Sugar Land Veterinary Specialty and Emergency Traumatic Brain Injury Causes Pathophysiology Neurologic assessment Therapeutic Approach Status
Rhonda Dixon, DVM Section Head, Emergency and Critical Care Sugar Land Veterinary Specialty and Emergency Traumatic Brain Injury Causes Pathophysiology Neurologic assessment Therapeutic Approach Status
BRAIN TRAUMA THERAPEUTIC RECOMMENDATIONS
 1 BRAIN TRAUMA THERAPEUTIC RECOMMENDATIONS Richard A. LeCouteur, BVSc, PhD, Dip ACVIM (Neurology), Dip ECVN Professor Emeritus, University of California, Davis, California, USA Definitions Hemorrhage:
1 BRAIN TRAUMA THERAPEUTIC RECOMMENDATIONS Richard A. LeCouteur, BVSc, PhD, Dip ACVIM (Neurology), Dip ECVN Professor Emeritus, University of California, Davis, California, USA Definitions Hemorrhage:
CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2
 CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2 M1 Objectives To understand how resuscitation techniques should be modified in the special circumstances of: Hypothermia Immersion and submersion Poisoning Pregnancy
CARDIAC ARREST IN SPECIAL CIRCUMSTANCES 2 M1 Objectives To understand how resuscitation techniques should be modified in the special circumstances of: Hypothermia Immersion and submersion Poisoning Pregnancy
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
PROTOCOL 1 Endotracheal Intubation (Adult and Pediatric) REQUEST EMT-P RESPONSE DO NOT DELAY TRANSPORT
 PROTOCOL 1 Endotracheal Intubation (Adult and Pediatric) 1. Basic Life Support airway management procedures are initiated. 2. Endotracheal Intubation is indicated under any of the following conditions:
PROTOCOL 1 Endotracheal Intubation (Adult and Pediatric) 1. Basic Life Support airway management procedures are initiated. 2. Endotracheal Intubation is indicated under any of the following conditions:
Lecture Notes. Chapter 9: Smoke Inhalation Injury and Burns
 Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
Lecture Notes Chapter 9: Smoke Inhalation Injury and Burns Objectives List the factors that influence mortality rate Describe the nature of smoke inhalation and the fire environment Recognize the pulmonary
SHOCK AETIOLOGY OF SHOCK (1) Inadequate circulating blood volume ) Loss of Autonomic control of the vasculature (3) Impaired cardiac function
 SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
SHOCK Shock is a condition in which the metabolic needs of the body are not met because of an inadequate cardiac output. If tissue perfusion can be restored in an expeditious fashion, cellular injury may
IV Fluids. I.V. Fluid Osmolarity Composition 0.9% NaCL (Normal Saline Solution, NSS) Uses/Clinical Considerations
 IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT.
 HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
HOW LOW CAN YOU GO? HYPOTENSION AND THE ANESTHETIZED PATIENT. Donna M. Sisak, CVT, LVT, VTS (Anesthesia/Analgesia) Seattle Veterinary Specialists Kirkland, WA dsisak@svsvet.com THE ANESTHETIZED PATIENT
STANDARDS of CARE. Pulmonary edema is defined as the effusion of serous fluid into the EMERGENCY AND CRITICAL CARE MEDICINE
 Visit us at www.vetlearn.com AUGUST 2003 VOL 5.7 STANDARDS of CARE EMERGENCY AND CRITICAL CARE MEDICINE FROM THE PUBLISHER OF COMPENDIUM NONCARDIOGENIC PULMONARY EDEMA Sarah Haldane, BVSC, MACVSc Resident
Visit us at www.vetlearn.com AUGUST 2003 VOL 5.7 STANDARDS of CARE EMERGENCY AND CRITICAL CARE MEDICINE FROM THE PUBLISHER OF COMPENDIUM NONCARDIOGENIC PULMONARY EDEMA Sarah Haldane, BVSC, MACVSc Resident
Acute tumor lysis syndrome (ATLS), although
 ACUTE TUMOR LYSIS SYNDROME Michele Cohen, DVM, DACVIM (Oncology) College of Veterinary Medicine Auburn University Auburn, Alabama Acute tumor lysis syndrome (ATLS), although uncommon, can be a serious
ACUTE TUMOR LYSIS SYNDROME Michele Cohen, DVM, DACVIM (Oncology) College of Veterinary Medicine Auburn University Auburn, Alabama Acute tumor lysis syndrome (ATLS), although uncommon, can be a serious
Understanding the pediatric patient and basics of pediatric emergencies. Dr. Alenka Hrovat Vernik DrVetMed PhD MRCVS
 Understanding the pediatric patient and basics of pediatric emergencies Dr. Alenka Hrovat Vernik DrVetMed PhD MRCVS Stages of development Neonatal period - from birth till 3 rd -4 th week Weaning period
