Introduction. Methods
|
|
|
- Logan Sutton
- 5 years ago
- Views:
Transcription
1 Europace (2015) 17, doi: /europace/euu332 CLINICAL RESEARCH Cardiac electrophysiology Electrophysiological studies in patients with paroxysmal supraventricular tachycardias but no electrocardiogram documentation: findings from a prospective registry Joerg Lauschke 1 *, Julia Schneider 1, Ralph Schneider 1, Catharina Nesselmann 2, Tina Tischer 1, Aenne Glass 3, and Dietmar Bänsch 1 1 Department of Cardiology, University Medical Center, Ernst-Heydemann-Str. 6, Rostock 18059, Germany; 2 Department of Cardiac Surgery, University Medical Center, Schillingallee 35, Rostock 18057, Germany; and 3 Institute for Biostatistics and Informatics in Medicine and Ageing Research, University Medical Center, Ernst-Heydemann-Str. 8, Rostock 18057, Germany Received 24 April 2014; accepted after revision 17 October 2014 Aims A significant proportion of patients presenting with paroxysmal supraventricular tachycardia (PSVT) has no electrocardiogram (ECG) documentation. In these patients an electrophysiological study (EPS) may be performed to facilitate the diagnosis.... Methods In a prospective registry we compared the prevalence of inducible arrhythmias and the clinical outcome in 525 patients and results with and without ECG documentation. Compared with patients with a documented PSVT a smaller but substantial proportion of patients (63.7%) without ECG documentation had inducible supraventricular tachycardias (SVT). Atrioventricular nodal reentrant tachycardia was the most common type in both groups. Patients with an inducible SVT and no documentation were significantly younger, had a shorter episode duration and a lower hospitalization rate, which may be the cause for the lacking documentation. Similar to patients with documented PSVTs most of these patients (90.0%) were asymptomatic or clinically improved after the EPS. Even 43% of patients without an inducible tachycardia improved clinically, probably due to a placebo effect of the EPS. In particular, patients between 31 and 60 years of age seemed to benefit from an EPS because they were more likely to have inducible SVTs that could be cured by radiofrequency ablation.... Conclusion Our data show that a substantial proportion of patients with suspected paroxysmal tachycardia, but without ECG documentation, have inducible SVTs and obtain a clear clinical benefit from an EPS. Thus, our data provide justification for using EPS for patients in this category. To the best of our knowledge, ours is the first prospective registry that supports this approach Keywords Paroxysmal supraventricular tachycardia PSVT SVT ECG Ablation Introduction An electrophysiological study (EPS) is recommended for patients with documented symptomatic paroxysmal supraventricular tachycardia (PSVT). 1 However, in clinical practice, a significant proportion of patients with a typical clinical history, but with no previous electrocardiogram (ECG) documentation of the tachycardia, may be referred for an EPS in order to facilitate a definitive diagnosis; however, the outcomes for these patients are unknown. Using a prospective registry, we compared the frequency of inducible and ablated supraventricular tachycardias (SVT) as well as the clinical outcomes among patients referred for suspected paroxysmal supraventricular tachycardia, either with or without ECG documentation. Methods Patients Five hundred and twenty-five consecutive patients, referred to the Rostock University Medical Center for suspected paroxysmal supraventricular * Corresponding author. Tel: ; fax: , address: joerg.lauschke@uni-rostock.de Both authors contributed equally to this work. Published on behalf of the European Society of Cardiology. All rights reserved. & The Author For permissions please journals.permissions@oup.com.
2 802 J. Lauschke et al. What s new? A substantial proportion of patients with suspected paroxysmal supraventricular tachycardias but without an electrocardiogram documentation have inducible tachycardias that are curable by ablation. These patients clearly benefit from an electrophysiological study. The clinical outcome is comparable to patients with a documented tachycardia. tachycardia between 2009 and 2013, were included in the prospective registry. All of them presented with a history of paroxysmal regular tachycardia (regular palpitations, on/off-phenomenon, termination after vagal manoeuvres), either with or without ECG documentation, as assessed by 12 lead ECG, Holter, or an implantable loop recorder. All patients received at least one 24 h Holter by the referring physician. After confirmation of typical symptoms, a physical examination, a 12-lead-ECG, a routine laboratory test, and an EPS were performed in all patients. All patients gave written informed consent prior to the EPS. Patients with overt pre-excitation were excluded from the registry because the diagnosis of atrio-ventricular reentrant tachycardia (AVRT) could be made from the resting 12 lead ECG without an ECG-documented tachycardia. Patients with irregular palpitations highly suggestive of paroxysmal atrial fibrillation were also excluded. Electrophysiological study The EPS was performed under conscious sedation. An octapolar catheter (Webster D-Type, Biosense Webster) was advanced to the coronary sinus (CS) via the left subclavian vein. A second octapolar catheter was placed at the bundle of His via the right femoral vein. A quadripolar catheter (Soloist, Medtronic) was placed in the right ventricular apex via the left femoral vein. For SVT induction, programmed ventricular and atrial stimulation was performed (basic cycle length: 600 ms, 1 3 extra stimuli, stimulation at the Wenckebach point). In the absence of inducible SVT, stimulation was repeated under isoprenaline and atropine. However, when a sustained SVT was induced reproducibly, differentiation of the type of tachycardia was achieved by overdrive ventricular pacing (using atrial entrainment as a proof of principle for reentrant tachycardias), His synchronous PVCs during tachycardia (preceding the A in case of AVRT) and the response to entrainment (VAV vs. VAAV). For right atrial tachycardia, an additional 10 polar catheter was placed in the high right atrium or along the crista terminalis, as required. As a standard procedure, the site of earliest activation under atrial tachycardia (AT) was mapped with a 4 mm tip ablation catheter guided by fluoroscopy. If these attempts failed, a 3D activation map was achieved using Carto 3 (Biosense Webster, Diamond Bar). Ablation of accessory pathways, AV-node modulation, ablation of AT, or atrial flutter was performed according to current guidelines. 1 All ablation catheters had a 4 mm platinum tip. For atrio-ventricular nodal reentrant tachycardia (AVNRT) and AT ablation a non-irrigated catheter was used with a power of W, and a temperature limit of 558C. For ablation of accessory pathways, a non-irrigated catheter with a power of W and a temperature limit of 558C was used. For atrial flutter and atrial fibrillation, an irrigated catheter was used with 40 W/458C and W/438C, respectively. Post-ablation, the stimulation protocol described above was repeated. Follow-up Clinical follow-ups were scheduled in our outpatient clinic at 6, 12, and 18 months after the ablation. Patients who lived far away were monitored by referring physicians who provided reports to our institution. Patients were advised to schedule additional visits if symptoms recurred. Long-term data on the clinical course following the ablation were collected through additional phone calls with the patients, and the patient records were updated accordingly. A recurrent PSVT after ablation was defined as any PSVT lasting longer than 10 s. These recurrences were differentiated into the initially ablated PSVT and other types of PSVT not diagnosed during the first procedure. In the case of a recurrent symptomatic PSVT, a re-ablation was performed if appropriate. Patients who declined a second procedure were treated medically. Statistics Statistical analysis was performed with IBM SPSS Statistics for Windows, version 21.0 (IBM Corp). Descriptive statistics were computed for variables of interest. The statistics computed included means and standard deviations of continuous variables, frequencies, and relative frequencies of categorical factors. Because of no normal distributions, testing for differences of continuous variables between two study groups was accomplished by the Mann Whitney U test by ranks. For categorical factors comparisons between groups were performed by Fisher s exact test or x 2 test. For all tests a ¼ 0.05 was set as statistically significant. For 65 patients with an inducible SVT, but without any documentation, the logistic regression model was used to assess the independence of SVT inducibility from the prognostic factors age, gender, structural heart disease, duration and frequency of symptoms. First, bivariate analyses were performed to look for a significant influence of variables on SVT inducibility. For the parameter episode duration, a dichotomy value of 50 min was used because this was the mean episode duration in 65 patients with inducible SVTs but without ECG documentation. Second, variables yielding P values 0.20 in the bivariate analysis were entered into the multivariate models to highlight some possible associations between the outcome and some covariates that were of borderline significance. All P values resulted from two-sided statistical tests and P 0.05 was considered to be significant. Results In this study, 423 of 525 patients (80.6%) presented with an ECGdocumented PSVT, while 102 patients (19.4%) had a typical history of a PSVT but without any ECG-documented tachycardia. Patients without any ECG documentation had shorter episodes of PSVT (P ¼ 0.02), were younger at presentation for EPS (P, 0.01) and less frequently hospitalized (P, 0.01) than patients with an ECG documented PSVT. The duration of symptoms did not differ significantly between the two groups (P ¼ 0.17). Both groups included more women than men (61.5% in the group with ECG documentation; 70.6% in the group without), but this difference was not statistically significant (P ¼ 0.11). All baseline characteristics are presented in Tables 1 and 2. The mean follow-up period was 30 months. Complete follow-up was recorded for 467 patients (89%). Supraventricular tachycardias could be induced during the EPS in 378 of 423 (89.4%) patients with ECG documentation. The most common type of induced SVTs were AVNRT (249 patients, 58.9%) followed by AVRT (87 patients, 20.6%) and AT (28 patients, 6.6%). The foci of AT were crista terminalis (13 patients, 46.4%), lateral free wall of the right atrium (three patients, 10.7%), right atrial
