ACE Standards. for Peripheral Vascular Intervention (PVI) Accreditation
|
|
|
- Jocelin McCoy
- 5 years ago
- Views:
Transcription
1 ACE Standards for Peripheral Vascular Intervention (PVI) Accreditation Accreditation for Cardiovascular Excellence Quality in Invasive Cardiovascular Care th St. NW, Ste 330 Washington D.C Accreditation for T: Cardiovascular Excellence (2014)
2 ACE Standards for Peripheral Vascular Intervention (PVI) Accreditation Table of Contents 1. STANDARDS: Facility Related STANDARDS: Personnel Related STANDARDS: Quality Assurance STANDARDS: Radiation Safety STANDARDS: Reporting of Results STANDARDS: Patient Indications STANDARDS: Patient Outcomes Performance Metrics...12 References...13 Published Oct Accreditation for Cardiovascular Excellence (2014)
3 1. STANDARDS: Facility Related 1.1. Each hospital department or section (cath lab, operating room, radiology suite, etc) performing Peripheral Angiography and Interventions (PVI) must document that they have the resources to perform the procedure in a safe manner Equipment Digital subtraction angiography( 12-in image intensifier preferred) with on-line image storage and retrieval capabilities Advanced physiologic monitoring with real-time and archived physiologic, hemodynamic and rhythm monitoring equipment with support staff capable of interpreting results and responding appropriately Large inventory of disposable supplies for vascular access management, diagnostic angiography and peripheral vascular intervention The inventory should include devices and drugs to assist in the management of emergent complications including allergic reactions, arterial thrombosis, thromboembolism or vessel rupture and dissection All staff should be trained in the appropriate use of these devices Emergency management equipment and systems must be readily available in the interventional suite. This includes resuscitation equipment, a defibrillator, vasoactive and antiarrhythmic drugs, endotracheal intubation, and personnel familiar with their indications and use There must be a process documenting routine preventive maintenance and testing of laboratory equipment, including a comprehensive radiation safety program such as outlined by The Society for Cardiovascular Angiography and/or the American College of Radiology. 2. STANDARDS: Personnel Related 2.1. Each Department within the Institution (cath lab, radiology, and surgery) performing PVI must have: A licensed, board-certified physician in an appropriate specialty and/or sub-specialty as a Medical Director A Technical Director (licensed technologist or registered nurse) with a minimum of 5 years experience working in an invasive angiographic imaging laboratory A clearly delineated program for the initial granting of privileges with physician operators meeting the peer-reviewed national societal training standards appropriate for the individual s specialty. The initial granting of privileges should be free of conflict of interest A standard operating procedure for monitoring peri-procedural, in-hospital and 30-day outcomes. ACE Standards for Peripheral Vascular Intervention (PVI) Accreditation 3
4 2.2. Maintenance of physician privileges Physicians must obtain 30 hours of Category 1 continuing medical education credits per year period with a minimum of 20 hours in the field of endovascular diagnosis and therapy of non-cardiac vascular diseases The institution must have a defined process for re-credentialing which should be based on volume, outcomes, fulfillment of CME requirements and other quality parameters and should be uniform for all operators irresective of specialty. These may develop over time and be implemented in a later version of these standards Recertification criteria for individual practitioners should be decided by each institution but guidelines should include documentation for fulfillment of CME requirements as outlined in and participation in at least 50%of Morbidity and Mortality and/or case review meetings An operator s complication rates should not exceed those defined in publications by professional societies or the following thresholds Mortality 1% Stroke 1% Major complications: emergency surgery, transfusion, unplanned amputation, dialysis composite of 3% Minor complications: Hematoma, AV fistula 3% Hospital privileges and state licensing should be maintained throughout the period of certification for all operators. Any loss of either hospital privileges or state license shall be reported to ACE with an explanation from the Medical Director, CEO or CMO or institutional leader at the facility For adult laboratories, physicians must maintain ACLS certification and follow facility standards for radiation safety Other Health Care Professionals Skilled allied health professionals in the laboratory (advanced practice clinicians, nurses and technicians) must be trained and experienced in evaluating patients before and after catheter-based interventional procedure. State requirements for performance and roles of personnel must be supplied and facilities will be reviewed for compliance based on these standards Documentation of training of nursing personnel in the recognition and management of acute cardiovascular syndromes and endovascular complications is required Documentation of training of support staff to interpret results from physiologic, hemodynamic and rhythm monitoring equipment All personnel with direct patient care responsibilities should be ACLS certified Facilities should have policies regarding the supervising role of the primary operating physician during the procedure when secondary operators are performing the procedure and direct the nonphysician provider or fellow in addition to providing all clinical decision making. 4 Accreditation for Cardiovascular Excellence (2014)
5 3. STANDARDS: Quality Assurance 3.1. A quality monitoring program must include a multidisciplinary peer-review conference with randomly selected PVI procedures reviewed for their indications, imaging quality, documentation, and complications. The quality oversight committee should also review outcomes and make privileging recommendations All major complications should be reviewed A regularly scheduled quality monitoring conference must occur no less than quarterly. All operators must have documented participation in a minimum of 50% of the quality review meetings The quality oversight committee for this program should be representative of the individual specialties involved, and the Chair of the committee should rotate on a regular basis A cath lab/or/endovascular specific quality assurance (QA) monitoring program must be present and integrated with the facility quality improvement program (CQI) effort A QA program should include structural, process and outcomes indicators Structural indicators may include: a) credentialing and re-credentialing criteria, b) completion of accurate and informative reports, c) documentation of CME participation Process indicators may include: a) quality of angiographic studies, b) completion of accurate and informative reports, c) emergency response times, d) total procedure and fluoroscopy times, e) contrast usage, f) radiation dose, and g) other criteria Outcome indicators assessed should be part of an overall QA program The quality assurance program must include a peer-review process with randomly selected diagnostic and interventional procedures representing all operators performing cases. These should be reviewed for their indications and complications, and include a periodic review of all major laboratory/or/endovascular complication rates The QA program must include an assessment of: a) the rate of non-obstructive peripheral disease, b) an assessment of overall and vascular complication rates for all types of procedures performed, and c) an assessment of the diagnostic accuracy and adequacy of angiograms The oversight committee should be empowered to identify the minimum case volume for primary operators to maintain privileges, as well as a threshold complication rate to trigger activation of measures for remediation or potential suspension of privileges Major events such as [30 day] Death, Major Stroke, and unplanned amputation rates should not exceed 1% of the patient volume, or established thresholds. ACE Standards for Peripheral Vascular Intervention (PVI) Accreditation 5
