ISPUB.COM. Hypertrophic Cardiomyopathy. L Hull-Grommesh CLINICAL DESCRIPTION INCIDENCE/PREVALENCE
|
|
|
- Marilynn Parsons
- 5 years ago
- Views:
Transcription
1 ISPUB.COM The Internet Journal of Advanced Nursing Practice Volume 10 Number 2 L Hull-Grommesh Citation L Hull-Grommesh.. The Internet Journal of Advanced Nursing Practice Volume 10 Number 2. Abstract Hypertrophic cardiomyopathy is a common, genetically transmitted cardiovascular disease affecting 1 in 500 persons. Patients with hypertrophic cardiomyopathy can be asymptomatic. Often the first presenting symptom is sudden cardiac death. The nurse practitioner must be aware of the diagnostic impact of hypertrophic cardiomyopathy on the patient and family, the importance of early diagnosis, and current management and treatment options. The purpose of this article is to review hypertrophic cardiomyopathy and increase awareness of this disease among nurse practitioners. CLINICAL DESCRIPTION Hypertrophic cardiomyopathy (HCM) is a familial, genetic, cardiovascular disorder affecting 1 in 500 persons (1). Dr. Robert Donald Teare was one of the first physicians to recognize HCM. Over 50 years ago, he observed characteristic asymmetrical thickening of the ventricular septum and sudden cardiac death in a group of patients from the same family (1). As asymmetric ventricular hypertrophy involving the septum is only one feature of HCM, healthcare professionals now know that other features include atrial enlargement, myocyte disarray, and interstitial fibrosis (1). HCM causes stiffening and delayed relaxation of the ventricles, thus requiring higher pressure to expand with the inflow of blood (1). As a consequence diastolic heart failure develops and may progress to a dilated or systolic heart failure. HCM can be non-obstructive or obstructive to blood flow. Non-obstructive HCM is the more common form and is characterized by ventricular muscle thickening without impedance of blood flow out of the left ventricle. Left ventricular outflow obstruction is seen in 25% of patients with HCM and is often referred to as hypertrophic obstructive cardiomyopathy (HOCM) (2). In the past, HOCM was known as idiopathic hypertrophic subaortic stenosis (IHSS). Obstruction of blood flow out of the left ventricular outflow tract generates rapid ejection of blood, resulting in the pulling the anterior leaflet of the mitral valve toward the thickened septum. The pulling motion is called systolic anterior motion (SAM), and constant pulling of the mitral valve leaflet leads to mitral regurgitation. The blood flow obstruction seen in HOCM can be transient or persistent (3, 4). HCM varies widely among patients in both the severity of the disease and the complications that may occur. Most patients with HCM are asymptomatic or have very few symptoms. Clinical progression of the disease is slow, and medications help. HCM takes one of four different paths (5). The first path is sudden cardiac death from ventricular arrhythmias that occur due to the myocte disarray of the cardiac cells which causes disturbances in the normal conduction of the electrical activity of the heart. The second path presents progressive symptoms of dyspnea on exertion, chest pain, pre-syncope, dizziness, and syncope. The third path is the progression of the HCM to heart failure followed by a dilated form of cardiomyopathy which occurs in 10 to 15% of patients (2). The fourth path is comprised of complications related to the development of atrial fibrillation secondary to HCM (5). Atrial fibrillation and the loss of atrial kick associated with atrial fibrillation decreases cardiac output and presents symptoms in patients who were originally asymptomatic. The fact that many patients with HCM are asymptomatic suggests that the incidence and prevalence of HCM may be under estimated (6). INCIDENCE/PREVALENCE Although HCM is the most common inherited cardiac disorder, no differences in incidence exist between genders (7). HCM is also a common cause of exercise-related sudden cardiac death in athletes less than 35 years old, and the most common cause of death in athletic events (2). For adults, the peak incidence of HCM is in the second decade of life, while the peak distribution is in the fourth through the sixth 1 of 6
2 decades of life (7). The prevalence of HCM in the general population is 0.2% (12). The annual rate of sudden cardiac death secondary to HCM ranges from 0.5% to 1.5% (3). Four-percent of patients with HCM die each year (7). Although most deaths occur from sudden cardiac death secondary to arrhythmias, heart failure is less likely to be the cause of death. A recent study of 2155 patients with HCM in Japan found that patients with a low ventricular ejection fraction, a left bundle branch block on the electrocardiogram, or a high cardiothoracic ratio on a chest x-ray had poorer prognoses (8). GENETICS HCM has an autosomal-dominant mode of inheritance, where autosomal refers to a mutation on one of the numbered chromosomes (9). When a mutation is passed on in a dominant way, only one mutation is sufficient to cause the condition, and a person with one dominant mutation of HCM will develop HCM (9). A child of a person with HCM has a 50% chance of getting the mutation. Despite the identification of genetic mutations leading to HCM, this disorder remains genetically diverse with more than 450 known mutations in 13 genes (10). In the past HCM was considered idiopathic, but is now recognized as a disorder resulting from dominant mutations in genes encoding the proteins of the contractile apparatus (8). HCM can be caused by mutations in genes encoding cardiac myosin heavy chain BMHC, MyBPC, cardiac troponin T, cardiac troponin I, essential light chains, regulatory light chains, and cardiac actin (11). The variability in clinical course may be explained by the different roles that mutant proteins play in the sarcomere (10). Mutations in the gene-encoding cardiac myosin heavy chain were the first to be identified as a cause of familial HCM. The genes of HCM may present early in life, and is believed to cause severe hypertrophy, increase the risk of outflow obstruction, and increase the risk of sudden death. The cardiac myosin-binding protein C (MyBPC) mutations often cause late onset HCM and have a favorable prognosis (8). The variability in HCM is also affected by the coexistence of hypertension or ischemic heart disease. Tsoutsman and colleagues found Tnl-203/MHC-403 double mutant mice developed a severe cardiac phenotype characterized by heart failure and early death (10). The authors concluded that the presence of two disease-causing mutations predisposes individuals to a greater risk of developing severe heart failure than human HCM caused by a single gene mutation. Genetic testing for HCM has been limited by costs (1). Mutation analysis for eight sarcomeric genes is now commercially available for clinical testing (9). However, the test costs over $4000, and many insurance companies do not pay for testing. Due to the heterogeneity of HCM, false negative test results may occur, although a negative test does not exclude the possibility that the individual s HCM is caused by a mutation that was not tested (9). The lack of specific genetic testing does not prevent testing with standard diagnostics, such as echocardiography and electrocardiogram. The traditional recommended screening interval/follow-up for patients and families with HCM is every 12 to 18 months (2). Screening involves performing both echocardiogram and electrocardiogram (7). Testing of family members should begin at age 12, and, if no evidence of hypertrophy throughout the years develops, testing may conclude at age 21 (7). However, the guideline is controversial. As substantial molecular diversity and heterogeneity of HCM, some believe testing should continue into mid-life (6). DIAGNOSIS Early identification and evaluation of the subtle symptoms related to HCM by the NP may avoid the initial presentation of sudden cardiac death. A comprehensive physical examination and review of symptoms by the nurse practitioner may lead to a diagnosis of HCM. The most common symptoms of HCM are dyspnea, chest pain, fatigue, palpitations, dizziness, and syncope. Syncope can result from inadequate cardiac output secondary to left ventricular outflow obstruction or from ventricular arrhythmias and may be provoked by exertion or exercise. Ventricular arrhythmias occur in 75% of HCM patients undergoing ambulatory monitoring (2). Chest pain and heart failure symptoms also develop from diastolic dysfunction and from outflow obstruction, which causes mitral regurgitation and fluid backs up into the left atrium and lungs. Significant shortness of breath occurs if the mitral regurgitation and or outflow obstruction worsens. A careful patient and family history by the NP also may reveal clues to HCM. However, a physical exam and history may not provide any signs of HCM. A diagnosis of HCM may be suspected if the patient has a history of syncope or a family history of sudden death. Patients with HCM often have a harsh, systolic crescendo-decrescendo murmur at the left 2 of 6
