Thrombus Localization with Emergency Cerebral CT
|
|
|
- Madeline Alexander
- 5 years ago
- Views:
Transcription
1 Thrombus Localization with Emergency Cerebral CT Thomas Tomsick, ' Thomas Brott, William Barsan, Joseph Broderick, E. Clarke Haley, and Judith Spilker Purpose: To determine the prevalence of the hyperdense middle cerebral artery sign (HMCAS) in an acute stroke population (treated with intravenous tissue plasminogen activator (tpa) within 90 minutes of stroke onset); to correlate the presence/absence of the sign with arteriographic findings; and to correlate the HMCAS with the volume of subsequent infarction. Patients and Methods: patients wtih acute ischemic stroke underwent CT to exclude cerebral hemorrhage and were then treated with intravenous tpa. The neuroradiologist, blinded to the clinical and arteriographic data, sought the HMCAS on the initial and subsequent scans. Results: The HMCAS was detected by CT in 9 of (.%) patients (one false positive). Arteriograms in of the true positive patients confirmed the CT -predicted middle cerebral artery segment in. The patients developed infarcts larger than patients not exhibiting the sign ( cc vs cc, P <.00). Conclusion: The HMCAS does predict middle cerebral artery occlusion and subsequent development of a large infarct. Index terms: Arteries, cerebral, middle (MCA); Brain, infarction; Arteries, stenosis and occlusion AJNR :7-6, January / February 99 The hyperdense middle cerebral artery sign (HMCAS) on computed tomography (CT) has been shown to be a marker for thrombus in the middle cerebral artery (MCA) (-). In two previous stroke therapy studies, six patients exhibiting the sign (HMCAS+ patients) developed larger infarcts, on average, than patients not exhibiting the sign (HMCAS- patients) (). Based on those observations, we hypothesized that the sign might occur frequently enough in an acute stroke population to allow some prediction of infarct volume. Furthermore, the sign might hold promise as a marker to predict patterns of response to thrombolytic therapy, including such adverse effects as hemorrhagic transformation Received March 6, 99; revision requested April 6; revision received August 9; final acceptance August. Presented in part at the th International Joint Conference on Stroke and Cerebral Circulation, Orlando, FL, 990. This work was supported by National Institute of Neurological and Communicative Disorders and Stroke grant NOl-NS--. Departments of Radiology, Neurology, Emergency Medicine, University of Cincinnati, Cincinnati, OH Address reprint requests to T. Tomsick, Department of Radiology, University of Cincinnati, Bethesda Avenue, Cincinnati, OH University of Virginia, Charlottesville, VA 90. AJNR :7-6, Jan/ Feb / 9/ 0-07 American Society of Neuroradiology 7 (, 6) in successfully recanalized vessels (7). If the HMCAS can offer this information, its status would be elevated from an observational curiosity to a useful clinical tool. The purpose of this study was: ) to determine the prevalence of the HMCAS in an acute stroke population; ) to correlate the presence or absence of the sign with subsequent arteriographic findings where possible; and ) to correlate the HMCAS with the volume of subsequent infarction. Methods Fifty-five patients with acute ischemic stroke had a CT scan to exclude cerebral hemorrhage and then were treated with intravenous tpa within 90 minutes of symptom onset. The tpa was administered over minutes according to a dose-escalation design, and, accordingly, some patients received low doses and others received higher doses (mean dose 7.96 mg; interquartile range -70 mg). Patients were excluded from the study () if they were patients older than age 0, had severe hypertension, were using anticoagulants, or had only an isolated sensory deficit or ataxia. Patients were not excluded on the basis of the presumed ischemic stroke type (eg, Lacunar stroke patients were eligible), but those with only a sensory deficit or with isolated ataxia were excluded. The neuroradiologist, blinded to clinical and arteriographic data, sought the HMCAS on the initial scan, and examined subsequent scans for its
2 AJNR:, January / February 99 Fig.. CT categories I-IV on the left, from above downward, in patients 9,, 9, and, respectively. persistence or disappea rance. The initial scans were performed with a slice thickness of 0 mm in 9 patients, with 9 mm in one patient, with mm in nine patients, and with mm in six patients. The HMCAS (MCA denser than its counterpart, and denser than any visualized artery or vein), was categorized according to the most proximal MCA segment thought to be involved on CT: CT category I, proximal M segment; CT category II, distal M or M -M junction; CT category Ill, multiple M segments; CT category IV, single M segm ent (Figs., A, A, A, and A). Subsequent arteriagrams were examined for thromboembolism, and the segm ents of vessel occlusion were classified, modified according to the m ethod of Saito: pattern, proximal MCA (M ) occlusion; pattern, MCA trunk (M ) distal to lenticulostriate arteries; pattern, two or more M segment occlusions; pattern, single M occlusion; pattern, single or multiple M occlusions (9). Infarct/edema volumes in surviving patients were measured using a pen-trace technique (0) on subsequent scans at - hours, 7-0 days, and months (Fig. 6). Clinically, the subjects were examined neurologically with a standardized examination scale (NIH Stroke Scale) () prior to tpa treatment and six times following the initiation of treatment, including at seven days. Statistical analysis was performed with nonparametric techniques, including the Wilcoxan rank sum test. Results The HMCAS was present in 9 patients (Table ). One of the determinations was falsely positive, being localized to the hemisphere contralateral to the clinically involved hemisphere and the angiographically-identified M thrombus. The mean infarct volume in the true-positive HMCAS was cc (interquartile range 7- cc). The mean infarct volume in the HMCAS- was cc (interquartile range 0-6 cc). This difference is statistically significant (P <.00). Table summarizes infarct volumes according to CT category of MCA segment involved. Mean volumes were generally higher the more proximal the MCA segment involved, but statistical correlation could not be established. Table summarizes arteriographic correlation in the HMCAS+ patients who underwent cerebral arteriography. Perfect correlation (presence of occlusion on arteriogram in the exact segment of MCA predicted) was present in / arteriagrams performed a mean. days (range -7) post-treatment. Table summarizes data on arteriograms performed in 7 HMCAS- patients that exhibited: two vertebral and one basilar artery occlusion; two internal carotid artery (ICA) occlusions extending into the M and M segments, respectively; one embolic proximal M ; four distal M ; two M; and five M occlusions. Discussion The prevalence of the HMCAS in this study was.% (9/). As previously shown, identification of the HMCAS by CT is a subjective exercise that lacks universal agreement. The specificity and positive predictive value have been shown to be high despite lack of total interobserver agreement (). Certain individual case-examples provide clear, unequivocal evidence of thromboembolism. Arteriographic correlation was obtained in patients, including / true-positive HMCAS+ patients. Arteriographic occlusion correlated with HMCAS+ CT category in / arteriograms (Table ). One discrepancy occurred in a CT category IV patient whose arteriogram on day exhibited M emboli, while her 7-day CT exhibited infarction, including the lenticulostriate distribution. The other exception occurred in act category I patient who exhibited distal M narrowing and M occlusions on day. It is postulated that the more proximal embolus suspected on CT
3 A B c Fig.. A, CT ca tegory I HMCAS (arrow) on the left (patient ). B, Pattern occlusion of proximal M, segment. C, Corticocortical collaterals fill the M segments within sec. D, Seven-day infarct in the lenticulostriate distribution of 6 cc. D A B Fig.. A, CT category I HMCAS on left (patient ). B, Anteroposterior RCC arteriogram documents poor collateral flow into the occluded MCA-ICA system at hr. C, Seven-day infarct of 7 cc. c
4 60 AJNR:, January / February 99 Fig.. A, CT category II HMCAS on right (patient 0)., A nteroposterior RCC arteriogram shows near complete distal M, occlusion, extending into M segments, on day. Some lenticulostriate branches opacify, while others are occluded. C, Seven-day infarct volume of 6 cc includes the lenticulostriate distributions, with minimal petechial hemorrhagic change. A c either lysed or passed distally prior to arteriography in both these patients. Of the HMCAS- patients who underwent arteriography, seven showed no intracranial occlusion, and three had vertebrobasilar occlusions. Thus proven thrombi/emboli in the MCA of patients evaded CT detection. Therefore the negative predictive value of an absent HMCAS in excluding MCA thrombus is low (0/ =.6%). Mean CT infarct volume of HMCASpatients with proven MCA occlusive disease was 0 cc (range 0- cc). The frequencies of arteriographically documented ICA occlusion (7 /,.%) and MCA occlusion (/,.%) in all patients who underwent arteriography are within the range of occurrence in other stroke studies (7,,, ). The presence of the HMCAS does predict development of a large infarct with few exceptions, despite treatment with intravenous tpa. CT category I (proximal M ) involvement predicted an infarct of 00 cc or greater in eight of nine patients. Infarct patterns involved the central
