Clinical Study Safety and Complications of Medical Thoracoscopy
|
|
|
- Amos Simon
- 5 years ago
- Views:
Transcription
1 Advances in Medicine Volume 2016, Article ID , 6 pages Clinical Study Safety and Complications of Medical Thoracoscopy Shimaa Nour Moursi Ahmed, 1,2 Hideo Saka, 1 Hamdy Ali Mohammadien, 2 Ola Alkady, 2 Masahide Oki, 1 Yoshimasa Tanikawa, 3 Rie Tsuboi, 1 Masahiro Aoyama, 3 and Keiji Sugiyama 1 1 Department of Respiratory Medicine, National Hospital Organization Nagoya Medical Center, Nagoya, Aichi , Japan 2 Department of Respiratory Medicine, Sohag University Hospital, Nasr City Street, Sohag 82524, Egypt 3 Department of Respiratory Medicine and Clinical Immunology, Toyota Kosei Hospital, Ibohara Josuicho, Toyota-Shi , Japan Correspondence should be addressed to Hideo Saka; saka@med.nagoya-u.ac.jp Received 3 May 2016; Revised 1 June 2016; Accepted 2 June 2016 Academic Editor: Isamu Sugawara Copyright 2016 Shimaa Nour Moursi Ahmed et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Objectives.To highlight the possible complications of medical thoracoscopy (MT) and how to avoid them. Methods. Aretrospective and prospective analysis of 127 patients undergoing MT in Nagoya Medical Center (NMC) and Toyota Kosei Hospital. The data about complications was obtained from the patients, notes on the computer system, and radiographs. Results. The median age was 71.0 (range, ) years and 101 (79.5%) were males. The median time with chest drain after procedure was 7.0 (range, ) days and cases with talc poudrage were 30 (23.6%). Malignant histology was reported in 69 (54.3%), including primary lung cancer in 35 (27.5), mesothelioma in 18 (14.2), and metastasis in 16 (12.6). 58 (45.7%) revealed benign pleural diseases and TB was diagnosed in 15 (11.8%). 21 (16.5%) patients suffered from complications including lung laceration in 3 (2.4%), fever in 5 (3.9%) (due to hospital acquired infection (HAI) in 2, talc poudrage in 2, and malignancy in 1), HAI in 2 (1.6%), prolonged air-leak in 14 (11.0%), and subcutaneous emphysema in 1 (0.8%). Conclusions. MT is generally a safe procedure. Lung laceration is the most serious complication and should be managed well. HAI is of low risk and can be controlled by medical treatment. 1. Introduction MT is used increasingly by chest physicians and has become, after bronchoscopy, the second most important endoscopic technique in respiratory medicine [1]. It is considered to be oneofthemainareasofinterventionalpulmonologyandan important part of a specialist pleural disease service [2, 3]. Thoracoscopy is the oldest invasive interventional technique in the recent history of respiratory medicine. It was initially performed in 1910 by an internist from Sweden, Hans- Christian Jacobaeus. Jacobaeus was the first to use the term thoracoscopy that he described as replacing fluid with air in order to examine the pleural surfaces of two patients with tuberculous pleurisy. Jacobaeus later developed a therapeutic application for thoracoscopy by using thermocautery to lyse adhesions and create a pneumothorax to treat tuberculosis (Jacobaeus operation) [4]. At the end of the 1990s, semirigid (or flex-rigid) thoracoscope was successfully introduced as a new instrument for thoracoscopy [5]. Pulmonologists who used to work with a flexible bronchoscope found it more familiar. It allows easy lateral vision or even retro visualization of the point of entry, but its main limitations are small biopsies taken through the smallworkingchannelandthedifficultytolysetheadhesions [6]. The application of MT is mainly for diagnosing pleural effusion and for performing talc poudrage pleurodesis in malignant pleural effusion and recurrent spontaneous pneumothorax [7]. For the diagnosis of malignant pleural disease, MT has consistently been demonstrated to be superior to fluid cytology and blind closed needle biopsy [8 10] with a sensitivity of up to 95% [11]. A recent study comparing MT with CT-guided Abrams needle biopsy demonstrated no significant difference with the two techniques, although
2 2 Advances in Medicine the advantage of thoracoscopy remains that pleurodesis can be performed after pleural fluid removal during the procedure [12]. It also plays a crucial role in staging non-small-cell lung cancer and guiding treatment and prognosis, as the documentation of pleural metastasis renders the patient inoperable (stage M1a) [13]. It can be useful as well to provide large biopsies required for the application of molecular techniques, such as the use of molecular markers, for example, epidermal growth factor receptor; these markers participate in the modern staging of malignant diseases and provide possibilities for potential therapies [14]. Other nonroutine and more complex applications of MT are in the treatment of empyema, in lung biopsy with forceps, and in cervical sympathectomy; these procedures are considered advanced, need more experience, and should definitely be performed by experts and highly trained thoracoscopists [15]. MT in the hands of experienced physicians is safe with mortality of 0.35% (95% confidence interval (CI) %) and likely to be less if diagnostic procedures alone are performed [16]. This compares favorably with mortality from transbronchial biopsy ( %) [17] and mediastinoscopy (0.17%) [18]. Pain is frequently reported after the procedure and may be more common when using talc poudrage for pneumothorax when compared with malignant effusion [19]. There has been previous concern with respect to the development of acute respiratory distress syndrome (ARDS) following talc poudrage, [20] which was likely to be from the grade of talc utilized [21]. Major complications (empyema, hemorrhage, port site tumor growth, bronchopleural fistula and/or persistent air leak, postoperative pneumothorax, and pneumonia)occurin1.8%(95%ci %)andminorcomplications (subcutaneous emphysema, minor hemorrhage, operative skin site infection, fever, and atrial fibrillation) occur in 7.3% (95% CI %) [16]. TheaimofthisstudyistoevaluatethesafetyofMTand the possible complications that can occur during and after the procedure. 2. Materials and Methods 2.1. Patients. We performed a retrospective and prospective analysis of 127 patients undergoing MT for diagnostic and therapeutic purposes in NMC during the period of 2007 to 2015andToyotaKoseiHospitalduringtheperiodof2011to The retrospective analysis included patients during the period of 2007 to 2013 in NMC and during the period of 2011 to 2013 in Toyota Kosei Hospital and prospective analysis included the patients during 2014 and 2015 for both. During the period of our study, the total number of patients was 139 but we excluded 10 patients due to defective data required for analysis and the other 2 patients were excluded due to failure to complete MT. The patients data was obtained from the hospital computerized system. The case notes were examined for any report of complications and radiographs were examined for outcome. The histology and relevant microbiology reports were obtained from the laboratory computerized system MT and Chest Tube Management. MT was performed by experienced physicians using The Olympus semirigid LTF- 260 thoracoscopy. The patients were in the lateral position with local anesthesia and conscious sedation using midazolam and fentanyl in NMC and only local anesthesia in Toyota Kosei Hospital, with ECG and pulse oximetry monitoring throughout. About 5 to 10 biopsies were taken from the parietal pleura depending on the macroscopic findings and 4 g of graded talc (Steritalc, Novatech, La Ciotat, France) poudrage was used during pleurodesis. All patients had 16 F chest drains after the procedurethroughthesameentryportasthethoracoscopy. Intercostal drains were connected to an underwater seal and negative suction ( 10 to 20 cm/h 2 O) was used till the drainedfluidbecomeslessthan150ml/day Prethoracoscopic Investigations. All patients were subjected to pleural fluid analysis, chest X-ray, chest CT, chest ultrasonography (US), ECG, and routine liver and kidney functions Thoracoscopic Technique Premedication. Midazolam 0.4 mg together with fentanyl 0.2 mg was administered to the patients just before the procedure through intravenous line and sometimes during the procedure if it lasted for long time. Oxygen via nasal cannula was administered during the entire procedure to maintain SpO 2 >90%. After premedication, the combined scope and forceps were inserted, under local anesthesia, through a trocar with an outer diameter of 10 mm and without valve, in an intercostal space, with the patient resting on the healthy side. A sterile catheter was introduced through the trocar and the residual effusion was taken under sterile conditions. After the pleural cavity had been emptied, the lung and pleura were examined by way of the thoracoscope and any abnormality like adhesions, fibrin deposition, discoloration of the pleura, hyperemia, tuberculous nodules, formation of tumors, and so forth was observed. Whenever feasible, biopsies were taken, placed immediately in formalin, and sent for microscopic examination. About 5 to 10 biopsies were taken from each patient from the parietal pleura depending on the macroscopic findings Statistical Analysis. Statistical analyses were processed by statistical software program (PASW Statistics 16; SPSS Inc., Chicago, IL, USA). Data were statistically described in terms of frequencies (number of cases), percentages, median, and rangewhenappropriate. 3. Results Thetotalnumberofcaseswas127withmedianageof71.0 (range, ) years and 101 (79.5%) were males; as regards smoking, 36 (28.3%) cases were current smokers. The median duration of drainage by intercostal tube after MT was 7.0 (range, ) days and cases of talc poudrage
