Talc pleurodesis: Comparison of talc slurry instillation with thoracoscopic talc insufflation for malignant pleural effusions
|
|
|
- Shona Robbins
- 6 years ago
- Views:
Transcription
1 Journal of BUON 11: , Zerbinis Medical Publications. Printed in Greece ORIGINAL ARTICLE Talc pleurodesis: Comparison of talc slurry instillation with thoracoscopic talc insufflation for malignant pleural effusions A. Debeljak, P. Kecelj, N. Triller, S. Letonja, I. Kern, L. Debevec, A. Rozman University Clinic of Respiratory and Allergic Diseases Golnik, Golnik, Slovenia Summary Purpose: Pleurodesis can relieve dyspnea in patients with malignant pleural effusions. We retrospectively compared the success rate of talc slurry instillation pleurodesis with thoracoscopic talc powder insuffl ation pleurodesis. Patients and methods: From 2000 to 2005, two methods of talc pleurodesis were performed in 71 patients with symptomatic massive malignant pleural effusions: a) through the pleural drain (24F), 50 ml of a slurry containing 4-5 g of Luzenac talc in saline with 20 ml 1% lidocaine were instilled. The drain was clamped for 1 h; b) insufflation of 3-5 g of talc powder was performed via videothoracoscope using local anaesthesia. The drain was left in the pleural space until the daily secretion of pleural fl uid was under 100 ml. Pleurodesis was considered successful when the patient was without dyspnea and did not need pleural fluid evacuation and the pleural fl uid did not re-accumulate in the 1st month after pleurodesis. Results: The success rate of talc slurry pleurodesis was 78% (38/49). Excluding 8 patients who died in the first month, the success rate increased to 93% (38/41). Thoracoscopic pleurodesis was successful in 77% (17/22) of patients. Excluding one patient who died in the first month, the success rate increased to 81% (17/21) (intergroup difference non signifi cant). Complications were observed in 41% (20/49) vs. 73% (16/22) of patients in the talc slurry group and thoracoscopic group, respectively (p=0.013). Conclusion: Pleurodesis with instillation of talc slurry and with insuffl ation of talc during thoracoscopy were equally successful in patients with massive malignant pleural effusions. However, thoracoscopic pleurodesis is accompanied with considerably more complications, rather as a result of the thoracoscopy itself and not as a consequence of pleurodesis. Key words: diagnostic thoracoscopy, massive malignant pleural effusion, pleurodesis, talc slurry Introduction Pleurodesis is carried out to achieve symphysis between the visceral and parietal pleural surfaces in dyspneic patients with massive, usually malignant pleural effusions. Relief of dyspnea is its primary indication [1]. Received ; Accepted Author and address for correspondence: Andrej Debeljak, MD, PhD University Clinic of Respiratory and Allergic Diseases Golnik Golnik 36 SI 4204 Golnik Slovenia Tel: Fax: andrej.debeljak@klinika-golnik.si Pleurodesis is indicated in patients with malignant pleural effusion without other therapeutic possibilities or when other therapies are contraindicated or unsuccessful. The clinical indication for pleurodesis is dyspnea, rapid accumulation of pleural effusion and frequent thoracocenteses (more than one per week). Patients should be in relatively good general health status with expected survival greater than 3 months. A trapped lung should be excluded [2]. Lung cannot expand because of extensive malignant or in flammatory changes in the pleura. In patients with bronchial carcinoma, central tumor with extensive atelectasis should be excluded [3]. In these conditions, pleural therapeutic thoracocentesis can result in lack of lung re-expansion and development of a fluid pneumothorax. The application of thoracocentesis in some pa-
2 464 tients with abundant malignant pleural effusion and dyspnea because of trapped lung is therapeutic. A high success rate with low morbidity and mortality has been reported in patients with good general health status and surgical implantation of pleuro-peritoneal shunts [4]. Before pleurodesis after therapeutic thoracocentesis, it is necessary to confirm dyspneic relief. Chest X-ray should confirm appropriate re-expansion of the lung and substantial decrease of the pleural effusion without pneumothorax. There are over 30 different sclerosing agents. Among them, the most frequently used are: talc, tetracycline hydrochloride, nitrogen mustard, bleomycin, doxorubicin, 5-fluorouracil, thiotepa, quinacrine, corynebacterium parvum, interferon gamma, silver nitrate and sodium hydroxide. The best rate of success has been reported with talc pleurodesis [5]. Talc slurry can be applied through a pleural drain or talc powder insufflation through thoracoscope. Before pleurodesis as much as possible pleural fluid should be removed. In an prospective randomised trial pleurodesis with talc slurry and talc poudrage had similar efficiency [6]. Thoracotomy with parietal pleurectomy, though effective, should not be used without careful consideration because of considerable mortality [7]. In patients with good general health status video-assisted thoracic surgery (VATS) with partial pleurectomy or abrasion of the parietal pleura can be applied. In patients with poor general condition and a short expected survival (less than 3 months), an indwelling pleural catheter connected to a bottle or a bag is the method of choice. A series of patients treated with an indwelling catheter (PleurX Denver Biomedical) with a valve preventing the uncontrolled movement of air and fluid was reported. Patients used catheters for 1-6 months with 70-80% symptomatic relief. This method is convenient because patients generally need no hospitalisation [8]. With the same method, dyspnea was controlled in 100% and pleurodesis was achieved in 58% of patients [9]. When the patient s general health status is poor and expected survival is short, repeated therapeutic thoracocenteses can be an acceptable choice. The important shortcoming of repeated thoracocenteses is discomfort, deterioration of quality of life and depletion of proteins and electrolytes. Patients and methods From 2000 to 2005, we performed pleurodesis in 71 patients with massive malignant, quickly accumulating pleural effusion. Their average age was 62.2 ± 12.2 years. Because of massive pleural effusion all patients were dyspneic. Before pleurodesis, they had 3-10 therapeutic thoracocenteses with L of fluid removed at each procedure. The patients coagulation parameters were within normal limits and they experienced no respiratory insufficiency. Two patients had bilateral pleural effusions. Talc slurry pleurodesis was performed in patients with known malignant pleural effusion confirmed cytologically. Before pleurodesis, a pleural drain was inserted. The place for introduction was chosen according to clinical, chest X-ray and ultrasound examination (usually in the 6th intercostal space in the mid-axillary line). After local anaesthesia with ml of 1% lidocaine, a 24 F plastic drain was inserted through the incision into the pleural space. The drain was fixed with suture to the skin. Before talc slurry instillation, all pleural effusions were evacuated. For each procedure, 3-5 g of sterile talc (Luzenac, Toulouse, France) were used. Talc was mixed in a 50 ml syringe with 20 ml of 1% lidocaine and 30 ml of 0.9% saline solution. The syringe was vigorously agitated to achieve an even distribution of talc. The talc slurry was instilled and the drain was clamped for 1 h. The drain was connected to the underwater seal drainage system Ocean (Atrium Medical Corporation, USA), with negative pressure of 20 cm of water. Tramadol hydrochloride 100 mg b.i.d and, in case of pain, tramadol hydrochloride 50 mg or fentanyl 0.1 mg intravenously were administered. Diagnostic thoracoscopy was performed in patients with suspicion for malignant pleural effusion in whom 3 cytological examinations of pleural fluid were negative for malignant cells. We used Olympus videothoracoscope A5252A. Patients were pre-medicated with 1 mg of atropine sulphate subcutaneously. Local anaesthesia was administered with 30 ml of 1% lidocaine and fentanyl 0.1 mg was given intravenously. Before the introduction of the thoracoscope, a pneumothorax with a Veress needle and Erka pneumothorax apparatus was created under chest X-ray control (Phillips BV 29). The extention of the pneumothorax was controlled with a needle. We used 1 port in the 6th intercostal space in the mid-axillary line. The pleural fluid was completely aspirated to achieve better visualisation of the pleural surfaces. Forceps biopsies (11±4) were performed from the macroscopically pathological pleural sites. Samples were imprinted on slides for cytological examination and sent to the histological laboratory in 10% formalin. In patients with abundant pleural effusion and macroscopically malignant changes, pleurodesis was performed with insufflation of 3-5 g of talc under optical control with
