NIH Public Access Author Manuscript J Pediatr. Author manuscript; available in PMC 2012 March 1.
|
|
|
- Rafe Bates
- 5 years ago
- Views:
Transcription
1 NIH Public Access Author Manuscript Published in final edited form as: J Pediatr March ; 158(3): doi: /j.jpeds He's Dizzy when he Stands Up. An Introduction to Initial orthostatic Hypotension Julian M. Stewart, M.D., Ph.D. 1,2 and Debbie Clarke, B.S. 1,2 1 Department of Pediatrics, New York Medical College Valhalla, NY Department of Physiology, New York Medical College Valhalla, NY Keywords rapid standing; head-up tilt; orthostatic intolerance; syncope Introduction to the patient and the most frequent orthostatic complaint The most frequent orthostatic complaint in young people is lightheadedness or dizziness on rapid standing, sometimes from a seated position, most often from a supine position after hours of recumbency(1,2). The most common complainant is an adolescent in the middle of a growth spurt. Often the patient is already tall or is growing rapidly. Similar complaints are seen among young people of both sexes, particularly in patients of slender build and reduced blood volume (3). The complaints relate to normal physiology shared by people of all ages and have been identified by students of orthostasis in the past (1,2,4 6). Typically, there is transient pallor, perhaps some loss of postural tone, blurred vision or even loss of vision (black out, white out, spots), and less commonly, loss of consciousness. Symptoms instantly disappear with recumbency and are reduced or even abolished by standing up more slowly or in stages (7). Symptoms and signs peak soon after standing, in synchrony with a transient and substantial decrease in blood pressure which has its nadir at approximately 8 15 seconds after standing as shown in Figure 1. Heart rate increases as BP falls. These findings can be demonstrated using beat-to-beat finger arterial photoplethysmography (Finapres, Finometer, TNO Amsterdam) (2,8,9) or other means for beat-to-beat assessment. The BP decrements are usually not apparent by auscultatory or oscillometric blood pressure measurement, having a far too rapid and fleeting time course to be detected by these methods (10). Thus, the clinician needs to rely on clinical history and perhaps observation of the patient. The history is that of rapid-onset, short-lived dizziness and other symptoms on rapidly standing upright. If the patient can remain upright or can be held upright, all symptoms abate and disappear within 60 seconds and usually within less than 30 seconds (11). After recovery, the patient is usually entirely well and is free of subsequent fainting and of 2010 Mosby, Inc. All rights reserved Address for Correspondence: Julian M. Stewart M.D., Ph.D. Professor of Pediatrics, Physiology, Medicine The Center for Hypotension Suite Bradhurst Avenue New York Medical College Hawthorne, New York Telephone: Fax: stewart@nymc.edu. Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final citable form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain. The authors declare no conflicts of interest.
2 Stewart and Clarke Page 2 symptoms of orthostatic symptoms. The patient is otherwise entirely healthy. This stands in contrast with the clinical entity of instantaneous orthostatic hypotension (INOH) described by Tanaka and coworkers (2) in which recovery from hypotension was prolonged or ineffectual. Many sufferers report successfully holding themselves upright until the unpleasant sensations pass. There appears to be no relationship between this transient hypotension and the degree of orthostatic tolerance demonstrated in a laboratory setting in normal young subjects (9). These studies should be cautiously interpreted because they excluded subjects with known OI. However, they do demonstrate that IOH need not cause more pernicious forms of OI. This short-lived hypotension is different from simple faint, in which maintaining the patient in the upright position makes the faint persistent and the patient often becomes much worse, clinically (12). Can it occur on a tilt table? We often observe the phenomenon as tilt commences. However, the decrease in BP is generally of smaller magnitude compared with standing. This is shown in Figure 2 in the same subject who had standing and upright tilt to 70 performed separately on the same morning. The magnitude of BP decrease may depend on the rapidity of upright tilt. Also, during active standing, alterations in BP and HR are more closely related to skeletal muscle activity, abdominal compression and responsive reflex changes (13). In addition, there is an anticipatory increase in both heart rate and blood pressure seconds prior to the stand which is absent during the tilt. This is due to a phenomenon called central command in which higher neurological centers engage the autonomic nervous system in order to prepare the body for exercise (14). Initial Orthostatic Hypotension (IOH) Initial orthostatic hypotension (IOH), aptly named by Wieling and other students of orthostatic intolerance because of early, transient, orthostatic (standing up) hypotension (1,4,6,15,16) which can be substantial and symptomatic. However, unlike true orthostatic hypotension, with its relentlessly progressive fall in blood pressure while the subject remains upright, IOH is short-lived and blood pressure recovery always occurs. As defined by consensus (17), true orthostatic hypotension (OH) is a sustained reduction of systolic blood pressure of at least 20 mm Hg or diastolic blood pressure of at least 10 mm Hg within 3 minutes of standing or upright tilting to 60 or more. On one hand, true orthostatic hypotension is often associated with autonomic failure or severe autonomic dysfunction which can be life threatening (18). On the other hand, IOH is associated with autonomic integrity and usually has few, if any, consequences. In those of slight build and small blood volume, mean arterial pressure may decrease by nearly 50% (Figure 1) with comparable changes in cerebral blood flow leading to unconsciousness. Such extremes are relatively rare (1/100 young patients seen in our syncope center over last 10 years), but can occur and require medical attention. However, an estimated 50% of adolescents and somewhat fewer young patients in their twenties, experience this difficulty during the first half of life. IOH, again, becomes common and more dangerous in the elderly, especially those patients taking vasoactive medications or those patients with medical problems placing them at increased risk (6). Dehydration is also a potentiating factor. Otherwise, in the young, IOH is evanescent, improves with time as teens age, and can be clinically remediated through preventative or responsive aversive maneuvers (6,15,19). IOH is almost always due to normal rather than abnormal physiology. There is no autonomic dysfunction. Merely a [normal] delay in compensation for gravitational loading during postural change (20). But is it Orthostatic Intolerance? It is, by definition, but it is not autonomic dysfunction. Orthostatic intolerance (OI) is defined as the development of symptoms and signs when upright that are relieved by
3 Stewart and Clarke Page 3 recumbence (21,22). Even so, other forms of brief OI are facts of everyday life and may be thought to be normal aspects of life which are not necessarily harmful. For example, the experiences of postural lightheadedness during states of dehydration or fever are universal. More life-affecting forms of orthostatic intolerance are also common and include simple postural faint (vasovagal faint, neurocardiogenic syncope, reflex syncope, (23,24)) as a prevalent form of acute orthostatic intolerance in which transient loss of consciousness and postural tone occurs as the result of cerebral hypoperfusion (25). This almost always results from hypotension occurring while upright. Chronic orthostatic intolerance occurs as well and includes the postural tachycardia syndrome (POTS) (26 28), and neurally mediated hypotension (29 31) which may occur alone or as part of chronic fatigue syndrome (32). Postural hyperventilation has also been reported (33). Simple faint and chronic OI are related by the common feature of reduced cardiac filling, and therefore early reflex tachycardia is common to both (34,35). Estimates of lifetime incidence of at least one fainting episode may reach 40 50% approximately half occurring during childhood (36). Fainting, NMH, POTS, or postural hyperpnea may be provoked in virtually any healthy subject in the laboratory with sufficient central hypovolemia using a tilt table and lower body negative pressure together to profoundly unload the heart (37). Therefore, these are not diseases in a strict sense; autonomic dysfunction is not necessary for their occurrence. Rather, these problems represent circulatory inadequacy in efficiently coping with physiological stressors, with varying response thresholds, in different individuals. Nevertheless, syncope and chronic OI can interfere with quality of life and thus require remediation. Is Initial Orthostatic Hypotension different from simple faint? The hallmark of IOH is its immediacy and transient nature, with restoration of blood pressure in less than a minute, although the extent of associated hypotension may be occasionally sufficient to produce transient loss of consciousness. This is distinguished from simple postural faint which is not immediate but occurs after some minutes of upright stance. Also, the young patient with IOH will usually recover normal blood pressure even if upright stance is artificially maintained by propping the patient up. This is not at all the case for simple faint which, if standing is artificially maintained, progresses to complete loss of blood pressure and often severe bradycardia or asystole (38) with potentially pernicious outcome (12). Finally, and characteristically, simple postural faint in the young is almost always vasovagal faint which means that after a sufficient time upright, there is a hypotension (vasodilation) followed almost immediately by vagally mediated relative bradycardia (39). This contrasts with observations during IOH. Figure 3 shows blood pressure and heart rate in a patient with a history of postural fainting who upon upright tilt has IOH, recovers, and then goes on to suffer a typical vasovagal episode. It is clear that the hypotension of IOH is accompanied by tachycardia, and the delayed hypotension of the vasovagal faint is accompanied by bradycardia. In the first instance (IOH), tachycardia is a reflex response to hypotension. In the second instance (vasovagal faint), early upright reflex tachycardia does occur in relation to blood volume shifts in the upright position (40). However, subsequent hypotension is associated with bradycardia which would seem physiologically inappropriate. The inappropriate bradycardia reflects baroreflex failure at faint; the tachycardia of IOH reflects physiologically appropriate baroreflex function.
