Citation Hepato-Gastroenterology, 55(86-87),
|
|
|
- Dylan Little
- 5 years ago
- Views:
Transcription
1 NAOSITE: Nagasaki University's Ac Title Author(s) Combined pancreatic resection and p multiple lesions of the pancreas: i of the pancreas concomitant with du Kuroki, Tamotsu; Tajima, Yoshitsugu Tomohiko; Kanematsu, Takashi Citation Hepato-Gastroenterology, 55(86-87), Issue Date URL Right Copyright 2008 Thieme Publishing This document is downloaded
2 Surgical Technique Combined pancreatic resection and pancreatic duct-navigation surgery for multiple lesions of the pancreas: intraductal papillary mucinous neoplasm of the pancreas concomitant with ductal carcinoma of the pancreas Running title: Combined pancreatic resection and pancreatic duct-navigation surgery Tamotsu Kuroki, Yoshitsugu Tajima, Noritsugu Tsuneoka, Tomohiko Adachi, Takashi Kanematsu Department of Surgery, Nagasaki University, Graduate School of Biomedical Sciences, Sakamoto, Nagasaki , Japan Correspondence to: Tamotsu Kuroki, Department of Surgery, Nagasaki University, Graduate School of Biomedical Sciences, Sakamoto, Nagasaki , Telephone: Fax:
3 SUMMARY When a branch-type IPMN of the uncinate process is concomitant with ductal carcinoma of the body of the pancreas, total pancreatectomy may be recommended. However, a decrease in quality of life becomes a serious problem after total pancreatectomy because of the abolition of endocrine and exocrine pancreatic function. We proposed the combined resection, which is consists of resection of the uncinate process of the pancreas with distal pancreatectomy. This surgical procedure of combined resection is most suitable for preservation of the pancreatic functions. In addition, we recommend the pancreatic duct-navigation surgery enable us to prevent the injury of the main pancreatic duct, and to dissect at the optimal cutting point of the pancreatic branch duct. Key words: combined resection; Multiple lesions; Intraductal papillary mucinous neoplasm; Pancreatic carcinoma; pancreatic duct-navigation surgery 2
4 INTRODUCTION Recent improvements in surgical devices and advances in knowledge of the pancreatic anatomy have allowed surgeons to approach the minimal resection of the pancreas. In addition, many benign and low-grade malignant pancreatic lesions, including intraductal papillary mucinous neoplasms (IPMNs) and mucinous cystic neoplasms, have been detected by the improving diagnostic modalities. Therefore, several new surgical procedures for minimal resection of the pancreas with pancreatic functional reserve have been proposed, including duodenum-preserving pancreatic head resection (DPPHR), medial pancreatectomy, inferior head resection and inferior branch preserving superior head resection of the pancreas. Especially, the branch type IPMN is a good candidate for such less invasive surgery, because it is more frequently located in the head of the pancreas, and shows less malignant potential. Although several surgical techniques and devices have been advocated to avoid complications following pancreatic surgery, the incidence of pancreatic fistula is still high. In particular, the incidence of pancreatic fistula following partial resection of the pancreas is high (1, 2). A pancreatic 3
5 fistula is one of the most frequent complications and still responsible for most morbidity and mortality after pancreatic surgery, leading to an intra-abdominal abscess and/or a lethal bleeding. We report herein a case of successful combined resection for a branch-type IPMN concomitant with ductal carcinoma of the pancreas under a pancreatic duct-navigation surgery for the prevention of postoperative pancreatic fistula. 4
6 PATIENT AND TECHNIQUE A 59-year-old Japanese woman was diagnosed as having a branch-type IPMN, 3cm in diameter, in the uncinate process of the pancreas at a local hospital 2 years ago. The IPMN was followed by an abdominal computed tomography (CT) every 6 months. A follow-up CT depicted a pancreatic body tumor, 2cm in diameter, as a new lesion, and thus the patient was referred to our hospital in July 2007 for further evaluation of the two tumors of the pancreas detected by CT. On admission, serum level of carbohydrate antigen 19-9 was elevated at 194 U/mL (normal, <37). Another tumor marker, carcinoembryonic antigen, was within the normal limit. Laboratory tests, including serum levels of amylase and total bilirubin, were normal. Abdominal ultrasonography (US) and CT demonstrated a multilobular cystic lesion, 3 cm in diameter, in the uncinate process of the pancreas and a solid tumor, 2 cm in diameter, in the body of the pancreas. Endoscopic retrograde pancreatography (ERP) showed a cystic lesion communicating with the main pancreatic duct and stenosis of the main pancreatic duct in the body of the pancreas together with dilated distal pancreatic duct (Fig. 1). Consequently, the cystic lesion was diagnosed as a 5
7 branch-type IPMN concomitant with ductal carcinoma of the pancreas, and the patient was considered to be a candidate for surgery. A distal pancreatectomy/splenectomy with the resection of the uncinate process was performed using the technique of pancreatic duct-navigation surgery. Under general anesthesia, an incision was made in the upper midline of the abdomen, 8 cm in diameter, and a disk for hand-assisted laparoscopic surgery (HALS) (Lap-Disk; Hakko, Tokyo, Japan) was placed. First, the gastrocolic ligament was divided by using an ultrasonic device and the pancreas was exposed. The retroperitoneum was incised along the superior and inferior borders of the pancreas, and then an adequate margin of the pancreas was mobilized under direct view through the Lap-Disk. Splenic artery and vein were divided separately and ligated. A 7 mm width Penrose drain was brought under the pancreas as a hanging maneuver. Using the Penrose drain, the pancreas could be retracted away from the retroperitoneum for the prevention of vessel and/or other organ injuries. Then, the pancreatic parenchyma of the body of the pancreas was transected with an ultrasonic device. The main pancreatic duct was isolated from the pancreatic parenchyma, and 6
8 a catheter for pancreatography was inserted into the main pancreatic duct at the cut surface of the remnant pancreas (Fig. 2). This catheter was served as an important device for the pancreatic duct-navigation surgery when the IPMN in the uncinate process was removed. Following the resection of the pancreatic body, a distal pancreatectomy with spleen was done using HALS technique. The first 12-mm trocar for the 30 0 angled laparoscope was introduced at the umbilicus under direct vision. Under a condition of pneumoperitoneum, two additional 12-mm and 5-mm trocars were placed in the left side of the abdomen. The splenocolic/splenogastric ligaments and the remaining splenic peritoneal attachments were divided to mobilized the pancreas and spleen completely. This resection involved dissection of the regional lymph nodes. The distal pancreas and spleen were extracted through the Lap-Disk. Under direct vision, the resection of the uncinate process was performed. Mobilization of the duodenum was not done. The communicating branches between the cystic lesion and the main pancreatic duct were carefully evaluated by using intraoperative US and pancreatography. The uncinate process was dissected from 7