6 4. STANDARDS: Radiation Safety 4.1. There must be a procedure in place to document radiation exposure of the patients and staff. Patients with excessive radiation exposure or clinically evident radiation damage (skin burns, alopecia, etc.) will be counseled by the radiation safety office The radiation safety program should be considered a component of the overall PVI facility quality assurance (QA) process with the Vascular Intervention program QA individual(s) actively involved with this process Each PVI facility must establish a radiation safety education program either in conjunction with the hospital Health Physics Department/ Medical Physicist and/ or an outside consultant and/or assistance from a web-based tutorial. Documentation of this training must be provided. This program should have the following mandated components: a) initial training or verification of prior training for all physicians and staff using fluoroscopy in the peripheral intervention facility; b) annual updates on radiation safety; c) hands on training for new operators in a facility and existing operators on newly purchased equipment Patient radiation dose needs to be monitored and recorded This should include the fluoroscopic time (FT, min) and total air kerma at the interventional reference point (Ka, r, Gy) and/or air kerma area product (PKA, Gycm2). Peak skin dose should be included if technology permits its measurement A surveillance program should be in place for patients whose recorded total air kerma at the interventional reference point (Ka, r) is 5 Gy or greater, PKA of 500 Gycm2, and/or fluoroscopy doses that exceed 60 minutes. This program should include the dose and a reason for this dose, patient notification, medical physicist/health physics involvement for Ka, r >10Gy, and a mechanism for patient follow up of potential adverse effects from radiation. Physician must wear radiation exposure badges, monthly dosages calculated, and yearly totals reviewed. The radiation safety officer is responsible for the monitoring of this process. 5. STANDARDS: Reporting of Results 5.1. The reporting standards of The Joint Commission (TJC) for operative procedures must be followed. These include: Preliminary procedure reports must be written or dictated immediately after the procedure. Final reports should be posted to the medical record within 72 hours There must be enough information in the record immediately after the procedure to manage the patient throughout the post-procedure period. This information could be entered as the procedure report or as a hand-written operative progress note. 6 Accreditation for Cardiovascular Excellence (2014)
7 If the procedure report is not placed in the medical record immediately after the procedure due to transcription or filing delay, then a progress note should be entered in the medical record immediately after the procedure to provide pertinent information for anyone required to attend the patient. Immediately after the procedure is defined as upon completion of procedure, before the patient is transferred to the next level of care The procedure progress note should contain at a minimum information including: a) name of the operator, b) procedures performed and description of each procedure, c) findings, d) estimated blood loss, e) specimens removed if appropriate, f) complications, g) post-operative diagnosis, and h) recommendations All procedure reports at a facility should be individualized to the institution but be consistent with the HPS for structured reporting, standardized among operators and contain relevant content on each of the following topics: Patient demographics, primary and assisting operator(s) and supporting staff present and procedures performed Indications for each component of the procedure (i.e. left femoral angiography, etc.) Appropriate supporting pertinent history, physical findings, and laboratory findings The time frame and procedural events with technical comments for example, Interventional procedures performed and any issues of concern Access site information and closure method All catheters, sheaths, guide wires, and interventional equipment used should be reported in a procedural section Drugs and doses given during the procedure, type and amount of radiographic contrast used, and estimation of radiation exposure should be included in the procedure report A clear description of any complications or a positive statement that there were no apparent complications Minimum requirements for reporting the peripheral diagnostic angiography are: 1) a description of the aorta and the vessels selected for arteriography, 2) a notation of the size, extent of distribution, tortuosity, and visual estimate of the degree of any narrowing, 3) patency of runoff vessels, 4) anatomic variations, 5) presence and severity of calcification, 6) presence and description of collaterals For interventional procedures a complete description of the procedure, key equipment used, in lab results such as point-of-care ACT measurements, complications occurring and outcome of the intervention. Technical comments are helpful should future interventions be necessary If performed, findings of intravascular ultrasound (IVUS) or OCT examinations and translesional pressure measurements or FFR should be reported within the procedure report. ACE Standards for Peripheral Vascular Intervention (PVI) Accreditation 7
8 The minimum content of an IVUS report includes: a) appropriate patient demographic information and date with reference to the accompanying angiographic and/or interventional reports; b) indication for the procedure; c) brief description of the IVUS procedure, including equipment used, the level of anticoagulation achieved and the peripheral vessels imaged; d) basic findings of the IVUS pullback, including any measurements that were performed such as minimum lumen diameter, minimum stent area, or plaque burden; e) any notable morphological plaque features such as dissection, calcium, or thrombus; f) changes in therapy that resulted from the information provided by IVUS; g) IVUS related complications and any consequent subsequent. A complete report would also include an analysis of three essential cross-sectional images a distal reference segment, the most severe lesion site, and a proximal reference segment. Lumen and external elastic lamina areas, calculated plaque plus media area, plaque burden, and area stenosis can be reported. If a stent is present, minimum diameter stenosis, lumen area of the stent and a description of strut apposition should be included If FFR and or pressure gradients are determined these must be documented IVUS images must be archived for subsequent review Standardized reports for new imaging techniques should be developed as needed and must include pertinent information similar to that described above for IVUS Summary of major findings or diagnosis Disposition of the patient as a result of the procedure and comments, including plans for follow-up care including medical therapy, imaging, and anticipated further interventions. 6. STANDARDS: Patient Indications 6.1. The indication for the peripheral vascular intervention must be documented according to accepted societal standards and be consistent with published guidelines, expert consensus documents, or appropriate use criteria (AUC) (15, 16, 17). Interventions for asymptomatic or non-threatening conditions are generally not warranted and must be fully supported by documented justification for performing the procedure There must be sufficient clinical information available in the procedure report and medical record to determine the indication for the procedure If the specific clinical scenario is not included in the AUC or if in the judgment of the physician the procedure is justified despite the AUC score, clear documentation of the reasoning should be included both in the medical record and in the procedure report Elective patients with claudication should have failed or be intolerant of a trial of medical therapy (cilostazol) and exercise (preferably supervised). 8 Accreditation for Cardiovascular Excellence (2014)
9 6.2. Interventional indications based on Fontaine or Rutherford chronic limb ischemia criteria. Rutherford Classification for Peripheral Arterial Disease Stage 0 Asymptomatic Stage 1 Mild claudication Stage 2 Moderate claudication Stage 3 Severe claudication Stage 4 Rest pain Stage 5 Ischemic ulceration not exceeding ulcer of the digits of the foot Stage 6 Severe ischemic ulcers or frank gangrene Fontaine Classification Stage 1 Asymptomatic Stage 2A Claudication pain walking more than two hundred meters Stage 2B Claudication pain walking less than two hundred meters Stage 3 Ischemic rest pain Stage 4 Necrosis and/or gangrene of the limb Measurement and documentation of disease severity Percent diameter stenosis: Severe = stenosis diameter > 70% Moderate = 50-69% Mild = < 50% By ultrasound using the following criteria: 0-49%, 50-99%, Occluded By ABI and TBI By MRA/CTA by degree of stenosis By Digital Subtraction Angiography (DSA) The degree of peripheral stenosis shall be measured by duplex ultrasound or peripheral angiography and recorded in the patient s procedure report. If the degree of stenosis is measured prior to the procedure, then the degree of stenosis must be confirmed by angiography at the start of the procedure All patients shall have an angiogram clearly documenting pre and post lesion assessment > 90% of cases should meet these criteria for stenosis 6.6. All treated patients shall have a post procedure peripheral angiogram to evaluate flow and the occurrence of distal embolization Pre-treatment peripheral anatomy may be evaluated by CTA, MRA, Ultrasound, or DSA but if so, documentation of these findings should be included as part of the pre-procedure evaluation. Otherwise, pre-procedure peripheral angiography should be performed as part of the initial angiographic lesions and anatomic assessment Residual stenosis should be < 30%. If not achieved, explanation such as severe calcification, etc should be included in the report. ACE Standards for Peripheral Vascular Intervention (PVI) Accreditation 9