3 Advances in Medicine 3 Table 1: Characteristics of patients undergoing medical thoracoscopy. The total Characteristics number of patients 127 Age, median (range), year 71.0 ( ) Sex, no. (%) Male 101 (79.5) Female 26 (20.5) Smoking status, number (%) Nonsmoker 44 (34.6) Smoker 36 (28.3) Ex-smoker 47 (37) The affected side, number (%) Right 69 (54.3) Left 55 (43.3) Bilateral 3 (2.4) Nature of pleural fluid analysis, number (%) Exudate 124 (97.6) Transudate 3 (2.3) Duration of ICT drainage, median (range), days 7.0 ( ) Talc poudrage, number (%) 30 (23.6) ICT: intercostals tube. NB: 10 of the cases of exudate were purulent and one was hemorrhagic fluid. Table 2: Diagnostic outcome of medical thoracoscopy in 127 patients. Malignant (n =69;54.3%of Primary lung cancer 35 (27.5% of Metastasis to pleura 16 (12.6% of Mesothelioma 18 (14.2% of Benign (n =58; 45.7% of Nonspecific pleuritis 27 (21.3% of Tuberculosis 15 (11.8% of Empyema 10 (7.9% of Hypoalbuminemia 2 (1.6% of Uremic pleuritis 2 (1.6% of Drug induced pleuritis 1 (0.9% of Ruptured bulla 1 (0.9% of NB: Cases of empyema were diagnosed before doing MT; they were not postprocedure complications. were 30 (23.6%). The details of patients characteristics are shown in Table 1. Benign pleural disease was diagnosed in 58 (45.7%), including tuberculosis in 15 (11.8%), empyema in 10 (7.9%), the nonspecific pleuritis in 27 (21.3%), hypoalbuminemia in 2 (1.6%), uremic pleuritis in 2 (1.6%), drug induced pleuritis in1(0.9%),andrupturedbullain1(0.9%of.thedetails are shown in Table 2. Malignant histology was reported in 69 (54.3%) including primary lung cancer in 35 (27.5%), metastasis in 16 (12.6%), Table 3: The secondary pleural cancers, differentiation, and origins. (a) Differentiation of the primary lung cancers (n =35) Type Number (%) of lung cancer Adenocarcinoma 29 (82.9) Squamous cell carcinoma 4 (11.4) Small-cell lung cancer 2 (5.7) (b) Primary origin of the metastases (n =16) Type Number (%) of metastases Lymphoma 4 (25) Kidney 2 (12.5) Prostate 2 (12.5) Ovary 2 (12.5) Pancreas 2 (12.5) Pharynx 1 (6.3) Colon 1 (6.3) Bladder 1 (6.3) Thymus 1 (6.3) Table 4: Thoracoscopic complications. Total number of patients 127, patients with complications 21 (16.5%) Type N (%) of total Lung laceration 3 (2.4) Fever 5 (3.9) HAI 2 (1.6) Prolonged air leak 14 (11.0) Subcutaneous emphysema 1 (0.8) Bleeding 0 ARDS 0 Mortality due to procedure 0 HAI, hospital acquired infection; ARDS, acute respiratory distress syndrome. and mesothelioma in 18 (14.2%). The frequency of different histological types of lung cancer was adenocarcinoma in 29 (82.9%), squamous-cell carcinoma in 4 (11.4%), and smallcellcarcinomain2(5.7%).themostcommonsourceof metastasis was lymphoma in 4 (25%). The details are shown in Tables 2 and 3. No mortality was related to the procedure of MT. No major bleeding from the biopsy sites or hemoptysis was observed. Complications occurred in 21 (16.5%) cases including lung lacerations in 3 (2.4%), fever in 5 (3.9%) (due to HAI in 2, talc poudrage in 2, and malignancy in 1), HAI in 2 (1.6%), prolonged air leak in 14 (11.0%), and subcutaneous emphysema in 1 (0.8%). The details are shown in Table 4. MT failed in two cases: the first case was due to extensive adhesions which rendered introducing the MT and the second one was a case of left primary spontaneous haemopneumothorax due to continuous bleeding from the ruptured emphysematous bulla.
4 4 Advances in Medicine Figure 1: Lung laceration in one of the patients following introducing the trocar. 4. Discussion Although this study was done on a large number of patients (127), the rate of complications was not so severe 16.5% (n = 21). The most serious complication was lung laceration which occurred in 3 cases, all of them occurred during introducing the trocar and did not exceed 1.5 cm in length as illustrated in Figure 1. Two of them were managed during performing MT by calling the cardiothoracic surgeon and the application of polyglycolic acid (PGA) mesh and fibrin glue over the site of the laceration under local anesthesia without any complications during and after the procedure but the third case was neglected during the procedure and that resulted in air leak and subcutaneous emphysema after procedure which increased and indicated urgent surgical intervention to close the laceration. To prevent the occurrence of lung laceration, some authors advocate the creation of pneumothorax a few hours or even the day before the thoracoscopy. However, direct introduction of a blunt trocar into the thoracic wall without prior induction of pneumothorax is safe and effective, especiallyifthereisenoughpleuralfluid.thetrocarshouldalways be inserted perpendicular to the chest wall with a rotating motion. It is safer to locate the tip over the border of the inferior rib at the chosen port of entry, in order to prevent damage to the intercostal vessels and nerves. The introduction of the trocar can be troublesome especially in cases of pleural adhesions. When the physician is not sure about the presence of tight adhesions between the lung and the chest wall at the chosen site of entry, a digital dissection and direct exploration of the port of entry with the telescope may be helpful [22]. Chest US can be also very helpful to identify loculations in thepleuralcavityandtolocatethebestentrysiteforthoracoscopy [23]. Actually, US was done before MT in the 3 cases complicated with lung lacerations, pneumothorax was created before introducing MT, and there were no extensive adhesions which may play a role in the occurrence of lung laceration, but the main cause was vigorous maneuver during introducing the trocar. The second and important complication in this study was fever; it occurred in 5 cases due to different causes. Fever was grade 1 in all cases according to Common Terminology Criteria for Adverse Events (CTCAE) version 4.0. Two of them occurred after talc poudrage and lasted only for two days and improved with antipyretics. The third case developed fever due to malignancy; this patient was diagnosed as pleural metastasis from renal cell carcinoma and did not improve with antipyretics or antibiotics. Already the patient presented with fever before performing MT, and it lasted with him until the discharge with exclusion of other causes. The fourth and fifth cases developed HAI in the form of worsening of the already diagnosed empyema after improvement following MT which was done for drainage and adhesiolysis; the fourth patient was of old age (70 years old) with bad general condition and stayed in hospital for one month; he developed fever two days after the procedure and improved after one week with antibiotics. The fifth patient has the same situation like the fourth one (being 76 years old, bad general condition, and long hospital stay for 33 days). He was complicated with septicemia and developed fever three days after the procedure which lasted for 2 days and then the patient died. Prolonged hospital stay with the bad general condition may play important role in the development of HAI. There were 11 cases of death but not related to MT; the main cause was malignancy and the presence of other comorbidities as hepatic and renal diseases. The median time for drainage by intercostal tube after procedure was 7.0 (range, ) days. In this study, long drainage time was due to prolonged air leak and incomplete lung reexpansion especially in neoplastic patients and patients diagnosed as empyema with other comorbidities and bad general condition. Cases complicated with prolonged air leak were 14 (11.0%) including 7 cases with malignancy, 6 cases with empyema, and one case with TB. With respect to developing postprocedure infections, this represents an area that can potentially be modified by improved patient management immediately after the procedure including active chest physiotherapy and early mobilization to reduce basal atelectasis, all practices that can be learnt