4 Stewart and Clarke Page 4 A few words about Physiology Supine Physiology While supine, arterial blood and venous reservoirs are at the same height. There is no net gravitational force acting on blood. Neurovascular mechanisms, such as peripheral vasoconstriction and venoconstriction, local and humoral vasoactive factors (e.g. epinephrine, angiotensin-ii, vasopressin, nitric oxide) are in their tonic resting conditions. The supine arterial vasculature is relatively vasodilated compared with its state when upright. While supine, the dependent venous pools are relatively underfilled having cranially redistributed blood while supine (41,42). Compensated Upright Physiology Upright posture requires rapid circulatory and neurologic compensation in order to maintain blood pressure and consciousness. If these are ineffective or if there is insufficient blood volume, the location of the brain above the heart and the presence of large venous reservoirs below the heart causes cardiac filling and blood pressure to decrease rapidly with consequent cerebral malperfusion and loss of consciousness (42). This describes the steady condition that is impaired in simple faint and autonomic failure. The transition from supine to upright The transition to the steady upright condition, that is, from supine to standing up, is not included in this description. The physiology changes radically when someone stands up. An ensemble of anti-gravity, anti-orthostatic physiological responses are evoked during standing up including the skeletal muscle pump (43) and arterial and cardiopulmonary baroreflexes (44,45). Actual vasodilation does not occur (46), although the literature suggests that the more vasodilated you are prior to orthostasis, the greater the initial hypotensive effect (20,47). Observations of increasing vasodilation are based on calculated total peripheral resistance (TPR) = MAP/CO. As MAP decreases transiently, CO increases as shown in Figure 1. This occurs before effective vasoconstriction can occur. The traditional calculation of TPR fails to factor in the abrupt onset of an additional force, gravity, which effectively propels blood caudally (48). The initial force of gravity is not effectively counterbalanced by skeletal muscle pumping because the leg veins are initially underfilled for the upright position. Later, during steady state standing, the effect of gravity is compensated by a pressure difference equal and opposite to gravitational force (ρgh) conferring mechanical equilibrium. Such equilibrium is initially absent upon rapid standing (49). Estimates of the initial pressure gradient for the subject of Figure 1 taking into consideration the average height of the hemostatic column from heart to splanchnic bed (approximately 20 cms) and from heart to mid thigh (approximately 80 cms) yields an average estimated height <h> of 50 cms of blood. This corresponds to a pressure of ρg<h> or roughly mmhg /cm blood *50cms = 39 mmhg for the subject of Figure 1. When TPR is recalculated as TPR = (MAP+ ρg<h>)/co the apparent initial decrease in TPR disappears as shown in the bottom right hand panel of Figure 1. This has been aptly described as a virtual conductance by Sheriff and others (46,47). Thus, at least initially, blood is propelled by uncompensated gravity, and is also pumped by the heart in declining amounts as cardiac venous return decreases until vasoconstriction occurs and a mechanical equilibrium is reached. The lungs and pulmonary venous return help to support left ventricular filling but this is unable to maintain BP. For those technically minded, the effect resembles a periodically driven (pressure generated by cardiac contraction, ~CP), resistance damped (blood vessel vasoconstriction, R) harmonic oscillator upon which a constant force (G) is suddenly applied (50). The
5 Stewart and Clarke Page 5 characteristic modes of operation of such a system can be found among the responses to standing and appear in Figure 4. Treatment of the young with IOH Summary Acknowledgments References Often reassurance is all that is needed, particularly if there is no loss of postural tone and the episodes are brief. Standing up more rapidly comes with youth and departs with age which may account for the maturational diminution of IOH. Rising more slowly may be sufficient therapy. Situations or illnesses that promote a contraction of blood volume can often be treated or avoided. Measures to increase blood volume such as enhanced salt and water intake may be of help. For more debilitating forms of IOH preventiveand treatment options currently favor physical maneuvers. Bilateral handgrip for 15 seconds before rising forestalls IOH by evoking the exercise pressor reflex which can substantially increase blood pressure (11). Lower body muscle contraction while seated (e.g. pumping calf muscles) can also help as a preemptive maneuver. Also, lower body muscle tensing of legs, buttocks and abdomen particularly attenuates the transient arterial blood pressure decrease once standing has occurred (15) and can be potentiated by handgrip. Recumbence and squatting are general measures used to remediate all forms of orthostatic intolerance. I have never had a patient who required more than physical aversive measures for IOH. Initial orthostatic hypotension is a normal short-lived response to rapid standing caused by a sudden increase of gravitational force. It is not a form of autonomic disease or maladaptation and is distinct in signs and symptoms from vasovagal faint. In some young subjects, the extent of hypotension may be large enough to produce symptoms. If symptoms impair the quality of life treatment in the form of aversive maneuvers should be employed. Supported by the National Heart, Lung, and Blood Institute (grants RO1HL074873, RO1HL087803, and R21HL091948). 1. Wieling W, Krediet CT, van Dijk N, Linzer M, Tschakovsky ME. Initial orthostatic hypotension: review of a forgotten condition. Clin Sci (Lond) 2007;112: [PubMed: ] 2. Tanaka H, Yamaguchi H, Matushima R, Tamai H. Instantaneous orthostatic hypotension in children and adolescents: a new entity of orthostatic intolerance. Pediatr Res 1999;46: [PubMed: ] 3. Owens PE, Lyons SP, O'Brien ET. Arterial hypotension: prevalence of low blood pressure in the general population using ambulatory blood pressure monitoring. J Hum Hypertens 2000;14: [PubMed: ] 4. Borst C, van Brederode JF, Wieling W, van Montfrans GA, Dunning AJ. Mechanisms of initial blood pressure response to postural change. Clin Sci (Lond) 1984;67: [PubMed: ] 5. Lewis T. A lecture on vasovagal syncope and the carotid sinus mechanism with comments on Gowers's and Nothangel's syndrome. BMJ 1932;1: Ref Type: Journal (Full). [PubMed: ] 6. Wieling W, Harms MP, Kortz RA, Linzer M. Initial orthostatic hypotension as a cause of recurrent syncope: a case report. Clin Auton Res 2001;11: [PubMed: ] 7. Postural hypotension. Faintness upon standing. Mayo Clin Health Lett 1999;17:6. 8. Tanaka H, Thulesius O, Borres M, Yamaguchi H, Mino M. Blood pressure responses in Japanese and Swedish children in the supine and standing position. Eur Heart J 1994;15: [PubMed: ]
6 Stewart and Clarke Page 6 9. Thomas KN, Cotter JD, Galvin SD, Williams MJ, Willie CK, Ainslie PN. Initial orthostatic hypotension is unrelated to orthostatic tolerance in healthy young subjects. J Appl Physiol 2009;107: [PubMed: ] 10. Pickering TG, Hall JE, Appel LJ, Falkner BE, Graves J, Hill MN, et al. Recommendations for blood pressure measurement in humans and experimental animals: Part 1: blood pressure measurement in humans: a statement for professionals from the Subcommittee of Professional and Public Education of the American Heart Association Council on High Blood Pressure Research. Hypertension 2005;45: [PubMed: ] 11. Clarke DA, Medow MS, Taneja I, Ocon AJ, Stewart JM. Initial orthostatic hypotension in the young is attenuated by static handgrip. J Pediatr 2010;156: [PubMed: ] 12. Folino AF, Buja GF, Martini B, Miorelli M, Nava A. Prolonged cardiac arrest and complete AV block during upright tilt test in young patients with syncope of unknown origin--prognostic and therapeutic implications. Eur Heart J 1992;13: [PubMed: ] 13. Pancheva MV, Panchev VS, Suvandjieva AV. Improved orthostatic tolerance by leg crossing and muscle tensing: indisputable evidence for the arteriovenous pump existence. J Appl Physiol 2006;101: [PubMed: ] 14. Mitchell JH. Cardiovascular control during exercise: central and reflex neural mechanisms. Am J Cardiol 1985;55:34D 41D. 15. Krediet CT, Go-Schon IK, Kim YS, Linzer M, Van Lieshout JJ, Wieling W. Management of initial orthostatic hypotension: lower body muscle tensing attenuates the transient arterial blood pressure decrease upon standing from squatting. Clin Sci (Lond) 2007;113: [PubMed: ] 16. Wieling W, Shepherd JT. Initial and delayed circulatory responses to orthostatic stress in normal humans and in subjects with orthostatic intolerance. Int Angiol 1992;11: [PubMed: ] 17. Consensus statement on the definition of orthostatic hypotension, pure autonomic failure, and multiple system atrophy. Neurology ;46: Smit AA, Halliwill JR, Low PA, Wieling W. Pathophysiological basis of orthostatic hypotension in autonomic failure. J Physiol 1999;519(Pt 1):1 10. [PubMed: ] 19. Krediet CT. Initial orthostatic hypotension in a 37-year old horse rider. Clin Auton Res 2002;12:404. [PubMed: ] 20. Stewart JM. Transient orthostatic hypotension is common in adolescents. J Pediatr 2002;140: [PubMed: ] 21. Robertson D, Biaggioni I, Ertl AC, Robertson RM, Diedrich A, Blakely RD, et al. Orthostatic intolerance: emerging genetic and environmental etiologies. J Gravit Physiol 1999;6: Stewart JM. Orthostatic intolerance in pediatrics. J Pediatr 2002;140: [PubMed: ] 23. Grubb BP. Neurocardiogenic syncope and related disorders of orthostatic intolerance. Circulation 2005;111: [PubMed: ] 24. Sutton R, Benditt D, Brignole M, Moya A. Syncope: diagnosis and management according to the 2009 guidelines of the European Society of Cardiology. Pol Arch Med Wewn 2010;120:42 7. [PubMed: ] 25. Thomas KN, Galvin SD, Williams MJ, Willie CK, Ainslie PN. Identical pattern of cerebral hypoperfusion during different types of syncope. J Hum Hypertens Raj SR. The Postural Tachycardia Syndrome (POTS): pathophysiology, diagnosis & management. Indian Pacing Electrophysiol J 2006;6: [PubMed: ] 27. Robertson D. The epidemic of orthostatic tachycardia and orthostatic intolerance. Am J Med Sci 1999;317:75 7. [PubMed: ] 28. Stewart JM. Chronic orthostatic intolerance and the postural tachycardia syndrome (POTS). J Pediatr 2004;145: [PubMed: ] 29. Bou-Holaigah I, Rowe PC, Kan J, Calkins H. The relationship between neurally mediated hypotension and the chronic fatigue syndrome. JAMA 1995;274: [PubMed: ] 30. Goldstein DS, Eldadah B, Holmes C, Pechnik S, Moak J, Sharabi Y. Neurocirculatory abnormalities in chronic orthostatic intolerance. Circulation 2005;111: [PubMed: ]