9 the superior mesenteric vein, and it was separated from the third portion of the duodenum. During the resection of the uncinate process, the catheter in the main pancreatic duct was clearly and easily detected by intraoperative US, and thus both the direction and position of the main pancreatic duct and the correlation between the cystic lesion and main pancreatic duct were correctly identified (Fig. 3). At the final step of subsequent pancreatic parenchymal transection, communicating pancreatic duct was fully exposed and encircled with radiopaque marker filament, which was obtained from surgical gauze. Using this marker with intraoperative pancreatography (Fig.4), the uncinate process was dissected at the optimal cutting point of the pancreatic branch duct, and then the pancreatic branch duct was ligated. After removal of the uncinate process, pancreatography was performed and revealed no injury to the main pancreatic duct or leakage from the transected pancreatic branch ducts. Because a mixture of indigocarmine and contrast material was used for the pancreatography, we were able to detect any minor pancreatic leakage as a blue spot at the cut surface of the pancreas and close the leaking points appropriately with 4-0 absorbable monofilament 8
10 sutures. After removal of the pancreatic catheter, the main pancreatic duct was ligated at the cut surface. Intraoperative frozen section histological examination of the dissected pancreatic ducts revealed a disease-free margin. Under direct vision, the cut edge of the proximal pancreas was detached approximately 3 cm from the retroperitoneum. Furthermore, the cut surface was fixed to the posterior wall of the gastric body for the prevention of the pancreatic leakage from the pancreatic duct including small pancreatic branch ducts. The fixation was constructed by interrupted-suturing between the pancreatic parenchyma and the seromuscular layer of the stomach with 4-0 absorbable monofilament sutures. As a consequence, the stump of the pancreas was completely covered by the gastric wall. So we called gastric wall-covering method for the term of the new method for the prevention of the pancreatic leakage (3). Operating time was 9 hours, and blood loss was 480 ml. The final pathological diagnosis was noninvasive intraductal papillary mucinous carcinoma of the uncinate process with invasive ductal carcinoma of the pancreatic body. The surgical margin was free of cancer cells. Her postoperative course was uneventful. The 9
11 drain was withdrawn on the 5th postoperative day and she was discharged home on the 15th postoperative day. 10
12 DISCUSSION IPMN of the pancreas is classified into two types: main pancreatic duct type and branch type. The incidence of carcinoma in IPMN is much higher in the main pancreatic duct type than in the branch type. Although the branch type of IPMN of the pancreas shows a favorable prognosis, it is accompanied by malignant diseases of the other organs and pancreatic adenocarcinoma (4). Yamaguchi et al. (5) proposed that clinicians should pay attention to the possible presence of ductal carcinoma of the pancreas in male patients with branch-type IPMN in their 6 th to 8 th decades. Thus, IPMN may be a sentinel for the diagnosis of carcinoma in situ of the pancreas (5). Tanaka et al. (6) recommended the 3-6 monthly follow-up for branch type IPMN if lesions is >20 mm in size. In the present case, the branch-type IPMN was followed by CT every 6 months. Nevertheless, an invasive ductal carcinoma of the pancreas developed in the body of the pancreas. In addition, Serikawa et al. (7) recommended to measure telomerase activity in the pancreatic juice to judge whether or not surgery is indicated. Pancreaticoduodenectomy or distal pancreatectomy has been 11
13 indicated for the treatment of patients with ductal carcinoma of the pancreas. In addition, when a branch-type IPMN is concomitant with ductal carcinoma of the pancreas as the present case, total pancreatectomy may be recommended. However, a decrease in quality of life becomes a serious problem after total pancreatectomy because of the abolition of endocrine and exocrine pancreatic function. Therefore, we conducted a resection of the uncinate process of the pancreas combined with distal pancreatectomy for the present case. The branch type IPMN shows lower malignant potential than invasive ductal adenocarcinoma of the pancreas. In the benign or low-grade malignant IPMN, complete tumor resection is sufficient for a cure. Therefore, several pancreas-preserving surgical procedures, including the resection of the uncinate process, have been advocated in the surgical treatment for the branch type IPMN in the head of the pancreas. Resection of the uncinate process of the pancreas is an ultimately less invasive surgical procedure for branch-type IPMN of the uncinate process, which is most suitable for the preservation of pancreatic functions. However, the incidence of the complications following the pancreas-preserving surgical procedures is high, 12
14 such as pancreatic fistula (1, 2). In the present case, the insertion of a pancreatic catheter via the stump of the main pancreatic duct was useful for identifying the pancreatic ductal system in order to avoid intraoperative injury to the main pancreatic duct. The pancreatic catheter in the main pancreatic duct is easily detectable using intraoperative US, and facilitative for an intraoperative pancreatography. The additional benefit of this technique is that the identification of the anatomical relationship between the cystic lesions and main pancreatic duct can be confirmed not only by a radiological image, but also by a direct palpation. In addition, we used radiopaque marker filament for encircling the communicating pancreatic duct with intraoperative pancreatography prior to the removal of the uncinate process. These surgical inventions for pancreatic duct-navigation surgery enable us to prevent the injury to the main pancreatic duct, and to dissect at the optimal cutting point of the targeting pancreatic branch duct. In conclusion, the resection of the uncinate process together with the distal pancreas, so called combined pancreatic resection, is the most ideal, least invasive pancreatic resection 13
15 for a branch-type IPMN of the uncinate process concomitant with ductal carcinoma of the body of the pancreas. Pancreatic duct-navigation surgery is an improved technique that allows the surgeon to more accurately determine the precise location and correlation of tumors and pancreatic ducts. 14
16 REFERENCES 1. Kuroki T, Tajima Y, Kanematsu T. Surgical management for the prevention of pancreatic fistula following distal pancreatectomy. J Hepatobiliary Pancreat Surg 2005; 12: Nakagohri T, Kenmochi T, Kainuma O, Tokoro Y, Kobayashi S, Asano T. Inferior head resection of the pancreas for intraductal papillary mucinous tumors. Am J Surg 2000; 179: Kuroki T, Tajima Y, Tsutsumi R, Tsuneoka N, Fukuda K, Haraguchi M, Furui J, Kanematsu T. Gastric wall-covering method for the prevention of pancreatic fistula after pancreatic resection. Hepatogastroenterology 2007; 54: Tanaka M. Intraductal papillary mucinous neoplasm of the pancreas: Diagnosis and treatment. Pancreas 2004; 28: Yamaguchi K, Ohuchida J, Ohtsuka T, Nakano K, Tanaka M. Intraductal papillary-mucinous tumor of the pancreas concomitant with ductal carcinoma of the pancreas. Pancreatology 2002; 2: Tanaka M, Chari S, Adsay V, Fernandez-del Castillo C, Falconi M, Shimizu M, Yamaguchi K, Yamao K, Matsuno S. International 15
17 consensus guidelines for management of intraductal papillary mucinous neoplasms and mucinous cystic neoplasms of the pancreas. Pancreatology 2006; 6: Serikawa M, Sasaki T, Fujimoto Y, Kuwahara K, Chayama K. Management of intraductal papillary-mucinous neoplasm of the pancreas: treatment strategy based on morphologic classification. J Clin Gastroenterol 2006; 40: FIGURE LEGENDS 16
18 Figure 1. Endoscopic retrograde pancreatography showed a cystic lesion communicating with the main pancreatic duct (arrow head), and stenosis of the main pancreatic duct in the body of the pancreas (arrow). Figure 2. A catheter for pancreatography was inserted into the main pancreatic duct. Figure 3. The catheter in the main pancreatic duct was clearly and easily detected by intraoperative ultrasonography (arrows). Figure 4. At the final step of subsequent pancreatic parenchymal transection, communicating pancreatic duct is fully exposed and encircled with radiopaque marker filament (arrow). 17