5 Advances in Medicine 5 Competing Interests The authors declare no competing interests regarding the publication of this paper. Acknowledgments The authors are grateful to Dr. Akiko Kada, MD, Ph.D., from the clinical research center in NMC for helping them in the statistical analysis of the data. Figure 2: Obliteration of the pleural space due to extensive adhesions and pleural thickening. from our surgical colleagues [23, 24]. The use of a one-off dose of intravenous broad spectrum antibiotic at the time of the procedure may also lead to a reduction of infections following thoracoscopy, although this practice varies among physicians and was not routine practice during the study period. The rates in this study of empyema, pneumonia, and 1-month mortality compare favorably with other large thoracoscopy series [25, 26]. MT failed in two cases: the first case was due to the presence of severe adhesions which rendered introducing MT so we gave up MT for the safety of the patient and thoracotomy was done. Chest US was used to determine the best site for introducing the trocar but the presence of extensive adhesions caused obliteration of the pleural cavity as illustrated in Figure 2. The second was a case of primary left haemopneumothorax due to spontaneous rupture of an emphysematous bulla, which was diagnosed before MT by chest CT. This indicated the presence of large amount of left pleural effusion with a rim of pneumothorax and a large apical emphysematous bulla, and thoracocentesis revealed hemorrhagic pleural effusion. The findings of bloody pleural effusion and normal pleura were observed during the procedure.activebleedingwasnotclearbutover2,000mlofhemorrhagic fluid was drained. A semiurgent video assisted thoracoscopic surgery (VATS) was indicated after the procedure, which was done on the next day for resection of the bulla. 5. Conclusions In conclusion, medical thoracoscopy is generally a safe procedure. Lung laceration is the most serious complication andshouldbemanagedwell.haiisoflowriskandcanbe controlled by medical treatment. Abbreviations MT: Medical thoracoscopy HAI: Hospital acquired infection ARDS: Acute respiratory distress syndrome US: Ultrasonography. References [1] R. Loddenkemper, P. N. Mathur, M. Noppen et al., Medical Thoracoscopy/Pleuroscopy. Manual and Atlas, Thieme, Stuttgart, Germany, [2] L. M. Seijo and D. H. Sterman, Interventional pulmonology, New England Medicine,vol.344,no.10,pp , [3]C.E.Hooper,Y.C.G.Lee,andN.A.Maskell, Settingupa specialist pleural disease service, Respirology, vol.15,no.7,pp , [4] H. C. Jacobaeus, The cauterization of adhesions in artificial pneumothorax treatment of pulmonary tuberculosis under thoracoscopic control, Proceedings of the Royal Society of Medicine, vol. 16, pp , [5] A.N.McLean,S.R.Bicknell,L.G.McAlpine,andA.J.Peacock, Investigation of pleural effusion: an evaluation of the new Olympus LTF semiflexible thoracofiberscope and comparison with Abram s needle biopsy, Chest, vol.114,no.1,pp , [6] P. Lee and H. G. Colt, Rigid and semirigid pleuroscopy: the future is bright, Respirology, vol. 10, no. 4, pp , [7] J.-M. Tschopp, R. Rami-Porta, M. Noppen, and P. Astoul, Management of spontaneous pneumothorax: stae of the art, European Respiratory Journal,vol.28,no.3,pp ,2006. [8] R. Loddenkemper and C. Boutin, Thoracoscopy: present diagnostic and therapeutic indications, European Respiratory Journal,vol.6,no.10,pp ,1993. [9] C. Boutin, J. R. Viallat, P. Cargnino, and P. Farisse, Thoracoscopy in malignant pleural effusions, American Review of Respiratory Disease,vol.124,no.5,pp ,1981. [10] R. Menzies and M. Charbonneau, Thoracoscopy for the diagnosis of pleural disease, Annals of Internal Medicine, vol. 114, no. 4, pp , [11] H. E. Davies, J. E. Nicholson, N. M. Rahman, E. M. Wilkinson, R. J. O. Davies, and Y. C. G. Lee, Outcome of patients with nonspecific pleuritis/fibrosis on thoracoscopic pleural biopsies, European Cardio-Thoracic Surgery, vol.38,no.4,pp , [12] M. Metintas, G. Ak, E. Dundar et al., Medical thoracoscopy vs CT scan-guided abrams pleural needle biopsy for diagnosis of patients with pleural effusions: a randomized, controlled trial, Chest,vol.137,no.6,pp ,2010. [13] M. E. Froudarakis, Diagnosis and management of pleural effusion in lung cancer, in Pleural Diseases, D. Bouros, Ed., pp , Informa, New York, NY, USA, 2nd edition, [14] M. E. Froudarakis, Thoracoscopy one century later: the oldest interventional technique of modern pneumonology, with great future prospects, Pneumon,vol.23,no.1,pp.28 33,2010.
6 6 Advances in Medicine [15]G.F.Tassi,R.J.O.Davies,andM.Noppen, Advancedtechniques in medical thoracoscopy, European Respiratory Journal, vol. 28, pp. 1 9, [16] N. M. Rahman, N. J. Ali, G. Brown et al., Local anaesthetic thoracoscopy: British Thoracic Society pleural disease guideline 2010, Thorax, vol. 65, supplement 2, pp. ii54 ii60, [17] D. C. Zavala, Pulmonary hemorrhage in fiberoptic transbronchial biopsy, Chest, vol. 70, no. 5, pp , [18] C. P. Wall, E. A. Gaensler, C. B. Carrington, and J. A. Hayes, Comparison of transbronchial and open biopsies in chronic infiltrative lung diseases, American Review of Respiratory Disease,vol.123,no.3,pp ,1981. [19]J.-R.Viallat,F.Rey,P.Astoul,andC.Boutin, Thoracoscopic talc poudrage pleurodesis for malignant effusions: a review of 360 cases, Chest,vol.110,no.6,pp ,1996. [20] D. H. Rehse, R. W. Aye, and M. G. Florence, Respiratory failure following talc pleurodesis, American Surgery,vol.177, no. 5, pp , [21] M. Noppen, Who s (still) afraid of talc? European Respiratory Journal,vol.29,no.4,pp ,2007. [22] F. Rodríguez-Panadero and B. R. Romero, Complications of thoracoscopy, in Thoracoscopy for Pulmonologists: A Didactic Approach, P. Astoul, G. Tassi, and J.-M. Tschopp, Eds., pp , Springer, Berlin, Germany, [23] A. R. L. Medford, Additional cost benefits of chest physicianoperated thoracic ultrasound (TUS) prior to medical thoracoscopy (MT), Respiratory Medicine, vol.104,no.7,pp , [24] J. A. Brooks-Brunn, Postoperative atelectasis and pneumonia: risk factors, AmericanJournalofCriticalCare,vol.4,no.5,pp , [25] J. A. Brooks-Brunn, Postoperative atelectasis and pneumonia, Heart and Lung,vol.24,no.2,pp ,1995. [26] K. Viskum and B. Enk, Complications of thoracoscopy, Poumon et le Coeur,vol.37,no.1,pp.25 28,1981.
7 MEDIATORS of INFLAMMATION The Scientific World Journal Gastroenterology Research and Practice Diabetes Research International Endocrinology Immunology Research Disease Markers Submit your manuscripts at BioMed Research International PPAR Research Obesity Ophthalmology Evidence-Based Complementary and Alternative Medicine Stem Cells International Oncology Parkinson s Disease Computational and Mathematical Methods in Medicine AIDS Behavioural Neurology Research and Treatment Oxidative Medicine and Cellular Longevity
The Portsmouth thoracoscopy experience, an evaluation of service by retrospective case note analysis
 Respiratory Medicine (2007) 101, 1021 1025 The Portsmouth thoracoscopy experience, an evaluation of service by retrospective case note analysis Sophie V. Fletcher,1, Robin J. Clark Respiratory Centre,
Respiratory Medicine (2007) 101, 1021 1025 The Portsmouth thoracoscopy experience, an evaluation of service by retrospective case note analysis Sophie V. Fletcher,1, Robin J. Clark Respiratory Centre,
Medical Thoracoscopy When to Choose Over a General Anaesthetic VATS
 Medical Thoracoscopy When to Choose Over a General Anaesthetic VATS SpR Training Day 07.07.14 Dr Alex West Consultant Chest/Pleural Physician Guy s and St Thomas Hospital Medical Thoracoscopy? No Just
Medical Thoracoscopy When to Choose Over a General Anaesthetic VATS SpR Training Day 07.07.14 Dr Alex West Consultant Chest/Pleural Physician Guy s and St Thomas Hospital Medical Thoracoscopy? No Just
Chapter 8. Other Important Tests and Procedures. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 8 Other Important Tests and Procedures 1 Introduction Additional important diagnostic studies include: Sputum examination Skin tests Endoscopic examination Lung biopsy Thoracentesis Hematology,
Chapter 8 Other Important Tests and Procedures 1 Introduction Additional important diagnostic studies include: Sputum examination Skin tests Endoscopic examination Lung biopsy Thoracentesis Hematology,
PAKISTAN JOURNAL OF CHEST MEDICINE. Volume 18, No 1, January-March REVIEW ARTICLE MEDICAL PLEUROSCOPY
 82 REVIEW ARTICLE MEDICAL PLEUROSCOPY Pyng Lee MD,* Henri G Colt,**Ali I. Musani MD*** ABSTRACT Pleuroscopy or medical thoracoscopy are terms used interchangeably to describe a minimally invasive procedure
82 REVIEW ARTICLE MEDICAL PLEUROSCOPY Pyng Lee MD,* Henri G Colt,**Ali I. Musani MD*** ABSTRACT Pleuroscopy or medical thoracoscopy are terms used interchangeably to describe a minimally invasive procedure
WHAT WE NEED FOR THORACOSCOPY
 WHAT WE NEED FOR THORACOSCOPY Medical School Marios Froudarakis, MD Department of Pneumonology University Hospital of Alexandroupolis mfroud@med.duth.gr Democritus University of Thrace Dedicated Course
WHAT WE NEED FOR THORACOSCOPY Medical School Marios Froudarakis, MD Department of Pneumonology University Hospital of Alexandroupolis mfroud@med.duth.gr Democritus University of Thrace Dedicated Course
Clinical Study The Incidence and Management of Pleural Injuries Occurring during Open Nephrectomy
 Advances in Urology Volume 2009, Article ID 948906, 4 pages doi:10.1155/2009/948906 Clinical Study The Incidence and Management of Pleural Injuries Occurring during Open Nephrectomy Ali Fuat Atmaca, Abdullah
Advances in Urology Volume 2009, Article ID 948906, 4 pages doi:10.1155/2009/948906 Clinical Study The Incidence and Management of Pleural Injuries Occurring during Open Nephrectomy Ali Fuat Atmaca, Abdullah
Malignant Effusions. Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital
 Malignant Effusions Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital Malignant Effusions Definition: Presence of malignant cells in the pleural space 75% are caused by
Malignant Effusions Anantham Devanand Respiratory and Critical Care Medicine Singapore General Hospital Malignant Effusions Definition: Presence of malignant cells in the pleural space 75% are caused by
Correspondence should be addressed to Haris Kalatoudis;
 Hindawi Case Reports in Critical Care Volume 2017, Article ID 3092457, 4 pages https://doi.org/10.1155/2017/3092457 Case Report Bronchopleural Fistula Resolution with Endobronchial Valve Placement and
Hindawi Case Reports in Critical Care Volume 2017, Article ID 3092457, 4 pages https://doi.org/10.1155/2017/3092457 Case Report Bronchopleural Fistula Resolution with Endobronchial Valve Placement and
Bronchogenic Carcinoma
 A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
A 55-year-old construction worker has smoked 2 packs of ciggarettes daily for the past 25 years. He notes swelling in his upper extremity & face, along with dilated veins in this region. What is the most
