Early computed tomographic (CT) ischemic change in the
|
|
|
- Neal Jenkins
- 5 years ago
- Views:
Transcription
1 Hyperdense Sylvian Fissure MCA Dot Sign A CT Marker of Acute Ischemia Philip A. Barber, MRCP(UK); Andrew M. Demchuk, FRCPC; Mark E. Hudon, FRCPC; J.H. Warwick Pexman, FRCPC; Michael D. Hill, FRCPC; Alastair M. Buchan, FRCP(Edin) Background and Purpose The hyperdense appearance of the main middle cerebral artery (HMCA) is now a familiar early warning of large cerebral infarction, brain edema, and poor prognosis. This article describes the hyperdensity associated with embolic occlusion of branches of the middle cerebral artery in the sylvian fissure (MCA dot sign). We define it and determine its incidence, diagnostic value, and reliability. Methods CT scans performed on patients with acute ischemic stroke within 3 hours of symptom onset were analyzed for signs of thromboembolic stroke and evidence of early CT ischemia. Two neuroradiologists and 2 stroke neurologists initially blinded to all clinical information and then with knowledge of the affected hemisphere evaluated scans for the presence of the MCA dot sign, the HMCA sign, and early MCA territory ischemic changes. Results Of 100 consecutive patients who presented within 3 hours of symptom onset, 91 were considered at symptom onset to have anterior circulation stroke syndromes. Early CT ischemia was seen in 74% of these baseline CT scans. The HMCA sign was seen in 5% of CT scans, whereas the MCA dot sign was seen in 16%. All patients then received intravenous tissue plasminogen activator. All 5 patients with an HMCA sign, including 2 with an associated MCA dot sign, were either dead or dependent at 3 months. The 14 patients with an MCA dot sign alone were independent at 3 months in 64% of cases, compared with 50% without the sign (Fisher s exact test P 0.79). Balanced statistics for both the HMCA and the MCA dot sign were in the moderate to good range when the stroke symptom side was given. Conclusions The MCA dot sign is an early marker of thromboembolic occlusion of the distal MCA branches seen in the sylvian fissure and is associated with better outcome than the HMCA sign. (Stroke. 2001;32:84-88.) Key Words: acute ischemic stroke computed tomography middle cerebral artery Early computed tomographic (CT) ischemic change in the territory of the middle cerebral artery (MCA) has diagnostic and prognostic value. 1,2 These changes are subtle, however, and therefore have variable reliability. 1 6 Noncontrast CT scans may show a hyperdense MCA (HMCA) sign that represents thromboembolism within the artery and is associated with large MCA territory infarction. 7,8 The HMCA sign has been associated with severe neurological deficit, extensive brain damage, and poor clinical outcome. 9 In this study, we describe the MCA dot sign, a hyperdensity in the distal MCA and its branches seen in the sylvian fissure. The recognition of such vascular information may be important in defining why some patients respond to thrombolysis and others do not and may help in decision making when further interventional therapies are being considered. We define the MCA dot sign and describe its incidence and its association with initial neurological severity and early parenchymal ischemic CT change seen in patients with acute stroke. We report the outcome after treatment with tissue plasminogen activator (tpa). We assumed that the hyperdensity seen within these smaller-caliber vessels is less likely to represent calcified atheromatous plaque than that in larger intracranial vessels, such as the carotid artery, MCA main stem, and basilar artery, as shown in previously detailed pathological studies. 10,11 Subjects and Methods One hundred patients who presented within 3 hours of symptom onset were treated with intravenous tpa between March 1996 and November Demographic data, stroke risk factors, baseline National Institutes of Health Stroke Scale (NIHSS), and stroke type according to the Oxford Community Stroke Project (OCSP) 12 were recorded. The outcome measures were functional outcome defined by the Rankin scale at 3 months, dichotomized into independence (0 to 2), dependence (3 to 5), and death, and symptomatic intracerebral hemorrhage. Patients had pretreatment noncontrast CT brain scans (baseline) and a second CT at 24 hours. CT scans were performed on a fourth-generation Toshiba Express scanner. Section thickness was 6 mm through the posterior fossa and 6 to 10 mm for the cerebral hemispheres. All CT scans were independently reviewed by 4 clinicians, 2 neuroradiologists (M.E.H., J.H.W.P.), and 2 stroke neurologists (A.M.D., P.A.B.). One of them had had only 2 months of experience of interpreting CT ischemic changes and applying the Alberta Stroke Received June 5, 2000; final revision received September 20, 2000; accepted September 20, From the Department of Clinical Neurosciences, University of Calgary, Seaman Family Magnetic Research Center, Calgary, Alberta, Canada. Correspondence to Dr A.M. Demchuk, Assistant Professor, Calgary Regional Stroke Program, Department of Clinical Neurosciences, University of Calgary, Calgary, Alberta, Canada American Heart Association, Inc. Stroke is available at 84
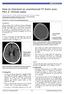
2 Barber et al Hyperdense Sylvian Fissure MCA Dot Sign 85 superior margin of the ganglionic structures, such that these structures were not visible. The MCA territory is allotted 10 points: caudate nucleus; lentiform nucleus; posterior limb of the internal capsule; insular ribbon; anterior MCA cortex (M1); MCA cortex lateral to the insular ribbon (M2); posterior MCA cortex (M3); and the anterior (M4), lateral (M5), and posterior MCA (M6) territories immediately superior to M1, M2, and M3, rostral to the basal ganglia. A single point was subtracted for an area of early ischemic change, such as focal swelling, or parenchymal hypoattenuation, for each of the defined regions. A normal CT scan received ASPECTS of 10 points. A score of 0 indicated diffuse ischemic involvement throughout the MCA territory. ASPECTS is presented both as ordinal data and dichotomized into 7 and 7. Proportions were compared by Fisher s exact test. Figure 1. A and B, Baseline CT scan on an 80-year-old woman (patient 74) who presented with aphasia, dense right hemiparesis, and right hemianopia within 3 hours of symptom onset. The CT scan shows a hyperdensity of an M2 branch in the sylvian fissure (MCA dot sign), which also appears plumper than the contralateral side (black arrow). It is associated with loss of gray-white differentiation and parenchymal hypodensity in the temporal and parietal lobes (white arrows). C and D, Area of confirmed infarction at 24 hours. The MCA dot sign remains visible (black arrow). Program Early CT Score (ASPECTS), compared with the 2 years of experience of the others. The scans were initially read with the researchers blinded to all clinical information, the follow-up CT scan, and outcome data. On a separate occasion, they read them again knowing the side of the body of the stroke symptoms. Each scan was assessed specifically for the presence of the following CT signs: an MCA dot sign, an HMCA sign, and evidence of early CT ischemic change. When there was complete disagreement about the presence of a CT sign, a consensus was reached by a panel of CT readers (M.E.H., P.A.B.). The interobserver agreement for the HMCA, the MCA dot sign, and the presence of early CT ischemic change was assessed between each observer. Balanced statistics, 13 which correct for the prevalence of a particular observation, were used to assess the evidence for agreement between observers. The MCA dot sign was defined as the hyperdensity of an arterial structure (seen as a dot) in the sylvian fissure relative to the contralateral side or to other vessels within the sylvian fissure (Figure 1). The HMCA was defined as an MCA denser than its counterpart. Positive MCA dot and HMCA signs were considered appropriate if associated with CT ischemic change on either the baseline or 24-hour CT scan. Hyperdense signs contralateral to the symptomatic hemisphere or the final area of infarction were considered false-positive by the reading panel. Early CT ischemic change was considered to be when there was either loss of discrimination between gray and white matter, tissue hypodensity, or swelling of brain tissue resulting in compression of local cerebrospinal fluid spaces relative to other structures or to the contralateral hemisphere. 1 ASPECTS was used to define and quantify early CT ischemic change, and this has been described previously. 2 ASPECTS was determined from 2 standardized axial CT cuts, 1 at the level of the thalamus and basal ganglia and 1 adjacent to the most Results One hundred consecutive patients were assessed. The mean age was 68.6 years (SD 14 years). There were 53 men. For all patients, the median baseline NIHSS was 16. The OCSP stroke classifications were 53 total anterior circulation syndrome (TACS), 31 partial anterior circulation syndrome (PACS), 9 posterior occipital circulation syndrome (POCS), and 7 lacunar anterior circulation syndrome (LACS). Median baseline AS- PECTS was 8.5. At 3 months, 51.5% of the patients were independent. There were 8 symptomatic hemorrhages. Seventyfour percent of the baseline CT scans showed evidence of early CT ischemic change. This rose to 85% on the follow-up 24-hour CT scan. MCA dot signs were identified in 16 patients and HMCA signs in 5 (2 of whom had associated MCA dot signs) by the reading panel (Figure 2). Figure 2. CT scan at baseline (A, B) and 24 hours (C, D) of a 74-year-old woman presenting with a dense left hemiparesis, neglect, and hemianopia (NIHSS 17). Black arrows demonstrate the HMCA and MCA dot signs (A, B) and residual MCA dot sign (D) on the 24-hour scan.