3 Electrophysiological studies in patients with paroxysmal supraventricular tachycardias 803 Table 1 Baseline characteristics of all patients recruited in the clinical cohort Characteristic All (mean + SD) ECG documentation No ECG documentation P values (mean + SD) (mean + SD)... Gender Female, n (%) 332 (63.2) 260 (61.5) 72 (70.6) 0.11 a Duration of symptoms (years) b Episodes per month b Episode duration (min) b Age at EPS (years) ,0.01 b Age at first symptomatic episode (years) b Hospitalizations ,0.01 b Emergency calls ,0.01 b a Fisher s exact test. b Mann Whitney U test. Table 2 Prevalence of structural heart disease Structural heart disease All (n 5 525) ECG documentation No ECG documentation (n 5 423) (n 5 102)... CAD 57 (10.8%) 50 (11.8%) 7 (6.9%) DCM 4 (0.8%) 4 (1.0%) 0 HCM 2 (0.4%) 2 (0.5%) 0 Other 4 (0.8%) 3 (0.7%) 1 (1.0%) None 452 (86.1%) 361 (85.3%) 91 (89.2%) No data available 6 (1.1%) 3 (0.7%) 3 (2.9%) Distribution not significantly different between patients with and without ECG documentation (x 2 test, P ¼ 0.47). CAD, coronary artery disease; DCM, dilated cardiomyopathy; HCM, hypertrophic cardiomyopathy. appendage (two patients, 7.1%), atrial septum (two patients, 7.1%), CS ostium (one patient, 3.6%), sinus node area (one patient, 3.6%), and mitral annulus (six patients, 21.5%). Supraventricular tachycardia could not be induced in 45 patients (10.6%). Supraventricular tachycardia was reproducibly induced in 65 of 102 patients without any documentation (63.7%). As with the ECGdocumented patient group, AVNRT was found to be the most common SVT (57 patients, 55.9%) among those without documentation. We found low AVRT (two patients, 2.0%), but a comparable rate of AT (five patients, 4.9%). The foci of AT were crista terminalis (three patients, 60%), lateral free wall of the right atrium (1 patient, 20%), and multiple right atrial sites in one patient (20%). In conclusion, the distribution of inducible SVTs differed between patients with and without ECG documentation (x 2 test for the whole 6 2 contingency table, P, 0.01, Table 3). For individual types of inducible SVTs, we found for AVRT and for none significant differences in probabilities between both groups (Fisher s exact test, P, 0.01). In the group with ECG-documented PSVTs, 376 patients (88.9%) were ablated: [249 for AVNRT (58.9%), 87 for concealed accessory pathways (20.6%), 25 for AT (5.9%)]. Fifteen patients (3.5%) received a cavo-tricuspid isthmus ablation for common type atrial flutter, whereas two patients (0.5%) received a pulmonary vein isolation plus lines for left atrial reentrant tachycardias and atrial fibrillation. Thirty-seven of 249 patients ablated for AVNRT (14.8%) presented with a recurrent PSVT, and four of these (1.6%) were AVNRT. Thirtythree patients had other types of PSVT not previously documented or induced: mostly AT and atrial fibrillation. All patients with a recurrent AVNRT were successfully reablated. Sixteen of 87 patients (18.4%) ablated for accessory pathways presented with a recurrent PSVT, 5 of them (5.7%) with the initiallyablatedavrt, and 11 patients with other types of PSVT, mostly AF. Two of the five patients with ablated AVRT were successfully reablated. In one patient, two ablations remained ineffective, whereas two other patients did not show up for a second repetition. Nine of 25 patients (36%) ablated for AT presented with a recurrent PSVT. However, none of these recurrent PSVTs were documented or initially ablated. Most of them had atrial fibrillation or atrial flutter. All 15 patients ablated for common type atrial flutter remained free of atrial flutter. However, five of these developed atrial fibrillation. Two hundred seventy-six patients (71.1%) were free of any symptoms during follow-up, whereas 70 patients (18.0%) had milder symptoms, and 42 patients (10.8%) did not improve clinically (Figure 1). Sixty-four of the 102 patients (62.7%) without ECG documentation were ablated [57 for AVNRT (55.9%), two for a concealed accessory pathway (2.0%) and five for AT (4.9%)]. Eight of the 57 patients (14%) ablated for AVNRT presented with a recurrent PSVT. Seven of
4 804 J. Lauschke et al. Table 3 Types and frequencies of induced SVTs All (n 5 525) ECG documentation No ECG documentation P values a (n 5 423) (n 5 102)... AVNRT 306 (58.3%) 249 (58.9%) 57 (55.9%) 0.66 AVRT 89 (17.0%) 87 (20.6%) 2 (2.0%),0.01 AT 33 (6.3%) 28 (6.6%) 5 (4.9%) AFlut 12 (2.3%) 12 (2.8%) AFib 3 (0.6%) 2 (0.5%) 1 (1.0%) none 82 (15.6%) 45 (10.6%) 37 (36.2%),0.01 Significantly different distribution between patients with and without ECG documentation (chi-square test for the 6 2 contingency table, P, 0.01). AFlut, atrial flutter; AFib, atrial fibrillation. a Fisher s exact test. Number of patients (%) 11% 11% 10% 19% 18% 70% 71% 26% 64% All ECG docu No ECG docu Asymptomatic Improved No change Figure 1 Clinical outcomes in all patients and those with or without ECG documentation. these recurrences were different types of PSVT not addressed in the initial procedure. One patient had a recurrent AVNRT and was successfully reablated. Overall, the recurrence rate after AVNRT ablation was 1.8%. Patients ablated for an accessory pathway were free of any recurrent arrhythmia. One of five patients ablated for AT presented with a recurrent PSVT which was not the initially ablated tachycardia. Supraventricular tachycardia could not be induced in 37 patients (36.2%) without any ECG documentation. Interestingly, 16 (43.2%) of these patients showed no symptoms or milder symptoms after the EP study. Fifty patients (63.7%) were asymptomatic during follow-up, and 21 patients (26.3%) improved clinically. However, eight patients (10.0%) did not show clinical improvement (Figure 1). For all 102 patients without ECG documentation, we compared the markers of age at EPS, and duration of symptoms, between the groups of patients with and without an inducible SVT. Patients with an inducible SVT were significantly older ( vs years, P ¼ 0.01), and were symptomatic for a longer period ( vs years, P, 0.01; Figure 2). Figures 3 and 4 show the inducibility rates for SVTs with respect to age at EPS and the duration of symptoms. Since we were looking for markers of SVT inducibility, we used a logistic regression model for age, gender, structural heart disease, duration, and frequency of symptoms in the group of 65 patients with an inducible SVT, but without any documentation. Additionally, multivariate analysis was performed for the parameters of age at EPS, and duration of symptoms. In patients between 31 and 60 yearsof age at the time of EPS, an inducible SVTwassignificantly more likely than in patients younger than 31 years or older than 60 years of age (odds ratio 3.27, P ¼ 0.03). For the marker duration of symptoms, the differences were not significant. Likewise, no clear differences were noted for all other parameters mentioned above (Tables 4 and 5; Figures 3 and 4). Discussion Compared with patients with a documented PSVT, a smaller but still substantial proportion of patients (63.7%) without ECG documentation had inducible SVTs which could eventually be cured with radiofrequency (RF) ablation. Atrio-ventricular nodal reentrant tachycardia was the most common type of inducible SVT in both groups. Patients with an inducible SVT but with no ECG documentation were significantly younger and also had shorter episode durations and lower hospitalization rates, which may be the cause for the lack of ECG documentation. Among the patients with documented PSVTs, 89.0% were asymptomatic or clinically improved after the EPS. In the group without documentation 90% of patients were asymptomatic or clinically improved after the EPS. Interestingly, 43% of patients without PSVT documentation and without inducible SVT also improved clinically, probably due to a placebo effect from the reassuring information provided by the EPS that no tachycardia could be induced. Considering the clinical outcome following the EPS, 90.0% of all patients who presented with a typical history of paroxysmal SVT, but without a tachycardia ECG showed a clear benefit. In particular, patients between 31 and 60 years of age seem to have benefited most from an EPS, because they were more likely to have inducible SVTs. Surprisingly, our approach did not shorten the time between first symptoms and therapy as the patients without a documented tachycardia probably had milder symptoms. In addition, there was no electrophysiological laboratory available in the area prior to 2009, and patients might have accumulated over a long period of time. The clinical outcome in our registry (AVNRT recurrence rate: 1.8%, AVRT recurrence rate: 5.7%) is in line with published data from a single-centre study and meta-analyses. Feldman et al. 2 reported an acute success rate of 98.1% for AVNRT ablation.