Diagnostic Utility of Indigenous Technique of Pleuroscopy in Undiagnosed Cases of Exudative Pleural Effusions
 Journal of Health Science 6 (2018) 304-309 doi: 10.17265/2328-7136/2018.04.009 D DAVID PUBLISHING Diagnostic Utility of Indigenous Technique of Pleuroscopy in Undiagnosed Cases of Exudative Pleural Effusions
Journal of Health Science 6 (2018) 304-309 doi: 10.17265/2328-7136/2018.04.009 D DAVID PUBLISHING Diagnostic Utility of Indigenous Technique of Pleuroscopy in Undiagnosed Cases of Exudative Pleural Effusions
Thoracic Surgery; An Overview
 Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Thoracic Surgery What we see Thoracic Surgery; An Overview James P. Locher, Jr, MD Methodist Cardiovascular and Thoracic Surgery Lung cancer Mets Fungus and TB Lung abcess and empyema Pleural based disease
Initial experience of medical pleuroscopy via the peel-away introducer of the indwelling pleural catheter using a thin bronchoscope
 Surgical Technique of Interventional Pulmonology Corner Initial experience of medical pleuroscopy via the peel-away introducer of the indwelling pleural catheter using a thin bronchoscope Kassem Harris
Surgical Technique of Interventional Pulmonology Corner Initial experience of medical pleuroscopy via the peel-away introducer of the indwelling pleural catheter using a thin bronchoscope Kassem Harris
Computer Tomography of the Thorax Selection of
 Diagnostic and Therapeutic Endoscopy, 1995, Vol. 2, pp. 89-92 Reprints available directly from the publisher Photocopying permitted by license only (C) 1995 Harwood Academic Publishers GmbH Printed in
Diagnostic and Therapeutic Endoscopy, 1995, Vol. 2, pp. 89-92 Reprints available directly from the publisher Photocopying permitted by license only (C) 1995 Harwood Academic Publishers GmbH Printed in
APPROACH TO PLEURAL EFFUSIONS. Raed Alalawi, MD, FCCP
 APPROACH TO PLEURAL EFFUSIONS Raed Alalawi, MD, FCCP CASE 65-year-old woman with H/O breast cancer presented with a 1 week H/O progressively worsening exersional dyspnea. Physical exam: Diminished breath
APPROACH TO PLEURAL EFFUSIONS Raed Alalawi, MD, FCCP CASE 65-year-old woman with H/O breast cancer presented with a 1 week H/O progressively worsening exersional dyspnea. Physical exam: Diminished breath
Medical Thoracoscopy: Experiences in Siriraj Hospital
 Medical Thoracoscopy: Experiences in Siriraj Hospital Jamsak Tscheikuna MD* * Division of Respiratory Disease and Tuberculosis, Department of Medicine, Faculty of Medicine, Siriraj Hospital, Mahidol University
Medical Thoracoscopy: Experiences in Siriraj Hospital Jamsak Tscheikuna MD* * Division of Respiratory Disease and Tuberculosis, Department of Medicine, Faculty of Medicine, Siriraj Hospital, Mahidol University
Image: reproduced from Eur Respir Mon 2010; 48: with permission from the publisher.
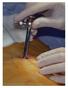 Image: reproduced from Eur Respir Mon 2010; 48: 119 132 with permission from the publisher. R. Loddenkemper 1 P. Lee 2 M. Noppen 3 P.N. Mathur 4 1 German Central Committee against Tuberculosis (DZK), Lungenklinik
Image: reproduced from Eur Respir Mon 2010; 48: 119 132 with permission from the publisher. R. Loddenkemper 1 P. Lee 2 M. Noppen 3 P.N. Mathur 4 1 German Central Committee against Tuberculosis (DZK), Lungenklinik
Adam J. Hansen, MD UHC Thoracic Surgery
 Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Adam J. Hansen, MD UHC Thoracic Surgery Sometimes seen on Chest X-ray (CXR) Common incidental findings on computed tomography (CT) chest and abdomen done for other reasons Most lung cancers discovered
Alper Toker, MD. VATS decortication. Istanbul University, Istanbul Medical School Department of Thoracic Surgery
 VATS decortication Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery Pleural space infection is a common pathology causing morbidity and mortality. It is a collection
VATS decortication Alper Toker, MD Istanbul University, Istanbul Medical School Department of Thoracic Surgery Pleural space infection is a common pathology causing morbidity and mortality. It is a collection
R. F. Falkenstern-Ge, 1 S. Bode-Erdmann, 2 G. Ott, 2 M. Wohlleber, 1 and M. Kohlhäufl Introduction. 2. Histology
 Case Reports in Oncological Medicine Volume 2013, Article ID 167585, 4 pages http://dx.doi.org/10.1155/2013/167585 Case Report Late Lung Metastasis of a Primary Eccrine Sweat Gland Carcinoma 10 Years after
Case Reports in Oncological Medicine Volume 2013, Article ID 167585, 4 pages http://dx.doi.org/10.1155/2013/167585 Case Report Late Lung Metastasis of a Primary Eccrine Sweat Gland Carcinoma 10 Years after
A randomized trial comparing the diagnostic yield of rigid and semirigid thoracoscopy in undiagnosed pleural effusions
 0 0 0 A randomized trial comparing the diagnostic yield of rigid and semirigid thoracoscopy in undiagnosed pleural effusions [Running title: RISE trial] Sahajal Dhooria Navneet Singh Ashutosh N Aggarwal
0 0 0 A randomized trial comparing the diagnostic yield of rigid and semirigid thoracoscopy in undiagnosed pleural effusions [Running title: RISE trial] Sahajal Dhooria Navneet Singh Ashutosh N Aggarwal
Diagnostic value of medical thoracoscopy for undiagnosed pleural effusions
 4590 Diagnostic value of medical thoracoscopy for undiagnosed pleural effusions RUI LIN CHEN, YONG QING ZHANG, JUN WANG, HUA WU and SHU MEI YANG Department of Respiratory Medicine, Shaanxi Provincial People's
4590 Diagnostic value of medical thoracoscopy for undiagnosed pleural effusions RUI LIN CHEN, YONG QING ZHANG, JUN WANG, HUA WU and SHU MEI YANG Department of Respiratory Medicine, Shaanxi Provincial People's
Pneumothorax. Defined as air in the pleural space which can occur through a number of mechanisms
 Pneumothorax Defined as air in the pleural space which can occur through a number of mechanisms Traumatic pneumothorax Penetrating chest trauma Common secondary to bullet or knife penetration Chest tube
Pneumothorax Defined as air in the pleural space which can occur through a number of mechanisms Traumatic pneumothorax Penetrating chest trauma Common secondary to bullet or knife penetration Chest tube
Procedure: Chest Tube Placement (Tube Thoracostomy)
 Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Procedure: Chest Tube Placement (Tube Thoracostomy) Basic Information: The insertion and placement of a chest tube into the pleural cavity for the purpose of removing air, blood, purulent drainage, or
Pneumothorax Post CT-guided Fine Needle Aspiration Biopsy for Lung Nodules: Our Experience in King Hussein Medical Center
 Pneumothorax Post CT-guided Fine Needle Aspiration Biopsy for Lung Nodules: Our Experience in King Hussein Medical Center Ala Qayet MD*, Laith Obaidat MD**, Mazin Al-Omari MD*, Ashraf Al-Tamimi MD^, Ahmad
Pneumothorax Post CT-guided Fine Needle Aspiration Biopsy for Lung Nodules: Our Experience in King Hussein Medical Center Ala Qayet MD*, Laith Obaidat MD**, Mazin Al-Omari MD*, Ashraf Al-Tamimi MD^, Ahmad
Management of Pleural Effusion
 Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
Management of Pleural Effusion Development of Pleural Effusion pulmonary capillary pressure (CHF) capillary permeability (Pneumonia) intrapleural pressure (atelectasis) plasma oncotic pressure (hypoalbuminemia)
Case Report Complete Obstruction of Endotracheal Tube in an Infant with a Retropharyngeal and Anterior Mediastinal Abscess
 Hindawi Case Reports in Pediatrics Volume 2017, Article ID 1848945, 4 pages https://doi.org/10.1155/2017/1848945 Case Report Complete Obstruction of Endotracheal Tube in an Infant with a Retropharyngeal
Hindawi Case Reports in Pediatrics Volume 2017, Article ID 1848945, 4 pages https://doi.org/10.1155/2017/1848945 Case Report Complete Obstruction of Endotracheal Tube in an Infant with a Retropharyngeal
A Randomized Trial Comparing the Diagnostic Yield of Rigid and Semirigid Thoracoscopy in Undiagnosed Pleural Effusions
 A Randomized Trial Comparing the Diagnostic Yield of Rigid and Semirigid Thoracoscopy in Undiagnosed Pleural Effusions Sahajal Dhooria MD DM, Navneet Singh MD DM, Ashutosh N Aggarwal MD DM, Dheeraj Gupta
A Randomized Trial Comparing the Diagnostic Yield of Rigid and Semirigid Thoracoscopy in Undiagnosed Pleural Effusions Sahajal Dhooria MD DM, Navneet Singh MD DM, Ashutosh N Aggarwal MD DM, Dheeraj Gupta
Thoracoscopic Management of Complicated Parapneumonic Effusions in Young Children. Saeed Al Hindi, MD, CABS, FRCSI*
 Bahrain Medical Bulletin, Vol. 31, No. 4, December 2009 Thoracoscopic Management of Complicated Parapneumonic Effusions in Young Children Saeed Al Hindi, MD, CABS, FRCSI* Objective: To evaluate the role
Bahrain Medical Bulletin, Vol. 31, No. 4, December 2009 Thoracoscopic Management of Complicated Parapneumonic Effusions in Young Children Saeed Al Hindi, MD, CABS, FRCSI* Objective: To evaluate the role
Pneumothorax and Chest Tube Problems
 Pneumothorax and Chest Tube Problems Pneumothorax Definition Air accumulation in the pleural space with secondary lung collapse Sources Visceral pleura Ruptured esophagus Chest wall defect Gas-forming
Pneumothorax and Chest Tube Problems Pneumothorax Definition Air accumulation in the pleural space with secondary lung collapse Sources Visceral pleura Ruptured esophagus Chest wall defect Gas-forming
The diagnosis and management of pneumothorax
 Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Respiratory 131 The diagnosis and management of pneumothorax Pneumothorax is a relatively common presentation in patients under the age of 40 years (approximately, 85% of patients are younger than 40 years).