10 7. STANDARDS: Patient Outcomes 7.1. Hospital-based outcomes, prior to discharge Lesion success adequate inflow and appropriate outflow are required to keep the revascularized segment functioning Procedural success rate should be > 90% of cases Complications Access site complications Requires re-intervention or surgical correction Thromboembolism Infection requiring antibiotics or drainage Results in prolonged hospital stay Requires any transfusion of PRBSs or platelets Bleeding per Bleeding Academic Research Consortium (BARC) Criteria Type 0 - No bleeding Type 1 - Bleeding that is not actionable and does not cause the patient to seek treatment Type 2 - Any clinically overt sign of hemorrhage that is actionable and requires diagnostic studies, hospitalization, or treatment by a health care professional Type 3 - a. Overt bleeding plus Hgb drop of 3 to < 5 g/dl (provided the drop is related to bleed); transfusion with overt bleeding b. Overt bleeding plus Hgb drop < 5 g/dl (provided the drop is related to bleed); cardiac tamponade; bleeding requiring surgical intervention for control; bleeding requiring IV vasoactive agents. c. Intracranial hemorrhage confirmed by autopsy, imaging, or lumbar puncture; intraocular bleed compromising vision. Type 4 - Surgery-related bleeding within 48 hours Type 5 - a. Probable fatal bleeding b. Definite fatal bleeding (overt, autopsy or imaging confirmation) Target site complications: dissection, occlusion, extravasation Renal failure (need for dialysis, doubling serum Cr, 25% increase from baseline or absolute increase of 0.5 mg/dl within 48 hours of contrast administration) Access site complication not requiring intervention Hematoma Percutaneous repair (thrombin injection, ultrasound-guided compression) of pseudoaneurysm AV fistula not requiring further treatment 10 Accreditation for Cardiovascular Excellence (2014)
11 Other procedure related complications, including cardiovascular or pulmonary compromise, radiation or other injury, and other events warranting clinical management or observation. Procedure related complications occur within 48 hours of the procedure or during the same hospitalization The procedure progress note should contain at a minimum information including: a) name of the operator, b) procedures performed and description of each procedure, c) findings, d) estimated blood loss, e) specimens removed if appropriate f) complications, g) post-operative diagnosis and h) recommendations Follow-up Outcomes to 30 days (3 to 6 weeks post-procedure) Symptomatic, functional, quality of life improvement Target lesion/vessel revascularization Wound healing Day Adverse Event Death Myocardial Infarction Stroke All amputations, (planned and unplanned, reported separately) End-organ damage or renal failure 7.3. Follow-up Outcomes 180 days Symptomatic improvement Target lesion/vessel revascularization/primary assisted patency/secondary patency Wound healing Day Adverse Event Death Myocardial Infarction Stroke All amputations, (planned and unplanned, reported separately) End-organ damage or renal failure ACE Standards for Peripheral Vascular Intervention (PVI) Accreditation 11
12 7.4. Follow-up Outcomes 360 days Symptomatic improvement Target lesion/vessel revascularization/primary assisted patency/secondary patency Wound healing Day Adverse Event Death Myocardial Infarction Stroke All amputations, (planned and unplanned, reported separately) End-organ damage or renal failure 8. Performance Metrics As part of the ACE application, performance metrics from the NCDR PVI Registry Executive Summary will be reviewed. The specific performance metrics examined and their source are shown in the table below. Lower Extremity (LE) Process Metrics Source Line Measurement of ABI prior to procedure NCDR PVI Registry 27 Smoking cessation intervention prior to discharge NCDR PVI Registry 28 Antiplatelet therapy prescribed at discharge NCDR PVI Registry 29 Statins prescribed at discharge NCDR PVI Registry 30 LE Outcome Metrics Angiographic success NCDR PVI Registry 31 Incidence of bleeding or any vascular complications NCDR PVI Registry 32 Incidence of any major adverse event NCDR PVI Registry Accreditation for Cardiovascular Excellence (2014)
13 References 1. Norgren, L., Hiatt, W.R., Dormandy, J.A., Nehler, M.R., Harris, K.A., and Fowkes, F.G.R. Inter-Society Consensus for the Management of Peripheral Arterial Disease (TASC II). Journal of Vascular Surgery, January 2007; 45(1): S5A- S67A. 2. Balter S, M. J. (2007). Managing Patient Dose in Interventional Cardiology. Catheterization and Cardiovascular Interventions, 70: Rooke, T. W., et al. (2011). ACCF/AHA Focused Update of the Guideline for the Management of Patients With Peripheral Artery Disease (Updating the 2005 Guideline): A Report of the American College of Cardiology Foundation/ American Heart Association Task Force on Practice Guidelines. Circulation. 2011; 124: Hirshfeld, J. M., et al. (2004). ACC/ACP/SCAI/SVMB/SVS Clinical Competence Statement on Vascular Medicine and Catheter- Based Peripheral Vascular Interventions. J Am Coll Cardiol, 44: White, C.J., Gray, W.A., Endovascular Therapies for Peripheral Arterial Disease: An Evidence-Based Review. Circulation, 2007; 116: Stecker, M. M., & Balter, S. P. (2009). Guidelines for Patient Radiation Dose Management. J Vasc Interv Radiol, 20:S263-S Stephen Balter, P. (2006). Radiation Management for Interventional Fluoroscopy Staff Safety. 8. Aihara H, Soga Y, Iida O, et al. Long-Term Outcomes of Endovascular Therapy for Aortoiliac Bifurcation Lesions in the Real-Al Registry. Journal of Endovascular Therapy, 2014;21:25: Park KB, Do YS, Kim, DI, et al. The TransAtlantic Inter-Society Consensus (TASC) Classification System in Iliac Arterial Stent Placement: Long-term Patency and Clinical Limitations. Journal of Vascular Interventional Radiology, February 2007, 18:2, Olin JW, Allie DE, Belkin M, et al. ACCF/AHA/ACR/SCAI/SIR/SVM/SVN/SVS 2010 Performance Measures for Adults With Peripheral Artery Disease: A Report of the American College of Cardiology Foundation/American Heart Association Task Force on Performance Measures, the American College of Radiology, the Society for Cardiac Angiography and Interventions, the Society for Interventional Radiology, the Society for Vascular Medicine, the Society for Vascular Nursing, and the Society for Vascular Surgery, Circulation, 2010; 122: Siracuse JJ, Gill HL, Cassidy SP, et al. Endovascular treatment of lesions in the below-knee popliteal artery, Journal of Vascular Surgery, 2014 Mar 17. Doi: /j.jvs/ Zhang F, Zhang H, Luo X, et al. Catheter-directed thrombolysis-assisted angioplasty for chronic lower-limb ischemia, Annals of Vascular Surgery, Apr 2014; 28(3): Hodgkiss-Harlow KD, Bandyk DF. Interpretation of arterial duplex testing of lower-extremity arteries and interventions, Seminars in Vascular Surgery, Jun-Sep 2013; 26(2-3): National Coverage Determination (NCD) for Percutaneous Transluminal Angioplasty (PTA) (20.7)100-3 (9), 12/9/ Klein AJ, Pinto DS, Gray BH, et al. Appropriate Use Criteria: A Society for Cardiovascular Angiography and Interventions (SCAI) Consensus Statement for Femoral-Popliteal Arterial Intervention, Catheterization and Cardiovascular Interventions, Klein AJ, Feldman DN, Aronow HD, et al. Appropriate Use Criteria: A Society for Cardiovascular Angiography and Interventions (SCAI) Consensus Statement for Aorto-Iliac Arterial Intervention. Catheterization and Cardiovascular Interventions, Gray BH, Diaz-Sandoval LJ, Dieter RS, et al. Appropriate Use for Infrapopliteal Arterial Intervention: An expert consensus document from the Society for Cardiovascular Angiography And Intervention (SCAI), 2014, in press. 18. Jones WS, Schmit KM, Vemulapalli V, et al. Treatment Strategies for Patients With Peripheral Artery Disease, Comparative Effectiveness Reviews, No.118, May Sanborn TA, Tcheng JE, Anderson HV, Chambers CE, Cheatham SL, DeCaro MV, Durack JC, Everett AD, Gordon JB, Hammond WE, Hijazi ZM,Kashyap VS, Knudtson M, Landzberg MJ, Martinez-Rios MA, Riggs LA, SimKH, Slotwiner DJ, Solomon H, Szeto WY, Weiner BH, Weintraub WS, Windle JR. ACC/AHA/SCAI 2014 health policy statement on structured reporting for the cardiac catheterization laboratory: a report of the American College of Cardiology Clinical Quality Committee. J Am Coll Cardiol 2014;63: ACE Standards for Peripheral Vascular Intervention (PVI) Accreditation 13
14 Notes 14 Accreditation for Cardiovascular Excellence (2014)
15 Notes ACE Standards for Peripheral Vascular Intervention (PVI) Accreditation 15
16 Accreditation for Cardiovascular Excellence Quality in Invasive Cardiovascular Care th St. NW, Ste 330 Washington D.C T:
ACE Standards. for Carotid Artery Stenting Accreditation. Accreditation for Cardiovascular Excellence Quality in Invasive Cardiovascular Care