3 465 a TH insufflator (Karel Storz Tuttlingen, Germany). At the end of the procedure a 24 F drain was inserted, fixed with a suture to the skin and connected to the underwater seal drainage system. The drain was left intrapleurally until the daily exudate was under 100 ml. In 11 patients, a talc slurry of 3-5 g was instilled twice because the daily exudation did not fall under 100 ml. Pleurodesis was considered successful when, in the first month after the procedure, the patient was not dyspneic, did not need therapeutic thoracocentesis and chest X-ray showed total or partial ( 50%) resolution of the previous pleural effusion. The success of pleurodesis in the two groups was compared by Pearson Chi-Square test. A p-value less than 0.05 was considered statistically significant. Results Pleurodesis was performed unilaterally on the right and left sides in 35 patients; bilateral pleurodesis was performed in 1 patient. Talc slurry pleurodesis was performed in 49 patients and thoracoscopic talc insufflation pleurodesis in 22 patients. Diagnoses of the group of patients with talc slurry pleurodesis are shown in Table 1. Diagnoses of the patients in the group with talc insufflation are presented in Table 2. Overall success was achieved in 77% (55/71) of the patients. In the first month, 9 patients died because of progressive malignant diseases: 8 in the group with talc slurry pleurodesis and 1 in the group with thoracoscopic talc insufflation. Excluding the patients that died in the first month, the success rate increased to 89% (55/62). In the group of patients with talc slurry pleurodesis, success was achieved in 78% (38/49) of them. Table 2. Types of malignant disease in 22 patients with thoracoscopic talc insufflation pleurodesis Patients, n (%) Mesothelioma 16 (73) Adenocarcinoma of unknown origin 2 (9) Osteosarcoma of tibia 1 (4.5) Lung adenocarcinoma 1 (4.5) Pancreatic adenocarcinoma 1 (4.5) Renal cell carcinoma 1 (4.5) Excluding the dead patients, the success rate was 93% (38/41). The drain was left in place for 4.8 ± 3.5 days. In one patient, the drain was left permanently connected to the disposable bag. The success of pleurodesis in each group according to cancer types is presented in Tables 3 and 4. The success rate of talc powder insufflation was 77% (17/22) (Figure 1). Excluding the dead patient, Figure 1. Thoracoscopic image after insufflation of 4 g of talc in a patient with epitheloid mesothelioma. Table 1. Types of malignant disease in 49 patients with talc slurry instillation pleurodesis Patients, n Patients, n (%) (%) Lung cancer 13 (26.5) Ovarian cancer 2 (4) adenocarcinoma 10 (20.5) Large bowel adenocarcinoma 1 (2) squamous cell 1 (2) Renal cell carcinoma 1 (2) small cell 1 (2) Pancreatic adenocarcinoma 1 (2) unspecified 1 (2) Malignant thymoma 1 (2) Adenocarcinoma of unknown origin 11 (22) Testicular seminoma/teratoma 1 (2) Breast cancer 9 (18.5) Salivary gland adenocarcinoma 1 (2) Mesothelioma 8 (16.5)
4 466 Table 3. Success of pleurodesis in 49 patients with talc slurry instillation Patients/success n (%) Lung cancer 13/10 (77) Adenocarcinoma of unknown origin 11/9 (82) Breast cancer 9/8 (89) Other extrapulmonary tumors 8/4 (50) Mesothelioma 8/7 (88) Table 4. Success of pleurodesis in 22 patients with thoracoscopic talc powder insufflation Patients/success n (%) Mesothelioma 16/12 (75) Extrapulmonary tumors 3/3 (100) Adenocarcinoma of unknown origin 2/2 (100) Lung cancer 1/0 (0) the success rate was 81% (17/21). The drain was left in place for 5.1 ± 4.3 days. Comparison of the success rate of talc slurry (38/49 and 38/41) and thoracoscopic talc powder insufflation pleurodesis (17/22 and 17/21), showed a non-significant difference (p=0.979 and p=0.167, respectively). Repeated talc slurry pleurodesis was successful in 55% (6/11) of the patients. During thoracoscopy we did not perform pleurodesis with talc insufflation in 12 patients, but 2-4 days after thoracoscopy we performed talc slurry pleurodesis through the drain because of abundant exudation (greater than 100 ml per day). These patients were included into the group of talc slurry pleurodesis. In 2 of them, pleurodesis was not successful. Two breast cancer patients had bilateral pleural fluid. In one of them, talc slurry pleurodesis was performed bilaterally. Her pleural effusions dropped to less than 50% of the initial amount, so the patient did not need additional therapeutic thoracocentesis. However, she became hypoxemic and needed long-term oxygen therapy. The second patient had talc slurry pleurodesis performed on the right side and therapeutic thoracocentesis performed on the left side. She also had carcinomatous pericarditis and died within the first month after pleurodesis. After talc slurry pleurodesis complications were observed in 41% (20/49) of the patients: pain (7), fever (6), pneumothorax (3), pleural empyema (2), subcutaneous emphysema (1), and confusion (1). Complications of thoracoscopic pleurodesis were observed in 73% (16/22) of the patients: pain (5), fever (4), pneumothorax (3), subcutaneous emphysema (1), pulmonary oedema (1), pleural empyema (1), and hypotension with respiratory insufficiency (1). Complications were significantly more frequent in the group with thoracoscopic pleurodesis (p=0.013). Discussion The success rate of pleurodesis in our group of patients is comparable to the success of pleurodesis observed in our patients performed in earlier years when thoracoscopic pleurodesis with talc insufflation was the only method used [10,11]. According to data from the literature, talc slurry pleurodesis is as efficient as thoracoscopic talc insufflation [12]. In a randomised study, researchers observed a lower success rate of talc slurry instillation relative to talc powder insufflation [13]. Results of another randomised study [6] and our present study do not support these findings. We did not randomly place patients into talc slurry and thoracoscopic pleurodesis groups. We selected patients with known diagnosis of malignant pleural disease for talc slurry pleurodesis and patients with suspicion for malignant pleural disease for thoracoscopy. The malignant infiltration of the pleura was more extensive in patients with known diagnosis in the talc slurry group relative to patients with 3 negative cytological examinations of pleural effusion in the thoracoscopic group. This could explain why more patients died in the first month in the talc slurry group. Shorter survival and lower success rates of pleurodesis can be expected in patients with more extensive malignant pleural infiltration. The other explanation could be that in the talc insufflation group more patients had mesotheliomas. The median survival of mesothelioma patients is more favorable (6 months) than patients with pleural carcinomatosis (2.3-5 months, depending on the origin of malignancy) [14]. It seems that the decision for pleurodesis should be made early, when the pleural effusion is not loculated and the pleura is not thickened because of inflammation or malignant tissue, which subsequently prevents the appropriate re-expansion of the lung, resulting in a trapped lung. Although we wanted to select patients with an expected survival of 2-3 months, 9 patients died in the first month because of malignant disease. It is obvious that it is difficult to predict prognosis in a group of very frail patients with malignant infiltration of the pleura. The Consensus Statement of the American Thoracic Society and European Respiratory Society [15] defines pleurodesis as successful when it relieves dyspnea due to pleural effusion and when the fluid does not
