Treatment of May-Thurner Syndrome with Catheter-Guided Local Thrombolysis and Stent Insertion
|
|
|
- Blanche Kelly
- 6 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE Treatment of May-Thurner Syndrome with Catheter-Guided Local Thrombolysis and Stent Insertion Jong-Youn Kim, MD 1, Donghoon Choi, MD 1, Young Guk Ko, MD 1 Sungha Park, MD 1, Yangsoo Jang, MD 1 and Do Yun Lee, MD 2 1 Cardiology Division, Yonsei Cardiovascular Center and Cardiovascular Research Institute, 2 Department of Diagnostic Radiology, Yonsei University College of Medicine, Seoul, Korea ABSTRACT Background:May-Thurner syndrome is an uncommon disease entity in which the left common iliac vein is compressed by the right common iliac artery, with the subsequent development of deep vein thrombosis and chronic venous insufficiency. Herein, our experience on the treatment of extensive iliofemoral deep venous thrombosis due to May-Thurner syndrome, using endovascular techniques, is reported. Methods:Twenty-one symptomatic patients, 8 men and 13 women, with a mean age of 51 years, were referred for treatment. Eighteen of these patients were treated with catheter-guided thrombolysis, but three, with short segment involvement, did not require thrombolysis. After completion of the thrombolytic therapy, the residual venous narrowing was treated by balloon angioplasty and/or self-expandable stent placement. Patients were then followed-up by clinic visits and venography. Results:The mean total dose of urokinase and duration of infusion were 4.28±1.89 million units and 72±35 hours, respectively. Eighteen of the 21 patient received stent deployments. The mean diameter of the stents was 12.9±2.0 mm. Initial technical success, with immediate symptom resolution, was achieved in 20 of the 21 patients (95%). Among the patients who received stent implantation, two had recurrent thrombotic occlusion during the follow-up period. (mean 10.8 months); all three patients who did not receive stent implantation had recurrent thromboses There were no major bleeding complications, with the exception of one patient who developed a retroperitoneal hematoma. Conclusions:Catheter-guided thrombolysis and angioplasty with stent implantation are safe and effective for the treatment of May-Thurner syndrome. (Korean Circulation J 2004;34 (7): ) KEY WORDS:Venous thrombosis;thrombolytic therapy;stents. Introduction Received:February 11, 2004 Accepted:May 18, 2004 Correspondence:Donghoon Choi, MD, Cardiology Division, Yonsei Cardiovascular Center and Research Institue, Yonsei University College of Medicine, 134 Shinchon-dong, Seodaemungu, Seoul , Korea Tel: , Fax: cdhlyj@yumc.yonsei.ac.kr In 1956, May and Thurner first described a spur-like formation of the left common iliac vein in 22% of autopsies. 1) Chronic pulsatile compression of the left common iliac vein, between the right common iliac artery and the lumbar vertebral body, may induce excessive local intimal proliferation, resulting in impaired venous return and massive venous thrombosis. 2) Usually, these patients present with left leg edema, pain or deep vein thrombosis. Because of the chronic physical compression by the right common iliac artery and the large size of the thrombus that develops at the iliac vein, anticoagulation alone is usually ineffective in resolving the deep vein thrombosis and the subsequent prevention of pulmonary embolisms. Previous reports have shown anticoagulation alone, and a thrombectomy combined with prospective anticoagulation, to have rethrombosis rates of up to 73% in patients with a venous spur. 3) Therefore, corrective treatment is indicated to prevent the development of a pulmonary embolism and the long-term complications of post-thrombotic syndrome, including chronic leg edema, pain, hyperpigmentation and skin ulcers. Recently, catheter-directed 655
2 Treatment of May-Thurner Syndrome thrombolysis and endovascular angioplasty with stents have been used to treat DVT in these patients. Herein, our experience and treatment efficacy of endovascular venous angioplasty in patients with deep vein thrombosis due to May-Thurner syndrome is reported. Methods A retrospective analysis was performed on 21 patients diagnosed with May-Thurner syndrome, and treated with catheter guided local thrombolysis and endovascular venous angioplasty, between August 1999 and December Sixteen patients presented with acute iliofemoral venous thrombosis and 5 with chronic venous outflow obstruction. The characteristic May-Turner syndrome lesion was diagnosed with a venogram. These lesions are defined by stenosis of the proximal left common iliac vein, including the portion underlying the right common iliac artery, as well as the presence of significant venous collateral vessels (Figure 1). After an ipsilateral puncture of the popliteal vein by a modified Seldinger s method (Early in this series, other access sites were utilized, including the right internal jugular (n=2), right common femoral vein (n=1), left common femoral vein (n=2), a 6.5 F hemostatic sheath was inserted. Through the hemostatic sheath, a 5F multi-sideport infusion catheter (60 cm, COOK, Bloomington, USA) was inserted and passed through the thrombotic occlusion of the left common iliac vein. In the case of total occlusion, the infusion catheter was placed just distal to the occlusion, through which urokinase infusion was performed. When the lesion was partially reanalyzed at follow-up, the infusion catheter was passed across the lesion and the urokinase infusion continued. In addition to urokinase infusion, heparin infusion was performed through the hemostatic sheath to maintain the aptt between 60 to 90 second. A venogram was performed daily to assess the status of the thrombotic occlusion. The endpoints of thrombolytic therapy were near clot dissolution, lytic stagnation (no interval change for 24 hours) or development of a major complication (in one case, retroperitoneal bleeding developed). Residual stenosis combined with an organic change of the vein was treated by angioplasty and stent implantation (Figure 2). The stent size was determined by measuring the diameter of patent distal common iliac vein, with the stenting performed through an 8 F hemostatic A B Figure 1. Digital subtraction angiography (DSA) on admission showed a total occlusion of the left iliac and femoral veins (A). Follow-up DSA after urokinase infusion for 3 days showed remaining thrombi and an obstructive lesion at the left common iliac vein (arrow), with extensive cross-pelvic and hypogastric collateralization (B). 656
3 Jong-Youn Kim, et al A B Figure 2. After deployment of 2 Wallstents (12 46 mm and mm)(a). Completion digital subtraction angiography showed a satisfactory angiographic result, with abolition of collaterals and the rapid in-line flow, superiorly, into the inferior vena cava (B). sheath exchanged for the 6.5 F sheath. Through the sheath, a inch hydrophilic guidewire was passed across the lesion, and angioplasty with stent implantation performed with self expanding Wallstent (Boston Scientific, Waterstone, Massachusetts, USA) with average profile of 12.9±2 mm and length of 65.4±18.2 mm unit of heparin was administered at the start of the procedure, and systemic heparinization performed after the procedure to maintain the aptt between 60 to 90 seconds for 5 days. Coumadization was simultaneously started with heparinization to maintain an INR of 2-3, and performed for 6 months. A venogram was performed 1 week after the procedure, immediately before discharge and 6 months after the procedure, to assess the patency rate. Results Out of the 21 patients, there were 8 males and 13 female, with an average age of 51 years. Three of the patients demonstrated complications due to pulmonary thromboembolism on a lung perfusion scan and a further 3 did not undergo catheter guided thrombolysis due to the short length of their lesion. The average infusion rate and total dose of urokinase were 92000±30000 IU/hr and 4,280,000± IU, respectively, with a total infusion time of 72±35 hours. For the treatment of residual stenosis, balloon angioplasty alone was performed on 3 patients, and stent implantation on 18. Wallstent (Boston Scientific, Waterstone, Massachusetts, USA) was used for stent implantation in all the patients, with an average profile of 12.9±2 mm and length of 65.4± 18.2 mm. After the procedure, all patients had good patency of the common iliac vein. The follow-up venogram, performed 7-10 days after the procedure, showed absence of residual thrombi in all 18 patients implanted with stents, with resolution of the leg edema. One of the 3 patients who underwent balloon angioplasty alone showed severe residual stenosis, but his colon cancer was in the terminal stage, so no further management, only IVC filter insertion was performed. There was a single case of major bleeding as a complication that resulted in a retroperitoneal hematoma, which resolved spontaneously in 13 days. After the procedure, all 21 patients showed no evidence of newly developed pulmonary embolism in the follow-up lung perfusion scans performed within 7 days of the procedure. The follow-up rate was high, with follow-up venogram performed on 17 of the 18 patients 657