 2015 ACE Standards for Carotid Artery Stenting Accreditation Accreditation for Cardiovascular Excellence Quality in Invasive Cardiovascular Care 1100 17th St. NW, Ste 330 Washington D.C. 20036 1 Accreditation
2015 ACE Standards for Carotid Artery Stenting Accreditation Accreditation for Cardiovascular Excellence Quality in Invasive Cardiovascular Care 1100 17th St. NW, Ste 330 Washington D.C. 20036 1 Accreditation
ACE Standards. for Electrophysiology (EP) and Implantable Cardioverter Defibrillators (ICD) Accreditation
 2015 ACE Standards for Electrophysiology (EP) and Implantable Cardioverter Defibrillators (ICD) Accreditation Accreditation for Cardiovascular Excellence Quality in Invasive Cardiovascular Care 1100 17th
2015 ACE Standards for Electrophysiology (EP) and Implantable Cardioverter Defibrillators (ICD) Accreditation Accreditation for Cardiovascular Excellence Quality in Invasive Cardiovascular Care 1100 17th
ACE Standards. for Carotid Artery Stenting Accreditation. Accreditation for Cardiovascular Excellence Quality in Invasive Cardiovascular Care
 2010 ACE Standards for Carotid Artery Stenting Accreditation Accreditation for Cardiovascular Excellence Quality in Invasive Cardiovascular Care 2400 N Street NW, Suite 500 Washington, D.C. 20037-1153
2010 ACE Standards for Carotid Artery Stenting Accreditation Accreditation for Cardiovascular Excellence Quality in Invasive Cardiovascular Care 2400 N Street NW, Suite 500 Washington, D.C. 20037-1153
Data Requirements. Accreditation for Cardiovascular Excellence Quality in Invasive Cardiovascular Care
 2011 Data Requirements Accreditation for Cardiovascular Excellence Quality in Invasive Cardiovascular Care 2400 N Street NW, Suite 500 Washington, D.C. 20037-1153 T: 202-657-6859 1 1. 2. It is required
2011 Data Requirements Accreditation for Cardiovascular Excellence Quality in Invasive Cardiovascular Care 2400 N Street NW, Suite 500 Washington, D.C. 20037-1153 T: 202-657-6859 1 1. 2. It is required
Imaging Strategy For Claudication
 Who are the Debators? Imaging Strategy For Claudication Duplex Ultrasound Alone is Adequate to Select Patients for Endovascular Intervention - Pro: Dennis Bandyk MD No Disclosures PRO - Vascular Surgeon
Who are the Debators? Imaging Strategy For Claudication Duplex Ultrasound Alone is Adequate to Select Patients for Endovascular Intervention - Pro: Dennis Bandyk MD No Disclosures PRO - Vascular Surgeon
Making the difference with Live Image Guidance
 Live Image Guidance 2D Perfusion Making the difference with Live Image Guidance In Peripheral Arterial Disease Real-time results, instant assessment Severe foot complications the result of hampered blood
Live Image Guidance 2D Perfusion Making the difference with Live Image Guidance In Peripheral Arterial Disease Real-time results, instant assessment Severe foot complications the result of hampered blood
Peripheral Vascular Disease
 Peripheral artery disease (PAD) results from the buildup of plaque (atherosclerosis) in the arteries of the legs. For people with PAD, symptoms may be mild, requiring no treatment except modification of
Peripheral artery disease (PAD) results from the buildup of plaque (atherosclerosis) in the arteries of the legs. For people with PAD, symptoms may be mild, requiring no treatment except modification of
Peripheral Arterial Disease: the growing role of endovascular management
 Peripheral Arterial Disease: the growing role of endovascular management Poster No.: C-1931 Congress: ECR 2012 Type: Educational Exhibit Authors: E. M. C. Guedes Pinto, E. Rosado, D. Penha, P. Cabral,
Peripheral Arterial Disease: the growing role of endovascular management Poster No.: C-1931 Congress: ECR 2012 Type: Educational Exhibit Authors: E. M. C. Guedes Pinto, E. Rosado, D. Penha, P. Cabral,
PAD Characterization Within A Healthcare System" RAPID Face-to-Face Meeting Schuyler Jones, MD September 14, 2016
 PAD Characterization Within A Healthcare System" RAPID Face-to-Face Meeting Schuyler, MD September 14, 2016 Interventional Cardiology and Cath Labs Disclosures Research Grants: Agency for Healthcare Research
PAD Characterization Within A Healthcare System" RAPID Face-to-Face Meeting Schuyler, MD September 14, 2016 Interventional Cardiology and Cath Labs Disclosures Research Grants: Agency for Healthcare Research
STONY BROOK UNIVERSITY HOSPITAL VASCULAR CENTER CREDENTIALING POLICY BROCHURE
 STONY BROOK UNIVERSITY HOSPITAL VASCULAR CENTER CREDENTIALING POLICY BROCHURE Per Medical Board decision March 18, 2008: These credentialing standards do NOT apply to peripheral angiography performed in
STONY BROOK UNIVERSITY HOSPITAL VASCULAR CENTER CREDENTIALING POLICY BROCHURE Per Medical Board decision March 18, 2008: These credentialing standards do NOT apply to peripheral angiography performed in
John E. Campbell, MD Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division
 John E. Campbell, MD Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division John Campbell, MD For the 12 months preceding this CME activity,
John E. Campbell, MD Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division John Campbell, MD For the 12 months preceding this CME activity,
PAD and CRITICAL LIMB ISCHEMIA: EVALUATION AND TREATMENT 2014
 PAD and CRITICAL LIMB ISCHEMIA: EVALUATION AND TREATMENT 2014 Van Crisco, MD, FACC, FSCAI First Coast Heart and Vascular Center, PLLC Jacksonville, FL 678-313-6695 Conflict of Interest Bayer Healthcare
PAD and CRITICAL LIMB ISCHEMIA: EVALUATION AND TREATMENT 2014 Van Crisco, MD, FACC, FSCAI First Coast Heart and Vascular Center, PLLC Jacksonville, FL 678-313-6695 Conflict of Interest Bayer Healthcare
DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service
 M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
M AY. 6. 2011 10:37 A M F D A - C D R H - O D E - P M O N O. 4147 P. 1 DEPARTMENT OF HEALTH & HUMAN SERVICES Public Health Service Food and Drug Administration 10903 New Hampshire Avenue Document Control
Carotid Artery Stenting
 Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
Carotid Artery Stenting JESSICA MITCHELL, ACNP CENTRAL ILLINOIS RADIOLOGICAL ASSOCIATES External Carotid Artery (ECA) can easily be identified from Internal Carotid Artery (ICA) by noticing the branches.
Current Vascular and Endovascular Management in Diabetic Vasculopathy
 Current Vascular and Endovascular Management in Diabetic Vasculopathy Yang-Jin Park Associate professor Vascular Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine Peripheral artery
Current Vascular and Endovascular Management in Diabetic Vasculopathy Yang-Jin Park Associate professor Vascular Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine Peripheral artery
Clinical and morphological features of patients who underwent endovascular interventions for lower extremity arterial occlusive diseases
 Original paper Clinical and morphological features of patients who underwent endovascular interventions for lower extremity arterial occlusive diseases Sakir Arslan, Isa Oner Yuksel, Erkan Koklu, Goksel
Original paper Clinical and morphological features of patients who underwent endovascular interventions for lower extremity arterial occlusive diseases Sakir Arslan, Isa Oner Yuksel, Erkan Koklu, Goksel
Introduction. Risk factors of PVD 5/8/2017
 PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
Version 4.4. Institutional Outcomes Report 2014Q3. National Outcomes Report Aggregation Date: Jan 12, :59:59 PM
 Version 4.4 Institutional Outcomes Report 2014Q3 National Outcomes Report 999997 Aggregation Date: Jan 12, 2015 11:59:59 PM Publish Date: Jan 29, 2015 If User desires to publish or otherwise distribute
Version 4.4 Institutional Outcomes Report 2014Q3 National Outcomes Report 999997 Aggregation Date: Jan 12, 2015 11:59:59 PM Publish Date: Jan 29, 2015 If User desires to publish or otherwise distribute
Carotid Stenting Certification
 Carotid Stenting Certification Disclosures Founding Board Member ICACSF SVIN Representative to ICACSF No financial interest Intersocietal Accreditation Commission (IAC) Accreditation is IAC s only business
Carotid Stenting Certification Disclosures Founding Board Member ICACSF SVIN Representative to ICACSF No financial interest Intersocietal Accreditation Commission (IAC) Accreditation is IAC s only business
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE)
 Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2)
 Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
BC Vascular Day. Contents. November 3, Abdominal Aortic Aneurysm 2 3. Peripheral Arterial Disease 4 6. Deep Venous Thrombosis 7 8
 BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
LIBERTY 360 Study. 15-Jun-2018 Data 1. Olinic Dm, et al. Int Angiol. 2018;37:
 LIBERTY 360 Study LIBERTY is a prospective, observational, multi-center study to evaluate procedural and long-term clinical and economic outcomes of endovascular device interventions in patients with symptomatic