7 Stewart and Clarke Page Rowe PC, Bou-Holaigah I, Kan JS, Calkins H. Is neurally mediated hypotension an unrecognised cause of chronic fatigue? Lancet 1995;345: [PubMed: ] 32. Rowe PC. Orthostatic intolerance and chronic fatigue syndrome: New light on an old problem. J Pediatr 2002;140: [PubMed: ] 33. Stewart JM, Medow MS, Cherniack NS, Natelson BH. Postural hypocapnic hyperventilation is associated with enhanced peripheral vasoconstriction in postural tachycardia syndrome with normal supine blood flow. Am J Physiol Heart Circ Physiol 2006;291:H904 H913. [PubMed: ] 34. Stewart JM. Postural tachycardia syndrome and reflex syncope: similarities and differences. J Pediatr 2009;154: [PubMed: ] 35. Taneja I, Medow MS, Glover JL, Raghunath NK, Stewart JM. Increased vasoconstriction predisposes to hyperpnea and postural faint. Am J Physiol Heart Circ Physiol 2008;295:H372 H381. [PubMed: ] 36. Moya A, Sutton R, Ammirati F, Blanc JJ, Brignole M, Dahm JB, et al. Guidelines for the diagnosis and management of syncope (version 2009): the Task Force for the Diagnosis and Management of Syncope of the European Society of Cardiology (ESC). Eur Heart J 2009;30: [PubMed: ] 37. LeLorier P, Klein GJ, Krahn A, Yee R, Skanes A, Shoemaker JK. Combined head-up tilt and lower body negative pressure as an experimental model of orthostatic syncope. J Cardiovasc Electrophysiol 2003;14: [PubMed: ] 38. Grubb BP, Gerard G, Roush K, Temesy-Armos P, Elliott L, Hahn H, et al. Differentiation of convulsive syncope and epilepsy with head-up tilt testing. Ann Intern Med 1991;115: [PubMed: ] 39. Morillo CA, Eckberg DL, Ellenbogen KA, Beightol LA, Hoag JB, Tahvanainen KU, et al. Vagal and sympathetic mechanisms in patients with orthostatic vasovagal syncope. Circulation 1997;96: [PubMed: ] 40. Rowell, LB. Human Cardiovascular Control. Oxford University Press; NY, NY.: Maw GJ, Mackenzie IL, Taylor NA. Redistribution of body fluids during postural manipulations. Acta Physiol Scand 1995;155: [PubMed: ] 42. Rowell, LB. Human Cardiovascular Control. Oxford University Press; NY, NY.: The Passive Effects of Gravity. 43. Ten Harkel AD, Van Lieshout JJ, Wieling W. Effects of leg muscle pumping and tensing on orthostatic arterial pressure: a study in normal subjects and patients with autonomic failure. Clin Sci (Colch) 1994;87: [PubMed: ] 44. Jacobsen TN, Morgan BJ, Scherrer U, Vissing SF, Lange RA, Johnson N, et al. Relative contributions of cardiopulmonary and sinoaortic baroreflexes in causing sympathetic activation in the human skeletal muscle circulation during orthostatic stress. Circ Res 1993;73: [PubMed: ] 45. Victor RG, Mark AL. Interaction of cardiopulmonary and carotid baroreflex control of vascular resistance in humans. J Clin Invest 1985;76: [PubMed: ] 46. Halliwill JR. Virtual conductance, real hypotension: what happens when we stand up too fast? J Appl Physiol 2007;103: [PubMed: ] 47. Sheriff DD, Nadland IH, Toska K. Hemodynamic consequences of rapid changes in posture in humans. J Appl Physiol 2007;103: [PubMed: ] 48. Hill L. The influences of the force of gravity on the circulation of the blood. J Physiol (London) 1951;18: Clark JR, Hooker DR, Weed LH. The hydrostatic factor in venous pressure measurements. American Journal of Physiology 1932;109: Ref Type: Journal (Full). 50. Klepner, D.; Kolekow, RJ. An Introduction to Mechanics. Cambridge University press; Cambridge, UK: The Harmonic Oscillator. The Forced harmonic oscillator; p
8 Stewart and Clarke Page 8 Figure 1. Rapid standing results in initial orthostatic hypotension in a representative subject. Blood pressure (BP) is shown in the left upper panel, heart rate (HR) in the left middle panel, and cardiac output measured by Modelflow (CO) in the left lower panel. Cerebral blood flow velocity (CBFv) is shown in the right upper panel, total peripheral resistance (TPR) calculated as MAP/CO in the right middle panel, and TPR calculated as (MAP+ ρg<h>)/co to include the effects of gravity, is shown in the right lower panel. BP, CBFv, and TPR decrease while HR and CO increase transiently during the stand. TPR corrected for gravity increases shortly after BP falls.
9 Stewart and Clarke Page 9 Figure 2. Rapid standing (black lines) is compared with upright tilt (gray lines) to 70 in the same subject. The upper panel shows changes in blood pressure (BP) and the lower panel shows changes in heart rate (HR). There is a greater fall in BP and rise in HR with standing compared with tilt. Also, both BP and HR increase in anticipation of standing - a phenomenon called central command.
10 Stewart and Clarke Page 10 Figure 3. Initial orthostatic hypotension at the onset of upright tilt is compared with vasovagal faint in a representative patient. The upper panel shows blood pressure (BP) and the lower panel shows heart rate (HR). HR increases with IOH but decreases with fainting.
11 Stewart and Clarke Page 11 Figure 4. The right panels show blood pressure responses to rapid standing of 3 separate patients. The top panel, labeled critically damped shows a rapid recovery phase, the middle panel shows a slower recovery that can be best fit by two exponential functions and the bottom panel labeled underdamped shows an oscillatory BP recovery. These are characteristic modes of a damped harmonic oscillator modeled in the left hand side of the figure. The oscillator originally driven by a periodic cardiac rhythm (~C) upon which is abruptly superimposed the effects of a gravitational force (G). R corresponds to vascular resistance (the damping) and VCap is the vascular capacitance.
University of Groningen
 University of Groningen Initial orthostatic hypotension in teenagers and young adults van Wijnen, Veera; Harms, Mark; Go-Schon, I. K.; Westerhof, B. E.; Krediet, C. T. P.; Stewart, J.; Wieling, W. Published
University of Groningen Initial orthostatic hypotension in teenagers and young adults van Wijnen, Veera; Harms, Mark; Go-Schon, I. K.; Westerhof, B. E.; Krediet, C. T. P.; Stewart, J.; Wieling, W. Published
Veins. VENOUS RETURN = PRELOAD = End Diastolic Volume= Blood returning to heart per cardiac cycle (EDV) or per minute (Venous Return)
 Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
SYNCOPE. Sanjay P. Singh, MD Chairman & Professor, Department of Neurology. Syncope
 SYNCOPE Sanjay P. Singh, MD Chairman & Professor, Department of Neurology. Syncope Syncope is a clinical syndrome characterized by transient loss of consciousness (TLOC) and postural tone that is most
SYNCOPE Sanjay P. Singh, MD Chairman & Professor, Department of Neurology. Syncope Syncope is a clinical syndrome characterized by transient loss of consciousness (TLOC) and postural tone that is most
June 8, 2018, London UK TREATMENT OF VASOVAGAL SYNCOPE
 June 8, 2018, London UK TREATMENT OF VASOVAGAL SYNCOPE Where to go for help Syncope: HRS Definition Syncope is defined as: a transient loss of consciousness, associated with an inability to maintain postural
June 8, 2018, London UK TREATMENT OF VASOVAGAL SYNCOPE Where to go for help Syncope: HRS Definition Syncope is defined as: a transient loss of consciousness, associated with an inability to maintain postural
Neurocardiogenic syncope
 Neurocardiogenic syncope Syncope Definition Collapse,Blackout A sudden, transient loss of consciousness and postural tone, with spontaneous recovery Very common Syncope Prevalence All age groups (particularly
Neurocardiogenic syncope Syncope Definition Collapse,Blackout A sudden, transient loss of consciousness and postural tone, with spontaneous recovery Very common Syncope Prevalence All age groups (particularly
Orthostatic Intolerance (OI) In the Young. (orthostasis = standing) (OI= Can t remain standing)
 Orthostatic Intolerance (OI) In the Young (orthostasis = standing) (OI= Can t remain standing) Gravitational Blood Distribution in Man and Beast Unconstrained Pooling Causes Rapid Loss of BP Circulatory
Orthostatic Intolerance (OI) In the Young (orthostasis = standing) (OI= Can t remain standing) Gravitational Blood Distribution in Man and Beast Unconstrained Pooling Causes Rapid Loss of BP Circulatory
POSTURAL ORTHOSTATIC TACHYCARDIA SYNDROME (POTS) IT S NOT THAT SIMPLE
 POSTURAL ORTHOSTATIC TACHYCARDIA SYNDROME (POTS) IT S NOT THAT SIMPLE POTS Irritable heart syndrome. Soldier s heart. Effort syndrome. Vasoregulatory asthenia. Neurocirculatory asthenia. Anxiety neurosis.
