Assistant Professor Dr. Tavga A Baban PhD Pharmacology & Toxicology 1/3/2019 1
|
|
|
- Clara Hunter
- 5 years ago
- Views:
Transcription
1 Assistant Professor Dr. Tavga A Baban PhD Pharmacology & Toxicology 1/3/2019 1
2 Pathophysiology Cardiovascular system (CVS) consist of:- 1. Myocardium. 2. Vascular vessels (arteries, veins and capillaries). Both has important functions in:- 1. Supplying the tissues and cells of the body with nutrients, respiratory gases, hormones and metabolites. 1/3/2019 2
3 2. Removing the waste products of tissue and cellular metabolism as well as foreign materials such as microorganisms. 3. Maintain the optimal internal homeostasis of the body temperature and cellular PH. 4. Play a critical role in well-being and survival of other major organs of the body especially high vascularized organs that are depend on nutrients and O2. 1/3/2019 3
4 1/3/2019 4
5 General Mechanisms of toxicity 1. Interference with Ion Homeostasis A. Inhibition of Na +,K + -ATPase B. Na + Channel Blockade C. K + Channel Blockade D. Ca 2+ Channel Blockade 2. Altered Coronary Blood Flow A. Coronary Vasoconstriction B. Ischemia-Reperfusion Injury 1/3/2019 5
6 1/3/2019 6
7 1/3/2019 7
8 General Mechanisms of toxicity 3. Oxidative Stress 4. Organellar dysfunction:- A. Sarcolemmal Injury, SR Dysfunction, and Ca 2+ Overload. B. Mitochondrial Injury 5. Apoptosis and Oncosis 1/3/2019 8
9 Drugs produce CVS toxicity Drug classes that affect this system:- 1. Digitalis glycosides. 2. Beta-adrenergic blockers. 3. Calcium channel blockers. 4. Diuretics, vasodilators and angiotensin blockers. 1/3/2019 9
10 Digitalis glycosides Used in the treatment of congestive heart failure. Management of certain supraventricular rhythm disturbances. Used by 15% of hospitalized persons % of patient taking digitalis will experience toxicity. This drug posses narrow therapeutic index. 1/3/
11 Digitalis toxicity Therapeutic dose of digoxin is ng/ml Toxic dose is only 2-3 times greater. Mortality rate with toxic doses is reported to be as great as 25%. 1/3/
12 Factors enhance digoxin toxicity Concurrent administration of a diuretic that induces potassium loss is the most cause of toxicity. Narrow therapeutic index: ng/ml. Drug-drug interaction : quinidine and verapamil. The anaerobic microorganism Eubacterium lentum affect digitalis level?????? Renal disease Electrolyte imbalance (hypokalemia) Enhanced sympathomimetic amine release, example: during period of stress such as dental office visits. 1/3/
13 Pharmacokinetics Measurement Digoxin Digitoxin Onset time (oral ingestion) 1.5-6hr 3-6hr Peak Half life Protein binding 4-6hr 31-40hr 20-25% 6-12hr 4-6days 90-97% Volume of distribution 7-8L/kg 0.6L/kg Route of elimination Renal, 75% Hepatic, 80% Toxic blood levels 2.4ng/ml Over 30ng/ml Enterohepatic cycling Small Large (6.6%/day) 1/3/
14 Mechanism of toxicity A toxic dose of digitalis interferes with transport of Na + and Ca +2. It binds with high affinity to an inhibitory site on the portion of the NaK-ATPase structure that faces the outside of the cell, thus Na + and K + transport are blocked. Since K + transport back into the cells is blocked, its concentration in the extracellular fluid increases. Positive inotropic effect from elevated intracellular (cytosolic) Ca during systole. Digitals overdose causes a reduction in resting membrane potentials and cardiac pacemaker cells cannot function properly. Peripheral vasodilation and reduced afterload. 1/3/
15 1/3/
16 1/3/
17 Characteristics of Poisoning The symptoms involve not only the heart, but also the GIT and CNS. Early manifestations occur in 50% of all cases involve:- 1. CVS:- Dysarrhythmias, atrioventricular block and severe bradycardia 2. GIT disturbance: anorexia, abdominal pain; nausea and vomiting? 3. Blurred vision: loss of visual acuity, greenyellow halos 4. CNS effects: a variety of neuropsychiatric disturbances 1/3/
18 General Management Discontinue digoxin, gastrointestinal decontamination, especially with AC. Orogastric lavage preferred to emesis in a digoxin-toxic patient already vomiting. AC and sorbitol, then MDAC up to 1 g/kg every 2 4 hours. Slow absorption and an enterohepatic circulation make digoxin very amenable to decontamination, with both AC and MDAC. Steroid-binding resins: Cholestyramine and colestipol to bind digoxin and interrupt enterohepatic circulation along with MDAC. Hemoperfusion and hemodialysis ineffective due to high molecular weight and increased volume of distribution. 1/3/
19 Specific Management Digoxin-specific antibody fragments Fabs (DigiBind ): Will decrease free digoxin but elevate total serum digoxin levels; Fabs will also decrease levels of K and increase excretion of Fab-bound digoxin. K > 5 meq/l: Fab > insulin and glucose > NaHCO3 > sodium polystyrene sulfonate. Supraventricular tachycardia (SVT): Fab preferred over β-blockers. Tachy or bradyarrhythmia associated with hypokalemia can be treated with K supplement only. 1/3/
20 Specific Management Atrial and ventricular arrhythmia that do not respond to K therapy should be treated with phynetoin and lidocaine. We can not use quinidine and procainamide?? Ventricular tachycardia (VT)/ventricular fibrillation (VF): Cardioversion/defibrillation preferred over Fab, phenytoin, and lidocaine. 1/3/
21 Contraindicated medications 1) Catecholamines may precipitate more serious ectopic arrhythmias 2) calcium, due to increased intracellular calcium stores. 3) Potassium in digitalis induced hyperkalemia?? Heart block terminating in sinus arrest. 1/3/
22 Digoxin-Specific Fabs Indication Rising K or K > 5 meq/l at any time. Severe ventricular dysrhythmias: VT and VF Progressive bradydysrhythmias refractory to atropine. Serum [dig] > ng/ml anytime. Ingestion of > 4 mg of digoxin by a child; and > 10 mg by adult. 1/3/
23 Beta-Blockers Indications Hypertension: β1-selective > nonselectives. Angina: Reduce anginal attacks and decrease post-myocardial infarction mortality. Tachydysrhythmias: Used in theophylline overdose. Tremor: Propranolol. Hyperthyroidism: β-blockers moderate the sympathetic, hyperdynamic effects of thyroid storm. Open-angle glucoma. 1/3/
24 1/3/
25 Mechanism of toxicity It bind to beta receptors and block the actions of beta agonists. In overdoses the membrane stabilizing activity or quinidine like action predominant. This is responsible for severe myocardial depression which lead to heart block and CNS effect. ISA cause HT and tachycardia. High lipid solubility increase CNS effects. Toxicity occur after 20 min. post ingestion but usually appear after 1-2 hrs. 1/3/
26 Mechanism of action 1/3/
27 Characteristics of poisoning The major features of beta-adrenergic blocker toxicity are related to their antagonistic action on cardiac beta receptors. Produce bradycardia in 92% and severe hypotension in 77% leads to cardiogenic shock. ECG changes include AV block (prolonged PR interval ), QRS widening, absence of P waves, and prolongation of QT interval. 1/3/
28 Characteristics of poisoning CNS effects involves seizures results from hypoglycemia, cerebral hypoxia, or from membrane-stabilizing effect. It occurs in 58% of patients following the ingestion of more than 1600 mg propranolol. 1/3/
29 Cardiac CNS Others Arrhythmias Bradycardia AV block Hypotension Sleepiness Dizziness Unconsciousness Coma Bronchospasm Pulmonary edema Hypoglycemia Hyperkalemia Tachycardia Shock Seizures Respiratory depression 1/3/
30 General management Asymptomatic: No ipecac, AC preferred over lavage. Mild toxicity: AC and atropine for bradycardia and fluid bolus for hypotension. Moderate toxicity: All of the above and glucagon (hormone secreted by pancreatic α cells in response to decreased levels of glucose and elevated catechols); administer 2 5 mg bolus of glucagon IV push to bypass β-receptors and to increase intracellular camp; CaCl2 IV up to 1 g; consider 1/3/2019 more atropine, up to 3 mg IV. 30
31 Specific Management of Severe Toxicity General management and invasive monitoring. Catecholamine infusion: Dobutamine (β1) preferred over norepinephrine (NE) (α and β) and isoproterenol. Isoproterenol is the least preferred catecholamine due to peripheral vasodilation with hypotension (from β2 stimulation). 1/3/
32 Specific Management of Severe Toxicity Add a phosphodiesterase inhibitor: Amrinone or milrinone and theophylline to bypass β-receptors and increase intracellular camp restoring cardiac contractility. Consider IV insulin( positive inotropic activity) and glucose therapy. Hemodialysis or Hemoperfusion may be indicated when the toxicity due to Nadolol or Atenolol specially when there are sign of renal failure. Other b- blockers are poor candidate for HD & HP. Why? 1/3/2019 Protein binding & volume of distribution. 32
33 The major action of these drugs is to diminish the inward movement of Ca 2+ through the L-type voltage-dependent Ca 2+ channels located in sarcolemma. These drugs are also termed Ca 2+ channel blockers.