5 467 re-accumulate until the patient s death. Success should be evaluated with and without the inclusion of patients who die within the first month after pleurodesis. It is possible that in the non-dyspneic patient who does not experience pleural fluid re-accumulation, success can be of short duration because of early death of the patient. We think that the time interval without dyspnea, without therapeutic thoracocentesis and without pleural fluid re-accumulation should be defined. Similar to other authors, we delineated an one-month interval [6,16]. Complications in our patients were similar with those described by other authors. Complications were more frequent in the group with thoracoscopic talc pleurodesis, possibly because pain, fever, pneumothorax and subcutaneous emphysema are additional complications of thoracoscopy itself and not a consequence of pleurodesis. We never observed acute respiratory distress, as some other authors did [17]. This complication is supposedly connected with advanced malignant disease, chronic obstructive lung disease, great quantity of applied talc, the use of non-sterile talc, talc with small particles or pleural abrasion or numerous thoracoscopic pleural biopsies [18]. To prevent the possibility of acute respiratory distress, we used sterile Lusenac talc, with large particles (> 30 microns) and we never used more than 10 g of talc. Nine of our patients who died in the first month had advanced malignant disease and 34 patients had 11 pleural forceps biopsies and none of them had acute respiratory distress. Our observation does not support advanced malignant disease or numerous thoracoscopic pleural biopsies as the etiology of acute respiratory distress after talc pleurodesis. In conclusion, talc pleurodesis is a successful procedure in patients with abundant malignant pleural effusion. Pleurodesis with thoracoscopic talc insufflation has a similar success rate as pleurodesis with talc slurry instillation. Thoracoscopic insufflation of talc under direct optical control is the best diagnostic and therapeutic method in patients with suspicious massive malignant pleural effusions or without a definitive diagnosis. In patients with known malignant infiltration of the pleura, talc slurry instillation can be applied. Serious complications are rare. Patients selected for pleurodesis should be in relatively good general condition with an expected survival duration greater than 2-3 months. References 1. Sahn SA. Malignancy metastatic to the pleura. Clin Chest Med 1998; 19: Sahn SS. Malignant pleural effusion. In: Bouros D (ed): Pleural disease: Lung biology in health and disease. Marcel Dekker, New York, Basel, 2004, Vol 186, pp Rodriguez-Panadero F. Pleurodesis. In: Bouros D (ed): Pleural disease: Lung biology in health and disease. Marcel Dekker, New York, Basel, 2004, Vol 186, pp Genc O, Petrou P, Ladas G, Goldstraw P. The long term morbidity of pleuro-peritoneal shunts in the management of recurrent malignant effusions. Eur J Cardio-thorac Surg 2000; 18: Walker-Renard PB, Vaughan LM, Sahn SA. Chemical pleurodesis for malignant plural effusions. Ann Intern Med 1994; 120: Dresler CM, Olak J, Herndon JE. Phase III intergroup study of talc poudrage vs. talc slurry sclerosis for malignant pleural effusion. Chest 2005; 127: Bernard A, Bernard de Dompsure R, Hagry O, Favre JP. Early and late mortality after pleurodesis for malignant pleural effusion. Ann Thorac Surg 2002; 74: van den Toorn LM, Schaap E, Surmont VFM, Pouw EM, van Rijt KCD, van Klaveren RJ. Management of recurrent malignant pleural effusions with chronic indwelling pleural catheter. Lung Cancer 2005; 50: Musani AI, Haas AR, Seijo L, Wilby M, Sterman DH. Outpatient management of malignant pleural effusions with small-bore tunneled pleural catheters. Respiration 2004; 71: Turel M, Debeljak A, Kecelj P: Thoracoscopic talc pleurodesis for malignant pleural effusion. Endoscopic Rev 1998; 3: Debeljak A, Kecelj P, Kern I, Vidmar S, Rott T. Medical thoracoscopy: Experience with 212 patients. J BUON 2000; 5: Yim AP, Chan AT, Lee TW, Wan IY, Ho JK. Thoracoscopic talc insufflation versus talc slurry for symptomatic malignant pleural effusions. Ann Thorac Surg 1996; 62: Maρes N, Rodriguez-Panadero F, Bravo JL, Hernandez H, Alix A. Talc pleurodesis: prospective and randomised study. Clinical follow up. Chest 2000; 118, 4 (Suppl): 131S. 14. Heffner JE, Nietert PJ, Barbieri C. Pleural fluid ph as a predictor of survival of patients with malignant pleural effusions. Chest 2000; 117: Antony VB, Loddenkemper R, Astoul P et al. Management of malignant pleural effusions. Am J Respir Crit Care Med 2000; 162: Sarikos G, Baka S, Galaktidou G, Valla V, Kortsaris AH. Intrapleural interferon-γ administration in the treatment of malignant pleural effusions. J BUON 2001; 6: Rehse DH, Aye RW, Florence MG. Respiratory failure following talc pleurodesis. Am J Surg 1999; 177: Bouros D, Froudarakis M, Siafakas NM. Pleurodesis: everything flows. Chest 2000; 118:
A comparison between two types of indwelling pleural catheters for management of malignant pleural effusions
 Original Article A comparison between two types of indwelling pleural catheters for management of malignant pleural effusions Sushilkumar Satish Gupta 1, Charalampos S. Floudas 2, Abhinav B. Chandra 3
Original Article A comparison between two types of indwelling pleural catheters for management of malignant pleural effusions Sushilkumar Satish Gupta 1, Charalampos S. Floudas 2, Abhinav B. Chandra 3
Medical Thoracoscopy When to Choose Over a General Anaesthetic VATS
 Medical Thoracoscopy When to Choose Over a General Anaesthetic VATS SpR Training Day 07.07.14 Dr Alex West Consultant Chest/Pleural Physician Guy s and St Thomas Hospital Medical Thoracoscopy? No Just
Medical Thoracoscopy When to Choose Over a General Anaesthetic VATS SpR Training Day 07.07.14 Dr Alex West Consultant Chest/Pleural Physician Guy s and St Thomas Hospital Medical Thoracoscopy? No Just
APPROACH TO PLEURAL EFFUSIONS. Raed Alalawi, MD, FCCP
 APPROACH TO PLEURAL EFFUSIONS Raed Alalawi, MD, FCCP CASE 65-year-old woman with H/O breast cancer presented with a 1 week H/O progressively worsening exersional dyspnea. Physical exam: Diminished breath
APPROACH TO PLEURAL EFFUSIONS Raed Alalawi, MD, FCCP CASE 65-year-old woman with H/O breast cancer presented with a 1 week H/O progressively worsening exersional dyspnea. Physical exam: Diminished breath
Rapid pleurodesis is an outpatient alternative in patients with malignant pleural effusions: a prospective randomized controlled trial
 Original Article Rapid pleurodesis is an outpatient alternative in patients with malignant pleural effusions: a prospective randomized controlled trial Serkan Özkul, Akif Turna, Ahmet Demirkaya, Burcu
Original Article Rapid pleurodesis is an outpatient alternative in patients with malignant pleural effusions: a prospective randomized controlled trial Serkan Özkul, Akif Turna, Ahmet Demirkaya, Burcu
10th European Congress Perspectives in Lung Cancer Brussels March 6-7, Speaker Information and Disclosure
 10th European Congress Perspectives in Lung Cancer Brussels March 6-7, 2009 Speaker Information and Disclosure 10th European Congress Perspectives in Lung Cancer Brussels March 6-7, 2009 Management of
10th European Congress Perspectives in Lung Cancer Brussels March 6-7, 2009 Speaker Information and Disclosure 10th European Congress Perspectives in Lung Cancer Brussels March 6-7, 2009 Management of
Chapter 8. Other Important Tests and Procedures. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 8 Other Important Tests and Procedures 1 Introduction Additional important diagnostic studies include: Sputum examination Skin tests Endoscopic examination Lung biopsy Thoracentesis Hematology,
Chapter 8 Other Important Tests and Procedures 1 Introduction Additional important diagnostic studies include: Sputum examination Skin tests Endoscopic examination Lung biopsy Thoracentesis Hematology,
Journal of American Science 2014;10(4)
 Povidone-iodine Pleurodesis versus Talc Pleurodesis in Preventing Recurrence of Malignant Pleural Effusion Islam M. Ibrahim (MD) 1 ; Mohammed F. Eltaweel (MBBCh) 1 ; Alaa A. El-Sessy (MD) 2 and Ahmed L.
Povidone-iodine Pleurodesis versus Talc Pleurodesis in Preventing Recurrence of Malignant Pleural Effusion Islam M. Ibrahim (MD) 1 ; Mohammed F. Eltaweel (MBBCh) 1 ; Alaa A. El-Sessy (MD) 2 and Ahmed L.
Povidone-iodine pleurodesis versus talc pleurodesis in preventing recurrence of malignant pleural effusion
 Ibrahim et al. Journal of Cardiothoracic Surgery (2015) 10:64 DOI 10.1186/s13019-015-0270-5 RESEARCH ARTICLE Open Access Povidone-iodine pleurodesis versus talc pleurodesis in preventing recurrence of
Ibrahim et al. Journal of Cardiothoracic Surgery (2015) 10:64 DOI 10.1186/s13019-015-0270-5 RESEARCH ARTICLE Open Access Povidone-iodine pleurodesis versus talc pleurodesis in preventing recurrence of
The Portsmouth thoracoscopy experience, an evaluation of service by retrospective case note analysis
 Respiratory Medicine (2007) 101, 1021 1025 The Portsmouth thoracoscopy experience, an evaluation of service by retrospective case note analysis Sophie V. Fletcher,1, Robin J. Clark Respiratory Centre,
Respiratory Medicine (2007) 101, 1021 1025 The Portsmouth thoracoscopy experience, an evaluation of service by retrospective case note analysis Sophie V. Fletcher,1, Robin J. Clark Respiratory Centre,
EFFECTIVENESS OF TALC SLURRY IN PRODUCING PLEURODESIS: A STUDY IN RABBITS
 Trakia Journal of Sciences, Vol. 5, No. 3-4, pp 7-11, 2007 Copyright 2007 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution EFFECTIVENESS OF TALC SLURRY IN
Trakia Journal of Sciences, Vol. 5, No. 3-4, pp 7-11, 2007 Copyright 2007 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution EFFECTIVENESS OF TALC SLURRY IN
Some clinical conditions such as congestive heart failure, cirrhosis, acute. Bleomycin in the treatment of 50 cases with malignant pleural effusion
 Original Article Bleomycin in the treatment of 5 cases with malignant pleural effusion Novin Nikbakhsh (MD) *1 Ali Pourhasan Amiri (MD) 2 Danial Hoseinzadeh (MD) 3 1- Department of Surgery, Babol University
Original Article Bleomycin in the treatment of 5 cases with malignant pleural effusion Novin Nikbakhsh (MD) *1 Ali Pourhasan Amiri (MD) 2 Danial Hoseinzadeh (MD) 3 1- Department of Surgery, Babol University