5 AJNR:, January / February 99 6 Fig.. A, CT ca tegory IV HMCAS on left (arrow) (patient )., Recanalizing occlusion in angular artery (arrows) at hr. C, Seven-day infarct = 7 cc. basal ganglia region in all patients, indicating lenticulostriate-distribution occlusion, and infarct patterns involved the cortical regions, indicating cortical branch-distribution involvement with inadequate cortical collaterals, in eight of nine patients. The smallest infarct (6 cc) developed in a patient with an M embolus and excellent corticocortical anastomoses from both the anterior cerebral artery and posterior cerebral artery (Fig. ). The largest infarct occurred in a patient with ICA occlusion extending into the M segment and poor corticocortical anastomoses (Fig. ). Positive correlation of arteriographic findings with infarct location and size has been previously noted (9,. 6). CT category II (distal M -M junction) involvement in four patients also presaged a large infarct (-cc mean volume, range 7- cc). Again infarct volume was smallest with incomplete M occlusion, combined with good distal corticocortical anastomosis (Figs. and ). CT category Ill (multiple M ) involvement occurred in only one patient, but the volume of 0 cc is virtually identical to the CT category II (distal M ) mean volume (Figs. and 6). Four CT category IV patients developed mean infarct volume
6 6 AJNR:, January/February 99 Fig. 6. CT category Ill patient 9 (Fig. ), demonstrates 7-day volume = 0 cc, with petechial hemorrhagic change. TABLE : 7-Day infarct volume and arteriographic findings in 9 HMCAS patients Patient Scan Section Thickness 7 -Day Infarct Volume (cc) Pattern Arteriographic Occlusion Arteriogram Day. SB. MP. EG. MM. ws 6. JV 7. JB. NE 9. LM 0. DG. sc. JP. NC. AA. WH 6. AB 7. JC'. VB 9. AE ICA+ ICA+ ICA+ ICA+ ICA+ N/A 7 Note.-Outline of patient population: CT slice thickness; infarct volume within 7 days; pattern of arteriographic occlusion (ICA = internal carotid artery occlusion; = M proximal; = M distal to lenticulostriates; = multiple M ; = single M ; = distal M, M ; PCA = posterior cerebral artery); arteriogram day ( = no arteriogram). False+: HMCAS suspected on side opposite MCA occlusion. of approximately half that of CT category lll, as might theoretically be expected (Figs. and ). Therefore, a predictable pattern of infarct volumes do occur depending on the MCA segment involved (Table ), as well as on the collateral flow. This analysis suggests that the relatively frequent HMCAS correlates with arteriographic findings and is associated with development of large infarcts despite tpa therapy, volumetrically predictable based on identification of the MCA segment involved on CT. That such excellent angio-
7 AJNR:, January / February 99 6 TABLE : Summary of mean and range volumes of infarct/edema at 7-0 days in each HMCAS category Category Number Mean Volume (cc) Range (cc) II 7- Ill 0 0 IV patients less likely to achieve a satisfactory outcome with standard therapy, or even with experimental intravenous thrombolysis. The HMCAS combined with an immediate arteriogram to demonstrate inadequacy of collateral flow may indicate the need for more aggressive therapy, such as intraarterial thrombolysis. TABLE : Arteriographic correlation indicating the number of arteriograms performed in each CT category and the number confirming the CT-predicted location of the filling defect CT Category II Ill IV No. of Arteriograms 7 Correlation TABLE : Arteriographic findings in arteriogram s performed in 7 HMCAS-patients MCA occlusion Pattern and ICA occlusion Pattern and ICA occlusion Pattern Pattern Pattern Pattern Pattern ICA stenosis (dissection) Vertebrobasilar occlusion Normal Total graphic correlation was obtained raises the question that intravenous tpa in doses used may be inefficient in recanalizing occluded cerebral arteries. Other questions that need to be answered regarding the HMCAS and thrombolytic therapy include: Is there any differences between HMCAS+ and HMCAS- patients in their response to treatment? Does the HMCAS, as prima facie evidence of arterial occlusion, predispose to hemorrhagic transformation in the recanalization phase ()? Several randomized trials of thrombolytic therapy for acute ischemic stroke are underway. The radiographic and clinical comparisons of the treated patients to the control patients may provide some answers. The concept that an immediate CT finding can help predict infarct size and possibly predict response to therapy has important implications. This might allow selection of a subgroup of stroke 6 6 Acknowledgment The authors wish to acknowledge Vicki S. Hertzberg for her help in statistical analysis. References. Gacs G, Fox AJ, Barnett HJM, Vinuela F. CT visualization of intracranial arterial thromboembolism. Stroke 9; : Pressman BD, Tourje EJ, T hompson JR. An early CT sign of ischemic infarction: increased density in a cerebral artery. AJNR 97;: 6-6. Schuierer G, Huk W. The unilateral hyperdense m iddle cerebral artery: an early CT-sign of embolism or thrombosis. Neuroradiology 9;0: 0-.. Tomsick T A, Brott TG, Olinger CP, et al. Hyperdense middle cerebral artery: incidence and quantitative significance. Neuroradio/ogy 99;:-. Fisher M, Adams RD. Observations on brain embolism with special reference to mechanism of hemorrhagic infarction. J Neuropatho/ Exp Neuro/ 9; 0: Okada Y, Yamaguchi T, Minematsu K, et al. Hemorrhagic transformation in cerebral embolism. Stroke 99;9: tpa Acute Stroke Study Group. An open multicenter study of the safety and efficacy of va rious doses of tpa in patients with acute stroke: a progress report (abstr). Stroke 990;:. Brott T, Haley C, Levy D, et al. Safety and potential efficacy of tissue plasminogen activator (tpa) for stroke (abstr). Stroke 990; : 9. Saito I, Segawa H, Shiokawa Y, Taniyuchi M, Tsutsumi K. Middle cerebral artery occlusion: correlation of computed tomography and angiography with clinical outcome. S troke 97; : Brott T, Marler JR, Olinger CP, et al. Measurements of acute cerebral infarction: lesion size by computed tomography. Stroke 99;0: 7-7. Brott T, Adams HP, Olinger CP, et al. Measurements of acute cerebral infarction: a clinical exam scale. S troke 99;0:6-70. Tomsick T A, Brott TG, Chambers AA, et al. Hyperdense middle cerebral artery sign on CT : efficacy in detecting middle cerebral artery thrombosis. AJNR 990; :7-77. Solis OJ, Roberson GR, Taveras JM, Mohr J, Pessin M. Cerebral angiography in acute cerebral infa rction. Rev ln teram Radio/ 977;:9-. Olsen TS, Skriver EB, Herning M. Cause of cerebral infarction in the ca rotid territory: its relation to the size and the location of the infarct and to the underlying vascular lesion. Stroke 9; 6:9-66. Fieschi C, Argentino C, Lenzi GL, Sacchetti ML, Toni D, Bozzao L. Clinical and instrumental evaluation of patients with ischemic stroke within the first six hours. J Neural Sci 99;9 :- 6. Bozzao L, Bastianello J, Fantozzi LM, Angelon V, Argentino C, Fieschi C. Correlation of angiographic and sequential CT findings in patients with evolving cerebral infarction. AJNR 99;0:-
Prognostic Value of the Hyperdense Middle Cerebral Artery Sign and Stroke Scale Score before Ultraearly Thrombolytic Therapy
 Prognostic Value of the Hyperdense Middle Cerebral Artery Sign and Stroke Scale Score before Ultraearly Thrombolytic Therapy Thomas Tomsick, Thomas Brott, William Barsan, Joseph Broderick, E. Clarke Haley,
Prognostic Value of the Hyperdense Middle Cerebral Artery Sign and Stroke Scale Score before Ultraearly Thrombolytic Therapy Thomas Tomsick, Thomas Brott, William Barsan, Joseph Broderick, E. Clarke Haley,
Neuro-- radiology 9 Springer-Verlag 1991
 Neuroradiology (1991) 33:207-211 Neuro-- radiology 9 Springer-Verlag 1991 Hyperdense middle cerebral artery CT sign Comparison with angiography in the acute phase of ischemic supratentorial infarction
Neuroradiology (1991) 33:207-211 Neuro-- radiology 9 Springer-Verlag 1991 Hyperdense middle cerebral artery CT sign Comparison with angiography in the acute phase of ischemic supratentorial infarction
Early Angiographic and CT Findings in Patients with Hemorrhagic Infarction in the Distribution of the Middle Cerebral Artery
 1115 Early Angiographic and CT Findings in Patients with Hemorrhagic Infarction in the Distribution of the Middle Cerebral Artery L. Bozzao 1 U. Angeloni S. Bastianello L. M. Fantozzi A. Pierallini C.
