DOWNLOAD PDF AORTOILIAC OCCLUSIVE DISEASE
|
|
|
- Owen Hawkins
- 5 years ago
- Views:
Transcription
1 Chapter 1 : Diagnosing Aortoiliac Occlusive Disease NYU Langone Health Aortoiliac occlusive disease is the blockage of the aorta, the main blood vessel in your body, or the iliac arteries. The iliac arteries are the branches that your aorta divides into around the level of the belly button to provide blood to your legs and the organs in your pelvis. What Is Aortoiliac Occlusive Disease? Aortoiliac occlusive disease occurs when your iliac arteries become narrowed or blocked. These branches are called the iliac arteries. The iliac arteries go through your pelvis into your legs, where they divide into many smaller arteries that run down to your toes. Aortoiliac disease is considered a type of peripheral arterial disease PAD because it affects arteries, which are blood vessels that carry blood away from your heart to your limbs. Your arteries are normally smooth and unobstructed on the inside, but as you age, a sticky substance called plaque can build up in the walls of your arteries. Plaque is made up of cholesterol, calcium, and fibrous tissue. As more plaque builds up, it causes your arteries to narrow and stiffen. This process is called atherosclerosis, or hardening of the arteries. Eventually, enough plaque builds up to interfere with blood flow in your iliac arteries or leg arteries. Physicians call this aortoiliac occlusive disease because it involves the aortoiliac arteries. What Are The Symptoms? Early in the disease, you may feel pain, cramping, or fatigue in your lower body when you walk or exercise. The pain with walking usually occurs in your buttocks, thighs, and legs. This symptom is called intermittent claudication because it stops when you rest. As the disease worsens, you may find that pain occurs when you walk for shorter distances. Ultimately, as the disease progresses, you may feel pain, usually in your toes or feet, even when you are resting. Some men who have aortoiliac occlusive disease also experience erectile dysfunction, the inability to have or maintain an erection. Aortoiliac disease may worsen if it is not treated. Signs that it has advanced include: Severe pain, coldness, and numbness in a limb; Sores on your toes, heels, or lower legs; Dry, scaly, cracked skin on your foot. Major cracks, or fissures, may become infected if left untreated; Weakened muscles in your legs; and Gangrene tissue death, which may require amputation. What Causes Aortoiliac Occlusive Disease? Atherosclerosis, or hardening of the arteries, causes most cases of aortoiliac occlusive disease. Risk factors for hardening of the arteries include: Smoking; High cholesterol levels in the blood; High blood pressure; Having a family history of heart disease. Diagnosis To diagnose aortoiliac disease, a physician may order a variety of tests, including: Pulse tests; Blood pressure testing in the leg; Doppler ultrasound; and Arteriography, in which a contrast dye is injected into the arteries and x rays are taken. Treatment Options If the disease is mild or moderate, a physician may prescribe the following: Maintain a healthy body weight Follow a physician-approved walking program Eat a low-fat and high-fiber diet Stop smoking and all forms of tobacco use Receive regular foot care from a healthcare professional to reduce the risk of foot ulcers Medication to improve blood flow in the lower extremities If the disease is severe, treatments may include: Angioplasty and stenting Bypass surgery to replace or bypass blocked arteries with a segment of synthetic blood vessel Angioplasty or Surgery If you have severe aortoiliac occlusive disease, particularly if it does not improve with the measures described above, your physician may recommend a minimally invasive treatment called angioplasty to improve the circulation in your legs. For more extensive blockages or those that cannot be treated with angioplasty, surgery to bypass or clear your blocked arteries may be required. During an angioplasty procedure, which is sometimes performed at the same time as an angiogram, a long, thin, flexible tube, called a catheter, is inserted into a small puncture over an artery in your leg and is guided through your arteries to the blocked area. Once there, a special balloon attached to the catheter is inflated and deflated several times. The balloon pushes the plaque in your artery against your artery walls, widening the vessel. In some circumstances, a tiny mesh-metal tube called a stent may then be placed into the narrowed area of your artery to keep it open. The stent remains permanently in your artery. After successful angioplasty, blood flows more freely through your artery. For more information, medical assessment and medical quote as attachment to Contact Center Tel. IST Only for international patients seeking treatment in India. Page 1
2 Chapter 2 : Aortoiliac Occlusive Disease Causes Symptoms Treatment Prevention Diagnosis In medicine, aortoiliac occlusive disease, also known as Leriche's syndrome and Leriche syndrome, is a form of central artery disease involving the blockage of the abdominal aorta as it transitions into the common iliac arteries. Intermittent claudication â pain in muscles when walking or using the affected muscles that is relieved by resting those muscles. This is due to the unmet oxygen demand in muscles with use in the setting of inadequate blood flow. Critical limb ischemia, consisting of: Rest pain, a pain in the soles of the feet, particularly when the feet are elevated, such as when in bed. Tissue loss, consisting of arterial insufficiency ulcers, which are sores or wounds that heal slowly or not at all, and gangrene. Medical signs of PAD in the legs, due to inadequate perfusion, include: Noticeable change in color â blueness, or in temperature coolness when compared to the other limb. Diminished hair and nail growth on affected limb and digits Causes[ edit ] The illustration shows how PAD can affect arteries in the legs. Figure A shows a normal artery with normal blood flow. The inset image shows a cross-section of the normal artery. The inset image shows a cross-section of the narrowed artery. Risk factors contributing to PAD are the same as those for atherosclerosis: Smokers have up to a tenfold increase in relative risk for PAD in a dose-response relationship. Smokers are 2 to 3 times more likely to have lower extremity peripheral arterial disease than coronary artery disease. Hypertension increased the risk of intermittent claudication 2. Peripheral arterial disease is more common in the following populations of people: All people aged 65 years and over regardless of risk factor status. All people between the age of 50 to 69 and who have a cardiovascular risk factor particularly diabetes or smoking. Age less than 50 years, with diabetes and one other atherosclerosis risk factor smoking, dyslipidemia, hypertension, or hyperhomocysteinemia. Individuals with an abnormal lower extremity pulse examination. Those with known atherosclerotic coronary, carotid, or renal artery disease. You can assist by editing it. September Learn how and when to remove this template message Measuring the ankle-brachial index Upon suspicion of PAD, the first-line study is the ankleâ brachial index ABI, which is the ratio of blood pressure in the ankle to blood pressure in the upper arm. When the blood pressure readings in the ankles is lower than that in the arms, blockages in the arteries which provide blood from the heart to the ankle are suspected. An ABI range of 1. ABI values of 0. These relative categories have prognostic value. A base line ABI is obtained prior to exercise. The patient is then asked to exercise usually patients are made to walk on a treadmill at a constant speed until claudication pain occurs or a maximum of 5 minutes, following which the ankle pressure is again measured. Such results and suspicions merit further investigation and higher level studies. Other imaging can be performed by angiography, [22] where a catheter is inserted into the common femoral artery and selectively guided to the artery in question. While injecting a radiodense contrast agent an X-ray is taken. Any flow limiting stenoses found in the x-ray can be identified and treated by atherectomy, angioplasty or stenting. Contrast angiography is the most readily available and widely used imaging technique. Modern multislice computerized tomography CT scanners provide direct imaging of the arterial system as an alternative to angiography. Magnetic resonance angiography MRA is a noninvasive diagnostic procedure that uses a combination of a large magnet, radio frequencies, and a computer to produce detailed images to provide pictures of blood vessels inside the body. The advantages of MRA include its safety and ability to provide high-resolution three-dimensional 3D imaging of the entire abdomen, pelvis and lower extremities in one sitting. Asymptomatic, incomplete blood vessel obstruction Stage II: Mild claudication pain in limb Stage IIA: Claudication when walking a distance of greater than meters Stage IIB: Claudication when walking a distance of less than meters Stage III: Rest pain, mostly in the feet Stage IV: Rutherford, consists of four grades and seven categories: Asymptomatic Grade I, Category 1: Mild claudication Grade I, Category 2: Moderate claudication Grade I, Category 3: Severe claudication Grade II, Category 4: Minor tissue loss; Ischemic ulceration not exceeding ulcer of the digits of the foot Grade IV, Category 6: Management of high cholesterol, and medication with antiplatelet drugs. Medication with aspirin, clopidogrel and statins, which reduce clot formation and cholesterol levels, respectively, can help with disease progression and address the other cardiovascular risks that the affected person is likely to have. Regular exercise for those with claudication Page 2
3 helps open up alternative small vessels collateral flow and the limitation in walking often improves. Treadmill exercise 35 to 50 minutes, 3 to 4 times per week [22] has been reviewed as another treatment with a number of positive outcomes including reduction in cardiovascular events and improved quality of life. Supervised exercise programs increase pain-free walking time and the maximum walking distance in people with PAD. Medication[ edit ] Cilostazol or pentoxifylline can improve symptoms in some. The benefit of revascularization is thought to correspond to the severity of ischemia and the presence of other risk factors for limb loss such as wound and infection severity. Other criteria that affect outcome following revascularization are length of lesion, and number of lesions. The great saphenous vein is used as a conduit if available, although artificial Gore-Tex or PTFE material is often used for long grafts when adequate venous conduit is unavailable. When gangrene has set in, amputation is required to prevent infected tissues from causing sepsis, a life-threatening illness. Guidelines[ edit ] An updated consensus guideline from the American College of Cardiology and American Heart Association for the diagnosis and treatment of lower extremity, renal, mesenteric and abdominal aortic PAD was compiled in, combining the and guidelines. In the USA peripheral arterial disease affects 12â 20 percent of Americans age 65 and older. Approximately 10 million Americans have PAD. Despite its prevalence and cardiovascular risk implications, only 25 percent of PAD patients are undergoing treatment. The incidence of symptomatic PAD increases with age, from about 0. The prevalence of PAD varies considerably depending on how PAD is defined, and the age of the population being studied. Diagnosis is critical, as people with PAD have a four to five times higher risk of heart attack or stroke. Prospective Diabetes Study trials, in people with type 1 and type 2 diabetes, respectively, demonstrated that glycemic control is more strongly associated with microvascular disease than macrovascular disease. It may be that pathologic changes occurring in small vessels are more sensitive to chronically elevated glucose levels than is atherosclerosis occurring in larger arteries. Page 3