34 PHARMACOLOGY AND CLINICAL USE Ca2+ channel antagonists affect the contractility of both smooth and cardiac muscle cells. At least three distinct mechanisms have been suggested to lead to increased levels of cytosolic Ca 2+ and the subsequent contraction of smooth muscle: (1) extracellular Ca2+ influx through voltage-sensitive Ca2+ channels in response to the depolarization of the membrane; (2) second messenger- (i.e., inositol triphosphate) mediated release of a Ca2+ from the SR; and (3) influx of extracellular Ca2+ via receptor-operated Ca2+ channels in response to receptor occupancy. 1/3/
35 1/3/
36 1/3/
37 Clinical uses Ca2+ channel antagonists are efficacious in the treatment of various types of CV disorders, including 1. Hypertension 2. angina pectoris 3. myocardial infarction 4. cardiac arrhythmias. 1/3/
38 Mechanism of toxicity Ca2+ channel antagonists inhibit the voltagedependent Ca2+ channels in vascular smooth muscle cells inducing relaxation of vascular smooth muscle, leading to vasodilation. The contraction of cardiac muscle is dependent on the influx of extracellular Ca2+ through the L- type channels, and the subsequent Ca2+-induced Ca2+ release from the SR. Thus, Ca2+ channel antagonists exert a negative inotropic effect on myocardium. 1/3/
39 In the SA and AV nodes, depolarization is largely dependent on the influx of extracellular Ca2+ through the L-type channels. Therefore, Ca2+ channel antagonists have the potential to depress the rate of sinus node pacemaker and slow AV conduction. In addition, all approved Ca2+ channel antagonists are able to decrease coronary vascular resistance and thereby increase coronary blood flow. 1/3/
40 CLINICAL MANIFESTATIONS OF TOXICITY Excessive vasodilation. These effects may be manifest as dizziness, hypotension, headache, flushing, and nausea. Patients may also experience constipation, peripheral edema, coughing, wheezing, and pulmonary edema. With severe overdoses that result in dramatic Ca2+ channel blockage, all Ca2+ channel antagonists exert a negative inotropic effect with depressed cardiac contraction, conduction blockage, hypotension, and shock. 1/3/
41 Metabolic acidosis with hyperglycemia(the mechanism is related to the suppressive effect by Ca2+ channel antagonists on pancreatic B cell insulin release coupled with whole-body insulin resistance). 1/3/
42 Clinical management of intoxication (1) providing supportive care. (2) decreasing drug absorption, and decontamination of the GI tract via the use of activated charcoal is crucial (3) augmenting myocardial function with cardiotonic agents. Intravenous injection of calcium salts is the first-line treatment of Ca2+ channel antagonist overdoses(multiple IV boluses of 10 cc of 10% calcium chloride every minutes to keep the serum calcium between meq/l is reasonable). 1/3/
43 Because there is no specific antidote,. Other cardiotonic drugs may include glucagon(the inotropic action of glucagon seems to be related to an increase of camplevels in the myocardium), atropine, and catecholamines. The other line agent is amrinone, which is a noncatecholamine inotropic agent that increases camp intracellularly 1/3/
44 Vasodilators This class includes a broad spectrum of medications that dilate peripheral arteries and veins, producing BP e.g alpha-adrenergic blockers and direct acting agents (Hydralazine, Minoxidil sulfate, Diazoxide) and nitroprusside represent another class of antihypertensive drugs in addition to nitrite. These drugs produce vascular smooth muscle relaxation independent of innervation or known pharmacological receptors. 1/3/
45 Nitrate and Nitrite Nitrate Sources:- 1. Synthetic nitrogen-gassed fertilizers. 2. Food production. 3. Food processing. 4. As a main or by product during manufacture of different chemicals and drugs. 5. Animal waste products. All these result in high level of nitrate. 1/3/
46 Nitrite Sources:- Recreational drugs: amyl, butyl, and isobutyl nitrite. Nitrite undergo nitrosation with amines producing nitrosamines (carcinogenic chemicals). Nitrate convert to nitrite, and this may be subjected to nitrosation in vivo (animal study). Antioxidants like vitamins E & C, butylated hydroxytoluene and butylated hydroxyanisole are added to nitrite-treated foods and some drug products 1/3/
47 Mechanism of Nitrate toxicity The drug affect the myocardium and the vascular system. It produce aging of the vessels. This drug is NO donor and this will increase cgmp (by activating guanylyl cyclase) which is responsible for smooth muscle relaxation including vasculature, as a result fall in blood pressure will occur. 1/3/
48 1/3/
49 Mechanism of Nitrate toxicity During toxicity excessive amount of nitrate produce intense vasodilation, which can precipitate several bad outcomes staring with throbbing headache passing through flushing and rapid fall in blood pressure ending with cardiogenic shock. The heart will compensate by:- 1. Baroreceptor stimulation. 2. Reflex sympathetic activation. Through these reflex mechanisms result in increase heart rate and force of contraction. 1/3/
50 Mechanism of Nitrate toxicity The second important mechanism of toxicity is the production of methemoglobin. The drug will cause oxidation of ferrous (HbFe +2 ) iron in hemoglobin to the ferric (HbFe +3 ) state. Methemoglobin is unable to transport oxygen so cyanosis will occur. 1/3/
51 1/3/
52 Characteristic of poisoning The characteristic mainly due to the formation of methemoglobinemia:- 1. Arterial blood is chocolate-brown in color. 2. Gray cyanosis not respond to oxygen therapy. 3. Easy fatigability. 4. Dyspnea; respiratory distress. 5. Tachycardia. 6. Dizziness with exertion. 7. Decreased oxygen carrying capacity. 1/3/
53 Methemoglobinemia Many chemical agents contribute to the production of methemoglobinemia like dapsone, aniline, sulfonamide, local anesthetic..etc. table 5.3 page 101. Nitrites are more potent than nitrates in producing methemoglobin. Hem oxidation also occur spontaneously from environment or from certain foods. 1% -2% of total hemoglobin are present in methemoglobin form without inducing any pathogenesis. 1/3/