LIBERTY 360 Study LIBERTY is a prospective, observational, multi-center study to evaluate procedural and long-term clinical and economic outcomes of endovascular device interventions in patients with symptomatic
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Treatment Strategies For Patients with Peripheral Artery Disease
 Treatment Strategies For Patients with Peripheral Artery Disease Presented by Schuyler Jones, MD Duke University Medical Center & Duke Clinical Research Institute AHRQ Comparative Effectiveness Review
Treatment Strategies For Patients with Peripheral Artery Disease Presented by Schuyler Jones, MD Duke University Medical Center & Duke Clinical Research Institute AHRQ Comparative Effectiveness Review
UPMC 1 Delineation of Privileges Request Criteria Summary Sheet. Specialty: MEDICINE. Successful Completion of an ACGME/AOA, accredited program
 UPMC 1 Facility: UPMC St. Margaret Specialty: MEDICINE KNOWLEDGE Successful Completion of an ACGME/AOA, accredited program TRAINING The successful completion of an approved (ACGME/AOA) post graduate residency
UPMC 1 Facility: UPMC St. Margaret Specialty: MEDICINE KNOWLEDGE Successful Completion of an ACGME/AOA, accredited program TRAINING The successful completion of an approved (ACGME/AOA) post graduate residency
(EU), FACC (USA), FSCAI (USA)
 How to reduce vascular complications of TAVI Paul TL Chiam MBBS (S pore), MMed, MRCP (UK), FAMS FRCP (Edin), FESC (EU), FACC (USA), FSCAI (USA) Cardiologist Mount Elizabeth Hospital Singapore Definition
How to reduce vascular complications of TAVI Paul TL Chiam MBBS (S pore), MMed, MRCP (UK), FAMS FRCP (Edin), FESC (EU), FACC (USA), FSCAI (USA) Cardiologist Mount Elizabeth Hospital Singapore Definition
Peripheral Arterial Disease: A Practical Approach
 Peripheral Arterial Disease: A Practical Approach Sanjoy Kundu BSc, MD, FRCPC, DABR, FASA, FCIRSE, FSIR The Scarborough Hospital Toronto Endovascular Centre The Vein Institute of Toronto Scarborough Vascular
Peripheral Arterial Disease: A Practical Approach Sanjoy Kundu BSc, MD, FRCPC, DABR, FASA, FCIRSE, FSIR The Scarborough Hospital Toronto Endovascular Centre The Vein Institute of Toronto Scarborough Vascular
Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP)
 Kasr El Aini Journal of Surgery VOL., 11, NO 3 September 2010 31 Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP) Farghaly A,
Kasr El Aini Journal of Surgery VOL., 11, NO 3 September 2010 31 Thrombin injection vs Conventional Surgical Repair in Treatment of Iatrogenic Post-cath Femoral Artery Pseudoaneurysm (IFAP) Farghaly A,
How to manage TAVI related vascular complications. Paul TL Chiam MBBS, FRCP, FESC, FACC, FSCAI
 How to manage TAVI related vascular complications Paul TL Chiam MBBS, FRCP, FESC, FACC, FSCAI Definition VARC-2 consensus statement Complications caused by: Wire Catheter Anything related to vascular access
How to manage TAVI related vascular complications Paul TL Chiam MBBS, FRCP, FESC, FACC, FSCAI Definition VARC-2 consensus statement Complications caused by: Wire Catheter Anything related to vascular access
Step by step Hybrid procedures in peripheral obstructive disease. Holger Staab, MD University Hospital Leipzig, Germany Clinic for Vascular Surgery
 Step by step Hybrid procedures in peripheral obstructive disease Holger Staab, MD University Hospital Leipzig, Germany Clinic for Vascular Surgery Disclosure Speaker name: H.H. Staab I have the following
Step by step Hybrid procedures in peripheral obstructive disease Holger Staab, MD University Hospital Leipzig, Germany Clinic for Vascular Surgery Disclosure Speaker name: H.H. Staab I have the following
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant INDICATION: Abdominal aortic aneurysm. INTERVENTIONAL RADIOLOGIST:
The Utility of Atherectomy and the Jetstream Atherectomy System
 The Utility of Atherectomy and the Jetstream Atherectomy System William A. Gray, MD Columbia University Medical Center 2014 Boston Scientific Corporation or its affiliates. All rights reserved. IMPORTANT
The Utility of Atherectomy and the Jetstream Atherectomy System William A. Gray, MD Columbia University Medical Center 2014 Boston Scientific Corporation or its affiliates. All rights reserved. IMPORTANT
Diagnosis and Management of Femoral Access Site Complications IV: Novel Techniques for Endovascular Rescue
 Diagnosis and Management of Femoral Access Site Complications IV: Novel Techniques for Endovascular Rescue Robert M. Bersin, M.D. Director, Endovascular Services Seattle Cardiology and the Cardiovascular
Diagnosis and Management of Femoral Access Site Complications IV: Novel Techniques for Endovascular Rescue Robert M. Bersin, M.D. Director, Endovascular Services Seattle Cardiology and the Cardiovascular
The present status of selfexpanding. for CLI: Why and when to use. Sean P Lyden MD Cleveland Clinic Cleveland, Ohio
 The present status of selfexpanding and balloonexpandable tibial BMS and DES for CLI: Why and when to use Sean P Lyden MD Cleveland Clinic Cleveland, Ohio Disclosure Speaker name: Sean Lyden, MD I have
The present status of selfexpanding and balloonexpandable tibial BMS and DES for CLI: Why and when to use Sean P Lyden MD Cleveland Clinic Cleveland, Ohio Disclosure Speaker name: Sean Lyden, MD I have
The Role of Lithotripsy in Solving the Challenges of Vascular Calcium. Thomas Zeller, MD
 The Role of Lithotripsy in Solving the Challenges of Vascular Calcium Thomas Zeller, MD 1 1 Disclosure Speaker name: Thomas Zeller... I have the following potential conflicts of interest to report: X X
The Role of Lithotripsy in Solving the Challenges of Vascular Calcium Thomas Zeller, MD 1 1 Disclosure Speaker name: Thomas Zeller... I have the following potential conflicts of interest to report: X X
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
2-YEAR DATA SUPERA POPLITEAL REAL WORLD
 2-YEAR DATA SUPERA POPLITEAL REAL WORLD Enrique M. San Norberto. Angiology and Vascular Surgery. Valladolid University Hospital. Valladolid. Spain. Disclosure Speaker name: ENRIQUE M. SAN NORBERTO I have
2-YEAR DATA SUPERA POPLITEAL REAL WORLD Enrique M. San Norberto. Angiology and Vascular Surgery. Valladolid University Hospital. Valladolid. Spain. Disclosure Speaker name: ENRIQUE M. SAN NORBERTO I have
Peripheral Arterial Disease. Westley Smith MD Vascular Fellow
 Peripheral Arterial Disease Westley Smith MD Vascular Fellow Background (per 10,000) Goodney P, et al. Regional intensity of vascular care and lower extremity amputation rates. JVS. 2013; 6: 1471-1480.
Peripheral Arterial Disease Westley Smith MD Vascular Fellow Background (per 10,000) Goodney P, et al. Regional intensity of vascular care and lower extremity amputation rates. JVS. 2013; 6: 1471-1480.
2015 ARDMS Physicians Vascular Interpretation Job Task Analysis Summary Report
 P a g e 1 2015 ARDMS Physicians Vascular Interpretation Job Task Analysis Summary Report American Registry for Diagnostic Medical Sonography (ARDMS) P a g e 2 Table of Contents ABOUT THE REPORT... 3 METHODOLOGY...
P a g e 1 2015 ARDMS Physicians Vascular Interpretation Job Task Analysis Summary Report American Registry for Diagnostic Medical Sonography (ARDMS) P a g e 2 Table of Contents ABOUT THE REPORT... 3 METHODOLOGY...
Evolving Challenges in the Evaluation and Treatment of Lower Extremity PAD -- The Peripheral Academic Research Consortium (PARC)
 Evolving Challenges in the Evaluation and Treatment of Lower Extremity PAD -- The Peripheral Academic Research Consortium (PARC) W. Schuyler Jones, MD FACC Director, Adult Cardiac Catheterization Laboratory
Evolving Challenges in the Evaluation and Treatment of Lower Extremity PAD -- The Peripheral Academic Research Consortium (PARC) W. Schuyler Jones, MD FACC Director, Adult Cardiac Catheterization Laboratory
Endovascular and Hybrid Treatment of TASC C & D Aortoiliac Occlusive Disease
 Endovascular and Hybrid Treatment of TASC C & D Aortoiliac Occlusive Disease Arash Bornak, MD FACS Vascular & Endovascular Surgery University of Miami Miller School of Medicine No disclosure BACKGROUND
Endovascular and Hybrid Treatment of TASC C & D Aortoiliac Occlusive Disease Arash Bornak, MD FACS Vascular & Endovascular Surgery University of Miami Miller School of Medicine No disclosure BACKGROUND
Dealing with Calcification in BTK Arteries: Is Lithoplasty the Answer?
 Dealing with Calcification in BTK Arteries: Is Lithoplasty the Answer? Andrew Holden, MBChB, FRANZCR, EBIR Director of Interventional Radiology Auckland, New Zealand LINC 2017 January 25 th 2017 Disclosure
Dealing with Calcification in BTK Arteries: Is Lithoplasty the Answer? Andrew Holden, MBChB, FRANZCR, EBIR Director of Interventional Radiology Auckland, New Zealand LINC 2017 January 25 th 2017 Disclosure
V.A. is a 62-year-old male who presents in referral
 , LLC an HMP Communications Holdings Company Clinical Case Update Latest Trends in Critical Limb Ischemia Imaging Amit Srivastava, MD, FACC, FABVM Interventional Cardiologist Bay Area Heart Center St.
, LLC an HMP Communications Holdings Company Clinical Case Update Latest Trends in Critical Limb Ischemia Imaging Amit Srivastava, MD, FACC, FABVM Interventional Cardiologist Bay Area Heart Center St.