5 Electrophysiological studies in patients with paroxysmal supraventricular tachycardias 805 Age at EPS (years) Not inducible Inducible Not inducible Inducible Figure 2 Comparison of age at EPS (left panel) and duration of symptoms (right panel) between patients with and without an inducible SVT among patients without ECG documentation (n ¼ 102). Shown are the median, the interquartile range (IQR), and minimum and maximum values that are no outliers. Values beyond the quartiles by.1.5 IQRs were defined as outliers, by more than 3.0 IQRs as extreme outliers. Inducibility rate (%) < 31 years years years Age at EPS (years) Figure 3 Inducibility rates for SVTs in 102 patients without ECG documentation according to age at EPS (P ¼ 0.06). Inducibility rate (%) < 11 years years > 20 years Duration of symptoms (years) Figure 4 Inducibility rates for SVTs in 102 patients without ECG documentation according to duration of symptoms (P ¼ 0.20). A meta-analysis by Spector et al 3 found a single-procedure success rate of 93.2% for AVNRT and AVRT ablation, and 91.7% for ablation of atrial flutter with recurrence rates of 6.5% and 13.2%, respectively. Single-centre data published by Schlaepfer and Fromer 4 showed Duration of symptoms (years) Table 4 Univariate logistic regression analysis of predictors of inducibility in 102 patients without ECG documentation Parameter OR 95% CI P values... Duration of symptoms vs. 10 years a vs. 10 years a Episodes per month vs. 1 a vs. 1 a vs. 1 a Episode duration vs. 50 min a Gender 0.34 Female vs. male a Age at EPS vs. 30 years a vs. 30 years a Age at first symptomatic episode vs. 30 years a vs. 30 years a Structural heart disease 0.53 Yes vs. no a OR, odds ratio; CI, confidence interval. a Reference category. that 93% of patients who underwent accessory pathway ablation were asymptomatic or showed clinical improvement during a mean follow-up period of 48 months. They reported a recurrence rate of 4%. In our registry, we noted symptomatic improvement in 89.1% of patients with documented PSVT, and in 90.0% of patients without documented PSVTs, respectively. These results are comparable to the data published by Bathina et al., 5 who reported symptomatic improvement in 84% of patients who underwent RF ablation for documented PSVTs. These findings therefore seem to justify the use of an EP study, even if no paroxysmal SVT has been documented.
6 806 J. Lauschke et al. Table 5 Multivariate logistic regression analysis of predictors of inducibility in 102 patients without ECG documentation Parameter Adjusted 95% CI P values OR... Duration of symptoms vs. 10 years a vs. 10 years a Age at EPS vs. 30 years a vs. 30 years a OR, odds ratio; CI, confidence interval. a Reference category. We observed a recurrence rate for PSVTs not inducible and therefore not ablated in the first procedure (mainly AT, atrial flutter and atrial fibrillation) of 15.4% in patients with and of 12.5% in patients without ECG documentation, respectively. These rather high rates may be due to the strict definition of PSVT recurrence which was any PSVT lasting longer than 10 seconds. Additionally, 33% of patients in our cohort were older than 60 years. Therefore, one might expect a higher incidence of atrial flutter and atrial fibrillation during follow-up. Alternative strategies to force ECG documentation could include either telemetry or an implantable loop recorder (ILR). Although telemetry is non-invasive, the use of telemetry or ILR may be time consuming and the use of ILR in particular may cause additional costs. Conclusion Our data show that a substantial proportion of patients with suspected paroxysmal tachycardias, but without ECG documentation, have inducible SVTs and obtain a clear clinical benefit from an EP study. Thus, our data provide justification for using EPS for patients in this category. To the best of our knowledge, ours is the first prospective registry which supports this approach. Conflict of interest: None declared. References 1. Blomstroem-Lundqvist C, Scheinman MM, Aliot EM, Alpert JS, Calkins H, Camm AJ et al. European Society of Cardiology Committee, NASPE-Heart Rhythm Society. ACC/AHA/ESC guidelines for the management of patients with supraventricular arrhythmias executive summary. A report of the American College of Cardiology/ American Heart Association Task Force on Practice Guidelines and the European Society Of Cardiology Committee For Practice Guidelines (writing committee to develop guidelines for the management of patients with supraventricular arrhythmias) developed in collaboration with NASPE-Heart Rhythm Society. J Am Coll Cardiol 2003; 42: Feldman A, Voskoboinik A, Kumar S, Spence S, Morton JB, Kistler PM et al. Predictors of acute and long-term success of slow pathway ablation for atrioventricular nodal reentrant tachycardia: a single centre series of 1,419 consecutive patients. Pacing Clin Electrophysiol 2011;34: Spector P, Reynolds MR, Calkins H, Sondhi M, Xu Y, Martin A et al. Meta-analysis of ablation of atrial flutter and supraventricular tachycardia. Am J Cardiol 2009; 104: SchlaepferJ, FromerM. Lateclinicaloutcomeaftersuccessful radiofrequencycatheter ablation of accessory pathways. Eur Heart J 2001;22: Bathina MN, Mickelsen S, Brooks C, Jaramillo J, Hepton T, Kusumoto FM. Radiofrequency catheter ablation versus medical therapy for initial treatment of supraventricular tachycardia and its impact on quality of life and healthcare costs. Am J Cardiol 1998;82:
LONG RP TACHYCARDIA MAPPING AND RF ABLATION
 LONG RP TACHYCARDIA MAPPING AND RF ABLATION Dr. Hayam Eldamanhoury Ain shams univeristy Arrhythmia is a too broad topic SVT is broadly defined as narrow complex ( unless aberrant conduction ) Requires
LONG RP TACHYCARDIA MAPPING AND RF ABLATION Dr. Hayam Eldamanhoury Ain shams univeristy Arrhythmia is a too broad topic SVT is broadly defined as narrow complex ( unless aberrant conduction ) Requires
What s new in my specialty?
 What s new in my specialty? Jon Melman, MD Heart Rhythm Specialists McKay-Dee Hospital some would say some would say my specialty 1 some would say my specialty First pacemaker 1958 some would say my specialty
What s new in my specialty? Jon Melman, MD Heart Rhythm Specialists McKay-Dee Hospital some would say some would say my specialty 1 some would say my specialty First pacemaker 1958 some would say my specialty
Case 1 Left Atrial Tachycardia
 Case 1 Left Atrial Tachycardia A 16 years old woman was referred to our institution because of recurrent episodes of palpitations and dizziness despite previous ablation procedure( 13 years ago) of postero-septal
Case 1 Left Atrial Tachycardia A 16 years old woman was referred to our institution because of recurrent episodes of palpitations and dizziness despite previous ablation procedure( 13 years ago) of postero-septal
WPW syndrome and AVRT
 WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
WPW syndrome and AVRT Myung-Yong Lee, MD, PhD Division of Cardiology Department of Internal Medicine School of Medicine Dankook University, Cheonan, Korea Supraventricular tachycardia (SVT) Paroxysmal
Basic Electrophysiology Protocols
 Indian Journal of Cardiology ISSN-0972-1622 2012 by the Indian Society of Cardiology Vol. 15, (3-4), 27-37 [ 27 Review Article Shomu Bohora Assistant Professor, Deptt. of Cardiology, U.N. Mehta Institute
Indian Journal of Cardiology ISSN-0972-1622 2012 by the Indian Society of Cardiology Vol. 15, (3-4), 27-37 [ 27 Review Article Shomu Bohora Assistant Professor, Deptt. of Cardiology, U.N. Mehta Institute
A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence
 www.ipej.org 125 Case Report A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence Miguel A. Arias MD, PhD; Eduardo Castellanos MD, PhD; Alberto Puchol MD;
www.ipej.org 125 Case Report A Narrow QRS Complex Tachycardia With An Apparently Concentric Retrograde Atrial Activation Sequence Miguel A. Arias MD, PhD; Eduardo Castellanos MD, PhD; Alberto Puchol MD;
How to ablate typical slow/fast AV nodal reentry tachycardia
 Europace (2000) 2, 15 19 Article No. eupc.1999.0070, available online at http://www.idealibrary.com on OW TO... SERIES ow to ablate typical slow/fast AV nodal reentry tachycardia. eidbüchel Department
Europace (2000) 2, 15 19 Article No. eupc.1999.0070, available online at http://www.idealibrary.com on OW TO... SERIES ow to ablate typical slow/fast AV nodal reentry tachycardia. eidbüchel Department
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
Supraventricular Tachycardia (SVT) Bruce Stambler, MD Piedmont Heart Atlanta, GA Supraventricular Tachycardia Objectives Types and mechanisms AV nodal reentrant tachycardia (AVNRT) AV reciprocating tachycardia
Case Report Simultaneous Accessory Pathway and AV Node Mechanical Block
 185 Case Report Simultaneous Accessory Pathway and AV Node Mechanical Block Daniel Garofalo, MD, FRACP, Alfonso Gomez Gallanti, MD, David Filgueiras Rama, MD, Rafael Peinado Peinado, PhD, FESC Unidad de