54 Erythrocytes contain several enzyme systems that reduce methemoglobin back to hemoglobin. These are diaphorase I and diaphorase II which are methemoglobin reductase enzyme. These two enzymes dependent on concentration of NADH & NADPH. When MetHb increase diaphorase II activity can increase 60 fold. Normal erythrocytic MetHb. Reductase can reduce methemoglobin to hemoglobin at a rate 250 times its rate of formation. 1/3/
55 Toxicity occur when these enzymatic system become saturated, when the person ingest large amounts of oxidizing agent. Toxic MetHb. can result from a congenital disorder, hereditary MetHb. This condition characterized by absence of NADH-dependent MetHb. reductase. The condition characterized by cyanosis at birth. 1/3/
56 Nitrate induced MetHb. In infants is of special concern for several reason:- 1. Gastric ph is less acidic. 2. Fetal Hb. Is more susceptible to oxidation to MetHb. than is adult Hb. Why? 3. Incomplete hepatic microsomal enzyme system. 1/3/
57 Management of MetHb. Methylene blue (tetramethylthionine chloride) is the specific antidote for MetHb. It is a dye that serves as an intermediate in electron transfer between methemoglobin reductase (diaphorase II) and methemoglobin. If MetHb is less than 30%:- 1. Remove the toxic agent. 2. Give oxygen 100%. 1/3/
58 If MetHb exceed 30% :- Methylene blue 1% solution is administered at 1-2mg/kg intravenously. Other reducing agent may be used such as ascorbic acid as a substitute for methylene blue. Methylene blue should be used with caution since larger doses may actually produce MetHb. A dose of 5mg/kg has been reported to increase methemoglobin level. Doses greater than 15mg/kg are associated with hemolysis. 1/3/
59 Mechanism of action of Methylene blue Explain the mechanism of action of methylene blue in methemoglobinemia, support your answer by figure. Determine the dose of methylene blue that produce hemolysis. At which concentration of MetHb. Methylene blue is indicated? 1/3/
60 Explain Why? 1. Gastric ph in infant affect Nitrate poisoning. 2. Person with genetically absence NADH-dependent methemoglobin reductase experience more toxicity after i.v. dose of sodium nitrite than normal subject. 1/3/
Clinical Toxicology Toxicity of Digitalis Glycosides 5 th Year (Lab 3)
 Clinical Toxicology Toxicity of Digitalis Glycosides 5 th Year (Lab 3) Lecturer: Rua Abbas Al-Hamdy Department of Pharmacology & Toxicology University of Al-Mustansiriyah 2017-2018 Introduction: Digitalis
Clinical Toxicology Toxicity of Digitalis Glycosides 5 th Year (Lab 3) Lecturer: Rua Abbas Al-Hamdy Department of Pharmacology & Toxicology University of Al-Mustansiriyah 2017-2018 Introduction: Digitalis
Heart Failure (HF) Treatment
 Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Heart Failure (HF) Treatment Heart Failure (HF) Complex, progressive disorder. The heart is unable to pump sufficient blood to meet the needs of the body. Its cardinal symptoms are dyspnea, fatigue, and
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Heart Failure. Dr. Alia Shatanawi
 Heart Failure Dr. Alia Shatanawi Left systolic dysfunction secondary to coronary artery disease is the most common cause, account to 70% of all cases. Heart Failure Heart is unable to pump sufficient blood
Heart Failure Dr. Alia Shatanawi Left systolic dysfunction secondary to coronary artery disease is the most common cause, account to 70% of all cases. Heart Failure Heart is unable to pump sufficient blood
Drugs Used in Heart Failure. Assistant Prof. Dr. Najlaa Saadi PhD pharmacology Faculty of Pharmacy University of Philadelphia
 Drugs Used in Heart Failure Assistant Prof. Dr. Najlaa Saadi PhD pharmacology Faculty of Pharmacy University of Philadelphia Heart Failure Heart failure (HF), occurs when cardiac output is inadequate to
Drugs Used in Heart Failure Assistant Prof. Dr. Najlaa Saadi PhD pharmacology Faculty of Pharmacy University of Philadelphia Heart Failure Heart failure (HF), occurs when cardiac output is inadequate to
ANTI - ARRHYTHMIC DRUGS
 ANTI - ARRHYTHMIC DRUGS CARDIAC ACTION POTENTIAL K Out Balance Ca in/k out Na in K Out GENERATION OF ARRHYTHMIAS Four mechanisms of arrhythmia generation; Increased normal automaticity Abnormal automaticity
ANTI - ARRHYTHMIC DRUGS CARDIAC ACTION POTENTIAL K Out Balance Ca in/k out Na in K Out GENERATION OF ARRHYTHMIAS Four mechanisms of arrhythmia generation; Increased normal automaticity Abnormal automaticity
Atrial fibrillation in the ICU
 Atrial fibrillation in the ICU Atrial fibrillation Preexisting or incident (new onset) among nearly one in three critically ill patients Formation of arrhythogenic substrate usually fibrosis (CHF, hypertension,
Atrial fibrillation in the ICU Atrial fibrillation Preexisting or incident (new onset) among nearly one in three critically ill patients Formation of arrhythogenic substrate usually fibrosis (CHF, hypertension,
Mr. Eknath Kole M.S. Pharm (NIPER Mohali)
 M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
M.S. Pharm (NIPER Mohali) Drug Class Actions Therapeutic Uses Pharmacokinetics Adverse Effects Other Quinidine IA -Binds to open and inactivated Na+ -Decreases the slope of Phase 4 spontaneous depolarization
Antihypertensive drugs SUMMARY Made by: Lama Shatat
 Antihypertensive drugs SUMMARY Made by: Lama Shatat Diuretic Thiazide diuretics The loop diuretics Potassium-sparing Diuretics *Hydrochlorothiazide *Chlorthalidone *Furosemide *Torsemide *Bumetanide Aldosterone
Antihypertensive drugs SUMMARY Made by: Lama Shatat Diuretic Thiazide diuretics The loop diuretics Potassium-sparing Diuretics *Hydrochlorothiazide *Chlorthalidone *Furosemide *Torsemide *Bumetanide Aldosterone
Antihypertensive Agents Part-2. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
Antihypertensive Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Agents that block production or action of angiotensin Angiotensin-converting
Cardiac Drugs: Chapter 9 Worksheet Cardiac Agents. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate.
 Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Complete the following. 1. drugs affect the rate of the heart and can either increase its rate or decrease its rate. 2. drugs affect the force of contraction and can be either positive or negative. 3.