Malignant Effusions. Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital
 Malignant Effusions Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital Malignant Effusions Definition: Presence of malignant cells in the pleural space 75% are caused by
Malignant Effusions Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital Malignant Effusions Definition: Presence of malignant cells in the pleural space 75% are caused by
The diagnosis and management of pneumothorax
 Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Indwelling Pleural Catheters in Malignant and Non-Malignant Disease
 Indwelling Catheters in Malignant and Non-Malignant Disease 20th Hellenic Conference November 2011 Najib Rahman Clinical Lecturer Oxford Centre for Respiratory Medicine University of Oxford, UK Najib.rahman@ndm.ox.ac.uk
Indwelling Catheters in Malignant and Non-Malignant Disease 20th Hellenic Conference November 2011 Najib Rahman Clinical Lecturer Oxford Centre for Respiratory Medicine University of Oxford, UK Najib.rahman@ndm.ox.ac.uk
Management of Pleural Effusion
 Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
Talc poudrage versus talc slurry in the treatment of malignant pleural effusion. A prospective comparative study
 European Journal of Cardio-thoracic Surgery 30 (2006) 827 832 www.elsevier.com/locate/ejcts Talc poudrage versus talc slurry in the treatment of malignant pleural effusion. A prospective comparative study
European Journal of Cardio-thoracic Surgery 30 (2006) 827 832 www.elsevier.com/locate/ejcts Talc poudrage versus talc slurry in the treatment of malignant pleural effusion. A prospective comparative study
Pleural Effusion. Exudative pleural effusion - Involve an increase in capillary permeability and impaired pleural fluid resorption
 Pleural Effusion Definition of pleural effusion Accumulation of fluid between the pleural layers Epidemiology of pleural effusion Estimated prevalence of pleural effusion is 320 cases per 100,000 people
Pleural Effusion Definition of pleural effusion Accumulation of fluid between the pleural layers Epidemiology of pleural effusion Estimated prevalence of pleural effusion is 320 cases per 100,000 people
Long term results of pleurodesis in malignant pleural effusions: Doxycycline vs Bleomycin
 Original Article Long term results of pleurodesis in malignant pleural effusions: Doxycycline vs Bleomycin Rahmatollah Rafiei, Behnam Yazdani, Sayed Milad Ranjbar, Zahra Torabi, Sedigheh Asgary 1, Somayeh
Original Article Long term results of pleurodesis in malignant pleural effusions: Doxycycline vs Bleomycin Rahmatollah Rafiei, Behnam Yazdani, Sayed Milad Ranjbar, Zahra Torabi, Sedigheh Asgary 1, Somayeh
Alper Toker, MD. VATS decortication. Istanbul University, Istanbul Medical School Department of Thoracic Surgery
 VATS decortication Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery Pleural space infection is a common pathology causing morbidity and mortality. It is a collection
VATS decortication Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery Pleural space infection is a common pathology causing morbidity and mortality. It is a collection
Supplementary Online Content
 Supplementary Online Content Rahman NM, Pepperell J, Rehal S, et al. Effect of opioids vs NSAIDs and larger vs smaller chest tube size on pain control and pleurodesis efficacy among patients with malignant
Supplementary Online Content Rahman NM, Pepperell J, Rehal S, et al. Effect of opioids vs NSAIDs and larger vs smaller chest tube size on pain control and pleurodesis efficacy among patients with malignant
Management of malignant pleural effusions
 Eur Respir J 2001; 18: 402 419 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 ERS ATS STATEMENT Management of malignant pleural effusions
Eur Respir J 2001; 18: 402 419 Printed in UK all rights reserved Copyright #ERS Journals Ltd 2001 European Respiratory Journal ISSN 0903-1936 ERS ATS STATEMENT Management of malignant pleural effusions
Pneumothorax and Chest Tube Problems
 Pneumothorax and Chest Tube Problems Pneumothorax Definition Air accumulation in the pleural space with secondary lung collapse Sources Visceral pleura Ruptured esophagus Chest wall defect Gas-forming
Pneumothorax and Chest Tube Problems Pneumothorax Definition Air accumulation in the pleural space with secondary lung collapse Sources Visceral pleura Ruptured esophagus Chest wall defect Gas-forming
Study of Predictors for Successful Pleurodesis in Patients with Malignant Pleural Effusion
 Med. J. Cairo Univ., Vol. 85, No. 1, March: 11-20, 2017 www.medicaljournalofcairouniversity.net Study of Predictors for Successful Pleurodesis in Patients with Malignant Pleural Effusion TALAT A. ARAFA,
Med. J. Cairo Univ., Vol. 85, No. 1, March: 11-20, 2017 www.medicaljournalofcairouniversity.net Study of Predictors for Successful Pleurodesis in Patients with Malignant Pleural Effusion TALAT A. ARAFA,
EVIDENCE THAT MESOTHELIAL CELLS MAY REGULATE THE ACUTE INFLAMMATORY RESPONSE IN TALC PLEURODESIS
 ERJ Express. Published on July 26, 2006 as doi: 10.1183/09031936.06.00037906 EVIDENCE THAT MESOTHELIAL CELLS MAY REGULATE THE ACUTE INFLAMMATORY RESPONSE IN TALC PLEURODESIS Marchi E, MD; Vargas FS, MD;
ERJ Express. Published on July 26, 2006 as doi: 10.1183/09031936.06.00037906 EVIDENCE THAT MESOTHELIAL CELLS MAY REGULATE THE ACUTE INFLAMMATORY RESPONSE IN TALC PLEURODESIS Marchi E, MD; Vargas FS, MD;
Pleural fluid glucose: A predictor of unsuccessful pleurodesis in a preselected cohort of patients with malignant pleural effusion
 JBUON 2014; 19(4): 1018-1023 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Pleural fluid glucose: A predictor of unsuccessful pleurodesis in
JBUON 2014; 19(4): 1018-1023 ISSN: 1107-0625, online ISSN: 2241-6293 www.jbuon.com E-mail: editorial_office@jbuon.com ORIGINAL ARTICLE Pleural fluid glucose: A predictor of unsuccessful pleurodesis in
CHEST DRAIN PROTOCOL
 CHEST DRAIN PROTOCOL Rationale The pleural membranes have an important role in effective lung expansion. The visceral pleura is a thin, smooth, serous membrane covering the surface of the lungs and is
CHEST DRAIN PROTOCOL Rationale The pleural membranes have an important role in effective lung expansion. The visceral pleura is a thin, smooth, serous membrane covering the surface of the lungs and is
Malignant pleural effusion (MPE) is frequently encountered
 ORIGINAL ARTICLE Thoracoscopic Assessment of Pleural Tumor Burden in Patients with Malignant Pleural Effusion Prognostic and Therapeutic Implications Lama Sakr, MD,* Fabien Maldonado, MD, Laurent Greillier,
ORIGINAL ARTICLE Thoracoscopic Assessment of Pleural Tumor Burden in Patients with Malignant Pleural Effusion Prognostic and Therapeutic Implications Lama Sakr, MD,* Fabien Maldonado, MD, Laurent Greillier,
Tunneled pleural catheters for management of malignant pleural effusions: a 2-year review of outcomes at a high-volume center
 Original Article Page 1 of 8 Tunneled pleural catheters for management of malignant pleural effusions: a 2-year review of outcomes at a high-volume center Amit K. Mahajan 1,2, Devon T. Collins 1, Christiana
Original Article Page 1 of 8 Tunneled pleural catheters for management of malignant pleural effusions: a 2-year review of outcomes at a high-volume center Amit K. Mahajan 1,2, Devon T. Collins 1, Christiana
Louis Saffran, MD; David E. Ost, MD, FCCP; Alan M. Fein, MD, FCCP; and Mark J. Schiff, MD
 Outpatient Pleurodesis of Malignant Pleural Effusions Using a Small-Bore Pigtail Catheter* Louis Saffran, MD; David E. Ost, MD, FCCP; Alan M. Fein, MD, FCCP; and Mark J. Schiff, MD Study objective: Patients
Outpatient Pleurodesis of Malignant Pleural Effusions Using a Small-Bore Pigtail Catheter* Louis Saffran, MD; David E. Ost, MD, FCCP; Alan M. Fein, MD, FCCP; and Mark J. Schiff, MD Study objective: Patients
Department of Thoracic Surgery, Dr. Carol Davila Central Emergency University Military Hospital Bucharest, Romania b
 Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Minimally Invasive Surgical Treatment of Malignant Pleural Effusions Adrian CIUCHE, MD a ; Claudiu NISTOR, PhD a ; Daniel PANTILE, MR a ; Prof. Teodor
Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Minimally Invasive Surgical Treatment of Malignant Pleural Effusions Adrian CIUCHE, MD a ; Claudiu NISTOR, PhD a ; Daniel PANTILE, MR a ; Prof. Teodor
Manejo Práctico del Derrame Pleural
 Manejo Práctico del Derrame Pleural San José, Costa Rica Junio 29, 2017 Rodrigo Cartín Ceba, MD, MSc Consultant, Pulmonary and Critical Care Medicine Associate Professor of Medicine Mayo Clinic 2010 MFMER
Manejo Práctico del Derrame Pleural San José, Costa Rica Junio 29, 2017 Rodrigo Cartín Ceba, MD, MSc Consultant, Pulmonary and Critical Care Medicine Associate Professor of Medicine Mayo Clinic 2010 MFMER
EMPYEMA. Catheter Based Treatment vs. VATS. UCHSC Department of Surgery Grand Rounds August 27 th, Jeremy Hedges, M.D.