3 86 Stroke January 2001 Balanced Statistics Between 4 Pairs of Observers for the Sylvian Fissure MCA Dot Sign, Hyperdense MCA, and ASPECTS Balanced Statistics Blind to clinical information MCA Dot Sign Hyperdense MCA ASPECTS 7 and 7 Observer 1 vs observer Observer 1 vs observer Observer 1 vs observer Observer 2 vs observer Observer 2 vs observer Observer 3 vs observer Knowledge of stroke side Observer 1 vs observer Observer 1 vs observer Observer 1 vs observer Observer 2 vs observer Observer 2 vs observer Observer 3 vs observer The balanced statistic is a measure of agreement between the 2 observers (stroke neurologists and experienced neuroradiologists). A value of 0 indicates agreement no better than chance, and a value of 1 indicates perfect agreement. Values of 0 to 0.2 indicate poor agreement; 0.21 to 0.40, fair agreement; 0.41 to 0.61, moderate agreement; 0.61 to 0.81, good agreement; and 0.81 to 1, excellent agreement. 13 Two more cases of MCA dot signs were considered by some of the independent readers to probably represent falsepositive signs, because they were not associated with CT ischemic change on the 24-hour scan or were not related to the anatomic locality of the patient s symptoms. The interobserver reliability for the MCA dot sign and HMCA sign and the recognition of early CT ischemic change are summarized in the Table. This table shows that the reliability with ASPECTS improves when clinical information is available. It reveals that observer 4 has less experience than the others with this method of interpretation. The recognition of the HMCA sign did not change when clinical information was provided. The scores converge when clinical information is available during the assessment of the MCA dot sign, suggesting that it helps the less experienced. For cases in which an MCA dot sign was identified, the artery was considered plumper by the observers in 12 of the 16 cases. The median NIHSS was 15 for patients with an MCA dot sign, 15 when no occlusion was identified, and 18 for an HMCA sign (comparisons between groups were not statistically significant). The OCSP stroke types were 7 TACS and 9 PACS. As expected, the presence of an MCA dot sign was strongly associated with cortical symptoms and signs (TACS or PACS versus POCS and LACS, P 0.001). In addition, there is no significant difference between patients with the MCA dot sign and patients in whom no occlusion was seen in terms of functional outcome at 3 months (Fisher s exact test P 0.56). The presence of an HMCA sign was not statistically associated with a greater probability of dependence or death than when no hyperdense artery sign was seen or an MCA dot sign was present (Fisher s exact test P 0.054). This may relate to the small number of HMCA signs seen in this study. All 5 of these patients were dead or dependent at 3 months. However, an MCA dot sign was associated with better outcomes at 3 months than an HMCA sign was (Fisher s exact test P 0.033). We also found that the presence of either an MCA dot sign or an HMCA sign correlated well with the degree of CT ischemia quantified by ASPECTS (dichotomized score 7 versus 7). 2 Three of 14 patients with MCA dot signs had ASPECTS 7, compared with 5 of 5 with HMCA signs (Fisher s exact test P 0.005). No statistical difference was seen for ASPECTS when the MCA dot sign was compared with the group in which no vascular occlusion was identified (Fisher s exact test P 1.0). The clinical characteristics and 24-hour cerebral infarcts of patients with an MCA dot are presented in Figure 3. These results of this figure are summarized for pattern recognition in Figure 4. Discussion Early CT ischemic change has been shown to have prognostic use in predicting functional outcome and symptomatic intracerebral hemorrhage before thrombolysis is administered. 1,2 It can also provide information regarding vascular thromboembolic occlusions. 7 Much has been written about the HMCA sign and its association with large MCA infarction. 7,9 The reliability of this sign is uncertain. Thrombosis can be confused with calcified artery walls, particularly in the elderly, and with a slice showing the MCA very well in the symptomatic hemisphere but not so ideally on the opposite side. Consequently, the incidence of the HMCA sign has been reported to be as high as 41%, 7 but others found the hyperdense artery sign in only 5% of patients with acute ischemic stroke. 14 In this study, we describe the phenomenon of hyperdensity of the MCA branches observed within the sylvian fissure, the MCA dot sign. Previous pathological studies suggest that atherosclerosis mainly affects the larger extracranial and intracranial cerebral vessels, and therefore hyperdensity within the smaller sylvian M2 branches is more likely to be representative of embolic material than calcified atheromatous plaque. 10,11 The incidence of the MCA dot sign in this group of consecutive patients treated with thrombolysis was 16%, a finding similar to the incidence of distal MCA branch (M2 or M3 segments) in the analysis of CT findings from ECASS I. 9 The frequency of the MCA dot sign in this study was greater than that of the HMCA sign; the dot sign, therefore, may be a more useful indicator of thromboembolic stroke. The characteristics of the MCA dot sign have not been described previously. We defined the sign as the hyperdensity of MCA branches (either M2 or M3) beyond the MCA bifurcation seen in the sylvian fissure compared with other arteries in the contralateral sylvian fissure. The dot sign is characteristically associated with confirmed infarction typically affecting the insular cortex in 12 of our patients and
4 Barber et al Hyperdense Sylvian Fissure MCA Dot Sign 87 Figure 3. CT scan findings with hyperdense sylvian fissure MCA dot sign. Associated HMCA signs (patients 48 and 88), baseline NIHSS, and functional outcome are labeled for each case. adjacent temporal and frontal parietal cortices, corresponding to the ASPECTS areas M2 and M5 (Figures 1, 3, and 4). Many of the cases in which isolated MCA dot signs were present produced infarction in the basal ganglia (most commonly the lentiform nucleus). There are 3 possible explanations for this: first, the thrombus caused proximal MCA occlusion, resulting in reduced blood flow in the lenticulostriate arteries, and later migrated to a more distal position; second, an associated HMCA occlusion was not visible for technical reasons (eg, slice thickness); and third, the lateral lenticulostriate vessels may originate distal to the MCA bifurcation. We observed on occasion that the thrombosed Figure 4. The pattern of CT infarction at 24 hours in cases in which an MCA dot sign was observed. The sign is most commonly associated with CT infarction in the insula (n 12), M2 (n 11), and M5 (n 9) regions, according to the ASPECTS system. artery appeared to be not only more hyperdense but also plumper than adjacent arteries in the sylvian fissure and the contralateral side. This may be due to clot within the vessel, distending it. Two cases that were considered by some of the independent observers to show MCA dot signs were later labeled as false-positives by the panel of CT readers, because the signs were not related to the area of ischemia. One was in the contralateral hemisphere and the other in the brain stem. Neither was associated with ipsilateral CT ischemic change on the follow-up CT. One case, however, in which an MCA dot sign was observed contralateral to the symptomatic side, produced confirmed infarction in the basal ganglia on the follow-up CT scan. This patient was in atrial fibrillation and developed bilateral hemispheric strokes of cardioembolic origin. The presence of the MCA dot sign was associated with severe stroke (median NIHSS 15). Although the natural history of the sign cannot be commented on because all patients received intravenous tpa, the functional outcome with treatment is generally good, with 64% independent at 3 months. This contrasts with the 5 patients with HMCA signs who died or were dependent at 3 months. This may support the concept that branch MCA occlusions (of either the M2 or M3 branches) respond better to intravenous thrombolysis than larger vessels, such as the MCA.15 The interobserver reliability for the sign was in the moderate to good range. The poorer results were associated with observer 4, who was the least experienced of the readers. It is hoped that the recognition of the MCA dot sign, with its