1115 Early Angiographic and CT Findings in Patients with Hemorrhagic Infarction in the Distribution of the Middle Cerebral Artery L. Bozzao 1 U. Angeloni S. Bastianello L. M. Fantozzi A. Pierallini C.
Correlation of Early CT Signs in the Deep Middle Cerebral Artery Territories with Angiographically Confirmed Site of Arterial Occlusion
 AJNR Am J Neuroradiol 22:65 659, April 2 Correlation of Early CT Signs in the Deep Middle Cerebral Artery Territories with Angiographically Confirmed Site of Arterial Occlusion Shinichi Nakano, Tsutomu
AJNR Am J Neuroradiol 22:65 659, April 2 Correlation of Early CT Signs in the Deep Middle Cerebral Artery Territories with Angiographically Confirmed Site of Arterial Occlusion Shinichi Nakano, Tsutomu
The occurrence and magnitude of infarctions in
 735 Early Collateral Blood Supply and Late Parenchymal Brain Damage in Patients With Middle Cerebral Artery Luigi Bozzao, MD, Luigi Maria Fantozzi, MD, Stefano Bastianello, MD, Alessandro Bozzao, MD, and
735 Early Collateral Blood Supply and Late Parenchymal Brain Damage in Patients With Middle Cerebral Artery Luigi Bozzao, MD, Luigi Maria Fantozzi, MD, Stefano Bastianello, MD, Alessandro Bozzao, MD, and
Potential of CT Angiography in Acute Ischemic Stroke
 Potential of CT Angiography in Acute Ischemic Stroke Michael Knauth, Rüdiger von Kummer, Olav Jansen, Stefan Hähnel, Arnd Dörfler, and Klaus Sartor PURPOSE: To study the ability of CT angiography to show
Potential of CT Angiography in Acute Ischemic Stroke Michael Knauth, Rüdiger von Kummer, Olav Jansen, Stefan Hähnel, Arnd Dörfler, and Klaus Sartor PURPOSE: To study the ability of CT angiography to show
Comparison of Five Major Recent Endovascular Treatment Trials
 Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
ACUTE STROKE TREATMENT IN LARGE NIHSS PATIENTS. Justin Nolte, MD Assistant Profession Marshall University School of Medicine
 ACUTE STROKE TREATMENT IN LARGE NIHSS PATIENTS Justin Nolte, MD Assistant Profession Marshall University School of Medicine History of Presenting Illness 64 yo wf with PMHx of COPD, HTN, HLP who was in
ACUTE STROKE TREATMENT IN LARGE NIHSS PATIENTS Justin Nolte, MD Assistant Profession Marshall University School of Medicine History of Presenting Illness 64 yo wf with PMHx of COPD, HTN, HLP who was in
Essentials of Clinical MR, 2 nd edition. 14. Ischemia and Infarction II
 14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
Early computed tomographic (CT) ischemic change in the
 Hyperdense Sylvian Fissure MCA Dot Sign A CT Marker of Acute Ischemia Philip A. Barber, MRCP(UK); Andrew M. Demchuk, FRCPC; Mark E. Hudon, FRCPC; J.H. Warwick Pexman, FRCPC; Michael D. Hill, FRCPC; Alastair
Hyperdense Sylvian Fissure MCA Dot Sign A CT Marker of Acute Ischemia Philip A. Barber, MRCP(UK); Andrew M. Demchuk, FRCPC; Mark E. Hudon, FRCPC; J.H. Warwick Pexman, FRCPC; Michael D. Hill, FRCPC; Alastair
Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report
 Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report BY JIRI J. VITEK, M.D., JAMES H. HALSEY, JR., M.D., AND HOLT A. McDOWELL, M.D. Abstract: Occlusion of All Four
Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report BY JIRI J. VITEK, M.D., JAMES H. HALSEY, JR., M.D., AND HOLT A. McDOWELL, M.D. Abstract: Occlusion of All Four
IMAGING IN ACUTE ISCHEMIC STROKE
 IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
IMAGING IN ACUTE ISCHEMIC STROKE
 IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
Collateral Circulation and Outcome after Basilar Artery Thrombolysis
 AJNR Am J Neuroradiol 19:1557 1563, September 1998 Collateral Circulation and Outcome after Basilar Artery Thrombolysis DeWitte T. Cross, III, Christopher J. Moran, Paul T. Akins, Edward E. Angtuaco, Colin
AJNR Am J Neuroradiol 19:1557 1563, September 1998 Collateral Circulation and Outcome after Basilar Artery Thrombolysis DeWitte T. Cross, III, Christopher J. Moran, Paul T. Akins, Edward E. Angtuaco, Colin
Angiographic Assessment of Pial Collaterals as a Prognostic Indicator Following Intra-arterial Thrombolysis for Acute Ischemic Stroke
 AJNR Am J Neuroradiol 26:1789 1797, August 2005 Angiographic Assessment of Pial Collaterals as a Prognostic Indicator Following Intra-arterial Thrombolysis for Acute Ischemic Stroke Gregory A. Christoforidis,
AJNR Am J Neuroradiol 26:1789 1797, August 2005 Angiographic Assessment of Pial Collaterals as a Prognostic Indicator Following Intra-arterial Thrombolysis for Acute Ischemic Stroke Gregory A. Christoforidis,
Acute stroke. Ischaemic stroke. Characteristics. Temporal classification. Clinical features. Interpretation of Emergency Head CT
 Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
The National Institutes of Health Stroke Scale (NIHSS)
 National Institutes of Health Stroke Scale Score and Vessel Occlusion in 252 Patients With Acute Ischemic Stroke Mirjam R. Heldner, MD; Christoph Zubler, MD; Heinrich P. Mattle, MD; Gerhard Schroth, MD;
National Institutes of Health Stroke Scale Score and Vessel Occlusion in 252 Patients With Acute Ischemic Stroke Mirjam R. Heldner, MD; Christoph Zubler, MD; Heinrich P. Mattle, MD; Gerhard Schroth, MD;
Advances in Neuro-Endovascular Care for Acute Stroke
 Advances in Neuro-Endovascular Care for Acute Stroke Ciarán J. Powers, MD, PhD, FAANS Associate Professor Program Director Department of Neurological Surgery Surgical Director Comprehensive Stroke Center
Advances in Neuro-Endovascular Care for Acute Stroke Ciarán J. Powers, MD, PhD, FAANS Associate Professor Program Director Department of Neurological Surgery Surgical Director Comprehensive Stroke Center
The Oxfordshire Community Stroke Project (OCSP) devised
 Relationship Between Pattern of Intracranial Artery Abnormalities on Transcranial Doppler and Oxfordshire Community Stroke Project Clinical Classification of Ischemic Stroke G.E. Mead, MD; J.M. Wardlaw,
Relationship Between Pattern of Intracranial Artery Abnormalities on Transcranial Doppler and Oxfordshire Community Stroke Project Clinical Classification of Ischemic Stroke G.E. Mead, MD; J.M. Wardlaw,
Intracranial Balloon Angioplasty of Acute Terminal Internal Carotid Artery Occlusions
 AJNR Am J Neuroradiol 23:1308 1312, September 2002 Case Report Intracranial Balloon Angioplasty of Acute Terminal Internal Carotid Artery Occlusions Joon K. Song, Edwin D. Cacayorin, Morgan S. Campbell,
AJNR Am J Neuroradiol 23:1308 1312, September 2002 Case Report Intracranial Balloon Angioplasty of Acute Terminal Internal Carotid Artery Occlusions Joon K. Song, Edwin D. Cacayorin, Morgan S. Campbell,