OCT Guided Atherectomy: Initial Results of the VISION Trial Using the Pantheris Catheter. Patrick Muck, MD
 OCT Guided Atherectomy: Initial Results of the VISION Trial Using the Pantheris Catheter Patrick Muck, MD Chief, Division of Vascular Surgery Good Samaritan Hospital Cincinna
OCT Guided Atherectomy: Initial Results of the VISION Trial Using the Pantheris Catheter Patrick Muck, MD Chief, Division of Vascular Surgery Good Samaritan Hospital Cincinna
Case Report Successful Implantation of a Coronary Stent Graft in a Peripheral Vessel
 Case Reports in Vascular Medicine Volume 2015, Article ID 725168, 4 pages http://dx.doi.org/10.1155/2015/725168 Case Report Successful Implantation of a Coronary Stent Graft in a Peripheral Vessel Alexander
Case Reports in Vascular Medicine Volume 2015, Article ID 725168, 4 pages http://dx.doi.org/10.1155/2015/725168 Case Report Successful Implantation of a Coronary Stent Graft in a Peripheral Vessel Alexander
Update on Tack Optimized Balloon Angioplasty (TOBA) Below the Knee. Marianne Brodmann, MD Medical University Graz Graz, Austria
 Update on Tack Optimized Balloon Angioplasty (TOBA) Below the Knee Marianne Brodmann, MD Medical University Graz Graz, Austria Critical Limb Ischemia Infrapopliteal arterial disease is a leading source
Update on Tack Optimized Balloon Angioplasty (TOBA) Below the Knee Marianne Brodmann, MD Medical University Graz Graz, Austria Critical Limb Ischemia Infrapopliteal arterial disease is a leading source
Registry Assessment of Peripheral Interventional Devices (RAPID)
 Registry Assessment of Peripheral Interventional Devices (RAPID) Adding Data Sources May 2, 2018 W. Schuyler Jones, MD Duke Clinical Research Institute Duke Heart Center Disclosures Research Grants: Agency
Registry Assessment of Peripheral Interventional Devices (RAPID) Adding Data Sources May 2, 2018 W. Schuyler Jones, MD Duke Clinical Research Institute Duke Heart Center Disclosures Research Grants: Agency
MICHAEL R. JAFF, DO MASSACHUSETTS, UNITED STATES. Medtronic Further. Together
 DRUG-COATED BALL0ON TREATMENT FOR PATIENTS WITH INTERMITTENT CLAUDICATION: INSIGHTS FROM THE IN.PACT GLOBAL FULL CLINICAL COHORT MICHAEL R. JAFF, DO MASSACHUSETTS, UNITED STATES Medtronic Further. Together
DRUG-COATED BALL0ON TREATMENT FOR PATIENTS WITH INTERMITTENT CLAUDICATION: INSIGHTS FROM THE IN.PACT GLOBAL FULL CLINICAL COHORT MICHAEL R. JAFF, DO MASSACHUSETTS, UNITED STATES Medtronic Further. Together
Christian Wissgott MD, PhD Assistant Director, Radiology Westküstenkliniken Heide
 2-Year Results Of The Tack Optimized Balloon Angioplasty (TOBA) Trial For Fem- Pop Lesions Demonstrates Safety and Efficacy Of The Tack Endovascular System In Repairing Focal Post-PTA Dissections Christian
2-Year Results Of The Tack Optimized Balloon Angioplasty (TOBA) Trial For Fem- Pop Lesions Demonstrates Safety and Efficacy Of The Tack Endovascular System In Repairing Focal Post-PTA Dissections Christian
DURABLE. CONSISTENT. SAFE. IN.PACT Admiral Drug-Coated Balloon
 DURABLE. CONSISTENT. SAFE. Drug-Coated Balloon THE SCIENCE BEHIND THE OUTCOMES DCB has proven, long-term durable outcomes across multiple clinical trials, as well as across complex patient and lesion types.
DURABLE. CONSISTENT. SAFE. Drug-Coated Balloon THE SCIENCE BEHIND THE OUTCOMES DCB has proven, long-term durable outcomes across multiple clinical trials, as well as across complex patient and lesion types.
Subject Area Modules. Subject Area Modules. Subject Area Modules Published on Society for Vascular Surgery (
 Purchasing the VESAP3 comprehensive package provides access to all 10 VESAP3 modules, in learning and exam mode, for $151 less than the cost of purchasing all modules individually. Click here to learn
Purchasing the VESAP3 comprehensive package provides access to all 10 VESAP3 modules, in learning and exam mode, for $151 less than the cost of purchasing all modules individually. Click here to learn
DISRUPT PAD. (( Data Summary )) DISRUPT PAD Data Summary SPL Rev. B 2016 Shockwave Medical Inc. All rights reserved.
 DISRUPT PAD (( Data Summary )) DISRUPT PAD Data Summary SPL 60971 Rev. B 1 Summary of the key findings from the DISRUPT PAD Study 99% of femoropopliteal lesions treated were moderately or severely calcified.
DISRUPT PAD (( Data Summary )) DISRUPT PAD Data Summary SPL 60971 Rev. B 1 Summary of the key findings from the DISRUPT PAD Study 99% of femoropopliteal lesions treated were moderately or severely calcified.
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease
 Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Pre-and Post Procedure Non-Invasive Evaluation of the Patient with Carotid Disease Michael R. Jaff, D.O., F.A.C.P., F.A.C.C. Assistant Professor of Medicine Harvard Medical School Director, Vascular Medicine
Coronary angiography and PCI
 Coronary arteries Coronary angiography and PCI Samo Granda, Franjo Naji Department of Cardiology Clinical department of internal medicine University clinical centre Maribor Coronary arteries Atherosclerosis
Coronary arteries Coronary angiography and PCI Samo Granda, Franjo Naji Department of Cardiology Clinical department of internal medicine University clinical centre Maribor Coronary arteries Atherosclerosis
Accurate Vessel Sizing Drives Clinical Results. IVUS In the Periphery
 Accurate Vessel Sizing Drives Clinical Results IVUS In the Periphery Discussion Iida O, et. al. Study Efficacy of Intravascular Ultrasound in Femoropopliteal Stenting for Peripheral Artery Disease With
Accurate Vessel Sizing Drives Clinical Results IVUS In the Periphery Discussion Iida O, et. al. Study Efficacy of Intravascular Ultrasound in Femoropopliteal Stenting for Peripheral Artery Disease With
2019 ABBOTT REIMBURSEMENT GUIDE CMS Physician Fee Schedule
 ABBOTT REIMBURSEMENT GUIDE CMS Physician Fee Schedule This document and the information contained herein is for general information purposes only and is not intended and does not constitute legal, reimbursement,
ABBOTT REIMBURSEMENT GUIDE CMS Physician Fee Schedule This document and the information contained herein is for general information purposes only and is not intended and does not constitute legal, reimbursement,
Current Status of Endovascular Therapies for Critical Limb Ischemia
 Current Status of Endovascular Therapies for Critical Limb Ischemia Bulent Arslan, MD Associate Professor of Radiology Director, Vascular & Interventional Radiology Rush University Medical Center bulent_arslan@rush.edu
Current Status of Endovascular Therapies for Critical Limb Ischemia Bulent Arslan, MD Associate Professor of Radiology Director, Vascular & Interventional Radiology Rush University Medical Center bulent_arslan@rush.edu
Case Discussion. Disclosures. Critical Limb Ischemia: A Selective Approach to Revascularization Works Best 4/28/2012. None. 58 yo M, DM, CAD, HTN
 Critical Limb Ischemia: A Selective Approach to Revascularization Works Best None Disclosures Michael S. Conte MD, FACS Division of Vascular and Endovascular Surgery Co-Director, Heart and Vascular Center
Critical Limb Ischemia: A Selective Approach to Revascularization Works Best None Disclosures Michael S. Conte MD, FACS Division of Vascular and Endovascular Surgery Co-Director, Heart and Vascular Center
Introduction 3. What is Peripheral Vascular Disease? 5. What Are Some of the Symptoms of Peripheral Vascular Disease? 6
 Patient Information Table of Contents Introduction 3 What is Peripheral Vascular Disease? 5 What Are Some of the Symptoms of Peripheral Vascular Disease? 6 What Causes Peripheral Vascular Disease? 7 How
Patient Information Table of Contents Introduction 3 What is Peripheral Vascular Disease? 5 What Are Some of the Symptoms of Peripheral Vascular Disease? 6 What Causes Peripheral Vascular Disease? 7 How