5 88 Stroke January 2001 associated pattern of infarction, most commonly the insular cortex, and the ASPECTS cortical areas M2 and M5 (Figure 4), will help the less experienced to detect ischemia on the baseline CT scan. The weakness of this study is the absence of a gold standard. Therefore, we were unable to calculate the sensitivity or specificity of the sign. Further studies should attempt to validate this CT finding with either high-resolution MR angiography of the distal MCA branches or formal angiography. As with the HMCA sign, the sensitivity of the MCA dot sign is likely to be poor. It is necessary to develop reliable and accessible noninvasive imaging modalities in acute ischemic stroke, such as MR angiography, CT angiography, and transcranial Doppler. Understanding why acute ischemic stroke resolves rapidly in some patients but not in others is of importance when considering acute stroke therapies, such as thrombolysis. Intravenous tpa is an important therapeutic option that may be appropriate for some occlusive disease, such as MCA branch occlusions, whereas other large-artery occlusions may not be as responsive. 15,16 The identification of thromboembolic occlusions has become even more pertinent after the publication of the positive PROACT II trial. 17 Because time is of the essence in the treatment of acute ischemic stroke, it is reassuring for the treating clinician that an occlusive lesion can be identified rapidly and noninvasively. The MCA dot sign can facilitate this process. We conclude that the recognition of the MCA dot sign may help in the diagnosis and treatment of thromboembolic MCA branch occlusion and CT infarction. This sign is not infrequently seen in hyperacute stroke, and it has a better prognosis than the HMCA sign. Acknowledgments Dr Buchan was funded in part by the Medical Research Council of Canada, the Heart and Stroke Foundation of Alberta/NWT, and the Alberta Heritage Foundation for Medical Research. References 1. von Kummer R, Allen KL, Holle R, Bozzao L, Bastianello S, Manelfe C, Bluhmki E, Ringleb P, Meier DH, Hacke W. Acute stroke: usefulness of early CT findings before thrombolytic therapy. Radiology. 1997;205: Barber PA, Demchuk AM, Zhang J, Buchan AM, for the ASPECTS Study Group. The validity and reliability of a novel quantitative CT score in predicting outcome in hyperacute stroke prior to thrombolytic therapy. Lancet. 2000;355: Dippel DWJ, Du RY, van Beest Holle M, van Kooten F, Moseley ME, Cohen Y, Mintorovitch J, Chilewitt L, Shimiza H, Kucharcyck J, Wedland MF, Weinstein PR. The validity and reliability of early infarct signs on CT in acute ischaemic stroke. Cerebrovasc Dis. 1997;7(suppl 4): Schriger D, Kalafut M, Starkman S, Krueger M, Saver J. Cranial computed tomography interpretation in acute stroke: physician accuracy in determining eligibility for thrombolytic therapy. JAMA. 1998;279: Grotta J, Chiu D, Lu M, Patel S, Levine SR, Tilley B, Brott TG, Haley EC, Lyden PD, Kothari R, Frankel M, Lewandowski CA, Libman R, Kwiatkowski T, Broderick JP, Marler JR, Corrigan J, Huff S, Mitsias P, Talati S, Tanne D. Agreement and variability in the interpretation of early CT changes in stroke patients qualifying for intravenous rtpa. Stroke. 1999;30: Wardlaw JM, Dorman PJ, Lewis SC, Sandercock PAG. Can stroke physicians and neurologists identify signs of early cerebral infarction on CT? J Neurol Neurosurg Psychiatry. 1999;67: Leys D, Pruvo JP, Godefroy O, Randepierre, Leclerc X. Prevalence and significance of hyperdense middle cerebral artery in acute stroke. Stroke. 1992;23: von Kummer R, Holle R, Grzyska U, Hofmann E, Jansen O, Peterson D, Schumacher M, Sartor K. Interobserver agreement in assessing early CT signs of middle cerebral artery infarction. AJNR Am J Neuroradiol. 1996;17: Manelfe C, Larrue V, von Kummer R, Bozzao L, Ringleb P, Bastianello S, Iweins F, Lasaffre E. Association of hyperdense middle cerebral artery sign with clinical outcome in patients with tissue plasminogen activator. Stroke. 1999;30: Baker A, Iannone A. Cerebrovascular disease, I: the large arteries of the circle of Willis. Neurology. 1959;9: Fisher CM, Gore I, Okabe N. Atherosclerosis of the carotid and vertebral arteries: extracranial and intracranial. J Neuropathol Exp Neurol. 1965; 24: Bamford J, Sandercock PAJ, Dennis M, Burn J, Warlow CP. Classification and natural history of clinically identifiable subtypes of cerebral infarction. Lancet. 1991;337: Lantz C, Nebenzehl E. Behavior and interpretation of the K statistic: resolution of the two paradoxes. J Clin Epidemiol. 1996;49: Yang SS, Ryu SJ, Wu CL. Early CT diagnosis of cerebral ischemia. Stroke. 1990;21(suppl I):I Yamaguchi T, Mori E, Minematsu K, del Zoppo, eds. Thrombolytic Therapy in Acute Ischemic Stroke 111. Tokyo, Japan: Springer-Verlag; Caplan LR, Mohr JP, Kistler JP, Koroshetz, Grotta J. Clinical debate: should thrombolytic therapy be the first-line treatment for acute ischemic stroke? N Engl Med. 1997;337: Furlan A, Higashida R, Wechsler L, Gent M, Rowley H, Kase C, Pessin M, Ahuja A, Callahan F, Clarke W, Silver F, Rivera F, for the PROACT Investigators. Intra-arterial prourokinase for acute ischemic stroke: the PROACT II study: a randomised controlled trial. JAMA. 1999;282:
I schaemic stroke is currently the third leading cause
 1426 PAPER The probability of middle cerebral artery MRA flow signal abnormality with quantified CT ischaemic change: targets for future therapeutic studies P A Barber, A M Demchuk, M D Hill, J H Warwick
1426 PAPER The probability of middle cerebral artery MRA flow signal abnormality with quantified CT ischaemic change: targets for future therapeutic studies P A Barber, A M Demchuk, M D Hill, J H Warwick
Noncontrast computed tomography (CT) reliably distinguishes
 Extent of Early Ischemic Changes on Computed Tomography (CT) Before Thrombolysis Prognostic Value of the Alberta Stroke Program Early CT Score in ECASS II Imanuel Dzialowski, MD; Michael D. Hill, MD, MSc,
Extent of Early Ischemic Changes on Computed Tomography (CT) Before Thrombolysis Prognostic Value of the Alberta Stroke Program Early CT Score in ECASS II Imanuel Dzialowski, MD; Michael D. Hill, MD, MSc,
Interrater Reliability and Sensitivity of CT Interpretation by Physicians Involved in Acute Stroke Care
 Detection of Early CT Signs of >1/3 Middle Cerebral Artery Infarctions Interrater Reliability and Sensitivity of CT Interpretation by Physicians Involved in Acute Stroke Care Mary A. Kalafut, MD; David
Detection of Early CT Signs of >1/3 Middle Cerebral Artery Infarctions Interrater Reliability and Sensitivity of CT Interpretation by Physicians Involved in Acute Stroke Care Mary A. Kalafut, MD; David
IMAGING IN ACUTE ISCHEMIC STROKE
 IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
Use of the Alberta Stroke Program Early CT Score (ASPECTS) for Assessing CT Scans in Patients with Acute Stroke
 AJNR Am J Neuroradiol 22:1534 1542, September 2001 Use of the Alberta Stroke Program Early CT Score (ASPECTS) for Assessing CT Scans in Patients with Acute Stroke J. H. Warwick Pexman, Philip A. Barber,
AJNR Am J Neuroradiol 22:1534 1542, September 2001 Use of the Alberta Stroke Program Early CT Score (ASPECTS) for Assessing CT Scans in Patients with Acute Stroke J. H. Warwick Pexman, Philip A. Barber,
IMAGING IN ACUTE ISCHEMIC STROKE
 IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
IMAGING IN ACUTE ISCHEMIC STROKE Timo Krings MD, PhD, FRCP (C) Professor of Radiology & Surgery Braley Chair of Neuroradiology, Chief and Program Director of Diagnostic and Interventional Neuroradiology;
Agreement and Variability in the Interpretation of Early CT Changes in Stroke Patients Qualifying for Intravenous rtpa Therapy
 Agreement and Variability in the Interpretation of Early CT Changes in Stroke Patients Qualifying for Intravenous rtpa Therapy James C. Grotta, MD; David Chiu, MD; Mei Lu, PhD; Suresh Patel, MD; Steven
Agreement and Variability in the Interpretation of Early CT Changes in Stroke Patients Qualifying for Intravenous rtpa Therapy James C. Grotta, MD; David Chiu, MD; Mei Lu, PhD; Suresh Patel, MD; Steven
Acute stroke. Ischaemic stroke. Characteristics. Temporal classification. Clinical features. Interpretation of Emergency Head CT
 Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Prognostic Value of the Hyperdense Middle Cerebral Artery Sign and Stroke Scale Score before Ultraearly Thrombolytic Therapy
 Prognostic Value of the Hyperdense Middle Cerebral Artery Sign and Stroke Scale Score before Ultraearly Thrombolytic Therapy Thomas Tomsick, Thomas Brott, William Barsan, Joseph Broderick, E. Clarke Haley,
Prognostic Value of the Hyperdense Middle Cerebral Artery Sign and Stroke Scale Score before Ultraearly Thrombolytic Therapy Thomas Tomsick, Thomas Brott, William Barsan, Joseph Broderick, E. Clarke Haley,
Even in the era of diffusion and perfusion-weighted MRI,
 The Hyperdense Posterior Cerebral Artery Sign A Computed Tomography Marker of Acute Ischemia in the Posterior Cerebral Artery Territory Timo Krings, MD; Dagmar Noelchen, MD; Michael Mull, MD; Klaus Willmes,
The Hyperdense Posterior Cerebral Artery Sign A Computed Tomography Marker of Acute Ischemia in the Posterior Cerebral Artery Territory Timo Krings, MD; Dagmar Noelchen, MD; Michael Mull, MD; Klaus Willmes,
Validation of Computed Tomographic Middle Cerebral Artery Dot Sign. An Angiographic Correlation Study
 Validation of Computed Tomographic Middle Cerebral Artery Dot Sign An Angiographic Correlation Study Megan C. Leary, MD; Chelsea S. Kidwell, MD; J. Pablo Villablanca, MD; Sidney Starkman, MD; Reza Jahan,
Validation of Computed Tomographic Middle Cerebral Artery Dot Sign An Angiographic Correlation Study Megan C. Leary, MD; Chelsea S. Kidwell, MD; J. Pablo Villablanca, MD; Sidney Starkman, MD; Reza Jahan,
Lack of Clinical Significance of Early Ischemic Changes on Computed Tomography in Acute Stroke JAMA. 2001;286:
 ORIGINAL CONTRIBUTION Lack of Clinical Significance of Early Ischemic Changes on Computed Tomography in Acute Stroke Suresh C. Patel, MD Steven R. Levine, MD Barbara C. Tilley, PhD James C. Grotta, MD
ORIGINAL CONTRIBUTION Lack of Clinical Significance of Early Ischemic Changes on Computed Tomography in Acute Stroke Suresh C. Patel, MD Steven R. Levine, MD Barbara C. Tilley, PhD James C. Grotta, MD
How well does the Oxfordshire Community Stroke Project classification predict the site and size of the infarct on brain imaging?