Understanding the pediatric patient and basics of pediatric emergencies Dr. Alenka Hrovat Vernik DrVetMed PhD MRCVS Stages of development Neonatal period - from birth till 3 rd -4 th week Weaning period
ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments
 ADENOSINE Paroxysmal SVT 1 st Dose 6 mg rapid IV 2 nd & 3 rd Doses 12 mg rapid IV push Follow each dose with rapid bolus of 20 ml NS May cause transient heart block or asystole. Side effects include chest
ADENOSINE Paroxysmal SVT 1 st Dose 6 mg rapid IV 2 nd & 3 rd Doses 12 mg rapid IV push Follow each dose with rapid bolus of 20 ml NS May cause transient heart block or asystole. Side effects include chest
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Evidence- Based Medicine Fluid Therapy
 Evidence- Based Medicine Fluid Therapy Ndidi Musa M.D. Assosciate Professor of Pediatrics Medical College of Wisconsin/ Children s Hospital of Wisconsin Disclosures A. I have no relevant financial relationships
Evidence- Based Medicine Fluid Therapy Ndidi Musa M.D. Assosciate Professor of Pediatrics Medical College of Wisconsin/ Children s Hospital of Wisconsin Disclosures A. I have no relevant financial relationships
Proceeding of the LAVECCS
 Close this window to return to IVIS Proceeding of the LAVECCS Congreso Latinoamericano de Emergencia y Cuidados Intensivos Ju1. 28-30, 2011 Santiago de Chile, Chile www.laveccs.org Reprinted in IVIS with
Close this window to return to IVIS Proceeding of the LAVECCS Congreso Latinoamericano de Emergencia y Cuidados Intensivos Ju1. 28-30, 2011 Santiago de Chile, Chile www.laveccs.org Reprinted in IVIS with
SHOCK Susanna Hilda Hutajulu, MD, PhD
 SHOCK Susanna Hilda Hutajulu, MD, PhD Div Hematology and Medical Oncology Department of Internal Medicine Universitas Gadjah Mada Yogyakarta Outline Definition Epidemiology Physiology Classes of Shock
SHOCK Susanna Hilda Hutajulu, MD, PhD Div Hematology and Medical Oncology Department of Internal Medicine Universitas Gadjah Mada Yogyakarta Outline Definition Epidemiology Physiology Classes of Shock
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials
 Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
Neonatal Life Support Provider (NLSP) Certification Preparatory Materials NEONATAL LIFE SUPPORT PROVIDER (NRP) CERTIFICATION TABLE OF CONTENTS NEONATAL FLOW ALGORITHM.2 INTRODUCTION 3 ANTICIPATION OF RESUSCITATION
MANAGEMENT OF THORACIC TRAUMA. Luis H. Tello MV, MS DVM, COS Portland Hospital Classic Banfield Pet Hospital - USA
 MANAGEMENT OF THORACIC TRAUMA Luis H. Tello MV, MS DVM, COS Portland Hospital Classic Banfield Pet Hospital - USA luis.tello@banfield.com Chest Trauma: Big threat!!!! CAUSES OF THORACIC TRAUMA Blunt Trauma
MANAGEMENT OF THORACIC TRAUMA Luis H. Tello MV, MS DVM, COS Portland Hospital Classic Banfield Pet Hospital - USA luis.tello@banfield.com Chest Trauma: Big threat!!!! CAUSES OF THORACIC TRAUMA Blunt Trauma
Preparing for your upcoming PALS course
 IU Health PALS Study Guide Preparing for your upcoming PALS course UPDATED November 2016 Course Curriculum: 2015 American Heart Association (AHA) Guidelines for Pediatric Advanced Life Support (PALS) AHA
IU Health PALS Study Guide Preparing for your upcoming PALS course UPDATED November 2016 Course Curriculum: 2015 American Heart Association (AHA) Guidelines for Pediatric Advanced Life Support (PALS) AHA
How Normal Body Processes Are Altered By Disease and Injury
 1 Chapter 4, GENERAL PRINCIPLES OF PATHOPHYSIOLOGY. Part 1 How Normal Body Processes Are Altered By Disease and Injury 2 How Cells Respond to Change and Injury 3 Pathology & Pathophysiology : the study
1 Chapter 4, GENERAL PRINCIPLES OF PATHOPHYSIOLOGY. Part 1 How Normal Body Processes Are Altered By Disease and Injury 2 How Cells Respond to Change and Injury 3 Pathology & Pathophysiology : the study
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 6.1 Define key terms introduced in this chapter. Slides 11, 15, 17, 26, 27, 31, 33, 37, 40 42, 44, 45, 51, 58 6.2 Describe the basic roles and structures
Introduction to Emergency Medical Care 1 OBJECTIVES 6.1 Define key terms introduced in this chapter. Slides 11, 15, 17, 26, 27, 31, 33, 37, 40 42, 44, 45, 51, 58 6.2 Describe the basic roles and structures
Respiratory Failure. Causes of Acute Respiratory Failure (ARF): a- Intrapulmonary:
 Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
Respiratory failure exists whenever the exchange of O 2 for CO 2 in the lungs cannot keep up with the rate of O 2 consumption & CO 2 production in the cells of the body. This results in a fall in arterial
Right-Sided Congestive Heart Failure Basics
 Right-Sided Congestive Heart Failure Basics OVERVIEW Failure of the right side of the heart to pump blood at a sufficient rate to meet the needs of the body or to prevent blood from pooling within the
Right-Sided Congestive Heart Failure Basics OVERVIEW Failure of the right side of the heart to pump blood at a sufficient rate to meet the needs of the body or to prevent blood from pooling within the
ANESTHETIZING DISEASED PATIENTS: URINARY; NEUROLOGICAL; TRAUMATIZED
 ANESTHETIZING DISEASED PATIENTS: URINARY; NEUROLOGICAL; TRAUMATIZED Lyon Lee DVM PhD DACVA Patients with Urinary Tract Diseases General considerations Three main factors to consider in anesthetizing urinary
ANESTHETIZING DISEASED PATIENTS: URINARY; NEUROLOGICAL; TRAUMATIZED Lyon Lee DVM PhD DACVA Patients with Urinary Tract Diseases General considerations Three main factors to consider in anesthetizing urinary
Trauma Patient. Trauma Patient. Anesthesia of the Acute Trauma Patient
 Anesthesia of the Acute Trauma Patient Stuart Clark Price, DVM, MS, DACVIM, DACVAA University of Illinois College of Veterinary Medicine Trauma Patient Unique challenge to veterinary facility Resource
Anesthesia of the Acute Trauma Patient Stuart Clark Price, DVM, MS, DACVIM, DACVAA University of Illinois College of Veterinary Medicine Trauma Patient Unique challenge to veterinary facility Resource
CHANGES FOR DECEMBER 2008 PREHOSPITAL CARE MANUAL
 CHANGES FOR DECEMBER 2008 PREHOSPITAL CARE MANUAL Item Changed Airway Management Procedure Oral Intubation Procedure Tube Confirmation and Monitoring Procedure C10 Chest Pain/ACS M2 Allergic Reaction/Anaphylaxis
CHANGES FOR DECEMBER 2008 PREHOSPITAL CARE MANUAL Item Changed Airway Management Procedure Oral Intubation Procedure Tube Confirmation and Monitoring Procedure C10 Chest Pain/ACS M2 Allergic Reaction/Anaphylaxis
KASHVET VETERINARIAN RESOURCES FLUID THERAPY AND SELECTION OF FLUIDS
 KASHVET VETERINARIAN RESOURCES FLUID THERAPY AND SELECTION OF FLUIDS INTRODUCTION Formulating a fluid therapy plan for the critical small animal patient requires careful determination of the current volume
KASHVET VETERINARIAN RESOURCES FLUID THERAPY AND SELECTION OF FLUIDS INTRODUCTION Formulating a fluid therapy plan for the critical small animal patient requires careful determination of the current volume
PALS Case Scenario Testing Checklist Respiratory Case Scenario 1 Upper Airway Obstruction
 Respiratory Case Scenario 1 Upper Airway Obstruction Directs administration of 100% oxygen or supplementary oxygen as needed to support oxygenation Identifies signs and symptoms of upper airway obstruction
Respiratory Case Scenario 1 Upper Airway Obstruction Directs administration of 100% oxygen or supplementary oxygen as needed to support oxygenation Identifies signs and symptoms of upper airway obstruction
Shock. Perfusion. The cardiovascular system s circulation of blood and oxygen to all the cells in different tissues and organs of the body
 Shock Chapter 10 Shock State of collapse and failure of the cardiovascular system Leads to inadequate circulation Without adequate blood flow, cells cannot get rid of metabolic wastes The result- hypoperfusion
Shock Chapter 10 Shock State of collapse and failure of the cardiovascular system Leads to inadequate circulation Without adequate blood flow, cells cannot get rid of metabolic wastes The result- hypoperfusion
How Normal Body Processes Are Altered By Disease and Injury
 1 Chapter 4, General Principles of Pathophysiology Part 1 How Normal Body Processes Are Altered By Disease and Injury 2 How Cells Respond to Change and Injury 3 Pathology & Pathophysiology : the study
1 Chapter 4, General Principles of Pathophysiology Part 1 How Normal Body Processes Are Altered By Disease and Injury 2 How Cells Respond to Change and Injury 3 Pathology & Pathophysiology : the study
Dry body skin has a ( higher / lower ) resistance to the flow of the electric current than the internal organs of the body.