185 Case Report Simultaneous Accessory Pathway and AV Node Mechanical Block Daniel Garofalo, MD, FRACP, Alfonso Gomez Gallanti, MD, David Filgueiras Rama, MD, Rafael Peinado Peinado, PhD, FESC Unidad de
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
Declaration of conflict of interest NONE
 Declaration of conflict of interest NONE Transatlantic Electrophysiology Lessons for and from Iberoamerica European Society of Cardiology Mexican Society of Cardiology Wolff-Parkinson-White Syndrome in
Declaration of conflict of interest NONE Transatlantic Electrophysiology Lessons for and from Iberoamerica European Society of Cardiology Mexican Society of Cardiology Wolff-Parkinson-White Syndrome in
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology
 EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
EHRA Accreditation Exam - Sample MCQs Invasive cardiac electrophysiology Dear EHRA Member, Dear Colleague, As you know, the EHRA Accreditation Process is becoming increasingly recognised as an important
Looks Like VT But Isn't - Successful Ablation Of A Left Free Wall Accessory Pathway With Mahaim-like Properties
 www.ipej.org 112 Case Report Looks Like VT But Isn't - Successful Ablation Of A Left Free Wall Accessory Pathway With Mahaim-like Properties Faizel Osman MD MRCP 1, Peter J Stafford BSc MD FRCP 2, G Andre
www.ipej.org 112 Case Report Looks Like VT But Isn't - Successful Ablation Of A Left Free Wall Accessory Pathway With Mahaim-like Properties Faizel Osman MD MRCP 1, Peter J Stafford BSc MD FRCP 2, G Andre
Bernard Belhassen, MD; Roman Fish, MD; Sami Viskin, MD; Aharon Glick, MD; Michael Glikson, MD; Michael Eldar, MD
 www.ipej.org 3 Original Article Incidence of Dual AV Node Physiology Following Termination of AV Nodal Reentrant Tachycardia by Adenosine-5'-Triphosphate: A Comparison with Drug Administration in Sinus
www.ipej.org 3 Original Article Incidence of Dual AV Node Physiology Following Termination of AV Nodal Reentrant Tachycardia by Adenosine-5'-Triphosphate: A Comparison with Drug Administration in Sinus
Dysrhythmias 11/7/2017. Disclosures. 3 reasons to evaluate and treat dysrhythmias. None. Eliminate symptoms and improve hemodynamics
 Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
the ECG, 6 mg of intravenous adenosine was administered as a fast bolus through a large bore intravenous cannula in
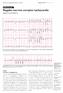 (arrows). Electrocardiography Series Singapore Med.1 2011, 52(3) 146 CME Article Regular narrow complex tachycardia Singh D, Teo S G, Poh K K V Hr JL1 11 VL VF WA, Fig. I ECG shows regular narrow complex
(arrows). Electrocardiography Series Singapore Med.1 2011, 52(3) 146 CME Article Regular narrow complex tachycardia Singh D, Teo S G, Poh K K V Hr JL1 11 VL VF WA, Fig. I ECG shows regular narrow complex
Topographic Distribution of Focal Left Atrial Tachycardias Defined by Electrocardiographic and Electrophysiological Data
 Circ J 2005; 69: 205 210 Topographic Distribution of Focal Left Atrial Tachycardias Defined by Electrocardiographic and Electrophysiological Data Hitoshi Hachiya, MD; Sabine Ernst, MD; Feifan Ouyang, MD;
Circ J 2005; 69: 205 210 Topographic Distribution of Focal Left Atrial Tachycardias Defined by Electrocardiographic and Electrophysiological Data Hitoshi Hachiya, MD; Sabine Ernst, MD; Feifan Ouyang, MD;
Asymptomatic patient with WPW
 Asymptomatic patient with WPW Dimosthenis Avramidis, MD. Arrythmiologist Mitera Children s Hospital Athens Greece Scientific Associate 1st Cardiology Dpt Evangelismos Hospital Athens Greece Preexcitation
Asymptomatic patient with WPW Dimosthenis Avramidis, MD. Arrythmiologist Mitera Children s Hospital Athens Greece Scientific Associate 1st Cardiology Dpt Evangelismos Hospital Athens Greece Preexcitation
Time to recurrence of atrial fibrillation influences outcome following catheter ablation
 Time to recurrence of atrial fibrillation influences outcome following catheter ablation Larraitz Gaztañaga, MD, David S. Frankel, MD, Maria Kohari, MD, Lavanya Kondapalli, MD, Erica S. Zado, PA-C, FHRS,
Time to recurrence of atrial fibrillation influences outcome following catheter ablation Larraitz Gaztañaga, MD, David S. Frankel, MD, Maria Kohari, MD, Lavanya Kondapalli, MD, Erica S. Zado, PA-C, FHRS,
Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing
 Hellenic J Cardiol 2008; 49: 446-450 Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing ELEFTHERIOS GIAZITZOGLOU, DEMOSTHENES G. KATRITSIS Department of Cardiology, Athens
Hellenic J Cardiol 2008; 49: 446-450 Case Report Wide-QRS Tachycardia Inducible by Both Atrial and Ventricular Pacing ELEFTHERIOS GIAZITZOGLOU, DEMOSTHENES G. KATRITSIS Department of Cardiology, Athens
CATHETER ABLATION FOR TACHYCARDIAS
 190 CATHETER ABLATION FOR TACHYCARDIAS MASOOD AKHTAR, M.D. T ACHY ARRHYTHMIAS constitute a major cause of mortality and morbidity. The most serious manifestation of cardiac arrhythmia is sudden cardiac
190 CATHETER ABLATION FOR TACHYCARDIAS MASOOD AKHTAR, M.D. T ACHY ARRHYTHMIAS constitute a major cause of mortality and morbidity. The most serious manifestation of cardiac arrhythmia is sudden cardiac
480 April 2004 PACE, Vol. 27
 Incremental Value of Isolating the Right Inferior Pulmonary Vein During Pulmonary Vein Isolation Procedures in Patients With Paroxysmal Atrial Fibrillation HAKAN ORAL, AMAN CHUGH, CHRISTOPH SCHARF, BURR
Incremental Value of Isolating the Right Inferior Pulmonary Vein During Pulmonary Vein Isolation Procedures in Patients With Paroxysmal Atrial Fibrillation HAKAN ORAL, AMAN CHUGH, CHRISTOPH SCHARF, BURR
EP WIRE on Management Preexcitation syndromes
 EP WIRE on Management Preexcitation syndromes 1. Is your Institution: A University Hospital 70.7% 41 A Private Hospital 13.8% 8 Other Type of Hospital 15.5% 9 Institution name: 50 answered question 58
EP WIRE on Management Preexcitation syndromes 1. Is your Institution: A University Hospital 70.7% 41 A Private Hospital 13.8% 8 Other Type of Hospital 15.5% 9 Institution name: 50 answered question 58
Debate: Asymptomatic Patients with Ventricular Preexcitation Require EP Testing for Risk Stratification. Carlo Pappone, MD, PhD, FACC
 Debate: Asymptomatic Patients with Ventricular Preexcitation Require EP Testing for Risk Stratification Carlo Pappone, MD, PhD, FACC The Wolff-Parkinson-White Syndrome Demographics Δ waves detectable on
Debate: Asymptomatic Patients with Ventricular Preexcitation Require EP Testing for Risk Stratification Carlo Pappone, MD, PhD, FACC The Wolff-Parkinson-White Syndrome Demographics Δ waves detectable on
Ankara, Turkey 2 Department of Cardiology, Division of Arrhythmia and Electrophysiology, Yuksek Ihtisas
 258 Case Report Electroanatomic Mapping-Guided Radiofrequency Ablation of Adenosine Sensitive Incessant Focal Atrial Tachycardia Originating from the Non-Coronary Aortic Cusp in a Child Serhat Koca, MD
258 Case Report Electroanatomic Mapping-Guided Radiofrequency Ablation of Adenosine Sensitive Incessant Focal Atrial Tachycardia Originating from the Non-Coronary Aortic Cusp in a Child Serhat Koca, MD
Atrial Fibrillation and Common Supraventricular Tachycardias. Sunil Kapur MD
 Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
Atrial Fibrillation and Common Supraventricular Tachycardias Sunil Kapur MD Cardiac Electrophysiology Brigham and Women s Hospital Instructor, Harvard Medical School No disclosures Cardiac Conduction:
Since pulmonary veins (PVs) have
 Case Report Hellenic J Cardiol 2011; 52: 371-376 Left Atrial-Pulmonary Vein Reentrant Tachycardia Following Pulmonary Vein Isolation Dionyssios Leftheriotis, Feifan Ouyang, Karl-Heinz Kuck II. Med. Abteilung,
Case Report Hellenic J Cardiol 2011; 52: 371-376 Left Atrial-Pulmonary Vein Reentrant Tachycardia Following Pulmonary Vein Isolation Dionyssios Leftheriotis, Feifan Ouyang, Karl-Heinz Kuck II. Med. Abteilung,
Succesful Radiofrequency Ablation of Atrial Tachycardia Arising From Within the Coronary Venous Sinus
 Succesful Radiofrequency Ablation of Atrial Tachycardia Arising From Within the Coronary Venous Sinus The Harvard community has made this article openly available. Please share how this access benefits
Succesful Radiofrequency Ablation of Atrial Tachycardia Arising From Within the Coronary Venous Sinus The Harvard community has made this article openly available. Please share how this access benefits
Ablation Update and Case Studies. Lawrence Nair, MD, FACC Director of Electrophysiology Presbyterian Heart Group
 Ablation Update and Case Studies Lawrence Nair, MD, FACC Director of Electrophysiology Presbyterian Heart Group Disclosures No financial relationships to disclose Objectives At the conclusion of this activity,
Ablation Update and Case Studies Lawrence Nair, MD, FACC Director of Electrophysiology Presbyterian Heart Group Disclosures No financial relationships to disclose Objectives At the conclusion of this activity,
Catheter ablation of atrial fibrillation: Indications and tools for improvement of the success rate of the method. Konstantinos P.