 558 Neurosciences Trials Unit, Department of Clinical Neurosciences, Western General Hospital, Edinburgh EH4 2XU, UK G E Mead S C Lewis J M Wardlaw M S Dennis C P Warlow Correspondence to: Dr S C Lewis,
558 Neurosciences Trials Unit, Department of Clinical Neurosciences, Western General Hospital, Edinburgh EH4 2XU, UK G E Mead S C Lewis J M Wardlaw M S Dennis C P Warlow Correspondence to: Dr S C Lewis,
Correlation of Early CT Signs in the Deep Middle Cerebral Artery Territories with Angiographically Confirmed Site of Arterial Occlusion
 AJNR Am J Neuroradiol 22:65 659, April 2 Correlation of Early CT Signs in the Deep Middle Cerebral Artery Territories with Angiographically Confirmed Site of Arterial Occlusion Shinichi Nakano, Tsutomu
AJNR Am J Neuroradiol 22:65 659, April 2 Correlation of Early CT Signs in the Deep Middle Cerebral Artery Territories with Angiographically Confirmed Site of Arterial Occlusion Shinichi Nakano, Tsutomu
ACUTE STROKE IMAGING
 ACUTE STROKE IMAGING Mahesh V. Jayaraman M.D. Director, Inter ventional Neuroradiology Associate Professor Depar tments of Diagnostic Imaging and Neurosurger y Alper t Medical School at Brown University
ACUTE STROKE IMAGING Mahesh V. Jayaraman M.D. Director, Inter ventional Neuroradiology Associate Professor Depar tments of Diagnostic Imaging and Neurosurger y Alper t Medical School at Brown University
Thrombus Localization with Emergency Cerebral CT
 Thrombus Localization with Emergency Cerebral CT Thomas Tomsick, ' Thomas Brott, William Barsan, Joseph Broderick, E. Clarke Haley, and Judith Spilker Purpose: To determine the prevalence of the hyperdense
Thrombus Localization with Emergency Cerebral CT Thomas Tomsick, ' Thomas Brott, William Barsan, Joseph Broderick, E. Clarke Haley, and Judith Spilker Purpose: To determine the prevalence of the hyperdense
Thrombolytic Therapy in Clinical Practice The Norwegian Experience
 Thrombolytic Therapy in Clinical Practice The Norwegian Experience Thomassen Lars Thomassen, Ulrike Waje-Andreassen, Halvor Næss ABSTRACT Background: Awaiting the European approval of thrombolysis, we
Thrombolytic Therapy in Clinical Practice The Norwegian Experience Thomassen Lars Thomassen, Ulrike Waje-Andreassen, Halvor Næss ABSTRACT Background: Awaiting the European approval of thrombolysis, we
Stroke School for Internists Part 1
 Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
Stroke School for Internists Part 1 November 4, 2017 Dr. Albert Jin Dr. Gurpreet Jaswal Disclosures I receive a stipend for my role as Medical Director of the Stroke Network of SEO I have no commercial
New therapies directed at acute middle cerebral artery
 Regional Angiographic Grading System for Collateral Flow Correlation With Cerebral Infarction in Patients With Middle Cerebral Artery Occlusion Jane J. Kim, MD; Nancy J. Fischbein, MD; Ying Lu, PhD; Daniel
Regional Angiographic Grading System for Collateral Flow Correlation With Cerebral Infarction in Patients With Middle Cerebral Artery Occlusion Jane J. Kim, MD; Nancy J. Fischbein, MD; Ying Lu, PhD; Daniel
Subscriptions: Information about subscribing to Stroke is online at
 Selection of Acute Ischemic Stroke Patients for Intra-Arterial Thrombolysis With Pro-Urokinase by Using ASPECTS Michael D. Hill, Howard A. Rowley, Felix Adler, Michael Eliasziw, Anthony Furlan, Randall
Selection of Acute Ischemic Stroke Patients for Intra-Arterial Thrombolysis With Pro-Urokinase by Using ASPECTS Michael D. Hill, Howard A. Rowley, Felix Adler, Michael Eliasziw, Anthony Furlan, Randall
Downloaded from by on January 15, 2019
 Alberta Stroke Program Early Computed Tomography Score to Select Patients for Endovascular Treatment Interventional Management of Stroke (IMS)-III Trial Michael D. Hill, MD, FRCPC; Andrew M. Demchuk, MD,
Alberta Stroke Program Early Computed Tomography Score to Select Patients for Endovascular Treatment Interventional Management of Stroke (IMS)-III Trial Michael D. Hill, MD, FRCPC; Andrew M. Demchuk, MD,
Potential of CT Angiography in Acute Ischemic Stroke
 Potential of CT Angiography in Acute Ischemic Stroke Michael Knauth, Rüdiger von Kummer, Olav Jansen, Stefan Hähnel, Arnd Dörfler, and Klaus Sartor PURPOSE: To study the ability of CT angiography to show
Potential of CT Angiography in Acute Ischemic Stroke Michael Knauth, Rüdiger von Kummer, Olav Jansen, Stefan Hähnel, Arnd Dörfler, and Klaus Sartor PURPOSE: To study the ability of CT angiography to show
[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]
![[(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD] [(PHY-3a) Initials of MD reviewing films] [(PHY-3b) Initials of 2 nd opinion MD]](/thumbs/89/98619893.jpg) 2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
2015 PHYSICIAN SIGN-OFF (1) STUDY NO (PHY-1) CASE, PER PHYSICIAN REVIEW 1=yes 2=no [strictly meets case definition] (PHY-1a) CASE, IN PHYSICIAN S OPINION 1=yes 2=no (PHY-2) (PHY-3) [based on all available
ORIGINAL CONTRIBUTION. Multiphasic Helical Computed Tomography Predicts Subsequent Development of Severe Brain Edema in Acute Ischemic Stroke
 ORIGINAL CONTRIBUTION Multiphasic Helical Computed Tomography Predicts Subsequent Development of Severe Brain Edema in Acute Ischemic Stroke Soo Joo Lee, MD; Kwang Ho Lee, MD; Dong Gyu Na, MD; Hong Sik
ORIGINAL CONTRIBUTION Multiphasic Helical Computed Tomography Predicts Subsequent Development of Severe Brain Edema in Acute Ischemic Stroke Soo Joo Lee, MD; Kwang Ho Lee, MD; Dong Gyu Na, MD; Hong Sik
Cerebrovascular Disease lll. Acute Ischemic Stroke. Use of Intravenous Alteplace in Acute Ischemic Stroke Louis R Caplan MD
 Cerebrovascular Disease lll. Acute Ischemic Stroke Use of Intravenous Alteplace in Acute Ischemic Stroke Louis R Caplan MD Thrombolysis was abandoned as a stroke treatment in the 1960s due to an unacceptable
Cerebrovascular Disease lll. Acute Ischemic Stroke Use of Intravenous Alteplace in Acute Ischemic Stroke Louis R Caplan MD Thrombolysis was abandoned as a stroke treatment in the 1960s due to an unacceptable
Imaging of the brain in acute ischaemic stroke: comparison of computed tomography and magnetic resonance diffusion-weighted imaging
 1528 PAPER Imaging of the brain in acute ischaemic stroke: comparison of computed tomography and magnetic resonance diffusion-weighted imaging P A Barber, M D Hill, M Eliasziw, A M Demchuk, J H W Pexman,
1528 PAPER Imaging of the brain in acute ischaemic stroke: comparison of computed tomography and magnetic resonance diffusion-weighted imaging P A Barber, M D Hill, M Eliasziw, A M Demchuk, J H W Pexman,
Analysis of DWI ASPECTS and Recanalization Outcomes of Patients with Acute-phase Cerebral Infarction