4 Treatment of May-Thurner Syndrome who underwent stent implantation, with 2 patients showing recurrent thrombi formation. All 3 patients that underwent balloon angioplasty alone showed recurrent thrombotic occlusion, with 2 of these developing signs of postthrombotic syndrome, resulting in debilitating pain, leg edema and recurrent ulcer formation. One patient implanted with stent showed leg edema, with postthrombotic syndrome, despite the absence of recurrent thrombi. Discussion May and Thurner syndrome is a spur-like formation of the left common iliac vein due to chronic pulsatile compression of the left common iliac vein, between the right common iliac artery and the lumbar vertebral body, resulting in excessive local intimal proliferation, impaired venous return and venous thrombosis. 1)2) This may account for the higher frequency of left rather than right side common iliac vein thromboses. 6) Chronic vibratory pulsation of the common iliac artery on the venous wall may result in frictional damage of the intimal wall, which may result in subsequent intimal proliferation and venous thrombosis. 5) This disease is reported to be more frequent in women, which was also the case in our study. 7) Because of the chronic nature of the disease process, patients typically present with symptoms and signs of postthrombotic syndrome, such as pigmentation, varicose vein, chronic leg pain, phlebitis and recurrent skin ulcers. 2) Also, acute thrombosis may develop in patients at high risk of developing deep vein thrombosis, such as in patients undergoing orthopedic surgery. 2) In our study, sixteen patients presented with acute deep vein thrombosis, 5 had a history of cerebrovascular disease or trauma resulting in prolonged immobilization and 4 were in an early postoperative state following surgical treatment for malignancies. The two major treatment goals with deep vein thrombosis are the prevention of pulmonary embolism and postthrombotic syndrome development. The pathogenesis of postthrombotic syndrome is known to be due to chronic venous obstruction and venous valve insufficiency due to the formation of thrombi. Previous, Eklof and Kistner showed that patients with deep vein thrombosis treated by thrombectomy showed no evidence of post thrombotic syndrome, whereas 18% of those treated with anticoagulation showed signs of post thrombotic syndrome after 4 years of follow-up. 8) The results of that study show that it is imperative to remove the thrombi as early as possible. Thrombolytics are an effective treatment for the resolution of venous thrombi, with systemic thrombolytic therapy reported as being superior to anticoagulation in preventing postthrombotic syndrome. 9) However, the use of systemic thrombolytic therapy is limited by the possibility of severe bleeding complications, which make it contraindicatory for patients at a high risk of deep vein thrombosis formation, such as in pregnancy, surgery and cerebrovascular disease. 10)11) Localized thrombolytic therapy is commonly being performed to decrease the risk of major bleeding. Theoretically, local infusion of thrombolytic agents at the site of thrombotic occlusion maximizes the therapeutic effect while minimizing the risk of major bleeding. The successful treatment of deep vein thrombosis with local thrombolytic therapy has already been shown. 12)13) Urokinase is used in our catheter laboratory because of its lower cost and lower rate of bleeding complications compared to t-pa. All the patients in the study group showed successful recanalization, with only one case of major bleeding resulting in a retroperitoneal hematoma, which resolved uneventfully. The popliteal vein is the usual site of access used by us, with the internal jugular vein (n=2) and right common femoral vein (n=1) being the other sites used. Use of these sites entails passing catheters in a retrograde fashion, so infusion of the thrombolytic drug may be less effective. Direct puncture of the left common femoral vein is inadvisable as thrombolysis or intervention will some-times involve the access site. In 6 cases of this study, the left common femoral vein had a thrombus and required stent insertion. Therefore, the common femoral vein is used as the access site only when the involved site is short and limited within the femoral vein. 658
5 Jong-Youn Kim, et al The rationale for angioplasty with stent implantation in residual stenosis is that the implant of a stent is effective therapy for a venous obstruction 14) and superior to balloon dilatation alone. 15) The possible problem of valve destruction by the stents, and the subsequent development of venous insufficiency, does not apply to femoral veins due to the absence of valves in the femoral veins. Complete resolution of the residual stenosis may not be possible with balloon angioplasty, which may result in higher risk of rethrombosis. In fact, all 3 patients who underwent balloon angioplasty alone showed restenosis and rethrombosis, which reemphasizes the importance of complete resolution of the residual stenosis. This was demonstrated by the fact that only 2 of the 17 patients showed thrombus formation at the site of stent implantation at follow-up. Because of the inherent thrombogenicity of metallic stents before endothelization and the high risk of recurrent venous thrombosis, all the patients received standard prophylactic treatment with coumadine for 6 months. It is our belief the duration of treatment is adequate unless there are associated conditions requiring prolonged or indefinite anticoagulation. There was a single case of major bleeding complication that resulted in a retroperitoneal hematoma, which resolved spontaneously in 13 days. After the procedure, all 21 patients showed no evidence of newly developed pulmonary embolism in the follow-up lung perfusion scans performed within 7 days of the procedure. This study has demonstrated the safety of local catheter guided thrombolysis and stenting, with minimal risk of major bleeding complications and iatrogenic embolism during the procedure. This study has shown excellent immediate results and patency rates, with minimal complications, using localized catheter-guided thrombolysis plus angioplasty with stent implantation. Further studies will be needed to demonstrate the long term patency rate in a larger population of patients. REFERENCES 1) May R, Thurner J. Ein Gef ssporn in der vena iliaca communis sinistra als wahrscheinliche ursache der überwiegende linksseitigen beckenvenenthrombose. Z Kreisl-Forsch 1956; 45: ) Baron HC, Sharms J, Wayne M. Iliac vein compression syndrome: a new method of treatment. Am Surg 2000;66: ) Burroughs KE. New considerations in the diagnosis and therapy of deep vein thrombosis. South Med J 1999;92: ) Binkert CA, Schoch C, Stuckmann G, Largiader J, Wigger P, Schoepke W, et al. Treatment of pelvid venous spur(may- Thurner syndrome) with self-ezpanding metallic endoprostheses. Cardiovasc Intervent Radiol 1998;21: ) Gerarld JO, Charles PS, Craig B, Stephen TK, Manmood KR, Daniel YS, et al. Endovascular management of iliac vein compression(may-thurner) syndrome. JVIR 2000;11: ) Heijmen RH, Bollen TL, Duyndam DA, Overtoom TT, Van den Berg JC, Moll FL. Endovascular venous stenting in May- Thurner syndrome. J Cardiovasc Surg 2001;42: ) Steinberg JB, Jacocks MA. May-Thurner syndrome. a previously unreported variant. Ann Vasc Surg 1993;7: ) Eklof B, Kistner RL. Is there a role for thrombectomy in iliofemoral venous thrombolysis? Semin Vase Surg 1996;9: ) O Donnell TF Jr, Browse NL, Burnand KG, Thomas ML. The socioeconomic effects of iliofemoral thrombosis. J Surg Res 1987;22: ) Strandness ED, Manzo RA, Markel A. Is there a role for thrombolytic treatment of deep vein thrombosis? Cardiol Board Rev 1993;10: ) Sherry S. Thrombolytic therapy for DVT. Semin Interv Radiol 1985;2: ) Jung IH, Choi DH, Kim HJ, Kyung HD, Koo BK, Cho SY, et al. A case of eosinophilia associated with massive deep vein thrombosis treated with local urokinase infusion. Korean Circ J 2001;31: ) Kim HJ, Chung IH, Cho DK, Cho JR, Choi DH, Koo BK, et al. May-Thurner syndrome: two cases treated with catheter-directed thrombolysis and stent placement. Korean Circ J 2001:31: ) Nazarian GK, Bjarnason H, Dietz CA, Bernadas CA, Hunter DW. Iliofemoral venous stenosis: effectiveness of treatment with metallic endovascular stents. Radiology 1996;200: ) Whittemore AD, Donaldson MC, Polak JF, Mannick JA. Limitations of balloon angioplasty for vein graft stenosis. J Vasc Surg 1991;14:
Interventional Treatment VTE: Radiologic Approach
 Interventional Treatment VTE: Radiologic Approach Hae Giu Lee, MD Professor, Dept of Radiology Seoul St. Mary s Hospital The Catholic University of Korea Introduction Incidence High incidence: 250,000-1,000,000/year
Interventional Treatment VTE: Radiologic Approach Hae Giu Lee, MD Professor, Dept of Radiology Seoul St. Mary s Hospital The Catholic University of Korea Introduction Incidence High incidence: 250,000-1,000,000/year
How to best approach chronic venous occlusions?