3 sternal border (7). The murmur must be carefully assessed, as the systolic murmur of HCM may be misinterpreted to be the systolic murmur of aortic stenosis. Typically, the intensity of the systolic murmur diminishes with squatting and increases with standing (5). Radiating, systolic murmurs along the carotid arteries are most likely to be the systolic murmur of aortic stenosis. NPs must provide a comprehensive work-up and thorough history and physical with attention to the review of symptoms in the attempt to identify those patients at risk for HCM. As a result, providing early interventions may prevent the sequela of complications associated with HCM. The awareness of the NP of how HCM is diagnosed and knowledge of the risk factors for sudden death are key in helping to prevent complications of HCM. All patients with HCM should be assessed for risk of sudden cardiac death according to the American College of Cardiology/European Society of Cardiology guidelines (Table 1) (2). Figure 1 Table 1: Risk Factors for Sudden Cardiac Death in Patients with HCM An echocardiogram is gold standard and used to confirm the diagnosis of HCM (6). More specifically, a left ventricular wall thickness greater than 15 mm establishes HCM (2). The echocardiogram also identifies outflow obstruction. The electrocardiogram may be normal in patients with HCM, but typically shows ST-segment and T-wave abnormalities, and giant negative T-waves in the precordial leads may be seen (2). Holter monitoring is also used to detect any arrhythmias. Differential diagnoses for HCM include disorders that cause hypertrophy of the left ventricle. These disorders include the athlete s heart syndrome, left ventricular hypertrophy secondary to hypertension, and cardiac amyloidosis (11). Whereas the hypertrophy seen in HCM is asymmetrical, the hypertrophy seen in hypertension, cardiac amyloidosis, and athlete s heart syndrome is concentric. Once the diagnosis of HCM is made or suspected, the NP must individualize the patient s treatment plan. MANAGEMENT/TREATMENT Medical management is directed towards reducing symptoms and preventing complications. The treatment and management is often difficult because of the heterogeneous nature of the disorder and the lack of randomized controlled trials. Recent guidelines on HCM published by the American College of Cardiology and the European Society of Cardiology help clinicians in decision making. Currently, no specific algorithm is available to guide treatment and assess prognosis so treatment plans must be individualized. Management and treatments include beta blocker therapy, calcium channel blocker therapy, antiarrhythmic therapy, internal cardiac defibrillator (ICD) placement, alcohol ablation of the intraventricular septum, septal myectomy surgery, and surveillance. The most common medications used are beta blockers which slow the heart rate, enhance diastolic filling, and decrease myocardial oxygen demand (3). The use of beta blockers helps the heart to contract and relax. Calcium channel blockers also help to relax the stiff left ventricle and increase filling of the ventricles. An antiarrhythmic drug, such as amiodarone, is commonly used in patients found to have ventricular arrhythmias on holter monitoring. Medications that decrease afterload of the heart should be avoided as these agents cause a further reduction in the filling pressures, a fall in blood pressure and syncope. The prophylactic treatment of asymptomatic HCM patients with ICDs is controversial. An ICD can be life saving to the patient with HCM and ventricular arrhythmias as sudden cardiac death is most commonly caused by ventricular arrhythmias. Rapid defibrillation is critical to the patient s survival. ICD placement is indicated in high risk HCM patients, such as those that have a decreased blood pressure with exercise, history of cardiac arrest or ventricular tachycardia, family history of cardiac arrest, history of unexplained syncope, and or severe muscle thickening. Takagi, Yamakado, and Nakano studied both completely asymptomatic and symptomatic patients with HCM and found that patients who were completely asymptomatic have a significantly lower mortality rate than those with symptoms (0.9 % vs. 1.9 % respectively, p<0.05) (12). ICD insertion in young patients may be lifesaving, yet invoke many psychosocial issues. Maron and colleagues examined the clinical risk profile of sudden cardiac death from ventricular arrhythmias and the 3 of 6
4 use of ICDs (7). These authors studied 506 patients with HCM who underwent ICD placement for primary or secondary prevention of sudden cardiac death. The mean age of the participants was 42 years, and all patients were followed for four years. The authors found that the ICD successfully terminated ventricular arrhythmias in 20% of the patients. The researchers also discovered that patients who received an internal cardiac defibrillator for only one risk factor had a similar incidence of internal cardiac defibrillator firings. The authors looked at four risk factors, which included a family history of sudden death due to HCM, massive left ventricular hypertrophy, non-sustained ventricular tachycardia on holter monitoring, and prior unexplained syncope (7). The conclusion was that a single risk factor for sudden cardiac death in HCM may be enough to justify implantation of an internal cardiac defibrillator as primary prevention. Approximately 20 to 40 % of patients with HOCM who develop heart failure symptoms will be refractory to medical therapy. Alcohol septal ablation (ASA) of the intraventricular septum can be performed via alcohol infused into the septal coronary artery that supplies blood to the septum. The alcohol causes death of that area of the septum and reduces the hypertrophy. The reduction in the septal hypertrophy decreases the left ventricular outflow obstruction. A systematic review of 42 ASA studies by Alam, Dokainish, and Lakkis found that ASA offers good outcomes to patients with HCOM (13). Patients who had ASA performed had an increase in exercise tolerance and decrease in the diameter of the basal septum. The mortality within 30 days of the procedure was 1.5% and the mortality after 30 days was 0.5%. Although ASA is a percutaneous procedure and much less invasive than surgery, complete heart block during and after the procedure may require permanent pacemaker insertion. Another treatment option for HCM patients who are refractory to medical treatment is surgical septal myectomy which involves re-sectioning a small amount of the ventricular septum (6). Surgery may also involve repair of the mitral valve. Surgery is much more invasive than ASA. Education regarding activity, medications and follow-up is critical. Patients must be instructed to avoid hypovolemia which may reduce the filling pressures of the heart and increase the risk of syncope. Patients with HCM should avoid strenuous activities and competitive sports. The NP is in a unique position to educate the patient and family members about HCM. Education regarding all aspects of HCM is critical, including the risk of sudden cardiac death. The diagnosis of HCM impacts not only the patient, but the family. Family members, as well as patients with HCM, may feel anxiety about the possible development of HCM. The patient with HCM may live in fear of sudden cardiac death. The NP can provide support for the patients and family and help to relieve their anxieties. Education regarding a home automated external defibrillator and cardiopulmonary resuscitation should be included. CONCLUSION HCM is a common inherited cardiovascular disorder, yet is often under-recognized. Nurse practitioners must be aware of HCM and how the condition is diagnosed. The NP can play a major role in identifying patients with HCM. The importance of assessing risk and relaying treatments options to patients is an important role. The NP also plays a critical part in the symptom management, family evaluation and prevention of sudden cardiac death in patients with HCM. Patients with HCM can be identified through a complete history and physical examination. Individualized care can then be developed for each patient with HCM, as HCM varies in the severity of symptoms and complications. The nurse practitioner is in a key position to provide education on activity, risk factors for sudden cardiac death, genetic testing, and follow-up for the patient and family. In the future, genetic testing and identification of genes will continue to help clarify the treatment and management of patients with HCM. ACKNOWLEGEMENTS The author would like to thank the following individuals for their support, encouragement, and review of this manuscript: Monique Lambert, DNP, RN; Nina Selz, PhD; Susan D. Ruppert, PhD, RN, ANP-BC, NP-C, FCCM, FAANP; and Oscar Rosales, MD. References 1. Keren, A, Syrris, P, McKenna, WJ. Hypertrophic cardiomyopathy: The genetic determinants of clinical disease expression. Nat Clin Pract. 2008;5(3): Maron, BJ. Sudden death in young athletes. N Engl J Med. 2003;349: Miller, MA, Gomes, JA, & Fuster, V. Risk stratification of sudden cardiac death in hypertrophic cardiomyopathy. Nat Clin Pract. 2007;4(12): Adabag, S, Kuskowski, M, & Maron, B. Abstract 3600: Identification of hypertrophic cardiomyopathy in the community and the value of preparticipation sports examinations. Circulation, 2006;114, II Yao, EF. Hypertrophic cardiomyopathy. Aviat Space Environ Med. 2008;79(2): Maron, BJ, Seidman, JG, Seidman, CE. Proposal for 4 of 6