 J Med Dent Sci 2012; 59: 57-63 Original Article Analysis of DWI ASPECTS and Recanalization Outcomes of Patients with Acute-phase Cerebral Infarction Keigo Shigeta 1,2), Kikuo Ohno 1), Yoshio Takasato 2),
J Med Dent Sci 2012; 59: 57-63 Original Article Analysis of DWI ASPECTS and Recanalization Outcomes of Patients with Acute-phase Cerebral Infarction Keigo Shigeta 1,2), Kikuo Ohno 1), Yoshio Takasato 2),
Background. Recommendations for Imaging of Acute Ischemic Stroke: A Scientific Statement From the American Heart Association
 for Imaging of Acute Ischemic Stroke: A Scientific Statement From the American Heart Association An Scientific Statement from the Stroke Council, American Heart Association and American Stroke Association
for Imaging of Acute Ischemic Stroke: A Scientific Statement From the American Heart Association An Scientific Statement from the Stroke Council, American Heart Association and American Stroke Association
Review Article Differentiating between Hemorrhagic Infarct and Parenchymal Intracerebral Hemorrhage
 Hindawi Publishing Corporation Radiology Research and Practice Volume 2012, Article ID 475497, 11 pages doi:10.1155/2012/475497 Review Article Differentiating between Hemorrhagic Infarct and Parenchymal
Hindawi Publishing Corporation Radiology Research and Practice Volume 2012, Article ID 475497, 11 pages doi:10.1155/2012/475497 Review Article Differentiating between Hemorrhagic Infarct and Parenchymal
Symptomatic intracerebral hemorrhage (sich) after
 Reduced Pretreatment Ipsilateral Middle Cerebral Artery Cerebral Blood Flow Is Predictive of Symptomatic Hemorrhage Post Intra-Arterial Thrombolysis in Patients With Middle Cerebral Artery Occlusion Rishi
Reduced Pretreatment Ipsilateral Middle Cerebral Artery Cerebral Blood Flow Is Predictive of Symptomatic Hemorrhage Post Intra-Arterial Thrombolysis in Patients With Middle Cerebral Artery Occlusion Rishi
Intra-arterial thrombolysis (IAT) has the potential to rescue
 Published September 3, 2008 as 10.3174/ajnr.A1276 ORIGINAL RESEARCH G.A. Christoforidis C. Karakasis Y. Mohammad L.P. Caragine M. Yang A.P. Slivka Predictors of Hemorrhage Following Intra-Arterial Thrombolysis
Published September 3, 2008 as 10.3174/ajnr.A1276 ORIGINAL RESEARCH G.A. Christoforidis C. Karakasis Y. Mohammad L.P. Caragine M. Yang A.P. Slivka Predictors of Hemorrhage Following Intra-Arterial Thrombolysis
Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients
 AJNR Am J Neuroradiol 0:7, January 999 Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients Birgit Ertl-Wagner, Tobias Brandt, Christina Seifart,
AJNR Am J Neuroradiol 0:7, January 999 Diagnostic and Therapeutic Consequences of Repeat Brain Imaging and Follow-up Vascular Imaging in Stroke Patients Birgit Ertl-Wagner, Tobias Brandt, Christina Seifart,
Essentials of Clinical MR, 2 nd edition. 14. Ischemia and Infarction II
 14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
14. Ischemia and Infarction II Lacunar infarcts are small deep parenchymal lesions involving the basal ganglia, internal capsule, thalamus, and brainstem. The vascular supply of these areas includes the
What to expect on post mechanical thrombectomy CT - a guide to correct diagnosis.
 What to expect on post mechanical thrombectomy CT - a guide to correct diagnosis. Poster No.: C-2257 Congress: ECR 2017 Type: Educational Exhibit Authors: T. Buende Tchokouako, H. Nejadhamzeeigilani, A.
What to expect on post mechanical thrombectomy CT - a guide to correct diagnosis. Poster No.: C-2257 Congress: ECR 2017 Type: Educational Exhibit Authors: T. Buende Tchokouako, H. Nejadhamzeeigilani, A.
Translent CT hyperattenuation after intraarterial thrombolysis in stroke. Contrast extravasation or hemorrhage
 Translent CT hyperattenuation after intraarterial thrombolysis in stroke. Contrast extravasation or hemorrhage Poster No.: C-0053 Congress: ECR 2013 Type: Scientific Exhibit Authors: A. Losa Palacios,
Translent CT hyperattenuation after intraarterial thrombolysis in stroke. Contrast extravasation or hemorrhage Poster No.: C-0053 Congress: ECR 2013 Type: Scientific Exhibit Authors: A. Losa Palacios,
Early Angiographic and CT Findings in Patients with Hemorrhagic Infarction in the Distribution of the Middle Cerebral Artery
 1115 Early Angiographic and CT Findings in Patients with Hemorrhagic Infarction in the Distribution of the Middle Cerebral Artery L. Bozzao 1 U. Angeloni S. Bastianello L. M. Fantozzi A. Pierallini C.
1115 Early Angiographic and CT Findings in Patients with Hemorrhagic Infarction in the Distribution of the Middle Cerebral Artery L. Bozzao 1 U. Angeloni S. Bastianello L. M. Fantozzi A. Pierallini C.
Diffusion-Weighted Imaging Results in Higher Accuracy and Lower Interrater Variability in the Diagnosis of Hyperacute Ischemic Stroke
 CT and Diffusion-Weighted MR Imaging in Randomized Order Diffusion-Weighted Imaging Results in Higher Accuracy and Lower Interrater Variability in the Diagnosis of Hyperacute Ischemic Stroke J.B. Fiebach,
CT and Diffusion-Weighted MR Imaging in Randomized Order Diffusion-Weighted Imaging Results in Higher Accuracy and Lower Interrater Variability in the Diagnosis of Hyperacute Ischemic Stroke J.B. Fiebach,
Stroke: clinical presentations, symptoms and signs
 Stroke: clinical presentations, symptoms and signs Professor Peter Sandercock University of Edinburgh EAN teaching course Burkina Faso 8 th November 2017 Clinical diagnosis is important to Ensure stroke
Stroke: clinical presentations, symptoms and signs Professor Peter Sandercock University of Edinburgh EAN teaching course Burkina Faso 8 th November 2017 Clinical diagnosis is important to Ensure stroke
Neuro-- radiology 9 Springer-Verlag 1991
 Neuroradiology (1991) 33:207-211 Neuro-- radiology 9 Springer-Verlag 1991 Hyperdense middle cerebral artery CT sign Comparison with angiography in the acute phase of ischemic supratentorial infarction
Neuroradiology (1991) 33:207-211 Neuro-- radiology 9 Springer-Verlag 1991 Hyperdense middle cerebral artery CT sign Comparison with angiography in the acute phase of ischemic supratentorial infarction
Neurological Deterioration in Acute Ischemic Stroke
 Neurological Deterioration in Acute Ischemic Stroke Potential Predictors and Associated Factors in the European Cooperative Acute Stroke Study (ECASS) I A. Dávalos, MD; D. Toni, MD; F. Iweins, MSc; E.
Neurological Deterioration in Acute Ischemic Stroke Potential Predictors and Associated Factors in the European Cooperative Acute Stroke Study (ECASS) I A. Dávalos, MD; D. Toni, MD; F. Iweins, MSc; E.