The Predictive Value of Early CT and Angiography for Fatal Hemispheric Swelling in Acute Stroke
 AJNR Am J Neuroradiol 19:839 846, May 1998 The Predictive Value of Early CT and Angiography for Fatal Hemispheric Swelling in Acute Stroke Thomas Kucinski, Christoph Koch, Ulrich Grzyska, Heinz-Jörg Freitag,
AJNR Am J Neuroradiol 19:839 846, May 1998 The Predictive Value of Early CT and Angiography for Fatal Hemispheric Swelling in Acute Stroke Thomas Kucinski, Christoph Koch, Ulrich Grzyska, Heinz-Jörg Freitag,
Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke
 Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Validation of Computed Tomographic Middle Cerebral Artery Dot Sign. An Angiographic Correlation Study
 Validation of Computed Tomographic Middle Cerebral Artery Dot Sign An Angiographic Correlation Study Megan C. Leary, MD; Chelsea S. Kidwell, MD; J. Pablo Villablanca, MD; Sidney Starkman, MD; Reza Jahan,
Validation of Computed Tomographic Middle Cerebral Artery Dot Sign An Angiographic Correlation Study Megan C. Leary, MD; Chelsea S. Kidwell, MD; J. Pablo Villablanca, MD; Sidney Starkman, MD; Reza Jahan,
UPDATES IN INTRACRANIAL INTERVENTION Jordan Taylor DO Metro Health Neurology 2015
 UPDATES IN INTRACRANIAL INTERVENTION Jordan Taylor DO Metro Health Neurology 2015 NEW STUDIES FOR 2015 MR CLEAN ESCAPE EXTEND-IA REVASCAT SWIFT PRIME RECOGNIZED LIMITATIONS IV Alteplase proven benefit
UPDATES IN INTRACRANIAL INTERVENTION Jordan Taylor DO Metro Health Neurology 2015 NEW STUDIES FOR 2015 MR CLEAN ESCAPE EXTEND-IA REVASCAT SWIFT PRIME RECOGNIZED LIMITATIONS IV Alteplase proven benefit
Cerebrovascular Disease lll. Acute Ischemic Stroke. Use of Intravenous Alteplace in Acute Ischemic Stroke Louis R Caplan MD
 Cerebrovascular Disease lll. Acute Ischemic Stroke Use of Intravenous Alteplace in Acute Ischemic Stroke Louis R Caplan MD Thrombolysis was abandoned as a stroke treatment in the 1960s due to an unacceptable
Cerebrovascular Disease lll. Acute Ischemic Stroke Use of Intravenous Alteplace in Acute Ischemic Stroke Louis R Caplan MD Thrombolysis was abandoned as a stroke treatment in the 1960s due to an unacceptable
NEURORADIOLOGY DIL part 4
 NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
11/1/2018. Disclosure. Imaging in Acute Ischemic Stroke 2018 Neuro Symposium. Is NCCT good enough? Keystone Heart Consultant, Stock Options
 Disclosure Imaging in Acute Ischemic Stroke 2018 Neuro Symposium Keystone Heart Consultant, Stock Options Kevin Abrams, M.D. Chief of Radiology Medical Director of Neuroradiology Baptist Hospital, Miami,
Disclosure Imaging in Acute Ischemic Stroke 2018 Neuro Symposium Keystone Heart Consultant, Stock Options Kevin Abrams, M.D. Chief of Radiology Medical Director of Neuroradiology Baptist Hospital, Miami,
MEET 2007: Evaluation and treatment of the stroke and TIA patient for the non-neurointerventionist. neurointerventionist
 MEET 2007: Evaluation and treatment of the stroke and TIA patient for the non-neurointerventionist neurointerventionist Steve Ramee, MD Ochsner Medical Center New Orleans DISCLOSURE Nothing Nothing to
MEET 2007: Evaluation and treatment of the stroke and TIA patient for the non-neurointerventionist neurointerventionist Steve Ramee, MD Ochsner Medical Center New Orleans DISCLOSURE Nothing Nothing to
On Call Guide to CT Perfusion. Updated: March 2011
 On Call Guide to CT Perfusion Updated: March 2011 CT Stroke Protocol 1. Non contrast CT brain 2. CT perfusion: contrast 40cc bolus dynamic imaging at 8 slice levels ~ 60 sec creates perfusion color maps
On Call Guide to CT Perfusion Updated: March 2011 CT Stroke Protocol 1. Non contrast CT brain 2. CT perfusion: contrast 40cc bolus dynamic imaging at 8 slice levels ~ 60 sec creates perfusion color maps
Even in the era of diffusion and perfusion-weighted MRI,
 The Hyperdense Posterior Cerebral Artery Sign A Computed Tomography Marker of Acute Ischemia in the Posterior Cerebral Artery Territory Timo Krings, MD; Dagmar Noelchen, MD; Michael Mull, MD; Klaus Willmes,
The Hyperdense Posterior Cerebral Artery Sign A Computed Tomography Marker of Acute Ischemia in the Posterior Cerebral Artery Territory Timo Krings, MD; Dagmar Noelchen, MD; Michael Mull, MD; Klaus Willmes,
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Thrombolytic Therapy in Acute Occlusion of the Intracranial Internal Carotid Artery Bifurcation
 Thrombolytic Therapy in Acute Occlusion of the Intracranial Internal Carotid Artery Bifurcation Olav Jansen, Rüdiger von Kummer, Michael Forsting, Werner Hacke, and Klaus Sartor PURPOSE: To evaluate efficacy
Thrombolytic Therapy in Acute Occlusion of the Intracranial Internal Carotid Artery Bifurcation Olav Jansen, Rüdiger von Kummer, Michael Forsting, Werner Hacke, and Klaus Sartor PURPOSE: To evaluate efficacy
EMBOLIC OCCLUSION OF THE SUPERIOR AND IN- FERIOR DIVISIONS OF THE MIDDLE CEREBRAL ARTERY WITH ANGIOGRAPHIC-CLINICAL CORRELATION*
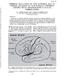 MARCH, 1976 Pre EMBOLIC OCCLUSION OF THE SUPERIOR AND IN- FERIOR DIVISIONS OF THE MIDDLE CEREBRAL ARTERY WITH ANGIOGRAPHIC-CLINICAL CORRELATION* ABSTRACT: Superior Rolandlc rolandic By L. REED ALTEMUS,
MARCH, 1976 Pre EMBOLIC OCCLUSION OF THE SUPERIOR AND IN- FERIOR DIVISIONS OF THE MIDDLE CEREBRAL ARTERY WITH ANGIOGRAPHIC-CLINICAL CORRELATION* ABSTRACT: Superior Rolandlc rolandic By L. REED ALTEMUS,
The National Institute of Neurological Disorders and Stroke
 ORIGINAL RESEARCH A. Srinivasan M. Goyal P. Stys M. Sharma C. Lum Microcatheter Navigation and Thrombolysis in Acute Symptomatic Cervical Internal Carotid Occlusion BACKGROUND AND PURPOSE: The treatment
ORIGINAL RESEARCH A. Srinivasan M. Goyal P. Stys M. Sharma C. Lum Microcatheter Navigation and Thrombolysis in Acute Symptomatic Cervical Internal Carotid Occlusion BACKGROUND AND PURPOSE: The treatment
Brain Attack. Strategies in the Management of Acute Ischemic Stroke: Neuroscience Clerkship. Case Medical Center
 Brain Attack Strategies in the Management of Acute Ischemic Stroke: Neuroscience Clerkship Stroke is a common and devastating disorder Third leading antecedent of death in American men, and second among
Brain Attack Strategies in the Management of Acute Ischemic Stroke: Neuroscience Clerkship Stroke is a common and devastating disorder Third leading antecedent of death in American men, and second among
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
Although moyamoya disease, a rare cerebrovascular occlusive