POSTURAL ORTHOSTATIC TACHYCARDIA SYNDROME (POTS) IT S NOT THAT SIMPLE POTS Irritable heart syndrome. Soldier s heart. Effort syndrome. Vasoregulatory asthenia. Neurocirculatory asthenia. Anxiety neurosis.
DECLARATION OF CONFLICT OF INTEREST
 DECLARATION OF CONFLICT OF INTEREST The Management of Syncope remains a challenge: Clues from the History Richard Sutton, DSc Emeritus Professor of Cardiology Imperial College, St Mary s Hospital, London,
DECLARATION OF CONFLICT OF INTEREST The Management of Syncope remains a challenge: Clues from the History Richard Sutton, DSc Emeritus Professor of Cardiology Imperial College, St Mary s Hospital, London,
Summary and conclusions
 Summary and conclusions Syncope is an extremely common symptom with a life time prevalence of 30 to 40% in the general population. 52,81,212 In common with its frequent occurrence, syncope accounts for
Summary and conclusions Syncope is an extremely common symptom with a life time prevalence of 30 to 40% in the general population. 52,81,212 In common with its frequent occurrence, syncope accounts for
Responses to Changes in Posture QUESTIONS. Case PHYSIOLOGY CASES AND PROBLEMS
 64 PHYSIOLOGY CASES AND PROBLEMS Case 12 Responses to Changes in Posture Joslin Chambers is a 27-year-old assistant manager at a discount department store. One morning, she awakened from a deep sleep and
64 PHYSIOLOGY CASES AND PROBLEMS Case 12 Responses to Changes in Posture Joslin Chambers is a 27-year-old assistant manager at a discount department store. One morning, she awakened from a deep sleep and
Findings from the 2015 HRS Expert Consensus Document on Postural Tachycardia Syndrome (POTS) and Inappropriate Sinus Tachycardia (IST)
 Findings from the 2015 HRS Expert Consensus Document on Postural Tachycardia Syndrome (POTS) and Inappropriate Sinus Tachycardia (IST) Ahmad Hersi, MBBS, MSc, FRCPC Professor of Cardiac Sciences Consultant
Findings from the 2015 HRS Expert Consensus Document on Postural Tachycardia Syndrome (POTS) and Inappropriate Sinus Tachycardia (IST) Ahmad Hersi, MBBS, MSc, FRCPC Professor of Cardiac Sciences Consultant
C. T. Paul Krediet, Ingeborg K. Go-Schön, Yu-Sok Kim, Mark Linzer, Johannes J. Van Lieshout, Wouter Wieling, C. T. Paul Krediet
 Management of initial orthostatic hypotension: lower body muscle tensing attenuates the transient arterial blood pressure decrease upon standing from squatting C. T. Paul Krediet, Ingeborg K. Go-Schön,
Management of initial orthostatic hypotension: lower body muscle tensing attenuates the transient arterial blood pressure decrease upon standing from squatting C. T. Paul Krediet, Ingeborg K. Go-Schön,
Faculty Disclosure. Sanjay P. Singh, MD, FAAN. Dr. Singh has listed an affiliation with: Consultant Sun Pharma Speaker s Bureau Lundbeck, Sunovion
 Faculty Disclosure Sanjay P. Singh, MD, FAAN Dr. Singh has listed an affiliation with: Consultant Sun Pharma Speaker s Bureau Lundbeck, Sunovion however, no conflict of interest exists for this conference.
Faculty Disclosure Sanjay P. Singh, MD, FAAN Dr. Singh has listed an affiliation with: Consultant Sun Pharma Speaker s Bureau Lundbeck, Sunovion however, no conflict of interest exists for this conference.
Syncope: Evaluation of the Weak and Dizzy
 Syncope: Evaluation of the Weak and Dizzy William M. Miles, MD, FACC, FHRS Professor of Medicine Silverstein Chair for Cardiovascular Education University of Florida College of Medicine Disclosures Medtronic,
Syncope: Evaluation of the Weak and Dizzy William M. Miles, MD, FACC, FHRS Professor of Medicine Silverstein Chair for Cardiovascular Education University of Florida College of Medicine Disclosures Medtronic,
SYMPATHETIC STRESSORS AND SYMPATHETIC FAILURES
 SYMPATHETIC STRESSORS AND SYMPATHETIC FAILURES Any discussion of sympathetic involvement in circulation, and vasodilation, and vasoconstriction requires an understanding that there is no such thing as
SYMPATHETIC STRESSORS AND SYMPATHETIC FAILURES Any discussion of sympathetic involvement in circulation, and vasodilation, and vasoconstriction requires an understanding that there is no such thing as
Tilt training EM R1 송진우
 Tilt training 2006.7.15. EM R1 송진우 Introduction North American Vasovagal Pacemaker Study Randomized, controlled trial Reduction in the likelihood of syncope by dual chamber pacing with rate drop response
Tilt training 2006.7.15. EM R1 송진우 Introduction North American Vasovagal Pacemaker Study Randomized, controlled trial Reduction in the likelihood of syncope by dual chamber pacing with rate drop response
Exercise Training for PoTS and Syncope
 B 140 120 100 80 60 40 20 0 Blood Pressure (mm Hg) Blood Pressure Heart Rate 60 degree Head Up Tilt Time 140 120 100 80 60 40 20 0 Heart Rate (beats.min -1 ) Exercise Training for PoTS and Syncope C Blood
B 140 120 100 80 60 40 20 0 Blood Pressure (mm Hg) Blood Pressure Heart Rate 60 degree Head Up Tilt Time 140 120 100 80 60 40 20 0 Heart Rate (beats.min -1 ) Exercise Training for PoTS and Syncope C Blood
Syncope: Evaluation of the Weak and Dizzy
 Syncope: Evaluation of the Weak and Dizzy William M. Miles, MD, FACC, FHRS Professor of Medicine Silverstein Chair for Cardiovascular Education University of Florida College of Medicine Disclosures Medtronic,
Syncope: Evaluation of the Weak and Dizzy William M. Miles, MD, FACC, FHRS Professor of Medicine Silverstein Chair for Cardiovascular Education University of Florida College of Medicine Disclosures Medtronic,
Tilt Table Testing. Dr. Prateek Suri
 Tilt Table Testing Dr. Prateek Suri Background Syncope is very commonly seen in the population Among the various causes of syncope vasovagal syncope is the most common cause There is an absence of a gold
Tilt Table Testing Dr. Prateek Suri Background Syncope is very commonly seen in the population Among the various causes of syncope vasovagal syncope is the most common cause There is an absence of a gold
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1
 BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
Tilt Table Testing MM /01/2015. HMO; PPO; QUEST Integration 09/22/2017 Section: Medicine Place(s) of Service: Office, Outpatient
 Tilt Table Testing Policy Number: Original Effective Date: MM.02.024 01/01/2015 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 09/22/2017 Section: Medicine Place(s) of Service:
Tilt Table Testing Policy Number: Original Effective Date: MM.02.024 01/01/2015 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST Integration 09/22/2017 Section: Medicine Place(s) of Service:
Syncope Guidelines: What s New?