 EMPYEMA Catheter Based Treatment vs. VATS UCHSC Department of Surgery Grand Rounds August 27 th, 2007 Jeremy Hedges, M.D. OVERVIEW Empyema Pathogenesis Treatment Catheter based treatment Fibrinolytics
EMPYEMA Catheter Based Treatment vs. VATS UCHSC Department of Surgery Grand Rounds August 27 th, 2007 Jeremy Hedges, M.D. OVERVIEW Empyema Pathogenesis Treatment Catheter based treatment Fibrinolytics
Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20,
 Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20, 521-525 Empyema thoracis Original Article Singh DR 1, Joshi MR 2, Thapa P 2, Nath S 3 1 Assistant Professor, 2 Lecturer, 3 Professor,
Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20, 521-525 Empyema thoracis Original Article Singh DR 1, Joshi MR 2, Thapa P 2, Nath S 3 1 Assistant Professor, 2 Lecturer, 3 Professor,
Diagnostic and Prognostic Implications of Pleural Adhesions in Malignant Effusions
 ORIGINAL ARTICLE Diagnostic and Prognostic Implications of Pleural Adhesions in Malignant Effusions Silvia Bielsa, MD,* José Martín-Juan, MD, José M. Porcel, MD,* and Francisco Rodríguez-Panadero, MD Background
ORIGINAL ARTICLE Diagnostic and Prognostic Implications of Pleural Adhesions in Malignant Effusions Silvia Bielsa, MD,* José Martín-Juan, MD, José M. Porcel, MD,* and Francisco Rodríguez-Panadero, MD Background
CHRONIC PLEURAL CHANGES AFTER INTRAPLEURAL INSTILLATION OF IODPOVIDONE EXPERIMENTAL STUDY IN RABBITS
 Trakia Journal of Sciences, Vol. 9, No 1, pp 17-23, 2011 Copyright 2011 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) ISSN 1313-3551 (online) Original Contribution
Trakia Journal of Sciences, Vol. 9, No 1, pp 17-23, 2011 Copyright 2011 Trakia University Available online at: http://www.uni-sz.bg ISSN 1313-7050 (print) ISSN 1313-3551 (online) Original Contribution
Diagnostic Approach to Pleural Effusion
 Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
Diagnostic Approach to Pleural Effusion Objectives Define the leading causes of pleural effusion Classify the type of effusion Identify procedures and tests associated with diagnosis 2 Agenda Basic anatomy
Table 2: Outcomes measured. Table 1: Intrapleural alteplase instillation therapy protocol
 ORIGINAL RESEARCH ARTICLE Intrapleural F brinolytic Therapy with Alteplase in Empyema Thoracis in Children conducted in the Department of Pediatric critical care and Pulmonology unit at our institution
ORIGINAL RESEARCH ARTICLE Intrapleural F brinolytic Therapy with Alteplase in Empyema Thoracis in Children conducted in the Department of Pediatric critical care and Pulmonology unit at our institution
ASEPT -System ASEPT Pleural/Peritoneal. ASEPT Drainage Kits (600 ml + 1,200 ml) Accessories. Quality and Experience
 Quality and Experience ASEPT -System ASEPT Pleural/Peritoneal Drainage System ASEPT Drainage Kits (600 ml + 1,200 ml) Accessories Recurring pleural effusions or malignant ascites can be treated on an outpatient
Quality and Experience ASEPT -System ASEPT Pleural/Peritoneal Drainage System ASEPT Drainage Kits (600 ml + 1,200 ml) Accessories Recurring pleural effusions or malignant ascites can be treated on an outpatient
Aspiration versus tube drainage in primary spontaneous pneumothorax: a randomised study
 Eur Respir J 2006; 27: 477 482 DOI: 10.1183/09031936.06.00091505 CopyrightßERS Journals Ltd 2006 CLINICAL FORUM Aspiration versus tube drainage in primary spontaneous pneumothorax: a randomised study A.K.
Eur Respir J 2006; 27: 477 482 DOI: 10.1183/09031936.06.00091505 CopyrightßERS Journals Ltd 2006 CLINICAL FORUM Aspiration versus tube drainage in primary spontaneous pneumothorax: a randomised study A.K.
Video-assisted thoracoscopic PlasmaJet ablation for malignant pleural mesothelioma
 Case Report on Thoracic Surgery Page 1 of 5 Video-assisted thoracoscopic PlasmaJet ablation for malignant pleural mesothelioma Periklis Perikleous, Nizar Asadi, Vladimir Anikin Department of Thoracic Surgery,
Case Report on Thoracic Surgery Page 1 of 5 Video-assisted thoracoscopic PlasmaJet ablation for malignant pleural mesothelioma Periklis Perikleous, Nizar Asadi, Vladimir Anikin Department of Thoracic Surgery,
laboratory and animal investigations Distribution of Calibrated Talc After Intrapleural Administration*
 laboratory and animal investigations Distribution of Calibrated Talc After Intrapleural Administration* An Experimental Study in Rats Anne Fraticelli, MD; Andrée Robaglia-Schlupp, MD; Helene Riera, BS;
laboratory and animal investigations Distribution of Calibrated Talc After Intrapleural Administration* An Experimental Study in Rats Anne Fraticelli, MD; Andrée Robaglia-Schlupp, MD; Helene Riera, BS;
To Drain or Not to Drain: An Evidence-Based Approach to Palliative Procedures for the Management of Malignant Pleural Effusions
 Vol. 44 No. 2 August 2012 Journal of Pain and Symptom Management 301 Palliative Care Rounds Edited by Erik K. Fromme, MD, and Robert M. Arnold, MD, on behalf of Society of General Internal Medicine End-of-Life
Vol. 44 No. 2 August 2012 Journal of Pain and Symptom Management 301 Palliative Care Rounds Edited by Erik K. Fromme, MD, and Robert M. Arnold, MD, on behalf of Society of General Internal Medicine End-of-Life
Pancreatic Cancer And Malignant Pleural Effusion. N Barbetakis, M Krikeli, M Vassiliadis, N Lyratzopoulos, A Efstathiou, C Tsilikas
 ISPUB.COM The Internet Journal of Surgery Volume 6 Number 2 Pancreatic Cancer And Malignant Pleural Effusion N Barbetakis, M Krikeli, M Vassiliadis, N Lyratzopoulos, A Efstathiou, C Tsilikas Citation N
ISPUB.COM The Internet Journal of Surgery Volume 6 Number 2 Pancreatic Cancer And Malignant Pleural Effusion N Barbetakis, M Krikeli, M Vassiliadis, N Lyratzopoulos, A Efstathiou, C Tsilikas Citation N
Clinical Study Safety and Complications of Medical Thoracoscopy
 Advances in Medicine Volume 2016, Article ID 3794791, 6 pages http://dx.doi.org/10.1155/2016/3794791 Clinical Study Safety and Complications of Medical Thoracoscopy Shimaa Nour Moursi Ahmed, 1,2 Hideo
Advances in Medicine Volume 2016, Article ID 3794791, 6 pages http://dx.doi.org/10.1155/2016/3794791 Clinical Study Safety and Complications of Medical Thoracoscopy Shimaa Nour Moursi Ahmed, 1,2 Hideo
ASEPT. Pleural Drainage System INSTRUCTIONS FOR USE REF LOT STERILE EO. Manufactured for: 824 Twelfth Avenue Bethlehem, PA
 ASEPT Pleural Drainage System LS-00116-01-AB 017-11 INSTRUCTIONS FOR USE Do not reuse STERILIZE Do not resterilize 30 C Rx only 15 C REF Store at controlled room temperature 15-30 C (59-86 F) Keep away
ASEPT Pleural Drainage System LS-00116-01-AB 017-11 INSTRUCTIONS FOR USE Do not reuse STERILIZE Do not resterilize 30 C Rx only 15 C REF Store at controlled room temperature 15-30 C (59-86 F) Keep away
Easwaramangalath Venugopal Krishnakumar*, Muhammed Anas, Davis Kizhakkepeedika Rennis, Vadakken Devassy Thomas, Babu Vinod
 International Journal of Research in Medical Sciences Krishnakumar EV et al. Int J Res Med Sci. 2015 Nov;3(11):3177-3181 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20151158
International Journal of Research in Medical Sciences Krishnakumar EV et al. Int J Res Med Sci. 2015 Nov;3(11):3177-3181 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20151158
Review Article. Pleurodesis: technique and indications*
 Pleurodesis: technique and indications 347 Review Article Pleurodesis: technique and indications* MARCELO COSTA VAZ 1, EVALDO MARCHI 2, FRANCISCO SUSO VARGAS 3 ABSTRACT Recurrent pleural effusion, which