Recommendations for Follow-up After Vascular Surgery Arterial Procedures SVS Practice Guidelines
 Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Imaging for Peripheral Vascular Disease
 Imaging for Peripheral Vascular Disease James G. Jollis, MD Director, Rex Hospital Cardiovascular Imaging Imaging for Peripheral Vascular Disease 54 year old male with exertional calf pain in his right
Imaging for Peripheral Vascular Disease James G. Jollis, MD Director, Rex Hospital Cardiovascular Imaging Imaging for Peripheral Vascular Disease 54 year old male with exertional calf pain in his right
Intercepting PAD. Playbook for Cardiovascular Care 2018 February 24, Jonathan D Woody, MD, FACS. University Surgical Vascular
 Intercepting PAD Playbook for Cardiovascular Care 2018 February 24, 2018 Jonathan D Woody, MD, FACS University Surgical Vascular Attending Vascular Surgeon - Piedmont Athens Regional Adjunct Clinical Associate
Intercepting PAD Playbook for Cardiovascular Care 2018 February 24, 2018 Jonathan D Woody, MD, FACS University Surgical Vascular Attending Vascular Surgeon - Piedmont Athens Regional Adjunct Clinical Associate
Patient Brochure. Clearstream Technologies, Ltd. Moyne Upper Enniscorthy Co. Wexford, Ireland. PK Rev. 0 05/17
 Patient Brochure Clearstream Technologies, Ltd. Moyne Upper Enniscorthy Co. Wexford, Ireland PK1411100 Rev. 0 05/17 LIFESTREAM Patient Brochure If you or a member of your family has been diagnosed with
Patient Brochure Clearstream Technologies, Ltd. Moyne Upper Enniscorthy Co. Wexford, Ireland PK1411100 Rev. 0 05/17 LIFESTREAM Patient Brochure If you or a member of your family has been diagnosed with
Abdominal and thoracic aneurysm repair
 Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Disclosures. Critical Limb Ischemia. Vascular Testing in the CLI Patient. Vascular Testing in Critical Limb Ischemia UCSF Vascular Symposium
 Disclosures Vascular Testing in the CLI Patient None 2015 UCSF Vascular Symposium Warren Gasper, MD Assistant Professor of Surgery UCSF Division of Vascular Surgery Critical Limb Ischemia Chronic Limb
Disclosures Vascular Testing in the CLI Patient None 2015 UCSF Vascular Symposium Warren Gasper, MD Assistant Professor of Surgery UCSF Division of Vascular Surgery Critical Limb Ischemia Chronic Limb
2017 Cardiology Survival Guide
 2017 Cardiology Survival Guide Chapter 2: Angioplasty/Atherectomy/Stent The term angioplasty literally means "blood vessel repair." During an angioplasty procedure, the physician inserts a catheter, with
2017 Cardiology Survival Guide Chapter 2: Angioplasty/Atherectomy/Stent The term angioplasty literally means "blood vessel repair." During an angioplasty procedure, the physician inserts a catheter, with
Adult Cardiology Clinical Privileges
 Name: Effective from / / to / / Initial privileges (initial appointment) (reappointment) Renewal of privileges All new applicants should meet the following requirements as approved by the governing body,
Name: Effective from / / to / / Initial privileges (initial appointment) (reappointment) Renewal of privileges All new applicants should meet the following requirements as approved by the governing body,
Tom Eisele, Benedikt M. Muenz, and Grigorios Korosoglou. Department of Cardiology & Vascular Medicine, GRN Hospital Weinheim, Weinheim, Germany
 Case Reports in Vascular Medicine Volume 2016, Article ID 7376457, 4 pages http://dx.doi.org/10.1155/2016/7376457 Case Report Successful Endovascular Repair of an Iatrogenic Perforation of the Superficial
Case Reports in Vascular Medicine Volume 2016, Article ID 7376457, 4 pages http://dx.doi.org/10.1155/2016/7376457 Case Report Successful Endovascular Repair of an Iatrogenic Perforation of the Superficial
Endovascular Therapy vs. Open Femoral Endarterectomy Rationale and Design of the Randomized PESTO Trial
 Endovascular Therapy vs. Open Femoral Endarterectomy Rationale and Design of the Randomized PESTO Trial Prof. Thomas Zeller, MD Department Angiology Clinic for Cardiology and Angiology II University Heart-Center
Endovascular Therapy vs. Open Femoral Endarterectomy Rationale and Design of the Randomized PESTO Trial Prof. Thomas Zeller, MD Department Angiology Clinic for Cardiology and Angiology II University Heart-Center
Role of ABI in Detecting and Quantifying Peripheral Arterial Disease
 Role of ABI in Detecting and Quantifying Peripheral Arterial Disease Difference in AAA size between US and Surgeon 2 1 0-1 -2-3 0 1 2 3 4 5 6 7 Mean AAA size between US and Surgeon Kathleen G. Raman MD,
Role of ABI in Detecting and Quantifying Peripheral Arterial Disease Difference in AAA size between US and Surgeon 2 1 0-1 -2-3 0 1 2 3 4 5 6 7 Mean AAA size between US and Surgeon Kathleen G. Raman MD,
CHALLENGING ILIAC ACCESSES AND THROMBOSIS PREVENTION
 CHALLENGING ILIAC ACCESSES AND THROMBOSIS PREVENTION ARMANDO MANSILHA MD, PhD, FEBVS UNIVERSITY HOSPITAL - PORTO Disclosure of Interest Speaker name: ARMANDO MANSILHA I have the following potential conflicts
CHALLENGING ILIAC ACCESSES AND THROMBOSIS PREVENTION ARMANDO MANSILHA MD, PhD, FEBVS UNIVERSITY HOSPITAL - PORTO Disclosure of Interest Speaker name: ARMANDO MANSILHA I have the following potential conflicts
Larry Diaz, MD, FSCAI Mehdi H. Shishehbor, DO, FSCAI
 PAD Diagnosis Larry Diaz, MD, FSCAI Metro Health / University of Michigan Health, Wyoming, MI Mehdi H. Shishehbor, DO, FSCAI University Hospitals Harrington Heart & Vascular Institute, Cleveland, OH PAD:
PAD Diagnosis Larry Diaz, MD, FSCAI Metro Health / University of Michigan Health, Wyoming, MI Mehdi H. Shishehbor, DO, FSCAI University Hospitals Harrington Heart & Vascular Institute, Cleveland, OH PAD:
Stratifying Management Options for Patients with Critical Limb Ischemia: When Should Open Surgery Be the Initial Option for CLI?
 Stratifying Management Options for Patients with Critical Limb Ischemia: When Should Open Surgery Be the Initial Option for CLI? Peter F. Lawrence, M.D. Gonda Vascular Center Division of Vascular Surgery
Stratifying Management Options for Patients with Critical Limb Ischemia: When Should Open Surgery Be the Initial Option for CLI? Peter F. Lawrence, M.D. Gonda Vascular Center Division of Vascular Surgery
CAROTID ARTERY ANGIOPLASTY
 CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
The Struggle to Manage Stroke, Aneurysm and PAD
 The Struggle to Manage Stroke, Aneurysm and PAD In this article, Dr. Salvian examines the management of peripheral arterial disease, aortic aneurysmal disease and cerebrovascular disease from symptomatology
The Struggle to Manage Stroke, Aneurysm and PAD In this article, Dr. Salvian examines the management of peripheral arterial disease, aortic aneurysmal disease and cerebrovascular disease from symptomatology
Corporate Medical Policy
 Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Corporate Medical Policy Endovascular Therapies for Extracranial Vertebral Artery Disease File Name: Origination: Last CAP Review: Next CAP Review: Last Review: endovascular_therapies_for_extracranial_vertebral_artery_disease
Access strategy for chronic total occlusions (CTOs) is crucial
 Learn How Access Strategy Impacts Complex CTO Crossing Arthur C. Lee, MD The Cardiac & Vascular Institute, Gainesville, Florida VASCULAR DISEASE MANAGEMENT 2018;15(3):E19-E23. Key words: chronic total
Learn How Access Strategy Impacts Complex CTO Crossing Arthur C. Lee, MD The Cardiac & Vascular Institute, Gainesville, Florida VASCULAR DISEASE MANAGEMENT 2018;15(3):E19-E23. Key words: chronic total
The VGH Interventional Cardiology Fellowship program has successfully trained 38 interventional fellows since 1993.