4 Chapter 3 : Aortoiliac Occlusive Disease SIU School of Medicine Aortoiliac occlusive disease may be a significant cause of lower-extremity ischemic symptoms. In the past, most patients have been treated with a variety of open surgical procedures, including aortobifemoral and extra-anatomic bypasses. Basic Facts Aortoiliac occlusive disease is the narrowing or blockage of the main arteries in the pelvis, which supply blood to the legs. It is a type of peripheral arterial disease, or PAD, which affects arteries that carry blood away from the heart to the head, torso, arms, and legs. Aortoiliac disease can prevent blood from reaching parts of the buttocks, groin, legs and feet. A lack of blood can cause discomfort or weakness in the hips or legs while walking, sores on the legs, feet, and toes, known as ulcers, and even gangrene. The most common symptom of aortoiliac disease is a discomfort in the legs during activity, called intermittent claudication. Male patients with aortoiliac disease often experience erectile dysfunction. Aortoiliac disease, also called aortoiliac occlusive disease, refers to disorders of the two major blood vessels that feed the lower half of the body? Aortoiliac disease occurs in one or more of the following locations: The lower abdominal aorta; The iliac arteries; or The point where the aorta divides and becomes the iliac arteries. Impaired circulation in these arteries can result in disorders of the pelvic organs, legs, or the kidneys, which causes a condition called renal artery disease. Additionally, aortoiliac disease can result in an aortic abdominal aneurysm AAA, a dangerous health condition. Risk factors for atherosclerosis include: Smoking; High blood pressure, or hypertension; Obesity; High cholesterol or hyperlipidemia; and A family history of cardiovascular disease. The primary symptoms of aortoiliac disease are pain, cramping, or tiredness called intermittent claudication, which occur when a person walks or exercises. Male patients with aortoiliac disease also often experience erectile dysfunction. Eventually, severe symptoms can occur in the lower extremities, including: Severe pain, coldness, and numbness in a limb; Sores on the toes, heels, or lower leg called ulcers ; Muscle atrophy wasting ; and Symptoms of renal artery disease include: Hypertension; Symptoms of kidney failure; and An abnormal sound or murmur, called a bruit. Most people with AAA do not feel any symptoms. Others, however, may experience symptoms including: A rhythmic, pulsating feeling in the abdomen, similar to a heartbeat; Deep pain in the abdomen or lower back; and Severe, sudden abdominal or back pain, which may indicate imminent rupture. Patients with a ruptured abdominal aortic aneurysm, which requires immediate emergency medical attention, usually feel sudden and intense weakness, dizziness, or pain, and may lose consciousness. Page 4
5 Chapter 4 : Aortoiliac Disease Aortoiliac occlusive disease occurs when your iliac arteries become narrowed or blocked. The aorta, your body's main artery, splits into branches at about the level of your belly button. These branches are called the iliac arteries. You may have varied symptoms or no symptoms at all and still have aortoiliac occlusive disease. As the disease progresses, these symptoms may occur after walking very short distances. The most common cause of aortoiliac disease is atherosclerosis hardening of the arteries. Hardening of the arteries may be caused by smoking, high cholesterol, high blood pressure, genetic predisposition or obesity. Radiation to the pelvis may cause progressive inflammation in the arterial wall leading to blockages of the arteries. Diagnosis See a vascular surgeon You will be asked questions about symptoms and medical history, including questions about family members. The vascular surgeon will also perform a physical exam. Tests may be recommended Initially an ankle-brachial index test and a duplex ultrasound may be recommended. If further testing is needed a CT angiogram, MR angiogram, or a catheter-directed angiogram are options. These studies use different types of dye to help identify where blockages in the arteries are located to plan further treatment. With a catheter-directed angiogram, dye is injected through a thin tube catheter inserted in an artery. Treatments Aortoiliac occlusive disease may be managed by: Risk factor modification, such as quitting smoking, controlling cholesterol or high blood pressure, managing diabetes and regular exercise. Medication may be prescribed, such as an aspirin or another medication to prevent platelets from clotting in the blood. A statin drug may help control cholesterol and also help prevent plaque progression. If further treatment is needed, a minimally invasive procedure or a surgical bypass may be considered. The most common minimally invasive treatment is the placement of a stent in your aorta or iliac arteries. This procedure is commonly done at the same time as a catheter-directed angiogram test. The stent is a small device that compacts the plaque against the walls of the arteries to create a wider path for blood flow to the lower half of your body. An angioplasty, in which an inflatable balloon device is inserted through the catheter to further assist in opening up the arteries, can be added to the treatment. A surgical bypass is the creation of a detour around the blockage. The detour may start in the aorta near your heart and may end either in the iliac arteries in your pelvis, or in an artery in your groin. A bypass may be performed either on one or both sides at the same time. For severe disease that includes the aorta and both iliac arteries, a bypass typically runs from the aorta to the groin arteries, usually using an artificial graft. If there is not a suitable artery to originate the bypass in the aorta, or if you are not healthy enough to undergo an aortic-based procedure, the bypass generally starts at the axillary artery underneath the collarbone and ends in one or both legs. Staying Healthy The best way to prevent development of aortoiliac occlusive disease is to not smoke, and manage cholesterol, blood pressure and diabetes. If you do smoke, ask your vascular surgeon to help you find a smoking cessation program that will work for you. Page 5
6 Chapter 5 : Aortoiliac Occlusive Disease in Adults NYU Langone Health Aortoiliac occlusive disease (AIOD) is a condition that arises as a result of two other blood disorders: peripheral arterial disease (PAD) and atherosclerosis. After the blood vessels in the upper leg, the aorta and iliac arteries are the second most commonly affected blood vessels by PAD. Volume 9 - Issue 2 - February Abstract Aortoiliac stenting is the treatment of choice for aortoiliac occlusive disease. After reviewing treatment techniques, research shows that outcomes are similar for balloon expandable and self-expanding stents. Covered stents are now being studied but no published benefit exists over uncovered stenting. Secondary patency of aortoiliac intervention rivals open surgery through 3 years. In, Andreas Gruentzig described the first percutaneous angioplasty. Within the next decade, endovascular treatment of iliac occlusive disease began to gain momentum as patients and radiologists fueled interest. Simultaneously in the s, surgery was considered the gold standard therapy for aortoiliac occlusive disease AIOD. The well documented long-term outcomes of aortofemoral bypass AFB were thought to have solidified the use of surgical therapy as the sole definitive therapy for this disease. The first article describing results of iliac angioplasty in the Journal of Vascular Surgery was not published until and was done by an interventional radiologist. Aortobifemoral bypass ABF is still common for TASC D lesions, but in some practices, it has become a rarely performed operation, relegated to the uncommon patient after failed endovascular therapy. Evaluation of Disease Patients with aortoiliac occlusive disease will commonly complain of hip, buttock, or thigh muscle group heaviness, achiness or pain with ambulation or exercise. Leriche syndrome describes the triad of hip or buttock claudication, impotence, and diminished femoral pulses, a hallmark of the patient with aortoiliac occlusive disease. Atheroembolism from unstable plaque can occlude the distal circulation leading to blue toe syndrome. Some patients will present with concomitant distal occlusive disease and will have calf or foot claudication, rest pain, tissue loss, or gangrene depending on the severity of the blockages. Identification of AOID will be identified in most patients with simple physical exam and pulse palpation. Diminished femoral pulses are noted in many, but some with significant disease may still have femoral pulses at rest. Bruits or thrills over the aortoiliac and femoral vessels are common. Noninvasive imaging should start with segmental limb pressures with plethysmography. High thigh pressures should normally be higher than brachial pressure. In the setting of AIOD the high thigh pressure will be lower and pulse volume recordings will show diminished waveforms. Some patients may have normal ankle pressures that drop only after exercise. Duplex ultrasonography is commonly used to show the level and degree of disease in the iliac and femoral vessels. Limitation of this technology can be poor visualization of the vessels in obese patients and patients with gas-filled intestine. The study quality relies on the skill of the technician obtaining the study. Computed tomographic angiography CTA has recently emerged as a popular noninvasive imaging modality that can show the amount of calcification, areas of stenosis, and occlusions as well as the current collateral circulation. Identification of the amount of occlusive disease in the femoral vessels is critical to improving the success of iliac intervention, as open surgical treatment of femoral vessels improves outcomes. The 2 biggest limitations of CTA are the risk of radiation and intravenous contrast related problems such as allergic response and contrast-induced nephropathy. Diabetic patients have a higher risk of contrast related nephropathy. In patients with impaired creatinine clearance, precontrast hydration with intravenous isotonic solutions can minimize this risk. Magnetic resonance angiography MRA can also be used to image the aortoiliac segment. A limitation of MRA is that it is really a flow study, and low flow situations and previously stented vessels can cause signal drop out, falsely appearing as occlusions. In the setting of chronic total occlusions CTO, several techniques can be used to cross the lesion. Spinning a hydrophilic guide wire with catheter or balloon support is the most commonly used method. Use of braided catheters and dedicated crossing catheters Quick-Cross, Spectranetics has diminished the need for using angioplasty balloons for support. When attempting to cross an iliac occlusion from an ipsilateral retrograde femoral approach the greatest difficulty comes in re-entry back into the true lumen Figure 1. Often due to dense calcification at the aortic bifurcation, the catheter and wire will want to pass subintimally up the aorta and will not re-enter the true lumen. In this situation, contralateral Page 6
7 retrograde femoral access can be helpful to start a new plane to direct a wire cranially across the occlusion. Once the wire is able to get through the proximal cap and within the subintimal channel, many times the wires will enter the same subintimal plane created from below and allow capture with a snare. This technique of snaring the wire will ensure true lumen to true lumen access above and below the occlusion. In the setting of a flush iliac occlusion with the aortic bifurcation, contralateral access is often unsuccessful in crossing the occlusion due to lack of pushability in the direction of the vessel. In these situations, brachial access is usually successful. By placing a long 5 Fr or 6 Fr sheath to the level of the aortic bifurcation, coupled with an angled catheter and stiff hydrophilic wire most CTOs are easily crossed. Several options exist when re-entry into the true lumen after crossing a CTO has not occurred. In the patient with concomitant femoral occlusive disease, open distal external iliac and common femoral endarterectomy will allow communication to the true lumen with open retrieval of the wire through the endarterectomized vessel, or snaring of the wire after completion of the vessel patch and accessing through the patch with a sheath. The other method of gaining access back into the true lumen is by use of a re-entry device such as the Outback LTD Cordis Corporation or Pioneer catheter Medtronic Medical. The technique has been described as locate, tune, and deploy. Once the needle is advanced into the true lumen flow channel, the 0. The Pioneer device uses Volcano intravascular ultrasound Volcano Corporation to locate the true lumen flow channel. The depth of penetration of the needle can be set to allow directed passage into the true lumen allowing a second 0. Treatment with angioplasty is acceptable, however multiple views may be necessary to ensure flow-limiting dissection does not exist. Pressure measurement across the area of treatment with a vasodilator challenge can unmask residual disease, which may not be apparent on angiography. Intravascular ultrasound has also been used to ensure adequate luminal expansion after interventional therapy. Despite many successful cases with angioplasty, the use of stents has become the most common treatment due to excellent long-term results. Although no outcome difference exists between self-expanding and balloon expandable stents, several engineering differences exist. Self-expanding stents most commonly used today are made out of nitinol and do not foreshorten with placement. They have chronic outward force and are typically oversized 1 mm larger than the reference vessel they are intended to treat. Nitinol self-expanding stents are flexible, making them ideal for external iliac disease. In the setting of severe calcific