Pleurodesis: technique and indications 347 Review Article Pleurodesis: technique and indications* MARCELO COSTA VAZ 1, EVALDO MARCHI 2, FRANCISCO SUSO VARGAS 3 ABSTRACT Recurrent pleural effusion, which
ASEPT. Pleural Drainage System INSTRUCTIONS FOR USE. Rx only REF LOT. STERILE EO Sterilized using ethylene oxide
 ASEPT Pleural Drainage System INSTRUCTIONS FOR USE L1171/D REV 2014-02 2 Do not reuse 2 STERILIZE Do not resterilize Store at room temperature STERILE EO Sterilized using ethylene oxide Rx only Do not
ASEPT Pleural Drainage System INSTRUCTIONS FOR USE L1171/D REV 2014-02 2 Do not reuse 2 STERILIZE Do not resterilize Store at room temperature STERILE EO Sterilized using ethylene oxide Rx only Do not
Pneumothorax lecture no. 3
 Pneumothorax lecture no. 3 Is accumulation of air in a pleural space or accumulation of extra pulmonary air within the chest, Is uncommon during childhood, may result from external trauma, iatrogenic,
Pneumothorax lecture no. 3 Is accumulation of air in a pleural space or accumulation of extra pulmonary air within the chest, Is uncommon during childhood, may result from external trauma, iatrogenic,
Thoracoscopic Talc Versus Tunneled Pleural Catheters for Palliation of Malignant Pleural Effusions
 ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
Pneumothorax. Defined as air in the pleural space which can occur through a number of mechanisms
 Pneumothorax Defined as air in the pleural space which can occur through a number of mechanisms Traumatic pneumothorax Penetrating chest trauma Common secondary to bullet or knife penetration Chest tube
Pneumothorax Defined as air in the pleural space which can occur through a number of mechanisms Traumatic pneumothorax Penetrating chest trauma Common secondary to bullet or knife penetration Chest tube
In patients with solid organ cancers, malignant pleural effusion
 ORIGINAL ARTICLE Palliation and Pleurodesis in Malignant Pleural Effusion The Role for Tunneled Pleural Catheters Kei Suzuki, MD,* Elliot L. Servais, MD,* Nabil P. Rizk, MD, FACS,* Stephen B. Solomon,
ORIGINAL ARTICLE Palliation and Pleurodesis in Malignant Pleural Effusion The Role for Tunneled Pleural Catheters Kei Suzuki, MD,* Elliot L. Servais, MD,* Nabil P. Rizk, MD, FACS,* Stephen B. Solomon,
Clinical Study The Effect of Silver Nitrate Pleurodesis after a Failed Thoracoscopic Talc Poudrage
 Hindawi Publishing Corporation BioMed Research International Volume 2013, Article ID 295890, 5 pages http://dx.doi.org/10.1155/2013/295890 Clinical Study The Effect of Silver Nitrate Pleurodesis after
Hindawi Publishing Corporation BioMed Research International Volume 2013, Article ID 295890, 5 pages http://dx.doi.org/10.1155/2013/295890 Clinical Study The Effect of Silver Nitrate Pleurodesis after
Treatment of recurrent malignant pleural effusion by iodized talc pleurodesis1
 Treatment of recurrent malignant pleural effusion by iodized talc pleurodesis1 GLYNNE R. JONES rom Sully Hospital (Thoracic Centre), Penarth, Glamorgan Thorax (1969), 24, 69. Chemical pleurodesis using
Treatment of recurrent malignant pleural effusion by iodized talc pleurodesis1 GLYNNE R. JONES rom Sully Hospital (Thoracic Centre), Penarth, Glamorgan Thorax (1969), 24, 69. Chemical pleurodesis using
Pleural Fluid Analysis: Back to Basics
 Pleural Fluid Analysis: Back to Basics Tonya L. Page, MSN, RN, ACNP-BC Patrick A. Laird, DNP, RN, ACNP-BC 70 y/o female with complaints of shortness of breath and orthopnea for 1 month. Symptoms have worsened
Pleural Fluid Analysis: Back to Basics Tonya L. Page, MSN, RN, ACNP-BC Patrick A. Laird, DNP, RN, ACNP-BC 70 y/o female with complaints of shortness of breath and orthopnea for 1 month. Symptoms have worsened
Post-Graduate ERS Seminar on Medical Thoracoscopy. October 13-15, Alexandroupolis, Greece
 Post-Graduate ERS Seminar on Medical Thoracoscopy October 13-15, 2011 - Alexandroupolis, Greece Invited speakers Subjects Robert Loddenkemper, Berlin, Germany YC Gary Lee, Perth Australia Wolfgang Frank,
Post-Graduate ERS Seminar on Medical Thoracoscopy October 13-15, 2011 - Alexandroupolis, Greece Invited speakers Subjects Robert Loddenkemper, Berlin, Germany YC Gary Lee, Perth Australia Wolfgang Frank,
WHAT WE NEED FOR THORACOSCOPY
 WHAT WE NEED FOR THORACOSCOPY Medical School Marios Froudarakis, MD Department of Pneumonology University Hospital of Alexandroupolis mfroud@med.duth.gr Democritus University of Thrace Dedicated Course
WHAT WE NEED FOR THORACOSCOPY Medical School Marios Froudarakis, MD Department of Pneumonology University Hospital of Alexandroupolis mfroud@med.duth.gr Democritus University of Thrace Dedicated Course
Original Article. Abstract
 Original Article How VATS has changed the Management of Spontaneous Pneumothorax in the 21st century Saulat Hasnain Fatimi, 1 Hashim Muhammad Hanif, 2 Shahida Aziz, 3 Sana Mansoor, 4 Marium Muzaffar 5
Original Article How VATS has changed the Management of Spontaneous Pneumothorax in the 21st century Saulat Hasnain Fatimi, 1 Hashim Muhammad Hanif, 2 Shahida Aziz, 3 Sana Mansoor, 4 Marium Muzaffar 5
Image: reproduced from Eur Respir Mon 2010; 48: with permission from the publisher.
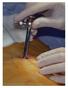 Image: reproduced from Eur Respir Mon 2010; 48: 119 132 with permission from the publisher. R. Loddenkemper 1 P. Lee 2 M. Noppen 3 P.N. Mathur 4 1 German Central Committee against Tuberculosis (DZK), Lungenklinik
Image: reproduced from Eur Respir Mon 2010; 48: 119 132 with permission from the publisher. R. Loddenkemper 1 P. Lee 2 M. Noppen 3 P.N. Mathur 4 1 German Central Committee against Tuberculosis (DZK), Lungenklinik
Routine chest drainage after patent ductus arteriosis ligation is not necessary
 Original Article Brunei Int Med J. 2010; 6 (3): 126-130 Routine chest drainage after patent ductus arteriosis ligation is not necessary Amy THIEN, Samuel Kai San YAPP, Chee Fui CHONG Department of Surgery,
Original Article Brunei Int Med J. 2010; 6 (3): 126-130 Routine chest drainage after patent ductus arteriosis ligation is not necessary Amy THIEN, Samuel Kai San YAPP, Chee Fui CHONG Department of Surgery,
Efficacy of pleurodesis for malignant pleural effusions in breast cancer patients
 Eur Respir J 2011; 38: 1425 1430 DOI: 10.1183/09031936.00171610 CopyrightßERS 2011 Efficacy of pleurodesis for malignant pleural effusions in breast cancer patients T. Hirata*, K. Yonemori*, A. Hirakawa
Eur Respir J 2011; 38: 1425 1430 DOI: 10.1183/09031936.00171610 CopyrightßERS 2011 Efficacy of pleurodesis for malignant pleural effusions in breast cancer patients T. Hirata*, K. Yonemori*, A. Hirakawa
Viscum Album Versus Bleomycin for Pleurodesis among Patients with Malignant Pleural Effusion
 American Journal of Cardiovascular Disease Research, 2014, Vol. 2, No. 2, 17-22 Available online at http://pubs.sciepub.com/ajcdr/2/2/1 Science and Education Publishing DOI:10.12691/ajcdr-2-2-1 Viscum
American Journal of Cardiovascular Disease Research, 2014, Vol. 2, No. 2, 17-22 Available online at http://pubs.sciepub.com/ajcdr/2/2/1 Science and Education Publishing DOI:10.12691/ajcdr-2-2-1 Viscum
DISCOVER NEW HORIZONS IN FLUID DRAINAGE. Bringing Safety and Convenience to Fluid Drainage Management
 DISCOVER NEW HORIZONS IN FLUID DRAINAGE Bringing Safety and Convenience to Fluid Drainage Management DRAIN ASEPT Pleural and Peritoneal Drainage Catheter System 600mL or 1,000mL Evacuated Drainage Bottle
DISCOVER NEW HORIZONS IN FLUID DRAINAGE Bringing Safety and Convenience to Fluid Drainage Management DRAIN ASEPT Pleural and Peritoneal Drainage Catheter System 600mL or 1,000mL Evacuated Drainage Bottle