Case Report PET/CT Imaging in Oncology: Exceptions That Prove the Rule
 Case Reports in Oncological Medicine Volume 2013, Article ID 865032, 4 pages http://dx.doi.org/10.1155/2013/865032 Case Report PET/CT Imaging in Oncology: Exceptions That Prove the Rule M. Casali, 1 A.
Case Reports in Oncological Medicine Volume 2013, Article ID 865032, 4 pages http://dx.doi.org/10.1155/2013/865032 Case Report PET/CT Imaging in Oncology: Exceptions That Prove the Rule M. Casali, 1 A.
Pleural Effusion. Exudative pleural effusion - Involve an increase in capillary permeability and impaired pleural fluid resorption
 Pleural Effusion Definition of pleural effusion Accumulation of fluid between the pleural layers Epidemiology of pleural effusion Estimated prevalence of pleural effusion is 320 cases per 100,000 people
Pleural Effusion Definition of pleural effusion Accumulation of fluid between the pleural layers Epidemiology of pleural effusion Estimated prevalence of pleural effusion is 320 cases per 100,000 people
Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication for Repeat Metastasectomy
 Respiratory Medicine Volume 2015, Article ID 570314, 5 pages http://dx.doi.org/10.1155/2015/570314 Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication
Respiratory Medicine Volume 2015, Article ID 570314, 5 pages http://dx.doi.org/10.1155/2015/570314 Clinical Study Metastasectomy of Pulmonary Metastases from Osteosarcoma: Prognostic Factors and Indication
Lung Surgery: Thoracoscopy
 Lung Surgery: Thoracoscopy A Problem with Your Lungs Your doctor has told you that you need surgery called thoracoscopy for your lung problem. This surgery alone may treat your lung problem. Or you may
Lung Surgery: Thoracoscopy A Problem with Your Lungs Your doctor has told you that you need surgery called thoracoscopy for your lung problem. This surgery alone may treat your lung problem. Or you may
Supplementary Online Content
 Supplementary Online Content Rahman NM, Pepperell J, Rehal S, et al. Effect of opioids vs NSAIDs and larger vs smaller chest tube size on pain control and pleurodesis efficacy among patients with malignant
Supplementary Online Content Rahman NM, Pepperell J, Rehal S, et al. Effect of opioids vs NSAIDs and larger vs smaller chest tube size on pain control and pleurodesis efficacy among patients with malignant
Current Management of Postpneumonectomy Bronchopleural Fistula
 Current Management of Postpneumonectomy Bronchopleural Fistula Shaf Keshavjee MD MSc FRCSC FACS Surgeon-in-Chief, University Health Network James Wallace McCutcheon Chair in Surgery Professor, Division
Current Management of Postpneumonectomy Bronchopleural Fistula Shaf Keshavjee MD MSc FRCSC FACS Surgeon-in-Chief, University Health Network James Wallace McCutcheon Chair in Surgery Professor, Division
CHEST INJURIES. Jacek Piątkowski M.D., Ph. D.
 CHEST INJURIES Jacek Piątkowski M.D., Ph. D. CHEST INJURIES 3-4% of all injuries 8% of patients hospitalized due to injuries 65% of patients who died at the accident place CLASSIFICATION OF THE CHEST INJURIES
CHEST INJURIES Jacek Piątkowski M.D., Ph. D. CHEST INJURIES 3-4% of all injuries 8% of patients hospitalized due to injuries 65% of patients who died at the accident place CLASSIFICATION OF THE CHEST INJURIES
Talc pleurodesis: Comparison of talc slurry instillation with thoracoscopic talc insufflation for malignant pleural effusions
 Journal of BUON 11: 463-467, 2006 2006 Zerbinis Medical Publications. Printed in Greece ORIGINAL ARTICLE Talc pleurodesis: Comparison of talc slurry instillation with thoracoscopic talc insufflation for
Journal of BUON 11: 463-467, 2006 2006 Zerbinis Medical Publications. Printed in Greece ORIGINAL ARTICLE Talc pleurodesis: Comparison of talc slurry instillation with thoracoscopic talc insufflation for
Case Report Internal Jugular Vein Thrombosis in Isolated Tuberculous Cervical Lymphadenopathy
 Volume 2016, Article ID 5184196, 4 pages http://dx.doi.org/10.1155/2016/5184196 Case Report Internal Jugular Vein Thrombosis in Isolated Tuberculous Cervical Lymphadenopathy Sanjay Khaladkar, Avadhesh
Volume 2016, Article ID 5184196, 4 pages http://dx.doi.org/10.1155/2016/5184196 Case Report Internal Jugular Vein Thrombosis in Isolated Tuberculous Cervical Lymphadenopathy Sanjay Khaladkar, Avadhesh
Interventional Pulmonology
 Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
The Role of Thoracoscopy in the Diagnosis of Pleural Effusion of Unknown Origin
 Short Communication J Babol Univ Med Sci Vol 20, Issu 8; Aug 2018. P:31-36 The Role of Thoracoscopy in the Diagnosis of Pleural Effusion of Unknown Origin R. Mahmodlou (MD) 1, J. Sarbazzadeh (MD) 1, S.A.
Short Communication J Babol Univ Med Sci Vol 20, Issu 8; Aug 2018. P:31-36 The Role of Thoracoscopy in the Diagnosis of Pleural Effusion of Unknown Origin R. Mahmodlou (MD) 1, J. Sarbazzadeh (MD) 1, S.A.