 How to best approach chronic venous occlusions? Prof. Nils Kucher Director Venous Thromboembolism Reseach Group University Hospital Bern nilskucher.com Disclosure Speaker name: Nils Kucher X X I have the
How to best approach chronic venous occlusions? Prof. Nils Kucher Director Venous Thromboembolism Reseach Group University Hospital Bern nilskucher.com Disclosure Speaker name: Nils Kucher X X I have the
Percutaneously Inserted AngioVac Suction Thrombectomy for the Treatment of Filter-Related. Iliocaval Thrombosis
 Percutaneously Inserted AngioVac Suction Thrombectomy for the Treatment of Filter-Related Iliocaval Thrombosis Faiz D. Francis, DO; Gianvito Salerno, MD; Sabbah D. Butty, MD Abstract In the setting of
Percutaneously Inserted AngioVac Suction Thrombectomy for the Treatment of Filter-Related Iliocaval Thrombosis Faiz D. Francis, DO; Gianvito Salerno, MD; Sabbah D. Butty, MD Abstract In the setting of
Venous interventions in DVT
 Venous interventions in DVT Sriram Narayanan Chief of Vascular and Endovascular Surgery, Tan Tock Seng Hospital A/Prof of Surgery, National University of Singapore ANTI-COAGULATION LMWH Warfarin x 6m Acute
Venous interventions in DVT Sriram Narayanan Chief of Vascular and Endovascular Surgery, Tan Tock Seng Hospital A/Prof of Surgery, National University of Singapore ANTI-COAGULATION LMWH Warfarin x 6m Acute
Intervention for Deep Venous Thrombosis and Pulmonary Embolus
 Intervention for Deep Venous Thrombosis and Pulmonary Embolus Michael R. Jaff, DO Paul and Phyllis Fireman Endowed Chair in Vascular Medicine Massachusetts General Hospital Professor of Medicine Harvard
Intervention for Deep Venous Thrombosis and Pulmonary Embolus Michael R. Jaff, DO Paul and Phyllis Fireman Endowed Chair in Vascular Medicine Massachusetts General Hospital Professor of Medicine Harvard
Chronic Iliocaval Venous Occlusive Disease
 none Chronic Iliocaval Venous Occlusive Disease David Rigberg, M.D. Clinical Professor of Surgery Division of Vascular Surgery University of California Los Angeles Chronic Venous Occlusive Disease Chronic
none Chronic Iliocaval Venous Occlusive Disease David Rigberg, M.D. Clinical Professor of Surgery Division of Vascular Surgery University of California Los Angeles Chronic Venous Occlusive Disease Chronic
Michael Meuse, M.D. Vascular and Interventional Radiology
 Michael Meuse, M.D. Vascular and Interventional Radiology Iliac Vein Compression Syndrome Left CIV compressed by right CIA Virchow 1851: DVT L>R May and Thurner 1954: venous spurs Cockett and Thomas 1965:
Michael Meuse, M.D. Vascular and Interventional Radiology Iliac Vein Compression Syndrome Left CIV compressed by right CIA Virchow 1851: DVT L>R May and Thurner 1954: venous spurs Cockett and Thomas 1965:
Straub Endovascular System &
 Straub Endovascular System & S t r a u b E n d o v a s c u l a r To o l s Straub Endovascular System Effective debulking in occluded arteries and veins Effective debulking in many indications Rotarex
Straub Endovascular System & S t r a u b E n d o v a s c u l a r To o l s Straub Endovascular System Effective debulking in occluded arteries and veins Effective debulking in many indications Rotarex
VIRTUS: Trial Design and Primary Endpoint Results
 VIRTUS: Trial Design and Primary Endpoint Results Mahmood K. Razavi, MD St. Joseph Cardiac and Vascular Center Orange, CA, USA IMPORTANT INFORMATION: These materials are intended to describe common clinical
VIRTUS: Trial Design and Primary Endpoint Results Mahmood K. Razavi, MD St. Joseph Cardiac and Vascular Center Orange, CA, USA IMPORTANT INFORMATION: These materials are intended to describe common clinical
Surgical approach for DVT. Division of Vascular Surgery Department of Surgery Seoul National University College of Medicine
 Surgical approach for DVT Seung-Kee Min Division of Vascular Surgery Department of Surgery Seoul National University College of Medicine Treatment Options for Venous Thrombosis Unfractionated heparin &
Surgical approach for DVT Seung-Kee Min Division of Vascular Surgery Department of Surgery Seoul National University College of Medicine Treatment Options for Venous Thrombosis Unfractionated heparin &
1234 MATSUDA A et al.
 1234 MATSUDA A et al. Circulation Journal ORIGINAL ARTICLE Official Journal of the Japanese Circulation Society http://www.j-circ.or.jp Peripheral Vascular Disease Early and Long-Term Outcomes of Venous
1234 MATSUDA A et al. Circulation Journal ORIGINAL ARTICLE Official Journal of the Japanese Circulation Society http://www.j-circ.or.jp Peripheral Vascular Disease Early and Long-Term Outcomes of Venous
MAY-THURNER SYNDROME A CONTROVERSIAL VASCULAR ANOMALY
 Medical interventions MAY-THURNER SYNDROME A CONTROVERSIAL VASCULAR ANOMALY Shepherd E Alexandra 1, Shepherd S Caterina 1 1. BSc, University College London, UK Corresponding author: aeshep@gmail.com The
Medical interventions MAY-THURNER SYNDROME A CONTROVERSIAL VASCULAR ANOMALY Shepherd E Alexandra 1, Shepherd S Caterina 1 1. BSc, University College London, UK Corresponding author: aeshep@gmail.com The
NOTE: Deep Vein Thrombosis (DVT) Risk Factors
 Deep Vein Thrombosis (DVT) Deep Vein Thrombosis (DVT) is the formation of a blood clot, known as a thrombus, in the deep leg vein. It is a very serious condition that can cause permanent damage to the
Deep Vein Thrombosis (DVT) Deep Vein Thrombosis (DVT) is the formation of a blood clot, known as a thrombus, in the deep leg vein. It is a very serious condition that can cause permanent damage to the
Not all Leg DVT s are the Same: Which Patients Benefit from Interventional Therapy? Case 1:
 12/16/2015 Not all Leg DVT s are the Same: Which Patients Benefit from Interventional Therapy? Constantino S.Peña, FSIR, FSCCT, FAHA Interventional Radiologist Medical Director, Vascular Imaging Miami
12/16/2015 Not all Leg DVT s are the Same: Which Patients Benefit from Interventional Therapy? Constantino S.Peña, FSIR, FSCCT, FAHA Interventional Radiologist Medical Director, Vascular Imaging Miami
Clinical Guide - Inferior Vena Cava Filters (Reviewed 2006)
 Clinical Guide - Inferior Vena Cava Filters (Reviewed 2006) Principal Developer: V. Oliva Secondary Developers: W. Geerts Background The treatment of choice for deep venous thrombosis (DVT) and pulmonary
Clinical Guide - Inferior Vena Cava Filters (Reviewed 2006) Principal Developer: V. Oliva Secondary Developers: W. Geerts Background The treatment of choice for deep venous thrombosis (DVT) and pulmonary
BC Vascular Day. Contents. November 3, Abdominal Aortic Aneurysm 2 3. Peripheral Arterial Disease 4 6. Deep Venous Thrombosis 7 8
 BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
BC Vascular Day Contents Abdominal Aortic Aneurysm 2 3 November 3, 2018 Peripheral Arterial Disease 4 6 Deep Venous Thrombosis 7 8 Abdominal Aortic Aneurysm Conservative Management Risk factor modification
Pulmonary Emboli without Leg Symptoms, May-Thurner syndrome. Case Report and Review
 ISPUB.COM The Internet Journal of Internal Medicine Volume 9 Number 2 Pulmonary Emboli without Leg Symptoms, May-Thurner syndrome. Case Report and Review A Hamo, M Alyaseen, F Alkhankan, T Gress Citation
ISPUB.COM The Internet Journal of Internal Medicine Volume 9 Number 2 Pulmonary Emboli without Leg Symptoms, May-Thurner syndrome. Case Report and Review A Hamo, M Alyaseen, F Alkhankan, T Gress Citation
VIVO-EU Results: Prospective European Study of the Zilver Vena TM Venous Stent in the Treatment of Symptomatic Iliofemoral Venous Outflow Obstruction
 VIVO-EU Results: Prospective European Study of the Zilver Vena TM Venous Stent in the Treatment of Symptomatic Iliofemoral Venous Outflow Obstruction Gerard J O Sullivan, M.D. and Jennifer McCann-Brown,
VIVO-EU Results: Prospective European Study of the Zilver Vena TM Venous Stent in the Treatment of Symptomatic Iliofemoral Venous Outflow Obstruction Gerard J O Sullivan, M.D. and Jennifer McCann-Brown,
Technique de recanalisation: mon expérience avec Aspirex
 JFICV 2017, Deauville Thrombose veineuse profonde aiguë en 2017 Technique de recanalisation: mon expérience avec Aspirex Romaric LOFFROY Département de Radiologie Diagnostique et Thérapeutique CHU Hôpital