Instruct patient and caregivers: Need for constant monitoring Potential complications of drug therapy
 Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Assessment Prior to administration: Assess patient for chest pain, dysrhythmias, and vital signs (initially and throughout therapy) Obtain complete medical history, including allergies, especially heart
Dysrhythmias. Dysrythmias & Anti-Dysrhythmics. EKG Parameters. Dysrhythmias. Components of an ECG Wave. Dysrhythmias
 Dysrhythmias Dysrythmias & Anti-Dysrhythmics Rhythm bad in the heart: Whitewater rafting Electrical impulses coordinate heart Reduction in Cardiac Output PEA Asystole Components of an ECG Wave EKG Parameters
Dysrhythmias Dysrythmias & Anti-Dysrhythmics Rhythm bad in the heart: Whitewater rafting Electrical impulses coordinate heart Reduction in Cardiac Output PEA Asystole Components of an ECG Wave EKG Parameters
Chapter 26. Media Directory. Dysrhythmias. Diagnosis/Treatment of Dysrhythmias. Frequency in Population Difficult to Predict
 Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Chapter (9) Calcium Antagonists
 Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
Chapter (9) Calcium Antagonists (CALCIUM CHANNEL BLOCKERS) Classification Mechanism of Anti-ischemic Actions Indications Drug Interaction with Verapamil Contraindications Adverse Effects Treatment of Drug
WRITER TRISTAN WALKER TABLE OF CONTENTS. The Basics of cardiac pharmacology 2007
 WRITER TRISTAN WALKER TABLE OF CONTENTS 1. WHAT ARE THE MAJOR CLASSES OF CARDIAC DRUGS?...2 2. HOW DO THEY WORK?...3 3. CONSIDERATIONS FOR THE PEDIATRIC PATIENT...7 4. SUMMARY TABLE...10 REFERENCES...14
WRITER TRISTAN WALKER TABLE OF CONTENTS 1. WHAT ARE THE MAJOR CLASSES OF CARDIAC DRUGS?...2 2. HOW DO THEY WORK?...3 3. CONSIDERATIONS FOR THE PEDIATRIC PATIENT...7 4. SUMMARY TABLE...10 REFERENCES...14
Heart failure. Failure? blood supply insufficient for body needs. CHF = congestive heart failure. increased blood volume, interstitial fluid
 Failure? blood supply insufficient for body needs CHF = congestive heart failure increased blood volume, interstitial fluid Underlying causes/risk factors Ischemic heart disease (CAD) 70% hypertension
Failure? blood supply insufficient for body needs CHF = congestive heart failure increased blood volume, interstitial fluid Underlying causes/risk factors Ischemic heart disease (CAD) 70% hypertension
7/21/2017. Learning Objectives. Current Cardiovascular Pharmacology. Epinephrine. Cardiotonic Agents. Epinephrine. Epinephrine. Arthur Jones, EdD, RRT
 Learning Objectives Current Cardiovascular Pharmacology Arthur Jones, EdD, RRT Explain the actions, effects, indications, adverse effects, & precautions for agents from the following drug categories Cardiotonic
Learning Objectives Current Cardiovascular Pharmacology Arthur Jones, EdD, RRT Explain the actions, effects, indications, adverse effects, & precautions for agents from the following drug categories Cardiotonic
Arrhythmias. Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium.
 Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
Arrhythmias Simple-dysfunction cause abnormalities in impulse formation and conduction in the myocardium. However, in clinic it present as a complex family of disorders that show variety of symptoms, for
Document 3 Summary of Data and Guidance for Medical Professionals
 Document 3 Summary of Data and Guidance for Medical Professionals Anvirzel Anvirzel is a novel antitumor compound extracted from the plant Nerium oleander, which belongs to the family Apocynaceae. Anvirzel
Document 3 Summary of Data and Guidance for Medical Professionals Anvirzel Anvirzel is a novel antitumor compound extracted from the plant Nerium oleander, which belongs to the family Apocynaceae. Anvirzel
Antiarrhythmic Drugs
 Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
ALS MODULE 7 Pharmacology
 ALS MODULE 7 Pharmacology Relates to HLT404C Apply Advanced Resuscitation Techniques Introduction There are no studies that addressed the order of drug administration. There is inadequate evidence to define
ALS MODULE 7 Pharmacology Relates to HLT404C Apply Advanced Resuscitation Techniques Introduction There are no studies that addressed the order of drug administration. There is inadequate evidence to define
Arrhythmias. 1. beat too slowly (sinus bradycardia). Like in heart block
 Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Angina Pectoris. Edward JN Ishac, Ph.D. Smith Building, Room
 Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth University
Angina Pectoris Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth University
Pharmacology. Drugs affecting the Cardiovascular system (Antianginal Drugs)
 Lecture 7 (year3) Dr Noor Al-Hasani Pharmacology University of Baghdad College of dentistry Drugs affecting the Cardiovascular system (Antianginal Drugs) Atherosclerotic disease of the coronary arteries,
Lecture 7 (year3) Dr Noor Al-Hasani Pharmacology University of Baghdad College of dentistry Drugs affecting the Cardiovascular system (Antianginal Drugs) Atherosclerotic disease of the coronary arteries,
METOTRUST XL-25/50 Metoprolol Succinate Extended-Release Tablets
 METOTRUST XL-25/50 Metoprolol Succinate Extended-Release Tablets COMPOSITION Each film-coated tablet of Metotrust XL-25 contains: Metoprolol Succinate USP 23.75 mg equivalent to Metoprolol Tartrate 25
METOTRUST XL-25/50 Metoprolol Succinate Extended-Release Tablets COMPOSITION Each film-coated tablet of Metotrust XL-25 contains: Metoprolol Succinate USP 23.75 mg equivalent to Metoprolol Tartrate 25
Heart Failure. Subjective SOB (shortness of breath) Peripheral edema. Orthopnea (2-3 pillows) PND (paroxysmal nocturnal dyspnea)
 Pharmacology I. Definitions A. Heart Failure (HF) Heart Failure Ezra Levy, Pharm.D. HF Results when one or both ventricles are unable to pump sufficient blood to meet the body s needs There are 2 types
Pharmacology I. Definitions A. Heart Failure (HF) Heart Failure Ezra Levy, Pharm.D. HF Results when one or both ventricles are unable to pump sufficient blood to meet the body s needs There are 2 types
PHARMACOLOGY OF ARRHYTHMIAS
 PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
PHARMACOLOGY OF ARRHYTHMIAS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 27, 2012 Materials on: Exam #5 Required reading: Katzung, Chapter 14 1 CARDIAC ARRHYTHMIAS Abnormalities
Antiarrhythmic Drugs. Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018
 Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018 2 Ion Permeability Changes Potential Changes Genes and Proteins 3 Cardiac Na+ channels 5 6
Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2018 2 Ion Permeability Changes Potential Changes Genes and Proteins 3 Cardiac Na+ channels 5 6
Angina pectoris due to coronary atherosclerosis : Atenolol is indicated for the long term management of patients with angina pectoris.
 Lonet Tablet Description Lonet contains Atenolol, a synthetic β1 selective (cardioselective) adrenoreceptor blocking agent without membrane stabilising or intrinsic sympathomimetic (partial agonist) activity.
Lonet Tablet Description Lonet contains Atenolol, a synthetic β1 selective (cardioselective) adrenoreceptor blocking agent without membrane stabilising or intrinsic sympathomimetic (partial agonist) activity.
DRUGS USED IN ANGINA PECTORIS
 DRUGS USED IN ANGINA PECTORIS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 16, 2010 Materials on: Exam #7 Required reading: Katzung, Chapter 12 1 TYPES OF ISCHEMIC HEART DISEASE
DRUGS USED IN ANGINA PECTORIS Course: Integrated Therapeutics 1 Lecturer: Dr. E. Konorev Date: November 16, 2010 Materials on: Exam #7 Required reading: Katzung, Chapter 12 1 TYPES OF ISCHEMIC HEART DISEASE
Chapter 14. Agents used in Cardiac Arrhythmias
 Chapter 14 Agents used in Cardiac Arrhythmias Cardiac arrhythmia Approximately 50% of post-myocardial infarction fatalities result from ventricular tachycarida (VT) or ventricular fibrillation (VF). These
Chapter 14 Agents used in Cardiac Arrhythmias Cardiac arrhythmia Approximately 50% of post-myocardial infarction fatalities result from ventricular tachycarida (VT) or ventricular fibrillation (VF). These
Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms. Introduction to the Algorithms
 Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Introduction to the Algorithms Cardiac Arrest Algorithms Prehospital Medication Profiles Perspective regarding the EMT- Intermediate
Emergency Cardiovascular Care: EMT-Intermediate Treatment Algorithms Introduction to the Algorithms Cardiac Arrest Algorithms Prehospital Medication Profiles Perspective regarding the EMT- Intermediate
Antiarrhythmic Drugs. Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2017
 Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2017 Types of Cardiac Arrhythmias Abnormalities of Impulse Formation: Rate disturbances. Triggered
Antiarrhythmic Drugs Munir Gharaibeh MD, PhD, MHPE School of Medicine, The University of Jordan November 2017 Types of Cardiac Arrhythmias Abnormalities of Impulse Formation: Rate disturbances. Triggered
Congestive Heart Failure (CHF) Edward JN Ishac, Ph.D.