disease, nitinol stents may not generate sufficient chronic outward force to achieve expansion of a diseased segment. In this setting, balloon expandable stents have a unique advantage. I prefer to use balloon expandable stents for common iliac disease due to accuracy of placement and the fact that most common iliac ostial disease has a component of calcified aortic plaque. Currently most balloon expandable stents are made from stainless steel and have greater hoop strength to keep a calcified lesion expanded after dilation. More recently work has been done with cobalt chromium and platinum to decrease the strut thickness to lower profile while maintaining visibility. Depending on the cell design, a balloon expandable stent will foreshorten to varying degrees with dilation above the designed diameter for use. The cell design limits the maximum size you can dilate a stent. Most commercially available premounted stents in the U. Due to the limitation of diameter, I use self-expanding large diameter stents for aortic disease. Nitinol self-expanding stents can be very accurately placed but are limited at 14 mm in maximum diameter. However this size is generally adequate to treat occlusive disease to get an adequate hemodynamic result. Only when severe calcific disease is present I will use unmounted giant balloon expandable stents. I reserve the use of covered stents for rupture of the treated vessel. Depending on location, I use balloon expandable covered stents for aortic and common iliac locations and self-expanding covered stents for external iliac locations. Others perform parallel or kissing stents, which in effect raises the bifurcation. The large disadvantage of this approach is that the ability to cross from one femoral artery to the contralateral side is eliminated. This can make treatment of infrainguinal disease more difficult in future encounters. A hybrid technique of crossing the struts of a self-expanding stent placed from the aorta to one iliac artery by a balloon expandable stent from the contralateral side has been described as an alternative to the classic kissing stent technique. For flush aortic occlusions, the use of thrombolysis from a brachial approach can allow dissolution of chronic thrombus and allow successful endovascular treatment Figures 2A and 2B. Typically, a catheter is used to cross into one iliac artery to the open vessel distally. Subintimal passage of the wire should be avoided. Thrombolysis is then Page 7
8 initiated. After establishing flow into the aorta and one iliac artery, the catheter can be repositioned to the opposite iliac artery. After dissolution of the clot, endovascular treatment with stenting of residual disease is performed Figures 3A and 3B. Treatment Outcomes The treatment of aortoiliac occlusive disease began with angioplasty. The introduction of the Palmaz balloon expandable stent Cordis significantly altered the interventional landscape providing an option to achieve success when angioplasty alone did not have optimal results and led to approval of the P stent for iliac use in The 6-month mean percent luminal diameter loss was Primary patency was Despite improved results in single-center series the randomized Dutch Iliac Stent Trial failed to show improved outcomes of primary stenting over selective stenting. In cases where the residual mean pressure gradient was greater than 10 mmhg across the treated site, patients with iliac artery disease were randomly assigned to undergo primary stent placement or percutaneous transluminal angioplasty with selective stent placement. The Wallstent Boston Scientific was the first self-expanding stent to achieve approval for iliac use in the U. Martin reported the 2-year results of the FDA phase II, multicenter trial of the Wallstent in the iliac and femoral arteries. One of the first self-expanding nitinol stents to be used was the Strecker stent Boston Scientific. Primary patency at 12 months was Jaff reported the 2-year outcomes of safety and effectiveness in the iliac artery with patency and ABI measurements showing improvement at 2 years as compared with preprocedure measurements. Most of these series do not describe what types of stents were used. In Sullivan reported on patients who underwent PTA and primary stenting of the common iliac, Variables associated with better patency included stenosis rather than occlusion, shorter lesion length, older age, and limb-threatening ischemia. Increased confidence in outcomes treating short occlusions and long stenoses with stents led physicians to treat more difficult lesions with interventional therapy. The technical success rate of SA was lower than that of IA There was no difference in primary patency rates for either technique. Patency for SA and IA was Page 8
9 Chapter 6 : Aortoiliac Occlusive Disease Society for Vascular Surgery The authors concluded that endovascular treatment of extensive aortoiliac occlusive disease can be performed successfully by experienced interventionists in selected patients. Aortoiliac occlusive disease occurs when your iliac arteries become narrowed or blocked. These branches are called the iliac arteries. The iliac arteries go through your pelvis into your legs, where they divide into many smaller arteries that run down to your toes. Aortoiliac disease is considered a type of peripheral arterial disease PAD because it affects arteries, which are blood vessels that carry blood away from your heart to your limbs. Your arteries are normally smooth and unobstructed on the inside, but as you age, a sticky substance called plaque can build up in the walls of your arteries. Plaque is made up of cholesterol, calcium, and fibrous tissue. As more plaque builds up, it causes your arteries to narrow and stiffen. This process is called atherosclerosis, or hardening of the arteries. Eventually, enough plaque builds up to interfere with blood flow in your iliac arteries or leg arteries. Physicians call this aortoiliac occlusive disease because it involves the aortoiliac arteries. When your iliac arteries narrow or become blocked, your legs may not receive the blood and oxygen they need. This lack of oxygen is called ischemia and it can cause pain. In severe cases, sores or gangrene can develop, which can result in losing a limb. However, these developments are uncommon unless the process is not treated and is allowed to progress. What are the symptoms? Early in the disease, you may feel pain, cramping, or fatigue in your lower body when you walk or exercise. The pain with walking usually occurs in your buttocks, thighs, and legs. This symptom is called intermittent claudication because it stops when you rest. As the disease worsens, you may find that pain occurs when you walk for shorter distances. Ultimately, as the disease progresses, you may feel pain, usually in your toes or feet, even when you are resting. Some men who have aortoiliac occlusive disease also experience erectile dysfunction, the inability to have or maintain an erection. Aortoiliac disease may worsen if it is not treated. Signs that it has advanced include: Severe pain, coldness, and numbness in a limb Sores on your toes, heels, or lower legs Dry, scaly, cracked skin on your foot. Major cracks, or fissures, may become infected if left untreated Weakened muscles in your legs Gangrene tissue death, which may require amputation If you experience any of these advanced symptoms, it usually means that your leg arteries are blocked in more than one place. Robbins may need to treat more than one site to prevent gangrene or limb loss. What causes aortoiliac occlusive disease? Atherosclerosis, or hardening of the arteries, causes most cases of aortoiliac occlusive disease. Risk factors for hardening of the arteries include: It is caused by inflammation in the arteries. What tests will I need? Robbins asks you questions about your general health, medical history, and symptoms. In addition, He conducts a physical exam. Together these are known as a patient history and exam. As part of your history and exam, Dr. Robbins will ask you if you smoke or have high blood pressure. Robbins will also want to know when your symptoms occur and how often. A pulse examination that checks your pulse in several places in your legs for weak or absent pulses is part of your physical exam. For this test, Dr. Robbins will simply place his or her fingers over pulse points. After the history and exam, if Dr. Robbins suspects you may have aortoiliac disease, he or she may perform tests to further define its extent and severity, such as: The vascular technician will compare the two numbers to determine your ABI. Normally, the blood pressures in your ankle and arm should be about equal. But if your ankle pressure is half your arm pressure or lower, your leg arteries are probably narrowed. To perform the ABI, Dr. The ABI helps Dr. Robbins diagnose aortoiliac disease, but it does not identify which specific arteries are blocked. Doppler ultrasound Doppler ultrasound is another non-invasive test that uses high-frequency sound waves that bounce off of blood cells and blood vessels to show blood flow and problems with the structure of blood vessels. This test better identifies specific arteries that are blocked. Angiography There are three types of arteriography that may be performed: Contrast arteriography usually provides better resolution but is a more invasive test. Robbins injects a contrast dye into your arteries and then takes x-ray images. The structure of your arteries appears on the x-ray pictures because x-rays themselves cannot pass through the dye. This test finds the exact location and pattern of blockages. The dye is later passed from your body through your kidneys. If a blockage is identified and is appropriate for treatment by Page 9
10 angioplasty and a stent, this procedure may be carried out at the same time. How is aortoiliac occlusive disease treated? Lifestyle Changes In mild to moderate cases, Dr. Robbins may recommend that you change certain aspects of your lifestyle. If you are a smoker, the most important step you can take is to quit smoking. Chemicals in tobacco can damage your arteries. These chemicals can also increase your chance of having complications from aortoiliac occlusive disease. In addition to quitting smoking, Dr. Robbins may recommend that you maintain a healthy weight, follow a structured walking program at least 3 or 4 times a week, and eat a low-fat and high-fiber diet. These changes help slow hardening of the arteries. Robbins may prescribe medications to lower high cholesterol. If you have high blood pressure, regular monitoring of your blood pressure and compliance in taking medication if prescribed is important. If you have diabetes, you need to control your blood sugar levels with diet and medication. In addition, if you have diabetes, you may develop impaired sensation in your feet, a condition called neuropathy. Robbins may recommend that you receive foot care from a qualified healthcare professional and learn the basics of caring for your feet at home. This includes practicing foot hygiene, wearing protective, well fitting, and cushioned footwear, and avoiding injuries to your foot. This type of care can be very important because, as you lose the protective feeling in your feet, you can develop sores on them that may be difficult to heal. Medications If you do not have a disqualifying medical condition, such as heart failure, Dr. Robbins may also prescribe cilostazol Pletal, which may improve the distance you are able to walk without pain. Other drugs your physician may prescribe include aspirin or clopidogrel Plavix, either of which can lower your chances of blood clots. Statins are a class of medications that Dr. Robbins may use to control your cholesterol levels. Angioplasty or Surgery If you have severe aortoiliac occlusive disease, particularly if it does not improve with the measures described above, Dr. Robbins may recommend a minimally invasive treatment called angioplasty to improve the circulation in your legs. For more extensive blockages or those that cannot be treated with angioplasty, surgery to bypass or clear your blocked arteries may be required. During an angioplasty procedure, which is sometimes performed at the same time as an angiogram, a long, thin, flexible tube, called a catheter, is inserted into a small puncture over an artery in your leg and is guided through your arteries to the blocked area. Once there, a special balloon attached to the catheter is inflated and deflated several times. The balloon pushes the plaque in your artery against your artery walls, widening the vessel. In some circumstances, a tiny mesh-metal tube called a stent may then be placed into the narrowed area of your artery to keep it open. The stent remains permanently in your artery. After successful angioplasty, blood flows more freely through your artery. Bypass surgery, usually done through abdominal or leg incisions depending upon the location of the blockage, creates a detour around the narrowed or blocked sections of your artery. A Y-shaped tube made of synthetic fabric, called a graft, is attached to your aorta above the blockage. The two branches of the graft are then attached to either your left and right iliac arteries or other major arteries in each leg called the femoral arteries. Although more invasive, bypass surgery restores blood flow in about 85 percent of patients. Results are commonly maintained for 10 or more years. An endarterectomy is a way for Dr. Robbins to remove the plaque from your artery. To perform an endarterectomy, your Dr. Robbins makes an incision in your leg or abdomen, depending upon the location of the blockage in the artery, and removes the plaque contained in the inner lining of the diseased artery. This leaves a wide-open artery and restores blood flow through your leg artery. The best choice of the treatment depends upon the pattern of blockage as well as how much blockage you have. Robbins will help you determine which method of treatment is best for your particular situation. Page 10