19 Fig. 1 Kuroki et al.
20 Fig. 2 Kuroki et al.
21 Fig. 3 Kuroki et al.
22 Fig. 4 Kuroki et al.
Citation American Journal of Surgery, 196(5)
 NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
NAOSITE: Nagasaki University's Ac Title Author(s) Multifocal branch-duct pancreatic i neoplasms Tajima, Yoshitsugu; Kuroki, Tamotsu Amane; Adachi, Tomohiko; Mishima, T Kanematsu, Takashi Citation American
Yoshitsugu; Kanematsu, Takashi; Kur
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Laparoscopic Middle Pancreatectomy Surgery Kitasato, Amane; Adachi, Tomohiko; Yoshitsugu; Kanematsu, Takashi; Kur Hepato-Gastroenterology, 59(120),
Title. region. Author(s) Citation Surgery, 145(3), pp ; Issue Date
 NAOSITE: Nagasaki University's Ac Title Author(s) Huge pancreatic pseudocyst migratin region. Tajima, Yoshitsugu; Mishima, Takehi Taiichiro; Adachi, Tomohiko; Tsuneo Citation Surgery, 145(3), pp.341-342;
NAOSITE: Nagasaki University's Ac Title Author(s) Huge pancreatic pseudocyst migratin region. Tajima, Yoshitsugu; Mishima, Takehi Taiichiro; Adachi, Tomohiko; Tsuneo Citation Surgery, 145(3), pp.341-342;
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Citation Transplantation Proceedings, 47(3),
 NAOSITE: Nagasaki University's Ac Title Author(s) Hybrid Procedure in Living Donor Li Soyama, Akihiko; Takatsuki, Mitsuhi Tomohiko; Kitasato, Amane; Kinoshit Baimakhanov, Zhassulan; Kuroki, Tam Citation
NAOSITE: Nagasaki University's Ac Title Author(s) Hybrid Procedure in Living Donor Li Soyama, Akihiko; Takatsuki, Mitsuhi Tomohiko; Kitasato, Amane; Kinoshit Baimakhanov, Zhassulan; Kuroki, Tam Citation
Outline. Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review 4/6/2017. Case Example Background Classification Histology Guidelines
 Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
Intraductal Papillary Mucinous Neoplasm (IPMN) Guideline Review The Nurse Practitioner Association New York State Capital Region Teaching Day Matthew Warndorf MD Case Example Background Classification
Intraductal Papillary Mucinous Neoplasm of the Pancreas. Masao Tanaka Editor
 Intraductal Papillary Mucinous Neoplasm of the Pancreas Masao Tanaka Editor Intraductal Papillary Mucinous Neoplasm of the Pancreas Masao Tanaka Editor Intraductal Papillary Mucinous Neoplasm of the Pancreas
Intraductal Papillary Mucinous Neoplasm of the Pancreas Masao Tanaka Editor Intraductal Papillary Mucinous Neoplasm of the Pancreas Masao Tanaka Editor Intraductal Papillary Mucinous Neoplasm of the Pancreas
Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas.
 Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist)
Pancreas (Exocrine) Protocol applies to all carcinomas of the exocrine pancreas. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist)
Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases
 Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Jichi Medical University Journal Chronic pancreatitis mimicking intraductal papillary mucinous neoplasm of the pancreas; Report of tow cases Noritoshi Mizuta, Hiroshi Noda, Nao Kakizawa, Nobuyuki Toyama,
Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
 Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Langenbecks Arch Surg (2009) 394:209 213 DOI 10.1007/s00423-008-0330-6 CURRENT CONCEPT IN CLINICAL SURGERY Congenital dilatation of the common bile duct and pancreaticobiliary maljunction clinical implications
Pancreas Quizzes c. Both A and B a. Directly into the blood stream (not using ducts)
 Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Pancreas Quizzes Quiz 1 1. The pancreas produces hormones. Which type of hormone producing organ is the pancreas? a. Endocrine b. Exocrine c. Both A and B d. Neither A or B 2. Endocrine indicates hormones
Intraductal Papillary-Mucinous Neoplasm of the Pancreas Penetrating to the Stomach and the Common Bile Duct
 CASE REPORT Intraductal Papillary-Mucinous Neoplasm of the Pancreas Penetrating to the Stomach and the Common Bile Duct Norihiro Goto 1, Masahiro Yoshioka 1, Motohito Hayashi 1, Toshinao Itani 1, Jun Mimura
CASE REPORT Intraductal Papillary-Mucinous Neoplasm of the Pancreas Penetrating to the Stomach and the Common Bile Duct Norihiro Goto 1, Masahiro Yoshioka 1, Motohito Hayashi 1, Toshinao Itani 1, Jun Mimura
Objectives. Intraoperative Consultation of the Whipple Resection Specimen. Pancreas Anatomy. Pancreatic ductal carcinoma 11/10/2014
 Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Intraoperative Consultation of the Whipple Resection Specimen Pathology Update Faculty of Medicine, University of Toronto November 15, 2014 John W. Wong, MD, FRCPC Department of Anatomical Pathology Sunnybrook
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
ORIGINAL ARTICLE. Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm
 ONLINE FIRST ORIGINAL ARTICLE Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm A Longitudinal Level II Cohort Study Toshiyuki Moriya, MD, PhD; L. William Traverso,
ONLINE FIRST ORIGINAL ARTICLE Fate of the Pancreatic Remnant After Resection for an Intraductal Papillary Mucinous Neoplasm A Longitudinal Level II Cohort Study Toshiyuki Moriya, MD, PhD; L. William Traverso,
Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms of pancreas
 Korean J Hepatobiliary Pancreat Surg 2014;18:152-158 http://dx.doi.org/10.14701/kjhbps.2014.18.4.152 Original Article Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms
Korean J Hepatobiliary Pancreat Surg 2014;18:152-158 http://dx.doi.org/10.14701/kjhbps.2014.18.4.152 Original Article Surgical outcomes of multifocal branch duct intraductal papillary mucinous neoplasms