 RESISTANCE OF INTERNAL ORGANS (SUCH AS HEART, LUNGS, LIVER, ETC.) Dry body skin has a ( higher / lower ) resistance to the flow of the electric current than the internal organs of the body. 19. Electricity
RESISTANCE OF INTERNAL ORGANS (SUCH AS HEART, LUNGS, LIVER, ETC.) Dry body skin has a ( higher / lower ) resistance to the flow of the electric current than the internal organs of the body. 19. Electricity
Prehospital Care Bundles
 Prehospital s The MLREMS Prehospital s have been created to provide a simple framework to help EMS providers identify the most critical elements when caring for a patient. These bundles do not replace
Prehospital s The MLREMS Prehospital s have been created to provide a simple framework to help EMS providers identify the most critical elements when caring for a patient. These bundles do not replace
Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida
 Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida Reprinted in the IVIS website with the permission of the NAVC http:/// The North American Veterinary Conference
Proceeding of the NAVC North American Veterinary Conference Jan. 8-12, 2005, Orlando, Florida Reprinted in the IVIS website with the permission of the NAVC http:/// The North American Veterinary Conference
Michael Avant, M.D. The Children s Hospital of GHS
 Michael Avant, M.D. The Children s Hospital of GHS OVERVIEW ER to ICU Transition Early Management Priorities the First 48 hours Organ System Support Complications THE FIRST 48 HOURS Communication Damage
Michael Avant, M.D. The Children s Hospital of GHS OVERVIEW ER to ICU Transition Early Management Priorities the First 48 hours Organ System Support Complications THE FIRST 48 HOURS Communication Damage
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02
 PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
PEDIATRIC TREATMENT GUIDELINES - CARDIAC VENTRICULAR FIBRILLATION - PULSELESS VENTRICULAR TACHYCARDIA (SJ-PO1) effective 05/01/02 Revision #5 04/19/02 Identify Dysrhythmia DEFIBRILLATE: 2 J/kg, 4 J/kg,
Steven Berkowitz, DVM Chief, Emergency and Critical Care Saint Francis Veterinary Center
 Steven Berkowitz, DVM Chief, Emergency and Critical Care Saint Francis Veterinary Center Outline Anatomy Common Diseases Interventions Oxygen Therapy Medications Nebulization Coupage Respiratory Tract
Steven Berkowitz, DVM Chief, Emergency and Critical Care Saint Francis Veterinary Center Outline Anatomy Common Diseases Interventions Oxygen Therapy Medications Nebulization Coupage Respiratory Tract
Z19.2 Cross Reference to Patient Care Maps & Clinical Care Procedures
 2017-04-07 Old version G1 Code of Ethics G2 Scope and Function G3 Scene Assessment G4 Triage G5 Primary Survey G6 Shock G7 Load and Go G8 Secondary Survey G9 Unconscious Patient G10A Obstructed Airway
2017-04-07 Old version G1 Code of Ethics G2 Scope and Function G3 Scene Assessment G4 Triage G5 Primary Survey G6 Shock G7 Load and Go G8 Secondary Survey G9 Unconscious Patient G10A Obstructed Airway
PALS Review 2015 Guidelines
 PALS Review 2015 Guidelines BLS CPR BLS CPR changed in 2010. The primary change is from the ABC format to CAB. 1. Scene Safety 2. Establish Unresponsiveness 3. Check for breathing if absent or agonal (No
PALS Review 2015 Guidelines BLS CPR BLS CPR changed in 2010. The primary change is from the ABC format to CAB. 1. Scene Safety 2. Establish Unresponsiveness 3. Check for breathing if absent or agonal (No
Updated Policies and Procedures # s 606, 607, 610, 611, 612, 613, 625, 628, 630, 631, and 633 (ACLS Protocols and Policies)
 SLO County Emergency Medical Services Agency Bulletin 2012-09 PLEASE POST Updated Policies and Procedures # s 606, 607, 610, 611, 612, 613, 625, 628, 630, 631, and 633 (ACLS Protocols and Policies) July
SLO County Emergency Medical Services Agency Bulletin 2012-09 PLEASE POST Updated Policies and Procedures # s 606, 607, 610, 611, 612, 613, 625, 628, 630, 631, and 633 (ACLS Protocols and Policies) July
Calcium (Ca 2+ ) mg/dl
 Quick Guide to Laboratory Values Use this handy cheat-sheet to help you monitor laboratory values related to fluid and electrolyte status. Remember, normal values may vary according to techniques used