JFICV 2017, Deauville Thrombose veineuse profonde aiguë en 2017 Technique de recanalisation: mon expérience avec Aspirex Romaric LOFFROY Département de Radiologie Diagnostique et Thérapeutique CHU Hôpital
Challenging Case of Pulse Infusion Thrombolysis Using a Unique Pump System for a Patient With Deep Vein Thrombosis: A Case Report
 J Cardiol 2002 Feb; 39 2 : 115 119 Challenging Case of Pulse Infusion Thrombolysis Using a Unique Pump System for a Patient With Deep Vein Thrombosis: A Case Report MD Seiji Taro Katsuo Yasushi Fumiyuki
J Cardiol 2002 Feb; 39 2 : 115 119 Challenging Case of Pulse Infusion Thrombolysis Using a Unique Pump System for a Patient With Deep Vein Thrombosis: A Case Report MD Seiji Taro Katsuo Yasushi Fumiyuki
The hallmark of percutaneous thrombus management
 Treating Venous Thromboembolism Without Lytic Medications What the present and the near future will bring in terms of techniques and devices to remove venous thrombus. BY CONSTANTINO S. PEÑA, MD; RIPAL
Treating Venous Thromboembolism Without Lytic Medications What the present and the near future will bring in terms of techniques and devices to remove venous thrombus. BY CONSTANTINO S. PEÑA, MD; RIPAL
Catheter-Directed Thrombolysis for Acute Limb Ischemia. Hwan Jun Jae MD Seoul National University Hospital Seoul, Korea
 Catheter-Directed Thrombolysis for Acute Limb Ischemia Hwan Jun Jae MD Seoul National University Hospital Seoul, Korea Disclosure Speaker name: Hwan Jun Jae... I have the following potential conflicts
Catheter-Directed Thrombolysis for Acute Limb Ischemia Hwan Jun Jae MD Seoul National University Hospital Seoul, Korea Disclosure Speaker name: Hwan Jun Jae... I have the following potential conflicts
Percutaneous Mechanical Thrombectomy for Acute Iliofemoral DVT with the Aspirex Catheter: The Dijon Experience
 JFICV 2018, Beaune Percutaneous Mechanical Thrombectomy for Acute Iliofemoral DVT with the Aspirex Catheter: The Dijon Experience Prof. Romaric LOFFROY, MD, PhD, FCIRSE Chief, Department of Vascular and
JFICV 2018, Beaune Percutaneous Mechanical Thrombectomy for Acute Iliofemoral DVT with the Aspirex Catheter: The Dijon Experience Prof. Romaric LOFFROY, MD, PhD, FCIRSE Chief, Department of Vascular and
Meissner MH, Gloviczki P, Comerota AJ, Dalsing MC, Eklof BG, Gillespie DL, et al. J Vasc Surg. 2012;55:
 Early thrombus removal strategies for acute deep venous thrombosis: Clinical Practice Guidelines of the Society for Vascular Surgery and the American Venous Forum Meissner MH, Gloviczki P, Comerota AJ,
Early thrombus removal strategies for acute deep venous thrombosis: Clinical Practice Guidelines of the Society for Vascular Surgery and the American Venous Forum Meissner MH, Gloviczki P, Comerota AJ,
Pharmaco-mechanical techniques stand alone procedures? Peter Neglén, MD, PhD SP Vascular Center Limassol Cyprus
 Pharmaco-mechanical techniques stand alone procedures? Peter Neglén, MD, PhD SP Vascular Center Limassol Cyprus Faculty Disclosure Peter Neglén, M.D., Ph.D Stockholder/Founder of Veniti, Inc. Member, Medical
Pharmaco-mechanical techniques stand alone procedures? Peter Neglén, MD, PhD SP Vascular Center Limassol Cyprus Faculty Disclosure Peter Neglén, M.D., Ph.D Stockholder/Founder of Veniti, Inc. Member, Medical
RadRx Your Prescription for Accurate Coding & Reimbursement Copyright All Rights Reserved.
 Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Interventional Radiology Coding Case Studies Prepared by Stacie L. Buck, RHIA, CCS-P, RCC, CIRCC, AAPC Fellow President & Senior Consultant Week of June 4, 2018 Thrombolysis, Thrombectomy & Angioplasty
Iliofemoral DVT: Miminizing Post-Thrombotic Syndrome
 Iliofemoral DVT: Miminizing Post-Thrombotic Syndrome Catherine K. Chang, MD FACS Vascular Surgery San Diego Southern California Permanente Medical Group Acute Deep Venous Thrombosis Incidence & Outcomes
Iliofemoral DVT: Miminizing Post-Thrombotic Syndrome Catherine K. Chang, MD FACS Vascular Surgery San Diego Southern California Permanente Medical Group Acute Deep Venous Thrombosis Incidence & Outcomes
Treatment of Chronic DVT with EKOS: Reproducing ACCESS PTS Data in Every Day Clinical Practice
 Treatment of Chronic DVT with EKOS: Reproducing ACCESS PTS Data in Every Day Clinical Practice Mert Dumantepe, MD Acibadem Altunizade Hospital, Istanbul, Turkey Department of Cardiovascular Surgery Disclosure
Treatment of Chronic DVT with EKOS: Reproducing ACCESS PTS Data in Every Day Clinical Practice Mert Dumantepe, MD Acibadem Altunizade Hospital, Istanbul, Turkey Department of Cardiovascular Surgery Disclosure
VERNACULAR Trial & Clinical Experience with the VENOVO Venous Stent
 Stephen Black, MD VERNACULAR Trial & Clinical Experience with the VENOVO Venous Stent 1 Speaker Disclaimers The speakers presentation today is on behalf of Bard Peripheral Vascular, Inc. Any discussion
Stephen Black, MD VERNACULAR Trial & Clinical Experience with the VENOVO Venous Stent 1 Speaker Disclaimers The speakers presentation today is on behalf of Bard Peripheral Vascular, Inc. Any discussion
A rare case of May-Thurner-like syndrome in an elderly lady
 CASE REPORT A rare case of May-Thurner-like syndrome in an elderly lady Chris Pui Yan Yee 1, Kapil Sahnan 2, Robert Hywel Thomas 1, Kaji Sritharan 1 1. Department of Vascular Surgery, St Mary's Hospital,
CASE REPORT A rare case of May-Thurner-like syndrome in an elderly lady Chris Pui Yan Yee 1, Kapil Sahnan 2, Robert Hywel Thomas 1, Kaji Sritharan 1 1. Department of Vascular Surgery, St Mary's Hospital,
On Which Criteria Do You Select Your Stent for Ilio-femoral Venous Obstruction? North American Point of View
 On Which Criteria Do You Select Your Stent for Ilio-femoral Venous Obstruction? North American Point of View Peter Gloviczki, MD Ying Huang, MD, PhD Division of Vascular and Endovascular Surgery, Mayo
On Which Criteria Do You Select Your Stent for Ilio-femoral Venous Obstruction? North American Point of View Peter Gloviczki, MD Ying Huang, MD, PhD Division of Vascular and Endovascular Surgery, Mayo
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of Interventional procedure overview of ultrasound-enhanced, catheterdirected thrombolysis
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of Interventional procedure overview of ultrasound-enhanced, catheterdirected thrombolysis
Clinical results of venous stents. Michael K. W. Lichtenberg MD, FESC
 Clinical results of venous stents Michael K. W. Lichtenberg MD, FESC Conflict of Interest - Disclosure Within the past 12 months, I or my spouse/partner have had a financial interest/arrangement or affiliation
Clinical results of venous stents Michael K. W. Lichtenberg MD, FESC Conflict of Interest - Disclosure Within the past 12 months, I or my spouse/partner have had a financial interest/arrangement or affiliation
Aggressive endovascular management of ilio-femoral DVT. thrombotic syndrome. is the key in preventing post
 CACVS 2017 Aggressive endovascular management of ilio-femoral DVT is the key in preventing post thrombotic syndrome ALI AMIN MD, FACS,FACC, RVT CHIEF OF ENDOVASCULAR INTERVENTIONS READING HEALTH SYSTEM
CACVS 2017 Aggressive endovascular management of ilio-femoral DVT is the key in preventing post thrombotic syndrome ALI AMIN MD, FACS,FACC, RVT CHIEF OF ENDOVASCULAR INTERVENTIONS READING HEALTH SYSTEM
DOPPLER ULTRASOUND OF DEEP VENOUS THROMBOSIS
 TOKUDA HOSPITAL SOFIA DOPPLER ULTRASOUND OF DEEP VENOUS THROMBOSIS MILENA STANEVA, MD, PhD Department of vascular surgery and angiology Venous thromboembolic disease continues to cause significant morbidity
TOKUDA HOSPITAL SOFIA DOPPLER ULTRASOUND OF DEEP VENOUS THROMBOSIS MILENA STANEVA, MD, PhD Department of vascular surgery and angiology Venous thromboembolic disease continues to cause significant morbidity
SAMPLE CHAPTERS UNESCO-EOLSS MANAGEMENT OF SUBCLAVIAN VEIN THROMBOSIS KNOWN AS PAGET-SCHROETTER SYNDROME
 MANAGEMENT OF SUBCLAVIAN VEIN THROMBOSIS KNOWN AS PAGETSCHROETTER SYNDROME J. Ernesto Molina University of Minnesota, Minneapolis, Minnesota, U.S.A. Keywords: Thoracic outlet, Venous disease Contents 1.