 Ioannina 2015 Catheter ablation of atrial fibrillation: Indications and tools for improvement of the success rate of the method Konstantinos P. Letsas, MD, FESC SECOND DEPARTMENT OF CARDIOLOGY LABORATORY
Ioannina 2015 Catheter ablation of atrial fibrillation: Indications and tools for improvement of the success rate of the method Konstantinos P. Letsas, MD, FESC SECOND DEPARTMENT OF CARDIOLOGY LABORATORY
Clinical Cardiac Electrophysiology
 Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Clinical Cardiac Electrophysiology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of
Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh
 Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh Arrhythmias and Heart Failure Ventricular Supraventricular VT/VF Primary prevention
Arrhythmias and Heart Failure Dr Chris Lang Consultant Cardiologist and Electrophysiologist Royal Infirmary of Edinburgh Arrhythmias and Heart Failure Ventricular Supraventricular VT/VF Primary prevention
Cardiac Arrhythmias. For Pharmacists
 Cardiac Arrhythmias For Pharmacists Agenda Overview of the normal Classification Management Therapy Conclusion Cardiac arrhythmias Overview of the normal Arrhythmia: definition From the Greek a-, loss
Cardiac Arrhythmias For Pharmacists Agenda Overview of the normal Classification Management Therapy Conclusion Cardiac arrhythmias Overview of the normal Arrhythmia: definition From the Greek a-, loss
Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC
 Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC Professor of Medicine Director of Cardiac Electrophysiology Temple University Health System Plumbing Electrical System Bradyarrhythmias Sinus Node
Arrhythmia Management Joshua M. Cooper, MD, FHRS, FACC Professor of Medicine Director of Cardiac Electrophysiology Temple University Health System Plumbing Electrical System Bradyarrhythmias Sinus Node
A request for a log book extension must be put in writing and sent to BHRS, Unit 6B, Essex House, Cromwell Business Park, Chipping Norton,
 7 7. A request for a log book extension must be put in writing and sent to BHRS, Unit 6B, Essex House, Cromwell Business Park, Chipping Norton, Oxfordshire OX7 5SR. E-mail: admin@bhrs.com. Tel: 01789 867
7 7. A request for a log book extension must be put in writing and sent to BHRS, Unit 6B, Essex House, Cromwell Business Park, Chipping Norton, Oxfordshire OX7 5SR. E-mail: admin@bhrs.com. Tel: 01789 867
Case-Based Practical ECG Interpretation for the Generalist
 Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Case-Based Practical ECG Interpretation for the Generalist Paul D. Varosy, MD, FACC, FAHA, FHRS Director of Cardiac Electrophysiology VA Eastern Colorado Health Care System Associate Professor of Medicine
Ectopic Atrial Tachycardia
 Europace Madrid, 26-29 June 2011 Ectopic Atrial Tachycardia P. Loh, MD, PhD University of Utrecht Division Heart & Lungs Epidemiology Nonsustained atrial tachycardia Frequent finding on holter registrations
Europace Madrid, 26-29 June 2011 Ectopic Atrial Tachycardia P. Loh, MD, PhD University of Utrecht Division Heart & Lungs Epidemiology Nonsustained atrial tachycardia Frequent finding on holter registrations
Supraventricular Tachycardia (SVT)
 Supraventricular Tachycardia (SVT) Daniel Frisch, MD Cardiology Division, Electrophysiology Section Thomas Jefferson University Hospital daniel.frisch@jefferson.edu Short RP Are these the Mid same RP tachycardias?
Supraventricular Tachycardia (SVT) Daniel Frisch, MD Cardiology Division, Electrophysiology Section Thomas Jefferson University Hospital daniel.frisch@jefferson.edu Short RP Are these the Mid same RP tachycardias?
TACHYARRHYTHMIAs. Pawel Balsam, MD, PhD
 TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
TACHYARRHYTHMIAs Pawel Balsam, MD, PhD SupraVentricular Tachycardia Atrial Extra Systole Sinus Tachycardia Focal A. Tachycardia AVRT AVNRT Atrial Flutter Atrial Fibrillation Ventricular Tachycardia Ventricular
CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint
 CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Clinical Cardiac Electrophysiology MOC exam blueprint Based on feedback
CLINICAL CARDIAC ELECTROPHYSIOLOGY Maintenance of Certification (MOC) Examination Blueprint ABIM invites diplomates to help develop the Clinical Cardiac Electrophysiology MOC exam blueprint Based on feedback
Catheter Ablation for Cardiac Arrhythmias
 Catheter Ablation for Cardiac Arrhythmias Policy Number: 2.02.01 Last Review: 5/1/2018 Origination: 05/2015 Next Review: 5/1/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide
Catheter Ablation for Cardiac Arrhythmias Policy Number: 2.02.01 Last Review: 5/1/2018 Origination: 05/2015 Next Review: 5/1/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide
Differential diagnosis and pacing in maneuvers narrow QRS tachycardia. Richard Schilling
 Differential diagnosis and pacing in maneuvers narrow QRS tachycardia Richard Schilling Differential diagnosis of narrow complex QRS tachycardia Anything that activates the ventricle normally via the His
Differential diagnosis and pacing in maneuvers narrow QRS tachycardia Richard Schilling Differential diagnosis of narrow complex QRS tachycardia Anything that activates the ventricle normally via the His
PARA-HISSIAN CONCEALED ACCESSORY PATHWAY
 PARA-HISSIAN CONCEALED ACCESSORY PATHWAY Anamnestic Findings 41 y.o. man with normal cardiac findings on echocardiography, suffering for paroxysmal supra-ventricular tachycardia since 1982 with rapid onset
PARA-HISSIAN CONCEALED ACCESSORY PATHWAY Anamnestic Findings 41 y.o. man with normal cardiac findings on echocardiography, suffering for paroxysmal supra-ventricular tachycardia since 1982 with rapid onset
Focal Atrial Tachycardia Originating From the Non-Coronary Aortic Sinus Electrophysiological Characteristics and Catheter Ablation
 Journal of the American College of Cardiology Vol. 48, No. 1, 2006 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.02.053
Journal of the American College of Cardiology Vol. 48, No. 1, 2006 2006 by the American College of Cardiology Foundation ISSN 0735-1097/06/$32.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2006.02.053
Paroxysmal Supraventricular Tachycardia PSVT.
 Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Supraventricular Tachycardia: From Fetus to Adult. Mohamed Hamdan, MD
 Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
Raphael Rosso MD, Yuval Levi Med. Eng., Sami Viskin MD Tel Aviv Sourasky Medical Center
 Radiofrequency Ablation of Atrial Fibrillation: Comparison of Success Rate of Circular Ablation vs Point-by-Point Ablation with Contact Force Assessment in Paroxysmal and Persistent Atrial Fibrillation
Radiofrequency Ablation of Atrial Fibrillation: Comparison of Success Rate of Circular Ablation vs Point-by-Point Ablation with Contact Force Assessment in Paroxysmal and Persistent Atrial Fibrillation
ACCESSORY PATHWAYS AND SVT. Neil Grubb Royal Infirmary of Edinburgh
 ACCESSORY PATHWAYS AND SVT Neil Grubb Royal Infirmary of Edinburgh Bypass tracts - properties accessory AV connections usually endocardial may exhibit unidirectional conduction conduction properties similar
ACCESSORY PATHWAYS AND SVT Neil Grubb Royal Infirmary of Edinburgh Bypass tracts - properties accessory AV connections usually endocardial may exhibit unidirectional conduction conduction properties similar
APPROACH TO TACHYARRYTHMIAS
 APPROACH TO TACHYARRYTHMIAS PROF.DR.MD.ZAKIR HOSSAIN PROFESSOR AND HEAD DEPARTMENT OF MEDICINE SZMCH TACHYARRYTHMIA Cardiac arrythmia is a disturbance of electrical rhythm of heart. Cardac arrythmia with
APPROACH TO TACHYARRYTHMIAS PROF.DR.MD.ZAKIR HOSSAIN PROFESSOR AND HEAD DEPARTMENT OF MEDICINE SZMCH TACHYARRYTHMIA Cardiac arrythmia is a disturbance of electrical rhythm of heart. Cardac arrythmia with
Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
 Journal of Geriatric Cardiology (2018) 15: 193 198 2018 JGC All rights reserved; www.jgc301.com Case Report Open Access Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
Journal of Geriatric Cardiology (2018) 15: 193 198 2018 JGC All rights reserved; www.jgc301.com Case Report Open Access Repetitive narrow QRS tachycardia in a 61-year-old female patient with recent palpitations
AF Today: W. For the majority of patients with atrial. are the Options? Chris Case
 AF Today: W hat are the Options? Management strategies for patients with atrial fibrillation should depend on the individual patient. Treatment with medications seems adequate for most patients with atrial
AF Today: W hat are the Options? Management strategies for patients with atrial fibrillation should depend on the individual patient. Treatment with medications seems adequate for most patients with atrial
Successful treatment of tachycardia-induced cardiomyopathy secondary to dual atrioventricular nodal nonreentrant tachycardia using cryoablation
 Successful treatment of tachycardia-induced cardiomyopathy secondary to dual atrioventricular nodal nonreentrant tachycardia using cryoablation Harold Rivner, MD, * Chris Healy, MD, Raul D. Mitrani, MD,
Successful treatment of tachycardia-induced cardiomyopathy secondary to dual atrioventricular nodal nonreentrant tachycardia using cryoablation Harold Rivner, MD, * Chris Healy, MD, Raul D. Mitrani, MD,
Measuring the refractory period threshold of AV-node after Radiofrequency ablation
 J. Appl. Environ. Biol. Sci., 6(3)146-151, 2016 2016, TextRoad Publication ISSN: 2090-4274 Journal of Applied Environmental and Biological Sciences www.textroad.com Measuring the refractory period threshold
J. Appl. Environ. Biol. Sci., 6(3)146-151, 2016 2016, TextRoad Publication ISSN: 2090-4274 Journal of Applied Environmental and Biological Sciences www.textroad.com Measuring the refractory period threshold
CATHETER ABLATION CODING & REIMBURSEMENT GUIDE. Updated September 2018
 CATHETER ABLATION CODING & REIMBURSEMENT GUIDE Updated September 2018 TABLE OF CONTENTS Diagnosis Codes...3 ICD-10-CM Diagnosis Codes Coverage for Catheter Ablation Procedures....4 Medicare Other Payers
CATHETER ABLATION CODING & REIMBURSEMENT GUIDE Updated September 2018 TABLE OF CONTENTS Diagnosis Codes...3 ICD-10-CM Diagnosis Codes Coverage for Catheter Ablation Procedures....4 Medicare Other Payers
Mechanism of Immediate Recurrences of Atrial Fibrillation After Restoration of Sinus Rhythm
 Mechanism of Immediate Recurrences of Atrial Fibrillation After Restoration of Sinus Rhythm AMAN CHUGH, MEHMET OZAYDIN, CHRISTOPH SCHARF, STEVE W.K. LAI, BURR HALL, PETER CHEUNG, FRANK PELOSI, JR, BRADLEY
Mechanism of Immediate Recurrences of Atrial Fibrillation After Restoration of Sinus Rhythm AMAN CHUGH, MEHMET OZAYDIN, CHRISTOPH SCHARF, STEVE W.K. LAI, BURR HALL, PETER CHEUNG, FRANK PELOSI, JR, BRADLEY
Is cardioversion old hat? What is new in interventional treatment of AF symptoms?
 Is cardioversion old hat? What is new in interventional treatment of AF symptoms? Joseph de Bono Consultant Electrophysiologist University Hospitals Birmingham Atrial Fibrillation (AF) Affects 2% of the
Is cardioversion old hat? What is new in interventional treatment of AF symptoms? Joseph de Bono Consultant Electrophysiologist University Hospitals Birmingham Atrial Fibrillation (AF) Affects 2% of the
CARDIOINSIGHT TM NONINVASIVE 3D MAPPING SYSTEM CLINICAL EVIDENCE SUMMARY
 CARDIOINSIGHT TM NONINVASIVE 3D MAPPING SYSTEM CLINICAL EVIDENCE SUMMARY April 2017 SUPPORTING EVIDENCE RHYTHM AF VT PUBLICATIONS Driver Domains in Persistent Atrial Fibrillation (Haissaiguerre, et al)
CARDIOINSIGHT TM NONINVASIVE 3D MAPPING SYSTEM CLINICAL EVIDENCE SUMMARY April 2017 SUPPORTING EVIDENCE RHYTHM AF VT PUBLICATIONS Driver Domains in Persistent Atrial Fibrillation (Haissaiguerre, et al)
WPW in Athletes Should we treat all? age? RAMI FOGELMAN SCHNEIDER CHILDREN MEDICAL CENTER OF ISRAEL
 WPW in Athletes Should we treat all? age? RAMI FOGELMAN SCHNEIDER CHILDREN MEDICAL CENTER OF ISRAEL W.P.W Clues in sinus rhythm No Q in Lt chest leads (WPW 88%, control 5%) PR < 100msec (WPW 80%, control
WPW in Athletes Should we treat all? age? RAMI FOGELMAN SCHNEIDER CHILDREN MEDICAL CENTER OF ISRAEL W.P.W Clues in sinus rhythm No Q in Lt chest leads (WPW 88%, control 5%) PR < 100msec (WPW 80%, control
«Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ.
 «Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ» the primary mechanism of SCD in patients with WPW is the rapid conduction
«Aσθενής με ασυμπτωματικό WPW και παροξυσμική κολπική μαρμαρυγή» Χάρης Κοσσυβάκης Επιμελητής A Καρδιολογικό Τμήμα Γ.Ν.Α. «Γ. ΓΕΝΝΗΜΑΤΑΣ» the primary mechanism of SCD in patients with WPW is the rapid conduction
COMPLEX CASE STUDY INNOVATIVE COLLECTIONS. Case presentation
 The Journal of Innovations in Cardiac Rhythm Management, 3 (2012), 939 943 INNOVATIVE COLLECTIONS COMPLEX CASE STUDY Subtle Changes in Electrogram Morphology During Para-Hisian Pacing Performed on IV Adenosine:
The Journal of Innovations in Cardiac Rhythm Management, 3 (2012), 939 943 INNOVATIVE COLLECTIONS COMPLEX CASE STUDY Subtle Changes in Electrogram Morphology During Para-Hisian Pacing Performed on IV Adenosine:
Catheter ablation techniques in managing arrhythmias
 THEME Arrhythmias Peter M Kistler MBBS, PhD, FRACP, is a cardiologist and electrophysiologist, Department of Cardiology, The Alfred Hospital, and Department of Clinical Electrophysiology Research, The
THEME Arrhythmias Peter M Kistler MBBS, PhD, FRACP, is a cardiologist and electrophysiologist, Department of Cardiology, The Alfred Hospital, and Department of Clinical Electrophysiology Research, The
Accepted Manuscript. Inadvertent Atrial Dissociation Following Catheter Ablation: A Demonstration of Cardiac Anisotropy and Functional Block
 Accepted Manuscript Inadvertent Atrial Dissociation Following Catheter Ablation: A Demonstration of Cardiac Anisotropy and Functional Block Shashank Jain, MD, Sajid Mirza, MD, Gunjan Shukla, MD, FHRS PII:
Accepted Manuscript Inadvertent Atrial Dissociation Following Catheter Ablation: A Demonstration of Cardiac Anisotropy and Functional Block Shashank Jain, MD, Sajid Mirza, MD, Gunjan Shukla, MD, FHRS PII:
Supplementary Online Content
 Supplementary Online Content Verma A, Champagne J, Sapp J, et al. Asymptomatic episodes of atrial fibrillation before and after catheter ablation: a prospective, multicenter study. JAMA Intern Med. Published
Supplementary Online Content Verma A, Champagne J, Sapp J, et al. Asymptomatic episodes of atrial fibrillation before and after catheter ablation: a prospective, multicenter study. JAMA Intern Med. Published
Incessant Tachycardia Using a Concealed Atrionodal Bypass Tract
 191 Incessant Tachycardia Using a Concealed Atrionodal Bypass Tract ADAM ZIVIN, M.D., atid FRED MORADY, M.D. From the Division of Cardiology. Department of Internal Medicine, University of Michigan Medical
191 Incessant Tachycardia Using a Concealed Atrionodal Bypass Tract ADAM ZIVIN, M.D., atid FRED MORADY, M.D. From the Division of Cardiology. Department of Internal Medicine, University of Michigan Medical