5 contemporary screening strategies in families with hypertrophic cardiomyopathy. J Am Coll Cardiol. 2004;44(11): Maron, BJ, Spirito, P, Shen, WK, Haas, TS, Formisano, F, Link, MS, et al. Implantable cardioverter-defibrillators and prevention of sudden cardiac death in hypertrophic cardiomyopathy. J Am Coll Cardiol, 2007;298(4): Nasermoaddeli, A, Katsuyuki, M, Matsumori, A, Soyama, Y, Morikawa, Y, Kitabatake, A, et al. Prognosis and prognostic factors in patients with hypertrophic cardiomyopathy in Japan: Results from a nationwide study. Heart. 2007; 93: Robin, NH, Tabereaux, PB, Benza, R, & Korf, BR. Genetic testing in cardiovascular disease. J Am Coll Cardiol. 2007;50(8): Tsoutsman, T, Kelly, M, Dominic, CH, Tan, JE, Tu, E, Lam, L, et al. Severe heart failure and early mortality in a double-mutation mouse model of familial hypertrophic cardiomyopathy. Circulation. 2008;117(14): Arad, M, Seidman, JG, & Seidman, CE. Phenotypic diversity in hypertrophic cardiomyopathy. Hum Mol Genet. 2002;11(20): Takagi, E, Yamakado, T, & Nakano, T. Prognosis of completely asymptomatic 13. J Am Coll Cardiol. 1999;33: Alam, M, Dokainigh, H, Lakkis, N. Alcohol septal ablation for hypertrophic obstructive cardiomyopathy: A systematic review of published studies. J Interv Cardiol. 2006;19(4): of 6
6 Author Information Lori Hull-Grommesh, DNP, RN, CCRN, ACNP-BC Acute Care Nurse Practitioner Cardiology, Memorial Hermann Hospital-Texas Medical Center Houston, Texas 6 of 6
Treatment of Hypertrophic Cardiomyopathy in Bruce B. Reid, MD
 Treatment of Hypertrophic Cardiomyopathy in 2017 Bruce B. Reid, MD Disclosures I have no conflicts of interest to disclose I will not be discussing any off label medications and/or devices Objectives 1)
Treatment of Hypertrophic Cardiomyopathy in 2017 Bruce B. Reid, MD Disclosures I have no conflicts of interest to disclose I will not be discussing any off label medications and/or devices Objectives 1)
Medical Policy and and and and
 ARBenefits Approval: 10/12/2011 Effective Date: 01/01/2012 Revision Date: Code(s): 93799, Unlisted cardiovascular service or procedure Medical Policy Title: Percutaneous Transluminal Septal Myocardial
ARBenefits Approval: 10/12/2011 Effective Date: 01/01/2012 Revision Date: Code(s): 93799, Unlisted cardiovascular service or procedure Medical Policy Title: Percutaneous Transluminal Septal Myocardial
Hypertrophic Cardiomyopathy
 019-CardioCase:019-CardioCase 4/16/07 1:39 PM Page 19 Hypertrophic Cardiomyopathy Abdullah Alshehri, MD; and Andrew Ignaszewski, MD, FRCPC CardioCase presentation Presley s check-up Presley, 37, discovered
019-CardioCase:019-CardioCase 4/16/07 1:39 PM Page 19 Hypertrophic Cardiomyopathy Abdullah Alshehri, MD; and Andrew Ignaszewski, MD, FRCPC CardioCase presentation Presley s check-up Presley, 37, discovered
Index of subjects. effect on ventricular tachycardia 30 treatment with 101, 116 boosterpump 80 Brockenbrough phenomenon 55, 125
 145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
145 Index of subjects A accessory pathways 3 amiodarone 4, 5, 6, 23, 30, 97, 102 angina pectoris 4, 24, 1l0, 137, 139, 140 angulation, of cavity 73, 74 aorta aortic flow velocity 2 aortic insufficiency
The Management of HOCM: What are the Surgical Options
 The Management of HOCM: What are the Surgical Options Konstadinos A Plestis, MD System Chief of Cardiac Thoracic and Vascular Surgery Main Line Health Care System Professor Sidney Kimmel Medical College
The Management of HOCM: What are the Surgical Options Konstadinos A Plestis, MD System Chief of Cardiac Thoracic and Vascular Surgery Main Line Health Care System Professor Sidney Kimmel Medical College
Cardiomyopathy: The Good, the Bad.and the Insurable?
 Cardiomyopathy: The Good, the Bad.and the Insurable? WAHLU Spring Seminar 2014 Joy Geiger, RN, BSN, ALMI Medical Consultant The Northwestern Mutual Life Insurance Company Milwaukee, WI Objectives Overview
Cardiomyopathy: The Good, the Bad.and the Insurable? WAHLU Spring Seminar 2014 Joy Geiger, RN, BSN, ALMI Medical Consultant The Northwestern Mutual Life Insurance Company Milwaukee, WI Objectives Overview
Managing Hypertrophic Cardiomyopathy with Imaging. Gisela C. Mueller University of Michigan Department of Radiology
 Managing Hypertrophic Cardiomyopathy with Imaging Gisela C. Mueller University of Michigan Department of Radiology Disclosures Gadolinium contrast material for cardiac MRI Acronyms Afib CAD Atrial fibrillation
Managing Hypertrophic Cardiomyopathy with Imaging Gisela C. Mueller University of Michigan Department of Radiology Disclosures Gadolinium contrast material for cardiac MRI Acronyms Afib CAD Atrial fibrillation
HYPERTROPHIC CARDIOMYOPATHY
 HYPERTROPHIC CARDIOMYOPATHY Most often diagnosed during infancy or adolescence, hypertrophic cardiomyopathy (HCM) is the second most common form of heart muscle disease, is usually genetically transmitted,
HYPERTROPHIC CARDIOMYOPATHY Most often diagnosed during infancy or adolescence, hypertrophic cardiomyopathy (HCM) is the second most common form of heart muscle disease, is usually genetically transmitted,
Apical Hypertrophic Cardiomyopathy With Hemodynamically Unstable Ventricular Arrhythmia Atypical Presentation
 Cronicon OPEN ACCESS Hemant Chaturvedi* Department of Cardiology, Non-Invasive Cardiology, Eternal Heart Care Center & research Institute, Rajasthan, India Received: September 15, 2015; Published: October
Cronicon OPEN ACCESS Hemant Chaturvedi* Department of Cardiology, Non-Invasive Cardiology, Eternal Heart Care Center & research Institute, Rajasthan, India Received: September 15, 2015; Published: October
Cardiac Issues in the Adolescent Athlete. Sean Levchuck, M.D. St. Francis Hospital- The Heart Center
 Cardiac Issues in the Adolescent Athlete Sean Levchuck, M.D. St. Francis Hospital- The Heart Center Sudden Cardiac Death Incidence is.6-6.2 % per 100,000 children in the US 20-25 % of the deaths occur
Cardiac Issues in the Adolescent Athlete Sean Levchuck, M.D. St. Francis Hospital- The Heart Center Sudden Cardiac Death Incidence is.6-6.2 % per 100,000 children in the US 20-25 % of the deaths occur
Steel vs Alcohol. Or Neither. Management of Hypertrophic Cardiomyopathy. Josh Doll, MD January 24, 2015
 Steel vs Alcohol Or Neither Management of Hypertrophic Cardiomyopathy Josh Doll, MD January 24, 2015 47yo Male, Mr. L Severe progressive dyspnea on exertion and weight gain Previous avid Cross-Fit participant
Steel vs Alcohol Or Neither Management of Hypertrophic Cardiomyopathy Josh Doll, MD January 24, 2015 47yo Male, Mr. L Severe progressive dyspnea on exertion and weight gain Previous avid Cross-Fit participant
Anaesthesia for non-cardiac surgery in patients left ventricular outflow tract obstruction (LVOTO)
 Anaesthesia for non-cardiac surgery in patients left ventricular outflow tract obstruction (LVOTO) Dr. Siân Jaggar Consultant Anaesthetist Royal Brompton Hospital London UK Congenital Cardiac Services
Anaesthesia for non-cardiac surgery in patients left ventricular outflow tract obstruction (LVOTO) Dr. Siân Jaggar Consultant Anaesthetist Royal Brompton Hospital London UK Congenital Cardiac Services
Cardiomyopathy Consequences. function of the myocardium for any reason. This is a serious disease in which the heart muscle
 Becki Simmons Cardiomyopathy Consequences Cardiomyopathy, which literally means "heart muscle disease," is the deterioration of the function of the myocardium for any reason. This is a serious disease
Becki Simmons Cardiomyopathy Consequences Cardiomyopathy, which literally means "heart muscle disease," is the deterioration of the function of the myocardium for any reason. This is a serious disease
What s new in Hypertrophic Cardiomyopathy?