MANAGEMENT OF SUBCLAVIAN VEIN THROMBOSIS KNOWN AS PAGETSCHROETTER SYNDROME J. Ernesto Molina University of Minnesota, Minneapolis, Minnesota, U.S.A. Keywords: Thoracic outlet, Venous disease Contents 1.
Spontaneous Tilting after Placement of the Gu nther-tulip Inferior Vena Caval Filter: A Case Report 1
 Spontaneous Tilting after Placement of the Gu nther-tulip Inferior Vena Caval Filter: Case Report 1 Tae-Seok Seo, M.D., In-Ho Cha, M.D., Hae Young Seol, M.D., Cheol Min Park, M.D. Tilting of a deployed
Spontaneous Tilting after Placement of the Gu nther-tulip Inferior Vena Caval Filter: Case Report 1 Tae-Seok Seo, M.D., In-Ho Cha, M.D., Hae Young Seol, M.D., Cheol Min Park, M.D. Tilting of a deployed
DEEP VEIN THROMBOSIS (DVT): TREATMENT
 DEEP VEIN THROMBOSIS (DVT): TREATMENT OBJECTIVE: To provide an evidence-based approach to treatment of patients presenting with deep vein thrombosis (DVT). BACKGROUND: An estimated 45,000 patients in Canada
DEEP VEIN THROMBOSIS (DVT): TREATMENT OBJECTIVE: To provide an evidence-based approach to treatment of patients presenting with deep vein thrombosis (DVT). BACKGROUND: An estimated 45,000 patients in Canada
A Dedicated Venous Self-expanding Oblique Hybrid Nitinol Stent (Sinus-Obliquus Stent)
 A Dedicated Venous Self-expanding Oblique Hybrid Nitinol Stent (Sinus-Obliquus Stent) Anna Stuck, Rolf P. Engelberger, Nils Kucher Division of Angiology Cantonal Hospital Fribourg & Bern University Hospital
A Dedicated Venous Self-expanding Oblique Hybrid Nitinol Stent (Sinus-Obliquus Stent) Anna Stuck, Rolf P. Engelberger, Nils Kucher Division of Angiology Cantonal Hospital Fribourg & Bern University Hospital
The hallmark of percutaneous thrombus management
 Treating Venous Thromboembolism Without Lytic Medications What the present and the near future will bring in terms of techniques and devices to remove venous thrombus. BY CONSTANTINO S. PEÑA, MD; RIPAL
Treating Venous Thromboembolism Without Lytic Medications What the present and the near future will bring in terms of techniques and devices to remove venous thrombus. BY CONSTANTINO S. PEÑA, MD; RIPAL
Copy Here. The Easy One.. What is the Role of Thrombus Removal in Acute Proximal DVT after ATTRACT? Deep Venous Thrombosis Spectrum
 What is the Role of Thrombus Removal in Acute Proximal DVT after ATTRACT? Mitchell J. Silver DO FACC FSVM RPVI Director, Center for Critical Limb Care Riverside Methodist Hospital Ohio Health Heart and
What is the Role of Thrombus Removal in Acute Proximal DVT after ATTRACT? Mitchell J. Silver DO FACC FSVM RPVI Director, Center for Critical Limb Care Riverside Methodist Hospital Ohio Health Heart and
Use of EKOS Catheter in the management of Venous Mr. Manoj Niverthi, Mr. Sarang Pujari, and Ms. Nupur Dandavate, The GTF Group
 Use of EKOS Catheter in the management of Venous Thromboembolism @ Mr. Manoj Niverthi, Mr. Sarang Pujari, and Ms. Nupur Dandavate, The GTF Group Introduction Georgia Thrombosis Forum (GTF, www.gtfonline.net)
Use of EKOS Catheter in the management of Venous Thromboembolism @ Mr. Manoj Niverthi, Mr. Sarang Pujari, and Ms. Nupur Dandavate, The GTF Group Introduction Georgia Thrombosis Forum (GTF, www.gtfonline.net)
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of Interventional procedure overview of ultrasound-enhanced, catheterdirected thrombolysis
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of Interventional procedure overview of ultrasound-enhanced, catheterdirected thrombolysis
THERE IS NO ROLE FOR SURGICAL THERAPY FOR DVT
 THERE IS NO ROLE FOR SURGICAL THERAPY FOR DVT Tara D. Balint, MD FACS Sentara RMH Thursday, June 14, 2018 1 Objectives of treatment for DVT Prevent death from PE Prevent recurrent VTE Prevent post-thrombotic
THERE IS NO ROLE FOR SURGICAL THERAPY FOR DVT Tara D. Balint, MD FACS Sentara RMH Thursday, June 14, 2018 1 Objectives of treatment for DVT Prevent death from PE Prevent recurrent VTE Prevent post-thrombotic
Case Report May-Thurner Syndrome: A Case Report and Review of the Literature
 Case Reports in Vascular Medicine Volume 2013, Article ID 740182, 5 pages http://dx.doi.org/10.1155/2013/740182 Case Report May-Thurner Syndrome: A Case Report and Review of the Literature Shivani Kalu,
Case Reports in Vascular Medicine Volume 2013, Article ID 740182, 5 pages http://dx.doi.org/10.1155/2013/740182 Case Report May-Thurner Syndrome: A Case Report and Review of the Literature Shivani Kalu,
Catheter direct thrombolysis: Role of actilyse in treatment of acute deep venous thrombosis
 The Egyptian Journal of Radiology and Nuclear Medicine (2013) 44, 57 62 Egyptian Society of Radiology and Nuclear Medicine The Egyptian Journal of Radiology and Nuclear Medicine www.elsevier.com/locate/ejrnm
The Egyptian Journal of Radiology and Nuclear Medicine (2013) 44, 57 62 Egyptian Society of Radiology and Nuclear Medicine The Egyptian Journal of Radiology and Nuclear Medicine www.elsevier.com/locate/ejrnm
Venous stent experience in Arnsberg Michael K. W. Lichtenberg MD, FESC
 Venous stent experience in Arnsberg Michael K. W. Lichtenberg MD, FESC IMPORTANT INFORMATION: These materials are intended to describe common clinical considerations and procedural steps for the on-label
Venous stent experience in Arnsberg Michael K. W. Lichtenberg MD, FESC IMPORTANT INFORMATION: These materials are intended to describe common clinical considerations and procedural steps for the on-label
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE)
 Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
Comparison Of Primary Long Stenting Versus Primary Short Stenting For Long Femoropopliteal Artery Disease (PARADE) Young-Guk Ko, M.D. Severance Cardiovascular Hospital, Yonsei University Health System,
J Jpn Coll Angiol, 2009, 49:
 Online publication August 27, 2009 1 2 J Jpn Coll Angiol, 2009, 49: 247 254 deep vein thrombosis, thrombolytic therapy, catheter-directed thrombolysis, inferior vena cava filter, pulmonary thromboembolism
Online publication August 27, 2009 1 2 J Jpn Coll Angiol, 2009, 49: 247 254 deep vein thrombosis, thrombolytic therapy, catheter-directed thrombolysis, inferior vena cava filter, pulmonary thromboembolism
Improved clinical outcomes Evidence on venous thrombectomy followed by stenting
 Improved clinical outcomes Evidence on venous thrombectomy followed by stenting Michael K. W. Lichtenberg, MD, FESC Vascular Centre Arnsberg, Germany Venous Centre Arnsberg, Germany Disclosure Speaker
Improved clinical outcomes Evidence on venous thrombectomy followed by stenting Michael K. W. Lichtenberg, MD, FESC Vascular Centre Arnsberg, Germany Venous Centre Arnsberg, Germany Disclosure Speaker
Tom Eisele, Benedikt M. Muenz, and Grigorios Korosoglou. Department of Cardiology & Vascular Medicine, GRN Hospital Weinheim, Weinheim, Germany