Quick Guide to Laboratory Values Use this handy cheat-sheet to help you monitor laboratory values related to fluid and electrolyte status. Remember, normal values may vary according to techniques used
Adult Drug Reference. Dopamine Drip Chart. Pediatric Drug Reference. Pediatric Drug Dosage Charts DRUG REFERENCES
 Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
Atrial Fibrillaton. Key: RA: right atrium RV: right ventricle PA: pulmonic artery LA: left atrium LV: left ventricle AO: aorta
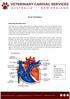 Atrial Fibrillaton How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job of the right
Atrial Fibrillaton How does the heart work? The heart is the organ responsible for pumping blood to and from all tissues of the body. The heart is divided into right and left sides. The job of the right
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of
 Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Objectives. Initial Burn Care and Fluid Resuscitation 6/5/2015 INITIAL MANAGEMENT
 Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Initial Burn Care and Fluid Resuscitation Sarah Taylor MSN, RN, ACNS-BC Clinical Nurse Specialist Trauma Burn Center University of Michigan Health System Ann Arbor, MI Objectives Discuss the initial assessment
Seizures Emergency Treatment
 Seizures Emergency Treatment Emergency Seizures SEIZURE CLASSIFICATION Cluster seizures - 2 or more generalized convulsive seizures in 24 hours Simon R. Platt BVM&S MRCVS Dipl. ACVIM (Neurology) Dipl.ECVN
Seizures Emergency Treatment Emergency Seizures SEIZURE CLASSIFICATION Cluster seizures - 2 or more generalized convulsive seizures in 24 hours Simon R. Platt BVM&S MRCVS Dipl. ACVIM (Neurology) Dipl.ECVN
Nassau Regional Emergency Medical Services. Advanced Life Support Pediatric Protocol Manual
 Nassau Regional Emergency Medical Services Advanced Life Support Pediatric Protocol Manual 2014 PEDIATRIC ADVANCED LIFE SUPPORT PROTOCOLS TABLE OF CONTENTS Approved Effective Newborn Resuscitation P 1
Nassau Regional Emergency Medical Services Advanced Life Support Pediatric Protocol Manual 2014 PEDIATRIC ADVANCED LIFE SUPPORT PROTOCOLS TABLE OF CONTENTS Approved Effective Newborn Resuscitation P 1
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
MICHIGAN. State Protocols. Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.
 MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator
 Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Pediatric Burn Management Justin D. Klein, MD Associate Burn Director Lisa C. Vitale, RN Burn Program Coordinator Lecture Overview Burn statistics and etiologies Pre-hospital evaluation Anatomy of a burn
Cleveland Clinic Regional Hospitals EMS Protocol DRAFT Release Notes. Global Changes
 Cleveland Clinic Regional Hospitals EMS Protocol 2014 DRAFT Release Notes Global Changes Added cautions and stops with selected high risk medications / procedures on protocol tree page for safety Individual
Cleveland Clinic Regional Hospitals EMS Protocol 2014 DRAFT Release Notes Global Changes Added cautions and stops with selected high risk medications / procedures on protocol tree page for safety Individual
a central pulse located at the apex of the heart Apical pulse Apical-radial pulse a complete absence of respirations Apnea
 Afebrile absence of a fever Apical pulse a central pulse located at the apex of the heart Apical-radial pulse measurement of the apical beat and the radial pulse at the same time Apnea a complete absence
Afebrile absence of a fever Apical pulse a central pulse located at the apex of the heart Apical-radial pulse measurement of the apical beat and the radial pulse at the same time Apnea a complete absence
Traumatic Brain Injury
 Traumatic Brain Injury Mark J. Harris M.D. Associate Professor University of Utah Salt Lake City USA Overview In US HI responsible for 33% trauma deaths. Closed HI 80% Missile / Penetrating HI 20% Glasgow
Traumatic Brain Injury Mark J. Harris M.D. Associate Professor University of Utah Salt Lake City USA Overview In US HI responsible for 33% trauma deaths. Closed HI 80% Missile / Penetrating HI 20% Glasgow
Medical APMLE. Podiatry and Medical.