 What s new in Hypertrophic Cardiomyopathy? Dr Andris Ellims HCM Clinic @ The Alfred Hypertrophic Cardiomyopathy = otherwise unexplained LV hypertrophy* 1 in 500 prevalence most common inherited cardiovascular
What s new in Hypertrophic Cardiomyopathy? Dr Andris Ellims HCM Clinic @ The Alfred Hypertrophic Cardiomyopathy = otherwise unexplained LV hypertrophy* 1 in 500 prevalence most common inherited cardiovascular
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders
 C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
C1: Medical Standards for Safety Critical Workers with Cardiovascular Disorders GENERAL ISSUES REGARDING MEDICAL FITNESS-FOR-DUTY 1. These medical standards apply to Union Pacific Railroad (UPRR) employees
Pediatrics. Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment. Overview
 Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Hypertrophic Cardiomyopathy: beyond gradient and wall thickness
 Hypertrophic Cardiomyopathy: beyond gradient and wall thickness Michael H. Picard, M.D. Massachusetts General Hospital Harvard Medical School no disclosures special thanks to A. Baggish 1 Hypertrophic
Hypertrophic Cardiomyopathy: beyond gradient and wall thickness Michael H. Picard, M.D. Massachusetts General Hospital Harvard Medical School no disclosures special thanks to A. Baggish 1 Hypertrophic
Hereditary Cardiovascular Conditions. genetic testing for undiagnosed diseases
 Hereditary Cardiovascular Conditions genetic testing for undiagnosed diseases What is Hypertrophic Cardiomyopathy (HCM)? normal heart heart with hcm Extra or thick heart muscle Typically in the left ventricle
Hereditary Cardiovascular Conditions genetic testing for undiagnosed diseases What is Hypertrophic Cardiomyopathy (HCM)? normal heart heart with hcm Extra or thick heart muscle Typically in the left ventricle
Cardiomyopathy. Jeff Grubbe MD FACP, Chief Medical Director, Allstate Life & Retirement
 Cardiomyopathy Jeff Grubbe MD FACP, Chief Medical Director, Allstate Life & Retirement Nebraska Home Office Life Underwriters Association March 20, 2018 1 Cardiomyopathy A myocardial disorder in which
Cardiomyopathy Jeff Grubbe MD FACP, Chief Medical Director, Allstate Life & Retirement Nebraska Home Office Life Underwriters Association March 20, 2018 1 Cardiomyopathy A myocardial disorder in which
Sudden cardiac death: Primary and secondary prevention
 Sudden cardiac death: Primary and secondary prevention By Kai Chi Chan Penultimate Year Medical Student St George s University of London at UNic Sheba Medical Centre Definition Sudden cardiac arrest (SCA)
Sudden cardiac death: Primary and secondary prevention By Kai Chi Chan Penultimate Year Medical Student St George s University of London at UNic Sheba Medical Centre Definition Sudden cardiac arrest (SCA)
cardiomyopathy. INTRODUCTION NONISCHEMIC CARDIOMYOPATHY
 FACTS ABOUT Cardiomyopathy INTRODUCTION Ischemic cardiomyopathy typically refers to heart muscle damage that results from coronary artery disease, such as heart attack, Cardiomyopathy is a disease of the
FACTS ABOUT Cardiomyopathy INTRODUCTION Ischemic cardiomyopathy typically refers to heart muscle damage that results from coronary artery disease, such as heart attack, Cardiomyopathy is a disease of the
How NOT to miss Hypertrophic Cardiomyopathy? Adaya Weissler-Snir, MD University Health Network, University of Toronto
 How NOT to miss Hypertrophic Cardiomyopathy? Adaya Weissler-Snir, MD University Health Network, University of Toronto Introduction Hypertrophic cardiomyopathy is the most common genetic cardiomyopathy,
How NOT to miss Hypertrophic Cardiomyopathy? Adaya Weissler-Snir, MD University Health Network, University of Toronto Introduction Hypertrophic cardiomyopathy is the most common genetic cardiomyopathy,
December 2018 Tracings
 Tracings Tracing 1 Tracing 4 Tracing 1 Answer Tracing 4 Answer Tracing 2 Tracing 5 Tracing 2 Answer Tracing 5 Answer Tracing 3 Tracing 6 Tracing 3 Answer Tracing 6 Answer Questions? Contact Dr. Nelson
Tracings Tracing 1 Tracing 4 Tracing 1 Answer Tracing 4 Answer Tracing 2 Tracing 5 Tracing 2 Answer Tracing 5 Answer Tracing 3 Tracing 6 Tracing 3 Answer Tracing 6 Answer Questions? Contact Dr. Nelson
HEART CONDITIONS IN SPORT
 HEART CONDITIONS IN SPORT Dr. Anita Green CHD Risk Factors Smoking Hyperlipidaemia Hypertension Obesity Physical Inactivity Diabetes Risks are cumulative (multiplicative) Lifestyles predispose to RF One
HEART CONDITIONS IN SPORT Dr. Anita Green CHD Risk Factors Smoking Hyperlipidaemia Hypertension Obesity Physical Inactivity Diabetes Risks are cumulative (multiplicative) Lifestyles predispose to RF One
Clinical Policy: Holter Monitors Reference Number: CP.MP.113
 Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
Clinical Policy: Reference Number: CP.MP.113 Effective Date: 05/18 Last Review Date: 04/18 Coding Implications Revision Log Description Ambulatory electrocardiogram (ECG) monitoring provides a view of
Cardiac Conditions in Sport & Exercise. Cardiac Conditions in Sport. USA - Sudden Cardiac Death (SCD) Dr Anita Green. Sudden Cardiac Death
 Cardiac Conditions in Sport & Exercise Dr Anita Green Cardiac Conditions in Sport Sudden Cardiac Death USA - Sudden Cardiac Death (SCD)
Cardiac Conditions in Sport & Exercise Dr Anita Green Cardiac Conditions in Sport Sudden Cardiac Death USA - Sudden Cardiac Death (SCD)
Hypertrophic Cardiomyopathy: basics and management
 Hypertrophic Cardiomyopathy: basics and management Bette Kim, MD Program Director, Cardiomyopathy Program Director, Roosevelt Hospital Echocardiography Lab Assistant Professor of Clinical Medicine Mount
Hypertrophic Cardiomyopathy: basics and management Bette Kim, MD Program Director, Cardiomyopathy Program Director, Roosevelt Hospital Echocardiography Lab Assistant Professor of Clinical Medicine Mount
Cardiac hypertrophy and how it may break an athlete s heart e the Cypriot case
 Eur J Echocardiography (2005) 6, 301e307 Cardiac hypertrophy and how it may break an athlete s heart e the Cypriot case C.E. Chee a,1, C.P. Anastassiades a,1, A.G. Antonopoulos b, A.A. Petsas b, L.C. Anastassiades
Eur J Echocardiography (2005) 6, 301e307 Cardiac hypertrophy and how it may break an athlete s heart e the Cypriot case C.E. Chee a,1, C.P. Anastassiades a,1, A.G. Antonopoulos b, A.A. Petsas b, L.C. Anastassiades
THE CARDIOVASCULAR SYSTEM
 THE CARDIOVASCULAR SYSTEM AND RESPONSES TO EXERCISE Mr. S. Kelly PSK 4U North Grenville DHS THE HEART: A REVIEW Cardiac muscle = myocardium Heart divided into two sides, 4 chambers (L & R) RS: pulmonary
THE CARDIOVASCULAR SYSTEM AND RESPONSES TO EXERCISE Mr. S. Kelly PSK 4U North Grenville DHS THE HEART: A REVIEW Cardiac muscle = myocardium Heart divided into two sides, 4 chambers (L & R) RS: pulmonary
Hypertrophic Cardiomyopathy
 Hypertrophic Cardiomyopathy From Genetics to ECHO Alexandra A Frogoudaki Second Cardiology Department ATTIKON University Hospital Athens University Athens, Greece EUROECHO 2010, Copenhagen, 11/12/2010
Hypertrophic Cardiomyopathy From Genetics to ECHO Alexandra A Frogoudaki Second Cardiology Department ATTIKON University Hospital Athens University Athens, Greece EUROECHO 2010, Copenhagen, 11/12/2010
Etiology, Classification & Management. Sheba Medical Center Cardiology Department Matthew Wright St. George s University of London
 Etiology, Classification & Management Sheba Medical Center Cardiology Department Matthew Wright St. George s University of London Introduction World Health Organization (1995): Diseases of myocardium (heart
Etiology, Classification & Management Sheba Medical Center Cardiology Department Matthew Wright St. George s University of London Introduction World Health Organization (1995): Diseases of myocardium (heart
Pre-participation Screening for the Prevention of sudden Cardiac Death in Young Athletes. Thomas W. Allen, DO, MPH
 Pre-participation Screening for the Prevention of sudden Cardiac Death in Young Athletes Thomas W. Allen, DO, MPH Cardiovascular disorders are the leading cause of sudden death in young athletes accounting
Pre-participation Screening for the Prevention of sudden Cardiac Death in Young Athletes Thomas W. Allen, DO, MPH Cardiovascular disorders are the leading cause of sudden death in young athletes accounting
Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009
 www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers MANAGEMENT
www.ivis.org Proceedings of the 34th World Small Animal Veterinary Congress WSAVA 2009 São Paulo, Brazil - 2009 Next WSAVA Congress : Reprinted in IVIS with the permission of the Congress Organizers MANAGEMENT
HYPERTROPHIC CARDIOMYOPATHY (HCM) PRESENTED AS UNSTABLE ANGINA COMPLICATED BY SERIOUS VENTRICULAR ARRHYTHMIAS CASE REPORT AND REVIEW LITERATURE
 HYPERTROPHIC CARDIOMYOPATHY (HCM) PRESENTED AS UNSTABLE ANGINA COMPLICATED BY SERIOUS VENTRICULAR ARRHYTHMIAS CASE REPORT AND REVIEW LITERATURE Lusyun Kumar Yadav * and Jin li Jun Department of Cardiology,
HYPERTROPHIC CARDIOMYOPATHY (HCM) PRESENTED AS UNSTABLE ANGINA COMPLICATED BY SERIOUS VENTRICULAR ARRHYTHMIAS CASE REPORT AND REVIEW LITERATURE Lusyun Kumar Yadav * and Jin li Jun Department of Cardiology,
marked increase in thickness of walls of heart in patient with HCM.