 Case Reports in Vascular Medicine Volume 2016, Article ID 7376457, 4 pages http://dx.doi.org/10.1155/2016/7376457 Case Report Successful Endovascular Repair of an Iatrogenic Perforation of the Superficial
Case Reports in Vascular Medicine Volume 2016, Article ID 7376457, 4 pages http://dx.doi.org/10.1155/2016/7376457 Case Report Successful Endovascular Repair of an Iatrogenic Perforation of the Superficial
Optimal Utilization of Thrombolytics
 April 8-9, 2011 New York LaGuardia Marriott COMPLETE MANAGEMENT OF VENOUS DISEASE Optimal Utilization of Thrombolytics Anthony J. Comerota, MD, FACS, FACC Director, Jobst Vascular Institute Adjunct Professor
April 8-9, 2011 New York LaGuardia Marriott COMPLETE MANAGEMENT OF VENOUS DISEASE Optimal Utilization of Thrombolytics Anthony J. Comerota, MD, FACS, FACC Director, Jobst Vascular Institute Adjunct Professor
Techniques for thrombus removal in acute DVT Benefits of an Endovascular Approach for Rapid Flow Restoration in DVT
 Techniques for thrombus removal in acute DVT Benefits of an Endovascular Approach for Rapid Flow Restoration in DVT Michael K. W. Lichtenberg, MD, FESC Vascular Centre Arnsberg, Germany Disclosure Speaker
Techniques for thrombus removal in acute DVT Benefits of an Endovascular Approach for Rapid Flow Restoration in DVT Michael K. W. Lichtenberg, MD, FESC Vascular Centre Arnsberg, Germany Disclosure Speaker
I-Ming Chen, MD. Endovascular Stenting for Palliative Treatment of Superior Vena Cava Syndrome in End-Stage Lung Cancer
 Endovascular Stenting for Palliative Treatment of Superior Vena Cava Syndrome in End-Stage Lung Cancer I-Ming Chen, MD Division of CardioVascular Surgery Taipei Veterans General Hospital, Taiwan (Live
Endovascular Stenting for Palliative Treatment of Superior Vena Cava Syndrome in End-Stage Lung Cancer I-Ming Chen, MD Division of CardioVascular Surgery Taipei Veterans General Hospital, Taiwan (Live
Image-Guided Approach to Treatment of Patients with Nonthrombotic
 Image-Guided Approach to Treatment of Patients with Nonthrombotic May Thurner Syndrome Brian DeRubertis, MD, FACS Associate Professor of Surgery Division of Vascular Surgery UCLA School of Medicine Los
Image-Guided Approach to Treatment of Patients with Nonthrombotic May Thurner Syndrome Brian DeRubertis, MD, FACS Associate Professor of Surgery Division of Vascular Surgery UCLA School of Medicine Los
Emerging Tools for Lytic-Free, Single-Session Treatment of Venous Thromboembolic Disease
 FEATURED TECHNOLOGY THE CLOTTRIEVER AND FLOWTRIEVER SYSTEMS Emerging Tools for Lytic-Free, Single-Session Treatment of Venous Thromboembolic Disease The ClotTriever Outcomes (CLOUT) registry principal
FEATURED TECHNOLOGY THE CLOTTRIEVER AND FLOWTRIEVER SYSTEMS Emerging Tools for Lytic-Free, Single-Session Treatment of Venous Thromboembolic Disease The ClotTriever Outcomes (CLOUT) registry principal
Acoustic Pulse Thrombolysis Treatment
 Acoustic Pulse Thrombolysis Treatment BTGVascular.com SETTING THE STANDARD FOR VASCULAR THERAPIES Quickly & safely dissolve thrombus with the EKOS System. The Acoustic Pulse Difference Acoustic Pulse Thrombolysis
Acoustic Pulse Thrombolysis Treatment BTGVascular.com SETTING THE STANDARD FOR VASCULAR THERAPIES Quickly & safely dissolve thrombus with the EKOS System. The Acoustic Pulse Difference Acoustic Pulse Thrombolysis
Intravascular ultrasound scan evaluation of the obstructed vein
 Intravascular ultrasound scan evaluation of the obstructed vein Peter Neglén, MD, PhD, and Seshadri Raju, MD, Jackson, Miss Purpose: The purpose of this study was the comparison of intravascular ultrasound
Intravascular ultrasound scan evaluation of the obstructed vein Peter Neglén, MD, PhD, and Seshadri Raju, MD, Jackson, Miss Purpose: The purpose of this study was the comparison of intravascular ultrasound
Introduction. Case CASE REPORTS ABSTRACT
 CASE REPORTS Arrhythmia 2015;16(4):226-231 doi: http://dx.doi.org/10.18501/arrhythmia.2015.038 Massive Deep Vein Thrombosis Underlying Unexpected Iliac Vein Compression Syndrome (May-Thurner Syndrome)
CASE REPORTS Arrhythmia 2015;16(4):226-231 doi: http://dx.doi.org/10.18501/arrhythmia.2015.038 Massive Deep Vein Thrombosis Underlying Unexpected Iliac Vein Compression Syndrome (May-Thurner Syndrome)
Bare Metal Stents vs Stent Grafts
 Bare Metal Stents vs Stent Grafts ASDIN 12th Annual Scientific Meeting Phoenix, AZ, February 20, 2016 Dirk Hentschel, MD Director, Interventional Nephrology Brigham and Women s Hospital Disclosure Consultant:
Bare Metal Stents vs Stent Grafts ASDIN 12th Annual Scientific Meeting Phoenix, AZ, February 20, 2016 Dirk Hentschel, MD Director, Interventional Nephrology Brigham and Women s Hospital Disclosure Consultant:
Venous Thrombosis. Magnitude of the Problem. DVT 2 Million PE 600,000. Death 60,000. Estimated Cost of VTE Care $1.5 Billion/year.
 Venous Thrombosis Magnitude of the Problem DVT 2 Million Postthrombotic Syndrome 800,000 PE 600,000 Death 60,000 Silent PE 1 Million Pulmonary Hypertension 30,000 Estimated Cost of VTE Care $1.5 Billion/year
Venous Thrombosis Magnitude of the Problem DVT 2 Million Postthrombotic Syndrome 800,000 PE 600,000 Death 60,000 Silent PE 1 Million Pulmonary Hypertension 30,000 Estimated Cost of VTE Care $1.5 Billion/year
Post-thrombotic syndrome (PTS), often the
 Revascularization of Chronic Venous Occlusion in the Setting of Post-Thrombotic Syndrome Jon George, MD; Deepakraj Gajanana; Sean Janzer; Vincent Figueredo; Dennis Morris From the Einstein Heart and Vascular
Revascularization of Chronic Venous Occlusion in the Setting of Post-Thrombotic Syndrome Jon George, MD; Deepakraj Gajanana; Sean Janzer; Vincent Figueredo; Dennis Morris From the Einstein Heart and Vascular
Recanalization of the Left Common Iliac Vein for MayeThurner Syndrome Associated with Arteriovenous Fistula
 EJVES Short Reports (2015) 29, 3e7 SHORT REPORT Recanalization of the Left Common Iliac Vein for MayeThurner Syndrome Associated with Arteriovenous Fistula H. Yuan a, J. Sun b,h.t.qi c, X. Jin a, X.J.
EJVES Short Reports (2015) 29, 3e7 SHORT REPORT Recanalization of the Left Common Iliac Vein for MayeThurner Syndrome Associated with Arteriovenous Fistula H. Yuan a, J. Sun b,h.t.qi c, X. Jin a, X.J.
Endovascular Treatment for Iliac Vein Compression Syndrome: a Comparison between the Presence and Absence of Secondary Thrombosis
 Endovascular Treatment for Iliac Vein Compression Syndrome: a Comparison between the Presence and Absence of Secondary Thrombosis Wen-Sheng Lou, MD Jian-Ping Gu, MD Xu He, MD Liang Chen, MD Hao-Bo Su,
Endovascular Treatment for Iliac Vein Compression Syndrome: a Comparison between the Presence and Absence of Secondary Thrombosis Wen-Sheng Lou, MD Jian-Ping Gu, MD Xu He, MD Liang Chen, MD Hao-Bo Su,
Should We Be More Aggressive in the Treatment of Acute DVT?