According to the international consensus guidelines for
 ORIGINAL ARTICLE Natural History of Branch Duct Intraductal Papillary Mucinous Neoplasm With Mural Nodules A Japan Pancreas Society Multicenter Study Go Kobayashi, MD, PhD,* Naotaka Fujita, MD, PhD,* Hiroyuki
ORIGINAL ARTICLE Natural History of Branch Duct Intraductal Papillary Mucinous Neoplasm With Mural Nodules A Japan Pancreas Society Multicenter Study Go Kobayashi, MD, PhD,* Naotaka Fujita, MD, PhD,* Hiroyuki
Takayuki; Eguchi, Susumu; Kanematsu. Citation Pediatric surgery international, 27
 NAOSITE: Nagasaki University's Ac Title Author(s) Endoscopic balloon dilatation for c jejunum in an infant. Mochizuki, Kyoko; Obatake, Masayuki Takayuki; Eguchi, Susumu; Kanematsu Citation Pediatric surgery
NAOSITE: Nagasaki University's Ac Title Author(s) Endoscopic balloon dilatation for c jejunum in an infant. Mochizuki, Kyoko; Obatake, Masayuki Takayuki; Eguchi, Susumu; Kanematsu Citation Pediatric surgery
A large mural nodule in branch duct intraductal papillary mucinous adenoma of the pancreas: a case report
 Haruki et al. Surgical Case Reports (2015) 1:20 DOI 10.1186/s40792-014-0009-x CASE REPORT Open Access A large mural nodule in branch duct intraductal papillary mucinous adenoma of the pancreas: a case
Haruki et al. Surgical Case Reports (2015) 1:20 DOI 10.1186/s40792-014-0009-x CASE REPORT Open Access A large mural nodule in branch duct intraductal papillary mucinous adenoma of the pancreas: a case
Multiple Primary Quiz
 Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Multiple Primary Quiz Case 1 A 72 year old man was found to have a 12 mm solid lesion in the pancreatic tail by computed tomography carried out during a routine follow up study of this patient with adult
Branch duct intraductal papillary mucinous neoplasm of the pancreas: single-center experience with 324 patients who underwent surgical resection
 Korean J Hepatobiliary Pancreat Surg 2015;19:113-120 http://dx.doi.org/10.14701/kjhbps.2015.19.3.113 Original Article Branch duct intraductal papillary mucinous neoplasm of the pancreas: single-center
Korean J Hepatobiliary Pancreat Surg 2015;19:113-120 http://dx.doi.org/10.14701/kjhbps.2015.19.3.113 Original Article Branch duct intraductal papillary mucinous neoplasm of the pancreas: single-center
Pancreaticoduodenectomy the anatomy and the surgical approaches
 Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Pancreaticoduodenectomy the anatomy and the surgical approaches Paul BS LAI Division of Hepato biliary and Pancreatic Surgery Department of Surgery The Chinese Univesity of Hong Kong Whipple s operation
Prevention Of Pancreaticojejunal Fistula After Whipple Procedure
 ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
ISPUB.COM The Internet Journal of Surgery Volume 4 Number 2 Prevention Of Pancreaticojejunal Fistula After Whipple Procedure N Barbetakis, K Setsiz Citation N Barbetakis, K Setsiz. Prevention Of Pancreaticojejunal
PANCREAS DUCTAL ADENOCARCINOMA PDAC
 CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
CONTENTS PANCREAS DUCTAL ADENOCARCINOMA PDAC I. What is the pancreas? II. III. IV. What is pancreas cancer? What is the epidemiology of Pancreatic Ductal Adenocarcinoma (PDAC)? What are the risk factors
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES
 JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
Title. Author(s) Takatsuki, Mitsuhisa; Eguchi, Susum. Citation Pancreatology, 14(6), pp ; 2. Issue Date
 NAOSITE: Nagasaki University's Ac Title Author(s) Laparoscopic spleen-preserving dist splenic vessel preservation: The ro Matsushima, Hajime; Kuroki, Tamotsu Amane; Hirabaru, Masataka; Hidaka, Takatsuki,
NAOSITE: Nagasaki University's Ac Title Author(s) Laparoscopic spleen-preserving dist splenic vessel preservation: The ro Matsushima, Hajime; Kuroki, Tamotsu Amane; Hirabaru, Masataka; Hidaka, Takatsuki,
Index (SIRS), 158, 173
 Index A Acute pancreatitis surgery abdominal compartment syndrome, 188 adjuvant treatment, 194 anterior approach, 175 antibiotic prophylaxis, 166 167, 197 Atlanta classification, 181 classification of
Index A Acute pancreatitis surgery abdominal compartment syndrome, 188 adjuvant treatment, 194 anterior approach, 175 antibiotic prophylaxis, 166 167, 197 Atlanta classification, 181 classification of
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts
 Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
Evaluation of AGA and Fukuoka Guidelines for EUS and surgical resection of incidental pancreatic cysts Authors Alexander Lee 1, Vivek Kadiyala 2,LindaS.Lee 3 Institutions 1 Texas Digestive Disease Consultants,
A Multicentric Development Of Intraductal Papillary Mucinous Neoplasm Treated By Repeated Pancreatectomy
 ISPUB.COM The Internet Journal of Surgery Volume 7 Number 2 A Multicentric Development Of Intraductal Papillary Mucinous Neoplasm Treated By Repeated T Matsumoto, K Iwaki, H Uchida, K Yada, K Shibata,
ISPUB.COM The Internet Journal of Surgery Volume 7 Number 2 A Multicentric Development Of Intraductal Papillary Mucinous Neoplasm Treated By Repeated T Matsumoto, K Iwaki, H Uchida, K Yada, K Shibata,
Case Scenario 1. Discharge Summary
 Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Case Scenario 1 Discharge Summary A 69-year-old woman was on vacation and noted that she was becoming jaundiced. Two months prior to leaving on that trip, she had had a workup that included an abdominal