11 Chapter 7 : Peripheral artery disease - Wikipedia Aortoiliac occlusive disease is a common circulatory disorder in which the iliac arteries become narrow or blocked. The iliac arteries branch from the aorta (a large artery that is the body's primary supplier of blood) to carry oxygen-rich blood into your legs. Aortoiliac occlusive disease also known as AIOD is a medical condition characterised by blockage of the aorta which is the most important blood vessel in the body or the iliac arteries. The iliac arteries are the branches of the aorta which supplies blood to the lower portion of the body including the lower limbs and other organs in the pelvic region. The iliac arteries branches around the level of belly button before supplying the above mentioned areas. It has been seen that the iliac arteries and the aorta are the second most common blood vessels to be affected by peripheral arterial disease; the most commonly affected one being the blood vessels of the thigh. It is characterised by a classical triad of: Absence or reduced femoral pulses Claudication in the buttock or thigh region Erectile dysfunction. Symptoms of Aortoiliac Occlusive Disease Symptoms of aortoiliac occlusive disease are varied in nature. Some patients may have multiple symptoms while some may not have any symptoms but still have aortoiliac occlusive disease. The following symptoms are known to be associated with aortoiliac occlusive disease: Pain and Discomfort along with Cramping while Walking: There may be pain and discomfort in the lower portion of the body associated with generalised fatigue and weakness. The symptoms are mild to moderate when felt over the regions of buttocks, thighs or calves. As the disease progresses, the affected individual may experience pain or cramping after walking for short distances. Some male patients may experience erectile dysfunction which in turn affects their sexual health. The severely progressed cases, one pain experience pain in the lower legs including toes while at rest. There may be sensitivity to temperature changes, coldness or numbness in the lower limbs. In extreme cases, it may be associated with soreness or wounds on legs and feet and even gangrene in some cases, which if left untreated, can lead to tissue death in the feet. Possible Causes of Aortoiliac Occlusive Disease The most common causes of aortoiliac occlusive disease are discussed below: Atherosclerosis also known as hardening of the arteries is one of the most common causes of aortoiliac occlusive disease. Atherosclerosis is commonly caused by excessive smoking, high cholesterol, elevated blood pressure, obesity, or genetic inheritance. Excessive exposure to radiation may lead to inflammation in the walls of the arteries leading to blockage in them. Diagnosis of Aortoiliac Occlusive Disease Aortoiliac occlusive disease is treated by a vascular surgeon. A thorough case history is obtained by a vascular surgeon followed by a physical examination. Diagnostic tests include ankle brachial index test and duplex ultrasound study. In some cases, CT angiogram, MR angiogram or catheter directed angiogram are obtained. Different types are used to detect the severity and location of blockage. In cases of catheter angiogram, the dye in injected using a catheter inserted in an artery. Treatment and Management of Aortoiliac Occlusive Disease In most of the cases, the treatment modality includes the following: Lowering Blood Pressure and Sugar Levels: Identification of the associated risk factors and controlling the same such as limiting smoking, regulating cholesterol levels, controlling blood pressure, management of diabetes, following a healthy lifestyle and regular exercising. Blood Thinners to Reduce Blood Clotting: Prescription of anti-platelet medicines such as Aspirin is often helpful in this condition. It prevents clotting of platelets in the blood. This also helps in regulating cholesterol level and prevents development of plaque. Anti-platelet medicines help in reducing risk of myocardial infarction, vascular death and stroke. In advanced cases, surgical intervention may be needed. A surgical bypass which is a minimally invasive procedure is often considered if the condition has advanced. This procedure involves placement of a stent in the aorta or the iliac arteries. In most of the cases, the stenting procedure is done at the same time of doing catheter directed angiogram test. In stenting, the stent usually compresses the plaque against the artery walls, thus creating more space for the blood to flow through them. Over a period of time, the plaque gets crushed or gets dissipated. In cases of angioplasty, an inflatable balloon is introduced in the blocked arteries with the help of a catheter which helps in widening the lumen of the artery. Surgical bypass is a procedure, where a detour is created around the blocked vessel. In these cases, a detour is created from the aorta, near the heart to either an Page 11
12 artery in the groin or iliac arteries in the pelvis. It may be done unilaterally or bilaterally at the same time. An artificial graft is often used in this procedure. In unfavourable conditions, a bypass may start from the axillary artery underneath the collarbone and end in one or both legs. In most of the cases, the outcome of the treatment is long lasting and good; but needs follow up at regular intervals. It is advised to follow up every 3 to 6 months for the first year and every 6 to 12 months after that. In cases, where a prosthetic implant has been grafted, a lifelong risk of developing graft infection exists. Besides these, appropriate oral prophylaxis is recommended prior to any dental treatment, sigmoidoscopy, urologic instrumentation or any other gastro-intestinal surgical procedures. Prevention of Aortoiliac Occlusive Disease Aortoiliac occlusive disease is associated with unhealthy lifestyle and can be prevented by living a healthy life. Leading an active life with being physically active and regular exercises can help in preventing this condition. Regular physical activity can help in management of increased cholesterol level, elevated blood pressure and increased blood glucose level. Refraining from smoking is also beneficial. It is recommended to enrol in smoking cessation program which can help is quitting smoking if you are unable to do it on your own or if there is a relapse. Besides this, following a healthy balanced diet is also essential. It is recommended to follow a low fat diet. Page 12
13 Chapter 8 : Aortoiliac occlusive disease - Wikipedia Treatment of patients with peripheral arterial disease (PAD) has two goals. The first and foremost goal is to reduce the risk of vascular events (myocardial infarction [MI], stroke, vascular death) that occur at an alarmingly high rate in patients with PAD. Aortoiliac Occlusive Disease What is aortoiliac occlusive disease? The aorta and iliac arteries are the blood vessels in the abdomen through which nutrient rich blood that flows to the legs must pass. Aortoiliac occlusive disease occurs when these arteries become narrowed or blocked by atherosclerotic plaque hardening of the arteries which is largely made of cholesterol. Aortoiliac disease is considered a type of peripheral arterial disease PAD because it affects arteries, which are blood vessels that carry blood away from your heart to your limbs. When your iliac arteries narrow or become blocked, your legs may not receive the blood and oxygen they need. This lack of oxygen is called ischemia and it can cause pain. In severe cases, sores or gangrene can develop, which can result in losing a limb. However, these developments are uncommon unless the process is not treated and is allowed to progress. What are the symptoms? Early in the disease, you may feel pain, cramping, or fatigue in your legs when you walk or exercise. The pain with walking usually occurs in your buttocks, thighs, and legs and goes away if you stop walking. As the disease worsens, you may find that pain occurs when you walk for shorter distances. Some men with aortoiliac occlusive disease also experience erectile dysfunction, the inability to have or maintain an erection. What causes aortoiliac occlusive disease? Atherosclerosis, or hardening of the arteries, causes most cases of aortoiliac occlusive disease and is related to smoking, high cholesterol levels in the blood, high blood pressure, obesity, and having a family history of heart disease. What tests will I need? First your physician asks you questions about your general health, medical history, and symptoms and will perform a physical exam. Your physician will want to know if you smoke and when your symptoms occur. If your physician suspects you may have aortoiliac disease, he or she may perform tests to further define its severity, such as measuring the blood pressure in your arms, ankles, and toes. Your physician may also use ultrasound to try to locate the exact area of blockage. If your symptoms are severe enough to warrant treatment your vascular surgeon will perform angiography to obtain more precise information about the location and severity of your blockages to better guide your treatment. Angiography There are three types of angiography that may be performed: Contrast arteriography usually provides better resolution but is a more invasive test. Your physician injects a contrast dye into your arteries and then takes x-ray images. This test finds the exact location and pattern of blockages. The dye is excreted from your body through your kidneys. If a blockage is identified and is appropriate for treatment by angioplasty and stenting, this procedure may be carried out at the same time. CTA and MRA are alternative less invasive methods to look for blockages, but do not provide the same quality of imaging or the opportunity to treat with angioplasty and stenting. How is aortoiliac occlusive disease treated? Lifestyle Changes In mild to moderate cases, your physician may recommend that you change certain aspects of your lifestyle like quitting smoking, maintain a healthy weight, following a structured walking program at least 3 or 4 times a week, and eating a low-fat and high-fiber diet. If necessary, your physician may prescribe medications to lower high cholesterol. If you have diabetes, you need to control your blood sugar levels with diet and medication. Medications If you do not have a disqualifying medical condition, such as heart failure, your physician may also prescribe cilostazol Pletal, which may improve the distance you are able to walk without pain, or aspirin or clopidogrel Plavix, either of which can lower your chances of blood clots. Statins are a class of medications that your physician may use to control your cholesterol levels. None of these medications will "cure" you of the disease, but are important at relieving some of your symptoms, and may help protect your arteries from developing further disease. Angioplasty or Surgery If you have severe aortoiliac occlusive disease, particularly if it does not improve with the measures described above, your physician may recommend a minimally invasive treatment called angioplasty to improve the circulation in your legs. For more extensive blockages or those that cannot be treated with angioplasty, surgery to bypass or clear your blocked arteries may be required. During an angioplasty procedure, which is sometimes performed at the same time as an angiogram, a balloon is inflated Page 13
Lower Extremity Arterial Disease
 Lower Extremity Arterial Disease Circulating the Facts About Peripheral Disease Brought to you by the Education Committee of the Society for 1 www.svnnet.org Peripheral Artery Disease (PAD) Many people
Lower Extremity Arterial Disease Circulating the Facts About Peripheral Disease Brought to you by the Education Committee of the Society for 1 www.svnnet.org Peripheral Artery Disease (PAD) Many people
Introduction What Causes Peripheral Vascular Disease? How Do Doctors Treat Peripheral Vascular Disease?... 9
 Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
Patient Information Table of Contents Introduction... 3 What is Peripheral Vascular Disease?... 5 What Are Some of the Symptoms of Peripheral Vascular Disease?... 7 What Causes Peripheral Vascular Disease?...