Persistent Spontaneous Pneumothorax for Four Years: A Case Report
 303) Persistent Spontaneous Pneumothorax for Four Years: A Case Report Mizuno Y., Iwata H., Shirahashi K., Matsui M., Takemura H. Department of General and Cardiothoracic Surgery, Graduate School of Medicine,
303) Persistent Spontaneous Pneumothorax for Four Years: A Case Report Mizuno Y., Iwata H., Shirahashi K., Matsui M., Takemura H. Department of General and Cardiothoracic Surgery, Graduate School of Medicine,
How to do it: ultrasoundguided
 How to do it: ultrasoundguided pleural biopsy Background Malignancy is the cause of 40,000 pleural effusions in the UK and 175,000 in the USA [1], with pleural fluid cytology able to diagnose, at best,
How to do it: ultrasoundguided pleural biopsy Background Malignancy is the cause of 40,000 pleural effusions in the UK and 175,000 in the USA [1], with pleural fluid cytology able to diagnose, at best,
Proceedings of the World Small Animal Veterinary Association Sydney, Australia 2007
 Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress THE LAST GASP II: LUNGS AND THORAX David Holt, BVSc, Diplomate ACVS University of Pennsylvania School of Veterinary
Proceedings of the World Small Animal Sydney, Australia 2007 Hosted by: Next WSAVA Congress THE LAST GASP II: LUNGS AND THORAX David Holt, BVSc, Diplomate ACVS University of Pennsylvania School of Veterinary
Medical Thoracoscopy in Pleural Disease: Experience from a One-Center Study
 ORIGINAL ARTICLE https://doi.org/10.4046/trd.2017.80.2.194 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2017;80:194-200 Medical Thoracoscopy in Pleural Disease: Experience from a One-Center
ORIGINAL ARTICLE https://doi.org/10.4046/trd.2017.80.2.194 ISSN: 1738-3536(Print)/2005-6184(Online) Tuberc Respir Dis 2017;80:194-200 Medical Thoracoscopy in Pleural Disease: Experience from a One-Center
Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax
 Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax I. Kalnins, M.B., T. A. Torda, F.F.A.R.C.S,, and J. S. Wright, F.R.A.C.S. ABSTRACT Bilateral pleurodesis by median
Bilateral Simultaneous Pleurodesis by Median Sternotomy for Spontaneous Pneumo thorax I. Kalnins, M.B., T. A. Torda, F.F.A.R.C.S,, and J. S. Wright, F.R.A.C.S. ABSTRACT Bilateral pleurodesis by median
Endoscopy. Pulmonary Endoscopy
 Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
Ultrasound-Guided Medical Thoracoscopy in the Absence of Pleural Effusion
 [ Original Research Pulmonary Procedures ] Ultrasound-Guided Medical Thoracoscopy in the Absence of Pleural Effusion Giampietro Marchetti, MD, FCCP ; Alberto Valsecchi, MD ; Davide Indellicati, MD ; Sabrina
[ Original Research Pulmonary Procedures ] Ultrasound-Guided Medical Thoracoscopy in the Absence of Pleural Effusion Giampietro Marchetti, MD, FCCP ; Alberto Valsecchi, MD ; Davide Indellicati, MD ; Sabrina
Routine chest drainage after patent ductus arteriosis ligation is not necessary
 Original Article Brunei Int Med J. 2010; 6 (3): 126-130 Routine chest drainage after patent ductus arteriosis ligation is not necessary Amy THIEN, Samuel Kai San YAPP, Chee Fui CHONG Department of Surgery,
Original Article Brunei Int Med J. 2010; 6 (3): 126-130 Routine chest drainage after patent ductus arteriosis ligation is not necessary Amy THIEN, Samuel Kai San YAPP, Chee Fui CHONG Department of Surgery,
A Repeat Case of Idiopathic Spontaneous Hemothorax
 Case Report A Repeat Case of Idiopathic Spontaneous Hemothorax Felix R. Gaw, MD Jack H. Bloch, MD, PhD, FACS Nolan J. Anderson, MD, FACS Spontaneous hemothorax, a collection of blood in the pleural cavity
Case Report A Repeat Case of Idiopathic Spontaneous Hemothorax Felix R. Gaw, MD Jack H. Bloch, MD, PhD, FACS Nolan J. Anderson, MD, FACS Spontaneous hemothorax, a collection of blood in the pleural cavity
Case Study #2. Case Study #1 cont 9/28/2011. CAPA 2011 Christy Wilson PA C. LH is 78 yowf with PMHx of metz breast CA presents
 Case Study #1 CAPA 2011 Christy Wilson PA C 46 yo female presents with community acquired PNA (CAP). Her condition worsened and she was transferred to the ICU and placed on mechanical ventilation. Describe
Case Study #1 CAPA 2011 Christy Wilson PA C 46 yo female presents with community acquired PNA (CAP). Her condition worsened and she was transferred to the ICU and placed on mechanical ventilation. Describe
Post-Graduate ERS Seminar on Medical Thoracoscopy. October 13-15, Alexandroupolis, Greece
 Post-Graduate ERS Seminar on Medical Thoracoscopy October 13-15, 2011 - Alexandroupolis, Greece Invited speakers Subjects Robert Loddenkemper, Berlin, Germany YC Gary Lee, Perth Australia Wolfgang Frank,
Post-Graduate ERS Seminar on Medical Thoracoscopy October 13-15, 2011 - Alexandroupolis, Greece Invited speakers Subjects Robert Loddenkemper, Berlin, Germany YC Gary Lee, Perth Australia Wolfgang Frank,
Case Report Two Cases of Small Cell Cancer of the Maxillary Sinus Treated with Cisplatin plus Irinotecan and Radiotherapy
 Case Reports in Otolaryngology Volume 2013, Article ID 893638, 4 pages http://dx.doi.org/10.1155/2013/893638 Case Report Two Cases of Small Cell Cancer of the Maxillary Sinus Treated with Cisplatin plus
Case Reports in Otolaryngology Volume 2013, Article ID 893638, 4 pages http://dx.doi.org/10.1155/2013/893638 Case Report Two Cases of Small Cell Cancer of the Maxillary Sinus Treated with Cisplatin plus
Flex-rigid pleuroscopic biopsy with the SB knife Jr is a novel technique for diagnosis of malignant or benign fibrothorax
 Case Report Flex-rigid pleuroscopic biopsy with the SB knife Jr is a novel technique for diagnosis of malignant or benign fibrothorax Xiao-Bo Wang 1, Yan Yin 1, Yuan Miao 2, Ralf Eberhardt 3, Gang Hou
Case Report Flex-rigid pleuroscopic biopsy with the SB knife Jr is a novel technique for diagnosis of malignant or benign fibrothorax Xiao-Bo Wang 1, Yan Yin 1, Yuan Miao 2, Ralf Eberhardt 3, Gang Hou
Role of medical Thoracoscopy in the Management of Multiloculated Empyema
 Sumalani et al. BMC Pulmonary Medicine (2018) 18:179 https://doi.org/10.1186/s12890-018-0745-y RESEARCH ARTICLE Role of medical Thoracoscopy in the Management of Multiloculated Empyema Kamran Khan Sumalani
Sumalani et al. BMC Pulmonary Medicine (2018) 18:179 https://doi.org/10.1186/s12890-018-0745-y RESEARCH ARTICLE Role of medical Thoracoscopy in the Management of Multiloculated Empyema Kamran Khan Sumalani
Pleural Fluid Analysis: Back to Basics
 Pleural Fluid Analysis: Back to Basics Tonya L. Page, MSN, RN, ACNP-BC Patrick A. Laird, DNP, RN, ACNP-BC 70 y/o female with complaints of shortness of breath and orthopnea for 1 month. Symptoms have worsened
Pleural Fluid Analysis: Back to Basics Tonya L. Page, MSN, RN, ACNP-BC Patrick A. Laird, DNP, RN, ACNP-BC 70 y/o female with complaints of shortness of breath and orthopnea for 1 month. Symptoms have worsened
Case Report Bilateral Distal Femoral Nailing in a Rare Symmetrical Periprosthetic Knee Fracture
 Case Reports in Orthopedics, Article ID 745083, 4 pages http://dx.doi.org/10.1155/2014/745083 Case Report Bilateral Distal Femoral Nailing in a Rare Symmetrical Periprosthetic Knee Fracture Marcos Carvalho,
Case Reports in Orthopedics, Article ID 745083, 4 pages http://dx.doi.org/10.1155/2014/745083 Case Report Bilateral Distal Femoral Nailing in a Rare Symmetrical Periprosthetic Knee Fracture Marcos Carvalho,
Pleural fluid analysis
 Pleural fluid analysis Dr Akash Verma Senior Consultant- Department of Respiratory and Critical Care Medicine Tan Tock Seng Hospital, Singapore 308433 Adj A/Professor- Lee Kong Chian School of Medicine
Pleural fluid analysis Dr Akash Verma Senior Consultant- Department of Respiratory and Critical Care Medicine Tan Tock Seng Hospital, Singapore 308433 Adj A/Professor- Lee Kong Chian School of Medicine
Case Report Renal Cell Carcinoma Metastatic to Thyroid Gland, Presenting Like Anaplastic Carcinoma of Thyroid
 Case Reports in Urology Volume 2013, Article ID 651081, 4 pages http://dx.doi.org/10.1155/2013/651081 Case Report Renal Cell Carcinoma Metastatic to Thyroid Gland, Presenting Like Anaplastic Carcinoma
Case Reports in Urology Volume 2013, Article ID 651081, 4 pages http://dx.doi.org/10.1155/2013/651081 Case Report Renal Cell Carcinoma Metastatic to Thyroid Gland, Presenting Like Anaplastic Carcinoma
Thoracoscopy for Lung Cancer
 Thoracoscopy for Lung Cancer Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your doctor may have recommended an operation to remove your lung cancer. The
Thoracoscopy for Lung Cancer Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your doctor may have recommended an operation to remove your lung cancer. The
Bao-An Gao 1, Gang Zhou 2 *, Li Guan 1, Ling-Yun Zhang 1, Guang-Ming Xiang 1. Introduction
 Original Article Effectiveness and safety of diagnostic flexi-rigid thoracoscopy in differentiating exudative pleural effusion of unknown etiology: a retrospective study of 215 patients Bao-An Gao 1, Gang
Original Article Effectiveness and safety of diagnostic flexi-rigid thoracoscopy in differentiating exudative pleural effusion of unknown etiology: a retrospective study of 215 patients Bao-An Gao 1, Gang
Case Report Formation of a Tunnel under the Major Hepatic Vein Mouths during Removal of IVC Tumor Thrombus
 Case Reports in Urology Volume 2013, Article ID 129632, 4 pages http://dx.doi.org/10.1155/2013/129632 Case Report Formation of a Tunnel under the Major Hepatic Vein Mouths during Removal of IVC Tumor Thrombus
Case Reports in Urology Volume 2013, Article ID 129632, 4 pages http://dx.doi.org/10.1155/2013/129632 Case Report Formation of a Tunnel under the Major Hepatic Vein Mouths during Removal of IVC Tumor Thrombus
Case Report Five-Year Survival after Surgery for Invasive Micropapillary Carcinoma of the Stomach
 Case Reports in Surgery Volume 2013, Article ID 560712, 4 pages http://dx.doi.org/10.1155/2013/560712 Case Report Five-Year Survival after Surgery for Invasive Micropapillary Carcinoma of the Stomach Shigeo
Case Reports in Surgery Volume 2013, Article ID 560712, 4 pages http://dx.doi.org/10.1155/2013/560712 Case Report Five-Year Survival after Surgery for Invasive Micropapillary Carcinoma of the Stomach Shigeo
1. Referral. 2. Clinical Evaluation
 VCAWLAspecialty.com 1. Referral Moose, a 13-year-old Labrador Retriever, first came to the Internal Medicine Department at for evaluation of a 1 month history of progressive hacking/retching, increased
VCAWLAspecialty.com 1. Referral Moose, a 13-year-old Labrador Retriever, first came to the Internal Medicine Department at for evaluation of a 1 month history of progressive hacking/retching, increased
Modern Approaches to Empyema
 Modern Approaches to Empyema Amit Bhargava, MD Attending Thoracic Surgeon Assistant Professor Department of Cardiovascular and Thoracic Surgery 1 Principles of Treatment Adequate drainage Sterilization
Modern Approaches to Empyema Amit Bhargava, MD Attending Thoracic Surgeon Assistant Professor Department of Cardiovascular and Thoracic Surgery 1 Principles of Treatment Adequate drainage Sterilization
Thoracoscopy: medical versus surgical in the management of pleural diseases
 Review Article on Pleural Disease Thoracoscopy: medical versus surgical in the management of pleural diseases Samira Shojaee 1, Hans J. Lee 2 1 Virginia Commonwealth University, Richmond, VA 23219, USA;
Review Article on Pleural Disease Thoracoscopy: medical versus surgical in the management of pleural diseases Samira Shojaee 1, Hans J. Lee 2 1 Virginia Commonwealth University, Richmond, VA 23219, USA;
Thoracoscopy for the Diagnosis of Pleural Disease Richard Menzies, MD, MSc; and Marc Charbonneau, MD
 Thoracoscopy for the Diagnosis of Pleural Disease Richard Menzies, MD, MSc; and Marc Charbonneau, MD Objective: To assess the accuracy and safety of thoracoscopy for the evaluation of pleural disease.