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Intraductal papillary mucinous neoplasm (IPMN) is a distinct
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:815 819 Evaluation of the Guidelines for Management of Pancreatic Branch-Duct Intraductal Papillary Mucinous Neoplasm RAYMOND S. TANG,* BENJAMIN WEINBERG,
Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas
 Korean J Hepatobiliary Pancreat Surg 2011;15:27-22 Original Article Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas Dae Young Jun 1, Hyung Jun Kwon 2, Sang Geol
Korean J Hepatobiliary Pancreat Surg 2011;15:27-22 Original Article Predictive factors for invasive intraductal papillary mucinous neoplasm of the pancreas Dae Young Jun 1, Hyung Jun Kwon 2, Sang Geol
Topics: Staging and treatment for pancreatic cancer. Staging systems for pancreatic cancer: Differences between the Japanese and UICC systems
 M. J Hep Kobari Bil Pancr and S. Surg Matsuno: (1998) Staging 5:121 127 system for pancreatic cancer 121 Topics: Staging and treatment for pancreatic cancer Staging systems for pancreatic cancer: Differences
M. J Hep Kobari Bil Pancr and S. Surg Matsuno: (1998) Staging 5:121 127 system for pancreatic cancer 121 Topics: Staging and treatment for pancreatic cancer Staging systems for pancreatic cancer: Differences
CASE REPORT. Abstract. Introduction. Case Report
 CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
CASE REPORT Branch Duct Intraductal Papillary Mucinous Neoplasms of the Pancreas Involving Type 1 Localized Autoimmune Pancreatitis with Normal Serum IgG4 Levels Successfully Diagnosed by Endoscopic Ultrasound-guided
Cover Page. The following handle holds various files of this Leiden University dissertation:
 Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Cover Page The following handle holds various files of this Leiden University dissertation: http://hdl.handle.net/1887/6119 Author: Spruit, E.N. Title: Increasing the efficiency of laparoscopic surgical
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma
 Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Intraductal papillary mucinous neoplasm of the bile ducts: a rare form of premalignant lesion of invasive cholangiocarcinoma Authors: R. Revert Espí, Y. Fernandez Nuñez, I. Carbonell, D. P. Gómez valencia,
Middle segment-preserving pancreatectomy for metachronous intraductal papillary mucinous neoplasm after pancreatoduodenectomy: a case report
 Yamada et al. Surgical Case Reports (2017) 3:28 DOI 10.1186/s40792-017-0306-2 CASE REPORT Middle segment-preserving pancreatectomy for metachronous intraductal papillary mucinous neoplasm after pancreatoduodenectomy:
Yamada et al. Surgical Case Reports (2017) 3:28 DOI 10.1186/s40792-017-0306-2 CASE REPORT Middle segment-preserving pancreatectomy for metachronous intraductal papillary mucinous neoplasm after pancreatoduodenectomy:
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts
 ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
ACG Clinical Guideline: Diagnosis and Management of Pancreatic Cysts Grace H. Elta, MD, FACG 1, Brintha K. Enestvedt, MD, MBA 2, Bryan G. Sauer, MD, MSc, FACG (GRADE Methodologist) 3 and Anne Marie Lennon,
MATERIALS AND METHODS Patients
 Yonago Acta medica 216;59:232 236 Original Article Usefulness of T-Shaped Gauze for Precise Dissection of Supra-Pancreatic Lymph Nodes and for Reduced Postoperative Pancreatic Fistula in Patients Undergoing
Yonago Acta medica 216;59:232 236 Original Article Usefulness of T-Shaped Gauze for Precise Dissection of Supra-Pancreatic Lymph Nodes and for Reduced Postoperative Pancreatic Fistula in Patients Undergoing
FDG-PET Findings of Intraductal Oncocytic Papillary Neoplasms of the Pancreas: Two Case Reports
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2005;3:S53 S57 The Use of Pancreatoscopy in the Diagnosis of Intraductal Papillary Mucinous Tumor Lesions of the Pancreas KENJIRO YASUDA, MUNEHIRO SAKATA, MOOSE
MULTIMEDIA ARTICLE - Clinical Imaging. Brian KP Goh 1, Yaw-Fui Alexander Chung 1,4, David CE Ng 2, Sathiyamoorthy Selvarajan 3, Khee-Chee Soo 1,4
 MULTIMEDIA ARTICLE - Clinical Imaging Positron Emission Tomography with 2-Deoxy-2-[ 18 F] Fluoro-D- Glucose in the Detection of Malignancy in Intraductal Papillary Mucinous Neoplasms of the Pancreas Brian
MULTIMEDIA ARTICLE - Clinical Imaging Positron Emission Tomography with 2-Deoxy-2-[ 18 F] Fluoro-D- Glucose in the Detection of Malignancy in Intraductal Papillary Mucinous Neoplasms of the Pancreas Brian
General Surgery PURPLE SERVICE MUHC-RVH Site
 Preamble HPB is a clinical teaching unit with several different vocations: It regroups all solid organ Transplantation as well as most advanced Hepatobiliary and Pancreatic clinical activities performed
Preamble HPB is a clinical teaching unit with several different vocations: It regroups all solid organ Transplantation as well as most advanced Hepatobiliary and Pancreatic clinical activities performed
WHICH LYMPH NODES SHOULD BE
 Y.K.: 82 Y.O. WOMAN WITH ANEMIA No GI symptoms. Chronic AF taking coumadin: INR=2.1. HCT=24. Anemia persists despite Rx. Colonoscopy: tumor in ascending colon. Bx: adenocarcinoma. Rx: Laparoscopic right
Y.K.: 82 Y.O. WOMAN WITH ANEMIA No GI symptoms. Chronic AF taking coumadin: INR=2.1. HCT=24. Anemia persists despite Rx. Colonoscopy: tumor in ascending colon. Bx: adenocarcinoma. Rx: Laparoscopic right
Case Scenario 1. The patient has now completed his neoadjuvant chemoradiation and has been cleared for surgery.
 Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Accessory Glands of Digestive System
 Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Accessory Glands of Digestive System The liver The liver is soft and pliable and occupies the upper part of the abdominal cavity just beneath the diaphragm. The greater part of the liver is situated under
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair BACKGROUND EPIDEMIOLOGY 9/11/2018
 Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
Journal of Interventional Gastroenterology A Combination of Snare Polypectomy and APC Therapy for Prolapsing Common Bile Duct Adenoma
 Journal of Interventional Gastroenterology A Combination of Snare Polypectomy and APC Therapy for Prolapsing Common Bile Duct Adenoma --Manuscript Draft-- Manuscript Number: Full Title: Article Type: Section/Category:
Journal of Interventional Gastroenterology A Combination of Snare Polypectomy and APC Therapy for Prolapsing Common Bile Duct Adenoma --Manuscript Draft-- Manuscript Number: Full Title: Article Type: Section/Category:
SETTING Fudan University Shanghai Cancer Center. RESPONSIBLE PARTY Haiquan Chen MD.
 OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
OFFICIAL TITLE A Phase Ⅲ Study of Left Side Thoracotomy Approach (SweetProcedure) Versus Right Side Thoracotomy Plus Midline Laparotomy Approach (Ivor-Lewis Procedure) Esophagectomy in Middle or Lower
PersPeCTIves. Controversies in the management of pancreatic ipmn. Masao Tanaka
 PersPeCTIves OpiniOn Controversies in the management of pancreatic ipmn Masao Tanaka Abstract Although considerable progress has been made in our understanding of intraductal papillary mucinous neoplasm
PersPeCTIves OpiniOn Controversies in the management of pancreatic ipmn Masao Tanaka Abstract Although considerable progress has been made in our understanding of intraductal papillary mucinous neoplasm
Inagaki M, Obara M, Kino S, Goto J, Suzuki S, Ishizaki A, Tanno S, Kohgo Y, Tokusashi Y, Miyokawa N, Kasai S.
 Journal of Hepato-Biliary-Pancreatic Surgery (2007) 14(3):264-269. Pylorus-preserving total pancreatectomy for an intraductal papillarymucinous neoplasm of the pancreas. Inagaki M, Obara M, Kino S, Goto
Journal of Hepato-Biliary-Pancreatic Surgery (2007) 14(3):264-269. Pylorus-preserving total pancreatectomy for an intraductal papillarymucinous neoplasm of the pancreas. Inagaki M, Obara M, Kino S, Goto
The Pancreas. Basic Anatomy. Endocrine pancreas. Exocrine pancreas. Pancreas vasculature. Islets of Langerhans. Acinar cells Ductal System
 SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
SGNA: Back to Basics Rogelio G. Silva, MD Assistant Clinical Professor of Medicine University of Illinois at Chicago Department of Medicine Division of Gastroenterology Advocate Christ Medical Center GI
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY 2013/12/21
 THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer
 Review Article Page 1 of 5 Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer Wei Wang*, Wejun Xiong*, Qiqi Peng, Shanao Ye, Yansheng Zheng, Lijie
Review Article Page 1 of 5 Laparoscopic spleen-preserving complete splenic hilum lymphadenectomy for advanced proximal gastric cancer Wei Wang*, Wejun Xiong*, Qiqi Peng, Shanao Ye, Yansheng Zheng, Lijie
Evaluation of Suspected Pancreatic Cancer
 Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
Evaluation of Suspected Pancreatic Cancer October 15, 2015 If you experience technical difficulty during the presentation: Contact WebEx Technical Support directly at: US Toll Free: 1-866-779-3239 Toll
Pancreatobiliary Frozen Section Nightmares
 Pancreatobiliary Frozen Section Nightmares Aatur D. Singhi, MD PhD Assistant Professor University of Pittsburgh Medical Center Department of Pathology singhiad@upmc.edu Objectives Briefly give an overview
Pancreatobiliary Frozen Section Nightmares Aatur D. Singhi, MD PhD Assistant Professor University of Pittsburgh Medical Center Department of Pathology singhiad@upmc.edu Objectives Briefly give an overview
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
P resently, pancreaticoduodenectomy is widely accepted as the standard surgical procedure for patients with
 OPEN SUBJECT AREAS: CANCER THERAPY PANCREATIC CANCER GASTROINTESTINAL CANCER OUTCOMES RESEARCH Received 13 May 2013 Accepted 3 June 2013 Published 25 June 2013 Correspondence and requests for materials
OPEN SUBJECT AREAS: CANCER THERAPY PANCREATIC CANCER GASTROINTESTINAL CANCER OUTCOMES RESEARCH Received 13 May 2013 Accepted 3 June 2013 Published 25 June 2013 Correspondence and requests for materials
Intraductal papillary mucinous neoplasm in an annular pancreas: a case report
 Kobayashi et al. Surgical Case Reports (2015) 1:68 DOI 10.1186/s40792-015-0068-7 CASE REPORT Intraductal papillary mucinous neoplasm in an annular pancreas: a case report Shinichiro Kobayashi 1, Yukio
Kobayashi et al. Surgical Case Reports (2015) 1:68 DOI 10.1186/s40792-015-0068-7 CASE REPORT Intraductal papillary mucinous neoplasm in an annular pancreas: a case report Shinichiro Kobayashi 1, Yukio
PAPER. Experience With 208 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas
 PAPER Experience With 0 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas Thomas Schnelldorfer, MD; Michael G. Sarr, MD; David M. Nagorney, MD; Lizhi Zhang, MD; Thomas C. Smyrk, MD;
PAPER Experience With 0 Resections for Intraductal Papillary Mucinous Neoplasm of the Pancreas Thomas Schnelldorfer, MD; Michael G. Sarr, MD; David M. Nagorney, MD; Lizhi Zhang, MD; Thomas C. Smyrk, MD;
ABDOMEN - GI. Duodenum
 TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
TALA SALEH ABDOMEN - GI Duodenum - Notice the shape of the duodenum, it looks like capital G shape tube which extends from the pyloroduodenal junction to the duodenojejunal junction. - It is 10 inches
Pancreatic Cysts. Darius C. Desai, MD FACS St. Luke s University Health Network
 Pancreatic Cysts Darius C. Desai, MD FACS St. Luke s University Health Network None Disclosures Incidence Widespread use of cross sectional imaging Seen in over 2% of patients having abdominal imaging
Pancreatic Cysts Darius C. Desai, MD FACS St. Luke s University Health Network None Disclosures Incidence Widespread use of cross sectional imaging Seen in over 2% of patients having abdominal imaging
Management A Guideline Based Approach to the Incidental Pancreatic Cysts. Common Cystic Pancreatic Neoplasms.
 Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
Management 2016 A Guideline Based Approach to the Incidental Pancreatic Cysts ISMRM 2016 Masoom Haider, MD, FRCP(C) Professor of Radiology, University of Toronto Clinician Scientist, Ontario Institute
Neoplasias Quisticas del Páncreas
 SEAP -Aproximación Práctica a la Patología Gastrointestinal- Madrid, 26 de mayo, 2006 Neoplasias Quisticas del Páncreas Gregory Y. Lauwers, M.D. Director, Service Massachusetts General Hospital Harvard
SEAP -Aproximación Práctica a la Patología Gastrointestinal- Madrid, 26 de mayo, 2006 Neoplasias Quisticas del Páncreas Gregory Y. Lauwers, M.D. Director, Service Massachusetts General Hospital Harvard
Select problems in cystic pancreatic lesions
 Disclosure Select problems in cystic pancreatic lesions Five Prime Therapeutics shareholder Adicet Bio shareholder Bristol-Meyer Squibb advisory board grace.kim@ucsf.edu Pancreatic cystic lesions Intraductal
Disclosure Select problems in cystic pancreatic lesions Five Prime Therapeutics shareholder Adicet Bio shareholder Bristol-Meyer Squibb advisory board grace.kim@ucsf.edu Pancreatic cystic lesions Intraductal
Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS
 Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS Brooklyn VAMC September 21 st GI Grand Rounds - What is it? - Clinical entity that has emerged from
Intraductal Papillary Mucinous Neoplasms: We Still Have a Way to Go! Francesco M. Serafini, MD, FACS Brooklyn VAMC September 21 st GI Grand Rounds - What is it? - Clinical entity that has emerged from
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Pancreas Case Scenario #1
 Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Pancreas Case Scenario #1 An 85 year old white female presented to her primary care physician with increasing abdominal pain. On 8/19 she had a CT scan of the abdomen and pelvis. This showed a 4.6 cm mass
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Pylorus Preserving Pancreaticoduodenectomy
 REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
REVIEW Pylorus Preserving Pancreaticoduodenectomy Jacqueline M. Garonzik-Wang, M. B. Majella Doyle Pancreaticoduodenectomy (PD) has become the standard of care for resectable pancreatic cancer and premalignant
ORIGINAL ARTICLE. The Impact of Laparoscopy and Laparoscopic Ultrasound on the Management of Pancreatic
 ORIGINAL ARTICLE The Impact of Laparoscopy and Laparoscopic Ultrasound on the Management of Pancreatic Cystic Lesions Pinhas P. Schachter, MD; Yona Avni, MD; Gabriela Gvirtz, MD; Ada Rosen, MD; Abraham
ORIGINAL ARTICLE The Impact of Laparoscopy and Laparoscopic Ultrasound on the Management of Pancreatic Cystic Lesions Pinhas P. Schachter, MD; Yona Avni, MD; Gabriela Gvirtz, MD; Ada Rosen, MD; Abraham
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds
 Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Dr Claire Smith, Consultant Radiologist St James University Hospital Leeds Imaging in jaundice and 2ww pathway Image protocol Staging Limitations Pancreatic cancer 1.2.4 Refer people using a suspected
Surgical Treatment for Periampullary Carcinoma A Study of 129 Patients*)
 Hiroshima Journal of Medical Sciences Vol. 33, No. 2, 179,...183, June, 1984 HJM 33-24 179 Surgical Treatment for Periampullary Carcinoma A Study of 129 Patients*) Tsuneo TAN AKA, Motomu KODAMA, Rokuro
Hiroshima Journal of Medical Sciences Vol. 33, No. 2, 179,...183, June, 1984 HJM 33-24 179 Surgical Treatment for Periampullary Carcinoma A Study of 129 Patients*) Tsuneo TAN AKA, Motomu KODAMA, Rokuro
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
of bile leakage after liver resecti
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Percutaneous embolization with n-bu of bile leakage after liver resecti Kuroki, Tamotsu; Kitasato, Amane; T Hiroaki; Taniguchi, Ken; Maeda, Shi
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Percutaneous embolization with n-bu of bile leakage after liver resecti Kuroki, Tamotsu; Kitasato, Amane; T Hiroaki; Taniguchi, Ken; Maeda, Shi
Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer
 Masters of Surgery Page 1 of 5 Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer Tingsong Yang 1, Fairweather Mark
Masters of Surgery Page 1 of 5 Cattell-Braasch maneuver combined with superior mesenteric artery first approach for resection of borderline resectable pancreatic cancer Tingsong Yang 1, Fairweather Mark
Laparoscopy-assisted D2 radical distal subtotal gastrectomy
 Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Masters of Gastrointestinal Surgery Laparoscopy-assisted D2 radical distal subtotal gastrectomy Xiaogeng Chen, Weihua Li, Jinsi Wang, Changshun Yang Department of Tumor Surgery, Fujian Provincial Hospital,
Virtual MR Pancreatoscopy in the Evaluation of the Pancreatic Duct in Chronic Pancreatitis
 MULTIMEDIA ARTICLE - Videoclips Virtual MR Pancreatoscopy in the Evaluation of the Pancreatic Duct in Chronic Pancreatitis Rakesh Kalapala 1, Lingareddy Sunitha 2, Reddy D Nageshwar 1, Guduru V Rao 1,
MULTIMEDIA ARTICLE - Videoclips Virtual MR Pancreatoscopy in the Evaluation of the Pancreatic Duct in Chronic Pancreatitis Rakesh Kalapala 1, Lingareddy Sunitha 2, Reddy D Nageshwar 1, Guduru V Rao 1,
An investigation of pancreatic volume by disease using pancreatic volumetry
 Yamagata Med J (ISSN 0288-030X)2015;33(2):71-76 DOI 10.15022/00003469 An investigation of pancreatic volume by disease using pancreatic volumetry Tsuyoshi Fukumoto, Toshihiro Watanabe, Koji Tezuka, Akiko
Yamagata Med J (ISSN 0288-030X)2015;33(2):71-76 DOI 10.15022/00003469 An investigation of pancreatic volume by disease using pancreatic volumetry Tsuyoshi Fukumoto, Toshihiro Watanabe, Koji Tezuka, Akiko
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
Three-dimensional computed tomography simulation for laparoscopic lymph node dissection in the treatment of proximal gastric cancer
 Review Article Three-dimensional computed tomography simulation for laparoscopic lymph node dissection in the treatment of proximal gastric cancer Hideki Sunagawa, Takahiro Kinoshita Gastric Surgery Division,
Review Article Three-dimensional computed tomography simulation for laparoscopic lymph node dissection in the treatment of proximal gastric cancer Hideki Sunagawa, Takahiro Kinoshita Gastric Surgery Division,
5/17/2013. Pancreatic Cancer. Postgraduate Course in General Surgery CASE 1: CASE 1: Overview. Case presentation. Differential diagnosis
 Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
Overview Case presentation Postgraduate Course in General Surgery Differential diagnosis Diagnosis and therapy Eric K. Nakakura Koloa, HI March 26, 2013 Outcomes CASE 1: CASE 1: A 78-year-old man developed
An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein
 J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
J Gastrointest Surg (2007) 11:425 431 DOI 10.1007/s11605-007-0131-1 An Innovative Option for Venous Reconstruction After Pancreaticoduodenectomy: the Left Renal Vein Rory L. Smoot & John D. Christein &
Endoscopic Ultrasonography Assessment for Ampullary and Bile Duct Malignancy
 Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Diagnostic and Therapeutic Endoscopy, Vol. 3, pp. 35-40 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam B.V.