 Surgical Management of Hypertrophic Obstructive Cardiomyopathy Hani K. Najm MD, Msc, FRCSC, FRCS (Glasg Glasg), FACC, FESC President of Saudi Heart Association King Abdulaziz Cardiac Centre Riyadh, Saudi
Surgical Management of Hypertrophic Obstructive Cardiomyopathy Hani K. Najm MD, Msc, FRCSC, FRCS (Glasg Glasg), FACC, FESC President of Saudi Heart Association King Abdulaziz Cardiac Centre Riyadh, Saudi
12 Lead ECG Interpretation
 12 Lead ECG Interpretation Julie Zimmerman, MSN, RN, CNS, CCRN Significant increase in mortality for every 15 minutes of delay! N Engl J Med 2007;357:1631-1638 Who should get a 12-lead ECG? Also include
12 Lead ECG Interpretation Julie Zimmerman, MSN, RN, CNS, CCRN Significant increase in mortality for every 15 minutes of delay! N Engl J Med 2007;357:1631-1638 Who should get a 12-lead ECG? Also include
Hypertrophic Cardiomyopathy Ud Din Shah, MD; DM; FICC; FESC; FACC
 3 Article 1 Physicians Academy January 2018 Hypertrophic Cardiomyopathy Mehraj Ud Din Shah, MD; DM; FICC; FESC; FACC Hypertrophic Cardiomyopathy (HCM) is a genetic disorder which causes clinically unexplained
3 Article 1 Physicians Academy January 2018 Hypertrophic Cardiomyopathy Mehraj Ud Din Shah, MD; DM; FICC; FESC; FACC Hypertrophic Cardiomyopathy (HCM) is a genetic disorder which causes clinically unexplained
HYPERTROPHIC CARDIOMYOPATHY: Severe Heart Failure. Paolo Spirito, Genoa, Italy
 HYPERTROPHIC CARDIOMYOPATHY: Severe Heart Failure Paolo Spirito, Genoa, Italy Clinical Substrates for Heart Failure Symptoms in HCM Diastolic dysfunction Atrial fibrillation LV outflow obstruction Evolution
HYPERTROPHIC CARDIOMYOPATHY: Severe Heart Failure Paolo Spirito, Genoa, Italy Clinical Substrates for Heart Failure Symptoms in HCM Diastolic dysfunction Atrial fibrillation LV outflow obstruction Evolution
Inspiratory Right Ventricular Outflow Obstruction in a Patient with Hypertrophic Cardiomyopathy
 Case Reports Inspiratory Right Ventricular Outflow Obstruction in a Patient with Hypertrophic Cardiomyopathy Kazufumi TSUCHIHASHI, M.D., Akihito TSUCHIDA, M.D., Nobuichi HIKITA, M.D., Shuji YONEKURA, M.D.,
Case Reports Inspiratory Right Ventricular Outflow Obstruction in a Patient with Hypertrophic Cardiomyopathy Kazufumi TSUCHIHASHI, M.D., Akihito TSUCHIDA, M.D., Nobuichi HIKITA, M.D., Shuji YONEKURA, M.D.,
If you woke up breathing this morning, Congratulations! You get another chance. Use it wisely!
 Seton Medical Center Austin, Texas Cynthia Webner DNP, RN, CCNS, CCRN-CMC, CHFN www.cardionursing.com RULES OF LIFE If you woke up breathing this morning, Congratulations! You get another chance. Use it
Seton Medical Center Austin, Texas Cynthia Webner DNP, RN, CCNS, CCRN-CMC, CHFN www.cardionursing.com RULES OF LIFE If you woke up breathing this morning, Congratulations! You get another chance. Use it
Cardiac Considerations and Care in Children with Neuromuscular Disorders
 Cardiac Considerations and Care in Children with Neuromuscular Disorders - importance of early and ongoing treatment, management and available able medications. Dr Bo Remenyi Department of Cardiology The
Cardiac Considerations and Care in Children with Neuromuscular Disorders - importance of early and ongoing treatment, management and available able medications. Dr Bo Remenyi Department of Cardiology The
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
AF in the ER: Common Scenarios CASE 1. Fast facts. Diagnosis. Management
 AF in the ER: Common Scenarios Atrial fibrillation is a common problem with a wide spectrum of presentations. Below are five common emergency room scenarios and the management strategies for each. Evan
AF in the ER: Common Scenarios Atrial fibrillation is a common problem with a wide spectrum of presentations. Below are five common emergency room scenarios and the management strategies for each. Evan
Echocardiographic Evaluation of the Cardiomyopathies. Stephanie Coulter, MD, FACC, FASE April, 2016
 Echocardiographic Evaluation of the Cardiomyopathies Stephanie Coulter, MD, FACC, FASE April, 2016 Cardiomyopathies (CMP) primary disease intrinsic to cardiac muscle Dilated CMP Hypertrophic CMP Infiltrative
Echocardiographic Evaluation of the Cardiomyopathies Stephanie Coulter, MD, FACC, FASE April, 2016 Cardiomyopathies (CMP) primary disease intrinsic to cardiac muscle Dilated CMP Hypertrophic CMP Infiltrative
IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT JANUARY 24, 2012
 IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT201203 JANUARY 24, 2012 The IHCP to reimburse implantable cardioverter defibrillators separately from outpatient implantation Effective March 1, 2012, the
IHCP bulletin INDIANA HEALTH COVERAGE PROGRAMS BT201203 JANUARY 24, 2012 The IHCP to reimburse implantable cardioverter defibrillators separately from outpatient implantation Effective March 1, 2012, the
Congestive Heart Failure or Heart Failure
 Congestive Heart Failure or Heart Failure Dr Hitesh Patel Ascot Cardiology Group Heart Failure Workshop April, 2014 Question One What is the difference between congestive heart failure and heart failure?
Congestive Heart Failure or Heart Failure Dr Hitesh Patel Ascot Cardiology Group Heart Failure Workshop April, 2014 Question One What is the difference between congestive heart failure and heart failure?
