Hepatic Artery Reconstruction with Double- Needle Microsuture in Living-Donor Liver Transplantation
|
|
|
- Daisy Ross
- 5 years ago
- Views:
Transcription
1 LIVER TRANSPLANTATION 12:46 50, 2006 ORIGINAL ARTICLE Hepatic Artery Reconstruction with Double- Needle Microsuture in Living-Donor Liver Transplantation Mutsumi Okazaki, 1 Hirotaka Asato, 1 Akihiko Takushima, 3 Takashi Nakatsuka, 4 Shunji Sarukawa, 1 Keita Inoue, 1 Kiyonori Harii, 3 Yasuhiko Sugawara, 2 and Masatoshi Makuuchi 2 1 Department of Plastic and Reconstructive Surgery and 2 Artificial Organ and Transplantation Division, Department of Surgery, Graduate School of Medicine, University of Tokyo, Bunkyo-ku, Tokyo, Japan; 3 Department of Plastic and Reconstructive Surgery, Kyorin University, School of Medicine, Mitaka-City, Tokyo, Japan; and 4 Department of Plastic and Reconstructive Surgery, Saitama Medical School, Irumagun, Saitama, Japan In living-donor liver transplantation (LDLT), reconstruction of the hepatic artery is challenging because the recipient artery is located deep in the abdominal cavity and the operating field is limited. Also, the hepatic artery of the graft is short and the recipient artery is occasionally damaged. To overcome these difficulties, we developed a double-needle microsuture technique for artery reconstruction. A total of 161 adult patients received 163 LDLTs using this new technique. The first suture was placed at the most difficult point in the artery to be visualized through the microscope. Each stitch was placed from the inner side of the arterial wall to the outer side. The posterior stitch was tied pulling toward the back. The subsequent sutures were advanced anteriorly on either side adjacent to the previous suture. Hepatic artery thrombosis occurred in 4 patients (2.5%), only 2 (1.2%) of which were associated with arterial reconstruction. Intimal dissection developed in the recipient artery in 2 patients (1.2%). Three (50%) of these 6 complications occurred more than 10 days after LDLT. In conclusion, this suturing technique allows for safe intimal adaptation even when the arterial tunica intima is separated from the tunica media, because all stitches are carried from inside of the vessel to the outside, contributing to more satisfactory results. Liver Transpl 12:46 50, AASLD. Received July 5, 2005; accepted July 5, Hepatic arterial thrombosis (HAT) after liver transplantation is a life-threatening event associated with a high rate of graft loss or death. 1 The incidence of HAT during the first 30 days has been reduced to approximately 5% by recent technical advances. 2 HAT is more common, however, in split or living-donor liver transplantation (LDLT). 3 One of the most important processes in LDLT is hepatic artery reconstruction, which in our institute is performed chiefly by plastic microsurgeons using an operating microscope. Anastomosed hepatic arteries in LDLT are larger (2-4 mm) in diameter than those used in the common free flap transfer (1-2 mm). Hepatic artery reconstruction in LDLT is, however, often challenging because the recipient artery is located deep in the abdominal cavity, the operating field is narrow, and the hepatic artery of the graft is short. In addition, the recipient artery is occasionally damaged by severe atherosclerosis, transarterial chemoembolization, or previous surgery (especially hepatectomy and Kasai s operation). In the conventional method of microvascular anasto- Abbreviations: HAT, hepatic artery thrombosis; LDLT, living-donor liver transplantation. Research from the Ministry of Education, Culture, Sports, Science and Technology of Japan and Grants-in-Aid for Research on HIV/AIDS, a multicenter pilot clinical study to compare the safety and efficacy of a steroid-free immunosuppression protocol with monoclonal anti-il2r antibody in hepatitis C virus-positive living-donor liver transplantation, and Research on Measures for Intractable Diseases from the Ministry of Health, Labor and Welfare of Japan. Address reprint requests to Yasuhiko Sugawara, MD, Artificial Organ and Transplantation Division, Department of Surgery, Graduate School of Medicine, University of Tokyo, Hongo, Bunkyo-ku, Tokyo, , Japan. Telephone: ; FAX: ; yasusuga-tky@umin.ac.jp DOI /lt Published online in Wiley InterScience ( American Association for the Study of Liver Diseases.
2 HA RECONSTRUCTION WITH DOUBLE-NEEDLE SUTURE 47 mosis, the arteries were held with a double clamp with 2 stay sutures, which must be rotated for posterior wall anastomosis. 4 A posterior-wall-first anastomotic technique 5,6 has significant advantages for hepatic artery reconstruction in LDLT. In the technique, microsutures are placed in the back wall of the vessel first, and turning over of the microclamp is eliminated. To make the technique easier, we devised a 9-0 nylon thread (4 cm) with a double needle and adopted it in the posteriorwall-first anastomotic technique and named it the double-needle microsuture technique. We analyzed our experience of hepatic artery reconstruction using this method and discuss its problems from the microsurgeon s point of view. PATIENTS AND METHODS Patients The subjects were 161 adult patients who underwent 163 LDLTs from January 2000 to June 2004 using the double-needle microsuture technique. They were the subjects of the study. There were 83 men and 78 women, ranging in age from yr, with a mean of 48 yr. The indications for LDLT included hepatitis virusrelated cirrhosis in 65, cholestatic liver disease including primary biliary cirrhosis and auto immune hepatitis in 50, fulminant hepatitis in 21, biliary atresia in 7, retransplantation in 2, and others in 18. There were 57 patients with hepatocellular carcinoma, 37 of which had a history of transcatheter arterial chemoembolization before LDLT. Liver graft types included right liver with (n 22) or without (n 68) middle hepatic vein, left liver with (n 51) or without (n 5) middle hepatic vein, and right lateral sector (n 17). The graft type selection criteria and donor hepatectomy procedure were described previously. 7,8 In all the LDLTs, the graft artery was anastomosed end-to-end to the recipient artery. The recipient artery was selected according to its patency, the extent of intimal damage, and caliber consistency with that of the graft artery. Surgical Technique For hepatic artery reconstruction, the operating microscope was placed on the right cranial side of the patient. The microsurgeon was positioned at the right side of the operating field and the assistant microsurgeon at the left and the second assistant at the right cranial side for retraction of the liver. A suction drain was placed at the subphrenic space to continuously remove blood and ascites to clear the operating field. The present technique was indicated when it was difficult to turn over the graft artery. A 9-0 monofilament nylon microsuture with double needles (W10V43-9N; Keisei Medical Industrial, Tokyo, Japan; Fig. 1) was specially devised for this technique. Different from the conventional double-needle microsuture, our suture has a short thread (4 cm), which provides the prompt interrupted sutures. The details of our procedure for Figure 1. The 9-0 monofilament nylon microsuture with double needles. The needle is 3/8 circle, 4 mm in length and 0.1 mm in diameter, and the nylon thread is 4 cm in length. the anastomosis are shown in Figure 2. The recipient and graft arteries were clamped with single microclamps to temporarily halt blood flow (Fig. 2A). The first suture was placed at the most difficult point (usually at the middle of the posterior wall) in the artery to be visualized through the microscope. Each stitch was always placed from the inner side of the arterial wall to the outer side (Fig. 2B). The posterior stitch was tied pulling toward the back (Fig. 2C). The subsequent sutures were advanced anteriorly on either side adjacent to the previous suture (Fig. 2D). The anterior vessel wall was sutured with a regular 9-0 microsuture with a single needle (Fig. 2E). When there was a discrepancy in diameter between the graft and recipient artery, each suture was placed to gradually compensate for the discrepancy. Monitoring Patency After reconstruction, the intrahepatic arterial signals were checked using color Doppler ultrasonography. 9 When the graft had multiple arterial stumps, backbleeding from the nonanastomosed stump was checked after reconstruction was complete. When there was sufficient hepatic arterial blood flow in the nonanastomosed stump, no additional arterial reconstruction was performed. 10 Postoperative anticoagulant therapy was administered as described previously. 3 Color Doppler ultrasonography was performed twice a day for 2 weeks to confirm the patency of the intrahepatic arteries. RESULTS Arteries Anastomosed (Table 1) For the recipient artery, the trunks of the right, left, or middle hepatic artery were used in 89 patients (55%), and the branches of the right hepatic artery or left hepatic artery were used in 73 patients (45%). In 1