 Medical APMLE Podiatry and Medical http://killexams.com/exam-detail/apmle Question: 290 Signs and symptoms of hemolytic transfusion reactions include: A. Hypothermia B. Hypertension C. Polyuria D. Abnormal
Medical APMLE Podiatry and Medical http://killexams.com/exam-detail/apmle Question: 290 Signs and symptoms of hemolytic transfusion reactions include: A. Hypothermia B. Hypertension C. Polyuria D. Abnormal
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Cor pulmonale. Dr hamid reza javadi
 1 Cor pulmonale Dr hamid reza javadi 2 Definition Cor pulmonale ;pulmonary heart disease; is defined as dilation and hypertrophy of the right ventricle (RV) in response to diseases of the pulmonary vasculature
1 Cor pulmonale Dr hamid reza javadi 2 Definition Cor pulmonale ;pulmonary heart disease; is defined as dilation and hypertrophy of the right ventricle (RV) in response to diseases of the pulmonary vasculature
Burn Priorities of Care: Triage/Treatment/Transfer. Via Christi Regional Burn Center Sarah Fischer, MSN, RN
 Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Burn Priorities of Care: Triage/Treatment/Transfer Via Christi Regional Burn Center Sarah Fischer, MSN, RN Disclosure I have nothing to disclose Objectives Identify American Burn Association referral criteria
Proceedings of the 36th World Small Animal Veterinary Congress WSAVA
 www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
www.ivis.org Proceedings of the 36th World Small Animal Veterinary Congress WSAVA Oct. 14-17, 2011 Jeju, Korea Next Congress: Reprinted in IVIS with the permission of WSAVA http://www.ivis.org 14(Fri)
Prehospital Resuscitation for the 21 st Century Simulation Case. VF/Asystole
 Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Prehospital Resuscitation for the 21 st Century Simulation Case VF/Asystole Case History 1 (hypovolemic cardiac arrest secondary to massive upper GI bleed) 56 year-old male patient who fainted in the presence
Competency Title: Continuous Positive Airway Pressure
 Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Pediatric Resuscitation
 Pediatric Resuscitation Section 24 Pediatric Cardiac Arrest Protocol The successful resuscitation of a child in cardiac arrest is dependent of a systematic approach of initiating life-saving CPR, recognition
Pediatric Resuscitation Section 24 Pediatric Cardiac Arrest Protocol The successful resuscitation of a child in cardiac arrest is dependent of a systematic approach of initiating life-saving CPR, recognition
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
MICHIGAN. Table of Contents. State Protocols. Adult Treatment Protocols
 MICHIGAN State Protocols Protocol Number Protocol Name Adult Treatment Protocols Table of Contents 3.1 Altered Mental Status 3.2 Stroke/Suspected Stroke 3.3 Respiratory Distress 3.4 Seizures 3.5 Sepsis
MICHIGAN State Protocols Protocol Number Protocol Name Adult Treatment Protocols Table of Contents 3.1 Altered Mental Status 3.2 Stroke/Suspected Stroke 3.3 Respiratory Distress 3.4 Seizures 3.5 Sepsis
INDUCED HYPOTHERMIA. F. Ben Housel, M.D.
 INDUCED HYPOTHERMIA F. Ben Housel, M.D. Historical Use of Induced Hypothermia 1950 s - Moderate hypothermia (30-32º C) in open heart surgery to protect brain against global ischemia 1960-1980 s - Use of
INDUCED HYPOTHERMIA F. Ben Housel, M.D. Historical Use of Induced Hypothermia 1950 s - Moderate hypothermia (30-32º C) in open heart surgery to protect brain against global ischemia 1960-1980 s - Use of
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ACLS Prep. Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep.
 November, 2013 ACLS Prep Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep. ACLS Prep Preparation is key to a successful ACLS experience.
November, 2013 ACLS Prep Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep. ACLS Prep Preparation is key to a successful ACLS experience.
Lesson 4-3: Cardiac Emergencies. CARDIAC EMERGENCIES Angina, AMI, CHF and AED
 Lesson 4-3: Cardiac Emergencies CARDIAC EMERGENCIES Angina, AMI, CHF and AED THREE FAMILIAR CARDIAC CONDITIONS Angina Pectoris Acute Myocardial Infarction Congestive Heart Failure ANGINA PECTORIS Chest
Lesson 4-3: Cardiac Emergencies CARDIAC EMERGENCIES Angina, AMI, CHF and AED THREE FAMILIAR CARDIAC CONDITIONS Angina Pectoris Acute Myocardial Infarction Congestive Heart Failure ANGINA PECTORIS Chest
June 2011 Bill Streett-Training Section Chief
 Capnography 102 June 2011 Bill Streett-Training Section Chief Terminology Capnography: the measurement and numerical display of end-tidal CO2 concentration, at the patient s airway, during a respiratory
Capnography 102 June 2011 Bill Streett-Training Section Chief Terminology Capnography: the measurement and numerical display of end-tidal CO2 concentration, at the patient s airway, during a respiratory
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Acute Severe Asthma Document Control Information Author E Randle Author Position CATS Consultant Document Owner E Polke Document Owner Position Co-ordinator
Children s Acute Transport Service Clinical Guidelines Acute Severe Asthma Document Control Information Author E Randle Author Position CATS Consultant Document Owner E Polke Document Owner Position Co-ordinator
LeMone & Burke Ch 30-32
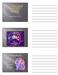 LeMone & Burke Ch 30-32 2 Right side- Low oxygenation Low pressure Light workload Goes toward the lungs Left side High oxygenation Thick walled high pressure Heavier workload Carries oxygenation blood
LeMone & Burke Ch 30-32 2 Right side- Low oxygenation Low pressure Light workload Goes toward the lungs Left side High oxygenation Thick walled high pressure Heavier workload Carries oxygenation blood
Pet owners are often very anxious about veterinary procedures that involve anesthesia. This handout attempts to alleviate some of these concerns.