Diastolic Heart Failure
 Diastolic Heart Failure Presented by: Robert Roberts, M.D., FRCPC, MACC, FAHA, FRSC Professor of Medicine and Chair ISCTR University of Arizona, College of Medicine Phoenix Scientist Emeritus and Advisor,
Diastolic Heart Failure Presented by: Robert Roberts, M.D., FRCPC, MACC, FAHA, FRSC Professor of Medicine and Chair ISCTR University of Arizona, College of Medicine Phoenix Scientist Emeritus and Advisor,
Citation for published version (APA): Christiaans, I. (2010). Hypertrophic cardiomyopathy: towards an optimal strategy
 UvA-DARE (Digital Academic Repository) Hypertrophic cardiomyopathy: towards an optimal strategy Christiaans, I. Link to publication Citation for published version (APA): Christiaans, I. (2010). Hypertrophic
UvA-DARE (Digital Academic Repository) Hypertrophic cardiomyopathy: towards an optimal strategy Christiaans, I. Link to publication Citation for published version (APA): Christiaans, I. (2010). Hypertrophic
ORIGINAL PAPER. R. C. Steggerda & J. C. Balt & K. Damman & M. P. van den Berg & J. M. ten Berg
 Neth Heart J (2013) 21:504 509 DOI 10.1007/s12471-013-0453-4 ORIGINAL PAPER Predictors of outcome after alcohol septal ablation in patients with hypertrophic obstructive cardiomyopathy. Special interest
Neth Heart J (2013) 21:504 509 DOI 10.1007/s12471-013-0453-4 ORIGINAL PAPER Predictors of outcome after alcohol septal ablation in patients with hypertrophic obstructive cardiomyopathy. Special interest
Sudden Death (SD) and hypertrophic cardiomyopathy (HCM) Attempt of risk stratification
 Sudden Death (SD) and hypertrophic cardiomyopathy (HCM) Attempt of risk stratification 84th Annual Scientific Meeting of the Aerospace Medical Association May 12-16, 2013 Sheraton Chicago Hotel & Towers,
Sudden Death (SD) and hypertrophic cardiomyopathy (HCM) Attempt of risk stratification 84th Annual Scientific Meeting of the Aerospace Medical Association May 12-16, 2013 Sheraton Chicago Hotel & Towers,
Consequences of Cardiomyopathy. thickened and stiff, the left ventricle is most often affected. This results in a lack of pumping
 Roseanne Baird March 30, 2010 BI 104 Dr. Hammoudi Consequences of Cardiomyopathy Cardiomyopathy is a disease in which the myocardium of the heart becomes enlarged, thickened and stiff, the left ventricle
Roseanne Baird March 30, 2010 BI 104 Dr. Hammoudi Consequences of Cardiomyopathy Cardiomyopathy is a disease in which the myocardium of the heart becomes enlarged, thickened and stiff, the left ventricle
Hypertrophic Cardiomyopathy
 Hypertrophic Cardiomyopathy IMPORTANT For the majority of affected individuals, Hypertrophic Cardiomyopathy is a condition which will not limit the quality or duration of life. A minority, however experience
Hypertrophic Cardiomyopathy IMPORTANT For the majority of affected individuals, Hypertrophic Cardiomyopathy is a condition which will not limit the quality or duration of life. A minority, however experience
HYPERTROPHIC CARDIOMYOPATHY RISK STRATIFICATION WHAT IS NEW?
 HYPERTROPHIC CARDIOMYOPATHY RISK STRATIFICATION WHAT IS NEW? Division of Inherited Cardiac Diseases Heart Center for the Young and Athletes A Dpt of Cardiology University of Athens LANCET 2013 ESC HCM
HYPERTROPHIC CARDIOMYOPATHY RISK STRATIFICATION WHAT IS NEW? Division of Inherited Cardiac Diseases Heart Center for the Young and Athletes A Dpt of Cardiology University of Athens LANCET 2013 ESC HCM
HISTORY. Question: What category of heart disease is suggested by the fact that a murmur was heard at birth?
 HISTORY 23-year-old man. CHIEF COMPLAINT: Decreasing exercise tolerance of several years duration. PRESENT ILLNESS: The patient is the product of an uncomplicated term pregnancy. A heart murmur was discovered
HISTORY 23-year-old man. CHIEF COMPLAINT: Decreasing exercise tolerance of several years duration. PRESENT ILLNESS: The patient is the product of an uncomplicated term pregnancy. A heart murmur was discovered
Pathophysiology: Heart Failure
 Pathophysiology: Heart Failure Mat Maurer, MD Irving Assistant Professor of Medicine Outline Definitions and Classifications Epidemiology Muscle and Chamber Function Pathophysiology Heart Failure: Definitions
Pathophysiology: Heart Failure Mat Maurer, MD Irving Assistant Professor of Medicine Outline Definitions and Classifications Epidemiology Muscle and Chamber Function Pathophysiology Heart Failure: Definitions
Slide 1. Slide 2. Slide 3. Sudden Cardiac Death In Athletes. Epidemiology. Epidemiology. Shaun McMurtry, MD Primary Care Sports Medicine
 Slide 1 Sudden Cardiac Death In Athletes Shaun McMurtry, MD Primary Care Sports Medicine Slide 2 Epidemiology College and Professional Athletes 500,000 participants each year Competitive Athletics Estimated
Slide 1 Sudden Cardiac Death In Athletes Shaun McMurtry, MD Primary Care Sports Medicine Slide 2 Epidemiology College and Professional Athletes 500,000 participants each year Competitive Athletics Estimated
NON-INVASIVE TREATMENT OPTIONS IN HYPERTROPHIC CARDIOMYOPATHY
 NON-INVASIVE TREATMENT OPTIONS IN HYPERTROPHIC CARDIOMYOPATHY SGK, 2015 Christiane Gruner University Heart Center, Zurich Department of Cardiology NONINVASIVE TREATMENT OPTIONS: TOPICS 1. LVOT obstruction
NON-INVASIVE TREATMENT OPTIONS IN HYPERTROPHIC CARDIOMYOPATHY SGK, 2015 Christiane Gruner University Heart Center, Zurich Department of Cardiology NONINVASIVE TREATMENT OPTIONS: TOPICS 1. LVOT obstruction
Outline. Pathophysiology: Heart Failure. Heart Failure. Heart Failure: Definitions. Etiologies. Etiologies
 Outline Pathophysiology: Mat Maurer, MD Irving Assistant Professor of Medicine Definitions and Classifications Epidemiology Muscle and Chamber Function Pathophysiology : Definitions An inability of the
Outline Pathophysiology: Mat Maurer, MD Irving Assistant Professor of Medicine Definitions and Classifications Epidemiology Muscle and Chamber Function Pathophysiology : Definitions An inability of the
Valvular Heart Disease
 Valvular Heart Disease MITRAL STENOSIS Pathophysiology rheumatic fever. calcific degeneration, malignant carcinoid disease, congenital mitral stenosis. SLE. The increased pressure gradient across the mitral
Valvular Heart Disease MITRAL STENOSIS Pathophysiology rheumatic fever. calcific degeneration, malignant carcinoid disease, congenital mitral stenosis. SLE. The increased pressure gradient across the mitral
Ischemia results from a number of factors: 1. Impaired vasodilator reserve
 Hypertrophic Cardiomyopathy (HCM) February 24, 2018 Henry Green, MD, FACC, FACP Clinical Professor of Medicine, Wayne State University http://sites.google.com/site/theheartsite Definition Hypertrophic
Hypertrophic Cardiomyopathy (HCM) February 24, 2018 Henry Green, MD, FACC, FACP Clinical Professor of Medicine, Wayne State University http://sites.google.com/site/theheartsite Definition Hypertrophic
HISTORY. Question: How do you interpret the patient s history? CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: 45-year-old man.
 HISTORY 45-year-old man. CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: His dyspnea began suddenly and has been associated with orthopnea, but no chest pain. For two months he has felt
HISTORY 45-year-old man. CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: His dyspnea began suddenly and has been associated with orthopnea, but no chest pain. For two months he has felt
Echocardiography as a diagnostic and management tool in medical emergencies
 Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
9/17/2010. Phidippides. Phidippides. Sudden Death in the Young Athlete. What is the extent of the problem? Can we prevent it?