3 48 OKAZAKI ET AL. TABLE 1. Artery Anastomosed Recipient No. Graft No. Right 56 Right 90 Paramedian branch 32 Lateral branch 17 of right of right Left 28 Left 48 Lateral branch of 27 Branch of left 7 right Branch of left 14 Middle 1 Middle 5 Gastroduodenal 1 juice leakage after splenectomy. This was treated with open drainage on postoperative day 9. There was no hepatic arterial flow in the graft by Doppler ultrasonography on postoperative day 14, which was suspected to be thrombosed. It spontaneously revascularized, however, after the administration of anticoagulants. 11 Patient 3 had simultaneous arterial and portal vein thrombosis, could not receive retransplantation, and died. Patient 4 received LDLT twice before in another institution and received a third LDLT in our hospital. The hepatic artery of the liver graft was anastomosed to the posterior branch of the right hepatic artery of the previous graft. The postoperative course was uneventful for the first 2 weeks. On postoperative day 17, however, there was an intraperitoneal abscess, probably due to bile leakage, and HAT was discovered. In spite of repeated percutaneous drainage of the abscess and administration of anticoagulants and antibiotics, the graft became necrotic and the patient died. In addition to HAT, subintimal hemorrhage developed in the recipient artery due to the intimal dissection in 2 patients (1.2%; Table 2). Figure 2. Schematics of the microvascular anastomosis. (A) The view of the operating field. The recipient and graft arteries are clamped by single microclamps. (B) The first suture is placed at the posterior wall. (C) The posterior stitch is tied, pulling toward the back for good intima adaptation. (D) The subsequent sutures are placed on either side adjacent to the previous suture. (E) The sutures of the anterior wall can be performed with common single-needle microsutures. patient, the gastroduodenal artery was anastomosed because of severe intimal damage due to arterial embolization in the hepatic arteries. There was 1 graft artery in 142 patients (87%), 2 in 20 (12%), and 3 in 1. In all patients, a single arterial reconstruction was performed. 6 Vascular interposition grafts were not used in the series. Hepatic Artery Thrombosis The incidence of HAT was 2.5% (4/163). HAT was detected 8 hours after anastomosis (patient 1), 14 days (patient 2), 3 days (patient 3), and 17 days (patient 4) postoperatively (Table 2). The graft was salvaged in patient 1 by prompt thrombectomy and reanastomosis. Patient 2 received a left liver graft and had pancreatic DISCUSSION The double-needle microsuture technique does not require that the arteries be turned over, which allows for anastomosis of the arteries in situ. The first stitch can be placed at any point along the posterior wall. The next stitch can be advanced along either side of the previous suture. Turnover of the microclip might lacerate the intima, 12 which might cause intimal dissection. This technique is helpful for arteries in which the tunica intima is separated from the tunica media due to serious atherosclerosis or damage resulting from embolization because all stitches are carried from inside of the vessel to the outside, and intimal adaptation can be performed more safely (Fig. 3). In this technique, the surgeon needs to change the needle holder from one needle to the other. This hazard is overcome with experience. In our institute, hepatic artery reconstruction has been performed chiefly by plastic microsurgeons, who had experienced more than 50 free-flap transfers with microvascular anastomosis. Our double-needle microsuture is employed also for the end-to-side anastomosis between flap artery and external carotid artery in head and neck reconstruction using free flap. 13 In
4 HA RECONSTRUCTION WITH DOUBLE-NEEDLE SUTURE 49 TABLE 2. Cases with Arterial Complication No. Age/ gender Disease Complication Onset Graft Graft artery Recipient artery Complication Course 1 46F AIH HAT 8 hours RLS LBr A5 None Salvaged 2 40M HCV HAT 14 POD L C LHA LHA Pancreatic juice leakage Spontaneous revascularization 3 58F PBC HAT 3 POD RLS LBr LBr Portal vein Not salvaged thrombosis 4 31M PSC HAT 17 POD R RHA PBr Liver abscess Not salvaged 5 59M HCV SIH 2 hours L C LHA LHA None Salvaged 6 39M PBC SIH 12 POD L C LHA RHA None Salvaged Abbreviations: HCV, hepatitis C viral cirrhosis; PBC, primary biliary cirrhosis; PSC, primary sclerosing cholangitis; POD, postoperative day; AIH, autoimmune hepatitis; LSRL, lateral sector of right liver; L C, left liver with caudate lobe; RHA, right hepatic artery; LHA, left hepatic artery; LBr, lateral branch of right hepatic artery; PBr, paramedian branch of right hepatic artery; HAT, hepatic artery thrombosis; SIH, subintimal hemorrhage. Figure 3. Schematics of the technique when the tunica intima was separated from the tunica media. All stitches were carried from inside of the vessel to the outside (left panel), allowing for secure sutures with good intima adaptation (right). most cases in LDLT, the hepatic artery anastomosis was completed in about 30 minutes. In hepatic artery reconstruction in LDLT, the complications tend to occur later than those after common free tissue transfers. In common free tissue transfers, more than 80% of vascular thromboses occur within the first 3 postoperative days. 14,15 Serious impairments of the coagulation system in patients with end-stage liver disease might prevent HAT in the early postoperative days. A hypercoagulable state occurs following LDLT due to acceleration of the coagulation system and delayed recovery of the fibrinolytic system. 16 The risk of HAT might increase as liver function recovers. Early diagnosis of HAT and consequent revascularization will lead to graft salvage. 8 Our results suggest that verification of the patency of the intrahepatic arteries with color Doppler ultrasonography is necessary for at least 3 weeks postoperatively. Intimal dissection of the recipient artery is one complication of artery reconstruction, particularly after LDLT. To minimize the incidence of intimal dissection, careful dissection and preparation of the recipient artery are mandatory, in addition to careful adaptation of the tunica intima during arterial anastomosis. Careful selection of an appropriate recipient artery is key to a successful reconstruction. The use of an artery other than hepatic arteries for the recipient is one strategy, including the right gastroepiploic, 17 left gastric, or gastroduodenal artery. Even slight oozy bleeding at the anastomotic site after removal of the microclamp is not negligible in LDLT because most patients have a seriously impaired coagulation system. When oozy bleeding is noted, spontaneous hemostasis cannot be expected, so additional sutures are indicated for hemostasis. If the bleeding is from the posterior wall, the bleeding point from the anastomosis is difficult to control. It is thus recommended that the sutures be inserted close to each other, especially in the posterior wall. Biphasic movements of the vessels, caused by ventilation and heart movement, are another problem. The movement due to ventilation appears problematic; the upper abdominal organs together with the recipient artery move in accordance with ventilation. Handling of the microforceps or needle holders should be adjusted to the ventilation movements. Respiration can be withheld during suture placement as the need arises. Active movement of the recipient artery is easy to overcome, but the large-amplitude movement caused passively by heart movement is occasionally problematic. Quick insertion and release of the needle into the arterial wall is necessary so that the arterial wall is not injured by the needle. The incidence of HAT in LDLT is 2 to 5%, 13,18 20 which is equivalent with our results (2.5%, 4/163). Of the 4 patients with HAT, only 2 (patients 1 and 3) were assumed to be associated with arterial reconstruction. For a lower morbidity rate, it is necessary to create an adequate operating field, select the appropriate recipient artery, and use suitable microinstruments. We believe that our newly developed double-needle microsuture technique is helpful for easier and safer hepatic artery reconstruction in LDLT.