Adenosine Mapping for Adenosine-Dependent Accessory Pathway Ablation
 Adenosine Mapping for Adenosine-Dependent Accessory Pathway Ablation MARTIN J. LAPAGE, M.D., M.S.,* MICHAEL J. WALSH, M.D., JOHN H. REED, M.D., M.P.H., and J. PHILIP SAUL, M.D. From the *Department of
Adenosine Mapping for Adenosine-Dependent Accessory Pathway Ablation MARTIN J. LAPAGE, M.D., M.S.,* MICHAEL J. WALSH, M.D., JOHN H. REED, M.D., M.P.H., and J. PHILIP SAUL, M.D. From the *Department of
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Case Report. Sumito Narita MD 1;3, Takeshi Tsuchiya MD, PhD 1, Hiroya Ushinohama MD, PhD 2, Shin-ichi Ando MD, PhD 3
 Case Report Identification and Radiofrequency Catheter Ablation of a Nonsustained Atrial Tachycardia at the Septal Mitral Annulus with the Use of a Noncontact Mapping System: A Case Report Sumito Narita
Case Report Identification and Radiofrequency Catheter Ablation of a Nonsustained Atrial Tachycardia at the Septal Mitral Annulus with the Use of a Noncontact Mapping System: A Case Report Sumito Narita
Post-ablation Management: Drug therapy, Anticoagulation and long-term Monitoring
 Catheter Ablation of Atrial Fibrillation: State of the Art Post-ablation Management: Drug therapy, Anticoagulation and long-term Monitoring Dipen Shah Service de Cardiologie Hospital Cantonal de Genève
Catheter Ablation of Atrial Fibrillation: State of the Art Post-ablation Management: Drug therapy, Anticoagulation and long-term Monitoring Dipen Shah Service de Cardiologie Hospital Cantonal de Genève
Interventional solutions for atrial fibrillation in patients with heart failure
 Interventional solutions for atrial fibrillation in patients with heart failure Advances in Cardiovascular Arrhythmias Great Innovations in Cardiology Matteo Anselmino, MD PhD Division of Cardiology Department
Interventional solutions for atrial fibrillation in patients with heart failure Advances in Cardiovascular Arrhythmias Great Innovations in Cardiology Matteo Anselmino, MD PhD Division of Cardiology Department
Recurrent Implantable Defibrillator Discharges (ICD) Discharges ICD Storm
 Recurrent Implantable Defibrillator Discharges (ICD) Discharges ICD Storm Guy Amit, MD, MPH Soroka University Medical Center Ben-Gurion University of the Negev Beer-Sheva, Israel Disclosures Consultant:
Recurrent Implantable Defibrillator Discharges (ICD) Discharges ICD Storm Guy Amit, MD, MPH Soroka University Medical Center Ben-Gurion University of the Negev Beer-Sheva, Israel Disclosures Consultant:
Case Report Mahaim Fiber Accelerated Automaticity and Clues to a Mahaim Fiber Being Morphologically an Ectopic or a Split AV Node
 www.ipej.org 62 Case Report Mahaim Fiber Accelerated Automaticity and Clues to a Mahaim Fiber Being Morphologically an Ectopic or a Split AV Node Shomu Bohora, Narayanan Namboodiri, Santosh Dora, VK Ajit
www.ipej.org 62 Case Report Mahaim Fiber Accelerated Automaticity and Clues to a Mahaim Fiber Being Morphologically an Ectopic or a Split AV Node Shomu Bohora, Narayanan Namboodiri, Santosh Dora, VK Ajit
Clinical Value of Noninducibility by High-Dose Isoproterenol Versus Rapid Atrial Pacing After Catheter Ablation of Paroxysmal Atrial Fibrillation
 13 Clinical Value of Noninducibility by High-Dose Isoproterenol Versus Rapid Atrial Pacing After Catheter Ablation of Paroxysmal Atrial Fibrillation THOMAS CRAWFORD, M.D., AMAN CHUGH, M.D., ERIC GOOD,
13 Clinical Value of Noninducibility by High-Dose Isoproterenol Versus Rapid Atrial Pacing After Catheter Ablation of Paroxysmal Atrial Fibrillation THOMAS CRAWFORD, M.D., AMAN CHUGH, M.D., ERIC GOOD,
Case Report Catheter ablation of Atrial Incisional Tachycardia mistaken for Atrial flutter
 www.ipej.org 134 Case Report Catheter ablation of Atrial Incisional Tachycardia mistaken for Atrial flutter Ottaviano L 1,2, Muto C 1, Carreras G 1, Canciello M 1, Tuccillo B 1. 1 Department of Cardiology,
www.ipej.org 134 Case Report Catheter ablation of Atrial Incisional Tachycardia mistaken for Atrial flutter Ottaviano L 1,2, Muto C 1, Carreras G 1, Canciello M 1, Tuccillo B 1. 1 Department of Cardiology,
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
Catheter ablation of atrial macro re-entrant Tachycardia - How to use 3D entrainment mapping -
 Catheter ablation of atrial macro re-entrant Tachycardia - How to use 3D entrainment mapping - M. Esato, Y. Chun, G. Hindricks Kyoto Ijinkai Takeda Hosptial, Department of Arrhythmia, Japan Kyoto Koseikai
Catheter ablation of atrial macro re-entrant Tachycardia - How to use 3D entrainment mapping - M. Esato, Y. Chun, G. Hindricks Kyoto Ijinkai Takeda Hosptial, Department of Arrhythmia, Japan Kyoto Koseikai
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD
 Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
Patient Resources: Arrhythmias and Congenital Heart Disease
 Patient Resources: Arrhythmias and Congenital Heart Disease Overview Arrhythmias (abnormal heart rhythms) can develop in patients with congenital heart disease (CHD) due to thickening/weakening of their
Patient Resources: Arrhythmias and Congenital Heart Disease Overview Arrhythmias (abnormal heart rhythms) can develop in patients with congenital heart disease (CHD) due to thickening/weakening of their
Electrophysiology and Cathether Ablation: Historical Evolution. Saverio Iacopino, MD, FACC, FESC
 Electrophysiology and Cathether Ablation: Historical Evolution Saverio Iacopino, MD, FACC, FESC Historical Evolution ü 1967 ü 1968 ü 1969 ü 1973 ü 1979 Durrer D et al. first described initiation and termination
Electrophysiology and Cathether Ablation: Historical Evolution Saverio Iacopino, MD, FACC, FESC Historical Evolution ü 1967 ü 1968 ü 1969 ü 1973 ü 1979 Durrer D et al. first described initiation and termination
Original Article. Tehran Heart Center, Tehran University of Medical Sciences, Tehran, Iran.
 TEHRAN HEART CENTER Original Article Radiofrequency Catheter Ablation of Atrioventricular Nodal Reentrant Tachycardia: Success Rates and Complications during 14 Years of Experience Ahmad Yaminisharif,
TEHRAN HEART CENTER Original Article Radiofrequency Catheter Ablation of Atrioventricular Nodal Reentrant Tachycardia: Success Rates and Complications during 14 Years of Experience Ahmad Yaminisharif,
Medicine. Dynamic Changes of QRS Morphology of Premature Ventricular Contractions During Ablation in the Right Ventricular Outflow Tract
 Medicine CLINICAL CASE REPORT Dynamic Changes of QRS Morphology of Premature Ventricular Contractions During Ablation in the Right Ventricular Outflow Tract A Case Report Li Yue-Chun, MD, Lin Jia-Feng,
Medicine CLINICAL CASE REPORT Dynamic Changes of QRS Morphology of Premature Ventricular Contractions During Ablation in the Right Ventricular Outflow Tract A Case Report Li Yue-Chun, MD, Lin Jia-Feng,
Atrial Fibrillation: Electrophysiological Mechanisms and the Results of Interventional Therapy
 Vol. 8, No. 3, September 2003 185 Atrial Fibrillation: Electrophysiological Mechanisms and the Results of Interventional Therapy A.SH. REVISHVILI Bakoulev Research Centre for Cardiovascular Surgery, Russian
Vol. 8, No. 3, September 2003 185 Atrial Fibrillation: Electrophysiological Mechanisms and the Results of Interventional Therapy A.SH. REVISHVILI Bakoulev Research Centre for Cardiovascular Surgery, Russian
In certain cases of supraventricular
 Case Report Hellenic J Cardiol 2013; 54: 469-473 A Tachycardia with Varying QRS Morphology and RP Intervals: Differential Diagnosis and Therapy Socrates Korovesis, Eleftherios Giazitzoglou, Demosthenes
Case Report Hellenic J Cardiol 2013; 54: 469-473 A Tachycardia with Varying QRS Morphology and RP Intervals: Differential Diagnosis and Therapy Socrates Korovesis, Eleftherios Giazitzoglou, Demosthenes
The pulmonary veins have been demonstrated to often
 Pulmonary Vein Isolation for Paroxysmal and Persistent Atrial Fibrillation Hakan Oral, MD; Bradley P. Knight, MD; Hiroshi Tada, MD; Mehmet Özaydın, MD; Aman Chugh, MD; Sohail Hassan, MD; Christoph Scharf,
Pulmonary Vein Isolation for Paroxysmal and Persistent Atrial Fibrillation Hakan Oral, MD; Bradley P. Knight, MD; Hiroshi Tada, MD; Mehmet Özaydın, MD; Aman Chugh, MD; Sohail Hassan, MD; Christoph Scharf,
Arrhythmia 341. Ahmad Hersi Professor of Cardiology KSU
 Arrhythmia 341 Ahmad Hersi Professor of Cardiology KSU Objectives Epidemiology and Mechanisms of AF Evaluation of AF patients Classification of AF Treatment and Risk stratification of AF Identify other
Arrhythmia 341 Ahmad Hersi Professor of Cardiology KSU Objectives Epidemiology and Mechanisms of AF Evaluation of AF patients Classification of AF Treatment and Risk stratification of AF Identify other
Tachycardia-induced heart failure - Does it exist?