 DISCLOSURES Consultant Penumbra, Inc. UCSF Vascular Surgery Symposium April 6, 2017 K. Pallav Kolli, MD Assistant Professor of Clinical Radiology University of California, San Francisco 17 yo male, DVT
DISCLOSURES Consultant Penumbra, Inc. UCSF Vascular Surgery Symposium April 6, 2017 K. Pallav Kolli, MD Assistant Professor of Clinical Radiology University of California, San Francisco 17 yo male, DVT
IVUS is strongly recommanded before treating a venous femoro-iliac obstruction CONS. F Thony CHU Grenoble
 IVUS is strongly recommanded before treating a venous femoro-iliac obstruction CONS F Thony CHU Grenoble Disclosure Speaker name: Frédéric THONY I do not have any potential conflict of interest Introduction
IVUS is strongly recommanded before treating a venous femoro-iliac obstruction CONS F Thony CHU Grenoble Disclosure Speaker name: Frédéric THONY I do not have any potential conflict of interest Introduction
Complex Iliocaval Reconstruction PNEC. Seattle WA. Bill Marston MD Professor, Div of Vascular Surgery University of N.
 Complex Iliocaval Reconstruction 2017 PNEC. Seattle WA Bill Marston MD Professor, Div of Vascular Surgery University of N. Carolina DISCLOSURES William Marston, MD Consultant/Advisory Board: Veniti, Cardinal
Complex Iliocaval Reconstruction 2017 PNEC. Seattle WA Bill Marston MD Professor, Div of Vascular Surgery University of N. Carolina DISCLOSURES William Marston, MD Consultant/Advisory Board: Veniti, Cardinal
Aspirex for Upper and Lower Extremity DVT
 Aspirex for Upper and Lower Extremity DVT Steven Kum MD Vascular & Endovascular Surgeon Director of Vascular Service Changi General Hospital Singapore Disclosure Speaker name:... I have the following potential
Aspirex for Upper and Lower Extremity DVT Steven Kum MD Vascular & Endovascular Surgeon Director of Vascular Service Changi General Hospital Singapore Disclosure Speaker name:... I have the following potential
Vascular Surgery and Transplant Unit University of Catania. Pierfrancesco Veroux
 Vascular Surgery and Transplant Unit University of Catania Pierfrancesco Veroux Bologna-Palazzo dei Congressi, 23 Ottobre 2017 Disclosure Speaker name: Prof. Pierfrancesco Veroux I have the following potential
Vascular Surgery and Transplant Unit University of Catania Pierfrancesco Veroux Bologna-Palazzo dei Congressi, 23 Ottobre 2017 Disclosure Speaker name: Prof. Pierfrancesco Veroux I have the following potential
Innovative Endovascular Approach to Pulmonary Embolism by Ultrasound Enhanced Thrombolysis. Prof. Ralf R.Kolvenbach MD,PhD,FEBVS
 Innovative Endovascular Approach to Pulmonary Embolism by Ultrasound Enhanced Thrombolysis Prof. Ralf R.Kolvenbach MD,PhD,FEBVS Catheter-based thrombolysis Local administration of lytic agent Higher local
Innovative Endovascular Approach to Pulmonary Embolism by Ultrasound Enhanced Thrombolysis Prof. Ralf R.Kolvenbach MD,PhD,FEBVS Catheter-based thrombolysis Local administration of lytic agent Higher local
PEARL Registry Update Overview Venous Arterial AV Access
 PEARL Registry Update Overview Venous Arterial AV Access PEARL Registry Overview (as of 10 Sep12*) Overview Venous Arterial AV Access HOME Topic Data Support Comments Study Design Prospective, non-randomized,
PEARL Registry Update Overview Venous Arterial AV Access PEARL Registry Overview (as of 10 Sep12*) Overview Venous Arterial AV Access HOME Topic Data Support Comments Study Design Prospective, non-randomized,
Treatment of Axillosubclavian Vein Thrombosis: A Novel Technique for Rapid Removal of Clot Using Low-Dose Thrombolysis
 J ENDOVASC THER 733 RAPID COMMUNICATION Treatment of Axillosubclavian Vein Thrombosis: A Novel Technique for Rapid Removal of Clot Using Low-Dose Thrombolysis Frank R. Arko, MD; Paul Cipriano, MD; Eugene
J ENDOVASC THER 733 RAPID COMMUNICATION Treatment of Axillosubclavian Vein Thrombosis: A Novel Technique for Rapid Removal of Clot Using Low-Dose Thrombolysis Frank R. Arko, MD; Paul Cipriano, MD; Eugene
AV ACESS COMPLICATIONS. Ass. Prof. Dr. Habas
 AV ACESS COMPLICATIONS Ass. Prof. Dr. Habas COMPLICATION AVF IS CONSIDERED A MINOR PROCEDURE INCIDENCE OF COMPLICATION- 20-27% MANY A COMPLICATION LEADS TO FAILURE OF FISTULA LOSS OF SITE AND VEIN FOR
AV ACESS COMPLICATIONS Ass. Prof. Dr. Habas COMPLICATION AVF IS CONSIDERED A MINOR PROCEDURE INCIDENCE OF COMPLICATION- 20-27% MANY A COMPLICATION LEADS TO FAILURE OF FISTULA LOSS OF SITE AND VEIN FOR
Deep Venous Pathology. Eberhard Rabe Department of Dermatology University of Bonn Germany
 Deep Venous Pathology Eberhard Rabe Department of Dermatology University of Bonn Germany Disclosures None for this presentation Consultant: Sigvaris, EUROCOM Speakers bureau: Bayer Vital, Aspen, Boehringer,
Deep Venous Pathology Eberhard Rabe Department of Dermatology University of Bonn Germany Disclosures None for this presentation Consultant: Sigvaris, EUROCOM Speakers bureau: Bayer Vital, Aspen, Boehringer,
Interventional Radiology in Trauma. Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital
 Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
Management of Acute DVT Extending From the Tibial Veins to the Common Iliac Vein Using the AngioJet Thrombectomy System
 FEATURED TECHNOLOGY: ANGIOJET THROMBECTOMY SYSTEM Sponsored by Boston Scientific Corporation Management of Acute DVT Extending From the Tibial Veins to the Common Iliac Vein Using the AngioJet Thrombectomy
FEATURED TECHNOLOGY: ANGIOJET THROMBECTOMY SYSTEM Sponsored by Boston Scientific Corporation Management of Acute DVT Extending From the Tibial Veins to the Common Iliac Vein Using the AngioJet Thrombectomy
Case Study of Implantation of a VICI VENOUS STENT - Combined NIVL and PTS Stenting
 Case Study of Implantation of a VICI VENOUS STENT - Combined NIVL and PTS Stenting Courtesy of Mr. Stephen Black United kingdom Patient History 25 y/o female 2011: Conservatively treated ilio-femoral DVT
Case Study of Implantation of a VICI VENOUS STENT - Combined NIVL and PTS Stenting Courtesy of Mr. Stephen Black United kingdom Patient History 25 y/o female 2011: Conservatively treated ilio-femoral DVT
Improved clinical outcomes Evidence on venous mechanical thrombectomy followed by stenting
 Improved clinical outcomes Evidence on venous mechanical thrombectomy followed by stenting Michael K. W. Lichtenberg, MD, FESC Vascular Centre Arnsberg, Germany German Venous Centre Arnsberg, Germany Disclosure
Improved clinical outcomes Evidence on venous mechanical thrombectomy followed by stenting Michael K. W. Lichtenberg, MD, FESC Vascular Centre Arnsberg, Germany German Venous Centre Arnsberg, Germany Disclosure
Understanding of the importance of venous
 The Critical Need for an Iliofemoral Venous Obstruction Classification System An overview of a potential classification system to better identify and treat iliofemoral venous outflow obstruction. BY WILLIAM
The Critical Need for an Iliofemoral Venous Obstruction Classification System An overview of a potential classification system to better identify and treat iliofemoral venous outflow obstruction. BY WILLIAM
Re-intervention for occluded iliac vein stents
 Review Article Re-intervention for occluded iliac vein stents Stacey Black 1, Amy Janicek 2, M. Grace Knuttinen 3 1 University of Arizona, Tucson, Arizona, USA; 2 Arizona State Radiology, Tucson, Arizona,
Review Article Re-intervention for occluded iliac vein stents Stacey Black 1, Amy Janicek 2, M. Grace Knuttinen 3 1 University of Arizona, Tucson, Arizona, USA; 2 Arizona State Radiology, Tucson, Arizona,
Anticoagulation therapy following endovascular treatment of iliofemoral deep vein thrombosis
 Anticoagulation therapy following endovascular treatment of iliofemoral deep vein thrombosis Tim Sebastian, M.D. University Hospital Zurich Clinic for Angiology Disclosure Speaker name: Tim Sebastian I
Anticoagulation therapy following endovascular treatment of iliofemoral deep vein thrombosis Tim Sebastian, M.D. University Hospital Zurich Clinic for Angiology Disclosure Speaker name: Tim Sebastian I
Sample page. POWER UP YOUR CODING with Optum360, your trusted coding partner for 32 years. Visit optum360coding.com.