Thoracoscopy for the Diagnosis of Pleural Disease Richard Menzies, MD, MSc; and Marc Charbonneau, MD Objective: To assess the accuracy and safety of thoracoscopy for the evaluation of pleural disease.
Research Article The Cost of Prolonged Hospitalization due to Postthyroidectomy Hypocalcemia: A Case-Control Study
 Advances in Endocrinology, Article ID 954194, 4 pages http://dx.doi.org/10.1155/2014/954194 Research Article The Cost of Prolonged Hospitalization due to Postthyroidectomy Hypocalcemia: A Case-Control
Advances in Endocrinology, Article ID 954194, 4 pages http://dx.doi.org/10.1155/2014/954194 Research Article The Cost of Prolonged Hospitalization due to Postthyroidectomy Hypocalcemia: A Case-Control
Introduction to Interventional Pulmonology
 Introduction to Interventional Pulmonology Alexander Chen, M.D. Director, Interventional Pulmonology Assistant Professor of Medicine and Surgery Divisions of Pulmonary and Critical Care Medicine and Cardiothoracic
Introduction to Interventional Pulmonology Alexander Chen, M.D. Director, Interventional Pulmonology Assistant Professor of Medicine and Surgery Divisions of Pulmonary and Critical Care Medicine and Cardiothoracic
Indwelling Pleural Catheters in Malignant and Non-Malignant Disease
 Indwelling Catheters in Malignant and Non-Malignant Disease 20th Hellenic Conference November 2011 Najib Rahman Clinical Lecturer Oxford Centre for Respiratory Medicine University of Oxford, UK Najib.rahman@ndm.ox.ac.uk
Indwelling Catheters in Malignant and Non-Malignant Disease 20th Hellenic Conference November 2011 Najib Rahman Clinical Lecturer Oxford Centre for Respiratory Medicine University of Oxford, UK Najib.rahman@ndm.ox.ac.uk
Table 2: Outcomes measured. Table 1: Intrapleural alteplase instillation therapy protocol
 ORIGINAL RESEARCH ARTICLE Intrapleural F brinolytic Therapy with Alteplase in Empyema Thoracis in Children conducted in the Department of Pediatric critical care and Pulmonology unit at our institution
ORIGINAL RESEARCH ARTICLE Intrapleural F brinolytic Therapy with Alteplase in Empyema Thoracis in Children conducted in the Department of Pediatric critical care and Pulmonology unit at our institution
Case Report Ruptured Hydatid Cyst with an Unusual Presentation
 Case Reports in Surgery Volume 2011, Article ID 730604, 4 pages doi:10.1155/2011/730604 Case Report Ruptured Hydatid Cyst with an Unusual Presentation Deepak Puri, Amit Kumar Mandal, Harinder Pal Kaur,
Case Reports in Surgery Volume 2011, Article ID 730604, 4 pages doi:10.1155/2011/730604 Case Report Ruptured Hydatid Cyst with an Unusual Presentation Deepak Puri, Amit Kumar Mandal, Harinder Pal Kaur,
Original Research. Mummadi, Srinivas; Pack, Sasheen; Hahn, Peter
 The Official Journal of the International Society of Pleural Diseases Original Research The Use of Bronchoscopic Oxygen Insufflation to Isolate Persistent Air Leaks in Secondary Pneumothorax Due to COPD
The Official Journal of the International Society of Pleural Diseases Original Research The Use of Bronchoscopic Oxygen Insufflation to Isolate Persistent Air Leaks in Secondary Pneumothorax Due to COPD
Video-Mediastinoscopy Thoracoscopy (VATS)
 Surgical techniques Video-Mediastinoscopy Thoracoscopy (VATS) Gunda Leschber Department of Thoracic Surgery ELK Berlin Chest Hospital, Berlin, Germany Teaching Hospital of Charité Universitätsmedizin Berlin
Surgical techniques Video-Mediastinoscopy Thoracoscopy (VATS) Gunda Leschber Department of Thoracic Surgery ELK Berlin Chest Hospital, Berlin, Germany Teaching Hospital of Charité Universitätsmedizin Berlin
Clinically Resectable Lung Tumors
 Diagnostic and Therapeutic Endoscopy, 1996, Vol. 2, pp. 151-155 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam
Diagnostic and Therapeutic Endoscopy, 1996, Vol. 2, pp. 151-155 Reprints available directly from the publisher Photocopying permitted by license only (C) 1996 OPA (Overseas Publishers Association) Amsterdam
Research Article Predictions of the Length of Lumbar Puncture Needles
 Computational and Mathematical Methods in Medicine, Article ID 732694, 5 pages http://dx.doi.org/10.1155/2014/732694 Research Article Predictions of the Length of Lumbar Puncture Needles Hon-Ping Ma, 1,2
Computational and Mathematical Methods in Medicine, Article ID 732694, 5 pages http://dx.doi.org/10.1155/2014/732694 Research Article Predictions of the Length of Lumbar Puncture Needles Hon-Ping Ma, 1,2
Charles Mulligan, MD, FACS, FCCP 26 March 2015
 Charles Mulligan, MD, FACS, FCCP 26 March 2015 Review lung cancer statistics Review the risk factors Discuss presentation and staging Discuss treatment options and outcomes Discuss the status of screening
Charles Mulligan, MD, FACS, FCCP 26 March 2015 Review lung cancer statistics Review the risk factors Discuss presentation and staging Discuss treatment options and outcomes Discuss the status of screening
Case Report Overlap of Acute Cholecystitis with Gallstones and Squamous Cell Carcinoma of the Gallbladder in an Elderly Patient
 Case Reports in Surgery Volume 2015, Article ID 767196, 4 pages http://dx.doi.org/10.1155/2015/767196 Case Report Overlap of Acute Cholecystitis with Gallstones and Squamous Cell Carcinoma of the Gallbladder
Case Reports in Surgery Volume 2015, Article ID 767196, 4 pages http://dx.doi.org/10.1155/2015/767196 Case Report Overlap of Acute Cholecystitis with Gallstones and Squamous Cell Carcinoma of the Gallbladder
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis)
 Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
Lung Cancer Resection
 Lung Cancer Resection Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your health care provider may have recommended an operation to remove your lung cancer.
Lung Cancer Resection Introduction The occurrence of lung cancer has increased dramatically over the last 50 years. Your health care provider may have recommended an operation to remove your lung cancer.