5 50 OKAZAKI ET AL. REFERENCES 1. Sheiner PA, Varma CV, Guarrera JV, Cooper J, Garatti M, Emre S, et al. Selective revascularization of hepatic artery thromboses after liver transplantation improves patient and graft survival. Transplantation 1997;64: Settmacher U, Stange B, Haase R, Heise M, Steinmuller T, Bechstein WO, et al. Arterial complications after liver transplantation. Transpl Int 2000;13: Sugawara Y, Kaneko J, Akamatsu N, Imamura H, Kokudo N, Makuuchi M. Anticoagulant therapy against hepatic artery thrombosis in living donor liver transplantation. Transplant Proc 2002;34: Furuta S, Ikegami T, Nakazawa Y, Hashikura Y, Matsunami H, Kawasaki S, et al. Hepatic artery reconstruction in living donor liver transplantation from the microsurgeon s point of view. Liver Transpl Surg 1997;3: Harris GD, Finseth F, Buncke HJ. Posterior-wall-first microvascular anastomotic technique. Br J Plast Surg 1981; 34: Yamamoto Y, Sugihara T, Sasaki S, Furukawa H, Furukawa H, Okushiba S, et al. Microsurgical reconstruction of the hepatic and superior mesenteric arteries using a back wall technique. J Reconstr Microsurg 1999;15: Sugawara Y, Makuuchi M. Advances in adult living donor liver transplantation: a review based on reports from the 10th anniversary of the adult-to-adult living donor liver transplantation meeting in Tokyo. Liver Transpl 2004;10: Sakamoto Y, Takayama T, Nakatsuka T, Asato H, Sugawara Y, Sano K, et al. Advantage in using living donors with aberrant hepatic artery for partial liver graft arterialization. Transplantation 2002;74: Kasai H, Makuuchi M, Kawasaki S, Ishizone S, Kitahara S, Matsunami H, et al. Intraoperative color Doppler ultrasonography for partial-liver transplantation from the living donor in pediatric patients. Transplantation 1992;54: Ikegami T, Kawasaki S, Matsunami H, Hashikura Y, Nakazawa Y, Miyagawa S, et al. Should all hepatic arterial branches be reconstructed in living-related liver transplantation? Surgery 1996;119: Sugawara Y, Ohtsuka H, Kaneko J, Imamura H, Makuuchi M. Spontaneous revascularization of arterial thrombosis after living donor liver transplantation. Abdom Imaging 2002;27: Uchiyama H, Hashimoto K, Hiroshige S, Harada N, Soejima Y, Nishizaki T, et al. Hepatic artery reconstruction in living-donor liver transplantation: a review of its techniques and complications. Surgery 2002;131(1 Suppl): S200 S Okazaki M, Asato H, Takushima A, Nakatsuka T, Sarukawa S, Harii K. Availability of end-to-side arterial anastomosis to the external carotid artery in free-flap transfer for head and neck reconstruction. Jpn J Head Neck Cancer 2004;30: Kroll SS, Schusterman MA, Reece GP, Miller MJ, Evans GR, Robb GL, et al. Timing of pedicle thrombosis and flap loss after free-tissue transfer. Plast Reconstr Surg 1996; 98: Salgado CJ, Smith A, Kim S, Higgins J, Behnam A, Herrera HR, et al. Effects of late loss of arterial inflow on free flap survival. J Reconstr Microsurg 2002;18: Hashikura Y, Kawasaki S, Okumura N, Ishikawa S, Matsunami H, Ikegami T, et al. Prevention of hepatic artery thrombosis in pediatric liver transplantation. Transplantation 1995;60: Itabashi Y, Hakamada K, Narumi S, Toyoki Y, Totsuka E, Umehara Y, et al. A case of living-related partial liver transplantation using the right gastroepiploic artery for hepatic artery reconstruction. Hepatogastroenterology 2000;47: Wei WI, Lam LK, Ng RW, Liu CL, Lo CM, Fan ST, et al. Microvascular reconstruction of the hepatic artery in live donor liver transplantation: experience across a decade. Arch Surg 2004;139: Turrion VS, Alvira LG, Jimenez M, Lucena JL, Ardaiz J. Incidence and results of arterial complications in liver transplantation: experience in a series of 400 transplants. Transplant Proc 2002;34: Hatano E, Terajima H, Yabe S, Asonuma K, Egawa H, Kiuchi T, et al. Hepatic artery thrombosis in living related liver transplantation. Transplantation 1997;64:
Hepatic Artery Reconstruction in Living Donor Liver Transplant Experience at King Hussein Medical Center
 Hepatic Artery Reconstruction in Living Donor Liver Transplant Experience at King Hussein Medical Center Khaldoun J. Haddadin MD FRCS (Eng)*, Nasser Q. Ahmad MD MRCSI*, Abdelhamid M. Aladwan MD ** ABSTRACT
Hepatic Artery Reconstruction in Living Donor Liver Transplant Experience at King Hussein Medical Center Khaldoun J. Haddadin MD FRCS (Eng)*, Nasser Q. Ahmad MD MRCSI*, Abdelhamid M. Aladwan MD ** ABSTRACT
Successful Application of Supraceliac Aortohepatic Conduit Using Saphenous Venous Graft in Right Lobe Living Donor Liver Transplantation
 LETTERS FROM THE FRONTLINE Successful Application of Supraceliac Aortohepatic Conduit Using Saphenous Venous Graft in Right Lobe Living Donor Liver Transplantation TO THE EDITOR: Hepatic artery (HA) reconstruction
LETTERS FROM THE FRONTLINE Successful Application of Supraceliac Aortohepatic Conduit Using Saphenous Venous Graft in Right Lobe Living Donor Liver Transplantation TO THE EDITOR: Hepatic artery (HA) reconstruction
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
All-in-one sleeve patch graft venoplasty for multiple hepatic vein reconstruction in living donor liver transplantation
 DOI:10.1111/j.1477-2574.2012.00442.x HPB Technical Report All-in-one sleeve patch graft venoplasty for multiple hepatic vein reconstruction in living donor liver transplantation Chao-Long Chen*, Anthony
DOI:10.1111/j.1477-2574.2012.00442.x HPB Technical Report All-in-one sleeve patch graft venoplasty for multiple hepatic vein reconstruction in living donor liver transplantation Chao-Long Chen*, Anthony
Outcome Analysis in Adult-to-Adult Living Donor Liver Transplantation Using the Left Lobe. Patients
 Outcome Analysis in Adult-to-Adult Living Donor Liver Transplantation Using the Left Lobe Yuji Soejima, Mitsuo Shimada, Taketoshi Suehiro, Shoji Hiroshige, Mizuki Ninomiya, Satoko Shiotani, Noboru Harada,
Outcome Analysis in Adult-to-Adult Living Donor Liver Transplantation Using the Left Lobe Yuji Soejima, Mitsuo Shimada, Taketoshi Suehiro, Shoji Hiroshige, Mizuki Ninomiya, Satoko Shiotani, Noboru Harada,
Liver Transplantation in Children: Techniques and What the Surgeon Wants to Know from Imaging
 Liver Transplantation in Children: Techniques and What the Surgeon Wants to Know from Imaging Jaimie D. Nathan, MD Associate Professor of Surgery and Pediatrics Associate Surgical Director, Liver Transplant
Liver Transplantation in Children: Techniques and What the Surgeon Wants to Know from Imaging Jaimie D. Nathan, MD Associate Professor of Surgery and Pediatrics Associate Surgical Director, Liver Transplant
Characterization of the Middle Hepatic Artery and Its Relevance to Living Donor Liver Transplantation
 LIVER TRANSPLANTATION 16:736-741, 2010 ORIGINAL ARTICLE Characterization of the Middle Hepatic Artery and Its Relevance to Living Donor Liver Transplantation Shaofa Wang, 1,3 Xiaoshun He, 1 * Ziping Li,
LIVER TRANSPLANTATION 16:736-741, 2010 ORIGINAL ARTICLE Characterization of the Middle Hepatic Artery and Its Relevance to Living Donor Liver Transplantation Shaofa Wang, 1,3 Xiaoshun He, 1 * Ziping Li,
ORIGINAL ARTICLE. Characteristics of Liver Grafts in Living-Donor Adult Liver Transplantation
 ORIGINAL ARTICLE Characteristics of Liver Grafts in Living-Donor Adult Liver Transplantation Comparison Between Right- and Left-Lobe Grafts Mitsuo Shimada, MD, PhD; Satoko Shiotani, MD; Mizuki Ninomiya,
ORIGINAL ARTICLE Characteristics of Liver Grafts in Living-Donor Adult Liver Transplantation Comparison Between Right- and Left-Lobe Grafts Mitsuo Shimada, MD, PhD; Satoko Shiotani, MD; Mizuki Ninomiya,