Brain Attack. Strategies in the Management of Acute Ischemic Stroke: Neuroscience Clerkship. Case Medical Center
 Brain Attack Strategies in the Management of Acute Ischemic Stroke: Neuroscience Clerkship Stroke is a common and devastating disorder Third leading antecedent of death in American men, and second among
Brain Attack Strategies in the Management of Acute Ischemic Stroke: Neuroscience Clerkship Stroke is a common and devastating disorder Third leading antecedent of death in American men, and second among
Since the National Institute of Neurologic Disorders and
 ORIGINAL RESEARCH R.M. Sugg E.A. Noser H.M. Shaltoni N.R. Gonzales M.S. Campbell R. Weir E.D. Cacayorin J.C. Grotta Intra-Arterial Reteplase Compared to Urokinase for Thrombolytic Recanalization in Acute
ORIGINAL RESEARCH R.M. Sugg E.A. Noser H.M. Shaltoni N.R. Gonzales M.S. Campbell R. Weir E.D. Cacayorin J.C. Grotta Intra-Arterial Reteplase Compared to Urokinase for Thrombolytic Recanalization in Acute
Intravenous tpa has been a mainstay of acute stroke
 J Neurosurg 115:359 363, 2011 Aggressive intervention to treat a young woman with intracranial hemorrhage following unsuccessful intravenous thrombolysis for left middle cerebral artery occlusion Case
J Neurosurg 115:359 363, 2011 Aggressive intervention to treat a young woman with intracranial hemorrhage following unsuccessful intravenous thrombolysis for left middle cerebral artery occlusion Case
ASPECTS on CTA Source Images Versus Unenhanced CT Added Value in Predicting Final Infarct Extent and Clinical Outcome
 ASPECTS on CTA Source Images Versus Unenhanced CT Added Value in Predicting Final Infarct Extent and Clinical Outcome Shelagh B. Coutts, MBChB; Michael H. Lev, MD; Michael Eliasziw, PhD; Luca Roccatagliata,
ASPECTS on CTA Source Images Versus Unenhanced CT Added Value in Predicting Final Infarct Extent and Clinical Outcome Shelagh B. Coutts, MBChB; Michael H. Lev, MD; Michael Eliasziw, PhD; Luca Roccatagliata,
Non-contrast Computed Tomography in Acute Ischaemic Stroke: A Pictorial Review
 CONTINUING MEDICAL EDUCATION Non-contrast Computed Tomography in Acute Ischaemic Stroke: A Pictorial Review H Radhiana*, S O Syazarina**, M M Shahizon Azura**, H Hilwati***, M A Sobri** *Department of
CONTINUING MEDICAL EDUCATION Non-contrast Computed Tomography in Acute Ischaemic Stroke: A Pictorial Review H Radhiana*, S O Syazarina**, M M Shahizon Azura**, H Hilwati***, M A Sobri** *Department of
The Role of Neuroimaging in Acute Stroke. Bradley Molyneaux, HMS IV
 The Role of Neuroimaging in Acute Stroke Bradley Molyneaux, HMS IV Patient CR 62 yo F w/ 2 wk h/o altered mental status Presents to ED w/ confusion following a fall 1 day prior New onset left facial droop
The Role of Neuroimaging in Acute Stroke Bradley Molyneaux, HMS IV Patient CR 62 yo F w/ 2 wk h/o altered mental status Presents to ED w/ confusion following a fall 1 day prior New onset left facial droop
ACUTE ISCHEMIC STROKE. Current Treatment Approaches for Acute Ischemic Stroke
 ACUTE ISCHEMIC STROKE Current Treatment Approaches for Acute Ischemic Stroke EARLY MANAGEMENT OF ACUTE ISCHEMIC STROKE Rapid identification of a stroke Immediate EMS transport to nearest stroke center
ACUTE ISCHEMIC STROKE Current Treatment Approaches for Acute Ischemic Stroke EARLY MANAGEMENT OF ACUTE ISCHEMIC STROKE Rapid identification of a stroke Immediate EMS transport to nearest stroke center
The National Institutes of Health Stroke Scale (NIHSS)
 National Institutes of Health Stroke Scale Score and Vessel Occlusion in 252 Patients With Acute Ischemic Stroke Mirjam R. Heldner, MD; Christoph Zubler, MD; Heinrich P. Mattle, MD; Gerhard Schroth, MD;
National Institutes of Health Stroke Scale Score and Vessel Occlusion in 252 Patients With Acute Ischemic Stroke Mirjam R. Heldner, MD; Christoph Zubler, MD; Heinrich P. Mattle, MD; Gerhard Schroth, MD;
CT and MR Imaging in Young Stroke Patients
 CT and MR Imaging in Young Stroke Patients Ashfaq A. Razzaq,Behram A. Khan,Shahid Baig ( Department of Neurology, Aga Khan University Hospital, Karachi. ) Abstract Pages with reference to book, From 66
CT and MR Imaging in Young Stroke Patients Ashfaq A. Razzaq,Behram A. Khan,Shahid Baig ( Department of Neurology, Aga Khan University Hospital, Karachi. ) Abstract Pages with reference to book, From 66
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases
 How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
Stroke Update. Lacunar 19% Thromboembolic 6% SAH 13% ICH 13% Unknown 32% Hemorrhagic 26% Ischemic 71% Other 3% Cardioembolic 14%
 Stroke Update Michel Torbey, MD, MPH, FAHA, FNCS Medical Director, Neurovascular Stroke Center Professor Department of Neurology and Neurosurgery The Ohio State University Wexner Medical Center Objectives
Stroke Update Michel Torbey, MD, MPH, FAHA, FNCS Medical Director, Neurovascular Stroke Center Professor Department of Neurology and Neurosurgery The Ohio State University Wexner Medical Center Objectives
Intravenous or intra-arterial thrombolysis for acute ischemic
 ORIGINAL RESEARCH C. Tanaka T. Ueguchi E. Shimosegawa N. Sasaki T. Johkoh H. Nakamura J. Hatazawa Effect of CT Acquisition Parameters in the Detection of Subtle Hypoattenuation in Acute Cerebral Infarction:
ORIGINAL RESEARCH C. Tanaka T. Ueguchi E. Shimosegawa N. Sasaki T. Johkoh H. Nakamura J. Hatazawa Effect of CT Acquisition Parameters in the Detection of Subtle Hypoattenuation in Acute Cerebral Infarction:
Thrombus hounsfield unit on CT predicts vascular recanalization in stroke patients
 Thrombus hounsfield unit on CT predicts vascular recanalization in stroke patients Poster No.: C-2616 Congress: ECR 2010 Type: Scientific Exhibit Topic: Neuro Authors: H. F.Termes, J. Puig, J. Daunis-i-Estadella,
Thrombus hounsfield unit on CT predicts vascular recanalization in stroke patients Poster No.: C-2616 Congress: ECR 2010 Type: Scientific Exhibit Topic: Neuro Authors: H. F.Termes, J. Puig, J. Daunis-i-Estadella,
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Automated CT Segmentation and Analysis for Acute Middle Cerebral Artery Stroke
 AJNR Am J Neuroradiol :1050 1055, June/July 001 Automated CT Segmentation and Analysis for Acute Middle Cerebral Artery Stroke Joseph A. Maldjian, Julio Chalela, Scott E. Kasner, David Liebeskind, and
AJNR Am J Neuroradiol :1050 1055, June/July 001 Automated CT Segmentation and Analysis for Acute Middle Cerebral Artery Stroke Joseph A. Maldjian, Julio Chalela, Scott E. Kasner, David Liebeskind, and
Clinical benefit of tissue plasminogen activator (tpa) in
 Thrombolysis in Brain Ischemia (TIBI) Transcranial Doppler Flow Grades Predict Clinical Severity, Early Recovery, and Mortality in Patients Treated With Intravenous Tissue Plasminogen Activator Andrew
Thrombolysis in Brain Ischemia (TIBI) Transcranial Doppler Flow Grades Predict Clinical Severity, Early Recovery, and Mortality in Patients Treated With Intravenous Tissue Plasminogen Activator Andrew
NEURORADIOLOGY DIL part 4
 NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
An intravenous thrombolysis using recombinant tissue
 ORIGINAL RESEARCH I. Ikushima H. Ohta T. Hirai K. Yokogami D. Miyahara N. Maeda Y. Yamashita Balloon Catheter Disruption of Middle Cerebral Artery Thrombus in Conjunction with Thrombolysis for the Treatment
ORIGINAL RESEARCH I. Ikushima H. Ohta T. Hirai K. Yokogami D. Miyahara N. Maeda Y. Yamashita Balloon Catheter Disruption of Middle Cerebral Artery Thrombus in Conjunction with Thrombolysis for the Treatment
Imaging for Acute Stroke
 Imaging for Acute Stroke Nine case studies detailing the impact of imaging on stroke therapy. BY ANSAAR T. RAI, MD Ischemic stroke is a dynamic process, and the term stroke in evolution precisely underscores
Imaging for Acute Stroke Nine case studies detailing the impact of imaging on stroke therapy. BY ANSAAR T. RAI, MD Ischemic stroke is a dynamic process, and the term stroke in evolution precisely underscores
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
An Updated Systematic Review of rt-pa in Acute Ischaemic Stroke
 Wardlaw An Updated Systematic Review of rt-pa in Acute Ischaemic Stroke Joanna M Wardlaw COMPETING INTERESTS The author is on the Steering Committees of the Third International Stroke Trial (IST3) and