A comparison between two types of indwelling pleural catheters for management of malignant pleural effusions
 Original Article A comparison between two types of indwelling pleural catheters for management of malignant pleural effusions Sushilkumar Satish Gupta 1, Charalampos S. Floudas 2, Abhinav B. Chandra 3
Original Article A comparison between two types of indwelling pleural catheters for management of malignant pleural effusions Sushilkumar Satish Gupta 1, Charalampos S. Floudas 2, Abhinav B. Chandra 3
Pleuroscopy offers physicians a unique opportunity for the
 STATE OF THE ART: CONCISE REVIEW State of the Art: Pleuroscopy Pyng Lee, MD,* and Henri G. Colt, MD, FCCP The terms pleuroscopy, thoracoscopy, medical thoracoscopy, and video-assisted thoracic surgery
STATE OF THE ART: CONCISE REVIEW State of the Art: Pleuroscopy Pyng Lee, MD,* and Henri G. Colt, MD, FCCP The terms pleuroscopy, thoracoscopy, medical thoracoscopy, and video-assisted thoracic surgery
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20,
 Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20, 521-525 Empyema thoracis Original Article Singh DR 1, Joshi MR 2, Thapa P 2, Nath S 3 1 Assistant Professor, 2 Lecturer, 3 Professor,
Kathmandu University Medical Journal (2007), Vol. 5, No. 4, Issue 20, 521-525 Empyema thoracis Original Article Singh DR 1, Joshi MR 2, Thapa P 2, Nath S 3 1 Assistant Professor, 2 Lecturer, 3 Professor,
Medical thoracoscopy for exudative pleural effusion: an eight-year experience from a country with a young population
 Thomas et al. BMC Pulmonary Medicine (2017) 17:151 DOI 10.1186/s12890-017-0499-y RESEARCH ARTICLE Medical thoracoscopy for exudative pleural effusion: an eight-year experience from a country with a young
Thomas et al. BMC Pulmonary Medicine (2017) 17:151 DOI 10.1186/s12890-017-0499-y RESEARCH ARTICLE Medical thoracoscopy for exudative pleural effusion: an eight-year experience from a country with a young
Navigational Bronchoscopy with Transbronchial Radiofrequency Ablation
 Navigational Bronchoscopy with Transbronchial Radiofrequency Ablation Katie S. Nason, MD MPH AATS Focus on Thoracic: Mastering Surgical Innovation October 28, 2017 No disclosures Radiofrequency ablative
Navigational Bronchoscopy with Transbronchial Radiofrequency Ablation Katie S. Nason, MD MPH AATS Focus on Thoracic: Mastering Surgical Innovation October 28, 2017 No disclosures Radiofrequency ablative
Thoracoscopy in the diagnosis of pleural effusion
 Thorax, 1977, 32, 550-554 Thoracoscopy in the diagnosis of pleural effusion A. CANTO, E. BLASCO, M. CASILLAS, A. G. ZARZA. J. PADILLA, J. PASTOR, V. TARAZONA, AND F. PARfS From the Thoracic Surgery Service,
Thorax, 1977, 32, 550-554 Thoracoscopy in the diagnosis of pleural effusion A. CANTO, E. BLASCO, M. CASILLAS, A. G. ZARZA. J. PADILLA, J. PASTOR, V. TARAZONA, AND F. PARfS From the Thoracic Surgery Service,
Diagnostic and Prognostic Implications of Pleural Adhesions in Malignant Effusions
 ORIGINAL ARTICLE Diagnostic and Prognostic Implications of Pleural Adhesions in Malignant Effusions Silvia Bielsa, MD,* José Martín-Juan, MD, José M. Porcel, MD,* and Francisco Rodríguez-Panadero, MD Background
ORIGINAL ARTICLE Diagnostic and Prognostic Implications of Pleural Adhesions in Malignant Effusions Silvia Bielsa, MD,* José Martín-Juan, MD, José M. Porcel, MD,* and Francisco Rodríguez-Panadero, MD Background
THORACIK RICK. Lungs. Outline and objectives Richard A. Malthaner MD MSc FRCSC FACS
 THORACIK RICK Outline and objectives Lungs Management of a solitary lung nodule Mediastinum Management of a mediastinal mass Pleura Management of a pleural fluid & pneumothorax Esophagus & Stomach Management
THORACIK RICK Outline and objectives Lungs Management of a solitary lung nodule Mediastinum Management of a mediastinal mass Pleura Management of a pleural fluid & pneumothorax Esophagus & Stomach Management
Department of Thoracic Surgery, Dr. Carol Davila Central Emergency University Military Hospital Bucharest, Romania b
 Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Minimally Invasive Surgical Treatment of Malignant Pleural Effusions Adrian CIUCHE, MD a ; Claudiu NISTOR, PhD a ; Daniel PANTILE, MR a ; Prof. Teodor
Mædica - a Journal of Clinical Medicine ORIGINAL PAPERS Minimally Invasive Surgical Treatment of Malignant Pleural Effusions Adrian CIUCHE, MD a ; Claudiu NISTOR, PhD a ; Daniel PANTILE, MR a ; Prof. Teodor
Image: reproduced from Eur Respir Mon 2010; 48: with permission from the publisher.
 Image: reproduced from Eur Respir Mon 2010; 48: 119 132 with permission from the publisher. R. Loddenkemper 1 P.N. Mathur 2 P. Lee 3 M. Noppen 4 1 German Central Committee against Tuberculosis (DZK), Lungenklinik
Image: reproduced from Eur Respir Mon 2010; 48: 119 132 with permission from the publisher. R. Loddenkemper 1 P.N. Mathur 2 P. Lee 3 M. Noppen 4 1 German Central Committee against Tuberculosis (DZK), Lungenklinik
The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL
 The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL Conflict of Interest This presentation is supported by AstraZeneca Two main steps before
The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL Conflict of Interest This presentation is supported by AstraZeneca Two main steps before
Research Article Prognostic Factors in Advanced Non-Small-Cell Lung Cancer Patients: Patient Characteristics and Type of Chemotherapy
 SAGE-Hindawi Access to Research Lung Cancer International Volume 2011, Article ID 152125, 4 pages doi:10.4061/2011/152125 Research Article Prognostic Factors in Advanced Non-Small-Cell Lung Cancer Patients:
SAGE-Hindawi Access to Research Lung Cancer International Volume 2011, Article ID 152125, 4 pages doi:10.4061/2011/152125 Research Article Prognostic Factors in Advanced Non-Small-Cell Lung Cancer Patients:
Dr. A.Torossian, M.D., Ph. D. Department of Respiratory Diseases
 Pleural effusions Dr. A.Torossian, M.D., Ph. D. Department of Respiratory Diseases A pleural effusion is an abnormal collection of fluid in the pleural space resulting from excess fluid production or decreased
Pleural effusions Dr. A.Torossian, M.D., Ph. D. Department of Respiratory Diseases A pleural effusion is an abnormal collection of fluid in the pleural space resulting from excess fluid production or decreased
Interventional Pulmonary Case Based Discussions (ATS) Ali Imran Saeed, MD University of New Mexico
 Interventional Pulmonary Case Based Discussions (ATS) Ali Imran Saeed, MD University of New Mexico Objectives Interventional Pulmonary in New Mexico Interventional Pulmonary and Advanced Diagnostic Cases
Interventional Pulmonary Case Based Discussions (ATS) Ali Imran Saeed, MD University of New Mexico Objectives Interventional Pulmonary in New Mexico Interventional Pulmonary and Advanced Diagnostic Cases
UNDERSTANDING SERIES LUNG CANCER BIOPSIES LungCancerAlliance.org
 UNDERSTANDING SERIES LUNG CANCER BIOPSIES 1-800-298-2436 LungCancerAlliance.org CONTENTS What is a Biopsy?...2 Non-Surgical Biopsies...3 Surgical Biopsies...5 Biopsy Risks...6 Biopsy Results...6 Questions
UNDERSTANDING SERIES LUNG CANCER BIOPSIES 1-800-298-2436 LungCancerAlliance.org CONTENTS What is a Biopsy?...2 Non-Surgical Biopsies...3 Surgical Biopsies...5 Biopsy Risks...6 Biopsy Results...6 Questions
Surgical indications: Non-malignant pulmonary diseases. Punnarerk Thongcharoen
 Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
Surgical indications: Non-malignant pulmonary diseases Punnarerk Thongcharoen Non-malignant Malignant as a pathological term: Cancer Non-malignant = not cancer Malignant as an adjective: Disposed to cause
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Eisuke Nomura, Hisatada Hiraoka, and Hiroya Sakai. 1. Introduction. 2. Case Report
 Case Reports in Orthopedics Volume 2016, Article ID 1026861, 5 pages http://dx.doi.org/10.1155/2016/1026861 Case Report Spontaneous Recurrent Hemarthrosis of the Knee: A Report of Two Cases with a Source
Case Reports in Orthopedics Volume 2016, Article ID 1026861, 5 pages http://dx.doi.org/10.1155/2016/1026861 Case Report Spontaneous Recurrent Hemarthrosis of the Knee: A Report of Two Cases with a Source
(SKILLS/HANDS-ON) Chest Tubes. Rebecca Carman, MSN, ACNP-BC. Amanda Shumway, PA-C. Thomas W. White, MD, FACS, CNSC
 (SKILLS/HANDS-ON) Chest Tubes Rebecca Carman, MSN, ACNP-BC Nurse Practitioner, Trauma Services, Intermountain Medical Center, Intermountain Healthcare Amanda Shumway, PA-C APC Trauma and Critical Care
(SKILLS/HANDS-ON) Chest Tubes Rebecca Carman, MSN, ACNP-BC Nurse Practitioner, Trauma Services, Intermountain Medical Center, Intermountain Healthcare Amanda Shumway, PA-C APC Trauma and Critical Care