 Congestive Heart Failure (CHF) Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Congestive Heart Failure (CHF) Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia Campus of Virginia Commonwealth
Leading Causes of Death in the U.S. Congestive Heart Failure (CHF) Edward JN Ishac, Ph.D. Blood flow at rest and exercise
 Congestive Heart Failure (CHF) Leading Causes of Death in the U.S Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia
Congestive Heart Failure (CHF) Leading Causes of Death in the U.S Edward JN Ishac, Ph.D. Smith Building, Room 742 eishac@vcu.edu 828-2127 Department of Pharmacology and Toxicology Medical College of Virginia
WHAT DO YOU SEE WHEN YOU STIMULATE BETA
 CARDIAC DRUG REVIEW WHAT DO YOU SEE WHEN YOU STIMULATE BETA VASODILATE BRONCHODILATE +CHRONOTROPE +INOTROPE EPI S OTHER NAME? ADRENALIN WHAT DOES EPI DO THAT NOREPI AND DOPAMINE DO NOT DO? BETA 2 BRONCHODILATOR
CARDIAC DRUG REVIEW WHAT DO YOU SEE WHEN YOU STIMULATE BETA VASODILATE BRONCHODILATE +CHRONOTROPE +INOTROPE EPI S OTHER NAME? ADRENALIN WHAT DOES EPI DO THAT NOREPI AND DOPAMINE DO NOT DO? BETA 2 BRONCHODILATOR
B. 14 Antidysrhythmic drugs. a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification
 B. 14 Antidysrhythmic drugs a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification I II III IV membrane stabilizers all ERP, ERP/APD, all except c APD classified
B. 14 Antidysrhythmic drugs a. Classify antidysrhythmics by their electrophysiological actions. Vaughan-Williams classification I II III IV membrane stabilizers all ERP, ERP/APD, all except c APD classified
HEART FAILURE PHARMACOLOGY. University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D
 HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
HEART FAILURE PHARMACOLOGY University of Hawai i Hilo Pre- Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 1 LEARNING OBJECTIVES Understand the effects of heart failure in the body
Drug Treatment of Ischemic Heart Disease
 Drug Treatment of Ischemic Heart Disease Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014 Categories of Ischemic Heart Disease Fixed "Stable, Effort Angina Variant
Drug Treatment of Ischemic Heart Disease Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014 Categories of Ischemic Heart Disease Fixed "Stable, Effort Angina Variant
Antihypertensives. Antihypertensive Classes. RAAS Inhibitors. Renin-Angiotensin Cascade. Angiotensin Receptors. Approaches to Hypertension Treatment
 Approaches to Hypertension Treatment Antihypertensives Inhibit Sympathetic impulses Inhibit contractility Inhibit heart rate Inhibit vasoconstriction Inhibit smooth muscle function Inhibit RAAS Inhibit
Approaches to Hypertension Treatment Antihypertensives Inhibit Sympathetic impulses Inhibit contractility Inhibit heart rate Inhibit vasoconstriction Inhibit smooth muscle function Inhibit RAAS Inhibit
Antiarrhythmic Drugs 1/31/2018 1
 Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
Antiarrhythmic Drugs 1/31/2018 1 Normal conduction pathway: 1- SA node generates action potential and delivers it to the atria and the AV node 2- The AV node delivers the impulse to purkinje fibers Other
PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker
 PACKAGE INSERT Pr PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker ACTIONS AND CLINICAL PHARMACOLOGY Phentolamine produces an alpha-adrenergic
PACKAGE INSERT Pr PHENTOLAMINE MESYLATE INJECTION SANDOZ STANDARD 5 mg/ ml THERAPEUTIC CLASSIFICATION Alpha-adrenoreceptor Blocker ACTIONS AND CLINICAL PHARMACOLOGY Phentolamine produces an alpha-adrenergic
Objectives: This presentation will help you to:
 emergency Drugs Objectives: This presentation will help you to: Five rights for medication administration Recognize different cardiac arrhythmias and determine the common drugs used for each one List the
emergency Drugs Objectives: This presentation will help you to: Five rights for medication administration Recognize different cardiac arrhythmias and determine the common drugs used for each one List the
Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs
 Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs Blood Pressure Normal = sys
Introductory Clinical Pharmacology Chapter 41 Antihypertensive Drugs Blood Pressure Normal = sys
Antiarrhythmic Drugs Öner Süzer
 Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 09.11.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
Antiarrhythmic Drugs Öner Süzer www.onersuzer.com osuzer@istanbul.edu.tr Last update: 09.11.2009 1 Süzer Farmakoloji 3. Baskı 2005 2 1 Süzer Farmakoloji 3. Baskı 2005 3 Figure 14 1 Schematic representation
DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS)
 DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS) Beta-blockers have been widely used in the management of angina, certain tachyarrhythmias and heart failure, as well as in hypertension. Examples
DRUG CLASSES BETA-ADRENOCEPTOR ANTAGONISTS (BETA-BLOCKERS) Beta-blockers have been widely used in the management of angina, certain tachyarrhythmias and heart failure, as well as in hypertension. Examples
Angina Pectoris Dr. Shariq Syed
 Angina Pectoris Dr. Syed 1 What is Angina Pectoris (AP)? Commonly known as angina is chest pain often due to ischemia of the heart muscle, Because of obstruction or spasm of the coronary arteries 2 What
Angina Pectoris Dr. Syed 1 What is Angina Pectoris (AP)? Commonly known as angina is chest pain often due to ischemia of the heart muscle, Because of obstruction or spasm of the coronary arteries 2 What
Chapter 23. Media Directory. Cardiovascular Disease (CVD) Hypertension: Classified into Three Categories
 Chapter 23 Drugs for Hypertension Slide 37 Slide 41 Media Directory Nifedipine Animation Doxazosin Animation Upper Saddle River, New Jersey 07458 All rights reserved. Cardiovascular Disease (CVD) Includes
Chapter 23 Drugs for Hypertension Slide 37 Slide 41 Media Directory Nifedipine Animation Doxazosin Animation Upper Saddle River, New Jersey 07458 All rights reserved. Cardiovascular Disease (CVD) Includes
Drug Treatment of Ischemic Heart Disease
 Drug Treatment of Ischemic Heart Disease Munir Gharaibeh, MD, PhD, MHPE School of Medicine, The University of Jordan November, 2017 Categories of Ischemic Heart Disease Fixed "Stable, Effort Angina Variant
Drug Treatment of Ischemic Heart Disease Munir Gharaibeh, MD, PhD, MHPE School of Medicine, The University of Jordan November, 2017 Categories of Ischemic Heart Disease Fixed "Stable, Effort Angina Variant