 2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
Complications of endovascular treatment of May-Thurner syndrome George Geroulakos
 Complications of endovascular treatment of May-Thurner syndrome George Geroulakos Professor of Vascular Surgery, National and Kapodistrian University of Athens Director, Department of Vascular Surgery,
Complications of endovascular treatment of May-Thurner syndrome George Geroulakos Professor of Vascular Surgery, National and Kapodistrian University of Athens Director, Department of Vascular Surgery,
Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases
 Chin J Radiol 2003; 28: 137-142 137 Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases SHE-MENG CHENG SUK-PING NG FEI-SHIH YANG SHIN-LIN SHIH Department
Chin J Radiol 2003; 28: 137-142 137 Interventional Treatment for Complete Occlusion of Arteriovenous Shunt: Our Experience in 39 cases SHE-MENG CHENG SUK-PING NG FEI-SHIH YANG SHIN-LIN SHIH Department
The evidence for venous interventions is evolving- many patients do actually benefit. Nils Kucher University Hospital Bern Switzerland
 The evidence for venous interventions is evolving- many patients do actually benefit Nils Kucher University Hospital Bern Switzerland Disclosure Speaker name: Nils Kucher X X I have the following potential
The evidence for venous interventions is evolving- many patients do actually benefit Nils Kucher University Hospital Bern Switzerland Disclosure Speaker name: Nils Kucher X X I have the following potential
Endovascular treatment of acquired arteriovenous fistula with severe hemodynamic effects: a case report
 Endovascular treatment of acquired arteriovenous fistula with severe hemodynamic effects: a case report The Leipzig Interventional Course, January 24 27, 2017 El Samman K., Šedivý P., Šnajdrová A., Přindišová
Endovascular treatment of acquired arteriovenous fistula with severe hemodynamic effects: a case report The Leipzig Interventional Course, January 24 27, 2017 El Samman K., Šedivý P., Šnajdrová A., Přindišová
Primary to non-coronary IVUS
 codes 2018 2018 codes Primary to non-coronary IVUS Page 2 All coding, coverage, billing and payment information provided herein by Philips is gathered from third-party sources and is subject to change.
codes 2018 2018 codes Primary to non-coronary IVUS Page 2 All coding, coverage, billing and payment information provided herein by Philips is gathered from third-party sources and is subject to change.
(This is a sample cover image for this issue. The actual cover is not yet available at this time.)
 (This is a sample cover image for this issue. The actual cover is not yet available at this time.) This is an open access article which appeared in a journal published by Elsevier. This article is free
(This is a sample cover image for this issue. The actual cover is not yet available at this time.) This is an open access article which appeared in a journal published by Elsevier. This article is free
Starting with deep venous treatment
 Starting with deep venous treatment Carsten Arnoldussen, MD Interventional Radiologist Maastricht University Medical Centre, Maastricht VieCuri Medical Centre, Venlo The Netherlands Background Maastricht
Starting with deep venous treatment Carsten Arnoldussen, MD Interventional Radiologist Maastricht University Medical Centre, Maastricht VieCuri Medical Centre, Venlo The Netherlands Background Maastricht
Role of Interventional Cardiologists in Lower Limb Swelling/DVT -Case Series on May-Thurner Syndrome and its Variants
 J Cardiovasc Disease Res., 2018; 9(2):92-98 A Multifaceted Peer Reviewed Journal in the field of Cardiology www.jcdronline.org www.journalonweb.com/jcdr Case Series Role of Interventional Cardiologists
J Cardiovasc Disease Res., 2018; 9(2):92-98 A Multifaceted Peer Reviewed Journal in the field of Cardiology www.jcdronline.org www.journalonweb.com/jcdr Case Series Role of Interventional Cardiologists
Iliofemoral stenting for venous occlusive disease
 From the Society for Vascular Surgery Iliofemoral stenting for venous occlusive disease Jessica M. Titus, MD, Mireille A. Moise, MD, James Bena, MS, Sean P. Lyden, MD, and Daniel G. Clair, MD, Cleveland,
From the Society for Vascular Surgery Iliofemoral stenting for venous occlusive disease Jessica M. Titus, MD, Mireille A. Moise, MD, James Bena, MS, Sean P. Lyden, MD, and Daniel G. Clair, MD, Cleveland,
ENHANCING YOUR OPTIONS
 ANGIOJET ULTRA Thrombectomy System ENHANCING YOUR OPTIONS FOR RESTORING FLOW When you need the versatility and power to restore flow Refined from experience in over 700,000 cases worldwide, today s AngioJet
ANGIOJET ULTRA Thrombectomy System ENHANCING YOUR OPTIONS FOR RESTORING FLOW When you need the versatility and power to restore flow Refined from experience in over 700,000 cases worldwide, today s AngioJet
Brachytherapy for In-Stent Restenosis: Is the Concept Still Alive? Matthew T. Menard, M.D. Brigham and Women s Hospital Boston, Massachussetts
 Brachytherapy for In-Stent Restenosis: Is the Concept Still Alive? Matthew T. Menard, M.D. Brigham and Women s Hospital Boston, Massachussetts Disclosure Speaker name: Matthew T. Menard... x I do not have
Brachytherapy for In-Stent Restenosis: Is the Concept Still Alive? Matthew T. Menard, M.D. Brigham and Women s Hospital Boston, Massachussetts Disclosure Speaker name: Matthew T. Menard... x I do not have
BY DAVID GILLESPIE, MD; MARCIA JOHANSSON, RN, MS; AND CAROLYN GLASS, MD
 Stent Placement fter DVT Thrombolysis/ Mechanical Thrombectomy Which patients should be stented and which should not? Y DVID GILLESPIE, MD; MRCI JOHNSSON, RN, MS; ND CROLYN GLSS, MD It is an exciting time
Stent Placement fter DVT Thrombolysis/ Mechanical Thrombectomy Which patients should be stented and which should not? Y DVID GILLESPIE, MD; MRCI JOHNSSON, RN, MS; ND CROLYN GLSS, MD It is an exciting time
Case 37 Clinical Presentation
 Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Case 37 73 Clinical Presentation The patient is a 62-year-old woman with gastrointestinal (GI) bleeding. 74 RadCases Interventional Radiology Imaging Findings () Image from a selective digital subtraction
Regardless of whether you are a vascular surgeon,
 C A S E R E P O R T The Versatility of the GORE VIABAHN Endoprosthesis Several case reports highlighting its unique design and why it is a valuable tool for the interventionist. BY PETER WAYNE, MD Regardless
C A S E R E P O R T The Versatility of the GORE VIABAHN Endoprosthesis Several case reports highlighting its unique design and why it is a valuable tool for the interventionist. BY PETER WAYNE, MD Regardless
As with any intervention, selection of an appropriate
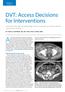 DVT: ccess Decisions for Interventions ssessing the advantages and disadvantages of venous access options is crucial for safe and successful DVT intervention. Y JOHN. KUFMN, MD, MS, FSIR, FH, FCIRSE, EIR
DVT: ccess Decisions for Interventions ssessing the advantages and disadvantages of venous access options is crucial for safe and successful DVT intervention. Y JOHN. KUFMN, MD, MS, FSIR, FH, FCIRSE, EIR
Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents
 Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents Jesus Contreras, D.O. PGY-4 John Yasmer, D.O. Department of Radiology No Disclosures Objectives Introduce
Introduction to the Native Arteriovenous Fistula: A primer for medical students and radiology residents Jesus Contreras, D.O. PGY-4 John Yasmer, D.O. Department of Radiology No Disclosures Objectives Introduce
- Our patients with iliofemoral DVT - Effective thrombus removal with purely mechanical thrombectomy can lead to better outcomes
 - Our patients with iliofemoral DVT - Effective thrombus removal with purely mechanical thrombectomy can lead to better outcomes Michael K. W. Lichtenberg, FESC Conflict of Interest - Disclosure Within
- Our patients with iliofemoral DVT - Effective thrombus removal with purely mechanical thrombectomy can lead to better outcomes Michael K. W. Lichtenberg, FESC Conflict of Interest - Disclosure Within
TEACHING CASE # 5. Reocclusion Of Transverse And Sigmoid Venous Sinuses Mechanical and Chemical Thrombectomy
 TEACHING CASE # 5 Reocclusion Of Transverse And Sigmoid Venous Sinuses Mechanical and Chemical Thrombectomy CASE PRESENTATION 22M with right transverse and sigmoid venous sinuses occlusion s/p transvenous
TEACHING CASE # 5 Reocclusion Of Transverse And Sigmoid Venous Sinuses Mechanical and Chemical Thrombectomy CASE PRESENTATION 22M with right transverse and sigmoid venous sinuses occlusion s/p transvenous