 VGH Interventional Cardiology Fellowship Program 1. Introduction: The VGH interventional cardiology training program is a competitive, high-volume, fellowship training program that instructs trainees on
VGH Interventional Cardiology Fellowship Program 1. Introduction: The VGH interventional cardiology training program is a competitive, high-volume, fellowship training program that instructs trainees on
Abdominal Aortic Aneurysms. A Surgeons Perspective Dr. Derek D. Muehrcke
 Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
PATIENT SPECIFIC STRATEGIES IN CRITICAL LIMB ISCHEMIA. Dr. Manar Trab Consultant Vascular Surgeon European Vascular Clinic DMCC Dubai, UAE
 PATIENT SPECIFIC STRATEGIES IN CRITICAL LIMB ISCHEMIA Dr. Manar Trab Consultant Vascular Surgeon European Vascular Clinic DMCC Dubai, UAE Disclosure Speaker name: DR. Manar Trab I have the following potential
PATIENT SPECIFIC STRATEGIES IN CRITICAL LIMB ISCHEMIA Dr. Manar Trab Consultant Vascular Surgeon European Vascular Clinic DMCC Dubai, UAE Disclosure Speaker name: DR. Manar Trab I have the following potential
Surgical Options for revascularisation P E T E R S U B R A M A N I A M
 Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
Surgical Options for revascularisation P E T E R S U B R A M A N I A M The goal Treat pain Heal ulcer Preserve limb Preserve life The options Conservative Endovascular Surgical bypass Primary amputation
Management of In-stent Restenosis after Lower Extremity Endovascular Procedures
 Management of In-stent Restenosis after Lower Extremity Endovascular Procedures Piotr Sobieszczyk, MD Associate Director, Cardiac Catheterization Laboratory Cardiovascular Division and Vascular Medicine
Management of In-stent Restenosis after Lower Extremity Endovascular Procedures Piotr Sobieszczyk, MD Associate Director, Cardiac Catheterization Laboratory Cardiovascular Division and Vascular Medicine
Challenging of contrast agent-free endovascular treatment using 3D imaging
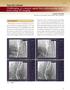 AC17-0010 Challenging of contrast agent-free endovascular treatment using 3D imaging Amane Kozuki Department of Cardiology, Osaka Saiseikai Nakatsu Hospital Introduction With advances in devices and techniques,
AC17-0010 Challenging of contrast agent-free endovascular treatment using 3D imaging Amane Kozuki Department of Cardiology, Osaka Saiseikai Nakatsu Hospital Introduction With advances in devices and techniques,
The incidence of peripheral artery disease (PAD)
 Pharmacologic Options for Treating Restenosis The role of cilostazol in the treatment of patients with infrainguinal lesions. By Osamu Iida, MD, and Yoshimitsu Soga, MD The incidence of peripheral artery
Pharmacologic Options for Treating Restenosis The role of cilostazol in the treatment of patients with infrainguinal lesions. By Osamu Iida, MD, and Yoshimitsu Soga, MD The incidence of peripheral artery
National Vascular Registry
 National Vascular Registry Bypass Patient Details Patient Consent* 2 Not Required If patient not consented: Date consent recorded / / (DD/MM/YYYY) Do not record NHS number, NHS number* name(s) or postcode.
National Vascular Registry Bypass Patient Details Patient Consent* 2 Not Required If patient not consented: Date consent recorded / / (DD/MM/YYYY) Do not record NHS number, NHS number* name(s) or postcode.
National Vascular Registry
 National Vascular Registry Angioplasty Patient Details Patient Consent* 2 Not Required If patient not consented: Date consent recorded / / (DD/MM/YYYY) Do not record NHS number, NHS number* name(s) or
National Vascular Registry Angioplasty Patient Details Patient Consent* 2 Not Required If patient not consented: Date consent recorded / / (DD/MM/YYYY) Do not record NHS number, NHS number* name(s) or
CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments
 CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) In CY2015 and in an effort to help pay providers for quality, not
CY2017 Hospital Outpatient: Vascular Procedure APCs and Complexity Adjustments Comprehensive Ambulatory Payment Classifications (c-apcs) In CY2015 and in an effort to help pay providers for quality, not
Introduction What Causes Peripheral Vascular Disease? How Do Doctors Treat Peripheral Vascular Disease?... 9
 Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
The results of EVT for Chronic Aortic Occlusion - a multicenter retrospective study - Taku Kato, MD Rakuwakai Otowa Hospital, Kyoto, Japan
 The results of EVT for Chronic Aortic Occlusion - a multicenter retrospective study - Taku Kato, MD Rakuwakai Otowa Hospital, Kyoto, Japan COI disclosure Disclosure Speaker name: Taku Kato... I have the
The results of EVT for Chronic Aortic Occlusion - a multicenter retrospective study - Taku Kato, MD Rakuwakai Otowa Hospital, Kyoto, Japan COI disclosure Disclosure Speaker name: Taku Kato... I have the
Rotarex mechanical debulking: The Leipzig experience in patients
 Rotarex mechanical debulking: The Leipzig experience in 1.200+ patients Dierk Scheinert, MD Division of Interventional Angiology University-Hospital Leipzig, Germany Disclosure Speaker name: Dierk Scheinert
Rotarex mechanical debulking: The Leipzig experience in 1.200+ patients Dierk Scheinert, MD Division of Interventional Angiology University-Hospital Leipzig, Germany Disclosure Speaker name: Dierk Scheinert
CPT Code Details
 CPT Code 93572 Details Code Descriptor Intravascular Doppler velocity and/or pressure derived coronary flow reserve measurement (coronary vessel or graft) during coronary angiography including pharmacologically
CPT Code 93572 Details Code Descriptor Intravascular Doppler velocity and/or pressure derived coronary flow reserve measurement (coronary vessel or graft) during coronary angiography including pharmacologically
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Managing Conditions Resulting from Untreated Cardiometabolic Syndrome
 Managing Conditions Resulting from Untreated Cardiometabolic Syndrome Matthew P. Namanny DO, FACOS Vascular/Endovascular Surgery Saguaro Surgical/AZ Vascular Specialist Tucson Medical Center Critical Limb
Managing Conditions Resulting from Untreated Cardiometabolic Syndrome Matthew P. Namanny DO, FACOS Vascular/Endovascular Surgery Saguaro Surgical/AZ Vascular Specialist Tucson Medical Center Critical Limb
Popliteal Artery Aneurysms: Diagnosis and Repair Options
 Deepak N. Deshmukh DO April 27, 2018 Popliteal Artery Aneurysms: Diagnosis and Repair Options No Disclosures Popliteal Artery Aneurysms (PAAs) Male Predominanace Most common peripheral Aneurysm (70%) 30-50%
Deepak N. Deshmukh DO April 27, 2018 Popliteal Artery Aneurysms: Diagnosis and Repair Options No Disclosures Popliteal Artery Aneurysms (PAAs) Male Predominanace Most common peripheral Aneurysm (70%) 30-50%
The Accuracy of a Volume Plethysmography System as Assessed by Contrast Angiography
 Research imedpub Journals http://www.imedpub.com/ DOI: 10.21767/2572-5483.100036 Journal of Preventive Medicine The Accuracy of a Volume Plethysmography System as Assessed by Contrast Angiography Andrew
Research imedpub Journals http://www.imedpub.com/ DOI: 10.21767/2572-5483.100036 Journal of Preventive Medicine The Accuracy of a Volume Plethysmography System as Assessed by Contrast Angiography Andrew
TAVR : Caring for your patients before and after TAVR
 TAVR : Caring for your patients before and after TAVR Zubair Ahmed MD FSCAI Interventional Cardiologist Washington Regional Medical Center / Walker Heart Institute What is Aortic Valve Stenosis? AVA ~4
TAVR : Caring for your patients before and after TAVR Zubair Ahmed MD FSCAI Interventional Cardiologist Washington Regional Medical Center / Walker Heart Institute What is Aortic Valve Stenosis? AVA ~4
Patient Information. Peripheral Arterial Disease and the Lutonix 035 Balloon. Advancing Lives and the Delivery of Health Care
 Patient Information Peripheral Arterial Disease and the Lutonix 035 Balloon Advancing Lives and the Delivery of Health Care Contents Peripheral Arterial Disease (PAD) Peripheral Arterial Disease (PAD)
Patient Information Peripheral Arterial Disease and the Lutonix 035 Balloon Advancing Lives and the Delivery of Health Care Contents Peripheral Arterial Disease (PAD) Peripheral Arterial Disease (PAD)
Assurant Cobalt Iliac BALLOON EXPANDABLE STENT SYSTEM
 Assurant Cobalt Iliac BALLOON EXPANDABLE STENT SYSTEM Innovating for life. CONFORMABILIT Y 6 F S H E AT H C O M PAT I B I L I T Y THE ASSURANT COBALT ILIAC STENT, WITH ITS UNIQUE COBALT CHROMIUM MODULAR
Assurant Cobalt Iliac BALLOON EXPANDABLE STENT SYSTEM Innovating for life. CONFORMABILIT Y 6 F S H E AT H C O M PAT I B I L I T Y THE ASSURANT COBALT ILIAC STENT, WITH ITS UNIQUE COBALT CHROMIUM MODULAR