 Printable Version Anesthesia for Cats Pet owners are often very anxious about veterinary procedures that involve anesthesia. This handout attempts to alleviate some of these concerns. The word anesthesia
Printable Version Anesthesia for Cats Pet owners are often very anxious about veterinary procedures that involve anesthesia. This handout attempts to alleviate some of these concerns. The word anesthesia
Basic Fluid and Electrolytes
 Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Acute Respiratory Distress: The Blue Patient
 E m e rg e n c y M e d i c i n e R E S P I R A T O R Y Peer Reviewed Stacey Leach, DVM, & Deborah Fine, DVM, MS, Diplomate ACVIM University of Missouri Acute Respiratory Distress: The Blue Patient PROFILE
E m e rg e n c y M e d i c i n e R E S P I R A T O R Y Peer Reviewed Stacey Leach, DVM, & Deborah Fine, DVM, MS, Diplomate ACVIM University of Missouri Acute Respiratory Distress: The Blue Patient PROFILE
Brachycephalic Airway Syndrome (Upper Airway Problems Seen in Short-Nosed Breeds) Basics
 Brachycephalic Airway Syndrome (Upper Airway Problems Seen in Short-Nosed Breeds) Basics OVERVIEW Partial upper airway obstruction in short-nosed, flat-faced (brachycephalic) breeds of dogs and cats caused
Brachycephalic Airway Syndrome (Upper Airway Problems Seen in Short-Nosed Breeds) Basics OVERVIEW Partial upper airway obstruction in short-nosed, flat-faced (brachycephalic) breeds of dogs and cats caused
Fundamentals of Pharmacology for Veterinary Technicians Chapter 19
 Figure 19-1 Figure 19-2A Figure 19-2B Figure 19-3 Figure 19-4A1 Figure 19-4A2 Figure 19-4B Figure 19-4C Figure 19-4D Figure 19-5 Figure 19-6A Figure 19-6B A Figure 19-7A B Figure 19-7B C Figure 19-7C D
Figure 19-1 Figure 19-2A Figure 19-2B Figure 19-3 Figure 19-4A1 Figure 19-4A2 Figure 19-4B Figure 19-4C Figure 19-4D Figure 19-5 Figure 19-6A Figure 19-6B A Figure 19-7A B Figure 19-7B C Figure 19-7C D
1 Chapter 10 Shock 2 Shock Shock: Inadequate State of collapse and failure of the system Leads to inadequate circulation Without adequate blood flow,
 1 Chapter 10 Shock 2 Shock Shock: Inadequate State of collapse and failure of the system Leads to inadequate circulation Without adequate blood flow, cannot get rid of metabolic wastes Results in hypoperfusion
1 Chapter 10 Shock 2 Shock Shock: Inadequate State of collapse and failure of the system Leads to inadequate circulation Without adequate blood flow, cannot get rid of metabolic wastes Results in hypoperfusion
Ventricular Tachycardia Basics
 Ventricular Tachycardia Basics OVERVIEW Ventricular refers to the ventricles of the heart; tachycardia is the medical term for rapid heart rate The heart of the dog or cat is composed of four chambers;
Ventricular Tachycardia Basics OVERVIEW Ventricular refers to the ventricles of the heart; tachycardia is the medical term for rapid heart rate The heart of the dog or cat is composed of four chambers;
The ALS Algorithm and Post Resuscitation Care
 The ALS Algorithm and Post Resuscitation Care CET - Ballarat Health Services Valid from 1 st July 2018 to 30 th June 2020 2 Defibrillation Produces simultaneous mass depolarisation of myocardial cells
The ALS Algorithm and Post Resuscitation Care CET - Ballarat Health Services Valid from 1 st July 2018 to 30 th June 2020 2 Defibrillation Produces simultaneous mass depolarisation of myocardial cells
Pediatric Code Blue. Goals of Resuscitation. Focus Conference November Ensure organ perfusion
 Pediatric Code Blue Focus Conference November 2015 Duane C. Williams, MD Pediatric Critical Care Department of Pediatrics Children s Hospital of Richmond at VCU Goals of Resuscitation Ensure organ perfusion
Pediatric Code Blue Focus Conference November 2015 Duane C. Williams, MD Pediatric Critical Care Department of Pediatrics Children s Hospital of Richmond at VCU Goals of Resuscitation Ensure organ perfusion
Dyspnea. Stephanie Lindsay
 Dyspnea Stephanie Lindsay What is dyspnea? An unpleasant sensation of difficult, labored breathing Shortness of air Dyspnea is not the same as tachypnea therefore patients may not present with rapid breathing