Matthew McCollough, M.D. April 9, 2009 University of Louisville
 Matthew McCollough, M.D. April 9, 2009 University of Louisville List the differential diagnosis for pancreatic cysts Review the epidemiology Illustrate the types of cysts through case discussions Discuss
Matthew McCollough, M.D. April 9, 2009 University of Louisville List the differential diagnosis for pancreatic cysts Review the epidemiology Illustrate the types of cysts through case discussions Discuss
Hepatobiliary and Pancreatic Malignancies
 Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
Hepatobiliary and Pancreatic Malignancies Gareth Eeson MD MSc FRCSC Surgical Oncologist and General Surgeon Kelowna General Hospital Interior Health Consultant, Surgical Oncology BC Cancer Agency Centre
Appendix 9: Endoscopic Ultrasound in Gastroenterology
 Appendix 9: Endoscopic Ultrasound in Gastroenterology This curriculum is intended for clinicians who perform endoscopic ultrasonography (EUS) in gastroenterology. It includes standards for theoretical
Appendix 9: Endoscopic Ultrasound in Gastroenterology This curriculum is intended for clinicians who perform endoscopic ultrasonography (EUS) in gastroenterology. It includes standards for theoretical
Terumitsu; Nagayasu, Takeshi
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation A rare case of segmental ulcerative Tominaga, Tetsuro; Nonaka, Takashi; Shuichi; Kunizaki, Masaki; Sumida, Terumitsu; Nagayasu, Takeshi Acta medica
NAOSITE: Nagasaki University's Ac Title Author(s) Citation A rare case of segmental ulcerative Tominaga, Tetsuro; Nonaka, Takashi; Shuichi; Kunizaki, Masaki; Sumida, Terumitsu; Nagayasu, Takeshi Acta medica
Contaminated Wound: Report of a Cas
 NAOSITE: Nagasaki University's Ac Title Author(s) Citation Endovascular Treatment of a Carotid Contaminated Wound: Report of a Cas Yamaguchi, Nimpei; Kaneko, Kenichi; Takahashi, Haruo Acta medica Nagasakiensia,
NAOSITE: Nagasaki University's Ac Title Author(s) Citation Endovascular Treatment of a Carotid Contaminated Wound: Report of a Cas Yamaguchi, Nimpei; Kaneko, Kenichi; Takahashi, Haruo Acta medica Nagasakiensia,
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
A A-a 1. Adachi T, Tajima Y, Kuroki T, Mishima T, Kitasato A, Tsuneoka N, Kanematsu T: Chemopreventive effects of a selective cyclooxygenase-2
 A A-a 1. Adachi T, Tajima Y, Kuroki T, Mishima T, Kitasato A, Tsuneoka N, Kanematsu T: Chemopreventive effects of a selective cyclooxygenase-2 inhibitor (etodolac) on chemically induced intraductal papillary
A A-a 1. Adachi T, Tajima Y, Kuroki T, Mishima T, Kitasato A, Tsuneoka N, Kanematsu T: Chemopreventive effects of a selective cyclooxygenase-2 inhibitor (etodolac) on chemically induced intraductal papillary
Robot Assisted Rectopexy
 1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
1. Abdominal cavity approach 1A Trocars Introduce Introduce five trocars to gain access to the abdominal cavity (in da Vinci Si type; In Xi type the trocar placement may differ slightly). First the camera
Duodenum retroperitoneal
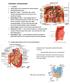 Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Intraabdominal Roux-en-Y reconstruction with a novel stapling technique after laparoscopic distal gastrectomy
 Gastric Cancer (2009) 12: 164 169 DOI 10.1007/s10120-009-0520-0 Technical note 2009 by International and Japanese Gastric Cancer Associations Intraabdominal Roux-en-Y reconstruction with a novel stapling
Gastric Cancer (2009) 12: 164 169 DOI 10.1007/s10120-009-0520-0 Technical note 2009 by International and Japanese Gastric Cancer Associations Intraabdominal Roux-en-Y reconstruction with a novel stapling
Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble?
 Korean Journal of HBP Surgery Case Report Vol. 15, No. 2, May 2011 Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble? Serous cystic neoplasm (SCN) of the pancreas is considered a benign
Korean Journal of HBP Surgery Case Report Vol. 15, No. 2, May 2011 Serous Cystic Neoplasm: Do We Have to Wait Till It Causes Trouble? Serous cystic neoplasm (SCN) of the pancreas is considered a benign
Pancreatic Disorders & Therapy
 ISSN: 2165-7092 rpancreatic Disorders & The apy Review Article Pancreatic Disorders & Therapy Kimura and Tezuka, 2015, 5:1 DOI: 10.4172/2165-7092.1000148 Open Access Acute Pancreatitis is a Predictive
ISSN: 2165-7092 rpancreatic Disorders & The apy Review Article Pancreatic Disorders & Therapy Kimura and Tezuka, 2015, 5:1 DOI: 10.4172/2165-7092.1000148 Open Access Acute Pancreatitis is a Predictive
Pancreatic Cancer. What is pancreatic cancer?
 Scan for mobile link. Pancreatic Cancer Pancreatic cancer is a tumor of the pancreas, an organ that is located behind the stomach in the abdomen. Pancreatic cancer does not always cause symptoms until
Scan for mobile link. Pancreatic Cancer Pancreatic cancer is a tumor of the pancreas, an organ that is located behind the stomach in the abdomen. Pancreatic cancer does not always cause symptoms until
ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP
 ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP 3-4 November 2017 at the AMC in Amsterdam Organizing committee: Mo Abu Hilal, Professor of Surgery at Southampton University Marc Besselink, Professor
ADVANCED LAPAROSCOPIC PANCREAS SURGERY A HANDS-ON WORKSHOP 3-4 November 2017 at the AMC in Amsterdam Organizing committee: Mo Abu Hilal, Professor of Surgery at Southampton University Marc Besselink, Professor