 Renal Artery Lesions in Patients With Moyamoya Disease Angiographic Findings Ichiro Yamada, MD; Yoshiro Himeno, MD; Yoshiharu Matsushima, MD; Hitoshi Shibuya, MD Background and Purpose Renal artery lesions
Renal Artery Lesions in Patients With Moyamoya Disease Angiographic Findings Ichiro Yamada, MD; Yoshiro Himeno, MD; Yoshiharu Matsushima, MD; Hitoshi Shibuya, MD Background and Purpose Renal artery lesions
Endovascular Treatment for Acute Ischemic Stroke
 ular Treatment for Acute Ischemic Stroke Vishal B. Jani MD Assistant Professor Interventional Neurology, Division of Department of Neurology. Creighton University/ CHI health Omaha NE Disclosure None 1
ular Treatment for Acute Ischemic Stroke Vishal B. Jani MD Assistant Professor Interventional Neurology, Division of Department of Neurology. Creighton University/ CHI health Omaha NE Disclosure None 1
AMSER Case of the Month: March 2019
 AMSER Case of the Month: March 2019 62 year-old male with left-sided weakness Ashley Graziano OMS IV, Lake Erie College of Osteopathic Medicine Erik Yannone MD, Charles Q. Li MD, Warren Chang MD, Matthew
AMSER Case of the Month: March 2019 62 year-old male with left-sided weakness Ashley Graziano OMS IV, Lake Erie College of Osteopathic Medicine Erik Yannone MD, Charles Q. Li MD, Warren Chang MD, Matthew
I schaemic stroke is currently the third leading cause
 1426 PAPER The probability of middle cerebral artery MRA flow signal abnormality with quantified CT ischaemic change: targets for future therapeutic studies P A Barber, A M Demchuk, M D Hill, J H Warwick
1426 PAPER The probability of middle cerebral artery MRA flow signal abnormality with quantified CT ischaemic change: targets for future therapeutic studies P A Barber, A M Demchuk, M D Hill, J H Warwick
Acute Ischemic Stroke Imaging. Ronald L. Wolf, MD, PhD Associate Professor of Radiology
 Acute Ischemic Stroke Imaging Ronald L. Wolf, MD, PhD Associate Professor of Radiology Title of First Slide of Substance An Illustrative Case 2 Disclosures No financial disclosures Off-label uses of some
Acute Ischemic Stroke Imaging Ronald L. Wolf, MD, PhD Associate Professor of Radiology Title of First Slide of Substance An Illustrative Case 2 Disclosures No financial disclosures Off-label uses of some
Intra-arterial thrombolysis (IAT) has the potential to rescue
 Published September 3, 2008 as 10.3174/ajnr.A1276 ORIGINAL RESEARCH G.A. Christoforidis C. Karakasis Y. Mohammad L.P. Caragine M. Yang A.P. Slivka Predictors of Hemorrhage Following Intra-Arterial Thrombolysis
Published September 3, 2008 as 10.3174/ajnr.A1276 ORIGINAL RESEARCH G.A. Christoforidis C. Karakasis Y. Mohammad L.P. Caragine M. Yang A.P. Slivka Predictors of Hemorrhage Following Intra-Arterial Thrombolysis
NHL Journal of Medical Sciences/July 2014/Vol 3/Issue 2 18
 Research article NIHSS Score: A handy tool to predict vascular occlusion in acute ischemic stroke Ronak Shah*, Chintal Vyas**, Jyoti Vora*** *Senior Resident, **Assistant Professor, ***Associate Professor,
Research article NIHSS Score: A handy tool to predict vascular occlusion in acute ischemic stroke Ronak Shah*, Chintal Vyas**, Jyoti Vora*** *Senior Resident, **Assistant Professor, ***Associate Professor,
Mechanical thrombectomy in Plymouth. Will Adams. Will Adams
 Mechanical thrombectomy in Plymouth Will Adams Will Adams History Intra-arterial intervention 1995 (NINDS) iv tpa improved clinical outcome in patients treated within 3 hours of ictus but limited recanalisation
Mechanical thrombectomy in Plymouth Will Adams Will Adams History Intra-arterial intervention 1995 (NINDS) iv tpa improved clinical outcome in patients treated within 3 hours of ictus but limited recanalisation
Significant Relationships
 Opening Large Vessels During Acute Ischemic Stroke Significant Relationships Wade S Smith, MD, PhD Director UCSF Neurovascular Service Professor of Neurology Daryl R Gress Endowed Chair of Neurocritical
Opening Large Vessels During Acute Ischemic Stroke Significant Relationships Wade S Smith, MD, PhD Director UCSF Neurovascular Service Professor of Neurology Daryl R Gress Endowed Chair of Neurocritical
Judicious use of thrombolytic agents has greatly improved the
 Predictors of Clinical Improvement, Angiographic Recanalization, and Intracranial Hemorrhage After Intra-Arterial Thrombolysis for Acute Ischemic Stroke J.I. Suarez, MD; J.L. Sunshine, MD; R. Tarr, MD;
Predictors of Clinical Improvement, Angiographic Recanalization, and Intracranial Hemorrhage After Intra-Arterial Thrombolysis for Acute Ischemic Stroke J.I. Suarez, MD; J.L. Sunshine, MD; R. Tarr, MD;
Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients
 AJNR Am J Neuroradiol 0:7, January 999 Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients Birgit Ertl-Wagner, Tobias Brandt, Christina Seifart,
AJNR Am J Neuroradiol 0:7, January 999 Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients Birgit Ertl-Wagner, Tobias Brandt, Christina Seifart,
ACUTE STROKE IMAGING
 ACUTE STROKE IMAGING Mahesh V. Jayaraman M.D. Director, Inter ventional Neuroradiology Associate Professor Depar tments of Diagnostic Imaging and Neurosurger y Alper t Medical School at Brown University
ACUTE STROKE IMAGING Mahesh V. Jayaraman M.D. Director, Inter ventional Neuroradiology Associate Professor Depar tments of Diagnostic Imaging and Neurosurger y Alper t Medical School at Brown University
New therapies directed at acute middle cerebral artery
 Regional Angiographic Grading System for Collateral Flow Correlation With Cerebral Infarction in Patients With Middle Cerebral Artery Occlusion Jane J. Kim, MD; Nancy J. Fischbein, MD; Ying Lu, PhD; Daniel
Regional Angiographic Grading System for Collateral Flow Correlation With Cerebral Infarction in Patients With Middle Cerebral Artery Occlusion Jane J. Kim, MD; Nancy J. Fischbein, MD; Ying Lu, PhD; Daniel
Giant Serpentine Aneurysms: Radiographic Features and Endovascular Treatment
 Giant Serpentine Aneurysms: Radiographic Features and Endovascular Treatment Michel E. Mawad and Richard P. Klucznik PURPOSE: To describe the characteristic CT, MR, and angiographic features of giant serpentine
Giant Serpentine Aneurysms: Radiographic Features and Endovascular Treatment Michel E. Mawad and Richard P. Klucznik PURPOSE: To describe the characteristic CT, MR, and angiographic features of giant serpentine
Distal arterial emboli may be sequelae of intravenous (IV)