 Syncope Guidelines: What s New? Dr. Samuel Asirvatham Professor of Medicine and Pediatrics Mayo Clinic College of Medicine Medical Director, Electrophysiology Laboratory Program Director, EP Fellowship
Syncope Guidelines: What s New? Dr. Samuel Asirvatham Professor of Medicine and Pediatrics Mayo Clinic College of Medicine Medical Director, Electrophysiology Laboratory Program Director, EP Fellowship
Leg intravenous pressure during head-up tilt
 J Appl Physiol 105: 811 815, 2008. First published July 17, 2008; doi:10.1152/japplphysiol.90304.2008. Leg intravenous pressure during head-up tilt Jan T. Groothuis, 1,5 Fleur Poelkens, 1,2 Constantijn
J Appl Physiol 105: 811 815, 2008. First published July 17, 2008; doi:10.1152/japplphysiol.90304.2008. Leg intravenous pressure during head-up tilt Jan T. Groothuis, 1,5 Fleur Poelkens, 1,2 Constantijn
Rehabilitation for Postural Tachycardia Syndrome (POTS)
 Rehabilitation for Postural Tachycardia Syndrome (POTS) Satish R Raj MD MSCI FACC FHRS FRCPC Associate Professor of Cardiac Sciences University of Calgary Adjunct Associate Professor of Medicine Autonomic
Rehabilitation for Postural Tachycardia Syndrome (POTS) Satish R Raj MD MSCI FACC FHRS FRCPC Associate Professor of Cardiac Sciences University of Calgary Adjunct Associate Professor of Medicine Autonomic
Death after Syncope: Can we predict it? Daniel Zamarripa, MD Senior Medical Director December 2013
 Death after Syncope: Can we predict it? Daniel Zamarripa, MD Senior Medical Director December 2013 Death after Syncope: Can we predict it? Those who suffer from frequent and severe fainting often die suddenly
Death after Syncope: Can we predict it? Daniel Zamarripa, MD Senior Medical Director December 2013 Death after Syncope: Can we predict it? Those who suffer from frequent and severe fainting often die suddenly
Key Words: Autonomic, syncope, orthostatic tachycardia, orthostatic hypotension,
 Update on the theory and management of orthostatic intolerance and related syndromes in adolescents and children. Julian M. Stewart Departments of Physiology, Pediatrics and Medicine New York Medical College,
Update on the theory and management of orthostatic intolerance and related syndromes in adolescents and children. Julian M. Stewart Departments of Physiology, Pediatrics and Medicine New York Medical College,
Microgravity and the Circulatory System. Mina Iscandar Kevin Morgan
 Microgravity and the Circulatory System Mina Iscandar Kevin Morgan Outline Introduction Circulatory System on Earth Changes Due to Microgravity Side effects Upon Return to Earth Possible Countermeasures
Microgravity and the Circulatory System Mina Iscandar Kevin Morgan Outline Introduction Circulatory System on Earth Changes Due to Microgravity Side effects Upon Return to Earth Possible Countermeasures
INTRODUCTION POTS is: Poorly understood Rarely considered SIGNIFICANT morbidity Appropriate initial diagnosis & care will expedite management of POTS
 Learning objectives At the end of this presentation the learner should: Define POTS & identify the various etiologies of POTS Be able to differentiate POTS from other causes of orthostatic intolerance
Learning objectives At the end of this presentation the learner should: Define POTS & identify the various etiologies of POTS Be able to differentiate POTS from other causes of orthostatic intolerance
Distinguishing Cardiac from Non- Cardiac Syncope
 10 th Annual International SADS Foundation Conference Toronto Distinguishing Cardiac from Non- Cardiac Syncope Shubhayan Sanatani, MD, FRCPC Head, Division of Cardiology, BC Children s Hospital Director,
10 th Annual International SADS Foundation Conference Toronto Distinguishing Cardiac from Non- Cardiac Syncope Shubhayan Sanatani, MD, FRCPC Head, Division of Cardiology, BC Children s Hospital Director,
La sincope vasovagale come difesa
 La sincope vasovagale come difesa Paolo Alboni www.gimsi.it Sezione di Cardiologia e «Syncope Unit» Ospedale Privato Quisisana Ferrara Vasovagal reflex Vasovagal syncope Vasovagal reflex Afferent part
La sincope vasovagale come difesa Paolo Alboni www.gimsi.it Sezione di Cardiologia e «Syncope Unit» Ospedale Privato Quisisana Ferrara Vasovagal reflex Vasovagal syncope Vasovagal reflex Afferent part
Diagnostic and therapeutic management of the patient with syncope M. Brignole Arrhythmologic Centre and Syncope Unit Lavagna, Italy
 Diagnostic and therapeutic management of the patient with syncope M. Brignole Arrhythmologic Centre and Syncope Unit Lavagna, Italy Eur Heart J. 2009 Nov;30(21):2631-71 Available on www.escardio.org/guidelines
Diagnostic and therapeutic management of the patient with syncope M. Brignole Arrhythmologic Centre and Syncope Unit Lavagna, Italy Eur Heart J. 2009 Nov;30(21):2631-71 Available on www.escardio.org/guidelines
Clinical Studies 129
 Clinical Studies 129 Syncope in migraine. The population-based CAMERA study Roland D. Thijs, 1* Mark C. Kruit, 2* Mark A. van Buchem, 2 Michel D. Ferrari, 1 Lenore J. Launer, 3,4 and J. Gert van Dijk
Clinical Studies 129 Syncope in migraine. The population-based CAMERA study Roland D. Thijs, 1* Mark C. Kruit, 2* Mark A. van Buchem, 2 Michel D. Ferrari, 1 Lenore J. Launer, 3,4 and J. Gert van Dijk
Orthostatic Hypotension (Postural Hypotension)
 Orthostatic Hypotension (Postural Hypotension) Authors: SCIRE Community Team Reviewed by: Darryl Caves, PT Last updated: April 9, 2018 Changes to blood pressure control after spinal cord injury (SCI) may
Orthostatic Hypotension (Postural Hypotension) Authors: SCIRE Community Team Reviewed by: Darryl Caves, PT Last updated: April 9, 2018 Changes to blood pressure control after spinal cord injury (SCI) may
Blood Pressure. a change in any of these could cause a corresponding change in blood pressure
 Blood Pressure measured as mmhg Main factors affecting blood pressure: 1. cardiac output 2. peripheral resistance 3. blood volume a change in any of these could cause a corresponding change in blood pressure
Blood Pressure measured as mmhg Main factors affecting blood pressure: 1. cardiac output 2. peripheral resistance 3. blood volume a change in any of these could cause a corresponding change in blood pressure
:{ic0fp'16. Geriatric Medicine: Blood Pressure Monitoring in the Elderly. Terrie Ginsberg, DO, FACOI
 :{ic0fp'16 ACOFP 53 rd Annual Convention & Scientific Seminars Geriatric Medicine: Blood Pressure Monitoring in the Elderly Terrie Ginsberg, DO, FACOI Blood Pressure Management in the Elderly Terrie B.
:{ic0fp'16 ACOFP 53 rd Annual Convention & Scientific Seminars Geriatric Medicine: Blood Pressure Monitoring in the Elderly Terrie Ginsberg, DO, FACOI Blood Pressure Management in the Elderly Terrie B.
Syncope By Remus Popa
 Syncope By Remus Popa A 66 years old male is brought to the ED from a restaurant where he fainted while dining out with his family. He complained of nausea and stood up to go to the restroom but immediately
Syncope By Remus Popa A 66 years old male is brought to the ED from a restaurant where he fainted while dining out with his family. He complained of nausea and stood up to go to the restroom but immediately
Research Article Cerebral Blood Flow, Heart Rate, and Blood Pressure Patterns during the Tilt Test in Common Orthostatic Syndromes
 Neuroscience Journal Volume 216, Article ID 612734, 2 pages http://dx.doi.org/1.1155/216/612734 Research Article Cerebral Blood Flow, Heart Rate, and Blood Pressure Patterns during the Test in Common Orthostatic
Neuroscience Journal Volume 216, Article ID 612734, 2 pages http://dx.doi.org/1.1155/216/612734 Research Article Cerebral Blood Flow, Heart Rate, and Blood Pressure Patterns during the Test in Common Orthostatic
I ngestion of water increases seated blood pressure (BP) in
 1737 PAPER The effects of water ingestion on orthostatic hypotension in two groups of chronic autonomic failure: multiple system atrophy and pure autonomic failure T M Young, C J Mathias... See end of
1737 PAPER The effects of water ingestion on orthostatic hypotension in two groups of chronic autonomic failure: multiple system atrophy and pure autonomic failure T M Young, C J Mathias... See end of
The diagnosis of orthostatic intolerance (OI) and postural tachycardia syndrome (POTS) is based on a symptomatic, excessive
 Postural Tachycardia in Children and Adolescents: What is Abnormal? Wolfgang Singer, MD 1, David M. Sletten, BA 1, Tonette L. Opfer-Gehrking, LPN 1, Chad K. Brands, MD 2, Philip R. Fischer, MD 2, and Phillip
Postural Tachycardia in Children and Adolescents: What is Abnormal? Wolfgang Singer, MD 1, David M. Sletten, BA 1, Tonette L. Opfer-Gehrking, LPN 1, Chad K. Brands, MD 2, Philip R. Fischer, MD 2, and Phillip
Special circulations, Coronary, Pulmonary. Faisal I. Mohammed, MD,PhD
 Special circulations, Coronary, Pulmonary Faisal I. Mohammed, MD,PhD 1 Objectives Describe the control of blood flow to different circulations (Skeletal muscles, pulmonary and coronary) Point out special
Special circulations, Coronary, Pulmonary Faisal I. Mohammed, MD,PhD 1 Objectives Describe the control of blood flow to different circulations (Skeletal muscles, pulmonary and coronary) Point out special
Cerebral and cardiovascular dynamics in response to orthostatic stress Harms, M.P.M.
 UvA-DARE (Digital Academic Repository) Cerebral and cardiovascular dynamics in response to orthostatic stress Harms, M.P.M. Link to publication Citation for published version (APA): Harms, M. P. M. (2008).