Dyspnea Stephanie Lindsay What is dyspnea? An unpleasant sensation of difficult, labored breathing Shortness of air Dyspnea is not the same as tachypnea therefore patients may not present with rapid breathing
ENVIRONMENTAL EMERGENCIES
 Joanna Jakubaszko-Jabłońska ENVIRONMENTAL EMERGENCIES Chair of Emergency Medicine Wroclaw Medical University Emergency treatment of near-drowning victims Clinical findings: The victim may present with
Joanna Jakubaszko-Jabłońska ENVIRONMENTAL EMERGENCIES Chair of Emergency Medicine Wroclaw Medical University Emergency treatment of near-drowning victims Clinical findings: The victim may present with
SHOCK. Pathophysiology
 SHOCK Dr. Ahmed Saleem FICMS TUCOM / 3rd Year / 2015 Shock is the most common and therefore the most important cause of death of surgical patients. Death may occur rapidly due to a profound state of shock,
SHOCK Dr. Ahmed Saleem FICMS TUCOM / 3rd Year / 2015 Shock is the most common and therefore the most important cause of death of surgical patients. Death may occur rapidly due to a profound state of shock,
Acute Respiratory Distress Syndrome (ARDS) An Update
 Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Acute Respiratory Distress Syndrome (ARDS) An Update Prof. A.S.M. Areef Ahsan FCPS(Medicine) MD(Critical Care Medicine) MD ( Chest) Head, Dept. of Critical Care Medicine BIRDEM General Hospital INTRODUCTION
Introduction (1 of 3)
 Chapter 10 Shock Introduction (1 of 3) Shock (hypoperfusion) means a state of collapse and failure of the cardiovascular system. In the early stages, the body attempts to maintain homeostasis. As shock
Chapter 10 Shock Introduction (1 of 3) Shock (hypoperfusion) means a state of collapse and failure of the cardiovascular system. In the early stages, the body attempts to maintain homeostasis. As shock
Printed copies of this document may not be up to date, obtain the most recent version from
 Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
Children s Acute Transport Service Clinical Guidelines Septic Shock Document Control Information Author Claire Fraser P.Ramnarayan Author Position tanp CATS Consultant Document Owner E. Polke Document
3/10/15. Summary. Anatomy Larynx. Anatomy Trachea
 Summary Anatomy Brachycephalic Airway Syndrome (BCAS) Crisis Anatomy Larynx Anatomy Trachea Tracheal rings are incomplete, C-shaped cartilage with the dorsal membrane being completed by tracheal muscle
Summary Anatomy Brachycephalic Airway Syndrome (BCAS) Crisis Anatomy Larynx Anatomy Trachea Tracheal rings are incomplete, C-shaped cartilage with the dorsal membrane being completed by tracheal muscle
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv
 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) Rv.8.18.18 ACUTE RESPIRATORY DISTRESS SYNDROME (ARDS) SUDDEN PROGRESSIVE FORM OF ACUTE RESPIRATORY FAILURE ALVEOLAR CAPILLARY MEMBRANE BECOMES DAMAGED AND MORE
Nursing Process Focus: Patients Receiving Dextran 40 (Gentran 40)
 Assess for presence/history of hypovolemia, shock, venous thrombosis. Assess vital signs: Hypovolemic shock secondary to surgery, burns, hemorrhage, other serious condition PT and PTT abnormalities Venous
Assess for presence/history of hypovolemia, shock, venous thrombosis. Assess vital signs: Hypovolemic shock secondary to surgery, burns, hemorrhage, other serious condition PT and PTT abnormalities Venous
IFT1 Interfacility Transfer of STEMI Patients. IFT2 Interfacility Transfer of Intubated Patients. IFT3 Interfacility Transfer of Stroke Patients
 IFT1 Interfacility Transfer of STEMI Patients IFT2 Interfacility Transfer of Intubated Patients IFT3 Interfacility Transfer of Stroke Patients Interfacility Transfer Guidelines IFT 1 TRANSFER INTERFACILITY
IFT1 Interfacility Transfer of STEMI Patients IFT2 Interfacility Transfer of Intubated Patients IFT3 Interfacility Transfer of Stroke Patients Interfacility Transfer Guidelines IFT 1 TRANSFER INTERFACILITY