EDUCATION. Peripheral Artery Disease
 EDUCATION Peripheral Artery Disease Peripheral Artery Disease You may have circulation problems that have to do with your blood vessels. You may feel aches, pains, cramps, numbness or muscle fatigue when
EDUCATION Peripheral Artery Disease Peripheral Artery Disease You may have circulation problems that have to do with your blood vessels. You may feel aches, pains, cramps, numbness or muscle fatigue when
Patient Brochure. Clearstream Technologies, Ltd. Moyne Upper Enniscorthy Co. Wexford, Ireland. PK Rev. 0 05/17
 Patient Brochure Clearstream Technologies, Ltd. Moyne Upper Enniscorthy Co. Wexford, Ireland PK1411100 Rev. 0 05/17 LIFESTREAM Patient Brochure If you or a member of your family has been diagnosed with
Patient Brochure Clearstream Technologies, Ltd. Moyne Upper Enniscorthy Co. Wexford, Ireland PK1411100 Rev. 0 05/17 LIFESTREAM Patient Brochure If you or a member of your family has been diagnosed with
Introduction 3. What is Peripheral Vascular Disease? 5. What Are Some of the Symptoms of Peripheral Vascular Disease? 6
 Patient Information Table of Contents Introduction 3 What is Peripheral Vascular Disease? 5 What Are Some of the Symptoms of Peripheral Vascular Disease? 6 What Causes Peripheral Vascular Disease? 7 How
Patient Information Table of Contents Introduction 3 What is Peripheral Vascular Disease? 5 What Are Some of the Symptoms of Peripheral Vascular Disease? 6 What Causes Peripheral Vascular Disease? 7 How
DON T LET LEG PAIN BECOME A REAL THREAT.
 DON T LET LEG PAIN BECOME A REAL THREAT. These three words have the power to change lives. Between 8 to 10 million Americans are estimated to suffer from poor blood flow to the legs and feet potentially
DON T LET LEG PAIN BECOME A REAL THREAT. These three words have the power to change lives. Between 8 to 10 million Americans are estimated to suffer from poor blood flow to the legs and feet potentially
Leg artery disease. Information for patients Sheffield Vascular Institute
 Leg artery disease Information for patients Sheffield Vascular Institute page 2 of 12 You have been diagnosed as having leg artery disease. This leaflet explains more about leg artery disease and answers
Leg artery disease Information for patients Sheffield Vascular Institute page 2 of 12 You have been diagnosed as having leg artery disease. This leaflet explains more about leg artery disease and answers
ANGIOPLASTY AND STENTING
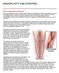 ANGIOPLASTY AND STENTING What is angioplasty and stenting? During an angioplasty, your vascular surgeon inflates a small balloon inside a narrowed blood vessel. This balloon helps to widen your blood vessel
ANGIOPLASTY AND STENTING What is angioplasty and stenting? During an angioplasty, your vascular surgeon inflates a small balloon inside a narrowed blood vessel. This balloon helps to widen your blood vessel
Abdominal Exam: The examination of the abdomen used by physicians to detect an abdominal aortic aneurysm.
 Glossary of Terms Abdominal Exam: The examination of the abdomen used by physicians to detect an abdominal aortic aneurysm. Angiogram: A diagnostic test requiring the insertion of a catheter into an artery
Glossary of Terms Abdominal Exam: The examination of the abdomen used by physicians to detect an abdominal aortic aneurysm. Angiogram: A diagnostic test requiring the insertion of a catheter into an artery
Atherosclerosis. Atherosclerosis happens when the blood vessels
 Atherosclerosis Atherosclerosis happens when the blood vessels that carry oxygen and nutrients from your heart to the rest of your body (arteries) become thick and stiff sometimes restricting blood flow
Atherosclerosis Atherosclerosis happens when the blood vessels that carry oxygen and nutrients from your heart to the rest of your body (arteries) become thick and stiff sometimes restricting blood flow
Learning About. Peripheral Artery Disease
 SM A C P S P E C I A L R E P O R T Learning About Peripheral Artery Disease What Is Peripheral Artery Disease? Peripheral artery disease (PAD) is a form of atherosclerosis the hardening and narrowing of
SM A C P S P E C I A L R E P O R T Learning About Peripheral Artery Disease What Is Peripheral Artery Disease? Peripheral artery disease (PAD) is a form of atherosclerosis the hardening and narrowing of
Aortic and Iliac Artery Occlusive Disease (Updated 10.08)
 S PATIENT INFORMATION oregon surgical specialists Aortic and Iliac Artery Occlusive Disease (Updated 10.08) Abdominal aortic and iliac artery occlusive disease occurs when the arteries in your abdomen
S PATIENT INFORMATION oregon surgical specialists Aortic and Iliac Artery Occlusive Disease (Updated 10.08) Abdominal aortic and iliac artery occlusive disease occurs when the arteries in your abdomen
Introduction. Risk factors of PVD 5/8/2017
 PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
PATHOPHYSIOLOGY AND CLINICAL FEATURES OF PERIPHERAL VASCULAR DISEASE Dr. Muhamad Zabidi Ahmad Radiologist and Section Chief, Radiology, Oncology and Nuclear Medicine Section, Advanced Medical and Dental
Patient Information. Peripheral Arterial Disease and the Lutonix 035 Balloon. Advancing Lives and the Delivery of Health Care
 Patient Information Peripheral Arterial Disease and the Lutonix 035 Balloon Advancing Lives and the Delivery of Health Care Contents Peripheral Arterial Disease (PAD) Peripheral Arterial Disease (PAD)
Patient Information Peripheral Arterial Disease and the Lutonix 035 Balloon Advancing Lives and the Delivery of Health Care Contents Peripheral Arterial Disease (PAD) Peripheral Arterial Disease (PAD)
Imaging for Peripheral Vascular Disease
 Imaging for Peripheral Vascular Disease James G. Jollis, MD Director, Rex Hospital Cardiovascular Imaging Imaging for Peripheral Vascular Disease 54 year old male with exertional calf pain in his right
Imaging for Peripheral Vascular Disease James G. Jollis, MD Director, Rex Hospital Cardiovascular Imaging Imaging for Peripheral Vascular Disease 54 year old male with exertional calf pain in his right
A Healthy Heart. IN BRIEF: Your Guide to
 IN BRIEF: Your Guide to A Healthy Heart If you re like most people, you may think of heart disease as a problem for other folks. If you re a woman, you may believe that being female protects you from heart
IN BRIEF: Your Guide to A Healthy Heart If you re like most people, you may think of heart disease as a problem for other folks. If you re a woman, you may believe that being female protects you from heart
Understanding Peripheral
 Patient Information Guide Understanding Peripheral Artery Disease Innova Vascular Self-Expanding Stent System Table of Contents Glossary... 2 What is Peripheral Artery Disease?... 4 Treating Peripheral
Patient Information Guide Understanding Peripheral Artery Disease Innova Vascular Self-Expanding Stent System Table of Contents Glossary... 2 What is Peripheral Artery Disease?... 4 Treating Peripheral
Peripheral Vascular Disease Patient Awareness
 Peripheral Vascular Disease Patient Awareness Interventional Radiology: your minimally invasive alternative www.cirse.org Cardiovascular and Interventional Radiological Society of Europe Cardiovascular
Peripheral Vascular Disease Patient Awareness Interventional Radiology: your minimally invasive alternative www.cirse.org Cardiovascular and Interventional Radiological Society of Europe Cardiovascular
Objectives. Abdominal Aortic Aneuryms 11/16/2017. The Vascular Patient: Diagnosis and Conservative Treatment
 The Vascular Patient: Diagnosis and Conservative Treatment Ferrell-Duncan Clinic Zachary C. Schmittling, M.D., F.A.C.S. Vascular and General Surgery Ferrell-Duncan Clinic Cox Health Systems Objectives
The Vascular Patient: Diagnosis and Conservative Treatment Ferrell-Duncan Clinic Zachary C. Schmittling, M.D., F.A.C.S. Vascular and General Surgery Ferrell-Duncan Clinic Cox Health Systems Objectives
Practical Point in Diabetic Foot Care 3-4 July 2017
 Diabetic Foot Ulcer : Role of Vascular Surgeon Practical Point in Diabetic Foot Care 3-4 July 2017 Supapong Arworn, MD Division of Vascular and Endovascular Surgery Department of Surgery, Chiang Mai University
Diabetic Foot Ulcer : Role of Vascular Surgeon Practical Point in Diabetic Foot Care 3-4 July 2017 Supapong Arworn, MD Division of Vascular and Endovascular Surgery Department of Surgery, Chiang Mai University
Role of ABI in Detecting and Quantifying Peripheral Arterial Disease
 Role of ABI in Detecting and Quantifying Peripheral Arterial Disease Difference in AAA size between US and Surgeon 2 1 0-1 -2-3 0 1 2 3 4 5 6 7 Mean AAA size between US and Surgeon Kathleen G. Raman MD,
Role of ABI in Detecting and Quantifying Peripheral Arterial Disease Difference in AAA size between US and Surgeon 2 1 0-1 -2-3 0 1 2 3 4 5 6 7 Mean AAA size between US and Surgeon Kathleen G. Raman MD,
Carotid Stenosis (carotid artery disease)
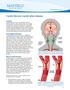 1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
1 Carotid Stenosis (carotid artery disease) Overview Carotid stenosis is a narrowing of the carotid arteries, the two major arteries that carry oxygenrich blood from the heart to the brain. Also called
Peripheral Vascular Disease
 Peripheral artery disease (PAD) results from the buildup of plaque (atherosclerosis) in the arteries of the legs. For people with PAD, symptoms may be mild, requiring no treatment except modification of
Peripheral artery disease (PAD) results from the buildup of plaque (atherosclerosis) in the arteries of the legs. For people with PAD, symptoms may be mild, requiring no treatment except modification of