HYPERTENSION: Sustained elevation of arterial blood pressure above normal o Systolic 140 mm Hg and/or o Diastolic 90 mm Hg
 Lecture 39 Anti-Hypertensives B-Rod BLOOD PRESSURE: Systolic / Diastolic NORMAL: 120/80 Systolic = measure of pressure as heart is beating Diastolic = measure of pressure while heart is at rest between
Lecture 39 Anti-Hypertensives B-Rod BLOOD PRESSURE: Systolic / Diastolic NORMAL: 120/80 Systolic = measure of pressure as heart is beating Diastolic = measure of pressure while heart is at rest between
Adenosine. poison/drug induced. flushing, chest pain, transient asystole. Precautions: tachycardia. fibrillation, atrial flutter. Indications: or VT
 Adenosine Indications: 1. Narrow complex PSVT 2. Does not convert atrial fibrillation, atrial flutter or VT 1. Side effects include flushing, chest pain, transient asystole 2. May deteriorate widecomplex
Adenosine Indications: 1. Narrow complex PSVT 2. Does not convert atrial fibrillation, atrial flutter or VT 1. Side effects include flushing, chest pain, transient asystole 2. May deteriorate widecomplex
Section 3, Lecture 2
 59-291 Section 3, Lecture 2 Diuretics: -increase in Na + excretion (naturesis) Thiazide and Related diuretics -decreased PVR due to decreases muscle contraction -an economical and effective treatment -protect
59-291 Section 3, Lecture 2 Diuretics: -increase in Na + excretion (naturesis) Thiazide and Related diuretics -decreased PVR due to decreases muscle contraction -an economical and effective treatment -protect
Cardiotoxic Medications
 Cardiotoxic Medications Dean Olsen, DO Faculty, New York City Poison Control Center Director Emergency Medicine Residency Nassau University Medical Center Assistant Professor Pharmacology, Toxicology New
Cardiotoxic Medications Dean Olsen, DO Faculty, New York City Poison Control Center Director Emergency Medicine Residency Nassau University Medical Center Assistant Professor Pharmacology, Toxicology New
POSITIVE INOTROPIC AGENTS
 POSITIVE INOTROPIC AGENTS Positively inotropic agents increase the strength of contraction of heart muscle (myocardial contractility). Drugs of this group include: Cardioactive inotropes (digoxin, digitoxin);
POSITIVE INOTROPIC AGENTS Positively inotropic agents increase the strength of contraction of heart muscle (myocardial contractility). Drugs of this group include: Cardioactive inotropes (digoxin, digitoxin);
ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments
 ADENOSINE Paroxysmal SVT 1 st Dose 6 mg rapid IV 2 nd & 3 rd Doses 12 mg rapid IV push Follow each dose with rapid bolus of 20 ml NS May cause transient heart block or asystole. Side effects include chest
ADENOSINE Paroxysmal SVT 1 st Dose 6 mg rapid IV 2 nd & 3 rd Doses 12 mg rapid IV push Follow each dose with rapid bolus of 20 ml NS May cause transient heart block or asystole. Side effects include chest
MWLCEMS SYSTEM Continuing Education Packet Management of the Acute MI Patient
 MWLCEMS SYSTEM Continuing Education Packet Management of the Acute MI Patient In this CE we will discuss the patient presenting with an acute ST-Elevation Myocardial Infarction (STEMI) Definition: Myocardial
MWLCEMS SYSTEM Continuing Education Packet Management of the Acute MI Patient In this CE we will discuss the patient presenting with an acute ST-Elevation Myocardial Infarction (STEMI) Definition: Myocardial
Chapter 13. Learning Objectives. Learning Objectives 9/11/2012. Poisonings, Overdoses, and Intoxications
 Chapter 13 Poisonings, Overdoses, and Intoxications Learning Objectives Discuss use of activated charcoal in treatment of poisonings List treatment options for acetaminophen overdose List clinical manifestations
Chapter 13 Poisonings, Overdoses, and Intoxications Learning Objectives Discuss use of activated charcoal in treatment of poisonings List treatment options for acetaminophen overdose List clinical manifestations
Cardiac arrhythmias. Janusz Witowski. Department of Pathophysiology Poznan University of Medical Sciences. J. Witowski
 Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
DIGOXIN TOXICITY: A REVIEW
 DIGOXIN TOXICITY: A REVIEW Dr. Laxmi Narayan Goit 1* and Prof. Dr. Yang Shaning 2 1 Department of Cardiology, the first affiliated Hospital of Yangtze University, Jingzhou, Hubei, P.R China. 2 Department
DIGOXIN TOXICITY: A REVIEW Dr. Laxmi Narayan Goit 1* and Prof. Dr. Yang Shaning 2 1 Department of Cardiology, the first affiliated Hospital of Yangtze University, Jingzhou, Hubei, P.R China. 2 Department
DOBUTamine INJECTION, USP R x only
 DOBUTamine INJECTION, USP R x only DESCRIPTION Dobutamine Injection, USP is 1,2-benzenediol, 4-[2-[[3-(4-hydro-xyphenyl)-1- methylpropyl]amino]ethyl]-hydrochloride, (±). It is a synthetic catecholamine.
DOBUTamine INJECTION, USP R x only DESCRIPTION Dobutamine Injection, USP is 1,2-benzenediol, 4-[2-[[3-(4-hydro-xyphenyl)-1- methylpropyl]amino]ethyl]-hydrochloride, (±). It is a synthetic catecholamine.
Congestive Heart Failure
 Congestive Heart Failure (CHF) Congestive Heart Failure - 2007 Edward JN Ishac. Ph.D. Associate Professor, Dept. Pharmacology & Toxicology Office: Smith 742; Tel: 828 2127 eishac@vcu.edu Heart failure:
Congestive Heart Failure (CHF) Congestive Heart Failure - 2007 Edward JN Ishac. Ph.D. Associate Professor, Dept. Pharmacology & Toxicology Office: Smith 742; Tel: 828 2127 eishac@vcu.edu Heart failure:
Fundamentals of Pharmacology for Veterinary Technicians Chapter 8
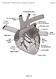 Figure 8-1 Figure 8-2 Figure 8-3 Figure 8-4 Figure 8-5 Figure 8-7 Figure 8-8 Figure 8-9 TABLE 8-1 Blood Flow Through the Heart The right atrium receives blood from all tissues, except the lungs, through
Figure 8-1 Figure 8-2 Figure 8-3 Figure 8-4 Figure 8-5 Figure 8-7 Figure 8-8 Figure 8-9 TABLE 8-1 Blood Flow Through the Heart The right atrium receives blood from all tissues, except the lungs, through
Composition Each ml of Ventol solution for inhalation contains 5 mg Salbutamol (as sulphate).
 VENTOL Composition Each ml of Ventol solution for inhalation contains 5 mg Salbutamol (as sulphate). Respiratory Solution Action Salbutamol is a short-acting, relatively selective beta2-adrenoceptor agonist.
VENTOL Composition Each ml of Ventol solution for inhalation contains 5 mg Salbutamol (as sulphate). Respiratory Solution Action Salbutamol is a short-acting, relatively selective beta2-adrenoceptor agonist.