 Tachycardia-induced heart failure - Does it exist? PD Dr Etienne Delacrétaz Clinique Cecil et Hôpital de Fribourg SSC Cardiology meeting 2015 Zürich Rapid atrial fibrillation is a common cause of heart
Tachycardia-induced heart failure - Does it exist? PD Dr Etienne Delacrétaz Clinique Cecil et Hôpital de Fribourg SSC Cardiology meeting 2015 Zürich Rapid atrial fibrillation is a common cause of heart
Debate-STAR AF 2 study. PVI is not enough
 Debate-STAR AF 2 study PVI is not enough Debate about STAR AF 2 trial STAR AF trial Substrate and Trigger Ablation for Reduction of Atrial Fibrillation EHJ 2010 STAR-AF 2 trial One Size Fits All? PVI is
Debate-STAR AF 2 study PVI is not enough Debate about STAR AF 2 trial STAR AF trial Substrate and Trigger Ablation for Reduction of Atrial Fibrillation EHJ 2010 STAR-AF 2 trial One Size Fits All? PVI is
Concealed Accessory Pathway in Late Presentation Wolff-Parkinson-White Syndrome
 CASE REPORT Concealed Accessory Pathway in Late Presentation Wolff-Parkinson-White Syndrome Stephanie Rose1, Richard Armstrong2, David Moore2 Third year medicine, Trinity College Dublin Department of Cardiology,
CASE REPORT Concealed Accessory Pathway in Late Presentation Wolff-Parkinson-White Syndrome Stephanie Rose1, Richard Armstrong2, David Moore2 Third year medicine, Trinity College Dublin Department of Cardiology,
Peri-Mitral Atrial Flutter with Partial Conduction Block between Left Atrium and Coronary Sinus
 Accepted Manuscript Peri-Mitral Atrial Flutter with Partial Conduction Block between Left Atrium and Coronary Sinus Ryota Isogai, MD, Seiichiro Matsuo, MD, Ryohsuke Narui, MD, Shingo Seki, MD;, Michihiro
Accepted Manuscript Peri-Mitral Atrial Flutter with Partial Conduction Block between Left Atrium and Coronary Sinus Ryota Isogai, MD, Seiichiro Matsuo, MD, Ryohsuke Narui, MD, Shingo Seki, MD;, Michihiro
Catheter Ablation of Atrial Tachycardia Originating from the Tip of Right Atrial Appendage
 Case Report Catheter Ablation of Atrial Tachycardia Originating from the Tip of Right Atrial Appendage Masaru Inoue MD, Takao Matsubara MD, Toshihiko Yasuda MD, Kenji Miwa MD, Tadatsugu Gamou MD, Hounin
Case Report Catheter Ablation of Atrial Tachycardia Originating from the Tip of Right Atrial Appendage Masaru Inoue MD, Takao Matsubara MD, Toshihiko Yasuda MD, Kenji Miwa MD, Tadatsugu Gamou MD, Hounin
Right and Left Atrial Flutter: How To Differentiate Them on the Basis of Surface Electrocardiogram?
 Right and Left Atrial Flutter: How To Differentiate Them on the Basis of Surface Electrocardiogram? G. INAMA, C. PEDRINAZZI,O.DURIN,P.GAZZANIGA,P.AGRICOLA Introduction Atrial flutter is a common arrhythmia
Right and Left Atrial Flutter: How To Differentiate Them on the Basis of Surface Electrocardiogram? G. INAMA, C. PEDRINAZZI,O.DURIN,P.GAZZANIGA,P.AGRICOLA Introduction Atrial flutter is a common arrhythmia
Department of Cardiology, Athens Euroclinic, Athens, Greece. of typical slow-fast atrioventricular
 Hellenic J Cardiol 2010; 51: 407-412 Original Research Slow-Pathway Ablation for Atrioventricular Nodal Re-Entrant Tachycardia with No Risk of Atrioventricular Block Eleftherios Gi a z i t z o g l o u,
Hellenic J Cardiol 2010; 51: 407-412 Original Research Slow-Pathway Ablation for Atrioventricular Nodal Re-Entrant Tachycardia with No Risk of Atrioventricular Block Eleftherios Gi a z i t z o g l o u,
Ji-Eun Ban, MD, Sang-Weon Park, MD, Hyun-Soo Lee, MPH, Jong-Il Choi, MD, and Young-Hoon Kim, MD
 Case Report Print SSN 1738-5520 On-line SSN 1738-5555 Korean Circulation Journal Swallowing-nduced Atrial Tachyarrhythmias Successfully Ablated at the Left Posterior nteratrial Septum in Patient with Wolff-Parkinson-White
Case Report Print SSN 1738-5520 On-line SSN 1738-5555 Korean Circulation Journal Swallowing-nduced Atrial Tachyarrhythmias Successfully Ablated at the Left Posterior nteratrial Septum in Patient with Wolff-Parkinson-White
Pediatrics. Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment. Overview
 Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Arrhythmia/Electrophysiology
 Arrhythmia/Electrophysiology Atrioventricular Nodal Reentrant Tachycardia in Patients Referred for Atrial Fibrillation Ablation Response to Ablation That Incorporates Slow-Pathway Modification William
Arrhythmia/Electrophysiology Atrioventricular Nodal Reentrant Tachycardia in Patients Referred for Atrial Fibrillation Ablation Response to Ablation That Incorporates Slow-Pathway Modification William
Differentiating Junctional Tachycardia and Atrioventricular Node Re-Entry Tachycardia Based on Response to Atrial Extrastimulus Pacing
 Journal of the American College of Cardiology Vol. 52, No. 21, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.08.030
Journal of the American College of Cardiology Vol. 52, No. 21, 2008 2008 by the American College of Cardiology Foundation ISSN 0735-1097/08/$34.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2008.08.030
Radiofrequency Catheter Ablation of Atrioventricular Nodal Reentrant Tachycardia in Patient with Interruption of Inferior Vena Cava
 Suzuki K AVNRT ablation in patient with interruption of IVC Case Report Radiofrequency Catheter Ablation of Atrioventricular Nodal Reentrant Tachycardia in Patient with Interruption of Inferior Vena Cava
Suzuki K AVNRT ablation in patient with interruption of IVC Case Report Radiofrequency Catheter Ablation of Atrioventricular Nodal Reentrant Tachycardia in Patient with Interruption of Inferior Vena Cava
Pre-excitation on the ECG what next? Kevin M W Leong Specialty Registrar in Cardiology
 Pre-excitation on the ECG what next? Kevin M W Leong Specialty Registrar in Cardiology Nicholas F Kelland Consultant in Cardiology and Electrophysiology Northern General Hospital Sheffield Teaching Hospitals
Pre-excitation on the ECG what next? Kevin M W Leong Specialty Registrar in Cardiology Nicholas F Kelland Consultant in Cardiology and Electrophysiology Northern General Hospital Sheffield Teaching Hospitals
Catheter Ablation for Cardiac Arrhythmias. Description
 Subject: Catheter Ablation for Cardiac Arrhythmias Page: 1 of 21 Last Review Status/Date: December 2016 Catheter Ablation for Cardiac Arrhythmias Description Catheter ablation is a technique to eliminate
Subject: Catheter Ablation for Cardiac Arrhythmias Page: 1 of 21 Last Review Status/Date: December 2016 Catheter Ablation for Cardiac Arrhythmias Description Catheter ablation is a technique to eliminate
Comparative Effectiveness of Radiofrequency Catheter Ablation for Atrial Fibrillation Executive Summary
 Number 15 Effective Health Care Comparative Effectiveness of Radiofrequency Catheter Ablation for Atrial Fibrillation Executive Summary Background The Agency for Healthcare Research and Quality commissioned
Number 15 Effective Health Care Comparative Effectiveness of Radiofrequency Catheter Ablation for Atrial Fibrillation Executive Summary Background The Agency for Healthcare Research and Quality commissioned
Case Report Electroanatomical Mapping and Ablation of Upper Loop Reentry Atrial Flutter
 Hellenic J Cardiol 46: 74-78, 2005 Case Report Electroanatomical Mapping and blation of Upper Loop Reentry trial Flutter POSTOLOS KTSIVS, PNGIOTIS IONNIDIS, CHRLMOS VSSILOPOULOS, THIN GIOTOPOULOU, THNSIOS
Hellenic J Cardiol 46: 74-78, 2005 Case Report Electroanatomical Mapping and blation of Upper Loop Reentry trial Flutter POSTOLOS KTSIVS, PNGIOTIS IONNIDIS, CHRLMOS VSSILOPOULOS, THIN GIOTOPOULOU, THNSIOS