Wardlaw An Updated Systematic Review of rt-pa in Acute Ischaemic Stroke Joanna M Wardlaw COMPETING INTERESTS The author is on the Steering Committees of the Third International Stroke Trial (IST3) and
Acute stroke imaging
 Acute stroke imaging Aims Imaging modalities and differences Why image acute stroke Clinical correlation to imaging appearance What is stroke Classic definition: acute focal injury to the central nervous
Acute stroke imaging Aims Imaging modalities and differences Why image acute stroke Clinical correlation to imaging appearance What is stroke Classic definition: acute focal injury to the central nervous
Significance of Large Vessel Intracranial Occlusion Causing Acute Ischemic Stroke and TIA
 Significance of Large Vessel Intracranial Occlusion Causing Acute Ischemic Stroke and TIA Wade S. Smith, MD, PhD; Michael H. Lev, MD, FAHA; Joey D. English, MD, PhD; Erica C. Camargo, MD, MMSc; Maggie
Significance of Large Vessel Intracranial Occlusion Causing Acute Ischemic Stroke and TIA Wade S. Smith, MD, PhD; Michael H. Lev, MD, FAHA; Joey D. English, MD, PhD; Erica C. Camargo, MD, MMSc; Maggie
CT INTERPRETATION COURSE
 CT INTERPRETATION COURSE Refresher Course ASTRACAT October 2012 Stroke is a Clinical Diagnosis A clinical syndrome characterised by rapidly developing clinical symptoms and/or signs of focal loss of cerebral
CT INTERPRETATION COURSE Refresher Course ASTRACAT October 2012 Stroke is a Clinical Diagnosis A clinical syndrome characterised by rapidly developing clinical symptoms and/or signs of focal loss of cerebral
Judicious use of thrombolytic agents has greatly improved the
 Predictors of Clinical Improvement, Angiographic Recanalization, and Intracranial Hemorrhage After Intra-Arterial Thrombolysis for Acute Ischemic Stroke J.I. Suarez, MD; J.L. Sunshine, MD; R. Tarr, MD;
Predictors of Clinical Improvement, Angiographic Recanalization, and Intracranial Hemorrhage After Intra-Arterial Thrombolysis for Acute Ischemic Stroke J.I. Suarez, MD; J.L. Sunshine, MD; R. Tarr, MD;
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIUTION Usefulness of Triphasic Perfusion Computed Tomography for Intravenous Thrombolysis With Tissue-Type Plasminogen Activator in Acute Ischemic Stroke Kwang Ho Lee, MD; Soo Joo Lee, MD;
ORIGINAL CONTRIUTION Usefulness of Triphasic Perfusion Computed Tomography for Intravenous Thrombolysis With Tissue-Type Plasminogen Activator in Acute Ischemic Stroke Kwang Ho Lee, MD; Soo Joo Lee, MD;
Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke
 Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Original Contribution Spontaneous Recanalization after Complete Occlusion of the Common Carotid Artery with Subsequent Embolic Ischemic Stroke Abstract Introduction: Acute carotid artery occlusion carries
Arterial Occlusion Revealed by CT Angiography Predicts NIH Stroke Score and Acute Outcomes after IV tpa Treatment
 AJNR Am J Neuroradiol 26:246 251, February 2005 Arterial Occlusion Revealed by CT Angiography Predicts NIH Stroke Score and Acute Outcomes after IV tpa Treatment John R. Sims, Guy Rordorf, Eric E. Smith,
AJNR Am J Neuroradiol 26:246 251, February 2005 Arterial Occlusion Revealed by CT Angiography Predicts NIH Stroke Score and Acute Outcomes after IV tpa Treatment John R. Sims, Guy Rordorf, Eric E. Smith,
AMSER Case of the Month: March 2019
 AMSER Case of the Month: March 2019 62 year-old male with left-sided weakness Ashley Graziano OMS IV, Lake Erie College of Osteopathic Medicine Erik Yannone MD, Charles Q. Li MD, Warren Chang MD, Matthew
AMSER Case of the Month: March 2019 62 year-old male with left-sided weakness Ashley Graziano OMS IV, Lake Erie College of Osteopathic Medicine Erik Yannone MD, Charles Q. Li MD, Warren Chang MD, Matthew
Hyperperfusion syndrome after MCA embolectomy a rare complication?
 ISSN 1507-6164 DOI: 10.12659/AJCR.889672 Received: 2013.08.13 Accepted: 2013.09.11 Published: 2013.11.29 Hyperperfusion syndrome after MCA embolectomy a rare complication? Authors Contribution: Study Design
ISSN 1507-6164 DOI: 10.12659/AJCR.889672 Received: 2013.08.13 Accepted: 2013.09.11 Published: 2013.11.29 Hyperperfusion syndrome after MCA embolectomy a rare complication? Authors Contribution: Study Design
Direct Percutaneous Transluminal Angioplasty for Acute Middle Cerebral Artery Trunk Occlusion. An Alternative Option to Intra-arterial Thrombolysis
 Direct Percutaneous Transluminal Angioplasty for Acute Middle Cerebral Artery Trunk Occlusion An Alternative Option to Intra-arterial Thrombolysis Shinichi Nakano, MD; Tsutomu Iseda, MD; Takumi Yoneyama,
Direct Percutaneous Transluminal Angioplasty for Acute Middle Cerebral Artery Trunk Occlusion An Alternative Option to Intra-arterial Thrombolysis Shinichi Nakano, MD; Tsutomu Iseda, MD; Takumi Yoneyama,
The Predictive Value of Early CT and Angiography for Fatal Hemispheric Swelling in Acute Stroke
 AJNR Am J Neuroradiol 19:839 846, May 1998 The Predictive Value of Early CT and Angiography for Fatal Hemispheric Swelling in Acute Stroke Thomas Kucinski, Christoph Koch, Ulrich Grzyska, Heinz-Jörg Freitag,
AJNR Am J Neuroradiol 19:839 846, May 1998 The Predictive Value of Early CT and Angiography for Fatal Hemispheric Swelling in Acute Stroke Thomas Kucinski, Christoph Koch, Ulrich Grzyska, Heinz-Jörg Freitag,
ISCHEMIC STROKE IMAGING
 ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
BY MARILYN M. RYMER, MD
 Lytics, Devices, and Advanced Imaging The evolving art and science of acute stroke intervention. BY MARILYN M. RYMER, MD In 1996, when the US Food and Drug Administration (FDA) approved the use of intravenous
Lytics, Devices, and Advanced Imaging The evolving art and science of acute stroke intervention. BY MARILYN M. RYMER, MD In 1996, when the US Food and Drug Administration (FDA) approved the use of intravenous
Imaging Stroke: Is There a Stroke Equivalent of the ECG? Albert J. Yoo, MD Director of Acute Stroke Intervention Massachusetts General Hospital
 Imaging Stroke: Is There a Stroke Equivalent of the ECG? Albert J. Yoo, MD Director of Acute Stroke Intervention Massachusetts General Hospital Disclosures Penumbra, Inc. research grant (significant) for
Imaging Stroke: Is There a Stroke Equivalent of the ECG? Albert J. Yoo, MD Director of Acute Stroke Intervention Massachusetts General Hospital Disclosures Penumbra, Inc. research grant (significant) for
NHL Journal of Medical Sciences/July 2014/Vol 3/Issue 2 18
 Research article NIHSS Score: A handy tool to predict vascular occlusion in acute ischemic stroke Ronak Shah*, Chintal Vyas**, Jyoti Vora*** *Senior Resident, **Assistant Professor, ***Associate Professor,
Research article NIHSS Score: A handy tool to predict vascular occlusion in acute ischemic stroke Ronak Shah*, Chintal Vyas**, Jyoti Vora*** *Senior Resident, **Assistant Professor, ***Associate Professor,
EFFICACY AND SAFETY OF INTRA-ARTERIAL THROMBOLYTIC
 Open Access Research Journal Medical and Health Science Journal, MHSJ www.pradec.eu ISSN: 1804-1884 (Print) 1805-5014 (Online) Volume 10, 2012, pp. 2-9 EFFICACY AND SAFETY OF INTRA-ARTERIAL THROMBOLYTIC
Open Access Research Journal Medical and Health Science Journal, MHSJ www.pradec.eu ISSN: 1804-1884 (Print) 1805-5014 (Online) Volume 10, 2012, pp. 2-9 EFFICACY AND SAFETY OF INTRA-ARTERIAL THROMBOLYTIC
Published April 17, 2014 as /ajnr.A3931
 Published April 17, 2014 as 10.3174/ajnr.A3931 ORIGINAL RESEARCH BRAIN Relative Filling Time Delay Based on CT Perfusion Source Imaging: A Simple Method to Predict Outcome in Acute Ischemic Stroke W. Cao,
Published April 17, 2014 as 10.3174/ajnr.A3931 ORIGINAL RESEARCH BRAIN Relative Filling Time Delay Based on CT Perfusion Source Imaging: A Simple Method to Predict Outcome in Acute Ischemic Stroke W. Cao,
Michael Horowitz, MD Pittsburgh, PA
 Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
Michael Horowitz, MD Pittsburgh, PA Introduction Cervical Artery Dissection occurs by a rupture within the arterial wall leading to an intra-mural Hematoma. A possible consequence is an acute occlusion
The administration of intravenous tissue plasminogen
 Intravenous Tissue Plasminogen Activator for Acute Ischemic Stroke A Canadian Hospital s Experience Kristine M. Chapman, MD; Andrew R. Woolfenden, MD; Douglas Graeb, MD; Dean C.C. Johnston, MD; Jeff Beckman,