 ORIGINAL RESEARCH S. King P. Khatri J. Carrozella J. Spilker J. Broderick M. Hill T. Tomsick, for the IMS & IIMS II Investigators Anterior Cerebral Artery Emboli in Combined Intravenous and Intra-arterial
ORIGINAL RESEARCH S. King P. Khatri J. Carrozella J. Spilker J. Broderick M. Hill T. Tomsick, for the IMS & IIMS II Investigators Anterior Cerebral Artery Emboli in Combined Intravenous and Intra-arterial
An intravenous thrombolysis using recombinant tissue
 ORIGINAL RESEARCH I. Ikushima H. Ohta T. Hirai K. Yokogami D. Miyahara N. Maeda Y. Yamashita Balloon Catheter Disruption of Middle Cerebral Artery Thrombus in Conjunction with Thrombolysis for the Treatment
ORIGINAL RESEARCH I. Ikushima H. Ohta T. Hirai K. Yokogami D. Miyahara N. Maeda Y. Yamashita Balloon Catheter Disruption of Middle Cerebral Artery Thrombus in Conjunction with Thrombolysis for the Treatment
Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery
 2011 65 4 239 245 Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery a* a b a a a b 240 65 4 2011 241 9 1 60 10 2 62 17 3 67 2 4 64 7 5 69 5 6 71 1 7 55 13 8 73 1
2011 65 4 239 245 Carotid Endarterectomy for Symptomatic Complete Occlusion of the Internal Carotid Artery a* a b a a a b 240 65 4 2011 241 9 1 60 10 2 62 17 3 67 2 4 64 7 5 69 5 6 71 1 7 55 13 8 73 1
ACUTE ISCHEMIC STROKE. Current Treatment Approaches for Acute Ischemic Stroke
 ACUTE ISCHEMIC STROKE Current Treatment Approaches for Acute Ischemic Stroke EARLY MANAGEMENT OF ACUTE ISCHEMIC STROKE Rapid identification of a stroke Immediate EMS transport to nearest stroke center
ACUTE ISCHEMIC STROKE Current Treatment Approaches for Acute Ischemic Stroke EARLY MANAGEMENT OF ACUTE ISCHEMIC STROKE Rapid identification of a stroke Immediate EMS transport to nearest stroke center
Small Vessel Stroke. Domenico Inzitari Careggi University Hospital Florence (Italy)
 Small Vessel Stroke Domenico Inzitari Careggi University Hospital Florence (Italy) Topics Lacunar stroke The small vessel conundrum Small and large Conclusions Fisher s lacunar syndromes Pure motor hemiparesis
Small Vessel Stroke Domenico Inzitari Careggi University Hospital Florence (Italy) Topics Lacunar stroke The small vessel conundrum Small and large Conclusions Fisher s lacunar syndromes Pure motor hemiparesis
Anatomic Evaluation of the Circle of Willis: MR Angiography versus Intraarterial Digital Subtraction Angiography
 Anatomic Evaluation of the Circle of Willis: MR Angiography versus Intraarterial Digital Subtraction Angiography K. W. Stock, S. Wetzel, E. Kirsch, G. Bongartz, W. Steinbrich, and E. W. Radue PURPOSE:
Anatomic Evaluation of the Circle of Willis: MR Angiography versus Intraarterial Digital Subtraction Angiography K. W. Stock, S. Wetzel, E. Kirsch, G. Bongartz, W. Steinbrich, and E. W. Radue PURPOSE:
Combined Intravenous and Intra-Arterial r-tpa Versus Intra-Arterial Therapy of Acute Ischemic Stroke
 Combined Intravenous and Intra-Arterial r-tpa Versus Intra-Arterial Therapy of Acute Ischemic Stroke Emergency Management of Stroke (EMS) Bridging Trial Christopher A. Lewandowski, MD; Michael Frankel,
Combined Intravenous and Intra-Arterial r-tpa Versus Intra-Arterial Therapy of Acute Ischemic Stroke Emergency Management of Stroke (EMS) Bridging Trial Christopher A. Lewandowski, MD; Michael Frankel,
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine
 Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Vivek R. Deshmukh, MD Director, Cerebrovascular and Endovascular Neurosurgery Chairman, Department of Neurosurgery Providence Brain and Spine Institute The Oregon Clinic Disclosure I declare that neither
Disclosure. Advances in Interventional Neurology. Disclosure. Natural History of Disease 3/15/2018. Vishal B. Jani MD
 Advances in Interventional Neurology Disclosure Vishal B. Jani MD Medical Director Vascular Neurology Consultant Interventional Neurology CHI Health Assistant Professor, Creighton University School of
Advances in Interventional Neurology Disclosure Vishal B. Jani MD Medical Director Vascular Neurology Consultant Interventional Neurology CHI Health Assistant Professor, Creighton University School of
Imaging Stroke: Is There a Stroke Equivalent of the ECG? Albert J. Yoo, MD Director of Acute Stroke Intervention Massachusetts General Hospital
 Imaging Stroke: Is There a Stroke Equivalent of the ECG? Albert J. Yoo, MD Director of Acute Stroke Intervention Massachusetts General Hospital Disclosures Penumbra, Inc. research grant (significant) for
Imaging Stroke: Is There a Stroke Equivalent of the ECG? Albert J. Yoo, MD Director of Acute Stroke Intervention Massachusetts General Hospital Disclosures Penumbra, Inc. research grant (significant) for
Extra- and intracranial tandem occlusions in the anterior circulation - clinical outcome of endovascular treatment in acute major stroke.
 Extra- and intracranial tandem occlusions in the anterior circulation - clinical outcome of endovascular treatment in acute major stroke. Poster No.: C-1669 Congress: ECR 2014 Type: Scientific Exhibit
Extra- and intracranial tandem occlusions in the anterior circulation - clinical outcome of endovascular treatment in acute major stroke. Poster No.: C-1669 Congress: ECR 2014 Type: Scientific Exhibit
Historical. Medical Policy
 Medical Policy Subject: Mechanical Embolectomy for Treatment of Acute Stroke Policy #: SURG.00098 Current Effective Date: 01/01/2016 Status: Revised Last Review Date: 08/06/2015 Description/Scope This
Medical Policy Subject: Mechanical Embolectomy for Treatment of Acute Stroke Policy #: SURG.00098 Current Effective Date: 01/01/2016 Status: Revised Last Review Date: 08/06/2015 Description/Scope This
Measurements of Acute Cerebral Infarction: Lesion Size by Computed Tomography
 87 Measurements of Acute Cerebral Infarction: Lesion Size by Computed Tomography Thomas Brott, MD, John R. Marler, MD, Charles P. Olinger, MD, Harold P. Adams Jr., MD, Thomas Tomsick, MD, William G. Barsan,
87 Measurements of Acute Cerebral Infarction: Lesion Size by Computed Tomography Thomas Brott, MD, John R. Marler, MD, Charles P. Olinger, MD, Harold P. Adams Jr., MD, Thomas Tomsick, MD, William G. Barsan,
Neurological Deterioration in Acute Ischemic Stroke
 Neurological Deterioration in Acute Ischemic Stroke Potential Predictors and Associated Factors in the European Cooperative Acute Stroke Study (ECASS) I A. Dávalos, MD; D. Toni, MD; F. Iweins, MSc; E.
Neurological Deterioration in Acute Ischemic Stroke Potential Predictors and Associated Factors in the European Cooperative Acute Stroke Study (ECASS) I A. Dávalos, MD; D. Toni, MD; F. Iweins, MSc; E.