Intravenous Infusions
 Intravenous Infusions 1) An IV insulin infusion can be used for patients: a) with out of control diabetes b) with DKA (Diabetic Ketoacidosis) c) after a heart attack 2) Hyperglycemia is an adaptive response
Intravenous Infusions 1) An IV insulin infusion can be used for patients: a) with out of control diabetes b) with DKA (Diabetic Ketoacidosis) c) after a heart attack 2) Hyperglycemia is an adaptive response
PEDIATRIC SVT MANAGEMENT
 PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias
 1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
1. Antihypertensive agents 2. Vasodilators & treatment of angina 3. Drugs used in heart failure 4. Drugs used in arrhythmias Only need to know drugs discussed in class At the end of this section you should
DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE
 DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE Mefri Yanni, MD Bagian Kardiologi dan Kedokteran Vaskular RS.DR.M.Djamil Padang The 3rd Symcard Padang, Mei 2013 Outline Diagnosis Diagnosis Treatment options
DIAGNOSIS AND MANAGEMENT OF ACUTE HEART FAILURE Mefri Yanni, MD Bagian Kardiologi dan Kedokteran Vaskular RS.DR.M.Djamil Padang The 3rd Symcard Padang, Mei 2013 Outline Diagnosis Diagnosis Treatment options
Treatment of T Angina reatment of By Ali Alalawi
 Treatment of Angina By Ali Alalawi Determinants of Oxygen Demand Need to improve ratio of: Coronary blood flow / cardiac work Or Cardiac O2 Supply / Cardiac Requirement Coronary Circulation vs Other Circulation
Treatment of Angina By Ali Alalawi Determinants of Oxygen Demand Need to improve ratio of: Coronary blood flow / cardiac work Or Cardiac O2 Supply / Cardiac Requirement Coronary Circulation vs Other Circulation
Systemic Pharmacology Lecture 7: Neuropharmacology
 Systemic Pharmacology Lecture 7: Neuropharmacology Drugs act on Sympathetic NS (adrenergic system) Adrenergic Drugs (Sympathomimetics), adrenergic agonists, or alpha- and beta-adrenergic agonists Antiadrenergic
Systemic Pharmacology Lecture 7: Neuropharmacology Drugs act on Sympathetic NS (adrenergic system) Adrenergic Drugs (Sympathomimetics), adrenergic agonists, or alpha- and beta-adrenergic agonists Antiadrenergic
HTEC 91. Performing ECGs: Procedure. Normal Sinus Rhythm (NSR) Topic for Today: Sinus Rhythms. Characteristics of NSR. Conduction Pathway
 HTEC 91 Medical Office Diagnostic Tests Week 3 Performing ECGs: Procedure o ECG protocol: you may NOT do ECG if you have not signed up! If you are signed up and the room is occupied with people who did
HTEC 91 Medical Office Diagnostic Tests Week 3 Performing ECGs: Procedure o ECG protocol: you may NOT do ECG if you have not signed up! If you are signed up and the room is occupied with people who did
Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood:
 Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood: Cardiac Output (CO) CO=SVxHR (stroke volume x heart rate) Cardiac output: The amount of blood
Towards a Greater Understanding of Cardiac Medications Foundational Cardiac Concepts That Must Be Understood: Cardiac Output (CO) CO=SVxHR (stroke volume x heart rate) Cardiac output: The amount of blood
β adrenergic blockade, a renal perspective Prof S O McLigeyo
 β adrenergic blockade, a renal perspective Prof S O McLigeyo Carvedilol Third generation β blocker (both β 1 and β 2 ) Possesses α 1 adrenergic blocking properties. β: α blocking ratio 7:1 to 3:1 Antioxidant
β adrenergic blockade, a renal perspective Prof S O McLigeyo Carvedilol Third generation β blocker (both β 1 and β 2 ) Possesses α 1 adrenergic blocking properties. β: α blocking ratio 7:1 to 3:1 Antioxidant
Autonomic Nervous System (ANS) وحدة اليوزبكي Department of Pharmacology- College of Medicine- University of Mosul
 Autonomic Nervous System (ANS) د. م. أ. وحدة اليوزبكي Department of Pharmacology- College of Medicine- University of Mosul Sympathetic (Adrenergic) nervous system 3 Objectives At end of this lecture, the
Autonomic Nervous System (ANS) د. م. أ. وحدة اليوزبكي Department of Pharmacology- College of Medicine- University of Mosul Sympathetic (Adrenergic) nervous system 3 Objectives At end of this lecture, the
Adrenergic Receptor as part of ANS
 Adrenergic Receptor as part of ANS Actions of Adrenoceptors Beta-1 adrenergic receptor Located on the myocytes of the heart Specific actions of the β1 receptor include: 0 Increase cardiac output, by 0
Adrenergic Receptor as part of ANS Actions of Adrenoceptors Beta-1 adrenergic receptor Located on the myocytes of the heart Specific actions of the β1 receptor include: 0 Increase cardiac output, by 0
BETALOL Esmolol hydrochloride HIKMA PHARMACEUTICALS
 09-15 BETALOL Esmolol hydrochloride HIKMA PHARMACEUTICALS ACTION Esmolol hydrochloride is a beta 1-selective (cardioselective) adrenergic receptor blocking agent with rapid onset, a very short duration
09-15 BETALOL Esmolol hydrochloride HIKMA PHARMACEUTICALS ACTION Esmolol hydrochloride is a beta 1-selective (cardioselective) adrenergic receptor blocking agent with rapid onset, a very short duration
Respiratory Pharmacology. Manuel Otero Lopez Department of Anaesthetics and Intensive Care Hôpital Européen Georges Pompidou, Paris, France
 Respiratory Pharmacology Manuel Otero Lopez Department of Anaesthetics and Intensive Care Hôpital Européen Georges Pompidou, Paris, France Programme Bronchomotor tone Drugs and factors influencing airway
Respiratory Pharmacology Manuel Otero Lopez Department of Anaesthetics and Intensive Care Hôpital Européen Georges Pompidou, Paris, France Programme Bronchomotor tone Drugs and factors influencing airway
Vasoactive Medications. Matthew J. Korobey Pharm.D., BCCCP Critical Care Clinical Specialist Mercy St. Louis
 Vasoactive Medications Matthew J. Korobey Pharm.D., BCCCP Critical Care Clinical Specialist Mercy St. Louis Objectives List components of physiology involved in blood pressure Review terminology related
Vasoactive Medications Matthew J. Korobey Pharm.D., BCCCP Critical Care Clinical Specialist Mercy St. Louis Objectives List components of physiology involved in blood pressure Review terminology related
EKG Competency for Agency
 EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
EKG Competency for Agency Name: Date: Agency: 1. The upper chambers of the heart are known as the: a. Atria b. Ventricles c. Mitral Valve d. Aortic Valve 2. The lower chambers of the heart are known as
Titrating Critical Care Medications
 Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
Titrating Critical Care Medications Chad Johnson, MSN (NED), RN, CNCC(C), CNS-cc Clinical Nurse Specialist: Critical Care and Neurosurgical Services E-mail: johnsoc@tbh.net Copyright 2017 1 Learning Objectives
sympatholytics sympatholytics sympatholytics
 sympatholytics sympatholytics sympatholytics CNS-ACTING SYMPATHOPLEGICS Sympathetic brain signals Doesn t affect baroreceptor reflex (no orthostatic hypotension) Methyldopa α-methylne crosses BBB (+) α-adrenoreceptors
sympatholytics sympatholytics sympatholytics CNS-ACTING SYMPATHOPLEGICS Sympathetic brain signals Doesn t affect baroreceptor reflex (no orthostatic hypotension) Methyldopa α-methylne crosses BBB (+) α-adrenoreceptors
Core Safety Profile. Pharmaceutical form(s)/strength: Film-coated tablets 1.25 mg, 2.5 mg, 3.75 mg, 5 mg, 7.5 mg and 10 mg. Date of FAR:
 Core Safety Profile Active substance: Bisoprolol Pharmaceutical form(s)/strength: Film-coated tablets 1.25 mg, 2.5 mg, 3.75 mg, 5 mg, 7.5 mg and 10 mg P - RMS: FI/H/PSUR/0002/002 Date of FAR: 13.12.2011
Core Safety Profile Active substance: Bisoprolol Pharmaceutical form(s)/strength: Film-coated tablets 1.25 mg, 2.5 mg, 3.75 mg, 5 mg, 7.5 mg and 10 mg P - RMS: FI/H/PSUR/0002/002 Date of FAR: 13.12.2011
Prof dr Aleksandar Raskovic DIRECT VASODILATORS
 Prof dr Aleksandar Raskovic DIRECT VASODILATORS Direct vasodilators Minoxidil (one of the most powerful peripheral arterial dilators) Opening of KATP channels, efflux of K, lose of Ca and smooth muscle
Prof dr Aleksandar Raskovic DIRECT VASODILATORS Direct vasodilators Minoxidil (one of the most powerful peripheral arterial dilators) Opening of KATP channels, efflux of K, lose of Ca and smooth muscle
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
BLOCADRIL. Composition Blocadril 10 Tablets Each tablet contains Propranolol hydrochloride 10 mg.