TIAN AND OTHERS common hepatic artery. For LDLT, a microvascular technique was employed to anastomose the donor artery to either the right or left hep
 Original Article Treatment of Hepatic Artery Thrombosis After Orthotopic Liver Transplantation Ming Guo Tian, Wai Kuen Tso, 1 Chung Mau Lo, Chi Leung Liu and Sheung Tat Fan, Departments of Surgery and
Original Article Treatment of Hepatic Artery Thrombosis After Orthotopic Liver Transplantation Ming Guo Tian, Wai Kuen Tso, 1 Chung Mau Lo, Chi Leung Liu and Sheung Tat Fan, Departments of Surgery and
Biliary Anatomy in Living-related Liver Transplantation
 The 5th IHPBA Congress - Istanbul Biliary Anatomy in Living-related Liver Transplantation biliary trees hilar plate Assessment for Vascular Anatomy 1. 3DCT portal vein hepatic vein hepatic artery 2. No
The 5th IHPBA Congress - Istanbul Biliary Anatomy in Living-related Liver Transplantation biliary trees hilar plate Assessment for Vascular Anatomy 1. 3DCT portal vein hepatic vein hepatic artery 2. No
In-Hospital Mortality in Adult Recipients of Living Donor Liver Transplantation: Experience of 576 Consecutive Cases at a Single Center
 LIVER TRANSPLANTATION 15:1420-1425, 2009 ORIGINAL ARTICLE In-Hospital Mortality in Adult Recipients of Living Donor Liver Transplantation: Experience of 576 Consecutive Cases at a Single Center Toshimi
LIVER TRANSPLANTATION 15:1420-1425, 2009 ORIGINAL ARTICLE In-Hospital Mortality in Adult Recipients of Living Donor Liver Transplantation: Experience of 576 Consecutive Cases at a Single Center Toshimi
Evaluation of Tissue Blood Flow of the Gastric Tube after Vessel Anastomosis for Esophageal Reconstruction
 Kobe J. Med. Sci., Vol. 57, No. 3, pp. E87-E97, 2011 Evaluation of Tissue Blood Flow of the Gastric Tube after Vessel Anastomosis for Esophageal Reconstruction HITOSHI FUKUYAMA 1, HAJIME IKUTA 1, DAISUKE
Kobe J. Med. Sci., Vol. 57, No. 3, pp. E87-E97, 2011 Evaluation of Tissue Blood Flow of the Gastric Tube after Vessel Anastomosis for Esophageal Reconstruction HITOSHI FUKUYAMA 1, HAJIME IKUTA 1, DAISUKE
Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps
 e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
e50 Case Report THIEME Novel Interpositional Vein Grafting for Pedicle Extension of Island Pedicle Flaps Shuhei Yoshida, MD 1 Isao Koshima, MD 1 Shogo Nagamatsu, MD 2 Kazunori Yokota, MD 2 Shuji Yamashita,
Title. Author(s)Kondo, S.; Katoh, H.; Hirano, S.; Ambo, Y.; Tanaka, CitationBritish Journal of Surgery, 90(6): Issue Date
 Title Portal vein resection and reconstruction prior to he hepatobiliary cancer. Author(s)Kondo, S.; Katoh, H.; Hirano, S.; Ambo, Y.; Tanaka, CitationBritish Journal of Surgery, 90(6): 694-697 Issue Date
Title Portal vein resection and reconstruction prior to he hepatobiliary cancer. Author(s)Kondo, S.; Katoh, H.; Hirano, S.; Ambo, Y.; Tanaka, CitationBritish Journal of Surgery, 90(6): 694-697 Issue Date
ORIGINAL ARTICLE. Received April 30, 2007; accepted June
 LIVER TRANSPLANTATION 13:1405-1413, 2007 ORIGINAL ARTICLE Human Leukocyte Antigen and Adult Living- Donor Liver Transplantation Outcomes: An Analysis of the Organ Procurement and Transplantation Network
LIVER TRANSPLANTATION 13:1405-1413, 2007 ORIGINAL ARTICLE Human Leukocyte Antigen and Adult Living- Donor Liver Transplantation Outcomes: An Analysis of the Organ Procurement and Transplantation Network
Variations in portal and hepatic vein branching of the liver
 Yamagata Med J (ISSN 0288-030X)2015;33(2):115-121 DOI 10.15022/00003476 Variations in portal and hepatic vein branching of the liver Wataru Kimura, Tsuyoshi Fukumoto, Toshihiro Watanabe, Ichiro Hirai First
Yamagata Med J (ISSN 0288-030X)2015;33(2):115-121 DOI 10.15022/00003476 Variations in portal and hepatic vein branching of the liver Wataru Kimura, Tsuyoshi Fukumoto, Toshihiro Watanabe, Ichiro Hirai First
LEE AND OTHERS Annual LDLT (n) year Total Adult-to-adult Paedi
 ADULT-TO-ADULT LIVING DONOR LIVER TRANSPLANTATION Asian Journal of Surgery Excerpta Medica Asia Ltd Adult-to-Adult Living Donor Liver Transplantation at the Asan Medical Center, Korea S.G. Lee, 1 K.M.
ADULT-TO-ADULT LIVING DONOR LIVER TRANSPLANTATION Asian Journal of Surgery Excerpta Medica Asia Ltd Adult-to-Adult Living Donor Liver Transplantation at the Asan Medical Center, Korea S.G. Lee, 1 K.M.
CLINICAL EXPERIENCE OF A MICROVASCULAR VENOUS COUPLER DEVICE IN FREE TISSUE TRANSFERS
 CLINICAL EXPERIENCE OF A MICROVASCULAR VENOUS COUPLER DEVICE IN FREE TISSUE TRANSFERS Kao-Ping Chang, Sin-Daw Lin, and Chung-Sheng Lai Faculty of Medicine, College of Medicine, Kaohsiung Medical University,
CLINICAL EXPERIENCE OF A MICROVASCULAR VENOUS COUPLER DEVICE IN FREE TISSUE TRANSFERS Kao-Ping Chang, Sin-Daw Lin, and Chung-Sheng Lai Faculty of Medicine, College of Medicine, Kaohsiung Medical University,
Endoscopic Management of Postoperative Biliary Complications in Donors for Living Donor Liver Transplantation
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2003;1:183 188 Endoscopic Management of Postoperative Biliary Complications in Donors for Living Donor Liver Transplantation KAZUNORI HASEGAWA,* SHUJIRO YAZUMI,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2003;1:183 188 Endoscopic Management of Postoperative Biliary Complications in Donors for Living Donor Liver Transplantation KAZUNORI HASEGAWA,* SHUJIRO YAZUMI,*
Key words: gastric cancer, postoperative complication, total gastrectomy
 Key words: gastric cancer, postoperative complication, total gastrectomy 115 (115) Fig. 1 Technique of esophagojejunostomy (Quotation from Shimotsuma M and Nakamura R')). A, Technique for hand suture for
Key words: gastric cancer, postoperative complication, total gastrectomy 115 (115) Fig. 1 Technique of esophagojejunostomy (Quotation from Shimotsuma M and Nakamura R')). A, Technique for hand suture for
Liver transplantation is a gold standard of therapy. Estimation of Standard Liver Volume for Liver Transplantation in the Korean Population
 Estimation of Standard Liver Volume for Liver Transplantation in the Korean Population Hee Chul Yu, 1,2 Heecheon You, 3 Ho Lee, 4 Zhe-Wu Jin, 1 Jang Il Moon, 5 and Baik Hwan Cho 1,2 The standard liver
Estimation of Standard Liver Volume for Liver Transplantation in the Korean Population Hee Chul Yu, 1,2 Heecheon You, 3 Ho Lee, 4 Zhe-Wu Jin, 1 Jang Il Moon, 5 and Baik Hwan Cho 1,2 The standard liver
Venous Outflow Reconstruction Using an Expanded Polytetrafluoroethylene Vascular Graft in Living-Donor Liver Transplant: A Single-Center Experience
 ARTICLe Venous Outflow Reconstruction Using an Expanded Polytetrafluoroethylene Vascular Graft in Living-Donor Liver Transplant: A Single-Center Experience Chia-Yu Lai, 1 Shao-Min Han, 2 Yi-Ju Chen, 1
ARTICLe Venous Outflow Reconstruction Using an Expanded Polytetrafluoroethylene Vascular Graft in Living-Donor Liver Transplant: A Single-Center Experience Chia-Yu Lai, 1 Shao-Min Han, 2 Yi-Ju Chen, 1
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Liver transplant for biliary atresia
 Jean de Ville de Goyet ISMETT Director of the Department for the Treatment and Study of Pediatric Abdominal Diseases and Abdominal Transplantation The first human liver transplant was performed on a pediatric
Jean de Ville de Goyet ISMETT Director of the Department for the Treatment and Study of Pediatric Abdominal Diseases and Abdominal Transplantation The first human liver transplant was performed on a pediatric
Hepatic venous congestion (HVC) from deprivation
 Cryopreserved Iliac Artery is Indispensable Interposition Graft Material for Middle Hepatic Vein Reconstruction of Right Liver Grafts Shin Hwang, Sung-Gyu Lee, Chul-Soo Ahn, Kwang-Min Park, Ki-Hun Kim,