UvA-DARE (Digital Academic Repository) Cerebral and cardiovascular dynamics in response to orthostatic stress Harms, M.P.M. Link to publication Citation for published version (APA): Harms, M. P. M. (2008).
Rapid Access Clinics for Transient Loss of Consciousness
 Rapid Access Clinics for Transient Loss of Consciousness Michael Gammage Department of Cardiovascular Medicine University of Birmingham and University Hospital Birmingham NHS Foundation Trust Those who
Rapid Access Clinics for Transient Loss of Consciousness Michael Gammage Department of Cardiovascular Medicine University of Birmingham and University Hospital Birmingham NHS Foundation Trust Those who
CASE 13. What neural and humoral pathways regulate arterial pressure? What are two effects of angiotensin II?
 CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
Disclosures. Adult Postural Orthostatic Tachycardia Syndrome (POTS) Topics. Objectives. Definition/Terminology. Epidemiology 2/2/2017
 Disclosures Adult Postural Orthostatic Tachycardia Syndrome (POTS) Nothing to disclose (no financial or pharmaceutical affiliations) All discussed pharmacologic treatments are off-label Juan J. Figueroa,
Disclosures Adult Postural Orthostatic Tachycardia Syndrome (POTS) Nothing to disclose (no financial or pharmaceutical affiliations) All discussed pharmacologic treatments are off-label Juan J. Figueroa,
Repeated tilt testing in patients with tilt-positive neurally mediated syncope
 Europace (25) 7, 628e633 Repeated tilt testing in patients with tilt-positive neurally mediated syncope Hugo Ector a, *, Rik Willems a, Hein Heidbüchel a, Tony Reybrouck b,c a Department of Cardiology,
Europace (25) 7, 628e633 Repeated tilt testing in patients with tilt-positive neurally mediated syncope Hugo Ector a, *, Rik Willems a, Hein Heidbüchel a, Tony Reybrouck b,c a Department of Cardiology,
ORTHOSTATIC INTOLERANCE AN EXPRESSION OF AUTONOMIC DISFUNCTION IN PARKINSON S DISEASE
 Rev. Med. Chir. Soc. Med. Nat., Iaşi 2014 vol. 118, no. 1 INTERNAL MEDICINE - PEDIATRICS ORIGINAL PAPERS ORTHOSTATIC INTOLERANCE AN EXPRESSION OF AUTONOMIC DISFUNCTION IN PARKINSON S DISEASE Emilia-Lidia
Rev. Med. Chir. Soc. Med. Nat., Iaşi 2014 vol. 118, no. 1 INTERNAL MEDICINE - PEDIATRICS ORIGINAL PAPERS ORTHOSTATIC INTOLERANCE AN EXPRESSION OF AUTONOMIC DISFUNCTION IN PARKINSON S DISEASE Emilia-Lidia
Središnja medicinska knjižnica
 Središnja medicinska knjižnica Adamec I., Klepac N., Milivojević I., Radić B., Habek M. (2012) Sick sinus syndrome and orthostatic hypotension in Parkinson's disease. Acta Neurologica Belgica, 112 (3).
Središnja medicinska knjižnica Adamec I., Klepac N., Milivojević I., Radić B., Habek M. (2012) Sick sinus syndrome and orthostatic hypotension in Parkinson's disease. Acta Neurologica Belgica, 112 (3).
Figure 1 Uncontrolled state where ZPFV is increased by 500 ml.
 Question 1 Part I Description The initial venous zero pressure filling volume was 2500 ml. The heart rate was fixed at 72 beats/min. The systemic arterial pressure (SAP) was 114/75 mmhg (average = 94 mmhg).
Question 1 Part I Description The initial venous zero pressure filling volume was 2500 ml. The heart rate was fixed at 72 beats/min. The systemic arterial pressure (SAP) was 114/75 mmhg (average = 94 mmhg).
Clinical Policy Title: Tilt table testing
 Clinical Policy Title: Tilt table testing Clinical Policy Number: 09.01.13 Effective Date: October 1, 2016 Initial Review Date: July 20, 2016 Most Recent Review Date: August 17, 2017 Next Review Date:
Clinical Policy Title: Tilt table testing Clinical Policy Number: 09.01.13 Effective Date: October 1, 2016 Initial Review Date: July 20, 2016 Most Recent Review Date: August 17, 2017 Next Review Date:
Cardiac Pathophysiology
 Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
Syncope and TLOC overview
 PART 1 Syncope and TLOC overview 1 2 CHAPTER 1 Definition and classification of syncope and transient loss of consciousness Jean-Jacques Blanc Syncope is a common complaint responsible for up to 1% of
PART 1 Syncope and TLOC overview 1 2 CHAPTER 1 Definition and classification of syncope and transient loss of consciousness Jean-Jacques Blanc Syncope is a common complaint responsible for up to 1% of
The Exercise Pressor Reflex
 The Exercise Pressor Reflex Dr. James P. Fisher School of Sport, Exercise & Rehabilitation Sciences College of Life & Environmental Sciences University of Birmingham, UK Copenhagen, 2018 Based on work
The Exercise Pressor Reflex Dr. James P. Fisher School of Sport, Exercise & Rehabilitation Sciences College of Life & Environmental Sciences University of Birmingham, UK Copenhagen, 2018 Based on work
Cerebral Blood Flow Velocity Declines Before Arterial Pressure in Patients With Orthostatic Vasovagal Presyncope
 Journal of the American College of Cardiology Vol. 39, No. 6, 2002 2002 by the American College of Cardiology Foundation ISSN 0735-1097/02/$22.00 Published by Elsevier Science Inc. PII S0735-1097(02)01719-9
Journal of the American College of Cardiology Vol. 39, No. 6, 2002 2002 by the American College of Cardiology Foundation ISSN 0735-1097/02/$22.00 Published by Elsevier Science Inc. PII S0735-1097(02)01719-9
Orthostatic hypotension: a new classification system
 Europace (2007) 9, 937 941 doi:10.1093/europace/eum177 Orthostatic hypotension: a new classification system B.M.T. Deegan 1,2 *, M. O Connor 3, T. Donnelly 3, S. Carew 3, A. Costelloe 3, T. Sheehy 3, G.
Europace (2007) 9, 937 941 doi:10.1093/europace/eum177 Orthostatic hypotension: a new classification system B.M.T. Deegan 1,2 *, M. O Connor 3, T. Donnelly 3, S. Carew 3, A. Costelloe 3, T. Sheehy 3, G.
EHA Physiology: Challenges and Solutions Lab 1 Heart Rate Response to Baroreceptor Feedback
 Group No. Date: Computer 5 Names: EHA Physiology: Challenges and Solutions Lab 1 Heart Rate Response to Baroreceptor Feedback One of the homeostatic mechanisms of the human body serves to maintain a fairly
Group No. Date: Computer 5 Names: EHA Physiology: Challenges and Solutions Lab 1 Heart Rate Response to Baroreceptor Feedback One of the homeostatic mechanisms of the human body serves to maintain a fairly
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions
 Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
Chapter 14 Blood Vessels, Blood Flow and Pressure Exam Study Questions 14.1 Physical Law Governing Blood Flow and Blood Pressure 1. How do you calculate flow rate? 2. What is the driving force of blood
Prolonged Asystole during Head-Up Tilt Test in a Patient with Malignant Neurocardiogenic Syncope
 Case Report Prolonged Asystole during Head-Up Tilt Test in a Patient with Malignant Neurocardiogenic Syncope Takashi Tokano MD 1, Yuji Nakazato MD 2, Akitoshi Sasaki MD 3, Gaku Sekita MD 3, Masayuki Yasuda
Case Report Prolonged Asystole during Head-Up Tilt Test in a Patient with Malignant Neurocardiogenic Syncope Takashi Tokano MD 1, Yuji Nakazato MD 2, Akitoshi Sasaki MD 3, Gaku Sekita MD 3, Masayuki Yasuda
UNIVERSITY HOSPITALS OF LEICESTER NHS TRUST CARDIAC INVESTIGATIONS PAEDIATRIC & CONGENITAL SYNCOPE INVESTIGATIONS/QUESTIONNAIRE PROTOCOL
 UNIVERSITY HOSPITALS OF LEICESTER NHS TRUST CARDIAC INVESTIGATIONS PAEDIATRIC & CONGENITAL SYNCOPE INVESTIGATIONS/QUESTIONNAIRE PROTOCOL Written Date: 2009 by Dr Duke, then updated by Dr Sarita Makam 12/4/2016
UNIVERSITY HOSPITALS OF LEICESTER NHS TRUST CARDIAC INVESTIGATIONS PAEDIATRIC & CONGENITAL SYNCOPE INVESTIGATIONS/QUESTIONNAIRE PROTOCOL Written Date: 2009 by Dr Duke, then updated by Dr Sarita Makam 12/4/2016
Note: At the end of the instructions, you will find a table which must be filled in to complete the exercise.