 Phidippides Phidippides Sudden Death in the Young Athlete What is the extent of the problem? Can we prevent it? 1 Number of cardiovascular (CV), trauma-related, and other sudden death events in 1866 young
Phidippides Phidippides Sudden Death in the Young Athlete What is the extent of the problem? Can we prevent it? 1 Number of cardiovascular (CV), trauma-related, and other sudden death events in 1866 young
Hypertrophic Cardiomyopathy: Patient Management in 2018
 Hypertrophic Cardiomyopathy: Patient Management in 2018 Mackram F. Eleid, MD Giornate Cardiologeche Torinesi October 26, 2018 2018 MFMER slide-1 Disclosures No relevant financial relationships to disclose
Hypertrophic Cardiomyopathy: Patient Management in 2018 Mackram F. Eleid, MD Giornate Cardiologeche Torinesi October 26, 2018 2018 MFMER slide-1 Disclosures No relevant financial relationships to disclose
Appropriate Use Criteria for Initial Transthoracic Echocardiography in Outpatient Pediatric Cardiology (scores listed by Appropriate Use rating)
 Appropriate Use Criteria for Initial Transthoracic Echocardiography in Outpatient Pediatric Cardiology (scores listed by Appropriate Use rating) Table 1: Appropriate indications (median score 7-9) Indication
Appropriate Use Criteria for Initial Transthoracic Echocardiography in Outpatient Pediatric Cardiology (scores listed by Appropriate Use rating) Table 1: Appropriate indications (median score 7-9) Indication
INTRODUCTION. left ventricular non-compaction is a sporadic or familial cardiomyopathy characterized by
 A Rare Case of Arrhythmogenic Right Ventricular Cardiomyopathy Co-existing with Isolated Left Ventricular Non-compaction NS Yelgeç, AT Alper, Aİ Tekkeşin, C Türkkan INTRODUCTION Arrhythmogenic right ventricular
A Rare Case of Arrhythmogenic Right Ventricular Cardiomyopathy Co-existing with Isolated Left Ventricular Non-compaction NS Yelgeç, AT Alper, Aİ Tekkeşin, C Türkkan INTRODUCTION Arrhythmogenic right ventricular
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
Index Note: Page numbers of article titles are in boldface type. A Acute coronary syndrome(s), anticoagulant therapy in, 706, 707 antiplatelet therapy in, 702 ß-blockers in, 703 cardiac biomarkers in,
PIONEER-HCM Cohort B Results:
 PIONEER-HCM Cohort B Results: Reduction in left ventricular outflow tract gradient with mavacamten in symptomatic obstructive hypertrophic cardiomyopathy patients D Jacoby 1, S Lester 2, A Owens 3, A Wang
PIONEER-HCM Cohort B Results: Reduction in left ventricular outflow tract gradient with mavacamten in symptomatic obstructive hypertrophic cardiomyopathy patients D Jacoby 1, S Lester 2, A Owens 3, A Wang
ECG Workshop. Nezar Amir
 ECG Workshop Nezar Amir Myocardial Ischemia ECG Infarct ECG in STEMI is dynamic & evolving Common causes of ST shift Infarct Localisation Left main artery occlusion: o diffuse ST-depression with ST elevation
ECG Workshop Nezar Amir Myocardial Ischemia ECG Infarct ECG in STEMI is dynamic & evolving Common causes of ST shift Infarct Localisation Left main artery occlusion: o diffuse ST-depression with ST elevation
Utility of Echocardiography
 Hypertrophic Cardiomyopathy and Beyond- Echo Hawaii 2018 Lawrence Rudski MD FRCPC FACC FASE Professor of Medicine Director, Division of Cardiology and Azrieli Heart Center Jewish General Hospital, McGill
Hypertrophic Cardiomyopathy and Beyond- Echo Hawaii 2018 Lawrence Rudski MD FRCPC FACC FASE Professor of Medicine Director, Division of Cardiology and Azrieli Heart Center Jewish General Hospital, McGill
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Implantable cardioverter defibrillators for the treatment of arrhythmias and cardiac resynchronisation therapy for the treatment of heart failure (review
Hypertrophic Cardiomyopathy
 Hypertrophic Cardiomyopathy A Presentation for the MUD meeting January, 2018 Reviewed by Bill Rooney MD VP/Medical Director 1 https://commons.wikimedia.org/wiki/file:blausen_0166_cardiomyopathy_hypertrophic.p
Hypertrophic Cardiomyopathy A Presentation for the MUD meeting January, 2018 Reviewed by Bill Rooney MD VP/Medical Director 1 https://commons.wikimedia.org/wiki/file:blausen_0166_cardiomyopathy_hypertrophic.p
Hypertrophic Obstructive Cardiomyopathy
 The new england journal of medicine clinical practice Hypertrophic Obstructive Cardiomyopathy Rick A. Nishimura, M.D., and David R. Holmes, Jr., M.D. This Journal feature begins with a case vignette highlighting
The new england journal of medicine clinical practice Hypertrophic Obstructive Cardiomyopathy Rick A. Nishimura, M.D., and David R. Holmes, Jr., M.D. This Journal feature begins with a case vignette highlighting
Pre-Participation Athletic Cardiac Screening
 Pre-Participation Athletic Cardiac Screening Kimberly A Krabill, MD Pediatric and Fetal Cardiologist Northwest Congenital Heart Care, Division of MedNax Cardiology Update for Primary Care Symposium July
Pre-Participation Athletic Cardiac Screening Kimberly A Krabill, MD Pediatric and Fetal Cardiologist Northwest Congenital Heart Care, Division of MedNax Cardiology Update for Primary Care Symposium July
CCRN Review Cardiovascular
 CCRN Review Cardiovascular Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Angina Definition discomfort that occurs when oxygen demand
CCRN Review Cardiovascular Leanna R. Miller, RN, MN, CCRN-CMC, PCCN-CSC, CEN, CNRN, CMSRN, NP Education Specialist LRM Consulting Nashville, TN Angina Definition discomfort that occurs when oxygen demand
In the Thick of It: Hypertrophic Cardiomyopathy
 In the Thick of It: Hypertrophic Cardiomyopathy Munir S. Janmohamed M.D. FACC Assistant Clinical Professor of Medicine Director, Heart Failure Outreach Department of Medicine, Division of Cardiology Advanced
In the Thick of It: Hypertrophic Cardiomyopathy Munir S. Janmohamed M.D. FACC Assistant Clinical Professor of Medicine Director, Heart Failure Outreach Department of Medicine, Division of Cardiology Advanced
Ablative Therapy for Ventricular Tachycardia
 Ablative Therapy for Ventricular Tachycardia Nitish Badhwar, MD, FACC, FHRS 2 nd Annual UC Davis Heart and Vascular Center Cardiovascular Nurse / Technologist Symposium May 5, 2012 Disclosures Research
Ablative Therapy for Ventricular Tachycardia Nitish Badhwar, MD, FACC, FHRS 2 nd Annual UC Davis Heart and Vascular Center Cardiovascular Nurse / Technologist Symposium May 5, 2012 Disclosures Research
CME Article Brugada pattern masking anterior myocardial infarction
 Electrocardiography Series Singapore Med J 2011; 52(9) : 647 CME Article Brugada pattern masking anterior myocardial infarction Seow S C, Omar A R, Hong E C T Cardiology Department, National University
Electrocardiography Series Singapore Med J 2011; 52(9) : 647 CME Article Brugada pattern masking anterior myocardial infarction Seow S C, Omar A R, Hong E C T Cardiology Department, National University
Index. cardiacep.theclinics.com. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A AEDs. See Automated external defibrillators (AEDs) AF. See Atrial fibrillation (AF) Age as factor in SD in marathon runners, 45 Antiarrhythmic
Note: Page numbers of article titles are in boldface type. A AEDs. See Automated external defibrillators (AEDs) AF. See Atrial fibrillation (AF) Age as factor in SD in marathon runners, 45 Antiarrhythmic
REtrive. REpeat. RElearn Design by. Test-Enhanced Learning based ECG practice E-book
 Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning based ECG practice E-book REtrive REpeat RElearn Design by S I T T I N U N T H A N G J U I P E E R I Y A W A
Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning based ECG practice E-book REtrive REpeat RElearn Design by S I T T I N U N T H A N G J U I P E E R I Y A W A
I n 490 BC, Pheidippides, the renowned Athenean
 710 REVIEW Risk of competitive sport in young athletes with heart disease S Firoozi, S Sharma, W J McKenna... The majority of sudden deaths in young athletes occur in the context of underlying inherited
710 REVIEW Risk of competitive sport in young athletes with heart disease S Firoozi, S Sharma, W J McKenna... The majority of sudden deaths in young athletes occur in the context of underlying inherited
Left ventricular non-compaction: the New Cardiomyopathy on the Block
 Left ventricular non-compaction: the New Cardiomyopathy on the Block Aamir Jeewa MB BCh, FAAP, FRCPC Section Head, Cardiomyopathy & Heart Function Program The Hospital for Sick Children Assistant Professor
Left ventricular non-compaction: the New Cardiomyopathy on the Block Aamir Jeewa MB BCh, FAAP, FRCPC Section Head, Cardiomyopathy & Heart Function Program The Hospital for Sick Children Assistant Professor