Cryopreserved Iliac Artery is Indispensable Interposition Graft Material for Middle Hepatic Vein Reconstruction of Right Liver Grafts Shin Hwang, Sung-Gyu Lee, Chul-Soo Ahn, Kwang-Min Park, Ki-Hun Kim,
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Living Donor Liver Transplantation Wits Donald Gordon Medical Centre
 Living Donor Liver Transplantation Wits Donald Gordon Medical Centre J Loveland, J Botha, R Britz, B Strobele, A Mahomed, B Bobat, S Rambarran, F van der Schyff et al The First 1963 C Henry Kempe presented
Living Donor Liver Transplantation Wits Donald Gordon Medical Centre J Loveland, J Botha, R Britz, B Strobele, A Mahomed, B Bobat, S Rambarran, F van der Schyff et al The First 1963 C Henry Kempe presented
Citation Transplantation Proceedings, 47(3),
 NAOSITE: Nagasaki University's Ac Title Author(s) Hybrid Procedure in Living Donor Li Soyama, Akihiko; Takatsuki, Mitsuhi Tomohiko; Kitasato, Amane; Kinoshit Baimakhanov, Zhassulan; Kuroki, Tam Citation
NAOSITE: Nagasaki University's Ac Title Author(s) Hybrid Procedure in Living Donor Li Soyama, Akihiko; Takatsuki, Mitsuhi Tomohiko; Kitasato, Amane; Kinoshit Baimakhanov, Zhassulan; Kuroki, Tam Citation
Synthetic Graft for Reconstruction of Middle Hepatic Vein Tributaries in Living-Donor Liver Transplant
 POSter PreSeNtAtION Synthetic Graft for Reconstruction of Middle Hepatic Vein Tributaries in Living-Donor Liver Transplant Refaat Kamel, 1 Yasser Hatata, 2 Karim Hosny, 3 Khaled Amer, 4 Mohamed Taha 5
POSter PreSeNtAtION Synthetic Graft for Reconstruction of Middle Hepatic Vein Tributaries in Living-Donor Liver Transplant Refaat Kamel, 1 Yasser Hatata, 2 Karim Hosny, 3 Khaled Amer, 4 Mohamed Taha 5
Variations in Surgical Anatomy of the Portal Vein in Living Donor Liver Transplantation
 Kasr El Aini Journal of Surgery VOL., 9, NO 3 January 2008 19 Variations in Surgical Anatomy of the Portal Vein in Living Donor Liver Transplantation A. Ayad ; W. Tobar; M.Hassan; A.Hosny; M.El Shazly;
Kasr El Aini Journal of Surgery VOL., 9, NO 3 January 2008 19 Variations in Surgical Anatomy of the Portal Vein in Living Donor Liver Transplantation A. Ayad ; W. Tobar; M.Hassan; A.Hosny; M.El Shazly;
Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated with stent failure
 Kato et al. BMC Surgery (2017) 17:11 DOI 10.1186/s12893-017-0209-y RESEARCH ARTICLE Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated
Kato et al. BMC Surgery (2017) 17:11 DOI 10.1186/s12893-017-0209-y RESEARCH ARTICLE Portal vein stent placement for the treatment of postoperative portal vein stenosis: long-term success and factor associated
Liver retransplantation for adult recipients
 Korean J Hepatobiliary Pancreat Surg 2013;17:1-7 Review Article Liver retransplantation for adult recipients Shin Hwang, Chul-Soo Ahn, Ki-Hun Kim, Deok-Bog Moon, Tae-Yong Ha, Gi-Won Song, Dong-Hwan Jung,
Korean J Hepatobiliary Pancreat Surg 2013;17:1-7 Review Article Liver retransplantation for adult recipients Shin Hwang, Chul-Soo Ahn, Ki-Hun Kim, Deok-Bog Moon, Tae-Yong Ha, Gi-Won Song, Dong-Hwan Jung,
An Artificial Vascular Graft Is a Useful Interpositional Material for Drainage of the Right Anterior Section in Living Donor Liver Transplantation
 LIVER TRANSPLANTATION 13:1159-1167, 2007 ORIGINAL ARTICLE An Artificial Vascular Graft Is a Useful Interpositional Material for Drainage of the Right Anterior Section in Living Donor Liver Transplantation
LIVER TRANSPLANTATION 13:1159-1167, 2007 ORIGINAL ARTICLE An Artificial Vascular Graft Is a Useful Interpositional Material for Drainage of the Right Anterior Section in Living Donor Liver Transplantation
Yurong Liang, Jing Wang, Xianjie Shi, Jiahong Dong, and Wanqing Gu. 1. Introduction. 2. Patients and Methods
 Gastroenterology Research and Practice Volume 2015, Article ID 934565, 4 pages http://dx.doi.org/10.1155/2015/934565 Clinical Study Application of a Gastroduodenal Artery Graft for Reconstruction of the
Gastroenterology Research and Practice Volume 2015, Article ID 934565, 4 pages http://dx.doi.org/10.1155/2015/934565 Clinical Study Application of a Gastroduodenal Artery Graft for Reconstruction of the
Hepatic Artery Thrombosis After Orthotopic Liver Transplant: A Review of the Same Institute 5 Years Later
 ARtıCle Hepatic Artery Thrombosis After Orthotopic Liver Transplant: A Review of the Same Institute 5 Years Later Linwei Wu, 1 Jianwei Zhang, 2 Zhiyong Guo, 1 Qiang Tai, 1 Xiaoshun He, 1 Weiqiang Ju, 1
ARtıCle Hepatic Artery Thrombosis After Orthotopic Liver Transplant: A Review of the Same Institute 5 Years Later Linwei Wu, 1 Jianwei Zhang, 2 Zhiyong Guo, 1 Qiang Tai, 1 Xiaoshun He, 1 Weiqiang Ju, 1
Impact Of Reconstructing A Single Hepatic Artery On Small-For-Size Grafts In Living Donor Liver Transplantation
 ISPUB.COM The Internet Journal of Surgery Volume 31 Number 2 Impact Of Reconstructing A Single Hepatic Artery On Small-For-Size Grafts In Living Donor Liver K, A, B, C Citation K, A, B, C.. The Internet
ISPUB.COM The Internet Journal of Surgery Volume 31 Number 2 Impact Of Reconstructing A Single Hepatic Artery On Small-For-Size Grafts In Living Donor Liver K, A, B, C Citation K, A, B, C.. The Internet
Portal vein arterialization: a salvage procedure for a totally de-arterialized liver. The Paul Brousse Hospital experience
 DOI:10.1111/hpb.12200 HPB ORIGINAL ARTICLE Portal vein arterialization: a salvage procedure for a totally de-arterialized liver. The Paul Brousse Hospital experience Prashant Bhangui 1, Chady Salloum 2,
DOI:10.1111/hpb.12200 HPB ORIGINAL ARTICLE Portal vein arterialization: a salvage procedure for a totally de-arterialized liver. The Paul Brousse Hospital experience Prashant Bhangui 1, Chady Salloum 2,
Anatomical study. Clinical study. R. Ogawa, H. Hyakusoku, M. Murakami, R. Aoki, K. Tanuma* and D. G. Pennington?
 British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
British Journal of Plastic Surgery (2002) 55, 396-40 I 9 2002 The British Association of Plastic Surgeons doi: 10.1054/bjps.2002.3877 PLASTIC SURGERY An anatomical and clinical study of the dorsal intercostal
Adult-to-adult living donor liver transplantation Triumphs and challenges
 Falk Symposium No. 163 on Chronic Inflammation of Liver and Gut Adult-to-adult living donor liver transplantation Triumphs and challenges ST Fan, MS, MD, PhD, DSc Professor Sun CY Chair of Hepatobiliary
Falk Symposium No. 163 on Chronic Inflammation of Liver and Gut Adult-to-adult living donor liver transplantation Triumphs and challenges ST Fan, MS, MD, PhD, DSc Professor Sun CY Chair of Hepatobiliary
Sinusoidal Perfusion in the Veno-Occlusive Region of Living Liver Donors Evaluated by Indocyanine Green and Near-Infrared Spectroscopy
 LIVER TRANSPLANTATION 14:872 880, 2008 ORIGINAL ARTICLE Sinusoidal Perfusion in the Veno-Occlusive Region of Living Liver Donors Evaluated by Indocyanine Green and Near-Infrared Spectroscopy Takuya Hashimoto,
LIVER TRANSPLANTATION 14:872 880, 2008 ORIGINAL ARTICLE Sinusoidal Perfusion in the Veno-Occlusive Region of Living Liver Donors Evaluated by Indocyanine Green and Near-Infrared Spectroscopy Takuya Hashimoto,
Biliary Reconstruction for Infantile Living Donor Liver Transplantation: Roux-en-Y Hepaticojejunostomy or Duct-to-Duct Choledochocholedochostomy?
 LIVER TRANSPLANTATION 14:1761-1765, 2008 ORIGINAL ARTICLE Biliary Reconstruction for Infantile Living Donor Liver Transplantation: Roux-en-Y Hepaticojejunostomy or Duct-to-Duct Choledochocholedochostomy?
LIVER TRANSPLANTATION 14:1761-1765, 2008 ORIGINAL ARTICLE Biliary Reconstruction for Infantile Living Donor Liver Transplantation: Roux-en-Y Hepaticojejunostomy or Duct-to-Duct Choledochocholedochostomy?