 Autonomic Nervous System Theoretical foundations and instructions for conducting practical exercises carried out during the course List of practical exercises 1. Deep (controlled) breath test 2. Cold pressor
Autonomic Nervous System Theoretical foundations and instructions for conducting practical exercises carried out during the course List of practical exercises 1. Deep (controlled) breath test 2. Cold pressor
Department of Paediatrics Clinical Guideline. Syncope Guideline
 Department of Paediatrics Clinical Guideline Syncope Guideline Definition Transient, self-limited loss of consciousness (TLOC), usually leading to falling. Onset is relatively rapid. Recovery is spontaneous,
Department of Paediatrics Clinical Guideline Syncope Guideline Definition Transient, self-limited loss of consciousness (TLOC), usually leading to falling. Onset is relatively rapid. Recovery is spontaneous,
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Adenosine in idiopathic AV block, 445 446 Adolescent(s) syncope in, 397 409. See also Syncope, in children and adolescents AECG monitoring.
Index Note: Page numbers of article titles are in boldface type. A Adenosine in idiopathic AV block, 445 446 Adolescent(s) syncope in, 397 409. See also Syncope, in children and adolescents AECG monitoring.
Blood pressure. Formation of the blood pressure: Blood pressure. Formation of the blood pressure 5/1/12
 Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
On the Track of Syncope induced by Orthostatic Stress - Feedback Mechanisms Regulating the Cardiovascular System
 Proceedings of the 7th IFAC Symposium on Modelling and Control in Biomedical Systems On the Track of Syncope induced by Orthostatic Stress - Feedback Mechanisms Regulating the Cardiovascular System Ottesen
Proceedings of the 7th IFAC Symposium on Modelling and Control in Biomedical Systems On the Track of Syncope induced by Orthostatic Stress - Feedback Mechanisms Regulating the Cardiovascular System Ottesen
Evaluation of Dizziness and Fainting in Children and Adolescents
 Evaluation of Dizziness and Fainting in Children and Adolescents Collin Cowley, MD - Pediatric Cardiology Lynne Kerr, MD, PhD Pediatric Neurology Chuck Norlin, MD General Pediatrics Bettina Smith Edmondson,
Evaluation of Dizziness and Fainting in Children and Adolescents Collin Cowley, MD - Pediatric Cardiology Lynne Kerr, MD, PhD Pediatric Neurology Chuck Norlin, MD General Pediatrics Bettina Smith Edmondson,
"Non-Epileptic Paroxysmal Events (NEPE) Erick Sell, M.D Neurology Division Children s Hospital of Eastern Ontario
 "Non-Epileptic Paroxysmal Events (NEPE) Erick Sell, M.D Neurology Division Children s Hospital of Eastern Ontario Objectives Learn the clinical presentation of some examples of non-epileptic paroxysmal
"Non-Epileptic Paroxysmal Events (NEPE) Erick Sell, M.D Neurology Division Children s Hospital of Eastern Ontario Objectives Learn the clinical presentation of some examples of non-epileptic paroxysmal
Cardiac Output MCQ. Professor of Cardiovascular Physiology. Cairo University 2007
 Cardiac Output MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 90- Guided by Ohm's law when : a- Cardiac output = 5.6 L/min. b- Systolic and diastolic BP
Cardiac Output MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 90- Guided by Ohm's law when : a- Cardiac output = 5.6 L/min. b- Systolic and diastolic BP
Key Words: Head-up tilt test, Neurally mediated syncope, Unexplained syncope
 203 Original Article Randomized Prospective Comparison of Two Protocols for Head-up Tilt Testing in Patients with Normal Heart and Recurrent Unexplained Syncope Mohammad Alasti, MD 1, Mohammad Hosein Nikoo,
203 Original Article Randomized Prospective Comparison of Two Protocols for Head-up Tilt Testing in Patients with Normal Heart and Recurrent Unexplained Syncope Mohammad Alasti, MD 1, Mohammad Hosein Nikoo,
REGULATION OF CARDIOVASCULAR SYSTEM
 REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
REGULATION OF CARDIOVASCULAR SYSTEM Jonas Addae Medical Sciences, UWI REGULATION OF CARDIOVASCULAR SYSTEM Intrinsic Coupling of cardiac and vascular functions - Autoregulation of vessel diameter Extrinsic
Evaluation copy. Heart Rate Response to Baroreceptor Feedback. Computer
 Heart Rate Response to Baroreceptor Feedback Computer 5 One of the homeostatic mechanisms of the human body serves to maintain a fairly constant blood pressure. Major determinants of blood pressure are
Heart Rate Response to Baroreceptor Feedback Computer 5 One of the homeostatic mechanisms of the human body serves to maintain a fairly constant blood pressure. Major determinants of blood pressure are
Vasovagal syncope in 2016: the current state of the faint
 Interventional Cardiology Vasovagal syncope in 2016: the current state of the faint In this article, we will review the challenges in defining syncope and the evolution of its definition over the past
Interventional Cardiology Vasovagal syncope in 2016: the current state of the faint In this article, we will review the challenges in defining syncope and the evolution of its definition over the past
Computational Models of Cardiovascular Function for Analysis of Post-Flight Orthostatic Intolerance
 Computational Models of Cardiovascular Function for Analysis of Post-Flight Orthostatic Intolerance Thomas Heldt, Eun B. Shim, Roger D. Kamm, and Roger G. Mark Massachusetts Institute of Technology Background:
Computational Models of Cardiovascular Function for Analysis of Post-Flight Orthostatic Intolerance Thomas Heldt, Eun B. Shim, Roger D. Kamm, and Roger G. Mark Massachusetts Institute of Technology Background:
EFFECTS OF SUDDEN AND PROLONGED STANDING FROM SUPINE POSTURE ON HEART RATE, ECG-PATTERN AND BLOOD PRESSURE
 J. Human Ergol.,17: 3-12,1988 Center for Academic Publications Japan. Printed in Japan. EFFECTS OF SUDDEN AND PROLONGED STANDING FROM SUPINE POSTURE ON HEART RATE, ECG-PATTERN AND BLOOD PRESSURE Satipati
J. Human Ergol.,17: 3-12,1988 Center for Academic Publications Japan. Printed in Japan. EFFECTS OF SUDDEN AND PROLONGED STANDING FROM SUPINE POSTURE ON HEART RATE, ECG-PATTERN AND BLOOD PRESSURE Satipati
Hemodynamic effects of intermittent compression as a countermeasure to orthostatic stress
 Hemodynamic effects of intermittent compression as a countermeasure to orthostatic stress by Travis Gibbons A thesis presented to the University of Waterloo in fulfillment of the thesis requirement for
Hemodynamic effects of intermittent compression as a countermeasure to orthostatic stress by Travis Gibbons A thesis presented to the University of Waterloo in fulfillment of the thesis requirement for
Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to
 Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to 90 mmhg. These pressures are called Normal blood pressure
Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to 90 mmhg. These pressures are called Normal blood pressure
Syncope Guidelines Update. Bernard Harbieh, FHRS AUBMC-KMC Beirut-Lebanon
 Syncope Guidelines Update Bernard Harbieh, FHRS AUBMC-KMC Beirut-Lebanon New Syncope Guidelines Increase the volume of information on diagnosis and management Incorporation of emergency specialists, neurologists,
Syncope Guidelines Update Bernard Harbieh, FHRS AUBMC-KMC Beirut-Lebanon New Syncope Guidelines Increase the volume of information on diagnosis and management Incorporation of emergency specialists, neurologists,
Therefore MAP=CO x TPR = HR x SV x TPR
 Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Management of syncope in 2014 Role of tilt test
 Gdansk BEATA Symposium October 10-11, 2014 Management of syncope in 2014 Role of tilt test Antonio Raviele, MD, FESC, FHRS ALFA Alliance to Fight Atrial fibrillation, Mestre Venice, Italy Protocols /
Gdansk BEATA Symposium October 10-11, 2014 Management of syncope in 2014 Role of tilt test Antonio Raviele, MD, FESC, FHRS ALFA Alliance to Fight Atrial fibrillation, Mestre Venice, Italy Protocols /
Autonomic Variation of Blood Pressure in Middle Aged Diabetics: A Prospective Study
 Original Article DOI: 10.17354/ijss/2016/16 Autonomic Variation of Blood Pressure in Middle Aged Diabetics: A Prospective Study M Usharani 1, K Chandini 2 1 Professor and Head, Department of Physiology,
Original Article DOI: 10.17354/ijss/2016/16 Autonomic Variation of Blood Pressure in Middle Aged Diabetics: A Prospective Study M Usharani 1, K Chandini 2 1 Professor and Head, Department of Physiology,
Valutazione iniziale e stratificazione del rischio
 Valutazione iniziale e stratificazione del rischio Paolo Alboni Sezione di Cardiologia Ospedale Privato Quisisana Ferrara DEFINITION OF SYNCOPE Syncope is a transient loss of consciousness due to global
Valutazione iniziale e stratificazione del rischio Paolo Alboni Sezione di Cardiologia Ospedale Privato Quisisana Ferrara DEFINITION OF SYNCOPE Syncope is a transient loss of consciousness due to global
Incidence, Clinical Presentation. and Outcome in Patients with Long. Asystole Induced by Head-up Tilt Test
 2005 16 134-138 Incidence, Clinical Presentation and Outcome in Patients with Long Asystole Induced by Head-up Tilt Test Ming-Ting Chou, Chen-Chuan Cheng, Wen-Shiann Wu, and Tseui-Yuen Huang Division of
2005 16 134-138 Incidence, Clinical Presentation and Outcome in Patients with Long Asystole Induced by Head-up Tilt Test Ming-Ting Chou, Chen-Chuan Cheng, Wen-Shiann Wu, and Tseui-Yuen Huang Division of
Exercise hemodynamics in Parkinson s Disease and autonomic dysfunction
 Exercise hemodynamics in Parkinson s Disease and autonomic dysfunction David A. Low 1,2,3*, Ekawat Vichayanrat 2,3, Valeria Iodice 2,3 and Christopher J. Mathias 2,3 1 Research Institute of Sport and Exercise
Exercise hemodynamics in Parkinson s Disease and autonomic dysfunction David A. Low 1,2,3*, Ekawat Vichayanrat 2,3, Valeria Iodice 2,3 and Christopher J. Mathias 2,3 1 Research Institute of Sport and Exercise
Clinical Case 1 A patient with a syncope Panos E. Vardas President Elect of the ESC, Prof of Cardiology, University Hospital of Crete
 Clinical Case 1 A patient with a syncope Panos E. Vardas President Elect of the ESC, Prof. of Cardiology, University Hospital of Crete Case presentation A 64-year-old male smoker, with arterial hypertension
Clinical Case 1 A patient with a syncope Panos E. Vardas President Elect of the ESC, Prof. of Cardiology, University Hospital of Crete Case presentation A 64-year-old male smoker, with arterial hypertension
Control of blood tissue blood flow. Faisal I. Mohammed, MD,PhD
 Control of blood tissue blood flow Faisal I. Mohammed, MD,PhD 1 Objectives List factors that affect tissue blood flow. Describe the vasodilator and oxygen demand theories. Point out the mechanisms of autoregulation.