Neuro-vascular Intervention in Stroke. Will Adams Consultant Neuroradiologist Plymouth Hospitals NHS Trust
 Neuro-vascular Intervention in Stroke Will Adams Consultant Neuroradiologist Plymouth Hospitals NHS Trust Stroke before the mid 1990s Swelling Stroke extension Haemorrhagic transformation Intravenous thrombolysis
Neuro-vascular Intervention in Stroke Will Adams Consultant Neuroradiologist Plymouth Hospitals NHS Trust Stroke before the mid 1990s Swelling Stroke extension Haemorrhagic transformation Intravenous thrombolysis
/ / / / / / Hospital Abstraction: Stroke/TIA. Participant ID: Hospital Code: Multi-Ethnic Study of Atherosclerosis
 Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Multi-Ethnic Study of Atherosclerosis Participant ID: Hospital Code: Hospital Abstraction: Stroke/TIA History and Hospital Record 1. Was the participant hospitalized as an immediate consequence of this
Sinus Venous Thrombosis
 Sinus Venous Thrombosis Joseph J Gemmete, MD FACR, FSIR, FAHA Professor Departments of Radiology and Neurosurgery University of Michigan Hospitals Ann Arbor, MI Outline Introduction Medical Treatment Options
Sinus Venous Thrombosis Joseph J Gemmete, MD FACR, FSIR, FAHA Professor Departments of Radiology and Neurosurgery University of Michigan Hospitals Ann Arbor, MI Outline Introduction Medical Treatment Options
Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke
 Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke Tetsuyoshi Horiuchi, Junpei Nitta, Shigetoshi Ishizaka, Kohei Kanaya, Takao Yanagawa, and Kazuhiro Hongo. Department of Neurosurgery,
Emergency EC-IC bypass for symptomatic atherosclerotic ischemic stroke Tetsuyoshi Horiuchi, Junpei Nitta, Shigetoshi Ishizaka, Kohei Kanaya, Takao Yanagawa, and Kazuhiro Hongo. Department of Neurosurgery,
Perils of Mechanical Thrombectomy in Acute Asymptomatic Large Vessel Occlusion
 Perils of Mechanical Thrombectomy in Acute Asymptomatic Large Vessel Occlusion Aman B. Patel, MD Robert & Jean Ojemann Associate Professor Director, Cerebrovascular Surgery Director, Neuroendovascular
Perils of Mechanical Thrombectomy in Acute Asymptomatic Large Vessel Occlusion Aman B. Patel, MD Robert & Jean Ojemann Associate Professor Director, Cerebrovascular Surgery Director, Neuroendovascular
CEREBRO VASCULAR ACCIDENTS
 CEREBRO VASCULAR S MICHAEL OPONG-KUSI, DO MBA MORTON CLINIC, TULSA, OK, USA 8/9/2012 1 Cerebrovascular Accident Third Leading cause of deaths (USA) 750,000 strokes in USA per year. 150,000 deaths in USA
CEREBRO VASCULAR S MICHAEL OPONG-KUSI, DO MBA MORTON CLINIC, TULSA, OK, USA 8/9/2012 1 Cerebrovascular Accident Third Leading cause of deaths (USA) 750,000 strokes in USA per year. 150,000 deaths in USA
Occlusio Supra Occlusionem: Intracranial Occlusions Following Carotid Thrombosis as Diagnosed by Cerebral Angiography
 Occlusio Supra Occlusionem: Intracranial Occlusions Following Carotid Thrombosis as Diagnosed by Cerebral Angiography BY B. ALBERT RING, M.D. Abstract: Occlusio Supra Occlusionem: Intracranial Occlusions
Occlusio Supra Occlusionem: Intracranial Occlusions Following Carotid Thrombosis as Diagnosed by Cerebral Angiography BY B. ALBERT RING, M.D. Abstract: Occlusio Supra Occlusionem: Intracranial Occlusions
Michael Horowitz, MD Pittsburgh, PA
 Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
Transcranial Doppler ultrasonography (TCD)
 532 Transcranial Doppler Ultrasound Findings in Middle Cerebral Artery Occlusion M. Kaps, MD, M.S. Damian, MD, U. Teschendorf, and W. Dorndorf, MD We evaluated the efficacy of transcranial Doppler ultrasonography
532 Transcranial Doppler Ultrasound Findings in Middle Cerebral Artery Occlusion M. Kaps, MD, M.S. Damian, MD, U. Teschendorf, and W. Dorndorf, MD We evaluated the efficacy of transcranial Doppler ultrasonography
Analysis of DWI ASPECTS and Recanalization Outcomes of Patients with Acute-phase Cerebral Infarction
 J Med Dent Sci 2012; 59: 57-63 Original Article Analysis of DWI ASPECTS and Recanalization Outcomes of Patients with Acute-phase Cerebral Infarction Keigo Shigeta 1,2), Kikuo Ohno 1), Yoshio Takasato 2),
J Med Dent Sci 2012; 59: 57-63 Original Article Analysis of DWI ASPECTS and Recanalization Outcomes of Patients with Acute-phase Cerebral Infarction Keigo Shigeta 1,2), Kikuo Ohno 1), Yoshio Takasato 2),
Stroke/TIA. Tom Bedwell
 Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
Blood Supply. Allen Chung, class of 2013
 Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
Blood Supply Allen Chung, class of 2013 Objectives Understand the importance of the cerebral circulation. Understand stroke and the types of vascular problems that cause it. Understand ischemic penumbra
Distal hyperintense vessels on FLAIR An MRI marker for collateral circulation in acute stroke?
 Distal hyperintense vessels on FLAIR An MRI marker for collateral circulation in acute stroke? K.Y. Lee, MD, PhD L.L. Latour, PhD M. Luby, PhD A.W. Hsia, MD J.G. Merino, MD, MPhil S. Warach, MD, PhD Address
Distal hyperintense vessels on FLAIR An MRI marker for collateral circulation in acute stroke? K.Y. Lee, MD, PhD L.L. Latour, PhD M. Luby, PhD A.W. Hsia, MD J.G. Merino, MD, MPhil S. Warach, MD, PhD Address
Acute Stroke Treatment: Current Trends 2010
 Acute Stroke Treatment: Current Trends 2010 Helmi L. Lutsep, MD Oregon Stroke Center Oregon Health & Science University Overview Ischemic Stroke Neuroprotectant trials to watch for IV tpa longer treatment
Acute Stroke Treatment: Current Trends 2010 Helmi L. Lutsep, MD Oregon Stroke Center Oregon Health & Science University Overview Ischemic Stroke Neuroprotectant trials to watch for IV tpa longer treatment
Translent CT hyperattenuation after intraarterial thrombolysis in stroke. Contrast extravasation or hemorrhage
 Translent CT hyperattenuation after intraarterial thrombolysis in stroke. Contrast extravasation or hemorrhage Poster No.: C-0053 Congress: ECR 2013 Type: Scientific Exhibit Authors: A. Losa Palacios,
Translent CT hyperattenuation after intraarterial thrombolysis in stroke. Contrast extravasation or hemorrhage Poster No.: C-0053 Congress: ECR 2013 Type: Scientific Exhibit Authors: A. Losa Palacios,
The DAWN of a New Era for Wake-up Stroke
 The DAWN of a New Era for Wake-up Stroke Alan H. Yee, D.O. Stroke and Critical Care Neurology Department of Neurology University of California Davis Medical Center Objectives Review Epidemiology and Natural
The DAWN of a New Era for Wake-up Stroke Alan H. Yee, D.O. Stroke and Critical Care Neurology Department of Neurology University of California Davis Medical Center Objectives Review Epidemiology and Natural
Imaging of Moya Moya Disease
 Abstract Imaging of Moya Moya Disease Pages with reference to book, From 181 To 185 Rashid Ahmed, Hurnera Ahsan ( Liaquat National Hospital, Karachi. ) Moya Moya disease is a rare disease causing occlusion
Abstract Imaging of Moya Moya Disease Pages with reference to book, From 181 To 185 Rashid Ahmed, Hurnera Ahsan ( Liaquat National Hospital, Karachi. ) Moya Moya disease is a rare disease causing occlusion
Hrushchak N.M. The Pharma Innovation Journal 2014; 3(9): 38-42
 2014; 3(9): 38-42 ISSN: 2277-7695 TPI 2014; 3(9): 38-42 2013 TPI www.thepharmajournal.com Received: 10-10-2014 Accepted: 23-11-2014 Ivano-Frankivsk national medical university Kalush regional hospital.
2014; 3(9): 38-42 ISSN: 2277-7695 TPI 2014; 3(9): 38-42 2013 TPI www.thepharmajournal.com Received: 10-10-2014 Accepted: 23-11-2014 Ivano-Frankivsk national medical university Kalush regional hospital.
Patients are said to require emergency surgery in the
 Intraluminal Thrombus in the Cerebral Circulation Implications for Surgical Management 681 Alastair Buchan, MRCP, FRCPC, Peter Gates, MB, BS, David Pelz, MD, FRCPC, and Henry J.M. Barnett, MD, FRCPC Thrombi
Intraluminal Thrombus in the Cerebral Circulation Implications for Surgical Management 681 Alastair Buchan, MRCP, FRCPC, Peter Gates, MB, BS, David Pelz, MD, FRCPC, and Henry J.M. Barnett, MD, FRCPC Thrombi
Acute brain vessel thrombectomie: when? Why? How?