Current status of hepatic surgery in Korea
 Korean J Hepatol. 2009 Dec; 15(Suppl 6):S60 - S64. DOI: 10.3350/kjhep.2009.15.S6.S60 Current status of hepatic surgery in Korea Kyung Sik Kim Department of Surgery, Severance Hospital, Yonsei University
Korean J Hepatol. 2009 Dec; 15(Suppl 6):S60 - S64. DOI: 10.3350/kjhep.2009.15.S6.S60 Current status of hepatic surgery in Korea Kyung Sik Kim Department of Surgery, Severance Hospital, Yonsei University
Single-Center Experience and Long-Term Outcomes of Duct-to-Duct Biliary Reconstruction in Infantile Living Donor Liver Transplantation
 LIVER TRANSPLANTATION 20:347 354, 2014 ORIGINAL ARTICLE Single-Center Experience and Long-Term Outcomes of Duct-to-Duct Biliary Reconstruction in Infantile Living Donor Liver Transplantation Hidekazu Yamamoto,
LIVER TRANSPLANTATION 20:347 354, 2014 ORIGINAL ARTICLE Single-Center Experience and Long-Term Outcomes of Duct-to-Duct Biliary Reconstruction in Infantile Living Donor Liver Transplantation Hidekazu Yamamoto,
Surgical Injuries of Postmortem Donor Livers: Incidence and Impact on Outcome After Adult Liver Transplantation
 LIVER TRANSPLANTATION 12:1365-1370, 2006 ORIGINAL ARTICLE Surgical Injuries of Postmortem Donor Livers: Incidence and Impact on Outcome After Adult Liver Transplantation Danielle M. Nijkamp, 1 Maarten
LIVER TRANSPLANTATION 12:1365-1370, 2006 ORIGINAL ARTICLE Surgical Injuries of Postmortem Donor Livers: Incidence and Impact on Outcome After Adult Liver Transplantation Danielle M. Nijkamp, 1 Maarten
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A ACLF. See Acute-on-chronic liver failure (ACLF) Acute kidney injury (AKI) in ACLF patients, 967 Acute liver failure (ALF), 957 964 causes
Index Note: Page numbers of article titles are in boldface type. A ACLF. See Acute-on-chronic liver failure (ACLF) Acute kidney injury (AKI) in ACLF patients, 967 Acute liver failure (ALF), 957 964 causes
Percutaneous Microwave Coagulation Therapy for Hepatocellular Carcinoma
 Hiroshima J. Med. Sci. Vol. 47, No.4, 151~155, December, 1998 HIJM47-2 151 Percutaneous Microwave Coagulation Therapy for Hepatocellular Carcinoma Toshimasa ASAHARA1l, Hideki NAKAHARA1l, Toshikatsu FUKUDA1l,
Hiroshima J. Med. Sci. Vol. 47, No.4, 151~155, December, 1998 HIJM47-2 151 Percutaneous Microwave Coagulation Therapy for Hepatocellular Carcinoma Toshimasa ASAHARA1l, Hideki NAKAHARA1l, Toshikatsu FUKUDA1l,
OPERATIVE TECHNIQUES AND HAZARDS
 OPERATIVE TECHNIQUES AND HAZARDS CHRIS O SULLIVAN MD FRCSI CONSULTANT HBP AND LIVER TRANSPLANT SURGEON FREEMAN HOSPITAL, N-UPON-TYNE CAVAL RECONSTRUCTION IN ORTHOTOPIC LIVER TRANSPLANTATION RESECTION OF
OPERATIVE TECHNIQUES AND HAZARDS CHRIS O SULLIVAN MD FRCSI CONSULTANT HBP AND LIVER TRANSPLANT SURGEON FREEMAN HOSPITAL, N-UPON-TYNE CAVAL RECONSTRUCTION IN ORTHOTOPIC LIVER TRANSPLANTATION RESECTION OF
Doppler Ultrasound Findings in the Hepatic Artery Shortly After Liver Transplantation
 Gastrointestinal Imaging Pictorial Essay García-riado et al. Hepatic rtery fter Liver Transplantation Gastrointestinal Imaging Pictorial Essay FOUS ON: Ángeles García-riado 1 Rosa Gilabert nnalisa erzigotti
Gastrointestinal Imaging Pictorial Essay García-riado et al. Hepatic rtery fter Liver Transplantation Gastrointestinal Imaging Pictorial Essay FOUS ON: Ángeles García-riado 1 Rosa Gilabert nnalisa erzigotti
Open Access. Noriaki Sadanaga 1*, Keigo Morinaga 2 and Hiroshi Matsuura 1
 Sadanaga et al. Surgical Case Reports (2015) 1:22 DOI 10.1186/s40792-015-0020-x Open Access Secondary reconstruction with a transverse colon covered with a pectoralis major muscle flap and split thickness
Sadanaga et al. Surgical Case Reports (2015) 1:22 DOI 10.1186/s40792-015-0020-x Open Access Secondary reconstruction with a transverse colon covered with a pectoralis major muscle flap and split thickness
Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy
 LETTERS FROM THE FRONTLINE Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy TO THE EDITOR: Despite advances
LETTERS FROM THE FRONTLINE Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy TO THE EDITOR: Despite advances
Paediatric Liver Transplant Programme Wits Donald Gordon Medical Centre
 Paediatric Liver Transplant Programme Wits Donald Gordon Medical Centre J Loveland, J Botha, R Britz, B Strobele, S Rambarran, A Terblanche, C Kock, P Walabh, M Beretta, M Duncan et al 1817 reveal the
Paediatric Liver Transplant Programme Wits Donald Gordon Medical Centre J Loveland, J Botha, R Britz, B Strobele, S Rambarran, A Terblanche, C Kock, P Walabh, M Beretta, M Duncan et al 1817 reveal the
Liver Transplantation
 1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
The Journal of Thoracic and Cardiovascular Surgery
 Accepted Manuscript Commentary: NO FLOW? QUICK, RE-SEW Ross M. Bremner, MD, PhD PII: S0022-5223(19)30560-4 DOI: https://doi.org/10.1016/j.jtcvs.2019.02.092 Reference: YMTC 14240 To appear in: The Journal
Accepted Manuscript Commentary: NO FLOW? QUICK, RE-SEW Ross M. Bremner, MD, PhD PII: S0022-5223(19)30560-4 DOI: https://doi.org/10.1016/j.jtcvs.2019.02.092 Reference: YMTC 14240 To appear in: The Journal
HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein
 Journal of Surgical Oncology 2006;93:338 342 HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein MARCEL AUTRAN C. MACHADO, MD, 1,2 * PAULO
Journal of Surgical Oncology 2006;93:338 342 HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein MARCEL AUTRAN C. MACHADO, MD, 1,2 * PAULO
PUT YOUR BEST FOOT FORWARD
 PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
PUT YOUR BEST FOOT FORWARD Bala Ramanan, MBBS 1 st year vascular surgery fellow Introduction The epidemic of diabetes and ageing of our population ensures critical limb ischemia will continue to grow.
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Management of Extensive Portal Vein Thrombosis
 Management of Extensive Portal Vein Thrombosis Deok-Bog Moon, Sung-Gyu Lee, Chul-Soo Ahn, Shin Hwang, Ki-Hun Kim, Gi-Won Song, Dong-Hwan Jung, Gil-Chun Park, Kyu-Bo Sung 1, Gi- Young Ko 1, Dong-Il Kweon
Management of Extensive Portal Vein Thrombosis Deok-Bog Moon, Sung-Gyu Lee, Chul-Soo Ahn, Shin Hwang, Ki-Hun Kim, Gi-Won Song, Dong-Hwan Jung, Gil-Chun Park, Kyu-Bo Sung 1, Gi- Young Ko 1, Dong-Il Kweon
Erratum to: Int J Hematol (2014) 99: DOI /s
 Int J Hematol (216) 13:725 729 DOI 1.17/s12185-16-1987-1 ERRATUM Erratum to: Prolonged thrombocytopenia after living donor liver transplantation is a strong prognostic predictor irrespective of history
Int J Hematol (216) 13:725 729 DOI 1.17/s12185-16-1987-1 ERRATUM Erratum to: Prolonged thrombocytopenia after living donor liver transplantation is a strong prognostic predictor irrespective of history
INTRODUCTION. Toshihiko Satake 1, Jun Sugawara 2, Kazunori Yasumura 1, Taro Mikami 2, Shinji Kobayashi 3, Jiro Maegawa 2. Idea and Innovation
 Mini-Flow-Through Deep Inferior Epigastric Perforator Flap for Breast Reconstruction with Preservation of Both Internal Mammary and Deep Inferior Epigastric Vessels Toshihiko Satake 1, Jun Sugawara 2,
Mini-Flow-Through Deep Inferior Epigastric Perforator Flap for Breast Reconstruction with Preservation of Both Internal Mammary and Deep Inferior Epigastric Vessels Toshihiko Satake 1, Jun Sugawara 2,
Supplementary Digital Content
 Geissler et al: Sirolimus and Hepatocellular Carcinoma in Liver Transplantation Page 1 of 10 Supplementary Digital Content Supplementary Table 1. Surgical procedures used Total Transplant technique Piggy
Geissler et al: Sirolimus and Hepatocellular Carcinoma in Liver Transplantation Page 1 of 10 Supplementary Digital Content Supplementary Table 1. Surgical procedures used Total Transplant technique Piggy
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms
 J Neurosurg 97:486 491, 2002 Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms Technical note DAVID
J Neurosurg 97:486 491, 2002 Intracranial-to-intracranial vascular anastomosis created using a microanastomotic device for the treatment of distal middle cerebral artery aneurysms Technical note DAVID
of bile leakage after liver resecti
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Percutaneous embolization with n-bu of bile leakage after liver resecti Kuroki, Tamotsu; Kitasato, Amane; T Hiroaki; Taniguchi, Ken; Maeda, Shi
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Percutaneous embolization with n-bu of bile leakage after liver resecti Kuroki, Tamotsu; Kitasato, Amane; T Hiroaki; Taniguchi, Ken; Maeda, Shi
ProCol Vascular Bioprosthesis
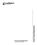 ProCol Vascular Bioprosthesis Instructions for use - English ProCol Vascular Bioprosthesis ProCol Vascular Bioprosthesis (Catalog Numbers HJL016-10-N, HJL016-25-N, HJL016-30-N, HJL016-40-N) Instructions
ProCol Vascular Bioprosthesis Instructions for use - English ProCol Vascular Bioprosthesis ProCol Vascular Bioprosthesis (Catalog Numbers HJL016-10-N, HJL016-25-N, HJL016-30-N, HJL016-40-N) Instructions
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps
 Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Breast Reconstruction with Superficial Inferior Epigastric Artery Flaps: A Prospective Comparison with TRAM and DIEP Flaps Pierre M. Chevray, M.D., Ph.D. Houston, Texas Breast reconstruction using the
Informed Consent for Liver Transplant Patients
 Informed Consent for Liver Transplant Patients Evaluation Process You will be evaluated with consultations, lab tests and various procedures to determine the medical appropriateness of liver transplant.