Intercepting PAD. Playbook for Cardiovascular Care 2018 February 24, Jonathan D Woody, MD, FACS. University Surgical Vascular
 Intercepting PAD Playbook for Cardiovascular Care 2018 February 24, 2018 Jonathan D Woody, MD, FACS University Surgical Vascular Attending Vascular Surgeon - Piedmont Athens Regional Adjunct Clinical Associate
Intercepting PAD Playbook for Cardiovascular Care 2018 February 24, 2018 Jonathan D Woody, MD, FACS University Surgical Vascular Attending Vascular Surgeon - Piedmont Athens Regional Adjunct Clinical Associate
Percutaneous Transluminal Angioplasty (PTA) and Stenting For PVS Patients
 Percutaneous Transluminal Angioplasty (PTA) and Stenting For PVS Patients There are two types of blood vessels in the body arteries and veins. Arteries carry blood rich in oxygen from the heart to all
Percutaneous Transluminal Angioplasty (PTA) and Stenting For PVS Patients There are two types of blood vessels in the body arteries and veins. Arteries carry blood rich in oxygen from the heart to all
PROCEDURES FOR PERIPHERAL ARTERIAL DISEASE
 PROCEDURES FOR PERIPHERAL ARTERIAL DISEASE Improving Blood Flow and Relieving Pain Learning About PAD Your doctor has told you that you have peripheral arterial disease (PAD). This means the arteries in
PROCEDURES FOR PERIPHERAL ARTERIAL DISEASE Improving Blood Flow and Relieving Pain Learning About PAD Your doctor has told you that you have peripheral arterial disease (PAD). This means the arteries in
Intermittent Claudication
 Intermittent Claudication Exceptional healthcare, personally delivered Ask 3 Questions Preparation for your Appointments We want you to be active in your healthcare. By telling us what is important to
Intermittent Claudication Exceptional healthcare, personally delivered Ask 3 Questions Preparation for your Appointments We want you to be active in your healthcare. By telling us what is important to
Index. cardiology.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ABI. See Ankle-brachial index (ABI). Afterload, deconstructing of, in ventricular vascular interaction in heart failure, 449 Air plethysmography
Index Note: Page numbers of article titles are in boldface type. A ABI. See Ankle-brachial index (ABI). Afterload, deconstructing of, in ventricular vascular interaction in heart failure, 449 Air plethysmography
Heart Disease (Coronary Artery Disease)
 Heart Disease (Coronary Artery Disease) Understanding how the heart works To understand heart disease, you must first know how the heart works. The heart is like any other muscle, requiring blood to supply
Heart Disease (Coronary Artery Disease) Understanding how the heart works To understand heart disease, you must first know how the heart works. The heart is like any other muscle, requiring blood to supply
BC Vascular Day. Contents. November 3, Abdominal Aortic Aneurysm 2 3. Peripheral Arterial Disease 4 6. Deep Venous Thrombosis 7 8
 BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
Coronary angioplasty and stents
 Tests and Procedures Coronary angioplasty and stents By Mayo Clinic Staff Coronary angioplasty (AN-jee-o-plas-tee), also called percutaneous coronary intervention, is a procedure used to open clogged heart
Tests and Procedures Coronary angioplasty and stents By Mayo Clinic Staff Coronary angioplasty (AN-jee-o-plas-tee), also called percutaneous coronary intervention, is a procedure used to open clogged heart
Peripheral Arterial Disease: A Practical Approach
 Peripheral Arterial Disease: A Practical Approach Sanjoy Kundu BSc, MD, FRCPC, DABR, FASA, FCIRSE, FSIR The Scarborough Hospital Toronto Endovascular Centre The Vein Institute of Toronto Scarborough Vascular
Peripheral Arterial Disease: A Practical Approach Sanjoy Kundu BSc, MD, FRCPC, DABR, FASA, FCIRSE, FSIR The Scarborough Hospital Toronto Endovascular Centre The Vein Institute of Toronto Scarborough Vascular
Garland Green, MD Interventional Cardiologist. Impact of PAD: Prevalence, Risk Factors, Testing, and Medical Management
 Garland Green, MD Interventional Cardiologist Impact of PAD: Prevalence, Risk Factors, Testing, and Medical Management Peripheral Arterial Disease Affects over 8 million Americans Affects 12% of the general
Garland Green, MD Interventional Cardiologist Impact of PAD: Prevalence, Risk Factors, Testing, and Medical Management Peripheral Arterial Disease Affects over 8 million Americans Affects 12% of the general
Introduction to Peripheral Arterial Disease. Stacey Clegg, MD Interventional Cardiology August
 Introduction to Peripheral Arterial Disease Stacey Clegg, MD Interventional Cardiology August 20 2014 Outline (and for the ABIM board exam * ** ***) Prevalence* Definitions Lower Extremity: Aorta*** Claudication***
Introduction to Peripheral Arterial Disease Stacey Clegg, MD Interventional Cardiology August 20 2014 Outline (and for the ABIM board exam * ** ***) Prevalence* Definitions Lower Extremity: Aorta*** Claudication***
Peripheral Arterial Disease
 UFS Peripheral Arterial Disease A problem of supply and demand Larry Rhoads, Associate Chief Underwriter November 8, 2011 PAD Two categories of these circulation disorders: Functional peripheral vascular
UFS Peripheral Arterial Disease A problem of supply and demand Larry Rhoads, Associate Chief Underwriter November 8, 2011 PAD Two categories of these circulation disorders: Functional peripheral vascular
Treatment Strategies For Patients with Peripheral Artery Disease
 Treatment Strategies For Patients with Peripheral Artery Disease Presented by Schuyler Jones, MD Duke University Medical Center & Duke Clinical Research Institute AHRQ Comparative Effectiveness Review
Treatment Strategies For Patients with Peripheral Artery Disease Presented by Schuyler Jones, MD Duke University Medical Center & Duke Clinical Research Institute AHRQ Comparative Effectiveness Review
Peripheral Arterial Disease. Westley Smith MD Vascular Fellow
 Peripheral Arterial Disease Westley Smith MD Vascular Fellow Background (per 10,000) Goodney P, et al. Regional intensity of vascular care and lower extremity amputation rates. JVS. 2013; 6: 1471-1480.
Peripheral Arterial Disease Westley Smith MD Vascular Fellow Background (per 10,000) Goodney P, et al. Regional intensity of vascular care and lower extremity amputation rates. JVS. 2013; 6: 1471-1480.
Carotid Artery Stenting
 Disclaimer This movie is an educational resource only and should not be used to manage cardiovascular health. All decisions about the management of Carotid Artery Disease must be made in conjunction with
Disclaimer This movie is an educational resource only and should not be used to manage cardiovascular health. All decisions about the management of Carotid Artery Disease must be made in conjunction with
Global Peripheral Artery Disease Market: Trends & Opportunities ( ) February 2016
 Global Peripheral Artery Disease Market: Trends & Opportunities (2015-2020) February 2016 Global Peripheral Artery Disease Market Report Scope of the Report This report entitled Global Peripheral Artery
Global Peripheral Artery Disease Market: Trends & Opportunities (2015-2020) February 2016 Global Peripheral Artery Disease Market Report Scope of the Report This report entitled Global Peripheral Artery
Cordis S.M.A.R.T. and S.M.A.R.T. CONTROL Nitinol System For the Iliac Arteries
 Endovascular Cordis S.M.A.R.T. and S.M.A.R.T. CONTROL Nitinol System For the Iliac Arteries A Patient s Guide to Peripheral Vascular Disease in the Iliac Arteries this guidebook... This guidebook is proudly
Endovascular Cordis S.M.A.R.T. and S.M.A.R.T. CONTROL Nitinol System For the Iliac Arteries A Patient s Guide to Peripheral Vascular Disease in the Iliac Arteries this guidebook... This guidebook is proudly
Vascular Disease. Conditions & Treatments
 Vascular Disease Conditions & Treatments Vascular Disease Expertise That s Second-to-None Vascular disease refers to a variety of conditions affecting the blood vessels (i.e., the arteries and veins) that
Vascular Disease Conditions & Treatments Vascular Disease Expertise That s Second-to-None Vascular disease refers to a variety of conditions affecting the blood vessels (i.e., the arteries and veins) that
CORONARY ARTERY BYPASS GRAFT
 CORONARY ARTERY BYPASS GRAFT Coronary artery disease develops because of hardening of the arteries (arteriosclerosis) that supply blood to the heart muscle. In the diagnosis of coronary artery disease,
CORONARY ARTERY BYPASS GRAFT Coronary artery disease develops because of hardening of the arteries (arteriosclerosis) that supply blood to the heart muscle. In the diagnosis of coronary artery disease,
Imaging Strategy For Claudication
 Who are the Debators? Imaging Strategy For Claudication Duplex Ultrasound Alone is Adequate to Select Patients for Endovascular Intervention - Pro: Dennis Bandyk MD No Disclosures PRO - Vascular Surgeon
Who are the Debators? Imaging Strategy For Claudication Duplex Ultrasound Alone is Adequate to Select Patients for Endovascular Intervention - Pro: Dennis Bandyk MD No Disclosures PRO - Vascular Surgeon
Steven Hadesman, MD Chief Medical Officer, MeridianRx Internal Medicine Physician, St. John Hospital
 Steven Hadesman, MD Chief Medical Officer, MeridianRx Internal Medicine Physician, St. John Hospital Deep Venous Thrombosis Varicose Veins Venous insufficiency Phlebitis Lymphedema Elephantiasis nostras
Steven Hadesman, MD Chief Medical Officer, MeridianRx Internal Medicine Physician, St. John Hospital Deep Venous Thrombosis Varicose Veins Venous insufficiency Phlebitis Lymphedema Elephantiasis nostras
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
urhealth May 2018 Nu Mu Lambda...