Historical Notes: Clinical Exercise Testing in the Athlete. An Efficient Heart. Structural Changes, Cont. Coronary Arteries
 Clinical Exercise Testing in the Athlete The athlete s heart Sudden cardiac death in athletes Screening athletes for cardiovascular disease Historical Notes: Giovanni Lancisi (father of cardiology), 17
Clinical Exercise Testing in the Athlete The athlete s heart Sudden cardiac death in athletes Screening athletes for cardiovascular disease Historical Notes: Giovanni Lancisi (father of cardiology), 17
Preventing Sudden Death in Young Athletes. Outline. Scope of the Problem. Causes of SCD in Young Athletes. Sudden death in the young athlete
 Preventing Sudden Death in Young Athletes Ronn E. Tanel, MD Director, Pediatric Arrhythmia Service UCSF Children s Hospital Associate Professor of Pediatrics UCSF School of Medicine Outline Sudden death
Preventing Sudden Death in Young Athletes Ronn E. Tanel, MD Director, Pediatric Arrhythmia Service UCSF Children s Hospital Associate Professor of Pediatrics UCSF School of Medicine Outline Sudden death
Cardiac hypertrophy : differentiating disease from athlete
 Cardiac hypertrophy : differentiating disease from athlete Ario Soeryo Kuncoro, MD, Cardiologist Echocardiography Division, National Cardiovascular Centre Harapan Kita-Jakarta Departement of Cardiology
Cardiac hypertrophy : differentiating disease from athlete Ario Soeryo Kuncoro, MD, Cardiologist Echocardiography Division, National Cardiovascular Centre Harapan Kita-Jakarta Departement of Cardiology
TSDA Boot Camp September 13-16, Introduction to Aortic Valve Surgery. George L. Hicks, Jr., MD
 TSDA Boot Camp September 13-16, 2018 Introduction to Aortic Valve Surgery George L. Hicks, Jr., MD Aortic Valve Pathology and Treatment Valvular Aortic Stenosis in Adults Average Course (Post mortem data)
TSDA Boot Camp September 13-16, 2018 Introduction to Aortic Valve Surgery George L. Hicks, Jr., MD Aortic Valve Pathology and Treatment Valvular Aortic Stenosis in Adults Average Course (Post mortem data)
Management of HOCM: Non-Surgical Options
 Management of HOCM: Non-Surgical Options Howard C. Herrmann, MD, FACC, MSCAI John Bryfogle Professor of Cardiovascular Medicine and Surgery Health System Director for Interventional Cardiology Director,
Management of HOCM: Non-Surgical Options Howard C. Herrmann, MD, FACC, MSCAI John Bryfogle Professor of Cardiovascular Medicine and Surgery Health System Director for Interventional Cardiology Director,
In Vivo Animal Models of Heart Disease. Why Animal Models of Disease? Timothy A Hacker, PhD Department of Medicine University of Wisconsin-Madison
 In Vivo Animal Models of Heart Disease Timothy A Hacker, PhD Department of Medicine University of Wisconsin-Madison Why Animal Models of Disease? Heart Failure (HF) Leading cause of morbidity and mortality
In Vivo Animal Models of Heart Disease Timothy A Hacker, PhD Department of Medicine University of Wisconsin-Madison Why Animal Models of Disease? Heart Failure (HF) Leading cause of morbidity and mortality
8/8/2011. CARDIAC RESYCHRONIZATION THERAPY for Heart Failure. Case Presentation. Case Presentation
 CARDIAC RESYCHRONIZATION THERAPY for Heart Failure James Taylor, DO, FACOS Cardiothoracic and Vascular surgery San Angelo Community Medical Center San Angelo, TX Case Presentation 64 year old female with
CARDIAC RESYCHRONIZATION THERAPY for Heart Failure James Taylor, DO, FACOS Cardiothoracic and Vascular surgery San Angelo Community Medical Center San Angelo, TX Case Presentation 64 year old female with
Mitral Regurgitation
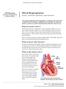 UW MEDICINE PATIENT EDUCATION Mitral Regurgitation Causes, symptoms, diagnosis, and treatment This handout describes mitral regurgitation, a disease of the mitral valve. It explains how this disease is
UW MEDICINE PATIENT EDUCATION Mitral Regurgitation Causes, symptoms, diagnosis, and treatment This handout describes mitral regurgitation, a disease of the mitral valve. It explains how this disease is
8 th ANNUAL CLINICAL CARDIOLOGY COURSE Nashville, TN
 8 th ANNUAL CLINICAL CARDIOLOGY COURSE Nashville, TN Mark your Calendar for July 26-29, 2018 to Attend the Only Available Comprehensive Review of Clinical Cardiology Practice designed for Nurse Practitioners
8 th ANNUAL CLINICAL CARDIOLOGY COURSE Nashville, TN Mark your Calendar for July 26-29, 2018 to Attend the Only Available Comprehensive Review of Clinical Cardiology Practice designed for Nurse Practitioners
Presenter: Steven Brust, HCS-D, HCS-H Product Manager, Home Health Coding Center
 Presenter: Steven Brust, HCS-D, HCS-H Product Manager, Home Health Coding Center Pinpoint & properly assign the appropriate heart failure codes Left- vs. Right-sided Left ventricular failure (LVF) may
Presenter: Steven Brust, HCS-D, HCS-H Product Manager, Home Health Coding Center Pinpoint & properly assign the appropriate heart failure codes Left- vs. Right-sided Left ventricular failure (LVF) may
Skin supplied by T1-4 (medial upper arm and neck) T5-9- epigastrium Visceral afferents from skin and heart are the same dorsal root ganglio
 Cardio 2 ECG... 3 Cardiac Remodelling... 11 Valvular Diseases... 13 Hypertension... 18 Aortic Coarctation... 24 Erythropoiesis... 27 Haemostasis... 30 Anaemia... 36 Atherosclerosis... 44 Angina... 48 Myocardial
Cardio 2 ECG... 3 Cardiac Remodelling... 11 Valvular Diseases... 13 Hypertension... 18 Aortic Coarctation... 24 Erythropoiesis... 27 Haemostasis... 30 Anaemia... 36 Atherosclerosis... 44 Angina... 48 Myocardial
Systolic Anterior Motion of Mitral Valve Subchordal Apparatus: A Rare Echocardiographic Pattern in Non- Obstructive Hypertrophic Cardiomyopathy
 Case Report Cardiol Res. 2017;8(5):258-264 Systolic Anterior Motion of Mitral Valve Subchordal Apparatus: A Rare Echocardiographic Pattern in Non- Obstructive Hypertrophic Cardiomyopathy Jezreel L. Taquiso
Case Report Cardiol Res. 2017;8(5):258-264 Systolic Anterior Motion of Mitral Valve Subchordal Apparatus: A Rare Echocardiographic Pattern in Non- Obstructive Hypertrophic Cardiomyopathy Jezreel L. Taquiso
Common Codes for ICD-10
 Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Common Codes for ICD-10 Specialty: Cardiology *Always utilize more specific codes first. ABNORMALITIES OF HEART RHYTHM ICD-9-CM Codes: 427.81, 427.89, 785.0, 785.1, 785.3 R00.0 Tachycardia, unspecified
Jonathan Kim MD, FACC
 Jonathan Kim MD, FACC Assistant Professor, Division of Cardiology, Emory University Adjunct Assistant Professor, School of Applied Physiology, Georgia Tech Team Cardiologist, Sports Medicine, Emory University
Jonathan Kim MD, FACC Assistant Professor, Division of Cardiology, Emory University Adjunct Assistant Professor, School of Applied Physiology, Georgia Tech Team Cardiologist, Sports Medicine, Emory University
ESC Guidelines on Hypertrophic Cardiomyopathy
 2014 version ES Guidelines on Hypertrophic ardiomyopathy Pr Michel KOMAJDA Dept of ardiology HU PTE SALPETRERE University Pierre et Marie urie PARS FRANE European Heart Journal (2014):doi:10.1093/eurheartj/ehu284
2014 version ES Guidelines on Hypertrophic ardiomyopathy Pr Michel KOMAJDA Dept of ardiology HU PTE SALPETRERE University Pierre et Marie urie PARS FRANE European Heart Journal (2014):doi:10.1093/eurheartj/ehu284
2019 Qualified Clinical Data Registry (QCDR) Performance Measures
 2019 Qualified Clinical Data Registry (QCDR) Performance Measures Description: This document contains the 18 performance measures approved by CMS for inclusion in the 2019 Qualified Clinical Data Registry
2019 Qualified Clinical Data Registry (QCDR) Performance Measures Description: This document contains the 18 performance measures approved by CMS for inclusion in the 2019 Qualified Clinical Data Registry
CARDIOMYOPATHY IN CT. Hans- Christoph Becker Professor of Radiology
 CARDIOMYOPATHY IN CT Hans- Christoph Becker Professor of Radiology 1 Cardiomyopathy Heart muscle disease Deterioration of the heart function, heart failure Dyspnea, peripheral edema Risk of arrhythmia,
CARDIOMYOPATHY IN CT Hans- Christoph Becker Professor of Radiology 1 Cardiomyopathy Heart muscle disease Deterioration of the heart function, heart failure Dyspnea, peripheral edema Risk of arrhythmia,
Cardiac Sarcoidosis. Millee Singh DO Non Invasive Cardiology First Coast Heart and Vascluar
 Cardiac Sarcoidosis Millee Singh DO Non Invasive Cardiology First Coast Heart and Vascluar Introduction Multisystem granulomatous disease of unknown etiology characterized by noncaseating granulomas in
Cardiac Sarcoidosis Millee Singh DO Non Invasive Cardiology First Coast Heart and Vascluar Introduction Multisystem granulomatous disease of unknown etiology characterized by noncaseating granulomas in