ASEPT System ASEPT Pleural/Peritoneal. ASEPT Drainage Kits (600 ml ml) Accessories. Quality and Experience
 Quality and Experience ASEPT System ASEPT Pleural/Peritoneal Drainage System ASEPT Drainage Kits (600 ml + 000 ml) Accessories Recurring pleural effusions or malignant ascites can be treated on an outpatient
Quality and Experience ASEPT System ASEPT Pleural/Peritoneal Drainage System ASEPT Drainage Kits (600 ml + 000 ml) Accessories Recurring pleural effusions or malignant ascites can be treated on an outpatient
A prospective, randomised trial of pneumothorax therapy: Manual aspiration versus conventional chest tube drainage
 Respiratory Medicine (2012) 106, 1600e1605 Available online at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed A prospective, randomised trial of pneumothorax therapy: Manual aspiration
Respiratory Medicine (2012) 106, 1600e1605 Available online at www.sciencedirect.com journal homepage: www.elsevier.com/locate/rmed A prospective, randomised trial of pneumothorax therapy: Manual aspiration
ASEPT Pleural Drainage System
 ORDERING INFORMATION ASEPT Drainage PRODUCTS (Provided separately, see package label for contents) ASEPT Pleural Drainage System 622289 (1 each) (includes ASEPT Pleural drainage catheter and insertion
ORDERING INFORMATION ASEPT Drainage PRODUCTS (Provided separately, see package label for contents) ASEPT Pleural Drainage System 622289 (1 each) (includes ASEPT Pleural drainage catheter and insertion
Intrapleural Instillation of Qllinacrjne for Treatment of Recurrent Spontaneous Pneumothorax
 Intrapleural Instillation of Qllinacrjne for Treatment of Recurrent Spontaneous Pneumothorax Alberto J. Larrieu, M.D., G. Frank. Tyers, M.D., Edward H. Williams, M.D., Martin J. O'Neill, M.D., and John
Intrapleural Instillation of Qllinacrjne for Treatment of Recurrent Spontaneous Pneumothorax Alberto J. Larrieu, M.D., G. Frank. Tyers, M.D., Edward H. Williams, M.D., Martin J. O'Neill, M.D., and John
PLEURODESIS IN MALIGNANT PLEURAL EFFUSION WITH SPECIAL EMPHASIS ON TETRACYCLINE AS THE SCLEROSING AGENT
 PLEURODESIS IN MALIGNANT PLEURAL EFFUSION WITH SPECIAL EMPHASIS ON TETRACYCLINE AS THE SCLEROSING AGENT K. Viskum. Department of Pulmonary Medicine. Bispebjerg Hospital. Copenhagen. Denmark. INTRODUCTION
PLEURODESIS IN MALIGNANT PLEURAL EFFUSION WITH SPECIAL EMPHASIS ON TETRACYCLINE AS THE SCLEROSING AGENT K. Viskum. Department of Pulmonary Medicine. Bispebjerg Hospital. Copenhagen. Denmark. INTRODUCTION
Thoracic surgeons are aware that video-assisted thoracic surgery
 General Thoracic Surgery Migliore Efficacy and safety of single-trocar technique for minimally invasive surgery of the chest in the treatment of noncomplex pleural disease Marcello Migliore, MD, PhD, FETCS
General Thoracic Surgery Migliore Efficacy and safety of single-trocar technique for minimally invasive surgery of the chest in the treatment of noncomplex pleural disease Marcello Migliore, MD, PhD, FETCS
BTS GUIDELINES FOR THE MANAGEMENT OF SPONTANEOUS PNEUMOTHRAX 2003
 BTS GUIDELINES FOR THE MANAGEMENT OF SPONTANEOUS PNEUMOTHRAX 2003 GRADING OF PRIMARY LITERATURE(The Bibliographies) Ia Meta-analysis analysis of randomised trials Ib Randomised controlled trial IIa Well
BTS GUIDELINES FOR THE MANAGEMENT OF SPONTANEOUS PNEUMOTHRAX 2003 GRADING OF PRIMARY LITERATURE(The Bibliographies) Ia Meta-analysis analysis of randomised trials Ib Randomised controlled trial IIa Well
Thoracic Surgery; An Overview
 Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
PAKISTAN JOURNAL OF CHEST MEDICINE. Volume 18, No 1, January-March REVIEW ARTICLE MEDICAL PLEUROSCOPY
 82 REVIEW ARTICLE MEDICAL PLEUROSCOPY Pyng Lee MD,* Henri G Colt,**Ali I. Musani MD*** ABSTRACT Pleuroscopy or medical thoracoscopy are terms used interchangeably to describe a minimally invasive procedure
82 REVIEW ARTICLE MEDICAL PLEUROSCOPY Pyng Lee MD,* Henri G Colt,**Ali I. Musani MD*** ABSTRACT Pleuroscopy or medical thoracoscopy are terms used interchangeably to describe a minimally invasive procedure
Pneumothorax has long been listed as one of the
 Pneumothorax in Cystic Fibrosis* Patrick A. Flume, MD, FCCP Spontaneous pneumothorax is a common complication in patients with cystic fibrosis (CF). It is thought to occur more frequently in patients with
Pneumothorax in Cystic Fibrosis* Patrick A. Flume, MD, FCCP Spontaneous pneumothorax is a common complication in patients with cystic fibrosis (CF). It is thought to occur more frequently in patients with
North West London Trauma Network. Management of Chest Drains
 North West London Trauma Network Management of Chest Drains Contents Introduction... 2 What is a chest drain?... 2 Indications for insertion:... 2 Insertion of drain:... 3 Equipment:... 3 Procedure...
North West London Trauma Network Management of Chest Drains Contents Introduction... 2 What is a chest drain?... 2 Indications for insertion:... 2 Insertion of drain:... 3 Equipment:... 3 Procedure...
Prognostic Factors in Patients With Spontaneous
 Diagnostic and Therapeutic Endoscopy, 1995, Vol. 2, pp. 1-5 Reprints available directly from the publisher Photocopying permitted by license only (C) 1995 Harwood Academic Publishers GmbH Printed in Singapore
Diagnostic and Therapeutic Endoscopy, 1995, Vol. 2, pp. 1-5 Reprints available directly from the publisher Photocopying permitted by license only (C) 1995 Harwood Academic Publishers GmbH Printed in Singapore
original article Management of malignant pleural effusions with indwelling pleural catheters or talc pleurodesis
 original article Management of malignant pleural effusions with indwelling pleural catheters or talc pleurodesis Nadim Srour MD MSc 1,2, Kayvan Amjadi MD 1,3, Alan John Forster MD MSc 1,2,3,4,5, Shawn
original article Management of malignant pleural effusions with indwelling pleural catheters or talc pleurodesis Nadim Srour MD MSc 1,2, Kayvan Amjadi MD 1,3, Alan John Forster MD MSc 1,2,3,4,5, Shawn
Management of spontaneous pneumothorax: British Thoracic Society pleural disease guideline 2010
 1 Respiratory Medicine, Royal Infirmary of Edinburgh, UK 2 Department of Respiratory Medicine, Castle Hill Hospital, Cottingham, East Yorkshire, UK 3 North Bristol Lung Centre, Southmead Hospital, Bristol,
1 Respiratory Medicine, Royal Infirmary of Edinburgh, UK 2 Department of Respiratory Medicine, Castle Hill Hospital, Cottingham, East Yorkshire, UK 3 North Bristol Lung Centre, Southmead Hospital, Bristol,
Top Tips for Pleural Disease in 2012
 Top Tips for Pleural Disease in 2012 The unilateral pleural effusion on the Post Take Ward Round Pleural Effusion on CXR Bedside ultrasound + Pleural aspirate Empyema Nil evidence infection Admit IV antibiotics
Top Tips for Pleural Disease in 2012 The unilateral pleural effusion on the Post Take Ward Round Pleural Effusion on CXR Bedside ultrasound + Pleural aspirate Empyema Nil evidence infection Admit IV antibiotics
Trust Guideline for the management of Parapneumonic Effusion in children
 A clinical guideline recommended for use For Use in: By: For: Division responsible for document: Buxton ward, Children s Assessment Unit (CAU) All staff Children with parapneumonic effusion Women and Children
A clinical guideline recommended for use For Use in: By: For: Division responsible for document: Buxton ward, Children s Assessment Unit (CAU) All staff Children with parapneumonic effusion Women and Children
Pleurodesis. What is a pleurodesis?