Intravenous Tissue Plasminogen Activator for Acute Ischemic Stroke A Canadian Hospital s Experience Kristine M. Chapman, MD; Andrew R. Woolfenden, MD; Douglas Graeb, MD; Dean C.C. Johnston, MD; Jeff Beckman,
Stroke/TIA. Tom Bedwell
 Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
Stroke/TIA Tom Bedwell tab1g11@soton.ac.uk The Plan Definitions Anatomy Recap Aetiology Pathology Syndromes Brocas / Wernickes Investigations Management Prevention & Prognosis TIAs Key Definitions Transient
Site of Arterial Occlusion Identified by Transcranial Doppler Predicts the Response to Intravenous Thrombolysis for Stroke
 Site of Arterial Occlusion Identified by Transcranial Doppler Predicts the Response to Intravenous Thrombolysis for Stroke Maher Saqqur, MD, FRCPC; Ken Uchino, MD; Andrew M. Demchuk, MD, FRCPC; Carlos
Site of Arterial Occlusion Identified by Transcranial Doppler Predicts the Response to Intravenous Thrombolysis for Stroke Maher Saqqur, MD, FRCPC; Ken Uchino, MD; Andrew M. Demchuk, MD, FRCPC; Carlos
Thrombolytic therapy for ischemic stroke A review. Part II Intra-arterial thrombolysis, vertebrobasilar stroke, phase IV trials, and stroke imaging
 Thrombolytic therapy for ischemic stroke A review. Part II Intra-arterial thrombolysis, vertebrobasilar stroke, phase IV trials, and stroke imaging Peter D. Schellinger, MD; Jochen B. Fiebach, MD; Alexander
Thrombolytic therapy for ischemic stroke A review. Part II Intra-arterial thrombolysis, vertebrobasilar stroke, phase IV trials, and stroke imaging Peter D. Schellinger, MD; Jochen B. Fiebach, MD; Alexander
Without reperfusion therapy, almost 80% of patients with
 ORIGINAL RESEARCH V. Puetz P.N. Sylaja M.D. Hill S.B. Coutts I. Dzialowski U. Becker G. Gahn R. von Kummer A.M. Demchuk CT Angiography Source Images Predict Final Infarct Extent in Patients with Basilar
ORIGINAL RESEARCH V. Puetz P.N. Sylaja M.D. Hill S.B. Coutts I. Dzialowski U. Becker G. Gahn R. von Kummer A.M. Demchuk CT Angiography Source Images Predict Final Infarct Extent in Patients with Basilar
The principal goal in treating acute ischemic stroke is rapid
 ORIGINAL RESEARCH S. Sugiura K. Iwaisako S. Toyota H. Takimoto Simultaneous Treatment with Intravenous Recombinant Tissue Plasminogen Activator and Endovascular Therapy for Acute Ischemic Stroke Within
ORIGINAL RESEARCH S. Sugiura K. Iwaisako S. Toyota H. Takimoto Simultaneous Treatment with Intravenous Recombinant Tissue Plasminogen Activator and Endovascular Therapy for Acute Ischemic Stroke Within
One of the most important issues a clinician must consider
 Defining Clinically Relevant Cerebral Hemorrhage After Thrombolytic Therapy for Stroke Analysis of the National Institute of Neurological Disorders and Stroke Tissue-Type Plasminogen Activator Trials Neal
Defining Clinically Relevant Cerebral Hemorrhage After Thrombolytic Therapy for Stroke Analysis of the National Institute of Neurological Disorders and Stroke Tissue-Type Plasminogen Activator Trials Neal
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT
 Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
ACUTE STROKE TREATMENT IN LARGE NIHSS PATIENTS. Justin Nolte, MD Assistant Profession Marshall University School of Medicine
 ACUTE STROKE TREATMENT IN LARGE NIHSS PATIENTS Justin Nolte, MD Assistant Profession Marshall University School of Medicine History of Presenting Illness 64 yo wf with PMHx of COPD, HTN, HLP who was in
ACUTE STROKE TREATMENT IN LARGE NIHSS PATIENTS Justin Nolte, MD Assistant Profession Marshall University School of Medicine History of Presenting Illness 64 yo wf with PMHx of COPD, HTN, HLP who was in
Significant Relationships
 Opening Large Vessels During Acute Ischemic Stroke Significant Relationships Wade S Smith, MD, PhD Director UCSF Neurovascular Service Professor of Neurology Daryl R Gress Endowed Chair of Neurocritical
Opening Large Vessels During Acute Ischemic Stroke Significant Relationships Wade S Smith, MD, PhD Director UCSF Neurovascular Service Professor of Neurology Daryl R Gress Endowed Chair of Neurocritical
The Oxfordshire Community Stroke Project (OCSP) devised
 Relationship Between Pattern of Intracranial Artery Abnormalities on Transcranial Doppler and Oxfordshire Community Stroke Project Clinical Classification of Ischemic Stroke G.E. Mead, MD; J.M. Wardlaw,
Relationship Between Pattern of Intracranial Artery Abnormalities on Transcranial Doppler and Oxfordshire Community Stroke Project Clinical Classification of Ischemic Stroke G.E. Mead, MD; J.M. Wardlaw,
Intracranial Balloon Angioplasty of Acute Terminal Internal Carotid Artery Occlusions
 AJNR Am J Neuroradiol 23:1308 1312, September 2002 Case Report Intracranial Balloon Angioplasty of Acute Terminal Internal Carotid Artery Occlusions Joon K. Song, Edwin D. Cacayorin, Morgan S. Campbell,
AJNR Am J Neuroradiol 23:1308 1312, September 2002 Case Report Intracranial Balloon Angioplasty of Acute Terminal Internal Carotid Artery Occlusions Joon K. Song, Edwin D. Cacayorin, Morgan S. Campbell,
NEURO IMAGING OF ACUTE STROKE
 1 1 NEURO IMAGING OF ACUTE STROKE ALICIA RICHARDSON, MSN, RN, ACCNS-AG, ANVP-BC WENDY SMITH, MA, RN, MBA, SCRN, FAHA LYNN HUNDLEY, APRN, CNRN, CCNS, ANVP-BC 2 2 1 DISCLOSURES Alicia Richardson: Stryker
1 1 NEURO IMAGING OF ACUTE STROKE ALICIA RICHARDSON, MSN, RN, ACCNS-AG, ANVP-BC WENDY SMITH, MA, RN, MBA, SCRN, FAHA LYNN HUNDLEY, APRN, CNRN, CCNS, ANVP-BC 2 2 1 DISCLOSURES Alicia Richardson: Stryker
Trial Design and Reporting Standards for Intra-Arterial Cerebral Thrombolysis for Acute Ischemic Stroke
 Trial Design and Reporting Standards for Intra-Arterial Cerebral Thrombolysis for Acute Ischemic Stroke Randall T. Higashida, MD; Anthony J. Furlan, MD; for the Technology Assessment Committees of the
Trial Design and Reporting Standards for Intra-Arterial Cerebral Thrombolysis for Acute Ischemic Stroke Randall T. Higashida, MD; Anthony J. Furlan, MD; for the Technology Assessment Committees of the
Comparison of Five Major Recent Endovascular Treatment Trials
 Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Comparison of Five Major Recent Endovascular Treatment Trials Sample size 500 # sites 70 (100 planned) 316 (500 planned) 196 (833 estimated) 206 (690 planned) 16 10 22 39 4 Treatment contrasts Baseline
Introduction. Abstract. Michael Yannes 1, Jennifer V. Frabizzio, MD 1, and Qaisar A. Shah, MD 1 1
 Reversal of CT hypodensity after acute ischemic stroke Michael Yannes 1, Jennifer V. Frabizzio, MD 1, and Qaisar A. Shah, MD 1 1 Abington Memorial Hospital in Abington, Pennsylvania Abstract We report
Reversal of CT hypodensity after acute ischemic stroke Michael Yannes 1, Jennifer V. Frabizzio, MD 1, and Qaisar A. Shah, MD 1 1 Abington Memorial Hospital in Abington, Pennsylvania Abstract We report
Stroke is a strongly age-related disease, and the number of
 ORIGINAL RESEARCH D. Kim G.A. Ford C.S. Kidwell S. Starkman F. Vinuela G.R. Duckwiler R. Jahan J.L. Saver, for the UCLA Intra- Arterial Thrombolysis Investigators Intra-Arterial Thrombolysis for Acute
ORIGINAL RESEARCH D. Kim G.A. Ford C.S. Kidwell S. Starkman F. Vinuela G.R. Duckwiler R. Jahan J.L. Saver, for the UCLA Intra- Arterial Thrombolysis Investigators Intra-Arterial Thrombolysis for Acute
Principles Arteries & Veins of the CNS LO14
 Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Collateral Circulation and Outcome after Basilar Artery Thrombolysis
 AJNR Am J Neuroradiol 19:1557 1563, September 1998 Collateral Circulation and Outcome after Basilar Artery Thrombolysis DeWitte T. Cross, III, Christopher J. Moran, Paul T. Akins, Edward E. Angtuaco, Colin
AJNR Am J Neuroradiol 19:1557 1563, September 1998 Collateral Circulation and Outcome after Basilar Artery Thrombolysis DeWitte T. Cross, III, Christopher J. Moran, Paul T. Akins, Edward E. Angtuaco, Colin
Update on Emergency Imaging of Acute Ischemic Stroke
 Update on Emergency Imaging of Acute Ischemic Stroke Daniel Kawakyu-O Connor, M.D. Division of Emergency Imaging, University of Rochester Medical Center, Rochester, NY Introduction The term acute stroke
Update on Emergency Imaging of Acute Ischemic Stroke Daniel Kawakyu-O Connor, M.D. Division of Emergency Imaging, University of Rochester Medical Center, Rochester, NY Introduction The term acute stroke