 BLOCADRIL Composition Blocadril 10 Tablets Each tablet contains Propranolol hydrochloride 10 mg. Tablets Blocadril 40 Tablets Each tablet contains Propranolol hydrochloride 40 mg. Action Propranolol is
BLOCADRIL Composition Blocadril 10 Tablets Each tablet contains Propranolol hydrochloride 10 mg. Tablets Blocadril 40 Tablets Each tablet contains Propranolol hydrochloride 40 mg. Action Propranolol is
CSI Skills Lab #5: Arrhythmia Interpretation and Treatment
 CSI 202 - Skills Lab #5: Arrhythmia Interpretation and Treatment Origins of the ACLS Approach: CSI 202 - Skills Lab 5 Notes ACLS training originated in Nebraska in the early 1970 s. Its purpose was to
CSI 202 - Skills Lab #5: Arrhythmia Interpretation and Treatment Origins of the ACLS Approach: CSI 202 - Skills Lab 5 Notes ACLS training originated in Nebraska in the early 1970 s. Its purpose was to
Clinical Pathway: Management Of The Life-Threatening Overdose
 Clinical Pathway: Management Of The Life-Threatening Overdose Intravenous access Oxygen Pulse oximetry n-invasive blood pressure monitoring Accu-Check ECG monitoring and ECG Chest x-ray Respiratory depression?
Clinical Pathway: Management Of The Life-Threatening Overdose Intravenous access Oxygen Pulse oximetry n-invasive blood pressure monitoring Accu-Check ECG monitoring and ECG Chest x-ray Respiratory depression?
a lecture series by SWESEMJR
 Electrolyte disturbances Hypokalaemia Decreased extracellular potassium increases excitability in the myocardial cells and consequently the effect of very severe hypokalaemia is ventricular arrhythmia.
Electrolyte disturbances Hypokalaemia Decreased extracellular potassium increases excitability in the myocardial cells and consequently the effect of very severe hypokalaemia is ventricular arrhythmia.
RESPIRATORY PHARMACOLOGY - ASTHMA. Primary Exam Teaching - Westmead ED
 RESPIRATORY PHARMACOLOGY - ASTHMA Primary Exam Teaching - Westmead ED Sympathomimetic agents MOA: relax airway smooth muscle and inhibit broncho constricting mediators from mast cells May also inhibit
RESPIRATORY PHARMACOLOGY - ASTHMA Primary Exam Teaching - Westmead ED Sympathomimetic agents MOA: relax airway smooth muscle and inhibit broncho constricting mediators from mast cells May also inhibit
DRUGS USED TO TREAT HYPERTENSION BY ALI ALALAWI
 DRUGS USED TO TREAT HYPERTENSION BY ALI ALALAWI 3. Vasodilators Drugs which dilate blood vessels ( decrease peripheral vascular resistance) by acting on smooth muscle cells through non-autonomic mechanisms:
DRUGS USED TO TREAT HYPERTENSION BY ALI ALALAWI 3. Vasodilators Drugs which dilate blood vessels ( decrease peripheral vascular resistance) by acting on smooth muscle cells through non-autonomic mechanisms:
TELEMETRY EXAM. 1. Match the numeral in the right column with the correct drug in the left column. a. Pronestyl 1. Hypotension
 TELEMETRY EXAM 1. Match the numeral in the right column with the correct drug in the left column. a. Pronestyl 1. Hypotension b. Digitalis 2. Tachycardias c. Potassium 3. Assists in repolarization d. Inderal
TELEMETRY EXAM 1. Match the numeral in the right column with the correct drug in the left column. a. Pronestyl 1. Hypotension b. Digitalis 2. Tachycardias c. Potassium 3. Assists in repolarization d. Inderal
Basic Fluid and Electrolytes
 Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Cardiovascular Disorders. Heart Disorders. Diagnostic Tests for CV Function. Bio 375. Pathophysiology
 Cardiovascular Disorders Bio 375 Pathophysiology Heart Disorders Heart disease is ranked as a major cause of death in the U.S. Common heart diseases include: Congenital heart defects Hypertensive heart
Cardiovascular Disorders Bio 375 Pathophysiology Heart Disorders Heart disease is ranked as a major cause of death in the U.S. Common heart diseases include: Congenital heart defects Hypertensive heart
Salicylate (Aspirin) Ingestion California Poison Control Background 1. The prevalence of aspirin-containing analgesic products makes
 Salicylate (Aspirin) Ingestion California Poison Control 1-800-876-4766 Background 1. The prevalence of aspirin-containing analgesic products makes these agents, found in virtually every household, common
Salicylate (Aspirin) Ingestion California Poison Control 1-800-876-4766 Background 1. The prevalence of aspirin-containing analgesic products makes these agents, found in virtually every household, common
Adult Drug Reference. Dopamine Drip Chart. Pediatric Drug Reference. Pediatric Drug Dosage Charts DRUG REFERENCES
 Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
Adult Drug Reference Dopamine Drip Chart Pediatric Drug Reference Pediatric Drug Dosage Charts DRUG REFERENCES ADULT DRUG REFERENCE Drug Indication Adult Dosage Precautions / Comments ADENOSINE Paroxysmal
TILAZEM. Diltiazem hydrochloride 240 mg
 Tilazem Capsules Page 1 of 9 TILAZEM Diltiazem hydrochloride SCHEDULING STATUS: S3 PROPRIETARY NAME (AND DOSAGE FORM): TILAZEM 180 CR (controlled-release capsule) TILAZEM 240 CR (controlled-release capsule)
Tilazem Capsules Page 1 of 9 TILAZEM Diltiazem hydrochloride SCHEDULING STATUS: S3 PROPRIETARY NAME (AND DOSAGE FORM): TILAZEM 180 CR (controlled-release capsule) TILAZEM 240 CR (controlled-release capsule)
ANTI-ARRHYTHMICS AND WARFARIN. Dr Nithish Jayakumar
 ANTI-ARRHYTHMICS AND WARFARIN Dr Nithish Jayakumar Contents 1. Anti-arrhythmics Pacemaker and myocardial potentials Drug classes mechanisms; s/e; contra-indications Management of common arrhythmias 2.
ANTI-ARRHYTHMICS AND WARFARIN Dr Nithish Jayakumar Contents 1. Anti-arrhythmics Pacemaker and myocardial potentials Drug classes mechanisms; s/e; contra-indications Management of common arrhythmias 2.
7/7/ CHD/MI LVH and LV dysfunction Dysrrhythmias Stroke PVD Renal insufficiency and failure Retinopathy. Normal <120 Prehypertension
 Prevalence of Hypertension Hypertension: Diagnosis and Management T. Villela, M.D. Program Director University of California, San Francisco-San Francisco General Hospital Family and Community Medicine
Prevalence of Hypertension Hypertension: Diagnosis and Management T. Villela, M.D. Program Director University of California, San Francisco-San Francisco General Hospital Family and Community Medicine
Drug Therapy of Heart Failure. Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014
 Drug Therapy of Heart Failure Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014 Drug Therapy of Heart Failure Definition of Heart Failure Causes Classifications
Drug Therapy of Heart Failure Munir Gharaibeh, MD, PhD, MHPE Faculty of Medicine, The University of Jordan November, 2014 Drug Therapy of Heart Failure Definition of Heart Failure Causes Classifications
Antihypertensives. Diagnostic category
 Measurement of blood pressure At first assessment, take both arms then choose the one with the higher reading. Beware of orthostatic hypotension. Measure BP in sitting position, and repeat after patient
Measurement of blood pressure At first assessment, take both arms then choose the one with the higher reading. Beware of orthostatic hypotension. Measure BP in sitting position, and repeat after patient