 2014 Pleurodesis Pleurodesis What is a pleurodesis? Pleurodesis is a procedure which involves a doctor or nurse practitioner putting a special solution in your chest. This solution is placed between the
2014 Pleurodesis Pleurodesis What is a pleurodesis? Pleurodesis is a procedure which involves a doctor or nurse practitioner putting a special solution in your chest. This solution is placed between the
PLEURAL EFFUSION. Prof. G. Zuliani
 PLEURAL EFFUSION Prof. G. Zuliani Anatomy of pleural membrane and pleural space Pleural membrane consists of parietal pleura and visceral pleura A space situated between parietal and visceral pleura is
PLEURAL EFFUSION Prof. G. Zuliani Anatomy of pleural membrane and pleural space Pleural membrane consists of parietal pleura and visceral pleura A space situated between parietal and visceral pleura is
The Imaging Journey of Patients with Malignant Pleural Mesothelioma: Experience of a Tertiary Mesothelioma MDT
 The Imaging Journey of Patients with Malignant Pleural Mesothelioma: Experience of a Tertiary Mesothelioma MDT V. Lam, J. Brozik, A. J. Sharkey, A. Bajaj, D. T. Barnes Glenfield Hospital, Leicester, United
The Imaging Journey of Patients with Malignant Pleural Mesothelioma: Experience of a Tertiary Mesothelioma MDT V. Lam, J. Brozik, A. J. Sharkey, A. Bajaj, D. T. Barnes Glenfield Hospital, Leicester, United
Malignant Pleural Effusion: Medical Approaches for Diagnosis and Management
 REVIEW http://dx.doi.org/10.4046/trd.2014.76.5.211 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;76:211-217 Malignant Pleural Effusion: Medical Approaches for Diagnosis and Management
REVIEW http://dx.doi.org/10.4046/trd.2014.76.5.211 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2014;76:211-217 Malignant Pleural Effusion: Medical Approaches for Diagnosis and Management
F.M.N.H. Schramel*, T.G. Sutedja*, J.C.E. Braber*, J.C. van Mourik**, P.E. Postmus*
 Eur Respir J, 1996, 9, 1821 1825 DOI: 10.1183/09031936.96.09091821 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 0903-1936 Cost-effectiveness of
Eur Respir J, 1996, 9, 1821 1825 DOI: 10.1183/09031936.96.09091821 Printed in UK - all rights reserved Copyright ERS Journals Ltd 1996 European Respiratory Journal ISSN 0903-1936 Cost-effectiveness of
Pleural effusion occurs in up to 89% of patients
 Symptomatic Persistent Post-Coronary Artery Bypass Graft Pleural Effusions Requiring Operative Treatment* Clinical and Histologic Features Y. C. Gary Lee, MBChB; Marcelo A. C. Vaz, MD; Kim A. Ely, MD;
Symptomatic Persistent Post-Coronary Artery Bypass Graft Pleural Effusions Requiring Operative Treatment* Clinical and Histologic Features Y. C. Gary Lee, MBChB; Marcelo A. C. Vaz, MD; Kim A. Ely, MD;
Modern Approaches to Empyema
 Modern Approaches to Empyema Amit Bhargava, MD Attending Thoracic Surgeon Assistant Professor Department of Cardiovascular and Thoracic Surgery 1 Principles of Treatment Adequate drainage Sterilization
Modern Approaches to Empyema Amit Bhargava, MD Attending Thoracic Surgeon Assistant Professor Department of Cardiovascular and Thoracic Surgery 1 Principles of Treatment Adequate drainage Sterilization
Persistent Spontaneous Pneumothorax for Four Years: A Case Report
 303) Persistent Spontaneous Pneumothorax for Four Years: A Case Report Mizuno Y., Iwata H., Shirahashi K., Matsui M., Takemura H. Department of General and Cardiothoracic Surgery, Graduate School of Medicine,
303) Persistent Spontaneous Pneumothorax for Four Years: A Case Report Mizuno Y., Iwata H., Shirahashi K., Matsui M., Takemura H. Department of General and Cardiothoracic Surgery, Graduate School of Medicine,
Comment / Changes / Approval. Initial version for consultation
 Document Control Title Pleural Procedures Guidelines Author Respiratory Consultant Directorate Medicine Date Version Issued 0.1 Aug 2011 0.2 Sep 2011 0.3 Sep 2011 0.4 Oct 2011 1.0 Oct 2011 Status Draft
Document Control Title Pleural Procedures Guidelines Author Respiratory Consultant Directorate Medicine Date Version Issued 0.1 Aug 2011 0.2 Sep 2011 0.3 Sep 2011 0.4 Oct 2011 1.0 Oct 2011 Status Draft
Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax
 Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax I. Kalnins, M.B., T. A. Torda, F.F.A.R.C.S,, and J. S. Wright, F.R.A.C.S. ABSTRACT Bilateral pleurodesis by median
Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax I. Kalnins, M.B., T. A. Torda, F.F.A.R.C.S,, and J. S. Wright, F.R.A.C.S. ABSTRACT Bilateral pleurodesis by median
CONTEMPORARY MANAGEMENT OF MALIGNANT PLEURAL EFFFUSION -Shailesh Agrawal 16/3/2018
 CONTEMPORARY MANAGEMENT OF MALIGNANT PLEURAL EFFFUSION -Shailesh Agrawal 16/3/2018 Overview Problem statement Etiology Diagnosis Approach to treatment Treatment modalities Repeated thoracocentesis ICD
CONTEMPORARY MANAGEMENT OF MALIGNANT PLEURAL EFFFUSION -Shailesh Agrawal 16/3/2018 Overview Problem statement Etiology Diagnosis Approach to treatment Treatment modalities Repeated thoracocentesis ICD
Pleural fluid analysis
 Pleural fluid analysis Dr Akash Verma Senior Consultant- Department of Respiratory and Critical Care Medicine Tan Tock Seng Hospital, Singapore 308433 Adj A/Professor- Lee Kong Chian School of Medicine
Pleural fluid analysis Dr Akash Verma Senior Consultant- Department of Respiratory and Critical Care Medicine Tan Tock Seng Hospital, Singapore 308433 Adj A/Professor- Lee Kong Chian School of Medicine
Clinical predictors of successful and earlier pleurodesis with a tunnelled pleural catheter in malignant pleural effusion: a cohort study
 Clinical predictors of successful and earlier pleurodesis with a tunnelled pleural catheter in malignant pleural effusion: a cohort study OPEN Pen Li MD, Alison Graver MD, Sarah Hosseini MD, Sunita Mulpuru
Clinical predictors of successful and earlier pleurodesis with a tunnelled pleural catheter in malignant pleural effusion: a cohort study OPEN Pen Li MD, Alison Graver MD, Sarah Hosseini MD, Sunita Mulpuru
EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC CHANGES
 Trakia Journal of Sciences, Vol. 3, No. 2, pp 61-65, 2005 Copyright 2005 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC
Trakia Journal of Sciences, Vol. 3, No. 2, pp 61-65, 2005 Copyright 2005 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution EXPERIMENTAL PLEURAL EMPYEMA PATHOLOGIC
BGS Autumn The wet lung - Pleural effusions. Nick Maskell. BGS Autumn Meeting November 2017
 The wet lung - Pleural effusions BGS Autumn Meeting November 2017 Nick Maskell Professor of Respiratory Medicine Bristol University, Bristol Conflicts of interest Prof Maskell has sat on advisory boards
The wet lung - Pleural effusions BGS Autumn Meeting November 2017 Nick Maskell Professor of Respiratory Medicine Bristol University, Bristol Conflicts of interest Prof Maskell has sat on advisory boards
(SKILLS/HANDS-ON) Chest Tubes. Rebecca Carman, MSN, ACNP-BC. Amanda Shumway, PA-C. Thomas W. White, MD, FACS, CNSC
 (SKILLS/HANDS-ON) Chest Tubes Rebecca Carman, MSN, ACNP-BC Nurse Practitioner, Trauma Services, Intermountain Medical Center, Intermountain Healthcare Amanda Shumway, PA-C APC Trauma and Critical Care
(SKILLS/HANDS-ON) Chest Tubes Rebecca Carman, MSN, ACNP-BC Nurse Practitioner, Trauma Services, Intermountain Medical Center, Intermountain Healthcare Amanda Shumway, PA-C APC Trauma and Critical Care
Spontaneous pneumothorax
 Follow the link from the online version of this article to obtain certified continuing medical education credits Spontaneous pneumothorax Oliver Bintcliffe, Nick Maskell Academic Respiratory Unit, School
Follow the link from the online version of this article to obtain certified continuing medical education credits Spontaneous pneumothorax Oliver Bintcliffe, Nick Maskell Academic Respiratory Unit, School
Surgical pleurodesis for Vanderschueren s stage III primary spontaneous pneumothorax
 Eur Respir J 2008; 31: 837 841 DOI: 10.1183/09031936.00140806 CopyrightßERS Journals Ltd 2008 Surgical pleurodesis for Vanderschueren s stage III primary spontaneous pneumothorax O. Rena*, F. Massera #,
Eur Respir J 2008; 31: 837 841 DOI: 10.1183/09031936.00140806 CopyrightßERS Journals Ltd 2008 Surgical pleurodesis for Vanderschueren s stage III primary spontaneous pneumothorax O. Rena*, F. Massera #,
Endoscopy. Pulmonary Endoscopy
 Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
SURGERY FOR GIANT BULLOUS EMPHYSEMA
 SURGERY FOR GIANT BULLOUS EMPHYSEMA Dr. Carmine Simone Head, Division of Critical Care & Thoracic Surgeon Department of Surgery December 15, 2006 OVERVIEW Introduction Classification Patient selection
SURGERY FOR GIANT BULLOUS EMPHYSEMA Dr. Carmine Simone Head, Division of Critical Care & Thoracic Surgeon Department of Surgery December 15, 2006 OVERVIEW Introduction Classification Patient selection
Lung biopsy (mucosal/transbronchial/open lung)
 Lung biopsy (mucosal/transbronchial/open lung) Ernst Eber, MD Respiratory and Allergic Disease Division, Paediatric Department, Medical University of Graz, Austria ERS Task Force. Eur Respir J 2003;22:698-708.
Lung biopsy (mucosal/transbronchial/open lung) Ernst Eber, MD Respiratory and Allergic Disease Division, Paediatric Department, Medical University of Graz, Austria ERS Task Force. Eur Respir J 2003;22:698-708.