 May 2018 1 Health & Wellness Committee Bro. Trenton Taylor Committee Chair Bro. William J. Bennett, M.D., Ph.D. Medical Editor Contents Carotid Artery A Disease 3-24 Bro. Antonio Pruitt, PT, DPT, MPA Editor,
May 2018 1 Health & Wellness Committee Bro. Trenton Taylor Committee Chair Bro. William J. Bennett, M.D., Ph.D. Medical Editor Contents Carotid Artery A Disease 3-24 Bro. Antonio Pruitt, PT, DPT, MPA Editor,
Peripheral Arterial Disease Extremity
 Peripheral Arterial Disease Lower Extremity 05 Contributor Dr Steven Chong Advisors Dr Ashish Anil Dr Tay Jam Chin Introduction Risk Factors Clinical Presentation Classification History PHYSICAL examination
Peripheral Arterial Disease Lower Extremity 05 Contributor Dr Steven Chong Advisors Dr Ashish Anil Dr Tay Jam Chin Introduction Risk Factors Clinical Presentation Classification History PHYSICAL examination
Diagnosis and Endovascular Treatment of Critical Limb Ischemia: What You Need to Know S. Jay Mathews, MD, MS, FACC
 Diagnosis and Endovascular Treatment of Critical Limb Ischemia: What You Need to Know S. Jay Mathews, MD, MS, FACC Interventional Cardiologist/Endovascular Specialist Bradenton Cardiology Center Bradenton,
Diagnosis and Endovascular Treatment of Critical Limb Ischemia: What You Need to Know S. Jay Mathews, MD, MS, FACC Interventional Cardiologist/Endovascular Specialist Bradenton Cardiology Center Bradenton,
Recommendations for Follow-up After Vascular Surgery Arterial Procedures SVS Practice Guidelines
 Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Arterial Bypass Grafts to the Legs and Femoral Endarterectomy
 Patient Information Arterial Bypass Grafts to the Legs and Femoral Endarterectomy We expect you to make a rapid recovery after your operation and to experience no serious problems. However, it is important
Patient Information Arterial Bypass Grafts to the Legs and Femoral Endarterectomy We expect you to make a rapid recovery after your operation and to experience no serious problems. However, it is important
PAD and CRITICAL LIMB ISCHEMIA: EVALUATION AND TREATMENT 2014
 PAD and CRITICAL LIMB ISCHEMIA: EVALUATION AND TREATMENT 2014 Van Crisco, MD, FACC, FSCAI First Coast Heart and Vascular Center, PLLC Jacksonville, FL 678-313-6695 Conflict of Interest Bayer Healthcare
PAD and CRITICAL LIMB ISCHEMIA: EVALUATION AND TREATMENT 2014 Van Crisco, MD, FACC, FSCAI First Coast Heart and Vascular Center, PLLC Jacksonville, FL 678-313-6695 Conflict of Interest Bayer Healthcare
Step by step Hybrid procedures in peripheral obstructive disease. Holger Staab, MD University Hospital Leipzig, Germany Clinic for Vascular Surgery
 Step by step Hybrid procedures in peripheral obstructive disease Holger Staab, MD University Hospital Leipzig, Germany Clinic for Vascular Surgery Disclosure Speaker name: H.H. Staab I have the following
Step by step Hybrid procedures in peripheral obstructive disease Holger Staab, MD University Hospital Leipzig, Germany Clinic for Vascular Surgery Disclosure Speaker name: H.H. Staab I have the following
Abdominal Aortic Aneurysms. A Surgeons Perspective Dr. Derek D. Muehrcke
 Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Abdominal Aortic Aneurysms A Surgeons Perspective Dr. Derek D. Muehrcke Aneurysm Definition The abnormal enlargement or bulging of an artery caused by an injury or weakness in the blood vessel wall A localized
Guide to Cardiology Care at Scripps
 Guide to Cardiology Care at Scripps Cardiology is the word in health care associated with heart, but the body s vascular system is also an important part of heart care. Your body has more than 60,000 miles
Guide to Cardiology Care at Scripps Cardiology is the word in health care associated with heart, but the body s vascular system is also an important part of heart care. Your body has more than 60,000 miles
Intervention for Lower Extremity PAD: When, why and what?! Robert F Cuff, MD FACS RVT RPVI
 Intervention for Lower Extremity PAD: When, why and what?! Robert F Cuff, MD FACS RVT RPVI 1 Disclosures I have no financial disclosures related to this talk Objectives 1. Discuss indications for intervention
Intervention for Lower Extremity PAD: When, why and what?! Robert F Cuff, MD FACS RVT RPVI 1 Disclosures I have no financial disclosures related to this talk Objectives 1. Discuss indications for intervention
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE)
 Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of November 19, 2018 Abdominal Aortogram, Bilateral Runoff
Lower limb angioplasty and stenting. Information for patients Sheffield Vascular Institute
 Lower limb angioplasty and stenting Information for patients Sheffield Vascular Institute Why have I been given this leaflet? You have been given this leaflet because you need a procedure known as an angioplasty
Lower limb angioplasty and stenting Information for patients Sheffield Vascular Institute Why have I been given this leaflet? You have been given this leaflet because you need a procedure known as an angioplasty
Copyright HMP Communications
 Ocelot With Wildcat in a Complicated Superficial Femoral Artery Chronic Total Occlusion Soundos K. Moualla, MD, FACC, FSCAI; Richard R. Heuser, MD, FACC, FACP, FESC, FSCAI From Phoenix Heart Center, Phoenix,
Ocelot With Wildcat in a Complicated Superficial Femoral Artery Chronic Total Occlusion Soundos K. Moualla, MD, FACC, FSCAI; Richard R. Heuser, MD, FACC, FACP, FESC, FSCAI From Phoenix Heart Center, Phoenix,
Angiogram and angioplasty
 Angiogram and angioplasty The femoral arteries run from the groin to the thigh, delivering blood to your legs. When there is a narrowing or blockage in these arteries, the blood supply to the legs is reduced,
Angiogram and angioplasty The femoral arteries run from the groin to the thigh, delivering blood to your legs. When there is a narrowing or blockage in these arteries, the blood supply to the legs is reduced,
UNDERSTANDING ATHEROSCLEROSIS
 UNDERSTANDING ATHEROSCLEROSIS UNDERSTANDING ATHEROSCLEROSIS ARTERIES Arteries are blood vessels that carry oxygenated blood to all the organs of the body. Arteries are made up of three important layers:
UNDERSTANDING ATHEROSCLEROSIS UNDERSTANDING ATHEROSCLEROSIS ARTERIES Arteries are blood vessels that carry oxygenated blood to all the organs of the body. Arteries are made up of three important layers:
Angioplasty and Vascular Stenting
 Scan for mobile link. Angioplasty and Vascular Stenting Angioplasty uses imaging guidance to insert a balloon-tipped catheter into a narrow or blocked blood vessel where the balloon is inflated to open
Scan for mobile link. Angioplasty and Vascular Stenting Angioplasty uses imaging guidance to insert a balloon-tipped catheter into a narrow or blocked blood vessel where the balloon is inflated to open
Carotid Angioplasty and Stenting
 Carotid Angioplasty and Stenting Your Carotid Artery Problem The carotid arteries are blood vessels in the neck that carry blood to the brain. One or both of your carotids is narrowed due to a buildup
Carotid Angioplasty and Stenting Your Carotid Artery Problem The carotid arteries are blood vessels in the neck that carry blood to the brain. One or both of your carotids is narrowed due to a buildup
INL No. A0083 Project Medtronic Thoracic patients guide Description Version 18
 INL No. A0083 Project Medtronic Thoracic patients guide Description Version 18 www.inl-agency.com PATIENT INFORMATION BOOKLET Endovascular Stent Grafts: A treatment for Thoracic Aortic disease Table of
INL No. A0083 Project Medtronic Thoracic patients guide Description Version 18 www.inl-agency.com PATIENT INFORMATION BOOKLET Endovascular Stent Grafts: A treatment for Thoracic Aortic disease Table of
Disclosures. Critical Limb Ischemia. Vascular Testing in the CLI Patient. Vascular Testing in Critical Limb Ischemia UCSF Vascular Symposium
 Disclosures Vascular Testing in the CLI Patient None 2015 UCSF Vascular Symposium Warren Gasper, MD Assistant Professor of Surgery UCSF Division of Vascular Surgery Critical Limb Ischemia Chronic Limb
Disclosures Vascular Testing in the CLI Patient None 2015 UCSF Vascular Symposium Warren Gasper, MD Assistant Professor of Surgery UCSF Division of Vascular Surgery Critical Limb Ischemia Chronic Limb
Abdominal Vascular Arterial Disease
 Abdominal Vascular Arterial Disease Abdominal Vascular Arterial Disease People take better care of their health when they know what s going on in their bodies. For those with abdominal vascular arterial
Abdominal Vascular Arterial Disease Abdominal Vascular Arterial Disease People take better care of their health when they know what s going on in their bodies. For those with abdominal vascular arterial
INL No. A0075 Project Medtronic Patient Information Leaflet Description 16 page booklet
 INL No. A0075 Project Medtronic Patient Information Leaflet Description 16 page booklet www.inl-agency.com PATIENT INFORMATION BOOKLET Endovascular stent grafts: A treatment for Abdominal Aortic Aneurysms
INL No. A0075 Project Medtronic Patient Information Leaflet Description 16 page booklet www.inl-agency.com PATIENT INFORMATION BOOKLET Endovascular stent grafts: A treatment for Abdominal Aortic Aneurysms
Peripheral Arterial Disease: Who has it and what to do about it?
 Peripheral Arterial Disease: Who has it and what to do about it? Seth Krauss, M.D. Alaska Annual Nurse Practitioner Conference September 16, 2011 Scope of the Problem Incidence: 20%
Peripheral Arterial Disease: Who has it and what to do about it? Seth Krauss, M.D. Alaska Annual Nurse Practitioner Conference September 16, 2011 Scope of the Problem Incidence: 20%
Stratifying Management Options for Patients with Critical Limb Ischemia: When Should Open Surgery Be the Initial Option for CLI?
 Stratifying Management Options for Patients with Critical Limb Ischemia: When Should Open Surgery Be the Initial Option for CLI? Peter F. Lawrence, M.D. Gonda Vascular Center Division of Vascular Surgery
Stratifying Management Options for Patients with Critical Limb Ischemia: When Should Open Surgery Be the Initial Option for CLI? Peter F. Lawrence, M.D. Gonda Vascular Center Division of Vascular Surgery
Peripheral Arterial. Disease
 Peripheral Arterial Disease Peripheral Arterial Disease People take better care of their health when they know what s going on in their bodies. For those with peripheral arterial occlusive disease, this
Peripheral Arterial Disease Peripheral Arterial Disease People take better care of their health when they know what s going on in their bodies. For those with peripheral arterial occlusive disease, this
The Struggle to Manage Stroke, Aneurysm and PAD
 The Struggle to Manage Stroke, Aneurysm and PAD In this article, Dr. Salvian examines the management of peripheral arterial disease, aortic aneurysmal disease and cerebrovascular disease from symptomatology
The Struggle to Manage Stroke, Aneurysm and PAD In this article, Dr. Salvian examines the management of peripheral arterial disease, aortic aneurysmal disease and cerebrovascular disease from symptomatology
Rapid Recovery Hyperbarics 9439 Archibald Ave. Suite 104 Rancho Cucamonga CA,
 Foot at risk Age Well By Dr LIEW NGOH CHIN Are limb amputations due to diabetes preventable? DIABETES mellitus is a major global health problem and has reached epidemic proportions in many developed and
Foot at risk Age Well By Dr LIEW NGOH CHIN Are limb amputations due to diabetes preventable? DIABETES mellitus is a major global health problem and has reached epidemic proportions in many developed and
Heart Disease. Signs and Symptoms
 Heart Disease The term "heart disease" refers to several types of heart conditions. The most common type is coronary artery disease, which can cause heart attack, angina, heart failure, and arrhythmias.
Heart Disease The term "heart disease" refers to several types of heart conditions. The most common type is coronary artery disease, which can cause heart attack, angina, heart failure, and arrhythmias.
Femoro-femoral bypass surgery. Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England.
 Femoro-femoral bypass surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Femoro-femoral bypass surgery Brought to you in association with EIDO Healthcare and endorsed by the Royal College of Surgeons England. Discovery has made every effort to ensure that we obtained the information
Non-invasive examination
 Non-invasive examination Segmental pressure and Ankle-Brachial Index (ABI) The segmental blood pressure (SBP) examination is a simple, noninvasive method for diagnosing and localizing arterial disease.
Non-invasive examination Segmental pressure and Ankle-Brachial Index (ABI) The segmental blood pressure (SBP) examination is a simple, noninvasive method for diagnosing and localizing arterial disease.
Peripheral Arterial Disease (PAD): Presentation, Diagnosis, and Treatment
 Peripheral Arterial Disease (PAD): Presentation, Diagnosis, and Treatment Prepared and Presented by Jon Manocchio, Pharm D Blanchard Valley Hospital October 2011 Introduction PAD is a condition that is
Peripheral Arterial Disease (PAD): Presentation, Diagnosis, and Treatment Prepared and Presented by Jon Manocchio, Pharm D Blanchard Valley Hospital October 2011 Introduction PAD is a condition that is
V.A. is a 62-year-old male who presents in referral
 , LLC an HMP Communications Holdings Company Clinical Case Update Latest Trends in Critical Limb Ischemia Imaging Amit Srivastava, MD, FACC, FABVM Interventional Cardiologist Bay Area Heart Center St.
, LLC an HMP Communications Holdings Company Clinical Case Update Latest Trends in Critical Limb Ischemia Imaging Amit Srivastava, MD, FACC, FABVM Interventional Cardiologist Bay Area Heart Center St.
all about your heart...