 Acute brain vessel thrombectomie: when? Why? How? Didier Payen, MD, Ph D Université Paris 7 Département Anesthesiologie-Réanimation Univ Paris 7; Unité INSERM 1160 Hôpital Lariboisière AP-HParis current
Acute brain vessel thrombectomie: when? Why? How? Didier Payen, MD, Ph D Université Paris 7 Département Anesthesiologie-Réanimation Univ Paris 7; Unité INSERM 1160 Hôpital Lariboisière AP-HParis current
Since the National Institute of Neurologic Disorders and
 ORIGINAL RESEARCH R.M. Sugg E.A. Noser H.M. Shaltoni N.R. Gonzales M.S. Campbell R. Weir E.D. Cacayorin J.C. Grotta Intra-Arterial Reteplase Compared to Urokinase for Thrombolytic Recanalization in Acute
ORIGINAL RESEARCH R.M. Sugg E.A. Noser H.M. Shaltoni N.R. Gonzales M.S. Campbell R. Weir E.D. Cacayorin J.C. Grotta Intra-Arterial Reteplase Compared to Urokinase for Thrombolytic Recanalization in Acute
Reduction of flow velocities in patients with ischemic events in the middle cerebral artery long-term follow-up with ultrasound
 Acta Neurol. Belg., 20,, -5 Original articles Reduction of flow velocities in patients with ischemic events in the middle cerebral artery long-term follow-up with ultrasound Christine Kremer and Kasim
Acta Neurol. Belg., 20,, -5 Original articles Reduction of flow velocities in patients with ischemic events in the middle cerebral artery long-term follow-up with ultrasound Christine Kremer and Kasim
CT and MR Imaging in Young Stroke Patients
 CT and MR Imaging in Young Stroke Patients Ashfaq A. Razzaq,Behram A. Khan,Shahid Baig ( Department of Neurology, Aga Khan University Hospital, Karachi. ) Abstract Pages with reference to book, From 66
CT and MR Imaging in Young Stroke Patients Ashfaq A. Razzaq,Behram A. Khan,Shahid Baig ( Department of Neurology, Aga Khan University Hospital, Karachi. ) Abstract Pages with reference to book, From 66
In cerebral embolism, recanaiization occurs very
 680 Case Reports Recanaiization of Intracranial Carotid Occlusion Detected by Duplex Carotid Sonography Haruhiko Hoshino, MD, Makoto Takagi, MD, Ikuo Takeuchi, MD, Tsugio Akutsu, MD, Yasuyuki Takagi, MD,
680 Case Reports Recanaiization of Intracranial Carotid Occlusion Detected by Duplex Carotid Sonography Haruhiko Hoshino, MD, Makoto Takagi, MD, Ikuo Takeuchi, MD, Tsugio Akutsu, MD, Yasuyuki Takagi, MD,
What to expect on post mechanical thrombectomy CT - a guide to correct diagnosis.
 What to expect on post mechanical thrombectomy CT - a guide to correct diagnosis. Poster No.: C-2257 Congress: ECR 2017 Type: Educational Exhibit Authors: T. Buende Tchokouako, H. Nejadhamzeeigilani, A.
What to expect on post mechanical thrombectomy CT - a guide to correct diagnosis. Poster No.: C-2257 Congress: ECR 2017 Type: Educational Exhibit Authors: T. Buende Tchokouako, H. Nejadhamzeeigilani, A.
Clinical Study Circle of Willis Variants: Fetal PCA
 Stroke Research and Treatment Volume 2013, Article ID 105937, 6 pages http://dx.doi.org/10.1155/2013/105937 Clinical Study Circle of Willis Variants: Fetal PCA Amir Shaban, 1 Karen C. Albright, 2,3,4,5
Stroke Research and Treatment Volume 2013, Article ID 105937, 6 pages http://dx.doi.org/10.1155/2013/105937 Clinical Study Circle of Willis Variants: Fetal PCA Amir Shaban, 1 Karen C. Albright, 2,3,4,5
How to Interpret CT/CTA for Acute Stroke in the Age of Endovascular Clot Retrieval
 How to Interpret CT/CTA for Acute Stroke in the Age of Endovascular Clot Retrieval Peter Howard MD FRCPC Disclosures No conflicts to disclose How to Interpret CT/CTA for Acute Stroke in the Age of Endovascular
How to Interpret CT/CTA for Acute Stroke in the Age of Endovascular Clot Retrieval Peter Howard MD FRCPC Disclosures No conflicts to disclose How to Interpret CT/CTA for Acute Stroke in the Age of Endovascular
ENDOVASCULAR THERAPIES FOR ACUTE STROKE
 ENDOVASCULAR THERAPIES FOR ACUTE STROKE Cerebral Arteriogram Cerebral Anatomy Cerebral Anatomy Brain Imaging Acute Ischemic Stroke (AIS) Therapy Main goal is to restore blood flow and improve perfusion
ENDOVASCULAR THERAPIES FOR ACUTE STROKE Cerebral Arteriogram Cerebral Anatomy Cerebral Anatomy Brain Imaging Acute Ischemic Stroke (AIS) Therapy Main goal is to restore blood flow and improve perfusion
The hyperdense vessel sign on CT predicts successful recanalization with the Merci device in acute ischemic stroke
 Editor s choice Scan to access more free content 1 Neuro Interventional Service, University of Iowa, Carver College of Medicine, Iowa City, Iowa, USA 2 Division of Interventional Neuroradiology, UCLA,
Editor s choice Scan to access more free content 1 Neuro Interventional Service, University of Iowa, Carver College of Medicine, Iowa City, Iowa, USA 2 Division of Interventional Neuroradiology, UCLA,
Update on Early Acute Ischemic Stroke Interventions
 Update on Early Acute Ischemic Stroke Interventions Diana Goodman MD Lead Neurohospitalist Maine Medical Center Assistant Professor of Neurology, Tufts University School of Medicine I have no disclosures
Update on Early Acute Ischemic Stroke Interventions Diana Goodman MD Lead Neurohospitalist Maine Medical Center Assistant Professor of Neurology, Tufts University School of Medicine I have no disclosures
ACUTE STROKE INTERVENTION: THE ROLE OF THROMBECTOMY AND IA LYSIS
 Associate Professor of Neurology Director of Neurointerventional Services University of Louisville School of Medicine ACUTE STROKE INTERVENTION: THE ROLE OF THROMBECTOMY AND IA LYSIS Conflict of Interest
Associate Professor of Neurology Director of Neurointerventional Services University of Louisville School of Medicine ACUTE STROKE INTERVENTION: THE ROLE OF THROMBECTOMY AND IA LYSIS Conflict of Interest
Trial Design and Reporting Standards for Intra-Arterial Cerebral Thrombolysis for Acute Ischemic Stroke
 Trial Design and Reporting Standards for Intra-Arterial Cerebral Thrombolysis for Acute Ischemic Stroke Randall T. Higashida, MD; Anthony J. Furlan, MD; for the Technology Assessment Committees of the
Trial Design and Reporting Standards for Intra-Arterial Cerebral Thrombolysis for Acute Ischemic Stroke Randall T. Higashida, MD; Anthony J. Furlan, MD; for the Technology Assessment Committees of the
Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography
 Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography Kazumi Kimura, Yoichiro Hashimoto, Teruyuki Hirano, Makoto Uchino, and Masayuki Ando PURPOSE: To determine
Diagnosis of Middle Cerebral Artery Occlusion with Transcranial Color-Coded Real-Time Sonography Kazumi Kimura, Yoichiro Hashimoto, Teruyuki Hirano, Makoto Uchino, and Masayuki Ando PURPOSE: To determine
Tae Hong Lee, MD, Kyung Pil Park, MD 2, Chang Hwa Choi, MD 3, Hak Jin Kim, MD, Chang Won Kim, MD
 Case Report Urgent Recanalization Using Stents for Acute Internal Carotid Artery Occlusion in Progressive Stroke Patients with Contralateral Chronic Carotid Occlusion Tae Hong Lee, MD, Kyung Pil Park,
Case Report Urgent Recanalization Using Stents for Acute Internal Carotid Artery Occlusion in Progressive Stroke Patients with Contralateral Chronic Carotid Occlusion Tae Hong Lee, MD, Kyung Pil Park,
Although plaque morphology of patients with
 1740 Short Communications Rupture of Atheromatous Plaque as a Cause of Thrombotic Occlusion of Stenotic Internal Carotid Artery Jun Ogata, MD, Junichi Masuda, MD, Chikao Yutani, MD, and Takenori Yamaguchi,
1740 Short Communications Rupture of Atheromatous Plaque as a Cause of Thrombotic Occlusion of Stenotic Internal Carotid Artery Jun Ogata, MD, Junichi Masuda, MD, Chikao Yutani, MD, and Takenori Yamaguchi,