Control of blood tissue blood flow Faisal I. Mohammed, MD,PhD 1 Objectives List factors that affect tissue blood flow. Describe the vasodilator and oxygen demand theories. Point out the mechanisms of autoregulation.
For more information
 For more information www.escardio.org/guidelines ESC GUIDELINES FOR THE DIAGNOSIS AND MANAGEMENT OF SYNCOPE Task Force for the Diagnosis and Management of Syncope of the European Society of Cardiology
For more information www.escardio.org/guidelines ESC GUIDELINES FOR THE DIAGNOSIS AND MANAGEMENT OF SYNCOPE Task Force for the Diagnosis and Management of Syncope of the European Society of Cardiology
Syncope is defined by rapid onset of transient loss of
 Mechanisms of Vasovagal Syncope in the Young: Reduced Systemic Vascular Resistance Versus Reduced Cardiac Output Julian M. Stewart, MD, PhD; Marvin S. Medow, PhD; Richard Sutton, MB, BS, DSc; Paul Visintainer,
Mechanisms of Vasovagal Syncope in the Young: Reduced Systemic Vascular Resistance Versus Reduced Cardiac Output Julian M. Stewart, MD, PhD; Marvin S. Medow, PhD; Richard Sutton, MB, BS, DSc; Paul Visintainer,
The management of vasovagal syncope
 QJM: An International Journal of Medicine, 2016, 767 773 doi: 10.1093/qjmed/hcw089 Advance Access Publication Date: 23 June 2016 Review Sir William Osler Medicine Masterclass REVIEW SIR WILLIAM OSLER MEDICINE
QJM: An International Journal of Medicine, 2016, 767 773 doi: 10.1093/qjmed/hcw089 Advance Access Publication Date: 23 June 2016 Review Sir William Osler Medicine Masterclass REVIEW SIR WILLIAM OSLER MEDICINE
P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp , , , I. Major Functions of the Circulatory System
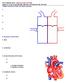 P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp 360-390, 395-404, 410-428 433-438, 441-445 I. Major Functions of the Circulatory System 1. 2. 3. 4. II. Structure of the Heart 1. atria 2. ventricles
P215 SPRING 2019: CIRCULATORY SYSTEM Chaps 13, 14 & 15: pp 360-390, 395-404, 410-428 433-438, 441-445 I. Major Functions of the Circulatory System 1. 2. 3. 4. II. Structure of the Heart 1. atria 2. ventricles
HEART SOUNDS & BLOOD PRESSURE
 LABORATORY HANDBOOK HEART SOUNDS & BLOOD PRESSURE For the course Systems Biology Karolinska Institutet Department of Physiology and Pharmacology Physiology Education Postal address: 171 77 Stockholm Visiting
LABORATORY HANDBOOK HEART SOUNDS & BLOOD PRESSURE For the course Systems Biology Karolinska Institutet Department of Physiology and Pharmacology Physiology Education Postal address: 171 77 Stockholm Visiting
Utility of a Single-Stage Isoproterenol Tilt Table Test in Adults A Randomized Comparison With Passive Head-Up Tilt
 Journal of the American College of Cardiology Vol. 33, No. 4, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(98)00658-5 Utility
Journal of the American College of Cardiology Vol. 33, No. 4, 1999 1999 by the American College of Cardiology ISSN 0735-1097/99/$20.00 Published by Elsevier Science Inc. PII S0735-1097(98)00658-5 Utility
Cardiovascular Responses to Exercise
 CARDIOVASCULAR PHYSIOLOGY 69 Case 13 Cardiovascular Responses to Exercise Cassandra Farias is a 34-year-old dietician at an academic medical center. She believes in the importance of a healthy lifestyle
CARDIOVASCULAR PHYSIOLOGY 69 Case 13 Cardiovascular Responses to Exercise Cassandra Farias is a 34-year-old dietician at an academic medical center. She believes in the importance of a healthy lifestyle
Contempo GIMSI Cosa cambia alla luce della letteratura in tema di terapia farmacologica
 Contempo GIMSI 2015-2017 Cosa cambia alla luce della letteratura in tema di terapia farmacologica Dott.ssa Diana Solari Centro Aritmologico e Sincope Unit, Lavagna www.gimsi.it POST 2 (Prevention of Syncope
Contempo GIMSI 2015-2017 Cosa cambia alla luce della letteratura in tema di terapia farmacologica Dott.ssa Diana Solari Centro Aritmologico e Sincope Unit, Lavagna www.gimsi.it POST 2 (Prevention of Syncope
Treatment of orthostatic hypotension in Multiple System Atrophy New Clinical Studies
 Treatment of orthostatic hypotension in Multiple System Atrophy New Clinical Studies Cyndya A. Shibao, M.D., F.A.H.A. Assistant Professor of Medicine Division of Clinical Pharmacology Disclosure Lundbeck
Treatment of orthostatic hypotension in Multiple System Atrophy New Clinical Studies Cyndya A. Shibao, M.D., F.A.H.A. Assistant Professor of Medicine Division of Clinical Pharmacology Disclosure Lundbeck
Disclosures. Where We Are Going. My Goals for Giving This Talk. Diagnosis and Management of Dysautonomia in the Pediatric Population
 Diagnosis and Management of Dysautonomia in the Pediatric Population Disclosures David M Bush, MD, PhD Pediatric Cardiology/Electrophysiology Pediatric Cardiology Associates of San Antonio Adjunct Associate
Diagnosis and Management of Dysautonomia in the Pediatric Population Disclosures David M Bush, MD, PhD Pediatric Cardiology/Electrophysiology Pediatric Cardiology Associates of San Antonio Adjunct Associate
Increased Postural Sway in Control Subjects With Poor Orthostatic Tolerance
 Journal of the American College of Cardiology Vol. 46, No. 7, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2005.07.011
Journal of the American College of Cardiology Vol. 46, No. 7, 2005 2005 by the American College of Cardiology Foundation ISSN 0735-1097/05/$30.00 Published by Elsevier Inc. doi:10.1016/j.jacc.2005.07.011
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders
 C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
droxidopa (Northera )
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Presentation of transient loss of consciousness
 Presentation of transient loss of consciousness Definition of transient loss of consciousness Transient loss of consciousness: sudden onset, complete loss of consciousness of brief duration with relatively
Presentation of transient loss of consciousness Definition of transient loss of consciousness Transient loss of consciousness: sudden onset, complete loss of consciousness of brief duration with relatively
For the Faint of Heart
 For the Faint of Heart Developing a Simple Consistent Approach to Diagnosis of Syncope/PoTS R. Austin Raunikar, MD, FAAP, FACC Clinical Associate Professor, USCSOM Greenville Pediatric Cardiology, GHS
For the Faint of Heart Developing a Simple Consistent Approach to Diagnosis of Syncope/PoTS R. Austin Raunikar, MD, FAAP, FACC Clinical Associate Professor, USCSOM Greenville Pediatric Cardiology, GHS
Reduced baroreflex sensitivity in patients with vasovagal syncope
 DOI: 10.4149/BLL_2015_113 CLINICAL STUDY Reduced baroreflex sensitivity in patients with vasovagal syncope Mitro P, Simurda M, Evin L, Murin P, Muller E Cardiology Clinic, Safarik University and VUSCH
DOI: 10.4149/BLL_2015_113 CLINICAL STUDY Reduced baroreflex sensitivity in patients with vasovagal syncope Mitro P, Simurda M, Evin L, Murin P, Muller E Cardiology Clinic, Safarik University and VUSCH