 For a healthy heart If you smoke, stop smoking. Eat lots of fruit and vegetables and less fat. Be more active every day. Be a healthy weight. Relax take time out for yourself. Local contact: For more information
For a healthy heart If you smoke, stop smoking. Eat lots of fruit and vegetables and less fat. Be more active every day. Be a healthy weight. Relax take time out for yourself. Local contact: For more information
Peripheral Vascular/Arterial Disease (PVD/PAD) Patient Guide. Guide contents: 2 What Is PVD/PAD? 3 The Risks 3 Diagnosing the Condition
 Guide contents: 2 What Is PVD/PAD? 3 The Risks 3 Diagnosing the Condition 4 Medication & Treatment 5 Key Questions to Ask Your Cardiologist 6 Symptom Tracker 7 Appointment Calendar 8 Health Journal 9 Your
Guide contents: 2 What Is PVD/PAD? 3 The Risks 3 Diagnosing the Condition 4 Medication & Treatment 5 Key Questions to Ask Your Cardiologist 6 Symptom Tracker 7 Appointment Calendar 8 Health Journal 9 Your
2017 Cardiology Survival Guide
 2017 Cardiology Survival Guide Chapter 2: Angioplasty/Atherectomy/Stent The term angioplasty literally means "blood vessel repair." During an angioplasty procedure, the physician inserts a catheter, with
2017 Cardiology Survival Guide Chapter 2: Angioplasty/Atherectomy/Stent The term angioplasty literally means "blood vessel repair." During an angioplasty procedure, the physician inserts a catheter, with
Your heart is a muscular pump about the size of your fist, located
 How Your Heart Works Your heart is a muscular pump about the size of your fist, located slightly to the left and behind your breastbone. Its function is to pump blood throughout your body. As your heart
How Your Heart Works Your heart is a muscular pump about the size of your fist, located slightly to the left and behind your breastbone. Its function is to pump blood throughout your body. As your heart
Boca Raton Regional Hospital Grand Rounds September 13, 2016
 Boca Raton Regional Hospital Grand Rounds September 13, 2016 W. Anthony Lee, MD, FACS Chief, BocaCare Vascular Surgery Christine E. Lynn Heart and Vascular Institute Boca Raton, Florida Disclosures No
Boca Raton Regional Hospital Grand Rounds September 13, 2016 W. Anthony Lee, MD, FACS Chief, BocaCare Vascular Surgery Christine E. Lynn Heart and Vascular Institute Boca Raton, Florida Disclosures No
Understanding Peripheral
 Patient Information Guide Understanding Peripheral Artery Disease ELUVIA Drug-Eluting Vascular Stent System Table of Contents Glossary...2 What is Peripheral Artery Disease?...4 Treating Peripheral Artery
Patient Information Guide Understanding Peripheral Artery Disease ELUVIA Drug-Eluting Vascular Stent System Table of Contents Glossary...2 What is Peripheral Artery Disease?...4 Treating Peripheral Artery
Coronary Artery Disease
 Coronary Artery Disease This information is at http://www.nhlbi.nih.gov/health/dci/diseases/cad/cad_all.html and is provided by the NHLBI, one of the Institutes of the National Institutes of Health. To
Coronary Artery Disease This information is at http://www.nhlbi.nih.gov/health/dci/diseases/cad/cad_all.html and is provided by the NHLBI, one of the Institutes of the National Institutes of Health. To
Access strategy for chronic total occlusions (CTOs) is crucial
 Learn How Access Strategy Impacts Complex CTO Crossing Arthur C. Lee, MD The Cardiac & Vascular Institute, Gainesville, Florida VASCULAR DISEASE MANAGEMENT 2018;15(3):E19-E23. Key words: chronic total
Learn How Access Strategy Impacts Complex CTO Crossing Arthur C. Lee, MD The Cardiac & Vascular Institute, Gainesville, Florida VASCULAR DISEASE MANAGEMENT 2018;15(3):E19-E23. Key words: chronic total
What s New in the Management of Peripheral Arterial Disease
 What s New in the Management of Peripheral Arterial Disease Sibu P. Saha, MD, MBA Professor of Surgery Chairman, Directors Council Gill Heart Institute University of Kentucky Lexington, KY Disclosure My
What s New in the Management of Peripheral Arterial Disease Sibu P. Saha, MD, MBA Professor of Surgery Chairman, Directors Council Gill Heart Institute University of Kentucky Lexington, KY Disclosure My
Aortoiliac occlusive disease
 Role of endovascular therapy in TASC II C & D inflow disease Per the TASC II Document: Surgery is the treatment of choice for type D lesions Aortoiliac occlusive disease Bala Ramanan, MBBS 1 st year vascular
Role of endovascular therapy in TASC II C & D inflow disease Per the TASC II Document: Surgery is the treatment of choice for type D lesions Aortoiliac occlusive disease Bala Ramanan, MBBS 1 st year vascular
CAROTID ARTERY ANGIOPLASTY
 CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
CAROTID ARTERY ANGIOPLASTY Coverage for services, procedures, medical devices and drugs are dependent upon benefit eligibility as outlined in the member's specific benefit plan. This Medical Coverage Guideline
SCAI Fall Fellows Course Subclavian/Innominate Case Presentation
 SCAI Fall Fellows Course 2012 Subclavian/Innominate Case Presentation Daniel J. McCormick DO, FACC, FSCAI Director, Cardiovascular Interventional Therapy Pennsylvania Hospital University of Pennsylvania
SCAI Fall Fellows Course 2012 Subclavian/Innominate Case Presentation Daniel J. McCormick DO, FACC, FSCAI Director, Cardiovascular Interventional Therapy Pennsylvania Hospital University of Pennsylvania
Disclosures. Iliac Stenting: How could I mess this up? Surgery vs. Stenting: Gold Standard?
 Disclosures Boston Scientific, Medical Advisory Board Endologix Corp., Consultant and trainer, AFX Aorto-Iliac Disease: Bare Metal, Covered or Stent Grafts How I Decide John S. Lane III MD, FACS Professor
Disclosures Boston Scientific, Medical Advisory Board Endologix Corp., Consultant and trainer, AFX Aorto-Iliac Disease: Bare Metal, Covered or Stent Grafts How I Decide John S. Lane III MD, FACS Professor
Disclosures. Tips and Tricks for Tibial Intervention. Tibial intervention overview
 Tips and Tricks for Tibial Intervention Donald L. Jacobs, MD C Rollins Hanlon Endowed Professor and Chair Chair of Surgery Saint Louis University SSM-STL Saint Louis University Hospital Disclosures Abbott
Tips and Tricks for Tibial Intervention Donald L. Jacobs, MD C Rollins Hanlon Endowed Professor and Chair Chair of Surgery Saint Louis University SSM-STL Saint Louis University Hospital Disclosures Abbott
Peripheral arterial disease for primary care Ed Aboian, MD
 Peripheral arterial disease for primary care Ed Aboian, MD Division of Vascular and Endovascular Surgery Palo Alto Medical Foundation, Burlingame Ca Disclosures Nothing to disclose Clinical presentation
Peripheral arterial disease for primary care Ed Aboian, MD Division of Vascular and Endovascular Surgery Palo Alto Medical Foundation, Burlingame Ca Disclosures Nothing to disclose Clinical presentation
Current Vascular and Endovascular Management in Diabetic Vasculopathy
 Current Vascular and Endovascular Management in Diabetic Vasculopathy Yang-Jin Park Associate professor Vascular Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine Peripheral artery
Current Vascular and Endovascular Management in Diabetic Vasculopathy Yang-Jin Park Associate professor Vascular Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine Peripheral artery
Current Status of Endovascular Therapies for Critical Limb Ischemia
 Current Status of Endovascular Therapies for Critical Limb Ischemia Bulent Arslan, MD Associate Professor of Radiology Director, Vascular & Interventional Radiology Rush University Medical Center bulent_arslan@rush.edu
Current Status of Endovascular Therapies for Critical Limb Ischemia Bulent Arslan, MD Associate Professor of Radiology Director, Vascular & Interventional Radiology Rush University Medical Center bulent_arslan@rush.edu
BC Vascular Surgery Day
 BC Vascular Surgery Day November 4, 2017 1 Table of Contents Abdominal Aortic Aneurysm 3 4 Acute DVT 5 6 Peripheral Arterial Disease 7 9 Varicose Veins 10 11 Diabetic Foot Ulcers 12 13 Carotid Stenosis
BC Vascular Surgery Day November 4, 2017 1 Table of Contents Abdominal Aortic Aneurysm 3 4 Acute DVT 5 6 Peripheral Arterial Disease 7 9 Varicose Veins 10 11 Diabetic Foot Ulcers 12 13 Carotid Stenosis
John E. Campbell, MD Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division
 John E. Campbell, MD Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division John Campbell, MD For the 12 months preceding this CME activity,
John E. Campbell, MD Assistant Professor of Surgery and Medicine Department of Vascular Surgery West Virginia University, Charleston Division John Campbell, MD For the 12 months preceding this CME activity,
ARTERIAL BYPASS GRAFTS IN THE LEG
 The Christchurch Department of Vascular Surgery is actively involved in research projects aimed at improving treatment for patients with arterial disease. Marilyn Ollett Department of Surgery Christchurch
The Christchurch Department of Vascular Surgery is actively involved in research projects aimed at improving treatment for patients with arterial disease. Marilyn Ollett Department of Surgery Christchurch
A PATIENT`S GUIDE TO CORONARY ARTERY DISEASE. AND YOUR NIRxcell CoCr CORONARY Stent on RX System
 A PATIENT`S GUIDE TO CORONARY ARTERY DISEASE AND YOUR NIRxcell CoCr CORONARY Stent on RX System TABLE OF CONTENTS ABOUT THIS BOOKLET PAGE 3 WHAT IS CORONARY ARTERY DISEASE (CAD) CORONARY ARTERY DISEASE
A PATIENT`S GUIDE TO CORONARY ARTERY DISEASE AND YOUR NIRxcell CoCr CORONARY Stent on RX System TABLE OF CONTENTS ABOUT THIS BOOKLET PAGE 3 WHAT IS CORONARY ARTERY DISEASE (CAD) CORONARY ARTERY DISEASE
Intravascular Ultrasound
 Scan for mobile link. Intravascular Ultrasound Intravascular ultrasound (IVUS) uses a transducer or probe to generate sound waves and produce pictures of the coronary arteries. IVUS can show the entire
Scan for mobile link. Intravascular Ultrasound Intravascular ultrasound (IVUS) uses a transducer or probe to generate sound waves and produce pictures of the coronary arteries. IVUS can show the entire
Lessons for Successful Subintimal Angioplasty in SFA CTO
 Lessons for Successful Subintimal Angioplasty in SFA CTO John R. Laird Professor of Medicine Medical Director of the Vascular Center UC Davis Medical Center CTOs in the Periphery Presence of Total Occlusion
Lessons for Successful Subintimal Angioplasty in SFA CTO John R. Laird Professor of Medicine Medical Director of the Vascular Center UC Davis Medical Center CTOs in the Periphery Presence of Total Occlusion