Informed Consent for Liver Transplant Patients Evaluation Process You will be evaluated with consultations, lab tests and various procedures to determine the medical appropriateness of liver transplant.
Biliary complications after right lobe living donor liver transplantation: a single-centre experience
 DOI:10.1111/j.1477-2574.2011.00401.x HPB ORIGINAL ARTICLE Biliary complications after right lobe living donor liver transplantation: a single-centre experience Onur Yaprak 1, Murat Dayangac 1, Murat Akyildiz
DOI:10.1111/j.1477-2574.2011.00401.x HPB ORIGINAL ARTICLE Biliary complications after right lobe living donor liver transplantation: a single-centre experience Onur Yaprak 1, Murat Dayangac 1, Murat Akyildiz
Original article: new surgical approaches to the Klatskin tumour
 Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Information for patients (and their families) waiting for liver transplantation
 Information for patients (and their families) waiting for liver transplantation Waiting list? What is liver transplant? Postoperative conditions? Ver.: 5/2017 1 What is a liver transplant? Liver transplantation
Information for patients (and their families) waiting for liver transplantation Waiting list? What is liver transplant? Postoperative conditions? Ver.: 5/2017 1 What is a liver transplant? Liver transplantation
CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion
 CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion Julien Pauchot, MD, PhD, a Emilie Ducroux, MD, b Grégoire Leclerc, MD, a Laurent Obert,
CASE REPORT Omentum Free Flap Anastomosed to Arterial Bypass in Open Knee Dislocation: Case Report and Discussion Julien Pauchot, MD, PhD, a Emilie Ducroux, MD, b Grégoire Leclerc, MD, a Laurent Obert,
What Is the Real Gain After Liver Transplantation?
 LIVER TRANSPLANTATION 15:S1-S5, 9 AASLD/ILTS SYLLABUS What Is the Real Gain After Liver Transplantation? James Neuberger Organ Donation and Transplantation, NHS Blood and Transplant, Bristol, United Kingdom;
LIVER TRANSPLANTATION 15:S1-S5, 9 AASLD/ILTS SYLLABUS What Is the Real Gain After Liver Transplantation? James Neuberger Organ Donation and Transplantation, NHS Blood and Transplant, Bristol, United Kingdom;
Microvascular free tissue transfer is a standard
 ORIGINAL ARTICLE INTERNAL MAMMARY ARTERY AND VEIN: RECIPIENT VESSELS FOR FREE TISSUE TRANSFER TO THE HEAD AND NECK IN THE VESSEL-DEPLETED NECK Mark L. Urken, MD, 1 Kevin M. Higgins, MD, 2 Bryant Lee, MD,
ORIGINAL ARTICLE INTERNAL MAMMARY ARTERY AND VEIN: RECIPIENT VESSELS FOR FREE TISSUE TRANSFER TO THE HEAD AND NECK IN THE VESSEL-DEPLETED NECK Mark L. Urken, MD, 1 Kevin M. Higgins, MD, 2 Bryant Lee, MD,
The Synovis GEM COUPLER
 The Synovis GEM COUPLER e Synovis product portfolio includes Coupler, Flow Coupler and GeM MicroClip. ese products are used for joining small diameter vessels during autologous tissue breast reconstruction;
The Synovis GEM COUPLER e Synovis product portfolio includes Coupler, Flow Coupler and GeM MicroClip. ese products are used for joining small diameter vessels during autologous tissue breast reconstruction;
Liver Transplantation for Alcoholic Liver Disease in the United States: 1988 to 1995
 Liver Transplantation for Alcoholic Liver Disease in the United States: 1988 to 1995 Steven H. Belle, Kimberly C. Beringer, and Katherine M. Detre T he Scientific Liver Transplant Registry (LTR) was established
Liver Transplantation for Alcoholic Liver Disease in the United States: 1988 to 1995 Steven H. Belle, Kimberly C. Beringer, and Katherine M. Detre T he Scientific Liver Transplant Registry (LTR) was established
Key words: celiac occlusive disease, pancreaticoduodenectomy, abdominal aorta-celiac bypass
 Key words: celiac occlusive disease, pancreaticoduodenectomy, abdominal aorta-celiac bypass 51(2023) Table 1 Laboratory data on admission Fig. 2 Percutaneous transhepatic cholangiogram shows tapering obstruction
Key words: celiac occlusive disease, pancreaticoduodenectomy, abdominal aorta-celiac bypass 51(2023) Table 1 Laboratory data on admission Fig. 2 Percutaneous transhepatic cholangiogram shows tapering obstruction
ORIGINAL ARTICLE ORIGINAL ARTICLE 887. Liver Transplantation AASLD. Received January 25, 2017; accepted April 13, 2017.
 ORIGINAL ARTICLE LI ET AL. Hepatic Artery Reconstruction in Living Donor Liver Transplantation Using Surgical Loupes: Achieving Low Rate of Hepatic Arterial Thrombosis in 741 Consecutive Recipients Tips
ORIGINAL ARTICLE LI ET AL. Hepatic Artery Reconstruction in Living Donor Liver Transplantation Using Surgical Loupes: Achieving Low Rate of Hepatic Arterial Thrombosis in 741 Consecutive Recipients Tips
Expansion of the oral end of free revascularised jejunum with a jejunal patch flap rotated like a folding fan
 British Journal of Plastic Surgery (1998), 51, 103-108 9 1998 The British Association of Plastic Surgeons BRITISH JOURNAL OF ~ PLASTIC SURGERY Expansion of the oral end of free revascularised jejunum with
British Journal of Plastic Surgery (1998), 51, 103-108 9 1998 The British Association of Plastic Surgeons BRITISH JOURNAL OF ~ PLASTIC SURGERY Expansion of the oral end of free revascularised jejunum with
Extending Indication: Role of Living Donor Liver Transplantation for Hepatocellular Carcinoma
 LIVER TRANSPLANTATION 13:S48-S54, 27 SUPPLEMENT Extending Indication: Role of Living Donor Liver Transplantation for Hepatocellular Carcinoma Satoru Todo, 1 Hiroyuki Furukawa, 2 Mitsuhiro Tada, 3 and the
LIVER TRANSPLANTATION 13:S48-S54, 27 SUPPLEMENT Extending Indication: Role of Living Donor Liver Transplantation for Hepatocellular Carcinoma Satoru Todo, 1 Hiroyuki Furukawa, 2 Mitsuhiro Tada, 3 and the
A New Porcine Model of Autologous Living-donor Liver Transplantation
 Jichi Medical University Journal A New Porcine Model of Autologous Living-donor Liver Transplantation Nobuyuki Hojo, Toshimitsu Ishibashi, Toshihiko Yasuda, Yasunaru Sakuma, Taketo Fujiwara, Yoshikazu
Jichi Medical University Journal A New Porcine Model of Autologous Living-donor Liver Transplantation Nobuyuki Hojo, Toshimitsu Ishibashi, Toshihiko Yasuda, Yasunaru Sakuma, Taketo Fujiwara, Yoshikazu
CLINICAL LIVER, PANCREAS, AND BILIARY TRACT
 GASTROENTEROLOGY 2008;134:1908 1916 BILIARY TRACT Neither Multiple Tumors Nor Portal Hypertension Are Surgical Contraindications for Hepatocellular Carcinoma TAKEAKI ISHIZAWA, KIYOSHI HASEGAWA, TAKU AOKI,
GASTROENTEROLOGY 2008;134:1908 1916 BILIARY TRACT Neither Multiple Tumors Nor Portal Hypertension Are Surgical Contraindications for Hepatocellular Carcinoma TAKEAKI ISHIZAWA, KIYOSHI HASEGAWA, TAKU AOKI,
The first liver transplant in a human was performed
 Liver Transplantation With Monosegments. Technical Aspects and Outcome: A Meta-Analysis Marcelo Enne, 1 Lucio Pacheco-Moreira, 1 Elizabeth Balbi, 2 Alexandre Cerqueira, 1 Giuseppe Santalucia, 3 and José
Liver Transplantation With Monosegments. Technical Aspects and Outcome: A Meta-Analysis Marcelo Enne, 1 Lucio Pacheco-Moreira, 1 Elizabeth Balbi, 2 Alexandre Cerqueira, 1 Giuseppe Santalucia, 3 and José
Citation Hepato-Gastroenterology, 55(86-87),
 NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko;
Surgical anatomy of the biliary tract
 HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
AATS Focus on Thoracic Surgery: Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017?
 AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
AATS Focus on Thoracic Surgery: Mastering Surgical Innovation Las Vegas, NV October 28, 2017 Session VIII: Video Session Minimally Invasive Esophagectomy: Are We Still Getting Better in 2017? James D.
ORIGINAL ARTICLE. Summary
 Transplant International ISSN 0934-0874 ORIGINAL ARTICLE Thrombotic and nonthrombotic hepatic artery complications in adults and children following primary liver transplantation with long-term follow-up
Transplant International ISSN 0934-0874 ORIGINAL ARTICLE Thrombotic and nonthrombotic hepatic artery complications in adults and children following primary liver transplantation with long-term follow-up
Living donor liver transplantation: Eastern experiences
 Living donor liver transplantation: Eastern experiences K Tanaka 1, Y Ogura 1, T Kiuchi 1, Y Inomata 2, S Uemoto 3 and H Furukawa 4 "Deportment of Transplantation and Immunology, Kyoto University Hospital,
Living donor liver transplantation: Eastern experiences K Tanaka 1, Y Ogura 1, T Kiuchi 1, Y Inomata 2, S Uemoto 3 and H Furukawa 4 "Deportment of Transplantation and Immunology, Kyoto University Hospital,
Heart Transplantation for Patients with a Fontan Procedure
 Heart Transplantation for Patients with a Fontan Procedure Kirk R. Kanter MD Professor of Surgery Pediatric Cardiac Surgery Emory University School of Medicine Children s Healthcare of Atlanta Atlanta,
Heart Transplantation for Patients with a Fontan Procedure Kirk R. Kanter MD Professor of Surgery Pediatric Cardiac Surgery Emory University School of Medicine Children s Healthcare of Atlanta Atlanta,
Anatomical relationship between arteries and veins in the paraumbilical region q
 The British Association of Plastic Surgeons (2003) 56, 552 556 Anatomical relationship between arteries and veins in the paraumbilical region q N. Imanishi a, *, H. Nakajima b, T. Minabe c, H. Chang d,
The British Association of Plastic Surgeons (2003) 56, 552 556 Anatomical relationship between arteries and veins in the paraumbilical region q N. Imanishi a, *, H. Nakajima b, T. Minabe c, H. Chang d,
Minimally Invasive Esophagectomy
 American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
American Association of Thoracic Surgery (AATS) 95 th Annual Meeting Seattle, WA April 29, 2015 General Thoracic Masters of Surgery Video Session Minimally Invasive Esophagectomy James D. Luketich MD,
Living Donor Hepatectomy: The Importance of the Residual Liver Volume
 LIVER TRANSPLANTATION 17:1404-1411, 2011 ORIGINAL ARTICLE Living Donor Hepatectomy: The Importance of the Residual Liver Volume Trevor W. Reichman, Charbel Sandroussi, Solomon M. Azouz, Lesley Adcock,
LIVER TRANSPLANTATION 17:1404-1411, 2011 ORIGINAL ARTICLE Living Donor Hepatectomy: The Importance of the Residual Liver Volume Trevor W. Reichman, Charbel Sandroussi, Solomon M. Azouz, Lesley Adcock,
Reconstruction of axillary scar contractures retrospective study of 124 cases over 25 years
 British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
British Journal of Plastic Surgery (2003), 56, 100 105 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00035-3 Reconstruction
Home Intravenous Antibiotic Treatment for Intractable Cholangitis in Biliary Atresia
 Home Intravenous Antibiotic Treatment for Intractable Cholangitis in Biliary Atresia Hye Kyung Chang, Jung-Tak Oh, Seung Hoon Choi, Seok Joo Han Division of Pediatric Surgery, Department of Surgery, Yonsei
Home Intravenous Antibiotic Treatment for Intractable Cholangitis in Biliary Atresia Hye Kyung Chang, Jung-Tak Oh, Seung Hoon Choi, Seok Joo Han Division of Pediatric Surgery, Department of Surgery, Yonsei
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options
 Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
Post-operative complications following hepatobiliary surgery: imaging findings and current radiological treatment options Poster No.: C-1501 Congress: ECR 2015 Type: Educational Exhibit Authors: A. Hadjivassiliou,
Step-by-step isolated resection of segment 1 of the liver using the hanging maneuver
 The American Journal of Surgery (2009) 198, e42 e48 HowIDoIt Step-by-step isolated resection of segment 1 of the liver using the hanging maneuver Rafael López-Andújar, Ph.D.*, Eva Montalvá, Ph.D., Marcos
The American Journal of Surgery (2009) 198, e42 e48 HowIDoIt Step-by-step isolated resection of segment 1 of the liver using the hanging maneuver Rafael López-Andújar, Ph.D.*, Eva Montalvá, Ph.D., Marcos
Transplant Hepatology
 Transplant Hepatology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified
Transplant Hepatology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified
An Algorithm to Guide Recipient Vessel Selection in Cases of Free Functional Muscle Transfer for Facial Reanimation
 An Algorithm to Guide Recipient Vessel Selection in Cases of Free Functional Muscle Transfer for Facial Reanimation Original Article Francis P Henry, Jonathan I Leckenby, Daniel P Butler, Adriaan O Grobbelaar
An Algorithm to Guide Recipient Vessel Selection in Cases of Free Functional Muscle Transfer for Facial Reanimation Original Article Francis P Henry, Jonathan I Leckenby, Daniel P Butler, Adriaan O Grobbelaar
Contaminated Wound: Report of a Cas
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Endovascular Treatment of a Carotid Contaminated Wound: Report of a Cas Yamaguchi, Nimpei; Kaneko, Kenichi; Takahashi, Haruo Acta medica Nagasakiensia,
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Endovascular Treatment of a Carotid Contaminated Wound: Report of a Cas Yamaguchi, Nimpei; Kaneko, Kenichi; Takahashi, Haruo Acta medica Nagasakiensia,
Pediatric Liver Transplantation Outcomes in Korea
 ORIGINAL ARTICLE Cell Therapy & Organ Transplantation http://dx.doi.org/6/jkms.8..4 J Korean Med Sci 0; 8: 4-47 Pediatric Liver Transplantation Outcomes in Korea Jong Man Kim,, * Kyung Mo Kim,, * Nam-Joon
ORIGINAL ARTICLE Cell Therapy & Organ Transplantation http://dx.doi.org/6/jkms.8..4 J Korean Med Sci 0; 8: 4-47 Pediatric Liver Transplantation Outcomes in Korea Jong Man Kim,, * Kyung Mo Kim,, * Nam-Joon
Living donor liver transplantation without the use of blood products. Liu, CL; Fan, ST; Lo, CM; Wei, WI; Yong, BH; Lai, CL; Wong, J
 Title Living donor liver transplantation without the use of blood products. Author(s) Liu, CL; Fan, ST; Lo, CM; Wei, WI; Yong, BH; Lai, CL; Wong, J Citation Hong Kong Medical Journal = Xianggang Yi Xue
Title Living donor liver transplantation without the use of blood products. Author(s) Liu, CL; Fan, ST; Lo, CM; Wei, WI; Yong, BH; Lai, CL; Wong, J Citation Hong Kong Medical Journal = Xianggang Yi Xue
